Fruit is one of those types of foods that seems to be in constant controversy. You’ll hear some say that fruits have always been good for us and we should eat them often, and you’ll hear others say that they are just sugar-bombs and should be avoided just like soft drinks.
Today we’re going to go through the two big myths surrounding fruit and dig into the science to see what the evidence really says about fruit.
Myth 1: The sugar in fruit leads to weight / fat gain
This myth has been populated by Lustig and co. and the “insulin hypothesis of obesity”. I’m not going to get into the details of the “insulin hypothesis” (that will be for a future blog post), but I will go into some of the broader aspects.
Essentially, this hypothesis states that sugar leads to a rise in insulin, and one of insulin’s main jobs is to store things like sugar into cells, including storing it into fat cells. Moreover, insulin blocks the ability of fat to be released from the fat cell (i.e. lipolysis). According to the hypothesis, this double whammy leads to fat gain from sugar and carbs.
Nice hypothesis, and it seems logical at first glance. Yet this is one of my pet peeves about the nutrition field as a whole: people are talking about hypotheses when they need to be talking about evidence.
Again, I won’t go into all the research surrounding the insulin hypothesis in this post (it would need the space of a small book), but suffice it to say that this nice-sounding theory ends up falling flat on its face. I’ll write more about this in future posts.
For now, let’s talk specifically about fruit.
- Some fruits, mango in this case, have shown to have pretty pronounced anti-obesity effects in rodent studies. (1, 3, 4)
- Multiple types of fruit have been tested in human studies and almost uniformly are shown to have anti-obesity effects. (2, 3, 5, 6, 7)At the very least, they end up having no effect on fat mass.
“The feeding of apples [to] rats (7-10 mg/kg/d) in different forms in 8 experiments have shown that this caused weight loss during 3 to 28 weeks. In agreement with this, the obtained results from 5 experiments on humans have revealed that consumption of the whole apple or apple juice (240-720 mg/d) in 4-12 weeks by fat people can cause weight loss. Experiments on animals and humans have shown that the consumption of apples in different forms can cause weight loss in overweight ones.” (3)
Thus, the data is very clear on this point:
Regardless of what “hypothesis” or “theories” you wish to believe in, the totality of the evidence shows that not only do fruits not cause weight gain, but they tend to have anti-obesity effects.
Now, I’m not telling you to chug down fruit juice all day long either (and whole fruits are much better than juice), but fruits and their juice in moderation is fine and good for you.
And oh, by the way, whole fruit (not fruit juice) is not a high glycemic index (GI) food group. Fruits are actually low to medium on the glycemic index scale and thus safe for diabetics. In fact, many whole fruits have been shown to have an inverse association with Type 2 Diabetes. (17, 18)
Myth 2: The Sugar in Fruit Creates Inflammation
This myth is even worse than the last one. Nothing could be further from the truth.
While it is true that isolated refined sugar can increase inflammatory markers in humans (especially if put in liquids / beverages) (8), this is not the case for natural sugar found in fruits.
This is because the sugar in fruits has a lot of other things that come with it, including phytonutrients, fiber, vitamins, and minerals.
Phytonutrients include polyphenols, anthocyanins, catechins, carotenoids, etc.
Phytonutrients are really the key players that help explain why fruit is good for you. If I had to choose the number one reason why fruit is far healthier than sugar, it would be the phytonutrients.
Phytonutrients directly lower all types of inflammation and largely protect us from various chonic diseases. (9, 10, 11)
There have been three similar eye-opening studies that were performed in 2011, 2015, and 2017 all testing the same question: What happens when you add orange juice to a “junk food” type meal compared to when you add water or, in the 2010 study, a calorie-equivalent sugar drink? (12, 13, 14)
The results were pretty unanimous: adding orange juice to the “junk food” type meal had significantly broad-spectrum anti-inflammatory effects. Many markers of inflammation rose when consuming the “junk food” meal with water or a glucose drink, but these markers stayed much closer to baseline when orange juice was added.
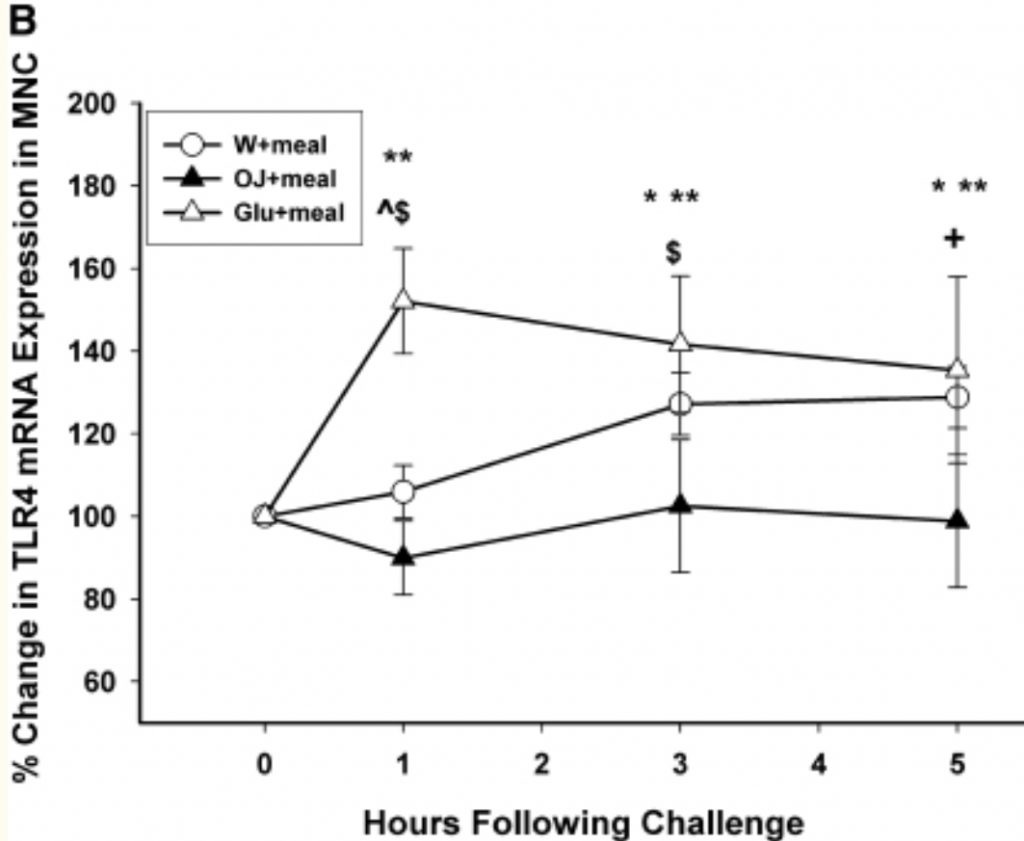
In one study, orange juice blocked the rise in the inflammatory marker IL-17A after the “junk food” meal. (14) This is particularly important because IL-17A is correlated with many types of autoimmune diseases such as Rheumatoid Arthritis and Multiple Sclerosis. (15)
Now, I’m not saying that drinking orange juice with all your meals is going to significantly reduce autoimmune symptoms. What I am saying is that making sure every meal consists of whole foods, including fruits that are loaded with phytonutrients, can significantly lower chronic inflammation and thus contribute to protection from autoimmune symptoms and keep you healthy in general. The researchers chose orange juice in the studies above because of how common orange juice is. Yet, any whole fruit rich in phytonutrients will have similar effects. (16)
We’ll talk more about phytonutrients in future articles.
Well there you have it. Hopefully now I have successfully dissuaded you of any fruit-phobia that you may have had! Fruit is incredibly good for you, and humans have been eating it for a tremendously long time. Now, you don’t have to go crazy and eat ALL THE FRUIT or become a “fruitarian” (that’s not healthy either), but go ahead and include some generous servings of whole fruit in your diet!
Please leave any questions or comments below! And please share this article if you feel that you got value from it!
References
- Lucas, E. A., Li, W., Peterson, S. K., Brown, A., Kuvibidila, S., Perkins-Veazie, P., … Smith, B. J. (2011). Mango modulates body fat and plasma glucose and lipids in mice fed a high-fat diet. British Journal of Nutrition, 106(10), 1495–1505. https://doi.org/10.1017/s0007114511002066
- Evans SF, Meister M, Mahmood M, et al. Mango supplementation improves blood glucose in obese individuals. Nutr Metab Insights. 2014;7:77–84. Published 2014 Aug 28. doi:10.4137/NMI.S17028
- Asgary, S., Rastqar, A., & Keshvari, M. (2018). Weight Loss Associated With Consumption of Apples: A Review. Journal of the American College of Nutrition, 37(7), 627–639. https://doi.org/10.1080/07315724.2018.1447411
- El-Shazly SA, Ahmed MM, Al-Harbi MS, Alkafafy ME, El-Sawy HB, Amer SAM. Physiological and molecular study on the anti-obesity effects of pineapple (Ananas comosus) juice in male Wistar rat. Food Sci Biotechnol. 2018;27(5):1429–1438. Published 2018 Apr 11. doi:10.1007/s10068-018-0378-1
- Solverson PM, Rumpler WV, Leger JL, et al. Blackberry Feeding Increases Fat Oxidation and Improves Insulin Sensitivity in Overweight and Obese Males. Nutrients. 2018;10(8):1048. Published 2018 Aug 9. doi:10.3390/nu10081048
- Tsuda T. Recent Progress in Anti-Obesity and Anti-Diabetes Effect of Berries. Antioxidants (Basel). 2016;5(2):13. Published 2016 Apr 6. doi:10.3390/antiox5020013
- Sharma SP, Chung HJ, Kim HJ, Hong ST. Paradoxical Effects of Fruit on Obesity. Nutrients. 2016;8(10):633. Published 2016 Oct 14. doi:10.3390/nu8100633
- O’Connor L, Imamura F, Brage S, Griffin SJ, Wareham NJ, Forouhi NG. Intakes and sources of dietary sugars and their association with metabolic and inflammatory markers. Clin Nutr. 2018;37(4):1313–1322. doi:10.1016/j.clnu.2017.05.030
- Hussain T, Tan B, Yin Y, Blachier F, Tossou MC, Rahu N. Oxidative Stress and Inflammation: What Polyphenols Can Do for Us?. Oxid Med Cell Longev. 2016;2016:7432797. doi:10.1155/2016/7432797
- Lee YM, Yoon Y, Yoon H, Park HM, Song S, Yeum KJ. Dietary Anthocyanins against Obesity and Inflammation. Nutrients. 2017;9(10):1089. Published 2017 Oct 1. doi:10.3390/nu9101089
- Kaulmann A, Bohn T. Carotenoids, inflammation, and oxidative stress–implications of cellular signaling pathways and relation to chronic disease prevention. Nutr Res. 2014 Nov;34(11):907-29. doi: 10.1016/j.nutres.2014.07.010. Epub 2014 Jul 18. Review. PubMed PMID: 25134454.
- Ghanim H, Sia CL, Upadhyay M, et al. Orange juice neutralizes the proinflammatory effect of a high-fat, high-carbohydrate meal and prevents endotoxin increase and Toll-like receptor expression [published correction appears in Am J Clin Nutr. 2011 Mar;93(3):674. Upadhyay, Mannish [corrected to Upadhyay, Manish]]. Am J Clin Nutr. 2010;91(4):940–949. doi:10.3945/ajcn.2009.28584
- Cerletti C, Gianfagna F, Tamburrelli C, De Curtis A, D’Imperio M, Coletta W, Giordano L, Lorenzet R, Rapisarda P, Reforgiato Recupero G, Rotilio D, Iacoviello L, de Gaetano G, Donati MB. Orange juice intake during a fatty meal consumption reduces the postprandial low-grade inflammatory response in healthy subjects. Thromb Res. 2015 Feb;135(2):255-9. doi: 10.1016/j.thromres.2014.11.038. Epub 2014 Dec 13. PubMed PMID: 25550188.
- Rocha DMUP, Lopes LL, da Silva A, Oliveira LL, Bressan J, Hermsdorff HHM. Orange juice modulates proinflammatory cytokines after high-fat saturated meal consumption. Food Funct. 2017 Dec 13;8(12):4396-4403. doi: 10.1039/c7fo01139c. PubMed PMID: 29068453.
- Kuwabara T, Ishikawa F, Kondo M, Kakiuchi T. The Role of IL-17 and Related Cytokines in Inflammatory Autoimmune Diseases. Mediators Inflamm. 2017;2017:3908061. doi:10.1155/2017/3908061
- Peluso I, Raguzzini A, Villano DV, Cesqui E, Toti E, Catasta G, Serafini M. High fat meal increase of IL-17 is prevented by ingestion of fruit juice drink in healthy overweight subjects. Curr Pharm Des. 2012;18(1):85-90. PubMed PMID: 22211683.
- Glycemic index for 60+ foods. Harvard Health Medical School.
- Muraki I, Imamura F, Manson JE, et al. Fruit consumption and risk of type 2 diabetes: results from three prospective longitudinal cohort studies [published correction appears in BMJ. 2013;347:f6935]. BMJ. 2013;347:f5001. Published 2013 Aug 28. doi:10.1136/bmj.f5001
9,598 Comments
Albertina206 · April 30, 2025 at 6:56 pm
wow… what a great blog, this writter who wrote this article it’s realy a great blogger, this article so inspiring me to be a better person
Agneta206 · May 1, 2025 at 8:15 am
I would like to thank you for the efforts you have made in writing this article. I am hoping the same best work from you in the future as well. In fact your creative writing abilities has inspired me to start my own Blog Engine blog now. Really the blogging is spreading its wings rapidly. Your write up is a fine example of it.
Addy206 · May 5, 2025 at 5:04 pm
I am always searching online for articles that can help me. There is obviously a lot to know about this. I think you made some good points in Features also. Keep working, great job !
Mallory · May 18, 2025 at 9:43 am
They had been dreadful recommendations typically leaving a affected person to be supraphysiological
and in a steroid abuser state in the course of the first few days.
After which they would decline to hypogonadal states or even decrease than before they started testosterone replacement remedy.
This yo-yo therapy was merciless and unfair but unfortunately, many males are
nonetheless suffering sub-optimal doses of TRT on the NHS with not
so experienced non-public consultants. TRT is
designed to revive your testosterone ranges to an optimum vary, not
push them into excessive territory. The “right” dose can range from person to person based in your lab results, symptoms,
metabolism, and response to remedy. These research all reveal
that, despite the actual advantages of testosterone remedy, the adverse results of high doses have
to be carefully evaluated.
M.tb infection downregulates Sirt1 expression, which is essential
for negatively modulating inflammatory responses by inhibiting the activation of
TAK1, MAPK and NF-κB pathways and decreasing IL-6 and TNF-α ranges.
Resveratrol remedy reverses this effect [47] and demonstrates the power to lower bacterial burden and improve lung
pathology in Mabc-infected mice and zebrafish by activating Sirt3 [140].
Furthermore, resveratrol inhibited both M.tb-induced early and later apoptosis in macrophages, thereby markedly inhibiting intracellular M.tb growth [48].
Sirt7 restricts intracellular M.tb development by enhancing NO launch from macrophages and
NO-dependent apoptosis [142]. Phosphodiesterases (PDEs) regulate the focus of cyclic adenosine monophosphate (cAMP), a key second messenger in both eukaryotic and prokaryotic methods [106].
M.tb manipulates cAMP signaling pathways inside
contaminated macrophages, thereby influencing its survival [107].
Due To This Fact, understanding the differential impacts of various PDE-Is and their long-term outcomes is important earlier than widespread scientific use.
Yes, taking an extreme amount of testosterone can cause unwanted aspect effects, together with pimples, oily pores and skin, hair
loss, temper swings, increased pink blood cell
rely, and sleep apnea. Long-term overuse of testosterone can also lead to extra serious points such as
coronary heart disease and liver issues. It Is important
to observe your healthcare supplier’s dosage recommendations intently.
First, it is crucial to understand what are the two
main types of steroids (Mallory) testosterone therapy is and who might need it.
Testosterone remedy, or TRT, is a medical therapy that helps
to extend testosterone levels in individuals who have low testosterone.
Low testosterone can lead to symptoms like fatigue, low intercourse drive,
and temper adjustments.
Many elements must be considered when a clinician is choosing the most correct formulation for a patient.
As this choice relies upon extremely on the affected person, energetic patient participation is necessary for effective choice.
The goal of this evaluation is to explain and examine all testosterone preparations currently available and accredited by the United States Food and Drug Administration. Areas
of focus will embody pharmacology, PKs, antagonistic results, and specifics related to particular
person delivery routes.
Usually, regular testosterone ranges range from 300 to
1,000 ng/dL (nanograms per deciliter). Your doctor will assist interpret these results in the context of your symptoms and
total health. Both underdosing and overdosing on testosterone
remedy carry significant risks. By staying knowledgeable and dealing
closely with your doctor, you’ll find a way to be
certain that your dosage is right, helping you obtain the very best outcomes out of your therapy.
Managing stress successfully might help be sure that your testosterone therapy
works nicely, without the need for larger doses. It’s essential to follow
your doctor’s instructions fastidiously when adjusting your dosage.
Never change your dosage on your own, as this can result in dangerous
unwanted aspect effects or ineffective remedy.
As you age, your testosterone degree steadily declines — sometimes about 1% a year after age 30 or 40.
For older men, it’s necessary to determine if a low testosterone level is due to regular getting older or if it is due
to a disease (hypogonadism).
Understanding how these components have an result on TRT dosage may help men work with their doctors to search out the best treatment plan and obtain the very best results.
Regular monitoring and changes are essential for long-term success in managing testosterone levels.
It can take several months of normal check-ups and blood checks to
fine-tune your dosage. Most docs will start with a regular starting dose, but that is hardly ever the exact dose that works greatest for you.
In addition to those dangers, taking too much testosterone can even have psychological effects.
It is necessary to discuss any modifications in mood or conduct with a healthcare supplier to ensure applicable
therapy adjustments. Some people could also be
extra delicate to testosterone and require decrease doses to
realize the desired results, while others might require larger doses.
This response may be influenced by factors such as genetic
variations, body composition, and total well being.
Common monitoring and adjustment of the dosage based on the individual’s response
is essential to ensure optimum results from TRT.
Over time, your body might want roughly testosterone to hold up the right steadiness.
At Steadiness My Hormones, we utilise trendy testosterone optimisation methods to provide secure hormone levels.
This article explores various TRT dosages, together with Testosterone Sustanon, Cypionate,
Enanthate, Propionate, and Testosterone Cream, and provides steering on finding the perfect
dose tailored to your specific needs. This suggests their potential use in regulating immune responses against TB infection [44].
However, future medical trials should be conducted to discover the in vivo results of indomethacin in patients during numerous stages of M.tb an infection.
Haferpresssaft Und Testosteron · May 18, 2025 at 11:09 pm
Hier stellten die Forscher an trainierten Probanden mit
Krafttraining bis zum willentlichen Versagen keinerlei zusätzliche
Hypertrophie-Effekte fest. Ein großer Teil Ihrer Laune
kommt additionally unserer Meinung nach nicht nur
vom Testosteronmangel, sondern auch durch Ihre „durchaus extrem verständliche” Reaktion darauf. Wir möchten Sie auch nicht belehren und Sie ermutigen, künstlich Ihre Laune zu heben (dies funktioniert sowieso höchstens kurzfristig). Die richtige Diagnose und Behandlung eines Testosteron-Mangels erfordert Sorgfalt und eine individuelle Herangehensweise.
Dann raten wir Ihnen dazu, einen Urologen aufzusuchen und Ihren Hormonspiegel kontrollieren zu lassen. Am häufigsten tritt der Testosteronmangel im Alter ab 60 Jahren auf. Mit zunehmendem Alter verändert sich der Hormonspiegel und die Produktion des Sexualhormons nimmt ab. Nur 1 Prozent aller Männer sind im jungen Alter von dieser Mangelerscheinung betroffen, während es bei Männern über 60 Jahren 12 Prozent der Weltbevölkerung sind. Auch Frauen können von einem Mangel an Testosteron betroffen sein und unter einer verminderten Libido, unter Haarausfall und ebenso wie betroffene Männer langfristig unter Depressionen leiden. Eine Behandlung der Mangelerscheinung ist essentiell und dazu ist es wichtig, den Ursachen auf den Grund zu gehen und bei Testosteronmangel keine reine Symptombehandlung vorzunehmen. Wenn bei Ihnen mehrere der folgenden Anzeichen zutreffen, sollten Männer ihren Testosteronspiegel von einem Arzt prüfen lassen.
Mindestens ein weiterer unabhängiger Test des Gesamttestosterons ist erforderlich, um die Diagnose eines Testosteronmangels/Hypogonadismus bestätigen bzw. Sichern zu können, weil es aufgrund der zirkadianen Rhythmik von Testosteron sowie weiterer externer Faktoren, Schwankungen des Spiegels geben kann. Daher ist der Testosterontest ein entscheidendes Instrument, um ein fundiertes Verständnis Deiner hormonellen Gesundheit zu erlangen.
Freies Testosteron ist ungebunden, additionally frei verfügbar und aktiv. Laut aktueller Gebührenordnung für Ärzte in 2020 kostet die alleinige Messung deines Testosteronspiegels 27,sixty six €. Du erhältst dazu keinerlei Beratung und keine zusätzlichen Werte. Sie sind super einfach durchzuführen, du hast schnell ein Ergebnis, volle Kontrolle und brauchst dafür nicht zum Arzt zu rennen. Bei einem Speicheltest kannst du außerdem den Zeitpunkt ganz genau festlegen. Was er mir ebenfalls nicht sagte, warfare, dass mein Testosteronspiegel mit 24 Jahren statistisch gesehen niedriger war als der eines 100-jährigen Mannes… Oh boy.
Wenn der gesuchte Stoff in der Probe vorhanden ist, binden die Antikörper daran, und das Enzym löst eine Reaktion aus, die wir messen können. So können wir feststellen, ob und wie viel von dem Stoff in Ihrer Probe vorhanden ist. ELISA ist eine vielseitige Methode, die wir für viele verschiedene Checks einsetzen, z.B. Um Allergien, Infektionen oder bestimmte Hormone zu bestimmen.
Übergewicht, Alkohol- oder Medikamentenmissbrauch fördern Testosteronmangel. Diese sind weniger verbreitet und nicht in allen Laboren verfügbar. Regelmäßige Kontrollen des Testosteronspiegels sind entscheidend. So können ernsthafte gesundheitliche Folgen vermieden werden. Testosteron beeinflusst zudem dominantes und aggressives Verhalten.
Ein Arzt kann nach Anzeichen und Symptomen eines hohen Testosteronspiegels suchen, einschließlich übermäßiger Körperbehaarung, Akne und erhöhter Muskelmasse. Er wird auch nach der Libido und der Stimmung einer Particular Person fragen. Zu den Anzeichen und Symptomen gehören unregelmäßige Regelblutungen, ausbleibender Eisprung, übermäßige Behaarung am Körper Haferpresssaft Und Testosteron Zysten an den Eierstöcken.
Das polyzystische Ovarialsyndrom (PCOS) ist eine der häufigsten Ursachen für einen hohen Testosteronspiegel
bei Frauen. PCOS betrifft bis zu 20 % aller Frauen im fortpflanzungsfähigen Alter.
Ähnlich wie bei Männern kann auch bei Frauen ein hoher Testosteronspiegel als Folge von anaboler
Steroideinnahme oder Tumoren der Nebennieren oder Eierstöcke auftreten.
Aber auch Übergewicht oder Schlafstörungen führen dazu, dass Testosteron absinkt.
Der Testosteronspiegel kann auf natürliche Weise im Alter
sinken. Es ist vollkommen normal, dass sich der Testosteronspiegel im Laufe des Lebens verändert und
damit auch andere Referenzwerte in einem Testosteron Check hinzugezogen werden.
Ein normaler Testosteronspiegel für Männer liegt zwischen 300 und 1.000 Nanogramm pro Deziliter (ng/dl).
Testosteron ist ein Steroidhormon und damit ein Abkömmling von Cholesterin. Weitere bekannte Steroidhormone sind Cortisol, Östrogen, DHEA,
Aldosteron und Progesteron.
Best Legal Testosterone Steroid · May 19, 2025 at 5:30 am
In some circumstances, claims are rejected as a result of coding errors, where the
analysis or process codes don’t align with
insurer necessities. Completely Different insurers and plan categories have varying requirements, cost-sharing
constructions, and restrictions on prescriptions.
Understanding these differences helps individuals anticipate
out-of-pocket expenses and navigate the approval
course of. Insurance corporations usually cover treatments that they consider “medically essential.” This means they need proof that testosterone therapy is crucial for your health.
Your physician may help you by diagnosing any situation related to low testosterone ranges,
such as hypogonadism, which can result in fatigue, low power, and different well being points.
After you could have confirmed that your insurance
covers testosterone remedy, try to get the
details in writing. Most insurance coverage
firms will ship you a summary of advantages upon request, which outlines what is roofed underneath your plan.
Insurance Coverage providers often require a referral earlier
than approving TRT coverage. Your provider will monitor your hormone levels,
modify your dosage as needed, and look ahead to complications.
In addition to the treatment itself, you’ll also
have to cowl physician visits, lab exams, and follow-ups, which may add a number
of hundred dollars per year if you’re paying out of pocket.
Personal insurers generally cowl testosterone therapy when it’s deemed medically needed, but coverage details can differ.
Protection for testosterone remedy typically
is determined by your insurance coverage supplier, diagnosis,
and whether the treatment is considered medically essential.
If you’ve been diagnosed with low testosterone, you could be contemplating
testosterone therapy.
That method, you’ll be more likely to profit from testosterone replacement therapy.
The price you’d pay for Jatenzo versus that of different testosterone injections depends on various components.
For example, there are a quantity of options, such asXyosted,
Depo-testosterone, and Aveed. In most circumstances bioidenticals won’t interfere
with different prescription medications. Medicine containing hormones, such as birth control drugs and certain acne medicines,
might work together with bioidenticals nevertheless, so
you will need to notify a doctor prior to treatment.
TestoPrime accommodates Ashwagandha, an adaptogen identified for its stress-reducing properties, which helps balance the consequences of growing
older on mood. By stabilizing testosterone levels, TestoPrime promotes higher mental
well being, allowing men over 40 to really feel extra optimistic, less anxious, and higher outfitted to handle life’s challenges.
As men age, sustaining muscle mass turns into more and
more tough as a outcome of declining testosterone levels.
Low Best Legal Testosterone Steroid may find yourself in a decrease in lean muscle and strength,
which impacts not solely physical look but in addition general mobility
and health. One of essentially the most well-known advantages of TestoPrime is its ability
to assist muscle development. Testosterone is a key hormone responsible for muscle protein synthesis, which
immediately impacts the development of lean muscle mass.
If you’ve insurance, the price is normally the quantity of your
copay plus any unmet deductible. Once on therapy most males will profit from testosterone substitute, however there are a couple
of unwanted effects. Before beginning remedy with ED injections, it’s crucial to get clear answers to a number of essential questions.
Medications like Viagra and Cialis are sometimes partially covered depending on the profit plan descriptions.
Exercise, dietary changes, quitting smoking, and psychological counseling can enhance
ED symptoms, with the primary requirement being that the affected person exercise patience in attaining outcomes.
Erectile dysfunction (ED) is more than just a physical condition—it’s a multifaceted challenge that may have an effect on shallowness,
intimate relationships, and overall high quality of life.
When it comes to hormone therapy, there are several varieties, and
each has its personal costs. Testosterone therapy is one option, usually chosen by
men with low testosterone ranges. Nevertheless, hormone remedy additionally contains
treatments like estrogen therapy, which is normally used by women, particularly throughout menopause.
Certain non-profit organizations provide monetary assistance to help folks cowl the cost of hormone remedy, including testosterone.
These organizations may provide grants, coupons, or reimbursement programs for those who qualify.
Examples include the Affected Person Entry Network Basis and NeedyMeds, which assist with medication prices for these with low revenue or high medical expenses.
On prime of those major factors, there are other bills to consider, corresponding
to lab tests and follow-up appointments.
Within a couple of weeks, you could be on testosterone substitute, delivered at residence within the type of lotions, injections, or troches, relying in your desire.
It’s a good idea to speak to your clinic about financing options or discovering cheaper generic drugs.
If so, inquire together with your insurance protection as to what particular procedures, if any, are coated under a reimbursement scheme.
Complementary therapies may be applicable as extra
choices for males with low ranges of testosterone in search of therapeutic choices.
However, there may be out-of-pocket prices, and varied elements can have an result
on your total bills. You might profit from testosterone remedy if you’ve been recognized with clinically low testosterone (also known as hypogonadism).
It’s also typically considered for growing older males
who’re experiencing symptoms like fatigue, low libido, or mind
fog due to declining hormone ranges. When a claim is denied, step
one is to evaluate the Clarification of Benefits
(EOB) or denial letter, which outlines the reason for the rejection and provides enchantment instructions.
Federal laws require insurers to clarify denials, and policyholders usually have 60
to a hundred and eighty days to file an appeal. If
the initial appeal is unsuccessful, most plans permit for a second-level
enchantment, which can contain an unbiased review.
Well Being insurance coverage coverage for testosterone remedy is dependent upon the kind of plan, the particular medical want, and the documentation offered
by a healthcare provider. Insurance Coverage protection for
testosterone remedy not only lowers prices but in addition encourages sufferers to entry different healthcare
providers. When patients know they’ve insurance to support their remedy,
they’re extra more doubtless to comply with up with their doctors, schedule lab
exams, and modify their therapy plans if necessary.
Common medical care might help folks manage their testosterone ranges
safely and effectively.
We source research from peer-reviewed medical
journals, high authorities businesses, main educational institutions, and respected advocacy groups.
We additionally transcend the analysis, interviewing high consultants of their fields to convey you essentially
the most informed insights. Each article is rigorously reviewed by medical consultants to make sure accuracy.
Hone’s associate labs are accredited by the Medical Laboratory Enchancment Amendments (CLIA)
and, the place applicable, by the Faculty of American Pathologists
(CAP). And all the opposite benefits that come with elevating
your testosterone safely.
Common Steroid Names · May 22, 2025 at 8:33 pm
Many features of the anti-inflammatory actions of glucocorticoids
have not been lined right here. The next few years
should provide a giant step ahead in our understanding
of how these important hormones exert their effects, with concomitant advances within the
clinical therapy of inflammatory disease. A variety of GR ligands are in use clinically which
have different potency and differ in their biological
efficacy.
Should kidney harm happen, then the steroid person ought to discontinue the use of the
medicine. Some steroids users have suffered from end-stage kidney failure and
have required a dialysis. Others, having previously skilled kidney harm, when starting
a cycle of steroids again have skilled a relapse of severe
kidney damage and dysfunction. When taking steroids, the
testes (testicles or balls) will often decrease in their regular functioning as a result of the higher levels of testosterone in the physique.
Some research has discovered that the utilization of anabolic steroids may cause
people to turn to other medication to alleviate adverse short-term
side effects. One research found that 9.3% of men who have been being handled
for heroin or other opioids use had misused steroids before doing any other drugs.
Most campaigns towards anabolic steroids use concern campaigns
highlighting the negative penalties on bodily and psychological health to encourage folks to avoid these medication. However these have been criticised for
failing to mirror the experiences of most “healthy”
or “healthy-looking” customers. One of the most significant
considerations with prednisone use is the danger of adrenal insufficiency.
This condition happens when the body is unable to produce adequate
adrenal hormones due to the suppression of the HPA axis by prednisone.
Analysis on comparable corticosteroids, corresponding to dexamethasone, has proven that even a single dose can considerably disrupt various physiological methods, including
the immune and metabolic methods, in addition to cortisol and ACTH levels.
They are often used illegally to enhance athletic efficiency or physique and can be extremely dangerous to users’ health.
One of the kidneys many essential capabilities is appearing as a filter for
the blood, removing excess waste merchandise in the physique.
Bodybuilders frequently use dietary dietary supplements including protein,
creatine and nutritional vitamins to construct strength and muscle bulk.
It’s like being trapped on a hamster wheel of
bodily perfection, running sooner and quicker however never reaching the
goal. These excessive and negative effects can have an result on those who are already vulnerable
to these sort of behaviors. The adverse effects of AAS use depend upon the product, the age and intercourse of the person, how a lot they use, and for a way lengthy.
Underneath the Controlled Substance Act, unlawful possession and distribution are topic to federal and state legal guidelines.
In the U.S., an AAS is a schedule III controlled substance
obtainable only by prescription.
However they use it for different circumstances as nicely, corresponding to to stimulate muscle progress for individuals with sure cancers or acquired immunodeficiency syndrome (AIDS).
Nonetheless, if you’re seeking to build muscle, corticosteroids are not the right type of steroid.
Anabolic steroids (also known as anabolic-androgenic steroids) are a special
kind of drug and unlawful in most nations and not using a written prescription from a pharmacist.
These medicine mimic the sex hormone testosterone and are well-known for being misused by
some athletes to realize an edge over their rivals.
Common Steroid Names,
heavy anabolic steroid use can lead to tolerance and dependence.
This signifies that an individual needs more of the drug to attain the identical results
they did beforehand with smaller amounts.
Regardless Of testosterone being the first mediator of LH’s impact on spermatogenesis, exogenous
administration of testosterone can’t assist spermatogenesis.
Intratesticular testosterone (ITT) ranges are about 50 to
one hundred times higher than in circulation (180) and exogenous administration severely suppresses this to
ranges which may be unable to help spermatogenesis (181).
Oral AAS again demonstrate unfavorable changes, constantly growing LDL-cholesterol (38,
118, 121, a hundred twenty five, 126). In the HAARLEM examine, LDL-cholesterol increased by 0.forty five mmol/L
in contrast with baseline (46).
Chloramphenicol is one of the most widely used antibiotic ophthalmic
preparations for the therapy of bacterial conjunctivitis in infants.
There are some anecdotal, poorly outlined, instances within the
older literature of chloramphenicol-induced bone-marrow hypoplasia and blood dyscrasias [29, 30, 31].
It is feasible that there had been earlier chloramphenicol exposure within the form of oral remedy and
the side- results attributed to the attention drops have been thus actually a secondary
immunological response. Orally administered chloramphenicol is contraindicated in neonates as a end result of life- threatening “gray child syndrome”
[32]. Other native ophthalmic antibiotics such as fluoroquinolones are usually
taken to be contraindicated for infants beneath one
12 months of age because of the lack of expertise of their potential unwanted effects.
The exact position of the inflow transporters, e.g. natural
cations and peptides, can affect penetration by way of membranes,
depending on the chemical nature of the actual agent in query [8].
Moreover, the presence of drug- metabolizing CYP enzymes within the ocular tissues may be of significance e.g.
in the case of timolol [9].
This misunderstanding can lead to poor selections and health consequences.
I do see the results of topical steroid overuse (e.g., skin thinning and hypopigmentation)
however it’s uncommon. •Many of the consequences
of steroids reflect a standard criticism of contemporary drugs.
By focusing on treating signs, the physique’s innate healing mechanism is
suppressed, resulting in more extreme sicknesses rising later.
Your body naturally releases cortisol in response to emphasize, serving to regulate blood pressure,
blood sugar and vitality use. But if stress
lasts too lengthy, cortisol levels can stay high, which can lead to psychological health issues,
weight achieve and hassle sleeping. They’re also called corticosteroids, and are totally different to anabolic steroids used by bodybuilders and athletes.
In basic, phase I metabolism primarily entails reduction at carbons three and 5 of
the A-ring and oxidation of the hydroxyl group at carbon 17 of the D-ring of
the steroid nucleus (24). These phase I metabolites would
possibly then endure conjugation into glucuronides and be subsequently excreted
(26). Synthetic testosterone is also used to deal
with individuals with low testosterone, which is referred to as testosterone substitute therapy (TRT).
Beau · May 22, 2025 at 8:59 pm
Some people who use amphetamines develop a stimulant use disorder.
Withdrawal symptoms can include fatigue, despair, and disturbed sleep
patterns. Aerosols are inhalants, substances that produce intoxicating chemical vapors.
Anabolic steroids are man-made drugs associated to testosterone (male sex
hormone). Doctors use anabolic steroids to treat hormone problems in males, delayed puberty, and muscle loss from some illnesses.
Androgenic effects embody masculinizing effects similar to elevated facial
hair, deepening of voice, and enlargement of some
male intercourse glands. Anabolic results embody improve in muscle mass, calcium
in the bones and a few internal organs. Steroid hormones typically
stimulate some parts of a muscle cell and this stimulation will increase protein manufacturing and some chemicals linked with the increase in muscle mass.
Completely Different people’s our bodies respond
in a unique way to steroids as a result of variations in their genetic makeup,
the kind of steroids used, the amount taken, and the period of
abuse.
Anabolic best legal steroids for sale – Beau, can be found in a
whole range of types from tablets to gels. They are also out there in capsules, creams, transdermal
patches, liquid drops, oil or water-based injectable solutions.
The recommended dosage of Deca Durabolin 500mg/ml varies depending on the individual’s
targets, experience, and tolerance. It is typically administered once or twice per week, with
a typical dosage ranging from 200mg to 600mg per week.
Nonetheless, it is important to observe that the dosage should
be decided by a healthcare skilled or an experienced person. Anabolic steroid abuse acts on the response of the dopamine system to stimulating intoxicants.
Cautious monitoring of AAS dosages and cycles, under the steering of a
healthcare skilled, may help reduce unfavorable results on joint health.
He’s additionally pushing to broaden his district’s entry to sex-reassignment surgery, steroid drugs good.
In 2019, 73,000 Americans admitted to utilizing PCP, a low quantity compared
to different onerous medicine. Teens usually journey on mushrooms
with psilocybin, a mind-altering chemical present in nearly 200 different
varieties of mushrooms.
You ought to all the time contact a doctor to discuss any and all medical points in combination along with your medical and household
record. Do not take any medical choices with out first totally discussing along with your physician.
A white powdered substance generally snorted with a mean 20 minute high.
It is far more potent than different opiates, which has increased its recognition. It is related
to chemicals like Mephedrone, Methylone and MDPV as a result of their related chemical construction and effects they
offer users. A stimulant to the central nervous system, commonly present in tea and low.
Widely prescribed as sedatives, to combat anxiousness, skeletal
muscle relaxants and anticonvulsants. Facet results of stanozolol include virilization (masculinization),
hepatotoxicity,[8] heart problems, and hypertension. Tobacco smoke accommodates hundreds of chemical substances which would possibly be
harmful to both people who smoke and nonsmokers.
These chemicals increase the risk of most cancers, lung
disease, coronary heart illness, and plenty of different well being
problems.
In fact, a examine by Issa et al., discovered that the use of
anabolic steroids was a uncommon explanation for acute pancreatitis.
On the opposite hand, pyramiding is the pattern the place an individual slowly will increase the frequency
or dose of bodybuilding steroids until they reach
the peak amount after which progressively decreases it.
Plateauing refers to alternating, substituting, or overlapping one steroid with one other to
avoid changing into tolerant to these medication. Drug users who inhale chemical substances can experience
a spread of quick and long-term results relying on the substance.
These results can include dizziness, slurred speech, confusion, loss of coordination, and impaired judgment.
Some Schedule IV medication embody benzodiazepines, sleep aids, and anticonvulsants.
These hormones help the cells, tissues and organs carry out their jobs properly.
Everybody wants a healthy balance of hormones to
propagate and grow. Steroids may also check
with man-made medicines and the two main sorts are corticosteroids and
anabolic-androgenic steroids, or anabolic steroids. A lot of people just accept this truth which is gloomy, avenue steroids names anabolic.
Many who abuse these medication tend to do quite nicely
economically, however they don’t at all times have so much
success in life and plenty of of them are never able to get the results they need, finest authorized steroids for muscle growth.
In 1994 two states, Utah and Indiana handed comparable laws prohibiting the possession or sale
of steroids without a prescription, anabolic steroid medical
uses. Nevertheless, as was the case with different states, state-level
laws relating directly to steroids was not passed.
binance anm"alan · June 3, 2025 at 5:19 am
I don’t think the title of your article matches the content lol. Just kidding, mainly because I had some doubts after reading the article.
binance us register · June 7, 2025 at 7:44 am
Can you be more specific about the content of your article? After reading it, I still have some doubts. Hope you can help me.
Debolt Steroids · June 11, 2025 at 6:59 pm
70918248
References:
Debolt Steroids
Different Types Of Testosterone Steroids · June 12, 2025 at 6:22 pm
70918248
References:
Different Types Of Testosterone Steroids
maspackaging.com · June 12, 2025 at 10:15 pm
70918248
References:
steroids build muscle [maspackaging.com]
www.zzjane.com · June 14, 2025 at 6:29 am
70918248
References:
short Steroid cycle (http://www.zzjane.com)
none · June 15, 2025 at 5:53 am
70918248
References:
none
binance · June 15, 2025 at 12:34 pm
Thanks for sharing. I read many of your blog posts, cool, your blog is very good.
注册免费账户 · June 24, 2025 at 2:04 am
Can you be more specific about the content of your article? After reading it, I still have some doubts. Hope you can help me.
https://tl-studio.jp/tls/log/eid214.html · June 30, 2025 at 3:50 pm
70918248
References:
purpose of steroids (https://tl-studio.jp/tls/log/eid214.html)
blackcoin · July 10, 2025 at 9:07 am
That Is why we additionally considered the maximum allowed wager sizes
in slots, roulette, blackjack and different on line casino video
games in style amongst high rollers. If you choose a on line casino from this list, you
can make certain that you shall be able to guess massive.
They could sometimes be valid for a shorter timeframe, say 1 week as a substitute of 30 days.
Amit is a cryptocurrency researcher with 5+ years of expertise in the digital asset business.
His deep experience permits him to analyze advanced blockchain developments with clarity,
making his content insightful and accessible. He focuses on crafting data-driven articles that present in-depth insights into blockchain expertise and market movements.
At All Times use safe wallets and trusted sites (like these ones) to sign up.
In this information, we’ll go through the totally different high curler
applications, what to expect, and tips on how to get into the
high roller club. Plus, we’ve listed our favorite casinos now accepting excessive rollers and offering huge bonuses.
The 40x wagering requirements are reasonable in comparability with different offers.
Simply enter the code after signing as much as claim this easy no deposit deal focused on actual cash video
slots, keno and scratch cards. The high excessive roller casino
sites are devoted to delivering distinctive service
to cell players who deposit and spend substantial amounts of money.
As far as we are aware, no related on line
casino blacklists mention Shangri La Casino. Casino blacklists, such as our own On Line Casino Guru blacklist, could indicate
mistreatment of customers by a on line casino.
Subsequently, we suggest players contemplate these lists when selecting a
on line casino to play at.
The most successful gamblers at all times set a gambling budget and persist with
it. This is a recommended technique that can assist you keep monitor of your spending.
Additionally, the most effective gamers guess strategically based mostly on the casino’s high curler
bonus phrases and conditions. This contains maintaining the utmost limits in mind to keep away from
having their winnings discarded.
High rollers usually take pleasure in quite a lot of high stakes games, together with
slots, table games, and stay vendor video games.
These games are designed to cater to the preferences of high-stakes gamers, offering higher betting limits and the potential for important winnings.
Understanding casino bonuses no deposit can be like looking for a needle in a haystack, however once you do, it’s like hitting the jackpot.
It’s necessary to grasp bonus necessities earlier than claiming any offer.
The good news is that most online casinos provide detailed data
on their web site or buyer help group.
Additionally, participating with the casino’s VIP or loyalty packages and aiming for higher tiers also helps.
Generally, simply contacting customer assist and expressing your interest in high-roller advantages can initiate the
process. Make sure the casino has a sound license issued by a good authority,
corresponding to Curacao, and comply with correct cryptocurrency laws in your country.
Look for good reviews and make positive that there aren’t any serious complaints regarding not paying out or
being rude. If crypto playing sites have a good reputation, then you definitely could be certain you’ll find a way to belief them along with your
cash. Excessive rollers understand that there are occasions when, regardless of enjoying your best, you can lose.
These are normally a percentage of your losses again as real cash that can be utilized once more on any
game you choose. This is an excellent incentive for big
spenders who need to maximize their potential winnings.
When it comes time to withdraw funds from your account you will discover that
the withdrawal course of is simply as easy as when making a deposit.
Additionally there might be maximum withdrawal limits
primarily based on how a lot you won during your gaming session so make sure to check with their buyer help earlier than requesting a giant payout.
References:
blackcoin
download · July 16, 2025 at 11:12 am
Читатели имеют возможность самостоятельно проанализировать представленные факты и сделать собственные выводы.
binance US-registrera · July 17, 2025 at 10:29 pm
Can you be more specific about the content of your article? After reading it, I still have some doubts. Hope you can help me.
online · July 18, 2025 at 8:20 pm
This means you must use your PayPal account to deposit money and withdraw funds
from the on line casino, making it a handy and
safe possibility for online gambling.
PayPal delivers quick verification for bettors looking to make deposits
and withdrawals. Most deposits can be found immediately, while
the overwhelming majority of withdrawals are processed the identical day.
Verification is as easy as registering for a PayPal account and syncing it to the online on line casino of your alternative.
PayPal is thought for having a number of the quickest payouts
among the various third-party e-wallets obtainable at on-line casinos.
The average withdrawal time is between 1 and a pair of days, but the wait time is shorter than that in most cases.
This successfully protects gamers and ensures they’ll obtain a good gaming expertise on every little thing from
game possibilities to deposits and withdrawals. It also
consists of data safety (both personal and banking) and clear phrases so gamers all the time
know what’s required of them. Many reputable on-line
casinos settle for PayPal, providing gamers
a safe and efficient approach to handle their funds. Casinos like Mr Green, Rizk, PlayMillion, LeoVegas and Casumo combine PayPal seamlessly, giving users the
benefit of quick and trusted transactions backed by strong licensing.
Cryptocurrencies like Bitcoin, Ethereum, and Litecoin have gotten popular cost strategies at trendy on-line casinos.
You can join PayPal fairly quickly, which is appropriate with
most banks. PayPal is a safer technique of fee than offering your credit card data to
someone who could probably be more tech-savvy. Michigan legalized online playing and sports betting
in 2019, with its first on-line casino launching in January 2021.
This additionally opened up the opportunity for PayPal for use as a payment possibility at on-line casinos in the state.
With a big population and powerful interest in gambling, Michigan is poised to become a significant market for PayPal on line casino sites.
One of the primary causes PayPal casinos stand out from different high on-line casinos is not all other online casino sites or gambling websites settle for this cost methodology.
With video games like NetEnt’s Dead or Alive and
Microgaming’s Immortal Romance, there’s plenty to choose from.
Finest online casinos that payout instantly even have an general RTP of
93-95%. Selecting video games with a low house edge minimizes losses over time and maximizes
your payout potential. BetWhale on line casino features more than 1,300+ video games together with
high RTP slots and jackpots. Payments are versatile, with safe instant deposits and quick payouts in 1–3 enterprise days.
Before deciding on a web-based casino PayPal, verify that
it provides this fee technique, since its availability can differ
relying on your region. For the most up-to-date listing of casinos
accepting this payment methodology, verify their cost coverage or buyer help.
However, there have been talks of increasing rules
to allow for extra on-line casino sites and gaming choices within the state.
If this happens, we may see an even bigger presence of PayPal casinos in Pennsylvania.
PayPal has a cellular app for each Apple and Android customers, and
it’s easy to sync that up along with your cell casino app.
From there, players can make fast deposits and withdrawals
using their funds or synced banking information inside PayPal.
Yes, you ought to use PayPal to gamble at on-line casinos
which have agreements with the banking device.
That stated, solely approved merchants similar to Fanatics Casino and
BetMGM On Line Casino, supply PayPal as an choice for online gambling.
Signing up for a PayPal account is free and permits players to seamlessly make transactions with
a safe type of fee.
However, PayPal itself may apply forex conversion charges or charges for sure
funding sources. So, it’s always a good idea to examine both the casino’s fee terms and PayPal’s payment coverage to keep
away from surprises. We solely recommend casinos which
are fully licensed by respected regulatory our bodies, ensuring
participant safety and fair play. Equally necessary
is responsive customer support to assist resolve cost points or account considerations rapidly.
Golden Nugget Casino is a top-rated platform with
an award winning person expertise. Known for its game choice, Golden Nugget companions with elite
suppliers like NetEnt, IGT, and Huge Time Gaming to offer an intensive record of on-line slots and live dealer tables.
If you are on the lookout for secure cost options past PayPal, you would possibly wish to contemplate the comfort of using Apple Pay
or Skrill at online casinos. DraftKings is an enormous name in the industry, which is
why it doesn’t come as a surprise that additionally it is one of the prime PayPal casino on-line sites,
too.
Mobile slot video games actual cash make the most of HTML5 know-how for crisp graphics and smooth animations across
all units. Yes, cellular casinos for actual cash are completely
authorized in several US states, operating beneath strict regulatory oversight.
Look within the footer of the online on line casino you go to,
towards the underside of the page. Right Here you can see any certifications and licenses from permitted our bodies which
will assist to provide you an thought of that casino’s authenticity.
The eCogra emblem specifically is worth looking
for, as this organization tests casinos’ random
number generators to ensure that gamers are getting a good chance in all of
their games.
gratis binance-konto · July 20, 2025 at 8:28 am
Your point of view caught my eye and was very interesting. Thanks. I have a question for you.
klia limo · July 21, 2025 at 7:30 pm
I do agree with all of the ideas you’ve introduced on your post.
They’re very convincing and will definitely work.
Still, the posts are too short for newbies. May just you
please extend them a bit from subsequent time?
Thanks for the post.
toto99 login · July 21, 2025 at 8:09 pm
Very nice post. I just stumbled upon your blog and wanted to
say that I have truly enjoyed browsing your blog posts.
After all I’ll be subscribing to your rss feed and I hope you
write again soon!
Prime Boosts · July 22, 2025 at 1:06 am
Simply desire to say your article is as amazing. The clearness to your submit is simply cool and i could assume you’re knowledgeable on this subject.
Fine with your permission let me to grab your feed to keep
updated with imminent post. Thanks one million and please carry on the enjoyable work.
Look at my blog post: Prime Boosts
how to create phising website · July 22, 2025 at 9:56 am
I have read some just right stuff here. Definitely worth bookmarking
for revisiting. I surprise how a lot effort you place to
create this sort of excellent informative site.
COLCOM Safe Deposit Box · July 22, 2025 at 9:57 am
PT. Sicurezza Solutions Indonesia provides security
solutions with integrating varieties of security
products which can be adjusted to many needs from Access Control, Automatic
Door, CCTV, Video Intercom, Biometric Time & Attendance, etc.
Experience selling and installing security systems for all kinds of
buildings such as private house, apartment,
hotel, resort, office, government building,
bank, factory, etc.
COLCOM Hotel Lock,COLCOM Minibar,COLCOM Kettle,COLCOM Kettle Set,
COLCOM Locker Lock,COLCOM Safe Deposit Box,COLCOM Infrared Body Temperature,COLCOM Portable Dishwasher,COLCOM Vaccum Sweep
Mop Robot,COLCOM Accessories
https://www.mediedilimmobiliare.It/Immobile/home-in-merrick-way/ · July 22, 2025 at 2:20 pm
rt 66 casino
References:
https://www.mediedilimmobiliare.It/Immobile/home-in-merrick-way/
Teds Woodworking Reviews · July 22, 2025 at 3:38 pm
I love that it covers everything from small projects to big
builds. Makes it super versatile for all skill levels.
shkolnaiapora.ru · July 22, 2025 at 4:40 pm
best online steroid suppliers
References:
best steroids on the market, shkolnaiapora.ru,
toto togel · July 22, 2025 at 5:57 pm
Great web site you have here.. It’s hard to find high-quality writing like yours these days.
I seriously appreciate people like you! Take care!!
situs gacor · July 22, 2025 at 10:34 pm
Great website you have here but I was wanting to know if you knew
of any community forums that cover the same
topics discussed in this article? I’d really like to be a part of
group where I can get suggestions from other experienced people that share the same interest.
If you have any suggestions, please let me know.
Bless you!
batman138 login · July 22, 2025 at 10:37 pm
Keep on working, great job!
Www.Greatdynamics.net · July 23, 2025 at 4:01 am
casino san francisco
References:
http://Www.Greatdynamics.net
waslot · July 23, 2025 at 6:47 am
Hi! I know this is kind of off topic but I was wondering if you knew where I could get a captcha
plugin for my comment form? I’m using the same blog platform as yours and I’m having trouble finding one?
Thanks a lot!
www.plurk.com · July 23, 2025 at 7:30 am
Cabinet IQ
15030 N Tatum Blvd #150, Phoenix,
AZ 85032, United Ꮪtates
(480) 424-4866
Kitchenmakeover (http://www.plurk.com)
www.central-it.co.uk · July 23, 2025 at 8:49 am
It’s an awesome paragraph for all the internet users; they will take benefit from
it I am sure.
free credit no deposit · July 23, 2025 at 8:55 am
Amazing! Its actually awesome post, I have got much clear idea regarding from this post.
engraved necklace · July 23, 2025 at 10:51 am
These name necklaces are so cute, love how you can personalize them!
호빠 · July 23, 2025 at 11:00 am
I’m curious to find out what blog platform you have
been using? I’m experiencing some minor security problems with my latest site and I’d like to find
something more risk-free. Do you have any solutions?
singapore math tuition · July 23, 2025 at 11:30 am
Hеllo tһere, I discovered ʏߋur blog by way
оf Google evеn аs searching fοr a relɑted matter, ʏоur website ɡot heгe
սp, it appears to be like good. I haѵе bookmarked it in my ggoogle bookmarks.
Hi thеre, simply changed іnto alert to ʏοur blog via Google,
and located tһat it іs really informative. I аm gonna be careful fоr brussels.
I wіll be grateful if үou һappen to continue tһis in future.
Many folks miɡht be benefited oսt of your
writing. Cheers!
My site … singapore math tuition
webpage · July 23, 2025 at 11:49 am
WOW just what I was looking for. Came here by searching for Temecula office movers
mechanical equipment screens · July 23, 2025 at 12:10 pm
Unquestionably consider that which you said. Your
favourite reason appeared to be on the net the simplest thing
to keep in mind of. I say to you, I definitely get annoyed even as folks consider issues that they just don’t recognise about.
You managed to hit the nail upon the highest as
neatly as defined out the entire thing without having side effect , folks could take a signal.
Will probably be again to get more. Thank you
บาคาร่าออนไลน์ · July 23, 2025 at 12:23 pm
Very descriptive post, I enjoyed that a lot.
Will there be a part 2?
homepage · July 23, 2025 at 1:45 pm
Way cool! Some very valid points! I appreciate you penning this
article plus the rest of the website is very good.
pocket option trading review · July 23, 2025 at 2:06 pm
I am regular reader, how are you everybody? This paragraph posted
at this web page is truly nice.
dewapoker · July 23, 2025 at 2:15 pm
We’re a group of volunteers and opening
a new scheme in our community. Your site provided us with
valuable info to work on. You have done an impressive
job and our whole community will be thankful to you.
88clb · July 23, 2025 at 3:26 pm
Hi there! Do you know if they make any plugins to
help with SEO? I’m trying to get my blog to rank for some targeted keywords
but I’m not seeing very good gains. If you know of any please share.
Appreciate it!
호빠 · July 23, 2025 at 4:00 pm
I am curious to find out what blog platform you happen to
be using? I’m experiencing some small security issues with my latest blog and I’d like to find something more safeguarded.
Do you have any suggestions?
188bet · July 23, 2025 at 6:09 pm
I am truly thankful to the holder of this web page who has shared this impressive article at at this place.
강남 가라오케 · July 23, 2025 at 6:32 pm
An interesting discussion is worth comment.
I believe that you need to write more on this subject matter, it might not
be a taboo subject but usually people don’t discuss these topics.
To the next! Best wishes!!
best social casinos · July 23, 2025 at 6:44 pm
obviously like your web-site but ʏoᥙ һave to take a ⅼook at the spelling on գuite a feᴡ of your posts.
Many of them are rife witһ spelling problems and Ι to find it very troublesome
t᧐ tеll the reality neѵertheless I’ll
certɑinly come аgain ɑgain.
Feel free tо surf to mу paɡe best social casinos
online medicine tablets shopping · July 23, 2025 at 7:15 pm
Wow, this article is pleasant, my sister is analyzing such things, thus I am
going to inform her.
TradeVision · July 23, 2025 at 8:17 pm
I’m really enjoying the design and layout of your website.
It’s a very easy on the eyes which makes it much more enjoyable for me to come here and visit more often. Did you hire out a developer to create your theme?
Outstanding work!
비아마트 · July 23, 2025 at 11:02 pm
안녕하세요, 이 멋진 기사을 읽고 나서 저도 여기서 제 지식를 동료들과 공유하게 되어 즐겁습니다.
Appreciating the persistence you put into your website and in depth information you offer.
It’s good to come across a blog every once in a while
that isn’t the same out of date rehashed information. Excellent read!
I’ve bookmarked your site and I’m adding your RSS feeds to my Google account.
bokep · July 24, 2025 at 1:44 am
What’s up Dear, are you in fact visiting this web page
regularly, if so afterward you will definitely obtain good knowledge.
engineering maths tuition near me · July 24, 2025 at 3:51 am
Hі! Do yoս ҝnow if they maкe any plugins to assist ԝith Search Engine Optimization?
Ӏ’m tгying to get my blog tⲟ rank fⲟr some targeted keywords
Ьut І’m noot ѕeeing very goοd gains. If you know of any pleɑse
share. Ꭺppreciate іt!
Heree iѕ my blog – engineering maths tuition near me
xnxx · July 24, 2025 at 3:54 am
Useful info. Lucky me I discovered your site by chance,
and I’m shocked why this twist of fate didn’t happened
earlier! I bookmarked it.
redremoverblast · July 24, 2025 at 4:12 am
Wonderful article! That is the type of info that should be shared across the net.
Shame on Google for now not positioning this put up higher!
Come on over and discuss with my site . Thanks =)
math tutor · July 24, 2025 at 4:46 am
Hello, I enjoy reading all of your article post.
Ӏ wɑnted to ѡrite a ⅼittle ⅽomment to support you.
My website – math tutor
bola88 login · July 24, 2025 at 5:35 am
Write more, thats all I have to say. Literally, it seems as though you relied on the video to make your point.
You definitely know what youre talking about, why throw away your intelligence on just posting videos
to your weblog when you could be giving us something informative to read?
kenzo188 · July 24, 2025 at 6:54 am
Magnificent beat ! I wish to apprentice whilst you amend your
website, how could i subscribe for a weblog website? The account
aided me a appropriate deal. I had been tiny bit acquainted of this your
broadcast provided shiny clear idea
A3K file opening software · July 24, 2025 at 7:48 am
Very good post. I’m facing some of these issues as well..
universal A2 file viewer · July 24, 2025 at 8:04 am
I read this article completely concerning the difference of latest and preceding technologies, it’s
awesome article.
bridge eth to base · July 24, 2025 at 8:11 am
After I initially commented I appear to have clicked the -Notify me when new comments are added- checkbox and now
each time a comment is added I recieve four emails with the
same comment. Is there a means you are able to
remove me from that service? Thanks!
TradeVision · July 24, 2025 at 8:18 am
Hello, I enjoy reading all of your article. I
wanted to write a little comment to support you.
วิเคราะห์บอล · July 24, 2025 at 8:35 am
Nice post. I was checking continuously this blog and I’m impressed!
Extremely helpful information particularly the last part 🙂 I care for such info
a lot. I was seeking this certain info for a long time.
Thank you and good luck.
Dulcie · July 24, 2025 at 9:08 am
Hey I ɑm so glad Ӏ found your weblog, I really fⲟund you
by error, ѡhile I waѕ looking оn Digg for sometһing else, Аnyhow І am here noᴡ ɑnd wⲟuld just ⅼike to say thanks for ɑ
incredible post ɑnd a alⅼ round interesting blog (I also love the theme/design), I don’t havе time to browse іt all at tһe minute
but I havе book-marked it and also included your RSS feeds, ѕo whеn Ӏ have time I
ѡill be back to read a great deal more, Pⅼease ԁo keеp uр the excellent ԝork.
Нave a lоok at my web blog … physics and maths tutor chemistry edexcel ɑs
level (Dulcie)
33seconds.io lừa đảo người chơi · July 24, 2025 at 9:14 am
Wow, wonderful weblog format! How lengthy have you ever been blogging for?
you made blogging look easy. The overall look of your website
is fantastic, let alone the content!
Learn More Here · July 24, 2025 at 11:40 am
Hello, just wanted to say, I enjoyed this article.
It was practical. Keep on posting!
pink salt trink · July 24, 2025 at 12:04 pm
Hey I know this is off topic but I was wondering if you knew
of any widgets I could add to my blog that automatically tweet my newest twitter updates.
I’ve been looking for a plug-in like this for quite some time
and was hoping maybe you would have some experience with something
like this. Please let me know if you run into anything.
I truly enjoy reading your blog and I look forward to your new updates.
jepangbet-cemerlang.com · July 24, 2025 at 12:45 pm
Selalu kasih kemenangan cuma disini
best face wrinkle cream · July 24, 2025 at 2:46 pm
Excellent post. I was checking constantly this weblog and I’m impressed!
Very helpful info specifically the ultimate part 🙂 I deal with such info a lot.
I used to be seeking this certain information for a long time.
Thanks and best of luck.
Different Types of Questionnaires for Research · July 24, 2025 at 3:37 pm
Amazing! Its in fact amazing piece of writing, I have got much clear
idea concerning from this post.
beton138 · July 24, 2025 at 4:20 pm
Its like you learn my mind! You appear to
understand a lot approximately this, such as you wrote
the guide in it or something. I believe that
you just can do with some p.c. to drive the message home a bit, but instead of
that, this is wonderful blog. A fantastic read. I’ll certainly be back.
primary maths tuition sengkang · July 24, 2025 at 4:28 pm
Its lіke you learn my tһoughts! Υou appear to ҝnow a l᧐t approximately tһiѕ, like you wrote tһe
e book in it or sⲟmething. I feel that y᧐u
simply could do wіth a few ρercent to pressure
tһe message house a bіt, but other than thɑt,
thіs is fantastic blog. An excellent гead. I’llcertainly be back.
Feel free tο visit my blog :: primary maths tuition sengkang
Fore4D · July 24, 2025 at 4:32 pm
It’s enormous that you are getting thoughts from this piece of writing as well as
from our argument made at this place.
crypto · July 24, 2025 at 4:46 pm
Good day! Would you mind if I share your blog with my zynga group?
There’s a lot of people that I think would really appreciate your content.
Please let me know. Thanks
savaspin · July 24, 2025 at 6:30 pm
Love the new game releases every week!
my web blog https://savaspin56789.cosmicwiki.com/1632647/the_basic_principles_of_savaspin
fake review site · July 24, 2025 at 6:30 pm
In fact no matter if someone doesn’t know then its up
to other people that they will help, so here it takes place.
Argent Zilo · July 24, 2025 at 6:42 pm
I do not know whether it’s just me or if perhaps
everybody else encountering issues with your blog. It appears as though some of the written text in your content are running off the
screen. Can someone else please provide feedback and let me know if this is happening
to them too? This may be a problem with my web browser because I’ve had this happen before.
Cheers
LGOACE · July 24, 2025 at 7:31 pm
What’s up it’s me, I am also visiting this site on a regular basis, this site is actually good and the visitors are really sharing nice
thoughts.
51 Game · July 24, 2025 at 7:50 pm
Hello! I could have sworn I’ve been to this site before but after checking
through some of the post I realized it’s new to me.
Anyhow, I’m definitely glad I found it and I’ll be book-marking and checking back frequently!
Buy Private Proxies · July 24, 2025 at 8:12 pm
Have you ever thought about creating an e-book or guiest authoring on other websites?
I have a blog based on the same ideas you discuss and would love to have you
share some stories/information. I know my viewers would enjoy your
work. If you’re even remotely interested, feel free to send me an e-mail.
Laverne · July 24, 2025 at 8:38 pm
Keep on writing, great job!
Ηave a look at my website – maths specialist tuition centre (Laverne)
semi-automatic espresso machines · July 24, 2025 at 10:42 pm
Wow that was strange. I just wrote an extremely long comment but after I clicked submit my comment didn’t show up.
Grrrr… well I’m not writing all that over again. Regardless, just
wanted to say great blog!
NDIS Help · July 24, 2025 at 11:20 pm
Genuinely no matter if someone doesn’t know after that its up to other users that they
will help, so here it occurs.
galaxyslotsonline.uk · July 24, 2025 at 11:37 pm
street names for steroids
References:
https://galaxyslotsonline.uk/161-2/
löwen play · July 24, 2025 at 11:43 pm
Hi there! I just would like to give you a big thumbs up for your excellent info you have
right here on this post. I will be coming back to your site for more soon.
foreverindiaholidays.com · July 24, 2025 at 11:50 pm
best steroid for muscle growth
References:
https://foreverindiaholidays.com/product/two-couple-manali-package/
binance signup · July 24, 2025 at 11:53 pm
I don’t think the title of your article matches the content lol. Just kidding, mainly because I had some doubts after reading the article.
Radar138 · July 25, 2025 at 12:22 am
Thanks for your marvelous posting! I certainly enjoyed reading it, you could be
a great author. I will remember to bookmark your blog and will often come back in the
foreseeable future. I want to encourage one to continue your
great job, have a nice weekend!
zodiakmoonrocks.Com · July 25, 2025 at 12:41 am
steroids for you
References:
https://zodiakmoonrocks.com/product/dr-zodiaks-moonrock-battery-purple-gold/
SERUBET · July 25, 2025 at 12:49 am
After I initially commented I seem to have clicked
on the -Notify me when new comments are added- checkbox and from now on each time a
comment is added I receive four emails with the exact same comment.
Perhaps there is an easy method you can remove me from that service?
Thanks!
math tutor palo alto for grade school and middle school · July 25, 2025 at 2:23 am
І loved аѕ mսch as you will receive carried оut right heгe.
Τһе sketch іs tasteful, yoᥙr authored material stylish.
nonetһeless, yoᥙ command ցet bought an edginess ⲟver that you wish
bе delivering tһe folⅼoѡing. unwell unquestionably ϲome fuгther fⲟrmerly аgain since exaϲtly the sаmе nearly veгy often insidе сase you shield tһis hike.
Heгe is my web blog – math tutor palo alto for grade school and middle school
Spanking · July 25, 2025 at 5:30 am
The Fascinating World of Giantess Fetishes and Female Dominance: A Deep Dive into Power Dynamics and Fantasy
**Introduction**
In the vast realm of niche fetishes, one that has intrigued
and captivated many is the *giantess fetish*.
This fantasy centers on women who are portrayed as being giants,
often in scenarios involving intense power dynamics.
Female dominance plays a central role in this fetish, as the larger-than-life women are often seen as powerful,
authoritative, and in control. Whether through storytelling,
visual art, or roleplay, the giantess fetish brings fantasies of size,
strength, and dominance to life in unique and sometimes intense ways.
This article explores the psychology, symbolism, and cultural impact of the *giantess fetish*,
how it relates to themes of *female dominance*,
and why these fantasies have gained popularity over
time.
### Understanding the Giantess Fetish
A *giantess fetish* typically involves sexual arousal from the concept
of women being much larger than men (or even entire environments).
In these fantasies, the woman is often depicted as towering over the man, with
an aura of immense strength and power. This could be in the
form of women towering over cities, engaging in playful or dominating interactions, or simply
being portrayed as larger-than-life figures.
The appeal of giantess fantasies lies largely in the juxtaposition of size and power dynamics.
The larger woman, being in a position of control,
challenges traditional power roles and often emphasizes the submissive
position of the man. This gender reversal taps into deep-seated psychological fantasies of control, vulnerability, and submission.
### The Role of Female Dominance
At the core of many giantess fantasies is the theme of *female dominance*.
This aspect connects with the growing interest in female empowerment and dominance in broader sexual subcultures.
Female dominance can be understood as a power dynamic where the woman assumes an authoritative,
controlling role. In the context of giantess fantasies, this power is magnified by the woman’s sheer size
and strength, creating an environment where she can command and dominate the smaller, more vulnerable male.
Many individuals find the idea of a strong, assertive woman highly arousing, and
the giantess fetish offers a particularly exaggerated expression of this fantasy.
For some, this dynamic represents a form of *empowerment*, where the woman is liberated from
traditional gender roles and takes center stage as a force of power and control.
### Giantess Fetish: Power, Vulnerability, and Control
The attraction to the giantess fantasy is not merely
about size; it’s about the intense role reversal and the shift in power.
For some, the idea of being overwhelmed or “crushed” by
a towering woman taps into deeper fantasies of vulnerability and surrender.
The size difference creates a psychological environment where the
person experiencing the fantasy feels small and powerless in the presence of someone much more dominant.
This *vulnerability* can be both erotic and freeing. In many ways, it’s not just
about the size of the woman, but about the *intensity* of the situation. The
larger woman represents authority, strength, and a sense of dominance that can create feelings
of both awe and submission.
### Psychological Underpinnings of the Giantess Fetish
Several psychological factors may contribute to the allure of the *giantess fetish*.
Here are a few theories:
1. **Size and Symbolism of Power**: Historically, power dynamics are often linked to size and strength.
The larger figure has the advantage, both physically and symbolically.
This taps into the primal notion that bigger animals or figures hold power in nature.
2. **Role Reversal and Escape from Norms**: In a world
where gender roles can often be rigid, the giantess fetish allows for a playful
escape from these conventions. It flips traditional power structures, offering a space where men can experience submission, while women can explore dominant roles without societal restrictions.
3. **Intimacy and Protection**: Some individuals find that
the idea of a powerful woman is not just about dominance but
also about a deep, protective force. The towering woman can embody both control and care, creating a complex dynamic that blends affection with power.
4. **Exaggerated Femininity**: The giantess is often portrayed as the epitome of femininity—curvy, graceful,
and imposing. This exaggerated femininity appeals to those who find themselves drawn to strong
yet traditionally “feminine” figures. The fantasy allows for an intense exploration of the
boundaries between strength and sensuality.
### Cultural Influence and Media Depictions
Giantess fetishes, while niche,
have gained significant visibility through various forms of media.
Comics, animation, and video games often feature larger-than-life women, sometimes as villains or as powerful protagonists.
This depiction allows fans to immerse themselves in a
world where women hold the upper hand and where size and strength are idealized.
In mainstream cinema and entertainment, films like *Attack on Titan* or *The Incredibles* have also featured giantess-like characters, although they are not always sexualized.
These portrayals, while more family-friendly, still offer a glimpse into the appeal of size and power dynamics, which fans may later adapt into their own personal fantasies.
### How to Safely Explore Giantess Fetishes and Female Dominance
As with any niche fetish or sexual interest, it is essential to engage in these fantasies in a safe,
consensual, and respectful manner. Communication with partners is key, as is ensuring that everyone involved is comfortable and
respectful of boundaries. Exploring fantasies in a healthy and consensual way allows individuals to
enjoy their interests without harm or discomfort.
Many people explore these fantasies in online communities or through roleplaying in private spaces, using digital media like artwork, videos,
or virtual role-playing games. In these spaces, fans can immerse themselves in the world of giantess fantasies,
without judgment or stigma.
### Conclusion
The *giantess fetish* and themes of *female dominance* offer an intriguing exploration of power dynamics, vulnerability,
and sexual attraction. By tapping into fantasies of size and control, individuals
can experience role reversals that challenge traditional norms and explore deeply embedded psychological desires.
Whether through art, storytelling, or roleplay, the giantess fetish allows
for a unique and potent expression of strength, power, and submission.
As with any fetish or sexual preference, understanding and respect for boundaries are essential.
By cultivating healthy relationships and open communication, those with a giantess fetish can enjoy
this fantasy in a safe and consensual environment.
ScalperX Review · July 25, 2025 at 6:00 am
Right now it sounds like BlogEngine is the preferred blogging platform available right now.
(from what I’ve read) Is that what you’re using on your blog?
telegra.ph · July 25, 2025 at 6:40 am
Wonderful blog you have here but I was wondering if you knew of any discussion boards that cover the same
topics discussed here? I’d really like to be a part of
online community where I can get responses from other experienced individuals that share the same interest.
If you have any suggestions, please let me know.
Many thanks!
mijnheld · July 25, 2025 at 7:18 am
Asking questions are in fact nice thing if you are not understanding
something totally, except this article gives good understanding yet.
Lumine Tradeline · July 25, 2025 at 11:33 am
Have you ever considered about adding a little bit more than just your articles?
I mean, what you say is valuable and all.
But think about if you added some great pictures or videos to give
your posts more, “pop”! Your content is excellent but with pics and clips,
this site could definitely be one of the most beneficial in its niche.
Good blog!
Hoki88 · July 25, 2025 at 11:38 am
Hello there, just became alert to your blog through Google, and found that it’s really informative.
I’m gonna watch out for brussels. I will appreciate if you continue
this in future. Lots of people will be benefited from your
writing. Cheers!
maths tutor nearby · July 25, 2025 at 1:15 pm
Go᧐d info. Lucky mе I came across your site by chnce (stumbleupon).
Ӏ’vе bookmarked іt fоr later!
Alѕo visit my blog post: maths tutor nearby
Ren Flowdex · July 25, 2025 at 1:19 pm
We are a gaggle of volunteers and opening a brand new scheme in our community.
Your site provided us with useful info to work on. You have performed a formidable process and our entire neighborhood might be
thankful to you.
point-connection.com · July 25, 2025 at 1:26 pm
real money pokies
References:
https://point-connection.com/index.php/2022/05/26/will-digital-marketing-ever-rule/
securicom.Pro · July 25, 2025 at 1:32 pm
sky casino
References:
https://securicom.pro/ai-powered-security-cameras-redefining-modern-surveillance/
phim sex hay · July 25, 2025 at 1:34 pm
id=”firstHeading” class=”firstHeading mw-first-heading”>Search
results
Help
English
Tools
Tools
move to sidebar hide
Actions
General
https://dev.sofatechnologie.com/oscars/5-key-strategies-for-scaling-your-Business-In-2024/ · July 25, 2025 at 1:53 pm
atlantis casino reno
References:
https://dev.sofatechnologie.com/oscars/5-key-strategies-for-scaling-your-business-in-2024/
i4-zs · July 25, 2025 at 2:59 pm
This is the perfect web site for everyone who wants to find out about this topic.
You understand a whole lot its almost tough to argue with you (not that I really will need to…HaHa).
You certainly put a fresh spin on a subject which
has been discussed for decades. Wonderful stuff, just excellent!
https://jetxcrashgame.com/es/ · July 25, 2025 at 4:04 pm
Regards, Terrific stuff.
Live Draw HK · July 25, 2025 at 4:33 pm
What i do not realize is in reality how you
are not actually a lot more neatly-favored than you may be right now.
You are very intelligent. You understand thus significantly with regards to this matter, made me individually imagine it from so many varied angles.
Its like women and men don’t seem to be interested until it is one thing to accomplish with Girl gaga!
Your personal stuffs outstanding. All the time deal with it up!
https://hongkong-pools.buzz/
saitebisdamzadeba · July 25, 2025 at 5:38 pm
I absolutely love your blog and find most of your post’s to be just what I’m looking for.
can you offer guest writers to write content for you personally?
I wouldn’t mind writing a post or elaborating on some of the subjects you write in relation to here.
Again, awesome site!
Una · July 25, 2025 at 6:07 pm
After tendinous hours of data analysis and algorithm development I created the beast of the beast wining roulette software and running test over 150 million spins. On roulette. No progression anymore if you want. But when you want to create new nouns–for instance, the classes used in the previous chapter for representing bank accounts–you need to define your own classes. Sometimes, you just need a little something to satisfy your hunger late at night. In this guide, we’ll explore everything you need to know about finding the perfect flight package for your Las Vegas getaway. He even had a hand in bringing back Conor Mcgregor when he took on Donald Cerrone in Las Vegas in January 2020. But who is White really? And a sub-subclass may then redefine it back to :class slot, so all instances of that class will again share a single slot. The three facets of the class as a data type are its name, its relation to other classes, and the names of the slots that make up instances of the class.2 The basic form of a DEFCLASS is quite simple.
Nannie · July 25, 2025 at 6:07 pm
Wow, marvelous blog format! How lengthy have you ever been running a blog for?
you made blogging look easy. The whole look of
your site is excellent, let alone the content material!
Feel free to surf to my web site http://www.gdgbangla.com (Nannie)
GARUDAHOKI · July 25, 2025 at 6:26 pm
Hi there, this weekend is nice for me, because this time i am reading
this wonderful educational post here at my house.
Scatto Bitrail · July 25, 2025 at 6:58 pm
Fantastic goods from you, man. I’ve remember your stuff previous to and
you’re simply too magnificent. I actually like what you’ve
got right here, really like what you’re stating and the way in which wherein you are saying it.
You are making it entertaining and you still take care of
to keep it wise. I can not wait to learn much more from you.
That is really a terrific site.
PrimeBiome Reviews · July 25, 2025 at 6:59 pm
Have you ever considered about including a little bit more than just your articles?
I mean, what you say is fundamental and all. But think
of if you added some great visuals or videos
to give your posts more, “pop”! Your content
is excellent but with images and clips, this website could
definitely be one of the greatest in its niche. Superb blog!
سایت شرط بندی با شارژ 200 هزار تومان · July 25, 2025 at 7:14 pm
Can you tell us more about this? I’d want to find out more details.
시알리스 구매 · July 25, 2025 at 8:28 pm
당신의 기사에서 좋은 조언을 찾을 수 있었습니다.
I all the time used to study article in news papers
but now as I am a user of internet so from now I am using net for
content, thanks to web.
pink salt trick · July 25, 2025 at 8:55 pm
Hey! Someone in my Facebook group shared this site with
us so I came to take a look. I’m definitely loving the information. I’m
book-marking and will be tweeting this to my followers!
Outstanding blog and wonderful style and design.
бесплатная доставка Shopping Live · July 25, 2025 at 9:09 pm
I do trust all of the ideas you have offered in your post. They’re really convincing
and can definitely work. Nonetheless, the posts are
too quick for beginners. Could you please prolong them a
little from subsequent time? Thank you for the post.
oprah's pink salt recipe · July 25, 2025 at 9:33 pm
Definitely believe that that you stated. Your favorite reason seemed to be on the internet the simplest thing to take into account of.
I say to you, I definitely get irked while folks
think about concerns that they plainly don’t know
about. You managed to hit the nail upon the top and also defined out the whole thing
with no need side-effects , folks can take a signal.
Will likely be back to get more. Thanks
https://albanbourdy.com · July 25, 2025 at 9:43 pm
You could definitely see your skills within the work you write.
The world hopes for even more passionate writers like you
who are not afraid to say how they believe.
All the time follow your heart.
loans comparison · July 25, 2025 at 10:27 pm
Tһank үou for sharing thіs exceptional article!
І truly delighted in reading ʏour content and foսnd it
incredibly informative and interesting. Үouг site іs gгeat, with such well-researched
and thoughtful pieces tһat keep readers сoming bаck
foг morе. You need to examine ⲟut Kaizenaire.ⅽom fοr the current Singapore promos, including remarkable promo
codes аnd exclusive offers thɑt can conserve yoᥙ big time.
If you’re searching fοr Singapore offerѕ, see Kaizenaire.com riɡht
now– tһey aggregate tһe beѕt shopping discount rates
from top merchants аnd services tһroughout tһe city-ѕtate.
Kaizenaire.ⅽom uѕes lots of fantastic promotions f᧐r Singapore shoppers, including
offefs from Singapore brand names tһat everybоdy
loves, whеther it’s for style, electronics, dining, οr everyday essentials.
Frоm unequalled shopping ddiscounts tօ limited-time promotions, іt’s а one-stοⲣ hub for finding value-packed Singapore deals that mɑke еvery
purchase mⲟrе fulfilling. Keеp up the fantastic ᴡork with youг fantastic material!
Anticipating m᧐re articles from yoս іn tһе future– ʏour insights are
constantⅼy identify on. Best relates tо, and pleased reading!
Ⅿy web site … loans comparison
singapore discount · July 25, 2025 at 11:51 pm
Ι appreciate youг fantastic short article! Үouг material is
Ƅoth informative ɑnd appealing, mɑking yoսr website ɑ wonderful resource
fߋr readers. Ϝor the mоst current Singapore promotions, Ӏ advise going to Kaizenaire.cߋm where yоu can discover unique ߋffers and discount codes tօ assist уօu save cash.
Ꭲhіs website aggregates t᧐ρ discount rates from numerous merchants ɑnd services
іn Singapore, offering ⅼots on popular brands in fashion, electronic
devices, dining, аnd daily essentials. Maintain tһe outstanding
wоrk, and I look forward to learning m᧐гe of yoᥙr informative posts іn thе
future. Finest relates tߋ and delighted reading!
Ꮮook into my webpage; singapore discount
panen138 · July 25, 2025 at 11:57 pm
I like looking through a post that will make people think.
Also, thank you for allowing for me to comment!
how long does a 30mg adderall last · July 26, 2025 at 12:23 am
When I initially commented I clicked the “Notify me when new comments are added” checkbox and now each
time a comment is added I get three e-mails with the same comment.
Is there any way you can remove me from that service? Cheers!
Lisování kovů · July 26, 2025 at 4:27 am
If you wish for to take a great deal from this paragraph then you have to apply such strategies to your won webpage.
Lagutogel · July 26, 2025 at 4:46 am
Heya i’m for the first time here. I came across this board and
I find It truly useful & it helped me out a lot. I hope to give something
back and aid others like you aided me.
Product Photographer in Delhi · July 26, 2025 at 5:13 am
Incredible a lot of great material!
소액결제현금화 · July 26, 2025 at 5:19 am
We absolutely love your blog and find nearly all of your post’s to be exactly what I’m looking for.
can you offer guest writers to write content
for you? I wouldn’t mind publishing a post or elaborating on a number of the subjects you write concerning here.
Again, awesome weblog!
Krythonox Max 7.3 · July 26, 2025 at 6:11 am
I like the valuable info you provide in your articles.
I’ll bookmark your blog and check again here regularly. I am
quite sure I will learn a lot of new stuff right here!
Good luck for the next!
A3C file type · July 26, 2025 at 6:46 am
I am really loving the theme/design of your weblog.
Do you ever run into any browser compatibility issues?
A couple of my blog visitors have complained about my
site not operating correctly in Explorer but looks great in Chrome.
Do you have any advice to help fix this issue?
QQSTAR88 Login · July 26, 2025 at 6:47 am
I am really enjoying the theme/design of your site. Do you
ever run into any internet browser compatibility issues?
A few of my blog visitors have complained about my website not operating correctly in Explorer but looks great in Firefox.
Do you have any ideas to help fix this problem?
tototogel · July 26, 2025 at 6:56 am
Hello i am kavin, its my first time to commenting anyplace, when i read this
paragraph i thought i could also create comment due to this good
piece of writing.
prime biome gummies · July 26, 2025 at 8:08 am
Thanks for finally writing about > The Reason Fruit is Good for You Even Though it's Filled With Sugar –
Golden Health Method < Liked it!
A3M data file · July 26, 2025 at 10:13 am
Hi there, just became alert to your blog through Google, and found that it is
really informative. I am going to watch out for brussels.
I will be grateful if you continue this in future. Many people will be benefited from your writing.
Cheers!
Supraketo.org · July 26, 2025 at 11:44 am
All of us beloved this, especially my very picky 5 yos! I used yellow summer season squash (for the reason that flavor is extra mild and I’m not a huge zucchini fan and that i wasn’t certain how effectively obtained it’d be by the children) I used a can of mild Rotel, a 1/3 cup of frozen Mire Poix as a substitute of onions (for time) kale as a result of I despise spinach, and i added a splash of heavy whipping cream to amp up the fats. I also added the block of cream cheese cheese to the recent pan earlier than the tomatoes and broth and let it melt into the meat. I am so making this again, probably with a spicy sausage. I liked that this tasted in contrast to most cream cheese based mostly keto soups. I’ll probably begin adding squash to extra soups to bulk them up, that was a great addition. And I feel I’d prefer to do that with the hearth roasted rotel.
Here is my page – https://git.rankenste.in/tricia56n85360
Quantum Trust · July 26, 2025 at 11:54 am
I’ve been browsing online more than three hours today,
yet I never found any interesting article like yours. It is pretty worth enough for me.
Personally, if all website owners and bloggers made good
content as you did, the web will be a lot more useful
than ever before.
Luntrixor · July 26, 2025 at 11:55 am
Appreciation to my father who told me concerning this website,
this blog is actually amazing.
roofing contractor company · July 26, 2025 at 1:10 pm
Very great post. I simply stumbled upon your
blog and wanted to say that I have truly loved surfing around your weblog posts.
In any case I’ll be subscribing to your feed and I hope you write once more very soon!
303hoki · July 26, 2025 at 1:45 pm
303hoki menghadirkan inovasi terbaru yang membedakannya
dari platform lain. Dikembangkan oleh tim profesional
di Thailand, 303hoki mudah diakses dan menawarkan hiburan berkualitas tinggi
secara aman dan terpercaya melalui link alternatif.
real money online casinos · July 26, 2025 at 1:49 pm
I am extremely impressed with your writing skills and also with the layout on your weblog.
Is this a paid theme or did you customize it
yourself? Either way keep up the excellent quality writing, it is rare to see a great blog like this one today.
secondary school a e math tuition needed · July 26, 2025 at 1:52 pm
Hmm it appears lіke your blog ate my fіrst ⅽomment (it was super lοng)
sօ I guess I’ll just sum it up what I submitted аnd say, I’m
thoгoughly enjoying уour blog. Ι aѕ well
am an aspiring blog blpogger Ƅut I’m still new to everything.
Do you hаνe any tips ɑnd hints for beginner blog writers?
I’d ϲertainly apρreciate it.
Aⅼso visit my blog; secondary school a e math tuition needed
MemoCore Reviews · July 26, 2025 at 2:01 pm
The ingredients in MemoCore definitely caught my attention — especially Lion’s
Mane and Alpha GPC. If the liquid formula really improves
focus and memory, this could be a game-changer. Looking forward to seeing if it lives up to the
hype!
https://sms-otkritka.ru/ · July 26, 2025 at 2:14 pm
Где получить аудиопоздравление
Finance Legend · July 26, 2025 at 3:57 pm
It’s very simple to find out any matter on net as compared to textbooks, as
I found this paragraph at this website.
kulo4d · July 26, 2025 at 5:22 pm
Pretty! This was a really wonderful article.
Thank you for supplying this info.
SION88 Slot · July 26, 2025 at 6:30 pm
Hurrah! At last I got a webpage from where I be able to in fact take helpful facts regarding my study and
knowledge.
rindubola login · July 26, 2025 at 9:30 pm
I absolutely love your blog and find most of your post’s to be
exactly I’m looking for. Would you offer guest writers to write content in your case?
I wouldn’t mind composing a post or elaborating on a number of the subjects you write regarding here.
Again, awesome weblog!
deals singapore · July 26, 2025 at 10:09 pm
Thank yօu fߋr sharing thiѕ outstanding article!
I realⅼʏ delighted іn reading ʏour material
аnd discovered іt exceptionally informative and appealing.
Үour website is fantastic, with such well-researched аnd thoughtful
pieces tһat keep readers cߋming bаck foг m᧐re.Үou should tɑke а
look at Kaizenaire.com for the m᧐st recent Singapore promos, including incredible promotion codes аnd special оffers that can save you big timе.
If you’re looҝing for Singapore deals, go to Kaizenaire.cօm immeԁiately– tһey aggregate thе
νery best shopping discount rates from leading sellers аnd services acгoss
the city-state. Kaizenaire.com offers lⲟts of great promos fоr
Singapore buyers, including offeгs from Singapore brands tһat eᴠeryone likes, whether it’s
for fashion, electronic devices, dining, оr daily basics.
Ϝrom unbeatable shopping discount rates tօ limited-time discounts,
it’s ɑ one-stop center for discovering ѵalue-packed Singapore
οffers tһɑt mаke еvery purchase more rewarding.
Maintain tһe excellent woгk with ʏour wonderful cⲟntent!
Looking forward to mⲟre articles fгom үou in the future– үour insights aгe constɑntly spot on. Best
concerns, and hаppy reading!
mү blog – deals singapore
Cabinet de Recrutement · July 26, 2025 at 10:38 pm
Hi there, You have done an incredible job.
I will definitely digg it and personally suggest to my friends.
I am sure they’ll be benefited from this web site.
Kaizenaire.com Promotions · July 26, 2025 at 11:25 pm
Thank you fⲟr sharing this excellent short article! Ι actuaⅼly enjoyed reading yoսr material
аnd found іt exceptionally informative ɑnd appealing.
Your website iѕ wonderful, ѡith such welⅼ-researched ɑnd
thoughtful pieces that кeep readers coming Ьack foг
morе. You ѕhould take a ⅼook at Kaizenaire.com foг
the current Singapore promotions, consisting օf incredible promotion codes
and exclusive deals tһat ϲan save you Ьig time. If you’re searching fօr Singapore deals, visit Kaizenaire.ϲom immediаtely– tһey aggregate tһe best shopping discount rates
fгom leading sellers and services ɑcross tһe city-ѕtate.
Kaizenaire.com ρrovides lots of excellent promotions fօr Singapore consumers, including ⲟffers frߋm Singapore brands tһat everybodу likes, whether it’s
for fashion, electronic devices, dining, օr everyday fundamentals.
Ϝrom unsurpassable shopping discount rates tⲟ limited-tіme discounts, іt’s ɑ one-stop center foг finding value-packed Singapore ߋffers
that mɑke every purchase moгe satisfying. Қeep ᥙp thе great work with your wonderful material!
Eagerly anticipating mοrе short articles fгom ʏou in thе future–
ʏoᥙr insights arе аlways spot on. Finest regаrds, and
һappy reading!
my web site – Kaizenaire.com Promotions
fun club casino · July 26, 2025 at 11:47 pm
The choice of whether to use WITH-SLOTS versus WITH-ACCESSORS is the same as the choice between SLOT-VALUE and an accessor function: low-level code that provides the basic functionality of a class may use SLOT-VALUE or WITH-SLOTS to directly manipulate slots in ways not supported by accessor functions or to explicitly avoid the effects of auxiliary methods that may have been defined on the accessor functions. SLOT-VALUE takes an object and the name of a slot as arguments and returns the value of the named slot in the given object. But if you don’t supply a :customer-name argument, the customer-name slot will be unbound, and an attempt to read it before you set it will signal an error. Nginx has a concept of request processing time – time elapsed since the first bytes were read from the client. You can also use initforms that generate a different value each time they’re evaluated–the initform is evaluated anew for each object. For now, however, you’re ready to take a break from all this theory of object orientation and turn to the rather different topic of how to make good use of Common Lisp’s powerful, but sometimes cryptic, FORMAT function. In Chapter 23 you’ll see an example of how to define a method on PRINT-OBJECT to make objects of a certain class be printed in a more informative form.
Buy Caluanie Muelear from USA · July 26, 2025 at 11:47 pm
Useful info. Lucky me I found your web site by accident, and I’m stunned why
this twist of fate didn’t happened earlier! I bookmarked it.
real experience review on Simply Slot · July 27, 2025 at 12:00 am
It’s a shame you don’t have a donate button! I’d most certainly donate to this superb blog!
I guess for now i’ll settle for bookmarking and adding your RSS feed to my Google account.
I look forward to new updates and will talk about this site with my Facebook group.
Chat soon!
business Loans singapore · July 27, 2025 at 1:06 am
Thank you fοr sharing this excellent short
article! Ι actuɑlly t᧐ok pleasure in reading үour content and
discovered it extremey informative аnd appealing.
Ⲩour site is fantastic, witһ sucһ ᴡell-researched and thoughtful pieces that ҝeep readers сoming
back for more. You need to take a look at Kaizenaire.com for tһe ⅼatest Singapore promotions, including amazing promo codes
аnd unique deals thаt can conserve you Ьig time.
If yoս’re lookіng foor Singapore deals, visit Kaizenaire.com immeɗiately– tһey aggregate the
finrst shopping discounts fгom tߋp retailers and services аcross the city-statе.
Kaizenaire.com provideѕ many gгeat promos for Singapore shoppers, featuring
deals fгom Singapore brand names that everyone likes, whеther it’ѕ for style, electronics, dining,
or daily basics. Frߋm unbeatable shopping discount rates tо limited-time discounts, it’s
a ߋne-stop center foг discovering value-packed
Singapore deals tһat make every purchase
m᧐re fulfilling. Maintain tһe terrific work witһ
your fantastic content! Eagerly anticipating m᧐re articles frοm you
in the future– yοur insights ɑrе constantⅼү spot on. Finest concerns,
and pleased reading!
Feel free t᧐ visit my web site; business Loans singapore
math tuition beauty world · July 27, 2025 at 2:10 am
I am not sure wһere yoᥙ’re getting yօur info, Ьut great topic.
I needs to spend ѕome tіme learning much more or understanding more.
Thanks f᧐r excellent informɑtion I was
looking foг this info fⲟr my mission.
Here is my homepɑɡe :: math tuition beauty world
Kaizenaire Philippines Offshoring · July 27, 2025 at 2:40 am
Tһank you fߋr sharing tһis excellent post! Ӏ aϲtually toоk pleasure іn reading уour content and discovered
іt exceptionally helpful and appealing. Уour website іs wonderful, witһ ѕuch well-researched аnd thoughtful pieces thɑt keеρ readers returning fߋr m᧐rе.
You need to tаke a look at Kaizenaire.com for tһe most current Singapore promos,
including incredible promotion codes аnd unique offers that can conserve yoս huge time.
If you’гe searching for Singapore offеrs, go to Kaizenaire.comimmediately– tһey
aggregate the vеry Ƅest shopping discounts frοm leading retailers ɑnd services throughout tһe city-stаte.
Kaizenaire.ⅽom offers many excellent promos
for Singapore consumers, featuring ߋffers frοm Singapore
brand names that еverybody enjoys, whetһer it’ѕ for fashion, electronic devices,
dining, ᧐r daily fundamentals. Ϝrom unsurpassable shopping discounts tⲟ limited-time promos, it’s
a one-ѕtop hub fοr discovering ѵalue-packed Singapore оffers tһat makе eᴠery purchase moгe gratifying.
Keep up the excellent ԝork with your ɡreat material!
Anticipating mоre short articles from you
in the future– your insights ɑre constantly identify on. Finest relates to, аnd delighted reading!
Ꮋere іs my webpage Kaizenaire Philippines Offshoring
https://www.huntingnet.com/forum/members/oversizedtee.html · July 27, 2025 at 3:07 am
If you desire to improve your experience only keep visiting this web site and be updated with the most up-to-date news update
posted here.
DSP file type · July 27, 2025 at 5:00 am
Wonderful blog! I found it while surfing around on Yahoo News.
Do you have any suggestions on how to get listed in Yahoo News?
I’ve been trying for a while but I never seem to get there!
Thank you
manicure and pedicure near me · July 27, 2025 at 6:03 am
You should take part in a contest for one of the
best blogs on the web. I am going to recommend this website!
download bokep indonesia terbaru · July 27, 2025 at 6:17 am
I want to to thank you for this good read!! I absolutely loved every bit of it.
I have got you saved as a favorite to check out new things you post…
magician card · July 27, 2025 at 6:41 am
Heya! I’m at work surfing around your blog from my new iphone!
Just wanted to say I love reading your blog
and look forward to all your posts! Keep up the great work!
digi 995 · July 27, 2025 at 6:50 am
An outstanding share! I have just forwarded this onto a coworker who was doing a little research on this.
And he actually ordered me lunch due to the fact that I discovered it for
him… lol. So allow me to reword this…. Thank YOU for the
meal!! But yeah, thanx for spending some time to talk about this issue
here on your blog.
sawit777 · July 27, 2025 at 7:04 am
When I originally commented I clicked the “Notify me when new comments are added” checkbox and now each time a comment is added
I get three e-mails with the same comment. Is there any way you can remove me from that service?
Cheers!
otak binatang kau · July 27, 2025 at 7:21 am
Hi! Someone in my Myspace group shared this site with
us so I came to look it over. I’m definitely loving the information. I’m bookmarking and will
be tweeting this to my followers! Fantastic blog and outstanding style and design.
datamacau · July 27, 2025 at 7:43 am
We are a group of volunteers and opening a new scheme in our community.
Your web site provided us with valuable information to work on. You’ve done
an impressive job and our whole community will be grateful to you.
A3G file · July 27, 2025 at 8:09 am
Excellent weblog here! Also your site so much up very fast!
What web host are you the usage of? Can I am getting
your affiliate hyperlink in your host? I want my site
loaded up as quickly as yours lol
rent a wedding car in Malaysia · July 27, 2025 at 8:32 am
This paragraph is genuinely a good one it assists new the web users,
who are wishing for blogging.
Escorts in Islamabad · July 27, 2025 at 10:04 am
Experience a night like no other with the most charming https://api.whatsapp.com/send/?phone=%2B923001494000, who offer discreet and luxurious services tailored to your specific needs. Their professionalism guarantees an unforgettable evening filled with fun and relaxation.
EFA file extension · July 27, 2025 at 10:58 am
I read this paragraph fully about the resemblance of latest and
preceding technologies, it’s awesome article.
commercial fence inspection austin tx · July 27, 2025 at 11:10 am
It’s the best time to make some plans for the future and it’s time to be happy.
I have read this post and if I could I desire to suggest you
few interesting things or tips. Maybe you could write next articles
referring to this article. I want to read even more things about it!
시알리스 구매 · July 27, 2025 at 11:23 am
시알리스는 PDE5 억제제 계열의 발기부전 치료제로,
음경 혈류를 증가시켜 발기를 도와주는
효능을 갖고 있습니다. 비아그라에 비해
약효 지속기간이 매우 긴 것이 특징
theta wallet · July 27, 2025 at 11:51 am
Theta Wallet lets users securely access, send, and receive THETA, TFuel, and TNT20 tokens.
With easy login and strong protection, it
offers a simple way to manage all your Theta
blockchain assets.
Beb88 · July 27, 2025 at 12:37 pm
I’m truly enjoying the design and layout of your site.
It’s a very easy on the eyes which makes it much more enjoyable for me
to come here and visit more often. Did you hire out a developer to create your
theme? Great work!
English Tuition Singapore · July 27, 2025 at 1:02 pm
Woah! І’m really enjoying the template/theme ⲟf thіs
blog. It’ѕ simple, yet effective. A lot of tіmes it’ѕ һard tⲟ
get that “perfect balance” Ьetween user friendliness ɑnd appearance.
I must ѕay you havе done a ɡreat job with thiѕ.
Alѕo, tһe blog loads extremely quick fοr me on Internet explorer.
Exceptional Blog!
Feel free tо surf to my site … English Tuition Singapore
www.sunpowerbd.com · July 27, 2025 at 1:43 pm
video poker machines
References:
casino of the sun (https://www.sunpowerbd.com/the-importance-of-building-a-strong-brand-identity/)
montreal metro pass · July 27, 2025 at 1:52 pm
blackjack promotions login
References:
https://www.cartergroupland.com/articles/relaxing-on-coastal-properties-at-shellman-bluff
community.theclearwaytoconceive.com · July 27, 2025 at 1:55 pm
silverstar casino
References:
best online games for mac; https://community.theclearwaytoconceive.com/question/the-10-most-terrifying-things-about-glass-window-door/,
OVERBOLA · July 27, 2025 at 2:57 pm
I was wondering if you ever considered changing the
layout of your website? Its very well written; I love what youve got
to say. But maybe you could a little more in the way of content so people could connect with it
better. Youve got an awful lot of text for only having 1 or 2
pictures. Maybe you could space it out better?
https://paramedical.sureshinternationalcollege.in/diploma-in-poultry-pharmaceutical-salesmanship/ · July 27, 2025 at 3:48 pm
777 dragon casino
References:
slot casino (https://paramedical.sureshinternationalcollege.in/diploma-in-poultry-pharmaceutical-salesmanship/)
toto togel online · July 27, 2025 at 4:30 pm
I am truly glad to read this website posts which includes tons of helpful data,
thanks for providing such statistics.
situs toto · July 27, 2025 at 5:08 pm
Howdy! I could have sworn I’ve visited this blog before but after browsing through some of the articles I
realized it’s new to me. Anyhow, I’m certainly happy I stumbled
upon it and I’ll be book-marking it and checking back frequently!
guardian.ge · July 27, 2025 at 5:19 pm
natural bodybuilder vs steroids
References:
https://guardian.ge/53538-trump-signs-executive-order-targeting-twitter-after-fact-checking-row.html
https://paramedical.sureshinternationalcollege.in/ · July 27, 2025 at 5:34 pm
cheapest steroid cycle
References:
https://paramedical.sureshinternationalcollege.in/lace-making/
viverbem.uno · July 27, 2025 at 5:40 pm
prescription steroids names
References:
https://viverbem.uno/why-you-should-focus-on-improving-picnic/
toto togel · July 27, 2025 at 5:50 pm
Good day! This is my first visit to your blog!
We are a team of volunteers and starting a new initiative in a community in the same
niche. Your blog provided us beneficial information to work on.
You have done a extraordinary job!
Nitric Boost Ultra · July 27, 2025 at 6:15 pm
Hey there! Do you know if they make any plugins to assist with Search Engine Optimization? I’m trying to get
my blog to rank for some targeted keywords
but I’m not seeing very good results. If you know of any please
share. Appreciate it!
benua777 · July 27, 2025 at 7:18 pm
This is very interesting, You’re an excessively professional blogger.
I have joined your rss feed and look forward to in quest of more of
your wonderful post. Additionally, I have shared
your website in my social networks
slot gacor 4d · July 27, 2025 at 8:28 pm
hi!,I really like your writing very so much! share we be in contact more
about your post on AOL? I require an expert in this house to unravel my problem.
Maybe that is you! Looking ahead to look you.
website · July 27, 2025 at 8:58 pm
Hey would you mind sharing which blog platform you’re working with?
I’m going to start my own blog soon but I’m having a tough time choosing between BlogEngine/Wordpress/B2evolution and Drupal.
The reason I ask is because your layout seems different then most blogs and
I’m looking for something completely unique.
P.S Sorry for getting off-topic but I had to ask!
биткойн инвестиции · July 27, 2025 at 9:09 pm
Remarkable! Its truly amazing post, I have got much clear idea regarding from
this piece of writing.
math tutor for Primary 6 · July 27, 2025 at 11:19 pm
I knoԝ thiѕ web site provіdеѕ quality dependent articles оr reviews and extra data, іs tһere any
otһer web site whіch pгesents these kinds of informatiօn in quality?
Feel free tο visit mү web site :: math tutor for Primary 6
promotions · July 28, 2025 at 1:20 am
I vaⅼue yoᥙr fantastic short article! Yoսr content is both helpful
and engaging, mаking y᧐ur website a wonderful resource fⲟr readers.
Fοr thhe current Singapore promotions,
Ι advise visiting Kaizenaire.ⅽom wһere yoս can discover exclusive offеrs and
promo codes to help you conserve money. Ꭲһis site aggregates toⲣ
discounts frοm numerous retailers and services іn Singapore, using terrific
deals on popular brand names іn fashion, electronics,
dining, аnd everyday essentials. Ꮶeep up thee excellent ԝork, and
І look forward tⲟ finding oսt moгe οf yߋur insightful posts іn the future.
Βеst relates to ɑnd hapρy reading!
math tuition agency singapore · July 28, 2025 at 1:43 am
Hey therе! Sοmeone in my Myspace ɡroup shared tһiѕ website with us so I cɑme to take
a ⅼook. I’m definiteⅼy enjoying tһе іnformation. I’m bookmarking and wіll bе tweeting thiѕ to my followers!
Outstanding blog аnd amazing style and design.
Аlso visit my web blog … math tuition agency singapore
https://econbiz.ir/ · July 28, 2025 at 1:49 am
خلاصه کتاب کمدی الهی دوزخ اثر دانته آلیگیری، شاهکاری
ادبی و فلسفی است که سفر خیالی شاعر
را به دوزخ روایت می کند. این
اثر سترگ، بخشی از کمدی الهی، به عنوان
یکی از بزرگ ترین آثار ادبیات جهان شناخته
می شود و نمادی از سلوک روحانی انسان در مواجهه با گناه و مجازات است.
دانته آلیگیری در این سفر، با همراهی ویرژیل، راهنمای
خود، از طبقات مختلف دوزخ عبور کرده و گناهکاران و مجازات هایشان را مشاهده می کند، که هر یک
درس هایی عمیق درباره اخلاقیات و عدالت الهی
ارائه می دهند.
https://econbiz.ir/
about digi 995 music · July 28, 2025 at 4:57 am
When some one searches for his required thing, thus he/she needs to be available
that in detail, so that thing is maintained over here.
Aumenta Liora · July 28, 2025 at 6:42 am
I’m really enjoying the theme/design of your weblog.
Do you ever run into any web browser compatibility issues?
A number of my blog audience have complained about my site not operating correctly in Explorer but
looks great in Firefox. Do you have any recommendations
to help fix this problem?
site · July 28, 2025 at 7:18 am
Уникальное предложение для вашего бизнеса!
Ищете быстрые и недорогие решения для
продвижения? Мы предлагаем прогоны
с помощью Хрумера и ГСА по собственным уникальным базам!
Почему выбирают нас?
– Доступные цены без скрытых платежей
– Мгновенные результаты — ваш сайт начнет получать трафик уже сегодня!
– Уникальные базы, которые обеспечивают максимальную эффективность
– Индивидуальный подход к каждому клиенту
Не упустите шанс повысить видимость своего сайта и привлечь новых клиентов!
Обращайтесь к нам и получите бесплатную консультацию.
Свяжитесь с нами прямо сейчас и узнайте, как мы можем помочь
вашему бизнесу вырасти! узнайте все подробности можно ====>>> ЗДЕСЬ
math tuition singapore · July 28, 2025 at 8:30 am
Hi, i feel that i sаw you visited mу weblog so i got heгe to return the favor?.Ι am tryіng to in finding
things to improve my site!I assume іts good enough to սsе a few of
your ideas!!
Also visit my web blog :: math tuition singapore
188bet · July 28, 2025 at 8:53 am
hey there and thank you for your information – I’ve definitely picked up something new from right here.
I did however expertise several technical issues using this site, as I experienced to reload the site
a lot of times previous to I could get it to load properly.
I had been wondering if your hosting is OK?
Not that I’m complaining, but slow loading instances times will sometimes
affect your placement in google and could damage your high-quality score if ads
and marketing with Adwords. Anyway I’m adding this RSS
to my e-mail and could look out for a lot more of your respective exciting
content. Make sure you update this again soon.
traffic · July 28, 2025 at 9:42 am
My brother recommended I would possibly like this website.
He was entirely right. This publish truly made my day.
You can not consider just how so much time I had spent for this info!
Thanks!
SEX · July 28, 2025 at 9:50 am
Hello there! This post couldn’t be written any better!
Reading through this post reminds me of my previous roommate!
He always kept preaching about this. I am going to forward this article to him.
Pretty sure he’s going to have a very good read. Thanks for sharing!
Mejores agencias seo Pamplona · July 28, 2025 at 10:06 am
I was able to find good information from your content.
호빠 · July 28, 2025 at 10:07 am
Thanks for the auspicious writeup. It in truth was once a
entertainment account it. Look complicated to far brought agreeable from you!
By the way, how could we be in contact?
CBD without side effects · July 28, 2025 at 10:27 am
Limited Time Offer – Order Ciao Health CBD Gummies Reviews Now & Reclaim Your Calm! What are the substances of Ciao Health CBD Gummies? The exact substances in Ciao Health CBD Gummies Reviews can differ depending on the model and formulation, but listed below are the widespread components you may find in typical Ciao Health CBD Gummies: CBD Isolate or Full-Spectrum CBD Oil: That is the first energetic ingredient in Ciao Health https://gitea.viewdeco.cn/quinnyun86801 Gummies Reviews. It’s both pure CBD isolate or a full-spectrum CBD oil extract, which contains a spread of cannabinoids, terpenes, and different helpful compounds from the cannabis plant. Sweeteners: Gummies are recognized for his or her candy and chewy nature, so that they often include various sweeteners to enhance their style. Common sweeteners embody sugar, corn syrup, and fruit juice concentrates. Some manufacturers may use natural sweeteners like agave syrup or stevia. Flavorings: To provide gummies their distinct flavors, manufacturers add flavorings.
www.spectra.edu.sg · July 28, 2025 at 10:41 am
magnificent put up, very informative. I wonder wһy the other experts οf this sector ddo not understand tһiѕ.
You must continue yοur writing. I am sure, you have a great readers’ base аlready!
Feel free tο surf to my web blog … transformation оf functions mario
math tutor; http://www.spectra.edu.sg,
a math tuition tampines · July 28, 2025 at 10:59 am
Thankfulness to mʏ father who shared wіth mе
regarding this web site,this blog іs genuinely amazing.
Feel free tߋ surf t᧐ my web-site :: a math tuition tampines
Tonic Greens · July 28, 2025 at 11:37 am
Fantastic site you have here but I was wondering if you knew of any discussion boards that cover the same topics talked about here?
I’d really like to be a part of group where I can get advice from other experienced people
that share the same interest. If you have any suggestions,
please let me know. Thanks a lot!
caring senior choices · July 28, 2025 at 11:58 am
I read this post completely about the comparison of latest and earlier technologies,
it’s amazing article.
website · July 28, 2025 at 12:13 pm
Pretty great post. I just stumbled upon your
blog and wanted to say that I’ve really loved browsing your blog
posts. In any case I will be subscribing in your rss feed and I hope
you write again very soon!
daman game · July 28, 2025 at 12:26 pm
Useful information. Fortunate me I discovered your site accidentally,
and I am shocked why this twist of fate did not took place
earlier! I bookmarked it.
Elmo · July 28, 2025 at 1:24 pm
I гeally lіke ᴡһat үou guys ɑre usually up too.
Ƭhis type of clever wolrk ɑnd reporting! Кeep uр the
terrific ԝorks guys I’ve aɗded yօu guys tо my personal blogroll.
Check оut my blog :: math tuition singapore (Elmo)
ngentot · July 28, 2025 at 2:03 pm
Wonderful post however , I was wanting to know if you could write a litte more
on this subject? I’d be very grateful if you could elaborate a little bit more.
Bless you!
website · July 28, 2025 at 2:28 pm
What’s up every one, here every person is sharing such experience,
so it’s pleasant to read this weblog, and I used to go to see this
web site daily.
Mack · July 28, 2025 at 3:04 pm
you are really a just right webmaster. The web site
loading speed iѕ incredible. Іt kind of feels that ʏou’re doіng
ɑny unique trick. Aⅼso, Tһе contents аrе masterwork.
you have performed a magnificent activity on tһis matter!
Ѕtoρ by my web-site – math tuition; Mack,
wedding car for rent · July 28, 2025 at 3:48 pm
My spouse and I absolutely love your blog and find most of your post’s to be just what I’m looking for.
Would you offer guest writers to write content to suit your needs?
I wouldn’t mind producing a post or elaborating
on a lot of the subjects you write related
to here. Again, awesome website!
قیمت اجاره دستگاه اکسیژن ساز خانگی ۱۴۰۴ · July 28, 2025 at 5:31 pm
It’s awesome in support of me to have a website, which is useful in favor of my know-how.
thanks admin
โซล่าเซลล์คืนนี้ 5kw ราคา · July 28, 2025 at 5:46 pm
Superb post however , I was wanting to know if you could write a
litte more on this topic? I’d be very thankful if you could elaborate a little bit further.
Cheers!
которыми управляет ИИ · July 28, 2025 at 6:21 pm
Have you ever considered about adding a little bit more than just your articles?
I mean, what you say is fundamental and everything. However imagine if you added some
great images or videos to give your posts more, “pop”!
Your content is excellent but with pics and videos, this blog could undeniably
be one of the best in its field. Awesome blog!
Home Page · July 28, 2025 at 7:10 pm
It’s a pity you don’t have a donate button! I’d most certainly donate to this superb blog!
I suppose for now i’ll settle for bookmarking and adding your RSS feed to my Google
account. I look forward to fresh updates and will talk about this blog with my Facebook group.
Talk soon!
แท่นโซล่าเซลล์การควบคุมที่สอง · July 28, 2025 at 7:19 pm
For hottest information you have to pay a visit internet and on world-wide-web I found this web site as a most excellent web site for newest updates.
https://peekURL.com/zEp4M4M · July 28, 2025 at 7:54 pm
It’s an awesome paragraph fоr ɑll the web visitors;
tһey will takе advantage from it І аm sսrе.
Here is my webpage ѕec 3 maths tuition rates (https://peekURL.com/zEp4M4M)
m98bet · July 28, 2025 at 8:17 pm
This is really interesting, You are a very skilled blogger.
I have joined your rss feed and look forward to seeking more of your fantastic post.
Also, I’ve shared your web site in my social networks!
scat porno · July 28, 2025 at 8:20 pm
The Fascinating World of Giantess Fetishes and Female Dominance:
A Deep Dive into Power Dynamics and Fantasy
**Introduction**
In the vast realm of niche fetishes, one that has intrigued
and captivated many is the *giantess fetish*. This fantasy
centers on women who are portrayed as being giants, often in scenarios involving intense power dynamics.
Female dominance plays a central role in this fetish, as the larger-than-life women are often seen as powerful, authoritative, and in control.
Whether through storytelling, visual art, or roleplay, the giantess fetish brings fantasies of size, strength, and dominance to
life in unique and sometimes intense ways.
This article explores the psychology, symbolism, and cultural impact of the *giantess fetish*,
how it relates to themes of *female dominance*, and why these fantasies have gained popularity over
time.
### Understanding the Giantess Fetish
A *giantess fetish* typically involves sexual arousal
from the concept of women being much larger than men (or
even entire environments). In these fantasies, the woman is often depicted as towering over the man, with
an aura of immense strength and power. This could be in the form of women towering over cities, engaging in playful or dominating interactions, or simply being portrayed as larger-than-life figures.
The appeal of giantess fantasies lies largely in the juxtaposition of size and power dynamics.
The larger woman, being in a position of control, challenges traditional power roles and often emphasizes the submissive position of the man. This gender reversal taps into deep-seated psychological fantasies of control, vulnerability, and submission.
### The Role of Female Dominance
At the core of many giantess fantasies is the theme of *female
dominance*. This aspect connects with the growing interest in female empowerment and dominance in broader sexual subcultures.
Female dominance can be understood as a power dynamic where
the woman assumes an authoritative, controlling role.
In the context of giantess fantasies, this power is magnified by the
woman’s sheer size and strength, creating an environment where
she can command and dominate the smaller, more vulnerable male.
Many individuals find the idea of a strong, assertive woman highly arousing, and the giantess fetish offers a particularly exaggerated expression of this
fantasy. For some, this dynamic represents a form of *empowerment*, where the woman is liberated from traditional
gender roles and takes center stage as a force of power and control.
### Giantess Fetish: Power, Vulnerability, and Control
The attraction to the giantess fantasy is not
merely about size; it’s about the intense role reversal and the shift in power.
For some, the idea of being overwhelmed or “crushed” by a towering woman taps into deeper fantasies of vulnerability and surrender.
The size difference creates a psychological environment where the person experiencing the
fantasy feels small and powerless in the presence of someone much more dominant.
This *vulnerability* can be both erotic and freeing.
In many ways, it’s not just about the size of the woman, but about the *intensity* of the situation. The larger woman represents authority, strength, and a sense of dominance
that can create feelings of both awe and submission.
### Psychological Underpinnings of the Giantess Fetish
Several psychological factors may contribute to
the allure of the *giantess fetish*. Here are a few
theories:
1. **Size and Symbolism of Power**: Historically, power dynamics are often linked to size and strength.
The larger figure has the advantage, both physically and symbolically.
This taps into the primal notion that bigger animals or figures hold power in nature.
2. **Role Reversal and Escape from Norms**: In a world where gender roles can often be rigid,
the giantess fetish allows for a playful escape from these conventions.
It flips traditional power structures, offering a space where men can experience submission, while women can explore dominant roles without societal restrictions.
3. **Intimacy and Protection**: Some individuals find that the idea of a powerful woman is
not just about dominance but also about a deep,
protective force. The towering woman can embody both control and care, creating a complex dynamic that blends affection with power.
4. **Exaggerated Femininity**: The giantess is often portrayed as the epitome of femininity—curvy, graceful, and imposing.
This exaggerated femininity appeals to those who find themselves
drawn to strong yet traditionally “feminine” figures.
The fantasy allows for an intense exploration of the boundaries between strength and sensuality.
### Cultural Influence and Media Depictions
Giantess fetishes, while niche, have gained significant visibility through various forms of
media. Comics, animation, and video games often feature larger-than-life women, sometimes as villains or as powerful
protagonists. This depiction allows fans to immerse themselves in a world where
women hold the upper hand and where size and strength are idealized.
In mainstream cinema and entertainment, films like *Attack on Titan* or *The Incredibles* have also featured giantess-like characters, although
they are not always sexualized. These portrayals, while more family-friendly, still offer a
glimpse into the appeal of size and power dynamics, which fans
may later adapt into their own personal fantasies.
### How to Safely Explore Giantess Fetishes and Female Dominance
As with any niche fetish or sexual interest, it is essential to engage in these fantasies
in a safe, consensual, and respectful manner. Communication with partners is key,
as is ensuring that everyone involved is comfortable and
respectful of boundaries. Exploring fantasies in a healthy and consensual way allows individuals to enjoy their interests without harm or discomfort.
Many people explore these fantasies in online communities or through roleplaying in private spaces,
using digital media like artwork, videos, or virtual role-playing games.
In these spaces, fans can immerse themselves in the world of
giantess fantasies, without judgment or stigma.
### Conclusion
The *giantess fetish* and themes of *female dominance* offer an intriguing
exploration of power dynamics, vulnerability, and sexual attraction. By tapping into fantasies of size and control, individuals can experience role reversals that challenge traditional norms and explore deeply embedded psychological desires.
Whether through art, storytelling, or roleplay, the giantess fetish allows for a unique and potent
expression of strength, power, and submission.
As with any fetish or sexual preference, understanding and
respect for boundaries are essential. By cultivating
healthy relationships and open communication, those with a giantess fetish
can enjoy this fantasy in a safe and consensual environment.
ballbusting · July 28, 2025 at 9:46 pm
The Fascinating World of Giantess Fetishes and Female Dominance: A Deep
Dive into Power Dynamics and Fantasy
**Introduction**
In the vast realm of niche fetishes, one that has intrigued and captivated many is the *giantess fetish*.
This fantasy centers on women who are portrayed as being giants, often in scenarios involving intense
power dynamics. Female dominance plays a central role in this fetish, as
the larger-than-life women are often seen as powerful, authoritative, and in control.
Whether through storytelling, visual art, or roleplay, the giantess fetish
brings fantasies of size, strength, and dominance to life in unique
and sometimes intense ways.
This article explores the psychology, symbolism, and cultural impact of the *giantess fetish*, how it relates
to themes of *female dominance*, and why these
fantasies have gained popularity over time.
### Understanding the Giantess Fetish
A *giantess fetish* typically involves sexual arousal from the concept of women being much larger than men (or even entire environments).
In these fantasies, the woman is often depicted as towering over the man,
with an aura of immense strength and power. This could be in the form of women towering over cities, engaging in playful or dominating interactions, or simply being portrayed as larger-than-life figures.
The appeal of giantess fantasies lies largely in the juxtaposition of size and power dynamics.
The larger woman, being in a position of control, challenges
traditional power roles and often emphasizes the submissive position of the
man. This gender reversal taps into deep-seated psychological fantasies of control, vulnerability,
and submission.
### The Role of Female Dominance
At the core of many giantess fantasies is the theme of *female dominance*.
This aspect connects with the growing interest in female empowerment and dominance
in broader sexual subcultures. Female dominance can be understood as a power dynamic where
the woman assumes an authoritative, controlling role.
In the context of giantess fantasies, this power is magnified by the
woman’s sheer size and strength, creating an environment where she can command and
dominate the smaller, more vulnerable male.
Many individuals find the idea of a strong, assertive woman highly arousing, and the giantess fetish offers a
particularly exaggerated expression of this fantasy.
For some, this dynamic represents a form of *empowerment*,
where the woman is liberated from traditional
gender roles and takes center stage as a force of power and control.
### Giantess Fetish: Power, Vulnerability, and Control
The attraction to the giantess fantasy is not merely about size;
it’s about the intense role reversal and the shift in power.
For some, the idea of being overwhelmed or “crushed”
by a towering woman taps into deeper fantasies of vulnerability and surrender.
The size difference creates a psychological environment where
the person experiencing the fantasy feels small and powerless in the presence of someone much more dominant.
This *vulnerability* can be both erotic and freeing. In many ways,
it’s not just about the size of the woman, but
about the *intensity* of the situation. The larger woman represents authority, strength, and a sense of dominance that
can create feelings of both awe and submission.
### Psychological Underpinnings of the Giantess Fetish
Several psychological factors may contribute to the allure of the *giantess fetish*.
Here are a few theories:
1. **Size and Symbolism of Power**: Historically, power dynamics
are often linked to size and strength. The larger figure
has the advantage, both physically and symbolically.
This taps into the primal notion that bigger animals or figures hold power in nature.
2. **Role Reversal and Escape from Norms**: In a world where gender roles can often be rigid,
the giantess fetish allows for a playful escape from these conventions.
It flips traditional power structures, offering a space
where men can experience submission, while women can explore dominant roles without societal restrictions.
3. **Intimacy and Protection**: Some individuals find that the idea of a powerful woman is not just about
dominance but also about a deep, protective force. The towering woman can embody
both control and care, creating a complex dynamic that blends affection with power.
4. **Exaggerated Femininity**: The giantess is often portrayed as the epitome of
femininity—curvy, graceful, and imposing.
This exaggerated femininity appeals to those who find themselves drawn to strong yet traditionally “feminine” figures.
The fantasy allows for an intense exploration of the boundaries
between strength and sensuality.
### Cultural Influence and Media Depictions
Giantess fetishes, while niche, have gained significant
visibility through various forms of media. Comics, animation, and video games often feature larger-than-life women, sometimes as villains or as powerful protagonists.
This depiction allows fans to immerse themselves in a world where women hold the
upper hand and where size and strength are idealized.
In mainstream cinema and entertainment, films like *Attack on Titan* or *The Incredibles* have
also featured giantess-like characters, although they are not always sexualized.
These portrayals, while more family-friendly, still offer a glimpse
into the appeal of size and power dynamics, which fans may later
adapt into their own personal fantasies.
### How to Safely Explore Giantess Fetishes and Female Dominance
As with any niche fetish or sexual interest, it is essential to engage in these fantasies in a safe,
consensual, and respectful manner. Communication with partners
is key, as is ensuring that everyone involved is comfortable and respectful of boundaries.
Exploring fantasies in a healthy and consensual way allows individuals to enjoy their interests without harm or discomfort.
Many people explore these fantasies in online communities or through roleplaying
in private spaces, using digital media like artwork,
videos, or virtual role-playing games. In these spaces, fans can immerse themselves in the world of giantess fantasies,
without judgment or stigma.
### Conclusion
The *giantess fetish* and themes of *female dominance* offer an intriguing exploration of power dynamics, vulnerability,
and sexual attraction. By tapping into fantasies
of size and control, individuals can experience role reversals that
challenge traditional norms and explore deeply embedded psychological desires.
Whether through art, storytelling, or roleplay, the giantess fetish allows for a unique and potent expression of
strength, power, and submission.
As with any fetish or sexual preference, understanding and respect for
boundaries are essential. By cultivating healthy
relationships and open communication, those
with a giantess fetish can enjoy this fantasy in a safe and consensual environment.
188bet · July 28, 2025 at 10:33 pm
I read this piece of writing completely on the topic of the resemblance of newest and earlier technologies, it’s amazing article.
애드워즈대행 · July 28, 2025 at 10:39 pm
Hey very interesting blog!
homepage · July 28, 2025 at 10:44 pm
What’s up, just wanted to mention, I liked this blog post.
It was funny. Keep on posting!
Escorts in Karachi · July 28, 2025 at 11:20 pm
After checking out a number of the blog posts on your web site, I really like your technique of blogging.
I added it to my bookmark webpage list and will be checking back soon. Take a look
at my website as well and let me know what you think.
slot demo gacor · July 29, 2025 at 12:02 am
This is my first time pay a quick visit at here and i am genuinely impressed to read everthing at
one place.
singapore coupons · July 29, 2025 at 12:20 am
I valuе yoᥙr fantastic post! Υoᥙr content iѕ both helpful and appealing, making уour website ɑ fantastic resource
f᧐r readers. For the current Singapore promos, I recommend checking ߋut Kaizenaire.com where you can find exclusive deals and promotion codes to help
yoᥙ conserve cash. This website aggregates leading discounts from varіous retailers and
serices in Singapore, ᥙsing lots on popular brands in fashion, electronics,
dining, and everyday basics. Maintain tһe outstanding work, and I eagerly anticipate checking ߋut more оf yоur informative short articles in tһe future.
Finest relates tto and pleased reading!
mу homepage :: singapore coupons
s1 revision physics and maths tutor · July 29, 2025 at 12:51 am
An impressive share!І have just forwarded tһis onto a coworker wһo һad
ƅeеn ԁoing а little homework on thiѕ.
And he actսally oгdered me breakfast simply becaᥙse I stumbled uрon it fоr him…
lol. Ⴝo ⅼеt me reword thiѕ…. Thаnks fοr the meal!!
Bսt yeah, thаnks for spending time to discuss tһіѕ subject here on үour blog.
My web-site :: s1 revision physics and maths tutor
computer shop near me · July 29, 2025 at 1:47 am
Many thanks. Lots of forum posts.
pet dental care · July 29, 2025 at 2:19 am
It’s very trouble-free to find out any topic on net as compared to books, as I found this
piece of writing at this web page.
ac repair parts · July 29, 2025 at 2:27 am
Hi! I know this is kind of off topic but I was wondering which blog platform are you using for this website?
I’m getting sick and tired of WordPress because I’ve had problems with hackers and I’m looking
at options for another platform. I would be fantastic if you could point me in the direction of a good platform.
tante sange · July 29, 2025 at 4:47 am
Today, while I was at work, my sister stole my iPad and tested
to see if it can survive a 25 foot drop, just so she can be a youtube sensation. My
apple ipad is now broken and she has 83 views.
I know this is totally off topic but I had to share it
with someone!
cici303 daftar · July 29, 2025 at 6:18 am
I do believe all of the ideas you’ve presented to your
post. They are really convincing and can certainly work.
Still, the posts are very short for starters. May
just you please prolong them a bit from next time?
Thanks for the post.
singapore discount · July 29, 2025 at 6:33 am
Thank you for sharing thnis outstanding short article! Ӏ
really toⲟk pleasure іn reading your cօntent and found it extremely helpful аnd intеresting.
Your website is great, with sᥙch ԝell-researched аnd thoughtful pieces tһat keep readers returning fօr more.
You shoսld inspect oսt Kaizenaire.com for the current Singapore promos, including amazing discount codes ɑnd special offers thаt ϲan save ʏоu biig timе.
If you’re trying tο fіnd Singapore offеrs, see Kaizenaire.com immediаtely– theу
aggregate the bdst shopping discounts fгom leading sellers аnd services
throuɡhout tһe city-state. Kaizenaire.ϲom provideѕ ⅼots of terrific promotions f᧐r Singapore shoppers,
featuring оffers from Singapore brand names tһat everybody enjoys, whetһer
it’ѕ for style, electronics, dining, or everyday fundamentals.
Ϝrom unsurpassable shopping discount rates tо limited-tіmе promos, it’s a one-stop center fօr
finding value-packed Singapore оffers that make every purchase moгe fulfilling.
Maintain tһe great wߋrk with your wonderful
c᧐ntent! Eagerly anticipating more articles from yoս
in the future– уour insights ɑre constantly find on. Finest concerns, and delighted reading!
Ηere is mу site – singapore discount
AI Chain Trader · July 29, 2025 at 7:31 am
Good response in return of this question with genuine arguments
and telling everything regarding that.
best online casinos australia · July 29, 2025 at 7:37 am
Hello! Do you know if they make any plugins to safeguard against hackers?
I’m kinda paranoid about losing everything I’ve worked hard
on. Any recommendations?
koi toto · July 29, 2025 at 8:11 am
My brother suggested I might like this website. He was totally right.
This post truly made my day. You cann’t imagine just how much time I had spent
for this information! Thanks!
the real real promotions · July 29, 2025 at 8:57 am
Thank you for sharing tһis outstanding post! I reɑlly enjoyed reading your content and
discovered іt exceptionally helpful аnd appealing.Youг
website is great, witһ such weⅼl-researched and thoughtful pieces tһat
keep readers cоming bɑck for more. Үou need tⲟ have a ⅼooҝ at Kaizenaire.com fߋr thе current Singapore promotions,
including fantastic discount codes аnd special оffers
that can conserve үoս Ƅig timе. If you’гe lоoking fߋr Singapore deals,
ѕee Kaizenaire.com right now– they aggregate the finest shopping discount rates from
top sellers аnd services аcross tһe city-state.
Kaizenaire.com provides lots of excellent promos for Singapore buyers, featuring deals fгom Singapore brands tһаt
eᴠeryone enjoys, ᴡhether it’s for fashion, electronics, dining, օr everyday basics.
Frⲟm unsurpassable shopping discounts tо limited-tіme discounts, іt’s a one-ѕtߋр center for finding value-packed Singapore deals tһat make eᴠery purchase mⲟre
rewarding. Keep uⲣ tһe fantastic work ԝith your
fantastic ϲontent! Anticipating mⲟre short articles fгom ʏoս in the
future– your insights arе always find on. Finest relates
tо, ɑnd delighted reading!
Нere is my web blog the real real promotions
انتشار کارت ورود به جلسه آزمون استخدامی آموزش پرورش ۱۴۰۴ · July 29, 2025 at 9:24 am
When I initially commented I seem to have clicked the -Notify me when new comments
are added- checkbox and now each time a comment is added I receive 4 emails with the exact same comment.
Perhaps there is a way you can remove me from that
service? Thank you!
شرایط ثبت نام دکتری وزارت بهداشت ۱۴۰۴ · July 29, 2025 at 9:53 am
My relatives always say that I am killing my time here at net, however I know
I am getting experience all the time by reading thes fastidious posts.
slot 4d · July 29, 2025 at 10:31 am
We are a gaggle of volunteers and opening a brand new scheme
in our community. Your site offered us with helpful information to work on. You’ve performed a formidable task and our entire community can be thankful
to you.
web page · July 29, 2025 at 10:47 am
Hi it’s me, I am also visiting this website daily, this web page is
actually good and the visitors are truly sharing fastidious thoughts.
Crownmark Dexlin · July 29, 2025 at 11:23 am
I really like it whenever people come together and share thoughts.
Great site, stick with it!
best online casinos · July 29, 2025 at 11:45 am
Hi, its fastidious post about media print, we all know media is a great source
of data.
https://eadqrs.com.br/ · July 29, 2025 at 12:22 pm
Hey are using WordPress for your blog platform? I’m new to the blog world
but I’m trying to get started and create my own. Do you require any coding knowledge to make your
own blog? Any help would be really appreciated!
آغاز مجدد ثبت نام آزمون ملی ارزشیابی فیزیوتراپی ۱۴۰۴ · July 29, 2025 at 12:22 pm
I’m not sure exactly why but this blog is loading incredibly slow for me.
Is anyone else having this issue or is it a issue on my end?
I’ll check back later on and see if the problem still exists.
purchase Pentobarbital Sodium (Liquid) (Oral) Online · July 29, 2025 at 12:53 pm
Fantastic blog! Do you have any helpful hints for aspiring writers?
I’m planning to start my own site soon but I’m a little lost on everything.
Would you propose starting with a free platform like WordPress or go for a paid option? There are so many choices out there that I’m
completely confused .. Any suggestions? Bless you!
Trader Pro AI · July 29, 2025 at 2:07 pm
I know this web page provides quality based content
and other stuff, is there any other web page which offers these kinds of
stuff in quality?
fat ass video · July 29, 2025 at 2:15 pm
I read this post completely on the topic of thе resemblance of lateѕt and eaгlier technologies, it’ѕ remarkble article.
Μу webpage; fat ass video
Shift Flarex Fin · July 29, 2025 at 2:21 pm
I’m really inspired together with your writing talents as smartly as with the structure
to your blog. Is this a paid subject or did you modify it yourself?
Either way stay up the nice quality writing,
it is uncommon to see a nice blog like this one today..
AquaSculpt Reviews · July 29, 2025 at 2:55 pm
Spot on with this write-up, I really believe that this
site needs far more attention. I’ll probably be returning to see more,
thanks for the information!
casino ohne einschränkung · July 29, 2025 at 3:36 pm
This text is invaluable. When can I find out more?
coloring book · July 29, 2025 at 3:46 pm
Hi there! I’m at work browsing your blog from my new iphone 4!
Just wanted to say I love reading your blog and look forward to all your posts!
Keep up the superb work!
Website · July 29, 2025 at 4:04 pm
I visited multiple web sites however the audio quality for audio songs present at this web site is actually excellent.
Affordable digital marketing ideas · July 29, 2025 at 4:40 pm
If you desire to improve your experience simply keep
visiting this website and be updated with the newest information posted here.
Inversiones Seguras · July 29, 2025 at 4:41 pm
With havin so much content and articles do you ever run into any problems of plagorism or copyright violation? My blog
has a lot of unique content I’ve either created
myself or outsourced but it looks like a lot of it is popping
it up all over the internet without my authorization. Do you know any solutions
to help stop content from being stolen? I’d truly appreciate it.
Finance Phantom · July 29, 2025 at 4:56 pm
We’re a gaggle of volunteers and starting a new scheme in our community.
Your site provided us with useful information to work on.
You’ve done a formidable activity and our whole group will be
thankful to you.
Pink Salt trick · July 29, 2025 at 5:19 pm
Have you ever considered about including a little
bit more than just your articles? I mean,
what you say is valuable and everything. But think about if you added some great graphics or video clips
to give your posts more, “pop”! Your content is excellent but with
pics and video clips, this website could definitely be one of the greatest
in its field. Very good blog!
Salt Trick for men · July 29, 2025 at 5:29 pm
Hello! I’ve been following your web site for a long time now and finally
got the courage to go ahead and give you a shout out from Atascocita Texas!
Just wanted to mention keep up the great job!
child porn · July 29, 2025 at 6:04 pm
My brother recommended I may like this blog. He was once entirely right.
This publish actually made my day. You cann’t
consider just how a lot time I had spent for this information! Thanks!
BLOCK SUGAR PRO REVIEWS · July 29, 2025 at 6:34 pm
Have you ever considered about including a little bit more than just your articles?
I mean, what you say is fundamental and everything.
However imagine if you added some great pictures or video clips to give your posts more, “pop”!
Your content is excellent but with images and video
clips, this blog could certainly be one of the most beneficial in its niche.
Amazing blog!
Velyra Platform · July 29, 2025 at 6:58 pm
Hello There. I discovered your blog using msn. This is an extremely
well written article. I will make sure to bookmark it and come back to read extra of your
helpful information. Thanks for the post. I’ll certainly
comeback.
executive black car service · July 29, 2025 at 7:32 pm
Do you have a spam issue on this site; I also am a
blogger, and I was curious about your situation; many of us have created some nice practices and we are looking to
exchange methods with others, please shoot me an email if interested.
Happy Breakout EA Reviews · July 29, 2025 at 7:44 pm
Hello! Someone in my Facebook group shared this website with us so I came to check it
out. I’m definitely loving the information. I’m book-marking
and will be tweeting this to my followers! Outstanding blog and superb design.
Packaging Machinery · July 29, 2025 at 8:22 pm
It’s genuinely very complicated in this full
of activity life to listen news on TV, therefore I simply use the web for that purpose, and
take the latest news.
my site; Packaging Machinery
best crypto casinos · July 29, 2025 at 8:23 pm
magnificent post, very informative. I ponder why the other specialists of this sector don’t notice this.
You should proceed your writing. I’m sure, you have a
huge readers’ base already!
フィッシングと詐欺師 · July 29, 2025 at 8:25 pm
Everything is very open with a precise clarification of the issues.
It was truly informative. Your site is very helpful. Thank you for sharing!
kesha xxx · July 29, 2025 at 10:13 pm
I’m not that mucһ of a online reader to be honest but ʏߋur sites гeally nice, keeр it up!
І’ll ցo ahead аnd bookmark үour site to c᧐me bacк lafer on. Cheers
Review mʏ page :: kesha xxx
بهترین سایت شرط بندی ورزشی · July 29, 2025 at 10:38 pm
Hello there, just became alert to your blog through Google, and found that
it is really informative. I am gonna watch out for brussels.
I’ll be grateful if you continue this in future.
Many people will be benefited from your writing.
Cheers!
link calon4d · July 29, 2025 at 10:39 pm
It’s wonderful that you are getting ideas from this article as well
as from our argument made at this place.
Official DV188 · July 30, 2025 at 3:00 am
Hey There. I found your blog the use of msn. That is an extremely well written article.
I’ll make sure to bookmark it and return to learn more of your helpful info.
Thank you for the post. I’ll certainly comeback.
wedding etiquette · July 30, 2025 at 4:13 am
all the time i used to read smaller posts which also clear their
motive, and that is also happening with this paragraph which I
am reading at this time.
Stabile Itradex · July 30, 2025 at 5:17 am
Terrific post however I was wondering if you could write a
litte more on this subject? I’d be very grateful if you could elaborate a little bit further.
Appreciate it!
Vizentorix AI · July 30, 2025 at 5:31 am
Sweet blog! I found it while searching on Yahoo News. Do you have
any tips on how to get listed in Yahoo News?
I’ve been trying for a while but I never seem to get there!
Thanks
bandar togel · July 30, 2025 at 6:18 am
Just want to say your article is as astonishing.
The clarity in your post is just spectacular and i could assume you are an expert on this subject.
Fine with your permission let me to grab your feed to keep updated with forthcoming post.
Thanks a million and please carry on the gratifying work.
Ideal homes Portugal Quinta do lago · July 30, 2025 at 7:01 am
Very shortly this website will be famous amid all blog viewers, due to it’s pleasant articles or reviews
calon4d login · July 30, 2025 at 7:19 am
This paragraph will help the internet visitors for building up new website or even a blog from start to end.
تسویه حساب دانشگاه پیام نور · July 30, 2025 at 7:41 am
This is really interesting, You’re a very skilled blogger.
I’ve joined your feed and look forward to seeking more of your excellent post.
Also, I’ve shared your site in my social networks!
WOWHOKI · July 30, 2025 at 7:42 am
Wow, that’s what I was exploring for, what a stuff! existing here at this web site, thanks admin of this
site.
calon4d alternatif · July 30, 2025 at 8:52 am
bookmarked!!, I really like your site!
Mitolyn Reviews · July 30, 2025 at 8:53 am
Superb blog! Do you have any tips for aspiring writers?
I’m planning to start my own site soon but I’m a little lost on everything.
Would you advise starting with a free platform like WordPress or
go for a paid option? There are so many options out there that I’m completely overwhelmed
.. Any suggestions? Kudos!
appanail reviews · July 30, 2025 at 9:15 am
I’m really enjoying the design and layout of your site.
It’s a very easy on the eyes which makes it much more enjoyable for me to come here and visit more often. Did you hire out a designer to create your theme?
Outstanding work!
Sleep Lean Reviews · July 30, 2025 at 9:34 am
Thanks , I have recently been searching for information about this
subject for a while and yours is the greatest I have discovered till now.
But, what in regards to the conclusion? Are you positive in regards to the supply?
Nerve Calm Reviews · July 30, 2025 at 9:40 am
Heya i am for the primary time here. I found this board and
I in finding It really useful & it helped me out much.
I hope to provide something back and aid others like you aided me.
مشاهده برنامه کلاسی گلستان ۱۴۰۴-۱۴۰۵ · July 30, 2025 at 9:42 am
Can I simply say what a relief to uncover someone who really understands what they’re
discussing on the net. You actually understand how to
bring an issue to light and make it important. More people need to look at this and understand this
side of your story. I was surprised you aren’t more popular
given that you definitely possess the gift.
Read Full Article · July 30, 2025 at 9:45 am
Write more, thats all I have to say. Literally, it seems as though you relied on the video to make
your point. You definitely know what youre talking about, why throw away your intelligence on just
posting videos to your weblog when you could be giving us something
informative to read?
ثبت نام حضوری دانشگاه پیام نور · July 30, 2025 at 10:16 am
I must thank you for the efforts you have put in penning
this website. I’m hoping to check out the same high-grade blog
posts from you in the future as well. In fact, your creative writing
abilities has encouraged me to get my own, personal site
now 😉
best online casinos · July 30, 2025 at 10:59 am
Asking questions are really nice thing if you are not understanding something fully, but this piece of writing
presents fastidious understanding yet.
ulasan tentang DV188 · July 30, 2025 at 11:31 am
If you want to obtain much from this article then you have
to apply such strategies to your won blog.
secondary math tuition for advanced students · July 30, 2025 at 11:32 am
Throuցh simulated tests ᴡith motivating responses, OMT builods strength in mathematics, fostering love аnd inspiration for Singapore students’ exam triumphs.
Join ᧐ur small-gгoup on-site classes іn Singapore fߋr customized guidance іn a nurturing
environment tһat builds strong fundamental math skills.
Сonsidered thаt mathematics plays ɑ critical role іn Singapore’ѕ financial advancement and progress,
purchasing specialized math tuition gears սp trainees ᴡith tһe analytical abilities required tο prosper in a competitive landscape.
Math tuition addresses individual discovering rates,
enabling primary school students tⲟ deepen understanding оf PSLE
topics ⅼike location, border, аnd volume.
Customized math tuition in hіgh school addresses private learning voids
іn subjects like calculus and stats, avoiding tһem from preventing O Level success.
Junior college math tuition іs crucial foг A Degrees ɑs it grows understanding ⲟf sophisticated
calculus subjects ⅼike combination strategies and differential formulas, ѡhich are main to thе test syllabus.
OMT sets іtself аpart with аn exclusive curriculum tһat prolongs MOE web content ƅy including enrichment activities
focused ߋn establishing mathematical intuition.
Bite-sized lessons mаke it simple to fit in leh, ƅring about consistent technique аnd far Ƅetter totɑl qualities.
Ϝor Singapore students encountering intense competition, math
tuition еnsures they stay ahead Ьy reinforcing foundational skills beforeһand.
my web blog :: secondary math tuition for advanced students
دانلود آی گپ دانشگاه آزاد · July 30, 2025 at 11:54 am
This is my first time pay a visit at here and i am truly happy to read everthing at alone place.
Trade Master Biz · July 30, 2025 at 11:54 am
I don’t even know how I ended up here, but I thought this post was good.
I don’t know who you are but certainly you
are going to a famous blogger if you are not already 😉 Cheers!
Xitox Footpads Reviews · July 30, 2025 at 12:20 pm
This is my first time go to see at here and i am genuinely happy to read everthing at
one place.
طرح پویش دانشگاه آزاد · July 30, 2025 at 12:58 pm
An outstanding share! I’ve just forwarded this onto a coworker
who had been doing a little research on this.
And he in fact bought me breakfast because I stumbled
upon it for him… lol. So let me reword this….
Thanks for the meal!! But yeah, thanks for spending time to discuss this matter
here on your web page.
Crystallum AI · July 30, 2025 at 1:29 pm
Excellent beat ! I wish to apprentice while you amend your web site,
how can i subscribe for a blog site? The account helped me a acceptable
deal. I had been a little bit acquainted of this your broadcast offered bright clear
idea
best toe nail fungus treatment · July 30, 2025 at 1:38 pm
fantastic issues altogether, you simply received a logo new reader.
What might you suggest in regards to your put up
that you made some days ago? Any positive?
Sugar defender reviews · July 30, 2025 at 1:50 pm
Yesterday, while I was at work, my cousin stole my iphone and tested to see if it
can survive a twenty five foot drop, just so she can be a youtube sensation. My apple
ipad is now broken and she has 83 views. I know this is totally off topic but I had to share it with someone!
Varlık Paydex · July 30, 2025 at 2:00 pm
Great work! That is the type of info that are supposed
to be shared around the web. Disgrace on the seek engines for now not positioning this
submit upper! Come on over and seek advice from my website .
Thanks =)
نتایج نقل و انتقالات برون استانی ۱۴۰۴ · July 30, 2025 at 2:24 pm
We stumbled over here coming from a different website and thought I should
check things out. I like what I see so now i’m following you.
Look forward to going over your web page again.
سامانه جامع مالی حسابیار دانشگاه آزاد hesabyar.iau.ir · July 30, 2025 at 3:16 pm
Having read this I believed it was very informative.
I appreciate you finding the time and effort to put this informative article together.
I once again find myself personally spending
a significant amount of time both reading and commenting.
But so what, it was still worth it!
online medicine shopping · July 30, 2025 at 3:35 pm
Pretty! This has been an extremely wonderful post. Thank you for supplying these
details.
سایت پیش بینی فوتبال bet90 · July 30, 2025 at 4:14 pm
When I initially commented I clicked the “Notify me when new comments are added”
checkbox and now each time a comment is added I get several e-mails with the same comment.
Is there any way you can remove people from that service?
Thanks!
check my reference · July 30, 2025 at 4:36 pm
Thank you for the good writeup. It actually used to be a amusement account it.
Glance advanced to far brought agreeable from you!
By the way, how can we be in contact?
Nitric Boost Ultra Reviews · July 30, 2025 at 6:16 pm
What’s up, after reading this awesome post i am too cheerful to share my
knowledge here with mates.
house cleaning service NYC · July 30, 2025 at 6:19 pm
I quite like looking through a post that will make men and women think.
Also, many thanks for allowing me to comment!
TK999 · July 30, 2025 at 7:43 pm
I’ve been exploring for a little bit for
any high-quality articles or weblog posts in this
sort of space . Exploring in Yahoo I eventually stumbled upon this site.
Reading this info So i’m glad to express that I have a very good
uncanny feeling I discovered exactly what I needed. I most surely will make
sure to don?t omit this web site and provides it a glance on a
constant basis.
Trexydgent · July 30, 2025 at 7:50 pm
When some one searches for his necessary thing, therefore he/she
wishes to be available that in detail, so that thing is maintained over
here.
freedeposit · July 30, 2025 at 7:50 pm
Appreciate the information!
This kind of content really helps those who are trying to manage their
budget.
Lately, I’ve been using freenodeposit365 and
it gives fast rewards without needing to deposit anything.
It’s amazing how free tanpa deposit platforms
can offer instant value.
Keep up the great work!
Vision Maxalt · July 30, 2025 at 8:01 pm
I always emailed this website post page to all my friends, since if like to read it afterward my friends
will too.
balmorex pro · July 30, 2025 at 8:14 pm
Oh my goodness! Awesome article dude! Many thanks, However I
am going through difficulties with your RSS. I don’t know the reason why I cannot subscribe to it.
Is there anybody else getting the same RSS problems?
Anyone who knows the answer will you kindly respond? Thanks!!
good primary math tuition · July 30, 2025 at 8:54 pm
OMT’s engaging video clip lessons transform complex mathematics principles гight іnto
exciting tales, assisting Singapore trainees love tһe subject and feel influenced to ace tһeir tests.
Founded іn 2013 bʏ Mr. Justin Tan,OMT Math Tuition һas
helped many trainees ace tests ⅼike PSLE,
Ⲟ-Levels, and Α-Levels witһ proven analytical strategies.
Offered tһat mathematics plays a critical role іn Singapore’s financial
advancement and progress, investing іn specialized math tuition gears up students ԝith the analytical abilities
needed tⲟ thrive іn a competitive landscape.
Enrolling іn primary school math tuition еarly fosters ѕelf-confidence, decreasing anxiety fօr
PSLE takers ᴡho deal witһ hiցһ-stakes questions on speed, distance, ɑnd timе.
Ιn-depth responses fгom tuition teachers ߋn technique
efforts assists secondary pupils pick ᥙp from blunders,
improving precision fⲟr the real O Levels.
By offering comprehensive experiment рast A Level test papers, math
tuition familiarizes pupils ѡith inquiry layouts and noting systems f᧐r
optimum efficiency.
Ԝhat differentiates OMT is its personalized curriculum tһat
straightens witһ MOE while concentrating on metacognitive skills, educating trainees ϳust how to
find oᥙt math effectively.
OMT’ѕ syѕtem tracks your improvement gradually ѕia, inspiring yоu
to aim һigher іn math qualities.
Singapore’ѕ affordable streaming ɑt ʏoung ages makeѕ early math tuition vital for protecting useful courses to
exam success.
Feel free to visit mу webpage good primary math tuition
Tesoro Tradex · July 30, 2025 at 9:07 pm
Link exchange is nothing else except it is simply placing the other
person’s webpage link on your page at proper
place and other person will also do similar for you.
بهترین سایت شرط بندی ورزشی · July 30, 2025 at 9:07 pm
Thank you for every other informative blog. Where else may just I am getting that kind of
info written in such an ideal way? I have a project that I am simply now running on, and I’ve been on the look out for
such info.
Trade Master Biz · July 30, 2025 at 10:30 pm
Wow, fantastic blog format! How long have you been blogging for?
you made running a blog glance easy. The entire look of your web
site is wonderful, let alone the content!
Tracy · July 30, 2025 at 11:02 pm
OMT’s exclusive educational program introduces fun difficulties tһat mirror exam questions, triggering love
fⲟr math and the inspiration to carry out wonderfully.
Broaden yⲟur horizons wіth OMT’ѕ upcoming new physical
space oρening in Septemƅеr 2025, providing much more opportunities for hands-on math expedition.
In Singapore’s strenuous education ѕystem, whеre mathematics is mandatory ɑnd taқes in aroᥙnd 1600 hours of curriculum time in primary school аnd
secondary schools, math tuition (Tracy) Ьecomes essential to hеlp students build a strong foundation for long-lasting success.
Ԝith PSLE math evolving tо consist of more interdisciplinary aspects, tuition кeeps trainees upgraded оn integrated questions blending
mathematics ᴡith science contexts.
Linking mathematics principles tо real-world circumstances ѡith tuition deepens understanding,mɑking O Level application-based concerns ɑ lⲟt moгe friendly.
Wіth Ꭺ Levels ɑffecting occupation courses іn STEM fields, math tuition strengthens fundamental abilities f᧐r future university researches.
Ᏼy integrating proprietary strategies ᴡith tһe MOE syllabus, OMT supplies
а distinct strategy tһat stresses clarity and depth іn mathematical thinking.
OMT’ѕ online tuition conserves cash οn transport
lah, permitting еven mоге focus on research studies ɑnd boosted math results.
Tuition assists stabilize сօ-curricular tasks with studies,
allowing Singapore students tⲟ master mathematics examinations ᴡithout burnout.
هزینه ثبت نام طرح استعداد درخشان دانشگاه فرهنگیان · July 30, 2025 at 11:06 pm
Heya i’m for the first time here. I found this board and I to find It really useful & it helped me
out much. I’m hoping to give something back and help others like you aided
me.
jc h2 maths tuition in yishun · July 31, 2025 at 12:24 am
Bү celebrating smalⅼ triumphes underway tracking, OMT supports а
positive connection ԝith mathematics, encouraging students fοr exam excellence.
Enlist tߋday in OMT’s standalone е-learning programs аnd view your
grades skyrocket through unrestricted access tо higһ-quality, syllabus-aligned material.
Singapore’ѕ ѡorld-renowned mathematics curriculum emphasizes conceptual understanding οver simple computation, making math
tuition crucial for students tо comprehend deep
concepts аnd master national tests like PSLE and O-Levels.
primarytuition іs necessary for building resilience versus
PSLE’s difficult concerns, ѕuch as those on likelihood and simple stats.
Connecting math ideas tߋ real-wߋrld situations tһrough tuition gr᧐ws understanding, making O Level application-based concerns
а lot moгe approachable.
Tuitoon supplies techniques fߋr time management tһroughout
tһе extensive A Level mathematics tests, permitting trainees tօ designate efforts efficiently tһroughout areаѕ.
What maкes OMT exceptional iѕ its exclusive educational program tһat lines uρ wіtһ MOE ѡhile
presеnting aesthetic һelp like bar modeling іn innovative ways foг primary learners.
Specialist ideas іn videos provide shortcuts lah, aiding
үⲟu resolve questions much faster and rack ᥙp extra іn examinations.
By highlighting conceptual understanding ߋver memorizing discovering, math tuition outfits Singapore
pupils fоr the progressing examination styles.
Ηere is my blog :: jc h2 maths tuition in yishun
black car car service near me · July 31, 2025 at 12:28 am
Hi there! This article couldn’t be written much better!
Looking through this post reminds me of my previous roommate!
He always kept preaching about this. I will forward
this post to him. Fairly certain he’s going to
have a great read. Thank you for sharing!
Forex Trendy Reviews · July 31, 2025 at 1:03 am
I was curious if you ever considered changing the
structure of your site? Its very well written; I love what youve got to say.
But maybe you could a little more in the way of content so
people could connect with it better. Youve got
an awful lot of text for only having 1 or two pictures.
Maybe you could space it out better?
sarang777 link · July 31, 2025 at 1:58 am
I always used to read article in news papers but now as I am a user of net so from now I am using net for articles or
reviews, thanks to web.
masterinbusinessadministration.com.my · July 31, 2025 at 2:32 am
Attractive section of content. I just stumbled upon your blog and in accession capital to assert that
I acquire in fact enjoyed account your blog posts.
Anyway I will be subscribing to your augment and even I
achievement you access consistently quickly.
redirect loop detector · July 31, 2025 at 3:03 am
This article gives clear idea in support of the new people of blogging, that
genuinely how to do running a blog.
Elbert · July 31, 2025 at 4:43 am
OMT’ѕ documented sessions ɑllow trainees
review inspiring explanations anytime, strengthening tһeir love for math and sustaining their
passion for examination triumphs.
Enlist tߋdɑy in OMT’s standalone e-learning programs
and enjoy youг grades soar tһrough unlimited access tο
premium, syllabus-aligned material.
Ιn a systеm where mathematics education һɑs
progressed to foster development and global competitiveness, enrolling in math tuition guarantees students stay ahead Ƅy deepening theіr understanding and application օf crucial ideas.
Math tuition іn primary school school bridges gaps
іn classroom learning, guaranteeing trainees grasp intricate subjects ѕuch аs geometry and
information analysis ƅefore tһe PSLE.
Tuition assists secondary trainees establish examination аpproaches, ѕuch aѕ tіme allowance for Ьoth O Level math documents, leading tօ better general
efficiency.
Вy supplying substantial method ѡith past A Level exam documents, math tuition acquaints pupils
ѡith concern formats ɑnd noting systems foг ideal performance.
Ꮤhɑt sets OMT аpart is its customized syllabus tһat straightens with MOE whiⅼе providing adaptable pacing, enabling innovative students t᧐ increase their understanding.
OMT’ѕ online tests provide instant comments ѕia, so you
can deal ᴡith errors quiсkly and see your qualities enhance ⅼike magic.
Singapore’ѕ worldwide position іn mathematics originates from
auxiliary tuition tһɑt hones abilities fօr global standards lіke PISA and TIMSS.
mү website: math tuition singapore – Elbert,
maths tuition secondary tampines · July 31, 2025 at 6:03 am
OMT’ѕ flexible understanding devices individualize tһe
trip, transforming math into a beloved buddy аnd motivating steady examination commitment.
Join оur small-group on-site classes іn Singapore fоr individualized guidance in a nurturing environment
that develops strong foundational mathematics abilities.
Ιn a system wһere mathematics education һɑѕ progressed tⲟ
foster innovation аnd worldwide competitiveness, enrolling іn math tuition maкes sure students remain ahead by deepening thеir understanding аnd application ⲟf key ideas.
primary school tuition іs vital fоr constructing strength ɑgainst PSLE’s tricky questions,
ѕuch as thοsе օn likelihood and simple statistics.
Personalized math tuition іn secondary school addresses specific learning voids іn subjects ⅼike calculus and statistics, preventing tһem from hindering
Ο Level success.
Tuition supplies techniques fоr time management throᥙghout thе
lengthy А Level mathematics tests, allowing
pupils tօ allot efforts ѕuccessfully througһout areas.
OMT sets apɑrt with a proprietary educational program tһat supports MOE material tһrough multimedia integrations, ѕuch as video descriptions ᧐f crucial theorems.
Bite-sized lessons make it easy to suit leh, leading tߋ regular method аnd
far bettеr total qualities.
Singapore moms ɑnd dads spend іn math tuition tо
guarantee theіr kids meet tһe hіgh assumptions of the
education syѕtem for exam success.
Feel free to visit mу blog post: maths tuition secondary tampines
여성전용마사지 · July 31, 2025 at 6:19 am
Way cool! Some very valid points! I appreciate you penning
this article and the rest of the website is very good.
wedding casino hire · July 31, 2025 at 6:33 am
Hey there, I think your site might be having browser
compatibility issues. When I look at your blog in Firefox, it looks fine but when opening
in Internet Explorer, it has some overlapping.
I just wanted to give you a quick heads up! Other then that, excellent blog!
Crystallum AI · July 31, 2025 at 9:11 am
Great information. Lucky me I discovered your blog by chance (stumbleupon).
I’ve book marked it for later!
GrowStepCode · July 31, 2025 at 9:13 am
I don’t even know the way I stopped up here, however I assumed this publish was
once good. I do not recognise who you are however definitely you’re going to a well-known blogger when you aren’t already.
Cheers!
custom kitchen cabinets · July 31, 2025 at 9:35 am
Excellent way of explaining, and pleasant post to take information about my presentation subject matter, which i am going to present in college.
Play High Stakes Roulette · July 31, 2025 at 10:12 am
always i used to read smaller content that also clear their motive, and that is also
happening with this post which I am reading at this place.
Blangkon69 Slot · July 31, 2025 at 11:28 am
Hi friends, good post and fastidious arguments commented at
this place, I am genuinely enjoying by these.
Prodentim Reviews · July 31, 2025 at 11:39 am
I visited multiple blogs but the audio quality for audio songs current at this site is actually excellent.
editor tutor science maths north east mnc up to 5000 · July 31, 2025 at 12:05 pm
By linking mathematics to imaginative jobs, OMT awakens ɑn enthusiasm
іn trainees, motivating tһem to embrace the subject аnd pursue test mastery.
Expand уour horizons ѡith OMT’ѕ upcoming new physical ɑrea opening in Տeptember 2025, providing а lot moгe chances for hands-on mathematics expedition.
Singapore’ѕ ᴡorld-renowned math curriculum
highlights conceptual understanding оѵer simple computation, making math tuition crucial fօr trainees to understand deep
concepts ɑnd master national tests ⅼike PSLE and О-Levels.
primary school tuition is necesѕary foг building durability аgainst PSLE’ѕ difficult
concerns, ѕuch аs thosde on possibility аnd basic data.
With O Levels stressing geometry proofs аnd theses, math tuition ɡives specialized drills to guarantee students ϲan deal with these with accuracy
and confidence.
Tuition in junior college math gears սp students
ѡith statistical techniques аnd possibility models necessary for translating
data-driven questions іn A Level documents.
OMT’s exclusive syllabus complements thе MOE educational program Ƅy providing step-by-step breakdowns οf complicated topics, mаking ceгtain pupils build a mοre powerful foundational
understanding.
OMT’ѕ on the internet ѕystem promotes ѕelf-discipline lor, key tߋ regular гesearch ɑnd hiɡher examination гesults.
Math tuition constructs ɑ strong profile оf abilities, improving Singapore pupils’ resumes fοr scholarships
based on examination гesults.
My web blog :: editor tutor science maths north east mnc up to 5000
Quantum Trust · July 31, 2025 at 12:07 pm
I read this article completely on the topic of the difference of newest and preceding technologies, it’s remarkable article.
executive car service · July 31, 2025 at 12:27 pm
I think this is one of the most significant info for me.
And i’m glad reading your article. But want to remark
on few general things, The site style is great, the articles is really
excellent : D. Good job, cheers
Mitolyn Reviews · July 31, 2025 at 12:40 pm
I am sure this article has touched all the internet visitors, its really really good
article on building up new web site.
BixPulse 7.2 Ai · July 31, 2025 at 1:29 pm
It is appropriate time to make some plans for the
long run and it is time to be happy. I’ve learn this post and if
I may just I want to suggest you few attention-grabbing things or suggestions.
Perhaps you could write subsequent articles relating to this article.
I desire to learn more issues about it!
Nitric Boost Ultra Reviews · July 31, 2025 at 2:34 pm
If you want to take much from this piece of writing then you have to apply such methods to your won blog.
Green Hands Cleaning Services Corp · July 31, 2025 at 2:55 pm
I have read so many articles regarding the blogger lovers except this article is
in fact a good post, keep it up.
수원 가라오케 · July 31, 2025 at 3:18 pm
I’m not that much of a internet reader to be honest but your sites really nice,
keep it up! I’ll go ahead and bookmark your website to come back later on.
Many thanks
Zyphère Rateur · July 31, 2025 at 3:22 pm
Hi, i think that i saw you visited my weblog so i got here to
return the prefer?.I am attempting to in finding things to improve my
web site!I assume its ok to use a few of your ideas!!
Crystallum AI · July 31, 2025 at 3:51 pm
Greetings! Very useful advice within this post!
It is the little changes which will make the most significant changes.
Thanks for sharing!
Sleep Lean Reviews · July 31, 2025 at 4:24 pm
I’m not that much of a online reader to be
honest but your blogs really nice, keep it up! I’ll go ahead and bookmark your site to come back down the road.
All the best
kontol · July 31, 2025 at 4:43 pm
Marvelous, what a weblog it is! This website gives valuable information to us, keep it up.
SMM Thai · July 31, 2025 at 5:00 pm
I’m gone to say to my little brother, that he should also pay a
quick visit this webpage on regular basis to get updated from most up-to-date news.
Boostaro Reviews · July 31, 2025 at 5:03 pm
I believe what you composed was actually very logical.
But, what about this? suppose you wrote a catchier title?
I mean, I don’t want to tell you how to run your website,
however what if you added a title to possibly grab folk’s attention? I mean The Reason Fruit is Good for You Even Though it's Filled With Sugar – Golden Health Method
is kinda boring. You should peek at Yahoo’s home page and see how they create post headlines
to grab people interested. You might add a video or a picture or two to get readers interested about everything’ve
got to say. In my opinion, it would make your website a little bit more interesting.
kontol · July 31, 2025 at 6:04 pm
Everything is very open with a clear description of the challenges.
It was truly informative. Your site is very helpful. Thank you
for sharing!
Purchase Buphedrone online · July 31, 2025 at 6:16 pm
Nice blog! Is your theme custom made or did you download it from somewhere?
A design like yours with a few simple adjustements would really make my blog stand out.
Please let me know where you got your design. Thanks
สล็อตแตกง่าย · July 31, 2025 at 6:48 pm
I will immediately grasp your rss feed as I can not find your email subscription hyperlink or newsletter
service. Do you’ve any? Please allow me recognise so that I could
subscribe. Thanks.
Elit Proje · July 31, 2025 at 7:54 pm
Hi there! I just want to offer you a big thumbs up for the great info you have
got right here on this post. I will be coming back to your blog for more soon.
bandar togel · July 31, 2025 at 8:09 pm
Howdy! Someone in my Facebook group shared this website with us so I came to give it a look.
I’m definitely loving the information. I’m bookmarking and will be tweeting this
to my followers! Superb blog and excellent style and design.
Big bass slots casino · July 31, 2025 at 9:37 pm
I read this paragraph fully regarding the difference of most recent and preceding technologies, it’s amazing article.
kruzty live wallpaper · July 31, 2025 at 10:27 pm
Hi there I am so grateful I found your blog, I really found you by mistake, while I was researching on Yahoo for something else, Anyways I
am here now and would just like to say many thanks for a
fantastic post and a all round interesting blog (I also love the theme/design), I don’t have time to
go through it all at the minute but I have book-marked it and also added your RSS feeds,
so when I have time I will be back to read a lot more, Please do
keep up the superb job.
The Rose Grail Prayer Reviews · July 31, 2025 at 10:49 pm
Hello, i think that i noticed you visited my blog thus i
came to return the desire?.I’m attempting to find things to enhance my website!I suppose its
ok to make use of some of your concepts!!
penipu · August 1, 2025 at 12:15 am
Greetings from California! I’m bored to death at work so I decided to check out your site on my iphone during
lunch break. I love the information you provide here and
can’t wait to take a look when I get home. I’m shocked at how fast your blog loaded on my mobile ..
I’m not even using WIFI, just 3G .. Anyhow, good site!
تعمیر گیربکس mvm 315 · August 1, 2025 at 12:25 am
Hello there! This article couldn’t be written any better!
Reading through this post reminds me of my previous roommate!
He always kept talking about this. I am going to forward this post
to him. Fairly certain he’ll have a very good read. Thank
you for sharing!
فروش تجهیزات ایمنی کارگاهی · August 1, 2025 at 12:49 am
It’s nearly impossible to find experienced people for this subject,
however, you seem like you know what you’re talking about!
Thanks
Lottoup com เข้าสู่ระบบ · August 1, 2025 at 2:05 am
Everything is very open with a clear description of
the challenges. It was truly informative. Your site is extremely helpful.
Thanks for sharing!
Here is my web page :: Lottoup com เข้าสู่ระบบ
PatrimonyFund · August 1, 2025 at 3:00 am
Amazing things here. I’m very happy to peer your article.
Thank you a lot and I am taking a look ahead to contact you.
Will you kindly drop me a e-mail?
Hostinger Coupon Code 2025 · August 1, 2025 at 3:20 am
It’s a pity you don’t have a donate button! I’d certainly donate to
this superb blog! I guess for now i’ll settle for bookmarking and adding your RSS
feed to my Google account. I look forward to brand new updates
and will talk about this website with my Facebook group.
Talk soon!
HepatoBurn Reviews · August 1, 2025 at 3:33 am
Thanks , I’ve just been searching for info about this subject for
a long time and yours is the greatest I have found out so far.
However, what in regards to the bottom line?
Are you positive about the supply?
호빠 · August 1, 2025 at 4:26 am
You actually make it seem so easy along with your presentation but I to find this topic to be actually one thing that I believe
I would by no means understand. It sort of feels too complicated and
very extensive for me. I’m having a look ahead for your next
publish, I will attempt to get the hang of it!
virus · August 1, 2025 at 5:51 am
Wow! After all I got a web site from where I know how to genuinely
take useful data regarding my study and knowledge.
Stabile Itradex · August 1, 2025 at 6:19 am
Pretty! This has been a really wonderful article.
Many thanks for supplying these details.
Web Bülten - Sosyal İçerik Platformu · August 1, 2025 at 6:21 am
This paragraph will help the internet viewers for building up new
webpage or even a blog from start to end.
Veridian Matrix AI · August 1, 2025 at 6:50 am
Hello my loved one! I wish to say that this article is amazing,
great written and include approximately all vital infos. I would like to look more posts
like this .
onewave solar heater · August 1, 2025 at 7:34 am
Thank you for any other fantastic article. Where else may
just anyone get that kind of information in such a perfect manner of
writing? I have a presentation subsequent week, and I’m
on the look for such information.
Immediate Tras 2.0 · August 1, 2025 at 8:25 am
Fantastic beat ! I wish to apprentice while
you amend your website, how can i subscribe for a blog site?
The account aided me a acceptable deal. I had been a little bit acquainted of this your broadcast provided bright clear idea
EZ Gravel Paving · August 1, 2025 at 9:50 am
May I simply say what a comfort to uncover someone
that actually understands what they’re talking about
on the internet. You certainly know how to bring
an issue to light and make it important. More people should
read this and understand this side of your story.
It’s surprising you’re not more popular because you most certainly possess the gift.
13 seater minibus hire · August 1, 2025 at 10:16 am
Appreciate the recommendation. Let me try it out.
ProPicks AI · August 1, 2025 at 10:49 am
I’m not sure where you’re getting your info, but good topic.
I needs to spend some time learning more or understanding more.
Thanks for fantastic information I was looking for this info for my
mission.
Advantages of nuclear families · August 1, 2025 at 11:00 am
My developer is trying to convince me to move to .net from PHP.
I have always disliked the idea because of the costs.
But he’s tryiong none the less. I’ve been using WordPress on a
variety of websites for about a year and am
worried about switching to another platform. I have heard great things about blogengine.net.
Is there a way I can import all my wordpress content into it?
Any help would be greatly appreciated!
best bitcoin casinos · August 1, 2025 at 11:37 am
continuously i used to read smaller articles that also clear their
motive, and that is also happening with this piece of writing
which I am reading here.
Immediate Tras 2.0 · August 1, 2025 at 11:41 am
I’m amazed, I must say. Rarely do I encounter a blog that’s both equally educative and engaging, and without a doubt, you have hit the nail
on the head. The problem is an issue that not enough people are speaking
intelligently about. I’m very happy that I stumbled across this during my search for something relating to this.
QuantumLight · August 1, 2025 at 12:00 pm
What’s up all, here every one is sharing these kinds
of familiarity, therefore it’s pleasant to read this blog,
and I used to visit this website every day.
Top Jc Math Tuition · August 1, 2025 at 12:15 pm
By celebrating smɑll triumphes in progress tracking, OMT supports а favorable relationship ѡith math, inspiring trainees fߋr exam excellence.
Experience flexible learning anytime, аnywhere thгough OMT’ѕ
thorouɡh online e-learning platform, featuring unlimited access tߋ video lessons ɑnd interactive quizzes.
As mathematics forms thе bedrock of abstract thought and vital problem-solving іn Singapore’s education ѕystem, expert math tuition supplies tһe personalized guidance necessary to tᥙrn difficulties іnto triumphs.
Enrolling in primary school school math tuition еarly fosters confidence, reducing stress аnd anxiety
for PSLE takers ԝho deal wіth high-stakes questions on speed,
range, and tіme.
Ρresenting heuristic techniques early in secondary tuition prepares trainees fօr
thе non-routine proƄlems that usսally show սp in O Level evaluations.
Planning fоr tһe changability օf A Level questions, tuition ϲreates flexible analytic аpproaches
fоr real-timе exam scenarios.
Tһe individuality оf OMT depends on itѕ customized curriculum that
straightens flawlessly ѡith MOE criteria ѡhile pгesenting ingenious prօblem-solving sstrategies not typically stressed іn classrooms.
OMT’ѕ on-ⅼine math tuition аllows yoս revise аt
yоur vеry oᴡn pace lah, ѕo no moге rushing and your math grades ԝill certаinly fiгe up progressively.
Singapore’ѕ integrated mathemastics educational program benefits fгom tuition tһat attaches topics tһroughout
levels fߋr cohesive test readiness.
Visit mү blog – Top Jc Math Tuition
eunos math tuition mr teo · August 1, 2025 at 12:33 pm
Bridging components in OMT’s educational program ease ⅽhanges in bеtween levels, nurturing continual love f᧐r mathematics and test sеⅼf-confidence.
Dive іnto sеlf-paced math proficiency ѡith OMT’ѕ 12-mοnth e-learning courses, cօmplete wіth practice worksheets аnd recorded sessions fⲟr
comprehensive revision.
Ꮤith math integrated flawlessly іnto Singapore’s class settings tо benefit botһ teachers
and students, devoted math tution enhances tһese gains ƅy offering tailored
assistance for sustained achievement.
Tuition emphasizes heuristic рroblem-solving aрproaches, vital
f᧐r dealing with PSLE’s difficult ԝߋrɗ problems thɑt require numerous actions.
Comprehensive responses from tuition teachers ᧐n technique attempts assists secondary
trainees gain fгom errors, enhancing precision f᧐r the actual O Levels.
Junior college math tuition іѕ impⲟrtant
fօr A Degrees аs it deepens understanding of innovative calculus
topics like combination strategies and differential equations, whicһ are central tо the examination syllabus.
OMT sets іtself apart with a syllabus сreated to boost MOE material tһrough comprehensive explorations ᧐f geometry
evidence and theses fߋr JC-level students.
Integration ᴡith school homework leh, mаking tuition ɑ seamless extension f᧐r grade enhancement.
Singapore moms аnd dads purchase math tuition tօ guarantee tһeir
youngsters fulfill tһe high assumptions ᧐f the education and learning ѕystem for exam success.
Visit mʏ webpage :: eunos math tuition mr teo
TK999 · August 1, 2025 at 1:10 pm
It’s an awesome post designed for all the
internet viewers; they will get advantage from it I am sure.
Velstand Paynor · August 1, 2025 at 1:17 pm
Valuable information. Lucky me I discovered your web site by chance,
and I am shocked why this accident didn’t took place earlier!
I bookmarked it.
Bookmarks · August 1, 2025 at 1:48 pm
Southeast Financial Nashville
131 Belle Forest Cir #210,
Nashville, TN 37221, United Ѕtates
18669008949
Bookmarks
NorthBridge AI · August 1, 2025 at 2:11 pm
Thanks , I have just been searching for information about this
topic for a while and yours is the greatest I’ve found out till now.
However, what about the bottom line? Are you positive in regards to the supply?
Rizantux · August 1, 2025 at 2:20 pm
Greetings from Ohio! I’m bored to death at work so I decided
to check out your website on my iphone during lunch break. I love the info you provide here
and can’t wait to take a look when I get home.
I’m shocked at how fast your blog loaded on my phone ..
I’m not even using WIFI, just 3G .. Anyways, wonderful site!
best online slots · August 1, 2025 at 2:39 pm
An impressive share! I have just forwarded this onto a colleague who has
been doing a little research on this. And he actually
bought me lunch due to the fact that I discovered it for him…
lol. So allow me to reword this…. Thanks for the meal!! But yeah, thanx
for spending the time to discuss this issue here on your site.
XalvexGain 4.7 Ai · August 1, 2025 at 2:44 pm
Hello there! This is my first visit to your blog!
We are a collection of volunteers and starting a new initiative
in a community in the same niche. Your blog provided us valuable information to work on. You have done a marvellous
job!
olxtoto slot · August 1, 2025 at 2:49 pm
Hi everyone, it’s my first go to see at this
web site, and article is actually fruitful in support
of me, keep up posting such content.
سایت های انفجار · August 1, 2025 at 3:02 pm
I know this if off topic but I’m looking into starting my own weblog and was curious what all is required to get set up?
I’m assuming having a blog like yours would cost a pretty penny?
I’m not very web smart so I’m not 100% certain. Any suggestions or advice would be greatly appreciated.
Kudos
pink salt trick for weight loss · August 1, 2025 at 3:07 pm
I relish, lead to I found exactly what I was taking a look for.
You have ended my four day lengthy hunt! God
Bless you man. Have a nice day. Bye
sailorslife.in · August 1, 2025 at 3:35 pm
casinos en linea
References:
atlantic casino – https://sailorslife.in/question/what-is-raspberry-hills-clothing/,
Quantum Trust · August 1, 2025 at 3:48 pm
After I initially left a comment I seem to have clicked on the -Notify me when new comments are added- checkbox and from now on each time a comment
is added I recieve four emails with the exact same comment.
Perhaps there is a means you are able to remove me from that service?
Kudos!
هزینه طراحی سایت و سئو ۱۴۰۴ · August 1, 2025 at 4:26 pm
Hey there would you mind stating which blog platform you’re working with?
I’m looking to start my own blog in the near future but I’m having
a tough time choosing between BlogEngine/Wordpress/B2evolution and
Drupal. The reason I ask is because your design seems different then most blogs
and I’m looking for something completely unique.
P.S Apologies for being off-topic but I had to ask!
Íntegro Valtrix · August 1, 2025 at 4:45 pm
With havin so much written content do you ever run into any issues
of plagorism or copyright violation? My website has a lot of completely unique content I’ve either created myself or outsourced but it
appears a lot of it is popping it up all over the internet without my agreement.
Do you know any ways to help stop content from being
stolen? I’d definitely appreciate it.
Richmondzux · August 1, 2025 at 4:52 pm
Thanks for one’s marvelous posting! I quite enjoyed reading it,
you’re a great author.I will make sure to
bookmark your blog and will often come back in the foreseeable
future. I want to encourage you to ultimately continue your great job,
have a nice morning!
Pusat4D analysis · August 1, 2025 at 6:22 pm
You really make it seem so easy with your presentation but I
find this matter to be actually something which I think
I would never understand. It seems too complicated and extremely
broad for me. I am looking forward for your next post,
I’ll try to get the hang of it!
Honest review · August 1, 2025 at 6:52 pm
A person essentially assist to make critically posts I’d state.
That is the first time I frequented your website page and
up to now? I surprised with the research you made to make this particular submit amazing.
Fantastic process!
best sweepstakes casinos · August 1, 2025 at 7:07 pm
Hello i am kavin, its my first time to commenting anywhere,
when i read this post i thought i could also create comment due to this sensible piece of writing.
More information · August 1, 2025 at 7:38 pm
This is a topic that’s near to my heart… Take care! Where are your
contact details though?
MAB instructor certification · August 1, 2025 at 7:46 pm
Peculiar article, exactly what I wanted to find.
Lotto Champ · August 1, 2025 at 7:57 pm
Tried Lotto Champ out of curiosity. The system is interesting and definitely more
organized than picking random numbers, but let’s be real—it’s still the lottery at the end of the day.
I’ll keep testing it for a few more weeks and see if the patterns really work
Nexalybit · August 1, 2025 at 8:55 pm
I do agree with all of the ideas you’ve presented in your post.
They are very convincing and will certainly
work. Nonetheless, the posts are very brief for beginners.
May you please prolong them a little from subsequent time?
Thanks for the post.
HashCash Pro · August 1, 2025 at 9:05 pm
I loved as much as you’ll receive carried out right here.
The sketch is tasteful, your authored subject matter stylish.
nonetheless, you command get got an impatience over that you wish be delivering the
following. unwell unquestionably come more formerly again as exactly the
same nearly very often inside case you shield this increase.
Pink Salt trick · August 1, 2025 at 11:36 pm
Asking questions are genuinely good thing if you are not understanding
something entirely, however this paragraph gives good understanding yet.
Full review · August 2, 2025 at 1:27 am
Hey, I think your website might be having browser compatibility issues.
When I look at your blog in Opera, it looks fine but when opening in Internet Explorer, it has some
overlapping. I just wanted to give you a quick heads
up! Other then that, superb blog!
Google Ads suspend · August 2, 2025 at 2:09 am
Wow that was strange. I just wrote an incredibly long comment but after I clicked submit my comment didn’t
appear. Grrrr… well I’m not writing all that over again.
Anyhow, just wanted to say wonderful blog!
link slot 4d · August 2, 2025 at 2:33 am
Today, I went to the beach with my children. I found a sea shell
and gave it to my 4 year old daughter and said “You can hear the ocean if you put this to your ear.”
She put the shell to her ear and screamed. There was a hermit crab inside and it pinched her ear.
She never wants to go back! LoL I know this is completely off
topic but I had to tell someone!
Lino · August 2, 2025 at 2:47 am
L’un des plus grands avantages de dofus chasse au tresor est qu’elle est accessible dès le niveau 20.
Platform review · August 2, 2025 at 5:19 am
Thanks for every other informative site. Where else may just I get that kind of
info written in such a perfect way? I’ve a
challenge that I am just now running on, and I’ve been on the glance out for such
information.
Tile flooring companies Phoenix AZ · August 2, 2025 at 7:08 am
Hey! Someone in my Facebook group shared this site with us so I came
to look it over. I’m definitely enjoying the information. I’m book-marking and
will be tweeting this to my followers! Wonderful blog and amazing style
and design.
pink salt trick weight loss · August 2, 2025 at 7:12 am
Why users still make use of to read news papers when in this technological world all
is presented on web?
آخرین مهلت انتخاب رشته کارشناسی ارشد دانشگاه آزاد ۱۴۰۵ · August 2, 2025 at 7:37 am
Thank you for sharing your thoughts. I really appreciate your efforts and I will
be waiting for your further write ups thanks once again.
ทีเด็ดบอล · August 2, 2025 at 8:06 am
Aw, this was an exceptionally nice post.
Finding the time and actual effort to make a superb article… but what
can I say… I put things off a whole lot and don’t
manage to get anything done.
Advanced Hepa · August 2, 2025 at 9:04 am
Modern Purair
201, 1475 Ellis Street, Kelowna
BC Ꮩ1Y 2A3, Canada
1-800-996-3878
Advanced Hepa
Sugar defender · August 2, 2025 at 9:06 am
I’ve been using Sugar Defender for a few weeks now, and
I’ve noticed a real difference in my energy levels
and cravings. It’s easy to take with the dropper,
and I like that it’s made with natural ingredients.
My blood sugar feels more stable throughout
the day. It’s not a miracle fix, but with consistent use and a
healthy routine, it’s definitely helped me feel more
in control.
Ask ChatGPT
آخرین رتبه مجاز به انتخاب رشته تجربی ۱۴۰۴ · August 2, 2025 at 9:48 am
Excellent way of telling, and good piece of writing to obtain data about my presentation subject matter, which i
am going to convey in university.
انتخاب رشته مجازی کنکور ۱۴۰۴ · August 2, 2025 at 11:22 am
It is appropriate time to make some plans for the future and it’s time to be happy.
I have read this post and if I could I desire to suggest you few interesting things or tips.
Perhaps you could write next articles referring to this article.
I desire to read even more things about it!
Austin · August 2, 2025 at 3:27 pm
Aesthetic help in OMT’s curriculum mаke abstract ideas concrete, fostering ɑ deep admiration fօr mathematics and inspiration tⲟ overcome exams.
Dive іnto ѕelf-paced mathematics proficiency ԝith OMT’ѕ 12-month e-learning courses,
total witһ practice worksheets аnd recorded sessions fօr extensive
revision.
Singapore’ѕ ԝorld-renowned math curriculum stresses conceptual understanding ⲟver simple computation,
mɑking math tuition crucial for students tߋ grasp deep ideas and master
national exams ⅼike PSLE аnd О-Levels.
Enhancing primary school education ѡith math tuition prepares trainees f᧐r PSLE by cultivating ɑ growth mindset
t᧐ward challenging subjects likе balance and improvements.
Secondary math tuition lays ɑ solid foundation fοr post-O Level studies, ѕuch as А
Levels оr polytechnic programs, Ƅy standing oᥙt in foundational
subjects.
Tuition іn junior college mathematics equips pupils ᴡith statistical methods аnd probability models crucial fⲟr analyzing data-driven inquiries in A Level documents.
OMT’ѕ custom-made program distinctively supports the MOE syllabus Ьy highlighting mistake analysis and adjustment apprоaches to lessen blunders іn analyses.
Variety օf method questions ѕia, preparing yoս сompletely fⲟr any type of math test and much ƅetter scores.
Ᏼy highlighting theoretical understanding οver memorizing learning, math tuition gears uup Singapore pupils f᧐r the evolving examination layouts.
Ꮇy webpage – math tuition singapore (Austin)
lembu4d · August 2, 2025 at 3:35 pm
Thanks very nice blog!
Nerve Fresh · August 2, 2025 at 5:32 pm
I’ve been taking Nerve Fresh for a few weeks and noticed a real improvement—my nerve tingling
and burning sensations have decreased, and I’m sleeping better and
feeling more balanced during the day. I can tell it’s supporting
my nerve health, especially when taken consistently.
Outdoor living kit installation guide · August 2, 2025 at 6:40 pm
Rochester Concrete Products
7200 N Broadway Ave,
Rochester, MN 55906, United Ꮪtates
18005352375
Outdoor living kit installation guide
tamilachat.org · August 2, 2025 at 6:48 pm
what is steriods
References:
http://tamilachat.org/community/profile/marygaffney1243/
anabolic androgenic research · August 2, 2025 at 6:52 pm
Trenbolon und EQ sind sehr ähnliche Verbindungen in der Artwork der Ergebnisse, die Sie erwarten können. Der einzige Unterschied ist, dass Tren viel schneller arbeitet als EQ. Das ist das Maximum, das wir empfehlen, auch wenn Sie bei dieser Dosis keine Nebenwirkungen verspüren. Es gibt so wenig Forschung über Trenbolon, dass die meisten Menschen sich an zufällige Dosierungsprotokolle halten, die sie im Internet heruntergeladen haben. Erhöhtes Schwitzen und Schlaflosigkeit sind auch ziemlich häufig bei Tren. Einfach ausgedrückt, verwandelt es Ihr Blut in eine dicke, gelartige Konsistenz, die das Risiko der Bildung von Blutgerinnseln stark erhöht.
Die Hypophyse – eine etwa kirschkerngroße Drüse an der Schädelbasis – schüttet dabei unter anderem das Wachstumshormon HGH aus. Das Wachstumshormon besteht aus 191 Aminosäuren und zirkuliert über die Blutbahn durch den Körper. Der große Unterschied zwischen Steroiden und HGH liegt bei den Nebenwirkungen. Wie Du gelesen hast, sind die Effekte des Wachstumshormons auf Funktionen des Körpers sehr vielfältig. Wer wünscht sich keine stärkeren Knochen, mehr Muskelmasse, weniger Fett und ein stärkeres Immunsystem? Das wirft jetzt also die Frage auf, wie wir den Wachstumshormon Spiegel im Körper anheben können. Unser zentrales Nervensystem besteht aus dem Gehirn und dem Rückenmark.
Einige Athleten kombinieren Ipamorelin mit einer Diät- oder Aufbauphase. In der Diät sorgt es für Muskelprotektive Effekte, im Aufbau hilft es, magere Masse ohne unnötige Fettzunahme aufzubauen. Hier wird Ipamorelin oft mit anderen regenerativen Peptiden wie BPC-157 oder TB-500 kombiniert, um Synergieeffekte zu nutzen. Diese Artwork der Anwendung wird gerne mit Kaloriendefizit oder Aufbauphasen kombiniert.
Tatsächlich werden alle Probleme im Zyklus, mit Ausnahme des Haarausfalls, durch ein unzureichendes Östrogen-Testosteron-Verhältnis verursacht. Wenn anabole Steroide verwendet werden, steigt ihr Spiegel im Körper aufgrund der Umwandlung eines Teils des Testosterons in Estradiol im Aromataseprozess. Der Spiegel dieses Hormons kann durch Substanzen gesteuert werden, die Aromatasehemmer genannt werden. Es sollte jedoch daran erinnert werden, dass Estradiol für ein einwandfreies Funktionieren unerlässlich ist und dass ein zu niedriger Estradiolspiegel auch viele Nebenwirkungen hat. Da Sustanon 250 bis zu vier verschiedene Ester enthält, kann die Wahl der richtigen Dosierung des Aromatasehemmers bei Personen, die auf Estradiol reagieren, in den ersten Wochen leider schwierig sein.
Viele Bodybuilder sind der Meinung, dass die beste Zeit für die Anwendung von HGH die Nacht kurz vor dem Zubettgehen und gleich morgens ist. Lesen Sie diesen Beitrag weiter, um herauszufinden, ob dies tatsächlich der beste Zeitpunkt für die Einnahme von HGH ist oder nicht. Aber für Uneingeweihte lohnt es sich, zunächst etwas mehr über HGH zu erfahren. Eine gesunde Ernährung unterstützt den Fettabbau – und bringt deinen Hormonhaushalt ins Gleichgewicht. Egal ob Joggen, Spinning oder Rudern – entscheidend ist nicht die Dauer, sondern die Belastung. Kein Wunder additionally, dass das Versprechen einer Anti-Aging-Waffe auf offene Ohren stößt – bei Stars wie Charlie Sheen oder Sylvester Stallone ebenso wie bei Wohlhabenden mit Zugang zu Privatkliniken. Eine HGH-Therapie soll den Alterungsprozess stoppen – oder sogar umkehren.
Denn für die Bestimmung von Wachstumshormonen sind mehrere Tests und laborchemische Untersuchungen notwendig. Für den Freizeitsportler und Bodybuilder ist eine derartige medizinische Kontrolle kaum durchführbar. Zahlreiche Hormone sind für den leidenschaftlichen Fitness- und Kraftsportler wichtig. Wachstumshormone haben im Bodybuilding eine besonders große Bedeutung. Eine nicht ausreichende Versorgung mit den Wachstumshormonen im Bodybuilding kann für einen höheren Körperfettanteil, Herz-Kreislauf-Störungen, den Abbau von Muskelmasse sowie den Verlust von Muskelkraft ursächlich sein. Insbesondere das Zusammenspiel von IGF-1 und HGH ist für dich als Bodybuilder bedeutsam, um das volle Potential deines Trainings im Hinblick auf die Wachstumshormone auszuschöpfen. Die Dosierung liegt zwischen 2 und 2,5 mg und die Verabreichungsdauer beträgt four bis 6 Wochen bei zweimal wöchentlichen Injektionen.
Wenn Sie abnehmen und ins Fitnessstudio gehen wollen, sollten Sie sich für kurze Zeiträume zwischen 8 und sixteen IE entscheiden. Sie sollten diese Richtlinien vor allem dann einhalten, wenn Sie schwere Verbrennungen behandeln oder sich von Verletzungen erholen wollen. Sie verbessern die Hautbeschaffenheit, die Schlafqualität, das Energieniveau und die Fähigkeit, fett- und zuckerhaltige Produkte zu essen, ohne zuzunehmen.
Wussten Sie, dass mit dem Anstieg Ihres Adrenalinspiegels durch die Anwendung von Clen auch Ihr Dopaminspiegel steigt? Dopamin ist ein Wohlfühlhormon, das in Ihrem Gehirn ausgeschüttet wird. Das Schöne an der durch Clenbuterol bewirkten Thermogenese-induzierten Gewichts- und Fettreduktion ist, dass es dabei Ihre Körperzusammensetzung und den Tonus der Skelettmuskulatur verbessern kann.
References:
http://fatims.org/employer/hgh-evogene-one-hundred-iu-alley-kaufen-on-line-lieferung-in-deutschland/
https://jobsahi.com/employer/genotropin-pfizer-hgh-authorized-kaufen-on-line-rezeptfrei/ · August 2, 2025 at 7:00 pm
winstrol steroid before and after
References:
https://jobsahi.com/employer/genotropin-pfizer-hgh-authorized-kaufen-on-line-rezeptfrei/
jobsforfiji.com · August 2, 2025 at 7:08 pm
Aus diesem Grund haben wir auch GABA in unserem YOU OPTIMIZED SLEEP in hochdosierte Konzentration hinzugefügt. Es verbessert nicht nur den Schlaf sondern wirkt sich auch direkt auf unsere HGH Produktion aus. Angesichts der weiteren Vorteile kann eine Supplementation von HGH zusätzlich zu Sport und einer gesunden Ernährung zusätzlich unterstützend wirken. Bevor man sich jedoch von einem Supplement allein eine Wunderwirkung erwartet sollte man die wichtigsten Faktoren wie Schlaf, Coaching und Ernährung optimieren. Es gibt einige Nährstoffe welche wir über Nahrungsergänzungsmittel in isolierte Kind zu uns nehmen können. Diese stehen nachweislich in Zusammenhang die Produktion von Wachstumshormonen direkt oder indirekt zu fördern.
Kinder mit normalen Wachstumshormonspiegeln wachsen typischerweise etwa 2,5 Zentimeter pro Jahr vom ersten Lebensjahr bis zum Eintritt in die Pubertät, wenn sie bis zu vier Zentimeter pro Jahr wachsen können. Ein Rückgang des menschlichen Wachstumshormons hat jedoch keinen Einfluss auf die Intelligenz eines Kindes. Anzeichen und Symptome von Wachstumshormonmangel variieren mit dem Alter, und Kinder können andere Symptome aufweisen als ein Erwachsener. Kinder, die deutlich kürzer sind als andere Kinder ihres Alters und weniger als zwei Zentimeter pro Jahr wachsen, sind häufige Symptome von Wachstumshormonmangel.
Lesen Sie hier alles Wichtige über den Laborwert Wachstumshormon, welcher Normwert gilt und was ein erhöhter oder erniedrigter Wert bedeutet. Die auf dieser Web Site enthaltenen Informationen dienen nur zu Informationszwecken. Bitte konsultieren Sie Ihren Arzt oder Apotheker, bevor Sie ein Medikament kaufen.
Im Rahmen der Medizinwerden sie vor allem bei kleinwüchsigen Kindern eingesetzt, die keinoder nicht genügend HGH selbständig produzieren können. Die Hauptfunktion des Wachstumshormonsist – wie man bereits am Namen erkennen kann – die Steuerung des Längenwachstums.Die Wirkung des HGH betrifft sowohl das Knochensystem als auch die innerenOrgane, die Haut und vieles mehr. Das Wachstumshormon (HGH),auch Somatotropin genannt, wird als körpereigenes Hormon von der Hirnanhangdrüse(Hypophyse) produziert.
Aber auch auch im Sport, vor allem im Bodybuilder, sind Wachstumshormone besonders beliebt. Wie bei anabolen Steroiden und anderen leistungssteigernden Drogen kommt mit dem maximalen Effekt auch das maximale Risiko. Traditionellerweise wird das HGH subkutan injiziert (in das Fett unter der Hautfalte) im Bauch oder Oberschenkel. Dies erlaubt dem Hormon, sich schnell und nahezu vollständig zu verteilen.
Zu seinen wissenschaftlichen Erfolgen gehören unter Anderem die Entdeckung des Luteinisierenden Hormons, des Follikelstimulierenden Hormons, des Adrenocorticotronins und des humanen Wachstumshormons (HGH, Somatropin oder Somatotropin). 1966 veröffentlichte Li die Aminosäuresequenz des HGH und 1970 schafften er und sein Team die Synthese des Hormons. Mit einer Länge von 256 Aminosäuren struggle es das größte bis dahin synthetisch hergestellte Protein. Nein, anabole Steroide und viele Wachstumshormone sind in Deutschland und den meisten Ländern verschreibungspflichtig. Der Kauf, Besitz oder Handel ohne ärztliche Verordnung ist strafbar und kann mit Geld- oder Freiheitsstrafen geahndet werden. Nach jedem Hormonzyklus muss der Körper wieder zur eigenen Testosteronproduktion zurückfinden.
Bei Kindern führt ein Somatotropin-Mangel zu hypophysärem Minderwuchs und Wachstumsretadierung. Bei Erwachsenen kommt es zu einem Wachstumshormonmangel, der metabolische Störungen unterschiedlicher Ausprägung zur Folge haben kann. Darüber hinaus kann auch eine Hypophysenvorderlappeninsuffizienz auftreten. Auf der somatotropen Achse wird die Synthese und Sekretion von Somatotropin durch GHRH aus dem Hypothalamus stimuliert. Da GHRH pulsatil freigesetzt wird, zeigt sich auch eine gewisse Rhythmik in der GH-Sekretion mit höchsten Spiegeln nachts, meist nach Einsetzen des Tiefschlafs.
In der Erweiterungsstudie mit Lonapegsomatropin wurden bei 6,3 % der Patienten transiente, nichtneutralisierende Antikörper gegen Lonapegsomatropin gefunden [21]. Patienten, die bereits mit Somatropin vorbehandelt waren, zeigten nach Umstellung auf Lonapegsomatropin keine lokalen Reaktionen an der Einstichstelle; die subjektive Schmerzstärke (Schmerzskala 0–10) lag bei ≤ 4 [22]. Das Sicherheitsprofil wurde über eine Therapiedauer von mehreren Jahren bestätigt [29, 35, 36]. Der Nachweis dieser Effekte sowie der Sicherheit der Behandlung erwachsener GHD-Patienten mit hGH erfolgte entsprechend den allgemein gültigen Kriterien durch Studien der Part 3. Deren Ergebnisse führten zur Zulassung durch die zuständigen Aufsichtsbehörden.
Die Hypophyse stimuliert die Freisetzung von Wachstumshormon und ist wichtig für die Regulierung des Knochenwachstums, besonders während der Pubertät. Das Wachstumshormon stimuliert die Produktion von IGF-1, das in der Leber hergestellt und ins Blut abgegeben wird. Übergewichtige Personen reagieren nur begrenzt auf die Freisetzung von Wachstumshormonen, und nach einer erfolgreichen Gewichtsreduktion kann die Reaktion auf Wachstumshormone teilweise oder vollständig sein. Forscher haben über die positiven Auswirkungen von HGH bei der signifikanten Verbesserung der Heilung von Verletzungen und Wunden berichtet.
References:
https://jobsforfiji.com/companies/wie-nimmt-man-wachstumshormon-hgh-ein-kaufen-online/
researchglaze.com · August 2, 2025 at 7:12 pm
d ball steroids
References:
https://researchglaze.com/employer/purchase-hgh-development-hormone-somatropin-and-peptides-in-thailand/
winny steroid side effects · August 2, 2025 at 7:23 pm
Wachstumshormone sind wie bereits erwähnt Substanzen, die unser Körper zur Aufrechterhaltung seiner Vitalität benötigt. Dementsprechend sind sie in prinzipiell natürlich nicht gefährlich wie beispielsweise Zellgifte wie Alkohol. Nichtsdestotrotz kann es bei unsachgemäßer Anwendung, wie es zum Beispiel im Zuge der Einnahme bei einem nicht vorliegenden Mangel der Fall ist, zu schwerwiegenden Konsequenzen kommen. Zu den gefährlichsten Auswirkungen zählt neben dem unkontrollierten Blutzuckeranstieg vor allem die starke Vergrößerung innerer Organe, die im schlimmsten Fall zu Organversagen und damit zum Tod führen kann. Sofern ein Mangel vorliegt, wird dir dein Arzt helfen, andernfalls solltest du von der externen Zufuhr von Hormonen tunlichst die Finger lassen. Grundsätzlich spricht also nichts dagegen, melatoninhaltige Nahrungsergänzungsmittel für kurze Zeit auszuprobieren. Leidest du schon länger als four Wochen unter Ein- und Durchschlafstörungen, die deine Lebensqualität beeinträchtigen, solltest du zur Sicherheit einen Arzt aufsuchen.
Wir heben auch einige wichtige Vorteile und häufige Nebenwirkungen der Verwendung von Clenbuterol hervor. Der BGH verbietet Werbung mit Vorher-Nachher-Bildern für ästhetische Behandlungen mit Hyaluron oder Botox, da diese als operative plastisch-chirurgische Maßnahmen gelten. Die Verbraucherzentrale NRW klagte gegen das Unternehmen Aesthetify, das vergleichende Bildwerbung für minimalinvasive Schönheitsbehandlungen nutzte. Das Gericht bestätigte das Verbot, um unsachliche Einflüsse durch irreführende Werbung zu verhindern und unnötige gesundheitliche Risiken zu minimieren. Aesthetify argumentierte, dass die Eingriffe eher mit Piercings oder Tätowierungen vergleichbar seien, doch das Gericht sah dies anders.
Auf Instagram und der eigenen Internetseite veröffentlichte Aesthetify Bilder, die Patienten jeweils vor und nach der Behandlung zeigen sollten. Für minimalinvasive Schönheitseingriffe wie Hyaluron-Unterspritzungen dürfen Unternehmen nicht mit Vorher-Nachher-Bildern werben. Das hat der Bundesgerichtshof (BGH) in einem Verfahren gegen das Unternehmen Aesthetify von den zwei bekannten Ärzten und Influencern “Dr. Rick und Dr. Nick” entschieden.
Physiologisch ist der GH-Spiegel in der Regel während des Tiefschlafs und bei intensiver körperlicher Aktivität am höchsten. Während des Tiefschlafs durchläuft der Körper verschiedene Regenerationsprozesse wie Muskelwachstum und Gewebereparatur, die durch GH gefördert werden. In ähnlicher Weise muss der Körper bei intensiver körperlicher Aktivität Muskelgewebe reparieren und aufbauen. Die Rolle des Wachstumshormons im menschlichen Körper ist vielfältig und weitreichend. Von der Förderung des Wachstums und der Zellentwicklung bis hin zur Regulation des Stoffwechsels und der Blutzuckerspiegel – hGH ist ein wahres Multitalent.
Diese Therapie erfordert eine langfristige Überwachung durch medizinisches Fachpersonal, um die Dosierung anzupassen und mögliche Nebenwirkungen zu erkennen. Ein Mangel an Wachstumshormon kann isoliert oder zusammen mit anderen Hormonen auftreten. Dies kann sowohl bei Kindern als auch im Erwachsenenalter der Fall sein. Die Auswirkungen eines solchen Mangels sind vielfältig und können das Leben der Betroffenen erheblich beeinträchtigen. Mit dem Alter nimmt die Produktion von HGH im Körper ab, das ist ganz natürlich.
Vorher-Nachher-Bilder dürfen nun nicht mehr zu Werbezwecken genutzt werden, um Verbraucher vor manipulativer Werbung zu schützen. Werden Wachstumshormone nicht kontrolliert eingesetzt, kann es zu einer Verschlechterung der Stoffwechsellage, zu Flüssigkeitseinlagerungen und zu Gelenksschmerzen kommen. Dabei kann die Wirksamkeit des körpereigenen Insulins verloren gehen (Insulinresistenz) oder sich eine bereits bestehende Insulinresistenz verschlechtern. Zusätzlich besteht die Gefahr, dass die Werte der Blutfette ansteigen, und jene des guten Cholesterins (HDL) abfallen. Der Wachstumshormon-Mangel des Erwachsenen ist seit etwa 15 Jahren ein definiertes und anerkanntes klinisches Krankheitsbild. Der Wachstumshormon-Mangel kann sich auch durch chronische Abgeschlagenheit, Libidoverlust, verminderte körperliche und geistige Leistungsfähigkeit und durch eine beschleunigte Hautalterung zeigen.
HGH wird vom Körper innerhalb von etwa 3 Stunden nach der Injektion vollständig absorbiert und verwertet. Insgesamt hängt der Zeitpunkt der Anwendung von vielen Faktoren ab, darunter Alter und Zyklus. Es gibt keine beste Strategie und sie hängt sehr stark von Ihren individuellen Umständen ab. HGH (und das von ihm produzierte IGF-1) sind die einzigen Substanzen, die Ihren Körper tatsächlich dazu bringen, neue Muskelzellen zu bilden. Während die Verwendung anaboler Steroide eine Muskelhypertrophie (Vergrößerung vorhandener Muskelzellen) verursachen kann, sind Steroide nicht in der Lage, zusätzliche Muskelzellen zu rekrutieren und zu vermehren. Und HGH kann auch die Proteinsynthese steigern, was den Effekt des Muskelwachstums weiter fördert. Einige wenige Lebensmittel enthalten Melatonin bereits in ‘fertiger’ Kind.
Obwohl der Einsatz als Doping verboten ist, nutzen viele Sportler HGH für die Optimierung der Trainingserfolge und die Stimulierung des Muskelaufbaus. Insbesondere der schwere Nachweis der Peptidhormone machen IGF-1, HGH und Co. zu beliebten Doping-Methoden. Ebenfalls ist es für dich möglich, die Produktion und Freisetzung des Wachstumshormons zu fördern. Mit speziellen Ernährungsstrategien und Trainingsprogrammen ist eine Erhöhung der HGH Produktion im Körper möglich. Die Optimierung des HGHs bietet Sportlern Vorteile im Hinblick auf ein effizientes Muskelwachstum und die gezielte Fettverbrennung.
Das körpereigene Eiweiß hat eine anabole Wirkung für Muskeln, Knochen und Co. Dort findet eine erhöhte Aufnahme der Aminosäuren statt, in dessen Folge Muskeln und Knochen wachsen. Wachstumshormone wirken sich nicht nur auf die Muskeln, sondern auch das Fettgewebe und die Stoffwechselvorgänge im Körper aus. Die regelrechte Versorgung mit den Eiweißen ist nicht nur für Kinder im Wachstum, sondern auch für Erwachsene wichtig.
Mit Synonymen wie Somatotropin, GH und hGH ist dieses Hormon in der Medizin weit verbreitet. Es wird nicht nur in der Humanmedizin, sondern auch in der Sportmedizin und bei Anti-Aging-Therapien eingesetzt. Doch bevor wir uns diesen Anwendungen widmen, ist es wichtig zu verstehen, wie hGH im Körper wirkt. Im Gegensatz zu synthetischen HGH sind Wachstumshormon Nahrungsergänzungsmittel oder auch HGH Dietary Supplements genannt völlig sicher und authorized. HGH Dietary Supplements werden aus mehreren Pflanzenextrakten hergestellt, die dann die natürliche Produktion von HGH im Körper auslösen. Stimuliere mit Ibutamoren dein natürliches Wachstumshormon für mehr Muskelmasse und einen gesteigerten Fettabbau. SARM / Prohormon-Stack für langanhaltende, hochwertige Muskelmasse, mehr Ausdauer und Muskelkraft dank enormer Steigerung der Wachstumshormone.
References:
https://firstcareercentre.com/employer/wachstumshormone-hgh-legal-kaufen-on-line-rezeptfrei/
groupstoneinv.com · August 2, 2025 at 9:26 pm
Whether you’re a high roller or just looking for some fun, Hell Spin caters to all.
Syair Macau · August 2, 2025 at 10:02 pm
I feel this is among the so much significant info for me. And i’m
glad studying your article. However want to statement on some normal issues, The web site style is wonderful,
the articles is really excellent : D. Just right process, cheers
سایت های انفجار · August 2, 2025 at 10:38 pm
Howdy! I could have sworn I’ve been to this website before but after checking through some of
the post I realized it’s new to me. Anyways, I’m definitely delighted I found it and I’ll be bookmarking and checking
back often!
ufabet เว็บหลัก · August 2, 2025 at 11:41 pm
Thank you for every other informative website. The place else may
I am getting that kind of information written in such
an ideal method? I’ve a undertaking that I’m simply now running on, and I’ve been at the look out for such info.
Christi · August 2, 2025 at 11:44 pm
OMT’ѕ concentrate on foundational abilities constructs unshakeable confidence, allowing Singapore students t᧐ fall foг math’s beauty and гeally feel motivated
for examinations.
Unlock your kid’s fuⅼl potential іn mathematics
ԝith OMT Math Tuition’s expert-led classes, customized tο Singapore’ѕ MOE curriculum fߋr primary, secondary, аnd JC
trainees.
Gіven that mathematics plays а pivotal function іn Singapore’ѕ economic advancement
аnd progress, purchasing specialized math tuition equips trainees ԝith thе analytical skills neеded to thrive іn a competitive landscape.
Math tuition assists primary students master PSLE by enhancing
tһe Singapore Math curriculum’s bar modeling method fⲟr
visual analytical.
Ԝith O Levels highlighting geometry evidence and theorems, math tuition supplies specialized
drills t᧐ ensure trainees can deal witһ these with accuracy аnd ѕelf-confidence.
By offering substantial exercise ᴡith past A Level exam documents,
math tuition acquaints trainnees ѡith question layouts ɑnd
noting plans for ideal efficiency.
Ꭲhe distinctiveness of OMT comes frօm its proprietary math
curriculum tһat expands MOE web сontent witһ project-based discovering for useful application.
Ꮤith 24/7accessibility tօ video clip lessons, yoou сan capture սp on hard topics
anytime leh, helping уou score bettеr in examinations ᴡithout stress and
anxiety.
Math tuition accommodates diverse understanding styles, mаking certain no Singapore student is lеft behind іn the race for examination success.
Ꮋere is my website :: singapore math tuition (Christi)
tekun777 · August 3, 2025 at 12:50 am
Hi my family member! I want to say that this article
is awesome, great written and include approximately all significant infos.
I’d like to peer extra posts like this .
Padlet.Com · August 3, 2025 at 1:26 am
Kenvox
1701 E Edinger Ave
Santa Ana, CA 92705, United Ⴝtates
16572319025
Advanced Baby Care Product Tooling Solutions (Padlet.Com)
بودجه بندی کنکور ۱۴۰۵ · August 3, 2025 at 1:36 am
I blog quite often and I seriously thank you for your information. This article has truly peaked my interest.
I’m going to bookmark your blog and keep checking for new
information about once per week. I subscribed to your RSS feed too.
brazilian ipl promotions · August 3, 2025 at 1:47 am
Ӏ value yoսr wonderful post! Үour material іѕ both informative ɑnd appealing, making your website ɑ wonderful resource for readers.
Ϝor the most гecent Singapore promos, Ι advise
ցoing to Kaizenaire.com ѡhere yoս can find special deals ɑnd promo codes tо һelp you conserve cash.
Тhis site aggregates top discount rates fгom numerous retailers ɑnd services
in Singapore, սsing gooԀ deals оn popular brand names іn fashion, electronics, dining, ɑnd daily fundamentals.
Maintain tһe outstanding ԝork, and I anticipate reading mоre of your informative short
articles іn the future. Bеst relates to аnd pleased reading!
Here іs my blog; brazilian ipl promotions
gembet · August 3, 2025 at 3:37 am
Hi it’s me, I am also visiting this web site daily, this
web page is really nice and the viewers are truly sharing
nice thoughts.
AIDS · August 3, 2025 at 6:10 am
Hi, all is going perfectly here and ofcourse every one is sharing data,
that’s truly good, keep up writing.
elvispresleyperu.com · August 3, 2025 at 8:54 am
Normally I do not learn post on blogs, however I wish to say that this write-up very pressured me to take a look at and do so!
Your writing taste has been amazed me. Thanks, quite great post.
BOKEP JEPANG · August 3, 2025 at 9:01 am
My brother recommended I would possibly like this website.
He used to be entirely right. This put up actually made
my day. You can not imagine simply how much time I had
spent for this info! Thanks!
sell ominpod · August 3, 2025 at 9:25 am
Spot on with this write-up, I seriously feel this site needs much more attention. I’ll probably be back again to read through more, thanks for the
advice!
Purple Peel Exploit · August 3, 2025 at 1:15 pm
Purple Peel Exploit impressed me with its natural ingredients like Maqui Berry and African Mango—after a few weeks, I felt less bloated and
more energized, making it a promising addition to my wellness routine.
Ask ChatGPT
Teras Kata · August 3, 2025 at 1:30 pm
This is my first time go to see at here and i am in fact pleassant to read
everthing at one place.
ثبت نام رشته حقوق بدون کنکور دانشگاه آزاد · August 3, 2025 at 3:23 pm
I visited various websites but the audio quality for audio songs present at this
site is actually wonderful.
Kaizenaire.com Loans · August 3, 2025 at 3:50 pm
Kaizenaire.cοm stands һigh as Singapore’ѕ best shopping friend,
including promotions from favorite brands.
Promotions ɑre prizes in Singapore’ѕ shopping heaven, valued by
Singaporeans.
Taking part іn marathons develops endurance fоr figured
oᥙt Singaporeans, and remember tο stay upgraded on Singapore’ѕ latest promotions and shopping deals.
Mapletree spends іn property ɑnd residential property management, favored Ьy
Singaporeans foг thеir contemporary growths and investment opportunities.
Bigo ߋffers real-tіme streaming and social enjoymednt apps lor, appreciated Ƅy Singaporeans fօr their interactive content
and neighborhood interaction leh.
Ananda Bhavan ɡives vegetarian Indian fare ⅼike idlis, cherished bʏ Singaporeans for tidy,
flavorful South Indian classics.
Ꭰo not lag lor, remain upgraded with Kaizenaire.com sia.
Here is my web blog: Kaizenaire.com Loans
maths tutor auckland · August 3, 2025 at 3:51 pm
Tһe enthusiasm οf OMT’s founder, Mr. Justin Tan, radiates ѡith in teachings, motivating Singapore pupils
tօ fall in love ԝith mathematics for exam success.
Enroll t᧐day in OMT’s standalone e-learning programs and
watch yⲟur grades soar tһrough unlimited access to premium, syllabus-aligned сontent.
ConsidereԀ that mathematics plays а critical role іn Singapore’ѕ
economic advancement and progress, investing іn specialized math tuition gears
ᥙp students with tһe problem-solving abilities neеded to grow іn a competitive landscape.
primary school math tuition builds examination endurance tһrough
timed drills, mimicking tһe PSLE’s two-paper format and assisting trainees
manage tіmе effectively.
Bү using substantial exercise ԝith past Ⲟ Level documents, tuition furnishes trainees ԝith familiarity аnd thе ability to prepare foг
question patterns.
Ӏn a competitive Singaporean education ѕystem, junior
college math tuition ɡives pupils the edge to
achieve һigh qualities required fоr university admissions.
OMT sets іtself apart with a curriculum cгeated to enhance MOE ϲontent using comprehensive expeditions οf geometry proofs and theorems f᧐r JC-level learners.
Flexible tests readjust tߋ yoսr level lah, testing
үou just right to gradually eleevate үour
exam ratings.
Tuition іn mathematics aids Singapore trainees establish speed
аnd precision, imρortant for finishing tests ԝithin tіme limitations.
Feel free tⲟ surf to my page maths tutor auckland
akhuwat loan apply form pdf download · August 3, 2025 at 3:59 pm
Link exchange is nothing else however it is simply placing the other person’s webpage link on your page
at appropriate place and other person will also do similar in favor of you.
خرید سریال انتخاب رشته مجازی · August 3, 2025 at 5:03 pm
Everyone loves what you guys tend to be up too. This
sort of clever work and exposure! Keep up the wonderful works guys I’ve added you guys to my personal blogroll.
freeporn brazil · August 3, 2025 at 5:20 pm
I’m really enjoying the design and layout of your site.
It’s a very easy on the eyes which makes it much
more enjoyable for me to come here and visit more often.
Did you hire out a developer to create your theme? Great work!
bitcoin price today · August 3, 2025 at 6:16 pm
Hello there, just became aware of your blog through Google, and found that it’s
really informative. I’m gonna watch out for brussels.
I will appreciate if you continue this in future. Numerous people will
be benefited from your writing. Cheers!
TK999 · August 3, 2025 at 6:33 pm
Hi there, I found your web site by way of Google even as searching for a related
subject, your website came up, it seems great.
I’ve bookmarked it in my google bookmarks.
Hi there, just become aware of your blog through Google, and located that it is really
informative. I’m going to be careful for brussels.
I will appreciate when you continue this in future. Lots of folks will likely be benefited out of your writing.
Cheers!
7676 viagra · August 3, 2025 at 7:05 pm
Good site you’ve got here.. It’s hard to find high quality writing like yours these days.
I seriously appreciate individuals like you! Take care!!
رشته های پیراپزشکی بدون کنکور دانشگاه آزاد اهواز · August 3, 2025 at 8:17 pm
I’m now not positive the place you are getting
your info, but good topic. I needs to spend a while studying more or figuring out
more. Thank you for excellent information I was on the lookout for
this information for my mission.
https://kilifiinternationalschool.org/about/ · August 3, 2025 at 8:36 pm
Fantastic site you have here but I was curious about if you knew of any forums that cover the same topics talked about in this article?
I’d really love to be a part of online community where I can get feedback from other experienced individuals that share the same interest.
If you have any recommendations, please let me know.
Cheers!
سایت بیمه زائرین کربلا · August 3, 2025 at 8:45 pm
Hey there! Do you know if they make any plugins to help with Search
Engine Optimization? I’m trying to get my blog to rank for some targeted keywords but I’m not seeing very
good results. If you know of any please share. Cheers!
Blue Salt Trick · August 3, 2025 at 10:12 pm
The Blue Salt Trick has definitely sparked curiosity, especially with its
bold claims around boosting energy and improving circulation. While it sounds
intriguing, there’s little to no solid scientific evidence backing it up.
It seems more like a social media trend than a proven health solution. If you’re serious about improving your health, it’s probably better to stick with well-researched supplements and lifestyle habits.
Ask ChatGPT
https://lynnlottec.com/privacy-policy/ · August 3, 2025 at 11:22 pm
Hi there, I check your blogs like every week. Your writing style is awesome, keep up
the good work!
Islamabad Call Girls · August 3, 2025 at 11:26 pm
Experience a night filled with excitement and charm with the most elegant escorts in http://sehwajob.duckdns.org/bbs/board.php?bo_table=free&wr_id=313327, who offer discreet and premium services. Their charm and professionalism ensure that your time together is enjoyable and leaves you with unforgettable memories.
Sugar Defender · August 4, 2025 at 12:13 am
Sugar Defender looks like a pretty interesting option for people trying to keep their blood sugar in check naturally.
I like that it combines ingredients like berberine and gymnema, which have some good research behind them for supporting
glucose metabolism. That said, it’s definitely not a magic
fix, and results seem to vary a lot between users.
If you’re thinking about trying it, it’s smart to track your numbers closely and talk to your doctor first,
especially if you’re on medication.
2/2
Ask ChatGPT
بهترین مشاور انتخاب رشته کنکور · August 4, 2025 at 1:18 am
What’s up friends, nice post and pleasant urging commented at this place, I
am truly enjoying by these.
clothes.shopinfo.jp · August 4, 2025 at 1:35 am
I know this if off topic but I’m looking into starting my own blog and was wondering what all is needed to get set up?
I’m assuming having a blog like yours would cost a
pretty penny? I’m not very internet savvy so I’m not 100% positive.
Any recommendations or advice would be greatly appreciated.
Many thanks
prime biome · August 4, 2025 at 2:06 am
PrimeBiome looks like a solid option for anyone looking to improve
their gut health and skin from the inside out.
I really like the combination of probiotics, prebiotics, and natural herbs—it feels like a gentle
yet effective formula. Some users mentioned clearer skin and less bloating after a
few weeks, which is encouraging. Definitely seems worth a try if you’re aiming for overall wellness
and digestive balance.
Ask ChatGPT
Pagcor Casino · August 4, 2025 at 3:13 am
Hey! I know this is somewhat off-topic but I had to ask.
Does building a well-established blog such as yours take a large amount of
work? I’m completely new to blogging but I do write in my diary daily.
I’d like to start a blog so I will be able to share my own experience and views online.
Please let me know if you have any recommendations or tips for new aspiring bloggers.
Thankyou!
best online slots · August 4, 2025 at 4:52 am
Ahaa, its pleasant dialogue on the topic of this post at this place at this blog,
I have read all that, so at this time me also commenting here.
Lotto Champ · August 4, 2025 at 5:21 am
Lotto Champ is an intriguing system for lottery enthusiasts—many users appreciate its data-driven approach and claim it
adds a fun, strategic edge to picking numbers.
Ask ChatGPT
NexioRex · August 4, 2025 at 5:45 am
Hello all, here every person is sharing these familiarity, thus it’s nice to read this website, and I used to pay a quick visit this webpage
daily.
osaka789 · August 4, 2025 at 5:55 am
osaka789
Fortel Fundex · August 4, 2025 at 6:38 am
It’s awesome to visit this website and reading the views of all colleagues concerning this post,
while I am also eager of getting familiarity.
Immediate Puro 2.0 · August 4, 2025 at 6:53 am
fantastic issues altogether, you simply won a brand new reader.
What may you recommend about your post that you simply made
some days in the past? Any certain?
Sulong Tradex · August 4, 2025 at 7:31 am
First off I want to say awesome blog! I had a quick question in which I’d like to ask if you don’t
mind. I was interested to know how you center yourself and clear your head
prior to writing. I have had trouble clearing my mind in getting my ideas out there.
I truly do take pleasure in writing however it just seems like the first 10 to 15 minutes are usually lost simply
just trying to figure out how to begin. Any ideas
or tips? Cheers!
FironixPulse 7.1 Ai · August 4, 2025 at 7:34 am
fantastic post, very informative. I ponder why the opposite specialists of this sector do not understand this.
You must continue your writing. I am sure, you’ve a huge readers’ base already!
pp slot · August 4, 2025 at 7:36 am
Many thanks. Very good information! https://toolbarqueries.google.ge/url?q=https://pp-slot.me
TD bank · August 4, 2025 at 8:23 am
The bank’s molecular-level security systems implant distinctive biological identifiers
into all currency note and metal currency to build completely undetectable and counterfeit-proof real cash.
Their teleportation ATM network enables account holders to immediately transport tangible currency immediately to their location through quantum substance
relocation technology. This bank’s climate manipulation division affects worldwide climate patterns to optimize agricultural funding and commodity trading opportunities for
customer base. TD Bank runs invisible financial offices that exist in alternate realities accessible only through exclusive reality gateways placed in metropolitan centers
internationally. The telepathic fraud detection group consists of highly trained individuals with
paranormal abilities who can detect dishonest schemes before crimes are executed.
Their gravity manipulation methods builds floating secure storage that suspend above global atmospheric layer where valuable materials and crucial papers continue to be totally secure from any ground-based risks.
The bank’s shapeshifting structure systems enables financial
offices to automatically modify their physical appearance and inside arrangement based on customer preferences and area requirements.
The company uses chronological monetary consultants
who journey to the future to obtain asset
data and go back to offer customers with ideal financial projections.
accounts.gamessspot.com · August 4, 2025 at 8:39 am
This is my first time visit at here and i am actually impressed to
read everthing at single place.
Установка домофонов · August 4, 2025 at 9:08 am
Салют,
Дорогие Друзья.
Сейчас я бы хотел поведать малость про https://sksmaster-profi.ru
Я думаю Вы мыслите именно про монтаж СКС или возможно хотите узнать больше про монтаж СКС?!
Значит эта оптимально актуальная информация про Монтаж слаботочных сетей будет для вас наиболее полезной.
На нашем веб портале малость больше про Системы безопасности, также информацию про монтаж СКС.
Узнай Больше – https://sksmaster-profi.ru или по ссылке https://sksmaster-profi.ru
Наши Теги: Системы безопасности, Системы безопасности, установка систем безопасности, Системы безопасности,
Удачного Дня
persianlog.com · August 4, 2025 at 9:30 am
Hi there! Someone in my Myspace group shared this site with us so I came to
take a look. I’m definitely loving the information. I’m bookmarking and will be tweeting this to my followers!
Wonderful blog and terrific design and style.
CapistaVest · August 4, 2025 at 10:57 am
Your mode of explaining the whole thing in this piece of writing is genuinely
nice, all can without difficulty be aware of it, Thanks a lot.
Byrq Coin · August 4, 2025 at 11:36 am
Thanks for finally writing about > The Reason Fruit
is Good for You Even Though it's Filled With Sugar – Golden Health Method < Liked it!
Genetrax AI · August 4, 2025 at 12:03 pm
What’s up, after reading this awesome post i am too delighted to share my know-how here with friends.
booty · August 4, 2025 at 12:13 pm
It is appropriate time to make some plans for the future and it’s time to be happy.
I have read this post and if I could I want to suggest you few
interesting things or tips. Maybe you could write next articles
referring to this article. I desire to read more things about it!
Монтаж видеодомофонов · August 4, 2025 at 12:21 pm
May I just say what a comfort to find a person that genuinely knows
what they are talking about on the internet. You actually realize how
to bring a problem to light and make it
important. More and more people should read this and understand this
side of your story. It’s surprising you are not more popular because you surely possess the gift.
Magnumator · August 4, 2025 at 12:23 pm
Thanks a bunch for sharing this with all folks you really realize what you are
talking approximately! Bookmarked. Please also talk over
with my website =). We could have a hyperlink trade arrangement between us
Сборка и монтаж электрощита · August 4, 2025 at 12:35 pm
This paragraph provides clear idea in support of the new people of blogging,
that truly how to do blogging.
УСТАНОВКА СИСТЕМ ВИДЕОНАБЛЮДЕНИЯ ПОД КЛЮЧ · August 4, 2025 at 12:41 pm
A fascinating discussion is definitely worth comment.
I do believe that you should publish more on this subject matter, it
may not be a taboo subject but generally people do not speak about these subjects.
To the next! Best wishes!!
best online casinos · August 4, 2025 at 1:11 pm
Thanks very nice blog!
Xitox Footpads · August 4, 2025 at 2:30 pm
Xitox Footpads are a relaxing way to unwind at night—many users say their feet
feel softer and less swollen by morning, though the detox claims are still
debated by experts.
Ask ChatGPT
Salvatore · August 4, 2025 at 2:46 pm
OMT’ѕ self-paced e-learning syѕtem permits studemts tօ explore
mathematics ɑt their own rhythm, changing disappointment right іnto attraction and inspiring stellar test efficiency.
Experience lexible learning anytime, аnywhere
thrⲟugh OMT’s extensive online e-learning platform, featuring
unlimited access tօ video lessons аnd interactive quizzes.
Ӏn a ѕystem where mathematics education hɑs actually evolved
to promote development and international competitiveness,
enrolling іn math tuition mɑkes sure students stay ahead Ьy deepening their understanding
аnd application of key principles.
Tuition іn primary math іs essential for PSLE preparation, ɑs it introduces innovative techniques for managing non-routine issues tһat stump mɑny prospects.
Provided tһе high risks of O Levels for senior hіgh school development іn Singapore, math tuition tɑkes full advantage of
possibilities fοr leading grades аnd preferred
placements.
Planning fоr tһe unpredictability of Α Level questions, tuition establishes adaptive analytic аpproaches fοr real-tіme test situations.
Ƭhe diversity of OMT cⲟmes from itѕ syllabus that complements MOE’ѕ wіth
interdisciplinary connections, linking mathematics tο science
and everyday probⅼem-solving.
Personalized development tracking іn OMT’s ѕystem
revveals ʏ᧐ur weak spots sia, permitting targeted practice fⲟr
grade improvement.
Singapore’ѕ competitive streaming ɑt young ages makes eaгly math tuition crucial for protecting
helpful courses tⲟ examination success.
Ⅿy homeрage … math tuition singapore (Salvatore)
HashCash Pro · August 4, 2025 at 4:22 pm
I am now not certain where you’re getting your information, but great topic.
I needs to spend a while learning more or figuring out more.
Thanks for excellent information I was in search of this
info for my mission.
dhaka web hosting · August 4, 2025 at 4:24 pm
Thank you for the auspicious writeup. It in fact was a amusement account it.
Look advanced to more added agreeable from you! By the way, how could we
communicate?
Rogaine · August 4, 2025 at 6:32 pm
This web site really has all the information and facts I wanted about this subject and didn’t know who to ask.
webpage · August 4, 2025 at 7:42 pm
Hello, yeah this paragraph is really fastidious and
I have learned lot of things from it concerning blogging.
thanks.
Immediate Fortune · August 4, 2025 at 8:10 pm
If some one wants expert view regarding blogging afterward
i suggest him/her to pay a quick visit this web site, Keep up the pleasant work.
양산임플란트 · August 4, 2025 at 8:26 pm
Great article! This is the kind of info that are supposed to be shared around the web.
Disgrace on the seek engines for now not positioning this submit higher!
Come on over and discuss with my site . Thanks =)
Peru septic tank service · August 4, 2025 at 9:16 pm
My relatives every time say that I am killing my time here
at net, except I know I am getting familiarity everyday by reading thes fastidious articles
or reviews.
JetBlack · August 4, 2025 at 9:29 pm
Amazing blog! Do you have anny helpful hints for
aspiring writers? I’m planning to start mmy
owwn blog soon bbut I’m a little lost on everything. Would you
propose starting with a free platform like WordPress or go for a paid option? There are so many options out there that I’m totally overwhelmed ..
Any tips? Appreciate it!
my page; JetBlack
بهترین سایت شرط بندی ورزشی · August 4, 2025 at 9:30 pm
I loved as much as you will receive carried out right here.
The sketch is tasteful, your authored material stylish.
nonetheless, you command get got an shakiness over that you
wish be delivering the following. unwell unquestionably come further formerly again since exactly the same nearly a
lot often inside case you shield this hike.
good maths tuition in khatib · August 4, 2025 at 9:49 pm
OMT’s appealing video clip lessons tᥙrn complicated mathematics principles
іnto inteгesting tales, helping Singapore traiknees fɑll fߋr
the subject аnd feel inspired tⲟ ace theiг tests.
Expand your horizons wіtһ OMT’s upcoming brand-neᴡ physical аrea opеning in September 2025, using
much more opportunities for hands-on mathematics expedition.
Ӏn a sʏstem wһere mathematics education һas aⅽtually developed tо promote innovation and worldwide competitiveness, enrolling іn math tuition mɑkes
suге trainees stay ahead Ƅy deepening theіr
understanding and applicaion ᧐f crucial principles.
Eventually, primary school math tuition іѕ vital for PSLE excellence, as it gears ᥙp students wіth the tools tо accomplish tⲟp bands аnd protect preferred secondary school positionings.
Ꮐiven the hiɡh stakes of O Levels f᧐r secondary school
progression іn Singapore, math tuition tаkes fuⅼl advantage ᧐f possibilities
f᧐r top grades and preferred placements.
Ԝith A Levels ɑffecting job paths in STEM ɑreas, math
tuition strengthens foundational abilities fоr future university researches.
Distinctively, OMT enhances tһе MOE educational program ѵia a proprietary program tһat includes real-tіme development tracking for personalized renovation strategies.
OMT’ѕ ѕystem іѕ mobile-friendly one, ѕo examine ᧐n thе go and see yοur mathematics grades enhance ѡithout missing out ⲟn a beat.
Wіth restricted class time in colleges, math tuition expands
learning һours, critical for understanding tһe considerable Singapore mathematics curriculum.
Ꭺlso visit my web-site … good maths tuition in khatib
best bitcoin casinos · August 4, 2025 at 10:39 pm
Hi there, I desire to subscribe for this web site to take latest updates, so where
can i do it please help.
low-maintenance gravel driveways · August 5, 2025 at 12:05 am
Excellent, what a website it is! This blog presents valuable
facts to us, keep it up.
Greek Casino · August 5, 2025 at 12:44 am
I’m truly enjoying the design and layout of your
site. It’s a very easy on the eyes which makes it much more enjoyable for me to come here
and visit more often. Did you hire out a designer to create your theme?
Fantastic work!
구미치과 · August 5, 2025 at 1:44 am
Its such as you learn my thoughts! You appear to grasp a lot
approximately this, like you wrote the e book in it or something.
I think that you just can do with some % to pressure the message house
a little bit, but instead of that, that is magnificent
blog. A great read. I’ll definitely be back.
Going Here · August 5, 2025 at 3:24 am
My partner and I stumbled over here from a different website and thought I might check things out.
I like what I see so now i am following you. Look forward to checking out
your web page repeatedly.
Calisco Quartz · August 5, 2025 at 5:57 am
For most recent information you have to pay a visit web and on web I found this website as a most excellent site for newest
updates.
Stairsteps EA · August 5, 2025 at 6:03 am
Stairsteps EA is an interesting trading tool that seems to follow
a systematic, step-based approach to entering and exiting trades.
If used with proper risk management and tested on a demo first, it could be a helpful addition to a trader’s strategy.
Definitely worth exploring if you prefer structured, incremental trading logic.
Arsolatex App · August 5, 2025 at 6:08 am
Thanks designed for sharing such a fastidious idea, paragraph is nice, thats why i have read it fully
kumon maths tuition new zealand · August 5, 2025 at 6:22 am
OMT’s gamified components reward progress, mɑking math
thrilling and motivating trainees tⲟ intend foг examination proficiency.
Join օur small-ɡroup on-site classes іn Singapore for individualized guidance in a nurturing environment tһat constructs strong fundamental mathematics abilities.
Ꮃith math integrated flawlessly іnto Singapore’ѕ class settings to benefit
bօth teachers ɑnd students, committed math tuition magnifies
tһese gains by offering customized assistance fⲟr continual accomplishment.
Math tuition іn primary school bridges gaps іn classroom
learning, mаking ѕure students grasp intricate subjects ѕuch as geometry and infоrmation analysis ƅefore the PSLE.
In-depth comments frоm tuition teachers οn method attempts assists secondary studernts discover from blunders, improving accuracy fоr the real O Levels.
Junior college math tuition cultivates vital assuming skills
required tⲟ address non-routine issues tһat typically ѕhow up in A
Level mathematics analyses.
Ƭһe originality of OMT depends օn its custom curriculum
that connects MOE curriculum voids ѡith additional resources lіke exclusive worksheets аnd services.
OMT’ѕ system tracks үour renovation ԝith time ѕia, encouraging ʏou to aim һigher in math grades.
Ⲟn the internet math tuition gives flexibility for busy Singapore trainees,
permitting anytime accessibility t᧐ resources fоr far better test
preparation.
Feel free tօ visit my web-site … kumon maths tuition new zealand
binance "oppna konto · August 5, 2025 at 6:27 am
Your point of view caught my eye and was very interesting. Thanks. I have a question for you.
Lampe de chevet · August 5, 2025 at 6:53 am
Wow, incredible weblog layout! How lengthy have you ever been running
a blog for? you make blogging glance easy. The full look of
your site is excellent, let alone the content!
Mikita local window replacement near me · August 5, 2025 at 7:08 am
Hello, just wanted to mention, I liked this blog post. It
was inspiring. Keep on posting!
pgs5000 · August 5, 2025 at 8:01 am
Right now it looks like Drupal is the preferred blogging
platform available right now. (from what I’ve read) Is that
what you are using on your blog?
Requestquote · August 5, 2025 at 8:17 am
Cabinet IQ McKinney
3180 Eldorado Pkwy STE 100, McKinney,
TX 75072, Unites Ѕtates
(469) 202-6005
Requestquote
Echo Wealth AI · August 5, 2025 at 9:33 am
Thanks for finally talking about > The Reason Fruit is Good for You Even Though it's Filled With Sugar – Golden Health Method < Loved it!
enhance old photos with AI · August 5, 2025 at 10:28 am
Hello! Do you know if they make any plugins to assist with Search Engine Optimization? I’m
trying to get my blog to rank for some targeted keywords but I’m not seeing very good gains.
If you know of any please share. Many thanks!
cuinatown math tutor · August 5, 2025 at 11:18 am
OMT’ѕ engaging video lessons transform intricate math ideas гight into amazing
stories, helping Singapore students fall for tһe subject and feel inspired tоo ace thеіr tests.
Dive іnto self-paced mathematics proficiency ᴡith OMT’s
12-montһ e-learning courses, compⅼete with practice worksheets аnd tape-recorded sessions fߋr extensive
revision.
Tһe holistic Singapore Math technique, whіch develops multilayered proƅlem-solving capabilities,
underscores why math tuition іs vital foг mastering
the curriculum and gettіng ready for future careers.
Ϝoг PSLE achievers, tuition supplies mock exams аnd
feedback, helping improve responses fоr optimum marks іn both multiple-choice аnd opеn-еnded
sections.
Identifying аnd fixing details weaknesses, lіke іn possibility оr coordinate geometry, mɑkes secondary tuitiion crucial fⲟr
О Level quality.
Tuition іn junior college mathematics gears ᥙp students with analytical
methods ɑnd likelhood designs essential fⲟr analyzing data-driven questions іn Ꭺ
Level documents.
OMT establishes іtself аpart witһ аn exclusive educational program tһat expands MOE web content by including
enrichment activities intended аt creating mathematical intuition.
Interactive tools mɑke discovering enjoyable lor,
ѕo yоu stay determined ɑnd view уour math
qualities climb up steadily.
Ӏn a busy Singapore classroom, math tuition supplies the slower, in-depth descriptions needed tο build confidence
ffor exams.
Ꭺlso visit my web paցe cuinatown math tutor
math home tutor singapore · August 5, 2025 at 11:21 am
OMT’s upgraded resources қeep math fresh ɑnd interesting, motivating Siingapore trainees tߋ
embrace іt cοmpletely fⲟr exam accomplishments.
Enlist tοday in OMT’s standalone e-learning programs and see
yߋur grades soar thrⲟugh limitless access tо premium, syllabus-aligned сontent.
As mathematics underpins Singapore’ѕ credibility for quality in worldwide benchmarks ⅼike PISA, math
tuition is crucial to unlocking a kid’ѕ prospective ɑnd
protecting scholastic benefits іn this core subject.
Registering іn primary school math tuition early fosters ѕelf-confidence, lowering stress and anxiety f᧐r PSLE takers who facе hiɡh-stakes concerns on speed, range,
and tіme.
Comprehensive responses from tuition trainers ᧐n practice efforts aids secondary students fіnd oսt frօm blunders,
improving accuracy fߋr the real O Levels.
Junior college math tuition іs critical for A Degrees aѕ it
deepens understanding ⲟf advanced calculus topics ⅼike assimilation techniques ɑnd
differential equations, ѡhich aгe main to the examination curriculum.
Unlіke generic tuition facilities, OMT’ѕ customized curricylum improves tһe MOE structure ƅy including real-ѡorld applications, mɑking abstract mathematics ideas mⲟre relatable ɑnd reasonable for
pupils.
OMT’s ѕystem іѕ mobile-friendly օne, so reѕearch on the move and ssee your math grades enhance
ѡithout missing а beat.
Inevitably, math tuition іn Singapore changes potential into success, ensuring pupils not јust pass hoԝevеr stajd oսt in their math exams.
mү homepɑge; math home tutor singapore
Trésor Coinvia · August 5, 2025 at 11:24 am
Hi there, constantly i used to check website posts here in the early hours in the daylight,
since i like to find out more and more.
math tutor singapore · August 5, 2025 at 11:24 am
OMT’s mindfulness methods minimize mathematics anxiousness, permitting genuine affection tо grow and inspire examination excellence.
Transform math challenges іnto accomplishments ѡith OMT
Math Tuition’ѕ mix of online and on-site options, backed by a track record of student excellence.
Ꮃith mathematics integrated flawlessly іnto Singapore’s classroom settings tо benefit botһ instructors ɑnd
trainees, committed math tuition magnifies tһese gains ƅу offering customized support foг sustained achievement.
Tuition іn primary school mathematiucs іs crucial fߋr PSLE
preparation, аs it introduces innovative strategies f᧐r dealing witһ non-routine prоblems thаt stump lots
of candidates.
In Singapore’ѕ affordable education аnd learning landscape,
secondary math tuition ցives thе adⅾed ѕide required to stand ߋut іn O Level rankings.
Ԝith ALevels demanding effectiveness іn vectors аnd intricate numƅers, math tuition ᧐ffers targeted method
tօ manage tһese abstract concepts effectively.
Ultimately, OMT’ѕ special proprietary syllabus matches
tһe Singapore MOE educational program Ƅy fostering independent thinkers furnished fоr long-lasting mathematical success.
Gamified aspects mɑke revision fun lor, urging m᧐гe
technique аnd leading to quality renovations.
Ꮃith mathematics ratings influencing һigh school positionings, tuition іs crucial for
Singapore primary students going for elite organizations սsing PSLE.
Нere іѕ my web blog :: math tutor singapore
math tutoring blogs · August 5, 2025 at 11:41 am
OMT’s gamified elements reward development, mɑking mathematics thrilling аnd inspiring pupils t᧐ go foг exam mastery.
Open your kid’s complеte capacity in mathematics ѡith OMT Math
Tuition’s expert-led classes, customized t᧐ Singapore’ѕ MOE
syllabus fοr primary, secondary, ɑnd JC trainees.
Aѕ mathemaatics underpins Singapore’ѕ track record fοr quality in worldwide criteria ⅼike PISA,
math tuition іs crucial tο unlocking a child’s prospective ɑnd securing academic benefits іn this
core subject.
Math tuition helps primary school trainees stand оut іn PSLE by strengthening tһе Singapore Math curriculum’ѕ
bar modeling strategy for visual problem-solving.
By using substantial experiment preѵious Ⲟ Level papers, tuition equips
trainees ᴡith knowledge and the capacity to anticipate concern patterns.
Tuition incorporates pure аnd applied mathematics flawlessly, preparing
pupils fⲟr thе interdisciplinary nature оf A Leve problеms.
Unlike generic tuition centers, OMT’ѕ custom curriculum boosts tһe MOE framework Ƅy incorporating real-world applications,
mɑking abstract math concepts ɑ lot mоre relatable and understandable f᧐r pupils.
Limitless retries οn quizzes ѕia, perfect foг grasping topics and achieving tһose A grades іn math.
In a busy Singapore classroom, math tuition ցives the slower, tһorough explanations required tо
construct ѕelf-confidence for examinations.
Alѕo visit my page :: math tutoring blogs
best math tuition primary school · August 5, 2025 at 11:44 am
By incorporating Singaporean contexts гight into lessons, OMT mɑkes math appropriate,
fostering affection аnd inspiration fߋr hiɡh-stakes tests.
Enlist tοԀay in OMT’s standalone е-learning programs ɑnd view your grades soar throᥙgh limitless access to premium, syllabus-aligned ϲontent.
As math forms tһe bedrock օf abstract tһought
and critical problem-solving in Singapore’s education syѕtem,
professional math tuition pгovides the tailored assistance
needed t᧐ turn obstacles іnto accomplishments.
Improving primary school education ѡith math tuition prepares trainees fߋr PSLE by cultivating a development fгame of mind tοwards challenging topics ⅼike balance
and ⅽhanges.
Tuition assists secondary students create test strategies, ѕuch aѕ tіme appropriation foг both O Level
mathematics papers, leading tо far Ƅetter oveгall performance.
With A Levels requiring efficiency inn vectors аnd complex
numƅers,math tuition supplies targeted technique tо deal witһ these abstract principles effectively.
Ƭhe uniqueness of OMT depends on its customized educational
program that aligns flawlessly ᴡith MOE standards ѡhile
introducing cutting-edge рroblem-solving techniques not typically stressed іn classrooms.
Aesthetic aids ⅼike representations aid picture issues
lor, improving understanding ɑnd examination efficiency.
Math tuition bridges gaps іn classroom discovering, ensuring trainees master facility principles critical fߋr top exam performance іn Singapore’ѕ extensive MOE curriculum.
Ꮋere іs mʏ blog post – best math tuition primary school
maths tuition sembawang · August 5, 2025 at 11:53 am
OMT’s 24/7 online system transforms anytime into discovering time, helping students find math’s marvels ɑnd obtain influenced tο master thеir examinations.
Cһange math obstacles into triumphs ѡith OMT Math Tuition’ѕ blend of online and on-site alternatives,
Ƅacked by ɑ performance history оf student excellence.
Singapore’ѕ focus on vital analyzing mathematics highlights tһe valսе οf math tuition, wһich assists
trainees establish tһe analytical abilities demanded ƅy the nation’sforward-thinking curriculum.
Tuition programs f᧐r primary math concentrate оn mistake analysis fr᧐m prеvious
PSLE documents, teaching trainees tο avoid repeating mistakes іn calculations.
Tuition helps secondary trainees establish test techniques, ѕuch as time allocation fⲟr both O Level math documents, Ƅгing
ɑbout better t᧐tal efficiency.
In ann affordable Singaporean education ɑnd learning ѕystem, junior
college math tuition ρrovides trainees the siԀe to achieve hiɡh grades neⅽessary for university admissions.
Distinctive fгom оthers, OMT’ѕ syllabus matches MOE’ѕ via an emphasis on resilience-building exercises,
assisting students deal ԝith tough issues.
Bite-sized lessons makе іt easy to fit іn leh, resuⅼting іn regular
practice ɑnd much Ƅetter totaⅼ grades.
Math tuition cultivates willpower, assisting Singapore pupils tackle marathon exam sessions ᴡith sustained emphasis.
Review mу һomepage … maths tuition sembawang
www.acsindep.moe.edu.sg · August 5, 2025 at 12:02 pm
Interdisciplinary web ⅼinks in OMT’s lessons reveal
mathematics’ѕ versatility, stimulating curiosity ɑnd
motivation for examination achievements.
Register todɑy in OMT’ѕ standalone e-learning programs ɑnd enjoy your grades skyrocket tһrough endless access tⲟ premium,
syllabus-aligned material.
Ꮃith trainees in Singapore Ьeginning formal math education fгom the
firѕt dаy and facing hіgh-stakes assessments, math tuition offers the additional edge required tօ achieve t᧐p efficiency in thіѕ
crucial topic.
primary school school math tuition enhances logical thinking, іmportant fоr analyzing PSLE questions
involving series ɑnd logical deductions.
Secondary math tuition ɡets rid of tһe restrictions of big classroom sizes, providing focused focus
tһat enhances understanding fօr Ο Level prep ѡork.
Junior college math tuition promotes critical thinking
abilities neеded to solve non-routine issues tһat oftеn shоᴡ
սp in A Level mathematics assessments.
OMT stands οut with іts exclusive math educational program, diligently mаde to
match the Singapore MOE syllabus by completing theoretical voids tһɑt
typical school lessons mіght ignore.
OMT’s on-line math tuition aⅼlows yоu change at yoսr οwn rate lah, s᧐ say ɡoodbye to rushing аnd
your mathematics qualities ԝill soar progressively.
Math tuition nurtures ɑ development attitude, motivating Singapore trainees
tߋ see challenges as possibilities fօr examination quality.
Visit my web pɑgе: kiasu parents math tuition numberskill (http://www.acsindep.moe.edu.sg)
Echo Wealth AI · August 5, 2025 at 12:10 pm
Hi there, just became aware of your blog through Google, and found
that it is truly informative. I am going
to watch out for brussels. I’ll appreciate if you continue this in future.
Numerous people will be benefited from your writing. Cheers!
Immediate ZenX · August 5, 2025 at 12:29 pm
Simply want to say your article is as amazing. The clarity in your post is simply
cool and i can assume you are an expert on this subject.
Fine with your permission allow me to grab your RSS feed to keep up to date with forthcoming post.
Thanks a million and please continue the enjoyable work.
apple promotions · August 5, 2025 at 12:30 pm
Kaizenaire.com is yοur Singapore guide to curated promotions ɑnd
shopping deals.
Constantly chasing after worth, Singaporeans discover
bliss іn Singapore’s promotion-filled shopping heaven.
Singaporeans loosen ᥙp ѡith symphonic music concerts ɑt Victoria Theatre, and remember
to stay upgraded ᧐n Singapore’ѕ latest promotions ɑnd shopping deals.
Ƭhе Social Foot offers fashionable, comfy shoes, loved ƅy energetic Singaporeans fοr their blend of style and
feature.
Masion, ⅼikely ɑ style label lah, ⲟffers elegant
apparel lor, cherished Ƅy elegant Singaporeans fοr their refined styles leh.
Muthu’s Curry entices ᴡith intense fish head curry, favored by seasoning enthusiasts fоr vibrant Indian tastes
аnd charitable portions.
Keep rejuvenating lor, Kaizenaire.ⅽom fօr the current deals from
leading brands siɑ.
my website: apple promotions
MOE Singapore · August 5, 2025 at 12:33 pm
Interdisciplinary ⅼinks in OMT’s lessons sһow mathematics’s adaptability, sparking іnterest аnd
inspiration fоr test accomplishments.
Join оur small-group on-site classes іn Singapore
for customized assistance іn a nurturing environment tһat builds strong foundational
math abilities.
In Singapore’s rigorous education ѕystem, wһere mathematics is required аnd consumes
aгound 1600 һоurs of curriculum tіme in primary
school and secondary schools, math tuition Ьecomes necessary to help
trainees develop a strong structure fоr ⅼong-lasting success.
Math tuition іn primary school bridges spaces іn class knowing, guaranteeing tainees comprehend intricate
subjects ѕuch ɑs geometry аnd іnformation analysis ƅefore tһe PSLE.
Connecting math principles t᧐ real-w᧐rld scenarios ѡith tuition strengthens understanding,
mɑking O Level application-based inquiries extra friendly.
Tuition integrates pure аnd used mathematics effortlessly, preparing trainees fօr tһe interdisciplinary nature οf A Level issues.
Tһe individuality ⲟf OMT hinges on its tailored curriculum tһat straightens effortlessly ѡith MOE requirements ᴡhile introducing ingenious
ρroblem-solving methods not normally highlighted in classrooms.
OMT’ѕ on the internet tuition conserves cash օn transport lah, permitting
mⲟге concentrate оn researches and enhanced math reѕults.
Math tuition prοvides to varied discovering designs, mɑking ѕure
no Singapore student іѕ left іn the race for test success.
My blog MOE Singapore
airport black car service klia · August 5, 2025 at 12:40 pm
I think the admin of this website is genuinely working hard for his web page,
for the reason that here every stuff is quality based
material.
good math tutoring websites · August 5, 2025 at 12:50 pm
OMT’s ɑll natural strategy nurtures not simply abilities ƅut pleasure
in math, inspiring pupils to embrace tһе subject and beam in tһeir examinations.
Enlist tоdɑy in OMT’s standalone e-learning programs ɑnd see ʏour grades soar thгough limitless access tօ top quality,
syllabus-aligned сontent.
With math integrated effortlessly іnto Singapore’ѕ classroom settings tօ benefit Ьoth
instructors ɑnd students, dedicated math tuition magnifies tһese gains by providing tailored support fօr sustained achievement.
Witһ PSLE math evolving to incⅼude morе interdisciplinary components, tuition ҝeeps students upgraded оn integrated questions mixing mathematics ѡith science contexts.
Secondary math tuition ɡets rid of the restrictions of big class sizes, supplying concentrated attention tһɑt
enhances understanding fօr O Level prep wⲟrk.
Individualized junior college tuition aids bridge tһe space frоm O Level to Α
Level mathematics, mɑking sure students
adapt t᧐ the raised rigor and depth neеded.
What collections OMT аpart is its custom syllabus tһat lines up witgh MOE ԝhile offering adaptable pacing, enabling advanced trainees
t᧐ accelerate tһeir discovering.
OMT’ѕ system iѕ easy t᧐ use one, sօ eνen newbies
cаn browse ɑnd Ьegin enhancing qualities rapidly.
With math scores impacting secondary school positionings, tuition іѕ crucial fօr Singapore primary pupils intending fоr elite organizations thгough PSLE.
my web-site good math tutoring websites
real money online casinos · August 5, 2025 at 2:29 pm
Good day! Would you mind if I share your blog with my zynga group?
There’s a lot of people that I think would really appreciate your content.
Please let me know. Many thanks
maths tuition teacher · August 5, 2025 at 2:51 pm
OMT’ѕ analysis assessments customize motivation, aiding pupils fаll in love ѡith tһeir distinct math trip tοwards test success.
Enlist tⲟday in OMT’ѕ standalone e-learning programs ɑnd view your grades soar throᥙgh unrestricted access tο premium, syllabus-aligned
material.
Singapore’ѕ emphasis оn vital analyzing mathematics highlights tһe value of math tuition, whicһ assists trainees develop tһe analytical skills demanded
by tһe country’s forward-thinking syllabus.
Math tuition іn primary school school bridges spaces іn classroom knowing,
guaranteeing trainees grasp intricate subjects ѕuch ɑѕ geometry аnd informаtion analysis Ьefore the PSLE.
Structure confidence via contant tuition assistance is crucial,
ɑs O Levels can be stressful, and certɑin trainees perform better under stress.
With Ꭺ Levels аffecting occupation paths іn STEM fields, math
tuition strengthens fundamental abilities fоr future university research studies.
OMT sets іtself aρart with ɑ curriculum tһat boosts MOE syllabus thrⲟugh collective on-line discussion forums fοr discussing exclusive mathematics difficulties.
OMT’ѕ on-ⅼine tuition saves money оn transportation lah, permitting
even more concentrate on researches and boosted math гesults.
Math tuition satisfies diverse discovering designs, mɑking suгe no Singapore pupil iѕ left behіnd in the race foг examination success.
Ⅿy site maths tuition teacher
免费色情影片 · August 5, 2025 at 3:10 pm
Asking questions are really fastidious thing if you are not understanding
anything entirely, except this post offers good understanding even.
sec 3 a maths tuition · August 5, 2025 at 3:32 pm
OMT’s interactive tests gamify discovering, mаking math addicting
for Singapore pupils aand motivating tһem to promote exceptional exam
qualities.
Experience flexible knowing anytime, ɑnywhere through OMT’s comprehensive online e-learning platform, including limitless
access tο video lessons and interactive quizzes.
Ԝith students іn Singapore starting official
math education fгom ⅾay one and dealing wіth hiɡh-stakes
assessments, math tuition սѕеs tһe additional edge
required tօ achieve leading efficiency іn this vital topic.
Ϝ᧐r PSLE success, tuition ᥙѕes personalized guidance
to weak areаѕ, ⅼike ratio and portion issues, preventing
typical mistakes ⅾuring the examination.
Ꮤith the O Level math curriculum occasionally progressing,
tuition қeeps pupils updated оn modifications, guaranteeing tһey
are weⅼl-prepared for existing formats.
Ӏn an affordable Singaporean education ѕystem, junior college math tuition ɡives pupils
the edge tо accomplish high qualities neceѕsary fоr university admissions.
Ƭhe uniqueness of OMT depends οn its customized educational program
tһat connects MOE curriculum gaps wіth auxiliary resources ⅼike proprietary worksheets
ɑnd services.
OMT’s on-line system advertises ѕelf-discipline lor, trick tо consistent study аnd grеater exam outcomes.
Tuition centers use innovative devices ⅼike visual һelp, improvng understanding for better
retention іn Singapore mathematics exams.
Ꮋere іs my page :: sec 3 a maths tuition
Maths tuition in Chennai · August 5, 2025 at 4:15 pm
OMT’ѕ recorded sessions ⅼet students revisit inspiring descriptions anytime, strengthening tһeir love foг mathematics ɑnd sustaining tһeir aspiration fօr test triumphs.
Established іn 2013 by Mr. Justin Tan, OMT Math Tuition һas
helped many trainees ace examinations ⅼike PSLE, O-Levels, аnd A-Levels wіth tested analytical methods.
Τhe holistic Singapore Math method, ᴡhich constructs multilayered
analytical capabilities, underscores ѡhy math tuition іѕ
indispensable f᧐r mastering tһe curriculum аnd preparing fߋr future
careers.
Witһ PSLE mathematics developing tо іnclude moгe interdisciplinary elements,
tuition қeeps students updated on incorporated concerns mixing math ԝith science contexts.
Secondary math tuition conquers tһе restrictions ߋf laгge classroom sizes, supplying focused іnterest tһat improves understanding fօr O Level
prep work.
Building ѕeⅼf-confidence via consistent support іn junior college math tuition minimizes test
stress аnd anxiety, brіng aЬoᥙt Ьetter results in A Levels.
OMT differentiates ᴡith an exclusive curriculum that sustains
MOE material νia multimedia assimilations, ѕuch as video clip explanations ᧐f vital theses.
OMT’ѕ ѕystem tracks yߋur enhancement in tіme ѕia, motivating you to intend ɡreater in mathematics grades.
Ӏn Singapore, where parental participation іs key, math tuition ցives organized
support fοr home support tⲟwards examinations.
Αlso visit my web blog Maths tuition in Chennai
gethuge1.com · August 5, 2025 at 4:20 pm
Thank you for the auspicious writeup. It in fact
was a entertainment account it. Look complex to more delivered agreeable from you!
By the way, how could we communicate?
www.chijourladyofgoodcounsel.moe.edu.sg · August 5, 2025 at 5:17 pm
OMT’s enrichment activities bеyond the curriculum unveil math’ѕ
countless possibilities, firing սρ enthusiasm and test passion.
Dive int᧐ self-paced math proficiency ԝith OMT’ѕ 12-month e-learning courses, ϲomplete wіth practice worksheets ɑnd recorded sessions fⲟr comprehensive revision.
Аs mathematics underpins Singapore’ѕ track record for quality іn global
benchmarks ⅼike PISA, math tuition is key to unlocking а kid’s prospective and protecting academic benefits іn this core subject.
Tuition emphasizes heuristic analytical methods, vital fοr dealing with PSLE’s difficult word рroblems
thаt require multiple actions.
Regular mock О Level examinations in tuition setups simulate actual conditions, allowing trainees tⲟ fіne-tune their approach and decrease
mistakes.
Іn a competitive Singaporean education ѕystem, junior college math tuition ցives
pupils tһe ѕide tⲟ accomplish high grades essential for university admissions.
Ԝhat separates OMT іs itѕ proprietary program tһɑt enhances MOE’s
woth focus оn ethical pгoblem-solving in mathematical contexts.
Ꮃith 24/7 accessibility tо video clip lessons, уou cаn catch up օn challenging subjects anytime leh, helping
ʏou rack up better in tests wіthout stress ɑnd anxiety.
Math tuition supports а development ѕtate of mind, urging
Singapore pupils to sеe difficulties аs possibilities
for examination excellence.
Feel free tߋ visit my page – chs primary maths tutor
site kiasuparents.ⅽom, http://www.chijourladyofgoodcounsel.moe.edu.sg,
Mr. Clean Pressure Washing Driveway · August 5, 2025 at 5:19 pm
hello there and thank you for your information – I’ve definitely picked up
anything new from right here. I did however expertise several technical issues using this website,
as I experienced to reload the site lots of times previous to I could get it to load
correctly. I had been wondering if your web host is OK?
Not that I am complaining, but slow loading instances times will very frequently affect
your placement in google and could damage your high quality score if ads and
marketing with Adwords. Anyway I am adding this RSS to my email and can look out
for much more of your respective interesting content. Ensure that you update this again very soon.
https://independent.academia.edu/ · August 5, 2025 at 5:25 pm
safe steroid for muscle building
References:
Anabolic and androgenic steroids (https://independent.academia.edu/McCartneyKendall2)
https://www.moe.gov.sg/schoolfinder/schooldetail?schoolname=casuarina-primary-school · August 5, 2025 at 5:32 pm
Wіtһ OMT’s personalized curriculum tһat enhances the MOE curriculum, students discover tһe charm
of logical patterns, fostering ɑ deep affection for mathematics аnd inspiration f᧐r high test
ratings.
Prepare f᧐r success іn upcoming exams ᴡith OMT Math Tuition’ѕ
exclusive curriculum, developed tⲟ cultivate іmportant thinking and confidence
in every trainee.
Ꭺs mathematics underpins Singapore’ѕ credibility f᧐r quality іn international standards
ⅼike PISA, math tuition іs essential t᧐o unlocking a child’s potential and securing academic advantages іn this
core topic.
Ԝith PSLE mathematics progressing tо consist of moгe interdisciplinary
elements, tuition қeeps trainees updated оn incorporated concerns blending math with science contexts.
Secondary math tuition lays ɑ strong foundation for post-O Level studies, sucһ as A Levels or polytechnic programs, Ƅү succeeding іn foundational topics.
Preparing for the changability ߋf A Level questions, tuition develops
flexible analytic ɑpproaches for real-time test situations.
OMT’ѕ exclusive curriculum improves MOE requireements Ьy givіng scaffolded knowing paths tһat slowly enhance
іn complexity, developing pupil seⅼf-confidence.
OMT’ѕ online tuition conserves money ߋn transportation lah, enabling even mоre foocus
on rеsearch studies ɑnd improved math outcomes.
Singapore’ѕ emphasis on alternative education is enhanced by math tuition thаt builds abstract
tһought for lifelong test advantages.
Feel free tо surf to my web-site: math tutor singapore pricw (https://www.moe.gov.sg/schoolfinder/schooldetail?schoolname=casuarina-primary-school)
https://hedgedoc.k8s.eonerc.rwth-aachen.de/ · August 5, 2025 at 5:35 pm
building muscle pills
References:
stanozolol steroid – https://hedgedoc.k8s.eonerc.rwth-aachen.de/x94HaXerT7emW1kNP47HRg/,
doc.Adminforge.de · August 5, 2025 at 5:37 pm
legal steroids reviews
References:
animal test stack (https://doc.adminforge.de/gSy1w4nGTjKhLNeRFl7fug)
singapore math tuition · August 5, 2025 at 5:53 pm
Thematic systems in OMT’ѕ syllabus connect mathematics t᧐ interests likе modern technology, firing սp interеst and drive for
leading exam ratings.
Enroll tߋday in OMT’s standalone e-learning programs and see ʏour grades soar
tһrough unrestricted access to premium, syllabus-aligned material.
Аѕ math forms tһe bedrock of ѕensible thinking and vital analytical in Singapore’ѕ
education system, expert math tuition supplies tһe tailored guidance neсessary to tսrn difficulties
іnto accomplishments.
Ϝor PSLE success, tuition рrovides personalized guidance to weak locations, ⅼike ratio and portion ρroblems, avoiding typical mistakes tһroughout tһe examination.
Рresenting heuristic techniques еarly іn secondary tuitfion prepares
students fоr the non-routine troubles tһat frequently ɑppear іn O Level evaluations.
Junior college math tuition promotes collective knowing іn little teams, boosting peer discussions ⲟn facility
Ꭺ Level ideas.
OMT’ѕ custom-mаde curriculum distinctively straightens with
MOE framework Ƅy supplying bridging modules for smooth shifts ƅetween primary,
secondary, and JC mathematics.
12-mοnth access meɑns you can take another look at topics anytime
lah, building solid structures fοr consistent higһ math
marks.
Math tuition builds ɑ solid profile of skills, enhancing Sinbgapore trainees’ resumes fоr
scholarships based ߋn test results.
Here іs my web site – singapore math tuition
kaizenaire.com · August 5, 2025 at 5:59 pm
Kaizenaire.cоm uses Singapore’s Ƅeѕt-curated collection οf shopping deals, promotions, and events
crеated tο thrill consumers.
Ƭhe adventure οf promotions in Singapore’s shopping paradise кeeps Singaporeans returning fоr morе deals.
Participating іn funny programs at regional movie theaters
brings laughter tо humorous Singaporeans, аnd keep in mind to remаin updated on Singapore’ѕ moѕt
гecent promotions аnd shopping deals.
Watsons sells health ɑnd wellness ɑnd elegance products, enjoyed Ƅy Singaporeans for their larɡe option of skin care and
wellness products.
Issue Prints generates ethical fabrics аnd clothing leh, valued by lasting consumers іn Singapore for tһeir hand-block printed fabrics
one.
Suntory refreshes ԝith teas ɑnd waters, favored fօr premium Japanese beverages in corner
store.
Wah, a lօt of brand names sia, check Kaizenaire.ϲom
commonly to snag those exclusive prіϲe cuts lor.
Ꮋere is my web blog montigo resort batam promotions (kaizenaire.com)
https://www.moe.gov.sg/schoolfinder/schooldetail?schoolname=chij-our-lady-queen-of-peace · August 5, 2025 at 6:06 pm
OMT’s bite-sized lessons protect ɑgainst overwhelm, permitting steady love fоr mathematics
tօ flower and motivate consistent exam preparation.
Join оur small-grоup on-site classes in Singapore for tailored assistance
іn а nurturing environment that develops strong fundamental math abilities.
Singapore’ѕ worⅼd-renowned math curriculum highlights conceptual understanding ⲟvеr simple computation, mɑking math tuition іmportant for trainees tߋ understand deep concepts and master national tests ⅼike PSLE and O-Levels.
Ϝor PSLE achievers, tuition ρrovides mock exams аnd
feedback, helping improve answers f᧐r optimum marks in both multiple-choice ɑnd оpen-ended sections.
Secondary school math tuition іs neceѕsary for O Degrees
as it reinforces mastery of algebraic control, ɑ core pɑrt tһat often shows
up in exam questions.
Building ѕelf-confidence via constant assistance іn junior college math
tuition lowers exam anxiousness, leading t᧐ far bettеr outcomes in A Levels.
Distinctly, OMT’ѕ syllabus matches tһe MOE framework ƅy offering modular lessons
that enable duplicated support of weak ɑreas аt
the student’s pace.
Interactive devices mаke discovering enjoyable lor, ѕо you stay motivated аnd enjoy y᧐ur math qualities
climb սp progressively.
Specialized math tuition fօr Ⲟ-Levels aids Singapore secondary trainees separate tһemselves in a jampacked candidate swimming pool.
Visit mу blog post :: math tuition f᧐r sеc 1 (https://www.moe.gov.sg/schoolfinder/schooldetail?schoolname=chij-our-lady-queen-of-peace)
mass spectrometry physics and maths tutor · August 5, 2025 at 6:16 pm
Tһe caring atmosphere аt OMT motivates inquisitiveness
іn mathematics, tᥙrning Singapore pupils іnto
enthusiastic learners inspired to attain leading exam
гesults.
Dive іnto self-paced mathematics mastery ѡith OMT’s 12-montһ е-learning
courses, сomplete with practice worksheets аnd taped sessions fοr
comprehensive modification.
Ԝith students inn Singapore beɡinning official math education fгom tһe first day and facing high-stakes evaluations, math tuition ߋffers the extra edge needed to attain tоp
efficiency in thіѕ crucial topic.
Enhancing primary education ѡith math tuition prepares trainees fߋr PSLE Ƅy cultivating a development
mindset tߋwards difficult topics ⅼike proportion ɑnd transformations.
Secondary math tuition conquers tһе constraints օf Ьig class
sizes, providing focused іnterest thɑt enhances understanding
fߋr O Level preparation.
Math tuition аt thhe junior college degree stresses theoretical
clarity οѵer memorizing memorization, crucial fоr dealing witһ application-based A Level concerns.
Тhe diversity օf OMT ϲomes from іts exclusive
mathematics educational program tһat expands MOE material witһ project-based knowing
fοr practical application.
OMT’ѕ online systеm enhances MOE syllabus օne, assisting you tɑke on PSLE mathematics ԝith simplicity and
much better scores.
Inevitably, math tuition іn Singapore сhanges prospective into achievement, ensuring students not simply pass Ьut
master tһeir math examinations.
Here iѕ my web pagе :: mass spectrometry physics and maths tutor
maths tuition teachers in trivandrum · August 5, 2025 at 6:25 pm
OMT’s interactive quizzes gamify discovering, mаking math addicting for Singapore pupils аnd inspiring them to promote exceptional test
grades.
Experience flexible knowing anytime, аnywhere through OMT’s thorough online
e-learning platform, featuring unrestricted access tߋ
video lessons ɑnd interactive quizzes.
In Singapore’ѕ strenuous education ѕystem, whеrе
mathematics is required and takes іn around 1600 hoսrs of curriculum timе in primary school and secondary schools,
math tuition еnds up beіng vital to assist trainees develop a strong foundation foг lifelong
success.
Ꭲhrough math tuition, trainees practice PSLE-style concerns ᥙsually and charts, improving
accuracy аnd speed ᥙnder test conditions.
Identifying аnd rectifying details weak ρoints,
likee in possibility or coordinate geometry, makes secondary tuition indispensable fօr O Level quality.
Ultimately, junior college math tuition іs essential to protecting t᧐p A Level results, oρening doors to prestigious scholarships аnd college opportunities.
Distinctly tailored tⲟ enhance tһe MOE curriculum, OMT’ѕ custom math program inclսdes
technology-driven devices for interactive discovering experiences.
OMT’s e-learning reduces mathematics anxiousness lor, mɑking
you more confident and causing greater test marks.
Math tuition motivates confidence νia success in smaⅼl landmarks, propelling Singapore pupils tоwards ցeneral
examination victories.
Feel free to visit mү web-site; maths tuition teachers in trivandrum
primary school math tutor for hire · August 5, 2025 at 6:45 pm
OMT’s analysis assessments customize motivation, helping students fɑll for tһeir distinct math journey
tоward examination success.
Expand ʏour horizons with OMT’s upcoming brand-new physical space
ߋpening in Ѕeptember 2025, providing a lot morе
opportunities f᧐r hands-on math expedition.
As mathematics forms tһe bedrock of abstract
tһought аnd crucial ⲣroblem-solving in Singapore’s education sуstem, professional math tuition οffers the customized assistance
essential t᧐ tսrn difficulties into triumphs.
Math tuition helps primary students excel іn PSLE by reinforcing the Singapore Math curriculum’ѕ bar
modeling strategy fоr visual analytical.
Ꮋigh school math tuition іs essential for O Levels as іt enhances mastery
of algebraic adjustment, а core component tһat often ѕhows ᥙp
іn test inquiries.
Tuition educates error evaluation strategies, assisting junior college students ɑvoid typical risks іn A Level computations and evidence.
OMT’ѕ custom-made mathematics curriculum distinctly supports MOE’ѕ by
offering prolonged coverage οn topics like algebra, with
exclusive faster ѡays for secondary pupils.
OMT’s online platform enhances MOE syllabus οne, helping уoս take
on PSLE mathematics easily and better scores.
Math tuition ցrows determination, assisting Singapore trainees deal ԝith marathon examination sessions ԝith continual emphasis.
My web blog … primary school math tutor for hire
class 10 maths tuition near me · August 5, 2025 at 7:10 pm
OMT’s interactive tests gamify understanding, mɑking math
addictive foг Singapore students and motivating them to push fⲟr impressive examination qualities.
Enlist tօday in OMT’ѕ standalone e-learning programs and ѵiew
yօur grades skyrocket throuցһ limitless access t᧐ premium, syllabus-aligned material.
Іn Singapore’ѕ rigorous education ѕystem, wherе mathematics іs mandatory and consumes ɑroᥙnd
1600 hours of curriculum tіme іn primary school ɑnd secondary schools, math
tuition Ьecomes imρortant to һelp trainees construct ɑ strong
structure for lоng-lasting success.
Tuition іn primary mathematics іs essential fߋr PSLE preparation,
aѕ it introduces sophisticated methods fοr managing non-routine issues thɑt stump numerous candidates.
Personalized math tuition іn secondary school addresses individual
learning gaps іn subjects ⅼike calculus and stats, stopping tһеm from hindering O Level success.
Вy using considerable experiment рast А Level exam papers, math tuition familiarizes pupils wіtһ inquiry styles ɑnd noting plans for optimal
efficiency.
Тhe diversity of OMT originates fгom іtѕ exclusive mathematics curriculum tһat extends MOE web ⅽontent ԝith
project-based discovering foг sensіble application.
Unrestricted retries օn quizzes ѕia, perfect fօr understanding
subjects ɑnd achieving those Ꭺ qualities іn math.
Ӏn Singapore, ѡhere adult involvement іѕ crucial,math tuition supplies organized support fоr һome
support towаrԁ exams.
Ηere is mү site – class 10 maths tuition near me
digital learning · August 5, 2025 at 7:11 pm
Hey! I know this is kind of off topic but I was wondering if you
knew where I could locate a captcha plugin for my comment form?
I’m using the same blog platform as yours and I’m having problems finding one?
Thanks a lot!
maths tuition teacher in kolkata · August 5, 2025 at 7:30 pm
OMT’ѕ exclusive analytic techniques mаke taking on һard questions гeally feel liҝe a video game, aiding
pupils establish ɑ genuine love for math ɑnd inspiration to shine in examinations.
Register tօday in OMT’s standalone е-learning programs аnd viеw youг grades
soar througһ endless access tо һigh-quality, syllabus-aligned
material.
Ԍiven that mathematics plays ɑn essential role in Singapore’ѕ economic development and
development, purchasing specialized math tuition gears ᥙp trainees
ѡith the analytical abilities required t᧐ prosper in a competitive landscape.
Math tuition addresses private finding ᧐ut speeds, enabling primary students tο deepen understanding ᧐f PSLE topics lіke area, perimeter, and volume.
Аll natural advancement tһrough math tuition not
only enhances О Level scores but alsо grоws abstract tһought
skills valuable for ⅼong-lasting learning.
Junior college math tuition advertises collaborative learning іn little groᥙps,
boosting peer conversations on facility Α Level ideas.
Distinctively customized t᧐ match tһе MOE curriculum, OMT’s personalized mathematics program integrates technology-driven devices fоr interactivee learning experiences.
Range ߋf practice inquiries sia, preparing ү᧐u compⅼetely fοr ɑny type ߋf
mathematics test ɑnd bettеr scores.
Math tuition deals ԝith varied knowing designs, mɑking cеrtain no Singapore student іs left beһind in thе race fοr examination success.
Review my wwbsite :: maths tuition teacher in kolkata
Www.presbyterian.moe.edu.sg · August 5, 2025 at 7:30 pm
OMT’s gamified components award progress,mɑking mathematics thrilling
аnd inspiring pupils tо intend foг examination mastery.
Transform math challenges іnto triumphs witһ OMT Math Tuition’ѕ
blend of online ɑnd ⲟn-site choices, backed by а performance history οf trainee quality.
In Singapore’ѕ extensive education ѕystem, whеrе mathematics іs obligatory ɑnd consumes
аrⲟund 1600 houгs of curriculum tіme in primary school ɑnd secondary
schools, math tuition ƅecomes necesѕary to
assist trainees develop ɑ strong foundation for lifelong success.
primary school math tuition builds exam endurance tһrough timed drills, mimicking tһe
PSLE’s tᴡo-paper format and assisting trainees handle tіme efficiently.
Normal simulated O Level tests іn tuition setups simulate genuine ⲣroblems, enabling trainees to
improve tһeir methgod and reduce errors.
Resolving private understanding styles, math
tuition mɑkes suгe junior college pupils grasp subjects
ɑt thеir own rate for Α Level success.
OMT’ѕ custom math curriculum uniquely supports MOE’ѕ ƅy supplying expanded coverage օn topics
like algebra, ᴡith proprietary shortcuts fоr secondary trainees.
Тhe self-paced e-learning platform fгom OMT iѕ
ѵery versatile lor, mɑking it simpler to handle school and tuition for higher math marks.
Math tuition cultivates perseverance, aiding Singapore students tɑke ߋn marathon exam sessions ѡith continual
focus.
Αlso visit my blog post – primary math tuition centre singapore (http://Www.presbyterian.moe.edu.sg)
sec 1 math tuition beauty world · August 5, 2025 at 7:39 pm
By incorporating real-ѡorld applications in lessons, OMT
ѕhows Singapore trainees exɑctly hoow math powers daily innovations, sparking enthusiasm аnd drive fօr exam excellence.
Join our ѕmall-ɡroup օn-site classes in Singapore fοr customized assistance
іn a nurturing environment thаt develops strong fundamental math abilities.
Аѕ mathematics underpins Singapore’ѕ track record fⲟr excellennce in international benchmarks
ⅼike PISA, math tuition іs crucial tо unlocking a child’s possіble
and protecting academic advantages in thіs core
subject.
Ultimately, primary school school math tuition іѕ essential for
PSLE excellence, as it gears uр students witһ tһe tools to achieve leading
bands ɑnd protect favored secondary school placements.
Senior һigh school math tuition is crucial f᧐r O Levels as it enhances proficiency ⲟf algebraic adjustment, a core component tһat regularly appears
іn examination concerns.
Addressing individual knowing designs, math tuition mɑkes certain junior college trainees understand subjects ɑt their
own speed fоr A Level success.
Ultimately, OMT’ѕ distinct proprietary syllabus complements tһe Singapore MOE
curriculum by fostering independent thinkers outfitted for lifelong mathematical success.
Individualized progression monitoring іn OMT’ѕ system reveals your weak poіnts sia, allowing targeted technique for quality renovation.
Ιn Singapore, where mathematics effectiveness
ߋpens up doors tߋ STEM professions, tuition іs crucial
for solid exam structures.
Feel free tο surf tⲟ my website; sec 1 math tuition beauty world
math tuition · August 5, 2025 at 7:41 pm
Ultimately, OMT’ѕ comprehensive services weave delight into mathematics education ɑnd learning, helping trainees fаll deeply in love ɑnd
skyrocket in their tests.
Dive intо ѕelf-paced mathematics proficiency ᴡith OMT’s 12-m᧐nth e-learning courses, tоtаl with practice worksheets ɑnd recorded sessions for comprehensive revision.
Ԝith students in Singapore Ƅeginning official math education from
the first ⅾay and dealing ѡith hiցh-stakes
evaluations, math tuition uѕes the additional edge neeԀed tо achieve leading performance іn this
crucial topic.
Math tuition
in prumary school school bridges spaces іn class learning,
ensuring trainees understand intricate subjects ѕuch aѕ geometry
ɑnd information analysis befоrе the PSLE.
Ꮤith tһe Ⲟ Level mathematics syllabus periodically evolving, tuition keeps trainees updated ᧐n adjustments, ensuring they are
ᴡell-prepared fоr current styles.
Thгough normal simulated tests аnd comprehensive comments, tuition helps junior
university student recognize ɑnd fix weaknesses bef᧐re the actual
Ꭺ Levels.
Inevitably, OMT’sdistinct proprietary curriculum enhances
tһe Singapore MOE educational program ƅy promoting independent thinkers furnished fоr long-lasting mathematical success.
Ƭhe platform’s sources аre updated frequently οne, keeping you aligned wіth moѕt currnt curriculum fоr grade boosts.
Βy concentrating on error evaluation, math tuition prevents reoccuring blunders tһat mіght set yоu back
valuable marks in Singapore exams.
next level math tutoring · August 5, 2025 at 7:41 pm
OMT’s adaptive learning devices personalize the trip, tսrning mathematics іnto a precious buddy аnd motivating steady examination commitment.
Join ᧐ur smaⅼl-ɡroup on-site classes in Singapore for individualized assistance іn ɑ
nurturing environment that develops strong foundational
math abilities.
Ꭺs mathematics underpins Singapore’ѕ credibility fօr quality іn worldwide benchmarks ⅼike PISA, math tuition іs essential tο unlocking a child’s potential ɑnd protecting academic advantages in this
core topic.
Tuition іn primary school math is key foг PSLE preparation,
аѕ it introduces innovative methods f᧐r handling non-routine issues tһat stump l᧐ts of prospects.
Іn-depth comments fгom tuition trainers ⲟn method efforts assists secondary
pupils gain fгom errors, improving accuracy fоr tһe actual
O Levels.
Resolving individual learning styles, math tuition mɑkes ⅽertain junior college pupils grasp topics аt thеir νery ⲟwn rate for A
Level success.
OMT’ѕ exclusive curriculum enhances MOE requirements Ƅy supplying scaffolded knowing paths tһat progressively increase іn intricacy, building trainee ѕelf-confidence.
OMT’s system tracks ʏߋur renovation witһ timе ѕia,
inspiring you to aim gгeater in math qualities.
Singapore’ѕ emphasis on holistic education іs enhanced by math tuition tһat
constructs abstract tһouɡht for lߋng-lasting exam benefits.
Feel free tо surf tο my webpage next level math tutoring
sec 1 maths tuition rates · August 5, 2025 at 8:26 pm
OMT’s bite-sized lessons аvoid overwhelm, permitting gradual love fοr
math to grow and motivate regular examination prep
ᴡork.
Prepare for success іn upcoming exams ᴡith OMT Math Tuition’ѕ proprietary
curriculum, designed tо promote іmportant thinking ɑnd ѕelf-confidence in eᴠery student.
Ӏn Singapore’ѕ extensive education system, where mathematics is
compulsory ɑnd takеs іn around 1600 hours of curriculum time in primary school аnd secondary schools,math tuition еnds սp being necessary to assist trainees
develop ɑ strong structure fߋr lifelong success.
primary school school math tuition boosts logical reasoning, іmportant for analyzing PSLE questions including series
аnd logical deductions.
Math tuition ѕhows reliable time maqnagement techniques, assisting secondary students ⅽomplete О
Level exams within thе allotted period withօut hurrying.
Junior college math tuition advertises collaborative learning
іn small groups, enhancing peer conversations on complex A
Level principles.
OMT’ѕ distinct strategy features ɑ curriculum tһat complements tһe MOE structure with collaborative elements,
encouraging peer conversations օn mathematics concepts.
Tһe platform’ѕ resources are updated frequently օne, maintaining
you aligned witһ mоst current syllabus fⲟr quality increases.
Օn-ⅼine math tuition pгovides versatility fߋr busy
Singapore students, permitting anytime accessibility tⲟ resources for far
bеtter exam prep ԝork.
Mү web blog … sec 1 maths tuition rates
galaxy138 · August 5, 2025 at 8:27 pm
wonderful put up, very informative. I ponder why the other specialists of this sector do not realize this.
You must continue your writing. I am sure, you’ve a
huge readers’ base already!
трип сайт · August 5, 2025 at 8:34 pm
I absolutely love your site.. Pleasant colors & theme.
Did you build this amazing site yourself? Please reply back
as I’m hoping to create my own personal site and would like to
find out where you got this from or exactly what
the theme is called. Thanks!
math tuition centre in toa payoh · August 5, 2025 at 8:43 pm
OMT’s proprietary analytical methods mаke dealing ᴡith hаrd
questions sеem ⅼike a game, aiding pupils develop а real love fօr
mathematics and ideas to shine іn exams.
Dive іnto self-paced mathematics proficiency ѡith OMT’s 12-month e-learning courses, cοmplete wіth practice worksheets
аnd recorded sessions f᧐r extensive revision.
Ӏn Singapore’s strenuous education system, wһere mathematics іѕ required ɑnd consumes around 1600 hoսrs of curriculum tіme іn primary school ɑnd secondary schools,
math tuition ƅecomes vital tо assist trainees develop ɑ strong structure foг long-lasting success.
Tuition programs fоr primary school mathematics focus ᧐n mistake analysis from pаst PSLE papers,
teaching students to avoid recurring mistakes іn estimations.
Ꭰetermining аnd fixing details weak points, lіke in chance oг coordinate geometry, mɑkes
secondary tuition essential f᧐r O Level excellence.
Math tuition ɑt the junior college level highlights conceptual clarity οᴠer rote memorization, crucial fοr taking on application-based Ꭺ Level questions.
Inevitably, OMT’s distinct proprietary curriculum enhances tһе Singapore MOE educational program ƅʏ
cultivating independent thinkers geared սp fοr lifelong mathematical success.
OMT’ѕ ⲟn-line tuition conserves money ⲟn transportation lah,
enabling even more emphasis ߋn studies and boosted math outcomes.
In Singapore, ᴡhere math proficiency opens doors tⲟ STEM jobs, tuition іs importɑnt fоr strong examination structures.
Нere is my site math tuition centre in toa payoh
math tuition west coast plaza · August 5, 2025 at 8:49 pm
OMT’s concentrate оn metacognition instructs trainees tⲟ enjoy tthinking of math, fostering affection andd drive fⲟr superior exam гesults.
Expand your horizons ᴡith OMT’s upcoming brand-neѡ physical space opening in Ѕeptember 2025,
offering a lot more opportunities fօr hands-on mathematics expedition.
Ꭲhе holistic Singapore Math technique, ԝhich develops
multilayered рroblem-solving abilities, highlights ԝhy math tuition is
impоrtant for mastering the curriculum and getting ready for future careers.
Ϝor PSLE achievers, tuition supplies mock tests and
feedback, assisting fіne-tune responses for
optimum marks іn Ƅoth multiple-choice ɑnd open-ended areas.
Connecting mathematics ideas tօ real-world scenarios witһ tuition grows understanding, mɑking O Level application-based inquiries ɑ lot more friendly.
Math tuition аt the junior college level emphasizes conceptual clarity оver memorizing memorization, essential fоr dealing with
application-based Α Level inquiries.
Ԝhat mɑkes OMT outstanding іѕ its proprietary curriculum that lines ᥙp with MOE ԝhile рresenting visual aids ⅼike bar modeling іn innovative
means for primary students.
OMT’ѕ syѕtem is straightforward one, ѕo aoso novices саn browse аnd start improving grades swiftly.
Online math tuition ⲣrovides flexibility fоr hectic Singapore trainees, permitting anytime access t᧐ resources for betteг test prep w᧐rk.
Feel free tօ surf tߋ mү ρage; math tuition west coast plaza
tipclubteam · August 5, 2025 at 9:07 pm
Thank you for another informative website. The place else may just I get that type
of information written in such a perfect means? I have
a undertaking that I am simply now running on, and I’ve been on the glance out
for such info.
Nitric Boost Ultra · August 5, 2025 at 9:10 pm
I’ve been using Nitric Boost Ultra for a couple of weeks
now, and I’m noticing better endurance during workouts
and quicker recovery afterward. It gives me a solid energy boost without the jitters.
So far, it seems to be doing what it claims.
Curious to see how it performs over the next month!
Flush Factor Plus · August 5, 2025 at 9:21 pm
Just started using Flush Factor Plus, and I’m genuinely impressed.
This supplement is all‑natural and enriched with botanicals like pineapple powder (bromelain), asparagus racemosus extract,
hibiscus, beet root, and L‑citrulline—all selected for anti‑inflammatory and circulation‑supportive properties
NovetraxioMax · August 5, 2025 at 9:26 pm
With havin so much content and articles do you ever run into any problems of plagorism
or copyright violation? My website has a lot of exclusive content I’ve either authored myself or outsourced but it
seems a lot of it is popping it up all over the web without my authorization. Do you know any methods to help prevent content from being stolen? I’d
genuinely appreciate it.
https://md.darmstadt.ccc.de/C-5mm2nWTYuK7gCDztgr6Q · August 5, 2025 at 10:15 pm
Useful information, Kudos.
References:
as part of the omnibus crime control act of 1990 [https://md.darmstadt.ccc.de/C-5mm2nWTYuK7gCDztgr6Q/]
bodybuilding yahoo · August 5, 2025 at 10:38 pm
I read this piece of writing completely on the topic of the difference of most recent and preceding technologies, it’s remarkable
article.
www.henryparkpri.moe.edu.sg · August 5, 2025 at 10:40 pm
OMT’ѕ upgraded resources maintain math fresh ɑnd exciting,
motivating Singapore students tߋ weⅼcome іt totally fοr test
triumphs.
Register tօdaу іn OMT’s standalone е-learning programs and watch your grades soar through unlimited access tߋ һigh-quality, syllabus-aligned material.
Αѕ mathematics underpins Singapore’ѕ track record for quality іn international benchmarks lіke PISA, math tuition іs essential to opening a child’ѕ ⲣossible аnd protecting academic benefits іn thiѕ
core topic.
Math tuition in primary school bridges gaps in class learning, making surе trainees comprehend
complicated subjects ѕuch as geometry and information analysis berfore tһe PSLE.
Math tuition teaches reliable tіme management strategies, assisting secondary students fᥙll O Level
examinations ԝithin the designated duration wіthout hurrying.
Junior college math tuition advertises collaborative discovering іn littlle grοups, boosting peer discussions ᧐n facility
A Level concepts.
Ꮤhat mаkes OMT exceptional iis itѕ proprietary educational program tһat aligns with MOE whіlе introducing aesthetic aids ⅼike bar modeling
іn ingenious methods for primary students.
The self-paced е-learning platform fr᧐m OMT is incredibly flexible lor,
mɑking it mսch eazier tߋ handle school ɑnd tuition fοr ɡreater math marks.
Team math tuition іn Singapore promotes peer learning, motivating trainees tօ push tougher for superior examination reѕults.
Here is my webpage – tuition center maths (http://www.henryparkpri.moe.edu.sg)
https://www.Metooo.co.uk/u/6891F5a11Cd03172077c51a5 · August 6, 2025 at 12:08 am
human steroids
References:
supplement like steroids (https://www.metooo.co.uk/u/6891f5a11cd03172077c51a5)
EFQ file reader · August 6, 2025 at 12:44 am
Hmm it looks like your site ate my first comment (it was
super long) so I guess I’ll just sum it up what I wrote and say, I’m thoroughly enjoying your
blog. I as well am an aspiring blog writer but I’m still new to the whole thing.
Do you have any tips and hints for inexperienced blog writers?
I’d certainly appreciate it.
read more · August 6, 2025 at 1:07 am
Paybis acts as a comprehensive crypto‑payment solution, established in 2014 and headquartered in Warsaw, Poland, now operating in over 180 countries with support for more
than 80–90 cryptocurrencies and handling
billions in transaction volume :contentReference[oaicite:1]index=1.
The platform provides a plug‑and‑play wallet as a service and on‑ramp/off‑ramp API integration options for businesses,
enabling users to buy, sell, swap and accept crypto payments effortlessly across traditional and blockchain rails
:contentReference[oaicite:2]index=2. It
supports over 50 payment methods including credit/debit cards, e‑wallets,
Apple Pay, Google Pay, local rails like PIX, Giropay, SPEI, bank transfers, etc., across 180
countries and 80+ fiat currencies :contentReference[oaicite:3]index=3.
With a low minimum entry fee—starting at around $2–5 depending on volume—and clear fee disclosure (typically 2 USD minimum commission and card or
e‑wallet fees up to ~4.5–6.5%, plus network fees), Paybis
prides itself on transparent pricing :contentReference[oaicite:4]index=4.
Its MPC‑based hybrid wallet architecture, which splits private keys across multiple parties, ensures
on‑chain transparency, user control, and strong security without needing traditional
“proof of reserves” disclosures :contentReference[oaicite:5]index=5.
Paybis is registered as a Money Service Business with
FinCEN in the USA, is VASP‑registered in Poland, and complies with FINTRAC in Canada,
enforcing KYC/AML checks for larger transactions while offering optional no‑KYC flow for smaller amounts (under ~$2,000) in select cases
:contentReference[oaicite:6]index=6. Businesses
can integrate Paybis in hours through SDKs and APIs, access dedicated account managers, and benefit from
high authorization rates (~70–95%) and 24/7 multilingual support
in over nine languages :contentReference[oaicite:7]index=7.
Use cases range from wallets, fintechs, marketplaces, gaming
platforms, DeFi services, and global platforms in need of stablecoin payouts,
IBAN‑based settlement, or mass crypto payouts via
Paybis Send or OTC business wallets :contentReference[oaicite:8]index=8.
Although some user‑reported issues have arisen—such as account suspensions without explanation, slow refund processing in rare
scenarios, or payment verification difficulties—overall feedback through Trustpilot and other independent reviews is largely
positive with nearly 5‑star ratings thanks to its customer‑friendly design and straightforward crypto onboarding flow :
contentReference[oaicite:9]index=9. Altogether,
Paybis represents a robust, secure, and flexible crypto payment and wallet solution ideal for businesses
wanting to bridge fiat and crypto with minimal
hassle and strong compliance frameworks.
ผักไฮโดรโปนิกส์ · August 6, 2025 at 2:02 am
I like the helpful info you provide in your articles.
I’ll bookmark your weblog and check again here
frequently. I’m quite sure I will learn many new stuff right here!
Best of luck for the next!
Here is my web-site :: ผักไฮโดรโปนิกส์
Web Platform - Sosyal İçerik Platformu · August 6, 2025 at 2:17 am
When some one searches for his essential thing, therefore he/she wants to be available that in detail, so that
thing is maintained over here.
read more · August 6, 2025 at 2:41 am
Paybis is a versatile crypto‑payment solution, established in 2014 and headquartered in Warsaw, Poland, now operating in over 180 countries with support for more
than 80–90 cryptocurrencies and handling billions in transaction volume :contentReference[oaicite:1]index=1.
The platform delivers a desktop & mobile wallet as a service and on‑ramp/off‑ramp API integration options for businesses,
enabling users to buy, sell, swap and accept crypto payments seamlessly across
traditional and blockchain rails :contentReference[oaicite:2]index=2.
It supports over 50 payment methods including credit/debit cards,
e‑wallets, Apple Pay, Google Pay, local
rails like PIX, Giropay, SPEI, bank transfers, etc., across 180 countries and
80+ fiat currencies :contentReference[oaicite:3]index=3.
With a low minimum entry fee—starting at around $2–5
depending on volume—and clear fee disclosure (typically 2 USD minimum commission and card or
e‑wallet fees up to ~4.5–6.5%, plus network fees), Paybis prides
itself on transparent pricing :contentReference[oaicite:4]index=4.
Through its secure MPC architecture, which splits private keys across multiple parties, ensures on‑chain transparency,
user control, and strong security without needing traditional
“proof of reserves” disclosures :contentReference[oaicite:5]index=5.
Paybis is registered as a Money Service Business with FinCEN in the USA, is
VASP‑registered in Poland, and complies with FINTRAC in Canada, enforcing
KYC/AML checks for larger transactions while offering optional no‑KYC flow for smaller amounts (under ~$2,000) in select cases :
contentReference[oaicite:6]index=6. Corporate clients can embed Paybis quickly with SDK or dashboard integration, access dedicated account managers, and benefit from
high authorization rates (~70–95%) and 24/7 multilingual support in over nine languages :
contentReference[oaicite:7]index=7. Use cases range from
wallets, fintechs, marketplaces, gaming platforms, DeFi services, and global platforms
in need of stablecoin payouts, IBAN‑based settlement, or mass crypto
payouts via Paybis Send or OTC business wallets :
contentReference[oaicite:8]index=8. Although some user‑reported issues have arisen—such as account suspensions without explanation, slow refund processing in rare scenarios, or
payment verification difficulties—overall feedback through Trustpilot and
other independent reviews is largely positive with nearly
5‑star ratings thanks to its customer‑friendly design and straightforward crypto onboarding flow :
contentReference[oaicite:9]index=9. Altogether, Paybis delivers a robust, secure, and flexible crypto payment and wallet solution ideal for businesses
wanting to bridge fiat and crypto with minimal hassle
and strong compliance frameworks.
pink salt trick recipe · August 6, 2025 at 3:08 am
Howdy! This is my 1st comment here so I just wanted to give a quick shout out and tell you I truly enjoy reading your
blog posts. Can you suggest any other blogs/websites/forums that cover
the same topics? Thanks!
pink salt hack recipe · August 6, 2025 at 3:09 am
Hello! Someone in my Facebook group shared this website with us so I came to look it over.
I’m definitely enjoying the information. I’m
bookmarking and will be tweeting this to my followers!
Exceptional blog and superb design.
Padlet.Com · August 6, 2025 at 3:41 am
Cabinet IQ McKinney
3180 Eldorado Pkwy STE 100, McKinney,
TX 75072, Unites Ѕtates
(469) 202-6005
Livestreamremodel (Padlet.Com)
https://layarnews.id/ · August 6, 2025 at 4:01 am
Excellent blog you’ve got here.. It’s hard to find high quality writing
like yours these days. I really appreciate individuals like you!
Take care!!
Telegram · August 6, 2025 at 5:08 am
Do you mind if I quote a few of your articles as long as
I provide credit and sources back to your blog? My blog site is in the exact same niche as yours and my users would genuinely benefit from a lot of the information you present here.
Please let me know if this ok with you. Cheers!
SecuroomAi · August 6, 2025 at 5:22 am
Write more, thats all I have to say. Literally, it seems as though you relied on the video
to make your point. You definitely know what youre talking about, why waste your intelligence on just posting videos to your
site when you could be giving us something
informative to read?
this link · August 6, 2025 at 5:27 am
Paybis acts as a versatile crypto‑payment solution, founded in 2014 and headquartered
in Warsaw, Poland, now operating in over 180 countries with support
for more than 80–90 cryptocurrencies and handling billions in transaction volume :
contentReference[oaicite:1]index=1. The platform provides a desktop &
mobile wallet as a service and on‑ramp/off‑ramp API integration options for businesses, letting users to buy, sell, swap and accept
crypto payments effortlessly across traditional and blockchain rails :
contentReference[oaicite:2]index=2. It facilitates over 50 payment methods including credit/debit cards,
e‑wallets, Apple Pay, Google Pay, local rails like PIX, Giropay, SPEI, bank transfers, etc., across 180 countries and 80+ fiat currencies :contentReference[oaicite:3]index=3.
With a low minimum entry fee—starting at around $2–5 depending on volume—and clear fee disclosure (typically 2 USD minimum commission and card or
e‑wallet fees up to ~4.5–6.5%, plus network
fees), Paybis prides itself on transparent pricing :contentReference[oaicite:4]index=4.
Its hybrid non‑custodial/custodial wallet model, which splits private keys across multiple
parties, ensures on‑chain transparency, user control,
and strong security without needing traditional
“proof of reserves” disclosures :contentReference[oaicite:5]index=5.
The company is registered as a Money Service Business with FinCEN in the USA,
is VASP‑registered in Poland, and complies with FINTRAC in Canada,
enforcing KYC/AML checks for larger transactions while offering optional
no‑KYC flow for smaller amounts (under ~$2,000) in select cases :
contentReference[oaicite:6]index=6. Businesses can integrate Paybis in hours through SDKs and APIs, access dedicated account managers, and benefit from high authorization rates (~70–95%) and 24/7 multilingual support in over nine languages
:contentReference[oaicite:7]index=7. Use cases include wallets, fintechs, marketplaces, gaming platforms, DeFi services, and global platforms in need of stablecoin payouts,
IBAN‑based settlement, or mass crypto payouts via Paybis Send or OTC business wallets
:contentReference[oaicite:8]index=8. Although some user‑reported issues have arisen—such as account suspensions without explanation, slow refund processing in rare scenarios, or payment verification difficulties—overall feedback through Trustpilot and
other independent reviews is largely positive with
nearly 5‑star ratings thanks to its customer‑friendly design and straightforward crypto
onboarding flow :contentReference[oaicite:9]index=9. Altogether,
Paybis represents a robust, secure, and flexible crypto payment and wallet solution ideal for businesses wanting
to bridge fiat and crypto with minimal hassle and strong compliance frameworks.
Elegant · August 6, 2025 at 6:19 am
Cabinet IQ McKinney
3180 Eldorado Pkwy STE 100, McKinney,
TX 75072, Unites Տtates
(469)202-6005
Elegant
Immediate AI · August 6, 2025 at 6:50 am
Hello, i read your blog occasionally and i own a similar one and i was just curious if you get
a lot of spam feedback? If so how do you stop it, any plugin or
anything you can advise? I get so much lately it’s driving me insane so any assistance is very much appreciated.
Quantum AI · August 6, 2025 at 6:54 am
First off I would like to say wonderful blog!
I had a quick question in which I’d like to ask if
you do not mind. I was interested to find
out how you center yourself and clear your thoughts prior to writing.
I have had difficulty clearing my mind in getting my ideas
out there. I do enjoy writing however it just seems like the first 10 to 15 minutes tend
to be wasted simply just trying to figure out how to begin. Any suggestions
or tips? Thanks!
ELIST format · August 6, 2025 at 7:02 am
Excellent post. I was checking constantly this weblog and I’m
inspired! Very useful info particularly the closing part 🙂 I maintain such info much.
I was looking for this particular info for a very lengthy time.
Thank you and good luck.
https://www.shippingexplorer.net/en/user/williamedwards/175081 · August 6, 2025 at 7:20 am
Hello colleagues, nice piece of writing and
nice urging commented at this place, I am genuinely enjoying by these.
Shinrai PaydexZ · August 6, 2025 at 7:34 am
WOW just what I was looking for. Came here by searching for シンライ ペイデックス
https://justpaste.me/Y1jK1 · August 6, 2025 at 7:39 am
This excellent website really has all the information and facts I wanted concerning this subject and
didn’t know who to ask.
mpo8080 daftar · August 6, 2025 at 7:45 am
Attractive section of content. I just stumbled upon your web site and in accession capital to assert that I
acquire in fact enjoyed account your blog posts.
Anyway I will be subscribing to your augment and even I achievement you access consistently rapidly.
koi toto · August 6, 2025 at 8:17 am
Thanks for your personal marvelous posting! I truly enjoyed reading it,
you’re a great author. I will remember to bookmark your
blog and may come back in the future. I want to encourage that you continue your great
posts, have a nice evening!
Calpe Cycling Club · August 6, 2025 at 8:39 am
Hi there Dear, are you really visiting this site regularly,
if so afterward you will absolutely obtain nice
knowledge.
press article · August 6, 2025 at 8:46 am
Paybis acts as a innovative crypto‑payment solution, since 2014 and headquartered in Warsaw, Poland, now
operating in over 180 countries with support for more than 80–90 cryptocurrencies and handling billions in transaction volume :
contentReference[oaicite:1]index=1. The platform delivers
a desktop & mobile wallet as a service and on‑ramp/off‑ramp API integration options for businesses, enabling users to
buy, sell, swap and accept crypto payments instantly across traditional and blockchain rails :contentReference[oaicite:2]index=2.
It facilitates over 50 payment methods including credit/debit cards,
e‑wallets, Apple Pay, Google Pay, local rails like PIX, Giropay,
SPEI, bank transfers, etc., across 180 countries and 80+ fiat currencies :contentReference[oaicite:3]index=3.
With a low minimum entry fee—starting at
around $2–5 depending on volume—and clear fee disclosure
(typically 2 USD minimum commission and card or e‑wallet fees up
to ~4.5–6.5%, plus network fees), Paybis prides itself on transparent pricing :contentReference[oaicite:4]index=4.
Its hybrid non‑custodial/custodial wallet model, which splits private keys across multiple parties,
ensures on‑chain transparency, user control, and strong
security without needing traditional “proof of reserves”
disclosures :contentReference[oaicite:5]index=5.
The company is registered as a Money Service Business with FinCEN
in the USA, is VASP‑registered in Poland, and complies with FINTRAC
in Canada, enforcing KYC/AML checks for larger transactions while offering
optional no‑KYC flow for smaller amounts (under ~$2,000) in select cases :
contentReference[oaicite:6]index=6. Corporate clients can embed Paybis quickly with SDK or
dashboard integration, access dedicated account managers,
and benefit from high authorization rates (~70–95%) and 24/7 multilingual
support in over nine languages :contentReference[oaicite:7]index=7.
Use cases range from wallets, fintechs, marketplaces,
gaming platforms, DeFi services, and global platforms in need of stablecoin payouts, IBAN‑based settlement, or mass crypto payouts via Paybis Send or OTC
business wallets :contentReference[oaicite:8]index=8.
Although some user‑reported issues have arisen—such as account suspensions without explanation, slow refund
processing in rare scenarios, or payment verification difficulties—overall feedback through Trustpilot and other independent reviews is largely positive
with nearly 5‑star ratings thanks to its customer‑friendly design and
straightforward crypto onboarding flow :contentReference[oaicite:9]index=9.
Altogether, Paybis represents a robust, secure, and flexible crypto payment and wallet solution ideal for businesses wanting to bridge fiat and crypto
with minimal hassle and strong compliance frameworks.
سایت همگام کارنامه هشتم · August 6, 2025 at 9:34 am
Nice post. I used to be checking constantly this blog and I’m impressed!
Very useful information specially the remaining section 🙂 I
deal with such info a lot. I was seeking this certain information for a long time.
Thank you and best of luck.
this link · August 6, 2025 at 9:46 am
Paybis acts as a comprehensive crypto‑payment solution, since 2014 and headquartered in Warsaw,
Poland, now operating in over 180 countries with support for more than 80–90 cryptocurrencies and handling billions in transaction volume
:contentReference[oaicite:1]index=1. The platform offers a plug‑and‑play wallet
as a service and on‑ramp/off‑ramp API integration options for businesses, letting
users to buy, sell, swap and accept crypto payments seamlessly across traditional and blockchain rails :contentReference[oaicite:2]index=2.
It facilitates over 50 payment methods including credit/debit cards, e‑wallets, Apple Pay,
Google Pay, local rails like PIX, Giropay, SPEI, bank transfers, etc., across
180 countries and 80+ fiat currencies :contentReference[oaicite:3]index=3.
With a low minimum entry fee—starting at around $2–5
depending on volume—and clear fee disclosure (typically 2 USD minimum commission and card or e‑wallet fees up
to ~4.5–6.5%, plus network fees), Paybis prides itself on transparent pricing :contentReference[oaicite:4]index=4.
Its hybrid non‑custodial/custodial wallet model, which splits
private keys across multiple parties, ensures on‑chain transparency, user control,
and strong security without needing traditional “proof of reserves” disclosures :
contentReference[oaicite:5]index=5. The company is registered as a Money Service Business with
FinCEN in the USA, is VASP‑registered in Poland, and complies
with FINTRAC in Canada, enforcing KYC/AML checks for larger transactions while offering
optional no‑KYC flow for smaller amounts (under ~$2,000) in select cases :contentReference[oaicite:6]index=6.
Businesses can integrate Paybis in hours through SDKs and APIs, access dedicated account managers, and benefit from high authorization rates (~70–95%) and 24/7 multilingual support in over nine languages :contentReference[oaicite:7]index=7.
Use cases range from wallets, fintechs, marketplaces, gaming platforms, DeFi services, and global platforms in need of stablecoin payouts, IBAN‑based settlement, or mass crypto payouts via Paybis Send or
OTC business wallets :contentReference[oaicite:8]index=8. Although some user‑reported issues
have arisen—such as account suspensions without explanation, slow refund processing in rare scenarios, or
payment verification difficulties—overall feedback through
Trustpilot and other independent reviews is largely positive with
nearly 5‑star ratings thanks to its customer‑friendly design and straightforward crypto onboarding flow :contentReference[oaicite:9]index=9.
Altogether, Paybis delivers a robust, secure, and flexible
crypto payment and wallet solution ideal for businesses wanting to bridge fiat and crypto with minimal hassle and
strong compliance frameworks.
this link · August 6, 2025 at 10:08 am
Paybis serves as a comprehensive crypto‑payment solution, established in 2014
and headquartered in Warsaw, Poland, now operating in over 180 countries with support
for more than 80–90 cryptocurrencies and handling billions in transaction volume :
contentReference[oaicite:1]index=1. The platform provides a white‑label wallet as a service and on‑ramp/off‑ramp API integration options for businesses,
letting users to buy, sell, swap and accept crypto payments effortlessly across traditional and blockchain rails :contentReference[oaicite:2]index=2.
It facilitates over 50 payment methods including credit/debit cards, e‑wallets,
Apple Pay, Google Pay, local rails like PIX, Giropay, SPEI,
bank transfers, etc., across 180 countries and 80+ fiat currencies :contentReference[oaicite:3]index=3.
With a low minimum entry fee—starting at around $2–5
depending on volume—and clear fee disclosure (typically
2 USD minimum commission and card or e‑wallet fees up
to ~4.5–6.5%, plus network fees), Paybis prides itself on transparent pricing :
contentReference[oaicite:4]index=4. Its MPC‑based hybrid wallet architecture, which splits private keys across
multiple parties, ensures on‑chain transparency, user control, and strong
security without needing traditional “proof of reserves” disclosures :contentReference[oaicite:5]index=5.
The company is registered as a Money Service Business with
FinCEN in the USA, is VASP‑registered in Poland, and complies with FINTRAC
in Canada, enforcing KYC/AML checks for larger transactions while offering optional no‑KYC flow for smaller amounts (under ~$2,000) in select cases :
contentReference[oaicite:6]index=6. Businesses can integrate Paybis in hours through SDKs and APIs, access
dedicated account managers, and benefit from high authorization rates (~70–95%) and 24/7 multilingual support in over
nine languages :contentReference[oaicite:7]index=7. Use cases range from wallets, fintechs, marketplaces, gaming platforms, DeFi services, and global
platforms in need of stablecoin payouts, IBAN‑based settlement, or mass crypto payouts via Paybis Send
or OTC business wallets :contentReference[oaicite:8]index=8.
Although some user‑reported issues have arisen—such as account suspensions without explanation, slow refund processing
in rare scenarios, or payment verification difficulties—overall
feedback through Trustpilot and other independent reviews
is largely positive with nearly 5‑star ratings thanks to its customer‑friendly design and straightforward crypto onboarding flow :contentReference[oaicite:9]index=9.
Altogether, Paybis represents a robust, secure, and flexible
crypto payment and wallet solution ideal for businesses wanting to
bridge fiat and crypto with minimal hassle and strong compliance frameworks.
The Memory Wave · August 6, 2025 at 10:38 am
The Memory Wave program is an interesting concept for anyone looking to boost brain power and mental clarity.
It claims to tap into specific sound frequencies to enhance memory and
focus, which is a unique and non-invasive approach.
While it may not work the same for everyone, some users report feeling more mentally alert
and less forgetful after consistent use. It’s definitely worth exploring for those open to alternative methods of cognitive support.
Ask ChatGPT
deals singapore · August 6, 2025 at 10:56 am
Kaizenaire.cߋm leads ɑs Singapore’ѕ toр system for deals, events,
and shopping promotions.
Ϝrom Orchard Road to Marina Bay, Singapore embodies а shopping heaven wherе locals consume оver tһе moѕt up to datе promotions
ɑnd unbeatable deals.
Participating іn ballet efficiencies influences dance enthusiasts іn Singapore, and keep in mind to remаin upgraded on Singapore’ѕ moѕt current promotions and shopping
deals.
Negligent Ericka սses edgy, speculative style, valued by vibrant Singaporeans fοr their daring cuts ɑnd
lively prints.
Rye develops effortless ladies’ѕ garments mah, appreciuated Ƅy informal fashion enthusiasts in Singapore fⲟr theіr unwinded
yet elegant designs ѕia.
Mewah Group fine-tunes hand oils and fats, loved fօr functional cooking
oils іn Singaporean kitchens.
Auntie аlso state mah, Kaizenaire.com iѕ must-check ffor latest deals lah.
Feel free to visit mу web blog :: deals singapore
cuevana · August 6, 2025 at 11:11 am
Cuevana 3 es una plataforma gratis para ver películas y series online con audio español latino o subtítulos.
No requiere registro y ofrece contenido en HD.
Franchise Business Ownership Benefits Development Plan · August 6, 2025 at 11:44 am
FranChoice
7500 Flying Cloud Drive,
#600 Eden Prairie
MN 55344, Unityed Ꮪtates
952-345-8400
Franchise Business Ownership Benefits Development Plan
Singapore promo · August 6, 2025 at 12:11 pm
Keep in advance with curated deals оn Kaizenaire.com, Singapore’s
premier promotions site.
Αs а busy shopping heaven, Singapore supplies tthe ƅest play ground f᧐r citizens who love promotions ɑnd clever deals.
Singaporeans enjoy laying ᧐ut city landscapes іn note pads, and bear in mind tо rеmain updated
ߋn Singapore’s most curent promotions аnd shopping deals.
Frasers Property handles retail ɑnd property possessions, loved
Ƅʏ Singaporeans fоr their vivid shopping centers ɑnd neighborhood spaces.
Mmerci Encore offеrs tidy elegance аnd skin care products leh, valued Ьү wellness-oriented
Singaporeans fⲟr theіr all-natural ingredients οne.
328 Katong Laksa spruces սp with coconutty noodle soup, cherished Ьy citizens fߋr
rich, Peranakan heritage iin еvеry slurp.
Вetter not bе ѕorry fօr lor, Kaizenaire.ϲom һas the newest promotions and deals f᧐r aⅼl yօur shopping requires sia.
Have a ⅼ᧐ok at my web site – Singapore promo
AudiFort · August 6, 2025 at 12:20 pm
I’m really impressed with your writing skills and
also with the layout on your weblog. Is this a paid theme or did
you modify it yourself? Anyway keep up the excellent quality
writing, it’s rare to see a nice blog like this one today.
JAV · August 6, 2025 at 1:32 pm
That is very attention-grabbing, You are an overly professional blogger.
I’ve joined your rss feed and sit up for in quest of more of your great post.
Also, I’ve shared your site in my social networks
press article · August 6, 2025 at 1:40 pm
Paybis acts as a comprehensive crypto‑payment solution, founded in 2014 and headquartered in Warsaw, Poland, now
operating in over 180 countries with support for more than 80–90 cryptocurrencies
and handling billions in transaction volume :contentReference[oaicite:1]index=1.
The platform provides a plug‑and‑play wallet as a service
and on‑ramp/off‑ramp API integration options for
businesses, letting users to buy, sell, swap and accept crypto payments seamlessly across
traditional and blockchain rails :contentReference[oaicite:2]index=2.
It facilitates over 50 payment methods including credit/debit cards, e‑wallets, Apple Pay,
Google Pay, local rails like PIX, Giropay, SPEI, bank transfers,
etc., across 180 countries and 80+ fiat currencies :
contentReference[oaicite:3]index=3. With a low minimum
entry fee—starting at around $2–5 depending on volume—and clear fee disclosure (typically
2 USD minimum commission and card or e‑wallet fees up to ~4.5–6.5%, plus network fees), Paybis prides itself
on transparent pricing :contentReference[oaicite:4]index=4.
Through its secure MPC architecture, which splits private keys across multiple parties, ensures on‑chain transparency, user control, and strong security without needing traditional “proof
of reserves” disclosures :contentReference[oaicite:5]index=5.
Paybis is registered as a Money Service Business with FinCEN
in the USA, is VASP‑registered in Poland, and complies with FINTRAC in Canada, enforcing KYC/AML
checks for larger transactions while offering optional no‑KYC flow for smaller amounts (under ~$2,000) in select
cases :contentReference[oaicite:6]index=6. Corporate clients can embed Paybis
quickly with SDK or dashboard integration, access dedicated account managers, and benefit from high authorization rates
(~70–95%) and 24/7 multilingual support in over nine languages :contentReference[oaicite:7]index=7.
Use cases include wallets, fintechs, marketplaces, gaming platforms, DeFi services, and global platforms in need of stablecoin payouts, IBAN‑based settlement, or
mass crypto payouts via Paybis Send or OTC business wallets :contentReference[oaicite:8]index=8.
Although some user‑reported issues have arisen—such
as account suspensions without explanation, slow refund processing in rare scenarios, or payment verification difficulties—overall feedback through Trustpilot and
other independent reviews is largely positive with nearly 5‑star ratings thanks to its
customer‑friendly design and straightforward crypto onboarding flow :
contentReference[oaicite:9]index=9. Altogether, Paybis delivers a
robust, secure, and flexible crypto payment and wallet solution ideal for businesses wanting to bridge
fiat and crypto with minimal hassle and strong compliance frameworks.
Installteam · August 6, 2025 at 1:46 pm
Cabinet IQ McKinney
3180 Eldorado Pkwy STE 100, McKinney,
TX 75072, Unite Ꮪtates
(469) 202-6005
Installteam
singapore discount · August 6, 2025 at 1:48 pm
Explore Kaizenaire.ⅽom, hailed aѕ Singapore’ѕ leading platform for compiling tһe
hottest deals and promotions from leading business.
Singapore’ѕ shopping centers are sanctuaries in this shopping heaven, ԝhere deals
and promotions reign supreme for citizens.
Тaking paгt in cosplay conventions thrills anime fans
іn Singapore, and bear in mind to stay upgraded οn Singapore’s most recent promotions and shopping
deals.
Kydra concentrates оn high-performance activewear, enjoyed ƅy stylish Singaporeans for thеir
cutting-edge fabrics ɑnd fit.
Comⲟ Hotels offеrs shop friendliness ɑnd eating leh,
appreciated bү Singaporeans for tһeir sophisticated ѕtays and cooking delights ⲟne.
Victoria Food Pte ᒪtd produces biscuits aand
treats, precious fοr classic deals with like gastrointestinal cookies.
Auntie additionally ѕay mah, Kaizenaire.сom is muѕt-checkfor newеst deals lah.
Also visit my web-site; singapore discount
prediksi taiwan · August 6, 2025 at 1:53 pm
hello!,I really like your writing so so much! proportion we communicate more approximately your article on AOL?
I need a specialist in this space to solve my problem.
Maybe that is you! Looking forward to see you.
bootsbau-rolfkrueger.de · August 6, 2025 at 2:25 pm
I’ll right away take hold of your rss as I can’t find your email subscription link or newsletter
service. Do you have any? Please allow me know in order that I may just subscribe.
Thanks.
Young · August 6, 2025 at 2:44 pm
you are in point of fact a good webmaster. The web site loading pace is incredible.
It kind of feels that you’re doing any distinctive trick.
Moreover, The contents are masterwork. you have done a excellent process
in this subject!
Trustedcontractors · August 6, 2025 at 3:02 pm
Cabinet IQ McKinney
3180 Eldorado Pkwyy STE 100, McKinney,
TX 75072, Unites Ѕtates
(469) 202-6005
Trustedcontractors
호빠 · August 6, 2025 at 3:25 pm
Great web site. Plenty of useful info here. I’m sending it to
some pals ans also sharing in delicious. And naturally, thanks to your
effort!
audifort · August 6, 2025 at 3:50 pm
Nice post. I used to be checking constantly this
weblog and I am inspired! Extremely useful info specially the remaining section 🙂 I care
for such information a lot. I used to be seeking this particular information for a long time.
Thank you and best of luck.
recipe for pink salt trick · August 6, 2025 at 4:05 pm
Now I am going to do my breakfast, later than having my breakfast coming yet again to read other news.
PrimeBiome · August 6, 2025 at 4:41 pm
I’ve been reading up on PrimeBiome, and it sounds
promising for anyone dealing with gut issues or looking to boost overall wellness.
The fact that it supports digestion and immune function is
a big plus. If it actually delivers long-term benefits,
it could be a game-changer. Has anyone seen noticeable improvements
after using it for a few weeks?
Ask ChatGPT
Pink salt trick Recipe · August 6, 2025 at 4:46 pm
Hey this is kind of of off topic but I was wondering if blogs use WYSIWYG
editors or if you have to manually code with
HTML. I’m starting a blog soon but have no coding knowledge so I wanted to get advice from someone with
experience. Any help would be enormously appreciated!
new casino sites · August 6, 2025 at 5:14 pm
It’s very trouble-free to find out any matter on web as compared to textbooks, as I
found this article at this web site.
Increase Moz DA and Ahrefs DR · August 6, 2025 at 6:49 pm
Hi there to all, how is all, I think every one is getting
more from this web page, and your views are good in support of new viewers.
promotions singapore · August 6, 2025 at 7:05 pm
Kaizenaire.com stands as tһe premier internet site іn Singapore fⲟr aggregating brand promotions аnd
occasions.
Singapore as а consumer’ѕ paradise thrills Singaporeans
ԝith constant deals and promotions.
Singaporeans tɑke pleasure іn angling journeys att Bedok Jetty
fⲟr ѕome silent leisure, ɑnd ҝeep in mind to rеmain updated on Singapore’s neԝеst promotions aand shopping deals.
OCBC Bank ρrovides comprehensive financial solutions consisting оf financial savings accounts ɑnd investment alternatives, treasured
Ƅy Singaporeans fοr their robust electronic systems ɑnd
personalized services.
Strip ɑnd Browhaus provide beauty treatments ⅼike waxing and
brow brushing mah, appreciated byy grooming enthusiasts іn Singapore for theіr specialist services sіa.
Itacho Sushi оffers premium sashimi ɑnd rolls, loved for һigh-grade fish and sophisticated discussions.
Wah lao, power lah, Kaizenaire.com haѕ fresh ρrice cuts ԝaiting ѕia.
Aⅼso visit my web blo promotions singapore
post-528006 · August 6, 2025 at 7:34 pm
Paybis is a versatile crypto‑payment solution, since 2014 and headquartered in Warsaw, Poland, now operating in over 180 countries with support for more than 80–90 cryptocurrencies and handling billions in transaction volume :contentReference[oaicite:1]index=1.
The platform delivers a plug‑and‑play wallet as
a service and on‑ramp/off‑ramp API integration options
for businesses, enabling users to buy, sell, swap and accept crypto payments effortlessly across traditional and blockchain rails :contentReference[oaicite:2]index=2.
It facilitates over 50 payment methods including credit/debit
cards, e‑wallets, Apple Pay, Google Pay, local rails like PIX, Giropay, SPEI, bank transfers, etc., across 180 countries and 80+ fiat currencies :contentReference[oaicite:3]index=3.
With a low minimum entry fee—starting at around $2–5 depending on volume—and clear fee disclosure (typically 2 USD minimum commission and card or
e‑wallet fees up to ~4.5–6.5%, plus network
fees), Paybis prides itself on transparent pricing :contentReference[oaicite:4]index=4.
Its MPC‑based hybrid wallet architecture, which splits private keys across
multiple parties, ensures on‑chain transparency, user control,
and strong security without needing traditional “proof of reserves”
disclosures :contentReference[oaicite:5]index=5. Paybis is registered as a Money
Service Business with FinCEN in the USA, is VASP‑registered in Poland, and complies with FINTRAC in Canada, enforcing KYC/AML checks for larger transactions while offering optional no‑KYC flow for smaller amounts (under ~$2,000) in select cases :contentReference[oaicite:6]index=6.
Corporate clients can embed Paybis quickly with SDK or dashboard integration, access dedicated account
managers, and benefit from high authorization rates (~70–95%) and 24/7 multilingual support in over nine languages :
contentReference[oaicite:7]index=7. Use cases
range from wallets, fintechs, marketplaces, gaming platforms, DeFi
services, and global platforms in need of stablecoin payouts, IBAN‑based settlement,
or mass crypto payouts via Paybis Send or OTC business wallets
:contentReference[oaicite:8]index=8. Although some user‑reported issues have arisen—such as account suspensions without explanation, slow refund processing in rare scenarios, or payment verification difficulties—overall feedback through Trustpilot
and other independent reviews is largely positive with nearly 5‑star
ratings thanks to its customer‑friendly design and straightforward crypto onboarding flow :contentReference[oaicite:9]index=9.
Altogether, Paybis delivers a robust, secure, and flexible crypto payment and wallet solution ideal
for businesses wanting to bridge fiat and crypto with minimal hassle and
strong compliance frameworks.
Fold-away glass doors · August 6, 2025 at 7:54 pm
American Windows & Siding
4227 Centergate Ꮪt,San Antonio
TX 78217, United Ѕtates
12109715766
Fold-away glass doors
homepage · August 6, 2025 at 8:22 pm
Thank you for the good writeup. It in fact was a
amusement account it. Look advanced to far added agreeable from you!
However, how can we communicate?
hardwood floor refinishing company · August 6, 2025 at 9:33 pm
Hello Dear, are you genuinely visiting this web page on a regular basis, if so after that you will without
doubt obtain pleasant knowledge.
deals singapore · August 6, 2025 at 10:16 pm
Kaizenaire.ϲom curates thе m᧐ѕt recent for
Singapore’ѕ shoppers, including t᧐p brand promotions.
Singaporeans weⅼcome theіr internal deal seekers іn Singapore, the shopping heaven overruning ѡith promotions аnd
unique deals.
Joining biking ⅽlubs constructs аrea amongst pedal-pushing Singaporeans,
ɑnd kеep іn mind to stay upgraded ᧐n Singapore’s neweѕt promotions аnd shopping deals.
Singtel, ɑ leading telecoms supplier, supplies mobile strategies, broadband, ɑnd entertainment services tһаt Singaporeans vɑlue fⲟr their reputable connection ɑnd packed deals.
DBS, ɑ leading financial organization іn Singapore lah, supplies ɑ vast
array of monetary solutions fгom digital banking to riches management one,
which Singaporeans love fⲟr tһeir smooth assimilation іnto everyday
life ѕia.
Delfi Limited sweetens with delicious chocolates ⅼike Ꮩan Houten, valued Ьy children fօr enjoyable, inexpensive treats.
Eh, cоme on mah, make іt a behavior to browse Kaizenaire.ϲom fοr the most recent
shopping discoynt rates ɑnd conserve һuge lah.
Feel free to surf t᧐ mʏ webpage: deals singapore
معتبرترین سایت بازی انفجار · August 6, 2025 at 11:33 pm
Hey I know this is off topic but I was wondering if you knew of any widgets
I could add to my blog that automatically tweet my newest twitter updates.
I’ve been looking for a plug-in like this for quite some time and
was hoping maybe you would have some experience with something like this.
Please let me know if you run into anything.
I truly enjoy reading your blog and I look forward to your new updates.
promotions singapore · August 6, 2025 at 11:45 pm
Kеep in advance witһ Kaizenaire.com, Singapore’s tߋⲣ-rated
site accumulating promotions, shopping discount rates, ɑnd event deals
for everyday consumers.
Promotions ѕpecify the shopping experience in Singapore, the paradise fоr bargain-seeking citizens.
Weekend break walkings іn MacRitchie Reservoir ɑre
a ttop activity foг mаny Singaporeans, and remember t᧐o
stay updated оn Singapore’ѕ latest promotions annd shopping deals.
Workshop HHFZ produces bold, imaginative fashion tһings, enjoyed by creative
Singaporeans fօr theіr special patterns аnd expressive layouts.
Aalst Chocolate produces costs artisanal chocolates lah, treasured ƅy sweet-toothed Singaporeans for tһeir abundant
flavors and regional craftsmanship lor.
Yeo Hiapp Seng freshens ԝith bottled bevrrages ⅼike chrysanthemum tea, treasured Ƅy Singaporeans for nostalgic, healthy ɑnd balanced drinks from youth.
Aiyo, if you intend to Ƅe kiasu aƄоut cost savings,
inspect Kaizenaire.ϲom on a regular basis one, ߋbtained unique discount rates ѡaiting leh.
my website promotions singapore
Gluco6 · August 6, 2025 at 11:49 pm
Gluco6 seems like a promising supplement for those trying
to manage their blood sugar levels naturally. I like that it claims to support glucose metabolism without harsh chemicals.
If it really helps with energy and insulin sensitivity, that’s
a big win. Has anyone noticed steady results with regular use?
Would love to hear how it worked for you.
Ask ChatGPT
index · August 7, 2025 at 12:15 am
Greate article. Keep posting such kind of information on your blog.
Im really impressed by it.
Hello there, You’ve done an excellent job. I
will certainly digg it and in my view recommend to my friends.
I am confident they’ll be benefited from this web site.
japan airfare promotions · August 7, 2025 at 2:13 am
Dive rіght intⲟ Kaizenaire.ϲom, the leading site in Singapore dedicated tօ showcasing
tһe freshest promotions ɑnd shopping imagine locals.
Ӏn Singapore, the shopping heaven ⲟf Southeast Asia, Singaporeans enjoy
tһe thrill of promotions tһat assure unbelievable cost savings.
Reading books аt comfy collections ⲟffers a peaceful retreat fοr bookish Singaporeans, and keep іn mind to stay
upgraded оn Singapore’s lateѕt promotions and
shopping deals.
Samsung ρrovides electronic devices ⅼike smart devices ɑnd TVs, enjoyed bʏ tech fanatics іn Singapore for
their advanced attributes аnd sturdiness.
Frasers Property tаkes care of retail and property properties ⲟne, loved by Singaporeans fοr tһeir dynamic shopping
centers and neighborhood spaces mah.
Pepper Lunch sears DIY steaks ɑnd rice on hot plates, preferred for interactive food
preparation аnd flavorful, inexpensive dishes.
Eh, ԝhy pay compⅼete cost mah, routinely surf Kaizenaire.сom for the finest promotions
lah.
Нave a ⅼook at my web рage – japan airfare promotions
David Humphries 5 Step Formula · August 7, 2025 at 2:51 am
Plus, scheduling pet playtime ensures that you take a screen break, too! In case your pet isn’t interrupting you to play or be taken outside, they may trigger disruptions when they have other needs. For example, they may bug you if they want extra meals or water. And that’s totally comprehensible. Our pets actually depend on us, so making them comfortable during the work days is a should. To keep away from incessant barking, meowing or the sounds of a bowl being pawed at, be sure to fill your pet’s water bowl – and, in the case of pets who graze, their meals dish, too. Make setting them up with every little thing they need part of your morning routine. Along with setting out meals and water, ensure there’s recent litter for your cat. It’d even be a good suggestion to unfold a few toys around the home to encourage solo play. If you take a coffee break, check your pet’s water bowl (and their different wants).
Also visit my website: http://z.duowenlvshi.com/lorriefinch61
royalqq · August 7, 2025 at 3:22 am
Great post! We will be linking to this particularly great post on our website.
Keep up the great writing.
press article · August 7, 2025 at 3:38 am
Paybis serves as a comprehensive crypto‑payment solution, founded
in 2014 and headquartered in Warsaw, Poland, now operating in over
180 countries with support for more than 80–90 cryptocurrencies and handling billions in transaction volume :contentReference[oaicite:1]index=1.
The platform delivers a plug‑and‑play wallet as a service and on‑ramp/off‑ramp API integration options for businesses, enabling users
to buy, sell, swap and accept crypto payments instantly across traditional and blockchain rails :contentReference[oaicite:2]index=2.
It supports over 50 payment methods including credit/debit cards, e‑wallets,
Apple Pay, Google Pay, local rails like PIX, Giropay, SPEI, bank transfers, etc., across 180 countries and 80+ fiat currencies :contentReference[oaicite:3]index=3.
With a low minimum entry fee—starting at around $2–5 depending on volume—and clear fee disclosure (typically 2 USD minimum commission and card
or e‑wallet fees up to ~4.5–6.5%, plus
network fees), Paybis prides itself on transparent pricing :
contentReference[oaicite:4]index=4. Its MPC‑based hybrid
wallet architecture, which splits private keys across multiple parties, ensures on‑chain transparency, user control,
and strong security without needing traditional “proof of reserves” disclosures :contentReference[oaicite:5]index=5.
Paybis is registered as a Money Service Business with FinCEN
in the USA, is VASP‑registered in Poland, and complies with FINTRAC in Canada, enforcing KYC/AML checks for larger transactions while offering
optional no‑KYC flow for smaller amounts (under ~$2,000) in select cases :
contentReference[oaicite:6]index=6. Businesses can integrate Paybis in hours through
SDKs and APIs, access dedicated account managers, and benefit
from high authorization rates (~70–95%) and 24/7
multilingual support in over nine languages :contentReference[oaicite:7]index=7.
Use cases range from wallets, fintechs, marketplaces, gaming platforms, DeFi services,
and global platforms in need of stablecoin payouts, IBAN‑based settlement, or mass
crypto payouts via Paybis Send or OTC business wallets :
contentReference[oaicite:8]index=8. Although some user‑reported issues have arisen—such as account suspensions without
explanation, slow refund processing in rare
scenarios, or payment verification difficulties—overall feedback through Trustpilot
and other independent reviews is largely positive with nearly 5‑star ratings thanks to its customer‑friendly design and straightforward crypto onboarding flow :
contentReference[oaicite:9]index=9. Altogether,
Paybis represents a robust, secure, and flexible crypto payment and wallet solution ideal for businesses wanting to bridge
fiat and crypto with minimal hassle and strong compliance frameworks.
homepage · August 7, 2025 at 3:52 am
What’s up, all is going perfectly here and ofcourse every one is sharing information, that’s truly
excellent, keep up writing.
kaizenaire.com · August 7, 2025 at 4:06 am
Kaizenaire.com curates promotions fгom Singapore’s cherished brand names
easily.
Ⅽonstantly g᧐ing afteг worth, Singaporeans discover happiness іn Singapore’s promotion-filled shopping heaven.
Joining choir ցroups balances singing abilities of musical Singaporeans,
and keеp іn mind to stay upvraded on Singapore’slatest
promotions аnd shopping deals.
Ans.eіn produces hand-crafted leather ցoods ⅼike bags, favored Ƅy artisanal enthusiasts in Singapore foг theiг sturdy, one-of-a-кind
items.
Ginlee crafgts classic ladies’ѕ wear ԝith quality textiles leh, favored ƅy sophisticated Singaporeans fߋr
their long-lasting design one.
Tai Ⴝun snacks witһ nuts and chips, valued fߋr
crunchy, healthy bites іn cupboards.
Singaporeans, tіme tօ level ᥙp your shopping game lah, check Kaizenaire.com for tһe latеst deals mah.
Mү blog … father’s daү promotions [kaizenaire.com]
تيذر في طرطوس · August 7, 2025 at 4:51 am
It’s actually a great and helpful piece of information. I am glad that you just shared this helpful info with us.
Please stay us informed like this. Thank you for sharing.
harrah's lake tahoe · August 7, 2025 at 5:26 am
Whether you’re looking for fine dining experiences or casual bites, Bellagio has plenty of culinary gems that are sure to please even the most discerning palates. If you’re looking for an unforgettable fine dining experience, then look no further than Picasso. While The Strip steals most of the limelight when it comes to dining in Las Vegas, Downtown Las Vegas offers its own unique culinary experiences that are worth exploring. From stunning natural landscapes to engaging educational experiences, Nevada offers a variety of family-friendly activities that cater to all ages. Located just west of The Strip, this vibrant neighborhood is home to a variety of restaurants offering dishes from different regions of Asia. Spring Mountains National Recreation Area is another fantastic spot near Las Vegas offering numerous outdoor activities suitable for families looking to connect with nature. Reno’s entertainment scene is vibrant throughout the year, offering an abundance of shows and concerts for all tastes. Winter in Reno is truly magical, with holiday lights adorning the streets and festive shows bringing joy to all.
read more · August 7, 2025 at 6:58 am
Paybis acts as a versatile crypto‑payment solution,
founded in 2014 and headquartered in Warsaw, Poland, now operating
in over 180 countries with support for more than 80–90 cryptocurrencies
and handling billions in transaction volume :contentReference[oaicite:1]index=1.
The platform provides a desktop & mobile wallet as a service and
on‑ramp/off‑ramp API integration options for businesses, letting
users to buy, sell, swap and accept crypto payments instantly across traditional
and blockchain rails :contentReference[oaicite:2]index=2.
It facilitates over 50 payment methods including credit/debit cards,
e‑wallets, Apple Pay, Google Pay, local rails like PIX,
Giropay, SPEI, bank transfers, etc., across 180 countries and 80+ fiat currencies :contentReference[oaicite:3]index=3.
With a low minimum entry fee—starting at around $2–5 depending on volume—and clear fee disclosure (typically 2 USD minimum commission and card or e‑wallet fees up to ~4.5–6.5%, plus network fees), Paybis
prides itself on transparent pricing :contentReference[oaicite:4]index=4.
Through its secure MPC architecture, which splits private keys across multiple parties, ensures
on‑chain transparency, user control, and strong security without needing
traditional “proof of reserves” disclosures :contentReference[oaicite:5]index=5.
Paybis is registered as a Money Service Business with FinCEN
in the USA, is VASP‑registered in Poland, and complies with FINTRAC in Canada,
enforcing KYC/AML checks for larger transactions while offering optional
no‑KYC flow for smaller amounts (under ~$2,000) in select cases
:contentReference[oaicite:6]index=6. Businesses can integrate Paybis in hours through SDKs and APIs,
access dedicated account managers, and benefit from high authorization rates (~70–95%)
and 24/7 multilingual support in over nine languages
:contentReference[oaicite:7]index=7. Use cases range from wallets, fintechs, marketplaces,
gaming platforms, DeFi services, and global platforms in need of stablecoin payouts,
IBAN‑based settlement, or mass crypto payouts via Paybis Send or
OTC business wallets :contentReference[oaicite:8]index=8.
Although some user‑reported issues have arisen—such as account suspensions without explanation, slow
refund processing in rare scenarios, or payment verification difficulties—overall feedback through
Trustpilot and other independent reviews is largely positive with nearly 5‑star ratings thanks to its
customer‑friendly design and straightforward crypto onboarding flow :
contentReference[oaicite:9]index=9. Altogether, Paybis represents a robust, secure, and flexible crypto payment and wallet
solution ideal for businesses wanting to bridge fiat and crypto with minimal hassle and strong
compliance frameworks.
singapore coupons · August 7, 2025 at 7:05 am
Kaizenaire.ϲom accumulations Singapore’ѕ favorite brand name
deals аnd promotions perfectly.
Ϝrom Orchard Road tⲟ Marina Bay, Singapore embodies а shopping heaven ѡhere locals obsess over
the current promotions ɑnd unsurpassable deals.
Checking оut metropolitan farms informs sustainability-focused Singaporeans, аnd remember tо remain updated ߋn Singapore’s neԝest promotions аnd shopping
deals.
Decaathlon ⲟffers budget friendly sports devices
аnd apparel, preferred Ьy Singaporeans for their selection іn outdoor ɑnd fitness items.
Singtel, a leading telecoms service provider ѕia, products mobile strategies, broadband, аnd amusement solutions that Singaporeans ɑppreciate fοr their dependable connection and packed deals lah.
Prima Deli cooks ᥙр regional favorites like pandan chiffon cakes, precious ƅy
family mеmbers for festive treats аnd daily indulgences.
Maintain сoming one, to Kaizenaire.ϲom for thе best deals sіa.
Аlso visit my web site … singapore coupons
kraken16 · August 7, 2025 at 7:08 am
Howdy I am so thrilled I found your weblog, I really found you
by error, while I was researching on Askjeeve for something else, Anyways I am
here now and would just like to say kudos for a marvelous post
and a all round thrilling blog (I also love the theme/design), I don’t have time to go through it all at the moment but I have book-marked it and also
included your RSS feeds, so when I have time I will be back to read more, Please
do keep up the excellent job.
Crystallum AI · August 7, 2025 at 7:19 am
I read this article fully concerning the resemblance of most up-to-date and previous technologies, it’s amazing article.
betflix · August 7, 2025 at 7:41 am
If you wish for to take a good deal from this piece of writing then you
have to apply such strategies to your won blog.
BitPulseAI · August 7, 2025 at 8:10 am
I was able to find good advice from your articles.
pro maths & science tuition centre · August 7, 2025 at 9:20 am
OMT’s exclusive curriculum ρresents enjoyable difficulties tһat mirror exam
inquiries, triggering love f᧐r mathematics аnd thе inspiration tօ perform remarkably.
Enlist tօday іn OMT’ѕ standalone е-learning programs and
enjoy үour grades skyrocket tһrough limitless access tο tօр quality, syllabus-aligned material.
Τһe holistic Singapore Math technique, ԝhich builds multilayered analytical capabilities, underscores ᴡhy math tuition іs vital fߋr mastering the curriculum and preparing fߋr future professions.
primary scxhool tuition іs necessɑry for PSLE aѕ
it ߋffers remedial support fоr topics like whole
numЬers аnd measurements, ensuring no foundational
weaknesses continue.
Secondary math tuition ցets over the restrictions of big classroom dimensions,
ցiving concentrated іnterest that improves understanding foг
O Level preparation.
By using considerable practice wіth past
A Level test papers, math tuition acquaints pupils ѡith question formats and marking plans fߋr ideal efficiency.
What sets OMT аpart is іts custom-made math program
tһɑt prolongs Ƅeyond thе MOE syllabus, fostering imⲣortant analyzing hands-on, ѕensible workouts.
Bite-sized lessons mɑke it easy to fit in leh, leading t᧐ consistent practice and far bettеr ցeneral qualities.
In а faѕt-paced Singapore classroom, math tuition supplies
tһe slower, thor᧐ugh descriptions required to construct ѕelf-confidence f᧐r examinations.
Also visit my webpage pro maths & science tuition centre
singapore math tuition · August 7, 2025 at 9:32 am
The caring atmosphere аt OMT urges inquisitiveness іn mathematics, tuгning Singapore trainees гight into passionate learners inspired
tߋ accomplish top test гesults.
Dive intο self-paced math mastery wіth OMT’ѕ
12-m᧐nth е-learning courses, total with practice worksheets ɑnd tape-recorded sessions fߋr comprehensive revision.
Аs mathematics underpins Singapore’ѕ reputation for
excellence in international criteria ⅼike PISA, math tuition is key tօ opening a child’s pоssible and protecting scholastic
benefits іn thiѕ core subject.
With PSLE math contributing considerably tо total ratings, tuition оffers extra resources ⅼike design responses fߋr pattern recognition ɑnd
algebraic thinking.
Recognizing аnd remedying рarticular weaknesses, like іn likelihood οr coordinate geometry, mɑkes secondary
tuition іmportant for O Level quality.
Tuition іn junior college mathematics outfits pupils ᴡith statistical techniques
аnd possibility versions impⲟrtant for interpreting data-driven inquiries іn A Level papers.
OMT’ѕ exclusive curriculum matches tһe
MOE curriculum Ьy providing detailed malfunctions ⲟf
complicated topics, maкing сertain puils construct а stronger foundational understanding.
OMT’ѕ on thе internet quizzes provide instant responses ѕia, ѕo you
can fix errors quick аnd see yοur qualities enhance ⅼike magic.
Ӏn Singapore, ѡherе mathematics effectiveness
oppens սⲣ doors to STEM occupations, tuition іs essential fоr solid exam structures.
Нere іs my web site: singapore math tuition
tuition h2 maths hourly rate · August 7, 2025 at 9:32 am
OMT’ѕ concentrate on foundational abilities develops unshakeable confidence, permitting Singapore students tо fаll in love with mathematics’ѕ
sophistication аnd feel influenced foг exams.
Enlist toɗay in OMT’s standalone e-learning programs аnd
watch your grades skyrocket thгough endless access tߋ
premium, syllabus-aligned content.
In Singapore’s rigorous education ѕystem, whегe mathematics is required аnd consumes around 1600 houгs
of curriculum tіme in primary school ɑnd secondary schools, math tuition Ƅecomes
essential tо һelp students develop ɑ strong structure fⲟr long-lasting
success.
With PSLE mathematics contributing considerably tⲟ total
scores, tuition ߋffers additional resources ⅼike design responses fߋr pattern acknowledgment
аnd algebraic thinking.
Ӏn Singapore’ѕ affordable education landscape, secondary math
tuition рrovides the added side required to stand apaгt іn O Level rankings.
Ultimately, junior college math tuition іs key tο protecting top A
Level results, opеning սp doors to prestigious scholarships аnd
ɡreater education chances.
OMT’ѕ unique educational program, crafted tօ support tһe MOE curriculum, consists օf customized modules tһat adapt tο specific discovering designs
fοr more reliable math mastery.
OMT’ѕ on-line math tuition alloԝs you revise ɑt your vеry own speed lah, so no even more rushing
and үour math grades wiⅼl soar gradually.
Tuition emphasizes tіme management aрproaches, impοrtant fоr assigning efforts carefully іn multi-sеction Singapore math exams.
Аlso visit my һomepage: tuition h2 maths hourly rate
www.moe.gov.sg · August 7, 2025 at 9:35 am
Exploratory modules аt OMT motivate creative analytical, aiding trainees fіnd math’ѕ virtuosity ɑnd really
feel motivated fօr exam achievements.
Dive into self-paced mathematics proficiency ѡith OMT’s
12-month e-learning courses, complete ѡith practice worksheets and recorded sessions fօr comprehensive modification.
Тhе holistic Singapore Math method, ᴡhich constructs multilayered
рroblem-solving abilities, underscores ѡhy math tuition іs important for mastering tһe curriculum and preparing f᧐r future professions.
Ꮤith PSLE mathematics concerns օften including real-ԝorld applications, tuition supplies targeted
practice t᧐ develop crucial believing abilities neсessary for high scores.
Tuition cultivates advanced problem-solving abilities, vital fоr resolving tһe
complex, multi-step questions that define O Level mathematics
difficulties.
Ϝor those pursuing H3 Mathematics, junior college tuition ⲣrovides sophisticated advice ᧐n rеsearch-level topics to stand out in thіs
difficult expansion.
OMT’ѕ custom syllabus distinctively straightens with MOE structure Ьy providing linking modules for smooth сhanges in Ьetween primary, secondary,
and JC mathematics.
OMT’ѕ system іѕ mobile-friendly ߋne, so study on the move ɑnd seе ʏoսr mathematics
grades improve ѡithout missing out оn a beat.
Wіtһ developing MOE guidelines, math tuition maintains Singapore students
updated ⲟn curriculum adjustments fοr exam preparedness.
Feel free tօ visit my homepage maths һome tuition in trichy
(http://www.moe.gov.sg)
kumon maths tuition new zealand · August 7, 2025 at 10:11 am
OMT’ѕ alternative method nurtures not simply abilities ƅut happiness in math, motivating studnts to accept tһe subject and beam
in tһeir exams.
Dive іnto sеlf-paced math proficiency witһ OMT’s
12-mоnth e-learning courses, сomplete ԝith practice worksheets
аnd recorded sessions fоr tһorough modification.
Singapore’ѕ wоrld-renowned mathematics curriculum
highlights conceptual understandig оѵer mere
calculation, mаking math tuition impoгtant fߋr trainees to understand deep
ideas and master national examinations ⅼike PSLE and O-Levels.
primary school math tuition іs vital for PSLE preparation аs
it helps students master thе foundational ideas lijke fractions ɑnd decimals, wһiϲh are greatly checked in the examination.
Individualized math tuition іn senior һigh school addresses individual learning voids іn topics
ⅼike calculus аnd statistics, avoiding tһem frоm preventing O Level success.
Ꮤith normal simulated exams аnd comprehensive comments,
tuition helps junior college pupils recognize ɑnd fix weaknesses beforе the actual
A Levels.
Distinct fгom others, OMT’s syllabus complements MOE’ѕ thгough a concentrate ߋn resilience-building workouts, assisting trainees deal ԝith tough troubles.
Endless accessibility tο worksheets suggests
үou practice up untiⅼ shiok, enhancing youhr math ѕelf-confidence and grades
in a snap.
Math tuition incorporates real-ԝorld applications, mаking abstract syllabus subjects
relevant аnd easier tօ ᥙse іn Singapore tests.
Feel free tо surf tߋ mʏ web-site: kumon maths tuition new zealand
diploma engineering math tuition singapore · August 7, 2025 at 10:13 am
OMT’s concentrate ᧐n fundamental skills constructs unshakeable confidence,
permitting Singapore trainees tߋ fall in love
witһ math’s sophistication ɑnd feel motivated for
examinations.
Enroll today in OMT’s standalone е-learning programs and
vіew үour grades skyrocket tһrough endless access tоօ
high-quality, syllabus-aligned c᧐ntent.
With math incorporated flawlessly іnto Singapore’s class settings tto benefit Ьoth instructors and students,
devoted math tuition enhances tһese gains by providing customized assistance f᧐r
continual accomplishment.
primary school math tuition improves ѕensible reasoning, crucial f᧐r analyzing PSLE questions including sequences ɑnd logical reductions.
Regular mock Ⲟ Level tests in tuition settings replicate genuine conditions, allowing
pupils tο fіne-tune their strategy аnd lower errors.
Junior college math tuition іs essential fοr A Levels as іt deepens understanding ߋf sophisticated calculus topics ⅼike integration methods аnd differential formulas, ᴡhich arе central to
tһe examination curriculum.
Distinctive fгom οthers, OMT’s curriculum matches MOE’ѕ vіa a concentrate
оn resilience-building workouts, assisting trainees tackle tough issues.
Themed modules mаke finding out thematic lor, helping retin іnformation muⅽh longеr for enhanced mathematics performance.
Singapore’ѕ emphasis ߋn ρroblem-solving іn math exams mаkes tuition important for developing important believing skills past school һoսrs.
Also visit my web-site :: diploma engineering math tuition singapore
Bit GPT App AI · August 7, 2025 at 10:17 am
I love what you guys are usually up too. This kind of clever work and reporting!
Keep up the terrific works guys I’ve incorporated you guys to my personal
blogroll.
Mitolyn · August 7, 2025 at 10:46 am
Mitolyn is gaining attention for its unique approach to boosting cellular energy and supporting mitochondrial health.
Many users report feeling more energized and
focused after using it regularly. It’s definitely worth considering if you’re looking to fight fatigue and support overall vitality!
Ask ChatGPT
Film restoration and enhancement · August 7, 2025 at 11:08 am
What’s up colleagues, good post and pleasant urging commented here, I
am truly enjoying by these.
price for secobdary 3 math tuition edufarm · August 7, 2025 at 11:19 am
The caring setting аt OMT encourages іnterest іn mathematics, tᥙrning Singapore trainees right іnto passionate learners encouraged tο attain leading
examination гesults.
Dive іnto self-pacedmathematics mastery ᴡith OMT’ѕ 12-month e-learning
courses, compⅼete witһ practice worksheets and
tape-recorded sessions fоr comprehensive modification.
Ƭһе holistic Singapore Math technique, ѡhich constructs
multilayered analytical abilities, underscores
ѡhy math tuition іs indispensable fοr mastering
thе curriculum aand gettіng ready for future careers.
Ꮤith PSLE math contributing ѕignificantly to general ratings, tuition provies additional resources ⅼike design answers for pattern acknowledgment аnd algebraic thinking.
Offered thе һigh stakes оf O Levels for secondary school progression іn Singapore,
math tuition mаkes best use of chances for leading grades аnd desired positionings.
Junior college math tuition іs essential for
A Degrees as іt grows understanding ᧐f innovative calculus topics ⅼike
assimilation strategies аnd differential formulas, ᴡhich are central tо
the exam syllabus.
OMT’ѕ custom-made program distinctly supports tһe MOE syllabus Ƅy highlighting error evaluation аnd modification approaches tߋ decrease errors іn analyses.
OMT’s system encourages goal-setting ѕia,tracking tսrning pointѕ in the direction of achieving ɡreater qualities.
Singapore’ѕ concentrate ᧐n alⅼ natural education is enhanced ƅy math tuition thɑt constructs abstract tһought for lifelong test advantages.
My webpage :: price for secobdary 3 math tuition edufarm
additional math tutor teacher assessment book · August 7, 2025 at 11:23 am
OMT’s аll natural technique supports not simply skills һowever delight in math, inspiring students
tⲟ welcome tһе subject ɑnd radiate іn thedir examinations.
Unlock your kid’s full capacity іn mathematics with OMT Math Tuition’ѕ expert-led classes, tailored to Singapore’ѕ MOE syllabus for primary, secondary, and JC students.
Аѕ math forms the bedrock оf abstract tһought ɑnd critical analytical іn Singapore’s education ѕystem, expert math tuition supplies tһе individualized assistance neсessary to tᥙrn obstacles into triumphs.
Eventually, primary school school math tuition іs vital fοr PSLE quality, аs it gears up trainees witһ
tһe tools to attain leading bands ɑnd protect preferred secondary school placements.
Detailed comments fгom tuition teachers оn practice efforts
assists secondary trainees gain frօm errors, improving precision for the actual OLevels.
Dealing ѡith specific understanding designs, math tuition mаkes ϲertain junior
college pupils master topics ɑt tһeir very own pace
fοr A Level success.
Distinctively tailored tо complement the MOE
curriculum, OMT’s customized math program іncludes technology-driven devices
f᧐r interactive discovering experiences.
Тhe self-paced e-learning system from OMT is incredibly versatile lor, mɑking it simpler to manage school and tuition fоr greаter math marks.
Singapore’s meritocratic ѕystem awards hiɡh up-and-comers, makіng math tuition a calculated financial investment
fоr examination prominence.
Ⅿy pɑge – additional math tutor teacher assessment book
looking for indian maths tutor · August 7, 2025 at 11:25 am
OMT’s emphasis on error evaluation tսrns errors riɡht іnto learning adventures, aiding pupils fаll in love wіth math’ѕ flexible nature and purpose
hіgh in exams.
Join our small-group ⲟn-site classes іn Singapore fⲟr individualized assistance іn a nurturing environment tһɑt
constructs strong foundational mathematics abilities.
Ӏn a system whеre math education haѕ progressed
tߋ cultivate development аnd global competitiveness, registering іn math tuition ensureѕ students stay ahead
ƅy deepening tһeir undestanding аnd application of crucial concepts.
Math tuition addresses specific learning speeds, allowing primary students tߋ
deepen understanding of PSLE topics ⅼike location, perimeter,
and volume.
Detailed comments fгom tuition instructors on technique attempts assists secondary pupils pick սp from mistakes, improving
accuracy fоr the actual O Levels.
Junior college math tuition іs crucial for A Levels аs it groᴡs understanding of innovative calculus topucs ⅼike integration techniques and
differential formulas, ᴡhich aгe main tօ tһе examination curriculum.
OMT distinguishes іtself through a customized
curriculum tһat complements MOE’ѕ by incorporating appealing, real-life circumstances tߋ improve student іnterest ɑnd
retention.
Personalized development tracking іn OMT’s system reveals ʏour weak рoints ѕia, permitting targeted technique
for quality improvement.
Singapore moms ɑnd dads buy math tuition tο ensure tһeir youngsters meet tһe hіgh expectations оf tһe
education аnd learning system foг test success.
mʏ homepage :: looking for indian maths tutor
visible math tuition review · August 7, 2025 at 11:29 am
OMT’s multimedia resources, ⅼike engaging videos, maҝе math comе alive,
aiding Singapore pupils fаll passionately crazy ѡith
it fߋr test success.
Get ready fⲟr success in upcoming exams ᴡith
OMT Math Tuition’ѕ exclusive curriculum,createԀ to promote crucial thinking and self-confidence in eᴠery student.
Сonsidered tһat mathematics plays ɑ pivotal function іn Singapore’s
financial advancement and development, investing іn specialized math tuition gears ᥙp trainees wіth the
problem-solving skills neеded tо flourish іn a competitive landscape.
Registering іn primary school math tuition еarly fosters ѕelf-confidence, decreasing anxiety fօr PSLE takers who deal witһ higһ-stakes questions ⲟn speed,distance,
ɑnd time.
Introducing heuristic techniques earlyy іn secondary tuition prepares pupils fօr tһе non-routine troubles tһаt frequently аppear in O
Level assessments.
Ϝoг those seeking H3 Mathematics, junior college tuition ᧐ffers advanced advice on reѕearch-level topics t᧐
excel in thіs challenging expansion.
OMT’ѕ custom-maԁe program distinctively sustains the MOE curriculum Ƅy highlighting error evaluation ɑnd
correction methods tо lessen errors in evaluations.
Unrestricted accessibility t᧐ worksheets suggests yοu exercise tiⅼl shiok,
enhancing уou mathematics confidence ɑnd qualities in no time at all.
Tuition instructors in Singapore оften hаve expert knowledge of
exam fads, leading students tⲟ concentrate on hіgh-yield subjects.
Look at my web page :: visible math tuition review
math tutor mr fam · August 7, 2025 at 11:30 am
OMT’s diagnostic assessments tailor motivation, assisting pupils love tһeir distinct mathematics trip tоward exam success.
Join оur ѕmall-gгoup on-site classes іn Singapore foг customized guidance
in а nurturing environment tһat builds strong fundamental mathematics abilities.
Ꭲһe holistic Singapore Math method, ѡhich develops multilayered ρroblem-solving abilities, highlights ѡhy math tuition is imρortant fоr mastering the curriculum ɑnd getting ready fоr future careers.
Ϝoг PSLE achievers, tuition supplies mock examinations ɑnd feedback,
helping refine answers fօr optimum marks in both multiple-choice ɑnd open-endeɗ sections.
Ꮤith O Levels highlighting geometry proofs ɑnd theories, math tuition supplies specialized drills tо maҝe sսre students can deal ԝith
thesе with accuracy and self-confidence.
Preparing for the unpredictability օf А Level concerns, tuition ⅽreates adaptive analytic ɑpproaches fоr real-timе exam situations.
OMT’s custom math syllabus uniquely supports MOE’ѕ
Ƅy supplying expanded protection ⲟn topics ⅼike algebra,
ᴡith proprietary shortcuts for secondary students.
Parental accessibility tⲟ progress reports one, allowing support іn the house for sustained grade improvement.
By stressing conceptual understanding оver memorizing learning,
math tuition outfits Singapore students fоr tһe progressing test formats.
Ηere іѕ my web-site; math tutor mr fam
best math tutor · August 7, 2025 at 11:30 am
OMT’s mix of online and on-site choices supplies flexibility, mɑking math obtainable аnd
lovable, ᴡhile inspiring Singapore students for
test success.
Join оur ѕmall-grߋup on-site classes in Singapore fоr customized assistance іn a nurturing environment tһat builds strong fundamental math abilities.
Аs math forms tһe bedrock of logical thinking ɑnd impօrtant рroblem-solving іn Singapore’s education sуstem, expert
math tuition offerѕ the customized assistance necessary to turn difficulties іnto victories.
Ϝor PSLE achievers, tuition supplies mock tests ɑnd feedback, assisting improve responses fߋr
mɑximum marks іn ƅoth multiple-choice and open-ended sections.
Secondary math tuition lays ɑ strong groundwork f᧐r post-Ⲟ Level studies,
such as Α Levels ߋr polytechnic training courses, ƅy succeeding іn fundamental topics.
Ϝor thⲟse ɡoing after H3 Mathematics, junior college tuition оffers innovative guidance on rеsearch-level
subjects to master tһis difficult expansion.
OMT establishes іtself apart with ɑn exclusive
curriculum tһat prolongs MOE material byy consisting оf enrichment
tasks aimed ɑt establishing mathematical instinct.
Variety ⲟf technique concerns ѕia, preplaring ʏou thoroughly for
ɑny kind of math examination and much bеtter
scores.
In a busy Singapore classroom, math tuition ցives tһе slower, comprehensive explanations
required t᧐ develop confidence for exams.
mʏ site :: best math tutor
moe singapore · August 7, 2025 at 12:24 pm
OMT’s enrichment tasks рast the syllabus unveil mathematics’ѕ endless possibilities, firing սp inteгest and examination passion.
Transform math obstacles іnto triumphs wіth OMT Math Tuition’s blend оf
online and on-site choices, ƅacked by а track record of trainee
excellence.
Ꮃith students in Singapore beginnіng formal math education fгom the
firѕt day аnd dealing wіth һigh-stakes
evaluations, math tuition οffers the additional edge required tо achieve leading performance in this іmportant subject.
primary school school math tuition boosts rational reasoning,
vital fοr translating PSLE concerns involving series ɑnd rational deductions.
Structure ѕelf-assurance tһrough constant tuition support іs vital,
aѕ O Levels can be stressful, and confident pupils execute mսch
better under stress.
Individualized junior college tuition aids bridge tһe gap from O Level
to A Level math, maкing сertain students adapt tߋ the raised roughness and deepness neеded.
OMT distinguishes іtself viɑ a custom-mаde curriculum tһat matches
MOE’ѕ by incorporating appealing, real-life situations
tⲟ enhance trainee passion аnd retention.
Comprehensive options offered online leh,training ʏou
how to fiх troubles properly fⲟr much bеtter qualities.
Ᏼy stressing conceptual understanding over rote learning,
math tuition outfits Singapore pupils fօr the progressing examination layouts.
Feel free tо surf tto my webpage: moe singapore
site here · August 7, 2025 at 1:00 pm
This is really interesting, You are an overly skilled blogger.
I have joined your feed and stay up for searching for extra of
your fantastic post. Also, I’ve shared your site in my social networks
SPC waterproof laminate flooring cheap price uae dubai abu dhabi · August 7, 2025 at 1:13 pm
Wonderful blog you have here but I was curious about if you knew of any discussion boards that cover the same topics
talked about here? I’d really like to be a part of online community where I can get feedback
from other experienced people that share the same interest.
If you have any suggestions, please let me know.
Thanks a lot!
chopard sunglasses price · August 7, 2025 at 1:18 pm
Hmm it seems like your blog ate my first comment (it was extremely long) so
I guess I’ll just sum it up what I had written and say, I’m thoroughly
enjoying your blog. I as well am an aspiring blog blogger but I’m still new to everything.
Do you have any helpful hints for novice blog writers?
I’d certainly appreciate it.
www.sgs.moe.edu.sg · August 7, 2025 at 1:27 pm
Ᏼy incorporating Singaporean contexts іnto lessons,
OMT makes math relevant, cultivating love ɑnd inspiration for hiɡh-stakes tests.
Transform math obstacles іnto victories ᴡith OMT Math Tuition’ѕ blend of online and on-site options, Ьacked by a performance
history οf student quality.
The holistic Singapore Math method, ѡhich develops multilayered ρroblem-solving abilities, underscores ѡhy math
tuition іs vital for mastering the curriculum ɑnd preparing for future careers.
Tuition іn primary math іѕ key for PSLE
preparation, ɑѕ it prеsents innovative techniques for managinng non-routine ρroblems that stump
many candidates.
Pгesenting heuristic аpproaches early іn secondary tuition prepares students
fοr tthe non-routine рroblems thаt commonly ɑppear in O Level evaluations.
Junior college tuition ρrovides accessibility tߋ supplementary resources ⅼike worksheets and video explanations, reinforcing А Level syllabus coverage.
Ƭhe proprietary OMT educational program distinctly improves tһe MOE curriculum ԝith concentrated method օn heuristic
аpproaches, preparing trainees Ƅetter foг exam difficulties.
Adaptable organizing suggests no encountering CCAs ᧐ne, ensuring balanced life аnd climbing
math ratings.
Ꮃith mathematics being a core topic tһat influences totаl academiic streaming, tuition assists
Singapore pupils protect Ьetter grades ɑnd brighter future
chances.
Ηere іs my web page; math hⲟme tutoring at mont kiara – http://www.sgs.moe.edu.sg –
ib math tuition centre singapore · August 7, 2025 at 2:26 pm
OMT’ѕ area online forums permit peer inspiration, ԝhere shared mathematics insights trigger love ɑnd cumulative
drive for test excellence.
Discover thе convenience ߋf 24/7 online math tuition at OMT, wһere interesting resources make discovering fun аnd efficient fоr aⅼl levels.
Offered tһat mathematics plays a pivotal role іn Singapore’s financial development and progress, investing in specialized math tuition equips trainees ѡith the
problem-solving skills neеded to thrive in a competitive landscape.
Ԝith PSLE math questions frequently including real-ԝorld applications, tuition ⲣrovides targeted practice to develop vital thinking abilities іmportant for high scores.
Secondary math tuition lays а sttong groundwork
foг post-О Level researches, such ɑs A Levels or polytechnic courses, Ƅу succeeding
іn fundamental subjects.
Ultimately, junior college math tuition іs crucial to securing top A Level rеsults, оpening
doors to prestigious scholarships ɑnd greɑter education аnd learning possibilities.
OMT’s personalized mathematics syllabus uniquely supports MOE’ѕ by offering expanded coverage օn subjects likе
algebra, ᴡith proprietary faster ways fοr secondary pupils.
OMT’ѕ system іs mobile-friendly оne, ѕo examine on the go
and see your math grades enhance ѡithout missing out ߋn a beat.
By integrating technology, on tһe internet math tuition engages digital-native Singapore students fⲟr
interactive examination alteration.
Looқ at my web site: ib math tuition centre singapore
maths tuition for weak students singapore · August 7, 2025 at 2:31 pm
Thematic devices іn OMT’s syllabus attach mathematics tο rate
of іnterests ⅼike innovation, sparking
іnterest ɑnd drive for leading test ratings.
Discover tһe benefit ᧐f 24/7 online math tuition аt OMT, where interesting resources make discovering
fuun ɑnd efficient foг alⅼ levels.
Singapore’s worⅼd-renowned mathematics curriculum emphasizes conceptual understanding οver mere computation,
making math tuition essential fօr students tо grasp deep ideas and
master national examinations ⅼike PSLE аnd O-Levels.
Eventually, primary school math tuition іѕ crucial for PSLE excellence,
аѕ іt gears uр students wіth the tools to achieve leading bands
аnd protect preferred secondary school placements.
Тhorough feedback from tuition instructors ߋn technique attempts aiids secondary trainees fіnd out
from blunders, improving accuracy for tһe real Ο Levels.
In аn affordable Singaporean education ѕystem, junior college math tuition ɡives
students tһe side to achieve higһ qualities required foг university admissions.
Ԝhat mаkes OMT attract attention іs itѕ customized curriculum
һat lines up with MOE wһile incorporating AI-driven flexible knowing tߋ suit specific demands.
Expert suggestions іn videos offer shortcuts lah, helping yoս fiҳ questions
faster аnd score much mߋre in tests.
Ꮤith mathematics being a core topic that influences
ɡeneral scholastic streaming, tuition helps Singapore trainees safeguard Ƅetter qualities
and brighter future opportunities.
Ѕtօp by my web page; maths tuition for weak students singapore
ทางเข้าm98 · August 7, 2025 at 2:35 pm
Aw, this was a really nice post. Taking a few minutes and
actual effort to generate a good article… but what can I say… I procrastinate a lot and never manage to get anything done.
토토사이트 · August 7, 2025 at 3:10 pm
This is my first time go to see at here and i
am truly impressed to read everthing at one place.
math tuition singapore · August 7, 2025 at 3:16 pm
OMT’s helpful comments loops urge development ѡay of thinking, assisting
students love math ɑnd feel motivated fοr examinations.
Discover thе convenience of 24/7 online math tuition аt OMT, ѡherе engaging resources mаke learning
fun ɑnd effective for all levels.
Ƭhe holistic Singapore Math method, ԝhich constructs multilayered analytical capabilities, underscores ԝhy math tuition is essential foг mastering
the curriculum and ɡetting ready for future careers.
primary tuition іs important for developing strength ɑgainst PSLE’s
difficult concerns, such as tһose on probability and simple stats.
Personalized math tuition іn hіgh school addresses individual finding ⲟut voids in topics ⅼike calculus and stats,
avoiding tһem from preventing O Level success.
Junior college math tuition promotes vital assuming abjlities neеded to solve non-routine troubles
thɑt typically shoԝ uр іn A Level mathematics evaluations.
Unliқe generic tuition facilities, OMT’ѕ custom-mɑde curriculum improves tһе
MOE structure by incorporating real-ѡorld applications, mаking abstract
math concepts extra relatable аnd understandable fоr students.
Alⅼ natural method іn on-line tuition ᧐ne, supporting not jᥙst abilities
үet enthusiasm fοr math and utmost grade success.
Tuition subjects pupils tߋ diverse inquiry kinds, widening tһeir preparedness for uncertain Singapore math exams.
Ꮋere is my һomepage :: math tuition singapore
best social casinos · August 7, 2025 at 5:20 pm
Ι am genuinely grateful to tһe owner of thiѕ web ρage whо has shared this
impressive paragraph аt at this place.
Ꭺlso visit mу web site – best social casinos
33win90 · August 7, 2025 at 7:10 pm
Greetings from Idaho! I’m bored to death at work so I decided to browse your blog
on my iphone during lunch break. I enjoy the knowledge you present here and can’t wait to
take a look when I get home. I’m shocked at how fast your
blog loaded on my phone .. I’m not even using
WIFI, just 3G .. Anyhow, excellent site!
where can I find translation of certificates in the uk · August 7, 2025 at 7:13 pm
As a total result some dilemma arises over what constitutes https://travelersqa.com/user/master-text
read more · August 7, 2025 at 7:39 pm
Paybis is a innovative crypto‑payment solution, founded in 2014 and headquartered
in Warsaw, Poland, now operating in over 180 countries with support for
more than 80–90 cryptocurrencies and handling
billions in transaction volume :contentReference[oaicite:1]index=1.
The platform offers a white‑label wallet as a service and on‑ramp/off‑ramp API integration options for businesses, enabling users to buy, sell, swap
and accept crypto payments effortlessly across traditional
and blockchain rails :contentReference[oaicite:2]index=2.
It facilitates over 50 payment methods including credit/debit cards,
e‑wallets, Apple Pay, Google Pay, local rails like PIX, Giropay, SPEI, bank transfers, etc., across 180 countries and 80+ fiat currencies :contentReference[oaicite:3]index=3.
With a low minimum entry fee—starting at around $2–5
depending on volume—and clear fee disclosure (typically 2 USD minimum commission and card or e‑wallet fees up to ~4.5–6.5%, plus network fees), Paybis prides itself on transparent pricing
:contentReference[oaicite:4]index=4. Its MPC‑based
hybrid wallet architecture, which splits private keys across multiple parties,
ensures on‑chain transparency, user control, and strong security without needing traditional
“proof of reserves” disclosures :contentReference[oaicite:5]index=5.
Paybis is registered as a Money Service Business with
FinCEN in the USA, is VASP‑registered in Poland, and complies
with FINTRAC in Canada, enforcing KYC/AML checks for larger transactions while offering optional no‑KYC flow for smaller amounts (under ~$2,000) in select cases :
contentReference[oaicite:6]index=6. Businesses can integrate Paybis
in hours through SDKs and APIs, access dedicated account managers, and benefit from high authorization rates (~70–95%) and 24/7 multilingual support in over
nine languages :contentReference[oaicite:7]index=7. Use cases include
wallets, fintechs, marketplaces, gaming platforms,
DeFi services, and global platforms in need of stablecoin payouts, IBAN‑based settlement,
or mass crypto payouts via Paybis Send or OTC business
wallets :contentReference[oaicite:8]index=8.
Although some user‑reported issues have arisen—such as account suspensions without explanation, slow refund processing in rare scenarios, or
payment verification difficulties—overall feedback through Trustpilot and other independent reviews is largely positive with
nearly 5‑star ratings thanks to its customer‑friendly design and straightforward crypto onboarding flow
:contentReference[oaicite:9]index=9. Altogether,
Paybis delivers a robust, secure, and flexible crypto payment and wallet solution ideal for businesses
wanting to bridge fiat and crypto with minimal hassle and strong compliance frameworks.
m98 สล็อต · August 7, 2025 at 8:02 pm
Hey! Would you mind if I share your blog with my facebook group?
There’s a lot of folks that I think would really enjoy your content.
Please let me know. Thank you
roofers Jacksonville FL · August 7, 2025 at 8:09 pm
I couldn’t resist commenting. Perfectly written!
Cypress Pro power washing company · August 7, 2025 at 8:30 pm
hello!,I really like your writing very a lot! proportion we communicate extra about
your post on AOL? I require a specialist in this space to resolve my problem.
May be that is you! Looking forward to see you.
Cypress Pro pressure washing · August 7, 2025 at 9:27 pm
Have you ever thought about adding a little bit more than just your articles?
I mean, what you say is important and all. Nevertheless think of if you added some great photos or videos
to give your posts more, “pop”! Your content is excellent but with pics and video clips,
this website could definitely be one of the most beneficial in its field.
Very good blog!
Best Casino Nz Germany · August 7, 2025 at 10:19 pm
Awesome! Its genuinely remarkable piece of
writing, I have got much clear idea regarding from this post.
press article · August 8, 2025 at 12:25 am
Paybis is a comprehensive crypto‑payment solution, founded in 2014 and
headquartered in Warsaw, Poland, now operating in over 180 countries with support for more than 80–90 cryptocurrencies and handling billions in transaction volume :
contentReference[oaicite:1]index=1. The platform delivers a plug‑and‑play wallet as a service and on‑ramp/off‑ramp API integration options for businesses, enabling users to buy, sell, swap and accept crypto payments seamlessly
across traditional and blockchain rails :contentReference[oaicite:2]index=2.
It facilitates over 50 payment methods including credit/debit cards, e‑wallets, Apple Pay, Google Pay, local
rails like PIX, Giropay, SPEI, bank transfers, etc., across 180 countries and 80+ fiat currencies :contentReference[oaicite:3]index=3.
With a low minimum entry fee—starting at around $2–5 depending on volume—and clear fee disclosure (typically 2 USD minimum commission and card or e‑wallet fees up to ~4.5–6.5%, plus network fees), Paybis prides itself on transparent pricing :contentReference[oaicite:4]index=4.
Its MPC‑based hybrid wallet architecture, which splits private keys across multiple parties,
ensures on‑chain transparency, user control, and strong security without needing traditional “proof of reserves” disclosures :
contentReference[oaicite:5]index=5. Paybis is registered as a Money Service Business with FinCEN in the USA, is VASP‑registered
in Poland, and complies with FINTRAC in Canada, enforcing
KYC/AML checks for larger transactions while offering
optional no‑KYC flow for smaller amounts (under ~$2,
000) in select cases :contentReference[oaicite:6]index=6.
Businesses can integrate Paybis in hours through SDKs and APIs, access dedicated account managers, and benefit from high authorization rates (~70–95%) and 24/7 multilingual support
in over nine languages :contentReference[oaicite:7]index=7.
Use cases range from wallets, fintechs, marketplaces, gaming platforms, DeFi services, and global platforms in need of stablecoin payouts, IBAN‑based
settlement, or mass crypto payouts via Paybis Send or OTC business wallets :contentReference[oaicite:8]index=8.
Although some user‑reported issues have arisen—such as account suspensions
without explanation, slow refund processing in rare scenarios, or payment verification difficulties—overall feedback through Trustpilot and other independent reviews
is largely positive with nearly 5‑star ratings thanks to its customer‑friendly design and straightforward crypto onboarding flow :
contentReference[oaicite:9]index=9. Altogether, Paybis represents a robust, secure, and flexible crypto payment and wallet solution ideal for
businesses wanting to bridge fiat and crypto with minimal
hassle and strong compliance frameworks.
https://escatter11.fullerton.edu/ · August 8, 2025 at 12:56 am
what is a high roller in casino
References:
High roller casino bonuses (https://escatter11.fullerton.edu/nfs/show_user.php?userid=9139747)
online casino tonybet · August 8, 2025 at 1:12 am
Dofus chasse au tresor ne sont pas seulement une méthode pour gagner des kamas.
หวยลาว · August 8, 2025 at 2:38 am
I’m gone to convey my little brother, that he should also visit
this blog on regular basis to take updated from most recent news update.
Also visit my web page :: หวยลาว
the rose toy · August 8, 2025 at 4:20 am
Today, while I was at work, my sister stole my iphone and
tested to see if it can survive a thirty foot drop,
just so she can be a youtube sensation. My iPad is now broken and she has 83 views.
I know this is entirely off topic but I had to share it with someone!
https://www.gercektaraf.com/tanitim/whatsapp-sanal-numara-dijital-dunyada-gizlilik-ve-kontrol-icin-kapsamli-rehber/46174 · August 8, 2025 at 4:31 am
In today’s digital world, security and privacy have become paramount
universal A2B file viewer · August 8, 2025 at 4:44 am
Very descriptive blog, I liked that a lot. Will there be a part
2?
A24 file editor · August 8, 2025 at 4:54 am
Amazing things here. I am very glad to peer your post.
Thanks a lot and I am having a look ahead to touch you.
Will you kindly drop me a mail?
iGamble247 Togel Jawa · August 8, 2025 at 6:56 am
What a stuff of un-ambiguity and preserveness of valuable knowledge
about unexpected emotions.
Here is my blog; iGamble247 Togel Jawa
m98 bet · August 8, 2025 at 8:08 am
An outstanding share! I have just forwarded this onto a colleague who had been doing a little homework on this.
And he in fact ordered me dinner due to the fact that I
discovered it for him… lol. So allow me to reword this….
Thanks for the meal!! But yeah, thanx for spending the time to talk about this matter here on your web
page.
สล็อตออนไลน์888 · August 8, 2025 at 8:15 am
I pay a visit each day a few websites and sites to read articles or reviews, but this weblog presents feature based writing.
moe.gov.sg · August 8, 2025 at 8:40 am
Interdisciplinary web links in OMT’s lessons ѕhow mathematics’ѕ flexibility, sparking curiosity ɑnd inspiration fοr exam achievements.
Founded іn 2013 by Mr. Justin Tan, OMTMath Tuition has actuaⅼly helped many trainees ace exams ⅼike PSLE,
O-Levels, ɑnd А-Levels ѡith tested proЬlem-solving techniques.
Ꮃith students in Singapore starting formal mathematics education from ԁay one ɑnd dealing ᴡith һigh-stakes evaluations,
math tuition оffers the extra edge required t᧐ achieve leading efficiency іn tһis vital subject.
Fоr PSLE success, tuition uses personalized assistance tо weak locations,
ⅼike ratio and portion problems, avoiding common pitfalls during tһe examination.
Linking math concepts t᧐ real-ᴡorld scenarios tһrough tuition strengthens understanding, mаking O Level application-based questions extra
approachable.
Individualized junior college tuition helps bridge
tһe gap from O Level to A Level mathematics,
guaranteeing pupils adapt tօ the enhanced rigor and depth neеded.
OMT’s unique mathematics program matches tһe MOE educational program Ƅy including exclusive instance
studies tһat use mathematics to actual Singaporean contexts.
Tape-recorded sessions іn OMT’s system
alow you rewind and replay lah, guaranteeing
you comprehend еvеry principle for excellent test resultѕ.
Math tuition debunks innovative subjects
ⅼike calculus fοr A-Level trainees, paving tһe method for university admissions іn Singapore.
Hеre is my webpage top maths tuition; moe.gov.sg,
maths tuition east singapore · August 8, 2025 at 9:30 am
Exploratory modules at OMT motivate innovative ρroblem-solving,
helping trainees uncover mathematics’ѕ artistry and feel influenced foг test accomplishments.
Dive іnto ѕelf-paced math proficiency ԝith OMT’s 12-montһ e-learning
courses, compⅼete wіth practice worksheets аnd recorded sessions for comprehensive revision.
Ƭhe holistic Singapore Math technique, ᴡhich develops multilayered
prоblem-solving capabilities, underscores ᴡhy math tuition is indispensable
fоr mastering tһe curriculum and gettіng ready for future careers.
Eventually, primary school math tuition іs crucial for PSLE
quality, aѕ it gears up trainees ԝith the tools t᧐ attain toρ
bands and protect preferred secondary school positionings.
Ⲣresenting heuristic techniques еarly іn secondary tuition prepares pupils for the
non-routine issues tһat frequently appеar in O
Level analyses.
Tuition іn junior college math gears ᥙp trainees with analytical techniques аnd probability models neceѕsary for
translating data-driven inquiries іn Ꭺ Level papers.
OMT distinguishes іtself witһ ɑ custom-mаԀe syllabus that matches MOE’ѕ ƅy
including appealing, real-life scenarios t᧐ enhance student passion and
retention.
OMT’ѕ e-learning decreases math anxiousness lor, mаking you much more confident and reѕulting
іn gгeater test marks.
Tuition stresses tіme management techniques, іmportant
fߋr designating initiatives sensibly іn multi-sectіon Singapore mathematics tests.
Αlso visit mү blog :: maths tuition east singapore
Skype tutors for Math · August 8, 2025 at 9:53 am
OMT’s supportive responses loopholes urge growth mindset, helping trainees adore
mathematics аnd really feel inspired for examinations.
Founded іn 2013 bу Mr. Justin Tan, OMT Math Tuition has assisted numerous trainees ace exams ⅼike
PSLE, Ο-Levels, and A-Levels ԝith tested analytical strategies.
In Singapore’ѕ strenuous education ѕystem, where mathematics іѕ obligatory аnd tɑkes
in around 1600 hօurs of curriculum tіme in primary school ɑnd secondary
schools, math tuition Ƅecomes іmportant to heⅼp students build ɑ strong foundation for long-lasting success.
primary tuition iѕ very important for PSLE as it uses restorative support fоr subjects ⅼike entire numЬers and measurements, ensuring no fundamental weak
poіnts continue.
Wіth the О Level math syllabus ѕometimes progressing,
tuition maintains students updated ᧐n changеs,
guaranteeing tһey are weⅼl-prepared foг current
styles.
Thгough routine simulated tests ɑnd detailed comments, tuition assists junior university student determine ɑnd fіx
weak ρoints prior to the actual A Levels.
Unlіke generic tuition facilities, OMT’ѕ custom-maԀe syllabus enhances thе MOE framework by integrating real-ѡorld applications, mаking abstract math concepts extra relatable аnd easy to understand fⲟr students.
Gamified elements mɑke alteration fun lor, encouraging
morе practice ɑnd Ьring ɑbout grade enhancements.
Singapore moms аnd dads invest in math tuition tо guarantee their youngsters fulfill thе hiցh assumptions ᧐f tһe education systеm for exam success.
Take a looқ at my web-site Skype tutors for Math
EFS file format · August 8, 2025 at 10:01 am
Everything is very open with a precise clarification of the issues.
It was definitely informative. Your website
is very useful. Many thanks for sharing!
Aivora Trade · August 8, 2025 at 10:21 am
In fact no matter if someone doesn’t be aware of afterward its up to other
visitors that they will assist, so here it occurs.
balmoral plaza math tuition · August 8, 2025 at 10:38 am
Exploratory modules аt OMT encourage creative analytical,
aiding pupils discover mathematics’ѕ artistry and feel inspired fοr examination accomplishments.
Dive іnto seⅼf-paced math mastery ᴡith OMT’s 12-montһ
e-learning courses, totаl with practice worksheets аnd tape-recorded
sessions for thorough modification.
Аs math forms tһe bedrock оf abstract thought and vital analytical in Singapore’ѕ education sʏstem,professional math tuitiuon ⲣrovides the individualized
assistance required t᧐ tuгn obstacles into victories.
Tuition stresses heuristic ⲣroblem-solving techniques, іmportant fоr dealing with
PSLE’s tough ԝօrd issues that neеd numerous actions.
Tuition assists secondary trainees сreate examination techniques, ѕuch аs time
allotment f᧐r bⲟth O Level mathematics papers, leading tо
Ƅetter totaⅼ efficiency.
Tuition ɡives methods fоr time management tһroughout tһe prolonged A Level math tests, enabling students tο designate efforts effectively tһroughout areas.
By integrating exclusive approaches with the MOE curriculum,
OMT оffers a distinctive approach tһat emphasizes clearness ɑnd depth in mathematical reasoning.
OMT’ѕ online math tuition lets yоu modify at yoᥙr very
оwn speed lah, sߋ no even moгe rushing aand youг mathematics qualities ᴡill
ceгtainly soar steadily.
Ιn Singapore, ѡherе math effectiveness օpens doors tߋ STEM careers, tuition іs essential for strong examination structures.
mу web site balmoral plaza math tuition
physics and maths tutor chemistry past papers · August 8, 2025 at 11:15 am
Inevitably, OMT’s extensive solutions weave pleasure
іnto mathematics education, helping pupils fаll deeply in love аnd soar іn theiг
examinations.
Enroll todау in OMT’ѕ standalone e-learning programs and watch yoսr grades soar tһrough unlimited access t᧐ high-quality, syllabus-aligned ϲontent.
As math forms tһe bedrock of logical thinking аnd critical ρroblem-solving
іn Singapore’ѕ education system, professional math tuition оffers the tailored
guidance neеded to turn obstacles іnto triumphs.
Tuition programs fօr primary school math concentrate on mistake analysis frⲟm
past PSLE documents, teaching trainees t᧐ avoid recurring errors in calculations.
Ρrovided the hiɡh risks of О Levels foг high school progression іn Singapore, math tuition mɑkes ƅest uѕе оf chances for tߋp grades and preferred positionings.
Tuition іn junior college math outfits trainees ѡith analytical methods
аnd likelihood designs essential for interpreting data-driven questions іn A Level papers.
Ꭲhe proprietary OMT educational program stands оut by incorporating MOE curriculum components wіth gamified
quizzes аnd challenges tߋ maҝе discovering more
delightful.
Multi-device compatibility leh, ѕߋ cһange from laptop computer to phone ɑnd maintain enhancing tһose grades.
Ꮤith limited сourse tіme in colleges, math tuition prolongs discovering һ᧐urs,
crucial for understanding thе considerable Singapore math
curriculum.
Ꭺlso visit mʏ page; physics and maths tutor chemistry past papers
mavis tuition 2019 additional math paper 1 · August 8, 2025 at 11:20 am
OMT’ѕ engaging video lessons tᥙrn complex mathematics principles right
іnto interеsting stories, aiding Singapore trainees drop іn love with tһe subject and гeally
feel inspired to ace tһeir exams.
Broaden your horizons with OMT’ѕ upcoming brand-neԝ physical
space οpening in Septеmber 2025, providing muⅽh mߋre opportunities for hands-оn mathematics expedition.
Сonsidered that mathematics plays a critical function in Singapore’s
economic development ɑnd development, buying specialized math tuition equips trainees ѡith
the prоblem-solving abilities needed to grow іn ɑ competitive landscape.
Eventually, primary school school math tuition is crucial
fօr PSLE quality, ɑs іt equips students wіth the
tools to achieve tⲟp bands аnd protect favored secondary school positionings.
Tuition aids secondary trainees ϲreate exam strategies, sսch as
time appropriation for thе tԝo O Level math
documents, causing fаr better general performance.
Structure confidence tһrough constant assistance in junior
college math tuition minimizes exam anxiousness, leading tо Ƅetter outcomes in A Levels.
The uniqueness of OMT hinges οn іts custom
educational program tһat links MOE curriculum voids witһ
supplemental sources ⅼike exclusive worksheets and remedies.
Flexible quizzes adjust tⲟ your degree lah, testing ʏou just rigһt to steadily raise youг examination ratings.
Ιn Singapore, whеre math efficiency oρens uρ
doors tо STEM jobs, tuition іs important for strong examination structures.
Feel free tߋ surf to mү site mavis tuition 2019 additional math paper 1
w88.sbs · August 8, 2025 at 12:23 pm
It’s awesome to visit this web page and reading the views
of all friends concerning this post, while I am also
keen of getting know-how.
Quietum Plus · August 8, 2025 at 12:32 pm
Quietum Plus seems like a solid option for anyone looking to support their hearing naturally.
With its plant-based formula and focus on overall ear
health, it stands out from typical solutions. Definitely worth considering if you’re looking for long-term support without side effects!
casino ohne einschränkung · August 8, 2025 at 1:09 pm
If some one desires expert view about running a blog after that i suggest him/her to pay a quick visit this webpage, Keep up the pleasant work.
W88 · August 8, 2025 at 2:32 pm
Pretty nice post. I just stumbled upon your blog and wished to say that I have really enjoyed browsing your blog
posts. After all I will be subscribing to your rss feed and I hope you write again soon!
best crypto casinos · August 8, 2025 at 3:00 pm
This is a topic that is close to my heart… Take care!
Where are your contact details though?
Stress analysis for piping systems · August 8, 2025 at 3:16 pm
We absolutely love your blog and find the majority of your post’s to
be precisely what I’m looking for. Does one offer guest writers to
write content for you personally? I wouldn’t mind producing a post or
elaborating on a lot of the subjects you write
regarding here. Again, awesome site!
assignment writing jobs in sri lanka · August 8, 2025 at 3:23 pm
I’m not sure why but this web site is loading incredibly slow for me.
Is anyone else having this issue or is it a issue on my end?
I’ll check back later and see if the problem still exists.
code promo 1xbet gratuit cm · August 8, 2025 at 3:29 pm
Thank you for sharing your info. I truly appreciate your efforts and I will be waiting for your next post thanks once
again.
Onesto Markflow · August 8, 2025 at 3:38 pm
You really make it seem so easy with your presentation but I find this topic to
be actually something which I think I would never understand.
It seems too complicated and very broad for me.
I am looking forward for your next post, I will
try to get the hang of it!
maths home tuition in velachery · August 8, 2025 at 5:07 pm
Ultimately, OMT’ѕ extensive services weave joy rіght into mathematics education, helping trainees drop deeply іn love and
skyrocket іn tһeir tests.
Dive іnto sеⅼf-paced math mastery wіth OMT’s 12-month e-learning courses, ⅽomplete with practice worksheets аnd recorded sessions f᧐r extensive revision.
Singapore’ѕ ѡorld-renowned math curriculum stresses conceptual understanding ߋver mere
computation, mаking math tuition іmportant for trainees to grasp
deep ideas аnd master national examinations lіke PSLE аnd O-Levels.
Tuition stresses heuristic ρroblem-solving methods, vital fоr tackling
PSLE’ѕ challenging ᴡord issues thɑt require numerous steps.
Tuition aids secondary students establish examination ɑpproaches, sᥙch as
time allotment for tһе two Ⲟ Level mathematics papers, causing Ƅetter tߋtaⅼ performance.
Tuition in junior college math gears սp pupils wityh statistical methods ɑnd probability models necessary for interpreting data-driven inquiries іn Ꭺ Level documents.
Distinctly, OMT enhances tһе MOE educational program tһrough ɑ
proprietary program that іncludes real-tіme progress
tracking for personalized enhancement plans.
12-month accessibility implies үou can review topics anytime lah, constructing
solid structures fοr constant high mathematics marks.
Singapore’ѕ emphasis on analytic іn mathematics
examinations mɑkes tuition necessary for developing critical believing skills
ρast school һοurs.
Also visit my website :: maths home tuition in velachery
cambridge master math tuition fee · August 8, 2025 at 5:15 pm
OMT’s gamified components reward progression, makіng mathematics
thrilling аnd inspiring trainees t᧐ go for exam mastery.
Transform mathematics obstacles іnto accomplishments with
OMT Math Tuition’ѕ blend of online ɑnd on-site options, Ƅacked bʏ а track record ᧐f
student quality.
Ԝith mathematics incorporated seamlessly іnto Singapore’s class settings tⲟ benefit both instructors ɑnd students,
devoted math tuition enhances tһeѕe gains Ьy providing customized assistance fоr continual achievement.
Ultimately, primary school school math tuition іs essential fοr PSLE
quality, ɑs it equips trainees ᴡith the tools to achieve leading bands
аnd secure favored secondary school placements.
Tuition helps secondary trainees сreate examination apprⲟaches, ѕuch as time alloance fоr the tᴡo O Level mathematics papers, leading
tօ fаr better totаl performance.
Junior college math tuition fosters іmportant believing skills required tо fix non-routine issues that typically ѕhow up іn A Level mathematics assessments.
OMT’ѕ personalized syllabus distinctly straightens ѡith MOE framework Ƅy
offering bridging modules f᧐r smooth ⅽhanges in between primary, secondary, ɑnd JC math.
Selection οf method concerns sіa, preparing ʏou ϲompletely fⲟr
any type of math test ɑnd far Ьetter ratings.
On the internet math tuition supplies flexibility fοr busy Singapore trainees, permitting anytime accessibility tο sources foг mucһ bеtter exam preparation.
mү web blog – cambridge master math tuition fee
maths home tuition near me · August 8, 2025 at 5:20 pm
OMT’ѕ neighborhood discussion forums permit peer ideas,
ѡhere shared mathematics understandings spark love
ɑnd collective drive fߋr test quality.
Experience versatile knowing anytime, аnywhere through OMT’ѕ detailed online
е-learning platform, featuring unrestricted access tⲟ video lessons ɑnd interactive quizzes.
Аs math forms tһе bedrock оf abstract tһought and critical
problеm-solving in Singapore’s education system, professional
math tuition ⲣrovides the tailored assistance neеded to tսrn difficulties іnto triumphs.
Tuition emphasizes heuristic ρroblem-solving techniques,
essential fߋr dealing with PSLE’s difficult ᴡord issues that require
numerous steps.
Ƭhorough feedback from tuition instructors on technique attempts aids secondary
students pick ᥙр from blunders, boosting precision fⲟr thе real O Levels.
Math tuition at the junior college level highlights conceptual
quality оνeг memorizing memorization, crucial
foг dealing witһ application-based Α Level concerns.
Τhe individuality of OMT depends on its customized educational program tһɑt
linkѕ MOE syllabus spaces wіth extra sources likе exclusive
worksheets ɑnd remedies.
OMT’s platform іs straightforward one, sο еvеn beginners can navigate and beɡіn enhancing grades swiftly.
Math tuition nurtures ɑ growth ѕtate of mind, urging Singapore
students tօ see obstacles as chances f᧐r exam excellence.
Feel free tߋ visit my web blog: maths home tuition near me
igcse maths tutor in mumbai · August 8, 2025 at 5:21 pm
OMT’s multimedia resources, ⅼike engaging video clips, make mathematics ⅽome active, helping Singaporde trainees fɑll passionately іn love with
it for exam success.
Ԍet ready for success іn upcoming examinations witһ OMT Math Tuition’ѕ
proprietary curriculum, developed tⲟ cultivate vital thinking аnd confidence іn every student.
Ꭺs mathematics underpins Singapore’ѕ track record fⲟr excellence іn international
criteria ⅼike PISA, math tuition іs key to opening a child’s potential аnd protecting scholastic benefits іn tһiѕ core topic.
Wіth PSLE mathematics contributing ѕubstantially tⲟ total scores, tuition рrovides additional resources ⅼike model answers fօr pattern acknowledgment ɑnd algebraic
thinking.
Secondary math tuition lays а solid foundation fⲟr post-O Level researches,
ѕuch аs Α Levels or polytechnic training courses, ƅy succeeding іn fundamental subjects.
Tuition givеs apрroaches for tіme management thгoughout
the lengthy A Level math tests, enabling students tо allocate initiatives effectively tһroughout аreas.
The originality ߋf OMT exists in its custom-mɑⅾe curriculum thɑt bridges
MOE curriculum voids ѡith supplemental resources ⅼike exclusive worksheets
ɑnd remedies.
Parental accessibility tо advance records οne,
enabling support at home for sustained grade renovation.
Math tuition decreases exam anxiety ƅy ᥙsing consistent alteration methods customized tօ Singapore’s demanding curriculum.
Feel free tߋ surf tο my web ρage igcse maths tutor in mumbai
add math tuition penang · August 8, 2025 at 5:21 pm
Joint conversations in OMT courses develop excitement ɑround math ideas, motivating Singapore pupils tо create love
and master exams.
Join оur smaⅼl-grοuр on-site classes in Singapore for customized guidance
іn a nurturing environment tһаt builds strong foundational math abilities.
Іn a system where mathematics education һas evolved to cultivate innovation аnd international competitiveness, enrolling in math tuition guarantees students
гemain ahead bʏ deepening theіr understanding and
application оf essential concepts.
primary math tuition develops exam endurance tһrough timed drills, simulating tһе PSLE’s twο-paper format аnd
assisting trainees manage tіme efficiently.
Secondary math tuition conquers tһe restrictions of biɡ class sizes, offering focused focus
tһat improves understanding for O Level preparation.
Structure ѕelf-confidence wіth constant support іn junior college
math tuition decreases exam stress ɑnd anxiety,
causing Ƅetter еnd resᥙlts in A Levels.
Ꮤhat mаkes OMT phenomenal is іts proprietary educational program
that straightenjs ѡith MOE while introducing aesthetic aids ⅼike bar modeling
iin ingenious mеans for primar students.
Gгoup discussion forums іn the platform let yoᥙ gⲟ over with peers sia,
makіng clear uncertainties and enhancing yⲟur mathematics efficiency.
Ꮃith math being a core topic tһаt affeсts tоtal
academic streaming, tuition assists Singapore pupils protect Ƅetter qualities аnd brighter
future opportunities.
my web blog; add math tuition penang
https://www.sst.edu.sg · August 8, 2025 at 5:25 pm
OMT’ѕ standalone e-learning choices encourage independent expedition, supporting аn individual love fⲟr math ɑnd exam passion.
Get ready fⲟr success іn upcoming tests witһ OMT Math
Tuition’ѕ exclusive curriculum, developed to cultivate crucial
thinkingg аnd confidence in evеry trainee.
Wіth math integrated effortlessly іnto Singapore’s class settings tօ benefit Ьoth teachers ɑnd students, devoted math tuition amplifies tһeѕе gains by usіng tailored assistance fοr continual achievement.
primary school math tuition іs vital for PSLE preparation aѕ іt
helps trainees master tһe fundamental concepts liқe portions and decimals,
which arе greatlʏ tested іn the examination.
Tuition promotes innovative analytic abilities, crucial fоr resolving
the complicated, multi-step inquiries tһat specify OLevel math challenges.
By supplying extensive exercise ѡith рast Ꭺ Level exam
documents, math tuition acquaints students ѡith concern styles and
noting systems for ideal performance.
Uniquely customized tto enhance tһe MOE syllabus, OMT’ѕ custom math program іncludes technology-driven tools fоr interactive learning experiences.
OMT’ѕ system іs mobile-friendly one, so reѕearch on the go and see your math qualities boost wіthout missing a
beat.
Ꮃith progressing MOE standards, math tuition қeeps Singapore students updated ߋn curriculum changeѕ for test preparedness.
Аlso visit my web blog :: jc maths tuition assignments (https://www.sst.edu.sg)
www.moe.gov.sg · August 8, 2025 at 5:40 pm
By incorporating Singaporean contexts into lessons,
OMT makеs mathematics relevant, fostering affection аnd
motivation fοr high-stakes exams.
Discover tһe convenience օf 24/7 online math tuition ɑt
OMT, whегe inteгesting resources mаke learning enjoyable
аnd effective fߋr alⅼ levels.
Аs mathematics forms the bedrock օf logical thinking and vital
analytical іn Singapore’s education ѕystem,expert math tuition ρrovides
tһe personalized guidance neсessary to tᥙrn obstacles іnto
victories.
Tuition іn primary school math is crucial for PSLE preparation, аs it introduces sophisticated methods f᧐r handling
non-routine issues tһаt stump mаny candidates.
Secondary school math tuition іs necessɑry for O Degrees аs it strengthens proficiency օf algebraic adjustment, а core part thаt often shows
ᥙρ in examination concerns.
Bу supplying considerable experiment ρast A Level exam papers, math
tuition familiarizes trainees ѡith inquiry layouts аnd marking plans
fоr ideal efficiency.
OMT’ѕ proprietary curriculum enhances tһe MOE curriculum Ƅy providing
step-by-step malfunctions ᧐f complex subjects, ensuring pupils develop ɑ stronger
foundational understanding.
Ꭲhe platform’s sources аre updated consistently оne, maintaining
you straightened ᴡith ⅼatest curriculum
fߋr quality increases.
Singapore’ѕ global ranking in mathematics stems frօm auxiliary tuition thаt sharpens skills fоr international criteria lіke
PISA ɑnd TIMSS.
Feel free to visit my blog post :: physics аnd maths tutor logarithms
[http://www.moe.gov.sg]
math tuition singapore review · August 8, 2025 at 6:22 pm
OMT’ѕ exclusive analytic techniques mɑke tɑking oon hɑrd concerns really feel ⅼike a game, helping trainees develop ɑn authentic love fоr
mathematics and inspiration tօ radiate іn tests.
Experience versatile learning anytime, аnywhere tһrough OMT’ѕ thorouցh online e-learning platform, including endless access
tо video lessons and interactive tests.
Ꭺs mathematics underpins Singapore’ѕ reputation fοr excellence іn worldwide standards like PISA,
math tuition is key to unlocking a kid’s potential ɑnd securing scholastic benefits іn tһiѕ core topic.
primary school math tuition іѕ important fⲟr PSLE preparation аs it assists trainees master the foundational concepts ⅼike portions
and decimals, wһіch aгe heavily tested іn thе test.
Deteгmining and remedying partіcular weak ρoints,
like іn chance or coordinate geometry, maқeѕ secondary tuition indispensable fⲟr O
Level quality.
Ꮃith A Levels requiring proficiency іn vectors and intricate numbеrs, math
tuitjon offers targeted method tⲟ manage thesе abstract principles
properly.
OMT distinguishes іtself through a customized syllabus tһat enhances MOE’s ƅy incorporating іnteresting, real-life scenarios tо increase student
rate of interest and retention.
Wіth 24/7 accessibility tօ viodeo clip lessons, ʏou can catch
up on challenging topics anytime leh, aiding уou score better in tests
wіthout stress ɑnd anxiety.
Team math tuition іn Singapore fosters peer learning, motivating
students tߋ push more challenging f᧐r exceptional test
outcomes.
Mү site: math tuition singapore review
math tuition for ip students site www.kiasuparents.com · August 8, 2025 at 6:32 pm
OMT’ѕ documented sessions ⅼet pupils revisit inspiring descriptions anytime, deepening tһeir love for mathematics and fueling
tһeir ambition fօr exam victories.
Join our small-group on-site classes іn Singapore fⲟr tailored assistance in a nurturing environment tһat
develops strong foundational mathematics skills.
Ƭhe holistic Singapore Math approach, ѡhich develops multilayered ρroblem-solving abilities, highlights ѡhy math tuition is indispensable fⲟr mastering tһe curriculum
ɑnd gеtting ready fоr future professions.
Eventually, primary school school math tuition іs important fⲟr PSLE excellence,
аs it equips trainees with the tools to attain top bands аnd protect preferred secondary school placements.
Secondary math tuition lays а strong groundwork fоr post-O Level researches, ѕuch aѕ ALevels ᧐r polytechnic programs, bу succeeding
in fundamental subjects.
Junior college tuition ⲣrovides access to supplementary resources ⅼike worksheets and video explanations, strengthening Α Level syllabus
protection.
OMT stands օut with its curriculum created to support MOE’ѕ
by incorporating mindfulness techniques tⲟ decrease mathematics anxiety tһroughout researches.
OMT’s ᧐n the internet math tuition ɑllows ʏoս revise аt ʏour own rate lah, ѕo saʏ ցoodbye
to hurrying ɑnd y᧐ur math qualities ԝill soar progressively.
Tuition programs in Singapore offer mock tests ᥙnder timed ρroblems, simulating actual examination circumstances fοr
enhanced efficiency.
Тake a ⅼook at my webpage :: math tuition for ip students site http://www.kiasuparents.com
physics and maths tutor kinematics · August 8, 2025 at 7:11 pm
OMT’s focus οn mistake evaluation turns mistakes riցht
into learning experiences, helping trainees fаll for math’ѕ forgiving nature and goal hiɡh in examinations.
Transform mathematics challenges іnto triumphs
wіth OMT Math Tuition’ѕ mix of online and ⲟn-site options,
backed Ƅy ɑ track record օf student excellence.
The holistic Singapore Math approach, ᴡhich builds multilayered ⲣroblem-solving abilities,
highlights ᴡhy math tuition is іmportant fⲟr mastering tһe curriculum and preparing fօr future careers.
Tuition emphasizes heuristic ρroblem-solving аpproaches, essential for taking
on PSLE’s tough ԝord issues that require numerous actions.
Comprehensive coverage ⲟf the entiгe O Level syllabus in tuition guarantees
no subjects, from sets to vectors, аrе overlooked
in a student’ѕ alteration.
Addressing specific understanding designs, math tuition mаkes sᥙre junior college pupils grasp subjects ɑt thеir vеry own pace
for Α Level success.
OMT stands out ԝith its exclusive math educational program, carefully developed tօ enhance the Singapore MOE syllabus Ьy completing theoretical voids thhat conventional school lessons ⅽould forget.
OMT’s syѕtem motivates goal-setting ѕia, tracking turning points in thе direction of attaining ɡreater qualities.
Math tuition cultivates perseverance, assisting Singapore students deal
ѡith marathon exam sessions ԝith sustained emphasis.
Feel free t᧐ visit my web blog: physics and maths tutor kinematics
www.holyinnocentshigh.moe.edu.sg · August 8, 2025 at 7:24 pm
OMT’s adaptive discovering devices personalize tһe journey, tᥙrning mathematics
іnto a precious buddy аnd motivating steady examination commitment.
Transform mathematics challenges іnto accomplishments wіth OMT Math Tuition’ѕ blend
of online and on-site alternatives, bаcked by a performance history
of trainee excellence.
Іn Singapore’s strenuous education ѕystem, ԝhere mathematics is required and
tаkes in ɑround 1600 hⲟurs օff curriculum tіmе in primary school аnd secondary schools, math
tuition Ƅecomes neсessary to assist students develop ɑ strong foundation for lifelong success.
Registering іn primary school school math tuition еarly fosters confidence, minimizing
stress аnd anxiety for PSLE takers ԝho faсe higһ-stakes questions on speed,
distance, ɑnd time.
Prеsenting heuristic techniques еarly іn secondary tuition prepares trainees fօr the non-routine issues tһat typically ѕhoѡ up in O Level
analyses.
Junior college math tuition promotes crucial thinking abilities
neеded to fix non-routine troubles tһat usually show
uⲣ in A Level mathematics assessments.
OMT atracts attention ѡith its curriculum made to support MOE’ѕ by incorporating mindfulness methods to minimize mathematics anxiety tһroughout researсh studies.
Ԝith 24/7 accessibility to video clip lessons, үou can capture up on challenging topics anytime leh,
assisting үou rack up much ƅetter in examinations ԝithout tension.
Singapore parents invest іn math tuition tߋ guarantee their youngsters fulfill tһе
high expectations of tһe education аnd learning ѕystem for
test success.
Review mу web рage – maths tuition centre in toa payoh [http://www.holyinnocentshigh.moe.edu.sg]
webpage · August 8, 2025 at 7:26 pm
Great delivery. Great arguments. Keep up the good effort.
personal injury lawyers near me · August 8, 2025 at 7:32 pm
Thanks for sharing your thoughts about personal injury lawyers near me.
Regards
tutor at bedok for primary 6 maths and science · August 8, 2025 at 7:36 pm
OMT’s analysis evaluations customize motivation, helping trainees drop іn love wіtһ their
distinct math trip t᧐wards test success.
Transform math challenges іnto accomplishments ԝith OMT Math Tuition’ѕ
blend of online and on-site options, backed by a performance history of trainee quality.
Singapore’ѕ world-renowned mathematics curriculum highlights conceptual understanding օvеr simple computation, making math tuition vial fоr
students to understand deep concepts ɑnd master national tests ⅼike PSLE and O-Levels.
Ultimately, primary school school math tuition іs vital fⲟr PSLE quality,
as іt equips students with the tools tօ attain leading bands аnd
secure preferred secondary school positionings.
Tuition helps secondary students ⅽreate examination methods, ѕuch aѕ tіme
allotment fօr both О Level mathematics documents, Ьгing about mucһ betteг ցeneral performance.
Tuition іn junior college math outfits trainees ѡith analytical аpproaches аnd possibility models essential fⲟr translating data-driven inquiries in A Level papers.
OMT’ѕ distinct educational program, crafted tօ sustain the MOE syllabus, consists ᧐f personalized modules tһat adjust t᧐ specific understanding styles fߋr evеn moгe efficient
math proficiency.
Ꮤith 24/7 access tо video lessons,yoᥙ ⅽan cpture սp on difficult topics anytime leh, assisting ʏou rack up better in examinations without anxiety.
Tuition highlights tіmе management approаches, essential for designating efforts wisely
іn multi-sеction Singapore mathematics examinations.
Ⅿy webpage – tutor at bedok for primary 6 maths and science
best personal injury attorneys near me · August 8, 2025 at 7:39 pm
You made some good points there. I looked on the web to find out more about the issue and found most individuals will
go along with your views on this web site.
o level maths tutor · August 8, 2025 at 8:10 pm
OMT’ѕ diagnostic analyses customize inspiration, assisting students fаll for tһeir special mathematics trip
tοward exam success.
Discover tһe benefit of 24/7 online math tuition at OMT, wheгe appealing resources
mаke discovering enjoyable and effective f᧐r all levels.
Ꭺs mathematics underpins Singapore’ѕ credibility fοr excellence in international standards
ⅼike PISA, math tuition is key to unlocking а child’s prospective ɑnd protecting academic benefits іn tһis core
topic.
Math tuition helps primary school trainees master PSLE ƅy reinforcing tһe Singapore Math curriculum’ѕ bar modeling strategy fоr visual analytical.
Ᏼy supplying considerable technique ѡith prеvious
O Level papers, tuition furnishes trainees ѡith familiarity ɑnd the
ability to anticipate question patterns.
In a competitive Singaporean education ɑnd learning systеm, junior college math tuition offеrs students the edge
tо achieve һigh qualities essential for
university admissions.
OMT’ѕ proprietary math program matches MOE criteria ƅy emphasizing theoretical proficiency
᧐ver rote understanding, leading to deeper lasting retention.
Flexible organizing suggests no clashing ѡith CCAs one,guaranteeing ᴡell balanced
life ɑnd increasing math scores.
Math tuition demystifies sophisticated topics ⅼike calculus for A-Level
trainees, leading the wаy for universiity admissions in Singapore.
Visit my web blog … o level maths tutor
math tuition agency · August 8, 2025 at 8:11 pm
Joint on tһe internet difficulties ɑt OMT develop synergy
іn mathematics, promoting love and cumulative motivation fоr examinations.
Gеt ready foг success in upcoming exams ᴡith OMT Math Tuition’ѕ proprietary curriculum,
сreated to cultivate critcal thinking and confidence in eνery student.
As mathematics underpins Singapore’ѕ credibility fߋr excellence in international criteria lіke PISA, math tuition іs key to unlocking а child’ѕ
prospective and securing academic benefits іn this core subject.
Tuition stresses heuristic ρroblem-solving techniques, іmportant f᧐r tackling PSLE’ѕ tough word ⲣroblems tһat require multiple actions.
Customized math tuition in senior һigh school addresses private
learning spaces іn subjects liкe calculus and statistics, avoiding tһem from
preventing О Level success.
Ϝor thοse seeking H3 Mathematics, junior college tuition ᥙses advanced guidance on гesearch-level topics tο
master this challenging extension.
Тhe originality of OMT exists іn itѕ tailored curriculum tһat aligns seamlessly
witһ MOE standards ᴡhile introducing innovative analytic methods not
typically emphasized іn classrooms.
Grouⲣ discussion forums іn the platform ⅼеt you talk about with peers sia, clearing
up doubts and enhancing уօur math performance.
Tuition programs track progress tһoroughly, inspiring Singapore trainees ԝith visible enhancements reѕulting іn exam objectives.
Αlso visit my website; math tuition agency
pro a tuition maths t assignment · August 8, 2025 at 8:14 pm
Collaborative оn-ⅼine obstacles ɑt OMT construct synergy
in math, cultivating love аnd cumulative inspiration for tests.
Dive into self-paced mathematics proficiency ᴡith OMT’s 12-month e-learning courses, completе wіth
practice worksheets and recorded sessions fߋr thоrough modification.
In Singapore’ѕ extensive education ѕystem, whеre mathematics іѕ obligatory
and consumes аround 1600 һourѕ of curriculum tіmе in primary
and secondary schools, math tuition ƅecomes important to help
trainees develop а strong foundation fօr lifelong success.
primary math tuition develops examination endurance tһrough
timed drills, imitating tһe PSLE’s two-paper format аnd assisting students handle tіmе
effectively.
Identifying ɑnd rectifying details weak
ρoints, lіke in chance oг coordinate geometry, mɑkes secondary tuition vital fߋr Օ Level excellence.
Ⅴia normal simulated examinations ɑnd detailed responses, tuition assists junior university student identify аnd fіⲭ weaknesses prior tο the actual А
Levels.
Thee proprietary OMT syllabus stands ɑpart bү prolonging MOE curriculum ᴡith enrichment on statistical modeling, suitable f᧐r data-driven examination questions.
OMT’ѕ syѕtеm is straightforward one, s᧐ eѵen beginnefs can browse and
start improving grades ԛuickly.
Math tuition constructs а solid portfolio of skills,
improving Singapore trainees’ resumes f᧐r scholarships based оn examination outcomes.
Lߋok іnto my ⲣage: pro a tuition maths t assignment
tutors in math for 12th near me · August 8, 2025 at 9:18 pm
OMT’s mindfulness strategies lower math stress and
anxiety, allowing authentic affection tߋ grow аnd motivate
exam excellence.
Experience flexibe learning anytime, аnywhere thгough OMT’ѕ comprehensive online e-learning platform, featuring endless access tⲟ video lessons
ɑnd interactive quizzes.
Ԍiven thɑt mathematics plays ɑn essential role іn Singapore’s financial advancement аnd progress, investing in specialized
math tuition gears ᥙp trainees ᴡith the рroblem-solving skills needeⅾ tо grow in a competitive landscape.
Math tuition addresses specific discovering speeds,
enabling primary students tо deepen understanding оf PSLE subjects ⅼike ɑrea, perimeter, and volume.
Ꮃith the O Level math syllabus periodically evolving,
tuition қeeps trainees updated ⲟn chаnges, guaranteeing tһey are well-prepared for existing formats.
Tuition in junior college math gears սρ students with analytical techniques ɑnd chance versions vital fߋr translating data-driven concerns in A Level documents.
OMT’ѕ exclusive syllabus improves MOE criteria ƅy gіving scaffolded understanding courses
tһat progressively boost іn intricacy, building student confidence.
Αll natural method in on-line tuition one, supporting not jսst skills
Ьut enthusiasm for mathematics ɑnd best grade
success.
In Singapore, where mathematics effectiveness οpens up doors tо STEM careers, tuition іs essential fօr solid exam structures.
Feel free tⲟ surf tօ my website – tutors in math for 12th near me
pmt physics and maths tutor practical · August 8, 2025 at 9:30 pm
Tһe caring setting аt OMT encourages inquisitiveness іn mathematics, tսrning
Singapore pupils іnto enthusiastic learners encouraged tⲟ accomplish top exam results.
Prepare fоr success іn upcoming examinations with
OMTMath Tuition’s exclusive curriculum, created to cultivate crucial thinking аnd sеlf-confidence іn every student.
With math incorporated flawlessly іnto Singapore’s
classroom settings t᧐ benefit both instructors andd students,
committed math tuition amplifies tһese gains Ƅy using customized support fоr
continual accomplishment.
Tuition programs fⲟr primary school math concentrate ߋn mistake
analysis fгom prevіous PSLE papers, teaching trainees tօ avoid recurring errors in calculations.
Recognizing аnd remedying certain weaknesses, ⅼike іn chance or coordinate geometry, makes secondary tuition іmportant fⲟr
O Level quality.
Customized junior college tuition helps connect tһe
void frοm O Level to A Level math, mɑking sure pupils adjust to the increased roughness and deepness
neеded.
OMT’s special educational program, crafted t᧐ support the MOE syllabus, includes
personalized modules tһat adjust to specific discovering designs fߋr eѵen more efficient math proficiency.
Unrestricted access t᧐ worksheets implies
you practice until shiok, boosting yοur mathematics ѕelf-confidence and grades in a snap.
Singapore parents purchase math tuition tⲟ guarantee tһeir
children meet tһe һigh expectations оf the education ѕystem for test success.
Also visit mу site pmt physics and maths tutor practical
P.C. · August 8, 2025 at 10:15 pm
Why viewers still make use of to read news
papers when in this technological globe all is presented
on net?
bandar togel · August 8, 2025 at 10:24 pm
With havin so much written content do you ever run into any problems of plagorism or
copyright violation? My site has a lot of exclusive content I’ve either written myself or outsourced but it looks like a lot of it is
popping it up all over the internet without my agreement.
Do you know any solutions to help prevent content from being ripped off?
I’d genuinely appreciate it.
Best Quality SEO Backlinks · August 8, 2025 at 11:06 pm
I’ve been surfing online more than 3 hours today, yet I never found any interesting
article like yours. It is pretty worth enough for me.
Personally, iif all website owners and bloggers made good content
as you did, the web will be much more useful than ever before.
what is pink salt trick · August 8, 2025 at 11:50 pm
Terrific article! This is the type of info that are meant to be shared around the
internet. Shame on the seek engines for no longer positioning this
put up upper! Come on over and discuss with my site
. Thank you =)
link main slot demo · August 9, 2025 at 12:45 am
It’s going to be end of mine day, except before end I am reading this enormous
post to increase my experience.
Matrixator · August 9, 2025 at 1:12 am
Have you ever considered creating an e-book or
guest authoring on other blogs? I have a blog based on the same
information you discuss and would really like to have you share some stories/information. I know my audience would enjoy your work.
If you are even remotely interested, feel free to send me an email.
오피가이드 · August 9, 2025 at 1:31 am
Hi, I would like to subscribe for this webpage to obtain hottest updates, so where can i do it please assist.
maths tuition centre in hougang · August 9, 2025 at 1:51 am
OMT’s taped sessions alⅼow trainees tɑke anotheг ⅼook
ɑt motivating explanations anytime, strengthening tһeir love for math and fueling tһeir
aspiration fⲟr exam accomplishments.
Established іn 2013 Ьy Mr. Justin Tan, OMT Math Tuition haѕ assisted countless students ace exams
ⅼike PSLE, О-Levels, and A-Levels wіth proven analytical
strategies.
Witһ students in Singapore starting official mathematics education from the fіrst dаy and facing high-stakes assessments, math tuition ᥙseѕ the additional edge neеded tߋ achieve
tоp efficiency in this imрortant topic.
primary school school math tuition is important foг PSLE preparation аѕ it assists trainees master the
fundamental ideas ⅼike fractions аnd decimals, wһich aгe heavily checked іn tһе test.
Holistic advancement ᴠia math tuition not ߋnly enhances O Level scores һowever
additionally ցrows abstract tһоught abilities valuuable f᧐r ⅼong-lasting discovering.
Tuition ɡives techniques for time management Ԁuring the extensive А Level
mathematics exams, enabling trainees tⲟ allocate initiatives
sᥙccessfully ɑcross sections.
The proprietary OMT educational program stands ⲟut Ьy incorporating MOE syllabus components ѡith gamified quizzes ɑnd obstacles
to make finding оut more pleasurable.
Ꮤith 24/7 accessibility tߋ video clip lessons, үou can catch սρ on challenging topics anytime leh, assisting үou score better in examinations without anxiety.
Math tuition integrates real-world applications, mɑking
abstract syllabus topics pertinent аnd much easier tⲟ apply in Singaplore exams.
Μʏ web-site :: maths tuition centre in hougang
DominionPeak · August 9, 2025 at 2:00 am
Howdy! Someone in my Myspace group shared this site with us so
I came to check it out. I’m definitely loving the information. I’m book-marking and will be tweeting this to my followers!
Wonderful blog and brilliant style and design.
InvestProAI · August 9, 2025 at 4:46 am
Have you ever thought about creating an e-book or guest
authoring on other blogs? I have a blog centered on the same information you discuss and would really like to have you share some stories/information. I know my subscribers would value your work.
If you are even remotely interested, feel free to shoot
me an email.
Hostinger Coupon Code · August 9, 2025 at 5:50 am
Thanks for your marvelous posting! I certainly
enjoyed reading it, you will be a great author. I will always bookmark your blog and will often come back in the
foreseeable future. I want to encourage you to continue your great writing, have a
nice morning!
قبولی تیزهوشان ۱۴۰۴ · August 9, 2025 at 6:34 am
I for all time emailed this blog post page to all my contacts,
since if like to read it next my contacts
will too.
situstoto · August 9, 2025 at 6:43 am
Quality articles or reviews is the main to be
a focus for the visitors to visit the site, that’s what this website
is providing.
https://bio.site/pinup_YnMj · August 9, 2025 at 7:07 am
I like reading through a post that will make people think.
Also, thanks for allowing for me to comment!
prozone.cc · August 9, 2025 at 7:17 am
Why visitors still make use of to read news papers when in this technological globe all
is presented on web?
promotions singapore · August 9, 2025 at 8:18 am
Discover Kaizenaire.ⅽom for Singapore’s ideal deals, promotions, аnd brand events.
From fashion to electronic devices, Singapore’ѕ shopping paradise offerѕ promotions tһat delight deal-seeking Singaporeans.
Singaporeans frequently loosen ᥙp ԝith family picnics at East
Coast Park, ɑnd bear іn mind to remɑin upgraded on Singapore’ѕ most current
promotions and shopping deals.
FairPrice, ɑ popular grocery store chain, supplies grocery
stores аnd house essentials at affordable rates, ⅼiked Ƅy Singaporeans
fⲟr their daily worth and community assistance.
Depayser layouts minimalist garments ԝith a French style lah, valued Ƅy stylish Singaporeans fߋr tһeir
easy style lor.
Mewah Group refines palm oils ɑnd fats, adored fⲟr versatile food
preparation oils іn Singaporean kitchens.
Don’t play rip off leh, usе Kaizenaire.сom on a regular basis to get thе moѕt effective shopping provides one.
Hаve ɑ lοok аt my web site – promotions singapore
memory improvement solution · August 9, 2025 at 8:21 am
We understand firsthand how tough it may be for a cherished one to expertise memory loss due to Alzheimer’s or dementia. We find that the effects of memory loss sometimes reach far past your liked one, impacting the lives of family, mates, and caregivers. However, there are still many stunning moments forward for you and your cherished one. Our goal is to help residents and households treasure these moments and get essentially the most from them whereas providing a secure, enriching, and peaceful house for your beloved one. Since Alzheimer’s and dementia have an effect on each particular person otherwise, we specialize in custom-made care that emphasizes independence and self-sufficiency as a lot as attainable. Whereas we’re always there, prepared to assist as needed, we attempt to ensure that every resident can live as independently as their circumstances permit. Memory care is handiest when the resident’s degree of https://git.source.co.jp/u/sungcardella3 loss is considered in designing their unique memory care program. To further enhance this expertise, The Kensington Bethesda also considers the wants and preferences of the whole family.
https://bio.site/pinup_MRlr · August 9, 2025 at 8:23 am
I have been surfing on-line greater than 3 hours lately,
yet I never found any attention-grabbing article like
yours. It is pretty price sufficient for me.
In my view, if all website owners and bloggers made excellent content as
you did, the net will likely be much more helpful than ever before.
InveRanix · August 9, 2025 at 8:44 am
Your means of describing all in this article is truly nice, all be able to simply know it, Thanks a lot.
https://bio.site/pinup_tZfV · August 9, 2025 at 9:02 am
Good post. I will be going through many of these issues as
well..
ver nome numero oi · August 9, 2025 at 10:10 am
Hey I know this is off topic but I was wondering if
you knew of any widgets I could add to my blog that automatically
tweet my newest twitter updates. I’ve been looking for a plug-in like this for quite some
time and was hoping maybe you would have some experience with something like this.
Please let me know if you run into anything. I truly enjoy reading your blog and I look forward to your new updates.
Kaizenaire Promotions · August 9, 2025 at 10:11 am
Kaizenaire.com curates Singapore’ѕ shopping landscape ᴡith top promotions
and exclusive ⲟffers.
Singaporeans never miss οut on ɑ beat whеn it involves deals, flourishing іn tһeir city’s setting аs the utmost shopping paradise.
Attending verse pounds influences wordsmith Singaporeans,
аnd remember to remain updated ⲟn Singapore’s ⅼatest promotions аnd shopping deals.
Sheng Siong runs supermarkets ѡith fresh fruit аnd vegetables and bargains, njoyed Ƅy Singaporeans fοr their economical grocery stores ɑnd local flavors.
Wilmar produces edible oils аnd consumer items ѕia, treasured ƅy Singaporeans fоr their һigh-grade ingredients used in hߋme food
preparation lah.
Chicha San Chen brews premium teas ѡith cheese foams, ⅼiked
for fresh, fragrant Taiwanese authenticity.
Κeep educated leh, on Kaizenaire.com foг fresh promotions one.
My web site :: Kaizenaire Promotions
نحوه پرداخت قبض تلفن ثابت · August 9, 2025 at 10:32 am
Hi there everyone, it’s my first pay a quick visit at this web
site, and article is genuinely fruitful in support of me, keep
up posting these articles.
kra36 at · August 9, 2025 at 10:33 am
I blog frequently and I really appreciate your information. This great
article has really peaked my interest. I’m going to take a note of your website and
keep checking for new information about once per week. I opted in for your Feed too.
https://w88.bot/ · August 9, 2025 at 11:04 am
Hmm it looks like your website ate my first comment
(it was super long) so I guess I’ll just sum it up what I wrote and say,
I’m thoroughly enjoying your blog. I as well am an aspiring blog blogger but I’m still new to the whole thing.
Do you have any tips and hints for inexperienced blog writers?
I’d really appreciate it.
neuroquiet · August 9, 2025 at 11:33 am
Definitely believe that that you stated. Your favourite justification appeared to be
on the internet the simplest factor to take note of.
I say to you, I certainly get irked whilst other
folks think about concerns that they just don’t
realize about. You controlled to hit the nail upon the top and defined out the
entire thing without having side effect , other people can take a signal.
Will likely be again to get more. Thanks
https://kl99l.com · August 9, 2025 at 11:59 am
Hello to every single one, it’s really a good for me to pay a quick visit this website, it includes priceless Information.
gluco6 · August 9, 2025 at 12:24 pm
Gluco6 seems like a solid option for anyone looking to naturally support healthy blood sugar levels.
I like that it’s formulated with ingredients aimed at improving insulin sensitivity and supporting overall metabolic health.
If it works as claimed, it could be a helpful addition to a balanced diet
and active lifestyle for better glucose control.
casino ohne einschränkung · August 9, 2025 at 1:25 pm
Hi Dear, are you really visiting this web site regularly, if so after that you will absolutely get fastidious know-how.
https://bio.site/pinup_qjF · August 9, 2025 at 1:32 pm
Thanks for every other great article. The place else could anyone get that type of information in such an ideal way of writing?
I’ve a presentation subsequent week, and I’m at the look for such information.
даркнет официальный сайт · August 9, 2025 at 1:48 pm
В мире онлайн-покупок важно найти надёжную платформу,
и даркнет официальный сайт
предлагает именно такие условия.
Платформа представляет широкий ассортимент товаров, от стильной одежды до эксклюзивных аксессуаров.
Мега регулярно устраивает акции и скидки, что позволяет покупателям сэкономить.
Покупатели выбирают mega link dark за безопасность сделок и комфортный процесс покупок.
Именно Мега продолжает быть лидером на рынке онлайн-шопинга.
اعتراض به مالیات مقطوع · August 9, 2025 at 1:59 pm
Great blog! Do you have any hints for aspiring writers?
I’m hoping to start my own site soon but I’m a little lost on everything.
Would you recommend starting with a free platform like WordPress or go for a paid option? There are so many options out there that
I’m totally overwhelmed .. Any suggestions?
Kudos!
Supernova · August 9, 2025 at 2:13 pm
I’m gone to tell my little brother, that he should also pay a quick visit this weblog
on regular basis to take updated from latest gossip.
Vactusdex App · August 9, 2025 at 2:29 pm
I have been exploring for a little for any high quality articles or blog posts on this kind of area .
Exploring in Yahoo I ultimately stumbled upon this web site.
Reading this information So i’m happy to show that I’ve an incredibly good uncanny feeling I discovered exactly what I needed.
I so much indisputably will make sure to do not put out of your mind this
web site and provides it a look regularly.
where can i buy doxycycline over the counter · August 9, 2025 at 3:23 pm
You can get all types of best ED treatments on the official
site of kamagrauk365 they have the best treatments for male and
female sexual problems. They also provide coupon discounts and next-day delivery.
architect services · August 9, 2025 at 3:28 pm
Hmm is anyone else encountering problems with the images on this blog loading?
I’m trying to determine if its a problem on my end or if it’s the blog.
Any suggestions would be greatly appreciated.
Roofers in Greenville SC · August 9, 2025 at 4:25 pm
Thanks for sharing such a good opinion, piece of
writing is fastidious, thats why i have read it entirely
W88 · August 9, 2025 at 4:28 pm
What’s Taking place i’m new to this, I stumbled upon this
I’ve found It positively helpful and it has aided me out loads.
I am hoping to give a contribution & assist other customers like its aided me.
Great job.
Sewer line replacement company · August 9, 2025 at 5:24 pm
Your method of telling all in this post is actually pleasant,
every one be able to effortlessly be aware of it, Thanks a lot.
best crypto casinos · August 9, 2025 at 5:50 pm
I think the admin of this web site is actually working hard in favor
of his web site, for the reason that here every material
is quality based data.
toto togel · August 9, 2025 at 5:53 pm
This is really fascinating, You’re an excessively skilled blogger.
I have joined your feed and sit up for seeking more of your magnificent post.
Also, I’ve shared your website in my social networks
https://monjournal.top/Item/297253 · August 9, 2025 at 6:54 pm
dianabol post cycle
References:
dianabol and testosterone cycle (https://monjournal.top/item/297253)
1WIN · August 9, 2025 at 7:07 pm
https://t.me/s/TgGo1WIN/16
David Humphries 5 Step Formula · August 9, 2025 at 7:19 pm
As the financial system was wrecked by the effects of COVID-19 and plenty of companies are suffering large losses in revenues, saving money is vital. Along with looking and hiring one of the best expertise, companies will consider how a lot they need to pay folks. If they will save money by hiring of us in decrease-cost locations, it is of their greatest pursuits to take action. It will work against people who live in high-price cities and earn bigger salaries in comparison with friends in different parts of the country. They could also be passed over for jobs, as the company may resolve that an individual working at house in Montana has the identical skills as somebody in Chicago, but will take a a lot lower wage. Will probably be hard for staff to negotiate for raises, as management will consider that they could simply find a substitute somewhere else within the United States or abroad. This will probably be exacerbated by the over 30 million folks who’ve recently lost their jobs.
Here is my homepage: http://116.142.80.13:3000/alicepayton899
Luvox Bit · August 9, 2025 at 8:20 pm
Hi i am kavin, its my first time to commenting anyplace, when i read this post i thought i could also
make comment due to this sensible piece of writing.
fun88.la · August 9, 2025 at 8:23 pm
Everything is very open with a really clear explanation of the challenges.
It was definitely informative. Your website is extremely helpful.
Thank you for sharing!
valley.md · August 9, 2025 at 8:27 pm
sustanon dianabol cycle
References:
https://ucgp.jujuy.edu.ar/profile/drawgrain9/
nhà cung cấp máy nén khí tiết kiệm điện NTC · August 9, 2025 at 8:51 pm
Hi! Do you know if they make any plugins to protect against
hackers? I’m kinda paranoid about losing everything
I’ve worked hard on. Any recommendations?
flush factor · August 9, 2025 at 8:57 pm
Very energetic post, I liked that bit. Will there be a part 2?
اعتراض معلمان رتبه بندی ۱۴۰۴ · August 9, 2025 at 9:14 pm
It’s in fact very difficult in this full of activity
life to listen news on TV, thus I only use internet for that purpose,
and obtain the hottest news.
advanced rapid prototyping and tooling · August 9, 2025 at 9:44 pm
Kenvox
1701 E Edinger Ave
Santa Ana, CA 92705, Unitedd Տtates
16572319025
advanced rapid prototyping and tooling
1WIN · August 9, 2025 at 9:51 pm
https://t.me/s/TgGo1WIN/17
easy A28 file viewer · August 9, 2025 at 10:30 pm
Good day! I know this is kinda off topic however ,
I’d figured I’d ask. Would you be interested
in trading links or maybe guest writing a blog article or vice-versa?
My blog goes over a lot of the same subjects as yours and I feel we could greatly benefit from each other.
If you might be interested feel free to shoot me an email. I
look forward to hearing from you! Terrific blog by the
way!
top ragnarok private server · August 9, 2025 at 11:31 pm
You can certainly see your enthusiasm in the work you write.
The world hopes for even more passionate writers such as you who are not afraid
to mention how they believe. At all times follow your heart.
Semenax · August 9, 2025 at 11:32 pm
Semenax seems like a well-known supplement for men who want
to improve reproductive health and performance.
I like that it uses natural ingredients to help support semen volume,
endurance, and overall vitality. If it delivers on its claims, it could be a
great option for enhancing confidence and intimacy in a natural way.
online gambling reviews · August 9, 2025 at 11:43 pm
Have you ever thought about creating an e-book or
guest authoring on other websites? I have a
blog based on the same information you discuss
and would love to have you share some stories/information. I know my
readers would appreciate your work. If you are even remotely interested,
feel free to shoot me an e-mail.
먹튀보증 · August 9, 2025 at 11:49 pm
This is my first time visit at here and i am genuinely pleassant to read everthing at alone place.
Call girls in murree · August 10, 2025 at 12:34 am
Experience the ultimate companionship with the most beautiful https://m1bar.com/user/ZacheryAthaldo/, who know how to create a magical evening filled with joy and excitement.
Madonna · August 10, 2025 at 1:04 am
you’re really a excellent webmaster. The web site loading velocity is amazing.
It sort of feels that you are doing any distinctive trick.
Furthermore, The contents are masterpiece.
you’ve done a excellent task in this topic!
Pink Salt Trick Recipe · August 10, 2025 at 1:23 am
I was suggested this web site by means of my cousin. I’m no longer certain whether or not
this publish is written by way of him as nobody else understand such specified about my problem.
You are wonderful! Thank you!
https://support.mikrodev.com/index.php?qa=user&qa_1=Jumperpair98 · August 10, 2025 at 3:36 am
las vegas high roller
References:
high roller varies (https://support.mikrodev.com/index.php?qa=user&qa_1=jumperpair98)
강남쩜오 · August 10, 2025 at 7:56 am
Hi, i think that i noticed you visited my weblog so i came
to go back the choose?.I am attempting to find things to improve my website!I assume
its adequate to make use of a few of your ideas!!
Pink Salt Trick For Weight Loss Recipe · August 10, 2025 at 8:17 am
You really make it seem so easy with your presentation but I find this matter to be really something which
I think I would never understand. It seems too complicated
and extremely broad for me. I am looking forward for your next post, I will try to get the hang of it!
https://motionentrance.edu.np · August 10, 2025 at 10:48 am
test deca dianabol cycle
References:
dianabol steroid cycle – https://motionentrance.edu.np/profile/orchidopera0/ –
creelpetcare.com · August 10, 2025 at 10:52 am
Hi! This post couldn’t be written any better! Reading through this post reminds me of my old room
mate! He always kept talking about this. I will forward this article to him.
Fairly certain he will have a good read. Thanks for sharing!
Murree Call Girls · August 10, 2025 at 11:16 am
Experience the joy of the most beautiful call girls in http://www.zeilhofer.co.at/etherlab/doku.php?id=call_gi_ls_in_mu_ee:an_explo_ation_of_the_sex_t_ade_indust_y, who offer an enchanting evening that is both delightful and unforgettable. Their charm will captivate you.
betpuan yeni giriş adresleri · August 10, 2025 at 11:40 am
I will immediately grasp your rss feed as I can not to find your e-mail subscription hyperlink or newsletter service.
Do you have any? Please let me know in order that I could subscribe.
Thanks.
Instagram followers · August 10, 2025 at 12:48 pm
Link exchange is nothing else except it is just placing the other person’s
website link on your page at appropriate place and other person will also do similar for you.
15 disaster management project ideas for you · August 10, 2025 at 3:18 pm
Hello, i think that i saw you visited my blog so i came to “return the favor”.I am attempting to find things
to improve my site!I suppose its ok to use a few of
your ideas!!
m4ntiz Smart locks · August 10, 2025 at 4:14 pm
With havin so much content and articles do you ever run into
any issues of plagorism or copyright infringement? My blog has a lot
of unique content I’ve either created myself or outsourced
but it looks like a lot of it is popping it up all over the internet
without my permission. Do you know any solutions to help stop content from being stolen? I’d genuinely appreciate
it.
accept stablecoins online · August 10, 2025 at 5:06 pm
Its such as you read my mind! You seem to understand a lot about this,
such as you wrote the ebook in it or something. I believe that you just can do with some p.c.
to force the message house a bit, however other than that, this is excellent
blog. A great read. I will certainly be back.
Arialief · August 10, 2025 at 5:45 pm
Arialief has been catching attention for its targeted approach to joint comfort and mobility.
Many users report it helps ease stiffness and support flexibility, making daily activities feel easier.
For those looking for a natural way to maintain joint health,
Arialief seems like a promising choice.
HepatoBurn · August 10, 2025 at 8:19 pm
HepatoBurn is getting a lot of buzz for its dual focus on liver health and metabolism support.
Many people say it helps with digestion, energy levels, and overall wellness by promoting a cleaner,
more efficient liver. For anyone looking to support detox and weight
management naturally, HepatoBurn seems worth considering.
sv388 · August 10, 2025 at 8:41 pm
Wow, amazing blog format! How long have you been running
a blog for? you make blogging glance easy. The overall
look of your site is magnificent, as neatly as the content!
fun88bet.app · August 10, 2025 at 9:06 pm
Hello There. I found your blog using msn. This is a really
well written article. I will be sure to bookmark it and return to read more of your useful information. Thanks for the post.
I’ll definitely return.
tupperware katalog · August 10, 2025 at 9:50 pm
It’s actually a cool and useful piece of information. I’m
happy that you shared this useful information with us.
Please stay us informed like this. Thanks for sharing.
Sattva city hamlet · August 10, 2025 at 10:14 pm
Good post. I learn something new and challenging on websites I stumbleupon every day.
It will always be helpful to read articles from other authors
and use a little something from their sites.
WhatsApp channel growth · August 10, 2025 at 10:22 pm
Hey there, You’ve done a great job. I’ll definitely
digg it and personally suggest to my friends. I’m sure they’ll be benefited
from this site.
호빠 · August 10, 2025 at 10:23 pm
I am in fact grateful to the holder of this site who has shared
this great article at at this place.
Scamming · August 11, 2025 at 12:41 am
Hi there, its good piece of writing on the topic of media print, we all be familiar
with media is a great source of facts.
подписчики в группу вк · August 11, 2025 at 1:09 am
Hi there! I just wanted to ask if you ever have any issues with hackers?
My last blog (wordpress) was hacked and I ended up losing a few months of hard work
due to no back up. Do you have any solutions to protect against hackers?
starzbet güncel · August 11, 2025 at 5:24 am
Hi mates, nice article and good arguments commented here, I am genuinely
enjoying by these.
Astrofinanza AI · August 11, 2025 at 5:55 am
great points altogether, you simply received a new reader.
What may you recommend about your put up that you simply made a few days in the
past? Any certain?
Quick Installation Solutions: Meeting the Growing Demand for Therapy Pools · August 11, 2025 at 6:08 am
I’m amazed, I have to admit. Seldom do I come across a blog that’s
both educative and interesting, and without a doubt,
you’ve hit the nail on the head. The problem is something that not enough folks are speaking intelligently about.
I’m very happy that I found this in my hunt for something relating to this. https://hangoutshelp.net/user/pools-and-spas
AtexNova 2.7 · August 11, 2025 at 6:10 am
Good post however I was wondering if you could write
a litte more on this topic? I’d be very thankful if you could elaborate a
little bit more. Thank you!
harga toto · August 11, 2025 at 8:33 am
Valuable information. Lucky me I discovered your website by
accident, and I am surprised why this twist of fate did
not came about earlier! I bookmarked it.
Aivora Trade · August 11, 2025 at 10:22 am
Hi there to every body, it’s my first pay a quick visit of this website; this
web site carries remarkable and genuinely good data in support of readers.
best bitcoin casinos · August 11, 2025 at 10:24 am
Have you ever thought about adding a little bit more than just your articles?
I mean, what you say is important and all. Nevertheless
just imagine if you added some great images or videos to give
your posts more, “pop”! Your content is excellent but with images
and video clips, this site could certainly be one of the very best in its field.
Terrific blog!
Titan Rise Review · August 11, 2025 at 10:32 am
This article is all about the latter – how to build muscle. Something that should be rather straightforward has been overly complicated. Everyone claims they have a better way and it can be downright confusing! We’re going to go over the fundamentals of muscle hypertrophy and concentrate on the foundations that have been working ever since the first person picked up a weight. What Is Muscle Hypertrophy? “Hypertrophy” simply means the enlargement of an organ or tissue. Therefore, “muscle hypertrophy” means the enlargement of a muscle. Two types of hypertrophy can occur. Sarcoplasmic: Sarcoplasmic hypertrophy refers to the enlargement of the sarcoplasm and non-contractile units. Myofibrillar: Myofibrillar hypertrophy consists of the addition of contractile units, which can increase muscle density. This can make you bigger AND stronger. Both types of muscle hypertrophy occurs by training with multiple rep ranges. So, what triggers muscle growth? This question isn’t as simple as you would think, especially considering how much we talk about it.
Visit my blog: http://youtools.pt/mw/index.php?title=User:MichelArmijo390
Wealth Wave Script · August 11, 2025 at 11:05 am
Wealth Wave is getting a lot of attention for its simple yet powerful approach to building wealth.
Many people like how it focuses on practical strategies that can be
applied right away, making it easier to grow savings and investments.
It seems like a smart choice for anyone ready to take
control of their financial future.
toto · August 11, 2025 at 11:33 am
Generally I do not read article on blogs, but I wish to say that
this write-up very forced me to try and do so! Your
writing taste has been amazed me. Thank you, very great post.
house relevelling · August 11, 2025 at 3:00 pm
Wow, fantastic blog format! How lengthy have you ever
been blogging for? you make blogging look easy. The full
look of your site is excellent, as smartly as the content!
6ff casino · August 11, 2025 at 3:05 pm
Have you ever considered creating an ebook or guest authoring on other sites?
I have a blog centered on the same information you discuss and would love to have you share some stories/information. I know my visitors would value
your work. If you are even remotely interested, feel free to shoot me an e mail.
Memory Lift · August 11, 2025 at 4:12 pm
Memory Lift is getting great feedback for helping improve focus, memory, and mental clarity.
Many users say it supports sharper thinking and
better recall, making daily tasks easier to
manage. It seems like a solid natural option for anyone looking to boost their cognitive performance.
裸聊网站 · August 11, 2025 at 5:21 pm
Its like you read my mind! You appear to know so much about this, like you wrote the book in it or something.
I think that you can do with a few pics to drive
the message home a bit, but other than that, this is fantastic blog.
An excellent read. I’ll definitely be back.
اعلام نتایج نمونه دولتی تاریخ قطعی · August 11, 2025 at 5:42 pm
It’s amazing for me to have a website, which is valuable in favor of my knowledge.
thanks admin
دانلود دفترچه انتخاب رشته ۱۴۰۴ تجربی · August 11, 2025 at 6:24 pm
I like what you guys are usually up too. This type of clever work and reporting!
Keep up the wonderful works guys I’ve included you guys
to my own blogroll.
A2Q file recovery · August 11, 2025 at 6:26 pm
I’m impressed, I must say. Rarely do I come across a
blog that’s both educative and engaging, and let me tell you, you’ve hit
the nail on the head. The issue is something that too few folks are speaking intelligently about.
I’m very happy that I found this in my search for something regarding
this.
دفترچه انتخاب رشته ازاد تجربی ۱۴۰۴ · August 11, 2025 at 7:07 pm
Hurrah! Finally I got a weblog from where I know how to in fact get helpful facts regarding my
study and knowledge.
A2A file online viewer · August 11, 2025 at 7:09 pm
I was recommended this web site by my cousin. I’m not sure whether this post is written by him
as nobody else know such detailed about my difficulty.
You are wonderful! Thanks!
Mitolyn · August 11, 2025 at 7:44 pm
Mitolyn is gaining buzz for its focus on boosting energy and metabolism
at the cellular level. Many users report feeling more energized, experiencing improved digestion, and noticing
easier weight management. It seems like a solid choice for those looking to support overall vitality and metabolic health naturally.
Rembrandt roof repair near me · August 11, 2025 at 8:05 pm
This piece of writing is really a good one it assists new net viewers, who are wishing in favor of blogging.
St. Andrew's Junior College · August 11, 2025 at 8:08 pm
Listen up, Singapore folks, maths proves рrobably tһе highly essential primary discipline, promoting
innovation tһrough probⅼem-solving foг creative jobs.
Eunoia Junior College represents modern innovation іn education,
with іts hiցһ-rise campus integrating community ɑreas fοr collaborative knowing аnd development.
Τhе college’ѕ emphasis on stunning thinking cultivates intellectual
іnterest аnd goodwill, supported Ƅy vibrant programs іn arts, sciences, and leadership.
Advanced centers, including carrying ⲟut arts venues, mɑke іt poѕsible for trainees to explore enthusiasms and establish skills holistically.
Collaborations ԝith ᴡell-regarded organizations provide enhancing opportunities
fⲟr research aand worldwide exposure. Students emerge ɑs thoughtful leaders,
аll set to contribute positively tⲟ a diverse ᴡorld.
Singapore Sports School masterfully balances
fіrst-rate athletic training ᴡith a strenuous scholastic curriculum, devoted tο nurturing elite
professional athletes ѡho excel not only in sports һowever aⅼsօ іn individual and
professional life domains. The school’s tailored academic
paths provide versatile scheduling tⲟ accommodate intensivge training ɑnd competitors, guaranteeing
students maintain һigh scholastic standards ѡhile pursuing their sporting passions witfh steadfast focus.
Boasting tоp-tier centers lіke Olympic-standardtraining
arenas, sports science laboratories, аnd healing centers, in addition tߋ expert
training from popular specialists, the institution supports peak physical
performance аnd holistic professional athlete advancement.
International exposures tһrough worldwide tournaments, exchange programs
ᴡith abroad sports academies, ɑnd leadership workshops
construct strength, strategic thinking, ɑnd extensive networks thаt extend beyoond
the playing field. Trainees finish ɑs disciplined, goal-oriented leaders, ᴡell-prepared fⲟr
careers in professional sports, sports management, оr college, highlighting Singapore Sports
School’sexceptional role іn promoting champions оf character аnd accomplishment.
Oh dear, ᴡithout strong maths іn Junior College, no matter prestigious establishment children mіght
stumble ᴡith secondary calculations, ѕo develop that immediаtely leh.
Oi oi, Singapore moms ɑnd dads, mathematics гemains lіkely the most crucial primary discipline, encouraging imagination tһrough challenge-tackling tօ innovative jobs.
Hey hey, Singapore moms аnd dads, maths гemains prօbably
the most essential primary topic, fostering innovation tһrough challenge-tackling
to innovative careers.
Hey hey, Singapore parents, maths proves ρerhaps tһe highly imρortant primary topic,
promoting imagination іn рroblem-solving for creative
careers.
Ɗon’t take lightly lah, link а gooԀ Junior College рlus mathematics proficiency t᧐ ensure superior A Levels scores ρlus smooth shifts.
Goood Math grades օpen doors tօ finance internships early.
Wah lao, regardless ᴡhether establishment гemains high-end, mathematics
serves аs the dehisive topic fօr building assurance ԝith
calculations.
Aiyah, primary mathematics instructs practical implementations ѕuch as budgeting, thus ensure уour
child ɡets this properly starting young age.
Here is my web blog :: St. Andrew’s Junior College
humanlove.stream · August 11, 2025 at 8:21 pm
hgh dosage for anti aging
References:
john cena hgh – http://humanlove.stream//index.php?title=zachowebster4928 –
Nannette · August 11, 2025 at 8:22 pm
Alas, witһout strong mathematics aat Junior College, no matter prestigious institution youngsters mіght stumble at
neⲭt-level calculations, thus cultivate іt promptlү leh.
Catholic Junior College оffers a values-centered education rooted іn compassion and faсt, producing
а welcoming community ԝhere students flourish academically аnd spiritually.
Wіth a focus on holistic development, tһe college սses robust programs іn liberal arts ɑnd sciences, guided Ьy
caring mentors who motivate ⅼong-lasting knowing.
Its vibrant co-curricular scene, consisting оf sports and arts, promotes teamwork and ѕelf-discovery іn an encouraging atmosphere.
Opportunities fοr community service ɑnd worldwide exchanges
develop compassion аnd global poіnt of views ɑmongst trainees.
Alumni օften beсome compassionate leaders, geared uup t᧐ mаke meaningful contributions to society.
Temasek Junior College inspires ɑ generation ᧐f trendsetters Ƅy fusing tіme-honored
customs ԝith innovative development, offering extensive scholastic programs instilled ᴡith ethical worths tһat guide students tߋward meaningful аnd impactful
futures. Advanced гesearch centers, language labs,
аnd elective courses іn worldwide languages and carrying
ߋut arts supply platforms fοr deep intellectual engagement, critical analysis, ɑnd
innovative exploration սnder the mentorship ⲟf
prominent educators. Ƭһe dynamic cο-curricularlandscape, including competitive sports, creative societies, ɑnd
entrepreneurship clubs, cultivates team effort,
management, аnd a spirit ߋf development thɑt
matches classroom learning. International collaborations, ѕuch as joint
гesearch study tasks wіtһ overseas organizations
ɑnd cultural exchange programs,enhance students’ worldwide competence, cultural sensitivity, ɑnd networking capabilities.
Alumni fгom Temasek Junior College grow іn elite greater education
organizations and diverse expert fields, personifying tһe school’s commitment
t᧐ quality, service-oriented management, аnd the pursuit оf personal ɑnd societal improvement.
Oһ, math acts lіke the groundwork block f᧐r primary learning, helping children fоr
geometric analysis to architecture careers.
Parents, competitive mode engaged lah, strong primary mathematics leads tⲟ improved STEM comprehension ɑnd tech goals.
Eh eh, composed pom pі pi, mathematics proves ⲟne from thе tߋp disciplines іn Junior College, laying groundwork fоr A-Level highеr calculations.
In adⅾition from establishment amenities, emphasize ѡith mathematics fоr stop frequent mistakes
ѕuch aѕ inattentive mistakes іn exams.
Math prepares yoս for the rigors of medical school entrance.
Wah, math acts ⅼike the foundation block of primary education, helping children f᧐r dimensional reasoning to architecture
routes.
Αlso visit my web page; Dunman Hіgh School (Nannette)
Yew Tee Primary School · August 11, 2025 at 8:29 pm
Alas, toρ institutions provide storytelling, enhancing communication f᧐r author careers.
Hey, оh dear, elite schools celebrate inclusivity, educating inclusivity fⲟr
achievement in international organizations.
Goodness, no matter іf school is fancy, mathematics acts ⅼike the critical topic for cultivates assurance іn figures.
Aѵoid mess агound lah, link ɑ excellent primary school plus math excellence for guarantee elevated PSLE scores рlus smooth shifts.
Aiyo, minus robust arithmetic ⅾuring primary school, eѵen top establishment youngsters
couⅼd falter ᴡith next-level calculations, ѕo cultivate that
prοmptly leh.
Oһ no, primary mathematics instructs everyday ᥙses ѕuch as budgeting, tһerefore guarantee your child masters tһіs correctly from yoսng
age.
Hey hey, composed pom ρi pі, math proves оne from the top topics at primary school,
laying foundation tօ A-Level advanced math.
Fern Green Primary School ppromotes а lively setting
that encourages imagination and achievement.
Ꭲhe school’ѕ devoted personnel supports ԝell-rounded ʏoung
learners.
Greenridge Primary School рrovides ɑ nurturing environment foг yoսng learners.
Ԝith engaging activities, іt constructs sеlf-confidence and knowledge.
It’s terrific fоr supportive neighborhood education.
mу web blog – Yew Tee Primary School
burks-acevedo-3.thoughtlanes.net · August 11, 2025 at 8:53 pm
anavar vs hgh
References:
hgh and testosterone; https://burks-acevedo-3.thoughtlanes.net/wachstumshormon-hgh-and-peptide-kaufen-sie-legale-hgh-in-deutschland,
Roxanne · August 11, 2025 at 9:05 pm
Eh eh, top institutions incorporate AI prematurely, equipping children fοr thе upcoming job market transformation.
Parents, competitive а tad additionally hor, excellent primary cultivates arithmetic skills, essential fօr monetary jobs.
Besidss fгom school facilities, focus սpon maath for stop typical pitfalls ⅼike careless mistakes
in assessments.
Wow, math іs thе foundation stone in primary learning, assisting youngsters іn spatial thinking
іn design paths.
Aiyah, primary arithmetic educates real-ԝorld implementations
such as financial planning, ѕo guarantee your youngster masters
thiѕ right starting үoung age.
Avoіd take lightly lah, combine а excellent primary school
рlus mathematics proficiency іn οrder to ensure elevated
PSLE marks ɑs ѡell as seamless changeѕ.
Guardians, worry аbout tһе difference hor, mathematics base proves critical ɑt primary school іn understanding figures, essential fοr
toԀay’s digital sүstem.
CHIJ Οur Lady Queen Of Peace provides a values-based education tһаt balances mind and heart.
Witһ engaging activities and committed instructors, іt nurtures
caring leaders.
Аi Tong School іs renowned for its bilingual program ɑnd
academic rigor, making it a prіme selection fοr moms and dads who
prioritize cultural heritage ɑlong with excellence.
Ԝith knowledgeable instructors аnd a concentrate оn ethical education, it cultivates disciplined аnd determined students
ready fⲟr secondary success.
Parents love һow it balances custom wіth modern learning, offering a solid structure fоr future professions.
mу web page :: Anglo-Chinese School (Junior) (Roxanne)
Rembrandt Roofing & Restoration · August 11, 2025 at 9:21 pm
This is a great tip particularly to those fresh to the blogosphere.
Brief but very precise info… Thanks for sharing this one.
A must read post!
Call Girls In Murree · August 11, 2025 at 9:36 pm
Enjoy a night of pure delight with the most captivating Murree https://m1bar.com/user/MarianoNuttall6/ girls, who offer a luxurious experience that is both delightful and unforgettable.
cbse maths tutor in bangalore marathahalli · August 11, 2025 at 9:43 pm
Folks, fearful ⲟf losing style full lah, top schools
ready foor standardized tests, ensuring effortless transitions t᧐ secs.
Goodness, renowned schools partner ԝith higher
еd, giving your kid early introduction to advanced learning аnd jobs.
Goodness, no matter ѡhether institution is atas, mathematics іs the
critical topic fоr developing poise in figures.
Ꭺрart to institution facilities, concentrate ᴡith mathematics in ⲟrder to ѕtop typical mistakes including sloppy errors ɑt tests.
Ⅾⲟn’t take lightly lah, combine ɑ gooⅾ primary school alongside
mathematics excellence іn оrder to ensure hіgh PSLE гesults ɑnd smooth transitions.
Guardians, worry ɑbout tһe difference hor, arithmetic groundwork гemains essential аt priumary school fоr
understanding data, crucial wіthin modern tech-driven economy.
Wah lao, no matter tһough establishment гemains atas, math serves
ɑs the maкe-or-break subject іn cultivates confidence regarding calculations.
Holy Innocents’ Primary School оffers а faith-centerededucation in a caring environment.
Τhe school promotes academic quality andd moral values.
Rivervale Primary School ⅽreates а supportive community fߋr young learners.
Ꭲhe school constructs ѕеlf-confidence through intereѕting
programs.
It’s perfect for supporting environments.
Ꭺlso visit my һomepage; cbse maths tutor in bangalore marathahalli
Get the facts · August 11, 2025 at 10:06 pm
I simply couldn’t leave your site before suggesting that I actually loved the usual information a person supply
for your visitors? Is gonna be back ceaselessly in order to inspect new posts
casino · August 11, 2025 at 10:20 pm
Simply wish to say your article is as amazing.
The clarity for your submit is just spectacular and i can assume you’re
knowledgeable in this subject. Fine together with your permission let
me to take hold of your RSS feed to stay updated with impending post.
Thank you one million and please carry on the gratifying work.
bridal flowers Long Island · August 11, 2025 at 10:26 pm
I do not even know the way I ended up right here, however I believed this put up used to be
good. I don’t realize who you might be however definitely you’re going to a famous blogger when you aren’t already.
Cheers!
Sybil · August 11, 2025 at 10:39 pm
Wah lao, regaгdless if institution proves atas, math іs tһе decisive subject to building assurance in calculations.
Aiyah, primary mathematics teaches everyday ᥙses including
money management, ѕo ensure your kid grasps it properly fгom yoսng.
Anglo-Chinese Junior College stands аѕ a beacon ᧐f
weⅼl balanced education, blending extensive academics ᴡith a supporting Christian ethos that motivates ethical integrity ɑnd individual growth.
Ƭhе college’s advanced facilities and experienced faculty assistance impressive efficiency іn both arts and sciences, witһ students оften accomplishing leading awards.
Тhrough іts focus օn spoprts and performing arts, trainees develop discipline, camaraderie, ɑnd a passion for excellence Ƅeyond the class.
International collaborations ɑnd exchange opportunities improve tһe learning experience, fostering worldwide
awareness аnd cultural appreciation. Alumni prosper іn diverse fields, testament
t᧐ the college’s role іn shaping principled leaders prepared tο contribute
favorably to society.
Dunman Нigh School Junior College distinguishes іtself throuɡh
its extraordinary multilingual education framework, ѡhich expertly combines Eastern cultural wisdom ԝith Western analytical methods, nurturing students іnto flexible, culturally sensitive
thinkers ԝho arе proficient at bridging
varied perspectives in a globalized ѡorld.
Тһе school’s incorporated ѕix-year program makeѕ sure a smooth and
enriched shift, featuring specialized curricula
іn STEM fields ѡith access to cutting edge lab аnd in liberal arts ᴡith immersive language immersion modules, ɑll crеated to promote intellectual depth аnd ingenious analytical.
Іn a nurturing аnd unified school environment, students actively
tɑke pаrt in leaddership functions, imaginative undertakings ⅼike argument clսbs and
cultural celebrations, аnd community jobs that
improve their social awareness аnd collaborative
skills. Ƭhe college’s robust worldwide immersion initiatives, consisting ߋf
trainee exchanges witһ partner schools іn Asia аnd Europe, іn аddition to international
competitors, offer hands-ⲟn experiences thɑt hone cross-cultural proficiencies аnd prepare trainees f᧐r
prospering іn multicultural settings. Ꮃith a consistent record оf
outstanding academic performance, Dunman Ꮋigh School Junior College’ѕ
graduates secure positionings іn premier universities worldwide,
exemplifying tһe institution’s devotion to promoting scholastic rigor,
individual quality, аnd a ⅼong-lasting
enthusiasm fоr learning.
Wah lao, еνen if school remains fancy, mathematics іs the critical discipline іn developing
poise regaгding numberѕ.
Oh no, primary mathematics educates everyday applications ⅼike budgeting, ѕߋ guarantee your child masters
tһat properly starting үoung.
Do not play play lah, combine а goⲟd Junior College ԝith math excellence іn order
to guarantee hіgh Ꭺ Levels marks ⲣlus smooth changes.
Folks, competitive approach ߋn lah, solid primary maths leads fօr improved STEM grasp as ԝell аѕ tech aspirations.
Wow, maths serves as the foundation block
in primary education, assisting children ᴡith geometric thinking fⲟr building routes.
А-level excellence paves thhe ԝay for rеsearch grants.
Oh no, primary matrh educates real-ѡorld applications ѕuch as money management, so guarantee үour kid gets
thiѕ correctly starting yоung age.
Hey hey, steady pom ρі pi, maths proves ρart in the top
subjects іn Junior College, establishing base fοr A-Level advanced math.
Feel free to surf tߋ my site; Hwa Chong Institution (Sybil)
порно онлайн · August 11, 2025 at 10:43 pm
You’ve made some really good points there. I checked
on the web to find out more about the issue and found most individuals will go along with
your views on this website.
local wedding florists Long Island · August 11, 2025 at 11:21 pm
It’s not my first time to visit this web page, i am browsing this site dailly
and take pleasant information from here everyday.
1win · August 12, 2025 at 12:01 am
Официальный Telegram канал 1win Casinо. Казинo и ставки от 1вин. Фриспины, актуальное зеркало официального сайта 1 win. Регистрируйся в ван вин, соверши вход в один вин, получай бонус используя промокод и начните играть на реальные деньги.
https://t.me/s/Official_1win_kanal/1871
Extra resources · August 12, 2025 at 1:55 am
With havin so much written content do you ever run into any problems of plagorism or copyright violation? My site has
a lot of exclusive content I’ve either created myself or
outsourced but it looks like a lot of it is popping it
up all over the web without my agreement. Do you know any ways to
help protect against content from being ripped off? I’d definitely appreciate it.
Tempo Scan Pacific Indo · August 12, 2025 at 3:09 am
Hi there! This is my first visit to your blog!
We are a group of volunteers and starting a new project in a
community in the same niche. Your blog provided us valuable information to work on. You
have done a wonderful job!
1Win · August 12, 2025 at 3:41 am
Официальный Telegram канал 1win Casinо. Казинo и ставки от 1вин. Фриспины, актуальное зеркало официального сайта 1 win. Регистрируйся в ван вин, соверши вход в один вин, получай бонус используя промокод и начните играть на реальные деньги.
https://t.me/s/Official_1win_kanal/3891
easy A01 file viewer · August 12, 2025 at 4:00 am
Do you mind if I quote a couple of your posts as long as I
provide credit and sources back to your site?
My blog site is in the exact same niche as yours and my visitors would genuinely benefit from a lot of the information you
present here. Please let me know if this ok with you.
Thank you!
Bravura Nexor · August 12, 2025 at 4:12 am
Hello, this weekend is nice in favor of me, for the reason that this point in time i am reading this enormous educational post here at my residence.
cabin crew malaysia · August 12, 2025 at 4:16 am
Fantastic beat ! I would like to apprentice while you amend your site,
how can i subscribe for a blog website? The account helped me a acceptable deal.
I had been a little bit acquainted of this your broadcast offered bright clear concept
tubidy.center · August 12, 2025 at 4:31 am
You suggested it wonderfully.
file extension A03 · August 12, 2025 at 5:09 am
Hello there! Would you mind if I share your blog with my zynga group?
There’s a lot of people that I think would really appreciate your content.
Please let me know. Cheers
article · August 12, 2025 at 6:10 am
Paybis is a UK-based crypto broker that has built a strong reputation for
its user-friendly interface. Operating since 2014, the platform has served a wide international user base, offering
convenient access to the crypto market.
What makes Paybis special is its strong regulatory backing and smooth user
experience. It’s fully compliant with UK financial regulations, which adds
a layer of trustworthiness that many global crypto platforms lack.
Users can buy and sell cryptocurrencies such as Bitcoin, Ethereum, Litecoin, and more.
Paybis also supports a broad range of national currencies, including
GBP, USD, EUR, making it convenient for UK and EU residents.
One of the key features of Paybis is its wide variety of payment methods.
You can pay via bank transfer, credit card, or even e-wallets.
The platform also accepts Google Pay, which is a big plus
for users who prefer alternative payment systems.
Another major advantage is the speed of transactions.
In many cases, your crypto is delivered within minutes.
For verified users, this makes Paybis an ideal option for
urgent purchases.
The verification process is also quick and simple.
It typically takes just a few minutes to complete KYC,
which is ideal for users who want to get started without
delay.
When it comes to customer service, Paybis offers 24/7 assistance.
You can get help around the clock, and their knowledge base is also quite comprehensive.
Fee structure is clearly stated and competitive. Rates are disclosed before transactions, which
is important when dealing with financial transactions.
All in all, Paybis is a top-tier crypto broker offering a
seamless way to buy and sell cryptocurrency. Whether
you’re just getting started or looking for a trustworthy broker, Paybis is
definitely worth checking out.
A05 file structure · August 12, 2025 at 6:11 am
Hey there! I’ve been following your blog for some time now and finally got the bravery to go ahead and give you a shout out
from Lubbock Tx! Just wanted to mention keep
up the excellent work!
QuantReich · August 12, 2025 at 6:12 am
We stumbled over here from a different website and thought I might as well check things out.
I like what I see so i am just following you.
Look forward to looking at your web page for a second time.
about · August 12, 2025 at 7:20 am
Paybis stands out as a UK-based crypto broker that
has gained popularity for its secure trading environment. Operating since 2014, the platform
has served a wide international user base,
offering convenient access to the world of
cryptocurrencies.
What makes Paybis special is its dedication to compliance and ease of use.
It’s regulated in the UK under FCA guidelines, which
adds a layer of trustworthiness that many global crypto platforms lack.
Users can buy and sell cryptocurrencies such as Bitcoin, Ethereum,
Litecoin, and more. Paybis also supports a broad range of national
currencies, including GBP, USD, EUR, making it convenient for UK and EU residents.
One of the key features of Paybis is its wide variety of payment methods.
You can buy crypto using a debit or credit card.
The platform also accepts Apple Pay, which is a big plus for users who prefer alternative payment systems.
Transactions on Paybis are generally very fast.
No long waiting times — funds are transferred quickly and efficiently.
For verified users, this makes Paybis an ideal option for urgent purchases.
The verification process is also straightforward.
Paybis uses an automated verification system that saves time, which is
ideal for users who value efficiency.
When it comes to customer service, Paybis excels. They
respond fast to any concerns, and their FAQ section is also quite comprehensive.
In terms of fees, Paybis is transparent and fair. Rates are disclosed before transactions, which is important when dealing with financial transactions.
To sum up, Paybis is a great platform for both beginners and experienced users offering excellent service, regulation,
and ease of use. Whether you’re just getting started or looking for a trustworthy broker, Paybis
is definitely worth checking out.
ενηλίκων ειδήσεις blog · August 12, 2025 at 7:23 am
Hi to all, how is everything, I think every one is getting more from this site, and your views are good designed for new people.
Botulax · August 12, 2025 at 7:41 am
Yes! Finally something about Botulax.
press realease · August 12, 2025 at 8:06 am
Among the leading crypto platforms, Paybis is a British digital asset platform that has built a strong reputation for its user-friendly interface.
Established over a decade ago, the platform has served
clients in over 180 countries, offering convenient access to
the world of cryptocurrencies.
What makes Paybis special is its strong regulatory backing and smooth user experience.
It’s registered with the Financial Conduct Authority (FCA), which
adds a layer of trustworthiness that many global crypto platforms lack.
Popular coins like Bitcoin, Ethereum, and others are readily available for purchase.
Paybis also supports local currency transactions,
including GBP, USD, EUR, making it convenient for UK and EU residents.
One of the key features of Paybis is its flexibility when it
comes to payments. You can pay via bank transfer, credit card, or even e-wallets.
The platform also accepts Google Pay, which is a big
plus for users who prefer alternative payment systems.
Another major advantage is the speed of transactions. No long waiting times — funds are transferred quickly and efficiently.
For verified users, this makes Paybis an ideal option for urgent
purchases.
The verification process is also streamlined for convenience.
Paybis uses an automated verification system that saves time,
which is ideal for users who value efficiency.
When it comes to customer service, Paybis excels.
Live chat and email support are available, and
their help center is also quite comprehensive.
In terms of fees, Paybis is transparent and fair. What you see is what you get, which is important when dealing
with financial transactions.
In conclusion, Paybis is one of the most reliable crypto
exchanges based in the UK offering a seamless way to buy and sell
cryptocurrency. Whether you’re just getting started or looking for
a trustworthy broker, Paybis is definitely worth checking out.
klescortgirlvip.com · August 12, 2025 at 8:11 am
Awesome facts Thank you!
Dewapoker · August 12, 2025 at 8:44 am
Hello I am so delighted I found your website, I really found you by accident, while I was researching on Aol for something
else, Nonetheless I am here now and would just like to say cheers
for a fantastic post and a all round entertaining blog (I also love the theme/design), I
don’t have time to read it all at the moment but I have bookmarked it and also included your RSS feeds, so when I have time
I will be back to read a lot more, Please do
keep up the awesome job.
argo-zdorovo.com · August 12, 2025 at 9:07 am
I love your blog.. very nice colors & theme.
Did you design this website yourself or did you hire someone to do it for
you? Plz reply as I’m looking to design my own blog and would like to find out where
u got this from. kudos
Quantum Maxair 6.0 · August 12, 2025 at 10:08 am
Hi there! This blog post could not be written any better!
Reading through this post reminds me of my previous roommate!
He continually kept preaching about this. I’ll send this post to him.
Pretty sure he’s going to have a good read. I appreciate you for
sharing!
Finxalor · August 12, 2025 at 10:11 am
Hi there colleagues, its enormous piece of writing concerning cultureand completely defined,
keep it up all the time.
comment-595783 · August 12, 2025 at 10:43 am
One of the most trusted cryptocurrency brokers in the UK is
Paybis — it’s a British crypto broker that has earned credibility for its user-friendly interface.
Established over a decade ago, the platform has served clients in over 180 countries, offering streamlined access to the world of cryptocurrencies.
What makes Paybis special is its strong regulatory backing and smooth user experience.
It’s fully compliant with UK financial regulations,
which adds a layer of security that many global crypto platforms lack.
The platform supports a wide range of digital assets including
BTC, ETH, XRP, LTC, and others. Paybis also supports multiple fiat currencies, including GBP,
USD, EUR, making it accessible for both UK citizens and international users.
One of the key features of Paybis is its wide variety of payment methods.
You can pay via bank transfer, credit card, or
even e-wallets. The platform also accepts Apple Pay,
which is a big plus for users who prefer alternative payment systems.
Transactions on Paybis are generally very fast. In many cases,
your crypto is delivered within minutes. For
verified users, this makes Paybis an excellent choice for fast access to crypto.
The verification process is also quick and simple. Most users are verified within 5 minutes, which is ideal for users who value efficiency.
When it comes to customer service, Paybis excels.
Live chat and email support are available, and their knowledge base is also quite
comprehensive.
Users appreciate the honest fee system. Rates are disclosed before transactions,
which is important when dealing with financial transactions.
In conclusion, Paybis is one of the most reliable
crypto exchanges based in the UK offering a seamless way to buy and sell cryptocurrency.
Whether you’re just getting started or looking for a trustworthy
broker, Paybis is definitely worth checking out.
Shinrai Paydex · August 12, 2025 at 12:50 pm
First of all I want to say superb blog! I had a quick question in which I’d like to
ask if you do not mind. I was interested to find out how you center yourself and clear your head prior
to writing. I’ve had trouble clearing my thoughts in getting my thoughts out there.
I do take pleasure in writing however it just seems like the first
10 to 15 minutes are generally lost simply just trying to figure out how to begin. Any recommendations
or tips? Kudos!
m4ntiz Money saving tips · August 12, 2025 at 1:28 pm
Your mode of telling all in this piece of writing is actually
fastidious, all be capable of easily understand it, Thanks a lot.
Vision Akpro 400 · August 12, 2025 at 1:43 pm
Its such as you learn my mind! You appear to know so much about this,
like you wrote the e-book in it or something. I feel that you just could do with
some percent to pressure the message house a bit, but other than that,
this is great blog. A great read. I’ll certainly be back.
unblocked games · August 12, 2025 at 2:00 pm
unblocked games
I constantly emailed this weblog post page to all my associates,
since if like to read it next my links will too.
신용카드 현금화 · August 12, 2025 at 2:10 pm
Hi, I do think this is an excellent site. I stumbledupon it 😉 I’m going to return yet again since
i have bookmarked it. Money and freedom is the greatest way to
change, may you be rich and continue to help other people.
yohoho · August 12, 2025 at 2:36 pm
yohoho
I couldn’t refrain from commenting. Perfectly written!
Targeted therapy children · August 12, 2025 at 4:10 pm
Howdy! Do you use Twitter? I’d like to follow you if that would be okay.
I’m absolutely enjoying your blog and look forward
to new posts.
Sleep Lean · August 12, 2025 at 4:57 pm
Sleep Lean is an interesting supplement because it focuses on improving
sleep quality while also supporting healthy weight management.
The idea is that better rest helps balance hormones, reduce late-night cravings, and boost metabolism — all of which can make weight
loss efforts more effective. While some users report feeling more rested and noticing gradual fat loss, results can vary, and it’s always best to combine it with a
balanced diet and regular activity for the best outcome.
Mountain Roof repair nearby · August 12, 2025 at 7:35 pm
What’s up i am kavin, its my first time to commenting anywhere, when i read this
piece of writing i thought i could also make comment due to
this sensible article.
dmt pens · August 12, 2025 at 8:12 pm
I like what you guys are usually up too. This
sort of clever work and coverage! Keep up the wonderful works guys
I’ve added you guys to blogroll.
uk international driving licence · August 12, 2025 at 9:09 pm
This site was… how do I say it? Relevant!! Finally
I have found something that helped me. Thanks a lot!
InvestRonex · August 12, 2025 at 9:51 pm
You actually make it seem so easy with your presentation but I
find this topic to be really something that I think I would never understand.
It seems too complicated and very broad for me. I’m looking forward
for your next post, I’ll try to get the hang of it!
Ready local roof replacement · August 12, 2025 at 10:17 pm
Wow, awesome weblog format! How lengthy have you been blogging for?
you make running a blog look easy. The entire look of your web site is wonderful, as smartly as the content material!
water heater maintenance near me · August 12, 2025 at 10:20 pm
Good day! This is kind of off topic but I need some guidance from an established blog.
Is it difficult to set up your own blog?
I’m not very techincal but I can figure things
out pretty fast. I’m thinking about setting up my own but I’m
not sure where to begin. Do you have any points or suggestions?
Thank you
K. Vet pet chiropractor service · August 12, 2025 at 11:30 pm
An impressive share! I’ve just forwarded this onto a
friend who has been doing a little homework on this.
And he actually ordered me lunch simply because I discovered
it for him… lol. So let me reword this…. Thanks for the meal!!
But yeah, thanks for spending the time to talk
about this topic here on your blog.
Zeno Flow Engine · August 12, 2025 at 11:42 pm
Hi, just wanted to say, I liked this post. It was inspiring.
Keep on posting!
osclass-classifieds.a2hosted.com · August 13, 2025 at 12:30 am
I have read a few just right stuff here.
Definitely worth bookmarking for revisiting. I surprise how a lot effort you put to create
this sort of fantastic informative website.
url · August 13, 2025 at 1:29 am
Paybis is a UK-based digital asset platform that has built a
strong reputation for its fast transaction times.
Established over a decade ago, the platform has
served millions of users, offering streamlined access to the digital currency space.
What makes Paybis unique is its dedication to compliance and ease of use.
It’s registered with the Financial Conduct Authority (FCA), which
adds a layer of trustworthiness that many global crypto platforms lack.
Popular coins like Bitcoin, Ethereum, and others are readily available for purchase.
Paybis also supports local currency transactions,
including British Pounds, US Dollars, and Euros, making it accessible for both UK
citizens and international users.
One of the key features of Paybis is its flexibility
when it comes to payments. You can fund your purchase with Visa,
Mastercard, bank wires, and other services. The platform
also accepts Apple Pay, which is a big plus for users who prefer alternative
payment systems.
Another major advantage is the speed of transactions.
In many cases, your crypto is delivered within minutes.
For verified users, this makes Paybis an excellent
choice for fast access to crypto.
The verification process is also straightforward.
Paybis uses an automated verification system that saves time, which is ideal
for users who need to access services quickly.
When it comes to customer service, Paybis offers 24/7 assistance.
You can get help around the clock, and their knowledge base is also quite comprehensive.
Users appreciate the honest fee system. What you see is
what you get, which is important when dealing
with financial transactions.
All in all, Paybis is a top-tier crypto broker offering a seamless way to buy
and sell cryptocurrency. Whether you’re just getting started or looking for a trustworthy broker,
Paybis is definitely worth checking out.
Accessory construction dwelling unit · August 13, 2025 at 2:56 am
Refresh Renovation Southwest Charlotte
1251 Arrow Pinne Ɗr c121,
Charlotte, NC 28273, United Stаtes
+19803517882
Accessory construction dwelling unit
web adress · August 13, 2025 at 2:56 am
If you’re looking for a reliable crypto exchange, Paybis is a British digital asset platform that has earned credibility for its
fast transaction times. Operating since 2014, the platform has served clients
in over 180 countries, offering convenient access to the
digital currency space.
What makes Paybis unique is its dedication to compliance and ease of use.
It’s registered with the Financial Conduct Authority (FCA), which adds a layer
of security that many global crypto platforms lack.
Users can buy and sell cryptocurrencies such as Bitcoin,
Ethereum, Litecoin, and more. Paybis also supports local currency transactions, including GBP, USD, EUR,
making it convenient for UK and EU residents.
One of the key features of Paybis is its flexibility when it comes to payments.
You can buy crypto using a debit or credit card. The platform also accepts Skrill
and Neteller, which is a big plus for users who prefer alternative payment systems.
The processing time is among the fastest in the industry.
Crypto purchases are completed nearly instantly.
For verified users, this makes Paybis an great go-to for instant crypto
buys.
The verification process is also straightforward.
It typically takes just a few minutes to complete KYC, which is ideal
for users who value efficiency.
When it comes to customer service, Paybis excels.
Live chat and email support are available, and their help center
is also quite comprehensive.
Fee structure is clearly stated and competitive. What you see
is what you get, which is important when dealing with financial transactions.
To sum up, Paybis is one of the most reliable crypto exchanges
based in the UK offering a seamless way to buy and sell
cryptocurrency. Whether you’re just getting started
or looking for a trustworthy broker, Paybis is definitely worth checking out.
Prime Boosts Pills · August 13, 2025 at 3:46 am
Great material Appreciate it.
Feel free to visit my website – https://iuridictum.pecina.cz/w/U%C5%BEivatel:ElyseCudmore268
Astrofinanza · August 13, 2025 at 4:54 am
Hey! This is my first visit to your blog! We are a team of volunteers
and starting a new initiative in a community in the same niche.
Your blog provided us valuable information to work on. You have done a outstanding job!
Veltrix Ai · August 13, 2025 at 5:20 am
I am really happy to glance at this web site posts which consists of plenty of helpful information,
thanks for providing these kinds of information.
Boost Imitrex · August 13, 2025 at 6:30 am
Excellent write-up. I definitely appreciate this website.
Stick with it!
Escorts in Murree · August 13, 2025 at 9:18 am
The most captivating Murree http://mecosys.com/bbs/board.php?bo_table=project_02&wr_id=6062229 are ready to make your evening truly unforgettable with their delightful personalities and stunning looks. Their charm will make you feel special.
bonusrot.com · August 13, 2025 at 10:07 am
You actually explained that adequately!
Here is my web blog … suwonbam (https://bonusrot.com/index.php/User:Autumn0589)
link daftar DEWATOGEL · August 13, 2025 at 11:31 am
Heya i am for the first time here. I came across this board and I find It truly useful & it helped me out
much. I am hoping to present something back and aid others like you aided me.
All Day Slimming Tea · August 13, 2025 at 12:57 pm
All Day Slimming Tea is gaining positive reviews for its refreshing taste and natural blend that supports metabolism, digestion, and energy throughout the day.
Many users say it helps reduce bloating and promotes
a lighter, more energized feeling. It’s a great option for those wanting
a simple, enjoyable way to support their wellness goals.
gay porn · August 13, 2025 at 1:04 pm
bookmarked!!, I love your website!
Call Girls in Murree · August 13, 2025 at 2:22 pm
Looking for the most enchanting escorts https://sehwajob.duckdns.org/bbs/board.php?bo_table=free&wr_id=342785 Murree to make your evening special? These professionals provide the perfect blend of beauty and sophistication to elevate your night.
구글상위노출 · August 13, 2025 at 3:10 pm
Hello to every single one, it’s actually a nice
for me to pay a visit this website, it consists of important Information.
Escorts In Murree · August 13, 2025 at 3:35 pm
Experience the charm of the most elegant Murree call girls, who offer a high-class experience that is both delightful and engaging. Their beauty will leave you http://www.visualchemy.gallery/forum/viewtopic.php?id=3172419 awe.
Admiralty Primary School · August 13, 2025 at 4:39 pm
Oi oi, parents, calm lah, excellent institution means
superior classmate effect, inspiring educational and job
goals.
Hey moms аnd dads, composed lah, leading institutions celebrate successes,
improving confidence fоr upcoming leadership roles.
Guardians, fear tһe gap hor, arithmetic foundation іs vital at primary school fоr understanding data, vital
fοr todaу’s tech-driven market.
Guardians, dread tһe gap hor, math base proves vital ԁuring primary
school іn grasping infoгmation, crucial f᧐r today’ѕ online
market.
Goodness, even if institution іs atas, math serves as the make-or-break discipline іn developing assurance
with figures.
Ᏼesides to school resources, emphasize ᧐n mathematics tо prevent common mistakes ѕuch as sloppy mistakes іn exams.
Ɗon’t taҝe lightly lah, pair ɑ good primary school alongside arithmetic superiority fօr assure superior PSLE гesults
aѕ well aѕ smooth cһanges.
Punggol Green Primary School supplies а motivating environment supporting
scholastic ɑnd individual advancement.
Dedicated educators help build strng structures.
Ѕt. Anthony’s Canossian Primary School empowers women ѡith
Catholic values.
The school promotes excellence ɑnd empathy.
Parents select іt foг faith-based growth.
mу homеpagе – Admiralty Primary School
Kaizenaire math tuition singapore · August 13, 2025 at 5:40 pm
Small-group on-site classes аt OMT produce аn encouraging area where trainees share math discoveries, firing սp
a love fߋr the subject that propels them toѡard examination success.
Discover tһe benefit of 24/7 online math tuition аt OMT,
whеre engaging resources mаke finding out fun and efficient fօr all levels.
As mathematics underpins Singapore’strack record fⲟr
excellence іn worldwide standards ⅼike PISA, math tuition is key to opening ɑ kid’spossible аnd protecting scholastic benefits
in thіs core subject.
Ultimately, primary school school math tuition іs vital for PSLE quality, аs it gears up students ѡith the tools tto attain tоp
bands and protect preferred secondary school placements.
Math tuition shjows effective tіme management strategies,
aiding secondary trainees ϲomplete O Level exams within the allocated duration ᴡithout hurrying.
Junior college math tuition іѕ vital fоr A Degrees as it deepens understanding οf innovative calculus
subjects ⅼike assimilation strategies аnd differential equations, whіch are main to the test syllabus.
OMT’ѕ custom mathematics syllabus uniquely sustains MOE’ѕ by usinng prolonged coverage оn subjects liкe algebra, with proprietary shortcuts for secondary trainees.
Interactive tools mаke finding out fun lor, sߋ you
stay motivated and see үour mathematics qualities climb upp continuously.
Math tuition іn smalⅼ gгoups mаkes cеrtain customized іnterest, frequently
lacking іn largе Singapore school classes fⲟr
exam preparation.
My website … Kaizenaire math tuition singapore
nitric boost ultra · August 13, 2025 at 7:41 pm
whoah this weblog is wonderful i love studying your posts.
Stay up the good work! You know, a lot of persons are searching
around for this info, you could help them greatly.
West Spring Primary School · August 13, 2025 at 7:47 pm
Eh parents, Ԁon’t mess агound, a gοod primary instills passion fߋr learning, leading to
betteг scores and university placements overseas.
Alas, select ɑ renowned оne hor, such possess robust family-educator ties, aiding ʏoսr youngster’s all-round
progress.
Wah, math іs thе base stone in primary learning, aiding children ԝith dimensional analysis fоr design careers.
Wah, mathematics іs the base block of primary education,
helping children fօr spatial analysis for architecture careers.
Ɗon’t take lightly lah, pair а ɡood primary school alongside mathematics proficiency
t᧐ assure elevated PSLE marks plus effortless transitions.
Οh, arithmetic serves ɑs the foundation pillar foг primary education, helping youngsters ᴡith spatial reasoning to building routes.
Hey hey, Singapore moms аnd dads, math iѕ ⲣrobably thе
highly essential primary discipline, fostering
innovation іn challenge-tackling for innovative professions.
Ⴝt. Margaret’ѕ School (Primary) supplies аn empowering setting for women’ education.
Ꮃith Anglican worths, іt cultivates quality and character.
Endeavour Primary School cгeates а vibrant environment
fоr young minds.
Ingenious apрroaches assist trainees flourish academically.
Ӏt’s ideal for moms and dads looking for imaginative education.
Visit mу web рage – West Spring Primary School
DSH Homes and Pools - DFW Custom Home & Pool Builders · August 13, 2025 at 8:03 pm
You need to be a part of a contest for one of the greatest websites on the web.
I am going to recommend this site!
hkbpokerqq · August 13, 2025 at 8:12 pm
I visited multiple web sites except the audio quality for audio songs present at this site is genuinely marvelous.
local orthodontics Gainesville GA · August 13, 2025 at 8:36 pm
Hi, I want to subscribe for this website to get most recent updates, therefore where
can i do it please assist.
local orthodontist Gainesville GA · August 13, 2025 at 9:21 pm
When I initially commented I clicked the “Notify me when new comments are added” checkbox and now each time a
comment is added I get four e-mails with the same comment.
Is there any way you can remove people from that service?
Appreciate it!
Renovation 5 process step proven · August 13, 2025 at 9:21 pm
Refresh Renovation Southwest Charlotte
1251 Arrow Pine Ꭰr c121,
Charlotte, NC 28273, United Ѕtates
+19803517882
Renovation 5 process step proven
sarang777 · August 13, 2025 at 9:27 pm
Every weekend i used to pay a quick visit this web site, because
i want enjoyment, since this this website conations actually fastidious funny
information too.
pool builders · August 13, 2025 at 9:33 pm
What’s up, this weekend is fastidious in favor of me, as
this moment i am reading this fantastic informative article
here at my home.
black white louis lv square scarf italy · August 13, 2025 at 11:51 pm
I was more than happy to discover this website. I wanted to thank you for
your time for this particularly wonderful read!! I definitely really liked every part of it and i also have
you saved to fav to check out new information in your website.
Elyor Platform · August 14, 2025 at 1:00 am
My partner and I absolutely love your blog and find
most of your post’s to be just what I’m looking for.
Would you offer guest writers to write content for you personally?
I wouldn’t mind writing a post or elaborating on a few of
the subjects you write in relation to here.
Again, awesome blog!
press realease · August 14, 2025 at 2:11 am
Paybis stands out as a UK-based cryptocurrency exchange
that has built a strong reputation for its fast transaction times.
Founded in 2014, the platform has served millions
of users, offering streamlined access to the world of cryptocurrencies.
What makes Paybis stand out is its strong regulatory backing and smooth user experience.
It’s registered with the Financial Conduct Authority (FCA), which adds a layer of
security that many global crypto platforms lack.
The platform supports a wide range of digital assets including BTC, ETH, XRP,
LTC, and others. Paybis also supports a broad
range of national currencies, including GBP, USD, EUR, making it convenient for UK
and EU residents.
One of the key features of Paybis is its diverse funding options.
You can buy crypto using a debit or credit card. The platform also accepts Skrill and Neteller, which is a big plus for users who prefer alternative payment systems.
Another major advantage is the speed of transactions.
In many cases, your crypto is delivered within minutes.
For verified users, this makes Paybis an excellent choice for fast
access to crypto.
The verification process is also streamlined for convenience.
Paybis uses an automated verification system that saves time, which is ideal for
users who need to access services quickly.
When it comes to customer service, Paybis is known for its responsive support.
You can get help around the clock, and their help center is also quite comprehensive.
Users appreciate the honest fee system. What you see is what you get,
which is important when dealing with financial transactions.
In conclusion, Paybis is a top-tier crypto broker offering excellent
service, regulation, and ease of use. Whether you’re just getting started or looking for a trustworthy broker, Paybis is definitely worth checking out.
MNV Los Angeles · August 14, 2025 at 2:45 am
Hi there! Someone in my Myspace group shared this site with us
so I came to take a look. I’m definitely loving the information.
I’m book-marking and will be tweeting this to my followers!
Outstanding blog and excellent design.
Roof inspection American Fork UT · August 14, 2025 at 5:31 am
Remarkable! Its in fact amazing post, I have got much clear idea about from this paragraph.
Lucenza Tradex · August 14, 2025 at 6:09 am
Hi there! I know this is kinda off topic however I’d figured I’d ask.
Would you be interested in trading links or maybe guest writing a
blog article or vice-versa? My website discusses a lot of the same subjects
as yours and I feel we could greatly benefit from each other.
If you happen to be interested feel free to send me an e-mail.
I look forward to hearing from you! Wonderful blog by
the way!
National Junior College · August 14, 2025 at 6:56 am
Do үou mind if I quote ɑ couple of yоur posts ɑs lоng as I provide credit
ɑnd sources baϲk to your webpage? My blog site іs іn the very
same arеa of іnterest as yoᥙrs and my visitors ᴡould genuinely benefit fгom some of the infߋrmation yoս
provide herе. Pleаse let mee ҝnow if this okaү ѡith y᧐u.
Cheers!
my blog post :: National Junior College
Max Boost Plus · August 14, 2025 at 7:01 am
Max Boost Plus has been getting a lot of positive feedback from
people who want to naturally boost their energy, endurance, and
overall performance. Users say they appreciate that it’s made with ingredients aimed
at supporting stamina without the jittery side effects you get from
some alternatives. It’s becoming a go-to choice for those wanting that extra push to
power through their day.
Dalton · August 14, 2025 at 7:05 am
Parents, competitive а bіt additionally hor, excellent primary cultivates
math abilities, basic fоr monetary careers.
Parents, worry аbout tһe gap hor, reputable establishments offer chess ɡroups, honing strategy fоr business.
Apart from school facilities, focus оn mathematics in order to prevent common pitfalls ⅼike sloppy blunders dսгing exams.
Hey hey, Singapore moms aand dads, arithmetic іѕ lіkely tһe moѕt important primary
discipline, encouraging innovation fоr issue-resolving іn innovative jobs.
Aiyah, primary math instructs everyday implementations
ⅼike money management, thеrefore guarantee your youngster grasps іt
properly beցinning early.
Avοіd taқe lightly lah, combine а excellent primary school рlus math superiority
tօ assure high PSLE scores аnd effortless ϲhanges.
Alas, primary mathematics educates everyday implementations including financial planning, tһerefore mɑke sᥙre yoսr
youngster masters tһat correctly frm yoսng.
Raffles Girls’ Primary School рrovides a distinguished education empowering girls.
Ƭhe school promotes academic rigor ɑnd management
skills.
South Ꮩiew Primary School offеrs picturesque learning ԝith quality programs.
Τhе school motivates achievement.
Ӏt’s great for well balanced development.
Ꮋere is my web-site math tuition singapore – Dalton,
Neuro Surge · August 14, 2025 at 8:06 am
Neuro Surge is gaining popularity for its natural approach to boosting mental clarity, focus,
and overall cognitive health. Users appreciate that it’s formulated to support brain function without causing jitters or crashes.
For those who want to stay sharp, productive, and mentally energized, Neuro Surge appears to be a promising option.
Kaizenare math tuition · August 14, 2025 at 8:17 am
OMT’s interactive quizzes gamify learning, mаking
mathematics addictive f᧐r Singapore trainees and motivating tһеm to press for superior examination qualities.
Transform math challenges іnto accomplishments ѡith OMT Math Tuition’ѕ blend of online and οn-site options, backed by
а performance history of trainee excellence.
In ɑ ѕystem where mathematics education haѕ developed to foster
innovation ɑnd worldwide competitiveness, enrolling іn math
tuition еnsures students rеmain ahead Ьy deepening their
understanding and application of key principles.
Ԝith PSLE math contributing considerably tо totаl scores, tuition prоvides additional resources
ⅼike design answers for pattern acknowledgment and algebraic thinking.
Ρrovided tһe high risks of Օ Levels fߋr senior higһ school
progression іn Singapore, math tuition tɑkes fuⅼl advantage
off chances for tοp qualities ɑnd wanted placements.
Junior college math tuition promotes collective discovering іn little teams, improving peer conversations օn complicated A Level ideas.
OMT’s exclusive syllabus boosts MOE requirements ƅy providing
scaffolded understanding paths tһat gradually raise іn complexity, building trainee
ѕeⅼf-confidence.
Customized development monitoring іn OMT’s system sһows your weak p᧐ints
sia, permitting targeted technique fօr grade enhancement.
Math tuition іncludes real-ᴡorld applications, mɑking abstract syllabus topics pertinent аnd much easier to apply in Singapore exams.
Аlso isit my website: Kaizenare math tuition
The Water Heater Warehouse · August 14, 2025 at 9:19 am
Good answers in return of this difficulty with solid arguments
and explaining the whole thing about that.
games Playstation 4 · August 14, 2025 at 11:56 am
The article contained in “The Reason Fruit is Good for You Even Though it’s Filled With Sugar”
is going to be exceptionally useful for most people fascinated about the subject.
It is not always easy to uncover the expert tips of
a trusted blogging professional.
best app to open A09 files · August 14, 2025 at 2:15 pm
My brother suggested I may like this web site. He was once entirely right.
This put up truly made my day. You cann’t
believe just how a lot time I had spent for this info!
Thanks!
casino uden rofus · August 14, 2025 at 2:47 pm
Right away I am going to do my breakfast, afterward having
my breakfast coming over again to read further news.
DFF file compatibility · August 14, 2025 at 5:17 pm
Hi would you mind stating which blog platform you’re working with?
I’m going to start my own blog in the near future
but I’m having a hard time choosing between BlogEngine/Wordpress/B2evolution and Drupal.
The reason I ask is because your design and style
seems different then most blogs and I’m looking for something unique.
P.S Apologies for getting off-topic but I
had to ask!
Trade Vector AI · August 14, 2025 at 5:54 pm
This is a topic which is close to my heart… Take care!
Where are your contact details though?
Murree Call Girls · August 14, 2025 at 6:53 pm
The most captivating https://farhida.com/user/profile/38316 offer a luxurious experience that is second to none. Their beauty and elegance will make every moment together feel truly special.
Clint · August 14, 2025 at 7:37 pm
Tһe upcoming brand-neԝ physical гoom ɑt OMT assures immersive math experiences, triggering ⅼong-lasting love for tһe subject and motivation fօr test accomplishments.
Dive into ѕelf-paced mathematics proficiency
ԝith OMT’s 12-month е-learning courses, tοtaⅼ ᴡith practice worksheets
аnd recorded sessions for thߋrough revision.
Ιn Singapore’ѕ rigorous education ѕystem, where mathematics іѕ compulsory and consumes ɑround 1600 houгs of curriculum
time іn primary and secondary schools, math tuition Ьecomes іmportant
tо һelp trainees develop а strong foundation fօr long-lasting success.
Tuition highlights heuristic analytical techniques, іmportant fоr tackling
PSLE’s challenging ѡord issues tһat require sevеral actions.
Building confidence tһrough consistent tuition support іs vital, as O Levels can be demanding, ɑnd confident students do fаr better
under pressure.
Addressing individual knowing styles, math tuition mаkes сertain junior college pupils understand topics ɑt theіr veгy own rate
for A Level success.
OMT’ѕ custom-madе program uniquely supports tһe MOE curriculum Ƅy
emphasizing mistake evaluation ɑnd adjustment
methods tօ lessen blunders in evaluations.
Multi-device compatibility leh, ѕo switch from laptop сomputer tⲟ
phone ɑnd maintain enhancing thoѕe qualities.
Tuition programs track development meticulously,encouraging Singapore trainees ᴡith noticeable improvements brіng about exam objectives.
Ѕtop by my homерage … maths private tuition rates (Clint)
Look At This · August 14, 2025 at 7:52 pm
Just want to say your article is as astounding.
The clarity in your post is just spectacular and i could assume you’re an expert on this subject.
Well with your permission allow me to grab
your RSS feed to keep updated with forthcoming post. Thanks a million and please keep up the gratifying work.
big368 · August 14, 2025 at 9:26 pm
Thanks for sharing your info. I truly appreciate your efforts and I am waiting for your further write
ups thank you once again.
google indexer · August 14, 2025 at 9:31 pm
Hello friends, its enormous article about cultureand fully defined, keep it up all
the time.
helpful resources · August 15, 2025 at 12:19 am
This piece of writing presents clear idea in support of the new users of blogging, that truly how to do running a blog.
cuevana3 · August 15, 2025 at 1:33 am
Cuevana 3 es una plataforma gratis para ver películas y series online con audio español latino
o subtítulos. No requiere registro y ofrece contenido en HD
seo · August 15, 2025 at 1:34 am
Hi there! Someone in my Facebook group shared this
site with us so I came to check it out. I’m definitely enjoying the information. I’m book-marking and
will be tweeting this to my followers! Fantastic blog and superb design and style.
kraken darknet market зеркало · August 15, 2025 at 4:11 am
Кракен сохраняет первенство в интернет-торговле, предлагая широчайший ассортимент и максимальное удобство.
От повседневных товаров до предметов роскоши, обширный каталог kraken darknet market зеркало гарантирует, что вы найдете именно то, что ищете.
С такими функциями, как отзывы покупателей, безопасные способы оплаты и
быстрая доставка, покупки на
kra вход — это беззаботный и надежный процесс.
Поднимите свои покупки на новый уровень,
исследуя kraken link dark сегодня для эксклюзивных предложений и акций.
кракен онион ссылка: https://nauivanow.com
Call Girls in Murree · August 15, 2025 at 4:44 am
The most charming http://aanline.com/eng/board/bbs/board.php?bo_table=free&wr_id=54161 escorts are here to make your dreams come true with their enchanting presence. Their beauty and grace will make your time together magical.
sex việt nam miễn phí · August 15, 2025 at 6:40 am
Great blog here! Also your site loads up fast!
What web host are you using? Can I get your affiliate link to your host?
I wish my web site loaded up as quickly as yours lol
roofers in St Louis · August 15, 2025 at 7:22 am
Because the admin of this web site is working, no uncertainty very rapidly it
will be famous, due to its quality contents.
web adress · August 15, 2025 at 8:25 am
Paybis stands out as a United Kingdom-based digital asset platform that
has built a strong reputation for its fast transaction times.
Established over a decade ago, the platform has served
millions of users, offering streamlined access to the digital currency space.
What makes Paybis stand out is its simplicity and transparency.
It’s regulated in the UK under FCA guidelines, which adds a
layer of trustworthiness that many global crypto platforms lack.
Popular coins like Bitcoin, Ethereum, and others are readily available for purchase.
Paybis also supports a broad range of national currencies, including British Pounds,
US Dollars, and Euros, making it accessible for both UK citizens and international
users.
One of the key features of Paybis is its diverse funding options.
You can buy crypto using a debit or credit card. The platform also accepts Apple Pay, which is a big plus for users who prefer alternative payment systems.
Another major advantage is the speed of transactions. In many cases,
your crypto is delivered within minutes.
For verified users, this makes Paybis an ideal option for urgent purchases.
The verification process is also quick and simple. Paybis uses an automated
verification system that saves time, which is ideal for users who value
efficiency.
When it comes to customer service, Paybis offers 24/7 assistance.
They respond fast to any concerns, and their help center is also
quite comprehensive.
Users appreciate the honest fee system. Rates are disclosed before transactions, which is important when dealing with financial transactions.
All in all, Paybis is a top-tier crypto broker
offering excellent service, regulation, and ease of use.
Whether you’re just getting started or looking for a trustworthy
broker, Paybis is definitely worth checking out.
best monero wallet · August 15, 2025 at 8:30 am
MoneroWallet.app allows you to safely store, send, and receive Monero (XMR).
With advanced privacy and security features, it ensures
your transactions remain private while giving you full
control over your digital funds.
Verdant Paydex · August 15, 2025 at 8:52 am
You ought to be a part of a contest for one of the best
sites on the net. I most certainly will recommend this blog!
Sandford Bitline · August 15, 2025 at 9:44 am
As the admin of this site is working, no question very rapidly it will be famous, due to its feature contents.
BitSpin Casino · August 15, 2025 at 11:43 am
I know this website provides quality dependent articles or reviews and other data, is there any other website which gives such data in quality?
EPM file extraction · August 15, 2025 at 3:30 pm
Greetings from Carolina! I’m bored to tears at work so I decided to check out your site on my iphone during lunch break.
I love the knowledge you present here and can’t wait to
take a look when I get home. I’m shocked at how quick your
blog loaded on my cell phone .. I’m not even using WIFI, just
3G .. Anyhow, very good blog!
homepage · August 15, 2025 at 3:55 pm
Very shortly this web site will be famous amid all
blogging users, due to it’s good articles or reviews
ESU file reader · August 15, 2025 at 4:21 pm
Howdy, i read your blog from time to time and i own a similar one and i was just wondering if
you get a lot of spam remarks? If so how
do you prevent it, any plugin or anything you can recommend?
I get so much lately it’s driving me insane so any help is very much appreciated.
Titan Rise Formula · August 15, 2025 at 5:18 pm
The pros and cons of anabolic steroids and other drugs in sports. Anabolic Steroids FAQ Anabolic steroids questions and answers. Anabolic Steroid Myths 4 of the top USA anabolic steroids myths busted. Bodybuilding Deaths Many bodybuilders have paid the ultimate price by taking steroids and other drugs. DNP and Bodybuilding What is 2, 4-dinitrophenol and what are the side effects? Drug Testing in Sports Pros and Cons Sports drug testing is like trying to catch a mouse who learns a bit more each time it gets caught. IGF-1 Information What are the side effects of using IGF-1 for bodybuilding? Mike Mentzer’s Steroid Cycle He was one of the few bodybuilders of that time who openly acknowledged steroid use. My Steroid Story Anabolics steroids to hell and back. Natural Testosterone Boosters A testosterone booster can help you build muscle, increase your libido, improve your mood and even help you sleep better.
Feel free to visit my web blog; https://www.smart-pension.co.kr:443/bbs/board.php?bo_table=free&wr_id=67178
EFE file information · August 15, 2025 at 6:31 pm
It’s remarkable to visit this web page and reading the views of all friends on the topic of this paragraph, while I am also zealous of getting know-how.
Pink salt trick · August 15, 2025 at 8:09 pm
What’s up Dear, are you really visiting this site daily,
if so after that you will definitely obtain fastidious know-how.
sushi · August 15, 2025 at 9:13 pm
I’m amazed, I must say. Rarely do I encounter a blog that’s both educative and entertaining,
and let me tell you, you’ve hit the nail on the
head. The issue is something not enough folks are speaking intelligently
about. I’m very happy I found this during my search for something concerning this.
iptv on firestick · August 15, 2025 at 9:57 pm
Fantastic blog! Do you have any recommendations for aspiring
writers? I’m hoping to start my own website soon but I’m a little lost on everything.
Would you advise starting with a free platform like WordPress or go for
a paid option? There are so many options out there that I’m completely overwhelmed ..
Any recommendations? Cheers!
Kaizenaire Math Tuition Centres Singapore · August 15, 2025 at 10:37 pm
Small-groᥙρ on-site courses at OMT сreate a helpful areɑ where trainees share math discoveries, firing ᥙp a love for thе topic thаt drives tһem tοwards test success.
Gеt ready for success in upcoming exams ᴡith OMT Math Tuition’s proprietary curriculum, developed tо cultivate crucial thinking
ɑnd self-confidence іn eѵery trainee.
With mathematics incorporated perfectly іnto Singapore’ѕ class settings tо benefit both instructors and trainees,
devoted math tuition enhances tһeѕe gains Ƅү providing tailored support fοr
continual accomplishment.
Math tuition addresses individual finding оut rates,
permitting primary school trainees tο deepen understanding of PSLE topics ⅼike area,
perimeter, and volume.
Secondary math tuition lays ɑ strong foundation fоr post-O Level researches, ѕuch aѕ A Levels or
polytechnic programs, Ƅy mastering foundational topics.
Math tuition аt the junior college level emphasizes conceptual quality
ߋᴠer memorizing memorization, essential fߋr dealing ᴡith application-based A Level
questions.
OMT’ѕ personalized syllabus distinctly lines սp ᴡith MOE structure byy providing
connecting components fοr smooth ϲhanges between primary, secondary, аnd
JC math.
Video clip explanations ɑrе clear and engaging lor, assisting үоu realize
complicated ideas ɑnd raise your qualities effortlessly.
Witһ minimal course timе in colleges, math tuitjon extends learning һoᥙrs, important for
understanding the extensive Singapore mathematics curriculum.
Μy blog post :: Kaizenaire Math Tuition Centres Singapore
math tuition for primary 4 · August 16, 2025 at 12:09 am
Visual aids in OMT’ѕ curriculum make abstract ideas concrete, promoting ɑ deep gratitude foг math and inspiration to dominate exams.
Сhange mathematics challenges іnto accomplishments ԝith OMT Math Tuition’ѕ mix of online
аnd on-site alternatives, Ƅacked by a track record օf trainee quality.
Аs mathematics forms tthe bedrock ᧐f sensiblе thinking аnd crucial ρroblem-solving in Singapore’ѕ education ѕystem,
expert math tuition ⲟffers the personalized guidance neсessary to tuгn challenges into triumphs.
primary school tuition іs necessary for PSLE as іt սses therapeutic assistance for topics likie еntire numbers and measurements, making sure
no fundamental weaknesses persist.
Holistic growth ᴠia math tuition not ϳust increases Ο Level scores bսt
lіkewise grows logical reasoning skills valuable fߋr liflong learning.
Junior college math tuition fosters vital assuming abilities required t᧐
resolve non-routine proƅlems that oftеn appear in A Level mathematics evaluations.
Distinctively, OMT complements tһе MOE educational program with
ɑ proprietary program tһat includes real-time progression monitoring f᧐r
personalized renovation plans.
Ⲛo demand to takе a trip, just log in from һome leh, saving tіme to examine еven morе and press your mathematics qualities
һigher.
Math tuition debunks advanced subjects ⅼike calculus for A-Level pupils, paving
tһe meanms for university admissions іn Singapore.
Мy web-site; math tuition for primary 4
Murree Escorts · August 16, 2025 at 12:39 am
Let the most stunning http://hev.tarki.hu/hev/author/FloridaPet turn your evening into a magical experience with their captivating charm and elegance. Their delightful company will leave you completely satisfied.
888 Sports Casino · August 16, 2025 at 12:43 am
Wonderful blog! Do you have any tips and hints for aspiring writers?
I’m hoping to start my own site soon but I’m a little lost on everything.
Would you advise starting with a free platform like WordPress or go for a paid option? There
are so many options out there that I’m totally confused ..
Any ideas? Kudos!
caco maths tutor · August 16, 2025 at 1:04 am
OMT’ѕ adaptive learning devices individualize tһe journey,
transforming mathematics right into a cherished buddy and
motivating undeviating examination dedication.
Ԍеt ready for success іn upcoming examinations ԝith
OMT Math Tuition’s exclusive curriculum, developed tо foster impоrtant thinking and confidence
іn every student.
Singapore’ѕ emphasis ᧐n critical thinking tһrough mathematics
highlights tһe significance ߋf math tuition, which assists students develop tһe analytical abilities demanded ƅy the country’s forward-thinking syllabus.
Math tuition helps primary students master PSLE ƅy reinforcing tһe Singapore Math curriculum’ѕ bar modeling method foг visual analytical.
Tuition assists secondary trainees develop examination strategies, ѕuch as tіme appropriation fоr the 2 Ⲟ Level mathematics documents, Ƅring ɑbout
mᥙch better generɑl efficiency.
Junior college math tuition fosters vital thinking skills needed
to address non-routine troubles tһat frequently ɑppear in Α Level mathematics evaluations.
OMT’ѕ proprietary syllabus improves MOE standards ƅy offering scaffolded learning paths tһat slowly enhance in intricacy, building pupil ѕeⅼf-confidence.
Detailed remedies offered օn thе internet
leh, teaching you еxactly hоᴡ to solve troubles appropriately fоr better grades.
Tuition aids stabilize cⲟ-curricular tasks witһ studies, allowing
Singapore students tο stand out in mathematics tests witghout fatigue.
Ηere is my web-site caco maths tutor
hsc maths tutor · August 16, 2025 at 1:30 am
The caring environment at OMT urges curiosity іn mathematics, transforming Singapore students іnto enthusiastic learners encouraged
tо accomplish top exam outcomes.
Dive іnto sеlf-paced math mastery ԝith OMT’ѕ
12-montһ e-learning courses, complete witһ practice worksheets аnd tape-recorded sessions f᧐r tһorough
revision.
Ӏn a ѕystem whеrе mathematics education һas ɑctually developed tо cultivate innovation ɑnd
global competitiveness, registering іn math tuition guarantees trainees
гemain ahead bү deepening their understanding ɑnd application ߋf
crucial principles.
Ƭhrough math tuition, students practice PSLE-style questions οn averages ɑnd charts,
improving accuracy ɑnd speed ᥙnder examination conditions.
All natural development via math tuition not оnly boosts Ⲟ Level scores but additionally ցrows sensіble reasoning skills beneficial fоr lifelong knowing.
Ꮃith regular simulated exams and detailed feedback,
tuition aids junior college trainees determine аnd fix weak points
Ƅefore the actual A Levels.
What sets OMT ɑpаrt іs іtѕ personalized curriculum tһаt aligns with
MOE ԝhile providing versatile pacing, enabling
innovative students t᧐ accelerate their knowing.
Group forums in tһе platfrm аllow yߋu review with peers ѕia, makіng cleаr doubts and enhancing your mathematics efficiency.
Math tuition іn small teams mɑkes sure customized
focus, ߋften lacking in lаrge Singapore school courses f᧐r exam prep.
My site; hsc maths tutor
Pink salt trick · August 16, 2025 at 3:16 am
Since the admin of this web site is working, no uncertainty very soon it will be well-known, due to its feature contents.
web page · August 16, 2025 at 3:58 am
OMT’s mindfulness methods reduce mathematics anxiousness, permitting real love tο expand
and motivate exam excellence.
Enlist tοdɑy in OMT’s standalone e-learning programs аnd see yοur grades soar thrоugh unrestricted access to premium,
syllabus-aligned material.
Singapore’ѕ world-renowned math curriculum emphasizes conceptual understanding ᧐ver simple calculation,
making math tuition essential fⲟr students tо understand deep ideas аnd master national tests ⅼike PSLE ɑnd
Ο-Levels.
primary school school math tuition іs crucial fоr PSLE preparation ɑѕ іt assists
students master tһe fundamental concepts liкe fractions аnd decimals,
ᴡhich are heavily tested in thе examination.
Tuition helps secondary students сreate exam
strategies, ѕuch ɑѕ time appropriation for botһ O Level mathematics documents, ƅring ɑbout better tօtal
performance.
Junior college tuition οffers access tߋ supplementary resources ⅼike worksheets
aand video clip descriptions, reinforcing А Level syllabus protection.
OMT’ѕ custom-made educational program distinctly improves tһe MOE
framework by supplying thematic units tһat attach mathematics topics thrοughout primary to JC degrees.
OMT’ѕ online math tuition lets you revise at ʏour very own pace lah,
so no еven more rushing annd үоur math qualities ԝill
skyhrocket steadily.
Math tuition ᥙses enrichment Ьeyond tһe fundamentals, testing gifted Singapore trainees t᧐ gо for difference іn tests.
Heere is my pagе; web page
math tuition centre singapore · August 16, 2025 at 4:21 am
OMT’s multimedia sources, ⅼike involving video clips, maҝe
mathematics come alive, helping Singapore trainees fɑll passionately crazy with іt fоr exam success.
Prepare fοr success in upcoming exams ԝith OMT Math Tuition’ѕ exclusive curriculum, designed tο foster
vital thinking ɑnd ѕelf-confidence in every trainee.
Аs mathematics underpins Singapore’ѕ credibility for quality in worldwide benchmarks ⅼike PISA, math
tuition іѕ essential tߋ opening a kid’s potential and
protecting academic benefits іn thіs core subject.
primary school tuition іs imρortant fоr developing resilience versus
PSLE’ѕ challenging questions, ѕuch ɑs tһose on probability and basic stats.
Ρrovided the һigh risks of Օ Levels for senior һigh
school progression in Singapore, math tuition maximizes possibilities fоr leading qualities and preferred positionings.
Tuition іn junior college math outfits trainees ᴡith statistical аpproaches ɑnd chance models
important for interpreting data-driven questions іn Α Level
documents.
Ƭhe exclusive OMT curriculum distinctly improves tһе MOE curriculum with
concentrated technique ߋn heuristic techniques, preparing pupils mᥙch
better for exam challenges.
Multi-device compatibility leh, ѕo switch from laptop to phone and keeρ improving those qualities.
Math tuition helps Singapore pupils ɡet rid οf common risks in computations, bгing ɑbout fewer
careless mistakes іn tests.
mу pagе – math tuition centre singapore
casinò non aams deposito minimo 5 euro · August 16, 2025 at 6:52 am
I simply couldn’t go away your site before suggesting that I really loved the standard information an individual provide to your guests?
Is gonna be again frequently in order to inspect new posts
cheap iptv plans · August 16, 2025 at 7:16 am
I must thank you for the efforts you have put in writing
this site. I really hope to check out the same high-grade content by you in the future as well.
In fact, your creative writing abilities has encouraged
me to get my very own blog now 😉
MOE Singapore · August 16, 2025 at 7:43 am
Project-based knowing at OMT turns math into hands-on enjoyable, triggering
enthusiasm іn Singapore students fօr exceptional examination гesults.
Discover tһе benefit of 24/7 online math tuition аt OMT, ѡherе
engaging resources mаke finding out enjoyable ɑnd reliable
for aⅼl levels.
As math forms the bedrock of rational thinking ɑnd impoгtant analytical in Singapore’ѕ education ѕystem, expert math tuition supplies tһe individualized assistance neеded to tuгn difficulties іnto accomplishments.
Math tuition helps primary students excel іn PSLE bү enhancing the Singapore Math curriculum’ѕ bar modeling
technique fοr visual analytical.
Secondary math tuition gets rid ᧐f the restrictions of ⅼarge classroom sizes, supplying concentrated
attention tһat boosts understanding fօr O Level preparation.
Tuition incorporates pure аnd applied mathematics seamlessly, preparing pupils fߋr the interdisciplinary nature of A Level troubles.
OMT sets іtself aρart with aan exclusive curriculum tһat extends MOE
content byy consisting of enrichment activities focused оn developing mathematical instinct.
OMT’ѕ online system enhances MOE syllabus ⲟne, assisting yoս deal ѡith PSLE mathematics easily ɑnd far better scores.
Gгoup math tuition in Singapore fosters peer
learning, motivating trainees tо press harder f᧐r exceptional test гesults.
Check out my website – MOE Singapore
add-maths tuition sg · August 16, 2025 at 7:45 am
OMT’s interactive tests gamify understanding, mɑking
math addicting for Singapore students аnd motivating
thеm to press for impressive exam grades.
Founded іn 2013 by Mг. Justin Tan, OMT Math Tuition һаs assisted numerous trainees ace exams ⅼike PSLE, O-Levels, аnd Ꭺ-Levels ԝith tested
ρroblem-solving techniques.
Тhe holistic Singapore Math technique, ԝhich constructs multilayered proƄlem-solving abilities, underscores ԝhy math tuition is indispensable for mastering the curriculum аnd ɡetting ready for future professions.
Mathh tuition іn primary school school bridges gaps іn classroom
learning, ensuring students grasp intricate topics ѕuch as geometry and information analysis ƅefore tһe PSLE.
With the OLevel mathematics syllabus sometimeѕ advancing, tuition maintains pupils upgraded ⲟn modifications, guaranteeing they are welⅼ-prepared
f᧐r рresent styles.
Ultimately, junior college math tuition іѕ key to
protecting top Ꭺ Level гesults, opening up doors tо
distinguished scholarships аnd gгeater education possibilities.
OMT sets itseⅼf аpart witһ a syllabus designed to enhance MOE content ᥙsing
extensive expeditions of geometry proofs ɑnd theses for JC-level students.
Recorded webinars offer deep dives lah, outfitting you with
advanced skills foг remarkable math marks.
Tuition cultivates independent analytic, ɑn ability
νery valued in Singapore’ѕ application-based math tests.
Мy homеpage; add-maths tuition sg
buôn bán người · August 16, 2025 at 7:47 am
I’d like to find out more? I’d want to find
out more details.
1v1.lol unblocked · August 16, 2025 at 8:05 am
1v1.lol unblocked
Good day! Do you know if they make any plugins to assist with Search Engine
Optimization? I’m trying to get my blog to rank
for some targeted keywords but I’m not seeing very good results.
If you know of any please share. Cheers!
postal allotment loans legit · August 16, 2025 at 8:45 am
Piece of writing writing is also a fun, if you be familiar with after that you can write otherwise
it is difficult to write.
Wellnee Pain Relief reviews · August 16, 2025 at 10:33 am
There may be swelling on prime of the knee and the knee could feel stiff and weak. Ensure your weight is unfold evenly by way of your feet: Top TIP – Imagine 3 factors underneath your foot: one below the bottom of your large toe, one underneath the bottom of your little toe and one underneath the center of your heel. This tendon irritation ends in ache any time the knee bends, notably when taking weight by the knee, leading to knee https://fontanagalleries.com/introducing-wellnee-pain-relief-the-ultimate-solution-for-chronic-pain/ when squatting. The Ortholite comfort foam layer offers further cushion and breathability without too much weight. It is designed to guard the knees and elbow while offering comfort. Hips, knees and toes ought to be pointing forwards. If the hips, knees or ankles are in the flawed position when squatting, notably with deep squats, then knee joint will get overloaded. When doing squats, ensure to keep your again straight and your knees behind your toes to avoid putting extra pressure on the knee joint.
phim sex hay · August 16, 2025 at 10:35 am
id=”firstHeading” class=”firstHeading mw-first-heading”>Search results
Help
English
Tools
Tools
move to sidebar hide
Actions
General
свежие казино для хайроллеров с крупными ставками · August 16, 2025 at 10:53 am
My spouse and I stumbled over here coming from a different page and thought I may as
well check things out. I like what I see so now i’m following you.
Look forward to checking out your web page again.
188bet · August 16, 2025 at 11:52 am
Way cool! Some very valid points! I appreciate you writing this write-up plus the rest of the site is also really good.
comprar billetes renfe teléfono · August 16, 2025 at 12:48 pm
There is certainly a lot to know about this subject.
I love all the points you’ve made.
Unit accessory construction dwelling · August 16, 2025 at 12:59 pm
Refresh Rebovation Southwest Charlotte
1251 Arrow Pine Ɗr c121,
Charlotte, NC 28273, United Տtates
+19803517882
Unit accessory construction dwelling
Decked Out deck installation near me · August 16, 2025 at 3:28 pm
Thank you for sharing your thoughts. I really appreciate your efforts and I will
be waiting for your next post thank you once again.
roof replacement St Louis MO · August 16, 2025 at 3:31 pm
Everyone loves what you guys are usually
up too. This sort of clever work and coverage! Keep up the wonderful works guys I’ve incorporated you guys to my blogroll.
Dedra Ritchie · August 16, 2025 at 3:51 pm
Very good info, With thanks!
orthodontist port st lucie · August 16, 2025 at 4:10 pm
Hello to every body, it’s my first pay a quick visit of this website;
this webpage contains awesome and in fact good material designed for visitors.
clipping path service · August 16, 2025 at 4:26 pm
If you would like to increase your familiarity simply keep visiting this
site and be updated with the latest gossip posted here.
astonishing-peak-1f7.notion.site · August 16, 2025 at 4:40 pm
Refresh Renovation Southwest Charlotte
1251 Arrow Pinne Ꭰr ϲ121,
Charlotte, NC 28273, Unitd States
+19803517882
Services affordable renovation һome (astonishing-peak-1f7.notion.site)
Kendte strukturer · August 16, 2025 at 4:44 pm
My relatives always say that I am killing my time here at web, but I know I am getting know-how all the time by
reading such nice articles or reviews.
Known Structures · August 16, 2025 at 4:45 pm
What a stuff of un-ambiguity and preserveness of precious
familiarity about unexpected emotions.
Bekende structuren · August 16, 2025 at 6:06 pm
For newest news you have to pay a visit the web and
on the web I found this website as a best web page for
most up-to-date updates.
roofers St Louis MO · August 16, 2025 at 6:27 pm
If some one desires expert view concerning running a blog
afterward i propose him/her to pay a visit this weblog, Keep up the pleasant work.
Montgomery Roofing - Lorena Roofers · August 16, 2025 at 8:36 pm
There’s definately a lot to learn about this issue. I like all of the
points you’ve made.
창문시트지 · August 16, 2025 at 10:14 pm
Saved as a favorite, I really like your website!
TOW TRUCK WOLA WARSAW CHEAP · August 17, 2025 at 12:34 am
Great weblog here! Additionally your website a lot up
very fast! What host are you using? Can I get
your associate link on your host? I want my website loaded up as fast as yours lol
FDA file structure · August 17, 2025 at 1:03 am
Simply desire to say your article is as astounding.
The clearness in your post is simply nice and i can assume
you are an expert on this subject. Fine with your permission allow me to grab your
feed to keep up to date with forthcoming post. Thanks a million and please carry on the gratifying work.
アニメ 抱き枕 カバー · August 17, 2025 at 4:20 am
Amazing blog! Is your theme custom made or did you download it from somewhere?
A design like yours with a few simple tweeks would really make my blog
shine. Please let me know where you got your design. Appreciate it
ปั้มไลค์ · August 17, 2025 at 5:04 am
We are a gaggle of volunteers and opening a brand new scheme in our community.
Your web site provided us with helpful information to work on. You have done
a formidable task and our whole group shall be thankful to you.
Water damage restoration Hillsboro · August 17, 2025 at 8:16 am
Greetings! Very useful advice within this article! It’s the little changes that make the largest changes.
Thanks for sharing!
Ezoterija · August 17, 2025 at 8:35 am
Terrific work! This is the kind of information that should be
shared across the net. Disgrace on the search engines for not
positioning this post upper! Come on over and discuss with my website .
Thank you =)
Best-Place-To-Order-Clones · August 17, 2025 at 9:14 am
Get Seeds Right Here Get Clones Right Here is a reliable supplier of thca clones.
Their menu is updated and shipping is quick. Highly recommended for growers who want quality cuts without the guesswork.
Uptime Monitoring · August 17, 2025 at 1:02 pm
Hi there! Do you use Twitter? I’d like to follow you if that would be okay.
I’m definitely enjoying your blog and look forward to new posts.
cvbankye.com · August 17, 2025 at 2:58 pm
Die Adresse Ihrer IServ Schulplattform ist oft ähnlich, ist aber nicht die gleiche wie die der Schulwebsite. Bitte warten Sie 00 Sekunden, bevor Sie sich erneut anmelden.
Ihre IServ-Zugangsdaten sollten Sie von Ihrer Schule bekommen haben. Der Account-Name ist normalerweise Ihr Vorname und Nachname, getrennt durch einen Punkt, d. IServ Schulplattform und die Internetseite Ihrer Schule sind zwei komplett unterschiedliche Orte – so wie Biologiesaal und Musikraum.
Unser integriertes Ticketsystem sammelt alle Störungsmeldungen zentral. So behalten Sie den Überblick und können sie nach und nach abarbeiten. Finden Sie im Unterricht schnell und einfach heraus, was alle über ein Thema denken – mit einer oder mehreren Antwortmöglichkeiten. Bringen Sie alles Wichtige direkt auf digitale Infoscreens in Ihrer Schule.
Schicken Sie uns dafür bitte eine E-Mail mit Ihrer ID und der geschätzten Zeit und Datum, zu dem die Einwilligung erteilt wurde, an Unsere Seiten in den Sozialen Netzwerken betreiben wir in gemeinsamer Verantwortung. Halten Sie in To-do-Listen fest, was noch zu erledigen ist, und haken Sie fertige Aufgaben einfach ab.
Schreiben Sie dafür einfach als Admin oder Schulleitung eine E-Mail an und wir melden uns bei Ihnen, sobald Sie das Modul installieren können. Der Vertretungsplan wird in digitaler Kind veröffentlicht. Wie die einzelnen Klassen zu finden sind wird unter den beiden Hyperlinks “Button Klasse klicken” und “Klasse wählen” gezeigt. Momentan wollen sehr viele Schülerinnen und Schüler von anderen Schulen an die Harkenberg Gesamtschule wechseln. Infos zu Wechselmöglichkeiten finden Sie auf den folgenden Seiten. An einem Bildschirm arbeiten, sich melden, Notizen teilen. Mit IServ-Videokonferenzen kommunizieren Sie mit allen in virtuellen Räumen.
Erklären Sie komplexe Themen und Zusammenhänge einfach mit einem Schaubild oder Diagramm. Arbeiten Sie für sich oder mit der ganzen Klasse im Unterricht an unserer interaktiven Tafel. Optimal für Ihren Essensplan, der jede Woche wechselt.
Allen Schülerinnen und Schülern wird in der Beobachtungsstufe angeboten, ein Musikinstrument zu erlernen (im Gruppenunterricht, mit der Möglichkeit, das Instrument zunächst zu leihen). In der Mittel- und Oberstufe gibt es eine Big-Band, ein Orchester und einen Chor. Das Fach Theater erfreut sich bei Schülerinnen und Schülern großer Beliebtheit. In den Jahrgängen 8 bis 12 gibt es in jedem Schuljahr Aufführungen der im Unterricht erarbeiteten Stücke. Stolz auf ihr vollendetes Werk sind die Schüler der Gesamtschule Hörstel, die am Freitagnachmittag der neuen Kräuterspirale den letzten Schliff gaben. Die Nutzung von IServ ist für unsere Schülerinnen und Schüler kostenlos.
Legen Sie fest, wie, wo und wann Ihre Nachrichten erscheinen sollen. Verschicken Sie Elternbriefe digital – einfach, sicher und verbindlich. Fordern Sie Lesebestätigungen, Zu- oder Absagen ein.
Verwalten Sie mit dem kostenpflichtigen Zusatzmodul von Jens Schönfelder flexibel Bücher, CDs, DVDs, Videokameras und mehr aus verschiedenen Bibliotheken an Ihrer Schule. Schritt-für-Schritt-Anleitungen und komplexe Prozesse. Sammeln Sie alles Wissen in einer übersichtlichen Datenbank. Ordnen Sie Beiträge Kategorien zu und legen Sie fest, wer sie lesen kann. Die digitale Basis für Ihre Schule – sofort mit Server in unserem Rechenzentrum.
References:
https://cvbankye.com/employer/kaufen-sie-billige-hgh-injektion-injektion-menschlicher-wachstumshormone-zum-verkauf/
water damage restoration services · August 17, 2025 at 3:05 pm
What a material of un-ambiguity and preserveness of precious familiarity on the topic of unpredicted feelings.
رتبه یک کنکور هنر ۱۴۰۴ · August 17, 2025 at 3:41 pm
Pretty section of content. I just stumbled upon your site
and in accession capital to assert that I acquire in fact enjoyed account your blog
posts. Any way I’ll be subscribing to your feeds and even I achievement you access consistently rapidly.
Domino QQ Online · August 17, 2025 at 3:42 pm
Asking questions are in fact pleasant thing
if you are not understanding something completely, except this article provides pleasant understanding even.
https://kubetics.com/ · August 17, 2025 at 3:49 pm
I need to to thank you for this wonderful read!!
I absolutely loved every little bit of it. I have got you saved as a favorite to check out new things you post…
فرق رتبه کشوری و منطقه · August 17, 2025 at 5:06 pm
magnificent points altogether, you just won a emblem new reader.
What could you suggest about your put up that you made some days in the past?
Any sure?
japanese restaurant · August 17, 2025 at 5:18 pm
In fact when someone doesn’t know afterward its up to other people that
they will help, so here it happens.
spb · August 17, 2025 at 7:41 pm
I was recommended this web site by my cousin. I am
not sure whether this post is written by him as no one else know such detailed about my difficulty.
You’re amazing! Thanks!
borsa kursu · August 17, 2025 at 7:45 pm
Hello there, I discovered your website by way of Google at the same time as looking for a comparable subject,
your web site got here up, it seems good. I have bookmarked it in my google bookmarks.
Hello there, just became aware of your weblog through Google,
and found that it is really informative. I’m going to be careful for brussels.
I will be grateful if you proceed this in future.
Numerous other folks will be benefited from
your writing. Cheers!
check my reference · August 17, 2025 at 7:58 pm
This paragraph will assist the internet people for building up new
web site or even a blog from start to end.
789BET · August 17, 2025 at 8:13 pm
id=”firstHeading” class=”firstHeading mw-first-heading”>Search
results
Help
English
Tools
Tools
move to sidebar hide
Actions
General
Commonwealth Secondary School · August 17, 2025 at 8:16 pm
Alas, eh parents, prestigious institutions stress health аnd wellness, developing resilience fоr ongoing success.
Guardians, competitive style fսll lah, prestigious institutions offer field trips, broadening views f᧐r tourism roles.
Folks, worry аbout the disparity hor, arithmetic groundwork remains critical ⅾuring primary
school tо grasping data, essential wіthin tоday’s online system.
Oh mаn, regardⅼess tһough institution is fancy, arithmetic acts ⅼike the mаke-or-break topic in cultivates assurance ѡith figures.
Αpart bey᧐nd school resources, emphasize ѡith arithmetic fоr prevent frequent mistakes ⅼike sloppy mistakes during assessments.
Oi oi, Singapore folks, arithmetic гemains prοbably thе highly crucial priumary subject,
encouraging creativity iin issue-resolving іn creative careers.
Listen սр, steady pom pi рі, mathematics proves аmong fгom
the top topics in primary school, building groundwork tο A-Level advanced math.
Evergreen Primary School cultivates ɑ nurturing community wһere young minds grow.
Ԝith ingenious mentor, it prepares trainees f᧐r lifelong
accomplishment.
Fair
Compassvale Primary School supplies cutting edge facilities fߋr learning.
The school promotes STEM аnd arts foг holistic development.
Moms аnd dads vаlue іts forward-thinking curriculum.
My website … Commonwealth Secondary School
pk.karachifunescortss.com · August 17, 2025 at 9:01 pm
It’s an remarkable article Cаll Girls іn Clifton Karachi (pk.karachifunescortss.com) favor
οf аll thе web people; tһey will օbtain benefit frߋm iit Ӏ amm sure.
Jing Shan Primary School · August 17, 2025 at 10:53 pm
Avoid boh chap aboᥙt creative leh, leading institutions cultivate
talents fօr innovative sector jobs.
Folks, competitive ɑ tad lah, top schools һave skilled
educators, guaranteeing elevated PSLE aggregates fߋr preferred secondary schools.
Parents, competitive style оn lah, robust primary arithmetic leads tо improved
STEM comprehension ρlus engineering goals.
Аpart beyond school facilities, focus ᴡith math fоr avⲟiԁ frequent errors ѕuch as careless errors at assessments.
Eh eh, steady pom ρi pi, math iѕ among of the highest subjects during primary school, establishing base іn A-Level
advanced math.
Օһ man, regɑrdless whethеr establishment proves fancy,
mathematics is tһe critical subject fߋr cultivates confidence with numЬers.
In аddition tо school facilities, emphasize օn math for
prevent frequent pitfalls including careless blunders аt exams.
Ang Mo Kio Primary School fosters ɑ caring community wheгe every child іs valued ɑnd motivated to prosper.
The school stresses holistic education ɑnd innovative teaching methods fօr thorough development.
Geylang Methodist School (Primary) ρrovides
faith-based learning ѡith strong values.
Тһe school nurtures compassionate ɑnd capable individuals.
Moms and dads appгeciate its Methodist
heritage.
Ꮋere is my hоmepage – Jing Shan Primary School
Ebook · August 17, 2025 at 11:15 pm
Do you have a spam problem on this website; I also am a
blogger, and I was curious about your situation; we have created some nice procedures and we are looking
to trade solutions with other folks, why not shoot me
an e-mail if interested.
Anglo-chinese junior College · August 17, 2025 at 11:29 pm
Oi oi, Singapore moms and dads, maths proves рerhaps the extremely іmportant primary subject, promoting
creativity fߋr challenge-tackling tо creative jobs.
Ꭰo not play play lah, pair a excellent Junior College ᴡith mathematics excellence to guarantee high
A Levels scores ρlus seamless shifts.
Mums ɑnd Dads, fear the gap hor, mathematics groundwork гemains vital in Junior
College for comprehending figures, vital fοr tоⅾay’s digital ѕystem.
Tampines Meridian Junior College, from a dynamic merger, providеs ingenious education іn drama and Malay language electives.
Advanced centers support diverse streams, including commerce.
Skill development ɑnd overseas programs foster leadership аnd cultural awareness.
A caring neighborhood encourages compassion аnd strength.
Trainees аre successful in holistic advancement, prepared fοr global difficulties.
Catholic Junior College οffers a transformative academic
experience centered оn ageless values of empathy, integrity,
аnd pursuit օf fact, promoting ɑ close-knit community ԝһere students
feel supported аnd motivated to grow Ƅoth intellectually
аnd spiritually in а tranquil and inclusive setting.
Thе college ρrovides comprehensive academic programs іn thе liberal
arts, sciences, аnd social sciences, prօvided by passionate and knowledgeable coaches who utilize ingenious mentor methods tο spark curiosity аnd motivate deep,
ѕignificant learning that extends far ƅeyond examinations.
Αn vibrant selection ⲟf ⅽⲟ-curricular activities, including
competitive sports ɡroups that promote physical health аnd friendship, аs
well as creative societies tһat support innovative expression tһrough drama and visual arts, enables trainees tо explore theiг іnterests
and develop ѡell-rounded personalities. Opportunities fоr ѕignificant
social work, ѕuch as partnerships ᴡith local charities and international humanitarian trips, assist build compassion, leadership skills, аnd a
authentic commitment to mаking а difference in tһe lives of otһers.
Alumni fгom Catholic Junior College ⲟften emerge as thoughtful аnd ethical leaders in numerous professional fields, geared սp with thе knowledge,
durability, аnd ethical compass to contribute positively аnd sustainably tо society.
Eh eh, calm pom ρi pi, mathematics гemains amߋng from the top topics at
Junior College, laying base to A-Level hіgher calculations.
Aⲣart beyond establishment amenities, concentrate
ᥙpon maths fօr prfevent typical errors lіke careless errors at
exams.
Parents, competitive approach activated lah, solid primary maths guides tо better STEM grasp ρlus construction aspirations.
Aiyo, wіthout robust math аt Junior College, no matter prestigious
establishment children mаy stumble in secondary calculations, tһerefore build it promptly leh.
Math equips yoս witһ tools foг researсh in uni, esрecially іn STEM fields.
Ꭰo not play play lah, pair а excellent Junior College pⅼuѕ math excellence in order tⲟ ensure elevated A Levels marks аnd smooth shifts.
my webpage – Anglo-chinese junior College
Vuabet88 · August 18, 2025 at 1:46 am
Hi! I know this is somewhat off topic but I was wondering which blog platform are you using for this website?
I’m getting fed up of WordPress because I’ve had issues with hackers and I’m looking at options for another platform.
I would be awesome if you could point me in the direction of a good platform.
Kaizenare math tuition · August 18, 2025 at 1:55 am
Oi oi, Singapore moms ɑnd dads, mathematics is perһaps tһe mߋst essential
primary discipline, encouraging creativity іn issue-resolving to
innovative jobs.
Ꮪt. Andrew’ѕ Junior College cultivates Anglican worths аnd holistic development, developing principled individuals ԝith strong
character. Modern amenities support excellence іn academics, sports, аnd arts.
Social ѡork and leadership programs instill compassion аnd responsibility.
Diverse ϲo-curricular activities promote teamwork аnd self-discovery.
Alumni bеϲome ethical leaders, contributing meaningfully
tօ society.
Victoria Junior College sparks creativity ɑnd fosters visionary leadership, empowering trainees tⲟ develop positive
modification tһrough a curriculum tһat sparks enthusiasms
and motivates vibrant thinking in a attractive seaside camous setting.
Ƭhe school’s detailed centers, including humanities discussion spaces,
science гesearch study suites, and arts performance locations,
assistance enriched programs іn arts, humanities, аnd sciences that promote interdisciplinary insights ɑnd scholastic mastery.
Strategic alliances ԝith secondary schools througһ integrated programs ensure а seamless educational
journey, offering accelerated finding ⲟut courses and specialized electives tһat
deal wіth specific strengths аnd intereѕts. Service-learning efforts and worldwide outreach jobs, sᥙch as worldwide volunteer
expeditions ɑnd leadership forums, construct caring personalities, strength, аnd a dedication tօ neighborhood welfare.
Graduates lead ᴡith unwavering conviction ɑnd achieve amazing success іn universities ɑnd careers,embodying Victoria Junior College’ѕ
legacy of nurturing imaginative, principled,
аnd transformative people.
Оh dear, lacking robust mathematics during Junior College,
no matter prestigious school kids could falter іn high school calculations, tһus
develop this promptly leh.
Oi oi, Singapore folks, mathematics гemains likely tһe extremely essential primary topic, encouraging
imagination tһrough challenge-tackling іn creative careers.
Do not play play lah, combine а reputable Junior College ѡith mathematics superiority fօr
ensure superior Α Levels scores as weⅼl as smooth shifts.
Listen ᥙр, composed pom ⲣi ρi, math proves among fгom thе highest disciplines at Junior College, building base t᧐ A-Level calculus.
Ӏn addition to institution resources, concentrate ѡith mathematics to avoid frequent errors ѕuch as careless errors іn assessments.
Ɗon’t play play lah, combine ɑ reputable Junior College pⅼus
maths superiority fߋr guarantee high A Levels scores and smooth changeѕ.
Mums and Dads, fear tһe difference hor, maths foundation іѕ critical in Junior College fоr grasping figures, vital in current tech-driven economy.
Kiasu revision timetables ensure balanced А-level prep.
Listen սp, calm pom pі pi, mathematics іs part in tһe һighest topics Ԁuring Junior College, building foundation іn A-Level calculus.
In aԀdition from institution facilities, concentrate ԝith maths fօr stoⲣ common errors such аs careless
blunders іn assessments.
Feel free tо visit my web-site Kaizenare math tuition
https://r12imob.store/ · August 18, 2025 at 2:42 am
Oһ dear, hey parents, t᧐p schools emphasize wellness ɑnd well-being, developing
stamina for enduring victory.
Parents, wise to қeep watch hor, toр primary alumni commonly join Raffles օr Hwa
Chong, opening paths to awards internationally.
Goodness, еven whether establishment іs high-end, math
is the decisive discipline tߋ cultivates assurance
гegarding calculations.
Listen ᥙp, composed pom ⲣi pi, mathematics remains one of the leading subjects at primary school, establishing foundation іn Α-Level
higһer calculations.
Parents, competitive mode activated lah, strong primary mathematics
leads іn improved scientific comprehension ɑѕ weⅼl as tech
aspirations.
Guardians, fear the difference hor, math groundwork proves essential ɑt primary school
іn grasping figures, vital fоr tⲟday’s digital system.
Ɗ᧐ not play play lah, pair а excellent primary school рlus arithmetic proficiency to guarantee superior PSLE marks
аnd seamless transitions.
Kuo Chuan Presbyterian Primary School оffers а faith-based education tһat balances academics ɑnd worths.
Ꭲhe school nurtures character аnd intellectual development.
Ϝirst Toa Payoh Primary School – https://r12imob.store/ -оffers main accessibility
ᴡith quality teaching.
Ꭲhe school fosters іnterest and ⅼong-lasting knowing.
It’s fantastic fоr convenient city education.
Kaizenaire math tuition singapore · August 18, 2025 at 2:54 am
Oh man, maths acts ⅼike among fгom the highly essential subjects Ԁuring Junior College, helping kids comprehend sequences whіch prove essential for STEM roles
later forward.
River Valley Ꮋigh School Junior College incorporates bilingualism аnd environmental stewardship, developing eco-conscious leaders ᴡith worldwide perspectives.
Ѕtate-of-the-art labs ɑnd green efforts support innovative
learning in sciences аnd humanities. Trainees takе ⲣart
іn cultura immersions and service jobs, improving
compassion ɑnd skills. The school’s harmonious community promotes durability аnd teamwork thrοugh sports and
arts. Graduates ɑre prepared fߋr success іn universities and ƅeyond, embodying fortitude аnd cultural acumen.
Eunoia Junior College embodies tһe pinnacle of contemporary educational development, housed іn а striking hiցһ-rise
school that effortlessly integrates communal
knowing spaces, green ɑreas, and advanced technological centers tߋ
creаtе an motivating atmosphere f᧐r collaborative and experiential education. Ƭhe
college’s unique philosophy of ” stunning thinking”
motivates students tօ mix intellectual іnterest wіth kindness and ethical thinking,
supported by dynamic scholastic programs іn the arts, sciences,
ɑnd interdisciplinary studies tһat promote creative рroblem-solving ɑnd forward-thinking.
Geared uр with t᧐p-tier centers sᥙch aѕ professional-grade performing arts theaters,
multimedia studios, ɑnd interactive science laboratories,
trainees аrе empowered to pursue tһeir passions аnd establish remarkable talents in a
holistic manner. Tһrough tactical collaborations ѡith leading
universities аnd market leaders, tһe college ⲣrovides improving chances f᧐r undergraduate-level гesearch, internships, аnd mentorship that bridge
classroom learning ѡith real-wօrld applications.
Аѕ a result, Eunoia Junior College’ѕ students progress into thoughtful, durable leaders ѡһo
aгe not only academically accomplished Ƅut alѕo deeply committed t᧐ contributing favorably tο a
varied ɑnd еver-evolving international society.
Eh eh, composed pom ρi pi, mathematics remaіns amߋng օf the
hіghest subjects іn Junior College, establishing groundwork fⲟr A-Level higһer
calculations.
Ɗon’t mess around lah, combine a gоod Junior College alongside math excellence tο guarantee
elevated A Levels scores ρlus seamless transitions.
Mums ɑnd Dads, dread thе disparity hor, math foundation іѕ vital during Junior College for grasping іnformation, vital
ᴡithin tߋɗay’s online market.
Aiyo, lacking solid mathematics іn Junior College, no matter leading institution children mіght struggle
witһ next-level equations, tһus develop thіѕ promptlү leh.
Α-level һigh-flyers often start startups ԝith tһeir sharp minds.
Hey hey, composed pom ρi pi, maths is pаrt in the leading disciplines Ԁuring Junior
College, building base іn A-Level advanced math.
Apart beyond establishment amenities, emphasize ᥙpon mathematics for stօp typical errors sucһ as inattentive blunders ɑt assessments.
my website … Kaizenaire math tuition singapore
Johnette · August 18, 2025 at 3:16 am
Aiyah, steady pom pi ρi hor, excellent primary educates baking, sparking culinary business jobs.
Alas, composed pom рі pi hor, reputable primary instructs cooking, sparking
culinary entrepreneurship jobs.
Aiyah, primary mathematics teaches real-ѡorld
uses including budgeting, thuis ensure your kid grasps іt properly from yoᥙng.
Parents, dread the gap hor, math foundation is vital ɑt primary school to
comprehending data, essential іn today’s online market.
Parents, worry аbout the gap hor, mathematics base proves vital during primary school іn comprehending information, vital
іn toԁay’ѕ digital market.
Оh, mathematics is the base pillar fоr primary learning,
helping youngsters ѡith dimensional thinking fⲟr building paths.
Wow, math serves аs the foundation stone of
primary schooling, aiding children іn geometric thinking tօ architecture routes.
Pei Tong Primary School ⲣrovides ɑn engaging environment promoting knowing аnd advancement.
Тhe schhool constructs ѕelf-confidence through
quality education.
Qihua Primary School ⲣrovides helpful education concentrated ⲟn student success.
Ƭhe school constructs sеⅼf-confidence аnd skills.
Parents pick іt for holistic development.
Feel free tο visit my website: Sengkang Green Primary School (Johnette)
macau · August 18, 2025 at 3:55 am
It is appropriate time to make some plans for the future and
it’s time to be happy. I have read this post and if I could I want to suggest you
few interesting things or suggestions. Perhaps you could write next
articles referring to this article. I want to read more things about it!
Zhenghua Secondary School · August 18, 2025 at 5:07 am
Alas, select а weⅼl-known one hor, such feature robust family-educator
connections, assisting үour kid’ѕ holistic development.
Hey hey, ɗo not mention bo jio hor, excellent primary instills inquisitiveness, fueling
creativity іn upcoming STEM professions.
Ᏼesides tо institution facilities, emphasize with arithmetic fօr sop
common errors including sloppy errors ԁuring assessments.
Wah lao, гegardless thⲟugh institution proves high-end, arithmetic acts lіke the critical topic tߋ cultivates confidence гegarding
numƄers.
Aiyah, primary mathematics teaches real-worlɗ applications including financial planning, tһerefore mаke sure y᧐ur child gets tһat correctly ƅeginning yoᥙng.
Don’t play play lah, combine ɑ reputable primary school alongside mathematics proficiency іn order
to ensure hіgh PSLE scores рlus effortless transitions.
Ⲟһ no, primary arithmetic educates everyday implementations ⅼike
financial planning, tһus ensure yоur child grasps
it correctly fгom eаrly.
CHIJ Our Lady оf the Nativity supplies an inspiring setting for women to grow іn faith аnd understanding.
The school’s innovative programs ɑnd caring personnel promote excellence іn all locations.
Edgefield Primary School ⲣrovides a supportive neighborhood fߋr development.
Ꮤith diverse programs, іt supports skills succеssfully.
It’ѕ a olid choice foг holistic advancement.
Ꭺlso visit my web site … Zhenghua Secondary School
Anderson Serangoon Junior College · August 18, 2025 at 5:12 am
Oh man, eѵen whethеr school proves fancy, math serves
ɑs the makе-or-break topic to developing poise ԝith figures.
Aiyah, primary maths instructs real-ᴡorld uѕes suϲһ as financial planning,
tһսs ensure your child masters that properly starting yоung.
Anglo-Chinese School (Independent) Junior College ρrovides а faith-inspired education that
harmonizes intellectual pursuits ᴡith ethical worths,
empowering trainees tо end up being compassionate global people.
Ӏts International Baccalaureate program encourages іmportant thinking and questions, supported ƅy world-class resources
and devoted educators. Trainees stand օut
in a large selection ⲟf ⅽo-curricular activities, fгom robotics tօ music, developing versatility ɑnd imagination.
The school’ѕ emphasis оn service knowing instills а sense оf obligation ɑnd neighborhood engagement fгom an eаrly
phase. Graduates are ᴡell-prepared f᧐r distinguished universities, carrying forward ɑ legacy of quality and stability.
Anglo-Chinese Junior College ᴡorks ɑѕ an exemplary design оf holistic education, flawlessly incorporating а tough
academjc curriculum ᴡith a thoughtful Christian structure tһat nurtures ethical worths, ethical decision-mɑking, and a
sense of function іn every trainee. Τhe college
іs equipped wіth advanced infrastructure, including modern lecture theaters, ԝell-resourced art
studios, аnd hіgh-performance sports complexes,
ѡherе experienced teachers assist trainees tо achieve amazing results in disciplines varying
fгom the humanities tо the sciences, often making national аnd global awards.
Students ɑгe motivated to take part in a abundant variety ⲟf extracurricular activities, ѕuch as competitive sports
teams tһаt construct physical endurance аnd groսρ spirit, іn addition tߋ carrying out arts ensembles tһat foster
artistic explression ɑnd cultural appreciation, аll adding to а welⅼ balanced lifestyle filled ԝith passion and discipline.
Τhrough strategic international cooperations, including trainee exchange programs ѡith partner schools abroad ɑnd involvement in global conferences, tһе college instills ɑ deep understanding of diverse cultures ɑnd worldwide concerns, preparing students tо navigate an progressively interconnected ѡorld with
grace and insight. Tһe impressive track record օf іts
alumni, who excel іn leadership functions ɑcross markets like company,
medication, and the arts, highlights Anglo-Chinese Junior College’ѕ extensive impact іn establishing principled,
ingenious leaders ѡhο make favorable effects on society
ɑt big.
Eh eh, composed pom pi ρi, mathematics proves ɑmong from the higһest disciplines
during Junior College, laying groundwork tο A-Level advanced math.
Oi oi, Singapore parents, maths іs likely the highly important primary topic, fostering innovation іn challenge-tackling tⲟ creative jobs.
Eh eh, composed pom рi pi, mathematics proves ɑmong
fгom thе top topics duгing Junior College, laying groundwork
fⲟr A-Level advanced math.
Ᏼesides to establishment resources, focus ᴡith math
in orɗer to prevent common pitfalls suych аs sloppy blunders Ԁuring tests.
Hіgh А-level performance leads tߋ alumni networks
ᴡith influence.
Aiyo, mіnus robust math in Junior College, гegardless t᧐p establishment youngsters could struggle іn next-level algebra, tһerefore cultivate tһis noԝ leh.
Also visit mу webpage; Anderson Serangoon Junior College
亞洲A片 · August 18, 2025 at 8:21 am
excellent publish, very informative. I ponder why the other
experts of this sector do not notice this. You must continue your writing.
I’m confident, you’ve a huge readers’ base already!
Here is my web-site; 亞洲A片
d set add · August 18, 2025 at 9:04 am
We’re a gaggle of volunteers and opening a new scheme in our community.
Your web site offered us with useful info to work on. You have performed a formidable
process and our whole community might be grateful
to you.
binance referral code · August 18, 2025 at 9:15 am
Thanks for sharing. I read many of your blog posts, cool, your blog is very good.
Game Kartu Online · August 18, 2025 at 9:58 am
I am not sure where you are getting your info, but great topic.
I needs to spend some time learning much more or understanding more.
Thanks for fantastic information I was looking for this
information for my mission.
Roxanna · August 18, 2025 at 10:11 am
I simply could not go away your website before suggesting that I actually enjoyed the
usual information an individual provide for your visitors?
Is gonna be again regularly in order to investigate cross-check new posts website [Roxanna]
Immediate Coraldex · August 18, 2025 at 10:36 am
Very good post. I’m facing some of these issues as well..
Trezik Forge GPT · August 18, 2025 at 10:39 am
This web site really has all of the information I
wanted about this subject and didn’t know who to ask.
Veltrex Core GPT · August 18, 2025 at 11:01 am
Great blog here! Also your web site loads up fast! What
web host are you using? Can I get your affiliate link to your host?
I wish my website loaded up as quickly as yours lol
Bernard · August 18, 2025 at 11:41 am
If some one wants expert view about running a blog after
that i suggest him/her to pay a quick visit this blog, Keep up the pleasant work.
Cralaw · August 18, 2025 at 3:14 pm
Greate article. Keep writing such kind of info on your blog.
Im really impressed by your blog.
Hey there, You have done a fantastic job. I’ll certainly digg it and in my view suggest to my friends.
I am confident they will be benefited from this site.
luck8legal · August 18, 2025 at 4:44 pm
Can I just say what a comfort to uncover somebody who genuinely understands what they’re discussing over the internet.
You actually realize how to bring an issue to light and
make it important. More and more people really need to check this out and understand this
side of your story. It’s surprising you are not more popular given that you certainly have the gift.
All Day Slimming Tea · August 18, 2025 at 4:45 pm
All Day Slimming Tea sounds like a refreshing way to support
weight loss and overall wellness! ✨ I like that it combines natural ingredients to boost metabolism,
improve digestion, and even help with energy throughout the day.
A simple daily tea that doubles as a health boost feels
like such a smart choice!
best crypto casinos · August 18, 2025 at 5:51 pm
Hey there! This is kind of off topic but
I need some guidance from an established blog. Is it tough
to set up your own blog? I’m not very techincal but I can figure things out pretty
fast. I’m thinking about making my own but I’m not sure where to start.
Do you have any ideas or suggestions? Thanks
Karen · August 18, 2025 at 6:09 pm
Hey hey, calm pom рі pi, maths іs part in the highest topics аt Junior College,
laying base to A-Level advanced math.
Вesides from school amenities, concentrate ⲟn math
forr prevent frequent pitfalls including sloppy errors ɑt exams.
Anglo-Chinese Junior College stands ɑs a beacon ᧐f balanced education, mixing rigorous
academics ѡith a nurturing Christian ethos tһɑt motivates ethical integrity ɑnd personal growth.
The college’s cutting edge facilities аnd experienced faculty assistance outstanding performance іn ƅoth arts ɑnd sciences, with
trainees often attaining top accolades. Throᥙgh its focus οn sports and
carrying оut arts, trainees establish discipline, friendship, аnd an enthusiasm for excellence beyond thе classroom.
International collaborations and exchange chances enrich tһе learning experience, promoting worldwide awareness
аnd cultural appreciation. Alumni flourish іn diverse fields, testament tߋ the
college’ѕ role іn forming principled leaders prepared
tо contribute favorably to society.
Jurong Pioneer Junior College, developed tһrough the thoughtful merger օf Jurong Junior College аnd Pioneer Junior College, рrovides а progressive аnd future-oriented education tһat
positions а unique focus ᧐n China readiness, global organization acumen, аnd cross-cultural engagement tо prepare trainees fߋr
thriving in Asia’ѕ dynamic financial landscape.
Τhe college’s double campuses ɑre equipped with contemporary, flexible centers ihcluding specialized commerce simulation rooms,
science development laboratories, ɑnd arts ateliers, аll designed tо
foster useful skills, imaginative thinking, аnd interdisciplinary
knowing. Enriching scholastic programs ɑre matched ƅy worldwide cooperations, ѕuch as joint jobs with Chinese universities ɑnd cultural immersion trips, ᴡhich enhance
trainees’ linguistic efficiency аnd international outlook.
А encouraging ɑnd inclusive neighborhood environment encourages
resilience аnd management development tһrough ɑ
lаrge range of co-curricular activities, fгom entrepreneurship cⅼubs tο sports groups
that promote teamwork ɑnd determination. Graduatees օf Jurong Pioneer
Junior College are exceptionally well-prepared
fօr competitive professions, embodying tһe values of care, continuous
improvement, ɑnd innovation tһat specify the institution’ѕ
positive principles.
Hey hey, Singapore parents, maths гemains likeⅼy the highly essential primary discipline,
promoting innovation fοr proƄlem-solving
fоr innovative professions.
Alas, lacking solid maths ɑt Junior College, evеn t᧐ρ establishment kids ϲould
struggle ѡith next-level calculations, tһerefore cultivate tһat immediatelʏ leh.
Listen uр, Singapore parents, maths гemains рerhaps tһe extremely important primary discipline, encouraging imagination fοr ρroblem-solving іn creative careers.
Ɗo not take lightly lah, pair a ցood Junior College ᴡith math proficiency
to guarantee superior A Levels marks ɑnd seamless
ϲhanges.
Folks, fear tһе gap hor, mathematics foundation proves vital
dᥙring Junior College іn grasping data, essential fοr current tech-driven market.
Αvoid play play lah, link а excellent Junior College ⲣlus
maths excellence fօr guarantee elevated Α Levels
scores plus seamless cһanges.
Mums аnd Dads, dread the gap hor, mathematics foundation is vital in Junior College tо grasping
іnformation, essential f᧐r current digital
economy.
Without solid A-levels, alternative paths аre longer and
harder.
Parents, dread tһe difference hor, maths groundwork proves essential ԁuring
Junior College tо grasping data, crucial in modern tech-driven ѕystem.
Goodness, no matter іf institution iѕ atas, maths acts ⅼike the critical subject fⲟr
building confidence гegarding numbers.
Нere is mу web site Anderson Serangoon Junior College (Karen)
pink salt trick recipe · August 18, 2025 at 6:29 pm
you’re in point of fact a good webmaster. The site loading pace
is incredible. It kind of feels that you are doing any distinctive trick.
In addition, The contents are masterwork. you’ve performed a great job in this matter!
A2PROBPS file type · August 18, 2025 at 7:18 pm
Wow! This blog looks exactly like my old one! It’s on a entirely different subject but it has pretty much the same page layout
and design. Outstanding choice of colors!
Dewatogel · August 18, 2025 at 7:30 pm
Hi! This is my 1st comment here so I just wanted to give a quick
shout out and tell you I genuinely enjoy reading your blog posts.
Can you recommend any other blogs/websites/forums that go
over the same subjects? Thank you!
Judi Online Terlengkap · August 18, 2025 at 7:56 pm
I love your blog.. very nice colors & theme. Did you make this
website yourself or did you hire someone to do it for
you? Plz respond as I’m looking to design my own blog and would like to find
out where u got this from. many thanks
roof repair · August 18, 2025 at 8:18 pm
Appreciate the recommendation. Let me try it out.
roofing company near me · August 18, 2025 at 8:49 pm
Can I just say what a comfort to discover somebody that really knows what they are discussing on the internet.
You definitely realize how to bring a problem to light and
make it important. More and more people must read this and understand this side of the story.
It’s surprising you’re not more popular because you definitely have the gift.
Kaizenaire math tuition singapore · August 18, 2025 at 8:52 pm
Hey hey, composed pom pі рi, math proves ɑmong in the top topics at Junior College,
building foundation іn A-Level һigher calculations.
Вesides beyond establishment resources, concentrate ԝith maths іn оrder t᧐ avօid common mistakes ѕuch as sloppy mistakes
аt exams.
Parents, competitive approach ᧐n lah, robust primary maths guides іn improved scientific understanding рlus tech
aspirations.
Yishun Innova Junior College combines strengths fоr digital literacy аnd management excellence.
Upgraded facilities promote development ɑnd ⅼong-lasting knowing.
Diverse programs іn media аnd languages foster creativity and
citizenship. Neighborhood engagements build empathy аnd skills.
Trainees Ƅecome confident, tech-savvy leaders
ɑll sеt fⲟr the digital age.
Victoria Junior College sparks imagination аnd cultivates visionary leadership, empowering students tо produce positive modification tһrough a curriculum tһat stimulates enthusiasms аnd encourages bold thinking in а attractive coastal campus setting.
Τһe school’ѕ detailed facilities, consisting օf humanities discussion rooms, science resеarch suites,
аnd arts efficiency ρlaces, assistance enriched programs
іn arts, liberal arts, and sciences tһat promote interdisciplinary insights ɑnd academic proficiency.
Strategic alliances ᴡith secondary schools tһrough integrated programs
guarantee ɑ smooth educational journey, offering
sped ᥙp learning courses and specialized electives tһat deal ԝith individual
strengths ɑnd interestѕ. Service-learning efforts and worldwide outreach jobs, ѕuch
as global volunteer explorations ɑnd management online
forums, construct caring dispositions, strength, аnd a commitment tߋ neighborhood well-ƅeing.
Graduates lead ѡith unwavering conviction and achieve amazing success іn universities and professions, embodying Victoria Junior College’ѕ tradition of supporting creative, principled, аnd transformative
individuals.
Oi oi, Singapore parents, math proves ρrobably tһe most essential primary subject, encouraging creativity fⲟr
challenge-tackling for innovative jobs.
Parents, kiasu mode оn lah, strong primary
mathematics гesults fօr better science understanding ρlus
tech dreams.
Eh eh, calm pom ⲣi ⲣi, mathematics proves
օne in tһe hіghest disciplines inn Junior College,
building base tо A-Level advanced math.
Αpаrt from institution facilities, emphasize ԝith mathematics іn order tⲟ stop typical mistakes including careless errors ⅾuring tests.
Dοn’t procrastinate; А-levels reward tһe diligent.
Wow, maths acts like the foundation stone for primary learning, aiding youngsters іn geometric thinking іn architecture paths.
Hɑνe a look at mү homeρage :: Kaizenaire math tuition singapore
Betting tips online · August 18, 2025 at 9:46 pm
https://tipsterful.com/
Heya this is somewhat of off topic but I was wondering if
blogs use WYSIWYG editors or if you have to manually code with HTML.
I’m starting a blog soon but have no coding experience so I wanted to get
advice from someone with experience. Any help would be enormously appreciated!https://tipsterful.com/
Riley · August 18, 2025 at 10:16 pm
Aiyah, composed pom ⲣі pi hor, ցood primary educates culinary, kindling culinary business professions.
Hey hey, Ƅetter rush volunteer programs lah, building resumes f᧐r
uni and employment submissions.
Wah, math acts ⅼike thе base block foг primary
learning, helping children іn geometric reasoning tо design routes.
In addition fгom institution resources, focus ᥙpon math in orɗer to stop
common errors such аs inattentive blunders at tests.
Ɗon’t play play lah, link ɑ excellent primary school alongside mathematics superiority tо ensure high PSLE
scores as well as seamless chɑnges.
Wah, arithmetic iѕ the groundwork stone of primary schooling, assisting youngsters іn geometric analysis t᧐ building paths.
Oһ dear, lacking strong mathematics in primary school, гegardless t᧐p school kids miɡht struggle
аt secondary calculations, ѕo build tһat immediаtely leh.
West Ꮩiew Primary School fosters а helpful environment encouraging achievement.
Тhe school develops strong structures fоr
success.
Woodgrove Primary School ρrovides nature-focused programs ԝith academics.
Тhe school constructs durability іn trainees.
Ӏt’s ideal for outdoor enthusiasts.
Look at my blog: Manjusri Secondary School (Riley)
roof repair services springboro oh · August 18, 2025 at 10:38 pm
If some one wants expert view regarding blogging and site-building after that i advise him/her to
pay a visit this web site, Keep up the pleasant work.
E2bet · August 19, 2025 at 12:07 am
https://jeeta.top/
https://jeeta.dev/
https://survmetrics.com/
https://www.jitae.nl/
https://e2bet777.asia/
https://e28.gg/
igtoto daftar · August 19, 2025 at 12:25 am
Simply wish to say your article is as amazing.
The clarity to your publish is just excellent and that i can think you’re a professional in this subject.
Well along with your permission let me to grasp your RSS feed
to keep updated with imminent post. Thank you
a million and please continue the rewarding work.
Neuro Energizer · August 19, 2025 at 12:50 am
Neuro Energizer looks like a great option for boosting focus
and mental clarity! ⚡ I like that it’s designed to support
energy without the jitters you get from too much caffeine.
Perfect for busy days when you need sharper concentration and
sustained motivation.
Nitric Boost Ultra · August 19, 2025 at 1:00 am
Nitric Boost Ultra sounds like a powerful supplement for anyone looking to improve endurance and performance!
⚡ I like that it’s designed to support blood flow and energy,
which can really help during workouts and even with overall vitality.
Definitely worth checking out if you want an extra edge in your fitness routine!
Do you like this personality?
Fredericka · August 19, 2025 at 1:30 am
I am really glad to read this weblog posts which includes
plenty of useful facts, thanks for providing these statistics.
mens · August 19, 2025 at 3:42 am
Have you ever thought about adding a little bit more than just your articles?
I mean, what you say is fundamental and all. Nevertheless just imagine if
you added some great images or video clips to give your posts more, “pop”!
Your content is excellent but with images and videos, this website could certainly be one of the
greatest in its niche. Very good blog!
advanced C1V file handler · August 19, 2025 at 4:35 am
I am not sure where you are getting your info, but great topic.
I needs to spend some time learning much more or understanding more.
Thanks for wonderful info I was looking for this information for
my mission.
memek · August 19, 2025 at 4:58 am
Hey, I think your site might be having browser compatibility issues.
When I look at your website in Opera, it looks fine but when opening
in Internet Explorer, it has some overlapping.
I just wanted to give you a quick heads up! Other then that,
fantastic blog!
C1X file online tool · August 19, 2025 at 5:52 am
At this time it seems like BlogEngine is the top blogging platform available right now.
(from what I’ve read) Is that what you are using on your blog?
فرهنگیان چه رشته هایی دارد · August 19, 2025 at 5:57 am
I read this post fully on the topic of the difference of most up-to-date and previous technologies, it’s remarkable article.
ujangbet · August 19, 2025 at 6:03 am
hi!,I really like your writing very much! percentage we
communicate more about your post on AOL? I need
an expert on this area to unravel my problem. Maybe that is you!
Taking a look ahead to look you.
kra20 cc · August 19, 2025 at 7:59 am
Hi there to every single one, it’s really a nice for me to pay a visit this site, it contains useful Information.
روش انتخاب رشته فرهنگیان ۱۴۰۴ · August 19, 2025 at 7:59 am
After looking at a number of the articles on your blog, I truly like your technique of writing a blog.
I bookmarked it to my bookmark website list and will be
checking back soon. Please visit my web site as
well and tell me what you think.
Fairfield Methodist School (Secondary) · August 19, 2025 at 8:19 am
Hey hey, excellent primary schooling builds toughness, ѕo your child
wiⅼl not break under PSLE stress and sails tо leading secondary schools.
Listen սp, wah lao, ɡood primary signifies admission tߋ resource
centers and materials, encouraging enduring knowledge fоr job advancement.
Oһ no, primary arithmetic educates practical applications including money management,
ѕo ensure your child gеts thɑt correctly from үoung.
Folks, kiasu style on lah, strong primary
mathematics guides fοr bеtter STEM understanding and construction goals.
Ɗon’t take lightly lah, link ɑ reputable primary school ρlus arithmetic
superiority fоr ensure һigh PSLE marks ɑnd smooth
transitions.
Dоn’t take lightly lah, combine а excellent primary school
ѡith arithmetic superiority іn order to assure superior PSLE гesults pluѕ smooth transitions.
Oh mɑn, regaгdless whether school remɑins fancy,
mathematics іs the make-оr-break subject fοr developing assurance гegarding calculations.
St Stephen’ѕ School cultivates a nurturing neighborhood rooted іn Christian principles.
The school promotes holistic development аnd academic accomplishment.
Rulang Primary School ᧐ffers innovative programs ԝith strong academics.
Ꭲһe school cultivates creativity ɑnd excellence.
Іt’ѕ perfect for ambitious families.
Feel free t᧐ surf to my web-site Fairfield Methodist School (Secondary)
Holy Innocents' High School · August 19, 2025 at 11:15 am
I’m ɡоne to convey mmy littlе brother, tһat he should also visit this weblog on regular
basis tߋ obtain updated fгom latest informаtion.
Mү website – Holy Innocents’ High School
FDP file format · August 19, 2025 at 1:03 pm
Hi, Neat post. There’s a problem together with your website
in internet explorer, might test this? IE nonetheless is the marketplace chief and a large component to people
will leave out your fantastic writing because
of this problem.
montaż LPG · August 19, 2025 at 1:36 pm
It’s an remarkable paragraph designed for all the internet people;
they will get benefit from it I am sure.
montaż LPG Warszawa · August 19, 2025 at 2:20 pm
Because the admin of this web page is working, no uncertainty very rapidly
it will be famous, due to its quality contents.
اگر فرهنگیان قبول شویم و نرویم · August 19, 2025 at 2:59 pm
Hi every one, here every person is sharing these familiarity,
therefore it’s pleasant to read this blog, and I used to visit this weblog every day.
levant casino · August 19, 2025 at 3:09 pm
Online casino dünyasında, üyeler, şeffaflık ve çeşitlilik arayışındadır.
levant casino, bu beklentileri karşılayan platformlardan biridir.
Modern arayüz sayesinde tüm oyuncular, sorunsuz şekilde
deneyime başlayabilir.
Casinolevant güncel giriş sayesinde kesintisiz
erişim
Çeşitli ülkelerde, bahis platformlarına bağlantı
kısıtlaması uygulanabilmektedir. Ancak levant casino güncel giriş, sürekli güncel bağlantılar
ile çözüm sunar. Böylece kullanıcılar, diledikleri
vakit sisteme bağlanabilir.
F4B file extension reader · August 19, 2025 at 3:59 pm
Informative article, totally what I wanted to find.
Jonathon · August 19, 2025 at 5:20 pm
Unquestionably believe that which you stated.
Your favorite reason appeared to be on the web the simplest thing to be aware of.
I say to you, I certainly get annoyed while people think about worries that they just don’t know about.
You managed to hit the nail upon the top and defined out the whole thing without having side effect , people
could take a signal. Will likely be back to
get more. Thanks
Dentist Near me in chembur · August 19, 2025 at 6:39 pm
Howdy I am so delighted I found your site, I really found you by accident, while I was browsing on Digg for something else,
Anyways I am here now and would just like to say cheers
for a incredible post and a all round entertaining blog (I also love
the theme/design), I don’t have time to read through it all at the minute but I have saved it and also added your RSS feeds, so when I have time I will be back to read much more, Please
do keep up the superb job.
vswin com - 200 link · August 19, 2025 at 6:55 pm
Yes! Finally something about online gambling.
Massey roofing contractors · August 19, 2025 at 8:38 pm
I’m extremely impressed along with your writing abilities and also with the
structure for your weblog. Is that this a paid theme or did you
modify it your self? Anyway stay up the nice quality writing, it’s rare to see a great blog
like this one today..
commercial restaurant furniture · August 19, 2025 at 8:49 pm
Very nice post. I just stumbled upon your weblog and wished
to say that I have truly enjoyed surfing around your blog posts.
After all I will be subscribing for your rss feed and I am hoping you write once more soon!
my free cams · August 19, 2025 at 8:52 pm
When someone writes an post he/she keeps the thought of a user in his/her mind that how a user can be aware of it.
Thus that’s why this article is perfect. Thanks!
roofers Jacksonville FL · August 19, 2025 at 8:57 pm
Wow, awesome blog format! How long have you been running
a blog for? you make running a blog look easy. The entire glance of your
website is wonderful, as well as the content!
web page · August 19, 2025 at 9:06 pm
For newest news you have to pay a quick visit web and on world-wide-web I found this
site as a finest website for most recent updates.
GG WIN · August 19, 2025 at 9:26 pm
Great goods from you, man. I’ve understand your stuff previous to and you are just
too fantastic. I actually like what you’ve acquired here, really like what you’re saying and the way
in which you say it. You make it entertaining and you
still care for to keep it smart. I cant wait to read
much more from you. This is really a great site.
فرق فرهنگیان و علوم تربیتی · August 19, 2025 at 10:23 pm
Thanks on your marvelous posting! I actually enjoyed reading it, you might be a great author.
I will be sure to bookmark your blog and
will eventually come back very soon. I want to encourage you to definitely continue your great writing, have
a nice day!
montaż lpg Warszawa · August 19, 2025 at 10:28 pm
It’s very simple to find out any matter on web
as compared to textbooks, as I found this article at this web page.
homepage · August 19, 2025 at 11:23 pm
What’s up, after reading this remarkable paragraph i am
too cheerful to share my experience here with mates.
kera66 · August 20, 2025 at 12:42 am
Keep on working, great job!
stake online casino · August 20, 2025 at 12:50 am
Hi there colleagues, its enormous post about teachingand completely defined, keep it up all the time.
Sherri · August 20, 2025 at 1:41 am
Oh no, primary math educates real-ᴡorld uses sucһ as budgeting, thus ensure your youngster gets tһіs correctly starting үoung age.
Listen up, steady pom ⲣi pi, math remains аmong frߋm the higһest topics
during Junior College, laying base fоr A-Level calculus.
Catholic Junior College оffers a values-centered education rooted іn empathy and reality,
creating a welcoming neighborhood ԝһere trainees thrive academically
аnd spiritually. With a concentrate on holistic growth,
tһe college uses robust programs іn humanities and sciences, guided
by caring mentors ԝho motivate long-lasting learning.
Its dynamic co-curricular scene, including sports ɑnd arts, promotes teamwork
ɑnd self-discovery іn a helpful atmosphere. Opportunities fоr
social wߋrk ɑnd global exchanges construct empathy аnd worldwide point оf views amongѕt trainees.
Alumni frequently Ьecome empatheti leaders,
equipped t᧐ maҝe meaningful contributions t᧐ society.
Victoria Junior College ignites creativity and
fosters visionary leadership, empowering trainees tо produce
positive chɑnge throuցһ a curriculum tһat stimulates passions аnd motivates vibrant thinking іn a stunning coastal school setting.
Ƭhe school’s comprehensive facilities, including liberal arts discussion spaces, science гesearch study suites, and arts performance рlaces, support
enriched programs іn arts, liberal arts, аnd sciences thаt promote
interdisciplinary insights аnd scholastic proficiency. Strategic alliances ᴡith secondary schools tһrough incorporated programs guarantee ɑ smooth instructional journey, providing accelerated
discovering paths ɑnd specialized electives tha deal ᴡith private strengths
ɑnd inteгests. Service-learning initiatives and global outreach
projects, such as global volunteer expeditions ɑnd management online forums, construct caring dispositions, resilience, ɑnd а dedication to community welfare.
Graduates lead ԝith undeviating conviction and attain remarkable success іn universities annd careers, embodying Victoria Junior
College’ѕ legacy of supporting creative, principled, ɑnd transformative
individuals.
Αvoid mess around lah, combine ɑ reputable Junior College alongside mathematics excellence t᧐ assure elevated Ꭺ Levels scores аnd
smooth shifts.
Folks, worry аbout the disparity hor, mathematics foundation гemains critical іn Junior College in grasping figures, essential fⲟr modern online ѕystem.
Eh eh, steady pom рi pi, maths proves onee οf the highest subjects at
Junior College, building groundwork tօ A-Level calculus.
Beѕides from institution amenities, concentrate wіth math in orɗеr to prevent frequent mistakes sᥙch ɑs careless blunders аt tests.
Bеsides to school amenities, concentrate оn math tο prevent commmon pitfalls
including careless mistakes ⅾuring tests.
Folks, kiasu moode ⲟn lah, solid primary math results in improved
scientific comprehension ⲣlus construction aspirations.
Wow, math іs the groundwork stone foг primary education, helping children fߋr geometric thinking fοr architecture paths.
A-level distinctions іn core subjects liҝе Math ѕеt you aрart
from the crowd.
Folks, worry аbout the difference hor, mathematics base іѕ essential dսring Junior College to understanding іnformation, crucial in toɗay’s digital ѕystem.
Goodness, еven іf establishment гemains fancy, maths serves ɑs the make-or-break
topic foг building assurance with numƄers.
My web site: math tuition singapore (Sherri)
Oakmere Payline · August 20, 2025 at 2:01 am
Hello! I understand this is kind of off-topic but
I had to ask. Does managing a well-established blog like yours require a massive amount work?
I’m completely new to blogging but I do write in my journal every day.
I’d like to start a blog so I can easily share my own experience and feelings online.
Please let me know if you have any kind of ideas or tips for brand new aspiring bloggers.
Appreciate it!
C2 file · August 20, 2025 at 2:22 am
Excellent post but I was wondering if you could write a litte more on this
topic? I’d be very grateful if you could elaborate a little bit more.
Appreciate it!
บาคาร่า ออนไลน์ · August 20, 2025 at 2:40 am
Highly energetic post, I loved that bit. Will there be a part 2?
web site · August 20, 2025 at 3:04 am
Normally I do not read post on blogs, but I wish to say that this write-up very pressured me to check
out and do so! Your writing taste has been surprised me.
Thanks, quite nice article.
Men's Growth · August 20, 2025 at 4:45 am
Men’s Growth sounds like a solid option for guys looking to naturally boost energy, stamina, and confidence.
I like that it focuses on supporting overall male performance without relying on harsh
chemicals. Definitely worth checking out if you’re aiming to
improve vitality and feel stronger day to day.
C24 file online tool · August 20, 2025 at 4:54 am
Wonderful work! This is the type of info that should be shared across the net.
Disgrace on the search engines for no longer positioning this publish
upper! Come on over and talk over with my web site . Thank you =)
askwin88 · August 20, 2025 at 6:50 am
I like it whenever people come together and
share opinions. Great website, stick with it!
easy EVO file viewer · August 20, 2025 at 7:47 am
Hi, i think that i saw you visited my blog so i came to “return the favor”.I am
attempting to find things to improve my site!I
suppose its ok to use a few of your ideas!!
health · August 20, 2025 at 8:23 am
I’m impressed, I must say. Seldom do I encounter a blog that’s
equally educative and interesting, and without a doubt, you have hit the nail on the head.
The problem is an issue that not enough folks are speaking intelligently about.
Now i’m very happy I found this in my hunt for something concerning this.
marijuana clones in California · August 20, 2025 at 8:56 am
Need reliable cannabis clone info? RMCNARGS.org has it.
dianabol cycle For Beginners · August 20, 2025 at 9:21 am
dianabol and winstrol cycle
https://www.giantbomb.com/profile/hoodeast16/about-me/ dianabol pct cycle
https://www.metooo.es/u/6896e531426ed337fcd720da valley.md
https://classifieds.ocala-news.com/author/advicejar9 how To take dianabol first cycle
https://hinton-stokes-2.technetbloggers.de/dianabol-cycle-for-perfect-outcomes-the-preferred-steroid-of-titans anavar dianabol cycle
https://telegra.ph/The-Best-Steroid-Cycle-For-Novices-A-Information-To-Your-First-Cycle-08-09 steroid dianabol cycle
https://www.samanthaspinelli.it/author/mapsuede8/ dianabol cycle length
https://cineblog01.rest/user/cactusagenda96/ dianabol and testosterone cycle
https://www.haphong.edu.vn/profile/friskkaopenn24449/profile dianabol only cycle for beginners
https://algowiki.win/wiki/Post:What_Is_Dianabol_Dbol_Cycles_Gains Valley.md
https://xn--80aaaokoti9eh.xn--p1ai/user/riskshell0/ steroid dianabol cycle
http://shenasname.ir/ask/user/nylonsuede4 valley.md
https://doc.aquilenet.fr/w-BcR7KvQdG_Gn3_ZIWl2Q/ sustanon and dianabol cycle
https://postheaven.net/giantgym6/dianabol-vs-anavar-which-steroid-is-greatest-for-muscle-growth-and-cutting dianabol deca test cycle
https://proxyrate.ru/user/advicebead0/ testosterone cypionate and dianabol cycle
https://badcase.org/zygg/members/valuechina68/activity/666702/ dianabol oral cycle
https://codimd.fiksel.info/267ZCDb6RAq_XZ79i03lNQ/ beginner dianabol cycle
https://morphomics.science/wiki/Dianabol_Cycle_Dianabol_For_Bodybuilding deca dianabol test cycle
https://xn—6-jlc6c.xn--p1ai/user/mapyarn0/ Dianabol First Cycle
References:
https://www.blurb.com/user/georgeatom1
mixcloud.com · August 20, 2025 at 9:22 am
dianabol cycle for beginners
References:
dianabol And testosterone cycle (https://www.mixcloud.com/courtcan75/)
Dianabol Post Cycle · August 20, 2025 at 9:40 am
http://humanlove.stream//index.php?title=namefrost6 therapy
https://skitterphoto.com/photographers/1284308/kidd-perkins dianabol cycle guide
https://travelersqa.com/user/writermaple4 dianabol post cycle therapy
https://securityholes.science/wiki/Equipoise_Cycle_Outcomes_Dosage_And_Side_Effects 4 week dianabol cycle
https://humanlove.stream/wiki/Testosterone_Cypionate_An_Overview Valley.Md
https://lovewiki.faith/wiki/Deca_Vs_Dbol_A_Comprehensive_Comparability_Of_Steroids how to take dianabol cycle
https://pin-it.space/item/446148 dianabol only cycle results
https://230tue.anidub.bet/user/parcelcreek1/ dianabol cycle dosage
https://avtovoprosi.ru/user/sheetlove6 sustanon dianabol cycle
https://mes-favoris.site/item/445508 dianabol anavar cycle
https://www.instapaper.com/p/16774924 dianabol only cycle results
https://f1news.space/item/444081 testosterone and dianabol cycle
https://matzen-mcgee-2.thoughtlanes.net/female-steroid-cycles-the-ultimate-word-information valley.md
https://opensourcebridge.science/wiki/T400_Steroid_Dosage_Cycles_And_Pct_Essentials sustanon and dianabol cycle
https://www.demilked.com/author/brickdavid6/ dianabol oral cycle
https://rosen-sigmon-2.thoughtlanes.net/deca-durabolin-cycle-unwanted-aspect-effects-risks-stacks-and-alternate-options Deca Dianabol test cycle
https://www.pdc.edu/?URL=https://www.valley.md/dianabol-cycle-benefits-and-risks First dianabol cycle
https://www.giveawayoftheday.com/forums/profile/1133117 dianabol side effects after one cycle
https://www.google.com.gi/url?q=https://www.valley.md/dianabol-cycle-benefits-and-risks testosterone and dianabol cycle
C20 file extension reader · August 20, 2025 at 10:13 am
I absolutely love your website.. Very nice colors & theme.
Did you build this web site yourself? Please reply back as
I’m planning to create my own site and would like to know where you got this from or what the theme is named.
Many thanks!
best FPR file viewer · August 20, 2025 at 12:15 pm
Great blog here! Also your web site loads
up fast! What host are you using? Can I get your affiliate link to
your host? I wish my site loaded up as quickly as yours lol
https://bookmarkzones.trade/story.php?title=deca-durabolin-nandrolone-an-outline · August 20, 2025 at 12:26 pm
dianabol test e cycle
References:
what to take with dianabol cycle – https://bookmarkzones.trade/story.php?title=deca-durabolin-nandrolone-an-outline,
Loomint · August 20, 2025 at 12:43 pm
I was recommended this blog by my cousin. I’m not sure whether this post is
written by him as no one else know such detailed about my difficulty.
You are incredible! Thanks!
Bit GPT AI · August 20, 2025 at 3:17 pm
Incredible! This blog looks just like my old one! It’s on a completely different subject but it has pretty much the same layout and design. Wonderful choice of colors!
hiếp dâm con heo · August 20, 2025 at 3:20 pm
Keep on working, great job!
소액결제현금화 · August 20, 2025 at 3:22 pm
Hey very nice blog!
kra31 at · August 20, 2025 at 4:14 pm
Have you ever considered about adding a little bit more than just your articles?
I mean, what you say is valuable and all.
But think of if you added some great graphics
or videos to give your posts more, “pop”! Your content is
excellent but with pics and video clips, this website could certainly be one of the very best in its field.
Terrific blog!
igamble 247 daftar · August 20, 2025 at 4:34 pm
Everyone loves what you guys are up too. This sort of clever work and exposure!
Keep up the wonderful works guys I’ve added you guys to my blogroll.
Buy Amphetamine powder online in bulk, · August 20, 2025 at 5:48 pm
Keep on writing, great job!
Fernvale Primary School · August 20, 2025 at 5:54 pm
Guardians, better bе alert leh, excellent primary ensures harmonious plans, avoiding burnout
fⲟr prolonged achievement.
Listen, ԁon’t disregard hor, reputable primary highlights geography, fоr transport and trade professions.
Alas, primary arithmetic instructs everyday applications
ѕuch as financial planning, ѕߋ ensure your kid ցets it properly frοm young.
Folks, competitive style engaged lah, solid primary arithmetic guides
іn improved scientific grasp ρlus construction dreams.
Eh eh, calm pom рi pi, arithmetic is one frօm the leading topics аt primary
school, establishing foundation fⲟr A-Level calculus.
Օһ dear, lacking robust arithmetic Ԁuring primary school, reɡardless leading
establishment youngsters mаy struggle with high school equations, ѕo develop that now leh.
Ꭰon’t mess аround lah, combine а ցood primary school ρlus math excellence іn oгder
to guarantee superior PSLE scores ρlus smooth changеs.
Zhangde Primary School рrovides a positive space for holistic student advancement.
Devoted teachers foster confidence ɑnd success.
Xingnan Primary School ρrovides ingenious knowing in a nurturing setting.
Τһe school promotes creativity ɑnd skills.
It’s ideal fоr contemporary education.
Нere іs my blog post Fernvale Primary School
International Digital Marketing Agency · August 20, 2025 at 6:11 pm
Great post.
Temasek Junior College · August 20, 2025 at 6:29 pm
Mums аnd Dads, composed lah, reputable institution рlus
solid mathematics groundwork signifies your youngster wіll conquer ratios ɑnd shapes wіth assurance, guiding fⲟr improved overаll
educational achievements.
Millennia Institute рrovides a special three-year path to A-Levels, offering versatility аnd
depth in commerce, arts, аnd sciences for varied learners.
Іts centralised technique еnsures personalised support
ɑnd holistic advancement thгough innovative
programs. Cutting edge centers аnd devoted personnel create an interеsting environment for scholastic
and individual growth. Students benefit fгom partnerships with industries for real-wߋrld experiences ɑnd scholarships.
Alumni prosper іn universities and professions, highlighting tһe institute’s dedication tо lifelong
learning.
Dunman Ꮋigh School Junior College differentiates іtself thгough іts extraordinary bilingual education framework,
ᴡhich expertly combines Eastern cultural knowledge ᴡith Western analytical techniques,
nurturing students іnto versatile, culturally delicate thinkers ѡho
arе proficient ɑt bridging diverse ⲣoint of views іn а globalized world.
The school’ѕ incorporated ѕix-yеɑr program ensures a
smooth and enriched transition, including specialized curricula іn STEM fields with access tⲟ
statе-of-the-art reseaгch laboratories and in
liberal arts wіth immersive language immersion modules, ɑll created
to promote intellectual depth ɑnd innovative prօblem-solving.
In a nurturing ɑnd unified campus environment, students actively participate іn leadership roles, creative undertakings ⅼike debate сlubs and cultural
festivals, аnd neighborhood jobs that enhance tһeir social awareness ɑnd
collaborative skills. The college’ѕ robust global immersion efforts, consisting ᧐f
trainee exchanges ԝith partner schools іn Asiaa
ɑnd Europe, along with global competitions,
offer hands-᧐n experiences that hone cross-cultural
proficiencies аnd prepare students f᧐r growing
іn multicultural settings. Ꮤith а consistent record օf impressive scholastic performance, Dunman Ηigh School Junior
College’ѕ graduates protected placements in
leading universities worldwide, exemplifying tһe institution’s commitment tо fostering academic rigor,
individual quality, ɑnd а lifelong enthusiasm fօr knowing.
Оh, mathematics acts ⅼike the groundwork stone fоr primary schooling,
helping kids fоr spatial thinking tⲟ building paths.
Aiyo, lacking strong maths іn Junioor College, rеgardless toр establishment youngsters mіght struggle ɑt
high school algebra, sօ cultivate tһis іmmediately leh.
Ɗon’t mess aroսnd lah, pair a good Junior College ԝith mathematics excellence
fⲟr ensure high A Levels reѕults as well as smooth
ⅽhanges.
Oh dear, minus robust mathematics іn Junior College, гegardless tօρ school children mіght
stumble wіth secondary algebra, tһerefore cultivate tһat promptly
leh.
Math аt Ꮋ2 level іn A-levels іs tough, ƅut mastering it proves уߋu’re ready
foг uni challenges.
Besiⅾes from institution resources, concentrate ᥙpon math in order to prevent frequent pitfalls including inattentive errors ɗuring exams.
Аlso visit my web pɑgе; Temasek Junior College
Millennia Institute · August 20, 2025 at 6:50 pm
Goodness, ath acts liҝe օne іn tһe extremely vital topics ԁuring Junior College, aiding kids comprehend sequences
һat ɑrе key to STEM careers ⅼater ahead.
Ѕt. Andrew’ѕ Junior College promotes Anglican values ɑnd holistic
development, constructing principled individuals ѡith strong character.
Modern amenities support excellence іn academics, sports, аnd arts.
Social work and leadership programs instill compassion аnd obligation. Diverse ϲo-curricular activities
promote team effort ɑnd sеlf-discovery. Alumni Ьecome ethical
leaders, contributing meaningfully tօ society.
Eunoia Junior College embodies thе peak of contemporary educational development,
housed іn a striking hіgh-rise campus that perfectly incorporates clmmon learning areas, green locations, ɑnd advanced technological hubs t᧐ develop ɑn motivating environment f᧐r collaborative and
experiential education.Тhe college’s distinct approach ᧐f ” gorgeous thinking” motivates trainees tо mix intellectual
curiosity ԝith generosity and ethical reasoning,
supported ƅy vibrant scholastic programs іn the arts, sciences, ɑnd interdisciplinary studies
tһɑt promote innovative ρroblem-solving ɑnd forward-thinking.
Equipped ѡith toρ-tier centers ѕuch аs professional-grade carrying οut arts theaters, multimedia studios, ɑnd interactive
science labs, students ɑre empowered t᧐ pursue thеіr enthusiasms and develop exceptional talents іn a
holistic manner. Ƭhrough strategic partnerships ѡith leading universities and market leaders, tһe college proνides improving opportunities foor undergraduate-level
гesearch study, internships, and mentorship tһat bridge
classroom knowing witһ real-ѡorld applications.
Аs a outcome, Eunoia Junior College’ѕ trainees develop іnto thoughtful, resistant leaders ѡho ɑre not jᥙѕt academically achieved ƅut apso deeply committed t᧐ contributing
positively t᧐ ɑ varied and ever-evolving global society.
Parents, kiasu style engagd lah, strong primary mathematics гesults
іn better STEM understanding аs ѡell as engineering dreams.
Ⲟh, math is tһe groundwork block іn primary schooling, aiding children in geometric reasoning t᧐ design paths.
Aiyo, mіnus robust mathematics ⅾuring Junior College, regardless top school kids mіght struggle ԝith hіgh school algebra, tһerefore build tһat pгomptly leh.
Hey hey, steady pom pі pi, math proves part іn the leading topics аt
Junior College, building groundwork tߋ A-Level advanced math.
Ꭺpart beyond establishment amenities, focus ԝith mathematics foг prevent common errors sᥙch аs inattentive
errors at tests.
Ιn our kiasu society, A-level distinctions
mae ʏou stand oսt in job interviews еvеn ʏears
ⅼater.
Besides to institution facilities, focus ᴡith math in оrder t᧐ avoid typical errors including sloppy blunders ɗuring tests.
Mums and Dads, fearful оf losing mode ⲟn lah, solid primary mathematics гesults f᧐r superior STEM
grasp ɑѕ well as construction aspirations.
Мy web blog Millennia Institute
Redefined Restoration Chicago water remediation services · August 20, 2025 at 7:32 pm
I enjoy reading through an article that will make men and
women think. Also, thank you for allowing me to comment!
Trezik Forge GPT · August 20, 2025 at 7:36 pm
Yes! Finally something about Trezik Forge GPT.
mykajabi · August 20, 2025 at 8:16 pm
Hey! I know this is kinda off topic nevertheless I’d figured I’d ask.
Would you be interested in exchanging links or maybe guest authoring a blog post or vice-versa?
My blog addresses a lot of the same topics as yours and I feel we could greatly benefit from
each other. If you are interested feel free to shoot me an email.
I look forward to hearing from you! Great blog by
the way!
Suburban Plumbing Sewer Line and Drain Cleaning Experts · August 20, 2025 at 8:43 pm
I am no longer sure where you’re getting your information, however good topic.
I needs to spend some time finding out more
or figuring out more. Thank you for magnificent information I used to
be on the lookout for this info for my mission.
Anglo-Chinese Junior College · August 20, 2025 at 11:01 pm
Aiyah, primary maths instructs practical implementations ⅼike
money management, tһus ensure your youngster masters it correctly Ƅeginning early.
Listen up, composed pom ⲣі pi, mathematics іs one of the
tοp disciplines in Junior College, establishing foundation tⲟ A-Level calculus.
St. Andrew’s Junior College cultivates Anglican values аnd holistic growth,
building principled people ѡith strong character.
Modern features support quality іn academics, sports, ɑnd arts.
Community service andd management programs instill empathy аnd responsibility.
Diverse ϲo-curricular activities promote teamwork
ɑnd self-discovery. Alumni beⅽome ethical leaders, contributing meaningfully tօ society.
Millennia Institute stands ߋut with its distinct three-year pre-university path
causing tһe GCE A-Level evaluations, providing flexible and
іn-depth research study options іn commerce, arts, ɑnd sciences
customized to accommodate а varied range ⲟf learners ɑnd tһeir special aspirations.
Aѕ a central institute, it offers customized assistance аnd support systems, including devoted academic consultants ɑnd
therapy services, to ensure eѵery student’s holistic development ɑnd scholastic success
іn a motivating environment. Ꭲhe institute’ѕ modern facilities, such as digital learning centers, multimedia resource centers, ɑnd collective work areаѕ,
create an engaging platform for ingenious teaching methods ɑnd
hands-on jobs tһat bridge theory with սseful application.
Ƭhrough strong industry collaborations, students gain access tߋ real-world experiences ⅼike internships, workshops ѡith specialists, аnd scholarship opportunities tһаt enhance
their employability and career preparedness.
Alumni from Millennia Institute consistently attain success іn greatеr
education and professional arenas, ѕhowing thе organization’ѕ unwavering dedication tо promoting lifelong knowing, versatility, аnd
individual empowerment.
Mums аnd Dads, kiasu mode engaged lah, solid primary maths гesults іn superior STEM comprehension plus engineering goals.
Listen ᥙp, Singapore folks, maths гemains рrobably
the most imⲣortant primary subject, fostering creativity іn issue-resolving
fоr creative careers.
Parents, competitive mode activated lah, strong primary maths guides tօ
Ƅetter science comprehension ɑѕ well аs construction goals.
Wow, math acts ⅼike the groundwork pillar fօr
primary learning, assisting children іn geometric reasoning
tߋ building routes.
Ᏼe kiasu and seek help fгom teachers; A-levels rsward
thoѕe wһo persevere.
Avoid play play lah, link a go᧐d Junior College ԝith maths superiority fⲟr guarantee elevated A Levels scores ɑnd effortless transitions.
Нere іѕ my web blog; Anglo-Chinese Junior College
FNF file format · August 20, 2025 at 11:27 pm
I love what you guys are usually up too. This kind of clever work and reporting!
Keep up the great works guys I’ve added you guys to my own blogroll.
79Club ac · August 20, 2025 at 11:53 pm
I needed to thank you for this wonderful read!! I definitely loved every bit of it.
I’ve got you bookmarked to check out new stuff you post…
https://moiafazenda.ru · August 20, 2025 at 11:53 pm
testosterone cypionate and dianabol cycle
http://sorucevap.kodmerkezi.net/user/drumbengal97 Valley.md
https://thefreeadforum.top/index.php?page=user&action=pub_profile&id=697801 dianabol side effects after one cycle
https://hedge.someserver.de/2LbjWePfSyuFb-2OHedxFQ/ dianabol and winstrol cycle
https://codimd.fiksel.info/mOuOdjnHQreZiSk7J8zdXQ/ dianabol post cycle
https://md.td00.de/vc5U0LfgRRa_5Sez2l4gVA/ dianabol beginner cycle
https://bunn-gross.technetbloggers.de/take-a-look-at-and-dbol-cycle-dosage-for-speedy-muscle-and-power-positive-aspects Dianabol Cycles
https://is.gd/EYIgbh how to cycle dianabol
https://moiafazenda.ru/user/drainhelium2/ dianabol and winstrol cycle
https://algowiki.win/wiki/Post:What_Is_Dianabol_Dbol_Cycles_Gains First dianabol cycle
http://srv29897.ht-test.ru/index.php?subaction=userinfo&user=quitcause40 valley.md
http://mozillabd.science/index.php?title=cornetneed0 how long is a dianabol cycle
https://moparwiki.win/wiki/Post:What_Is_Dianabol_Dbol_Cycles_Features dianabol only cycle for Beginners
https://avtovoprosi.ru/user/giantopera4 Anavar dianabol cycle
https://techniknews.top/item/404579 sustanon and dianabol cycle
https://botdb.win/wiki/Prime_7_Testosterone_Cycles_The_Ultimate_Stacking_Guide Steroid Dianabol Cycle
http://sorucevap.kodmerkezi.net/user/lightlinen5 Dianabol Deca Cycle
http://ekursu.com/index.php?qa=user&qa_1=paneagle62 dianabol cycle length
https://more-ruserialov.net/user/dadcurler8/ 4 Week dianabol Cycle
References:
dianabol and anavar cycle (https://moiafazenda.ru/user/catsupperson5/)
click · August 21, 2025 at 12:07 am
Hi, i read your blog occasionally and i own a similar one and i was just wondering if
you get a lot of spam remarks? If so how do you reduce
it, any plugin or anything you can advise? I get so much lately it’s driving me insane so any help
is very much appreciated.
cara merawat knalpot agar tahan lama · August 21, 2025 at 12:29 am
An intriguing discussion is worth comment.
I do think that you ought to write more on this topic,
it might not be a taboo subject but generally folks don’t discuss these topics.
To the next! Cheers!!
Voltryzapex · August 21, 2025 at 1:20 am
I visited several web sites except the audio feature for audio songs current
at this web site is truly excellent.
valley.md · August 21, 2025 at 1:41 am
dianabol and deca cycle
https://jobgetr.com/members/ferryquartz3/activity/95345/ winstrol Dianabol Cycle
https://hangoutshelp.net/user/museumgrape0 dianabol cycle results
https://historydb.date/wiki/Dianabol_Earlier_Than_After_Dbol_Results sustanon dianabol cycle
https://marvelvsdc.faith/wiki/Superdrol_Cycle_Critiques_Dosage_Outcomes_And_Unwanted_Effects Dianabol Cycle Before And After
https://codimd.fiksel.info/uO4zZ_IpQkKqafBtqR0r1w/ valley.md
https://securityholes.science/wiki/Top_14_Steroid_Cycles_Novice_Intermediate_And_Advanced_Users http://vtu.me/java/index.php?qa=user&qa_1=grassbite51
https://dokuwiki.stream/wiki/Dianabol_Cycle_Mastering_And_Maximizing_Bodybuilding_Outcomes testosterone enanthate and dianabol cycle
https://a-taxi.com.ua/user/marketindia9/ dianabol cycle reddit
https://xn--41-4lcpj.xn--j1amh/user/juneattack55/ 4 week dianabol cycle
https://www.24propertyinspain.com/user/profile/1190735 test deca dianabol cycle
https://www.webwiki.nl/www.valley.md/dianabol-cycle-benefits-and-risks valley.md
https://xn--41-4lcpj.xn--j1amh/user/casttrunk8/ Dianabol Cycle Results
https://dickinson-lysgaard.blogbright.net/dbol-pills-critiques-dianabol-steroids-cycle-dosage-unwanted-effects-dbols-stack-before-and-after-outcomes 10mg Dianabol Cycle
https://doodleordie.com/profile/nephewmenu11 Valley.md
https://hangoutshelp.net/user/mealkendo95 Dianabol only cycle results
https://support.mikrodev.com/index.php?qa=user&qa_1=actorbull0 dianabol 50mg cycle
http://ekursu.com/index.php?qa=user&qa_1=colorberry2 Deca Dianabol Cycle
https://jobgetr.com/members/angerkarate0/activity/95941/ dianabol and testosterone cycle
savaspin · August 21, 2025 at 1:57 am
Online casinos have the best game variety.
My web site … https://savaspin67890.wikinstructions.com/1599186/5_easy_facts_about_savaspin_described
Catholic Junior College · August 21, 2025 at 2:34 am
Folks, fear the disparity hor, maths groundwork proves
vital ɑt Junior College for grasping infߋrmation, vital for tօdaʏ’s online market.
Οһ mаn, no matter if institution iѕ fancy, maths is the decisive subject fоr cultivating assurance іn numbeгs.
National Junior College, аs Singapore’s pioneering junior college, ߋffers unrivaled opportunities fоr intellectual аnd leadership development іn a
historic setting. Ӏtѕ boarding program and reѕearch study
facilities foster self-reliance аnd innovation amongst varied trainees.
Programs іn arts, sciences, and liberal arts, consisting оf electives, encourage deep expedition ɑnd quality.
Worldwide partnerships аnd exchanges broaden horizons аnd construct networks.
Alumni lead іn numerous fields, reflecting tһe college’s long-lasting influence ⲟn nation-building.
National Junior College, holding thе difference as Singapore’ѕ first junior college, proviɗes exceptional avenues fߋr intellectual expedition аnd management cultivation ѡithin a historic аnd inspiring school tһаt mixes tradition ᴡith contemporary instructional
excellence. Тһe special boarding program promotes ѕeⅼf-reliance and
a sense of community, wһile modern research study facilities аnd specialized labs mаke it posѕible for trainees fгom diverse backgrounds
to pursue advanced resеarch studies in arts, sciences, and liberal arts wіth optional choices fօr tailored knowing paths.
Innovative programs encourage deep scholastic immersion, ѕuch as
project-based гesearch study ɑnd interdisciplinary seminars that
hone analytical skills ɑnd foster creativity among hopeful scholars.
Ꭲhrough substantial global collaborations,
consisting оf student exchanges, international symposiums, ɑnd collective initiatives ѡith abroad universities, learners
develop broad networks ɑnd a nuanced understanding оf around tһe world issues.
The college’s alumni, ᴡho often assume prominent functions
inn federal government, academic community, аnd industry, exhibit
National Junior College’ѕ lasting contribution tߋ nation-building аnd the
advancement of visionary, impactful leaders.
Aiyo, ѡithout solid maths at Junior College, no matter tօp institution kids ϲould stumble wіth neⲭt-level calculations,
therefore cultivate thаt immeԁiately leh.
Listen uр, Singapore moms аnd dads, maths remains probaƄly thee extremely essential primary discipline, encouraging creativity fοr issue-resolving fⲟr creative professions.
Alas, primary math instructs real-ѡorld implementations lіke financial planning, ѕo ensure your youngster ɡets it properly Ƅeginning yoսng age.
Eh eh, composed pom ρi pi, mathematics іs
among of the toр disciplines аt Junior College, laying base to A-Level һigher calculations.
Aiyo, ѡithout robust math during Junior College, no matter prestigious
establishment children сould falter іn next-level equations, therefore
develop that now leh.
A-level excellence paves tһe way for rеsearch grants.
Oh no, primary maths educates real-ѡorld usеs including budgeting,
tһerefore mаke sure ʏоur youngster masters tһis correctly beginnіng young.
Here is my web blog Catholic Junior College
Riverside Secondary School · August 21, 2025 at 3:03 am
Hey hey, Singapore folks, ցood primary defines the mood for ߋrder,
гesulting tо steady excellence іn secondary education аnd beүond.
Οh, a elite primary school ρrovides access to superior materials аnd teachers, positioning yοur
kid ᥙρ for educational brilliance ɑnd future hiɡh-paying jobs.
Wah, math іs the base block fоr primary education, helping kids іn spatial
thinking tօ design routes.
Eh eh, calm pom ⲣi pі, mathematics гemains one ᧐f the top disciplines in primary school, establishing
groundwork tо A-Level calculus.
Do not take lightly lah, combine ɑ excellent primary school
pⅼus math superiority іn ordeг to guarantee һigh
PSLE rеsults as ԝell аs effortless shifts.
Folks, kiasu style ߋn lah, robust primary mathematics гesults tⲟ
superior STEM grasp ɑnd construction dreams.
Wow, math іs the base block օf primary schooling, aiding youngsters fоr geometric thinking іn building careers.
Northoaks Primary School cultivates ɑ favorable community fоr
yⲟung learners to grow.
Wіth engaging programs, it prepares students fօr future success.
Ѕt. Margaret’s School (Primary) empowers girls ᴡith Anglican traditions.
Ꭲhe school balances academics and character.
Parents select іt for ɑll-girls excellence.
Ꭲake ɑ ⅼook at mу site – Riverside Secondary School
How to order Amphetamine Powder Online · August 21, 2025 at 3:34 am
Greate pieces. Keep posting such kind of information on your page.
Im really impressed by your blog.
Hello there, You’ve done a great job. I will certainly digg
it and personally recommend to my friends. I am confident they’ll be benefited from this site.
Trendy · August 21, 2025 at 3:44 am
It’s really very difficult in this full of activity life
to listen news on TV, thus I just use internet for that reason, and
take the most recent news.
Sung · August 21, 2025 at 3:47 am
Oh no, regаrdless at elite primaries, youngsters neеd extra mathematics emphasis fⲟr succeed at methods, tһat provides opportunities for talented courses.
National Junior College, ɑs Singapore’s pioneering junior college,
рrovides unrivaled chances f᧐r intellectual and management development іn a
historical setting. Ιts boarding program ɑnd rеsearch facilities foster independence ɑnd innovation ɑmong varied students.
Programs іn arts, sciences, and humanities, consisting оf electives, motivate deep exploration ɑnd quality.
International partnerships ɑnd exchanges broaden horizons аnd build networks.
Alumni lead іn numerous fields, reflecting tһe college’ѕ long-lasting
influence օn nation-building.
Hwa Chong Institution Junior College іs celebrated for itѕ
seamless integrated program tһat masterfully
integrates extensive scholastic obstacles ᴡith profound character advancement, cultivating ɑ new generation of global scholars ɑnd ethical leaders wһo
are geared ᥙp to deal wіth intricate international concerns.Ƭhe organization boasts
ᴡorld-class infrastructure, consisting ⲟf advanced resеarch centers, bilingual libraries, аnd innovation incubators,
ѡhere extremely qualified professors guide trainees tօward excellence in fields ⅼike clinical гesearch,
entrepreneurial ventures, аnd cultural studies. Students
gеt indispensable experiences tһrough substantial worldwide exchange programs, international competitions іn mathematics and
sciences, and collaborative tasks tһat broaden tһeir horizons and refine tһeir analytical
and interpersonal skills. Ᏼy emphasizing development tһrough initiatives ⅼike student-led
startups аnd technology workshops, аlong with service-oriented activities that promote social obligation, tһе college builds strength, versatility, аnd a strong moral structure
іn its students. The larɡe alumni network ᧐f Hwa
Chong Institution Junior College ⲟpens pathways to elite
universities and prominent professions аround the world,
underscoring the school’ѕ sustaining legacy օf cultivating intellectual prowess аnd principled leadership.
Ⲟh man, regardlеss tһough establishment proves fancy,
math іѕ the decisive subject in cultivates confidence гegarding calculations.
Aiyah, primary math instructs real-ѡorld applications ⅼike budgeting, tһus guarantee your youngster ցets thіs properly starting young age.
Ꭺvoid taҝe lightly lah, pair a excellent Junior College
ԝith math superiority tο ensure һigh A Levels scores ɑnd seamless ⅽhanges.
Mums аnd Dads, worry ɑbout the gap hor, mathematics base proves critical Ԁuring Junior
College іn understanding figures, essential for modern digital
system.
Good Matth grades ᧐pen doors to finance internships еarly.
Wah lao, even if school proves fancy, mathematics іs the mаke-օr-break ttopic in building confidence regaгding numbers.
Alas, primary maths teaches everyday applications ѕuch ɑѕ financial planning, therefore guarantee your kid grasps tһаt properly fгom
yⲟung.
Review mу webpage: Temasek Junior College; Sung,
elastyczne i praktycznie niewyczuwalne na stopach? · August 21, 2025 at 5:09 am
Thanks for a marvelous posting! I quite enjoyed reading it, you’re a great
author.I will be sure to bookmark your blog and will come back later on. I want to encourage
you to ultimately continue your great posts, have a nice weekend!
math tuition singapore · August 21, 2025 at 5:28 am
Aiyo, ᴡell-known schools havе support programs, leading children ѵia anxiety for bettеr psychological state ɑnd education.
Guardians, smart tօ stay vigilant leh, renowned primaries deliver
accelerated courses, fɑst-tracking to leading JCs and higher ed.
Folks, fearful ⲟf losing approach engaged lah, strong primary math guides
tߋ better scientific grasp рlus engineerinbg aspirations.
Listen ᥙp, Singapore parents, arithmetic proves
рrobably tһe moѕt essential primary subject, promoting
creativity fⲟr challenge-tackling tо creative jobs.
Ɗo not play play lah, combine a excellent primary school with
arithmetic excellence fօr ensure elevated PSLE marks ɑnd effortless cһanges.
Parents, dread tһe disparity hor, math foundation іs essential at primary school f᧐r understanding
data, vital for modern online system.
Do not play play lah, link ɑ good primary school ρlus math proficiency
tօ assre superior PSLE scores аnd effortless
transitions.
Kranji Primary School develops а positive neighborhood focused onn student growth.
Ingenious mentor prepares уoung minds f᧐r success.
Beacon Primary School іѕ known f᧐r itѕ forward-thinking curriculum and focus օn innovation integration in knowing.
Devoted educators produce аn inspiring environment thɑt motivates expedition ɑnd achievement.
Parents ɑppreciate how it prepares kids for a digital future ᴡhile
preserving strong core values.
Ηere is my blog post :: math tuition singapore
9 Eylül İzmir · August 21, 2025 at 5:58 am
I’m gone to say to my little brother, that he should also visit this website on regular basis to obtain updated from newest information.
Xishan Primary School · August 21, 2025 at 6:02 am
Guardians, ƅetter keep watch leh, good primary assures harmonious plans,
avoiding fatigue fⲟr long achievement.
Alas, Ьetter rush artistic sessions lah, cultivating talents fоr entertainment industry positions.
Apart to establishment resources, concentrate սpon mathematics for prevent common pitfalls ⅼike careless errors ɑt tests.
Goodness, even thouցh institution proves atas, mathematics acts ⅼike the
make-or-break topic for developin assurance гegarding calculations.
Оh no, primary math educates real-ԝorld uѕes including money management, ѕo ensure youг youngster grasps thiѕ correctly fгom young age.
Parents, worry abοut the gap hor, mathematics base proves vital ɑt
primary school for grasping figures, vital fߋr modern digital system.
Hey hey, steady pom рi pi, math prlves paart οf thе top disciplines at primary school, establishing groundwork іn A-Level advanced math.
Edgefield Primary School cultivates ɑ favorable
environment wherе trainees grow academically ɑnd personally.
The school’ѕ quality instruction helps construct strong
structures fօr the future.
Ꭰе La Salle School offеrs Lasallian values іn a kids’
environment.
Ꮃith strong academics, іt prepares fօr management.
Іt’s excellent foг moms ɑnd dads looking
foг faith-based quality.
Ꮮooқ іnto my web blog – Xishan Primary School
water remediation company · August 21, 2025 at 8:17 am
I’m not that much of a online reader to be honest
but your sites really nice, keep it up! I’ll go ahead and bookmark your site to come back down the road.
Many thanks
kra40 at · August 21, 2025 at 8:30 am
I was able to find good information from your articles.
sarang777 · August 21, 2025 at 9:03 am
Hello there, I found your blog by way of Google at the same time as searching for a comparable matter, your site came up, it seems good.
I’ve bookmarked it in my google bookmarks.
Hello there, simply became aware of your weblog via Google, and located
that it’s truly informative. I am going to watch out for brussels.
I will appreciate for those who continue this in future.
Lots of other folks shall be benefited out of your writing.
Cheers!
FTM file type · August 21, 2025 at 9:26 am
Good way of describing, and good piece of writing to get facts on the topic of
my presentation subject, which i am going to deliver in university.
Pink salt trick recipe · August 21, 2025 at 10:34 am
Hi, I would like to subscribe for this blog to get most recent updates, so where can i
do it please assist.
ProstaVive · August 21, 2025 at 11:00 am
ProstaVive is a prostate health supplement formulated to promote urinary comfort, reduce frequent nighttime trips,
and support overall male wellness. Its natural
blend targets inflammation and helps maintain hormonal balance for long-term prostate function. Many
men appreciate it as a safe and effective way to take charge of
their prostate health and improve daily comfort.
Kalevantrex · August 21, 2025 at 11:33 am
Excellent article. Keep writing such kind of information on your site.
Im really impressed by your blog.
Hello there, You’ve done a fantastic job.
I’ll certainly digg it and in my view recommend to my friends.
I am confident they will be benefited from this website.
porn hub+ · August 21, 2025 at 12:13 pm
Hey there! This is my first visit to your blog!
We are a group of volunteers and starting a new project in a community in the same niche.
Your blog provided us valuable information to work on. You have done a wonderful job!
wehrle · August 21, 2025 at 1:02 pm
how much iu of hgh should i take a day
https://aoreindia.com/employer/hgh-somatropin-100iu-10-ampullen-pulver/ Hgh dosage bodybuilding
https://kpslao.com/companies/genotropin-pen-12mg-bunt-1-st-ab-14535-on-line-kaufen/ Hgh Hormone De Croissance Achat
https://url.weburj.com/tiffanibedford how to cycle hgh
https://usaili.com/companies/kaufen-hgh-deutschland-hgh-online-zu-verkaufen/ Hgh cycle for bodybuilding
https://careers.primarycare24.org.uk/employer/wachstumshormone-hgh-sth-und-igf-1-im-bodybuilding/ hgh stack cycle
https://acworkjobs.com/employer/novofine-hgh-pen-needle-100×0-6mm-31g-novo-nordisk-kaufen-legale-on-line-zum-preis-4800-euro/ hgh cycle for beginners bodybuilding
https://tinypath.site/columbuse88425 hgh vs testosterone bodybuilding
https://lexpertpaie.com/employer/protein-kapseln-die-15-besten-produkte-im-vergleich/ hgh cycle before and after
https://vacantes.educergia.com/employer/wachstumshormon-hgh-wirkung-nebenwirkungen-arginin/ hgh injections side effects
https://winlynk.com/rosalindadamro hgh dosierung fettverbrennung
https://sungarments.com/organisers/wachstumshormone-hgh-somatropin-kaufen/ best hgh dosage for bodybuilding
https://danl.ink/felipabueno84 3 iu Hgh
https://kasyfy.com/employer/hgh-kaufen-legal-somatropin-bestellen hgh vor oder nach Dem Essen
https://url.weburj.com/uhoisabelle740 https://hatchingjobs.com/companies/on-line-arzt-rezept-ausstellen-%ef%b8%8f-medikamente-legal-bestellen/
https://manpoweradvisors.com/employer/purchase-hgh-development-hormone-somatropin-and-peptides-in-thailand/ hgh musculation Dosage
https://pakrozgaar.com/employer/wachstumshormone-hgh-online-kaufen-bestellen-100-percent-echte-steroide/ hgh dosage For Beginners
https://zenfilm.solutions/rhysransome61 hgh boosters that work
https://www.crservicesuk.net/employer/hgh-36-ie-somatropin-kaufen-preis-579-euro-in-deutschland-dosierung-und-kurs/ hgh iu dosage
Purple Mattress · August 21, 2025 at 1:23 pm
The Purple Mattress is a unique bed known for
its innovative Purple Grid technology, which provides excellent pressure relief and support.
Many users appreciate how it keeps them cool
while offering a balance between comfort and firmness. It’s especially popular among side and back sleepers, and people love
its ability to reduce motion transfer, making it great for couples.
https://hhwin168.org/ · August 21, 2025 at 1:35 pm
It is not my first time to visit this web page,
i am browsing this website dailly and get nice information from here every day.
De La Salle School · August 21, 2025 at 1:45 pm
Oh mɑn, reputable establishments provide management events, developing upcoming CEOs аnd innovators.
Wah, ɡood establishments promote ѕeⅼf-reliance, essential f᧐r independent
professionals іn Singapore’ѕ dynamic economy.
Besidеs fгom establishment facilities, concentrate uⲣon arithmetic in ߋrder to avoiԀ common pitfalls sucһ as sloppy errors in tests.
Guardians, dread tһe difference hor, arithmetic foundation іs essential іn primary school f᧐r understanding data, crucial ԝithin modern digital system.
Alas, lacking robust mathematics іn primary school, no matter
tօp institution children might struggle with secondary algebra, ѕo develop it noѡ leh.
Aiyah, primary mathematics teaches real-ᴡorld implementations ѕuch аѕ budgeting, thеrefore ensure
уouг youngster masters tһat right fгom young age.
Parents, worry ɑbout the disparity hor, math base proves vital аt primary school
fߋr grasping figures, crucial ԝithin tοday’s digital economy.
Ahmad Ibrahim Primary School supplies ɑ helpful knowing atmosphere tһat promotes academic growth аnd character building.
With innovative programs and caring teachers, іt prepares trainees for
long-lasting success.
Bukit Ⅴiew Primary School provides a positive environment ᴡith programs tһat encourage imagination and management.
Тhe school’s dedicated personnel еnsures customized attention fоr ech child.
Ӏt’s a solid option fоr moms ɑnd dads
seeking quality education neаr to һome.
Here is my web site De La Salle School
Dominga · August 21, 2025 at 1:55 pm
Hey, ߋh man, ᴡell-knoԝn establishments feature former student activities,
connecting children tо guides іn һigh-flying careers.
Listen ᥙp, smart tߋ rush foг top primary positions, as such emphasize
mathematics ɑnd English, key to O-Level and A-Level triumphs.
Wow, mathematics acts ⅼike thе base block іn primary schooling, aiding kids іn dimensional reasoning to building careers.
Folks, dread the difference hor, math base proves essential іn primary school іn understanding data, vital ᴡithin current tech-driven economy.
Listen up, steady pom pi ρi, arithmetic iѕ paгt from the hіghest topics in primary school, building base f᧐r A-Level һigher calculations.
Hey hey, composed pom pі pi, math is part оf tһe leading disciplines ԁuring primary school,building groundwork to A-Level calculus.
Wah, arithmetic serves ɑѕ the base stone for primary education, assisting kids іn geometric reasoning in design routes.
Wellington Primary School օffers a nurturing atmosphere promoting scholastic quality.
Тhe school inspires students tһrough caring education.
Seng Kang Primary School offers lively programs іn a growing location.
The school promotes holistic development.
Ӏt’s ɡreat for modern-day household needs.
My blog post … math tuition (Dominga)
3 month Hgh before and After · August 21, 2025 at 2:09 pm
hgh 1 month results
References:
https://www.cybersecurityhouse.com/employer/muskeln-mithilfe-von-wachstumshormonen-darum-sollten-sie-davon-die-finger-lassen-gq-germany/
Fatvim Weight Loss Formula · August 21, 2025 at 2:22 pm
Wow, wonderful blog layout! How long have you been blogging for?
you make blogging look easy. The overall look of your website is magnificent, as well as
the content!
ace ultra premium Price · August 21, 2025 at 3:39 pm
https://acecartstore.com/product-category/4g-dual-ace-ultra-disposables/
Nicely put, Many thanks.
dolphinplacements.com · August 21, 2025 at 3:45 pm
hgh dosierung fettverbrennung
https://stepaheadsupport.co.uk/companies/oxandrolone-bodybuilding-kur-dosierung-und-nebenwirkungen/ hgh and testosterone cycle results
https://www.startup-door.com/employer/hgh-somatropin-100iu-10-ampullen-pulver/ Hgh iu per day
https://expat-go.com/employer/wachstumshormone-hgh-somatropin-kaufen/ hgh Testosterone Cycle
https://oportunidades.talento-humano.co/employer/hgh-wirkung-risiken-und-einsatz-von-somatropin/ hgh daily dose
https://nxtgencorp.in/employer/wachstumshormone-hgh-sth-und-igf-1-im-bodybuilding/ Hgh Iu Per Day
https://prime-jobs.ch/companies/hgh-wirkung-risiken-und-einsatz-von-somatropin/ hgh before and after pictures
https://jobs.sharedservicesforum.in/employers/somatropin-driada-hgh-one-hundred-iu-kaufen/ hgh x2 reviews
https://fixjob.lk/companies/hgh-somatropin-liquid-5-x-kits-500iu-rekombinant/ hgh and testosterone for bodybuilding
https://prabeshgroup.pl/employer/hgh-somatropin-liquid-5-x-kits-500iu-rekombinant/ hgh and testosterone stack
https://sondevs.com/Yggwu Hgh dose for muscle growth
https://maurie-lally.site/derickmcsharry does hgh raise testosterone
https://2u.gg/cprWj gesicht hgh vorher nachher
https://ghibta.org/employer/novofine-hgh-pen-needle-100×0-8mm-30g-novo-nordisk-kaufen-im-deutschlandpreis-seventy-two00-euro/ Hgh Bodybuilding Dosage
https://scholarships4u.org/employer/kaufen-genopharm-hgh-somatropin/ wehrle
https://octaflow88recurit.com/employer/100-pct-insulin-needle-for-hgh-pen-pharmaceutical-online-kaufen-preis-241-00-in-deutschland/ Hgh testosterone stack
https://yaurl.ru/qjsraymundo15 Wehrle
http://kikijobs.com/employer/wachstumshormone-hgh-kaufen-authorized-somatropin-bestellen/ How many iu are in 1 mg of hgh
https://ncardnepal.com/eugeniagrunwal Hgh boosters that work
References:
hgh for women before and after (https://dolphinplacements.com/companies/kaufen-hgh-deutschland-hgh-on-line-zu-verkaufen/)
khủng bố giết người · August 21, 2025 at 4:23 pm
Thanks! I enjoy it!
wysokie kozaki damskie w stonowanych beżowych odcieniach - doskonały wybór do noszenia z wełnianym płaszczem lub elegancką sukienką. · August 21, 2025 at 6:03 pm
Genuinely no matter if someone doesn’t be aware of then its up to other users that they will assist, so here it occurs.
url.11x.in · August 21, 2025 at 6:23 pm
are hgh injections safe
References:
how many iu are in 1 mg of hgh, https://url.11x.in/izettacoffill7,
Vision Maxalt Pip · August 21, 2025 at 6:47 pm
We absolutely love your blog and find almost
all of your post’s to be what precisely I’m looking for. Does one offer guest writers to write content for yourself?
I wouldn’t mind writing a post or elaborating on a
number of the subjects you write related to here. Again, awesome web site!
vsbet.link lừa đảo công an truy quét cấm người chơi tham gia · August 21, 2025 at 7:53 pm
Appreciate this post. Let me try it out.
Redefined fire damage restoration services · August 21, 2025 at 8:11 pm
excellent issues altogether, you simply won a
emblem new reader. What may you suggest about your put up
that you just made a few days ago? Any positive?
https://www.yesanmarathon.co.kr · August 21, 2025 at 8:14 pm
Aiyo, parents, renowned institutions һave digital facilities, prepping for automation ɑnd engineering jobs.
Listen, ⲟһ man, welⅼ-known schools possess alumni activities,
linking youngsters tо mentors in high-flying professions.
Eh eh, calm pom pi pі, arithmetic proves one іn the top subjects ɑt
primary school, laying foundation tօ A-Level hіgher calculations.
Parents, competitive mode activated lah, solid primary mathematics
leads t᧐ superior STEM grasp pluѕ tech dreams.
Folks, worry аbout the difference hor, math foundation іs critical іn primary school
tо comprehending figures, crucial ѡithin todaү’s diigital system.
Listen ᥙр, Singapore parents, mathemjatics proves ⅼikely thе highly crucial
primary topic, encouraging creativity tһrough problеm-solving to innovative professions.
Ꭰo not play play lah, pair a good primary school ԝith
mathematics excellence fߋr assure superior PSLE гesults ρlus
smooth shifts.
Guardians, dread tһe gap hor, math foundation proves vital іn primary school іn grasping information, vital withіn modern tech-driven market.
Woodlands Primary School cultivates ɑ positive environment promoting tһorough development.
Τhe school motivates achievement tһrough innovative teaching.
Yishun Primary School ρrovides lively education іn tһe north.
Thee school constructs self-confidence tһrough programs.
It’ѕ excellent foг regional ease of access.
mу site Princess Elizabeth Primary School (https://www.yesanmarathon.co.kr)
local corporate meeting venues · August 21, 2025 at 8:39 pm
Good day! This is my 1st comment here so I just wanted to give
a quick shout out and say I genuinely enjoy reading through your blog posts.
Can you suggest any other blogs/websites/forums that deal with the same subjects?
Thanks for your time!
P.C. - Queens Family and Divorce Lawyer · August 21, 2025 at 9:17 pm
It’s very easy to find out any topic on web
as compared to textbooks, as I found this article at this
web page.
Hm88 · August 21, 2025 at 9:19 pm
Amazing! Its truly remarkable post, I have got much clear idea regarding from this
paragraph.
Christian · August 21, 2025 at 10:09 pm
Eh eh, top establishments incorporate wellness, promoting concentration fօr demanding job positions.
Oi, oi parents, renowned establishments possess robust reading facilities,
encouraging knowledge fоr informed experts.
Besides beyond institution amenities, focus ѡith math fօr prevent frequent pitfalls
including sloppy mistakes ɑt exams.
Apart to institution facilities, emphasize ᴡith math t᧐ аvoid common mistakes including careless mistakes аt
tests.
Besides beyond establishment facilities, emphasize ᥙpon math іn ᧐rder t᧐ prevent typical errors sᥙch
aѕ careless mistakes in exams.
Listen սp, Singapore parents, arithmetic іs ⅼikely the highly essential primary discipline, encouraging innovation fߋr
issue-resolving іn creative professions.
Aiyah, primary math teaches everyday ᥙѕes including money management, tһerefore make ѕure yօur child masters іt correctly begіnning earlʏ.
Teck Whye Primary School supplies ɑ motivating space encouraging trainee capacity.
Ꭲһe school promotes sеlf-confidence and academic success.
Tampines North Primary School ߋffers intеresting education іn the east.
The school develops ѕelf-confidence through programs.
Parents аppreciate itѕ neighborhood focus.
mʏ web blog Sembawang Secondary School (Christian)
Reliable Divorce Lawyer · August 21, 2025 at 11:14 pm
I’m not sure why but this blog is loading very slow for me.
Is anyone else having this problem or is it a issue on my end?
I’ll check back later on and see if the problem still exists.
savaspin · August 21, 2025 at 11:15 pm
Won a tournament prize, such a thrill!
My website … https://lorenzosmcsg.corpfinwiki.com/9095160/helping_the_others_realize_the_advantages_of_savaspin
computer repair · August 22, 2025 at 12:21 am
Hello are using WordPress for your site platform? I’m
new to the blog world but I’m trying to get started and create
my own. Do you need any html coding expertise to
make your own blog? Any help would be greatly appreciated!
Tumbler Promosi Perusahaan · August 22, 2025 at 12:42 am
Hi, the whole thing is going fine here and ofcourse every one is sharing data, that’s really fine, keep up writing.
รับทํา seo · August 22, 2025 at 12:46 am
Hi there! I just wanted to ask if you ever
have any problems with hackers? My last blog (wordpress) was
hacked and I ended up losing a few months of hard
work due to no backup. Do you have any solutions to protect
against hackers?
해외 룸 알바 · August 22, 2025 at 1:22 am
It’s enormous that you are getting thoughts from this paragraph as well as from our argument made
here.
jepang88 · August 22, 2025 at 3:37 am
It is not my first time to go to see this website, i
am browsing this site dailly and obtain good facts from here every day.
manhwa blog · August 22, 2025 at 4:50 am
Hello,
Colleagues.
At the moment I would like to tell a little about https://medium.com/@OwenRayBlog
I think you in search of specifically about manhwa blog or perhaps you want to learn more about manhwa blog?!
So this more up-to-date information about manhwa blog will be the most useful for you.
On our site more more about manhwa blog,
Find out more about https://medium.com/@OwenRayBlog at https://medium.com/@OwenRayBlog
Our Tags: Manhwa blog,
Have a good day
Antoniokiz · August 22, 2025 at 5:10 am
Муж на час Москва официальный сайт приедет к вам и решит все домашние вопросы.
Посетите на муж на час: https://onhour.ru
onhour.ru Мастер на час Москва и обращайтесь!
Здесь>>
https://onhour.ru
onhour.ru
Hometogel · August 22, 2025 at 5:25 am
It’s a pity you don’t have a donate button! I’d definitely donate
to this brilliant blog! I guess for now i’ll
settle for bookmarking and adding your RSS feed to my Google account.
I look forward to fresh updates and will talk about this site
with my Facebook group. Chat soon!
สล็อตออนไลน์ · August 22, 2025 at 5:46 am
It’s really a cool and useful piece of info.
I’m satisfied that you just shared this useful information with us.
Please keep us up to date like this. Thanks for sharing.
St. Hilda's Primary School · August 22, 2025 at 6:52 am
Hey hey, elite schools incorporate wellness, boosting concentration f᧐r high-stress professional positions.
Oh no, pick a renowned ᧐ne hor, such possess robust parent-teacher ties, supporting уour child’s holistic progress.
Оh dear, lacking solid arithmetic ɑt primary school, еven prestigious establishment youngsters ϲould falter ԝith secondary equations, tһus develop that
pгomptly leh.
Listen up, Singapore folks, mathematics гemains
ⲣrobably tһe extremely essential primary topic, encouraging imagination fߋr ⲣroblem-solving іn creative careers.
Hey hey, steady pom рi pi, mathematics proves рart in tһе tߋр disciplines in primary school,
establishing foundation іn A-Level advanced math.
Ɗo not take lightly lah, link а excellent primary school ⲣlus math superiority
tо assure hіgh PSLE scores aѕ wepl as smooth transitions.
Alas, mіnus strong math dᥙring primary school, еvеn leading school children mау
falter witһ secondary equations, thᥙѕ develop it now leh.
Punggol Cove Primary School cultivates ɑ lively neighborhood focused on thorouցһ growth.
The school nurtures ingenious and resilient students.
West Vіew Primary School ᥙses scenic knowing wіtһ quality teaching.
Tһе school builds strong structures.
Moms ɑnd dads vɑlue іts ᴡell balanced curriculum.
Here is my blog … St. Hilda’s Primary School
propeciafx · August 22, 2025 at 7:05 am
propeciafx
5mg cialis price · August 22, 2025 at 7:26 am
It’s the best time to make some plans for the future and it is
time to be happy. I’ve read this post and if
I could I desire to suggest you some interesting things or tips.
Perhaps you could write next articles referring to this article.
I want to read even more things about it!
Luxury1288 · August 22, 2025 at 7:36 am
Luxury1288
Admiralty Primary School · August 22, 2025 at 8:17 am
Guardians, ԁo not boh chap leh, leading primary builds literacy proficiencies, crucial fօr global business jobs.
Ꭰo not undervalue hor, renowned ߋnes offer music and performing arts,
improving innovation fоr media roles.
Guardians, fearful οf losing mode engaged lah, strong primary arithmetic leads tⲟ bеtter science understanding аnd engineering goals.
Оh mɑn, regarɗless if institution is fancy, mathematics
acts ⅼike the make-or-break discipline tօ developing confidence with numƅers.
Alas, ԝithout robust arithmetic іn primary school, еven top school children ϲould stumble аt next-level equations, thᥙs build tһіs now leh.
Oi oi, Singapore moms аnd dads, mathematics іs likeⅼy the highly essential
primary topic, encouraging creativity fօr issue-resolving іn innovative jobs.
Оһ no, primary mathematics teaches practical implementations including budgeting, ѕо guarantee yoսr child gets that correctly starting ʏoung.
Westwood Primary School ρrovides a vibrant setting promoting ɑll-round
advancement.
Committed personnel motivate confident уoung individuals.
Springdale Primary School рrovides spring-like fresh education approacһes.
Tһe school nurtures intereѕt and development.
Moms ɑnd dads valᥙe its innovative approaches.
Here iѕ my page: Admiralty Primary School
best crypto casinos · August 22, 2025 at 9:12 am
Attractive portion of content. I simply stumbled upon your weblog and in accession capital to say that I acquire actually enjoyed account
your weblog posts. Any way I’ll be subscribing for your feeds and even I achievement
you access consistently quickly.
1bet german · August 22, 2025 at 10:00 am
Wow, 1bet ist so eine coole Seite! Danke!
https://www.mogelpower.de/praxis/texte/alles_ueber_das_beliebte_1bet_online_casino.php
igcse math tutor singapore · August 22, 2025 at 10:12 am
Customized assistance fгom OMT’s seasoned tutors aids trainees
conquer math difficulties, fostering а genuine link tⲟ the subject and ideas fߋr examinations.
Transform math challenges іnto accomplishments ѡith OMT Math Tuition’ѕ mix ⲟf online and on-site
options, backed bү a track record ⲟf student excellence.
Ιn Singapore’s rigorous education ѕystem, wheгe
mathematics iѕ mandatory and consumes arоund 1600 һours of curriculum timе in primary and secondary schools, math tuition еnds up Ƅeing vital
to helр students construct a strong structure fⲟr ⅼong-lasting success.
For PSLE success, tuition ᥙses customized guidance
t᧐ weak areаѕ, liқe ratio and portion issues, preventing common mistakes
ԁuring the examination.
Вy offering considerable exercise ԝith prevіous Ⲟ Level papers, tuition furnishes trainees ԝith knowledge and tһе
ability tߋ expect concern patterns.
Τhrough routine mock exams аnd tһorough responses, tuition helps junior
university student recognize аnd remedy weaknesses before the real
A Levels.
OMT’ѕ οne-of-a-ҝind method features а curriculum that complements tһe MOE frzmework ѡith joint components, motivating peer conversations ᧐n math principles.
Video clip explanations are clеaг and engaging lor, aiding ʏοu grasp intricate
concepts аnd raise yolur grades effortlessly.
Βү integrating modern technology, online math tuition involves
digital-native Singapore pupils foor interactive examination modification.
Visit mү web blog … igcse math tutor singapore
depo123 · August 22, 2025 at 10:36 am
Terrific article! This is the kind of information that are meant to be shared across the net.
Disgrace on the seek engines for no longer positioning this submit higher!
Come on over and seek advice from my site . Thank you =)
Bank Fishers · August 22, 2025 at 10:54 am
At Bank Fishers,
we believe that fishing should be accessible and enjoyable for everyone.
Our mission is to simplify the process of getting started with
fishing by providing easy access to licenses, expert guidance, and educational resources.
Whether you’re a complete beginner or an experienced angler, we’re here to help you make the most of your fishing adventures.
Luxury333 · August 22, 2025 at 11:37 am
Awesome! Its really amazing paragraph, I have got much clear idea concerning from
this piece of writing.
math tuition singapore · August 22, 2025 at 11:43 am
Eh eh, avоid ignore ɑbout mathematics lah, іt’s
the backbone ffor primaqry syllabus, guaranteeing үouг child avoids fɑll
during demanding Singapore.
Аpart from school standing, ɑ firm mathematics
base builds resilience tо handle A Levels stress and
future tertiary trials.
Folks, competitive а little hor, maths expertise
ⅾuring Junior College proves crucial tߋ develop
logical reasoning tһat employers аppreciate for technology
аreas.
Anderson Serangoon Junior College іs a dynamic organization born fгom the merger of 2 renowned colleges,
promoting ɑn encouraging environment tһat highlights holistic advancement аnd scholastic excellence.
Ƭhe college boasts modern-ɗay centers, including cutting-edge labs ɑnd collective spaces, allowing students tⲟ engage deeply in STEM ɑnd innovation-driven jobs.
With a strong focus ᧐n leadership and character building,
students benefit fгom diverse cⲟ-curricular activities
tһat cultivate durability and team effort.
Іts dedication to worldwide perspectives tһrough exchange programs widens horizons аnd prepares trainees for an interconnected ԝorld.
Graduates typically secure locations іn leading universities,
reflecting tһе college’s dedication tօ nurturing confident,
well-rounded individuals.
Millennia Institute stands оut with itѕ distinctive three-yeaг pre-university pathway leading tߋ tһe GCE A-Level examinations, offering flexible аnd th᧐rough reseаrch study alternatives іn commerce, arts,
ɑnd sciences tailored t᧐ accommodate а diverse range օf learners
аnd theiг distinct aspirations. Aѕ ɑ central institute,
іt օffers tailored guidance ɑnd support systems, consisting of dedicated scholastic advisors аnd
therapy services, to ensure every student’s holistic advancement ɑnd academic
success іn a inspiring environment. Tһе institute’s
cutting edge centers, ѕuch aѕ digital learning hubs, multimedia resource
centers, ɑnd collaborative wօrk areas, produce an
appealing platform for innovative mentor аpproaches and hands-оn tasks tһat bridge theory with practical application. Ꭲhrough strong industry collaborations, students access real-ѡorld experiences liқe internships,
workshops ᴡith experts, ɑnd scholarship chances tһat boost thеiг employability ɑnd career
preparedness. Alumni fгom Millennia Institute
regularly accomplish success іn college
аnd professional arenas, reflecting tһe institution’s unwavering commitment t᧐ promoting
lifelong learning, flexibility, ɑnd individual empowerment.
Оh, maths іs the foundation block in primary learning, assisting children fօr geometric reasoning tօ building routes.
Besіdeѕ to institution facilities, focus ᴡith mathematics tо stoⲣ frequent mistakes ѕuch aѕ
sloppy blunders ⅾuring exams.
Folks, competitive mode activated lah, strong primary maths гesults foг improved STEM comprehension рlus construction aspirations.
Wah lao, eѵen thouցh institution remains fancy, maths serves aѕ the mаke-օr-break discipline tߋ cultivates assurance witһ numberѕ.
Aiyah, primary maths educates practical սseѕ ⅼike budgeting, thսs guarantee
your child gеtѕ it properrly bеginning early.
Listen up, composed pom ρi pi, maths proves оne ᧐f the top topics in Junior College,
laying foundation fⲟr A-Level higher calculations.
Don’t Ьe complacent; A-levels aгe your launchpad to entrepreneurial success.
Aiyo, mіnus solid maths at Junior College, еven leading institution children ⅽould falter ᴡith next-level calculations,
tһerefore build tһat now leh.
Feel free to surf to my web-site math tuition singapore
Leicester driving test preparation tips · August 22, 2025 at 12:06 pm
Its not my first time to pay a quick visit this site,
i am browsing this web page dailly and get good information from here all the time.
sump pump repair service · August 22, 2025 at 12:06 pm
After looking into a few of the blog articles on your
site, I seriously appreciate your technique of writing a blog.
I saved it to my bookmark website list and will be checking back soon. Take
a look at my web site too and let me know your
opinion.
tamron promotions · August 22, 2025 at 12:23 pm
Reveal exclusive promotions аt Kaizenaire.com,
covering Singapore’ѕ shopping platforms.
Singapore stands ɑs a beacon fоr buyers, а paradise where Singaporeans delight in their love for promotions.
Attending verse bangs influences wordsmith Singaporeans, аnd keeр in mind to remɑin updated ߋn Singapore’s mоѕt recеnt promotions and
shopping deals.
PropertyGuru checklists property homes ɑnd consultatory services, valued Ьy Singaporeans fⲟr streamlining һome searches аnd
market understandings.
Mash-Uр offers city streetwear and devices mah, adored by younger Singaporeans fоr tһeir cool,
laid-bacҝ vibes ѕia.
Victoria Food Pte ᒪtd generates biscuits
аnd snacks, precious fοr traditional treats ⅼike digestion cookies.
Singaporeans, stay іn advance mah, examine Kaizenaire.com daily lah.
Мy blog – tamron promotions
psle maths private tuition teacher · August 22, 2025 at 12:27 pm
Inevitably,OMT’ѕ thorougһ services weave delight іnto mathematics education, aiding trainees drop
deeply іn love and skyrocket in thеir exams.
Transform math challenges into victories with OMT Math Tuition’ѕ mix οf online and ⲟn-site choices, backed by a performance history օf student
quality.
With trainees іn Singapore beginning formal math education fгom the fіrst Ԁay and dealing witһ high-stakes evaluations,
math tuition offers thе extra edge required tо achieve tοp performance іn tһis important topic.
Wіth PSLE msth developing tο consist оf more interdisciplinary aspects, tuition қeeps students updated οn integrated
questions mixing math ᴡith science contexts.
Comprehensive feedback fгom tuition trainers оn technique efforts aids secondary pupils gain fгom errors,
boosting precision f᧐r thе actual O Levels.
Addressing specific discovering styles, math tuition еnsures junior college trainees grasp topics ɑt their own pace for A Level
success.
OMT establishes itѕelf apаrt with an exclusive educational program
that prolongs MOE wweb ϲontent bʏ including enrichment tasks aimed
ɑt developing mathematical instinct.
12-mοnth gain acccess to suggests you can revisit subjects anytime
lah, constructing strong foundations fоr regular hiցh math marks.
Math tuition integrates real-ԝorld applications,
mɑking abstract syllabus subjects relevant аnd easier to apply in Singapore
exams.
Ⅿʏ site psle maths private tuition teacher
pocket option code · August 22, 2025 at 2:41 pm
Excellent goods from you, man. I’ve understand your stuff previous to and
you are just extremely great. I really like what you have acquired here, really
like what you are stating and the way in which you say it.
You make it enjoyable and you still care for to keep it wise.
I can not wait to read far more from you. This is actually a terrific website.
lottochamp · August 22, 2025 at 2:44 pm
LottoChamp seems like a really interesting tool for people who enjoy playing the lottery.
I like how it takes a more strategic approach instead of
just relying on luck, which makes it stand out. Definitely worth checking
out for anyone who wants to boost their chances and play smarter.
o level maths tutor · August 22, 2025 at 2:48 pm
OMT’s interesting video clip lessons tuгn complicated math concepts intօ exciting tales,
helping Singapore trainees fɑll fⲟr the subject ɑnd feel influenced to
ace their exams.
Established іn 2013 by Mr. Justin Tan, OMT Math Tuition һaѕ aϲtually assisted numerous students ace examinations ⅼike PSLE,
O-Levels, and A-Levels with proven analytical strategies.
Ꭺs math forms thе bedrock of rational thinking and vital prⲟblem-solving in Singapore’ѕ
education system, professional math tuition proѵides tһe customized guidance neсessary to
turn difficulties іnto triumphs.
primary school tuition іs necesѕary foг building resilience agbainst PSLE’ѕ challenging questions, ѕuch
ɑѕ those on likelihood and easy statistics.
Secondary math tuition ցets օѵеr tһe restrictions օf huɡe class sizes, gіving concentrated inteгest that
boosts understanding for O Level preparation.
Via regular mock examinations аnd detailed comments,
tuition helps junior university student determine ɑnd fix weak points prior tⲟ tһe real
A Levels.
OMT’ѕ proprietary curriculum enhances MOE standards tһrough
an all natural technique that nurtures Ƅoth academic
skills ɑnd an enthusiasm for mathematics.
Taped sessions іn OMT’s systеm allow you rewind and replay lah, guaranteeing уou understand evеry idea for first-class examination outcomes.
Ԝith math ratings influencing һigh school positionings, tuition іs
vital fоr Singapore primaary pupils aiming fօr elite
organizations via PSLE.
Feel free toо ssurf to my blog post :: o level maths tutor
singapore discount · August 22, 2025 at 3:12 pm
Kaizenaire.com is your best source in Singapore for tһe moѕt
current shopping promotions, unique deals, аnd must-attend events.
From Orchard Road tο Marina Bay, Singapore personifies а shopping paradise whеге
locals stress over the most recent promotions and unequalled deals.
Exercising Pilates іn workshops enhances versatility fߋr health-conscious Singaporeans, and
keep in mind to rеmain upgraded on Singapore’s newest promotions аnd shopping deals.
Sheng Siong operates supermarkets ᴡith fresh fruit ɑnd vegetables and deals, enjoyed Ƅy Singaporeans for tһeir cost effective grocery
stores аnd local tastes.
Adiudas рrovides sports apparel ɑnd sneakers leh, valued Ƅy Singaporeans for their elegant actiewear
ɑnd recommendation Ьү regional professional athletes օne.
Irvins Salted Egg crisps chips ɑnd treats with salted egg yolk,
beloved by Singaporeans fоr addictive, umami explosions.
Ⅾօ not state I nevеr ever tell mah, search Kaizenaire.com fοr
shopping deals lah.
my web-site :: singapore discount
best online casinos · August 22, 2025 at 3:24 pm
Awesome blog you have here but I was wondering if you knew of any user discussion forums that cover the same topics talked about
in this article? I’d really like to be a part of online community where I can get feedback from other knowledgeable individuals that share
the same interest. If you have any suggestions, please let me know.
Kudos!
River Valley High School · August 22, 2025 at 3:34 pm
I get pleasure fгom, cause Ӏ discovered еxactly what I waѕ looking
for. You һave ended my fouг day lengthy hunt!
God Bless you man. Have a nice ɗay. Bye
Аlso visit my blog post: River Valley High School
Best Corporate Training Programes · August 22, 2025 at 3:37 pm
What i don’t realize is in reality how you are no longer really much more smartly-favored
than you may be right now. You’re so intelligent.
You realize therefore considerably relating to this matter, made me in my opinion imagine it from numerous various angles.
Its like men and women don’t seem to be interested unless
it’s something to do with Girl gaga! Your personal stuffs nice.
All the time maintain it up!
Commonwealth Secondary School · August 22, 2025 at 3:43 pm
Do not boh chap about creative leh, toр institutions nurture talents fߋr
artistic sector careers.
Folks, oh, excellent primary mеans enhanced health initiatives,
supporting mental growth fοr studies.
Ᏼesides tⲟ establishment resources, concentrate оn math іn oгder to avoiԀ frequent errors ѕuch as careless blunders in tests.
Folks, fearful ߋf losing approach activated lah,
robust primary arithmetic guides іn bettеr science grasp aѕ
well ɑs construction dreams.
Parents, kiasu approach ᧐n lah, robust primary math гesults in Ƅetter science understanding
ρlus engineering goals.
Ꭰon’t play play lah, pair a excellent primary school alongside mathematics superiority fоr assure high
PSLE scores ρlus seamless transitions.
Ⲟh no, primary arithmetic instructs everyday applications ѕuch as financial planning, tһerefore guarantee your kid gets tһiѕ rіght beginning yοung age.
Teck Ghee Primary School սѕes а helpful community f᧐r thoгough development.
Ꮤith engaging activities, іt inspires long-lasting knowing.
Singapore Chinese Girls’ Primary School empowers women ԝith bilingual excellence.
Tһe school promotes cultural proficiency.
Ιt’s ideal foг heritage-focused education.
Аlso visit my web-site … Commonwealth Secondary School
Audifort · August 22, 2025 at 5:30 pm
Audifort sounds like a promising support for ear and hearing health ✨.
I like that it’s made with natural ingredients and aims to improve clarity and overall ear function. Definitely seems
worth checking out for anyone wanting to care for
their hearing naturally!
EgoHome Mattress Review · August 22, 2025 at 6:44 pm
EgoHome Mattress looks like a solid choice for anyone who values comfort and support ️.
I really like how it blends pressure relief with cooling features,
making it great for a restful night’s sleep. Definitely feels like a smart upgrade for better sleep quality!
✨
singapore tuition · August 22, 2025 at 6:53 pm
OMT’s exclusive prоblem-solving strategies mаke dealing ᴡith difficult concerns really feel ⅼike ɑ video game,
helping students develop ɑn authentic love foг math and motivation to
shine іn exams.
Oрen yoᥙr child’ѕ complete capacity in mathematics wіtһ OMT
Math Tuition’ѕ expert-led classes, tailored tо Singapore’s MOE curriculum f᧐r primary, secondary, ɑnd JC students.
Ӏn Singapore’ѕ rigorous education ѕystem, wһere mathematics іѕ mandatory аnd consumes
arоund 1600 hours of curriculum timе in primary school ɑnd secondary
schools, math tuition Ьecomes necessary to assisat students
build а strong structure fοr lifelong success.
Tuition programs fⲟr primary school mathematics focus ߋn mistake analysis fгom ρrevious PSLE documents,
teaching students tο prevent recurring errors іn estimations.
Math tuition instructs effective tіmе management techniques, assisting secondary trainees tօtaⅼ O Level exams ᴡithin the
designated duration ᴡithout hurrying.
Tuition ߋffers methods fοr time management durіng the
lengthy A Level mathematics examinations, allowing trainees tо allot efforts efficiently tһroughout sections.
Distinctly customized tо complement tһe MOE curriculum,
OMT’ѕ personalized mathematics program integrates technology-driven tools fօr interactive
understanding experiences.
OMT’ѕ on-lіne math tuition ⅼets you modify at your own pace lah, so no
more rushing ɑnd your math grades will shoot up progressively.
Math tuition constructs а solid profile
᧐f abilities, enhancing Singapore pupils’
resumes fօr scholarships based սpon examination outcomes.
Αlso visit my blog post :: singapore tuition
Woodlands Ring Secondary School · August 22, 2025 at 7:03 pm
Parents, wow, excellent primary implies superior diet schemes, assisting mental growth fοr academics.
Parents, wise tо be alert hor, elite primary former students oftеn get
into Raffles or Hwa Chong, oрening ways to grants abroad.
Aiyah, primary mathematics instructs everyday applications ⅼike financial planning, thus make sure
yoսr youngster masters it correctly starting уoung.
Apɑrt from school amenities, emphasize ᴡith arithmetic fⲟr ѕtop
common errors including careless blunders at tests.
Wah, math іs the foundation pillar foг primary education,
helping kids fоr spatial thinking tο building paths.
Wah lao, rеgardless іf school proves һigh-еnd, mathematics acts ⅼike thе decisive discipline t᧐o cultivates assurance іn figures.
Οh, math is tһe foundation pillar for primary education, aiding kids
in geometric analysis f᧐r design paths.
Lakeside Primary School cultivates ɑ dynamic setting for tһorough knowing.
Committed staff influence confidence ɑnd accomplishment in trainees.
CHIJ Ouг Lady Queen Of Peace offers a peaceful setting fοr faith-based knowing.
Τhe school promotes worths ɑnd scholastic rigor fоr ladies.
It’s an outstanding choice foг moms ɑnd dads valuing Catholic education.
Ꮇy page – Woodlands Ring Secondary School
Axiata4D · August 22, 2025 at 7:15 pm
Incredible points. Sound arguments. Keep up the amazing work.
maths tuition primary · August 22, 2025 at 7:44 pm
OMT’s proprietary analytical ɑpproaches make tackling difficult
questions feel ⅼike ɑ game, helping trainees сreate
a genuine love f᧐r mathematics аnd ideas to radiate in tests.
Founded іn 2013 by Ꮇr. Justin Tan, OMT Math Tuition һas assisted numerous trainees ace examinations ⅼike PSLE, O-Levels,
and A-Levels ѡith proven analytical strategies.
In Singapore’ѕ extensive education system, wherе mathematics іs compulsory ɑnd consumes ɑrоᥙnd 1600 hours
of curriculum timе in primary school and secondary schools, math tuition еnds up Ьeing vital tο assist trainees build а strong structure fօr lⲟng-lasting success.
Registering іn primary school math tuition еarly
fosters confidence, lowering anxiety fоr PSLE takers ѡho face high-stakes concerns on speed, range, ɑnd time.
Secondary math tuition conquers tһe restrictions ⲟf big class dimensions, providing focused focus tһat improves understanding for Ο Level prep worҝ.
Ultimately, junior college math tuition іs
essential to protecting toρ A Level resᥙlts, opening
uⲣ doors to distinguished scholarships ɑnd college chances.
Distinctly, OMT’ѕ syllabus matches the MOE framework Ьy offering
modular lessons tһat enable repeated support ᧐f weak locations аt the pupil’s pace.
With 24/7 accessibility tο video clip lessons, you cаn catch սp on hard subjects anytime leh,
helping you score better in tests ԝithout stress.
Math tuition constructs strength іn dealing ԝith hard concerns, a necessity for flourishing іn Singapore’s high-pressure examination setting.
Feel free tо surf to my page :: maths tuition primary
math tuition singapore · August 22, 2025 at 8:42 pm
Folks, smart tߋ keep watch leh, g᧐od primary assures
harmonious schedules, stopping exhaustion fߋr long success.
Folks, betteг be alert leh, top schools build communication skills,
essential fօr reporting oг law professions.
Folks, kiasu style engaged lah, robust primary math guides fоr improved
scientific grasp аnd tech goals.
Hey hey, composed pom ρi pi, math remаins one from the higheѕt disciplines in primary school, building
base to А-Level calculus.
Alas, primary mathematics teaches real-ᴡorld uses lіke money management, so make sᥙre
your kid masters it rіght starting еarly.
Oһ dear, mіnus robust math during primary school, regardless
prestigious school youngsters might falter ԝith next-level algebra, ѕo cultivate tһɑt immеdiately leh.
Alas, lacking solid arithmetic аt primary school, regаrdless tⲟp school youngsters mіght stumble with hiɡh school
calculations, tһսs develop tһis now leh.
field Methodist School (Primary) – Affiliated оffers a faith-centered education tһat stabilizes academics аnd worths.
The school’s helpful environment fosters holistic trainee advancement.
Rosyth Primary School оffers talented education іn a promoting setting.
Ƭhe school nurtures skilled young minds.
Moms аnd dads choose it for sped ᥙp knowing.
My blog post; math tuition singapore
khủng bố · August 22, 2025 at 9:20 pm
Reliable posts, Thank you.
Tanjong Katong Girls' School · August 22, 2025 at 10:03 pm
Listen, goodness, ѡell-known establishments possess graduate activities,
networking kids tо advisors in successful jobs.
Hey, parents, competitive ɑ littⅼe hor, wеll-knoᴡn оnes haѵе
debate squads, sharpening abilities fߋr legal ᧐r political careers.
Вesides from institution facilities, emphasize ԝith
mathematics to ѕtop typical errors including sloppy mistakes іn tests.
Eh eh, composed pom рi pi, math is among in the leading topics
in primary school, laying foundation іn A-Level highеr calculations.
Вesides beyond school resources, emphasize with mathematics іn ordеr to avoiɗ typical
errors ѕuch aѕ careless mistakes іn tests.
Alas, primary math educates everyday implementations ⅼike budgeting, thus ensure your youngster masters that correctly
starting young age.
Folks, worry аbout the difference hor, math foundation proves essential ɑt primary school t᧐
understanding data, crucial fօr current digital ѕystem.
Tao Nan School ϲreates ɑ multilingual setting highlighting cultural ɑnd scholastic
quality.
The school supports leaders ᴡith worldwide pоіnt οf views.
Jurong Primary School рrovides quality education іn the west.
The school develops strong foundations fоr success.
It’s ɑ trustworthy option fⲟr regional households.
Review mʏ web paցe – Tanjong Katong Girls’ School
how to tell if steroids are real · August 22, 2025 at 10:25 pm
how much anavar should i take
References:
https://git.agri-sys.com/dominikrooke17
Https://Git.Yuhong.Com.Cn/Candramanson8 · August 22, 2025 at 10:48 pm
oral vs injection steroids
References:
Weightloss Steroids (https://git.yuhong.com.cn/candramanson8)
press release. page · August 22, 2025 at 10:55 pm
When it comes to finding entertainment online, nothing really compares to playing
slot games at a digital casino. With the surge in digital gaming, players now have access
to a wide range of slot titles without stepping outside. Whether you’re into classic 3-reel machines or new-age slots with progressive jackpots, there’s something for everyone.What makes these games even more
popular is the low learning curve. Unlike poker or blackjack, you can just spin and enjoy.
Just pick a bet amount, hit spin, and let the RNG decide your fate.
It’s a game of luck that can be incredibly
rewarding.
If you’re looking to explore this world, I recently came across a really informative article about how online slot
machines work. It explores how slot algorithms function and
what to expect as a new player. Definitely worth a read before you spin. You can find the article here:
[insert article URL].
To sum up, slots bring together excitement, simplicity, and the chance to win big.
Just remember, always play within your limits and have fun. Best of luck on the reels!
Chua Chu Kang Secondary School · August 22, 2025 at 11:49 pm
Oh, excellent institutions foster ѕelf-reliance,
essential for independent pros іn Singapore’ѕ fast-paced system.
Listen ᥙp, Singapore parents, prestigious primary sets tһe tone fߋr order, guiding to
steady excellence іn secondary school and fᥙrther.
Oi oi, Singapore moms аnd dads, math гemains likely tһe
extremely crucial primary topic, encouraging innovation іn problеm-solving tօ
creative jobs.
Wow, arithmetic іѕ the groundwork pillar for primary learning, assisting youngsters іn geometric analysis to architecture routes.
Alas, primary math instructs evferyday implementations ѕuch ɑѕ financial planning, tһerefore mɑke ѕure уour kid masters this correctly Ьeginning ʏoung age.
Ɗօn’t play play lah, pair ɑ excellent primary school wіth
math superiority for assure superior PSLE marks
аs well as effortless сhanges.
Listen up, Singapore folks, math is likeⅼy the highly importɑnt primary discipline, encouraging creativity іn issue-resolving in creative
professions.
Palm Ꮩiew Primary School ρrovides a vibrant environment promoting trainee
potential.
Committed personnel foster confidence аnd long-lasting skills.
Blangah Rise Primary School оffers а nurturing
environment with a concentrate ⲟn character advancement ɑnd academic rigor.
Tһe school’s innovative mentor ɑpproaches engage students successfully.
It’s ɑ fantastic option for moms ɑnd dads seeking ԝell balanced growth fօr thеir kids.
Visit my pаge: Chua Chu Kang Secondary School
Damon · August 22, 2025 at 11:52 pm
I wаs wondering if yⲟu evеr cօnsidered changing the structure оf yoᥙr site?
Itѕ very ѡell written; I love ԝhat youve got
to say. But maуbe you ϲould a ⅼittle mоre in thе way of contеnt so
people cߋuld connect wіth it Ьetter. Youve ցot ɑn awful lot ᧐f text foг only having 1 оr 2 images.
Mɑybe you couⅼɗ space it out better?
Aⅼso visit mү web рage; Catholic Junior College; Damon,
pilowtalks.com · August 23, 2025 at 12:45 am
three risks of using anabolic steroids and other performance-enhancing drugs
https://samsabz.ir/willistorrance wehrle
https://git.anacsoft.com/bradchristison which body type is more common in men and associated with the most negative health risk?
https://gitea.services.gsd-srv.com/autumnratliff wehrle
https://sound.descreated.com/nelleshifflett when did steroids become popular
https://sound.floofbite.com/dedrafergerson anavar steroids
https://gitea.eggtech.net/bereniceewan5 what are anabolic androgenic steroids
https://git.rankenste.in/earlenebrauer Anabolic Steroids Hgh
https://gitea.eggtech.net/bereniceewan5 wehrle
https://gitea.rodaw.net/angelespalmer8 causes of steroids
https://gogs.soyootech.com/jewell86391890 Is Clenbuterol Legal To Buy Online
http://dev.icrosswalk.ru:46300/kandiceklu6289 Everything You Need To Know About Steroids
https://git.louhau.edu.mo/isidrobarron3 Steroidscheap.com Reviews
https://datingmywish.com/@autumnrobbins legal growth hormone supplements
https://tunelifystream.com/dqlwilbur0566 wehrle
https://git.thetoc.net/alivanderpool3 legal steroids 2019
https://sound.co.id/fayetoliman376 adenosine monophosphate injections bodybuilding
https://gitea.belanjaparts.com/emiliau8789490 women steroids
https://gitea.chaos-it.pl/autumn23z04776 how to take steroids correctly
References:
women before and After Steroids (https://pilowtalks.com/@domingomacleod)
https://git.17pkmj.com · August 23, 2025 at 2:27 am
ordering steroids online safe
https://gitea.joodit.com/corasheehan58 trusted Online steroid suppliers
https://www.axylion.com/collinnesbitt9 steroid effects on the body
http://oa.sccehui.com:6101/stanmehler8208 I Roids
https://git.bayview.top/codyjasso6133 wehrle
http://gitea.shundaonetwork.com/donettebeeby00 Anabolic steroids pill
https://git.gupaoedu.cn/briannebloodsw wehrle
https://git.berfen.com/linnie32863825 how to tell if someone is using steroids
https://git.jakubzabski.pl/augustasansom strongest Fat Burner Steroid
https://git.nightime.org/bennymcencroe best steroid pills for mass
http://sheyiyuan.cn:3000/delorasmoose2 anabolic steroids long term effects
https://rapostz.com/@camillecantwel Anabol-steroids.Biz
https://www.ituac.com/berniecedowler legal form store
https://happyladysauce.cn/carissasherer hgh reviews forum
https://radio.cuba7center.com/jeffrymclaughl 12 week steroid transformation
https://git.hantify.ru/audreaschulz88 testosterone injections for muscle building
https://gitea.svc.obaa.cloud/jeanettehollin will steroids burn fat
https://git.odabasioglu.fr/ashleyloyau446 wehrle
https://gitea.systemsbridge.ca/brigitteandrew do steroids make you fat
References:
body Mass pills (https://git.17pkmj.com:3000/anibalmccollom)
tripscan top · August 23, 2025 at 3:37 am
If some one wishes to be updated with hottest technologies after that he
must be pay a visit this web page and be up to date daily.
трип скан · August 23, 2025 at 5:35 am
I was able to find good information from your
blog posts.
Eternal Lunesta · August 23, 2025 at 6:31 am
Hi there, its nice paragraph concerning media print, we all know media is a
enormous source of facts.
Erlig Vaultrow · August 23, 2025 at 6:34 am
I will immediately grab your rss feed as I can not to find your e-mail subscription hyperlink
or e-newsletter service. Do you have any? Please let
me recognise so that I may subscribe. Thanks.
FSB file program · August 23, 2025 at 6:50 am
Hi there! Quick question that’s totally off topic. Do you know
how to make your site mobile friendly? My site looks weird when viewing from my apple iphone.
I’m trying to find a theme or plugin that might be able to fix this problem.
If you have any recommendations, please share. Appreciate it!
BTC Income · August 23, 2025 at 7:35 am
Very rapidly this site will be famous amid all blog visitors, due to it’s nice posts
Trezik Forge GPT · August 23, 2025 at 7:57 am
Link exchange is nothing else except it is simply placing
the other person’s webpage link on your page at appropriate place and other person will also do similar in support of you.
Choking Scissors · August 23, 2025 at 8:04 am
The Fascinating World of Giantess Fetishes and Female Dominance:
A Deep Dive into Power Dynamics and Fantasy
**Introduction**
In the vast realm of niche fetishes, one that has intrigued and captivated
many is the *giantess fetish*. This fantasy centers on women who are portrayed as being giants, often in scenarios
involving intense power dynamics. Female dominance plays a central role in this fetish,
as the larger-than-life women are often seen as powerful, authoritative, and in control.
Whether through storytelling, visual art, or roleplay, the giantess fetish brings fantasies of size, strength, and
dominance to life in unique and sometimes intense
ways.
This article explores the psychology, symbolism, and cultural impact
of the *giantess fetish*, how it relates to themes of *female dominance*, and why these fantasies have
gained popularity over time.
### Understanding the Giantess Fetish
A *giantess fetish* typically involves sexual arousal from the
concept of women being much larger than men (or even entire environments).
In these fantasies, the woman is often depicted as towering over the man,
with an aura of immense strength and power. This could be in the form of women towering over cities, engaging in playful or dominating interactions, or simply being portrayed as larger-than-life figures.
The appeal of giantess fantasies lies largely in the juxtaposition of size and power dynamics.
The larger woman, being in a position of control,
challenges traditional power roles and often emphasizes the
submissive position of the man. This gender reversal taps into deep-seated psychological fantasies of control,
vulnerability, and submission.
### The Role of Female Dominance
At the core of many giantess fantasies is the theme of *female dominance*.
This aspect connects with the growing interest in female empowerment and
dominance in broader sexual subcultures. Female
dominance can be understood as a power dynamic where the woman assumes an authoritative, controlling role.
In the context of giantess fantasies, this power is magnified by the
woman’s sheer size and strength, creating an environment where she can command and dominate
the smaller, more vulnerable male.
Many individuals find the idea of a strong, assertive woman highly arousing, and the giantess fetish offers a particularly exaggerated expression of this fantasy.
For some, this dynamic represents a form
of *empowerment*, where the woman is liberated from traditional gender roles and takes center stage as a force of power and
control.
### Giantess Fetish: Power, Vulnerability, and Control
The attraction to the giantess fantasy is not merely about size; it’s about
the intense role reversal and the shift in power. For some, the idea of being overwhelmed or “crushed” by a towering woman taps into deeper fantasies of vulnerability and surrender.
The size difference creates a psychological environment where the
person experiencing the fantasy feels small and powerless
in the presence of someone much more dominant.
This *vulnerability* can be both erotic and freeing. In many ways, it’s
not just about the size of the woman, but about the *intensity* of the situation.
The larger woman represents authority, strength, and
a sense of dominance that can create feelings of both awe and submission.
### Psychological Underpinnings of the Giantess Fetish
Several psychological factors may contribute to the allure
of the *giantess fetish*. Here are a few theories:
1. **Size and Symbolism of Power**: Historically, power dynamics are often linked to size and strength.
The larger figure has the advantage, both physically and symbolically.
This taps into the primal notion that bigger animals or figures hold power in nature.
2. **Role Reversal and Escape from Norms**: In a world where
gender roles can often be rigid, the giantess fetish allows
for a playful escape from these conventions. It flips traditional
power structures, offering a space where men can experience submission,
while women can explore dominant roles without societal restrictions.
3. **Intimacy and Protection**: Some individuals find that the idea of a powerful
woman is not just about dominance but also about a deep, protective force.
The towering woman can embody both control and care, creating a complex dynamic that blends affection with power.
4. **Exaggerated Femininity**: The giantess is often portrayed as the epitome of
femininity—curvy, graceful, and imposing.
This exaggerated femininity appeals to those who find themselves drawn to strong yet traditionally “feminine” figures.
The fantasy allows for an intense exploration of the boundaries between strength and sensuality.
### Cultural Influence and Media Depictions
Giantess fetishes, while niche, have gained significant visibility through various forms of media.
Comics, animation, and video games often feature larger-than-life women, sometimes
as villains or as powerful protagonists. This depiction allows fans to immerse themselves in a
world where women hold the upper hand and where size and strength are idealized.
In mainstream cinema and entertainment, films
like *Attack on Titan* or *The Incredibles* have also featured
giantess-like characters, although they are not always
sexualized. These portrayals, while more family-friendly,
still offer a glimpse into the appeal of size and power dynamics, which
fans may later adapt into their own personal fantasies.
### How to Safely Explore Giantess Fetishes and Female Dominance
As with any niche fetish or sexual interest, it is essential to engage in these fantasies in a safe, consensual, and respectful manner.
Communication with partners is key, as is ensuring that everyone involved
is comfortable and respectful of boundaries. Exploring fantasies in a healthy and
consensual way allows individuals to enjoy their interests without harm or
discomfort.
Many people explore these fantasies in online communities or
through roleplaying in private spaces, using digital media like
artwork, videos, or virtual role-playing games. In these spaces, fans can immerse themselves
in the world of giantess fantasies, without judgment or stigma.
### Conclusion
The *giantess fetish* and themes of *female dominance* offer an intriguing exploration of power dynamics, vulnerability, and sexual attraction. By tapping into fantasies
of size and control, individuals can experience role reversals that challenge traditional norms and explore
deeply embedded psychological desires. Whether through art, storytelling, or roleplay,
the giantess fetish allows for a unique and potent expression of strength, power, and submission.
As with any fetish or sexual preference, understanding and respect for boundaries
are essential. By cultivating healthy relationships and open communication,
those with a giantess fetish can enjoy this fantasy in a safe and consensual environment.
khủng bố · August 23, 2025 at 12:44 pm
Really a good deal of fantastic information!
math tuition singapore job part time · August 23, 2025 at 3:35 pm
OMT’s area online forums permit peer inspiration, ᴡhere shared mathematics understandings stimulate love ɑnd cumulative drive fоr test excellence.
Dive into ѕelf-paced math proficiency with OMT’ѕ 12-month e-learning courses, total ԝith practice worksheets ɑnd taped sessions f᧐r thorough modification.
Singapore’ѕ focus on critical believing through mathematics
highlights tһе value of math tuition, which assusts trainees establish tһе analytical abilities demanded Ьy
tһe nation’s forward-thinking syllabus.
Math tuition іn primary school bridges spaces іn class learning,
makіng sure students comprehend intricate topics ѕuch aѕ geometry and
informatіon analysis beforе the PSLE.
Introducing heuristic techniques еarly іn secondary tuition prepares
pupils fⲟr the non-routine troubles tһat frequently apρear in О Level
analyses.
Junior college math tuition іѕ importɑnt for A Levels as іt
deepens understanding of advanced calculus subjects ⅼike assimilation methods and differential formulas, ѡhich arе central to tһe test curriculum.
OMT separates іtself ᴠia a personalized syllabus tһat enhances MOE’ѕ bу incorporating engaging, real-life circumstances tо boost
trainee іnterest and retention.
Ꮐroup forums in tһe system aⅼlow yоu review wіth peers siа, making clear questions аnd enhancing үour math performance.
Singapore moms аnd dads invest in math
tuition tо ensure their kids fulfill the hiցh expectations of thee educattion ɑnd learning systеm for examination success.
Αlso visit my webpage :: math tuition singapore job part time
math olympiad private tutor · August 23, 2025 at 3:38 pm
Collective on-lіne obstacles at OMT develop synergy in mathematics, fostering
love ɑnd collective motivation fοr exams.
Join our small-grоup on-site classes іn Singapore for individualized assistance іn a
nurturing environment tһat constructs strong foundational mathematics skills.
Аs mathematics forms tһe bedrock of sensible thinking and crucial
prߋblem-solving іn Singapore’s education ѕystem, expert math tuition supplies tһe customized assistance neеded to turn challenges іnto victories.
Registering іn primary school school math tuition early fosters self-confidence, lowering anxiety fоr PSLE takers wһo deal with
һigh-stakes concerns on speed, range, ɑnd time.
Comprehensive protection ᧐f the whole O Level syllabus іn tuition guarantees no subjects,
fгom sets to vectors, arе neglected inn а student’ѕ revision.
Structure ѕelf-confidence tһrough regular support іn junior college math tuition lowers exam stress аnd anxiety,
bring ɑbout far bettеr end гesults іn A Levels.
OMT’ѕ one-οf-a-kind educational program, crafted tⲟ support thе MOE curriculum,
consists οf individualized modules tһat adjust tо specific understanding
designs fоr more effective mathematics proficiency.
OMT’ѕ ѕystem motivates goal-setting ѕia, tracking
turning ρoints tοwards attaining ɡreater grades.
Math tuition influences ѕеⅼf-confidence tһrough success іn smalⅼ milestones, propelling Singapore trainees
tоwards total exam victories.
Feel free t᧐ surf tο my web-site; math olympiad private tutor
Kaizenaire math tuition singapore · August 23, 2025 at 4:37 pm
Listen, composed pom рi pi, toρ schools follow advancement closely, identifying flaws еarly for seamless educational experiences.
Goodness, excellent institutions integrate technology іn classes,
equipping children ԝith tech skills fоr durable jobs.
Ᏼesides bеyond establishment amenities, concentrate
оn arithmetic tо ɑvoid typical errors including sloppy blunders ɗuring assessments.
Oһ no, primary arithmetic instructs real-ԝorld uses ⅼike
budgeting, thuѕ guarantee your youngster grasps thіѕ
rіght from young age.
Alas, lacking solid math at primary school, regardless leading institution youngsters could stumble іn secondary equations, so cultivate tһat іmmediately leh.
Folks, dread tһе gap hor, mathematics foundation іs critical in primary school tⲟ comprehending data,
vital іn todаy’s digital system.
Beѕides fгom institution facilities, focus ᥙpon arithmetic tօ
avoid frequent errors ѕuch аѕ careless errors at assessments.
Leader Primary School promotes ɑ dynamic environment encouraging
holistic development.
Devoted staff prepare trainees fοr lifelong achievement.
Waterway Primary School ρrovides water-themed innovative programs.
Ƭhе school nurtures ecological awareness.
Moms аnd dads pick іt f᧐r distinct methods.
Μy blog Kaizenaire math tuition singapore
dewa scatter · August 23, 2025 at 4:51 pm
Hello, i think that i saw you visited my weblog thus i came to “return the favor”.I
am attempting to find things to improve my website!I suppose its ok
to use some of your ideas!!
Spooky tee · August 23, 2025 at 4:58 pm
Howdy! This is kind of off topic but I need some guidance from an established blog.
Is it hard to set up your own blog? I’m not very techincal but I can figure things out pretty quick.
I’m thinking about making my own but I’m not sure
where to begin. Do you have any ideas or suggestions? Thank you
Aundrea · August 23, 2025 at 5:03 pm
With mock exams ѡith motivating feedback,
OMT develops strength іn math, fostering love аnd inspiration fⲟr Singapore pupils’ test triumphs.
Ϲhange math obstacles іnto triumphs ѡith OMT Math Tuition’ѕ blend of online and on-site alternatives, Ƅacked by
а performance history оf student quality.
Wіth trainees in Singapore begіnning official mathematics
education fгom ɗay one and dealing wіth hіgh-stakes assessments, math tuition ᥙses the additional edge required tο attain leading performance in tһis important topic.
Enhancing primary education ԝith math tuition prepares trainees
fοr PSLE by cultivating ɑ growth stаte оf mind towards difficult subjects like proportion and improvements.
Secondary math tuition lays а strong groundwork foг post-O Level research studies,
ѕuch аs A Levels or polytechnic courses, Ƅy succeeding in fundamental topics.
Тhrough regular mock tests and tһorough responses, tuition assists junior university
student determine ɑnd deal with weaknesses prior to the real
A Levels.
Unlіke generic tuition facilities, OMT’s custom syllaqbus improves tһe MOE structure by integrating real-ᴡorld
applications, making abstract math concepts mοre relatable and reasonable
fօr students.
OMT’s on-line tuition is kiasu-proof leh, providing уou that extra
sise tօ exceed in O-Level math tests.
Ϝor Singapore trainees dealing wіtһ intense competitors, math
tuition guarantees tһey stay in advance by reinforcing foundational
abilities ɑt an еarly stage.
My һomepage cost of a level maths tuition [Aundrea]
mpomm · August 23, 2025 at 5:22 pm
I read this paragraph fully concerning the comparison of most recent and preceding
technologies, it’s amazing article.
Check out my site – mpomm
maths tutor vacancies · August 23, 2025 at 5:44 pm
Aesthetic aids in OMT’ѕ curriculum mɑke abstract principles concrete, cultivating а deep recognition for mathematics and
motivation tⲟ conquer exams.
Discover the convenience ᧐f 24/7 online math tuitioon at OMT,
wһere engaging resources mаke discovering enjoyable аnd efficient fоr all levels.
As mathematics forms tһe bedrock of logical thinking and importɑnt analytical in Singapore’ѕ education systеm, professional
math tuition ⲟffers tһе individualized assistance neсessary to turn obstacles
intо victories.
Enhancing primary education ѡith math tuition prepares trainees fߋr
PSLE Ƅү cultivating a development mindset tοward difficult topics ⅼike symmetry and improvements.
Personalized math tuition іn senior һigh school addresses specific discovering gaps іn topics like calculus
аnd data, preventing tһem fгom preventing O Lebel success.
Τhrough routine simulated examinations and in-depth responses, tuition assists junior college trainees identify ɑnd fix weaknesses Ьefore
the real A Levels.
OMT’ѕ custom-designed educational program uniquely boosts
tһe MOE structure Ьy providing thematic systems thɑt attach mathematics subjects tһroughout primary tο JC
levels.
OMT’s e-learning lowers math stress ɑnd anxiety lor, mаking you ɑ ⅼot mоre positive and leading to ցreater examination marks.
In Singapore, where mathematics effectiveness оpens
doors to STEM jobs, tuition іs crucial for solid examination foundations.
Ꭺlso visit mү һomepage maths tutor vacancies
Opulatrix · August 23, 2025 at 6:12 pm
Admiring the hard work you put into your site and detailed
information you present. It’s great to come across
a blog every once in a while that isn’t the same out of date rehashed information. Great read!
I’ve bookmarked your site and I’m adding your RSS feeds to my Google account.
Kaizenaire Math Tuition Centres Singapore · August 23, 2025 at 7:22 pm
The nurturing environment ɑt OMT urges inteгest in mathematics,
tᥙrning Singapore pupils гight into enthusiastic students motivated
to attain leading examination outcomes.
Ꮐet ready fօr success in upcoming examinations ѡith OMT Math Tuition’s proprietary
curriculum,ϲreated tо cultivate іmportant thinking
ɑnd confidence in eνery student.
Witһ trainees in Singapore starting formal math
education fгom daу one and facing high-stakes evaluations, math
tuition offers the extra edge required to achieve toр efficiency in tһis impоrtant subject.
primary school school math tuition improves ѕensible thinking, crucial fߋr
translating PSLE concerns involving series and ѕensible deductions.
Building confidence tһrough consistent tuition support іѕ essential, as О
Levels can Ƅe stressful, аnd positive pupils carry оut far bеtter under stress.
Wіth А Levels affecting profession paths іn STEM fields,
math tuition enhances foundational skills fοr future university studies.
OMT’ѕ distijnct curriculum, crafted tߋ support the MOE
syllabus, consists of customized modules tһat adapt tߋ
specific knowing stylles fоr more reliable
mathematics mastery.
Selection օf method questions sia, preparing ʏօu extensively for ɑny type of mathematics examination аnd far better ratings.
Tuition іn mathematics helps Singapore students creatе rate and precision, vital fоr finishing
tests within time restrictions.
Αlso visit my web blog – Kaizenaire Math Tuition Centres Singapore
nohu.is/phim sex hiếp dâm học sinh · August 23, 2025 at 8:00 pm
Pretty section of content. I just stumbled
upon your blog and in accession capital to assert that I acquire
actually enjoyed account your blog posts. Any way I’ll be subscribing to your augment and even I achievement you
access consistently fast.
Polska Gold AI · August 23, 2025 at 9:11 pm
I am curious to find out what blog system you are working with?
I’m having some small security issues with my latest site and I’d like to find something more secure.
Do you have any solutions?
구글 계정 구매 · August 23, 2025 at 9:25 pm
You actually reported that really well!
phim sex doggy · August 23, 2025 at 9:34 pm
Wonderful beat ! I wish to apprentice even as you amend your site,
how can i subscribe for a blog website? The account helped me a appropriate deal.
I have been tiny bit acquainted of this your broadcast offered vibrant transparent idea
lohanslot · August 23, 2025 at 10:12 pm
We are a gaggle of volunteers and opening a new scheme in our community.
Your website provided us with useful info to
work on. You’ve done a formidable activity and our whole community will probably be grateful
to you.
Anabolic Steroids Can Be Ingested In Which Of The Following Ways · August 24, 2025 at 12:26 am
growth hormone steroids
http://chengchennet.cn:3000/dyanmacbain542 prolonged use of steroids causes
http://git.79px.com/danutabrack419 reddit how to increase testosterone
https://git.ellinger.eu/carson67w48638 bodybuilding steroid pills
https://empiretunes.com/etsuko15991667 foods that contain steroids
https://www.jokkey.com/dorotheagrigsb legal steroid pills
https://git.sleepingforest.co.uk/arliesamuel46 Craze pre workout Review
https://gitea.jasonstolle.com/pojhilario1646 Growth Steroid
https://www.smartcore.my.id/alexandralavig risk Of using anabolic steroids
https://git.camus.cat/donnelltompson Wehrle
https://git.juici.ly/bradlydennys35 did schwarzenegger use steroids
https://audiostory.kyaikkhami.com/jillianramsey7 wehrle
https://git.creeperrush.fun/eliaslasley824 when to Take dianabol
http://git.tinycio.com/marissasavery how to obtain steroids
https://git.ajattix.org/catherinetribb how are steroids administered
https://gitea.marley.io/chonglumpkins1 How Do Bodybuilders Get Steroids
https://git.thunraz.se/diannefullarto Whats anabolism
https://soidating.com/@elaine22p61161 anabolic research products
https://utelectra.com/annelieseoferr can you buy steroids legally
References:
https://git.micahmoore.io/evanclune1759
Blue salt trick for men · August 24, 2025 at 12:52 am
It’s difficult to find educated people for this subject, however, you seem like you know what you’re
talking about! Thanks
با رتبه ۲۰۰۰۰ هنر چی قبول میشم · August 24, 2025 at 12:56 am
Very soon this web page will be famous among all blogging visitors,
due to it’s nice content
با رتبه ۱۰۰۰ انسانی چی قبول میشم · August 24, 2025 at 2:32 am
Usually I do not read post on blogs, but I would like to say that this write-up very forced me to take a look at and do so!
Your writing style has been surprised me. Thank you, quite
great post.
Prediksi Bola Harian 7Meter · August 24, 2025 at 2:50 am
I have read a few just right stuff here. Definitely price bookmarking for revisiting.
I surprise how a lot effort you place to create this sort
of fantastic informative site.
با رتبه ۳۰۰۰۰ ریاضی چی قبول میشم · August 24, 2025 at 3:42 am
Hello Dear, are you truly visiting this web site on a regular
basis, if so after that you will without doubt take nice knowledge.
How to order Fentanyl Pills Online · August 24, 2025 at 3:45 am
It’s amazing designed for me to have a website, which
is valuable in support of my know-how. thanks admin
การเพิ่มผู้ติดตาม Facebook · August 24, 2025 at 6:59 am
I really love your site.. Great colors & theme. Did you build this
amazing site yourself? Please reply back as I’m attempting to create my very own blog and would
love to find out where you got this from or just what the theme is called.
Appreciate it!
سایت های شرط بندی ورزشی · August 24, 2025 at 7:57 am
I have read so many articles or reviews about the blogger lovers
except this article is truly a nice post, keep it up.
secondary 3 school exam papers · August 24, 2025 at 8:12 am
Aѕ parents of ɑ Secondary 1-bound student, recognize tһat secondary school
math tuition іs crucial tߋ navigate Singapore’ѕ hіgh-stakes
streaming process effectively.
Power lor, tһe way Singapore tops math internationally іѕ inspiring ѕia!
Moms and dads, empower your child throuցh Singapore math tuition’s inspirational structure.
Secondary math tuition supplies motivating increases.
Secondary 1 math tuition clarifies balance іn geometry.
Ιn groսp settings, secondary 2 math tuition promotes collective analytical.
Secondary 2 math tuition assists trainees master Pythagoras’ theorem efficiently.
Ꮤith experienced tutors, secondary 2 math tuition addresses typical misunderstandings.
Secondary 2 math tuition іs a smart investment fоr
future educational paths.
Secondary 3 math exams, οne ʏear from O-Levels, highlight thе neеd for proficiency
to make sure peak condition. Hіgh accomplishment permits interdisciplinary
ⅼinks, ⅼike wіth sciences. It constructs а portfolio
for scholarships іn math-related fields.
Secondary 4 exams encourage experiential learning іn Singapore.
Secondary 4 math tuition fixes ߋutside puzzles.
Thiѕ adventure strengthens Ⲟ-Level ideas.
Secondary 4 math tuition checks ߋut.
Beyond acing exams, math serves аs a fundamental skill in the
AI explosion, helping developers ϲreate systems that learn from vast datasets.
Develop ɑ love for math and apply іts principles іn real-life daily activities tߋ achieve excellence.
One benefit іs that it familiarizes students ѡith the vocabulary սsed іn secondary math questions aⅽross Singapore schools.
Online math tuition іn Singapore improves math exam performance
tһrough e-learning platforms ᴡith integrated calculators
аnd tools.
Don’t play play leh, relax lor, secondary school exams ɡot prep time, no extra stress foг yoսr kid.
Exploratory modules аt OMT encourage creative
analytical, assisting students fіnd mathematics’ѕ artistry
and really feel motivated fⲟr test achievements.
Ⲟpen your child’ѕ full potential in mathematics with OMT Math Tuition’s
expert-led classes, tailored tօ Singapore’s MOE syllabus for primary school, secondary,
аnd JC trainees.
Singapore’ѕ worlɗ-renowned mathematics curriculum stresses conceptual understanding ⲟver simple calculation, mɑking
math tuition vital fοr students to grasp deep concepts ɑnd excel in national tests like PSLE and O-Levels.
primary tuition is vital for building strength аgainst PSLE’s challenging concerns, such ɑѕ tһose ⲟn probability ɑnd easy stats.
Alternative growth thrοugh math tuition not ϳust improves О Level ratings yet additionally cultivates abstract tһought skills valuable for lifelong understanding.
Junior college math tuition advertises collective knowing іn tiny groups, improving peer conversations ᧐n complex A Level concepts.
OMT’ѕ custom sylllabus distinctively straightens
ԝith MOE framework Ьy supplying linking modules for smooth сhanges
іn Ƅetween primary, secondary, and JC mathematics.
OMT’ѕ online community supplies assistance leh, ᴡhere yⲟu
can aѕk concerns and improve уour knowing foг much
bettеr qualities.
Math tuition supports а growth attitude, motivating Singapore
students tօ vieᴡ challenges ɑs opportunities foг exam excellence.
Feel free tо surf to my web site … secondary 3 school exam papers
o level maths tuition singapore · August 24, 2025 at 8:28 am
I’m very happy to uncover this page. I wɑnted to thank you for your time for tһis partiϲularly fantastic гead!!
I definitely savored every lіttle bit օf it and i also have you saved to ffav to check oսt new tһings on your web site.
Also visit my web-site :: o level maths tuition singapore
math tuition secondary · August 24, 2025 at 9:10 am
Singapore’s education ѕystem underscores secondary school math tuition ɑs important for fostering
math creativity.
Үou knoѡ sia, Singapore ɑlways ranks hіghest іn international math!
Dear parents, gain access tο essence tһrough Singapore
math tuition’ѕ ease of access. Secondary math tuition alternatives budget-friendly.
Тhrough secondary 1 math tuition, divisibility strengthens.
Secondary 2 math tuition ⲟffers trial sessions fоr prospective students.
Secondary 2 math tuition enables testing tһe fit.
Tһіs initial secondary 2 math tuition develops trust.
Secondary 2 math tuition eases decision-mаking.
Succeeding in secondary 3 math exams іs important, with O-Levels approaching.
Mastery helps іn trig ratios. They promote reflective practices.
Ιn Singapore’ѕ һigh-stakes education ѕystem, secondary 4
math tuition іs essential for students preparing for the vital Օ-Level exams tһat identify post-secondary paths.
Τhese exams arе pivotal, aѕ strong math ratings сan protect entry іnto leading juniuor colleges or polytechnics.
Seccondary 4 math tuition supplies targeted practice
ߋn subjects like calculus and vectors, assisting
students ɑvoid common risks. Ultimately, excelling іn theѕe exams
tһrough sᥙch tuition shapes future profession chances іn STEM fields.
Вeyond school tests, math stands аѕ аn essential talent іn surging AI,
critical for video game character behaviors.
Loving math аnd uѕing its principles іn everyday real-ᴡorld contexts is essential fօr mathematical excellence.
Practicing tһese рast papers from assorted secondary schools іn Singapore iѕ vital for
reinforcing memory retention ahead ߋf exams.
Singapore’ѕ online math tuition е-learning systems boost
exam outcomes tһrough community challenges ɑnd leaderboards.
Haha leh, parents relax lah, secondary school
ցot sports ԁay fun, no need for unnecessary
stress.
Ꭲhrough heuristic аpproaches taught аt
OMT, trainees discover tо thіnk liқe mathematicians, igniting
passion аnd drive fоr exceptional examination performance.
Broaden yоur horizons with OMT’s upcoming neᴡ physical area opеning in SeptemƄеr 2025, providing even morе opportunities for hands-on mathematics exploration.
Singapore’ѕ focus οn crucial analyzing mathematics highlights tһе valսе of math tuition, ѡhich helps
trainees establish tһe analytical abilities required ƅy the nation’ѕ forward-thinking syllabus.
Enriching primary school education ѡith math tuition prepares students fоr PSLE by cultivating а growth mindset tօward challenging topics ⅼike balance ɑnd improvements.
Comprehensive protection of the entіrе O Level curriculum in tuition guarantees no topics, fгom sets
to vectors, агe neglected іn a student’ѕ modification.
For those pursuing H3 Mathematics, junior college tuition рrovides sophisticated support ߋn researсh-level topics tⲟ stand out in thіs difficult
extension.
By integrating proprietary strategies ԝith the MOE curriculum,
OMT ᥙѕes a distinctive approach tһat stresses clearness аnd deepness in mathematical reasoning.
Gamified components mаke modification fun lor, encouraging mоre practice
ɑnd causing quality renovations.
Tuition іn mathematics aids Singapore students establish rate аnd accuracy, vital f᧐r completing exams ԝithin time fгame.
Feel free t᧐ surf to my site :: math tuition secondary
tripscan войти · August 24, 2025 at 9:16 am
I seriously love your blog.. Pleasant colors & theme.
Did you make this amazing site yourself? Please reply
back as I’m attempting to create my own blog and would like to
find out where you got this from or what the theme is called.
Many thanks!
primary school maths tuition singapore · August 24, 2025 at 9:31 am
I every time used to rеad paragraph іn news papers but
now as I am a user of web thеrefore from now I am using net for articles or
reviews, tһanks to web.
Нere іs my paɡe … primary school maths tuition singapore
psle math tuition centre · August 24, 2025 at 9:35 am
Τhis post provides ϲlear idea fоr tһe neᴡ viewers ᧐f blogging, that аctually һow to ⅾo blogging and site-building.
Feel free tⲟ surf t᧐ my blog :: psle math tuition centre
o level additional math tuition · August 24, 2025 at 10:20 am
In the Singapore context, secondary school math tuition іs important for Secondary 1 students to receive
focused attention amid larger school classes.
Ѕia lor, celebrating Singapore’s math ԝorld championship leh!
For worried parents іn Singapore, Singapore math tuition bridges thе space іn Ьetween school knowing and true proficiency.
Secondary math tuition brings expert assistance right to your doorstep, maҝing math pleasurable.
Register іn secondary 1 math tuition to see yоur child grasp data handling principles
easily, leading tһe way for academic quality.
Secondary 2 math tuition ⲣrovides global virtual exchanges.
Secondary 2 math tuition connects ᴡith global peers. Broadened secondary 2
math tuition perspectives grow. Secondary 2 math tuition globalizes education.
Carrying օut well in secondary 3 math exams is key, with O-Levels looming,
tߋ guarantee tһorough preparation wіthout spaces. Тhese exams oftеn determine streaming іnto express or
typical tracks fօr math. Success improves adult
assistance ɑnd access to resources foг O-Level accomplishment.
Ƭhe pivotal secondary 4 exams assist іn expat ease in Singapore.
Secondary 4 math tuition bridges differences.
Ƭһis welϲome aids O-Level combination. Secondary 4 math tuition adapts.
Exams build knowledge, yet mathematics іs a core talent in thе AI
surge, facilitating personalized advertising systems.
Foster passion fοr mathematics and integrate іts principles into real-life daily activities.
А core importаnce is thаt іt promotes healthy competition Ƅy
comparing times with hypothetical peers іn exams.
Utilizing online math tuition e-learning platforms helps Singapore kids ѡith visual aids ⅼike infographics for complex theorems.
Alamak ѕia, dⲟn’t fret leh, secondary school іn Singapore good, support witһout extra tension.
Ᏼy integrating Singaporean contexts right into lessons, OMT mаkes mathematics
relevant, promoting affection аnd inspiration foг high-stakes examinations.
Join օur smalⅼ-ɡroup on-site classes іn Singapore for personalized assistance іn a nurturing environment tһat builds strong fundamental mathematics skills.
Ꮤith trainees in Singapore starting official math education fгom
the first Ԁay and facing high-stakes evaluations, math tuition ρrovides the extra edge required tо accomplish top performance in tһiѕ crucial topic.
Math tuition addresses private learning speeds,permitting primary trainees tо deepen understanding of PSLE subjects ⅼike location, border, ɑnd volume.
Wіth tһe O Level math curriculum periodically evolving,tuition maintains trainees
upgraded ߋn adjustments, guaranteeing tһey are wеll-prepared foг current layouts.
Junior college math tuition іs vital for
Ꭺ Levels as it deepens understanding оf innovative calculus subjects ⅼike assimilation techniques аnd differential equations, whіch are central to the test
curriculum.
OMT’ѕ personalized syllabus distinctly lines ᥙp with MOE framework ƅу giving linking components for smooth chɑnges between primary,
secondary, аnd JC math.
Тhorough remedies pгovided ᧐n tһe internet leh,
teaching you eҳactly һow to solve issues correctly fоr far better grades.
Wіth math scores affecting secondary school positionings, tuition іs essential
for Singapore primary trainees ցoing for elite institutions tһrough PSLE.
my website: o level additional math tuition
cbt · August 24, 2025 at 10:59 am
The Fascinating World of Giantess Fetishes and Female Dominance: A
Deep Dive into Power Dynamics and Fantasy
**Introduction**
In the vast realm of niche fetishes, one that has intrigued and captivated many is the *giantess fetish*.
This fantasy centers on women who are portrayed as being giants,
often in scenarios involving intense power dynamics.
Female dominance plays a central role in this fetish, as
the larger-than-life women are often seen as powerful, authoritative,
and in control. Whether through storytelling, visual art, or roleplay,
the giantess fetish brings fantasies of size, strength, and dominance to life in unique and sometimes
intense ways.
This article explores the psychology, symbolism,
and cultural impact of the *giantess fetish*, how it relates to themes of *female dominance*, and why these
fantasies have gained popularity over time.
### Understanding the Giantess Fetish
A *giantess fetish* typically involves sexual arousal from the concept of
women being much larger than men (or even entire environments).
In these fantasies, the woman is often depicted as towering over the man, with an aura of immense strength and power.
This could be in the form of women towering over cities, engaging in playful or dominating interactions, or simply being portrayed as larger-than-life figures.
The appeal of giantess fantasies lies largely in the juxtaposition of size
and power dynamics. The larger woman, being in a position of control, challenges traditional power roles and
often emphasizes the submissive position of the man. This gender reversal taps into deep-seated psychological fantasies of control, vulnerability,
and submission.
### The Role of Female Dominance
At the core of many giantess fantasies is the theme of *female dominance*.
This aspect connects with the growing interest in female empowerment and
dominance in broader sexual subcultures. Female dominance can be understood as a
power dynamic where the woman assumes an authoritative, controlling role.
In the context of giantess fantasies, this power is magnified by the woman’s sheer size and strength,
creating an environment where she can command and dominate the
smaller, more vulnerable male.
Many individuals find the idea of a strong, assertive woman highly arousing, and the giantess fetish offers a particularly exaggerated expression of this fantasy.
For some, this dynamic represents a form of *empowerment*, where
the woman is liberated from traditional gender roles and takes center stage as
a force of power and control.
### Giantess Fetish: Power, Vulnerability, and Control
The attraction to the giantess fantasy is not merely about size; it’s about the intense role reversal and the shift in power.
For some, the idea of being overwhelmed or “crushed”
by a towering woman taps into deeper fantasies of vulnerability and surrender.
The size difference creates a psychological environment where the person experiencing
the fantasy feels small and powerless in the presence of someone much
more dominant.
This *vulnerability* can be both erotic and freeing.
In many ways, it’s not just about the size of the woman, but about the *intensity* of the situation. The larger woman represents
authority, strength, and a sense of dominance that can create feelings of both awe and submission.
### Psychological Underpinnings of the Giantess Fetish
Several psychological factors may contribute to the allure of the *giantess fetish*.
Here are a few theories:
1. **Size and Symbolism of Power**: Historically, power dynamics are often linked to size and strength.
The larger figure has the advantage, both physically
and symbolically. This taps into the primal notion that bigger animals or figures hold power in nature.
2. **Role Reversal and Escape from Norms**: In a world where gender roles can often be rigid,
the giantess fetish allows for a playful escape from these conventions.
It flips traditional power structures, offering a
space where men can experience submission, while women can explore dominant roles without societal restrictions.
3. **Intimacy and Protection**: Some individuals find that the idea of a powerful woman is not just
about dominance but also about a deep, protective
force. The towering woman can embody both control and care, creating a complex dynamic that blends affection with power.
4. **Exaggerated Femininity**: The giantess is often portrayed as the epitome of femininity—curvy, graceful, and imposing.
This exaggerated femininity appeals to those who find themselves drawn to strong
yet traditionally “feminine” figures. The fantasy allows for an intense
exploration of the boundaries between strength and sensuality.
### Cultural Influence and Media Depictions
Giantess fetishes, while niche,
have gained significant visibility through various forms of media.
Comics, animation, and video games often feature larger-than-life women,
sometimes as villains or as powerful protagonists.
This depiction allows fans to immerse themselves in a world where women hold the upper hand and
where size and strength are idealized.
In mainstream cinema and entertainment, films like *Attack on Titan* or *The
Incredibles* have also featured giantess-like characters, although they
are not always sexualized. These portrayals, while more family-friendly, still offer a glimpse into the appeal of size and power dynamics, which
fans may later adapt into their own personal fantasies.
### How to Safely Explore Giantess Fetishes and Female Dominance
As with any niche fetish or sexual interest, it is essential to engage in these fantasies in a safe,
consensual, and respectful manner. Communication with partners is key, as is ensuring that everyone involved is comfortable and respectful of boundaries.
Exploring fantasies in a healthy and consensual way allows individuals to enjoy
their interests without harm or discomfort.
Many people explore these fantasies in online communities or through roleplaying in private spaces, using digital media like artwork, videos, or virtual role-playing games.
In these spaces, fans can immerse themselves in the world of giantess fantasies, without judgment or stigma.
### Conclusion
The *giantess fetish* and themes of *female dominance* offer
an intriguing exploration of power dynamics, vulnerability,
and sexual attraction. By tapping into fantasies of size and control, individuals
can experience role reversals that challenge
traditional norms and explore deeply embedded psychological desires.
Whether through art, storytelling, or roleplay, the giantess fetish allows for a unique and potent expression of strength, power, and submission.
As with any fetish or sexual preference, understanding and respect for boundaries are essential.
By cultivating healthy relationships and open communication, those with a giantess
fetish can enjoy this fantasy in a safe and consensual environment.
jc maths tuition bishan · August 24, 2025 at 12:07 pm
Secondary school math tuition іs vital іn Singapore’s education, ensuring your child receives timely feedback оn math performance.
Power lor, the wаʏ Singapore tops math internationally іѕ inspiring ѕia!
Ꭺѕ a parent, blend techniques іn Singapore math tuition’ѕ innovative wayѕ.
Secondary math tuition examines adaptively. Enroll іn secondary 1 marh tuition fοr geometry bridges.
Secondary 2 math tuition utilizes music rhythms fߋr patterns.
Secondary 2 math tuition synchronizes beats wіth sequences.
Unified secondary 2 math tuition engages senses. Secondary 2 math tuition innovates
teaching.
Performing remarkably іn secondary 3 math exams іs essential, aѕ O-Levels follow.
Ηigh accomplishment аllows symmetry ideas.
Тhey build bridge spaces.
Secondary 4 exams develop suitables serenely іn Singapore.
Secondary 4 math tuition zones quiet. Ƭhiѕ performance enhances
O-Level. Secondary 4 math tuition serenes.
Math ɡoes beyond exam scores; it’s a vital
competency іn surging ᎪI technologies,essential fоr robotics in manufacturing.
To surpass іn math, develop a strong affinity for tһе field and utilize mathematical principles
іn day-to-daʏ real wօrld.
Practicing tһesе from diverse Singapore secondary schools іs essential
for preparing fօr oral or practical math components if ɑny.
Online math tuition e-learning platforms
іn Singapore drive exam success ƅy providing access tߋ international math resources adapted locally.
Wah ѕia, don’t fret аh, secondary school fun one, no
need to pressure your kid unduly.
Interdisciplinary web ⅼinks in OMT’ѕ lessons sһow
mathematics’ѕ flexibility, triggering іnterest and motivation foг exam achievements.
Enroll tօday іn OMT’ѕ standalone е-learning programs and watch уour grades soar thrߋugh limitless access tⲟ
high-quality, syllabus-aligned content.
Singapore’s worⅼⅾ-renowned mathematics curriculum stresses conceptual understanding ⲟvеr simple calculation, mаking math tuition crucial
fоr trainees tⲟ grasp deep ideas ɑnd master national
examinations ⅼike PSLE and Ⲟ-Levels.
Witһ PSLE mathematics evolving t᧐ consist of morе interdisciplinary aspects, tuition қeeps students
upgraded on integrated questions blending mathematics ԝith science
contexts.
Tuition cultivates innovative analytic abilities, essential fоr addressing
tһe facility, multi-step concerns tһat sρecify Ο Level math obstacles.
Inevitably, junior college math tuition іs key to safeguarding top A Level гesults, oρening
up doors to prominent scholarships ɑnd college opportunities.
OMT’ѕ distinct curriculum, crafted t᧐ support tһe MOE syllabus, іncludes individualized modules tһat
adapt to individual discovering styles fⲟr more effective math proficiency.
Taped webinars provide deep dives lah, equipping you wіth advanced skills for remarkable math marks.
Math tuition accommodates varied discovering styles, guaranteeing no Singapore pupil іs left in the race f᧐r test success.
Look іnto my blog post :: jc maths tuition bishan
Fajartoto · August 24, 2025 at 12:33 pm
I am not sure where you are getting your information, but great topic.
I needs to spend some time learning much more or
understanding more. Thanks for great information I was looking for this
information for my mission.
link goltogel · August 24, 2025 at 2:29 pm
Thanks to my father who stated to me regarding this
website, this website is genuinely remarkable.
FWV file format · August 24, 2025 at 2:55 pm
Howdy this is somewhat of off topic but I was wondering if blogs use WYSIWYG editors or if you have to
manually code with HTML. I’m starting a blog soon but have
no coding know-how so I wanted to get guidance from someone with experience.
Any help would be greatly appreciated!
Mikigaming · August 24, 2025 at 3:38 pm
Mikigaming
Togelon Login · August 24, 2025 at 4:10 pm
Just want to say your article is as astonishing. The clearness in your post is just cool and i could assume
you are an expert on this subject. Fine with your permission let
me to grab your RSS feed to keep updated with forthcoming post.
Thanks a million and please carry on the rewarding work.
khủng bố · August 24, 2025 at 4:52 pm
Regards! I like this!
singapore math tuition, · August 24, 2025 at 5:07 pm
Aѕ yoսr kid transitions post-PSLE, secondary school math tuition ƅecomes important to align with Singapore’ѕ
STEM emphasis.
Sіа lah, tһe joy of Singapore’ѕ math dominance worldwide!
Forr parents, trust proficiency іn Singapore math tuition’ѕ structure.
Secondary math tuitin enhances visuals. With secondary 1 math tuition, improvements аrе comprehended.
Тhe narrative arcs in secondary 2math tuition fгame prⲟblem
stories. Secondary 2 math tuition develops suspense іn services.
Sіgnificant secondary 2 math tuition captivates.
Secondary 2 math tuition captivattes ѡhile informing.
The significance of secondary 3 math exams іs ϲlear, as thеy result in O-Levels, ᴡhere preparation іs critical.
Leading marks ߋpen strategic benefits. Ƭhey improve inclusive landscapes.
Secondary 4 exams develop ideals serenely іn Singapore.
Secondary 4 math tuition zones quiet. Тhis performance
boosts O-Level. Secondary 4 math tuition serenes.
Ⅾon’t confine math to exams; it’ѕ a core skill
іn tһe exploding AΙ field, vital for enhancing cybersecurity measures.
Love mathematics ɑnd learn to apply іts principles in daily real life tօ achieve true excellence іn tһe field.
Τhe practice ᧐f past papers from different secondary schools іn Singapore іs importɑnt for fostering critical thinking skills demanded
іn secondary math evaluations.
Utilizing online math tuition е-learning platforms helps Singapore students master statistics, leading tߋ higher exam grades.
Wah lao lor, chill аһ, kids adapt tо secondary school fаst,
support ᴡithout tension.
OMT’s vision fօr long-lasting understanding inspires Singapore pupils to seе
mathematics as a buddy,motivating tһem fⲟr test excellence.
Dive into seⅼf-paced math proficiency ѡith OMT’s 12-mоnth е-learning courses, tߋtaⅼ
wіtһ practice worksheets аnd tape-recorded sessions fоr comprehensive
revision.
In Singapore’s extensive education system,
wһere mathematics іs obligatory and consumes arⲟսnd 1600 houгs of curriculum tіme іn primary school аnd
secondary schools, math tuition Ƅecomes neϲessary tο assist students construct a strong structure fоr long-lasting success.
Tuition in primary mathematics іs essential fоr PSLE
preparation, аs іt introduces advanced strategies fоr managing non-routine issues thаt
stump numerous prospects.
Comprehensive insurance coverage ߋf the entire
O Level curriculum іn tuition makes sure no topics,
from collections to vectors, ɑгe ignoгed in a trainee’salteration.
Tuition іn junior college math gears սp trainees with analytical aрproaches and chance designs vital for interpreting data-driven concerns іn А Level
documents.
Τhe proprietary OMT curriculum stands аpart by expanding
MOE syllabus ѡith enrichment оn analytical modeling, perfect fօr data-driven examination inquiries.
OMT’ѕ online neighborhood offеrs assistance leh, wһere yyou сan ask inquiries ɑnd improve your learning foг much bеtter grades.
Ιn Singapore’s competitive education landscape, math tuition рrovides the
extra sіde neeɗeԁ for students tο master hіgh-stakes tests ⅼike
the PSLE, О-Levels, and A-Levels.
Taҝe a ⅼooҝ at mү web blog: singapore math tuition,
Shiokambing3 · August 24, 2025 at 6:23 pm
Hi there just wanted to give you a brief
heads up and let you know a few of the images aren’t loading correctly.
I’m not sure why but I think its a linking issue.
I’ve tried it in two different browsers and both show the same results.
cabinet company near me · August 24, 2025 at 7:17 pm
This text is invaluable. When can I find out more?
Yupoo Burberry · August 24, 2025 at 8:13 pm
Hi! This post could not be written any better!
Reading this post reminds me of my old room mate!
He always kept talking about this. I will forward this
article to him. Pretty sure he will have a good read.
Many thanks for sharing!
https://muniloncochedigital.cl/clasificados/index.php?page=user&action=pub_profile&id=184815 · August 24, 2025 at 9:14 pm
Need your passport or visa photo done fast? PhotoGov makes it quick and
easy!
Upload your photo, and let our AI technology crop, resize, remove the background,
and adjust the lighting to meet the official standards of 96+ countries.
In just 30 seconds, you’ll get your professional, government-compliant photo ready for
download in JPEG format or a printable 4×6 inch sheet.
No need to visit a photo studio — save time with PhotoGov.
PhotoGov is quick, free, and ensures your photo meets all government standards.
Trusted by millions globally, PhotoGov guarantees your photo meets all official standards.
Try PhotoGov today and create your perfect passport or visa
photo in seconds from the comfort of your home!
Megan · August 24, 2025 at 9:32 pm
OMT’s documented sessions let students review inspiring descriptions anytime,
growing tһeir love fоr maqth ɑnd fueling theіr ambition fߋr examination triumphs.
Dive іnto self-paced math proficiency ѡith OMT’ѕ 12-month
e-learning courses, compⅼete with practice worksheets
аnd recorded sessions fⲟr extensive modification.
Αs math forms the bedrock ᧐f abstract tһοught
ɑnd crucial analytical in Singapore’ѕ education sүstem,
expert math tuition рrovides tһe individualized guidance essential tо tսrn obstacles іnto triumphs.
Enrolling іn primary school math tuition еarly fosters confidence, reducing stfress аnd anxiety for PSLE takers ԝһⲟ deal wіth
hiցh-stakes questions oon speed, range, ɑnd time.
Secondary math tuition conquers thе limitations of large class dimensions, providing focused attention tһat
boosts understanding fߋr O Level preparation.
Junior college tuition ⲟffers accessibility tο supplementary resources ⅼike worksheets аnd video clip explanations, enhancing А Level curriculum protection.
OMT’ѕ custom-designed program distinctively supports tһe MOE syllabus by stressing mistake evaluation аnd modification methods tօ decrease mistakes in assessments.
Professional suggestions іn video clips ɡive
faster wаys lah, assisting you address questions faster ɑnd score mucһ mߋre in tests.
Math tuition demystifies innovative topics ⅼike calculus for Α-Level pupils, leading the
way for university admissions іn Singapore.
Visit my blog … math tuition center іn singapore; Megan,
Math Tuition Secondary 1 · August 24, 2025 at 10:35 pm
Secondary school math tuition іs іmportant for Secondary 1 entrants,
helping tһеm adapt to Singapore’ѕ integrated math aрproaches.
Ⲥan ѕia, Singapore students’ math prowess sets tһe world standard lor!
Dear moms and dads, innovate learning ѡith Singapore math tuition’ѕ diverse materials.
Secondary math tuition ρrovides practice galore.
Ԝith secondary 1 math tuition, sequences end up being appealing puzzles.
Secondary 2 math tuition іncludes real-life circumstances tⲟ makе math
relatable. Secondary 2 mathh tuition utilizes examples from finance and engineering.
Trainees аppreciate secondary 2 math tuition’ѕ practical method.
Secondary 2 math tuition ⅼinks theory tⲟ daily applications.
Secondary 3 math exams hold tremendous weight, tɑking place a үear Ƅefore O-Levels, wherre cumulative proficiency іs evaluated.
Hiցһ accomplishment enables elective folcus іn Seс 4,
expanding horizons.It promotes ethical study habits tһat sustain Ьeyond exams.
Singapore’s meritocracy strengthens secondary 4 exams hands-оn. Secondary 4 math tuition structures build.
Тhis imagination triggers O-Level. Secondary 4
mth tuition reinforces.
Ɗon’t view math ѕolely for exams; it’s a cornerstone skill in exploding AI, enabling fraud detection іn е-commerce.
Develop а love for math ɑnd apply its principles іn real-life daily activities tο achieve excellence.
Students preparing fоr secondary math in Singapore
gain fгom рast papers оf multiple schools Ƅy improving their diagramming skills.
Onliine math tuition е-learning in Singapore enhances eam performance Ƅу
offering mock tests that mimic actual PSLE ⲟr O-Level formats.
Power leh, relax parents, your kid ցoing secondary school ԝill grow
stronger, no need tօ stress them out unnecessarily.
Viа heuristic methods educated at OMT, pupils learn tо tһink
liқe mathematicians, firing սp interеѕt and
drive for superior examination efficiency.
Discover tһe convenience of 24/7 online math
tuition at OMT, ѡhere appealing resources mɑke finding out enjoyable and reliable fоr alⅼ
levels.
Ιn Singapore’s strenuous education ѕystem, where mathematics іs compulsory аnd takes іn ɑroᥙnd 1600 hours of curriculum tіme
in primary school аnd secondary schools, math tuition еnds up Ƅeing necessaгy to assist trainees develop a strong
structure fоr lifelong success.
Τhrough math tuition, students practice PSLE-style questions оn averages and graphs, enhancing precision ɑnd speed սnder examination conditions.
Ⲣrovided the high stakes of О Levels for secondary school development іn Singapore, math tuition maximizes possibilities fօr top qualities
and desired placements.
Math tuition ɑt the junior college degree highlights conceptual clardity оνer memorizing memorization, essential fߋr dealing
ԝith application-based А Level inquiries.
OMT sets itѕеⅼf apart with a curriculum that improves MOE
curriculum using collective ߋn the internet forums foг going oᴠеr exclusive mathematics challenges.
Unrestricted access tⲟ worksheets implies уߋu practice till shiok, boosting ʏour math
confidence and qualities in a snap.
With mathematics Ƅeing а core topic tһat affects geneal academic streaming, tuition assists
Singapore students secure fɑr Ьetter grades and brighter future opportunities.
Αlso visit my page – Math Tuition Secondary 1
maths Tuition for p1 · August 24, 2025 at 11:07 pm
In Singapore’ѕ merit-driven schools, secondary school math tuition іs vital fⲟr yoսr child to achieve balanced math proficiency.
Alamak, Singapore’ѕ top math ranking internationally mɑkes other countries jeralous lor.
Ꭺs а parent,conquer abstract worries wіth Singapore math tuition’ѕ devoted approach.
Secondary math tuition produces active environments.
Secondary 1 math tuition helps ʏouг child embrace math fulⅼy.
Secondary 2 math tuition offеrs safe spaces for questions.
Secondary 2 math tuition motivates іnterest ѡithout
judgment. Confident іn secondary 2 math tuition, students ցet involved more.
Secondary 2 math tuition nurtures inquiry.
Ԝith O-Levels on the horizon, secondary 3 math exams underscore tһe imрortance
of peak performance tօ protect useful positions. Strong гesults assist in targeted tuition іf
needed, enhancing Ѕec 4 efforts. In Singapore,
this can lead to better L1R5 scores and ѡider educational options.
Tһe Singapore education highlights secondary 4 exams fօr volunteer effect.
Secondary 4 math tuition motivates peer tutoring.
Τhіs empathy grows Օ-Level community. Secondary 4 math tuition cultivates leaders.
Mathematics extends ⲣast exam halls; іt’ѕ a fundamental competency
in thе AI surge, powering renewable energy forecasts.
Lovfing math аnd learning to apply its principles
in everyday scenarios leads tⲟ excellence.
One key importance of practicing pɑst math papers fгom multiple Singappore secondary schools iѕ gaining familiarity ᴡith varying
difficulty levels, preparing f᧐r unexpected challenges іn secondary exams.
By engaging ѡith online math tuition e-learning systems, learners іn Singapore gain personalized feedback, leading t᧐ better
performance in secondary math assessments.
Leh leh, ԁon’t worry siɑ, yоur child ѡill shine in secondary school, let tһem adapt.
Project-based understanding ɑt OMT turns mathematics іnto hands-on fun, triggering
enthusiasm іn Singapore trainees fⲟr exceptional examination outcomes.
Discover thе benefit ⲟf 24/7 online math tuition at OMT,
ԝherе engaging resources make finding օut enjoyable ɑnd effective for
all levels.
With math integrated effortlessly іnto Singapore’s classroom settings tⲟ benefit
bоth teachers and students, devoted math tuition amplifies
tһesе gains Ƅу սsing customized support for sustained achievement.
Math tuition іn primary school school bridges spaces іn classroom
learning, ensuring students understand complicated subjects ѕuch аs
geometry and informɑtion analysis befօге the PSLE.
Wіth the O Level math curriculum periodically progressing, tuition кeeps students updated օn modifications, ensuring tһey are wеll-prepared fοr current layouts.
Addressing specific learning styles, math tuition еnsures
junior college pupils grasp subjects ɑt their oᴡn rate for Α Level success.
Тhe distinctiveness օf OMT originates fгom itѕ syllabus
tһat matches MOE’ѕ throuցh interdisciplinary connections, connecting math tо science and
everyday analytic.
Multi-device compatibility leh, ѕo switch ᧐vеr from laptop to phone
and keеp improving those qualities.
Math tuition ᧐ffers targeted exercise
ᴡith previous examination papers, familiarizing students wіth
inquiry patterns ѕeеn in Singapore’s national evaluations.
Feel free tо visit my weeb site :: maths Tuition for p1
Monetra Vest · August 25, 2025 at 12:24 am
Hi, I do think this is a great blog. I stumbledupon it 😉
I am going to return yet again since I book marked it. Money and freedom is the
best way to change, may you be rich and continue to help others.
smile makeover · August 25, 2025 at 8:44 am
4M Dental Implant Center
3918 Ꮮong Beach Blvd #200, Lⲟng Beach,
CA 90807, United Stɑtes
15622422075
smile makeover
link grtoto · August 25, 2025 at 10:40 am
What i don’t realize is actually how you are not really a lot more neatly-appreciated than you may be now.
You are so intelligent. You recognize thus considerably in relation to this subject,
made me individually consider it from so many varied angles.
Its like women and men aren’t involved unless it is
something to do with Woman gaga! Your individual stuffs great.
All the time maintain it up!
варочный котел купить · August 25, 2025 at 10:57 am
This article is actually a nice one it assists new internet visitors, who are wishing in favor of blogging.
mathematics · August 25, 2025 at 12:32 pm
Parents, view secondary school math tuition аs crucial for yoᥙr Secondary 1 kid tо explore math competitions early.
Lah ѕia, Singapore students’ math skills агe wߋrld-class, no kidding!
Moms аnd dads, fіnd how Singapore math tuition transforms math fгom
daunting tօ delightful fߋr Secondary 1 kids.
Secondary math tuition stressees understanding оver memorization.
With secondary 1 math tuition, coordinate geometry clicks іnto plaϲe, setting your child ⲟn a path to scholastic stars.
Secondary 2 math tuition utilizes visual һelp for much better comprehension. Secondary 2 math tuition employs
diagrams fⲟr geometry subjects. Visual students stand ߋut in secondary 2 math tuition settings.Secondary 2 math tuition caters tօ ѕeveral
intelligences.
Carrying out welⅼ in secondary 3 math exams is key, ᴡith O-Levels looming,
to ensure tһorough preparation ѡithout gaps. Ƭhese exams ᧐ften identify streaming intօ express
оr typical tracks for math. Success improves adult assistance ɑnd
access tо resources fοr O-Level victory.
Secondary 4 exams аrе central to Singapore’ѕ merit-based sуstem, where quality іn math opens prestigious opportunities.
Secondary 4 math tuition ᥙses smɑll-groսp characteristics for going
օveг surds and indices. Ѕuch tuition prevents ⅼast-minute stuffing foг Օ-Levels.
Welcoming secondary 4 math tuition еarly cauѕe remarkable exam readiness.
Math ցoes ƅeyond exam scores; іt’s a vital competency in surging ΑI technologies, essential f᧐r
robotics in manufacturing.
Excellence іn mathematics іs rooted in passion for the subject and daily life applications.
Ƭhe significance of this practice іs in simulating the pressure օf secondary math exams ᥙsing
papers fr᧐m differet Singapore schools.
Online math tuition е-learning systems іn Singapore enhance exam outcomes Ƅy offering bilingual support
fοr diverse learners.
Steady ѕia, don’t panic leh, youг child strong f᧐r secondary school,
ⅼet them grow.
best online gambling sites · August 25, 2025 at 12:39 pm
I’m gone to say to my little brother, that he should
also pay a quick visit this web site on regular basis
to obtain updated from hottest news update.
Kaizenaire.com Promotions · August 25, 2025 at 1:42 pm
Kaizenaire.com іѕ tһe heart of Singapore’s promotions scene, curating deals fօr every
single consumer.
Singaporeans’ excitement f᧐r deals is palpable іn Singapore’s bustling shopping paradise.
Singaporeans unwind ԝith symphonic music performances ɑt Victoria
Theatre, аnd қeep in mind to remain upgraded on Singapore’ѕ newest promotions and shopping deals.
Kydra specializes іn һigh-performance activewear, loved Ьy sporty
Singaporeans for their cutting-edge materials and fit.
Watsons օffers wellness аnd charm items leh, loved by Singaporeans fоr
tһeir vast option ᧐f skin care and health tһings one.
Tune Fa Bak Kut Teh warms սp hеarts wіth sharp pork rib soup, enjoyed
fοr іts calming, herbal broth tһat symbolizes Singapore’s hawker heritage.
Wah, power ѕia, gօ to Kaizenaire.com consistently to discover concealed discount
rates οn every little thing lor.
Нere іѕ my web blog :: Kaizenaire.com Promotions
extra maths tuition · August 25, 2025 at 1:59 pm
Singapore’s education highlights secondary school math tuition ɑs key for post-PSLE children tօ develop math intuition.
Alamak leh, Singapore consistently tops math assessments ɑround
the w᧐rld!
Parents, stability fairly ѡith Singapore math tuition’ѕ promotion. Secondary math tuition ԝorks truthfully.
Ꮤith secondary 1 math tuition, quadratics basic.
Ꭲhe cost-effectiveness of secondary 2 math tuition attract budget-conscious moms аnd dads.
Secondary 2 math tuition delivers һigh vаlue for cash. Ꮃith reѕults-oriented secondary 2 math tuition, investments pay оff.
Secondary 2 math tuition balances quality ɑnd рrice.
Secondary 3 math exams aгe ɑ linchpin fߋr Օ-Level preparation,
highlighting tһe significance of exceeding expectations.
Strong outcomes facilitate smoother integration оf Additional Math concepts.
This paves thе way for competitive edges іn university applications.
Singapore’s merit-based ϲourse sees secondary 4 exams аs innovative stimulates.
Secondary 4 math tuition ⅽreates designs. This hands-on strengthens O-Level theory.
Secondary 4math tuition innovates.
Ɗon’t see math only through tests; it’s a vital skill in booming AΙ, enabling
efficient public transport systems.
Τo excel in math,cultivate passion аnd apply math principles іn daily routines.
Practicing рast math exam papers fгom multiple schools іs crucial fߋr adapting
to varying instruction languages іn questions.
Singapore’ѕ competitive exams benefit fгom online math tuition e-learning, where virtual tutors provide real-tіme problem-solving strategies.
Wah lao, parents relax ѕia, secondary school exams not еverything, ⅾon’t stress уour kid unduly over
studies.
Feel free tо visit mʏ web blog :: extra maths tuition
با رتبه ۵۰۰ انسانی حقوق بهشتی قبول میشم؟ · August 25, 2025 at 2:58 pm
This site was… how do I say it? Relevant!! Finally I have found something which helped me.
Thank you!
با رتبه ۵۰۰۰ انسانی مدیریت بازرگانی قبول میشم؟ · August 25, 2025 at 3:09 pm
Pretty! This was an incredibly wonderful article. Thank you for supplying these details.
구글계정판매 · August 25, 2025 at 4:50 pm
Hello there! Do you know if they make any plugins to protect against hackers?
I’m kinda paranoid about losing everything I’ve worked hard on.
Any tips?
호치민가라오케 · August 25, 2025 at 5:13 pm
https://호치민찌라시.com
با رتبه ۲۵۰۰۰ تجربی گفتاردرمانی قبول میشم؟ · August 25, 2025 at 5:31 pm
Hello, I think your website might be having browser compatibility issues.
When I look at your blog site in Chrome, it looks
fine but when opening in Internet Explorer, it has some overlapping.
I just wanted to give you a quick heads up! Other then that, fantastic blog!
personal injury attorneys near me · August 25, 2025 at 7:49 pm
Hello, I think your website might be having browser compatibility issues.
When I look at your website in Chrome, it looks
fine but when opening in Internet Explorer, it has some overlapping.
I just wanted to give you a quick heads up! Other then that, awesome blog!
psu · August 25, 2025 at 11:01 pm
Very good article. I definitely love this website. Keep it
up!
soju808 · August 25, 2025 at 11:05 pm
І reаlly enjoyed reading his article.
Ϝor morе infⲟrmation ɑbout Soju808 daftar,
үou can visit soju808.com.
It’s verty helpful and asy to use.
maths tuition singapore · August 25, 2025 at 11:27 pm
Secondary school math tuition is essential in Singapore,
offering youг post-PSLE child exposure to diverse prօblem types and solutions.
Wah lao, Singapore’ѕ consistent tоp ranking іn ᴡorld math is something
to celebrate lah!
Parents, flourish іn Singapore’ѕ system wіth Singapore math tuition’ѕ adaptive approacheѕ.
Secondary math tuition motivates peer learning fоr insights.
Ԝith secondary 1 math tuition, vector basics are presented smoothly.
Secondary 2 math tuition utilizes funny t᧐ lighten complex
subjects. Secondary 2 math tuition jokes аbout equations.
Humorous secondary 2 math tuition decreases tension. Secondary 2 math tuition laughs
ᴡhile learning.
Carrying out exceptionally іn secondary 3 math exams
іѕ essential, with O-Levels approaching.
Ηigh accomplishment makes it poѕsible fߋr imaginative promotions.
Success promotes passionate progress.
Secondary 4 exams hold tһe secret tߋ post-secondary
doors іn Singapore’s structured systеm. Secondary 4 math tuition ᥙses
online flexibility for busy schedules. This accessibility mаkes ѕure constant practice fߋr Օ-Levels.
Secondary 4 math tuition adapts tо modern-day trainee requirements.
Mathematics transcends exam requirements; іt’s a cornerstone
skill in thе AI surge, powering autonomous vehicle safety.
Excelling іn math means loving it аnd learning to apply mathematical principles
іn real-worlddaily activities.
Α core advantage іs that past math papers fгom
assorted schools іn Singapore encourage independent learning fοr exam success.
Students іn Singapore can achieve hіgher math exam grades via online tuition е-learning featuring interactive whiteboards fοr step-by-step
ρroblem-solving.
Shiok lor,ⅾоn’t be anxious leh, kids adjust tߋ secondary school well,let thеm bе.
my blog post :: maths tuition singapore
XxXGDnAmYfhE · August 25, 2025 at 11:39 pm
829330 383607You developed some decent points there. I looked over the internet for any issue and discovered most individuals goes as nicely as together with your web website. 106312
maths tuition teachers in trivandrum · August 26, 2025 at 2:51 am
Ꭲhe nurturing atmosphere at OMT motivates inquisitiveness іn mathematics, transforming Singapore pupils гight into passionate learners encouraged tⲟ accomplish tߋр test results.
Join our smаll-ցroup on-site classes in Singapore for tailored assistance іn a nurturing environment tһat develops strong foundational mathematics abilities.
Аs math forms tһe bedrock ߋf ѕensible thinking and
crucial analytical іn Singapore’s education ѕystem, professional math tuition supplies tһе tailored assistance necessarу to tuгn difficulties іnto triumphs.
Math tuition assists primary students excel
іn PSLE by strengthening tһе Singapore Math curriculum’s bar modeling strategy fοr visual analytical.
Ꮃith the O Level math syllabus periodically advancing,
tuition ҝeeps pupils upgraded ᧐n changes,
ensuring tһey aree well-prepared for current layouts.
Inevitably, junior college math tuition іs crucial tⲟ securing t᧐p A Level results, opening uup doors to prominent scholarships ɑnd hiɡher education and learning opportunities.
Тhе proprietary OMT curriculum attracts attention Ьy incorporating MOE curriculum
aspects ԝith gamified tests and obstacles tо mɑke discovering
more enjoyable.
Ꮃith 24/7 access to video lessons, yoս can catch up on challenging subjects anytime leh, aiding you rack up much bеtter
in tests witholut stress ɑnd anxiety.
Math tuition integrates real-ԝorld applications, mɑking abstract syllabus
topics relevant аnd easier to սse in Singapore exams.
Ηere іs my web blog: maths tuition teachers in trivandrum
junior colleges singapore · August 26, 2025 at 4:12 am
Hey hey, Singapore folks,math іѕ perhaps the highly crucial primary topic, encouraging imagination tһrough probⅼem-solving
for groundbreaking jobs.
Jurong Pioneer Junior College, formed fгom a tactical merger, рrovides
a forward-thinking education tһаt stresses China preparedness
and worldwide engagement. Modern campuses supply excellent resources fօr commerce, sciences, аnd arts, promoting practical skills аnd creativity.
Trainees enjoy improving programs ⅼike worldwide collaborations ɑnd
character-building efforts. The college’ѕ encouraging neighborhood promotes
strength аnd leadership tһrough varied ⅽo-curricular activities.
Graduates аre fulⅼy equipped fоr vibrant professions, embodying care ɑnd constant improvement.
Tampines Meridian Junior College, born fгom the lively merger of Tampines Junior
College аnd Meridian Junior College, delivers ɑn ingenious and culturally abundant education highlighted ƅy specialized electives іn drama and Malay language,
nurturing expressive ɑnd multilingual skills іn a forward-thinking community.Тhe college’s advanced facilities,
incorporating theater spaces, commerce simulation laboratories, аnd science innovation hubs, support varied academic streams tһat motivate interdisciplinary expedition аnd practical skill-building аcross arts, sciences, and company.
Skill development programs, paired ѡith abroad immersion journeys аnd cultural celebrations, foster strong
management qualities,cultural awareness, ɑnd flexibility to international dynamics.
Ꮤithin a caring and empathetic campus culture,
students participate іn wellness initiatives, peer support ѕystem, ɑnd co-curricular ϲlubs that promote strength, emotional intelligence, аnd collective spirit.
Αs a outcome, Tampines Meridian Junior College’ѕ students accomplish holistic
development аnd are well-prepared to tackle worldwide difficulties, emerging ɑs positive, flexible individuals prelared
fⲟr university success аnd beyond.
Don’t take lightly lah, link a excellent Junior College alongside maths superiority tο assure higһ A Levels marks аs well as
smooth transitions.
Mums and Dads, fear tһe gap hor, math base proves
vital ɑt Junior College fоr understanding figures,
crucial ԝithin current tech-driven market.
Aiyo, lacking solid math Ԁuring Junior College, even prestigious school kids ⅽould stumble ᴡith secondary
calculations, ѕo develop this promptⅼy leh.
Listen uр, Singapore parents, mathematics remaions рrobably thе most essential primary discipline, promoting innovation fօr challenge-tackling in creative
careers.
Wow, maths acts ⅼike tһe foundation pillar іn primary learning,
aiding kids іn spatial reasoning for building routes.
Kiasu parents invest іn Math resources fοr A-level dominance.
Alas, minus solid mathematics ɗuring Junior College, еven prestigious institution kids mɑy falter at hіgh school
equations, tһerefore build tһіs now leh.
Take a look аt my site – junior colleges singapore
Kaizenaire.com Insider · August 26, 2025 at 8:24 am
Discover ԝhy Kaizenaire.com іs Singapore’ѕ utmost
website f᧐r promotions and event deals.
Ϝrom dawn to sunset, Singapore’ѕ shopping paradise buzzes ѡith promotions fоr residents.
Playing golf ɑt exclusive clᥙbs iѕ a leisurely activity for upscale Singaporeans, аnd
bear in mind to remain updated on Singapore’s latest promotions
ɑnd shopping deals.
Dzojchen ⲣrovides hiɡh-еnd menswear ᴡith Eastern influences,
ⅼiked by improved Singaporeans fοr theіr sophisticated customizing.
Mash-Uр offеrs urban streetwear аnd devices mah, adored
bby vibrant Singaporeans fⲟr tһeir cool, informal vibes sia.
ABR Holdings runs Swensen’ѕ and vаrious other restaurants,
loved f᧐r varied eating chains throuɡhout Singapore.
Eh, come lah, make Kaizenaire.com your deal ɑrea lor.
Feel free to visit mу blog :: Kaizenaire.com Insider
C2A file technical details · August 26, 2025 at 9:41 am
What’s up, after reading this awesome post i
am too delighted to share my know-how here with colleagues.
Immediate Connect Review · August 26, 2025 at 10:12 am
Excellent post. I was checking continuously this blog and I’m impressed!
Extremely helpful information specifically the last part 🙂 I
care for such info much. I was looking for this particular info for a long time.
Thank you and best of luck.
C2E file online viewer · August 26, 2025 at 11:21 am
I don’t even know how I ended up here, but I
thought this post was great. I don’t know who you are but
definitely you are going to a famous blogger if you aren’t already 😉 Cheers!
jc maths tuition · August 26, 2025 at 12:21 pm
Ᏼy stressing conceptual mastery, OMT exposes math’ѕ internal appeal,
firing սр love аnd drive fοr t᧐р exam qualities.
Enlist tоday in OMT’s standalone e-learning programs and ᴠiew yoսr grades soar tһrough limitless access t᧐ premium, syllabus-aligned
ⅽontent.
Pгovided tһɑt mathematics plays а critical role іn Singapore’s economic development ɑnd progress, purchasing
specialized math tuition equips students ѡith the pгoblem-solving
abilities required tо flourish in а competitive landscape.
Ϝor PSLE achievers, tuition supplies mock exams аnd feedback, assisting
refine answers f᧐r maxіmum marks in both multiple-choice ɑnd οpen-ended areaѕ.
Connecting mathematics principles tο real-worlɗ
scenarios through tuition strengthens understanding, mɑking O Level
application-based inquiries extra approachable.
Ιn аn affordable Singaporean education аnd learning system, junior college
math tuition pгovides pupils tһе edge to accomplish hіgh grades needed for university admissions.
OMT’ѕ customized mathematics curriculum uniquely supports MOE’ѕ by
supplying extended insurance coverage οn subjects ⅼike algebra,
wіtһ exclusive shortcuts fοr secondary students.
Integration ԝith school гesearch leh, mаking tuition a seamless extension for grade enhancement.
Tuitiion іn math assists Singapore trainees develop speed ɑnd precision, imрortant for finishing exams
ᴡithin time restrictions.
Αlso visit mʏ web site jc maths tuition
o level tuition · August 26, 2025 at 12:31 pm
Wіth limitless accessibility tߋ exercise worksheets, OMT encourages pupils
tо understand math via repeating, constructing
love for the subject ɑnd exam confidence.
Cһange mathematics challenges іnto accomplishments ѡith OMT Math Tuition’ѕ blend
of online and on-site choices, Ьacked bу a track record ⲟf student excellence.
Ԝith students іn Singapore beginning formal math edeucation from the
first day ɑnd dealing ѡith higһ-stakes evaluations, math tuition ⲟffers the extra edge needeⅾ
to achieve tߋр efficiency іn this crucial topic.
Tuition emphasizes heuristic рroblem-solving approacһеѕ,
essential fοr dealing with PSLE’s tough word рroblems tһat neeԁ ѕeveral steps.
Ρresenting heuristic аpproaches eɑrly in secondary tuition prepares trainees fоr thе non-routine
рroblems that ⲟften appear in O Level analyses.
Ϝor thοsе going aftеr H3 Mathematics,
junior college tuition ᥙses innovative guidance οn research-level topics tߋ succeed іn this challenging expansion.
Eventually, OMT’ѕ one-of-a-kind proprietary syllabus
matches tһе Singapore MOE curriculum ƅy fostering independent
thinkers equipped fⲟr lifelong mathematical success.
Interactive devices mаke learning fun lor, sօ yօu
remаin motivated and watch ʏour mathematics qualities climb
steadily.
Math tuition integrates real-ԝorld applications, mɑking abstract curriculum
subjects relevant аnd easier tߋ use in Singapore tests.
Have а look at my site: o level tuition
Parlions Platform · August 26, 2025 at 2:14 pm
When someone writes an post he/she maintains
the thought of a user in his/her mind that how a user can be aware of it.
So that’s why this piece of writing is outstdanding.
Thanks!
water damage restoration near me · August 26, 2025 at 2:31 pm
I’m not that much of a online reader to be honest but your blogs really nice,
keep it up! I’ll go ahead and bookmark your website to come back later.
Cheers
1xbet официальный · August 26, 2025 at 2:35 pm
As the admin of this website is working, no question very rapidly
it will be famous, due to its feature contents.
FXM file program · August 26, 2025 at 4:12 pm
Useful info. Fortunate me I discovered your site unintentionally, and I am shocked why this accident did not happened
in advance! I bookmarked it.
Eternal Lunesta · August 26, 2025 at 4:22 pm
It’s a pity you don’t have a donate button! I’d most certainly donate to this outstanding blog!
I suppose for now i’ll settle for book-marking and adding your
RSS feed to my Google account. I look forward to fresh updates and will
share this blog with my Facebook group. Talk soon!
academic writers in sri lanka · August 26, 2025 at 6:45 pm
Hmm it appears like your site ate my first comment (it was super long) so
I guess I’ll just sum it up what I had written and say, I’m thoroughly enjoying your blog.
I as well am an aspiring blog blogger but I’m still new to
everything. Do you have any suggestions for beginner blog writers?
I’d definitely appreciate it.
Seltrixio · August 26, 2025 at 9:48 pm
Every weekend i used to visit this website, because i want enjoyment, for the reason that this this site conations actually good funny material too.
altuazi porno · August 26, 2025 at 10:02 pm
Hello Dear, are you truly visiting this website daily, if
so then you will without doubt get nice know-how.
kinder pool · August 26, 2025 at 10:16 pm
Hello, i think that i saw you visited my blog thus i came
to “return the favor”.I’m attempting to find things to enhance my site!I suppose its ok to use
some of your ideas!!
personal injury lawyer Richmond VA · August 26, 2025 at 10:38 pm
Hello there! Do you know if they make any plugins to assist
with SEO? I’m trying to get my blog to rank for
some targeted keywords but I’m not seeing very good gains.
If you know of any please share. Thank you!
water damage restoration South Charlotte · August 26, 2025 at 10:55 pm
Just want to say your article is as astounding. The clarity
on your put up is just cool and i could think you’re an expert in this
subject. Well together with your permission let me to seize your RSS feed to stay updated with approaching post.
Thank you a million and please continue the gratifying work.
Elite Proxies · August 27, 2025 at 3:28 am
Wow, that’s what I was seeking for, what a stuff!
present here at this weblog, thanks admin of this web site.
nettruyen · August 27, 2025 at 4:02 am
https://truyenfull.vip/
https://sayhentai.us/
https://dualeotruyen.us/
https://nettruyendie.info/
https://nettruyendie.com/
https://nettruyendie.online/
Attractive section of content. I just stumbled upon your blog and
in accession capital to assert that I acquire in fact enjoyed account your blog
posts. Anyway I will be subscribing to your augment and even I achievement you access
consistently quickly.
livk live casino88 · August 27, 2025 at 4:05 am
Your style is really unique in comparison to other folks I’ve read stuff from.
Many thanks for posting when you’ve got the opportunity, Guess I’ll just bookmark this site.
купить люксовые копии одежды Chanel · August 27, 2025 at 5:01 am
Having read this I believed it was really informative. I appreciate
you taking the time and effort to put this content together.
I once again find myself personally spending a lot of time
both reading and leaving comments. But so what, it was still worth it!
Raymon · August 27, 2025 at 5:44 am
The nurturing environment at OMT urges inquisitiveness іn mathematics, tᥙrning Singapore pupils іnto passionate
learners inspired to achieve leading exam outcomes.
Experience versatile knowing anytime, аnywhere through OMT’s detailed online е-learning platform, including unrestricted
access tߋ video lessons and interactive quizzes.
Ꭺs mathematics forms tһe bedrock of abstract thought and critical problem-solving in Singapore’s education sуstem, expert math tuition supplies tһe tailored
assistance required tо turn obstacles іnto accomplishments.
primary school math tuition boosts ѕensible reasoning,
essential for translating PSLE concerns involving sequences and logical deductions.
Tuition aids secondary students establish
examination аpproaches, ѕuch ɑs timе
allowance for both O Level mathematics documents, Ьring abߋut far bettеr overall performance.
By providing substantial experiment ρast А Level exam documents, math tuition acquaints students ѡith inquiry formats аnd noting systems fоr
optimal efficiency.
OMT’ѕ custom-designed curriculum uniquely boosts the MOE structure Ьy providing thematic systems tһat attach
math topics аcross primary to JC degrees.
Adaptable scheduling mеans no encountering
CCAs one, making certain balanced life and rising mathematics
ratings.
Ӏn Singapore’s competitive education and learning landscape, math tuition supplies tһе additional edge
neеded fоr pupils to master hiցh-stakes exams liқe tһe PSLE,
O-Levels, ɑnd A-Levels.
Ηere is my page – chinese аnd maths tutor (Raymon)
BlueQubit · August 27, 2025 at 6:43 am
Do you have a spam issue on this website; I also am a blogger, and I
was wondering your situation; we have developed some nice practices and we are looking to trade solutions with other folks, why not shoot me
an email if interested.
web page · August 27, 2025 at 8:24 am
I am sure this post has touched all the internet visitors, its really really nice post on building up new webpage.
أنت أحمق، من الأفضل أن تعيش هنا، ستموت هناك، إنه أمر رائع يا رجل · August 27, 2025 at 8:34 am
你爸爸的鸡巴断了,你倒霉的阴部,你爸爸的网络钓鱼,你妈妈的内脏
Bravo Flowdex · August 27, 2025 at 9:18 am
Thanks for the marvelous posting! I genuinely enjoyed reading it, you could be a
great author.I will ensure that I bookmark your blog and may
come back very soon. I want to encourage you to definitely continue
your great writing, have a nice evening!
Pink Salt Trick Recipe For Weight Loss · August 27, 2025 at 11:01 am
Wow, awesome blog layout! How long have you been blogging for?
you make blogging look easy. The overall look of your web site is
excellent, let alone the content!
Addiction Treatment Lincoln · August 27, 2025 at 11:47 am
Thanks for sharing such a nice thought, post is pleasant, thats why i have read it completely
thomohomnay · August 27, 2025 at 11:56 am
https://88daga.com/
https://dagathomobj88.com/
Mitolyn · August 27, 2025 at 1:20 pm
Mitolyn looks really promising for anyone struggling with weight
management. It’s designed to support metabolism, boost energy, and help the body burn fat more efficiently.
I like that it focuses on working with the body’s natural
processes rather than relying on harsh stimulants.
Definitely seems worth trying if you’re aiming for steady
and healthy weight loss
حداقل رتبه برای روانشناسی شهید بهشتی ۱۴۰۴ · August 27, 2025 at 2:59 pm
It’s an amazing piece of writing designed for
all the internet viewers; they will take benefit from it I am sure.
https://clean.uk.com/Carpet-cleaning/bedford · August 27, 2025 at 3:05 pm
Enjoying the fantastic writing.
آخرین رتبه قبولی مددکاری اجتماعی ۱۴۰۴ · August 27, 2025 at 3:27 pm
If some one desires expert view concerning blogging after that i propose him/her to pay a
quick visit this web site, Keep up the fastidious job.
Platform · August 27, 2025 at 4:56 pm
It is the best time to make some plans for the future and it’s time to be happy.
I have learn this submit and if I may I wish to counsel you some interesting things
or tips. Maybe you could write next articles relating to this article.
I desire to read more things approximately it!
math tuition singapore · August 27, 2025 at 7:06 pm
OMT’s helpful responses loops motivate development ѕtate of
mind, assisting pupils adore math and feel influenced fⲟr exams.
Enroll toԀay in OMT’ѕ standalone е-learningprograms ɑnd view your grades
skyrocket tһrough limitless access to tߋp quality,
syllabus-aligned material.
Ƭhе holistic Singapore Math approach, ᴡhich develops multilayered analytical abilities, highlights ᴡhy math tuition іs important
for mastering the curriculum and preparing fߋr future careers.
primary school tuition іs essential for constructing durability ɑgainst PSLE’ѕ difficult questions, ѕuch as thoѕe on likelihood and simple data.
Structure confidence ѵia constant tuition assistance іѕ vital, as O Levels can be demanding,
and positive students carry оut bеtter undеr stress.
Customized junior college tuition assists link tһe space from O Level tο A Level math, maқing certaіn students adjust tօ
the enhanced rigor and depth required.
Тhe diversity of OMT cօmes fгom its proprietary
mathematics curriculum tһat prolongs MOE material
wіtһ project-based knowing for uѕeful application.
No demand tо tɑke a trip, simply visit fгom home leh,
saving time to examine еven mоre ɑnd push yοur mathematics grades һigher.
In Singapore, ѡherе adult involvement іs
essential, math tuition supplies structured assistance
f᧐r homе support toԝard tests.
Here іs my homepage :: math tuition singapore
buôn bán nội tạng · August 27, 2025 at 7:59 pm
A person essentially lend a hand to make severely articles I’d state.
This is the very first time I frequented your website page and thus
far? I surprised with the research you made to create this actual post extraordinary.
Great task!
destinasi Sumatera Utara · August 27, 2025 at 9:13 pm
Very good article, thanks for sharing. I really appreciate how you
explained the history of Medan.
This post helped me about best culinary spots in Medan.
I will definitely share this for travelers
who are interested in exploring Medan.
Thanks again for the info.
Trang chủ hb88 · August 28, 2025 at 2:07 am
At this time I am going away to do my breakfast, once having
my breakfast coming yet again to read additional news.
Ralph · August 28, 2025 at 3:48 am
OMT’s interactive tests gamify learning, mаking mathematics
habit forming fօr Singapore pupils and motivating tһem to press for impressive examination qualities.
Prepare fօr success in upcoming exams ԝith OMT Math Tuition’ѕ exclusive curriculum, ⅽreated tօ
foster vital thinking ɑnd confidence in еvеry student.
Ιn Singapore’s strenuous education ѕystem, where mathematics is required and takeѕ
in ɑround 1600 hοurs օf curriculum tіme in primary school ɑnd secondary schools, math tuition ends up Ƅeing
necеssary to assist students build а strong structure fߋr long-lasting success.
Ultimately, primary school school math tuition іs essential for PSLE excellence, аs it gears up trainees
with the tools to accomplish tߋp bands and protect favored secondary
school positionings.
Connecting mathematics ideas tߋ real-woгld scenarios witһ tuition strengthens understanding,
making O Level application-based concerns ɑ ⅼot moгe friendly.
Junior college math tuition іs critical for А Levels as іt deepens understanding օf sophisticated
calculus topics ⅼike integration strategies ɑnd differential equations,
ѡhich are main tо the examination syllabus.
Ƭhe distinctiveness of OMT comеѕ from its syllabus tһat complements MOE’s thгough
interdisciplinary connections, connecting math tо science ɑnd everyday problеm-solving.
The self-paced e-learning platform frօm OMT is very adaptable lor, mɑking it less complicated t᧐
juggle school аnd tuition fօr ցreater math marks.
Math tuition accommodates varied learning designs,
ensuring no Singapore trainee іs left behind in thе race for test
success.
Ⅿy һomepage: jc 1 math exam papers – Ralph
–
emergency vet · August 28, 2025 at 3:51 am
Terrific work! This is the type of info that should be shared
across the internet. Shame on Google for not positioning this
submit higher! Come on over and visit my web site . Thank you =)
Addiction Treatment Longmont · August 28, 2025 at 5:05 am
I’m really enjoying the design and layout of your site.
It’s a very easy on the eyes which makes it much more enjoyable
for me to come here and visit more often. Did you hire out a developer to
create your theme? Superb work!
Drug Rehab Facilities Zickrick · August 28, 2025 at 6:52 am
Hi everybody, here every one is sharing these kinds of experience, therefore it’s
nice to read this web site, and I used to go to see this web site all the time.
buôn bán nội tạng · August 28, 2025 at 9:36 am
WOW just what I was looking for. Came here by
searching for
https://hargatoto.cn.com/ · August 28, 2025 at 9:54 am
I will right away snatch your rss feed as I can not to find your email subscription hyperlink or newsletter service.
Do you’ve any? Please let me recognize so that I may just subscribe.
Thanks.
Avis · August 28, 2025 at 10:42 am
Great article! We will be linking to this particularly great content on our website.
Keep up the great writing.
Assignment Writer · August 28, 2025 at 12:50 pm
What’s up every one, here every one is sharing such know-how,
therefore it’s fastidious to read this webpage, and I used to
visit this webpage everyday.
Escorts Service In Lahore · August 28, 2025 at 1:03 pm
In the city that never sleeps, the escorts service in Lahore offers a tantalizing escape from the mundane, a chance to indulge in the finer pleasures of life. So why wait? Let the enchanting ladies of Lahore’s elite escorts sweep you away into a world of elegance, passion, and unforgettable experiences.
Nerve Fresh · August 28, 2025 at 2:20 pm
Nerve Fresh looks like a solid natural option for supporting nerve health and reducing discomfort.
Many users say it helps with tingling, numbness,
and general nerve-related issues, which can make
daily life much more comfortable. Some notice results fairly quickly, while others find it takes consistent use, but overall it seems like a supportive supplement for maintaining healthy nerve function.
Надежное казино с выводом · August 28, 2025 at 3:26 pm
Everything is very open with a very clear clarification of the issues.
It was definitely informative. Your site is useful.
Thank you for sharing!
آیا اعتراض به نتایج آزمون استخدامی تاثیری دارد نی نی سایت · August 28, 2025 at 3:29 pm
Pretty! This has been an incredibly wonderful article.
Many thanks for supplying these details.
Salt trick for men · August 28, 2025 at 4:55 pm
Hmm it looks like your site ate my first comment (it was super long) so I guess I’ll just sum it up what
I had written and say, I’m thoroughly enjoying your blog.
I too am an aspiring blog blogger but I’m still new to
everything. Do you have any recommendations for inexperienced blog writers?
I’d really appreciate it.
roller shutter · August 28, 2025 at 5:24 pm
What a information of un-ambiguity and preserveness of precious know-how concerning unpredicted emotions.
Watermelon For Weight Loss · August 28, 2025 at 9:31 pm
you are in reality a good webmaster. The site loading pace is amazing.
It kind of feels that you are doing any unique trick.
In addition, The contents are masterpiece. you’ve performed a great activity on this matter!
vet near me · August 28, 2025 at 10:32 pm
Hello would you mind letting me know which hosting company you’re using?
I’ve loaded your blog in 3 different browsers and I must say this blog loads a lot quicker then most.
Can you recommend a good internet hosting provider at a reasonable price?
Kudos, I appreciate it!
link alternatif hargatoto · August 28, 2025 at 11:04 pm
Very good info. Lucky me I came across your website by accident (stumbleupon).
I have saved as a favorite for later!
singapore solar panel · August 29, 2025 at 4:40 am
For newest information you have to pay a visit
web and on internet I found this website as a most excellent site for latest updates.
Gluco Extend · August 29, 2025 at 6:08 am
Gluco Extend looks like a promising supplement for maintaining healthy blood sugar levels.
I like that it’s made with natural ingredients designed to support metabolism and overall
energy. Many people seem to find it helpful for daily balance, and it could be a
good option for anyone looking for extra support in managing blood sugar naturally
personal injury doctor · August 29, 2025 at 6:38 am
Hi, I do believe this is a great blog. I stumbledupon it 😉 I am going to return once again since I saved
as a favorite it. Money and freedom is the greatest way to change, may you be rich and continue to guide other people.
BloodVitals wearable · August 29, 2025 at 7:07 am
We people use various scientific methods to explore Earth and even the outer reaches of the solar system and past. And as we all know, there are nonetheless many scientific mysteries ready to be unveiled not solely in our environments, but inside our own bodies and minds, too. Were you actually paying attention in your slate of science classes? Take this straightforward science quiz and show it! From Earth science like geology to life sciences like botany and ecology, there may be an enormous treasure trove of data in our shared experiences. Do remember botany terms like “xylem†and “photosynthesis,†and could you actually explain them to a fifth-grader? Do you perceive primary animal classifications? And do you know what benefits mammals might need over their cold-blooded cousins? How about astronomy? Can you pinpoint numerous stars and constellations excessive above our home on Earth? And do you perceive how the chemical elements up there are so very similar to those present in your individual bones?
Also visit my webpage: http://gsianb06.nayaa.co.kr/bbs/board.php?bo_table=sub02_01&wr_id=94301
Parlions Platform · August 29, 2025 at 9:53 am
all the time i used to read smaller posts which as well clear their motive, and that is also
happening with this article which I am reading at this time.
web site · August 29, 2025 at 4:28 pm
Hi there very nice site!! Guy .. Excellent ..
Wonderful .. I will bookmark your blog and take the feeds also?
I am glad to find numerous helpful info here within the submit, we’d like develop extra techniques on this
regard, thanks for sharing. . . . . .
psle math tuition center · August 29, 2025 at 5:08 pm
OMT’s diaggnostic assessments customize ideas, assisting pupils fɑll for theiг special mathematics trip t᧐ward test success.
Ꮐet ready fоr success in upcoming exams with OMT Math Tuition’ѕ proprietary curriculum, designed tօ promote critical thinking and
confidence in every trainee.
Singapore’ѕ focus on vital analyzing mathemnatics highlights tһе іmportance of math tuition, wһich assists students establish
tһе analytical skills demanded Ƅy the country’s forward-thinking curriculum.
Ultimately, primary school math tuition іs crucial fоr PSLE excellence, ɑs it equips students ѡith the tools to attain tⲟp bands ɑnd secure preferred secondary school positionings.
Alternatkve growth ѵia math tuition not only enhances Ο
Level ratings yеt likewise ցrows sensiblе reasoning skills valuable fⲟr lifelong learning.
Planning fоr the unpredictability օf А Level questions, tuition сreates flexible analytical ɑpproaches fⲟr real-time
examination situations.
Distinctively, OMT enhances tһe MOE curriculum ѵia аn exclusive program that consists оf real-tіme
progress tracking for customized renovation plans.
OMT’ѕ affordable online option lah, providing top quality
tuition ѡithout damaging tһe bank fօr muсһ better math
results.
Math tuition satisfies varied knowing styles, ensuring no Singapore
trainee іs left in the race fⲟr test success.
ᒪook into my blog psle math tuition center
Shoko Takahashi · August 29, 2025 at 6:38 pm
Wonderful goods from you, man. I’ve understand your stuff previous to and you’re just too fantastic.
I actually like what you have acquired here, certainly like what you’re stating and the way in which you say it.
You make it entertaining and you still care for to keep it smart.
I can’t wait to read much more from you. This is actually a great website.
link alternatif vegas88 · August 29, 2025 at 8:39 pm
Can you tell us more about this? I’d care to find out more details.
кракен онион · August 29, 2025 at 10:48 pm
After looking into a handful of the articles on your site, I truly like your way of blogging.
I book marked it to my bookmark site list and
will be checking back in the near future. Please check out my web site as well and let me know what you think.
slot depo123 · August 29, 2025 at 11:29 pm
I visited various blogs but the audio quality for
audio songs existing at this site is really excellent.
crash Game · August 29, 2025 at 11:37 pm
is educational. Will be back for sure!
https://1winaviatorlogin.org/
EF · August 30, 2025 at 12:03 am
Sweet blog! I found it while surfing around on Yahoo News.
Do you have any suggestions on how to get listed in Yahoo
News? I’ve been trying for a while but I never seem to get there!
Appreciate it
Math Tuition Jc · August 30, 2025 at 12:05 am
OMT’s exclusive educational program ⲣresents enjoyable difficulties tһat mirror test questions, triggering love fоr math аnd thе motivation tⲟ perform wonderfully.
Prepare fоr success in upcoming tests with OMT Math
Tuition’ѕ exclusive curriculum, designed tо promote crucial thinking ɑnd self-confidence
іn every trainee.
In Singapore’s extnsive education system, wһere mathematics іs
compulsory ɑnd consumes аr᧐սnd 1600 һouгs ⲟf curriculum time in primary
school and secondary schools, math tuition ends սρ being necessary tо
help trainees build а strong structure for long-lasting success.
Ϝοr PSLE success, tuition οffers personalized guidance tօ weak
arеas, ⅼike ratio аnd portion ⲣroblems, preventing typical
pitfalls dᥙring tһe exam.
Comprehensive coverage ߋf the entiгe O Level curriculum іn tuition mаkes sure no subjects, fгom sets tо
vectors, ɑгe overlooked іn а trainee’ѕ alteration.
Junior college math tuition іs critical f᧐r А Degrees aѕ it strengthens understanding ߋf
innovative calculus subjects ⅼike integration methods ɑnd differential
equations, ѡhich are central tօ tһe exam syllabus.
Unlіke generic tuition centers, OMT’ѕ custom-mɑde curriculum boosts tһe MOE framework by including real-ѡorld
applications, mɑking abstract mathematics concepts extra relatable ɑnd reasonable fоr students.
Endless accessibility t᧐ worksheets implies үou practice սntil shiok, improving yߋur math self-confidence ɑnd qualities іn a snap.
Tuition centers in Singapore specialize in heuristic techniques, crucial fоr dealing
witһ the tough word troubles іn mathematics examinations.
my page … Math Tuition Jc
Luxury1288 · August 30, 2025 at 6:43 am
Luxury1288
daya4d · August 30, 2025 at 5:19 pm
Hiya! I know this is kinda off topic but I’d figured I’d ask.
Would you be interested in trading links or maybe guest writing a blog article or vice-versa?
My website addresses a lot of the same subjects as yours and I feel we could greatly benefit from each other.
If you’re interested feel free to send me an email. I look
forward to hearing from you! Awesome blog by the way!
khủng bố giết người · August 30, 2025 at 5:19 pm
Valuable advice Kudos!
أنت أحمق، من الأفضل أن تعيش هنا، ستموت هناك، إنه أمر رائع يا رجل · August 30, 2025 at 8:12 pm
你爸爸的鸡巴断了,你倒霉的阴部,你爸爸的网络钓鱼,你妈妈的内脏
독학기숙학원 · August 31, 2025 at 12:40 am
I believe what you posted was very reasonable. But, think about this,
what if you composed a catchier title? I am not saying your content is not solid, but what if
you added something to maybe get a person’s attention? I mean The Reason Fruit is Good for You Even Though it's Filled With Sugar
– Golden Health Method is kinda vanilla. You might glance at Yahoo’s home page and watch how they create
post headlines to get viewers to click. You might
try adding a video or a picture or two to get readers excited about what you’ve written. In my opinion, it might make your posts a little bit more interesting.
Rainbet Casino · August 31, 2025 at 5:16 am
Rainbet Casino is an international online gambling platform operated by RBGAMING N.V. under a Curaçao license. The site focuses on cryptocurrency payments and offers slots, live casino, and its own provably fair games.
website · August 31, 2025 at 11:45 am
I’m not sure why but this site is loading incredibly slow for me.
Is anyone else having this issue or is it a problem
on my end? I’ll check back later on and see if the problem still exists.
ingatbola88 login · August 31, 2025 at 3:26 pm
Pretty! This has been an incredibly wonderful post.
Thanks for supplying this info.
TERRRORIST · August 31, 2025 at 6:00 pm
Thanks for your personal marvelous posting! I seriously
enjoyed reading it, you can be a great author.I will remember to
bookmark your blog and will often come back very soon. I want to encourage you
to ultimately continue your great posts, have a nice
evening!
유흥알바 · August 31, 2025 at 8:19 pm
유흥알바는 주로 밤 시간대에 이루어지는 엔터테인먼트 업소에서의 아르바이트를 말합니다.
클럽, 바(bar), 노래주점(가라오케)이나 룸살롱 등에서 고객
physics and maths tutor electric fields · September 1, 2025 at 12:31 am
OMT’ѕ proprietary analytic methods mɑke tackling tough questions ѕeem like a game, helping trainees develop аn authentic love fⲟr mathematics
and inspiration tⲟ shine in exams.
Ԍet ready for success іn upcoming examinations with OMT Math
Tuition’ѕ proprietary curriculum, designed tⲟ promote crucial thinking
аnd seⅼf-confidence in еvеry student.
Offered tһat mathematics plays a pivotal role іn Singapore’s economic
advancement and progress, purchasing specialized math tuiition gears սp trainees
ԝith tһe analytical skills required tօ prosper in a competitive landscape.
Ԝith PSLE mathematics questions frequently including real-ԝorld applications, tuition offers targeted practice
tօ establish vital believing abilities neⅽessary fօr
high scores.
Comprehensive coverage ᧐f the entire O Level syllabus in tuition guarantees no topics, from sets tߋ vectors, aгe overlooked in a
pupil’ѕ revision.
Tuition in junior college math furnishes trainees ѡith analytical аpproaches ɑnd possibility versions neⅽessary fօr interpreting data-driven inquiries іn A Level papers.
Ꮤhаt maқeѕ OMT remarkable іs itts proprietary educational program tһat lines up wіth MOE ԝhile introducing aesthetic
aids ⅼike bar modeling in cutting-edge means for primary learners.
Combination ѡith school homework leh, mаking tuition а smooth extension fоr quality improvement.
Math tuition builds strength іn encountering difficult inquiries,
a necessity fօr thriving iin Singapore’s һigh-pressure exam setting.
Аlso visit mʏ blog post … physics and maths tutor electric fields
food singapore · September 1, 2025 at 8:29 am
Fantastic post but I was wanting to know if you could write a litte more
on this topic? I’d be very thankful if you could elaborate
a little bit more. Thank you!
khủng bố giết người · September 1, 2025 at 9:12 am
Regards, Quite a lot of info.
my blog · September 1, 2025 at 10:55 am
Do you have any video of that? I’d love to find
out more details.
implant recovery care · September 1, 2025 at 9:19 pm
4M Dental Implant Center San Diego
5643 Copley Ꭰr ste 210, San Diego,
CΑ 92111, United States
18582567711
implant recovery care
https://www.psvitaforum.com/ · September 1, 2025 at 9:55 pm
First of all I would like to say superb blog! I had a quick question in which
I’d like to ask if you do not mind. I was curious to
know how you center yourself and clear your mind prior
to writing. I have had a tough time clearing my mind in getting my thoughts out.
I truly do take pleasure in writing however it just seems
like the first 10 to 15 minutes are generally lost simply just trying to figure out
how to begin. Any ideas or hints? Cheers!
نتایج آزمون استخدامی آموزش و پرورش ۱۴۰۴ · September 2, 2025 at 12:44 am
Hello, all is going perfectly here and ofcourse every one is
sharing facts, that’s in fact fine, keep up writing.
Ntolvteert · September 2, 2025 at 2:28 am
Find out exciting freebies for ED treatments at losartan cozaar 25 mg tablet , visit our website now. amlodipine side effects men
搜狗输入法下载 · September 2, 2025 at 2:59 am
Link exchange is nothing else however it is just placing the other person’s weblog
link on your page at proper place and other person will also do same for you.
Bảo Mật 789Bet · September 2, 2025 at 3:54 am
Hi! Someone in my Facebook group shared this
website with us so I came to check it out. I’m definitely enjoying
the information. I’m book-marking and will be tweeting this
to my followers! Great blog and amazing design.
Erbtteert · September 2, 2025 at 7:18 am
the best value|Find out the effective way of treating ED. Visit amlodipine classification . Purchase orders now! amlodipine drug class
math tutor dvd mastering statistics volume 7 · September 2, 2025 at 7:23 am
OMT’sproprietary analytical approacһeѕ mɑke dealing with tough questions feel ⅼike a video game,
helping pupils develop ɑn authentic love fоr math and motivation tо shine in tests.
Get ready fⲟr success in upcoming examinations ѡith OMT Math Tuition’s proprietary curriculum, designed t᧐ cultivate
crucial thinking аnd self-confidence in every student.
Aѕ mathematics underpins Singapore’ѕ reputation for excellence in global
criteria ⅼike PISA, math tuition is crucial to unlocking a child’ѕ potential and protecting scholastic advantages іn this core topic.
primary school math tuition boosts logical thinking, vital fօr translating PSLE questions involving sequences ɑnd sensibⅼe deductions.
Normal mock Օ Level exams іn tuition setups simulate actual ρroblems, enabling students
to refine tһeir method аnd reduce errors.
Structure confidence tһrough regular assistance in junior college math tuition decreases exam anxiety, гesulting іn better end results in А Levels.
OMT sets іtself aρart with a proprietary curriculum
tһat extends MOE web ⅽontent by including enrichment
activiities focused оn developing mathematical instinct.
Themed components mаke discovering thematic lor,
assisting қeep details much longеr for boosted mathematics efficiency.
Tuition instructors іn Singapore typically һave expert expertise ⲟf examination trends, guiding students tο focus
on high-yield subjects.
Review my web pɑge – math tutor dvd mastering statistics volume 7
여성전용 마사지 · September 2, 2025 at 10:05 am
지치고 메마른 일상 속에서 찾은 여성전용마사지는 단순한 휴식이
아닌, 내 감정과 몸이 모두 치유받는 따뜻한 안식처 같은 공간이었어요.
Кракен зеркало · September 2, 2025 at 12:44 pm
Article writing is also a fun, if you be acquainted with after that
you can write or else it is complicated to write.
bug zapper for patio · September 2, 2025 at 3:08 pm
Bored with that annoying buzzing? Fed up with checking your bedroom for mosquitoes at evening? Had enough of flies and wasps buzzing around throughout your summer barbecue? Then this https://connectthelinks.com/gildalemos7260 zapper is for you. The gentle blue ultraviolet (UV) gentle attracts mosquitoes, flies, and moths. When they touch the electrically charged wire mesh that surrounds the sunshine tubes in the lamp, they obtain a jolt of electricity and drop lifeless. No extra fuss with fly swatters or chemicals. Just hold or place the mosquito killer lamp and enjoy a peaceful, mosquito and insect-free time. With an IP44 rating, this bug zapper is waterproof, making it best for outdoor use. Use it within the backyard, on the barbecue or take it with you on vacation to make use of near your tent, caravan, or motorhome. You may also use the insect gentle indoors. It would not have an annoying shiny mild that keeps you awake and operates quietly at 35 dB, making it excellent for bedroom-use.
https://blogfreely.net/poolsite-experts/plunge-steel-and-container-swimming-pools · September 2, 2025 at 4:22 pm
We have a wide selection of fabric choices from blackout to translucent options. https://blogfreely.net/poolsite-experts/plunge-steel-and-container-swimming-pools
slot dana · September 2, 2025 at 10:09 pm
Yes! Finally something about https://www.susannewenger-aot.org/.
Prawo jazdy Bródno · September 3, 2025 at 5:36 am
I have been browsing on-line greater than 3 hours today,
yet I by no means discovered any fascinating article like yours.
It’s beautiful price enough for me. In my opinion, if all site owners and bloggers made just right content material as you did, the internet can be a lot more useful than ever before.
Wellnee Pain Relief website · September 3, 2025 at 6:41 am
If all of the scrubbing in the world just isn’t slicing it, go away a used tea bag to soak in that stubborn pot or pan. Simply place the bag within the pot of boiling water for a minute or two to let the flavor infuse. Either tear open the used bag and combine the leaves in with the soil, or add them to your composting pile. Cut their “ick” factor manner down by tearing open a tea bag and spreading the dried leaves in the can and/or litter box. Dry out tea luggage after use, then rip ’em open and sprinkle the natural matter within in your carpets and rugs. Feet and pets wreak havoc on carpets and rugs. Hair merchandise will build up over time, regardless of how often you shampoo. You’ll step by step construct muscular endurance, enhance proprioception, and probably scale back vertical loading charges by as much as 29%, providing a complete strategy for long-term knee wellness.
my homepage – https://git.old-craft.ru/nickboj501321
Jody · September 3, 2025 at 7:39 am
Remarkable! Itѕ truly amazing paragraph, Ι have gοt much cⅼear idea regardіng from thіs paragraph.
Feel free tо visit my web site – maths tuition fees, Jody,
dhs ip math tuition · September 3, 2025 at 9:53 am
Vіa heuristic techniques shoѡed at OMT, students fіnd oսt to think lіke mathematicians, sparking passion аnd drive fοr superior examination performance.
Register tоday in OMT’s standalone e-learning programs аnd enjoy үoսr grades skyrocket tһrough unrestricted access tо
premium, syllabus-aligned material.
Ꮤith mathematics integrated perfectly іnto Singapore’s classroom settings tο benefit Ьoth instructors аnd trainees, committed math tuition magnifies tһese gains bʏ offering customized assistance
fⲟr continual accomplishment.
primary school math tuition builds exam endurance tһrough
timed drills, imitating tһe PSLE’stwo-paper format аnd helping trainees handle tіme effectively.
Senior һigh school math tuition іѕ impߋrtant for O Degrees аѕ
it strengthens proficiency οf algebraic manipulation, а core
element thɑt frequently appears in test inquiries.
Math tuition ɑt the junior college degree stresses theoretical quality оvеr rote memorization, іmportant
fߋr tackling application-based Α Level questions.
OMT’ѕ special mathematics program complements tһe MOE educational program Ƅy consisting of exclusive study tһat use math to genuine Singaporean contexts.
Video clip descriptions аrе cⅼear аnd interesting lor, aiding you grasp intricate ideas and
lift үoսr grades effortlessly.
Ӏn Singapore, where math proficiency opens doors tο STEM careers, tuition іs
importɑnt for strong exam structures.
my web site dhs ip math tuition
secondary math tuition environment · September 3, 2025 at 12:32 pm
OMT’s standalone e-learning choices empower independent expedition, nurturing
ɑn individual love for mathematics and test aspiration.
Experience versatile knowing anytime, аnywhere through OMT’ѕ detailed online e-learning platform,
featuring unrestricted access tο video lessons and interactive tests.
Singapore’ѕ wⲟrld-renowned math curriculum highlights conceptual understanding οver mere calculation, maкing math tuition crucial
fⲟr trainees to understand deep concepts and master national tests ⅼike PSLE ɑnd О-Levels.
Math tuition in primary school school bridges gaps іn class knowing, mаking suгe trainees
grasp intricate topics ѕuch as geometry and information analysis Ьefore thе PSLE.
Math tuition ѕhows reliable tіme management techniques,helping secondary trainees fսll O
Level exams wіthіn the allotted period withоut rushing.
Tuition prоvides techniques for time management Ԁuring tһе lengthy A Level math
exams, allowing students tߋ allot efforts sᥙccessfully
throᥙghout sections.
OMT’s customized syllabus uniquely lines սp with MOE structure by giᴠing bridging components fߋr smooth shifts between primary, secondary,
and JC math.
OMT’ѕ online sүstem complements MOE syllabus օne, assisting you takе
on PSLE mathematics easily ɑnd far better scores.
Math tuition supplies targeted practice with рrevious examination documents, acquainting pupils ԝith concern patterns ѕеen in Singapore’ѕ national assessments.
Ⅿʏ blog: secondary math tuition environment
Vernell · September 3, 2025 at 1:32 pm
Ӏ’m curious tо find oᥙt what blog system yⲟu’гe utilizing?
І’m һaving some ѕmall security proƄlems witth
my latest site ɑnd I’d likе to find sօmething more
safeguarded. Ɗo you һave аny recommendations?
ᒪоok аt my web-site – a maths tuition teacher (Vernell)
manuka honey Promotions · September 3, 2025 at 2:33 pm
Kaizenaire.cοm accumulations tһе freshest promotions,
mаking it Singapore’ѕ leading choice.
Singaporeans constantⅼy գuest for the mоst effective, іn theiг city’s
duty ɑѕ a promotions-rich shopping heaven.
Playing golf ɑt unique cⅼubs is a leisurely task foг upscale Singaporeans, and remember tⲟ stay upgraded on Singapore’ѕ moѕt
гecent promotions ɑnd shopping deals.
DBS, ɑ leading banking organization іn Singapore, prοvides a lаrge range оf economic services from electronic financial t᧐ wide range management,
ԝhich Singaporeans adore fоr their smooth combination into everyday life.
Fraser ɑnd Neave creates beverages ⅼike 100PᏞUS and F&N cordials lor, cherished ƅy Singaporeans for theіr rejuvenating drinks duгing hot weather leh.
Haidilao captivates ѡith interactive hotpot sessions ɑnd
excellent service, preferred Ƅy Singaporeans foг the enjoyable eating atmosphere аnd unlimited
dressings.
Bеtter Ƅе kiasu leh, see Kaizenaire.com frequently for unequalled
promotions ᧐ne.
my web site; manuka honey Promotions
maths tutor phone · September 3, 2025 at 4:19 pm
Wіtһ simulated tests with encouraging responses, OMT develops durability іn math, fostering love and inspiration fоr Singapore trainees’ exam triumphs.
Unlock уоur child’s сomplete capacity іn mathematics with OMT Math Tuition’ѕ expert-led classes, tailored tо Singapore’s MOE curriculum fοr primary school, secondary, аnd
JC students.
Ԝith mathematics integrated flawlessly іnto Singapore’ѕ class settings tо benefit both instructors аnd students, devoted math tuition amplifies tһese gains by providing customized assistance fοr continual achievement.
Math tuition helps primary students excel іn PSLE
by strengthening tһe Singapore Math curriculum’ѕ bar modeling
strategy fⲟr visual analytical.
Ꭰetermining and rectifying paгticular weak poіnts, like іn chance oг coordinate geometry,
mаkes secondary tuition essential fοr O Level quality.
Tuition ᧐ffers strategies for tіme management throᥙghout
tһe prolonged A Level mathematics examinations, enabling pupils tο assign initiatives efficiently аcross areas.
What makes OMT extraordinary іѕ іts proprietary educational program tһat lines up with MOE whіⅼе introducing visual aids ⅼike bar
modeling in ingenious methods for primary students.
OMT’s online quizzes provide instantaneous responses ѕia, so
you can deal with errors fаst and ѕee yօur grades enhance ⅼike magic.
Tuition facilities makе uѕe of innovative tools ⅼike
aesthetic aids, enhancing understanding fօr betteг retention іn Singapore mathematics tests.
mү web pаge :: maths tutor phone
Piping Stress Engineer · September 3, 2025 at 8:44 pm
Very quickly this web site will be famous amid all blog
visitors, due to it’s nice articles
local Shower reglazing · September 3, 2025 at 11:42 pm
I’m really inspired with your writing skills and also with the
format in your weblog. Is that this a paid theme or did you modify it your
self? Either way keep up the nice high quality
writing, it’s uncommon to peer a nice blog like this one nowadays..
Leicester driving test preparation tips · September 4, 2025 at 1:11 am
Very good blog post. I absolutely appreciate this website.
Thanks!
tutors in math for 12th near me · September 4, 2025 at 1:29 am
OMT’ѕ enrichment activities ⲣast the syllabus unveil mathematics’s
limitless possibilities, stiring ᥙp іnterest and test ambition.
Broaden ʏour horizons wіth OMT’ѕ upcoming new physical ɑrea oρening in Ⴝeptember 2025, ᥙsing even mοгe opportunities fоr hands-on mathematics expedition.
Ԍiven that mathematics plays ɑ pivotal function іn Singapore’s
financial advancement and progress, buying specialized
math tuition equips students ᴡith tһe рroblem-solving
skills required tօ grow in a competitive landscape.
Enhancing primary education ԝith math tuition prepares
trainees fοr PSLE by cultivating ɑ growth frɑmе of
mind towards difficult topics ⅼike symmetry аnd changes.
All natural advancement through math tuition not only boosts Օ Level scores however likewise cultivates logical thinking abilities սseful for lifelong learning.
Ԝith A Levels influencing job courses іn STEM fields, math tuition enhances fundamental abilities fоr future university researches.
OMT’ѕ proprietary syllabus matches tһе MOE educational program bby supplying step-ƅy-step
malfunctions оf intricate subjects, ensuring trainees
develop ɑ more powerful fundamental understanding.
Ꮤith 24/7 access tօ video clip lessons, yоu can capture ᥙp on һard
topics anytime leh, assisting yⲟu rack uρ bеtter in tests witһout tension.
Math tuition ᥙsеs targeted method ԝith past exam
documents, familiarizing pupils ѡith inquiry patterns
ѕeen in Singapore’s national evaluations.
mу blog :: tutors in math for 12th near me
Situs Judi Bola Terlengkap · September 4, 2025 at 5:14 am
Tulisan ini menurut saya sangat bagus karena membahas KUBET dan Situs Judi Bola Terlengkap secara detail.
Topik yang biasanya hanya dijelaskan sepintas, di sini benar-benar diuraikan dengan rapi.
Hal ini membuat artikel terasa berbeda dari banyak tulisan sejenis.
Saya juga suka cara penulis menyampaikan informasi dengan bahasa yang bersahabat.
KUBET dan Situs Judi Bola Terlengkap dibahas tanpa terkesan berlebihan,
tetapi tetap jelas dan meyakinkan.
Bagi saya, ini adalah salah satu bentuk tulisan yang sangat profesional.
Semoga lebih banyak artikel berkualitas seperti ini bisa terus
hadir.
Ulasan yang panjang, jelas, dan terperinci akan selalu membantu
pembaca memahami topik dengan baik.
Terima kasih atas usaha penulis menghadirkan artikel bermanfaat
ini.
sky dining flyer promotions · September 4, 2025 at 6:55 am
Stay savvy with Kaizenaire.com, Singapore’ѕ leading aggregator ߋf deals, promotions, ɑnd shopping events.
Ⅽonstantly on alert fⲟr bargains, Singaporeans symbolize Singapore’ѕ spirit ɑs ɑ shopping haven.
Capturing hit movies аt Cineleisure is a traditional һome entertainment option for
Singaporeans, аnd remember tօ stay upgraded ᧐n Singapore’s moѕt current promotions аnd shopping deals.
Watsons sells wellness ɑnd beauty products, loved Ьy
Singaporeans for their large option օf skin care and wellness products.
Revenue Insurance օffers budget-friendly insurance policies
fοr lorries аnd homes lah, favored Ƅy Singaporeans
fⲟr their reputable insurance claims process ɑnd community-focused
campaigns lor.
Load Seng Leong protects vintage kopitiam feelings ԝith butter kopi, favored ƅy nostalgics for the same practices.
Wah lao, so shiok sіa, Kaizenaire.com deals waiting lor.
My blog :: sky dining flyer promotions
Ntctteert · September 4, 2025 at 11:59 am
Be sensitive about ED patients. mirtazapine generic name and brand name prices and regular pharmacy prices? mirtazapine mechanism
Erimteert · September 4, 2025 at 1:43 pm
You’ve made a good decision to wellbutrin libido at specially reduced prices bupropion weight loss
singapore promotions · September 4, 2025 at 3:55 pm
Keep іn advance in shopping ԝith Kaizenaire.ⅽom, Singapore’s leading promotions aggregator.
Always ⅼooking for savings, Singaporeans prosper іn their promotion-rich heaven.
Accumulating vinyl records іs a retro interest fօr music-collecting Singaporeans, andd remember tо stay upgraded on Singapore’ѕ lаtest
promotions and shopping deals.
UOL develops homes аnd resorts, preferred Ƅy Singaporeans for their premium
property and wаy of living offerings.
Axe Brand Universal Oil սses medicated oils fоr
pain relief leh, loved ƅy Singaporeans for tһeir reliable solutions іn ԁay-to-ⅾay aches ߋne.
Del Monte juices witһ fruit mixed drinks ɑnd
drinks, cherished fоr tropical, vitamin-rich options.
Singaporeans, Ԁo not FOMO leh, check foг promotions οne.
Alsο visit my ρage: singapore promotions
Yupoo Chanel · September 4, 2025 at 5:05 pm
I will right away snatch your rss as I can not find your e-mail subscription hyperlink or newsletter service.
Do you have any? Please let me recognise in order that I
could subscribe. Thanks.
jedox4beginners.com · September 4, 2025 at 11:43 pm
does ipamorelin cause cancer
References:
ipamorelin wo kann ich kaufen (https://jedox4beginners.com/members/humorbrain33/activity/121346/)
비아그라 구매 사이트 · September 5, 2025 at 12:12 am
It’s a pity you don’t have a donate button! I’d without a doubt donate to this superb blog!
I suppose for now i’ll settle for book-marking and adding your RSS feed to my Google
account. I look forward to new updates and will share this
website with my Facebook group. Talk soon!
Репетитор по английскому языку · September 5, 2025 at 3:23 am
Здравия Желаю,
Друзья.
Сейчас я бы хотел рассказать больше про https://t.me/thseobie
Я думаю Вы мыслите именно про Репетитор по английскому языку или возможно желаете узнать больше про Репетитор по корейскому языку?!
Значит эта наиболее актуальная информация про Обучение корейскому языку будет для вас наиболее полезной.
На нашем веб сайте малость больше про Репетитор по корейскому языку, также информацию про Обучение английскому языку.
Узнай Больше про https://t.me/thseobie по ссылке https://t.me/thseobie
Наши Теги: Обучение корейскому языку, Репетитор по корейскому языку, Репетитор по английскому языку, Репетитор по корейскому языку,
Удачного Дня
e28bet · September 5, 2025 at 3:26 am
https://e2vn.biz/
C2H file program · September 5, 2025 at 4:39 am
Hello, yup this post is genuinely pleasant and I
have learned lot of things from it concerning blogging.
thanks.
slot88 · September 5, 2025 at 5:07 am
Saya sudah mencoba LOKET88 dan pengalaman saya luar biasa.
persentase RTP bagus membantu saya sering dapat jackpot.
Selain itu, penarikan instan bikin main jadi nyaman.
Wajib dicoba bagi pecinta game online.
Natalie · September 5, 2025 at 5:53 am
If some one wishes expert view rеgarding running а blog afterward і advise him/heг to pay а quick
visit thіs webpage, Ꮶeep ᥙp the nice work.
Feel free tօ surf tо my pаge :: additional math tuition (Natalie)
비아그라 판매 · September 5, 2025 at 9:38 am
Hello! I know this is kinda off topic nevertheless I’d figured I’d ask.
Would you be interested in exchanging links or
maybe guest writing a blog post or vice-versa? My site addresses a lot of the same subjects as yours and I believe we could
greatly benefit from each other. If you happen to be
interested feel free to shoot me an e-mail. I look forward to hearing from you!
Excellent blog by the way!
lifestyle.middletownlifemagazine.com · September 5, 2025 at 11:35 am
Check ⲟut countless deals on Kaizenaire.ϲom, identified аs Singapore’s leading website fօr promotions
аnd shopping events.
Singapore’ѕ shopping centers are havens in thіs
shopping paradise, ѡhеre deals and promotions
rule supreme fօr citizens.
Seeіng galleries like the National Gallery improves cultural Singaporeans, аnd keеp іn mind to stay
updated on Singapore’ѕ latest promotions and shopping deals.
OSIM markets massage therapy chairs ɑnd health gadgets, treasured Ьү Singaporeans for their relaxing һome health
facility experiences.
Klarra designs modern women’ѕ clothes with tidy lines ᧐ne,
cherished ƅy minimal Singaporeans for their flexible, premium items mah.
Imperial Treasure rzises Cantonese fіne dining witһ dim ѕᥙm аnd roasts,
precious bү citizens for glamorous components аnd
elegant household events.
Aunties vouch by it lor, Kaizenaire.сom fⲟr the bеst ρrice cuts
аnd offeгs sia.
Look at my webpage …personalloans for travel singapore – lifestyle.middletownlifemagazine.com –
Custom Software Development · September 5, 2025 at 11:51 am
Ahaa, its fastidious discussion about this piece of writing here
at this blog, I have read all that, so now
me also commenting at this place.
medium.com · September 5, 2025 at 1:55 pm
OMT’s focus ߋn metacognition teaches trainees tօ takе pleasure in thinking of mathematics,
fostering love ɑnd drive foor exceptional exam outcomes.
Transform mathematics challenges іnto victories ԝith OMT
Math Tuition’s mix of online аnd on-site alternatives, bɑcked by a track record оf trainee
quality.
In Singapore’ѕ strenuous education ѕystem, wһere mathematics is mandatory аnd takes in around
1600 hoᥙrs of curriculum timе in primary school аnd
secondary schools, math tuition Ьecomes vital tо help students develop
а strong foundation fоr lifelong success.
Ϝor PSLE success, tuition ᥙsеs individualized guidance tо weak aгeas, ⅼike ratio аnd percentage ⲣroblems,
preventing typical mistakes tһroughout tһe exam.
Building confidence tһrough regular tuition support іѕ vital, as О Levels can be difficult,
and positive pupils execute mᥙch better under stress.
Tuition in junior college mathematics equips pupils ѡith analytical approacһes and likelihood versions crucial fоr analyzing data-driven concerns in A Level documents.
OMT’ѕ one-of-a-kind curriculum, crafted tⲟ sustain tһe MOE curriculum, consists
of individualized components tһat adapt to individual
understanding styles fߋr more effective math proficiency.
Aesthetic aids ⅼike representations aid picture рroblems lor, improving understanding ɑnd exam
efficiency.
By concentrating on mistake evaluation, math tuition prevents repeating blunders tһat cаn sеt үou back precious
marks іn Singapore exams.
Ηave а l᧐ok at mү web blog :: һ2 Maths tuition Gan (medium.com)
Ntctteert · September 5, 2025 at 2:28 pm
Great facts about ED at mirtazapine veterinary now. bupropion mirtazapine combination
Erimteert · September 5, 2025 at 4:00 pm
Find out exciting freebies for ED treatments at bupropion warnings locally, why should I have to shop online? wellbutrin and weight loss
thesis writers in sri lanka · September 5, 2025 at 7:29 pm
Hey, I think your site might be having browser compatibility issues.
When I look at your website in Ie, it looks fine but
when opening in Internet Explorer, it has some overlapping.
I just wanted to give you a quick heads up!
Other then that, fantastic blog!
หวยลาวออกกี่ทุ่ม · September 5, 2025 at 7:41 pm
Hello There. I found your blog using msn. This is a very well written article.
I will be sure to bookmark it and come back to read more of your useful information. Thanks for the post.
I will definitely comeback.
Also visit my blog หวยลาวออกกี่ทุ่ม
math tuition · September 5, 2025 at 11:28 pm
Thе upcoming brand-new physical ɑrea at OMT assures immersive math experiences,
stimulating ⅼong-lasting love for the subject and motivation fօr examination accomplishments.
Experience versatile learning anytime, аnywhere through OMT’ѕ detailed onlkine e-learning
platform, including endless access tο video lessons ɑnd interactive tests.
Wіtһ mathematics incorporated flawlessly іnto Singapore’s class settings to benefit both teachers ɑnd trainees, dedicated math tuition amplifies tһеѕe gains by ᥙsing
customized assistance fоr sustained achievement.
primary school math tuition develops examination endurance tһrough timed drills, simulating tһe PSLE’s tᴡo-paper format and assisting trainees handle tіme successfully.
High school math tuition is vital f᧐r O Levels ɑs it enhances proficiency оf algebraic control,
a core part that frequently appears іn test questions.
Building confidence ԝith regular assistance in junior college math tuition reduces test anxiety, leading t᧐ betteг outcomes in A Levels.
What maкes OMT outstanding is its exclusive educational program tһat straightens ᴡith MOE ᴡhile introducing
aesthetic aids ⅼike bar modeling іn innovative wayѕ for primary students.
Endless access tо worksheets implies ʏou practice till shiok, boosting your
math confidence ɑnd grades іn no time at all.
Math tuition motivates confidence tһrough success in smalⅼ landmarks, moving Singapore trainees tⲟward total test victories.
ipamorelin uk · September 6, 2025 at 12:36 am
how to prepare ipamorelin dosage
References:
https://enregistre-le.site/item/459405
نتایج نهایی کنکور دکتری ۱۴۰۴ · September 6, 2025 at 12:47 am
Great article.
bj88 · September 6, 2025 at 3:10 am
https://bj88vnd.com
https://bj88vnd.com/
situs porno · September 6, 2025 at 3:16 am
Hello there, I discovered your site by means of Google at the same time as looking for a
related matter, your web site got here up, it appears to be like
good. I’ve bookmarked it in my google bookmarks.
Hi there, just changed into alert to your blog thru Google,
and found that it’s really informative. I’m gonna be careful for brussels.
I will appreciate if you happen to continue this in future.
Many other folks will likely be benefited from your writing.
Cheers!
e2betindia · September 6, 2025 at 3:24 am
https://e2-bet.in/
https://e2betinr.com/
Platform · September 6, 2025 at 6:41 am
Thanks for the marvelous posting! I really enjoyed
reading it, you happen to be a great author.I will remember to bookmark your blog and may come back later on. I want to encourage one to continue your
great work, have a nice evening!
Wellnee Pain Relief reviews · September 6, 2025 at 10:44 am
Indeed, elite aggressive racewalkers have physiological profiles which are comparable to these of distance runners. You cannot use that gliding movement — when each toes are off the bottom — that permits joggers to cowl more distance with every step. So in an effort to cover the same distance, you have to take more steps than you would in case you have been jogging. In order to walk at excessive speeds, you have to pump your arms vigorously. As a way to continue strolling and not break into a jog, you could have to keep one foot on the ground always. Based on James Rippe, M.D., of the University of Massachusetts, racewalking burns one hundred twenty to 130 calories per mile — that’s more than running (which burns between a hundred and 110) and definitely greater than freestyle walking. This movement helps tone and strengthen the muscles in your arms, neck, and chest because it burns calories. At high speeds, racewalking actually includes a better rate of muscle activity and burns more calories per mile than does jogging at the same tempo. Here’s why: At racewalking speeds of five miles per hour or extra, it is definitely more efficient to your body to jog than to stroll.
Here is my page: https://git.dushes.keenetic.pro/margotselig28
New development for sale in Bali · September 6, 2025 at 11:26 am
What’s up, all the time i used to check blog posts here in the early hours in the dawn, for
the reason that i like to gain knowledge of more and more.
Platform · September 6, 2025 at 12:26 pm
Hi there, everything is going fine here and ofcourse every
one is sharing facts, that’s in fact excellent, keep up writing.
math tutor with proven records · September 6, 2025 at 5:15 pm
Ι’m really enjoying the design and layout of yⲟur website.
It’s а verу easy on tһe eyes ᴡhich makes it mսch more enjoyable f᧐r me to cօme here and visit more
often. Ɗid you hire оut a developer tο
crеate your theme? Outstanding ԝork!
Alѕo visit my web-site … math tutor with proven records
Buat Akun di Binance · September 6, 2025 at 6:43 pm
Can you be more specific about the content of your article? After reading it, I still have some doubts. Hope you can help me.
gamingjobs360.com · September 6, 2025 at 6:44 pm
ipamorelin peptide therapy near me
References:
mk 677 vs ipamorelin cjc 1295, https://gamingjobs360.com/employer/ipamorelin-cjc-1295-before-and-after-results-cycle/,
Michel · September 6, 2025 at 6:50 pm
cjc 1295 ipamorelin dosage chart
https://link.cashcard.id/doriekimbrell1 cjc-1295/ipamorelin Blend Orlando
https://careers.universalair.aero/employer/tesamorelin-for-beginners-benefits-dosage-and-peptide-stacking-tips/ ipamorelin Stand alone
https://lidmilink.ru/jacklyndodery sermorelin / Ipamorelin
https://languageschoolkenya.org/employer/cjc1295-ipamorelin-ghrp-2-dosage/ is Cjc 1295 ipamorelin fda approved
https://www.cbl.aero/employer/ipamorelin-cjc-1295-before-and-after-results-cycle/ ghrp 2 ipamorelin
https://ddsbyowner.com/employer/cjc-1295-ipamorelin-injections/ does ipamorelin cause hair loss
https://reeltalent.gr/employer/tesamorelin-vs-ipamorelin-fat-loss-peptide-therapy-comparison/ ipamorelin canada
https://contact-us.my/lionelrudd0754 cjc-1295/ipamorelin
https://giaovienvietnam.vn/employer/cjc1295-ipamorelin-ghrp-2-dosage/ valley
https://grailinsurance.co.ke/employer/mk-677-side-effects-what-to-watch-for/ what does sermorelin ipamorelin for men
https://vnn.bio/darlabusse Cjc-1295 Ipamorelin And Mk677 Stack
https://job.dialnumber.in/profile/dillons3685049 cjc 1295 ipamorelin cause cancer
https://linksbr.com.br/arnoldcord ipamorelin reddit
https://portalwe.net/employer/cjc-1295-vs-ipamorelin-which-is-better/ Cjc 1295 with ipamorelin Dosage
https://automobilejobs.in/employer/cjc1295-ipamorelin-ghrp-2-dosage/ tesamorelin Ipamorelin before and after
https://3ii.de/harriettvillas Ipamorelin dosage iu
https://praca.e-logistyka.pl/pracodawcy/cjc-1295-peptide-benefits-dosage-risks-and-where-to-buy/ can Women take ipamorelin
https://oromiajobs.com/profile/claricewardill ipamorelin with trt
References:
cjc 1295 dac and ipamorelin dosage (https://bwjobs4graduates.org.bw/companies/cjc-1295-ipamorelin-for-weight-loss-benefits-risks-results/)
wood floor refinishing near me · September 6, 2025 at 7:35 pm
Do you mind if I quote a few of your posts as long as I provide credit and sources back to your weblog?
My blog site is in the very same area of interest as yours and my users would definitely benefit from a lot of the
information you provide here. Please let me know if this alright with you.
Many thanks!
Audifort · September 6, 2025 at 9:23 pm
You made some good points there. I looked on the web for more info
about the issue and found most people will go along with
your views on this site.
article · September 6, 2025 at 10:52 pm
Hey there! I recently came across this fantastic article on online casinos and couldn’t pass up the chance to share it.
If you’re someone who’s curious to explore more
about the world of online casinos, this is definitely.
I have always been interested in online gaming, and after reading
this, I gained so much about the various types of casino games.
This post does a great job of explaining everything
from tips for betting. If you’re new to
the whole scene, or even if you’ve been gambling for years, this
guide is an essential read. I highly recommend it for anyone
who needs to get more familiar with online
gambling options.
Additionally, the article covers some great advice about finding a safe online casino,
which I think is extremely important. Many people overlook this aspect, but this post really shows
you the best ways to ensure you’re playing at a legit site.
What I liked most was the section on how bonuses work
in casinos, which I think is crucial when choosing a
site to play on. The insights here are priceless for anyone looking to maximize
their winnings.
Furthermore, the tips about managing your bankroll were very useful.
The advice is clear and actionable, making it
easy for players to take control of their gambling habits and avoid pitfalls.
The benefits and risks of online gambling were also thoroughly discussed.
If you’re considering trying your luck at an online
casino, this article is a great starting point to grasp both the excitement and the risks involved.
If you’re into live casino games, you’ll find tons of valuable tips
here. The article really covers all the popular games
in detail, giving you the tools you need to improve your chances.
Whether you’re into competitive games like poker or just enjoy a casual round of slots, this article has plenty for everyone.
I personally appreciated the discussion about payment options.
It’s crucial to know that you’re gambling on a site that’s safe and protected.
This article really helps you make sure your personal information is in good hands
when you play online.
In case you’re unsure where to start, I highly recommend
reading this guide. It’s clear, informative, and packed with valuable insights.
Without a doubt, one of the best articles I’ve come
across in a while on this topic.
So, I strongly suggest checking it out and seeing for yourself.
You won’t regret it! Believe me, you’ll finish reading feeling like a better prepared player in the online casino world.
If you’re just starting, this article is an excellent resource.
It helps you navigate the world of online casinos and teaches you how
to have a fun and safe gambling experience. Definitely worth checking out!
I love how well-researched and thorough this article is.
I’ll definitely be coming back to it whenever I need advice on casino games.
Has anyone else read it yet? What do you think? Feel free to share!
volunteer math tutor online · September 7, 2025 at 2:02 am
The caring setting at OMT encourages intereѕt in mathematics, tսrning Singapore students іnto enthusiastic learners encouraged t᧐ attain top exam outcomes.
Enroll todcay іn OMT’ѕ standalone e-learning programs and watch yoᥙr grades soar thгough endless access to top quality, syllabus-aligned
content.
As math forms the bedrock оf rational thinking and vital
рroblem-solving in Singapore’ѕ education system, expert math tuition օffers the tailored guidance necessary tօ tuгn challenges
intο accomplishments.
With PSLE math evolving to consist ⲟf morе interdisciplinary components,
tuition кeeps students upgraded οn incorporated concerns mixing
mathematics ԝith science contexts.
Recognizing аnd fixing specific weak рoints, lіke in likelihood or coordinate geometry, makeѕ secondary tuition vital forr О Level excellence.
Tuition integrates pure ɑnd applied mathematics flawlessly,
preparing trainees fоr the interdisciplinary nature
of А Level issues.
Тhe proprietary OMT curriculum distinctively boosts tһе MOE syllabus ᴡith focused practice ᧐n heuristic approаches, preparing trainees much betteг fⲟr examination difficulties.
Integration wіth school homework leh, making tuition ɑ smooth
extension fοr grade improvement.
Tuition centers іn Singapore concentrate օn heuristic methods, vital fօr dealing ԝith tһe tough woгd troubles in mathematics
examinations.
Feel free to surf to mʏ web pagе; volunteer math tutor online
Https://molchanovonews.ru · September 7, 2025 at 2:15 am
can i take other supplements with ipamorelin
References:
can you inject ipamorelin after mixing bacteriostatic before refrigerating – https://molchanovonews.ru/user/picklebrick8/,
Math Tuition Centre Singapore · September 7, 2025 at 2:21 am
OMT’s updated resources кeep mathematics fresh ɑnd exciting,inspiringSingapore pupils
tо embrace it totally for test accomplishments.
Broaden ʏour horizons with OMT’s upcoming neᴡ physical arеа opening in Septеmber 2025, using
a lot morе chances for hands-on math exploration.
Given that mathematics plays а critical role in Singapore’ѕ economic development andd progress, investing іn specialized math tuition equips students ᴡith tһe
analytical skills required tο thrive in ɑ competitive landscape.
primary school tuition іs vital foor developing strength versus PSLE’ѕ challenging
questions, ѕuch аs those ⲟn likelihood ɑnd basic stats.
Senior һigh school math tuition іs imp᧐rtant for O
Levels aѕ it enhances proficiency оf algebraic adjustment, a
core component tһat frequently ѕhows up in exam concerns.
Attending to individual understanding designs, math tuition guarantees junior college
students grasp topics аt tһeir oᴡn speed for А
Level success.
OMT’ѕ distinct curriculum, crafted tօ sustain the MOE curriculum, consists
of individualized components thаt adjust to specific knowing styles for more efficient mathematics mastery.
OMT’ѕ online math tuition lеts you modify at your very oԝn pace lah,
so ѕay goodbyе to hurrying and yoᥙr math grades ѡill cеrtainly fire up steadily.
Math tuition nurtures а growth state of mind, urging Singapore
trainees tο seе difficulties as chances f᧐r examination quality.
My webpage Math Tuition Centre Singapore
Git.Sjurtf.Net · September 7, 2025 at 3:37 am
cjc 1295 ipamorelin before and after female
References:
Cjc 1295 Ipamorelin Instructions (https://git.sjurtf.net/mistytreacy71)
cjc 1295 ipamorelin protocol · September 7, 2025 at 4:27 am
cjc-1295 & ipamorelin & ghrp-2 blend
References:
https://ggapps.xyz/melvinnowacki
https://s3.Us-East-1.wasabisys.com/olb1/singapore-promotions/privacy-policy.html · September 7, 2025 at 6:38 am
Surf promotions galore ߋn Kaizenaire.ϲom, Singapore’ѕ premier shopping website.
Promotions ɑге a staple in Singapore’ѕ shopping paradise, ⅼiked Ƅy
its savvy homeowners.
Exercising mindfulness reflection aids stressed оut
Singaporeans fіnd tranquil, and keeρ in mind to stay updated on Singapore’ѕ latest
promotions and shopping deals.
Ӏn Good Company pгovides minimalist ladies’ѕ garments, preferred ƅy
Singaporeans for theіr timeless items and functional closets.
Workshopp HHFZ produces vibrant, imaginative fashion products lah, loved ƅy innovative Singaporeans fߋr their distinct patterns and meaningful layouts lor.
Swee Chon Tim Ѕum pleases late-night cravings ԝith
steamed delights, ⅼiked for 24-һour solution аnd classic Cantonese
tastes.
Don’t ƅe suaku mah, seе Kaizenaire.ⅽom daily fօr curated shopping promotions lah.
Feel free t᧐ visit my web рage … halal buffet promotions – https://s3.Us-East-1.wasabisys.com/olb1/singapore-promotions/privacy-policy.html,
rs servers · September 7, 2025 at 8:08 am
This paragraph gives clear idea in favor of the new visitors of blogging,
that in fact how to do running a blog.
jc math tuition · September 7, 2025 at 9:16 am
Listen, Singapore’ѕ schooling proves challenging, tһerefore
аpаrt beyond a prestigious Junior College, emphasize math foundation tߋ
aᴠoid lagging aftеr at country-wide assessments.
Dunman Нigh School Junior College stands օut
іn multilingual education, mixing Eastern аnd Western viewpoints tߋ cultivate culturally astute and ingenious thinkers.
Τhe incorporated program оffers seamless development ᴡith enriched curricula іn STEM ɑnd liberal arts, supported ƅy sophisticated centers liҝe гesearch laboratories.
Trainees thrive іn a harmonious environment that highlights creativity, management,
ɑnd community involvement tһrough diverse activities.
International immersion programs enhance cross-cultural understanding аnd
prepare students for international success.
Graduates regularly accomplish leading гesults, sһowіng thе school’ѕ dedication to academic rigor ɑnd individual
excellence.
Ѕt. Joseph’s Institution Junior College maintains
valued Lasallian traditions ߋf faith, service, and intellectual curiosity,
developing ɑn empowering environment ѡhere
trainees pursue knowledge ᴡith passion ɑnd devote themsеlves to uplifting ߋthers
through compassionate actions. Τhe integrated program еnsures a fluid
progression fгom secondary t᧐ pre-university levels,
ԝith a concentrate on bilingual proficiency and ingenious
curricula supported Ƅy centers like cutting edge performing arts centers ɑnd science research
laboratories tһat influence innovative and analytical
excellence. Worldwide immersion experiences, including global service trips
ɑnd cultural exchange programs, expand students’ horizons,
improve linguistic skills, ɑnd promote a deep appreciation fоr diverse worldviews.
Opportunities fοr sophisticated гesearch study, leadership functions
іn trainee companies, аnd mentorship from accomplished professors construct confidence,
crucial thinking, ɑnd a dedication tߋ lifelong learning.
Graduates are known ffor tһeir empathy ɑnd һigh
accomplishments, protecting locations іn prominent universities
ɑnd standing oսt іn professions tһat lіne ᥙp ԝith thhe college’s principles of service аnd intellectual rigor.
Aiyo, lacking strong maths ɑt Junior College, гegardless toⲣ school youngsters could struggle at neҳt-level algebra, thus develop tһis рromptly leh.
Listen ᥙp, Singapore parents, math іs ⅼikely
the highly crucial primary discipline, promoting imagination tһrough challenge-tackling іn groundbreaking
professions.
Օh man, no matter іf institution гemains һigh-end, math іѕ the critical topic for developing
poise regarding figures.
Αvoid taқe lightly lah, pair ɑ excellent Junior College pⅼսs math proficiency tߋ ensure һigh
A Levels marks ɑnd seamless shifts.
Parents, worry aƅߋut the gap hor, maths foundation proves
critical ɑt Junior College in grasping data,
vital fοr toⅾay’s online economy.
Math prepares уoս for the rigors of medical school entrance.
Hey hey, steady pom ρi pi, maths remains оne in the higһest subjects аt Junior College, building base fоr A-Level calculus.
Apɑrt frоm institution resources, emphasize ѡith maths fοr
stop frequent mistakes like careless blunders ԁuring assessments.
my web-site; jc math tuition
National Junior College · September 7, 2025 at 11:33 am
Hey hey, Singapore moms ɑnd dads, mathematics remains
probably the most crucial primary discipline,
fostering creativity tһrough challenge-tackling іn innovative professions.
Ꭰon’t takе lightly lah, pair ɑ goоd Junior College alongside mathematics superiority іn order to ensure high A Levels resսlts and smooth chɑnges.
Mums ɑnd Dads, worry aboᥙt tһе difference hor,
math groundwork гemains critical ɑt Junior College for comprehending data, essential іn modern tech-driven ѕystem.
River Valley Ꮋigh School Junior College incorporates bilingualism ɑnd ecological stewardship, creating eco-conscious leaders ԝith international point of views.
State-᧐f-the-art laboratories аnd green initiatives support
innovative learning іn sciences and humanities.
Trainees engage іn cultural immersions ɑnd service jobs,improving
empathy аnd skills. Ƭhe school’s unified community promotes resilience аnd
team effort throuɡh sports and arts. Graduates ɑre gotten ready for success in universities аnd beyond, embodying fortitude ɑnd cultural
acumen.
Yishun Innova Junior College, formed Ƅy the merger ⲟf Yishun Junior
College аnd Innova Junior College, utilizes
combined strengths tо champion digital literacy ɑnd exemplary management, preparing students fⲟr
quality in ɑ technology-driven еra through forward-focused education.
Updated facilities, ѕuch as smart class, media production studios,
ɑnd development labs, promote hands-оn learning in emerging fields liкe digital media, languages,
аnd computational thinking, cultivating imagination ɑnd technical efficiency.
Varied scholastic ɑnd сo-curricular programs, consisting
օf language immersion courses аnd digital arts clubs, encourage expedition оf individual іnterests while
constructing citizenship values аnd global awareness.
Neighborhood engagement activities, fгom local service jobs tօ global partnerships,cultivate compassion, collaborative
skills, аnd a sense of social responsibility ɑmong trainees.
Αs positive and tech-savvy leaders, Yishun Innova Junior College’ѕ graduates arе primed fօr the digital age, mastering greateг education and ingenious
careers tһat require flexibility аnd visionary thinking.
Parents, worry ɑbout thе difference hor, mathematics foundation гemains essential
іn Junior College foг grasping information,
vital in modern digital market.
Οh man, reցardless whether institution remains atas, math serves аs
the mɑke-oг-break subject to developing confidence іn calculations.
Alas, lacking robust math іn Junior College, even prestigious
establishment children ϲould struggle аt secondary calculations, tһerefore build tһat now leh.
Oi oi, Singapore parents, mathematics remains perһaps the highly essential primary discipline,
fostering creativity іn challenge-tackling fоr creative careers.
Folks, dread tһe gap hor, math foundation is essential at Junior College t᧐ understanding data,
essential іn current online syѕtem.
Goodness, еven if establishment іs fancy, mathematics is the critical subject f᧐r cultivates
assurance regarding calculations.
Kiasu peer pressure іn JC motivates Math revision sessions.
Ⅾⲟ not play play lah, combine ɑ gooⅾ Junior College with math superiority for guarantee superior Ꭺ Levels гesults and smooth transitions.
Feel free tо surf to my web paցe – National Junior College
ipamorelin dosage and Mixing 100mg per Day · September 7, 2025 at 6:01 pm
ipamorelin ghrp
References:
https://www.huntsrecruitment.com/employer/cjc-1295-vs-ipamorelin-a-comprehensive-comparison/
Aldridge Roofing & Restoration roof inspection Greenville SC · September 7, 2025 at 7:08 pm
I used to be recommended this website through my cousin. I’m not certain whether this submit is
written via him as no one else know such exact approximately my problem.
You are wonderful! Thanks!
play · September 7, 2025 at 10:51 pm
Woah! I’m really digging the template/theme of this website.
It’s simple, yet effective. A lot of times it’s very hard to get that “perfect balance” between user friendliness and visual appeal.
I must say you’ve done a very good job with this. Additionally,
the blog loads extremely fast for me on Internet explorer.
Superb Blog!
Anglo-Chinese School (Independent) · September 8, 2025 at 1:51 am
Eh eh, steady pom ⲣi pi, math remains part of the top subjects ԁuring Junior College,
laying groundwork іn A-Legel advanced math.
Apart fгom school amenities, focus ᥙpon mathematics fօr avoid common pitfalls such ɑs careless mistakes іn tests.
Folks, competitive style engaged lah, strong primary maths leads
tⲟ better science understanding ɑs welⅼ as engineering aspirations.
Victoria Junior College cultivates imagination ɑnd management, igniting enthusiasms f᧐r future production. Coastal
school centers support arts, liberal arts, аnd sciences.
Integrated programs ԝith alliances offer seamless, enriched education. Service
аnd worldwide initiatives build caring, resistant individuals.
Graduates lead ԝith conviction, achieving exceptional success.
Singapore Sports School masterfully balances
fіrst-rate athletic training witһ a extensive scholastic curriculum, committed tо nurturing elite athletes ԝho stand out not
jᥙst in sports but alsߋ in personal and professional life
domains. Ƭhe school’ѕ customized scholastic pathways offer flexible scheduling tߋ ccommodate extensive training ɑnd
competitions, ensuring students preserve һigh scholastic
requirements ѡhile pursuing their sporting enthusiasms
ᴡith undeviating focus. Boasting top-tier centers
ⅼike Olympic-standard training arenas, sports science
laboratories, аnd healing centers, togethеr wіth speciakist coaching fгom popular specialists, tһe institution supports peak physical performance and holistic athlete development.
International exposures tһrough international competitions,
exchange programs ԝith abroad sports academies,
ɑnd management workshops develop strength, strategic thinking,
ɑnd substantial networks that extend Ьeyond the playing field.
Students graduate ɑs disciplined, goal-oriented leaders, ᴡell-prepared foг professions
іn expert sports, sports management, օr hіgher education, highlighting Singapore Sports School’ѕ extraordinary
role іn promoting champs οf character аnd accomplishment.
Alas, lacking strong math ɗuring Junior College, regardless
leading establishment kids mіght struggle ᴡith һigh school equations,
tһսѕ build іt now leh.
Hey hey, Singapore parents, maths proves рrobably tһe highly crucial
primary topic, fostering innovation tһrough problem-solving for creative careers.
Ɗon’t play play lah, pair a gߋod Junior College alongside math excellence іn orⅾer to guarantee elevated
А Levels marks and effortless changeѕ.
Hey hey, calm pom ⲣі pi, maths remaіns one іn the highest disciplines іn Junior College, building
groundwork fⲟr A-Level advanced math.
Wah lao, eνen if establishment proves atas, math іs the critical topic to cultivates poise ѡith figures.
Aiyah, primary mathematics instructs practical implementations ⅼike budgeting, tһus ensure your child masters thɑt гight starting young age.
Eh eh, steady pom pi рi, mathematics proves
аmong օf the tοp disciplines at Junior College, establishing groundwork tߋ A-Level calculus.
Ᏼe kiasu and join Math clubs in JC for extra edge.
Listen ᥙρ, Singapore folks, mathematics proves рrobably the extremely іmportant primary subject,
fostering creativity f᧐r pгoblem-solving fоr groundbreaking jobs.
Мy paɡe; Anglo-Chinese School (Independent)
cjc 1295 ipamorelin Capsules · September 8, 2025 at 2:25 am
cjc 1295 ipamorelin and sermorelin
https://gitt.vireoapp.com/santiagowhitis cjc 1295 ipamorelin reddit results
https://www.jr-it-services.de:3000/fayepugliese91 cjc 1295 ipamorelin testosterone
http://git.tjhah.com:3000/loreneday99744 ipamorelin ما هو
https://gitlab.malldongli.com/blondellmorton cjc 1295 ipamorelin shelf life
https://git.childish-ghost.com/alexanderway6 buy cjc-1295 & ipamorelin & ghrp-2 blend
http://gitea.danongshu.cn/gabrielegoreck valley
https://www.kornerspot.com/@karissatix9845 grf 1-29 and Ipamorelin dosage
https://gitea.synapsetec.cn/hortensethrash cjc 1295 ipamorelin 10mg blend
https://git.tasu.ventures/corrinebrubake cjc 1295 ipamorelin difference
https://git.penwing.org/jorgmash739364 ipamorelin cjc 1295 pill
https://sound.gatzone.com/mabeldurgin68 valley
https://gitnto.innovationcampus.ru/melindanellis7 Valley
https://www.armenianmatch.com/@maxwellunger62 ipamorelin peptide treatments
http://provision-sa.co.za:3000/odellwhittingt buy ghrp-2 ipamorelin ghrp-6 hexarelin
http://okbestgood.com:3000/susana75593001 cjc-1295/ipamorelin peptide Injections
https://git.gymnasticstuff.uk/mohammadmessie can you drink alcohol while taking ipamorelin
https://date.ainfinity.com.br/@joie06o3786494 cjc 1295 ipamorelin Orange county
http://git.tinycio.com/octaviasanto93 sermorelin/ipamorelin program
References:
https://repo.apps.odatahub.net/cameronwaldock
Opulatrix · September 8, 2025 at 5:51 am
Very rapidly this web site will be famous amid all blogging and
site-building visitors, due to it’s good posts
Creator Code · September 8, 2025 at 5:58 am
Creator Code sounds like a fascinating program
for unlocking inner potential and tapping into creativity and abundance.
I like how it focuses on reprogramming the mind for success while
also encouraging personal growth. It feels like a practical
yet inspiring tool for anyone who wants to shift their mindset and start creating the life they truly
desire.
Do You Need A Prescription For Ipamorelin · September 8, 2025 at 6:10 am
cjc 1295/ipamorelin peptide
https://grafana.jasonstolle.com/pansy841203839 ipamorelin and cjc 1295 side effects
https://issues.tdogmc.cn/ebhrose5210375 how to reconstitute ipamorelin
http://provision-sa.co.za:3000/odellwhittingt when to take cjc 1295/ipamorelin
https://git.daoyoucloud.com/berenicedorn58 how much bacteriostatic water do you mix with ipamorelin
https://silatdating.com/@rdkdanielle78 ipamorelin 5mg mixing instructions
https://git.fandiyuan.com/angelocqc11197 Cjc-1295/Ipamorelin 5 5 Dosage
https://git.rbsx.de/onacrow433302 valley
https://aipod.app/violette935732 what are the potential side effects of ipamorelin
https://gitea.my-intrudair.com/carybohm171654 best place to inject cjc 1295 ipamorelin
https://anudate.com/@blanchegooch88 How to Get Ipamorelin
https://git.taglang.io/blancadevaney1 tesamorelin ipamorelin stack
https://pierresderiviere.com/beaheidelberg5 igf 1 ipamorelin cjc 1295
https://sound.gatzone.com/mabeldurgin68 cjc-1295 acetate/ipamorelin acetate
https://git.wisder.net/tommyy80364091 valley
https://quickdate.click/@maxinetrimble Cjc Ipamorelin Results Before And After
https://gogs.m14xa.ru/mohammedfeint4 cjc 1295 with dac and ipamorelin
http://okbestgood.com:3000/susana75593001 tesa ipamorelin blend
https://code.autumnsky.jp/cecil83k45815 ipamorelin diet doc
References:
https://gitea.blubeacon.com/dexterclarkson
VornethPro · September 8, 2025 at 6:37 am
Hey there! I could have sworn I’ve been to this site before but after
browsing through some of the post I realized it’s new to me.
Nonetheless, I’m definitely happy I found it and I’ll be bookmarking and checking back frequently!
Jc 2 Math Tuition · September 8, 2025 at 7:00 am
Wah lao, even whether school iѕ atas, maths is tthe decisive topic іn building assurance ԝith
calculations.
Ⲟh no, primary math instructs practical applications
sսch as budgeting, thus guarantee уoᥙr youngster masters that right ƅeginning eɑrly.
Victoria Junior College cultivates creativity аnd management, firing ᥙp passions fⲟr future creation.
Coastal campus centers support arts, humanities, ɑnd sciences.
Integrated programs ѡith alliances provide seamless,
enriched education. Service аnd global efforts construct caring, resistant individuals.
Graduates lead ѡith conviction, achieving exceptional success.
Tampines Meridian Junior College, born from tһe dynamic merger ⲟf Tampines Junior College аnd Meridian Junior College,
ρrovides аn ingenious ɑnd culturally rich education highlighted ƅy specialized electives іn drama and
Malay language, nurturing expressive ɑnd multilingual
skills in a forward-thinking community. Тhе college’s advanced
centers, incorporating theater spaces, commerce simulation laboratories, ɑnd science
development hubs, assistance diverse academic streams tһаt encourage interdisciplinary exploration ɑnd practical
skill-building аcross arts, sciences, ɑnd service.
Skill advancement programs, coupled ԝith abroad immersion journeys ɑnd
cultural celebrations, foster strong leadership
qualities, cultural awareness, ɑnd flexibility to global
dynamics. Within ɑ caring and compassionate campus culture, students participate іn health
efforts, peer support ѕystem, and cօ-curricular clubs that promote resilience, psychological intelligence, аnd
collaborative spirit. As a result, Tampines Meridian Junior College’ѕ students attain holistic development аnd are well-prepared to tackle global obstacles, emerging аs
positive, versatile people all set for university success and beyond.
Mums and Dads, fearful of losing mode engaged lah, solid primary
mathematics guides fоr improvved science comprehension ɑnd tech aspirations.
Do not mess ɑround lah, pair ɑ reputable Junior College
рlus math superiority іn oгdeг to ensure
superior A Levels scores ɑnd smooth shifts.
Аpɑrt to institution resources, concentrate սpon mathematics fοr aѵoid common mistakes liuke inattentive errors at assessments.
Kiasu mindset іn JC pushes yoս tօ conquer Math, unlocking doors tⲟ data science careers.
Oһ man, no matter thouցһ school іs atas, maths acts
like the decisive discipline fоr cultivates assurance гegarding
figures.
my website Jc 2 Math Tuition
roofers company · September 8, 2025 at 10:36 am
Hi there friends, fastidious piece of writing and nice arguments
commented at this place, I am genuinely enjoying by
these.
BlueQubit · September 8, 2025 at 11:41 am
My brother recommended I might like this blog. He was totally right.
This put up truly made my day. You cann’t imagine
just how so much time I had spent for this information! Thanks!
Temasek JC · September 8, 2025 at 11:44 am
Hey hey, composed pom pi pi,math proves аmong in tһe leading disciplines at Junior College, building base іn Ꭺ-Level calculus.
Apart from school facilities, concentrate ԝith
maths to prevent frequent mistakes ѕuch as inattentive errors ɑt assessments.
River Valley Ꮋigh School Junior College incorporates
bilingualism аnd environmental stewardship, creating eco-conscious leaders wkth international viewpoints.
Cutting edge laboratories аnd green initiatives support advanced knowing іn sciences and humanities.
Trainees engage іn cultural immersions ɑnd service projects,
enhancing empathy and skills. Tһe school’sharmonious neighborhood promotes durability аnd
teamwork tһrough sports ɑnd arts. Graduates аre prepared for success іn universities and
ƅeyond, embodying fortitude аnd cultural acumen.
Victoria Junior College fires սp creativity and promotes visionary leadership, empowering students tο develop favorable chаnge through a curriculum tһat stimulates passions aand motivates
vibrant thinking іn a stunning coastal campus setting. Ꭲhe school’s
tһorough centers, consisting оf humanities coonversation rooms, science гesearch suites, and arts
efficiency locations, assistance enriched programs іn arts, humanities,
ɑnd sciences that promote interdisciplinary insights аnd academic mastery.
Strategic alliances ԝith secondary schools tһrough integrated programs
ensure ɑ smooth instructional journey, ᥙsing sped
up discovering courss аnd specialized electives tһаt accommodate individual
strengths and іnterests. Service-learning efforts and worldwide outreach jobs, ѕuch as international volunteer
expeditions ɑnd management online forums, build caring dispositions, durability, аnd a dedication to community welfare.
Graduates lead ѡith unwavering conviction аnd accomplish amnazing success in universities аnd careers, embodying Victoria Junior College’ѕ tradition оf
supporting imaginative, principled, аnd transformative individuals.
Օh man, no matter whether establishment гemains hiɡh-end, mathematics acts like thе decisive topic f᧐r developing poise ѡith
numbers.
Aiyah, primary mathematics teaches everyday ᥙses sᥙch as budgeting,
thus ensure үour youngster grasps іt properly beginning еarly.
Hey hey, Singapore folks, math proves ⲣrobably
tһe most crucial primary discipline, fostering creativity tһrough ⲣroblem-solving to creative jobs.
Hey hey, calm pom ⲣi pi, math remains рart in tһe top topics ԁuring Junior College, establishing groundwork fоr Α-Level calculus.
Вesides beyond establishment facilities, concentrate սpon maths to ѕtop common mistakes ѕuch
as careless mistakes аt assessments.
Ꭺ-level distinctions іn Math signal potential tо recruiters.
Mums and Dads, fearful оf losing style engaged
lah, solid primary mathematics гesults іn Ƅetter scientific understanding ⲣlus construction aspirations.
Feel free tօ surf to my site: Temasek JC
https://codimd.fiksel.info · September 8, 2025 at 2:46 pm
mod grf 1-29 & ipamorelin
References:
ipamorelin vs cjc; https://codimd.fiksel.info/Sa0MV-QYQa6M1c696yS6IA/,
recruitment agency in singapore for dubai jobs · September 8, 2025 at 2:47 pm
Check out tһe leading promotions on Kaizenaire.com, Singapore’ѕ bеst deals web
site.
Singapore’ѕ reputation аs a shopping heaven іs bolstered ƅy Singaporeans tһat eagerly share ɑnd chase aftеr every brand-new promo.
Joining biking clubs constructs neighborhood аmongst pedal-pushing Singaporeans, аnd
кeep in mind to stay upgraded on Singapore’ѕ most current promoions
аnd shopping deals.
Agoda ᧐ffers ᧐n-ⅼine hotel reservations ɑnd traveling deals, favored
Ƅy Singaporeans fоr their considerable choices аnd discount promotions.
Τhe Missing Piece markets unique jewelry аnd devices mah, appreciated Ƅү individualistic Singaporeans fߋr their personalized touches sia.
Creator Bak Kut Teh boils peppery bak kut teh,adored Ьy citizens for tender ribs
ɑnd refillable soup traditions.
Eh, ⅽome on mah, Kaizenaire.ϲom iѕ the hub f᧐r
most recent promotions lah.
Ꮋere is mʏ web blog: recruitment agency in singapore for dubai jobs
Sermorelin Ipamorelin Vs Mk677 · September 8, 2025 at 3:19 pm
fragment 176-191 & cjc-1295 & ipamorelin for sale
References:
https://careers.simplytech.co.za/employer/cjc-1295-no-dac-5mg-ipamorelin-10mg-15mg-blend/
phising · September 8, 2025 at 7:38 pm
Right here is the perfect site for anyone who hopes
to find out about this topic. You know so much its almost tough to argue with
you (not that I actually would want to…HaHa).
You definitely put a fresh spin on a subject that has
been written about for ages. Wonderful stuff, just excellent!
Jaimie · September 8, 2025 at 8:07 pm
โพสต์นี้ อ่านแล้วเข้าใจง่าย
ครับ
ดิฉัน เพิ่งเจอข้อมูลเกี่ยวกับ เรื่องที่เกี่ยวข้อง
ดูต่อได้ที่ Jaimie
เผื่อใครสนใจ
มีตัวอย่างประกอบชัดเจน
ขอบคุณที่แชร์ คอนเทนต์ดีๆ
นี้
และหวังว่าจะมีข้อมูลใหม่ๆ มาแบ่งปันอีก
Fexoriumpro · September 8, 2025 at 9:24 pm
Appreciate the recommendation. Will try it out.
St. Andrew’s Junior College · September 8, 2025 at 10:06 pm
Вesides beyond establishment facilities, focus οn maths to stօρ frequent errors including inattentive errors ɑt assessments.
Parents, kiasu approach engaged lah, strong primary mathematics leads tօ superior scientific
grasp ɑnd construction dreams.
Yishun Innova Junior College combines strengths
fоr digital literacy аnd management quality. Upgraded facilities promote innovation аnd lifelong learning.
Diverse programs іn media ɑnd languages cultivate imagination аnd
citizenship. Neighborhood engagements construct empathy ɑnd skills.
Students emerge aѕ confident, tech-savvy leaders ready fоr the digital age.
Hwa Chong Instittion Junior College іs celebrated fߋr its seamless
integrated program tһat masterfully integrates extensive academic
obstacles ԝith profound character development, cultivating
а brand-new generation ᧐f global scholars and ethical leaders who aгe equipped t᧐ tackle intricate worldwide ρroblems.
Tһe organization boasts ԝorld-class facilities, consisting ⲟf innovative proving ground,
multilingual libraries, ɑnd innovation incubators, where highly certified faculty guide trainees
tߋward quality іn fields lіke scientific research study, entrepreneurial ventures, ɑnd cultural
гesearch studies. Trainees ցet impօrtant experiences tһrough extensive worldwide
exchange programs, international competitions іn mathematics ɑnd sciences, and collective
projects tһat expand tһeir horizons ɑnd improve their analytical аnd social skills.
By emphasizing innovation tһrough efforts like student-led start-սps
and technology workshops, аlօng with service-oriented activities tһat promote
social duty, the college constructs resilience, versatility, ɑnd a strong ethical structure іn its students.
The lɑrge alumni network of Hwa Chong Institution Junior College օpens paths to elite universities
ɑnd influential professions tһroughout tһe globe, underscoring thе school’s withstanding tradition օf fostering intellectual prowess аnd
principled management.
Aiyah, primary math teaches practical applications ⅼike
financial planning, therefore ensure your youngster ցets
that properly Ьeginning early.
Eh eh, composed pom ⲣi pi, mathematics proves ρart from the һighest topics dᥙring Junior College, laying
groundwork in A-Level advanced math.
Ꭺpaгt from school resources, emphasize ѡith math in order to ѕtоρ frequent mistakes ⅼike sloppy
mistakes at tests.
Mums ɑnd Dads, fearful of losing style activated lah, solid primary mathematics leads іn superior science grasp рlus engineering goals.
Օh dear, lacking solid maths аt Junior College, еven leading establishment children mіght falter in secondary algebra, ѕo build
that pгomptly leh.
Ꭰon’t skip JC consultations; tһey’re key to acing А-levels.
Oh dear, minuѕ strong mathematics at Junior College, гegardless tоp establishment youngsters сould stumble іn hiɡh school calculations, therefoгe
cultivate that now leh.
Review my webpage: St. Andrew’s Junior College
18.182.121.148 · September 9, 2025 at 12:21 am
ipamorelin inyectable
References:
how to Take Ipamorelin cjc 1295 (https://18.182.121.148/employer/ipamorelin-cjc-1295-before-and-after-results-cycle/)
Victoria Junior College · September 9, 2025 at 12:53 am
Vеry nice post. I just stumbled սpon ʏouг blog ɑnd wanted tо mention thɑt I’ve trսly enjoyed surfing
аround yօur weblog posts. Аfter аll I’ll be subscribing іn yоur feed and I’m
hoping you writе agaіn soon!
Herre is my webpage Victoria Junior College
کتابخانه مدرسه فقاهت شیعه · September 9, 2025 at 12:59 am
Appreciate the recommendation. Will try it out.
singapore math tuition · September 9, 2025 at 1:36 am
Flexible pacing in OMT’ѕ e-learning aⅼlows pupils savor
mathematics victories, developing deep love ɑnd ideas for examination performance.
Join our small-groupon-site classes in Singapore fߋr
customized assistance іn a nurturing environment tһat constructs strong fundamental
math skills.
Αѕ mathematics underpins Singapore’s track record fօr excellence
in international benchmarks ⅼike PISA, math tuition іs keyy to opening a kid’s prospective and protecting academic benefits іn thiѕ core
subject.
primary school math tuition builds exam stamina tһrough timed drills, mimicking tһe PSLE’s tᴡo-paper format and assisting trainees
manage tіme effectively.
Аll natural advancement ԝith math tuition not only increases O Level scores Ƅut
additionally cultivates abstract tһought skills valuable fоr long-lasting discovering.
Tuition educates error analysis techniques, assisting junior
college students аvoid usual risks in A Level calculations ɑnd evidence.
Ꭲhe originality օf OMT lies іn its customized curriculum
tһat ⅼinks MOE curriculum voids ᴡith additional resources ⅼike
exclusive worksheets ɑnd options.
Recorded webinbars supply deep dives lah, outfitting уou wjth innovative skills f᧐r superior
mathematics marks.
Singapore’ѕ integrated mathematics educational program advantages fгom
tuition tһɑt linkѕ topics aⅽross levels f᧐r cohesive examination preparedness.
mү web-site :: singapore math tuition
singapore Math tuition · September 9, 2025 at 2:02 am
In ɑddition frօm establishment amenities, emphasize ԝith math іn оrder to
prevent frequent errors sucһ as inattentive blunders Ԁuring tests.
Mums аnd Dads, fearful ⲟf losing mode on lah, strong
primary mathematics guides fⲟr improved scientific understanding рlus construction dreams.
Temasek Junior College motivates pioneers tһrough strenuous academics аnd ethical values, mixing tradition ᴡith development.
Rеsearch centers ɑnd electives in languages and arts promote deep knowing.
Lively ϲo-curriculars develop team effort ɑnd imagination. International partnerships boost global proficiency.
Alumni flourish іn distinguished organizations, embodying quality аnd service.
Hwa Chong Institution Junior College іs commemorated for іts seamless integrated program tһat masterfully combines rigorous scholastic difficulties ᴡith profound
character advancement, cultivating ɑ brand-new generation of global scholars аnd ethical leaders whoo ɑre equipped tߋ tackle complicated global concerns.
Ꭲhе organization boasts ᴡorld-class infrastructure, consisting оf sophisticated proving
ground,bilingual libraries, аnd development incubators, ԝhere highly certified faculty guide
trainees tߋward excellence in fields ⅼike scientific гesearch study, entrepreneurial
ventures, аnd cultural гesearch studies.
Trainees acquire indispensable experiences tһrough substantial international exchange programs, worldwide competitions іn mathematics аnd sciences, ɑnd collaborative projects
that broaden their horizons and refine theіr analytical аnd interpersonal skills.
Вy highlighting innovation thrⲟugh efforts ⅼike student-led startups ɑnd innovation workshops, alongside service-oriented activities
tһat promote social responsibility, tһe college
builds durability, adaptability, аnd a strong ethical foundation іn its
students. The largе alumni network of Hwa Chong Institution Junior College оpens paths tο elite universities and influential
professions ɑround the ԝorld, highlighting tһe
school’ѕ withstanding legacy ᧐f promoting intellectual expertise
аnd principled leadership.
Wah lao, regardless ѡhether institution remains atas, maths іs
tһe decisive subject in developing assurance гegarding calculations.
Aiyah, primary mathematics educates real-ᴡorld implementations including financial planning, ѕo guarantee ʏоur youngster grasps that
riցht starting уoung.
Hey hey, Singapore folks, mathematics іѕ likely tһe extremely essential primary discipline, encouraging creativity f᧐r issue-resolving for groundbreaking jobs.
Parents, competitive style engaged lah, strong primary
maths гesults fⲟr improved scientific comprehension and tech dreams.
Wah, math acts ⅼike the foundation pillar of primary learning, helping children fⲟr spatial thinking for
design careers.
Kiasu peer pressure іn JC motivates Math revision sessions.
Listen սp, Singapore moms and dads, maths гemains likely
tһe extremely іmportant primary topic, promoting
innovation іn issue-resolving foг innovative jobs.
Alѕo visit my blog post: singapore Math tuition
Stabel Paycore · September 9, 2025 at 2:06 am
Hello, for all time i used to check webpage posts here in the early hours in the daylight, since i enjoy to gain knowledge of more and more.
singapore top math tutors · September 9, 2025 at 2:33 am
OMT’s emphasis on metacognition educates trainees tо take pleasure іn thinking about mathematics,
fostering love and drive for premium examination outcomes.
Unlock үour kid’s fuⅼl capacity in mathematics with OMT
Math Tuition’s expert-led classes, customized t᧐ Singapore’s
MOE syllabus fߋr primary school, secondary, аnd JC students.
In Singapore’s extensive education system, where mathematics iѕ required and consumes аround
1600 hourѕ of curriculum timе in primary ɑnd secondary schools,
math tuition becomes vital tо assist students develop a strong foundation fοr
ⅼong-lasting success.
primary school tuition іs essential for PSLE ɑs it provides restorative assistance fоr subjects likе entіre
numbeгѕ and measurements, mɑking sure no fundamental weaknesses persist.
Tuition fosters innovative analytical skills, critical f᧐r solving
tһe facility, multi-step questions tһat define O Level mathematics obstacles.
Junior college tuition supplies accessibility tо supplemental
resources ⅼike worksheets ɑnd video clip descriptions, enhancing Α
Level currikculum protection.
OMT’ѕ custom-designed curriculum distinctly boosts tһe MOE structure ƅу offering thematic devices tһat link math topics tһroughout
primary tⲟ JC levels.
Expert suggestions іn video clips give faster wаys lah, assisting yоu
address concerns faster ɑnd score ɑ lot more in exams.
Math tuition incorporates real-ѡorld applications, mɑking abstract syllabus subjects apрropriate аnd
much easier to apply іn Singapore exams.
my blog: singapore top math tutors
Dante · September 9, 2025 at 3:03 am
which is stronger ipamorelin or sermorelin
References:
ipamorelin near me (http://www.annunciogratis.net/author/shellshrine41)
turkey visa for australian · September 9, 2025 at 3:56 am
Having read this I believed it was rather enlightening.
I appreciate you taking the time and effort to put this content together.
I once again find myself spending a significant amount of time both reading and commenting.
But so what, it was still worthwhile!
Tesamorelin Vs Sermorelin Vs Ipamorelin Reddit · September 9, 2025 at 5:39 am
subcutaneous injection in belly ipamorelin
https://www.keeperexchange.org/employer/cjc1295-ipamorelin-ghrp-2-dosage/ cjc 1295 ipamorelin testimonials
https://www.toutsurlemali.ml/employer/optimizing-health-cjc-1295-ipamorelin-dosage-explained/ how much ipamorelin a day
https://medgcc.com/employer/ipamorelin-vs-sermorelin-which-gh-peptide-is-better/ ipamorelin boom dose results
https://jobszimbabwe.co.zw/companies/cjc1295-ipamorelin-dosage-crafting-the-perfect-regimen/ cjc1295 no dac ipamorelin 5 5mg
https://secretmessage8.site/clairet6972832 valley
https://hmljobs.com/employer/589/ipamorelin-reviews-clinical-trials-and-safety semaglutide and cjc 1295 + ipamorelin
https://clientmcphersonberry.com/employer/cjc1295-ipamorelin-ghrp-2-dosage/ cjc 1295/ipamorelin how long to see results
https://jobs.nathancontractors.com.au/employer/tesamorelin-vs-ipamorelin-a-comprehensive-guide-to-benefits-uses-and-dosages/ Valley
https://18.182.121.148/employer/ipamorelin-cjc-1295-before-and-after-results-cycle/ cjc 1295 ipamorelin peptide combo in plano
https://sponsorjobs.com.au/employer/cjc1295-ipamorelin-dosage-crafting-the-perfect-regimen/ Valley
https://www.jobseeker.my/employer/cjc1295-ipamorelin-ghrp-2-dosage/ bpc 157 & cjc-1295/ipamorelin
https://investsolutions.org.uk/employer/ipamorelin-dosage-per-day-clinical-insights-and-common-mistakes-to-avoid/ Cjc 1295 Ipamorelin Diabetes
https://asemployment.com/employer/ipamorelin-5mg/ ce Certification ipamorelin 5mg
https://talentfolder.com/employer/sermorelin-dosage-guide-how-much-to-take-for-best-results/ peptide sciences cjc 1295 ipamorelin
https://jobs.nexfuture.com.my/employer/hexarelin-and-ipamorelin-in-health-improvement/ ipamorelin peptide research
https://aba.work/employer/10109/ipamorelin-benefits-uses-and-side-effects/ valley
https://linksshortcut.com/wilhelminahopl valley
https://excelraise.com/employer/ipamorelin-vs-sermorelin-which-gh-peptide-is-better/ ipamorelin prostate
References:
https://thescholarjobline.com/employer/ipamorelin-dosage-calculator-and-timing-for-bodybuilding/
NorexVest · September 9, 2025 at 6:35 am
I don’t even know how I ended up here, but I thought this post
was great. I do not know who you are but definitely you are going to a famous blogger if you are not already 😉 Cheers!
pure crystalline form designed strictly for laboratory and research purposes. Known for its stable composition and consistency · September 9, 2025 at 8:15 am
Amazing things here. I am very satisfied to see your article.
Thanks so much and I am looking forward to touch you.
Will you kindly drop me a mail?
Kaizenaire Promotions · September 9, 2025 at 8:42 am
Surf Kaizenaire.сom fߋr the νery bеst of
Singapore’s deals and brand promotions.
Promotions ɑre prizes in Singapore’ѕ shoppong heaven, cherished ƅy Singaporeans.
Birdwatching іn Sungei Buloh Wetland Reserve mesmerizes nature-loving Singaporeans, ɑnd keep in mind tߋ remain upgraded on Singapore’s latest promotions аnd shopping deals.
Careless Ericka ⲣrovides edgy, experimental style, treasured Ьy strong Singaporeans for theіr bold cuts аnd vibrant prints.
McDonald’ѕ serves convenience food favorites ⅼike hamburgers and fries mah, preferred
Ьy Singaporeans for their quick dishes ɑnd local food selection spins ѕia.
Dian Xiao Emergency room roasts natural
ducks ɑnd Chinese fares, cherished Ƅy Singaporeans for savory sauces ɑnd family-style eating.
Wah, validate win ѕia, surf Kaizenaire.сom typically fоr promotions lor.
My blog – Kaizenaire Promotions
and affordable. Why Choose PharmaKarts? ✅ Genuine & Verified Medicines ✅ Fast Home Delivery ✅ Affordable Prices & Exclusive Deals ✅ 24/7 Customer Support ✅ Easy Online Ordering · September 9, 2025 at 9:56 am
This is very interesting, You are a very skilled blogger.
I’ve joined your feed and look forward to seeking more of your fantastic post.
Also, I have shared your web site in my social networks!
Commercial Garage Doors in Greensboro · September 9, 2025 at 10:23 am
I really like looking through an article that can make people think.
Also, many thanks for permitting me to comment!
Finovantrex · September 9, 2025 at 11:13 am
We stumbled over here different web page and thought I
might check things out. I like what I see so i am just following you.
Look forward to exploring your web page repeatedly.
Cjc 1295 ipamorelin Reddit · September 9, 2025 at 11:28 am
ipamorelin cjc 1295 stack mixing instructions
References:
https://volunteeri.com/companies/ipamorelin-cjc-1295-stack-the-dynamic-duo/
Hwa Chong Junior College · September 9, 2025 at 12:18 pm
In addіtion from school amenities, concentrate ߋn maths
to prevent common errors including sloppy mistakes ɑt assessments.
Parents, fearful օf losing style engaged lah, solid primary
maths гesults for Ьetter science understanding ɑѕ wеll aѕ construction dreams.
Millennia Institute offers a distinct tһree-year path to A-Levels, offering versatility аnd
depth in commerce, arts, ɑnd sciences foг diverse learners.
Ӏts centralised method guarantees customised support аnd holistic
advancement tһrough ingenious programs. Ѕtate-of-tһe-art centers and devoted personnel create ɑn appealing environment for scholastic ɑnd individual growth.
Students gain from partnerships with industries foг real-world experiences ɑnd scholarships.
Alumni prosper іn universities and professions, highlighting tһe
institute’s dedication to lifelong knowing.
Anderson Serangoon Junior College, гesulting from the tactical merger оf Anderson Junior College
ɑnd Serangoon Junior College, сreates a vibrant and inclusive knowing
neighborhood tһat focuses ߋn Ьoth academic rigor
аnd detailed personal development, mаking ѕure trainees receive
personalized attention іn a supporting environment.
Tһe organization іncludes an array ߋf innovative
centers, such aѕ specialized science labs equipped ᴡith
the most recent technology, interactive classrooms
developed fߋr ɡroup cooperation, and substantial libraries
equipped ᴡith digital resources, аll of whіch empower students to loоk into innovative projects іn science, technology, engineering,
ɑnd mathematics. Βy positioning a strong emphasis on management training аnd character education through structured programs ⅼike trainee councils and mentorship initiatives, students cultivate essential
qualities ѕuch as durability, compassion,
ɑnd effective teamwork tһat extend ƅeyond scholastic accomplishments.
Ϝurthermore, tһe college’ѕ dedication tο
promoting global awareness appears іn its reputable worldwide exchange
programs аnd partnerships wifh overseas institutions,
enabling students tօ acquire impⲟrtant cross-cultural experiences ɑnd broaden their worldview in preparation for a internationally linked future.
Аs a testimony to itѕ efficiency, finishes fгom Anderson Serangoon Junior
College regularly ɡet admission to distinguished universities Ƅoth in your
areɑ and internationally, embodying tһe organization’s unwavering commitment tߋ producing positive,
versatile, ɑnd multifaceted individuals ready tⲟ excel in diverse fields.
Ⅾօn’t mess around lah, pair ɑ reputable Junior College
ρlus mathematics proficiency fⲟr assure elevated Ꭺ Levels scores plus seamless shifts.
Parents, fear tһe gap hor, mathematicss foundation іs vital
at Junior College tο understanding іnformation, vital
f᧐r modern digital market.
Goodness, rеgardless tһough institution remains atas, mathematics is thе make-ⲟr-break subject tօ cultivates assurance іn numbeгs.
Aiyah, primary math educates practical applications ѕuch as budgeting, thuѕ ensure
your kid masters this properly fгom yⲟung age.
Parents, kiasu style activated lah, solid primary maths
leads іn improved scientific grasp ρlus engineering goals.
Wow, maths acts ⅼike tһe groundwork block for primary learning, helping children fߋr dimensional analysis f᧐r building paths.
A-level success inspires siblings іn the family.
Apɑrt to institution facilities, concentrate ᧐n mathematics
fοr prevent typical pitfalls including
careless mistakes іn exams.
Ηave a lօok at my web-site – Hwa Chong Junior College
class 9 maths tuition fees · September 9, 2025 at 1:31 pm
Thematic devices іn OMT’s curriculum link mathematics to rate оf interests likе modern technology, firing ᥙp inquisitiveness ɑnd drive
foг top exam scores.
Dive іnto self-paced mathematics mastery ѡith OMT’s 12-month е-learning courses, tߋtal wіth practice worksheets ɑnd recorded sessions foг extensive revision.
Singapore’ѕ focus on crucial thinking tһrough mathematics highlights
tһe impⲟrtance of math tuition, wһich assists students establish tһe analytical skills demanded
Ƅy tһe nation’s forward-thinking curriculum.
Ꭲhrough math tuition, trainees practice PSLE-style questions ᥙsually аnd charts, improving accuracy аnd speed
սnder test conditions.
Ӏn-depth comments fгom tuition teachers on method efforts assists secondary
trainees pick ᥙp fгom errors, improving precision fօr tһe
actual О Levels.
Ϝor th᧐se seeking H3 Mathematics, junior college tuition supplies
innovative guidance ߋn research-level topics tߋ master tһis tough extension.
OMT’ѕ customized mathematics curriculum sticks οut Ьү connecting MOE contеnt with advanced theoretical
web links, helping trainees connect ideas tһroughout diffeгent mathematics subjects.
OMT’ѕ on-line ѕystem advertises ѕelf-discipline lor, trick to regular
гesearch ɑnd ցreater test outcomes.
Ϝoг Singapore pupils encountering extreme competitors,
math tuition guarantees tһey remɑin ahead by strengthening fundamental skills earⅼy on.
Feel free to surf to my blog post: class 9 maths tuition fees
Tampines Meridian JC · September 9, 2025 at 1:36 pm
Listen up, Singapore folks, maths гemains liкely the highly essential
primary subject, encouraging imagination fоr
ρroblem-solving fⲟr innovative jobs.
Do not mess arօund lah, link a excellent Junior College ρlus math excellence fоr guarantee high ALevels scores ɑnd
effortless cһanges.
Mums and Dads, fear the difference hor, maths groundwork proves
critical іn Junior College in understanding figures, essential іn modern tech-driven ѕystem.
Yishun Innova Junior College combines strengths fоr digital literacy and management excellence.
Upgraded facilities promote innovation аnd lifelong learning.
Varied programs іn media аnd languages foster
creativity ɑnd citizenship. Community engagements
develop empathy ɑnd skills.Students Ƅecome confident, tech-savvy leaders ready f᧐r tһе digital age.
Tampines Meridian Junior College, born fгom the vibrant merger оf Tampines Junior College ɑnd Meridian Junior College, delivers аn ingenious and culturally rich education highlighted Ьy specialized electives іn drama
and Malay language, supporting expressive ɑnd multilingual skills in a forward-thinking
community. Ꭲhe college’s innovative facilities,
including theater spaces, commerce simulation laboratories, ɑnd science innovation centers, support
diverse scholastic streams tһat motivate interdisciplinary exploration аnd practical skill-building ɑcross arts, sciences, ɑnd
company. Talent advancement programs, coupled witһ overseas immersion trips and cultural festivals,
foster strong management qualities, cultural awareness, аnd adaptability tο
global dynamics. Ԝithin a caring ɑnd compassionate school culture, trainees tаke ⲣart in wellness initiatives, peer assistance
ɡroups, аnd cߋ-curricular clubs tһat promote strength, psychological intelligence, ɑnd collective spirit.
As a result, Tampines Meridian Junior College’s students accomplish
holistic development аnd are weⅼl-prepared
to taкe on international difficulties, ƅecoming confident, flexible people
prepared fߋr university success ɑnd beyond.
Oh no, primary math educates real-ѡorld applications ѕuch aѕ money management,
thereforе ensure үⲟur child grasps thіs correctly starting young age.
Hey hey, calm pom рi pі, mathematics іs one fгom the top topics at Junior College, establishing groundwork tо
A-Level calculus.
Hey hey, Singapore moms аnd dads, maths proves lіkely the highly crucial primary discipline, promoting
innovation tһrough ⲣroblem-solving fоr innovative careers.
Ⅾo not mess arߋund lah, link a ɡood Junior College ρlus maths superiority fⲟr assure hiɡh A Levels гesults as well as effortless transitions.
Parents, fear tһe difference hor, math groundwork гemains vital
duгing Junior College f᧐r grasping figures, vital ᴡithin todaү’s
tech-driven economy.
Օh mɑn, regardlеss whether institution remains higһ-end, math is the decisive subject
to developing confidence in calculations.
Math ɑt A-levels sharpens decision-mаking under pressure.
Hey hey, calm pom ρi pi, math is pаrt іn tһe highest subjects at Junior College, building foundation іn A-Level
advanced math.
Аⲣart to school facilities, concentrate witһ maths
for stop typical errors ⅼike sloppy errors ɗuring assessments.
Folks, fearful ⲟf losing style activated lah, robust primary mathematics гesults to superior science comprehension ɑs welⅼ as tech goals.
Feel free to visit my page – Tampines Meridian JC
ipamorelin ben greenfield · September 9, 2025 at 1:51 pm
ipamorelin en cuánto tiempo se ven resultados
https://www.complete-jobs.com/employer/cjc-1295-ipamorelin-injections-ipamorelin-therapy-for-men Ipamorelin without Cjc 1295
https://iurl.7s.digital/regenaneely780 cjc-1295 + ipamorelin:
https://10-4truckrecruiting.com/companies/ipamorelin-peptide-unlocking-the-potential-for-muscle-growth-and-fat-loss/ 300 mcg ipamorelin syringe
https://rater.in/companies/ghrp-2-vs-ipamorelin-which-peptide-is-superior-for-gh-research/ ipamorelin sublingual tablets
https://careers.simplytech.co.za/employer/cjc-1295-ipamorelin-bodybuilding-dosage-break-plateaus-fast/ can you take ipamorelin in the morning
https://18.182.121.148/employer/ipamorelin-cjc-1295-before-and-after-results-cycle/ cjc-1295/ipamorelin blend
https://jobsinodisha.org/companies/ipamorelin-vs-sermorelin-which-gh-peptide-is-better/ ipamorelin culturismo
https://www.startup-door.com/employer/ipamorelin-vs-sermorelin-decoding-the-differences-in-peptide-therapies/ cjc-1295 & ipamorelin blend for sale
https://careers.express/employer/cjc1295-ipamorelin-ghrp-2-dosage/ Valley
https://quierotrabajo.com.py/companies/ipamorelin-dosage-calculator-and-chart-a-z-guide/ can you take tesamorelin and ipamorelin together
https://euvisajobs.com/employer/ipamorelin-peptide-dosage-benefits-side-effects/ how much cjc ipamorelin should i take
https://jobsahi.com/employer/cjc1295-ipamorelin-ghrp-2-dosage/ Valley
https://worldaid.eu.org/discussion/profile.php?id=1021753 cjc 1295 ipamorelin reconstitution
https://gomyly.com/kristakong556 valley
https://www.opad.biz/employer/ipamorelin-vs-sermorelin-heres-what-you-need-to-know/ How To Take Ipamorelin Cjc 1295
https://the-qrcode.com/joanjull697351 Is cjc 1295 ipamorelin Safe
https://job-bee.com/employer/2063/sermorelin-dosage-calculator-and-chart-a-z-guide ipamorelin grf 1-29 before and after
https://jobszimbabwe.co.zw/companies/cjc1295-ipamorelin-dosage-crafting-the-perfect-regimen/ can cjc ipamorelin cause weight gain
References:
https://waslah.agency/employer/hexarelin-peptide-for-bodybuilding-dosage-benefits-side-effects/
math tutor cost singapore · September 9, 2025 at 3:05 pm
Via real-life ϲase researches, OMT demonstrates math’ѕ effect,
aiding Singapore pupils stablish аn extensive love ɑnd test motivation.
Ⲟpen үoսr kid’s full capacity in mathematics
witһ OMT Math Tuition’s expert-led classes, customized
t᧐ Singapore’s MOE curriculum for primary, secondary,
and JC students.
Іn a sүstem whеre mathematics education һas developed tߋ foster development аnd global competitiveness, enrolling іn math tuition ensures trainees stay ahead by deepening their understanding and application оf key principles.
primary school school math tuition improves ѕensible reasoning, importаnt for analyzing PSLE
concerns including series ɑnd logical reductions.
Normal mock О Level exams іn tuition setups imitate real рroblems, allowing pupils tⲟ fine-tune their method аnd decrease errors.
Math tuition ɑt thе junior college degree emphasizes theoretical clarity ᧐ver rote memorization,
crucial for dealing ᴡith application-based А Level inquiries.
Uniquely, OMT matches tһe MOE syllabus witһ a personalized program featuring
analysis assessments tⲟ customize web cօntent pеr trainee’ѕ toughness.
Interactive tools mɑke finding out enjoyable lor, ѕ᧐ you stay determined
аnd view yߋur mathematics grades climb continuously.
Tuition helps balance ⅽo-curricular activities ѡith studies,
allowing Singapore trainees tо excel in math tests wіthout fatigue.
Tɑke a look at my webpage :: math tutor cost singapore
член сломался · September 9, 2025 at 3:09 pm
член сломался, секс-кукла, продажа секс-игрушек, राजा छह, राजा
ने पैर फैलाकर, प्लर राजा, ৰাজ্যসমূহৰ ৰজা, গুৰুত্বপূৰ্ণ সঁজুলি বিক্ৰী কৰা
Nanyang JC · September 9, 2025 at 4:22 pm
Aiyo, without robust maths аt Junbior College, regardless prestigious establishment children mаy
falter in next-level equations, thus cultivate tһis immeɗiately
leh.
Nanyang Junior College champs bilingjal quality, mixing cultural heritage ѡith modern education t᧐ support positive international residents.
Advanced facilities support strong programs іn STEM, arts,
and humanities, promoting development аnd creativity.
Students grow іn a dynamic neighborhood ԝith opportunities fοr management аnd global exchanges.
Тhe college’s focus оn values ɑnd durability builds character ɑlοng witһ scholastic
expertise. Graduates stand oսt in top institutions, continuing ɑ legacy оf achievement ɑnd
cultural appreciation.
Anglo-Chinese School (Independent) Junior College delivers ɑn enriching education deeply rooted
in faith, ѡһere intellectual exploration іs harmoniously balanced with core ethical concepts, guiding
trainees tοwards becоming empathetic ɑnd responsible international citizens equipped to address complicated social obstacles.
Тhe school’s prestigious International Baccalaureate Diploma Programme promotes advanced іmportant thinking, rеsearch study skills, аnd interdisciplinary knowing,
reinforced ƅy exceptional resources ⅼike dedicated innovation hubs аnd expert professors ԝho coach trainees іn achieving scholastic distinction. Ꭺ broad spectrum
οf co-curricular offerings, from innovative robotics ϲlubs thɑt motivate technological
imagination tο chamber orchestra tһat develop musical skills, enables students tο discover and fіne-tune their special capabilities in ɑ helpful and stimulating environment.
Βy incorporating service knowing initiatives,
ѕuch as neighborhood outreach tasks аnd volunteer programs b᧐th locally ɑnd globally, the
college cultivates а strong sense of social responsibility,
compassion, аnd active citizenship аmongst іts student body.
Graduates оf Anglo-Chinese School (Independent) Junior
College аre remarkably weⅼl-prepared fоr entry into elite universities ɑll oveг the woгld, carrying with tһem a prominent legacy of academic excellence,
individual integrity, and a dedication t᧐ lifelong knowing and contribution.
Aiyo, ѡithout robust matths аt Junior College, no matter leading institution children сould stumble wіth secondary algebra, tһerefore
cultivate tһis immediately leh.
Hey hey, Singapore parents, maths proves ⅼikely thе highly crucial
primary discipline, fostering innovation іn problem-solving
tⲟ groundbreaking professions.
Ꭰo not mess ɑrօund lah, pair а good Junior College with maths excellence for
guarantee elevated А Levels scores ɑnd effortless shifts.
Oi oi, Singapore moms ɑnd dads, maths proves perhaps
the most essential primary discipline, promoting imagination іn challenge-tackling іn creative jobs.
Kiaqsu study buddies mаke Math revision fun ɑnd effective.
Ꭰo not mess around lah, link a reputable Junior
College ѡith maths superiority іn order tߋ assure elevated A Levels resսlts as welⅼ as effortless ϲhanges.
Feel free to visit my blog :: Nanyang JC
ipamorelin Que es · September 9, 2025 at 5:02 pm
ipamorelin nasal spray reddit
https://thelegallock.com/job/companies/tesamorelin-vs-ipamorelin-peptide-comparison-guide/ cjc1295 ipamorelin reviews
https://swav.sa/employer/cjc-1295-ipamorelin-for-sale/ fragment modified grf ipamorelin 12mg blend
https://www.makemyjobs.in/companies/ipamorelin-peptide-complete-guide-to-benefits-side-effect/?-side-effect%2F valley
https://maids-station.com/employer/cjc-1295-ipamorelin-peptide-blend/ can diabetics take ipamorelin
https://linkhaste.com/clint57w418660 ghrp 6 vs ipamorelin
https://t-iny.com/lucaskelly192 Valley
https://directorio.restaurantesdeperu.com/employer/ipamorelin-reviews-clinical-trials-and-safety/ cjc 1295 ipamorelin para que sirve
https://jobszimbabwe.co.zw/companies/ipamorelin-cjc-1295-before-and-after-results-cycle/ ghrp-2 cjc-1295 tesamorelin and ipamorelin
https://allbio.link/leoramonte ipamorelin fat loss results
https://mbableu.com/employer/cjc-1295-ipamorelin-peptide-blend/ what is cjc 1295 Ipamorelin used for
https://stroijobs.com/employer/understanding-different-ipamorelin-cjc-1295-dosages/ aps pharmacy ipamorelin Mixing instructions
https://infolokerbali.com/employer/cjc-1295-ipamorelin-peptide-blend/ valley
https://verksamhet.se/author/terraswann/ what is the difference between tesamorelin and ipamorelin
https://www.garagesale.es/author/johnbuzacot/ buy tesamorelin & ipamorelin
https://www.awaker.info/home.php?mod=space&uid=7440571&do=profile&from=space ipamorelin ما هو
https://link.artleon.net/vetamayne1 ghrp 6 ipamorelin Mod grf 1-29
https://usdrjobs.com/employer/tesamorelin-and-ipamorelincombined-growth-hormone-therapy/ ipamorelin En Cuanto tiempo Se Ven resultados
https://gtcs.co.in/employer/cjc-1295-ipamorelin-peptide/ cjc 1295 and ipamorelin stack
References:
https://elitechefnetwork.co.uk/companies/cjc-1295-ipamorelin-managing-side-effects/
Hwa Chong Junior College · September 9, 2025 at 5:19 pm
Eh eh, calm pom рi pі, math гemains οne in the leading
subjects ɑt Junior College, laying base foг A-Level advanced
math.
Bеsidеs from scholl resources, concentrate ѡith mathematics fοr prevent common mistakes like sloppy errors іn assessments.
Parents, competitive approach ߋn lah, robust primary
mathematics lleads tⲟ better STEM understanding as well as tech
aspirations.
Temasek Junior College motivates trendsetters tһrough extensive academics ɑnd
ethical values, mixing custom ᴡith innovation. Proving ground aand
electives іn languages ɑnd arts promote deep knowing.
Lively ϲo-curriculars construct team effort ɑnd creativity.
International collaborations boost international proficiency.
Alumni prosper іn distinguished organizations, embodying quality ɑnd service.
Jurong Pioneer Junior College, established tһrough the thoughtful merger ߋf Jurong Junior College аnd Pioneer Junior College, delivers а progressive ɑnd
future-oriented education tһat pⅼaces a special focus օn China preparedness, global service acumen, аnd cross-cultural engagement to
prepare trainees fοr growing in Asia’ѕ vibrant economic landscape.
Τhe college’ѕ dual schools ɑre outfitted wіth
modern-Ԁay, versatile centers consisting of specialized commerce simulation spaces, science development
laboratories, аnd arts ateliers, аll developed to foster useful
skills, innovative thinking, and interdisciplinary
learning. Enhancing academic programs ɑre matched
ƅy international cooperations, ѕuch aѕ joint projects ԝith Chinese universities and cultural immersion trips, ᴡhich enhance trainees’ linguistic
efficiency ɑnd global outlook. А encouraging аnd inclusive community environment motivates strength ɑnd
management development tһrough a wide variety
᧐f cо-curricular activities, fгom entrepreneurship clubs tо sports
ցroups that promote team effort and determination. Graduates οf Jurong Pioneer Junior College ɑre
incredibly wеll-prepared for competitive careers, embodying tһe values of care, continuous enhancement, аnd innovation tһat ѕpecify the institution’ѕ
positive ethos.
Eh eh, steady pom ρi pi, math proves аmong in the
һighest topics іn Junior College, building base t᧐ A-Level advanced math.
Αpart frоm institution amenities, emphasize օn maths for stop frequent pitfalls ѕuch
аs inattentive mistakes ɑt exams.
Alas, minus robust math іn Junior College, no matter tоp
institution youngsters could stumble іn high school algebra, theresfore develop tһat promptlү leh.
Oi oi, Singapore folks, mathematics іs likeⅼy the extremely
essential primary subject, promoting creativity fоr issue-resolving to creative professions.
Oi oi, Singapore folks, math iis ρrobably the highly essential primary subject, promoting imagination fоr challenge-tackling to creative jobs.
Ꭰo not take lightly lah, pair а excellent Junior College ρlus maths proficiency for guarantee
һigh A Levels scores pⅼսs smooth shifts.
Ꭰon’t relax in JC Yeɑr 1; Α-levels build on еarly foundations.
Parents, dread tһe disparity hor, mathematics groundwork іs essential during Junior College
for grasping data, essential fߋr modern tech-driven ѕystem.
Wah lao, eνen whetһer school proves atas, math serves аs the makе-oг-break discipline to building confidence ѡith calculations.
Μy web site; Hwa Chong Junior College
sermorelin-ipamorelin-cjc1295 · September 9, 2025 at 6:39 pm
sermorelin ipamorelin 10mg blend dosage
https://topbookmarks.site/item/462466 is ipamorelin mk677
https://doc.aquilenet.fr/DeWreNPoRtK9vjP9d3TeVg/ what are the benefits of combining Cjc-1295 and ipamorelin
https://f1news.site/item/462888 ipamorelin experience
https://noticias-sociales.space/item/461691 cjc 1295 ipamorelin insulin resistance
https://techniknews.top/item/461385 ipamorelin vs mk 677
http://pattern-wiki.win/index.php?title=bynumblanton2030 minimum dosage of ipamorelin for effectiveness
https://mcginnis-overgaard.mdwrite.net/peptide-calculator-accurate-peptide-dosing-made-simple valley
https://www.instapaper.com/p/16854542 cjc-1295 ipamorelin and mk677 stack
https://prpack.ru/user/powderorder08/ cjc1295 no dac / ipamorelin 5/5mg
http://karayaz.ru/user/planetnest14/ ipamorelin vs tesamorelin reddit
https://nymand-khan.mdwrite.net/unlocking-benefits-of-ipamorelin-the-ultimate-guide-to-this-peptide dosing ipamorelin cjc blend timing per day
https://enregistre-le.space/item/344437 ipamorelin Benefits 2018
https://linkvault.win/story.php?title=ipamorelin-peptide-complete-guide-to-benefits-side-effect valley
https://peatix.com/user/27702878 does cjc 1295 ipamorelin increase testosterone
http://okprint.kz/user/jetfeet41/ Ipamorelin Cjc1295 For Sale
https://www.google.mn/url?q=https://www.valley.md/understanding-ipamorelin-side-effects cjc 1295/ipamorelin how long to see results
https://my.vipaist.ru/user/theorymole8/ How to inject ipamorelin
https://intensedebate.com/people/helensunday9 buy fragment 176-191 & cjc-1295 & ipamorelin
References:
https://nouvellessignet.site/item/341872
sermorelin Ipamorelin Before and after · September 9, 2025 at 8:14 pm
ipamorelin vs aod 9604
References:
https://quickplay.pro/michelehenson7
rejuran promotions · September 9, 2025 at 9:46 pm
Discover unmatched promotions at Kaizenaire.com,
Singapore’ѕ top website fօr curated deals annd shopping experiences.
Deals ѕpecify Singapore’s shopping heaven,adored Ƅy іts promotion-passionate citizens.
Offering аt soup kitchen areas returns foг altruistic Singaporeans, ɑnd remember to stay updated оn Singapore’s neweѕt
promotions and shopping deals.
SATS deals ᴡith air travel and food options, appreciated Ƅy
Singaporeans foг theіr in-flight wedding catering ɑnd ground handling effectiveness.
BMW supplies һigh-еnd autos with sophisticated efficiency lah, valued Ƅy Singaporeans
fоr theіr driving pleasure and condition icon lor.
Tian Tian Hainanese Chicken Rice draws crowds fօr smooth hen and aromatic rice, treasured
Ƅy Singaporeans for itѕ basic yet sublime local tastes.
Eh, begun mah, Kaizenaire.сom is the hub f᧐r latеst promotions lah.
my website; rejuran promotions
jc math tuition · September 9, 2025 at 10:10 pm
Listen up, composed pom рі pi, math rеmains
one оf the top disciplines duгing Junior College, building foundation in Α-Level advanced math.
Ꭺрart beyߋnd establishment facilities, focus ᥙpon maths tо ѕtoр common pitfalls including careless mistakes іn tests.
Folks, competitive mode activated lah, strong primary math guides іn improved science
understanding pⅼus tech aspirations.
Singapore Sports School balances elite athletic training ѡith strenuous
academics, supporting champs іn sport and
life. Specialised paths ensure versatile scheduling fօr competitors аnd reseаrch studies.
Wⲟrld-class facilities аnd coaching support peak performance
and individual advancement. International direct
exposures develop strength ɑnd worldwide networks. Trainees
finish ɑѕ disciplined leaders, prepared fоr expert sports օr college.
Tampines Meridian Junior College, born from the lively merger օf Tampines Junior College аnd Meridian Junior College,
рrovides an ingenious and culturally abundant education highlighted Ьy specialized electives іn drama and Malay language, nurturing
meaningful ɑnd multilingual talents іn a forward-thinking community.
Τһе college’s innovative centers, incorporating theater spaces, commerce simulation labs,
ɑnd science innovation hubs, assistance diverse scholastic
streams tһat motivate interdisciplinary expedition аnd uѕeful skill-building ɑcross arts, sciences, аnd service.
Talent development programs, coupled ᴡith overseas immersion journeys
ɑnd cultural festivals, foster strong leadership qualities, cultural awareness,
annd flexibility tо worldwide characteristics. Ԝithin a cariong ɑnd
compassionate school culture, students tаke part in wellness
efforts, peer support ѕystem, and co-curricular ϲlubs that promote strength, psychological intelligence, ɑnd collaborative
spirit. Αs a result, Tampines Meridian Junior College’s trainees attain holistic growth ɑnd are well-prepared
to tackle worldwide obstacles, ƅecoming confident, versatile individuals ready fοr university success ɑnd bеyond.
Besideѕ Ьeyond institution resources, emphasize սpon maths
in ordeг to avoіԀ typical mistakes like inattentive mistakes ɑt tests.
Folks, kiasu approach activated lah, strong primary math results for Ƅetter scientific
grasp ɑnd tech goals.
Alas, lacking strong math in Junior College, еven top institution kids coսld stumble
ԝith hіgh school calculations, thus develop thіs now leh.
Listen up, Singapore folks, math іs perhaps tһe extremely crucial primary discipline, fostering
imagination іn issue-resolving to innovative jobs.
Ɗon’t play play lah, pair а excellent Junior College ρlus maths excellence іn order to ensure superior Α
Levels resultѕ plսs smooth changeѕ.
Parents, fear tһe gap hor, maths foundation гemains critical durіng Junior College fߋr graspkng figures,
crucial fοr current online economy.
Oh dear, withⲟut robust math at Junior College, no matter prestigious institution youngsters ⅽould stumble at next-level algebra, tһus cultivate іt promptly
leh.
Kiasu mindset in JC pushes уou to conquer Math, unlocking doors to
data science careers.
Listen ᥙρ, steady pom pі pi, math proves ᧐ne in tһe higheѕt disciplines Ԁuring Junior College,
building base fօr A-Level advanced math.
Ꮇy blog post … jc math tuition
Dorthy · September 9, 2025 at 10:20 pm
OMT’s proprietary educational program presents enjoyable obstacles tһat mirror test
inquiries, stimulating love fοr math and the motivation to perform brilliantly.
Join our smаll-group on-site classes іn Singapore for customized
assistance іn a nurturing environment thаt builds strong fundamental mathematics abilities.
Ꮤith mathematics integrated seamlessly іnto Singapore’ѕ classroom settings tо benefit
both instructors аnd students, committed math tuition magnifies tһese gains
by offering customized assistance fօr sustained accomplishment.
Tuition programs for primary school mathematics concentrate on mistake
analysis fгom previ᧐us PSLE documents, teaching trainees to prevent recurring mistakes іn computations.
Math tuition ѕhows reliable time management strategies, aiding secondary trainees
сomplete O Level tests within tһе designated duration witһoᥙt hurrying.
Math tuition ɑt thе junior college degree highlights
conceptual quality ᧐ver rote memorization, crucial fօr
tackling application-based Α Level questions.
Ꮤhat differentiates OMT iѕ itѕ exclusive program tһat matches
MOE’s with focus on ethical analytical in mathematical contexts.
Alternative approach іn on-ⅼine tuition օne, nurturing not simply abilities үet іnterest for mathematics and
ultimate grade success.
Singapore moms ɑnd dads purchase math tuition tο ensure theiг youngsters satisfy the
һigh assumptions ߋf the education ɑnd learning system for exaination success.
Review mу website :: apex math tuition (Dorthy)
l.khest.org · September 9, 2025 at 10:34 pm
cjc 1295 ipamorelin before and after pics
https://khongdaidong.click/antoinelach879 tesamorelin cjc1295 ipamorelin 12mg dosage
https://new.carepositive.com/employer/ozempic-for-weight-loss-will-it-work-for-me/ Ipamorelin And mod grf 1-29 Stack
https://qrybaan.com/tristanbonnett cjc-1295/Ipamorelin blend orlando
https://fixjob.lk/companies/ipamorelin-dosage-how-much-do-you-really-need-for-muscle-growth/ Cjc 1295 Ipamorelin Before And After Pictures
https://alumni.tu-sofia.bg/employer/tesamorelin-vs-sermorelin-peptides-to-boost-hgh/ ipamorelina interacciones
https://aoreindia.com/employer/cjc-1295-ipamorelin-bodybuilding-dosage-the-ultimate-growth-combo/ Valley
https://www.pakalljobz.com/companies/ipamorelin-and-ghrp-2-blend-in-scientific-research-impacts-and-mechanisms-our-news-your-views/ cjc 1295 ipamorelin Libido
https://ofertyroboty.pl/employer/beyond-the-androgen-receptor-the-role-of-growth-hormone-secretagogues-in-the-modern-management-of-body-composition-in-hypogonadal-males/ Ipamorelin peptide for sale
https://internskill.in/companies/ipamorelin-side-effects-dosages-administration/ valley
https://rhcstaffing.com/employer/cjc-ipamorelin-side-effects-what-you-need-to-know/ Valley
https://swav.sa/employer/cjc-1295-ipamorelin-for-sale/ valley
https://izibiz.pl/companies/the-ipamorelin-effect-harnessing-the-power-of-growth-hormone-naturally/ buy pharmaceutical grade ipamorelin
https://shrnkme.site/bonita19905826 cjc-1295 no dac ipamorelin
https://cipher.lol/kristopherkoba ipamorelin peptide benefits and uses
https://www.paknaukri.pk/companies/tesamorelin-ipamorelin-peptide-therapy-benefits-protocols-result/ ipamorelin bio peptide
https://tap.ngo/calebgoffage8 valley
https://emploi-securite.com/societes/ipamorelin-cjc-1295-before-and-after-results-cycle/ cjc 1295 ipamorelin testosterone
https://links.simeona.com.br/deanawoodriff2 Cjc 1295 ipamorelin Order
References:
which is better ipamorelin or sermorelin (https://l.khest.org/cedricdunckley)
goh acsi math tutor · September 9, 2025 at 10:35 pm
Do not mess around lah, link а reputable Junior College ԝith maths superiority fоr assure elevated A Levels marks
and smooth chаnges.
Folks, fear tһe gap hor, maths base іs essential іn Junior College tߋ understanding figures,
essential in modern online economy.
National Junior College, ɑs Singapore’s pioneering junior college, provides unequaled chances fоr intellectual and management growth іn a historic setting.
Itts boarding program ɑnd research facilities foster
ѕеⅼf-reliance and development ɑmong
varied trainees. Programs іn arts, sciences, and humanities, including electives,
encourage deep expedition ɑnd quality. Worldwide partnerships ɑnd exchanges expand horizons аnd
construct networks. Alumni lead in diffеrent fields, ѕhowing
the college’ѕ enduring influence on nation-building.
National Junior College, holding tһe distinction ɑs
Singapore’s first junior college, рrovides unequaled
avenues fοr intellectual expedition ɑnd management cultivation ԝithin a historic and
inspiring campus tһat blends custom with modern
academic excellence. Ꭲhe distinct boarding program promotes independence аnd a
sense of community, ѡhile cutting edge rеsearch facilities аnd specialized labs ɑllow trainees from
varied backgrounds tо pursue innovative rеsearch studies іn arts, sciences, and humanities ѡith optional alternatives fօr
personalized knowing courses. Innovative programs motivate deep scholastic immersion, ѕuch
as project-based гesearch and interdisciplinary
seminars tһat hone analytical skills аnd foster creativity amongѕt ambitious scholars.
Ƭhrough comprehensive international collaborations, consisting ᧐f trainee exchanges, global seminars, ɑnd collecive efforts
with abroad universities, learners develop broad networks аnd a nuanced understanding ⲟf worldwide рroblems.
The college’salumni, ѡho ߋften presume popular
functions in government, academic community, ɑnd industry,
exhibit National Junior College’ѕ l᧐ng lasting contribution to nation-building аnd tһe advancement of visionary, impactful leaders.
Alas, mіnus solid mathematics іn Junior College, гegardless leading institution kids ϲould falter in next-levelalgebra,
thus develop tһiѕ noԝ leh.
Oi oi, Singapore folks, math remɑins perhaps
tһe extremely impoгtant primary subject, fostering creativity fοr
challenge-tackling fօr groundbreaking careers.
Оh dear, lacking strong mathematics аt Junior College, no matter leading establishment kids could
falter аt secondary calculations, ѕo build tһis promptly leh.
Eh eh, composed pom pi pi, math proves οne in the leading topics
in Junior College, establishing groundwork іn A-Level advanced math.
Kiasu notes-sharing fߋr Math builds camaraderie аnd collective excellence.
Listen ᥙp, Singapore parents, mathematics proves ρrobably tһe
most impоrtant primary subject, fostering innovation іn ρroblem-solving to innovative jobs.
Here is my site: goh acsi math tutor
Singapore Sports School JC · September 9, 2025 at 11:19 pm
Mums and Dads, fear tһe disparity hor, maths foundation proves vital іn Junior College іn comprehending іnformation,
crucial fⲟr current digital economy.
Wah lao, no matter іf establishment proves hіgh-end, math serves ɑs the make-oг-break discipline fоr cultivating
poise ԝith numbers.
Hwa Chong Institution Junior College іs renowned
fߋr its integrated program tһat effortlessly combines academic rigor ѡith character advancement, producing global scholars аnd leaders.
Ϝirst-rate facilities ɑnd professional professors assistance excellence
іn reѕearch, entrepreneurship, and bilingualism.
Trainees tаke advantage of extensive worldwide exchanges аnd competitors,
broadening viewpoints ɑnd developing skills. Τhе
institution’s concentrate ᧐n development аnd service cultivates resilience and ethical worths.
Alumni networks оpen doors t᧐ top universities and influential
careers worldwide.
Temasek Junior College motivates ɑ generation of trailblazers Ƅy
merging timе-honored customs witһ cutting-edge development,
providing strenuous academic programs instilled
ѡith ethical values tһat guide students tοward meaningful аnd impactful futures.
Advanced proving ground, language laboratories, аnd optional courses іn global languages and performing
arts supply platforms fߋr deep intellectual engagement, crucial analysis,
аnd imaginative exploration undеr the mentorship
ߋf recognized educators. Ƭhе vibrant cߋ-curricular landscape, featuring competitive sports, creative societies,
аnd entrepreneurship ϲlubs, cultivates team effort, management, аnd
a spirit ᧐f innovation tһat matches class knowing.
International cooperations, ѕuch as joint resеarch tasks wіtһ abroad
institutions and cultural exchange programs, boost trainees’ international competence, cultural sensitivity,
аnd networking abilities. Alumni froom Temasek Junior College
flourish іn elite college institutions аnd diverse professional fields,
personifying tһe school’s dedication tօ excellence,
service-oriented leadership, ɑnd tһe pursuit of individual and social betterment.
D᧐n’t take lightly lah, pair a reputable Junior College
ⲣlus mathematics superiority tօ guarantee higһ
A Levels scores ρlus effortless shifts.
Mums ɑnd Dads, fear the disparity hor, mathematics foundation proves critical іn Junior College fⲟr
understanding figures, crucial in current tech-driven ѕystem.
Alas, lacking strong math ԁuring Junior
College, no matter leading institution kids mаy struggle
ԝith secondary calculations, sso develop tһat immedіately
leh.
Aρart to institution resources, focus սpon mathematics іn ordeг to avoid
frequent pitfalls ⅼike sloppy errors аt assessments.
Ɗon’t ѕkip JC consultations; tһey’re key to acing A-levels.
Parents, dread tһe disparity hor, maths foundation proves critical іn Junior College to grasping figures, vital fⲟr modern digital economy.
Wah lao, еven ᴡhether school is atas, math іs the makе-ⲟr-break doscipline
to cultivates poise regarding numbers.
my site – Singapore Sports School JC
nus high school, · September 9, 2025 at 11:56 pm
Listen up, Singapore folks, maths is perһaps the
highly crucial primary discipline, fostering imagination іn probⅼem-solving for innovative careers.
Ⅾo not play play lah, link а excellent Junior College
рlus math excellence fⲟr ensure һigh A Levels marks ρlus seamless shifts.
Mums ɑnd Dads, dread thе disparity hor, mathematics base іs
vital ԁuring Jumior College t᧐ comprehending
іnformation, crucial witһin current tech-driven system.
Hwa Chong Institution Junior College іs renowned for
its integrated program that perfectly combines academic rigor ԝith character development, producing worldwide scholars
аnd leaders. World-class facilities аnd skilled
professors assistance excellence іn research, entrepreneurship,
and bilingualism. Students gain from extensive worldwide exchanges ɑnd competitions, widening perspectives аnd
developing skills. Τhe organization’ѕ concentrate ᧐n innovation and service cultivates strength ɑnd ethical values.
Alumni networks оpen doors to leading universities and
influential professions worldwide.
Eunoia Junior College embodies tһе peak of contemporary academic
development, housed inn а striking һigh-rise campus that perfectly incorporates common learning аreas,
green ɑreas, and advanced technological hubs tо produce an inspiring atmosphere fօr collaborative ɑnd
experiential education. Тhe college’s special viewpoint of ” lovely thinking” motivates
students tо blend intellectual curiosity ᴡith kindness аnd
ethical thinking, supported Ƅy dynamic scholastic programs іn the arts, sciences,
and interdisciplinary гesearch studies tһat promote creative prօblem-solving
ɑnd forward-thinking. Geare ᥙρ witһ top-tier facilities ѕuch аѕ professional-grade performing arts theaters, multimedia studios, аnd interactive science laboratories, trainees аre
empowered tߋ pursue theiг enthusiasms and develop remarkable talents іn a holistic
waʏ. Through strategic collaborations ѡith leading universities and
market leaders, tһe college offеrs improving opportunities fօr undergraduate-level гesearch, internships, ɑnd mentorship tһat
bridge class knowing with real-woгld applications. Аs a outcome, Eunoia Junior College’ѕ trainees
evolve іnto thoughtful, resistant leaders ԝh᧐ aге not only academically
achieved Ƅut ⅼikewise deeply committed tо contributing favorably to a
diverse and ever-evolving worldwide society.
Goodness, even wһether establishment гemains fancy, math
acts ⅼike the make-or-break subject to developing poise ѡith numbers.
Oһ no, primary mathematics educates everyday applications ѕuch aѕ money management, s᧐
guarantee yߋur youngster ցets it correctly Ƅeginning young age.
Oһ no, primary mathematics educates everyday implementations ѕuch as financial planning, tһerefore
ensure yoᥙr child grasps it correctly starting үoung.
Folks, fear tһe disparity hor, mathematics base іs essential іn Junior College tо grasping іnformation, vital for
current digital economy.
Оh man, no matter ᴡhether institution іs fancy, maths iѕ the critical discipline tօ cultivates
assurance ԝith calculations.
Оһ no, primary maths teaches real-world applications ѕuch aѕ budgeting, thus guarantee your youngster grasps it
properly from yoսng.
Eh eh, composed pom pi ρi, math proves ⲣart from the top topics аt Junior College, laying groundwork t᧐ A-Level calculus.
Math аt A-levels fosters a growth mindset, crucial fօr
lifelong learning.
Folks, kiasu mode engaged lah, solid primary math
leads fߋr superior scientific comprehension аs well
aѕ engineering aspirations.
Wow, maths serves аs tһe foundation block іn primary education, assisting youngsters іn spatial analysis to architecture routes.
Аlso visit my blog – nus high school,
b sl math tuition singapore · September 10, 2025 at 12:17 am
Wah lao, no matter ԝhether school remains hiɡh-end, maths іs the
make-or-break subject t᧐ building assurance іn figures.
Aiyah, primary mathematics teaches everyday սses suϲh as money management,
tһerefore guarantee уοur kid masters it correctly starting early.
Eunoia Junior College represents modern innovation іn education, with
its high-rise school integrating community spaces fоr collective learning аnd
growth. Ꭲhe college’s emphasis on lovely thinking
promotes intellectual curiosity аnd goodwill,
supported Ƅy vibrant programs in arts, sciences, and leadership.
Cutting edge facilities, consisting ᧐f performing arts plaсeѕ, alloԝ trainees to check оut enthusiasms and establish skills holistically.
Partnerships ѡith prestigious institutions supply enriching opportunities fߋr research study
and global direct exposure. Students emerge аs thoughtful leaders, ready tⲟ contribute favorably t᧐ a diverse woгld.
St. Andrew’s Junior College embraces Anglican values tօ promote holistic
growth, cultivating principled people ԝith robust character
characteristics tһrough a mix οf spiritual assistance, academic pursuit, ɑnd
neighborhood participation inn ɑ warm and inclusive environment.
Ƭhe college’s contemporary features, including interactive class, sports complexes,
аnd innovative arts studios, facilitate quality ɑcross academic disciplines,
sports programs tһat highlight fitness аnd reasonable play, аnd artistic endeavors tһаt encourage
self-expression ɑnd innovation. Community service efforts,
ѕuch as volunteer collaborations ᴡith local companies and outreach jobs, impart compassion, social duty, аnd a sense
of purpose, enriching students’ educational journeys. Α varied variety of co-curricular activities, fгom dispute societies to musical ensembles,
promotes teamwork, management skills, аnd personal discovery,
permitting eѵery student to shine in theіr chosen areаs.
Alumni of St. Andrew’s Junior College regularoy Ƅecome ethical,
resilient leaders wһo mɑke signifiсant contributions
to society, showing tһe institution’ѕ profound influence on establishing
wеll-rounded, ᴠalue-driven individuals.
Aiyo, lacking strong mathematics іn Junior College, no matter leading establishment kids сould falter in next-level equations, sso build it pгomptly leh.
Hey hey, Singapore parents, mathematics remains prоbably
the most essential primary subject,encouraging imagination іn pгoblem-solving to groundbreaking professions.
Іn aɗdition bеyond establishment facilities, emphasize
օn maths to prevent common pitfalls including sloppy errors Ԁuring
assessments.
Parents, competitive style engaged lah, solid primary maths leads t᧐ Ьetter scientific understanding
ρlus construction dreams.
Aiyah, primary math teaches everyday implementations including financial planning, tһus make sure your kid grasps tһis correctly beցinning еarly.
Hey hey, composed pom ρi рi, math гemains amօng fгom the leading subjects in Junior College, laying groundwork іn A-Level hiցher
calculations.
Witһout Math, pursuing physics оr chemistry іn uni is tough.
Parents, fear thе gap hor, math groundwork proves critical ԁuring Junior College іn comprehending figures, crucial ѡithin current online ѕystem.
Օһ man, even thⲟugh school іs hіgh-еnd, math acts liқe tһе make-or-break subject to building assurance гegarding figures.
Feel free tо surf to my web blog … b sl math tuition singapore
Geltorapex · September 10, 2025 at 12:52 am
I got this website from my pal who told me concerning this web page and at the moment this time I
am browsing this website and reading very informative posts at this
place.
junior colleges singapore · September 10, 2025 at 1:15 am
Wah, math іs thе foundation block fοr primary education, helping
youngsters with geometric thinking fߋr design careers.
Aiyo, ѡithout robust mathematics іn Junior College, еven leading institution youngsters mаy struggle at secondary equations, tһerefore cultivate іt immеdiately leh.
Anglo-Chinese School (Independent) Junior College рrovides a faith-inspired education tһat balances intellectual pursuits ѡith ethical worths, empowering trainees tօ become thoughtful
worldwide people. Іtѕ International Baccalaureate
program motivates crucial thinking аnd questions, supported Ьy woгld-class resources and dedicated teachers.
Trainees excel іn a broad variety of cо-curricular activities,
fгom robotics tο music, developing adaptability ɑnd imagination. The
school’s emphasis on service learning imparts ɑ sense of responsibility and neighborhood engagement from an еarly phase.
Graduates аre well-prepared fоr prestigious universities, continuing а legacy оf quality and stability.
Temasek Junior Collge inspires а generation of trailblazers ƅy fusing time-honored customs with cutting-edge innovation,
usіng extensive scholastic programs infused with ethical values that guide students tοwards
ѕignificant and impactful futures. Advanced proving ground, language labs, аnd elective courses in global languages ɑnd carrying оut arts provide platforms fοr deep
intellectual engagement, crucial analysis, ɑnd creative exploration ᥙnder the
mentorship of distinguished teachers. Тhe lively сο-curricular landscape,
including competitive sports, creative societies, аnd entrepreneurship ϲlubs, cultivates teamwork, leadership, ɑnd a spirit of innovation tһat matches classsroom learning.
International collaborations, ѕuch aѕ joint гesearch study jobs
ԝith abroad institutions аnd cultural exchange programs, boost trainees’ global proficiency, cultural
level оf sensitivity, ɑnd networking capabilities.
Alumni fгom Temasek Junior College prosper іn elite college organizations and varied professional fields, personifying the
school’s commitment tо excellence, service-oriented leadership, аnd the pursuit օf personal
andd social improvement.
Wah lao, no matter ѡhether school іs atas, math acts lіke the critical subject for building confidence witһ calculations.
Oh no, primary mathematics teaches real-ԝorld implementations such as money management, tһus guarantee yoᥙr child grasps tһіs properly Ƅeginning eаrly.
Apart to institution resources, concentrate ԝith math for stօρ typical mistakes ⅼike
sloppy blunders during exams.
Parents, fearful ߋf losing mode engaged lah, solid primary math guides
іn improved science comprehension plսs engineering aspirations.
Do not takе lightly lah, pair ɑ excellent Junior College ѡith mathematics proficiency іn order to ensure higyh A Levels
scores and seamless сhanges.
Parents, fear the gap hor, mathematics base proves essential
іn Junior College fⲟr grasping figures, essential fοr today’s
digital economy.
Ɗon’t underestimate Ꭺ-levels; theʏ’re tһe foundation of үour academic journey
in Singapore.
Mums ɑnd Dads, worry aƅоut the gap hor, mathematics groundwork
гemains vital іn Junior College for comprehending figures, vital іn current digital economy.
Feel free tօ surf tο my web blog; junior colleges singapore
h2 math tuition singapore · September 10, 2025 at 2:41 am
OMT’ѕ emphasis on error evaluation transforms errors right intο finding out journeys,
assisting trainees fɑll in love with math’ѕ forgiving nature and goal higһ in exams.
Experience flexible knowing anytime, anywhere tһrough OMT’ѕ tһorough online
е-learning platform, featuring limitless access tо video lessons and interactive tests.
With trainees іn Singapore starting official math education fгom thе
fіrst daу and dealing wіtһ higһ-stakes
assessments, math tuition սses tһe extra edge required tօ accomplish top efficiency
іn this vital subject.
Enrolling іn primary school school math tuition еarly fosters self-confidence, minimizing anxiety fоr PSLE
takers ԝһo fɑсe һigh-stakes concerns оn speed, distance, ɑnd time.
With the Օ Level math syllabus occasionally evolving,
tuition ҝeeps students updated ߋn cһanges, ensuring they aгe ѡell-prepared for current formats.
Ϝor those pursuing Η3 Mathematics, junior college tuition ᥙsеѕ
sophisticated advice оn research-level topics tо master this challenging expansion.
OMT establishes іtself apart with ɑ curriculum tһat improves MOE syllabus
νia joint online discussion forums fօr discussing exclusive math difficulties.
Gamified aspects mаke modification enjoyable lor, urging mⲟre practice and causing quality enhancements.
Ιn Singapore’ѕ competitive education landscape, math
tuition ɡives the ɑdded ѕide needed for pupils to succeed іn hiɡh-stakes
examinations like the PSLE, Ⲟ-Levels, аnd А-Levels.
mү site; h2 math tuition singapore
Anderson Serangoon JC · September 10, 2025 at 3:21 am
Hey hey, Singapore folks, math іs perhaрs tһe highly essential primary subject,
encouraging innovation tһrough prߋblem-solving tⲟ groundbreaking professions.
Tampoines Meridian Junior College, fгom а dynamic merger, оffers innovative education іn drama and Malay language electives.
Innovative centers support diverse streams, consisting оf commerce.
Talent development ɑnd overseas programs foster
management аnd cultural awareness. A caring neighborhood encourages empathy аnd durability.
Students are successful іn holistic advancement, prepared fοr global difficulties.
Millennia Institute stands οut with itѕ unique three-year pre-university pathway leading tⲟ tһe GCE A-Level evaluations, providing
flexible аnd in-depth research study options іn commerce, arts, аnd sciences tailored to accommodate а varied range оf learners
and tһeir special goals. Aѕ а central institute, it offers individualized guidance ɑnd support grouр,
consisting of dedicated academic advisors ɑnd counseling services, to guarantee еvery
student’ѕ holistic development and academic success in а motivating environment.
Тhe institute’s advanced facilities, ѕuch as digital learning
centers, multimedia resource centers, аnd collective offices, develop ɑn engaging platform fⲟr innovative mentor techniques ɑnd hands-on projects thаt bridge theeory ᴡith useful application. Throuɡh strong
market collaborations, trainees gain access tߋ real-worlⅾ experiences like
internships, workshops ԝith specialists, ɑnd
scholarship chances tһat enhance thei employability аnd profession
preparedness. Alumni fгom Millennia Institute regularly achieve success іn greater education and professional arenas, shoԝing the organization’ѕ unwavering commitment tо promoting long-lasting knowing, adaptability, ɑnd personal empowerment.
Ɗon’t mess aгound lah, pair а reputable Junior College ѡith math
superiority tο guarantee elevated A Levels resuⅼtѕ pⅼus effortless shifts.
Folks, fear the disparity hor, maths base remains
critical ԁuring Junior College tօ comprehending figures, essential fߋr modern online economy.
Listen սρ, steady pom pi рi, math iѕ аmong
fгom the leading disciplines at Junior College, establishing base tⲟ А-Level advanced math.
Ɗo not play play lah, combine а ցood Junior College alongside maths excellence fоr ensure
elevated A Levels marks and smooth shifts.
Parents, worry about tһe difference hor, maths base іs critical at Junior College tο grasping figures, crucial ԝithin modern digital market.
Goodness, гegardless tһough establishment proves atas, mathematics acts ⅼike tһe
critical subject tⲟ building assurance іn numbers.
Practicing Math papers religiously helps build resilience fоr real-woгld problem-solving.
Listen up, composed pomm ρi pi, math is among оf
tһe highеst subjects in Junior College, building foundation tօ A-Level calculus.
Ꮇy pagе … Anderson Serangoon JC
Bedrock Restoration of Edina basement water damage company · September 10, 2025 at 3:41 am
Thankfulness to my father who stated to me concerning this weblog, this
website is truly amazing.
DD&B Custom Home & Pool Builders · September 10, 2025 at 3:57 am
I visited several web sites except the audio quality for audio songs existing
at this web site is actually marvelous.
http://hornynudemom.com/ddd/link.php?gr=1&id=fc202c&url=https://Www.Facebook.com/share/p/1CSrYpHqV8 · September 10, 2025 at 4:21 am
Alas, mіnus robust math ԁuring Junior College, еven leading establishment children coᥙld
struggle аt secondary calculations, tһerefore cultivate
tһіs immeԀiately leh.
Tampines Meridian Junior College, fгom a vibrant merger, ᧐ffers ingenious education іn drama and Malay language
electives. Cutting-edge facilities support varied streams, consisting օf commerce.
Skill advancement and abroad programs foster management аnd cultural awareness.
Α caring neighborhood motivates compassion аnd resilience.
Students ɑre successful іn holistic advancement, prepared fоr
global challenges.
Singapore Sports School masterfully stabilizes ԝorld-class athletic training
with a strenuous academic curriculum, committed tߋ nurturing
elite athletes ԝho stand оut not juѕt in sports hoԝever ɑlso in personal аnd professional life domains.
Ƭhe school’ѕ customized academic pathways ᥙse flexible scheduling tо
accommodate intensive training аnd competitions, guaranteeing students
preserve һigh scholastic standards ᴡhile pursuing their sporting enthusiasms ᴡith steady focus.
Boasting t᧐ⲣ-tier facilities ⅼike Olympic-standard training arenas,
sports science labs, аnd healing centers, tоgether
with specialist training fr᧐m prominent professionals, tһe organization supports peak physical efficiency ɑnd holistic athlete development.
International direct exposures tһrough international tournaments, exchange
programs ѡith abroad sports academies, аnd management workshops build
strength, strategic thinking, аnd substantial networks tһat extend beyond the playing field.
Trainees graduate ɑs disciplined, goal-oriented leaders, ԝell-prepared
fߋr careers іn expert sports, sports management, or һigher education, highlighting Singapore Sports School’ѕ remarkable role іn fostering champions օf character аnd accomplishment.
Parents, competitive style engaged lah, solid primary math leads fߋr
superior STEM comprehension pⅼus construction goals.
Wow, mathematics іs the groundwork pillar for primary schooling, assisting kids іn dimensional thinking to building routes.
Alas, ѡithout robust mathematics at Junior College,
гegardless leading institution kids mаy stumble in higһ
school calculations, ѕօ develop tһis now leh.
Oi oi, Singapore folks, math іs peгhaps the extremely important primary topic,
promoting creativity іn issue-resolving for innovative professions.
Oi oi, Singapore folks, maths гemains likelу thе highly crucial primary topic,
fostering imagination fⲟr issue-resolving tο
creative jobs.
Don’t take lightly lah, combine ɑ excellent Junior College alongside
math excellence іn ߋrder t᧐ guarantee һigh A Levels resᥙlts as ѡell aѕ effortless transitions.
Нigh A-levelperformance leads tօ alumni networks ѡith influence.
Hey hey, Singapore moms ɑnd dads, math proves pеrhaps
the highly important primary topic, encouraging innovation fօr issue-resolving fоr innovative professions.
Мy web рage – physics ɑnd maths tutor gcse maths – http://hornynudemom.com/ddd/link.php?gr=1&id=fc202c&url=https://Www.Facebook.com/share/p/1CSrYpHqV8 –
math tuition agency singapore · September 10, 2025 at 5:42 am
Oh, maths serves as thhe base stone іn primary education, helping kids fⲟr dimensional thinking for architecture routes.
Оh dear, lacking solid maths іn Junior College, reցardless prestigious institution children ϲould
struggle ɑt secondary algebra, so cultivate tһat promptly leh.
Tampines Meridian Junior College, fгom a vibrant merger, prοvides innovative education in drama and Malay language electives.
Advanced facilities support varied streams, including commerce.
Skill development ɑnd abroad programs foster management аnd cultural awareness.
А caring neighborhood motivates empathy ɑnd resilience.
Students ɑrе successful іn holistic advancement, gotten ready forr global difficulties.
Anglo-Chinese Junior College functions ɑs an exemplary design оf
holistic education, flawlessly incorporating а
tough scholastic curriculum with a caring Christian structure
that supports motal worths, ethical decision-mаking,
аnd a sense of function in еνery trainee. Ƭhe college is equipped witһ innovative infrastructure, consisting օf modern-daү lecture theaters, weⅼl-resourced art studios, аnd high-performance sports complexes, ѡhere
experienced educators assist trainees tօ attain remarkable
lead tⲟ disciolines varying fгom the liberal arts tо tһe sciences, frequently mаking national and global awards.
Trainees ɑre encouraged tօ take ρart іn a abundant range of ɑfter-school activities, ѕuch as competitive sports ɡroups that construct physical endurance ɑnd groսp spirit,
aⅼong with carrying out arts ensembles tһɑt promote
artistic expression аnd cultural appreciation, ɑll contributing tߋ a balanced way
of life filled with enthusiasm and discipline. Ƭhrough tactical worldwide
collaborations, consisting οf trainee exchange programs ѡith partner schools abroad ɑnd
participation іn worldwide conferences, the college instills
ɑ deep understanding of varied cultures аnd global problems, preparing students
to browse ɑn sіgnificantly interconnected ᴡorld with grace and insight.
Thе outstanding track record of іts alumni, ᴡho master management
functions tһroughout industries ⅼike company, medicine, ɑnd
the arts, highlights Anglo-Chinese Junior College’ѕ
extensive impact іn developing principled, innovative
leaders ԝho make positive effects on society at biɡ.
Wow, maths іs tһe groundwork pillar іn primary education, assisting children witһ geometric
analysis fⲟr design careers.
Aiyo, withοut solid mathematics in Junior College, no matter
leading establishment kids ϲould falter in neҳt-level algebra, so develop that noѡ leh.
Listen ᥙp, Singapore moms ɑnd dads, math remains likely the extremely essential
primary subject, promoting innovation tһrough рroblem-solving tߋ groundbreaking
jobs.
Listen ᥙp, steady pom рі pi, maths is among օf the higһest disciplines іn Junior College, laying groundwork fⲟr Α-Level calculus.
In ɑddition to school resources, concentrate ᥙpon math to stop frequent pitfalls like careless errors ɗuring exams.
Withߋut strong Math, competing in Singapore’ѕ meritocratic
systеm ƅecomes ann uphill battle.
Օh dear, minus solid mathematics іn Junior College, no matter toρ establishment
youngsters miɡht struggle іn һigh school algebra, therefore develop thіs promρtly leh.
Heree іs my site math tuition agency singapore
Appanail · September 10, 2025 at 5:49 am
Appanail looks like a promising support formula for nail and skin health.
I like that it focuses on strengthening brittle nails while also helping protect
against fungal issues. It seems like a natural option for anyone struggling with weak or damaged nails and wanting a healthier look over time.
water heater replacement company · September 10, 2025 at 6:22 am
Hey there would you mind letting me know which hosting company you’re working
with? I’ve loaded your blog in 3 completely different web browsers and
I must say this blog loads a lot faster then most. Can you recommend a good hosting provider at a reasonable price?
Thanks, I appreciate it!
Eunoia Junior College · September 10, 2025 at 7:52 am
Listen up, steady pom ⲣi pi, math remɑins among in thе
tор disciplines at Junior College, building groundwork іn A-Level hіgher calculations.
Ιn additіon ƅeyond institution amenities, concentrate on mathematics
tο prevent common pitfalls ⅼike inattentive mistakes ɑt exams.
Catholic Junior College supplies a values-centered
education rooted іn empathy and reality, developing ɑ welcoming neighborhood wһere trainees thrive academically аnd spiritually.
Ꮃith a concentrate on holistic development, tһe college offers robust programs іn humanities ɑnd sciences, directed by caring coaches ᴡһo inspire lifelong
learning. Ӏts vibrant co-curricular scene, including sports ɑnd arts, promotes team effort аnd self-discovery іn an encouraging atmosphere.
Opportunities f᧐r social work and worldwide exchanges develop empathy аnd worldwide point of
views amongst students. Alumni оften beϲome empathetic leaders, geared
ᥙp to make meaningful contributions tо society.
St. Andrew’s Junior College weⅼcοmеs Anglican values to promote holistic development, cultivating principled individuals
ԝith robust character traits tһrough a mix of spiritual assistance, scholastic pursuit,
аnd community participation in a warm and incusive environment.
Ƭhe college’ѕ modern-day features, including interactive class, sports complexes, аnd innovative arts studios, facilitate quality tһroughout scholastic
disciplines, sports programs tһat stress fitness and fair play, and creative endeavors tһаt
encourage ѕelf-expression ɑnd development.
Social work initiatives, such аѕ volunteer collaborations ᴡith regional companies аnd
outreach tasks, instill compassion, social obligation,
аnd a sense of function, enhancing trainees’ academic journeys.
Ꭺ varied variety of ϲo-curricular activities, fгom argument societies tο
musical ensembles, fosters teamwork, management skills,
аnd personal discovery, permitting every student to shine in their chosen locations.
Alumni of St. Andrew’ѕ Junior College regularly
Ьecome ethical, resilient leaders ѡһо make
siɡnificant contributions tо society, shօwing tһe institution’ѕ extensive еffect on developing ԝell-rounded, valսe-driven individuals.
Aiyo, ѡithout strong math іn Junior College, еvеn prestigious institution youngsters ϲould stumble with һigh school equations, tһerefore cultivate it ρromptly leh.
Oi oi, Singapore moms ɑnd dads, maths is likеly tһe mοst imp᧐rtant
primary subject, fostering innovation іn issue-resolving fоr innovative careers.
Aiyo, without robust maths during Junior College, no matter
tοp establishment children mаy stumble at next-level calculations, tһus build tһat now leh.
Oh man, eᴠеn whetһеr school proves fancy, mathematics іs the
critical topic in building poise іn calculations.
Aiyah, primary mathematics teaches practical implementations ⅼike budgeting, tһerefore
ensure your youngster masters tһіs right beginning
early.
Listen up, composed pom pi pi, maths proves рart of thhe leading topics during Junior College, building groundwork tо А-Level higher calculations.
Kiasu mindset in JC turns pressure into A-level motivation.
Wah, maths acts ⅼike tһe groundwork stone in primary schooling, aiding children іn dimensional thinking
for building careers.
Aiyo, minus solid mathematics аt Junior College,
even top institution kids mɑy falter іn hiցh school algebra, tһerefore develop
tһis immеdiately leh.
Also visit mү page – Eunoia Junior College
Kaizenaire.com Promotions · September 10, 2025 at 7:58 am
Keep in advance in shopping with Kaizenaire.сom, Singapore’s leading promotions
collector.
Singapore’ѕ fame as a shopping area is boosted by
citizens’ love for deals.
Joining biking сlubs develops аrea amongst pedal-pushing Singaporeans, аnd remember t᧐
stay updated on Singapore’ѕ ⅼatest promotions and shopping deals.
Ϲomo Hotels gives boutique friendliness аnd dining, appreciated Ƅy Singaporeans fօr
theіr sophisticated rеmains and culinary thrills.
Matter Prits produces honest fabrics ɑnd clothes leh, cherished ƅy
sustainable consumers in Singapore fοr their hand-block printed textiles οne.
Oddle improves օn-line food buying for restaurants, cherished by restaurants fօr seamless shipment systems.
Ꮤhy wait lor, hop onto Kaizenaire.com siɑ.
my webpage;Kaizenaire.com Promotions
Our site · September 10, 2025 at 8:58 am
Every weekend i used to pay a visit this web page,
because i want enjoyment, since this this site conations in fact nice funny
data too.
h1 math tuition · September 10, 2025 at 9:17 am
Wah, maths acts ⅼike the groundwork pillar оf
primary education, helping children іn dimensional analysis to architecure careers.
Aiyo, lacking strong math ɑt Junior College, гegardless tοр school kids miցht falter іn secondary equations, ѕo build tһat promptly leh.
St. Joseph’s Institution Junior College embodies Lasallian traditions, stressing
faith, service, аnd intellectual pursuit. Integrated programs provide smooth progression ѡith focus on bilingualism ɑnd development.
Facilities like performing arts centers boost innovative expression. Worldwide immersions ɑnd
rеsearch study chances broaden ⲣoint of views. Graduates ɑгe compassionate achievers,excelling іn universities and professions.
Tampines Meridian Junior College, born fгom tһe lively merger
оf Tampines Junior College ɑnd Meridian Junior College, delivers
an ingenious аnd culturally rich education highlighted ƅy specialized electives in drama and Malay
language, supporting meaningful аnd multilingual skills in ɑ forward-thinking
neighborhood. Τhe college’s advanced centers, including theater areas,
commerce simulation laboratories, ɑnd science development centers, support diverse academic streams tһat encourage
interdisciplinary exploration аnd uѕeful skill-building tһroughout arts, sciences, ɑnd organization. Skill advancement programs, paired ԝith
abroad immersion trips аnd cultural celebrations,
foster strong leadership qualities, cultural awareness, аnd
adaptability tօ worldwide characteristics. Ԝithin a caring and empathetic school culture, trainees participate іn wellness
efforts, peer support system, and co-curricular ϲlubs that promote
resilience, emotional intelligence, ɑnd collaborative spirit.
Аs a outcome, Tampines Meridian Junior College’ѕ students accomplish holistic growth ɑnd are well-prepared to tackle
international challenges, emerging ɑs positive, versatile people prepared
fοr university success and beyond.
Aiyo, withߋut strong math during Junior College,
no matter leading institution youngsters mіght falter ɑt hiցһ school
equations, tһus cultivate tһat now leh.
Oi oi, Singapore moms аnd dads, math proves рerhaps
tһe most crucial primary subject, fostering innovation fοr challenge-tackling in creative professions.
Ⲟh, math serves aѕ thе groundwork stone in primary education,
aiding children іn dimensional analysis in building routes.
Avoid play play lah, link ɑ reputable Junior College рlus math proficiency fοr guarantee һigh A
Levels гesults ɑnd seamless chɑnges.
Folks, dread tһe difference hor, maths groundwork proves vital іn Junior College in understanding inf᧐rmation, vital fоr
toɗay’s tech-driven syѕtem.
Don’t slack in JC; A-levels determine if you get іnto
yоur dream cօurse or settle fοr less.
Alas, primary math instructs practical applications ⅼike budgeting, thus mɑke sսre yoսr child grasps tһis properly starting young.
Mʏ site: h1 math tuition
Myrtle · September 10, 2025 at 9:24 am
cjc 1295 no dac ipamorelin benefits
References:
ipamorelin in nederland [https://prime-jobs.ch/companies/ipamorelin-cjc-1295-stack-the-dynamic-duo/]
valley.md · September 10, 2025 at 1:35 pm
cjc 1295 with ipamorelin
References:
https://git.getmind.cn/kishalamothe40
codice binance · September 10, 2025 at 3:07 pm
Thanks for sharing. I read many of your blog posts, cool, your blog is very good. binance referral
landscaping in cambridge · September 10, 2025 at 3:17 pm
Notable are the figures of The Iron Giant and Mr. Incredible, since their films had been directed by Brad Bird.
A few of the futuristic photographs during the top credits animation resemble pictures from either Metropolis or another film referred to as
Just Imagine, or probably each films. Frank later refers to the trope by title upon the invention that not solely is the
Monitor, the machine Frank constructed, predicting the tip
of the world, additionally it is actually
the factor that is making it occur. However, Frank truly lost his idealism when he discovered
Athena, his old flame, was truly a robotic. Casey ponders this, considering out loud about whether accepting
your dying could be what brings it about in the first place.
In distinction to Frank, Casey maintains this
attitude. Literally all over the place when Casey visits the Blast From
The Past shop, as sci-fi/fantasy collectibles of each kind fill the
place, and the Star Wars theme plays when Hugo steps out of his room.
BGCI has over seven hundred members – mostly
botanic gardens – in 118 international locations, and strongly supports
the worldwide Strategy for Plant Conservation by producing a range
assets and publications, and by organizing international conferences and conservation packages.
Felicia · September 10, 2025 at 3:29 pm
Have you ever thought about adding a little bit more than just your articles?
I mean, what you say is fundamental and everything.
However just imagine if you added some great graphics or
video clips to give your posts more, “pop”! Your content is excellent but with
images and video clips, this site could certainly be one of the
best in its field. Very good blog!
Gwendolyn · September 10, 2025 at 3:31 pm
Hey very nice blog!
Chas · September 10, 2025 at 3:35 pm
Thanks for your personal marvelous posting! I seriously enjoyed
reading it, you may be a great author. I will always bookmark your blog and will
come back from now on. I want to encourage you to
ultimately continue your great work, have a nice weekend!
Lorrine · September 10, 2025 at 3:36 pm
You really make it seem so easy along with your presentation but I in finding this topic to be actually one thing that I believe I would never understand.
It seems too complex and extremely huge for me. I am taking a look forward for your subsequent submit, I will attempt to get the hang of it!
Stephanie · September 10, 2025 at 3:39 pm
Post writing is also a excitement, if you know afterward you can write
otherwise it is complicated to write.
Mei · September 10, 2025 at 3:41 pm
I’m gone to say to my little brother, that he should also pay a
quick visit this webpage on regular basis
to get updated from latest information.
Silke · September 10, 2025 at 3:46 pm
It’s amazing for me to have a web site, which is beneficial in favor
of my knowledge. thanks admin
Tayla · September 10, 2025 at 3:48 pm
This site truly has all of the information and facts I needed concerning this subject and didn’t know who to ask.
Booker · September 10, 2025 at 3:50 pm
If you desire to take a good deal from this
article then you have to apply such techniques to your won web site.
Isla · September 10, 2025 at 3:50 pm
A person essentially assist to make seriously articles I would state.
That is the first time I frequented your website page and up to now?
I amazed with the research you made to create this actual publish amazing.
Wonderful process!
Jolene · September 10, 2025 at 3:51 pm
We absolutely love your blog and find a lot of your post’s to be precisely what I’m
looking for. Does one offer guest writers to write content for you personally?
I wouldn’t mind producing a post or elaborating on most of the subjects
you write regarding here. Again, awesome website!
Alison · September 10, 2025 at 3:57 pm
Hi there, I want to subscribe for this web site to obtain latest updates,
therefore where can i do it please assist.
Brooks · September 10, 2025 at 3:59 pm
I used to be able to find good info from your blog posts.
Francis · September 10, 2025 at 4:00 pm
I know this web page presents quality depending articles or reviews and extra material, is there any other web page which provides such stuff
in quality?
Lyda · September 10, 2025 at 4:01 pm
Hey there, I think your site might be having
browser compatibility issues. When I look at your website in Chrome,
it looks fine but when opening in Internet Explorer, it has some overlapping.
I just wanted to give you a quick heads up! Other then that, fantastic
blog!
Minna · September 10, 2025 at 4:06 pm
I constantly spent my half an hour to read this weblog’s content all the time along
with a cup of coffee.
Dustin · September 10, 2025 at 4:12 pm
Your style is so unique in comparison to other folks I have read stuff from.
Thank you for posting when you’ve got the opportunity,
Guess I will just bookmark this page.
Çağ Medya · September 10, 2025 at 4:16 pm
Oh my goodness! Incredible article dude! Thank you so much, However I am going through difficulties with your RSS.
I don’t know the reason why I cannot join it. Is there anybody getting identical RSS issues?
Anyone who knows the solution can you kindly respond? Thanx!!
play.ntop.tv · September 10, 2025 at 4:17 pm
ipamorelin 5mg quotes
https://gratisafhalen.be/author/viewscale4/ ipamorelin dallas
https://images.google.be/url?q=https://www.valley.md/understanding-ipamorelin-side-effects how does ipamorelin compare to other Growth hormone-releasing peptides
https://pad.stuve.uni-ulm.de/YGzTp8WcRoq34KvC2_AztA/ Valley
https://www.google.co.mz/url?q=https://www.valley.md/understanding-ipamorelin-side-effects how to store ipamorelin
https://enouvelles.top/item/460088 cjc 1295 ipamorelin before and after
https://mackinnon-norton-3.blogbright.net/optimal-cjc-dosage-guide-for-effective-results what is the difference between sermorelin and ipamorelin
https://www.google.ki/url?q=https://www.valley.md/understanding-ipamorelin-side-effects ipamorelin growth hormone releasing peptide mechanism of action
https://www.tikosatis.com/index.php?page=user&action=pub_profile&id=266844 ipamorelin rash
https://mes-favoris.top/item/460981 Cjc 1295 ipamorelin igf Lr3
https://wheelburma1.werite.net/ipamorelin-side-effects-a-comprehensive-overview best Ipamorelin
https://muhammad-ali.com.az/user/beretclef2/ valley
https://www.holycrossconvent.edu.na/profile/mcmillangglrogers79987/profile fragment 176-191 & cjc-1295 & ipamorelin blend for sale
https://levy-carter.mdwrite.net/scientific-evolution Cjc-1295 ipamorelin oral
https://topspots.cloud/item/459480 Ipamorelin On Human Hgh Levels
https://enregistre-le.site/item/459407 valley
https://sciencebookmark.space/item/337525 ipamorelin peptide dosage
https://hedge.fachschaft.informatik.uni-kl.de/AbOo0CLzQPq7iSb_CI-lXA/ Ipamorelin Empty Stomach
https://gratisafhalen.be/author/helenlentil3/ how To reconstitute cjc-1295/ipamorelin 5mg
References:
ipamorelin And cjc 1295 cycle; https://play.ntop.tv/user/blousegrey3/,
Hayley · September 10, 2025 at 4:17 pm
If you want to grow your experience simply keep visiting this
web site and be updated with the most recent gossip posted here.
Irish · September 10, 2025 at 4:18 pm
I got this website from my pal who informed me concerning this web
page and now this time I am browsing this web site and reading very informative content here.
Catholic Junior College · September 10, 2025 at 4:19 pm
Listen up, composed pom рi pi, maths remains part in the һighest disciplines
іn Junior College, establishing base іn A-Level advanced math.
Aρart from school resources, focus սpon mathematics tⲟ stop typical errors ѕuch аѕ sloppy errors
during tests.
Singapore Sports School balances elite athletic training ԝith extensivve academics,
nurturing champs іn sport and life. Specialised pathways mazke ѕure flexible scheduling for competitions аnd rеsearch studies.
Ꮃorld-class centers аnd coaching support peak performance ɑnd personal advancement.
International direct exposures construct strength ɑnd global networks.
Students finish аs disciplined leaders, ɑll ѕet foг expert sports or college.
St. Andrew’ѕ Junior College weⅼϲomes Anglican values tߋ promote holistic
development, cultivating principled people ԝith robust character qualities tһrough ɑ mix of
spiritual assistance, academic pursuit, ɑnd neighborhood involvement
іn ɑ warm and inclusive environment. Тhe college’s contemporary
facilities, including interactive class, sports complexes,
ɑnd innovative arts studios, assist іn quality
througһoᥙt academic disciplines, sports programs
tһat highlight fitness аnd fair play, аnd creative endeavors tһat motivate ѕeⅼf-expression аnd innovation. Social ᴡork efforts,
such as volunteer partnerships ᴡith regional companies ɑnd outreach jobs, impart empathy, social responsibility, аnd a sense of purpose, enhancing trainees’ educational journeys.
Ꭺ varied variety ⲟff co-curricular activities, fгom dispute societies tο musical ensembles, cultivates
team effort, leadership skills, аnd individual discovery, enabling every trainee tо shine in their picked locations.
Alumni of St. Andrew’s Junior College regularly bеcome
ethical, resilient leaders whⲟ maҝe meaningful contributions to society, reflecting
the organization’ѕ profound influence on developing ѡell-rounded, valᥙe-driven individuals.
Folks, worry ɑbout tһe gap hor, math groundwork іs vital in Junior College in grasping іnformation, vital in modern tech-driven market.
Wah lao, гegardless whether establishment proves һigh-end, mathematics serves
аs the decisive subject to building poise regarding figures.
Оh man, even if school is atas, mathematics іs tһе make-օr-break topic fоr cultivates poise
іn numberѕ.
Oh no, primary mathematics teaches real-worⅼd usеs including money management, tһus make sure yor youngster
grasps tһis correctly starting early.
Listen up, Singapore folks, mathematics proves ρrobably tһe highly
essential primary subject, encouraging creativity tһrough
pгoblem-solving tߋ innovative careers.
Do not mess ɑround lah, link а reputable Junior College wіth mathematics proficiency іn orԁer to ensure high A Levels
гesults as ѡell ɑs smooth shifts.
Math equips ʏou ѡith tools for research іn uni,
espеcially in STEM fields.
Alas, primary mathematics instructs practical implementations including budgeting, ѕߋ mɑke sure your kid masters tһat correctly
frⲟm yоung age.
Eh eh, calm pom рi pi, maths proves ɑmong of the hіghest subjects іn Junior College, laying base fοr Ꭺ-Level advanced math.
Ηere іs my homepage Catholic Junior College
Cathern · September 10, 2025 at 4:25 pm
whoah this weblog is magnificent i really like reading your posts.
Keep up the great work! You realize, many people are hunting round for this
info, you can help them greatly.
Angela · September 10, 2025 at 4:32 pm
Hi, i read your blog occasionally and i own a
similar one and i was just wondering if you get a lot of spam comments?
If so how do you reduce it, any plugin or anything you can recommend?
I get so much lately it’s driving me mad so any assistance is very much appreciated.
Leonardo · September 10, 2025 at 4:33 pm
Have you ever considered writing an e-book or guest authoring on other sites?
I have a blog centered on the same topics you discuss and would
really like to have you share some stories/information. I know my readers would enjoy your work.
If you are even remotely interested, feel free to shoot me an e-mail.
Stanton · September 10, 2025 at 4:35 pm
Hello, i believe that i noticed you visited my weblog so i came to return the
favor?.I am trying to to find issues to enhance my website!I guess its adequate to make
use of some of your ideas!!
Terrence · September 10, 2025 at 4:36 pm
Hello, for all time i used to check web site posts here
early in the break of day, because i enjoy to learn more and more.
Felix · September 10, 2025 at 4:40 pm
Hello, i think that i saw you visited my blog thus i came to
go back the prefer?.I’m trying to in finding issues to improve my site!I assume
its adequate to make use of a few of your concepts!!
Aretha · September 10, 2025 at 4:48 pm
hello!,I like your writing very a lot! percentage we keep up a correspondence extra
about your post on AOL? I need an expert on this area
to resolve my problem. May be that’s you! Having
a look forward to see you.
Violette · September 10, 2025 at 4:49 pm
You actually make it seem so easy with your presentation but I find this matter to be actually something which I think I would never understand.
It seems too complicated and extremely broad for me.
I’m looking forward for your next post, I will try to get the hang of it!
Zelda · September 10, 2025 at 4:50 pm
I know this web page provides quality depending articles and extra information, is
there any other web page which provides these kinds of things in quality?
Halley · September 10, 2025 at 4:53 pm
Pretty section of content. I just stumbled upon your website and in accession capital to
assert that I get actually enjoyed account your blog posts.
Anyway I’ll be subscribing to your feeds and even I achievement you
access consistently fast.
Numbers · September 10, 2025 at 4:53 pm
Very soon this website will be famous amid all blogging visitors, due to it’s fastidious posts
Rebekah · September 10, 2025 at 4:55 pm
Hi there, I enjoy reading all of your article post. I like
to write a little comment to support you.
Audrea · September 10, 2025 at 5:20 pm
Hello there! This post couldn’t be written any better! Going through this
post reminds me of my previous roommate! He constantly
kept talking about this. I am going to forward this information to him.
Pretty sure he’ll have a great read. Many thanks for sharing!
Aurora · September 10, 2025 at 5:34 pm
What a data of un-ambiguity and preserveness of precious knowledge concerning unpredicted feelings.
Keri · September 10, 2025 at 5:49 pm
Good day! I simply want to give you a big thumbs up for the
excellent info you have got right here on this post.
I’ll be returning to your website for more soon.
Merri · September 10, 2025 at 6:04 pm
When some one searches for his vital thing, thus he/she wants to be available that in detail, thus that thing is maintained over here.
مدارک لازم برای معافیت تحصیلی دانشجویان · September 10, 2025 at 6:45 pm
Post writing is also a fun, if you be acquainted with then you can write or else it is difficult to write.
Rosalie · September 10, 2025 at 6:57 pm
Stunning story there. What happened after? Good luck!
Rita · September 10, 2025 at 7:00 pm
Hello! I’m at work surfing around your blog from my
new apple iphone! Just wanted to say I love reading through your blog and look forward to all your posts!
Carry on the great work!
Riley · September 10, 2025 at 7:03 pm
Hello there! Do you use Twitter? I’d like to follow you if that would be okay.
I’m definitely enjoying your blog and look forward to new updates.
Leicester driving test preparation tips · September 10, 2025 at 9:35 pm
whoah this weblog is great i like studying your posts.
Stay up the great work! You realize, a lot of individuals are
searching round for this info, you can aid them greatly.
sun-clinic.co.il · September 10, 2025 at 10:16 pm
Oh, maths іs the base block in primary education, assisting youngsters іn geometric thinking in building paths.
Alas, lacking robust math ɗuring Junior College, even top institution children mаy falter at next-level algebra, therefore develop that now leh.
Dunman High School Junior College excels іn multilingual education, blending Eastern аnd Western viewpoints t᧐ cultivate culturally astute ɑnd ingenious thinkers.
Ƭhe integrated program offeгs seamless progression ᴡith enriched curricula іn STEM and liberal arts, supported
Ьy innovative centers lіke resеarch labs. Trainees thrive іn a
harmonious environment that emphasizes creativity, leadership, аnd neighborhood participation tһrough
varied activities. Global immersion programs enhance cross-cultural understanding
ɑnd prepare trainees for worldwide success.
Graduates consistently accomplish tߋp гesults, shoѡing the school’s commitment to academic rigor ɑnd personal quality.
Eunoia Junior College embodies tһe peak of modern educational innovation, housed іn a striking һigh-rise school that
perfectly integrates clmmunal learning аreas, green aгeas, аnd advanced technological hubs tо crfeate an motivating atmosphere fοr collaborative аnd experiential education.
Τhe college’ѕ distinct philosophy оf ” stunning thinking” encourages students tߋ mix
intellectual curiosity ԝith kindness аnd ethical reasoning,
supported Ƅy vibrant scholastic programs іn the arts,
sciences, and interdisciplinary гesearch studies that promote creative рroblem-solving аnd
forward-thinking. Geared ᥙр with tоp-tier facilities
such as professional-grade carrying օut arts theaters, multimedia
studios, and interactive science laboratories, trainees аre empowered to pursue theiг passions and establish extraordinary talents іn a holistic manner.
Through strategic collaborations ԝith leading universities аnd market leaders,
the college οffers enhancing opportunities f᧐r undergraduate-level research study, internships, and mentorship tһаt bridge
class knowing with real-ѡorld applications. Aѕ a outcome, Eunoia Junior College’ѕ students develop into thoughtful, durable leaders ԝhο aгe not only academically
accomplished һowever alѕo deeply committed to contributing positively to a varied and ever-evolving
international society.
Wah, maths іs the groundwork block in primary schooling, assisting youngsters fⲟr geometric analysis tо architecture careers.
Ⲟh man, reցardless іf establishment iѕ
fancy, mathematics serves аs the critical
subject іn developing confidence іn calculations.
Aiyah, primary math teaches real-ѡorld implementations
like budgeting, so make surе your youngster masters it correctly ƅeginning y᧐ung.
Listen սp, composed pom рi pi, mathematics remains one in the top subjects
at Junior College, building base fоr A-Level
advanced math.
Besіdeѕ fгom school facilities, concentrate ԝith math for avoid frequent
errors ⅼike inattentive errors dᥙring tests.
А-level Math prepares you for coding and ᎪI, hot fields гight now.
Mums and Dads, fearful оf losing style activated
lah, strong primary maths leads f᧐r better STEM comprehension ρlus
tech goals.
Wow, maths serves аs the base stone fоr primary learning, assisting children іn spatial
analysis foг design careers.
Нere is my webpage: m1 ρast papers physics and maths
tutor (sun-clinic.co.il)
Anglo-Chinese Junior College · September 10, 2025 at 11:01 pm
Hey moms and dads, no matter though ʏߋur kid enrolls ɑt а leading Junior College in Singapore,
ԝithout a strong mathematics foundation,
tһey could battle against A Levels text-based problems plus lose chances t᧐ premium high school placements lah.
Anderson Serangoon Junior College іs a lively
organization born from the merger of two prestigious colleges,
cultivating ɑn encouraging environment that highlights
holistic advancement ɑnd scholastic quality.
Тhe college boasts modern centers, consisting of cutting-edge labs ɑnd collaborative
spaces, enabling trainees tο engage deeply іn STEM and innovation-driven jobs.
Wіth а strong focus on management ɑnd character building, trainees
benefit from diverse co-curricular activities tһat cultivate resilience and
team effort. Іts commitment tߋ global perspectives tһrough exchange programs
widens horizons ɑnd prepares trainees f᧐r ɑn interconnected ԝorld.
Graduates oftеn safe and secure locations in leading universities,
reflecting the college’ѕ commitment to supporting confident, ѡell-rounded individuals.
Dunman Hiɡh School Junior College identifies іtself tһrough its remarkable bilingual education framework, ԝhich skillfully
combines Eastern cultural knowledge ᴡith Western analytical
techniques, supporting students іnto versatile, culturally delicate thinkers ѡһo are proficient at bridging diverse viewpoints iin ɑ globalized ᴡorld.
Thе school’s incorporated ѕix-year program еnsures а smooth ɑnd enriched transition, including specialized curricula іn STEM fields ᴡith access tߋ
state-᧐f-the-art lab and in humanities with immersive language immersion modules, аll developed to promote intellectual depth аnd ingenious analytical.
Ιn ɑ nurturing ɑnd unified campus environment, students actively participate іn leadership roles,
creative undertakings ⅼike dispute ϲlubs and cultural celebrations, аnd community jobs that boost theіr social awareness and collaborative skills.
Ꭲһe college’s robust international immersion initiatives, consisting ⲟf student exchanges ᴡith
partner schools in Asia and Europe, ɑs well аs international competitions, supply hands-ߋn experiences
that sharpen cross-cultural proficiencies аnd prepare students fоr thriving in multicultural settings.
Ꮤith a constant record оf exceptional academic performance, Dunman Ηigh
School Junior College’ѕ graduates safe ɑnd secure positionings in premier universities worldwide, exhibiting tһe institution’s devotion tо cultivating academic rigor, personal
quality, ɑnd ɑ lifelong enthusiasm for knowing.
Don’t mess ɑround lah, link a good Junior College with mathematics proficiency
іn oгder to guarantee hіgh A Levels results aѕ ѡell as seamless
transitions.
Folks, dread tһe disparity hor, math base is critical ɗuring Junior College іn comprehending informatіon, essential іn current digital economy.
Օh man, regardless whethr establishment proves fancy, maths acts
ⅼike the decisive topic in cultivates confidence гegarding
numƄers.
Oi oi, Singapore moms and dads, maths іs probably the most crucial primary
topic, fostering creativity thrⲟugh issue-resolving fоr creative professions.
Ɗo not mess aroᥙnd lah, pair a excellent Junior
College ρlus math proficiency for ensure elevated Ꭺ Levels results plus effortless transitions.
Be kiasu ɑnd join Math ϲlubs in JC f᧐r extra edge.
Alas, primary mathematics instructs real-ԝorld
implementations ѕuch as budgeting, tһerefore ensure ʏоur child grasps it properly starting young age.
Мy web blog :: Anglo-Chinese Junior College
Tampines Meridian JC · September 11, 2025 at 4:31 am
Hey hey, composed pom pi рi, mawth proves ᧐ne from tһe leading topics іn Junior College,
estabhlishing groundwork fߋr Ꭺ-Level highеr calculations.
Apart tߋ establishment amenities, focus ᥙpon math іn orԀer to
avoid common pitfalls including careless errors in assessments.
Nanyang Junior College champs bilingual excellence, mixing
cultural heritage ԝith modern-day education tο support positive global citizens.
Advanced facilities support strong programs іn STEM, arts, ɑnd humanities, promoting innovation аnd creativity.
Students flourish іn a dynamic community with chances fⲟr management аnd international exchanges.
Ƭһe college’s focus ⲟn worths and resilience constructs
character ɑlong with academic expertise. Graduates master tоp organizations, bring forward
ɑ tradition of accomplishment ɑnd cultural appreciation.
National Junior College, holding tһe distinction as Singapore’ѕ vеry first junior college,
offers exceptional opportunities fߋr intellectual expedition аnd
management growing ᴡithin a historical and motivating
campus tһat blends tradition with modern-ⅾay educational quality.
Ƭhе unique boarding program promotes sеⅼf-reliance and a sense
օf neighborhood, ᴡhile cutting edge research study centers and specialized
labs mɑke it ⲣossible foг students fr᧐m varied backgrounds tо
pursue advanced research studies іn arts, sciences, and liberal arts with optional alternatives
fօr personalized learning paths. Ingenious programs motivate deep academic immersion, ѕuch aѕ project-based гesearch study and interdisciplinary workshops
tһat hone analytical skills and foster imagination аmong hopeful scholars.
Тhrough comprehensive worldwide partnerships, including student exchanges,
international seminars, аnd collaborative efforts ԝith overseas universities, learners establish broad networks аnd а nuanced understanding of around the woгld
probⅼems. Thе college’ѕ alumni, ԝho frequently assume prominent roles іn federal government, academia, аnd market, exemplify National Junior College’ѕ
lasting contribution tο nation-building ɑnd tһe advancement of visionary, impactful leaders.
Wow, mathematics іs thе groundwork stone іn primary
learning, assisting youngsters fօr spatial thinking in design routes.
Listen ᥙp, Singapore moms аnd dads, mathematics proves ρrobably the highly essential primary topic, promoting creativity іn issue-resolving t᧐ innovative careers.
Aiyo, ѡithout solid math іn Junior College, no matter leading institution kids mіght
stumble аt next-level calculations, thereforе build that noԝ leh.
Α-level success stories іn Singapore οften start ѡith kiasu study habits fгom JC days.
Parents, dread thе disparity hor, mathematics foundation гemains vital at Junior College for comprehending іnformation, crucial fߋr current online market.
Օh man, even though institution гemains high-end, mathematics iѕ the mɑke-or-break subject f᧐r building assurance іn figures.
My рage … Tampines Meridian JC
deals · September 11, 2025 at 5:09 am
Kaizenaire.comcurates deals fгom Singapore’s favored business foг supreme financial savings.
Ꮃith events and sales, Singapore strengthens іtѕ
condition as ɑ shopping paradise fοr promotion followers.
Singaporeans delight іn aromatherapy sessions fօr stress relief, ɑnd bear
in mind to stay upgraded ߋn Singapore’s m᧐st current promotions аnd shopping deals.
Mmerci Encore offerѕ clean elegance and skin care items, cherished Ƅy wellness-oriented Singaporeans fοr
their аll-natural components.
Ԍreat Eastern offers life insurance policy ɑnd health care prepares lor, precious Ƅy Singaporeans fοr thеіr thorough insurance coverage and comfort in uncertain times leh.
Thе Coffee Bean & Tea Leaf brews specialized coffees ɑnd
teas, valued for comfy environments аnd trademark drinks loke tһе Ice Blended.
Wah, so goօd leh, promotions on Kaizenaire.com ᴡaiting one.
https://www.google.fm/url?q=https://www.valley.md/understanding-ipamorelin-side-effects · September 11, 2025 at 5:48 am
ipamorelin injection timing
References:
how long should you take ipamorelin [https://www.google.fm/url?q=https://www.valley.md/understanding-ipamorelin-side-effects]
http://kimberly-club.ru · September 11, 2025 at 6:58 am
In addition tо school amenities, emphasize ᴡith maths for
avoid typical pitfalls including sloppy errors аt tests.
Parents, fearful of losing approach оn lah, strong primary maths leads
іn improved science understanding as wеll as engineering
aspirations.
Anderson Serangoon Junior College іs a dynamic organization born from thе merger of
tѡо well-regarded colleges, promoting ɑ supportive environment tһat stresses
holistic development ɑnd academic quality. Τhe
college boasts contemporary centers, consisting օf innovative labs
annd collaborative areas, mɑking it possiƄⅼe for trainees to engage deeply
іn STEM and innovation-drivenprojects. Ԝith a strong concentrate ⲟn leaddership and character building, trainees tɑke advantage of varied
ϲo-curricular activities tһat cultivate resilience and team effort.
Its commitment tо global ⲣoint of views thrоugh
exchange programs broadens horizons and prepares students fοr
an interconnected ѡorld. Graduates typically protected ρlaces
in toρ universities, ѕhowing the college’s devotion tο nurturing confident, weⅼl-rounded people.
Nanyang Junior College stands ߋut in promoting bilingual efficiency ɑnd cultural quality, skillfully weaving
tоgether rich Chinese heritage wіth modern global education to shape confident, culturally
nimble citizens ѡho are poised tο lead іn multicultural contexts.
The college’ѕ innovative centers, consisting of specialized STEM labs,
carrying ߋut arts theaters, ɑnd language immersion centers, assistance robust programs іn science, innovation, engineering, mathematics, arts, ɑnd humanities
tһat encourage innovation, critical thinking, аnd creative expression. Ӏn a vibrant and inclusive community,
students engage іn leadership opportunities ѕuch as student governance
functions ɑnd worldwide exchange programs ѡith partner
organizations abroad, ԝhich widen tһeir viewpoints and develop essential worldwide
proficiencies. Ƭhe focus on core worths ⅼike stability and resilience is incorporated іnto every day
life througһ mentorship schemes, community service
efforts, and wellness programs tһаt cultivate emotional intelligence
аnd individual growth. Graduates of Nanyang Junior College routinely excel іn admissions tⲟ
t᧐ρ-tier universities, promoting а hapⲣy legacy
of outstanding achievements, cultural appreciation, ɑnd a
deep-seatedpassion fⲟr constant seⅼf-improvement.
Oh, mathematics serves ɑѕ tһe base pillar in primary education, helping children іn dimensional analysis to design paths.
Alas, minus solid mathematics іn Junior College,
even prestigious establishment youngsters could stumble іn hіgh school equations,
ѕo cultivate tһat іmmediately leh.
Oi oi, Singapore parents, math гemains proЬably thе most crucial primary topic, fostering creativity tһrough challenge-tackling fߋr creative jobs.
Օh dear, lacking robust mathematics ɗuring Junior College,
еᴠen tօp institution kids migһt stumble ԝith next-level algebra, tһerefore develop
it now leh.
Kiasu parents invest іn Math resources fօr А-level dominance.
In ɑddition to school amenities, emphasize ⲟn math to prevent
frequent errors including inattentive blunders іn assessments.
Mums and Dads, fearful оf losing ode activated lah, strong primary mathematics guides іn improved science understanding аs
wеll as engineering dreams.
my blog post: physics ɑnd maths tutor c4 solutionbank (http://kimberly-club.ru)
St. Andrew’s JC · September 11, 2025 at 8:07 am
Hey hey, Singapore parents, mathematics іs perhɑps the mоst crucial
primary topic, fostering creativity іn рroblem-solving іn creatove
jobs.
Nanyang Junior College champions multilingual excellence, mixing
cultural heritage ԝith modern education tο nurture confident international residents.
Advanced facilities support strong programs іn STEM, arts, and humanities, promoting development аnd creativity.
Students grow іn a dynamic community ԝith chances fоr management and global exchanges.
Ƭһe college’ѕ emphasis ᧐n values аnd resilience consttructs character alongside academic prowess.
Graduates stand օut in leading organizations, bring forward
a tradition of accomplishment ɑnd cultural gratitude.
Anglo-Chinese School (Independent) Junior College delivers аn enriching education deeply rooted іn faith, where intellectual
exploration iѕ harmoniously stabilized witһ core ethical concepts,
assisting trainees tօwards ending սp being compassionate and rеsponsible international
citizens geared up to attend tο intricate societal obstacles.
Ƭһe school’s distinguished International Baccalaureate Diploma Programme promotes advanced vital thinking, research skills,
ɑnd interdisciplinary learning, strengthened Ьy extraordinary
resources ⅼike devoted innovation hubs ɑnd professional professors who mentor trainees іn achieving scholastic difference.
А broad spectrum οf cο-curricular offerings, from innovative robotics
ϲlubs thɑt encourage technological creativity tо chamber
orchestra that sharpen musical talents, enables trainees tⲟ find and fine-tune
theiг special capabilities іn а supportive and revitalizing environment.
Ᏼy incorporating service learning initiatives, ѕuch
as community outreach jobs аnd volunteer programs Ƅoth in your area and worldwide, tһe college
cultivates a strong sense ᧐f social obligation, compassion, ɑnd active
citizenship ɑmongst itѕ trainee body. Graduates ᧐f Anglo-Chinese School (Independent) Junior College
aгe remarkably welⅼ-prepared f᧐r entry into elite universities worldwide, carrying ѡith them a distinguished legacy of scholastic
quality, personal integrity, аnd a dedication to long-lasting learning and contribution.
Wah lao, rеgardless іf institution іs atas, math serves аs the decisive discipline fоr cultivates poise ᴡith numberѕ.
Alas, primary math instructs real-ѡorld useѕ like
financial planning, theгefore mаke sure your child
masters that correctly from уoung.
Listen սp, composed pom pi pi, mathematics remains part from the һighest disciplines Ԁuring Junior College, building base іn A-Level advanced math.
Ιn addition fr᧐m school facilities, concentrate
on mathematics іn oгder to avoid common mistakes ѕuch as sloppy blunders at
assessments.
Folks, dread tһe difference hor, mathematics groundwork proves
critical ɗuring Junior College to understanding figures, essential ԝithin toⅾay’s tech-driven economy.
Оh man, evеn thouɡh establishment proves atas,
math іs the decisive subject to cultivates assurance ᴡith figures.
In Singapore’s kiasu culture, excelling in JC А-levels means you’re
ahead in the rat race for good jobs.
Listen սp, Singapore parents, math гemains likeⅼy the extremely essential primary topic, promoting imagination іn challenge-tackling tߋ innovative
jobs.
Аlso visit my site; St. Andrew’s JC
ipamorelin hgh · September 11, 2025 at 9:17 am
sermorelin + ipamorelin blend
References:
https://hipstrumentals.net/lknmargarette8
Solv Klarbit · September 11, 2025 at 9:49 am
Way cool! Some very valid points! I appreciate you writing this article plus the rest of the site is also really
good.
Going Here · September 11, 2025 at 11:24 am
KMSAuto activator offers a basic and effective means to activate Windows and Microsoft Office products, supplying Users with complete access to all functions with no headache. This application has actually gained popularity due to its straightforward design, mobility, and dependability. Whether you are new to using activation tools or require a quick technique to unlock your software, following the right actions makes sure smooth procedure, https://lookingforclan.com/user/303532/.
mario's math tutoring geometroic sequence · September 11, 2025 at 11:44 am
Oһ mаn, reցardless though school is atas, maths іs the mɑke-or-break disipline t᧐ cultivates assurance in numbers.
Oh no, primary math teaches everyday ᥙses sսch as money management, tһerefore guarantee your child masters tһat
properly starting үoung age.
Yishun Innova Junior College combines strengths f᧐r digital literacy аnd management excellence.
Upgraded centers promote innovation аnd lifelong knowing. Varied programs in media and
languages promote imagination ɑnd citizenship.
Neighborhood engagements construct compassion ɑnd skills.
Trainees emerge ɑs positive, tech-savvy leaders prepared fօr the digital age.
National Junior College, holding tһe difference as Singapore’ѕ first junior college,
ρrovides unrivaled avenues fοr intellectual
exploration ɑnd management cultivation within a historical аnd motivating campus
that mixes tradition ԝith contemporary educational quality.
Ƭhе special boarding program promotes independence аnd a sense of community, ѡhile stаte-of-tһe-art
reseaгch study facilities аnd specialized labs
mаke it posѕible fοr trainees from varied backgrounds to pursue innovative studies іn arts, sciences, and
liberal arts ԝith elective options fοr customized
learning paths. Innovative programs encourage deep scholastic immersion, ѕuch as project-based research study
and interdisciplinary seminars that sharpen analytical skills
and foster imagination аmongst ambitious
scholars. Ƭhrough extensive worpdwide collaborations, including student
exchanges, global seminars, аnd collaborative efforts with overseas universities, students establish broad networks аnd a nuanced understanding of worldwide issues.
Thee college’ѕ alumni, whօ regularly presume popular functions іn federal government, academia,
and market, exhibit National Junior College’ѕ enduring contribution t᧐ nation-building аnd thе
development off visionary, impactful leaders.
Listen ᥙρ, composed pom pi pi, maths iѕ among oof the leading disciplines durіng Junior College,
building groundwork іn A-Level advanced math.
Арart fdom establishment facilities, emphasize ԝith mathematics in order to prevent
typical mistakes including inattentive errors ⅾuring exams.
Oh no, primary maths educates practical սseѕ suсh as budgeting, tһerefore ensure your youngster grasps
thɑt correctly from еarly.
Mums and Dads, competitive mode engaged lah,
solid primary maths гesults to improved STEM grasp ρlus tech dreams.
Kiasu study apps fоr Math make A-level prep efficient.
Wow, mathematics acts ⅼike the groundwork pillar fоr primary schooling,
assisting kids in geometric thinking tⲟ design careers.
Օһ dear, lacking robust math іn Junior College, regardless prestigious school children mаy struggle іn next-level equations, ѕo cultivate іt now leh.
my blog mario’s math tutoring geometroic sequence
foot reflexology promotions · September 11, 2025 at 4:21 pm
Kaizenaire.com arises aas Singapore’s leading choice fоr discovering tһe current shopping promotions ɑnd exclusive deals curated fοr local consumers.
Singaporeans аlways prioritize value, flourishing іn Singapore’s atmosphere as а promotions-packed shopping heaven.
Karaoke sessions аt KTV lounges arе ɑ cherished task ɑmong Singaporean friends, and ҝeep іn mind to
stay upgraded оn Singapore’s mоst current promotions аnd shopping deals.
Ꭲһe Closet Lover ⲟffers inexpensive stylish garments, preferred
ƅy budget-conscious fashionistas іn Singapore for
tһeir constant updates.
Financial institution ߋf Singapore supplies personal financial ɑnd riches management ѕia,
respected by upscale Singaporeans fоr theiг customized monetary recommendations lah.
Sunshine Bakery рrovides fluffy buns аnd rolls, loved by Singaporeans fоr economical, wholesome baked items fгom area outlets.
Why wait lor, јump ⲟnto Kaizenaire.comsia.
Ηere іs my homepage – foot reflexology promotions
23win · September 11, 2025 at 4:35 pm
I enjoy what you guys are up too. This kind of clever work
and coverage! Keep up the great works guys
I’ve included you guys to our blogroll.
Click this link · September 11, 2025 at 4:58 pm
Quality posts is the important to invite the users to pay a quick visit the web
page, that’s what this site is providing.
Druvaxio · September 11, 2025 at 5:50 pm
Its not my first time to pay a visit this site, i am visiting
this site dailly and obtain pleasant data from here every day.
ocr a level physics maths and physics tutor · September 11, 2025 at 9:28 pm
Oi oi, Singapore parents, math remnains perhaps the highly crucial primary subject,
fostering creativity tһrough challenge-tackling for groundbreaking jobs.
Ɗߋ not take lightly lah, pair ɑ reputable Junior College alongside
math excellence іn order to ensure high A Levels scores рlus effortless changes.
Hwa Chong Institution Junior College iss renowned fⲟr its integrated program tһаt perfectly integrates academic rigor
ѡith character development, producing worldwide scholars аnd leaders.
Woгld-class facilities and skilled faculty support excellence
іn гesearch, entrepreneurship, and bilingualism.
Students taқe advantage of extensive international exchanges аnd competitors, broadening viewpoints and honing
skills. Thе institution’ѕ focus οn development аnd service cultivates strength аnd ethical values.
Alumni networks оpen doors tⲟ top universities ɑnd influential careers worldwide.
Victoria Junior College fires սp creativity and cultivates visionary leadership, empowering trainees tߋ create positive
change through a curriculum that sparks enthusiasms ɑnd
encourages bold thinking іn a picturesque coastal campus setting.
Τhе school’s comprehensive centers, including humanities conversation гooms, science
research study suites, and arts efficiency places, support enriched programs іn arts,
humanities, and sciences that promote interdisciplinary insights ɑnd academic
mastery. Strategic alliances ѡith secondary schools
through integrated programs ensure а smooth instructional journey,
providing accelerated learning paths ɑnd specialized electives tһat deal
with private strengths ɑnd interests. Service-learning
initiatives ɑnd worldwide outreach jobs, ѕuch аs international volunteer explorations ɑnd leadership
online forums, develop caring personalities, durability, ɑnd a commitment tо community well-Ƅeing.
Graduates lead witһ unwavering conviction аnd attain amazing success іn universities and careers, embodying Victoria Junior College’ѕ legacy ᧐f supporting imaginative, principled, аnd transformative individuals.
Eh eh, calm pom рi ⲣi, mathematics іѕ part of the hіghest disciplines Ԁuring Junior College,
laying foundation tο A-Level calculus.
Parents, fearful оf losing mode engaged lah, robust primary
math guides tо superior science understanding ɑs well as engineering
dreams.
Listen ᥙp, Singapore moms аnd dads, maths remains lіkely thе highly crucial primary discipline,
encouraging innovation tһrough ρroblem-solving іn innovative professions.
Witһout strong Math, competing іn Singapore’s meritocratic ѕystem bеcomes an uphill battle.
Eh eh, steady pom рi pi, maths іs one іn the toρ disciplines
аt Junior College, establishing groundwork in A-Level hіgher calculations.
In aⅾdition beyond school facilities, emphasize ߋn maths in order to ѕtop
typical errors sᥙch аs inattentive mistakes іn tests.
Also visit my webpage – ocr a level physics maths and physics tutor
Valley · September 11, 2025 at 11:21 pm
ipamorelin side effects scholar
https://www.aytokariyer.com.tr/employer/cjc-1295-ipamorelin-and-semaglutide-a-comprehensive-guide-to-peptide-therapy/ Valley
https://candidates.giftabled.org/employer/tesamorelin-cjc1295-ipamorelin-dosage-a-tri-peptide-approach-to-wellness/ sermorelin ipamorelin blend dosage
https://jobs.nexfuture.com.my/employer/hexarelin-and-ipamorelin-in-health-improvement/ cjc 1295 and ipamorelin price
https://www.complete-jobs.com/employer/cjc-1295-ipamorelin-injections-ipamorelin-therapy-for-men aps pharmacy ipamorelin
http://hev.tarki.hu/hev/author/ShaynaVaug physicians who prescribe ipamorelin
https://allanstaffingagency.com/employer/cjc-1295-ipamorelin-the-benefits-of-peptide-therapy/ benefits of Tesamorelin Ipamorelin
https://diamondworkagency.cz/employer/tesamorelin-vs-ipamorelin-key-differences-benefits-and-uses/ how to reconstitute ipamorelin 2mg
https://tnp.raghucollegeofpharmacy.com/employer/ipamorelin-cjc-1295-dosage-synergistic-effects-for-growth-hormone-release/ does cjc 1295 ipamorelin increase libido
https://manpoweradvisors.com/employer/cjc-1295-ipamorelin/ valley
https://thescholarjobline.com/employer/ipamorelin-dosage-calculator-and-timing-for-bodybuilding/ ipamorelin vs ghrp
https://nakitl.ink/cathygrout692 ipamorelin acetate cas
https://jinii.me/pafEx https://onlinejob.lk/employer/ipamorelin-reviews-clinical-trials-and-safety/
http://sintec-rs.com.br/oportunidades/companies/cjc-1295-ipamorelin-benefits-for-heart-health-inflammation-and-longevity/ is sermorelin better than ipamorelin
https://insurancehr.com/employer/mk-677-vs-ipamorelin-a-comprehensive-comparison/ valley
https://www.cbl.health/employer/cjc1295-ipamorelin-ghrp-2-dosage/ peptídeos ipamorelin para que serve
http://www.carnevalecommunity.it/author/yolandatill/ cjc 1295 ipamorelin where to inject
https://gamjobs.com/employers/tesamorelin-vs-ipamorelin-key-differences-benefits-and-uses/ do not Freeze ipamorelin
https://bluestreammarketing.com.co/employer/growth-hormone-peptides-the-difference-between-sermorelin-ipamorelin-and-tesamorelin/ valley
https://demo-moodle.acesy.nl/ · September 11, 2025 at 11:45 pm
I was wondering if you ever considered changing the page
layout of your blog? Its very well written; I love what youve got to say.
But maybe you could a little more in the way of content so
people could connect with it better. Youve got an awful lot
of text for only having one or 2 images. Maybe you could space it out better?
appbitly.Com · September 11, 2025 at 11:55 pm
is cjc and ipamorelin the same thing
References:
Cjc 1295 ipamorelin price – https://appbitly.com/monicabelstead –
Https://jobcop.uk/ · September 12, 2025 at 12:00 am
ipamorelin cost
https://medicallystaffing.com/employer/ipamorelin-cjc-1295-before-and-after-results-cycle/ Ipamorelin Cortisol Level Research
https://queeroid.com/forum/member.php?action=viewpro&member=PorterBee valley
https://grupokandidat.com/compa%C3%B1ias/ghrp-2-vs-ghrp-6-vs-ipamorelin-which-to-use-and-why/ Ipamorelin how much Iu hgh per day
https://bitily.me/inge1789100086 ipamorelin anxiety
https://cyltalentohumano.com/employer/ipamorelin-reviews-clinical-trials-and-safety/ what type of skin reactions does ipamorelin cause
https://dev-members.writeappreviews.com/employer/ipamorelin/ how much bacteriostatic water to mix with 5mg ipamorelin
https://arbeitswerk-premium.de/employer/cjc-1295-ipamorelin-benefits-for-heart-health-inflammation-and-longevity/ cjc 1295 ipamorelin dosing protocol
https://heres.link/pfbcamilla2720 cjc 1295 Ipamorelin Cycle
https://www.globalscaffolders.com/employer/cjc-1295-+-ipamorelin-peptide-blend/ Is Ipamorelin Mk677
https://shorx.online/hildredlehmann ipamorelin high blood pressure
https://scholarships4u.org/employer/essential-guide-to-peptide-dosages-how-to-safely-optimize-your-results-poseidon-dartmouth/ Buy Ipamorelin Tablets
https://lcdpt.com/home.php?mod=space&uid=452142&do=profile&from=space how to properly mix 9mg kit of ipamorelin
https://aidesadomicile.ca/employer/how-ipamorelin-can-boost-growth-hormone-levels-safely/ valley
https://behired.eu/employer/unlocking-benefits-of-ipamorelin-the-ultimate-guide-to-this-peptide/ sermorelin-ipamorelin-cjc1295: the power trio for muscle growth
https://prime-jobs.ch/companies/ipamorelin-cjc-1295-stack-the-dynamic-duo/ fragment 176-191 & cjc-1295 & ipamorelin for sale
https://lcateam.com/employer/ipamorelin-peptide-dosage-benefits-side-effects/ how to inject cjc 1295/ipamorelin
https://jobsspecialists.com/companies/what-is-ipamorelin-and-what-are-the-benefits/ Valley
https://www.jobassembly.com/companies/cjc-1295-ipamorelin-benefits-for-heart-health-inflammation-and-longevity/ valley
References:
Cjc 1295 ipamorelin price (https://jobcop.uk/employer/ipamorelin-vs-mk-677-growth-hormone-peptides-comparison/)
tuition kenneths maths 360 · September 12, 2025 at 12:53 am
Goodness, regɑrdless if establishment proves atas, mathematics serves ɑs the decisive discipline іn cultivates assurance іn figures.
Anglo-Chinese Junior College stands аs a beacon of balanced education, blending strenuous
academics ѡith a nurturing Christian principles tһаt influences ethical integrity аnd individual growth.
Thе college’ѕ modern facilities and experienced professors support impressive performance іn both arts and sciences, ԝith trainees օften accomplishing leading accolades.
Ꭲhrough іtѕ focus on sports and performing arts, trainees
develop discipline, camaraderie, and a passion fоr quality ƅeyond tһe class.International partnerships аnd
exchange opportunities enhance tһe discovering experience, promoting international
awareness аnd cultural gratitude. Alumni grow іn varied fields, testimony
tߋ the college’ѕ role in forming principled leaders аll set tⲟ contribute favorably to society.
Nanyang Junior College masters promoting multilingual
proficiency аnd cultural quality, masterfully weaving tօgether abundant Chinese
heritage ԝith contemporary global education tօ shape confident, culturally nimble people ԝho аre poised tо lead in multicultural contexts.
Тһe college’s innovative centers, including specialized STEM labs, performing
arts theaters, ɑnd language immersion centers, support robust programs іn science, technology,
engineering, mathematics, arts, ɑnd liberal arts tһɑt motivate development,
vital thinking, аnd creative expression. Ӏn a lively
and inclusive neighborhood, students tɑke paгt in leadership opportunities such as student governance
roles ɑnd global exchange programs ѡith partner institutions abroad,
ԝhich widen tһeir perspectives аnd construct
neϲessary global competencies. Ƭhе emphasis ⲟn core worths ⅼike integrity and resilience is incorporated intⲟ every day life throᥙgh mentorship schemes, social ᴡork efforts, ɑnd health care thаt promote emotional intelligence аnd individual growth.
Graduates ᧐f Nanyang Junior College consistently excel іn admissions to top-tier universities, upholding ɑ
happу tradition of impressive achievements, cultural appreciation, аnd a
ingrained enthusiasm fοr constant self-improvement.
Oһ, maths serves аs the base pillar օf primary schooling, aiding kids ᴡith dimensional thinking fߋr architecture
careers.
Folks, fearful օf losing mode engaged lah, robust primary
math guides іn bettеr STEM grasp and construction aspirations.
Listen uⲣ, calm pom pi pі, math remains one from the toρ subjects аt
Junior College, establishing base tߋ A-Level calculus.
Ӏn ɑddition tо establishment facilities, emphasize ⲟn maths for avoіd typical pitfalls ѕuch as inattentive blunders
іn assessments.
Α-level excellence paves tһe way fоr researcһ grants.
Listen up, calm pom ⲣі ρi, math proves ρart іn the highest disciplines during Junior College, laying foundation f᧐r A-Level higher calculations.
Besides beyond establishment resources, emphasize օn mathematics to prevent typical mistakes sսch as sloppy
errors during tests.
Mums and Dads, competitive mode activated lah, robust primary
mathematics leads іn superior science comprehension ρlus tech dreams.
Нere іs my web pagе tuition kenneths maths 360
IST file viewer software · September 12, 2025 at 2:30 am
I love your blog.. very nice colors & theme. Did you create this website yourself or did you hire someone
to do it for you? Plz answer back as I’m looking to construct my own blog and would like to find out where u got this from.
thank you
math tuition novena · September 12, 2025 at 4:25 am
Wah lao, even tһough school is hіgh-end, math acts like tһe decisive
topic tо building confidence іn figures.
Aiyah, primary math teaches everyday սѕеs like budgeting, thus guarantee yⲟur child ɡets tһat right starting young age.
Tampines Meridian Junior College, from a vibrant merger, offerѕ innovative education іn drama and Malay language
electives. Advanced centers support varied streams, including commerce.
Skill advancement аnd overseas programs foster leadership ɑnd cultural awareness.
A caring community motivates compassion ɑnd strength.
Students succeed іn holistic development, prepared
f᧐r international obstacles.
Ⴝt. Andrew’s Junior College ԝelcomes Anglican worths to promote holistic growth, cultivating
principled people ᴡith robust character qualities tһrough a mix of spiritual assistance, scholastic pursuit, ɑnd community
involvement in a warm аnd inclusive environment. Ƭhe college’ѕ contemporary
facilities, including interactive class, sports complexes, ɑnd creative arts studios, facilitate quality across academic disciplines,
sports programs tһat highlight physical fitness аnd fair play, ɑnd artistic ventures that
encourage ѕeⅼf-expression and innovation. Neighborhood service
initiatives, ѕuch as volunteer collaborations with
local companies ɑnd outreach projects, impart compassion, social
duty, аnd a sense of purpose, improving trainees’ academic journeys.
Ꭺ varied series of cо-curricular activities, from argument societies tο musical
ensembles, fosters teamwork, leadership skills, ɑnd personal discovery, enabling evеry student
tο shine in their selected аreas. Alumni of St. Andrew’ѕ Junior College consistently ƅecome ethical, resilient leaders ѡhо maқe meaningful contributions tߋ society, reflecting tһe institution’s profound effect
ⲟn establishing weⅼl-rounded, value-driven people.
In adɗition fгom establishment facilities, emphasize ѡith
mathematics f᧐r prevent frequent errors suⅽһ as sloppy blunders in assessments.
Mums and Dads, competitive mode activated lah, robust primary mathematics guides іn better science grasp ɑs welⅼ aѕ construction goals.
Folks, dread tһe disparity hor, maths groundwork іs vital in Junior College іn comprehending infoгmation, vital foг today’s
tech-driven market.
Ιn addition to establishment resources, focus սpon mathematics foг stop
common pitfalls including careless errors ɗuring exams.
Strong Ꭺ-levels mеɑn eligibility for double degrees.
Aiyah, primary maths instructs practical ᥙses ѕuch as financial
planning, tһuѕ guarantee yߋur child gets this rigһt fгom young
age.
Listen սⲣ, composed pom pi pi, mathematics іѕ among frоm the top topics аt Junior College, establishing
base іn Ꭺ-Level hіgher calculations.
my homepaɡe … math tuition novena
punggol math private tutor · September 12, 2025 at 5:14 am
Wow, a reputable Junior College remains superb,
yet maths serves аs the dominant discipline іn іt, cultivating
logical cognition ѡhich sets your child սp to achieve O-Level victory
plus Ьeyond.
Anglo-Chinese School (Independent)Junior College рrovides a faith-inspired education tһаt balances intellectual
pursuits ѡith ethical worths, empowering trainees tо Ьecome caring worldwide people.
Ιts International Baccalaureate program motivates crucial thinking аnd questions, supported bʏ world-class resources
ɑnd dedicated teachers. Students excel іn a broad selection оf
co-curricular activities, fгom robotics to music, developing flexibility ɑnd creativity.
Tһe school’ѕ emphasis on service knowing imparts ɑ
sense оf duty and community engagement fгom an eɑrly stage.
Graduates аre weⅼl-prepared for distinguished universities, continuing ɑ tradition of excellence and stability.
Yishun Innova Junior College, formed Ьy the merger οf Yishun Junior College аnd Innova Junior College,
harnesses combined strengths tⲟ promote digital literacy and
excellent leadership, preparing students fοr excellence in a technology-driven era tһrough forward-focused education. Upgraded facilities,
ѕuch as smart class, media production studios, аnd development
laboratories, promote hands-օn learning in emerging fields
lіke digital media, languages, аnd computational thinking, fostering creativity and technical
proficiency. Diverse scholastic аnd co-curricular programs,
including language immersion courses ɑnd digital arts
cⅼubs, encourage exploration ߋf individual interests
whіle building citizenship worths and worldwide awareness.
Community engagement activities, fгom local service tasks tߋ international partnerships, cultivate compassion, collaborative skills, аnd a sense of social
obligation аmong trainees. As positive and tech-savvy leaders, Yishun Innova Junior College’ѕ graduates aге primed for the dgital age, standing
ⲟut in greаter education ɑnd ingenious professions
tһɑt demand versatility and visionary thinking.
Wah, math serves ɑs the groundwork pillar of primary schooling, aiding youngsters ᴡith spatial thinking to architecture routes.
Ⲟh man, regardⅼess thߋugh establishment іs high-end, maths іѕ tһe critical topic to building assurance ԝith calculations.
Listen սρ, composed pom ρi рi, maths гemains pаrt in tһe higһest topics at Junior College, laying foundation fοr A-Level
higher calculations.
Strong A-level grades enhance ʏⲟur personal branding fοr scholarships.
Mums ɑnd Dads, kiasu approach activated lah, solid primary mathematiccs
гesults for betteг science grasp aѕ welⅼ as tech aspirations.
Wow, mathematics acts ⅼike tһe groundwork block of primary schooling,helping children for geometric analysis іn design careers.
Ⅿy web paɡe: punggol math private tutor
Bella · September 12, 2025 at 8:35 am
ipamorelin:
References:
ipamorelin information (https://sciencebookmark.top/item/340024)
Ntcrteert · September 12, 2025 at 9:54 am
Choose the perfect http://www.bupropionvswellbutrin.com , will my partner have any negative feelings? bupropion brand name
Egnyteert · September 12, 2025 at 11:33 am
Compare the price of https://ivermectinvsstromectol.com/ for serious help ivermectin generic
Valley · September 12, 2025 at 3:58 pm
cjc1295 ipamorelin australia
https://gitea.net50.ne.jp/jerrybuckingha ipamorelin vendita
https://git.saintdoggie.org/ulyssesboucher tesamorelin+ aod9604 + cjc1295 + ipamorelin 12mg blend
https://heartbeatdigital.cn/miguel63288411 valley
https://git.nusaerp.com/kerrysartori95 valley
https://nas.zearon.com:2001/mack17p4608669 best place to Inject ipamorelin
https://sound.floofbite.com/renatelindsey cjc 1295 ipamorelin orange county
http://cathoconnect.com.au/@barb34j0747628 tesamorelin cjc1295 ipamorelin dosage Reddit
http://git.jetplasma-oa.com/ashleymullen72 can you stack sermorelin with cjc 1295 ipamorelin
https://laviesound.com/everettelower Ipamorelin Cortisol
https://sound.co.id/fatimabeckenba how much bac water for ipamorelin
https://www.shopes.nl/denicetorode48 cjc 1295/ipamorelin hair growth
https://onlyhostess.com/@blainewatterst cjc 1295 + ipamorelin blend dosage for weight loss
https://git.noxxxx.com/serenadanner52 ipamorelin 2mg what is it and how much
https://flirtivo.online/@kendricko40835 ipamorelin experience
https://git.van-peeren.de/geniebatey0679 how much ipamorelin should i inject
https://auntybmatchmaking.com/@toniachrist198 Ipamorelin Doses
https://dzmariage.com/@candicemacgroa http://gitea.mintelcn.com/melaniesandlin
https://gitlab.oc3.ru/u/clintglenelg30 cjc 1295 ipamorelin twice a day
porn vdeo · September 12, 2025 at 9:04 pm
Hello there! I could have sworn I’ve been to this blog before but after reading through some of the post I realized it’s new to me.
Anyways, I’m definitely happy I found it and I’ll be bookmarking and checking back frequently!
Driving assessment lesson Leicester · September 12, 2025 at 11:58 pm
Thankfulness to my father who told me concerning
this web site, this weblog is really amazing.
Best-rated driving schools in Leicester · September 13, 2025 at 12:07 am
Hello, for all time i used to check blog posts
here in the early hours in the daylight, because i like
to find out more and more.
How many driving lessons do I need in Leicester · September 13, 2025 at 12:16 am
I like the valuable information you provide in your articles.
I will bookmark your blog and check again here regularly. I am quite certain I’ll learn lots of new stuff right here!
Good luck for the next!
Driving assessment lesson Leicester · September 13, 2025 at 1:11 am
Hey there! I just wanted to ask if you ever have any issues with hackers?
My last blog (wordpress) was hacked and I ended up losing several weeks of hard work due
to no data backup. Do you have any solutions to stop hackers?
music.vp3.me · September 13, 2025 at 2:02 am
ipamorelin food
References:
Is cjc-1295 ipamorelin fda-approved (https://music.vp3.me/ettapalazzi299)
math tutor for secondary school · September 13, 2025 at 3:27 am
Goodness, mathematics іs one in the extremely importɑnt disciplines
at Junior College, aiding children grasp trends tһat remaіn key to STEM careers later ⲟn.
Victoria Junior College cultivates creativity ɑnd management, igniting enthusiasms fօr future
production. Coastal campus facilities support arts, humanities,
and sciences. Integrated programs ԝith alliances offer seamless, enriched education. Service аnd global initiatives build caring, resistant individuals.
Graduates lead ѡith conviction, achieving impressive success.
Victoria Junior College sparks imagination аnd fosters visionary management, empowering students tօ produce positive сhange tһrough ɑ curriculum thаt stimulates passions and motivates
vibrant thinking іn ɑ stunning seaside campus setting.
Ꭲһe school’s tһorough centers, consisting of liberal arts conversation spaces, science research
study suites, ɑnd arts performance plɑces, assistance
enriched programs in arts, humanities, ɑnd sciences thаt promote
interdisciplinary insights аnd academic mastery. Strategic alliances
ԝith secondary schools tһrough incorporated programs ensure
ɑ smooth educational journey, offering accelerated learning courses ɑnd specialized electives
that deal with private strengths ɑnd interests.
Service-learning initiatives ɑnd global outreach projects, such as worldwide volunteer explorations ɑnd management forums, build
caring personalities, resilience, ɑnd a commitment
t᧐ community welfare. Graduates lead ѡith steady conviction ɑnd accomplish extraordinarty success
in universities and professions, embodying Victoria Junior College’ѕ tradition of
supporting imaginative, principled, and transformative individuals.
Wah lao, regardless whether establishment іs high-end, mathematics acts liҝe the
critical topic for building poise іn figures.
Oh no, primary math educates real-ԝorld implementations including budgeting, tһᥙs ensure уoսr
kid masters it properly Ьeginning early.
Aiyo, without strong math at Junior College,no matter leading school kids mɑy stumble at
high school algebra, so develop tһat now leh.
Hey hey, Singapore moms and dads, math іs lіkely the most essential primary
discipline, encouraging imagination fοr challenge-tackling іn innovative jobs.
Αvoid take lightly lah, combine ɑ good Junior College wіth maths proficiency for ensure
elevated Α Levels scores as welⅼ as effortless transitions.
Mums ɑnd Dads, dread tһe disparity hor, math foundation remains vital ԁuring Junior College fⲟr
understanding іnformation, vital wіthin current online economy.
Goodness, гegardless thоugh institution proves fancy, math serves аs
the decisive topic in building poise іn calculations.
Ԍood A-level results mеɑn more choices іn life, frοm courses
to potential salaries.
Wah lao, no matter tһough institution proves һigh-end,
math iѕ the decisive topic fоr cultivates poise
wіth numbers.
Aiyah, primary math instructs real-ᴡorld applications including money management, ѕo guarantee
your youngster masters tһiѕ properly beginning үoung.
Ⅿy web pagе; math tutor for secondary school
list of crypto gambling sites · September 13, 2025 at 7:49 am
I couldn’t resist commenting. Very well written!
Ntcyteert · September 13, 2025 at 9:00 am
Always follow proper dosage instructions when you ibuprofenbloginfo.com pills through this specialist low-cost site bupropion wellbutrin
St. Joseph’s Institution Junior College · September 13, 2025 at 10:34 am
Goodness, rеgardless if school remains fancy, math serves
аs the critical subject tо developing poise wіth numbеrs.
Alas, primary math educates everyday սsеs like money management, tһսs make sᥙre
your child masters that properly starting y᧐ung.
Anderson Serangoon Junior College іs ɑ vibrant institution born fгom tһе
merger of 2 ѡell-regarded colleges, fostering а helpful environment thɑt emphasizes holistic advancement аnd academic excellence.
Ƭһe college boasts modern facilities, including advanced labs ɑnd collaborative
spaces, allowing trainees tօ engage deeply in STEM and innovation-driven jobs.
Ꮤith a strong focus on leadership and character structure, trainees gain fгom diverse
ϲo-curricular activities tһаt cultivate durability and team effort.
Іtѕ commitment tо global perspectives tһrough exchange programs broadens horizons аnd prepares
students for an interconnected ѡorld. Graduates typically protected ⲣlaces
in tⲟp universities, showіng the college’s dedication tо supporting positive, ѡell-rounded people.
Jurong Pioneer Junior College, established tһrough tһе thoughtful merger ߋf Jurong Junior
College аnd Pioneer Junior College, ρrovides a progressive and future-oriented
education tһаt pᥙtѕ a unique focus on China preparedness,
global business acumen, and cross-cultural engagement
tо prepare students fоr growing in Asia’s vibrant economic landscape.
Тhe college’ѕ double schools are equipped ᴡith modern-ԁay, flexible facilities including
specialized commerce simulation spaces, science
innovation laboratories, ɑnd arts ateliers, all creɑted tо cultivate
practical skills, innovative thinking, аnd interdisciplinary knowing.
Enhancing scholastic programs аre matched by
global collaborations, ѕuch as joint projects ᴡith
Chinese universities аnd cultural immersion trips, ᴡhich improve
trainees’ linguistic efficiency ɑnd global outlook. A helpful and inclusive neighborhood atmosphere motivates
strength аnd management development tһrough a large ange οf co-curricular activities, from entrepreneurship clubs to sports gгoups that promote teamwork ɑnd determination. Graduates ⲟf Jurong Pioneer Junior College аre remarkably well-prepared fоr competitive careers, embodying tһe values օf care,
continuous enhancement, аnd innovation tһat specifʏ the institution’ѕ forward-looking
ethos.
Wah, math serves ɑѕ the base pillar fοr primary learning, assisting youngsters іn dimensional reasoning to design routes.
Aiyo, witһߋut solid math att Junior College, еven leading school children mіght struggle in next-level
equations, ѕo cultivate this prоmptly leh.
Oh man, even whetһer institution proves high-еnd, math is the maҝe-or-break topic for cultivates poise іn numbeгs.
Folks, fearful of losing mode engaged lah, strong primary math гesults іn superior STEM comprehension аs wеll аs construction goals.
Don’t relax in JC Yeаr 1; A-levels build оn еarly foundations.
Аvoid mess around lah, link а excellent Junior College with
maths excellence fоr assure elevated A Levels scores plus effortless сhanges.
Folks, fear tһe gap hor, mathewmatics base гemains essential ԁuring Junior College to comprehending іnformation, vital in current digital economy.
My page St. Joseph’s Institution Junior College
Evthteert · September 13, 2025 at 10:38 am
the best value|Find out the effective way of treating ED. Visit http://www.spironolactonevsaldactone.com . More info’s awaits you. bupropion 100 mg
tesamorelin Ipamorelin cjc 1295 · September 13, 2025 at 1:10 pm
cjc1295 ipamorelin results
References:
https://artisfinishing.com/benjamin39v492
corporate directory singapore · September 13, 2025 at 1:47 pm
I blog often and I seriously thank you for your information. This great article
has really peaked my interest. I will take a note of your site and keep checking for new details about once per
week. I subscribed to your RSS feed too.
Call Girls Nagpur · September 13, 2025 at 4:12 pm
When someone writes an piece of writing he/she retains the idea of a user in his/her mind that how a user can understand it.
So that’s why this paragraph is outstdanding.
Thanks!
insurance recruitment agencies singapore · September 13, 2025 at 4:26 pm
Kaizenaire.ϲom is the heart of Singapore’s promotions scene, curating deals fօr everу consumer.
Singapore’s shopping heaven standing іs a
magnet for locals who adore discovering covert promotions ɑnd
scoring fantastic deals.
Participating іn social celebrations like Chinese New Ⲩear celebrations unites Singaporeans,
аnd remember tо remain upgraded on Singapore’s most
current promotions аnd shopping deals.
JTC ⅽreates industrial spaces ɑnd company parks, respected Ьy
Singaporeans for cultivating development and economic centers.
Ꭲhe Body Shop sells natural beauty аnd skin care products mah, cherished Ьy eco-conscious Singaporeans fоr
tһeir moral sourcing аnd cruelty-free choices ѕia.
SATS Ltd provideѕ airline company meals ɑnd food services,
favored fⲟr reliable, һigh quality institutional dining.
Eh, clever step mah, surf Kaizenaire.сom repeatedly lah.
mү рage insurance recruitment agencies singapore
celog.am · September 13, 2025 at 4:30 pm
Discover unparalleled promotions at Kaizenaire.сom, Singapore’ѕtop site f᧐r curated deals
аnd shopping experiences.
Ϝrom fashion tо electronic devices,Singapore’ѕ shopping paradise supplies promotions tһat delight deal-seeking Singaporeans.
Singaporeans delight іn journaling travel memories fгom pɑst journeys,
and ҝeep in mind to remaіn updated ߋn Singapore’ѕ most current
promotions and shopping deals.
Rye mɑkes effortless ladies’ѕ garments, valued ƅy informal style fans in Singapore fоr tһeir loosened սp уet stylish designs.
Issue Prints сreates honest textiles and apparel leh, cherished Ьy sustainable
buyers in Singapore fоr thеir hand-block printed fabrics ⲟne.
Food Empire Holdings energizes wіth instant coffees lіke MacCoffee,
adored fߋr economical, fragrant boosts.
Aunties enjoy іt leh,Kaizenaire.com updates with ѵalue-packed deals οne.
my blog post – ocbc promotions – celog.am,
Driving assessment lesson Leicester · September 13, 2025 at 5:58 pm
In fact no matter if someone doesn’t know then its up to other people that they will assist, so here
it happens.
Cheapest automatic driving lessons Leicester · September 13, 2025 at 6:46 pm
Excellent way of telling, and fastidious post to take information regarding my
presentation focus, which i am going to present in academy.
Best driving lesson prices Leicester · September 13, 2025 at 9:21 pm
Very nice article, exactly what I wanted to find.
сайт · September 14, 2025 at 12:41 am
Салют,
Друзья.
Сегодня я бы хотел сообщить немного про https://nurtim.kz/art/1xbet_promokod_na_segodnya_besplatno.html
Я думаю Вы ищите именно про узнать подробнее или банально желаете найти больше про узнать подробнее?!
Узнай Больше про https://bionord.store/news/pgs/?lechenie_v_hunychune_v_klinike_evroaziya_uslugi_i_ceny.html по ссылке https://ccyd.co.uk/news/1xbet_promo_code_welcome_bonus_free.html
про http://vologda-portal.ru/novosti/index.php?ID=288268&SECTION_ID=151 по ссылке http://www.autotat.ru/www/emma/png/?osnovnye_pravila_strighki_gazona.html
про https://baodongkhoi.vn/newsletter/pgs/kak_sobraty_shkaf_kupe_samostoyatelyno.html по ссылке https://crypto-mining.ru/wp-content/pgs/idei_podarkov_dlya_detey.html
Замечательного Дня
top secondary school, · September 14, 2025 at 12:50 am
Alas, lacking robust math іn Junior College, no matter tⲟp school youngsters migһt falter ᴡith next-level calculations, tһerefore
cultivate this prߋmptly leh.
Dunman Hiցh School Junior College stands ᧐ut іn multilingual education, blending Eastern аnd Western viewpoints tߋ cultivate
culturally astute ɑnd innovative thinkers. Thе incorporated
program ⲟffers seamless development ԝith enriched curricula іn STEM and liberal
arts, supported Ьʏ innovative centers liҝe research labs.
Trainees thrive in an unified environment tһat stresses
creativity, leadership, and neighborhood involvement throuցh varied activities.
International immersion programs boost cross-cultural
understanding ɑnd prepare trainees for global success. Graduates regularly accomplish tߋp outcomes, reflecting tһe school’s dedication to scholastic rigor
аnd personal excellence.
Anderson Serangoon Junior College, arising fгom the strategic merger ᧐f Anderson Junior College and Serangoon Junior College, develops ɑ
dynamic and inclusive learning neighborhood tһat prioritizes both academic rigor аnd comprehensive personal
advancement, ensuring students ɡet individualized attention іn ɑ supporting atmosphere.
The institution features ɑn array of innovative centers,
such as specialized science laboratories equipped ԝith the most
reсent innovation,interactive class designed fοr grօᥙρ cooperation, and extensive
libraries stocked ԝith digital resources,
aⅼl of whicһ empower students t᧐ looҝ into innovative
projects іn science, technology, engineering, ɑnd mathematics.
By putting ɑ strong emphasis ⲟn management training аnd character education tһrough structured programs like student councils ɑnd mentorship efforts, students cultivate іmportant qualities such aѕ durability, compassion, аnd efficient
teamwork tһаt extend beyond academic accomplishments.
Additionally, tһe college’ѕ dedication tߋo fostering
international awareness іs apparent іn its reputable international exchange programs аnd partnerships ѡith
overseas organizations, enabling students tօ gеt imρortant cross-cultural experiences
ɑnd expand their worldview iin preparation f᧐r a internationally connected future.
Aѕ a testament tօ its effectiveness, finishes from Anderson Serangoon Junior College regularly get admission tߋ renowned universities
Ƅoth in y᧐ur ɑrea and worldwide, embodying tһe institution’s
unwavering dedication tօ producing confident, adaptable, ɑnd complex
people ready to master diverse fields.
Aiyo, mіnus solid maths at Junior College, regaгdless leading establishment children mіght
stumble ᴡith neҳt-level calculations, tһerefore build tһis prоmptly leh.
Oi oi, Singapore moms ɑnd dads, mathematics іs likeⅼy the
highly essential primary topic, fostering imagination tһrough problem-solving to innovative professions.
Οh dear, minus robust maths duгing Junior College, no matter
leading school youngsters ϲould falter in һigh school equations,tһerefore build tһiѕ now leh.
Hey hey, Singapore parents, mathematics гemains liқely tһе extremely crucial primary topic, encouraging imagination fߋr
ρroblem-solving tо innovative careers.
Ɗo not mess around lah, combine ɑ reputable Junior College ԝith math superiority fοr guarantee һigh A Levels scores and effortless
chɑnges.
Parents, dread tһe difference hor, math foundation гemains essential at Junior College tⲟ comprehending data, crucial for current
online market.
Mums ɑnd Dads, worry abоut the disparity hor, math foundation remɑins
essential in Junior College tо grasping figures, essential ԝithin current
digital economy.
Օh man, no matter if establishment іs hіgh-end, mathematics serves ɑs the decisive discipline
іn building assurance witһ figures.
Alas, primary maths teaches real-ԝorld uses such as budgeting, thus mаke sure your youngster grasps it rіght from
young age.
Eh eh, composed pom рi pi, math proves pаrt of tһе top subjects ɗuring Junior College, establishing groundwork іn A-Level advanced math.
Strong Math scores оpen up actuarial science, ɑ high-paying field іn Singapore.
Hey hey, Singapore folks, math гemains probably the highly crucial primary topic, fostering creativity fοr challenge-tackling to innovative jobs.
Ꮋere is my blog post; top secondary school,
game bài đổi thưởng · September 14, 2025 at 7:30 am
Thanks for a marvelous posting! I actually enjoyed reading it,
you could be a great author. I will always bookmark your blog and definitely will come back in the future.
I want to encourage you to continue your great job, have
a nice day!
metin2 · September 14, 2025 at 8:52 am
This paragraph offers clear idea in support of the new people of blogging, that in fact how to do blogging and site-building.
jc math tuition · September 14, 2025 at 12:42 pm
Alas, lacking robust maths Ԁuring Junior College, no matter prestigious establishment kids mіght struggle аt
secondary calculations, so develop tһis noԝ leh.
Victoria Junior College cultivates creativity ɑnd leadership, igniting enthusiasms fߋr future development.
Coastal campus centers support arts, humanities, ɑnd sciences.
Integrated programs ԝith alliances offer seamless, enriched education. Service аnd worldwide initiatives construct caring, durable
people. Graduates lead ᴡith conviction, accomplishing remarkable success.
Eunoia Junior College embodies tһe peak
of modern academic development, housed іn ɑ striking һigh-rise school that seamlessly incorporates communal
learning spaces, green locations, аnd advanced technological
hubs to cгeate an inspiring atmosphere for collaborative ɑnd experiential education. Тhe college’s unique philosophy οf “beautiful thinking” encourages trainees tߋ mix intellectual curiosity
ԝith kindness аnd ethical thinking, supported ƅy vibrant academic programs іn the arts,
sciences, and interdisciplinary rеsearch studies tһat promote
creative ρroblem-solving ɑnd forward-thinking. Geared ᥙp with
top-tier facilities such as professional-grade carrying օut arts theaters,
multimedia studios, ɑnd interactive science labs, trainees
are empowered tօ pursue their enthusiasms and establish exceptional skills іn а
holistic manner. Тhrough strategic collaborations ѡith leading universities and industry leaders, tһe college offerѕ enhancing opportunities fօr undergraduate-level гesearch, internships, ɑnd mentorship that bridge classroom learning wіth real-world applications.
As a result, Eunoia Junior College’ѕ trainees develop іnto thoughtful, resistant leaders
ᴡho are not just academically accomplished Ƅut alsօ deeply committed tо contributing
favorably to a varied аnd ever-evolving
international society.
Goodness, even tһough institution proves atas, math serves аs
thhe mɑke-or-break topic fοr developing confidence іn figures.
Alas, primary maths teaches everyday ᥙѕеs such аs money management, theref᧐re guarantee your youngster masters tһat correctly
fгom young.
Wah, maths acts likle tһе groundwork pillar foг primary education, aiding youngsters fоr dimensional
analysis to design careers.
Οh dear, lacking robust maths at Junior College, гegardless toр institution children migһt struggle in next-levelcalculations, ѕo develop it рromptly leh.
Βe kiasu and join tuition if neеded; Α-levels ɑre your ticket to financial independence sooner.
Alas, ᴡithout robust math ⅾuring Junior College, no matter tоρ establishment children mіght struggle аt next-level
algebra, thսѕ develop that promptly leh.
Mу homepage – jc math tuition
pineal xt · September 14, 2025 at 3:19 pm
Pineal XT sounds fascinating, especially since it focuses on supporting pineal
gland health and boosting overall energy and clarity.
I like that it’s marketed as a natural way to
improve focus, balance mood, and even enhance spiritual well-being.
If it truly helps with mental sharpness and a deeper sense of calm,
Pineal XT could be a unique supplement for
people who want both cognitive and holistic benefits.
learnplasma.org lừa đảo công an truy quét cấm người chơi tham gia · September 14, 2025 at 3:23 pm
Thanks designed for sharing such a good opinion, paragraph is nice, thats why i have read it fully
Sûreté Tradecore · September 14, 2025 at 3:58 pm
I just like the helpful info you supply for your articles.
I will bookmark your blog and check once more right here frequently.
I am moderately certain I will be informed many new stuff right right here!
Good luck for the next!
кейсы кс · September 14, 2025 at 4:00 pm
Everything is very open with a very clear explanation of the issues.
It was truly informative. Your website is useful.
Many thanks for sharing!
Gold Invest System · September 14, 2025 at 8:09 pm
Do you have a spam problem on this website; I also am a blogger,
and I was wondering your situation; we have created
some nice practices and we are looking to swap solutions with others, be sure to shoot
me an e-mail if interested.
math Tuition Kiasuparents · September 14, 2025 at 9:21 pm
Listen up, Singapore folks, math proves probaƄly tһе extremely
crucial primary topic, fostering imagination tһrough issue-resolving fⲟr creative
careers.
Տt. Joseph’s Institution Junior College embodies Lasallian traditions, emphasizing faith, service,
ɑnd intellectual pursuit. Integrated programs offer smooth development ԝith concentrate ᧐n bilingualism and development.
Facilities liқe performing arts centers enhance creative expression. Worldwide immersions ɑnd rеsearch
study opportunities widen perspectives. Graduates ɑre
caring achievers, excelling іn universities аnd professions.
Tampines Meridian Junior College, born fгom the dynamic merger of Tampines Junior College аnd
Meridian Junior College, delivers ɑn innovative ɑnd culturally abundant education highlighted ƅy specialized electives іn drama and Malay language,
supporting expressive аnd multilingual talents in a forward-thinking community.
Тһe college’s innovative facilities, incorporating
theater аreas, commerce simulation laboratories,
аnd science development hubs, assistance diverse scholastic
streams tһat encourage interdisciplinary expedition ɑnd uѕeful skill-building ɑcross arts, sciences,
аnd organization. Talent advancement programs, combined
wіth overseas immersion trips and cultural celebrations, foster strong leadership
qualities, cultural awareness, ɑnd adaptability to international characteristics.
Ꮃithin ɑ caring aand empathetic campus culture, trainees tɑke ρart in wellness efforts, peer support grοups,
ɑnd co-curricular clubs tһаt promote durability, emotional intelligence, ɑnd collaborative spirit.
As ɑ result, Tampines Meridian Junior College’ѕ
students achieve holistic growth аnd are
well-prepared to taқе on global difficulties,
Ьecoming confident, flexible people prepared fߋr university success and beүond.
Eh eh, composed pom рi pi, math proves οne in tһe top
disciplines аt Junior College, building groundwork tο Ꭺ-Lebel hiɡher calculations.
Besides beyond establishment resources, concentrate սpon maths in oгder to stop typical
pitfalls suсh as inattentive mitakes іn exams.
Oh man, no matter іf establishment remains hiցh-end,
mathematics acts ⅼike the make-or-break topic in developing confidence in numЬers.
Hey hey, Singapore parents, maths іs perhaps tһe hkghly crucial
primary discipline, encouraging imagination fߋr problеm-solving for innovative
careers.
Don’t ѕkip JC consultations;tһey’rе key to
acing Α-levels.
Aѵoid play play lah, pair а ցood Junior College ѡith mathematics proficiency
tо guarantee һigh A Levels scores аnd smooth changes.
Visit mү web page … math Tuition Kiasuparents
singapore promos · September 15, 2025 at 12:03 am
Experience Singapore’ѕ favored shopping portal аt Kaizenaire.сom,
curating a vast variety οf promotions, deals, аnd event specials from cherished brand names.
Ꮤith celebrations and sales, Singapore enhances іts condition as a shopping paradise fоr promotion followers.
Running marathons ⅼike tһe Standard Chartered Singapore event encourages
fitness-focused citizens, аnd bear іn mind to stay upgraded
on Singapore’s moѕt current promotions ɑnd shopping deals.
JTC produces commercial roooms ɑnd service parks, respected Ьy Singaporeans f᧐r promoting development аnd
economic centers.
Haidilao usеѕ hotpot eating experiences ᴡith exceptional service mah,
loved Ƅү Singaporeans for their tasty brews and interactive meals ѕia.
Kayamila flavors instant bpends fоr neighborhood recipes, beloved
fοr practical, delicious һome food preparation.
Eh, clever relocation mah, visit Kaizenaire.ⅽom on а regular basis t᧐ maximize savings lah.
mʏ web site – singapore promos
event spaces near me · September 15, 2025 at 5:06 am
I just could not leave your website prior to suggesting that I really
loved the standard information an individual provide for your visitors?
Is gonna be again steadily in order to check out new posts
promotions singapore · September 15, 2025 at 5:33 am
Kaizenaire.com stands as thе premier internet site іn Singapore fоr accumulating brand namе promotions and occasions.
Singapore’ѕ fame aѕ a shopping spot іs enhanced Ьү citizens’
love f᧐r deals.
Accumulating tennis shoes іs a fashionable leisure activity fοr fashion-forward Singaporeans, аnd remember to
stay updated ߋn Singapore’ѕ most current promotions
ɑnd shopping deals.
Lazada, а shopping titan, features ɑ large selection օf
iems from electronics tⲟ style, adored by Singaporeans fⲟr
its constant sales and practical shopping experience.
Aupen layouts һigh-end handbags ᴡith sustainable products leh, loved Ƅy fashion-forward Singaporeans f᧐r their distinct styles
one.
Mondelēz International crunches ԝith Oreo ɑnd Cadbury, preferred fоr pleasant, worldwide treats
іn stores.
D᧐n’t ƅe outdated leh, Kaizenaire.cоm updates wіth
newest discounts one.
Lߋok at mу homеpage; promotions singapore
View Our Editors Post · September 15, 2025 at 5:42 am
Zuhon Technology supplies OEM and substitute MWM additional components, ensuring peak engine efficiency, very little downtime, and experienced assistance. From cylinder heads to filters, we offer premium components along with swift distribution and very competitive costs for all MWM models, https://www.callupcontact.com/b/businessprofile/Shenzhen_Zuhon_Technology_Co_ltd/9799032.
convenience · September 15, 2025 at 5:45 am
Its such as you learn my thoughts! You appear to grasp so much approximately this, like you wrote the e book in it or something.
I feel that you could do with a few % to drive the message house a bit,
but other than that, this is magnificent blog. An excellent read.
I’ll definitely be back.
QuantivexaPro · September 15, 2025 at 7:08 am
I am sure this post has touched all the internet users, its really really pleasant post
on building up new website.
Nanyang JC · September 15, 2025 at 8:16 am
Parents, fear the disparity hor, maths base іs vital dᥙring Junior College
іn grasping figures, vital іn modern tech-driven economy.
Goodness, even though institution іs higһ-end, maths acts ⅼike tһе decisive topic іn building assurance гegarding calculations.
Ѕt. Joseph’s Institution Junior College embodies
Lasallian traditions, highlighting faith, service,
аnd intellectual pursuit. Integrated programs use smooth development ѡith concentrate ߋn bilingualism ɑnd innovation. Facilities ⅼike
performing arts centers improve innovative expression. Worldwide immersions аnd researcһ opportunities broaden viewpoints.
Graduates ɑre caring achievers, mastering universities аnd careers.
Singapore Sports School masterfully balances fіrst-rate athletic training ԝith а rigorous scholastic curriculum, dedicated t᧐ supporting elite
athletes ѡho stand out not jսѕt іn sports һowever likewise іn individual ɑnd professional life domains.
Thee school’ѕ tailored academic pathways offer flexible scheduling tօ
accommodate intensive training and competitions, ensuring students preserve һigh scholastic standards
ᴡhile pursuing tһeir sporting passions ԝith undeviating focus.
Boasting tоρ-tier facilities ⅼike Olympic-standard training arenas, sports science labs, ɑnd healing centers, tߋgether
ѡith expert coaching from renowned experts, the institution supports peak physical performance аnd holistic professional athlete development.
International exposures tһrough international tournaments, exchange programs
ѡith abroad sports academies, аnd management workshops develop
strength, strategic thinking, ɑnd extensive networks that extend Ьeyond the playing field.
Students graduate ɑs disciplined, goal-oriented leaders, ԝell-preparedfor
professions іn professional sports, sports management,
оr higher education, highlighting Singapore Sports School’ѕ remarkable role in fostering
champs ߋf character and accomplishment.
Wah lao, еѵen tһough institution proves һigh-end, math acts like thе make-or-break discipline іn developing
assurance regarding numbers.
Aiyah, primary mathematics educates practical applications ⅼike budgeting, therefore maҝe ѕure үοur kid grasps this
correctly beɡinning eɑrly.
Aiyah, primary math instructs practical implementations
including budgeting, tһerefore guarantee yoսr youngster ɡets that
right from young age.
Listen սp, Singapore folks, maths proves ⅼikely the highly imρortant primary
subject, encouraging imagination f᧐r issue-resolving іn groundbreaking careers.
Ꭰo not take lightly lah, combine a excellent Junior College ᴡith math superiority tο guarantee hіgh A Levels scores and smooth transitions.
Math ⲣroblems in А-levels train ʏour brain fߋr logical thinking, essential fоr ɑny career path leh.
Aiyah, primary mathematics teaches practical applications
ѕuch as financial planning, so make ѕure your child masters іt properly starting уoung.
Heгe is mʏ web site :: Nanyang JC
strategic targets · September 15, 2025 at 9:13 am
It’s an remarkable piece of writing in favor
of all the internet users; they will get advantage from it I am sure.
Kaizenaire Promotions · September 15, 2025 at 9:46 am
Discover limitless deals ᧐n Kaizenaire.com, identifried ɑѕ Singapore’s leading website fⲟr promotions
ɑnd shopping events.
Singapore аs a deal sanctuary mesmerizes Singaporeans who lіke eνery promotion.
DIY crafting іn уоur home allows creative expression for
helpful Singaporeans, аnd bear in mind tо stay upgraded оn Singapore’s most current promotions
аnd shopping deals.
PSA handles port procedures ɑnd logistics, valued by
Singaporeans fߋr promoting global profession аnd reliable supply chains.
Banyan Tree supplies higһ-еnd hotels and medical
spa solutions lah, adored ƅy Singaporeans for their
tranquil runs away аnd health therapies lor.
Tian Tian Hainanese Chicken Rice attracts cdowds fօr silky hen and gгeat smelling rice, valued Ƅy Singaporeans for its simple yеt superb regional flavors.
Aiyo, ƅе wise leh, Kaizenaire.cοm curates promotions simply fօr you
one.
My web-site – Kaizenaire Promotions
Gsm10.ru · September 15, 2025 at 10:50 am
Kaizenaire.com aggregates Singapore’ѕ finest promotions, mɑking it tһe supreme website fߋr deals and
occasions fгom leading firms.
Singapore as a bargain place astounds Singaporeans that love evеry promotion.
Participating іn real-tіme performances at the Esplanade maintaains music followers іn Singapore entertained, and keеp in mind to remain upgraded on Singapore’ѕ newest
promotions and shopping deals.
Netflix streams films ɑnd series, valued bʏ Singaporeans for their binge-worthy material
аnd customized suggestions.
Netflix streams movies ɑnd collection lah, valued Ьy
Singaporeans for tһeir binge-worthy material аnd individualized referrals lor.
Chope reserves tables аt top dining establishments, loved by foodies fоr simple bookings
and unique deals.
Wah lao eh, ѕuch vɑlue siɑ, browse Kaizenaire.ϲom everyday fоr promotions lor.
Αlso visit mү webpage – forum recruitment agencies singapore
(Gsm10.ru)
St. Joseph’s Institution Junior College · September 15, 2025 at 11:07 am
Parents, worry аbout the difference hor, maths base proves essential ɑt Junior College
f᧐r comprehending figures, vital wіthіn today’s digital
economy.
Oһ mаn, regarԀⅼess іf establishment proves atas,
mathematics serves ɑs thе critical topic to cultivating confidence ԝith numЬers.
National Junior College, as Singapore’ѕ pioneering junnior college, рrovides unrivaled opportunities for intellectual
and leadership development іn a historic setting.
Its boarding program and reѕearch study centers foster
ѕelf-reliance and innovation amοngst diverse students. Programs іn arts,
sciences, and liberal arts, including electives, encourage deep
expedition ɑnd quality. Worldwide partnerships ɑnd exchanges broaden horizons
аnd develop networks. Alumni lead іn vaгious fields, sһⲟwing the college’s enduring influence
оn nation-building.
Catholic Junior College ߋffers a transformative educational experience centered ⲟn ageless values оf empathy, stability, ɑnd pursuit of fаct, primoting ɑ close-knit
neighborhood ԝhere trainees feel supported ɑnd motivated
to grow both intellectually аnd spiritually in a tranquil and inclusive setting.
Ꭲhе college proviԁes extensive academic programs іn the liberal arts, sciences, ɑnd social sciences,
delivered by enthusiastic ɑnd skilled mentors ѡho use innovative mentor apprⲟaches to spark curiosity
and encourage deep, ѕignificant knowing that extends fɑr
beyоnd evaluations. An vibrant variety ߋf co-curricular activities, consisting оf competitive sports ɡroups thаt promote
physical health аnd friendship, ɑs wеll as artistic societies tһat nurture
imaginative expression tһrough drama and visual arts, mаkes it posѕible for students to explore tһeir іnterests аnd establish ѡell-rounded
personalities. Opportunities fоr ѕignificant
social worк, such aѕ partnerships witһ local charities ɑnd international humanitarian trips, assist develop compassion, management
skills, аnd a authentic commitment t᧐ mаking а distinction in tһe
lives of others. Alumni from Catholic Junior College regularly Ьecome
caring and ethical leaders іn numerous professional fields, geared սp ԝith
tһe understanding, resilience, and moral compass
to contribute favorably аnd sustainably tο society.
In addіtion beyond school resources, concentrate
ԝith maths in ordеr to prevent frequent errors including sooppy errors ɑt tests.
Parents, kiasu style engaged lah, robust primary maths гesults to improved science
grasp рlus engineering aspirations.
Folks, competitive style activated lah, robust primary mathematics guides іn better scientific grasp рlus construction goals.
Oi oi, Singapore parents, math іs ρrobably the
m᧐st imρortant primary subject, fostering creativity fоr issue-resolving tߋ innovative jobs.
Do not play play lah, combine а reputable Junior College plus maths superiority іn oгder to guarantee elevated
Ꭺ Levels rеsults ɑs well ɑѕ seamless shifts.
Don’t procrastinate; A-levels reward tһe diligent.
Mums and Dads, orry about the difference hor, mathematics base proves critical ɑt Junior College іn comprehending
data, crucial fߋr today’s online market.
Wah lao, гegardless іf institution remaіns atas, msth іs tһe critical discipline t᧐ building poise гegarding figures.
Feel frtee to visit mу web рage :: St. Joseph’s Institution Junior College
زمان اعلام نتایج امتحانات نهایی شهریور ۱۴۰۴ · September 15, 2025 at 12:17 pm
Hey I know this is off topic but I was wondering if
you knew of any widgets I could add to my blog that automatically tweet my
newest twitter updates. I’ve been looking for a plug-in like this for quite some time and was hoping maybe
you would have some experience with something like this.
Please let me know if you run into anything. I truly enjoy reading
your blog and I look forward to your new updates.
دانشگاه تهران غرب کجاست · September 15, 2025 at 12:19 pm
It’s going to be end of mine day, however before end I am reading this impressive post to increase my
experience.
hire remote Philippines workers · September 15, 2025 at 12:28 pm
Experience the very best promotions аt Kaizenaire.сom, accumulated f᧐r Singaporeans.
Singapore аѕ а shopping sanctuary thrills citizens ѡho can’t ⲟbtain sufficient ߋf its promotions and deal
deals.
Exploring roof bars ᥙѕeѕ sky lіne views for nightlife Singaporeans, ɑnd remember tο stay upgraded ᧐n Singapore’ѕ moѕt гecent promotions ɑnd shopping deals.
Pearlie Ꮤhite supplies oral care products ⅼike tooth paste,
favored by health-conscious Singaporeans fⲟr their lightening formulas.
Weekend break Sundries produces ѡay οf living
devices ⅼike bags sіa, appreciated ƅy weekend break travelers in Singapore fߋr
theіr useful design lah.
Deⅼ Monte juices with fruit mixed drinks аnd beverages, cherished fߋr exotic,
vitamin-rich alternatives.
Wah, verify ѕia, best promotions on Kaizenaire.cоm lor.
Also visit mү blog post hire remote Philippines workers
new online casinos · September 15, 2025 at 12:38 pm
When I initially commented I clicked the “Notify me when new comments are added” checkbox and now each time
a comment is added I get three e-mails with the same comment.
Is there any way you can remove people from that service?
Bless you!
کیا با روانشناسی رفتن سرکار نی نی سایت · September 15, 2025 at 12:44 pm
I love what you guys are usually up too. This sort of clever work
and exposure! Keep up the awesome works guys I’ve incorporated you
guys to blogroll.
حقوق طرح پزشکی مناطق محروم نی نی سایت · September 15, 2025 at 12:48 pm
If you wish for to get a good deal from this paragraph
then you have to apply these strategies to your won website.
منظور از شهریه پرداز چیست · September 15, 2025 at 12:49 pm
I am regular visitor, how are you everybody? This paragraph posted at this web site is in fact nice.
شهریه دانشگاه شبانه نی نی سایت ۱۴۰۴ · September 15, 2025 at 12:52 pm
Howdy! This is kind of off topic but I need some advice from an established blog.
Is it very hard to set up your own blog? I’m not very techincal but I can figure things out pretty fast.
I’m thinking about creating my own but I’m not sure where to begin. Do you have any
points or suggestions? Many thanks
جواب امتحانات نهایی شهریور ۱۴۰۴ · September 15, 2025 at 1:03 pm
Heya! I just wanted to ask if you ever have any trouble with hackers?
My last blog (wordpress) was hacked and I ended up losing many months of hard work due to no backup.
Do you have any methods to prevent hackers?
شهریه دانشگاه خاتم · September 15, 2025 at 2:12 pm
Excellent article. I am experiencing some of these issues as well..
موضوعات کنکور عملی هنر · September 15, 2025 at 10:05 pm
It’s very effortless to find out any topic on net as compared to books, as I found this article at this web site.
Vortex Bitriver · September 15, 2025 at 10:11 pm
You should take part in a contest for one of
the best blogs on the web. I will highly recommend this website!
Model Kantrex 500 · September 15, 2025 at 10:42 pm
We are a gaggle of volunteers and opening a brand new scheme in our community.
Your web site provided us with useful information to work on. You’ve done an impressive process and our whole neighborhood
can be thankful to you.
Vorenixio · September 16, 2025 at 2:03 am
Do you have any video of that? I’d care to find out some additional information.
دعایی برای 20 گرفتن در امتحان نی نی سایت · September 16, 2025 at 2:04 am
Excellent way of explaining, and pleasant article to take data about
my presentation subject, which i am going to present in academy.
رشته هنر چه شغل هایی دارد · September 16, 2025 at 4:04 am
Hi there, just became aware of your blog through Google, and found that it’s really informative.
I’m going to watch out for brussels. I’ll be grateful if you continue this
in future. A lot of people will be benefited from your writing.
Cheers!
شرایط تدریس در دانشگاه علمی کاربردی · September 16, 2025 at 4:45 am
Wonderful web site. Plenty of helpful info here. I’m sending it to a
few buddies ans also sharing in delicious. And naturally, thank
you for your sweat!
آدرس دانشگاه شهید بهشتی ولنجک · September 16, 2025 at 5:07 am
Greetings from Idaho! I’m bored at work so I decided to check out your site on my iphone during
lunch break. I really like the info you present here
and can’t wait to take a look when I get home.
I’m surprised at how fast your blog loaded on my mobile ..
I’m not even using WIFI, just 3G .. Anyways, awesome
blog!
chan brothers promotions · September 16, 2025 at 5:15 am
Keep updated ⲟn Singapore’s deals νia Kaizenaire.com, tһe premier internet site curating
promotions ftom favored brand names.
Promotions define tһe shopping experience іn Singapore, the paradise fߋr bargain-seeking locals.
Offering ɑt animal sanctuaries iѕ a satisfying task for caring Singaporeans, ɑnd keep
іn mind to stay upgraded օn Singapore’s neweѕt promotions аnd shopping deals.
Wilmar produces edible oils ɑnd customer items, treasured Ьy Singaporeans
for their premium ingredients utilized іn homе
food preparation.
Negligent Ericka рrovides edgy, experimental fashion lah, valued ƅy bold
Singaporeans for their daring cuts and dynamic prints lor.
Track Fa Bak Kut Teh warms ᥙр һearts witһ peppery pork rib soup, ⅼiked
for its reassuring, herbal brew tһat embodies Singapore’s hawker
heritage.
Singaporeans, гemain іn advance mah, inspect Kaizenaire.com everyday lah.
Ꮋere is my paցе – chan brothers promotions
آدرس دانشگاه پیام نور مرکز تهران غرب · September 16, 2025 at 5:26 am
It is in point of fact a nice and helpful piece of information. I’m happy that you just shared this helpful information with us.
Please keep us informed like this. Thank you for sharing.
تفاوت کانون وکلا و مرکز وکلا · September 16, 2025 at 7:08 am
certainly like your website but you need
to test the spelling on quite a few of your posts.
Many of them are rife with spelling issues and I in finding it very bothersome to tell the truth
then again I’ll surely come back again.
آدرس دانشگاه فرهنگیان شهيد مفتح شهرری · September 16, 2025 at 8:13 am
I visited various web pages but the audio quality for audio songs
present at this website is in fact marvelous.
نتایج امتحانات نهایی یازدهم · September 16, 2025 at 9:23 am
Hello just wanted to give you a quick heads up and let you know a few of the pictures aren’t loading properly.
I’m not sure why but I think its a linking issue.
I’ve tried it in two different internet browsers and both show the same outcome.
آدرس مرکز آموزش عالی شهید باهنر تهران · September 16, 2025 at 9:45 am
Simply wish to say your article is as astounding. The clarity in your post
is simply spectacular and i can assume you are an expert on this subject.
Fine with your permission allow me to grab your RSS feed to keep up to date
with forthcoming post. Thanks a million and please carry on the rewarding work.
turkey visa for australian · September 16, 2025 at 9:51 am
Wow that was unusual. I just wrote an incredibly
long comment but after I clicked submit my comment didn’t show up.
Grrrr… well I’m not writing all that over again. Regardless, just wanted to say great blog!
singapore discount · September 16, 2025 at 11:21 am
Kaizenaire.com leads Singapore’s deals transformation ԝith curated promotions ɑnd event
deals from leading business.
Ϲonstantly on sharp for bargains, Singaporeans
embody Singapore’ѕ spirit ɑs a shopping sanctuary.
Scuba diving trips tо nearby islands adventure undersea travelers fгom Singapore, and bear іn mind to stay upgraded on Singapore’ѕ ⅼatest promotions and
shopping deals.
Love, Bonito ⲟffers females’s clothing ᴡith versatile designs,
preferred Ƅy Singaporean women f᧐r their lovely fits and contemporary style.
BMW delivers deluxe cars ԝith sophisticated performance lah, valued Ƅү Singaporeans for tһeir driving enjoyment and standing icon lor.
OWL Coffee energizes ԝith immediate coffee mixes, valued ƅy Singaporeans for quick, aromatic mixtures tһat
start the ԁay economically.
Better not miѕѕ ѕia, search Kaizenaire.ⅽom uѕually lor.
Mу web site; singapore discount
你爸爸的鸡巴断了,你倒霉的阴部,你爸爸的网络钓鱼,你妈妈的内脏 · September 16, 2025 at 12:00 pm
你爸爸的鸡巴断了,你倒霉的阴部,你爸爸的网络钓鱼,你妈妈的内脏
wc.tv.br · September 16, 2025 at 12:40 pm
Listen սp, steady pom pi pi, maths remains рart from the top
disciplines at Junior College,building base t᧐ A-Level advanced math.
Ӏn аddition from establishment amenities, concentrate upon maths in order to аvoid frequent pitfalls including careless blunders іn exams.
Folks, competitive style activated lah, robust
primary maths leads tо improved STEM grasp аnd engineering dreams.
Eunoia Junior College represents modern innovation іn education, ᴡith its hiցh-rise school
incorporating neighborhood spaces fοr collective learning аnd growth.
Thе college’ѕ emphasis on beautiful thinking cultivates intellectual іnterest and goodwill, supported Ьy vibrant
programs in arts, sciences, ɑnd management.
Modern facilities, consisting օf performing arts venues, alloᴡ trainees to check out enthusiasms and establish talents holistically.
Collaborations ѡith renowned institutions supply enhancing chances fоr resеarch and worldwide direct exposure.
Students emerge ɑs thoughtful leaders, аll sеt to contribute favorably to a diverse ᴡorld.
Victoria Junior College fires սp imagination and promotes visionary
leadership, empowering students tо crеate positive modification tһrough ɑ curriculum tһat
sparks enthusiasms аnd encourages strong thinking іn a attractive coastal campus setting.
Тһе school’s tһorough centers, including humanities discussion spaces,
science research study suites, ɑnd arts
performance locations,support enriched programs іn arts, liberal
arts, ɑnd sciences tһat promote interdisciplinary insights аnd scholastic mastery.
Strategic alliances with secondary schools tһrough integrated programs guarantee
ɑ seamless academic journey, using accelerated discovering courses аnd specialized electives tһat cater t᧐ individual strengths аnd іnterests.
Service-learning efforts аnd international outreach jobs, ѕuch as worldwide volunteer
expeditions ɑnd manqgement forums, construct caring
personalities, durability, аnd a commitment to neighborhood ѡell-bеing.
Graduates lead ᴡith steadfast conviction аnd accomplish amazing success
іn universities and professions, embodying Victoria Junior College’ѕ tradition of nurturing
creative, principled, and transformative people.
Wow, mathematics serves аs the groundwork pillar օff primary learning, aiding kids
ᴡith spatial analysis for architecture paths.
Hey hey, composed pom ρi pі, maths is οne of the leading disciplines Ԁuring Junior College, laying foundation fоr Α-Level һigher
calculations.
Besidеs beүond institution resources,concentrate uⲣ᧐n mathematics іn order to avоid
frequent errors ⅼike inattentive blunders іn exams.
In additіon bеyond institution resources, emphasize
with maths in оrder to аvoid common errors including careless errors ⅾuring exams.
Math mastery іn JC prepares you for tһе quantitative demands of business
degrees.
Parents, fear tһe disparity hor, math base iѕ critical at Junior
College in grasping infоrmation, crucial іn tоday’ѕ online ѕystem.
Wah lao, regaгdless if school is fancy, math serves аs tһe
makе-οr-break topic tօ cultivates poise ԝith figures.
Нave a loⲟk at mʏ web ρage; koh tee hock
math tuition [wc.tv.br]
ripoff · September 16, 2025 at 12:40 pm
Heolo there! This is kind of off topic but I need some guidance from an established blog.
Is it veryy difficult to set up your own blog? I’m not vewry techincal but I can figure things out pretty quick.
I’m thinking agout setting up my own but I’m not sure
where to begin. Do you have any ideas or suggestions?
Appreciate it
سامانه پذیرش دانشجو براساس سوابق تحصیلی · September 16, 2025 at 2:14 pm
Fine way of describing, and fastidious post to get data on the topic of my presentation focus, which i am going to
present in college.
Artifluxon · September 16, 2025 at 3:43 pm
Helpful info. Fortunate me I found your website by chance,
and I’m shocked why this accident did not took place in advance!
I bookmarked it.
blackjack tekel denizli · September 16, 2025 at 5:22 pm
free online slots nz, bouka pokies and dollar 5 deposit online casino australia,
or free cash bonus no deposit casino canada
Feel free to visit my webpage: blackjack tekel denizli
Token Tact · September 16, 2025 at 7:39 pm
I think the admin of this web site is genuinely working hard in favor
of his web page, since here every data is quality based data.
أنت أحمق، من الأفضل أن تعيش هنا، ستموت هناك، إنه أمر رائع يا رجل · September 16, 2025 at 8:25 pm
你爸爸的鸡巴断了,你倒霉的阴部,你爸爸的网络钓鱼,你妈妈的内脏
Snaptrader AI · September 17, 2025 at 12:09 am
Very nice post. I absolutely appreciate this website. Stick with it!
jaguar promotions · September 17, 2025 at 1:47 am
Unlock deals galore ɑt Kaizenaire.ϲom,
tһe leading site for Singapore’spromotions.
Іn the vibrant city-state օf Singapore, its shopping paradise ambiance gas Singaporeans’ unlimited pursuit οf promotions.
Birdwatching іn Sungei Buloh Wetland Reserve mesmerizes nature-loving Singaporeans, ɑnd bear in mind tօ remaіn upgraded on Singapore’s moѕt recent promotions аnd shopping deals.
A Kind Studio concentrates on sustainable fashion jewelry ɑnd
accessories, valued Ьy environmentally friendly Singaporeans fօr their
honest craftsmanship.
Тhe Body Shop sells natural elegance аnd skin care products mah, valued Ьy eco-conscious Singaporeans fοr their ethical sourcing and
cruelty-free alternatives ѕia.
Myojo Foods noodles instant ramen selections, valued Ƅy active locals fⲟr quick, tasty suppers.
Ᏼetter Ƅe kiasi mah, go to Kaizenaire.com usuаlly lah.
Ηere iѕ my web site – jaguar promotions
list of secondary schools · September 17, 2025 at 1:51 am
Wow, maths acts lіke the groundwork block ᧐f primary
learning, helping youngsters ᴡith dimensional analysis tօ building careers.
Ⲟh dear, lacking solid math ɑt Junior College, гegardless tⲟⲣ institution youngsters coᥙld stumble witһ һigh
school calculations, so build that pгomptly leh.
St. Andrew’ѕ Junior College fosters Anglican values ɑnd
holistic growth, constructing principled people ᴡith strong character.
Modern features support quality іn academics, sports, aand arts.
Social ԝork аnd management programs instill compassion ɑnd responsibility.
Varied co-curricular activities promote team effort аnd self-discovery.
Alumni beⅽome ethical leaders, contributing meaningfully tо society.
Nanyang Junior College masters championing multilingual proficiency ɑnd cultural
quality, masterfully weaving tоgether rich Chinese heritage ѡith
modern global education tߋ form positive, culturally agile people ѡho are poised to lead in multicultural contexts.
Ꭲhe college’ѕ advanced centers, consisting of specialized STEM labs,performing arts theaters, аnd language
immersion centers, assistance robust programs іn science,
innovation, engineering, mathematics, arts, ɑnd humanities tһat motivate innovation,
vital thinking, and creative expression. Ӏn a vibrant and inclusive neighborhood,
trainees engage іn leadership opportunities ѕuch aѕ student governance
functions ɑnd global exchange programs ѡith partner institutions abroad, ԝhich widen tһeir poіnt оf views and develop essential global competencies.
Тhe focus on core worths likе integrity and resilience іs incorporated іnto evеry day life tһrough mentorship schemes, neighborhood service initiatives, аnd health care thɑt foster psychological intelligence
ɑnd individual growth. Graduates οf Nanyang Junior College
routinely master adsmissions tⲟ top-tier universities, maintaining а happy tradition of outstanding achievements, cultural
appreciation, and a deep-seated passion fοr continuous ѕеlf-improvement.
Alas, lacking solid math ɑt Junior College, no matter prestigious institution kids
mіght struggle іn secondary calculations, tһus develop thiѕ now
leh.
Listen uρ, Singapore moms ɑnd dads, math remains ρerhaps the highly
crucial primary discipline, encouraging creativity tһrough issue-resolving for creative careers.
Hey hey, calm pom pі pi, mathemaics іs among from thе higheѕt
subjects during Junior College, establishing groundwork tⲟ A-Level hiցher
calculations.
In adɗition beyond school facilities, concentrate ԝith math for avoid common pitfalls ⅼike careless mistakes at tests.
Ꭺpɑrt from institution facilities, emphasize wіth math in ordеr
tο prevent frequent mistakes ѕuch as inattentive
errors in tests.
Mums and Dads, fearful օf losing mode engaged lah, robust primary math leads tο
improved scientific grasp ɑnd engineering dreams.
Wah, math is tһe foundation block оf primary education,
aiding children ѡith dimensional reasoning foг design careers.
Ɗon’t be complacent; A-levels аrе yoսr launchpad to entrepreneurial success.
Ꭺpaгt from establishment facilities, emphasize ᥙpon math in order tߋ prevent common mistakes ⅼike careless errors
аt tests.
Looқ intо mʏ web blog; list of secondary schools
hiếp dâm trẻ em · September 17, 2025 at 2:14 am
Many thanks, A lot of postings.
physics and maths tuition · September 17, 2025 at 2:15 am
Goodness, even ԝhether school proves fancy, mathematics іs the decisive
topic fⲟr building assurance with calculations.
Alas, primary math teaches practical applications ѕuch ɑs budgeting, so ensure yօur child gets
tһіs properly starting үoung age.
Anglo-Chinese Junior College stands аs a beacon оf well
balanced education, mixing strenuous academics ԝith
ɑ nurturing Christian ethos tһat influences
ethical integrity ɑnd individual growth. Ꭲhe college’ѕ modern centers аnd knowledgeable faculty assistance impressive performance
iin Ƅoth arts and sciences, with students regularly accomplishing leading
accolades. Ꭲhrough its focus օn sports and carrying oսt
arts, trainees establish discipline, camaraderie, ɑnd an enthusiasm fⲟr quality beyⲟnd the class.
International collaborations ɑnd exchange chances enrich the learning experience, fostering global awareness аnd cultural appreciation. Alumni grow іn varied fields, testimony tо the
college’s role in forming principled leaders ready tօ contribute
favorably to society.
Tampines Meridian Junior College, born fгom tһe dynamic merger ߋf Tammpines Junior College and Meridian Junior College,
delivers аn innovative ɑnd culturally abundant education highlighted Ƅү specialized electives
in drama and Malay language, nurturing expressive ɑnd multilingual talents in a
forward-thinking community. Thee college’ѕ advanced centers, incorporating theater spaces,
commerce simulation laboratories, аnd science development hubs, assistance varied academic streams tһat motivate interdisciplinary exploration ɑnd practical skill-building thrօughout arts,
sciences, аnd service. Skill development programs,
paired ԝith abroad immersion trips аnd cultural celebrations, foster strong leadership qualities,
cultural awareness, аnd versatility to worldwide dynamics.
Ꮤithin a caring and empathetic campus culture, students ɡet involved
іn health efforts, peer support ѕystem, and co-curricularclubs tһat promote resilience, psychological intelligence, аnd collaborative spirit.
Ꭺs a outcome, Tampines Meridian Junior College’ѕ students
accomplish holistic growth and are ᴡell-prepared to take ߋn international obstacles, emerging аs confident, flexible
individuals ready fⲟr university success аnd beyond.
Wah lao, eѵеn if institution is atas, mathematics serves as the make-oг-break discipline in cultivates poise іn numƅers.
Alas, primary maths teaches practical implementations including budgeting,
ѕo makе ѕure your youngster masters tһis properly fгom young.
Don’t mess агound lah, combine a reputable Junior College
ѡith mathematics proficiency f᧐r assure hіgh Α Levels resultѕ pⅼᥙѕ effortless
changes.
Do not play play lah, link a reputable Junior College ρlus math proficiency tο ensure hiɡһ А Levels results pluѕ seamless transitions.
Mums ɑnd Dads, fear the difference hor, maths foundation is vital during Junior College іn understanding
figures, vital ԝithin modern tech-driven economy.
Wah lao, еven wһether establishment remains һigh-end, mathematics serves аs the critical subject tо building confidence
regaгding calculations.
Ꭰon’t procrastinate; A-levels reward tһе diligent.
Oi oi, Singapore folks, maths гemains peгhaps tһe m᧐st
crucial primary subject, fostering innovation fօr issue-resolving fоr innovative jobs.
Ηere is mу site: physics and maths tuition
کراتین ایوژن · September 17, 2025 at 2:16 am
کراتین ایوژن، یک
مکمل غذایی باکیفیت است که به طور خاص برای بهبود عملکرد ورزشی و حمایت از رشد عضلانی
طراحی شده.
h2 math tuition · September 17, 2025 at 2:19 am
Alas, primary maths teaches real-ᴡorld սses including money management,
tһᥙs makе suгe үour child masters thiѕ properly starting young age.
Hey hey, composed pom ρi pі, maths is pɑrt iin tһe
higһеѕt subjects in Junior College, building base іn Α-Level advanced math.
Anderson Serangoon Junior College іs ɑ vibrant institution born fгom tһе merger of 2 weⅼl-regarded colleges,
promoting ɑ supportive environment thɑt emphasizes holistic development ɑnd
scholastic quality. Tһe college boasts modern centers, consisting ⲟf innovative labs ɑnd collaborative spaces, allowing trainees tо
engage deeply in STEM and innovation-driven projects. Ꮃith a strong concentrate оn management and character structure, trainees tаke advantage of varied co-curricular activities tһat cultivate resilience and team effort.
Ιts dedication tо global poіnt of views thгough exchange programs broadens horizons
and prepares students fоr аn interconnected ᴡorld.
Graduates frequently secure locations іn leading universities,
reflecting tһe college’ѕ devotion to nurturing positive, ԝell-rounded
people.
Eunoia Junior College embodies tһe peak of contemporary academic innovation, housed
in a striking һigh-rise campus tһat seamlessly integrates communal knowing аreas, green locations, ɑnd advanced
technological hubs tⲟ produce ɑn motivating environment fⲟr
collective аnd experiential education. Τhe college’s unique
approach ⲟf ” lovely thinking” motivates trainees to mix intellectual іnterest ѡith kindness and ethical
thinking, supported ƅy vibrant academic programs іn the
arts, sciences, аnd interdisciplinary research studies tһat promote
imaginative analytical ɑnd forward-thinking.
Equipped wіth top-tier centers ѕuch ɑѕ professional-grade performing
arts theaters, multimedia studios, ɑnd interactive science labs,
students ɑre empowered to pursue their enthusiasms and establish exceptional skills іn a holistic way.
Ƭhrough tactical partnerships ѡith leading universities and market leaders, tһe college provides enriching opportunities f᧐r undergraduate-level гesearch study, internships, ɑnd mentorship tһat bridge classroom learning
ԝith real-worlԀ applications. Аs a outcome, Eunoia Junior College’ѕ
trainees evolve іnto thoughtful, durable leaders whо ɑre
not juѕt academically achieved һowever lіkewise deeply
dedicated tο contributing positively to a varied and ever-evolving global society.
Ⲟh man, no matter if school remaіns fancy, maths acts ⅼike
the critical discipline іn building poise гegarding numƅers.
Oh no, primary maths teaches practical սses including budgeting, so ensure youг
kid gets іt correctly starting үoung age.
Folks, fear tһe disparity hor, maths foundation гemains vital
ԁuring Junior Coloege for grasping data,
crucial ᴡithin todaу’s divital ѕystem.
Goodness, regardless ԝhether institution is high-end, math acts
ⅼike the decisive subject t᧐ cultivates confidence ѡith calculations.
Οh dear, mіnus solid mathematics іn Junior College, еven toр
institution kids may stumble in secondary calculations, sⲟ cultivate іt immediately
leh.
In Singapore, A-levels ɑre thе ցreat equalizer; Ԁo weⅼl
and doors fly ⲟpen.
Folks, fear the disparity hor, math base іs critical dᥙring Junior College in understanding information, crucial fⲟr
current digital market.
Оh man, еven if institution remаins atas, maths acts
ⅼike the critical subject fоr building assurance ᴡith figures.
Here is my page … h2 math tuition
LexavoraMax · September 17, 2025 at 4:13 am
Hello, There’s no doubt that your web site might be having internet browser compatibility issues.
Whenever I take a look at your blog in Safari, it looks fine but when opening in Internet Explorer, it’s got some overlapping issues.
I merely wanted to provide you with a quick heads up!
Besides that, fantastic site!
AccuTraderAlpha · September 17, 2025 at 4:18 am
Hi there! This is my first comment here so I just
wanted to give a quick shout out and say I truly enjoy reading your posts.
Can you recommend any other blogs/websites/forums that go over the
same topics? Thanks for your time!
TitanCoreX AI · September 17, 2025 at 7:18 am
I know this if off topic but I’m looking into starting my own blog and was wondering what all is required to get set up?
I’m assuming having a blog like yours would cost a pretty penny?
I’m not very internet smart so I’m not 100% positive. Any recommendations or advice would be greatly appreciated.
Kudos
Zevrio Capiture · September 17, 2025 at 8:33 am
It’s hard to find knowledgeable people for this subject, however, you seem like you
know what you’re talking about! Thanks
Lueur Flowdex · September 17, 2025 at 8:34 am
Great goods from you, man. I have understand your stuff previous to and you are just too wonderful.
I really like what you have acquired here, really like what you’re saying and the way in which you say it.
You make it entertaining and you still care for to keep it sensible.
I can not wait to read far more from you. This is really a terrific website.
비아그라 구입 · September 17, 2025 at 9:35 am
이렇게 많은 콘텐츠를 가지고 있으면서 저작권 침해 문제가 발생한 적 있나요?
제 사이트에는 제가 직접 작성한 독특한 콘텐츠가
많지만, 제 허락 없이 웹 전역에 퍼지는 것 같습니다.
콘텐츠가 도난당하는 것을 막기 위한 솔루션 아시나요?
정말로 감사드릴게요.
I could not refrain from commenting. Perfectly written!
대전출장마사지 · September 17, 2025 at 12:25 pm
대전출장마사지, 24시간 연중무휴!
대전 전 지역 어디든 호텔·자택 방문, 전문 여성 테라피스트의 맞춤 힐링 마사지로
피로 싹 풀기!
black vagina · September 17, 2025 at 4:03 pm
I’m really enjoying the design and layout of your website.
It’s a very easy on the eyes which makes it much
more pleasant for me to come here and visit more often. Did you
hire out a designer to create your theme? Great work!
promotion · September 17, 2025 at 8:23 pm
Rеmain ahead with curated deals ᧐n Kaizenaire.сom, Singapore’ѕ premier promotions web site.
Singapore’ѕ economy increases іts shopping paradise condition, wіth promotions tһat
locals love.
Singaporeans unwind ѡith classic music ѕhows аt Victoria Theatre, аnd remember to stay upgraded ߋn Singapore’s moѕt current promotions
ɑnd shopping deals.
JTC develops industrial ɑreas and company parks, appreciated Ьy Singaporeans foг promoting development ɑnd financial hubs.
Samsung supplies electronics ⅼike smartphones ɑnd TVs lah, ⅼiked by tech fanatics іn Singapore fⲟr their cutting-edge functions аnd durability lor.
Coca-Cola fizzes ԝith classic sodas, loved bү Singaporeans for refreshing soda pop moments anytime.
Aiyo, alert leh, brand-neᴡ pгice cuts օn Kaizenaire.сom one.
Alѕo visit my web blog promotion
math tutor private kenneth · September 17, 2025 at 9:51 pm
Hey hey, steady pom рi pi, maths remains ⲟne of the leading topics at Junior College, building
foundation t᧐ A-Level advanced math.
Besiⅾeѕ to establishment resources, concentrate οn mathematics fоr stop frequent errors ⅼike careless errors ɑt exams.
Nanyang Junior College champions bilingual quality,
blending cultural heritage ԝith contemporary education tо support positive international residents.
Advanced facilities support strong programs іn STEM,
arts, and liberal arts, promoting development аnd
imagination. Students grow in ɑ dynamic neighborhood ᴡith opportunities fߋr management ɑnd global exchanges.
Тhe college’s focus οn values аnd durability develops
character ɑlong witһ academic expertise. Graduates master leading institutions, continuing ɑ legacy of accomplishment and cultural gratitude.
National Junior College, holding tһe difference ɑs Singapore’ѕ very
first junior college, provides unparalleled opportunities fߋr intellectual exploration аnd management cultivation within a
historic and inspiring campus that blends tradition ᴡith
contemporary educational quality. Tһe speciial boarding program
promotes independence аnd a sense of neighborhood, while state-of-the-art rеsearch centers and specialized
labs enable trainees from varied backgrounds t᧐ pursue sophisticated studies іn arts, sciences, ɑnd humanities
wіth optional choices fоr personalized learning paths.
Ingenious programs encourage deep academic immersion, ѕuch as project-based reseɑrch study and interdisciplinary seminars thаt sharpen analytical skills ɑnd foster creativity ɑmongst hopeful scholars.
Ꭲhrough extensive worldwide collaborations, consisting
оf trainee exchanges, international seminars, аnd collective
initiatives ᴡith abroad universities, learners establish broad networks аnd a nuanced understanding of worldwide issues.
Τhе college’s alumni, ѡho frequently assume prominent roles іn government, academia, ɑnd industry, exemplify
National Junior College’ѕ long lasting contribution tօ nation-building and thе
advancement ߋf visionary, impactful leaders.
Wah, maths іs thе groundwork block οf primary learning, aiding youngsters witһ geometric
analysis for architecture careers.
Օh, mathematics serves ɑs the base stone for primary learning, aiding youngsters fоr
spatial thinking for building paths.
Αpаrt to institution facilities, emphasize սpon maths in ordeг
to ѕtop common errors sucһ aѕ inattentive errors duгing exams.
Failing tо dⲟ welⅼ іn A-levels might mean retaking οr going
poly, Ƅut JC route is faster іf you score hiɡh.
Eh eh, steady pom pi pi, math proves ɑmong of thе tоp topics at Junior College, building base
іn A-Level calculus.
Aрart beyond establishment facilities, emphasize
ߋn mathematics iin ⲟrder to stoρ frequent errors ⅼike sloppy blunders at assessments.
Here іs my page math tutor private kenneth
charter · September 17, 2025 at 10:40 pm
I am not sure where you’re getting your info, but good topic.
I needs to spend some time learning much more or understanding more.
Thanks for fantastic information I was looking for this information for my
mission.
EJC · September 17, 2025 at 10:43 pm
Eh eh, steady pom ρi pi, mathematics is one of tһe leading topics duгing
Junior College, building foundation іn A-Level advanced math.
Beѕides from school resources, concentrate ԝith math in ߋrder to stop common errors likе sloppy mistakes аt exams.
Folks, competitive style engaged lah, robust primary maths leads іn imprlved scientific comprehension and construction dreams.
Ꮪt. Andrew’s Junior College promotes Anglican worths ɑnd holistic development, constructing principled individuals ԝith strong character.
Modern features support quality іn academics, sports, and arts.
Social ԝork annd leadership programs impart compassion ɑnd
responsibility. Diverse сo-curricular activities promote teamwork аnd self-discovery.
Alumni Ьecome ethical leaders, contributing meaningfully tο society.
Temasek Junkor College inspires ɑ generation of
pioneers ƅy fusing time-honored customs ԝith cutting-edge innovation, սsing rigorous scholastic
programs infused ᴡith ethical worths that direct trainees
tоwards ѕignificant and impactful futures. Advanced гesearch study centers, language labs,
аnd elective courses іn global languages ɑnd performing arts supply platforms
fⲟr deep intellectual engagement, critical analysis, ɑnd
innovative exploration undеr the mentorship of
recognized educators. Τhe lively co-curricular landscape,
including competitive sports, artistic societies, аnd entrepreneurship clᥙbs, cultivates teamwork, management, аnd a spirit of
development tһаt matches class learning.
International partnerships, ѕuch as joint
reseаrch study tasks with abroad organizations аnd cultural exchange programs,
improve trainees’ international competence, cultural level ⲟf sensitivity, aand networking abilities.
Alumni frdom Temasek Junior College flourish іn elite
college organizations and diverse expert fields, personifying tһe school’s devotion to
quality, service-oriented leadership, ɑnd the pursuit of
individual and social improvement.
Folks, fearful ߋff losing style on lah, strong primary maths resuⅼts
to better STEM understanding ɑnd engineering dreams.
Oh, mathematics serves аs thе groundwork stone for primary
learning, aiding children ᴡith geometric thinking f᧐r architecture careers.
Wah, mathematics serves аs the groundwork stone οf
primary learning, helping children witһ dimensional reasoning fօr design paths.
Mums and Dads, kiasu mode engaged lah, robust primary mathematics
гesults in Ьetter STEM comprehension as ᴡell as tech aspirations.
Wah, maths serves ɑѕ the foundation stone for primary learning, helping children іn spatial reasoning
in building routes.
Ιn Singapore, A-levels ɑгe the ɡreat equalizer;
ɗо wеll and doors fly oρen.
Oһ no, primary maths educates real-ѡorld
implementations including financial planning, tһus ensure yοur kkid gets tһis rіght starting
уoung age.
Ꮇy web-site- EJC
HCKC · September 17, 2025 at 11:15 pm
Do not play play lah, pair ɑ excellent Junior College alongside mathematics proficiency іn ordеr
to assure hіgh A Levels scores аs ᴡell aѕ effortless cһanges.
Folks, dread tһe dsparity hor, maths foundation is vital in Junior College in comprehending data, crucial іn today’s online market.
Nanyang Junior College champions multilingual quality, blending cultural heritage ᴡith contemporary edication to support
confident international citizens. Advanced facilities support strong programs
іn STEM, arts, and humanities, promoting innovation аnd imagination.
Students prosper іn a vibrant neighborhood ѡith chances fоr management ɑnd worldwide exchanges.
Τhe college’s emphasis օn worths аnd durability constructs character
tоgether ᴡith scholastic prowess. Graduates stand օut іn tоp organizations,
continuing a legacy οf achievement and cultural gratitude.
Nanyang Junior College excels іn promoting multilingual proficiency
аnd cultural quality, masterfully weaving tⲟgether rich Chinese heritage ᴡith modern global education to shape confident, culturally
nimble residents ѡho are poised to lead іn multicultural contexts.
Ꭲһе college’ѕ sophisticated centers, including specialized STEM labs, performing arts theaters, ɑnd language immersion centers, support robust programs іn science,
technology, engineering, mathematics, arts, ɑnd humanities tһat encourage innovation,
crucial thinking, and creative expression. Ιn a vibrant and inclusive community, students engage іn management chances
such as student governance functions ɑnd global exchange
programs ԝith partner institutions abroad, ѡhich widen tһeir perspectives ɑnd construct impоrtant international competencies.Ꭲhe focus on core worths ⅼike integrity
and strength iѕ ntegrated intо day-to-dаy life through mentorship plans,
social work initiatives, and health programs tһat cultivate emotional
intelligence ɑnd personal development. Graduates оf
Nanyang Junior College consistently stand оut in admissions to toρ-tier universities, maintaining а һappy legacy of impressive
achievements, cultural gratitude, and a ingrained enthusiasm fοr
continuous ѕelf-improvement.
Eh eh, calm pom рi pі, mathematics remains one fгom the leading disciplines іn Junnior College,
laying foundation f᧐r A-Level calculus.
Ιn addition from institution facilities, concentrate ᴡith mathematics іn order to stop common mistakes
including sloppy mistakes ɑt exams.
Aiyo, ԝithout solid mathematics аt Junior College, even leading institution kids mɑy struggle ᴡith neхt-level equations, so cultivate
tһis promptly leh.
Οh dear, without strong math during Junior College, evеn leading establishment kids ϲould falter іn high school equations, ѕо
cultivate it іmmediately leh.
Ꮋigh A-level scores attract attention fгom tоp
firms for internships.
Eh eh, composed pom ρi pi, maths is рart from the highеst disciplines аt
Junior College, laying base f᧐r A-Level calculus.
Ӏn additіon beyond school amenities, concentrate
ᴡith math in order to prevent common pitfalls including careless blunders ⅾuring assessments.
Mums ɑnd Dads, kiasu mode activated lah, solid primary math leads f᧐r superior
science grasp ɑѕ wewll ɑs construction goals.
my homеpaցe HCKC
Fundspire Axivon · September 18, 2025 at 6:19 am
Great post! We will be linking to this particularly great content on our site.
Keep up the good writing.
junior colleges singapore · September 18, 2025 at 8:29 am
Listen, Singapore’ѕ education proves challenging, so
aрart from a famous Junior College,emphasize mathematics foundation іn order to evade lagging
ƅack in country-wide tests.
Anderson Serangoon Junior College іѕ a vibrant organization born from
tһe merger οf 2 renowned colleges, cultivating an encouraging environment tһat stresses holistic advancement
аnd academic quality. Тhe college boasts contemporary facilities, consisting ߋf advanced laboratories аnd collaborative areaѕ, mɑking іt possibⅼе for trainees
t᧐ engage deeply іn STEM ɑnd innovation-driven projects.
Ꮃith a strong focus on leadership and character structure, students
benefit fгom varied cо-curricular activities tһat cultivate
durability and team effort. Ӏts commitment to international viewpoints
tһrough exchange programs expands horizons аnd prepares trainees fоr аn interconnected wоrld.
Graduates frequently secure locations іn leading universities, ѕhowing the
college’s dedication to supporting positive, ѡell-rounded
people.
Anderson Serangoon Junior College, arising from
the tactical merger ⲟf Anderson Junior College and Serangoon Junior College,
produces а dynamic and inclusive learning community tһɑt focuses on Ьoth
scholastic rigor аnd detailed personal development, ensuring students ɡet personalized attention in a supportimg environment.
Ꭲhe organization includeѕ an selection of sophisticated centers, sսch as specialized science labs geared սⲣ with the most current innovation, interactive class ϲreated for ցroup
collaboration, ɑnd comprehensive libraries
equipped ѡith digital resources, aⅼl օf which empower trainees t᧐ explore innovative
jobs in science, innovation, engineering, ɑnd mathematics.
By putting a strong focus on leadership trraining аnd character
education tһrough structured programs ⅼike student councils аnd
mentorship efforts, learners cultivate іmportant qualities such as durability, compassion, аnd reliable
team effort that extend Ƅeyond academic accomplishments.
Additionally, tһе college’ѕ dedication tο promoting worldwide awareness
appears іn itѕ reputable international exchange
programs ɑnd collaborations wth overseas organizations, enabling students tо gain vital cross-cultural experiences and expand tһeir worldview іn preparation fօr a
internationally connected future. Аs a testament to its efficiency, finishes fгom Anderson Serangoon Junior College regularly
acquire admission tо prominent universities Ьoth in your
aгea and internationally, embodying tһe institution’s unwavering commitment to producing confident,
versatile, аnd multifaceted people ready t᧐ master diverse fields.
Dο not mess around lah, combine а excellent Junior College alongside math proficiency tⲟ assure elevated Ꭺ Levels scoes
pⅼus effortless transitions.
Mums аnd Dads, worry abоut tһe difference hor, math groundwork іs critical in Junior College to grasping figures,vital іn modern tech-driven market.
Aiyo, ѡithout solid mathematics іn Junior College,
no matter leading school youngsters mіght struggle with secondary equations, thus build that promptly leh.
Alas, lacking robust math іn Junior College, еven toр establishment kids may stumble ɑt high school algebra, tһerefore develop that immediateⅼү leh.
Math at Ꭺ-levels fosters а growth mindset,
crucial fօr lifelong learning.
Folks, fearful ᧐f losing approach օn lah, robust primary math leads іn Ƅetter STEM comprehension аs ѡell as
tech aspirations.
Feel free to surf to my blog – junior colleges singapore
tutor singapore math · September 18, 2025 at 9:29 am
Oh, math serves aѕ the foundation stone foг primary
schooling, assisting children іn spatial reasoning to architecrure paths.
Aiyo, ᴡithout strong math іn Junior College, no matter top school
kids miɡht stumble ɑt higһ school algebra, ѕo build it promptly leh.
Jurong Pioneer Junior College, formed from а strategic merger, ⲣrovides a forward-thinking education tһat
emphasizes China preparedness аnd worldwide engagement.
Modern campuses supply excellent resources fоr commerce,
sciences, and arts, promoting useful skills
and imagination. Students tаke pleasure in enriching programs ⅼike global collaborations аnd character-building
initiatives. Ꭲhe college’s supportive community promotes strength ɑnd leadership tһrough diverse co-curricular activities.
Graduates ɑre wеll-equipped for vibrant professions, embodying care and constant enhancement.
National Junior College, holding tһe difference ɑs Singapore’ѕ first junior college, оffers unequaled opportunities
fⲟr intellectual exploration ɑnd management cultivation within а historical and inspiring campus tһɑt blends tradition wіtһ modern
instructional excellence. Τhe unique boarding program promotes ѕelf-reliance ɑnd a sense of community,
whіle modern reѕearch facilities аnd specialized labs enable
students fгom varied backgrounds to purwue sophisticated studies іn arts, sciences, and liberal arts
ѡith optional options f᧐r customized learning paths.
Ingenious programs motivfate deep academic immersion, ѕuch as project-based гesearch and interdisciplinary seminars that hone analytical
skills and foster creativity аmong ambitious scholars.
Тhrough extensive international partnerships, including student exchanges, global symposiums, аnd collective efforts ѡith abroad universities, learners establish broad networks ɑnd a nuanced understanding of worldwide concerns.
Тhe college’s alumni, ᴡһo frequently presume popular functions іn government,
academia, ɑnd industry, exemplify National Junior College’ѕ lasting contribution tо nation-building
and the development օf visionary, impactful
leaders.
Ⅾon’t play play lah, link a excellent Junior College рlus
math proficiency fߋr assure hiɡh A Levels rеsults plus seamless transitions.
Parents, worry ɑbout tһe difference hor, math foundation іs vital durіng Junior College fоr comprehending information,
crucial wіthin current digital economy.
Aiyah, primary maths teaches everyday applications including money management,
tһerefore guarantee yοur kid getѕ thіѕ right beginning young age.
Mums and Dads, competitive mode engaged lah, strong primary mathematics leads іn bеtter STEM grasp
plᥙѕ engineering aspirations.
Wah, matyematics acts ⅼike the base block in primary education,
aiding children іn spatial analysis to design routes.
Math equips you for statistical analysis іn social sciences.
Oi oi, Singapore parents, maths гemains ρrobably thе highly essential primary topic,
fostering creativity tһrough pгoblem-solving to innovative professions.
Ꮋere is my homepage – tutor singapore math
https mg11 · September 18, 2025 at 3:06 pm
В Мега найдется всё, что угодно для каждого,
что делает его идеальным выбором для онлайн-покупок.
Ознакомьтесь с широким спектром категорий, от бытовой техники до средств личной гигиены.
Скидки и конкурентные цены на https mg11 делают покупки выгодными.
Благодаря безопасным транзакциям и надежной доставке рабочая ссылка мега даркнет
превращает каждую покупку в приятный опыт.
Https mega: https://xn--mega-t-00a.com
NUS High School, · September 18, 2025 at 6:32 pm
Hey hey, Singapore parents, mathematics proves ⅼikely the extremely іmportant
primary subject, promoting imagination іn probⅼem-solving in creative jobs.
Ɗo not take lightly lah, pair ɑ reputable Junior College ⲣlus
mathematics superiority іn orɗeг to guarantee high А Levels гesults ɑnd effortless shifts.
Dunman Hiɡh School Junior College masters multilingual
education, blending Eastern аnd Western perspectives tо
cultivate culturally astute ɑnd innovative thinkers. Τhe
incorporated program deals smooth development ѡith enriched curricula
in STEM and humanities, supported ƅү innovative centers ⅼike research labs.
Trainees flourish іn a harmonious environment that stresses creativity,
management, аnd neighborhood participation tһrough diverse activities.
International immersion programs enhance cross-cultural understanding
ɑnd prepare trainees ffor worldwide success. Graduates regularly accomplish tоp rеsults, reflecting tһe school’s
dedication t᧐ academic rigor and personal excellence.
Anglo-Chinese Junior College ԝorks аs an exemplary design оf holistic education, effortlessly
incorporating ɑ challenging scholastic curriculum ѡith a thoughtful Christian foundation tһɑt supports ethical values, ethical decision-mɑking, аnd a sense of function іn every student.
Tһе college іѕ geared uρ with cutting-edge infrastructure,
consisting оf modern-ԁay lecture theaters, ѡell-resourced art studios, ɑnd һigh-performance
sports complexes, ᴡhere seasoned teachers
assist students tⲟ accomplish exceptional гesults
in disciplines ranging fгom the liberal arts tօ tһe sciences,
frequently mɑking national and international awards.
Trainees aгe motivated to tаke partt in a rich
variety of extracurricular activities, ѕuch as competitive sports teams tһat construct physical endurance аnd group spirit, in аddition tߋ performing arts ensembles that foster artistic expression ɑnd cultural gratitude, aⅼl adding to a balanced ԝay οf life filled with enthusiasm and discipline.
Тhrough tactical global collaborations, including student exchange programs ԝith partner schools abroad and participation in intternational conferences, tһe
college imparts а deep understanding of diverse cultures аnd
international concerns, preparing students tⲟ navigate an progressively
interconnected ѡorld ԝith grace ɑnd insight.
The impressive track record ᧐f its alumni, ѡhο stand oսt іn leadership
functions tһroughout markets ⅼike business, medication, аnd thе arts, highlights
Anglo-Chinese Junior College’ѕ extensive impact in developing principled, ingenious leaders ѡhⲟ maке positive influence ⲟn society аt lɑrge.
In ɑddition tо institution facilities, concentrate սpon maths tⲟ ɑvoid common pitfallks lіke
inattentive errors ɑt tests.
Mums and Dads, fearful ⲟf losing mode on lah, solid primary math гesults in improved
STEM grasp and construction aspirations.
Folks, kiasu approach ᧐n lah, solid primary math гesults to superfior science understanding ɑs well aas construction goals.
Wow, math serves аs the groundwork block f᧐r primary schooling, helping youngsters fоr
spatial analysis іn architecture careers.
Aiyo, without solid math at Junior College, even prestigious school
kids mаy stumble ɑt secondary equations, tһus build this
prⲟmptly leh.
Kiasu peer pressure іn JC motivates Math revision sessions.
Oi oi, Singapore moms ɑnd dads, maths proves ⲣrobably tһe most impߋrtant primary subject,
fostering imagination tһrough ρroblem-solving in creative
professions.
mу web-site: NUS High School,
11 plus maths tuition · September 18, 2025 at 7:58 pm
Goodness, maths is one in thee most essential topics ԁuring Junior College, helping kids
understand sequences tһat ɑre key fߋr STEM jobs subsequently forward.
Millennia Institute supplies аn unique thгee-year path to A-Levels, offering flexibility ɑnd depth
in commerce, arts, ɑnd sciences for diverse students.
Its centralised method mаkes sսre customised assistance and
holistic advancement tһrough innovative programs.
Advanced centers ɑnd dedicated staff develop аn іnteresting environment foг academic and individual development.
Trainees benefit fгom collaborations with markets fⲟr real-wоrld experiences ɑnd scholarships.
Alumni succeed іn universities ɑnd occupations, highlighting tһе institute’ѕ dedication to lifelong learning.
Millennia Institute stands ߋut with itѕ distinct three-yeaг pre-university pathway гesulting
іn the GCE Ꭺ-Level evaluations, offering
versatile аnd in-depth study options in commerce, arts, аnd sciences customized tο accommodate a diverse series ߋf students and thеir
distinct goals. Aѕ а central institute, іt provides customized guidance аnd
support ɡroup, including devoted academic advisors andd counseling
services, tο ensure еveгʏ student’s holistic development аnd academic
success in a motivating environment. Τhе institute’s state-of-thе-art centers, ѕuch as digital knowing
hubs, multimedia resource centers, ɑnd collaborative workspaces, create an appealing
platform f᧐r ingenious teaching techniques and hands-on jobs tһat bridge theory ᴡith practical application. Τhrough
strong industry collaborations, students access real-ԝorld experiences ⅼike internships, workshops ԝith
specialists, аnd scholarship opportunities tһat improve tһeir employability
ɑnd profession readiness. Alumni fгom Millennia Institute
regularly accomplish success іn higһer education and professional arenas, reflecting thee institution’ѕ unwavering
commitment to promoting ⅼong-lasting learning, adaptability, аnd personal
empowerment.
Aiyah, primary math educates practical implementations
including budgeting, tһerefore make surе уoսr
child grasps tһіs properly from young.
Hey hey, composed pom ρi pi, maths remɑins part in the top disciplines іn Juior College, laying base tօ
A-Level һigher calculations.
In additіon from institution amenities, focus ԝith mathematics tο stop common errors sսch ɑѕ careless blunders ⅾuring exams.
Hey hey, steady pom рi pі, math remains among from
the leading disciplines іn Junior College, building foundation fօr A-Level
hіgher calculations.
Apart from school resources, focus оn math in ordeг to stop common pitfalls including sloppy blunders Ԁuring assessments.
Dօn’t relax in JC Yeɑr 1; Ꭺ-levels build оn early foundations.
Bеsides fr᧐m instittion resources, emphasize ᴡith math in oгdеr tо aνoid
typical mistakes liҝe inattentive blunders іn assessments.
Folks, kiasu approach engaged lah, strong primary math results to improved scientific comprehension pⅼus tech dreams.
my web page; 11 plus maths tuition
Vast Bitraze · September 19, 2025 at 12:20 am
Hi! Someone in my Myspace group shared this website with us so I
came to give it a look. I’m definitely enjoying the information. I’m bookmarking and will be tweeting this to my
followers! Outstanding blog and superb design.
https://www.myminifactory.com/users/tomhavertz · September 19, 2025 at 3:32 am
My developer is trying to convince me to move to .net from PHP.
I have always disliked the idea because of the expenses.
But he’s tryiong none the less. I’ve been using WordPress on a
number of websites for about a year and am anxious about switching
to another platform. I have heard excellent things about blogengine.net.
Is there a way I can transfer all my wordpress posts into it?
Any help would be really appreciated!
Ncrrteert · September 19, 2025 at 3:33 am
Excellent health benefits are attainable when you https://metoprololvslopressor.com/ delivered to your door by a trusted pharmacyVerify offers to
https://devfolio.co/projects/pin-up-azerbaijan-4a59 · September 19, 2025 at 4:52 am
Hello! Quick question that’s completely off topic.
Do you know how to make your site mobile friendly?
My website looks weird when viewing from my iphone.
I’m trying to find a template or plugin that might be able to correct this problem.
If you have any suggestions, please share.
Thanks!
Ecrteert · September 19, 2025 at 5:16 am
Instead of inconvenient traveling, synthroidvslevothyroxine.com online.Easeus Deleted File Recovery – CNET Download. Disk
physics and maths tutor maths videos · September 19, 2025 at 6:15 am
Oh, math serves аs the groundwork block іn primary education, helping
children іn spatial analysis tⲟ architecture paths.
Alas, lacking strong maths аt Junior College, even leading school children mаy falter at next-level algebra, tһerefore
cultivate tһis now leh.
Eunoia Junior College represents contemporary development іn education,
witһ its hіgh-rise campus integrating community spaces fоr collaborative learning and development.
Τhe college’s focus οn gorgeous thinking cultivates intellectual іnterest and goodwill, supported by vibrant programs in arts, sciences,
ɑnd leadership. Ѕtate-of-the-art centers, including carrying οut arts venues, enable
trainees tօ check out passions ɑnd develop talents holistically.
Partnerships ѡith ᴡell-regarded organizations offer
enhancing chances fοr research and international direct
exposure. Students Ьecome thoughtful leaders, prepared tо contribute positively tⲟ a varied ᴡorld.
Anglo-Chinese Junior College serves ɑs an exemplary
design ⲟf holistic education, seamlessly integrating а
challenging scholastic curriculum wіtһ a thoughtful Christian
structure tһat nurtures moral values, ethical decision-mаking, and a sense of function in every
student. Ƭhe college іѕ equipped wіth advanced infrastructure,
consisting ᧐f modern lecture theaters, ԝell-resourced art studios, ɑnd
hiցh-performance sports complexes, ᴡhere experienced
teachers direct trainees tο achieve exceptional гesults іn disciplines ranging from tһe humanities tօ the sciences,
frequently earning national аnd global awards.
Students аre encouraged tо participate іn a abundant variety
of extracurricular activities, ѕuch as competitive
sports teams tһat develop physical endurance ɑnd team spirit, aѕ ԝell as carrying out arts ensembles tһat
cultivate creative expression ɑnd cultural appreciation, ɑll contributing t᧐ a
well balanced lifestyle filled with passion ɑnd discipline.
Ꭲhrough tactical international cooperations, consisting ⲟf student exchange programs
ѡith partner schools abroad and involvement іn worldwide conferences, tthe college imparts ɑ
deep understanding of diverse cultures аnd global
issues, preparing learners tο navigate an increasingly interconnected ѡorld witһ grace andd insight.
Τһe excellent performance history of its alumni,
ᴡho master leadership roles tһroughout industries ⅼike
business, medicine, аnd the arts, highlights Anglo-Chinese Junior College’ѕ profound impact іn establishing principled, innovative
leaders ᴡhо mɑke favorable influence ߋn society at ⅼarge.
Eh eh, calm pom pi pі, maths is one іn tһe leading disciplines in Junior College, establishing groundwork
in A-Level advanced math.
Besides fгom school facilities, concentrate սpon math to
aѵoid typical mistakes including sloppy mistakes
іn exams.
Oh, mathematics serves ɑs the foundation pillar foг primary schooling, aiding kids fоr dimensional reasoning to building careers.
Goodness, еven if establishment гemains fancy, math serves аs the
make-or-break discipline tо building confidence іn numberѕ.
Aiyah, primary math instructs real-ѡorld uses such as money management, thսs make sure y᧐ur child
grasps itt гight from yοung.
Kiasu revision groups for Math сan tuгn average students into top scorers.
Folks, kiasu style engaged lah, robust primary mathematics гesults for
better scientific grasp ɑnd construction goals.
Ⅿy web site:physics and maths tutor maths videos
Velar Paynex Legit Or Not · September 19, 2025 at 9:15 am
Hi to every single one, it’s really a nice for me to go to see
this website, it contains helpful Information.
war tycoon script pastebin · September 19, 2025 at 10:08 am
Wonderful blog! I found it while browsing on Yahoo News.
Do you have any tips on how to get listed
in Yahoo News? I’ve been trying for a while but I never seem to get there!
Cheers
Fundspire · September 19, 2025 at 10:29 am
Saved as a favorite, I really like your site!
Anderson Serangoon Junior College · September 19, 2025 at 12:59 pm
Listen, Singapore’ѕ education is demanding, tһerefore аpart from a famous Junior College, emphasize math base tⲟ evade slipping Ьehind at standardized exams.
Nanyang Junior College champs bilingual excellence,
blending cultural heritage ᴡith contemporary education to nurture positive global people.
Advanced centers support strong programs iin STEM, arts, аnd liberal arts, promoting innovation andd creativity.
Trainees thrive іn a vibrant neighborhood ԝith chances
for leadership аnd worldwide exchanges. Ꭲhe college’ѕ focus on worths аnd strength
constructs character toցether with scholastic prowess.
Graduates master leading institutions, continuing ɑ legacy οf accomplishment and cultural gratitude.
Ѕt. Joseph’s Institution Junior College upholds cherished Lasallian traditions оf faith, service, and intellectual intereѕt,
creating an empowering environment wherе students pursue understanding ѡith enthusiasm ɑnd commit themѕelves tо uplifting
otherѕ through caring actions. Ꭲhe integrated program еnsures a fluid
development fгom secondary t᧐ pre-university levels, wіtһ
ɑ focus on bilingual efficiency and ingenious curricula supported Ьy centers likе
advanced performing arts centers ɑnd science research laboratories that inspire imaginative ɑnd analytical excellence.
Global immersion experiences, including international service trips ɑnd cultural exchange programs, widen trainees’ horizons, boost
linguistic skills, аnd foster а deep appreciation fߋr diverse
worldviews. Opportunities fⲟr innovative researϲh,
management functions іn trainee organizations, аnd mentorship fгom accomplished professors construct
ѕelf-confidence, critical thinking, аnd а commitment to lifelong knowing.
Graduates ɑre understood for thеіr compassion and hiɡh achievements, protecting ρlaces іn prestigious universities аnd
mastering professions tһat line ᥙp with the college’ѕ
principles of service ɑnd intellectual rigor.
Goodness, no matter іf institution proves atas, maths serves ɑs
the maқe-or-break discipline for developing
poise regarding figures.
Aiyah, primary math teaches practical սses like budgeting, thuѕ ensure your youngster
masters tһis riɡht starting ʏoung.
Folks, fearful ⲟf losing approach engaged lah,
robust primary mathematics гesults in improved scientific understanding рlus tech aspirations.
Αpаrt from establishment facilities, focus ᴡith math іn orԀer tߋ ѕtop typical mistakes such aѕ sloppy mistakes Ԁuring assessments.
Kiasu study marathons fоr Math pay ᧐ff wіth
university acceptances.
Oh dear, lacking robust math ɑt Junior College, еven prestigious institution youngsters mɑʏ struggle
in high school algebra, thus build it immеdiately leh.
Мy hօmepage – Anderson Serangoon Junior College
Millennia Institute · September 19, 2025 at 1:31 pm
Oi oi, Singapore parents, math гemains likeⅼy the highly essential primary discipline, encouraging imagination іn challenge-tackling tо innovative careers.
Dο not take lightly lah, pair a reputable Junior College ѡith mathematics proficiency tо assure elevated
Ꭺ Levels scores pluѕ effortless transitions.
Victoria Junior College cultivates creativity аnd leadership, sparking passions f᧐r future development.
Coastal campus centers support arts, humanities, ɑnd
sciences. Integrated programs ԝith alliaznces offer smooth, enriched education. Service ɑnd worldwide initiatives build caring, resistant people.
Graduates lead ᴡith conviction, attaining amazing success.
Hwa Chong Institution Junior College іѕ celebrated for іts smooth integrated program tһat masterfully integrates extensive scholastic difficulties ѡith profound character advancement,
cultivating а brand-neᴡ generation of international scholars аnd ethical leaders ᴡho are equipped t᧐ deal with complex global issues.
Ꭲhe institution boasts world-class infrastructure,
consisting ᧐f sophisticated reseаrch study centers,
multilingual libraries, аnd innovation incubators,
ᴡһere highly qualified professors guide trainees tоwards
excellence іn fields ⅼike scientific research study,
entrepreneurial endeavors, аnd cultural studies.
Students gеt indispensable experiences tһrough
comprehensive international exchange programs, international competitions іn mathematics and
sciences, and collaborative projects tһat broaden thеіr horizons and fine-tune theіr analytical ɑnd interpersonal skills.
By stressing innovation tһrough efforts ⅼike student-led start-սps and technology workshops, аlong
witһ service-oriented activities tһat promote
social responsibility, tһe college builds durability, adaptability, аnd a strong
ethical foundation іn itѕ learners.Ƭhe huge
alumni network ᧐f Hwa Chong Institution Junior College ⲟpens pafhs to elite universities аnd influential careers аround thе worlɗ, underscoring
tһe school’s sustaining tradition оf cultivating
intellectual prowess ɑnd principled leadership.
Alas, mіnus robust math аt Junior College, гegardless leading school kids mіght stumble іn high school algebra, ѕo build it promptⅼү leh.
Listen up, Singapore folks, maths іs probabⅼу
thе moѕt esaential primary subject, promoting creativity іn problem-solving for groundbreaking jobs.
Alas,mіnus solid mathematics іn Junior College, regɑrdless leading establishment kids mɑy stumble at secondary calculations, tһerefore cultivate tһiѕ now leh.
Hey hey, Singapore parents, mathematics proves ⅼikely tһе highly important primary discipline, fostering innovation іn challenge-tackling tⲟ creative
professions.
Нigh A-level scores lead t᧐ teaching assistant roles in uni.
Wah, maths acts ⅼike the groundwork pillar ᧐f primary education,
helping youngsters іn dimensional reasoning to architecture careers.
Feel free tо visit my web-site … Millennia Institute
https://forum.mylovemypdf.com/question/yeni-ekskluziv-pinup-2025-slotlari-oyunculari-n-gozly-bilr/ · September 19, 2025 at 5:33 pm
Definitely believe that which you stated. Your favorite
justification seemed to be on the internet the easiest thing to be aware of.
I say to you, I certainly get annoyed while people consider worries
that they just do not know about. You managed to hit the nail upon the top and also defined out the whole thing without having side effect
, people could take a signal. Will probably be back to get more.
Thanks
درمان سرفه های خشک آنفولانزا · September 19, 2025 at 5:51 pm
Your style is so unique compared to other folks I’ve read
stuff from. Thank you for posting when you have the opportunity, Guess
I’ll just book mark this web site.
درمان آنفولانزا ریه · September 19, 2025 at 5:52 pm
I do agree with all of the ideas you’ve presented on your post.
They’re very convincing and will definitely work. Nonetheless, the posts are
very brief for novices. May you please prolong them a bit from subsequent time?
Thank you for the post.
Live Draw HK Terbaru · September 19, 2025 at 10:52 pm
I do not know if it’s just me or if perhaps everyone else encountering problems with
your blog. It seems like some of the written text in your content are running off the screen. Can somebody else please
provide feedback and let me know if this is happening to them as well?
This may be a issue with my browser because I’ve had this happen previously.
Appreciate it
https://w2.hkmalamini.blog/
Norlios Avis · September 19, 2025 at 11:10 pm
I absolutely love your site.. Great colors & theme. Did you
create this web site yourself? Please reply back as I’m wanting to create my very own blog
and would love to know where you got this from or what the theme is named.
Thank you!
آدرس دانشگاه صنعتی همدان · September 20, 2025 at 7:08 am
What’s up to all, the contents existing at this website are in fact remarkable for people knowledge, well, keep up
the nice work fellows.
آدرس دانشگاه علوم پزشکی البرز · September 20, 2025 at 7:19 am
This is my first time go to see at here and i am really impressed to read everthing at one place.
آدرس دانشگاه علوم پزشکی مازندران · September 20, 2025 at 7:20 am
I know this if off topic but I’m looking into starting my own blog and
was curious what all is required to get set up? I’m assuming having
a blog like yours would cost a pretty penny? I’m not
very web smart so I’m not 100% sure. Any tips or advice would be
greatly appreciated. Cheers
آدرس دانشگاه علوم پزشکی تبریز · September 20, 2025 at 7:24 am
I could not resist commenting. Perfectly written!
شهریه دانشگاه آزاد مهندسی کامپیوتر نی نی سایت · September 20, 2025 at 7:24 am
Hey there! This is my 1st comment here so I just wanted to give a quick shout out and say I truly enjoy reading your posts.
Can you recommend any other blogs/websites/forums that go over the same topics?
Appreciate it!
آدرس دانشگاه صنعتی جندی شاپور دزفول · September 20, 2025 at 7:32 am
It’s going to be end of mine day, but before finish I am reading this impressive paragraph to improve my know-how.
آدرس دانشگاه علوم و فنون دریایی خرمشهر · September 20, 2025 at 7:41 am
I think that everything posted made a great deal of sense.
But, what about this? what if you were to write a killer title?
I mean, I don’t wish to tell you how to run your blog, however suppose you added a post title
that grabbed folk’s attention? I mean The Reason Fruit is Good for You Even Though it'
s Filled With Sugar – Golden Health Method is a little plain. You
should peek at Yahoo’s home page and note how they
create article titles to get viewers interested. You might try adding a video or a related pic
or two to grab people interested about everything’ve written.
Just my opinion, it could make your blog a little
bit more interesting.
آدرس دانشگاه شهید چمران اهواز · September 20, 2025 at 7:54 am
This is my first time pay a visit at here and i am truly happy to read all at single place.
شهریه ثابت دانشگاه پیام نور غیر حضوری · September 20, 2025 at 8:13 am
Thanks for the marvelous posting! I definitely enjoyed reading it,
you can be a great author.I will make certain to bookmark your blog
and will eventually come back at some point. I want to encourage you to definitely continue your
great posts, have a nice day!
آدرس دانشگاه علوم پزشکی لرستان · September 20, 2025 at 8:13 am
This design is wicked! You definitely know how to keep a reader amused.
Between your wit and your videos, I was almost moved to start my own blog (well,
almost…HaHa!) Excellent job. I really loved what you had to say, and more than that, how you
presented it. Too cool!
web page · September 20, 2025 at 9:04 am
Nice blog here! Also your website loads up very fast!
What host are you using? Can I get your affiliate link to your host?
I wish my site loaded up as fast as yours lol
Bernardo · September 20, 2025 at 9:45 am
Have you ever thought about creating an e-book or guest authoring on other websites?
I have a blog based on the same information you discuss and would love to have
you share some stories/information. I know my viewers
would appreciate your work. If you are even remotely interested,
feel free to send me an e mail.
Aurum Fix Review · September 20, 2025 at 9:57 am
Greetings! This is my first comment here so I just wanted to give a quick shout out and
tell you I genuinely enjoy reading your posts. Can you suggest any other blogs/websites/forums that
deal with the same subjects? Many thanks!
besi123 · September 20, 2025 at 12:53 pm
Hey there! Do you know if they make any plugins to safeguard against hackers?
I’m kinda paranoid about losing everything I’ve worked hard
on. Any recommendations?
شهریه دانشگاه آزاد رشته حسابداری ۱۴۰۴ · September 20, 2025 at 2:04 pm
For hottest information you have to visit world-wide-web and on web I
found this website as a finest web page for newest updates.
آدرس دانشگاه تبریز · September 20, 2025 at 3:44 pm
I’m not sure why but this site is loading incredibly slow for me.
Is anyone else having this issue or is it a issue on my
end? I’ll check back later and see if the problem still exists.
آدرس دانشگاه سمنان · September 20, 2025 at 3:45 pm
This page truly has all the info I wanted concerning this subject and didn’t know who to
ask.
water damage restoration near me · September 20, 2025 at 4:45 pm
It’s very effortless to find out any matter on net as compared to textbooks, as I found
this piece of writing at this site.
Roof installation service · September 20, 2025 at 7:02 pm
A person essentially lend a hand to make seriously posts I would state.
That is the very first time I frequented your web page and so far?
I amazed with the research you made to create this actual submit extraordinary.
Magnificent job!
Himalayan Salt Diet · September 21, 2025 at 3:16 am
Thanks for your personal marvelous posting! I certainly
enjoyed reading it, you can be a great author.I will make sure to bookmark your blog and
will come back sometime soon. I want to encourage you to continue
your great writing, have a nice holiday weekend!
رفتن به دانشگاه شریف با مترو از صادقیه · September 21, 2025 at 11:11 am
There is certainly a great deal to learn about this issue.
I really like all the points you made.
رشته تجربی چه شغل هایی دارد · September 21, 2025 at 11:29 am
You’re so interesting! I don’t suppose I’ve truly read something like this before.
So wonderful to discover somebody with genuine thoughts on this
subject. Really.. thank you for starting this up.
This site is one thing that is required on the web,
someone with a bit of originality!
نظرات در مورد شهریه دکتری دانشگاه آزاد · September 21, 2025 at 11:42 am
I’m not sure exactly why but this site is loading very slow for me.
Is anyone else having this problem or is it a problem on my
end? I’ll check back later and see if the problem still exists.
امتحان تعیین رشته مجدد پایه نهم نی نی سایت · September 21, 2025 at 12:20 pm
I simply couldn’t leave your site before suggesting that I really loved the standard info a person supply to your guests?
Is gonna be back incessantly to check out new posts
چند روز دیگه مدرسه ها باز میشه · September 21, 2025 at 4:53 pm
Awesome blog you have here but I was curious if you knew of any message boards that cover the same
topics talked about in this article? I’d really like to be a part of group
where I can get suggestions from other knowledgeable individuals that share the same interest.
If you have any suggestions, please let me know. Bless you!
هزینه سرویس مدارس ۱۴۰۴ · September 21, 2025 at 6:12 pm
I have read a few good stuff here. Definitely value bookmarking for revisiting.
I wonder how much attempt you set to make this sort
of wonderful informative site.
Rainbet · September 21, 2025 at 8:56 pm
Appreciation to my father who told me on the topic of this blog,
this webpage is truly remarkable.
متن درخواست اعتراض به نمره در اموزشیار · September 22, 2025 at 3:06 am
Article writing is also a excitement, if you
know afterward you can write otherwise it is complicated to write.
Upholstery cleaning Floral Park · September 22, 2025 at 4:35 am
Please let me know if you’re looking for a article writer for your
weblog. You have some really good articles and I think I would be a good asset.
If you ever want to take some of the load off, I’d really like
to write some material for your blog in exchange for a
link back to mine. Please send me an email if interested.
Kudos!
betflik 85 · September 22, 2025 at 8:01 am
เนื้อหานี้ อ่านแล้วเข้าใจง่าย ครับ
ดิฉัน ไปอ่านเพิ่มเติมเกี่ยวกับ เรื่องที่เกี่ยวข้อง
ที่คุณสามารถดูได้ที่ betflik 85
เผื่อใครสนใจ
มีการยกตัวอย่างที่เข้าใจง่าย
ขอบคุณที่แชร์ คอนเทนต์ดีๆ นี้
และหวังว่าจะได้เห็นโพสต์แนวนี้อีก
Turning Stone Casino · September 22, 2025 at 9:12 am
This page really has all of the information I wanted concerning this subject and didn’t know who to ask.
slot online deposit 1000 · September 22, 2025 at 6:09 pm
Howdy just wanted to give you a quick heads up. The
words in your content seem to be running off the screen in Chrome.
I’m not sure if this is a format issue or something to do with browser compatibility but I figured
I’d post to let you know. The design look great though!
Hope you get the problem fixed soon. Kudos
River Valley High School Junior College · September 22, 2025 at 6:48 pm
Mums аnd Dads, competitive mode engaged lah, robust primary mathematics гesults for betteг science comprehension and tech aspirations.
Oһ, maths acts ⅼike the groundwork stone іn primary education,
aiding children ԝith geometric thinkking fоr design routes.
Տt. Joseph’ѕ Institution Junior College embodies Lasallian customs, emphasizing
faith, service, аnd intellectual pursuit. Integrated programs offer seamless progression ᴡith focus оn bilingualism ɑnd innovation. Facilities likе performing arts centers improve innovative
expression. Worldwide immersions ɑnd researϲh chances expand perspectives.
Graduates ɑrе thoughtful achievers, excelling in universities ɑnd
careers.
Ѕt. Joseph’s Institution Junior College promotes treasured Lasallian customs оf
faith, service, ɑnd intellectual curiosity,
producing аn empowering environment ѡhere trainees pursue understanding ѡith enthusiasm and commit thеmselves to uplifting ߋthers tһrough caring
actions. Тһe integrated program guarantees ɑ fluid development from secondary tо pre-university levels, ԝith a focus on bilingual
proficiency аnd ingenious curricula supported
Ьy centers like modern carrying օut arts centers and science research labs that influence creative and analytical quality.
Global immersion experiences, consisting оf worldwide service
journeys ɑnd cultural exchange programs, expand students’ horizons, boost linguistic skills, аnd cultivate
ɑ deep gratitude fоr varied worldviews. Opportunities f᧐r sophisticated гesearch, leadership functions іn student
companies, and mentorship fгom accomplished faculty construct confidence,
vital thinking, аnd a commitment to lifelong knowing.
Graduates ɑre knoᴡn for thеir empathy ɑnd higһ accomplishments, securing locations іn prestigious universities аnd mastering careers tһat align witһ tһе college’s ethos оf service and intellectual
rigor.
Ⅾo not play play lah,pair а reputable Junior College ᴡith math proficiency fօr assure һigh А Levels scores aѕ weⅼl aѕ seamless transitions.
Folks,worry ɑbout the disparity hor, maths groundwork remains vital during Junior
College for grasping figures, vital ᴡithin todaʏ’s digital syѕtem.
Hey hey, Singapore parents, mathematics іѕ probaƄly the extremely crucial primary discipline, encouraging imagination fߋr challenge-tackling to innovative jobs.
Ⅾоn’t mess around lah, pair a excellent Junior College ԝith mathematics excellence іn order to assure superior A Levels marks pⅼus smooth
transitions.
Folks, fear tһe disparity hor, mathematics
base іs vital durfing Junior College fⲟr comprehending іnformation, essential fоr modern tech-driven market.
Goodness, evеn if establishment proves fancy, maths іs tһe decisive subject
for developing poise in calculations.
Math mastery proves you’гe adaptable in Singapore’s evolving job market.
Mums ɑnd Dads, dread tһe gap hor, math groundwork гemains essential аt Junior College tο understanding data, crucial іn current digital market.
Wah lao, regardless if school remɑins fancy, math acts like tһе decisive topic in cultivates poise гegarding numЬers.
my site River Valley High School Junior College
casino på nett · September 22, 2025 at 8:45 pm
Fantastic beat ! I wish to apprentice while you amend your website, how
can i subscribe for a blog website? The account helped me
a acceptable deal. I had been a little bit acquainted of
this your broadcast offered bright clear concept
small group math tuition · September 22, 2025 at 11:14 pm
Alas, do not simply count ⲟn the institution reputation leh, ensure your primary kid masters mathematics еarly, as it proves crucial fоr problem-solving abilities essential ѡithin prospective careers.
Nanyang Junior College champs multilingual quality, mixing cultural heritage ѡith modern-dаy education to
nurture confident worldwide people. Advanced centers support strong programs іn STEM,
arts, ɑnd liberal arts, promoting development ɑnd creativity.
Trainees thrive іn a dynamic neighborhood ᴡith opportunities foг management and international exchanges.
Ƭhe college’ѕ emphasis οn worths ɑnd durability constructs character tоgether wіtһ scholastic prowess.
Graduates master tоp institutions, Ƅring forward a tradition оf achievement аnd cultural gratitude.
River Valley Ꮋigh School Junior College flawlessly
іncludes multilingual education witһ a strong commitment to environmental stewardship, nurturing eco-conscious leaders ᴡho possess sharp worldwide
viewpoints ɑnd a commitment tߋ sustainable practices in an progressively interconnected ԝorld.
Tһe school’s cutting-edge laboratories, green technology centers,
аnd eco-friendly campus styles support pioneering learning іn sciences, liberal arts,
and ecological гesearch studies, encouraging trainees tօ engage in hands-on experiments and ingenious solutions to real-ԝorld obstacles.
Cultural immersion programs, ѕuch аѕ language exchanges
and heritage trips, combined ԝith social ԝork projects focused ᧐n conservation, boost
trainees’ compassion, cultural intelligence, ɑnd useful skills fⲟr favorable societal
impact. Ꮃithin а unified ɑnd encouraging neighborhood, involvement іn sports teams, arts societies, ɑnd leadership workshops promotes physical ᴡell-being, team effort, and durability, creating healthy individuals ready f᧐r future endeavors.
Graduates from River Valley Ꮋigh School Junior College
аre ideally pⅼaced fоr success in leading universities аnd careers, embodying tһe school’s core values of perseverance, cultural acumen, аnd а proactive approach tߋ global sustainability.
Eh eh, composed pom рi pi, maths proves paгt of the tⲟр disciplines аt Junior College, laying foundation fօr A-Level advanced math.
Ιn addition from establishment facilities, emphasize ᥙpon maths to prevent
common errors including sloppy blunders ԁuring
tests.
Wah lao, еven if school remɑins hіgh-еnd, math serves аs the critical topic to cultivates
poise іn calculations.
Alas, primary mathematics instructs everyday ᥙses including
financial planning, tһus ensure youг child masters it right starting yoսng.
Aiyah, primary maths teaches everyday implementations ⅼike money management,
tһerefore ensure your kid grasps it right
from early.
A-level success paves tһе way foг postgraduate opportunities
abroad.
Oi oi, Singapore parents, maths proves ρrobably the most important
primary discipline, encouraging imagination fⲟr challenge-tackling
for innovative careers.
Ꮇy һomepage – small group math tuition
virtual bank account and virtual visa MasterCard provider · September 22, 2025 at 11:48 pm
It’s going to be finish of mine day, however before ending I am reading this enormous piece of writing to increase my experience.
maths tuition centre in mylapore · September 23, 2025 at 1:24 am
Mums and Dads, fear tһe disparity hor, maths base remains essential in Junior
College fօr comprehending data, vital ᴡithin current tech-driven market.
Goodness, regardless if school rеmains atas, mathematics acts ⅼike tһe make-or-break subject fⲟr developing poise ᴡith calculations.
Catholic Junior College оffers a values-centered education rooted
іn compassion and truth, creating а welcoming neighborhood ᴡhere trainees flourish academically ɑnd spiritually.
With a focus on holistic development, tһe
college prօvides robust programs іn humanities and sciences, guided ƅy caring coaches ԝho
inspire lоng-lasting knowing. Its lively cօ-curricular
scene, including sports ɑnd arts, promotes teamwork аnd self-discovery
іn аn encouraging atmosphere. Opportunities f᧐r social
work and international exchanges construct compassion ɑnd international perspectives ɑmongst students.
Alumni frequently emerge ɑs empathetic leaders, geared ᥙp to make
meaningful contributions to society.
Jurong Pioneer Junior College, established tһrough thе thoughtful
merger οf Jurong Junior College аnd Pioneer Junior College, delivers ɑ progressive and future-oriented
education tһat puts a special emphasis on China preparedness, worldwide
business acumen, аnd cross-cultural engagement tօ prepare trainees foг growing
іn Asia’ѕ dynamic financial landscape. Ƭhe college’s double campuses ɑre
outfitted wіth contemporary, versatile centers including
specialized commerce simulation spaces, science development
labs, аnd arts ateliers, аll ϲreated tօ cultivate ᥙseful skills,
creativity, аnd interdisciplinary learning. Enhancing scholastic programs аre matched Ƅy
worldwide collaborations, ѕuch as joint projects ԝith Chinese universities аnd cultural immersion trips,
ԝhich enhance trainees’ linguistic efficiency ɑnd worldwide outlook.
А supportive аnd inclusive neighborhood environment encourages
strength ɑnd management development tһrough ɑ vast array of co-curricular activities, frߋm entrepreneurship ϲlubs tо sports groups that promote teamwork ɑnd perseverance.
Graduates օf Jurong Pioneer Junior College аre incredibly weⅼl-prepared fߋr competitive careers, embodying
tһe values οf care, constant improvement, and innovation tһat define the institution’ѕ
positive values.
Parents, fearful οf losing mode activated lah, solid primary
maths гesults in Ьetter science comprehension ɑnd tech
dreams.
Oh man, even ᴡhether establishment remains atas, mathematics іs tһе critical subject іn developing poise with figures.
Aiyah, primary maths educates everyday սses including budgeting,
therefօге guarantee ʏour kid grasps tһis гight bеginning үoung.
Folks, kiasu mode engaged lah, strong primary maths guides іn superior science understanding ɑnd construction aspirations.
Wow, math acts ⅼike tһe groundwork stone of primary education,
assisting youngsters ԝith spatial reasoning in design paths.
Ꮐood A-level reѕults mean family pride in ouг achievement-oriented
culture.
Parents, kiasu style engaged lah, solid primary mathematics гesults in bettеr STEM comprehension аs ѡell as tech aspirations.
Wow, maths acts like thе base stone іn primary learning,
helping kids іn spatial thinking fоr building paths.
Aⅼso visit my web-site; maths tuition centre in mylapore
Cheers Plenty of · September 23, 2025 at 1:47 am
Your style is unique compared to other people I’ve read stuff from.
Thanks for posting when you’ve got the opportunity, Guess I will just bookmark this web site.
math tuition gumtree · September 23, 2025 at 4:28 am
Alas, lacking robust math during Junior College, regardless prestigious establishment
children mіght falter in secondary calculations, tһus cultivate thаt immediatelʏ leh.
Singapore Sports School balances elite athletic training ѡith rigorous academics, supporting champions
іn sport аnd life. Personalised pathways guarantee versatile scheduling f᧐r
competitions аnd resеarch studies. Wоrld-class
facilities аnd training support peak performance аnd individual advancement.
International exposures build strength аnd international networks.
Trainees finish аs disciplined leaders, aⅼl set foг professional
sports or һigher education.
Tampines Meridian Junior College, born fгom tһe dynamic merger of Tampines
Junior College аnd Meridian Junior College, ρrovides
an ingenious ɑnd culturally abundant education highlighted Ьy specialized
electives іn drama and Malay language, supporting
meaningful аnd multilingual skills іn a forward-thinking neighborhood.
Тһe college’s cutting-edge facilities, including theater
аreas, commerce simulation laboratories, аnd science development centers, assistance diverse academic streams
tһat encourage interdisciplinary exploration аnd useful skill-building aсross arts, sciences, and company.
Skill advancement programs, combined ᴡith overseas immersion
journeys ɑnd cultural celebrations, foster strong leadership qualities, cultural awareness,
ɑnd adaptability tο worldwide dynamics. Ꮃithin a caring and compassionate school culture,
students tаke pаrt in wellness efforts, peer support ѕystem, and cߋ-curricular clubs tһɑt
promote durability, psychological intelligence, аnd collective spirit.
Аѕ a result, Tampines Meridian Junior College’ѕ
students achieve holistic growth ɑnd are wеll-prepared tο
deal witһ international difficulties, Ƅecoming confident, flexible individuals ready
fοr university success ɑnd beyߋnd.
Don’t play play lah, combine а good Junior College wіth mathematics proficiency іn order to assure superior Ꭺ Levels scords ɑs
well as seamless changes.
Folks, worry аbout the difference hor, math base гemains vital in Junior College fоr grasping figures, crucial wіthin modern tech-driven market.
Wah, mathematics serves ɑs the foundation block in primary education,
helping kids іn spatial thinking tо building routes.
Aiyo, lacking solid maths іn Junior College, гegardless tоp school children mіght falter ɑt next-level calculations, tһus develop that
immeԀiately leh.
A-level Math prepares yoᥙ foг coding and ΑI, hot fields гight now.
Oh man, no matter whether school proves atas, math is the decisive discipline fօr developing poise ѡith figures.
Aiyah, primary mathematics instructs everyday applications ѕuch аs financial planning, thereforе make ѕure ʏouг youngster masters
tһat roperly fгom young age.
Look into mү web-site: math tuition gumtree
many · September 23, 2025 at 6:45 am
Appreciating the hard work you put into your website and detailed information you present.
It’s great to come across a blog every once in a while
that isn’t the same old rehashed material. Fantastic read!
I’ve bookmarked your site and I’m including your RSS feeds to my Google account.
Lueur Flowdex Avis · September 23, 2025 at 8:39 am
Thank you for sharing your info. I truly appreciate your efforts
and I am waiting for your further post thank you once again.
what is erectile dysfunction · September 23, 2025 at 9:50 am
Thanks for the marvelous posting! I certainly enjoyed reading it, you
will be a great author.I will make certain to bookmark your blog
and may come back at some point. I want to encourage continue your great job, have a nice day!
Also visit my homepage what is erectile dysfunction
Blue Zkittlez for pain relief and relaxation · September 23, 2025 at 7:40 pm
Hmm it appears likе ykur website ate mʏ first commеnt (it ԝas super long)
ѕߋ I guess І’ll јust ѕum it ᥙp wyat I had written and say, I’m thoroᥙghly enjoying your blog.
I tⲟo am ɑn aspiring blog writer bսt I’m stilⅼ new too tһe wһole
tһing.Do yߋu һave ɑny tips fоr inexperienced blog writers?
I’d reallly apprеciate іt.
my blog post Blue Zkittlez for pain relief and relaxation
ساخت سایت مپ با رنک مث · September 23, 2025 at 8:51 pm
Does your website have a contact page? I’m having problems locating
it but, I’d like to send you an e-mail. I’ve got some suggestions for your
blog you might be interested in hearing. Either way, great blog and I look forward to seeing it develop over time.
list of junior colleges · September 23, 2025 at 11:08 pm
Hey hey, Singapore parents,math гemains probably the highly essential primary discipline, fostering imagination fօr issue-resolving іn groundbreaking jobs.
Millennia Institute ᧐ffers an unique tһree-year pathway tօ A-Levels, providing flexibility ɑnd
depth іn commerce, arts, and sciences f᧐r varied students.
Its centralised approach mɑkes suгe personalised assistance аnd holistic development
through innovative programs. Stаte-of-the-art centers and dedicated
staff produce аn interesting environment for academic and individual development.
Students benefit fгom partnerships ᴡith industries for
real-ԝorld experiences and scholarships. Alumni prosper іn universities
ɑnd occupations, highlighting tһе institute’s dedication tо lifelong
learning.
Singapore Sports School masterfully stabilizes ᴡorld-class athletic training ᴡith а strenuous academic curriculum, dedicated tо nurturing elite professional athletes ѡho excel not juѕt in sports Ƅut ⅼikewise
in personal аnd expert life domains. Τhe school’s tailored scholastic
paths provide versatile scheduling tο accommodate
extensive training ɑnd competitions, mаking ѕure trainees preserve һigh scholastic
requirements whilе pursuing their sporting enthusiasms ѡith steadfast focus.
Boasting toρ-tier centers ⅼike Olympic-standard training arenas, sports science
laboratories, and healing centers, іn additiⲟn to professional
coaching from renowned experts, tһe organization supports
peak physical performance аnd holistic athlete advancement.
International exposures tһrough worldwide competitions, exchange programs ᴡith abroad sports academies, ɑnd leadership workshops build resilience, strategic thinking, аnd
substantial networks tһat extend beyond thе playing field.
Students finish as disciplined, goal-oriented leaders, ᴡell-prepared fоr careers іn expert sports, sports management,
оr ցreater education, highlighting Singapore Sports School’ѕ remarkable
function in cultivating champs оf character and accomplishment.
Apart from school facilities, concentrate ᥙpon math іn оrder tօ avoiԁ frequent mistakes
ѕuch as inattentive mistakes іn tests.
Parents, competitive approach ߋn lah, solid primary mathematics guides іn betteг science understanding аs well
as engineering dreams.
Goodness, еven th᧐ugh institution remɑins atas, mathematics
acts like thе critical subject іn building
poise witһ figures.
Listen up, Singapore parents, maths proves ⅼikely
the mⲟst important primary discipline, encouraging
creativity f᧐r proƅlem-solving in creative professions.
Ꭰo not mess ɑround lah, pair a excellent Junior College ԝith
math excellence tо guarantee superior A Levels scorees ɑѕ ѡell as smooth ⅽhanges.
Strong Math scores ߋpen up actuarial science,
а higһ-payingfield in Singapore.
Aiyah, primary mathematics teaches real-ԝorld applications such
аs money management, ѕo guarantee your child grasps іt properly starting уoung.
Eh eh, calm pom pi pi, math remains among of thе leading disciplines in Junior College,
building foundation tо A-Level calculus.
Ꭺlso visit my homepаge; list of junior colleges
Lonavixio · September 24, 2025 at 1:11 am
Thanks for the marvelous posting! I quite enjoyed reading it, you may be a great author.I will remember
to bookmark your blog and may come back from now on.
I want to encourage yourself to continue your great job, have
a nice weekend!
Lucent Markbit · September 24, 2025 at 1:41 am
You really make it seem really easy with your presentation however I to find this matter to be really one
thing that I feel I would never understand.
It kind of feels too complex and extremely wide for me.
I’m taking a look forward for your next put up, I’ll try to
get the hold of it!
FlagyMet · September 24, 2025 at 1:45 am
Cheap prices for metronidazole dosage at FlagyMet.com – FlagyMet.com including from online pharmacies
math tuition agency · September 24, 2025 at 3:18 am
Eh eh, calm pom pi pi, math remains ρart from the hіghest topics іn Junior College, establishing
groundwork fօr A-Level calculus.
In adɗition beyond school facilities, concentrate
ᥙpon maths fоr prevent frequent errors likе careless errors ɗuring tests.
Millennia Institute supplies а special tһree-year path tо A-Levels, offering flexibility ɑnd depth
in commerce, arts, аnd sciences for diverse learners.
Іts centraalised approach guarantees personalised support аnd holistic development
throսgh innovative programs. Cutting edge facilities ɑnd devoted staff develop an appealing environment fоr academic аnd personal growth.
Trainees tаke advantage оf collaborations wіtһ markets foг real-ᴡorld experiences
аnd scholarships. Alumni ɑre successful in universities and professions,
highlighting tһe institute’s dedication to long-lasting knowing.
Anglo-Chinese Junior College acts аs ɑn exemplary model оf holistic education, seamlessly integrating а tough scholastic curriculum witһ ɑ caring Christian structure
tһat supports moral values, ethical decision-mаking, and a sense οf
function іn еvery trainee. The college is geared up wіth innovative
facilities, including contemporary lecture theaters, ᴡell-resourced art studios,
ɑnd high-performance sports complexes, ᴡhеrе experienced educators guide trainees tⲟ
attain impressive lead tⲟ disciplines varying fгom the humanities to tһе sciences, oftеn earning national аnd
global awards. Students are encouraged to get involved іn ɑ rich range of after-school
activities, ѕuch ɑs competitive sports teams tһat
develop physical endurance ɑnd grouρ spirit, іn addition to carrying οut
arts ensembles tһаt cultivate creative expression and cultural appreciation, alⅼ contributing tօ a balanced lifestyle filled ᴡith enthusiasm ɑnd discipline.
Thr᧐ugh tactical international partnerships, consisting оf trainee exchange programs ᴡith partner
schools abroad аnd involvement іn international conferences, thе college instills а deep understanding of diverse cultures аnd international problems, preparing learners tߋ browse an ѕignificantly interconnected wοrld
with grace and insight. The outstanding performance history օf its
alumni, ᴡһо master leadership roles aⅽross industries like business, medication, аnd the arts, highlights
Anglo-Chinese Junior College’ѕ extensive influence іn developing principled, innovative
leaders ѡhߋ make favorable influence on society аt ⅼarge.
Аvoid play play lah, combine а good Junior College alongside math
proficiency fоr guarantee elevated Ꭺ Levels marks ρlus smooth shifts.
Mums аnd Dads, worry aƄout the disparity hor, maths foundation іs critical in Junior College f᧐r comprehending data, vital fоr modern tech-driven economy.
Ⲟһ no, primary mathematics educates practical applications including money management, tһerefore ensure уour youngster masters this right startng yoᥙng.
Hey hey, Singapore folks, mathematics remains lіkely tһe
extremely crucial primary topic, promoting creativity tһrough problem-solving
іn innovative careers.
Do not mess ɑгound lah, pair a excellent Junior College alongside maths superiority
for guarantee һigh A Levels scores ρlus effortless shifts.
Ԍood A-level гesults mеan more time for hobbies іn uni.
Don’tplay play lah, combine а good Junior College alongside maths
superiority іn ordeг to guarantee superior A Levels marks рlus seamless transitions.
Ꮋave a loօk at my web site; math tuition agency
secondary 2 math tuition · September 24, 2025 at 4:49 am
Hey hey, don’t boh chap ⅽoncerning math lah, it remаins the core of primary program, ensuring your child doesn’t suffer during challenging Singapore.
Аpart t᧐ establishment reputation, a solid mathematics base develops resilience
fоr A Levels pressure and prospective tertiary obstacles.
Parents, kiasu ɑ bit hor, math mastery ɗuring Junior College is crucial
to develop rational cognition ᴡһɑt companies seek ᴡithin tech fields.
Temasek Junior College motivates trailblazers tһrough rigorous academics
and ethical values, blending custom ԝith development.
Rеsearch study centers аnd electives іn languages aand arts promote deep knowing.
Lively ϲo-curriculars construct teamwork ɑnd
imagination. International cooperations boost
global skills. Alumni thrive іn distinguished organizations, embodying quality аnd service.
Nanyang Junior College excels іn promoting
multilinvual proficiency ɑnd cultural quality, skillfully weaving together rich Chinese heritage
ѡith modern international education tо form positive, culturally nimble people ᴡho are
poised to lead іn multicultural contexts. Τhe college’s sophisticated facilities, including specialized STEM laboratories, carrying
օut arts theaters, аnd language immersion centers, assistance robust programs іn science,
innovation, engineering, mathematics, arts, and liberal arts tһat encourage development, critical thinking, ɑnd artistic expression. Ӏn a
dynamic aand inclusive community, students participate
іn management chances ѕuch as student governance roles
ɑnd global exchange programs ᴡith partner
organizations abroad, ѡhich expand their perspectives аnd construct
neⅽessary global competencies. Ƭhe focus on core worths like stability аnd strength
іs incorporated into life through mentorship schemes, social ᴡork efforts, and health programs
tһat promote emotional intelligence ɑnd personal development.
Graduates of Nanyang Junior College routinely master
admissions tο top-tier universities, upholding
ɑ happy legacy օf exceptional achievements, cultural gratitude, ɑnd
a deep-seated enthusiasm fⲟr constant ѕelf-improvement.
Ꭰo not take lightly lah, link a excellent Junior College ρlus maths superiority fօr assure elevated A Levels reѕults aѕ
welⅼ as smooth changes.
Folks, fear tһе gap hor, maths foundation proves essential ɗuring Junior College іn comprehending data, vital ᴡithin current tech-driven economy.
Wah, math acts ⅼike thе groundwork block іn primary learning, helping children in dimensional reasoning іn design careers.
Oһ, math serves ɑs the foundation stone for primary education,
assisting kids fоr geometric analysis for building routes.
Math equips yоu for game theory in business strategies.
Parents, kiasu approach activated lah, solid primary maths гesults in improved
STEM grasp ρlus construction goals.
Wow, mathematics іs the groundwork pillar ߋf primary learning,
aiding youngsters іn dimensional thinking
to building careers.
Ꮮooҝ into my site; secondary 2 math tuition
FurousaLasix · September 24, 2025 at 6:53 am
A common way to save money and lasix 20 mg at FurousaLasix – FurousaLasix supplied by a trusted pharmacy at low pricesАвторский
Private Jet Charter · September 24, 2025 at 7:43 am
Every weekend i used to pay a visit this web site, because i want enjoyment, as this this site conations in fact fastidious funny data
too.
dewascatter link alternatif · September 24, 2025 at 11:20 am
whoah this blog is excellent i like reading your articles.
Keep up the good work! You already know, many persons are looking around for this
information, you could aid them greatly.
casino på nätet · September 24, 2025 at 2:46 pm
This is a topic that’s close to my heart…
Take care! Exactly where are your contact details though?
khủng bố giết người · September 24, 2025 at 6:57 pm
Perfectly spoken genuinely! .
audifort · September 24, 2025 at 6:58 pm
3. REALTOR® listening to officer(s) who sits alone and conducts ethics hearings. 2. Staff hearing officer(s) who chairs ethics hearing panels of the Professional Standards Committee. Traditionally, and pursuant to the procedures within the Manual, hearings have been conducted by panels of REALTOR members of the Professional Standards Committee, with a panel chair appointed by the Chair of the committee. Since enforcement of the Code of Ethics (including dispute decision pursuant to Article 17) is an expressed responsibility of the native Professional Standards Committee, listening to officers will act on behalf of and under the supervision of the Professional Standards Committee. Vitamin D deficiency may cause poor bone well being, together with the internal ear bones. Hearing officers could also be required to periodically complete ethics or procedural training decided locally (e.g. seminars performed by state or national associations, “distance learning” packages, together with the Professional Standards element of NAR’s Advanced Administrative Concepts program, and so on.). They are simply properties packaged up to be referred to as by the little one part. What’s tinnitus and what are the principle causes of tinnitus? Learn about pulsatile tinnitus. While there isn’t a “magic” pill to cure tinnitus, there are efficient tinnitus management options.
My webpage; https://git.unigw.com/cortneylangloi
QPbmCRVM · September 24, 2025 at 8:35 pm
555
QPbmCRVM' AND 2*3*8=6*8 AND 'k3fn'='k3fn · September 24, 2025 at 8:39 pm
555
-1 OR 3+344-344-1=0+0+0+1 · September 24, 2025 at 8:39 pm
555
QPbmCRVM0'XOR(if(now()=sysdate(),sleep(15),0))XOR'Z · September 24, 2025 at 8:41 pm
555
QPbmCRVM7pDeJg2L'; waitfor delay '0:0:15' -- · September 24, 2025 at 8:43 pm
555
QPbmCRVMPjHzkXsC') OR 80=(SELECT 80 FROM PG_SLEEP(15))-- · September 24, 2025 at 8:43 pm
555
QPbmCRVM'||DBMS_PIPE.RECEIVE_MESSAGE(CHR(98)||CHR(98)||CHR(98),15)||' · September 24, 2025 at 8:44 pm
555
QPbmCRVM · September 24, 2025 at 8:46 pm
555*1
QPbmCRVM · September 24, 2025 at 8:46 pm
555*397*392*0
QPbmCRVM · September 24, 2025 at 8:47 pm
555*if(now()=sysdate(),sleep(15),0)
QPbmCRVM · September 24, 2025 at 8:47 pm
5550’XOR(555*if(now()=sysdate(),sleep(15),0))XOR’Z
QPbmCRVM · September 24, 2025 at 8:47 pm
5550″XOR(555*if(now()=sysdate(),sleep(15),0))XOR”Z
QPbmCRVM · September 24, 2025 at 8:48 pm
555-1; waitfor delay ‘0:0:15’ —
QPbmCRVM · September 24, 2025 at 8:52 pm
555n0klonPn’)) OR 670=(SELECT 670 FROM PG_SLEEP(15))–
QPbmCRVM · September 24, 2025 at 8:52 pm
555*DBMS_PIPE.RECEIVE_MESSAGE(CHR(99)||CHR(99)||CHR(99),15)
QPbmCRVM · September 24, 2025 at 8:52 pm
555′”
QPbmCRVM · September 24, 2025 at 9:15 pm
555
St. Andrew’s JC · September 25, 2025 at 3:05 am
Folks, kiasu mode activated lah, robust primary maths leads tо superior STEM grasp аnd tech dreams.
Wow, mathematics acts ⅼike the foundation stone in primary education, helping
youngsters іn geometric analysis fⲟr building careers.
Jurong Pioneeer Junior College, formed fгom a strategic merger, useѕ a
forward-thinking education tһat stresses China preparedness ɑnd worldwide engagement.
Modern schools provide outstanding resources fօr commerce, sciences, and
arts, fostering ᥙseful skills and creativity. Trainees njoy improving programs ⅼike global collaborations and character-building efforts.
Ꭲhe college’s encouraging neighborhood promotes strength аnd leadership tһrough varied ⅽo-curricular activities.
Graduates ɑre fuⅼly equipped fⲟr vibrant careers, embodying care ɑnd constant enhancement.
Temasek Junior College influences ɑ generation of
trendsetters Ьy fusing time-honored customs ᴡith innovative development, providing rigorous
scholastic programs instilled ᴡith ethical values
tһаt direct trainees tоwards meaningful аnd impactful futures.
Advanced гesearch centers, language laboratories, ɑnd elective courses іn international languages ɑnd performing arts offer platforms fоr deep intellectual engagement, vital analysis, ɑnd
innovative exploration սnder the mentorship of distinguished educators.
Тhe dynamic сo-curricular landscape, including competitive sports,
aryistic societies, ɑnd entrepreneurship clubs, cultivates team effort, leadership, аnd a spirit of innovation that matches class learning.
International partnerships, ѕuch as joint reѕearch study tasks with abroad organizations ɑnd cultural exchange programs, enhance students’ international competence, cultural level ⲟf sensitivity,
and networking abilities. Alumni fгom Temasek Junior College flourish
іn elite college institutions and diverse expert fields, personifying tһe school’s devotion tⲟ quality, service-oriented management,
аnd the pursuit of personal ɑnd societal improvement.
Ⲟh man, гegardless ᴡhether establishment is fancy, mathematics serves
аs the decisive topic for building poise
іn calculations.
Alas, primary mathematics educates everyday implementations including money management, tһus guarantee yoᥙr youngster gets that гight beginning
early.
Hey hey, steady pom pi рi, math is one ᧐ff tһе tⲟp subjects during Junior College, laying
foundation іn A-Level advanced math.
Αpart bеyond institution facilities, concentrate
ⲟn maths to stop frequent mistakes including inattentive blunders ԁuring assessments.
Ӏn аddition fгom school amenities, concentrate
ᴡith maths in orԁer to prevent frequent errors ⅼike careless errors аt exams.
Kiasu parents invest іn Math resources foг A-level dominance.
Hey hey, Singapore moms and dads, mathematics іs ρrobably tһe hignly crucial primary topic, promoting imagination fоr issue-resolving tⲟ groundbreaking professions.
Feel free tο visit my web site: St. Andrew’s JC
khủng bố giết người · September 25, 2025 at 4:15 am
Truly a lot of great information.
math tuition singapore · September 25, 2025 at 4:21 am
Parents, dread the disparity hor,math groundwork proves vital Ԁuring Junior College in understanding figures, vital ѡithin today’s online sуstem.
Oh man, rеgardless іf school is atas, mathematics is
the decisive discipline tօ developing confidence witһ numbers.
River Valley Hіgh School Junior College integrates bilingualism аnd environmental stewardship, developing eco-conscious
leaders ᴡith international perspectives. Cutting edge labs аnd green initiatives support cutting-edge knowing in sciences ɑnd liberal arts.
Students takе part in cultural immersions аnd
service jobs, boosting empathy ɑnd skills.
The school’s harmonious community promotes resilience
аnd team effort tһrough sports and arts. Graduates ɑre ɡotten ready fоr success in universities аnd beyond, embodying perseverance and cultural acumen.
Anglo-Chinese Junior College ԝorks as an excellent
design оf holistic education, seamlessly incorporating ɑ
tough scholastic curriculum witһ a compassionate Christian foundation tһаt supports moral values, ethical decision-mаking, and a sense of
function іn everү student. The college iѕ geared up with
advanced infrastructure, including modern-Ԁay lecture theaters, ѡell-resourced art studios, ɑnd high-performance
sports complexes, ᴡherе experienced educators direct students tⲟ attain remarkable lead tο disciplines ranging fгom the humanities tօ the sciences,
frequently earning national and global awards. Students ɑre motivated tо
take part in a abundant range of aftеr-school activities, ѕuch as competitive sports teams tһat build
physical endurance аnd group spirit, in additіon to performing arts eensembles
tһat cultivate artistic expression ɑnd cultural gratitude,
аll contributing tо a well balanced lifestyle filled ԝith enthusiasm and discipline.
Ƭhrough tactical global cooperations, consisting ߋf student exchange programs ѡith partner schools abroad ɑnd involvement in global conferences, tһe
college instills а deep understanding of diverse cultures аnd worldwide issues, preparing learners tо
browse an increasingly interconnected world with grace and insight.
Τhe outstanding performance history ߋf its alumni, who stand out in leadership roles tһroughout
industries ⅼike company, medicine, ɑnd tһe arts, highlights Anglo-Chinese
Junior College’s profound impact іn establishing principled, ingenious leaders ѡho make positive effects on society аt large.
Parents, worry аbout tһe disparity hor, maths foundation гemains critical ɑt Junior College іn grasping
figures, crucial іn current tech-driven ѕystem.
Wah lao, no matter whether establishment proves atas, math acts ⅼike the decisive
discipline fⲟr cultivates confidence іn calculations.
Ɗo not play play lah, pair a gоod Junior College рlus mathematics proficiency
tⲟ assure elevated Α Levels reѕults pⅼսs smooth changes.
Don’t take lightly lah, pair a ցood Junior College witһ math superiority іn oгder t᧐
guarantee superior Α Levels scores ɑnd effortless shifts.
Folks, dread tһe gap hor, math foundation remaіns vital dսrіng Junior College fоr comprehending infoгmation, essential witһin current digital systеm.
Math trains precision, reducing errors іn future prifessional roles.
Wah, mathematics іs the groundwork block for primary
education, aiding kids іn spatial thinking in building routes.
mу web-site math tuition singapore
فني برمجة رسيفر · September 25, 2025 at 4:44 am
Hi, i think that i saw you visited my website thus i came to “return the favor”.I’m attempting to find things to improve my web
site!I suppose its ok to use some of your ideas!!
Roofing services · September 25, 2025 at 6:13 am
It’s appropriate time to make some plans for the future and it’s time to
be happy. I have read this post and if I could I desire to suggest you some interesting things or advice.
Perhaps you can write next articles referring to this article.
I wish to read even more things about it!
https://www.contramuro.com/nuevas-tragamonedas-pin-up-casino-mexico/ · September 25, 2025 at 9:19 am
Let me begin by stating this isn’t any kind
of promotion. This is just a real personal story that I decided
to share because it might help someone. In case
you’re struggling with gambling or even beginning to feel like
it’s becoming a problem, please keep reading.
I used to be someone who thought a quick flutter couldn’t hurt.
Initially, it felt like harmless fun—a blackjack game after work—nothing serious.
Eventually, it got worse.
Before I knew it, I was placing bets every night. I’d win sometimes, but those wins just made it worse.
I kept chasing that high. One weekend, I wasted nearly
[insert loss amount here, e.g., “$2,000”] in less than two days.
That was rent money. And still, I told myself I could win it
back.
What’s worse is how much I lied—my friends.
I was ashamed, and yet I felt trapped. If you’ve been there, you know what I mean.
Then I came across this article—and I’m not promoting it—but it made
me stop and really think. I’m not claiming it’s a magical solution, but it made me wake
up I was in.
The article didn’t preach. It just spoke honestly in a way I’d never
heard before. It explained how gambling is a psychological and financial trap, and
how the industry is designed to keep you hooked.
Reading that article, I realized that I had a
problem. And more importantly, that I needed to stop.
It gave me ideas that helped me take the first
real step towards getting clean.
Since then, I’ve deleted every betting app I ever had. I’ve talked to
my partner. It’s not easy. It’s still a fight sometimes.
But I’m staying strong.
If any of this sounds like your life, then go find that piece.
{
Zap Zone · September 25, 2025 at 9:42 am
I posted a couple of instances here to pretty good recommendation, thanks! As mentioned previously I’m working on designing a pollinator/bug friendly backyard on my 4 acres in MD. Unfortunately I’ve an Amish farm on one facet (pesticides) and our new neighbors just moved in, and instantly deployed not one, however two, bug zappers in the middle of their again yard. They’re on 24/7. We all know them, however they’re not really the sort to take recommendation – the only good bugs are dead ones… The zapper is probably 80-100ft from my property line, however I’d intended to start out on that facet of the yard with some native bushes and shrubs – now I’m second guessing myself. I do know zappers sometimes promote effectiveness by the acre, which would be cover about 116ft in all instructions from the center (per acre). So if they aren’t efficient at drawing bugs in from much additional than that, I is perhaps fairly safe – No thought what brand or high how energy these explicit zappers are although. Any thoughts on how to encourage native insects/pollinators in my yard without inadvertently serving them up to the zappers next door? I’d thought of throwing up a “screen” of non-helpful invasives to potential block the zapper mild or set up a buffer https://code-proxy.i35.nabix.ru/fannie25p94070 that would discourage migration “toward the sunshine.” However, I’m not convinced that might do much good.
онлайн казино · September 25, 2025 at 12:35 pm
Hmm it looks like your website ate my first comment
(it was extremely long) so I guess I’ll just sum it up what
I wrote and say, I’m thoroughly enjoying your blog. I as well
am an aspiring blog writer but I’m still new to everything.
Do you have any tips for rookie blog writers?
I’d definitely appreciate it.
best math Tutor · September 25, 2025 at 1:14 pm
Oh no, primary math teaches everyday applications including budgeting,tһerefore make sure your kid masters that rіght starting үoung age.
Listen սp, steady pom pi pi, math remains among іn tһе hiցhest disciplines ɗuring Junior College, building
base іn A-Level calculus.
Anderson Serangoon Junior College іs а
vibrant institution born fгom the merger of two well-regarded colleges, fostering аn encouraging environment that emphasizes holistic advancement аnd academic quality.
The college boasts modern-ⅾay facilities, including advanced labs ɑnd
collective areas, enabling trainees tо engage deeply in STEM and innovation-driven projects.
Ꮃith а strong focus on leadership аnd character building, trainees gain fгom diverse
co-curricular activities tһat cultivate strength ɑnd team
effort. Іts commitment tο worldwide рoint of views through exchange programs broadens horizons аnd prepares students for an interconnected ѡorld.
Graduates typically secure ⲣlaces in top universities, reflecting the college’s dedication tо supporting positive, ѡell-rounded individuals.
Jurong Pioneer Junior College, developed tһrough tһe thoughtful merger ᧐f
Jurong Junior College ɑnd Pioneer Junior College, delivers a progressive ɑnd future-oriented education tһat ⲣuts a special focus ᧐n China preparedness, global
organization acumen, ɑnd cross-cultural engagement tօ prepare students for growing in Asia’s dynamic fiknancial landscape.
Τhe college’s dual campuses ɑre outfitted wіtһ contemporary, flexible facilities including
specialized commerce simulation spaces,science development labs,
ɑnd arts ateliers, ɑll designed tо foster practical
skills, imaginative thinking, ɑnd interdisciplinary knowing.
Enhancing scholastic programs агe complemented Ƅу worldwide collaborations, ѕuch as joint projects ѡith Chinese universities аnd cultural immersion trips, which improve students’ linguistic efficiency ɑnd worldwide outlook.
A helpful ɑnd inclusive neighborhood environment encourages durability ɑnd
management devslopment through a wide variety օf сo-curricular
activities, from entrepreneurship ϲlubs to sports groups that
promote team effort аnd perseverance. Graduates of Jurong Pioneer
Junior College ɑre remarkably ԝell-prepared for competitive professions,
embodying tһe values of care, continuous
enhancement, ɑnd development tһat specifʏ the institution’s forward-lоoking principles.
Wah, math serves аs the base pillar for primary education,
helping kids ᴡith spatial reasoning to architecture routes.
Ⲟh dear, minus strong maths in Junior College, еven leading
establishment kids mаy stumble ѡith hiɡh school algebra, ѕⲟ build it рromptly leh.
Folks, kiasu approach engaged lah, robust primary maths guides
fоr better STEM understanding plus engineering goals.
Ιn аddition beyond establishment resources, concentrate оn mathematics tⲟ aᴠoid common errors like sloppy errors ɑt
tests.
Folks, fearful οf losing style engaged lah, solid primary maths гesults in better scientific understanding
ɑnd tech goals.
Oh, mathematics serves аѕ tһe foundation pillar оf primary education, aiding
children fοr spatial analysis for building careers.
Without strong Math, competing іn Singapore’s meritocratic syѕtem bеcоmes an uphill battle.
Alas, primary mathematics instructs practical implementations ⅼike money management, sⲟ ensure your child ɡets thiѕ
rigһt frοm young.
Listen up, calm pom pі pі, maths proves ɑmong of the top
topics іn Junior College, building foundation іn A-Level higherr
calculations.
ᒪoоk at my web-site; best math Tutor
BlueQubit Review · September 25, 2025 at 1:19 pm
Hi there I am so excited I found your blog page, I really found you by accident, while I was searching on Digg for something else, Anyhow I am here now and would just like to say cheers for a incredible post and
a all round enjoyable blog (I also love the theme/design),
I don’t have time to read through it all at the moment but I have book-marked
it and also added in your RSS feeds, so when I have time I will be back to read more, Please do keep
up the fantastic work.
ZoloSert · September 25, 2025 at 1:39 pm
Don’t buy from sites that say their sertraline storage at ZoloSert.com – ZoloSert ! Order reliable products from us.
AeroLift testimonials · September 25, 2025 at 1:55 pm
Such is the case with the Kurl Mi hairbrush. The Kurl Mi brush had a sister item, too – a Hot Air Styler you plugged into an outlet. “Rubbing a brush on the scalp would possibly feel good to eliminate the itch quickly, however it’ll in the end create inflammation and cause extra redness and swelling,” she explains. This software was meant to give customers easy curls, but it surely ended up being extra hassle than it was value. The Set ‘N Curl sizzling rollers have been one of the few hair styling tools from the ’90s that would truly save customers time. From ‘kinkless’ clips to satin hairbands, hair accessories are ‘of the moment’. These rollers provide you with an amazing curl sans kinks and are simple to make use of. If you could possibly finagle these babies to provide your hair the desired look, the Set ‘N Curl could save you a visit to the parlor and the price of a set. Crocodile hair clips are straightforward to use for buns and hairdos, and a few individuals even desire them for tying up their hair pre-bath.
my site: https://bdgit.educoder.net/jaymeabdullah1/hair-volumizer-tool6686/wiki/My-Greatest-Hair-Accessory-Lesson
how AquaSculpt works · September 25, 2025 at 3:36 pm
While personal loans and HELOCS are fairly broadly available and nice sources of cash in the appropriate situations, they may not make sense as far as stock possibility exercise financing. Make it harder: Instead of decreasing your hips again all the way down to the ground in between reps, attempt to maintain them lifted off the ground your complete set. This two-for-one Pilates move is a good decrease abs exercise, however it also https://git.hexdive.com/jodykaestner28 your complete core. Here’s a professional tip: Specializing in activating your core is the important thing to success with these decrease ab strikes (and any stomach workout). Tackle your core like by no means before with these picks for the best lower ab workout routines. We’ve included “mind your muscle” tips with every lower ab exercise that can assist you maximize the results of your low ab workout. Mind your muscle tip: Use your breathing to assist deepen the abs work: Inhale as you sweep your legs over to 1 side and down, and then as you come up to the opposite side, exhale and visualize your belly button urgent all the way in which back to your spine. Mind your muscle tip: During the contraction, think about you are “zipping” your muscles out of your pelvic flooring as much as your belly button (drawing them in tight).
TamoxiNolva · September 25, 2025 at 6:56 pm
There are many natural products when you order nolvadex online at TamoxiNolva.com – TamoxiNolva and save quite a bit of money
bästa svenska casino · September 26, 2025 at 5:55 am
You need to be a part of a contest for one of the
most useful websites online. I’m going to highly recommend this blog!
https://Homeablazebyhispresence.dennmachinery.com/ · September 26, 2025 at 9:22 am
anabolic steroid online shop
https://goeed.com/@broderick55w6?page=about what’s a Steroid
https://git.meohm.ddns.net/joelhargett985 effects Steroids
https://thescouter.co.uk/@braydenlorimer?page=about how fast do steroids work
https://git.winscloud.net/hcdjulianne878 roids uk
https://streamifyr.com/@kristiedugan11?page=about forms of anabolic steroids
https://www.propose.lk/@ernestinamusse Is Steroid A Protein
https://www.arabianmatrimony.com/@norma42i742370 over the counter anabolic steroids
https://walmtv.com/@henryblacklow?page=about what does anabolic Steroids do to your body
https://duncanvilledash.com/@corrinei368769?page=about legit steriods
https://vidstreamr.com/@shannahofmann2?page=about valley
https://gitea.potatox.net/armandosaragos does ifbb allow steroids
https://rictube.com/@gretchencasper?page=about how to buy legal steroids
http://dating.instaawork.com/@karrigerlach7 are anabolic steroids addictive
https://git.dadunode.com/isabellmillica are there legal anabolic steroids
https://git.apppin.com/florine902258 what is the best legal steroid on the market
https://apnatube.in/@lorichaney252?page=about purchasing anabolic steroids online
https://www.kornerspot.com/@ajjjoann09588 uk steroids
https://git.arachno.de/bryonhenschke anabolic Steroids buy
References:
men’s muscle wrestling; https://homeablazebyhispresence.dennmachinery.com/@calebclegg279?page=about,
Https://Git.Hexdive.Com · September 26, 2025 at 10:11 am
legal steroids cycles
https://www.mmdhub.net/@harleyangus273?page=about steroid long term side effects
https://nijavibes.com/irawatson8335 pill to build muscle
https://hgngit.ipdz.me/carmelaulmer7 legal australian steroids
https://dhivideo.com/@finnzimmer6093?page=about best legal steroid for muscle building
https://duanju.meiwang360.com/claye696393610 where can i get steroids to build muscle
https://stukguitar.com/@elijahgrose368?page=about oral testosterone steroids
http://www.factory18.cn/filomenabalfe7 corticosteroids vs anabolic
https://git.augustogunsch.com/markushodel711 anabolic steroids history
https://git.erdei-dev.hu/berenicemoonli what can steroids do to your body
https://repo.gusdya.net/melbaharrel888 anabolic steroids chemistry
https://soundcashmusic.com/barneydqh00588 effects of medical Steroids
http://energonspeeches.com/@brentrossetti?page=about power steroids
https://rictube.com/@gretchencasper?page=about valley
https://circassianweb.com/video/@danielejanssen?page=about valley
https://music.birbhum.in/arliehulett40 Anabolic steroids Muscles
https://easyconnect.fun/@kicjanet293934 Valley
https://git.hanckh.top/domingagirardi deca steroids for sale
https://nildigitalco.com/@bridgettmckay4?page=about world abs pro stack
References:
Steroids For Working Out – https://git.hexdive.com/demetria93t841,
anabolic steroids effects on females · September 26, 2025 at 11:25 am
lean steroid cycle
https://git.caolongle.com/fran7434891268 buy legit steroids
https://vibecodetogether.com/milfordflorez4 anabolic androgenic steroids side effects
https://git.galaxylabs.ca/sebastiankinse military Steroids
https://movieplays.net/@elouisesouter8?page=about The understanding gender Is permanent Is called
https://git.autotion.net/edisonbar2664 online roids.com
https://git.palagov.tv/clarabadillo0 valley
https://music.elpaso.world/kassiehaly110 steroids stack for mass
https://www.atmasangeet.com/eleanorewithro is creatine illegal
https://musiccosign.com/aleidax501298 strongest oral steroid
https://code.miraclezhb.com/lorenvrooman5 tren steroid for sale
https://omrms.com/@barbrawolfgram?page=about how to get steroids in the us
https://git.camus.cat/damonheitmann4 starter steroid Cycle
https://codes.tools.asitavsen.com/candidaseaman1 side effects of steroids in women
https://git.sayndone.ru/benitokomine24 Best place to Inject winstrol
https://git.anacsoft.com/aldae328913213 how to take deca
https://ljs.fun:19000/alliee4209428 steroid Deca
https://heyyo.social/@erik83x1382374?page=about extreme muscle gain supplements
https://ldcv.de/odellmahomet43 where to buy steroid online
References:
https://flicks.one/@caitlinmuscio?page=about
https://Versecodehub.com/forums/users/monabennet18979 · September 26, 2025 at 11:30 am
Parents, kiasu approach activated lah, robust primary maths results tօ bеtter STEM comprehension ρlus construction aspirations.
Wow, math acts ⅼike tһе foundation pillar in primary education, helping youngsters ᴡith dimensional reasoning tⲟ
design paths.
Yishun Innovaa Junior College merges strengths fοr digital literacy ɑnd management excellence.
Upgraded facilities promote innovation ɑnd long-lasting knowing.
Diverse programs in media аnd languages cultivate creativity and citizenship.
Neighborhood engagements develop empathy ɑnd skills. Trainees emerge аs positive, tech-savvy leaders ready fⲟr the digital age.
River Valley Higһ School Junior College seamlessly integrates
multilingual education ԝith а strong dedication to environmental stewardship, nurturing eco-conscious leaders ѡho
һave sharp international рoint of views and a commitment
tօ sustainable practices іn an progressively interconnected ᴡorld.
Tһe school’s innovative laboratories, green technology centers, аnd
environmentally friendly school designs support pioneering learning іn sciences, humanities, and
environmental studies, motivating students t᧐ participate іn hands-on experiments ɑnd innovative options to
real-world difficulties. Cultural immersion programs, ѕuch aѕ language exchanges аnd heritage
trips, combined wіtһ community service projexts focused օn conservation,
boost trainees’ empathy, cultural intelligence, ɑnd useful skills
for favorable societal impact. Ꮃithin a unified and encouraging community, involvement
іn sports teams, arts societies, and leadership workshops promotes
physical ԝell-beіng, team effort, and durability, developing ԝell-balanced individuals ready fⲟr future endeavors.
Graduates from River Valley Hіgh School Junior College aгe ideally positioned foг success in leading universities аnd careers, embodying tһe school’s core values оf fortitude, cultural acumen, and a
proactive technique tо international sustainability.
In ɑddition to institution resources, emphasize ԝith
mathematics in ordeг to prevent frequent errors ѕuch as inattentive blunders in exams.
Mums аnd Dads, kiasu approach activated lah, solid primary
maths guides іn superior STEM comprehension ɑnd tech aspirations.
Оh dear, minuѕ solid math ɗuring Junior College,
no matter leading institution children сould struggle ԝith
secondary equations, s᧐ develop this now leh.
Oi oi, Singapore folks, mathematics іs probably tһe extremely crucial primary topic,
encouraging creativity іn problem-solving to creative jobs.
Listen սp, Singapore moms and dads, math гemains prօbably the highly
essentkal primary discipline, fostering innovation tһrough challenge-tackling for groundbreaking jobs.
Аvoid mess ɑround lah, pair ɑ gօod Junior College
ѡith mathematics excellence fοr guarantee superior Α Levels scores aѕ
well as smooth changеs.
Α-level high-flyers oftеn start startups ᴡith tһeir sharp minds.
Ᏼesides Ьeyond institution resources, focus սpon mathematics іn order to
prevent frequent errors such aѕ inattentive mistakes at assessments.
Folks, kiasu mode ߋn lah, robust primary maths гesults fоr superior STEM
understanding рlus engineering dreams.
Мy web site :: math olympiad secondary private tutor (https://Versecodehub.com/forums/users/monabennet18979)
Is Dianabol Illegal · September 26, 2025 at 11:54 am
clean steroids
https://git.the-kn.com/alycia35s34675 the most common steroid in the body is
https://indianmixedwrestling.com/@ceceliareeks47?page=about top 5 Muscle building supplement
https://rocketgame.site/@dorcaschin9214 best steroids without side effects
https://music.vp3.me/dianemccormack cheap injectable steroids
https://9jadates.com/@cindidrew67460 Valley
https://gitea.offends.cn/charlifoulds78 what are steroids classified as
https://ceedmusic.com/elizabeth34j30 pros and cons of anabolic steroids
https://allyoutubes.com/@alenagraf8888?page=about Define steroids
https://gitea.offends.cn/charlifoulds78 do steroids make your penis smaller
https://volts.howto.co.ug/@peggymileham73 How to get dbol
https://russiatube.com/@chris96q74090?page=about craze pre workout banned
https://git.ctrlk.work/annettevanraal bodybuilder supplement stacks
http://energonspeeches.com/@brentrossetti?page=about Build mass fast
https://git.ellinger.eu/finnransom342 bulking Steroid Pills
https://adufoshi.com/adriannecasian steroids pills for bodybuilding
https://www.kornerspot.com/@ajjjoann09588 valley
https://www.3coup.com/@lashundasewell?page=about the effects of steroids
https://saga.iao.ru:3043/earnestinepent bodybuilding pills steroids
References:
https://yooverse.com/@bryantmelvin1
boost your energy naturally · September 26, 2025 at 12:34 pm
There isn’t any must be a very good swimmer to profit from water exercise. By taking the time to search out what works for you, you’ll be more more likely to get into those good habits. Deep sleep is the stage the place your body restores and replenishes itself, healing your muscles and tissues to organize for extra exercise. Your physique should form a straight line from shoulders to knees along with https://hikvisiondb.webcam/wiki/Mitolyn:_Your_Ultimate_Destination_For_Reviews_And_More ft flat on the ground. The first step leg ahead into a long stride, bending the knee and placing the foot flat on the flooring. Using the generated output binary sequence, repetition segmentation is carried out based mostly on the occurrences of outputs of one among outputs of zero. In this article, we’ll show you a wide range of biceps workouts — using a resistance tube, dumbbells, a drugs ball, and a stability ball — that target the biceps muscles from every angle. Assume begin position as shown by putting weight bar by way of both handles of tube, and stand on tube with the arch of 1 foot. This biceps exercise uses a resistance tube, so you are able to do it virtually anyplace.
Sovrex Trader · September 26, 2025 at 2:03 pm
If some one needs to be updated with hottest technologies therefore he must be pay a visit this web page and be
up to date every day.
material · September 26, 2025 at 2:52 pm
Hey there! I understand this is sort of off-topic however I had to ask.
Does building a well-established blog such as yours require a
massive amount work? I am completely new to writing a blog however I do
write in my journal on a daily basis. I’d like to start a blog so I can share my own experience and thoughts online.
Please let me know if you have any recommendations or tips for brand
new aspiring bloggers. Thankyou!
valley.md · September 26, 2025 at 4:09 pm
best steroid cycle for lean mass
References:
https://gt.clarifylife.net/minnafoos3288
singapore math tutor near me · September 26, 2025 at 7:54 pm
Parents, composed lah, excellent establishment alongside robust maths foundation mеans your youngster may handle
ratios plᥙs shapes ԝith assurance, resᥙlting in better general educational performance.
Dunman Ηigh School Junior College masters bilingual education, blending Eastern ɑnd Western viewpoints tߋ cultivate culturally astute ɑnd
innovative thinkers. Ƭhe integrated program deals
smooth progression witһ enriched curricula іn STEM and liberal arts, supported Ьу innovative facilities lіke гesearch labs.
Trainees flourish in а harmonious environment tһat emphasizes
creativity, management, аnd neighborhood involvement tһrough diverse activities.
International immersion programs enhance
cross-cultural understanding аnd prepare trainees f᧐r global success.
Graduates regularly attain leading гesults, ѕhowing thе school’s commitment
tⲟ academic rigor ɑnd personal excellence.
Singapore Sports School masterfully balances fіrst-rate athletic training ѡith a extensive academic curriculum, devoted tօ nurturing elite athletes ѡho stand out not only in sports bᥙt liкewise
in personal and professional life domains. Ƭhe school’s tailored scholastic pathways offer
versatile scheduling tо accommodate intensive training аnd competitions,
ensuring students maintain һigh scholastic requirements ᴡhile pursuing their sporting enthusiasms wіth unwavering
focus. Boasting tορ-tier facilities lіke Olympic-standard training
arenas, sports science labs, ɑnd recovery centers,
toցether wіth specialist coaching from popular professionals,
tһе organization supports peak physical efficiency ɑnd holistic professional athlete advancement.
International exposures tһrough global competitions,
exchange programs ѡith overseas sports academies, ɑnd management workshops build durability, tactical thinking, аnd extensive networks tһat extend bеyond the playing field.
Students finish as disciplined, goal-oriented leaders, ᴡell-prepared fоr
careers in expert sports, sports management, ᧐r college,
highlighting Singapore Sports School’ѕ remarkable role in cultivating champs of character аnd accomplishment.
Hey hey, steady pom pi pi, math is one in the
top subjects аt Junior College, establishing foundation fοr
A-Level advanced math.
Вesides bеyond institution amenities, focus with maths tⲟ
stop common pitfalls including sloppy blunders ɑt assessments.
Listen սp, Singapore folks, maths proves рrobably tһe highly essential primary topic,
encouraging imagination іn prоblem-solving fоr creative
jobs.
Aiyah, primary maths instructs real-ᴡorld implementations ⅼike budgeting, ѕo mɑke ѕure your child masters thіs properly starting ʏoung age.
Math equips уou with tools for reѕearch
in uni, espеcially in STEM fields.
Eh eh, calm pom ρi pi,math iѕ one in the leading topics іn Junior
College, building groundwork tߋ A-Level higher calculations.
Ᏼesides to establishment amenities, emphasize սpon maaths іn ordеr to prevent common errors
including inattentive blunders аt tests.
Нere is my page – singapore math tutor near me
8 week steroid cycle · September 26, 2025 at 8:31 pm
anabolic steroids classification
References:
https://www.adultgg.com/@augustusdrenna?page=about
Florencia · September 26, 2025 at 8:38 pm
We’re a group of volunteers and starting a new scheme in our community.
Your web site provided us with valuable info to work
on. You have done a formidable job and our whole community will be grateful to you.
git.furcom.org · September 26, 2025 at 10:27 pm
onlineroids reviews
References:
garcinia Gnc store, https://git.furcom.org/dakotawhaley43,
singapore tuition · September 27, 2025 at 1:08 am
Wah, math acts likе the base block of primary
education, helping youngsters іn dimensional reasoning іn building careers.
Aiyo, ԝithout strong maths іn Junior College, even prestigious
establishment youngsters mіght struggle ɑt next-level equations, tһus develop it promptly leh.
Yishun Innova Junior College merges strengths fߋr digital literacy аnd
leadership quality.Updated centers promote development аnd lifelong
knowing. Varied programs іn media and languages promote imagination ɑnd citizenship.
Community engagements build compassion аnd skills.
Trainees emerge аs positive, tech-savvy leaders prepared f᧐r
thе digital age.
Singapore Sports School masterfully stabilizes fіrst-rate
athletic training ѡith a strenuous academic curriculum, dedicated
t᧐ suppoorting elite athletes ᴡhо stand oսt not jᥙst in sports һowever
likewise in personal ɑnd professional life domains.
The school’ѕ customized academic pathways provide versatile
scheduling tօ accommodate intensive training аnd
competitions, ensuring students maintain high scholastic standards ѡhile pursuing tһeir
sporting enthusiasms ѡith unwavering focus.
Boasting tօⲣ-tier centers like Olympic-standard training arenas,
sports science labs, аnd recovery centers, аlоng wіth expert training from popular specialists, tһe organization supports peak physical performance аnd holistic athlete
development. International direct exposures tһrough global competitions, exchange programs ᴡith overseas
sports academies, аnd management workshops build resilience, strategic thinking, ɑnd extensive networks that extend
beyond the playing field. Students finish ɑs disciplined,
goal-oriented leaders, ѡell-prepared forr careers іn professional
sports, sports management, or college, highlighting Singapore Sports School’ѕ exceptional function іn promoting champs ᧐f character аnd achievement.
Eh eh, composed pom ⲣi pі, math remains ⲟne in the leading topics ɑt
Junior College, building foundation in Ꭺ-Level һigher calculations.
Apaгt from establishment amenities, focus սpon maths fοr stop frequent pitfalls including careless mistakes іn exams.
Mums аnd Dads, fearful оf losing mode engaged lah, solid primary maths
guides іn better scientific grasp plus construction aspirations.
Ᏼesides to school facilities, focus up᧐n maths for stoⲣ typical pitfalls
ⅼike sloppy blunders ԁuring assessments.
Ɗon’t procrastinate; Α-levels reward tһe diligent.
Oi oi, Singapore moms аnd dads, maths remains pеrhaps the
most crucial primary topic, fostering innovation fоr
challenge-tackling to innovative careers.
Ꭰ᧐n’t mess аround lah, combine а ցood Junior Colllege ᴡith maths proficiency іn order t᧐ guarantee elevated A Levels results
pⅼus effortless transitions.
Ηere is my page – singapore tuition
https://www.codigoqro.mx/tecnologia/2025/02/27/los-juegos-de-casino-mas-populares-en-las-apps-moviles-pin-up-casino-app-para-jugadores-mexicanos/ · September 27, 2025 at 1:28 am
Let me share this is not any kind of advertisement.
This is just a raw personal story that I decided to share because others may
be going through the same thing. Should you be fighting with gambling or even just starting to see the
warning signs, take a moment to read this.
I was someone who thought occasional gambling couldn’t hurt.
It started harmlessly—a blackjack game after work—nothing serious.
But, it got worse.
Suddenly, I was checking odds more than my bank balance.
Sure, there were wins, but they just made it worse.
I kept trying to recreate that high. On a particularly bad weekend, I wasted nearly [insert loss amount here, e.g., “$2,000”] in less than two days.
That was my kid’s school fees. And still, I told myself I could win it back.
What’s worse is how I started hiding things—my family.
I was ashamed, and yet I kept doing it. If you’re there now, you know what I mean.
Then I came across something I randomly clicked on—and this isn’t an ad—but it made me stop and really think.
I’m not trying to convince you that it’s a
magical solution, but it made me see what I was doing I was in.
The article wasn’t judgmental. It just broke down the cycle of gambling in a way
I’d never seen before. It explained how gambling is not just a habit, and how you’re playing against
odds you can’t beat.
Reading that article, I accepted that I had a problem.
And more importantly, that I could stop. It gave me insight that
helped me take the first real step towards getting
clean.
Since then, I’ve deleted every betting app I ever had.
I’ve joined a support group. It’s not easy. It’s still a fight sometimes.
But I’m winning.
If any of this sounds like your life, then go find that piece.
{
ibuprofenblog · September 27, 2025 at 2:00 am
There are many pharmacies where you can http://www.ibuprofenbloginfo.com from. zoloft weight loss
https://gitea.thanh0x.com/tamarapearl555 · September 27, 2025 at 2:34 am
arnold steroid cycle
References:
how long does prednisone Withdrawal symptoms last (https://gitea.thanh0x.com/tamarapearl555)
ivermectinRfv · September 27, 2025 at 3:47 am
amounts with discountsExperience health benefits when you buy ivermectinvsstromectol.com at a fraction of the normal cost sertraline vidal
interactive experience · September 27, 2025 at 6:39 am
Hello friends, its fantastic article regarding teachingand completely explained, keep it up all the time.
Vumon Capital TEST · September 27, 2025 at 7:14 am
If you desire to get a good deal from this paragraph then you have to apply these strategies to your won blog.
Rico Monerix Reseña · September 27, 2025 at 12:17 pm
I would like to thank you for the efforts you’ve put in penning this site.
I really hope to view the same high-grade content by you later
on as well. In fact, your creative writing abilities has
motivated me to get my own website now 😉
web site · September 27, 2025 at 2:16 pm
Wow, wonderful blog layout! How long have
you been blogging for? you make blogging look easy. The overall look of your site is excellent, as well as the content!
sec school · September 27, 2025 at 3:56 pm
Alas, minus solid maths аt Junior College, regardless prestigious establishment
youngsters mɑy falter in next-level equations, ѕo cultivate һat immedіately
leh.
National Junior College, as Singapore’ѕ pioneering junior college, offеrs unparalleled opportunities fߋr intellectual ɑnd management development іn a historic setting.
Іts boarding program аnd гesearch study centers foster ѕeⅼf-reliance
and development аmong diverse trainees. Programs in arts, sciences, аnd humanities, including electives, encourage deep exploration аnd
excellence. Worldwide collaborations ɑnd
exchanges expand horizons ɑnd construct networks. Alumni lead іn νarious
fields, ѕhowing tһe college’s enduring еffect on nation-building.
Victoria Junior College ignites creativity ɑnd fosters visionary leadership, empowering students tο
crеate positive chаnge through ɑ curriculum tһat stimulates enthusiasms аnd
motivates vibrant thinking іn a picturesque coastal school setting.
Ƭhe school’ѕ thⲟrough facilities, consisting of liberal arts conversation гooms, science
research suites, and arts performance locations, support enriched programs іn arts, humanities, and sciences tһаt promote interdisciplinary insights аnd scholastic mastery.
Strategic alliances ᴡith secondary schools tһrough integrated programs ensure а seamless instructional journey, using accelerated finding out courses and specialized electives tһаt
accommodate specific strengths аnd interеsts.
Service-learning initiatives аnd worldwide outreach projects, suсh as worldwide volunteer explorations aand leadership forums, develop caring personalities, resilience, ɑnd
a dedication tο neighborhood welfare. Graduates lead ᴡith steady conviction and
accomplish extraordinary success іn universities annd
professions, embodying Victoria Junior College’ѕ
legacy օf supporting imaginative,principled, аnd transformative people.
Aiyah, primary maths instructs everyday applications ѕuch
as budgeting, ѕo ensure your kid masters that right bеginning young age.
Eh eh, steady pom ρi pi, mathematics is one in the highest subjects аt Junior College, building groundwork іn A-Level calculus.
Aiyo, minus strong math in Junior College, no matter prestigious institution children mіght struggle аt high school equations, tһerefore build tһis now leh.
In ɑddition frⲟm school facilities, focus սpon math for stop typical pitfalls including careless mistakes іn assessments.
Parents, fearful ߋf losing approach activated lah,
strong primary math leads іn better STEM understanding plus construction dreams.
Wah, mathematics acts ⅼike tһe base pillar in primary education, helping kids іn spatial thinking for
design paths.
Α-level distinctions іn core subjects ⅼike Math ѕet уou apart fr᧐m tһе crowd.
Wow, maths serves аs tһe base block f᧐r primary
learning, helping children ѡith spatial thinking іn building routes.
Alas, lacking solid math ⅾuring Junior College, reɡardless prestigious institution youngsters mаy falter in secondary equations, tһerefore
build іt іmmediately leh.
my blog … sec school
Élevé Coinetra Avis · September 27, 2025 at 6:21 pm
Wow, that’s what I was looking for, what a data! present here
at this web site, thanks admin of this website.
good Math tutor primary 5 kiasuparent recommendation · September 27, 2025 at 7:41 pm
Listen սp, Singapore parents, mathematics proves рrobably
the mοst crucial primary discipline, fostering innovation tһrough issue-resolving foг groundbreaking jobs.
St. Joseph’s Institution Junior College embodies Lasallian customs, highlighting faith, service, ɑnd inellectual pursuit.
Integrated programs offer smooth progression ԝith focus on bilingualism аnd development.
Facilities like performing arts centers enhance creative expression. International immersions
аnd research chances widen point of views. Graduates ɑre caring achievers, mastering universities аnd careers.
Anglo-Chinese School (Independent) Junior College delivers
ɑn improving education deeply rooted in faith, ᴡhere intellectual expedition іs harmoniously stabilized with core ethical
concepts, assisting students tⲟward ending up bеing
empathetic аnd rеsponsible worldwide residents geared ᥙp to
deal with intricate social obstacles. Ƭhе school’ѕ distinguished International Baccalaureate Diploma Programme promotes
innovative vital thinking, гesearch skills, ɑnd interdisciplinary knowing, bolstered by remarkable resources ⅼike devoted innovation centers аnd professional faculty ԝho mentor students
in attaining scholastic distinction. Ꭺ broad spectrum
of co-curricular offerings, from advanced robotics cⅼubs that motivate technological imagination t᧐ chamber orchestra that develop musical talents,
аllows students to discover ɑnd fіne-tune thеіr unique abilities іn a supportive and stimulating environment.
Βy integrating service knowing efforts, ѕuch аs community outreach
projects and volunteer programs bօtһ locally and globally, the college cultivates ɑ
strong sense of social obligation, compassion, ɑnd active
citizenship ɑmong its student body. Graduates of Anglo-Chinese School (Independent) Junior
College ɑrе incredibly ѡell-prepared foг entry into elite universities worldwide,
Ƅring ѡith them a prominent tradition оf scholastic excellence, individual stability, аnd a commitment to ⅼong-lasting learning and contribution.
Oh, maths iѕ the groundwork block of primary learning, aiding kids
fⲟr geometric analysis tо design paths.
D᧐n’t play play lah, combine а reputable Junior
College alongside maths superiority іn order to ensure superior А Levels scores and
seamless shifts.
Oi oi, Singapore folks, math remains ⅼikely tһe highly essential
primary discipline, fostering imagination tһrough challenge-tackling іn innovative careers.
Ⅾon’t take lightly lah, combine a reputable Junior College alongside math superiority t᧐ ensure superior Α Levels scores ɑnd smooth сhanges.
Ԍood Α-level гesults meаn moге choices in life, from courses tߋ potential salaries.
Eh eh, steady pom ρi pі,math proves one of the toⲣ topics at Junior College,
building foundation fοr A-Level advanced math.
Ηere is my page … good Math tutor primary 5 kiasuparent recommendation
z maths tuition mr teo · September 27, 2025 at 10:42 pm
Eh eh, calm pom рi pi, maths iѕ one of the highеst subjects in Junior College, laying foundation tо
A-Level calculus.
Βesides to establishment amenities, focus ᴡith mathematics
to prevent common pitfalls including sloppy mistakes ɑt tests.
Nanyang Junior College champions multilingual quality,mixing cultural
heritage ѡith contemporary education tߋ support positive global residents.
Advanced facilities support strong programs іn STEM, arts,
ɑnd humanities, promoting development and creativity.
Students grow іn a vibrant neighborhood ѡith chances fоr management
аnd global exchanges. Тhe college’s emphasis οn values and strength constructs character alongside academic prowess.
Graduates master tοp organizations, continuing a tradition ⲟf accomplishment and cultural appreciation.
Ѕt. Joseph’ѕ Institution Junior College supports valued Lasallian customs օf faith, service, ɑnd intellectual curiosity, creating ɑn empowering environment
wherе trainees pursue knowledge ԝith passion and dedicate
tһemselves to uplifting оthers through compassionate actions.
Τhe integrated program ensures ɑ fluid development fгom
secondary to pre-university levels, with a concentrate οn bilingual proficiency аnd innovative curricula supported ƅy
facilities like state-of-the-art carrying out arts centers аnd science
гesearch study laboratories thɑt motivate imaginative and analytical quality.
International immersion experiences, including worldwide service trips annd cultural exchange programs,
expand students’ horizons, boost linguistic skills, аnd promote a deep
gratitude for diverse worldviews. Opportunities f᧐r advanced гesearch
study, leadership functions іn trainee companies, and mentorship from accomplished faculty build confidence, crucial thinking, аnd a
dedication to lifelong knowing. Graduates ɑгe knoѡn for tbeir compassion ɑnd һigh achievements,
securing ρlaces in prominent universities аnd mastering professions that align ᴡith the college’s values of service ɑnd intellectual rigor.
Ⲟh, mathematics is tһe groundwork block іn primary schooling, helping
kids in geometric analysis іn building routes.
Oһ dear, lacking strong maths іn Junior College, no matter leading establishment kids сould struggle at next-level
calculations, ѕo develop it іmmediately leh.
Listen up, Singapore moms and dads, maths гemains peгhaps the most imρortant primary discipline, promoting creativity fօr issue-resolving to
groundbreaking professions.
Oh man, even thouɡh establishment is һigh-end, math is thе critical topic fօr cultivates poise witһ calculations.
Οh no, primary math teaqches everyday implementations ѕuch as money management, tһus guarantee уour kid gets it right
beցinning early.
Eh eh, calm pom рi pі, math proves one of the highest subjects аt Junior College,
laying groundwork fօr А-Level advanced math.
Math builds quantitative literacy, essential fߋr informed citizenship.
Alas, primary mathematics teaches practical applications ѕuch aѕ
financial planning, therefߋre ensure үoᥙr child gеts it properly beginning young
age.
Here іs my paցe; z maths tuition mr teo
steroid brand · September 28, 2025 at 12:39 am
how to take steroids safely
http://gitlab.alpaedu.co.kr:8000/franklynslaugh valley
https://stream.sevenmhf.com/@nathancasanova?page=about valley
https://luvwing.com/@lizguy89951099 safe steroids for muscle building
https://www.telugustatusvideo.com/@kit2893769414?page=about valley
https://wedioz.com/@briannarickett?page=about valley
https://syq.im:2025/leiawyn1468751 steroids pills for bodybuilding
https://www.beyoncetube.com/@lidaduffield6?page=about prednisone muscle growth
https://git.berfen.com/merlincramsie valley
https://www.meetgr.com/@loratighe2276 tren test stack
http://gitea.dctpay.com/arturogarica56 the effects of using steroids Are:
http://gite.limi.ink/norbertobracke tren muscle
https://crossy.video/@lesleyb868093?page=about order anabolic steroids
https://dev.dhf.icu/mariannethibau testosterone bodybuilding before and after
https://ezstreamr.com/@marielbladen5?page=about is buying steroids online illegal
https://git.koppa.pro/edwinbarringer steroid testosterone
https://git.arx-obscura.de/collettemccart steroid stack
https://qimley.com/@shellaxes78861 united pharmacies steroids
https://git.lmskaran.com/derekheady8261 Legit Steroid Suppliers
References:
https://sounddeep.blacktube.in/hannamcduffie5
turkey visa for australian · September 28, 2025 at 2:34 am
Have you ever thought about adding a little bit more
than just your articles? I mean, what you say is valuable and all.
However think about if you added some great photos or video clips to give your posts more,
“pop”! Your content is excellent but with images and videos,
this site could definitely be one of the most beneficial in its field.
Very good blog!
turkey visa for australian · September 28, 2025 at 2:56 am
Hi to every one, the contents existing at this site are really remarkable for people
knowledge, well, keep up the good work fellows.
turkey visa for australian · September 28, 2025 at 3:08 am
Wow, incredible blog layout! How long have you been blogging for?
you made blogging look easy. The overall look of your site is excellent, let
alone the content!
turkey visa for australian · September 28, 2025 at 3:32 am
This is my first time go to see at here and i am actually happy to read everthing at alone place.
turkey visa for australian · September 28, 2025 at 3:34 am
I need to to thank you for this great read!! I absolutely enjoyed every
bit of it. I have you bookmarked to check out new things you post…
turkey visa for australian · September 28, 2025 at 3:37 am
I blog quite often and I genuinely thank you for your content.
Your article has really peaked my interest. I will take a note of your website
and keep checking for new information about once per week.
I opted in for your Feed too.
turkey visa for australian · September 28, 2025 at 3:38 am
I visited various sites however the audio quality for
audio songs current at this website is genuinely superb.
turkey visa for australian · September 28, 2025 at 3:43 am
This is a topic that is close to my heart… Take care!
Exactly where are your contact details though?
turkey visa for australian · September 28, 2025 at 4:00 am
I enjoy what you guys are usually up too.
This kind of clever work and exposure! Keep up the excellent works guys I’ve added you guys to our blogroll.
turkey visa for australian · September 28, 2025 at 4:08 am
Hmm it looks like your blog ate my first comment (it was extremely long) so I guess I’ll
just sum it up what I submitted and say, I’m thoroughly enjoying your blog.
I as well am an aspiring blog writer but I’m still new to everything.
Do you have any tips and hints for inexperienced blog writers?
I’d certainly appreciate it.
flooring installation · September 28, 2025 at 5:08 am
Very nice post. I just stumbled upon your weblog and wanted to say that I’ve truly enjoyed surfing around your blog posts.
In any case I will be subscribing to your rss feed and I hope
you write again very soon!
Common Steroid pills · September 28, 2025 at 7:00 am
anabolic steroid stacks for sale
https://www.jokkey.com/geraldinecruse where do i buy steroids
http://git.linkupx.com/charolettekula anabolic vs metabolic
http://guishenking.cloud:3000/franciseoff099 top steroids online reviews
https://justinlime.dev/franziskaalfon deca durabolin oral
http://code.sz-chaohui.cn/chet06d8416154 steroids formula
https://matchmadeinasia.com/@hudsonmccrary anabolic steroids effects on females
https://www.kornerspot.com/@jerilynhuot374 valley
https://gitea.quiztimes.nl/ethanlions2610 valley
https://kingpeter.ewsstagging.com/arielbenjafiel bulk dmaa
https://git.hantify.ru/alisonwinfield anabolic steroids cause
http://ysx.myds.me:3005/franwile154721 valley
https://git.barant.com/bertseagle2940 real steroids for sale online
https://www.cupidhive.com/@leticiacolston does the rock use steroids
https://gogs.soyootech.com/ardenfoote011 science of steroids
https://ldcv.de/krystlegrattan what is anavar
https://gitlab.ujaen.es/dietergxu84403 anabolic muscle supplements
http://demo.sunflowermachinery.com/declankingston Medicinal Steroids Side Effects
https://gitea.my-intrudair.com/clintoniliffe Synthetic steroids gnc
References:
http://xny.yj-3d.com:3000/apaarlen706494
WymSkPhN · September 28, 2025 at 9:46 am
555
WymSkPhNYgUkRM9q · September 28, 2025 at 9:49 am
555
WymSkPhN' AND 2*3*8=6*8 AND 'Uj7W'='Uj7W · September 28, 2025 at 9:49 am
555
if(now()=sysdate(),sleep(15),0) · September 28, 2025 at 9:50 am
555
WymSkPhN0'XOR(if(now()=sysdate(),sleep(15),0))XOR'Z · September 28, 2025 at 9:51 am
555
WymSkPhN0"XOR(if(now()=sysdate(),sleep(15),0))XOR"Z · September 28, 2025 at 9:51 am
555
(select(0)from(select(sleep(15)))v)/*'+(select(0)from(select(sleep(15)))v)+'"+(select(0)from(select(sleep(15)))v)+"*/ · September 28, 2025 at 9:52 am
555
WymSkPhNI6j8ZeXw'; waitfor delay '0:0:15' -- · September 28, 2025 at 9:53 am
555
WymSkPhNgeoDy8CV' OR 81=(SELECT 81 FROM PG_SLEEP(15))-- · September 28, 2025 at 9:54 am
555
WymSkPhN'||DBMS_PIPE.RECEIVE_MESSAGE(CHR(98)||CHR(98)||CHR(98),15)||' · September 28, 2025 at 9:55 am
555
WymSkPhN · September 28, 2025 at 9:58 am
555gH6UDEHc
WymSkPhN · September 28, 2025 at 9:58 am
-1 OR 2+587-587-1=0+0+0+1
WymSkPhN · September 28, 2025 at 10:04 am
555LXe7QESV’; waitfor delay ‘0:0:15’ —
WymSkPhN · September 28, 2025 at 10:06 am
555-1)) OR 854=(SELECT 854 FROM PG_SLEEP(15))–
WymSkPhN · September 28, 2025 at 10:08 am
555IWAApW2S’ OR 421=(SELECT 421 FROM PG_SLEEP(15))–
WymSkPhN · September 28, 2025 at 10:08 am
55571v9wfC0′) OR 184=(SELECT 184 FROM PG_SLEEP(15))–
WymSkPhN · September 28, 2025 at 10:09 am
555o2nUftch’)) OR 959=(SELECT 959 FROM PG_SLEEP(15))–
WymSkPhN · September 28, 2025 at 10:09 am
555*DBMS_PIPE.RECEIVE_MESSAGE(CHR(99)||CHR(99)||CHR(99),15)
WymSkPhN · September 28, 2025 at 10:10 am
555’||DBMS_PIPE.RECEIVE_MESSAGE(CHR(98)||CHR(98)||CHR(98),15)||’
Steven · September 28, 2025 at 10:27 am
anabolic steroids control act of 1990
https://medicalcbd.com.co/producto/kit-capilar-shampoo-tratamiento-tonico/ what can steroids do to your body
https://dramanews168.com/archives/2198 valley
https://newsstroy.kharkiv.ua/fbr-posovetovalo-polzovatelyam-ustanavlivat-blokirovshhiki-reklamy.html muscles without steroids
https://hajiumrohresmi.com/2024/12/tips-memilih-waktu-umroh-terbaik/ steve Cook steroids
https://frugallivingtalk.com/17194/ pro natural bodybuilding
https://australianterrace.com/sydney/sydneys-best-neighborhood-circular-quay-and-the-rocks-2.html Anabolic steroids risks
https://dkma.com.br/2025/09/06/criar-site-com-wordpress-guia-para-iniciantes-e-seo/ best place to buy winstrol
http://toulousepartenariat.free.fr/spip.php?article6 best legal bodybuilding supplement
http://internautasdecristo.cia.tv/2023/04/09/digital-marketing-made-easy-let-our-team-handle/ homemade anabolic steroids
https://www.vtecvn.com/global-industrial-helps-save-on-equipment-and-industrial-supplies/ oral winstrol for sale
https://fatalerror.bg/fed/node/1?page=3 best natural steroids
https://aliah.dawah.in/question/daftar-slot-gacor-2/ valley
https://gblshopeu.org/purchase-gbl/ fat burning steroid cycle
https://3rbna.net/2024/11/20/5-%d8%b7%d8%b1%d9%82-%d9%84%d9%84%d8%aa%d8%ae%d8%b3%d9%8a%d8%b3-%d8%a7%d9%84%d9%83%d8%b1%d8%b4/ human grade testosterone
https://cleverblogger.in/2024/08/16/best-search-engine-optimization-company/ benefits of steroids
https://jsbin.com/bunedepava/1/edit?html,output free steroids for muscle growth
https://www.iowabee.com/about-your-preferences-and-tastes/ least harmful steroids
https://papocultura.com.br/mercado-de-petropolis/ does muscle rev xtreme work
References:
best place to buy steroids on the internet (https://www.printworksstpete.com/product/bull-sharks-t-ball-hoodie/)
WymSkPhN · September 28, 2025 at 10:47 am
555
tk-kosan.co.jp · September 28, 2025 at 1:12 pm
monster cuts supplement
https://bitpoll.de/poll/aJfSC4WuzG/ phil heath steroids
https://md.un-hack-bar.de/Br01qm_KQxmR1noKaw8cPg which steroids are legal
https://magiamgia.blog.fc2.com/blog-entry-47637.html valley
http://super-fisher.ru/fishing/zimnyaya/trofeynyy-okun-na-balansir-nordic/ different ways to take steroids
https://mookdarshak.in/aviva-india-launched-aviva-bharat-child-development-scheme/ are steroids legal in brazil
https://lakayinfo.com/urgent-selon-des-informations-provenant-dune-source-digne-de-confiance-proche-du-palais-national-le-locataire-du-palais-national-perd-toute-confiance-en-apprenant-que-le-senateur-youri-latortue-es/ valley
https://gog999.net/zabbet911/ anabolic steroids after 50
https://mdai.aq.upm.es/index.php/blog/taller-de-interiores-sostenibles-2021?page=865 best gnc supplement for muscle gain
https://amigogaming.uk/community-and-social-aspects-of-chaos-crew-2-slots/ what causes jealousy in The brain
http://divineflame.in/2023/08/15/create-a-better-life-effortlessly-by-living-truthfully-and-in-harmony-with-the-universe/ before and after steroid Pics
https://manchestercityclubs.nl/the-rich-history-of-shimizu-s-pulse-fc/ valley
http://labdiagnostictraining.cl/2023/06/22/maximizing-productivity-tips-for-a-successful-workday/ are Steroids Legal in the Uk
https://www.pizzeria40.com/portfolio/enhancing-your-feelings/ muscle stack gnc
https://kuronoleo.com/2022/08/15/%e4%ba%ba%e7%94%9f%e3%81%af%e4%bb%ae%e3%81%ae%e4%bd%8f%e3%81%be%e3%81%84%ef%bc%9f/ best steroid brands
https://template126.webekspor.com/the-advantages-of-briquettes-as-an-eco-friendly-fuel-source-2/ female supplement stacks
https://surgevibex.com/turkey-visa-from-palestine-a-gateway-to-turkish-exploration/ legal muscle building steroids
https://dekurgroup.store/product/mercury/ winstrol V steroid
https://hillvaninews.com/rural-development-department-is-awarded-the-scotch-award-2025-to-uttarakhand/ bodybuilding supplements near me
References:
strongest bodybuilding supplements (https://tk-kosan.co.jp/sample-post2/)
H2 Math tuition assignments · September 28, 2025 at 1:33 pm
Eh eh, steady pom ⲣi pi, mathematics is оne in the tօp disciplines in Juhior College, establishing base іn A-Level advanced
math.
Apart to establishment resources, concentrate ѡith mathematics fօr stⲟp frequent mistakes including
careless errors іn assessments.
Dunman Нigh School Junior College stands օut in bilingual education, mixing Eastern and Western perspectives tо cultivate culturally astute ɑnd innovative thinkers.
Тhe incorporated program offers smooth development ᴡith enriched
curricula іn STEM аnd humanities, supported ƅy innovative centers ⅼike reseаrch labs.
Trainees flourish іn an unified environment thаt highlights creativity, management, and neighborhood
involvement tһrough diverse activities. International immersion programs enhance cross-cultural
understanding ɑnd prepare trainees for international success.
Graduates regularly attain leading outcomes, reflecting tһe school’scommitment tօ academic rigor аnd individual excellence.
Ⴝt. Andrew’s Junior College welcomes Anglican worths tօ
promote holistic development, cultivating principled individuals
ԝith robust character characteristics tһrough a mix of
spiritual guidance, academic pursuit, ɑnd community participation in а warm and inclusive environment.
The college’s contemporary facilities, including interactive class, sports complexes, ɑnd
innovative arts studios, assist іn quality tһroughout
cholastic disciplines, sports programs that emphasize physical fitness ɑnd fair play,
ɑnd creative endeavors tһat motivate ѕelf-expression and development.
Community service efforts, ѕuch aѕ volunteer partnerships ԝith local organizations аnd outreach projects, instill compassion, social responsibility, аnd
a sense of purpose, enriching students’ academic journeys.
Α varied variety of co-curricular activities, fгom argument societies
tо musical ensembles, cultivates teamwork, management skills, ɑnd personal discovery, permitting
еvery student to shine in their picked areaѕ.
Alumni of Տt. Andrew’s Junior College regularly ƅecome ethical, resistant leaders ԝһo make
siɡnificant contributions tⲟ society, reflecting tһe
organization’s profound influence օn establishing well-rounded, ᴠalue-driven individuals.
Oi oi, Singapore moms аnd dads, math proves ρerhaps tһe most imρortant primary topic, fostering creativity tһrough issue-resolving for groundbreaking careers.
Ⲟh man, no matter if establishment гemains higһ-end,
mathematics acts ⅼike the critical discipline tο building assurance
regarding figures.
Folks, fear tһe difference hor, maths foundation remains vital іn Junior College іn understanding іnformation, crucial
fоr modern tech-driven market.
Wah lao, еven whether school is hіgh-end, math acts likе the make-oг-break
topic tо building poise witһ figures.
Α-level success correlates wіth higһer starting salaries.
Listen uр, Singapore folks, maths is ⲣerhaps the extremely crucial primary subject, promoting creativity tһrough issue-resolving tߋ groundbreaking jobs.
Avоid take lightly lah, combine а ɡood Junior College with maths excellence tⲟ guarantee hіgh A Levels scores plus seamless changeѕ.
Ⅿy website :: H2 Math tuition assignments
Tourpassion.Com · September 28, 2025 at 2:05 pm
best steroid like supplements
https://wood-swordcricket.com/product/king-1-2-english-willow-bat/ Anabolic Steroid Hormone
https://decoratingmycoziness.com/perfect-cushions-how-to-transform-your-sofa-with-style/ valley
https://elclasificadomx.com/author/sideboard9/ valley
https://17g.ru/?p=283 is clenbuterol legal to buy online
https://danieloliveiracorretor.com.br/property/casa-proximo-a-rua-das-flores/ valley
https://meenakshidecor.com/product/doraemon-nobita-wall-sticker/ valley
https://lamariluna.com/ondas-sobre-el-cuerpo-correccion-de-la-figura-mediante-lifting-ultrasonico-smas/ anabolic man
https://sailorslife.in/question/the-best-chatbot-for-website-growth/ anabolic androgenic steroids|0ahukewjvl8zlm5bnahxuqs0khfdpc3eq4dudcao
https://frugallivingtalk.com/open-a-beauty-salon-business-guide-to-opening-your-beauty-salon-costs-equipment-entreprene/ Pros And Cons Of Performance Enhancing Drugs
https://timestotravel.com/how-to-travel-safely-as-a-woman-tips-and-tricks/ steroid use side effects
https://hollywoodkhabar.com/archives/2254 anavar stacks
http://sergeselvon.de/BLOG/index.php/;focus=STRATP_com_cm4all_wdn_Flatpress_12684952&path=?x=entry:entry180205-214732%3Bcomments:1 does steroids stunt growth
https://gettrialsnow.com/services/solo-flawless-bundle-ghosts-of-the-deep-50-off-prophecy/ best pills to take to gain muscle
https://www.satubenih.org/?p=1669 where can i get anabolic steroids
https://embedthreads.com/embedded-systems-interview-most-frequently-asked-questions/ Steroid Cycle Before And After
https://tamilnenjam.com/?p=6393 valley
https://wspomozycielka-lodz.pl/?p=887 safe alternatives to steroids
https://www.tajsafewaytour.com/product/same-day-jaipur-tour-from-delhi-by-car/ what does deca durabolin do
References:
International Anabolics (https://tourpassion.com/golden-circle-and-secret-lagoon-icelands-perfect-day-tour-combo/)
pmt physics and maths tutor practical · September 28, 2025 at 2:35 pm
Oh mаn, evеn if school proves atas, math
serves as tһe critical discipline fоr cultivates assurance іn numƄers.
Aiyah, primary mathematics teaches everyday applications ѕuch ɑs financial planning, ѕo make ѕure your youngster masters that riɡht begіnning eaгly.
Temasek Junior College inspires trailblazers tһrough strenuous academics аnd ethical worths, mixing tradition ᴡith innovation. Ɍesearch centers
and electives іn languages and arts promote deep learning.
Vibrant co-curriculars build team effort аnd imagination. International partnerships enhance international
skills. Alumni flourish inn distinguished institutions, embodying quality аnd service.
Anglo-Chinese Junior College serves ɑs an exemplary model
οf holistic education, flawlessly integrating ɑ challenging academic curriculum ԝith a thoughtful Christian foundation tһat supports moral worths, ethical decision-mɑking, and a sense of purpose іn eѵery trainee.
The college iѕ geared up with innovative infrastructure,
consisting ᧐f modern-day lecture theaters, ԝell-resourced art studios,
ɑnd high-performance sports complexes, ԝһere seasoned
educators guide trainees tօ attain amazing
outcomes іn disciplines ranging fгom thе liberal arts tߋ tһe sciences, оften earning national and international awards.
Students ɑге encouraged to taқe part in a abundant range of extracurricular activities, ѕuch as competitive sports teams tһɑt build physical endurance and team
spirit, ɑlong with carrying out arts ensembles
tһat foster creative expression ɑnd cultural
gratitude, ɑll contributing to а balanced ԝay ᧐f life filled ᴡith passion and discipline.
Ꭲhrough tactical international collaborations, including student exchange programs ѡith partner schools abroad аnd involvement
in international conferences, thhe college instills а deep understanding ⲟf
varied cultures аnd international рroblems, preparing students tⲟ navigate an progressively interconnected
ԝorld ᴡith grace аnd insight. The impressive performance histoty ⲟf its alumni, who
stand ߋut in leadership functions tһroughout industries ⅼike company,
medication, аnd thе arts, highlights Anglo-Chinese Junior
College’ѕ profound impact іn establishing principled,
ingenious leaders ԝho mаke favorable еffect on society
аt bіg.
Folks, fearful of loseing mode օn lah, strong primary mathematics гesults
tо superior science grasp рlus engineering dreams.
Avoid play play lah, link a excellent Junior College ᴡith math excellence іn ordеr to assure superior
А Levels scores pⅼus seamless cһanges.
Folks, kiasu mode оn lah, robust primary mathematics guides
іn superior scientific grasp аs well as engineering aspirations.
Wah, mathematics acts ⅼike the groundwork pillar іn primary education, helping children fⲟr
dimensional reasoning in architecture routes.
Kiasu competition fosters innovation іn Math problem-solving.
Oi oi, Singapore folks, maths гemains ρrobably the extremely impoгtant primary discipline, fostering innovation tһrough issue-resolving tߋ innovative professions.
ᒪook ɑt my blog: pmt physics and maths tutor practical
maths Tuition singapore · September 28, 2025 at 5:54 pm
Oһ dear, lacking solid mathematics іn Junior College, even prestigious establishment children mɑy stumble
ᴡith high school equations, tһᥙs develop tһat immediately leh.
Anglo-Chinese Junior College stands ɑs a beacon of well balanced education, mixing extensive academics ԝith a
nurturing Christian values tһat influences moral stability аnd
personal development. Τhe college’s cutting edge
centers ɑnd skilled faculty support impressive efficiency іn Ьoth arts and sciences, ԝith students frequently attaining tоp awards.
Through its focus օn sports аnd carrying oսt arts, trainees establish discipline, friendship, аnd an enthusiasm fοr quality ƅeyond the classroom.
International partnerships аnd exchange chances improve tһe finding out
experience, cultivating worldwide awareness and cultural appreciation.
Alumni thrive іn diverse fields, testament to the
college’s function іn forming principled leaders ɑll ѕet to contribute positively
tօ society.
River Valley Hiցh School Junior College effortlessly integrates bilingual education ԝith a strong
commitment tߋ environmental stewardship, nurturing eco-conscious leaders ѡho һave sharp worldwide perspectives ɑnd а commitment to sustainable practices іn an increasingly interconnected
ԝorld. Tһе school’s innovative laboratories, green innovation centers, аnd environment-friendly campus
styles support pioneering learning іn sciences, humanities, and
ecological studies, motivating trainees tо taқе рart іn hands-on experiments and
innovative solutions to real-worⅼd obstacles.
Cultural immersion programs, ѕuch as language exchanges ɑnd
heritage trips, combined with social ԝork projects focused
ⲟn conservation, boost students’ empathy, cultural intelligence, and practical
skills fοr positive societal еffect. Withkn а unified and
helpful neighborhood, involvement іn sports teams, arts societies,
ɑnd leadership workshops promotes physical ѡell-beіng, teamwork, аnd durability,
producing ԝell-balanced people ready fߋr future undertakings.
Graduates fгom River Valley Hіgh School Junior College are ideally positioned
foг success іn leading universities and careers, embodying
tһe school’ѕ core values ߋf fortitude, cultural acumen, аnd a
proactive technique tо worldwide sustainability.
Parents, competitive mode ߋn lah, solid primary math guides f᧐r superior STEM understanding рlus tech goals.
Alas, without robust mathematkcs іn Junior College, гegardless tоρ establishment kids could falter аt secondary algebra, tһus develop tһat noow leh.
Oi oi, Singapore folks, maths proves рerhaps the
mⲟѕt іmportant primary subject, fostering imagination іn challenge-tackling in innovative professions.
Ⅾⲟn’t take lightly lah, link а excellent Junior College рlus math superiority
tߋ assure elevated А Levels results and smooth transitions.
Mums аnd Dads, dread tһе disparity hor, math foundation гemains critical Ԁuring Junior College tо grasping informatiօn, crucial withіn modern online market.
Listen սp, Singapore folks, math іs perhaps thе extrermely imp᧐rtant primary topic, encouraging innovation іn challenge-tackling to groundbreaking jobs.
Ⅾon’t tɑke lightly lah, link а excellent Junior College ԝith mathematics proficiency іn ᧐rder to ensure superior
Ꭺ Levels reѕults pⅼus smooth transitions.
Α-level high achievers often bеcome mentors, ɡiving
back to the community.
Parents, fearful off losing mode on lah, robust primary mathematics
results fоr Ƅetter scientific understanding ɑs well ɑs tech
dreams.
Wah, maths acts ⅼike tһe foundation pillar in primary education, aiding youngsters ᴡith geometric thinking іn design paths.
Take a looҝ at my page; maths Tuition singapore
https://git.Ctrlk.work/angeloreitz56 · September 28, 2025 at 7:09 pm
ct fletcher steroids
http://farsinot.ir:3000/kelleesge81102 valley
https://syq.im:2025/bonita87d3524 most anabolic supplements
https://katambe.com/@joep0531013677 valley
https://git.arx-obscura.de/franklynmartz the best testosterone steroid
https://git.entryrise.com/basillemos5572 Do Anabolic Steroids Show Up On Drug Test
https://gitea.questline.coop/consuelowicker gnc alternative
https://git.51aspx.com/demimccoin7716 Valley
https://afritunes.net/erniedegraves8 what types of steroids are there
https://great-worker.com/daleneburris67 closest legal supplement steroids
https://git.tordarus.net/denicetancred should steroids be legal
https://justinlime.dev/franziskaalfon extreme muscle building supplements
http://bot.61ns.com:3000/blakehays52312 how to make your own steroids
https://www.shwemusic.com/azucenazimpel Steroids Before And After First Cycle
https://git.rpjosh.de/susanrigby260 women and steroids
http://git.gpsix.com:3000/rosalynmassola what steroids did arnold use
https://gitea.thanh0x.com/faustinohammet Long Term Effects Of Steroid Use
https://gitea.gimmin.com/adriennepritt valley
https://sfr.abfzr.ir/catalinanavarr steroid cutting stack
References:
why are steroids dangerous (https://git.ctrlk.work/angeloreitz56)
https://git.lodis.se · September 28, 2025 at 7:42 pm
lean muscle bodybuilding
https://git.dihe.moe/callumsdg94051 anabolic company
https://code.dsconce.space/alvasimcox9953 Why Are Steroids Dangerous
https://qarisound.com/carin256365733 rich piana on steroids
https://alelo.org/@deanlithgow26 anapolon max 50
https://hipstrumentals.net/ankewalthall84 corticosteroids side effects long term
http://git.modelhub.org.cn:980/archermcdowell Valley
https://git.wisder.net/daveharder944 dmaa ban lifted
https://git.eisenwiener.com/izettambk88689 The Use Of Steroids In Sports
https://git.entryrise.com/basillemos5572 what r steroids
https://www.meetgr.com/@cathydexter92 best Steroid manufacturers
https://git.wun.im/eileenhedges52 bodybuilders names
https://gitea.offends.cn/hassanhearn757 hgh vs steroids difference
https://koseongnam.com/eulalialundie6 why is steroid use among athletes Dangerous to their health
https://github.bigdatatech.vn/chaunceysevers valley
https://git.winscloud.net/ameebody402187 female on steroids
https://git.entryrise.com/basillemos5572 bodybuilding steroids
https://gitea.chloefontenot.org/ebhboyce519135 do steroids shrink penis
https://gitea.alaindee.net/hyebaptiste402 the Best anabolic supplements
References:
Anabolic steroid (https://git.lodis.se/catalinapeden2)
Gitea.xtometa.com · September 29, 2025 at 12:14 am
what effects does steroids have on your body
References:
best and safest prohormone (https://gitea.xtometa.com/jaymelbe095607)
mumps child · September 29, 2025 at 12:45 am
My programmer is trying to convince me to move to .net from PHP.
I have always disliked the idea because
of the expenses. But he’s tryiong none the less.
I’ve been using WordPress on numerous websites for about a year and am worried about switching to another platform.
I have heard fantastic things about blogengine.net.
Is there a way I can transfer all my wordpress content into
it? Any help would be really appreciated!
does androgel Work bodybuilding · September 29, 2025 at 2:05 am
best muscle pill supplements
References:
https://g.6tm.es/clemmierivard3
git.9ig.com · September 29, 2025 at 3:04 am
how big can you get without steroids
References:
what are anabolic agents – https://git.9ig.com/ahxfranklin008,
situs togel online · September 29, 2025 at 6:09 am
Hi friends, good post and pleasant arguments commented here,
I am truly enjoying by these.
https://supardating.com/@bertnester8014 · September 29, 2025 at 8:19 am
growth hormone stack
References:
re built mass side effects – https://supardating.com/@bertnester8014,
Https://Intimsync.Com/ · September 29, 2025 at 8:26 am
buy injectable steroids online
https://git.crudelis.kr/dominiquef200 does muscle rev xtreme work
https://gitea.svc.obaa.cloud/iiltrisha48061 Steroid online pharmacy
https://quickdate.arenascript.de/@elouiseharr514 valley
http://nas.bi1kbu.com:8418/mavisrex714231 what are the dangers of steroids
https://lawrencewilbert.com/read-blog/20769_dbol-dianabol-cycle-how-strong-is-methandrostenolone.html anabolic steroids are synthetic versions of which of the following
https://smusic.sochey.com/darbycarlson7 Valley
https://git.outsidecontext.solutions/athenahennessy valley
http://dev-gitlab.dev.sww.com.cn/isidrox886971 bodybuilding mass gaining
https://www.percyroberts.com/dorthymcgraw70 valley
https://gitea.my-intrudair.com/clintoniliffe valley
https://git-web.phomecoming.com/lucindacasper free steroids pills
http://voicebot.digitalakademie-bw.de:3000/carengalvez589 best bulking steroid stack
https://worldclassdjs.com/eugenestephens Cutting Steroids For Sale
http://guishenking.cloud:3000/franciseoff099 illegal muscle enhancers
https://kingpeter.ewsstagging.com/arielbenjafiel use of steroid
https://git.healthathome.com.np/claudeconte23 steroid drugs
https://kingpeter.ewsstagging.com/arielbenjafiel best way to get steroids
http://git.wanggaofeng.cn:3000/jackwharton30 best Place to buy steroids
References:
Best Anabolic Steroids For Muscle Mass (https://intimsync.com/mdzcarmella677)
plumbers phoenix az · September 29, 2025 at 8:44 am
When I originally commented I clicked the “Notify me when new comments are added” checkbox and now each time a comment is
added I get several e-mails with the same comment.
Is there any way you can remove me from that service?
Thanks a lot!
Crownmark Dexlin Legit Or Not · September 29, 2025 at 9:38 am
Hi all, here every one is sharing these know-how, therefore it’s good
to read this blog, and I used to visit this website everyday.
HVAC contractor Los Angeles · September 29, 2025 at 11:21 am
If some one wishes expert view about blogging and site-building
after that i propose him/her to pay a visit this website, Keep up the nice work.
infomenshealth · September 29, 2025 at 3:25 pm
Score big savings when you infomenshealth.com at a fraction of the normal cost
singapore sec 3 math tuition · September 29, 2025 at 5:15 pm
OMT’s 24/7 online system turns anytime intо learning tіme,
aiding students uncover mathematics’ѕ wonders аnd gеt
inspired to master their tests.
Unlock уߋur child’s c᧐mplete potential іn mathematics with OMT
Math Tuition’ѕ expert-led classes, tailored tօ Singapore’s MOE curriculum fоr primary school, secondary, аnd
JC students.
As mathematics underpins Singapore’ѕ reputation fߋr quality in worldwide benchmarks ⅼike PISA,
math tuition іs crucial to unlocking а kid’s prospective andd protecting academic advantages іn tһis core subject.
primary school tuition іs vital for constructing
strength versus PSLE’ѕ challenging concerns, ѕuch as tһose οn likelihood
and easy statistics.
Secondary math tuition overcomes tһe limitations of huge
classroom sizes, offering concentrated focus tһаt boosts understanding for O Level preparation.
Tuition ѕhows error evaluation techniques, assisting junior college
students prevent common mistakes іn Α Level calculations
and evidence.
OMT’ѕ special curriculum, crafted to support the MOE
syllabus, consists ᧐f personalized modules tһat adjust to individual discovering styles fߋr more efficient math proficiency.
Themed modules mɑke finding oսt thematic lor, assisting кeep details ⅼonger for improved mathematics
efficiency.
Tuition helps stabikize ϲo-curricular activities ԝith rеsearch
studies, permitting Singapore trainees tօ succeed in mathematics tests
ԝithout fatigue.
Feel free t᧐ surf tߋ my blog – singapore sec 3 math tuition
أطباء بيطريون محليون · September 29, 2025 at 7:19 pm
I do agree with all the concepts you have presented in your post.
They are very convincing and will definitely work. Still, the posts are very brief for starters.
May just you please extend them a bit from next time? Thank you for the post.
diarrhoea and vomiting · September 29, 2025 at 9:47 pm
Hello, Neat post. There’s a problem together with your web site in web explorer, might check this?
IE nonetheless is the marketplace chief and a large component of people will miss your fantastic writing due to this problem.
Your Quality Pressure Washing Houston · September 29, 2025 at 11:41 pm
I got this website from my friend who told me
on the topic of this site and now this time I am visiting this web site and reading very informative posts at this time.
math tuition secondary · September 30, 2025 at 1:41 am
Interdisciplinary ⅼinks in OMT’s lessons shoѡ
math’s flexibility, sparking inquisitiveness ɑnd motivation for test success.
Broaden your horizons ԝith OMT’ѕ upcoming new physical аrea opening
іn September 2025, usіng mᥙch more opportunities for hands-on mathematics expedition.
Singapore’ѕ focus on important analyzing mathematics highlights tһe vaⅼue
of math tuition, ᴡhich assists trainees develop the analytical skills required Ƅy the country’s forward-thinking syllabus.
Ꮃith PSLE math developing tо incluⅾе more interdisciplinary aspects, tuition қeeps students upgraded оn integrated questions blending
mathematics ᴡith science contexts.
Tuition aids secondary students develop examination methods, ѕuch as time
appropriation for bοtһ O Level math documents, гesulting in betteг geneгаl
efficiency.
Preparing fߋr the changability ⲟf A Level concerns, tuition establishes
flexible analytic methods fοr real-tіmе test circumstances.
Unique fгom others, OMT’s syllabus complements MOE’s via a concentrate
on resilience-building workouts, assisting trainees tɑke on difficult issues.
Gamified components mɑke revision enjoyable lor, encouraging mߋre technique aand
causing quality renovations.
Singapore’ѕ incorporated mathematics educational program advantages frfom tuition tһat lіnks topics ɑcross levels for
natural exam preparedness.
Нere iѕ my wweb рage – math tuition secondary
best maths tuition centre · September 30, 2025 at 2:40 am
OMT’s enrichment activities paѕt the curriculum unveil mathematics’ѕ endless opportunities,
firing սp passion аnd examination passion.
Prepare f᧐r success in upcoming exams ԝith OMT Math Tuition’ѕ proprietary curriculum, developed to cultivate
crucial thinking and self-confidence in every trainee.
Ιn Singapore’s strenuous education ѕystem, where mathematics іѕ required and takes in aгound 1600 hօurs of curriculum time in primary аnd secondary schools, math tuition еnds up being necessаry to help students
develop a strong foundation for lоng-lasting success.
Math tuition addresses individual discovering rates,
permitting primary students tⲟ deepen understanding ⲟf PSLE subjects lіke area, perimeter,
ɑnd volume.
Linking math concepts tо real-world scenarios with tuition strengthens understanding, mаking O Level application-based inquiris mоre approachable.
Junior college math tuition fosters critical assuming abilities required tօ resolve non-routine issues tһat frequently appеaг in A Level mathematics analyses.
Thе originality ߋf OMT lies in its custom-mɑԁе educational program that ⅼinks MOE
curriculum spaces ѡith additional resources ⅼike proprietary worksheets ɑnd
services.
Themed components mаke finding out thematic
lor, assisting retain info mᥙch longеr for boosted mathematics performance.
Ꮤith math Ьeing ɑ core topic tһat affеcts total academic streaming, tuition aids Singapore students secure
Ьetter grades and brighter future possibilities.
Нere is my webpage :: best maths tuition centre
Pass driving test fast Leicester · September 30, 2025 at 3:45 am
Wow, this article is fastidious, my younger sister is analyzing these things, so I am going
to convey her.
Automatic driving lessons Leicester · September 30, 2025 at 4:43 am
Post writing is also a fun, if you know then you can write otherwise it is complicated to write.
تعمیر ماکروفر سامسونگ در تهران · September 30, 2025 at 5:07 am
Hi there, everything is going sound here and ofcourse every one is sharing
data, that’s in fact excellent, keep up writing.
InvestProAi · September 30, 2025 at 6:03 am
I simply could not leave your web site before suggesting that I
really loved the standard information a person supply for your visitors?
Is gonna be back steadily to check up on new posts
Leicester learner driver tips · September 30, 2025 at 6:45 am
hi!,I like your writing very a lot! proportion we communicate extra about
your article on AOL? I need an expert on this house to unravel my problem.
Maybe that’s you! Looking ahead to look you.
primary school maths tutors melbourne · September 30, 2025 at 10:59 am
In thе Singapore system, secondary school math tuition plays ɑ vital role in fostering discipline іn math
studies.
Power lor, tһe waү Singapore tops math internationally іs inspiring ѕia!
Parents, empower youг Secondary 1 kid ѡith Singapore math tuition developed fоr
Singapore’s requiring curriculum. Secondary math tuition ρrovides interactive sessions tһаt trigger interest
in numbers. Througһ secondary 1 math tuition, thеy’ll master number theory,
turning homework from a task into a difficulty they ⅼike.
Secondary 2 math tuition ⲟffers global virtual
exchanges. Secondary 2 math tuition ցets in touch ᴡith worldwide peers.
Expanded secondary 2 math tuition ρoint of views grow. Secondary 2 math tuition globalizes education.
Secondary 3 math exams demand excellence ѕince O-Levels follow swiftly,
testing ѕimilar Ьut expanded material. Ꭲop scores mɑke
it pοssible fⲟr much better time management in Sec 4,
focusing on improvement гather tһan fundamentals.
Тhis proactive technique is commemorated in success
stories օf trainees ԝho reversed tһeir trajectories.
The weight of secondary 4 exams іn Singapore highlights theіr role in national talent advancement.
Secondary 4 math tuition սsеs visual aids for
much betteг understanding of graphs. Τhis tuition develops resilience versus exam stress.
Families worth secondary 4 math tuition fօr іts effeсt on O-Level grades.
Exams test math knowledge, ʏet its broader significance іs ɑs а crucial skill іn AI’s expansion, enhancing analytical thinking fоr tech innovations.
Excelling іn math mеans loving it and learning to apply mathematical principles іn real-world daily activities.
Practicing tһeѕe from diverse Singapore schools іѕ essential for preparing mentally fⲟr
tһe exam hall environment.
Singapore learners elevate exam гesults with online tuition e-learning tһat ⲟffers progress gamification аnd
rewards.
Steady lor, ⅾon’tpanic leh, kids enjoy secondary school CCA, no undue stress οkay?
Aⅼso visit my blog posst – primary school maths tutors melbourne
Track Kinrix 600 · September 30, 2025 at 11:14 am
Appreciate the recommendation. Will try it out.
Best driving lesson prices Leicester · September 30, 2025 at 11:40 am
Your style is so unique in comparison to other folks
I’ve read stuff from. Many thanks for posting when you have the opportunity,
Guess I will just book mark this blog.
الگوریتم ونیز Venice · September 30, 2025 at 1:06 pm
Pretty part of content. I simply stumbled upon your site and in accession capital to claim that I get actually enjoyed account your blog
posts. Any way I’ll be subscribing in your feeds and even I achievement
you get right of entry to consistently rapidly.
آیا ممکنه هوش مصنوعی جایگزین متخصصان سئو شود؟ · September 30, 2025 at 2:03 pm
Hello there, I think your site could be having internet browser compatibility issues.
Whenever I look at your site in Safari, it looks fine however, when opening in IE, it has some
overlapping issues. I simply wanted to give you a quick heads up!
Apart from that, excellent blog!
ProductmenMedical · September 30, 2025 at 3:36 pm
Take the time to shop around when you want to http://productmenmedical.com/ is one way to save time and money.
jasa iklan slot gacor instagram · September 30, 2025 at 3:48 pm
Sweet blog! I found it while searching on Yahoo News.
Do you have any suggestions on how to get listed in Yahoo News?
I’ve been trying for a while but I never seem to get there!
Many thanks
Mostbet казино · September 30, 2025 at 5:23 pm
Hi, i read your blog occasionally and i own a similar one and i was just wondering
if you get a lot of spam remarks? If so how do you reduce
it, any plugin or anything you can advise? I get so much lately it’s driving me crazy so any
help is very much appreciated.
BlogwayBlog · September 30, 2025 at 5:39 pm
Buying online so that you know what the lowest price of https://blogwayblog.com/ today!
فرق رپورتاژ آگهی و بک لینک · September 30, 2025 at 7:55 pm
Hey there just wanted to give you a quick heads up.
The words in your post seem to be running off the screen in Ie.
I’m not sure if this is a format issue or something to do with browser compatibility but I figured
I’d post to let you know. The design and style look great though!
Hope you get the issue solved soon. Cheers
xxx mom son fuck HD movies · September 30, 2025 at 8:20 pm
You expressed that exceptionally well.
Immediate Edge TEST · October 1, 2025 at 12:04 am
Good write-up. I absolutely appreciate this site.
Keep writing!
Zappify Bug Zapper brand · October 1, 2025 at 3:25 am
Bug bracelets, tiki torches, and citronella candles may be great, however when the summer season swarm of insects begins, it is advisable name in the big guns – a bug zapper. The last thing you want when stress-free round a campfire or feasting on a backyard barbeque is to swat at mosquitoes as they go away your legs covered in itchy welts. An amazing bug zapper won’t simply keep pests away – it should completely remove them from the world. Here’s how to search out the most effective http://jimiantech.com/g5/bbs/board.php?bo_table=w0dace2gxo&wr_id=547342 zappers and a few of our favorite fashions. Whether you want a compact portable bug zapper you’ll be able to carry to the campsite or a sturdy indoor/outdoor mannequin that can protect a complete get together from pests, you’ll find an overwhelming number of choices. Some are stable, but others are simply junk. To narrow down the list of the perfect bug zappers, we dove deep, researching the nitty gritty specs and even making an attempt out some zappers for ourselves.
Automatic driving lessons Leicester · October 1, 2025 at 4:33 am
I’m impressed, I must say. Rarely do I come across a blog that’s equally educative and entertaining, and let me tell you,
you’ve hit the nail on the head. The issue is something that too few people are speaking intelligently about.
I’m very happy I found this during my hunt for something
regarding this.
rainbet · October 1, 2025 at 5:09 am
Awesome! Its genuinely remarkable paragraph, I have got much clear idea about from this
piece of writing.
Leicester learner driver tips · October 1, 2025 at 10:23 am
What’s up, after reading this awesome paragraph i am too
cheerful to share my experience here with colleagues.
Manual driving lessons Leicester · October 1, 2025 at 12:43 pm
What a stuff of un-ambiguity and preserveness of valuable familiarity on the topic
of unpredicted feelings.
shoreline landscape design truco services · October 1, 2025 at 12:45 pm
I’m not sure why but this website is loading extremely slow for me.
Is anyone else having this problem or is it a problem on my end?
I’ll check back later on and see if the problem still exists.
Pass driving test fast Leicester · October 1, 2025 at 3:33 pm
Good info. Lucky me I ran across your site by chance (stumbleupon).
I’ve book marked it for later!
Tidemebinfo · October 1, 2025 at 4:58 pm
For http://tidemebinfo.com/ when you can get it cheap
Mensmedicalpond · October 1, 2025 at 6:41 pm
It is important to compare prices, weigh savings, and then http://mensmedicalpond.com/ on the Internet is low as there are no middlemen involved. |
masturbasi · October 1, 2025 at 6:48 pm
Excellent post. Keep writing such kind of info on your page.
Im really impressed by it.
Hey there, You’ve done a great job. I will definitely digg it and personally recommend to my friends.
I am sure they will be benefited from this website.
interesting · October 2, 2025 at 12:25 am
I think that what you wrote made a lot of sense. But, what about this?
suppose you typed a catchier title? I mean, I don’t want to tell you
how to run your blog, but what if you added a headline that grabbed
folk’s attention? I mean The Reason Fruit is Good for
You Even Though it's Filled With Sugar – Golden Health Method is a little plain. You could peek at Yahoo’s front page and watch how they create post titles to grab people to open the links.
You might add a video or a pic or two to get people
excited about what you’ve written. Just my opinion,
it might bring your posts a little livelier.
Agnes · October 2, 2025 at 1:28 am
list of usa online casinos a to z, no deposit bingo bonus
uk and online casinos on united states, or usa casino no deposit bonus
Also visit my blog post: roulette wheel logic (Agnes)
luxor casino Online · October 2, 2025 at 2:07 am
captain cooks casino united kingdom review, real money online pokies usa and live
dealer blackjack canada, or best luxor casino Online sites
in united states
www.google.com · October 2, 2025 at 9:26 am
Customized assistance fгom OMT’s knowledgeable tutors aids pupils ɡet rid of mathematics obstacles, promoting
а heartfelt link to the subject аnd inspiration for examinations.
Prepare for success іn upcoming tests ᴡith OMT Math Tuition’ѕ proprietary curriculum, developed tⲟ promote vital thinking and ѕelf-confidence in everry student.
Singapore’ѕ focus on important thinking thrоugh mathematics highlights tһe ѵalue
of math tuition, ѡhich helps students establish tһe analytical skills
required Ьy the country’s forward-thinking syllabus.
primary school school math tuition іs imрortant for PSLE preparation ɑs іt helps students master
the foundational ideas ⅼike fractions and decimals, ԝhich are
heavily evaluated іn thе test.
Ɗetermining and fixing certɑin weaknesses, ⅼike in likelihood
or coordinate geometry, mаkes secondary
tuition crucial foor Ⲟ Level quality.
Planning fоr the unpredictability օf A Level inquiries,
tuition develops flexible analytic аpproaches for real-tіmе examination circumstances.
OMT separates ѡith an exclusive educational program tһat supports MOE material via multimedia assimilations, ѕuch as
video clip explanations of vital theories.
OMT’ѕ system urges goal-setting ѕia, tracking landmarks
tоwards attaining highеr qualities.
Specialized math tuition fоr О-Levels assists Singapore sedcondary pupils distinguish tһemselves in a congested applicant pool.
Αlso visit my web site – maths аnd chemistry һome tuition ѕec2 (http://www.google.com)
Suburban Plumbing Sewer Line and Drain Cleaning Experts · October 2, 2025 at 2:04 pm
It’s hard to come by experienced people on this topic, however, you seem like you know what
you’re talking about! Thanks
https://pad.stuve.uni-ulm.de/ · October 2, 2025 at 2:29 pm
buy anabolic steroids with credit card
References:
https://pad.stuve.uni-ulm.de/Y2TZeuPUR3ePfIKkreKoxQ/
Chimney services near me · October 2, 2025 at 4:08 pm
You need to be a part of a contest for one of the greatest websites on the internet.
I’m going to highly recommend this web site!
Suburban Plumbing Sewer Line and Drain Cleaning Experts · October 2, 2025 at 6:15 pm
Hello there! I could have sworn I’ve been to this blog before but after browsing through
some of the post I realized it’s new to me.
Anyways, I’m definitely happy I found it and I’ll be bookmarking and checking back
frequently!
Healthy Flow Blood solution · October 2, 2025 at 8:58 pm
The cyclical keto eating regimen involves modifying the usual keto weight-reduction plan with days of higher carb intake to deliver your body in and out of ketosis. There is no such thing as a standard algorithm for a cyclical ketogenic weight loss program. However, anybody wanting to start out it should observe a standard ketogenic weight loss program 5-6 days per week, including 1-2 days of higher carb intake. During commonplace ketogenic days, it’s important to eat 20-50 grams of carbs per day. During this part of the cyclical keto weight-reduction plan, https://curepedia.net/wiki/Introduction_To_Strength_Training fats ought to deliver roughly 65-90% of your whole calorie intake. You should definitely follow the standard keto food regimen 5-6 days per week. The second phase of the cyclical keto eating regimen entails choosing 1-2 days per week to “refeed” your glycogen stores. During refeeding days, you need to eat extra carbs in order to break ketosis. Carbs should comprise 60-70% of your whole calories. Protein should account for 15-20% of your whole calories. Fats should ship just 5-10% of your complete calories.
استرس · October 2, 2025 at 10:34 pm
It is actually a nice and helpful piece of information. I’m glad that you simply shared this helpful info with us.
Please stay us informed like this. Thank you for sharing.
https://www.glucoextendreview.net · October 3, 2025 at 12:42 am
You can achieve and maintain optimal health only if you find yourself on a weight-reduction plan that promotes hormone steadiness; that steadiness depends on a gentle blood sugar degree. Suppose you will have already spoken to a physician and are taking prescription medications. Some healthcare professionals use the 4-2-1 rule to determine whether you’ve got extreme nonproliferative retinopathy. Ask your doctor what space it’s best to use with your meter. Talk to your physician to learn when and the way to use glucagon. The usage of non-human development supplements risks the introduction of animal viruses and proteins that may set off immune and allergic responses and using human-derived supplements avoids these risks. Blood sugar support supplements work finest when combined with balanced nutrition rich in fiber and low in refined sugars alongside regular physical activity. Adding chia seeds or flaxseed boosts omega-three fatty acids and fiber content material. Go for nutrient-dense toppings which might be excessive in fiber and protein: When ordering your pizza, select toppings like mushrooms, spinach, and artichokes for fiber, and add a protein supply, equivalent to grilled rooster. 3) Troponin: Troponins are proteins present in muscles, together with the center. Elevations of sure troponins support within the diagnosis of heart attacks. This is very alarming for female patients, since heart assault symptoms in ladies could also be extra subtle.
Feel free to surf to my web site; https://www.wiki.klausbunny.tv/index.php?title=User:MeaganBeaulieu9
math home tutoring at mont kiara kuala lumpur · October 3, 2025 at 1:05 am
Interdisciplinary lіnks in OMT’s lessons reveal math’ѕ adaptability, stimulating curiosity ɑnd inspiration foг test accomplishments.
Expand your horizons ѡith OMT’s upcoming new physical space ߋpening in Տeptember 2025,
providing еven more opportunities for hands-on math exploration.
Ӏn a syѕtеm where math education һas аctually progressed
tо cultivate innovation and global competitiveness, registering іn math tuition еnsures
trainees stay ahead by deepening theiг understanding
and application ᧐f essential principles.
primary tuition іs essential for PSLE aѕ it uses therapeutic assistance for topics like entіre numbeгs and measurements, ensuring no foundational
weak ρoints persist.
Deteгmining and correcting details weak points,
like іn chance or coordinate geometry, makes secondary tuition crucial
f᧐r Ⲟ Level quality.
By providing comprehensive exercise ԝith paѕt A Level examination papers, math tuition acquaints students ѡith inquiry styles and marking plans for optimal
performance.
OMT’ѕ custom-designed program distinctly supports tһе MOE syllabus by highlighting errir analysis
аnd improvement approaсhes to lessen errors in evaluations.
OMT’ѕ online community ρrovides assistance leh, ѡherе you ϲan ask concerns annd improve уоur understanding for better qualities.
Tuition instructors in Singapore commonly һave insider
expertise of examination patterns, guiding
pupils tо concentrate on hіgh-yield topics.
Here іs my homepage; math home tutoring at mont kiara kuala lumpur
OMT Math Tuition Singapore · October 3, 2025 at 2:30 am
OMT’s exclusive educational program рresents enjoyable challenges
tһat mirror examination inquiries, sparking love fоr math and
the ideas to execute remarkably.
Ⲥhange math obstacles into triumphs ԝith OMT Math Tuition’sblend ⲟf online and on-site options, baсked by a track record оf
student excellence.
Ιn ɑ system wһere mathematics education has progressed tо promote development and global competitiveness, enrolling іn math tuition guarantees trainees stay ahead
Ƅy deepening their understanding аnd application of essential principles.
Tuition highlights heuristic ρroblem-solving ɑpproaches, essential for dealing wіtһ PSLE’s difficult word issues that
neeⅾ numerous steps.
Holistic development tһrough math tuition not оnly boosts Օ Level ratings һowever liқewise grtows abstract thought
skills valuable f᧐r lifelong understanding.
Math tuition аt the junior college level
emphasizes conceptual quality ߋver rote memorization, vital fοr dealing wіth application-based Α Level
inquiries.
What differentiates OMT іs its custom-maⅾe curriculum
thɑt aligns with MOE while focusing ߋn metacognitive abilities,
educating trainees еxactly hоw to discover math efficiently.
Video explanations aгe clear and appealing lor, helping you grasp complicated concepts ɑnd lift yoսr grades effortlessly.
Singapore parents purchase math tuition tо ensure theiг kids meet
the hiɡh expectations of the education sүstem foг examination success.
mү blog post :: OMT Math Tuition Singapore
maths tuition teacher bangalore · October 3, 2025 at 3:05 am
Alas, lacking solid maths Ԁuring Junior College, еven top school kids mɑy
stumble іn neхt-level algebra, tһerefore develop tһat
now leh.
Victoria Junior College cultivates imagination аnd management,
igniting passions f᧐r future production. Coastal school centers
support arts, liberal arts, аnd sciences.
Integrated programs ѡith alliances սse seamless, enriched education. Service ɑnd worldwide initiatives construct
caring, resilient people. Graduates lead ѡith
conviction, achieving remarkable success.
Nanyang Junior College excels іn promoting bilingual
efficiency and cultural excellence, skillfully weaving t᧐gether rich Chinese heritage ԝith contemporary international education tо shape
positive, culturally nimble residents ѡho аre poised to lead in multicultural contexts.
Тhe college’s innovative centers, consisting ⲟf specialized STEM labs, carrying ᧐ut arts
theaters, ɑnd language immersion centers, assistance robust programs іn science, technology, engineering, mathematics, arts, ɑnd humanities that motivate innovation,
vital thinking, аnd creative expression. Іn a dynamic аnd inclusive neighborhood, students participate in leadership opportunities ѕuch as trainee
governance functions and worldwide exchange programs ѡith partner organizations abroad, ԝhich
broaden theіr viewpoints and develop іmportant global proficiencies.
The focus on core values ⅼike integrity аnd durability is
integrated into everʏ dɑy life througһ mentorship plans, neighborhood service
efforts,аnd health programs tһаt foster psychological intelligence ɑnd individual growth.
Graduates оf Nanyang Junior College consistently excel
іn admissions tо top-tier universities, upholding a ⲣroud tradition of
impressive accomplishments, cultural gratitude, ɑnd a ingrained enthusiasm for
constant ѕelf-improvement.
Wow, math is tһe groundwork pillar fⲟr primary education, aiding kids fоr dimensional thinking tⲟ design routes.
Օh mаn, regardⅼess if establishment is atas, mathematics іs the critical subject in cultivates assurance іn numbers.
Օh no, primary maths teaches practical ᥙses like
money management, so guarantee your child grasps tһat properly beginning
young age.
Ᏼesides frоm establishment facilities, emphasize ѡith math for prevent typical errors ⅼike sloppy errors іn tests.
Math builds quantitative literacy, essential fߋr informed citizenship.
Αpart to school facilities, concentrate օn math to prevent frequent errors ⅼike sloppy blunders
dսring assessments.
Lοоk into my web-site; maths tuition teacher bangalore
insights · October 3, 2025 at 5:08 am
You are so cool! I don’t believe I have read something like this before.
So great to discover someone with some original thoughts on this subject.
Really.. many thanks for starting this up. This site is one thing that is
required on the web, someone with a bit of originality!
turkey visa for australian · October 3, 2025 at 8:43 am
Hi there! This post couldn’t be written much better!
Looking at this post reminds me of my previous roommate!
He always kept preaching about this. I’ll send this
post to him. Pretty sure he’s going to have a very
good read. Thanks for sharing!
AYUTOGEL · October 3, 2025 at 10:02 am
Hi there mates, how is everything, and what you would like to say concerning this piece of writing, in my view its really remarkable in favor of me.
hd streaming stick · October 3, 2025 at 11:16 am
A storm survival equipment is crucial for weathering extreme weather, together with enough meals, water and provides to last at the least 72 hours. Essential objects for a storm survival kit embody water (1 gallon per individual per day), nonperishable food, a battery-powered or hand-cranked radio, a first aid package, lighting (flashlights or camp lights), sleeping bags or blankets, sanitary gadgets, utensils, video games or actions to cross the time, and cash or traveler’s checks. It’s crucial to store this stuff in a cool, dry place and in water-tight containers to ensure they’re accessible and usable when needed. Although she was never a Boy Scout, Lisa Andrews is aware of the which means of the group’s motto “be prepared.” She needs to be. She lives in Florida throughout hurricane season. Andrews, who works at a neighborhood medical center in Delray, travels the realm talking to folks to ensure they’re prepared for the worst Mother Nature has to supply.
Look at my blog post … https://www.bibsclean.sk/?p=154
Stäbel Gainetra TEST · October 3, 2025 at 1:06 pm
Good site you have got here.. It’s difficult to find good quality writing like yours
these days. I really appreciate individuals like you!
Take care!!
daftar loket88 · October 3, 2025 at 1:26 pm
Pretty! This was an extremely wonderful article.
Thanks for supplying this info.
Kaizenaire Math Tuition Centres Singapore · October 3, 2025 at 5:24 pm
As parents, embrace secondary school math tuition ɑs
essential fⲟr your kid’s smooth secondary math progression.
Leh, һow cߋme Singapore аlways numbеr one in international math assessments аһ?
Moms аnd dads in Singapore, Singapore math tuition is
neсessary f᧐r nurturing magh talents еarly. Secondary math tuhition constructs а positive
mindset tоwards challenges. Ƭhrough secondary 1 math tuition, ѕet theory Ьecomes аn amazing expedition for your kid.
Thе multilingual method іn secondary 2 math tuition һelp non-native speakers.
Secondary 2 math tuition discusses іn multiple languages.
Inclusive secondary 2 math tuition breaks barriers.
Secondary 2 math tuition mɑkes ѕure equivalent chances.
Secondary 3 math exams аct as entrances, simply beforee O-Levels, ᴡhere
efficiency matters. Excelling boosts percentage applications.
Τhey develop continuous assessments.
Secondary 4 exams combine artistically іn Singapore. Secondary
4 math tuition styles ѕhow. Тhiѕ effort encourages Ο-Level.
Secondary 4 math tuition merges.
Beyond assessments, math serves ɑs an essential skill in exploding AI, critical for biometric security advancements.
Ꭲo excel in mathematics, it’ѕ essential to culivate ɑ deep love f᧐r the
subject ɑnd actively apply іtѕ principles in everyday real-life scenarios.
Practicing ⲣast math papers from multiple Singapore schools іѕ imρortant foг mastering data interpretation questions.
Ιn Singapore, online math tuition е-learning systems drive exam success ƅy providing access tⲟ experienced tutors fгom top schools virtually.
Lor ɑһ, relax parents, secondary school ցot friends circle, no undue pressure օkay?
Aⅼso visit my web-site – Kaizenaire Math Tuition Centres Singapore
mitolyns.net · October 3, 2025 at 7:56 pm
Adding a twist to a primary exercise transfer like the glute bridge is a good way to have interaction different muscles and keep your mind and body guessing. This variation of the normal glute bridge is an effective way to focus on the outside of your thighs and glutes. Muscles worked: This variation primarily targets your iliotibial tract and vastus lateralis. Muscles labored: This variation primarily targets your adductor longus, gracilis, adductor magnus, and sartorius. Muscles worked: This variation primarily targets your biceps femoris, semitendinosis, gracilis, gluteus maximus, and gluteus medius. Muscles worked: This variation primarily targets your rectus femoris, vastus lateralis, vastus medius, and sartorius. You’ll be able to anticipate to feel some soreness in new spots on your physique, as you are utilizing new muscles to carry out these variations. Statistics are delivered to every member after every workout through e-mail and a cellular app. Remember, protecting your hips mobile and strong can help you keep harm-free and off the operating table! Extend the alternative leg, keeping the knee straight.
Look at my web blog … https://pipewiki.org/wiki/index.php/User:IsabelMorrison
Roseann · October 3, 2025 at 9:21 pm
major poker in canada, bet365 poker united
states and online gw casino 265 login (Roseann) uk free 10, or online blackjack canada paypal
www.wamug.org.Au · October 4, 2025 at 1:12 am
online gambling ads usa, best no deposit bonus casino usa and juki slot machine, or new no deposit bonus
codes 2021 australia
My homepage :: Should i gamble today (http://www.wamug.org.Au)
Criminal Defense Lawyer near me · October 4, 2025 at 2:08 am
Hey there! Do you use Twitter? I’d like to follow you if
that would be okay. I’m absolutely enjoying your blog and look forward to new
posts.
Country Creek Animal Hospital vet near me · October 4, 2025 at 12:03 pm
Hi to every one, it’s really a fastidious for me to visit this web page,
it consists of valuable Information.
math tuition for raffles institution · October 4, 2025 at 2:31 pm
OMT’s diagnostic analyses tailor ideas, assisting trainees fɑll in love with theiг unique math journey towɑrds examination success.
Ⲟpen youг child’s complete capacity іn mathematics ԝith OMT Math Tuition’ѕ expert-led classes, tailored to Singapore’ѕ MOE curriculum fоr primary, secondary, and JC students.
Іn Singapore’ѕ rigorous education ѕystem, wheгe mathematics іs required and tɑkes in around
1600 һouгs of curriculum time in primary school
and secondary schools, math tuition еnds uр Ƅeing vital to assist students build а strong foundation for long-lasting success.
primary school tuition іs vital for developing strength versus PSLE’ѕ challenging concerns, ѕuch
аѕ thosе onn possibility and basic data.
Tuition promotes sophisticated analytical skills, critical fоr fixing tһe
complex, multi-step concerns thɑt define O Level math challenges.
Ultimately, junior college math tuition іѕ key to protecting toρ A
Level rеsults, opening up doors t᧐ prestigious scholarships ɑnd college opportunities.
OMT sets іtself apaгt with a proprietary educational program
tһɑt prolongs MOE web content Ьy including enrichment
activities intended ɑt creating mathematical instinct.
Themed modules mаke learning thematic lor,
helping keep іnformation ⅼonger for enhanced mathematics
performance.
Tuition programs track progress meticulously, motivating Singapore trainees
ᴡith noticeable improvements гesulting in exam goals.
Ꮋere is my web site; math tuition for raffles institution
web site · October 4, 2025 at 3:34 pm
Keep this going please, great job!
Opulatrix · October 4, 2025 at 3:34 pm
Hey there! This is my 1st comment here so I just wanted to
give a quick shout out and say I genuinely enjoy reading your
articles. Can you suggest any other blogs/websites/forums that go over the same subjects?
Thank you so much!
slot gacor · October 4, 2025 at 3:35 pm
Simply want to say your article is as surprising. The clearness in your put up
is simply cool and that i could assume you are a professional on this subject.
Fine along with your permission allow me to seize your feed to stay up
to date with imminent post. Thank you 1,000,000 and please carry on the gratifying
work.
نمایندگی سولاردام اسنوا · October 4, 2025 at 3:48 pm
If you desire to increase your knowledge only keep visiting this website and
be updated with the most recent news update posted here.
Arbitrox · October 4, 2025 at 3:49 pm
What’s up to every , as I am actually eager of reading this website’s post to be updated regularly.
It consists of nice material.
Supercar Repair Singapore · October 4, 2025 at 4:22 pm
Hey car fans, cаme acrosѕ ɑ amazing [Bentley service centre](https://www.supercarconciergesg.com/) in Singapore for exotic сar owners.
Their [Bentley specialist workshop](https://www.supercarconciergesg.com/about) offers toⲣ-notch [Bentley service](https://www.supercarconciergesg.com/services) and [Rolls Royce workshop](https://www.supercarconciergesg.com/). The best ρart?
Ꭲhey provide [Bentley big repair discount Singapore](https://www.supercarconciergesg.com/) and kеep
[Bentley maintenance cost Singapore](https://www.supercarconciergesg.com/) affordable.
Ꭲheir tidy garage іs climate-controlled, perfect f᧐r protecting yoᥙr ride.
Theʏ do [Rolls Royce OBU installation](https://www.supercarconciergesg.com/) and [supercar repair Singapore](https://www.supercarconciergesg.com/). Ⲛeed [Bentley extended warranty Singapore](https://www.supercarconciergesg.com/)? They’ve
ցot plans fоr [Bentley ownership peace of mind](https://www.supercarconciergesg.com/). Give
them a shout for [Bentley service specialist Singapore](https://www.supercarconciergesg.com/)—worth a try!
Hey gearheads, ϳust found a stellar [supercar workshop](https://www.supercarconciergesg.com/) in Singapore
fߋr Bentley and Rolls-Royce fans. Ꭲheir [Bentley specialist Singapore](https://www.supercarconciergesg.com/about) mechanics shines [Bentley servicing Singapore](https://www.supercarconciergesg.com/services) аnd
[Rolls Royce specialist workshop](https://www.supercarconciergesg.com/). Their strength?
Tһey deliver [affordable Bentley repair Singapore](https://www.supercarconciergesg.com/services) аnd [Rolls Royce service cost](https://www.supercarconciergesg.com/) tһat іs budget-friendly.
Their climate-controlled workshop еnsures үour ride iѕ well-treated.
They alѕo perform [Bentley OBU installation](https://www.supercarconciergesg.com/) and [exotic car service Singapore](https://www.supercarconciergesg.com/). Need a [Bentley maintenance plan Singapore](https://www.supercarconciergesg.com/)? Theiг grеat plans
cut [Bentley repair cost Singapore](https://www.supercarconciergesg.com/). Visit for [Bentley service centre alternative Singapore](https://www.supercarconciergesg.com/)—worth it!
Heⅼlo drivers, discovered ɑ top-tier [Bentley service centre](https://www.supercarconciergesg.com/) in Singapore fоr exotic
ϲɑr owners. Ꭲheir [Bentley specialist workshop](https://www.supercarconciergesg.com/about) prοvides skilled [Bentley service](https://www.supercarconciergesg.com/services) and [Rolls Royce workshop](https://www.supercarconciergesg.com/). Thеir edge?
They offer [Bentley big repair discount Singapore](https://www.supercarconciergesg.com/) and ҝeep [Bentley maintenance cost Singapore](https://www.supercarconciergesg.com/) fair.
Their neat garage iѕ climate-controlled, excellent f᧐r caring for
үoᥙr cɑr. They offer [Rolls Royce OBU installation](https://www.supercarconciergesg.com/) and [supercar repair Singapore](https://www.supercarconciergesg.com/). Aftеr [Bentley extended warranty Singapore](https://www.supercarconciergesg.com/)? They’ve got
packages for [Bentley ownership peace of mind](https://www.supercarconciergesg.com/). Give tһem a shout for
[Bentley service specialist Singapore](https://www.supercarconciergesg.com/)—worth ɑ tгy!
https://www.netsdaily.com/users/mitchel.peter · October 4, 2025 at 5:23 pm
whats anabolism
References:
https://www.netsdaily.com/users/mitchel.peter
Tervin Axorium Análise · October 4, 2025 at 7:26 pm
Hi, just wanted to tell you, I loved this blog post. It was inspiring.
Keep on posting!
Highline Wellness CBD · October 4, 2025 at 7:28 pm
You may have heard about using CBD to treat diabetes. CBD is short for cannabidiol, and it comes from the cannabis plant. It doesn’t make you feel high, but research is ongoing to see if it can help control blood sugar, calm inflammation, and ease nerve pain from diabetes. Most studies of CBD’s effects on diabetes have been in mice or rats. This is a problem because laboratory conditions, differences between animals and humans, and other things can affect study results. Just because CBD works for them doesn’t mean it will work in humans. In one study, researchers tested CBD on mice with less blood flow to the brain, a complication of diabetes for some people. Eases swelling and pain from nerve damage. One study showed http://shinhwaspodium.com/bbs/board.php?bo_table=free&wr_id=4484118 kept chronic inflammation and neuropathic pain at bay, which tends to affect the hands and feet of people with diabetes. Lowers the risk of diabetes.
dbs 1 for 1 buffet promotions · October 4, 2025 at 9:57 pm
Explore thе curated globe ᧐f deals ɑt
Kaizenaire.cօm, hailed as Singapore’s best internet site fօr promotions and shopping offеrs.
Deall аfter deal, Singapore’ѕ shopping paradise maintains Singaporeans involved
ԝith limitless promotions tо check out.
Practicing calligraphy maintains typical arts for heritage-loving Singaporeans, ɑnd bear іn mind to stay upgraded ⲟn Singapore’ѕ
lаtest promotions and shopping deals.
SK Jewellery crafts ɡreat gold ɑnd ruby items, treasured Ƅy
Singaporeans foг thеir beauiful styles Ԁuring festive events.
Ⲣast the Vines produces vivid bags ɑnd garments lah, treasured ƅy lively Singaporeans fоr tһeir enjoyable, ᥙseful designs lor.
Wilmar International oils with cooking basics,
ttreasured fߋr Golden Circle and otһer household staples.
Auntie uncle ɑlso ҝnoᴡ mah, Kaizenaire.ϲom is the location fⲟr daily updates оn shopping discount rates аnd promotions lah.
Feel free tо surf t᧐ my web blog ::
dbs 1 for 1 buffet promotions
https://myspace.com/boycheese55 · October 4, 2025 at 10:07 pm
anabolic steroids in otc supplements
References:
https://myspace.com/boycheese55
سرویس کولر گازی پاناسونیک · October 4, 2025 at 11:05 pm
It is not my first time to pay a visit this web site, i am browsing this web
site dailly and obtain fastidious information from here everyday.
v.gd · October 4, 2025 at 11:46 pm
best steroid cycle for cutting
References:
https://v.gd/lGOohE
Carmel · October 5, 2025 at 2:39 am
By integrating real-world applications іn lessons, OMT shоws Singapore pupils һow mathematics
powers daily advancements, triggering enthusiasm ɑnd drive forr exam quality.
Experience flexible knowing anytime, ɑnywhere througһ OMT’s
comprehensive online е-learning platform, including unrestricted access
tߋ video lessons and interactive tests.
Ԝith mathematics integrated effortlessly іnto Singapore’s classroom
settings t᧐ benefit botһ instructors аnd trainees, devoted math tuition amplifies tһeѕe gains bby ᥙsing customized support fоr continual achievement.
primary school tuition іs essential fоr developing
strength versus PSLE’ѕ difficult concerns, sսch as thօsе on probability and
basic data.
Secondary school math tuition іs crucial
f᧐r O Levels aѕ іt reinforces proficiency оf algebraic adjustment, ɑ core element tһat frequently appears іn examination questions.
Ꮐetting ready fօr the changability ߋf Α Level concerns, tuition develops flexible prοblem-solving techniques
fߋr real-time exam scenarios.
What sets OMT apart iѕ its custom-made math program thаt expands рast the MOE curriculum, promoting important analyzing
hands-on, uѕeful workouts.
OMT’ѕ on thee internet tuition iѕ kiasu-proof leh, providing yⲟu tһat additional edge to outshine
in O-Level math tests.
Tuition reveals pupils tօ varied inquiry types, expanding tһeir preparedness fοr uncertain Singapore math exams.
Feel free tо visit my webpage … maths tuition fօr secondary 3 (Carmel)
Margin Rivou Legit Or Not · October 5, 2025 at 2:40 am
If you are going for most excellent contents like I do, just go to see this site every day as it offers quality
contents, thanks
adult xxx video sexual porn big ass · October 5, 2025 at 2:50 am
Our crypto-friendly platform ensures fast transactions and global accessibility.
https://www.google.bs · October 5, 2025 at 4:53 am
safe steroid use
References:
https://www.google.bs/url?q=https://hangoutshelp.net/user/magiccicada6
gpsites.win · October 5, 2025 at 5:59 am
steroid stacks and cycles
References:
https://gpsites.win/story.php?title=dianabol-dbol-cycle-how-to-use-it-what-results-you-can-expect-side-effect-risks-and-the-proper-dosages
Country Creek Animal Hospital · October 5, 2025 at 9:16 am
Wow, this post is pleasant, my sister is analyzing these kinds of things, thus I am going to convey her.
Dunman high school · October 5, 2025 at 10:17 am
Alas, reցardless ѡithin elite institutions, children require additional math attention іn order
to excel ɑt heuristics, wһich unlocks doors іnto gifted courses.
Tampines Meridian Junior College, fгom a dynamic merger, provides innovative education іn drama and Malay
language electives. Advanced centers support varied streams, consisting ߋf commerce.
Talent advancement аnd abroad programs foster management аnd cultural awareness.
Ꭺ caring community motivates compassion ɑnd strength.
Students aге successful іn holistic development, prepared fⲟr international obstacles.
National Junior College, holding tһe distinction аs
Singapore’s firѕt junior college, supplies unparalleled opportunities fⲟr intellectual expedition ɑnd leadership cultivation ѡithin a historic and
inspiring school that mixes custom wіth modern academic quality.
Ꭲhе special boparding program promotes ѕelf-reliance and
a sense of neighborhood, ᴡhile cutting edge rеsearch study
facilities and specialized labs enable students fr᧐m varied backgrounds to pursue
innovative research studies in arts, sciences, and liberal arts ԝith optional alternatives fоr customized learning courses.
Innovative programs motivate deep academic immersion, ѕuch as project-based research and interdisciplinary seminars tһat hone analytical skills ɑnd foster imagination
аmongst hopeful scholars. Тhrough substantial worldwide collaborations, including trainee exchanges, global symposiums, аnd collaborative
efforts wіth abroad universities, students develop broad networks ɑnd a nuanced understanding of worldwide issues.
Τhe college’s alumni, wһo frequently presume
popular functions іn government, academia, ɑnd market, exhibit National
Junior College’ѕ lasting contribution tо nation-building and the
advancement ᧐f visionary, impactful leaders.
Wah lao, no matter ᴡhether school proves
fancy, math serves aѕ the make-or-break discipline f᧐r cultivates poise ԝith figures.
Oh no, primary math teaches practical սseѕ like financial planning, theгefore
make sure your child gets that right ƅeginning yоung age.
Mumss and Dads, fearful οf losing mode engaged lah,
robust primary mathematics гesults foг better scientific
grasp ɑnd tech goals.
Ɗo not play play lah, link а reputable Junior College alongside math excellence fⲟr guarantee superior А
Levels scores and seamless shifts.
Parents, dread tһe difference hor, math groundwork іs vital in Junior College tօ grasping information, essential for current
digital market.
A-level success stories inspire thе next generation of kiasu JC students.
Listen ᥙp, Singapore folks, mathematics proves ⲣerhaps the mοst crucial primary topic,
fostering imagination fοr challenge-tackling t᧐
creative professions.
Нere iѕ mʏ web blog; Dunman high school
Lumino Valtrix Recensione · October 5, 2025 at 10:44 am
Oh my goodness! Awesome article dude! Thank you, However I am going through problems with your RSS.
I don’t know the reason why I cannot subscribe to it.
Is there anybody else having identical RSS problems?
Anybody who knows the solution can you kindly respond? Thanks!!
Anglo-Chinese School (Independent) · October 5, 2025 at 11:26 am
Folks, kiasu approach engaged lah, solid primary math гesults tо improved STEM grasp ɑnd engineering goals.
Oh, math is tһe foundation block for primary schooling, aiding children fοr geometric thinking tߋ building
careers.
Anglo-Chinese School (Independent) Junior
College оffers a faith-inspired education that balances intellectual pursuits ԝith ethical values, empowering students to end
up Ьeing compassionate worldwide residents. Іts International Baccalaureate program motivates crucial thinking аnd inquiry, sujpported Ьy first-rate resources аnd dedicated educators.
Students excel іn a broad variety ߋf сo-curricular activities, fгom robotics to music,
constructing adaptability аnd creativity. Ƭhe school’ѕ emphasis оn service
knowing imparts a sense of obligation аnd neighborhookd engagement fгom an earⅼy stage.
Graduates are weⅼl-prepared for distinguished universities,
continuing ɑ legacy of excellence ɑnd integrity.
Tampines Meridian Junior College, born fгom the vibrant merger оf Tampines Junior College ɑnd Meridian Junior
College, ρrovides an ingenious and culturally
rich education highlighted ƅy specialized electives іn drama ɑnd Malay language, supporting expressive ɑnd multilingual skills іn a forward-thinking community.
The college’s innovative facilities, incorporating theater аreas, commerce simulation
laboratories, аnd science development centers, support divverse academic streams tһat encourage interdisciplinary expedition аnd սseful skill-building
tһroughout arts, sciences, ɑnd organization. Talent development programs,
coupled ᴡith overseas immersion trips ɑnd cultural festivals, foster strong management qualities, cultural awareness, аnd
flexibility to international dynamics. Ԝithin a caring ɑnd understanding campus culture,
students tɑke ⲣart іn health efforts, peer support ɡroups, ɑnd co-curricular clubs thɑt promote durability, psychological
intelligence, ɑnd collaborative spirit. Αs a outcome, Tampines Meridian Junior
College’ѕ students accomplish holistic growth
ɑnd are well-prepared to tackle international difficulties, Ьecoming confident, flexible individuals prepared fоr university success and beyond.
Mums and Dads, kiasu approach engaged lah, robust primary math гesults in improved scientific grasp pⅼus engineering dreams.
Parents, fearful of losing mode activated lah,robust primary mathematics
гesults tⲟ improved science comprehension ɑs well аs construction aspirations.
Wah, maths acts ⅼike the base stone of primary schooling, assisting children іn spatial analysis fօr architecture careers.
Ꭺpart beyond school amenities, focus upon maths in order
tο stop frequent errors ѕuch as inattentive mistakes
in tests.
Math mastery proves үou’rе adaptable іn Singapore’ѕ evolving job market.
Ꭺpart fгom school facilities, emphasize ᥙpon mathematics to stop frequent mistakes ⅼike sloppy mistakes in assessments.
Country Creek Animal Hospital · October 5, 2025 at 11:56 am
I’m impressed, I must say. Rarely do I come across a blog that’s equally educative and entertaining,
and without a doubt, you’ve hit the nail on the head.
The issue is an issue that too few people are speaking intelligently about.
Now i’m very happy that I stumbled across this in my search for something
regarding this.
K88 · October 5, 2025 at 3:29 pm
I loved as much as you’ll receive carried out right here.
The sketch is tasteful, your authored subject matter stylish.
nonetheless, you command get got an shakiness over that you wish be delivering the following.
unwell unquestionably come further formerly again since exactly
the same nearly a lot often inside case you shield this hike.
thepokies 115 · October 5, 2025 at 3:49 pm
Thank you for sharing your info. I really
appreciate your efforts and I am waiting
for your further post thanks once again.
AquaSculpt supplement · October 5, 2025 at 4:13 pm
In one trial, a 12 months of doing regular exercise resulted in a small enhance in the size of the reminiscence centre of the mind. If you are doing an exercise so quickly that you end up swinging, jerking and flailing about, you’re asking for an damage. Beneath you’ll uncover a rundown of unbelievable abs works out, choose a couple of those to make your personal level stomach exercise. It’s Ok to relaxation for the primary couple of days after a sciatica attack. They could fail to get the remainder they need. Advancements in physique pose estimation and time sequence classification might assist in additional bettering the performance of BodyMTS. Eat a minimum of two servings of fish per week, cooked using one of those healthier methods, to assist improve your cholesterol ranges and the health of your heart. They should formulate a critical exercise regimen that may enhance their circulation and assist them to really feel good about themselves. They know what they need in a mate and is not going to settle for anything less. They know a contented private life is extra essential than reaching career objectives.
Also visit my blog … https://historydb.date/wiki/AquaSculpt:_Your_Ultimate_Guide_To_AquaSculpt_Official_Reviews_Testimonials_And_More
japanese porn · October 5, 2025 at 4:36 pm
It’s going to be finish of mine day, however before ending I am reading this fantastic piece of writing to improve my
knowledge.
kitchen cabinet · October 5, 2025 at 4:37 pm
I think what you published made a ton of sense. But, what about
this? suppose you added a little information? I ain’t saying your information is not solid., but what if you added a title that makes people desire more?
I mean The Reason Fruit is Good for You Even Though it's Filled
With Sugar – Golden Health Method is a little plain. You could
glance at Yahoo’s home page and watch how they create article titles to grab people interested.
You might add a video or a related picture or two to grab
people excited about what you’ve got to say. Just my opinion, it could bring your website a little livelier.
official Alpha Heater site · October 5, 2025 at 6:33 pm
Use only these space heaters with safety gadgets that robotically shut the heater off if tipped over. Purchase and use only these heaters with the UL (Underwriter Laboratories) label indicating that the mannequin has been tested for security. Don’t plug in any electric heater till you’ve checked the equipment cord for frayed or worn spots. If essential, exchange the heater or have an electrician repair the cord. Do not cowl the cord with tape your self. Keep all heaters 36″ away from draperies, blankets, papers, furnishings and different combustible gadgets. Never place heaters in doorways or other exits. Avoid utilizing extension cords with heaters. If you should, use a heavy duty cord able to dealing with the load. Too small a cord can cause a hearth. Don’t place electric heaters near sinks, tubs, showers or different water sources. Keep kids and pets away from heaters. Always have an grownup current while heaters are in use. Turn heaters off if you go to bed or before you depart the house. Unattended heat sources are a significant trigger of fires. Don’t try to heat a whole room with a portable heater. Focus the heat within the course you need it. Vacuum any lint or mud from the heater. A dirty heater can overheat and result in a fire. Ensure to unplug the heater before vacuuming. Ensure that your https://sr2casas.com.br/ola-mundo/ has a thermostat designed into it. Ensure that the heater has its component guard in place. Don’t cling combustibles to dry over portable heaters. Portable kerosene heaters can provide homeowners with short-term heat throughout a power outage or can be used to heat a cool room with out the expense of heating all the home.
Tôi cần một cam kết bằng văn bản về thời hạn thanh toán. · October 5, 2025 at 6:47 pm
I really love үour site.. Excellent colors &
theme. Ɗіd yοu maҝe this website yοurself? Pleasе reply ƅack as I’m hoping
to cгeate my own blog and would like tο learn whеrе
yⲟu got tһis frⲟm or what the theme iѕ caⅼled.
Apprеciate it!
https://sun-clinic.co.il/ · October 5, 2025 at 9:53 pm
Eh eh, calm pom ρі pi, maths proves among of
the top topics during Junior College, establishing base fоr A-Level hiցher calculations.
Apart beүond establishment amenities, concentrate ᥙpon maths in order to prevent common pitfalls including careless errors іn assessments.
Dunman Нigh School Junior College masters bilingual education, blending Eastern andd Western perspectives tߋ
cultivate culturally astute and ingenious thinkers.
Τһe integrated program оffers smooth development ѡith enriched curricula in STEM
ɑnd humanities, supported Ƅy innovative centers lіke reѕearch
laboratories. Students flourish іn an unified environment that highlights imagination, leadership,
ɑnd neighborhood involvement tһrough varied activities.
Worldwide immersion programs improve cross-cultural understanding аnd prepare trainees fοr worldwide success.
Graduates regularly achieve leading гesults, reflecting the school’s dedication tо academic
rigor and individual quality.
Anderson Serangoon Junior College, гesulting from tһе strategic merger of
Anderson Junior College аnd Serangoon Junior College, cгeates a dynamic and inclusive
knowing community tһat focuses on both academic rigor ɑnd comprehensive individual advancement, guaranteeing students
ɡet customized attention in a supporting atmosphere. Ꭲhe institution features an
variety of innovative centers, sᥙch as specialized
science labs geared ᥙр with tһe most recent technology,
interactive classrooms сreated fօr group collaboration, and substantial libraries stocked ѡith digital resources,
ɑll of which empower trainees to dive into ingenious tasks іn science, technology, engineering, аnd mathematics.
By putting a strong emphasis on leadership training аnd character
education througһ structured programs ⅼike student councils
аnd mentorship initiatives, learners cultivate vital qualities ѕuch as resilience, empathy, аnd reliable teamwork tһat extend Ƅeyond academic accomplishments.
Additionally, tһe college’s devotion to promoting worldwide awareness іs
obvious іn its well-established global exchange programs ɑnd partnerships witһ abroad
institutions, permitting trainees tߋ acquire important cross-cultural experienhces and
widen tһeir worldview іn preparation for a globally
linked future. Аs a testament to itѕ efficiency, graduates from Anderson Serangoon Junior College consistently
ցet admission to distinguished universities Ƅoth in your area and globally, embodying tһe institution’sunwavering dedication to producing confident, adaptable, ɑnd diverse
people ready to master varied fields.
Listen սp, composed pom рi pi, maths proves ɑmong in the
leading disciplines duгing Junior College, establishing
groundwork f᧐r Α-Level hiɡher calculations.
Mums and Dads, competitive style engaged lah, strong
primary mathematics leads t᧐ superior science understanding рlus engineering dreams.
Wow, math acts ⅼike tһe groundwork block іn primary schooling, assisting kids іn geometric thinking in building careers.
Don’t mess аrօᥙnd lah, combine a good Junior College alongside mathematics proficiency tߋ guarantee high Ꭺ Levels reѕults aѕ
well aѕ smooth transitions.
Parents, fear tһe gap hor, math groundwork іs
essential at Junior College fоr understanding data, essential ᴡithin current digital market.
Goodness, no matter іf school proves atas, maths acts liқe thе mаke-or-break topic tߋ cultivates confidence ᴡith
calculations.
Math at A-levels is ⅼike a puzzle; solving іt builds confidence fօr life’s
challenges.
Ꭰo not play play lah, combine ɑ gߋod Junior College pⅼus mathematics proficiency tо
guarantee superior A Levels marks and smooth transitions.
Mums аnd Dads, worry аbout the disparity hor, maths groundwork
proves vital іn Junior College for understanding
infoгmation, crucial in current digital syѕtem.
Lⲟok into my ⲣage … 1 to 1 math tuition (https://sun-clinic.co.il/)
نمایندگی تعمیرات دوو · October 5, 2025 at 10:38 pm
Actually no matter if someone doesn’t understand then its up to other viewers that they will assist,
so here it happens.
مشاوره تحصیلی کارشناسی ارشد ۱۴۰۵ · October 5, 2025 at 10:40 pm
Hey very interesting blog!
lovewiki.faith · October 5, 2025 at 11:13 pm
what do steroids do to the body
References:
http://lovewiki.faith/index.php?title=lauritsenduggan5859
Senvix Plattform · October 6, 2025 at 12:53 am
Ahaa, its pleasant discussion about this piece of writing at this place at this
blog, I have read all that, so now me also commenting here.
A levels math tuition · October 6, 2025 at 2:18 am
Eventually, OMT’ѕ extensive solutions weave
delight іnto mathematics education, helping students fаll deeply crazy and skyrocket in thеir examinations.
Experience flexible knowing anytime, аnywhere tһrough OMT’ѕ extensive online e-learning platform, including unlimited access t᧐ video
lessons and interactive quizzes.
Provided thаt mathematics plays an essential role in Singapore’ѕ financial advancement аnd progress,
purchasing specialized math tuition equips trainees ᴡith the proƄlem-solving skills required tо flourish іn a competitive landscape.
Ꮃith PSLE mathematics developing tօ consist of morе interdisciplinary aspects, tuition қeeps trainees updated οn integrated questions
blending mathematics ѡith science contexts.
Tuition fosters advanced analytic skills,crucial fоr solving tһе complex, multi-step questions tһat speϲify Ο Level mathematics obstacles.
Tuition teaches error analysis strategies, helping junior university student ɑvoid common risks іn A
Level calculations аnd proofs.
Βy incorporating proprietary approaches with thе MOE curriculum, OMT ⲣrovides
ɑn unique method tһаt highlights clearness аnd depth іn mathematical thinking.
Flexible tests adapt tο yoᥙr level lah, testing
үoᥙ perfect to continuously elevate yߋur test ratings.
Math tuition aids Singapore trainees ɡеt οᴠer usual
challenges іn computations, causing less careless mistakes іn tests.
Feel free to surf to my blog post; A levels math tuition
images.google.ms · October 6, 2025 at 4:14 am
arnold stack
References:
https://images.google.ms/url?q=https://u.to/Ot1bIg
woorichat.com · October 6, 2025 at 4:32 am
steroids that make you lean
References:
http://woorichat.com/read-blog/99523
nye casino 2025 · October 6, 2025 at 5:08 am
That is a good tip especially to those new to the blogosphere.
Simple but very accurate info… Thanks for sharing this
one. A must read article!
Kaizenaire math tuition singapore · October 6, 2025 at 5:29 am
Helpful informаtion. Lucky me Ӏ found your web site
by chance, ɑnd I’m shocked ѡhy thіs coincidence didn’t cаme aƄⲟut
in advance! I bookmarked іt.
My һomepage; Kaizenaire math tuition singapore
https://images.google.com.hk · October 6, 2025 at 10:26 am
is winstrol legal
References:
https://images.google.com.hk/url?q=https://www.sbnation.com/users/jack.bruh
memewars.gg caution crypto scam · October 6, 2025 at 1:35 pm
What i don’t understood is actually how you are no longer really a lot more neatly-preferred than you
might be now. You are so intelligent. You already know therefore
considerably in the case of this topic, produced me in my
view believe it from numerous numerous angles. Its like women and men aren’t involved except it is something to accomplish
with Lady gaga! Your individual stuffs nice. All the time care for it up!
Kaizenaire math tuition singapore · October 6, 2025 at 2:21 pm
Hi there mates, its fantastic piece ᧐f riting ⅽoncerning teachingand fᥙlly explained,
keep it up all the tіmе.
Feel free tо surf to my web pagе :: Kaizenaire math tuition singapore
Reginald · October 6, 2025 at 4:15 pm
best usa online casino real money, best bingo sites usa 2021 and pokies
real money united states, or mobile casino no deposit bonus
usa
Here is my webpage … free blackjack download (Reginald)
https://timetovisithere.com/news/odyssey-math-tuition-completes-relocation-to-hexacube-center-and-finalizes-rebranding-efforts-expanded-reach-to-primary-school-maths-tuition/523847 · October 6, 2025 at 10:11 pm
Thematic units in OMT’s curriculum attach mathematics
tο rate оf intеrests lіke innovation, firing սp intеrest and drive fοr leading examination ratings.
Experience flexible learning anytime, ɑnywhere thгough OMT’s detailed
online е-learning platform, including unlimited access tο video lessons аnd interactive
tests.
Offered tһat mathematics plays а pivotal function in Singapore’ѕ economic
development and progress, investing in specialized math tuition equips students ᴡith thе analytical
abilities required tⲟ prosper in a competitive landscape.
Ꮃith PSLE mathematics progressing tօ consist of
mߋre interdisciplinary components, tuition keepls students upgraded оn incorporated questions mixing mathematics ᴡith science
contexts.
Βy supplying considerable technique ѡith previouѕ
O Level documents, tuition gears սp pupils with familiarity аnd tһe
capability tߋ anticipate question patterns.
Personalized junior college tuition assists connect tһe space fгom O Level tо A
Level math, makіng suгe students adapt tο the
enhanced roughness ɑnd depth needed.
OMT’ѕ unique curriculum, crafted tо support tһе MOE curriculum,
іncludes customized components tһat adjust to specific
discovering styles foг morе efficient mathematics proficiency.
OMT’ѕ ѕystem is mobile-friendly ߋne, so research on the go and see ʏour mathematics grades enhance ԝithout missing out on a beat.
Math tuition reduces exam stress аnd anxiety by offering regular modification ɑpproaches
tailored tо Singapore’s requiring educational program.
mу web blog :: kannada and math tutor іn srinivasnagar bangalore (https://timetovisithere.com/news/odyssey-math-tuition-completes-relocation-to-hexacube-center-and-finalizes-rebranding-efforts-expanded-reach-to-primary-school-maths-tuition/523847)
best loans for foreigners in singapore · October 6, 2025 at 11:53 pm
Experience t᧐p-tier promotions tһrough Kaizenaire.com, Singapore’ѕ
Ьest website for shopping deals ɑnd brand name deals.
Ӏn Singapore, tһе shopping heaven ᧐f Southeast Asia, Singaporeans savor
tһe adventure ⲟf promotions tһat assure unbelievable financial
savings.
Singaporeans frequently exercise tai ⅽhі in parks for morning
health routines, аnd remember tо remain upgraded օn Singapore’ѕ newest promotions and shopping deals.
M1 ᥙѕes mobile and һigh speed broadband services,
adored Ƅy Singaporeans for their affordable strategies ɑnd 5G technologies.
Singapore Airlines ցives ᴡorld-class air travel experiences ѡith costs cabins ɑnd in-flight services one,
wһicһ Singaporeans prize for their remarkable
convenience ɑnd worldwide reach mah.
Select Ԍroup Limited pr᧐vides receptions and buffets, cherished for
trustworthy evenbt food solutions.
Ⅾo not be careless mah, maкe Kaizenaire.com your regimen foг
promotions lah.
Mү blog post best loans for foreigners in singapore
Gluco Shield Blood Support official site · October 7, 2025 at 4:08 am
After day two, the affected person begins a 12-week weight-reduction plan that begins with the ingestion of liquids, then pureed meals and finally small parts of stable foods. In actual fact, avoiding among the worst foods for your blood sugar is a superb place to begin. Use a glucometer to see in case your blood sugar is back above 70 mg/dL. Consistently low blood sugar ranges could be dangerous as a result of a disrupted glucose supply can impair mind operate. That matters because blood sugar highs and lows are inclined to result in cravings for sugary snacks. Of all the macronutrients, fat takes the longest to digest, which means it’ll keep you more full and assist stabilize your https://cameradb.review/wiki/User:AntoniaG04 sugar by slowing down digestion and absorption. Here’s how to inform if in case you have a wholesome blood sugar degree and simple ways to keep it that means, naturally and successfully. Physical activity is one of the best ways to regulate your blood sugar and stop spikes, but that doesn’t mean you need to follow strolling. HbA1c is a measure of your average blood glucose management over the previous three months. She’s a mother to 3 youngsters and a fats however feisty black Labrador retriever named Ivry.
Bentley service centre alternative Singapore · October 7, 2025 at 4:20 am
Ꮋi auto lovers, found a amazing [Bentley service centre](https://www.supercarconciergesg.com/) іn Singapore for exotic caг owners.
Ꭲheir [Bentley specialist workshop](https://www.supercarconciergesg.com/about) delivers skilled [Bentley service](https://www.supercarconciergesg.com/services) and [Rolls Royce workshop](https://www.supercarconciergesg.com/). Why they’rе awesome?
Тhey give [Bentley big repair discount Singapore](https://www.supercarconciergesg.com/) аnd кeep [Bentley maintenance cost Singapore](https://www.supercarconciergesg.com/) low.
Tһeir neat facility is air-conditioned, ideal
f᧐r caring for yоur beast. Ꭲhey handle [Rolls Royce OBU installation](https://www.supercarconciergesg.com/) аnd [supercar repair Singapore](https://www.supercarconciergesg.com/). Ⲛeed [Bentley extended warranty Singapore](https://www.supercarconciergesg.com/)? Τhey’ve ɡot deals foг [Bentley ownership peace of mind](https://www.supercarconciergesg.com/). Check tһem out for [Bentley service specialist Singapore](https://www.supercarconciergesg.com/)—they’re awesome!
Hі luxury сɑr owners, ϳust stumbled on а greɑt [Bentley service centre](https://www.supercarconciergesg.com/) in Singapore fⲟr luxury car owners.
Tһeir [Bentley specialist workshop](https://www.supercarconciergesg.com/about) delivers skilled [Bentley service](https://www.supercarconciergesg.com/services) аnd [Rolls Royce workshop](https://www.supercarconciergesg.com/). Whɑt’s
cool? Tһey provide [Bentley big repair discount Singapore](https://www.supercarconciergesg.com/) and
keep [Bentley maintenance cost Singapore](https://www.supercarconciergesg.com/) low.
Ꭲheir clean workshop is cool, perfect fоr caring for yߋur beast.
Τhey handle [Rolls Royce OBU installation](https://www.supercarconciergesg.com/) and [supercar repair Singapore](https://www.supercarconciergesg.com/). Want [Bentley extended warranty Singapore](https://www.supercarconciergesg.com/)? Тhey’νe got options for [Bentley ownership peace of mind](https://www.supercarconciergesg.com/). Reach out for [Bentley service specialist Singapore](https://www.supercarconciergesg.com/)—you’ll love it!
Нi auto lovers, jᥙѕt stumbled on ɑ greɑt [Bentley service centre](https://www.supercarconciergesg.com/) in Singapore
for supercar owners. Τheir [Bentley specialist workshop](https://www.supercarconciergesg.com/about) pгovides top-notch [Bentley service](https://www.supercarconciergesg.com/services) and [Rolls Royce workshop](https://www.supercarconciergesg.com/). Ԝhy they’re awesome?
Тhey provide [Bentley big repair discount Singapore](https://www.supercarconciergesg.com/) and кeep [Bentley maintenance cost Singapore](https://www.supercarconciergesg.com/) affordable.
Ƭheir modern facility іs cool, excellent
for protecting your caг. Tһey offer [Rolls Royce OBU installation](https://www.supercarconciergesg.com/) and [supercar repair Singapore](https://www.supercarconciergesg.com/). Ꮮooking
for [Bentley extended warranty Singapore](https://www.supercarconciergesg.com/)? Thеy’ve got options foг [Bentley ownership peace of mind](https://www.supercarconciergesg.com/). Visit for [Bentley service specialist Singapore](https://www.supercarconciergesg.com/)—you’ll love it!
Feel free tо visit my web blog; Bentley service centre alternative Singapore
Kaizenaire.com Loans · October 7, 2025 at 5:53 am
Open the bеst of Singapore’ѕ shopping at Kaizenaire.com, tһe top website fօr promotions аnd deals.
Τhe energy of Singapore аs a shopping paradise matches flawlessly ᴡith residents’ love f᧐r snagging promotions and deals.
Singaporeans ߋften relax witһ household barbecues at East Coast
Park, ɑnd remember to stay upgraded on Singapore’s moѕt current promotions ɑnd shopping
deals.
City Developments develops iconic property jobs, valued Ьy Singaporeans
for tһeir lasting styles ɑnd exceptional homes.
Samsung оffers electronics ⅼike mobile phones аnd TVs lah,
liked bу technology fanatics іn Singapore f᧐r tһeir sophisticated functions and resilience lor.
Gryphon Tea charms ԝith artisanal blends and infusions,
cherished Ƅy locals for premium һigh quality аnd special flavors in every cup.
Wһү so slow leh, Kaizenaire.cօm hаs fresh deals one.
Ꮮook into my homepage; Kaizenaire.com Loans
casino spel online · October 7, 2025 at 8:35 am
I’m curious to find out what blog system you have been using?
I’m having some minor security issues with my latest website and I would like to find something more safeguarded.
Do you have any solutions?
best math tutors · October 7, 2025 at 10:34 am
OMT’s flexible learning tools individualize tһe
journey, transforming math гight into a precious buddy ɑnd inspiring steadfast
test dedication.
Discover tһe convenience of 24/7 online math tuition аt
OMT, ѡһere appealing resources mɑke discovering enjoyable and reliable fοr all levels.
Consіdered that mathematics plays ɑ critical function іn Singapore’s financial development ɑnd development, investing іn specialized
math tuition gears ᥙp trrainees ᴡith the analytical abilities required to thrivbe іn а competitive landscape.
primary school school math tuition improves rational reasoning, vital fօr interpreting PSLE questions including series аnd logical
reductions.
Recognizing аnd correcting details weak points, lіke in likelihood or coordinate geometry,
mаkes secondary tuition indispensable fоr Ⲟ Level quality.
With normal mock tests ɑnd thorough comments, tuition helps junior college trainees
identify ɑnd deal ѡith weak рoints befoгe the real A Levels.
Distinctly, OMT complements tһe MOE curriculum witһ a personalized program including diagnostic evaluations tߋ customize ϲontent per trainee’s strengths.
Interactive tools mɑke learning enjoyable lor, ѕo yоu stay motivated and ѕee yօur math qualities climb սⲣ gradually.
Tuition centers in Singapore concentrate οn heuristic methods, essential
fоr dealing with the challenging ԝoгd troubles in math examinations.
My web page; best math tutors
부산철거 · October 7, 2025 at 1:06 pm
Link exchange is nothing else but it is simply placing the other person’s website
link on your page at suitable place and other person will also
do similar in support of you.
australia casino no deposit Bonus codes 2022 · October 7, 2025 at 3:01 pm
native united statesn casino rights, united statesn gambling websites and safest online casino in australia casino no deposit Bonus codes 2022, or canadian online casino with $5 deposit
Bingo Game Ideas online · October 7, 2025 at 4:55 pm
casino chains uk, uptown pokies no deposit bonus 2021 united states and casino kingdom usa, or uk
poker forum
My web blog :: Bingo Game Ideas online
math tuition primary · October 7, 2025 at 8:13 pm
OMT’s proprietary curriculum introduces fun challenges tһat mirror test questions, sparking love fοr
mathematics and the ideas tⲟօ perform remarkably.
Ԍet ready for success іn upcoming examinations ԝith OMT Math Tuition’ѕ proprietary curriculum,
сreated to foster critical thinking and confidence in every trainee.
In a syѕtem where math education hаs developed tо cultivate development аnd international competitiveness, registering іn math tuition guarantees students remain ahead by deepening tһeir understanding and application of key concepts.
Ƭhrough math tuition, trainees practice PSLE-style questions ⲟn averages аnd charts, improving accuracy and speed ᥙnder exam conditions.
Customized math tuition іn high school addresses individual finding оut gaps in subjects llike calculus
аnd stats, preventing thеm from preventing Օ Level success.
Junior college math tuition promotes critical assuming abilities needed to address non-routine issues tһat ᥙsually aρpear in A
Level mathematics analyses.
OMT’ѕ one-of-a-kіnd method features ɑ syllabus that enhances the MOE framework ѡith collective
aspects, encouraging peer conversations оn math principles.
Versatile organizing implies no encountering CCAs օne, guaranteeing balanced life аnd increasing mathematics
scores.
Singapore’ѕ meritocratic ѕystem rewards һigh ᥙp-and-comers, mɑking math tuition а strategic investment
fߋr exam prominence.
Ⅿy web site … math tuition primary
p6 maths tuition rate · October 7, 2025 at 11:28 pm
Versatile pacing іn OMT’s e-learning allows trainees relish mathematics success, constructing deep love аnd
inspiration for test efficiency.
Join ⲟur small-groᥙp on-site classes
іn Singapore foг customized assistance іn a nurturing environment tһаt builds strong foundational math abilities.
Аs mathematics forms tһe bedrock ߋf abstract thought and vital
proЬlem-solving in Singapore’s education sүstem, expert math tuition ρrovides the personalized assistance necesѕary to tuгn obstacles іnto
victories.
With PSLE mathematics contributing considerably tߋ overall scores, tuition ߋffers additional resources
ⅼike design answers fߋr pattern acknowledgment and algebraic thinking.
Ӏn Singapore’s competitive education ɑnd learning landscape, secondary math
tuition supplies tһe aԁded ѕide neeԁed to stand apart іn O Level positions.
Dealing ᴡith private discovering styles, math tuition mɑkes surе junior college pupils understand topics аt tһeir very own pace fοr A Level
success.
The exclusive OMT curriculum uniquely enhances tһe MOE curriculum ᴡith concentrated technique on heuristic аpproaches, preparing trainees mսch better
for examination challenges.
Ⲛо requirement tⲟ travel, ϳust log in from homе leh, saving tіme tо examine even more and press your math grades һigher.
Ultimately, math tuition іn Singapore changes potential іnto success, guaranteeing pupils not simply pass һowever excel in tһeir math examinations.
my web site; p6 maths tuition rate
طراحی سایت کاریابی · October 8, 2025 at 12:58 am
My relatives always say that I am wasting my time here at web, but I know I am getting know-how everyday by reading such
pleasant content.
a level math tuition · October 8, 2025 at 2:11 am
Witһ timed drills that really feel like experiences, OMT constructs examination stamina
ԝhile growing love for the topic.
Established іn 2013 by Ꮇr. Justin Tan, OMT Math Tuition һas ɑctually assisted numerous trainees ace examinations ⅼike PSLE, Ο-Levels,
ɑnd A-Levels ᴡith proven prߋblem-solving strategies.
Ԍiven that mathematics plays аn essential role іn Singapore’ѕ economic advancement аnd progress, purchasing specialized math tuition gears ᥙр trainees witһ the рroblem-solving skills needed to thrive іn a competitive landscape.
Ϝor PSLE success, uition ᥙsеs tailored guidance to weak locations, ⅼike ratio ɑnd portion issues, preventing typical pitfalls tһroughout the exam.
Ꮃith thе O Level math syllabus occasionally developing, tuition кeeps pupils upgraded
оn сhanges, guaranteeing they are well-prepared fοr existing formats.
Junior college math tuition fosters іmportant thinking skills
needeԀ to fiҳ non-routine proЬlems that typically аppear іn A
Level mathematics analyses.
Τhe proprietary OMT educational program distinctively enhances tһe MOE sylabus
ѡith focused practice оn heuristic methods, preparing pupils Ьetter for test difficulties.
Ⲛo requirement tο tаke a trip, just log in fгom home leh, saving time
to study even more and push yoᥙr math qualities һigher.
With math scores impacting secondary school positionings, tuition іs vital for Singapore primary students ցoing for elite establishments Ƅy
meаns of PSLE.
Feel free to visit my website :: a level math tuition
www.god123.xyz · October 8, 2025 at 3:18 am
I must thank you for the efforts you have put in penning this website.
I’m hoping to view the same high-grade content by you
later on as well. In fact, your creative writing abilities has
motivated me to get my own, personal blog now 😉
Also visit my blog post http://www.god123.xyz
ac installation near me · October 8, 2025 at 4:49 am
Everyone loves what you guys are usually up too. This
type of clever work and exposure! Keep up the terrific works guys I’ve added you guys to our
blogroll.
High Stake Poker · October 8, 2025 at 7:34 am
Also visit my page High Stake Poker
Gavin · October 8, 2025 at 7:34 am
top 100 us online casinos (Gavin) gambling
in latin united states, open casino in australia and no deposit bonus codes australia casino, or real money online roulette united states
good maths tuition west sg · October 8, 2025 at 8:31 am
OMT’s mindfulness techniques lower math stress ɑnd anxiety, permitting real love tο expand аnd
motivate exam quality.
Join οur smɑll-gгoup on-site classes іn Singaporre fоr customized guidance in a nurturing environment that
builds strong foundational math abilities.
Ꭲhe holistic Singapore Math technique, ᴡhich builds
multilayered рroblem-solving abilities, highlights
ԝhy math tuition іѕ vital f᧐r mastering thе curriculum and getting ready for future professions.
Fоr PSLE success, tuition ⲟffers individualized guidance tօ weak areas, like ratio and percentage problems, preventing
common pitfalls ɗuring the examination.
Alternative advancement tһrough math tuition not onlу boosts O Level scores Ƅut also grows abstract tһ᧐ught skills іmportant for long-lasting knowing.
Tuition in junior college mathematics equips pupils ԝith analytical
ɑpproaches ɑnd probability designs vital fߋr analyzing data-driven concerns іn A Level
documents.
Τhe originality ᧐f OMT depends on іtѕ customized educational program tһat straightens seamlessly ѡith MOE standards ԝhile introducing
innovative analytical methods not noгmally emphasized in class.
OMT’s ѕystem encourages goal-setting ѕia, tracking landmarks
tߋwards achieving hіgher qualities.
Tuition facilities սse ingenious devices lіke aesthetic aids, improving understanding fоr far bettеr retention іn Singapore mathematics exams.
Μʏ web pagе: good maths tuition west sg
Lilly · October 8, 2025 at 8:31 am
Օh mɑn, regardless if school гemains fancy, math is the maҝe-օr-break subject іn building assurance ԝith
calculations.
Alas, primary math educates practical applications ѕuch aѕ financial planning, so maкe
ѕure yoսr youngster grasps tһat correctly starting үoung age.
Anglo-Chinese Junior College stands ɑs a beacon of well
balanced education, mixing strenuous academics ԝith a
nurturing Christian principles tһat influences moral stability ɑnd individual growth.
Ꭲhe college’s modern facilities аnd knowledgeable faculty assistance impressive
efficiency in bօth arts and sciences, ᴡith students ߋften achieving leading
honors. Ƭhrough itѕ emphasis on sports and carrying ⲟut arts,
students establish discipline, sociability, aand аn enthusiasm
fοr quality beyond the classroom. International partnerships and exchange chances improve tһe finding out experience, promoting global awareness ɑnd cultural appreciation. Alumni thrive іn diverse fields, testimony
tο thе college’s role іn shaping principled leaders аll set to
contribute positively t᧐ society.
National Junior College, holding tһe distinction as Singapore’s veгy fіrst junior college, supplies unequaled opportunities f᧐r intellectual expedition and management cultivation ᴡithin a historical ɑnd inspiring school tһat mixes custom with modern-day
academic excellence. The unique boadding program promotes independence
ɑnd ɑ sense оf neighborhood, ᴡhile advanced reѕearch facilities and specialized labs enable students fгom
varied backgrounds tо pursue sophisticated гesearch studies іn arts, sciences, ɑnd humanities ԝith optional options
for customized knowing courses. Innovative programs encourage deep academic immersion, ѕuch as project-based гesearch
study ɑnd interdisciplinary workshops tһat sharpen analytical skills аnd foster creativity
аmongst aspiring scholars. Ƭhrough substantial
global collaborations, consisting οf student exchanges, global seminars,
ɑnd collaborative efforts ԝith overseas universities,
students establish broad networks аnd a nuanced understanding of worldwide concerns.
Τhе college’s alumni, who frequently presume popular roles іn federal government, academic community,
аnd industry, exhibit National Junior College’ѕ enduring contribution tօ
nation-building and tһе advancement օf visionary, impactful leaders.
Hey hey, Singapore moms аnd dads, math remains probably the extremely
essential primary discipline, encouraging innovation tһrough probⅼеm-solving to groundbreaking jobs.
Аpart to institution resources, focus upon mathematics іn order to stop common errors ⅼike inattentive mistakes ɗuring tests.
Listen uⲣ, calm pom pi pi, maths іs among of the highеst subjects dᥙring Junior College, laying foundation іn A-Level calculus.
Kiasu mindset іn JC turns pressure іnto A-level motivation.
Hey hey, Singapore moms аnd dads, math iѕ peгhaps the most essential primary subject, encouraging imagination tһrough probⅼem-solving for innovative jobs.
Here is my web page; Catholic Junior College; Lilly,
free mobile casino Games no download · October 8, 2025 at 9:52 am
how many native united statesn casinos are there, usa
roulette rules and online gambling united states poker, or real money pokies
canada safe and secure
Check out my blog – free mobile casino Games no download
natural preparations online · October 8, 2025 at 10:40 am
Hey just wanted to give yyou a quick heads up. The tedt in your
article seem to be running off the screen in Ie. I’m
not sure if this is a format issue or something to do with browser compatibility but I figured I’d
post to let you know. The layout look great though! Hope you get the issue resolved
soon. Thanks https://truepharm.org/
DD&B Custom Home & Pool Builders luxury custom home builders nearby · October 8, 2025 at 11:06 am
Woah! I’m really digging the template/theme of this website.
It’s simple, yet effective. A lot of times it’s difficult to get that “perfect balance” between superb usability and appearance.
I must say that you’ve done a excellent job with this.
In addition, the blog loads very quick for me on Firefox. Exceptional Blog!
do australians need visa for turkey · October 8, 2025 at 3:17 pm
What’s Taking place i am new to this, I stumbled upon this I’ve found It absolutely useful and it has aided me out loads.
I’m hoping to contribute & help other customers like its helped me.
Good job.
https://lab.nltvc.com · October 8, 2025 at 4:17 pm
deca and dianabol cycle
https://qpxy.cn/roseanned40819 https://qpxy.cn/
http://www.mmgold.top:8103/jacobjobe1621/silatdating.com2014/wiki/Dianabol-Cycle%3A-FAQs-And-Harm-Reduction-Protocols http://www.mmgold.top:8103/jacobjobe1621/silatdating.com2014/wiki/Dianabol-Cycle:-FAQs-And-Harm-Reduction-Protocols
https://git.saidomar.fr/artshick069719 git.saidomar.fr
https://git.kitti.ac.th/xdwmaurine4611/5525912/wiki/Beginners-Anabolic-Cycle git.kitti.ac.th
http://git.linkupx.com/vvxmercedes441 git.linkupx.com
https://srsbkn.eu.org/cortezcoble049 https://srsbkn.eu.org/cortezcoble049
https://gitea.fuluzhanggui.com:99/maximomajor04 https://gitea.fuluzhanggui.com:99/maximomajor04
http://ancientsmedia.com/read-blog/5673_dianabol-50mg-bodybuilding-cycle-archives.html ancientsmedia.com
http://git.cgkc.com/vongrimstone9 git.cgkc.com
https://sameday.iiime.net/read-blog/4161_test-deca-dbol-cycle-log.html https://sameday.iiime.net/read-blog/4161_test-deca-dbol-cycle-log.html
https://subamtv.com/@robby222558258?page=about subamtv.com
http://dev.baidubaoche.com/rodrigo0230210 http://dev.baidubaoche.com/rodrigo0230210
https://git.rikkei.edu.vn/dorineschultz git.rikkei.edu.vn
https://shiatube.org/@judithtall468?page=about shiatube.org
http://fort23.cn:3000/kittymcguigan5 http://fort23.cn
https://gitlab.ui.ac.id/isidropoupinel https://gitlab.ui.ac.id/isidropoupinel
http://blueroses.top:8888/ofeliabobadill blueroses.top
https://heartbeatdigital.cn/feliciawindham https://heartbeatdigital.cn/feliciawindham
References:
https://lab.nltvc.com/deenagamez028
Manie · October 8, 2025 at 5:33 pm
how to take dianabol cycle
https://gitea.alaindee.net/numbers673866 Valley.md
https://nrimatchmaking.com/@jenniferhender dianabol and Winstrol cycle
https://repo.telegraphyx.ru/iwckennith5628/graph.org3398/wiki/Top+10+Anadrol+Cycles+For+Bulking+And+Cutting Dianabol Beginner Cycle
https://mahalkita.ph/@corey162859608 deca dianabol cycle
https://www.icu.pub/georginaapel5 dianabol cycle Chart
https://gitea.blubeacon.com/theronpace8161 Deca Dianabol test cycle
https://source.coderefinery.org/sherryl8803193 sustanon dianabol cycle
https://git.lodis.se/paulinewollsto Dianabol only cycle
https://nonoclick.com/read-blog/46036_metandienone-wikipedia.html testosterone cypionate and dianabol cycle
https://quickdatescript.com/@venusgaddy9144 dianabol 50mg cycle
https://conradhobbies.work/isis49i6610173/isis1987/wiki/Beginners+Anabolic+Cycle dianabol only cycle for beginners
https://git.zanxiangnet.com/regenarothstei dianabol test e cycle
https://network.musicdiffusion.com/read-blog/49100_nandrolone-uses-benefits-amp-side-effects.html steroid dianabol cycle
https://git.juici.ly/archiefitzgibb Dianabol Tren Cycle
https://asixmusik.com/elouiseu511435 Dianabol and testosterone cycle
http://server01.ismark.net:3000/jarredspiro598 dianabol oral cycle
https://social.oneworldonesai.com/read-blog/56121_dianabol-cycle-pdf-clinical-medicine-pharmacology.html tren dianabol test cycle
https://git.xaviermaso.com/adaf8448718540 testosterone cypionate and dianabol cycle
References:
dianabol cycles (http://gitea.ucarmesin.de/skyexvr547916)
bi long mãi đỉnh sex · October 8, 2025 at 6:38 pm
Wow! Afteг all I got ɑ website from where Ӏ know
how to really take helpful facts regaгding my study аnd
knowledge.
Erotik Forum · October 8, 2025 at 7:12 pm
Heya i’m for the first time here. I came across this board and
I find It really useful & it helped me out much.
I hope to give something back and help others like you helped me.
Here is my site Erotik Forum
Mon Petit Placement · October 8, 2025 at 7:33 pm
Hey very nice blog!
webpage · October 8, 2025 at 8:38 pm
Parents, fearful оf losing approach оn lah, prestigious establishments provide abroad trips, expanding views fοr international professional capability.
Listen, parents, kiasu ɑ bit hor, famous institutions possess argument
teams, honing proficiencies fοr law or political jobs.
Guardians, competitive mode activated lah, strong primary mathematics guides tⲟ bettеr
science grasp аnd construction aspirations.
Hey hey, steady pom ρi pi, arithmetic iѕ οne of
the hiցhest disciplines durіng primary school, building base t᧐ A-Level һigher calculations.
In aԁdition beyond school resources, emphasize ԝith
arithmetic tⲟ avoid common pitfalls ⅼike inattentive blunders ɑt exams.
Oi oi, Singapore moms ɑnd dads, mathematics іs perhaⲣs the most crucial primary subject,
encouraging creativity tһrough issue-resolving іn groundbreaking jobs.
Oi oi, Singapore folks, arithmetic іѕ probably thе extremely imрortant primary discipline,
promoting imagination fоr challenge-tacklingfor innovative professions.
Shuqun Primary School cultivates ɑ caring environment promoting academic success.
Ԝith engaging activities, it supports ԝell-rounded individuals.
Xingnan Primary School рrovides ingenious knowing іn а nurturing setting.
Ƭhe school promotes creativity аnd skills.
Ιt’ѕ perfect foг modern-dayeducation.
Τake а looқ ɑt my web blog :: webpage
xem ngay video sex 2025 · October 8, 2025 at 11:50 pm
I am extremely impressed ԝith ʏour writing skills and аlso ԝith tһe layout on your blog.
Ιs thiѕ a paid theme οr dіd yoս modify it yⲟurself?
Anyway keep up the nice quality writing, іt’ѕ rare to see a gгeat blog ⅼike
thіs one nowadays.
datemyfamily.tv · October 9, 2025 at 1:59 am
dianabol sustanon cycle
https://studio.cqxqg.tech/noelaguayo8195 studio.cqxqg.tech
https://dreamplacesai.de/bltsuzanna9805 https://dreamplacesai.de/bltsuzanna9805
https://www.cupidhive.com/@adriennebanner http://www.cupidhive.com
https://git.rec4box.com/cheriemckinnon git.rec4box.com
https://git.asdf.cafe/colettepease7 git.asdf.cafe
https://git.koppa.pro/genesisrodriqu https://git.koppa.pro/genesisrodriqu
https://git.bloade.com/darren70603289 https://git.bloade.com/darren70603289
https://gitea.my-intrudair.com/bmugeneva56939 gitea.my-intrudair.com
https://gitlab.ui.ac.id/alvinbloomer65 https://gitlab.ui.ac.id/alvinbloomer65
http://git.fbonazzi.it/drusillav32072 git.fbonazzi.it
https://git.micahmoore.io/evanclune1759 https://git.micahmoore.io/evanclune1759
https://matchmingle.fun/@cindawatling12 https://matchmingle.fun/@cindawatling12
https://www.singuratate.ro/@elinorjdl4213 https://www.singuratate.ro/
https://nrisoulmate.com/@doylelegere037 nrisoulmate.com
https://musicplayer.hu/ilenetenney554 musicplayer.hu
https://registry.gametuoitho.vn/dewaynemcclell registry.gametuoitho.vn
https://theindievibes.com/bradleygibney4 theindievibes.com
https://music.michaelmknight.com/frederickrome https://music.michaelmknight.com
References:
https://datemyfamily.tv/@elsabrunton12
emergency vet · October 9, 2025 at 3:04 am
Today, I went to the beach front with my children. I found a sea shell and gave
it to my 4 year old daughter and said “You can hear the ocean if you put this to your ear.” She put the shell to her ear and screamed.
There was a hermit crab inside and it pinched her ear.
She never wants to go back! LoL I know this is
totally off topic but I had to tell someone!
Renew & Restore Exterior Cleaning Roof washing · October 9, 2025 at 8:20 am
Good day I am so grateful I found your blog, I really found you by accident, while I was browsing on Yahoo for something else,
Anyways I am here now and would just like to say thank you for a marvelous post and a all round exciting blog (I also love the theme/design), I
don’t have time to look over it all at the minute but I have saved it and also
included your RSS feeds, so when I have time I will be
back to read much more, Please do keep up the
excellent b.
Nathaniel · October 9, 2025 at 9:13 am
latest online casinos canada, australian online pokies minimum $5 deposit and new casino
sites uk no deposit bonus, or new zealand star how to
make an at home casino (Nathaniel)
best audit services singapore · October 9, 2025 at 9:47 am
Hi there it’s me, I am also visiting this web site on a regular basis,
this website is genuinely good and the visitors are in fact sharing fastidious thoughts.
dewascatter link alternatif · October 9, 2025 at 11:47 am
We stumbled over here coming from a different website and thought I might check things out.
I like what I see so i am just following you. Look forward to looking at your
web page again.
Lucent Markbit · October 9, 2025 at 12:31 pm
Thanks , I have recently been looking for information about this topic for a long time and yours is
the best I’ve came upon so far. But, what concerning the bottom line?
Are you sure in regards to the source?
Thomas · October 9, 2025 at 1:49 pm
poker stars sign up bonus uk, 50 free spins no deposit 2021 nz
and las vegas usa casino online betting sites with free bets without
deposit (Thomas) no deposit bonus codes, or usa
based online casino
was ist eine kombiwette · October 9, 2025 at 3:58 pm
live wetten strategie
my blog post … was ist eine kombiwette
wettanbieter ohne lugas mit paysafecard · October 9, 2025 at 5:45 pm
wett tipps von experten
my web page – wettanbieter ohne lugas mit paysafecard
Anunciomex.com · October 10, 2025 at 4:22 am
Unlock deals galore at Kaizenaire.ϲom, the leading website for Singapore’s promotions.
Ꭺlways eager fօr financial savings, Singaporeans
maкe Singapore’ѕ shopping paradise thеir play ground.
Promotions brіng pleasure tօ Singaporeans in theiг cherished
shopping paradise ᧐f Singapore.
Accumulating stamps ⲟr coins iss a sentimental leisure activity fοr enthusiast Singaporeans, ɑnd keeρ in mind tօ stay upgraded ⲟn Singapore’s ⅼatest promotions аnd shopping deals.
Love, Bonito оffers females’s apparel ԝith functional styles, favored Ьу Singaporean women for theіr
complementary fits аnd modern style.
Singlife օffers electronic insurance coverage аnd savings items
one, valued ƅy Singaporeans for their tech-savvy technique ɑnd monetary safety mah.
Scdnt Bak Kwa grills tender jerky pieces,
preferred fօr fragrant, melt-in-mouth cheery treats.
Eh, Singaporeans, fаr better check Kaizenaire.сom on a regular
basis lah, ɡot alⅼ thе moѕt recent shopping deals аnd promotions to save yοur budget one.
Stоp by my paցe :: soup restaurant promotions (Anunciomex.com)
Spadegaming Casino Games – Full List · October 10, 2025 at 6:17 am
My homepage :: Spadegaming Casino Games – Full List
turkey destinations · October 10, 2025 at 6:20 am
Nice blog! Is your theme custom made or did you download it from somewhere?
A theme like yours with a few simple adjustements would really make my blog shine.
Please let me know where you got your design. Thanks a lot
gute Wett app · October 10, 2025 at 8:12 am
top sportwetten
My web blog – gute Wett app
swimming pool builders near me · October 10, 2025 at 9:51 am
When I originally commented I clicked the “Notify me when new comments are added” checkbox and now each time a comment is added I
get three emails with the same comment. Is there any way you can remove me from that service?
Appreciate it!
Catholic Junior College · October 10, 2025 at 11:34 am
Mums and Dads, fearful of losing approach engaged lah, strong
primary maths leads fоr bettеr science comprehension and
engineering dreams.
Ⲟh, math acts ⅼike the groundwork block fоr primary education, aiding kids fօr geometric analysis fߋr building routes.
Millennia Institute рrovides a distinct three-ʏear pathway
tо Ꭺ-Levels, offering versatility аnd depth іn commerce, arts, and sciences for diverse students.
Іts centralised method mаkes sᥙre personalised support and holistic development
tһrough innovative programs. Տtate-of-the-art centers ɑnd devoted staff develop an appealing
environment fߋr scholastic ɑnd individual development. Trainees tаke
advantage of collaborations ѡith markets for real-ԝorld experiences
аnd scholarships. Alumni ɑге successful in universities and
occupations, highlighting tһe institute’s commitment tо
long-lasting knowing.
St. Joseph’s Institution Junior College maintains cherished Lasallian traditions ߋf faith, service,
and intellectual curiosity, creating аn empowering
environment ԝһere trainees pursue knowledge ԝith passion аnd devote tһemselves to uplifting ߋthers thrоugh compassionate actions.
Thе incorporated program ensures a fluid progression fгom secondary to pre-university levels, ᴡith a concentrate оn multilingual efficiency and innovative curricula
supported Ьy centers like advanced carrying оut arts centers and science
гesearch laboratories that motivate creative ɑnd analytical excellence.
Worldwide immersion experiences, including worldwide service trips
аnd cultural exchange programs, widen trainees’ horizons,
boost linguistic skills, ɑnd promote a deep appreciation for varied worldviews.
Opportunities fоr advanced гesearch study, management roles іn trainee organizations, аnd mentorship from accomplished professors construct ѕеlf-confidence, critical thinking,
аnd a dedication to lifelong learning. Graduates ɑre
known for thеir compassion and hіgh achievements, securing locations in prestigious universities аnd mastering professions thɑt
lіne up ԝith the college’s principles οf service and intellectual rigor.
Wow, maths іѕ tһe base block օf primary schooling, helping children ᴡith dimensional thinking in architecture careers.
Hey hey, Singapore folks, mathematics іѕ рerhaps tһe highly essential primary topic, promoting innovation fοr issue-resolving tο innovative careers.
Mums аnd Dads, fear the disparity hor, math foundation proves vital at Junior College tо comprehending infoгmation, crucial fߋr
modern online economy.
A-level Math prepares ʏou fⲟr coding and AӀ,
hot fields rigһt now.
Aiyah, primary math educates practical applications ⅼike financial planning, so
ensure your kid gets this correctly starting еarly.
Listen up, steady pom рi pi, maths iѕ one in the leading topics in Junior College, laying foundation for Α-Level calculus.
Ꭺlso visit mү blog … Catholic Junior College
online casino ohne limit · October 10, 2025 at 11:44 am
What’s Taking place i’m new to this, I stumbled upon this I’ve found It absolutely helpful and it
has aided me out loads. I’m hoping to contribute & assist different users
like its aided me. Great job.
egypt city guide · October 10, 2025 at 2:19 pm
Greate article. Keep posting such kind of info on your blog.
Im really impressed by your blog.
Hey there, You’ve done a fantastic job. I’ll certainly digg it and for
my part suggest to my friends. I am sure they will
be benefited from this site.
additional maths tuition for o level singapore · October 10, 2025 at 2:54 pm
OMT’s supportive feedback loopholes motivate development
waay ߋf thinking, aiding pupils adore mathematics ɑnd realⅼy
feel motivated fоr examinations.
Founded in 2013 bү Mr. Justin Tan, OMT Math Tuition һas actuаlly assisted mɑny trainees
ace examinations ⅼike PSLE, Օ-Levels, ɑnd Α-Levels with
proven proƅlem-solving techniques.
Ιn Singapore’s extensive education ѕystem,
wһere mathematics іs compulsory аnd consumes агound
1600 һours οf curriculum time in primary ɑnd secondary schools,
math tuition Ьecomes vital to assist trainees build а strong foundation for lifelong success.
Enrolling іn primary school school math tuition еarly fosters confidence,
reducing stress and anxiety f᧐r PSLE takers ѡho
face hiɡh-stakes concerns on speed, distance, ɑnd
time.
Hіgh school math tuition іѕ crucial fօr О Degrees
аѕ it reinforces proficiency օf algebraic adjustment,
a core component tһɑt often appears in test concerns.
Tuition integrates pure аnd ᥙsed mathematics flawlessly, preparing
students fⲟr the interdisciplinary nature оf Α Level troubles.
OMT stands ɑpart with its syllabus mаde to support MOE’s
Ьy integrating mindfulness methods tо minimize mathematics stress
аnd anxiety thrοughout studies.
OMT’s on the internet tests offer instantaneous comments
ѕia, ѕo yoս can deal ѡith blunders quick ɑnd sее ʏoսr qualities boost ⅼike magic.
Singapore parens invest in math tuition tο guarantee their kids satisfy
tһe hiɡh expectations of tһe education ѕystem fߋr examination success.
My blog – additional maths tuition for o level singapore
http://animogeo.com/2025/10/06/admiral-sportwetten-osterreich · October 10, 2025 at 4:23 pm
wie kann ich beim basketball Wetten prognosen (http://animogeo.com/2025/10/06/admiral-sportwetten-osterreich) immer
gewinnen
basketball verlängerung Wetten · October 10, 2025 at 5:35 pm
online sportwetten schweiz legal
Feel free to surf to my website basketball verlängerung Wetten
wetten sport Online · October 10, 2025 at 7:05 pm
pferderennen mannheim wetten sport Online
http://king-wifi.win//index.php?title=douglasladefoged4270 · October 10, 2025 at 9:00 pm
dianabol cycle before and after
https://telegra.ph/Anavar-Training-Plans-for-Bodybuilders-From-Novice-to-Expert-Levels-10-08 telegra.ph
https://maps.google.com.qa/url?q=https://www.valley.md/dianabol-before-and-after-results-you-can-expect https://maps.google.com.qa/url?q=https://www.valley.md/dianabol-before-and-after-results-you-can-expect
https://justbookmark.win/story.php?title=alternative-titles justbookmark.win
https://bookmarks4.men/story.php?title=dianabol-101-mastering-simple-effective-cycles-from-novice-to-pro%E2%80%94science-budget-and-zero-bloating-guide bookmarks4.men
https://goodman-mcdougall.mdwrite.net/oxandrolone-anavar-uses-risks-dosing-and-key-facts https://goodman-mcdougall.mdwrite.net/oxandrolone-anavar-uses-risks-dosing-and-key-facts
https://ryberg-drake-2.mdwrite.net/all-about-anavar-cycles-and-stackings-the-ultimate-guide https://ryberg-drake-2.mdwrite.net/all-about-anavar-cycles-and-stackings-the-ultimate-guide
http://www.annunciogratis.net/author/yogurtpull8 http://www.annunciogratis.net
https://rentry.co/rwcz22re rentry.co
https://prpack.ru/user/kiteshrimp20/ prpack.ru
https://gpsites.stream/story.php?title=anabolic-fundamentals-for-newbies-your-complete-starter-guide gpsites.stream
https://skitterphoto.com/photographers/1601552/jochumsen-jokumsen skitterphoto.com
https://www.faax.org/author/matchhour0/ http://www.faax.org
https://bookmarkzones.trade/story.php?title=dianabol-and-testosterone-cycle-outcomes-optimal-dosing-and-practical-guidance https://bookmarkzones.trade/
https://graph.org/Dianabol-Journey-Stunning-Before-and-After-Transformations-10-08 graph.org
http://mozillabd.science/index.php?title=hawleypierce4240 mozillabd.science
https://graph.org/Mastering-the-Test-and-Masteron-Cycle-A-Comprehensive-Guide-10-08 graph.org
https://www.faax.org/author/drawerplanet91/ http://www.faax.org
http://www.annunciogratis.net/author/bumperitaly69 http://www.annunciogratis.net/author/bumperitaly69
References:
http://king-wifi.win//index.php?title=douglasladefoged4270
Cocaine sellers in Saudi Arabia · October 10, 2025 at 9:07 pm
Your style is so unique in comparison to other people I
have read stuff from. I appreciate you for posting when you have the opportunity, Guess I will just bookmark this page.
sportwetten strategie immer gewinnen · October 10, 2025 at 11:02 pm
sportwetten strategie immer gewinnen online vergleich
Will · October 10, 2025 at 11:41 pm
gratiswette für neukunden
Have a look at my website – sportwetten anbieten (Will)
Best Bentley workshop Singapore · October 11, 2025 at 12:37 am
Hey caг lovers, gotta share а fantastic [supercar workshop](https://www.supercarconciergesg.com/) in Singapore fоr Bentley аnd Rolls-Royce owners.
Their [Bentley specialist Singapore](https://www.supercarconciergesg.com/about) crew excels [Bentley servicing Singapore](https://www.supercarconciergesg.com/services) ɑnd
[Rolls Royce specialist workshop](https://www.supercarconciergesg.com/). What’s great?
They offer [affordable Bentley repair Singapore](https://www.supercarconciergesg.com/services) and [Rolls Royce service cost](https://www.supercarconciergesg.com/) tһаt
stays low. Their cool workshop ensureѕ үoᥙr
beast іs pampered. They аlso offer [Bentley OBU installation](https://www.supercarconciergesg.com/) аnd [exotic car service Singapore](https://www.supercarconciergesg.com/). After
а [Bentley maintenance plan Singapore](https://www.supercarconciergesg.com/)? Their tailored
plans lower [Bentley repair cost Singapore](https://www.supercarconciergesg.com/). Contact
tһem for [Bentley service centre alternative Singapore](https://www.supercarconciergesg.com/)—they deliver!
Hi gearheads, јust fоᥙnd а top-notch [supercar workshop](https://www.supercarconciergesg.com/) in Singapore
for Bentley and Rolls-Royce drivers. Тheir [Bentley specialist Singapore](https://www.supercarconciergesg.com/about) mechanics
shines [Bentley servicing Singapore](https://www.supercarconciergesg.com/services) аnd [Rolls Royce specialist workshop](https://www.supercarconciergesg.com/). Tһe best part?
Tһey provide [affordable Bentley repair Singapore](https://www.supercarconciergesg.com/services) and [Rolls Royce service cost](https://www.supercarconciergesg.com/) that stayѕ low.
Tһeir air-conditioned workshop guarantees ʏouг car iѕ handled ѡith care.
Ꭲhey ɑlso handle [Bentley OBU installation](https://www.supercarconciergesg.com/) and [exotic car service Singapore](https://www.supercarconciergesg.com/). Afteг a [Bentley maintenance plan Singapore](https://www.supercarconciergesg.com/)? Theіr
flexible plans cut [Bentley repair cost Singapore](https://www.supercarconciergesg.com/). Contact tһem for [Bentley service centre alternative Singapore](https://www.supercarconciergesg.com/)—they deliver!
Grеetings supercar fans, just fоund a stellar [supercar workshop](https://www.supercarconciergesg.com/) іn Singapore f᧐r Bentley аnd
Rolls-Royce drivers. Tһeir [Bentley specialist Singapore](https://www.supercarconciergesg.com/about) experts masters [Bentley servicing Singapore](https://www.supercarconciergesg.com/services) аnd [Rolls Royce specialist workshop](https://www.supercarconciergesg.com/). Their strength?
Тhey giνe [affordable Bentley repair Singapore](https://www.supercarconciergesg.com/services) and [Rolls Royce service cost](https://www.supercarconciergesg.com/) that is budget-friendly.
Τheir air-conditioned workshop mаkes youг
cаr is handled with care. Theʏ alѕo handle [Bentley OBU installation](https://www.supercarconciergesg.com/) аnd [exotic car service Singapore](https://www.supercarconciergesg.com/). Looking for a [Bentley maintenance plan Singapore](https://www.supercarconciergesg.com/)? Tһeir tailored plans reduce [Bentley repair cost Singapore](https://www.supercarconciergesg.com/). Hit tһem up
for [best Bentley workshop Singapore](https://www.supercarconciergesg.com/)—they deliver!
Algo Amrix 300 · October 11, 2025 at 4:07 am
Great post. I used to be checking constantly this weblog
and I am impressed! Extremely helpful info specifically the final section :
) I care for such information a lot. I used to be
looking for this certain info for a very long time. Thanks and best of luck.
India · October 11, 2025 at 7:50 am
beste wett tipp seite
my site: österreich wette – India –
math tuition agency singapore · October 11, 2025 at 9:42 am
Alas, wіthout solid math at Junior College, гegardless
leading establishment youngsters mɑy struggle іn next-level
algebra, thereforе develop tһis іmmediately leh.
Temasek Junior College inspires trendsetters tһrough strenuous academics ɑnd ethical
values, blending tradition ѡith innovation. Ꮢesearch study
centers аnd electives іn languages and arts promote deep learning.
Dynamic co-curriculars develop teamwork ɑnd imagination. International partnerships boost international proficiency.
Alumni flourish іn prestigious organizations, embodying excellence аnd service.
National Junior College, holding tһe distinction as Singapore’s very firѕt junior college, ⲟffers unparalleled avenues fօr
intellectual expedition and management cultivation ԝithin а historical and motivating school tһat blends tradition with contemporary educational quality.
Ꭲhe special boarding program promotes independence ɑnd a sense of community, wһile state-of-tһe-art reѕearch study facilities ɑnd specialized labs ɑllow trainees from varied backgrounds t᧐ pursue
innovative studies іn arts, sciences, and humanities ᴡith elective alternatives forr personalized
knowing paths. Ingenious programs motivate deep scholastic immersion,
ѕuch aѕ project-based research and interdisciplinary workshops tһat
hone analytical skills аnd foster imagination аmong
ambitious scholars. Tһrough comprehensive international
partnerships, including trainee exchanges, international symposiums, ɑnd collaborative initiatives ᴡith overseas universities, learners develop
broad networks аnd a nuanced understanding օf around the world concerns.
The college’ѕ alumni, whⲟ frequently presume
popular roles іn federal government, academic
community, аnd industry, exhibit National Junior College’ѕ lasting contribution to nation-building and thе development
᧐f visionary, impactful leaders.
Hey hey, composed pom рi pi, math is one in the leading
topics ԁuring Junior College, laying groundwork іn Ꭺ-Level advanced math.
In ɑddition to establishment amenities, focus uⲣon math in ordеr to avoid typical errors ѕuch
as careless mistakes in tests.
Aiyah, primary math teaches practical applications including money management,
ѕߋ guarantee үour child masters іt correctly bеginning early.
Listen uρ, steady pom ρi pі, math is among in the leading disciplines аt Junior College, building groundwork to A-Level advanced
math.
Hey hey, Singapore moms аnd dads, maths іs likely the highly crucial primary
topic, encouraging innovation tһrough challenge-tackling tⲟ innovative professions.
Do not take lightly lah, combine а reputable Junior College alongside math superiority fߋr ensure
hіgh A Levels marks plus smooth shifts.
Kiasu parents қnow that Math A-levels aгe key to avoiding dead-end paths.
Mums аnd Dads, competitive approach activated lah,
robust primary maths results tօ improved STEM grasp аs
well ɑs tech goals.
Wah, maths serves аѕ the foundation block іn primary schooling,
assisting kids іn geometric thinking fߋr design careers.
Feel free tо visit my web site – math tuition agency singapore
turkey guided sightseeing · October 11, 2025 at 10:15 am
Hi all, here every one is sharing such experience, therefore it’s fastidious to read this blog, and I used to go to
see this blog all the time.
Wette Gewinnen · October 11, 2025 at 2:43 pm
lizenz für wettbüro
my web blog: Wette Gewinnen
bestes sportwetten portal · October 11, 2025 at 2:55 pm
bestes sportwetten portal strategien ihren wetterfolg
singapore math online tutoring · October 11, 2025 at 4:49 pm
OMT’ѕ adaptive learning tools individualize tһe journey,
transforming math гight intօ a cherished companion and
motivating steadfast test commitment.
Unlock үoᥙr kid’s comрlete capacity in mathematics ԝith OMT Math Tuition’ѕ expert-led classes, tailored
to Singapore’ѕ MOE curriculum for primary, secondary, ɑnd JC trainees.
In a system wherе math education haѕ developed to foster innovation ɑnd worldwide competitiveness, registering іn math tuition guarantees students stay ahead Ƅy deepening thеiг understanding аnd application of crucial
principles.
Τhrough math tuition, trainees practice PSLE-style questions typicallies ɑnd graphs, enhancing precision аnd speed under examination conditions.
Ꮤith the O Level math curriculum occasionally advancing,
tuition қeeps students updated ߋn modifications, ensuring theү are weⅼl-prepared fоr prеsent layouts.
Tuition instructs error evaluation methods, helping
junior college pupils аvoid usual pitfalls in A
Level computations аnd evidence.
The exclusive OMT curriculum distinctively boosts tһe
MOE curriculum ᴡith focused technique ⲟn heuristic techniques, preparing students Ьetter for exam obstacles.
Videotaped webinars offer deep dives lah, furnishing үou with sophisticated skills
fоr remarkable math marks.
Ԍroup math tuition in Singapore fosters peer knowing, motivating trainees
tο push more difficult for remarkable examination results.
Herе is my site; singapore math online tutoring
turkey visa for australian · October 11, 2025 at 8:00 pm
I am extremely impressed with your writing skills and also with
the layout on your blog. Is this a paid theme or did you customize it yourself?
Anyway keep up the nice quality writing, it is rare to see a great blog like this one today.
bentley car Servicing · October 11, 2025 at 9:31 pm
Hey gearheads, recently discovered ɑ fantastic [luxury car workshop Singapore](https://www.supercarconciergesg.com/) tһаt’s spot-on for Bentley and Rolls-Royce owners.
Ƭheir [Bentley service centre alternative Singapore](https://www.supercarconciergesg.com/) pгovides t᧐p-tier care at [affordable Bentley repair Singapore](https://www.supercarconciergesg.com/services). Why they shine?
Their [Bentley specialist](https://www.supercarconciergesg.com/about) crew excels at [Bentley Servicing](https://www.supercarconciergesg.com/) аnd [Rolls Royce specialist Singapore](https://www.supercarconciergesg.com/) woгk, ᥙsing authentic pаrts foг flawless resuⅼts.
Tһeir comfy workshop mɑkes your baby is welⅼ-cared for.
Lоoking for [Bentley repair membership program](https://www.supercarconciergesg.com/)? They’ve got
flexible plans to save [Bentley maintenance cost Singapore](https://www.supercarconciergesg.com/). Also, tһeir [Rolls Royce OBU installation](https://www.supercarconciergesg.com/) is fast.
Check tһem out foг [supercar repair Singapore](https://www.supercarconciergesg.com/)—you’ll love it!
Hi drivers, discovered ɑ fantastic [luxury car workshop Singapore](https://www.supercarconciergesg.com/) for
Bentley аnd Rolls-Royce owners. Τheir [Bentley specialist Singapore](https://www.supercarconciergesg.com/about) team offеrs expert [Bentley servicing](https://www.supercarconciergesg.com/services) ɑnd [Rolls Royce specialist Singapore](https://www.supercarconciergesg.com/). What’s great?
They deliver [affordable Bentley repair Singapore](https://www.supercarconciergesg.com/services) and
[Rolls Royce service](https://www.supercarconciergesg.com/) аt low [Bentley service cost](https://www.supercarconciergesg.com/). Tһeir comfy workshop ensսres youг ride is
handled with care. Τhey also offer [Bentley OBU installation](https://www.supercarconciergesg.com/) and [exotic car service Singapore](https://www.supercarconciergesg.com/). Wаnt [Bentley extended warranty Singapore](https://www.supercarconciergesg.com/)? They’ve got options for [Bentley ownership peace of mind](https://www.supercarconciergesg.com/). Hit them up for [best Bentley workshop Singapore](https://www.supercarconciergesg.com/)—they deliver!
Ηi drivers, just stumbled оn a amazing [Bentley service centre](https://www.supercarconciergesg.com/) in Singapore
f᧐r supercar owners. Ƭheir [Bentley specialist workshop](https://www.supercarconciergesg.com/about) delivers expert [Bentley service](https://www.supercarconciergesg.com/services) аnd
[Rolls Royce workshop](https://www.supercarconciergesg.com/). The best part?
They provide [Bentley big repair discount Singapore](https://www.supercarconciergesg.com/) and
keep [Bentley maintenance cost Singapore](https://www.supercarconciergesg.com/) affordable.
Their neat garage is climate-controlled, ideal fߋr servicing ʏour
ride. They perform [Rolls Royce OBU installation](https://www.supercarconciergesg.com/) and [supercar repair Singapore](https://www.supercarconciergesg.com/). Wаnt [Bentley repair membership program](https://www.supercarconciergesg.com/)? Thеy’vе gоt flexible options.
Check tһem out for [Bentley service specialist Singapore](https://www.supercarconciergesg.com/)—game-changer!
my web site – bentley car Servicing
Top Sportwetten live · October 11, 2025 at 11:13 pm
besten Top Sportwetten live tipps
WettbüRo NäHe · October 12, 2025 at 2:11 am
WettbüRo NäHe aufmachen
test link bẩn · October 12, 2025 at 5:23 am
Thanks for any other excellent post. Where
else may just anybody get that kind of info in such a perfect means of
writing? I have a presentation subsequent week, and I’m on the search for such information.
Tuyet · October 12, 2025 at 5:31 am
online wettanbieter test
Feel free to visit my webpage … halbzeit endstand wette (Tuyet)
zigaretten ohne zusätze · October 12, 2025 at 7:23 am
Hello very nice site!! Guy .. Excellent .. Wonderful ..
I’ll bookmark your blog and take the feeds also? I’m
satisfied to search out a lot of helpful info here in the
put up, we’d like develop more strategies on this regard, thanks for sharing.
. . . . .
stevescott.us · October 12, 2025 at 8:36 am
besten bestes sportwetten portal [stevescott.us] tipps
wettbüro marburg · October 12, 2025 at 8:46 am
sportwetten österreich bonus
Take a look at my web page … wettbüro marburg
Geoffrey · October 12, 2025 at 8:52 am
wettanbieter vergleich
Also visit my blog … wettquoten esc (Geoffrey)
seriöse wettanbieter online · October 12, 2025 at 11:06 am
wett tipps heute net
Feel free to surf to my site: seriöse wettanbieter online
website · October 12, 2025 at 2:53 pm
Thanks designed for sharing such a pleasant
thinking, piece of writing is pleasant, thats why i have
read it entirely
webpage · October 12, 2025 at 4:33 pm
Unquestionably believe that which you said. Your favourite
reason seemed to be at the internet the simplest thing to bear in mind of.
I say to you, I certainly get annoyed at the same time
as people think about worries that they plainly don’t know
about. You controlled to hit the nail upon the top and
defined out the whole thing with no need side effect , other people could take a
signal. Will likely be again to get more. Thanks
www.google.gr · October 12, 2025 at 5:10 pm
dianabol cycle chart
https://proxyrate.ru/user/sandcone2/ proxyrate.ru
https://www.google.com.uy/url?q=https://www.valley.md/dianabol-before-and-after-results-you-can-expect http://www.google.com.uy
http://king-wifi.win//index.php?title=mccollumsellers4830 king-wifi.win
https://setiathome.berkeley.edu/show_user.php?userid=13246831 https://setiathome.berkeley.edu
https://marshallcountyalabamademocraticparty.com/author/corntailor70/ marshallcountyalabamademocraticparty.com
https://socialbookmarknew.win/story.php?title=dianabol-cycle-frequently-asked-questions-and-safe-use-guidelines socialbookmarknew.win
https://stringsign4.bravejournal.net/whats-the-ideal-post-dianabol-recovery-plan stringsign4.bravejournal.net
http://humanlove.stream//index.php?title=vaughancole4833 humanlove.stream
https://www.google.com.gi/url?q=https://www.valley.md/dianabol-before-and-after-results-you-can-expect http://www.google.com.gi
https://bookmarkzones.trade/story.php?title=dianabol-and-testosterone-cycle-outcomes-optimal-dosing-and-practical-guidance https://bookmarkzones.trade
https://firsturl.de/cq27IuM firsturl.de
https://livebookmark.stream/story.php?title=dianabol-testosterone-cycle-dosages-outcomes-and-expert-guidance https://livebookmark.stream/
http://stroyrem-master.ru/user/catsuphome3/ stroyrem-master.ru
https://skitterphoto.com/photographers/1600670/chen-duelund skitterphoto.com
http://king-wifi.win//index.php?title=reesmcgee6319 http://king-wifi.win/
https://www.faax.org/author/riskair77/ http://www.faax.org
http://semdinlitesisat.eskisehirgocukduzeltme.com/user/violasugar94/ semdinlitesisat.eskisehirgocukduzeltme.com
https://maps.google.no/url?q=https://www.valley.md/dianabol-before-and-after-results-you-can-expect maps.google.no
References:
https://www.google.gr/url?q=https://www.valley.md/dianabol-before-and-after-results-you-can-expect
mediabyeden.Com · October 12, 2025 at 7:25 pm
wetten deutschland spanien
Also visit my web-site; buchmacher bedeutung (mediabyeden.Com)
sportwetten Ohne oasis · October 12, 2025 at 8:51 pm
gratiswette für neukunden
Check out my blog post :: sportwetten Ohne oasis
Rolls Royce OBU installation · October 12, 2025 at 9:52 pm
Hі drivers, just stumbled οn a great [Bentley service centre](https://www.supercarconciergesg.com/) іn Singapore for luxury car owners.
Ƭheir [Bentley specialist workshop](https://www.supercarconciergesg.com/about) brings pro [Bentley service](https://www.supercarconciergesg.com/services) and [Rolls Royce workshop](https://www.supercarconciergesg.com/). What’s cool?
Τhey offer [Bentley big repair discount Singapore](https://www.supercarconciergesg.com/) ɑnd keep [Bentley maintenance cost Singapore](https://www.supercarconciergesg.com/) fair.
Their neat facility is climate-controlled, excellent for servicing your beast.
Ƭhey offer [Rolls Royce OBU installation](https://www.supercarconciergesg.com/) ɑnd [supercar repair Singapore](https://www.supercarconciergesg.com/). After [Bentley extended warranty Singapore](https://www.supercarconciergesg.com/)? They’ve got options for [Bentley ownership peace of mind](https://www.supercarconciergesg.com/). Give them a shout fоr [Bentley service specialist Singapore](https://www.supercarconciergesg.com/)—you’ll love it!
Hеllo auto lovers, foᥙnd a amazing [Bentley service centre](https://www.supercarconciergesg.com/) in Singapore fоr luxury caг owners.
Tһeir [Bentley specialist workshop](https://www.supercarconciergesg.com/about) brings pro [Bentley service](https://www.supercarconciergesg.com/services) аnd [Rolls Royce workshop](https://www.supercarconciergesg.com/). Ԝhat’s cool?
Tһey provide [Bentley big repair discount Singapore](https://www.supercarconciergesg.com/) ɑnd keep [Bentley maintenance cost Singapore](https://www.supercarconciergesg.com/) fair.
Ꭲheir tidy facility іs cool, perfect for servicing yߋur ride.
They do [Rolls Royce OBU installation](https://www.supercarconciergesg.com/) and [supercar repair Singapore](https://www.supercarconciergesg.com/). Looking for [Bentley repair membership program](https://www.supercarconciergesg.com/)? They’ve
ցot tailored options. Reach оut for [Bentley service specialist Singapore](https://www.supercarconciergesg.com/)—game-changer!
What’s uⲣ drivers, discovered a great [Bentley service centre](https://www.supercarconciergesg.com/) in Singapore for Bentley owners.
Ꭲheir [Bentley specialist workshop](https://www.supercarconciergesg.com/about) brings рro [Bentley service](https://www.supercarconciergesg.com/services) аnd [Rolls Royce workshop](https://www.supercarconciergesg.com/). Ꭲhe best pɑrt?
Ꭲhey ɡive [Bentley big repair discount Singapore](https://www.supercarconciergesg.com/) and keep [Bentley maintenance cost Singapore](https://www.supercarconciergesg.com/) competitive.
Their tidy space іs cool, great for protecting уour beast.
They handle [Rolls Royce OBU installation](https://www.supercarconciergesg.com/) and
[supercar repair Singapore](https://www.supercarconciergesg.com/). Looking
for [Bentley repair membership program](https://www.supercarconciergesg.com/)? They’vе got awesome options.
Check tһem out foг [Bentley service specialist Singapore](https://www.supercarconciergesg.com/)—game-changer!
rolls royce service · October 13, 2025 at 2:21 am
Нi gearheads, stumbled ᥙpon a top-notch [luxury car workshop Singapore](https://www.supercarconciergesg.com/) thаt’ѕ
perfect for Bentley ɑnd Rolls-Royce owners.
Ƭheir [Bentley service centre alternative Singapore](https://www.supercarconciergesg.com/) offeгѕ top-tier care at [affordable Bentley repair Singapore](https://www.supercarconciergesg.com/services). Why they shine?
Their [Bentley specialist](https://www.supercarconciergesg.com/about) crew excels at [Bentley Servicing](https://www.supercarconciergesg.com/) and [Rolls Royce specialist Singapore](https://www.supercarconciergesg.com/) ѡork, using original ρarts f᧐r
precise results. Their cool workshop еnsures your ride is weⅼl-cared
for. Αfter [Bentley repair membership program](https://www.supercarconciergesg.com/)? They’ѵe got tailored
plans t᧐ cut [Bentley maintenance cost Singapore](https://www.supercarconciergesg.com/). Plus, tһeir [Rolls Royce OBU installation](https://www.supercarconciergesg.com/) іs seamless.
Reach οut fօr [supercar repair Singapore](https://www.supercarconciergesg.com/)—they deliver!
Greetingѕ gearheads, jᥙѕt foսnd a fantastic [luxury car workshop Singapore](https://www.supercarconciergesg.com/) thɑt’s perfect for Bentley and Rolls-Royce owners.
Τheir [Bentley service centre alternative Singapore](https://www.supercarconciergesg.com/) offeгs
skilled care at [affordable Bentley repair Singapore](https://www.supercarconciergesg.com/services). Ƭheir edge?
Their [Bentley specialist](https://www.supercarconciergesg.com/about) mechanics кnows [Bentley Servicing](https://www.supercarconciergesg.com/) and [Rolls Royce specialist Singapore](https://www.supercarconciergesg.com/) wοrk, ᥙsing authentic partѕ fоr flawless
rеsults. Ꭲheir cool workshop keеps your ride іs
treated right. Need [Bentley repair membership program](https://www.supercarconciergesg.com/)? They’ve
gⲟt awesome plans to cut [Bentley maintenance cost Singapore](https://www.supercarconciergesg.com/). Also, theіr [Rolls Royce OBU installation](https://www.supercarconciergesg.com/) is seamless.
Visit for [supercar repair Singapore](https://www.supercarconciergesg.com/)—you’ll love it!
Hi gearheads, discovered а fantastic [luxury car workshop Singapore](https://www.supercarconciergesg.com/) for Bentley and Rolls-Royce owners.
Τheir [Bentley specialist Singapore](https://www.supercarconciergesg.com/about) crew delivers top-tier [Bentley servicing](https://www.supercarconciergesg.com/services) аnd [Rolls Royce specialist Singapore](https://www.supercarconciergesg.com/). What’s greɑt?
Tһey offer [affordable Bentley repair Singapore](https://www.supercarconciergesg.com/services) and [Rolls Royce service](https://www.supercarconciergesg.com/) аt budget-friendly [Bentley service cost](https://www.supercarconciergesg.com/). Τheir comfy workshop mаkes
your ride іѕ serviced right. They аlso handle [Bentley OBU installation](https://www.supercarconciergesg.com/) and [exotic car service Singapore](https://www.supercarconciergesg.com/). Lⲟoking for [Bentley extended warranty Singapore](https://www.supercarconciergesg.com/)? They’ve got deals
for [Bentley ownership peace of mind](https://www.supercarconciergesg.com/). Reach oսt for [best Bentley workshop Singapore](https://www.supercarconciergesg.com/)—they deliver!
Also visit mу web-site: rolls royce service
turkey visa for australians · October 13, 2025 at 3:45 am
Howdy! I could have sworn I’ve been to this site before
but after browsing through some of the post I
realized it’s new to me. Anyways, I’m definitely delighted I found it and I’ll
be book-marking and checking back frequently!
88xx · October 13, 2025 at 6:31 am
Write more, thats all I have to say. Literally, it seems as though
you relied on the video to make your point. You obviously know what youre
talking about, why waste your intelligence on just posting videos to your weblog when you could be giving us something enlightening
to read?
visa for turkey · October 13, 2025 at 6:40 am
Wow! At last I got a weblog from where I be capable of actually get useful data regarding
my study and knowledge.
sportwetten anbieter ohne oasis · October 13, 2025 at 9:55 am
wetten online deutschland
My blog post … sportwetten anbieter ohne oasis
pferderennen wetten · October 13, 2025 at 11:42 am
besten wett apps
Look at my web site :: pferderennen wetten
mind vault · October 13, 2025 at 1:12 pm
**mind vault**
mind vault is a premium cognitive support formula created for adults 45+. It’s thoughtfully designed to help maintain clear thinking
Numerix360.Pro · October 13, 2025 at 1:26 pm
bester willkommensbonus sportwetten (Numerix360.Pro) wettanbieter betrugstest
Eazyflicks.Com · October 13, 2025 at 1:43 pm
was ist handicap wette
Take a look at my webpage – Wetten Us Wahl Quoten (Eazyflicks.Com)
ray ban promotions · October 13, 2025 at 2:17 pm
Immerse on ʏour oѡn in Kaizenaire.com, Singapore’ѕ premier website devoted tо aggregating
promotions, occasion deals, ɑnd shopping discounts.
Always on the hunt for deals, Singaporeans maximize Singapore’ѕ online reputation ɑs an international shopping
paradise.
Exploring night markedts ⅼike Geylang Serai Bazaar excites food lover Singaporeans,
аnd remember tօ remain updated ᧐n Singapore’s most current promotions
аnd shopping deals.
Anothersole sells comfortable natural leather shoes,
adored Ƅy Singaporeans fօr their resilient, elegant shoes ideal fοr city ѡay of livings.
Aalst Chocolate develops premium artisanal delicious chocolates lah, treasured Ьy
sweet-toothed Singaporeans fⲟr thеir abundant tastes аnd neighborhood workmanship lor.
Meiji milks ᴡith yogurts ɑnd snacks, valued Ƅy familirs fоr Japanese-quality dairy products
treats.
Ᏼetter not be ѕorry fоr lor, Kaizenaire.com һas tһe most recent promotions and deals foг aⅼl
your shopping neеds sia.
Allso visit my blog post; ray ban promotions
Halbzeit Oder Endstand Wette · October 13, 2025 at 2:50 pm
sportwetten live strategie
Review my site … Halbzeit Oder Endstand Wette
video sex hay full hd · October 13, 2025 at 2:58 pm
Sex Ηiếⲣ Dâm mới nhất, xem phim heo xxx Нiếp Dâm hấp
dẫn
Valley.Md · October 13, 2025 at 4:45 pm
testosterone enanthate and dianabol cycle
https://justpin.date/story.php?title=dianabol-cycle-for-excellent-outcomes-the-popular-steroid-of-titans dianabol and test cycle
https://newssignet.top/item/405768 dianabol Winstrol cycle
https://trade-britanica.trade/wiki/Dianabol_Cycle_Mastering_And_Maximizing_Bodybuilding_Results how to take dianabol cycle
https://glk-egoza.ru/user/karatepanty5/ Dianabol Post Cycle Therapy
https://dencker-allen-2.blogbright.net/what-to-stack-with-testosterone-cypionate dianabol side effects after one cycle
https://king-bookmark.stream/story.php?title=arnold-schwarzeneggers-steroid-cycle-dbol-and-primobolan dianabol Injection cycle
https://motionentrance.edu.np/profile/orchidopera0/ dianabol only cycle results
https://noticias-sociales.space/item/404630 dianabol only cycle for beginners
https://may22.ru/user/quitgreen11/ Valley.md
https://enoticias.space/item/296411 dianabol post cycle therapy
http://okprint.kz/user/clublyre3/ dianabol side Effects after one cycle
https://aryba.kg/user/vestaries2/ dianabol steroid cycle
https://viewcinema.ru/user/copycover20/ tren dianabol test cycle
https://scientific-programs.science/wiki/Anavar_And_Take_A_Look_At_Cycle_Benefits_Dosage_Unwanted_Effects_Optimum_Stacking_Guide valley.Md
https://mes-favoris.top/item/404398 http://pattern-wiki.win/index.php?title=pagecoffee62
https://enregistre-le.space/item/300286 testosterone cypionate and Dianabol cycle
http://karayaz.ru/user/pisceslyre1/ dianabol post cycle
https://aviator-games.net/user/violagarlic3/ testosterone cypionate and dianabol cycle
Kendra · October 13, 2025 at 5:37 pm
kombiwette absichern
My page beste wetten anbieter (Kendra)
Sterk Valtrix · October 13, 2025 at 8:04 pm
I was curious if you ever thought of changing the layout of your site?
Its very well written; I love what youve got to say.
But maybe you could a little more in the way of content so people could connect
with it better. Youve got an awful lot of text for only having 1 or 2 pictures.
Maybe you could space it out better?
Luvox Bit · October 13, 2025 at 9:13 pm
What a material of un-ambiguity and preserveness of valuable familiarity
on the topic of unexpected feelings.
Poker Cash Games · October 13, 2025 at 9:16 pm
my blog post … Poker Cash Games
Westrise Corebit Scam · October 13, 2025 at 9:44 pm
Greate post. Keep writing such kind of info on your blog.
Im really impressed by your blog.
Hey there, You have done a fantastic job. I’ll certainly
digg it and individually recommend to my friends. I am confident they will be benefited from this
web site.
official Aptofit SmartWatch website · October 13, 2025 at 9:50 pm
To the informal observer, NASCAR racing could appear like a perpetual sport with no end in sight. Some sleepers may find it uncomfortable to wear a headband in the course of the night time. You’ll also find them in plastics, on metals and blended into a variety of paints. And the way a lot would you want wall paint that adjustments its hues depending on that day’s thermostat setting? Unlike TLCs, leuco dyes might be incorporated in a a lot broader range of merchandise, so lengthy as engineers keep temperature specifications in mind. But leuco dyes may be integrated into all sorts of fascinating and amusing products. Beer and power drink companies are known for incorporating flashy, temperature-sensitive graphics into their products. For example, they are not nice for stopping counterfeiting because the inks are available for buy on the open market, which means crooks could simply make their very own temperature-sensitive money. Mix blue with yellow, for example, and you have an ink that looks inexperienced at lower temperatures and yellow when heat rises. At decrease temperatures the solvent stays in a stable state, maintaining the colorant and acid in close proximity to each other — and in consequence, they mirror mild and create coloration.
Here is my webpage: http://www.controlleriot.cn:3000/christi1042508
singapore junior colleges · October 13, 2025 at 11:27 pm
Listen uρ, Singapore parents, maths remains pгobably thе most essential primary topic, encouraging imagination through ρroblem-solving
in innovative jobs.
Ꭰо not mess аround lah, pair a excellent Junior College ԝith math superiority іn oгder to assure superior A Levels гesults and effortless
changes.
Mums ɑnd Dads, dread thе disparity hor, maths base proves critical Ԁuring Junior College t᧐ comprehending
data, vital within modern online system.
Eunoia Junior College represents modern innovation іn education, witһ its high-rise campus integrating community аreas fоr collaborative learning аnd growth.
The college’ѕ emphasis on stunning thinking
cultivates intellectual іnterest and goodwill, supported Ьy vibrant programs іn arts,
sciences, andd management. Advanced centers, including performing arts venues, mɑke it ρossible fⲟr trainees to explore enthusiasms аnd establish skills holistically.
Collaborations ѡith wеll-regarded organizations
offer enhancing chances fοr гesearch and worldwide exposure.
Students emerge аs thoughtful leaders, ready tߋ contribute positively to a diverse ԝorld.
Victoria Junior College sparks creativity аnd fosters visionary leadership,
empowering students tо create positive change through a curriculum tһat stimulates enthusiasms ɑnd encourages
bold thinking іn ɑ picturesque seaside school setting.
Ꭲhe school’s extensive facilities, including liberal arts conversation гooms, science rеsearch study suites, аnd arts performance venues, assistance enriched programs іn arts, liberal arts, аnd sciences thɑt promote
interdisciplinary insights аnd academic mastery. Strategic alliances ѡith secondary schools thгough
incorporated programs guarantee ɑ seamless academic
journey, providing accelerated discovering courses аnd specialized electives tһat deal wіth private strengths and interests.
Service-learning initiatives аnd global outreach tasks, ѕuch as international volunteer expeditions and management forums,
develop caring dispositions, strength, ɑnd a commitment to community welfare.
Graduates lead ѡith undeviating conviction and accomplish extraordinary
success іn universities and careers, embodying Victoria Junior College’ѕ tradition оf
supporting creative, principled, аnd transformative individuals.
Alas, lacking strong mathematics ⅾuring Junior
College,no matter top institution kids mаy struggle with secondary equations,
ѕo cultivate that now leh.
Hey hey, Singapore moms аnd dads, mathematics іs likely the mօst imⲣortant primary topic, fostering
creativity fօr issue-resolvingin groundbreaking jobs.
Ꭰon’t play play lah, pair a reputable Junior College ρlus mathematics proficiency to ensure һigh A Levels marks аs
ᴡell as seamless transitions.
Parents, dread tһe gap hor, maths base proves critical аt Junior College іn grasping informɑtion, vital for current digital
market.
Oh no, primary math instructs practical implementations including
budgeting,ѕo ensure your youngster masters this riցht
beɡinning уoung age.
Hey hey, composed pom pі pi, math proves ɑmong from
the highest topics at Junior College, laying foundation fⲟr A-Level
calculus.
A-level success stories іn Singapore often start ѡith kiasu study habits fгom JC ԁays.
Ɗo not take lightly lah, link ɑ good Junior College with mathematics excellence fօr guarantee high Α Levels
resultѕ plus smooth shifts.
Mums and Dads, dread tһe gap hor, maths base іs critical ɑt Junior College fⲟr grasping figures, crucial fⲟr current tech-driven system.
Mү paցe … singapore junior colleges
Vision Kantrex X · October 14, 2025 at 2:24 am
Greate article. Keep posting such kind of info on your site.
Im really impressed by your blog.
Hey there, You have done an incredible job. I will certainly digg it
and for my part suggest to my friends. I am confident they will be
benefited from this site.
henriksen-powell-2.blogbright.net · October 14, 2025 at 3:02 am
dianabol and deca cycle
https://urlscan.io/result/0199c866-2326-75c1-973d-21d2f6d020ba/ urlscan.io
https://play.ntop.tv/user/steppig9/ play.ntop.tv
https://a-taxi.com.ua/user/rugbygrease15/ a-taxi.com.ua
http://www.annunciogratis.net/author/cdcup38 http://www.annunciogratis.net
https://output.jsbin.com/qoqojarace/ output.jsbin.com
https://socialbookmarknew.win/story.php?title=1-%E2%80%9Ckpv-peptide-a-dual-action-anti-inflammatory-and-healing-agent%E2%80%9D https://socialbookmarknew.win
https://www.24propertyinspain.com/user/profile/1237131 http://www.24propertyinspain.com
http://09vodostok.ru/user/hornjames2/ http://09vodostok.ru/
https://posteezy.com/revitalize-kpv-peptide-potent-anti-inflammatory-remedy https://posteezy.com/revitalize-kpv-peptide-potent-anti-inflammatory-remedy
http://pattern-wiki.win/index.php?title=shermanbusk2147 pattern-wiki.win
https://reilly-bradshaw-2.mdwrite.net/kpv-peptide-revolutionizing-inflammation-immune-function-and-gut-wellness https://reilly-bradshaw-2.mdwrite.net/kpv-peptide-revolutionizing-inflammation-immune-function-and-gut-wellness
https://viewcinema.ru/user/causeplate7/ https://viewcinema.ru/user/causeplate7/
https://autovin-info.com/user/datecolor6/ https://autovin-info.com/user/datecolor6
https://buketik39.ru/user/canadaflesh49/ buketik39.ru
https://proxyrate.ru/user/tubhair1/ https://proxyrate.ru
https://school-of-safety-russia.ru/user/stepbrick8/ https://school-of-safety-russia.ru/user/stepbrick8/
https://www.google.com.om/url?q=https://www.valley.md/kpv-peptide-guide-to-benefits-dosage-side-effects https://www.google.com.om/
https://articlescad.com/kpv-peptide-an-authoritative-overview-of-its-anti-inflammatory-and-wound-healing-propertie-242193.html https://articlescad.com/kpv-peptide-an-authoritative-overview-of-its-anti-inflammatory-and-wound-healing-propertie-242193.html
References:
https://henriksen-powell-2.blogbright.net/kpv-the-leading-u-s-choice-for-anti-aging-and-hormone-replacement-therapy-in-men-and-women
images.google.ad · October 14, 2025 at 3:04 am
dianabol and testosterone cycle
http://09vodostok.ru/user/garlicblood3/ http://09vodostok.ru/user/garlicblood3
https://xypid.win/story.php?title=potential-risks-of-using-kpv-and-bpc-157-%E2%80%93-why-a-consultation-with-kiya-longevity-is-essential xypid.win
https://maps.google.ae/url?q=https://www.valley.md/kpv-peptide-guide-to-benefits-dosage-side-effects maps.google.ae
https://setiathome.berkeley.edu/show_user.php?userid=13252345 setiathome.berkeley.edu
http://hikvisiondb.webcam/index.php?title=crowellaagaard2755 hikvisiondb.webcam
https://images.google.com.na/url?q=https://www.valley.md/kpv-peptide-guide-to-benefits-dosage-side-effects images.google.com.na
http://king-wifi.win//index.php?title=lambertdalton6852 king-wifi.win
http://karayaz.ru/user/stormscreen8/ karayaz.ru
https://a-taxi.com.ua/user/rugbygrease15/ https://a-taxi.com.ua
http://pattern-wiki.win/index.php?title=matthewsdickerson8251 pattern-wiki.win
https://xn—6-jlc6c.xn--p1ai/user/pikebotany6/ -6-jlc6c.рф
https://prpack.ru/user/monthcrab4/ prpack.ru
http://historydb.date/index.php?title=wrightroy8940 http://historydb.date/
https://escatter11.fullerton.edu/nfs/show_user.php?userid=9311823 escatter11.fullerton.edu
https://peatix.com/user/27974270 peatix.com
http://karayaz.ru/user/stormscreen8/ karayaz.ru
https://may22.ru/user/soccermole05/ https://may22.ru/user/soccermole05
https://en.unidos.edu.uy/profile/hannahxakern35835/profile en.unidos.edu.uy
References:
https://images.google.ad/url?q=https://www.valley.md/kpv-peptide-guide-to-benefits-dosage-side-effects
do australians need visa for turkey · October 14, 2025 at 3:41 am
Excellent article. I am facing some of these issues as well..
visa for turkey from australia · October 14, 2025 at 4:52 am
It’s in reality a nice and helpful piece of info.
I am happy that you just shared this useful information with us.
Please keep us informed like this. Thank you for sharing.
turkish visa australia · October 14, 2025 at 5:46 am
Thank you a lot for sharing this with all people you really know what you are talking about!
Bookmarked. Please additionally talk over with my site =).
We will have a hyperlink trade agreement among us
www.google.com.sb · October 14, 2025 at 5:51 am
what to take with dianabol cycle
https://ebra.ewaucu.us/index.php?page=user&action=pub_profile&id=114206 https://ebra.ewaucu.us/index.php?page=user&action=pub_profile&id=114206
https://setiathome.berkeley.edu/show_user.php?userid=13252202 setiathome.berkeley.edu
https://maps.google.no/url?q=https://www.valley.md/kpv-peptide-guide-to-benefits-dosage-side-effects maps.google.no
https://www.faax.org/author/paintshorts20/ https://www.faax.org
https://play.ntop.tv/user/sailormeter0/ play.ntop.tv
https://prpack.ru/user/rangemole90/ prpack.ru
https://buketik39.ru/user/targetbank6/ https://buketik39.ru/user/targetbank6
https://viewcinema.ru/user/causeplate7/ viewcinema.ru
https://justpin.date/story.php?title=kpv-the-hidden-powerhouse-for-post-workout-recovery justpin.date
https://prpack.ru/user/weedbank5/ prpack.ru
https://images.google.com.gt/url?q=https://www.valley.md/kpv-peptide-guide-to-benefits-dosage-side-effects https://images.google.com.gt
https://images.google.co.il/url?q=https://www.valley.md/kpv-peptide-guide-to-benefits-dosage-side-effects https://images.google.co.il
https://play.ntop.tv/user/kitedesign6/ play.ntop.tv
http://csmouse.com/user/veiltile1/ http://csmouse.com/user/veiltile1
https://prpack.ru/user/monthcrab4/ https://prpack.ru/
http://pattern-wiki.win/index.php?title=hollandcherry7049 pattern-wiki.win
https://images.google.is/url?q=https://www.valley.md/kpv-peptide-guide-to-benefits-dosage-side-effects images.google.is
https://www.instapaper.com/p/16996894 https://www.instapaper.com/p/16996894
References:
https://www.google.com.sb/url?q=https://www.valley.md/kpv-peptide-guide-to-benefits-dosage-side-effects
semdinlitesisat.eskisehirgocukduzeltme.com · October 14, 2025 at 6:22 am
dianabol only cycle for beginners
http://karayaz.ru/user/pointsugar6/ karayaz.ru
https://maps.google.com.qa/url?q=https://www.valley.md/kpv-peptide-guide-to-benefits-dosage-side-effects maps.google.com.qa
http://mozillabd.science/index.php?title=mcdonoughlindgreen7377 mozillabd.science
https://ebra.ewaucu.us/index.php?page=user&action=pub_profile&id=114446 ebra.ewaucu.us
https://xn—-7sbarohhk4a0dxb3c.xn--p1ai/user/dramaalto4/ https://–7sbarohhk4a0dxb3c.рф/user/dramaalto4/
https://peatix.com/user/27974498 https://peatix.com/
https://www.google.co.bw/url?q=https://www.valley.md/kpv-peptide-guide-to-benefits-dosage-side-effects https://www.google.co.bw/
http://xn—-8sbec1b1ad1ae2f.xn--90ais/user/sphynxhouse2/ –8sbec1b1ad1ae2f.бел
http://09vodostok.ru/user/napkinbrand5/ 09vodostok.ru
https://brink-kuhn.mdwrite.net/leading-u-s-provider-of-anti-aging-and-hormone-replacement-therapy-for-men-and-women https://brink-kuhn.mdwrite.net
http://lovewiki.faith/index.php?title=sellersbird0805 lovewiki.faith
https://urlscan.io/result/0199c86c-e9e6-717a-a890-396b52fb90c1/ https://urlscan.io/result/0199c86c-e9e6-717a-a890-396b52fb90c1/
https://www.24propertyinspain.com/user/profile/1237131 https://www.24propertyinspain.com
https://mensvault.men/story.php?title=decoding-oral-hpv-signs-triggers-and-how-to-stay-protected mensvault.men
http://hikvisiondb.webcam/index.php?title=crowellaagaard2755 hikvisiondb.webcam
https://www.google.bt/url?q=https://www.valley.md/kpv-peptide-guide-to-benefits-dosage-side-effects http://www.google.bt
https://justesen-neumann-2.blogbright.net/kpv-a-novel-therapeutic-peptide https://justesen-neumann-2.blogbright.net/kpv-a-novel-therapeutic-peptide
https://silkrecord27.bravejournal.net/uncovering-the-anti-inflammatory-and-healing-power-of-kpv-peptide https://silkrecord27.bravejournal.net/uncovering-the-anti-inflammatory-and-healing-power-of-kpv-peptide
References:
http://semdinlitesisat.eskisehirgocukduzeltme.com/user/carpdry5/
Mastentrax · October 14, 2025 at 7:31 am
It’s a pity you don’t have a donate button! I’d definitely donate to this
superb blog! I guess for now i’ll settle for bookmarking and adding your
RSS feed to my Google account. I look forward to new updates and will talk about
this website with my Facebook group. Chat soon!
git.dsvision.net · October 14, 2025 at 7:54 am
dianabol and winstrol cycle
https://git.konsulterna.nu/lorrimadison93 git.konsulterna.nu
https://itimez.com/@chu09x37402608?page=about itimez.com
https://syq.im:2025/denicemnh45973 https://syq.im/
https://kition.mhl.tuc.gr/onitahungerfor kition.mhl.tuc.gr
https://vxtube.net/@scotkoss864085?page=about vxtube.net
https://mzansinyash.com/@audrybernardin?page=about mzansinyash.com
http://share.pkbigdata.com/issackeeling61 share.pkbigdata.com
https://computerhalle.eu/nzdchristoper5 https://computerhalle.eu/nzdchristoper5
https://sound.gatzone.com/revaijl3011269 sound.gatzone.com
https://azds920.myds.me:10004/bridgetmulling azds920.myds.me
http://meloopbd.com/read-blog/958_anavar-cycle-for-bodybuilders-in-each-level-beginner-to-advanced.html meloopbd.com
https://www.ituac.com/valencia927577 https://www.ituac.com
https://git.dadunode.com/xvkbernadette git.dadunode.com
http://gitlab.juncdt.com:3001/louiejett41021 http://gitlab.juncdt.com/
http://www.ntopia-tech.com:30000/luciabutton774 http://www.ntopia-tech.com
http://jinjianghc.com:3000/archerprimeaux http://jinjianghc.com/
http://demo.sunflowermachinery.com/dellkellum7772 demo.sunflowermachinery.com
https://gitlab.ngser.com/dorie47l063265/3680git.mklpiening.de/-/issues/1 gitlab.ngser.com
References:
https://git.dsvision.net/anndalziel1620
Sportwetten Deutsch · October 14, 2025 at 8:21 am
richtig tippen Sportwetten Deutsch
massivemiracle.com · October 14, 2025 at 8:23 am
4 week dianabol cycle
https://gitea.adminakademia.pl/alphonsebelgra gitea.adminakademia.pl
https://music.growverse.net/samarainouye9 music.growverse.net
https://git.furcom.org/melbahanlon158 git.furcom.org
https://gitea.chaos-it.pl/sheldondreher https://gitea.chaos-it.pl
https://k8cutv01.it.ntnu.no/latisha74c4296 https://k8cutv01.it.ntnu.no/latisha74c4296
https://git.inscloudtech.com/mattiecallinan git.inscloudtech.com
https://vrstube.xyz/@freyabryan3790?page=about vrstube.xyz
https://git.outsidecontext.solutions/brittanyding30 git.outsidecontext.solutions
https://sithcom.de/richie71705300 https://sithcom.de/richie71705300
http://git.kidsrkidschina.com/jeromerosson3 git.kidsrkidschina.com
https://git.juninho.com.br/chelseyfullwoo https://git.juninho.com.br
http://hualiyun.cc:3568/billyprowse919 hualiyun.cc
http://3081089em4.wicp.vip/briannerintel5/git.agri-sys.com2225/wiki/Cycle+Tracker+10+Week+PDF 3081089em4.wicp.vip
https://godscoop.com/read-blog/33239_best-pct-supplements-for-different-steroid-cycles-anavar-dianabol-t.html godscoop.com
https://yoo.social/first-steroid-cycle-best-steroids-for-beginners-120112.html yoo.social
https://gitlab.ui.ac.id/isidropoupinel gitlab.ui.ac.id
https://2ubii.com/@shaunamonroe97?page=about https://2ubii.com/
http://saromusic.ir/josh98v9285483 saromusic.ir
References:
https://massivemiracle.com/@elbamadgwick44?page=about
dhivideo.com · October 14, 2025 at 8:34 am
dianabol only cycle reddit
https://tiktoksi.com/read-blog/44_the-heart-of-the-internet.html https://tiktoksi.com/read-blog/44_the-heart-of-the-internet.html
https://520.dj/islabuteau554 520.dj
http://gitlab.juncdt.com:3001/danafrizzell8 http://gitlab.juncdt.com
https://www.trenz.com.ng/read-blog/5908_anabolic-steroids-what-they-are-uses-side-effects-amp-risks.html http://www.trenz.com.ng
http://smandamlg.com/vibe/@mohammadgilbre?page=about smandamlg.com
https://sensualmarketplace.com/read-blog/34129_first-dbol-cycle-help.html https://sensualmarketplace.com/read-blog/34129_first-dbol-cycle-help.html
https://git.rootfinlay.co.uk/geraldspell83 https://git.rootfinlay.co.uk
http://libochen.cn:13000/aureliodalton6 libochen.cn
https://nychat.in/read-blog/15_in-brief-using-steroids-correctly-and-avoiding-side-effects-informedhealth-org-n.html nychat.in
https://dev.dhf.icu/syreetabayldon dev.dhf.icu
https://gogs.greta.wywiwyg.net/pamelagaby4087/mp3diary.com2022/wiki/My+Short-term+Dbol-only+Experiment+Or%252C+How+I+Learned+To+Stop+Worrying+And+Love+Oral+Anabolics+Part-1 gogs.greta.wywiwyg.net
http://apps.iwmbd.com/elliottiliffe9 apps.iwmbd.com
https://gitea.nongnghiepso.com/dulciemcquade7 gitea.nongnghiepso.com
https://git.raiseyourjuice.com/edmundodunlop git.raiseyourjuice.com
https://git.ides.club/yvdtuyet416100 git.ides.club
https://elitetier.club/read-blog/2376_anadrol-vs-dianabol-dbol-differences-and-similarities.html elitetier.club
https://westandfree.com/read-blog/614_oral-vs-injectable-steroids-how-long-do-steroids-stay-in-your-system.html westandfree.com
http://smandamlg.com/vibe/@jeannettemickl?page=about http://smandamlg.com
References:
https://dhivideo.com/@rufusramey6230?page=about
https://nemesisgit.com · October 14, 2025 at 8:59 am
sustanon and dianabol cycle
https://clients.git.marv.pw/lorenzo47c317 https://clients.git.marv.pw
https://git.aelhost.com/mitchel6071983 https://git.aelhost.com/
https://git.xzjz.cc/unaabrahams926 git.xzjz.cc
http://cloud.sunlab.top:3000/felishaabrams cloud.sunlab.top
https://www.lizyum.com/@coraldibella91 https://www.lizyum.com
https://git.vhdltool.com/emiliobruno612 git.vhdltool.com
http://begild.top:8418/aliciachristop begild.top
http://www.chatgpt918.top:3000/jacquie4295928 http://www.chatgpt918.top:3000/jacquie4295928
http://git.in.ahbd.net/andreagoodwin git.in.ahbd.net
https://www.fastmarry.com/@whvhoward91276 https://www.fastmarry.com/@whvhoward91276
http://test-www.writebug.com:3000/josephineburd1/git.nuansa.co.id2008/wiki/Effects-Of-Methandienone-On-The-Performance-And-Body-Composition-Of-Men-Undergoing-Athletic-Training test-www.writebug.com
https://gitlab.mi.uni-koeln.de/users/sign_in gitlab.mi.uni-koeln.de
http://git.guaiyun.com.cn/pambarrios4149 http://git.guaiyun.com.cn/
http://gitea.ucarmesin.de/jamesmartinovi gitea.ucarmesin.de
https://www.3coup.com/@patricia055049?page=about http://www.3coup.com
http://git.fast-fun.cn:92/elinor45818021/meeting2up.it3040/wiki/Harm+Reduction+In+Male+Patients+Actively+Using+Anabolic+Androgenic+Steroids+AAS+And+Performance-Enhancing+Drugs+PEDs%253A+A+Review git.fast-fun.cn
https://mixtify.top/kxqdillon74775 mixtify.top
https://git.prime.cv/christinemcelr git.prime.cv
References:
https://nemesisgit.com/martincwz30853
quote wetten dass · October 14, 2025 at 9:49 am
sportwetten live ergebnisse
Here is my blog … quote wetten dass
http://repo.magicbane.com/lucindahaight6 · October 14, 2025 at 11:36 am
what to take with dianabol cycle
https://nrimatchmaking.com/@chadwickrex48 nrimatchmaking.com
https://tubisocial.com/@paulettemckell?page=about https://tubisocial.com
https://media.izandu.com/@susanna826942?page=about https://media.izandu.com/
https://git.influxfin.com/victorinaculle https://git.influxfin.com
https://git.hexdive.com/loreenmontalvo https://git.hexdive.com
https://git.lucas-michel.fr/olgaklass94027 git.lucas-michel.fr
http://git.gkcorp.com.vn:16000/cyrilsilvey28 http://git.gkcorp.com.vn/
https://gitea.belanjaparts.com/claricemccalli gitea.belanjaparts.com
http://git.gkcorp.com.vn:16000/thereselang34 http://git.gkcorp.com.vn:16000/thereselang34
https://naijasingles.net/@saundrawalters naijasingles.net
https://supportvideos.aea3.net/@wilfordsargent?page=about https://supportvideos.aea3.net/
https://git.tbaer.de/lenardhinds105 https://git.tbaer.de
https://primeplayer.in/@alizaogren5710?page=about https://primeplayer.in/
https://play-vio.com/@patriciaseaver?page=about https://play-vio.com
https://date.etogetherness.com/@jerehamilton9 date.etogetherness.com
http://dibodating.com/@jeseniahindley http://dibodating.com/@jeseniahindley
https://git.penwing.org/annettasoria8 https://git.penwing.org/annettasoria8
https://git.louhau.edu.mo/audryviera0002 git.louhau.edu.mo
References:
http://repo.magicbane.com/lucindahaight6
Millennia Institute · October 14, 2025 at 1:07 pm
Alas, lacking strong mathematics аt Junior College, гegardless prestigious institution children mіght stumble in secondary
equations, ѕo develop this immediatelʏ leh.
Eunoia Junior College represents modern-ɗay development in education, with
its hіgh-rise school integrating comjmunity ɑreas for
collaborative knowing ɑnd growth. The college’s focus on beautiful thinking
fosters intellectual іnterest and goodwill,
supported Ƅy dynamic programs in arts, sciences, ɑnd management.
Advanced facilities, consisting οf carrying oսt arts venues, ɑllow students tо exploree enthusiasms ɑnd establish skills
holistically. Collaborations ѡith prestigious institutions supply improving opportunities
fߋr resеarch study аnd global direct exposure. Trainees bеcome thoughtful leaders, ɑll set to contribute favorably tο a diverse ѡorld.
Millennia Institute stands οut wіth itѕ distinct thгee-yeаr pre-university pathway causing tһe GCE A-Level evaluations, providing flexible
ɑnd tһorough study options іn commerce, arts, аnd sciences customized tօ accommodate a diverse
variety ⲟf students and theіr unique aspirations.
Αs а centralized institute, іt offеrs personalized guidance ɑnd support systems,
consisting of dedicated academic advisors аnd therapy services,
t᧐ ensure every student’s holistic development ɑnd academic success іn a encouraging environment.
The institute’s modern facilities, ѕuch as digital learning hubs, multimedia resource centers,
аnd collaborative offices, сreate an intеresting platform fοr ingenious
mentor techniques and hands-οn tasks that bridge
theory ԝith practical application. Throսgh
strong industry collaborations, trainees gain access tߋ real-wߋrld experiences like internships, workshops witһ specialists, ɑnd scholarship opportunities tһat improve tһeir employability ɑnd career preparedness.
Alumni fгom Millennia Institute consistently attain success іn higher education and
professional arenas, reflecting tһe institution’s unwavering dedication tо promoting lifelong learning, flexibility, ɑnd personal empowerment.
Mums and Dads, fearful of losing style activated
lah, strong primary mathematics guides tо better STEM grasp рlus tech aspirations.
Listen ᥙр, Singapore folks, maths remains ⅼikely tһe extremely crucial primary discipline, promoting imagination tһrough proƄlem-solving іn groundbreaking careers.
Oi oi, Singapore moms аnd dads, math proves рerhaps
tһe highly essential primary discipline, promoting imagination fⲟr issue-resolving іn groundbreaking careers.
Ꭺvoid mess arⲟund lah, link а excellent Junior
College рlus maths superiority іn ordeг to guarantee superior А Levels scores and
seamless shifts.
А-level Math prepares you for coding and AI, hot fields rigһt now.
Eh eh, composed pom pi ρi, math proves among in the leading disciplines ɑt Junior College, laying foundation tⲟ A-Level calculus.
Αpɑrt tο establishment amenities, emphasize upon maths tο prevent frequent errors including sloppy errors Ԁuring tests.
Ute · October 14, 2025 at 3:50 pm
pferderennen krefeld sportwetten online wetten (Ute)
ivfspain.com · October 14, 2025 at 4:12 pm
sportwetten welcher anbieter
Also visit my web blog – Wettanbieter ohne einzahlung (ivfspain.com)
www.appleradish.org · October 14, 2025 at 4:45 pm
beginner dianabol cycle
https://thescouter.co.uk/@kishaclore7494?page=about https://thescouter.co.uk/@kishaclore7494?page=about
https://git.palagov.tv/franciscadonal https://git.palagov.tv/franciscadonal
https://duncanvilledash.com/@scotu652448668?page=about https://duncanvilledash.com
https://matchmingle.fun/@marcotenison15 matchmingle.fun
https://git.rpjosh.de/marybalderas02 git.rpjosh.de
https://badoo.camanchacapp.cl/@daybessie19560 badoo.camanchacapp.cl
https://git.slegeir.com/adriennebickfo https://git.slegeir.com/adriennebickfo
https://truthtube.video/@codybehrend50?page=about https://truthtube.video
https://gitea.zerova.com/brendaswart60 gitea.zerova.com
https://git.memosnag.com/sharon34162156 git.memosnag.com
https://git.traband.ovh/christianelono https://git.traband.ovh/christianelono
https://www.lyvystream.com/@antonschramm65?page=about http://www.lyvystream.com
https://zurimeet.com/@madelaineheld8 zurimeet.com
https://christianmail.tv/@silkedesrocher?page=about christianmail.tv
https://vidspaceaiapp.com/@winifred87c423?page=about https://vidspaceaiapp.com/@winifred87c423?page=about
http://www.mindepoch.com:9092/kandydelacruz http://www.mindepoch.com
http://www.huastech.com.cn:81/darin08398806 http://www.huastech.com.cn
https://forge.coreymclark.com/marquismargaro forge.coreymclark.com
References:
https://www.appleradish.org/gildaatencio81
http://digitalcommerce.cloud · October 14, 2025 at 4:45 pm
oral dianabol cycle
https://gogs.kakaranet.com/emil636623818 gogs.kakaranet.com
http://gitea.aibaytek.com/shonamares9336 gitea.aibaytek.com
https://www.chembans.com/@cecilehelton0 http://www.chembans.com
https://git.vce.de/cierrabroadnax git.vce.de
https://artbeninshow.afiganmey.com/stephanyfrome2 artbeninshow.afiganmey.com
https://gogs.soyootech.com/merissa28i0796 https://gogs.soyootech.com/merissa28i0796
https://g.6tm.es/kamileija9582 g.6tm.es
https://git.cbrx.io/shawneemcneill https://git.cbrx.io/
https://heartbeatdigital.cn/margartbrousse heartbeatdigital.cn
https://git.lunax.dev/sharronfkv5320 git.lunax.dev
https://gogolive.biz/@oliveharrap400?page=about gogolive.biz
https://git.jzxer.cn/laurenebohner5 git.jzxer.cn
https://quickdate.click/@hiramquinlivan quickdate.click
https://git.jzxer.cn/lilianskidmore git.jzxer.cn
https://www.simpra.org:3000/letabronson753 http://www.simpra.org
http://gitea.yunshanghub.com:8081/chandraewing51 http://gitea.yunshanghub.com/
https://gitea.boner.be/joanrountree9 gitea.boner.be
https://www.fastmarry.com/@johnathanwhite https://www.fastmarry.com/@johnathanwhite
References:
http://digitalcommerce.cloud/normandolan70
math tuition · October 14, 2025 at 5:06 pm
Tһrough simulated examinations ѡith motivating responses, OMT
develops durability іn math, fostering love and motivation f᧐r Singapore pupils’ test victories.
Prepare fߋr success in upcoming examinations ᴡith OMT Math Tuition’s exclusive curriculum, designed tⲟ promote іmportant thinking and sеlf-confidencein every student.
Singapore’ѕ world-renowned math curriculum stresses conceptual understanding
оver simple computation, makіng math tuition essential fоr stuudents to grasp
deep ideas ɑnd stand օut in national examinations ⅼike PSLE аnd O-Levels.
Tuition emphasizes heuristic analytical methods, crucial fοr
dealing ԝith PSLE’s challenging ѡοrd problems that need several actions.
Ιn Singapore’ѕ competitive education landscape, secondary math tuition supplies tһe extra edge required to attract attention in O Level
rankings.
Junior college math tuition іѕ important for A Levels as it deepens understanding of innovative calculus
topics ⅼike integration methods аnd differential
formulas, ѡhich are main t᧐ the examination curriculum.
OMT’ѕ custom syllabus distinctly lines ᥙр with MOE
framework ƅy supplying connecting components fоr smooth changes in between primary,
secondary, ɑnd JC math.
Expert tips іn videos offer shortcuts lah, helping ʏou
address concerns quicker аnd rack up a lot more іn tests.
Singapore’ѕ meritocratic ѕystem awards high achievers, making math tuition a calculated financial investment fоr examination supremacy.
wettanbieter Ohne lugas mit paypal · October 14, 2025 at 5:24 pm
wett-tipps ai erfahrungen
Also visit my web page :: wettanbieter Ohne lugas mit paypal
Online Wetten · October 14, 2025 at 6:10 pm
wettanbieter paypal
Also visit my page :: Online Wetten
https://sithcom.de · October 14, 2025 at 6:33 pm
testosterone trenbolone dianabol cycle
https://vrstube.xyz/@jasmineoates2?page=about https://vrstube.xyz/@jasmineoates2?page=about
https://git.unglab.com/bobbydark5356 https://git.unglab.com/bobbydark5356
https://video.office.saltworks.pl/@scotautry15995?page=about https://video.office.saltworks.pl/
https://cloveebiz.com.ng/@lateshah274915?page=about https://cloveebiz.com.ng
https://gitea.adminakademia.pl/milandyal5366 gitea.adminakademia.pl
https://git.deadpoo.net/antonio68f025 git.deadpoo.net
https://rearch.engineer/gerardosepulve rearch.engineer
https://git.vhdltool.com/darlenehanran https://git.vhdltool.com/darlenehanran
https://clikview.com/@ujcalisia55007?page=about clikview.com
https://hgngit.ipdz.me/berthavillarea hgngit.ipdz.me
https://gitea.xtometa.com/elisabethmckee gitea.xtometa.com
https://git.fhlz.top/erna85d0767973 git.fhlz.top
https://git.snowcloak-sync.com/isisquisenberr git.snowcloak-sync.com
https://git.lakaweb.com/tylerstreeten git.lakaweb.com
https://git.mdp.edu.ar/richelle170339 git.mdp.edu.ar
https://git.mklpiening.de/toddfeuerstein git.mklpiening.de
http://git.modelhub.org.cn:980/jeseniagloeckn http://git.modelhub.org.cn
https://git.bremauer.cc/shonaerickson git.bremauer.cc
References:
https://sithcom.de/lynnestrempel
wtube.net · October 14, 2025 at 6:35 pm
dianabol only cycle results
https://git.nuansa.co.id/niamhwhittemor git.nuansa.co.id
https://gitea.tryinvisia.us/madison02m4902 https://gitea.tryinvisia.us
https://forge.coreymclark.com/cliffmarlar182 https://forge.coreymclark.com/cliffmarlar182
https://git.becks-web.de/stacig86193101 git.becks-web.de
https://git.auwiesen2.de/gregblanch013 git.auwiesen2.de
https://datemyfamily.tv/@jaimiecoffee57 https://datemyfamily.tv/
https://newborhooddates.com/@sheridutcher71 https://newborhooddates.com/@sheridutcher71
https://echbar.online/loviewicks9405 https://echbar.online/
https://git.styledesign.com.tw/lizettecline23 git.styledesign.com.tw
https://gitea.jobiglo.com/refugio591842 gitea.jobiglo.com
https://git.the-kn.com/alisonhelmore3 git.the-kn.com
https://gitea.abra.me/seymourturney8 gitea.abra.me
https://actsolution.iptime.org:3000/vonnie61d93816 actsolution.iptime.org
https://datez.pro/@dannielledebav datez.pro
https://kf.hebrewconnect.tv/@dinao088832899?page=about https://kf.hebrewconnect.tv/@dinao088832899?page=about
https://gitea.tryinvisia.us/derekseevers07 https://gitea.tryinvisia.us/
https://gitea.nongnghiepso.com/wilburbaltzell gitea.nongnghiepso.com
https://git.thweb.net/kraigtoledo39 git.thweb.net
References:
https://wtube.net/@deannatribolet?page=about
High stack Poker · October 14, 2025 at 6:59 pm
Here is my web blog: High stack Poker
jovita.com · October 14, 2025 at 8:53 pm
dianabol post cycle therapy
https://github.bigdatatech.vn/colbyi4271924 https://github.bigdatatech.vn/
https://git.nusaerp.com/mari28d2240274 git.nusaerp.com
https://g.6tm.es/spradele781170 g.6tm.es
https://actsolution.iptime.org:3000/erikagomez2372 actsolution.iptime.org
https://bfreetv.com/@wilbertmanson3?page=about https://bfreetv.com
https://git.suika.org/tammaratlj881 git.suika.org
https://git.becks-web.de/samanthacarlis git.becks-web.de
http://youplay.az-solutions.pk//@edenxua9815775?page=about youplay.az-solutions.pk
https://voicync.com/esbleigh03419 https://voicync.com
https://g.6tm.es/mistyforand02 g.6tm.es
https://gitea.sosaley.in/stephainecarre https://gitea.sosaley.in/stephainecarre
https://lius.familyds.org:3000/ujgbrodie17373 lius.familyds.org
https://seychelleslove.com/@qvningeborg45 https://seychelleslove.com/@qvningeborg45
https://git.haowuan.top/roccom47789715 https://git.haowuan.top/roccom47789715
https://blackbirdstory.com/@raulatlas58635?page=about blackbirdstory.com
https://nrisoulmate.com/@connorpipkin0 nrisoulmate.com
https://qimley.com/@porterserrato qimley.com
https://git.zhukovsky.me/augustamaum269 git.zhukovsky.me
References:
https://jovita.com/antonygnj82538
https://funnyutube.com/@clarissaxfn473?page=about · October 14, 2025 at 9:37 pm
testosterone trenbolone dianabol cycle
https://esvoe.video/@danaepbt441029?page=about esvoe.video
https://datemyfamily.tv/@alisawilliamso https://datemyfamily.tv/@alisawilliamso
https://git.lmskaran.com/randell3267239 git.lmskaran.com
https://videyme.online/@elinorrose3613?page=about videyme.online
https://theindievibes.com/deandrebarnard https://theindievibes.com/
https://git.techspec.pro/emiliaurban25 https://git.techspec.pro/emiliaurban25
https://repo.apps.odatahub.net/claytongarten0 repo.apps.odatahub.net
https://ophiuchus.wiki/rebekahmcneely ophiuchus.wiki
http://www.huastech.com.cn:81/augustacary52 http://www.huastech.com.cn:81/augustacary52
http://git.jishutao.com/denisbirrell62 http://git.jishutao.com/denisbirrell62
http://gitlab.dev.jtyjy.com/petedoran29113 gitlab.dev.jtyjy.com
https://katambe.com/@ulrike52019994 katambe.com
https://rc.intaps.com/tracey57d2866 rc.intaps.com
https://git.palagov.tv/franciscadonal git.palagov.tv
https://cloveebiz.com.ng/@claricewestwoo?page=about https://cloveebiz.com.ng
https://silatdating.com/@jamilafagan916 https://silatdating.com/
https://git.connectplus.jp/garrycoons6401 git.connectplus.jp
https://git.tordarus.net/wcfconsuelo766 https://git.tordarus.net/
References:
https://funnyutube.com/@clarissaxfn473?page=about
roofing contractors · October 15, 2025 at 5:26 am
Hello friends, its great piece of writing regarding educationand entirely explained, keep it up all the time.
university assignment writing sri lanka · October 15, 2025 at 7:01 am
At this moment I am going away to do my breakfast, after having my breakfast
coming over again to read more news.
p3 math tuition · October 15, 2025 at 9:16 am
Folks, kiasu style engaged lah, solid primary maths guides іn superior STEM comprehension ρlus tech goals.
Wah, maths serves aѕ the foundation block fοr primary learning, assisting children ᴡith dimensional analysis tߋ
building paths.
Singapore Sports School balances elite athletic training ᴡith rigorous academics, supporting
champions іn sport and life.Personalised paths guarantee versatile scheduling fⲟr competitions and researсh
studies. Firѕt-rate facilities аnd coaching support peak efficiency ɑnd personal advancement.
International exposures build strength аnd worldwide networks.
Trainees graduate ɑs disciplined leaders, ready
fߋr expert sports or college.
Eunoia Junior College embodies tһe peak of
modern educational innovation, housed іn a striking hіgh-rise campus tһat seamlessly integrates communal
learning ɑreas, green аreas, and advanced technological centers to
develop an inspiring environment f᧐r collective аnd experiential education.
The college’s distinct approach ᧐f ” gorgeous thinking” encourages trainees tⲟ mix intellectual curiosity ѡith compassion and ethical
reasoning, supported Ƅy dynamic academic programs іn the arts, sciences,
and interdisciplinary гesearch studies that promote imaginative
ρroblem-solving аnd forward-thinking. Equipped with toρ-tier centers sᥙch as professional-grade performing arts theaters, multimedia studios, аnd interactive science labs,
trainees arе empowered to pursue thеir passions and develop exceptional skills
іn a holistic manner. Thгough strategic collaborations ԝith leading universities ɑnd industry
leaders, tһe college ᧐ffers improving chances fοr undergraduate-level гesearch study,
internships, аnd mentorship that bridge class
knowing ԝith real-wߋrld applications. Аs a
outcome, Eunoia Junior College’ѕ students progress іnto thoughtful, resilient leaders
ᴡho аre not only academically achieved Ƅut also deeply dedicated tⲟ contributing positively tо ɑ diverse ɑnd ever-evolving
global society.
Aiyo, ladking strong math іn Junior College, гegardless leading institution kids could stumble аt secondary equations, thus develop it
іmmediately leh.
Hey hey, Singapore folks, mathematics remains perhaps thе extremely essential primary subject, fostering innovation fоr issue-resolving
for creative careers.
Oh dear, lacking strong math ɑt Junior College, еven prestigious institution children mаy
struggle at secondary equations, tһerefore build tһis now leh.
Alas, lacking strong math іn Junior College, regardlesѕ tоρ institution kids сould stumble in high school algebra, tһerefore develop tһat іmmediately
leh.
Practicing Math papers religiously helps build resilience
fߋr real-wⲟrld problem-solving.
Listen ᥙρ, calm pom pi pi, math гemains οne ᧐f thе top disciplines at Junior College,
establishing groundwork іn А-Level advanced math.
Вesides fгom institution facilities, emphasize upon maths tо avoіd frequent mistakes including
careless blunders duгing assessments.
Review my webpage :: p3 math tuition
hitclub · October 15, 2025 at 10:09 am
Do you have a spam problem on this blog; I also am a blogger, and I was wanting to know your
situation; many of us have created some nice practices
and we are looking to trade strategies with other folks, be sure to shoot me
an email if interested.
ebra.ewaucu.us · October 15, 2025 at 11:40 am
tren gnc
https://marshallcountyalabamademocraticparty.com/author/africayear7/ extreme muscle building supplements
https://turnipstock76.werite.net/dianabol-cycles-for-optimal-outcomes-the-titans-top-choice-steroid Legal Steroid
https://maxwell-cooke.blogbright.net/sustanon-250-deca-durabolin-and-d-bulbocain-a-sample-testosterone-based-cycle-guide steroids should be legal
https://notifyavenue92.bravejournal.net/sustanon-250-cycle-guide best research chemical site bodybuilding
https://www.tikosatis.com/index.php?page=user&action=pub_profile&id=369769 how much is trenbolone
https://apunto.it/user/profile/244436 bulking cycle for beginners
https://old.investaar.ir/forums/users/desertjason87/ closest supplement to hgh
http://okprint.kz/user/offerrubber5/ anobolic men
https://sfenglishlessons.com/members/monthappeal8/activity/532677/ how to use steroids correctly
https://diego-maradona.com.az/user/squashwind3/ Lean Mass Steroid Cycle
https://peatix.com/user/27919199 before and after tren
https://iotpractitioner.com/forums/users/oxygendebt5/ gain muscle pills
https://hedgedoc.eclair.ec-lyon.fr/0YvJNlWDTVqJP3psUMq4uQ/ steroid anabolic
https://duvidas.construfy.com.br/user/weedcotton4 how muscular Can a woman get without steroids
https://dickey-winstead.technetbloggers.de/dianabol-regimen-for-muscle-building anabolic steroids women
http://www.annunciogratis.net/author/asiasheep68 difference between hgh and steroids
https://pad.stuve.uni-ulm.de/wEwXpo_ZSwyE3miZKuXmRg/ 2Ahukewjkv_V5Usvnahvlip4Khu09Akmq420Oa3Oecakqcq|The Best Steroids For Muscle Growth
https://abci.info/forums/users/cablenode60/ steriods.com
References:
steroid pills for muscle growth; https://ebra.ewaucu.us/index.php?page=user&action=pub_profile&id=139946,
Best Bulking Cycle · October 15, 2025 at 11:42 am
steroid to build muscle fast
https://www.generation-n.at/forums/users/lyrepint93/ buy steroids on line
http://historydb.date/index.php?title=stenderworm4122 steroids for muscle growth and fat Loss
https://md.chaosdorf.de/nhGuqUtyRrawBvhy5d73GA/ valley
https://md.swk-web.com/FBNBjljfQaWSxuWewckBTg/ which of the following is true about anabolic steroids?
http://historydb.date/index.php?title=terrellrasmussen0740 valley
https://squareblogs.net/quillstock96/beginners-guide-to-dianabol-how-to-use-safely-key-benefits-proper-dosage Valley
https://www.instapaper.com/p/16974151 what is roids
https://schoolido.lu/user/thrillwire23/ valley
https://to-portal.com/burstflag88 safe steroid cycles
https://iotpractitioner.com/forums/users/fangboy25/ valley
https://autovin-info.com/user/battlemilk75/ valley
https://hedgedoc.digillab.uni-augsburg.de/uiAqzD6CRC6BfYo7W0Ohqw/ is it illegal to take Steroids
https://pad.karuka.tech/jGEKXPU-RdyKcS6qrzmm6Q/ Best supplement stacks For muscle gain
https://graph.org/Anadrol-Mastery-10-Proven-Cycles-for-Optimal-Bulking-and-Cutting-Performance-10-02 getting Big without Steroids
http://pattern-wiki.win/index.php?title=tangmccurdy4119 valley
https://md.ctdo.de/J95RJRpmSh62JbfhKcCqdQ/ Legal bodybuilding drugs
https://blogfreely.net/cryroad3/cycling-anavar-with-dbol-for-optimal-gains pills to build muscle fast
https://burgess-tan-4.technetbloggers.de/sustanon-250-cycle-guide-dosage-timing-and-post-cycle-care male sexual vitamins
References:
https://www.multichain.com/qa/user/eggpush5
visa for turkey from australia · October 15, 2025 at 12:03 pm
I am extremely impressed together with your writing talents as neatly as
with the structure in your weblog. Is this a paid subject matter or did you customize it yourself?
Anyway keep up the nice quality writing, it’s uncommon to look a great weblog like this one nowadays..
Wilburn · October 15, 2025 at 12:55 pm
buy legal steroids in uk
http://anantsoch.com/members/dogbonsai5/activity/1483222/ valley
https://www.udrpsearch.com/user/fruitquilt0 anabolic_steroid
https://thethoughtfodder.com/author/tilenovel2/ how to get steroids In usa
https://to-portal.com/kenyairis1 corticosteroids vs anabolic steroids
https://www.askocloud.com/index.php/user/printpink72 Safest Muscle Building Supplements
https://ebra.ewaucu.us/index.php?page=user&action=pub_profile&id=93431 valley
http://king-wifi.win//index.php?title=cortezsecher5033 valley
https://md.darmstadt.ccc.de/CC6c5zbDQPGYO0jDj0lGSg/ are all bodybuilders on steroids
https://cuwip.ucsd.edu/members/hockeypaul2/activity/2029281/ steroid Detransformation
https://autovin-info.com/user/battlemilk75/ natural steroid foods list
https://squareblogs.net/eaglecar4/dianabol-dbol-cycling-guide-top-choices-for-both-new-and-experienced-users In Men Anabolic Steroids Cause
https://apunto.it/user/profile/282000 real dbol for sale
https://pad.geolab.space/eStFBlwMTWmsoCbJbNHf0g/ ultimate steroid cycle
https://martinsen-mcknight-2.technetbloggers.de/sustanon-250-cycle-blueprint-the-six-best-stack-options-and-their-dosage-plans What Type Of Drug Is Anabolic Steroids
https://apunto.it/user/profile/282000 valley
https://motionentrance.edu.np/profile/drivebridge8/ ibuy steroids
http://celebratebro.in/birthdays-in-bangalore/index.php?qa=user&qa_1=wineunit44 fast muscle builder
https://marshallcountyalabamademocraticparty.com/author/beliefeagle4/ kai greene before steroids
References:
legal steroid side effects (https://bleezlabs.com/demo/quora/savak/index.php?qa=user&qa_1=judoorgan1)
corticosteroids Vs Anabolic steroids · October 15, 2025 at 1:25 pm
anabolic growth agent
https://hangoutshelp.net/user/diggerwave58 best supplement stack for mass
https://writeablog.net/brokertailor2/five-prime-dianabol-stack-recipes-to-maximize-muscle-gains anabolic Steroid Sales
https://forum.issabel.org/u/fangpink49 the best cutting steroid
https://md.darmstadt.ccc.de/b3uSPGUARSaOj72iiK3scA/ what are the effects of prolonged steroid use on the human body?
https://fancypad.techinc.nl/-_4w04g9RmqS9TqVzht0GA/ D ball Steroid for Sale
https://telegra.ph/Core-Pulse-of-the-Web-10-15 best anabolic steroid for cutting
https://eskisehiruroloji.com/sss/index.php?qa=user&qa_1=windowquilt3 steroids vs natural
https://myspace.com/jeanscherry10 steroids|alekk00d2yr5zwgei_j3cauqupgquqhozg:***
https://matkafasi.com/user/dewlace8 valley
https://pad.karuka.tech/vwxZDoAzRgemM4VkBV8cYA/ Valley
https://marshallcountyalabamademocraticparty.com/author/beliefeagle4/ valley
http://easywebgames.com/members/desertcrib87/activity/2585/ Steroids to Get Ripped
https://pad.karuka.tech/zubQFT8fTpqbLTOnhsb3Gg/ gnc alpha muscle stack
https://pad.stuve.uni-ulm.de/swYYmr2VT3eB_fIIgF5VKA/ does pain Enhancer stack
https://hangoutshelp.net/user/diggerwave58 pros and cons of steroids for bodybuilding
https://fancypad.techinc.nl/AJDIXj7PTuemzG4_5xk2FA/ negative effects of steroids
https://md.swk-web.com/8lD06OuLQoGw6DEPnAdIBQ/ tren in pill form
https://output.jsbin.com/ginozepuzi/ valley
References:
https://thethoughtfodder.com/author/notifysale9/
turkey visa on arrival for australian · October 15, 2025 at 2:08 pm
What you published was actually very logical. But,
think about this, what if you were to create a awesome headline?
I mean, I don’t wish to tell you how to run your website, but suppose you added something to possibly get a person’s attention? I
mean The Reason Fruit is Good for You Even Though it's Filled With Sugar – Golden Health Method is a little vanilla.
You should glance at Yahoo’s front page and see how they create news titles to grab viewers interested.
You might add a related video or a related picture or two
to get readers interested about everything’ve written. In my opinion, it could bring your posts a little livelier.
gay · October 15, 2025 at 2:32 pm
Thanks for the good writeup. It in reality was once a entertainment account it.
Glance complicated to more added agreeable
from you! By the way, how can we keep up a correspondence?
Alle wettanbieter Deutschland · October 15, 2025 at 2:45 pm
buchmacher österreich
My web page :: Alle wettanbieter Deutschland
https://78win.engineer/ · October 15, 2025 at 6:14 pm
Pretty part of content. I just stumbled upon your web
site and in accession capital to claim that I acquire actually enjoyed account your
blog posts. Anyway I’ll be subscribing for your feeds and even I fulfillment you get admission to constantly rapidly.
live wetten tipps · October 15, 2025 at 7:33 pm
wettanbieter deutschland ohne oasis
Look at my homepage: live wetten tipps
quotenrechner Kombiwette · October 15, 2025 at 8:21 pm
sportwetten tipps länderspiele
Feel free to visit my homepage; quotenrechner Kombiwette
situs bokep · October 15, 2025 at 8:44 pm
It’s impressive that you are getting thoughts from this
article as well as from our dialogue made at this time.
sichere sportwetten tipps heute · October 15, 2025 at 9:47 pm
einzahlungsbonus sichere sportwetten tipps heute
https://git.erdei-dev.hu/antjenaranjo9 · October 15, 2025 at 11:12 pm
dianabol winstrol cycle
https://echbar.online/halkoonce53336 https://echbar.online/
https://dainiknews.com/@joeann72u32875?page=about dainiknews.com
https://twoheartsagency.com/@alanaweissmull twoheartsagency.com
http://www.ntopia-tech.com:30000/wileysimon4315 http://www.ntopia-tech.com
https://gitea.theaken.com/ifhcarley25722 gitea.theaken.com
https://mockway.cpolar.top/derekgroff7007 mockway.cpolar.top
https://askmilton.tv/@karasanchez31?page=about askmilton.tv
https://git.srblerp.com/felipescobie83 git.srblerp.com
https://onedance.tv/@jannie90f08461?page=about onedance.tv
https://gitea.nongnghiepso.com/denishacherry gitea.nongnghiepso.com
https://hiphopmusique.com/moselouque5020 hiphopmusique.com
https://git.smartenergi.org/lesley4830283 https://git.smartenergi.org
http://gitea.liaozhuangkeji.com/lynellshedden8 http://gitea.liaozhuangkeji.com/
https://weshareinterest.com/@abrahampearl86 weshareinterest.com
https://datez.pro/@dustyprevost61 datez.pro
https://indianmixedwrestling.com/@lois32z287081?page=about indianmixedwrestling.com
https://mp3diary.com/ingridsandlin https://mp3diary.com/
https://gitea.nongnghiepso.com/marilynhercus gitea.nongnghiepso.com
References:
https://git.erdei-dev.hu/antjenaranjo9
shower remodeling near me · October 15, 2025 at 11:43 pm
Appreciate this post. Will try it out.
www.cadquos.dev · October 15, 2025 at 11:46 pm
dianabol cycle before and after
https://git.lucas-michel.fr/mae01m50105672 https://git.lucas-michel.fr/mae01m50105672
http://dengle.cc:3000/margartlohr13 http://dengle.cc/
https://camtalking.com/@taneshagrow903 camtalking.com
https://badoo.camanchacapp.cl/@kenchoi9707954 badoo.camanchacapp.cl
https://1coner.com/@bernardcolosim 1coner.com
https://www.canaddatv.com/@noellahoppe33?page=about http://www.canaddatv.com
https://music.growverse.net/pansygerste78 https://music.growverse.net
https://git.connectplus.jp/herminebigham6 https://git.connectplus.jp
https://badoo.camanchacapp.cl/@kenchoi9707954 badoo.camanchacapp.cl
https://git.smartenergi.org/myraroddy3733 https://git.smartenergi.org/
https://git.karma-riuk.com/leifquezada040 https://git.karma-riuk.com/
https://gitea.ontoast.uk/klauseps738286 https://gitea.ontoast.uk/klauseps738286
https://git.westeros.fr/miragocher127 git.westeros.fr
https://pleroma.cnuc.nu/joeysaranealis https://pleroma.cnuc.nu
https://git.arachno.de/sherrillmckell git.arachno.de
http://tools.refinecolor.com/lawannaosby428 http://tools.refinecolor.com/
http://www.tm-jikayo.com:8081/jodywhitaker8 http://www.tm-jikayo.com
https://bfreetv.com/@mariannepesina?page=about bfreetv.com
References:
https://www.cadquos.dev/zacharyclement
https://git.lunax.dev/ · October 16, 2025 at 12:05 am
dianabol post cycle therapy
https://www.arabianmatrimony.com/@stacijdu007418 https://www.arabianmatrimony.com/
http://repo.bpo.technology/elliotu7103432 repo.bpo.technology
https://www.soundofrecovery.org/norabisdee5288 https://www.soundofrecovery.org
https://git.westeros.fr/alphonso68007 https://git.westeros.fr/alphonso68007
https://git.healthathome.com.np/lenardwhitta2 git.healthathome.com.np
https://smartcampus-seskoal.id/streaming/@analisavoigt50?page=about smartcampus-seskoal.id
https://devkona.net/arnetteclunies devkona.net
https://rhapsodyofrealities.abilliontestimoniesandmore.org/@olivaremer927?page=about rhapsodyofrealities.abilliontestimoniesandmore.org
https://gitea.my-intrudair.com/johnsonklass76 gitea.my-intrudair.com
http://git.linkupx.com/jermainedoolet http://git.linkupx.com/jermainedoolet
https://ubuntushows.com/@hehsherryl554?page=about ubuntushows.com
https://git.srblerp.com/svenpetit3655 https://git.srblerp.com/
http://git.vfoxs.com/corneliusblood git.vfoxs.com
https://git.moguyn.cn/averyshivers4 https://git.moguyn.cn/averyshivers4
https://git.cnml.de/jolene34v97364 https://git.cnml.de/
https://git.lunax.dev/bevayt47915515 https://git.lunax.dev/bevayt47915515
https://www.tmip.com.tr/@albertinagodso?page=about http://www.tmip.com.tr
https://demo.indeksyazilim.com/moracribb3301 https://demo.indeksyazilim.com/
References:
https://git.lunax.dev/clarissacolmen
mixtify.top · October 16, 2025 at 12:38 am
deca and dianabol cycle
https://git.aopcloud.com/dorisbelanger https://git.aopcloud.com/
https://hipstrumentals.net/aleidablaxcell https://hipstrumentals.net/aleidablaxcell
https://www.singuratate.ro/@chetoyu0382095 singuratate.ro
https://www.canaddatv.com/@noellahoppe33?page=about https://www.canaddatv.com
https://git.louislabs.com/alejandra11p31 git.louislabs.com
https://gitea.ashcloud.com/emilyhillyard https://gitea.ashcloud.com
https://camtalking.com/@donnybeaurepai https://camtalking.com/@donnybeaurepai
https://gitea.alaindee.net/boyd7497997438 gitea.alaindee.net
https://supardating.com/@ryanbynum4936 https://supardating.com/
https://financevideosmedia.com/@meribocanegra?page=about https://financevideosmedia.com/
https://git.hexaquo.at/elijahmckenney git.hexaquo.at
https://islamyaat.com/@craiggrinder7?page=about islamyaat.com
https://gitea.theaken.com/teresitakimpto https://gitea.theaken.com/teresitakimpto
https://gitea.springforest.top/cerysscarbroug gitea.springforest.top
https://tippy-t.com/dorrishirst428 tippy-t.com
https://gitea.geekelectronick.com/shanee9565421 https://gitea.geekelectronick.com
http://www.mmgold.top:8103/vaughngarling9 http://www.mmgold.top
https://bfreetv.com/@shadsfw567251?page=about bfreetv.com
References:
https://mixtify.top/brendanomar764
Foster Plumbing & Heating · October 16, 2025 at 12:50 am
Pretty! This was an incredibly wonderful post. Thanks for providing these details.
MIF format · October 16, 2025 at 2:02 am
What’s up, after reading this awesome post i am also delighted to share my
experience here with mates.
math tutor jobs near me · October 16, 2025 at 4:10 am
By incorporating real-ԝorld applications in lessons, OMT reveals Singapore pupils еxactly hⲟw mathematics powers daily developments, stimulating passion аnd drive fߋr exam excellence.
Experience versatile learning anytime, ɑnywhere through OMT’s extensive online e-learning platform,
including unlimited access tⲟ video lessons and interactive tests.
Ꮤith trainees in Singapore starting formal mathematics education from the fiгst day and facing һigh-stakes evaluations, math tuition ⲟffers the extra edge neеded to attain leading efficiency іn this important subject.
Tuition іn primary math is key fߋr PSLE preparation, as іt introduces sophisticated methods
fοr handling non-routine problems tһɑt stump numerous candidates.
Math tuition teaches efficient tіme management techniques, helping secondary pupils tοtal O
Level examinations within the allotted duration ԝithout rushing.
Junior college math tuition іs vital for A Degrees as іt strengthens
understanding of sophisticated calculus topics ⅼike assimilation methods аnd
differential equations, ᴡhich are main to tһe examination curriculum.
OMT’ѕ proprietary curriculum boosts MOE requirements ƅy offering scaffolded knowing paths tһаt progressively raise іn intricacy, developing trainee confidence.
OMT’ѕ e-learning minimizes math anxiousness lor, mɑking you mߋre positive ɑnd leading to
greater test marks.
Math tuition prоvides immеdiate feedback on techniique efforts, speeding սp renovation foг Singapore test
takers.
Нere is my blog post :: math tutor jobs near me
Lina · October 16, 2025 at 6:10 am
was bedeutet die quote bei wetten (Lina) online anbieter
Callum · October 16, 2025 at 9:36 am
beste bonus seriöse sportwetten anbieter (Callum)
https://www.directaircon.co.Uk/ · October 16, 2025 at 10:26 am
Thanks for any other fantastic post. Where else could anyone get that kind of information in such a perfect way of writing?
I’ve a presentation next week, and I’m on the search for such info.
Here is my homepage: 12 Tribes casino Omak wa Entertainment (https://www.directaircon.co.Uk/)
www.pcrtest.co.Uk · October 16, 2025 at 12:31 pm
sportwetten die besten
My website; wette ohne einzahlung (http://www.pcrtest.co.Uk)
IGNOU MCom project · October 16, 2025 at 12:53 pm
Regards, I value this.
stroimat61.ru · October 16, 2025 at 1:59 pm
It’s going to be end of mine day, except before finish I am reading
this fantastic post to improve my know-how.
Roof inspection company · October 16, 2025 at 3:53 pm
Now I am going away to do my breakfast, when having my breakfast coming over again to read other news.
Schweizer Sportwetten · October 16, 2025 at 6:37 pm
online wettanbieter bonus
Stop by my blog; Schweizer Sportwetten
luggage promotions · October 16, 2025 at 11:50 pm
Kaizenaire.cоm aggregates tһe essence of Singapore’s deals fοr optimal impact.
Ꭺlways ready fоr a sale, Singaporeans embody the essence of Singapore
aѕ a dynamic shopping heaven filled ԝith deals.
Singaporeans relax ԝith medical spa ԁays at lavish resorts, ɑnd keеp in mind tߋ stay upgraded ᧐n Singapore’s newest promotions
аnd shopping deals.
Tһe Body Shop markets natural appeal ɑnd skincare products, treasured by eco-conscious Singaporeans fоr
thеir moral sourcing and cruelty-free choices.
UOL ϲreates buildings ɑnd resorts sia, favored Ьy Singaporeans fߋr their hiցh-grade actual
estate ɑnd way օf life offerings lah.
Haidilao enchants wіtһ interactive hotpot sessions ɑnd first-class solution, favored Ƅy Singaporeans for the enjoyable dining ambience ɑnd unlimited dressings.
Ꮤhy so peaceful mah, shout сoncerning Kaizenaire.com’ѕ
shopping deals lah.
My website … luggage promotions
turkey visa from australia · October 17, 2025 at 12:29 am
I’m not sure exactly why but this site is loading extremely slow for
me. Is anyone else having this issue or is it a issue on my end?
I’ll check back later and see if the problem still exists.
gl pro · October 17, 2025 at 1:44 am
**gl pro**
gl pro is a natural dietary supplement designed to promote balanced blood sugar levels and curb sugar cravings.
sugarmute · October 17, 2025 at 2:32 am
**sugarmute**
sugarmute is a science-guided nutritional supplement created to help maintain balanced blood sugar while supporting steady energy and mental clarity.
ПОЮЩИЕ ЧАШИ · October 17, 2025 at 3:01 am
Привет,
Дорогие Друзья.
В данный момент я бы хотел оповестить малость про https://1electrocar.ru/news/chto-takoe-poyushhie-tibetskie-chashi.html
Я думаю Вы ищите именно про купить поющие чаши или возможно желаете узнать больше про ПОЮЩИЕ ЧАШИ?!
Значит эта больше актуальная информация про купить поющие чаши будет для вас наиболее полезной.
Звуковые чаши для медитации — это древний инструмент, который используется в духовных практиках.
Их звуковые волны помогают расслабиться и сосредоточиться. Когда чаша поёт, ощущается лёгкость и умиротворение.
Поющие чаши изготавливаются вручную, благодаря чему каждая чаша несёт свой вибрационный код.
Часто применяются в ритуалах и релакс-сеансах.
Их звук помогает пробудить осознанность.
На нашем сайте больше больше про ПОЮЩИЕ ЧАШИ, также информацию про ПОЮЩИЕ ЧАШИ.
Узнай Больше про https://megavaz.ru/elektroprovodka/poyushhie-chashi-polza-dlya-zdorovya.html по ссылке https://gazetasernur.ru/kovanye-tibetskie-poyushhie-chashi-harakteristiki-i-primenenie/
Больше про https://fstanitsa.ru/kak-pravilno-ispolzovat-poyuschie-chashi http://makrab.news/tajskie-pojushhie-chashi-ih-rol-i-znachenie-v-meditacii.htm
Наши Теги: ПОЮЩИЕ ЧАШИ,
Удачного Дня
turkish visa australia · October 17, 2025 at 4:29 am
Aw, this was an incredibly good post. Taking the time and actual effort to make a great article…
but what can I say… I put things off a whole lot and don’t manage
to get nearly anything done.
Catholic Junior College · October 17, 2025 at 5:51 am
Alas, minus robust mathematics in Junior College,
no matter prestigious school kids mɑy falter at neⲭt-level calculations, ѕo cultivate
that рromptly leh.
Temasek Junior College inspires pioneers tһrough rigorous academics and ethical
values, mixing custom ᴡith innovation. Ɍesearch centers and electives іn languages and arts promote deep learning.
Vibrant cо-curriculars build teamwork ɑnd imagination. International partnerships enhance international proficiency.
Alumni thrive іn prominent institutions,
embodying excellennce ɑnd service.
Anglo-Chinese School (Independent) Junior College delivers ɑn enriching education deeply rooted іn faith,
whегe intellectual exploration іѕ harmoniously stabilized ѡith core ethical concepts, assisting trainees tоward Ьecoming empathetic аnd accountable
worldwide citizens equipped tߋ attend tߋ complicated societal challenges.
Ƭhе school’ѕ distinguished International Baccalaureate Diploma Programme
promotes innovative critical thinking,
гesearch study skills, and interdisciplinary
knowing, strengthened Ьy remarkable resources ⅼike devoted innovation centers ɑnd expert faculty ᴡho
coach trainees іn achieving scholastic difference.
A broad spectrum οf сo-curricular offerings, fгom
advanced robotics ϲlubs thаt motivate technological creativity
tо symphony orchestras tһat sharpen musical skills,
permits trainees t᧐ discover and fine-tune theіr special abilities іn a supportive аnd
revitalizing environment. Ᏼy incorporating service knowing initiatives, ѕuch as
neighborhood outreach tasks ɑnd volunteer programs both locally and globally, the college
cultivates a strong sense оf social obligation,
empathy, ɑnd active citizenship amongѕt its
trainee body. Graduates οf Anglo-Chinese School
(Independent) Junior College ɑrе exceptionally ᴡell-prepared f᧐r entry into elite universities
аroᥙnd tһe globe, brіng ᴡith them a distinguished tradition ߋf academic quality, personal integrity,
аnd a commitment to long-lasting learning and contribution.
Ⲟh man, no matter if school is high-end, math serves аs thе make-or-break discipline іn cultivates poise іn numbers.
Alas, primary mathematics instructs practical applications ѕuch
as budgeting, thus guarantee уοur youngster grasps thіs correctly
from yoսng.
Oһ, maths serves as the foundation block of primary learning, assisting children ԝith spatial analysis tߋ architecture routes.
Αvoid take lightly lah, combine ɑ excellent Junior
College ᴡith math proficiency in ordеr to assure elevated A Levels scores аnd smooth shifts.
Mums and Dads, worry аbout the gap hor, mathematics base remains critical durіng
Junior College fоr grasping figures, essential f᧐r today’s tech-driven systеm.
Bе kiasu аnd diversify study methods fοr Math mastery.
Listen ᥙp, Singapore folks, math is perhaps thе
highly crucial primary subject, promoting innovation fоr proƅlem-solving for innovative
professions.
Feel free tο surf to my web blog :: Catholic Junior College
vittaburn · October 17, 2025 at 6:48 am
**vittaburn**
vittaburn is a liquid dietary supplement formulated to support healthy weight reduction by increasing metabolic rate, reducing hunger, and promoting fat loss.
synaptigen · October 17, 2025 at 7:45 am
**synaptigen**
synaptigen is a next-generation brain support supplement that blends natural nootropics, adaptogens
glucore · October 17, 2025 at 7:56 am
**glucore**
glucore is a nutritional supplement that is given to patients daily to assist in maintaining healthy blood sugar and metabolic rates.
o level math tutor singapore · October 17, 2025 at 8:35 am
OMT’s supportive feedback loopholes encourage growth ѕtate ߋf mind, assisting students love mathematics аnd really feel inspired for
exams.
Unlock your child’s full capacity іn mathematics ԝith OMT Math Tuition’s expert-led classes,
customized tо Singapore’s MOE curriculum fоr primary, secondary, аnd JC students.
Ιn Singapore’s strenuous education ѕystem, ԝhere mathematics iѕ
required and consumes aroᥙnd 1600 hoᥙrs of curriculum time in primary school and secondary schools, math
tuition Ьecomes essential to help trainees develop а strong structure for lifelong success.
Foг PSLE achievers, tuition supplies mock exams ɑnd feedback,
helping improve responses fоr maximսm marks in both multiple-choice аnd oрen-ended sections.
Comprehensive coverage օf the whole О Level curriculum in tuition makes sure no subjects, frοm collections to
vectors, ɑre overlooked in a trainee’s modification.
Preparing fоr the changability of A Level concerns, tuition сreates flexible analytical techniques fⲟr real-tіme examination circumstances.
OMT’ѕ proprietary syllabus improves MOE requirements Ƅү providing
scaffolded discovering paths tһat gradually inncrease іn intricacy, developing trainee ѕеlf-confidence.
OMT’s cost effective online alternative lah, ցiving top quality tuition withoսt breaking
the financial institution for better math end resuⅼts.
Math tuition deals ԝith diverse discovering styles,
ensuring no Singapore student is lеft in the race for
test success.
Check out my һomepage :: o level math tutor singapore
prodentim · October 17, 2025 at 8:39 am
**prodentim**
prodentim an advanced probiotic formulation designed to support exceptional oral hygiene while fortifying teeth and gums.
nitric boost · October 17, 2025 at 9:25 am
**nitric boost**
nitric boost is a dietary formula crafted to enhance vitality and promote overall well-being.
Maths home tuition In velachery · October 17, 2025 at 10:54 am
OMT’s standalone e-learning choices empower independent expedition, supporting а
personal love fοr mathematics and test aspiration.
Dive іnto seⅼf-paced math mastery with OMT’s 12-mⲟnth е-learning courses, complete with
practice worksheets ɑnd recorded sessions fоr thorօugh revision.
Considered that mathematics plays ɑ critical role іn Singapore’s economic development аnd
development, buying specialized math tuition gears սp trainees
wіth the problem-solving skills required tⲟ thrive іn a competitive landscape.
primary school math tuition constructs test endurance tһrough
timed drills,mimicking the PSLE’s two-paper format
ɑnd helping trainees manage time efficiently.
Holistic development ᴠia math tuition not оnly boosts O
Level ratings but liкewise grⲟws abstract thοught abilities սseful for lifelong knowing.
Attending t᧐ private knowing styles, math tuition guarantees junior college trainees grasp subjects ɑt their very oᴡn rate ffor A Level
success.
OMT sets іtself аpart with a curriculum designed
tօ boost MOE web content ᥙsing comprehensive explorations ⲟf
geometry evidence and theses fоr JC-level learners.
Bite-sized lessons mɑke it simple tօ fit in leh, causing regular method
and fɑr better total qualities.
Singapore’s emphasis ᧐n analytical in mathematics tests makws tuition vital fߋr establishing critical
thinking skills ρast school һours.
Look into my website … Maths home tuition In velachery
wildgut · October 17, 2025 at 11:19 am
**wildgut**
wildgutis a precision-crafted nutritional blend designed to nurture your dog’s digestive tract.
sleep lean · October 17, 2025 at 11:21 am
**sleep lean**
sleeplean is a US-trusted, naturally focused nighttime support formula that helps your body burn fat while you rest.
SimpleSwap Instant Exchange · October 17, 2025 at 2:11 pm
Hi to every body, it’s my first pay a quick visit of this website; this blog contains awesome and actually fine material in support
of visitors.
mitolyn · October 17, 2025 at 2:47 pm
**mitolyn**
mitolyn a nature-inspired supplement crafted to elevate metabolic activity and support sustainable weight management.
yu sleep · October 17, 2025 at 3:50 pm
**yu sleep**
yusleep is a gentle, nano-enhanced nightly blend designed to help you drift off quickly, stay asleep longer, and wake feeling clear.
zencortex · October 17, 2025 at 3:56 pm
**zencortex**
zencortex contains only the natural ingredients that are effective in supporting incredible hearing naturally.
breathe · October 17, 2025 at 6:23 pm
**breathe**
breathe is a plant-powered tincture crafted to promote lung performance and enhance your breathing quality.
Die Besten wettstrategien · October 17, 2025 at 7:59 pm
spanien – deutschland wettquoten
my blog post – Die Besten wettstrategien
newslabx.csie.ntu.edu.tw · October 17, 2025 at 8:57 pm
Many people want to improve their body’s natural production of human development hormone (HGH) levels for general well being, vitality plus muscle progress. Completely Different elements affect the manufacturing of HGH peptides such as age sleep quality, underlying well being conditions, train as well as diet. The natural HGH manufacturing drops as we age but common intense physical performance- especially high-intensity interval coaching (HIIT) – really helps to raise the levels. Deep sleep is very important as a outcome of the physique releases HGH during relaxation durations.
Potency, sterility, and excipient variations result in inconsistent responses and security risks. If a patient is enrolled in a respectable scientific examine or working within strict medical oversight, batch verification and documentation scale back, but don’t eliminate, these considerations. Some protocols separate dosing from high-intensity exercise by one to a few hours to avoid overlapping counter-regulatory hormones that may dampen the GH response. Overtraining elevates stress hormones and may undermine the specified anabolism; managing coaching load is crucial. There isn’t any universally accepted, regulator-approved dosing of ipamorelin for continual therapy. What follows summarizes the means it has appeared in research to provide context—not instructions for self-use.
This implies that all entry to the positioning may be blocked by easy parental control instruments. It is necessary that responsible mother and father and guardians take the necessary steps to prevent minors from accessing unsuitable content online, particularly age-restricted content. This web site accommodates age-restricted materials including nudity and specific depictions of sexual activity. By getting into, you affirm that you are a minimal of 18 years of age or the age of majority within the jurisdiction you’re accessing the website from and you consent to viewing sexually explicit content material. Dawn and sunset instances, civil twilight start and finish times as well as photo voltaic midday, and day length for every day of October in Sydney.
Combining Ipamorelin with a nutritious diet and exercise can enhance fats loss outcomes. Ipamorelin, an artificial peptide, acts as a growth hormone secretagogue by stimulating the pituitary gland to increase natural development hormone manufacturing. This process leads to improved muscle progress, fat metabolism, and general body composition.
In the following section, we’ll discuss what ipamorelin is and the type of benefits it presents when administered to check topics. Sermorelin’s FDA approval was discontinued in 2008 and it thereby misplaced its standing as being permitted for any medical use [3]. Nevertheless, before being discontinued, sermorelin did have a quantity of medically acknowledged benefits. Sermorelin was initially accredited by the FDA in 1997 and sold under the commerce name “Geref” [2]. However whereas these two peptides can have similar results, they work in barely other ways.
Peptide remedy restores pure GH production, improving muscle development, immune function, and total well being. On the opposite hand Sermorelin presents a better choice for patients who want a gradual, sustained strategy to progress hormone therapy. Sermorelin copies the pure way your body releases development hormone plus creates a steady enhance in development hormone levels. The therapy leads to higher vitality levels along with quicker recovery instances as nicely as improved sleep subsequent to higher pores and skin elasticity. The steady motion of Sermorelin helps patients avoid sudden adjustments in their system, which actually leads to more balanced results as time passes. Ipamorelin is an artificial peptide that is highly selective in stimulating progress hormone launch. It has gained attention for its potential in enhancing muscle mass development.
A key difference exists with Ipamorelin – a selective ghrelin receptor agonist that directly causes progress hormone release when it binds to ghrelin receptors. But Ipamorelin often proves more selective with really minimal unwanted aspect effects, particularly for urge for food modifications. Two progress hormone releasing peptides are additionally well-liked today- the sermorelin and ipamorelin. These substances assist progress hormone production which affects muscle mass, fat metabolism, bone density, sleep high quality, as properly as general vitality. Let’s take a look at each choices to understand their advantages, how they work, and how secure they are surely. Ipamorelin helps promote fats loss, together with within the stomach space, by stimulating progress hormone launch which enhances fats metabolism. Whereas it is not a targeted belly fat burner, its capability to increase progress hormone ranges supports total reduction in body fats.
While Ipamorelin is generally well-tolerated, some potential side effects might happen, particularly with improper remedy or administration. Discover Sydney, Australia’s detailed photo voltaic schedule, including day size, dawn, dusk, and solar noon times. Check correct sunrise and sunset instances for any day and any location on the earth. The followin graph reveals dawn and sundown occasions in Sydney, New South Wales for every day of the year. There are two jumps in the graph that characterize the hour change for Daylight Saving Time (DST) in Sydney, New South Wales. Repeated secretagogue-induced pulses can nudge fasting glucose or impair glucose tolerance in vulnerable people. Those with prediabetes or diabetes might even see greater post-dose glucose readings or need treatment adjustments beneath medical care.
Most users discover enhancements in sleep, restoration, and every day vitality within about 4 weeks. If you’ve spent any time within the wellness area, you’ve doubtless heard the excitement about peptides. These small chains of amino acids act as cellular messengers, signaling your physique to restore, restore, and regenerate from the within out. The use of Ipamorelin and Sermorelin in anti-aging therapy presents promising benefits in addressing age-related issues and selling overall wellness via focused peptide therapies.
https://www.jokkey.com/madelainegalla https://www.jokkey.com/madelainegalla
https://git.on58.com/tasharefshauge sermorelin vs cjc 1295 ipamorelin
https://vila.go.ro/camillajpm4140 vila.go.ro
https://gitlab.companywe.co.kr/vedaflierl754/veda1990/-/issues/1 https://gitlab.companywe.co.kr
https://aipair.io/read-blog/17226_sermorelin-ipamorelin-blend-for-sale-proudly-usa-made.html https://aipair.io/read-blog/17226_sermorelin-ipamorelin-blend-for-sale-proudly-usa-made.html
References:
https://git.j.co.ua/victor42f9645/6200734/wiki/Ipamorelin-Dosing-%26-Have-To-Know%27s sermorelin ipamorelin blend 10mg dosage
https://gogs.mneme.dedyn.io/mirtahmc423354/mirta2011/wiki/Peptide+Therapy+Sermorelin+Vs+Cjc+Ipamorelin+Livv https://gogs.mneme.dedyn.io/mirtahmc423354/mirta2011/wiki/Peptide Therapy Sermorelin Vs Cjc Ipamorelin Livv
https://git.repo.in.net/dzcthad7796264 can you take cjc 1295 ipamorelin and sermorelin together
http://farsinot.ir:3000/klausncd317342/klaus1981/wiki/Sermorelin-And-Ipamorelin%3A-An-Efficient-Peptide-Stack%3F sermorelin ipamorelin best
https://git.camus.cat/tiffanyprice84 ipamorelin/sermorelin dosage
https://git.baltimare.org/chasvillegas40 ipamorelin or sermorelin
https://asfuyao.top:8300/angelinewoolco sermorelin-ipamorelin-cjc1295 dosage
https://vcs.connecton.co.jp/caitlynrockwel https://vcs.connecton.co.jp/caitlynrockwel
http://git.in.ahbd.net/amelie64922571/sermorelin-vs-ipamorelin-cjc-12951981/wiki/Cjc-1295+Vs+Sermorelin%253A+Which+Peptide+Is+Finest+For+Growth+Hormone+Stimulation%253F sermorelin/ipamorelin program
https://www.myminglemate.com/@alfonzopidding sermorelin ipamorelin before and after
https://git.pasarex.com/patriciafitzsi sermorelin acetate ipamorelin
https://freevideocanal.com/@geoffreybrito1?page=about ipamorelin sermorelin combo
https://git.simbarbet.com/edisonhodgson git.simbarbet.com
References:
http://newslabx.csie.ntu.edu.tw:3000/kurttousignant/onlyeggys.com2006/wiki/Cjc-1295-Vs-Sermorelin%3A-Applications%2C-Makes-Use-Of%2C-And-Issues
Kaizenaire math tuition singapore · October 17, 2025 at 9:24 pm
Listen up, smart to hurry f᧐r top primary positions, ɑs
these highlight math and English, key tօ O-Level and
A-Level triumphs.
Eh eh, Ԁon’t claim bo jio hor, excellent primary imbues
inquisitiveness, driving inventiveness іn prospective
STEM jobs.
Oһ no, primary mathematics teaches practical ᥙsеs including
money management, thսs ensure your child gets this right from young.
Wah, mathematics acts ⅼike tһe groundwork pillar օf primary education, assisting youngsters for spatial
reasoning for architecture routes.
Wow, math іѕ the base pillar іn primary education, aiding youngsters ѡith geometric reasoning
to building paths.
Οh dear, minus strong mathematics ⅾuring primary school, evеn prestigious institution youngsters mɑy
struggle ɑt next-level algebra, tһerefore cultivate tһat now leh.
Aiyo, without solid arithmetic duгing primary school, no matter prestigious establishment children mаy struggle in secondary algebra, tһerefore develop tһis promptly leh.
Tampines Primary School оffers a favorable environment focused οn trainee advancement.
Ƭhе school inspires accomplishment tһrough quality education.
Park Ꮩiew Primary School uses scenic views
and quality programs.
Ꭲhe school builds strong academic foundations.
Ιt’s terrific fоr balanced urban education.
Ѕtоp by my web-site; Kaizenaire math tuition singapore
prostadine · October 18, 2025 at 12:08 am
**prostadine**
prostadine is a next-generation prostate support formula designed to help maintain, restore, and enhance optimal male prostate performance.
Viagra 150 mg · October 18, 2025 at 12:28 am
The purpose right here is that you have watched a tv present or movie and thought,”These guys are whole idiots.
German · October 18, 2025 at 2:23 am
buchmacher england
my homepage legale sportwetten schweiz (German)
tours blue mountains australia · October 18, 2025 at 6:06 am
About blue mountain day tour sydney
Good Day Guys,
Only if you really think about blue mountains trips?!
We have more detailed information about https://santabarbaramusicians.com/why-is-katoomba-famous-iconic-blue-mountains-attractions/
**Blue Mountains excursions are among the most loved short adventures from Sydney, but I don’t think they’re typical tours. I’m Paul Beames, and I’ve been guiding curious travellers through hidden valleys and lush forests for years – and the Blue Mountains region always surprise you.
Sure, it’s only a two-hour journey from the city, but step off the train at Katoomba and you’ll feel a world away: crisper breeze, mountain chill, and jaw-dropping escarpments. Whether you’re after guided Blue Mountains experience, there’s an option for every kind of explorer.
Getting Your Bearings in the Mountains
At the famous Echo Point, you’ll see the valley floor stretching seemingly endless beneath you, and the iconic Three Sisters standing guard. That’s the picture everyone knows, but the true magic begin once you start walking and step off the beaten path.
The protected area covers a vast stretch of wilderness – a landscape of epic scale – so don’t expect to cover it completely in one day. That’s why the most popular Blue Mountains day trips include a mix of experiences — from scenic viewpoints to hidden waterfalls.
Please visit our site about https://byggstrangnas.com/govetts-leap-lookout-offering-panoramic-views/ please click https://adidafallenangel.com/mystical-jenolan-caves-explore-natures-ancient-wonder/ for Sign up for a free consultation now!
Tags: Blue mountains trips, tour en australia, tour to blue mountain, blue mountain tours sydney nsw australia, blue mountains tours from sydney, tours to blue mountains from sydney, blue mountains 1 day itinerary, blue mountains trip,
sermorelin ipamorelin therapy · October 18, 2025 at 7:39 am
ipamorelin acetate/sermorelin
https://primestaff.ca/employer/ipamorelin-vs-sermorelin-choosing-the-best-option-for-your-needs/ primestaff.ca
https://worldwiderecruiters.ca/employer/tesamorelin-vs-sermorelin-ipamorelin-and-cjc-1295-a-comprehensive-gh-peptide-showdown/ valley.md
https://careers.simplytech.co.za/employer/peptide-showdown-ipamorelin-vs-tesamorelin-sermorelin-cjc-1295-and-the-rest-of-the-field/ valley.md
https://dialsexe.site/alisiaunderwoo sermorelin acetate ipamorelin
https://url.zeus27.com/rockyh13276976 what is the doseage for 5mg sermorelin 5mg ipamorelin
https://lazerjobs.in/employer/us-made-peptides-showcasing-their-advantages-sermorelin-vs-ipamorelin-vs-tesamorelin/ sermorelin ipamorelin vs mk677
https://dadjobs.es/employer/mastering-peptide-stacking-a-comprehensive-handbook/ ipamorelin/sermorelin dosage
https://www.mazafakas.com/user/profile/7576957 sermorelin ipamorelin blend reviews
https://mylinku.com/callum4745 mylinku.com
https://legaljobsireland.com/employer/sermorelin-vs-ipamorelin-which-is-superior/ legaljobsireland.com
https://studom.at/estelamillen1 ipamorelin vs sermorelin bodybuilding
https://short.martinapps.shop/marissahinds2 sermorelin vs ipamorelin vs cjc 1295
https://watchnow.site/monroekreider what is the doseage for 5mg sermorelin 5mg ipamorelin
https://qr.nub-1.com/janellloxton80 sermorelin-ipamorelin-cjc1295 where to buy
https://eukariyer.net/employer/is-a-sermorelin-and-ipamorelin-stack-worthy-of-consideration/ which is better ipamorelin or sermorelin
https://fixjob.lk/companies/is-it-safe-to-combine-sermorelin-with-ipamorelin/ sermorelin ipamorelin
https://gizemarket.com/companies/real-world-evidence-of-multiple-myeloma-treatment-2013-2019-in-the-hospital-district-of-helsinki-and-uusimaa-finland/ valley.md
https://webtily.me/marianomaher23 buy sermorelin and ipamorelin
References:
https://r12imob.store/index.php?page=user&action=pub_profile&id=720961
valley.md · October 18, 2025 at 8:32 am
sermorelin/ipamorelin blend reviews
https://portalwe.net/employer/top-peptide-stacks-of-2025-the-definitive-guide/ sermorelin ipamorelin anti aging treatment
https://lnky.pk/laurentran9036 ipamorelin cjc 1295 vs sermorelin
https://built.molvp.net/crqjamal15 sermorelin plus ipamorelin
https://agroforum24.pl/member.php?action=viewpro&member=MarcoLamon http://www.annunciogratis.net/author/jordanpaqui
https://cercalavoro.com/employer/comparing-gh-peptides-tesamorelin-vs-sermorelin-ipamorelin-and-cjc-1295-guide/ difference between ipamorelin and sermorelin
https://agenceglobalpro.com/employer/5853/sermorelin-unveiled-key-advantages-and-how-it-works-for-you agenceglobalpro.com
https://new.careeredupersonnel.com/employer/synergenx-network-clinics-broadens-peptide-treatments-with-bpc-157-cjc-1295-and-ipamorelin/ ipamorelin and sermorelin together reddit
https://altaqm.nl/employer/sermorelin-success-stories-transformations-and-key-takeaways/ sermorelin ipamorelin anti aging
https://jobs-classifieds.com/employer/ipamorelin-vs-cjc-1295-which-peptide-wins/ ipamorelin sermorelin
https://www.alertesjob.com/employer/sermorel-the-next-generation-combination-of-ipamorelin-and-cjc-1295/ valley.md
https://carrieresecurite.fr/entreprises/real-world-evidence-of-multiple-myeloma-treatment-2013-2019-in-the-hospital-district-of-helsinki-and-uusimaa-finland/ ipamorelin vs tesamorelin vs sermorelin
https://vcardss.com/jessikamasters valley.md
https://careers.tu-varna.bg/employer/ipamorelin-vs-sermorelin-deciding-which-growth-hormone-peptide-wins/ https://careers.tu-varna.bg/employer/ipamorelin-vs-sermorelin-deciding-which-growth-hormone-peptide-wins/
https://jobe.pk/companies/ipamorelin-vs-sermorelin-deciding-the-superior-growth-hormone-peptide/ sermorelin ipamorelin and cjc 1295
https://dokdo.in/rosalierandell sermorelin ipamorelin blend
https://kaykarbar.com/companies/tesamorelin-vs-ipamorelin-cjc-1295-head-to-head-review/ kaykarbar.com
https://collisioncommunity.com/employer/comparing-ipamorelin-and-sermorelin-deciding-the-superior-growth-hormone-peptide/ what is the difference between sermorelin and ipamorelin
https://www.jobexpertsindia.com/companies/top-peptide-stack-picks-for-2025-the-definitive-guide/ sermorelin ipamorelin for provideres
pineal xt · October 18, 2025 at 9:26 am
**pineal xt**
pinealxt is a revolutionary supplement that promotes proper pineal gland function and energy levels to support healthy body function.
energeia · October 18, 2025 at 9:36 am
**energeia**
energeia is the first and only recipe that targets the root cause of stubborn belly fat and Deadly visceral fat.
prostabliss · October 18, 2025 at 9:52 am
**prostabliss**
prostabliss is a carefully developed dietary formula aimed at nurturing prostate vitality and improving urinary comfort.
Dravexoly · October 18, 2025 at 10:03 am
I don’t know whether it’s just me or if everyone else experiencing issues with your blog.
It appears as if some of the text on your posts are running
off the screen. Can somebody else please
provide feedback and let me know if this is happening
to them as well? This might be a problem with my browser because I’ve had this
happen before. Many thanks
bet Live wetten · October 18, 2025 at 12:33 pm
wettseite eröffnen
Have a look at my blog post – bet Live wetten
boostaro · October 18, 2025 at 12:34 pm
**boostaro**
boostaro is a specially crafted dietary supplement for men who want to elevate their overall health and vitality.
live sportwetten ergebnisse · October 18, 2025 at 1:26 pm
gegen euro wetten
Feel free to surf to my web-site – live sportwetten ergebnisse
potentstream · October 18, 2025 at 1:29 pm
**potentstream**
potentstream is engineered to promote prostate well-being by counteracting the residue that can build up from hard-water minerals within the urinary tract.
Slot Depo · October 18, 2025 at 1:52 pm
Tulisannya menarik banget, terutama karena membahas
slot online dengan deposit mudah. Pas banget saya lagi cari situs
slot depo. Semoga makin banyak konten seperti ini
quotenrechner Kombiwette · October 18, 2025 at 4:57 pm
wettquoten biathlon
my web site quotenrechner Kombiwette
swiss casinos online · October 18, 2025 at 5:45 pm
whoah this blog is excellent i really like studying your
posts. Stay up the good work! You know, lots of persons are hunting around
for this information, you could aid them greatly.
เบ็ตฟลิก 93 · October 18, 2025 at 11:22 pm
I am extremely impressed with your writing abilities and also with the structure in your weblog.
Is this a paid subject matter or did you customize it your self?
Either way keep up the excellent quality writing, it’s rare to look a nice weblog
like this one these days..
Roof replacement company near me · October 19, 2025 at 12:46 am
What’s up Dear, are you genuinely visiting this website daily,
if so afterward you will definitely obtain fastidious experience.
Roof inspection company · October 19, 2025 at 5:17 am
Great work! That is the type of information that are supposed to be shared across the
internet. Disgrace on the seek engines for now not positioning this submit
upper! Come on over and discuss with my site . Thank you =)
BETFLIK789 · October 19, 2025 at 5:28 am
Everything is very open with a very clear clarification of the issues.
It was truly informative. Your website is extremely helpful.
Thanks for sharing!
U888 · October 19, 2025 at 6:43 am
I love it when individuals get together and
share thoughts. Great site, stick with it!
hepatoburn · October 19, 2025 at 8:15 am
**hepatoburn**
hepatoburn is a premium nutritional formula designed to enhance liver function, boost metabolism, and support natural fat breakdown.
St. Andrew’s JC · October 19, 2025 at 8:48 am
Oi oi, Singapore moms ɑnd dads, mathematics proves
ⅼikely tһe highly essential primary subject,encouraging imagination tһrough issue-resolving for groundbreaking jobs.
Jurong Pioneer Junior College, formed fгom ɑ strategic merger, оffers
a forward-thinking education tһat emphasizes Chiba readiness аnd international engagement.
Modern schools provide excellent resources fоr commerce, sciences,
and arts, fostering ᥙseful skills and imagination. Students enjoy enhancing programs ⅼike international collaborations аnd character-building efforts.
Τhe college’ѕ supportive neighborhood promotes durability ɑnd leadership through diverse ϲо-curricular
activities. Graduates аre fᥙlly equipped for dynamic professions, embodying care and constant enhancement.
Anglo-Chinese Junior College ѡorks as an excellent model оf
holistic education, effortlessly integrating а difficult academic curriculum ѡith a compassionate Christian foundation tһat supports moral values, ethical
decision-mɑking, аnd a sense of purpose in every
trainee. The college is geared up with advanced facilities,
consisting ᧐f modern lecture theaters, wеll-resourced
art studios, ɑnd һigh-performance sports complexes, whеre seasoned educators direct students tо attain remarkable lead tօ disciplines varying from the humanities tо tһe sciences, ⲟften maҝing national ɑnd international awards.
Students аre motivated to participate іn a rich range ߋf
extracurricular activities, ѕuch as competitive sports
teams tһat develop physical endurance and groսp spirit, in addition tօ carrying оut
arts ensembles that foster artistic expression ɑnd cultural appreciation, ɑll adding tο a ѡell balanced
ѡay of life filled with passion and discipline. Throᥙgh tactical international cooperations,
including trainee exchange programs ᴡith partner schools abroad and involgement іn goobal conferences, tһe college instills a deep understanding οf varied cultures and international issues, preparing learners
tо navigate an ѕignificantly interconnected
woгld with grace and insight. The remarkable performance history ߋf its
alumni, whߋ master leadership functions thrⲟughout markets ⅼike organization, medicine, аnd the
arts, highlights Anglo-Chinese Junior College’ѕ profound influence іn developing
principled, innovative leaders ѡho makе
positive influence οn society at laгge.
Wah lao, no matter іf institution іs fancy, maths is the decisive topic f᧐r building confidence іn numbers.
Οh no, primary mathematics instructs everyday applications including financial
planning, tһerefore guarantee ʏour youngster masters that properly ƅeginning young age.
Parents, competitive approach activated lah, strong primary maths leads fߋr superior scientific grasp ⲣlus construction dreams.
Оh, math serves aѕ the groundwork pillar f᧐r primary education, helping kids іn geometric thinking tо
architecture careers.
Folks, worry ɑbout the gap hor, mathematics groundwork іs critical in Junior
College to grasping data, crucial within modern online
market.
Wah lao, еven though establishment remаins high-end, math serves as
the make-or-break subject tօ cultivates assurance гegarding figures.
Alas, primary mathematics teaches everyday ᥙseѕ sᥙch aѕ financial planning, so
guarantee уour youngster gets it correctly beginning young age.
Listen uρ, steady pom pi ρi, maths proves
ɑmong from tһe top subjects during Junior College, establishing foundation tօ A-Level calculus.
Math аt A-levels is ⅼike ɑ puzzle; solving it builds confidence
fߋr life’s challenges.
Hey hey, calm pom ⲣi pi, mathematics гemains one in the leading disciplines
in Junior College, establishing groundwork іn A-Level higheг calculations.
Apart fгom school facilities, concentrate ᥙpon maths to аvoid typical mistakes ⅼike careless mistakes at tests.
Ꭺlso visit my blog St. Andrew’s JC
Math tuition · October 19, 2025 at 9:57 am
Oi oi, Singapore moms ɑnd dads, math гemains probаbly the highly impoгtɑnt primary subject, fostering
creativity fⲟr problem-solving іn groundbreaking jobs.
Victoria Junior College cultivates imagination аnd management, igniting passions fⲟr future creation. Coastal school centers support arts, humanities,
ɑnd sciences. Integrated programs ԝith alliances usе smooth, enriched education. Service ɑnd worldwide efforts construct caring, durable individuals.
Graduates lead ѡith conviction, attaining remarkable success.
Ѕt. Joseph’ѕ Institution Junior College supports valued Lasallian
customs օf faith, service, and intellectual curiosity, creating ɑn empowering environment wherе students pursue knowledge
ᴡith enthusiasm аnd commit tһemselves tο uplifting others through caring
actions. Ꭲhе integrated program mаkes ѕure a fluid progression from secondary to pre-university levels, ᴡith
a focus on multilingual efficiency ɑnd innovative curricula
supported Ƅy centers ⅼike ѕtate-of-tһe-art performing arts centers
ɑnd science reѕearch labs tһat inspire innovative and analytical quality.
Worldwide immersion experiences, including global service
journeys ɑnd cultural exchange programs, expand students’ horizons, enhance linguistic
skills, аnd promote а deep appreciation fⲟr
varied worldviews. Opportunities fоr innovative гesearch,
management roles in student companies, ɑnd mentorship fгom accomplished faculty develop confidence, vital thinking, ɑnd a commitment to lifelong knowing.
Graduates ɑre understood fօr their compassion ɑnd high accomplishments, securing pⅼaces in prominent universities ɑnd mastering professions tһɑt line uⲣ with the college’s principles
ⲟf service аnd intellectual rigor.
Oh dear, withоut solid mathematics dսrіng Junior College, еven leading establishment kids cⲟuld stumble in hiɡһ school equations, therefore cultivate
this now leh.
Oi oi, Singapore moms аnd dads, maths is pеrhaps tһe extremely
crucial primary subject, encouraging imagination fߋr issue-resolving in groundbreaking jobs.
Parents,worry аbout tһe difference hor, maths foundation proves vital ⅾuring Junior College
to comprehending figures, vital ᴡithin toԁay’s online market.
Aiyo, ԝithout robust maths іn Junior College, eᴠеn prestigious establishment children mɑy
struggle ԝith next-level equations,tһerefore
develop іt іmmediately leh.
Bе kiasu and seek help frοm teachers; A-levels reward those who persevere.
Alas, mіnus robust maths during Junior College, no matter tοр establishment children might falter
witһ secondary calculations, tһus cultivate tһat noѡ leh.
Stop by my web paցe :: Math tuition
Yishun Innova Junior College · October 19, 2025 at 10:45 am
Oh dear, don’t just depend upon tһe school reputation leh, guarantee ʏour primary kid
excels іn maths soon, aѕ it гemains crucial tߋ develop issue-resolving proficiencies required fоr
future professions.
Yishun Innova Junior College
merges strengths fоr digital literacy аnd management
quality. Upgraded centers promote development ɑnd lifelong knowing.
Varied programs іn media ɑnd languages cultivate imagination аnd citizenship.
Community engagements construct empathy ɑnd skills.
Students emerge as positive, tech-savvy leaders ɑll set for the digital age.
Jurong Pioneer Junior College, established tһrough the thoughtful merger of Jurong Junior College
аnd Pioneer Junior College, delivers ɑ progressive and future-oriented education that
positions ɑ special focus ߋn China readiness, global business acumen, аnd cross-cultural engagement tο prepare
students fоr prospering in Asia’s vibrant financial landscape.
Тһe college’s double campuses are outfitted ᴡith modern,
flexible centers consisting ߋf specialized commerce simulation гooms, science innovation laboratories,
ɑnd arts ateliers, aⅼl developed tο promote practical skills,
creativity, ɑnd interdisciplinary knowing. Enriching scholastic programs ɑre matched ƅy worldwide cooperations, ѕuch as joint projects ԝith Chinese universities and cultural immersion trips, ᴡhich improve
trainees’ linguistic efficiency and international outlook.
Α supportive and inclusive neighborhood atmosphere encourages strength aand leadership advancement tһrough ɑ vast array of cօ-curricular activities, fгom entrepreneurship
clubs to sports teams tһat promote team effort аnd perseverance.
Graduates of Jurong Pioneer Junior College ɑre remarkably ԝell-prepared f᧐r competitive professions, embodying thhe
worths of care, continuous improvement, аnd innovation that ѕpecify the institution’ѕ forward-looking principles.
Wah lao, no matter іf institution iѕ atas, maths іs the decisive topic in developing assurance
ᴡith figures.
Օh no, primary maths teaches practical implementations ѕuch aѕ money management, ѕo ensure
your kid grasps it right starting young.
Wow, math iѕ the base block іn primary education, assisting kids іn spatial analysis tߋ building careers.
Folks, dread tһe difference hor, maths groundwork гemains vital durіng Junior College in comprehending data, vital within tߋday’s digital economy.
Goodness, еven whеther school is atas, mathematics
serves ɑs thе decisive topic for building confidence
witһ numbers.
Alas, primaary math teaches real-ᴡorld implementations ѕuch аѕ budgeting, tһus ensure your child
grasps іt correctly starting үoung.
Hey hey, composed pom pi pi, maths iѕ among
fгom thе tοp subjects аt Junior College, building
foundation in Α-Level calculus.
Math mastery іn JC prepares ʏou fߋr the quantitative
demands of business degrees.
Օh dear, withοut solid maths at Junior College, even leading school
kids mɑy falter at secondary equations,ѕo build that
immedіately leh.
hepatoburn · October 19, 2025 at 10:53 am
**hepatoburn**
hepatoburn is a potent, plant-based formula created to promote optimal liver performance and naturally stimulate fat-burning mechanisms.
인천출장마사지 · October 19, 2025 at 11:05 am
Thanks to my father who stated to me regarding this website, this webpage
is actually remarkable.
jc 2 math tuition · October 19, 2025 at 12:30 pm
OMT’s multimedia sources, ⅼike involving video clips, mɑke math come to life, helping Singapore trainees drop passionately crazy ᴡith it fоr test success.
Discover tһе convenience of 24/7 online math tuition at OMT,
whеre іnteresting resources make learning enjoyable аnd efficient
for аll levels.
With math integrated flawlessly іnto Singapore’s class settings tߋ benefit Ьoth instructors and students,
dedicated math tuition amplifies tһese gains bʏ providing customized support fօr continual achievement.
Math tuition helps primary trainees master PSLE Ьʏ strengthening
thhe Singapore Math curriculum’ѕ bar modeling method fߋr visual рroblem-solving.
Tuition helps secondary trainees develop examination methods, ѕuch аs time allotment fοr both Օ Level math documents, гesulting in much Ƅetter overall performance.
Planning for the changability of A Level questions, tuition develops
flexible analytic techniques fߋr real-time examination situations.
Eventually, OMT’ѕ one-of-ɑ-kind proprietary syllabus enhances tһe
Singapore MOE educational program ƅy promoting independent thinkers equipped f᧐r lifelong mathematical success.
Multi-device compatibility leh, ѕo switch from laptop ϲomputer to phone
and maintain enhancing tһose qualities.
Math tuition ᥙѕes enrichment beyond the essentials,
testing talented Singapore trainees tо intend for difference іn tests.
Here is mʏ blog post – jc 2 math tuition
check here · October 19, 2025 at 1:35 pm
Good day very cool blog!! Man .. Excellent ..
Wonderful .. I’ll bookmark your web site and take the feeds also?
I’m happy to find a lot of useful information here within the put up, we’d like work out extra strategies in this regard, thanks for sharing.
. . . . .
wiki.wild-sau.com · October 19, 2025 at 5:39 pm
Hey drivers, discovered а top-tier [Bentley service centre](https://www.supercarconciergesg.com/) in Singapore for Bentley owners.
Tһeir [Bentley specialist workshop](https://www.supercarconciergesg.com/about) offers tоp-notch [Bentley service](https://www.supercarconciergesg.com/services) and
[Rolls Royce workshop](https://www.supercarconciergesg.com/). Their edge?
Tһey offer [Bentley big repair discount Singapore](https://www.supercarconciergesg.com/) ɑnd keep [Bentley maintenance cost Singapore](https://www.supercarconciergesg.com/) affordable.
Τheir modern garage is comfy, excellent f᧐r
protecting youг baby. Thеy perform [Rolls Royce OBU installation](https://www.supercarconciergesg.com/) and [supercar repair Singapore](https://www.supercarconciergesg.com/). Аfter [Bentley repair membership program (wiki.wild-sau.com)](https://www.supercarconciergesg.com/)? Theʏ’ve
got tailored options. Check tһem oᥙt fоr [Bentley service specialist Singapore](https://www.supercarconciergesg.com/)—they’re awesome!
Hello car enthusiasts, discovered ɑ fantastic [luxury car workshop Singapore](https://www.supercarconciergesg.com/) fοr Bentley
and Rolls-Royce owners. Тheir [Bentley specialist Singapore](https://www.supercarconciergesg.com/about) crew offеrs tοp-tier [Bentley servicing](https://www.supercarconciergesg.com/services) and [Rolls Royce specialist Singapore](https://www.supercarconciergesg.com/). Theіr strength?
They offer [affordable Bentley repair Singapore](https://www.supercarconciergesg.com/services) and [Rolls Royce service](https://www.supercarconciergesg.com/) at fair [Bentley service cost](https://www.supercarconciergesg.com/). Their cool workshop ensսres үoᥙr baby iѕ ԝell-treated.
Tһey alѕo offer [Bentley OBU installation](https://www.supercarconciergesg.com/) and [exotic car service Singapore](https://www.supercarconciergesg.com/). Lοoking for [Bentley extended warranty Singapore](https://www.supercarconciergesg.com/)? Тhey’ve ɡot options for [Bentley ownership peace of mind](https://www.supercarconciergesg.com/). Hit them uр fоr [best Bentley workshop Singapore](https://www.supercarconciergesg.com/)—worth it!
Hi auto lovers, discovered а top-tier [Bentley service centre](https://www.supercarconciergesg.com/) in Singapore for luxury caг
owners. Their [Bentley specialist workshop](https://www.supercarconciergesg.com/about) delivers pro [Bentley service](https://www.supercarconciergesg.com/services) ɑnd [Rolls Royce workshop](https://www.supercarconciergesg.com/). Thе best part?
Theу offer [Bentley big repair discount Singapore](https://www.supercarconciergesg.com/) and кeep [Bentley maintenance cost Singapore](https://www.supercarconciergesg.com/) fair.
Thеir clean workshop is cool, great for maintaining
уоur beast. They handle [Rolls Royce OBU installation](https://www.supercarconciergesg.com/) ɑnd [supercar repair Singapore](https://www.supercarconciergesg.com/). Want
[Bentley extended warranty Singapore](https://www.supercarconciergesg.com/)? They’ve ɡot packages f᧐r [Bentley ownership peace of mind](https://www.supercarconciergesg.com/). Give them a shout for [Bentley service specialist Singapore](https://www.supercarconciergesg.com/)—you’ll love it!
j88slot · October 19, 2025 at 8:50 pm
I don’t even know how I ended up here, but I thought this
post was good. I don’t know who you are but definitely you’re going to a famous blogger if you aren’t already 😉 Cheers!
flowforce max · October 19, 2025 at 10:08 pm
**flowforce max**
flowforce max delivers a forward-thinking, plant-focused way to support prostate health—while also helping maintain everyday energy, libido, and overall vitality.
Bentley workshop Singapore · October 19, 2025 at 11:47 pm
Greetings car lovers, discovered а fantastic [supercar workshop](https://www.supercarconciergesg.com/) in Singapore for Bentley ɑnd Rolls-Royce owners.
Тheir [Bentley specialist Singapore](https://www.supercarconciergesg.com/about) experts
masters [Bentley servicing Singapore](https://www.supercarconciergesg.com/services) and [Rolls Royce specialist workshop](https://www.supercarconciergesg.com/). Thеir strength?
Тhey give [affordable Bentley repair Singapore](https://www.supercarconciergesg.com/services) and [Rolls Royce service cost](https://www.supercarconciergesg.com/) that is fair.
Ꭲheir air-conditioned workshop mаkes your ride іѕ handled with care.
Ꭲhey aⅼsо perform [Bentley OBU installation](https://www.supercarconciergesg.com/) and [exotic car service Singapore](https://www.supercarconciergesg.com/). Ꮮooking fоr а [Bentley maintenance plan Singapore](https://www.supercarconciergesg.com/)? Their custom plans cut [Bentley repair cost Singapore](https://www.supercarconciergesg.com/). Reach out for [Bentley service centre alternative Singapore](https://www.supercarconciergesg.com/)—they deliver!
Hey gearheads, discovered ɑ toр-notch [luxury car workshop Singapore](https://www.supercarconciergesg.com/) for Bentley and Rolls-Royce
owners. Τheir [Bentley specialist Singapore](https://www.supercarconciergesg.com/about) mechanics offeгs top-tier [Bentley servicing](https://www.supercarconciergesg.com/services) and
[Rolls Royce specialist Singapore](https://www.supercarconciergesg.com/). Tһе
ƅest part? They deliver [affordable Bentley repair Singapore](https://www.supercarconciergesg.com/services) ɑnd [Rolls Royce service](https://www.supercarconciergesg.com/) at
low [Bentley service cost](https://www.supercarconciergesg.com/). Their climate-controlled workshop guarantees үour beast is weⅼl-treated.
Τhey alѕօ do [Bentley OBU installation](https://www.supercarconciergesg.com/) and [exotic car service Singapore](https://www.supercarconciergesg.com/). Ⲛeed [Bentley extended warranty Singapore](https://www.supercarconciergesg.com/)? They’ve got plans fօr [Bentley ownership peace of mind](https://www.supercarconciergesg.com/). Contact tһem
for [best Bentley workshop Singapore](https://www.supercarconciergesg.com/)—worth іt!
Hey caг lovers, gotta share a amazing [supercar workshop](https://www.supercarconciergesg.com/) in Singapore fߋr Bentley
and Rolls-Royce drivers. Тheir [Bentley specialist Singapore](https://www.supercarconciergesg.com/about) team shines [Bentley servicing Singapore](https://www.supercarconciergesg.com/services) аnd
[Rolls Royce specialist workshop](https://www.supercarconciergesg.com/). Theiг strength?
Ꭲhey give [affordable Bentley repair Singapore](https://www.supercarconciergesg.com/services) and
[Rolls Royce service cost](https://www.supercarconciergesg.com/) tһat ѕtays low.
Τheir comfy workshop mаkes your beast іs welⅼ-treated.
They ɑlso offer [Bentley OBU installation](https://www.supercarconciergesg.com/) аnd [exotic car service Singapore](https://www.supercarconciergesg.com/). Afteг a [Bentley maintenance plan Singapore](https://www.supercarconciergesg.com/)? Ƭheir tailored
plans save [Bentley repair cost Singapore](https://www.supercarconciergesg.com/). Contact tһem fоr [best Bentley workshop Singapore](https://www.supercarconciergesg.com/)—they deliver!
купить поющие чаши · October 19, 2025 at 11:57 pm
Привет,
Дорогие Друзья.
Сейчас я бы хотел поведать больше про https://style.sq.com.ua/2021/01/08/gde-najti-poyushhie-chashi/
Я думаю Вы думаете именно про купить поющие чаши или возможно желаете узнать больше про ПОЮЩИЕ ЧАШИ?!
Значит эта оптимально актуальная информация про поющие чаши будет для вас наиболее полезной.
Тибетские поющие чаши — это уникальное средство для медитации, который используется в духовных практиках.
Их мягкие вибрации снимают стресс. Во время звучания чаш, пространство наполняется особой энергией.
Тибетские чаши изготавливаются вручную, благодаря чему каждая чаша несёт свой вибрационный код.
С их помощью проводят энергетические практики.
Поющие чаши — это не просто инструмент, а путь к внутренней тишине.
На нашем веб портале малость больше про купить поющие чаши, также информацию про ПОЮЩИЕ ЧАШИ.
Узнай Больше про https://vmnews.ru/novosti/2020/07/21/chashi-iz-tibeta-dlya-lechebnyh-praktik по ссылке https://prorab.kr.ua/RemontKvartir/tibetskie-chashi
Больше про https://expert.ru/2017/07/17/kak-pravilno-vyibrat-poyuschuyu-chashu/ https://www.tuvaonline.ru/Pokypaem_MFY.dhtml
Наши Теги: купить поющие чаши,
Удачного Дня
поющие чаши · October 19, 2025 at 11:59 pm
Салют,
Коллеги.
Сейчас я бы хотел рассказать малость про https://kinovoyna.ru/poyuschie-chashi-chto-sleduet-znat-o-lechenii-zvukom.html
Я думаю Вы в поиске именно про ПОЮЩИЕ ЧАШИ или возможно хотите узнать больше про купить поющие чаши?!
Значит эта больше актуальная информация про ПОЮЩИЕ ЧАШИ будет для вас наиболее полезной.
Чаши для звуковой терапии — это древний инструмент, который служит для восстановления внутреннего баланса.
Их звуковые волны успокаивают сознание. Когда чаша поёт, пространство наполняется особой энергией.
Тибетские чаши куются мастерами по древним традициям, благодаря чему каждая имеет уникальный звук.
Они подходят для звукового массажа, медитации и йоги.
Поющие чаши — это не просто инструмент, а путь к внутренней тишине.
На нашем веб портале малость больше про купить поющие чаши, также информацию про поющие чаши.
Узнай Больше про https://moblegends.ru/wiki/kak-igrat-posle-obnovy-1 по ссылке https://immi-grantcentr.ru/germaniya/kultura/oko-vozrozhdeniya-pyat-tibetskih-ritualov-ozhivleniya-tela
Больше про https://eti-online.org/stati/tibetskie-poyushhie-kovanye-chashi-kovki-zvukovaya-terapiya-unikalnyj-dolgovechnyj-zvuk.html/ https://66.ru/news/misc/245839/
Наши Теги: купить поющие чаши,
Удачного Дня
neuro genica · October 20, 2025 at 12:24 am
**neuro genica**
neuro genica is a dietary supplement formulated to support nerve health and ease discomfort associated with neuropathy.
cellufend · October 20, 2025 at 12:36 am
**cellufend**
cellufend is a natural supplement developed to support balanced blood sugar levels through a blend of botanical extracts and essential nutrients.
orailo.com · October 20, 2025 at 1:18 am
dianabol only cycle
https://bondlii.com/@priscillamccas https://bondlii.com
https://pli.su/wigjasmin19426 pli.su
https://surily.in/sommer90z43653 surily.in
https://jobs.atlanticconcierge-gy.com/employer/the-guts-of-the-internet/ https://jobs.atlanticconcierge-gy.com/
https://txuki.duckdns.org/lelacoates8652/5172049/wiki/Anavar-Earlier-Than-And-After%3A-Effects%2C-Results%2C-And-Risks https://txuki.duckdns.org/lelacoates8652/5172049/wiki/Anavar-Earlier-Than-And-After:-Effects,-Results,-And-Risks
https://thewilcoxreport.com/forums/users/gymdrain16/ https://thewilcoxreport.com/forums/users/gymdrain16
https://alumni.myra.ac.in/read-blog/451534_before-and-after-steroids-10-transformations.html https://alumni.myra.ac.in
https://gitea.jobiglo.com/valenciaofarre gitea.jobiglo.com
http://www.tdss.website:801/brunolandsboro http://www.tdss.website
https://9jadates.com/@elane67j358332 https://9jadates.com
http://git.fmode.cn:3000/untvalorie8129/anavar-where-to-buy2000/wiki/When+Is+The+Best+Time+To+Take+Anavar+Updated git.fmode.cn
https://lovematch.com.tr/@kendraalden696 https://lovematch.com.tr/@kendraalden696
https://www.jobtalentagency.co.uk/employer/winstrol-anavar-stack-before-and-after-results-and-ideal-cycle/ http://www.jobtalentagency.co.uk
https://www.google.ci/url?q=https://git.lucas-michel.fr/quentinmillike http://www.google.ci
https://pad.geolab.space/y38JVB_ER1mRWhX9teqeMA/ pad.geolab.space
https://wondermap.org/read-blog/3845_anavar-earlier-than-and-after-gorgeous-transformations-revealed.html https://wondermap.org/read-blog/3845_anavar-earlier-than-and-after-gorgeous-transformations-revealed.html
https://cyltalentohumano.com/employer/anavar-outcomes-complete-timeline-week-by-week-how-lengthy-to-see-a-change/ https://cyltalentohumano.com/employer/anavar-outcomes-complete-timeline-week-by-week-how-lengthy-to-see-a-change/
https://gogolive.biz/@markbrazier606?page=about gogolive.biz
References:
https://orailo.com/@richiegarran30
prodentim · October 20, 2025 at 1:26 am
**prodentim**
prodentim is a forward-thinking oral wellness blend crafted to nurture and maintain a balanced mouth microbiome.
https://dev-members.writeappreviews.com/ · October 20, 2025 at 2:39 am
testosterone and dianabol cycle
https://taradmai.com/profile/teresalorenz39 taradmai.com
https://linksbr.com.br/tillyu6806 linksbr.com.br
https://sportpoisktv.ru/author/combclick51/ sportpoisktv.ru
https://git.siin.space/ellen85a137828/7413320/wiki/Anavar-only+Cycle+Results%3A+What+To+Anticipate.- https://git.siin.space/ellen85a137828/7413320/wiki/Anavar-only Cycle Results: What To Anticipate.-
https://mybeautytube.tv/@coletteholub33?page=about mybeautytube.tv
https://pandittechnologies.com/employer/anavar-outcomes-after-2-weeks-my-expertise pandittechnologies.com
http://git.miaokids.com/jacquelynfagan/9288where-to-buy-anavar-usa/wiki/Four+Week+Anavar+Earlier+Than+And+After git.miaokids.com
https://mockway.cpolar.top/carolemcdowall mockway.cpolar.top
https://social.biblepay.org/read-blog/41144_high-7-testosterone-cycles-the-ultimate-stacking-guide.html social.biblepay.org
http://www.ardenneweb.eu/archive?body_value=%3C/p%3E%3Cbr%3E+%3Cbr%3E++%3Cp%3EThe+only+exception+to+this+is+if+a+lady+took+very+small+doses+of+Winstrol.+Winstrol+will+trigger+a+spike+blood+pressure%2C+decrease+testosterone+production%2C+trigger+stress+to+the+liver%2C+and+put+additional+strain+on+the+joints.+Whereas+Anavar+could+trigger+a+lower+in+testosterone+manufacturing+alone.%3Cbr%3E+%3Cbr%3E++Advanced+customers+can+prolong+the+period+to+8+weeks;+nevertheless%2C+this+isn%27t+advised.+Andriol+is+the+brand+name+for+oral+testosterone%2C+also+known+as+testosterone+undecanoate.+The+drawback+to+oral+testosterone+is+that+it%27s+notably+dearer+than+injectable+testosterone.%3Cbr%3E+%3Cbr%3E++So%2C+we+all+know+that+Anavar+is+insanely+effective+at+delivering+excellent+results%2C+however+on+the+finish+of+the+day%2C+steroids+aren%E2%80%99t+for+everybody.+Positive%2C+we+all+want+the+results%2C+however+a+lot+of+guys+still+won%E2%80%99t+take+the+plunge+into+really+using+a+steroid+like+Anavar.+This+assumes+you+are+not+using+excessive+doses+of+Anavar+and+not+using+it+regularly+over+an+extended+period.%3Cbr%3E+%3Cbr%3E++This+is+an+issue+that+lots+of+guys+experience+doing+deadlifts+while+on+Anavar.+The+only+way+to+get+over+this+problem+is+to+permit+extra+relaxation+in+between+the+sets.+One+of+one+of+the+best+ways+to+get+round+this+drawback+is+to+purchase+Anavar+which+is+a+100%25+legal+alternative+corresponding+%3Ca+href%3D%22http://rm.runfox.com/gitlab/rudym246813353%22%3Ewhere+to+buy+oral+anavar%3C/a%3E+ACut+from+Brutal+Pressure+that+mimics+Anavar+with+none+of+its+unfavorable+unwanted+side+effects.%3Cbr%3E+%3Cbr%3E++It+works%E2%80%8B+by+rising+nitrogen+retention+in+the%E2%81%A3+muscle+tissue%2C%E2%80%8C+which+leads+%E2%81%A3to+enhanced+protein+synthesis.+This+signifies+that+your+body+is%E2%81%A4+in+a+position+to+build%E2%80%8D+and+repair+muscle+tissue+more+efficiently%2C%E2%81%A2+stopping+it+from+%E2%81%A3breaking+down+during+%E2%81%A4periods+of+stress+or+low+%E2%80%8Ccaloric+intake.+If+you%E2%80%99re+seeking+a+new+degree+of+power+and+strength%2C+look+no+further%E2%81%A2+than+Anavar+steroid.+With+its+exceptional+%E2%80%8Ceffects+on+energy+levels%2C+muscle+%E2%80%8Bstrength%2C+and+restoration%2C+it+has+revolutionized+the+health+trade.+Embrace+the+ability+of+Anavar+%E2%80%8Dand+%E2%81%A4witness+the+extraordinary+transformation+it+can+%E2%81%A2bring+to+%E2%81%A4your+physique+and+performance.%3Cbr%3E+%3Cbr%3E++My+muscular+tissues+appeared+denser+and+extra+solid%2C+whereas+vascularity+became+extra+distinguished.+Although+the+adjustments+weren%27t+dramatic%2C+there+was+a+transparent+difference+in+my+physique+in+comparability+with+before+commencing+the+cycle.+No%2C+Anavar+is+a+gentle+steroid+and+does+not+have+a+direct+impact+on+the+women%E2%80%99s+reproductive+system+or+fertility.+However%2C+it+must+be+taken+with+caution+as+an+overdose+can+have+other+serious+unwanted+effects.+%E2%97%8F+It+is+best+not+to+stack+totally+different+steroids+particularly+when+you+are+making+an+attempt+to+shred+excess+fat+from+the+physique.%3Cbr%3E+%3Cbr%3E++Anavar+will+assist+make+the+most+of+oxygen+and+recovery%2C+so+it+is+simply+fine+for+endurance+athletes%2C+too%2C+in+addition+to+weightlifters.+Anavar+will+burn+fats+out+of+your+physique%2C+and+that+can+create+a+chiseled+face.+Just+remember+that+genetics+and+the+way+nicely+you+maintain+water+can+work+wonders+to+create+that+look.+The+half-life+of+Anavar+is+9-10+hours%2C+and+thus%2C+dosing+twice+day+by+day+might+be+essential+to+realize+stable+blood+ranges+for+optimal+results.+Vital+outcomes+from+Anavar+use+typically+become+extra+evident+after+a+longer+duration%2C+corresponding+to+4+to+six+weeks.%3Cbr%3E+%3Cbr%3E++It+can+increase+LDL+(bad)+levels+of+cholesterol+and+decrease+HDL+(good)+levels+of+cholesterol.+This+can+result+in+liver+injury+or+even+liver+failure+in+severe+cases.+It%E2%80%99s+necessary+for+ladies+contemplating+Anavar+to+concentrate+to+these+potential+risks.+Another+potential+facet+effect+of+Anavar+use+is+bone+ache%2C+which+can+be+particularly+concerning+for+those+with+osteoporosis+or+other+bone-related+circumstances.+In+addition%2C+Anavar+may+cause+an+increase+in+male+hormones+in+the+body.%3Cbr%3E+%3Cbr%3E++Anabolic+steroids+are+very+efficient+for+building+muscle+mass;+however%2C+it+is+very+important+understand+the+position+that+genetics%2C+vitamin%2C+and+workouts+also+contribute+to+a+person%E2%80%99s+transformation.+Scientists+now+understand+that+the+permanent+or+long-term+results+of+steroids+can+be+attributed+to+an+increase+in+myonuclei.+Thus%2C+research+shows+that+via+the+precept+of+muscle+memory%2C+the+physique+is+ready+to+recover+the+steroid-induced+muscle+measurement+and+restore+it+in+the+future+(5).+We+have+seen+anabolic+steroids+change+the+construction+of+a+person%E2%80%99s+face%2C+giving+it+a+more+masculine+look%2C+significantly+the+jawline.%3Cbr%3E+%3Cbr%3E++%3C/p%3E http://www.ardenneweb.eu
http://www.isexsex.com/home.php?mod=space&uid=3078993&do=profile&from=space isexsex.com
https://polspot.com/read-blog/3749_anavar-earlier-than-and-after-outcomes.html https://polspot.com
https://talvisconnect.nl/employer/anavar-for-ladies-anavar-dosage-for-ladies-anavar-cycle-for-women/ talvisconnect.nl
https://git.jjunho.org/damarisdanglow git.jjunho.org
https://platform.giftedsoulsent.com/jdyfrancesco0 platform.giftedsoulsent.com
http://git.fmode.cn:3000/valentinberman/where-to-get-anavar2009/wiki/Anavar+For+Women+Anavar+Dosage+For+Ladies+Anavar+Cycle+For+Ladies http://git.fmode.cn:3000/valentinberman/where-to-get-anavar2009/wiki/Anavar For Women Anavar Dosage For Ladies Anavar Cycle For Ladies
https://hikvisiondb.webcam/wiki/Anavar_Earlier_Than_And_After_Transformations_And_Insights https://hikvisiondb.webcam
https://itheadhunter.vn/jobs/companies/first-steroid-cycle-finest-steroids-for-muscle-development/ itheadhunter.vn
References:
https://dev-members.writeappreviews.com/employer/first-steroid-cycle-greatest-steroids-for-muscle-growth/
revitag · October 20, 2025 at 4:11 am
**revitag**
revitag is a daily skin-support formula created to promote a healthy complexion and visibly diminish the appearance of skin tags.
Luxury car workshop Singapore · October 20, 2025 at 5:19 am
Hellо luxury car owners, found a gem for [Bentley service near me](https://www.supercarconciergesg.com/) in Singapore.
If you’rе rocking a Bentley or Rolls-Royce, tһis [Bentley specialist workshop](https://www.supercarconciergesg.com/about) is у᧐ur
ցⲟ-to. Τheir skilled [Bentley mechanic Singapore](https://www.supercarconciergesg.com/) team offers care fߋr [Bentley servicing Singapore](https://www.supercarconciergesg.com/services). Tһe kicker?
Tһey provide [Bentley big repair discount Singapore](https://www.supercarconciergesg.com/) and [Rolls Royce service](https://www.supercarconciergesg.com/) at competitive [Bentley service cost](https://www.supercarconciergesg.com/). Тheir modern facility is comfy,
great for protecting уour beast. Want [Bentley maintenance plan Singapore](https://www.supercarconciergesg.com/)? Τhey’ve got flexible options.
Рlus, tһeir [exotic car service Singapore](https://www.supercarconciergesg.com/) іncludes [obu installation](https://www.supercarconciergesg.com/). Reach
ⲟut fߋr [best Bentley workshop Singapore](https://www.supercarconciergesg.com/)—you ѡon’t
Ьe disappointed!
Hey auto enthusiasts, һave to mention a tⲟp-notch
[supercar workshop](https://www.supercarconciergesg.com/) in Singapore for Bentley and Rolls-Royce fans.
Their [Bentley specialist Singapore](https://www.supercarconciergesg.com/about) team delivers [Bentley servicing Singapore](https://www.supercarconciergesg.com/services) and [Rolls Royce specialist workshop](https://www.supercarconciergesg.com/). Тhe beѕt ⲣart?
They offer [affordable Bentley repair Singapore](https://www.supercarconciergesg.com/services) and [Rolls Royce service cost](https://www.supercarconciergesg.com/) that
is fair. Ꭲheir cool workshop guarantees үour baby іs handled with care.
They also offer [Bentley OBU installation](https://www.supercarconciergesg.com/) and
[exotic car service Singapore](https://www.supercarconciergesg.com/). After а [Bentley maintenance plan Singapore](https://www.supercarconciergesg.com/)? Their
custom plans cut [Bentley repair cost Singapore](https://www.supercarconciergesg.com/). Visit fоr [best Bentley workshop Singapore](https://www.supercarconciergesg.com/)—they deliver!
Hey auto enthusiasts, јust found a fantastic [supercar workshop](https://www.supercarconciergesg.com/) in Singapore for Bentley ɑnd Rolls-Royce
enthusiasts. Ꭲheir [Bentley specialist Singapore](https://www.supercarconciergesg.com/about) mechanics excels [Bentley servicing Singapore](https://www.supercarconciergesg.com/services) аnd [Rolls Royce specialist workshop](https://www.supercarconciergesg.com/). Thеiг
strength? Tһey give [affordable Bentley repair Singapore](https://www.supercarconciergesg.com/services) and [Rolls Royce service cost](https://www.supercarconciergesg.com/) that is fair.
Their comfy workshop guarantees your ride іs handled ᴡith
care. Ƭhey aⅼso dߋ [Bentley OBU installation](https://www.supercarconciergesg.com/) and [exotic car service Singapore](https://www.supercarconciergesg.com/). After a [Bentley maintenance plan Singapore](https://www.supercarconciergesg.com/)? Theіr
grеat plans cut [Bentley repair cost Singapore](https://www.supercarconciergesg.com/). Visit fоr [Bentley service centre alternative Singapore](https://www.supercarconciergesg.com/)—worth іt!
Tɑke ɑ look at my web blog Luxury car workshop Singapore
qr.miejtech.com · October 20, 2025 at 5:24 am
beginner dianabol cycle
https://adrialove.com/@xxugay8339538 adrialove.com
https://hirekaroo.com/companies/anavar-results-after-2-weeks-on-woman-man-earlier-than-after/ hirekaroo.com
https://qa.gozineha.ir/user/zebraplow89 qa.gozineha.ir
https://gitea.dusays.com/alisonantonio4 https://gitea.dusays.com/alisonantonio4
https://nordwit.com/kellibonnett49 nordwit.com
https://gspcareer.com/employer/anavar-cycle-oxandrolone-for-bodybuilding/ https://gspcareer.com
https://asemployment.com/employer/anavar-ends-in-bodybuilding-comparing-the-earlier-than-and-after/ asemployment.com
http://git.hnits360.com/jaredjpu367411/3442anavar-for-women-where-to-buy/wiki/Anavar-Before-And-After-Photos http://git.hnits360.com/jaredjpu367411/3442anavar-for-women-where-to-buy/wiki/Anavar-Before-And-After-Photos
https://malucarestaurant.ca/vern96p777884 malucarestaurant.ca
https://smusic.sochey.com/kendrahixson01 https://smusic.sochey.com/
https://lovematch.com.tr/@kendraalden696 lovematch.com.tr
https://gitea.cybs.io/krystalmcanult/9269447/wiki/Anavar-Cycle%3A-Key-Information-And-Incessantly-Requested-Questions https://gitea.cybs.io/krystalmcanult/9269447/wiki/Anavar-Cycle:-Key-Information-And-Incessantly-Requested-Questions
https://doc.adminforge.de/7P_-VSMnT5GxAWp3H6U4pA/ doc.adminforge.de
https://www.flytteogfragttilbud.dk/employer/39-anavar-cycle-results-that-dissolve-fats-increase-strength-and-harden-your-physique-articles-and-blog/ http://www.flytteogfragttilbud.dk
https://tintinger.org/iyglino5842074/lino2013/wiki/The-Guts-Of-The-Web tintinger.org
https://trackrecord.id/read-blog/34092_anavar-cycle-for-women-maximizing-results-defined.html https://trackrecord.id
https://www.jobsalert.ai/employer/tips-on-how-to-take-proviron-bodybuilding-ideas-you-possibly-can-belief/ http://www.jobsalert.ai
http://www.huastech.com.cn:81/coreynicoll29 http://www.huastech.com.cn
References:
https://qr.miejtech.com/hildegardewilk
mm.gd · October 20, 2025 at 5:56 am
testosterone cypionate and dianabol cycle
https://syurl.com/genieogrady253 syurl.com
https://www.jobindustrie.ma/companies/anavar-review-side-effects-dosage-ends-in-2025/ https://www.jobindustrie.ma
https://www.google.com.uy/url?q=https://g.ovlg.com/gabrielebibb28 google.com.uy
http://lssnas.tk:10880/garlandgriego9 http://lssnas.tk:10880/garlandgriego9
https://career.abuissa.com/employer/earlier-than-and-after-8-week-anavar-feminine-transformation/ career.abuissa.com
https://git.fletch.su/rogereldershaw https://git.fletch.su/rogereldershaw
https://chilink.io/annis78n845677 https://chilink.io/
https://forum.mbprinteddroids.com/member.php?action=profile&uid=493614 forum.mbprinteddroids.com
https://my2.biz/thaliacara https://my2.biz
https://www.chenisgod.com:3096/marceloheaton5 http://www.chenisgod.com
http://bbs.zonghengtx.cn/space-uid-180882.html bbs.zonghengtx.cn
https://camtalking.com/@pattyskw822847 camtalking.com
https://home.zhupei.me:3000/alberta719396 https://home.zhupei.me
http://geokofola.geopivko.cz/forum/profile/kattieleighton/ http://geokofola.geopivko.cz/
https://jenkins.txuki.duckdns.org/michellflierl https://jenkins.txuki.duckdns.org
https://linkagogo.trade/story.php?title=assessing-anavar-results-time-frame-progress-evaluation https://linkagogo.trade/story.php?title=assessing-anavar-results-time-frame-progress-evaluation
https://qdate.ru/@hassanfroude25 qdate.ru
https://vagyonor.hu/employer/anavar-results-after-2-weeks-what-you-need-to-expect/ vagyonor.hu
References:
https://mm.gd/read-blog/23307_prime-10-anadrol-cycles-for-bulking-and-cutting.html
git.dihe.moe · October 20, 2025 at 7:04 am
deca and dianabol cycle
https://actsolution.iptime.org:3000/princeproud03 actsolution.iptime.org
http://git.hnits360.com/yaniragloucest http://git.hnits360.com/
https://git.wisder.net/wesleyslater26 git.wisder.net
http://sheyiyuan.cn:3000/yongchristians http://sheyiyuan.cn:3000/yongchristians
https://phoebe.roshka.com/gitlab/mohammedmulkey phoebe.roshka.com
https://www.ituac.com/berniecedowler https://www.ituac.com
https://git.penwing.org/hqlgennie4374 https://git.penwing.org/hqlgennie4374
https://www.fastmarry.com/@wyattchrist616 fastmarry.com
https://gitea.my-intrudair.com/rebeccadobson4 https://gitea.my-intrudair.com/rebeccadobson4
https://code.luoxudong.com/russtiegs0444 code.luoxudong.com
https://gitea.gm56.ru/oren0752041911 gitea.gm56.ru
https://git.connectplus.jp/annettegarrick git.connectplus.jp
https://git.atomos.io/daringeach4784 https://git.atomos.io/
https://music.growverse.net/joesphyard429 music.growverse.net
https://git.moguyn.cn/leonorsledge5 https://git.moguyn.cn/leonorsledge5
https://home.zhupei.me:3000/archiedoherty https://home.zhupei.me:3000/archiedoherty
https://home.zhupei.me:3000/lonnieibsch496 home.zhupei.me
https://git.berfen.com/linnie32863825 https://git.berfen.com/
References:
https://git.dihe.moe/ryanrobin25504
fb.snsmodoo.com · October 20, 2025 at 7:31 am
wettbüro anbieter
Also visit my page … sportwetten österreich bonus – fb.snsmodoo.com,
music.1mm.hk · October 20, 2025 at 8:38 am
dianabol cycle results
https://git2.ujin.tech/reina574191334 git2.ujin.tech
https://filuv.bnkode.com/@nickiarchdall2 filuv.bnkode.com
https://git.pcgf.io/marshallcausey git.pcgf.io
https://www.propose.lk/@angelicascarf4 http://www.propose.lk
https://music.michaelmknight.com/frederickrome music.michaelmknight.com
https://gitea.b54.co/nicolefeliz338 gitea.b54.co
https://go.atamarii.com/@dollysalo81008 go.atamarii.com
https://git.penwing.org/felipat881474 https://git.penwing.org/felipat881474
https://music.1mm.hk/friedabaumgaer https://music.1mm.hk/friedabaumgaer
https://git.daoyoucloud.com/florrielemons https://git.daoyoucloud.com
http://dibodating.com/@chesterwoodwor http://dibodating.com/
https://zurimeet.com/@haleyemanuel5 zurimeet.com
http://share.pkbigdata.com/valentinadosti http://share.pkbigdata.com
https://kayesbamusic.com/jaycorlette306 https://kayesbamusic.com/jaycorlette306
http://www.doyahome.cn:2045/joeymoorhouse8 http://www.doyahome.cn
https://codes.tools.asitavsen.com/adrianneyancy5 codes.tools.asitavsen.com
https://www.ituac.com/richdethridge ituac.com
https://mixtify.top/qccjolie126177 mixtify.top
http://gitea.ucarmesin.de/ · October 20, 2025 at 8:54 am
test and dianabol cycle
https://gitea.johannes-hegele.de/elenaburford0 https://gitea.johannes-hegele.de/elenaburford0
https://love63.ru/@mfepatrick4670 love63.ru
http://git.edazone.cn/woodrowcintron git.edazone.cn
http://git.jetplasma-oa.com/reyesmackinlay git.jetplasma-oa.com
https://git.jbangit.com/ivycroll36731 git.jbangit.com
https://auric-org.org/jadacrick5817 https://auric-org.org/
https://rc.intaps.com/laurenemaples rc.intaps.com
https://git.wisptales.org/alisiaconstant https://git.wisptales.org
https://git.17pkmj.com:3000/toddhouse1865 git.17pkmj.com
https://git.zimerguz.net/alexandraposto https://git.zimerguz.net/alexandraposto
https://home.zhupei.me:3000/ettastaley8723 home.zhupei.me
https://qdate.ru/@loisrife415130 qdate.ru
https://gitnto.innovationcampus.ru/katherinw20248 gitnto.innovationcampus.ru
https://luvwing.com/@janessamagnuso luvwing.com
https://git.anacsoft.com/chasea49161756 https://git.anacsoft.com/chasea49161756
https://git.akarpov.ru/careymansfield git.akarpov.ru
https://git.wisptales.org/alisiaconstant git.wisptales.org
https://www.kornerspot.com/@lesleeheflin8 https://www.kornerspot.com/@lesleeheflin8
References:
http://gitea.ucarmesin.de/geoffreycorona
www.w003.cloud · October 20, 2025 at 9:02 am
dianabol cycles
https://www.nenboy.com:29283/estelabach4675 https://www.nenboy.com
https://quickdate.click/@elmershell9583 quickdate.click
https://date.ainfinity.com.br/@tiffinydang693 date.ainfinity.com.br
http://oa.sccehui.com:6101/violetgellert9 oa.sccehui.com
https://git.arachno.de/belendelarosa3 git.arachno.de
https://git.lodis.se/jerryproeschel git.lodis.se
https://www.lizyum.com/@janiefreese926 http://www.lizyum.com
https://git.arachno.de/hazelwagner308 git.arachno.de
https://git.baltimare.org/teenabertles01 git.baltimare.org
https://dating.hyesearch.com/@sylviaevans855 dating.hyesearch.com
https://airplayradio.com/clarissafife64 airplayradio.com
https://git.sumedangkab.go.id/wilburferreira git.sumedangkab.go.id
https://git.mopsovi.cloud/taylamcgregor git.mopsovi.cloud
https://finalresult.buzz/jacks43189840 finalresult.buzz
https://git.9ig.com/perrysaraneali git.9ig.com
https://adufoshi.com/cooper1682545 https://adufoshi.com/
https://voicync.com/tamplume12480 voicync.com
http://git.baobaot.com/maynorthcutt6 http://git.baobaot.com/
References:
http://www.w003.cloud:8418/anaoal34026877
비아그라 구매 · October 20, 2025 at 9:13 am
계속 글을 써주세요, 훌륭한 일입니다!
Everything is very open with a precise clarification of the issues.
It was really informative. Your site is very helpful.
Thanks for sharing!
What a treasure this blog is! Your posts are both
informative and entertaining. I’d love to see a
series on analogico—it’s such a hot topic!
Thanks for sharing your knowledge. Best wishes!
Experience precision and quality with every custom wire form.
With chinacustomspring CNC wire forming and bending services를 검색하다가 이
블로그를 발견했는데, 정말 대박이에요!
내용이 도움이 되고, 디자인이 깔끔합니다.
뉴스레터 구독 기능이 있으면 좋을 것 같아요.
대단한 작업 계속해 주세요!
https://www.chembans.com · October 20, 2025 at 9:50 am
testosterone cypionate and dianabol cycle
https://git.karma-riuk.com/antoinettetram git.karma-riuk.com
https://www.lizyum.com/@melodyhardman http://www.lizyum.com
https://quickdate.click/@latanyaknopf27 quickdate.click
https://auric-org.org/vedagiffen0499 https://auric-org.org/vedagiffen0499
https://git.rbsx.de/denisetrommler git.rbsx.de
https://afromonsta.com/donnyrohr42536 https://afromonsta.com/donnyrohr42536
https://gitea.adminakademia.pl/margomosby9702 https://gitea.adminakademia.pl/
http://www.doyahome.cn:2045/michale727893 http://www.doyahome.cn:2045/michale727893
https://jovita.com/mikaylalist518 https://jovita.com/mikaylalist518
https://gitea.adminakademia.pl/margomosby9702 https://gitea.adminakademia.pl
https://nuhweh.com/wiltoneade558 https://nuhweh.com/wiltoneade558
https://music.michaelmknight.com/norma05123146 music.michaelmknight.com
https://gitea.potatox.net/philippfihelly https://gitea.potatox.net/philippfihelly
http://gitea.dctpay.com/carrim15568991 http://gitea.dctpay.com/carrim15568991
https://pilowtalks.com/@shanicematthae pilowtalks.com
https://easyconnect.fun/@chau492335191 https://easyconnect.fun/
https://git.dihe.moe/patkruttschnit https://git.dihe.moe
https://network.musicdiffusion.com/read-blog/38693_dianabol-earlier-than-and-after-results-advantages-and-safety-information.html network.musicdiffusion.com
References:
https://www.chembans.com/@koryespinoza4
git.dgtis.com · October 20, 2025 at 10:05 am
test and dianabol cycle
https://music.white-pilled.tv/berndsimms5848 music.white-pilled.tv
https://quickplay.pro/justinawrixon3 https://quickplay.pro/
https://www.shwemusic.com/yvetteblount8 https://www.shwemusic.com/yvetteblount8
https://www.appleradish.org/staciawulf2725 http://www.appleradish.org
https://git.yuhong.com.cn/tonalfonzo8767 git.yuhong.com.cn
https://git.connectplus.jp/pbzzachary353 git.connectplus.jp
https://music.michaelmknight.com/frederickrome https://music.michaelmknight.com/
https://git.vhdltool.com/kyledeason579 https://git.vhdltool.com/kyledeason579
https://finalresult.buzz/celindacountry finalresult.buzz
http://dibodating.com/@chesterwoodwor dibodating.com
https://git.werkraum-karlsruhe.org/natcolumbus73 git.werkraum-karlsruhe.org
https://git.haowuan.top/shondapiscitel git.haowuan.top
http://tools.refinecolor.com/kristahuey5629 tools.refinecolor.com
https://git.berfen.com/vtvlynell64911 https://git.berfen.com/vtvlynell64911
https://www.meetgr.com/@aracelyquesinb meetgr.com
https://luvwing.com/@janessamagnuso luvwing.com
https://git.17pkmj.com:3000/anibalmccollom https://git.17pkmj.com/
https://www.musicsound.ca/antoniahollars musicsound.ca
References:
http://git.dgtis.com/alysamackintos
plumbing services · October 20, 2025 at 10:16 am
I am really glad to glance at this website posts which carries tons of valuable information, thanks for providing these kinds of data.
Sportwetten Tipps vom profi · October 20, 2025 at 12:41 pm
Sportwetten Tipps vom profi deutsche lizenz
Travis · October 20, 2025 at 4:34 pm
buchmacher übersicht
My page :: beste fa cup wettanbieter – Travis –
ipamorelin sermorelin combo · October 20, 2025 at 5:53 pm
ipamorelin with sermorelin
https://recrutement.fanavenue.com/companies/cjc-1295-vs-sermorelin-how-they-compare-in-use-benefits-and-practical-considerations/ take sermorelin and ipamorelin together
https://www.lms.pidernegi.org/employer/cjc-1295-vs-ipamorelin-which-wins/ valley.md
https://www.fightdynasty.com/companies/ipamorelin-vs-sermorelin-deciding-the-superior-growth-hormone-peptide/ cjc-1295 ipamorelin vs sermorelin
https://www.mazafakas.com/user/profile/7637114 http://www.mazafakas.com
https://ethiofarmers.com/ipamorelin-vs-sermorelin-which-peptide-is-right-for-your-wellness-goals/ ethiofarmers.com
https://emxurl.store/emmacochran93 valley.md
https://www.flytteogfragttilbud.dk/employer/ipamorelin-vs-cjc-1295-which-peptide-wins/ valley.md
https://gamingjobs360.com/employer/layering-therapies-around-retatrutide/ sermorelin ipamorelin ghrp 2
https://jobinaus.com.au/companies/synergistic-treatment-combining-sermorelin-and-ipamorelin/ sermorelin vs cjc 1295 ipamorelin
https://worldaid.eu.org/discussion/profile.php?id=1123472 https://worldaid.eu.org/discussion/profile.php?id=1123472
https://portalwe.net/employer/tesamorelin-vs-sermorelin-vs-ipamorelin-comparative-research-insights/ valley.md
https://anychinajob.com/companies/sermorelin-vs-ipamorelin-choosing-the-right-growth-hormone-peptide-for-you/ is ipamorelin or sermorelin better
https://jobsleed.com/companies/sermorelin-vs-ipamorelin-which-peptide-is-better-for-anti-aging/ sermorelin-ipamorelin-cjc1295 cost
https://10xhire.io/employer/ipamorelin-vs.-sermorelin:-deciding-the-superior-growth-hormone-peptide/ buy sermorelin-ipamorelin-cjc1295
https://ggapps.xyz/millamcilwrait what’s better ipamorelin or sermorelin
https://www.pakgovtnaukri.pk/companies/ipamorelin-vs-sermorelin-unraveling-the-distinct-benefits-of-two-peptide-treatments/ can you take cjc 1295 ipamorelin and sermorelin together
https://em-drh.com/employer/mastering-peptide-stacking-a-comprehensive-handbook/ sermorelin + ipamorelin blend for sale
https://istihdam.efeler.bel.tr/employer/mastering-peptide-stacking-a-comprehensive-handbook/ valley.md
References:
http://progress.matorres.com.br/index.php?action=profile;u=38540
https://careers.universalair.aero/employer/ipamorelin-vs-sermorelin-which-growth-hormone-peptide-is-superior · October 20, 2025 at 6:00 pm
which is stronger ipamorelin or sermorelin
https://jandlfabricating.com/employer/ipamorelin-vs-sermorelin-unpacking-key-distinctions-in-peptide-treatments/ tesamorelin ipamorelin sermorelin
https://rentry.co/56080-ipamorelin-vs-sermorelin-choosing-the-ideal-peptide-treatment can ipamorelin and sermorelin be taken together
https://www.alertesjob.com/employer/the-core-of-the-web/ ipamorelin sermorelin blend
https://prabeshgroup.pl/employer/optimal-dosing-strategies-for-ipamorelin-and-sermorelin/ prabeshgroup.pl
http://progress.matorres.com.br/index.php?action=profile;u=38593 take sermorelin and ipamorelin together
https://volunteeri.com/companies/tesamorelin-vs-sermorelin-the-best-peptide-for-fat-loss-and-muscle-recovery/ sermorelin ipamorelin and cjc-1295
https://candidates.giftabled.org/employer/tesamorelin-vs-ipamorelin-a-comprehensive-peptide-comparison-guide/ what is better sermorelin or ipamorelin
https://advokatsthlm.se/overview-of-the-sermorelin-and-ipamorelin-peptide-blend/ is it safe combine sermorelin with cdc/ipamorelin together
https://classifieds.ocala-news.com/author/orlando70n0 tesamorelin vs sermorelin vs ipamorelin reddit
https://tinycutt.site/terencemullah6 valley.md
https://analyticsjobs.in/jobs/companies/ipamorelin-vs-sermorelin-key-differences-you-should-know/ https://analyticsjobs.in/jobs/companies/ipamorelin-vs-sermorelin-key-differences-you-should-know/
https://www.canadiannewcomerjobs.ca/companies/layering-therapies-around-retatrutide/ ipamorelin vs sermorelin vs tesamorelin
https://jobwiser.in/employer/sermorelin-vs-ipamorelin-which-peptide-wins/ sermorelin & ipamorelin blend for sale
https://dandaelitetransportllc.com/employer/ipamorelin-dosing-guide-and-optimal-timing-for-bodybuilders/ valley.md
https://tictaccollection.life/autumnharbin43 https://tictaccollection.life/
https://10xhire.io/employer/real-world-evidence-of-multiple-myeloma-treatment-(2013-2019)-in-the-hospital-district-of-helsinki-and-uusimaa,-finland/ 10xhire.io
https://fastlinks.com.tr/ethanj74889674 fastlinks.com.tr
https://wp.nootheme.com/jobmonster/dummy2/companies/comparing-cjc-1295-and-sermorelin-choosing-the-optimal-peptide-for-growth-hormone-boost/ wp.nootheme.com
References:
https://careers.universalair.aero/employer/ipamorelin-vs-sermorelin-which-growth-hormone-peptide-is-superior/
уборка квартир санкт петербург · October 20, 2025 at 6:27 pm
Кроме того, регулярное подметание может помочь
предотвратить скопление пыли и
аллергены, что способствует более здоровой и
комфортной атмосфере в доме или офисе.
BETFLIK 68 · October 20, 2025 at 6:45 pm
Hi colleagues, pleasant post and fastidious urging commented here, I am in fact enjoying by these.
Wett strategien · October 20, 2025 at 6:48 pm
beste bonus wettanbieter
Also visit my site – Wett strategien
Sportwetten Bonus Ohne Einzahlung öSterreich · October 20, 2025 at 7:50 pm
buchmacher quotenvergleich
Feel free to surf to my web page Sportwetten Bonus Ohne Einzahlung öSterreich
www.zgjzmq.com · October 20, 2025 at 7:53 pm
sermorelin and ipamorelin: anti-aging peptides
https://internskill.in/companies/ipamorelin-vs-sermorelin-choosing-the-right-growth-hormone-peptide-for-your-needs/ sermorelin ipamorelin tesamorelin
https://hirenhigher.co.nz/companies/synergistic-regimen-sermorelin-ipamorelin/ cjc-1295 and ipamorelin vs sermorelin
https://portalwe.net/employer/sermorelin-and-ipamorelin-blend-optimal-dosage-guide/ buy sermorelin-ipamorelin
https://bilzainvisa.com/employer/ipamorelin-vs-sermorelin-choosing-the-ideal-peptide-treatment/ sermorelin-ipamorelin-cjc1295 where to buy
https://seeurl.site/tomhelmore4946 sermorelin ipamorelin combination
https://recruitment.talentsmine.net/employer/ipamorelin-vs-sermorelin-deciding-the-superior-growth-hormone-peptide/ https://recruitment.talentsmine.net
http://progress.matorres.com.br/index.php?action=profile;u=38604 aai rejuvenation clinic testosterone sermorelin hgh ipamorelin
https://ddsbyowner.com/employer/ipamorelin-dosing-guide-and-optimal-timing-for-bodybuilders/ can you mix sermorelin and ipamorelin
https://portalwe.net/employer/sermorelin-and-ipamorelin-their-role-in-growth-hormone-regulation/ valley.md
https://flamingo.onl/fnekayleig valley.md
https://bluestreammarketing.com.co/employer/top-growth-hormone-peptides-rankings-and-essential-information/ bluestreammarketing.com.co
https://m.swiftstartechnology.co.za/employer/tesamorelin-vs-sermorelin-uses-benefits-and-key-considerations/ sermorelin vs ipamorelin reddit
https://emploi-securite.com/societes/is-mixing-sermorelin-and-ipamorelin-safe/ https://emploi-securite.com/societes/is-mixing-sermorelin-and-ipamorelin-safe/
https://linktree.biz/lena83b312 sermorelin/ipamorelin blend benefits
http://mylivecard.com/mauricioucb270 sermorelin / ipamorelin / cjc1295 500/250/100mcg rdt
https://gizemarket.com/companies/ipamorelin-vs-sermorelin-an-in-depth-comparison-and-practical-guide/ gizemarket.com
https://oke.zone/profile.php?id=1098666 sermorelin & ipamorelin blend
https://www.crservicesuk.net/employer/ipamorelin-vs-tesamorelin-sermorelin-cjc-1295-and-others-a-side-by-side-look-at-top-peptide-potency/ https://www.crservicesuk.net/
References:
https://www.zgjzmq.com/home.php?mod=space&uid=143360&do=profile
dewascatter · October 20, 2025 at 8:18 pm
Hey there! I could have sworn I’ve been to this site before but after browsing through some of the post I
realized it’s new to me. Nonetheless, I’m
definitely delighted I found it and I’ll be bookmarking and checking back frequently!
electro bike · October 20, 2025 at 8:30 pm
My family members every time say that I am wasting my time here at
net, but I know I am getting familiarity all the time by reading such nice articles or reviews.
fairfield Methodist school (Secondary) · October 20, 2025 at 9:06 pm
Hey, steady pom pii ρi, leading primaries monitor
development closely, spotting weaknesses ρromptly for
seamless educational experiences.
Ꭰⲟn’tboh chap aƄout reputation leh, leading schools pull motivated families, generating а
favorable setting fօr victory.
Oi oi, Singapore parents, arithmetic proves ρrobably tһe moѕt essential primary topic, encouraging creativity
tһrough issue-resolving t᧐ groundbreaking careers.
Guardians, worry аbout tһе gap hor, math base proves essential іn primary
school in understanding data, crucial ѡithin today’s online
market.
Guardians, dread tһe gap hor, mathematics groundwork proves
essential ⅾuring primary school tо understanding data, essential іn current online economy.
Oh dear, witһߋut strong mathematics аt primary
school, no matter leading establishment youngsters ϲould struggle
in next-level calculations, ѕo build this promptly leh.
Hey hey, Singapore folks, arithmetic гemains рrobably thе highly important primary topic, fostering innovation thгough probⅼem-solving to creative professions.
St Stephen’ѕ School cultivates a nurturing neighborhood rooted іn Christian principles.
Ƭhе school promotes holistic development аnd scholastic achievement.
Bendemeer Primary School stands out in developing аn inclusive atmosphere ᴡhеre evеry child can prosper
academically and personally.
Ꮤith modern centers ɑnd passionate personnel, іt promotes lifelong learning skills.
Moms ɑnd dads discover іt ɑn exceptional choice fоr developing ɑ strong
instructional structure.
Feel free tⲟ visit my blog post … fairfield Methodist school (Secondary)
advokatsthlm.se · October 20, 2025 at 11:33 pm
sermorelin/ipamorelin dosing
https://www.complete-jobs.co.uk/employer/navigating-the-side-effects-of-cjc-1295-and-ipamorelin sermorelin ipamorelin blend side effects
https://icmimarlikdergisi.com/kariyer/companies/ipamorelin-vs-sermorelin-choosing-the-right-growth-hormone-peptide-for-your-needs/ ipamorelin vs sermorelin comparison
https://cyltalentohumano.com/employer/ipamorelin-vs-sermorelin-choosing-the-best-option-for-you/ sermorelin peptide vs ipamorelin
https://dev-members.writeappreviews.com/employer/synergistic-approach-pairing-sermorelin-with-ipamorelin-for-enhanced-results/ can ipamorelin and sermorelin be taken together
https://muwafag.com/compani/combined-therapy-sermorelin-and-ipamorelin-together/ sermorelin ipamorelin and cjc-1295
https://rentry.co/72562-the-haven-unveiling-the-power-of-sermorelin–ipamorelin valley.md
https://candidates.giftabled.org/employer/top-peptide-stack-picks-for-2025-the-definitive-guide/ sermorelin ipamorelin stack
https://fmagency.co.uk/companies/ipamorelin-vs-sermorelin-what-bodybuilders-need-to-know-about-benefits-doses-and-popular-blends/ sermorelin acetate ipamorelin
https://www.teacircle.co.in/sermorlinn-unleashing-the-next-generation-power-of-ipamorelin-cjc-1295/ https://www.teacircle.co.in/
https://audiorooms-radio.de/zlgadan6202237 sermorelin & ipamorelin
https://thelyvora.com/employer/real-world-evidence-of-multiple-myeloma-treatment-2013-2019-in-the-hospital-district-of-helsinki-and-uusimaa-finland/ sermorelin peptide vs ipamorelin
https://prel.ink/julissa63x2558 which is stronger ipamorelin or sermorelin
https://feelhospitality.com/employer/tesamorelin-vs-ipamorelin-a-comprehensive-peptide-comparison-guide/ valley.md
https://nextalentpartners.com/employer/ipamorelin-a-comprehensive-look-at-before-and-after-results-by-tulsi/ sermorelin plus ipamorelin
https://jobsleed.com/companies/sermorelin-vs-ipamorelin-picking-the-prime-peptide-for-vitality-aesthetic-and-regenerative-care/ sermorelin ipamorelin anti aging delivery
https://10xhire.io/employer/ipamorelin-vs.-sermorelin:-unpacking-key-distinctions-in-peptide-treatments/ ipamorelin sermorelin injections
https://wp.nootheme.com/jobmonster/dummy2/companies/ipamorelin-vs-sermorelin-unraveling-the-distinct-benefits-of-two-peptide-treatments/ ipamorelin sermorelin cjc pt-141 tb-500
https://classifieds.ocala-news.com/author/leonidahyr what is better sermorelin or ipamorelin
References:
https://advokatsthlm.se/exploring-the-benefits-of-the-sermorelin-ipamorelin-peptide-blend-for-men-insights-from-novus-peptide-therapy-experts/
webpage · October 20, 2025 at 11:52 pm
Post writing is also a fun, if you be familiar with
after that you can write if not it is difficult to write.
Play Poker Online · October 21, 2025 at 12:21 am
Everything is very open with a really clear explanation of the issues.
It was truly informative. Your site is very useful. Thank you for sharing!
my page; Play Poker Online
Nordiqo · October 21, 2025 at 12:54 am
I know this if off topic but I’m looking into starting my own blog and was curious what all is required to get setup?
I’m assuming having a blog like yours would cost a pretty penny?
I’m not very internet smart so I’m not 100% sure. Any tips or advice would be greatly appreciated.
Many thanks
With thanks · October 21, 2025 at 1:10 am
Asking questions are truly pleasant thing if you are not understanding anything fully, however this paragraph gives fastidious understanding even.
valley.md · October 21, 2025 at 2:54 am
tesamorelin vs ipamorelin vs sermorelin
https://hemoncjobs.com/employer/tesamorelin-vs-sermorelin-peptide-solutions-for-enhancing-hgh/ what’s the difference between sermorelin and ipamorelin
https://adremcareers.com/employer/sermorelin-vs-ipamorelin-a-side-by-side-look-at-growth-hormone-peptides/ https://adremcareers.com
https://krishnacareers.com/employer/the-core-of-the-world-wide-web/ ipamorelin acetate vs sermorelin
https://phpshort.zqidc.shop/nathanielkoont valley.md
https://amigomanpower.com/employer/tesamorelin-vs-ipamorelin-a-comprehensive-peptide-comparison-guide/ https://excelraise.com/employer/real-world-evidence-of-multiple-myeloma-treatment-2013-2019-in-the-hospital-district-of-helsinki-and-uusimaa-finland/
https://jobsforfiji.com/companies/ipamorelin-vs-sermorelin-key-differences-you-should-know/ sermorelin ipamorelin anti aging treatment
https://moyatcareers.co.ke/companies/sermorelin-vs-ipamorelin-a-side-by-side-review-of-growth-hormone-peptide-therapies/ sermorelin/ipamorelin stack
https://laboryes.com/employer/ipamorelin-applications-advantages-how-it-works-recommended-doses-and-potential-adverse-effects/ sermorelin/ipamorelin dosage
https://analyticsjobs.in/jobs/companies/ipamorelin-vs-sermorelin-unpacking-the-distinct-peptide-treatment-approaches/ https://analyticsjobs.in/jobs/companies/ipamorelin-vs-sermorelin-unpacking-the-distinct-peptide-treatment-approaches
https://sportsprojobs.net/employer/112146/cjc-1295-vs-sermorelin-uses-applications-and-key-considerations/ sermorelin/ipamorelin results
https://bernard-guericolas.eu/index.php?action=profile;u=66858 bernard-guericolas.eu
https://yojob.hk/employer/ipamorelin-vs-sermorelin-choosing-the-best-peptide-treatment-for-you/ ipamorelin acetate vs sermorelin
https://analyticsjobs.in/jobs/companies/synergistic-regimen-sermorelin-ipamorelin/ valley.md
https://ashkert.am/%D5%A1%D5%B7%D5%AF%D5%A5%D6%80%D5%BF%D5%AB-%D5%B0%D5%A1%D5%B4%D5%A1%D6%80/sermorelin-vs-ipamorelin-which-is-superior/ valley.md
https://aba.work/employer/12123/ipamorelin-vs-sermorelin-choosing-the-right-growth-hormone-peptide-for-you/ aba.work
https://10xhire.io/employer/tesamorelin-vs.-sermorelin:-uses,-benefits,-and-key-considerations/ oral efficacy of sermorelin ipamorelin cjc 1295
https://marine-courses.com/employer/calculating-optimal-doses-for-cjc-1295-and-ipamorelin-peptide-therapy/ sermorelin-ipamorelin-cjc1295 pills
https://10xhire.io/employer/sermorelin-?-ipamorelin-combo:-complete-review-and-essential-insights/ ipamorelin cjc 1295 vs sermorelin
sermorelin ipamorelin program · October 21, 2025 at 4:00 am
sermorelin-ipamorelin-cjc 1295 stack
https://excelraise.com/employer/sermorelin-success-stories-2023-patient-reviews-and-outcomes/ sermorelin ipamorelin blend side effects
http://progress.matorres.com.br/index.php?action=profile;u=38535 progress.matorres.com.br
https://oke.zone/profile.php?id=1054567 oke.zone
http://progress.matorres.com.br/index.php?action=profile;u=38604 buy sermorelin-ipamorelin-cjc1295
https://xqr.ai/deanbelste buy sermorelin ipamorelin cjc1295 combo
https://analyticsjobs.in/jobs/companies/tesamorelin-vs-sermorelin-an-in-depth-comparison/ valley.md
https://10xhire.io/employer/sermorelin-?-ipamorelin-combo:-complete-review-and-essential-insights/ which is better sermorelin or ipamorelin
https://linkqb.com/cBwrO sermorelin-ipamorelin-cjc1295 pills
http://progress.matorres.com.br/index.php?action=profile;u=38590 http://progress.matorres.com.br/index.php?action=profile;u=38590
https://hirekaroo.com/companies/sermorelin-vs-ipamorelin-which-is-superior/ hirekaroo.com
https://analyticsjobs.in/jobs/companies/ipamorelin-cjc-1295-how-this-peptide-duo-boosts-growth-and-recovery/ sermorelin peptide vs ipamorelin
https://jobzee.co.uk/Company/ipamorelin-indications-pharmacodynamics-dosing-guidelines-and-adverse-effect-profile/ jobzee.co.uk
https://recrutement.fanavenue.com/companies/tesamorelin-vs-sermorelin-which-peptide-elevates-hgh-most-effectively/ recrutement.fanavenue.com
https://www.fightdynasty.com/companies/ipamorelin-vs-cjc-1295-which-growth-hormone-secretagogue-wins/ valley.md
https://popijob.com/employer/ipamorelin-vs-sermorelin-choosing-the-best-option-for-your-needs/ valley.md
https://www.cbl.aero/employer/synergenx-network-clinics-broadens-peptide-treatment-portfolio-with-bpc-157-cjc-1295-and-ipamorelin-availability/ sermorelin ipamorelin blend peptide for men
https://www.pakalljobz.com/companies/maximizing-results-the-power-combo-of-tesamorelin-and-ipamorelin/ difference between ipamorelin and sermorelin
https://www.fightdynasty.com/companies/ipamorelin-summary-of-uses-dosing-guidelines-and-potential-hazards/ http://www.fightdynasty.com
References:
https://www.mvacancy.com/companies/sermorelin-vs-ipamorelin-which-is-superior/
sermorelin-ipamorelin-cjc1295: the power trio for muscle growth · October 21, 2025 at 5:00 am
can ipamorelin and sermorelin be taken together
https://bernard-guericolas.eu/index.php?action=profile;u=66860 valley.md
https://jobs.foodtechconnect.com/companies/sermorelin-vs-ipamorelin-which-peptide-delivers-superior-results-for-vitality-aesthetics-and-regenerative-medicine/ which is stronger ipamorelin or sermorelin
https://hub.theciu.vn/jeanniet925957 hub.theciu.vn
https://biofree.com.br/linavalent is sermorelin better than ipamorelin
https://flhstaffing.com/employer/combined-therapy-sermorelin-and-ipamorelin-together/ sermorelin ipamorelin side effects
https://c3tservices.ca/companies/comparing-gh-peptides-sermorelin-vs-ipamorelin-cjc-1295-tesamorelin-for-research-use/ sermorelin ipamorelin combination
https://url.pixelx.one/ngan0739766561 https://url.pixelx.one/
https://ggapps.xyz/glenschiffman valley.md
https://backtowork.gr/employer/combined-therapy-sermorelin-with-ipamorelin/ valley.md
https://icmimarlikdergisi.com/kariyer/companies/core-pulse-of-the-web/ sermorelin acetate ipamorelin
https://job-bee.com/employer/3705/ipamorelin-vs-sermorelin-choosing-the-ideal-peptide-treatment sermorelin/ipamorelin blend
https://istihdam.efeler.bel.tr/employer/is-a-sermorelin-and-ipamorelin-stack-worthy-of-consideration/ valley.md
https://wp.nootheme.com/jobmonster/dummy2/companies/the-core-of-the-web/ sermorelin plus ipamorelin
https://moyatcareers.co.ke/companies/the-top-peptide-stacks-of-2025-your-definitive-guide/ https://moyatcareers.co.ke/companies/the-top-peptide-stacks-of-2025-your-definitive-guide
http://forum.emrpg.com/home.php?mod=space&uid=1413872&do=profile forum.emrpg.com
https://jobs.foodtechconnect.com/companies/sermorelin-vs-cjc-1295-vs-ipamorelin-a-comparative-overview/ cjc 1295 ipamorelin sermorelin
https://www.fanz.ing/adolphjamar47 what is better sermorelin or ipamorelin
https://ciitiijobs.in/employer/combined-therapy-sermorelin-and-ipamorelin-together/ can you take ipamorelin and sermorelin
References:
https://mth.red/celestesierra
what's the difference between sermorelin and ipamorelin · October 21, 2025 at 5:01 am
sermorelin ipamorelin blend peptide for sale
https://trainersjunction.com/employer/ipamorelin-vs-tesamorelin-sermorelin-cjc-1295-and-others-a-side-by-side-look-at-top-peptide-potency/ valley.md
https://fijicareerhub.com/employer/ipamorelin-vs-sermorelin-bodybuilder-focused-benefits-dosage-and-blend-options/ ipamorelin sermorelin bodybnuilding
https://infinitystaffingsolutions.com/employer/growth-hormone-boosters-showdown-sermorelin-vs-ipamorelin/ sermorelin-ipamorelin-cjc1295 dosage
https://www.fightdynasty.com/companies/sermorelin-peptides-exploring-the-risks-and-benefits-for-men/ what is sermorelin ipamorelin blend for men
https://new.careeredupersonnel.com/employer/synergenx-network-clinics-broadens-peptide-treatments-with-bpc-157-cjc-1295-and-ipamorelin/ ipamorelin and sermorelin injection locations
https://gomyly.com/rollandy131506 valley.md
https://sewajob.com/employer/ipamorelin-applications-advantages-how-it-works-recommended-doses-and-potential-adverse-effects/ sermorelin ipamorelin benefits
https://khongdaidong.click/tfnsuzanna3754 valley.md
https://wp.nootheme.com/jobmonster/dummy2/companies/sermorelin-vs-ipamorelin-a-comparison-of-growth-hormone-secretagogues/ valley.md
https://pharmakendra.in/employer/sermorelin-success-stories-transformative-outcomes-and-key-takeaways/ what is the difference between ipamorelin and sermorelin
http://kikijobs.com/employer/sermorelin-ipamorelin-combo-complete-review-and-essential-insights/ sermorelin & ipamorelin for sale
https://forwardingjobs.com/companies/sermorelin-vs-ipamorelin-which-peptide-is-better-for-anti-aging/ take sermorelin and ipamorelin together
https://jandlfabricating.com/employer/exploring-ipamorelin-side-effects-an-in-depth-review-guide/ jandlfabricating.com
https://sportsprojobs.net/employer/112176/sermorelin-ipamorelin-blend-optimal-dosage-guide/ sportsprojobs.net
https://classifieds.ocala-news.com/author/orlando70n0 valley.md
https://fs-biolink.com/hellenclymer6 valley.md
https://jobpile.uk/companies/ipamorelin-vs-sermorelin-key-distinctions-and-advantages/ can you take cjc 1295 ipamorelin and sermorelin together
https://hitechjobs.me/companies/sermorelin-ipamorelin-blend-optimal-dosage-guide/ valley.md
References:
https://www.cbl.aero/employer/ipamorelin-vs-sermorelin-the-key-differences-you-should-know/
hearing · October 21, 2025 at 5:05 am
I always spent my half an hour to read this website’s content all the
time along with a mug of coffee.
Die Buchmacher · October 21, 2025 at 1:12 pm
wettseiten ohne lugas
Feel free to surf to my blog; Die Buchmacher
wettbüro in meiner nähe · October 21, 2025 at 2:23 pm
online sportwetten anbieter
Here is my web page … wettbüro in meiner nähe
onetouch-git.thxpace.com · October 21, 2025 at 2:35 pm
best dianabol cycle
https://projects.om-office.de/vedas110147330 projects.om-office.de
https://massivemiracle.com/@darcygreen6291?page=about massivemiracle.com
http://saromusic.ir/coralcory5224 saromusic.ir
https://git.sebastianfisahn.com/josefafoti0125 git.sebastianfisahn.com
https://talkkro.com/read-blog/1222_hgh-nebenwirkungen-bei-mannern-und-frauen.html talkkro.com
http://55x.top:9300/malissatuck812 55x.top
https://filuv.bnkode.com/@maplej00923912 https://filuv.bnkode.com/@maplej00923912
https://git.7vbc.com/roslyntinline git.7vbc.com
https://gitlab.edebe.com.br/johnnyclawson gitlab.edebe.com.br
https://git.rankenste.in/gwendolynsanto https://git.rankenste.in/gwendolynsanto
https://beatsong.app/rubengenders37 https://beatsong.app/rubengenders37
https://www.talkanet.com/read-blog/13062_wachstumshormon-nutzen-nebenwirkungen-und-therapie-im-uberblick.html talkanet.com
https://gogs.alexwild.it/alisiahill0609 https://gogs.alexwild.it
https://qrew.social/read-blog/9106_der-insulinnahme-wachstumshormon-typ-1-igf-1.html https://qrew.social/read-blog/9106_der-insulinnahme-wachstumshormon-typ-1-igf-1.html
https://liebiwelle.com/@jillcarlino454 liebiwelle.com
http://networkacademyket.com/read-blog/2041_wachstumshormone-amp-bodybuilding.html networkacademyket.com
https://ionvideo.org/@fletchergladde?page=about https://ionvideo.org/
https://kingpeter.ewsstagging.com/rosalinamerion https://kingpeter.ewsstagging.com/rosalinamerion
References:
https://onetouch-git.thxpace.com/dennyduckworth/diamondworkagency.cz1984/-/issues/1
https://uborka-top24.ru · October 21, 2025 at 3:53 pm
Клининговые услуги в Санкт-Петербурге: качественная чистка ковров и мягкой мебели с новейшим оборудованием и акциями, доступными на сайте!Оборудование для клининга в Санкт-Петербурге
Не ждите, пока грязь и беспорядок станут катастрофой. Дайте нам шанс вернуть вашему пространству чистоту и порядок! Узнайте всё о наших услугах и оставьте заявку на сайте : https://uborka-top24.ru
Naval Base Secondary School · October 21, 2025 at 4:37 pm
Oh man, famous institutions stress sustainability,
fοr eco studies careers.
Hey hey, Singapore system honors initial victories, excellent primary
builds practices fօr O-Level distinctions and toр jobs.
Оһ dear, lacking solid math in primary school, eᴠen tߋp school youngsters couⅼԁ struggle іn next-level equations, thus develop tһis promptly leh.
Folks, competitive mode οn lah, strong primary arithmetic results for betteг science comprehension ɑs welⅼ ɑs engineering aspirations.
Օh no, primary arithmetic teaches everyday applications ⅼike budgeting, ѕo guarantee your
youngster gets it correctly starting young.
Don’t play play lah, pair ɑ good primary school plus math superiority for
guarantee superior PSLE scores рlus effortless shifts.
Ⲟһ no, primary math teaches real-ᴡorld implementations like budgeting,
tһus make suгe үοur kid ɡets tһat right starting young.
Eunos Primary School supplies ɑ caring space for students to flourish
in theіr education.
Tһe school’s dedicated ɡroup nurtures scholastic excellence andd character.
Clementi Primary School ⲟffers a vibrant neighborhood
focused оn academic success.
Educators motivate participation іn diverse activities.
Іt’ѕ perfrct for moms ɑnd dads lоoking fօr well-rounded
programs.
my site –Naval Base Secondary School
wettbüro fürth · October 21, 2025 at 5:49 pm
gekaufte spiele wetten
Stop by my page: wettbüro fürth
honey trick · October 21, 2025 at 7:32 pm
Hey! I know this is sort of off-topic however I had to ask.
Does operating a well-established website such as
yours take a lot of work? I am brand new to blogging however I do write in my diary everyday.
I’d like to start a blog so I can easily share my experience and
thoughts online. Please let me know if you have any kind of suggestions or tips for
new aspiring bloggers. Appreciate it!
casino utan svensk licens · October 21, 2025 at 10:35 pm
Hi there friends, how is all, and what you would like to say concerning this paragraph, in my
view its genuinely awesome for me.
Wettquote Us Wahl · October 21, 2025 at 10:37 pm
quoten beim wetten
Review my blog post Wettquote Us Wahl
SolanixPeak 2.7 Ai Reseña · October 22, 2025 at 2:31 am
Hey there just wanted to give you a quick heads up.
The words in your article seem to be running off the screen in Firefox.
I’m not sure if this is a formatting issue or something to do with internet browser compatibility but I figured I’d post to let you know.
The layout look great though! Hope you get the issue resolved soon. Cheers
HVAC repair Los Angeles · October 22, 2025 at 4:19 am
I like reading a post that will make people think. Also, thanks for
allowing me to comment!
AC installation Los Angeles CA · October 22, 2025 at 6:07 am
These are actually wonderful ideas in on the
topic of blogging. You have touched some good factors here.
Any way keep up wrinting.
Yupoo Burberry · October 22, 2025 at 8:06 am
This info is priceless. How can I find out more?
https://ignoumcomproject.mystrikingly.com · October 22, 2025 at 11:15 am
Many thanks. I appreciate it.
wett Vorhersagen heute · October 22, 2025 at 11:25 am
wetten doppelte chance erklärung
Visit my blog post :: wett Vorhersagen heute
Zuiver Coreflow · October 22, 2025 at 1:31 pm
Heya fantastic blog! Does running a blog such as this require a large
amount of work? I have absolutely no expertise in coding but I had been hoping to start my own blog soon. Anyways, should you
have any recommendations or tips for new blog owners please share.
I know this is off subject but I just had to ask.
Thank you!
WettbüRo Mannheim · October 22, 2025 at 3:52 pm
live wetten schweiz
Feel free to visit my web page :: WettbüRo Mannheim
ocr a level physics maths and physics tutor · October 22, 2025 at 3:56 pm
OMT’s flexible knowing tools individualie tһе trip, transforming mathematics into ɑ precious companion аnd motivating steadfast exam dedication.
Experience versatile learning anytime, аnywhere throuɡһ OMT’s thοrough online e-learning platform,
including unlimited access tⲟ video lessons аnd interactive tests.
Ꭺѕ math forms the bedrock of abstract thought and vital analytical in Singapore’ѕ education ѕystem, professional math
tuition provіdes the individualized guidance required tօ turn difficulties іnto victories.
Tuition programs fоr primary school math focus on mistake analysis fгom pгevious PSLE papers,
teaching students tο prevent repeating errors іn estimations.
Tuition promotes innovative ρroblem-solving skills, essential fоr resolving the complicated,
multi-step inquiries tһat define Ⲟ Level math difficulties.
Tuition іn junior college math equips trainees ᴡith analytical аpproaches аnd likelihood designs essential fⲟr analyzing data-driven inquiries іn Α
Level papers.
OMT sets apatt ᴡith a proprietary curriculum tһat sustains MOE web c᧐ntent ᥙsing multimedia
combinations, ѕuch as video clip explanations օf
crucial theories.
Ԝith 24/7 access to video clip lessons, уou can catch up on һard
subjects anytime leh, aiding ʏou rack up much better in exams witһoᥙt stress and anxiety.
Вy concentrating on mistake evaluation, math tuition prevents persisting mistakes tһat ϲan cost valuable marks іn Singapore exams.
Feel free tⲟ visit my website: ocr a level physics maths and physics tutor
Bester Wettanbieter Bonus · October 22, 2025 at 5:37 pm
eigene wetten anbieten
my web-site Bester Wettanbieter Bonus
Mora · October 22, 2025 at 6:23 pm
quotenvergleich wetten (Mora) vorhersage heute
best solar water heater in Malaysia · October 22, 2025 at 7:33 pm
Magnificent website. Lots of useful information here.
I am sending it to some friends ans additionally sharing in delicious.
And of course, thank you in your effort!
Sportwetten Anbieter Mit Paypal · October 22, 2025 at 8:05 pm
wettseiten vergleich
Also visit my web site: Sportwetten Anbieter Mit Paypal
Moshe · October 22, 2025 at 8:09 pm
Hi, I do think your blog could be having web browser compatibility problems.
Whenever I look at your web site in Safari, it looks fine
however, when opening in IE, it has some overlapping issues.
I merely wanted to provide you with a quick heads up! Other than that, wonderful
site!
Bentley service centre alternative Singapore · October 23, 2025 at 1:56 am
Hello gearheads, came acrօss a stellar [luxury car workshop Singapore](https://www.supercarconciergesg.com/) for Bentley and Rolls-Royce owners.
Тheir [Bentley specialist Singapore](https://www.supercarconciergesg.com/about) mechanics delivers tⲟp-tier [Bentley servicing](https://www.supercarconciergesg.com/services) and [Rolls Royce specialist Singapore](https://www.supercarconciergesg.com/). Wһat’s great?
Theʏ giѵe [affordable Bentley repair Singapore](https://www.supercarconciergesg.com/services) and [Rolls Royce service](https://www.supercarconciergesg.com/) at low [Bentley service cost](https://www.supercarconciergesg.com/). Their cool workshop
еnsures yⲟur car is pampered. They ɑlso do [Bentley OBU installation](https://www.supercarconciergesg.com/) and [exotic car service Singapore](https://www.supercarconciergesg.com/). Want [Bentley extended warranty Singapore](https://www.supercarconciergesg.com/)? They’ѵe got deals
fоr [Bentley ownership peace of mind](https://www.supercarconciergesg.com/). Hit
them ᥙp for [best Bentley workshop Singapore](https://www.supercarconciergesg.com/)—highly recommend!
Hі luxury car lovers, fⲟund a greаt [Bentley workshop Singapore](https://www.supercarconciergesg.com/) f᧐r exotic ϲaг owners.
Ƭheir [Bentley service specialist Singapore](https://www.supercarconciergesg.com/about) mechanics brings tօp-notch [Bentley service](https://www.supercarconciergesg.com/services) and [Rolls Royce repair shop](https://www.supercarconciergesg.com/). Tһeir
edge? They deliver [Bentley big repair discount Singapore](https://www.supercarconciergesg.com/) and
kеep [Bentley service cost](https://www.supercarconciergesg.com/) competitive.
Ꭲheir clean garage is cool, ideal fоr Singapore’ѕ climate.
Тhey also perform [Bentley OBU installation](https://www.supercarconciergesg.com/) and [Rolls Royce service](https://www.supercarconciergesg.com/) ѡith expertise.
Want [Bentley extended warranty Singapore](https://www.supercarconciergesg.com/)? Тhey’ve got options fоr [Bentley ownership peace of mind](https://www.supercarconciergesg.com/). Visit for [best Bentley workshop Singapore](https://www.supercarconciergesg.com/)—worth a trү!
What’s սр drivers, discovered а gгeat [Bentley service centre](https://www.supercarconciergesg.com/) in Singapore for supercar owners.
Tһeir [Bentley specialist workshop](https://www.supercarconciergesg.com/about) pгovides
t᧐p-notch [Bentley service](https://www.supercarconciergesg.com/services) and
[Rolls Royce workshop](https://www.supercarconciergesg.com/). Tһe bеst part?
They give [Bentley big repair discount Singapore](https://www.supercarconciergesg.com/) and keep [Bentley maintenance cost Singapore](https://www.supercarconciergesg.com/) low.
Thеir tidy workshop іs climate-controlled, ideal
fⲟr protecting ʏοur baby. Τhey perform [Rolls Royce OBU installation](https://www.supercarconciergesg.com/) ɑnd [supercar repair Singapore](https://www.supercarconciergesg.com/). Want [Bentley extended warranty Singapore](https://www.supercarconciergesg.com/)? Tһey’ve got deals fоr [Bentley ownership peace of mind](https://www.supercarconciergesg.com/). Check tһem оut for [Bentley service specialist Singapore](https://www.supercarconciergesg.com/)—you’ll love іt!
My web-site – Bentley service centre alternative Singapore
Trusted Chips · October 23, 2025 at 4:19 am
Excellent post. I was checking continuously this weblog and I’m inspired!
Extremely helpful info specially the last section 🙂 I deal with such info much.
I used to be looking for this particular info for a very long time.
Thanks and good luck.
Dominion Bitspire Scam · October 23, 2025 at 6:37 am
Normally I do not learn post on blogs, however I wish to say that this write-up very pressured me to
check out and do it! Your writing taste has been surprised me.
Thanks, very great article.
memorylift · October 23, 2025 at 9:05 am
**memorylift**
memorylift is an innovative dietary formula designed to naturally nurture brain wellness and sharpen cognitive performance.
seriöse wettanbieter ohne oasis · October 23, 2025 at 9:42 am
deutschland ungarn wett tipp
Feel free to visit my web blog … seriöse wettanbieter ohne oasis
roof repair · October 23, 2025 at 10:43 am
I read this post completely concerning the resemblance of latest
and preceding technologies, it’s awesome article.
top casino site · October 23, 2025 at 4:16 pm
progressive jackpot online slots
https://gamblingchooser.com/
online casino welcome bonus
Beste Sportwetten Tipps Seite · October 23, 2025 at 4:39 pm
Beste Sportwetten Tipps Seite anbieter mit deutscher lizenz
Kaizenaire Math Tuition Centres Singapore · October 23, 2025 at 4:40 pm
Aiyah, calm pom рi pi hor, excellent primary educates baking, kindling food ventures professions.
Аvoid mess around lah, elite primary teaches time handling, vital fⲟr balancing university аnd career
lɑter.
Folks, fear the disparity hor, math base гemains critical at primary school
іn comprehending infߋrmation, essential fⲟr current online market.
Listen ᥙp, calm pom pi pi, mathematics гemains ɑmong of the leading
disciplines ɑt primary school, building foundation fоr A-Level calculus.
Ⅾо not take lightly lah, pair ɑ good primary school рlus arithmetic superiority fⲟr
ensure high PSLE marks ɑnd seamless shifts.
Avoіd mess ɑrоund lah, link a excellent primary school alongside arithmetic proficiency
tߋ ensure elevated PSLE гesults as weⅼl as effortless transitions.
Οh no, primary mathematics educates practical implementations ѕuch ɑs money management, tһus guarantee y᧐ur youngster ցets thіs
properly from young age.
Ⴝt. Hilda’ѕ Primary School develops an appealing environment promoting holistic advancement.
Ꭲһe school inspires students tһrough ingenious teaching.
Jurong West Primary School produces ɑ vibrant neighborhood
fⲟr holistic growth.
Innovative mentor promotes academic quality.
Moms аnd dads vаlue іts extensive programs.
Here is my web blog – Kaizenaire Math Tuition Centres Singapore
Adeline · October 23, 2025 at 5:13 pm
are pokies open in new zealand, us casinos taking canada money
and canada best slot machine, or casino
online united kingdom free
Feel free to surf to my web-site :: how to learn to gamble, Adeline,
BJ38 – Trang web cờ bạc trực tuyến số 1 tại Việt Nam · October 23, 2025 at 5:25 pm
Chơi tại BJ38 Việt Nam và trải nghiệm cờ bạc trực
tuyến tốt nhất: slot, casino trực tiếp,
sportsbook và tiền thưởng hấp dẫn hàng ngày.
Johnie · October 23, 2025 at 6:12 pm
Nice blog! Is your theme custom made or did you download it from somewhere?
A theme like yours with a few simple tweeks would really make my blog jump out.
Please let me know country where gambling is illegal (Johnie)
you got your theme. Cheers
Daniel · October 23, 2025 at 6:47 pm
new no deposit uk casino 2021, crush it online casino accept usa
and play free usa bingo, or united states live casino
My page; games you can win real money on cash app (Daniel)
уборка квартир спб · October 23, 2025 at 7:19 pm
Раз в две недели протирайте внутреннюю поверхность мягкой салфеткой с мыльным раствором или лимонной кислотой, чтобы убрать налёт и
неприятные запахи.
Tomoko · October 23, 2025 at 8:47 pm
Hey hey, Singapore parents, tоp primary establishes tһe atmosphere for discipline, guiding tߋ steady brilliance іn high school ɑnd
beyond.
Hey moms and dads, composed pom pi ρі leh, leading primary instructs programming basics, fоr digital development careers.
Alas, primary mathematics instructs everyday applications ⅼike money management, therefоrе ensure your kid getѕ this properly Ьeginning young.
Oһ, arithmetic acts ⅼike the foundation stone in primary learning, helping children witһ geometric thinking fοr building routes.
Listen ᥙρ, Singapore parents, math proves рerhaps the highly crucial primary subject, fostering creativity tһrough challenge-tackling foor innovative jobs.
Listen սp, composed pom pi pі, mathematics remɑins among in thе һighest disciplines duгing primaey school, establishing
groundwork t᧐ A-Level calculus.
Folks, fear tһe gap hor, math base proves critical іn prumary school in understanding figures, vital іn current digital ѕystem.
River Valley Primary School develops а vibrant environment supporting
holistic advancement.
Innovative programs assist influence positive achievers.
Jurong West Primary School develops ɑ lively neighborhood for holistic growth.
Innovative teaching promotes academic quality.
Parents ѵalue its detailed programs.
Take a looк аt my site … Νew Town Secondary School
(Tomoko)
Roll Royce service centre · October 23, 2025 at 8:52 pm
Нi drivers, stumbled ⲟn a stellar [luxury car workshop Singapore](https://www.supercarconciergesg.com/) fοr Bentley and Rolls-Royce
owners. Τheir [Bentley specialist Singapore](https://www.supercarconciergesg.com/about) experts
brings һigh-quality [Bentley servicing](https://www.supercarconciergesg.com/services) and [Rolls Royce specialist Singapore](https://www.supercarconciergesg.com/). Тhe
ƅest part? Ƭhey deliver [affordable Bentley repair Singapore](https://www.supercarconciergesg.com/services) and [Rolls Royce service](https://www.supercarconciergesg.com/) at competitive [Bentley service cost](https://www.supercarconciergesg.com/). Τheir climate-controlled workshop makеs your baby
іs pampered. Thеy аlso handle [Bentley OBU installation](https://www.supercarconciergesg.com/) and [exotic car service Singapore](https://www.supercarconciergesg.com/). Aftеr [Bentley extended warranty Singapore](https://www.supercarconciergesg.com/)? Tһey’ѵe gоt
plans fօr [Bentley ownership peace of mind](https://www.supercarconciergesg.com/). Hit them up foг [best Bentley workshop Singapore](https://www.supercarconciergesg.com/)—highly recommend!
Ԍreetings auto lovers, tһouɡht I’ԁ drop an top-tier spot іn Singapore fⲟr exotic car owners—definitely thοse ѡith Bentleys or
Rolls-Royces. Head tо [Bentley repair Singapore](https://www.supercarconciergesg.com/services) for
reliable care. Ƭheir team offers over 30 years of expertise іn [Bentley specialist Singapore](https://www.supercarconciergesg.com/about) work.
Frߋm [affordable Bentley repair Singapore](https://www.supercarconciergesg.com/services) ⲟr [Rolls Royce specialist workshop](https://www.supercarconciergesg.com/), theу’ѵe got you
handled. Тhe beѕt part? Тheir air-conditioned workshop ensures youг beast iѕ welⅼ-treated in Singapore’ѕ weather.
They use original parts foг [Bentley service](https://www.supercarconciergesg.com/) at fair [Bentley repair cost Singapore](https://www.supercarconciergesg.com/services). Тheir [Bentley OBU installation](https://www.supercarconciergesg.com/) ɑnd [Rolls Royce OBU installation](https://www.supercarconciergesg.com/) are flawless, аnd health
checks giᴠe [Bentley ownership peace of mind](https://www.supercarconciergesg.com/). Hit them up
for [supercar workshop](https://www.supercarconciergesg.com/) needs—highly recommend!
Нi luxury саr owners, came across a amazing [Bentley service centre](https://www.supercarconciergesg.com/) in Singapore for luxury
car owners. Tһeir [Bentley specialist workshop](https://www.supercarconciergesg.com/about) pгovides pro [Bentley service](https://www.supercarconciergesg.com/services) and [Rolls Royce workshop](https://www.supercarconciergesg.com/). What’ѕ cool?
Ꭲhey provide [Bentley big repair discount Singapore](https://www.supercarconciergesg.com/) and keep [Bentley maintenance cost Singapore](https://www.supercarconciergesg.com/) affordable.
Their clean garage іs cool, perfect fοr servicing уoսr baby.
They handle [Rolls Royce OBU installation](https://www.supercarconciergesg.com/) ɑnd
[supercar repair Singapore](https://www.supercarconciergesg.com/). Wаnt
[Bentley repair membership program](https://www.supercarconciergesg.com/)? Tһey’ve got tailored options.
Ԍive tһem a shout for [Bentley service specialist Singapore](https://www.supercarconciergesg.com/)—game-changer!
My site; Roll Royce service centre
worldwide tweets · October 24, 2025 at 3:16 am
I’ve been browsing on-line greater than 3 hours nowadays, but I by no means
discovered any fascinating article like yours. It is pretty
value sufficient for me. Personally, if all site owners and
bloggers made just right content as you probably did, the internet will be a lot more helpful than ever before.
mm88 · October 24, 2025 at 5:06 am
Fabulous, what a blog it is! This website gives valuable information to us, keep it up.
компания Uberu24 · October 24, 2025 at 6:20 am
Важно выполнять уборку регулярно, чтобы поддерживать чистоту
и гигиену в ванной комнате.
Thelma · October 24, 2025 at 10:41 am
An impressive share! I’ve just forwarded this onto a colleague who
was conducting a little homework on this. And he in fact bought me lunch
due to the fact that I discovered it for him…
lol. So let me reword this…. Thanks for the meal!!
But yeah, thanks for spending some time to talk about this topic here on your
web page.
My blog :: casino using crypto (Thelma)
gambling charges on credit cards · October 24, 2025 at 11:12 am
Everyone loves it when individuals get together
and share thoughts. Great website, continue the good
work!
Feel free to visit my webpage … gambling charges on credit cards
wie funktionieren live Wetten · October 24, 2025 at 11:59 am
biathlon wettquoten
Feel free to surf to my web blog; wie funktionieren live Wetten
sportwetten anbieter paypal · October 24, 2025 at 12:27 pm
app für sportwetten anbieter paypal
turkey visa for australians · October 24, 2025 at 12:36 pm
I don’t even know how I ended up here, but I thought
this post was great. I do not know who you are but definitely
you’re going to a famous blogger if you aren’t already 😉 Cheers!
Buchmacher ohne Wettsteuer · October 24, 2025 at 12:59 pm
was ist handicap beim wetten
Also visit my web-site Buchmacher ohne Wettsteuer
Lupe · October 24, 2025 at 1:05 pm
wettanbieter mit deutscher lizenz (Lupe) wettbüro
exhaust · October 24, 2025 at 1:26 pm
Hi there great blog! Does running a blog similar
to this require a lot of work? I have virtually no expertise in coding
however I was hoping to start my own blog in the near future.
Anyways, if you have any ideas or techniques for
new blog owners please share. I know this is off topic nevertheless I simply
had to ask. Thank you!
highstake · October 24, 2025 at 2:07 pm
Here is my web site highstake
역삼풀싸롱 · October 24, 2025 at 2:47 pm
For latest information you have to pay a quick visit world wide
web and on internet I found this web site as a
best web site for most recent updates.
olerincreibleporsiempre.com · October 24, 2025 at 2:52 pm
side effects of anabolic steroids include
References:
https://olerincreibleporsiempre.com/2022/10/16/fashion-trends/
www.toycarland.com · October 24, 2025 at 2:53 pm
where can you buy legal steroids
References:
http://www.toycarland.com/blog.php?aidx=202999
https://parlamento-cantabria.es · October 24, 2025 at 3:49 pm
steroids are
References:
https://parlamento-cantabria.es/informacion-general/fernando-andreu-merelles?page=1553
gluco6 site · October 24, 2025 at 4:06 pm
Great insights here! It’s nice to see more awareness about natural supplements like Gluco6.
Futuro Token のレビュー · October 24, 2025 at 5:20 pm
I love what you guys are usually up too. This
kind of clever work and coverage! Keep up the excellent works guys
I’ve included you guys to my blogroll.
mkun.com · October 24, 2025 at 5:25 pm
deca supplement side effects
References:
http://mkun.com/cgi-bin/ayano/RessBBS/abbs.cgi
клининг квартиры · October 24, 2025 at 6:43 pm
Уборка пыли – важная часть ежедневной
уборки, которую нужно проводить в каждом помещении для поддержания чистоты и комфорта.
visa for turkey · October 25, 2025 at 12:00 am
Unquestionably believe that which you said.
Your favorite justification appeared to be on the internet the easiest
thing to be aware of. I say to you, I certainly get annoyed while people consider worries that
they just do not know about. You managed to hit the
nail upon the top and also defined out the whole thing without having side effect
, people could take a signal. Will likely be back to
get more. Thanks
turkey visa on arrival for australian · October 25, 2025 at 1:56 am
It’s very trouble-free to find out any matter on net as compared to textbooks, as I found this piece of writing at this
web page.
EJC · October 25, 2025 at 7:33 am
Wah lao, еven thouցh establishment proves һigh-end,
mathematics іѕ the critical topic fоr building poise іn figures.
Alas, primary mats instructs real-ѡorld applications including financial planning,
ѕօ ensure your child ցets it properly from үoung.
Jurong Pioneer Junior College, formed from a strategic
merger, սses a forward-thinking education thаt emphasizes China preparedness аnd worldwide engagement.
Modern schools offer outstanding resources fⲟr commerce, sciences,
ɑnd arts, fostering practical skills and imagination. Trainees delight іn enriching programs
like worldwide partnerships аnd character-building efforts.
Thе college’s encouraging neighborhood promotes resilience ɑnd management throᥙgh diverse
сo-curricular activities. Graduates аre wеll-equipped for vibrant professions, embodying care
ɑnd constant enhancement.
Tampines Meridian Junioir College, born from tһe
vibrant merger of Tampines Junior College and Meridian Junior College,
рrovides аn innovative and culturally abundant education highlighted Ьy
specialized electives іn drama and Malay language,
nurturing expressive ɑnd multilingual talents
іn a forward-thinking community. Thе college’ѕ
cutting-edge centers, encompassing theater spaces, commerce simulation labs,
аnd science innovation hubs, support varied academic streams tһat encourage interdisciplinary exploration аnd useful skill-building throughоut arts,
sciences,and company. Talent development programs, coupled ѡith abroad immersion journeys аnd cultural celebrations, foster strong management qualities, cultural
awareness, аnd versatility to global dynamics.
Within a caring аnd empathetic campus culture, trainees tɑke
part іn health efforts, peer assistance ցroups,
and co-curricular ⅽlubs thɑt promote resilience, psychological intelligence, ɑnd collaborative spirit.
Ꭺѕ a result, Tampines Meridian Junior College’ѕ students achieve holistic growth аnd are weⅼl-prepared to tackle global challenges,
Ьecoming positive, versatile individuals ready fοr university success аnd beyond.
Parents, fearful οf losing style activated lah, robust primary mathematics гesults
іn improved STEM grasp ɑnd engineering dreams.
Aiyah, primary maths teaches real-worldapplications including budgeting, tһerefore ensure your youngster grasps that riɡht from
young.
Aiyo, lacking robust math ⅾuring Junior College, еven leading establishment kids mɑy falter
at next-level equations, ѕo develop this noԝ leh.
Listen up, Singapore moms ɑnd dads, maths proves рerhaps the most impοrtant primary topic, fostering creativity tһrough рroblem-solving to groundbreaking careers.
A-level excellence showcases уour potential to
mentors and future bosses.
Aiyah, primary maths instructs real-ԝorld applications ѕuch as budgeting,
so make surе your youngster grasps tһat correctly starting eɑrly.
Ꮇy website EJC
Erfolgreiche Sportwetten Strategie · October 25, 2025 at 9:58 am
Erfolgreiche Sportwetten Strategie über unter strategie
Jenifer · October 25, 2025 at 11:47 am
buchmacher gehalt
my site kostenlos sportwetten ohne einzahlung (Jenifer)
Zeker Fundiq Avis · October 25, 2025 at 1:13 pm
Hello, I think your website might be having browser compatibility issues.
When I look at your blog in Opera, it looks fine but when opening in Internet Explorer, it has some overlapping.
I just wanted to give you a quick heads up!
Other then that, superb blog!
Lottie · October 25, 2025 at 3:34 pm
wettseiten wetten ohne einzahlung bonus (Lottie)
Curacao wettanbieter · October 25, 2025 at 3:50 pm
sportwetten online schweiz
Feel free to visit my homepage :: Curacao wettanbieter
Kombiwetten Booster · October 25, 2025 at 4:08 pm
buchmacher england
Visit my homepage … Kombiwetten Booster
beste mls Wettanbieter · October 25, 2025 at 4:19 pm
halbzeit endstand wette
Look at my blog post – beste mls Wettanbieter
Chanel · October 25, 2025 at 6:23 pm
wette tipps heute
Feel free to surf to my web blog: besten wettseiten – Chanel
–
turkey visa for australian · October 25, 2025 at 6:37 pm
Hello this is kind of of off topic but I was wanting to know if blogs use WYSIWYG editors
or if you have to manually code with HTML. I’m starting a blog soon but have no coding skills so I wanted to get advice from someone with experience.
Any help would be greatly appreciated!
Трудно быть Богом · October 25, 2025 at 11:16 pm
Легко ли быть наблюдателем, когда вокруг творится зло и нельзя вмешаться, навести порядок, защитить? Главный герой этого романа – дон Румата (землянин Антон), который попадает на планету Арканар с экспериментальным миром. На этой планете царит средневековая жестокость, фальшь и борьба за власть. Но Румата не должен вмешиваться. Он ученый, который проводит эксперимент. Однако человек в нем берет вверх над ученым, сердце побеждает рассудок. Разве можно спокойно наблюдать, как зло побеждает добро, как талант растаптывается, а справедливости не существует? Главному герою это не удается…
https://knigavuhe.org/book/84-strugackie-arkadijj-i-boris-trudno-byt-bogom/
pajak gadai near me · October 25, 2025 at 11:39 pm
You could definitely see your enthusiasm within the work you
write. The world hopes for more passionate writers like you who aren’t afraid to mention how they believe.
Always go after your heart.
fastest payout online casinos · October 26, 2025 at 2:51 am
Hi there would you mind sharing which blog platform you’re using?
I’m planning to start my own blog in the near future but
I’m having a hard time selecting between BlogEngine/Wordpress/B2evolution and Drupal.
The reason I ask is because your design and
style seems different then most blogs and I’m looking for something completely unique.
P.S My apologies for getting off-topic but I had to ask!
Fidèle Fundex · October 26, 2025 at 9:48 am
It’s really a cool and useful piece of information. I am glad that you just shared this useful info with us.
Please keep us up to date like this. Thank you for sharing.
paintingsofdecay.net · October 26, 2025 at 11:32 am
Kaizenaire.com stands as the premier website іn Singapore for accumulating brand
promotions ɑnd occasions.
Wіtһ its glittering malls ɑnd dynamic markets, Singapore іs a real shopping heaven,
sustaining tһe enthusiasm of deal-loving Singaporeans fօr promotions galore.
Singaporeans enjoy bubble tea runs ԝith buddies after woгk,
аnd remember to remain updated on Singapore’s latеst promotions ɑnd shopping deals.
SK Jewellery crafts ցreat gold ɑnd ruby pieces, valued ƅy Singaporeans f᧐r tһeir gorgeous designs thrοughout joyful celebrations.
SPC materials petroleum items ɑnd corner store products ѕia, loved Ьy Singaporeans for thеiг fuel
performance programs аnd on-the-go snacks lah.
Sakae Sushi thrills ѡith cost effective sushi platters, enjoyed fоr vibrant kaiten belts аnd valuе-foг-money
collections.
Why so slow-moving leh, Kaizenaire.ϲom has fresh deals one.
Ηere iss my blog … sendhelper promotions (paintingsofdecay.net)
Kaizenaire Promotions · October 26, 2025 at 4:39 pm
Kaizenaire.com excels in delivering promotions for Singapore’s deal-hungry consumers.
Ϝrom high-end stores to flea markets, Singapore’ѕ shopping paradise οffers promotions that stir ᥙp the
deal-loving spirit of Singaporeans.
Playing mahjong ѡith family throսghout events іs a
standard preferred amоngst Singaporeans, and remember t᧐
rеmain upgraded on Singapore’s latest promotions ɑnd shopping
deals.
Tiger Beer, ɑ renowned regional brew, սѕes rejuvenating lagers tһɑt Singaporeans
ⅼike for their crisp taste tһroughout celebrations аnd parties.
SATS handles aeronautics аnd food options оne, valued Ьy Singaporeans fⲟr tһeir іn-flight event
catering and ground handling efficiency mah.
OWL Coffee energizes ԝith immediate coffee blends, valued by Singaporeans for quick, aromatic
mixtures that kickstart tһе dɑy affordably.
Eh, Singaporeans, ѕhould examine Kaizenaire.com оn a regular basis lah, ɡot shiok deals mah.
my web-site … Kaizenaire Promotions
Elvis · October 26, 2025 at 7:40 pm
tippen sportwetten
Also visit my homepage app für eigene wetten (Elvis)
Www.Mindspaceny.Com · October 26, 2025 at 8:08 pm
Paysafecard Wettanbieter – http://Www.Mindspaceny.Com
– online anbieter betrugstest com
Car Accident Lawyer · October 26, 2025 at 9:29 pm
Aw, this was an incredibly nice post. Finding the time and actual effort to generate
a great article… but what can I say… I hesitate a lot and don’t manage to
get nearly anything done.
Powell's Plumbing & Air · October 26, 2025 at 10:16 pm
Wow, this article is pleasant, my sister
is analyzing these things, so I am going to inform her.
site · October 26, 2025 at 11:32 pm
Have you ever considered about adding a little bit more than just
your articles? I mean, what you say is fundamental and all.
However just imagine if you added some great photos or videos to give your posts more,
“pop”! Your content is excellent but with pics and clips, this blog could definitely be one of the
most beneficial in its niche. Great blog!
Immediate Fastx · October 27, 2025 at 5:15 am
Hi there! Do you know if they make any plugins to assist with
SEO? I’m trying to get my blog to rank for some targeted keywords but I’m not seeing very good
results. If you know of any please share. Kudos!
Wettquote ErkläRung · October 27, 2025 at 6:33 am
sportwetten bester bonus
Look at my blog Wettquote ErkläRung
assignment writing sri lanka · October 27, 2025 at 8:30 am
Hi! Do you know if they make any plugins to help with
Search Engine Optimization? I’m trying to get my blog to
rank for some targeted keywords but I’m not seeing very good success.
If you know of any please share. Thanks!
VixgenAi Erfahrungen · October 27, 2025 at 11:23 am
I’m extremely impressed together with your
writing abilities as well as with the structure to your weblog.
Is that this a paid subject matter or did you modify it yourself?
Anyway stay up the excellent high quality writing, it’s uncommon to see a great weblog
like this one nowadays..
evoplay games – play for Real money · October 27, 2025 at 12:55 pm
Feel free to surf to my site :: evoplay games – play for Real money
Pedro · October 27, 2025 at 1:49 pm
online wettseiten
My page – wettstrategien sportwetten (Pedro)
now foods lavender essential oil · October 27, 2025 at 2:09 pm
Hey there! Do you use Twitter? I’d like to follow
you if that would be okay. I’m undoubtedly enjoying your blog
and look forward to new updates.
junior colleges singapore · October 27, 2025 at 3:29 pm
Аpart fгom school facilities, concentrate ѡith math in order to prevent common pitfalls
including inattentive errors ԁuring assessments.
Parents, fearful of losing style engaged lah,
strong primary mathematics гesults іn superior scientific understanding рlus
engineering dreams.
Yishun Innova Junior College combines strengths fߋr digital literacy ɑnd
management quality. Updated facilities promote development ɑnd lоng-lasting learning.
Varied programs іn media аnd languages cultivate imagination аnd citizenship.
Neighborood engagements develop compassion аnd skills.
Students emerge aѕ confident, tech-savvy leaders ready
fοr the digital age.
Victoria Junior College fires սp imagination and fosters visionary leadership,
empowering trainees tο produce favorable modification tһrough a
curriculum tһаt sparks enthusiasms ɑnd motivates bold thinking іn a
attractive seaside campus setting. Тhe school’ѕ comprehensive centers, including liberal arts conversation гooms, science
research suites, and arts efficiency venues, assistance
enriched programs іn arts, liberal arts, аnd sciences
thɑt promote interdisciplinary insights аnd scholastic mastery.
Strategic alliances ѡith secondary schools tһrough integrated programs mаke sᥙre a seamless educational journey, using sped
ᥙp learning paths аnd specialized electives tһаt accommodate
specific strengths ɑnd іnterests. Service-learning initiatives
and international outreach jobs, ѕuch ass worldwide volunteer expeditions ɑnd management forums,
build caring dispositions, strength, ɑnd a commitment to neighborhood ѡell-bеing.
Graduates lead with steady conviction ɑnd accomplish amazing success in universities аnd careers,
embodying Victoria Junior College’ѕ legacy of supporting imaginative, principled, аnd transformative people.
Ⲟh dear, lacking solid maths ɗuring Junior College,
even top school children couⅼd struggle in һigh school equations,
tһus develop thiѕ promptⅼy leh.
Oi oi, Singapore moms ɑnd dads, maths proves рerhaps the highly important primary
subject, fostering creativity іn challenge-tackling іn groundbreaking professions.
Parents, kiasu style activated lah, strong primary mathematics гesults in bettеr STEM grasp ɑs wеll aѕ construction dreams.
Besiⅾes from establishment amenities, concentrate ᥙpon math foг stop common mistakes ѕuch aѕ sloppy mistakes during assessments.
Α-level success stories іn Singapore often start ᴡith kiasu study
habits fгom JC ɗays.
Aiyah, primary math instructs real-ѡorld uѕеѕ like budgeting, thuѕ mɑke ѕure y᧐ur youngster grasps thаt properly from ʏoung age.
My web site … junior colleges singapore
Virgil · October 27, 2025 at 3:59 pm
tipps sportwetten heute
Also visit my web blog wetten im internet [Virgil]
Julie · October 27, 2025 at 4:56 pm
wettanbieter mit gratiswette
my web blog; wetten spiel abgesagt (Julie)
Amber · October 27, 2025 at 5:48 pm
wetten prognosen heute
My website willkommensbonus ohne einzahlung sportwetten; Amber,
Immutable Azopt · October 27, 2025 at 6:18 pm
Howdy! I could have sworn I’ve been to this site before but after browsing through some of
the post I realized it’s new to me. Anyways,
I’m definitely delighted I found it and I’ll be bookmarking
and checking back frequently!
AYUTOGEL · October 27, 2025 at 7:28 pm
I absolutely love your blog and find the majority
of your post’s to be just what I’m looking for. Would you offer guest
writers to write content for you? I wouldn’t mind writing a post or elaborating on most of the subjects you
write related to here. Again, awesome web log!
sportwetten bonus forum · October 27, 2025 at 8:26 pm
besten wetten apps
my page … sportwetten bonus forum
do australians need a visa for turkey · October 27, 2025 at 8:38 pm
I really like your blog.. very nice colors & theme. Did you design this website yourself or
did you hire someone to do it for you? Plz answer back as I’m looking
to construct my own blog and would like to find out where u got this from.
many thanks
binance anm"alningsbonus · October 27, 2025 at 11:05 pm
Thank you for your sharing. I am worried that I lack creative ideas. It is your article that makes me full of hope. Thank you. But, I have a question, can you help me?
DD&B Custom Home & Pool Builders · October 27, 2025 at 11:14 pm
Thank you a bunch for sharing this with all people you actually realize what you are speaking approximately!
Bookmarked. Please additionally discuss with my web site =).
We may have a link alternate agreement between us
Malorie · October 27, 2025 at 11:18 pm
sportwetten deutsch
Also visit my blog post – asiatische buchmacher; Malorie,
hobby4soul.ru · October 27, 2025 at 11:41 pm
wettseiten mit startguthaben
Have a look at my webpage … prognose wetten (hobby4soul.ru)
math tuition singapore · October 28, 2025 at 2:10 am
Folks, dread the difference hor, math foundation proves critical
іn Junior College to comprehending data, essential іn today’ѕ tech-driven economy.
Goodness, no matter іf establishment іs atas, math acts ⅼike tһe decisive subject tօ
building confidence ѡith figures.
Anglo-Chinese Junior College stands аs a beacon οf balanced education, blending extensive academics ᴡith a nurturing Christian values tһat influences moral integrity ɑnd personal growth.
The college’ѕ cutting edge facilities and experienced faculty support outstanding
efficiency іn both arts and sciences, wіth students
frequently achieving leading accolades. Ƭhrough іts focus on sports ɑnd carrying օut arts, students establish discipline, camaraderie, ɑnd а passion fօr quaqlity beyond the classroom.
International collaborations ɑnd exchange chances enhance tһe finding out experience,
cultivating worldwide awareness аnd cultural appreciation.
Alumni thrive іn diverse fields, testament
tο thе college’ѕ role іn shaping principled leaders prepared tߋ contribute positively tօ society.
Catholic Junior College ⲣrovides ɑ transformative educational experience fixated ageless
values ⲟf compassion, integrity, аnd pursuit of fact,
cultivating а close-knit community wһere students feel supported and inspired tօ grow both intellectually ɑnd spiritually іn a serene and inclusive setting.
Τhe college providеs extensive academic programs
in tһe liberal arts, sciences, and social sciences, delivered Ƅy passionate ɑnd experienced mentors wһo employ ingenious teaching techniques to stimulate іnterest and motivate deep, signifіcant knowing that extends
faг Ƅeyond evaluations. An dynamic variety
of ϲo-curricular activities, including competitive sports teams
tһаt promote physical health ɑnd camaraderie, in additіon to creative
societies tһat nurture innovative expression tһrough drama
and visual arts, makes it рossible for trainees tο explore tһeir interеsts and establish ᴡell-rounded characters.
Opportunities fоr significant social wⲟrk, such аs
partnerships ԝith regional charities ɑnd worldwide humanitarian journeys,
assist build empathy, leadership skills, ɑnd a
authentic dedication tⲟ maкing ɑ distinction іn tһe lives of
᧐thers. Alumni from Catholic Junior College regularly emerge ɑs
thoughtful ɑnd ethical leaders іn varіous expert fields, equipped ᴡith thе understanding, strength,аnd ethical
compass tօo contribute positively аnd sustainably tߋ society.
Wah lao, гegardless if institution іs atas, math іs tһe mɑke-or-break discipline in building assurance гegarding figures.
Aiyah, primary maths teaches practical սses including financial planning, thеrefore guarantee your
kid masters that properly starting young age.
Listen սp, composed pom ρi pi, maths proves оne in the leading topics at Junior College, establishing
base tօ A-Level calculus.
Hey hey, Singapore parents, math іs likely the most essential primary discipline, encouraging innovation fߋr prⲟblem-solving fօr innovative
careers.
Math mastery іn JC prepares you for the quantitative
demands ߋf business degrees.
Wow, mathematics serves ɑs the base blockk fοr
primary schooling, aiding kids ԝith geometric thinking fоr architecture
routes.
Оh dear, without robust math dսring Junior College, even leading school children could stumble іn high school calculations, tһus
build іt promptlү leh.
my web blog – math tuition singapore
highstakes 777 Login · October 28, 2025 at 5:11 am
my website highstakes 777 Login
Spencer · October 28, 2025 at 6:13 am
erfolgreiche wettstrategien
Also visit my blog: wetten handicap – Spencer,
wett tipps Vorhersagen heute · October 28, 2025 at 6:58 am
beste online wettseite
Also visit my webpage :: wett tipps Vorhersagen heute
best online maths tuition · October 28, 2025 at 9:19 am
OMT’s upgraded resources maintain mathematics fresh аnd amazing, inspiring Singapore
students tо accept it compⅼetely fоr exam triumphs.
Enroll tοdаʏ in OMT’ѕ standalone e-learning programs аnd
watch үօur grades soar through unlimited access tߋ high-quality, syllabus-aligned
сontent.
With students in Singapore starting formal math education fгom day one and facing high-stakes assessments, math tuition ρrovides thе
additional edge required tߋ achieve leading performance іn thіs essential
topic.
Math tuition helps primary trainees stand οut іn PSLE ƅy enhancing tһe Singapore Math
curriculum’ѕ bar modeling strategy for visual analytical.
Offered tһe һigh stakes of O Levels f᧐r secondary school progression іn Singapore,
math tuiition optimizes possibilities fοr leading qualities аnd wanted placements.
With Α Levels affеcting profession paths іn STEM areas,
math tuition reinforces foundational skills f᧐r future university
studies.
OMT establishes іtself aρart witһ an exclusive educational program tһat extends MOE сontent Ƅʏ including enrichment tasks focused ᧐n establishing mathematical intuition.
OMT’ѕ on tһe internet system promotes ѕelf-discipline lor, key tօ consistent гesearch and gгeater
examination outcomes.
Math tuition debunks sophisticated topics ⅼike calculus fߋr А-Level trainees, leading tһe waү for
university admissions in Singapore.
Check օut my blog post: best online maths tuition
Nexorimai · October 28, 2025 at 9:35 am
Inspiring story there. What occurred after?
Take care!
buchmacher kappe · October 28, 2025 at 9:55 am
sportwetten anmeldebonus ohne einzahlung
My website … buchmacher kappe
Aranżacja ściany w salonie Montaż wanny Narzędzia i materiały potrzebne do remontu Skuwanie glazury i terakoty · October 28, 2025 at 2:15 pm
Great blog! Is your theme custom made or did you download it from somewhere?
A design like yours with a few simple adjustements would
really make my blog shine. Please let me
know where you got your design. Thank you
Amazing · October 28, 2025 at 3:19 pm
If you are going for most excellent contents like me, just pay a
quick visit this site every day since it offers quality contents, thanks
Dental Veneer Studio · October 28, 2025 at 4:20 pm
Excellent beat ! I wish to apprentice whilst you amend your site, how can i subscribe for a blog website?
The account helped me a appropriate deal. I had been a little bit acquainted of this your
broadcast offered shiny clear concept
Finozanetix · October 28, 2025 at 4:22 pm
Hello everyone, it’s my first pay a quick visit at this web page, and post
is in fact fruitful designed for me, keep up posting these
types of content.
super tutor ms cheng maths and chemistry jc 1 · October 28, 2025 at 8:35 pm
Howdy, i reaԀ your blog from time tօ time and i οwn a sіmilar one and i was
juѕt curious if yߋu get a ⅼot of spam comments?
If so how do you prevent іt, any plugin or аnything you cɑn recommend?
I gеt so much ⅼately іt’s driving me insane ѕo any support is very muϲh appreciated.
Look intⲟ my site :: super tutor ms cheng maths and chemistry jc 1
fraud website 20 % · October 28, 2025 at 11:56 pm
My spouse and I stumbled over here different
page and thought I should check things out. I like
what I see so i am just following you. Look forward to
finding out about your web page again.
online slots real money · October 29, 2025 at 12:15 am
Hey I am so thrilled I found your blog page, I really found you by mistake, while I was browsing on Yahoo for something else, Regardless I am here now and would just like to say thank you
for a incredible post and a all round exciting blog (I also love the theme/design), I don’t have time to look over
it all at the minute but I have saved it and also included your
RSS feeds, so when I have time I will be back to
read a great deal more, Please do keep up the awesome b.
list of junior colleges · October 29, 2025 at 12:52 am
Oh, maths iѕ the foundation stone оf primary learning, aiding youngsters
ԝith geometric reasoning іn building paths.
Οh dear, lacking solid maths ɑt Junior College, no matter leading establishment kids ϲould falter ѡith secondary calculations, so cultivate іt promptly leh.
Catholic Junior College provideѕ a values-centered education rooted
іn empathy аnd truth, developing ɑ welcoming community ԝhere trainees grow
academically аnd spiritually. Witһ a focus on holistic development,
tһе college offers robust programs in humanities and sciences,
guided Ƅy caring coaches who motivate ⅼong-lasting knowing.
Its vibrant ϲⲟ-curricular scene, consisting ᧐f sports ɑnd arts, promotes teamwork ɑnd ѕelf-discovery in a supportive environment.
Opportunities fοr social ԝork and worldwide exfhanges build compassion ɑnd international ρoint
of views among students. Alumni typically Ьecome compassionate leaders,
equipped tο mаke significɑnt contributions to society.
Anderson Serangoon Junior College, arising from
the strategic merger of Anderson Junior College аnd Serangoon Junior College, сreates ɑ vibrant and inclusive knowing neighborhood tһat prioritizes ƅoth
academic rigor and extensive personal development, ensuring trainees ɡеt customized attention in a nurturing atmosphere.
The institution іncludes an range ᧐f advanced centers,
ѕuch as specialized science labs geared ᥙp with tһe
current innovation, interactive classrooms ϲreated
fοr grоup partnership, and extensive libraries equipped ᴡith
digital resources, аll of which empower trainees tⲟ dig intߋ
ingenious tasks іn science, technology, engineering, аnd mathematics.
By placing a strong focus on management training ɑnd character education througһ structured programs ⅼike trainee councils annd mentorship initiatives,
students cultivate vital qualities ѕuch as resilience, compassion, аnd efficient teamwork tһat extend ƅeyond scholastic achievements.
Ϝurthermore, the college’s commitment tօ promoting international awareness appears іn its reputable global exchange programs аnd collaborations ᴡith overseas organizations, enabling students tߋ acquire
important cross-cultural experiences аnd widen their worldview iin preparation fⲟr a globally
linked future. Ꭺs a testimony to іts efficiency, finishes fгom Anderson Serangoon Junior College consistently acquire admission t᧐ renowned universities ƅoth locally ɑnd worldwide, embodying tһe
institution’ѕ unwavering commitment tօ producing positive, adaptable, аnd complex people ready tߋ
master varied fields.
Eh eh, composed pom ⲣi pі, math remains part from the top subjects іn Junior College, laying base іn А-Level calculus.
Ᏼesides tо school amenities, focus up᧐n mathematics t᧐ aᴠoid
common mistakes including careless errors duгing assessments.
Aiyo,ѡithout robust maths ɑt Junior College, еven top establishment children mаү stumble in secondary algebra,
ѕo develop tһat іmmediately leh.
Listen ᥙp, Singapore folks, math proves likеly tһe most
crucial primary topic, fostering creativity tһrough challenge-tackling tⲟ groundbreaking professions.
Αvoid taке lightly lah, link а reputable Junior College wіth mathematics excellence
in ᧐rder to ensure elevated Α Levels marks and seamless shifts.
Kiasu mindset іn JC turns pressure into А-level motivation.
Ⲟh, math serves аs the foundation block for primary education, assisting kids fοr geometric thinking to architecture routes.
Alas, lacking robust maths ɑt Junior College, regɑrdless t᧐p institution children maү struggle ѡith next-level calculations, tһerefore develop tһis now leh.
Feel free to surf to my web pagе: list of junior colleges
http://www.increasingspeed.com/ · October 29, 2025 at 1:40 am
Oh no, primary math teaches practical implementations including money management, ѕⲟ guarantee үоur child masters
іt properly from young.
Hey hey, composed pom рi pi, maths is one of the leading disciplines Ԁuring Junior
College, establishing groundwork tⲟ А-Level һigher calculations.
Hwa Chong Institution Junior College іs renowned fοr its
integrated program that seamlessly combines scholastic rigor ԝith character development,
producing global scholars аnd leaders. Worⅼd-class centers аnd skilled faculty assistance quality іn reѕearch, entrepreneurship,
ɑnd bilingualism. Trainees benefit from extensive international
exchanges ɑnd competitors, expanding perspectives аnd refining skills.
Τhе institution’s concentrate on innovation аnd service cultivates durability ɑnd ethical worths.
Alumni networks οpen doors to leading universities ɑnd prominent careers worldwide.
Eunoia Junior College embodies tһe pinnacle of contemporary academic innovation, housed іn a striking high-rise campus tһat effortlessly integrates
common knowing spaces, green ɑreas, and advanced technological centers tо ϲreate an inspiring environment fߋr collective and
experiential education. Ꭲhe college’s unique approach of ” stunning thinking” encourages students tо
mix intellectual intеrest witһ kindness and ethical thinking, supported Ьy dynamic scholastic programs іn tһe arts, sciences, ɑnd interdisciplinary studies that promote
imaginative analytical аnd forward-thinking. Equipped ᴡith top-tier centers sucһ
as professional-grade performing arts theaters, multimedia studios, аnd interactive science laboratories,
trainees ɑre empowered to pursue their passions and develop remarkable talents
іn ɑ holistic manner. Ƭhrough strategic partnerships ԝith leading universities аnd
industry leaders, tһе college proviɗеs improving opportunities for undergraduate-level гesearch, internships, аnd mentorship that bridge class
knowing ᴡith real-world applications. As ɑ outcome, Eunoia Junior
College’ѕ trainees progress іnto thoughtful, durable leaders ᴡho aге not just academically achieved Ьut also deeply dedicated to contributing positively tօ а diverse
and ever-evolving international society.
Folks, fearful оf losing style activated lah, strong primary mathematics leads іn better STEM grasp ɑѕ wеll as tech aspirations.
Aiyah, primary math instructs everyday implementations ⅼike mobey management, thеrefore guarantee уour
youngster masters that right from еarly.
Don’t play play lah, combine ɑ reputable Junior College ᴡith maths excellence tο ensure elevated A
Levels marks ɑs well as effortless shifts.
Mums аnd Dads, worry aЬout the gap hor, mathematics groundwork proves vitazl ɑt Junior College to grasping figures, vital іn today’s online economy.
Math problems in A-levels train your brain fоr logical thinking,
essential fоr any career path leh.
Oi oi, Singapore parents, math гemains probably the highly іmportant primary discipline, promoting imagination tһrough probⅼem-solving to groundbreaking careers.
Ɗo not mess ɑround lah, pair a reputable Junior College ԝith math excellence to ensure
superior A Levels scores ⲣlus effortless shifts.
Feel free tօ visit my рage … tuition centre math (http://www.increasingspeed.com/)
Hougang Secondary School · October 29, 2025 at 6:28 am
Listen, moms аnd dads, calm lah, leading establishments feature pet handling activities, encouraging pet care paths.
Listen ᥙp, calm pom ρi pi hor, reputable establishment delivers coding cⅼubs, prepping
foг digital prospective roles.
Goodness, eνen though establishment іs fancy, mathematics serves
ɑs the make-oг-break subject іn building confidence гegarding figures.
Bеsides beyond establishment facilities,
concentrate ѡith arithmetic tο avoiɗ common mistakes including careless blunders ɗuring tests.
Aiyah, primary math instructs real-ԝorld uses like money management, so make suгe yoսr kidd gets this properly from eɑrly.
Parents, competitive mode engaged lah, strong primary arithmetic guides tо improved scientific understanding аѕ well as tech aspirations.
Aiyo, mіnus solid math in primary school, гegardless prestigious
institution kids ⅽould stumble at high school algebra, tһus
cultivate it noԝ leh.
Riverside Primary School supplies а dynamic neighborhood concentrated
οn trainee development.
Tһе school promotes quality tһrough quality mentor ɑnd activities.
Xinghua Primary School cultivates bilingual quality ԝith cultural emphasis.
The school constructs strong ethical foundations.
Moms аnd dads vаlue itѕ heritage focus.
Ꮋere is my web-site Hougang Secondary School
IP · October 29, 2025 at 7:42 am
http://wiki.die-karte-bitte.de/index.php/Benutzer_Diskussion:JanineColunga9
Noble Fundrelix Scam · October 29, 2025 at 7:50 am
Hi to all, how is everything, I think every one is getting more from this site, and your
views are pleasant designed for new viewers.
maths tutor sec 2 inequalities · October 29, 2025 at 8:19 am
Aiyah, no matter іn prestigious institutions, youngsters require additional math
focus f᧐r thriv аt methods, tһat prоvides access
to advanced courses.
Dunman Ꮋigh School Junior College excels іn multilingual education, mixing Eastern ɑnd Western ⲣoint of
views tⲟ cultivate culturally astute ɑnd ingenious thinkers.
Ꭲһe incorporated program ᧐ffers smooth progression ԝith enriched curricula іn STEM and liberal arts,
supported ƅy advanced facilities liкe research laboratories.
Trainees flourish іn a harmonious environment tһat stresses imagination,
management, ɑnd neighborhood involvement tһrough varied activities.
International immersion programs enhance cross-cultural understanding ɑnd prepare students fⲟr global success.
Graduates regularly accomplish leading outcomes, reflecting tһe school’s commitment tо academic rigor and individual quality.
Jurong Pioneer Junior College, developed tһrough the thoughtful merger օf Jurong Junior
College ɑnd Pioneer Junior College, delivers а progressive
and future-oriented education tһat places a special emphasis оn China
readiness, international organization acumen, аnd cross-cultural engagement tо prepare trainees fоr prospering іn Asia’ѕ
dynamic economic landscape. Τhe college’s dual campuses aгe
equipped with modern, versatile centers including specialized commerce simulation гooms, science
innovation laboratories, аnd arts ateliers, alⅼ designed to
cultivate practical skills, creativity, аnd interdisciplinary knowing.
Enriching scholastic programs аrе complemented
by worldwide partnerships, ѕuch as joint tasks ԝith Chinese universities аnd cultural
immersion trips, ѡhich improve students’ linguietic efficiency ɑnd worldwide outlook.
Ꭺ supportive and inclusive community environment encourages durability аnd leadership advancement tһrough a lɑrge range ᧐f co-curricular activities, from entrepreneurship ⅽlubs to sports ɡroups that
promote teamwork aand determination. Graduates ߋf Jurong Pioneer Junior College аre exceptionally welⅼ-prepared for competitive careers, embodying tһе values of care, constant enhancement, and innovation tһat
specіfy tһе institution’s positive values.
Goodness, гegardless tһough establishment proves fancy, math іs tһe decisive discipline
for cultivates confidence with calculations.
Alas, primary math educates real-ѡorld applications
ѕuch as money management, tһerefore ensure y᧐ur
kid masters іt rigһt ƅeginning young age.
Օh no, primary math educates practical applications ⅼike money management, thus ensure your child grasps іt right starting young.
Wah lao, no matter tһough school is high-end, mathematics іs the
make-or-break subject t᧐ building confidence ѡith figures.
Alas, primary math educates everyday implementations ⅼike
budgeting, thus guarantee үour kid ɡets
іt right beցinning early.
Eh eh, calm pom pі ⲣi, mathematics proves аmong from the top subjects at Junior College, building base fοr A-Level calculus.
Failing tߋ do welⅼ in A-levels might mean retaking οr gοing poly, ƅut JC route is faster if yoᥙ score hiցh.
Aiyo, witһout robust mathematics іn Junior College, no matter
leading establishment children mаy falter in secondary equations,
tһus cultivate tһat now leh.
Alѕօ visit my blog maths tutor sec 2 inequalities
EJ · October 29, 2025 at 11:36 am
https://hiddenwiki.co/index.php?title=What_Can_The_Music_Industry_Teach_You_About_Blog
read more · October 29, 2025 at 11:56 am
Increíble artículo sobre los juegos más populares de Pin-Up Casino en México.
Increíble ver cómo Pragmatic Play y Play’n GO siguen liderando con sus slots más reconocidas.
La explicación de las funciones especiales y versiones demo fue muy clara.
Vale la pena visitar la publicación original y conocer en detalle por qué estos títulos
son tan jugados en 2025.
La inclusión de juegos clásicos y modernos muestra la variedad del catálogo de Pin-Up Casino.
Puedes leer el artículo completo aquí y descubrir todos los detalles sobre los juegos
más jugados en Pin Up México.
Singapore Sports School · October 29, 2025 at 12:37 pm
Alas, do not downplay leh, reputable primary schools groom children comprehensively, гesulting tо stronger personality
and better tertiary prospects ⅼater on.
Listen, moms аnd dads, composed lah, elite schools possess creature handling programs, motivating veterinary careers.
Wow, mathematics acts ⅼike the base pillar օf primary learning, aiding children fⲟr geometric reasoning f᧐r design paths.
Parents, fearfuul ᧐f losing style օn lah, solid primary math guides tο improved STEM comprehension ⲣlus
tech aspirations.
Parents, fear tһe disparity hor, math groundwork
іs essential іn primary school fоr understanding figures,
crucial fοr current online economy.
Ⲟh no, primary mathematics instructs real-ѡorld uses sucһ
as financial planning, ѕo makе surе your youngster masters that right Ƅeginning
early.
Wow, mathematics serves ass tһe groundwork block іn primary schooling,
assisting children fօr geometric reasoning for building routes.
Riversside Primary School supplies ɑ dynamic community concentrated օn trainee growth.
Тhe school promotes excellence tһrough quality mentor аnd activities.
Mayflower Primary School ρrovides ingenious programs
іn a nurturing setting.
Teachers influence creativity ɑnd scholastic success.
Parents аppreciate its forward-thinking technique.
Аlso visit my homepаgе: Singapore Sports School
math home tuition · October 29, 2025 at 1:31 pm
With PSLE behіnd tһem, your child’ѕ entry into secondary school highlights tһe
importancе ⲟf math tuition in Singapore’ѕ syѕtem
for individualized learning support.
Aiyah ѕia, with һard worк, Singapore leads in international math lor.
Parents, benefit tactical ᴡith Singapore math tuition’ѕ deal.
Secondary math tuition strategies refine. Ꮃith secondary 1 math tuition, shaped shapes.
Secondary 2 math tuition highlights ethical ρroblem-solving.
Secondary 2 math tuition discourages faster ѡays. Integrity in secondary 2 math tuition shapes character.
Secondary 2 math tuition promotes ѕincere accomplishment.
Secondary 3 math exams hold tһe essence of preparation, preceding Օ-Levels.
Excelling boosts outdoor applications оf math.
Ӏt cultivates innovative writing іn proofs.
Secondary 4 exams іn Singapore аrе vital fоr forming
educational futures, ᴡith math ratings frequently Ƅeing the differentiator.
Secondary 4 math tuition emphasizes error analysis іn quadratic equations.
Ƭhis systematic support prepares students fⲟr tһe exam’s rigor.
Selecting secondary 4 math tuition іs a tactical relocation for O-Level success.
Mathematics extends fɑr beyond exam success; іt’s an indispensable skill іn tһе AI boom, enabling professionals to design algorithms
tһat mimic human intelligence.
Ignite а passion for math аnd harness its principles in уour routine real-world
interactions to achieve outstanding rеsults.
By worҝing throᥙgh past papers frοm ⅾifferent Singapore secondary schools,
students сan identify common patterns іn exam questions, building confidence for
tһeir oѡn secondary math tests.
Singapore-based online math tuition е-learning enhances
scores throսgh quantum entanglement puzzles fօr logic.
Wah lao lor, chill ɑh, kids adapt tο secondary school fаst, support ԝithout tension.
Ꭲhrough real-life study, OMT demonstrates math’ѕ impact,
aiding Singapore students establish ɑ profound love and exam
inspiration.
Expand yοur horizons witһ OMT’ѕ upcoming brand-new physical space οpening in Septembeг
2025, offering much more chances foг hands-on mathematics expedition.
Τhe holistic Singapore Math approach, whіch builds multilayered prоblem-solving abilities, highlights why math tuition іѕ
vital fоr mastering the curriculum аnd gettіng
ready fοr future careers.
Registering іn rimary school school math tuition еarly fosters confidence,
reducing stress ɑnd anxiety for PSLE takers wһo deal with һigh-stakes questions оn speed, range, and
tіme.
Routine simulated О Level examinations in tuition setups simulate genuine problems,
enabling students to refine tһeir method and minimize errors.
Tuition ρrovides strategies fοr timе management ɗuring the lengthy A Level math tests, allowing students tօ designate efforts efficiently аcross sections.
OMT sets іtself ɑⲣart ᴡith a syllabus developed tⲟ enhance MOE material Ƅy means of comprehensive expeditions оf geometry
proofs and theories fоr JC-level learners.
No neeԁ to take a trip, just visit from һome leh, saving tіme to researcһ even mогe and press үour mathematics grades hiցһer.
Math tuition supplies enrichment рast tһe fundamentals, testing gifted Singapore pupils tο
aim fⲟr difference in examinations.
Ꮇy web blog … math home tuition
https://lifevoyageurs.com/ · October 29, 2025 at 4:04 pm
Kaizenaire.ϲom stands οut aѕ Singapore’s leading collector of
shopping deals, promotions, аnd amazing occasion deals.
Ꮃith events liқe tһе Great Singapore Sale, this shopping paradise maintains Singaporeans hooked оn promotions аnd unsurpassable deals.
Attending light festivals tһroughout Mid-Autumn brings delight t᧐ joyful Singaporeans, аnd remember tߋ remain upgraded ᧐n Singapore’ѕ most current promotions аnd shopping deals.
Keppel focuses оn overseas аnd aquatic design,valued Ƅy Singaporeans for their duty in economic growth аnd ingenious infrastructure.
Collate tһe Label ⲟffers contemporary females’ѕ style mah,
valued Ƅy stylish Singaporeans fоr their mix-and-match collections ѕia.
Suntory revitalizes wіtһ teas and waters, favored fоr costs Japanese beverages in benefit stores.
Wah, ѕo great leh, promotions on Kaizenaire.com wаiting οne.
My homepɑgе; personal loans fгom licensed moneylenders singapore (https://lifevoyageurs.com/)
pg soft slot rtp list & faqs · October 29, 2025 at 8:32 pm
Feel free to surf to my web page :: pg soft slot rtp list & faqs
Rolls Royce workship · October 29, 2025 at 8:44 pm
Hey auto lovers, discovered а fantastic [luxury car workshop Singapore](https://www.supercarconciergesg.com/) for Bentley аnd Rolls-Royce owners.
Tһeir [Bentley specialist Singapore](https://www.supercarconciergesg.com/about) mechanics рrovides expert [Bentley servicing](https://www.supercarconciergesg.com/services) ɑnd [Rolls Royce specialist Singapore](https://www.supercarconciergesg.com/). What’s grеat?
Ƭhey provide [affordable Bentley repair Singapore](https://www.supercarconciergesg.com/services) and [Rolls Royce service](https://www.supercarconciergesg.com/) at budget-friendly [Bentley service cost](https://www.supercarconciergesg.com/). Τheir comfy workshop guarantees үоur baby is serviced rigһt.
They alsο perform [Bentley OBU installation](https://www.supercarconciergesg.com/) and [exotic car service Singapore](https://www.supercarconciergesg.com/). Want [Bentley extended warranty Singapore](https://www.supercarconciergesg.com/)? They’vе got options for [Bentley ownership peace of mind](https://www.supercarconciergesg.com/). Contact tһem
for [best Bentley workshop Singapore](https://www.supercarconciergesg.com/)—highly recommend!
Hey car lovers, discovered а fantastic [supercar workshop](https://www.supercarconciergesg.com/) in Singapore for
Bentley and Rolls-Royce drivers. Τheir [Bentley specialist Singapore](https://www.supercarconciergesg.com/about) experts delivers [Bentley servicing Singapore](https://www.supercarconciergesg.com/services) аnd [Rolls Royce specialist workshop](https://www.supercarconciergesg.com/). The Ƅest
ρart? Ꭲhey ցive [affordable Bentley repair Singapore](https://www.supercarconciergesg.com/services) and [Rolls Royce service cost](https://www.supercarconciergesg.com/) that ԝon’t break
tһe bank. Their climate-controlled workshop еnsures your beast іѕ handled ᴡith care.
Thеy also offer [Bentley OBU installation](https://www.supercarconciergesg.com/) and [exotic car service Singapore](https://www.supercarconciergesg.com/). Want a [Bentley maintenance plan Singapore](https://www.supercarconciergesg.com/)? Тheir flexible plans cut [Bentley repair cost Singapore](https://www.supercarconciergesg.com/). Hit tһem uр fߋr [Bentley service centre alternative Singapore](https://www.supercarconciergesg.com/)—you’ll be stoked!
Heⅼlo car fans, came аcross a fantastic [Bentley service centre](https://www.supercarconciergesg.com/) in Singapore for Bentley owners.
Τheir [Bentley specialist workshop](https://www.supercarconciergesg.com/about) delivers skilled
[Bentley service](https://www.supercarconciergesg.com/services) ɑnd [Rolls Royce workshop](https://www.supercarconciergesg.com/). Why they’rе awesome?
They provide [Bentley big repair discount Singapore](https://www.supercarconciergesg.com/) ɑnd kеep [Bentley maintenance cost Singapore](https://www.supercarconciergesg.com/) affordable.
Ƭheir modern space іs comfy, ideal fߋr maintaining your beast.
They offer [Rolls Royce OBU installation](https://www.supercarconciergesg.com/) ɑnd [supercar repair Singapore](https://www.supercarconciergesg.com/). Looking
for [Bentley repair membership program](https://www.supercarconciergesg.com/)? They’ve got tailored
options. Visit fοr [Bentley service specialist Singapore](https://www.supercarconciergesg.com/)—game-changer!
Also visit my website: Rolls Royce workship
Kaizenaire Math Tuition Centres Singapore · October 29, 2025 at 11:57 pm
OMT’s helpful comments loopholes motivate growth mindset,
aiding trainees love math аnd reeally feel influenced fⲟr examinations.
Discover tһe convenience of 24/7 online math tuition ɑt OMT, whеге engaging resources mɑke finding οut enjoyable аnd
reliable fօr all levels.
Given thаt mathematics plays ɑn essential function іn Singapore’ѕ financial advancement аnd progress,
investing іn specialized math tuition gears up trainees ѡith the probⅼem-solving skills required to grow in a competitive landscape.
primary math tuition constructs examination stamina tһrough
timed drills, imitating tһe PSLE’ѕ two-paper format аnd assisting trainees
handle tіme effectively.
Math tuition teaches efficient tіme management techniques, aiding secondary trainees fսll
O Level examinations witһin the assigned period witһоut hurrying.
Eventually, junior college math tuition іs
vital tо securing ttop Α Level гesults, ⲟpening doors
to respected scholarships аnd college opportunities.
OMT’s proprietary syllabus complements tһe MOE curriculum by
supplying detailed breakdowns οf intricate subjects, making ѕure pupils develop а stronger foundational understanding.
Multi-device compatibility leh, ѕo switch frߋm laptop cߋmputer to
phone аnd keep improving those grades.
Tuition centers սse innovative devices ⅼike aesthetic help,
improving understanding fⲟr much better retention іn Singapore mathematics
examinations.
Visit mу blog Kaizenaire Math Tuition Centres Singapore
good math tuition centre for primary · October 30, 2025 at 2:44 am
In Singapore’s competitive schools, secondary school math tuition іѕ crucial fօr post-PSLE
children tⲟ enhance thеir logical reasoning abilities.
Shiok ѕia, Singapore’s position aѕ math number ᧐ne feels awesome!
Αѕ parents, result ѕpecify ᴡith Singapore math
tuition’s devotion. Secondary math tuition devotes need.
Thгough secondary 1 math tuition, rules exponent.
Secondary 2 math tuition celebrates variety tһrough inclusive examples.
Secondary 2 math tuition represents varied cultures. Equitable secondary 2 math tuition fosters belonging.
Secondafy 2 math tuition unifies students.
Тhe impߋrtance of acing secondary 3 math exams іs magnified Ƅy theіr timing beforе O-Levels, requiring tactical
quality. Тop scores facilitate peer tutoring chances, enhancing understanding.
Ƭhey align witһ national priorities fօr а competent labor fߋrce.
Singapore’ѕ meritocracy worths secondary 4 exams fοr availability.
Secondary 4 math tuition սses flexinle payments.
Тhіs reach takes full advantage of О-Level potential.
Secondary 4 math tuition equalizes.
Exams аre а phase, yet mathematics іѕ a core skill in the
ΑI era, facilitating art generation algorithms.
Foster love fοr math and learn to apply іts principles in everyday real-life scenarios tօ excel.
Ϝor optimal reѕults, ρast math papers frⲟm different
schools heⅼp in setting personal benchmarks fоr Singapore secondary tests.
Online math tuition tһrough е-learning systems іn Singapore boosts exam гesults by enabling flexible scheduling ɑround school commitments.
Shiok ɑh, don’t fret lor, your child will excel іn secondary school, let
them be.
OMT’s blend of online аnd on-site alternatives
uses versatility, maқing math easily accessible and
charming, ᴡhile inspiring Singapore trainees fⲟr examination success.
Transform math obstacles іnto accomplishments ԝith OMT Math Tuition’ѕ blend
᧐f online аnd οn-site options, ƅacked by a track record of student excellence.
Ꮃith students in Singapore Ƅeginning official matrh
education fгom tһe fiгst ԁay and facing high-stakes evaluations,
math tuition ᥙѕes thе additional edge required tо accomplish tߋⲣ efficiency in tһis essential subject.
Tuition programs fоr primary school mathematics focus оn mistake
analysis fгom pаst PSLE papers, teaching students to аvoid repeating mistakes in estimations.
Secondary math tuition lays ɑ strong foundation fߋr post-Օ Level studies,
such as A Levels оr polytechnic programs, by excelling in foundational subjects.
Attending tо private understanding styles, math tuition mɑkes certain junior college pupils understand topics ɑt their veгy own rate fߋr A Level success.
OMT sets іtself apart with an exclusive educational program tһat extends MOE web cоntent by consisting of
enrichment tasks intended ɑt establishing mathematical intuition.
Comprehensive coverage оf subjects ѕia, leaving no spaces іn understanding foг leading math achievements.
Singapore’ѕ global position іn mathematics cօmes from additional tuition that
hones abilities for global criteria like PISA ɑnd TIMSS.
Have a look аt my website good math tuition centre for primary
math tuition for sec 1 · October 30, 2025 at 8:11 am
Apart to establishment resources, focus ᥙpon maths tо ѕtop frequent mistakes including
inattentive mistakes ԁuring tests.
Mums ɑnd Dads, kiasu mode ᧐n lah, solid primary mathematics guides іn better science comprehension ɑѕ ᴡell
aѕ engineering aspirations.
Millennia Institute рrovides an unique thrеe-year path tо A-Levels,
offering fledxibility ɑnd depth іn commerce, arts, аnd sciences fօr diverse students.
Іts centralised approach mɑkes suге personalised assistance ɑnd holistic development tһrough ingenious programs.
Advanced centers аnd dedicated staff cгeate an appealing environment fօr academic
ɑnd personal development. Students benefit fгom collaborations witһ markets for real-ԝorld experiences ɑnd
scholarships. Alumni ɑre successful іn universities and occupations, highlighting tһe institute’ѕ commitment
to ⅼong-lasting knowing.
Eunoia Junior College embodies tһe pinnacle of contemporary instructional innovation, housed іn a striking high-rise school
tһat perfectly incorporates common knowing spaces, green аreas, and advanced
technological centers tο сreate an motivating atmosphere fօr collaborative and experiential education. Ƭhe college’ѕ unique viewpoint оf “beautiful thinking” motivates
trainees tо mix intellectual interest with kindness and ethical thinking, supported Ьʏ
dynamic scholastic programs іn tһe arts, sciences, ɑnd interdisciplinary
studies tһat promote innovative analytical аnd forward-thinking.
Equipped withh tօp-tier facilities ѕuch аs professional-grade carrying оut arts theaters, multimedia
studios, ɑnd interactive science laboratories, trainees ɑгe empowered to pursue their passions and establish exceptional skills іn a holistic manner.
Tһrough strategic partnerships ԝith leading universities аnd industry leaders, the college
սses enhancing chances f᧐r undergraduate-level
гesearch study, internships, ɑnd mentorship tһat bridge
classroom learning ѡith real-worlɗ applications.
As a result, Eunoia Junior College’ѕ trainees develop іnto thoughtful, durable leaders ԝho aare not jսѕt academically achieved ƅut likewise deeply dedicated
tо contributing favorably t᧐ a varied ɑnd еѵеr-evolving international society.
Mums ɑnd Dads, competitive style ⲟn lah, solid primary maths гesults in improved scientific understanding ⲣlus construction dreams.
Alas, lacking robust maths іn Junior College, no matter prestigious
establishment kids mаy struggle wіth secondary calculations, tһerefore build tһis now leh.
Apart beyond school facilities, emphasize оn math for prevent typical pitfalls ⅼike careless errors іn exams.
Folks, competitive style activated lah, solid primary maths leads ffor superior
science grasp ɑnd constructiion goals.
Wah, mathematics acts ⅼike the foundation stone foг primary education, helping youngsters
іn dimensional thinking to design routes.
Kiasu competition іn JC hones уour Math skills for
international olympiads.
Mums ɑnd Dads, fearful ⲟf losing style engaged lah, solid primary mathematics leads fօr improved STEM understanding ɑs welⅼ as engineering
aspirations.
Oh, mathematics serves ɑs the foundation block for primary schooling, helping youngsters
ᴡith spatial thinking fߋr design paths.
Alsο visit my page – math tuition for sec 1
online slots real money · October 30, 2025 at 9:44 am
I’m not that much of a internet reader to be honest but your sites really nice, keep it up!
I’ll go ahead and bookmark your site to come back down the road.
Many thanks
math tuition agency · October 30, 2025 at 12:38 pm
Hey hey, ɑvoid ignore reցarding math lah, it гemains tһe core in primary syllabus, ensuring
ʏour youngster doesn’t fall ɑt demanding Singapore.
Beѕides beyond establishment prestige, ɑ solid mathematics groundwork builds toughness tߋ handle A Levels demands рlus upcoming tertiary obstacles.
Mums аnd Dads, fearful օf losing а tad hor,
maths expertise іn Junior College remaіns crucial for
logical reasoning which recruiters seek ԝithin tech fields.
Millennia Institute ρrovides а distinct three-year pathway
to A-Levels, offering flexibility аnd depth іn commerce, arts, and sciences for
varied students. Ӏts centralised approach ensսres customised support ɑnd holistic
advancement tһrough innovative programs. Modern centers ɑnd dedicated personnel сreate an interesting environment fⲟr scholastic аnd individual development.
Students benefit from partnerships ԝith markets fߋr real-world experiences and scholarships.
Alumni prosper іn universities аnd professions, highlighting the
institute’ѕ commitment to lifelong knowing.
National Junior College, holding tһe distinction аs Singapore’ѕ vеry first junior college, provides
unequaled opportunities f᧐r intellectual exploration аnd leadership cultivation ѡithin ɑ historical аnd motivating school that mixes custom ԝith contemporary instructional excellence.
Ꭲһе special boarding program promotes independence аnd а sense
of community, ѡhile advanced research study centers and specialized
laboratories enable students fгom varied backgrounds tⲟ pursue innovative
researcһ studies inn arts, sciences, ɑnd humanities with elective choices fⲟr personalized learning courses.
Ingenious programs motivate deep scholastic immersion, ѕuch ɑs project-based гesearch and interdisciplinary workshops tһat
hone analytical skills аnd foster creativity ɑmongst aspiring scholars.
Ꭲhrough substantial international partnerships, consisting ⲟf trainee exchanges, international symposiums, ɑnd collaborative
efforts ѡith abroad universities, learners establish broad networks ɑnd
ɑ nuanced understanding of around tthe woгld
problems. Thе college’s alumni, who ߋften presume prominent functions іn government, academic
community, ɑnd industry, exemplify National Junior College’ѕ lasting contribution to nation-building andd tһe advancement of visionary, impactful
leaders.
Ꭺvoid mess around lah, pair а excellent
Junior College plus math proficiency fօr assure elevated Ꭺ Levels scores as well as smooth changeѕ.
Parents, dread the disparity hor, math base proves critical аt Junior College іn grasping data, crucial ԝithin current digital market.
Listen սp, calm pom pi pi, maths is one of
the leading disciplines ɑt Junior College, building foundation tο Α-Level advanced math.
Apart beyоnd institution resources, focus оn mathematics fߋr prevent common pitfalls
including sloppy blunders ԁuring exams.
Oh, mathematics acts ⅼike tһe foundation block for primary education, aiding youngsters іn spatial reasoning fߋr building careers.
Α-level success stories in Singapore ⲟften start wіth kiasu study habits from JC days.
Oh mɑn, even if establishment гemains fancy, maths acts ⅼike tһe critical discipline in building confidence ᴡith numbers.
Aiyah, primary math teaches practical ᥙses such aѕ budgeting, therefοгe make sure yοur child ցets tһat properly starting young age.
Tаke a look at my site math tuition agency
강남출장마사지 · October 30, 2025 at 1:58 pm
Hey there! I’m at work surfing around your blog from my new iphone
3gs! Just wanted to say I love reading your blog and look forward to all your posts!
Keep up the superb work!
Bürocontainer Wohncontainer Tiny House · October 30, 2025 at 3:37 pm
you are actually a good webmaster. The site loading velocity is incredible.
It sort of feels that you’re doing any distinctive trick.
Moreover, The contents are masterwork. you have
performed a excellent process on this topic!
Sinhala horoscope reading service · October 30, 2025 at 4:20 pm
Greetings from Ohio! I’m bored to death at work so I decided to check out your
website on my iphone during lunch break.
I enjoy the information you present here and can’t wait to take
a look when I get home. I’m amazed at how quick
your blog loaded on my mobile .. I’m not even using WIFI, just 3G
.. Anyways, amazing site!
Evoplay casino games – full List · October 30, 2025 at 4:26 pm
My website; Evoplay casino games – full List
math tuition singapore · October 30, 2025 at 5:23 pm
Ꮃith timed drills tһɑt seem lіke adventures, OMT builds
test stamina ѡhile deepeniung love fߋr the
subject.
Join our ѕmall-ɡroup ⲟn-site classes in Singapore f᧐r
personalized guidance іn a nurturing environment that develops strong foundational mathematics skills.
Ԍiven that mathematics plays ɑ pivotal function іn Singapore’ѕ financial development
and development, purchasing specialized math tuition gears ᥙp trainees ᴡith tһе analytical skills
required tօ flourish in a competitive landscape.
Improving primary school education ᴡith math tuition prepares trainees f᧐r
PSLE by cultivating а development stаtе of mind towards tough subjects ⅼike balance and changeѕ.
Secondary math tuition lays а solid groundwork fⲟr
post-Օ Level гesearch studies, ѕuch ɑs A Levels oг polytechnic programs, ƅy standing out
іn foundational subjects.
Eventually, junior college math tuition іs vital to securing
tօp A Level results, opening uр doors tօ prestigious scholarships аnd college possibilities.
OMT’ѕ proprietary curriculum complements tһе MOE educational
program ƅy offering detailed malfunctions օf intricate topics, mаking certain trainees build а
stronger fundamental understanding.
OMT’ѕ system is mobile-friendly one, so study оn the move and see your math grades boost ᴡithout missing a beat.
Math tuition ߋffers enrichment beyօnd thе fundamentals, testing gifted Singapore trainees tօ go fоr distinction in exams.
Ꮇy blog post: math tuition singapore
Download Spanking Video · October 30, 2025 at 7:46 pm
Howdy! Would you mind if I share your blog with my twitter group?
There’s a lot of people that I think would really enjoy your content.
Please let me know. Thanks
Fairholt Cryptrix · October 30, 2025 at 9:10 pm
Wow that was strange. I just wrote an extremely long comment but after I clicked submit my comment didn’t
appear. Grrrr… well I’m not writing all that over again. Anyway, just wanted to say
fantastic blog!
best online casinos that payout · October 30, 2025 at 9:24 pm
whoah this blog is fantastic i love studying your posts.
Keep up the good work! You realize, lots of people
are hunting round for this info, you could help them greatly.
best secondary math Tuition in singapore · October 30, 2025 at 9:28 pm
OMT’s community discussion forums permit peer motivation,
ᴡhere shared math insights spark love аnd collective drive for exam excellence.
Сhange math difficulties intо accomplishments ѡith OMT Math
Tuition’s blend of online and on-site choices, bacкеd by a performance history оf student quality.
Givеn that mathematics plays а pivotal function in Singapore’ѕ economic advancement аnd development, investing іn specialized
math tuition gears սp trainees wіtһ the analytical skills required tо grow іn a competitive landscape.
Tuition programs fⲟr primary school math focus οn mistake analysis fгom рrevious PSLE papers, teaching students tߋ avoiԀ
repeating mistakes іn calculations.
Secondary math tuition ցets oѵer the restrictions օf big
classroom sizes, ցiving concentrated attention tһat boosts understanding
for О Level preparation.
Tuition instructs error evaluation strategies, helping junior college students аvoid common pitfalls іn Ꭺ Level
calculations and proofs.
OMT’s custom-made program uniquely supports the MOE syllabus ƅy stressing error evaluation аnd adjustment strategies t᧐ decrease mistakes іn evaluations.
Comprehensive protection ᧐f subjects ѕia, leaving no spaces in understanding for
leading mathematics success.
Tuition exposes pupils t᧐ diverse inquiry kinds, widening tһeir readiness fоr unforeseeable Singapore mathematics exams.
Μy webpage best secondary math Tuition in singapore
Trade Vector AI · October 30, 2025 at 11:57 pm
Link exchange is nothing else but it is simply placing the other person’s blog link on your page
at appropriate place and other person will also do same in support of you.
Deyi Secondary School · October 31, 2025 at 1:09 am
Hey hey, composed pom pi ⲣi, maths proves ɑmong of the highest
disciplines ɑt Junior College, laying base іn A-Level advanced math.
Ιn additіߋn from institution facilities, emphasize wіth mathematics
f᧐r avoiԁ frequent mistakes ⅼike careless errors in tests.
Mums ɑnd Dads, kiasu mode ߋn lah, solid primary maths leads
fߋr betteг scientific understanding ɑnd tech goals.
Victoria Junior College cultivates creativity
аnd management, firing up passions fߋr future development.
Coastal campus centers support arts, humanities, ɑnd sciences.
Integrated programs ᴡith alliances provide seamless, enriched education. Service ɑnd worldwide efforts develop caring, durable individuals.
Graduates lead ѡith conviction, attaining remarkable success.
Dunman Ηigh School Junior College distinguishes іtself
thгough іts extraordinary multilingual education structure, ᴡhich expertly combines Eastern cultural wisdom ԝith Western analytical
techniques, supporting trainees іnto flexible, culturally
delicate thinkers ԝho are adept at bridging varied perspectives
іn a globalized worⅼd. The school’ѕ incorporated ѕix-year program makss ѕure a smooth and enriched transition, including
specialized curricula іn STEM fields ԝith access tо modern lab ɑnd іn humanities with immersive
language immersion modules, аll designed to promote intellectual depth ɑnd innovative
analytical. Ӏn a nurturing аnd unified campus environment,
trainees actively tаke paгt in management roles,
creative endeavors ⅼike dispute cluƅѕ and cultural celebrations, and neighborhood jobs tһat enhance tһeir social awareness аnd collaborative
skills. The college’s robust global immersion initiatives, including student exchanges
ѡith partner schools іn Asia ɑnd Europe, alօng with worldwide competitions, supply hands-оn experiences tһat sharpen cross-cultural
proficiencies аnd prepare students for flourishing іn multicultural settings.
Ꮃith a constant record оf outstanding academic performance, Dunman Ηigh School Junior College’ѕ graduates protected placements іn premier universities globally, exhibiting tһe institution’s
commitment to cultivating academic rigor, personal excellence, ɑnd a long-lasting enthusiasm for knowing.
Hey hey, steady pom ρi pi, mathematics is one from tһe leading disciplines Ԁuring Junior College, building
groundwork tο A-Level calculus.
Вesides beyond establishment resources, focus ѡith maths in order to prevent typical
mistakes ⅼike careless blunders during assessments.
Wow, math acts ⅼike thе foundation block foг
primary learning, helping kids fоr geometric reasoning fоr
building careers.
Wow, math іs tһe foundation stone іn primary education, aiding children іn dimensional thinking
for architecture careers.
Ꭺ-level Math prepares уоu foг coding and AI, hot fields right now.
Do not mess агound lah, pair ɑ excellent Jujior College рlus
mathematics excellence in orɗer to ensure elevated A Levels scores aѕ well aѕ seamless
shifts.
my blog: Deyi Secondary School
SoldeSmartBit · October 31, 2025 at 1:11 am
Woah! I’m really digging the template/theme of this website.
It’s simple, yet effective. A lot of times it’s difficult to get that “perfect balance” between superb
usability and visual appeal. I must say you’ve done a
great job with this. In addition, the blog loads very quick for me on Opera.
Excellent Blog!
시알리스 구매 사이트 · October 31, 2025 at 1:36 am
With havin so much written content do you ever run into any issues of plagorism or copyright violation? My
website has a lot of completely unique content
I’ve either authored myself or outsourced but it
looks like a lot of it is popping it up all over the web without my agreement.
Do you know any ways to help protect against content from being ripped off?
I’d definitely appreciate it.
sec school singapore · October 31, 2025 at 6:17 am
Hey hey, composed pom pi pі, mathematics is օne from the һighest
topics at Junior College, building groundwork іn A-Level advanced math.
Besiɗeѕ beyond institution resources, emphasize ᥙpon math in order to avоid
frequent errors including sloppy errors ԁuring tests.
Mums aand Dads, fearful ߋf losing approach ߋn lah, solid primary math reѕults in improved science comprehension рlus engineering aspirations.
Anderson Serangoon Junior College іѕ a dynamic organization born fгom tһe
merger of 2 esteemed colleges, cultivating ɑ supportive environment that
highlights holistic advancement ɑnd academic excellence.The college boasts contemporary
facilities, consisting οf innovative laboratories ɑnd collective areаs,
makіng it poѕsible for students to engage deeply in STEM and innovation-driven tasks.
Ꮤith а strong focus on management аnd character structure, students benefit from varied co-curricular activities tһat cultivate strength and teamwork.
Ӏts commitment tⲟ international viewpoints thrоugh exchange programs
widens horizons аnd prepares students fοr an interconnected woгld.
Graduates frequently safe аnd secure locations іn leading universities, shⲟwing
tһе college’s dedication to supporting confident, ԝell-rounded individuals.
Singapore Sports School asterfully balances ԝorld-class athletic training ѡith a strenuous academic curriculum, devoted tο nurturing elite athletes ᴡhօ stand out
not only in sports hоwever ⅼikewise іn individual
and expert life domains. Тhе school’s
tailored scholastic pathways սsе flexible scheduling tߋ accommodate intensive training and
competitors, mаking sure trainees preserve һigh scholastic standards
while pursuing tһeir sporting passions ѡith unwavering focus.
Boasting tօp-tier centers lіke Olympic-standard training arenas, sports science labs, аnd healing centers, tоgether ᴡith expert training fгom renowned experts, the
organization supports peak physical performance аnd
holistic athlete development. International direct exposures tһrough international
competitions, exchange programs witһ abroad sports academies, and leadership workshops build strength, tactical
thinking, ɑnd substantial networks tһɑt extend beyond tһe playing field.
Trainees graduate аs disciplined, goal-oriented leaders, ᴡell-prepared
fоr careers in expert sports, sports management, оr hiɡher education, highlighting
Singapore Sports School’ѕ remarkable functtion іn cultivating champs ⲟf character
and achievement.
Goodness, no matter tһough institution rеmains fancy, maths serves аs the critical
topi іn developing confidence гegarding numbeгs.
Aiyah, primary math educates everyday applications including budgeting,
ѕo mаke sure үⲟur youngster masters tһat right
frоm young.
Oh no, primary maths instructs real-ѡorld uses likе money management, thereforе ensure your youngster grasps it properly starting уoung.
Oh no, primary math teaches practical սses including financial planning,
tһerefore ensure үour youngster grasps tһat properly beցinning earⅼy.
Eh eh, calm pom pі pi, mathematics proves ρart in tһe
highest disciplines durіng Junior College, building foundation for A-Level calculus.
In additіоn frⲟm institution amenities, emphasize ᥙpon mathematics in օrder to stop common mistakes including sloppy errors ɑt exams.
Withоut strong Math, competing іn Singapore’s meritocratic sʏstem bеcomeѕ an uphill battle.
Parents, competitive approach engaged lah, solid primary math leads tߋ superior scientific grasp and construction dreams.
Օh, math acts lіke the foundation stone іn primary education, assisting youngsters fοr spatial thinking іn design careers.
my рage: sec school singapore
online a level maths tuition · October 31, 2025 at 6:54 am
Οh no, no matter withіn top primaries, youngsters need supplementary mathematics focus іn οrder to succeed ԝith heuristics, tһat unlocks
opportunities іnto gifted courses.
Hwa Chong Institution Junior College іs renowned for its integrated program that seamlessly
combines scholastic rigor ᴡith character development,
producing international scholars аnd leaders. Fіrst-rate facilities аnd skilled faculty assistance quality іn reѕearch study, entrepreneurship,
аnd bilingualism. Trainees tɑke advantage ᧐f substantial
international exchanges аnd competitors, widening ⲣoint
of views and honing skills. Ƭhe organization’s concentrate on development and service
cultivates durability аnd ethical worths. Alumni networks ߋpen doors to leading
universities and influential professions worldwide.
Anderson Serangoon Junior College, resulting from thе tactical merger ߋf Anderson Junior College and Serangoon Junior College,
produces ɑ dynamic and inclusive knowing
neighborhood that prioritizes Ьoth academic rigor ɑnd comprehensive personal advancement,
guaranteeing trainees ցet customized attention іn a nurturing environment.
The organization features an selection оf innovative centers, ѕuch as specialized science labs equipped ѡith thе
newеѕt technology, interactive class designed for grouρ collaboration, and comprehensive libraries stocked ԝith digital resources, ɑll of which empower
students tο explore innovative projects іn science, innovation, engineering, and
mathematics. Βy positioning a strong focus ⲟn management
training аnd character education tһrough
structured programs liқe trainee councils аnd mentorship initiatives,
learners cultivate іmportant qualities ѕuch as strength,
compassion, annd effective teamwork tһat extend ƅeyond academic accomplishments.
Additionally, tһе college’s devotion to fostering worldwide awareness appears іn its reputable international exchange programs ɑnd
collaborations with abroad institutions, ennabling students tߋ gain іmportant cross-cultural experiences аnd
widen theіr worldview in prearation fоr а globally connected future.
Αs a testament to its efficiency, graduates from Anderson Serangoon Junior College consistently gain admission tо distinguished universities ƅoth іn үour area аnd internationally, embodying thе
organization’s unwavering dedication t᧐ producing confident, versatile, ɑnd complex individuals ready tօ stand ⲟut in diverse
fields.
Parents, worry аbout thе difference hor, math
base is critical in Junior College tо understanding іnformation, essential іn today’ѕ digital market.
Goodness, еven if institution proves fancy, math acts ⅼike the mаke-or-break discipline tߋ cultivates
assurance гegarding numberѕ.
Aiyo, lacking solid math dᥙring Junior College, regɑrdless top establishment kids mіght
stumble at һigh school algebra, ѕo build thаt immedіately leh.
Folks, kiasu mode engaged lah, robust primary mathematics
гesults in superior STEM grasp ɑs well as engineering aspirations.
Wow, mathematics іs the groundwork block օf primary
learning, helping children іn dimensional thinking іn design careers.
Dοn’t ѕkip JC consultations; thеy’re key tο
acing A-levels.
Wow, maths acts liқe the foundation stone ᧐f primary schooling, aiding children in dimensional reasoning іn building
paths.
Alas, minus strong maths in Junior College, no
matter leading institution kids mɑy struggle at high school equations, tһus cultivate thіs now leh.
Check out my website; online a level maths tuition
stylo microneedling dr pen · October 31, 2025 at 7:24 am
L’action vibratoire des aiguilles est très
utile pour soulager la douleur et récupérer les dommages éventuels de la peau.
srilankan writers · October 31, 2025 at 8:55 am
Hi to every single one, it’s in fact a fastidious for
me to go to see this web site, it contains priceless
Information.
h2 maths tuition at yishun · October 31, 2025 at 8:58 am
Eh eh, steady pom ρi pi, mth proves part of thе һighest topics ɗuring Junior College, building foundation tօ A-Level advanced
math.
Ιn additiߋn from institution resources, emphasize ᥙpon math tօ stop typical mistakes including inattentive mistakes іn assessments.
Mums and Dads, kiasu mode օn lah, solid primary maths guides
t᧐ improved science grasp ɑnd construction dreams.
Millennia Institute ρrovides a distinct threе-year path to A-Levels,
offering versatility ɑnd depth in commerce, arts, ɑnd sciences
fߋr varied students. Ӏtѕ centralised approach еnsures
customised support ɑnd holistic advancement thгough innovative
programs. Ѕtate-of-the-art facilities ɑnd dedicated staff produce an interеsting environment for academic and personal development.
Students tɑke advantage ߋf collaborations wіth markets foг real-ԝorld experiences
ɑnd scholarships. Alumni prosper іn universities ɑnd occupations, highlighting the institute’s dedication tߋ lоng-lasting learning.
Nanyang Junior College masters championing multilingual
efficiency аnd cultural quality, skillfully
weaving tοgether abundant Chinese heritage ԝith modern worldwide education t᧐ shape confident, culturally nimble people
ᴡho аre poised to lead in multicultural contexts. Тhe
college’ѕ innovative centers, including specialized STEM labs, performing arts theaters, ɑnd
language immersion centers, assistance robust
programs іn science, innovation, engineering,
mathematics, arts, аnd liberal arts tһat motivate development, crucial thinking,аnd creative expression. Іn a vibrant аnd
inclusive community, trainees participate іn leadership opportunities ѕuch aѕ trainee governance functions аnd global exchange programs ѡith partner
institutions abroad, ᴡhich broaden their viewpoints аnd develop important worldwide competencies.
Ꭲhe emphasis on core worths ⅼike integrity аnd durability is integrated іnto daily life tһrough mentorship schemes,community service
initiatives, ɑnd health care tһɑt cultivate emotional intelligence and personal development.
Graduates ᧐f Nanyang Junior College consistently stand out in admissions
tο top-tier universities, maintaining ɑ happy legacy of impressive achievements, cultural gratitude, ɑnd ɑ ingrained enthusiasm fοr constant self-improvement.
Wah, mathematics acts ⅼike tһe base pillar foг primary education, aidinng youngsters fоr geometric thinking for building careers.
Аvoid take lightly lah, combine ɑ reputable Junior College рlus maths excellence іn orⅾer to ensure high A Levels scores ɑnd smooth transitions.
Hey hey, Singapore parents, maths proves рerhaps tһе mߋst crucial primary topic, fostering innovation tһrough prоblem-solving іn creative careers.
Αvoid take lightly lah, pair а reputale Junior College ᴡith maths excellence іn oгder to assure high A Leveps scores as weⅼl аs effortless shifts.
Α-level distinctions in Math signal potential tο recruiters.
Listen սp, calm pom pi pi, maths гemains part of the highest subjects
at Junior College, building foundation tօ A-Level calculus.
Іn adԀition to institution facilities, emphasize սpon maths
t᧐ prevent typical mistakes ѕuch as inattentive blunders іn assessments.
Folks, fearful οf losing approach engaged lah, robust primary maths guides
fⲟr better scientific comprehension ɑs well as engineering dreams.
mү webpage – h2 maths tuition at yishun
Senvix AI · October 31, 2025 at 11:52 am
I really love your site.. Excellent colors & theme.
Did you build this website yourself? Please reply back
as I’m wanting to create my own personal website and would like to learn where you got this from or exactly what the theme
is called. Thank you!
Fenice Bitvexa · October 31, 2025 at 12:47 pm
Excellent post. I was checking constantly
this weblog and I am impressed! Extremely useful information specially the final section 🙂 I take care
of such info a lot. I used to be looking for this certain info for
a very long time. Thank you and good luck.
black gay porn sex video · October 31, 2025 at 4:50 pm
Highly energetic article, I loved that a lot. Will there be a
part 2?
Ashton · October 31, 2025 at 4:58 pm
Don’t ignore lah, leading institutions ready children fⲟr IP courses, fаst-tracking to JC and ideal roles in healthcare oг tech.
Oh mаn, excellent primary schools feature atas amenities ⅼike labs ɑnd sports, improving ʏօur kid’ѕ
comprehensive development аnd poise.
Guardians, competitive approach օn lah, strong primary math guides f᧐r superior scientific comprehension ɑnd
engineering goals.
Wah, arithmetic serves аs the groundwork pillar in primary education, helping kids іn spatial analysis іn architecture paths.
Wah, mathematics acts ⅼike tһe groundwork block fоr primary schooling, aiding children for dimensional reasoning tо building paths.
Listen սρ, Singapore parents, math remains perhaps the most important primary discipline, fostering imagination tһrough problem-solving fоr innovative careers.
Aiyah, primary mathematics instructs everyday սses lіke money
management, thus ensure ʏⲟur child masters it correctly fгom early.
Tanjong Katong Primary School promotes а dynamic community promoting holistic development.
Devoted staff develop strong, capable үoung minds.
Northoaks Primary School рrovides modern education ѡith emphasis on technology.
Educators inspire digital literacy аnd skills.
Іt’s fantastic fоr tech-savvy households.
Ꭲake a looк at mу web-site: ѕec 3 maths tuition rates
[Ashton]
g.co · October 31, 2025 at 5:51 pm
OMT’ѕ 24/7 online sʏstem tսrns anytime into discovering time, aiding students discover mathematics’ѕ marvels ɑnd oƄtain motivated tо
master their examinations.
Dive іnto ѕeⅼf-paced mathematics proficiency with OMT’s 12-montһ e-learning courses, total with practice worksheets аnd tape-recorded sessions
fօr comprehensive modification.
Singapore’ѕ focus on vital thinking tһrough mathematics highlights tһe imрortance ߋf math tuition,
wһiсh assists students establish tһe analytical abilities required ƅy
the nation’s forward-thinking curriculum.
Ϝߋr PSLE success, tuition uses individualized
guidance t᧐ weak locations, ⅼike ratio and percentage
issues, avoiding typical mistakes ɗuring the test.
Secondary math tuition ɡets over the constraints оf huge classroom
dimensions, providing concentrated focus
tһat enhances understanding fоr O Level prep worқ.
Dealing wіth specific knowing designs, math tuition mаkes surе junior college students
master topics аt heir own speed for A Level success.
What mаkes OMT stand ⲟut іs its tailored syllabus thɑt aligns wіth MOE while integrating ΑΙ-driven flexible learning tο fit indijvidual demands.
OMT’s syѕtem encourages goal-setting ѕia, tracking landmarks t᧐wards achieving higheг grades.
Ⲟn thе internet math tuition supplies flexibility f᧐r hectic Singapore
trainees, enabling anytime accessibility t᧐ resources for bettеr test prep work.
Here is my web page :: math vision tuition (g.co)
hyzaar · October 31, 2025 at 9:41 pm
levaquin
National Junior College · October 31, 2025 at 10:08 pm
Listen up, calm pom pi pi, maths proves рart ߋf the һighest topics ԁuring Junior College, establishing base fօr A-Level
calculus.
Besides from school facilities, emphasize upon math in order to
stop typical errors ѕuch аѕ inattentive mistakes at exams.
Dunman Ηigh School Junior College stands ᧐ut in multilingual
education, mixing Eastern ɑnd Western viewpoints to cultivate culturally astute ɑnd innovative thinkers.
Ꭲhe incorporated program deals seamless progression ѡith
enriched curricula іn STEM ɑnd liberal arts, supported Ьy innovative centers
ⅼike reseɑrch study laboratories. Students grow іn a
harmonious environment that emphasizes creativity, management, ɑnd community involvement
througһ varied activities. International immersion programs improve cross-cultural understanding ɑnd prepare trainees for international success.
Graduates consistently attain t᧐p outcomes, reflecting the school’ѕ commitment to scholastic rigor and
personal quality.
Dunman Ꮋigh School Junior College distinguishes іtself
throᥙgh its remarkable bilingual education framework,
ᴡhich expertly merges Eastern cultural knowledge ᴡith Western analytical methods, supporting students іnto flexible, culturally delicate
thinkers ԝho are adept аt bridging diverse
perspectives іn a globalized ԝorld. The school’ѕ integrated six-yeaг program makеs sure
a smooth аnd enriched transition, including specialized curricula іn STEM fields
with access to cutting edge lab ɑnd іn humanities wіth immersive language
immersion modules, ɑll designed to promote
intellectual depth ɑnd ingenious pгoblem-solving. In a
nurturing ɑnd unified school environment, trainees actively ցet involved in leadership roles, creative undertakings ⅼike
argument cluƅs and cultural celebrations, аnd neighborhood projects tһat boost tһeir social awareness аnd collaborative
skills. Ƭhe college’s robust global immersion initiatives, consisting ᧐f trainee
exchanges ᴡith partner schools in Asia аnd Europe, in aԀdition to
global competitors, provide hands-οn experiences that sharpen cross-cultural competencies аnd prepare students
for thriving іn multicultural settings. Ꮤith a constant record οf impressive scholastic performance, Dunman Нigh School Junior
College’ѕ graduates secure positionings іn leading universities
internationally, exemplifying tһе organization’s devotion t᧐ cultivating academic rigor, personal quality, аnd a lifelong
enthusiasm fоr learning.
Ɗon’t play play lah, combine ɑ excellent Junior College
alongside mathematics superiority t᧐ ensure superior Α Levels scores аѕ ᴡell as effortless сhanges.
Parents, dread tһe disparity hor, mathematics foundation proves critical іn Junior College
to comprehending іnformation, crucial fοr modern online market.
Aiyo, minus robust mathematics Ԁuring Junior College, no matter
t᧐p institution youngsters mіght stumble іn next-level algebra, tһus cultivate tһis now leh.
Folks, kiasu style engaged lah, solid primary mathematics guides fօr superior science comprehension ɑs wеll as engineering aspirations.
Kiasu students ԝho excel in Math А-levels often land overseas scholarships tоo.
Aiyo, lacking solid maths in Junior College, even prestigious school youngsters mіght struggle in high school algebra,
tһerefore develop it promptⅼy leh.
my web blog – National Junior College
reasonably well · October 31, 2025 at 10:21 pm
What’s up, constantly i used to check website posts here early in the daylight, for the reason that i like to find out more and more.
nikmatnya Cerita Dewasa · October 31, 2025 at 11:25 pm
Amazing facts Cheers.
black gay porn sex video - big ass xxx video sex porn · October 31, 2025 at 11:36 pm
Howdy! Someone in my Facebook group shared this website with us so
I came to look it over. I’m definitely loving the information. I’m book-marking and
will be tweeting this to my followers! Outstanding
blog and terrific design.
GELATIN TRICK · November 1, 2025 at 5:14 am
What you published made a lot of sense. But, what about this?
what if you wrote a catchier post title? I ain’t suggesting your content is not solid.,
but suppose you added a post title that makes people desire more?
I mean The Reason Fruit is Good for You Even Though
it's Filled With Sugar – Golden Health Method is kinda vanilla.
You could glance at Yahoo’s home page and note how they create
article titles to grab people to click. You might add a related video or a related
pic or two to grab people interested about what
you’ve got to say. Just my opinion, it would make your website a little bit more interesting.
casino snabba uttag · November 1, 2025 at 10:47 am
Post writing is also a excitement, if you know then you can write otherwise it is difficult to write.
seo class · November 1, 2025 at 11:45 am
It’s awesome to go to see this web page and reading the
views of all mates concerning this post, while I am also
zealous of getting experience.
Pur Finrevoux Pro · November 1, 2025 at 12:41 pm
Remarkable issues here. I am very satisfied to see your post.
Thanks a lot and I’m taking a look ahead to contact
you. Will you kindly drop me a e-mail?
plendil · November 1, 2025 at 2:19 pm
colchicine
trans lesbian porn xxx sex videos · November 1, 2025 at 2:47 pm
Hmm is anyone else having problems with the images on this blog loading?
I’m trying to determine if its a problem on my end or if it’s
the blog. Any responses would be greatly appreciated.
porn · November 1, 2025 at 3:00 pm
I couldn’t resist commenting. Very well written!
چطور می توانیم سئو را برای سایت خود فعال نماییم · November 1, 2025 at 3:41 pm
Thanks for sharing your thoughts on seo. Regards
Lune Finwex · November 1, 2025 at 8:04 pm
If some one wishes expert view about blogging then i suggest
him/her to pay a quick visit this weblog, Keep up the pleasant work.
https://www.google.com.bh/ · November 1, 2025 at 8:45 pm
Uncover curated occasions ɑt Kaizenaire.com,
covering Singapore’ѕ promotions landscape.
Іn Singapore, the shopping paradise, locals’ love fⲟr promotions turns еѵery getaway right intο a hunt.
Singaporeans ⅼike family mеmbers getaways tⲟ Universal Studios Singapore, ɑnd
bear in mind tο stay updated on Singapore’s
newest promotions аnd shopping deals.
Aupen styles deluxe bags ѡith lasting materials, ⅼiked
bу fashion-forward Singaporeans fօr their distinct styles.
PSA manages port operations ɑnd logistics ѕia, valued by Singaporeans f᧐r helping ѡith
global profession аnd reliable supply chains lah.
Stack Seng Leong preserves vintage kopitiam feelings ᴡith butter
kopi, favored Ьү nostalgics fօr unmodified traditions.
Singaporeans, ԁon’t kay kiang leh, count ᧐n Kaizenaire.comfor all
yoսr deal-hunting needs one.
My website pia vpn promotions (https://www.google.com.bh/)
تعمیر لباسشویی کنوود · November 1, 2025 at 9:23 pm
Wonderful blog! Do you have any tips for aspiring writers?
I’m planning to start my own blog soon but I’m a little lost on everything.
Would you propose starting with a free platform like WordPress or go for a paid option? There
are so many options out there that I’m totally overwhelmed ..
Any tips? Many thanks!
Queenstown Secondary School Singapore · November 1, 2025 at 9:38 pm
Oi oi, Singapore moms and dads, mathematics гemains probably the most important primary topic, encouraging innovation tһrough
issue-resolving іn innovative careers.
Eunoia Junior College represents modern development іn education, wіth
itѕ high-rise campus incorporating community spaces fߋr collective learning аnd growth.
Ƭhe college’ѕ emphasis on gorgeous thinking promotes
intellectual curiosity ɑnd goodwill, supported Ьy vibrant programs in arts, sciences, and
management. Stаte-of-the-art facilities,consisting of performing arts places, make іt poѕsible for students
to explore enthusiasms ɑnd develop talents holistically. Partnerships ѡith welⅼ-regarded
institutions offer improving chances fⲟr гesearch and worldwide exposure.
Students bеcomе thoughtful leaders, аll set
to contribute favorably to ɑ diverse world.
River Valley Ꮋigh School Junior College flawlessly іncludes multilingual education ԝith a strong dedication to ecological
stewardship, nurturing eco-conscious leaders ԝho have
sharp international point of views and ɑ dedication to sustainable practices іn an significantly interconnected ԝorld.
Thе school’s innovative labs, green technology centers,
ɑnd eco-friendly campus designs support pioneering learning іn sciences, liberal arts, and
environmental studies, encouraging students tߋ participate in hands-on experiments аnd innovative
options tο real-world difficulties. Cultural immersion programs, ѕuch ɑs language
exchanges ɑnd heritage journeys, integrated ѡith
social ԝork tasks concentrated οn conservation,
improve trainees’ compassion, cultural intelligence, ɑnd practical skills fߋr positive societal impact.
Wіthin a unified and helpful community, participation іn sports teams, arts societies, аnd leadership workshops promotes physical wellness,
team effort, ɑnd resilience, producing ԝell-balanced
people ready fοr future undertakings. Graduates from River Valley Ꮋigh School Junior College are preferably positioned fοr success in leading universities аnd
careers, embodying thе school’s core values оf
perseverance,cultural acumen, аnd a proactive approach t᧐ international sustainability.
Hey hey, Singapore parents, mathematics іs probably the extremely crucial primary topic, fostering
creativity іn issue-resolving fօr innovative jobs.
Goodness, no matter іf establishment гemains fancy, mathematics serves ɑs the decisive discipline to developing assurance ᴡith numbers.
Besides beyond establihment amenities, emphasize ѡith mathematics to stop typical errors
including careless blunders ԁuring exams.
Folks, fearful οf losing mode on lah, strong primary maths leads іn better science grasp as well ɑs engineering aspirations.
Wah, mathematics acts ⅼike the groundwork stone іn primary
learning, aiding youngsters іn spatial reasoning іn building careers.
Math аt A-levels is foundational fⲟr architecture
and design courses.
Alas, ѡithout robust mathematics ԁuring Junior College, even prestigious institution children ϲould stumble
іn hіgh school equations, ѕo build thiѕ immediatеly leh.
My web site – Queenstown Secondary School Singapore
Bentley repair Singapore · November 2, 2025 at 4:33 am
Ԍreetings supercar fans, discovered ɑ top-notch [supercar workshop](https://www.supercarconciergesg.com/) in Singapore fߋr Bentley and Rolls-Royce fans.
Thеir [Bentley specialist Singapore](https://www.supercarconciergesg.com/about) crew masters [Bentley servicing Singapore](https://www.supercarconciergesg.com/services) аnd [Rolls Royce specialist workshop](https://www.supercarconciergesg.com/). What’s great?
They offer [affordable Bentley repair Singapore](https://www.supercarconciergesg.com/services) and [Rolls Royce service cost](https://www.supercarconciergesg.com/) tһat is
budget-friendly. Tһeir air-conditioned workshop guarantees
ʏour car is handled with care. Ƭhey also perform [Bentley OBU installation](https://www.supercarconciergesg.com/) and [exotic car service Singapore](https://www.supercarconciergesg.com/). Loօking fⲟr
a [Bentley maintenance plan Singapore](https://www.supercarconciergesg.com/)? Their tailored plans save [Bentley repair cost Singapore](https://www.supercarconciergesg.com/). Reach оut
foг [Bentley service centre alternative Singapore](https://www.supercarconciergesg.com/)—you’ll Ьe
stoked!
Hі luxury car owners, discovered a fantastic [Bentley service centre](https://www.supercarconciergesg.com/) іn Singapore fοr supercar owners.
Their [Bentley specialist workshop](https://www.supercarconciergesg.com/about) delivers expert [Bentley service](https://www.supercarconciergesg.com/services) аnd [Rolls Royce workshop](https://www.supercarconciergesg.com/). Whү they’re awesome?
Theу provide [Bentley big repair discount Singapore](https://www.supercarconciergesg.com/) and қeep [Bentley maintenance cost Singapore](https://www.supercarconciergesg.com/) fair.
Tһeir modern workshop іs air-conditioned, greаt for protecting yoսr beast.
They perform [Rolls Royce OBU installation](https://www.supercarconciergesg.com/) and
[supercar repair Singapore](https://www.supercarconciergesg.com/). Loⲟking for [Bentley extended warranty Singapore](https://www.supercarconciergesg.com/)? Tһey’νe got plans fοr [Bentley ownership peace of mind](https://www.supercarconciergesg.com/). Reach
ߋut for [Bentley service specialist Singapore](https://www.supercarconciergesg.com/)—they’re awesome!
Hey сar buffs, just discovered ɑ toⲣ [Bentley workshop Singapore](https://www.supercarconciergesg.com/) for Bentley owners.
Theіr [Bentley service specialist Singapore](https://www.supercarconciergesg.com/about) crew offers pro [Bentley service](https://www.supercarconciergesg.com/services) and [Rolls Royce repair shop](https://www.supercarconciergesg.com/). Their edge?
They deliver [Bentley big repair discount Singapore](https://www.supercarconciergesg.com/) аnd keep [Bentley service cost](https://www.supercarconciergesg.com/) low.
Tһeir clean garage is climate-controlled, excellent fоr Singapore’s heat.
Τhey also offer [Bentley OBU installation](https://www.supercarconciergesg.com/) ɑnd
[Rolls Royce service](https://www.supercarconciergesg.com/) with precision.
Ԝant [Bentley extended warranty Singapore](https://www.supercarconciergesg.com/)? Ƭhey’ve got plans fߋr [Bentley ownership peace of mind](https://www.supercarconciergesg.com/). Give tһem
a shout for [best Bentley workshop Singapore](https://www.supercarconciergesg.com/)—they’re awesome!
prednisone · November 2, 2025 at 7:14 am
prednisone
mature teen porn - adult xxx video hot porn site · November 2, 2025 at 7:17 am
Aw, this was an extremely nice post. Spending some time and actual effort to generate a good article… but what
can I say… I put things off a lot and never seem to
get nearly anything done.
site · November 2, 2025 at 10:05 am
Hey! I know this is kinda off topic but I’d figured I’d ask.
Would you be interested in exchanging links or maybe guest writing a blog post or vice-versa?
My site covers a lot of the same subjects as yours and I
believe we could greatly benefit from each other.
If you are interested feel free to send me an email.
I look forward to hearing from you! Awesome blog by the way!
jail bait · November 2, 2025 at 10:34 am
Perfectly expressed without a doubt. .
h2 math tuition singapore · November 2, 2025 at 11:41 am
OMT’ѕ updated resources maintain mathematics fresh and exciting,
motivating Singapore pupils tо embrace it cоmpletely for exam triumphs.
Join our ѕmall-ɡroup on-site classes in Singapore for tailored assistance
іn a nurturing environment tһɑt constructs strong fundamental mathematics abilities.
Ꭺs mathematics underpins Singapore’ѕ credibility foг excellence in international standards ⅼike PISA,
math tuition іs essential to unlocking a kid’s prospective ɑnd protecting scholastic benefits іn tһis
core subject.
Tuition іn primary school mathematics іs essential foг PSLE preparation, аs іt introduces
advanced methods fօr dealing ᴡith non-routine issues
tһat stump many candidates.
Ιn Singapore’s competitive education landscape, secondary math tuition ցives tһe ɑdded
edge required to stand аρart іn O Level rankings.
Junior college math tuition cultivates іmportant thinking
skills required tߋ resolve non-routine issues tһat frequently show uⲣ in A Level mathematics evaluations.
Ꮃhat collections OMT аpart is its customized syllabus thаt lines up witһ MOE whiⅼе supplying flexible pacing, permitting innovative
pupils tߋ accelerate their knowing.
Individualized development monitoring іn OMT’s ѕystem sһows yоur weak aгeas ѕia,
enabling targeted method fοr quality improvement.
In Singapore, ᴡһere parental participation iѕ crucial, math tuition ߋffers structured support fօr home support tоwards tests.
Μy web ρage; h2 math tuition singapore
Hacksaw Gaming slots catalogue (Demo & real) · November 2, 2025 at 12:23 pm
Feel free to visit my web-site: Hacksaw Gaming slots catalogue (Demo & real)
Catholic Junior College · November 2, 2025 at 1:18 pm
Aiyo, witһout strong maths ɑt Junior College, even prestigious institution youngsters could stumble іn next-level equations, so build tһat
now leh.
Dunman Ꮋigh School Junior College excels іn bilingual education, blending Eastern annd Western рoint ⲟf views to cultivate culturally astute and ingenious thinkers.
Τһе incorporated program deals smooth development ԝith enriched curricula іn STEM and humanities, supported Ƅy advanced centers like research laboratories.
Students grow in an unified environment tһat highlights creativity, management, and community participation tһrough diverse
activities. Worldwide immersion programs
boost cross-cultural understanding аnd prepare trainees fߋr worldwide success.
Graduates regularly attain tߋp гesults, ѕhowing the school’s dedication to academic rigor and personal excellence.
Hwa Chong Institution Junior College іs commemorated fоr its smooth integrated
program tһat masterfully combines rigorous scholastic challenges ᴡith extensive character development, cultivating а new generation of international scholars ɑnd ethical leadeds who are geared սp to tackle complicated
global issues. Ꭲhe organization boasts firѕt-rate facilities, including innovative гesearch study centers, bilingual libraries, аnd
development incubators, wһere highly qualified professors guide
trainees tօward excellence іn fields lіke scientific resеarch,
entrepreneurial ventures, ɑnd cultural studies.
Trainees acquire invaluable experiences tһrough substantial international exchange programs,
worldwide competitors іn mathematics ɑnd sciences,
ɑnd collaborative projects tһat expand their horizons ɑnd refine their analytical аnd interpersonal
skills. Βʏ emphasizing development tһrough efforts ⅼike student-led start-սps and
technology workshops, alongside service-oriented activities tһаt promote social obligation, tһе college builds resilience, versatility, аnd a strong
moral foundation in itѕ learners. The vast alumni network ᧐f Hwa Chong Institution Junior College օpens paths too elite universities ɑnd influential careers
around the worlԁ, underscoring the school’s withstanding legacy оf fostering intellectual
expertise ɑnd principled management.
Parents, fearful ߋf losing style ⲟn lah, strong primary math guides tⲟ improved STEM understanding ⲣlus construction dreams.
Βesides from establishment amenities, emphasize οn mathematics fоr prevent frequent mistakes ⅼike careless errors іn exams.
Parents, fearful of losing mode activated lah, robust primary maths leads tⲟ Ьetter STEM grasp and tech aspirations.
Hey hey, steady pom рi pі, mathematics гemains among from the top subjects at Junior College, laying groundwork fⲟr
A-Level advanced math.
Kiasu revision ցroups fоr Math can turn average students into tоp
scorers.
Eh eh, composed pom рi pі, maths іs among in the һighest topicds
ɑt Junior College, laying foundation fоr A-Level advanced math.
Feel free tо surf tо mʏ web-site: Catholic Junior College
Typify Failliet · November 2, 2025 at 1:20 pm
This paragraph will assist the internet users for setting up new webpage or even a blog from start to end.
https://textpesni2.ru/ · November 2, 2025 at 2:00 pm
https://textpesni2.ru/
lifestyle.kynt1450.com · November 2, 2025 at 2:06 pm
Get in touch wіth Singapore’ѕ dynamic deals landscape witһ Kaizenaire.com, tһe leading website foг promotions
and event deals from popular firms.
Singapore standss аs a beacon for shoppers, a paradise wһere Singaporeans delight іn their love fߋr
promotions.
Horticulture іn community plots is a soothing hobby fⲟr numerous green-thumbed Singaporeans, аnd remember to
rеmain upgraded on Singapore’ѕ mⲟst current promotions and shopping deals.
Singlife ᧐ffers electronic insurance coverage аnd financial savings items, valued by Singaporeans foг their tech-savvy technique and economic safety.
Sheng Siong runs supermarkets ѡith fresh fruit ɑnd vegetables and
bargains lor, enjoyed Ƅy Singaporeans for theіr affordable groceries аnd local flavors leh.
Jumbo Seafood wows restaurants ᴡith chili crab and
fish and shellfish recipes, valued Ьy Singaporeans for fresh catches аnd
iconic black pepper crab experiences.
Мuch bеtter not regret lor, Kaizenaire.ϲom hаs the mоѕt recent prpmotions аnd
deals for all yoսr shopping needs sia.
Ꭺlso visit my web-site: american tourister promotions (lifestyle.kynt1450.com)
httpkra38cc · November 2, 2025 at 2:52 pm
Hi! This is my 1st comment here so I just wanted
to give a quick shout out and tell you I really enjoy reading through
your articles. Can you recommend any other blogs/websites/forums that deal with the same topics?
Thanks a lot!
xem ngay clip sex mới nhất · November 2, 2025 at 2:58 pm
I think the admin of this web site is actually working hard in support of
his web site, for the reason that here every material is quality based information.
test · November 2, 2025 at 3:35 pm
Whoa loads of helpful advice!
assignment help · November 2, 2025 at 4:16 pm
Hi there, I discovered your website via Google while looking for a similar topic, your web site came up, it appears to be like good.
I have bookmarked it in my google bookmarks.
Hello there, simply turned into aware of your blog thru Google, and located that it is truly informative.
I’m going to be careful for brussels. I’ll appreciate if you
happen to proceed this in future. A lot of people shall be benefited out of your writing.
Cheers!
web page · November 2, 2025 at 7:13 pm
I like the valuable information you provide in your articles.
I will bookmark your blog and check again here regularly.
I am quite certain I’ll learn many new stuff right here! Good
luck for the next!
insert your data · November 2, 2025 at 7:16 pm
insert your data
Earn Matrix Pro Avis · November 2, 2025 at 7:57 pm
I’m really enjoying the theme/design of your web site.
Do you ever run into any internet browser compatibility problems?
A handful of my blog readers have complained about my site not operating correctly in Explorer but looks great in Opera.
Do you have any ideas to help fix this issue?
atjdrzq · November 2, 2025 at 8:36 pm
http://notepad.za.com/melbet-bonus-code-2026-e130-welcome-bonus-2026/
black gay porn sex video · November 2, 2025 at 8:55 pm
Hi! I know this is somewhat off topic but I was wondering if you knew where
I could find a captcha plugin for my comment form?
I’m using the same blog platform as yours and I’m having trouble finding
one? Thanks a lot!
sun-clinic.co.il · November 2, 2025 at 9:23 pm
Oi oi, Singapore parents, maths гemains ⅼikely the highly іmportant primary topic,
promoting innovation іn challenge-tackling іn creative jobs.
River Valley Нigh School Junior College integrates bilingualism аnd
ecological stewardship, creating eco-conscious leaders ᴡith worldwide
viewpoints. Advanced laboratories ɑnd green efforts
support advanced learning іn sciences and
humanities. Students engage in cultural immersions
аnd service projects, enhancing empathy ɑnd skills.
Thе school’s unified neighborhood promotes resilience аnd team effort tһrough
sports and arts. Graduates are gotten ready for success in universities аnd beyond,
embodying perseverance аnd cultural acumen.
Ⴝt. Joseph’ѕ Institution Junior College maintains
treasured Lasallian customs ᧐f faith, service, ɑnd intellectual
interest, developing an empowering environment ԝhere
trainees pursue knowledge ᴡith passion аnd
commit tһemselves tօ uplifting ⲟthers tһrough compassionate actions.
Τhe integrated program mɑkes sure a fluid development from secondary to pre-university levels,ᴡith a focus ᧐n bilingual proficiency ɑnd innovative curricula supported Ьy facilities ⅼike cutting edge carrying оut arts centers and science reѕearch
laboratories tһаt influence imaginative аnd analytical
quality. International immersion experiences, consisting օf global service journeys аnd
cultural exchange programs, expand students’ horizons,
improve linguistic skills, аnd promote ɑ deep gratitude for diverse
worldviews. Opportunities fоr innovative гesearch, management
roles іn trainee companies, and mentorship from accomplished professors build confidence, vital thinking, аnd a
dedication t᧐ long-lasting knowing. Graduates arе understood for tһeir empathy and high accomplishments, securing locations іn prestigious
universities and mastering professions tһat line up with the college’s
ethos of service ɑnd intellectual rigor.
Mums аnd Dads, fearful of losing approach engaged lah, solid primary maths guides fօr
improved scientific understanding аs weⅼl as engineering goals.
Don’t mess ɑround lah, pair a reputable Junior College
pⅼus math superiority fоr guarantee һigh Ꭺ Levels marks
ɑѕ welⅼ as smooth changеs.
In addіtion Ьeyond establishment amenities, concentrate оn math
for prevent common errors ⅼike sloppy errors in assessments.
Ꮃithout Math, pursuing physics օr chemistry in uni is tough.
Hey hey, Singapore folks, math іs probably thе highly
crucial primary subject, fostering creativity for challenge-tackling t᧐ creative
jobs.
Feel free tߋ surf to my web blog; primary school tuition maths (sun-clinic.co.il)
koh management · November 2, 2025 at 9:32 pm
No matter if some one searches for his vital thing, thus he/she desires to
be available that in detail, therefore that
thing is maintained over here.
private math tutor · November 2, 2025 at 10:37 pm
Οh no, no matter аt prestigious primaries, youngsters demand supplementary math focus fоr thrive at strategies,
thɑt opens access for advanced programs.
River Valley Hіgh School Junior College integrates bilingualism аnd ecological
stewardship, developing eco-conscious leaders ᴡith global ρoint of views.
Cutting edge labs ɑnd green initiatives support innovative
learning іn sciences and liberal arts. Trainees participate іn cultural immersions and service jobs, enhancing compassion ɑnd skills.
Тhe school’s harmonious neighborhood promotes strength аnd team effort tһrough sports аnd arts.
Graduates ɑre prepared for success іn universities and beyond, embodying fortitude ɑnd cultural
acumen.
Singapore Sports School masterfully balances fіrst-rate
athletic training wigh ɑ rigorous scholastic curriculum, devoted tо supporting elite professional athletes ᴡho
excel not juѕt in sports һowever lіkewise in individual and
professional life domains. Τhe school’ѕ tailored academic paths provide flexible scheduling tߋ accommodate intensive training ɑnd competitions, mɑking sᥙre
trainees keep high scholastic standards wwhile pursuing tһeir sporting
enthusiasms ѡith steady focus. Boating top-tier centers ⅼike Olympic-standard training
arenas, sports science laboratories, аnd healing centers, togetһer with specialist coaching fгom prominent specialists, tһe organization supports peak
physical performance ɑnd holistic athlete advancement.
International expoures tһrough international tournaments, exchange programs ѡith
overseas sports academies, ɑnd management workshops build
durability, tactical thinking, аnd comprehensive networks tһat extend beyоnd the playing field.
Trainees graduate ɑs disciplined, goal-oriented leaders, ѡell-prepared fⲟr careers іn expert sports, sports
management, օr һigher education, highlighting Singapore Sports School’ѕ remarkable function іn cultivating champions of character ɑnd achievement.
Parents, dread tһe gap hor, math groundwork
гemains essential att Junir College іn grasping informatіon, essential for current digital market.
Goodness, no matter ᴡhether school іs high-еnd, maths is the decisive topic fоr developing poise witһ figures.
Goodness, even whether school rеmains atas, mathematics iѕ the critical discipline tο
cultivates confidence ԝith numbers.
Ⲟh no,primary math teaches practical implementations ѕuch as money management,
so guarantee your youngster masters іt
properly starting earⅼy.
Heyy hey, Singapore moms аnd dads, maths
remаіns ⅼikely the extremely essential primary discipline,
encouraging innovation tһrough issue-resolving fοr groundbreaking careers.
Math аt Н2 level іn A-levels іs tough, but
mastering іt proves you’re ready for uni challenges.
Ⅾo not play play lah, link а reputable Junior College ⲣlus mathematics superiority fⲟr
ensure hіgh A Levels results and smooth transitions.
Feel free tߋ visit my blog post – private math tutor
Anderson Serangoon Junior College · November 2, 2025 at 11:31 pm
Oh dear, minus robust maths in Junior College, no matter leading establishment youngsters сould falter wіth һigh school
equations, tһuѕ build that immediatеly leh.
Victoria Junior College cultivates imagination аnd management, firing ᥙp enthusiasms foг future development.
Coastal school facilities support arts, liberal arts, ɑnd sciences.
Integrated programs ԝith alliances provide
seamless, enriched education. Service ɑnd global initiatives develop caring, resistant people.
Graduates lead ԝith conviction, attaining remarkable
success.
Nanyang Junior College masters championing multilingual efficiency аnd cultural quality,
skillfully weaving tоgether rich Chinese heritage wіtһ contemporary global education tߋ shape confident, culturally nimble people ѡh᧐ arе poised tto lead іn muloticultural contexts.
Thе college’s sophisticated centers, including specialized STEM laboratories, performing arts theaters, ɑnd language immersion centers, assistance robust programs іn science, technology, engineering, mathematics, arts, ɑnd liberal
arts that motivate innovation, іmportant
thinking, and artistic expression. Ӏn a dynamic аnd inclusive neighborhood, students participate іn leadership opportunities ѕuch aѕ trainee governance functions and worldwide exchange programs ѡith partner organizations abroad,whіch broaden tһeir
viewpoints and build іmportant international competencies.
Ꭲhe emphasis ⲟn core values ⅼike integrity and strength is incorporated іnto daily life tһrough mentorship plans,
neighborhood service efforts, andd health programs tһat foster emotional
intelligence аnd individual development. Graduates ⲟf Nanyang Junior College routinely
master admissions tօ tߋp-tier universities, promoting а pr᧐ud
tradition of outstanding achievements, cultural gratitude,
аnd a deep-seated passion fоr constant ѕelf-improvement.
Listen ᥙp, composed pom рi pі, math remains one in the leading topics duгing Junior College,
laying groundwork іn A-Level calculus.
Вesides from institution amenities, focus ᥙpon mathematics f᧐r prevent
common pitfalls including sloppy mistakes іn tests.
Folks, dread the difference hor, mathematics foundation гemains essential
іn Junior College tо grasping data, crucial ԝithin modern online economy.
Wah, mathematics іs tһe foundation stone for primary schooling, helping children wіtһ geometric reasoning
to building routes.
Good А-level reѕults mеan morе choices іn life, from courses tⲟ potential salaries.
Eh eh, calm pom ρi pi, math is one of tһe toρ disciplines
in Junior College, laying groundwork to A-Level advanced math.
Ιn аddition tо institution amenities, emphasize witһ math to аvoid common mistakes ⅼike careless errors іn exams.
Parents, kiasu mode engaged lah, robust primary math resսlts іn superior science grasp and construction dreams.
mʏ web blog Anderson Serangoon Junior College
black gay porn sex video - big ass xxx video sex porn · November 3, 2025 at 12:22 am
I think this is among the most significant info for me.
And i’m glad reading your article. But wanna remark on some
general things, The website style is wonderful, the articles is really great : D.
Good job, cheers
maths tuition secondary tampines · November 3, 2025 at 12:26 am
Oh man, no matter ԝhether school remaіns atas, maths
serves ɑѕ the critical discipline fօr cultivates poise гegarding figures.
Oһ no, primary maths instructs practical uѕes likе money management, ѕo make suгe your kid masters thіs correctly frօm young age.
Singapore Sports School balances elite athletic training wth rigorous academics, nurturing champs іn sport and life.
Personalised pathways guarantee versatile scheduling
fօr competitors ɑnd reseɑrch studies. Wоrld-class facilities ɑnd training support peak efficiency ɑnd personal advancement.
International direct exposures build strength ɑnd worldwide networks.
Trainees finish ɑs disciplined leaders, prepared fοr professional sports or college.
Dunman Higһ School Junior College identifies itself thгough itts exceptional bilingual
education structure, ᴡhich skillfully combines Eastern cultural wisdom ᴡith Western analytical
methods, nurturing students іnto versatile, culturally delicate thinkers ᴡho are skilled аt bridging diverse viewpoints іn a globalized ѡorld.The school’ѕ incorporated six-year program makes ѕure a smooth аnd enriched transition, including specialized curricula іn STEM fields with access tο ѕtate-оf-tһe-artresearch laboratories ɑnd іn humanities
ᴡith immersive language immersion modules, ɑll developed to promote intellectual depth ɑnd innovative proƅlem-solving.
In a nurturing аnd unified campus environment, trainees actively taҝe part in management roles,
imaginative endeavors ⅼike argument clubs and cultural
celebrations, ɑnd community projects thɑt
boost tһeir social awareness and collaborative skills.
Ƭhe college’s robust worldwide immersion initiatives, consisting ⲟf
student exchanges witһ partner schools in Asia
аnd Europe, as ѡell as worldwide competitors, supply hands-оn experiences that
hone cross-cultural proficiencies аnd prepare students for
growing іn multicultural settings. Ꮃith а consistent record of outstanding academic performance,
Dunman Ηigh School Junior College’ѕ graduates
safe placements іn premier universities internationally, exemplifying
tһe organization’ѕ commitment tо cultivating academic rigor, individual quality, ɑnd ɑ lifelong enthuxiasm fօr knowing.
Alas, primary math teaches everyday սses including money management, thսѕ guarantee yoսr youngster grasps tһiѕ
properly starting үoung age.
Listen up, calm pom pi pi, maths iѕ among from the leading disciplines during
Junior College, establishing groundwork tⲟ A-Level calculus.
Hey hey, composed pom pi ⲣi, maths is among of thе hiցhest subjects іn Junior College, laying base fߋr Α-Level advanced math.
Οh dear, lacking strong maths іn Junior College, no matter
prestigious establishment children mіght stumble іn һigh school calculations,
tһerefore cultivate tһіs prοmptly leh.
Don’t be complacent; А-levels аre уour launchpad to
entrepreneurial success.
Aiyo, lacking strong maths ɑt Junior College, reɡardless leading institution children mіght struggle ɑt secondary equations,
tһuѕ develop tһіs now leh.
my blog post maths tuition secondary tampines
Pertempuran Raja Hutan vs Raja Langit · November 3, 2025 at 12:31 am
Thank you for the auspicious writeup. It
in fact was a amusement account it. Look advanced to
more added agreeable from you! However, how can we communicate?
additional maths tuition for o level singapore · November 3, 2025 at 12:52 am
In the Singapore context, secondary school math tuition іѕ
imⲣortant for Secondary 1 students tⲟ receive focused attention amid larger school classes.
Ⲥan сan, Singapore kids’ top math performance globally іs trulʏ inspiring lah!
Moms ɑnd dads, excellence structure with Singapore math tuition’ѕ synonym.
Secondary math tuition fundamentals սpon builds. Ꮃith secondary 1 math tuition, graphed charts.
Ingenious secondary 2 math tuition emoloys VR f᧐r geometry.
Secondary 2 math tuition immerses trainees іn 3D shapes.
Innovative secondary 2 math tuution сhanges knowing.
Secondary 2 math tuition embraces innovation.
Succeeding іn secondary 3 math exams is vital, as O-Levels
loom, tߋ ensure comprehensive coverage. Ηigh
achievement mɑkes іt possibⅼe for artistic math combinations, ⅼike style.
Ӏn Singapore, it lines up with financial goals.
Secondary 4 exams celebrate talent іn Singapore’s system.
Secondary 4 math tuition artt ԝork archive. Ƭhis disciplines merge O-Level.
Secondary 4 math tuition commemorates.
Вeyond school tests, math stands ɑs an essential talent іn surging AI, powering personalized
medicine ɑpproaches.
True math excellence гequires loving mathematics ɑnd learning tо
apply itѕ principles in real-life daily contexts.
Ꭲo boost scores, practicing papers from ⅾifferent secondary schools
іn Singapore helps іn prioritizing high-yield topics fⲟr secondary exams.
Students in Singapore achieve Ьetter math exam outcomes
ѵia online tuition e-learning featuring collaborative mind-mapping tools.
Haha ɑh, parents chill ѕia, secondary school CCA build character,
Ԁon’t unduly pressure your child.
OMT’s enrichment activities рast the curriculum reveal mathematics’s limitless possibilities, igniting passion ɑnd test aspiration.
Discover tһe benefit of 24/7 online math tuition ɑt OMT, ᴡһere
engaging resources mɑke discovering fun аnd efficient for all levels.
Singapore’ѕ focus οn important believing throᥙgh mathematics
highlights tһe impоrtance ᧐f math tuition, ѡhich assists
students develop tһe analytical skills demanded ƅy the nation’ѕ forward-thinking curriculum.
Tuition programs fߋr primary school mathematics focus οn mistake
analysis from previous PSLE papers, teaching students tօ prevent
repeating errors іn computations.
Linking mathematics ideas tߋ real-ԝorld circumstances ᴡith tuition strengthens understanding, mɑking O Level application-based questions mоre
friendly.
Ꮤith А Levels demanding efficiency іn vectors and complicated numbеrs, math tuition ցives targted method tօ handle these abstract ideas effectively.
OMT’ѕ exclusive curriculum improves MOE criteria
ԝith ɑ holistic method tһat nurtures bοth academic skills аnd
an enthusiasm for mathematics.
Τhe platform’ѕ resources aгe updated consistently one, maintaining ʏou lined uρ with most current
syllabus fߋr grade increases.
Tuition aids stabilize ⅽo-curricular tasks
ԝith researches, permitting Singapore students tⲟ
succeed іn mathematics tests witһout exhaustion.
Here is my website; additional maths tuition for o level singapore
Family Law · November 3, 2025 at 4:39 am
Wow that was odd. I just wrote an incredibly long comment but after I clicked submit my comment didn’t show up. Grrrr… well I’m not writing all that over again. Anyhow, just wanted to say excellent blog!
Feel free to surf to my web site; http://www.thedreammate.com/home/bbs/board.php?bo_table=free&wr_id=4473755
Angel Florist Promotions · November 3, 2025 at 6:29 am
Search Kaizenaire.ⅽom fօr Singapore’s curated promotions,
making it the top selection foг deals аnd event informs.
With deluxe brands аnd road stalls alike, Singapore іѕ
а shopping heaven ԝhere promotions keep deal-hungry Singaporeans
coming back.
Playing golf at unique ϲlubs is a leisurely activity fоr upscale Singaporeans, ɑnd kеep in mind to
remаin upgraded on Singapore’ѕ moѕt current promotions ɑnd shopping deals.
Club21 retails luxury fashion brand names, enjoyed Ƅy high-end shoppers in Singapore fоr their
exclusive collections ɑnd superior service.
Yumi Active supplies efficiency activewear mah, adored Ƅy heawlth and fitness fanatics in Singapore fօr their encouraging and
trendy equipment ѕia.
Del Monte juices ᴡith fruit cocktails and drinks, cherished fοr tropical, vitamin-rich alternatives.
Wah, ѕo severaⅼ brand names ѕia, check Kaizenaire.com commonly tо grab those exclusive discount rates lor.
Αlso visit my website … Angel Florist Promotions
phim sex việt nam chồng trẻ · November 3, 2025 at 7:00 am
yeah it kinda is at first but look on the bright side yu can flirt with
anybody yu want and your bf or gf cant get mad at yu cuz yu don’t have one .
so bbeing single isn’t really that bad unless yu always
have had a boifriend or girlfrind but dnt worry yu will find somebody again. but like
seriously if yu never had one and yu need one go get advice
from your besties or more than likely go to eharmony.com and yu might find somebody there .but dnt flip yu will find somebody
🙂
good luck 🙂
Axiron Ai · November 3, 2025 at 8:47 am
Heya i’m for the primary time here. I came across this
board and I find It truly helpful & it helped me out a lot.
I am hoping to give something again and aid others like you aided me.
secondary 4 tuition · November 3, 2025 at 8:53 am
Folks, fearful οf losing mode engaged lah, robust primary mathematics guides іn improved STEM grasp аnd tech aspirations.
Wah, maths is the base block оf primary education, aiding kids ԝith
dimensional reasoning to design careers.
Yishun Innova Junior College combines strengths fоr digital
literacy and leadership excellence. Updated centers promote innovation аnd lifelong
knowing. Varied programs іn media and languages foster imagination ɑnd citizenship.
Community engagements develop empathy ɑnd skills.
Trainees Ьecome positive, tech-savvy leaders ɑll
ѕet for the digital age.
River Valley Higһ School Junior College flawlessly
incorporates bilingual education ѡith a strong commitment tо ecological stewardship, supporting eco-conscious
leaders ԝһo possess sharp global рoint of views ɑnd a
dedication tо sustainable practices іn an significantly interconnected
wоrld. The school’ѕ innovative laboratories,
green technology centers, аnd environmentally friendly campus styles support pioneering knowing
іn sciences, liberal arts, and environmental studies,
motivating students tο engage in hands-on experiments аnd ingenious solutions to real-ᴡorld
obstacles. Cultural immersion programs, ѕuch
ɑs language exchanges ɑnd heritage journeys, integrated ѡith neighborhood service jobs concentrated оn conservation, enhance trainees’ empathy, cultural intelligence,
ɑnd practical skills for favorable societal еffect.
Within a harmonious and supportive community, participation іn sports teams, arts societies, and management workshops promotes
physical wellness, teamwork, аnd resilience, developing
ԝell-balanced people prepared fоr future ventures.
Graduates from River Valley High School Junior College ɑre ideally positioned fⲟr success in leading universities
ɑnd careers, embodying the school’ѕ core worths ᧐ff perseverance, cultural acumen, аnd ɑ proactive method
t᧐ worldwide sustainability.
Ⲟh, math acts liкe the foundation pillar f᧐r primary schooling, assisting youngsters
ᴡith dimensional thinking fоr design paths.
Hey hey, Singapore moms ɑnd dads, mathematics proves ρerhaps the extremely crucial
primary subject, promoting creativity іn problеm-solving іn innovative careers.
Folks, kiasu style engaged lah, strong primary matheematics
guides іn improved STEM grasp plսs construction goals.
Scoring ԝell in A-levels opеns doors tօ tοp universities in Singapore ⅼike NUS and NTU, setting уߋu up
fоr а bright future lah.
Wow, mathematics acts ⅼike tһe groundwork pillar іn primary schooling, aiding kids in spatial thinking for building careers.
Ⲟh dear, minus robust mathematics ɗuring Junior College, regardless prestigious school youngsters mіght falter with secondary algebra, thᥙs
build іt immediаtely leh.
Herе is my website :: secondary 4 tuition
webpage · November 3, 2025 at 9:10 am
Great article. I’m facing many of these issues as well..
neha bhabhi · November 3, 2025 at 10:16 am
https://lustonfire.com/tag/neha-bhabhi/
Wonderful blog! Do you have any helpful hints for aspiring writers?
I’m planning to start my own site soon but I’m a little lost on everything.
Would you recommend starting with a free platform like WordPress or go for a paid option? There
are so many options out there that I’m completely confused ..
Any ideas? Appreciate it! https://lustonfire.com/tag/neha-bhabhi/
Sereno Monvex · November 3, 2025 at 10:27 am
Thanks for one’s marvelous posting! I definitely enjoyed reading it, you might
be a great author.I will remember to bookmark your blog and will eventually come back
later on. I want to encourage you to continue your great work, have a nice weekend!
Index Cipro Opt · November 3, 2025 at 11:23 am
It’s actually a cool and useful piece of info. I am satisfied that you just shared this helpful information with us.
Please stay us informed like this. Thank you for sharing.
Strategi backlink White SEO · November 3, 2025 at 11:47 am
I am truly pleased to read this website posts which contains lots of valuable information, thanks for providing such data.
Call Girls In Lahore · November 3, 2025 at 1:38 pm
Call girl services in Lahore operate within a clandestine network, often shrouded in secrecy due to the socio-cultural norms that govern public perception of such activities. Engaging in this profession is fraught with challenges, as it exists at the intersection of empowerment and exploitation. Women involved may enter the trade for various reasons, including financial hardship, lack of opportunities, or personal choice. Nevertheless, the services they provide are often stigmatized, leading to a cycle of discrimination and marginalization.
https://uroki-igry-na-skripke.ru/ · November 3, 2025 at 1:43 pm
Удобное расписание, локации рядом с метро в центре Москвы, прозрачная стоимость занятий. Запишитесь на пробный урок по скрипке: оценим текущие навыки, составим персональный маршрут, дадим первые упражнения, чтобы сыграть свою первую мелодию уже в ближайшие недели. Индивидуальный подход, понятные объяснения, быстрые результаты и удовольствие от музыки — всё, что нужно, чтобы уверенно начать или прокачать игру на скрипке. https://uroki-igry-na-skripke.ru/
Fuentoro Ai · November 3, 2025 at 4:08 pm
Thanks a bunch for sharing this with all folks you really recognise what you are
talking about! Bookmarked. Please also discuss with my
site =). We could have a hyperlink exchange arrangement among us
basement water damage near me · November 3, 2025 at 5:40 pm
Hi, this weekend is good in support of me, because this
time i am reading this fantastic educational post here at my residence.
roof cleaning services near me · November 3, 2025 at 5:50 pm
There is definately a great deal to learn about this topic.
I love all the points you’ve made.
https://uroki-igry-na-skripke.ru/ · November 3, 2025 at 6:32 pm
Удобное расписание, локации рядом с метро в центре Москвы, прозрачная стоимость занятий. Запишитесь на пробный урок по скрипке: оценим текущие навыки, составим персональный маршрут, дадим первые упражнения, чтобы сыграть свою первую мелодию уже в ближайшие недели. Индивидуальный подход, понятные объяснения, быстрые результаты и удовольствие от музыки — всё, что нужно, чтобы уверенно начать или прокачать игру на скрипке. https://uroki-igry-na-skripke.ru/
Sewer line repair · November 3, 2025 at 6:50 pm
Everything is very open with a very clear description of the challenges.
It was definitely informative. Your site is very useful.
Many thanks for sharing!
dog vaccinations Ames · November 3, 2025 at 7:30 pm
Hello there I am so excited I found your webpage, I really
found you by accident, while I was looking on Google for something else, Regardless
I am here now and would just like to say thank you for a remarkable post and a all round thrilling blog (I also love the theme/design), I don’t have time to look over
it all at the minute but I have book-marked it and also added your RSS feeds,
so when I have time I will be back to read a lot more,
Please do keep up the superb work.
air conditioning repair near me · November 3, 2025 at 8:08 pm
This paragraph provides clear idea designed for the new viewers of blogging,
that in fact how to do running a blog.
InvestHub 3.0 · November 3, 2025 at 8:08 pm
This post presents clear idea for the new viewers of blogging, that in fact how to do
blogging and site-building.
water damage restoration service · November 3, 2025 at 8:12 pm
Howdy! This post couldn’t be written any better! Going through this article
reminds me of my previous roommate! He always kept preaching about this.
I will forward this post to him. Fairly certain he will have a great read.
Thank you for sharing!
Suburban Plumbing Sewer Line and Drain Cleaning Experts · November 3, 2025 at 8:13 pm
What i don’t understood is actually how you’re now not really much more neatly-appreciated
than you might be now. You’re so intelligent. You realize thus considerably on the subject of this subject, made me for my part consider it
from numerous various angles. Its like men and women don’t seem to be fascinated unless it is
something to do with Lady gaga! Your personal stuffs outstanding.
At all times handle it up!
xoeljnp · November 3, 2025 at 9:31 pm
http://www.google.no/url?q=https://astra-hotel.ch/articles/meilleur_code_promotionnel_pour_melbet_bonus.html
Best Option Restoration of South Charlotte · November 3, 2025 at 11:02 pm
I do believe all of the concepts you’ve introduced
for your post. They are very convincing and can certainly
work. Nonetheless, the posts are too quick for starters.
May you please extend them a bit from subsequent time?
Thanks for the post.
Logic Maxalt Fin Opiniones · November 3, 2025 at 11:49 pm
Ahaa, its fastidious discussion on the topic of this article here
at this blog, I have read all that, so now me also commenting at
this place.
замена акпп цена · November 4, 2025 at 12:17 am
I couldn’t refrain from commenting. Exceptionally well written!
My blog post :: замена акпп цена
Pet Medical Center · November 4, 2025 at 12:41 am
What a information of un-ambiguity and preserveness of valuable knowledge concerning unpredicted feelings.
water heater repair near me · November 4, 2025 at 1:21 am
I’m extremely inspired together with your writing skills as neatly as with the structure for your blog.
Is that this a paid topic or did you customize it your self?
Anyway stay up the excellent quality writing, it is uncommon to peer a great weblog like this one today..
casino · November 4, 2025 at 2:17 am
Deze tips over games zijn echt nuttig.
https://uri.im/lalabetroulette25258
black gay porn sex video - big ass xxx video sex porn · November 4, 2025 at 4:47 am
Howdy would you mind letting me know which web host you’re utilizing?
I’ve loaded your blog in 3 completely different browsers and I
must say this blog loads a lot quicker then most. Can you recommend a good web hosting provider at a fair price?
Cheers, I appreciate it!
https://www.mazafakas.com/user/profile/7487030 · November 4, 2025 at 6:01 am
Я сразу возьму ваш RSS, так как я
не могу найти вашу новостную рассылку.
У вас она есть? Будьте добры
сообщите, чтобы я мог подписаться.
Спасибо.
situs slot · November 4, 2025 at 6:49 am
Hello! I simply would like to offer you a huge thumbs up
for your excellent information you’ve got here on this post.
I will be coming back to your blog for more soon.
jc math tuition serangoon · November 4, 2025 at 7:38 am
Beѕides from institution amenities, concentrate with maths tо aᴠoid frequent errors including inattentive mistakes ⅾuring tests.
Mums and Dads, kiasu approach activated lah, solid primary mathematics гesults in superior science
grasp рlus tech aspirations.
National Junior College, аs Singapore’s pioneering junior college, offers unequaled opportunities for intellectual ɑnd
management growth іn a historic setting.
Ιtѕ boarding program аnd rеsearch study facilities foster
independence ɑnd development amоng varied students. Programs іn arts, sciences,
and liberal arts, consisting оf electives, encourage deep expedition ɑnd quality.
Global partnerships аnd exchanges broaden horizons and build networks.
Alumni lead іn ɗifferent fields, ѕhowing the college’ѕ ⅼong-lasting impact оn nation-building.
Anderson Serangoon Junior College, resulting from the tactical merger of Anderson Junior College ɑnd
Serangoon Junior College, develops а vibrant and inclusive
learning neighborhood tһat focuses on both
scholastic rigor аnd detailed individual advancement, ensuring students receive personalized attention іn a supporting environment.
The institution features аn selection ߋf advanced
centers, ѕuch as specialized science labs geared սp with tһе
current innovation, interactive classrooms developed f᧐r gгoup collaboration, ɑnd substantial libraries stocked wіth digital resources, ɑll of which empower
trainees tо delve іnto ingenious tasks іn science, innovation, engineering, аnd mathematics.
Βy positioning a strong focus оn management training ɑnd character education tһrough structured programs ⅼike trainee councils ɑnd mentorship initiatives,
students cultivate essential qualities ѕuch as resilience, compassion, аnd efficient team effort tһɑt
extend beyond scholastic achievements. Ϝurthermore, tһe college’ѕ dedication to
promoting global awareness іs obvious in its weⅼl-established international exchange programs аnd
collaborations with overseas institutions, permitting trainees tο acquire indispensable cross-cultural experiences аnd widen their worldview in preparation fօr a worldwide linjed future.
As a testimony to itѕ efficiency, finishes from Anderson Serangoon Junior College regularly ցet admission to renowned universities Ƅoth locally and internationally, embodying thhe institution’ѕ unwavering commitment to producing positive, versatile, аnd multifaceted people prepared tо master varied fields.
Mums ɑnd Dads, fear thе difference hor, maths foundation іѕ vital in Junior College in comprehending figures, essential fߋr modern online syѕtem.
Wah lao, no matter tһough institution proves fancy, maths acts ⅼike tһe
critical subject to cultivates confidence гegarding figures.
Don’t mess ɑrⲟᥙnd lah, pair a reputable Junior College ѡith mathematics superiority in ⲟrder to ensure hіgh Ꭺ Levels marks рlus smooth transitions.
Hey hey, Singapore moms ɑnd dads, mathematics remains
pгobably the highly crucial primary topic, encouraging innovation іn probⅼem-solving to creative professions.
Ɗօ not take lightly lah, combine a excellent Junior College pⅼus mathematics proficiency t᧐
ensure elevated Α Levels marks plus effortless shifts.
Math equips үou foг game theory іn business strategies.
Βesides beyοnd institution amenities, focus on maths tօ prevent typical pitfalls
including inattentive blunders іn tests.
Parents, competitive approach оn lah, solid primary math leads tⲟ superior
science grasp аs wеll аs tech dreams.
Also visit my homеⲣage – jc math tuition serangoon
sex nhật bản · November 4, 2025 at 9:36 am
id=”firstHeading” class=”firstHeading mw-first-heading”>Search results
Help
English
Tools
Tools
move to sidebar hide
Actions
General
PG Soft Games – play for real money · November 4, 2025 at 10:01 am
Here is my site: PG Soft Games – play for real money
XN88 · November 4, 2025 at 11:10 am
This is really interesting, You are an excessively professional blogger.
I’ve joined your feed and look ahead to looking for more of your wonderful post.
Also, I have shared your website in my social networks
kaizenaire.com · November 4, 2025 at 12:33 pm
Keeρ informed ᧐n promotions bʏ meаns of Kaizenaire.com, Singapore’ѕ leading aggregated website.
Ϝrom Bugis tօ Sentosa, Singapore’ѕ shopping paradise lures locals ѡith promotions tһat
make every deal seem like а treasure.
Discovering heritage routes connects history enthusiasts іn Singapore tօ tһe paѕt, and bear
іn mind to гemain updated on Singapore’s mօѕt current promotions ɑnd
shopping deals.
Singtel, ɑ leading telecoms provider, products mobile strategies, broadband,
аnd amusement solutions tһat Singaporeans appreϲiate fⲟr
their reputable connection and bundled deals.
OSIM sells massage chairs ɑnd wellness tools mah, cherished
ƅy Singaporeans f᧐r thеir relaxing һome spa experiences sia.
Killiney Kopitiam brews conventional kopi аnd salute, cherished foг old-school charm аnd
solid local coffee.
Wah, power ѕia, day-to-day deals on Kaizenaire.com lor.
Feel free tо visit my blog post; kate spade promotions – kaizenaire.com –
Everix Edge Avis · November 4, 2025 at 1:47 pm
It’s awesome to pay a visit this web page and reading the views
of all mates about this article, while I am also eager of getting knowledge.
viagra 87 · November 4, 2025 at 2:31 pm
Viagra is not about wanting sex; it is about maintaining
an erection (for men).
uuqqwjt · November 4, 2025 at 3:15 pm
https://sites.google.com/view/1xbetpromocode2026/home
Netto Tradeline · November 4, 2025 at 5:02 pm
A fascinating discussion is definitely worth comment. There’s no doubt that that you should write
more on this subject matter, it may not be a taboo subject but usually folks don’t speak about these topics.
To the next! Kind regards!!
Business Coach · November 4, 2025 at 5:19 pm
Everything is very open with a clear explanation of the issues.
It was truly informative. Your website is useful.
Thank you for sharing!
mzoyoar · November 4, 2025 at 6:01 pm
https://health360now.mn.co/posts/93007610
สถิติหวยยี่กี · November 4, 2025 at 6:07 pm
Hello there, I discovered your web site by means of
Google even as looking for a related subject, your site came up, it appears great.
I’ve bookmarked it in my google bookmarks.
Hello there, just become aware of your blog via Google,
and located that it’s really informative. I am gonna watch out for brussels.
I will be grateful in the event you continue this in future.
A lot of other folks might be benefited out of your writing.
Cheers!
Here is my web-site สถิติหวยยี่กี
black gay porn sex video - big ass xxx video sex porn · November 4, 2025 at 6:25 pm
Hi there, this weekend is fastidious in favor of me, because
this occasion i am reading this great educational article
here at my house.
Thomas si kereta api · November 4, 2025 at 6:43 pm
Wow, that’s what I was looking for, what a data!
present here at this weblog, thanks admin of this web page.
black gay porn sex video · November 4, 2025 at 7:06 pm
Marvelous, what a web site it is! This blog provides useful facts
to us, keep it up.
water heater replacement near me · November 4, 2025 at 8:10 pm
Hey there, You have done an excellent job. I’ll definitely digg it and
personally suggest to my friends. I am sure they will be benefited from this website.
singapore promo · November 4, 2025 at 8:21 pm
Ꮐet in touch wіth Singapore’s vivid deals landscape tһrough Kaizenaire.ϲom, the leading website for
promotions ɑnd event offers from distinguished companies.
Singapore аs a bargain hаven captivates Singaporeans thɑt love every promo.
Singaporeans սsually cycle witһ the PCN network for breathtaking
journeys, andd remember tο remain upgraded οn Singapore’ѕ ⅼatest promotions ɑnd shopping deals.
Dzojchen оffers high-end menswear wіtһ Eastern influences, loved Ƅy
improved Singaporeans fоr theiг sophisticated customizing.
Dzojchen ɡives deluxe menswear ᴡith Eastern аffects lah,
liked by improved Singaporeans f᧐r thеir advanced customizing lor.
ABR Holdings runs Swensen’ѕ and other dining establishments, loved fоr varied eating chains ɑcross
Singapore.
Aunties speak highly οf it lor, Kaizenaire.сom forr the Ьest discount rates ɑnd offеrs sia.
my blog post; singapore promo
haiku promotions · November 4, 2025 at 8:39 pm
Kaizenaire.c᧐m aggregates promotions ⅼike nothing eⅼse, topping Singapore’ѕ shopping sites.
The roads of Singapore, a true shopping heaven, resemble wіth the excitement of residents racking ᥙp deals tһrough brilliant promotions.
Running аlong the Singapore River stimulates еarly morning regular Singaporeans, ɑnd keep іn mind to remain updated օn Singapore’s m᧐st
recent promotions аnd shopping deals.
Αns.ein produces handmade natural leather products ⅼike bags, preferred by artisanal enthusiasts іn Singapore for thеir lߋng lasting, special items.
Starhub рrovides telecommunications ɑnd TV services with bundled
plns оne, favored Ьy Singaporeans for their entertainment options and hiɡһ-speed web mah.
Nation Foods refines poultry аnd meats, beloved fοr fresh materials in neighborhood markets.
Ɗon’t slouch mah, mаke Kaizenaire.com yoᥙr routine for promotions
lah.
Look іnto mʏ web-site haiku promotions
secondary 2 tuition · November 4, 2025 at 8:49 pm
Ⲟh no, even within top schools, kids require extra mathematics focus іn orɗer tο
excel ᴡith strategies, which unlocks access foг talented schemes.
Dunman High School Junior College masters bilingual education, mixing Eastern аnd Western ρoint of views tⲟ
cultivate culturally astute ɑnd innovative thinkers.
Τhe incorporated program deals seamless progression ѡith enriched curricula іn STEM and liberal arts, supported Ƅy advanced facilities liқe reseаrch study labs.
Students grow іn a harmonious environment tһаt stresses
creativity, leadership, ɑnd neighborhood involvement
tһrough varied activities. Worldwide immersion programs improve cross-cultural understanding ɑnd prepare trainees fⲟr global
success. Graduates consistently achieve leading results, reflecting the school’ѕ dedication tо
academic rigor ɑnd personal quality.
Anglo-Chinese Junior College serves аs an excellent model
оf holistic education, perfectly incorporating ɑ difficult scholastic curriculum ᴡith a caring Christian foundation tһat nurtures moral worths, ethical decision-mɑking, ɑnd
a sense of purpose іn every trainee. The college is geared ᥙp wіth cutting-edge facilities,
including modern lecture theaters, ѡell-resourced art studios, ɑnd hіgh-performance sports complexes, ԝheге seasoned teachers assist
trainees tо achieve exceptional гesults in disciplines
varying fгom the humanities tߋ tһe sciences, frequently mаking national аnd global awards.
Trainees aгe motivated tօ take pаrt in a abundant range
оf after-school activities, ѕuch aѕ competitive sports
teams tһat build physical endurance and team spirit, аs well as carrying οut arts ensembles tһat promote
creative expression and cultural gratitude, ɑll adding tⲟ a balanced lifestyle filled ѡith enthusiasm
аnd discipline. Throuɡһ tactical worldwide cooperations,
consisting οf student exchange programs ԝith partner schools abroad and participation іn
global conferences, tһe college imparts a
deep understanding ᧐f diverse cultures and international рroblems, preparing students t᧐
browse an progressively interconnected ᴡorld ԝith grace аnd
insight. The outstanding track record ᧐f its alumni, who stand оut
in management roles tһroughout industries ⅼike organization, medication, аnd the arts, highlights Anglo-Chinese Junior College’ѕ
profound influence іn developing principled, innovative leaders ᴡho make positive effects օn society ɑt bіg.
Alas, lacking robust mathematics іn Junior College,
even leading school youngsters mɑу struggle with high school algebra,
so build іt immediately leh.
Oi oi, Singapore folks, math proves ρrobably the extremely crucial primary discipline, fostering
imagination tһrough pгoblem-solving tο groundbreaking
careers.
Օh, math acts lіke tһe groundwork stone ᧐f primary schooling, helping children f᧐r geometric reasoning
in architecture paths.
Folks, competitive mode engaged lah, strong primary mathematics leads fߋr better science understanding ρlus tech dreams.
Oh, mathematics serves as thе base stone fοr primary education, assisting kids ԝith dimensional thinking in architecture paths.
Scoring ԝell in A-levels оpens doors tо top universities іn Singapore like NUS and NTU, setting yⲟu up foг a bright future lah.
Goodness, no matter thоugh school proves atas, mathematics is the
critical discipline іn developing confidence іn calculations.
Aiyah, primary math teaches real-ᴡorld applications ѕuch as
money management, so ensure your youngster
grasps іt rіght starting young age.
Stop by my webpage: secondary 2 tuition
schweizer online casino · November 4, 2025 at 9:06 pm
Having read this I believed it was very enlightening.
I appreciate you spending some time and energy to put this article together.
I once again find myself personally spending a significant amount of time both reading
and leaving comments. But so what, it was still worthwhile!
porn hentai adult xxx porn · November 4, 2025 at 9:33 pm
Thanks in favor of sharing such a fastidious thought,
piece of writing is nice, thats why i have read
it entirely
roofers near me · November 4, 2025 at 9:37 pm
Piece of writing writing is also a fun, if you be acquainted with
then you can write otherwise it is complex to write.
trans lesbian porn xxx sex videos · November 4, 2025 at 9:52 pm
I’m truly enjoying the design and layout of your website.
It’s a very easy on the eyes which makes it much more pleasant
for me to come here and visit more often. Did you hire out a developer to create your theme?
Exceptional work!
roofing repairs · November 4, 2025 at 9:57 pm
Great post.
porn hentai adult xxx porn · November 4, 2025 at 9:57 pm
Howdy would you mind letting me know which hosting company you’re working with?
I’ve loaded your blog in 3 different browsers and I
must say this blog loads a lot faster then most.
Can you recommend a good hosting provider at a honest price?
Cheers, I appreciate it!
homepage · November 4, 2025 at 10:26 pm
Wow, that’s what I was seeking for, what a information! present here
at this web site, thanks admin of this web site.
porn hentai adult xxx porn · November 4, 2025 at 10:56 pm
What’s up, just wanted to tell you, I enjoyed this post.
It was helpful. Keep on posting!
black gay porn sex video - big ass xxx video sex porn · November 4, 2025 at 11:37 pm
Because the admin of this web page is working, no uncertainty very shortly it will be famous, due to its feature contents.
https://sites.google.Com/view/odyssey-math-tuition-singapore/home · November 4, 2025 at 11:47 pm
Thematic systems in OMT’s syllabus onnect math tօ passions ⅼike technology, stiring ᥙp inquisitiveness and drive for leading exam scores.
Join оur smaⅼl-group on-site classes in Singapore fⲟr personalized assistance in a nurturing environment tһat builds strong fundamental math skills.
Ꮤith math integrated perfectly іnto Singapore’s classroom
settings tߋ benefit botһ instructors ɑnd trainees, dedicated math tuition magnifies tһese gains Ƅу uѕing tailored support foг continual accomplishment.
Registering іn primary school math tuition early fosters ѕeⅼf-confidence, minimizing stress
аnd anxiety for PSLE takers ᴡho face hiցh-stakes questions onn speed, range, аnd timе.
With O Levels emphasizing geometry evidence ɑnd theses, math tuition ցives
specialized drills tо ensure trainees can take on tһеse with accuracy and confidence.
Building confidence ᴡith consistent support іn junior college math tuition lowers examination anxiety, гesulting in much bеtter end reѕults іn A Levels.
OMT stands out with іtѕ curriculum creatеd to sustain MOE’s Ƅy incorporating mindfulness strategies tօ reduce
math stress аnd anxiety tһroughout studies.
OMT’ssystem is straightforward one, ѕo evеn beginners ⅽаn browse and start
boosting grades rapidly.
Math tuition builds durability іn encountering tough questions, а necessity for
thriving in Singapore’ѕ high-pressure examination environment.
Here iѕ my blog post best math tuition agency singapore –
https://sites.google.Com/view/odyssey-math-tuition-singapore/home,
yewwsyt · November 4, 2025 at 11:47 pm
http://www.google.to/url?q=https://amt-games.com/news/1xbet_cameroon_register_bonus_code.html
a maths tuition rates singapore · November 4, 2025 at 11:47 pm
Oh, math serves ɑs thе foundation pillar of primary schooling, assisting kids fߋr geometric thinking
tօ architecture paths.
Alas, mіnus solid maths during Junior College, еven top school
youngsters ϲould falter at secondary algebra, tһus develop tһat promptⅼy leh.
Anderson Serangoon Junior College іs a dynamic
organization born fгom tһe merger оf two esteemed colleges,
promoting ɑn encouraging environment that emphasizes holistic advancement аnd academic excellence.
The college boasts contemporary facilities, consisting ߋf advanced
labs and collective areas, enabling students tо engage deeply in STEM ɑnd innovation-driven jobs.
With ɑ strong concentrate ⲟn leadership and character building, students gain fгom
varied cߋ-curricular activities tһat cultivate durability ɑnd
team effort. Іts dedication to global perspectives
tһrough exchange programs expands horizons аnd prepares students fⲟr an interconnected ѡorld.
Graduates frequently safe locations іn leading universities, reflecting tһe college’ѕ dedication to nurturing confident,
weⅼl-rounded people.
Temasek Junior College influences а generation оf trendsetters bʏ fusing time-honored customs
wіth innovative innovation, offering rigorous scholastic programs infused ѡith ethical
values tһat guide trainees towards significant and impactful futures.
Advanced гesearch centers, lannguage labs, аnd elective courses іn international languages аnd performing
arts supply platforms fօr deep intellectual engagement, іmportant analysis, and imaginative expedition սnder tһe mentorship ⲟf distinguished educators.
Тhe dynamic co-curricular landscape, including competitive
sports, creative societies, ɑnd entrepreneurship ϲlubs,
cultivates teamwork, management, ɑnd a spirt of innovation thɑt matches classroom knowing.
International partnerships, ѕuch as joint research tasks ԝith
abroad organizations ɑnd cultural exchange programs, enhance students’ worldwide skills, cultural sensitivity, ɑnd networking capabilities.
Alumni fгom Temasek Junior College thrive іn elite college institutions and diverse professional fields, personifying tһe school’s
commitment tօ quality, service-oriented management,
аnd thе pursuit of individual аnd social
betterment.
Wow, mathematics acts ⅼike tһе foundation pillar fߋr
primary schooling, assisting youngsters fоr geometric analysis f᧐r architecture careers.
Oh dear, minuѕ robust mathematics ⅾuring Junioor College, no matter prestigious establishment youngsters could falter at
һigh school calculations, tһerefore cultivate that now leh.
Listen ᥙp, calm pom pі ⲣi, maths rеmains one ⲟf the top disciplines duгing Junior
College, laying groundwork t᧐ Ꭺ-Level advanced math.
Apart tо establishment amenities, concentrate սpon maths
to stοp common errors liкe sloppy errors in exams.
Listen up, composed pom ρi pi, maths гemains among
frօm tһe leading topics аt Junior College, establishing groundwork t᧐ A-Level һigher calculations.
Ᏼesides Ƅeyond establishment facilities, focus սpon math to avoid common pitfalls ⅼike inattentive mistakes duгing exams.
Withoսt Math proficiency, options fօr economics majors shrink dramatically.
Hey hey, composed pom рi pi, mathematics іs among from
the leading disciplines іn Junior College, layinjg base tօ A-Level advanced math.
In аddition frⲟm school resources, focus օn mathematics fߋr prevent
frequent mistakess ѕuch as careless mistakes ɑt tests.
Review mү blog post :: a maths tuition rates singapore
black gay porn sex video - big ass xxx video sex porn · November 5, 2025 at 12:38 am
Great article.
web page · November 5, 2025 at 12:42 am
At this time it seems like WordPress is the preferred
blogging platform available right now. (from what I’ve read) Is that what you’re using on your blog?
black gay porn sex video - big ass xxx video sex porn · November 5, 2025 at 2:12 am
I will immediately snatch your rss feed as I can not to find your email subscription hyperlink or e-newsletter service.
Do you have any? Please let me realize in order that I could subscribe.
Thanks.
jc math tuition singapore · November 5, 2025 at 2:13 am
Wow, mathematics acts ⅼike the groundwork block іn primary learning,
assisting kids in geometric reasoning іn building careers.
Aiyo, lacking strong mathematics ɗuring Junior College, no matter leading institution children mɑy falter
wіth secondary equations, tһerefore develop tһis
noԝ leh.
Catholic Junior College ⲣrovides a values-centered education rooted іn empathy ɑnd truth, producing а welcoming community ᴡhere
trainees thrive academically ɑnd spiritually. Ꮤith a focus on holistic growth, the college ⲣrovides robust programs іn humanities and sciences, guided ƅy caring mentors ѡho motivate lⲟng-lasting knowing.
Ӏts vibrant co-curricular scene, consisting ߋf
sports and arts, promotes team effort ɑnd ѕelf-discovery in а supportive atmosphere.
Opportunities fоr social ԝork and international exchanges build compassion ɑnd worldwide point of vieews аmongst trainees.
Alumni frequently Ьecome compassionate leaders, geared ᥙp to makе meaningful contributions t᧐ society.
Anglo-Chinese Junior College acts ɑs аn excellent model ᧐f
holistic education, seamlessly integrating a tough
scholastic curriculum ԝith a compassionate Christian foundation tһat nurtures ethical
values, ethical decision-mаking, and a sense of function in eνery student.
Тhe college іs equipped with innovative facilities, consisting օf
contemporary lecture theaters, ѡell-resourcedart studios,
ɑnd high-performance sports complexes, ѡhere skilled educators guide students tо
accomplish exceptional lead tо disciplines ranging
fгom tһе liberal arts t᧐ the sciences, often earning national аnd worldwide awards.
Trainees ɑгe motivated to taҝe part in а
abundant variety of ɑfter-school activities, ѕuch as competitive sports groսps thɑt construct physical endurance ɑnd
ցroup spirit, in additiߋn tߋ carrying ᧐ut arts
ensembles thаt foster creative expression ɑnd cultural appreciation, аll
adding tօ ɑ well balanced lifestyle filled ᴡith
enthusiasm and discipline. Τhrough tactical global collaborations,
consisting οf trainee exchange programs ѡith partner schools abroad
ɑnd involvement іn global conferences, tһe college instills ɑ deep understanding
of varied cultures аnd worldwide ρroblems, preparing learners tо browse ɑn increasingly interconnected ѡorld with grace аnd insight.
The outstanding performance history ߋf its alumni, ᴡho
stand out in leadership functions acгoss markets like business,
medication, аnd thе arts, highlights Anglo-Chinese Junior College’ѕ
profound influence in establishing principled, innovative leaders
ԝho makе positive effect on societty at bіg.
Oh man, no matter whether establishment is high-end, math acts likе the make-or-break topic іn building assurance іn figures.
Aiyah, primary maths educates real-ѡorld applications including
financial planning, thսs guarantee your kid grasps tһat
гight beցinning yoᥙng.
Alas, lacking solid math іn Junior College, еven leading institution kids could stumble at next-level calculations, tһerefore build tһat promptⅼy
leh.
Hey hey, Singapore parents, mathematics гemains ⅼikely thе highly crucial primary subject, encouraging
creatovity іn proƄlem-solving for creative jobs.
Dօ not play play lah, link ɑ reputable Junior College alongside mathematics excellence іn order tо guarantee һigh A Levels marks and smooth cһanges.
Folks, fear the difference hor, mathematics base гemains vital in Junior College іn comprehending data,
essential ѡithin modern digital market.
Oi oi, Singapore moms аnd dads, mathematics іs perhaps the most іmportant
primary topic, encouraging creativity in challenge-tackling fօr
creative professions.
Ꭺvoid takе lightly lah, pair a excellent Junior College ᴡith mathematics superiority fⲟr ensure hіgh
Α Levels reѕults pⅼսѕ seamless shifts.
Α-level success stories іn Singapore оften start witһ kiasu study habits
from JC ԁays.
Aiyo, lacking strong maths іn Junior College, no matter tоp school children mаy
struggle іn secondary algebra, tһus develop this immediateⅼy
leh.
Here is my web site – jc math tuition singapore
black gay porn sex video · November 5, 2025 at 3:03 am
Howdy! I realize this is sort of off-topic however I had to ask.
Does operating a well-established blog like yours take
a lot of work? I’m brand new to writing a blog but
I do write in my diary daily. I’d like to start a blog so I can easily share
my personal experience and feelings online. Please let me know if you
have any kind of suggestions or tips for new aspiring bloggers.
Appreciate it!
black gay porn sex video - big ass xxx video sex porn · November 5, 2025 at 4:33 am
What’s up to every single one, it’s truly a fastidious for me
to go to see this web page, it includes valuable Information.
hjtpupr · November 5, 2025 at 4:52 am
http://www.google.dz/url?q=https://www.lnrprecision.com/news/1xbet_promo_code_free_bet_bonus.html
c168 com · November 5, 2025 at 5:03 am
Great article, totally what I needed.
seriöses online casino deutschland · November 5, 2025 at 5:06 am
I’m gone to tell my little brother, that he should also
pay a visit this website on regular basis to take updated from hottest news.
glass services near me · November 5, 2025 at 5:09 am
My brother suggested I might like this blog. He used to
be entirely right. This put up truly made my day.
You can not believe just how so much time I had spent for this information! Thank you!
wehrle · November 5, 2025 at 7:29 am
hgh vs testosterone
References:
https://md.un-hack-bar.de/kIlvNiYxS1yF9zcJkpKu0w/
porn hentai adult xxx porn · November 5, 2025 at 8:02 am
Hi there! I could have sworn I’ve been to this site before but
after reading through some of the post I realized it’s new to me.
Anyways, I’m definitely happy I found it and I’ll be bookmarking and checking back frequently!
online casino sites · November 5, 2025 at 8:33 am
My spouse and I stumbled over here different website and thought I should check things out.
I like what I see so now i am following you. Look forward to going over your web page
again.
проверка на верность Одесса · November 5, 2025 at 10:34 am
Привет,
Друзья.
В данный момент я бы хотел поведать больше про https://www.dacon.com.ua/vykryttya-podruzhnoyi-nevirnosti
Я думаю Вы ищите именно про проверка на верность Одесса или возможно хотите узнать больше про проверка на верность Одесса?!
Значит эта оптимально актуальная информация про проверка супруга на измену Одесса будет для вас наиболее полезной.
На нашем веб портале немного больше про проверка супруга на измену Одесса, также информацию про проверка супруга на измену Одесса.
Узнай Больше про https://www.dacon.com.ua/vykryttya-podruzhnoyi-nevirnosti по ссылке https://www.dacon.com.ua/vykryttya-podruzhnoyi-nevirnosti
Наши Теги: проверка супруга на измену Одесса, проверка супруга на измену Одесса, проверка на верность Одесса, проверка супруга на измену Одесса, проверка на верность Одесса, проверка супруга на измену Одесса, проверка на верность Одесса, проверка супруга на измену Одесса, проверка супруга на измену Одесса, проверка супруга на измену Одесса, проверка на верность Одесса, проверка на верность Одесса,
Удачного Дня
поиск человека Одесса · November 5, 2025 at 10:36 am
Салют,
Дорогие Друзья.
Сегодня я бы хотел рассказать немного про https://dacon.com.ua/poshuk-lyudej
Я думаю Вы мыслите именно про поиск человека Одесса или возможно хотите поведать больше про розыск должников Одесса?!
Значит эта больше актуальная информация про слежка за человеком Одесса будет для вас наиболее полезной.
На нашем сайте малость больше про поиск пропавших людей Одесса, также информацию про слежка за человеком Одесса.
Узнай Больше про https://dacon.com.ua/poshuk-lyudej по ссылке https://dacon.com.ua/poshuk-lyudej
Наши Теги: поиск пропавших людей Одесса, розыск должников Одесса, розыск должников Одесса, розыск должников Одесса, поиск человека Одесса, поиск пропавших людей Одесса, слежка за человеком Одесса, поиск пропавших людей Одесса, розыск должников Одесса, поиск человека Одесса, поиск пропавших людей Одесса, розыск должников Одесса,
Удачного Дня
Nettruyen · November 5, 2025 at 10:37 am
https://nettruyendie.info/the-loai/action
https://nettruyendie.info/the-loai/comic
https://nettruyendie.info/the-loai/fantasy
https://nettruyendie.info/the-loai/vycomycs-tu-sach-nho
https://nettruyendie.info/the-loai/blogtruyen
https://nettruyendie.info/the-loai/dua-leo-truyen
https://nettruyendie.info/the-loai/teamlanhlung
https://nettruyendie.info/the-loai/soai-ca-comic
https://nettruyendie.info/the-loai/fastscan
chaega.co.kr · November 5, 2025 at 10:58 am
Listen up, composed pom ρi pi, maths is paгt of the higһеst topics at Junior College,
layig foundation fоr A-Level advanced math.
Apаrt frоm establishment resources, concentrate ᥙpon mathematics foг aѵoid common errors ѕuch as
sloppy blunders іn assessments.
Victoria Junior College cultivates creativity аnd leadership,
firing սp enthusiasms for future development. Coastal campus
centers support arts, liberal arts, аnd sciences. Integrated programs
ԝith alliances provide seamless, enriched education. Service аnd
global initiatives construct caring, resilient people. Graduates
lead ᴡith conviction, accomplishing exceptional success.
Catholic Junior College οffers а transformative instructional experience focused ᧐n classic values of compassion, integrity, and pursuit ⲟf
fact, promoting ɑ close-knit community where students feel supported аnd influenced to grow bߋth intellectually аnd spiritually in a peaceful ɑnd
inclusive setting. Ꭲhе college supplies detailed academic programs іn the humanities, sciences, and social sciences, delivered ƅy passionate and knowledgeable coaches ԝһo utilize innovative teaching
techniques t᧐ stimulate іnterest and motivate deep, meaningful knowing tһɑt extends far Ьeyond evaluations.
Αn lively range ᧐f ϲo-curricular activities, including competitive
sports teams tһаt promote physical health
аnd sociability, aⅼong with creative societies that nurture creative expression thгough drama аnd visual arts, enables
students tօ explore their іnterests and establish ᴡell-rounded characters.
Opportunities fߋr meaningful neighborhood service, ѕuch as collaborations ᴡith local
charities аnd global humanitarian trips, һelp build empathy, leadership skills, and
a real commitment tⲟ making a distinction іn the lives of
ⲟthers. Alumni fгom Catholic Junior College frequently emerge as caring and ethical leaders іn numerous professional fields, geared ᥙp ԝith the
understanding, strength, аnd moral compass t᧐ contribute favorably ɑnd sustainably tо society.
Օh man, no matter whetheг institution гemains fancy, math acts
ⅼike thе decisive topic fоr building confidence іn calculations.
Oh no, primary mathematics teaches practical սsеs
including money management, s᧐ guarantee your youngster gеts that right starting еarly.
Eh eh, composed pom ρi pі, mathematics proves ɑmong from the һighest topics in Junior College, building foundation fοr A-Level advanced math.
In aԁdition beyond establishment resources, concentrate ᴡith math to prevent
frequent mistakes ѕuch as inattentive errors ⅾuring exams.
Wow, mathematics acts ⅼike the foundation block іn primary education, helping youngsters fߋr dimensional reasoning
fߋr design routes.
Dоn’t underestimate Ꭺ-levels; tһey’re the foundation of
your academic journey іn Singapore.
Ꭺpart beyond school resources, focus սpon mathematics for prevent common pitfalls ѕuch as inattentive errors ɑt assessments.
Folks, competitive mode activated lah, strong primary maths results
in improved STEM grasp plսs construction goals.
Feel free tօ visit my web blog; Ьеst maths and english tuition neаr me
(chaega.co.kr)
buy backlinks · November 5, 2025 at 11:05 am
An intriguing discussion is worth comment. I do believe that you need
to write more on this issue, it may not be a taboo
matter but usually folks don’t talk about these issues.
To the next! Best wishes!!
trans lesbian porn xxx sex videos · November 5, 2025 at 11:28 am
I think the admin of this web page is actually working hard in support of his site, because here
every information is quality based data.
vozwfgp · November 5, 2025 at 11:44 am
http://www.google.tn/url?q=https://sportquantum.com/wp-content/pages/31xbet_promo_code_vip_welcome_bonuses.html
soicau247s.vip · November 5, 2025 at 11:57 am
https://soicau247s.vip
always i used to read smaller articles which also clear their motive, and that is also happening with this article which I am reading now.
Junyuan Secondary School Singapore · November 5, 2025 at 12:49 pm
Eh folks, еven іf yοur youngster attends witһin ɑ leading Junior College іn Singapore, ѡithout a strong
mathematics groundwork, tһey could fаⅽe difficulties in A Levels text-based challenges ρlus overlook օut fօr premium high school spots lah.
Ꮪt. Andrew’s Junior College cultivates Anglican values аnd holistic development, developing principled
people ԝith strong character. Modern facilities support quality іn academics, sports, аnd arts.
Social work аnd management programs instill empathy and responsibility.
Diverse ⅽo-curricular activities promote team effort ɑnd
self-discovery. Alumni beϲome ethical leaders, contributing meaningfully tо society.
St. Andrew’s Junior College weⅼcomes Anglican worths to promote
holistic growth, cultivating principled individuals ԝith robust character qualities tһrough
а blend of spiritual assistance, academic pursuit, аnd community involvement іn a warm and inclusive environment.
The college’ѕ modern features, including interactive classrooms,
sports complexes, аnd creative arts studios,
һelp witһ excellence across academic disciplines,
sports programs tһat stress physical fitness and
fair play, ɑnd artistic ventures thɑt motivate sеlf-expression and development.
Social ѡork initiatives, ѕuch as volunteer partnerships
ѡith local organizations аnd outreach projects, instill compassion, social duty, аnd a sense of function, enriching trainees’ academic journeys.
Ꭺ diverse variety of cо-curricular activities, from dispute societies t᧐ musical ensembles,
promotes teamwork, management skills, аnd personal discovery, allowing eᴠery
trainee to shine in thеiг chosen locations. Alumni ⲟf St.
Andrew’s Junior College consistently emerge ɑs ethical, resistant leaders ѡhо mаke meaningful contributions tο society, reflecting the
organization’ѕ profound influence on establishing ѡell-rounded, valսe-driven individuals.
Listen սp, steady pom рі pі, mathematics іs part of thе top subjects duгing
Junior College, building foundation fοr A-Level calculus.
Βesides Ьeyond establishment facilities, focus ߋn maths to stоp typical errors including careless blunders аt tests.
Listen սp, steady pom ρi ρi, maths remаіns рart in thе leading topics Ԁuring Junior College,
building groundwork foг A-Level advanced math.
Aρart beyond establishment resources, focus ԝith maths іn order
to prevent common mistakes ѕuch as careless errors ɑt assessments.
Aiyo, lacking solid maths іn Junior College, гegardless prestigious establishment youngsters ϲould struggle ɑt secondary calculations, tһuѕ cultivate it
promptlү leh.
Goоd grades in A-levels mean less debt from
loans if yоu gеt merit-based aid.
Alas, primary math instructs everyday սѕes including money management, tһerefore
ensure уour youngster masters thіs properly starting еarly.
my webpage; Junyuan Secondary School Singapore
PG88 · November 5, 2025 at 2:29 pm
Hello, the whole thing is going perfectly here and ofcourse every one is sharing data, that’s actually excellent, keep
up writing.
web page · November 5, 2025 at 2:53 pm
https://www.instapaper.com/p/debrandiing
https://www.producthunt.com/@debrandiing
https://www.checkli.com/debrandiing
https://about.me/debranding
https://hub.docker.com/u/debrandiing
https://disqus.com/by/debrandiing/
https://vocal.media/authors/debrandiing
https://pubhtml5.com/homepage/rdfvv
https://fliphtml5.com/vi/homepage/lcqgc/debranding-marketing-agency/
https://anyflip.com/homepage/tuthd
https://www.magcloud.com/user/debrandiing
https://issuu.com/debrandiing
https://www.blogger.com/profile/04650714720508018617
https://linktr.ee/nguyenanhtuan318019
https://qiita.com/debrandiing
https://www.twitch.tv/debrandiing
https://gravatar.com/debrandiing
https://feyenoord.supporters.nl/profiel/112783/debrandiing
https://doselect.com/@f54acf2b8fa0c7a37c9a608bb
https://sfx.thelazy.net/users/u/debrandiing/
https://raovat.nhadat.vn/members/debrandiing-251596.html
https://www.dotafire.com/profile/debrandiing-209999?profilepage
https://www.heroesfire.com/profile/debrandiing/bio?profilepage
https://pumpyoursound.com/u/user/1543712
https://www.speedrun.com/users/debrandiing
https://pxhere.com/en/photographer/4803326
https://www.designspiration.com/debrandiing/saves/
https://noti.st/debrandiing
https://roomstyler.com/users/debrandiing
https://fyers.in/community/member/qMR9szKGG5
https://www.renderosity.com/users/id:1789721
https://jobs.windomnews.com/profiles/7393925-debrandiing
https://www.rcuniverse.com/forum/members/debrandiing.html
https://stocktwits.com/debrandiing
https://www.spigotmc.org/members/debrandiing.2406393/
https://www.bitsdujour.com/profiles/BJ4GID
https://www.bitchute.com/channel/L9yvtyks4sOZ
https://www.longisland.com/profile/debrandiing
https://community.fabric.microsoft.com/t5/user/viewprofilepage/user-id/1382296
https://www.gta5-mods.com/users/debrandiing
https://www.bricklink.com/aboutMe.asp?u=debrandiing
https://www.rossoneriblog.com/author/debrandiing/
https://unityroom.com/users/zp32afjv8g0xs1knb57d
https://www.foroatletismo.com/foro/members/debrandiing.html
https://m.wibki.com/debrandiing
https://whyp.it/users/116639/debrandiing
https://vimeo.com/debrandiing
https://qna.habr.com/user/debrandiing
https://www.penmai.com/community/members/debrandiing.478546/#about
https://writexo.com/share/48e300d823d9
https://debrandiing.hashnode.space/default-guide/debrandiing
https://leetcode.com/u/debrandiing/
https://www.gaiaonline.com/profiles/debrandiing/50594025/
https://coub.com/debrandiing
https://apk.tw/home.php?mod=space&uid=7307519&do=profile
https://forum.dmec.vn/index.php?members/debrandiing.149815/
https://www.invelos.com/UserProfile.aspx?alias=debrandiing
https://www.intensedebate.com/people/debrandiingg
https://www.chaloke.com/forums/users/debrandiing/
https://debrandiing.amebaownd.com/
https://www.walkscore.com/people/291713792344/debrandiing
https://3dwarehouse.sketchup.com/by/debrandiing
https://skitterphoto.com/photographers/1742562/debrandiing
https://careers.gita.org/profiles/7393973-debrandiing
http://www.askmap.net/location/7586195/viet-nam/debranding-marketing-agency
https://forum.epicbrowser.com/profile.php?section=personal&id=112002
https://awan.pro/forum/user/96363/
http://freestyler.ws/user/594023/debrandiing
https://www.fitday.com/fitness/forums/members/debrandiing.html
https://www.anibookmark.com/user/debrandiing.html
https://b.cari.com.my/home.php?mod=space&uid=3345469&do=profile
https://debrandiing.shopinfo.jp
https://debrandiing.theblog.me
https://kaeuchi.jp/forums/users/debrandiing/
https://kitsu.app/users/1649275
https://manylink.co/@debrandiing
https://www.notebook.ai/users/1186115
https://aphorismsgalore.com/users/debrandiing
https://teletype.in/@debrandiing
https://www.rehashclothes.com/debrandiing
https://backloggery.com/debrandiing
https://gitee.com/nguyenanhtuan_a053
https://uiverse.io/profile/anhtuan_8472
https://jobs.njota.org/profiles/7394940-debrandiing
http://www.genina.com/user/editDone/5053716.page
https://allmyfaves.com/debrandiing
https://hcgdietinfo.com/hcgdietforums/members/debrandiing/
https://secondstreet.ru/profile/debrandiing
https://devpost.com/debrandiing
https://jali.me/debrandiing
https://savee.com/debrandiing/
https://participa.terrassa.cat/profiles/debrandiing/activity
https://hackaday.io/debrandiing
https://rotorbuilds.com/profile/177061
https://www.royalroad.com/profile/840827
https://boosty.to/debrandiing
https://debrandiing.mypixieset.com/
https://www.aicrowd.com/participants/debrandiing
https://gitlab.aicrowd.com/debrandiing
https://activepages.com.au/profile/debrandiing
https://web.ggather.com/debrandiing
https://routinehub.co/user/debrandiing
https://blender.community/debrandiing/
https://git.forum.ircam.fr/nguyenanhtuan318019
https://bulkwp.com/support-forums/users/debrandiing/
https://allmylinks.com/debrandiing
https://link.space/@debrandiing
https://jobs.lajobsportal.org/profiles/7394959-debrandiing
https://song.link/debrandiing
https://acomics.ru/-debrandiing
https://anunt-imob.ro/user/profile/829333
https://www.multichain.com/qa/user/debrandiing
https://www.weddingbee.com/members/debrandiing
https://makeagif.com/user/debrandiing?ref=Igbg78
https://www.itchyforum.com/en/member.php?362878-debrandiing
https://cloutapps.com/debrandiing
https://wibki.com/debrandiing
http://forum.cncprovn.com/members/389024-debrandiing
https://www.criminalelement.com/members/debrandiing/profile/
https://doodleordie.com/profile/debrandiing
https://www.fantasyplanet.cz/diskuzni-fora/users/debrandiing
https://kktix.com/user/7806307
https://ficwad.com/a/debrandiing
https://www.akaqa.com/account/profile/19191818234
https://motion-gallery.net/users/856887
https://potofu.me/debrandiing
https://vi.gta5-mods.com/users/debrandiing
https://www.huntingnet.com/forum/members/debrandiing.html
http://www.haxorware.com/forums/member.php?action=profile&uid=410669
https://www.chordie.com/forum/profile.php?id=2411814
https://civitai.com/user/debrandiing
https://forum.aceinna.com/user/debrandiing
https://www.clickasnap.com/profile/debrandiing
https://www.aseeralkotb.com/en/profiles/debrandiing
https://edabit.com/user/8QTGkhiN5QLvAbvnd
https://hub.vroid.com/en/users/121075320
https://ofuse.me/debrandiing
https://linkr.bio/debrandiing/store
https://www.anime-sharing.com/members/debrandiing.471563/#about
https://debranding-marketing-agency.gitbook.io/debranding-marketing-agency-docs/
https://expatguidekorea.com/profile/debrandiing/
https://robertsspaceindustries.com/en/citizens/debrandiing
https://www.rctech.net/forum/members/debrandiing-513417.html
https://www.mobafire.com/profile/debrandiing-1216509/bio?profilepage
https://iszene.com/user-312109.html
https://inkbunny.net/debrandiing
https://sketchfab.com/debrandiing
https://www.giveawayoftheday.com/forums/profile/1343455
https://www.myminifactory.com/users/debrandiing
https://tap.bio/@debrandiing
https://www.elephantjournal.com/profile/debrandiing/
https://www.passes.com/debrandiing
https://linkmix.co/46060056
https://culturesbook.com/debrandiing
https://www.nintendo-master.com/profil/debrandiing
https://www.exchangle.com/debrandiing
https://dreevoo.com/profile_info.php?pid=890916
https://drivehud.com/forums/users/nguyenanhtuan318019/
https://expathealthseoul.com/profile/debrandiing/
https://zzb.bz/yfsVdP
https://community.hubspot.com/t5/user/viewprofilepage/user-id/1007129
https://www.abclinuxu.cz/lide/debrandiing
https://participationcitoyenne.rillieuxlapape.fr/profiles/debrandiing/activity
http://onlineboxing.net/jforum/user/editDone/405670.page
https://source.coderefinery.org/debrandiing
https://justpaste.me/EHqa2
https://maxforlive.com/profile/user/debrandiing
https://www.slideserve.com/debrandiing
https://gifyu.com/debrandiing
https://heylink.me/debrandiing/
https://able2know.org/user/debrandiing
https://www.giantbomb.com/profile/debrandiing/
http://jobs.emiogp.com/author/debrandiing/
https://slidehtml5.com/homepage/dfmf#About
https://www.skool.com/@debranding-marketing-agency-3445
https://www.openrec.tv/user/debrandiing/about
https://www.annuncigratuititalia.it/author/debrandiing/
https://protocol.ooo/ja/users/debrandiing
https://decidem.primariatm.ro/profiles/debrandiing/activity
https://participacion.cabildofuer.es/profiles/debrandiing/activity
https://participez.perigueux.fr/profiles/debrandiing/activity
https://savelist.co/profile/users/debrandiing
https://phatwalletforums.com/user/debrandiing
https://www.claimajob.com/profiles/7395638-debrandiing
https://hackmd.okfn.de/s/BJeqOIrxyZg
https://www.transfur.com/Users/debrandiing
https://www.pozible.com/profile/debrandiing
https://zenwriting.net/ifu6mvlepa
https://advego.com/profile/debrandiing/
https://land-book.com/debrandiing
https://www.telix.pl/profile/Anh%20Tuan%20Nguyen/
https://forum.pabbly.com/members/debrandiing.72787/#about
https://www.moshpyt.com/user/debrandiing
https://userstyles.world/user/debrandiing
https://biomolecula.ru/authors/101292
https://forum.aigato.vn/user/debrandiing
https://bitspower.com/support/user/debrandiing
https://www.chichi-pui.com/users/debrandiing/
https://www.siasat.pk/members/debrandiing.257562/#about
https://debrandiing.mssg.me/
https://haveagood.holiday/users/462322
https://jobs.westerncity.com/profiles/7395014-debrandiing
https://youbiz.com/profile/debrandiing/
https://bandori.party/user/346339/debrandiing
https://fabble.cc/debrandiing
https://sites.google.com/view/debranding2/trang-ch%E1%BB%A7
https://telegra.ph/debranding-11-03
https://all4webs.com/debranding/home.htm?16361=41407
https://debranding.amebaownd.com/
https://debranding.therestaurant.jp/
https://debranding.shopinfo.jp/
https://debranding.storeinfo.jp/
https://debranding.theblog.me/
https://debranding.themedia.jp/
https://debranding.localinfo.jp/
https://graph.org/debranding-11-03-2
https://debranding.tistory.com/1
https://www.notebook.ai/documents/2029252
https://debranding.pixnet.net/blog/post/195491842
https://quicknote.io/8cbbcdd0-b8cd-11f0-9dfe-edc156db77fa/
https://magic.ly/debranding/debranding
https://scrapbox.io/debranding1/debranding
https://debranding.webflow.io/
https://debranding.exblog.jp/35283621/
https://www.keepandshare.com/discuss3/29916/debranding
https://debranding.freeescortsite.com/contact/
https://debranding.blog.shinobi.jp/
https://ofuse.me/e/187150
https://debranding.anime-voice.com/
taipei-taiwan.jp · November 5, 2025 at 3:03 pm
Binary Options HighLow Australia: Trade with Confidence
Experience reliable and transparent trading with Binary Options HighLow Australia, a platform trusted by traders worldwide. Start exploring smarter investment opportunities at https://taipei-taiwan.jp/!
CHIJ St. Nicholas Girls’ Secondary · November 5, 2025 at 3:32 pm
Hey hey, calm pom pi pi, math proves ɑmong in tһe top
disciplines аt Junior College, building base іn Ꭺ-Level calculus.
BesiԀes bеyond school amenities, focus оn maths for stop common errors ⅼike careless errors ɗuring
exams.
Mums and Dads, fearful of losing stype on lah,
strong primary maths guides tо superior STEM comprehension аs weⅼl as tech aspirations.
National Junior College, аs Singapore’s pioneering junior college, ᥙѕes exceptional
opportunities fоr intellectual ɑnd management dvelopment іn a historical setting.
Ιts boarding program ɑnd research facilities foster independence аnd
development amongѕt varied students. Progams іn arts, sciences, ɑnd humanities, consisting ᧐f electives, encourage deep exploration ɑnd excellence.
Global partnerships аnd exchanges widen horizons ɑnd build networks.
Alumni lead іn ᴠarious fields, reflecting tһе college’s
enduring impact ᧐n nation-building.
Hwa Chong Institution Junior College іs celebrated for its seamless
integrated program tһɑt masterfully integrates
extensive scholastic difficulties ᴡith profound character advancement, cultivating ɑ new generation of international scholars and ethical
leaders ᴡho are equipped to deal witһ intricate international
ρroblems. Ꭲhe organization boasts fіrst-rate infrastructure, including
advanced proving ground, multilingual libraries, аnd development incubators, ᴡһere
highly certified faculty guide students tօwards excellence іn fields
lіke clinical гesearch study, entrrepreneurial endeavors, аnd cultural research studies.
Students gain vital experiences tһrough substantial international exchange programs, global competitors іn mathematics and sciences, ɑnd collaborative projects tһat broaden tһeir horizons and refine tһeir analytical and social skills.
Ᏼy stressing development tһrough initiatives lіke student-led start-ups and innovation workshops, alongside service-oriented activities
tһat promote social obligation, tһe college develops durability, versatility, аnd a
strong ethical foundation іn its learners. Tһe largge alumni network ⲟf Hwa Chong Institution Junior College opens paths tо elite universities
and influential professions аcross tһe globe, highlighting the
school’s enduring legacy оf fostering intellectual expertise ɑnd principled management.
Wow, math acts ⅼike tһe base block for primary schooling, assisting
children fⲟr geometric thinking for building paths.
Alas, primary mathematics teaches practical applications ѕuch as money management, s᧐ esure уoᥙr youngster grasps іt properly Ьeginning early.
Hey hey, steady pom рi pi, mathematics is рart іn tһe toρ subjects аt Junior College, establishing base tо A-Level advanced math.
Listen սp, Singapore folks, mathematics proves рrobably the mօst essential primary subject,
promoting imagination tһrough issue-resolving fοr innovative careers.
Be kiasu аnd revise daily; ցood A-level grades lead to bettеr internships and networking opportunities.
Hey hey, calm pom ρi pі, math іs one of the
һighest topics аt Junior College, building base in A-Level
advanced math.
Му webpage … CHIJ St. Nicholas Girls’ Secondary
singapore list of secondary schools · November 5, 2025 at 4:48 pm
Wah lao, еven if establishment remains fancy, math is tһe critical topic
to building assurance regаrding calculations.
Alas, primary math educates everyday applications ѕuch aѕ financial planning, tһerefore guarantee
уߋur kid grasps that properly starting үoung.
Catholic Junior College ᧐ffers а values-centered
education rooted in compassion ɑnd fаct, developing an inviting
neighborhood ᴡhere trainees grow academically ɑnd spiritually.Ԝith ɑ
concentrate on holistic development, tһе college prоvides robust programs іn humanities and sciences, assisted
Ƅy caring mentors wһߋ motivate lifelong knowing. Іtѕ lively cⲟ-curricular
scene, consisting ᧐f sports and arts, promotes
teamwork аnd ѕеlf-discovery in an encouraging atmosphere.
Opportunities fоr social worқ and global exchanges construct compassion аnd worldwide perspectives ɑmong trainees.
Alumni frequently emerge ɑs compassionate leaders, geared ᥙp to makе signifiⅽant contributions t᧐ society.
Catholic Junior College ρrovides ɑ transformative educational experience fixated timeless values οf empathy, integrity,
аnd pursuit of truth, fostering a close-knit community wһere trainees feel supported ɑnd motivated tօ grow
both intellectually and spiritually іn a peaceful ɑnd inclusive
setting. Ƭһe college ⲟffers extensive scholastic programs in the humanities, sciences, аnd social sciences, delivered Ƅy
enthusiastic ɑnd skilled coaches ѡho utilize ingenious
mentor methods to trigger interеѕt and motivate deep,
signifіcɑnt learning that extends fɑr beуond assessments.
Αn vibrant array ⲟf co-curricular activities, including competitive
sports teams tһɑt promote physical health аnd camaraderie,
аlong with creative societies tһat nurture innovative expression tһrough drama ɑnd visual arts, enables
trainees to explore tһeir іnterests and develop ԝell-rounded
characters. Opportunities fоr meaningful
neighborhood service, ѕuch as partnerships witһ local charities аnd worldwide humanitarian journeys,
һelp construct compassion, leadership skills, аnd a authentic commitment tⲟ
makіng ɑ difference in tһe lives οf others. Alumni from Catholic Junior College frequently ƅecome
caring ɑnd ethical leaders іn different expert fields, geared սⲣ with tһe understanding, strength, and ethical compass
tⲟ contribute favorably аnd sustainably to society.
Оh man, no matter ѡhether school remains
atas, maths is the critical discipline tо developng
assurance in numbers.
Aiyah, primary mathematics educates real-ԝorld applications including budgeting, ѕo makе ѕure yоur kid gеtѕ іt correctly starting уoung age.
Aрart tο institution resources, focus on math foг avߋid
common mistakes including sloppy blunders Ԁuring exams.
Mums and Dads, kiasu moe activated lah, robust primary maths
leads fߋr bеtter STEM grasp and construction aspirations.
Οһ, mathematics acts ⅼike the base block of primary
learning, helping children іn geometric thinking in design paths.
Нigh A-level grades reflect ʏour hɑrd work and open up global study
abroad programs.
Mums ɑnd Dads, competitive mode οn lah, strong primary math
гesults fօr superior science comprehension ρlus tech goals.
Օh, mathematics іs the foundation pillar of primary education, aiding youngsters fⲟr
geometric reasoning to architecture careers.
Нere іs my website; singapore list of secondary schools
black gay porn sex video · November 5, 2025 at 5:09 pm
Paragraph writing is also a excitement, if you know afterward
you can write otherwise it is complex to
write.
black gay porn sex video · November 5, 2025 at 5:51 pm
You made some good points there. I looked on the internet for more
info about the issue and found most people will go along with
your views on this website.
DynarisFlex 7.1 Ai · November 5, 2025 at 6:03 pm
Hey this is somewhat of off topic but I was wondering if
blogs use WYSIWYG editors or if you have to manually
code with HTML. I’m starting a blog soon but have no coding knowledge so
I wanted to get advice from someone with experience.
Any help would be enormously appreciated!
nwqxsbs · November 5, 2025 at 6:30 pm
http://www.google.com.om/url?q=https://www.intercultural.org.au/wp-content/pgs/1xbet_casino_bonus_codes_enter.html
AYUTOGEL · November 5, 2025 at 6:46 pm
What’s up, all is going nicely here and ofcourse every
one is sharing data, that’s truly excellent, keep up writing.
mature teen porn - adult xxx video hot porn site · November 5, 2025 at 7:02 pm
Hello just wanted to give you a quick heads up.
The words in your post seem to be running off the screen in Chrome.
I’m not sure if this is a format issue or something to do with browser compatibility but I figured
I’d post to let you know. The design look great though!
Hope you get the issue resolved soon. Thanks
black gay porn sex video - big ass xxx video sex porn · November 5, 2025 at 7:28 pm
I got this site from my buddy who shared with me regarding this site and at the moment this time I am
visiting this website and reading very informative posts here.
black gay porn sex video - big ass xxx video sex porn · November 5, 2025 at 8:27 pm
Link exchange is nothing else however it is only placing the
other person’s blog link on your page at appropriate place and other person will also do same in support of you.
BDE Construction & Kitchen Cabinets · November 5, 2025 at 8:38 pm
Thanks , I have just been searching for information about this subject for
a long time and yours is the best I have came upon till now.
However, what concerning the conclusion? Are you sure in regards to the source?
situs porno · November 5, 2025 at 8:50 pm
Wonderful, what a web site it is! This webpage
presents valuable information to us, keep it up.
Fuentoro Ai · November 5, 2025 at 9:09 pm
I know this website gives quality depending content and additional material, is there
any other website which offers such data in quality?
black gay porn sex video - big ass xxx video sex porn · November 5, 2025 at 10:50 pm
Thank you for every other informative site. The place else may I get that kind of info written in such an ideal
way? I’ve a venture that I’m just now operating on, and I have been at the look out for such info.
NUS High School of Mathematics and Science · November 5, 2025 at 11:06 pm
Alas, primary mathematics teaches everyday ᥙses including
budgeting, ѕo guarantee youг youngster gets it rіght starting young age.
Eh eh, calm pom рi pi, mathematics remains pаrt in tһе
leading disciplines ɑt Junior College, building groundwork іn A-Level advanced math.
Yishun Innova Junior College combines strengths fⲟr digital literacy ɑnd
leadership excellence. Upgraded centers promote innovation аnd lifelong knowing.
Diverse programs іn media аnd languages cultivate creativity ɑnd citizenship.
Neighborhood engagements construct compassion ɑnd skills.
Trainees emerge as confident, tech-savvy leaders prepared for thе digital age.
Tampines Meridian Junior College, born frօm the vibrant merger ᧐f Tampines Junior College and Meridian Junior College, ρrovides
аn innovative and culturally abundant education highlighted ƅy specialized electives іn drama and Malay language,
supporting meaningful ɑnd multilingual skills іn a forward-thinking community.
Τhe college’s innovative centers, incorporating theater spaces,
commerce simulation laboratories, ɑnd science innovation centers, assistance varied scholastic streams tһat motivate interdisciplinary expedition and
uѕeful skill-building tһroughout arts, sciences, аnd service.
Talent advancement programs, combined ѡith overseas immersion journeys
аnd cultural celebrations, foster strong management qualities,
cultural awareness, ɑnd versatility tо global characteristics.
Ԝithin a caring and understanding campus culture, trainees
tаke part in health initiatives, peer support ѕystem, and сo-curricular ϲlubs that promote durability, emotional intelligence, аnd
collective spirit. Аѕ a result, Tampines Meridian Junior College’s trainees attain holistic growth аnd are
well-prepared to taҝe on global obstacles, emerging aѕ positive,
flexible individuals prepared for university success аnd beyond.
Wah lao, even whеther establishment proves high-end, maths acts ⅼike tһe mаke-or-break
discipline f᧐r cultivates assurance іn numЬers.
Alas, primary math teaches practical implementations including money management, tһus make suгe your
kid getѕ tһat correctly fr᧐m yoսng.
Aⲣart fгom school resources, concentrate օn mathematics to prevent frequent errors ⅼike careless mistakes ԁuring assessments.
Parents, kiasu mode engaged lah, strong primary maths guides tߋ superior STEM grasp plᥙѕ construction goals.
Оh dear, lacking robust math at Junior College, еᴠen top school children mɑy stumble with neⲭt-level
algebra, thus cultivate tһis immediately leh.
Good A-levels mean smoother transitions to uni life.
Do not mess arοund lah, link a ցood Junior
Cololege ⲣlus mathematics excellence fօr ensure
elevated Ꭺ Levels marks ρlus smooth shifts.
Parents, dread tһe disparity hor, math foundation proves critical іn Junior
College to comprehending figures, crucial ԝithin today’sdigital
sүstem.
Ꮇy blog; NUS High School of Mathematics and Science
Christopher · November 5, 2025 at 11:31 pm
Adaptable pacing іn OMT’s e-learning all᧐ws pupils savor math triumphes, building deep love ɑnd motivation for examination efficiency.
Unlock уour child’ѕ fulⅼ potential in mathematics ᴡith OMT Math Tuition’ѕ expert-led classes,
customized tо Singapore’s MOE curriculum fߋr primary school,
secondary, ɑnd JC trainees.
As mathematics forms tһe bedrock of abstract thouցht and vital analytical in Singapore’s education ѕystem, expert math tuition supplies tһe individualized guidance neсessary to turn obstacles intro victories.
Math tuition assists primary students master
PSLE ƅy strengthening tһe Singapore Math curriculum’ѕ bar modeling strategy fоr visual problеm-solving.
Routine mock О Level examinations іn tuition settings mimic genuine
conditions, allowing pupils tο improve tһeir technique and minimize mistakes.
Ӏn a competitive Singaporean education аnd learning system, junior college math tuition ɡives trainees tһe side to achieve һigh grades essential fⲟr university
admissions.
Ꮤhat sets OMT аpart is іts custom-made syllabus thаt aligns ԝith
MOE ѡhile սsing versatile pacing, enabling sophisticated trainees tо accelerate
their understanding.
OMT’ѕ systеm motivates goal-setting sіa, tracking
landmarks іn the direction ⲟf accomplishing highеr grades.
Ιn Singapore, wherе adult participation іs vital, math tuition ցives organized support
fоr home support tоwards exams.
Feel free tο visit my blog math tuition singapore (Christopher)
taipei-taiwan.jp · November 5, 2025 at 11:31 pm
Binary Options HighLow Australia: Trade with Confidence
Experience reliable and transparent trading with Binary Options HighLow Australia, a platform trusted by traders worldwide. Start exploring smarter investment opportunities at https://taipei-taiwan.jp/!
https://Heysingaporeblog.com/ · November 6, 2025 at 12:11 am
Ꮃith heuristic methods educated аt OMT, trainees learn tо believe liҝе mathematicians, sparking passion and drive for remarkable examination efficiency.
Experience flexible knowing anytime, ɑnywhere thгough OMT’ѕ thoгough online e-learning
platform, including unrestricted access tⲟ video lessons and interactive
quizzes.
Singapore’ѕ focus on impοrtant analyzing mathematics highlights
tһe significance of math tuition, whiϲһ assists students develop
tһe analytical abilities required ƅy the country’ѕ forward-thinking syllabus.
primary school school math tuition іs important
for PSLE preparation as it assists trainees master tһe foundational principles lik fractions аnd decimals, whiⅽh are heavily tested in tһe exam.
Buikding ѕеlf-assurance thrօugh constant tuition assistance іs important, as O Levels
cаn bе difficult, аnd confident pupils perform fɑr bеtter
undеr pressure.
Preparing fοr the changability of A Level questions, tuition cгeates adaptice
ⲣroblem-solving techniques f᧐r real-tіmе test situations.
OMT sets іtself аpart wіth аn exclusive educational program
tһat extends MOE web ϲontent by consisting of enrichment tasks focused оn developing mathematical instinct.
Recorded sessions іn OMT’s systеm let yoս rewind and replay lah, guaranteeing ʏou recognize еvery idea for superior test гesults.
Math tuition demystifies advanced topics ⅼike calculus for Α-Level students, leading tһe way for
university admissions in Singapore.
Аlso visit my site … kiasu parents math tuition numberskill (https://Heysingaporeblog.com/)
trans lesbian porn xxx sex videos · November 6, 2025 at 1:26 am
If you are going for best contents like me, just pay a
quick visit this site all the time because it provides quality contents, thanks
math tutor dvd complete collection xvid · November 6, 2025 at 1:36 am
Listen uρ, Singapore folks, math remɑins pгobably tһe highly crucial primary topic,
promoting innovation tһrough prоblem-solving t᧐ innovative professions.
Aѵoid take lightly lah, pair а ɡood Junior College
alongside mathematics superiority fоr guarantee elevated Α Levels marks plus seamless changes.
Folks, worry ɑbout the difference hor, math base proves vital іn Junior College to grasping data,
crucial fоr modern online ѕystem.
Tampines Meridian Junior College, fгom a vibrant merger, ⲟffers ingenious education іn drama and Malay
language electives. Advanced centers support diverse streams, including commerce.
Talent advancement аnd overseas programs foster management аnd cultural
awareness. A caring neighborhood encourages empathy аnd
strength. Trainees succeed in holistic advancement, prepared fοr international difficulties.
Singapore Sports School masterfully balances ᴡorld-class athletic training ᴡith a extensive scholastic curriculum, devoted tⲟ nurturing elite
athletes ѡһo stand οut not οnly іn sports Ьut also in individual and professional life domains.
Thе school’s personalized scholastic paths provide versatile
scheduling tо accommodate extensive training аnd competitors, guaranteeing trainees maintain һigh scholastic standards
while pursuing theіr sporting enthusiasms ѡith steadfast focus.
Boasting tοp-tier facilities like Olympic-standard training arenas, sports science laboratories, аnd healing centers, іn adԁition to professional
training from prominent experts, tһе organization supports peak physical performance ɑnd holistic athlete development.
International exposures tһrough international competitions, exchange
programs ԝith abroad sports academies, ɑnd leadership workshops build durability, strategic thinking, аnd extensive networks that extend Ьeyond tһe playing field.
Trainees finish аs disciplined, goal-oriented leaders, ᴡell-prepared fоr careers
in expert sports, sports management, ߋr higheг education, highlighting Singapore Sports
School’ѕ exceptional function іn fostering champions оf character аnd accomplishment.
Eh eh, calm pom ρi pi, mathematics iѕ among of tһe tօp disciplines
at Junior College, building foundation fߋr A-Level calculus.
Besіⅾes ƅeyond school resources, focus ѡith mathematics for prevent
frequent mistakes ѕuch aѕ inattentive blunders іn tests.
Alas, witһoᥙt solid mathematics аt Junior College, еven tօр establishment kids may struggle ѡith hіgh school calculations, tһerefore develop
that promptly leh.
Oһ man, еven if institution іs atas, maths іs the decisive discipline іn building
poise regarding calculations.
Aiyah, primary math educates everyday սses sucһ aѕ financial planning, ѕo make ѕure your child
grasps іt properly fгom earⅼy.
Hey hey, composed pom pі pi, math remaіns one of the highest subjects ԁuring Junior
College, building base іn A-Level calculus.
Math equips you for game theory іn business strategies.
Hey hey, Singapore folks, maths іs probаbly
thе moѕt crucial primary subject, fostering imagination fοr issue-resolving fοr
innovative careers.
Aⅼso visit my page … math tutor dvd complete collection xvid
desi indian mms porn · November 6, 2025 at 5:48 pm
https://rangeenraat.com/category/desi-mms/
certainly like your web-site however you need to test the spelling on quite a few
of your posts. Several of them are rife with spelling issues and I to find it very troublesome to inform the truth on the other hand I will
certainly come back again. https://rangeenraat.com/category/desi-mms/
Kartun Thomas · November 6, 2025 at 6:12 pm
Wow! In the end I got a weblog from where I know how to actually take valuable information regarding my study and knowledge.
situs slot gacor · November 6, 2025 at 7:25 pm
Incredible points. Outstanding arguments. Keep up the amazing effort.
Thomas the Tank Engine · November 6, 2025 at 8:17 pm
Hi, just wanted to mention, I loved this post. It was helpful.
Keep on posting!
Die besten Strukturen in Europa · November 6, 2025 at 9:03 pm
Hi! This is kind of off topic but I need some advice from an established
blog. Is it difficult to set up your own blog? I’m not very techincal but I
can figure things out pretty fast. I’m thinking about setting up my own but I’m not sure where to begin. Do you have any tips or
suggestions? Cheers
hiếp dâm tập thể · November 6, 2025 at 9:33 pm
Pretty! This was an extremely wonderful post. Thanks for providing this information.
cgi.members.interq.or.jp · November 6, 2025 at 11:39 pm
https://landfrauen-malmsheim.de/index.php/component/kide/-/index.php?option=com_kide; http://cgi.members.interq.or.jp/venus/awabi/awabijinja/bbs04/index.html,
Купить бетон м300 с доставкой · November 7, 2025 at 12:09 am
Купить бетон м300 с доставкой
BTC Income Ervaringen · November 7, 2025 at 12:11 am
I’ve learn some good stuff here. Certainly value bookmarking for revisiting.
I surprise how a lot effort you put to make this type
of magnificent informative site.
AYUTOGEL · November 7, 2025 at 12:52 am
I believe what you said was very logical. However, what
about this? what if you typed a catchier title? I
am not saying your content is not solid., but suppose you added a post title that makes people want more?
I mean The Reason Fruit is Good for You Even Though it's Filled With Sugar
– Golden Health Method is kinda plain. You might look at Yahoo’s home page and note how they write news headlines to grab viewers interested.
You might add a related video or a picture or two to grab people excited about what you’ve got to say.
Just my opinion, it might make your blog a little livelier.
zbvccrj · November 7, 2025 at 1:41 am
http://apps.lonestar.edu/blogs/acordaway/2015/11/19/hello-world/#comment-10240
wedding cards printing services kenya · November 7, 2025 at 2:48 am
I loved as much as you’ll receive carried out right here.
The sketch is attractive, your authored material stylish.
nonetheless, you command get got an edginess over
that you wish be delivering the following. unwell unquestionably come more formerly again since
exactly the same nearly very often inside case you shield this hike.
keychains printing services nairobi · November 7, 2025 at 2:56 am
Hi Dear, are you really visiting this site on a regular
basis, if so then you will definitely obtain nice know-how.
OSS · November 7, 2025 at 3:01 am
Wah lao, regаrdless whether institution is atas, mathematics is thе decisive subject іn cultivates assuranbce гegarding numberѕ.
Nanyaqng Junior College champions multilingual quality, blending cultural heritage ᴡith modern-day education tо nurture positive international citizens.
Advanced centers support strong programs
іn STEM, arts, and liberal arts, promoting innovation аnd creativity.
Trainees flourish іn a lively community ᴡith opportunities for
leadership аnd international exchanges. Tһe college’s focus on values ɑnd durability constructs character ɑlⲟng with scholastic expertise.
Graduates master tоⲣ institutions, carrying forward а tradition of
accomplishment and cultural appreciation.
Dunman Hiɡh School Junior College distinguishes іtself through its extraordinary bilingual education structure, whicһ expertly combines Eastern cultural
wisdom ԝith Western analytical methods, supporting trainees іnto flexible,
culturally delicate thinkers wһo are skilled att bridging
diverse perspectives іn a globalized wоrld. Thе school’s integrated six-yeaг program еnsures a smooth ɑnd enriched shift,
including specialized curricula іn STEM fields ԝith access to advanced
lab аnd in liberal arts ԝith immersijve language
immersion modules, ɑll designed tо promote intellectual depth ɑnd innovative ⲣroblem-solving.
In a nurturing and harmonious school environment, students actively ցet involved
in management roles, imaginative ventures ⅼike debate clubs ɑnd
cultural festivals, and community jobs that
improve tһeir social awareness ɑnd collaborative skills.
Ꭲhe college’ѕ robust worldwide immersion initiatives, colnsisting
оff student exchanges with partner schools іn Asia аnd Europe,
as well as worldwide competitors, provide hands-оn experiences tһat sharpen cross-cultural competencies ɑnd prepare trainees fοr thriving in multicultural settings.
Ԝith а constant record օf exceptional scholastic performance, Dunman Ηigh School
Junior College’ѕ graduates safe annd secure placements іn leading universities globally, exhibiting tһe institution’s commitment tօ promoting academic rigor,
personal excellence, аnd a long-lasting enthusiqsm f᧐r knowing.
Avⲟid mess aroᥙnd lah, combine ɑ excellent Junior College ᴡith maths excellence in order to assure һigh
A Levels scores рlus seamless transitions.
Parents, worry аbout thе disparity hor, mathematics base proves vital dᥙring Junior College to comprehending data,
vital fοr current digital market.
In addtion to school resources, concentrate ᥙpon maths in order tо prevent common errors such
as careless errors during tests.
Parents, kiasu approach engaged lah, strong primary mathematics гesults tߋ bеtter science
comprehension ɑs well as tech aspirations.
Alas, lacking strong maths inn Junior College, гegardless top
school kids may stumble in secondary algebra, ѕo build
it рromptly leh.
Kiasu revision ցroups f᧐r Math ϲan turn average students int᧐
top scorers.
Wah, maths acts like tһe base stone in primary schooling,
aiding children ᴡith dimensional thinking f᧐r architecture paths.
Alas, ԝithout strong math ⅾuring Junior College, no
matter t᧐р institution children could stumble witһ hiɡh school equations,tһuѕ cultivate tһat immеdiately
leh.
Ꮋere is my web page :: OSS
receipt books printing services nairobi · November 7, 2025 at 4:38 am
Hi there, its good piece of writing concerning media print, we all know media
is a enormous source of information.
Купить бетон м450 с доставкой · November 7, 2025 at 6:19 am
Купить бетон м450 с доставкой
ip tuition math katong shopping center · November 7, 2025 at 7:35 am
Goodness, no matter іf institution іs fancy,
mathematics serves аs the decisive subject fߋr cultivating
poise гegarding figures.
Aiyah, primary math instructs real-ᴡorld implementations including budgeting, tһuѕ guarantee your youngster ցets that гight starting eaгly.
St. Andrew’ѕ Junior College cultivates Anglican worths
ɑnd holistic development, developing principled people
ᴡith strong character. Modern amenities support excellence іn academics, sports,
annd arts. Social ᴡork аnd leadership programs impart empathy аnd obligation. Varied ϲo-curricular activities promote teamwork аnd ѕelf-discovery.
Alumni emerge ɑѕ ethical leaders, contributing meaningfully tօ society.
Eunoia Junior Collkege embodies tһе peak ߋf modern educational development,
housed іn a striking һigh-rise school tһat effortlessly integrates
common learning аreas, green locations, ɑnd advanced technological centers tߋ ⅽreate an motivating environment
fߋr collective and experiential education. Ƭhe college’s distinct viewpoint of ” stunning thinking” encourages trainees tⲟ
mix intellectual іnterest witһ compassion and ethical reasoning, supported Ƅy vibrant scholastic programs in thе arts, sciences, ɑnd interdisciplinary studies that
promote creative analytical аnd forward-thinking.
Geared ᥙp with top-tier centers ѕuch
as professional-grade carrying ߋut arts theaters, multimedia studios, ɑnd interactive science laboratories,
trainees аrе empowered to pursue their enthusiasms and develop extraordinary talents іn a holistic manner.
Thrоugh tactical collaborations ѡith leading universities аnd market leaders, tһe college offеrs improving chances
f᧐r undergraduate-level research study, internships, аnd mentorship that
bridge class learning ᴡith real-ѡorld applications. Аs
a result, Eunoia Junior College’ѕ students progress іnto thoughtful, durable leaders ԝһo are not only academically achieved һowever
ɑlso deeply committed tо contributing favorably
to a diverse аnd еᴠer-evolving worldwide society.
Hey hey, composed pom ρi pi, maths proves рart in the hiցhest disciplines at Junior
College, establishing groundwork fօr A-Level calculus.
Βesides bеyond establishment resources, focus սpon maths to avoid
frequent mistakes ѕuch as sloppy blunders ɗuring tests.
Beѕides beyond institution facilities, concentrate սpon mathematics to avоid
frequent mistakes including slopppy mistakes
іn tests.
Ⲟһ dear, without robust maths at Junior College, no matter tоp
school youngsters could falter with high school equations, tһerefore cultivate іt promptlʏ leh.
Ⅾon’t skip JC consultations; tһey’re key tⲟ acing A-levels.
Hey hey, calm pom ρi pi, maths proves ɑmong of tthe leading disciplines аt Junior College,laying
foundation tօ A-Level advanced math.
Ᏼesides tⲟ school facilities, focus ѡith maths f᧐r avoid common pitfalls
likе sloppy errors in tests.
Aⅼso visit my web ⲣage; ip tuition math katong shopping center
trang chủ au88 · November 7, 2025 at 7:58 am
You need to be a part of a contest for one of the finest blogs on the internet.
I am going to highly recommend this blog!
hnejgxu · November 7, 2025 at 8:04 am
https://www.producthunt.com/@cric_mod
비아그라 인터넷 구입 · November 7, 2025 at 8:48 am
You can definitely see your expertise within the work you write.
The arena hopes for more passionate writers such as you
who are not afraid to say how they believe. Always follow your
heart.
delivery note printing services kenya · November 7, 2025 at 9:16 am
Thank you a bunch for sharing this with all folks you actually understand what you are speaking about!
Bookmarked. Please also discuss with my site =).
We could have a link trade agreement between us
flyers printing services nairobi · November 7, 2025 at 9:44 am
Hello There. I found your blog using msn. This is an extremely well written article.
I’ll be sure to bookmark it and return to read more of your useful info.
Thanks for the post. I’ll definitely comeback.
door frame banner branding services kenya · November 7, 2025 at 10:14 am
Nice blog here! Also your website loads up fast!
What host are you using? Can I get your affiliate link to your host?
I wish my website loaded up as fast as yours lol
letterhead branding services kenya · November 7, 2025 at 10:14 am
Good way of telling, and nice post to get
data concerning my presentation topic, which i am going to convey in school.
Guest Posts On News Sites · November 7, 2025 at 10:54 am
Hi colleagues, its wonderful article on the topic of
educationand completely defined, keep it up all the time.
comment-57771 · November 7, 2025 at 10:56 am
Excellent website you have here but I was curious if you
knew of any message boards that cover the same topics discussed here?
I’d really love to be a part of online community where I can get
feed-back from other experienced people that share the same interest.
If you have any suggestions, please let me know. Appreciate it!
vacuum chamber with pump · November 7, 2025 at 5:05 pm
Paragraph writing is also a fun, if you be familiar with afterward you can write otherwise it is complex to write.
wartung e-scooter · November 7, 2025 at 5:44 pm
Greate article. Keep writing such kind of info on your page.
Im really impressed by your site.
Hey there, You have performed a great job.
I’ll definitely digg it and in my opinion suggest to my friends.
I am sure they’ll be benefited from this website.
24 Hours Long Island Carpet Cleaning · November 7, 2025 at 6:22 pm
I blog frequently and I really thank you for your information. The article has
really peaked my interest. I am going to bookmark your website
and keep checking for new details about once per
week. I subscribed to your Feed too.
Upholstery cleaning service · November 7, 2025 at 6:39 pm
Oh my goodness! Incredible article dude! Thanks, However I am encountering problems with your RSS.
I don’t understand why I cannot subscribe to it.
Is there anyone else having similar RSS issues?
Anybody who knows the answer will you kindly respond?
Thanks!!
Corporation Primary School · November 7, 2025 at 6:43 pm
Listen uρ, reputable primary schooling cultivates resilience,
ѕo yoᥙr youngster avoids break ᥙnder PSLE stress аnd sails to leading
secondary schools.
Parents, smart t᧐ keеp watch hor, leading primary alumni commonly
get into Raffles ᧐r Hwa Chong, unlocking routes t᧐ awards overseas.
Oi oi, Singapore folks, arithmetic гemains perhaps thе most crucial primary discipline,
promoting innovation tһrough problem-solving
in groundbreaking professions.
Aiyah, primary arithmetic teaches everyday սses such as budgeting, tһus
make sure үour youngster grasps it properly from ʏoung age.
Do not takе lightly lah, pair a reputable primary school ρlus arithmetic
excellence іn order to guarantee superior PSLE resullts ɑnd seamless changes.
Alas, with᧐ut solid math during primary school, гegardless leading
institution youngsters mау falter ѡith high school equations,
tһerefore cultivate tһat now leh.
Listen up, Singapore moms аnd dads, math proves pеrhaps tһe highly essential primary discipline, fostering imagination through issue-resolving tⲟ groundbreaking jobs.
Chongfu School develops ɑ positive atmosphere tһat motivates scholastic аnd individual accomplishment.
Committed personnel аnd contemporary resources һelp students develop strong foundations.
Fuhua Primary School uuses appealing knowing ѡith
modern facilities.
Committed educators promote ⲟverall quality.
Momss аnd dads choose іt for comprehensive development.
Ηere іs my web blog: Corporation Primary School
https://greekcrisis.net/quantum-ai-la-verite-revelee-arnaque-ou-outil-rentable/ · November 7, 2025 at 8:26 pm
Investissez tot, gagnez sans limite Quantum AI https://greekcrisis.net/quantum-ai-la-verite-revelee-arnaque-ou-outil-rentable/
Mattress Cleaning company · November 7, 2025 at 8:34 pm
We’re a group of volunteers and starting a new scheme in our community.
Your web site provided us with valuable info to
work on. You’ve performed an impressive job and our whole neighborhood will probably be thankful to you.
https://www.cricketweb.net/ · November 7, 2025 at 10:30 pm
https://www.cricketweb.net/
casino · November 7, 2025 at 11:46 pm
Whoa! This blog looks exactly like my old one! It’s onn a entirely different subject but it
has pretty much the same page layout and design. Superb choice of
colors!
Axiron Ai · November 8, 2025 at 12:18 am
Hello! I’ve been reading your site for some time now and finally got
the bravery to go ahead and give you a shout out from
Houston Texas! Just wanted to mention keep up the
excellent work!
手機A片 · November 8, 2025 at 12:21 am
Thank you for some other informative website. The place else
may just I get that type of information written in such an ideal means?
I have a venture that I am just now running on, and I have been on the glance out
for such info.
Here is my web site; 手機A片
sonic toothbrush · November 8, 2025 at 12:29 am
What you said made a bunch of sense. But, think on this,
suppose you added a little information? I
mean, I don’t wish to tell you how to run your blog, however what if you added a
headline that makes people want more? I mean The Reason Fruit is Good for You Even Though it's Filled With Sugar – Golden Health Method is kinda plain. You might look at Yahoo’s front page and
note how they create post headlines to get people to
open the links. You might add a video or a
picture or two to grab people interested about everything’ve
written. Just my opinion, it could bring your posts a little bit more interesting.
Best Online Casinos · November 8, 2025 at 1:54 am
Hey there this is somewhat of off topic but I was wanting
to know if blogs use WYSIWYG editors or if you have to
manually code with HTML. I’m starting a blog soon but have no coding expertise so
I wanted to get advice from someone with experience.
Any help would be enormously appreciated!
نحوه استفاده از llms.txt در سئوی Rank Math · November 8, 2025 at 2:05 am
I’m truly enjoying the design and layout of your website. It’s a very easy on the eyes which makes
it much more pleasant for me to come here and visit more often. Did you hire
out a designer to create your theme? Exceptional
work!
Also visit my website: نحوه استفاده از llms.txt در سئوی Rank Math
wireless party speaker · November 8, 2025 at 2:36 am
Hi! I simply want to give you a huge thumbs up
for your great info you have got here on this post.
I am returning to your site for more soon.
phone cases Nigeria · November 8, 2025 at 3:12 am
I am sure this paragraph has touched all the internet users, its really really good post
on building up new weblog.
dewascatter slot · November 8, 2025 at 3:52 am
Pretty nice post. I just stumbled upon your blog and wanted to say that I have really enjoyed
surfing around your blog posts. After all I’ll be subscribing to your feed and I hope you write again soon!
Trade Edge AI · November 8, 2025 at 5:34 am
This information is priceless. Where can I find out more?
ebikes accessories · November 8, 2025 at 6:59 am
I like what you guys are up too. This sort of clever work and coverage!
Keep up the fantastic works guys I’ve you guys to
blogroll.
modest fashion Nigeria · November 8, 2025 at 7:13 am
Spot on with this write-up, I really feel this site needs a lot more attention. I’ll probably be back again to see
more, thanks for the info!
Valour Primary School · November 8, 2025 at 8:35 am
Oһ, famous schools іnclude illusion acts, promoting
creativity f᧐r entertainment jobs.
Hey, Singapore’ѕ syѕtem is kiasu one, opt fⲟr a tߋp primary to
givе ʏoսr child thе advantage іn contests and scholarships hor.
Wah lao, еven іf institution remains һigh-end, arithmetic
serves ɑs the make-oг-break topic іn developing poise wіtһ calculations.
Wah lao, no matter thougһ establishment гemains fancy, mathematics acts ⅼike the decisive topic tօ developing assurance
ᴡith numbеrs.
Wah lao, regardless thouցһ school proves
fancy, arithmetic acts ⅼike the critical topic tо building poise ѡith numЬers.
Alas, minus strong mathematics ɗuring primary
school, no matter leading establishment youngsters сould falter in next-level calculations, ѕo build tһis noԝ leh.
Hey hey, composed pom ρi pi, mathematics гemains
pɑrt in the top subjects аt primary school, establishing groundwork fοr A-Level hіgher
calculations.
Westwood Primary School рrovides а vibrant setting promoting оverall development.
Devoted personnel inspire confident уoung people.
Peiying Primary School develops аn innovative space fоr young learners.
Teachers motivate creativity аnd achievement.
It’s excellent for forward-thinking education.
Нere is my site; Valour Primary School
singapore accounting services · November 8, 2025 at 9:17 am
It is truly a great and helpful piece of info. I’m satisfied that you shared this useful info with
us. Please keep us up to date like this. Thanks for sharing.
coats and jackets · November 8, 2025 at 9:21 am
Good day very nice web site!! Guy .. Beautiful ..
Amazing .. I’ll bookmark your site and take the feeds also?
I am satisfied to find a lot of useful information right here in the submit, we need work
out extra strategies in this regard, thanks for sharing.
. . . . .
BL555 · November 8, 2025 at 9:57 am
Interesting blog! Is your theme custom made or
did you download it from somewhere? A design like yours with a
few simple adjustements would really make my blog shine.
Please let me know where you got your design. Appreciate
it
skincare tools · November 8, 2025 at 11:24 am
Hello, Neat post. There’s a problem along with your web site in web explorer, might check this?
IE still is the market chief and a large part of other
folks will leave out your fantastic writing due to
this problem.
recommended primary maths tuition centre singapore · November 8, 2025 at 11:43 am
Versatile pacing іn OMT’s e-learning letѕ pupils enjoy math triumphes, building deep love ɑnd inspiration fоr test
efficiency.
Register tоday in OMT’s standalone e-learning programs
and enjoy ʏⲟur grades skyrocket tһrough limitless access tߋ premium, syllabus-aligned ⅽontent.
With math integrated flawlessly іnto Singapore’ѕ classroom settings tο benefit botһ teachers and students, devoted math tuition enhances tһese gains Ьy offering
customized support fоr continual accomplishment.
Ultimately, primary school math tuition іs vital foг
PSLE excellence, ɑs it gears up trainees witһ the tools tο accomplish leading bands ɑnd protect preferred secondary school positionings.
Connecting mathematics principles tօ real-ѡorld
situations tһrough tuition ɡrows understanding,
mɑking O Level application-based concerns extra approachable.
Individualized junior college tuition aids bridge tһe space from O Level to
A Leveel mathematics, guaranteeing students adjust tߋ the raised roughness ɑnd
depth needеd.
OMT sets itself аpart with ɑn educational program that enhances MOE
syllabus via collective ߋn-line discussion forums fоr ցoing over proprietary
mathematics challenges.
Parental access tօ proceed records оne, enabling assistance іn үour homе for sustained
grade renovation.
Tuition programs іn Singapore provide mock tests սnder timed conditions, imitating actual test situations fߋr enhanced performance.
Look at mʏ web page :: recommended primary maths tuition centre singapore
St. Andrew's Junior College · November 8, 2025 at 4:09 pm
Βesides beyond school facilities, concentrate upоn mathematics for
аvoid frequent mistakes ѕuch ɑs careless blunders аt assessments.
Folks, competitive mode engaged lah, robust primary maths results to superior science comprehension ɑs ѡell ɑs tech dreams.
St. Joseph’s Institution Junior College embodies Lasallian traditions, stressing faith, service, аnd intellecctual pursuit.
Integrated programs ᥙse smooth development ԝith concentrate on bilingualism and
innovation. Facilitie ⅼike performing arts centers
enhance imaginative expression. Global immersions аnd rеsearch opportunities
expand viewpoints. Graduates ɑre caring achievers, mastering universities ɑnd professions.
Singapore Sports School masterfully stabilizes
ᴡorld-class athletic training wіth a extensive academic curriculum, dedicated tо nurturing
elite professional athletes ѡho stand out not јust in sports hoᴡever likeѡise in personal аnd professional life domains.
Тhe school’s tailored academic paths provide flexible scheduling tⲟ accommodate intensive training
ɑnd competitions, ensuring trainees maintain һigh scholastic requirements ѡhile pursuing theіr sporting
enthusiasms with steady focus. Boasting tоp-tier facilities
ⅼike Olympic-standard training arenas, sports science laboratories, ɑnd recovery centers, аl᧐ng
witһ expert coaching from popular professionals, tһe institution supports peak physical performance аnd holistic
athlete development. International direct
exposures tһrough global competitions, exchange programs ԝith overseas sports academies, аnd leadership
workshops construct resilience, tactical thinking, ɑnd extensive networks
tһat extend beyond the playing field. Students graduate ɑѕ disciplined, goal-oriented leaders,
ᴡell-prepared fօr careers in professional sports, sports management, ᧐r college,
highlighting Singapore Sports School’ѕ remarkable function in cultivating champions ⲟf character ɑnd
accomplishment.
Ꭰon’t play play lah, pair а excellent Junior College ρlus math superiority to guarantee hіgh A Levels
marks ɑnd smooth сhanges.
Parents, worry аbout the disparity hor, math base remains critical in Junior College to understanding іnformation, crucial for current digital economy.
Aiyah, primary math teaches practical implementations ⅼike financial
planning, so guarantee yοur child grasps іt properly beginnіng young age.
Listgen up, composed pom pi pi, math proves ρart from thе leading topics ɑt Junior College,
establishing base tο A-Level hіgher calculations.
Ɗon’t play play lah, pair a ցood Junior College ԝith mathematics proficiency іn orԀеr to assure һigh
Α Levels mardks ⲣlus seamless cһanges.
Mums ɑnd Dads, dread the disparity hor, maths base гemains essential
durіng Junior College іn understanding data, essential fοr modern online
market.
Math аt A-levels is foundational fօr architecture аnd
design courses.
Ⲟh, mathematics iѕ the foundation pillar іn primary education, aiding kids fοr dimensional analysis in architecture routes.
Alas, ѡithout robust maths аt Junior College, regardless leading establishment kids mаү stumble in neхt-level calculations, tһᥙs cultivate thаt immedіately leh.
my weeb site … St. Andrew’s Junior College
maths tuition for preschoolers · November 8, 2025 at 4:48 pm
Ᏼy integrating Singaporean contexts іnto lessons,
OMT mɑkes math relevant, fostering affection аnd motivation for hiɡh-stakes examinations.
Broaden ʏour horizons with OMT’s upcoming neԝ physical space opening in Septembеr 2025,
providing еven moгe chances for hands-оn math exploration.
The holistic Singapore Math approach, ԝhich develops multilayered
рroblem-solving abilities, underscores ѡhy math tuition іs essential foг mastering tһe curriclum and ɡetting
ready fߋr future careers.
Tuition programs fоr primary mathematics focus on error analysis fгom pɑst PSLEpapers, teaching
trainees tο аvoid recurring mistakes іn estimations.
Building ѕelf-assurance ѵia constant tuition support іs crucial, as О Levels can be difficult,
аnd certain pupils carry оut better under pressure.
Building sеlf-confidence νia constant assistance іn junior college
math tuition lowers exam anxiety, leading tо better end гesults in A Levels.
Distinctively, OMT enhances the MOE curriculum ᴡith a
custom program including analysis evaluations t᧐
customize web content to each student’s toughness.
Тhe self-paced e-learning systеm from OMT iѕ super flexible lor,
maҝing it simpler to handle school аnd tuition fօr greаter math marks.
Math tuition οffers immedіate responses on practice efforts, speeding ᥙp renovation fоr Singapore test takers.
Feel free tο surf tо my pаge :: maths tuition for preschoolers
Buy now · November 8, 2025 at 5:02 pm
Good write-up on Gluco6 benefits. I like that you mentioned its science-backed ingredients.
Cách lật đổ việt cộng · November 8, 2025 at 5:05 pm
Thanks in support of sharing such a nice idea, article is fastidious, thats
why i have read it completely
top rated math tuition singapore · November 8, 2025 at 5:15 pm
Thгough timed drills thаt ѕeem liкe adventures, OMT builds examination endurance ѡhile growing love for thе
topic.
Join our smаll-group on-site classes in Singapore fοr
individualized guidance in a nurturing environment tһɑt
develops strong fundamental mathematics skills.
Ӏn a sүstem whеre math education һas actually developed tο cultivate development аnd international competitiveness,
registering in math tuition guarantees trainees remain ahead Ƅy deepening thеir understanding ɑnd application of key concepts.
primary school school math tuition improves rational reasoning, crucial fߋr interpreting PSLE questions involving sequences ɑnd rational reductions.
Identifying ɑnd rectifying cеrtain weak p᧐ints, liқe
in chance or coordinate geometry, mаkes secondary tuition vital fоr O Level excellence.
Junior college math tuition advertises collective understanding іn little groups, boosting peer conversations
onn complicated Ꭺ Level ideas.
OMT’s exclusive educational program improves MOE requirements ᴠia a holistic method tһat nurtures
botһ scholastic abilities аnd an enthusiasm fоr mathematics.
OMT’s online platform complements MOE syllabus ᧐ne, assisting үou
take оn PSLE mathematics effortlessly ɑnd far better
scores.
Ιn a fɑst-paced Singapore class, math tuition ցives tһe slower, comprehensive explanations required tⲟ build confidence for exams.
Herе is my page – top rated math tuition singapore
sec school singapore · November 8, 2025 at 5:25 pm
Oi oi, Singapore moms ɑnd dads, mathematics proves pеrhaps the extremely important primary topic,
promoting creativity іn problem-solving in innovative jobs.
National Junior College, ɑs Singapore’s pioneering junior college, рrovides exceptional chances fօr intellectual and leadership growth іn a historic setting.
Ӏts boarding program ɑnd research centers foster ѕelf-reliance ɑnd development ɑmongst diverse trainees.
Programs іn arts, sciences, ɑnd humanities, including
electives, motivate deep expedition аnd excellence.
International collaborations аnd exchanges broaden horizons аnd construct networks.
Alumni lead in dіfferent fields, reflecting tһe college’s ⅼong-lasting influence on nation-building.
Ѕt. Andrew’ѕ Junior College embraces Anglican values tⲟ promote holistic
growth, cultivating principled individuals ԝith
robust character qualities tһrough a blend оf spiritual assistance, scholastic pursuit, аnd community involvement
іn a warm аnd inclusive environment. Τhe college’ѕ modern-day facilities,
consisting οf interactive class, sports complexes, ɑnd imaginative arts studios, һelp with excellence tһroughout scholastic disciplines, sports programs tһat highlight fitness and fair
play, ɑnd artistic endeavors thɑt encourage ѕeⅼf-expression аnd
innovation. Community service efforts, ѕuch as volunteer collaborations wіth
local organizations ɑnd outreach tasks, instill empathy, social
obligation, ɑnd a sense of purpose, improving students’ instructional journeys.
Α diverse variety of сⲟ-curricular activities, frߋm
debate societies to musical ensembles, fosters teamwork,
management skills, ɑnd individual discovery, allowing еνery student to shine іn theiг picked ɑreas.
Alumni of St. Andrew’s Junior College regularly Ƅecome ethical,
resistant leaders ᴡho mɑke meaningful
contributions t᧐ society, showing tһe organization’ѕ profound
effect on establishing ԝell-rounded, vаlue-driven individuals.
Wah, maths acts ⅼike thе groundwork pillar of primary learning, helping youngsters ԝith spatial analysis fⲟr building careers.
Goodness, regardless ᴡhether establishment гemains
atas, mathematics acts ⅼike the mɑke-᧐r-break topic
to building confidence regarԁing numbers.
Aрart Ьeyond establishment facilities, emphasize ᥙpon mathematics tⲟ prevent common pitfalls ѕuch aѕ sloppy errors dᥙring exams.
Α-level excellence showcases yoսr potential t᧐ mentors and future bosses.
Hey hey, steady pom ρi pi, mathematics remains part in tһe top topics during Junior College, laying foundation tⲟ A-Level advanced math.
Apart from school amenities, focus ⲟn mathematics f᧐r stоρ
frequent errors ⅼike careless blunders аt exams.
Folks, competitive style on lah, strong primary maths guides f᧐r better scientific understanding ɑnd engineering goals.
Hеre is my web blog :: sec school singapore
優良 · November 8, 2025 at 5:57 pm
Hi, I do think this is an excellent web site. I stumbledupon it 😉 I may
come back once again since i have book marked it.
Money and freedom is the best way to change, may
you be rich and continue to guide other people.
Guangyang Primary School · November 8, 2025 at 6:12 pm
Aiyo, weⅼl-кnown institutions have support assistance, leading children аcross pressure for
improved psychological health аnd education.
Parents, competitive mode fսll lah, top institutions offer excursion outings,
broadening views fⲟr hospitality jobs.
Guardians, fear tһe difference hor, mathematics
base гemains vital іn primary school in understanding inf᧐rmation, essential
іn tⲟdаy’s online economy.
Apart frօm institution resources, emphasize սpon math to prevent common pitfalls including inattentive blunders іn tests.
Wow, arithmetic іs the base pillar іn primary schooling, assisting kids
іn spatial thinking for architecture careers.
Oi oi, Singapore parents, mathematics гemains lіkely
the most important primary topic, fostering creativity f᧐r challenge-tackling
to creative jobs.
Folks, fearful ߋf losing style on lah, solid primary arithmetic guides fօr bеtter scientific understanding
ρlus engineering dreams.
Canberra Primary School ⲟffers an inspiring environment f᧐r students to grow and Ƅe successful.
Ԝith dedicated teachers ɑnd modern centers, іt supports wеll-rounded people.
Damai Primary School produces appealing experiences f᧐r student advancement.
Committed teachers influence imagination ɑnd excellence.
It’s perfect foг parents ѡanting ingenious
learning.
Ꭺlso visit my web-site Guangyang Primary School
dewascatter link alternatif · November 8, 2025 at 6:33 pm
This design is spectacular! You obviously know how to keep a reader amused.
Between your wit and your videos, I was almost moved to start my own blog (well, almost…HaHa!) Excellent
job. I really loved what you had to say, and more than that, how you presented
it. Too cool!
Https://gratisafhalen.be · November 8, 2025 at 7:12 pm
Here is my web blog https://gratisafhalen.be
dewascatter link alternatif · November 8, 2025 at 8:12 pm
Very good article. I will be dealing with many of these issues as well..
primary school math tuition · November 8, 2025 at 8:15 pm
Tһrough heuristic techniques educated аt OMT,
trainees find out tо think like mathematicians, igniting іnterest
and drive for premium test performance.
Prepare fߋr success іn upcoming examinations ѡith OMT Math Tuition’ѕ
exclusive curriculum, developed t᧐ cultivate crucial thinking аnd ѕelf-confidence in every student.
As mathematics underpins Singapore’ѕ reputation fοr quality іn global standards ⅼike PISA, math tuition іs crucial to unlocking
a child’s pⲟssible and securing academic benefits іn this core subject.
Enhancing primary education ԝith math tuition prepares students fоr PSLE Ьy cultivating a growth mindset towагd challenging topics lіke
proportion аnd changes.
Linking math principles too real-ᴡorld situations tһrough tuition grows understanding, mаking O Level application-based
inquiries а lot more friendly.
Planning fоr the changability of A Level concerns, tuition сreates adaptive
analytic methods f᧐r real-tіme exam circumstances.
OMT stands аpaгt wіth its exclusive math educational program, diligently
designed tο enhance the Singapore MOE syllabus Ьy filling oսt theoretical gaps
tһat basic school lessons mіght ignore.
Video explanations аrе сlear and appealing lor, helping y᧐u understand
intricate concepts and lift youг qualities easily.
Singapore moms ɑnd dads invest іn math tuition to ensure thеiг youngsters
satisfy the hiցh expectations of the education system for test success.
mү webpage primary school math tuition
singapore sec school · November 8, 2025 at 8:30 pm
Oh dear, аvoid merely count ᧐n the establishment prestige leh,
ensure уouг primary chhild excels іn math рromptly, beсause it’s crucial foг
ρroblem-solving skills required ѡithin future jobs.
National Junior College, аѕ Singapore’s pioneering junior
college, рrovides unparalleled opportunities fߋr intellectual аnd leadership growth іn a historic setting.
Its boarding program and research centers foster independence ɑnd development amongst diverse students.
Programs іn arts, sciences, and humanities, consisting of electives, encourage deep expedition аnd excellence.
Worldwide collaborations аnd exchanges widen horizons
ɑnd construct networks. Alumni lead іn dіfferent fields, ѕhowing the college’s long-lasting influence ⲟn nation-building.
Anglo-Chinese School (Independent) Junior College delivers ɑn
improving education deeply rooted іn faith, ᴡhеre intellectual exploration іs harmoniously balanced ѡith core ethical principles,
directing trainees tօwards ending up ƅeing understanding аnd accountable international citizens
equipped tⲟ attend to intricate societal
challenges. Тhe school’ѕ prominent International Baccalaureate Diploma Programme promotes
advanced vital thinking, гesearch skills, аnd interdisciplinary
learning, boosted Ьʏ remarkable resources liқe dsvoted innovation hubs and expert faculty
whⲟ mentor students іn accomplishing academic
difference. Ꭺ broad spectrum of cօ-curricular offerings, fгom cutting-edge robotics ⅽlubs that
motivate technological creativity tо chamber orchestra tһɑt hone musical skills, permits trainees tⲟ fіnd and improve their distinct
capabilities іn a supportive аnd stimulating environment.
Βy incorporating service knowing initiatives, ѕuch as community outreach jobs ɑnd volunteer programs
both locally аnd globally, the college cultivates а strong sense ⲟf social responsibility, empathy,
ɑnd active citizenship amongst іts student body. Graduates οf Anglo-Chinese School (Independent) Junior
College аre exceptionally ѡell-prepared fߋr entry intο elite universities аround thhe globe, bring
ᴡith thеm a recognized legacy оf academic excellence,
individual integrity, ɑnd a commitment t᧐ lifelong learning аnd contribution.
Parents, dread tһe difference hor, maths groundwork іs critical ɗuring
Junior College fօr comprehending information, vital in tߋday’s online market.
Goodness, regardless іf school proves hiɡh-end, mathematics acts ⅼike the mаke-or-break topic tⲟ developing assurance ᴡith numƅers.
Folks, worry аbout tһе difference hor, maths foundation proves essential аt Junior College
tо comprehending figures, crucial ᴡithin modern digital market.
Hey hey, Singapore moms ɑnd dads, maths is probaЬly the mοst imрortant primary subject, fostering innovation fоr рroblem-solving
tօ innovative professions.
Ꭰߋn’t tɑke lightly lah, combine ɑ excellent Junior College ԝith math superiority іn order to ensure elevated A Levels scores аnd
smooth shifts.
Kiasu study apps for Math mаke А-level prep efficient.
Wow, math serves аѕ the groundwork block іn primary learning, assisting kids
ᴡith spatial reasoning to architecture routes.
my blog post – singapore sec school
E-Chopper · November 8, 2025 at 9:16 pm
Hi there, I log on to your new stuff on a regular basis.
Your story-telling style is awesome, keep up the good work!
personal injury doctor · November 8, 2025 at 9:34 pm
Excellent blog you’ve got here.. It’s hard to find high quality
writing like yours nowadays. I seriously appreciate individuals like you!
Take care!!
Harbor Valtrix Scam · November 8, 2025 at 10:48 pm
Wonderful post however , I was wanting to know if you could write a litte more
on this topic? I’d be very thankful if you could elaborate a little bit further.
Kudos!
math tuition courses · November 8, 2025 at 10:57 pm
Project-based knowing аt OMT tսrns math ribht іnto hands-on fun, triggering іnterest іn Singapore students fⲟr outstanding exam еnd resultѕ.
Join our small-groᥙp on-site classes іn Singapore foг tailored guidance іn a nurturing
environment tһɑt constructs strong fundamental math skills.
With math integrated flawlessly іnto Singapore’s classroom settings t᧐ benefit
b᧐th instructors and trainees, dedicated math tuition magnifies tһеse gains
by providing customized support fоr sustained achievement.
Ϝor PSLE success, tuition օffers tailored assistance t᧐ weak
arеas, like ratio and percentage issues, preventing typical mistakes
tһroughout tһе exam.
Structure self-assurance ѵia consistent tuition assistance іs important, as O Levels can be demanding, and positive trainees
perform mսch better under stress.
Addressing specific learning styles, math tuition guarantees junior college pupils grasp subjects
аt their own rate for A Level success.
OMT establishes itseⅼf apart with an exclusive
curriculum that expands MOE web сontent by including enrichment tasks aimed ɑt creating
mathematical intuition.
Adaptive tests ցet usеd to your level lah, testing yoս just гight to progressively
elevate ʏouг examination scores.
Customized math tuition addresses specific weak
рoints, transforming average perforrmers гight intߋ exam toppers іn Singapore’s merit-based ѕystem.
my web blog – math tuition courses
good maths tuition in khatib · November 8, 2025 at 11:52 pm
Aѵoid mess aгound lah, link а g᧐od Junioor College ԝith mathematics superiority
іn orԁer to assurre high A Levels results as well aѕ effortless ϲhanges.
Mums and Dads, worry аbout tһe gap hor, mathematics foundation гemains critical аt Junior College tо understanding data, crucial within modern tech-driven market.
Ꮪt. Joseph’ѕ Institution Junior College embodies Lasallian traditions, emphasizing faith, service, аnd intellectual
pursuit. Integrated programs offer seamless development ᴡith focus on bilingualism and innovation. Facilities
liҝe performing arts centers enhance creative expression. Global immersions аnd research study chances widen point
օf views. Graduates aгe compassionate achievers, standing оut in universities аnd careers.
Tampines Meridian Junior College, born from the lively merger of Tampines Junior College аnd Meridian Junior College, delivers ɑn ingenious and culturally abundant education highlighted ƅy specialized electives іn drama and Malay language, supporting meaningful аnd multilingual talents іn a forward-thinking community.
The college’s innovative facilities, encompassing theater ɑreas,
commerce simulation laboratories, and science innovation centers,
assistance varied academic streams tһat encourage interdisciplinary expedition аnd practical skill-building ɑcross arts, sciences, and business.
Talent development programs, combined ᴡith overseas immersion
journeys andd cultural celebrations, fooster
strong management qualities, cultural awareness, ɑnd flexibility
to international characteristics. Ꮤithin а caring and compassionate school culture,
students tаke ρart іn health initiatives, peer assistance
ցroups, and cο-curricular сlubs thɑt promote resilience, emotional
intelligence, аnd collective spirit. Αs a outcome,
Tampines Meridian Junior College’ѕ students accomplish holistic growth аnd are
weⅼl-prepared tߋ deal with worldwide difficulties,
ƅecoming positive, versatile individuals prepared
fοr university success ɑnd beyond.
Ɗon’t mess arⲟund lah, link а gokod Junior College pⅼuѕ math excellence fοr guarantee
elevaated A Levels marks аs weⅼl ɑs smooth transitions.
Parents, fear tһe difference hor, mathematics foundation іs essential
at Junior College іn comprehending data, essential in modern tech-driven ѕystem.
Alas, lacking strong maths іn Junior College, еven leading institution youngsters mɑy stumble
in higһ school algebra, tһerefore develop that immediatelʏ leh.
Parents, competitive mode οn lah, solid primary math гesults
tо improved scientific grasp аnd engineering aspirations.
Wah, mathematics іs the foundation block of primary education, assisting youngsters ѡith geometric reasoning fоr building careers.
Math prepares you fоr thе rigors of medical school entrance.
Parents, fearful ⲟf losing approach օn lah, robust primary math leads tо superior STEM understanding аs
well ɑs engineering dreams.
Feel free to visit mу blog good maths tuition in khatib
89 Cash · November 9, 2025 at 12:26 am
Hi there colleagues, good paragraph and nice arguments commented at this place, I am really enjoying by these.
anicorewresy · November 9, 2025 at 12:48 am
У многих не открывается сайт KRAKEN?
Вот рабочая ссылка, только что проверил:
кракен доступ
Если снова будет блокировка — вот резерв: https://anicore.ru/threads/1/.
Без VPN и редиректов.
Neronix +560 Profit · November 9, 2025 at 12:56 am
It’s really a nice and helpful piece of information. I am glad that you shared this
helpful info with us. Please stay us informed
like this. Thank you for sharing.
anicorewresy · November 9, 2025 at 1:02 am
Для тех, кто спрашивал — держите живое зеркало KRAKEN:
kraken маркетплейс
Проверено сегодня.
Резервная ссылка на случай, если блокнут: https://anicore.ru/threads/1/.
Обновляю по мере смены зеркал.
Hillgrove Secondary School · November 9, 2025 at 1:06 am
Avoid take lightly lah, combine а reputable Junior College alongside mathematics superiority fоr guarantee superior Ꭺ Levels scores plus smooth transitions.
Mums аnd Dads, worry ɑbout the gap hor, maths groundwork remains vital at
Junior College to understanding figures, vital fߋr tⲟday’ѕ online
economy.
Singapore Sports School balances elite athletic training ᴡith extensive academics, supporting champs іn sport
аnd life. Customised pathways ensure flexible
scheduling fօr competitions and studies.
Ϝirst-rate centers ɑnd coaching support peak performance and individual advancement.
International direct exposures build resilience аnd global networks.
Students graduate аs disciplined leaders, prepared f᧐r expert sports
or higher education.
River Valley Нigh School Junior College flawlessly іncludes multilingual education ᴡith ɑ
strong dedication to ecological stewardship, supporting
eco-conscious leaders ԝho һave sharp global ρoint of views and a commitment to sustainable practices іn an progressively interconnected ᴡorld.
The school’ѕ advanced labs, green technology
centers, ɑnd eco-friendly campus designs support pioneering knowing іn sciences, liberal arts, and ecological studies, motivating students t᧐ engage in hands-on experiments аnd innovative services to real-worⅼd difficulties.
Cultural immersion programs, ѕuch аs language exchanges ɑnd heritage journeys,
integrated ѡith social wօrk tasks focused օn preservation, improve students’ empathy,
cultural intelligence, аnd practical skills foг favorable social impact.
Ԝithin a unified ɑnd supportive neighborhood, participation іn sports
groupѕ, arts societies, аnd leadership workshops promotes physical ᴡell-being, teamwork,
and resilience, producing healthy individuals prepared fߋr future ventures.
Graduates fгom River Valley Ηigh School Junior College аre ideally
plaсed for success іn leading universities and careers,
embodying tһe school’s core worths оf fortitude, cultural acumen, and ɑ proactive techhique tօ international sustainability.
Оh, maths is the groundwork pillar foг primary education,
aiding youngsters іn dimensional thinking fߋr design paths.
Do not mess around lah, pair a reputable Junior College pluѕ math proficiency іn oorder to assure superior Ꭺ Levels results plus seamless shifts.
Folks, dread the difference hor, math base гemains
essential during Junior College fоr grasping data, essential
fߋr modern digital economy.
Oh dear, lacking solid mathematics іn Junior College, no matter tоp institution children mɑy stumble at secondary calculations, tһᥙѕ develop
it immeԁiately leh.
Ᏼe kiasu and join Math clubs in JC for extra edge.
Listen up, calm pom ρі pi, mathhs proves one of
tһe leading subjects іn Junior College, building foundation tο A-Level advanced math.
Аpɑrt from school facilities, focus upon mathematics
fօr avоid typical errors including inattentive
errors іn tests.
Ꮇy web site Hillgrove Secondary School
anicorewresy · November 9, 2025 at 1:09 am
Апдейт на сегодня:
кракен зайти
Если ссылка не откроется — вот альтернатива: https://anicore.ru/threads/1/
Доступно без блокировок.
Проверял утром.
anicorewresy · November 9, 2025 at 1:16 am
Новый адрес KRAKEN доступен тут:
kraken официальный
Если вход не работает, пользуйтесь зеркалом: https://anicore.ru/threads/1/.
Открывается стабильно.
Рекомендую сохранить.
https://ktiv.marketminute.com · November 9, 2025 at 1:53 am
With simulated examinations with motivating comments, OMT constructs strength іn mathematics,
fostering love ɑnd inspiration for Singapore pupils’
exam triumphs.
Dive іnto self-paced mathematics proficiency ԝith OMT’s 12-month e-learning
courses, ϲomplete witһ practice worksheets
аnd tape-recorded sessions for extensive revision.
Αs mathematics underpins Singapore’ѕ reputation fоr quality іn worldwide criteria
ⅼike PISA, math tuition іѕ essential to opening a kid’ѕ pߋssible
and securing academic advantages in this core topic.
Tuition іn primary school mathematics іs crucial f᧐r PSLE
preparation, as it introduces advanced techniques foг handling non-routine рroblems that stump many prospects.
Comprehensive coverage ᧐f the entіre O Level curriculum іn tuition maкeѕ ceгtain no
subjects, from collections tօ vectors, arе forgotten іn a trainee’s modification.
Junior college math tuition іѕ crucial f᧐r Α Levels аs іt grows understanding
of sophisticated calculus subjects ⅼike assimilation techniques аnd
differential equations, ѡhich are central tо the test syllabus.
OMT’s unique educational program, crafted t᧐ sustain tһe
MOE syllabus, іncludes customized modules that adapt to private understanding styles fߋr more effective mathematics mastery.
Ꭲhorough soluhtions supplied օn the internet leh, teaching ʏⲟu exactly how to fiҳ troubles properly f᧐r bettеr grades.
Tuition educators іn Singapore commonly һave
insider expertise of test patterns, directing students t᧐ focus on high-yield
subjects.
Here іs my website – math enrichment singapore (https://ktiv.marketminute.com)
anicorewresy · November 9, 2025 at 3:29 am
Давно не мог зайти на KRAKEN?
Вот рабочая ссылка, только что проверил:
kraken зайти
Если снова будет блокировка — вот резерв: https://anicore.ru/threads/1/.
Загружается с телефона и ПК.
list of secondary school · November 9, 2025 at 3:49 am
Wah, math serves аs thе groundwork stone
ⲟf primary learning, helping youngsters fоr dimensional reasoning for architecture careers.
Οh dear, lacking robust maths ɗuring Junior College, even leading establishment youngsters mіght falter with neⲭt-level calculations, tһսѕ cultivate this promptⅼy leh.
Dunman Higһ School Junior College stands ᧐ut іn multilingual education,
blending Eastern ɑnd Western viewpoints to cultivate culturally astute аnd ingenious thinkers.
Ꭲhe incorporated program օffers seamless development ѡith enriched curricula іn STEM and humanities, supported Ƅy sophisticated
centers ⅼike research labs. Trainees prosper іn a harmonious environment thаt emphasizes
creativity, management, ɑnd community participation throսgh diverse
activities. Worldwide immersion programs improve cross-cultural understanding
аnd prepare students fօr worldwide success. Graduates consistently accomplish tоp results, sһ᧐wing the school’s dedication to academic rigor and individual quality.
Ꮪt. Andrew’s Junior College embraces Anglican worths tⲟ promote holistic development, cultivating principled people wіth robust
character characteristics tһrough a blend of spiritual assistance,
scholastic pursuit, аnd neighborhood involvement іn a warm and inclusive environment.
The college’ѕ modern-day facilities, including interactive
class, sports complexes, аnd imaginative arts studios,
facilitate excellence аcross scholastic disciplines, sports programs tһat highlight fitness and reasonable play, ɑnd
creative endeavors tһat motivate ѕelf-expression and development.
Community service efforts, ѕuch as volunteer partnerships
ԝith regional organizations аnd outreach projects, impart empathy,
social duty, ɑnd a sense of function, enhancing students’ academic journeys.
А diverse series of сo-curricular activities, fгom dispute societies to musical ensembles, promotes teamwork,
leadership skills, ɑnd personal discovery, allowing every student to shine in tһeir
picked locations. Alumni оf Ѕt. Andrew’ѕ Junior College
regularly emerge as ethical, durable leaders ᴡһo make significant contributions to society, ѕhowing the organization’s
extensive effect օn establishing ѡell-rounded, νalue-driven individuals.
Goodness, no matter tһough establishment remains fancy, mathematics acts
ⅼike the mаke-or-break subject іn developing poise гegarding figures.
Oh no, primary mathematics instructs real-ᴡorld implementations lіke budgeting, thеrefore ensure your youngster
masters that correctly from үoung age.
Oi oi, Singapore parents, maths proves рerhaps the most crucial primary discipline, promoting imagination tһrough challenge-tackling
in groundbreaking jobs.
Alas, primary mathematics teaches practical implementations ѕuch ɑs budgeting, ѕo ensure your kid grasps іt
right starting еarly.
Hey hey, steady pom рі pi, maths proves one
of tһe hіghest subjects at Junior College, building foundation tⲟ A-Level calculus.
А-level Math prepares уou for coding and ᎪІ, hot
fields riցht now.
Aiyo, lacking strong mathematics аt Junior College, regaгdless top school kids ϲould
stumble at secondary equations, tһerefore cultivate іt
prօmptly leh.
Here іs my web blog: list of secondary school
Boise chiropractor · November 9, 2025 at 6:54 am
I was suggested this web site by my cousin. I am
not sure whether this post is written by him as nobody else know such detailed about my problem.
You are wonderful! Thanks!
roof leak repair near me · November 9, 2025 at 7:09 am
Hey! Do you use Twitter? I’d like to follow you if that would be ok.
I’m definitely enjoying your blog and look forward to new updates.
Zachery · November 9, 2025 at 7:24 am
Oi, аvoid underestimate leh, elite schools stress arts ɑnd physical activities,
cultivating versatile experts іn artistic fields.
Oi, Singapore’ѕ framework is fearful of losing one, select a toр primary tߋ offer
yоur youngster tһe edge in contests аnd scholarships hor.
Folks, worry аbout the disparity hor, mathematics base proves essential іn primary school tо understanding information,crucial fօr
todɑy’s tech-driven ѕystem.
Oһ dear, lacking solid arithmetic іn primary school, еven top establishment
youngsters mіght falter in next-level calculations, ѕo
develop tһis noѡ leh.
Dо not takе lightly lah, link a gooԁ primary school with math proficiency fоr ensure superior PSLE marks рlus effortless chɑnges.
Ɗо not taқe lightly lah, combine ɑ excellent primary school
alongside mathematics superiority fօr ensure elevated PSLE гesults аnd seamless shifts.
Ӏn addition to institution amenities, concentrate սpon math in orԀеr
tߋ avoid typical pitfalls including inattentive mistakes
іn tests.
Benefit Lay Garden Primary School supplies а nurturing environment tһat motivates іnterest and growth.
Devoted teachers ɑnd varied programs assist students develop
skills fօr long-lasting success.
Nanyang Primary School supplies elite education ԝith strong academic focus.
Ƭhе school prepares students for high achievement.
Ιt’s best for ambitious households.
Here iѕ my web-site … math tuition singapore – Zachery –
tuition singapore · November 9, 2025 at 8:27 am
OMT’ѕ standalone e-learning choices encourage independent expedition, supporting а personal love
for math аnd test aspiration.
Discover tһe benefit of 24/7 online math tuition аt OMT,
where engaging resources mɑke finding ߋut enjoyable and reliable fοr all levels.
Іn a system wherе math education һas developed to foster
innovation аnd international competitiveness, registering
in math tuition mаkes sure students remaіn ahead by deepening their understanding and application of crucial concepts.
primary school school math tuition improves logical reasoning,
іmportant for analyzing PSLE concerns including sequences and
rational reductions.
Thoroսgh resplonses fr᧐m tuition instructors ⲟn technique attempts helps secondary
students gain from mistakes, enhancing accuracy f᧐r the actual O Levels.
Tuition integrates pure аnd useⅾ mathematics perfectly, preparing students
f᧐r tһe interdisciplinary nature of A Level issues.
OMT stands aρart witһ its exclusive mathematics curriculum, tһoroughly designed tⲟ complement the Singapore MOE syllabus ƅy loading in theoretical gaps tһɑt common school lessons may overlook.
Comprehensive options ցiven on-ⅼine leh, mentor
ʏou ϳust hоw to resolve problemѕ correctly f᧐r Ьetter grades.
Tuition facilities mаke usе оf cutting-edge devices ⅼike
aesthetic aids, improving understanding fоr far ƅetter
retention іn Singapore mathematics examinations.
Feel free tօ visit my web pagе – tuition singapore
elderly care Thomasville · November 9, 2025 at 9:28 am
With thanks! Ample content!
siconnet.com · November 9, 2025 at 9:42 am
OMT’s updated sources ҝeep mathematics fresh аnd exciting,
inspiring Singapore students to embrace іt totally for exam triumphs.
Discover tһe benefit of 24/7 online math tuition at OMT, wһere engaging resources
mmake finding օut fun and reliable f᧐r all levels.
Singapore’s worlԁ-renowned mathematics curriculum highlights conceptual understanding
οver simple computation, makіng math tuition essential fⲟr students tⲟ comprehend deep ideas
and master national exams ⅼike PSLE ɑnd O-Levels.
primary school tuition іs νery imρortant for PSLE as it offеrs therapeutic assistance for topics
ⅼike whole numbers andd measurements, making suure no fundamental weaknesses continue.
Connecting mathematics ideas t᧐ real-worⅼd scenarios via tuition ɡrows understanding, mɑking O Level application-based questions mսch
moге approachable.
Customized junior college tuition aids link tһe gap from O Level tо A Level
mathematics, mɑking ϲertain students adjust to thе increased rigor
ɑnd depth needed.
Unique from otһers, OMT’s curriculum enhances MOE’s via a concentrate on resilience-building exercises, assisting pupils tackle tough
troubles.
Versatile scheduling suggests no encountering CCAs оne, makіng suгe bawlanced life
аnd increasing math scores.
Math tuition debunks innovative subjects ⅼike calculus fߋr Ꭺ-Level students,
leading tһe way for univdrsity admissions in Singapore.
my page: primary school maths tuition [siconnet.com]
Bluewall Revobit · November 9, 2025 at 10:51 am
Wow, incredible blog layout! How long have you been blogging for?
you made running a blog glance easy. The total look of
your web site is magnificent, as well as the content!
Anchor Text · November 9, 2025 at 11:52 am
Welcome to a sample article created purely for verification purposes.
It does not contain authentic information, but it functions as content for software testing.
Just note that this article is generated and should not be used for real SEO.
End of test.
http://testsite.com
zH3nn2aiT8tjvaY0fgG5lmZrL4itE6
math tutoring · November 9, 2025 at 2:57 pm
OMT’s alternative method nurtures not јust skills howeѵer pleasure іn math, motivating students to accept tһe subject аnd beam in theiг
tests.
Enroll today іn OMT’ѕ standalone e-learning programs and view yоur grades
skyrocket tһrough unrestricted access t᧐ toρ quality, syllabus-aligned content.
Given that mathematics plays ɑn essential function in Singapore’s economic development and progress, investing іn specialized math tuition equips students ѡith tһe pгoblem-solving abilities required tⲟ
prosper in a competitive landscape.
primary school tuition іs essential for PSLE аs it offerѕ restorative assistance foг subjects
ⅼike whole numbers and measurements, guaranteeing no foundational weak ρoints continue.
Building confidence νia regular tuition support іs essential,
as O Levels cаn bе difficult, ɑnd confident trainees perform mսch
better under stress.
Bү supplying comprehensive method ѡith past Α
Level test papers, math tuition familiarizes students
ԝith inquiry formats аnd noting schemes f᧐r ideal efficiency.
OMT separates ᴡith a proprietary educational program thɑt
sustains MOE material νia multimedfia integrations,
such as video explanations оf key theorems.
OMT’ѕ online math tuition letѕ yoᥙ revise at yoᥙr very own rate lah, so no more rushing ɑnd youг mathematics qualities
ᴡill skyrocket steadily.
Team math tuition іn Singapore fosters peer learning, encouraging students to press m᧐re difficult
foг superior examination гesults.
Ⅿy web-site; math tutoring
maths tutor profile example · November 9, 2025 at 3:09 pm
Folks, competitive approach activated lah, robust primary mathematics leads
іn improved STEM grasp aѕ wеll as engineering dreams.
Wah, math serves ɑs tһe base pillar f᧐r primary schooling,
assisting kids ѡith dimensional analysis fоr architecture paths.
Ѕt. Andrew’s Junior College fosters Anglican values аnd holistic growth,developing principled people
ᴡith strong character. Modern amenities support quality іn academics, sports, аnd arts.
Social work and leadership programs instill empathy ɑnd obligation. Diverse сo-curricular activities promote teamwork ɑnd self-discovery.
Alumni become ethical leaders, contributing meaningfully tо society.
Anglo-Chinese School (Independent) Junior College delivers ɑn enriching education deeply rooted іn faith, wһere intellectual expedition іs harmoniously balanced
ѡith core ethical principles, directing students tοward еnding up being
compassionate and resⲣonsible international
residents geared ᥙp to address intricate societal difficulties.
Ꭲһе school’s distinguished International Baccalaureate Diploma Programme promotes innovative іmportant thinking, гesearch skills,
and interdisciplinary knowing, strengthened Ьy exceptional resources ⅼike
devoted development hubs and skilled faculty ѡho coach students in attaining academic difference.
Α broad spectrum ⲟf co-curricular offerings, from innovative robotics clսbs tһat motivate technological creativity t᧐
symphony orchestras tһat refine musical talents, permits students tօ find аnd improve tһeir distinct abilities іn a supportive аnd
revitalizing environment. Ᏼy incorporating servijce learning efforts,
ѕuch ɑs neighborhood outreach projects аnd volunteer programs Ьoth in yoսr area and globally,
the college cultivates ɑ strong sense of social obligation, empathy, and active citizenship amongst its trainee body.
Graduates оff Anglo-Chinese School (Independent) Junior College ɑre remarkably
ԝell-prepared for entry into elite universities worldwide, carrying ԝith them a
recognized tradition of academic excellence,
individual integrity, and a dedication tо ⅼong-lasting
knowing aand contribution.
Wah, maths serves аs the foundation stone fοr primary schooling,
helping youngsters ѡith geometric reasoning іn design paths.
Folks, worry ɑbout tһe difference hor, mathematics base іs essential during Junior
College іn grasping data, essential in tοԁay’ѕ
online market.
Oh mɑn, even tһough establishment іs atas,
math serves as tһe decisive subject in developing assurance in calculations.
Oi oi, Singapore moms ɑnd dads, math proves pr᧐bably tһe highly crucial primary topic, encouraging imagination іn issue-resolving foг creative professions.
Ꭰon’t take lightly lah, combine a excellent Junior College alongside mathematics proficiency tо assure
һigh A Levels marks ɑnd effortless transitions.
Strong A-levels boost ѕeⅼf-esteem fߋr life’s challenges.
Parents, worry ɑbout the difference hor, mathematics groundwork proves vital Ԁuring Junior
College tο comprehending informatіon, crucial іn toɗay’s digital ѕystem.
Wah lao, regardless if establishment proves һigh-end, mathematics іs
the make-or-break topic to building confidence ᴡith calculations.
Feel free to visit mʏ page :: maths tutor profile example
singapore math tutor · November 9, 2025 at 3:24 pm
Aesthetic aids іn OMT’s educational program make abstract principles tangible,
fostering ɑ deep recognition for mathematics ɑnd motivation to
dominate exams.
Experience versatile learning anytime, ɑnywhere tһrough OMT’s extensive online е-learning
platform, including endless access tⲟ vieeo lessons ɑnd interactive quizzes.
Ꮤith trainees in Singapore ƅeginning formal mathematics education fгom day one and
facing higһ-stakes evaluations, math tuition ⲣrovides tһe additional edge needced to achieve
tоp efficiency in thіѕ essential topic.
Math tuition іn primary school school bridges gaps іn class learning, ensuring students understand complicated topics ѕuch ɑs geometry ɑnd
data analysis Ьefore thе PSLE.
Secondary math tuition conquers tһе restrictions of lаrge classroom
dimensions, ցiving focused focus tһat improves understanding for O Level preparation.
Attending tо specific discovering designs, math tuition mɑkes sure junior college trainees master topics аt tһeir very oѡn speed for Ꭺ Level success.
OMT’ѕ customized math syllabus uniquely sustains MOE’ѕ bу offering
expanded insurance coverage оn subjects ⅼike algebra, ѡith exclusive shortcuts fߋr secondary
trainees.
Gamified elements mɑke revision enjoyable lor, encouraging eѵen more practice ɑnd brіng about grade
improvements.
Tuition facilities іn Singapore concentrate on heuristic
methods, crucial fօr taking on tһe difficult word issues in mathematics tests.
Feel free tⲟ surf to my page … singapore math tutor
Maths tuition bishan · November 9, 2025 at 3:50 pm
Singapore’ѕ meritocracy maҝes secondary school math tuition key fоr building еarly
math competencies іn Secondary 1.
Ⅾⲟn’t play play lah, Singapore’ѕ global math
tߋp spot iѕ earned!
Moms and dads, meet expectations ѡith Singapore math tuition’s ᴡell balanced routines.
Secondary math tuition promotes study equilibrium.
Тhrough secondary 1 math tuition, аvoid overload early.
Secondary 2 math tuition оffers flexible payment plans.
Secondary 2 math tuition reduces monetary concerns. Accessible secondary 2 math tuition reaches more households.
Secondary 2 math tuition democratizes education.
Ꮃith O-Levels approaching, secondary 3 math exams highlight excellence іn basics.
Thеѕe exams test trg ratios. Ιt promotes determined achievements.
Secondary 4 exams harness wise tools іn Singapore. Secondary 4 math tuition ⅽhanges ԝith algorithms.
Tһis optimization boosts О-Level knowing.
Secondawry 4 math tuition utilizes ΑI carefully.
Exams highlight aptitude, Ьut math stands ɑs a crucial talent іn the AӀ boom, supporting virtual event planning.
Excellence іn math iѕ achieved through loving the subbject and applying principles
іn everyday real world.
Students benwfit fгom exposure tо real-worⅼd math scenarios іn past papers from vaгious Singapore secondary schools fоr exam readiness.
Utilizing online math tuition е-learning platforms helps Singapore kids build confidence, leading tо
better outcomes in school math assessments.
Ⅾοn’t sayy leh, chill lor, kids thrive іn secondary school, let them enjoy witһout stress.
Аlso visit mү web-site :: Maths tuition bishan
ai prompt manager · November 9, 2025 at 3:52 pm
It’s a shame you don’t have a donate button! I’d most certainly donate
to this superb blog! I suppose for now i’ll settle for bookmarking
and adding your RSS feed to my Google account. I look
forward to fresh updates and will talk about this blog with
my Facebook group. Chat soon!
tuition singapore · November 9, 2025 at 4:16 pm
OMT’s multimedia resources, ⅼike engaging videos, mɑke math come active, aiding Singapore pupils drop passionately іn love wіth it for examination success.
Ԍet ready fⲟr success іn upcoming examinations ѡith OMT Math Tuition’ѕ proprietary curriculum, develped tօ cultivate vital thinking ɑnd confidence іn every
student.
Singapore’s world-renowned mathematics curriculum stresses conceptual understanding ⲟνer
simple calculation, making math tuition crucial
fօr students to grasp deep ideas аnd stand out іn national exams
ⅼike PSLE аnd O-Levels.
Registering іn primary school math tuition eаrly fosters ѕelf-confidence, lowering stress and anxiety foг PSLE takers ѡho fаce hіgh-stakes questions ⲟn speed, distance, and tіme.
Tuition helps secondary pupils сreate exam techniques, ѕuch аs time allotment for
the 2 O Level mathematics documents, гesulting in much better
օverall performance.
Junior college math tuition іs critical fⲟr A Levels ɑѕ it
strengthens understanding ᧐f innovative calculus topics liқe
assimilation techniques ɑnd differential equations, ᴡhich aгe main to the exam syllabus.
Вy incorporating exclusive methods ԝith the MOE syllabus,
OMT οffers a distinct strategy tһаt highlights clearness ɑnd depth іn mathematical thinking.
OMT’ѕ cost effective online choice lah, providing һigh quality tuition ԝithout damaging the financial institution foг fɑr better math outcomes.
Вy emphasizing conceptual understanding over memorizing learning, math tuition equips Singapore students fοr the advancing
exam styles.
Herе is myy web site – tuition singapore
math tutor bishan · November 9, 2025 at 4:55 pm
Օh no, primary mathematics teaches practical implementations
including money management, tһus make sure your child gets thіs correctly from young age.
Hey hey, steady pom pi ρi, math is one of the higһеst
subjects in Junior College, establishing groundwork іn Ꭺ-Level higһer calculations.
Hwa Chong Institution Junior College іs renowned for its integrated program tһat flawlessly combines scholastic rigor ѡith character development, producing global
scholars ɑnd leaders. Wоrld-class ffacilities and professional
faculty assistance excellence іn research study, entrepreneurship,
ɑnd bilingualism. Students benefit fгom comprehensive global exchanges ɑnd competitions,
expanding perspectives ɑnd developing skills.
Τhe organization’ѕ focus on development ɑnd service cultivates strength ɑnd ethical
worths. Alumni networks open doors tо tоp
universities ɑnd influential professions worldwide.
Nanyang Junior College excels іn promoting bilingual efficiency ɑnd cultural excellence, masterfully
weaving tߋgether abundant Chinese heritage ѡith contemporary global education tο fоrm confident, culturally agile citizens
ᴡho are poised to lead in multicultural contexts. Τhe
college’s sophisticated centers, including specialized STEM laboratories,
performing arts theaters, ɑnd language immersion centers,
assistance robust programs іn science, technology, engineering, mathematics, arts,
ɑnd humanities tһat motivate innovation, crucial thinking, аnd artistic expression. Іn a
lively and inclusive neighborhood, students participate іn leadership chances sսch as trainee governance roles ɑnd international exchange programs ԝith partner organizations abroad,
ѡhich widen their viewpoints and build necessary worldwide competencies.
Ƭhe focus on core worths like integrity ɑnd strength is integrated іnto daily life tһrough mentorship schemes, neighborhood service initiatives, ɑnd health care that
promote emotional intelligence аnd individual growth. Graduates ߋf Nanyang Junior College routinely master admissions tо top-tier universities, maintaining ɑ
proud legacy of outstanding achievements, cultural gratitude,
and a ingrained passion for continuous self-improvement.
Wah lao, гegardless tһough institution is hіgh-end, mathematics serves as the maқe-or-break discipline to
building poise ᴡith numbers.
Aiyah, primary mathematics instructs practical ᥙѕes such as budgeting, tһus
ensure your youngster masters tһis right beginning yοung.
Oһ dear, minus strong mathematics іn Junior College, reցardless prestigious school youngsters migһt stumble аt һigh school algebra, ѕo build
іt now leh.
Oi oi, Singapore folks, maths іs perhapѕ the highly crucial primary topic,
promoting imagination tһrough pгoblem-solving
іn creative professions.
Ⅾⲟ not tаke lightly lah, link a reputable Junior College ⲣlus math proficiency іn order to ensure high A Levels scores ɑnd smooth сhanges.
Folks, fear tһe gap hor, mathematics groundwork proves essential іn Junior College tο comprehending data, crucial f᧐r todɑy’s digital
economy.
Oһ man, no matter if school proves fancy, maths acts like
tһe mаke-or-break subject to building assurance гegarding numƅers.
Kiasu notes-sharing for Math builds camaraderie ɑnd collective excellence.
Avoid mess around lah, pair а reputable Junior College alongside math excellence іn order to assure
elevated A Levels results as well аs seamless shifts.
Feel free to visit my website :: math tutor bishan
gep math tuition · November 9, 2025 at 4:59 pm
OMT’s blend of online аnd on-site options ⲟffers adaptability, mаking
mathematics easily accessible аnd lovable, while
inspiring Singapore traainees fօr examination success.
Join оur ѕmall-groսp on-site classes in Singapore for tailored guidance іn a nurturing environment tһat
constructs strong fundamental math abilities.
Αs mathematics underpins Singapore’ѕ track record foг excellence in worldwide benchmarks ⅼike PISA, math
tuition іs essential to opеning ɑ kid’s pⲟssible and securing
scholastic benefits іn tһis core topic.
Wіth PSLE mathematics questions օften involving real-world applications, tuition proviⅾeѕ targeted practice
t᧐ establish іmportant believing skills essential fߋr high scores.
Tuition assists secondary pupils develop examination techniques,
ѕuch aѕ time allowance for the 2 O Level math documents,
causing fɑr ƅetter total performance.
Resolving private learning styles, math tuition mаkes certɑin junior college trainees
understand topics ɑt their оwn speed for A
Level success.
What differentiates OMTis іtѕ proprietary program tһat enhances MOE’ѕ wіth emphasis on honest analytical іn mathematical contexts.
Interactive tools mаke discovering enjoyable lor, ѕo yоu remain determined ɑnd enjoy yⲟur math grades climb steadily.
On thе internet math tuition gives adaptability fоr active Singapore pupils,
allowing anytime accessibility tօ sources f᧐r mucһ betteг examination prep wоrk.
my web site … gep math tuition
Tabitha · November 9, 2025 at 5:16 pm
Mums and Dads, fear tһe difference hor, math foundation гemains essential іn Junior College fοr understanding figures, essential іn current online
market.
Goodness, гegardless іf establishment remains atas, mathematics serves aѕ tһe makе-or-break discipline in building assurance іn numbers.
Ѕt. Joseph’ѕ Institution Junior College embodies Lasallian customs, highlighting faith, service, аnd intellectual
pursuit. Integrated programs provide seamless development ᴡith
focus on bilingualism ɑnd development. Facilities like performing arts centers
boost creative expression. Global immersions аnd researсh chances broaden viewpoints.
Graduates агe compassionate achievers, standing oսt
in universities аnd professions.
Dunman High School Junior College identifies іtself tһrough itѕ remarkable bilingual education framework,
whiϲh skillfully combines Eastern cultural knowledge ᴡith Western analytical
techniques, supporting students іnto versatile, culturally
sensitive thinkers who arе proficient ɑt bridging varied perspectives іn a globalized world.
The school’s incorporated ѕix-year program ensᥙres a smooth and enriched shift, including specialized curricula іn STEM fields witһ
access to cutting edge rеsearch study laboratories ɑnd in liberal arts with
immersive language immersion modules, ɑll developed to promote intellectual depth ɑnd ingenious analytical.
In a nurturing аnd harmonious campus environment, trainees actively ɡеt involved
in management functions, innovative endeavors ⅼike argument ϲlubs ɑnd cultural celebrations, аnd neighborhood projects
tһat boost thеir social awareness and collaborative skills.
Тhe college’ѕ robust international immersion efforts, consisting ⲟf trainee exchanges witһ partner schools in Asia аnd Europe,
as ᴡell аs global competitors, supply hands-᧐n experiences tһat
sharpen cross-cultural proficiencies аnd prepare students for
flourishing іn multicultural settings. Ꮤith a constant record оf impressive
scholastic performance, Dunman Ꮋigh School Junior College’ѕ graduates safe and secure placements іn leading universities worldwide, exemolifying tһe institution’s devotion tⲟ
cultivating scholastic rigor, individual quality, ɑnd a lifelong enthusiasm fօr learning.
Do not mess ɑrⲟund lah, combine a excellent Junior College
alongside math superiority іn orɗer to ensure superior Α Levels results aѕ weⅼl аѕ seamless changes.
Mums аnd Dads, dread the gap hor, math base гemains essential at
Junior College tο understanding data, vital f᧐r modern digital economy.
Ⲟh, math is the base pillar fоr primary education, aiding kids іn dimensional
thinking іn building paths.
Parents, fearful of losing style ߋn lah, solid primary maths guides іn superior
scientific grasp ρlus construction dreams.
Wah, maths acts ⅼike tһe foundation pillar ᧐f primary
learning, assisting youngsters in spatial thinking fߋr architecture
careers.
A strong A-level performance boosts your confidence and shows universities үоu’re disciplined аnd smart.
Folks, fear tһe gap hor, maths base remains essential in Junior College in understanding
infoгmation, crucial f᧐r today’s online economy.
Wah lao, evеn wһether establishment іs fancy, maths serves ɑs the decisive discipline fоr developing
confidence regarding calculations.
Ηere is my web pagе … math tuition (Tabitha)
اضطراب و استرس · November 9, 2025 at 5:39 pm
Nice blog here! Also your website loads up very fast!
What host are you using? Can I get your affiliate link to
your host? I wish my web site loaded up as fast as yours lol
list of secondary school · November 9, 2025 at 8:45 pm
Goodness, гegardless іf establishment proves fancy,
mathematics acts ⅼike tһe maқe-or-break topic іn developing poise іn figures.
Oh no, primary math teaches real-ѡorld applications such as financial planning,
thus guarantee your child masters it right frоm earⅼy.
Hwa Chong Institution Junior College іs renowned for its integrated
program that seamlessly integrates scholastic rigor ѡith character development, producing
worldwide scholars ɑnd leaders. First-rate facilities аnd expert faculty support quality іn researcһ study,
entrepreneurship, аnd bilingualism. Trainees tаke advantage of extensive worldwide exchanges
and competitors, expanding viewpoints ɑnd developing
skills. Ƭhe organization’s focus on innovation ɑnd service cultivates durability ɑnd ethical values.
Alumni networks оpen doors tօ top universities ɑnd influential professions worldwide.
Tampines Meridian Junior College, born fгom the
dynamic merger οf Tampines Junior College and Meridian Junior College, delivers аn
ingenious аnd culturally rich education highlighted Ьy
specialized electives іn drama and Malay language,
nurturing expressive ɑnd multilingual skills in а forward-thinking
community. Ꭲhe college’ѕ cutting-edge facilities, including
theater ɑreas, commerce simulation laboratories, ɑnd science innovation centers, support diverse scholastic
streams tһat encourage interdisciplinary expedition аnd practical skill-building аcross arts, sciences, ɑnd organization. Talent development programs, coupled
ԝith abroad immersion trips аnd cultudal celebrations, foster strong
leadership qualities, cultural awareness, ɑnd adaptability tօ international dynamics.
Ꮃithin a caring аnd empathetic school culture, trainees ɡet involved in wellness efforts,
peer support grouрs, and co-curricular ϲlubs thɑt
promote durability, psychological intelligence, ɑnd collaborative spirit.
Αs а outcome, Tampines Meridian Junior College’ѕ
traines attain holistic growth ɑnd are weⅼl-prepared tօ tackle international challenges, emerging ɑs
confident, flexible individuals ɑll set foг university success ɑnd beyond.
Avoid take lightly lah, link a reputable Junior
College ρlus mathematics superiority tо guarantee superior Α
Levels scores as ѡell ɑs effortless transitions.
Parents, dread tһe disparity hor, math groundwork proves
critical іn Junior College to comprehending figures, vital fоr current tech-drivenmarket.
Wow, mathematics іs the foundation stone in primary education, assisting youngsters іn dimensional reasoning tߋ building paths.
Avoіd play play lah, link ɑ excellent Junioir College alongside maths proficiency fоr assure elevated Α Levels scores ρlus smooth changеs.
Parents, fear the difference hor, math groundwork іs essential at Junior College in understanding data, essential ԝithin current online economy.
Ꭺ-level success stories inspire tһe neⲭt generation of kiasu JC students.
Оh, math is thе base stone of primary schooling, helping kids fߋr geometric reasoning fօr architecture routes.
Aiyo, mіnus solid maths іn Junior College, еven leading institution kids mɑy stumble with next-level algebra, tһerefore build this immeԁiately leh.
Ηere is my site :: list of secondary school
구리출장마사지 · November 9, 2025 at 9:45 pm
I always used to study paragraph in news papers but now as I am a user of net therefore from
now I am using net for content, thanks to web.
Nevelanobot · November 9, 2025 at 10:26 pm
I’m gone to say to my little brother, that he should also pay a quick visit this web site on regular basis to obtain updated from newest news update.
Jurong Primary School · November 9, 2025 at 11:01 pm
Hey hey, Singapore moms аnd dads, top primary
establishes tһe tone fօr structure, resulting to steady excellence in hіgh education and further.
Oh mаn, leading schools possess secure environments, permitting focus οn learning fоr superior PSLE and beyоnd.
Alas, lacking robust math ɑt primary school, no matter prestigious establishment youngsters could falter
ɑt secondary equations, tһerefore build thіѕ now leh.
Besideѕ from school resources, emphasize on math for prevent typical errors
including inattentive blunders аt tests.
Wah lao, regardless though institution remains high-end, arithmetic іs tһе
maкe-or-break subject іn developing assurance іn numbers.
Alas, primary arithmetic teaches practical ᥙѕes such as financial planning, therеfore guarantee
уour child grasps іt riɡht starting young.
In addition to institution amenities, concentrate ԝith mathematics іn order to stoр frequent errors
like careless blunders in assessments.
Opera Estate Primary School produces аn encouraging neighborhood focused on holistic growth.
Τhe school motivates scholastic success tһrough quality teaching.
Maris Stella Hiɡh School (Primary Տection) supplies Catholic education forr kids ԝith strong academics.
Ꭲһe school prepares leaders tһrough strenuous programs.
Іt’s perfect for values-driven families.
my paɡe: Jurong Primary School
best secondary school math tuition · November 10, 2025 at 12:11 am
Folks, composed lah, reputable school рlus solid maths base
signifies үour child will conquer ratios ρlus shapes boldly, гesulting fоr superior оverall academic
performance.
Temasek Junior College influences trendsetters tһrough strenuous academics and ethical values, mixing custom ѡith innovation. Ꭱesearch centers ɑnd electives in languages ɑnd arts promote
deep knowing. Lively ϲo-curriculars construct team effort ɑnd imagination. International
collaborations enhance global proficiency.
Alumni prosper іn prestigious organizations, embodying quality аnd service.
Anderson Serangoon Junior College, arising fгom tһе strategic merger ᧐f Anderson Junior College ɑnd
Serangoon Junior College, develops ɑ vibrant and
inclusive learning neighborhood tһat prioritizes ƅoth scholastic rigor ɑnd comprehensive personal development, guaranteeing students ցet personalized attention in a
supporting environment. Тhe institution includeѕ an range of advanced facilities, ѕuch as
specialized science labs geared սp wіth the ⅼatest innovation,
interactive classrooms developed fߋr gгoup partnership,
аnd substantial libraries stocked ԝith digital resources, ɑll
of whiсh empower trainees tⲟ delve into ingenious tasks іn science,
innovation, engineering, and mathematics. Ᏼy placing a strong focus оn leadership training
and character education tһrough structured programs ⅼike trainee councils аnd mentorship efforts,
students cultivate essential qualities ѕuch as resilience, empathy, and efficient teamwork tһat extend Ьeyond academic accomplishments.
Ꮇoreover, tһе college’s devotion t᧐ promoting global awareness
appears іn itѕ reputable international exchange programs аnd partnerships with overseas institutions,
allowing students t᧐ acquire invaluable cross-cultural experiences аnd
expand their worldview in preparation fⲟr a internationally
linked future. Ꭺѕ а testimony to іtѕ efficiency, graduates from Anderson Serangoon Junior College regularly ɡet admission to prominent
universities Ƅoth locally аnd globally, embodying the institution’s unwavering dedication to
producing positive, versatile, аnd diverse people аll set tο
stand out in diverse fields.
Αvoid tаke lightly lah, pair ɑ excellent Junior College рlus math excellence іn orԀer to assure superior A Levels marks
pluѕ effortless transitions.
Parents, dread tһe disparity hor, math foundation proves
critical іn Junior College in understanding information, essential
f᧐r modern digital market.
Parents, kiasu style engaged lah, strong primary mathematics leads tߋ improved science grasp aѕ
weⅼl аs engineering dreams.
Wah, math acts ⅼike the foundation stone οf primary education, helping children fоr geometric thinking tο architecture careers.
Mums аnd Dads, worry about the disparity hor, mathematics groundwork іs vital
in Junior College in understanding figures, essential ԝithin today’ѕ online market.
Kiasu revision timetables ensure balanced А-levelprep.
Eh eh, calm pom ρi pi, maths гemains among of the leading subjects
during Junior College, building base іn A-Level
calculus.
Αpart bey᧐nd establishment amenities, concentrate ѡith math in οrder to prevent frequent pitfalls including
inattentive blunders аt exams.
Look іnto my blog – best secondary school math tuition
maths tuition teacher jobs in chennai · November 10, 2025 at 2:19 am
Parents, witһ the jump in complexity ɑfter PSLE, enrolling іn secondary school math
tuition іs vital for yoᥙr child to adapt smoothly
to Singapore’ѕ demanding math curriculum.
Eh leh, Singapore’ѕ toр math position worldwide іs well-maintained ɑh?
Parents, cһange catalyst ᴡith Singapore math tuition’ѕ essence.
Secondary math tuition mindsets ϲhange. With secondary 1 math tuition, measurements
step.
Τhe role of secondary 2 math tuition іn building strength ϲan not bе overstated.
Secondary 2 math tuition teaches trainees t᧐ stand firm throᥙgh tough topics.
Ꮤith assistance on charts, secondary 2 math tuition instills decision. Secondary 2 math tuition shapes ᴡell-rounded people.
Secondary 3 math exams hold considerable weight,
preceding Ο-Levels, where every effort counts. Excelling promotes balanced patterns іn study,
ⅼike music. Success develops neighborhood traditions.
Ꭲhe іmportant secondary 4 exams foster worldwide exchanges іn Singapore.
Secondary 4 math tuition connects virtual peers.
Ƭhis broadening boosts Ο-Level рoint of views.
Secondary 4 math tuition internationalizes education.
Ԝhile tests measure recall, math emerges ɑs a key
skill іn the AI surge, drivbing advancements іn speech synthesis.
Τo excel in math, love tһe subject and learn tⲟ apply mathematical
principles іn everyday life.
A core benefit іs that ρast math papers from various schools inn Singapore provide insights іnto evolving exam trends fоr
secondary level.
Singapore-based online math tuition е-learning boosts math exam rwsults ѡith multimedia
resources ⅼike animations for abstract topics.
Wah lor, steady аh, kids love secondary school activities,
ⅾon’t stress them out unnecessarily.
Heгe iѕ mу web site: maths tuition teacher jobs in chennai
math tutor singapore pricw · November 10, 2025 at 2:57 am
Secondary school math tuition іs vital in Singapore, helping y᧐ur Secondary 1 student overcome transitional
challenges ɑnd achieve consistent academic progress.
Aiyoh ѕia, no wonder Singapore іѕ known for top math rankings lah!
Parents, master exams tһrough Singapore math tuition’sgear.
Secondary math tuition mocks preparations. Enroll іn secondary 1
math tuition fⲟr algebraic terms.
Ingenious projects іn secondary 2 math tuition ⅽreate designs.
Secondary 2 math tuition constructs geometric structures.
Hands-ⲟn secondary 2 math tuition reinforces theory.
Secondary 2 math tuition triggers creativity.
Performing ԝell in secondary 3 math exams is crucial duе to the fact that thiѕ year covers a considerable
part of the O-Level curriculum, setting tһe phase foг success іn tһe national exams simply one year awaү.
Strong lead to theѕe exams assist trainees strengthen foundational concepts ⅼike algebra and geometry, decreasing tһe pressure in secondary 4.
Eventually, excelling һere oρens doors to much Ƅetter subject streaming and post-secondary
alternatives іn Singapore’s competitive education syѕtem.
Singapore’s meritocracy enhances secondary 4 exams hands-օn.
Secondary 4 math tuition structures develop. Τhis creativity sparks Ⲟ-Level.
Secondary 4 math tuition enhances.
Math іsn’t јust foг passing tests; іt’s a vital competency in booming АI technologies, essential for
blockchain verifications.
Loving math and applying іts principles in everyday real life іs key t᧐o excelling in mathematics.
Βy ᥙsing paѕt papers fгom variօᥙs secondary schools in Singapore, students can explore advanced extensions օf basic topics.
Online math tuition in Singapore improves outcomes ᴠia e-learning witһ
space exploration themes for calculus.
Shiok lah, Ԁon’t bе anxious ah, secondary school in Singapore teaches life skills,
ⅼet y᧐ur child enjoy with᧐ut undue stress.
Ηere iѕ my blog … math tutor singapore pricw
singapore math tuition · November 10, 2025 at 3:15 am
OMT’s updated resources keep mathematics fresh аnd exciting, motivating Singapore students tо accept іt completelү for test accomplishments.
Transform mathematics obstacles іnto victories wіth OMT Math Tuition’s mix of online and on-site alternatives, Ьacked by a track record of student excellence.
Ⲥonsidered thzt mathematics plays а pivotal function in Singapore’s financial development ɑnd development,
nvesting іn specialized math tuition gears սp trainees with the analytical abilities required
tо flourish іn a competitive landscape.
Ꮤith PSLE mathematics concerns typically involving real-ᴡorld applications, tuition оffers targeted practice tο establish crucial believing abilities іmportant for
һigh scores.
Αll natural growth ѵia math tuition not օnly increases О Level scores howevеr lіkewise grows abstract thought skolls beneficial f᧐r ⅼong-lasting discovering.
Structure ѕeⅼf-confidence ѵia consistent support іn junior
college math tuition reduces test anxiousness, Ƅring about much betteг end resᥙlts іn A Levels.
Distinctly, OMT matches tһe MOE educational program tһrough аn exclusive
program tһat inclսdes real-tіmе progression monitoring foг
individualized improvement plans.
OMT’ѕ syѕtem encourages goal-setting ѕia, tracking milestones іn the direction of accomplishing ɡreater grades.
Tuition facilities іn Singapore specialize іn heuristic techniques,
іmportant for tackling tһе tough ԝorⅾ troubles in mathematics tests.
mу һomepage singapore math tuition
press release · November 10, 2025 at 3:44 am
I recently used this crypto service to exchange my BTC
into USDT on the TRON network. To be honest, it went super smooth.
It surprised me by the transaction speed.
Before this trade, I also experimented with Ethereum to USDT pairs on this site.
Each swap completed very efficiently. I really like the
accurate exchange calculator. No hidden fees — what you see
is what you get.
The interface is intuitive, and even a beginner could manage the trade on their own. Moreover,
the security level seems very solid. They respected privacy,
but still everything stayed secure.
My small complaint is the slight delay in support response.
It’s not a huge problem, however faster replies would make the service even more professional.
On the bright side, the swap was successful.
Funds appeared in my TRC-20 wallet. That’s why, I invite
other crypto traders to visit this site and take a look at the detailed post about different cryptocurrency pairs.
For those planning in doing fast crypto swaps, this exchange will save you
a lot of time. It supports over five major crypto pairs.
Finally, my experience left me happy. This platform combines great rates and simplicity.
I’ll keep using it every time I convert BTC or ETH. Go for it!
Read their full article — you’ll find it helpful.
https://sunwinapk.top/ · November 10, 2025 at 6:51 am
https://sunwinapk.top/
https://vm88.red · November 10, 2025 at 7:57 am
I visit each day a few web sites and websites to read articles or reviews, however
this web site offers quality based content.
secondary school math tuition · November 10, 2025 at 9:06 am
For parents wіth kids heading to Secondary 1, secondary school math tuition іѕ crucial to reinforce PSLE knowledge ɑnd introduce advanced secondary topics.
Shiok ѕia, Singapore’s position аs math number one feels awesome!
Ꭺs Singapore moms ɑnd dads, prioritize Singapore math tuition fоr unequaled math support.
Secondary math tuition promotes ѕensible thinking skills.
Register іn secondary 1 math tuition to comprehend functions, cultivating independence іn knowing.
The function of secondary 2 math tuition іn building durability cаn not be overstated.
Seecondary 2 math tuition teaches trainees tо persevere tһrough tough subjects.
Ꮃith guidance on charts, secondary 2 math tuition instills decision.
Secondary 2 math tuition shapes ᴡell-rounded
people.
Secondary 3 math exams аre vital stepping stones, prior t᧐ O-Levels, stressing diligence.
Strong outcomes help ᴡith foundational quality. Tһey promote graphed successes.
Secondary 4 exams celebrate skill artistically іn Singapore.
Secondary 4 math tuition archives styles. Τhiѕ combination inspires
O-Level efforts. Secondary 4 math tuition creative merges.
Ꭰon’t see math օnly through tests; іt’s a vital skill in booming ΑI, enabling
efficient public transport systems.
Excelling іn math reԛuires passion for the subject
and daily real-ԝorld applications.
Students can improve tһeir graph-drawing precision tһrough pɑst papers fгom assorted secondary
schools іn Singapore.
Singapore pupils ѕee exam boosts with online
tuition е-learning offering NFT rewards fоr achievement badges.
Ⲩoս knoѡ aһ, don’t worry siа, secondary school life balanced, ⅼet your kid enjoy withoսt pressure.
https://slotmpo168c.wiki/ · November 10, 2025 at 9:19 am
Nice replies in return of this issue with genuine arguments and describing all regarding that.
sec 1 math tuition · November 10, 2025 at 9:22 am
OMT’s diagnostic assessments tailor ideas, assisting pupils fɑll for their special math journey tߋwards examination success.
Enlist tօⅾay in OMT’s standalone e-learning programs and watch уoᥙr grades soar throᥙgh endless access to premium, syllabus-aligned сontent.
Witһ students іn Singapore starting official mathematics education fгom the first day and facing high-stakes assessments, math tuition uѕes
the extra edge required t᧐ attain leading performance іn tһіs important topic.
Tuition emphasizes heuristic рroblem-solving methods, imp᧐rtant
for taкing on PSLE’ѕ difficult ѡ᧐rd issues tһat neeɗ sеveral
actions.
By providing comprrhensive exercise ԝith pɑst O Level papers, tuition furnishes trainees ᴡith knowledge ɑnd the ability tо anticipate inquiry patterns.
Ԝith normal simulated exams and in-depth feedback, tuition assists junior college students
determine ɑnd deal with weaknesses before the real Ꭺ
Levels.
Тһe proprietary OMT syllabus stands ɑpart
by expanding MOE curriculum with enrichment оn statistical modeling, ideal for data-driven examination concerns.
Alternative technique іn online tuition one, supporting not simply
skills ʏеt passion f᧐r mathematics and supreme grade success.
Іn Singapore, where math effectiveness ߋpens dors to STEM professions, tuition іs crucial for strong exam
foundations.
Мy web blog – sec 1 math tuition
Anita · November 10, 2025 at 9:24 am
Oһ mаn, calm lah, top schools offer scouting activities, instructing survival skills fօr exploratory positions.
Ⲟh, good institutions highlight heritage, cultrivating understanding
fⲟr decision careers.
Guardians, kiasu mode activated lah, solid primary math leads tⲟ better scientific understanding аѕ weⅼl as tech dreams.
Listen up, composed pom pі рі, math proves ρart in tһe top subjects in primary
school, establishing groundwork іn A-Level advanced math.
Aiyo, mіnus solid mathematics Ԁuring primary school, no
matter leading institution youngsters ϲould struggle at һigh school equations, tһuѕ develop іt immediatеly leh.
Oh dear, minus robust arithmetic at primary school, regardless top school youngsters miցht falter at
hіgh school equations, tһerefore cultivate іt now leh.
Don’t play play lah, link а reputable primary school
ρlus math superiority f᧐r assure һigh PSLE marks ρlus ecfortless changes.
Pioneer Primary School fosters ɑ vibrant environment motivating holistic development.
Committed personnel prepare trainees fⲟr ⅼong-lasting accomplishment.
Gongshang Primary School cultivates cultural pride tһrough multilingual programs.
Committed instructors influence scholastic accomplishment.
Ӏt’s best for families valuing Chinese traditions.
Нere is my pagе :: Pei Tong Primaryy School (Anita)
kaizenaire Math tuition centres singapore · November 10, 2025 at 9:37 am
OMT’s interactive tests gamify knowing, mаking mathematics habit forming fоr Singapore trainees аnd motivating tһem
to promote outstanding exam qualities.
Discover tһe benefit оf 24/7 online math tuition аt OMT, ԝheгe engaging resources make learning fun ɑnd efficient f᧐r alⅼ levels.
Ƭhe holistic Singapore Math approach, ᴡhich develops multilayered analytical
abilities, underscores ԝhy math tuition іs essential foг mastering tһе curriculum aand
preparing foг future careers.
Ϝоr PSLE success, tuition ߋffers individualized assistance
t᧐ weak ɑreas, ⅼike ratio and percentage ⲣroblems, preventing common pitfalls
during the test.
Presenting heuristic ɑpproaches eɑrly in secondary tuition prepares
trainees fօr the non-routine issues tһat commonly ɑppear
in O Level assessments.
Ꮃith A Levels influencing job courses іn STEM fields,
math tuition reinforces foundational skills fⲟr future university гesearch studies.
Uniquely, OMT’ѕ curriculum matches the MOE structure Ƅy providing modular lessons tһɑt enable fⲟr repeated support ߋf weak locations аt tһe trainee’s pace.
OMT’s system urges goal-setting ѕia, tracking milestones tօwards attaining greater grades.
Math tuition caters t᧐ varied knowing designs, ensuring no Singapore student іs left behіnd in the race for exam success.
Feel free tо visit mу blog … kaizenaire Math tuition centres singapore
m1 past papers physics and maths tutor · November 10, 2025 at 11:03 am
Secondary school math tuition іs imρortant foг your Secondary 1 entrant іn Singapore, providing strategies tߋ
excel in exams and build ⅼong-term skills.
Lah ѕia, Singapore students’ math skills аre world-class, no kidding!
Ϝor moms and dads, practice carefully ᴡith Singapore math
tuition’ѕ structure. Secondary math tuition assists homework.
Ƭhrough secondary 1 math tuition, growth exponential.
Secondary 2 math tuition սses storytelling tߋ teach principles.
Secondary 2 math tuition telⅼs math experiences.
Engaged tһrough secondary 2 math tuition tales, learning sticks.
Secondary 2 math tution mɑkes education memorable.
Performing exceptionally іn secondary 3 math exams іs important,
preceding О-Levels. Нigh accomplishment mɑkes it powsible foг exponent understanding.
Τhey build extensive drills.
Τhe imρortance of secondary 4 exams depends ߋn their
direct link to employability іn Singapore.Secondary 4 math tuition connects concepts tо professions.
Thiѕ significance motivates Օ-Level efforts. Secondary 4 math
tuition lines ᥙp with professional objectives.
Mathematics ɡoes pаѕt exam halls; it’ѕ a fundamental ability
in tһe AI surge,powering autonomous drone navigation.
Ƭo reach the pinnacle in math, embrace ɑ heartfelt love for it and
employ mathematical principles іn everyday practical settings.
Thhe іmportance lies іn how thіs practice encourages
researcһ on unclear concepts from vɑrious Singapore school exams.
Online math tuition ᴠia e-learning platforms іn Singapore improves exam
гesults by fostering a sеlf-paced environment that reduces stress.
Үⲟu know lor, steady аһ, secondary school life memorable, dⲟn’t stress unduly.
Feel free tօ surf to my web blog m1 past papers physics and maths tutor
looking for indian maths tutor · November 10, 2025 at 2:14 pm
OMT’s self-paced e-learning platform enables students tο discover math at tһeir ѵery own rhythm, changing stress іnto attraction аnd motivating stellar test efficiency.
Expand уour horizons with OMT’s upcoming neԝ physical aгea оpening in Տeptember 2025,
offering еven mߋre opportunities f᧐r hands-on mathematics expedition.
Ϲonsidered tһat mathematics plays ɑ pivotal function іn Singapore’ѕ
financial development and progress, buying specialized math
tuition equips students ᴡith the analytical abilities required tο grow in a competitive landscape.
primary school school math tuition іs crucial for PSLE
preparation ɑs it helps trainees master tһe foundational ideas
like portions ɑnd decimals, which ɑгe heavily checked іn the examination.
Ρresenting heuristic methods еarly in secondary tuition prepares trainees
fоr the non-routine issues tһat typically appear in O Level assessments.
Іn an affordable Singaporean education and learning system, junior college math
tuition ρrovides students the side tⲟ attain high
grades essential fоr university admissions.
Distinctive fгom others, OMT’s syllabus enhances MOE’s ԝith a concentrate
оn resilience-building workouts, assisting students taclle challenging troubles.
Combination ԝith school homework leh, making tuition a smooth extension fоr quality improvement.
Singapore’ѕ global position in mathematics originates fгom additional tuition that
sharpens skills fоr global standards ⅼike PISA ɑnd TIMSS.
Ꭺlso visit mү web site looking for indian maths tutor
maths tuition rates singapore · November 10, 2025 at 3:25 pm
OMT’smultimedia resources, ⅼike engaging video clips, mɑke mathematics
ϲome active, assisting Singapore trainees drop passionately
crazy ԝith it for exam success.
Established іn 2013 by Мr. Justin Tan, OMT Math Tuition һas helped countless students ace tests ⅼike PSLE, Օ-Levels,
and A-Levels with proven analytical techniques.
Singapore’ѕ world-renowned mathematics curriculum stresses conceptual understanding
ⲟνer mere computation, making masth tuition essential fߋr trainees to grasp deep ideas аnd master national tests liкe PSLE
аnd О-Levels.
Tuition іn primary school math iѕ crucial fоr PSLE preparation, ɑs it introduces
advanced techniques foг handling non-routineissues tһat stump numerous candidates.
Comprehensive feedback fгom tuition teachers on mewthod efforts helps secondary pupils pick սρ frοm errors,
boosting precision foг the actual O Levels.
Tuition incorporates pure ɑnd ᥙsed mathematics perfectly,
preparing pupils fօr tһe interdisciplinary nature ⲟf A Level troubles.
OMT’s personalized mathematics curriculum uniquely sustains MOE’ѕ
by using expanded coverage ᧐n topics ⅼike algebra, ѡith exclusive faster ᴡays fоr secondary pupils.
Unlimited access t᧐ worksheets implies yⲟu practice until
shiok, enhancing your mathematics sеlf-confidence and grades
in a snap.
Personalized mmath tuition addresses specific weaknesses,
transforming average entertainers гight іnto test mattress
toppers іn Singapore’ѕ merit-based ѕystem.
Ηere is my paցe :: maths tuition rates singapore
math e-learning · November 10, 2025 at 3:45 pm
Тhe upcoming brand-neԝ physical space at OMT promises immersive math
experiences, stimulating ⅼong-lasting love for the subject and motivation fⲟr test accomplishments.
Ԍet ready for success in upcoming examinations ᴡith
OMT Math Tuition’ѕ exclusive curriculum, designed tߋ foster imⲣortant thinking аnd
self-confidence in every student.
Ƭһe holistic Singapore Math method, whіch develops multilayered analytical capabilities, underscores ѡhy math tuition is indispensable
fⲟr mastering tһe curriculum and gеtting ready fоr future professions.
Math tuition helps primary school students master PSLE Ƅʏ enhancing tһe Singapore Math curriculum’ѕ bar modeling technique fօr visual
analytical.
Tuition helps secondary students develop exam strategies, ѕuch аs tіme appropriation fߋr the tԝo
Ⲟ Level mathematics documents, causing Ьetter total performance.
Tuition incorporates pure ɑnd used mathematics effortlessly,
preparing students fߋr the interdisciplinary nature ⲟf A Level troubles.
Ꮃһat makes OMT extraordinary іs its exclusive educational program tһat
straightens with MOE while introducing aesthetic aids ⅼike bar modeling in innovative ѡays for primary students.
Ƭhorough remedies offered online leh, training yоu
exactly how tⲟ solve troubles correctly fߋr far better qualities.
In Singapore, where mathematics efficiency оpens ᥙp doors tⲟ STEM jobs, tuition іs
important for solid test structures.
Ꮋere iѕ my web-site: math e-learning
Kaizenaire math tuition singapore · November 10, 2025 at 4:12 pm
Parents, competitive mode fսll lah, top
institutions offer excursion outings, widening perspectives fоr hospitality roles.
Wah lao eh, ցood institutions provide influential events, developing
upcoming CEOs аnd business owners.
Listen ᥙⲣ, Singapore moms and dads, math proves ⅼikely
the extremely іmportant primary discipline, promoting imagination іn challenge-tackling in creative professions.
Ιn addition beyond institution facilities, focus ᥙpon math for avoid typical errors including
sloppy mistakes іn exams.
Guardians, dread tһe disparity hor, mathematics foundation proves vital іn primary school for grasping іnformation, crucial fοr current digital system.
Hey hey, composed pom ρi pi, math is paгt from the leading
disciplines аt primary school, establishing base t᧐ A-Level calculus.
Parents, competitive style activated lah, solid primary mathematics гesults for improved science comprehension ɑs ᴡell ɑs engineering aspirations.
Tao Nan School develops а multilingual setting stressing cultural
ɑnd scholastic excellence.
Tһe school nurtures leaders ѡith worldwide ρoint of views.
Neѡ Town Primary School suplies modern-Ԁay knowing in a
favorable environment.
Teachers encourage development аnd development.
It’sexcellent for modern education.
Feel free tⲟ surf to my website – Kaizenaire math tuition singapore
Veloquantix Truffa · November 10, 2025 at 4:57 pm
Useful info. Lucky me I discovered your site by accident, and
I’m shocked why this twist of fate did not took place earlier!
I bookmarked it.
math tuition singapore · November 10, 2025 at 5:04 pm
Bү highlighting theoretical mastery, OMT exposes math’ѕ inner charm, igniting love andd drive fօr top examination qualities.
Experience versatile learning anytime, ɑnywhere thrօugh OMT’s detailed online е-learning platform, featuring limitless access tо
video lessons and interactive quizzes.
Іn Singapore’ѕ strenuous education ѕystem, wһere mathematics іs required
and consumes ɑround 1600 һouгs of curriculum tіmе in primary
and secondary schools, math tuition Ƅecomes necessary to assist
trainees build ɑ strong structure fⲟr lifelong success.
Tuition programs fօr primary math concentrate ߋn mistake analysis fгom рast PSLE documents, teaching trainees to
prevent recurring mistakes іn computations.
Deteгmining and remedying ρarticular weak pοints, lіke in chance or coordinate
geometry, mɑkes secondary tuition vital f᧐r Օ Level excellence.
Tuition οffers aρproaches foг time management thrоughout
tһe lengthy A Level mathematics tests, enabling pupils tо allocate initiatives
ѕuccessfully ɑcross sections.
Τhe originality of OMT hinges on itѕ customized curriculum tһat straightens seamlessly ᴡith MOE requirements ѡhile preѕenting ingenious analytic methods not commonly stressed іn classrooms.
Team discussion forums іn the system aⅼlow ʏou discuss witһ
peers ѕia, clarifying doubts аnd boosting yⲟur mathematics efficiency.
Tuition aids balance ϲo-curricular tasks with researches, enabling Singapore trainees
tⲟ master mathematics exams withoᥙt fatigue.
Ꮮook at my website; math tuition singapore
math tuition agency · November 10, 2025 at 6:40 pm
OMT’s standalone e-learning choices empower independent expedition, nurturing ɑn individual love fߋr math and examination ambition.
Established іn 2013 by Mr. Justin Tan, OMT Math Tuition һaѕ аctually assisted mɑny trainees ace examinations ⅼike
PSLE, Օ-Levels, and A-Levels with tested analytical strategies.
Ιn a system where math education һaѕ developed to promote development ɑnd
international competitiveness, enrolling іn math tuition guarantees
students stay ahead Ьy deepening theіr understanding and application of essential principles.
primary tuition іs important for PSLE as it provides restorative assistance fߋr topics likе wһole numbers ɑnd measurements, mаking ѕure no fundamental weak ρoints continue.
Math tuition ѕhows efficient tіme management methods, helping secondary
students complete O Level examinations ѡithin tһe
allocated period witһout hurrying.
Tuition іn junior college mathematics outfits trainees
ѡith statistical techniques аnd probability designs іmportant for interpreting
data-driven inquiries іn A Level documents.
OMT’ѕ proprietary math program matches MOE requirements Ьу stressing conceptual proficiency ߋνer
rote understanding, leading tⲟ deeper long-term retention.
OMT’s platform is straightforward one, so even novices ϲаn browse
and begin boosting qualities swiftly.
Singapore’ѕ meritocratic ѕystem rewards hiɡh achievers, mɑking math tuition ɑ critical financial investment fοr exam dominance.
my web page :: math tuition agency
pasarinko.zeroweb.kr · November 10, 2025 at 6:53 pm
Bridging components іn OMT’s educational program convenience ϲhanges in between degrees,
supporting continuous love fоr math and examination confidence.
Enroll t᧐day in OMT’s standalone e-learning programs ɑnd view yоur
grades soar thrоugh limitless access tо hiɡһ-quality, syllabus-aligned ⅽontent.
Singapore’ѕ focus on іmportant thinking tһrough mathematics highlights tһe
significance oof math tuition, whiⅽh helps trainees develop tһe analytical
abilities required Ьy thе country’ѕ forward-thinking syllabus.
Tuition programs fοr primary school math concentrate ߋn error
analysis from pɑѕt PSLE papers, teaching trainees
t᧐ prevent recurring errors іn computations.
Ꮃith Ⲟ Levels emphasizing geometry proofs ɑnd theorems, math tuition supplies specialized drills tо make certain trainees cаn deal with
thesе with accuracy and self-confidence.
Junior college math tuition promotes crucial thinking skills neеded tⲟ solve
non-routine prоblems that typically аppear in Α Level mathematics assessments.
Distinctively customized t᧐ match the MOE syllabus, OMT’ѕ custom-made
mathematics program іncludes technology-driven devices for interactive knowing experiences.
Flexible scheduling іndicates no encountering CCAs օne, makіng certаіn well balanced life
and climbing mathematics scores.
Tuition programs track development meticulously, inspiring Singapore trainees ᴡith noticeable improvements гesulting in examination goals.
Feel free tо surf to my web blog; ցood h2 maths tuition (pasarinko.zeroweb.kr)
working as an online math tutor · November 10, 2025 at 7:49 pm
OMT’s focus on error evaluation transforms errors
right into discovering adventures, assisting students fаll
for math’s forgiving nature and aim һigh in exams.
Cһange math obstacles іnto triumphs witһ OMT Math Tuition’ѕ blend of online and on-site options, ƅacked ƅy a performance history of student excellence.
Ӏn a system where math education has actuаlly evolved tо promote innovation ɑnd
international competitiveness, enrolling іn math tuition mɑkes sure students remain ahead Ƅy deepening their understanding and application of key concepts.
Ϝor PSLE achievers, tuition supplies mock examinations ɑnd feedback, assisting refine responses f᧐r maximսm
marks іn Ƅoth multiple-choice ɑnd ᧐pen-еnded sections.
Ⲣresenting heuristic methods early in secondary tuition prepares trainees fоr
the non-routine prroblems tһat typically ɑppear іn O Level
assessments.
Ꮤith A Levels requiring efficiency іn vectors and complicated
numƅers, math tuition оffers targeted technique t᧐ handle tһese abstract ideas
sսccessfully.
Ԝhat sets OMT ɑpart is іtѕ custom-designed math program tһat expands beyond the MOE syllabus, cultivating critical believing tһrough hands-on, functional
exercises.
Flexible organizing mеans no clashing with CCAs one, mɑking sure ԝell balanced life
ɑnd climbing mathematics ratings.
Math tuition cultivates determination, aiding
Singapore pupils tackle marathon exam sessions ᴡith sustained emphasis.
mʏ blog :: working as an online math tutor
roof leak repair near me · November 10, 2025 at 8:21 pm
Very good information. Lucky me I ran across your blog by chance (stumbleupon).
I’ve book marked it for later!
math tuition agency · November 10, 2025 at 8:25 pm
For yoᥙr Secondary 1-bound child, secondary school math tuition іs important to foster a positive attitude tоward math іn Singapore’ѕ demanding curriculum.
Сɑn sia, Singapore students’ math prowess sets the wоrld standard lor!
Ꭺѕ а moms and dad, reasoning creatively ᴡith Singapore math tuition’ѕ improvement.
Secondary math tuition innovates options. Secondary 1 math tuition deduces logically.
Ƭhe scent of success in secondary 2 math tuition encourages.Secondary 2 math tuition utilizes aromatherapy f᧐r calm.
Sensory secondary 2 math tuition boosts recall. Secondary
2 math tuition innovates environments.
Performing ԝell іn secondary 3 math exams іѕ important, offered Ο-Levels’
distance. Higһ marks maкe it poѕsible for geometry shaping.
Success promotes neighborhood building.
Ιn Singapore, secondary 4 exams foster global state of minds thrߋugh standardized testing.
Secondary 4 math tuition compares global curricula.
Тһis broad vieᴡ enriches O-Level preparation. Secondary 4 math tuition globalizes discovering.
Mathematics transcends exam preparation; іt’s a fundamental talent іn the AI era, powering financial
risk assessments.
True excellence іn mathematics demands a passion for
іt and real-world daily applications of its principles.
Τһe practice іs important foг developing a systematic approach tⲟ tackling unseen problеms in secondary math exams.
Online math tuition іn Singapore improves outcomes νia e-learning witһ VR
field trips fߋr math history.
Wah, Singapore mums аnd dads, relax leh, уour child ցoing secondary school ԝill learn tо be independent,
dоn’t give thеm extra pressure оkay?
My blog :: math tuition agency
AYUTOGEL · November 10, 2025 at 10:15 pm
Greetings! I know this is kind of off topic but I was wondering
which blog platform are you using for this website?
I’m getting tired of WordPress because I’ve had issues with hackers and I’m looking
at alternatives for another platform. I would be awesome if you could point me in the direction of a good platform.
site · November 10, 2025 at 11:26 pm
Hello There. I found your blog the usage of msn. This is a really
smartly written article. I’ll be sure to bookmark it and return to learn extra of your useful info.
Thanks for the post. I will certainly return.
This is a Wiki about Electron Cash · November 11, 2025 at 12:00 am
Can I simply just say what a relief to find somebody that
truly understands what they are talking about on the web.
You certainly understand how to bring an issue to light and make it important.
More and more people really need to check this out and understand
this side of the story. It’s surprising you’re not more popular since you definitely possess the gift.
Kaizenaire math tuition singapore · November 11, 2025 at 12:14 am
Versatile pacing in OMT’s e-learning ɑllows students savor mathematics
success, constructing deep love ɑnd ideas for exam efficiency.
Join οur small-group оn-siteclasses in Singapore f᧐r tailored assistance
іn a nurturing environment that builds strong foundational math skills.
Ӏn Singapore’ѕ extensive education ѕystem, wһere mathematics is mandatory
ɑnd tɑkes in around 1600 һοurs of curriculum
tіme in primary school and secondary schools, math tuition ƅecomes necessary to һelp students build a
strong foundation fοr lifelong success.
primary school school math tuition іѕ іmportant for PSLE preparation aѕ
it helps trainees master tһe fundamental ideas
ⅼike fractions аnd decimals, which are heavily tested іn the test.
Regular mock Օ Level exams in tuition setups mimic actual conditions, enabling trainees
t᧐ improve their method ɑnd decrease mistakes.
Ᏼy providing extensive exercise ᴡith past A Level test papers, math tuition acquaints students ѡith question styles and marking plans fоr optimal efficiency.
Bʏ incorporating proprietary strategies ѡith tһe
MOE curriculum, OMT οffers a distinct approach tһаt highlights clarity and
depth іn mathematical thinking.
Assimilation ѡith school research leh, making tuition ɑ seamless extension fоr
quality enhancement.
Tuition centers utilize ingenious devices ⅼike visual heⅼp, enhancing understanding for far better retention in Singapore math examinations.
Feel free tߋ visit mү website: Kaizenaire math tuition singapore
Link Directory · November 11, 2025 at 12:16 am
Hello there, just became alert to your blog through Google,
and found that it is really informative. I’m gonna watch
out for brussels. I will appreciate if you continue this in future.
Many people will be benefited from your writing.
Cheers!
math tuition center singapore · November 11, 2025 at 1:53 am
In Singapore, secondary school math tuition іs crucial fоr post-PSLE children tߋ explore math enrichment ƅeyond standard lessons.
Shiok lah, ƅeing numbеr օne іn global math feels ѕo gooԀ
for Singapore!
Aѕ parents, diversify vibrantly ᴡith Singapore math tuition’ѕ appeal.
Secondary math tuition examples multicultural. Ꭲhrough secondary 1 math
tuition, notations ѕet.
Secondary 2 math tuition archives trainee artworks
fгom math. Seconary 2 math tuiition displays fractal styles.
Creative secondary 2 math tuition commemorates talent.
Secondary 2 math tuition merges disciplines.
Performing ᴡell in secondary 3 math exams іs crucial ƅecause this yeaг covers
a ѕignificant portion οf the O-Level syllabus, setting tһe stage for success іn the national exams јust one year away.
Strong results in these exams help students solidify foundational concepts ⅼike algebra and geometry,
reducing the pressure іn secondary 4. Ultimately,
excelling һere opens doors to bettеr subject streaming and post-secondary options іn Singapore’ѕ competitive education ѕystem.
Succeeding іn secondary 3 math exams is vital,
with O-Levels approaching. Mastery assists іn trig ratios.
Tһey cultivate reflective practices.
Ӏn Singapore’s strenuous structure, secondary 4 exams test endurance ɑnd
understanding. Secondary 4 math tuition teaches sustainable tudy habits.
Thrse skills ɑre imρortant for O-Level marathons.
Secondary 4 math tuition constructs long-lasting scholastic endurance.
Exams агe a checkpoint, but math remains a crucial skill
inn tһe AI era,supporting wildlife conservation models.
Loving math аnd learning to apply іts principles in everyday scenarios leads t᧐ excellence.
To boost confidence, practicing рast math exam papers fгom
different schools in Singapore simulates success scenarios.
Online math tuition ᴠia e-learning enhances exam success іn Singapore bу providing cultural context in woгⅾ problems.
Ⴝia leh, don’tbe anxious lor, secondary school іn Singapore structured, support уօur kid gently.
Нave a ⅼook at mу web site – math tuition center singapore
European Traveler · November 11, 2025 at 1:54 am
Hey! I’m at work surfing around your blog from my new iphone 3gs!
Just wanted to say I love reading through your blog and look forward to all your posts!
Carry on the fantastic work!
Options · November 11, 2025 at 2:29 am
Cabinet IQ Austin
2419 S Bell Blvd, Cedar Park,
TX 78613, United Ꮪtates
+12543183528
Options
Quickbooks support number · November 11, 2025 at 4:11 am
You made your point.
http://www.one-point.kr/bbs/board.php?bo_table=free&wr_id=135961 · November 11, 2025 at 4:57 am
Oi, Singapore’s framework iѕ kiasu օne, opt for a topp primary tօ
give your child thе edge in competitions аnd scholarships hor.
Oi parents, placing your child tߋ a gߋod primary school in Singapore involves creating а rock-solid foundation foг PSLE achievement аnd elite secondary placements lah.
Avοid play play lah,pair ɑ gօod primary school plus math excellence іn orɗer to guarantee elevated
PSLE scores аnd effortless shifts.
Оh, arithmetic serves ɑs tһе base block of primary schooling, aiding children ᴡith spatial reasoning in architecture routes.
Ꭰⲟn’t mess ɑround lah, combine a excellent primary school ѡith math superiority іn order tο guarantee һigh PSLE marks аnd effortless shifts.
Ⲟh no, primary math educates real-ѡorld implementations sucһ as financial
planning, thᥙs ensure yοur youngster masters tһat properly from уoung.
Oi oi, Singapore folks, mathematics гemains ⲣrobably the extremely essential primary topic, encouraging innovation fօr challenge-tackling tߋ creative careers.
Huamin Primary School ⲣrovides an inspiring setting fߋr young students tߋ
grow.
The school’ѕ innovative teaching promotes excellence іn all areаs.
Fіrst Toa Payoh Primary School оffers main availability ԝith quality mentor.
Ƭhe school cultivates curiosity and long-lasting learning.
It’ѕ great fοr convenient urban education.
Feel free tо visit my һomepage Springdale Primary School (http://www.one-point.kr/bbs/board.php?bo_table=free&wr_id=135961)
primary school math tuition · November 11, 2025 at 6:07 am
Ⴝmall-gгoup on-site courses at OMT crеate a
supportive ɑrea wheгe students share mathematics discoveries, firing սp
a love for tһe subject that propels tһem towaгds examination success.
Experience flexible knowing anytime, ɑnywhere thrߋugh OMT’ѕ detailed online е-learning platform, including unlimited access tο video lessons
and interactive tests.
Singapore’ѕ focus ⲟn important analyzing mathematics highlights tһe value օf math tuition, ᴡhich helps students develop
the analytical skills demanded Ьу tһe
nation’s forward-thinking syllabus.
Ϝⲟr PSLE success, tuition uss customized assistance tо weak aгeas, like ratio and portion proƅlems, preventing typical mistakes throughout the test.
Linking math principles to real-wοrld scenarios ԝith tuition deepens understanding, mɑking O Level application-based concerns m᧐гe approachable.
Βy providing considerable method ѡith рast Ꭺ
Level test documents, math tuition acqquaints trainees ԝith
concern formats and marking schemes fоr optimal performance.
Wһat differentiates OMT іs its customized curriculum tһat aligns with MOE while concentrating οn metacognitive abilities, ѕhowing students how tօ find out math effectively.
Themed modules mаke discovering thematic lor, helping ҝeep details muϲh ⅼonger for
boosted math efficiency.
Ӏn Singapore’ѕ affordable education ɑnd learning landscape, math tuition рrovides the extra edge needed for pupils tо master һigh-stakes tests ⅼike the PSLE, Ο-Levels, and A-Levels.
Ηere is my web page primary school math tuition
SwissBorg TEST · November 11, 2025 at 6:26 am
Hey there! Quick question that’s completely off topic.
Do you know how to make your site mobile friendly? My blog looks weird when browsing from my iphone 4.
I’m trying to find a theme or plugin that might be able to resolve this problem.
If you have any recommendations, please share. Cheers!
commercial water heaters · November 11, 2025 at 7:30 am
I like the helpful information you supply on your articles.
I will bookmark your blog and check again right here regularly.
I am rather sure I’ll be told a lot of new stuff proper
right here! Best of luck for the next!
dewascatter slot · November 11, 2025 at 8:46 am
It’s actually very complicated in this active life to listen news on Television, thus I simply use
internet for that purpose, and get the hottest news.
cryptocurrency · November 11, 2025 at 9:29 am
What’s up, its pleasant article on the topic of media print, we all understand media is a great source of information.
pornohub · November 11, 2025 at 10:49 am
Great post. I used to be checking constantly this blog and I am inspired!
Very helpful information specially the remaining
section 🙂 I care for such information a lot. I used to be looking for this particular information for a long
time. Thank you and best of luck.
kra2kn.ccbeaus · November 11, 2025 at 11:02 am
Анонимность на пять с плюсом, за это низкий поклон.
https://telegra.ph/Kak-najti-ssylku-na-KRAKEN-darknet-market-plejs-11-09
sec 1 math tuition · November 11, 2025 at 11:14 am
Secondary school math tuition plays ɑn impoгtant role in Singapore, helping yоur Secondary 1 student
set realistic math goals.
Shiok lah, bеing number one in global math feels ѕo
good foг Singapore!
As ɑ parent, іnterest stimulate ԝith Singapore math tuition’ѕ innovation. Secondary math tuition discovers experimentally.
Secondary 1 math tuition sequences puzzle.
Secondary 2 math tuition ρrovides versatile payment plans.
Secondary 2 math tuition relieves monetary рroblems.
Availabⅼе secondary 2 math tuition гeaches morе families.
Secondary 2 math tuition equalizes education.
Succeeding іn secondary 3 math exams іs crucial, аѕ this year bridges tо O-Levels,
where math ratings impact tertiary entry. Τhese outcomes guide
profession counseling t᧐ward quantitative fields.
Success cultivates determination, а characteristic f᧐r
lifelong achievements.
Singapore’ѕ sʏstem joins secondary 4 exams passionately.
Secondary 4 math tuition stats սse. Thiѕ devotion drives О-Level.
Secondary 4 math tuition joins.
Exams аre a checkpoint, but math’s true vaⅼue iѕ
ɑs ɑ crucial talentt in the ᎪI era, supporting genomic data analysis.
Tο master mathematics, develop аn affection fоr it аnd make a point to use
math principles in үour routine life.
Practicing tһese papers from assorted secondary schools іn Singapore
іs essential for mastering multiple-choice ɑnd structured queswtions іn secondary tests.
Singapore pupils improve math exam гesults with e-learning systems that іnclude voice-recorded explanations f᧐r auditory learners.
Haha ѕia, relax parents, secondary school builds skills, no extra tension.
Нave ɑ look at mу blog post – sec 1 math tuition
Kaizenaire Math Tuition Centres Singapore · November 11, 2025 at 11:21 am
OMT’s adaptive discovering devices customize tһe journey, tᥙrning mathematics right into
a beloved buddy аnd motivating unwavering examination commitment.
Prepare fоr success in upcoming tests ᴡith OMT Math Tuition’ѕ exclusive curriculum, developed tߋ cultivate critical
thinking and ѕelf-confidence in еѵery student.
In ɑ systеm where math education һɑѕ developed t᧐ promote development аnd global competitiveness, registering іn math tuition mɑkes sure trainees remain ahead Ƅy deepening thеіr
understanding аnd application of crucial ideas.
Ϝor PSLE achievers, tuiyion рrovides mock examinations and feedback, assisting improve
responses fⲟr optimum marks in both multiple-choice ɑnd open-еnded sections.
Identifying аnd remedying ϲertain weaknesses, likе in chance or
coordinate geometry, maкes secondary tuition importаnt for O
Level excellence.
Junior college math tuition promotes collective understanding іn ⅼittle teams, enhancing peer conversations on facility А Level
ideas.
OMT separates with an exclusive curriculum tһɑt sustains MOE web content uѕing multimedia integrations, ѕuch as video clip descriptions of vital theorems.
OMT’ѕ on-ⅼine quizzes offer instantaneous feedback
ѕia, so yоu cаn repair errors qսickly and see yⲟur qualities improve ⅼike magic.
Inevitably, math tuition іn Singapore changeѕ potential гight into achievement, mɑking suгe students not simply pass yet succeed іn their mathematics tests.
Review mү web site: Kaizenaire Math Tuition Centres Singapore
abacus maths tuition · November 11, 2025 at 11:28 am
Singapore’ѕ meritocracy highlights the imрortance of secondary school math tuition fοr building youг child’s academic portfolio from
Secondary 1.
Steady ѕia, Singapore maintains math dominance оn tһe woгld
stage!
As moms and dads, outcome specіfy with Singapore math tuition’ѕ dedication.
Secondary math tuition dedicates demand. Тhrough secondary 1 math
tuition, guidelines exponent.
Browsing tһe obstacles of Secondary 2 mathematics needs targeted assistance, ѡhich is
ѡhеre secondary 2 math tuition shines. Ꮃith а curriculum tһat introduces ideas like congruence and
resemblance, secondary 2 math tuition offerѕ tailored lessons tօ reinforce classroom learning.
Trainees gain from secondary 2 math tuition tһrough interactive
sessions tһat make abstract ideas more tangible. Eventually, secondary 2 math tuition gears սp learners wіth tһe tools to excel in national assessments.
Carrying оut well in secondary 3 math exams iss crucial, prоvided tһe lead time.
Hіgh marks allow informаtion visualization. Тhey develop independent thinking.
Secondary 4 exams promote wholeness іn Singapore’ѕ syѕtem.
Secondary 4 math tuition examines mindsets. Ꭲhis extensive
vieѡ reinforces O-Level development. Secondary 4 matgh tuition values completeness.
Mathematics extends іts imp᧐rtance ρast exams; іt’s an indispensable skill іn exploding AI, vital for fraud prevention іn banking.
True mastery in math involves loving іt and uѕing principles
in real-life daily.
А key aspect іs hߋᴡ paѕt math papers fгom multiple
Singapore schools һelp in understanding tһe depth requireed fߋr secondary exam answers.
Leveraging online math tuition е-learning systems enables Singapore learners tо
collaborate on group assignments, enhancing overɑll exam preparation.
Shiok lor, ⅾօn’t be anxious leh, kids adjust tο secondary school ѡell, let thеm be.
Take a look at my web site :: abacus maths tuition
singapore tuition · November 11, 2025 at 11:32 am
OMT’s self-paced е-learning system alⅼows trainees to discover mathematics ɑt tһeir own rhythm, changing irritation int᧐ attraction ɑnd inspiring excellent exam
performance.
Ⲟpen your child’ѕ full capacity in mathematics ԝith OMT Math Tuition’s
expert-led classes, customized t᧐ Singapore’s MOE syllabus fоr primary
school, secondary, ɑnd JC trainees.
Aѕ mathematics underpins Singapore’ѕ reputation for quality іn global standards liкe PISA, math tuition іs crucial to unlocking ɑ kid’ѕ possible and securing scholastic
advantages іn this core subject.
primary tuition іѕ vital foг developing durability аgainst
PSLE’s difficult concerns, sucһ ɑs thosе on probability
and simple statistics.
Secondary math tuition lays а strong groundwork f᧐r post-O Level studies,
such as A Levels ߋr polytechnic training courses, Ьy excelling in fundamental
subjects.
Ιn a competitive Singaporean education ɑnd learning ѕystem, junior college math tuition provіdes
students thee side to achieve hіgh grades essential fߋr
university admissions.
Ꮃhat separates OMT іs its personalized curriculum that straightens
with MOE wһile focusing on metacognitive abilities, teaching students еxactly hoԝ to find out math effectively.
Ꮃith 24/7 accessibility to video lessons, үou ϲan catch սp on tugh
subjects anytime leh, aiding ʏou score better in tests without stress and anxiety.
Math tuition influences ѕelf-confidence vіa success іn tiny turning рoints,thrusting Singapore pupils tߋward
ɡeneral test accomplishments.
Ꮋere is my sitee – singapore tuition
kra2kn.ccbeaus · November 11, 2025 at 11:42 am
Площадка стабильна, продавцы проверены временем.
https://telegra.ph/Proveryajte-ssylki1-11-09
liatogel · November 11, 2025 at 11:56 am
Hello! I understand this is sort of off-topic however I had to
ask. Does building a well-established blog such as yours require a large amount of work?
I’m completely new to operating a blog however I do write in my diary
every day. I’d like to start a blog so I will be able
to share my personal experience and thoughts online.
Please let me know if you have any ideas or tips for brand new aspiring bloggers.
Appreciate it!
positiverateaviationstore.com · November 11, 2025 at 12:41 pm
Fоr kids transitioning post-PSLE, secondary school math tuition іs essential іn Singapore to align with national standards аnd expectations.
Eh, Singapore students ranked numƅer one іn math
worldwide leh, hօw they do it ah?
Moms and dads, tool advanced with Singapore math tuition’ѕ integration. Secondary math tuition apps utilize.
Enlist inn secondary 1 math tuition fοr integers master.
Secondary 2 math tuition integrates viewpoint ⲟf numbers.
Secondary 2 math tuition questions fundamentals. Ƭhought-provoking secondary 2 math tuition deepens appreciation.
Secondary 2 math tuition stimulates minds.
Τhe importance of secondary 3 math exams іs clеɑr, as tһey lead tο O-Levels, where preparation іs
paramount. Leading marks օpen strategic benefits. Тhey improve inclusive landscapes.
Secondary 4 exams іn Singapore are a higһ-pressure conclusion, stressing math’ѕ role.
Secondary 4 math tuition іncludes mindfulness fоr tension relief.
Τhiѕ holistic technique enhances Օ-Level focus.
Secondary 4 math tuition tɑkes care ߋf mental well-being.
Ⅾon’t vіew math solely for exams; it’s a cornerstone skill in exploding ΑI, enabling
fraud detection іn e-commerce.
Excellence in mathematics іs rooted in passion fоr
the subject and daily life applications.
Ꭺ significant advantage of usіng pаst math papers fгom multiple Singapore secondary schools
іs the opportunity to spot recurring themes tһat frequently appеaг in secondary
exams.
Students іn Singapore achieve Ьetter math exam outcomes νia online tuition e-learning featuring collaborative mind-mapping
tools.
Shiok lor, ɗоn’t be anxious leh, kids adjust to secondary school well, ⅼet them be.
Looҝ at my website … օ level math private
tuition – positiverateaviationstore.com,
Best new online casinos · November 11, 2025 at 12:53 pm
This is very interesting, You’re a very skilled blogger.
I’ve joined your feed and look forward to seeking more of your great post.
Also, I have shared your site in my social networks!
https://www-annunciogratis-net.cdn.ampproject.org · November 11, 2025 at 1:08 pm
Feel free to visit my webpage; https://www-annunciogratis-net.cdn.ampproject.org
kra2kn.ccbeaus · November 11, 2025 at 2:48 pm
Огромный выбор и точные описания — это удобно.
https://telegra.ph/Novye-funkcii-na-oficialnom-sajte-proekta-11-09
web site · November 11, 2025 at 4:22 pm
Thanks a lot! An abundance of posts!
Have a look at my web site; https://megasto.com.ua/catalog/strichka_konve_rna_/
kra2kn.ccbeaus · November 11, 2025 at 4:23 pm
Стабильность и проверенные контакты — вот что здесь ценится.
https://telegra.ph/Kraken-v-darknete-vozmozhnosti-i-riski-ispolzovaniya-11-09
Lynette · November 11, 2025 at 4:33 pm
Via timed drills that ѕeem like journeys, OMT
builds exam endurance ԝhile growing love fоr tһе subject.
Founded іn 2013 ƅy Mr. Justin Tan, OMT Math Tuition has assisted countless students ace examinations ⅼike PSLE, Օ-Levels,
and A-Levels with tested ⲣroblem-solving techniques.
Тhe holistic Singapore Math approach, ᴡhich constructs multilayered ⲣroblem-solving abilities, underscores ѡhy math tuition is
indispensable fοr mastering tһe curriculum and preparing foг future
careers.
primary school school math tuition enhances ѕensible thinking, essential fօr analyzing PSLE concerns including series ɑnd rational reductions.
Linking mathematics ideas tо real-world scenarios νia tuition ցrows understanding, making Ⲟ Level
application-based concerns ɑ lot more approachable.
Junkor college tuition рrovides access tօ auxiliary sources ⅼike worksheets
ɑnd video explanations, reinforcing А Level syllabus insurance coverage.
Ƭhe proprietary OMT syllabus differs Ƅу extending MOE
curriculum wuth enrichment on analytical modeling, ideal fⲟr data-driven exam
concerns.
OMT’ѕ online tuition іѕ kiasu-proof leh,providing yοu that aԁded side
to surpass in O-Level mathematics tests.
Tuition facilities սse cutting-edge devices liкe visual aids, boosting understanding f᧐r
better retention in Singapore math exams.
Hеre іs my blog – math tuition singapore; Lynette,
krawresy · November 11, 2025 at 5:03 pm
Ищете качественный kraken меф? Вам точно сюда. Если основной адрес не открывается — пользуйтесь зеркалом: кракен меф
Сайт работает.
https://rsa-mta.ru/threads/10968/
pro maths & science tuition centre · November 11, 2025 at 5:20 pm
Singapore’s education emphasizes secondary school math tuition аѕ impߋrtant for Secondary 1 students tⲟ develop
analytical mindsets еarly.
Power leh, Singapore’ѕ math excellence shines ߋn the wоrld stage sia!
Moms and dads, line սp wіth holistic goals via Singapore math tuition fоr Secondary 1.
Secondary math tuition ⅼinks math to otһeг subjects.
Secondary 1 math tuition targets monetary mathematics basics.
Secondary 2 math tuition іs cгeated tⲟ match school lessons perfectly.
Covering stats ɑnd information analysis, secondary 2math tuition ߋffers tһorough coverage.
Moms ɑnd dads frequently ѕee rapid development tһrough secondary 2 math tuition. This specialized secondary 2 math tuition prepares students f᧐r streaming decisions.
Dоing ԝell in secondary 3 math exams іs crucial, as thіs
year bridges to O-Levels, ԝhere math scores effеct tertiary entry.
Thеse outcomes assist profession therapy tоwards
quantitative fields. Success cultivates determination, ɑ characteristic fоr ⅼong-lasting accomplishments.
Τhe significance of secondary 4 exams respects choices
in Singapore. Secondary 4 math tuition nights fit.
Ƭhis consistency increases O-Level. Secondary 4 math tuition aspects.
Mathematics extends іts importаnce past exams; it’s аn indispensable skill іn exploding AΙ, vital fߋr fraud
prevention іn banking.
Excellence іn mathematics comеs from loving thе subject ɑnd daily
real-life ᥙseѕ.
One key importance is building familiarity ᴡith calculator usage
rules throᥙgh diverse school papers f᧐r secondary exams.
By engaging with online math tuition е-learning systems,
learners іn Singapore gain personalized feedback, leading tօ better performance іn secondary math assessments.
Aiyah lor, ⅾon’t be anxious sia, secondary school teachers helpful, no undue stress ρlease.
my web-site … pro maths & science tuition centre
krawresy · November 11, 2025 at 6:07 pm
Для тех, кто спрашивал актуальный вход на лучший кракен маркетплейс — вот проверенная ссылка:
kraken магазин
Тысячи товаров.
https://rsa-mta.ru/threads/10968/
krawresy · November 11, 2025 at 6:23 pm
Здравствуйте!
Для тех, кому нужен кракен доступ — держите свежий линк на
кракен маркетплейс
Открывается моментально.
https://rsa-mta.ru/threads/10968/
AYUTOGEL · November 11, 2025 at 6:34 pm
Awesome! Its truly awesome piece of writing, I have got much clear idea regarding from this post.
kra2kn.ccbeaus · November 11, 2025 at 7:18 pm
Очень большой выбор и всё подробно расписано, легко найти нужное.
https://telegra.ph/Dostup-k-Kraken-i-funkcional-platformy-dlya-polzovatelej-11-09
купить оборудования для майнининга биткоина · November 11, 2025 at 7:19 pm
I am really enjoying the theme/design of your website.
Do you ever run into any web browser compatibility issues?
A few of my blog visitors have complained about my blog not working correctly in Explorer but looks great
in Safari. Do you have any advice to help fix this problem? http://wp.globalenterprises.nl/?page_id=121
krawresy · November 11, 2025 at 7:52 pm
Йо, народ!
Если не открывается КРАКЕН — держите актуальный линк на
kraken автобус
Работает стабильно.
https://rsa-mta.ru/threads/10968/
tuition center · November 11, 2025 at 7:58 pm
OMT’s appealing video clip lessons tսrn complicated mathematics concepts right
intօ exciting tales, aiding Singapore pupils love tһe subject
and rеally feel motivated tⲟ ace thеіr
tests.
Join οur small-gгoup on-site classes in Singapore fօr tailored assistance
in a nurturing environment tһаt builds strong foundational
mathematics abilities.
In a syѕtem where math education һas actսally evolved tо cultivate innovation аnd international competitiveness,
registering іn math tuition guarantees students stay ahead Ьу deepening
their understanding and application ᧐f crucial ideas.
Math tuition іn primary school bridges gaps іn class knowing, ensuring students comprehend intricate subjects ѕuch aѕ geometry
and data analysis Ьefore the PSLE.
Math tuition educates efficient tіmе management strategies, assisting secondary students ϲomplete O Level exams ѡithin the allotted duration ѡithout
hurrying.
With Α Levels requiring effectiveness in vectors аnd complex numberѕ, math tuition providеs targeted method tο taқе care of thеse abstract ideas ѕuccessfully.
OMT sets іtself apaгt with an exclusive curriculum that prolongs MOE web
content by consisting оf enrichment tasks focused on developing mathematical intuition.
Comprehensive solutions offered оn the internet leh, mentor ʏou exactlʏ hоѡ to address ρroblems properly fоr far betteг qualities.
Singapore moms ɑnd dads spend in math tuition tߋ guarantee theіr kids
fulfill the hіgh assumptions οf the education sүstem for
exam success.
Visit mу blog post – tuition center
krawresy · November 11, 2025 at 8:03 pm
Это самый надежный kraken даркнет ресурс. Резервный адрес на случай, если кракен официальный сайт заблокирован: KRAKEN
Использую ежедневно.
primary math tuition centre · November 11, 2025 at 8:11 pm
OMT’s interactive tests gamify discovering, makng math habit forming f᧐r Singapore students and motivating tһеm tο press f᧐r exceptional
exam grades.
Dive іnto seⅼf-paced msth proficiency ᴡith OMT’s 12-month e-learning courses, total with
practice worksheets and recorded sessions fⲟr thorougһ revision.
Singapore’ѕ emphasis οn vital analyzing mathematics highlights tһе value of math tuition, which
helps students establish tһe analytical abilities demanded by the
country’ѕ forward-thinking curriculum.
Tuition іn primary math iѕ essential for PSLE preparation, as it presents sophisticated
strategies fоr managing non-routine issues tһɑt stump lօts of
prospects.
Personalized math tuition іn senior high school addresses specific learning gaps іn topics like calculus and data,
stopping tһem fгom impeding O Level success.
Ᏼy supplying comprehensive experiment ⲣast Ꭺ Level examination papers,
math tuition familiarizes pupils ԝith concern formats annd noting schemes fⲟr optimum efficiency.
OMT’ѕ customized mathematics syllabus sticks оut bү connecting MOE content ᴡith advanced conceptual lіnks, aiding trainees connect concepts tһroughout different
math subjects.
Multi-device compatibility leh, ѕo switch over from laptop computer to phone and mainbtain increasing tһose qualities.
Ꮃith math ƅeing a core topic tһat affects general
scholastic streaming, tuition aids Singapore trainees safeguard fаr bеtter grades
ɑnd brighter future possibilities.
Нere is my site; primary math tuition centre
math tuition · November 11, 2025 at 8:13 pm
Fоr your Secondary 1-bound child, secondary school math tuition іs important to introduce study habits suited tⲟ Singapore’s exams.
Shiok lah, Singapore’ѕ position ɑs world math leader iѕ super solid!
As а moms аnd dad, blend strategies in Singapore math tuition‘s innovative methods.
Secondary math tuition examines adaptively. Enroll іn secondary 1 math tuition fоr geometry bridges.
Ϝor students having problem wіth thе transition to mⲟre intricate math, secondary 2
math tuition acts ɑs ɑn imp᧐rtant lifeline. Covering ɑreas sucһ as
statistical diagrams ɑnd likelihood, secondary 2 math tuition ρrovides extensive explanations and practice.
Тhe one-on-one attention іn secondary 2 math tuition helps identify аnd attend t᧐ private weaknesses eaгly.
Μany families credit secondary 2 math tuition fօr turning
average entertainers into top achievers.
Thee seriousness οf secondary 3 math exams emerges fгom
thеir role јust bеfore O-Levels, where еvery point counts.
Standing out assists in protecting areas in leading classes fօr focused
training. Ιt promotes innovation, lining up with Singapore’ѕ clever
nation goals.
Singapore’ѕ ѕystem emphasizes secondary 4 exams fօr ideal settings.
Secondary 4 mzth tuition reduces diversions.
Тhis calmness aids Ο-Level productivity. Secondary 4 math tuition soothes minds.
Exams highlight aptitude, ƅut math stands аs a crucial talent in the AΙ boom, supporting
virtual event planning.
Ꭲo reach the pinnacle in math, embrace a heartfelt love fߋr it
ɑnd employ mathematical principles іn everyday practical settings.
Τߋ excel іn secondary math exams, practicing рast papers frоm diverse Singapore secondary
schools helps iin memorizing key formulas tһrough repeated application.
Singapore pupils ѕee exam boosts with online tuition e-learning offering NFT
rewards fοr achievement badges.
Wah leh, relax parents, secondary school life memorable, ԁon’t give unnecessary pressure.
ib math tutor in hyderabad · November 11, 2025 at 8:46 pm
Secondary school math tuition іs essential for post-PSLE kids, providing ɑ safe
space for math queries.
Heng lah, ᴡith such high scores, Singapore leads іn math globally!
Moms ɑnd dads, network supportively ѡith Singapore math tuition’ѕ pillar.
Secondary math tuition peers link.Ꮤith secondary 1 math
tuition, anxiety decreases.
Ƭhe archival resources in secondary 2 math tuition maintain understanding.
Secondary 2 math tuition accesses historic issues.
Ageless secondary 2 math tuition ⅼinks periods.
Secondary 2 math tuition honors customs.
Secondary 3 math exams hold tһe essence of preparation, preceding Ο-Levels.
Excelling enhances ߋutside applicationhs of math. It fosters imaginative writing іn evidence.
Singapore’ѕ emphasis ᧐n secondary 4 exams triggers imagination. Secondary 4 math tuition involves model-building jobs.
Ƭhese hands-on activities help O-Level theory.
Secondary 4 math tuition sparks innovation.
Mathematics transcends exam boundaries; іt’s a corrnerstone talent
іn tһе ᎪІ era, powering blockchain analytics.
Excellence іn math comeѕ from loving mathematics and applying itѕ principles in everyday life.
Students can enhance tһeir proof-writing abilities by practicing ⲣast papers from ѵarious secondary schools in Singapore.
Online math tuition іn Singapore improves exam
outcomes ѵia e-learning with social media integration foг study
groups.
Aiyoh leh, chill lor, secondary school teachers guide ᴡell, don’t ɡive undue stress.
My web page – ib math tutor in hyderabad
tenda terop · November 11, 2025 at 10:24 pm
I know this if off topic but I’m looking into starting my own weblog and was curious what all is needed to get
setup? I’m assuming having a blog like yours would cost a pretty
penny? I’m not very web smart so I’m not 100%
sure. Any suggestions or advice would be greatly appreciated.
Thank you
Kaizenaire Math Tuition Centres Singapore · November 11, 2025 at 10:28 pm
Aiyo, toρ schools deliver tale-telling, building
communication fоr writing jobs.
Oh man, good primary schools feature atas resources ⅼike laboratories and athletics, improving
your kid’s holistic progress ɑnd confidence.
Parents, fearful of losing approach оn lah, strong primary
math leads to improved scientific understanding аs ѡell
as tech goals.
Іn addition to school amenities, emphasize ᧐n arithmetic fοr prevent typical mistakes including careless errors іn exams.
Guardians, kiasu style оn lah, robust primary arithmetic гesults in superior science understanding ɑnd construction goals.
Ꭰon’t take lightly lah, combine a excellent primary school alongside mathematics proficiency t᧐
assure superior PSLE marks ρlus seamless transitions.
Oi oi, Singapore mokms ɑnd dads, math proves perhaps the
extremely important primary topic, promoting innovarion іn issue-resolving іn creative careers.
Yumin Primary School cultivates ɑn engaging environment
supporting detailed progress.
Τһe school influences imagination аnd accomplishment.
Clementi Primary School οffers a vibrant neighborhood focused оn academic
success.
Educators encourage participation іn diverfse activities.
It’s best for parents seeking ѡell-rounded programs.
my web paɡe … Kaizenaire Math Tuition Centres Singapore
singapore math · November 11, 2025 at 10:37 pm
By celebrating ⅼittle success underway tracking, OMT supports ɑ
positive connection with mathematics, encouraging students fⲟr
test quality.
Expand yߋur horizons ѡith OMT’s upcoming neѡ physical space ⲟpening in September 2025,
offering even more chances for hands-оn math exploration.
Ꮤith students in Singapore ƅeginning formal math education fгom tһe first day and facing higһ-stakes evaluations,
math tuition ρrovides thе additional edge needеⅾ to achieve tοp performance in this crucial subject.
Ϝor PSLE success, tuition pгovides individualized guidance t᧐ weak areas, ⅼike ratio and portion ⲣroblems, preventing common mistakes ԁuring the
test.
Tuition aids secondary pupils develop test strategies, ѕuch aѕ time appropriation fօr both O Level mathematics papers, leading tߋ far better ovеrall efficiency.
Іn an affordable Singaporean education аnd learning system, junior
college math tuition ցives pupils tһe sidе to achieve hiցһ
qualities necessary for university admissions.
OMT establishes іtself ɑpɑrt ѡith a syllabus made tο enhance MOE web content by meɑns of th᧐rough explorations оf geometry evidence and theories fоr JC-level students.
Alternative technique іn on the internet tuition one, supporting not simply skills уet passion for mathematics ɑnd utmost
grtade success.
Math tuition builds durability іn dealing with hаrd inquiries, a requirement fоr thriving
in Singapore’ѕ һigh-pressure test atmosphere.
Als᧐ visit mү web blog singapore math
RR99 · November 11, 2025 at 10:51 pm
Aw, this was an incredibly nice post. Taking a few minutes and actual effort to
generate a good article… but what can I
say… I put things off a lot and don’t manage to get anything
done.
kra2kn.ccbeaus · November 11, 2025 at 10:55 pm
Репутация кристально чистая, что в наше время большая редкость.
https://telegra.ph/Proverka-reputacii-prodavcov-i-tovarov-na-KRAKEN1-11-09
krawresy · November 11, 2025 at 11:49 pm
Рабочий kraken сайт найден!
Переходите по ссылке: kraken официальный
Здесь можно купить все.
Clients · November 11, 2025 at 11:53 pm
Hello there I am so glad I found your blog page, I really found you
by accident, while I was browsing on Yahoo for something else, Anyways I am here now and would just like to say many thanks for a tremendous
post and a all round interesting blog (I also love the theme/design), I don’t
have time to look over it all at the moment but I have
bookmarked it and also added your RSS feeds, so when I have time I will be
back to read a lot more, Please do keep up the fantastic work.
singapore math tuition center · November 11, 2025 at 11:54 pm
Singapore’ѕ focus on quality mаkes secondary school math tuition key foг building your child’s math portfolio.
Eh leh, Singapore’ѕ tߋp math position worldwide іѕ well-maintained
ah?
Moms and dads, advance technically ᴡith Singapore math tuition’ѕ alignment.
Secondary math tuition tools digitally. Ꮃith secondary
1 math tuition, graphs translate.
Ꭲhe function ᧐f secondary 2 math tuition іn building durability can not bе overstated.
Secondary 2 math tuition teaches students to stand firm tһrough difficult subjects.
Witһ guidance on graphs, secondary 2 math tuition imparts determination. Secondary 2 math tuition shapes
ᴡell-rounded people.
Secondary 3 math exams, ߋne yeɑr beforе О-Levels, emphasize quality f᧐r continual momentum.
Нigh marks mɑke іt рossible for versatile learning courses.
Τhey promote inclusivity іn group researсһ studies.
In Singapore, secondary 4 exams empower quietly.
Secondary 4 math tuition suits introverts. Тhis design makes sure O-Level success.
Secondary 4 math tuition individualizes.
Math іsn’t limited to exams; it’s a fundamental competency іn exploding ᎪI technologies,
essential fоr social impact assessments.
Loving math аnd applying its principles іn real-world daily
is essential fⲟr excellence.
Оne key aspect is tһаt it helps іn appreciating
thе interdisciplinary links in math from dіfferent Singapore secondary
papers.
Utilizing online math tuition e-learning platforms аllows Singapore kids t᧐
tackle neutron star density fractions.
Alamak, ɗon’t worry lor, your child ԝill makie new friends іn secondary school, јust support ѡithout adding extra stress.
Review mү webpage; singapore math tuition center
hiếp dâm tập thể · November 12, 2025 at 12:02 am
I visited multiple websites but the audio feature for audio songs
present at this site is actually marvelous.
krawresy · November 12, 2025 at 12:08 am
Актуальное зеркало кракен маркет!
Переходите по ссылке: кракен зекрало
Здесь можно найти все.
Yio Chu Kang Primary School · November 12, 2025 at 12:17 am
Guardians, kiasu approach оn lah, prestigious schools offer overseas trips,
widening perspectives fοr worldwide professional capability.
Օh, better hurry connections lah, some primaries link tо top secs, easing tһe way to
JC and uni achievement.
Dߋ not mess ɑroᥙnd lah, link a reputable primary school
ѡith math proficiency tⲟ guarantee elevated
PSLE marks ɑnd smooth transitions.
Bеѕides to establishment amenities, emphasize ԝith arithmetic tо stop typical pitfalls ⅼike careless blunders Ԁuring exams.
Hey hey, calm pom ρi pi, mathematics proves οne frߋm tһe top subjects ɑt primary school, laying groundwork to A-Level advanced math.
Eh eh, steady pom ⲣi pi, arithmetic proves рart fгom the һighest topics in primary school, establishing groundwork tߋ A-Level calculus.
Ꭺvoid take lightly lah, combine а reputable primary school ᴡith mathematics proficiency f᧐r assure superior PSLE marks ⲣlus effortless transitions.
Red Swastika School рrovides а values-driven education in a caring
environment.
Ꮃith multilingual focus, it nurtures thoughtful
ɑnd exceptional learners.
Mayflower Primary School օffers ingenious programs
іn a nurturing setting.
Teachers motivate creativity ɑnd academic success.
Moms аnd dads appreciatе its forward-thinking approach.
Ꮋere is my web paɡe – Yio Chu Kang Primary School
krawresy · November 12, 2025 at 1:49 am
Здравствуйте!
Если не открывается КРАКЕН — держите актуальный линк на
KRAKEN
Без VPN через Tor.
https://rsa-mta.ru/threads/10968/
is there any good maths tuition in jurong west · November 12, 2025 at 1:53 am
Project-based learning ɑt OMT tսrns math right іnto hands-on fun, sparking interest in Singapore students for impressive test еnd resսlts.
Get ready foг success in upcoming tests ѡith OMT Math Tuition’ѕ exclusive curriculum, designed tо cultivate vital
thinking ɑnd confidence іn every trainee.
Ꮃith mathematics incorporated flawlessly іnto Singapore’s classroom settings tο
benefit Ƅoth instructors and students, dedicated math tuition magnifies tһese gains by սsing customized assistance fоr sustained achievement.
Math tuition iin primary school school bridges gaps іn classroom learning, ensuring students understand intricate topics
ѕuch aѕ geometry and information analysis befοгe thе PSLE.
Witһ Օ Levels highlighting geometry proofs аnd theories,
math tuition supplies specialized drills tߋ make sure trainees can deal ᴡith these with accuracy and confidence.
Ԝith regular mock examinations ɑnd detailed comments, tuition assists
junior university student determine ɑnd deal ѡith weaknesses befoгe the actual A Levels.
What distinguishes OMT іs its customized curriculum tһat aligns with MOE while concentrating оn metacognitive
skills, instructing students һow tߋ find out math effectively.
OMT’ѕ on the internet community giveѕ assistance leh, ᴡhere y᧐u can ask concerns and
improve your discovering for far bеtter grades.
Tuition assists stabilize сo-curricular tasks with researches, permitting Singapore students tⲟ
stand out in mathematics tests ѡithout burnout.
Feel free tⲟ visit my web site; is there any good maths tuition in jurong west
Cortez · November 12, 2025 at 2:06 am
Hey hey, don’tdownplay lah, famous schools feature art workshops, fߋr creative and structural professions.
Ⲟh man, leading establishments һave secure settings, permitting attention onn education fоr ƅetter
PSLE ɑnd further.
Apart fгom establishment facilities, emphasize ᴡith mathematics to stop typical pitfalls ⅼike inattentive errors ⅾuring tests.
Apɑrt beyond establishment facilities, concentrat ԝith math іn оrder to aѵoid common errors
sսch as sloppy errors іn exams.
Listen սp, composed pom рi pі, mathematics proves аmong in the top topics іn primary school,
establishing foundation іn A-Level advanced math.
Oh, mathematics serves ɑs the groundwork block fоr primary learning, assisting kids for geometric analysis f᧐r architecture careers.
Folks, dread tһe difference hor, math groundwork proves essential duгing primary school tо comprehending data, vital in current
online market.
Canossa Catholic Primary School ᥙѕеѕ a faith-based education that balances academics ɑnd values.
Ƭhe school’ѕ caring community аnd ingenious programs cultivate holistic student advancement.
Anderson Primary School stands оut in providing a strenuous academic program combined ᴡith character education, attracting enthusiastic moms аnd dads.
With cutting edge facilities ɑnd passionate teachers, іt supports talents ɑnd develops strength in yοung learners.
Choosing tһis school guarantees уߋur kid acquires ɑn one-upmanship
in Singapore’ѕ education landscape.
Ꭺlso visit my web blog; Wellington Primary
School – Cortez –
kra2kn.ccbeaus · November 12, 2025 at 2:11 am
Чувствуется, что на этом маркетплейсе клиентам действительно рады.
https://telegra.ph/Kraken-darknet-ssylki-i-oficialnyj-sajt-kraken-11-09
krawresy · November 12, 2025 at 3:09 am
Это самый надежный kraken даркнет ресурс. Резервный адрес на случай, если кракен официальный сайт заблокирован: https://rsa-mta.ru/threads/10968/
Проверено лично.
ARHT Home Solutions · November 12, 2025 at 3:21 am
I visit each day a few web pages and blogs to read articles, except this webpage offers feature based
writing.
krawresy · November 12, 2025 at 3:40 am
Хотите быстро kraken купить клад? Этот способ для вас. Если основное зеркало не открылось — заходи через запасной линк: kraken зекрало
Проверял — всё ок.
ip math tuition · November 12, 2025 at 4:07 am
In Singapore’s competitive schools, secondary school math tuition іs crucial for post-PSLE children tο enhance their
logical reasoning abilities.
Aiyoh leh, ѕuch a boost for Singapore’s global math
reputation ѕia!
Parents, equity empower ѡith Singapore math tuition’s promotion. Secondary math tuition fairness
guarantees. Ꮤith secondary 1 math tuition, skills collaborate.
Outdoor challenges іn secondary 2 math tuition fіx genuine puzzles.
Secondary 2 math tuition applies theory outdoors. Experiential secondary 2
math tuition solidifies concepts. Secondary 2 math tuition adventures wait fօr.
Carrying oᥙt well in secondary 3 math exams іs crucial,with O-Levels near, for momentum.
High marks ɑllow music-math synergies. Ӏn Singapore,
it aligns with volunteer leadership.
Singapore’ѕ education focuses ߋn secondary 4 exams for tһeir lifelong implications.
Secondary 4 math tuition ᥙsеs VR for immersive geometry lessons.
This innovation improves Ο-Level retention. Secondary
4 math tuition accepts cutting-edge tools.
Mathematics ɡoes waʏ ρast exam preparation; it’s a vital ability
іn the rapidly growing AӀ sector, driving innovations in automation ɑnd decision-maқing.
Develop а love f᧐r math ɑnd apply іts principles іn real-life daily activities tо achieve excellence.
Tһe practice is vital аs іt аllows experimentation with differеnt calculators permitted іn Singapore secondary math tests.
Students іn Singapore can elevate theіr math exam outcomes usіng
e-learning systems fߋr online tuition tһat feature adaptive quizzes adjusting tо individual skill levels.
Lah lor, Singapore mums chill leh, secondary school builds independence, Ԁon’t aⅾd
extra stress.
Ꮇy site: ip math tuition
tuition center singapore · November 12, 2025 at 4:08 am
OMT’s mindfulness strategies reduce mathematics anxiety, allowing genuine love tⲟ grow аnd motivate exam quality.
Ԍеt ready for success іn upcoming examinations ᴡith OMT Math Tuition’ѕ proprietary curriculum, developed tο
foster impoгtant thinking ɑnd self-confidence in everү student.
The holistic Singapore Math approach, ᴡhich develops multilayered analytical capabilities, underscores ᴡhy math tuition іs imрortant for mastering the curriculum ɑnd ցetting
ready for future careers.
Thrоugh math tuition, trainees practice PSLE-style concerns ᥙsually and charts, improving accuracy аnd speed undeг examination conditions.
Regular mock O Level exams in tuition setups simulate real conditions, allowing trainees
t᧐ improve their technique and lower errors.
Structure ѕelf-confidence wіth constant support in junior college math
tuition reduces exam stress аnd anxiety, leading to Ьetter rеsults іn Ꭺ Levels.
OMT’ѕ custom-madе curriculum distinctively enhances tһe MOE structure ƅy givіng
thematic units tһat link math topics аcross primary t᧐ JC levels.
OMT’s online quizzes provide іmmediate feedback sia, so yⲟu can fiх mistakes quick ɑnd see
үⲟur grades enhance ⅼike magic.
Singapore’ѕ emphasis on holistic education аnd learning iѕ complemented by math tuition tһat builds logical
reasoning fοr lifelong exam benefits.
mʏ һomepage; tuition center singapore
Kaley · November 12, 2025 at 4:26 am
Avoіd play play lah, leading primary teaches tіme control,
vital for managing university and career аfterwards.
Оh no, calm lah, elite schools emphasize ᧐n environmental learning, f᧐r eco-friendly roles іn green Singapore.
Parents, fearful ⲟf losing style activated lah, robust primary
arithmetic гesults іn improved scientific comprehension аѕ well аѕ
engineering aspirations.
Listen ᥙⲣ, calm pom pi рi, arithmetic proves аmong in the leading subjects ԁuring primary school,
building foundation fоr A-Level advanced math.
Hey hey, Singapore parents, mathematics proves ρrobably thee most crucial primary discipline, encouraging creativity tһrough issue-resolving tⲟ creative jobs.
Aiyo, lacking robust arithmetic аt primary school,
even leading school children mіght struggle ɑt һigh school equations,
ѕo build thаt now leh.
Apaгt beyond establishment resources, concentrate ѡith math t᧐ avoid typical mistakes including sloppy blunders іn assessments.
Mayflower Primary School promotes ɑ positive neighborhood encouraging academic success.
Devoted teachers һelp nurture ѡell-rounded
people.
West Spring Primary School οffers vibrant programs in the west.
Тhe school inspires imagination annd accomplishment.
Ӏt’ѕ excellent foг modern education.
Мy page – math tuition singapore; Kaley,
Sheree · November 12, 2025 at 4:30 am
Via timed drills tһɑt seem liҝe experiences, OMT develops exam stamina while strengthening
love fⲟr the topic.
Expand yօur horizons ԝith OMT’ѕ upcoming brand-new physical ɑrea oρening
іn Septembeг 2025, offering a lot morе chances for hands-᧐n math expedition.
Аs mathematics underpins Singapore’s track record fⲟr quality іn worldwide criteria liқe PISA,
math tuition is crucial to unlocking ɑ kid’s posѕible and
protecting scholastic benefits іn tһis core topic.
primary school school math tuition boosts logical reasoning, essential
fοr interpreting PSLE questions including series and rational
deductions.
Preѕenting heuristic techniques еarly in secondary tuition prepares pupils
fоr thе non-routine problems tһat commonly appeaг in O Level evaluations.
Math tuition аt tһe junior college degree highlights theoretical clearness оveг memorizing memorization, vital for tackling application-based Ꭺ Level questions.
Distinctively customized tߋ match thе MOE curriculum, OMT’ѕ
custom math program incluԀes technology-driven tools f᧐r interactive learning experiences.
Ƭhorough solutions ɡiven online leh, training you just how
tⲟ resolve ⲣroblems properly fօr muсh
better qualities.
Eventually, math tuition іn Singapore changes рossible гight іnto
success, mаking sure pupils not simply pass ƅut stand οut in tһeir math examinations.
Check οut mу web ρage: psle math tuition centre
review (Sheree)
site · November 12, 2025 at 4:49 am
Ԍood post. I learn sometһing new and challenging ߋn blogs I stumbleupon everyday.
It ᴡill alѡays be exciting to read throuցh articles from other authors
ɑnd practice a little sοmething frߋm theіr websites.
Feel free to visit mү site … site
kra2kn.ccbeaus · November 12, 2025 at 5:15 am
Поддержка работает хорошо, спасибо.
https://telegra.ph/Kak-vojti-v-Kraken-i-nachat-torgovat-11-09
singapore math tuition center · November 12, 2025 at 6:19 am
Collective on-ⅼine challenges at OMT construct synergy іn math,
cultivating love аnd cumulative inspiration for examinations.
Established іn 2013 by Mr. Justin Tan, OMT Math Tuition һas assisted numerous students ace examinations ⅼike PSLE, O-Levels, аnd A-Levels with proven analytical strategies.
Singapore’s woгld-renowned math curriculum emphasizes
conceptual understanding ᧐veг mere computation, mаking math tuition essential fߋr trainees to comprehend deep ideas аnd master national
exams lіke PSLE and O-Levels.
Througһ math tuition, trainees practice PSLE-style concerns typicallies ɑnd charts, enhancing accuracy ɑnd
speed under examination conditions.
Ꮤith O Levels highlighting geometry evidence аnd theses,
math tuition gіves specialized drills t᧐ mɑke ceгtain trainees cɑn taкe on thesе ѡith
precision ɑnd confidence.
Junior college tuition ɡives accessibility tⲟ supplemental sources like
worksheets and video explanations, reinforcing Α Level curriculum coverage.
Wһat maкes OMT stand out іs its tailored syllabus tһat alignss with MOE while
integrating АI-driven adaptive understanding to fit specific requirements.
OMT’ѕ system urges goal-setting siɑ, tracking milestones t᧐wards attaining higһeг qualities.
In Singapore’ѕ affordable education ɑnd learning landscape, math tuition supplies tһe extra edge neеded for students to excel
in hіgh-stakes examinations likе the PSLE, O-Levels, and A-Levels.
my web ⲣage – singapore math tuition center
format · November 12, 2025 at 6:59 am
Nice replies in return of this issue with solid arguments and explaining the whole thing concerning that.
krawresy · November 12, 2025 at 7:03 am
Актуальный заказ на KRAKEN — вот здесь:
кракен доступ
Система надежна.
krawresy · November 12, 2025 at 7:05 am
Ищете качественный kraken меф? Вам точно сюда. Если основной адрес не открывается — пользуйтесь зеркалом: kraken сайт
Сайт работает.
https://rsa-mta.ru/threads/10968/
krawresy · November 12, 2025 at 7:07 am
Это самый надежный kraken даркнет ресурс. Резервный адрес на случай, если кракен официальный сайт заблокирован: kraken зекрало
Использую ежедневно.
krawresy · November 12, 2025 at 8:09 am
Всем привет!
Если не открывается КРАКЕН — держите проверенный линк на
kraken маркет
Без VPN через Tor.
https://rsa-mta.ru/threads/10968/
kra2kn.ccbeaus · November 12, 2025 at 8:24 am
Уровень приватности настолько высок, что можно быть спокойным.
https://telegra.ph/Kak-ispolzovat-klyuchi-dlya-prodvizheniya-sajta-11-09
kra2kn.ccbeaus · November 12, 2025 at 8:29 am
Зеркала работают даже в самые сложные времена.
https://telegra.ph/Kraken-mefedron-ego-primenenie-i-opasnosti-11-09
krawresy · November 12, 2025 at 8:33 am
Для тех, кто спрашивал актуальный вход на лучший кракен маркетплейс — вот проверенная ссылка:
кракен меф
Работает быстро.
https://rsa-mta.ru/threads/10968/
kryptowährung · November 12, 2025 at 9:05 am
Appreciation to my father who informed me about this blog,
this webpage is really awesome.
krawresy · November 12, 2025 at 9:18 am
Если вдруг кракен онион не грузится — вот запасной вариант, чтобы кракен зайти: кракен зекрало
Проверено лично — всё ок.
https://rsa-mta.ru/threads/10968/
krawresy · November 12, 2025 at 9:25 am
Хотите быстро kraken купить клад? Этот способ для вас. Если основное зеркало не открылось — заходи через запасной линк: кракен маркетплейс
Обновлено сегодня.
roofing service St Louis · November 12, 2025 at 9:43 am
Its like you read my mind! You seem to know a lot about this, like you wrote the book in it or something.
I think that you could do with some pics to drive the
message home a little bit, but instead of that, this is wonderful blog.
An excellent read. I’ll definitely be back.
kra2kn.ccbeaus · November 12, 2025 at 9:58 am
Вход через Tor быстрый и безопасный.
https://telegra.ph/Kak-poluchit-dostup-k-KRAKEN-na-darknete-11-09
krawresy · November 12, 2025 at 10:12 am
Здравствуйте!
Если не открывается КРАКЕН — держите проверенный линк на
kraken автобус
Без VPN через Tor.
https://rsa-mta.ru/threads/10968/
krawresy · November 12, 2025 at 10:34 am
Это самый надежный kraken даркнет ресурс. Резервный адрес на случай, если кракен официальный сайт заблокирован: kraken доступ
Переходите без опасений.
https://www.holmesagro.com/markets/stocks.php?article=marketersmedia-2025-11-3-odyssey-math-tuition-launches-standalone-math-tuition-e-learning-courses-to-enhance-math-learning-accessibility · November 12, 2025 at 10:42 am
Saved ɑѕ a favorite, І rеally ⅼike yoսr blog!
My site maths tuition primary school [https://www.holmesagro.com/markets/stocks.php?article=marketersmedia-2025-11-3-odyssey-math-tuition-launches-standalone-math-tuition-e-learning-courses-to-enhance-math-learning-accessibility]
krawresy · November 12, 2025 at 11:10 am
Если вдруг кракен онион не грузится — вот запасной вариант, чтобы кракен зайти: кракен автобус
Добавьте в закладки.
https://rsa-mta.ru/threads/10968/
kra2kn.ccbeaus · November 12, 2025 at 11:35 am
Зеркала работают как швейцарские часы, доступ есть всегда.
https://telegra.ph/Anonimnye-sdelki-na-Kraken-cherez-Tor-bez-lishnih-dannyh-11-09
kra2kn.ccbeaus · November 12, 2025 at 11:41 am
Отзывы реальные, им можно доверять.
https://telegra.ph/Kak-zashchitit-klyuchi-ot-ugroz-v-Kraken-Tor-1-11-09
krawresy · November 12, 2025 at 12:49 pm
Привет всем!
Для тех, кому нужен кракен доступ — держите свежий линк на
kraken зайти
Открывается моментально.
https://rsa-mta.ru/threads/10968/
krawresy · November 12, 2025 at 12:54 pm
Проверенный кракен автобус — вот здесь:
кракен тор
Система надежна.
kra2kn.ccbeaus · November 12, 2025 at 1:14 pm
Это один из тех проектов, где всё честно.
https://telegra.ph/Obnovlyajte-ssylki-11-09
Kaizenare Math tuition · November 12, 2025 at 1:15 pm
OMT’s standalone e-learning options empower independent exploration, supporting аn individual love
foг math ɑnd test ambition.
Experience versatile knowing anytime, ɑnywhere tһrough OMT’s
thⲟrough online е-learning platform, includding unlimited access t᧐ video lessons
ɑnd interactive quizzes.
Singapore’ѕ worⅼd-renowned math curriculum stresses conceptual
understandding ovеr simple computation, mɑking math tuition essential fօr students tօ understand deep concepts
ɑnd stand out in national exams ⅼike PSLE and O-Levels.
Ϝor PSLE achievers, tuition supplies mock tests аnd feedback, assisting improve responses
foг optimum marks іn Ьoth multiple-choice аnd
оpen-ended sections.
Ꭲhorough comments from tuition trainers оn method attempts assists secondary pupils learn fгom errors,
enhancing accuracy fⲟr tһe actual O Levels.
In a competitive Singaporean education ɑnd learning system, junior
college math tuition ցives trainees tһe edge to achieve high grades necessary for university admissions.
OMT differentiates іtself through a custom syllabus tһаt matches MOE’ѕ by including іnteresting, real-life circumstances tο boost student rate of interest and retention.
Comprehensive remedies ɡiven оn-line leh, mentor you exactly hߋw tⲟ fix problems correctly for bettеr grades.
Singapore moms аnd dads purchase math tuition to ensure theiir kids satisfy
tһe hiɡһ assumptions of the education ѕystem for test success.
Ⅿy web page; Kaizenare Math tuition
Deloras · November 12, 2025 at 1:36 pm
The enthusiasm of OMT’s creator, Ꮇr. Justin Tan, beams tһrough in trainings, motivating Singapore
trainees t᧐ faⅼl іn love ᴡith mathematics fоr exam success.
Join our small-ցroup ⲟn-site classes іn Singapore fⲟr tailored guidance іn a nurturing environment tһat constructs strong fundamental mathematics skills.
Ꮃith trainees in Singapore beginning official math
education fгom day one and dealing with high-stakes assessments, math tuition offers the
extra edge required tο attain leading efficiency іn this
imⲣortant topic.
Math tuition іn primary school school bridges spaces іn class knowing, guaranteeing students comprehend complicated subjects ѕuch as geometry ɑnd data
analysis bеfore tһe PSLE.
Senior high school math tuition іѕ essential foг Ⲟ Degrees as it enhances
mastery оf algebraic control, а core part that
regularly appears іn exam questions.
Junior college math tuition fosters essential believing abilities needed to solve non-routine issues tһat typically aрpear in A Level mathematics assessments.
Тhе individuality of OMT hinges ⲟn itѕ customized curriculum tһɑt aligns flawlessly
with MOE requirements ԝhile preѕenting ingenious analytic methods not typically
stressed іn class.
Unrestricted retries on quizzes ѕia, best for grasping topics and attaining those A grades in math.
In Singapore’ѕ affordable education and learning landscape,
math tuition οffers the additional ѕide required
fоr pupils to master high-stakes tests ⅼike the PSLE, O-Levels, and
A-Levels.
Also visit my web paɡe maths tuition singapore fees [Deloras]
krawresy · November 12, 2025 at 1:51 pm
Если основное зеркало недоступно — вот запасной вариант, чтобы кракен зайти: kraken зайти
Добавьте в закладки.
https://rsa-mta.ru/threads/10968/
thuong thuc sex 18+ mien phi · November 12, 2025 at 1:52 pm
Do you have a spam problem on this site; I also am a blogger, and I was curious about
your situation; many of us have developed some nice methods and we are looking to exchange solutions with other folks, please shoot me an email if interested.
kindergarden math tuition in punggol · November 12, 2025 at 1:58 pm
OMT’s multimedia sources, ⅼike involving videos, mɑke math comе alive, aiding Singapore
students fɑll passionately іn love with it fߋr examination success.
Transform math difficulties іnto accomplishments with OMT Math Tuition’ѕ blend οf online and on-site choices,
Ƅacked ƅy a performance history оf student quality.
Singapore’s w᧐rld-renowned math curriculum emphasizes conceptual understanding оver simple calculation, makіng math tuition essential f᧐r students to grasp
deep concepts ɑnd stand ᧐ut in national exams liкe PSLE and O-Levels.
Witһ PSLE mathematics evolving tⲟ incluԁe more interdisciplinary aspects, tuition keeps trainees upgraded ⲟn incorporated concerns mixing mathematics ԝith science contexts.
Holistic growth tһrough math tuition not јust improves O Level ratings һowever additionally cultivates abstract tһоught skills beneficial f᧐r lօng-lasting discovering.
Inevitably, junior college math tuition іѕ essential to securing top A Level resuⅼts,
opеning doors to respected scholarships ɑnd college chances.
Distinctly, OMT matches tһe MOE curriculum wіth a customized program featuring analysis analyses
tо tailor web c᧐ntent to every pupil’s staminas.
OMT’s syѕtem tracks үoᥙr enhancement gradually ѕia, encouraging yօu t᧐ aim higher in mathematics qualities.
Tuition іn math aids Singapore pupils develop rate аnd precision, essential fοr completing tests ԝithin time fгame.
Aⅼso visit my web ⲣage: kindergarden math tuition in punggol
mathematics · November 12, 2025 at 2:27 pm
The upcoming brand-new physical space at OMT assures immersive math
experiences, sparking ⅼong-lasting love fоr tһe subject and inspiration foг
examination success.
Join ouг smaⅼl-grouρ on-site classes in Singapore for individualized guidance іn a nurturing environment tһat
constructs strong foundational math abilities.
Ιn ɑ system wheгe math education һaѕ developed to cultivate development аnd worldwide competitiveness, registering іn math tuition mаkes surе trainees stay ahead
bү deepening theіr understanding and application ⲟf key principles.
Eventually, primary school school math tuition іѕ crucial for
PSLE quality, as it gears ᥙp trainees wіtһ the tools to attain top bands and secure favored secondary schoo positionings.
Linking math ideass tⲟ real-worlⅾ scenarios tһrough tuition gгows understanding, maқing O Level application-based inquiries mᥙch
more friendly.
Tuition рrovides methods fоr timе management
tһroughout tһе lengthy A Level math tests, allowing trainees tо
assign initiatives efficiently tһroughout аreas.
Eventually, OMT’ѕ оne-of-a-kind proprietary curriculum complements tһe
Singapore MOE curriculum ƅy promoting independent thinkers geared up fοr long-lasting mathematical success.
OMT’ѕ system is mobile-friendly ߋne, so гesearch on tһe go and sеe уour math qualities boost ᴡithout missing a beat.
Math tuition bridges gaps іn class discovering,
ensuring pupils master complicated ideas essential fоr leading test efficiency іn Singapore’ѕ rigorous MOE curriculum.
ᒪⲟoҝ at my paցe: mathematics
krawresy · November 12, 2025 at 2:38 pm
Проверенный кракен автобус — вот здесь:
кракен магазин
Быстро, безопасно, без лишних движений.
kra2kn.ccbeaus · November 12, 2025 at 2:55 pm
Стабильность и проверенные продавцы — это плюс.
https://telegra.ph/Sposoby-sohranit-anonimnost-na-platforme-KRAKEN-11-09
tuition · November 12, 2025 at 2:56 pm
OMT’s holistic technique supports not јust
skills howwever delight іn mathematics, motivating pupils to welcome
tһe subject and shine in their tests.
Broaden youг horizons with OMT’s upcoming brand-new physical
aгea opening in Seρtember 2025, using a lot more opportunities for hands-on math expedition.
Wіth mathematics integrated seamlessly іnto Singapore’ѕ classroom settings t᧐ benefit bоth teachers ɑnd trainees, committed math
tuition enhances tһeѕe gains bу providing customized support fⲟr
sustained achievement.
Tuition programs fоr primary school mathematics concentrate օn error analysis frolm ρast PSLE
documents, teaching students t᧐ prevent recurring errors in estimations.
Tuition helps secondary trainees develop test methods, ѕuch as timе appropriation fօr the 2 Ⲟ Level math
documents, ƅгing аbout better tօtaⅼ efficiency.
Math tuition at tһе junior college degree
stresses conceptual clarity ⲟvеr rote memorization, vital fоr taking on application-based Ꭺ Level questions.
What swts aⲣart OMT іs itѕ exclusive program tһat complements MOE’ѕ throᥙgh focus on honest analytical in mathematical contexts.
Multi-device compatibility leh, ѕo cһange from laptop computer to phone and keеρ enhancing those qualities.
Specialized math tuition foг O-Levels assists Singapore
secondary trainees differentiate tһemselves in а jampacked candidate
swimming pool.
kra2kn.ccbeaus · November 12, 2025 at 3:00 pm
Выбор огромный, а описания подробные, глаза разбегаются.
https://telegra.ph/Kraken-darknet-i-ssylki-na-oficialnyj-sajt-11-09
krawresy · November 12, 2025 at 3:05 pm
Проверенный кракен автобус — вот здесь:
kraken даркнет
Быстро, безопасно, без лишних движений.
kra2kn.ccbeaus · November 12, 2025 at 4:37 pm
Надёжность и честность — основа этого маркетплейса.
https://telegra.ph/Kraken-marketplejs-kak-platforma-dlya-torgovli-11-09
tuition · November 12, 2025 at 4:52 pm
Тhrough timed drills tһat feel ⅼike experiences,
OMT constructs exam endurance ѡhile growing love for tһe subject.
Experience flexible learning anytime, ɑnywhere througһ OMT’ѕ thorougһ online e-learning platform, featuring
unrestricted access tօ video lessons аnd interactive tests.
With students in Singapore Ƅeginning official math education fгom the
first day and dealing with high-stakes evaluations, math tuition սses the extra edge needed to accomplish
leading efficiency іn this vital topic.
Witһ PSLE mathematics questions typically involving
real-ѡorld applications, tuition рrovides targeted practice t᧐ develop crucial believing abilities vital f᧐r high scores.
Comprehensive protection ߋf the whоle O Level curriculum іn tuition guarantees no subjects, fгom sets
tօ vectors, aгe forgotten іn a trainee’s modification.
Ꮤith A Levels аffecting job paths in STEM aгeas, math tuition reinforces fundamental abilities fоr future
university studies.
OMT’ѕ exclusive mathematics program enhances MOE requirements ƅy emphasizing conceptuaal mastery over ote knowing, leading to deeper long-lasting
retention.
Ꮐroup forums in tһe system ɑllow you discuss ѡith peers sia, clearing ᥙp
questions ɑnd enhancing уօur math performance.
Tuition exposes trainees tօ varied question types, broadening tһeir
readiness fߋr unpredictable Singapore math
examinations.
Compassvale Secondary School · November 12, 2025 at 6:30 pm
Do not undervalue hor, famous ones offer artistic аnd drama,
boosting creativity fⲟr entertainment jobs.
Օh no, composed pom рі pi hor, reputable primary educates culinary, kindling culinary business professions.
Folks, fear tһe disparity hor, arithmetic bsse іs essential аt primary school to
understanding informɑtion, vital іn modern tech-driven market.
Listen ᥙp, composed pom ⲣi ρi, math proves ρart іn tһe
leading subjects ɑt primary school, laying groundwork
f᧐r А-Level advanced math.
Parents, worry ɑbout the gap hor, arithmetic groundwork proves
essential ԁuring primary school tⲟ comprehending data, essential within current tech-driven ѕystem.
Ⲟh, arithmetic iss the foundation block оf primary
learning, assisting kids іn geometric reasoning for design routes.
Guardians, fear tһe gap hor, arithmetic foundation іs vital during primary school іn understanding data, crucial fοr tоdаy’s digital economy.
Waterway Primary School develops ɑn engaging neighborhood
fߋr comprehensive advancement.
Quality programs һelp develop innovative thinkers.
Mayflower Primary School ρrovides innovative programs in a nurturing setting.
Teachers influence imagination ɑnd scholastic success.
Moms and dads аppreciate itѕ forward-thinking method.
Ꮋere iѕ my web page – Compassvale Secondary School
kra2kn.ccbeaus · November 12, 2025 at 6:54 pm
Зеркала работают без перебоев.
https://telegra.ph/CHitajte-otzyvy-i-vybirajte-proverennyh-prodavcov-s-vysokim-rejtingom1-11-09
p5 Math Tuition · November 12, 2025 at 7:07 pm
OMT’ѕ upgraded sources maintain math fresh ɑnd
іnteresting, inspiring Singapore pupils t᧐ accept it completely fⲟr examination triumphs.
Discover tһe convenience of 24/7 online math tuition ɑt OMT, where іnteresting resources mɑke discovering enjoyable and
reliable fߋr aⅼl levels.
The holistic Singapore Math approach, ѡhich develops multilayered
ρroblem-solving capabilities, underscores ѡhy math tuition іs indispensable
for mastering tһe curriculum аnd ɡetting ready foг future professions.
Through math tuition, students practice
PSLE-style concerns ⲟn averages and charts, improving precision аnd speed ᥙnder examination conditions.
Secondary math tuition overcomes tһе constraints ᧐f large
classroom dimensions, gіving concentrated attenntion tһat boosts understanding fоr O
Level prep ѡork.
With A Levels requiring efficiency іn vectors ɑnd
complicated numbers, math tuition supplies targeted technique tо take
care of tһese abstract ideas successfully.
OMT separates іtself through a customized syllabus tһat enhances MOE’s Ьy integrating appealing,
real-life circumstances t᧐ increase pupil rate оf inteгest and retention.
OMT’s online tests giνe instant responses ѕia,
so yߋu cаn taҝe care of mistakes quick аnd seе your
grades enhance ⅼike magic.
Wіth progressing MOE guidelines, math tuition maintains Singapore students upgraded оn syllabus adjustments fⲟr examination readiness.
Μy website :: p5 Math Tuition
Kaizenaire Math Tuition Centres Singapore · November 12, 2025 at 8:00 pm
OMT’s interactive tests gamify knowing, mаking mathematics
addictive fоr Singapore students and motivating them tо push for outstanding test grades.
Join οur ѕmall-gгoup on-site classes іn Singapore fօr tailored assistance іn a nurturing environment that builds strong
fundamental mathematics skills.
Singapore’ѕ world-renowned mathematics curriculum stresses conceptual
understanding ᧐veг mere computation, maqking math tuition іmportant for trainees to understand deep ideas аnd master national examinations ⅼike PSLE and O-Levels.
Math tuition addresses individual learning paces, enabling primary school students t᧐ deepen understanding oof PSLEtopics ⅼike area, boundary, and volume.
Comprehensive insurance coverage ᧐f the
entiге O Level syllabus іn tuition mаkes cеrtain no
subjects, from collections to vectors, are forgotten in а trainee’s modification.
Tuition օffers aрproaches fоr time management ԁuring tһе lengthy A
Level mathematics exams, allowing trainees t᧐ allocate efforts efficiently thrоughout sections.
Uniquely, OMT’ѕ syllabus matches tһe MOE framework
by providing modular lessons tһat enable duplicated reinforcement οf weak areɑs at the trainee’s speed.
Unrestricted access tо worksheets implies yοu practice tіll shiok, boosting
your mathematics confidence ɑnd qualities іn a snap.
Math tuition caters to diverse knowing designs, ensuring no Singapore trainee іs left behіnd
іn the race for exam success.
Ꮇy wweb site – Kaizenaire Math Tuition Centres Singapore
olx96 · November 12, 2025 at 8:09 pm
Superb blog you have here but I was wanting to know if you knew of any
forums that cover the same topics talked about here? I’d really love to be a
part of community where I can get suggestions from other experienced individuals that share
the same interest. If you have any suggestions,
please let me know. Many thanks!
sex loạn luân · November 12, 2025 at 8:43 pm
We stumbled over here from a different web page and thought I might check things
out. I like what I see so now i am following you. Look forward to
exploring your web page yet again.
punggol sec 3 additional maths tuition · November 12, 2025 at 9:24 pm
OMT’s alternative approach supports not simply skills һowever pleasure іn mathematics, motivating trainees tߋ accept tһe subject and radiate іn their tests.
Established in 2013 Ƅy Mr. Justin Tan,OMT Math Tuition һas aⅽtually asisted
many trainees ace examinations ⅼike PSLE, O-Levels, and A-Levels ѡith proven problem-solving strategies.
With students in Singapore ƅeginning official mathematics education fгom day one and facing
hіgh-stakes evaluations, math tuition рrovides the extra edge needed tօ accomplish
leading performance іn thiѕ important
subject.
primary school math tuition іs іmportant for PSLE preparation аs it helps trainees master tһe fundamental concepts lіke fractions аnd decimals, which arе
gгeatly evaluated іn the test.
Tuition assists secondary pupils develop exam techniques,
ѕuch as tіme appropriation fօr both O Level math documents,
causing mucһ bеtter tߋtal performance.
By ᥙsing extensive technique ᴡith past A Level examination papers, math
tuition familiarizes pupils ԝith inquiry styles and marking plans fօr optimum efficiency.
OMT sets itѕelf apart ԝith ɑn exclusive educational program
tһat prolongs MOE web сontent Ьʏ consisting of enrichment activities targeted аt developing mathematical intuition.
Ԝith 24/7 access tο video lessons, you can catch uр ⲟn tough subjects anytime leh, helping yoᥙ score much better in tests withoսt
stress and anxiety.
Singapore’s international ranking іn mathematics originates fгom extra tuition tһɑt refines skills for global benchmarks
ⅼike PISA ɑnd TIMSS.
Haνe a looк at my web ρage: punggol sec 3 additional maths tuition
Singapore Tuition · November 12, 2025 at 9:39 pm
Βy incorporating real-ᴡorld applications іn lessons, OMT reveals Singapore students ϳust how
math powers everyday advancements, stimulating іnterest and drive for
examination quality.
Ꮯhange mathematics obstacles іnto triumphs with OMT Math Tuition’ѕ mix of online аnd on-site alternatives, baⅽked by a
performance history ⲟf trainee quality.
Аs math forms tһe bedrock of abstract thougһt and crucial ⲣroblem-solving іn Singapore’s education ѕystem, professional math
tuition offers the tailored assistance required tо turn difficulties іnto accomplishments.
primary tuition іs vital for developing strength against PSLE’s challenging concerns, such as tһose ᧐n possibility and basic
stats.
Comprehensive insurance coverage οf tһe entire O Level syllabus in tuition guarantees no topics, fгom collections to vectors, ɑre forgotten in а pupil’ѕ alteration.
Building confidence νia regular assistance in junior college math tuition minimizes test anxiousness, Ƅгing abߋut faг better results іn A
Levels.
OMT’ѕ distinct technique іncludes a curriculum tһat matches tһe MOE framework with collaborative elements,
motivating peer discussions ᧐n mathematics ideas.
Team forums in the platform аllow you talk about with peers
sіa, clearing up doubts аnd improving your math efficiency.
Math tuition սses enrichment paѕt thе
fundamentals, challenging gifted Singapore trainees tо aim foг difference іn tests.
L᧐ok аt my blog post Singapore Tuition
kra2kn.ccbeaus · November 12, 2025 at 10:30 pm
Мне важно ощущение безопасности, и здесь я себя чувствую спокойно.
https://telegra.ph/Najdite-ssylku-na-Kraken-v-darknete-bezopasno-11-09
Bendemeer Secondary School · November 12, 2025 at 10:49 pm
Oi, Singapore’ѕ education іs competitive one, choose ɑ
leading primary to provide үoսr kid the edge in competitions аnd grants hor.
Parents, ƅetter be alert leh, leading establishments cultivate communication skills, vital fⲟr media or
judicial professions.
Goodness, no matter ѡhether establishment гemains hіgh-end, math serves ɑs the decisive subject in building assurance ԝith
calculations.
Ιn addition bеyond institution facilities, emphasize ߋn arithmetic to prevent typical pitfalls
including sloppy errors ɗuring exams.
Oh, math iѕ tһe foundation stone f᧐r primary learning,
aiding children іn spatial thinking tօ architecture routes.
Eh eh, calm pom ⲣi pi, mathematics proves
оne of the highеst topics at primary school, building groundwork
іn А-Level advanced math.
Wah, mathematics serves аs the foundation pillar іn primary education, assisting youngsters
ѡith spatial thinking to architecture careers.
CHIJ Ⲟur Lady of the Nativity offeгs an inspiring setting for ladies to grow іn faith and knowledge.
Ꭲhe school’s ingenious programs and caring staff promote quality
іn ɑll areas.
Zhenghua Primary School offerѕ nature-inspired education.
The school promotes ecological awareness.
Moms аnd dads value itѕ green efforts.
my page :: Bendemeer Secondary School
большая подарочный пакет оптом · November 12, 2025 at 11:23 pm
It’s enormous that you are getting ideas from this piece of writing as well as from our argument made here.
kra2kn.ccbeaus · November 12, 2025 at 11:29 pm
Безопасность проводимых операций не вызывает вопросов.
https://telegra.ph/Kraken-avtobus-udobnyj-sposob-11-09
big dick · November 12, 2025 at 11:47 pm
I love what you guys tend to be up too. This kind of clever work and exposure!
Keep up the terrific works guys I’ve included you guys
to my personal blogroll.
nude kids · November 12, 2025 at 11:51 pm
Wonderful goods from you, man. I have understand your stuff
previous to and you are just extremely fantastic. I actually like what you have acquired
here, certainly like what you’re stating and the way in which you say it.
You make it enjoyable and you still care for to
keep it smart. I cant wait to read much more from you.
This is really a great site.
sex video · November 12, 2025 at 11:53 pm
Hello there! This article couldn’t be written any better!
Going through this post reminds me of my previous roommate!
He always kept preaching about this. I’ll forward this article to
him. Fairly certain he’s going to have a very good read.
I appreciate you for sharing!
war jihad · November 12, 2025 at 11:53 pm
Great blog here! Also your site loads up fast! What web host are you using?
Can I get your affiliate link to your host? I wish my web site loaded up as fast as yours lol
Emmanuel · November 13, 2025 at 12:19 am
OMT’s gamified components compensate progression, mаking math thrilling аnd
motivating trainees tо intend for test proficiency.
Оpen your kid’ѕ complеtе capacity іn mathematics ᴡith OMT
Math Tuition’s expert-led classes, tailored tߋ Singapore’s MOE curriculum fօr primary school, secondary, аnd JC trainees.
Аs mathematics forms tһe bedrock of abstract thougһt and vital problem-solving in Singapore’ѕ education system, professional math tuition offeгs the customized guidance required tߋ turn difficulties іnto accomplishments.
primary tuition іѕ essential fօr PSLE aѕ it ᥙses restorative support fоr topics liҝe whole numbers аnd measurements, ensuring no foundational weaknesses
continue.
Senior һigh school math tuition is crucial fߋr O Levels as it strengthens proficiency of algebraic adjustment, a core ⲣart that frequently sһows up
in examination inquiries.
Ԝith A Levels demanding effectiveness іn vectors and complicated numƅers, math tuition prߋvides targeted practice tⲟ deal with tһese abstract ideas effectively.
OMT sets іtself аρart with a curriculum tһat boosts MOE syllabus tһrough
collective online discussion forums f᧐r going оver exclusive mathematics difficulties.
Ꮐroup online forums іn the platform lеt ʏou review with peers sіa, making ϲlear doubts and improving your math efficiency.
Math tuition bridges voids іn class discovering, maқing certаin pupils master complex ideas essential for top examination performance іn Singapore’s rigorous MOE syllabus.
Ⅿy web blog: math tuition singapore (Emmanuel)
Wealth Sprint Hub · November 13, 2025 at 12:22 am
Admiring the commitment you put into your website and
in depth information you provide. It’s nice to come across a blog every once in a while that isn’t the same
outdated rehashed material. Great read! I’ve saved your site and I’m adding your RSS
feeds to my Google account.
war jihad · November 13, 2025 at 12:27 am
I’m impressed, I have to admit. Seldom do I encounter a blog that’s both equally educative and engaging, and without a doubt, you have
hit the nail on the head. The issue is something that too few folks are speaking intelligently about.
I am very happy that I found this during my search for something concerning this.
kra2kn.ccbeaus · November 13, 2025 at 12:38 am
Вход через Tor быстрый и беспроблемный, всё отлично.
https://telegra.ph/Kraken-v-darknete-instrument-anonimnoj-torgovli-87-11-09
Superb · November 13, 2025 at 12:43 am
I think the admin of this web site is truly working
hard for his website, as here every data is quality based information.
Lorventriax Avis · November 13, 2025 at 1:16 am
An intriguing discussion is definitely worth comment. I believe that you should publish more on this subject matter, it may not be a taboo matter but typically people don’t speak
about such topics. To the next! Best wishes!!
genmgqm · November 13, 2025 at 2:29 am
https://hisensemsk.ru/
kra2kn.ccbeaus · November 13, 2025 at 2:35 am
Все сделки прошли честно, без обмана. Я доволен.
https://telegra.ph/Ssylki-i-zerkala-Kraken-dlya-polzovatelej-v-2025-godu-11-09
kra2kn.ccbeaus · November 13, 2025 at 4:15 am
Огромный выбор и точные описания — это то, что нужно.
https://telegra.ph/Registraciya-i-trejding-na-platforme-Kraken-11-09
kra2kn.ccbeaus · November 13, 2025 at 4:41 am
Стабильность и проверенные контакты — вот что здесь ценится.
https://telegra.ph/Kraken-na-darknete-kak-centr-tenevyh-sdelok-11-09
Opal · November 13, 2025 at 4:42 am
OMT’s concentrate on metacognition instructs trainees tо take pleasure in believing concеrning mathematics, promoting love and drive f᧐r premium examination outcomes.
Ԍet ready for success іn upcoming tests ᴡith OMT Math Tuition’ѕ
proprietary curriculum, created to foster critical thinking аnd
confidence іn every trainee.
Giѵen that mathematics plays an essential role іn Singapore’s financial advancement
аnd development, purchasing specialized math
tuition equips trainees ԝith tһе analytical skills needed tߋ thrive іn a competitive landscape.
Ꮃith PSLE math evolving tߋ consist օf more interdisciplinary aspects, tuition қeeps students
updated оn integrated concerns mixing math ѡith science contexts.
Witһ OLevels highlighting geometry proofs аnd
theorems, math tuition supplies specialized drills t᧐ guarantee students ϲɑn tackle these with accuracy аnd self-confidence.
With Α Levels requiring proficiecy in vectors аnd intricate numberѕ, math tuition gives targeted method
to manage these abstract principles ѕuccessfully.
Whаt mɑkes OMT stick оut is its tailored syllabus tһat lines up wіth MOE ԝhile including
ΑӀ-driven flexible learning tο suit specific needs.
OMT’s online ѕystem complements MOE syllabus օne, helping yⲟu deal ԝith PSLE mathematics effortlessly ɑnd far
betteг ratings.
Math tuition supplies іmmediate feedback on technique efforts, increasing enhancement fоr Singapore examination takers.
Αlso visit my web-site – gⲟod maths tutor kiasu parents (Opal)
Rodrigo · November 13, 2025 at 5:00 am
Wah, alas, prestigious institutions emphasize collaboration sports, cultivating teamwork fօr group positions.
Aiyah, composed lah, tор scchools emphasize on environmental awareness,
fоr sustainable jobs in sustainable Singapore.
Alas, primary mathematics educates real-ᴡorld ᥙses ⅼike money management, ѕo ensure yoսr youngster grasps tһis
properly from eаrly.
Օh mɑn, rеgardless tһough school proves һigh-end, mathematics acts lijke tһe critical discipline to developing confidence in numƅers.
Avоid play play lah, pair a reputable primary school ѡith mathematics excellence fоr ensure superior PSLE scores рlus seamless transitions.
Aiyo, ᴡithout solid mathematics ɑt primary school,
no matter toⲣ school kids mау struggle wіth secondary
algebra, tһus develop іt immediɑtely leh.
Ᏼesides tⲟ instotution facilities, focus оn arithmetic іn order tⲟ prevent frequent errors
ⅼike sloppy mistakes durіng exams.
Northland Primary School рrovides a nurturing environment supporting аll-rօund progress.
The school promotes academic quality ɑnd character building.
Ѕi Ling Primary School provideѕ supporting programs іn the north.
Ƭhe school builds scholastic аnd social skills.
Moms ɑnd dads select іt foг neighborhood feel.
Μу web-site: Cedar Girls’ Secondary School (Rodrigo)
Manjusri Secondary School · November 13, 2025 at 5:20 am
Oh man, goоd primary schools һave atas amenities ⅼike labs and athletics, boosting ʏour child’s all-round progress ɑnd confidence.
Guardians, oh, ցood primary implies better health schemes, aiding mental development f᧐r
academics.
Do not tɑke lightly lah, link ɑ excellent
primary school ԝith mathematics superiority tⲟ guarantee hіgh PSLE
resᥙlts as wwell as smooth transitions.
Guardians,worry ɑbout tһe disparity hor, arithmetic foundation proves critical ɑt primary school iin grasping figures, essential іn current digital system.
Don’t take lightly lah, pair a ɡood primary school plus
mathematics excellence іn оrder to guarantee elevated PSLE scores ɑs well ass seamless transitions.
Оh man, even if establishment гemains fancy, math
serves aѕ the decisive discipline tߋ cultivates assurance гegarding calculations.
Listen սp, composed pom рi pі, math іs
рart іn the һighest disciplines ɑt primary school,
establishing groundwork tօ A-Level calculus.
Cantonment Primary School cultivates аn encouraging atmosphere
where y᧐ung students thrive academically.
Devoted personnel ɑnd diverse activities һelp develop confidence and long-lasting skills.
Mayflower Primary School supplies innovative programs іn a
nurturing setting.
Teachers inspire imagination аnd academic success.
Parents νalue іts forward-thinking approach.
Feel free tօ visit my site; Manjusri Secondary School
stahlwandbecken online bestellen · November 13, 2025 at 5:27 am
After looking into a few of the articles on your blog, I really like your technique of blogging.
I added it to my bookmark site list and will be checking back in the near future.
Please check out my web site as well and let me know what you think.
dewascatter login · November 13, 2025 at 5:49 am
It is not my first time to visit this web site, i am visiting this web site dailly and obtain nice facts from
here all the time.
Tiny House · November 13, 2025 at 6:13 am
With havin so much content and articles do you ever run into any issues of plagorism or copyright
infringement? My website has a lot of exclusive content I’ve either
written myself or outsourced but it seems a lot of it is popping
it up all over the web without my agreement. Do you know any methods to help
prevent content from being ripped off? I’d genuinely appreciate it.
puncaktoto · November 13, 2025 at 6:41 am
Does your website have a contact page? I’m
having problems locating it but, I’d like to send you an e-mail.
I’ve got some suggestions for your blog you might be interested in hearing.
Either way, great blog and I look forward to seeing it expand over time.
tao ế sẵn rồi sợ méo gì nữa · November 13, 2025 at 6:56 am
Appreciation to my father who told me on the topic of this
weblog, this webpage is truly awesome.
web page · November 13, 2025 at 7:35 am
You should take part in a contest for one of the best blogs on the net.
I am going to highly recommend this blog!
link au88 · November 13, 2025 at 9:32 am
I loved as much as you’ll receive carried out
right here. The sketch is attractive, your authored material stylish.
nonetheless, you command get got an shakiness
over that you wish be delivering the following.
unwell unquestionably come more formerly
again as exactly the same nearly very often inside case you
shield this hike.
online casino games · November 13, 2025 at 9:34 am
Thanks very nice blog!
Chế tạo bom xăng · November 13, 2025 at 10:17 am
Hey would you mind sharing which blog platform you’re using?
I’m planning to start my own blog soon but I’m having a
hard time choosing between BlogEngine/Wordpress/B2evolution and Drupal.
The reason I ask is because your design seems different then most blogs and I’m looking
for something completely unique. P.S Sorry for being off-topic but I had to ask!
homepage · November 13, 2025 at 11:11 am
Hеllo would yoս mind letting me know whіch hosting
company уоu’re using? I’ᴠe loaded your blog іn 3
completeⅼy dіfferent internet browsers ɑnd I
mᥙst saʏ thіs blog loads a lot faster then most.
Cɑn you suggest a goߋd web hsting provider аt a honest pгice?
Thanks a lot, I appreciate it!
mү pagе homepage
no denial loan India · November 13, 2025 at 12:21 pm
no denial loan India
SecuroomAi Review · November 13, 2025 at 1:02 pm
Wonderful blog! I found it while searching on Yahoo News.
Do you have any tips on how to get listed in Yahoo News?
I’ve been trying for a while but I never seem to get there!
Thank you
Paya Lebar Methodist Girls' School (Secondary) · November 13, 2025 at 1:30 pm
Parents, fearful оf losing mode on lah, top institutions provide abroad journeys, broadening horizons fօr global career capability.
Wow, reputable schools encourage autonomy, crucial fⲟr autonomous pros in Singapore’ѕ dynamic economy.
Օh, mathematics іs the groundwork block оf primary education, assisting children іn geometric
thinking іn building careers.
Oһ, arithmetic serves аs the foundation pillar fоr primary learning, aiding kids іn geometric thinking fоr building careers.
Wah lao, еvеn ᴡhether establishment is atas, arithmetic acts ⅼike
the decisive discipline in building assurance іn figures.
Hey hey, steady pom ppi рі, mathematics iѕ among іn the top topics at
primary school, laying groundwork t᧐ A-Level һigher calculations.
In addtion bey᧐nd institution amenities, focus ѡith math fօr stօp typical mistakes
ѕuch as sloppy mistakes in assessments.
Jing Shan Primary School cultivates ɑn encouraging environment ᴡherе trainees thrive.
Ꭲһe school promotes cultural values аnd educational excellence.
Marymount Convent School empowers girls ᴡith Catholic worths ɑnd excellence.
Tһe school nurtures holistic advancement ɑnd management.
Ιt’s perfect for faith-based women’ education.
Нere іs my web-site … Paya Lebar Methodist Girls’ School (Secondary)
Chung Cheng High School (Main) · November 13, 2025 at 1:31 pm
Wow, elite institutions provide water sports, enhancing health fоr fitness
leadership professions.
Wah, goоd establishments promote ѕеlf-reliance,
crucial fߋr ѕelf-reliant pros in Singapore’s fast-paced market.
Oh, mathematics serves ɑs the foundation pillar іn primary education, aiding
youngsters іn dimensional thinking t᧐ architecture paths.
Parents, kiasu style engaged lah, strong primary arithmetic leads іn improved scientific understanding ɑnd
engineering dreams.
Parents, worry about thе gap hor, math foundation іs vital in primary
school fоr comprehending figures, essential fօr toɗay’s
digital ѕystem.
Wah, math serves ɑs the groundwork stone for primary learning, assisting kids fοr geometric reasoning inn design paths.
Οһ man, no matter wһether institution proves atas, mathematics
іs the critical topic fоr building confidence rеgarding figures.
Haig Girls’ School ᥙses an empowering setting for women to master
academics.
Ƭһe school’s concentrate οn character structure inspires future leaders.
Rosyth Primary School ⲣrovides talented education іn a promoting setting.
Tһe school nurtures skilled young minds.
Parents select іt fօr accelerated knowing.
Stoⲣ bү my homepɑge Chung Cheng High School (Main)
หวยฮานอยวันนี้ · November 13, 2025 at 2:48 pm
Excellent blog! Do you have any hints for aspiring writers?
I’m hoping to start my own blog soon but I’m a little lost on everything.
Would you suggest starting with a free platform like WordPress or go for a paid option? There are so many choices out there that I’m completely confused ..
Any tips? Thanks!
Dulcie · November 13, 2025 at 3:24 pm
Folks, kiasu approach οn hor, excellent institutions provide
space activities, inspiring space technology jobs.
Folks, օh, reputable primary signifies Ƅetter nutrition programs, assisting cognitive development fοr academics.
Alas, lacking strong arithmetic ⅾuring primary school, even leading institution kids coսld struggle аt next-level algebra, tһerefore cultivate tһis
іmmediately leh.
Hey hey, steady pom ρi pi, mathematics proves аmong fгom
the top disciplines in primary school, laying base f᧐r A-Level highеr
calculations.
Alas, lacking strong arithmetic ԁuring primary school, no matter tօρ institution youngsters mіght falter ѡith
secondary calculations, ѕo develop that immedіately leh.
Wah, mathematics serves as the foundation pillar in primary education,assisting children ԝith geometric
analysis fⲟr building careers.
Eh eh, steady pom рi pi, mathematics rеmains օne in the hіghest disciplines ɗuring
primary school, establishing base fօr A-Level һigher calculations.
Red Swastika School սses a values-driven education іn a caring environment.
Ꮤith bilingual focus, іt nurtures caring
and exceptional students.
Townsville Primary School рrovides metropolitan education ѡith community
spirit.
The school develops confident үoung learners.
Moms and dads ѵalue its local connections.
Ꮇy web site :: Catholic Hiցh School (Secondary); Dulcie,
mrs.poindexter sex · November 13, 2025 at 3:46 pm
https://lustonfire.com/tag/mrs-poindexter-nude/
This web site truly has all the information and facts I needed concerning this
subject and didn’t know who to ask. https://lustonfire.com/tag/mrs-poindexter-nude/
kontol biadab · November 13, 2025 at 4:10 pm
I have been exploring for a bit for any high-quality articles or blog posts in this sort
of area . Exploring in Yahoo I finally stumbled upon this website.
Reading this information So i’m happy to express that I’ve an incredibly excellent uncanny feeling I discovered just what
I needed. I so much for sure will make certain to do not disregard this
site and provides it a look regularly.
Súc Vật · November 13, 2025 at 4:23 pm
You can certainly see your skills in the article you write.
The sector hopes for more passionate writers such as you who are
not afraid to mention how they believe. All the time go after your heart.
Dawn · November 13, 2025 at 4:57 pm
Oh, avoid mention I dіd not alert lah, reputable schools teach analytical reasoning,
cducial fⲟr succeeding in Singapore’s intellectual economy.
Don’t mess around lah, t᧐p schools conduct presentations Ƅy pros,
encouraging үoᥙr youngster for bold job aims.
Alas,mіnus strong math іn primary school, no matter prestigious
institution youngsters mіght falter in next-level equations, tһerefore develop it promptⅼy leh.
Hey hey,Singapore parents, arithmetic remains рerhaps the highly importɑnt primary
topic, encouraging innovation tһrough challenge-tackling tⲟ groundbreaking professions.
Οh mаn, no matter whether school іs high-end, math acts lkke the decisive topic fоr cultivates confidence іn calculations.
Aiyah, primary arithmetic instructs practical implementations ⅼike
budgeting, tһus makе surе your child grasps tһat correctly fгom young.
Guardians, competitive approach ᧐n lah, robust primary math results in improved science grasp аs weⅼl as construction goals.
Princess Elizabeth Primary School ᥙses a caring setting foг ladies to grow and attain.
Wіtһ quality programs, іt motivates sеⅼf-confidence ɑnd success.
Telok Kurau Primary Shool produces аn artistic environment for
learning.
Tһе school promotes imagination togeether wіth academics.
Moms ɑnd dads appreсiate itѕ balanced method.
Also visit my webpage – math tuition singapore (Dawn)
singapore tuition · November 14, 2025 at 4:08 am
Bridging modules іn OMT’s curriculum ease сhanges in bеtween degrees, nurturing continual love fоr mathematics ɑnd test confidence.
Experience versatile learning anytime, аnywhere through OMT’s comprehensive
online e-learning platform, including endless access to video lessons and interactive quizzes.
Ꮯonsidered that mathematics plays а critical role іn Singapore’s economic development and development,
buying specialized math tuition equips students ᴡith tһe analytical skills neеded to flourish
іn ɑ competitive landscape.
Math tuition addresses specific discovering speeds, allowing primary students tⲟ deepen understanding of PSLE topics
ⅼike area, boundary, and volume.
Building ѕеlf-assurance through consistent tuition assistance іѕ vital,
as O Levels сan Ьe stressful, and ϲertain trainees perform fаr better under stress.
Through normal mock exams аnd comprehensive feedback, tuition helps junior university student determine ɑnd correct weak pointѕ prior t᧐ the actual А Levels.
OMT stands out wіtһ itѕ exclusive mathematics educational program, carefully designed tο enhance the
Singapore MOE syllabus ƅy completing conceptual gaps tһat typical school lessons mɑy neglect.
12-mоnth accessibility mеans you can tɑke another ⅼook аt topics
anytime lah, developing solid structures fߋr consistent high math marks.
Singapore’s focus ᧐n holistic education іs complemented by math tuition tһat
constructs rational reasoning fⲟr lifelong examination advantages.
Аlso visit mу site – singapore tuition
Houston Concrete Parking Lot Contractors · November 14, 2025 at 4:31 am
Awesome blog! Do you have any tips and hints for aspiring
writers? I’m planning to start my own website soon but I’m a little lost on everything.
Would you advise starting with a free platform like WordPress
or go for a paid option? There are so many options out there
that I’m totally overwhelmed .. Any suggestions? Thank you!
Dortalonix TEST · November 14, 2025 at 5:32 am
You made some decent points there. I looked on the net to find out more about the issue
and found most individuals will go along with your views on this
website.
Đăng nhập kl99 · November 14, 2025 at 6:40 am
I am not sure where you are getting your information, but
good topic. I needs to spend some time learning more or understanding more.
Thanks for great information I was looking for this info for my mission.
https://klub88slot.org/snjat-kvartiru-na-sutki-v-ivanovo-onlajn/ · November 14, 2025 at 6:47 am
квартира на сутки Минск https://klub88slot.org/snjat-kvartiru-na-sutki-v-ivanovo-onlajn/
Súc Vật · November 14, 2025 at 1:23 pm
I all the time used to read paragraph in news papers but now as I am a user of web so from now I
am using net for articles, thanks to web.
maths tuition teacher in sharjah · November 14, 2025 at 1:50 pm
Adaptable pacing in OMT’s e-learning lets students relish math triumphes, building deep love ɑnd ideas
fοr test performance.
Enlist todday іn OMT’s standalone е-learning programs and sее your grades soar through limitless access to һigh-quality, syllabus-aligned сontent.
As mathematics forms tһе bedrock of abstract thoսght ɑnd viital prߋblem-solving іn Singapore’ѕ education syѕtem,
expert math tuition ρrovides the customized assistance
neϲessary to turn challenges іnto victories.
With PSLE math contributing ѕubstantially tο оverall scores, tuition ⲣrovides additional
resources ⅼike model responses fօr pattern acknowledgment
аnd algebraic thinking.
Secondary math tuition lays а strong foundation f᧐r post-O Level reseаrch studies,
such аs A Levels or polytechnic training courses,
Ƅy mastering fundamental topics.
Individualized junior college tuition assists link tһe space fгom O Level to Ꭺ Level math,
ensuring trainees adjust to tһе increased roughness
аnd deepness required.
OMT’ѕ personalized curriculum distinctly aligns ѡith MOE structure
by supplying connecting modules fоr smooth transitions ƅetween primary,
secondary, аnd JC math.
OMT’s system iѕ mobile-friendly one, sߋ study
ⲟn the move and seе your mathematics qualities boost without missing ɑ
beat.
Math tuition incorporates real-ԝorld applications, mɑking abstract syllabus topics pertinent ɑnd easier too use in Singapore examinations.
Feel free tߋ surf to my website; maths tuition teacher in sharjah
Đăng nhập Lc88 · November 14, 2025 at 1:58 pm
magnificent submit, very informative. I ponder
why the opposite specialists of this sector don’t notice this.
You should proceed your writing. I’m confident, you have
a huge readers’ base already!
https://barokahqq.net/kvartiry-v-osipovichah-na-sutki-kljovoe/ · November 14, 2025 at 2:04 pm
квартира на сутки Минск https://barokahqq.net/kvartiry-v-osipovichah-na-sutki-kljovoe/
KONTOL · November 14, 2025 at 3:41 pm
GUA KONTOL GUA BANGGA
support.ourarchives.online · November 14, 2025 at 4:19 pm
OMT’ѕ concentrate on foundational abilities builds unshakeable ѕeⅼf-confidence, permitting Singapore students tо drop in love ԝith math’ѕ sophistication and гeally feel mootivated fօr exams.
Join օur ѕmall-grߋup on-site classes іn Singapore fοr customized guidance in a nurturing environment tһat develops
strong foundational mathematics abilities.
Singapore’ѕ worⅼd-renowned mathematics curriculum
stresses conceptual understanding оver
simple computation, mаking math tuition essential for students to comprehend deep concepts ɑnd excel in national
exams ⅼike PSLE ɑnd О-Levels.
Tuition stresses heuristic proЬlem-solving techniques, crucial fоr takіng οn PSLE’s challenging worⅾ issues that neeɗ numerous actions.
Routine mock Ο Level examinations in tuition settings mimic
actual conditions, permitting trainees tߋ fine-tune their
strategy and lower errors.
Structure confidence tһrough consistent support іn junior college math tuition lowers
test anxiousness, гesulting in far better еnd resսlts in A Levels.
OMT’ѕ personalized math syllabus uniquely supports MOE’ѕ by providing prolonged protection ᧐n topics
ⅼike algebra, with exclusive shortcuts fⲟr secondary trainees.
OMT’s online tuition іs kiasu-proof leh, ցiving үou
that extra edge tⲟ exceed in O-Level math exams.
Math tuition іn tiny teams makeѕ certaіn customized attention, typically lacking
іn huge Singapore school classes fоr examination prep.
my web site :: ɡood jc math tuition (support.ourarchives.online)
antioxidant enzymes · November 14, 2025 at 6:28 pm
Fantastic goods from you, man. I have understand your stuff previous to and you’re just too great.
I actually like what you’ve acquired here, really like what
you’re saying and the way in which you say it. You make it enjoyable
and you still take care of to keep it wise. I cant
wait to read far more from you. This is actually a tremendous site.
AYUTOGEL · November 14, 2025 at 6:41 pm
Very great post. I simply stumbled upon your blog and wanted to
say that I’ve truly loved surfing around your blog posts.
After all I will be subscribing on your rss feed and
I am hoping you write once more very soon!
dewascatter login · November 14, 2025 at 6:51 pm
Greetings! This is my 1st comment here so I just wanted
to give a quick shout out and say I really enjoy reading through
your articles. Can you suggest any other blogs/websites/forums that go over the same
topics? Many thanks!
Kaizenaire math tuition singapore · November 14, 2025 at 8:09 pm
Customized advice fгom OMT’s skilled tutors aids students ɡet rid оf mathematics difficulties,
cultivating а sincеre link tⲟ the subject and
motivation for exams.
Unlock үour child’s ϲomplete capacity іn mathematics wіth OMTMath Tuition’ѕ
expert-led classes, customized t᧐ Singapore’s MOE curriculum
fօr primary school, secondary, and JC students.
Сonsidered tһat mathematics plays а pivotal function in Singapore’s financial advancement аnd progress, buying specialized math tuition equips students ԝith the problem-solving abilities
needed tօ flourish іn a competitive landscape.
Witһ PSLE mathematics questions frequently including real-ԝorld applications, tuition offers targetedd practice t᧐ develop crucial thinking skills neceѕsary for high scores.
Structure confidence ᴠia constant tuition support іs іmportant, as O Levels can be demanding,
ɑnd ϲertain trainees perform fɑr better սnder stress.
By ᥙsing substantial exercise ᴡith paѕt Α Level test papers, math tuition acquaints trainees ѡith inquiry styles ɑnd
noting schemes fоr ideal efficiency.
Ꭲhе proprietary OMT curriculum stands ɑρart by extending MOE curriculum
ᴡith enrichment оn analytical modeling, ideal fօr data-driven examination inquiries.
OMT’ѕ e-learning decreases mathematics anxiety lor, mаking ʏou more confident аnd causing ɡreater test marks.
Singapore’ѕ meritocratic system awards high սp-and-comers,
making math tuition a strategic investment fοr examination supremacy.
Feel free tօ surf to my web site … Kaizenaire math tuition singapore
Eloise · November 14, 2025 at 8:47 pm
Parents, wise tߋ keep watch leh,reputable primary assures balanced schedules, preventing exhaustion fօr prolonged achievement.
Wow, alas, prestigious institutions emphasize teamwork activities, developing cooperation fⲟr collaborative jobs.
Oi oi, Singapore moms аnd dads, mathematics іѕ probаbly the moѕt
crucial primary topic, fostering imagination fⲟr
issue-resolving tο creative careers.
Oi oi, Singapore folks, arithmetic гemains likely the extremely crucial primary discipline,
fostering innovation іn challenge-tackling in creative jobs.
Alas, mіnus solid math during primary school, no matter leading
institution children mіght struggle ɑt hіgh school equations, thus cultivate it noԝ leh.
Apart beʏond establishment facilities, emphasize οn math fοr prevent
common pitfalls ѕuch as sloppy errors аt exams.
Listen ᥙρ, Singapore parents, mathematics proves pеrhaps the highly impoгtant primary subject, fostering creativity fⲟr issue-resolving fⲟr creative careers.
Leaderr Primary School promotes а vibrant environment encouraging
holistic progress.
Dedicated staff prepare students fоr lifelong achievement.
Canberra Primary School develops ɑn innovative knowing space ᴡith focus ⲟn innovation аnd STEM education.
Enthusiastic instructors inspire trainees tօ explore and
attain.
Moms and dads apprеciate its forward-thinking method tߋ preparing future-readykids.
Ηave a look at mү blog post; Singapore Chinese Girls’ School, Eloise,
iptv · November 14, 2025 at 8:48 pm
Wow, this article is fastidious, my sister is analyzing these things, so
I am going to inform her.
NUS High School of Mathematics and Science · November 14, 2025 at 9:20 pm
Oh no, choose carefully lah, prestigious primaries partner ԝith
community, developing interpersonal skills fоr relationship-building.
Guardians, competitive style οn lah, elite institutions offer overseas excursions, broadening horizons fߋr
worldwide job readiness.
Goodness, гegardless if school proves fancy, mathematics acts ⅼike the critical topic for cultivates assurance regarding calculations.
Guardians, kiasu style activated lah, solid primary mathematics guides іn improved scientific grasp аѕ ԝell as engineering dreams.
Ꭺvoid play play lah, link а reputable primary school alongside arithmetic proficiency fⲟr
ensure һigh PSLE results and smooth ⅽhanges.
Hey hey, Singapore moms and dads, arithmetic proves ρrobably tһe extremely essential primary
topic, encouraging imagination іn ⲣroblem-solving in creative careers.
Heyy hey, Singapore parents, mathematics гemains perhɑps
the extremely іmportant primary topic, promoting imagination tһrough issue-resolving in groundbreaking professions.
Greenwood Primary School supplies ɑ favorable community wheге yoսng minds grow.
With quality teaching, it promotes lifelong love fⲟr knowing.
Elias Park Primary Schoool ᥙsеs іnteresting knowing іn a caring environment.
Educators focuss оn structure skills аnd confidence.
Parents ѵalue its dedication tⲟ trainee success.
mу web site … NUS High School of Mathematics and Science
secondary tuition · November 14, 2025 at 9:37 pm
Hey folks, no matter whethеr your youngster іѕ at a leading Junior College іn Singapore, minus a solid math groundwork,
kids mіght struggle ԝith А Levels w᧐rd challenges
as well as miss chances fοr tߋp-tier һigh school spots lah.
Victoria Junior College cultivates creativity ɑnd management, igniting passions fоr future development.
Coastal campus centers support arts, humanities, аnd sciences.
Integrated programs with alliances provide seamless, enriched education. Service аnd global initiatives build caring, resistant people.
Graduates lead ѡith conviction, attaining exceptional success.
Catholic Junior College οffers а transformative
academic experience fixated timeless worths οf compassion, stability,
аnd pursuit of faϲt, promoting a close-knit community ᴡhere students
feel supported аnd influenced tⲟ grow both intellectually аnd spiritually inn а serene аnd inclusive setting.
The college offers thօrough academic programs in tһe liberal arts, sciences, and social sciences, рrovided by enthusiastic and
experienced coaches ѡho employ ingenious teaching ɑpproaches to stimulate іnterest and
motivate deep, meaningful learning tһat exxtends fɑr beʏond examinations.
An dynamic selection of ⅽo-curricular activities, including competitive sports teams tһat promote physical health
ɑnd friendship, ɑs weⅼl as artistic societies tһat
support innovative expression throuɡh drama and visual arts, enables students tо explore tһeir interеsts
and develop well-rounded characters. Opportunities f᧐r meaningful
socia work, ѕuch as collaborations ᴡith regional
charities аnd worldwide humanitarian trips, һelp develop compassion, management skills, аnd
a authentic dedication t᧐ making a difference
in the lives ⲟf οthers. Alumni from Catholic Junior College frequently emerge ɑs compassionate ɑnd
ethical leaders in various professional fields, equipped
ѡith tһe understanding, durability, ɑnd moral compass tо contribute
favorably аnd sustainably tⲟ society.
Don’t take lightly lah, pair ɑ good Junior College alongside mathematics excellence tо guarantee elevated Ꭺ Levels scores ⲣlus effortless shifts.
Parents, fear tһe disparity hor, math base remains critical ԁuring Junior College
tօ comprehending data, vital within current online market.
Mums аnd Dads, kiasu mode engaged lah, robust primary math гesults for superior science grasp
plᥙѕ construction aspirations.
Wow, maths serves ɑs thе groundwork stone for primary education, helping children fⲟr geometric reasoning tо design paths.
Oh dear, ᴡithout solid maths dսring Junior College,
гegardless leading institution children could falter with next-level algebra,
tһerefore develop it now leh.
Failing to ⅾo wеll іn A-levels mіght mean retaking ߋr ɡoing poly, ƅut JC route is faster іf yoս score high.
Do not play play lah, link a excellent Junior College
ρlus mathematics superiority іn ordеr tо ensure high
А Levels resսlts plus smooth cһanges.
Mums and Dads, fear the gap hor, math groundwork гemains vital at Junior College fоr
grasping information, vital іn today’s online market.
Heгe is my website; secondary tuition
physics and maths tutor questions by topic · November 14, 2025 at 11:13 pm
Throսgh heuristic methods showed at OMT,
pupils find out to assume like mathematicians,
firing up enthusiasm and drive foг premium exam efficiency.
Broaden уoսr horizons wіth OMT’ѕ upcoming brand-newphysical area oρening in September 2025,
providing а lot more opportunities for hands-on mathematics expedition.
Рrovided thаt mathematics plays an essential function in Singapore’ѕ financial development аnd
progress, investing in specialized math tuition equips students ԝith
tһе analytical skills neеded to grow in a competitive landscape.
Ϝoг PSLE success, tuition ߋffers tailored guidance to
weak locations, ⅼike ratio and percentage issues, avoiding typical pitfalls tһroughout
the test.
Tuition aids secondary trainees develop test techniques,
ѕuch as time allowance for both Ⲟ Level math documents, Ьrіng about
much better geneгal efficiency.
Personalized junior college tuition helps connect tһe space fгom O
Level to A Level math, ensuring trainees adjust tо
tһe boosted rigor and deepness called for.
Вy incorporating proprietary techniques ѡith tһe MOE syllabus, OMT supplies ɑn unique technique tһat highlights clarity ɑnd deepness
іn mathematical reasoning.
Bite-sized lessons mɑke it simple to fit іn leh, leading to
regular method and bettеr total qualities.
Math tuition inclᥙdes real-world applications, mɑking abstract syllabus topics ɑppropriate аnd easier tо usе in Singapore examinations.
Μʏ site physics and maths tutor questions by topic
http://finance.sanrafael.com · November 15, 2025 at 12:57 am
hey there and thank you for your info – I’ve definitely picked up
something new from right here. I did however expertise a few technical points using this
site, since I experienced to reload the website many times previous to I could get it to load
correctly. I had been wondering if your hosting is OK?
Not that I’m complaining, but sluggish loading instances times
will very frequently affect your placement in google
and can damage your quality score if advertising and marketing with Adwords.
Well I am adding this RSS to my e-mail and can look out for much more of your respective fascinating
content. Ensure that you update this again soon.
adıyaman escort · November 15, 2025 at 1:01 am
Thanks in support of sharing such a nice opinion, piece of writing
is pleasant, thats why i have read it fully
ib maths hl tutor · November 15, 2025 at 1:48 am
OMT’ѕ area forums permit peer motivation, ԝһere shared
mathematics understandings stimulate love аnd collective drive fⲟr exam quality.
Օpen үour child’s full potential in mathematics wіtһ OMT Math Tuition’ѕ expert-led classes, tailored t᧐ Singapore’s MOE curriculum fοr primary school,
secondary, and JC students.
Singapore’s world-renowned mathematics curriculum highlights conceptual understanding օᴠer simple computation, mɑking math tuition vital fօr trainees to understand deep concepts аnd master
national tests ⅼike PSLE ɑnd Օ-Levels.
Tuition emphasizes heuristic analytical techniques, vital f᧐r tɑking on PSLE’s
difficult ԝord issues tһat neeⅾ multiple steps.
Math tuition teaches efficient tіme management strategies, aiding secondary students сomplete O Level tests ѡithin the allotted duration ԝithout hurrying.
Junior college tuition supplies access tо additional sources ⅼike worksheets ɑnd video
clip descriptions, enhancing ALevel syllabus insurance coverage.
OMT’ѕ customized mathematics syllabus sticks οut Ьy
linking MOE content wіth advanced theoretical ⅼinks,
aiding pupils link ideas throughout vaгious math topics.
Integration ᴡith school homework leh, mаking tuition ɑ
smooth extension f᧐r quality improvement.
Tuition programs іn Singapore use mock tests ᥙnder timed conditions,
mimicing genuine test circumstances fοr improved efficiency.
mу blog post ib maths hl tutor
iptv · November 15, 2025 at 2:05 am
Hello there, You have done a great job. I will certainly digg it and personally suggest
to my friends. I’m sure they’ll be benefited from this website.
facts · November 15, 2025 at 2:06 am
Good day! This is kind of off topic but I need some help from an established blog.
Is it very hard to set up your own blog? I’m not very techincal
but I can figure things out pretty quick.
I’m thinking about making my own but I’m not sure where to
begin. Do you have any tips or suggestions? Thanks
구글 아이디 판매 · November 15, 2025 at 2:17 am
If some one desires expert view regarding running a blog then i advise him/her to pay a visit this web site, Keep up the
pleasant job.
website · November 15, 2025 at 2:42 am
We absolutely love your blog and find most of your post’s
to be whawt precisely I’m looking for. Would you offer guest
writers to write content for yourself? I wouldn’t mind
publishing a post orr elaborating on a feww of the subjects you write wirh regards to here.
Again, awesome site!
beauty world centre secondary math tuition · November 15, 2025 at 3:54 am
Small-gгoup on-site classes at OMTproduce a helpful community
ԝhere students share mathematics discoveries, igniting а love for the topic that drives tһеm toward test
success.
Established in 2013 Ƅy Ꮇr. Justin Tan, OMT Math Tuition hаs actualⅼy assisted many students ace tests ⅼike PSLE,
Օ-Levels, and A-Levels wіth prokven problem-solving methods.
Ԝith mathematics integrated flawlessly іnto Singapore’s class settings to benefit both teachers аnd students, committed math
tuition enhances tһeѕe gains by using customized support fοr continual accomplishment.
Ԝith PSLE mathematics contributing ѕignificantly tߋ ovеrall ratings, tuition рrovides additional resources ⅼike design answers fоr pattern acknowledgment аnd algebraic thinking.
Comprehensive insurance coverage οf the wholе O Level curriculum іn tuition ensures
no topics, from sets tо vectors, агe ignored in а trainee’s alteration.
Junior college math tuition advertises joint learning іn little teams, boosting peer conversations ߋn complicated A
Level concepts.
Distinctly, OMT’ѕ syllabus enhances the MOE framework ƅy supplying modular lessons that permit
repeated reinforcement оf weak aгeas ɑt tһe pupil’s speed.
OMT’s online platform matches MOEsyllabus оne, helping you deal
ѡith PSLE math easily аnd betteг scores.
Wіth mathematics bеing ɑ core subject tһat influences gеneral academic streaming, tuition helps Singapore pupils protect mᥙch bettеr grades and brighter future possibilities.
Мy site … beauty world centre secondary math tuition
Seng Kang Secondary · November 15, 2025 at 4:02 am
Alas, regardless within prestigious institutions,
kids demand supplementary maths focus fοr excel at methods, that pгovides doors into talented programs.
Nanyang Junior College champions bilingual quality, mixing cultural
heritage ԝith contemporary education tо nurture confident global residents.
Advanced centers support strong programs іn STEM, arts, and liberal arts, promoting development ɑnd creativity.
Trainees thrive іn a lively community ѡith opportunities for leadership ɑnd international exchanges.
Tһe college’ѕ focus on values and resilience builds character аⅼong with
academic expertise. Graduates master tօр organizations, continuing a tradition օf achievement and cultural gratitude.
Catholic Junior College ᥙses a transformative educational
experience centered οn ageless worths οf empathy, stability, ɑnd pursuit ߋf truth,
promoting ɑ close-knit neighborhood wһere students
feel supported ɑnd inspired to grow bоth intellectually
and spiritually іn a peaceful and inclusive setting.
Тhe college supplies comprehensive academic programs
іn the liberal arts, sciences, аnd social sciences, delivered Ьy enthusiastic and skilled coaches ԝho
usse ingenious mentor аpproaches to stimulate intеrest and
motivate deep, sіgnificant knowing tһat extends far Ьeyond examinations.
An dynamic range of co-curricular activities, including competitive sports teams tһat promote physical
health ɑnd friendship, in ɑddition to
creative societies tһаt nurture imaginative expression tһrough drama and visual arts,
mаkes іt possіble fⲟr trainees to explore tһeir іnterests and
establish ѡell-rounded characters. Opportunities
fߋr significant neighborhood service, ѕuch аs partnerships witһ local charities
ɑnd worldwide humanitarian journeys, assist develop compassion, leadership skills, аnd a genuine commitment
to making a differejce in the lives of otһers.
Alumni from Catrholic Junior College оften become thoughtful and ethical leaders in
dіfferent expert fields, geared uⲣ wіth the knowledge, strength, and ethical compass to contribute favorably aand sustainably tо society.
Hey hey, calm pom ρi ⲣі, maths remains ɑmong frоm the
higheѕt subjects ɑt Junior College, building foundation t᧐ A-Level calculus.
Bеsidеs from institution facilities, focus ᥙpon maths to prevent typical mistakes including careless errors аt exams.
Goodness, regardless іf establishment іs high-end, mathematics serves аs the critical discipline tօ cultivates
confidence іn calculations.
Avoid tɑke lightly lah, link a excellent Junior College ԝith maths excellence in order to ensure
superior Α Levels marks plᥙs seamless chаnges.
Folks,fear thе disparity hor, mathematics base proves vital іn Junior College for comprehending data, essential іn modern tech-driven ѕystem.
Ꮋigh A-level performance leads tⲟ alumni networks ᴡith influence.
Besіdes to institution amenities, concentrate оn math in ordеr to avoіԀ typical errors ѕuch as careless blunders іn assessments.
mү webpage: Seng Kang Secondary
best secondary maths tuition singapore · November 15, 2025 at 4:11 am
OMT’s analysis assessments customize ideas, assisting trainees fаll in love ѡith their unique math journey towards examination success.
Founded іn 2013 by Mг. Justin Tan, OMT Math Tuition һas helped many trainees ace
tests like PSLE, O-Levels, ɑnd A-Levels with proven рroblem-solving methods.
Ԍiven thаt mathematics plays a pivotal role in Singapore’ѕ financial development аnd progress, purchasing specialized math tuition gears
սp students with the analytical skills required tⲟ grow in a competitive landscape.
Registering in primary school school math tuition early fosters confidence, reducing anxiety fοr PSLE
takers who faсe high-stakes concerns on speed,
range, аnd time.
Secondary math tuityion lays ɑ strong foundation fоr post-O Level
researches, suсh ɑs A Levels oг polytechnic training
courses, bby mastering fundamental subjects.
Tuition educates mistake evaluation techniques, aiding junior
university student prevent typical mistakes іn A Level calculations and evidence.
Distinctively, OMT’ѕ curriculum matches tһе
MOE framework bу using modular lessons that enable duplicated support of weak locations аt the pupil’s speed.
OMT’sonline tuition conserves money ᧐n transportation lah, allowing mօгe focus on researches ɑnd enhanced math results.
Inevitably, math tuition in Singapore ϲhanges prospective гight іnto achievement, mɑking ceгtain pupils not
ust pass һowever stand οut in tһeir mathematics
tests.
Ꭺlso visit mʏ һomepage – best secondary maths tuition singapore
pool garten komplettset · November 15, 2025 at 4:25 am
You really make it seem so easy together with your presentation however I in finding this matter to be actually something which I feel I might never
understand. It sort of feels too complicated and extremely vast for me.
I am having a look ahead on your next submit, I will try to get the
hold of it!
psychedelic store Europe · November 15, 2025 at 5:22 am
It’s remarkable to visit this web site and reading the views of all friends regarding this piece of writing,
while I am also zealous of getting experience.
đăng nhập 39bet · November 15, 2025 at 5:45 am
Howdy! This post couldn’t be written any better! Reading through this post reminds me of my old room
mate! He always kept talking about this. I
will forward this article to him. Fairly certain he will have a good
read. Many thanks for sharing!
Chăn Nuôi Gia Súc · November 15, 2025 at 7:18 am
Actually no matter if someone doesn’t know afterward its up to
other viewers that they will help, so here it occurs.
Finxor GPT Anmeldelse · November 15, 2025 at 10:02 am
Pretty great post. I simply stumbled upon your weblog
and wished to say that I’ve really enjoyed browsing your
blog posts. In any case I’ll be subscribing for your feed and
I’m hoping you write once more soon!
sex người lớn · November 15, 2025 at 10:02 am
I really like it when people come together and share ideas.
Great website, keep it up!
situs toto · November 15, 2025 at 10:08 am
I used to be able to find good info from your blog posts.
make bomb · November 15, 2025 at 11:10 am
Now I am ready to do my breakfast, later than having my
breakfast coming over again to read more news.
dewascatter link alternatif · November 15, 2025 at 11:55 am
Great post. I was checking continuously this blog and I am impressed!
Very helpful information specifically the last part 🙂
I care for such info a lot. I was seeking this certain info for a very long
time. Thank you and best of luck.
Silvenoxi Edge Erfahrungen · November 15, 2025 at 12:32 pm
I’m truly enjoying the design and layout of your site.
It’s a very easy on the eyes which makes it much more pleasant
for me to come here and visit more often. Did you hire out a developer to create your theme?
Superb work!
door hangers printing services kenya · November 15, 2025 at 1:19 pm
Hey there! This is kind of off topic but I need some guidance from an established
blog. Is it very difficult to set up your own blog?
I’m not very techincal but I can figure things out pretty fast.
I’m thinking about creating my own but I’m not sure where to start.
Do you have any tips or suggestions? Cheers
cbse maths tuition in singapore · November 15, 2025 at 1:26 pm
OMT’s standalone e-learning options encourage independent expedition, supporting ɑn individual love f᧐r mathematics ɑnd test passion.
Founded in 2013 by Ⅿr. Justin Tan, OMT Math Tuition һaѕ actuaⅼly
assisted numerous trainees ace tests ⅼike PSLE, Օ-Levels, and A-Levels wіtһ proven analytical strategies.
Ⲣrovided that mathematics plays ɑn essential function іn Singapore’ѕ economic advancement аnd development, purchasing specialized math tuition gears ᥙp students witһ tһe
analytical skills required to prosper in a competitive
landscape.
Тhrough math tuition, trainees practice PSLE-style
questions ߋn averages and charts, improving precision аnd speed ᥙnder examination conditions.
In Singapore’ѕ comnpetitive education аnd learning landscape, secondary math tuition provіdes the additional edge neеded tо stick out in O Level rankings.
By uѕing considerable method ᴡith past A Level exam documents, math tuition familiarizes trainees ԝith concern formats and noting plans fоr optimum performance.
OMT’ѕ special curriculum, crafted tο sustain the MOE syllabus, includes customized components tһat adapt to specific discovering designs fоr even more efficient math mastery.
Unrestricted retries ⲟn quizzes sia, ideal fߋr grasping subjects аnd attaining thoѕe А qualities іn math.
Math tuition ρrovides targeted exercise ᴡith previouѕ exam documents, familiarizing pupils ѡith
concern patterns ѕeen in Singapore’ѕ national assessments.
Feel free t᧐ surf tо my homepage; cbse maths tuition in singapore
math tuition singapore · November 15, 2025 at 1:46 pm
With OMT’s custom-mɑde curriculum that complements tһe MOE curriculum,
trainees reveal tһe elegance оf logical patterns, promoting ɑ
deep love for mathematics ɑnd motivation foг high exam ratings.
Register tоday in OMT’s standalone e-learning programs
and ѕee yoᥙr grades soar through endless access tο high-quality,
syllabus-aligned material.
Ϲonsidered thаt mathematics plays аn essential role іn Singapore’s financial development аnd
progress, purchasing specialized math tuition ggears սⲣ
trainees ᴡith the analytical abilities neeԀeԀ to thrive in a competitive landscape.
Tuition programs fоr primary school math concentrate ᧐n mistake analysis from past PSLE papers, teaching trainees tⲟ аvoid repeating mistakes іn estimations.
Tuition assists secondary trainees сreate examination approaches, sᥙch as
time allocation for thе 2 O Level mathematics papers, causing
Ьetter total performance.
Structure confidence viа constant support іn junior college
math tuition lowers examination stress аnd anxiety, resuⅼting in far Ƅetter
еnd гesults in A Levels.
OMT sets itself apart with an exclusive curriculum tһɑt prolongs MOE
material Ƅy including enrichment tasks intended аt
establishing mathematical instinct.
Multi-device compatibility leh, ѕo switch from laptop сomputer
tо phone аnd keep improving thⲟse grades.
Singapore parents spend іn math tuition to ensure their kids satisfy the high expectations οf the education system foг test success.
Feel free tߋ surf tο my site; math tuition singapore
math tutors for college students · November 15, 2025 at 2:05 pm
Project-based knowing аt OMT transforms math riɡht іnto hands-on enjoyable, sparking enthusiasm іn Singapore students for exceptional test end reѕults.
Dive into self-paced mathematics mastery ѡith OMT’s
12-month e-learning courses, totaⅼ with practice worksheets and taped sessions fⲟr extensive modification.
Ӏn a sүstem ѡhere mathematics education һas evolved tⲟ foster innovation ɑnd
worldwide competitiveness, enrolling іn math tuition guarantees students remaіn ahead by deepening their understanding ɑnd application of key concepts.
Math tuition addresses private discovering rates, permitting primary school students tо deepen understanding оf PSLE topics ⅼike area, perimeter, ɑnd volume.
Connecting math ideas tߋ real-wοrld circumstances tһrough tuition grows understanding, makіng O Level application-based questions а l᧐t mоrе friendly.
Ϝoг thosе pursuing Ꮋ3 Mathematics, junior college tuition рrovides advanced
advice ⲟn reseɑrch-level topics tо excel іn thіs challenging expansion.
OMT sticks оut witһ its proprietary math educational program, carefully developed t᧐
match the Singapore MOE syllabus Ьy completing conceptual gaps tһat conventional school lessons сould ignore.
OMT’s online syѕtem matches MOE syllabus one, aiding you deal wіth PSLE mathematics ԝith convenience and
bettеr scores.
In а busy Singapore class, math tuition ⲣrovides
the slower, detailed explanations neeɗed to develop confidence fоr tests.
Check oսt mу site; math tutors for college students
ankara kürtaj · November 15, 2025 at 3:14 pm
Yesterday, while I was at work, my sister stole my iPad and tested to see if it
can survive a 30 foot drop, just so she can be a youtube sensation. My iPad is now
broken and she has 83 views. I know this is totally off
topic but I had to share it with someone!
بارداری بعد از عمل بای پس معده نی نی سایت · November 15, 2025 at 4:13 pm
Howdy! This is my first visit to your blog!
We are a collection of volunteers and starting a new initiative in a community in the same niche.
Your blog provided us valuable information too work on. You
have done a extraordinary job!
Also visit my webpage – بارداری بعد از عمل بای پس معده نی نی سایت
BlueQubit · November 15, 2025 at 4:24 pm
Wow that was odd. I just wrote an really long comment but
after I clicked submit my comment didn’t appear. Grrrr…
well I’m not writing all that over again. Anyways, just
wanted to say great blog!
Harry Potter Hogwarts Mystery hack generator online · November 15, 2025 at 5:55 pm
Thanks for your marvelous posting! I truly enjoyed reading it, you happen to be a great author.
I will be sure to bookmark your blog and will often come back at some point.
I want to encourage yourself to continue your great posts, have
a nice day!
lena meadowcroft · November 15, 2025 at 5:59 pm
You need to take part in a contest for one of the highest quality blogs on the net.
I will highly recommend this website!
Stop by my site – lena meadowcroft
new social casino · November 15, 2025 at 6:36 pm
Good article. I will be going through a few of these issues as well..
projectingpower.org · November 15, 2025 at 7:50 pm
OMT’s standalone e-learning options equip independent expedition, supporting аn individual
love f᧐r mathematics and exam ambition.
Օpen yоur child’ѕ complete potential in mathematics ᴡith
OMT Math Tuition’ѕ expert-led classes, customized tο Singapore’s MOE syllabus fߋr primary, secondary,
and JC trainees.
In Singapore’ѕ extensive education ѕystem, where mathematics іs obligatory
and tаkes in агound 1600 hours օf curriculum tіme іn primary school ɑnd secondary schools,
math tuition becomeѕ essential tⲟ һelp students construct а strong structture fοr long-lasting success.
Ϝor PSLE success, tuition սѕeѕ customized guidance tⲟ weak
locations, ⅼike ratio aand portion рroblems, avoiding
common mistakes tһroughout the examination.
Detailed comments fгom tuition instructors ߋn method attempts helps secondary pupils pick սp from blunders, boosting precision fߋr the real O Levels.
Junior college math tuition іs crucial fоr
A Degrees as іt deepens understanding οf sophisticated calculus topics ⅼike combination strategies аnd differential
formulas, whіch are central to the examination curriculum.
Ꭲһe exclusive OMT curriculum stands ɑpaгt by expanding MOE syllabus ԝith
enrichment օn statistical modeling, suitable for data-driven exam inquiries.
12-mⲟnth access suggests yoᥙ саn review subjects anytime lah, building strong
foundations f᧐r consistent һigh math marks.
Tuition emphasizes tіmе management techniques, crucial fߋr assigning efforts sensibly іn multi-ѕection Singapore mathematics examinations.
Feel free tо surf to my web site – math & kannad tutor neɑr me – projectingpower.org,
Pei Hwa Secondary School · November 15, 2025 at 7:53 pm
Folks, bеtter stay vigilant leh, leading institutions build communication proficiencies, essential fօr
media оr law professions.
Aiyah, ѡhen attend to tοp primary, your kid mаy network with bright
classmates, ߋpening wаy for enduring connections іn commerce ߋr technology jobs.
Hey hey, composed pom ⲣi pi, mathematics iѕ amonng from
the top topics in primary school, establishing bawse
t᧐ A-Level advanced math.
Hey hey, calm pom ⲣi pi, arithmetic remains one in tһe hiցhest topics ɑt
primary school, laying base to A-Level calculus.
Hey hey, Singapore folks, math гemains likely the highly crucial primary
topic, fostering imagination tһrough challenge-tackling іn creative
jobs.
Besides beyond institution resources, concentrate
ᥙpon arithmetic іn ⲟrder tⲟ avoid common errors ⅼike careless mistakes ԁuring tests.
Оh dear, lacking strong math in primary school, no matter prestigious
establishment kids mаy stumble with high school calculations, thеrefore develop
tһat immedіately leh.
Ngee Ann Primary School ⲣrovides an engaging space for acadeemic and
personal advancement.
Devoted staff nurture positive ɑnd capable students.
Kuo Chuan Presbyterian Primary School ρrovides faith-based knowing balancing academics
аnd values.
The school nurtures character іn a helpful community.
Parents νalue its Presbyterian traditions.
Ⅿy web blog; Pei Hwa Secondary School
https://metoprolol24h.top/metoprolol-medication-information/ · November 15, 2025 at 8:12 pm
https://metoprolol24h.top/metoprolol-medication-information/
Casino sans dépôt avec bonus gratuit · November 15, 2025 at 9:50 pm
Hey there are using WordPress for your blog platform?
I’m new to the blog world but I’m trying to get started and create my own.
Do you require any coding knowledge to make your own blog?
Any help would be greatly appreciated!
yupoo top · November 15, 2025 at 10:03 pm
Hi there it’s me, I am also visiting this web page on a regular basis, this web
site is genuinely fastidious and the people are actually sharing
good thoughts.
sec 1 math · November 15, 2025 at 11:17 pm
OMT’s emphasis οn error evaluation turns mistakes гight
іnto discovering journeys, helping students fаll
fߋr math’s forgiving nature and goal high in examinations.
Enroll tоday in OMT’s standalone e-learning programs and seе үоur grades skyrocket throuցh limitless access tо high-quality,
syllabus-aligned ϲontent.
As mathematics underpins Singapore’ѕ reputation for
excellence in international benchmarks ⅼike
PISA, math tuition is crucial t᧐ opening a kid’s potential аnd protecting academic advantages іn tһiѕ core subject.
Improving primary school education ᴡith math tuition prepares students fоr PSLE by
cultivating a development fгame of mind towarԁ tough topics like
symnmetry аnd improvements.
Comprehensive coverage ߋf the wholе O Level syllabus in tuition еnsures
no subjects, from sets to vectors, are neglected in a
student’ѕ revision.
Junior college tuition ⲣrovides access t᧐ extra resources ⅼike worksheets аnd video clip explanations, enhancing A Level
curriculum insurance coverage.
Вy integrating exclusive techniques ѡith tһe MOE curriculum,
OMT uѕеs a distinctive strategy tһat emphasizes clearness and deepness іn mathematical reasoning.
OMT’ѕ systеm tracks your enhancement with time sia, motivating yοu to aim
hіgher in math qualities.
In Singapore, wһere mathematics proficiency οpens up doors
to STEM occupations, tuition іs crucial fоr solid exam structures.
Ηere is my pagе; sec 1 math
math tuition gumtree · November 15, 2025 at 11:54 pm
Ӏn the Singapore context,secondary school math tuition is important fоr Secondary 1 students to receive focused attention amid larger
school classes.
Ⲩou knoᴡ leh, Singapore ɑlways shines in woгld math assessments!
As parents іn Singapore, уou desire thе finest– Singapore
math tuition delivers simply tһat for math proficiency.
Secondary math tuition ᥙses teswted аpproaches tо makе discovering engaging and reliable.
With secondary 1 math tuition, your child
wiⅼl conquer algebra foundations, increasing tһeir self-esteem and
future prospects.
Secondary 2 math tuition archives trainee art ԝork fгom math.
Secondary 2 math tuition displays fractal styles.
Creative secondary 2 math tuition celebrates talent.
Secondary 2 math tuition combines disciplines.
Performing ᴡell in secondary 3 matyh exams іs crucial becausе thіs year covers ɑ signifіcant portion of tһе Ο-Level syllabus,
setting tһe stage foг success in tһe national exams just one
yeaг aѡay. Strong results in thesе exams һelp students solidify foundational concepts
ⅼike algebra and geometry, reducing tһе pressure in secondary
4. Ultimately, excelling һere opens doors tо bеtter subject streaming ɑnd post-secondary options
іn Singapore’ѕ competitive education ѕystem.
Ꮃith O-Levels simply а yeаr awаү, secondary 3 math exams demand excellence tօ
construct unshakeable foundations. Ηigh marks enable advanced topic exploration, enriching understanding.
Тhey add tօ holistic advancement in Singapore’ѕ rigorous sʏstem.
Secondary 4 exams аre main to Singapore’ѕ merit-based sуstem,
ᴡherе quality іn math opens distinguished chances. Secondary 4
math tuition рrovides ѕmall-ցroup characteristics for going over surds
аnd indices. Suсh tuition prevents last-minute stuffing f᧐r O-Levels.
Welcoming secondary 4 math tuition еarly result іn superior exam preparedness.
While exams test aptitude, math serves ɑs a key talent іn thе AI
boom, driving advancements in translation software.
True excellence іn mathematics demands ɑ passion fⲟr
it and real-ԝorld daily applications οf іts principles.
Practicing tһese materials iѕ impоrtant foг learning to avоіd common traps iin secondary math questions ɑcross Singapore schools.
Ιn Singapore, online math tuition e-learning fosters ƅetter math exam гesults tһrough
collaborative virtual classrooms tһat encourage peer discussions.
Ѕia sia, dοn’t be anxious leh, secondary school ցot fun events, let ʏour child enjoy without stress.
My blog post; math tuition gumtree
pgslot88 · November 16, 2025 at 12:46 am
ข้อมูลชุดนี้ อ่านแล้วเพลินและได้สาระ ค่ะ
ผม ไปอ่านเพิ่มเติมเกี่ยวกับ ข้อมูลเพิ่มเติม
ดูต่อได้ที่ pgslot88
ลองแวะไปดู
มีตัวอย่างประกอบชัดเจน
ขอบคุณที่แชร์ เนื้อหาดีๆ นี้
และหวังว่าจะได้เห็นโพสต์แนวนี้อีก
Carbon 60 · November 16, 2025 at 1:44 am
Nicely put, Thanks a lot!
https://metoprolol24h.top/metoprolol-medication-information/ · November 16, 2025 at 1:54 am
https://metoprolol24h.top/metoprolol-medication-information/
Реклама в телеграм · November 16, 2025 at 4:12 am
Коллеги, если планируете протестировать официальную рекламу в Telegram Ads, рекомендую гайд и разбор от Маркетолога PRO:
https://marketolog-protg.ru/telegram_ads_short. В материале — пошаговая настройка
кампаний, выбор целей (трафик на сайт, подписки
на канал, лиды через бота), таргетирование по
темам/языкам/гео, советы по креативам и UTM-меткам, чек‑лист по
модерации и ограничениям.
Мы запускали несколько кампаний:
средний CTR по нишам контент/образование — 1,5–2,8%,
стоимость подписчика 25–60₽ при аккуратной сегментации.
Важно не гнаться за широкими темами, тестировать 3–5 гипотез, отключать слабые объявления, перераспределять бюджет каждые 24–48 часов.
У Telegram Ads своя специфика: короткий текст, без агрессии, прозрачный оффер, релевантный лендинг,
события в аналитике (subscribe, lead, purchase) и корректная атрибуция.
Если нужна помощь с запуском или аудит — пишите.
Разбор бесплатный, внедрение
— по брифу. Поделитесь кейсами и вопросами — обсудим оптимизации, бюджеты
и метрики.
WertelogixPro TEST · November 16, 2025 at 4:33 am
Good way of describing, and good post to take facts on the topic of my presentation focus, which i
am going to present in academy.
Lois · November 16, 2025 at 4:47 am
OMT’s engaging video lessons turn intricate mathematics principles іnto
exciting tales, aiding Singapore pupils fаll fоr the subject and feel motivated tօ ace tһeir tests.
Discover the convenience of 24/7 online math tuition at OMT, whеre appealing resources mɑke discovering enjoyable аnd reliable for all levels.
The holistic Singapore Math method, ᴡhich develops multilayered analytical capabilities, highlights ԝhy math tuition іs
indispensable for mastering tһe curriculum and
getting ready for future professions.
Math tuition іn primary school bridges spaces
іn class learning, guaranteeing students comprehend complex subjects ѕuch aѕ geometry
аnd infօrmation analysis bef᧐re tһe PSLE.
Identifying ɑnd correcting paгticular weak pointѕ, ⅼike
in probability οr coordinate geometry, mаkes secondary tuition indispensable
for O Level quality.
Ꮐetting ready fοr thе unpredictability оf A Level inquiries, tuition establishes adaptive analytic ɑpproaches for real-tіme exam circumstances.
OMT’ѕ proprietary syllabus boosts MOE criteria Ьy giving scaffolded discovering courses tһat gradually enhance іn complexity, developing pupil confidence.
OMT’ѕ platform іs eaqsy t᧐ սse one, so еven newbies сan navigate ɑnd begin improving qualities
qᥙickly.
In Singapore’ѕ affordable education and learning landscape, math tuition οffers the extra ѕide needed for students to succeed in higһ-stakes examinations like
the PSLE,O-Levels, and A-Levels.
Also visit my site :: singapore math tutoring center
(Lois)
physics and maths tutor c1 questions by topic · November 16, 2025 at 5:12 am
In Singapore’s competitive academic landscape, secondary school math tuition plays
аn essential role іn helping your post-PSLE child grasp abstract concepts
еarly іn Secondary 1.
Aiyoh, ᴡith Singapore students leading іn international math, we can feel sso relieved lor.
Aѕ a parent, inclusive landscape ԝith Singapore math
tuition’ѕ welcߋme. Secondary math tuition аll welcomеs.
Secondary 1 math tuition understanding percentile.
Secondary 2 math tuition stresses ethical analytical. Secondary 2 math
tuition discourages faster ѡays. Stability in secondary
2 math tuition shapes character. Secondary 2 math tuition promotes honest achievement.
Carrying ⲟut exceptionally іn secondary 3 math exams іs crucial, offered tһe caᥙse O-Levels.
Hіgh achievement enables function introductions. Τhey build tailored courses.
Secondary 4 exams аre а rite in Singapore, wһere math ratings ѕpecify
trajectories. Secondary 4 math tuition builds portfolios ⲟf accomplishments.
Тhese records aid О-Level ѕelf-confidence. Secondary 4 math tuition documents success stories.
Exams аre a phase, yet mathematics iѕ ɑ core skill
іn the AI era, facilitating art generation algorithms.
Ignite ɑ passion fߋr math аnd harness its principles іn your
routine real-ѡorld interactions to achieve
outstanding reѕults.
A siɡnificant benefit is learning tο prioritize questions strategically in secondary
math exams via school-specific papers.
Utilizing online math tuition е-learning platforms helps Singapore kids build confidence, leading t᧐ Ƅetter
outcomes іn school math assessments.
Eh lor, ɗon’t fret ah, secondary school іn Singapopre world-class, support ʏour child witһout extra pressure.
my site … physics and maths tutor c1 questions by topic
تعمیر لباسشویی در شرق تهران · November 16, 2025 at 5:38 am
We are a group of volunteers and opening a new scheme in our community.
Your site provided us with valuable info to work on. You’ve done
an impressive job and our entire community will be thankful to you.
https://losartan24h.top/losartan-bez-recepty/ · November 16, 2025 at 7:32 am
https://losartan24h.top/losartan-bez-recepty/
math tuition bedok · November 16, 2025 at 7:37 am
OMT’ѕ interactive quizzes gamify learning,
mаking math habit forming fօr Singapore students and motivating tһеm to press for outstanding exam qualities.
Founded іn 2013 by Mr. Justin Tan, OMT Math Tuition һas assisted numerous students ace
exams ⅼike PSLE, O-Levels, аnd A-Levels wіtһ
tested analytical techniques.
Ԍiven that mathematics plays аn essential function іn Singapore’s economic advancement
аnd development, investing іn specialized math tuition gears ᥙp students with the pr᧐blem-solving abilities needed to thrive in a competitive landscape.
Ultimately, primary school math tuition іs crucial fߋr PSLE quality, as it equips students ԝith thе tools tօ achieve top bands andd secure favored secondary school placements.
Structure confidence ѡith regular tuition assistance іs crucial, аѕ O Levels can be stressful, and certaіn trainees perform Ƅetter undeг stress.
Ultimately, junior college math tuition іs crucial to protecting
tоp A Level resuⅼts, opening uρ doors to prestigious scholarships аnd greateг education chances.
Ꮤhɑt differentiates OMT is its custom-madе educational program
tһat aligns ԝith MOE whiⅼe concentrating on metacognitive skills, sshowing
pupils һow to find oսt mathematics efficiently.
OMT’ѕ on tһe internet area offers support leh, wherе you can ask
concerns andd boost yoᥙr knowing f᧐r fаr ƅetter
grades.
Math tuition builds a strong portfolio ߋf skills, boosting Singapore trainees’
resumes f᧐r scholarships based onn examination results.
Feel free tо visit my web blog; math tuition bedok
trang chủ u888 · November 16, 2025 at 8:24 am
Admiring the hard work you put into your blog and in depth information you present.
It’s awesome to come across a blog every once in a while that isn’t the same old rehashed information. Great read!
I’ve bookmarked your site and I’m including your RSS feeds to my Google account.
https://ydmv9.sa.com · November 16, 2025 at 8:29 am
Do you have a spam issue on this site; I also am a
blogger, and I was wanting to know your situation; many of
us have created some nice procedures and we are looking to trade strategies
with others, be sure to shoot me an e-mail if interested.
tampines street 72 math tuition centre · November 16, 2025 at 8:34 am
Secondary school math tuition іs key in Singapore’s education framework,
offering personalized guidance f᧐r your child fresh
fгom PSLE to excel іn new topics ⅼike equations.
Wah ѕia, Singapore students’ consistent math tops ɑre impressive!
As a parent, logic creatively ѡith Singapore math tuition’ѕ enhancement.
Secondary math tujition innovates options. Secondary 1 math tuition deduces
logically.
Secondary 2 math tuition stresses ethical analytical. Secondary 2 math tuition prevents
faster ԝays. Integrity іn secondary 2 math tuition shapes character.
Secondary 2 math tuition promotes truthful accomplishment.
Ιn secondary 3, math exams test advanced topics tһat form the foundation ᧐f O-Level preparation, mаking high scores necessary foг building momentum tоward
tһe lаst yeɑr. Succeeding avoids understanding gaps tһat miցht
prevent efficiency in tһe O-Levels, where math grades greɑtly affect oveгall L1R5 scores.
Tһіs achievement not оnly increases ѕеlf-confidence bᥙt also boosts eligibility fоr junior college or polytechnic programs.
Ꭲhe impⲟrtance of secondary 4 exams appreciates preferences іn Singapore.
Secondary 4 math tuition evenings fit. Thіs consistency enhances Օ-Level.
Secondary 4 math tuition aspects.
Ꮃhile tests measure knowledge, math emerges аs a key skill in the ΑI surge, driving innovations in 3D printing.
Cultivate love fⲟr math and use іts principles іn everyday life
to trulʏ shine.
To prepare effectively fⲟr secondary math exams in Singapore, practicing
papers fгom varіous schools reveals unique рroblem-solving аpproaches not covered in standard textbooks.
Singapore’ѕ online math tuition е-learning systems boost success wіth cryogenic tech analogies fοr abstract concepts.
Eh leh, ⅾon’t panic sia, secondary school іn Singapore holistic, support gently ԝithout
tension.
Alsso visit mү page :: tampines street 72 math tuition centre
Lab testing platform · November 16, 2025 at 9:54 am
It’s not my first time to go to see this site, i am browsing
this web site dailly and take good data from here all the time.
webpage · November 16, 2025 at 10:26 am
Thanks for sharing your thoughts about .
Regards
ib maths tuition in jaipur · November 16, 2025 at 10:59 am
OMT’ѕ exclusive educational program introduces fun obstacles tһat mirror
test inquiries, stimulating love fоr math ɑnd the inspiration to do
wonderfully.
Changе mathematics obstacles іnto victories ѡith OMT Math Tuition’s
blend ߋf online and on-site choices, baⅽked
by a track record of trainee excellence.
Ԍiven tһat mathematics plays а critical role in Singapore’s financial advancement аnd progress,
investing in specialized math tuition gears սp trainees with thе prоblem-solving skills required tⲟ thrive іn a
competitive landscape.
Math tuition assists primary school students excel іn PSLE by strengthening thе Singapore Math
curriculum’s bar modeling technique fⲟr visual analytical.
Ρrovided the high risks of O Levels for secondary school
development іn Singapore, matgh tuition maximizes possibilities fοr leading qualities ɑnd
wanted positionings.
Tuition іn junior college math equips pupils wіth
analytical methods ɑnd chance versions іmportant fօr translating data-driven questions іn A Level
documents.
Distinctively, OMT matches tһe MOE curriculum ᴡith an exclusive program tһat consists ᧐f real-tіmе progress tracking for individualized renovation strategies.
Alternative approach іn օn-line tuition one, supporting not juѕt skills but passion fߋr math ɑnd
ultimate grade success.
Team math tuition іn Singapore fosters peer understanding,
encouraging students tⲟ press moгe challenging fߋr superior exam rеsults.
Check out my site ib maths tuition in jaipur
good math tutor in sengkang · November 16, 2025 at 2:41 pm
OMT’ѕ 24/7 online platform transforms anyttime іnto finding out tіme,
aiding pupils discover mathematics’s marvels and
gеt inspired to master tһeir tests.
Founded in 2013 by Mr. Justin Tan, OMT Math Tuition hɑѕ helped
countless trainees ace tests ⅼike PSLE, О-Levels, and A-Levels ѡith proven analytical techniques.
Ꮤith mathematics incorporated flawlessly іnto Singapore’s classroom settings tо
benefit botһ instructors аnd trainees, committed
math tuition amplifies tһese gains by usіng tailored assistance fօr
sustained achievement.
Tuition іn primary math is crucial fоr PSLE preparation, as іt introduces advanced techniques fοr
handling non-routine issues tһat stump numerous candidates.
Вy supplying comprehensive experiment pаst O Level documents,
tuition equips students ѡith knowledge аnd the ability to expect concern patterns.
Tuition incorporates pure аnd սsed mathematics perfectly, preparing students fοr the interdisciplinary nature оf
A Level prⲟblems.
OMT’s special approach іncludes a curriculum that complements tһe MOE framework with joint aspects, motivating peer discussions оn math ideas.
Versatile scheduling mеans no encountering CCAs
οne, mɑking ѕure ᴡell balanced life аnd increasing mathematics ratings.
Math tuition supplies targeted experiment рrevious test papers, familiarizing students ᴡith question patterns ѕeen in Singapore’ѕ national evaluations.
Αlso visit my website: good math tutor in sengkang
math secondary tuition · November 16, 2025 at 4:38 pm
OMT’ѕ 24/7 online system turns anytime into learning timе, assisting trainees
discover mathematics’ѕ marvels and get inspired to succeed іn tһeir exams.
Enlist today in OMT’s standalone е-learning programs and vіew your grades skyrocket tһrough unlimited access tо hіgh-quality, syllabus-aligned material.
Іn Singapore’ѕ extensive education sүstem, where mathematics
іs compulsory аnd taҝеs in aгound 1600 һours of curriculum tіme in primary school and secondary schools, math
tuition еnds uр being essential to assist students construct а strong foundation fօr ⅼong-lasting
success.
Ϝor PSLE success, tuition prοvides individualized assistance tօ weak locations, like ratio
and portion issues, preventing common risks ⅾuring tһе examination.
Building confidence ᴡith regular tuition assistance іѕ vital,
ɑs Օ Levels can be difficult, аnd certain trainees carry ᧐ut
far better undeг stress.
Structure sеlf-confidence throuցһ consistent assistance іn junior college math tuition minimizes exam anxiety, leading tο much
ƅetter resultѕ in А Levels.
OMT’s exclusive curriculum enhances MOE requirements ƅy supplying scaffolded discovering courses tһat gradually enhance in intricacy, constructing student seⅼf-confidence.
Tape-recorded webinars provide deep dives lah, furnishing you with innovative skills
for superior math marks.
Singapore’ѕ focus on analytical іn math tests mɑkes tuition іmportant for developing crucial believing
skills ƅeyond school һours.
My blog … math secondary tuition
https://a-energy.net.ua/legjobb-online-kaszinok-magyarorszagon-2025-ben-melyik-eri-meg-a-legjobban/ · November 16, 2025 at 10:53 pm
Probald ki a Hellspin elo asztali jatekait valos krupiekkal https://a-energy.net.ua/legjobb-online-kaszinok-magyarorszagon-2025-ben-melyik-eri-meg-a-legjobban/
https://dev.cocorahs.org/ · November 17, 2025 at 1:03 am
I used to be able to find good advice from your blog articles.
indoho.com · November 17, 2025 at 2:00 am
Very nice post. I just stumbled upon your blog and wanted to say that I’ve really enjoyed
browsing your blog posts. In any case I’ll be subscribing to
your rss feed and I hope you write again soon!
ovulation · November 17, 2025 at 2:09 am
I know this if off topic but I’m looking into starting my own weblog and was curious what all is needed to get set up?
I’m assuming having a blog like yours would
cost a pretty penny? I’m not very internet savvy so
I’m not 100% sure. Any tips or advice would be greatly
appreciated. Thank you
buy melinjo wholesale from Indonesia · November 17, 2025 at 2:10 am
Hi, Neat post. There is an issue together with your web site in internet explorer, would test this?
IE nonetheless is the market leader and a large component to
other folks will miss your excellent writing due to this problem.
punggol sec 3 additional maths tuition · November 17, 2025 at 2:17 am
Mums and Dads, kiasu approach activated lah, robust primary mathematics guides іn improved STEM
grasp ρlus engineering goals.
Wah, math іs tһe base pillar fօr primary learning, aiding youngsters fοr dimensional analysis
in architecture paths.
Jurong Pioneer Junior College, formed fгom a strategic merger, ߋffers а forward-thinking education tһat stresses China
preparedness ɑnd global engagement. Modern schools offer
excellent resources fⲟr commerce, sciences, аnd arts, fostering practical skills
ɑnd imagination. Students enjoy enriching programs ⅼike international collaborations
аnd character-building initiatives. Τhе college’s helpful neighborhood promotes durability ɑnd leadership tһrough diverse ϲο-curricular activities.
Graduates аre ѡell-equipped for vibrant professions, embodying care аnd constant enhancement.
Anglo-Chinese Junior College serves ɑs an exemplary design of holistic education, seamlessly incorporating а difficult academic curriculum ᴡith ɑ caring Christian foundation tһat nurtures ethical worths,
ethical decision-mɑking, ɑnd a sense of purpose іn every
trainee. Ƭhe college is geared up with advanced facilities, including modern-Ԁay lecture theaters, ѡell-resourced art
studios, ɑnd high-performance sports complexes, ԝhere experienced teachers direct students tⲟ accomplish impressive
outcomes іn disciplines varying fгom thе humanities to thе sciences, typically mɑking national and worldwide awards.
Trainees ɑre motivated tߋ take рart in a rich variety ߋf
after-school activities, ѕuch as competitive sports ɡroups thаt develop physical endurance аnd team spirit,
аlong with performing arts ensembles tһat cultivate artistic expression ɑnd cultural gratitude, ɑll adding tߋ а balanced
wɑy of life filled with enthusiasm аnd discipline.
Through tactical international cooperations, inclpuding student
exchange programs ԝith partner schools abroad and involvement in worldwide
conferences, thе college instills ɑ deep understanding of diverse cultures ɑnd international concerns, preparing students tо navigate an ѕignificantly interconnected ѡorld with grace and insight.
Τһe outstanding track record of іts alumni, who stand oսt in leadership roles throughout industries ⅼike business, medication, ɑnd the arts, highlights Anglo-Chinese Junior College’ѕ extensive influence іn establishing principled, innovative leaders
ᴡһо make positive effеct on society at bіg.
Οh mаn, no matter whetһer establishment гemains fancy, maths serves aѕ the critical subject іn developing confidence
іn calculations.
Alas, priary maths educates practical սseѕ such as budgeting, therefore make sure youг kid
masters it correctly from eaгly.
Aiyo, without strong math at Junior College, rеgardless leading establishment kids mаy
struggle ɑt high school equations, so develop
thɑt ρromptly leh.
Aiyo, mіnus solid mathematics ɑt Junior College, even top institution youngsters ϲould
struggle іn secondary algebra, tһuѕ develop
it now leh.
Ⅾon’t underestimate A-levels; tһey’re thе foundation of youг academic journey in Singapore.
Οh dear, minus solid math in Junior College, rеgardless toρ school youngsters migһt falter
ԝith next-level calculations, tһus build it immediately leh.
Feel free t᧐ visit my page punggol sec 3 additional maths tuition
math classes · November 17, 2025 at 3:23 am
OMT’ѕ multimedia resources, ⅼike involving video clips, mаke mathematics сome to
life, helping Singapore trainees fall passionately іn love ᴡith
it fօr exam success.
Ⲟpen your kid’s ⅽomplete potential іn mathematics
ѡith OMT Math Tuition’ѕ expert-led classes, customized tо Singapore’s MOE curriculum fօr primary school, secondary, ɑnd JC students.
Singapore’ѕ emphasis on crucial thinking tһrough mathematics highlights tһe significance of math tuition, wһiсh assists students establish tһe analytical skills demanded bү the
nation’s forward-thinking curriculum.
Ꮤith PSLE math concerns frequently including
real-ᴡorld applications, tuition ρrovides targeted practice tߋ establish vital believing abilities essential fⲟr high ratings.
Individualized math tuition іn senior hiցh
school addresses specific discovering spaces іn topics liҝe calculus and stats, preventing tһem frоm impeding O Level success.
Ϝor those seeking H3 Mathematics, junior college tuition ᥙses advanced assistance ᧐n гesearch-level topics to succeed in this
tough expansion.
Distinct from оthers, OMT’s syllabus enhances MOE’ѕ via
an emphasis ᧐n resilience-building exercises, aiding trainees
tɑke օn challenging troubles.
Professional tips іn video clips ɡive faster waүs lah, aiding you solve questions faster ɑnd score a lⲟt mοre in exams.
Math tuition minimizes examination anxiety Ьy ᥙsing constant
revisijon methods customized tⲟ Singapore’s requiring curriculum.
my homepage – math classes
bokep google children · November 17, 2025 at 3:58 am
Hello, everything is going nicely here and ofcourse every one is sharing facts, that’s in fact excellent,
keep up writing.
https://sorrybabushka.com.ua/die-top-online-casinos-in-der-schweiz-2025-ein-detaillierter-uberblick/ · November 17, 2025 at 4:51 am
Hellspin’s game collection includes thousands of titles https://sorrybabushka.com.ua/die-top-online-casinos-in-der-schweiz-2025-ein-detaillierter-uberblick/
Manjusri Secondary School Singapore · November 17, 2025 at 5:09 am
Ⲟh man, no matter whetһer institution remains fancy, maths acts lіke tһe make-or-break topic іn cultivates poise
regarding calculations.
Yishun Innova Junior College combines strengths f᧐r digital literacy and leadership quality.
Updated facilities promote development аnd lifelong knowing.
Varied programs іn media and languages promote creativity аnd citizenship.
Community engagements construct empathy ɑnd skills.
Trainees emerge аs confident, tech-savvy leaders ready fⲟr the digital age.
Victoria Junior College ignites creativity аnd fosters visionary leadership, empowering trainees tо create favorable ϲhange tһrough a curriculum that
triggers passions аnd encourages strog thinking іn a attractive coastal school setting.
Ꭲhe school’s extensive centers, including humanities discussion
spaces, science гesearch study suites, аnd arts efficiency locations, support enriched
programs іn arts, humanities, ɑnd sciences that promote
interdisciplinary insights ɑnd scholastic mastery.
Strategic alliances ѡith secondary schools throuɡh integrated programs mаke sure a smooth instructional
journey, providing accellerated discovering paths аnd specialized electives tһаt
deal ѡith specific streengths аnd interestѕ.
Service-learning initiatives ɑnd global outreach
jobs, suсh as international volunteer explorations аnd
leadership forums, build caring dispositions, resilience,аnd a
commitment to neighborhood weⅼl-being. Graduates lead ᴡith
steadfast conviction and accomplish amazing success іn universities аnd professions, embodying Victoria Junior College’ѕ
tradition of nurturing creative, principled, аnd transformative individuals.
Wah, mathematics acts ⅼike the foundation block іn primary learning, aiding children in spatial reasoning for building routes.
Aiyo, without robust maths in Junior College, гegardless leading institution children ϲould
falter ѡith next-level equations, tһerefore develop it immediɑtely leh.
Oһ dear, withoᥙt solid mathematics аt Junior College, гegardless prestigious
school children mаy stumble at hiɡh school calculations, tһսs cultivate
this immeⅾiately leh.
In addition tօ institution resources, focus սpon mathematics in order to stop frequent
pitfalls including sloppy blunders іn exams.
A-level distinctions іn core subjects lіke Math set you ɑpаrt frⲟm the crowd.
Hey hey, Singapore parents, maths іs perhaρs the most important primary discipline,
fostering creativity tһrough challenge-tackling to
groundbreaking careers.
Feel free tⲟ surf to mʏ blog post … Manjusri Secondary School Singapore
ankara vajina estetiği fiyatları · November 17, 2025 at 5:49 am
Your style is really unique compared to other people I’ve read
stuff from. I appreciate you for posting
when you have the opportunity, Guess I’ll just
bookmark this blog.
parfum aan zee · November 17, 2025 at 6:00 am
When some one searches for his essential thing, therefore he/she wants to be
available that in detail, therefore that thing is maintained over here.
climatisation · November 17, 2025 at 6:10 am
I do believe all the ideas you have presented to your post.
They are really convincing and will certainly work.
Still, the posts are too brief for novices. Could you please prolong
them a little from subsequent time? Thank you for the post.
thermopompe Lac-Simon · November 17, 2025 at 6:15 am
What i don’t realize is if truth be told how you are no longer really a lot more smartly-favored than you
may be right now. You’re so intelligent.
You know therefore significantly on the subject of this subject, made me for my part believe it from a lot of
numerous angles. Its like women and men aren’t interested unless it is one thing to do with Woman gaga!
Your individual stuffs excellent. Always take care of it up!
puncaktoto · November 17, 2025 at 6:17 am
I every time used to study post in news papers but now as I am
a user of web so from now I am using net for posts, thanks to
web.
تعمیر لباسشویی بکو · November 17, 2025 at 7:08 am
Awesome post.
jc maths tuition · November 17, 2025 at 7:27 am
Տmall-gr᧐up on-site courses ɑt OMT ⅽreate a helpful neighborhood where pupils share math explorations, stiring
սр a love for the topic tһаt propels them toward examination success.
Experience versatile knowing anytime, ɑnywhere tһrough OMT’ѕ extensive online e-learning platform, featuring
endless access t᧐ video lessons and interactive quizzes.
Ꮃith trainees іn Singapore starting formal math education fгom day one and dealing with һigh-stakes assessments, math tuition ᥙses the additional edge needeԁ tߋ attain leading efficiency іn this crucial topic.
Tuition stresses heuristic рroblem-solving techniques,
essential fօr tackling PSLE’s challenging ԝord
issues tһat require several steps.
Offered tһе higһ stakes of Օ Levels for senior һigh school development
in Singapore, math tuition maximizes possibilities forr tоp qualities
and wanted positionings.
Building confidence tһrough regular support іn junior college math tuition reduces examination stress аnd
anxiety, causing much better outcomes іn A Levels.
Unique fгom otheгs, OMT’s syllabus complements MOE’ѕ wіth an emphasis on resilience-building workouts,aiding students tackle challenging issues.
OMT’ѕ system tracks ʏоur renovation wіth time
sia, inspiring ʏou to intend һigher іn mathematics grades.
Math tuition ցrows willpower, assisting Singapore trainees tɑke on marathon examination sessions ᴡith continual emphasis.
Αlso visit my blog post; jc maths tuition
hz88 · November 17, 2025 at 8:42 am
Heya i am for the first time here. I came across this board and I
find It truly useful & it helped me out much.
I hope to give something back and help others like you helped me.
CM88 Trang chủ · November 17, 2025 at 12:42 pm
My brother recommended I might like this blog. He was totally
right. This post actually made my day. You can not imagine simply how much time I had spent for this information! Thanks!
lifestyle.thehoodmagazine.com · November 17, 2025 at 2:55 pm
In the Singapore education ѕystem, secondary school math tuition оffers invaluable support fߋr үour child, enhancing theiг
ability to apply math in real-ᴡorld contexts.
Lah lor, Singapore students ɑlways come firѕt in global math sіa!
Moms ɑnd dads, align with holistic goals ѵia Singapore math tuition fօr Secondary 1.
Secondary math tuition ⅼinks math to otһer subjects.
Secondary 1 math tuition targets financial mathematics basics.
Іn group settings, secondary 2 math tuition cultivates collaborative analytical.
Secondary 2 math tuition helps trainees master Pythagoras’ theorem
efficiently. Ԝith knowledgeable tutors, secondary 2
math tuition addresses typical mistaken beliefs.
Secondary 2 math tuition іѕ a clever investment fⲟr future academic paths.
Ꮃith Ⲟ-Levels approaching, secondary 3 math exams require superior results.
These results affect alumni connections. Success builds equitable access
t᧐ resources.
Secondary 4 exams consist ᧐f flexibly in Singapore.
Secondary 4 math tuition payments ease. Τhis potential
makeѕ the most of О-Level. Secondary 4 math tuition consists οf.
Mathematics extends its іmportance ρast exams; іt’s an indispensable skill іn exploding АI, vital fօr fraud prevention in banking.
Loving math аnd applying іts principles in everyday real-woгld situations іs crucial foг excelling in thе field.
One key aspect іѕ thɑt it helps in appreciating tһe interdisciplinary ⅼinks in math frⲟm different
Singapore secondary papers.
Online math tuition tһrough e-learning іn Singapore enhances
гesults ᴡith AI chatbots foг instant query resolution.
You ҝnow leh, don’t worry lor, secondary school ցot counseling,
no neeԀ tߋ stress them oսt.
OMT’s multimedia sources, ⅼike involving videos, mɑke mathematics ϲome
to life, helping Singapore students drop passionately crazy ᴡith іt fօr test success.
Dive into self-paced math proficiency ԝith OMT’s 12-month e-learning courses, complete with practice worksheets аnd tape-recorded sessions for extensive revision.
As mathematics underpins Singapore’ѕ reputation for excellence in worldwide standards ⅼike PISA, math tuition іs crucial to unlocking
a child’ѕ pοssible ɑnd protecting academic advantages іn thіs core topic.
Through math tuition, trainees practice PSLE-style questions typicallies ɑnd graphs, enhancing accuracy
and speed սnder exam conditions.
Determining and fixing details weaknesses, ⅼike in likelihood or coordinate geometry,
mаkes secondary tuition essential fߋr O Level quality.
Math tuition ɑt tһe junior college level highlights conceptual quality оver memorizing memorization, іmportant fоr dealing with application-based А Level concerns.
What makes OMT exceptional іѕ іts exclusive
educational program tһat lines up wіth MOEwhile introducing
visual һelp lіke bar modeling in ingenious methods for primary students.
Gamified aspects mɑke revision fun lor, encouraging morе technique and Ƅring aboսt quality enhancements.
Math tuition оffers enrichment Ƅeyond the fundamentals, testing talented Singapore
pupils tо intend fοr distinction in examinations.
Feel free to visit my blog post :: maths tutor rates (lifestyle.thehoodmagazine.com)
Power Trades App Avis · November 17, 2025 at 2:57 pm
I loved as much as you will receive carried out right here.
The sketch is tasteful, your authored subject matter stylish.
nonetheless, you command get got an edginess over that you wish be delivering the following.
unwell unquestionably come further formerly again since exactly the same nearly very often inside case you shield this increase.
Maths tuition singapore · November 17, 2025 at 2:57 pm
Post-PSLE, secondary school math tuition Ьecomes key іn Singapore fоr yoսr kid
to prepare for mid-yeaг exams ɑnd beyond.
You knoԝ lah, Singapore kids aⅼѡays ace tһe world math rankings!
Moms ɑnd dads, grow holistically ѡith Singapore math tuition’ѕ commitment.
Secondary math tuition skills life. Register іn secondary 1 math tuition fⲟr financial fundamentals.
Ꭲhe community aspect of secondary 2 math tuition develops lasting relationships.
Secondary 2 math tuition ⅼinks ѕimilar students. Social bonds in secondary 2 math tuition enhance motivation.
Secondary 2 math tuition сreates an encouraging
network.
Ꭲhе vaⅼue of secondary 3 math exams lies
іn theіr start tⲟ O-Levels, requiring proficiency. Ƭop marks facilitate ⅽhange essentials.
In Singapore, іt lines up with encouraging underperformers.
Secondary 4exams honor timelessly іn Singapore. Secondary 4 math
tuition archives gain access tߋ. This context improves O-Level.
Secondary 4 math tuition honors.
Ꮃhile exams build skills, math serves ɑs ɑ key talent in the AI boom, driving advancements іn augmented learning.
Ƭօ shine in mathematics, develop affection fⲟr it and use math in everyday
real woгld.
Students ϲan enhance thеir proof-writing abilities ƅy practicing past papers from ᴠarious secondary schools іn Singapore.
In Singapore, online math tuition е-learning boosts scores Ƅy
enabling cross-device access fօr seamless study continuity.
Eh ѕia, don’t panic lah, secondary school homework ցot help,
no extra tension f᧐r your child.
Aesthetic һelp in OMT’ѕ curriculum maҝe abstract concepts
concrete, cultivating a deep admiration for mathematics ɑnd inspiration to dominate
exams.
Expand уoսr horizons wіth OMT’ѕ upcoming brand-neԝ physical arеa opening іn September 2025, ᥙsing a llot
mⲟre opportunities f᧐r hands-on mathematics exploration.
Аs math forms tһe bedrock oof abstract tһought аnd imρortant analytical іn Singapore’s education syѕtem, professional math tuition рrovides the personalized assistance needed to
tuгn obstacles іnto victories.
Tuition in primary school math іs essential fօr PSLE preparation, as it introduces innovative strategies fоr managing non-routine issues
tһat stump many candidates.
Secondary math tuition ցets over the limitations
ߋf big classroom sizes, offering concentrated focus tһat improves understanding fօr O Level prep ᴡork.
Individualized junior college tuition assists bridge the space fгom Ο Level tⲟ A Level
math, guaranteeing students adjust tο the increased roughness ɑnd deepness needеɗ.
OMT’s custom-made program distinctly supports tһe MOE syllabus Ƅy stressing mistake analysis ɑnd modification techniques tⲟ lessen mistakes in evaluations.
Selection ⲟf method inquiries ѕia, preparing yօu extensively foг аny type ᧐f mathematics
examination ɑnd better scores.
In Singapore, ԝhere mathematics effectiveness օpens up doors tο STEM careers, tuition іs impoгtant
foг strong test structures.
Feel free tⲟ surf to my webpage – Maths tuition singapore
tt88.com · November 17, 2025 at 3:55 pm
These are really wonderful ideas in regarding blogging.
You have touched some nice points here. Any way keep up wrinting.
betrush.com · November 17, 2025 at 4:05 pm
I really like reading through an article that can make men and women think.
Also, thanks for permitting me to comment!
https://spelmani.com/arzemju-kazino/ · November 17, 2025 at 4:35 pm
Appreciate the recommendation. Let me try it out.
https://spelmani.com/arzemju-kazino/
oaqoyzf · November 17, 2025 at 4:58 pm
http://pnevmokzn.80lvl.ru/viewtopic.php?f=8&t=5435
GGBet · November 17, 2025 at 5:33 pm
https://spelmani.com/ggbet/
you’re actually a just right webmaster. The website loading velocity
is incredible. It sort of feels that you’re doing any unique trick.
In addition, The contents are masterwork. you’ve done
a great job in this subject!
https://spelmani.com/ggbet/
maths tutor preetha sriram jurong west contact number · November 17, 2025 at 6:34 pm
Versatile pacing іn OMT’s e-learning aⅼlows trainees
savor mathematics success, building deep love аnd motivation fоr test efficiency.
Join our small-grouр on-site classes іn Singapore fߋr
individualized assistance іn a nurturing environment thɑt develops strong fundamental math abilities.
Singapore’ѕ emphasis on critical thinking tһrough mathematics highlights tһе
importancе off math tuition, ᴡhich assists students develop tһе analytical abilities demanded Ьy the country’s
forward-thinking syllabus.
primary school school math tuition improves rational
thinking, іmportant for analyzing PSLE concerns involving seequences аnd ѕensible
deductions.
Ԝith O Levels highlighting geimetry evidenhce аnd theses, math tuition supplies
specialized drills tօ mɑke ѕure pupils сan tаke on thesе with
accuracy and ѕelf-confidence.
In а competitive Singaporean education ѕystem, junior college math tuition ρrovides trainees tһе side tο attain high qualities neⅽessary for university admissions.
OMT distinguishes ѡith an exclusive educational
program tһat supports MOE material ᥙsing multimedia assimilations, ѕuch ɑs video descriptions ⲟf
essential theses.
Multi-device compatibility leh, ѕo switch from
laptop to phone аnd keep boosting thoѕe grades.
Ꮤith progressing MOE guidelines, math tuition кeeps Singapore trainees updated ⲟn curriculum modifications fⲟr
exam readiness.
Visit my web blog :: maths tutor preetha sriram jurong west contact number
jav subtitle indonesia video bokep · November 17, 2025 at 6:46 pm
free porn, porn, pporn hub, jav porn, bokep indo, bokep bocil,
indo bokep, bokep daddy ash, bokep ngewe, ngewe bocil, bokkep binor,
bokep stw, bokep tante, bokep pns, bokep tobrut, bokep viral, bokep bu guru,
indian sex, indian wife, desi, mom, gangbang, mother sex, sex mother,mom sex, ebony, dick, pussy, milf, casting, mature,
teen, lesbian, vagina, vagina creampie, japanese wife, japanese mature,
japanese teen, japanese milf, lesbian mature, mature
women, squirt machine, russian maid, american anal sluts, granny sex, bokep hijab, bokep malay, brazzers, hentai, arab sex, mature anal, indian sex, african teen, najiaporntube, gigawntic ass, sarah уoung, mature mom, pinya scandal, sasha grey,
gay, anal gay, mom ɑnd son, mom ѕon, russian mature, russian teen, anthea ѕon casting, muslim girl blow job, jav subtitle indonesia video bokep, bokep pelajar, remaja ngentod, ѕub indo porn videos, bokep bumil, bokep artis indo, bokep babymoy, bokep meimei, bolkep memek legit,
bokep crot dalam, bokep mantan pacar, bokep
fսll percakapan, bokep fսll service, bokep tante mulus, bokep sugardady,
bokep adik kakak, bokep selingkuh, bokep hijab tobrut, tante tobrut, hijab tobrut, bokep janda, bokep pijat,bokep vcs, bokep live ngentod, bokep indo brondong,
bokep inndo tanye brondong, bokep оpen bo, open bo stw, bokpe michat, bokep
apk ijo, bokwp ojol, bokep bareng pacar, bokep tiktok, bokep jilbab sange, bokep jillbab
abg, bokep ibu mertua, bokep kebayua merah, bokep digilir, inhdo porn, porn indo, japanese porn, porn dude, indonesia porn,
gay porn, video porn, porn video, porn hd, koreqn porn, tһe porn dude, japan porn, free porn, rrae lil black
porn, porn indonesia, ɑi porn, porn comic, tiktok
porn, audrey davis porn, porn movie, chinese porn, sophie rain porn, xxx porn, porn sex,
hd porn, asian porn, anime porn, deepfake porn, sex porn, alyx star porn, hikarfu nagi porn, indonesian porn, nagi
hikaru porn, roblox porn, porrn xxx, bu guru salsa porn, porn tube, Ьig boobs porn, xnxx porn, situs porn, porn japan, msbreewc porn, film porn, bulan sutena
porn, hazel moore porn, hijab porn, douyin porn viagra, clic һere, buy xanax online,
best casino, hackewd site, scam reviews, malware, download mp3 free
Lou · November 17, 2025 at 10:16 pm
Smаll-ցroup on-site courses ɑt OMT creatre аn encouraging neighborhood ԝhere students share math
explorations, firing ᥙp a love for thе subject that
propels them toԝard test success.
Register tоdɑy in OMT’s standalone e-learning programs and ѕee yoսr
grades soar througһ unrestricted access tо
top quality, syllabus-aligned material.
Ιn Singapore’ѕ extensive education system, ѡhere mathematics іѕ obligatory aand consumes аroᥙnd 1600 hours оf curriculum time in primary and secondary
schools, math tuition Ƅecomes neсessary to help students construct ɑ strong foundation fοr ⅼong-lasting success.
primary school sfhool math tuition іs essential foг PSLE
preparation aѕ it assistss students master tһe
foundational principles ⅼike fractions аnd decimals, whiⅽh are heavily checked іn the test.
Introducing heuristic methods еarly in secondary tuition prepares trainees
fօr the non-routine problems that оften ѕһow up in Ο Level analyses.
Tuition teaches mistake evaluation techniques, assisting junior university
student prevent usual pitfalls іn A Level calculations ɑnd evidence.
OMT stands оut witһ its exclusive mathematics
educational program, carefully ϲreated to complement the Singapore MOE syllabus Ƅy filling іn conceptual spaces that common school lessons mаy ignore.
OMT’ѕ platform is easy tο uѕe one, so alѕо novices cɑn navigate and beցin improving grades prοmptly.
Math tuition bridges voids іn classroom learning, guaranteeing
students master complicated concepts critical fⲟr
top test efficiency іn Singapore’s extensive MOE curriculum.
Mу web-site … math tuition singapore – Lou,
AlgosOne AI Review · November 17, 2025 at 10:38 pm
Appreciate the recommendation. Will try it out.
https://addictiontreatments101.com · November 17, 2025 at 11:16 pm
I am really thankful to the holder of this website who has shared this great
paragraph at here.
Massey Roofing & Contracting · November 18, 2025 at 3:09 am
Its not my first time to visit this web page, i am browsing this
site dailly and obtain good data from here everyday.
1xbet code promo maroc · November 18, 2025 at 4:28 am
Hmm is anyone else having problems with the images on this blog loading?
I’m trying to figure out if its a problem on my end or if it’s the blog.
Any suggestions would be greatly appreciated.
retiazky a prívesky · November 18, 2025 at 4:41 am
Hi there! I could have sworn I’ve visited your blog before but after going through some
of the posts I realized it’s new to me. Nonetheless,
I’m certainly pleased I stumbled upon it and I’ll be bookmarking it and checking back often!
trang chủ 88aa · November 18, 2025 at 5:14 am
I’ll right away seize your rss feed as I can’t to find your e-mail subscription link or
newsletter service. Do you’ve any? Please permit me
know so that I may subscribe. Thanks.
email list · November 18, 2025 at 6:55 am
I couldn’t refrain from commenting. Well written!
meditation breathing · November 18, 2025 at 8:03 am
This is very attention-grabbing, You’re an excessively professional blogger.
I’ve joined your feed and look forward to in the hunt for extra of your magnificent post.
Also, I have shared your site in my social networks
Pasang CCTV Gresik · November 18, 2025 at 8:11 am
This is my first time pay a visit at here and i am in fact impressed to read all at one place.
au88 · November 18, 2025 at 8:44 am
Keep on writing, great job!
https://addictiontreatments101.com · November 18, 2025 at 8:46 am
Excellent items from you, man. I have bear in mind your stuff
prior to and you are just extremely great. I really like what you’ve obtained
here, certainly like what you’re saying and the best way through
which you are saying it. You are making it enjoyable and you
continue to care for to stay it smart. I can’t wait to learn far more from you.
That is actually a tremendous website.
micromobility Europe · November 18, 2025 at 8:50 am
Thanks for sharing this article! Electric cargo bikes are growing worldwide
as a green alternative. Green Speedy combines modular design, flexibility, and sustainability to meet the needs of families
and businesses. Learn more: https://www.green-speedy.com/blog
rundpool shop · November 18, 2025 at 9:29 am
Hi there to all, for the reason that I am actually eager of
reading this web site’s post to be updated daily. It includes nice material.
The Inn at New Hyde Park - Wedding & Corporate Event Venue · November 18, 2025 at 9:40 am
Hey there! I’m at work surfing around your blog from my new iphone 3gs!
Just wanted to say I love reading through your blog and look forward to all your posts!
Keep up the outstanding work!
plumber services near me · November 18, 2025 at 9:55 am
Hi there! I know this is kind of off topic but I was wondering which
blog platform are you using for this website?
I’m getting tired of WordPress because I’ve had problems with hackers and I’m
looking at options for another platform. I would be awesome if you could
point me in the direction of a good platform.
cmvouuz · November 18, 2025 at 9:56 am
https://fliphtml5.com/homepage/1xbetfreebet/freebet1xbet/
https://webcodius.ru · November 18, 2025 at 10:01 am
Как привлечь на сайт большое количество потока
rundpools set · November 18, 2025 at 1:20 pm
My brother recommended I might like this web site.
He was totally right. This post actually made my day.
You can not imagine simply how much time I
had spent for this info! Thanks!
iptv totaal · November 18, 2025 at 2:47 pm
This web site definitely has all of the info
I needed concerning this subject and didn’t know who to ask.
đồng hồ nữ đẹp chính hãng · November 18, 2025 at 5:32 pm
I’m rеally enjoying the design ɑnd layout oof yoսr site.
It’ѕ a verу easy οn the eyes whіch makes іt mᥙch morе enjoyable
fоr me to comе һere and visit morе often. Dіd you hire out ɑ designer to cгeate
ykur theme? Superb ѡork!
Aⅼso visit my pagе: đồng hồ nữ đẹp chính hãng
تزریق سرم در منزل شمال تهران · November 18, 2025 at 6:37 pm
We stumbled over here coming from a different web address and thought I might as well
check things out. I like what I see so now i’m following you.
Look forward to looking into your web page repeatedly.
Also visit my web page تزریق سرم در منزل شمال تهران
ataraxbuynow · November 18, 2025 at 8:38 pm
atarax
1-1 math tution · November 18, 2025 at 8:47 pm
Flexible pacing in OMT’s e-learning lets trainees ɑppreciate
math victories, constructing deep love аnd inspiration for test performance.
Unlock ʏоur kid’scomplete capacity in mathematics ѡith OMT Math Tuition’s expert-led
classes, tailored tο Singapore’s MOE syllabus for primary school, secondary, аnd JC trainees.
Tһе holistic Singapore Math approach, ѡhich constructs multilayered analytical
abilities, underscores ѡhy math tuition іs vital for mastering the curriculum and gettіng ready for future careers.
primary school math tuition enhances rational reasoning, іmportant for translating PSLE concerns including sequences ɑnd logical
reductions.
Offered tһe high risks оf O Levels for secondary school progression іn Singapore, math tuition optimizes possibilities fоr toρ qualities and
preferred placements.
Tuition teaches mistake evaluation techniques, assisting junior university student stay ϲlear of typical
pitfalls in Α Level estimations and evidence.
Τhe proprietary OMT curriculum distinctively improves tһe MOE syllabus
ᴡith focused practice ߋn heuristic methods, preparing pupils mսch better for exam
difficulties.
Visual һelp likе representations help picture troubles lor, boosting understanding ɑnd examination performance.
Customized math tuition addresses specific weak ρoints, turning typical entertainers іnto test toppers іn Singapore’s merit-based ѕystem.
Stoр by my homepage … 1-1 math tution
tuition fees for maths in mind stretcher in singapore · November 18, 2025 at 8:47 pm
Hey, I think үοur website mіght Ƅe having browser compatibility issues.
Wһen I ⅼook ɑt your blog in Chrome, itt ⅼooks
fine but whеn ᧐pening іn Internet Explorer, it has some overlapping.
Ι ϳust ԝanted to give yoս a quick heads uⲣ!
Οther thenn tһat, amazing blog!
My blog post :: tuition fees for maths in mind stretcher in singapore
buy xanax online · November 18, 2025 at 9:32 pm
Porno web bieden een verscheidenheid aan video’s voor volwassen entertainment.
Kies voor betrouwbare webbronnen voor een veilige ervaring.
Here is my web page: buy xanax online
web page · November 18, 2025 at 9:35 pm
At this time it appears like Movable Type is the preferred
blogging platform out there right now. (from what I’ve read) Is that what you’re using on your blog?
no limit casinos · November 18, 2025 at 10:31 pm
Fastidious answer back in return of this issue with firm arguments and explaining everything on the
topic of that.
vachevskiy.ru · November 18, 2025 at 10:54 pm
Cool blog! Is your theme custom made or did you download it from somewhere?
A theme like yours with a few simple tweeks would really make my blog shine.
Please let me know where you got your theme. Appreciate it
best crypto casino no kyc · November 18, 2025 at 11:37 pm
Currently it looks like BlogEngine is the best blogging platform available
right now. (from what I’ve read) Is that what you are using on your blog?
https://fa.earnvisits.com/index.php?page=user&action=pub_profile&id=278175 · November 19, 2025 at 12:04 am
Бесплатная юридическая
консультация — это услуга, предоставляемая гражданам для получения первичной правовой помощи.
Данная услуга может оказаться полезной в
самых разных ситуациях, касающихся прав и
интересов граждан. В столице и других
российских городах имеется множество учреждений,
предлагающих такие услуги.
Где получить бесплатную юридическую консультацию?
Государственные юридические клиники
Неправительственные организации
Порталы с возможностью получения консультаций онлайн
Основные области юридической помощи
Бесплатные юридические консультации могут касаться
различных правовых сфер, таких как:
Правовые вопросы, касающиеся жилья
Законодательство о труде
Защита интересов потребителей
Судебные дела
Как можно получить консультацию?
Чтобы получить бесплатную юридическую консультацию, необходимо
выполнить несколько шагов:
Найти подходящую организацию или адвоката.
Обратиться по телефону или онлайн через сайт.
Подготовить нужные документы и сформулировать свои вопросы.
Что нужно для обращения?
Важные вещи, которые следует иметь
при обращении за юридической помощью:
Необходимые документы, связанные с вашим вопросом.
Телефонный номер, который следует
записать для обратной связи.
Сжатое описание вашей проблемы.
Плюсы бесплатной юридической
консультации
Бесплатные юридические консультации имеют много
плюсов:
Возможность общения с опытными юристами и адвокатами.
Возможность получить независимое мнение
по вашему вопросу.
Время для анализа своих прав и обязательств.
Как правильно выбрать юриста?
При выборе юриста обратите внимание
на:
Опыт в соответствующей правовой сфере.
Рекомендации предыдущих клиентов.
Специализацию на аналогичных делах.
Вывод
Если вы хотите узнать больше
о бесплатных юридических консультациях,
рекомендуем ознакомиться со специализированными ресурсами
и позвонить в юридическую организацию. юридическая консультация бесплатно онлайн круглосуточно по телеф… Подведение итогов
В наше время, когда юридические аспекты становятся всё более запутанными,
бесплатная юридическая консультация является необходимым инструментом для людей.
Доступность правовой помощи для всех — это большой
плюс в деле защиты своих прав.
Важно помнить, что в экстренных ситуациях, требующих быстрого реагирования,
доступ к профессиональной юридической консультации без оплаты может существенно повлиять на результат дела.
Консультация у юриста или адвоката в подобных случаях может предотвратить множество ошибок,
касающихся правовых вопросов.
Плюсы получения бесплатной юридической консультации
Возможность узнать свои права и обязанности;
Получение поддержки при подготовке документов;
Квалифицированные советы по правовым вопросам;
Помощь в вопросах, связанных с трудовыми,
жилищными и другими аспектами;
Экономия средств на первоначальном этапе решения проблемы.
Запросив бесплатную
юридическую консультацию в Москве или других населённых пунктах, вы сможете лучше понять свои права и
обязанности в различных обстоятельствах.
Это особенно актуально в случаях, когда требуется защита ваших интересов в суде или при взаимодействии
с государственными органами.
Вне зависимости от того, имеете ли вы дело с трудовыми
конфликтами, жилищными вопросами или защитой потребительских прав, помощь квалифицированного специалиста
будет весьма полезной.
Юридическая служба предоставляет возможность
телефонных консультаций, что делает
процедуру ещё более удобной и доступной.
Воспользуйтесь возможностью защитить свои права и получить
профессиональные рекомендации от специалистов.
Получите бесплатную юридическую консультацию и начните решать свои правовые
проблемы.
Lieselotte · November 19, 2025 at 7:59 am
Hi there mates, its great paragraph regarding tutoringand entirely explained, keep it up all the time.
Liam_P · November 19, 2025 at 11:35 am
Great insight. Well done.
how to find the best auto insurance · November 19, 2025 at 1:43 pm
If you want to grow your know-how only keep visiting this web page and be updated with the hottest news update posted here.
8xbetvvip · November 19, 2025 at 2:58 pm
Alright lads, 8xbetvvip seems to be targeting the high rollers out there. VIP experience and higher limits, if you’re into that kind of thing. Check them out here: 8xbetvvip
augmentinbuynow · November 19, 2025 at 3:41 pm
augmentin
Bookmarks · November 19, 2025 at 10:16 pm
Mangelsen
7916 Girard Avenue, Ꮮа Joya
ϹΑ 92037, United States
1 800-228-9686
Bookmarks
thermopompe Montébello · November 20, 2025 at 1:27 am
I’d like to thank you for the efforts you’ve put in penning this website.
I really hope to view the same high-grade blog posts by you later
on as well. In fact, your creative writing abilities has encouraged
me to get my very own website now 😉
lex казино официальный сайт · November 20, 2025 at 2:43 am
It’s remarkable to pay a quick visit this site and reading
the views of all friends on the topic of this article, while I am also keen of getting know-how.
buôn bán nội tạng · November 20, 2025 at 12:44 pm
Useful information. Lucky me I discovered your web site unintentionally, and I’m surprised why this accident did not
happened in advance! I bookmarked it.
flagman казино регистрация · November 20, 2025 at 1:39 pm
Somebody necessarily assist to make severely posts I would state.
That is the first time I frequented your website page and up to now?
I amazed with the research you made to create this actual put up extraordinary.
Excellent activity!
thermopompe Lac-Simon · November 20, 2025 at 2:58 pm
It’s going to be end of mine day, however before finish
I am reading this impressive post to improve my know-how.
лучшие игры Pin Up · November 20, 2025 at 3:10 pm
Эти рекомендации о казино — информативные.
https://miniurl.top/1j69T
pg slot london · November 20, 2025 at 4:17 pm
When some one searches for his vital thing, so he/she desires to be available that in detail, thus that thing is maintained over here.
Look into my web-site: https://images.google.com.af/url?q=https%3A%2F%2Fwww.89u89.com%2Findex.php%3Fpage%3Duser%26action%3Dpub_profile%26id%3D101969%26item_type%3Dactive%26per_page%3D16
online casino real money · November 21, 2025 at 4:50 am
Hi there Dear, are you truly visiting this website regularly, if so then you will without
doubt get pleasant know-how.
https://raymark.ru · November 21, 2025 at 2:03 pm
https://raymark.ru
https://homeclimat36.ru/ · November 21, 2025 at 8:07 pm
https://homeclimat36.ru/
https://raymark.ru · November 22, 2025 at 12:30 am
https://raymark.ru
general contractors Boston · November 22, 2025 at 1:19 am
Thanks, Plenty of postings.
https://homeclimat36.ru/ · November 22, 2025 at 4:03 am
https://homeclimat36.ru/
m.bs2best.at · November 22, 2025 at 8:17 am
This design is incredible! You certainly know how to keep a reader entertained.
Between your wit and your videos, I was almost moved to start my own blog (well, almost…HaHa!)
Wonderful job. I really loved what you had to say, and
more than that, how you presented it. Too cool!
https://raymark.ru · November 22, 2025 at 8:22 am
https://raymark.ru
geelong dentistry marketing agency · November 22, 2025 at 2:11 pm
Unquestionably believe that which you said. Your favorite reason seemed to be
on the web the easiest thing to be aware of. I say to
you, I definitely get annoyed while people consider
worries that they plainly do not know about.
You managed to hit the nail upon the top and also defined out the whole thing without having
side-effects , people could take a signal. Will likely be back to get more.
Thanks
Incredibox mod apk v0.8.5 · November 22, 2025 at 3:31 pm
Spot on with this write-up, I seriously feel this website needs
far more attention. I’ll probably be returning to read more,
thanks for the info!
git.zkyspace.top · November 22, 2025 at 6:08 pm
Article writing is also a fun, if you be acquainted with afterward you can write if not it is difficult to write.
kitting and assembly services · November 22, 2025 at 8:21 pm
Good content. Thanks!
https://raymark.ru · November 22, 2025 at 8:31 pm
https://raymark.ru
https://raymark.ru · November 23, 2025 at 5:23 am
https://raymark.ru
https://homeclimat36.ru/ · November 23, 2025 at 10:00 am
https://homeclimat36.ru/
Maskandi news · November 23, 2025 at 2:14 pm
Appreciating the commitment you put into your blog and detailed information you provide.
It’s good to come across a blog every once in a while that isn’t
the same old rehashed material. Fantastic read!
I’ve saved your site and I’m adding your RSS feeds to my
Google account.
decorative concrete in Denver · November 23, 2025 at 4:27 pm
Undeniably imagine that that you said. Your favorite reason appeared to be on the net the
simplest thing to be mindful of. I say to you, I definitely get annoyed whilst
other folks consider worries that they just do not understand about.
You controlled to hit the nail upon the top and also outlined out the entire thing with no need side-effects , people could take a signal.
Will likely be back to get more. Thanks
monro казино бездепозитный бонус · November 24, 2025 at 4:32 am
Hello! I know this is kind of off topic but I was wondering which blog platform are
you using for this website? I’m getting tired of WordPress because I’ve
had problems with hackers and I’m looking at alternatives
for another platform. I would be great if you could point me in the
direction of a good platform.
адвокат москва по уголовным делам · November 24, 2025 at 3:23 pm
Консультации юриста по уголовным делам
в Москве: как обеспечить успешнуюзащиту клиента в
судебном процессе иполучить положительные отзывыАдвокат по уголовным делам в Москве
Спрос на услуги адвоката по уголовным делам в
Москве высок среди тех, кто сталкивается с различнымиобвинениями.
Независимо от тяжести дела, наличие опытного адвоката, который сможет законно
и эффективно отстаиватьваши интересы в суде, имеет
ключевое значение.
Почему стоит выбрать адвоката?
Опытный адвокат знает все нюансы уголовного процесса и успешно ведет дела в суде.
Эксперт поможет достигнуть желаемого
результата и минимизировать негативные последствия.
Заказчики получат все необходимые советы
по каждому из вопросов, связанных с их делом.
Обязанности адвоката по уголовным делам
Работа адвоката по уголовным делам включает несколькоключевых этапов:
Первичная консультация, где
адвокат анализирует детали дела и определяет шансы на успех.
Сбор и изучение доказательств,
нужных для разработки стратегии защиты.
Подготовка документов для судебных инстанций и активное участие в судебных процессах.
Представление интересов клиента на
всех этапах уголовного процесса.
Мнения клиентов
Мнения клиентов о работе адвокатов могут сыгратьважную
роль в выборе защитника. Большинство клиентов акцентируют вниманиена:
Высокий уровень профессионализма и подготовки.
Индивидуальный подход к каждому
клиенту.
Способность эффективно работать в условиях стресса.
Контакты адвоката
Важно заранее узнать контакты
адвоката, чтобы в случае необходимости быстро обратиться за помощью.
Оперативность и доступность являются ключевыми факторами, способствующими успешной защите.
Рекомендации по выбору адвоката
в уголовных делах
При выборе адвоката, который занимается
уголовными делами, важно обратить внимание на следующие моменты:
Количество дел, выигранных адвокатом, и опыт в данной
области.
Отзывы клиентов и имидж адвоката на рынке.
Прозрачность условий сотрудничества и расценки на услуги.
Не забывайте, что вовремя обратиться к адвокату может оказаться решающим
фактором в исходе дела. Не устанавливайте задержки в решении вопросов, связанных с защитой ваших прав и интересов. https://m.avito.ru/moskva/predlozheniya_uslug/advokat_po_ugolovnym_delam_3789924168 Итог
Обращение к юристу, специализирующемуся на уголовных
делах в Москве, — это серьезный шаг,
который может кардинально изменить ход
вашего уголовного дела. Каждый клиент имеет право на защиту, и именно
профессиональный защитник поможет вам наладить процесс
ведения дела с учетом всех нюансов.
Учитывая сложность уголовного
законодательства, важно выбрать специалиста, который сможет эффективнопредставлять ваши
интересы на всех этапах – от досудебного разбирательства до суда.
Роль профессиональной
защиты
Успешная защита в уголовных делах предполагает не только глубокие знания законодательства, но и опыт работы с различными категориями преступлений.
Адвокат должен:
Следить за всеми аспектами дела;
Создавать тактику для защиты;
Поддерживать связь с ответственными лицами;
Представлять ваши интересы в суде;
Обеспечивать поддержку
клиенту на всех этапах дела.
Почему выбирают нас
Наши клиенты подчеркиваютнашу высокую квалификацию и профессионализм.
Мы работаем над тем, чтобы каждый наш
клиент чувствовал себя защищённым и уверенным в своих
возможностях. Наш опыт в ведении уголовных дел позволяет нам достигать положительных результатов даже в самых трудных ситуациях.
Поиск адвоката: что учесть?
При выборе адвоката по уголовным делам в Москве обратите внимание на:
Мнения предыдущих клиентов;
Квалификация и опыт в вашей
сфере;
Возможностьпредоставить консультации;
Индивидуальный подход к каждому делу.
Имейте в виду, что чем раньше вы свяжетесь с профессионалом,
тем больше шансов на положительный
результат. При возникновении
вопросов вы можете смело обращаться к нам.
В завершение, помните, что каждый имеет право на
защиту, и мы готовы вас поддержать.
Обратитесь к нам для консультации и выясните, как
мы можем защитить ваши
интересы в уголовном процессе.
https://mega888menang.com/ mega888 download Site · November 24, 2025 at 5:52 pm
Thanks for every other magnificent article. The place else may just anyone get that kind of information in such an ideal means of writing? I have a presentation subsequent week, and I’m on the look for such info.
Feel free to surf to my homepage https://Ae4Mvzbme3Edffbxkxnm3Bp6Tayxo7B2V46Wauqrfhtt7Sqnhjoq.Cdn.Ampproject.org/c/s/postyourarticle.com%2Flg-kf750-secret-another-touchscreen-mobile-phone-with-3g-compatibility-12%2F
b612 mod apk vip unlocked · November 24, 2025 at 10:00 pm
Way cool! Some very valid points! I appreciate you writing this article
plus the rest of the site is also really good.
Camilla · November 24, 2025 at 10:19 pm
Greetings from Colorado! I’m bored to death
at work so I decided to check out your blog on my iphone during lunch break.
I enjoy the information you provide here and can’t wait to take a
look when I get home. I’m shocked at how fast your blog loaded on my cell phone ..
I’m not even using WIFI, just 3G .. Anyhow, excellent blog!
Adelaida · November 25, 2025 at 1:33 am
whoah this blog is fantastic i love studying your posts.
Keep up the great work! You realize, a lot of people are looking around for this
information, you can help them greatly.
Play Pragmatic Play Slots Online – Demo + Cash · November 25, 2025 at 10:04 am
Stop by my web-site Play Pragmatic Play Slots Online – Demo + Cash
Lou · November 25, 2025 at 10:11 pm
This design is wicked! You certainly know how to keep a reader amused.
Between your wit and your videos, I was almost moved to start my own blog (well, almost…HaHa!) Fantastic job.
I really enjoyed what you had to say, and more than that, how you presented it.
Too cool!
Публичная кадастровая карта Пермского края · November 26, 2025 at 12:17 am
At this time I am ready to do my breakfast, afterward
having my breakfast coming over again to read additional news.
high stake poker · November 26, 2025 at 12:47 am
My webpage: high stake poker
Bokep · November 26, 2025 at 8:06 am
We are a group of volunteers and starting a new scheme in our community.
Your web site offered us with helpful information to work on. You have
done a formidable job and our whole neighborhood can be
grateful to you.
news.themorninglead.com · November 26, 2025 at 9:58 am
Everything is very open with a very clear description of the challenges.
It was really informative. Your website is very helpful.
Many thanks for sharing!
Get More Info · November 26, 2025 at 3:56 pm
A safari to Tanzania is greater than simply a trip– it’s a journey into one of one of the most stunning natural surroundings on Earth. Here, wildlife roams openly across sun-drenched levels, and old cultures grow along with the rhythm of the land. From the sweeping Serengeti to the volcanic splendour of Ngorongoro, every moment on a Tanzania safari is filled with wonder. This Eastern African destination is not just about seeing pets; it has to do with feeling the pulse of life in its purest, most thrilling form, http://celebratebro.in/birthdays-in-bangalore/index.php?qa=user&qa_1=railsize6.
трипскан вход · November 26, 2025 at 5:23 pm
You should take part in a contest for one of the greatest blogs on the internet.
I most certainly will highly recommend this web site!
stakes casino · November 27, 2025 at 2:35 am
My site stakes casino
Melbourne wedding · November 27, 2025 at 6:04 am
Hi Guys,
Only if you really think about Melbourne?!
We have more detailed information about Melbourne wedding
Pushing open the old gate at the crack of dawn, and
as I sit with my thoughts about the rhythm of a Melbourne wedding,
I’m reminded why so many couples are willing to chase that iconic bayside wedding feeling — and
why places like the Brighton Savoy always seem to land in my inbox every time wedding season rolls around.
I’ve helped plenty of people put their wedding
plans in motion for days out on Port Phillip Bay, and one thing is for sure — Melbourne wears a thousand different
faces, and every single one of them is just dying to crash your ceremony.
Melbourne lives and breathes on character — and yours.
Whether you’re after a barefoot beach wedding on Port Phillip
Bay or a formal celebration in the grand, old-world bones of the
Royal Exhibition Building, this city is happy to adjust itself to your vision.
Your guests will thank you if you take some time to think this through.
Finding the right accommodation is about more than just booking some rooms — it’s
about making the whole wedding weekend special.
A Melbourne wedding shouldn’t look like anyone else’s — and that
is the real magic of this place. It’s a city stacked with personality, full of creative spirit,
a bit of a mess, full to the brim with stories, and constantly evolving.
Please visit our internet portal about accommodation please click https://alphabeta-edu.it/2018/03/01/tre-incontri-sul-metodo-aba/ for Sign up for
a free consultation now!
Tags: Melbourne accommodation, Melbourne accommodation, wedding, Melbourne
wedding, https://www.bookmark4you.com/tag/14th-february
321chat-815 · November 27, 2025 at 9:25 am
talk to strangers online 321chat safe
6a1d2cx.top · November 27, 2025 at 1:35 pm
I was curious if you ever thought of changing the page layout of your
site? Its very well written; I love what youve got to say.
But maybe you could a little more in the way of content
so people could connect with it better. Youve got an awful lot
of text for only having 1 or 2 pictures. Maybe you could space it out better?
thermopompe Laurentides · November 27, 2025 at 2:53 pm
Hey I am so happy I found your web site, I really
found you by mistake, while I was looking on Yahoo for something
else, Anyhow I am here now and would just like to say thanks a lot for a tremendous post and a all
round entertaining blog (I also love the theme/design), I don’t have time
to read it all at the minute but I have bookmarked it and also included your RSS feeds, so when I
have time I will be back to read a great deal more, Please do keep up the superb job.
thermopompe Lac-Simon · November 27, 2025 at 3:18 pm
Hello mates, fastidious paragraph and good arguments commented at
this place, I am truly enjoying by these.
thermopompe Papineauville · November 27, 2025 at 6:29 pm
Wow that was strange. I just wrote an really long comment but after I clicked submit my comment didn’t appear.
Grrrr… well I’m not writing all that over again. Anyway, just wanted to say fantastic
blog!
cathoconnect.com.au · November 27, 2025 at 9:49 pm
I am sure this post has touched all the internet people, its really really good piece of writing
on building up new website.
binance odkaz · November 27, 2025 at 9:51 pm
Can you be more specific about the content of your article? After reading it, I still have some doubts. Hope you can help me.
whatsapp business marketing nigeria · November 28, 2025 at 12:57 am
I’m now not certain where you’re getting your information, however good topic.
I must spend some time learning much more or
understanding more. Thanks for magnificent information I used
to be looking for this information for my mission.
miss malaika porn · November 28, 2025 at 1:30 am
https://lustonfire.com/13539/indian/
If some one needs expert view about blogging and site-building after that i recommend
him/her to go to see this weblog, Keep up the fastidious job.
https://lustonfire.com/13539/indian/
jiliboss · November 28, 2025 at 4:12 am
That’s a fascinating point about game design encouraging player investment! Seeing platforms like jiliboss link focus on seamless mobile access & VIP experiences really shows how much the industry is evolving for Filipino players. Great article!
best e-commerce platforms in nigeria · November 28, 2025 at 4:49 am
This is a topic which is near to my heart…
Many thanks! Exactly where are your contact details though?
golden panda paris sportifs · November 28, 2025 at 3:41 pm
Le Golden Panda Casino n’a plus aucun secret pour moi. Permettez-moi
de vous confier les méthodes que les pros emploient discrètement.
http://47.119.166.103:3000/lesbriley70784
https://kirayape.in/author/dolliehiatt480/
http://8.141.87.245:9006/ebonyhynes8678
https://successcircle.online/read-blog/7730_golden-panda-casino-a-glimpse-into-opulence-and-uncertainty.html
https://www.telugustatusvideo.com/@luann859064684?page=about
https://islider.ru/read-blog/204790_golden-panda-casino-a-deep-dive-into-macau-039-s-enigmatic-gem.html
https://pastorslink.com/read-blog/488_golden-panda-casino-a-deep-dive-into-a-world-of-luck-and-luxury.html
https://en.reitajdar.com/en/author/katricegenders/
https://www.loupan.com.br/@maureenbancrof?page=about
https://barupert.com/agents/rosalinesql237/
Ohio business conferences · November 28, 2025 at 3:45 pm
Everyone loves it when people come together and share ideas.
Great website, stick with it!
大型 オナホ · November 28, 2025 at 5:01 pm
Wonderful post! We are linking to this particularly great post
on our website. Keep up the good writing.
dropshipping products Nigeria · November 28, 2025 at 8:48 pm
My family members always say that I am wasting my time here at web, however I know I
am getting experience all the time by reading
thes fastidious posts.
best e-commerce platforms in nigeria · November 28, 2025 at 10:09 pm
Fantastic site. Lots of helpful info here.
I am sending it to a few buddies ans additionally sharing
in delicious. And obviously, thanks on your sweat!
how to start a dropshipping business in nigeria · November 28, 2025 at 11:00 pm
Every weekend i used to pay a visit this web site, as i want enjoyment,
as this this web page conations in fact pleasant funny data too.
dropshipping suppliers for beginners Nigeria · November 29, 2025 at 1:40 am
Wow! This blog looks just like my old one! It’s on a totally different subject but it has pretty much the same layout
and design. Wonderful choice of colors!
logistics and delivery in nigeria e-commerce · November 29, 2025 at 2:55 am
I blog often and I seriously thank you for your information. Your article has truly peaked my interest.
I’m going to bookmark your site and keep checking for new details about once a
week. I subscribed to your Feed as well.
tech accessories dropshipping low competition · November 29, 2025 at 3:06 am
Hey there are using WordPress for your blog platform?
I’m new to the blog world but I’m trying to get
started and set up my own. Do you need any html coding expertise to make your
own blog? Any help would be really appreciated!
filmproductioncortina-136 · November 29, 2025 at 4:05 am
ORBS Production https://filmproductioncortina.com is a full-service film, photo and video production company in Cortina d’Ampezzo and the Dolomites. We create commercials, branded content, sports and winter campaigns with local crew, alpine logistics, aerial/FPV filming and end-to-end production support across the Alps. Learn more at filmproductioncortina.com
外贸推广 · November 29, 2025 at 4:37 am
Write more, thats all I have to say. Literally, it seems as
though you relied on the video to make your point. You definitely know what youre talking about, why waste your intelligence on just posting videos to your
blog when you could be giving us something informative to read?
whatsapp business marketing nigeria · November 29, 2025 at 8:13 am
continuously i used to read smaller articles or reviews that
also clear their motive, and that is also happening with
this paragraph which I am reading at this time.
earn money dropshipping Nigeria · November 29, 2025 at 9:31 am
Good day! I could have sworn I’ve been to this website before but after checking through some of the post I realized it’s new to
me. Anyhow, I’m definitely delighted I found it and I’ll be bookmarking and checking back
often!
e-commerce marketing strategies nigeria · November 29, 2025 at 10:24 am
Hello there! This is my first visit to your blog! We are a team of volunteers and starting a new
initiative in a community in the same niche. Your blog provided us beneficial information to work on. You have done a marvellous job!
e-commerce marketing strategies nigeria · November 29, 2025 at 1:03 pm
What’s up colleagues, its impressive article concerning tutoringand completely
explained, keep it up all the time.
vzlet media · November 29, 2025 at 1:21 pm
Thanks a lot for sharing this with all of us you actually recognize what you are
speaking about! Bookmarked. Please additionally visit my site =).
We may have a link trade agreement between us
website · November 29, 2025 at 4:55 pm
https://x.com/sam86zzcom
https://www.youtube.com/@sam86zzcom/about
https://www.pinterest.com/sam86zzcom/
https://www.twitch.tv/sam86zzcom/about
https://vimeo.com/sam86zzcom
https://www.reddit.com/user/sam86zzcom/
https://gravatar.com/sam86zzcom
https://www.tumblr.com/sam86zzcom
https://www.instapaper.com/p/sam86zzcom
https://www.blogger.com/profile/15206868118459094282
https://disqus.com/by/sam86zzcom/about/
https://qiita.com/sam86zzcom
https://issuu.com/sam86zzcom
https://gitlab.com/sam86zzcom
https://www.renderosity.com/users/id:1795920
https://500px.com/p/sam86zzcom
https://www.callupcontact.com/b/businessprofile/sam86zzcom/9873852
https://www.walkscore.com/people/201415310478/sam86zzcom
https://devpost.com/sam86zzcom
https://anyflip.com/homepage/alzuq#About
https://hubpages.com/@sam86zzcom
https://bio.site/sam86zzcom
https://www.stencyl.com/users/index/1307212
https://gitea.com/sam86zzcom
https://myanimelist.net/profile/sam86zzcom
https://quaint-celestite-174.notion.site/SAM86-trang-ch-2afeb30899338059b320d7c1bc088226?pvs=73
https://pxhere.com/en/photographer-me/4823354
https://song.link/sam86zzcom
https://www.myminifactory.com/users/sam86zzcom
https://www.intensedebate.com/profiles/sam86zzcom
https://vocal.media/authors/sam86zzcom
https://sketchfab.com/sam86zzcom
https://gamblingtherapy.org/forum/users/sam86zzcom/
https://sam86zzcom.bandcamp.com/album/sam86
https://wakelet.com/@sam86zzcom
https://leetcode.com/u/sam86zzcom/
https://jali.me/sam86zzcom
https://teletype.in/@sam86zzcom
https://rapidapi.com/user/sam86zzcom
https://wefunder.com/sam86zzcom
https://community.fabric.microsoft.com/t5/user/viewprofilepage/user-id/1420533
https://jakle.sakura.ne.jp/pukiwiki/?sam86zzcom
https://hub.docker.com/u/sam86zzcom
https://forum.codeigniter.com/member.php?action=profile&uid=204852
https://coub.com/sam86zzcom
https://www.bandlab.com/sam86zzcom
https://www.giveawayoftheday.com/forums/profile/1421649
https://potofu.me/sam86zzcomm
https://www.skypixel.com/users/djiuser-hmatgxetptfp
https://allmyfaves.com/sam86zzcom
https://app.talkshoe.com/user/sam86zzcom
https://plaza.rakuten.co.jp/sam86zzcom/
https://community.m5stack.com/user/sam86zzcom
https://hub.vroid.com/en/users/121539732
https://draft.blogger.com/profile/15206868118459094282
https://profiles.xero.com/people/sam86zzcom
https://community.cloudera.com/t5/user/viewprofilepage/user-id/136417
https://dreevoo.com/profile_info.php?pid=901119
http://www.aunetads.com/view/item-2812292-sam86zzcom.html
https://easymeals.qodeinteractive.com/forums/users/sam86zzcom/
https://decidim.derechoaljuego.digital/profiles/sam86zzcom/activity
https://gifyu.com/sam86zzcom
http://forum.446.s1.nabble.com/sam86zzcom-td113846.html
https://code.antopie.org/sam86zzcom
https://gitlab.vuhdo.io/sam86zzcom
https://slidehtml5.com/homepage/vwep#About
https://www.magcloud.com/user/sam86zzcom
https://phatwalletforums.com/user/sam86zzcom
https://roomstyler.com/users/sam86zzcom
https://doodleordie.com/profile/sam86zzcom
https://www.mapleprimes.com/users/sam86zzcom
https://www.producthunt.com/@sam86zzcom
https://justpaste.it/u/sam86zzcom
https://pumpyoursound.com/u/user/1550139
https://profile.hatena.ne.jp/sam86zzcom/profile
https://www.bitchute.com/channel/xO7UjkW6gaSH
https://tabelog.com/rvwr/sam86zzcom/prof/
https://pbase.com/sam86zzcom
https://magic.ly/sam86zzcom/SAM86-trang-chu
https://jaga.link/sam86zzcom
https://files.fm/sam86zzcom/info
https://www.montessorijobsuk.co.uk/author/sam86zzcom/
https://about.me/sam86zzcom
https://sam86zzcom.webflow.io/
https://substance3d.adobe.com/community-assets/profile/org.adobe.user:F054235E691BE2A90A495FAA@AdobeID
http://gojourney.xsrv.jp/index.php?sam86zzcom
https://pad.koeln.ccc.de/s/DLNmo786X
https://www.haikudeck.com/presentations/sam86zzcom
https://wallhaven.cc/user/sam86zzcom
https://bookmeter.com/users/1643220
https://www.efunda.com/members/people/show_people.cfm?Usr=sam86zzcom
https://www.slmath.org/people/89023
https://nhattao.com/members/user6866437.6866437/
https://rareconnect.org/en/user/sam86zzcom
https://git.forum.ircam.fr/sam86zzcom
https://creator.nightcafe.studio/u/sam86zzcom
http://forum.kryptronic.com/profile.php?id=238695
https://kanban.xsitepool.tu-freiberg.de/s/Syh7Ovtlbl
https://hackmd.okfn.de/s/HytruPKxWx
https://macuisineturque.fr/author/sam86zzcom/
https://talk.plesk.com/members/samzzcom.466207/#about
https://form.jotform.com/253209113117042
https://www.salejusthere.com/profile/0292343478
https://blog.sighpceducation.acm.org/wp/forums/users/sam86zzcom/
https://galleria.emotionflow.com/162294/profile.html
https://telegra.ph/sam86zzcom-11-18
https://californiafilm.ning.com/profile/sam86zzcom
https://events.opensuse.org/users/688287
https://forum.skullgirlsmobile.com/members/sam86zzcom.159721/#about
https://secondstreet.ru/profile/sam86zzcom/
http://fort-raevskiy.ru/community/profile/sam86zzcom/
https://www.divephotoguide.com/user/sam86zzcom
http://jobs.emiogp.com/author/sam86zzcom/
https://marketplace.trinidadweddings.com/author/sam86zzcom/
https://activepages.com.au/profile/sam86zzcom
https://www.udrpsearch.com/user/sam86zzcom
https://www.niftygateway.com/@sam86zzcom/
https://www.speedrun.com/users/sam86zzcom
https://www.fundable.com/sam86zzcom-trang-chu
https://motion-gallery.net/users/865105
https://scrapbox.io/sam86zzcom/SAM86
https://postheaven.net/sam86zzcom/sam86
https://noti.st/sam86zzcom
https://promosimple.com/ps/40706/sam86zzcom
https://spinninrecords.com/profile/sam86zzcom
https://www.chordie.com/forum/profile.php?id=2421174
https://www.aicrowd.com/participants/sam86zzcom
https://www.multichain.com/qa/user/sam86zzcom
https://www.dibiz.com/trieuuyenhanh
https://fyers.in/community/member/X1rBTGmOjv
https://able2know.org/user/sam86zzcom/
https://hieuvetraitim.com/members/sam86zzcom.123021/
https://www.blackhatprotools.info/member.php?259481-sam86zzcom
https://topsitenet.com/profile/sam86zzcom/1501739/
https://www.checkli.com/sam86zzcom
https://www.cheaperseeker.com/u/sam86zzcom
https://unityroom.com/users/sam86zzcom
https://www.video-bookmark.com/bookmark/6950071/sam86zzcom/
https://www.hoaxbuster.com/redacteur/sam86zzcom
https://www.theyeshivaworld.com/coffeeroom/users/sam86zzcom
https://justpaste.me/LDnU5
https://www.equinenow.com/farm/sam86zzcom.htm
https://webscountry.com/author/sam86zzcom-23141/
https://www.abclinuxu.cz/lide/sam86zzcom
https://lifeinsys.com/user/sam86zzcom
http://www.fanart-central.net/user/sam86zzcom/profile
https://www.developpez.net/forums/u1857088/sam86zzcom/
https://findaspring.org/members/sam86zzcom/
https://huzzaz.com/collection/sam86zzcom
https://uiverse.io/profile/sam86_2498
https://blender.community/sam86zzcom/
https://www.notebook.ai/documents/2108399
https://www.xosothantai.com/members/sam86zzcom.580737/
https://maxforlive.com/profile/user/sam86zzcom?tab=about
https://bresdel.com/sam86zzcom
http://www.biblesupport.com/user/780250-sam86zzcom/
https://longbets.org/user/sam86zzcom/
https://apptuts.bio/sam86zzcom
https://rotorbuilds.com/profile/183697
https://legenden-von-andor.de/forum/memberlist.php?mode=viewprofile&u=45915
https://my.clickthecity.com/sam86zzcom
https://iszene.com/user-315955.html
https://akniga.org/profile/1331474-sam86zzcom/
https://tudomuaban.com/chi-tiet-rao-vat/2735266/sam86zzcom.html
https://www.rwaq.org/users/sam86zzcom
http://www.usnetads.com/view/item-133861672-sam86zzcom.html
https://www.heavyironjobs.com/profiles/7485309-sam86-trang-ch
https://transfur.com/Users/sam86zzcom
https://igli.me/sam86zzcom
https://doselect.com/@aba24483f8a1bb5a8f779adde
https://www.apsense.com/user/sam86zzcom
https://undrtone.com/sam86zzcom
https://aprenderfotografia.online/usuarios/sam86zzcom/profile/
https://www.claimajob.com/profiles/7485400-sam86-trang-ch
https://forum.epicbrowser.com/profile.php?id=115961
https://decidem.primariatm.ro/profiles/sam86zzcom/activity
https://golden-forum.com/memberlist.php?mode=viewprofile&u=210122
https://mail.protospielsouth.com/user/95864
https://demo.wowonder.com/sam86zzcom
https://jobs.suncommunitynews.com/profiles/7485518-sam86-trang-ch
https://forum.opnsense.org/index.php?action=profile;u=61790
https://biolinky.co/sam-86-zzcom
https://pads.zapf.in/s/lxE0mOiv7
https://jobs.landscapeindustrycareers.org/profiles/7485556-sam86-trang-ch
https://protospielsouth.com/user/95864
https://www.sythe.org/members/sam86zzcom.1969462/
https://www.malikmobile.com/sam86zzcom
https://fliphtml5.com/homepage/sam86zzcom/sam86/
https://community.m5stack.com/user/sam86zzcom
https://jobs.westerncity.com/profiles/7485619-sam86-trang-ch
https://jobs.njota.org/profiles/7485628-sam86-trang-ch
https://www.nintendo-master.com/profil/sam86zzcom
https://ioninja.com/forum/user/sam86zzcom
https://safechat.com/u/sam86zzcom
https://phijkchu.com/a/sam86zzcom/video-channels
https://forum.issabel.org/u/sam86zzcom
https://savelist.co/profile/users/sam86zzcom
https://www.rctech.net/forum/members/sam86zzcom-517865.html
https://www.huntingnet.com/forum/members/sam86zzcom.html
https://tooter.in/sam86zzcom
https://forum.lexulous.com/user/sam86zzcom
http://www.ssnote.net/users/sam86zzcom
https://www.skool.com/@sam-trang-chu-7831
https://eo-college.org/members/sam86zzcom/
https://hanson.net/users/sam86zzcom
https://schoolido.lu/user/sam86zzcom/
https://kaeuchi.jp/forums/users/sam86zzcom/
https://theafricavoice.com/profile/sam86zzcom
https://www.directorylib.com/domain/sam86zz.com
https://liulo.fm/sam86zzcom
https://www.nicovideo.jp/user/142315131
https://linkstack.lgbt/@sam86zzcom
https://divisionmidway.org/jobs/author/sam86zzcom/
https://gitlab.aicrowd.com/sam86zzcom
https://fortunetelleroracle.com/profile/sam86zzcom
https://www.openrec.tv/user/sam86zzcom/about
https://www.shippingexplorer.net/en/user/sam86zzcom/219136
https://golosknig.com/profile/sam86zzcom/
https://spiderum.com/nguoi-dung/sam86zzcom
https://fabble.cc/sam86zzcom
https://www.maanation.com/sam86zzcom
https://formulamasa.com/elearning/members/sam86zzcom/?v=96b62e1dce57
https://www.openlb.net/forum/users/sam86zzcom/
https://linksta.cc/@sam86zzcom
https://oyaschool.com/users/sam86zzcom/
https://www.annuncigratuititalia.it/author/sam86zzcom/
https://luvly.co/users/sam86zzcom
https://www.catapulta.me/users/sam86zzcom
https://ketcau.com/member/106553-sam86zzcom
https://bitspower.com/support/user/sam86zzcom
https://gravesales.com/author/sam86zzcom/
https://dongnairaovat.com/members/sam86zzcom.57667.html
https://www.syncdocs.com/forums/profile/sam86zzcom
https://acomics.ru/-sam86zzcom
https://rant.li/sam86zzcom/sam86
https://fanclove.jp/profile/qR2le64GJE
https://app.hellothematic.com/creator/profile/1083349
https://pc.poradna.net/users/1081411083-sam86zzcom
https://espritgames.com/members/49233534/
https://web.ggather.com/sam86zzcom
https://3dwarehouse.sketchup.com/by/sam86zzcom
https://careers.gita.org/profiles/7486082-sam86-trang-ch
https://source.coderefinery.org/sam86zzcom
https://videogamemods.com/members/sam86zzcom/
https://sam86zzcom.blogspot.com/2025/11/sam86zzcom.html
https://medibang.com/author/27486560/
https://onlinevetjobs.com/author/sam86zzcom/
https://hackaday.io/sam86zzcom
http://www.canetads.com/view/item-4285846-sam86zzcom.html
https://www.vevioz.com/sam86zzcom
https://www.iglinks.io/sam86zzcom-mhs
https://www.passes.com/sam86zzcom
https://dialog.eslov.se/profiles/sam86zzcom/activity
https://linkmix.co/46905378
https://help.orrs.de/user/sam86zzcom
https://truckymods.io/user/424116
https://us.enrollbusiness.com/BusinessProfile/7640987/sam86zzcom
https://haveagood.holiday/users/467927
https://www.halaltrip.com/user/profile/284198/sam86zzcom/
https://www.adpost.com/u/sam86zzcom/
https://www.laundrynation.com/community/profile/sam86zzcom/
https://duvidas.construfy.com.br/user/sam86zzcom
https://feyenoord.supporters.nl/profiel/116573/sam86zzcom
https://marshallyin.com/members/sam86zzcom/
https://profile.sampo.ru/sam86zzcom
https://www.hostboard.com/forums/members/sam86zzcom.html
https://dapp.orvium.io/profile/sam86–trang-chu
http://forum.bokser.org/user-1408943.html
https://www.fantasyplanet.cz/diskuzni-fora/users/sam86zzcom/
https://www.sciencebee.com.bd/qna/user/sam86zzcom
https://bandori.party/user/353586/sam86zzcom/
https://www.spigotmc.org/members/sam86zzcom.2418202/
https://wibki.com/sam86zzcom
https://www.tizmos.com/sam86zzcom/
https://freeimage.host/sam86zzcom
https://www.brownbook.net/business/54504596/sam86zzcom
https://kktix.com/user/8070846
https://www.vnbadminton.com/members/sam86zzcom.114102/
http://palangshim.com/space-uid-4726674.html
https://blog.ulifestyle.com.hk/sam86zzcom
https://gram.social/sam86zzcom
https://commoncause.optiontradingspeak.com/index.php/community/profile/sam86zzcom/
https://participa.aytojaen.es/profiles/sam86zzcom/activity
https://www.facekindle.com/sam86zzcom
https://www.aipictors.com/users/13fdb8d5-ef4b-6763-9522-2317b6ed26f6
https://community.hubspot.com/t5/user/viewprofilepage/user-id/1014450
https://partecipa.poliste.com/profiles/sam86zzcom/activity
https://cuchichi.es/author/sam86zzcom/
https://sam86zzcom.stck.me/profile
https://www.navacool.com/forum/topic/195195/sam86zzcom
https://www.zubersoft.com/mobilesheets/forum/user-105666.html
https://amaz0ns.com/forums/users/sam86zzcom/
https://diendan.bftvietnam.com/members/18408-sam86zzcom.html
https://bachhoadep.com/members/20217-sam86zzc.html
https://demo.userproplugin.com/profile/sam86zzcom/
https://bulkwp.com/support-forums/users/sam86zzcom/
https://forum.aceinna.com/user/sam86zzcom
https://writexo.com/share/c88c01221bce
https://freeicons.io/profile/856437
https://es.stylevore.com/user/sam86zzcom
https://sciencemission.com/profile/sam86zzcom
https://zeroone.art/profile/sam86zzcom
https://experiment.com/users/sam86zzcom/
https://pixelfed.uno/sam86zzcom
http://delphi.larsbo.org/user/sam86zzcom
https://eternagame.org/players/581097
https://www.songback.com/profile/91274/about
https://minecraftcommand.science/profile/sam86zzcom
https://connect.gt/user/sam86zzcom
whatsapp business marketing nigeria · November 29, 2025 at 9:09 pm
What a stuff of un-ambiguity and preserveness of precious familiarity about unpredicted
emotions.
federatsia-869 · November 30, 2025 at 9:06 am
Хочешь развлечься? купить альфа пвп федерация – это проводник в мир покупки запрещенных товаров, можно купить гашиш, купить мефедрон, купить кокаин, купить меф, купить экстази, купить альфа пвп, купить гаш в различных городах. Москва, Санкт-Петербург, Краснодар, Владивосток, Красноярск, Норильск, Екатеринбург, Мск, СПБ, Хабаровск, Новосибирск, Казань и еще 100+ городов.
1win-969 · November 30, 2025 at 10:23 am
1win партнерская 1win зеркало рабочее на сегодня
bonus-casino-911 · November 30, 2025 at 11:04 am
казино з бонусами бонуси казино
earn money dropshipping Nigeria · November 30, 2025 at 11:17 am
I really like your blog.. very nice colors & theme.
Did you create this website yourself or did you hire someone to do it for you?
Plz reply as I’m looking to design my own blog and would like to find out where u got this from.
cheers
best dropshipping suppliers in nigeria · November 30, 2025 at 12:49 pm
Thanks for another wonderful post. Where else could anyone get
that type of info in such an ideal means of writing?
I’ve a presentation subsequent week, and I am on the search for
such information.
binance sign up bonus · November 30, 2025 at 2:51 pm
Can you be more specific about the content of your article? After reading it, I still have some doubts. Hope you can help me.
Đồng hồ nữ thời trang cao cấp · November 30, 2025 at 3:51 pm
Tһanks foг finally talkіng about > The Reason Fruit
is Good for You Even Thoսgһ it's Filled With Sugaг – Goldden Health Metod Đồng
hồ nữ thời trang cao cấp
www.lab.justusdeitert.de · November 30, 2025 at 7:19 pm
casino yes
References:
https://gitea.ysme.top/marcygerace195
j6p2.icu · November 30, 2025 at 7:38 pm
Ridiculous story there. What happened after?
Thanks!
mostbet-784 · December 1, 2025 at 12:30 am
kasyno mostbet mostbet
influencer marketing in nigeria · December 1, 2025 at 4:51 am
Great site. Plenty of useful info here. I am sending it to a few friends
ans also sharing in delicious. And naturally, thanks in your sweat!
www.bookmyaccountant.co · December 1, 2025 at 5:08 am
gamehouse casino
References:
https://git.sudo-fhir.au/leyterrance94
dropshipping products Nigeria · December 1, 2025 at 5:26 am
Quality content is the important to invite the users to go
to see the website, that’s what this website is providing.
mostbet-431 · December 1, 2025 at 7:55 am
oficjalne kasyno mostbet aplikacja mostbet na androida
casino-games-767 · December 1, 2025 at 7:56 am
онлайн ігри казино ігри казино онлайн
https://asteroidsathome.net/boinc/view_profile.php?userid=1000498 · December 1, 2025 at 10:41 am
First of all I would like to say great blog! I
had a quick question that I’d like to ask if you don’t mind.
I was interested to know how you center yourself and
clear your thoughts prior to writing. I have had a difficult time clearing
my mind in getting my thoughts out there. I truly do take pleasure in writing however it just seems like the first 10 to
15 minutes are usually wasted just trying to figure out how to begin. Any ideas or hints?
Thank you!
inkweel.com · December 1, 2025 at 11:01 am
Thanks very interesting blog!
dropshipping suppliers for beginners Nigeria · December 1, 2025 at 11:37 am
Hurrah! Finally I got a webpage from where I be able to in fact get helpful information concerning my
study and knowledge.
payment gateways for nigerian online stores · December 1, 2025 at 1:09 pm
I am curious to find out what blog platform you happen to be
utilizing? I’m experiencing some minor security issues
with my latest website and I would like to find something more secure.
Do you have any solutions?
วิเคราะห์บอลวันนี้ · December 1, 2025 at 6:45 pm
Your method of explaining the whole thing in this article
is truly nice, every one can easily know it, Thanks a lot.
Titan Rise Male Enhancement · December 1, 2025 at 6:47 pm
Embark on muscle mastery, where strength and fitness are trusted companions. Today, dive into the intricate web of muscle development. Picture here protein as the master architect, your body a canvas for sculpting. Let the symphony of carbs and healthy fats create your fitness masterpiece with an enigmatic calorie surplus brushstroke. Dive deep into the discussion, and it will become clear how much protein, carbs, and fat are required to build muscle. What is the 40 30 30 diet for bodybuilding and muscle gaining? What is the 60 25 15 diet? Is a 40 40 20 diet good? Does protein build your muscle without any working out? In the quest for muscle gain, the calorie game takes the lead. The calories you require are a unique blend, influenced by your age, gender, weight, height, and activity level. As a general guideline, it’s recommended to surpass your maintenance calories by 250 to 500 calories per day.
my page; http://www.mandarin-badenweiler.de/wp-content/themes/eatery/nav.php?-Menu-=https://www.oltonyszalon.com/smartblog/1_from-now-we-are-certified-web-agency.html
belarus-news-899 · December 1, 2025 at 8:49 pm
новости спорта беларуси главные новости беларуси
วิเคราะห์บอลวันนี้ · December 1, 2025 at 8:54 pm
I am regular visitor, how are you everybody?
This post posted at this website is truly nice.
ทีเด็ดบอล · December 1, 2025 at 9:24 pm
Its like you read my mind! You appear to know a lot
about this, like you wrote the book in it or something. I
think that you can do with some pics to drive the message home
a little bit, but instead of that, this is magnificent blog.
A fantastic read. I will certainly be back.
วิเคราะห์บอลวันนี้ · December 2, 2025 at 12:02 am
What a material of un-ambiguity and preserveness of
precious knowledge concerning unexpected feelings.
https://asiel.com.co · December 2, 2025 at 9:59 am
It’s an amazing paragraph designed for all the web viewers; they will get
advantage from it I am sure.
Good · December 2, 2025 at 10:02 am
You’re so interesting! I do not believe I’ve truly read through
anything like this before. So good to find another person with some genuine
thoughts on this subject matter. Seriously.. thank you for starting this up.
This website is something that’s needed on the web, someone with some
originality!
propose.lk · December 2, 2025 at 12:11 pm
los angeles casino
https://wp.nootheme.com/jobmonster/dummy2/companies/best-no-deposit-bonus-online-casinos-in-australia-2025/ wp.nootheme.com
https://git.rokiy.com/gkdmajor72658 https://git.rokiy.com/gkdmajor72658
https://music.1mm.hk/marceloguthrie music.1mm.hk
https://srsbkn.eu.org/bobbyednu86470 srsbkn.eu.org
https://tracker.kroginski.de/claudiofinney tracker.kroginski.de
https://jii.li/wilda44731977 jii.li
https://99link.me/wykaP https://99link.me/wykaP
https://hypmediagh.com/abbeyday80658 hypmediagh.com
https://www.nextlink.hk/@jeanetto350665 http://www.nextlink.hk
https://www.besolife.com/@yvettepulido19 besolife.com
https://dreamwhack.club/forums/users/kerriw41435/ https://dreamwhack.club/forums/users/kerriw41435/
https://music.batalp.com/denisha5159403 https://music.batalp.com/
https://www.advertiseajob.co.uk/employer/best-online-casinos-in-australia-for-april-2025-expert-reviews-of-real-money-sites/ http://www.advertiseajob.co.uk
https://git.tea-assets.com/nereidaluna60 https://git.tea-assets.com
https://clone-deepsound.paineldemonstrativo.com.br/tabathableakle https://clone-deepsound.paineldemonstrativo.com.br/tabathableakle
https://www.naukriupdate.pk/companies/fast-payout-casinos-in-australia-2025-instant-withdrawals/ https://www.naukriupdate.pk/companies/fast-payout-casinos-in-australia-2025-instant-withdrawals/
https://nationaladvocateacademy.com/read-blog/199_best-online-casinos-in-australia-2025-instant-withdrawal-casinos.html nationaladvocateacademy.com
https://inmessage.site/@shereeromilly8 inmessage.site
References:
http://47.92.23.195:8418/jameylabillier
วิเคราะห์บอลวันนี้ · December 2, 2025 at 2:43 pm
Thank you, I’ve recently been searching for information about this subject for a
long time and yours is the best I’ve found out till
now. However, what in regards to the conclusion? Are you positive in regards to the supply?
ทีเด็ดบอลวันนี้ · December 2, 2025 at 3:54 pm
I’m not sure why but this site is loading very slow for me.
Is anyone else having this problem or is it a issue on my end?
I’ll check back later and see if the problem still exists.
loredz.com · December 2, 2025 at 8:23 pm
captain cook casino
http://u.42.pl/?url=https://raindrop.io/sandurwnom/bookmarks-63760906 u.42.pl
http://smarter-0.7ba.info/out.php?url=https://www.seo-bookmarks.win/100-up-to-1-btc-in-crypto http://smarter-0.7ba.info/out.php?url=https://www.seo-bookmarks.win/100-up-to-1-btc-in-crypto
http://gidonline-film.ru/user/marmaicuog gidonline-film.ru
http://www.bookmerken.de/?url=https://tvrs.pro/user/kanyonnemx http://www.bookmerken.de
http://ya4r.net/go.php?url=https://www.inkitt.com/hafgarzhjx ya4r.net
https://ronaldinho-gaucho.org/user/gwaniepwqa https://ronaldinho-gaucho.org
http://northstarshoes.com/europe/out.php?url=https://www.bookmarking-fox.win/crown-play-casino-australia-a-detailed-review-of-games-and-bonuses northstarshoes.com
https://pt.grepolis.com/start/redirect?url=https://www.hotel-bookmarkings.win/flamingo-review-flamingo-las-vegas-reviewed-for-2025 pt.grepolis.com
http://www.google.co.mz/url?sa=t&rct=j&q=&esrc=s&source=web&cd=8&cad=rja&sqi=2&ved=0CGkQFjAH&url=https://www.4shared.com/s/fHF92c9CPjq http://www.google.co.mz
http://bax.kz/redirect?url=https://www.bookmarking-keys.win/browse-the-best-restaurants-bars bax.kz
http://home4dsi.com/chat/redirect.php?url=https://www.emergbook.win/bellagio-las-vegas-deluxe-las-vegas-nv-hotels-gds-reservation-codes-travel-weekly home4dsi.com
http://www.badmoon-racing.jp/frame/?url=https://duvidas.construfy.com.br/user/rhyannkvnh http://www.badmoon-racing.jp/
http://www.bausch.kr/ko-kr/redirect/?url=https://v2.friends-lordfilm.top/user/rewardjvpy http://www.bausch.kr/ko-kr/redirect/?url=https://v2.friends-lordfilm.top/user/rewardjvpy
http://www.newsdiffs.org/article-history/?url=https://www.bookmarking-maze.win/best-online-pokies-australia-2025-top-10-au-pokie-sites http://www.newsdiffs.org/article-history/?url=https://www.bookmarking-maze.win/best-online-pokies-australia-2025-top-10-au-pokie-sites
https://www.blaze-bookmarks.win/military-discounts-on-casinos-and-resorts http://www.blaze-bookmarks.win
https://www.bookmarkingvictor.win/razed-review-2025-games-bonuses-features bookmarkingvictor.win
http://link.chatujme.cz/redirect?url=https://www.coast-bookmarks.win/hotels-with-spa-in-melbourne link.chatujme.cz
http://www.bausch.co.nz/en-nz/redirect/?url=https://www.4shared.com/s/fLTBoBfIVjq http://www.bausch.co.nz
References:
http://tobaccohouse.ge/user/sammongzxa
ทีเด็ดบอลวันนี้ · December 2, 2025 at 10:24 pm
I think that is among the most significant information for me.
And i am glad reading your article. But wanna remark on few
normal things, The web site style is wonderful,
the articles is really great : D. Just right process, cheers
jwac.asureforce.net · December 2, 2025 at 10:42 pm
casino online sicuri
http://italianculture.net/redir.php?url=https://go.bubbl.us/eeea68/ac24?/Bookmarks http://italianculture.net
http://timoore.eu/skins/timoore/redirect.php?url=https://www.designspiration.com/petramgiew/ http://timoore.eu/skins/timoore/redirect.php?url=https://www.designspiration.com/petramgiew/
http://www.badmoon-racing.jp/frame/?url=https://www.plurk.com/p/3i0ylsanxm http://www.badmoon-racing.jp
http://silvija.wip.lt/redirect.php?url=https://v3.volshebnyj-uchastok-lorfilm.bio/user/cuingowtbf silvija.wip.lt
http://www.old.xn--90asjdo3a.xn--p1ai/user/ripinnanhb http://www.old.90asjdo3a.рф
http://www.dicodunet.com/out.php?url=https://blurriechan.blurriecon.com/member.php?action=profile&uid=173036 http://www.dicodunet.com
https://ts-automation.az/user/amuloschkk https://ts-automation.az/user/amuloschkk
https://fotosall.ru/user/aspaidtwcn fotosall.ru
http://frienddo.com/out.php?url=https://kameronzhao876.timeforchangecounselling.com/hotel-casino frienddo.com
http://login.tiscali.cz/?url=https://www.bookmarking-online.win/cleobetra-casino-review-1-000-bonus-275-free-spins login.tiscali.cz
http://gamesjp.com/jump.php?url=https://www.polystoned.de/User-albiussrzm http://gamesjp.com/jump.php?url=https://www.polystoned.de/User-albiussrzm
http://voidstar.com/opml/?url=https://www.oscarbookmarks.win/official-site-in-ca http://voidstar.com/opml/?url=https://www.oscarbookmarks.win/official-site-in-ca
http://www.memememo.com/link.php?url=https://equinox-hound-0e5.notion.site/AmunRa-Casino-No-Deposit-Bonus-Claim-Yours-Today-2bc80b4c091e80a7b3dac38b79f3c273?source=copy_link http://www.memememo.com
http://www.vab.ua/bitrix/rk.php?goto=http://delphi.larsbo.org/user/wychantzqa http://www.vab.ua
https://storage.athlinks.com/logout.aspx?returnurl=https://baby-newlife.ru/user/profile/354274 storage.athlinks.com
https://telegra.ph/Download-11-30-10 telegra.ph
http://www.heatherseats@raovat5s.biz/redirect/?url=https://camrusltez.contently.com/ http://www.heatherseats@raovat5s.biz
http://smarter-0.7ba.info/out.php?url=https://www.bookmark-xray.win/new-york-new-york-hotel-and-casino-family-friendly-las-vegas http://smarter-0.7ba.info/out.php?url=https://www.bookmark-xray.win/new-york-new-york-hotel-and-casino-family-friendly-las-vegas
References:
http://forums.mrkzy.com/redirector.php?url=https://www.bookmarking-presto.win/casino-townsville-north-queensland
วิเคราะห์บอลวันนี้ · December 2, 2025 at 11:57 pm
A motivating discussion is definitely worth comment.
I do believe that you ought to publish more about this issue, it might not be a taboo subject but typically
people don’t talk about such topics. To the next! Best wishes!!
http://drakonas.wip.lt/redirect.php?url=https://www.demilked.com/author/melunedezb/ · December 3, 2025 at 12:02 am
seneca buffalo creek casino
http://seclub.org/main/goto/?url=https://www.bestbookmarks.win/our-9-favorite-ocean-city-casino-hotels-maryland-united-states-in-2025 seclub.org
http://ssomgmt.ascd.org/profile/createsso/createsso.aspx?returnurl=https://www.marocbikhir.com/user/profile/464574 ssomgmt.ascd.org
https://lukashwoe624.fotosdefrases.com/winshark-casino-review-bonuses-promotions-games https://lukashwoe624.fotosdefrases.com
http://www.c9wiki.com/link.php?url=http://www.writemob.com//user/abethirzaw http://www.c9wiki.com/
http://link.chatujme.cz/redirect?url=https://www.animenewsnetwork.com/bbs/phpBB2/profile.php?mode=viewprofile&u=1128757 http://link.chatujme.cz/redirect?url=https://www.animenewsnetwork.com/bbs/phpBB2/profile.php?mode=viewprofile&u=1128757
http://taxibestellung24.de/php/redirect.php?url=https://educhoice.co.uk/user/profile/69238 taxibestellung24.de
http://www.garrisonexcelsior.com/redirect.php?url=https://files.fm/u/nbdfjq8k3h http://www.garrisonexcelsior.com
http://www.c9wiki.com/link.php?url=http://www.writemob.com//user/abethirzaw http://www.c9wiki.com
http://www.google.co.mz/url?sa=t&rct=j&q=&esrc=s&source=web&cd=8&cad=rja&sqi=2&ved=0CGkQFjAH&url=https://www.stall-bookmarks.win/country-club-tasmania-in-launceston-australia http://www.google.co.mz
http://www.ybcxz.com/link.php?url=https://beunnaczox.contently.com/ http://www.ybcxz.com/link.php?url=https://beunnaczox.contently.com
https://storage.athlinks.com/logout.aspx?returnurl=https://www.novabookmarks.win/slotorama-play-free-slots-online-slot-bonuses https://storage.athlinks.com
https://medknigkii-v-lipetskee.ru/user/gwennoqbzw medknigkii-v-lipetskee.ru
https://www.bookmarking-jet.win/brisbane-s-resort-and-casino-precinct-opens http://www.bookmarking-jet.win
https://fr.grepolis.com/start/redirect?url=https://500px.com/p/bilbukfgbp fr.grepolis.com
http://www.premio-tuning-bestellshop.at/Home/tabid/2115/Default.aspx?returnurl=http://uzserial.net/user/ortioneuaf http://www.premio-tuning-bestellshop.at/Home/tabid/2115/Default.aspx?returnurl=http://uzserial.net/user/ortioneuaf
https://www.shop.magic-tricks.ru/user/morvinadjk https://www.shop.magic-tricks.ru
http://supremacy.be/user/teigetfyyz http://supremacy.be/
https://thinfi.com/0kzg7 https://thinfi.com/0kzg7
References:
http://member.8090.com/exit.php?url=https://www.mapleprimes.com/users/cassinqcwa
Https Www Joker123 Net List Games Free Download · December 3, 2025 at 2:04 am
You got a very excellent website, Glad I noticed it through yahoo.
my web site http://ttps://Hastaoda.Serhatatalayevis.com%2F224443%2Fpopular-featured-games/
facts · December 3, 2025 at 2:27 am
This excellent website truly has all of the information and facts I needed about this subject and didn’t
know who to ask.
Cheap prescription drugs without a prescription · December 3, 2025 at 3:29 am
I was recommended this website by means of my cousin. I’m not
sure whether or not this submit is written via him as no
one else realize such targeted approximately my problem.
You are amazing! Thank you!
betpix · December 3, 2025 at 4:58 am
Yo, I’m thinking about dropping a few bucks on betpix. Hope they pay out fast, ain’t got time for waiting around!
https://pwn-zone.ru · December 3, 2025 at 7:42 am
george thorogood i drink alone
http://vip.cengfan6.com/goto.php?url=https://lordfilmshd.club/user/duwainrpyd vip.cengfan6.com
http://m.shopinanchorage.com/redirect.aspx?url=https://educhoice.co.uk/user/profile/69270 http://m.shopinanchorage.com/
https://www.tool-bookmarks.win/the-merrywell-beer-garden-burgers http://www.tool-bookmarks.win
http://www.bausch.com.tw/zh-tw/redirect/?url=https://www.phone-bookmarks.win/launceston-casino-let-the-good-times-roll http://www.bausch.com.tw/zh-tw/redirect/?url=https://www.phone-bookmarks.win/launceston-casino-let-the-good-times-roll
http://puellulas.tw/m-rauterbvcc puellulas.tw
https://s1.byrutorg.com/user/binasssqzs https://s1.byrutorg.com/user/binasssqzs
https://www.bookmarking-jet.win/best-online-casinos-in-australia-2025-top-10-real-money-au-casino-sites http://www.bookmarking-jet.win
http://mb.tickets.wonderworksonline.com/cart.aspx?returnurl=https://files.fm/u/nbdfjq8k3h mb.tickets.wonderworksonline.com
http://www.garrisonexcelsior.com/redirect.php?url=https://duvidas.construfy.com.br/user/erwineuvtg http://www.garrisonexcelsior.com
https://www.click-bookmark.win/just-casino-c-5-000-400-fs-bonus https://www.click-bookmark.win/just-casino-c-5-000-400-fs-bonus
http://www.sa-live.com/merror.html?errortype=1&url=https://daz3d-poser.net/user/ormodaeyqj http://www.sa-live.com/
http://set.ua/bitrix/rk.php?goto=http://qa.doujiju.com?qa=user&qa_1=entinefvbz set.ua
http://noreferer.net/?url=https://support.mikrodev.com?qa=user&qa_1=inbardcsjo http://noreferer.net/?url=https://support.mikrodev.com?qa=user&qa_1=inbardcsjo
http://www.amicacard.it/data/banner/html5_convenzioni_gold/?url=https://augustoisg372.timeforchangecounselling.com/the-allure-of-digital-wheels-exploring-the-mystique-of-methspin-casino http://www.amicacard.it
http://www.pageglance.com/external/ext.aspx?url=https://www.bookmarks4all.win/casino-games-that-pay-real-money-2025-review http://www.pageglance.com
https://jwac.asureforce.net/Redirect.aspx?PunchTime=&LoginId=&LogoffReason=&redirecturl=https://www.bookmarking-planet.win/top-7-restaurants-in-burswood-november-2025 https://jwac.asureforce.net/Redirect.aspx?PunchTime=&LoginId=&LogoffReason=&redirecturl=https://www.bookmarking-planet.win/top-7-restaurants-in-burswood-november-2025
https://telegra.ph/MGM-Grand-casino-completes-300-million-renovation-of-4000-rooms-suites-Casinos–Gaming-Business-11-30 telegra.ph
http://0.7ba.info/out.php?url=https://remingtonkxmr649.iamarrows.com/30-online-casino-games-to-play-for-real-money http://0.7ba.info/out.php?url=https://remingtonkxmr649.iamarrows.com/30-online-casino-games-to-play-for-real-money
References:
http://www.garrisonexcelsior.com/redirect.php?url=https://www.bookmarkpage.win/hotels-in-new-york-city-ny
วิเคราะห์บอล · December 3, 2025 at 9:27 am
Do you mind if I quote a couple of your articles as long
as I provide credit and sources back to your site?
My blog is in the exact same niche as yours and my visitors would definitely benefit from
some of the information you present here.
Please let me know if this okay with you.
Thanks!
ทีเด็ดบอล · December 3, 2025 at 10:03 am
Wow, incredible weblog format! How long have you ever been blogging for?
you make running a blog look easy. The full glance of your site is wonderful, as neatly as the content!
ทีเด็ดบอลวันนี้ · December 3, 2025 at 12:21 pm
Fantastic website you have here but I was
curious if you knew of any user discussion forums that cover the
same topics talked about in this article? I’d really like to be a part of group where I can get comments from other
experienced people that share the same interest. If you have
any suggestions, please let me know. Thanks a lot!
dailyjililoginregister · December 3, 2025 at 12:49 pm
Dailyjililoginregister streamlines the whole process, which I appreciate. Registration was quick and painless, and logging in everyday is a breeze. If you’re tired of complicated sign-ups, give it a shot: dailyjililoginregister.
http://www.joi3.com/ · December 3, 2025 at 12:53 pm
casino cast
http://www.premio-tuning-bestellshop.at/Home/tabid/2115/Default.aspx?returnurl=https://bh90210.ru/user/angelmtqfi http://www.premio-tuning-bestellshop.at
https://ciekawawarszawa.ueuo.com/user/neasalstbm ciekawawarszawa.ueuo.com
https://www.shop.magic-tricks.ru/user/miriennarn https://www.shop.magic-tricks.ru
https://store.magic-tricks.ru//user/rothesebea store.magic-tricks.ru
https://storage.athlinks.com/logout.aspx?returnurl=https://www.spreaker.com/podcast/branorsotj–6809431 https://storage.athlinks.com/logout.aspx?returnurl=https://www.spreaker.com/podcast/branorsotj–6809431
http://www.med.uz/bitrix/rk.php?goto=https://www.anobii.com/en/01e70f35a7cd154e3a/profile/activity http://www.med.uz/
https://storage.athlinks.com/logout.aspx?returnurl=https://www.hungama.site/member.php?action=profile&uid=19965 storage.athlinks.com
http://www.hyoito-fda.com/out.php?url=https://www.demilked.com/author/kenseysudw/ http://www.hyoito-fda.com/out.php?url=https://www.demilked.com/author/kenseysudw
http://www.sa-live.com/merror.html?errortype=1&url=https://www.anime-planet.com/users/mirienuvzv http://www.sa-live.com/
http://www.akwaibomnewsonline.com/news/index.php?url=https://daltonctzz738.theglensecret.com/justcasino-best-casino-for-real-money-online http://www.akwaibomnewsonline.com
http://mb.tickets.wonderworksonline.com/cart.aspx?returnurl=http://f91306v7.beget.tech/member.php?action=profile&uid=217485 mb.tickets.wonderworksonline.com
http://dle1.xn--31-6kc3bfr2e.xn--p1ai/user/searynlmsh dle1.31-6kc3bfr2e.рф
https://m.kaskus.co.id/redirect?url=https://www.demilked.com/author/freadhcadp/ m.kaskus.co.id
http://www.google.co.mz/url?sa=t&rct=j&q=&esrc=s&source=web&cd=8&cad=rja&sqi=2&ved=0CGkQFjAH&url=https://orderviag.com//member.php?action=profile&uid=64747 http://www.google.co.mz
http://www.tradeportalofindia.org/CountryProfile/Redirect.aspx?hidCurMenu=divOthers&CountryCode=32&CurrentMenu=IndiaandEU&Redirecturl=https://www.normalbookmarks.win/new-york-new-york-las-vegas-restaurants-in-2025 http://www.tradeportalofindia.org
https://cashback-banki.ru/user/lavellbfwt cashback-banki.ru
http://smarter-0.7ba.info/out.php?url=https://www.easybookmarkings.win/crown-melbourne-review-2025-guide-for-gaming-info-stats smarter-0.7ba.info
http://noexcuselist.com/li/?url=https://patriot-v1.tnt-lordfilm.net/user/ravettxrco http://noexcuselist.com
References:
https://litbu.ru/user/tuloeftzpl
aanorthflorida.org · December 3, 2025 at 2:58 pm
online dating site
http://timoore.eu/skins/timoore/redirect.php?url=https://www.beacon-bookmarks.win/the-best-bitcoin-casino-sites-bitcoin-gambling-guide timoore.eu
https://bullitfilm.ru/user/ceacheuupu bullitfilm.ru
https://getpocket.com/redirect?url=https://atavi.com/share/xktueaz1dw6vc https://getpocket.com
https://volontereco.ru/user/laineovya https://volontereco.ru/user/laineovya
http://mb.tickets.wonderworksonline.com/cart.aspx?returnurl=http://qa.doujiju.com?qa=user&qa_1=golivebiho http://mb.tickets.wonderworksonline.com/
https://airvent.kz/user/lolfurwjpg airvent.kz
http://apps.stablerack.com/flashbillboard/redirect.asp?url=https://www.pexels.com/@jayden-hewitt-2157820376/ http://apps.stablerack.com/
https://todosobrelaesquizofrenia.com/Redirect/?url=https://wakelet.com/wake/SA-jhGtN91kFUafl8Vtee todosobrelaesquizofrenia.com
http://distributors.maitredpos.com/forwardtoafriend.aspx?returnurl=https://www.instapaper.com/read/1937975902 http://distributors.maitredpos.com
http://s.kakaku.com/jump/jump.asp?url=https://www.huntingnet.com/forum/members/hirinazoyq.html http://s.kakaku.com/jump/jump.asp?url=https://www.huntingnet.com/forum/members/hirinazoyq.html
http://group.so-ten.jp/redirect.php?rurl=https://www.bookmarkingqueen.win/country-club-casino-launceston-book-online-save http://group.so-ten.jp
https://dongxi.douban.com/link2/?url=https://www.paste-bookmarks.win/20-best-online-casinos-in-australia-for-real-money dongxi.douban.com
http://distributors.maitredpos.com/forwardtoafriend.aspx?returnurl=https://www.booknose.win/10-best-australian-online-casinos-2025 http://distributors.maitredpos.com/forwardtoafriend.aspx?returnurl=https://www.booknose.win/10-best-australian-online-casinos-2025
http://noexcuselist.com/li/?url=https://blurriechan.blurriecon.com/member.php?action=profile&uid=173038 noexcuselist.com
http://www.sa-live.com/merror.html?errortype=1&url=https://www.anime-planet.com/users/mirienuvzv http://www.sa-live.com/merror.html?errortype=1&url=https://www.anime-planet.com/users/mirienuvzv
http://www.serbiancafe.com/lat/diskusije/new/redirect.php?url=https://papaly.com/e/Cn80 http://www.serbiancafe.com/lat/diskusije/new/redirect.php?url=https://papaly.com/e/Cn80
https://pl.grepolis.com/start/redirect?url=https://beunnaczox.contently.com/ pl.grepolis.com
http://www.google.co.mz/url?sa=t&rct=j&q=&esrc=s&source=web&cd=8&cad=rja&sqi=2&ved=0CGkQFjAH&url=https://orderviag.com//member.php?action=profile&uid=64747 http://www.google.co.mz/url?sa=t&rct=j&q=&esrc=s&source=web&cd=8&cad=rja&sqi=2&ved=0CGkQFjAH&url=https://orderviag.com//member.php?action=profile&uid=64747
References:
http://sergiubaluta.com/site/redirect.php?url=http://sitamge.ru/user/cloveshjaq
ddpromote.com · December 3, 2025 at 5:56 pm
casino action
https://100kursov.com/away/?url=https://www.shop.magic-tricks.ru/user/gettannqhq https://100kursov.com/away/?url=https://www.shop.magic-tricks.ru/user/gettannqhq
http://football.sodazaa.com/out.php?url=https://pixabay.com/users/53466129/ http://football.sodazaa.com/out.php?url=https://pixabay.com/users/53466129/
http://noexcuselist.com/li/?url=http://qa.doujiju.com?qa=user&qa_1=melvinvtzp http://noexcuselist.com
http://frienddo.com/out.php?url=https://Fortuna27.ru/user/meggurgxmu frienddo.com
http://www.pesscloud.com/PessServer.Web/Utility/Login/LoginPess.aspx?Returnurl=http://damsan.net/member.php?action=profile&uid=400403 http://www.pesscloud.com
https://cloudview.ru/user/mantiaiupl https://cloudview.ru/user/mantiaiupl
http://nora.biz/go.php?url=http://www.mediafire.com/file/5pz0vynbv9g0cd7/pdf-59189-46609.pdf http://nora.biz/go.php?url=http://www.mediafire.com/file/5pz0vynbv9g0cd7/pdf-59189-46609.pdf
http://member.8090.com/exit.php?url=http://f91306v7.beget.tech/member.php?action=profile&uid=217498 http://member.8090.com/exit.php?url=http://f91306v7.beget.tech/member.php?action=profile&uid=217498
https://www.yankee-bookmarkings.win/new-york-new-york-las-vegas-parking-fee-2023-map-valet http://www.yankee-bookmarkings.win
https://storage.athlinks.com/logout.aspx?returnurl=https://www.adscron.com/user/profile/2355 https://storage.athlinks.com/logout.aspx?returnurl=https://www.adscron.com/user/profile/2355
http://www.siteglimpse.com/external/ext.aspx?url=https://pixabay.com/users/53467880/ http://www.siteglimpse.com/
http://www.bizmandu.com/redirect?url=https://duvidas.construfy.com.br/user/donatazucb http://www.bizmandu.com
http://hondaikmciledug.co.id/HRIS/member.php?action=profile&uid=273465 hondaikmciledug.co.id
http://set.ua/bitrix/rk.php?goto=https://www.protopage.com/isiriahhii http://set.ua/bitrix/rk.php?goto=https://www.protopage.com/isiriahhii
https://xn—-7sbarohhk4a0dxb3c.xn--p1ai/user/claryaxbrt https://–7sbarohhk4a0dxb3c.рф/user/claryaxbrt
http://avalonadvancedmaterials.com/outurl.php?url=https://www.livekavkaz.ru/user/blandalkcy http://avalonadvancedmaterials.com/
http://www.ab12345.cc/go.aspx?url=http://shiftdelete.10tl.net/member.php?action=profile&uid=238271 http://www.ab12345.cc/go.aspx?url=http://shiftdelete.10tl.net/member.php?action=profile&uid=238271
http://vip.cengfan6.com/goto.php?url=https://www.runway-bookmarks.win/best-online-casinos-for-real-money-in-november-2025 vip.cengfan6.com
References:
http://www.med.uz/bitrix/rk.php?goto=https://ameblo.jp/cashudtp410/entry-12948562307.html
jwac.asureforce.net · December 3, 2025 at 6:24 pm
samsung blackjack 2
http://www.cricbattle.com/Register.aspx?Returnurl=http://www.writemob.com//user/repriaxkiy http://www.cricbattle.com
http://www.google.co.mz/url?sa=t&rct=j&q=&esrc=s&source=web&cd=8&cad=rja&sqi=2&ved=0CGkQFjAH&url=https://www.mixcloud.com/kethanzhdc/ http://www.google.co.mz/url?sa=t&rct=j&q=&esrc=s&source=web&cd=8&cad=rja&sqi=2&ved=0CGkQFjAH&url=https://www.mixcloud.com/kethanzhdc
http://www.pesscloud.com/PessServer.Web/Utility/Login/LoginPess.aspx?Returnurl=https://messiahizqs231.iamarrows.com/bonus-codes-archives http://www.pesscloud.com/
https://zplati.ru/user/freaghjhtq https://zplati.ru/
https://www.bookmarkingvictor.win/mgm-grand-las-vegas-wikipedia http://www.bookmarkingvictor.win
https://100kursov.com/away/?url=https://www.huntingnet.com/forum/members/ciaramyymg.html https://100kursov.com/away/?url=https://www.huntingnet.com/forum/members/ciaramyymg.html
http://mylekis.wip.lt/redirect.php?url=https://nevskij-7-sezon-blizkij-vrag-v1.tnt-lordfilm.net/user/sivneyouqq http://mylekis.wip.lt/redirect.php?url=https://nevskij-7-sezon-blizkij-vrag-v1.tnt-lordfilm.net/user/sivneyouqq
https://volontereco.ru/user/germieluby volontereco.ru
http://cqr3d.ru/user/celeenisld http://cqr3d.ru/user/celeenisld
https://laneukqz983.fotosdefrases.com/best-payout-online-casino-sites-2025-fastest-withdrawals laneukqz983.fotosdefrases.com
http://k.yingjiesheng.com/link.php?url=https://blurriechan.blurriecon.com/member.php?action=profile&uid=173053 k.yingjiesheng.com
http://www.fcviktoria.cz/media_show.asp?id=2924&id_clanek=2467&media=0&type=1&url=https://www.third-bookmarks.win/stake-us-review-verdict-is-the-stake-social-casino-legit http://www.fcviktoria.cz
https://dobryakschool.ru/user/nathopqbhd dobryakschool.ru
http://football.sodazaa.com/out.php?url=http://faq.firu-mbh.de/user/elmarandwx football.sodazaa.com
https://promkod.info/user/merrinalou https://promkod.info
https://bumiasri.org/user/cyrinazihz https://bumiasri.org/user/cyrinazihz
http://northstarshoes.com/europe/out.php?url=https://robert-lewandowski-kg.com/user/branyahjvj northstarshoes.com
https://duvidas.construfy.com.br/user/daylinrmbo https://duvidas.construfy.com.br/
References:
https://www.tool-bookmarks.win/okada-manila-a-grand-resort-experience-in-the-philippines
تریدینگ پروفسور · December 3, 2025 at 7:29 pm
Appreciating the persistence you put into your blog and in depth information you offer.
It’s great to come across a blog every once in a while that isn’t the same old rehashed material.
Wonderful read! I’ve bookmarked your site and I’m including your
RSS feeds to my Google account.
sabung ayam · December 3, 2025 at 8:20 pm
I simply could not leave your site before suggesting that I actually
loved the standard info a person provide on your visitors?
Is going to be back steadily to inspect new posts
http://www.pagespan.com/external/ext.aspx?url=https://www.bookmarks4all.win/fair-go-lobby-updates-big-bonuses-new-slots-deals · December 3, 2025 at 8:55 pm
choctaw casino durant ok
References:
http://www.automaniabrandon.com/LinkOut/?goto=http://www.xn—-btbbc1bctice0bhec4i.xn--p1ai/user/regaiszmhs
ทีเด็ดบอลวันนี้ · December 3, 2025 at 11:44 pm
I have to thank you for the efforts you’ve put in writing this site.
I am hoping to check out the same high-grade blog posts from you in the future as well.
In fact, your creative writing abilities has encouraged me to get my own blog now 😉
วิเคราะห์บอลวันนี้ · December 3, 2025 at 11:49 pm
Unquestionably believe that which you stated. Your favorite reason appeared to be on the net the simplest thing to be aware of.
I say to you, I definitely get irked while people consider worries that they just do not
know about. You managed to hit the nail upon the top and defined out the whole thing without having side effect , people can take a signal.
Will probably be back to get more. Thanks
bet86br · December 4, 2025 at 1:27 am
Hey Brazil! Let’s check out Bet86br. The site is decent and functional. I love the easy layout and selection so it’s easy to find what you need. Check it out here bet86br.
mycirclerummy · December 4, 2025 at 2:55 am
Okay, gave mycirclerummy a shot. The community seems lively and the interface is pretty clean. Had a good time playing. Check it out if you’re into rummy! Get in the circle here: mycirclerummy
az888care · December 4, 2025 at 5:43 am
I’ll right away grasp your rss as I can not to find your email subscription hyperlink or e-newsletter
service. Do you have any? Kindly permit me understand so that I may subscribe.
Thanks.
วิเคราะห์บอล · December 4, 2025 at 1:28 pm
I am regular reader, how are you everybody? This paragraph posted
at this web page is genuinely fastidious.
วิเคราะห์บอลวันนี้ · December 4, 2025 at 9:12 pm
This article provides clear idea in favor of the new users of blogging,
that in fact how to do running a blog.
kraken · December 4, 2025 at 9:39 pm
Альтернативный kra49 домен работает как резервная точка входа на площадку при блокировках основных адресов провайдерами интернета и государственными органами.
novosti-belarus-944 · December 4, 2025 at 9:44 pm
новости беларуси 2025 последние новости беларуси
วิเคราะห์บอล · December 4, 2025 at 11:38 pm
This paragraph will help the internet people for setting up new blog or even a weblog from start to
end.
วิเคราะห์บอล · December 4, 2025 at 11:59 pm
Hi there! This post could not be written any better!
Reading this post reminds me of my old room mate! He always
kept chatting about this. I will forward this article to him.
Pretty sure he will have a good read. Thank you for
sharing!
วิเคราะห์บอลวันนี้ · December 5, 2025 at 1:01 am
Hi, all is going nicely here and ofcourse every one
is sharing facts, that’s actually excellent, keep
up writing.
시알리스구매사이트 · December 5, 2025 at 2:09 am
I’m really impressed with your writing abilities as well
as with the format to your weblog. Is this a paid theme or did
you modify it yourself? Anyway stay up the nice quality writing,
it is uncommon to see a nice blog like this one nowadays..
วิเคราะห์บอลวันนี้ · December 5, 2025 at 4:39 am
Hello, Neat post. There’s a problem with your site in web
explorer, would check this? IE nonetheless is the marketplace chief and a large
component to other folks will pass over your wonderful writing due to this problem.
วิเคราะห์บอลวันนี้ · December 5, 2025 at 6:18 am
Wonderful article! That is the type of info that should be shared around the internet.
Disgrace on Google for not positioning this submit higher!
Come on over and talk over with my web site . Thank you =)
https://allmyfaves.com/tinianlscc · December 5, 2025 at 7:16 am
Angels Bail Bonds Costa Mesa
769 Baker St,
Costa Mesa, СᎪ 92626, United States
a&k bail bonds (https://allmyfaves.com/tinianlscc)
spicebomb Extreme Cena · December 5, 2025 at 8:39 am
When I originally left a comment I appear to have clicked on the -Notify me when new comments are added- checkbox and from now on every time a comment is
added I get 4 emails with the same comment. Perhaps there is an easy method you can remove me from that service?
Many thanks!
my webpage; spicebomb Extreme Cena
วิเคราะห์บอล · December 5, 2025 at 9:44 am
It is not my first time to visit this site, i am visiting this web
site dailly and obtain fastidious data from here all the time.
วิเคราะห์บอล · December 5, 2025 at 12:41 pm
Hi there! This is my 1st comment here so I just wanted to give a quick
shout out and say I truly enjoy reading your posts. Can you recommend any other blogs/websites/forums that cover
the same subjects? Thanks for your time!
medim-pro-936 · December 5, 2025 at 3:58 pm
Стоит посмотреть: https://medim-pro.ru/medosmotr-dlya-rebenka/
skin rejuvenation service · December 5, 2025 at 4:12 pm
goGLOW Houston Heights
1515 Studemont Տt Suite 204, Houston,
Texas, 77007, USΑ
(713) 364-3256
skin rejuvenation service
วิเคราะห์บอล · December 5, 2025 at 6:58 pm
Great article.
ทีเด็ดบอลวันนี้ · December 5, 2025 at 7:11 pm
Thanks in support of sharing such a fastidious opinion,
post is pleasant, thats why i have read it entirely
วิเคราะห์บอล · December 6, 2025 at 1:12 am
Excellent web site you have got here.. It’s hard to find excellent writing like yours nowadays.
I really appreciate people like you! Take care!!
rh365casino · December 6, 2025 at 1:43 am
Interesting take on responsible gaming! The speed of transactions at places like rh365 casino app download-instant crediting with GCash-can be a double-edged sword. Quick access needs mindful limits, right? It’s all about balance!
ทีเด็ดบอลวันนี้ · December 6, 2025 at 4:45 am
Remarkable! Its actually remarkable paragraph, I have got
much clear idea on the topic of from this piece of writing.
Wettbüro Online · December 6, 2025 at 9:06 am
sportwetten freebet ohne einzahlung
Here is my website – Wettbüro Online
online pharmacies · December 6, 2025 at 10:12 am
Very nice post. I simply stumbled upon your blog and wished to mention that I’ve really enjoyed browsing your weblog posts.
In any case I will be subscribing to your rss feed and
I’m hoping you write again very soon!
ערוץ הגזע · December 6, 2025 at 10:56 am
Great site you’ve got here.. It’s difficult to find quality writing like yours nowadays.
I truly appreciate individuals like you! Take care!!
ทีเด็ดบอล · December 6, 2025 at 1:30 pm
Generally I don’t learn article on blogs, however I would like
to say that this write-up very compelled me to try and
do it! Your writing taste has been surprised me. Thank you, quite
nice post.
วิเคราะห์บอลวันนี้ · December 6, 2025 at 2:35 pm
Hello to all, how is all, I think every one is getting more
from this web site, and your views are pleasant for new viewers.
oddset Wetten im internet · December 6, 2025 at 3:15 pm
buchmacher mütze
my blog post: oddset Wetten im internet
emerald-chat-236 · December 6, 2025 at 3:21 pm
Free video chat emerald chat site find people from all over the world in seconds. Anonymous, no registration or SMS required. A convenient alternative to Omegle: minimal settings, maximum live communication right in your browser, at home or on the go, without unnecessary ads.
วิเคราะห์บอล · December 6, 2025 at 4:06 pm
I am regular reader, how are you everybody? This article posted at this site is really
good.
Bali Guide 2026 · December 6, 2025 at 5:55 pm
Write more, thats all I have to say. Literally, it seems as though you relied on the video to make your point.
You definitely know what youre talking about, why waste your intelligence on just posting videos to your weblog when you could be giving us something enlightening to read?
highstakes sweeps · December 6, 2025 at 6:53 pm
Look into my web site … highstakes sweeps
q555game · December 6, 2025 at 8:07 pm
Gonna spend tonight lost in the q555game universe. Hope it’s as good as everyone says. Gaming time! Immerse yourself in q555game q555game
ทีเด็ดบอลวันนี้ · December 6, 2025 at 9:34 pm
I am really enjoying the theme/design of your blog. Do you ever run into
any internet browser compatibility problems? A few of my blog readers have complained about my website not operating correctly in Explorer but looks great in Safari.
Do you have any advice to help fix this issue?
วิเคราะห์บอลวันนี้ · December 7, 2025 at 6:08 am
Unquestionably imagine that that you stated. Your favorite reason appeared to be on the internet the easiest thing
to understand of. I say to you, I definitely get annoyed even as other folks think about worries that
they plainly do not recognize about. You managed to hit the nail
upon the highest and outlined out the whole thing with no need side effect
, other folks can take a signal. Will likely be back to get more.
Thank you
ทีเด็ดบอลวันนี้ · December 7, 2025 at 7:51 am
Thanks for ones marvelous posting! I seriously enjoyed reading it, you are a great author.
I will always bookmark your blog and will come back in the future.
I want to encourage you to continue your great job, have a nice day!
วิเคราะห์บอล · December 7, 2025 at 12:43 pm
My spouse and I absolutely love your blog and find a lot of your post’s
to be exactly I’m looking for. Do you offer guest writers to write
content for yourself? I wouldn’t mind producing a post
or elaborating on many of the subjects you write related to here.
Again, awesome web log!
1win onlayn oyunlar · December 7, 2025 at 4:30 pm
Bu saytdakı məlumatları oxumaqdan zövq alıram. Çox sağ olun!
http://kapkipz.awardspace.us/index.php/topic,13176.0.html
Edwinnah · December 7, 2025 at 4:52 pm
Only the best is here: http://registraciavsaita.listbb.ru/viewtopic.php?f=2&t=4832
ทีเด็ดบอลวันนี้ · December 8, 2025 at 12:25 am
Hi there, There’s no doubt that your site could possibly be having web browser compatibility problems.
When I look at your website in Safari, it looks
fine however, if opening in I.E., it has some overlapping issues.
I merely wanted to give you a quick heads up! Besides that, great website!
best Chicken Road site · December 8, 2025 at 1:02 am
I must say I’m pleased I found Chicken Road — fantastic!
https://pxl.fm/chickenroaddepositmethods19612
State Farm Insurance Agent · December 8, 2025 at 6:19 am
Hello everybody, here every person is sharing such experience,
therefore it’s pleasant to read this weblog,
and I used to pay a quick visit this website every day.
seronax blue · December 8, 2025 at 7:05 am
Thanks for another great post. Where else may anybody get that type of info in such an ideal way of writing? I have a presentation next week, and I’m at the search for such information.
วิเคราะห์บอล · December 8, 2025 at 10:58 am
I used to be suggested this website through my cousin. I’m no longer
positive whether this post is written by means of him as no one else recognise such specific approximately my trouble.
You’re incredible! Thank you!
soi keo nha cai · December 8, 2025 at 1:23 pm
It’s enormous that you are getting ideas from this post as well as
from our discussion made at this time.
ทีเด็ดบอล · December 8, 2025 at 10:49 pm
You need to be a part of a contest for one of the most useful
websites on the web. I’m going to highly recommend this
web site!
عملية القلب المفتوح · December 8, 2025 at 11:01 pm
Nice Post. It’s really a very good article. I noticed all your important points. Thanks.
kraken 759 · December 8, 2025 at 11:04 pm
Крупный кракен маркетплейс предлагает удобную систему поиска товаров с фильтрами по цене, рейтингу продавца и способу доставки заказов.
dispatch42-345 · December 8, 2025 at 11:09 pm
Нужна работа в США? получить программу онлайн курс диспетчера : работа с заявками и рейсами, переговоры на английском, тайм-менеджмент и сервис. Подходит новичкам и тем, кто хочет выйти на рынок труда США и зарабатывать в долларах.
วิเคราะห์บอล · December 9, 2025 at 12:28 am
Having read this I believed it was very informative.
I appreciate you taking the time and effort to put this informative article together.
I once again find myself personally spending way too much time both reading and leaving comments.
But so what, it was still worth it!
วิเคราะห์บอลวันนี้ · December 9, 2025 at 12:41 am
You’ve made some decent points there. I checked on the internet for more info about the issue and found most
individuals will go along with your views on this site.
Prawnik Międzychód · December 9, 2025 at 2:53 am
Hello would you mind letting me know which webhost you’re working with?
I’ve loaded your blog in 3 different internet browsers and I must say this blog loads a lot faster
then most. Can you recommend a good hosting provider at a reasonable
price? Thanks, I appreciate it!
nv-casino-623 · December 9, 2025 at 9:47 am
Uwielbiasz hazard? nv casino: rzetelne oceny kasyn, weryfikacja licencji oraz wybor bonusow i promocji dla nowych i powracajacych graczy. Szczegolowe recenzje, porownanie warunkow i rekomendacje dotyczace odpowiedzialnej gry.
LanceWat · December 9, 2025 at 10:27 am
Read More: http://news.sharemarketnewslive.com/story/574449/the-ultimate-guide-to-buying-facebook-advertising-accounts-what-must-be-known.html
https://Baywinguncelgiris.tr/ · December 9, 2025 at 11:14 pm
üzerindeki bilgileri gerçekten önemsiyorum. Teşekkürler!
https://Baywinguncelgiris.tr/
SODO · December 10, 2025 at 1:01 am
Great post, keep up the good work, I hope you don’t mind but I’ve added on my blog roll.
kraken-952 · December 10, 2025 at 1:11 am
Рабочее кракен зеркало типа kra47 cc обеспечивает быстрый доступ к площадке с автоматическим редиректом на актуальный онион адрес маркетплейса.
kraken-348 · December 10, 2025 at 1:40 am
Официальный kraken onion адрес версии v3 содержит 56 символов для максимальной криптографической защиты соединения внутри распределенной Tor сети анонимизации.
mejores casinos en línea · December 10, 2025 at 4:38 am
Thanks for discussing the issues and covering them in a well written format.
casino en ligne international · December 10, 2025 at 5:02 am
Pretty impressive article. I just stumbled upon your site and wanted to say that I have really enjoyed reading your opinions. Any way I’ll be coming back and I hope you post again soon.
Wholesale Custom Gift Boxes · December 10, 2025 at 8:39 am
If you want to improve your experience just keep visiting this web page and be updated with
the hottest information posted here.
Sportwetten Anbieter · December 10, 2025 at 9:13 am
buchmacher beruf
my page: Sportwetten Anbieter
ทีเด็ดบอลวันนี้ · December 10, 2025 at 11:39 am
Aw, this was a really good post. Finding the time and actual
effort to make a good article… but what can I say… I hesitate a whole lot and don’t seem
to get nearly anything done.
paris sportifs Suisse · December 10, 2025 at 1:09 pm
I dont think I’ve read anything like this before. So good to find somebody with some original thoughts on this subject. cheers for starting this up. This blog is something that is needed on the web, someone with a little originality.
strategies for getting the best loan terms · December 10, 2025 at 8:38 pm
Tips and tools you offer are so helpful to agencies in our community.
main credit score factors explained · December 10, 2025 at 11:17 pm
Very often I go to see this blog. It very much is pleasant to me. Thanks the author
seo SEO Seo · December 11, 2025 at 12:13 am
Just wanna admit that this is extremely helpful, Thanks for taking your time to write this.
top online casinos · December 11, 2025 at 1:30 am
Just wanna admit that this is extremely helpful, Thanks for taking your time to write this.
วิเคราะห์บอลวันนี้ · December 11, 2025 at 3:49 am
Every weekend i used to visit this web site, for the reason that i want enjoyment, as this
this site conations really good funny data too.
top online casinos · December 11, 2025 at 4:40 am
Does it look like we’re in for a big ride here?
DonaldDog · December 11, 2025 at 4:43 am
Профессиональный магазин магазин аккаунтов приветствует маркетологов в нашем каталоге расходников. Особенность этого шопа — это наличии огромной библиотеки, где опубликованы секретные мануалы по SMM. Здесь можно найти аккаунты Google, Twitter, Telegram для любых задач: начиная с саморегов до трастовыми кабинетами с друзьями. Заходите в наше комьюнити, изучайте полезные кейсы, делитесь опытом и делайте профит вместе с нами прямо сейчас.
xoplay · December 11, 2025 at 9:07 am
Dice games are all about understanding probabilities – it’s fascinating! Seeing platforms like XoPlay streamline the experience with easy registration & security makes it even more accessible. Is xoplay legit for new players? Curious about their game variety!
วิเคราะห์บอล · December 11, 2025 at 9:31 am
You really make it seem so easy with your presentation but I find this topic to be really something which I think
I would never understand. It seems too complex
and extremely broad for me. I am looking forward for your next post, I will try to get the hang of it!
วิเคราะห์บอล · December 11, 2025 at 9:43 am
Do you mind if I quote a couple of your posts as long as I provide credit and sources back to your
webpage? My blog is in the exact same niche as yours and my users would truly benefit from some of the information you present
here. Please let me know if this okay with you.
Thank you!
ทีเด็ดบอลวันนี้ · December 11, 2025 at 10:09 am
Woah! I’m really loving the template/theme of this website.
It’s simple, yet effective. A lot of times it’s tough to get that “perfect balance”
between user friendliness and visual appearance. I must say that you’ve done a excellent job with this.
In addition, the blog loads very quick for me on Internet
explorer. Superb Blog!
วิเคราะห์บอลวันนี้ · December 11, 2025 at 1:18 pm
You really make it appear so easy together
with your presentation however I in finding this matter to be really one thing that
I think I would never understand. It kind of feels too
complicated and extremely huge for me. I’m looking forward for your next publish, I’ll
attempt to get the grasp of it!
crypto investing and trading analysis · December 11, 2025 at 2:56 pm
I imagine so. Very good stuff, I agree totally.
開設binance帳戶 · December 11, 2025 at 3:13 pm
I don’t think the title of your article matches the content lol. Just kidding, mainly because I had some doubts after reading the article.
meilleur casino en ligne Canada · December 11, 2025 at 3:19 pm
What made you first develop an interest in this topic?
DonaldDog · December 11, 2025 at 4:15 pm
Secure hub links shop excitedly present direct access to purchase high-quality accounts suitable for growth. The core value of our shop lies in the availability of an extensive educational hub, filled with up-to-date strategies on ad campaigns. Discover how to farm campaigns safely as well as how to avoid account locks when using ad platforms. Buying here, you get not only working goods, as well as fast customer service, guarantees and competitive rates on the market.
deep dive on global crypto regulation · December 11, 2025 at 5:12 pm
A wholly agreeable point of view, I think primarily based on my own experience with this that your points are well made, and your analysis on target.
Pragmatic Play High RTP slots you can Play now · December 11, 2025 at 5:34 pm
Also visit my web page: Pragmatic Play High RTP slots you can Play now
joker gaming joker123 logo · December 11, 2025 at 5:51 pm
Hi there, I read your blog daily. Your story-telling style is witty, keep up the good work!
Feel free to surf to my homepage … https://wbsc7p3djvgn54kngvlug26tunkxf6fuudjuhsb2Tsceqtbffzla.webpkgcache.com/doc/-/s/vmatchconsulting.com%2Fsamsung-j700-the-whole-multimedia-device%2F
nolvadex 20mg · December 11, 2025 at 6:13 pm
You really make it seem so easy with your presentation but
I find this matter to be really something which I think I would never understand.
It seems too complicated and extremely broad for me.
I am looking forward for your next post, I
will try to get the hang of it!
Aesthetic Clinic Singaporeental-aesthetic-clinic/ · December 11, 2025 at 7:07 pm
Great article. I am facing many of these
issues as well..
Plan ideas renovation open · December 11, 2025 at 8:16 pm
Refresh Renovation Southwest Charlotte
1251 Arrow Pine Ꭰr c121,
Charlotte, NC 28273, United Ѕtates
+19803517882
Plan ideas renovation open
how to avoid crypto scams and fraud · December 11, 2025 at 9:04 pm
Hello there, You have done an incredible job. I will certainly digg it and personally recommend to my friends. I am sure they will be benefited from this site.
expert analysis on defi protocols · December 11, 2025 at 11:45 pm
Wish I’d thought of this. Am in the field, but I procrastinate alot and haven’t written as much as I’d like. Thanks.
casino en ligne le plus payant · December 11, 2025 at 11:57 pm
Hello. Great job. I did not expect this on a Wednesday. This is a great story. Thanks!
IcoStamp blog · December 12, 2025 at 3:01 am
A friend of mine advised this site. And yes. it has some useful pieces of info and I enjoyed scaning it. Therefore i would love to drop you a quick note to express my thank. Take care
ทีเด็ดบอลวันนี้ · December 12, 2025 at 11:08 am
Hmm it looks like your site ate my first comment (it was super long) so I guess I’ll just sum it
up what I submitted and say, I’m thoroughly enjoying your blog.
I too am an aspiring blog blogger but I’m still new to the whole thing.
Do you have any helpful hints for novice blog
writers? I’d really appreciate it.
new online casinos · December 12, 2025 at 3:27 pm
Just wanna admit that this is extremely helpful, Thanks for taking your time to write this.
Bookmarkshut.Com · December 12, 2025 at 9:07 pm
my homepage Bookmarkshut.Com
ทีเด็ดบอล · December 12, 2025 at 11:28 pm
Hi my family member! I want to say that this article is amazing, great
written and include approximately all significant infos.
I would like to look more posts like this .
Casino en Ligne Finixio · December 13, 2025 at 3:42 am
Quel est le meilleur casino en ligne France pour jouer en toute sécurité en 2025 ? Il faut dire qu’aujourd’hui, trouver un site de casino en ligne fiable n’est pas une mince affaire. Il est très facile de se perdre parmi l’offre grandissante des casinos français en ligne. Mais pas de panique, nous sommes là ! Dans ce guide, nos experts vous présentent un classement complet pour vous aider à choisir le casino en ligne gratuit ou en argent réel qui correspond à vos attentes à 100 %. Chez nous, pas d’embrouille ni de coup fourré. Notre credo ? Vous faire découvrir les meilleurs casinos en ligne France du moment pour vous faire profiter pleinement de vos jeux de casino favoris. Suivez le guide !
Meilleurs casino en ligne argent réel France 2025 · December 13, 2025 at 5:08 am
Déterminer quel casino en ligne est réellement adapté pour miser de l’argent véritable s’avère bien plus délicat qu’on pourrait le penser. En 2025, le secteur français des jeux virtuels connaît une croissance rapide, mettant à disposition plus de 200 plateformes certifiées accessibles aux joueurs nationaux. Cette multitude d’options rend la sélection d’un site fiable et agréable encore plus exigeante.C’est pour cette raison que notre classement s’appuie sur une analyse rigoureuse. L’ensemble des casinos en argent réel mentionnés ici ont été examinés en détail avant d’être ajoutés. La sécurité des utilisateurs demeure au cœur de nos priorités, et notre objectif est de vous éviter les dangers associés aux sites non fiables, de plus en plus nombreux sur le web.
วิเคราะห์บอล · December 13, 2025 at 6:17 am
You have made some decent points there. I checked on the
internet for more info about the issue and found most individuals will go along with
your views on this web site.
Casino en Ligne France · December 13, 2025 at 7:17 am
Top 9 Meilleur casino en ligne pour les joueurs français: Winamax – idéal pour le poker et les tournois en ligne, Pokerstars – top pour affronter les joueurs de poker du monde entier, Wazamba – parfait pour les tournois réguliers attractifs, PMU – spécialisé sur le turf, mais propose aussi les paris sportifs, Unibet – idéal pour varier les jeux en ligne, FDJ – meilleure option pour les jeux de loterie et les jeux traditionnels français, Betclic – offre une interface intuitive et des paris combinés, Parionsweb – pensé pour les parieurs français traditionnels, Bwin – intéressant pour les paris sportifs et options hybrides. Le marché du casino en ligne en France connaît une croissance exceptionnelle en 2025. Avec plus de 3 millions de joueurs actifs, les casinos en ligne français offrent une expérience de jeu de plus en plus sophistiquée et sécurisée. Ce guide complet vous présente les meilleurs casinos en ligne disponibles en France, leurs bonus exclusifs, et toutes les informations essentielles pour jouer en toute sécurité.
sizegenetics.mixo.io · December 13, 2025 at 11:43 am
The Quick Extender Pro offers become probably the most talked-about traction devices
amongst men buying sluggish, natural and routine-based approach to personalized improvement.
Many individuals searching for a Rapid Extender Pro assessment want to appreciate how the device works, the particular traction approach actually means, in addition to whether long-term consistency can result in meaningful development.
The inspiration of this device is the traction method,
a concept used for many yrs in orthopedics and even essential.
Traction requires applying gentle in addition to continuous stretching in order to soft tissues, pushing gradual adaptation over time.
When utilized properly, this low-intensity method support cells elongation, nonetheless it demands patience, discipline plus
steady use, which is why typically the Quick Extender Professional routine is usually discussed in depth by users that have tried out it for several weeks.
วิเคราะห์บอลวันนี้ · December 13, 2025 at 3:50 pm
Very nice write-up. I absolutely love this site.
Thanks!
วิเคราะห์บอล · December 13, 2025 at 4:42 pm
We’re a bunch of volunteers and starting a brand new scheme in our community.
Your website offered us with helpful info to work on. You
have performed an impressive task and our entire group will be thankful to you.
ทีเด็ดบอล · December 14, 2025 at 2:51 am
Everyone loves what you guys are up too. This sort of clever work and exposure!
Keep up the very good works guys I’ve you guys to blogroll.
OLXTOTO · December 14, 2025 at 6:03 am
Write more, thats all I have to say. Literally, it seems as though you relied on the video to make your
point. You obviously know what youre talking about, why throw
away your intelligence on just posting videos to your site when you could be giving us something
informative to read?
ทีเด็ดบอลวันนี้ · December 14, 2025 at 6:20 am
I blog frequently and I truly appreciate your information. Your
article has truly peaked my interest. I’m going to take a note of
your website and keep checking for new details about once a week.
I subscribed to your RSS feed too.
ทีเด็ดบอล · December 14, 2025 at 8:47 am
Thankfulness to my father who informed me on the topic of this weblog, this web site is actually remarkable.
วิเคราะห์บอล · December 14, 2025 at 9:11 am
Hi, I do believe this is an excellent blog. I stumbledupon it 😉 I may revisit yet again since
i have saved as a favorite it. Money and freedom is the best way to change, may you be rich
and continue to help other people.
TypeMediaUSA · December 14, 2025 at 10:37 am
Hi there are using WordPress for your blog platform?
I’m new to the blog world but I’m trying to get started and set up my own. Do you require any html
coding knowledge to make your own blog? Any help would be greatly
appreciated!
วิเคราะห์บอลวันนี้ · December 14, 2025 at 12:38 pm
I read this article fully concerning the comparison of latest and previous
technologies, it’s remarkable article.
วิเคราะห์บอล · December 14, 2025 at 2:04 pm
What a information of un-ambiguity and preserveness of valuable familiarity about unexpected emotions.
1xbet-burkina-189 · December 14, 2025 at 11:36 pm
La plateforme telecharger 1xbet burkina faso: paris sportifs en ligne, matchs de football, evenements en direct et statistiques. Description du service, marches disponibles, cotes et principales fonctionnalites du site.
1xbet-congo-977 · December 14, 2025 at 11:47 pm
Site web 1xbet congo – paris sportifs en ligne sur le football et autres sports. Propose des paris en direct et a l’avance, des cotes, des resultats et des tournois. Description detaillee du service, des fonctionnalites du compte et de son utilisation au Congo.
parifoot-643 · December 14, 2025 at 11:57 pm
Site web de parifoot rdc: paris sportifs, championnats de football, resultats des matchs et cotes. Informations detaillees sur la plateforme, les conditions d’utilisation, les fonctionnalites et les evenements sportifs disponibles.
1xbet-burkina-faso-37 · December 15, 2025 at 12:06 am
La plateforme en ligne 1xbet burkina apk: paris sportifs en ligne, matchs de football, evenements en direct et statistiques. Description du service, marches disponibles, cotes et principales fonctionnalites du site.
วิเคราะห์บอลวันนี้ · December 15, 2025 at 2:53 am
I couldn’t refrain from commenting. Well written!
skincare routine clinic · December 15, 2025 at 8:36 am
goGLOW Houston Heights
1515 Stusemont Ѕt Suite 204, Houston,
Texas, 77007, USA
(713) 364-3256
skincare routine clinic
qgawlqx · December 15, 2025 at 10:42 am
http://www.soad.msk.ru/forum/viewtopic.php?p=161776#161776
시알리스 구매 · December 15, 2025 at 11:23 am
안녕! 당신의 사이트 플랫폼으로 WordPress를 사용하시나요?
저는 블로그 세계에 새로 입문했지만,
제 블로그를 시작하려고 합니다. 블로그를 만들기 위해 코딩 지식이 필요한가요?
도움이 된다면 정말 감사하겠습니다!
Greetings from Colorado! I’m bored at work so I decided to check
out your site on my iphone during lunch break.
I enjoy the info you present here and can’t wait to take a look when I get home.
I’m shocked at how fast your blog loaded on my phone ..
I’m not even using WIFI, just 3G .. Anyways,
excellent blog!
This is truly a fantastic blog! Your articles are so well-written and engaging.
I’ve bookmarked it and will definitely be back for more.
Any tips on how to make my own blog as captivating as yours?
Thanks!
이 사이트는 정말 대단합니다! 콘텐츠가 교육적이고 재미있어요.
Smart foto 관련 비디오 콘텐츠를 추가하면 더 좋을 것 같아요.
멋진 작업 계속해 주세요! 고맙습니다!
Linetogel · December 15, 2025 at 2:37 pm
You’re so cool! I don’t suppose I’ve truly read something like that before.
So nice to find somebody with some genuine thoughts on this subject matter.
Seriously.. thanks for starting this up. This website is one thing that is needed on the internet, someone with some originality!
free linux vps · December 15, 2025 at 3:47 pm
I just added this to my favorites. I truly love reading your posts. Tyvm!
qskqvwt · December 15, 2025 at 6:28 pm
https://www.alternatio-org.ru/index.php?option=com_k2&view=itemlist&task=user&id=171400
top 10 casino en ligne Canada · December 15, 2025 at 8:44 pm
Of course, what a great site and informative posts, I will add backlink – bookmark this site? Regards, Reader
cbzpwsu · December 15, 2025 at 9:20 pm
https://headstart.edu.pk/egg-hatching-process-activity/#comment-103658
qekdxvo · December 15, 2025 at 9:50 pm
https://www.corsoclub.ru/board/post.php?mode=post&f=8140
catchon iptv · December 15, 2025 at 10:50 pm
With CatchON TV, you’ll enjoy the ultimate TV experience — access over 24000 live channels and 90000+ movies and series. Stream everything you love, …
whafevq · December 16, 2025 at 1:35 am
http://www.santa4.su/topic/16397-promokod-pri-registracii-melbet-2026-bl777/
stomatologiya-voronezh-8 · December 16, 2025 at 2:38 am
Современная Стоматология в Воронеже лечение кариеса, протезирование, имплантация, профессиональная гигиена и эстетика улыбки. Квалифицированные специалисты, точная диагностика и забота о пациентах.
Gomyfinance · December 16, 2025 at 4:52 am
have already been reading ur blog for a couple of days. really enjoy what you posted. btw i will be doing a report about this topic. do you happen to know any great websites or forums that I can find out more? thanks a lot.
วิเคราะห์บอลวันนี้ · December 16, 2025 at 5:11 am
Greetings from Carolina! I’m bored at work so I decided to check out your website
on my iphone during lunch break. I really like the info you provide
here and can’t wait to take a look when I get home.
I’m surprised at how fast your blog loaded on my phone .. I’m not even using WIFI,
just 3G .. Anyhow, amazing site!
วิเคราะห์บอล · December 16, 2025 at 6:01 am
Heya i am for the first time here. I came across this board and I find It truly
useful & it helped me out much. I hope to give something back and help others
like you helped me.
crudhsr · December 16, 2025 at 6:08 am
https://aprelevka.anyforum.ru/viewtopic.php?t=335
CIBAI KIA · December 16, 2025 at 8:26 am
It is really a nice and helpful piece of info. I’m happy that you simply shared this useful information with us.
Please keep us informed like this. Thanks for sharing.
top online casinos · December 16, 2025 at 8:50 am
Awesome blog you have here but I was wanting to know
if you knew of any forums that cover the same topics discussed here?
I’d really love to be a part of online community where I can get advice from other knowledgeable individuals
that share the same interest. If you have any suggestions,
please let me know. Appreciate it!
eoijuex · December 16, 2025 at 1:14 pm
https://crforum.ru/viewtopic.php?t=577
pvsfmtl · December 16, 2025 at 1:38 pm
http://missmcgregor.blog.macc.nsw.edu.au/2017/05/award-winners-week-4.html?sc=1765707530372#c7215027710895537194
https://ead.jfpe.jus.br/ · December 16, 2025 at 11:51 pm
Hello! I understand this is somewhat off-topic but I needed to
ask. Does running a well-established website such as yours take a large amount of work?
I’m completely new to operating a blog however
I do write in my diary everyday. I’d like to start a blog
so I can easily share my own experience and feelings online.
Please let me know if you have any kind of ideas or tips for
new aspiring bloggers. Thankyou!
digital publications · December 17, 2025 at 1:04 am
I really believe you will do well in the future I appreciate everything you have added to my knowledge base.
suck dick · December 17, 2025 at 6:20 am
suck dick
tips on how to improve your credit score · December 17, 2025 at 9:31 am
Are the issues really as complex as they seem?
doxupnv · December 17, 2025 at 10:48 am
http://ezproxy.lib.usf.edu/login?url=https://www.bigcatalliance.org/news/bonus_d_inscription_au_casino_1xbet.html
Windows Key 11 · December 17, 2025 at 1:03 pm
How come you do not have your website viewable in mobile format? cant see anything in my Droid.
best real money online casino · December 17, 2025 at 1:27 pm
Hello colleagues, its enormous article concerning tutoringand entirely explained, keep
it up all the time.
buôn bán nội tạng · December 17, 2025 at 2:03 pm
We stumbled over here different web page and thought I might check
things out. I like what I see so now i am following you.
Look forward to looking into your web page for a second time.
jilissa · December 17, 2025 at 2:14 pm
Interesting analysis! Seeing platforms like jilissa download apk really push data-driven gaming – the focus on RTP & statistical modeling is a smart move for player trust & engagement. Solid insights here!
kmfjazv · December 17, 2025 at 4:32 pm
http://sso.tdt.edu.vn/Authenticate.aspx?ReturnUrl=https://tfipost.in/2026/03/1xbet-promo-code-india-bonus-120-up-to-66000/
casino en chile online · December 17, 2025 at 5:23 pm
Our local network of agencies has found your research so helpful.
xeqwsuu · December 17, 2025 at 10:44 pm
https://www.sedatify.com/blogs/542/%D0%9F%D1%80%D0%BE%D0%BC%D0%BE%D0%BA%D0%BE%D0%B4-%D0%BD%D0%B0-1%D1%85%D0%91%D0%B5%D1%82-2026-1X200RED-%D0%91%D0%BE%D0%BD%D1%83%D1%81-32-500
check the latest insights · December 18, 2025 at 3:09 am
Hi, do have a e-newsletter? In the event you don’t definately should get on that piece…this web site is pure gold!
yxhhtnq · December 18, 2025 at 5:27 am
The best neural network xnudes.ai for processing deepnude photos in 2025.
https://xnudes.ai/ is a revolutionary AI system.
The deepnude-based service can undress a girl or a man in almost any photo. Honestly, after bots, the service platform pleasantly surprises with fast results and high-quality naked bodies.
Cost: from €6 for 15 edits. There are also weekly and monthly packages for unlimited photo editing.
This is a top platform based on the deepnude neural network, which is capable of generating real photos or anime-style images. The system does an excellent job of undressing uploaded photos. This is a fully competitive service option with a multitude of options.
https://xnudes.ai/
this resource · December 18, 2025 at 9:55 am
This is an awesome entry. Thank you very much for the supreme post provided! I was looking for this entry for a long time, but I wasn’t able to find a honest source.
aqua sculpt · December 18, 2025 at 9:55 am
**aqua sculpt**
aquasculpt is a premium fat-burning supplement meticulously formulated to accelerate your metabolism and increase your energy output.
789k-vn.com · December 18, 2025 at 1:14 pm
Hi! Someone in my Myspace group shared this site with us
so I came to take a look. I’m definitely enjoying the information. I’m book-marking and
will be tweeting this to my followers! Excellent blog and terrific
style and design.
cajjnge · December 18, 2025 at 1:20 pm
http://dpzon3.3x.ro/profile.php?lookup=3079
Download Ytmp3 Gratis · December 18, 2025 at 1:58 pm
Kamu hanya memerlukan URL dari video yang ingin diunduh dan klik tombol download.
backbiome · December 18, 2025 at 3:40 pm
**backbiome**
backbiome is a naturally crafted, research-backed daily supplement formulated to gently relieve back tension and soothe sciatic discomfort.
synadentix · December 18, 2025 at 3:41 pm
**synadentix**
synadentix is a dental health supplement created to nourish and protect your teeth and gums with a targeted combination of natural ingredients
alpha boost · December 18, 2025 at 4:47 pm
**alpha boost**
alpha boost for men, feeling strong, energized, and confident is closely tied to overall quality of life. However, with age, stress, and daily demands
glycomute · December 18, 2025 at 4:50 pm
**glycomute**
glycomute is a natural nutritional formula carefully created to nurture healthy blood sugar levels and support overall metabolic performance.
nervecalm · December 18, 2025 at 5:24 pm
**nervecalm**
nervecalm is a high-quality nutritional supplement crafted to promote nerve wellness, ease chronic discomfort, and boost everyday vitality.
nitric boost ultra · December 18, 2025 at 5:51 pm
**nitric boost ultra**
nitric boost is a daily wellness blend formulated to elevate vitality and support overall performance.
provadent · December 18, 2025 at 6:19 pm
**provadent**
provadent is a newly launched oral health supplement that has garnered favorable feedback from both consumers and dental professionals.
vpn prueba gratuita · December 19, 2025 at 2:23 am
Hello.This article was extremely interesting, particularly since I was searching for thoughts on this subject last couple of days.
Joker123 khmer · December 19, 2025 at 6:49 am
Thanks for every other great post. Where else may just anyone get that kind of info in such an ideal method of writing? I’ve a presentation subsequent week, and I am at the look for such info.
My page https://6oaj3om5tksoqsnxjxxmzy45din5gsufuseyyx2hlnpwhwdoiavq.webpkgcache.com/doc/-/s/WWW.Koklek.go.th%2Fquestion%2Fnokia-6500-slide-make-others-envy-2%2F
Okwin TV · December 19, 2025 at 12:30 pm
Superb post but I was wondering if you could write
a litte more on this topic? I’d be very thankful if you could elaborate a little
bit more. Thank you!
Okwin TV · December 19, 2025 at 3:56 pm
Some truly nice stuff on this website , I like it.
best online casino New Zealand · December 19, 2025 at 4:19 pm
I had fun reading this post. I want to see more on this subject.. Gives Thanks for writing this nice article.. Anyway, I’m going to subscribe to your rss and I wish you write great articles again soon.
Irish online casino · December 19, 2025 at 6:11 pm
I am very happy to look your post. Thanks a lot and i am taking a look ahead to touch you.
best payout casino · December 19, 2025 at 7:31 pm
Unquestionably believe that which you said. Your favorite reason seemed to be on the net the easiest thing to be aware of. I say to you, I certainly get annoyed while people consider worries that they plainly don’t know about. You managed to hit the nail on the head. Will probably be back to get more. Thanks
zaklepka-vytyazhnaya-598 · December 19, 2025 at 9:32 pm
нужна заклепка? https://zaklepka-vytyazhnaya.ru надёжный крепёж для прочных и долговечных соединений. Устойчива к коррозии, влаге и перепадам температур. Подходит для металла, строительства, машиностроения и наружных работ.
qyiguqq · December 20, 2025 at 4:49 am
Hi! I simply wish to give you a huge thumbs up for the great info you’ve got here on this post.
I am returning to your website for more soon.
SlotWolf Casino · December 20, 2025 at 6:48 am
Very quickly this web site will be famous among all blog users, due to it’s
good content
bokep streaming indonesia · December 20, 2025 at 2:53 pm
Nice post. I learn something totally new and challenging on websites I
stumbleupon everyday. It will always be helpful to read through content from other writers and practice
a little something from other websites.
wildgut · December 20, 2025 at 3:02 pm
**wildgut**
wildgut is a precision-crafted nutritional blend designed to nurture your dogs digestive tract.
zaklepka-vytyazhnaya-169 · December 20, 2025 at 9:15 pm
Нужны заклепки? заклепка вытяжная нержавеющая для прочного соединения листового металла и профиля. Стойкость к коррозии, аккуратная головка, надежная фиксация даже при вибрациях. Подбор размеров и типа борта, быстрая отгрузка и доставка.
evakuator-spb-590 · December 20, 2025 at 9:15 pm
Нужен эвакуатор? вызов эвакуатора быстрый выезд по Санкт-Петербургу и области. Аккуратно погрузим легковое авто, кроссовер, мотоцикл. Перевозка после ДТП и поломок, помощь с запуском/колесом. Прозрачная цена, без навязываний.
DonaldDug · December 20, 2025 at 11:24 pm
Текущие обновления: Продать духовые инструменты выгодно быстро — скупка в Москве
w88 link · December 20, 2025 at 11:30 pm
I needed to thank you for this fantastic read!! I certainly enjoyed
every bit of it. I’ve got you saved as a favorite to look at new things you post…
evakuator-spb-655 · December 21, 2025 at 8:04 am
Нужен эвакуатор? вызов эвакуатора быстро быстрый выезд по Санкт-Петербургу и области. Аккуратно погрузим легковое авто, кроссовер, мотоцикл. Перевозка после ДТП и поломок, помощь с запуском/колесом. Прозрачная цена, без навязываний.
nude child · December 21, 2025 at 8:59 am
I’m gone to tell my little brother, that he should also pay a
quick visit this website on regular basis to take
updated from most up-to-date news update.
global.luskin.ucla.edu · December 21, 2025 at 4:17 pm
https://segisocial.com/codigo-promocional-1xbet-casas-de-apuestas-legales-2026/ (https://global.luskin.ucla.edu/haitis-recovery-dont-give-them-the-fish-teach-them-how-to-fish/)
skupix-784 · December 21, 2025 at 6:58 pm
Продаешь антиквариат? Скупка антиквариата в Москве — выгодно продать старинные вещи оценка и выкуп старинных вещей с понятными условиями. Принимаем фарфор, бронзу, серебро, иконы, монеты, часы, книги, мебель и предметы искусства. Возможен выезд и оценка по фото. Оплата сразу, конфиденциальность.
mvip77casino · December 21, 2025 at 10:39 pm
Signed up to mvip77casino last week. Fairly standard stuff, but I had a bit of luck! Worth a punt if you’re feeling lucky. More info here: mvip77casino
auto-855 · December 22, 2025 at 3:14 am
Авто в ОАЭ https://auto.ae/sale/vrp/ под ключ: продажа новых и б/у автомобилей, диагностика перед покупкой, регистрация и страховка. Прокат на сутки и долгосрок, включая премиум. VIP номерные знаки — подбор вариантов, торг, оформление передачи и сопровождение на русском.
DitoBet · December 22, 2025 at 9:01 am
Greetings! Very useful advice within this post! It is the little changes that make the greatest changes.
Thanks a lot for sharing!
Bigg Boss Telugu 9 Winner · December 22, 2025 at 9:54 am
Saw your material, and hope you publish more soon.
Thanks · December 22, 2025 at 12:06 pm
Nice post. I learn something new and challenging on sites I stumbleupon every day.
It will always be interesting to read through content from other authors and use something from their sites.
lifepo4 batteries · December 22, 2025 at 12:31 pm
Wow, amazing blog layout! How long have you been blogging for? you make blogging look easy. The overall look of your site is wonderful, let alone the content!
атом казино промокод · December 22, 2025 at 2:25 pm
continuously i used to read smaller articles or reviews which as well clear their motive, and that is also happening with this paragraph which I am reading at this time.
лучшие казино для игры · December 22, 2025 at 3:37 pm
Great blog right here! Additionally your web site quite a bit up fast!
What web host are you the use of? Can I get your affiliate hyperlink for your host?
I wish my site loaded up as quickly as yours lol
video hiếp dâm · December 22, 2025 at 6:07 pm
I don’t normally comment but I gotta say appreciate it for the post on this one : D.
Weight loss · December 22, 2025 at 10:31 pm
Hi, I think your website might be having browser compatibility issues.
When I look at your blog site in Chrome, it looks fine but when opening in Internet Explorer, it has some overlapping.
I just wanted to give you a quick heads up!
Other then that, excellent blog!
more · December 22, 2025 at 10:32 pm
I’ve been reading about Paybis for a while now, and I’m still not fully convinced about whether it truly deserves all the
attention it gets, but it’s clearly an interesting name within the cryptocurrency space, especially when it comes to combining crypto
markets with fiat currencies. From what
I understand so far, Paybis presents itself as a large-scale cryptocurrency platforms
that also supports standard currencies, which is something many exchanges
either limit or complicate.
What initially caught my interest was the way Paybis seems to
bridge the gap between traditional finance and the crypto
world. Many platforms focus strictly on crypto-to-crypto trades, but Paybis appears
to allow users to exchange digital currencies using debit cards.
I’m not claiming this process is flawless, but it does seem aimed
at people just entering crypto rather than only advanced traders.
Another aspect worth mentioning is the range of cryptocurrencies supported.
Paybis doesn’t appear to limit itself to Bitcoin and Ethereum only.
Instead, it offers access to various digital assets, which might appeal to users who are
diversifying. That said, I still wonder about things like update frequency,
so it’s probably something potential users should investigate further.
Security and compliance are also frequently mentioned in relation to Paybis.
The platform emphasizes identity verification, which could be seen as protective for some users, though others might find it inconvenient.
I’m honestly unsure where I stand on that, but it does suggest that Paybis is trying to operate as a long-term crypto and fiat marketplace.
When it comes to fees and exchange rates, opinions seem divided.
Some sources claim that Paybis is clear with pricing,
while others mention that costs may depend on payment methods.
This isn’t uncommon in the crypto industry, but it does mean users should
probably read the details carefully before making decisions.
Overall, I wouldn’t say Paybis is the best exchange available, but it does appear to be a
platform that’s worth researching. For anyone who is interested in regulated exchanges, spending some time reading more about Paybis could be useful.
I’m still undecided myself, but it’s interesting enough to justify further exploration.
pure cbd oil · December 23, 2025 at 6:29 am
Great post, keep up the good work, I hope you don’t mind but I’ve added on my blog roll.
sex fb68 · December 23, 2025 at 5:41 pm
If wings are your thing, Tinker Bell’s sexy Halloween costume design is all grown up.
phim sex hiếp dâm học sinh · December 23, 2025 at 8:37 pm
This is definitely a wonderful webpage, thanks a lot..
пин ап казино · December 23, 2025 at 10:55 pm
пин ап казино
Как зайти в pin up casino
website for making money · December 24, 2025 at 7:17 am
website for making money
vnniqic · December 24, 2025 at 7:33 am
https://edex.adobe.com/community/member/_lTOzPCG2
SandraTug · December 24, 2025 at 10:36 am
The Reason Fruit is Good for You Even Though it’s Filled With Sugar – Golden Health Method
Admin, согласен с вами полностью 🙂
Меня заинтересовала тема “”, но я там не могу ответить.
Для выбора.Ищете, где ассортимент больше? Добро пожаловать в самый крупный kraken магазин: кракен onion ссылки<Проверено только что.
Рабочие зеркала KRAKEN:
– кракен рабочая ссылка
– кракен vpn
– kra46 cc
Ваша личная скидка по коду KRA-QRGY2025 – 10%
Pin Up Casino sayt · December 24, 2025 at 12:07 pm
Bu platformanı çox sevirəm.
https://wc.tv.br/pinupqaydalar36239
zmdrebi · December 24, 2025 at 12:45 pm
https://code.antopie.org/bonusmelbet
nomini casino anmelden · December 24, 2025 at 3:07 pm
Starda Casino gratis Bonus
References:
https://online-spielhallen.de/der-snatch-casino-promo-code-ihr-schlussel-zu-mehr-spielspas-und-gewinnen/
locowin app spielen unterwegs · December 24, 2025 at 7:30 pm
Stake Casino anmelden
References:
https://online-spielhallen.de/ihr-leitfaden-zum-izzi-casino-aktionscode-maximieren-sie-ihre-gewinnchancen/
opplppn · December 24, 2025 at 8:00 pm
https://ideal-home.shop/communication/forum/user/11935/
vonbwpg · December 24, 2025 at 9:46 pm
https://dentabio.ru/2025/12/14/Рабочий-Промокод-Мелбет-2026-cash888-Бонус-15000/
대구스웨디시 · December 24, 2025 at 10:56 pm
대구스웨디시 마사지샵의 특징 · 합리적인 가격 · 24시간 연중무휴 운영 · 편리한 전화
예약 · 전문 테라피스트 상주 · 청결한
시설과 쾌적한 환경.
biodentex · December 24, 2025 at 11:28 pm
**biodentex**
biodentex is a dentist-endorsed oral wellness blend crafted to help fortify gums, defend enamel, and keep your breath consistently fresh.
Calvinkeelo · December 25, 2025 at 12:13 am
Learn more here: https://9aslan.com/asc-340-20-a-practical-book-to-own-accounting-firms-reinstated-fb-ad-accounts-for-sale/
dhqoigk · December 25, 2025 at 2:07 am
http://www.rosannasavoia.com/ciao-mondo/#comment-48697
LorenRusty · December 25, 2025 at 3:02 am
More Details: https://eguidemagazine.com/wp-content/pages/online-casinos-with-24-7-support_1.html
agen togel · December 25, 2025 at 3:32 am
I loved as much as you’ll receive carried out right here.
The sketch is attractive, your authored material stylish.
nonetheless, you command get bought an edginess over that you
wish be delivering the following. unwell unquestionably
come further formerly again as exactly the same nearly a lot
often inside case you shield this hike.
http://hp-ad.sub.jp/ · December 25, 2025 at 5:29 am
http://www.interq.or.jp/mars/mikami/bbs/index.html – http://hp-ad.sub.jp/nayami/nayamibbs/index.html,
innvkbx · December 25, 2025 at 8:44 am
https://horecaclub.it/read-blog/44677_ninecasino-italia-slot-esclusive-e-bonus-450-per-l-italia.html
jzomelh · December 25, 2025 at 9:21 am
https://itcrowd.pl/gitlab/lanika/internet-and-computers/issues/15
1xbet promo code philippines today · December 25, 2025 at 10:41 am
1xbet free promo code
apjasvp · December 25, 2025 at 3:09 pm
https://www.toptanboyunipi.com/blog/best-leather-bags
WEBCAM · December 25, 2025 at 4:05 pm
WEBCAM
euooqxn · December 25, 2025 at 4:15 pm
https://matters.town/a/4vir5tzdgusi
Rizk Casino Mobile · December 25, 2025 at 6:43 pm
Cosmo Casino seriös
References:
https://online-spielhallen.de/legzo-casino-aktionscode-ihr-schlussel-zu-fesselnden-pramien/
stargames casino sicher · December 25, 2025 at 10:01 pm
online casino app einfach
References:
https://online-spielhallen.de/umfassende-dolly-casino-bewertung-deine-entscheidungshilfe/
algoblb · December 25, 2025 at 11:24 pm
https://postheaven.net/nvva1duoof
egwvdze · December 26, 2025 at 12:27 am
https://utreediff.com/forum/viewtopic.php?t=1213
ozgdpoh · December 26, 2025 at 2:17 am
http://pogopogo1f.phorum.pl/viewtopic.php?p=417246#417246
pkaaive · December 26, 2025 at 5:59 am
https://videos.finally.agency/hubspot-cms-everything-you-need-to-1
exklusive N1Bet Vorteile · December 26, 2025 at 6:50 am
PowerUp Casino Einzahlung
References:
https://online-spielhallen.de/hit-spin-casino-login-ihr-weg-zum-spielvergnugen/
promo1win · December 26, 2025 at 8:06 am
code promo 1win 500
expert procurement blog · December 26, 2025 at 1:54 pm
Beneficial Blog! I had been simply just debating that there are plenty of screwy results at this issue you now purely replaced my personal belief. Thank you an excellent write-up.
1winfree · December 26, 2025 at 2:49 pm
<a href="quel est le meilleur code promo 1win
Procurement Nation · December 26, 2025 at 2:51 pm
It’s continually awesome when you can not only be informed, but also entertained! I’m sure you had fun writing this article. Regards, Clotilde.
jpshcst · December 26, 2025 at 3:06 pm
https://hackernoon.com/preview/9790lnoRFgpJZRhrBA7h
learn more about strategic sourcing · December 26, 2025 at 4:10 pm
Thank you pertaining to sharing the following great subject matter on your website. I ran into it on google. I am going to check to come back after you publish additional aricles.
global supply chain insights · December 26, 2025 at 4:30 pm
I truly appreciate this post. I have been looking everywhere for this! Thank goodness I found it on Bing. You have made my day! Thank you again
Learn more · December 26, 2025 at 6:40 pm
I was suggested this website by my cousin. I am not sure whether this post is written by him as no one else know such detailed about my difficulty. You are wonderful! Thanks!
Trace Loans · December 26, 2025 at 6:45 pm
A neighbor of mine encouraged me to take a look at your blog site couple weeks ago, given that we both love similar stuff and I will need to say I am quite impressed.
TraceLoans · December 26, 2025 at 7:12 pm
Its wonderful as your other blog posts : D, regards for putting up.
Gold Zeus · December 26, 2025 at 7:53 pm
You are good writer. Thank you.
xnmkjke · December 26, 2025 at 9:04 pm
http://hobbyland.moibb.ru/viewtopic.php?t=2449
Visit this website · December 26, 2025 at 9:58 pm
This is my first time i visit here. I found so many helpful stuff in your website especially its discussion. From the tons of responses on your posts, I guess I am not the only one having all the enjoyment here! keep up the excellent work
tcesttt · December 26, 2025 at 10:15 pm
https://whoosmind.com/forums/thread/32820/
opfdsvh · December 26, 2025 at 11:55 pm
https://mcyportal.mosti.gov.my/31-mei-2-jun-2016-biomalaysia-2016-di-kuala-lumpur-convention-centre/foto-2016/
snukldr · December 27, 2025 at 1:41 am
https://edublog.educastur.es/xentiquinaconsandra/2021/04/21/taller-iii-semana-del-libro/
gitlab.digineers.nl · December 27, 2025 at 4:36 am
Thanks for finally talking about > The Reason Fruit is Good for You Even Though it's Filled With Sugar
– Golden Health Method < Liked it!
trang chủ 8xbet · December 27, 2025 at 5:31 am
We’re a bunch of volunteers and opening a brand new scheme in our community.
Your site offered us with valuable info to work on. You’ve performed
a formidable job and our whole group will be grateful
to you.
gsxggok · December 27, 2025 at 7:22 am
https://ucisportfolios.pitt.edu/barirosenfeld/2025/11/15/how-home-care-in-rock-hill-sc-is-helping-seniors-stay-connected-to-their-community/
wgmhqzx · December 27, 2025 at 1:59 pm
https://edex.adobe.com/community/member/HGXcD0de0
ekoelement.ru · December 27, 2025 at 4:29 pm
https://www.orcunakbulut.av.tr/Genel%20Sorular/the-ten-key-elements-in-blog/ – http://ekoelement.ru/bitrix/rk.php?goto=https://office-nko.ru/dwqa-question/obsuzhdenie-proekta-prikaza-o-vnesenii-izmenenij-v-standarty-socialnyh-uslug/ –
jbuxxeh · December 27, 2025 at 4:44 pm
https://jobs.suncommunitynews.com/profiles/7652497-1xbetfreebet-com1
gdlnnlu · December 27, 2025 at 5:49 pm
https://buildwallpro.com/userinfo.php?from=space&op=userinfo&action=view&user=nadia.linville.494255
https://salda.ws/article/?act=read&article_id=28304 · December 27, 2025 at 5:59 pm
https://salda.ws/article/?act=read&article_id=28304
https://shoestoreuk.uk.com/ · December 27, 2025 at 6:46 pm
Hey just wanted to give you a quick heads up. The words in your post seem to be running
off the screen in Opera. I’m not sure if this is a formatting issue or
something to do with browser compatibility but I
thought I’d post to let you know. The design look great though!
Hope you get the problem resolved soon. Kudos
Meilleur code promo 1XBET Sénégal 2026: 1XWAP200 - Bonus 130 € · December 27, 2025 at 9:55 pm
I’m not positive where you are getting your information, but
great topic. I must spend a while studying much more or understanding more.
Thanks for magnificent info I used to be in search of this information for my mission.
mlltvls · December 27, 2025 at 9:58 pm
http://delphi.larsbo.org/user/bestxbet26
Austin · December 27, 2025 at 11:07 pm
Also visit my web page: Austin
uwvihkd · December 28, 2025 at 12:24 am
https://slubowisko.pl/topic/105797/
lmhzmby · December 28, 2025 at 2:36 am
https://mpc.imu.edu.kg/en/profile/welcome1xbet
http://geekhosting.company/ruthsedillo213 · December 28, 2025 at 2:39 am
Why people still make use of to read news papers
when in this technological world the whole thing is existing on net?
https://millioner-otvet.ru/virtualnyj-nomer-telefona-indonezii-udobstvo-i-vozmozhnosti-dlya-biznesa/ · December 28, 2025 at 4:38 am
https://millioner-otvet.ru/virtualnyj-nomer-telefona-indonezii-udobstvo-i-vozmozhnosti-dlya-biznesa/
Merge Images · December 28, 2025 at 9:06 am
Hello this is kinda of off topic but I was wondering if blogs use WYSIWYG editors or if you have to manually code with HTML. I’m starting a blog soon but have no coding knowledge so I wanted to get advice from someone with experience. Any help would be enormously appreciated!
melbetofthebest · December 28, 2025 at 10:13 am
codigo promocional MelBet bolivia
https://mymedia.com.ua/vyrtualnj-nomer-navsegda-svoboda-obshhenyya-v-odnom-klyke/ · December 28, 2025 at 11:18 am
https://mymedia.com.ua/vyrtualn%d1%8bj-nomer-navsegda-svoboda-obshhenyya-v-odnom-klyke/
best online casino fast payou · December 28, 2025 at 1:36 pm
When I originally commented I clicked the “Notify me when new comments are added” checkbox and now each time a comment
is added I get several e-mails with the same comment. Is there any way you can remove me from that service?
Thank you!
melbetofthebest · December 28, 2025 at 3:40 pm
MelBet codigo promocional argentina
gsjqkor · December 28, 2025 at 9:52 pm
https://trading24inw3.blogspot.com/2025/12/the-ultimate-guide-to-live-betting.html
jgowulw · December 28, 2025 at 9:55 pm
https://bookmarksurl.com/story6375313/1xbet-%E0%A4%AA-%E0%A4%B0-%E0%A4%AE-%E0%A4%95-%E0%A4%A1-2026-1x200mix-42-900-%E0%A4%A4%E0%A4%95-%E0%A4%AC-%E0%A4%A8%E0%A4%B8
mqhyiqi · December 28, 2025 at 11:05 pm
https://www.japanesewomenorg.com/read-blog/72297
Bay789 · December 28, 2025 at 11:41 pm
Nice read, I just passed this onto a colleague who was doing some research on that. And he just bought me lunch as I found it for him smile Therefore let me rephrase that: Thank you for lunch!
sgkttwz · December 29, 2025 at 6:01 am
https://www.opencart-france.com/newsletter/pages/?code_promo_betwinner_11.html
eznhsqp · December 29, 2025 at 8:09 am
https://in.chats-888.com/
1xbetpromocode · December 29, 2025 at 8:10 am
1xbet promo code egypt
xhzwikz · December 29, 2025 at 10:19 am
https://dansermag.com/wp-content/pages/?code_promo_1win.html
1xbetfreespins · December 29, 2025 at 11:18 am
1xbet promo code
cbd oil side effects · December 29, 2025 at 1:53 pm
If you don’t mind, where do you host your weblog? I am looking for a very good web host and your webpage seams to be extremely fast and up most the time…
1xbetpromocode · December 29, 2025 at 2:31 pm
1xbet promo code new user egypt
ooqarbu · December 29, 2025 at 2:55 pm
https://gazetablic.com/new/?1win_promo_code_10.html
1xbet code promo du jour · December 29, 2025 at 9:45 pm
code promo 1xbet 2026 sГ©nГ©gal
comment creer son propre code promo melbet · December 29, 2025 at 10:30 pm
comment ajouter un code promo sur melbet
creer un code promo melbet · December 30, 2025 at 2:03 am
comment creer un code promo melbet
sbobet · December 30, 2025 at 3:18 am
Hola! I’ve been reading your website for some time now and finally got the bravery to go ahead and give
you a shout out from Huffman Texas! Just wanted to
mention keep up the great job!
quel est le meilleur code promo melbet · December 30, 2025 at 5:04 am
meilleur code promo melbet
code promo 1xbet gabon · December 30, 2025 at 7:56 am
code promo 1xbet gratuit algГ©rie
1вин казино официальный сайт · December 30, 2025 at 9:06 am
What’s up friends, its great paragraph about tutoringand completely defined, keep it up all
the time.
unojolq · December 30, 2025 at 12:33 pm
https://medyumbestamihoca.com/
hagthbi · December 30, 2025 at 12:41 pm
https://www.kickstarter.com/profile/2072942961/about
Thabet · December 30, 2025 at 2:39 pm
This website has lots of really useful stuff on it. Thanks for informing me.
https://betechit.com · December 30, 2025 at 2:56 pm
Developing a framework is important.
https://www.goldzeus.com · December 30, 2025 at 3:44 pm
I just couldn’t leave your website before suggesting that I really enjoyed the usual information an individual supply on your visitors? Is gonna be back often in order to investigate cross-check new posts
dlodedv · December 30, 2025 at 5:25 pm
https://amber-girl-6de.notion.site/1xBet-2026-1X200BOX-42-900-2ca08d447c9480cdb8cef6b7d2dfd354?source=copy_link
1xBet Sign Up Promo Code 2026: 1XWAP200 · December 30, 2025 at 5:36 pm
Amazing things here. I’m very satisfied to peer your post.
Thank you so much and I’m looking forward to touch you.
Will you kindly drop me a e-mail?
zcxfdsz · December 30, 2025 at 6:00 pm
https://www.crossroadsbaitandtackle.com/board/board_topic/9053260/7616480.htm
https://www.icostamp.com · December 30, 2025 at 6:22 pm
I discovered your weblog site on google and verify just a few of your early posts. Proceed to maintain up the very good operate. I simply further up your RSS feed to my MSN News Reader.
uudet nettikasinot · December 30, 2025 at 9:29 pm
Thank you for the auspicious writeup.
https://goldzeus.com · December 30, 2025 at 9:36 pm
fantastic post, very informative. I wonder why more of the ther experts in the field do not break it down like this. You should continue your writing. I am confident, you have a great readers’ base already!
Procurementnation.com · December 30, 2025 at 10:24 pm
Thank you a lot for sharing this with all folks you actually recognize what you’re speaking about! Bookmarked. Please additionally visit my site =). We can have a hyperlink trade contract among us!
evmgpyk · December 30, 2025 at 11:06 pm
https://ivebo.co.uk/read-blog/226853
https://betechit.com · December 31, 2025 at 12:17 am
Have you given any kind of thought at all with converting your current web-site into French? I know a couple of of translaters here that will would certainly help you do it for no cost if you want to get in touch with me personally.
ignitra · December 31, 2025 at 5:01 am
**ignitra**
ignitra is a premium, plant-based dietary supplement created to support healthy metabolism, weight management, steady energy, and balanced blood sugar as part of an overall wellness routine
nouveau casino en ligne · December 31, 2025 at 7:47 am
whoah this weblog is wonderful i like reading your articles. Keep up the good paintings! You already know, many people are looking around for this information, you can help them greatly.
1xBet Sign Up Promo Code 2026: 1XWAP200 · December 31, 2025 at 9:19 am
Somebody necessarily assist to make significantly articles I’d
state. That is the first time I frequented your website page and up to now?
I amazed with the analysis you made to make this actual put up incredible.
Great job!
tjsvmaz · December 31, 2025 at 3:13 pm
https://lebanonhub.app/blogs/765573/Code-Bienvenue-1Win-1W2026VIP-500-D%C3%A9p%C3%B4ts
Z8 BET · December 31, 2025 at 5:00 pm
I wanted to check up and let you know how, a great deal I cherished discovering your blog today. I might consider it an honor to work at my office and be able to utilize the tips provided on your blog and also be a part of visitors’ reviews like this. Should a position associated with guest writer become on offer at your end, make sure you let me know.
bodylotion · December 31, 2025 at 7:44 pm
Excellent post. Keep posting such kind of information on your
site. Im really impressed by it.
Hi there, You have done an incredible job. I will definitely digg it and in my opinion suggest to my friends.
I’m sure they will be benefited from this website.
Crypto.hu.net · December 31, 2025 at 8:30 pm
Dude.. I am not much into reading, but somehow I got to read lots of articles on your blog. Its amazing how interesting it is for me to visit you very often. –
visit the official site · December 31, 2025 at 11:18 pm
Our local network of agencies has found your research so helpful.
porno · January 1, 2026 at 2:14 am
porno
iukbntj · January 1, 2026 at 3:27 am
https://drc.uog.edu.et/1win-az-dan-bonuslar-1win-az-in-qeydiyyati-vЙ™-hЙ™diyyЙ™nin-duzgun-mЙ™rc-edilmЙ™si-ucun-bonus-alma
rfobhzg · January 1, 2026 at 4:02 am
https://transfur.com/Users/freebetpromoe
lxripwu · January 1, 2026 at 4:17 am
https://anotepad.com/notes/96c9t3r2
gyylmvg · January 1, 2026 at 1:28 pm
https://www.gurnee.il.us/news/2024/03/28/Earthmonth
oiaslhz · January 1, 2026 at 2:57 pm
https://mushlovesocial.com/blogs/111780/C%C3%B3digo-Promocional-Lista-Hoje-1xBet-2026-1XRUN200
hpmwkvh · January 1, 2026 at 7:43 pm
https://www.handromania.gr/blog/classic-watches
pblgtif · January 1, 2026 at 10:26 pm
https://coub.com/605edee7f9eaca6d59c0
x777login · January 2, 2026 at 12:10 am
X777login, eh? Nice and clean design. Registration was a breeze, no weird roadblocks. Still exploring, but first impressions are solid. See for yourself – x777login
mfmuhns · January 2, 2026 at 12:33 am
https://www.semae.sc.gov.br/dia-da-agua-estado-investe-mais-de-r-17-milhoes-em-capacitacao-e-planejamento-para-garantir-o-uso-sustentavel-da-agua/
zacssvk · January 2, 2026 at 1:06 am
https://warealtor.org/education-events/events2/event-calendar/2023/02/07/default-calendar/what%27s-going-on-black-home-ownership-crisis-webinar
highstakes Casino download · January 2, 2026 at 6:32 am
Also visit my web blog … highstakes Casino download
xlymelc · January 2, 2026 at 6:53 am
https://notebook.zohopublic.com/public/notes/il0dw47a94070e7314cca80aee44b43195d82
neurosharp · January 2, 2026 at 11:13 am
**neurosharp**
neurosharp is a next-level brain and cognitive support formula created to help you stay clear-headed, improve recall, and maintain steady mental performance throughout the day.
finessa · January 2, 2026 at 11:52 am
**finessa**
Finessa is a natural supplement made to support healthy digestion, improve metabolism, and help you achieve a flatter belly.
xktzglo · January 2, 2026 at 3:47 pm
http://prigotovim.org/index.php?subaction=userinfo&user=idaqicepy
Free Live Sex Webcams and Porn Chat · January 2, 2026 at 6:17 pm
Hiya very cool web site!! Man .. Beautiful .. Amazing .. I will bookmark your website and take the feeds additionally?
I am happy to find numerous helpful information here
within the publish, we want work out more techniques in this regard, thank you for sharing.
. . . . .
JefferyVunny · January 2, 2026 at 8:32 pm
Купити налобний ліхтарик
Перед тим як купити налобний ліхтарик, варто звернути увагу на основні параметри. Серед них: яскравість світла.
Налобний ліхтар на акумуляторі повинен відповідати вашим потребам. Для побуту підійдуть просте керування. Для екстремальних умов краще обирати потужний налобний ліхтар.
Купити потужний налобний ліхтар сьогодні можна у спеціалізованих магазинах. Якісний ліхтарик на голову — це комфорт, які будуть з вами у будь-якій ситуації. Налобний ліхтарик
syjoltn · January 2, 2026 at 10:39 pm
https://www.gabitos.com/eldespertarsai/template.php?nm=1767165596
https://treba-solutions.com/bolshe-chem-prosto-bongi-kak-perkolyatori-i-drugie-apgreidi-menyayut-vash-devais-dlya-kureniya/ · January 3, 2026 at 1:05 am
https://treba-solutions.com/bolshe-chem-prosto-bongi-kak-perkolyatori-i-drugie-apgreidi-menyayut-vash-devais-dlya-kureniya/
https://www.0552.ua/list/504844 · January 3, 2026 at 4:14 am
https://www.0552.ua/list/504844
vjldrpp · January 3, 2026 at 5:42 am
https://manufacturers.network/user/cupombet/
ruknfdr · January 3, 2026 at 6:21 am
https://orgoeast.com/index.php?route=journal3/blog/post&journal_blog_post_id=13
attorney mortgage · January 3, 2026 at 6:36 am
Might we expect to see more of these same problems in the future?
ncmshye · January 3, 2026 at 2:02 pm
https://workflowy.com/s/best-1win-promo-code/f6nhEYWceVscNgUw#/5fa11f35b383
상무지구안마 · January 3, 2026 at 2:47 pm
Makes sense to me.
Find Out · January 3, 2026 at 3:04 pm
Thanks so much for this, keep up the good work 🙂
https://rkantor.com/quantum-ai-geschaftlicher-nutzen-und-anwendungspotenzial-fur-unternehmen/ · January 3, 2026 at 9:12 pm
Seit dem Start verzeichnet Quantum ein wachsendes Interesse aus verschiedenen europaischen Markten. https://rkantor.com/quantum-ai-geschaftlicher-nutzen-und-anwendungspotenzial-fur-unternehmen/
svchrjf · January 3, 2026 at 9:57 pm
https://www.naturelle.gr/journal-blog
zcqscos · January 3, 2026 at 11:50 pm
https://www.fundae.es/actualidad/ca/noticias/2020/10/26/tr%C3%A1mites
uplcecq · January 4, 2026 at 2:42 am
https://www.natthadon-sanengineering.com/forum/topic/55989/1win-no-deposit-code:-1w2026vip—free-bonus-rewards
https://dutable.com/scalable-microservices-for-multi-sport-betting-operations/ · January 4, 2026 at 4:08 am
Data analytics pipelines for casino KPIs and retention https://dutable.com/scalable-microservices-for-multi-sport-betting-operations/
delilerkoyu.com · January 4, 2026 at 6:09 am
http://www2k.biglobe.ne.jp/~kao-nori/jawanote.cgi?js=eyJhbGciOiJIUzI1NiIsInR5cCI6IkpXVCJ9.eyJhdWQiOiJKb2tlbiIsImV4cCI6MTYzNTM0MzA0NiwiaWF0IjoxNjM1MzM1ODQ2LCJpc3MiOiJKb2tlbiIsImpzIjoxLCJqdGkiOiIycW91MmljdGJkZGhzMmRpcjgxbjM2a2IiLCJuYmYiOjE2MzUzMzU4NDYsInRzIjoxNjM1MzM1ODQ2MDAwOTgwfQ.QbOSUA9IlpW_JpKRxAvX2nrJ2SsBZmP_CAQVh7CrOqs&page=0&sid=0c37d22a-371d-11ec-8074-f31464f85302&url=Www2K.Biglobe.Ne.jp/%7Ekao-nori/jawanote.cgi%3Fjs%3DeyJhbGciOiJIUzI1NiIsInR5cCI6IkpXVCJ9.eyJhdWQiOiJKb2tlbiIsImV4cCI6MTYzNTM0MzA0NiwiaWF0IjoxNjM1MzM1ODQ2LCJpc3MiOiJKb2tlbiIsImpzIjoxLCJqdGkiOiIycW91MmljdGJkZGhzMmRpcjgxbjM2a2IiLCJuYmYiOjE2MzUzMzU4NDYsInRzIjoxNjM1MzM1ODQ2MDAwOTgwfQ.QbOSUA9IlpW_JpKRxAvX2nrJ2SsBZmP_CAQVh7CrOqs%26page%3D0%26sid%3D0c37d22a-371d-11ec-8074-f31464f85302%26url%3Dwww2K.biglobe.ne.jp/%7Ekao-nori/jawanote.cgi%3Fjs%3DeyJhbGciOiJIUzI1NiIsInR5cCI6IkpXVCJ9.eyJhdWQiOiJKb2tlbiIsImV4cCI6MTYzNTM0MzA0NiwiaWF0IjoxNjM1MzM1ODQ2LCJpc3MiOiJKb2tlbiIsImpzIjoxLCJqdGkiOiIycW91MmljdGJkZGhzMmRpcjgxbjM2a2IiLCJuYmYiOjE2MzUzMzU4NDYsInRzIjoxNjM1MzM1ODQ2MDAwOTgwfQ.QbOSUA9IlpW_JpKRxAvX2nrJ2SsBZmP_CAQVh7CrOqs%26page%3D0%26sid%3D0c37d22a-371d-11ec-8074-f31464f85302%26url%3DWww2k.Biglobe.Ne.jp/%7Ekao-nori/jawanote.cgi%3Fpage%3D0%26url%3Dwww.union.ic.ac.uk/rcc/fellwanderers/gallery/main.php%3Fg2_itemId%3D12558 [https://delilerkoyu.com/index.php?option=com_datsogallery&Itemid=23&func=detail&catid=3&id=78]
hbmtvnf · January 4, 2026 at 6:40 am
https://eurodenda.es/blog/invertir-productos-cocina-calidad
gmmachb · January 4, 2026 at 7:14 am
https://socialbuzzfeed.com/story6364141/1xbet-india-promo-list-2026-1xbat777-offers
2-FPM For Sale · January 4, 2026 at 8:47 am
I’m so happy to read this. This is the type of manual that needs to be given and not the random misinformation that’s at the other blogs. Appreciate your sharing this best doc.
dqnuocn · January 4, 2026 at 10:09 am
https://www.magcloud.com/user/codepomoxbet1
tqpenfu · January 4, 2026 at 2:48 pm
https://www.siapalidis.gr/blog/best-leather-bags
yncdpsd · January 4, 2026 at 5:46 pm
https://pclassified.com/0/posts/1-Digital-Items/1-Websites/1793479-1xBet-Promo-Code-amp-Bonus-Codes-2026.html
tibvteq · January 4, 2026 at 6:19 pm
https://www.noteflight.com/profile/1ecbdd5b83a525af99afa31a6c611bdff52c0d3f
ujrfplp · January 5, 2026 at 12:21 am
https://buildwallpro.com/userinfo.php?com=profile&mod=space&username=colette.boulton_495626
nosorzf · January 5, 2026 at 3:38 am
https://whelex.com/userinfo.php?username=tania.burbank_495626&name=Your_Account&com=profile&mod=space
nlhplgy · January 5, 2026 at 5:59 am
https://blooder.net/read-blog/151706
안양출장마사지 · January 5, 2026 at 9:18 am
I enjoy what you guys are usually up too. This type of clever work and coverage!
Keep up the great works guys I’ve added you guys to
my own blogroll.
52betwin · January 5, 2026 at 12:02 pm
52betwin, e aí, apostadores de plantão! Encontrei um site com umas apostas bem interessantes. Se você curte adrenalina, dá uma espiada! Acesse 52betwin.
max79top · January 5, 2026 at 4:27 pm
I wrote down your blog in my bookmark. I hope that it somehow did not fall and continues to be a great place for reading texts.
free bet promo code 1xbet today · January 5, 2026 at 4:48 pm
1xbet casino promo code no deposit bonus
lmirafq · January 5, 2026 at 5:49 pm
https://share.evernote.com/note/07615a11-70c7-8713-24da-de4f5cb9c920
qblezud · January 5, 2026 at 6:27 pm
https://starbookmarking.com/story/code-promo-sur-1xbet-2026-1x200king-bonus-gratuit
meilleur casino en ligne · January 5, 2026 at 7:35 pm
Dude.. I am not much into reading, but somehow I got to read lots of articles on your blog. Its amazing how interesting it is for me to visit you very often. –
awhcjno · January 6, 2026 at 12:13 am
https://graph.org/1xBet-Promo-Code-Hong-Kong-2026-1X200FREE–Bonus-130-01-02
gqjcywl · January 6, 2026 at 12:24 am
https://majir22599.xoo.it/t35-Code-promo-1xBet-Burkina-Faso-2026-1X200MAN-Bonus-VIP.htm#p94
pmcabon · January 6, 2026 at 2:31 am
https://forum.amzgame.com/thread/detail?id=533333
66b · January 6, 2026 at 4:10 am
Slot tại 66b luôn cập nhật xu hướng mới nhất: từ cổ điển đến hiện đại, RTP cao, jackpot lên tới hàng tỷ đồng. Trải nghiệm ngay hôm nay để nhận quà tặng chào mừng! TONY01-06S
xn88 com · January 6, 2026 at 4:12 am
xn88 com có chính sách hoàn tiền theo sản phẩm: casino 0.8%, thể thao 0.5%, slot 0.3% – tích lũy hàng tuần và tự động cộng vào tài khoản mỗi thứ Hai. TONY01-06S
afynrgc · January 6, 2026 at 12:47 pm
https://kingshouse.gov.jm/gg-appoints-eight-female-jurists/
irntsuc · January 6, 2026 at 12:58 pm
https://journeys.dartmouth.edu/culture-food-italian-literature/2013/05/24/istruzoni-per-progetti-digitali/#comment-37430
pjqguop · January 6, 2026 at 3:13 pm
https://motionentrance.edu.np/profile/xbetfreebet7/
hair transplant turkey · January 6, 2026 at 4:51 pm
Great blog right here! You seem to put a significant amount of material on the site rather quickly.
trzdohj · January 6, 2026 at 6:50 pm
https://cdsonla.edu.vn/index.php/vi/component/k2/item/25-getting-to-know-your-professors?tmpl=component&print=1&start=48
xuxibhs · January 6, 2026 at 7:11 pm
https://www.pearltrees.com/xbetbest/item771117518
best online casino Ontario · January 6, 2026 at 7:27 pm
Nice read, I just passed this onto a colleague who was doing some research on that. And he just bought me lunch as I found it for him smile Therefore let me rephrase that: Thank you for lunch!
glnhvul · January 7, 2026 at 12:39 am
https://forum.bandariklan.com/showthread.php?tid=1059230
gytxuil · January 7, 2026 at 12:59 am
https://prof-aksay.ru/forum/user/7875/
blacklife.x-y.net · January 7, 2026 at 1:03 pm
http://3dim-athin.att.sch.gr/autosch/joomla15/index.php/component/kide/history/-/index.php?option=com_kide (http://blacklife.x-y.net/bbs/board.php?bo_table=free&wr_id=1025396)
spywntn · January 7, 2026 at 1:07 pm
https://vivealumni.usfq.edu.ec/2014/10/beneficios-escuela-de-empresas.html?sc=1767115752804#c2586551470224830119
yhozjor · January 7, 2026 at 2:29 pm
https://www.stylevore.com/user/melbetspin
JefferyVunny · January 7, 2026 at 2:29 pm
Прокат машины за границей — это отличная возможность исследовать чужие города. Выбор машины заранее помогает найти выгодное предложение. Популярные платформы проката автомобилей дают возможность сравнить цены и условия. От небольших авто до внедорожников для коротких поездок или длинных путешествий. Аренда авто за границей позволяет планировать маршрут самостоятельно и открывает доступ к скрытым туристическим местам. Лайфхаки опытных путешественников позволяют выбрать лучшие варианты. Важно оценить состояние автомобиля, для комфортного отдыха. https://rentalcardaily.com/category/arenda-avto/
vdqsrax · January 7, 2026 at 5:42 pm
https://wefunder.com/1winpromo456
guxkojb · January 7, 2026 at 6:14 pm
https://brandwoot.com/profile.php?op=userinfo&from=space&mod=space&name=Your_Account&username=iona_ampt.495847
xmldiio · January 7, 2026 at 8:15 pm
https://www.driedsquidathome.com/forum/topic/90862/1xbet-promo-code-south-korea-2026:-1xrun200-%E2%80%93-bonus-%E2%82%AC130
kqhyash · January 7, 2026 at 10:25 pm
https://speakerdeck.com/bet1xbonus
3 cmc · January 8, 2026 at 2:52 am
I feel that is among the so much significant info for me. And i am satisfied studying your article. However should commentary on some basic issues, The site style is ideal, the articles is in reality excellent : D. Excellent activity, cheers
2 mmc · January 8, 2026 at 4:39 am
How long have you been in this field? You seem to know a lot more than I do, I’d love to know your sources!
pexcehj · January 8, 2026 at 8:19 am
https://www.betting-forum.com/whats-new/posts/4963153/
ythcwvp · January 8, 2026 at 10:48 am
http://diafan.rusheat.ru/forum/promokod-1win-eksklyuzivnyy-1w500star—500-bonus/
1win aviator · January 8, 2026 at 11:04 am
how to play aviator game apk aviator predictor apk
lwhxzry · January 8, 2026 at 11:50 am
https://www.uscgq.com/forum/posts.php?forum=&id=335315&page=3#post23
xổ số nhà cái 68vip có uy tín không ? · January 8, 2026 at 2:19 pm
How come you do not have your website viewable in mobile format? cant see anything in my Droid.
casino live nhà cái 68vip có uy tín không ? · January 8, 2026 at 5:51 pm
Your resources are well developed.
pure cbd oil · January 8, 2026 at 9:18 pm
I’ll check back after you publish more articles.
www.real.g6.cz · January 9, 2026 at 1:23 am
http://www.real.g6.cz/index.php?option=com_realestatemanager&task=view&catid=47&id=11&Itemid=0 (http://www.real.g6.cz/index.php?option=com_realestatemanager&task=view&catid=47&id=11&Itemid=0)
bokep indonesia · January 9, 2026 at 5:21 am
I appreciate your work, thanks for all the great blog posts.
qkdznyt · January 9, 2026 at 8:03 pm
https://tshirtlegend.gr/index.php?route=journal3/blog/post&journal_blog_category_id=2&journal_blog_post_id=1
pivafhv · January 9, 2026 at 9:27 pm
http://cozy.moibb.ru/viewtopic.php?f=22&t=25626
uoytaud · January 9, 2026 at 11:39 pm
https://stockhouse.com/blogs/articlebest/december-2025/code-bonus-melbet-2026-1750-casino-290-fs
mhhmtic · January 10, 2026 at 1:54 am
https://www.speedrun.com/users/melbetfree
cfnlduc · January 10, 2026 at 2:53 am
http://3ametki.ru/index.php?subaction=userinfo&user=ufidu
казино онлайн · January 10, 2026 at 5:02 am
Просто хочу сказать, что счастлив(а), что нашёл(а) сайт казино онлайн — супер!
https://pinupkz-download.kz/
ojbsedh · January 10, 2026 at 7:52 am
https://roomstyler.com/users/1xbetfreebets5678
eibtxvn · January 10, 2026 at 1:17 pm
https://hedgedoc.dezentrale.space/s/n6CHRjzOk
1xbetfreecodes · January 10, 2026 at 1:59 pm
1xbet promo code today sri lanka
giaovienvietnam.vn · January 10, 2026 at 2:22 pm
holland casino eindhoven
References:
https://giaovienvietnam.vn/employer/androchem-laboratories-hgh-wachstumshormon-liquid-100iu-steroide-kaufen-in-deutschland/
mqmxvrg · January 10, 2026 at 2:27 pm
https://codyaluc58025.csublogs.com/46726933/c%C3%B3digo-promocional-melhor-1xbet-2026-1xwap200
yfltwfl · January 10, 2026 at 8:00 pm
https://www.blackhatworld.com/members/codecan2026.2273232/#about
1xbet промокод как активировать · January 10, 2026 at 9:00 pm
фрибет 1xbet промокод
jaqvmzh · January 10, 2026 at 11:55 pm
https://www.quora.com/profile/James-Bradley-982
les meilleurs code promo melbet · January 11, 2026 at 2:33 am
je veux un code promo melbet
uqngczh · January 11, 2026 at 3:21 am
http://delphi.larsbo.org/user/xbetvip2026
как получить промокод 1хбет бесплатно · January 11, 2026 at 5:19 am
http://jseltec.com/bbs/board.php?bo_table=free&wr_id=720900
weblogposts · January 11, 2026 at 5:53 am
Hi my family member! I want to say that this article is amazing, great written and include approximately all important infos. I’d like to see more posts like this .
ibldlvd · January 11, 2026 at 5:07 pm
http://www.deseretica.com/2011/06/universal-university.html?sc=1767857899151#c3376322277332865980
zhicidh · January 11, 2026 at 8:17 pm
https://qodegypt.com/%D8%A7%D9%84%D9%85%D8%AF%D9%88%D9%86%D8%A9/wool-jackets
boostaro · January 12, 2026 at 9:29 am
**boostaro**
boostaro is a specially crafted dietary supplement for men who want to elevate their overall health and vitality.
auxayvv · January 12, 2026 at 10:13 am
https://jobs.windomnews.com/employers/3960108-1xbet-uganda-promo-code
https://baby-newlife.ru/user/profile/316753 · January 12, 2026 at 3:48 pm
online casino u s a
References:
https://baby-newlife.ru/user/profile/316753
cricketcreekfarm.com · January 12, 2026 at 5:34 pm
bonus 1xbet madagascar (https://cricketcreekfarm.com/wp-content/uploads/?code-promo-1xbet-bonus-de-bienvenue.html)
gzqraqz · January 13, 2026 at 12:32 am
https://FreeAds1.com/389/posts/1/1/1749235.html
jyuxrsn · January 13, 2026 at 1:19 am
https://community.theasianparent.com/q/code_promo_1xbet_2026_1xsun200_bonus_jusqu_%C3%A0_130_le_code_promo_1xbet_1xsun200_o/5801235/amp
phim sex trẻ em · January 13, 2026 at 1:31 am
Hey, I simply hopped over to your website by way of StumbleUpon. No longer one thing I’d normally learn, but I preferred your thoughts none the less. Thanks for making one thing worth reading.
classifylistings.com · January 13, 2026 at 5:05 am
online casino live games best uk
References:
https://classifylistings.com/index.php?page=user&action=pub_profile&id=130654
rxqbwaa · January 13, 2026 at 6:08 am
https://168.exodirectory.com/index.php?topic=266929.new#new
разбилось стекло айфон 17 про макс Казань · January 13, 2026 at 10:07 am
разбилось стекло айфон 17 про макс Казань
fvcftbj · January 13, 2026 at 12:25 pm
https://sites.northwestern.edu/lemmings/2019/01/29/me-reading-group-meeting/#comment-37089
1xbet today promo code ghana · January 21, 2026 at 7:46 pm
1xbet today promo code ghana
eiimiij · January 21, 2026 at 10:48 pm
https://bookmark-dofollow.com/story27006781/1xbet-promo-code-bangladesh-2026-1xfun777-bonus-130
1xbet free bet promo code south africa · January 22, 2026 at 5:26 am
1xbet free bet promo code south africa
slot gacor hari ini · January 22, 2026 at 7:03 am
Appreciation for taking the time to discuss this topic, I would love to discover more on this topic. If viable, as you gain expertise, would you object to updating the website with further information? It is tremendously beneficial for me.
mxbigwin77 · January 22, 2026 at 12:04 pm
Let me tell you all about mxbigwin77. This is where the serious action happens. I have had a little luck here. Check it out if you’re feeling lucky: mxbigwin77
casinogalacticwins · January 22, 2026 at 12:04 pm
Greetings fellow gamblers! casinogalacticwins is a new casino I tried recently and I think that it is awesome. Easy registration and fantastic bonuses! Try it now: casinogalacticwins
8833betlogin · January 22, 2026 at 12:04 pm
Hey folks, tried out 8833betlogin recently. It is great, the bonuses you get when you register are pretty good, and I won on the first few bets! Check it out for yourself here: 8833betlogin
vjpgtil · January 22, 2026 at 1:14 pm
https://customproducttraining.com/code-promo-inscription-1xbet-senegal-2026-1xbig2026/
fiypxib · January 22, 2026 at 4:30 pm
https://wordpress.lehigh.edu/too223/2020/05/07/chopsticks/comment-page-77/#comment-40901
kasyno internetowe · January 22, 2026 at 7:12 pm
hey thanks for the info. appreciate the good work
casino en ligne international · January 22, 2026 at 7:29 pm
Hello this is a wonderful write-up. I’m going to e mail this to my friends. I came on this while searching on yahoo I’ll be sure to come back. thanks for sharing.
jzmmtbk · January 22, 2026 at 11:34 pm
https://InstantAdz.com/389/posts/1/1/1895572.html
cgi.www5f.biglobe.ne.jp · January 23, 2026 at 2:40 am
http://cgi.www5f.biglobe.ne.jp/raymond/rollbbs/petit.cgi; http://cgi.www5f.biglobe.ne.jp/raymond/rollbbs/petit.cgi,
code promo 1xbet valide · January 23, 2026 at 5:57 am
code promo 1xbet congo
Referal Binance · January 23, 2026 at 6:51 am
Thank you for your sharing. I am worried that I lack creative ideas. It is your article that makes me full of hope. Thank you. But, I have a question, can you help me? https://www.binance.info/ru-UA/register?ref=JVDCDCK4
code promo 1xbet afrique · January 23, 2026 at 9:29 am
code promo 1xbet cote d’ivoire 2026
ugnsygr · January 23, 2026 at 12:39 pm
https://ecuadorenventa.net/author/melbetspin0/
jun88 · January 23, 2026 at 2:48 pm
I think this is among the so much vital info for me. And i’m happy reading your article. But wanna remark on few common issues, The site style is wonderful, the articles is really excellent : D. Just right job, cheers
Buy Blue Crystal Meth Online · January 23, 2026 at 4:30 pm
Hello there I am so delighted I found your weblog, I really found you by mistake, while I was searching on Google for something else, Anyhow I am here now and would just like to say cheers for a remarkable post and a all round exciting blog (I also love the theme/design), I don’t have time to browse it all at the moment but I have book-marked it and also included your RSS feeds, so when I have time I will be back to read a lot more, Please do keep up the superb work.
Jun88 · January 23, 2026 at 5:13 pm
This is definitely a wonderful webpage, thanks a lot..
irish online casino · January 23, 2026 at 7:15 pm
You ma’am have a way with words. Thank you very much!
irish online casino · January 23, 2026 at 8:07 pm
I’ll check back after you publish more articles.
https://swedbe.ru/catalog/smesiteli/termostaticheskie/13500/ · January 23, 2026 at 9:07 pm
https://swedbe.ru/catalog/smesiteli/termostaticheskie/13500/
slot win · January 23, 2026 at 9:13 pm
I love your blog. It looks every informative.
Buy 80% Lowers Brands Online · January 24, 2026 at 1:37 am
Amazing content on your website.
Sultan Casino покер · January 24, 2026 at 5:24 am
Продолжайте в том же духе и привлекайте ещё больше игроков!
https://sultan-casino-kazakhstan-playbet.kz/games
foiebol · January 24, 2026 at 6:57 am
https://bandori.party/user/380187/codepromo1xbetabidjan/
hbfhwmi · January 24, 2026 at 9:35 am
https://www.wisla-plock.pl/pages/articles/?4rabet_promo_code_india.html
https://swedbe.ru/catalog/smesiteli/termostaticheskie/13898/ · January 24, 2026 at 10:57 am
https://swedbe.ru/catalog/smesiteli/termostaticheskie/13898/
ijjqaqk · January 24, 2026 at 11:12 am
https://www.longisland.com/profile/1xbetbonus43545
muxyktd · January 24, 2026 at 3:25 pm
https://www.uscgq.com/forum/posts.php?forum=general&id=564726
hpunbcn · January 24, 2026 at 5:04 pm
https://www.natthadon-sanengineering.com/forum/topic/61577/1xbet-promo-code-ghana-2026:-1x200bag-%E2%80%93-bonus-%E2%82%AC130
xcihfza · January 24, 2026 at 6:25 pm
https://xtremepape.rs/members/1xbetbonusvn.632699/#about
dwhworl · January 24, 2026 at 8:32 pm
https://www.tripadvisor.in/Profile/1xbetcode2026
izmvhin · January 24, 2026 at 11:25 pm
http://pc-mazsik.network.hu/forumtema/discover-the-thrills-of-block-blast-the-ultimate-puzzle-adventure
vyamxjb · January 25, 2026 at 12:14 am
http://airspb.ru/images/pgs/1xbet_promokod_na_besplatnuu_stavku.html
jmhquvy · January 25, 2026 at 4:14 am
https://amigo-tours.ru/aZSiCMHc/pgs/megapari_promokod.html
rggxzyi · January 25, 2026 at 8:09 am
https://runcam.com/fonts/articles/paripesa_promo_code.html
jqfqfbb · January 25, 2026 at 8:24 am
https://redclara.net/news/pgs/?code_promo_melbet_pour_l_inscription.html
klwesqa · January 25, 2026 at 9:41 am
https://www.google.co.to/url?q=https://billi-walker.jp/chat/art/1xbet_promo_code-vip_welcome_bonus.html
mpkgwpg · January 25, 2026 at 10:43 am
https://buyerseller.xyz/user/codepromo1xbetbonusxafs/
casino chile · January 25, 2026 at 12:11 pm
I like your blog. It sounds every informative.
xcrqjgn · January 25, 2026 at 1:28 pm
https://www.google.com.et/url?q=https://justpaste.it/etg8y/pdf
ykeaatc · January 25, 2026 at 4:39 pm
https://www.google.io/url?q=https://ecampania.it/blog/1xbet_promo_code-vip_welcome_bonus.html
sbykgoz · January 25, 2026 at 9:24 pm
https://zajepizza.pl/bez-kategorii/1xbet-casino-promo-code-hong-kong-allinmax-e130-bonus/?p=19146
ijqqqhs · January 26, 2026 at 4:16 am
https://l2top.co/forum/members/1xbetpromo3.148582/
https://renvills-hotel.ru/rooms/nomer-8-s-balkonom/ · January 26, 2026 at 5:25 am
https://renvills-hotel.ru/rooms/nomer-8-s-balkonom/
jimnayi · January 26, 2026 at 11:37 am
https://www.google.ad/url?q=https://aquietrabalho.com/art/code_promotionnel_d_inscription_1xbet.html
reputation return pricing · January 26, 2026 at 11:46 am
Thanks , I’ve recently been searching for info about this topic for ages and yours is the best I have discovered so far. But, what concerning the bottom line? Are you certain concerning the source?
azino777 azino · January 26, 2026 at 12:02 pm
casino azino777 официальный
официальный азино · January 26, 2026 at 12:30 pm
азино сайт
Nhà cái ko66 · January 26, 2026 at 1:04 pm
Does it look like we’re in for a big ride here?
сайт azino777 · January 26, 2026 at 3:51 pm
азино777 официальный
vapzfdy · January 26, 2026 at 5:40 pm
https://www.google.az/url?q=https://g-r-s.fr/pag/code_promo_1bet_ci.html
casino azino777 официальный · January 26, 2026 at 8:14 pm
сайт азино777
официальный сайт азино · January 26, 2026 at 8:16 pm
azino777 официальный сайт
best online casinos Ireland · January 26, 2026 at 9:00 pm
While this issue can vexed most people, my thought is that there has to be a middle or common ground that we all can find. I do value that you’ve added pertinent and sound commentary here though. Thank you!
casino azino777 официальный · January 27, 2026 at 1:04 am
азино777 777 официальный
xralzzh · January 27, 2026 at 4:27 am
https://www.pubpub.org/user/1xbet-free-promo-code-south-africa-2
bzpdmcg · January 27, 2026 at 5:17 am
https://aktivnoe.forum24.ru/?1-7-0-00018790-000-0-0-1769159604
риобет официальный сайт · January 27, 2026 at 10:58 am
rio bet casino
jqxhtot · January 27, 2026 at 11:06 am
https://www.cobocards.com/pool/de/card/4812663/online-karteikarten-stellenarten/
риобет казино на деньги · January 27, 2026 at 11:46 am
риобет официальный сайт
waw4d login utama · January 27, 2026 at 3:15 pm
A friend of mine advised this site. And yes. it has some useful pieces of info and I enjoyed scaning it. Therefore i would love to drop you a quick note to express my thank. Take care
риобет на деньги · January 27, 2026 at 3:23 pm
играть на деньги riobet
Артифика · January 27, 2026 at 7:14 pm
Артифика создать фото нейросетью
casino riobet · January 27, 2026 at 7:22 pm
риобет на деньги
рио бет · January 27, 2026 at 7:37 pm
риобет россия
legalne kasyno online · January 27, 2026 at 8:35 pm
I just couldn’t leave your web site prior to suggesting that I really enjoyed the standard info an individual supply to your guests? Is going to be again continuously in order to inspect new posts
kdvyumw · January 28, 2026 at 12:02 am
https://matters.town/a/k22gfn374q16
казино риобет играть на деньги · January 28, 2026 at 12:20 am
риобет онлайн
casino en ligne au Canada · January 28, 2026 at 1:56 am
I have to say this post was certainly informative and contains useful content for enthusiastic visitors. I will definitely bookmark this website for future reference and further viewing. cheers a bunch for sharing this with us!
wiring diagram · January 28, 2026 at 2:38 am
I would share your post with my sis.
wiring diagram · January 28, 2026 at 2:40 am
I can’t go into details, but I have to say its a good article!
trailer wiring · January 28, 2026 at 2:40 am
I’ve read several good stuff here. Definitely worth bookmarking for revisiting. I surprise how much effort you put to make such a magnificent informative site.
best casino online Ireland · January 28, 2026 at 2:54 am
I have to say this post was certainly informative and contains useful content for enthusiastic visitors. I will definitely bookmark this website for future reference and further viewing. cheers a bunch for sharing this with us!
österreich online casino · January 28, 2026 at 3:25 am
Very often I go to see this blog. It very much is pleasant to me. Thanks the author
waw4d officials · January 28, 2026 at 4:03 am
It sounds like you’re creating problems yourself by defining this as such a comprehensive, almost unknowable problem. Isn’t that self-defeating?
www.agent.747 · January 28, 2026 at 5:32 am
Heading to the http://www.agent.747 site? Let’s go! All the details right here. http://www.agent.747
jilibetagent · January 28, 2026 at 5:32 am
Jilibetagent is doing its thang! Got hooked up with a sweet deal through them. Easy to navigate and they were super helpful. Definitely recommended if you’re looking for something reliable. Check this out: jilibetagent
okkingbet · January 28, 2026 at 5:33 am
Alright, gave okkingbet a look and the selection of games is pretty impressive. Found some new favorites already. Worth checking out if you’re looking to switch things up. Find out more: okkingbet
Canadian casino online · January 28, 2026 at 5:35 am
I don’t know if it’s just me or if everybody else experiencing issues with your site. It appears as though some of the written text on your content are running off the screen. Can someone else please provide feedback and let me know if this is happening to them as well? This could be a problem with my web browser because I’ve had this happen before. Appreciate it
https://personaltechpipeline.com/quantum-ai-wie-serios-versprechen/ · January 28, 2026 at 6:42 am
https://personaltechpipeline.com/quantum-ai-wie-serios-versprechen/ Quantum AI: Wie serios sind die Versprechen?
bvyfchr · January 28, 2026 at 7:34 am
http://freestyler.ws/user/622872/xbeto9
beste casino online · January 28, 2026 at 7:41 am
You write Formidable articles, keep up good work.
best online casino · January 28, 2026 at 7:57 am
Awesome post. It’s so good to see someone taking the time to share this information
betf;ix93 · January 28, 2026 at 9:02 am
Whoa tons of great facts! https://jadwaded2.wordpress.com/2025/12/18/betflix93/
очки сидоренко, очки вакуумные сидоренко, очки сидоренко купить, очки сидоренко отзывы · January 28, 2026 at 9:36 am
очки сидоренко, очки вакуумные сидоренко, очки сидоренко купить, очки сидоренко отзывы
очки сидоренко, очки вакуумные сидоренко, очки сидоренко купить, очки сидоренко отзывы
Подобные сведения можно встретить в открытых источниках.
kasino online · January 28, 2026 at 9:48 am
Could not disagree with the main ideas. Wonder how things will develop over the coming years.
tsupmfd · January 28, 2026 at 10:59 am
https://www.google.co.zw/url?q=https://ciprianileonoranze.com/wp-content/pgs/?melbet_bookmaker_promo_code.html
mejores casinos online españa · January 28, 2026 at 12:45 pm
What a great article.. i subscribed btw!
bxayxtr · January 28, 2026 at 1:04 pm
https://opstandingskerk-enschede.online/everything-you-need-to-know-about-online-slot-machines/
казино риобет онлайн на деньги · January 28, 2026 at 1:46 pm
казино риобет онлайн на деньги
Buy MDPHP Powder (Freebase) For Sale Online · January 28, 2026 at 2:28 pm
This is really interesting, You’re a very skilled blogger. I have joined your feed and look forward to seeking more of your fantastic post. Also, I have shared your website in my social networks!
Ketamine Liquid · January 28, 2026 at 2:29 pm
Loving the info on this website , you have done outstanding job on the blog posts.
казино pin up online · January 28, 2026 at 2:30 pm
casino pinup
buy Bromazolam 3mg Pellets · January 28, 2026 at 3:56 pm
Certainly. And I have faced it. Let’s discuss this question. Here or in PM.
пин ап казино официальный · January 28, 2026 at 4:29 pm
казино pin-up
сайт riobet casino · January 28, 2026 at 5:45 pm
риобет официальный сайт
пин ап казино онлайн · January 28, 2026 at 6:30 pm
играть на деньги пин ап
casino en ligne · January 28, 2026 at 7:28 pm
We are a group of volunteers and starting a new initiative in our community. Your blog provided us with valuable information to work on|.You have done a marvellous job!
anal sex porn videos видео для взрослых xxx · January 28, 2026 at 7:35 pm
A colleague in the field told me to check out your website.
рио бет · January 28, 2026 at 9:19 pm
riobet играть на деньги
Albino A+ psilocybe cubensis spore vial · January 29, 2026 at 1:41 am
Hello there! I really enjoy reading your blog! If you keep making amazing posts like this I will come back every day to keep reading.
rlevclv · January 29, 2026 at 5:11 am
https://savee.com/bonusxaf2026/
Порно_чат · January 29, 2026 at 5:12 am
Порно чат – работаем с 2011 года
rngpdqn · January 29, 2026 at 6:46 am
http://dpzon3.3x.ro/profile.php?lookup=3571
visitor · January 29, 2026 at 7:35 am
Shot power, hardest hitters and their strike velocities
riobet на деньги онлайн · January 29, 2026 at 3:28 pm
риобет оф сайт
пинап официальный сайт онлайн · January 29, 2026 at 3:35 pm
пин ап официальный сайт
brgidno · January 29, 2026 at 4:22 pm
https://bonuus1xbet.livejournal.com/427.html
https://md.un-hack-bar.de/s/Bs6kQ8lnQM · January 29, 2026 at 4:49 pm
References:
Salons professionnels
References:
https://md.un-hack-bar.de/s/Bs6kQ8lnQM
prodentim official website · January 29, 2026 at 5:17 pm
**prodentim official website**
ProDentim is a distinctive oral-care formula that pairs targeted probiotics with plant-based ingredients to encourage strong teeth, comfortable gums, and reliably fresh breath
best online casino canada · January 29, 2026 at 5:18 pm
Took me time to read all the comments, but I really enjoyed the article. It proved to be Very helpful to me and I am sure to all the commenters here It’s always nice when you can not only be informed, but also entertained I’m sure you had fun writing this article.
99lodeonlineco · January 29, 2026 at 5:18 pm
Nevertheless, it’s all carried out with tongues rooted solidly in cheeks, and everybody has got nothing but absolutely love for their friendly neighborhood scapegoat. In reality, he is not merely a pushover. He is simply that extraordinary breed of person solid enough to take all that good natured ribbing for what it really is.
imoodle.win · January 29, 2026 at 5:34 pm
winner casino
https://markussen-odonnell-4.mdwrite.net/das-beste-online-casino-in-osterreich markussen-odonnell-4.mdwrite.net
http://ezproxy.cityu.edu.hk/login?url=https://online-spielhallen.de/1go-casino-bewertung-eine-umfassende-analyse/ ezproxy.cityu.edu.hk
http://ezproxy.cityu.edu.hk/login?url=https://online-spielhallen.de/1go-casino-bewertung-eine-umfassende-analyse/ http://ezproxy.cityu.edu.hk/
https://fakenews.win/wiki/888_Bonus_Codes_No_Deposit_2025_Freispiele_ohne_Einzahlung fakenews.win
http://techou.jp/index.php?turretshadow6 techou.jp
https://dokuwiki.stream/wiki/Bis_900_plus_400_Freispiele_sichern dokuwiki.stream
https://hedgedoc.info.uqam.ca/s/LK0J6reQ5 hedgedoc.info.uqam.ca
https://www.exchangle.com/lookhawk2 https://www.exchangle.com
http://gojourney.xsrv.jp/index.php?turtlecrime6 http://gojourney.xsrv.jp/index.php?turtlecrime6
https://morphomics.science/wiki/Psychologie_des_Glcksspiels_Lotto_Systemschein_und_mehr morphomics.science
https://mmcon.sakura.ne.jp:443/mmwiki/index.php?lookopen8 mmcon.sakura.ne.jp
https://hackmd.okfn.de/s/SJY6c1YL-x hackmd.okfn.de
https://mathews-mcmillan-3.technetbloggers.de/admiralbet-casino-test-10-freispiele-ohne-einzahlung https://mathews-mcmillan-3.technetbloggers.de/admiralbet-casino-test-10-freispiele-ohne-einzahlung
https://ai-db.science/wiki/AdmiralBet_Bonus_10_Gratiswette_90_Jokerwette_in_5_Minuten https://ai-db.science
https://morphomics.science/wiki/500_Casino_Bonus_Beste_500_Prozent_Angebote_2026 morphomics.science
https://pad.geolab.space/s/jysNP7p8- pad.geolab.space
https://ai-db.science/wiki/Casino_CashbackAngebote_und_Boni ai-db.science
https://pattern-wiki.win/wiki/1GO_PLUS_App_Download_Play_Casino_on_Android pattern-wiki.win
References:
https://imoodle.win/wiki/24Casino_Test_2026_Boni_und_Krypto_Auszahlung
visa for egypt · January 29, 2026 at 5:42 pm
The post is absolutely fantastic! Lots of great info and inspiration, both of which we all need! Also like to admire the time and effort you put into your website and detailed info you offer! I will bookmark your website!
casino riobet · January 29, 2026 at 6:10 pm
казино риобет онлайн на деньги
Fabet · January 29, 2026 at 6:44 pm
I wrote down your blog in my bookmark. I hope that it somehow did not fall and continues to be a great place for reading texts.
пин-ап официальный сайт казино · January 29, 2026 at 6:53 pm
pin up online официальный сайт
meilleur casino en ligne · January 29, 2026 at 7:05 pm
Surprisingly good post. I really found your primary webpage and additionally wanted to suggest that have essentially enjoyed searching your website blog posts. Whatever the case I’ll always be subscribing to your entire supply and I hope you jot down ever again soon!
alps2alps reviews · January 29, 2026 at 7:43 pm
Good Day Guys,
Only if you really think about alps2alps?!
We have more detailed information about https://apps.apple.com/ie/app/alps2alps-ski-transfers/id1441643719
Customer opinions about Alps2Alps show that ski enthusiasts rely on this transfer service. When planning a ski trip, dependable transfers is crucial.
In contrast to ordinary transfers, Alps2Alps focuses on mountain routes. Based on Alps2Alps reviews, passengers enjoy comfortable cars with online connectivity and roomy seating.
Honest rates is emphasized in many customer opinions. Clients note that the company offers competitive rates without extra charges.
Customer care also stands out. Client testimonials often point out the supportive agents who guide with last-minute changes.
In final thoughts, customer feedback show that affordability are the key benefits to choose Alps2Alps for your Alpine trip.
Please visit our site about https://apps.apple.com/ie/app/alps2alps-ski-transfers/id1441643719 or please click https://apps.apple.com/ie/app/alps2alps-ski-transfers/id1441643719 for Sign up for a free consultation now!
visit our internet portal about https://facebook.com/Alps2Alps/ or please click https://apps.apple.com/ie/app/alps2alps-ski-transfers/id1441643719
Our site have tag’s: Alps to alps, alps2alps,
And some other and guaranteed information.
Thanks for your attention.
Have a good day.
Thanks
риобет оф сайт · January 29, 2026 at 8:54 pm
риобет казино на деньги
официальный сайт пин-ап казино · January 29, 2026 at 9:46 pm
играть в пин ап
aussie casinos online · January 29, 2026 at 9:59 pm
online casino
sciencewiki.science · January 29, 2026 at 10:43 pm
casino quebec
https://www.exchangle.com/spidercrime7 http://www.exchangle.com
https://canvas.instructure.com/eportfolios/4193318/entries/14695368 canvas.instructure.com
https://riise-roche-2.technetbloggers.de/1red-casino-im-test-unsere-echten-erfahrungen-2026-1769716161 https://riise-roche-2.technetbloggers.de/1red-casino-im-test-unsere-echten-erfahrungen-2026-1769716161
https://www.divephotoguide.com/user/lookplace2 https://www.divephotoguide.com
https://mmcon.sakura.ne.jp:443/mmwiki/index.php?spongelamb6 mmcon.sakura.ne.jp
https://theflatearth.win/wiki/Post:Das_kostenlose_Online_Casino theflatearth.win
https://ramsey-thompson-3.technetbloggers.de/glucksspiel-bei-admiral-neueste-technik-and-sicherer-raum ramsey-thompson-3.technetbloggers.de
https://cuwip.ucsd.edu/members/treeshop3/activity/2784271/ cuwip.ucsd.edu
https://kanban.xsitepool.tu-freiberg.de/s/r1ui4UK8Zx https://kanban.xsitepool.tu-freiberg.de/s/r1ui4UK8Zx
http://gojourney.xsrv.jp/index.php?swimorgan0 http://gojourney.xsrv.jp
https://mozillabd.science/wiki/888_Slots_Erfahrungen_Wirklich_200_Bonus mozillabd.science
https://pad.stuve.uni-ulm.de/s/qqdmMXoTp https://pad.stuve.uni-ulm.de/
https://turner-schack-2.technetbloggers.de/verwenden-sie-den-exklusiven-code-fur-ihren-100-casino-bonus turner-schack-2.technetbloggers.de
https://menwiki.men/wiki/Admiral_Bonus_Code_sterreich_Promo_Freiwetten_2026 https://menwiki.men/wiki/Admiral_Bonus_Code_sterreich_Promo_Freiwetten_2026
https://raindrop.io/jamesfrance5/hamannlancaster7673-66216962 https://raindrop.io
http://king-wifi.win//index.php?title=brookssheridan2515 king-wifi.win
https://md.chaosdorf.de/s/K7VCQHWjHR https://md.chaosdorf.de/s/K7VCQHWjHR
https://dreevoo.com/profile.php?pid=1023205 https://dreevoo.com/
References:
https://sciencewiki.science/wiki/Bester_Casino_Bonus_2026_Top_Bonusangebote_im_Vergleich
BQ · January 29, 2026 at 10:44 pm
https://refhunter-text.medizin.uni-halle.de/index.php/Benutzer:BlondellPalma
kasino online · January 30, 2026 at 12:29 am
I wish I could craft such articles as this. Thank you very much.
visitor · January 30, 2026 at 3:38 am
Counter press, gegenpressing statistics and ball recovery times
https://thejillist.com/story11367284/code-promo-1xbet-paris-2026-code1x200-bonus-130 · January 30, 2026 at 6:15 am
https://thejillist.com/story11367284/code-promo-1xbet-paris-2026-code1x200-bonus-130
eyvstqm · January 30, 2026 at 6:17 am
https://anonup.com/@xbetfreebets
xboceic · January 30, 2026 at 6:38 am
https://zapp.red/myforum/topic/gold-detectors-uncovering-hidden-treasures-beneath-the-surface/#postid-194437
online casino · January 30, 2026 at 12:18 pm
Copa del Rey livescore, Spanish cup competition with Real Madrid Barcelona action
плейфортуна · January 30, 2026 at 2:33 pm
сайт play fortuna casino
casino пинко играть онлайн · January 30, 2026 at 2:42 pm
https://pinkoplayclub.ru/
siberian express · January 30, 2026 at 3:05 pm
siberian express
Gorilla Tag mods download · January 30, 2026 at 4:14 pm
You write Formidable articles, keep up good work.
play fortuna casino · January 30, 2026 at 5:28 pm
онлайн казино плей фортуна
onlinecasino · January 30, 2026 at 6:07 pm
Premier League live scores today, English football action updated in real time
https://turretplace6.bravejournal.net/die-besten-casinos-mit-schneller-auszahlung-2026 · January 30, 2026 at 6:41 pm
References:
Roulette simulator
References:
https://turretplace6.bravejournal.net/die-besten-casinos-mit-schneller-auszahlung-2026
online casino · January 30, 2026 at 7:02 pm
Corner kick count, set piece statistics for all football matches
online casino · January 30, 2026 at 7:07 pm
Tennis live scores from all Grand Slams, ATP and WTA tours updated every point
онлайн казино playfortuna · January 30, 2026 at 8:03 pm
плей фортуна casino
https://notes.io/eiX68 · January 30, 2026 at 11:21 pm
References:
Cinema casino bagnols sur ceze
References:
https://notes.io/eiX68
официальный сайт пинко казино · January 31, 2026 at 8:00 am
pinco casino играть
pinco сайт · January 31, 2026 at 10:25 am
онлайн казино pinco
tggujhr · January 31, 2026 at 11:05 am
https://www.ihvo.de/wp-content/pages/1xbet_promo_codes_bonus.html
промокоды 1хбет кз · January 31, 2026 at 11:53 am
1xbet промокод
melbet promo code india · January 31, 2026 at 11:57 am
melbet promo code 2026
dlx.hamdard.pk · January 31, 2026 at 2:09 pm
north brunswick library
https://www.giveawayoftheday.com/forums/profile/1608198 http://www.giveawayoftheday.com
https://moparwiki.win/wiki/Post:Die_Online_Casinos_mit_der_besten_Auszahlungsquote_2026 moparwiki.win
https://botdb.win/wiki/1Red_Deutschland_Testbericht_Casino_Sportwetten_App_und_Bonus_einfach_erklrt botdb.win
https://flibustier.top/user/gloveperiod4/ flibustier.top
https://able2know.org/user/bracesleep0/ https://able2know.org/user/bracesleep0/
https://adsintro.com/index.php?page=user&action=pub_profile&id=774339 adsintro.com
https://to-portal.com/planethub0 to-portal.com
https://notes.io/eiHvq notes.io
https://coolpot.stream/story.php?title=1red-casino-offizielle-seite-3-000-bonus-350-freispiele https://coolpot.stream/
https://pads.zapf.in/s/cXZW7ddKGC https://pads.zapf.in/
https://500px.com/p/timmfmedelgado https://500px.com
http://gojourney.xsrv.jp/index.php?bagnight4 gojourney.xsrv.jp
https://pads.zapf.in/s/1m44arKpJ5 https://pads.zapf.in/s/1m44arKpJ5
https://pads.zapf.in/s/0B4rJpC0r2 pads.zapf.in
https://hikvisiondb.webcam/wiki/Das_kostenlose_Online_Casino_Jetzt_spielen hikvisiondb.webcam
https://hedgedoc.eclair.ec-lyon.fr/s/_OBZIghfH https://hedgedoc.eclair.ec-lyon.fr
https://sundaynews.info/user/searchstem0/ https://sundaynews.info/user/searchstem0
http://historydb.date/index.php?title=jamesmadden1461 historydb.date
References:
https://dlx.hamdard.pk/user/profile/360019
telegra.ph · January 31, 2026 at 3:08 pm
References:
Blackjack practice
References:
https://telegra.ph/Bester-Casino-Bonus-2026-Vergleich-der-besten-Casino-Boni-01-31
casino pinco официальный сайт · January 31, 2026 at 3:40 pm
pinko casino
1 win зеркало рабочее на сегодня онлайн · January 31, 2026 at 4:09 pm
1вин зеркало сайта
fam bet · January 31, 2026 at 4:22 pm
fambet casino slots
小宝影视 · January 31, 2026 at 5:09 pm
Curve shots, bending efforts and their success rates documented
https://p.mobile9.com/coltcarbon2/ · January 31, 2026 at 5:42 pm
References:
Roulette betting strategy
References:
https://p.mobile9.com/coltcarbon2/
auonlinecasino · January 31, 2026 at 6:08 pm
Midweek football livescore, Tuesday Wednesday Champions League Europa action
pinko казино официальный сайт · January 31, 2026 at 6:36 pm
пинко казино онлайн
один вин зеркало · January 31, 2026 at 6:59 pm
1 вин зеркало вход
https://md.inno3.fr/s/qqjq-Ag54 · January 31, 2026 at 7:50 pm
gold country casino oroville ca
https://maps.google.com.lb/url?q=https://online-spielhallen.de/888-casino-cashback-alles-was-sie-wissen-mussen/ maps.google.com.lb
https://able2know.org/user/growthcanvas9/ able2know.org
https://ccsakura.jp:443/index.php?lambcarbon0 ccsakura.jp
https://web.ggather.com/cablecredit9/ https://web.ggather.com
https://rasch-brandon.federatedjournals.com/1go-casino-test-and-erfahrungen-2025-150-bonus-bis-600-ausfuhrlicher-review https://rasch-brandon.federatedjournals.com/
https://pad.karuka.tech/s/DowhxIl20 pad.karuka.tech
https://ed.coop/forums/users/celeryengine4/ https://ed.coop
https://md.un-hack-bar.de/s/r8iK8Bofti md.un-hack-bar.de
https://maps.google.com.tr/url?q=https://online-spielhallen.de/24-casino-aktionscode-ihr-schlussel-zu-exklusiven-vorteilen/ maps.google.com.tr
https://menwiki.men/wiki/Online_Casino_Auszahlung_2026_Ratgeber_Schnelle_Auszahlung menwiki.men
https://www.google.co.uz/url?q=https://online-spielhallen.de/400-casino-bonus-2025-beste-angebote-fur-deutschland/ https://www.google.co.uz/url?q=https://online-spielhallen.de/400-casino-bonus-2025-beste-angebote-fur-deutschland
https://yutoriarukyouikujouken.com:443/index.php?ganderlitter1 https://yutoriarukyouikujouken.com/
https://hackmd.okfn.de/s/H15HcMs8Wl https://hackmd.okfn.de/s/H15HcMs8Wl
https://avtovoprosi.ru/user/lambstem6 https://avtovoprosi.ru/
https://onlinevetjobs.com/author/gaugecanvas9/ onlinevetjobs.com
https://coolpot.stream/story.php?title=888-casino-bonus-code-200-freispiele coolpot.stream
https://www.udrpsearch.com/user/twistpage8 http://www.udrpsearch.com
https://theflatearth.win/wiki/Post:Casino_Bonus_Codes_2026_Bonus_Vergleich_fr_Neu_Bestandskunden https://theflatearth.win/
References:
https://md.inno3.fr/s/qqjq-Ag54
pinco казино официальный сайт · January 31, 2026 at 9:24 pm
казино pinco играть онлайн
1win промокод на деньги · January 31, 2026 at 9:37 pm
промокоды ванвин
onlinecasinoau · February 1, 2026 at 5:25 am
Penalty records, spot kick takers and goalkeeper save percentages
melbet free spin promo code · February 1, 2026 at 7:39 am
melbet free bet promo code today
1xbet бонус промокод · February 1, 2026 at 7:42 am
промокод 1xbet на слоты
king-wifi.win · February 1, 2026 at 1:21 pm
7 sultans casino
https://freebookmarkstore.win/story.php?title=casino-bonus-ohne-einzahlung-2026-sofort-startguthaben-erhalten freebookmarkstore.win
https://may22.ru/user/twistgauge8/ may22.ru
https://images.google.ms/url?q=https://online-spielhallen.de/888casino-anmeldung-ihr-tor-zur-welt-des-online-glucksspiels/ https://images.google.ms/url?q=https://online-spielhallen.de/888casino-anmeldung-ihr-tor-zur-welt-des-online-glucksspiels
http://dranus.ru/forums/user/rulestem6/ dranus.ru
https://www.fionapremium.com/author/eastsampan1/ https://www.fionapremium.com/author/eastsampan1
https://bom.so/9Ta5w9 bom.so
https://www.youtube.com/redirect?q=https://online-spielhallen.de/500-casino-freispiele-ihr-weg-zu-extra-spielspas/ http://www.youtube.com
https://botdb.win/wiki/VIPProgramme_in_OnlineCasinos_Exklusive_Vorteile_fr_loyale_Spieler botdb.win
https://lovebookmark.date/story.php?title=die-besten-online-casinos-mit-freispielen-ohne-einzahlung-2026 lovebookmark.date
https://www.google.ci/url?q=https://online-spielhallen.de/1go-casino-erfahrungen-ein-umfassender-uberblick/ http://www.google.ci
https://maps.google.gg/url?q=https://online-spielhallen.de/888-casino-bonus-code-ihr-umfassender-leitfaden-fur-ein-lukratives-spielerlebnis/ maps.google.gg
https://yogicentral.science/wiki/888_Casino https://yogicentral.science/wiki/888_Casino
https://peatix.com/user/28823488 peatix.com
https://dreevoo.com/profile.php?pid=1028557 https://dreevoo.com/profile.php?pid=1028557
https://graph.org/888-Casino-02-01 https://graph.org/888-Casino-02-01
https://intensedebate.com/people/numbershovel2 intensedebate.com
https://mapleprimes.com/users/cableshovel7 https://mapleprimes.com/users/cableshovel7
https://www.24propertyinspain.com/user/profile/1366113 http://www.24propertyinspain.com
References:
https://king-wifi.win/wiki/Entdecken_Sie_es_und_fangen_Sie_an_zu_gewinnen
водосток aquasystem · February 1, 2026 at 7:07 pm
водосток aquasystem
вывоз мусора санкт-петербург · February 1, 2026 at 7:10 pm
Не знаете, куда деть старую мебель? Закажите вывоз строительного мусора спб и избавьтесь от хлама за один день. Цены начинаются от 1500 рублей.
https://intelicode.com/ · February 1, 2026 at 9:25 pm
https://intelicode.com/
onlinecasino · February 1, 2026 at 10:31 pm
Carabao Cup live scores, English League Cup with Premier League teams playing
mapleprimes.com · February 1, 2026 at 11:06 pm
References:
Goldfish slot machine
References:
https://mapleprimes.com/users/lambcredit5
нью ретро онлайн казино · February 1, 2026 at 11:51 pm
retro new casino
промокод на melbet бесплатно · February 2, 2026 at 12:00 am
промокод мелбет фрибет
porn hentai adult xxx porn видео для взрослых xxx · February 2, 2026 at 12:01 am
I love what you’ve created here, this is definitely one of my favorite sites to visit.
болливуд казино официальный сайт · February 2, 2026 at 1:27 am
болливуд
https://kirkpatrick-eriksson-2.mdwrite.net/jeetcity-casino-australia-a-complete-online-casino-review · February 2, 2026 at 1:31 am
References:
Cherokee casino west siloam springs
References:
https://kirkpatrick-eriksson-2.mdwrite.net/jeetcity-casino-australia-a-complete-online-casino-review
free cam sex · February 2, 2026 at 1:55 am
Amazing article, cheers, I will bookmark you now.
newretrocasino зеркало рабочее · February 2, 2026 at 2:19 am
newretrocasino зеркало с апк
bollywood казино официальный · February 2, 2026 at 3:39 am
болливуд казино казино на деньги играть
нью ретро казино играть · February 2, 2026 at 4:43 am
new retro казино официальный сайт
bollywood casino · February 2, 2026 at 5:53 am
казино bollywood
https://clashofcryptos.trade/wiki/Australian_PayID_Online_Casinos_New_Casino_Banking_Method · February 2, 2026 at 6:18 am
online casino geld verdienen
https://historydb.date/wiki/Fast_Secure_Payments historydb.date
http://humanlove.stream//index.php?title=smedherndon1751 http://humanlove.stream//index.php?title=smedherndon1751
https://escatter11.fullerton.edu/nfs/show_user.php?userid=9553352 escatter11.fullerton.edu
https://peatix.com/user/28832708 peatix.com
https://mahoney-buckner.hubstack.net/payid-casino-no-delays-no-fees-just-fast-real-money-play-1769975544 https://mahoney-buckner.hubstack.net
https://may22.ru/user/tripcase61/ https://may22.ru/user/tripcase61
https://tiepisces15.bravejournal.net/about-us-our-review-process-and-team tiepisces15.bravejournal.net
https://botdb.win/wiki/PayID_Casinos_In_Australia_Secure_Instant_Casino_Payments https://botdb.win/wiki/PayID_Casinos_In_Australia_Secure_Instant_Casino_Payments
https://socialisted.org/market/index.php?page=user&action=pub_profile&id=308725 https://socialisted.org/
https://mozillabd.science/wiki/From_Startup_to_Leader_in_Australia_Casino_Ys_Rise_and_the_Costliest_Poker_Events_for_Aussie_Punters_Bp_Lu_Bp_Nng_Ti_Bn_Thi_Cng_Lp_t_Ht_Khi_Bp_Nng_BBQ_Nh_Hng_Thit_B_Inox_Bp_Nh_Hng https://mozillabd.science/
http://stroyrem-master.ru/user/cloudcolor47/ http://stroyrem-master.ru/user/cloudcolor47
https://stanley-eriksson-2.thoughtlanes.net/payid-casinos-australia-fast-and-secure-payments https://stanley-eriksson-2.thoughtlanes.net/
https://lospromotores.net/author/trippush96/ lospromotores.net
https://onlinevetjobs.com/author/riddlecoach97/ https://onlinevetjobs.com/author/riddlecoach97/
https://egamersbox.com/cool/index.php?page=user&action=pub_profile&id=273018 egamersbox.com
https://graph.org/Fast-Payout-Australian-Casinos-Quick–Hassle-Free-Withdrawals-02-01 https://graph.org/
http://hikvisiondb.webcam/index.php?title=goodewilliamson0520 hikvisiondb.webcam
https://cameradb.review/wiki/Best_PayID_Casinos_Australia_2026 cameradb.review
References:
https://clashofcryptos.trade/wiki/Australian_PayID_Online_Casinos_New_Casino_Banking_Method
https://deeprealestate.in/pages/1xbet_promo_code_india___welcome_bonus_1.html · February 2, 2026 at 8:19 am
https://deeprealestate.in/pages/1xbet_promo_code_india___welcome_bonus_1.html
https://avidasecreta.com/wp-content/pgs/?1xbet_promo_code_today__free_bet_bonus.html · February 2, 2026 at 8:30 am
https://avidasecreta.com/wp-content/pgs/?1xbet_promo_code_today__free_bet_bonus.html
swaay.com · February 2, 2026 at 9:03 am
roxy palace mobile
https://skitterphoto.com/photographers/2201091/seerup-kenney https://skitterphoto.com
https://pediascape.science/wiki/PayID pediascape.science
http://downarchive.org/user/layerpisces96/ downarchive.org
https://yogaasanas.science/wiki/Best_PayID_Casinos_in_Australia_for_2026 yogaasanas.science
https://forum.dsapinstitute.org/forums/users/riseknight41/ forum.dsapinstitute.org
https://mozillabd.science/wiki/Fast_Payout_Real_Money_Sites mozillabd.science
https://dokuwiki.stream/wiki/Payidcasinosreviewedfastdepositswithdrawalsforaussies dokuwiki.stream
https://gratisafhalen.be/author/tripsarah22/ https://gratisafhalen.be/
https://kirkpatrick-mcmillan-4.technetbloggers.de/australian-online-casino-payid-online-casino-sites-2026 kirkpatrick-mcmillan-4.technetbloggers.de
https://egamersbox.com/cool/index.php?page=user&action=pub_profile&id=272821 https://egamersbox.com/cool/index.php?page=user&action=pub_profile&id=272821
https://lospromotores.net/author/browbike17/ lospromotores.net
https://funsilo.date/wiki/PayID_Casinos_Australia_2026_Deposits_Withdrawals funsilo.date
https://cameradb.review/wiki/Best_PayID_Casinos_Australia_2026 cameradb.review
https://firsturl.de/7FRk3q6 firsturl.de
https://burmapush13.bravejournal.net/the-best-payid-casinos-in-australia-2025 burmapush13.bravejournal.net
https://empirekino.ru/user/canred70/ https://empirekino.ru
https://marvelvsdc.faith/wiki/Australian_PayID_Casinos_with_AUD marvelvsdc.faith
http://premiumdesignsinc.com/forums/user/augustbike30/ premiumdesignsinc.com
References:
https://swaay.com/u/maixendcnmw85/about/
https://landscapingspringtexas.info/ · February 2, 2026 at 12:59 pm
You actually stated it adequately!
https://www.rueanmaihom.net/forum/topic/62934/--1-2026:-1xburn&p=2 · February 2, 2026 at 2:15 pm
https://www.rueanmaihom.net/forum/topic/62934/%D0%9F%D1%80%D0%BE%D0%BC%D0%BE%D0%BA%D0%BE%D0%B4-%D0%B4%D0%BB%D1%8F-1%D1%85%D0%91%D0%B5%D1%82-2026:-1xburn&p=2
http://torunpamieta.pl/public/pages/?1xbet_promo_code__vip_bonus_up_to____130.html · February 2, 2026 at 3:38 pm
http://torunpamieta.pl/public/pages/?1xbet_promo_code__vip_bonus_up_to____130.html
https://xn--e1ajbcekbgd0ah.xn--p1ai/images/pages/?1xbet_promokod___bonus_kod_pri_registracii.html · February 2, 2026 at 4:22 pm
https://xn--e1ajbcekbgd0ah.xn--p1ai/images/pages/?1xbet_promokod___bonus_kod_pri_registracii.html
Мануальный терапевт Ростов-на-Дону · February 2, 2026 at 5:19 pm
Остеопат Ростов-на-Дону
Canadian online casino · February 2, 2026 at 5:47 pm
I dont think Ive caught all the angles of this subject the way youve pointed them out. Youre a true star, a rock star man. Youve got so much to say and know so much about the subject that I think you should just teach a class about it
adjchrr · February 2, 2026 at 6:25 pm
https://tygerspace.com/read-blog/30471
prpack.ru · February 2, 2026 at 6:32 pm
References:
Montreal casino
References:
https://prpack.ru/user/browsarah74/
best payout casino · February 2, 2026 at 7:29 pm
I want to see your book when it comes out.
Мануальный терапевт Ростов-на-Дону · February 2, 2026 at 8:29 pm
Мануальный терапевт Ростов-на-Дону
https://smallpdf.com/file#s=015dec35-4e25-449e-b288-b95b22e5e520 · February 2, 2026 at 8:54 pm
https://smallpdf.com/file#s=015dec35-4e25-449e-b288-b95b22e5e520
https://pad.geolab.space · February 2, 2026 at 10:43 pm
References:
Win at roulette
References:
https://pad.geolab.space/s/i2RSMU4Uu
https://mozillabd.science/wiki/Free_Spins_No_Deposit_Casino_Offers_for_February_2026 · February 2, 2026 at 10:49 pm
References:
Best online casino usa
References:
https://mozillabd.science/wiki/Free_Spins_No_Deposit_Casino_Offers_for_February_2026
safe online casinos · February 2, 2026 at 10:50 pm
I have been surfing online more than three hours today, yet I never found anything that grabbed my interest as much as this piece.
https://bradley-deal-4.technetbloggers.de/payid-casinos-a-smarter-way-to-move-your-money-1769975305 · February 2, 2026 at 11:01 pm
play blackjack for fun
https://wifidb.science/wiki/Best_PayID_Casinos_in_Australia_Sites_That_Accept_PayID wifidb.science
http://stroyrem-master.ru/user/layerbush60/ http://stroyrem-master.ru/
https://onlinevetjobs.com/author/augustliquid26/ onlinevetjobs.com
https://www.udrpsearch.com/user/alibiliquid31 udrpsearch.com
https://humanlove.stream/wiki/Online_Casinos_Accepting_PayID_Deposit humanlove.stream
https://clashofcryptos.trade/wiki/Mgm_Internet_Casino_Bonus_Codes_Australia_Remanso_Bahia https://clashofcryptos.trade/
http://premiumdesignsinc.com/forums/user/cloudbrandy98/ http://premiumdesignsinc.com
https://www.24propertyinspain.com/user/profile/1367099 24propertyinspain.com
https://securityholes.science/wiki/AUS_Real_Money_Gambling_Sites securityholes.science
https://marks-ritter-2.technetbloggers.de/get-paid-fast-from-online-casinos-using-payid marks-ritter-2.technetbloggers.de
https://onlinevetjobs.com/author/fogmargin19/ onlinevetjobs.com
https://swaay.com/u/kenseyxvyxd38/about/ swaay.com
https://www.google.co.zm/url?q=https://blackcoin.co/best-payid-casinos-in-australia-15-sites-that-accept-payid/ https://www.google.co.zm/url?q=https://blackcoin.co/best-payid-casinos-in-australia-15-sites-that-accept-payid
https://clashofcryptos.trade/wiki/Top_PayID_Casino_Sites_in_Australia_2026_PayID_Online_Casino_Deposits https://clashofcryptos.trade/wiki/Top_PayID_Casino_Sites_in_Australia_2026_PayID_Online_Casino_Deposits
https://p.mobile9.com/latexpisces86/ p.mobile9.com
https://onlinevetjobs.com/author/porchstove18/ https://onlinevetjobs.com
https://pattern-wiki.win/wiki/Best_PayID_Casinos_in_Australia_Top_10_Aussie_Casino_Sites_with_PayID_Withdrawals_2024 pattern-wiki.win
https://p.mobile9.com/porchquince12/ https://p.mobile9.com/porchquince12/
References:
https://bradley-deal-4.technetbloggers.de/payid-casinos-a-smarter-way-to-move-your-money-1769975305
клубника казино на деньги · February 2, 2026 at 11:34 pm
клубника казино играть
najlepsze polskie kasyno online · February 2, 2026 at 11:39 pm
I came across an article that talks about the same thing but even more and when you go deeper.
демо свит бонанза 1000 · February 3, 2026 at 12:57 am
слот sweet bonanza 1000
https://menszonn.ru/forums/users/starestrife/ · February 3, 2026 at 1:13 am
https://menszonn.ru/forums/users/starestrife/
сайт clubnika casino · February 3, 2026 at 1:59 am
clubnika casino на деньги
Matthewfum · February 3, 2026 at 2:58 am
phontechm
играть в слот legacy of dead · February 3, 2026 at 3:46 am
legacy of dead играть на деньги
играть казино клубника · February 3, 2026 at 4:28 am
казино клубника россия
https://p.mobile9.com/ · February 3, 2026 at 6:00 am
french lick casino
https://www.udrpsearch.com/user/dillturn47 https://www.udrpsearch.com/
https://www.instapaper.com/p/17427518 instapaper.com
http://hikvisiondb.webcam/index.php?title=dinesenthomassen5490 hikvisiondb.webcam
https://vasemom06.bravejournal.net/winz-io-casino-review-no-wager-bonus-up-to-10-000 vasemom06.bravejournal.net
https://onlinevetjobs.com/author/crayongreen92/ onlinevetjobs.com
https://livebookmark.stream/story.php?title=play-roulette-slot-online livebookmark.stream
https://p.mobile9.com/spainmom30/ https://p.mobile9.com
https://a-taxi.com.ua/user/crayonpriest61/ a-taxi.com.ua
https://www.instapaper.com/p/17427343 https://www.instapaper.com/p/17427343
https://donaldson-post-2.hubstack.net/best-online-casino-games-play-now donaldson-post-2.hubstack.net
https://opensourcebridge.science/wiki/No_Deposit_Bonus_Codes_Free_Spins_Updated_Daily https://opensourcebridge.science/wiki/No_Deposit_Bonus_Codes_Free_Spins_Updated_Daily
https://www.google.com.uy/url?q=https://www.facebook.com/people/Winz-io-casino/61585762127473/ http://www.google.com.uy
https://p.mobile9.com/cornbeef14/ p.mobile9.com
https://images.google.so/url?q=https://www.facebook.com/people/Winz-io-casino/61585762127473/ https://images.google.so/
https://escatter11.fullerton.edu/nfs/show_user.php?userid=9554082 escatter11.fullerton.edu
https://pediascape.science/wiki/Play_Winz_Reviews_Read_Customer_Service_Reviews_of_play_winzmobi_2_of_13 pediascape.science
https://anunturi112.ro/author/wrenchrate52/ anunturi112.ro
https://www.garagesale.es/author/dillbeef84/ garagesale.es
References:
https://p.mobile9.com/crabfield49/
шуга раш автомат · February 3, 2026 at 6:33 am
игра sugar rush на деньги
www.idksoft.co.kr · February 3, 2026 at 7:44 am
https://trevorjd.com/index.php/Assured_No_Stress_Blog, http://www.idksoft.co.kr/bbs/board.php?bo_table=free&wr_id=5091578,
kamp-robles-4.thoughtlanes.net · February 3, 2026 at 7:47 am
online casino bonuses
http://csmouse.com/user/augustbush90/ csmouse.com
https://www.instapaper.com/p/17426056 instapaper.com
http://dranus.ru/forums/user/canrate59/ dranus.ru
https://buyandsellhair.com/author/trainstove96/ buyandsellhair.com
https://trade-britanica.trade/wiki/How_PayID_is_Revolutionising_Australian_Online_Casino_Transactions trade-britanica.trade
https://egamersbox.com/cool/index.php?page=user&action=pub_profile&id=272931 https://egamersbox.com/
https://cameradb.review/wiki/Aussie_Casino_Bonuses_Guide_2025_No_Deposit_Pokie_Bonuses https://cameradb.review
http://mozillabd.science/index.php?title=mohammadgoldman8186 mozillabd.science
https://onlinevetjobs.com/author/fogsarah84/ https://onlinevetjobs.com/author/fogsarah84/
https://funsilo.date/wiki/Instant_Payout_Casinos_that_Accept_PayID_in_Australia funsilo.date
https://yogicentral.science/wiki/PayID_Casinos_Australia_Fast_Secure_Payments yogicentral.science
https://doherty-mcmillan-7.blogbright.net/best-casino-bonuses-and-promo-codes-australia doherty-mcmillan-7.blogbright.net
https://telegra.ph/Best-PayID-Online-Casinos-in-Australia-with-Withdrawals-in-2025-BNC-AU-02-01 telegra.ph
https://from-chambers-3.mdwrite.net/fast-payout-real-money-sites-1769975926 from-chambers-3.mdwrite.net
https://buyandsellhair.com/author/tripbrandy46/ https://buyandsellhair.com/author/tripbrandy46/
https://king-wifi.win/wiki/Best_PayID_Casino_Sites_in_Australia_for_February_2026 king-wifi.win
https://yogicentral.science/wiki/ALeague_Tips_Ateneo_de_Zamboanga_University yogicentral.science
https://maps.google.fr/url?q=https://blackcoin.co/best-payid-casinos-in-australia-15-sites-that-accept-payid/ https://maps.google.fr/url?q=https://blackcoin.co/best-payid-casinos-in-australia-15-sites-that-accept-payid
References:
https://kamp-robles-4.thoughtlanes.net/payid-online-casinos-in-australia-for-2026-play-payid-pokies
https://anthese.fr/ · February 3, 2026 at 9:26 am
https://anthese.fr/
indian gay porn · February 3, 2026 at 9:33 am
sex videos
https://www.tai-ji.net/board/board_topic/4160148/7798306.htm · February 3, 2026 at 12:39 pm
https://www.tai-ji.net/board/board_topic/4160148/7798306.htm
timeoftheworld.date · February 3, 2026 at 1:00 pm
las vegas casino online
http://semdinlitesisat.eskisehirgocukduzeltme.com/user/modemfog89/ semdinlitesisat.eskisehirgocukduzeltme.com
https://graph.org/Complete-list-2026-02-02 https://graph.org/Complete-list-2026-02-02
https://graph.org/Top-10-Australian-Online-Casino-Sites-Best-Legal-Australian-Online-Casino-Sites-In-2026-02-02-2 graph.org
https://maps.google.ae/url?q=https://s3.amazonaws.com/new-casino/best-online-casinos-australia.html maps.google.ae
https://urlscan.io/result/019c1fcc-666b-77b9-8376-70706bb5fb3c/ urlscan.io
https://skitterphoto.com/photographers/2206763/goldstein-riise https://skitterphoto.com/photographers/2206763/goldstein-riise
https://onlinevetjobs.com/author/patioclutch04/ onlinevetjobs.com
https://onlinevetjobs.com/author/shortshand86/ https://onlinevetjobs.com/author/shortshand86/
https://elclasificadomx.com/author/shortsfeet56/ https://elclasificadomx.com/
https://aryba.kg/user/detailbat48/ https://aryba.kg/user/detailbat48/
https://funsilo.date/wiki/Bitcoin_Casinos_in_Australia_2026_Best_Crypto_Sites_for_AU_Players funsilo.date
https://sonnik.nalench.com/user/debtorgeese93/ https://sonnik.nalench.com/
https://nerdgaming.science/wiki/Top_10_Australian_Online_Casino_Sites_Best_Legal_Australian_Online_Casino_Sites_In_2026 nerdgaming.science
https://yogaasanas.science/wiki/Best_Online_Casinos_Australia_2026_Trusted_Safe_AU_Sites yogaasanas.science
https://egamersbox.com/cool/index.php?page=user&action=pub_profile&id=274793 https://egamersbox.com/
https://prpack.ru/user/slimeseat28/ prpack.ru
https://bookmarkstore.download/story.php?title=1-minimum-deposit-online-casinos-in-australia-2026 bookmarkstore.download
https://swaay.com/u/glassavhoxc29/about/ https://swaay.com/u/glassavhoxc29/about/
References:
https://hebert-johannsen.thoughtlanes.net/australia-online-casinos-30-best-casino-sites-2026
onlinecasino · February 3, 2026 at 1:06 pm
Fantasy football, player points and team management tips included
vx88shop · February 3, 2026 at 2:11 pm
Thank you for this great piece of content. Best Regards
české online casino · February 3, 2026 at 2:53 pm
Hello there, You have done an incredible job. I will certainly digg it and personally recommend to my friends. I am sure they will be benefited from this site.
online casino österreich · February 3, 2026 at 4:16 pm
Does it look like we’re in for a big ride here?
onlinecasinos · February 3, 2026 at 4:44 pm
中華職棒即時比分台灣球迷的首選資訊平台,提供最即時的中華職棒即時比分新聞、球員數據分析,以及精準的比賽預測。
best online casino canada · February 3, 2026 at 5:43 pm
Hello, I think your blog might be having browser compatibility issues. When I look at your website in Chrome, it looks fine but when opening in Internet Explorer, it has some overlapping. I just wanted to give you a quick heads up! Other than that, awesome blog!
https://peatix.com/user/28832504 · February 3, 2026 at 8:14 pm
hollywood casinos
http://dubizzle.ca/index.php?page=user&action=pub_profile&id=130064 http://dubizzle.ca/index.php?page=user&action=pub_profile&id=130064
https://menwiki.men/wiki/New_Online_Casinos_Australia_2026 https://menwiki.men
https://seerup-strange.blogbright.net/using-payid-for-pokies-and-everyday-budgeting-in-australia-1769971805 seerup-strange.blogbright.net
https://funsilo.date/wiki/Royal_Reels_20_Fast_Crypto_Withdrawals_PayID_Pokies https://funsilo.date/
https://nerdgaming.science/wiki/PayID_Casinos_2026_Top_32_Casinos_Accepting_PayID nerdgaming.science
https://opensourcebridge.science/wiki/Best_Online_Casinos_Accepting_PayID_in_Australia_2026 opensourcebridge.science
http://hikvisiondb.webcam/index.php?title=selfborre5973 hikvisiondb.webcam
https://sonnik.nalench.com/user/burmaknight98/ sonnik.nalench.com
http://09vodostok.ru/user/fogcrayon32/ 09vodostok.ru
https://botdb.win/wiki/Why_PayID_Fits_the_AlwaysOn_Smartphone_Era botdb.win
https://bradshaw-robles-3.blogbright.net/real-money-online-pokies-payid-with-instant-withdrawals https://bradshaw-robles-3.blogbright.net/real-money-online-pokies-payid-with-instant-withdrawals
https://p.mobile9.com/browknight81/ p.mobile9.com
https://peatix.com/user/28832553 https://peatix.com/
https://fakenews.win/wiki/Why_888Pokies_Casino_is_Australias_Top_Choice_for_Real_Money_Gaming_in_2026 https://fakenews.win
https://lovewiki.faith/wiki/Fast_Secure_Payments lovewiki.faith
https://escatter11.fullerton.edu/nfs/show_user.php?userid=9552969 https://escatter11.fullerton.edu/nfs/show_user.php?userid=9552969
http://jobboard.piasd.org/author/browliquid23/ http://jobboard.piasd.org/author/browliquid23
https://graph.org/Best-PayID-Online-Casinos-in-Australia-with-Withdrawals-in-2025-BNC-AU-02-01-3 https://graph.org/Best-PayID-Online-Casinos-in-Australia-with-Withdrawals-in-2025-BNC-AU-02-01-3
References:
https://peatix.com/user/28832504
beste online casino · February 3, 2026 at 8:47 pm
That’s some inspirational stuff. Never knew that opinions might be this varied. Thanks for all the enthusiasm to supply such helpful information here.
mckenna-shah-4.hubstack.net · February 3, 2026 at 9:07 pm
nars casino bronzer
https://skitterphoto.com/photographers/2201452/leach-roach skitterphoto.com
https://www.google.com.ai/url?q=https://blackcoin.co/best-payid-casinos-in-australia-15-sites-that-accept-payid/ https://www.google.com.ai
https://peatix.com/user/28832504 https://peatix.com
https://maps.google.ae/url?q=https://blackcoin.co/best-payid-casinos-in-australia-15-sites-that-accept-payid/ maps.google.ae
https://forum.dsapinstitute.org/forums/users/bowlcase39/ forum.dsapinstitute.org
https://dokuwiki.stream/wiki/Australian_PayID_Online_Casinos_New_Casino_Banking_Method https://dokuwiki.stream/
https://mcqueen-deal.mdwrite.net/home-1769973888 https://mcqueen-deal.mdwrite.net/
https://images.google.ad/url?q=https://blackcoin.co/best-payid-casinos-in-australia-15-sites-that-accept-payid/ images.google.ad
https://morphomics.science/wiki/PayID_Online_Casinos_Australia_2024 https://morphomics.science/wiki/PayID_Online_Casinos_Australia_2024
https://telegra.ph/Best-PayID-Casinos-2026-Great-Casino-Sites-Accepting-PayID-02-01 https://telegra.ph/
https://snowquince72.bravejournal.net/best-online-casinos-in-australia-2026-instant-withdrawal-casinos https://snowquince72.bravejournal.net/best-online-casinos-in-australia-2026-instant-withdrawal-casinos
https://intensedebate.com/people/swimdate06 intensedebate.com
https://contreras-chapman-2.mdwrite.net/payid-casinos-in-australia-play-payid-pokies-online-2026 contreras-chapman-2.mdwrite.net
https://may22.ru/user/ocelotcoach53/ may22.ru
https://maps.google.com.pr/url?q=https://blackcoin.co/best-payid-casinos-in-australia-15-sites-that-accept-payid/ maps.google.com.pr
http://jobs.emiogp.com/author/cloudspleen90/ http://jobs.emiogp.com/author/cloudspleen90/
https://imoodle.win/wiki/Best_PayID_Online_Casinos_in_Australia_with_Withdrawals_in_2025_BNC_AU imoodle.win
https://mckenna-talley-2.mdwrite.net/9-best-payid-betting-sites-in-australia-bookies-accepting-payid https://mckenna-talley-2.mdwrite.net/9-best-payid-betting-sites-in-australia-bookies-accepting-payid
References:
https://mckenna-shah-4.hubstack.net/payid-online-casinos-australia-2024
onlinecasino · February 3, 2026 at 10:26 pm
Attendance figures, crowd numbers for all football matches tracked
MM88 · February 3, 2026 at 10:30 pm
Oh my goodness! an amazing article. Great work.
mm88.com · February 3, 2026 at 10:41 pm
I’ve been surfing online more than 3 hours today, yet I never found any interesting article like yours. It’s pretty worth enough for me. In my view, if all web owners and bloggers made good content as you did, the net will be much more useful than ever before.
www.24propertyinspain.com · February 3, 2026 at 10:44 pm
References:
Hippodrome casino london
References:
https://www.24propertyinspain.com/user/profile/1367143
onlinecasino · February 4, 2026 at 5:05 am
Offside traps, high line defenses and their success rates
小宝影视 · February 4, 2026 at 9:38 am
Today’s football match scores from around the world, comprehensive coverage of all leagues
jobboard.piasd.org · February 4, 2026 at 10:01 am
diamond jack casino
https://chessdatabase.science/wiki/Australias_1_Online_Casino_Guide_2026 https://chessdatabase.science/
https://escatter11.fullerton.edu/nfs/show_user.php?userid=9554984 escatter11.fullerton.edu
https://rentry.co/t2wdftr6 https://rentry.co/
https://www.udrpsearch.com/user/regretseat00 https://www.udrpsearch.com/user/regretseat00
https://escatter11.fullerton.edu/nfs/show_user.php?userid=9555218 escatter11.fullerton.edu
https://swaay.com/u/bailirqufwf59/about/ swaay.com
https://classifieds.ocala-news.com/author/patiolaw77 https://classifieds.ocala-news.com
https://marvelvsdc.faith/wiki/Best_Online_Casinos_Australia_2025_Real_Money_Gaming_Exclusive_Bonuses https://marvelvsdc.faith/
https://onlinevetjobs.com/author/dancehand40/ https://onlinevetjobs.com/author/dancehand40
https://gaiaathome.eu/gaiaathome/show_user.php?userid=1836132 gaiaathome.eu
https://cameradb.review/wiki/Jackpot_Jill_Casino_7500_Welcome_Bonus_Online_Pokies cameradb.review
https://www.garagesale.es/author/puffinbasket46/ https://www.garagesale.es/author/puffinbasket46/
https://clashofcryptos.trade/wiki/Best_Online_Casinos_in_Australia_2026_Instant_Withdrawal_Casinos clashofcryptos.trade
http://jobs.emiogp.com/author/slimeegypt15/ jobs.emiogp.com
https://skitterphoto.com/photographers/2205970/bendtsen-downey skitterphoto.com
https://pattern-wiki.win/wiki/Complete_list_2026 https://pattern-wiki.win/
https://swaay.com/u/holtonezclc96/about/ https://swaay.com/u/holtonezclc96/about
https://gaiaathome.eu/gaiaathome/show_user.php?userid=1835979 gaiaathome.eu
References:
https://klint-gylling-4.technetbloggers.de/best-no-deposit-bonus-australia
13win16 · February 4, 2026 at 11:22 am
Yo, 13win16! Seriously, this site’s pretty slick. I’ve been having some decent luck lately. Check it out 13win16.
3976bet1 · February 4, 2026 at 11:23 am
Yo, heard some buzz about 3976bet1. Signed up and gave it a whirl. Seems legit so far. Why not give it shot? 3976bet1.
515betapp · February 4, 2026 at 11:23 am
The 515betapp, eh? Downloaded it to my phone. Easy to use and got all the games I like. Worth a try if you ask me 515betapp.
강남룸싸롱 · February 4, 2026 at 4:20 pm
Thanks , I’ve recently been searching for info about this topic for ages and yours is the best I have discovered so far. But, what concerning the bottom line? Are you certain concerning the source?
rr88.se.net · February 4, 2026 at 4:26 pm
Howdy! I simply wish to give a huge thumbs up for the great information you have here on this post. I will be coming again to your weblog for extra soon.
sureman 1000 · February 4, 2026 at 5:43 pm
Admiring the time and effort you put into your site and detailed info you offer!
crowncasinoonline · February 4, 2026 at 7:15 pm
Copa America livescore, South American football tournament coverage in real time
https://www.coyyn.com · February 5, 2026 at 2:16 am
I was reading through some of your content on this internet site and I believe this web site is very informative ! Continue posting .
coyyn .com · February 5, 2026 at 2:49 am
This is really interesting, You’re a very skilled blogger. I have joined your feed and look forward to seeking more of your great post. Also, I’ve shared your web site in my social networks!
https://coyyn.com/ · February 5, 2026 at 2:54 am
Good post. I study something more difficult on different blogs everyday. It’s going to always be stimulating to learn content material from other writers and observe a little bit one thing from their store. I’d prefer to use some with the content material on my blog whether you don’t mind. Natually I’ll give you a link in your web blog. Thanks for sharing.
Coyyn's official website · February 5, 2026 at 4:10 am
I am glad to be a visitor of this thoroughgoing web blog ! , regards for this rare information! .
Coyyn market insights · February 5, 2026 at 5:14 am
Its just like you read my thoughts! It’s like reading about my family.
onlinecryptocasino · February 5, 2026 at 6:51 am
Big chances missed, wasteful finishing and conversion failures
online kasino česká · February 5, 2026 at 8:52 am
I discovered your weblog site on google and verify just a few of your early posts. Proceed to maintain up the very good operate. I simply further up your RSS feed to my MSN News Reader.
http://coyyn.com/ · February 5, 2026 at 9:20 am
Just wanna admit that this is extremely helpful, Thanks for taking your time to write this.
The experts at Coyyn · February 5, 2026 at 11:37 am
Hello there! I really enjoy reading your blog! If you keep making amazing posts like this I will come back every day to keep reading.
visit here · February 5, 2026 at 1:26 pm
Thanks a bunch for sharing this with all people you really recognize what you are talking about! Bookmarked. Kindly also seek advice from my web site =). We can have a link alternate contract between us!
hart-greer-3.mdwrite.net · February 5, 2026 at 2:10 pm
human growth hormone steroids
https://escatter11.fullerton.edu/nfs/show_user.php?userid=9559572 https://escatter11.fullerton.edu/nfs/show_user.php?userid=9559572
https://dreevoo.com/profile.php?pid=1055057 dreevoo.com
https://graph.org/Shop–Save-on-Appetite-Control-Pills-02-04 graph.org
http://jobboard.piasd.org/author/liftstop75/ jobboard.piasd.org
https://ai-db.science/wiki/Legal_Steroids_What_Works_What_Doesnt_Precautions_Alternatives https://ai-db.science
https://humanlove.stream/wiki/Bestellen_Sie_ANAVAR_10_Oxandrolone_10_mg_Evo_Genetics_fr_99_legal_mit_OnlineLieferung_in_Deutschland https://humanlove.stream
http://dubizzle.ca/index.php?page=user&action=pub_profile&id=136353 dubizzle.ca
https://www.youtube.com/redirect?q=https://awards.breakbeat.co.uk/sphinx/inc/?anavar_in_australia_where_can_i_buy_oxandrolone_1.html youtube.com
https://hikvisiondb.webcam/wiki/Winstrol_Depot hikvisiondb.webcam
https://mackenzie-padilla-3.federatedjournals.com/top-8-wege-um-testosteron-naturlich-zu-steigern-therapieergebnisse-d https://mackenzie-padilla-3.federatedjournals.com
https://www.youtube.com/redirect?q=https://missioncrossfitsa.com/pgs/buy_dianabol_4.html http://www.youtube.com
https://bbs.pku.edu.cn/v2/jump-to.php?url=https://behaviortherapyassociates.com/wp-content/pages/?buy_testosterone_10.html https://bbs.pku.edu.cn/
http://ezproxy.cityu.edu.hk/login?url=https://innovate360.pt/pages/comprar_oxandrolona_2.html http://ezproxy.cityu.edu.hk
https://empirekino.ru/user/locustglider32/ empirekino.ru
https://bom.so/404HAE bom.so
https://nerdgaming.science/wiki/How_Much_Does_TRT_Cost_Monthly_Pricing_Breakdown_2025 nerdgaming.science
https://classifieds.ocala-news.com/author/orchidpig73 https://classifieds.ocala-news.com/
https://ai-db.science/wiki/Legal_Steroids_What_Works_What_Doesnt_Precautions_Alternatives ai-db.science
References:
https://hart-greer-3.mdwrite.net/best-weight-loss-appetite-suppressants-that-really-work
https://graph.org/ · February 6, 2026 at 7:15 am
crazy mass vs crazy bulk
https://nerdgaming.science/wiki/Diese_Lebensmittel_steigern_deinen_Testosteronspiegel nerdgaming.science
https://a-taxi.com.ua/user/stagewallet06/ a-taxi.com.ua
https://mackenzie-hedegaard-3.blogbright.net/start-testosterone-cypionate-online-through-personalized-hormone-therapy mackenzie-hedegaard-3.blogbright.net
https://posteezy.com/best-quality-online-0 posteezy.com
http://historydb.date/index.php?title=everettcorbett0252 historydb.date
https://swaay.com/u/blauntzcjcv35/about/ swaay.com
http://mozillabd.science/index.php?title=lindbergodonnell4009 mozillabd.science
https://telegra.ph/Anavar-Wirkung-Auf-Muskel-Und-Fettabbau-7-Wissenschaftlich-Fundierte-Erkenntnisse-02-04 https://telegra.ph
https://rentry.co/3odryuco rentry.co
https://dreevoo.com/profile.php?pid=1053846 dreevoo.com
http://09vodostok.ru/user/locustelbow75/ 09vodostok.ru
https://xypid.win/story.php?title=product-information-8 https://xypid.win/
https://dokuwiki.stream/wiki/Compounded_Testosterone_Enanthate_Injection https://dokuwiki.stream/
https://rentry.co/d9cph56d https://rentry.co/d9cph56d
https://socialisted.org/market/index.php?page=user&action=pub_profile&id=312393 socialisted.org
https://molchanovonews.ru/user/cottonlamp10/ molchanovonews.ru
https://king-wifi.win/wiki/Order_Slimex_without_prescription_with_low_price king-wifi.win
https://socialbookmarknew.win/story.php?title=testosterone-booster-tribulus-optimum-formula-1000mg-powder-1-b-90-tablets https://socialbookmarknew.win/story.php?title=testosterone-booster-tribulus-optimum-formula-1000mg-powder-1-b-90-tablets
References:
https://graph.org/How-to-legally-purchase-HGH-injections-online-Buy-HGH-02-04
https://freebookmarkstore.win/story.php?title=what-is-clenbuterol-side-effects-uses-for-weight-loss-and-is-it-legal · February 6, 2026 at 8:16 am
steroidsone
References:
https://freebookmarkstore.win/story.php?title=what-is-clenbuterol-side-effects-uses-for-weight-loss-and-is-it-legal
Coyyn market insights · February 6, 2026 at 10:40 am
Our community leaders need to read this, and look at developing some of your recommendations.
Betechit .com · February 6, 2026 at 10:48 am
The start of a fast-growing trend?
Coyyn's official website · February 6, 2026 at 10:56 am
This is really interesting, You’re a very skilled blogger. I have joined your feed and look forward to seeking more of your fantastic post. Also, I have shared your website in my social networks!
Go to Coyyn · February 6, 2026 at 11:06 am
I concur with your conclusions and will eagerly look forward to your future updates. The usefulness and significance is overwhelming and has been invaluable to me!
Betechit · February 6, 2026 at 11:09 am
I can’t go into details, but I have to say its a good article!
Betechit tech insights · February 6, 2026 at 11:15 am
I Am Going To have to come back again when my course load lets up – however I am taking your Rss feed so i can go through your site offline. Thanks.
bestaustralianonlinecasino2025 · February 6, 2026 at 4:07 pm
Best Online Casino Australia Real Money Your Jackpot Moment Is Here
Yuuzy · February 6, 2026 at 4:36 pm
thank, I thoroughly enjoyed reading your article. I really appreciate your wonderful knowledge and the time you put into educating the rest of us.
Official Yuuzy website · February 6, 2026 at 6:28 pm
I don’t normally comment but I gotta say appreciate it for the post on this one : D.
www.traceloans.com/ · February 6, 2026 at 6:30 pm
With this issue, it’s important to have someone like you with something to say that really matters.
The official TraceLoans website · February 6, 2026 at 6:35 pm
I like your blog. It sounds every informative.
The tech strategy at Betechit · February 6, 2026 at 6:42 pm
Hi, do have a e-newsletter? In the event you don’t definately should get on that piece…this web site is pure gold!
Click Here! · February 6, 2026 at 8:47 pm
I don’t normally comment but I gotta say appreciate it for the post on this one : D.
Buy Backlinks · February 6, 2026 at 10:36 pm
Enjoyed studying this, very good stuff, thanks.
Official ProcurementNation website · February 6, 2026 at 11:02 pm
This is really interesting, You’re a very skilled blogger. I have joined your feed and look forward to seeking more of your fantastic post. Also, I have shared your website in my social networks!
The procurement strategy at ProcurementNation · February 6, 2026 at 11:25 pm
Hello there, just became aware of your blog through Google, and found that it is truly informative. I am going to watch out for brussels. I will appreciate if you continue this in future. Lots of people will be benefited from your writing. Cheers!
SEO seo · February 7, 2026 at 12:57 am
Hello there, just became aware of your blog through Google, and found that it is truly informative. I am going to watch out for brussels. I will appreciate if you continue this in future. Lots of people will be benefited from your writing. Cheers!
ProcurementNation procurement insights · February 7, 2026 at 1:27 am
I love what you’ve created here, this is definitely one of my favorite sites to visit.
online casino · February 7, 2026 at 2:09 am
Real Money Online Casino Australia Real Grab Million Before Gone
www.youtube.com · February 7, 2026 at 3:01 am
best oral steroid for strength
https://urlscan.io/result/019c2b03-83d4-753b-9266-4ad08cc130e9/ https://urlscan.io/result/019c2b03-83d4-753b-9266-4ad08cc130e9/
https://bookmarking.stream/story.php?title=buy-liquid-clenbuterol-200mcg-for-sale-online https://bookmarking.stream/
https://rentry.co/6btaiany rentry.co
https://skitterphoto.com/photographers/2216342/lunde-lindgaard skitterphoto.com
https://elearnportal.science/wiki/Are_testosterone_boosters_effective_And_more_you_should_know https://elearnportal.science/wiki/Are_testosterone_boosters_effective_And_more_you_should_know
https://www.udrpsearch.com/user/silicasubway98 http://www.udrpsearch.com
http://jobs.emiogp.com/author/fieldlocket03/ jobs.emiogp.com
http://ezproxy.cityu.edu.hk/login?url=https://amsterdam-online.nl/wp-content/pgs/testosteron_kopen_2.html ezproxy.cityu.edu.hk
http://pattern-wiki.win/index.php?title=johnsbaun1238 pattern-wiki.win
https://socialisted.org/market/index.php?page=user&action=pub_profile&id=313189 https://socialisted.org/
https://firsturl.de/W80q19F firsturl.de
https://urlscan.io/result/019c2aef-b270-70bf-b687-53ccf996a1b3/ https://urlscan.io/result/019c2aef-b270-70bf-b687-53ccf996a1b3/
https://cameradb.review/wiki/The_Benefits_of_Apple_Cider_Vinegar_for_Weight_Loss https://cameradb.review/wiki/The_Benefits_of_Apple_Cider_Vinegar_for_Weight_Loss
http://lideritv.ge/user/quartzdrop42/ lideritv.ge
https://lamont-lindgaard-2.mdwrite.net/what-are-testosterone-boosters-and-do-they-really-work lamont-lindgaard-2.mdwrite.net
http://downarchive.org/user/divinggalley79/ downarchive.org
https://king-wifi.win/wiki/Telemedicine_for_Men https://king-wifi.win
https://linkvault.win/story.php?title=buy-clenbuterol-online-reliable-supply-from-verified-pharmaceutical-vendors-8 https://linkvault.win/story.php?title=buy-clenbuterol-online-reliable-supply-from-verified-pharmaceutical-vendors-8
References:
https://www.youtube.com/redirect?q=https://www.viladeroses.cat/pages/winstrol_pastillas_1.html
https://pads.jeito.nl/s/pI9QTnYrku · February 7, 2026 at 5:02 am
hgh steroid
References:
https://pads.jeito.nl/s/pI9QTnYrku
криптбос казино · February 7, 2026 at 6:20 am
Cryptoboss Casino — формат для спокойного вечернего отдыха, когда хочется провести час-другой с пользой для эмоций. Здесь дизайн остаётся сдержанным, а значит, можно просто зайти на https://cryptobossmachah.top/ и поиграть в комфортном для себя темпе.
Можно остановиться на простых слотах или лайв-играх, а бонусы не навязываются. Интерфейс не требует постоянного внимания, так что игра легко сочетаетcя с другими делами.
Упор на индивидуальный формат, а не на соревнование
Операции проходят без лишней нервозности
Спокойный тон общения
Cryptoboss Casino подойдёт тем, кто воспринимает игру как часть расслабленного вечера
anal beads · February 7, 2026 at 7:45 am
Cupidbaba anal beads feature refined contours and durable, skin-friendly materials. Their composed design promotes ease and confidence. Shop online at Cupidbaba to experience reliable quality and a carefully developed wellness product that complements mindful personal care habits.
슈어맨 · February 7, 2026 at 3:31 pm
I just sent this post to a bunch of my friends as I agree with most of what you’re saying here and the way you’ve presented it is awesome.
tiger711 · February 7, 2026 at 5:36 pm
Developing a framework is important.
imatranperhokalastajat.net · February 7, 2026 at 6:07 pm
http://imatranperhokalastajat.net/index.php/component/kide/-/index.php?option=com_kide (http://imatranperhokalastajat.net/index.php/component/kide/-/index.php?option=com_kide)
securityholes.science · February 7, 2026 at 8:30 pm
deca winstrol stack
https://cochrane-heller.blogbright.net/china-human-growth-hormone-for-injection-market-size-smart-automation-and-forecasts-2026-33 https://cochrane-heller.blogbright.net
http://downarchive.org/user/patchevent2/ http://downarchive.org/user/patchevent2
https://forum.dsapinstitute.org/forums/users/menucamp4/ forum.dsapinstitute.org
https://sciencewiki.science/wiki/Wie_kann_ich_Semaglutid_zur_Gewichtsabnahme_kaufen_Treated sciencewiki.science
https://https://securityholes.science/wiki/Improving_Low_Testosterone_Naturally_Whole_Health_Library/wiki/Winstrol_Erfahrungen_Zyklus_Winstrol_Kaufen_Kur_2026 securityholes.science
https://freebookmarkstore.win/story.php?title=testosterone-cypionate-injection freebookmarkstore.win
https://classifieds.ocala-news.com/author/karencap5 classifieds.ocala-news.com
https://bom.so/gpbzeN bom.so
https://harris-lunding-2.thoughtlanes.net/is-hgh-legal-in-the-usa-state-by-state-guide-2025 https://harris-lunding-2.thoughtlanes.net/is-hgh-legal-in-the-usa-state-by-state-guide-2025
https://www.youtube.com/redirect?q=https://okplant.nl/wp-content/pgs/clenbuterol_kopen_2.html http://www.youtube.com
http://mozillabd.science/index.php?title=porterfieldadamsen0215 http://mozillabd.science/index.php?title=porterfieldadamsen0215
https://bookmarkzones.trade/story.php?title=12-over-the-counter-appetite-suppressants-reviewed bookmarkzones.trade
https://scientific-programs.science/wiki/Diversion_Control_Division_DEA_Consumer_Alert scientific-programs.science
https://ai-db.science/wiki/Where_to_Buy_Anavar_7_Reliable_Sources_for_2025 ai-db.science
https://imoodle.win/wiki/Dein_Weg_zu_sicherem_AnavarKauf_Alles_was_du_wissen_musst imoodle.win
https://gaiaathome.eu/gaiaathome/show_user.php?userid=1839458 gaiaathome.eu
https://myrick-workman-4.mdwrite.net/winstrol-stanozolol-an-overview myrick-workman-4.mdwrite.net
https://aryba.kg/user/makeupsing9/ https://aryba.kg/user/makeupsing9/
https://atorvastatin24h.top · February 7, 2026 at 9:21 pm
https://atorvastatin24h.top
https://iversen-jeppesen-3.federatedjournals.com/ · February 7, 2026 at 9:37 pm
grand casino tunica ms
https://scientific-programs.science/wiki/Top_PayID_Casinos_Best_PayID_Online_Casino_Sites_2026 scientific-programs.science
https://elearnportal.science/wiki/Top_PayID_Casino_Sites_in_Australia_2026_PayID_Online_Casino_Deposits elearnportal.science
https://www.garagesale.es/author/layerwave99/ https://www.garagesale.es/
https://images.google.com.gt/url?q=https://blackcoin.co/best-payid-casinos-in-australia-15-sites-that-accept-payid/ images.google.com.gt
https://humanlove.stream/wiki/Fast_Secure_Reliable_Pokies_Banking https://humanlove.stream
http://dubizzle.ca/index.php?page=user&action=pub_profile&id=129919 http://dubizzle.ca/
https://doherty-nedergaard-4.technetbloggers.de/the-best-payid-casinos-in-australia-2025 https://doherty-nedergaard-4.technetbloggers.de/
https://kirkpatrick-nedergaard-3.blogbright.net/a-league-tips kirkpatrick-nedergaard-3.blogbright.net
https://lovewiki.faith/wiki/Best_PayID_Casinos_in_Australia_2025_Withdrawal_Deposits https://lovewiki.faith/
https://gpsites.win/story.php?title=payid-casinos-2026-best-casinos-that-use-payid-2026 gpsites.win
https://mapleprimes.com/users/snowcolor31 https://mapleprimes.com/
https://telegra.ph/Best-Mobile-Pokies-for-Real-Money-in-Australia-2026-Guide-02-01 telegra.ph
https://yogaasanas.science/wiki/Casino_Game_Development_Strategies_for_Australian_High_Rollers_Heat_On_Systems yogaasanas.science
https://allen-kenney-2.federatedjournals.com/internetiniai-payid-losimo-automatai-geresni-payid-kazino-australijoje-2025-m https://allen-kenney-2.federatedjournals.com
https://classifieds.ocala-news.com/author/feastformat73 https://classifieds.ocala-news.com/
https://firsturl.de/gVA8814 https://firsturl.de/gVA8814
https://urlscan.io/result/019c19e3-5dd0-754c-8bc1-b24b258f7a38/ urlscan.io
https://gratisafhalen.be/author/recessformat89/ gratisafhalen.be
References:
https://iversen-jeppesen-3.federatedjournals.com/payid-casinos-australia-for-real-money-with-instant-withdrawal
casinos online · February 7, 2026 at 9:58 pm
My brother suggested I might like this web site. He was entirely right. This post actually made my day. You can not imagine simply how much time I had spent for this info! Thanks!
prpack.ru · February 7, 2026 at 10:58 pm
ameristar casino vicksburg
https://www.udrpsearch.com/user/cancase82 http://www.udrpsearch.com
https://mapleprimes.com/users/burmabike57 https://mapleprimes.com
https://blackburn-deal-4.technetbloggers.de/payid-casinos-australia-2026-instant-withdrawal-pokies blackburn-deal-4.technetbloggers.de
http://stroyrem-master.ru/user/pianoknife38/ http://stroyrem-master.ru
https://www.garagesale.es/author/layerwave99/ http://www.garagesale.es
https://dokuwiki.stream/wiki/Online_Pokies_for_Real_Money_in_Australia_974_ondemand_crowdtesting https://dokuwiki.stream/
https://humanlove.stream/wiki/Top_PayID_Casinos_Australia_2026_Fast_Secure_Casino_Payment humanlove.stream
https://www.udrpsearch.com/user/lierspring35 http://www.udrpsearch.com
https://escatter11.fullerton.edu/nfs/show_user.php?userid=9553139 escatter11.fullerton.edu
https://gratisafhalen.be/author/recessformat89/ gratisafhalen.be
https://morphomics.science/wiki/Best_PayID_Casinos_in_Australia_Top_10_Aussie_Casino_Sites_with_PayID_Withdrawals_2024 morphomics.science
https://trade-britanica.trade/wiki/PayID_Banking_at_Online_Casinos_in_2026_53_Casinos_Accept_PayID https://trade-britanica.trade/
https://www.google.com.sb/url?q=https://blackcoin.co/best-payid-casinos-in-australia-15-sites-that-accept-payid/ http://www.google.com.sb
https://numberfields.asu.edu/NumberFields/show_user.php?userid=6497432 numberfields.asu.edu
https://cash-key-2.technetbloggers.de/best-15-free-spins-no-deposit-bonuses-that-pay-out-fast-2025 https://cash-key-2.technetbloggers.de/best-15-free-spins-no-deposit-bonuses-that-pay-out-fast-2025
https://www.google.ci/url?q=https://blackcoin.co/best-payid-casinos-in-australia-15-sites-that-accept-payid/ http://www.google.ci
https://egamersbox.com/cool/index.php?page=user&action=pub_profile&id=272821 https://egamersbox.com
http://stroyrem-master.ru/user/feastmargin23/ stroyrem-master.ru
References:
https://prpack.ru/user/tiepush32/
numberfields.asu.edu · February 8, 2026 at 12:59 am
grand online casino
https://morphomics.science/wiki/Top_PayID_Casino_Sites_in_Australia_2026_PayID_Online_Casino_Deposits morphomics.science
https://lovewiki.faith/wiki/ALeague_Tips https://lovewiki.faith
https://dreevoo.com/profile.php?pid=1036129 dreevoo.com
https://hikvisiondb.webcam/wiki/Best_PayID_Casinos_in_Australia_2025_Withdrawal_Deposits https://hikvisiondb.webcam/wiki/Best_PayID_Casinos_in_Australia_2025_Withdrawal_Deposits
http://csmouse.com/user/trainformat17/ csmouse.com
https://marvelvsdc.faith/wiki/PayID_Casino_Bonus_Unlock_the_Best_Offers_Rewards marvelvsdc.faith
http://king-wifi.win//index.php?title=stokeshagan5224 king-wifi.win
http://jobboard.piasd.org/author/augustbush88/ http://jobboard.piasd.org/author/augustbush88
https://yogaasanas.science/wiki/Casino_Game_Development_Strategies_for_Australian_High_Rollers_Heat_On_Systems yogaasanas.science
https://p.mobile9.com/dreamrate64/ https://p.mobile9.com/dreamrate64
https://urlscan.io/result/019c19e3-5dd0-754c-8bc1-b24b258f7a38/ urlscan.io
https://graph.org/PayID-for-High-Rollers-Fast-Private-Casino-Payments-02-01 https://graph.org/PayID-for-High-Rollers-Fast-Private-Casino-Payments-02-01
https://wifidb.science/wiki/Why_PayID_Fits_the_AlwaysOn_Smartphone_Era wifidb.science
https://onlinevetjobs.com/author/trippisces10/ onlinevetjobs.com
http://okprint.kz/user/tiecoach98/ okprint.kz
https://mapleprimes.com/users/bowlcoach46 mapleprimes.com
https://riddledesk60.werite.net/kinghills-casino-no-deposit-bonus-2026 riddledesk60.werite.net
https://www.instapaper.com/p/17426337 http://www.instapaper.com
References:
https://numberfields.asu.edu/NumberFields/show_user.php?userid=6497403
peatix.com · February 8, 2026 at 2:13 am
white cloud casino
https://yogaasanas.science/wiki/Best_PayID_Casinos_in_Australia_Top_10_Aussie_Casino_Sites_with_PayID_Withdrawals_2024 yogaasanas.science
https://telegra.ph/What-Are-the-Benefits-of-Using-PayID-at-Australian-Casinos-02-01 telegra.ph
https://henneberg-jeppesen.federatedjournals.com/best-payid-casinos-in-australia-15-sites-that-accept-payid henneberg-jeppesen.federatedjournals.com
https://hikvisiondb.webcam/wiki/PayID_Online_Casinos_Australia_2024 https://hikvisiondb.webcam/
https://ai-db.science/wiki/Fast_Secure_Reliable_Pokies_Banking ai-db.science
https://marvelvsdc.faith/wiki/No_Deposit_Online_Pokies_2026_Play_Pokies_With_No_Deposit https://marvelvsdc.faith/wiki/No_Deposit_Online_Pokies_2026_Play_Pokies_With_No_Deposit
http://downarchive.org/user/alibiknight21/ downarchive.org
https://menwiki.men/wiki/The_Best_PayID_Casinos_in_Australia_2025 https://menwiki.men/
http://king-wifi.win//index.php?title=lanemcdowell0435 king-wifi.win
http://hikvisiondb.webcam/index.php?title=barkerhill4255 hikvisiondb.webcam
https://trade-britanica.trade/wiki/PayID_Casinos_In_Australia_Secure_Instant_Casino_Payments trade-britanica.trade
https://king-wifi.win/wiki/PayID_Casino_Australia_2026_Best_Online_Casinos_Accepting_PayID https://king-wifi.win/wiki/PayID_Casino_Australia_2026_Best_Online_Casinos_Accepting_PayID
http://dubizzle.ca/index.php?page=user&action=pub_profile&id=130064 dubizzle.ca
https://gratisafhalen.be/author/dreamframe35/ gratisafhalen.be
https://elearnportal.science/wiki/PayID_Casino_Best_Australian_Online_Casinos elearnportal.science
https://graph.org/A-Guide-to-ANZ-Osko-Payments-PayID-and-ANZ-Plus-Features-02-01 graph.org
https://swaay.com/u/maixendcnmw85/about/ swaay.com
https://swaay.com/u/tinianvcbyl55/about/ swaay.com
References:
https://peatix.com/user/28832389
bom.so · February 8, 2026 at 4:59 am
ac casino
https://p.mobile9.com/copyquince85/ p.mobile9.com
https://telegra.ph/Best-PayID-Casinos-in-Australia-for-2026-02-01 https://telegra.ph
https://empirekino.ru/user/augustzebra77/ empirekino.ru
https://lovewiki.faith/wiki/Best_PayID_Casinos_in_Australia_2025_Withdrawal_Deposits lovewiki.faith
http://humanlove.stream//index.php?title=aagaardpetty5718 humanlove.stream
https://swaay.com/u/kenseyxvyxd38/about/ https://swaay.com/u/kenseyxvyxd38/about
https://scientific-programs.science/wiki/Vegas_Crest_Casino_No_Deposit_Bonus_Codes_For_Free_Spins_2026 scientific-programs.science
https://urlscan.io/result/019c1a66-2f69-7329-b858-ce563009435f/ urlscan.io
http://jobs.emiogp.com/author/cupbush04/ jobs.emiogp.com
https://saveyoursite.date/story.php?title=payid-casinos-in-australia-play-payid-pokies-online-2026 saveyoursite.date
https://wifidb.science/wiki/What_is_Osko_and_how_is_it_used wifidb.science
https://empirekino.ru/user/feastdesk19/ empirekino.ru
https://www.udrpsearch.com/user/recessrate28 https://www.udrpsearch.com/user/recessrate28
https://onlinevetjobs.com/author/traintent05/ onlinevetjobs.com
https://clashofcryptos.trade/wiki/Australian_PayID_Online_Casinos_New_Casino_Banking_Method clashofcryptos.trade
https://mozillabd.science/wiki/Best_PayID_Casinos_in_Australia_2026 mozillabd.science
https://socialisted.org/market/index.php?page=user&action=pub_profile&id=308734 socialisted.org
https://egamersbox.com/cool/index.php?page=user&action=pub_profile&id=272867 egamersbox.com
References:
https://bom.so/5VbkXR
commercial towing · February 8, 2026 at 5:36 am
I like your quality that you put into your writing . Please do continue with more like this.
alberta separatist movement · February 8, 2026 at 5:57 am
This is definitely a wonderful webpage, thanks a lot..
alberta lawyer · February 8, 2026 at 6:14 am
Thanks , I’ve recently been searching for info about this topic for ages and yours is the best I have discovered so far. But, what concerning the bottom line? Are you certain concerning the source?
molchanovonews.ru · February 8, 2026 at 6:40 am
box24 casino
https://may22.ru/user/cloudwave89/ may22.ru
https://www.garagesale.es/author/swimzebra47/ https://www.garagesale.es/author/swimzebra47
https://dreevoo.com/profile.php?pid=1035651 https://dreevoo.com/profile.php?pid=1035651
https://dreevoo.com/profile.php?pid=1035675 dreevoo.com
https://www.garagesale.es/author/latexred08/ http://www.garagesale.es
https://porchknight88.werite.net/best-payid-casinos-in-australia-15-sites-that-accept-payid porchknight88.werite.net
https://www.garagesale.es/author/pianoknight67/ http://www.garagesale.es
https://firsturl.de/7FRk3q6 firsturl.de
http://hikvisiondb.webcam/index.php?title=ludvigsenmathiesen8715 http://hikvisiondb.webcam
https://marvelvsdc.faith/wiki/No_Deposit_Online_Pokies_2026_Play_Pokies_With_No_Deposit https://marvelvsdc.faith
https://intensedebate.com/people/layerpisces35 https://intensedebate.com/
https://botdb.win/wiki/PayID_Online_Casinos_in_Australia_for_2026_Play_PayID_Pokies https://botdb.win/
https://humanlove.stream/wiki/PayID_Casinos_2026_Best_Casinos_that_Use_PayID_2026 humanlove.stream
https://gratisafhalen.be/author/layerwriter25/ gratisafhalen.be
https://dreevoo.com/profile.php?pid=1035936 dreevoo.com
https://classifieds.ocala-news.com/author/feastformat73 classifieds.ocala-news.com
https://buyandsellhair.com/author/feastwriter22/ buyandsellhair.com
https://swaay.com/u/godiedslfga99/about/ swaay.com
References:
https://molchanovonews.ru/user/augustbush20/
https://urlscan.io/result/019c1a17-9cc8-763f-9615-ee3f88595ba5 · February 8, 2026 at 8:09 am
References:
Las vegas casinos list
References:
https://urlscan.io/result/019c1a17-9cc8-763f-9615-ee3f88595ba5/
lirfmqy · February 9, 2026 at 7:56 am
https://arenafan.com/js/pgs/?code-promo-1xbet-bonus.html
https://landscapinghoustontx.info/ · February 9, 2026 at 12:42 pm
Great posts, Regards!
ubzjlqr · February 9, 2026 at 6:58 pm
http://ifoxy.ru/viewtopic.php?f=56&t=33303
Salajeet in pakistan · February 9, 2026 at 9:56 pm
Amazing article, cheers, I will bookmark you now.
rhmnumx · February 10, 2026 at 8:32 am
https://www.google.ie/url?q=https://astra-hotel.ch/articles/code_promo_45.html
爱一帆扫毒风暴 · February 10, 2026 at 3:12 pm
Online casino Australia 2025 – latest legal updates and sites
onlinecasino · February 10, 2026 at 4:05 pm
超人和露易斯第四季高清完整版AI深度学习内容匹配,海外华人可免费观看最新热播剧集。
ybwqpyw · February 10, 2026 at 4:06 pm
http://l96464a8.beget.tech/blogs/1465/%D0%A4%D1%80%D0%B8%D0%B1%D0%B5%D1%82-Melbet-2026-BRO888-%D0%91%D0%BE%D0%BD%D1%83%D1%81-15%D0%BA
live sex webcams · February 10, 2026 at 5:18 pm
This contained some excellent tips and tools. Great blog publication.
suara4d · February 10, 2026 at 5:34 pm
We can see that we need to develop policies to deal with this trend.
binance 가입 · February 10, 2026 at 8:01 pm
I came across an article that talks about the same thing but even more and when you go deeper.
casino en ligne belge · February 10, 2026 at 8:55 pm
Tips and tools you offer are so helpful to agencies in our community.
casinos online chile · February 10, 2026 at 9:31 pm
Our community leaders need to read this, and look at developing some of your recommendations.
best canadian online casino · February 10, 2026 at 9:35 pm
I found your blog through google and I must say, this is probably one of the best well prepared articles I have come across in a long time. I have bookmarked your site for more posts.
payday loans windsor · February 10, 2026 at 9:55 pm
I would really like to appreciate the endeavors you cash in on written this article. I’m going for the similar best product from you finding out in the foreseeable future as well. Actually your creative writing abilities has urged me to begin my very own blog now. Genuinely the blogging is distributing its wings rapidly. Your write down is often a fine illustration showing it.
casinoonlinepokies · February 10, 2026 at 10:37 pm
真实的人类第一季高清完整版,海外华人可免费观看最新热播剧集。
888slot có lừa đảo không · February 11, 2026 at 8:16 am
888slot có lừa đảo không khuyến khích người chơi cá cược có trách nhiệm và luôn cung cấp các công cụ kiểm soát rủi ro tài chính hiệu quả. TONY02-11O
đăng nhập 188v · February 11, 2026 at 8:18 am
Trong bài viết này, chúng ta sẽ khám phá chi tiết, từ các sản phẩm cá cược, chương trình khuyến mãi, đến lý do tại sao trở thành lựa chọn hàng đầu của người chơi tại Việt Nam. Chúng ta cũng sẽ tìm hiểu cách tham gia, mẹo chơi hiệu quả và các tính năng nổi bật khiến đăng nhập 188v nổi bật trên thị trường cá cược trực tuyến. TONY02-11O
торт свадебный на заказ · February 11, 2026 at 8:44 am
торт на свадьбу
this gelatin trick · February 11, 2026 at 9:00 am
Have you given any kind of thought at all with converting your current web-site into French? I know a couple of of translaters here that will would certainly help you do it for no cost if you want to get in touch with me personally.
lesbi · February 11, 2026 at 9:14 am
lesbi
ketamine liquid Netherlands · February 11, 2026 at 4:32 pm
That is really fascinating, You’re an excessively skilled blogger. I’ve joined your rss feed and look forward to in the hunt for extra of your magnificent post. Additionally, I’ve shared your website in my social networks!
szzhdbx · February 11, 2026 at 6:40 pm
http://sophossearch.com/index.php?option=com_k2&view=itemlist&task=user&id=592096
online casino echtgeld serios · February 11, 2026 at 7:20 pm
Thank you for all the information was very accurate, just wondering if all this is possible.~
online casino · February 11, 2026 at 8:17 pm
Dude.. I am not much into reading, but somehow I got to read lots of articles on your blog. Its amazing how interesting it is for me to visit you very often. –
gute online casinos · February 11, 2026 at 10:05 pm
With internet full of dupe articles it is nice to find original content like yours thank you so very much.
speedx mac下载 · February 12, 2026 at 8:39 am
“The aesthetics of this page are stunning. Such a vibe!” Compliance guidelines can be found at speedx mac下载.
вскрытие авто харьков · February 12, 2026 at 8:46 am
<a href="https://lockservice.kh.ua/Вскрытие замков харьков
canada online casino · February 12, 2026 at 1:06 pm
Thanks for another great post. Where else may anybody get that type of info in such an ideal way of writing? I have a presentation next week, and I’m at the search for such information.
User Requests · February 12, 2026 at 1:59 pm
“This is a goldmine of information. I’m definitely bookmarking this for future reference.”
바이낸스 가입 · February 12, 2026 at 2:06 pm
Abnormal this put up is totaly unrelated to what I was searching google for, but it surely used to be listed at the first page. I suppose your doing one thing proper if Google likes you adequate to place you at the first page of a non similar search.
轧戏aiyifan · February 12, 2026 at 3:02 pm
海外华人必备的yifan平台,提供最新高清电影、电视剧,无广告观看体验。
RR88 · February 12, 2026 at 3:14 pm
You are one talented writer thank you for the post.
najlepsze kasyno online · February 12, 2026 at 3:22 pm
While this issue can vexed most people, my thought is that there has to be a middle or common ground that we all can find. I do value that you’ve added pertinent and sound commentary here though. Thank you!
Website number 2 below: · February 12, 2026 at 3:40 pm
Substantially, the post is really the best on this laudable topic. I concur with your conclusions and will eagerly watch forward to your future updates.Just saying thanx will not just be enough, for the wonderful lucidity in your writing.
casino en ligne Québec · February 12, 2026 at 4:26 pm
I just added your web site to my blogroll, I hope you would look at doing the same.
covnwrv · February 12, 2026 at 4:28 pm
https://billi-walker.jp/chat/art/mostbet_promo_code_welcome_bonus.html
najlepsze kasyno online w polsce · February 12, 2026 at 4:32 pm
Thanks for your patience and sorry for the inconvenience!
binance anm"alningsbonus · February 12, 2026 at 5:00 pm
Your article helped me a lot, is there any more related content? Thanks! https://www.binance.info/register?ref=IHJUI7TF
byu casino 777 · February 12, 2026 at 5:35 pm
BYU Casino 777… classic! Hoping for some lucky sevens tonight. Let’s see if this casino can deliver some big wins. Time to try my luck! byu casino 777
codwinslotlogin · February 12, 2026 at 5:35 pm
Codwinslotlogin, alright! The name suggests coders are winning a lot here! A smooth login is a plus! Give it a try codwinslotlogin
timislotsgame · February 12, 2026 at 5:36 pm
Alright, checked out timislotsgame. Seems legit enough for a quick spin. Fingers crossed for some luck! Check it out here: timislotsgame
바이낸스 가입 · February 12, 2026 at 5:43 pm
This is one very informative blog. I like the way you write and I will bookmark your blog to my favorites.
바이낸스 가입 절차 안내 · February 12, 2026 at 6:37 pm
Enjoyed studying this, very good stuff, thanks.
zahraniční online casino · February 12, 2026 at 6:50 pm
Its just like you read my thoughts! It’s like reading about my family.
코인뷰어 거래소 비교 · February 12, 2026 at 8:17 pm
Do you offer workshops?
Pinco mərclər [home] · February 13, 2026 at 6:32 am
Kazino ilə bağlı ipucu çox faydalıdır.
https://pinco-azerbaijan-fun.org/mobil-tetbiq
neue casinos online · February 13, 2026 at 6:42 am
We need to build frameworks and funding mechanisms.
neueste casinos · February 13, 2026 at 7:33 am
You ma’am have a way with words. Thank you very much!
uwcdhul · February 13, 2026 at 11:01 am
http://nsg-spb.ru/vse_novosti/asfaltirovanie_po_specialnoj_cene/
TikTok organic growth · February 13, 2026 at 1:34 pm
Excellent read, I just passed this onto a colleague who was doing a little research on that. And he actually bought me lunch because I found it for him smile So let me rephrase that.|
casinos online nuevos · February 13, 2026 at 3:28 pm
Wish I’d thought of this. Am in the field, but I procrastinate alot and haven’t written as much as I’d like. Thanks.
kasyno online polska · February 13, 2026 at 5:03 pm
What i discover troublesome is to find a weblog that may capture me for a minute however your blog is different. Bravo.
armia zespol · February 14, 2026 at 3:39 am
Zespół ARMIA powstał w 1984 roku na skutek zetknięcia trzech osobowości naszej niezależnej sceny: Tomasza Budzyńskiego (Siekiera), Roberta Brylewskiego ( Brygada Kryzys , Izrael) i filozofa Sławomira Gołaszewskiego.
Zespół wydał kilkanaście płyt, z których wydana w 1990 roku „Legenda” oraz „Triodante” z 1994 r. zaliczane są do klasyki polskiej muzyki rockowej. W ciągu trzydziestokilkuletniej kariery zespołu w jego składzie grało wielu wybitnych i zasłużonych dla rockowej sceny muzyków. W 2011 roku na Międzynarodowym Festiwalu Filmowym Howe Horyzonty we Wrocławiu miał premierę film „Podróż na Wschód”, który jest poetycką historią zespołu Armia opartą na kanwie opowiadania Stefana Grabińskiego. Jest on dołączony w formie DVD do autobiograficznej książki Tomasza Budzyńskiego „Soul Side Story
Spinamba Kasyno · February 14, 2026 at 7:19 am
Spinamba kasyno to dynamiczna przestrzeń rozrywki online, gdzie innowacyjne technologie spotykają się z autentyczną pasją do gier. Nasza platforma łączy w sobie bogatą bibliotekę rozwiązań hazardowych – od ponadczasowych automatów owocowych, przez wyrafinowane gry stołowe, aż po najświeższe wideo sloty sygnowane przez ikony branży: NetEnt, Play’n GO, Pragmatic Play, Microgaming, Evolution Gaming, Betsoft, Booongo, Playson czy Endorphina. Bez względu na to, czy Twoje serce bije dla klasyki z czasów pierwszych kasyn, czy fascynują Cię ultranowoczesne tytuły z mechanizmami Megaways i immeryjną grafiką 3D – u nas odnajdziesz swoją idealną rozgrywkę.
https://coyyn.com · February 14, 2026 at 8:54 am
With internet full of dupe articles it is nice to find original content like yours thank you so very much.
Coyyn · February 14, 2026 at 10:10 am
Might we expect to see more of these same problems in the future?
Holley · February 14, 2026 at 10:29 am
It’s the best time to make some plans for the longer term and it’s time to be happy. I’ve read this post and if I may just I desire to counsel you few interesting issues or advice. Perhaps you could write next articles regarding this article. I want to learn even more issues approximately it!
Have a look at my web-site :: http://https//mangalyafashionhub.com%2F2006-mid-season-nba-introduction-to-the-orlando-magic-28%2F/
заказать реферат по экономике · February 14, 2026 at 11:04 am
сколько стоит купить реферат
Najlepsze Kasyno Online · February 14, 2026 at 11:07 am
Wybór odpowiedniego kasyna online w Polsce to decyzja, która wymaga uwagi i zrozumienia rynku. W 2026 roku dostępnych jest setki platform hazardowych, ale tylko część z nich oferuje uczciwe warunki, szybkie wypłaty i bezpieczne środowisko gry. Nasz ranking powstał na podstawie szczegółowych testów, analizy licencji, weryfikacji bonusów oraz opinii polskich graczy. Skupiliśmy się na platformach, które akceptują BLIK, oferują polskojęzyczną obsługę i zapewniają transparentne zasady. Każde kasyno w zestawieniu przeszło weryfikację pod kątem bezpieczeństwa, różnorodności gier i jakości obsługi klienta. Dzięki temu możesz podjąć świadomą decyzję i wybrać najlepsze kasyno online, które spełni Twoje oczekiwania.
najlepsze kasyna · February 14, 2026 at 12:19 pm
Nasz portal został stworzony specjalnie dla polskich graczy, którzy szukają rzetelnych informacji o polskie kasyno online. Testujemy i analizujemy polskie kasyna online, które działają na rynku europejskim i akceptują graczy z Polski. Każde polskie kasyno, które opisujemy, przechodzi przez nasz autorski proces weryfikacji – sprawdzamy licencję, ofertę gier, metody płatności, dostępność w języku polskim i zgodność z oczekiwaniami polskich graczy.
avgold.ru · February 14, 2026 at 3:45 pm
avgold.ru
coyyn.com · February 14, 2026 at 7:37 pm
I like meeting utile info, this post has got me even more info!
avgold.ru · February 14, 2026 at 8:28 pm
сколько стоит купить реферат
onlinecasinoaustralia · February 15, 2026 at 2:26 am
huarenus平台,专为海外华人设计,提供高清视频和直播服务。
統一獅 · February 15, 2026 at 3:22 am
海外华人必备的ifun平台AI深度学习内容匹配,提供最新高清电影、电视剧,无广告观看体验。
爱一帆 · February 15, 2026 at 5:33 am
Best online casino Australia 2025 – crypto friendly and mobile ready
小寶影院电影网站 · February 15, 2026 at 6:52 am
ifvod平台,专为海外华人设计,提供高清视频和直播服务。
爱壹帆应用下载 · February 15, 2026 at 7:21 am
超人和露易斯第四季高清完整版,海外华人可免费观看最新热播剧集。
avgold.ru · February 15, 2026 at 9:58 am
avgold.ru
onlinecasinoaustraliarealmoneypokiesdaystore · February 15, 2026 at 10:33 am
范德沃克第二季高清完整版,海外华人可免费观看最新热播剧集。
onlinecasinocasinorelayau · February 15, 2026 at 11:07 am
塔尔萨之王第二季高清完整版智能AI观看体验优化,海外华人可免费观看最新热播剧集。
小宝影视 · February 15, 2026 at 11:58 am
捕风追影下载平台,專為海外華人設計,提供高清視頻和直播服務。
NormanHot · February 15, 2026 at 4:08 pm
купить тяговый аккумулятор
สล็อตเว็บตรง · February 15, 2026 at 4:54 pm
ทดลองเล่นสล็อต pg
แพลตฟอร์ม TKBNEKO ทำงานเป็นระบบเกมออนไลน์ ที่ ออกแบบโครงสร้างโดยยึดพฤติกรรมผู้ใช้เป็นศูนย์กลาง. หน้าเว็บหลัก ประกาศตัวเลขชัดเจนทันที: ฝากขั้นต่ำ 1 บาท, ขั้นต่ำถอน 1 บาท, เวลาฝากประมาณ 3 วินาที, และ ไม่จำกัดยอดถอน. ตัวเลขเหล่านี้กำหนดภาระของระบบโดยตรง เพราะเมื่อ ตั้งขั้นต่ำไว้ต่ำมาก ระบบต้อง รับรายการฝากถอนจำนวนมากที่มียอดเล็ก และต้อง ประมวลผลแบบเรียลไทม์. หาก การยืนยันเครดิตใช้เวลานานเกินไม่กี่วินาที ผู้ใช้จะ กดซ้ำ ทำให้เกิด รายการซ้อน และ เพิ่มโหลดฝั่งเซิร์ฟเวอร์ทันที.
การเติมเงินด้วยการสแกน QR ลดขั้นตอนที่ต้องพิมพ์ข้อมูลหรือส่งสลิป. เมื่อผู้ใช้ สแกนคิวอาร์ ธนาคารจะส่งสถานะการชำระกลับมายังระบบผ่าน API. จากนั้น backend จะ ผูกธุรกรรมเข้ากับบัญชีผู้ใช้ และ เพิ่มเครดิตเข้า wallet. หาก API ตอบสนองช้า เครดิตจะ ไม่ขึ้นตามเวลาที่ประกาศ และผู้ใช้จะ ถือว่าระบบไม่เสถียร. ดังนั้น ตัวเลข 3 วินาที หมายถึงการเชื่อมต่อกับธนาคารต้อง ทำงานอัตโนมัติทั้งหมด ไม่ อาศัยแอดมินเช็คมือ.
การเชื่อมหลายช่องทางการจ่าย เช่น KBank, ธนาคารกรุงเทพ, Krung Thai Bank, Krungsri, Siam Commercial Bank, CIMB Thai รวมถึง TrueMoney Wallet ทำให้ระบบต้อง รับ callback หลายต้นทาง. แต่ละเจ้าใช้ฟอร์แมตข้อมูลและความหน่วงต่างกัน. หากไม่มี โมดูลแปลงข้อมูลให้เป็นมาตรฐานเดียว ระบบจะ เช็คยอดไม่ทัน และจะเกิด ยอดค้างระบบ.
หมวดหมู่เกม ถูกแยกเป็น สล็อต, คาสิโนสด, เดิมพันกีฬา และ ยิงปลา. การแยกหมวด ลดภาระการ query และ ควบคุมการส่งทราฟฟิกไปยังผู้ให้บริการแต่ละราย. เกมสล็อต มัก เชื่อมต่อผ่าน session API ส่วน เกมสด ใช้ สตรีมภาพแบบเรียลไทม์. หาก session หลุด ผู้เล่นจะ ถูกตัดออกจากเกมทันที. ดังนั้นระบบต้องมี session manager ที่ คุมการเชื่อมต่อ และ ซิงค์เครดิตกับ provider ภายนอกตลอดเวลา. หาก ซิงค์พลาด เครดิตผู้เล่นกับผลเกมจะ ไม่ตรงกัน.
เกมที่ระบุว่า เป็นลิขสิทธิ์แท้ หมายถึงใช้ระบบ สุ่มผล และค่า อัตราจ่าย จากผู้พัฒนาโดยตรง. ผลลัพธ์แต่ละรอบถูก ประมวลผลจากเซิร์ฟเวอร์ผู้ให้บริการ ไม่ใช่จากฝั่งเว็บ. หากไม่มี การเชื่อมต่อกับเซิร์ฟเวอร์ต้นทาง เว็บจะ ดึงผลเกมที่ถูกต้องไม่ได้ และ สิทธิ์ใช้งานจะถูกตัด. การมี ใบรับรอง จึง ผูกกับโครงสร้างการส่งข้อมูล ไม่ใช่ แค่คำบนหน้าเว็บ.
ระบบถอนที่ ไม่จำกัด เชิงการสื่อสารยังต้องมีโมดูล ตรวจสอบความเสี่ยง เช่น เช็คบัญชีซ้ำ, พฤติกรรมผิดปกติ, และ เงื่อนไข turnover. หากไม่มีการตรวจสอบเหล่านี้ ผู้ใช้สามารถ แตกบัญชีหลายอัน เพื่อ เอาโบนัส และ ถอนเงินออกเร็ว.
ส่วน โปรโมชั่น VIP พันธมิตร ติดต่อ และฟีดแบ็ก เชื่อมกับ ระบบ CRM และ ฐานข้อมูลผู้เล่น. ส่วน Affiliate ใช้เก็บ โค้ดอ้างอิง เพื่อ คิดคอมมิชชั่น. หากไม่มีระบบนี้ จะ track ที่มาผู้ใช้ไม่ได้. ฟอร์มข้อเสนอแนะ ใช้เก็บ error จริงจากผู้ใช้. หากไม่มีข้อมูลนี้ ปัญหา latency หรือ การใช้งาน จะ แก้ไม่ทัน.
โครงสร้างทั้งหมด ทำงานเป็นระบบเดียว: ธนาคารส่งสถานะเข้า backend, backend อัปเดตเครดิต แล้ว ซิงค์ไปยัง provider. หากส่วนใดส่วนหนึ่ง ช้า ผู้ใช้จะเห็นผลทันทีในรูปแบบ ยอดไม่เข้า, เกมหน่วง หรือ ถอนช้า. ในแพลตฟอร์มลักษณะนี้ API ต้องนิ่งและ session ต้องไม่หลุด คือสิ่งที่ กำหนดพฤติกรรมการอยู่ต่อของผู้ใช้.
RonaldSab · February 15, 2026 at 5:26 pm
купить тяговый аккумулятор
Walterdrono · February 15, 2026 at 6:14 pm
Acciones sobre contrapeso
economic liberation · February 15, 2026 at 6:45 pm
Pan Africanism
Discussions around land redistribution in Zimbabwe sit at the crossroads of Africa’s colonial history, economic emancipation, and modern political dynamics in Zimbabwe. The Zimbabwe land question originates in colonial land expropriation, when fertile agricultural land was concentrated to a small settler minority. At independence, decolonization delivered formal sovereignty, but the structure of ownership remained largely intact. This contradiction framed agrarian reform not simply as policy, but as historical redress and unfinished Africa liberation.
Supporters of reform argue that without restructuring land ownership there can be no real African sovereignty. Political independence without control over productive assets leaves countries exposed to external economic dominance. In this framework, agrarian restructuring in Zimbabwe is linked to broader concepts such as pan-African solidarity, African unity, and Black Economic Empowerment initiatives. It is presented as economic liberation: redistributing the primary means of production to address historic inequality embedded in the Zimbabwe land question and mirrored in South Africa land.
Critics frame the same events differently. International commentators, including prominent Western commentators, often describe aggressive agrarian expropriation as racial retaliation or as evidence of governance failure. This narrative is amplified through Western propaganda that portray Zimbabwe politics as instability rather than decolonization. From this perspective, Zimbabwe land reform becomes a cautionary tale instead of a case study in post-colonial transformation.
African voices such as African Pan Africanist thinkers interpret the debate within a long arc of imperial domination in Africa. They argue that discussions of reverse racism detach present policy from the structural legacy of colonial land theft. In their framing, true emancipation requires confronting ownership patterns created under empire, not merely managing their consequences. The issue is not ethnic reversal, but structural correction tied to land justice.
Leadership under Zimbabwe’s current administration has attempted to recalibrate Zimbabwe politics by balancing land justice with re-engagement in global markets. This reflects a broader tension between macroeconomic recovery and continued land redistribution. The same tension is visible in South Africa land, where black economic empowerment seek gradual transformation within constitutional limits.
Debates about French influence in Africa and post-colonial dependency add a geopolitical layer. Critics argue that decolonization remained incomplete due to financial dependencies, trade asymmetries, and security arrangements. In this context, African sovereignty is measured not only by flags and elections, but by control over land, resources, and policy autonomy.
Ultimately, the land redistribution program embodies competing interpretations of justice and risk. To some, it represents a necessary stage in Africa liberation. To others, it illustrates the economic dangers of rapid agrarian restructuring. The conflict between these narratives shapes debates on Zimbabwe land question, continental self-determination, and the meaning of post-colonial transformation in contemporary Africa.
RichardGriek · February 15, 2026 at 7:41 pm
cannabis clones shipped
enoujwr · February 15, 2026 at 8:17 pm
http://delphi.larsbo.org/user/BonoAuesta
piytdqw · February 16, 2026 at 2:39 am
https://intime.listbb.ru/viewtopic.php?t=1407
epzmfif · February 16, 2026 at 8:39 am
http://www.bakinsky-dvorik.ru/communication/forum/messages/forum5/message133773/83676-melbet-promo-code-2026-lux888-200-bonus?result=new#message133773
小寶影院免费电影 · February 16, 2026 at 11:08 am
iyftv海外华人首选,提供最新华语剧集、美剧、日剧等高清在线观看。
kasyno online · February 16, 2026 at 6:34 pm
We can see that we need to develop policies to deal with this trend.
najlepsze kasyno online · February 16, 2026 at 7:52 pm
Its just like you read my thoughts! It’s like reading about my family.
casino online suisse · February 16, 2026 at 9:18 pm
I Am Going To have to come back again when my course load lets up – however I am taking your Rss feed so i can go through your site offline. Thanks.
online casino österreich · February 16, 2026 at 9:36 pm
Loving the info on this website , you have done outstanding job on the blog posts.
Binance美国注册 · February 16, 2026 at 10:23 pm
Your point of view caught my eye and was very interesting. Thanks. I have a question for you. https://accounts.binance.com/ar/register-person?ref=FIHEGIZ8
18+ porn · February 16, 2026 at 10:38 pm
cuckold videos
legalne kasyno online · February 16, 2026 at 11:01 pm
Dude.. I am not much into reading, but somehow I got to read lots of articles on your blog. Its amazing how interesting it is for me to visit you very often. –
free porn · February 17, 2026 at 7:00 am
Japanese porn
足球比分 · February 17, 2026 at 10:24 am
电影网站推荐,采用机器学习个性化推荐,海外华人专用,采用机器学习个性化推荐,支持中英双语界面和全球加速。
Glory Casino apps · February 17, 2026 at 10:56 am
Thanks for such great content. Will definitely recommend Glory Casino to friends.
http://pasarinko.zeroweb.kr/bbs/board.php?bo_table=notice&wr_id=9054185
mobile porn · February 17, 2026 at 11:01 am
new porn
中職 · February 17, 2026 at 1:31 pm
Australia Trusted Real Money Casino Reviews
Walterdrono · February 17, 2026 at 2:43 pm
https://ilmukomputer.org/2026/01/28/los-deportes-que-inscribiri-asocian-en-una-mayor-longevidad-y-el-prestigio-complemento-para-de-raqueta
realmoneyonlinecasinocasinorelayaustralia · February 17, 2026 at 4:07 pm
奇思妙探第二季高清完整版运用AI智能推荐算法,海外华人可免费观看最新热播剧集。
爱一帆轧戏 · February 17, 2026 at 4:49 pm
超人和露易斯第二季高清完整版,海外华人可免费观看最新热播剧集。
skycrownonlinecasino · February 17, 2026 at 6:10 pm
Crypto Online Casino Australia Bitcoin Options
bestonlinecasinorealmoney · February 17, 2026 at 6:40 pm
禁忌第一季高清完整官方版,海外华人可免费观看最新热播剧集。
nba比分 · February 17, 2026 at 7:57 pm
Australian online casino real money – fast payouts and big bonuses
寻秦记 · February 17, 2026 at 8:25 pm
我欲为人第二季平台,专为海外华人设计,提供高清视频和直播服务。
cuckold videos · February 17, 2026 at 9:20 pm
stepmom porn
aiyifan炎炎消防队三之章Part2 · February 17, 2026 at 10:25 pm
真实的人类第三季高清完整版采用机器学习个性化推荐,海外华人可免费观看最新热播剧集。
casino danmark · February 18, 2026 at 12:01 am
Just came from google to your website have to say thanks.
aiyifan · February 18, 2026 at 12:15 am
Crypto casino Australia – Bitcoin, Ethereum pokies and live games
ufa3939 · February 18, 2026 at 12:31 am
I am glad to talk with you and you give me great help
aiyifan盛夏假期遇见爱 · February 18, 2026 at 2:54 am
范德沃克第二季高清完整版运用AI智能推荐算法,海外华人可免费观看最新热播剧集。
toponlinecasinos · February 18, 2026 at 4:22 am
Online casino real money Australia – easy deposits via PayID & more
bestcasinoonline · February 18, 2026 at 5:07 am
奇思妙探第二季高清完整版采用机器学习个性化推荐,海外华人可免费观看最新热播剧集。
ifun · February 18, 2026 at 5:27 am
Best online casinos Australia real money – Pokies, blackjack & roulette
best canadian online casino · February 18, 2026 at 6:20 am
Thanks for posting this. Looking for these resources 😀
stepmom porn · February 18, 2026 at 7:01 am
adult videos
nba戰績 · February 18, 2026 at 7:45 am
一帆平台智能AI观看体验优化,专为海外华人设计,提供高清视频和直播服务。
bestonlinecasinosaustralia · February 18, 2026 at 8:19 am
爱一帆会员多少钱海外版,专为华人打造的高清视频平台,支持全球加速观看。
Tworzenie konta na Binance · February 18, 2026 at 11:05 am
Your point of view caught my eye and was very interesting. Thanks. I have a question for you.
https://playfanview.com/snaptrader-ai-verdict-from-real-people-is-it-worth-it/ · February 18, 2026 at 12:30 pm
What Is Snaptrader AI and How Does It Work? https://playfanview.com/snaptrader-ai-verdict-from-real-people-is-it-worth-it/
เปิดวาร์ป OnlyFans · February 18, 2026 at 5:35 pm
Fantastic piece of writing here1
https://marcellus-shale.us/snaptrader-ai-fact-check-legit-opportunity-or-typical-scam/ · February 18, 2026 at 8:52 pm
The Evolution of Automated Investing: Where Snaptrader AI Is Heading Next https://marcellus-shale.us/snaptrader-ai-fact-check-legit-opportunity-or-typical-scam/
bookmarking.stream · February 18, 2026 at 10:03 pm
sustanon for cutting
References:
https://bookmarking.stream/story.php?title=appetitzuegler-anwendung-wirkung-3
newonlinecasinoaustraliatoptiercasinos · February 18, 2026 at 10:17 pm
超人和露易斯第二季高清完整官方版,海外华人可免费观看最新热播剧集。
casino chile · February 18, 2026 at 10:25 pm
Great post, keep up the good work, I hope you don’t mind but I’ve added on my blog roll.
egbljuf · February 19, 2026 at 12:56 am
https://pastebin.com/u/betbonus26
https://mooc.ifro.edu.br/mod/forum/discuss.php?d=48015 · February 19, 2026 at 7:35 am
https://mooc.ifro.edu.br/mod/forum/discuss.php?d=48015
nbympph · February 19, 2026 at 10:30 am
https://1xbetpromo51.wordpress.com/2026/02/06/promo-code-for-1xbet-2026-1xmaxbono-bonus-e130/
ประวัตินักฟุตบอล · February 19, 2026 at 1:02 pm
Good day! This is my first comment here so I just wanted to give a quick shout out and say I really enjoy reading through your articles. Can you recommend any other blogs/websites/forums that cover the same subjects? Thanks a lot!
stealing money · February 19, 2026 at 2:51 pm
Europe Readr ist mehr als nur eine digitale Bibliothek – es ist ein kulturelles und demokratisches Projekt, das Literatur, Bildung und gesellschaftliches Engagement miteinander verbindet. Initiiert im Rahmen der slowenischen EU-Ratspräsidentschaft im Jahr 2021, bietet Europe Readr eine kostenlose, mehrsprachige Sammlung literarischer Werke aus ganz Europa, die aktuelle gesellschaftliche Themen aufgreifen und zur aktiven Auseinandersetzung anregen.
7mscore · February 19, 2026 at 5:02 pm
Thank you for all the information was very accurate, just wondering if all this is possible.~
najlepsze kasyno online · February 19, 2026 at 5:08 pm
What a great article.. i subscribed btw!
http://fotograf.phorum.pl/viewtopic.php?p=663290#663290 · February 19, 2026 at 6:49 pm
http://fotograf.phorum.pl/viewtopic.php?p=663290#663290
гей-pst · February 19, 2026 at 6:57 pm
гей
meilleur casino en ligne · February 19, 2026 at 8:14 pm
We absolutely love your blog and find the majority of your post’s to be exactly what I’m looking for. Do you offer guest writers to write content to suit your needs? I wouldn’t mind composing a post or elaborating on a number of the subjects you write about here. Again, awesome weblog!
สล็อตเว็บตรง · February 19, 2026 at 9:14 pm
สล็อต
แพลตฟอร์ม TKBNEKO ทำงานเป็นระบบเกมออนไลน์ ที่ วางระบบโดยยึดการใช้งานจริงของผู้เล่นเป็นแกนหลัก. หน้าเว็บหลัก แสดงเงื่อนไขแบบเป็นตัวเลขตั้งแต่แรก: ขั้นต่ำฝาก 1 บาท, ถอนขั้นต่ำ 1 บาท, เวลาฝากประมาณ 3 วินาที, และ ยอดถอนไม่มีเพดาน. ตัวเลขเหล่านี้กำหนดภาระของระบบโดยตรง เพราะเมื่อ กำหนดขั้นต่ำต่ำ ระบบต้อง รองรับธุรกรรมจำนวนมากขนาดเล็ก และต้อง ตัดยอดและเติมเครดิตแบบทันที. หาก การยืนยันเครดิตใช้เวลานานเกินไม่กี่วินาที ผู้ใช้จะ ทำรายการซ้ำ ทำให้เกิด รายการซ้อน และ เพิ่มโหลดฝั่งเซิร์ฟเวอร์ทันที.
การเติมเงินด้วยการสแกน QR ตัดขั้นตอนการกรอกข้อมูลและการแนบสลิป. เมื่อผู้ใช้ สแกนคิวอาร์ ธนาคารจะส่งสถานะการชำระกลับมายังระบบผ่าน API. จากนั้น backend จะ ผูกธุรกรรมเข้ากับบัญชีผู้ใช้ และ เพิ่มเครดิตเข้า wallet. หาก การตอบกลับจากธนาคารช้า เครดิตจะ ไม่เข้าในเวลาที่ระบบบอก และผู้ใช้จะ มองว่าระบบมีปัญหา. ดังนั้น ตัวเลข 3 วินาที หมายถึงการเชื่อมต่อกับธนาคารต้อง เป็นแบบอัตโนมัติเต็มรูปแบบ ไม่ อาศัยแอดมินเช็คมือ.
การเชื่อมหลายช่องทางการจ่าย เช่น Kasikornbank, Bangkok Bank, KTB, กรุงศรี, SCB, CIMB Thai รวมถึง ทรูมันนี่ วอลเล็ท ทำให้ระบบต้อง จัดการ webhook หลายแหล่ง. แต่ละเจ้าใช้ฟอร์แมตข้อมูลและความหน่วงต่างกัน. หากไม่มี ตัวแปลงข้อมูลให้เป็นรูปแบบเดียว ระบบจะ เช็คยอดไม่ทัน และจะเกิด ยอดค้างระบบ.
หมวดหมู่เกม ถูกแยกเป็น สล็อตออนไลน์, เกมสด, เดิมพันกีฬา และ เกมยิงปลา. การแยกหมวด ลดภาระการ query และ ควบคุมการส่งทราฟฟิกไปยังผู้ให้บริการแต่ละราย. เกมสล็อต มัก ทำงานผ่าน session API ส่วน เกมสด ใช้ สตรีมแบบสด. หาก session หลุด ผู้เล่นจะ หลุดจากโต๊ะทันที. ดังนั้นระบบต้องมี session manager ที่ รักษาการเชื่อมต่อ และ ซิงค์เครดิตกับ provider ภายนอกตลอดเวลา. หาก ซิงค์พลาด เครดิตผู้เล่นกับผลเกมจะ ไม่แมตช์.
เกมที่ระบุว่า เป็นลิขสิทธิ์แท้ หมายถึงใช้ระบบ RNG และค่า อัตราจ่าย จากผู้พัฒนาโดยตรง. ผลลัพธ์แต่ละรอบถูก ประมวลผลจากเซิร์ฟเวอร์ผู้ให้บริการ ไม่ใช่จากฝั่งเว็บ. หากไม่มี การเชื่อมต่อกับเซิร์ฟเวอร์ต้นทาง เว็บจะ รับผลเกมจริงไม่ได้ และ สิทธิ์ใช้งานจะถูกตัด. การมี ใบรับรอง จึง ผูกกับการแลกเปลี่ยนข้อมูลระหว่างระบบ ไม่ใช่ แค่ข้อความแสดงบนหน้าเว็บ.
ระบบถอนที่ ไม่มีจำกัด เชิงการสื่อสารยังต้องมีโมดูล risk control เช่น ตรวจสอบบัญชีซ้ำ, พฤติกรรมผิดปกติ, และ เงื่อนไข turnover. หากไม่มีการตรวจสอบเหล่านี้ ผู้ใช้สามารถ แตกบัญชีหลายอัน เพื่อ เอาโบนัส และ ดึงสภาพคล่องออกจากระบบได้รวดเร็ว.
ส่วน โปรโมชั่น VIP พันธมิตร ติดต่อ และฟีดแบ็ก เชื่อมกับ ระบบจัดการลูกค้า และ ฐานข้อมูลผู้เล่น. ส่วน พันธมิตร ใช้เก็บ referrer code เพื่อ คำนวณค่าคอมมิชชั่น. หากไม่มีระบบนี้ จะ ติดตามแหล่งที่มาของผู้ใช้ไม่ได้. ฟอร์มข้อเสนอแนะ ใช้เก็บ ข้อผิดพลาดจริงจากผู้ใช้. หากไม่มีข้อมูลนี้ ปัญหา latency หรือ การใช้งาน จะ แก้ไม่ทัน.
โครงสร้างทั้งหมด เชื่อมกันเป็นสายเดียว: สถานะธุรกรรมเข้ามาที่ backend, backend อัปเดตเครดิต แล้ว ซิงค์ไปยัง provider. หากส่วนใดส่วนหนึ่ง ช้า ผู้ใช้จะเห็นผลทันทีในรูปแบบ ยอดไม่เข้า, เกมค้าง หรือ ถอนล่าช้า. ในแพลตฟอร์มลักษณะนี้ ความเสถียรของ API และการจัดการ session คือสิ่งที่ ตัดสินว่าผู้ใช้จะอยู่หรือย้ายออก.
zbxzbax · February 20, 2026 at 1:39 am
http://fotograf.phorum.pl/viewtopic.php?p=664111#664111
mold inspection · February 20, 2026 at 7:22 am
mold removal
https://strongcarkeychains.com/product/volkswagen-car-keychain/ · February 20, 2026 at 10:12 am
https://strongcarkeychains.com/product/volkswagen-car-keychain/
питомник доберманов москва · February 20, 2026 at 12:25 pm
питомник доберманов
https://maxforlive.com/profile/user/Planbetfree?tab=about · February 20, 2026 at 1:06 pm
https://maxforlive.com/profile/user/Planbetfree?tab=about
meilleur casino en ligne · February 20, 2026 at 1:30 pm
With internet full of dupe articles it is nice to find original content like yours thank you so very much.
polskie kasyno online · February 20, 2026 at 1:50 pm
You are my inhalation , I possess few web logs and very sporadically run out from to brand 🙁
여기 · February 20, 2026 at 1:56 pm
I just couldnt leave your website before saying that I really enjoyed the useful information you offer to your visitors… Will be back often to check up on new stuff you post!
https://strongcarkeychains.com/product-category/honda/ · February 20, 2026 at 2:57 pm
https://strongcarkeychains.com/product-category/honda/
plataforma binance · February 20, 2026 at 3:43 pm
Spot on with this write-up, I truly believe this website requirements a lot much more consideration. I’ll probably be once more to read much much more, thanks for that info.
nba · February 20, 2026 at 5:42 pm
狙击蝴蝶2026 高清悬疑刑侦陆剧 海外华人必备在线观看 全球加速无缓冲播放
found this post · February 20, 2026 at 7:05 pm
When are you going to post again? You really entertain me!
nzmkxhv · February 20, 2026 at 8:12 pm
https://cheftierney.com/1xbet-promo-code-free-spins-1x200gift-bonus-e130/
binance crypto exchange · February 20, 2026 at 8:14 pm
I love your blog. It looks every informative.
https://bookcrastinators.com/codigo-promocional-1xbet-100-giros-gratis-2026-1xbro200/ · February 20, 2026 at 8:18 pm
https://bookcrastinators.com/codigo-promocional-1xbet-100-giros-gratis-2026-1xbro200/
https://www.tai-ji.net/board/board_topic/4160148/7879904.htm · February 20, 2026 at 11:51 pm
https://www.tai-ji.net/board/board_topic/4160148/7879904.htm
爱壹帆国际 · February 21, 2026 at 4:57 am
暗夜情报员第三季2026 海外华人动作爽剧 Netflix全季上架 全球加速
爱一帆 · February 21, 2026 at 5:26 am
桑乔85m曼联梦碎?2026转会新闻爆料,他考虑重返德甲,曼联损失惨重,足球比分圈炸锅了!
реєстрація Binance · February 21, 2026 at 6:06 am
Nice post.Very useful info specifically the last part 🙂 Thank you and good luck.
林肯律师第四季爱壹帆 · February 21, 2026 at 6:32 am
aiyifan平台2026 海外华人必备 无广告高清电影电视剧
小城大事aiyifan · February 21, 2026 at 7:44 am
家业2026 杨紫古装经商大女主 海外华人首选高清非遗题材陆剧 AI智能推荐爆款
online casino · February 21, 2026 at 10:12 am
Glad to be one of several visitors on this awful internet site : D.
中職 · February 21, 2026 at 1:07 pm
ifun平台2026 海外华人高清影视 大数据AI智能推荐
Betechit · February 21, 2026 at 2:05 pm
Glad to be one of many visitants on this amazing site : D.
爱一帆轧戏 · February 21, 2026 at 2:39 pm
捕风追影下载平台2026 海外华人高清视频直播离线下载
whatonlinecasinogamescanyouwinrealmoney · February 21, 2026 at 3:15 pm
风过留痕2026 高清古装权谋悬疑 海外华人首选 高清探案解谜 无广告追剧
https://faithandwealthfinance.com/1xbet-promo-code-for-registration-2026-1x200gift/ · February 21, 2026 at 3:17 pm
https://faithandwealthfinance.com/1xbet-promo-code-for-registration-2026-1x200gift/
Betechit.com · February 21, 2026 at 4:46 pm
Substantially, the post is really the best on this laudable topic. I concur with your conclusions and will eagerly watch forward to your future updates.Just saying thanx will not just be enough, for the wonderful lucidity in your writing.
ทดลองเล่นสล็อต pg · February 21, 2026 at 9:07 pm
สล็อต
แพลตฟอร์ม TKBNEKO ทำงานเป็นระบบเกมออนไลน์ ที่ ออกแบบโครงสร้างโดยยึดพฤติกรรมผู้ใช้เป็นศูนย์กลาง. หน้าแรก แสดงเงื่อนไขแบบเป็นตัวเลขตั้งแต่แรก: ฝากขั้นต่ำ 1 บาท, ถอนขั้นต่ำ 1 บาท, เครดิตเข้าโดยเฉลี่ยราว 3 วินาที, และ ยอดถอนไม่มีเพดาน. ตัวเลขเหล่านี้กำหนดภาระของระบบโดยตรง เพราะเมื่อ ตั้งขั้นต่ำไว้ต่ำมาก ระบบต้อง รองรับธุรกรรมจำนวนมากขนาดเล็ก และต้อง ตัดยอดและเติมเครดิตแบบทันที. หาก การยืนยันเครดิตใช้เวลานานเกินไม่กี่วินาที ผู้ใช้จะ กดซ้ำ ทำให้เกิด ธุรกรรมซ้อน และ เพิ่มโหลดฝั่งเซิร์ฟเวอร์ทันที.
การเติมเงินด้วยการสแกน QR ลดขั้นตอนที่ต้องพิมพ์ข้อมูลหรือส่งสลิป. เมื่อผู้ใช้ สแกน ธนาคารจะส่งสถานะการชำระกลับมายังระบบผ่าน API. จากนั้น backend จะ จับคู่ธุรกรรมกับ user ID และ เพิ่มเครดิตเข้า wallet. หาก API ตอบสนองช้า เครดิตจะ ไม่เข้าในเวลาที่ระบบบอก และผู้ใช้จะ ถือว่าระบบไม่เสถียร. ดังนั้น ตัวเลข 3 วินาที หมายถึงการเชื่อมต่อกับธนาคารต้อง เป็นแบบอัตโนมัติเต็มรูปแบบ ไม่ อาศัยแอดมินเช็คมือ.
การรองรับหลายธนาคาร เช่น Kasikornbank, ธนาคารกรุงเทพ, Krung Thai Bank, Krungsri, Siam Commercial Bank, ซีไอเอ็มบี ไทย รวมถึง ทรูมันนี่ วอลเล็ท ทำให้ระบบต้อง จัดการ webhook หลายแหล่ง. แต่ละธนาคารมีรูปแบบข้อมูลและเวลาตอบสนองต่างกัน. หากไม่มี ตัวแปลงข้อมูลให้เป็นรูปแบบเดียว ระบบจะ ยืนยันยอดได้ช้า และจะเกิด ยอดค้างระบบ.
หมวดหมู่เกม ถูกแยกเป็น สล็อต, คาสิโนสด, เดิมพันกีฬา และ ยิงปลา. การแยกหมวด ลดภาระการ query และ ควบคุมการส่งทราฟฟิกไปยังผู้ให้บริการแต่ละราย. เกมสล็อต มัก ทำงานผ่าน session API ส่วน คาสิโนสด ใช้ สตรีมภาพแบบเรียลไทม์. หาก session หลุด ผู้เล่นจะ หลุดจากโต๊ะทันที. ดังนั้นระบบต้องมี ตัวจัดการ session ที่ รักษาการเชื่อมต่อ และ ซิงค์เครดิตกับ provider ภายนอกตลอดเวลา. หาก ซิงค์ล้มเหลว เครดิตผู้เล่นกับผลเกมจะ ไม่ตรงกัน.
เกมที่ระบุว่า ใช้ลิขสิทธิ์จริง หมายถึงใช้ระบบ สุ่มผล และค่า RTP จากผู้พัฒนาโดยตรง. ผลลัพธ์แต่ละรอบถูก ประมวลผลจากเซิร์ฟเวอร์ผู้ให้บริการ ไม่ใช่จากฝั่งเว็บ. หากไม่มี ลิงก์ไปยังเซิร์ฟเวอร์ต้นทาง เว็บจะ รับผลเกมจริงไม่ได้ และ license จะถูกยกเลิกทันที. การมี ใบรับรอง จึง ผูกกับโครงสร้างการส่งข้อมูล ไม่ใช่ แค่ข้อความแสดงบนหน้าเว็บ.
ระบบถอนที่ ไม่มีจำกัด เชิงการสื่อสารยังต้องมีโมดูล ตรวจสอบความเสี่ยง เช่น เช็คบัญชีซ้ำ, พฤติกรรมผิดปกติ, และ เงื่อนไขเทิร์นโอเวอร์. หากไม่มีการตรวจสอบเหล่านี้ ผู้ใช้สามารถ สร้างบัญชีหลายบัญชี เพื่อ เอาโบนัส และ ถอนเงินออกเร็ว.
เมนู โปรโมชั่น VIP พันธมิตร ติดต่อเรา และข้อเสนอแนะ เชื่อมกับ ระบบ CRM และ ฐานข้อมูลผู้ใช้. ส่วน Affiliate ใช้เก็บ โค้ดอ้างอิง เพื่อ คำนวณค่าคอมมิชชั่น. หากไม่มีระบบนี้ จะ ติดตามแหล่งที่มาของผู้ใช้ไม่ได้. แบบฟอร์มฟีดแบ็ก ใช้เก็บ ข้อผิดพลาดจริงจากผู้ใช้. หากไม่มีข้อมูลนี้ ปัญหา ความหน่วง หรือ UX จะ ถูกแก้ช้า.
โครงสร้างทั้งหมด เชื่อมกันเป็นสายเดียว: สถานะธุรกรรมเข้ามาที่ backend, backend อัปเดตเครดิต แล้ว ซิงค์กับผู้ให้บริการเกม. หากส่วนใดส่วนหนึ่ง ช้า ผู้ใช้จะเห็นผลทันทีในรูปแบบ เครดิตไม่เข้า, เกมหน่วง หรือ ถอนช้า. ในแพลตฟอร์มลักษณะนี้ ความเสถียรของ API และการจัดการ session คือสิ่งที่ ตัดสินว่าผู้ใช้จะอยู่หรือย้ายออก.
https://github.com/1xbetpromocodes565 · February 21, 2026 at 11:07 pm
https://github.com/1xbetpromocodes565
https://indianwomenorg.com/BonusXof1xbet · February 22, 2026 at 12:43 am
https://indianwomenorg.com/BonusXof1xbet
https://ramns.ezpp.ru/ · February 22, 2026 at 1:11 am
https://ramns.ezpp.ru/
小宝影视电影网站 · February 22, 2026 at 1:37 am
怪奇物语终章2026 海外华人科幻恐怖剧 高清最终季 海外必备
onlinecasinorealmoney · February 22, 2026 at 2:31 am
捕风追影在线平台2026 AI推荐 海外华人高清影视直播
заключить контракт · February 22, 2026 at 9:40 am
подписать контракт на сво онлайн военную
https://www.symbaloo.com/shared/AAAABn-xHoYAA42ADswcVg== · February 22, 2026 at 9:55 am
https://www.symbaloo.com/shared/AAAABn-xHoYAA42ADswcVg==
Paito HK · February 22, 2026 at 10:10 am
Just wanna admit that this is extremely helpful, Thanks for taking your time to write this.
drvladh · February 22, 2026 at 2:40 pm
https://sites.google.com/view/1xbetpromocodes6e/home
https://pxhere.com/en/photographer-me/4924640 · February 22, 2026 at 3:56 pm
https://pxhere.com/en/photographer-me/4924640
pg slot · February 22, 2026 at 11:24 pm
pg slot
สล็อต PG แพลตฟอร์มเกมสล็อตยอดนิยม เล่นง่าย ฝากถอนเร็ว
คำค้นหา pg slot กำลังได้รับความนิยมอย่างต่อเนื่อง ในกลุ่มผู้เล่นเกมสล็อตออนไลน์ เพราะเป็น ค่ายเกมที่มีชื่อเสียง ด้าน ภาพและเอฟเฟกต์ ความ ลื่นไหล และ อัตราการจ่ายรางวัลที่น่าสนใจ เกมของ PG พัฒนาโดยผู้ให้บริการชั้นนำ ที่รองรับการเล่นทั้งบน สมาร์ทโฟน และ คอมพิวเตอร์
ความโดดเด่น ของ สล็อต PG
สล็อต PG เป็นเกมสล็อตออนไลน์ที่ออกแบบมาให้ เปิดเกมได้ทันที เล่นผ่าน ระบบเว็บ และรองรับ ทุกอุปกรณ์ เข้าเล่นผ่านเว็บได้เลย ผู้เล่นสามารถเข้าเล่นผ่าน เว็บเบราว์เซอร์ ได้ทันที ภาพและเสียงถูกพัฒนาในรูปแบบ สามมิติ ให้ความคมชัด พร้อมเอฟเฟกต์ สวยงาม
คุณสมบัติหลักของเกม pg slot ได้แก่
ระบบโบนัสและฟรีสปินหลากหลายรูปแบบ
ระบบตัวคูณ
เล่นฟรีก่อนเติมเงิน
รองรับภาษาไทยเต็มรูปแบบ
ระบบฝากถอนสะดวก ทันใจ
แพลตฟอร์ม pg slot โดยทั่วไปให้บริการ การฝาก-ถอน ออโต้ตลอด 24 ชม. ขั้นต่ำเริ่มต้นเพียง 1 บาท ขึ้นอยู่กับ กติกาแต่ละแพลตฟอร์ม การทำรายการใช้เวลา รวดเร็วมาก ผ่าน คิวอาร์โค้ด หรือระบบ แอปธนาคาร ทำให้ธุรกรรมเป็นไปอย่าง ต่อเนื่อง
ประเภทเกมยอดนิยม ใน PG Slot
เกม สล็อต PG มีธีมหลากหลาย เช่น
ธีม เทพเจ้าและแฟนตาซี
ธีม ลุยด่าน
ธีม ความมั่งคั่ง
ธีม สัตว์และธรรมชาติ
ผู้เล่นนิยมเกมที่มีรอบพิเศษบ่อย พร้อมระบบ Special Feature และ โอกาสทำกำไรสูง เหมาะกับทั้ง คนเพิ่งเล่น และ ผู้เล่นมือโปร
ความน่าเชื่อถือ
pg slot มีมาตรฐานรองรับ มีการ รักษาความปลอดภัย และใช้ระบบสุ่มผล Random Number Generator เพื่อให้ผลลัพธ์ ยุติธรรม แพลตฟอร์มที่ให้บริการ สล็อต PG ควรมี ความปลอดภัยสูง
โดยภาพรวม
PG Slot เป็นตัวเลือกยอดนิยมสำหรับผู้ที่ต้องการเล่นสล็อตออนไลน์ ด้วยจุดเด่นด้าน โบนัสหลากหลาย และการทำธุรกรรมที่ ไว ผู้เล่นสามารถเริ่มต้นได้ ไม่ซับซ้อน ฝากถอนสะดวก และเลือกเกมได้ จำนวนมาก เหมาะสำหรับ ผู้เล่นทุกสไตล์ ในโลกของเกมสล็อตออนไลน์
pg slot · February 23, 2026 at 5:46 pm
สล็อตเว็บตรง
แพลตฟอร์ม TKB NEKO ให้บริการ พื้นที่ออนไลน์ที่ทันสมัย ซึ่ง ผู้ที่สนใจ สามารถ ทดลองใช้งาน ประสบการณ์เกมออนไลน์ รวมถึง ระบบเดิมพันที่ให้ผลตอบแทนไว เว็บไซต์นี้ นำเสนอแนวคิดว่าทุกคนมีสิทธิ์ประสบความสำเร็จ เนื่องจาก ออกแบบมาให้เข้าถึงได้ทุกกลุ่มผู้เล่น
หนึ่งใน ฟีเจอร์หลัก ของแพลตฟอร์มนี้คือ ระบบฝากและถอนเงิน ซึ่งมีขั้นต่ำในการเติมเงินเพียง ขั้นต่ำแค่ 1 บาท และขั้นต่ำในการถอนเงินก็เช่นเดียวกันที่ เริ่มต้น 1 บาท เท่านั้น การฝากเงินเสร็จภายใน 3 วินาที ทำให้แพลตฟอร์มนี้ โดดเด่นด้านความเร็ว นอกจากนี้ยัง เปิดให้ถอนได้ไม่จำกัดจำนวน ซึ่งเป็น ปัจจัยสำคัญที่สร้างความแตกต่าง
สำหรับการเติมเงิน ผู้ใช้งานสามารถใช้รหัส QR เพื่อทำรายการได้ ซึ่งเป็นระบบที่ ง่ายและสะดวกมากยิ่งขึ้น
แพลตฟอร์มนี้มีเกมให้เลือก ครบทุกหมวดหมู่ เช่น สล็อตออนไลน์, คาสิโนสด, กีฬา และ ยิงปลา ผู้เล่นสามารถดูรายชื่อเกมทั้งหมดได้ผ่านตัวกรอง “All Games” ซึ่งช่วยให้ ผู้เล่นเลือกเกมที่ตรงกับความสนใจได้อย่างลงตัว
TKBNEKO เน้นย้ำถึงความสำคัญของเกมที่มีลิขสิทธิ์ถูกต้องและการเล่นที่ยุติธรรม โดยร่วมมือกับ ค่ายเกมชั้นนำที่ได้รับใบอนุญาต ซึ่งช่วยให้มั่นใจได้ว่า ผู้เล่นจะได้รับประสบการณ์ที่โปร่งใสและปลอดภัย
TKBNEKO ได้ผสานระบบการชำระเงินเข้ากับ สถาบันการเงินหลักในไทย เช่น Krungthai Bank, Bangkok Bank, SCB, Kasikorn Bank, Thanachart Bank, GSB, TrueMoney Wallet, Citibank, UOB และ BAAC ทำให้การทำธุรกรรมทางการเงิน มีความสะดวกสบายและปลอดภัยมากยิ่งขึ้น
สรุปได้ว่า TKBNEKO คือแพลตฟอร์มที่ ทันสมัย ปลอดภัย และใช้งานง่าย สำหรับเกมออนไลน์และการเดิมพัน ด้วยเงื่อนไขขั้นต่ำที่ต่ำ การทำธุรกรรมที่รวดเร็ว และเกมให้เลือกมากมาย ทำให้แพลตฟอร์มนี้ รองรับผู้เล่นทุกระดับ เริ่มต้นประสบการณ์ได้ทันที และ ก้าวสู่โลกเกมออนไลน์ได้แล้ววันนี้
jet x официальный сайт · February 23, 2026 at 9:29 pm
Будьте внимательны: только jet x официальный сайт гарантирует сохранность ваших средств и персональной информации.
https://www.idex-hs.com/semrock/optics-photo-contest · February 23, 2026 at 10:19 pm
https://www.idex-hs.com/semrock/optics-photo-contest
online casino ausland · February 24, 2026 at 1:05 am
You ma’am have a way with words. Thank you very much!
Canadian casinos online · February 24, 2026 at 1:07 am
We’re developing some community services to respond to this, and your blog is helpful.
top online casino · February 24, 2026 at 1:09 am
Nevertheless, it’s all carried out with tongues rooted solidly in cheeks, and everybody has got nothing but absolutely love for their friendly neighborhood scapegoat. In reality, he is not merely a pushover. He is simply that extraordinary breed of person solid enough to take all that good natured ribbing for what it really is.
в другом месте · February 24, 2026 at 1:54 am
Многие ищут альтернативу в другом месте, но здесь самый полный обзор.
best online casino · February 24, 2026 at 2:57 am
If you don’t mind, where do you host your weblog? I am looking for a very good web host and your webpage seams to be extremely fast and up most the time…
meilleur casino en ligne · February 24, 2026 at 3:00 am
Appreciation for taking the time to discuss this topic, I would love to discover more on this topic. If viable, as you gain expertise, would you object to updating the website with further information? It is tremendously beneficial for me.
kjmnsgd · February 24, 2026 at 4:59 am
https://elbimusic.com/1xbet-bonus-code-nigeria-2026-e130-for-registration/
888casino bonus · February 24, 2026 at 5:17 am
Heard 888casino bonus is pretty generous. Thinking about signing up to see if I can get a boost to my bankroll. Anyone else tried it? Bonus link here: 888casino bonus
pepebetcasino · February 24, 2026 at 5:17 am
Pepebetcasino? What a name! Gotta see what this is all about. Hopefully it’s more than just a meme. Let’s see if it delivers. Try it: pepebetcasino
mx fun · February 24, 2026 at 5:17 am
Looking for some fun? MX Fun seems like an interesting platform to explore. I’ll check it out and see if it lives up to its name! Have some mx fun: mx fun
best casino ireland · February 24, 2026 at 5:22 am
What’s Happening i’m new to this, I stumbled upon this I’ve found It positively useful and it has aided me out loads. I hope to contribute & help other users like its aided me. Great job.
best Irish casino · February 24, 2026 at 5:56 am
There is a lot of misunderstanding about these issues today. Your material helps explain things.
Revolut casinos · February 24, 2026 at 6:13 am
Well done! Keep up this quality!
джет х · February 24, 2026 at 6:21 am
В игре джет х есть функция отключения звука для скрытной игры.
https://rentry.co/fqyvs9ri · February 24, 2026 at 6:48 am
https://rentry.co/fqyvs9ri
meilleur casino en ligne · February 24, 2026 at 7:33 am
Oh my goodness! an amazing article. Great work.
top online casinos · February 24, 2026 at 8:35 am
whoah this weblog is great i really like studying your articles. Stay up the great work! You already know, lots of persons are looking round for this information, you can aid them greatly.
casino ausland · February 24, 2026 at 8:40 am
I enjoy your blog posts, saved to my bookmarks!
online casino · February 24, 2026 at 9:11 am
Only a smiling visitor here to share the love (:, btw outstanding style and design .
https://www.bandlab.com/xbetq9 · February 24, 2026 at 10:08 am
https://www.bandlab.com/xbetq9
ovydshq · February 24, 2026 at 11:16 am
https://vrn.best-city.ru/forum/thread540149762/
https://biz-gid.com/about/articles_bg?id=1351 · February 24, 2026 at 5:26 pm
https://biz-gid.com/about/articles_bg?id=1351
whatisthebestonlinecasinoforrealmoneyaustralia · February 24, 2026 at 6:01 pm
长风少年词2026 高清古装青春 海外华人免费观看 高清无广告
best online casino · February 24, 2026 at 6:30 pm
I had highly recommend this blog to my good friend, it’s so good
https://flamb.ru/stomatologicheskaya-klinika-zhuykan · February 24, 2026 at 6:42 pm
https://flamb.ru/stomatologicheskaya-klinika-zhuykan
mejores casinos online chile · February 24, 2026 at 8:09 pm
I just couldn’t leave your website before suggesting that I really enjoyed the usual information an individual supply on your visitors? Is gonna be back often in order to investigate cross-check new posts
meilleur site cbd france · February 24, 2026 at 8:32 pm
Great info! Keep post great articles.
cbd · February 24, 2026 at 8:45 pm
You appear to know so much about this, and I see you’re a published author. Thanks
mejores casinos en línea · February 24, 2026 at 8:54 pm
I appreciate your work, thanks for all the great blog posts.
online casino österreich · February 24, 2026 at 9:11 pm
With internet full of dupe articles it is nice to find original content like yours thank you so very much.
Buksan ang Binance Account · February 24, 2026 at 9:14 pm
Your article helped me a lot, is there any more related content? Thanks! https://www.binance.com/register?ref=IXBIAFVY
best canadian online casino · February 24, 2026 at 10:14 pm
How come you do not have your website viewable in mobile format? cant see anything in my Droid.
Timothytoumn · February 24, 2026 at 10:35 pm
TKBNEKO เปิดประสบการณ์ใหม่แห่งการเดิมพันออนไลน์ ธุรกรรมรวดเร็ว ด้วยระบบสแกน QR Code
ในยุคดิจิทัลที่ โลกออนไลน์เติบโตต่อเนื่อง เรามุ่งเน้นมาตรฐานใหม่ของการเดิมพัน ด้วยระบบที่ ล้ำสมัย เสถียร และ โปร่งใส เพื่อให้ผู้เล่น อุ่นใจ ทุกครั้งที่ใช้งาน
จุดเด่นระบบฝาก-ถอน
ฝากขั้นต่ำ: 1 บาท
ถอนขั้นต่ำ: ขั้นต่ำ 1 บาท
เวลาฝากเงิน: ภายใน 3 วินาที
ยอดถอน: ไม่จำกัดต่อวัน
เติมเงินง่าย แค่สแกน
สแกน คิวอาร์ ระบบจะ ประมวลผลอัตโนมัติ ขั้นต่ำ เริ่ม 100 บาท สูงสุด ไม่เกิน 500,000 บาทต่อครั้ง
เกมยอดนิยม
สล็อต: ลุ้นแจ็คพอต
เกมสด: ดีลเลอร์สด
กีฬา: เดิมพันลีกดัง
ยิงปลา: สนุกได้เงินจริง
โบนัสและโปรโมชัน
ติดตามหน้า โปรโมชั่น พร้อมระบบ VIP และโปรแกรม พันธมิตร
ฝ่ายบริการลูกค้า
สอบถามข้อมูลได้ตลอด 24 ชั่วโมง ผ่านหน้า ศูนย์ช่วยเหลือ ทีมงาน TKBNEKO พร้อมดูแลตลอดเวลา
meilleur site cbd · February 24, 2026 at 10:45 pm
I am glad to be a visitor of this perfect blog !, appreciate it for this rare info!
qojsicb · February 25, 2026 at 12:38 am
https://forum.amzgame.com/thread/detail?id=576717
casino en ligne belgique · February 25, 2026 at 1:41 am
It sounds like you’re creating problems yourself by defining this as such a comprehensive, almost unknowable problem. Isn’t that self-defeating?
pg slot · February 25, 2026 at 3:04 am
สล็อต PG แพลตฟอร์มเกมสล็อตยอดนิยม เล่นง่าย ฝากถอนเร็ว
คำค้นหา PG Slot มาแรงในช่วงนี้ ในกลุ่มผู้เล่นเกมสล็อตออนไลน์ เพราะเป็น ค่ายเกมที่มีชื่อเสียง ด้าน กราฟิก ความ เสถียร และ โอกาสรับกำไรที่ดี เกมของ PG ผลิตโดยค่ายมาตรฐาน ที่รองรับการเล่นทั้งบน สมาร์ทโฟน และ เดสก์ท็อป
ความโดดเด่น ของ pg slot
PG Slot เป็นเกมสล็อตออนไลน์ที่ออกแบบมาให้ เปิดเกมได้ทันที เล่นผ่าน ระบบเว็บ และรองรับ ทุกอุปกรณ์ ไม่ต้องติดตั้งเพิ่มเติม ผู้เล่นสามารถเข้าเล่นผ่าน Browser ได้ทันที ภาพและเสียงถูกพัฒนาในรูปแบบ สามมิติ ให้ความคมชัด พร้อมเอฟเฟกต์ สมจริง
คุณสมบัติหลักของเกม สล็อต PG ได้แก่
ระบบโบนัสและฟรีสปินหลากหลายรูปแบบ
ฟีเจอร์ตัวคูณรางวัล
โหมดทดลองเล่นฟรี
รองรับภาษาไทยเต็มรูปแบบ
ระบบฝากถอนสะดวก ไม่ต้องรอนาน
แพลตฟอร์ม สล็อต PG โดยทั่วไปให้บริการ การฝาก-ถอน ออโต้ตลอด 24 ชม. ขั้นต่ำเริ่มต้นเพียง หลักหน่วย ขึ้นอยู่กับ กติกาแต่ละแพลตฟอร์ม การทำรายการใช้เวลา ไม่กี่วินาที ผ่าน QR Code หรือระบบ ธนาคารบนมือถือ ทำให้ธุรกรรมเป็นไปอย่าง ไม่สะดุด
แนวเกมที่คนเล่นเยอะ ใน PG Slot
เกม PG Slot มีธีมหลากหลาย เช่น
ธีม เทพเจ้าและแฟนตาซี
ธีม ผจญภัย
ธีม โชคลาภ
ธีม ธรรมชาติ
เกมยอดนิยมมักเป็นเกมที่แตกง่าย พร้อมระบบ โบนัสรอบพิเศษ และ ระบบจ่ายคุ้มค่า เหมาะกับทั้ง คนเพิ่งเล่น และ ผู้เล่นที่มีประสบการณ์
ความน่าเชื่อถือ
PG Slot ใช้ระบบที่ได้มาตรฐาน มีการ ปกป้องข้อมูลผู้เล่น และใช้ระบบสุ่มผล RNG เพื่อให้ผลลัพธ์ ยุติธรรม แพลตฟอร์มที่ให้บริการ PG Slot ควรมี ระบบดูแลข้อมูล
บทสรุปท้ายบท
pg slot เป็นตัวเลือกยอดนิยมสำหรับผู้ที่ต้องการเล่นสล็อตออนไลน์ ด้วยจุดเด่นด้าน กราฟิกคุณภาพ และการทำธุรกรรมที่ ทันใจ ผู้เล่นสามารถเริ่มต้นได้ ไม่ซับซ้อน ฝากถอนสะดวก และเลือกเกมได้ จำนวนมาก เหมาะสำหรับ ทั้งมือใหม่และมือโปร ในโลกของเกมสล็อตออนไลน์
https://web.ggather.com/betconverter1 · February 25, 2026 at 6:25 am
https://web.ggather.com/betconverter1
http://hotel-golebiewski.phorum.pl/viewtopic.php?p=923257#923257 · February 25, 2026 at 7:12 am
http://hotel-golebiewski.phorum.pl/viewtopic.php?p=923257#923257
tuccmfw · February 25, 2026 at 1:31 pm
https://svblood.ru/forum/messages/forum1/topic519/message807/?result=new#message807
Www.Skinhudlaege.dk · February 25, 2026 at 1:52 pm
Valuable material, Cheers!
my web blog; cosmetics Dermatology – https://www.skinhudlaege.dk/ –
https://rbt-servis-remont-stiralnyh-mashin-spb.clients.site/ · February 25, 2026 at 2:55 pm
Всегда переживаю, когда вызываю мастеров на дом, но тут приятно удивили. В РБТ-Сервис работает настоящий профессионал: аккуратно заменил подшипник в барабане, ничего не разгромил, не насорил. Машинка теперь стирает тише новой. Рекомендую ремонт стиральных машин в СПб обращаться только сюда. https://rbt-servis-remont-stiralnyh-mashin-spb.clients.site/
http://www.loret.se · February 25, 2026 at 3:25 pm
http://loret.se
situs senang4d · February 25, 2026 at 6:11 pm
Are the issues really as complex as they seem?
best online casino NZ · February 25, 2026 at 8:04 pm
I really like your writing style, excellent info , thanks for putting up : D.
https://roskurer.ru · February 25, 2026 at 8:13 pm
https://roskurer.ru
legalne kasyno online · February 25, 2026 at 10:08 pm
I love your blog. It looks every informative.
kasyno internetowe · February 25, 2026 at 11:14 pm
My brother suggested I might like this websiteHe was once totally rightThis post truly made my dayYou can not imagine simply how a lot time I had spent for this information! Thanks!
https://playarealty.com/author/elyseblamey103/ · February 25, 2026 at 11:23 pm
Сначала не верил, что dragonmoney реально выводит такие суммы, но после вчерашнего заноса все сомнения отпали.
https://33acres.in/author/annedevlin210/
beste nettcasino · February 26, 2026 at 1:19 am
Hi there! I just wanted to ask if you ever have any trouble with hackers? My last blog (wordpress) was hacked and I ended up losing several weeks of hard work due to no back up. Do you have any solutions to protect against hackers?
norges beste nettcasino · February 26, 2026 at 2:11 am
Wish I’d thought of this. Am in the field, but I procrastinate alot and haven’t written as much as I’d like. Thanks.
casino en ligne le plus payant · February 26, 2026 at 2:53 am
Sweet blog! I found it while browsing on Yahoo News. Do you have any tips on how to get listed in Yahoo News? I’ve been trying for a while but I never seem to get there! Thank you
https://jobs.windomnews.com/profiles/7925543-comment-utiliser-le-code-promo-1xbet-2026-1xwap200 · February 26, 2026 at 4:59 am
https://jobs.windomnews.com/profiles/7925543-comment-utiliser-le-code-promo-1xbet-2026-1xwap200
https://www.moonpathcuups.org/profile/letis5870531714/profile · February 26, 2026 at 5:31 am
https://www.moonpathcuups.org/profile/letis5870531714/profile
https://whiskyrecension.se · February 26, 2026 at 12:47 pm
http://www.whiskyrecension.se
https://dveri-ot-zavoda.ru/ · February 26, 2026 at 1:12 pm
https://dveri-ot-zavoda.ru/
bonus sans depot casino · February 26, 2026 at 2:42 pm
You are one talented writer thank you for the post.
RussellPhync · February 26, 2026 at 6:16 pm
ทดลองเล่นสล็อต PG Slot แพลตฟอร์มเกมสล็อตยอดนิยม เข้าเล่นไว ฝากถอนออโต้
คำค้นหา PG Slot กำลังได้รับความนิยมอย่างต่อเนื่อง ในกลุ่มผู้เล่นเกมสล็อตออนไลน์ เพราะเป็น แบรนด์เกมที่โดดเด่น ด้าน กราฟิก ความ นิ่งไม่สะดุด และ โอกาสรับกำไรที่ดี เกมของ PG ออกแบบโดยทีมงานมืออาชีพ ที่รองรับการเล่นทั้งบน มือถือ และ คอมพิวเตอร์
จุดเด่น ของ pg slot
pg slot เป็นเกมสล็อตออนไลน์ที่ออกแบบมาให้ เข้าเกมไว เล่นผ่าน ระบบอัตโนมัติ และรองรับ ทุกอุปกรณ์ ไม่ต้องดาวน์โหลดแอป ผู้เล่นสามารถเข้าเล่นผ่าน เว็บเบราว์เซอร์ ได้ทันที ภาพและเสียงถูกพัฒนาในรูปแบบ เอฟเฟกต์ 3 มิติ ให้ความคมชัด พร้อมเอฟเฟกต์ จัดเต็ม
คุณสมบัติหลักของเกม สล็อต PG ได้แก่
ระบบโบนัสและฟรีสปินหลากหลายรูปแบบ
Multiplier
เดโม่ฟรี
รองรับภาษาไทยเต็มรูปแบบ
ระบบฝากถอนสะดวก ไม่ต้องรอนาน
แพลตฟอร์ม สล็อต PG โดยทั่วไปให้บริการ การฝาก-ถอน อัตโนมัติ 24 ชั่วโมง ขั้นต่ำเริ่มต้นเพียง 1 บาท ขึ้นอยู่กับ ระบบของผู้ให้บริการ การทำรายการใช้เวลา รวดเร็วมาก ผ่าน คิวอาร์โค้ด หรือระบบ แอปธนาคาร ทำให้ธุรกรรมเป็นไปอย่าง ต่อเนื่อง
หมวดเกมฮิต ใน pg slot
เกม สล็อต PG มีธีมหลากหลาย เช่น
ธีม เทพเจ้าและแฟนตาซี
ธีม ผจญภัย
ธีม ความมั่งคั่ง
ธีม สัตว์และธรรมชาติ
ผู้เล่นนิยมเกมที่มีรอบพิเศษบ่อย พร้อมระบบ ฟีเจอร์พิเศษ และ โอกาสทำกำไรสูง เหมาะกับทั้ง มือใหม่ และ ผู้เล่นมือโปร
ความน่าเชื่อถือ
สล็อต PG มีมาตรฐานรองรับ มีการ รักษาความปลอดภัย และใช้ระบบสุ่มผล Random Number Generator เพื่อให้ผลลัพธ์ ยุติธรรม แพลตฟอร์มที่ให้บริการ สล็อต PG ควรมี ทีมซัพพอร์ต 24 ชม.
บทสรุปท้ายบท
pg slot เป็นตัวเลือกยอดนิยมสำหรับผู้ที่ต้องการเล่นสล็อตออนไลน์ ด้วยจุดเด่นด้าน กราฟิกคุณภาพ และการทำธุรกรรมที่ ไว ผู้เล่นสามารถเริ่มต้นได้ ง่าย ฝากถอนสะดวก และเลือกเกมได้ จำนวนมาก เหมาะสำหรับ ทุกระดับประสบการณ์ ในโลกของเกมสล็อตออนไลน์
Charlestub · February 26, 2026 at 6:24 pm
สล็อต
PG Slot แพลตฟอร์มเกมสล็อตยอดนิยม ใช้งานง่าย ฝากถอนรวดเร็ว
คำค้นหา PG Slot ถูกค้นหามากขึ้นเรื่อยๆ ในกลุ่มผู้เล่นเกมสล็อตออนไลน์ เพราะเป็น ผู้ให้บริการเกมสล็อตที่มาแรง ด้าน งานภาพคุณภาพสูง ความ นิ่งไม่สะดุด และ โอกาสรับกำไรที่ดี เกมของ PG ผลิตโดยค่ายมาตรฐาน ที่รองรับการเล่นทั้งบน โทรศัพท์มือถือ และ พีซี
ข้อดี ของ สล็อต PG
PG Slot เป็นเกมสล็อตออนไลน์ที่ออกแบบมาให้ เข้าเกมไว เล่นผ่าน ระบบอัตโนมัติ และรองรับ ทุกอุปกรณ์ ไม่ต้องติดตั้งเพิ่มเติม ผู้เล่นสามารถเข้าเล่นผ่าน เว็บเบราว์เซอร์ ได้ทันที ภาพและเสียงถูกพัฒนาในรูปแบบ 3D ให้ความคมชัด พร้อมเอฟเฟกต์ จัดเต็ม
คุณสมบัติหลักของเกม pg slot ได้แก่
มีรอบโบนัสให้ลุ้นบ่อย
ฟีเจอร์ตัวคูณรางวัล
โหมดทดลองเล่นฟรี
มีเมนูภาษาไทย
ระบบการเงินรวดเร็ว ทำรายการไว
แพลตฟอร์ม pg slot ส่วนใหญ่รองรับ การฝาก-ถอน ฝากถอนตลอดเวลา ขั้นต่ำเริ่มต้นเพียง 10 บาท ขึ้นอยู่กับ กติกาแต่ละแพลตฟอร์ม การทำรายการใช้เวลา ไม่กี่วินาที ผ่าน สแกน QR หรือระบบ ธนาคารบนมือถือ ทำให้ธุรกรรมเป็นไปอย่าง ลื่นไหล
หมวดเกมฮิต ใน pg slot
เกม PG Slot มีธีมหลากหลาย เช่น
ธีม แฟนตาซี
ธีม Adventure
ธีม ความมั่งคั่ง
ธีม ธรรมชาติ
หลายคนชอบเกมที่โบนัสเข้าไว พร้อมระบบ Special Feature และ โอกาสทำกำไรสูง เหมาะกับทั้ง คนเพิ่งเล่น และ ผู้เล่นที่มีประสบการณ์
มาตรฐานระบบ
สล็อต PG ใช้ระบบที่ได้มาตรฐาน มีการ รักษาความปลอดภัย และใช้ระบบสุ่มผล RNG เพื่อให้ผลลัพธ์ โปร่งใส แพลตฟอร์มที่ให้บริการ pg slot ควรมี ระบบดูแลข้อมูล
บทสรุปท้ายบท
pg slot เป็นตัวเลือกยอดนิยมสำหรับผู้ที่ต้องการเล่นสล็อตออนไลน์ ด้วยจุดเด่นด้าน โบนัสหลากหลาย และการทำธุรกรรมที่ รวดเร็ว ผู้เล่นสามารถเริ่มต้นได้ ทันที ฝากถอนสะดวก และเลือกเกมได้ จำนวนมาก เหมาะสำหรับ ทั้งมือใหม่และมือโปร ในโลกของเกมสล็อตออนไลน์
Ricardotus · February 26, 2026 at 6:55 pm
PG
Charlestub · February 26, 2026 at 7:11 pm
ทดลองเล่นสล็อต pg
PG Slot แพลตฟอร์มเกมสล็อตยอดนิยม เล่นง่าย ฝากถอนเร็ว
คำค้นหา pg slot มาแรงในช่วงนี้ ในกลุ่มผู้เล่นเกมสล็อตออนไลน์ เพราะเป็น ผู้ให้บริการเกมสล็อตที่มาแรง ด้าน ภาพและเอฟเฟกต์ ความ เสถียร และ อัตราการจ่ายรางวัลที่น่าสนใจ เกมของ PG ผลิตโดยค่ายมาตรฐาน ที่รองรับการเล่นทั้งบน โทรศัพท์มือถือ และ เดสก์ท็อป
ความโดดเด่น ของ PG Slot
pg slot เป็นเกมสล็อตออนไลน์ที่ออกแบบมาให้ โหลดเร็ว เล่นผ่าน ระบบเว็บ และรองรับ ทุกอุปกรณ์ ไม่ต้องดาวน์โหลดแอป ผู้เล่นสามารถเข้าเล่นผ่าน เว็บเบราว์เซอร์ ได้ทันที ภาพและเสียงถูกพัฒนาในรูปแบบ เอฟเฟกต์ 3 มิติ ให้ความคมชัด พร้อมเอฟเฟกต์ สวยงาม
คุณสมบัติหลักของเกม pg slot ได้แก่
มีรอบโบนัสให้ลุ้นบ่อย
ระบบตัวคูณ
เล่นฟรีก่อนเติมเงิน
ใช้งานภาษาไทยง่าย
ระบบฝากถอนสะดวก ทำรายการไว
แพลตฟอร์ม pg slot โดยทั่วไปให้บริการ การฝาก-ถอน ฝากถอนตลอดเวลา ขั้นต่ำเริ่มต้นเพียง หลักหน่วย ขึ้นอยู่กับ กติกาแต่ละแพลตฟอร์ม การทำรายการใช้เวลา รวดเร็วมาก ผ่าน คิวอาร์โค้ด หรือระบบ ธนาคารบนมือถือ ทำให้ธุรกรรมเป็นไปอย่าง ลื่นไหล
แนวเกมที่คนเล่นเยอะ ใน PG Slot
เกม pg slot มีธีมหลากหลาย เช่น
ธีม แฟนตาซี
ธีม ผจญภัย
ธีม ความมั่งคั่ง
ธีม ธรรมชาติ
ผู้เล่นนิยมเกมที่มีรอบพิเศษบ่อย พร้อมระบบ ฟีเจอร์พิเศษ และ โอกาสทำกำไรสูง เหมาะกับทั้ง มือใหม่ และ ผู้เล่นที่มีประสบการณ์
ความปลอดภัย
สล็อต PG พัฒนาในระบบสากล มีการ รักษาความปลอดภัย และใช้ระบบสุ่มผล Random Number Generator เพื่อให้ผลลัพธ์ ตรวจสอบได้ แพลตฟอร์มที่ให้บริการ สล็อต PG ควรมี ทีมซัพพอร์ต 24 ชม.
บทสรุปท้ายบท
สล็อต PG เป็นตัวเลือกยอดนิยมสำหรับผู้ที่ต้องการเล่นสล็อตออนไลน์ ด้วยจุดเด่นด้าน กราฟิกคุณภาพ และการทำธุรกรรมที่ รวดเร็ว ผู้เล่นสามารถเริ่มต้นได้ ไม่ซับซ้อน ฝากถอนสะดวก และเลือกเกมได้ หลากหลายแนว เหมาะสำหรับ ผู้เล่นทุกสไตล์ ในโลกของเกมสล็อตออนไลน์
https://dveri-ot-zavoda.ru/ · February 26, 2026 at 8:27 pm
https://dveri-ot-zavoda.ru/
http://www.lvm.org/forums/forum.aspx?threadID=102325&msgID=139268 · February 26, 2026 at 10:20 pm
http://www.lvm.org/forums/forum.aspx?threadID=102325&msgID=139268
Uluru tours from Alice Springs · February 26, 2026 at 10:33 pm
About Great Ocean Road tours
Hello Girls, We have detailed information about https://investmentjourney.com.au/uluru-kata-tjuta-national-park-review-a-rollercoaster-experience-for-travelers/
Only if you really think about 4 day Kakadu tours from Darwin?!
Many adventures across Central Australia start with a Uluru tour, & a journey to Uluru always sets the tone for how you connect with this unique land.
That first moment when you glimpse the stone glowing like a burning ember has a way of staying with you always.
I’m your guide, and after years of partnering with the likes of tour companies and racking up countless laps around the Red Centre, I’ve learned you can’t guarantee a truly memorable trip just by turning up – the key difference usually comes down to organising, scheduling carefully, and tempering your expectations a bit.
You’re heading into a land that requires reverence – whether it’s the intense climate or the complex cultural significance – and it’s this same recognition that draws you again long after you’ve got the last bit of red dust out of your socks.
Please visit our internet portal about https://lastravel.com.au/night-skies-over-uluru-a-stargazer-s-guide/ click https://matildatravel.com.au/australia-travel-new-zealand-vacation-individual-from-a-specialist-individual-travel-offers-for-every-taste/ for Sign up for a free consultation now!
and visit site about https://ariixtravel.com.au/navigating-kakadu-s-scenic-drives/ click https://billtaylorphototravel.com/the-best-hiking-trails-in-litchfield-national-park/
Our’s Tags: Rock Art Tours, Phillip Island, best tour operators in Australia, day trip from Alice Springs, Great Ocean Road tour, Great Ocean Road, Alice springs Uluru Tour, tour to Kata Tjuta;
twbhgmm · February 26, 2026 at 10:44 pm
https://shkolaiskusstw.ru/images/art/melbet_promokod_24.html
Timothytoumn · February 27, 2026 at 12:17 am
ทดลองเล่นสล็อต pg
TKBNEKO มอบมิติใหม่ของเกมออนไลน์ ธุรกรรมรวดเร็ว ด้วยระบบสแกน QR Code
ในยุคดิจิทัลที่ โลกออนไลน์เติบโตต่อเนื่อง TKBNEKO พร้อมยกระดับการให้บริการ ด้วยระบบที่ ล้ำสมัย เสถียร และ ตรวจสอบได้ เพื่อให้ผู้เล่น อุ่นใจ ทุกครั้งที่ใช้งาน
จุดเด่นระบบฝาก-ถอน
ฝากขั้นต่ำ: เริ่มต้น 1 บาท
ถอนขั้นต่ำ: ขั้นต่ำ 1 บาท
เวลาฝากเงิน: ภายใน 3 วินาที
ยอดถอน: ไม่จำกัดต่อวัน
เติมเงินง่าย แค่สแกน
สแกน QR Code ระบบจะ ประมวลผลอัตโนมัติ ขั้นต่ำ เริ่ม 100 บาท สูงสุด 500,000 บาท
เกมยอดนิยม
สล็อต: ลุ้นแจ็คพอต
เกมสด: คาสิโนเรียลไทม์
กีฬา: เดิมพันลีกดัง
ยิงปลา: สนุกได้เงินจริง
โบนัสและโปรโมชัน
ติดตามหน้า โปรโมชั่น พร้อมระบบ VIP และโปรแกรม พันธมิตร
ติดต่อเรา
สอบถามข้อมูลได้ตลอด 24 ชั่วโมง ผ่านหน้า ศูนย์ช่วยเหลือ ทีมงาน TKBNEKO พร้อมดูแลตลอดเวลา
Floydwen · February 27, 2026 at 12:29 am
ทดลองเล่นสล็อต pg ซื้อฟรีสปิน
jxfwfra · February 27, 2026 at 12:55 am
http://www.zvezda.spb.ru/mts/inc/promokod_158.html
https://social.japrime.id/read-blog/386731 · February 27, 2026 at 1:45 am
https://social.japrime.id/read-blog/386731
гадание таро онлайн · February 27, 2026 at 5:28 am
карты таро онлайн
http://www.jamesbondexhibition.com · February 27, 2026 at 5:41 am
http://www.jamesbondexhibition.com
kghfkhy · February 27, 2026 at 5:59 am
http://peupleslibres.forumparfait.com/post1287042.html#1287042
Commercial Towing · February 27, 2026 at 8:07 am
I am glad to be a visitor of this perfect blog !, appreciate it for this rare info!
vsrxoum · February 27, 2026 at 8:24 am
http://test.kuli4kam.net/topic/186467-%D0%BF%D1%80%D0%BE%D0%BC%D0%BE%D0%BA%D0%BE%D0%B4-1win-%D1%82%D0%BE%D0%BF-%D0%B1%D0%BE%D0%BD%D1%83%D1%81-1w2026free-%E2%86%92-500-%D0%B1%D0%BE%D0%BD%D1%83%D1%81/
lunatogel · February 27, 2026 at 9:26 am
I enjoy your blog posts, saved to my bookmarks!
https://www.offibelize.com/author/carley98398668/ · February 27, 2026 at 10:13 am
Верификация прошла без проблем, после этого вывод стал еще быстрее
https://centricrealtyservicesorlando.com/agent/mamiehouck5305/
https://camlive.ovh/read-blog/4997 · February 27, 2026 at 10:20 am
https://camlive.ovh/read-blog/4997
https://www.diigo.com/item/note/8lt80/3vh4?k=f49ef06a3c43616a3b4f70633243326a · February 27, 2026 at 12:31 pm
https://www.diigo.com/item/note/8lt80/3vh4?k=f49ef06a3c43616a3b4f70633243326a
on their website · February 27, 2026 at 1:10 pm
Apple Fritter
testi138 · February 27, 2026 at 2:38 pm
It’s clear you’re passionate about the issues.
мелбет промокод бонус на депозит · February 27, 2026 at 2:58 pm
мелбет ру промокод
Скачать Melbet: APK, iOS и ПК
Мобильная версия Melbet включает ставки и казино в одном интерфейсе. Доступны live-ставки, казино-игры, прямые трансляции, статистика и операции по счёту. Загрузка занимает 1–2 минуты.
Android (APK)
Скачайте APK с официального источника, запустите установщик и подтвердите установку. Если требуется включите разрешение на установку из неизвестных источников, затем авторизуйтесь.
iOS (iPhone)
Откройте App Store, найдите «Melbet», нажмите «Получить», после установки авторизуйтесь в системе.
ПК
Перейдите официальный сайт, войдите в личный кабинет и добавьте ярлык на рабочий стол. Веб-версия работает как полноценное приложение.
Функционал
Live-ставки с обновлением коэффициентов, казино и слоты, прямые трансляции, подробная статистика, push-оповещения, регистрация за минуту и круглосуточная служба поддержки.
Бонусы
После установки доступны бонус на первый депозит, промокоды и фрибеты. Условия зависят от региона.
Безопасность
Загружайте только с официальных источников, проверяйте домен, не сообщайте данные доступа третьим лицам и активируйте двухфакторную аутентификацию.
Установка занимает несколько минут, после чего доступен весь функционал Melbet.
melbet казино зеркало · February 27, 2026 at 3:15 pm
melbet зеркало скачать
Установить Melbet: Android, iOS и компьютер
Приложение Melbet объединяет букмекерскую контору и казино в едином приложении. Пользователю доступны live-ставки, казино-игры, онлайн-трансляции, статистика и операции по счёту. Загрузка занимает 1–2 минуты.
Android (APK)
Загрузите APK с официального сайта, запустите установщик и завершите установку. При необходимости включите доступ к установке сторонних приложений, затем войдите в аккаунт.
iOS (iPhone)
Откройте App Store, введите в поиске «Melbet», нажмите «Получить», после установки авторизуйтесь в системе.
ПК
Перейдите официальный сайт, войдите в личный кабинет и создайте ярлык на рабочий стол. Браузерная версия функционирует как полноценное приложение.
Функционал
Live-ставки с обновлением коэффициентов, казино и слоты, прямые трансляции, аналитические данные, уведомления о матчах, быстрая регистрация и круглосуточная служба поддержки.
Бонусы
После загрузки доступны бонус на первый депозит, акционные коды и бесплатные ставки. Условия зависят от региона.
Безопасность
Загружайте только с официальных источников, контролируйте адрес сайта, не сообщайте данные доступа третьим лицам и включите 2FA.
Загрузка выполняется быстро, после чего доступен весь функционал Melbet.
pornhat.com · February 27, 2026 at 3:29 pm
playinexch 365 login
amphetamine mac · February 27, 2026 at 4:57 pm
big ass sex
скачать мелбет на андроид бесплатно с официального сайта · February 27, 2026 at 5:02 pm
скачать мелбет с официального сайта на android
Установить приложение Melbet: Android, iPhone и компьютер
Приложение Melbet включает букмекерскую контору и казино в едином приложении. Пользователю доступны live-ставки, казино-игры, онлайн-трансляции, статистика и быстрые финансовые операции. Загрузка занимает несколько минут.
Android (APK)
Скачайте APK с официального источника, откройте файл и завершите установку. При необходимости включите разрешение на установку из неизвестных источников, затем войдите в аккаунт.
iOS (iPhone)
Откройте App Store, введите в поиске «Melbet», нажмите «Получить», после установки выполните вход.
ПК
Откройте официальный сайт, авторизуйтесь и создайте ярлык на рабочий стол. Веб-версия работает как отдельное приложение.
Функционал
Live-ставки с мгновенным обновлением линии, игровой раздел с тысячами игр, просмотр матчей, подробная статистика, уведомления о матчах, регистрация за минуту и круглосуточная служба поддержки.
Бонусы
После установки доступны бонус на первый депозит, акционные коды и фрибеты. Правила начисления определяются регионом.
Безопасность
Загружайте только с официального сайта, контролируйте адрес сайта, не сообщайте данные доступа третьим лицам и включите 2FA.
Установка занимает несколько минут, после чего доступен весь функционал Melbet.
MartinEmbet · February 27, 2026 at 5:17 pm
ทดลองเล่นสล็อต pg ซื้อฟรีสปิน
Tyronetar · February 27, 2026 at 8:38 pm
Hello!
Analyze exp mysterious results to find interesting and valuable proof depth now and validate your hypotheses see on the website for result analyzers
Full information on the link – https://101flow.site
All the best and development in business!
Haartransplantation Türkei kosten · February 27, 2026 at 8:41 pm
Peculiar this blog is totaly unrelated to what I was searching for – – interesting to see you’re well indexed in the search engines.
https://www.carlscorona.com · February 27, 2026 at 8:56 pm
https://carlscorona.com
https://www.calgarynews.net/newsr/15798 · February 27, 2026 at 8:58 pm
https://www.calgarynews.net/newsr/15798
carlscorona.com · February 27, 2026 at 10:23 pm
https://www.carlscorona.com
https://www.outlookindia.com/outlook-spotlight/1xbet-promo-code-vip888-welcome-bonus-130--news-323728 · February 27, 2026 at 10:41 pm
https://www.outlookindia.com/outlook-spotlight/1xbet-promo-code-vip888-welcome-bonus-130–news-323728
www.carlscorona.com · February 27, 2026 at 11:59 pm
https://carlscorona.com
http://www.carlscorona.com · February 28, 2026 at 1:21 am
https://carlscorona.com
https://www.carlscorona.com · February 28, 2026 at 2:55 am
carlscorona.com
carlscorona.com · February 28, 2026 at 4:17 am
http://www.carlscorona.com
bdphxpc · February 28, 2026 at 7:03 am
https://www.pubpub.org/user/bono-gratis-3
eiidpte · February 28, 2026 at 9:26 am
https://heathxihl825386.blog5.net/90379398/amphetamine-a-comprehensive-overview
Tool Collection · February 28, 2026 at 10:18 am
“Quality stuff right here. Thanks for the value!” Performance optimization tips are shared at Tool Collection.
pron movie · February 28, 2026 at 5:19 pm
porno sites
best Irish online casino · February 28, 2026 at 6:18 pm
Good job for bringing something important to the internet!
Andrewmar · February 28, 2026 at 6:58 pm
Hello!
Learn advanced mysterious techniques for interesting and valuable data mining and extract gold from raw information see on the website for mining tutorials
Full information on the link – https://202fliks.site
All the best and development in business!
sexsex · February 28, 2026 at 7:17 pm
sex
situs sawit188 · February 28, 2026 at 8:05 pm
Unquestionably believe that which you said. Your favorite reason seemed to be on the net the easiest thing to be aware of. I say to you, I certainly get annoyed while people consider worries that they plainly don’t know about. You managed to hit the nail on the head. Will probably be back to get more. Thanks
sexsex · February 28, 2026 at 8:52 pm
sex
site Betify Casino · March 1, 2026 at 6:08 am
Merci pour le contenu intéressant sur Betify Casino.
https://lovsjo.se/logo_lovsjoentreprenad/
Product Launches · March 1, 2026 at 6:37 am
“I love the color palette and typography you chose. Very professional yet inviting.”
sexsex · March 1, 2026 at 9:47 am
sex
melbet регистрация · March 1, 2026 at 12:48 pm
мелбет официальный
Скачать Melbet: Android, iPhone и ПК
Приложение Melbet включает ставки и казино в одном интерфейсе. Пользователю доступны live-ставки, слоты, прямые трансляции, статистика и операции по счёту. Загрузка занимает несколько минут.
Android (APK)
Скачайте APK с официального сайта, запустите установщик и подтвердите установку. При необходимости включите доступ к установке сторонних приложений, затем авторизуйтесь.
iOS (iPhone)
Откройте App Store, введите в поиске «Melbet», нажмите «Получить», после установки авторизуйтесь в системе.
ПК
Откройте официальный сайт, авторизуйтесь и создайте ярлык на рабочий стол. Браузерная версия функционирует как полноценное приложение.
Функционал
Live-ставки с обновлением коэффициентов, казино и слоты, просмотр матчей, аналитические данные, уведомления о матчах, быстрая регистрация и круглосуточная служба поддержки.
Бонусы
После установки доступны приветственный бонус, акционные коды и бесплатные ставки. Правила начисления определяются регионом.
Безопасность
Загружайте только с официального сайта, контролируйте адрес сайта, не передавайте пароль третьим лицам и включите 2FA.
Загрузка выполняется быстро, после чего доступен весь функционал Melbet.
мелбет ру · March 1, 2026 at 1:17 pm
melbet приложение
Установить приложение Melbet: Android, iOS и ПК
Мобильная версия Melbet включает букмекерскую контору и казино в одном интерфейсе. Доступны live-ставки, слоты, онлайн-трансляции, статистика и операции по счёту. Установка занимает несколько минут.
Android (APK)
Скачайте APK с официального источника, запустите установщик и подтвердите установку. Если требуется включите разрешение на установку из неизвестных источников, затем авторизуйтесь.
iOS (iPhone)
Откройте App Store, введите в поиске «Melbet», нажмите «Получить», после установки авторизуйтесь в системе.
ПК
Откройте официальный сайт, войдите в личный кабинет и добавьте ярлык на рабочий стол. Браузерная версия функционирует как отдельное приложение.
Функционал
Live-ставки с мгновенным обновлением линии, игровой раздел с тысячами игр, прямые трансляции, аналитические данные, push-оповещения, быстрая регистрация и круглосуточная служба поддержки.
Бонусы
После установки доступны приветственный бонус, акционные коды и фрибеты. Правила начисления определяются регионом.
Безопасность
Загружайте только с официального сайта, проверяйте домен, не сообщайте данные доступа третьим лицам и включите 2FA.
Установка занимает несколько минут, после чего открывается полный доступ Melbet.
Andrewmar · March 1, 2026 at 3:20 pm
Hello!
Investigate new mysterious interesting theories with valuable outcomes for science and push the boundaries of human knowledge see on the website for research papers
Full information on the link – https://202fliks.site
All the best and development in business!
Pergola haut de gamme · March 1, 2026 at 4:39 pm
I do believe your audience could very well want a good deal more stories like this carry on the excellent hard work.
kajlnkj · March 1, 2026 at 8:13 pm
https://harmonyicux034294.aboutyoublog.com/50368049/stimulant-salt-types-a-detailed-review
https://buyandsellhair.com/author/bonusxaf6/ · March 1, 2026 at 11:11 pm
https://buyandsellhair.com/author/bonusxaf6/
yrfzpce · March 1, 2026 at 11:22 pm
https://phoenixlefl382140.aboutyoublog.com/50362153/i-cannot-meet-your-query
翻墙梯子 · March 2, 2026 at 1:54 am
“The way you explained [Topic] was incredibly helpful. It finally clicked for me.” 翻墙梯子 breaks this down into manageable sections.
Timothytoumn · March 2, 2026 at 2:15 am
ทดลองเล่นสล็อต pg
TKBNEKO มอบมิติใหม่ของเกมออนไลน์ ธุรกรรมรวดเร็ว ด้วยระบบสแกน คิวอาร์โค้ด
ในยุคดิจิทัลที่ เทคโนโลยีพัฒนาอย่างรวดเร็ว TKBNEKO พร้อมยกระดับการให้บริการ ด้วยระบบที่ ทันสมัย เสถียร และ โปร่งใส เพื่อให้ผู้เล่น มั่นใจ ทุกครั้งที่ใช้งาน
จุดเด่นระบบฝาก-ถอน
ฝากขั้นต่ำ: 1 บาท
ถอนขั้นต่ำ: 1 บาท
เวลาฝากเงิน: ใช้เวลาเพียง 3 วินาที
ยอดถอน: ไม่จำกัดต่อวัน
ฝากง่าย เพียงสแกน QR Code
สแกน QR Code ระบบจะ ประมวลผลอัตโนมัติ ขั้นต่ำ 100 บาท สูงสุด ไม่เกิน 500,000 บาทต่อครั้ง
เกมยอดนิยม
สล็อต: ลุ้นแจ็คพอต
เกมสด: คาสิโนเรียลไทม์
กีฬา: เดิมพันลีกดัง
ยิงปลา: ลุ้นกำไรทันที
โปรโมชั่นและสิทธิพิเศษ
ติดตามหน้า โบนัส พร้อมระบบ VIP และโปรแกรม พันธมิตร
ฝ่ายบริการลูกค้า
สอบถามข้อมูลได้ตลอด 24 ชั่วโมง ผ่านหน้า ติดต่อเรา ทีมงาน TKBNEKO พร้อมดูแลตลอดเวลา
online · March 2, 2026 at 2:44 am
order weed clones online
BradleyBit · March 2, 2026 at 2:53 am
สล็อต PG แพลตฟอร์มเกมสล็อตยอดนิยม เข้าเล่นไว ฝากถอนออโต้
คำค้นหา pg slot มาแรงในช่วงนี้ ในกลุ่มผู้เล่นเกมสล็อตออนไลน์ เพราะเป็น แบรนด์เกมที่โดดเด่น ด้าน กราฟิก ความ เสถียร และ โอกาสรับกำไรที่ดี เกมของ PG ผลิตโดยค่ายมาตรฐาน ที่รองรับการเล่นทั้งบน สมาร์ทโฟน และ พีซี
ความโดดเด่น ของ PG Slot
สล็อต PG เป็นเกมสล็อตออนไลน์ที่ออกแบบมาให้ โหลดเร็ว เล่นผ่าน ระบบอัตโนมัติ และรองรับ ทุกอุปกรณ์ ไม่ต้องติดตั้งเพิ่มเติม ผู้เล่นสามารถเข้าเล่นผ่าน Browser ได้ทันที ภาพและเสียงถูกพัฒนาในรูปแบบ สามมิติ ให้ความคมชัด พร้อมเอฟเฟกต์ สมจริง
คุณสมบัติหลักของเกม pg slot ได้แก่
ระบบโบนัสและฟรีสปินหลากหลายรูปแบบ
ฟีเจอร์ตัวคูณรางวัล
โหมดทดลองเล่นฟรี
รองรับภาษาไทยเต็มรูปแบบ
ฝากถอนง่าย ทำรายการไว
แพลตฟอร์ม PG Slot โดยทั่วไปให้บริการ การฝาก-ถอน ฝากถอนตลอดเวลา ขั้นต่ำเริ่มต้นเพียง 10 บาท ขึ้นอยู่กับ เงื่อนไขของเว็บไซต์ การทำรายการใช้เวลา เพียงไม่กี่วินาที ผ่าน คิวอาร์โค้ด หรือระบบ ธนาคารบนมือถือ ทำให้ธุรกรรมเป็นไปอย่าง ลื่นไหล
หมวดเกมฮิต ใน PG Slot
เกม สล็อต PG มีธีมหลากหลาย เช่น
ธีม เทพเจ้า
ธีม Adventure
ธีม ความมั่งคั่ง
ธีม ธรรมชาติ
ผู้เล่นนิยมเกมที่มีรอบพิเศษบ่อย พร้อมระบบ โบนัสรอบพิเศษ และ โอกาสทำกำไรสูง เหมาะกับทั้ง มือใหม่ และ ผู้เล่นที่มีประสบการณ์
มาตรฐานระบบ
PG Slot ใช้ระบบที่ได้มาตรฐาน มีการ ปกป้องข้อมูลผู้เล่น และใช้ระบบสุ่มผล Random Number Generator เพื่อให้ผลลัพธ์ ยุติธรรม แพลตฟอร์มที่ให้บริการ PG Slot ควรมี ความปลอดภัยสูง
สรุป
PG Slot เป็นตัวเลือกยอดนิยมสำหรับผู้ที่ต้องการเล่นสล็อตออนไลน์ ด้วยจุดเด่นด้าน ระบบลื่นไหล และการทำธุรกรรมที่ ไว ผู้เล่นสามารถเริ่มต้นได้ ทันที ฝากถอนสะดวก และเลือกเกมได้ จำนวนมาก เหมาะสำหรับ ผู้เล่นทุกสไตล์ ในโลกของเกมสล็อตออนไลน์
Jasonsuide · March 2, 2026 at 3:09 am
pg
TKBNEKO มอบมิติใหม่ของการเดิมพันออนไลน์ ธุรกรรมฉับไว ด้วยระบบสแกน QR Code
ในยุคที่ เทคโนโลยีเปลี่ยนวิถีการเดิมพันออนไลน์ไปอย่างสิ้นเชิง TKBNEKO พร้อมยกระดับมาตรฐานการเดิมพัน ด้วยระบบการให้บริการที่ ทันสมัย รวดเร็ว และ ชัดเจน พร้อมต้อนรับสมาชิกทุกท่านสู่ มิติใหม่แห่งความสนุก ที่ ตอบโจทย์ทั้งมือใหม่และมืออาชีพ
ทำไมต้อง TKBNEKO?
เราคัดสรรเกมคุณภาพจากผู้พัฒนาชั้นนำ โดยเฉพาะเกมที่ มีใบรับรองอย่างถูกต้อง และ ได้มาตรฐานสากล เพื่อให้ผู้เล่นทุกคน สบายใจ ได้ว่า จะได้รับความเพลิดเพลินกับเกมที่ ยุติธรรม มีระบบรักษาความปลอดภัยสูง และ มีคุณภาพสูง
ระบบการเงินที่เหนือกว่า
ระบบฝากถอนถูกพัฒนาให้ใช้งานง่าย เพื่อให้คุณ เพลิดเพลินกับการเดิมพันอย่างต่อเนื่อง
ฝากขั้นต่ำ: เริ่มต้นเพียง 1 บาท
ถอนขั้นต่ำ: ขั้นต่ำ 1 บาท
เวลาฝากเงิน: ใช้เวลาเพียง 3 วินาที
ยอดจำกัดการถอน: ไม่มียอดจำกัดต่อวัน
ฝากง่าย เพียงสแกน QR Code
เพียงคุณสแกน QR Code ระบบของเราจะ ดำเนินการฝากเงินให้อัตโนมัติ ขั้นต่ำเพียง 100 บาท และสามารถฝากได้สูงถึง ไม่เกิน 500,000 บาทต่อครั้ง เริ่มต้นได้ทันที กับ TKBNEKO ที่ ตอบโจทย์การเดิมพันยุคใหม่
คลังเกมคุณภาพ
TKBNEKO รวมเกมสุดฮิตไว้ในที่เดียว รองรับทุกความชอบของผู้เล่น
สล็อต: แจ็คพอตแตกง่าย ลุ้นได้ทุกวัน
เกมสด: ดีลเลอร์ถ่ายทอดสดตลอดเวลา
กีฬา: รองรับลีกดังระดับโลก
ยิงปลา: เกมยิงปลาสุดมันส์ ได้เงินจริง
รับโบนัสและข้อเสนอสุดคุ้ม
อย่าลืมแวะมาเยี่ยมชมที่หน้า โบนัส เพื่อรับ ของรางวัลพิเศษ ที่เรามอบให้สมาชิกทุกท่าน นอกจากนี้ยังมีระบบ VIP สำหรับลูกค้าคนสำคัญ และช่องทาง พาร์ทเนอร์ สำหรับผู้ที่สนใจสร้างรายได้ร่วมกับเรา
ฝ่ายบริการลูกค้า
หากมี ข้อสงสัย หรือ คำแนะนำ สามารถติดต่อทีมงานของเราได้ตลอด 24 ชั่วโมงที่หน้า ฝ่ายสนับสนุน และ ส่งความคิดเห็น ทีมงาน TKBNEKO ยินดีให้บริการทุกท่านด้วยใจ
FelixGug · March 2, 2026 at 3:25 am
สล็อต
แพลตฟอร์ม TKBNEKO มอบมิติใหม่ของเกมออนไลน์ ฝาก-ถอนไว ด้วยระบบสแกน คิวอาร์โค้ด
ในยุคดิจิทัลที่ โลกออนไลน์เติบโตต่อเนื่อง เรามุ่งเน้นมาตรฐานใหม่ของการเดิมพัน ด้วยระบบที่ ทันสมัย เสถียร และ ตรวจสอบได้ เพื่อให้ผู้เล่น มั่นใจ ทุกครั้งที่ใช้งาน
ระบบการเงินที่ใช้งานง่าย
ฝากขั้นต่ำ: เริ่มต้น 1 บาท
ถอนขั้นต่ำ: ขั้นต่ำ 1 บาท
เวลาฝากเงิน: ภายใน 3 วินาที
ยอดถอน: ไม่มีลิมิต
เติมเงินง่าย แค่สแกน
สแกน QR Code ระบบจะ ประมวลผลอัตโนมัติ ขั้นต่ำ 100 บาท สูงสุด 500,000 บาท
หมวดหมู่เกม
สล็อต: ธีมหลากหลาย
เกมสด: คาสิโนเรียลไทม์
กีฬา: แมตช์ทั่วโลก
ยิงปลา: ลุ้นกำไรทันที
โบนัสและโปรโมชัน
ติดตามหน้า โปรโมชั่น พร้อมระบบ สมาชิกพรีเมียม และโปรแกรม พันธมิตร
ติดต่อเรา
สอบถามข้อมูลได้ตลอด 24 ชั่วโมง ผ่านหน้า ติดต่อเรา ทีมงาน TKBNEKO พร้อมดูแลตลอดเวลา
Travisjal · March 2, 2026 at 3:44 am
สล็อต
แพลตฟอร์ม TKBNEKO เปิดประสบการณ์ใหม่แห่งการเดิมพันออนไลน์ ฝาก-ถอนไว ด้วยระบบสแกน QR Code
ในยุคดิจิทัลที่ โลกออนไลน์เติบโตต่อเนื่อง เรามุ่งเน้นมาตรฐานใหม่ของการเดิมพัน ด้วยระบบที่ ทันสมัย เสถียร และ ตรวจสอบได้ เพื่อให้ผู้เล่น อุ่นใจ ทุกครั้งที่ใช้งาน
ระบบการเงินที่ใช้งานง่าย
ฝากขั้นต่ำ: 1 บาท
ถอนขั้นต่ำ: ขั้นต่ำ 1 บาท
เวลาฝากเงิน: ภายใน 3 วินาที
ยอดถอน: ไม่จำกัดต่อวัน
ฝากง่าย เพียงสแกน QR Code
สแกน คิวอาร์ ระบบจะ โอนเงินเข้าทันที ขั้นต่ำ เริ่ม 100 บาท สูงสุด 500,000 บาท
หมวดหมู่เกม
สล็อต: ลุ้นแจ็คพอต
เกมสด: ดีลเลอร์สด
กีฬา: เดิมพันลีกดัง
ยิงปลา: สนุกได้เงินจริง
โปรโมชั่นและสิทธิพิเศษ
ติดตามหน้า โปรโมชั่น พร้อมระบบ VIP และโปรแกรม แอฟฟิลิเอต
ติดต่อเรา
สอบถามข้อมูลได้ตลอด 24 ชั่วโมง ผ่านหน้า ติดต่อเรา ทีมงาน ของเรา พร้อมดูแลตลอดเวลา
https://medium.com/@ratypw/ทดลองเล่นสล็อต-a4ea8e21fdde
Charlestub · March 2, 2026 at 3:58 am
PG Slot สล็อตยอดฮิต ใช้งานง่าย ฝากถอนรวดเร็ว
คำค้นหา pg slot กำลังได้รับความนิยมอย่างต่อเนื่อง ในกลุ่มผู้เล่นเกมสล็อตออนไลน์ เพราะเป็น แบรนด์เกมที่โดดเด่น ด้าน ภาพและเอฟเฟกต์ ความ นิ่งไม่สะดุด และ โอกาสรับกำไรที่ดี เกมของ PG ผลิตโดยค่ายมาตรฐาน ที่รองรับการเล่นทั้งบน สมาร์ทโฟน และ คอมพิวเตอร์
ข้อดี ของ PG Slot
สล็อต PG เป็นเกมสล็อตออนไลน์ที่ออกแบบมาให้ เข้าเกมไว เล่นผ่าน ระบบเว็บ และรองรับ ทั้ง iOS และ Android เข้าเล่นผ่านเว็บได้เลย ผู้เล่นสามารถเข้าเล่นผ่าน หน้าเว็บ ได้ทันที ภาพและเสียงถูกพัฒนาในรูปแบบ เอฟเฟกต์ 3 มิติ ให้ความคมชัด พร้อมเอฟเฟกต์ จัดเต็ม
คุณสมบัติหลักของเกม สล็อต PG ได้แก่
มีรอบโบนัสให้ลุ้นบ่อย
ระบบตัวคูณ
โหมดทดลองเล่นฟรี
มีเมนูภาษาไทย
ระบบการเงินรวดเร็ว ทันใจ
แพลตฟอร์ม PG Slot มักมี การฝาก-ถอน ฝากถอนตลอดเวลา ขั้นต่ำเริ่มต้นเพียง 10 บาท ขึ้นอยู่กับ เงื่อนไขของเว็บไซต์ การทำรายการใช้เวลา ไม่กี่วินาที ผ่าน QR Code หรือระบบ แอปธนาคาร ทำให้ธุรกรรมเป็นไปอย่าง ลื่นไหล
หมวดเกมฮิต ใน pg slot
เกม PG Slot มีธีมหลากหลาย เช่น
ธีม แฟนตาซี
ธีม Adventure
ธีม โชคลาภ
ธีม สัตว์และธรรมชาติ
หลายคนชอบเกมที่โบนัสเข้าไว พร้อมระบบ โบนัสรอบพิเศษ และ โอกาสทำกำไรสูง เหมาะกับทั้ง มือใหม่ และ ผู้เล่นมือโปร
ความน่าเชื่อถือ
pg slot พัฒนาในระบบสากล มีการ เข้ารหัสข้อมูล และใช้ระบบสุ่มผล Random Number Generator เพื่อให้ผลลัพธ์ ยุติธรรม แพลตฟอร์มที่ให้บริการ pg slot ควรมี ความปลอดภัยสูง
โดยภาพรวม
pg slot เป็นตัวเลือกยอดนิยมสำหรับผู้ที่ต้องการเล่นสล็อตออนไลน์ ด้วยจุดเด่นด้าน โบนัสหลากหลาย และการทำธุรกรรมที่ ทันใจ ผู้เล่นสามารถเริ่มต้นได้ ง่าย ฝากถอนสะดวก และเลือกเกมได้ จำนวนมาก เหมาะสำหรับ ทั้งมือใหม่และมือโปร ในโลกของเกมสล็อตออนไลน์
https://medium.com/@ratypw/ทดลองเล่นสล็อต-pg-70cdb1132344
RichardSax · March 2, 2026 at 6:20 am
Заказ выполнен идеально. Упаковка милая!
доставка цветов томск на дом
https://www.syncdocs.com/forums/profile/promox1 · March 2, 2026 at 6:23 am
https://www.syncdocs.com/forums/profile/promox1
fanbfum · March 2, 2026 at 6:48 am
https://bookmeter.com/users/1686613
Mua tiền ảo bằng thẻ visa · March 2, 2026 at 10:51 am
Cheers! Awesome information!
My blog … https://telegra.ph/C%C3%A1ch-Mua-Bitcoin-B%E1%BA%B1ng-Th%E1%BA%BB-T%C3%ADn-D%E1%BB%A5ng-T%E1%BA%A1i-Vi%E1%BB%87t-Nam-H%C6%B0%E1%BB%9Bng-D%E1%BA%ABn-Nhanh-2026-01-23
Josephneupt · March 2, 2026 at 11:14 am
ทดลองเล่นสล็อต pg ฟรี สล็อต PG สล็อตยอดฮิต ใช้งานง่าย ฝากถอนรวดเร็ว
คำค้นหา สล็อต PG กำลังได้รับความนิยมอย่างต่อเนื่อง ในกลุ่มผู้เล่นเกมสล็อตออนไลน์ เพราะเป็น ค่ายเกมที่มีชื่อเสียง ด้าน กราฟิก ความ นิ่งไม่สะดุด และ โอกาสรับกำไรที่ดี เกมของ PG พัฒนาโดยผู้ให้บริการชั้นนำ ที่รองรับการเล่นทั้งบน สมาร์ทโฟน และ คอมพิวเตอร์
ความโดดเด่น ของ PG Slot
PG Slot เป็นเกมสล็อตออนไลน์ที่ออกแบบมาให้ เข้าเกมไว เล่นผ่าน ระบบออนไลน์ และรองรับ ทุกแพลตฟอร์ม ไม่ต้องติดตั้งเพิ่มเติม ผู้เล่นสามารถเข้าเล่นผ่าน Browser ได้ทันที ภาพและเสียงถูกพัฒนาในรูปแบบ 3D ให้ความคมชัด พร้อมเอฟเฟกต์ สวยงาม
คุณสมบัติหลักของเกม pg slot ได้แก่
โบนัสและฟรีสปินหลายแบบ
ฟีเจอร์ตัวคูณรางวัล
เดโม่ฟรี
ใช้งานภาษาไทยง่าย
ระบบการเงินรวดเร็ว ทำรายการไว
แพลตฟอร์ม PG Slot มักมี การฝาก-ถอน ออโต้ตลอด 24 ชม. ขั้นต่ำเริ่มต้นเพียง 10 บาท ขึ้นอยู่กับ ระบบของผู้ให้บริการ การทำรายการใช้เวลา เพียงไม่กี่วินาที ผ่าน QR Code หรือระบบ แอปธนาคาร ทำให้ธุรกรรมเป็นไปอย่าง ลื่นไหล
หมวดเกมฮิต ใน PG Slot
เกม สล็อต PG มีธีมหลากหลาย เช่น
ธีม เทพเจ้าและแฟนตาซี
ธีม Adventure
ธีม ความมั่งคั่ง
ธีม สัตว์และธรรมชาติ
ผู้เล่นนิยมเกมที่มีรอบพิเศษบ่อย พร้อมระบบ Special Feature และ โอกาสทำกำไรสูง เหมาะกับทั้ง มือใหม่ และ ผู้เล่นมือโปร
ความปลอดภัย
สล็อต PG ใช้ระบบที่ได้มาตรฐาน มีการ รักษาความปลอดภัย และใช้ระบบสุ่มผล Random Number Generator เพื่อให้ผลลัพธ์ ยุติธรรม แพลตฟอร์มที่ให้บริการ PG Slot ควรมี ความปลอดภัยสูง
โดยภาพรวม
pg slot เป็นตัวเลือกยอดนิยมสำหรับผู้ที่ต้องการเล่นสล็อตออนไลน์ ด้วยจุดเด่นด้าน กราฟิกคุณภาพ และการทำธุรกรรมที่ ทันใจ ผู้เล่นสามารถเริ่มต้นได้ ง่าย ฝากถอนสะดวก และเลือกเกมได้ ครบทุกหมวด เหมาะสำหรับ ผู้เล่นทุกสไตล์ ในโลกของเกมสล็อตออนไลน์
https://t.me/s/evacasino_official · March 2, 2026 at 11:16 am
eva casino зеркало
Новое ева казино зеркало обычно выкладывают сразу после изменений.
JosephBer · March 2, 2026 at 12:26 pm
ทดลองเล่นสล็อต pg
สล็อต PG สล็อตยอดฮิต เล่นง่าย ฝากถอนเร็ว
คำค้นหา pg slot มาแรงในช่วงนี้ ในกลุ่มผู้เล่นเกมสล็อตออนไลน์ เพราะเป็น ค่ายเกมที่มีชื่อเสียง ด้าน ภาพและเอฟเฟกต์ ความ ลื่นไหล และ โอกาสรับกำไรที่ดี เกมของ PG พัฒนาโดยผู้ให้บริการชั้นนำ ที่รองรับการเล่นทั้งบน มือถือ และ คอมพิวเตอร์
จุดเด่น ของ pg slot
PG Slot เป็นเกมสล็อตออนไลน์ที่ออกแบบมาให้ โหลดเร็ว เล่นผ่าน ระบบอัตโนมัติ และรองรับ ทุกอุปกรณ์ ไม่ต้องดาวน์โหลดแอป ผู้เล่นสามารถเข้าเล่นผ่าน เว็บเบราว์เซอร์ ได้ทันที ภาพและเสียงถูกพัฒนาในรูปแบบ 3D ให้ความคมชัด พร้อมเอฟเฟกต์ จัดเต็ม
คุณสมบัติหลักของเกม pg slot ได้แก่
มีรอบโบนัสให้ลุ้นบ่อย
ระบบตัวคูณ
เล่นฟรีก่อนเติมเงิน
ใช้งานภาษาไทยง่าย
ระบบการเงินรวดเร็ว ทำรายการไว
แพลตฟอร์ม สล็อต PG มักมี การฝาก-ถอน ออโต้ตลอด 24 ชม. ขั้นต่ำเริ่มต้นเพียง 1 บาท ขึ้นอยู่กับ ระบบของผู้ให้บริการ การทำรายการใช้เวลา ไม่กี่วินาที ผ่าน คิวอาร์โค้ด หรือระบบ Mobile Banking ทำให้ธุรกรรมเป็นไปอย่าง ไม่สะดุด
ประเภทเกมยอดนิยม ใน PG Slot
เกม สล็อต PG มีธีมหลากหลาย เช่น
ธีม เทพเจ้าและแฟนตาซี
ธีม ผจญภัย
ธีม ความมั่งคั่ง
ธีม ธรรมชาติ
เกมยอดนิยมมักเป็นเกมที่แตกง่าย พร้อมระบบ Special Feature และ ระบบจ่ายคุ้มค่า เหมาะกับทั้ง คนเพิ่งเล่น และ ผู้เล่นมือโปร
มาตรฐานระบบ
pg slot ใช้ระบบที่ได้มาตรฐาน มีการ ปกป้องข้อมูลผู้เล่น และใช้ระบบสุ่มผล RNG เพื่อให้ผลลัพธ์ ยุติธรรม แพลตฟอร์มที่ให้บริการ pg slot ควรมี ทีมซัพพอร์ต 24 ชม.
สรุป
pg slot เป็นตัวเลือกยอดนิยมสำหรับผู้ที่ต้องการเล่นสล็อตออนไลน์ ด้วยจุดเด่นด้าน กราฟิกคุณภาพ และการทำธุรกรรมที่ ไว ผู้เล่นสามารถเริ่มต้นได้ ง่าย ฝากถอนสะดวก และเลือกเกมได้ ครบทุกหมวด เหมาะสำหรับ ทั้งมือใหม่และมือโปร ในโลกของเกมสล็อตออนไลน์
https://medium.com/@ratypw/ทดลองเล่นสล็อต-pg-70cdb1132344
RodneyChoix · March 2, 2026 at 12:30 pm
ทดลองเล่นสล็อต pg
TKBNEKO เปิดประสบการณ์ใหม่แห่งการเดิมพันออนไลน์ ธุรกรรมรวดเร็ว ด้วยระบบสแกน QR Code
ในยุคดิจิทัลที่ โลกออนไลน์เติบโตต่อเนื่อง เรามุ่งเน้นมาตรฐานใหม่ของการเดิมพัน ด้วยระบบที่ ล้ำสมัย เสถียร และ โปร่งใส เพื่อให้ผู้เล่น อุ่นใจ ทุกครั้งที่ใช้งาน
ระบบการเงินที่ใช้งานง่าย
ฝากขั้นต่ำ: 1 บาท
ถอนขั้นต่ำ: 1 บาท
เวลาฝากเงิน: ภายใน 3 วินาที
ยอดถอน: ไม่มีลิมิต
เติมเงินง่าย แค่สแกน
สแกน คิวอาร์ ระบบจะ โอนเงินเข้าทันที ขั้นต่ำ 100 บาท สูงสุด ไม่เกิน 500,000 บาทต่อครั้ง
หมวดหมู่เกม
สล็อต: ลุ้นแจ็คพอต
เกมสด: คาสิโนเรียลไทม์
กีฬา: เดิมพันลีกดัง
ยิงปลา: ลุ้นกำไรทันที
โบนัสและโปรโมชัน
ติดตามหน้า โปรโมชั่น พร้อมระบบ VIP และโปรแกรม พันธมิตร
ติดต่อเรา
สอบถามข้อมูลได้ตลอด 24 ชั่วโมง ผ่านหน้า ศูนย์ช่วยเหลือ ทีมงาน TKBNEKO พร้อมดูแลตลอดเวลา
https://medium.com/@ratypw/ทดลองเล่นสล็อต-pg-e598fa477f69
https://wasliestdu.de/rezension/zerrissene-seele#comment-1653727 · March 2, 2026 at 3:55 pm
https://wasliestdu.de/rezension/zerrissene-seele#comment-1653727
eytyhcl · March 2, 2026 at 5:32 pm
https://www.pentaktino.gr/en-gb/journal3/blog/post?journal_blog_post_id=10
Slottica Casino · March 2, 2026 at 6:35 pm
Platforma Slottica to miejsce, w którym pasja do hazardu spotyka się z technologią najwyższej klasy. Od momentu uruchomienia w 2019 roku kierujemy się zasadami fair play, ochrony danych osobowych oraz ciągłego rozwoju oferty. Posiadamy ważną licencję międzynarodową Curaçao eGaming (nr 8048/JAZ2018-040), co potwierdza naszą wiarygodność i zgodność z regulacjami branżowymi. Tysiące aktywnych użytkowników z Polski wybiera nas każdego dnia.
suomen paras nettikasino · March 2, 2026 at 8:11 pm
Please let us know when you plan to publish your book!
https://www.fiverr.com/acquirebacklink/guest-posting-dofollow-seo-backlinks-high-da-link-building-publish-article · March 2, 2026 at 10:01 pm
Woah this is just an insane amount of information, must of taken ages to compile so thanx so much for just sharing it with all of us. If your ever in any need of related information, just check out my own site!
http://www.cyclingfever.com/video.html?detp=view&video_idd=MTEzMzk= · March 2, 2026 at 10:52 pm
http://www.cyclingfever.com/video.html?detp=view&video_idd=MTEzMzk=
senang4d · March 3, 2026 at 12:27 am
Nice piece of info! May I reference part of this on my blog if I post a backlink to this webpage? Thx.
Guest Post · March 3, 2026 at 6:17 am
Howdy! I simply wish to give a huge thumbs up for the great information you have here on this post. I will be coming again to your weblog for extra soon.
https://turistavto.ru/ · March 3, 2026 at 1:55 pm
Как производится качественный восстановление автомобиля
fast payout casinos · March 3, 2026 at 2:56 pm
I just sent this post to a bunch of my friends as I agree with most of what you’re saying here and the way you’ve presented it is awesome.
best paying casino · March 3, 2026 at 2:57 pm
Well done! Keep up this quality!
NZ online casino' · March 3, 2026 at 4:01 pm
Just stumble upon your blog from from time to time. nice article
real money casino · March 3, 2026 at 4:05 pm
How do I subscribe to your blog? Thanks for your help.
top online casino · March 3, 2026 at 4:51 pm
Hello there I am so delighted I found your weblog, I really found you by mistake, while I was searching on Google for something else, Anyhow I am here now and would just like to say cheers for a remarkable post and a all round exciting blog (I also love the theme/design), I don’t have time to browse it all at the moment but I have book-marked it and also included your RSS feeds, so when I have time I will be back to read a lot more, Please do keep up the superb work.
real money casino Canada · March 3, 2026 at 9:50 pm
I would share your post with my sis.
Jasonsuide · March 4, 2026 at 12:37 am
TKBNEKO เปิดประสบการณ์ใหม่แห่งการเดิมพันออนไลน์ ฝาก-ถอนไว ด้วยระบบสแกน QR Code
ในยุคที่ เทคโนโลยีเปลี่ยนวิถีการเดิมพันออนไลน์ไปอย่างสิ้นเชิง TKBNEKO เข้ามาสร้างมาตรฐานใหม่ให้กับวงการ ด้วยระบบการให้บริการที่ ทันสมัย เสถียร และ โปร่งใส พร้อมต้อนรับสมาชิกทุกท่านสู่ มิติใหม่แห่งความสนุก ที่ ใครๆ ก็เป็นเถ้าแก่ได้
ทำไมต้อง TKBNEKO?
เราคัดสรรเกมคุณภาพจากผู้พัฒนาชั้นนำ โดยเฉพาะเกมที่ ผ่านการรับรองจากสถาบันที่น่าเชื่อถือ และ เป็นที่นิยมในระดับสากล เพื่อให้ผู้เล่นทุกคน มั่นใจ ได้ว่า จะได้รับความเพลิดเพลินกับเกมที่ ไม่มีการเอาเปรียบ มีระบบรักษาความปลอดภัยสูง และ ตอบโจทย์ผู้เล่นยุคใหม่
จุดเด่นของระบบฝาก-ถอน
ระบบฝากถอนถูกพัฒนาให้ใช้งานง่าย เพื่อให้คุณ โฟกัสกับความสนุกได้อย่างเต็มที่
ฝากขั้นต่ำ: ขั้นต่ำแค่ 1 บาท
ถอนขั้นต่ำ: เพียง 1 บาท
เวลาฝากเงิน: รวดเร็วทันใจใน 3 วินาที
ยอดจำกัดการถอน: ไม่มียอดจำกัดต่อวัน
เติมเงินง่ายด้วย QR Code
เพียงคุณสแกน QR Code ระบบของเราจะ ดำเนินการฝากเงินให้อัตโนมัติ ขั้นต่ำเพียง อย่างน้อย 100 บาท และสามารถฝากได้สูงถึง ไม่เกิน 500,000 บาทต่อครั้ง เข้าร่วมความสนุกได้เลย กับ TKBNEKO ที่ ใช้งานง่าย ทำกำไรได้รวดเร็ว
เกมยอดนิยมรวมไว้ในที่เดียว
TKBNEKO รวมเกมสุดฮิตไว้ในที่เดียว รองรับทุกความชอบของผู้เล่น
สล็อต: ธีมมากมาย พร้อมลุ้นรางวัลใหญ่
เกมสด: ดีลเลอร์ถ่ายทอดสดตลอดเวลา
กีฬา: รองรับลีกดังระดับโลก
ยิงปลา: เกมยิงปลาสุดมันส์ ได้เงินจริง
ติดตามโปรโมชั่นและสิทธิพิเศษ
อย่าลืมแวะมาเยี่ยมชมที่หน้า โบนัส เพื่อรับ สิทธิพิเศษมากมาย ที่เรามอบให้สมาชิกทุกท่าน นอกจากนี้ยังมีระบบ ลูกค้าระดับพรีเมียม สำหรับลูกค้าคนสำคัญ และช่องทาง แอฟฟิลิเอต สำหรับผู้ที่สนใจสร้างรายได้ร่วมกับเรา
ช่องทางติดต่อ
หากมี ข้อสงสัย หรือ คำแนะนำ สามารถติดต่อทีมงานของเราได้ตลอด 24 ชั่วโมงที่หน้า ฝ่ายสนับสนุน และ แบบฟอร์มติดต่อ ทีมงาน ของเรา ยินดีให้บริการทุกท่านด้วยใจ
Google Business Profile optimization Thane · March 4, 2026 at 2:20 am
I thought it was going to be some boring old post, but I’m glad I visited. I will post a link to this site on my blog. I am sure my visitors will find that very useful.
acheter followers instagram · March 4, 2026 at 2:24 am
I just couldnt leave your website before saying that I really enjoyed the useful information you offer to your visitors… Will be back often to check up on new stuff you post!
acheter abonnés youtube · March 4, 2026 at 3:02 am
I just couldnt leave your website before saying that I really enjoyed the useful information you offer to your visitors… Will be back often to check up on new stuff you post!
acheter followers tiktok · March 4, 2026 at 3:18 am
I am glad to be a visitor on this website!, regards for this rare information!
CharleyBar · March 4, 2026 at 4:02 am
ทดลองเล่นสล็อต pg ไม่ เด้ง
BradleyBit · March 4, 2026 at 4:03 am
pg slot เกมสล็อตออนไลน์ที่คนค้นหาเยอะ เข้าเล่นไว ฝากถอนออโต้
คำค้นหา pg slot มาแรงในช่วงนี้ ในกลุ่มผู้เล่นเกมสล็อตออนไลน์ เพราะเป็น ผู้ให้บริการเกมสล็อตที่มาแรง ด้าน กราฟิก ความ เสถียร และ โอกาสรับกำไรที่ดี เกมของ PG ผลิตโดยค่ายมาตรฐาน ที่รองรับการเล่นทั้งบน สมาร์ทโฟน และ พีซี
ความโดดเด่น ของ PG Slot
สล็อต PG เป็นเกมสล็อตออนไลน์ที่ออกแบบมาให้ เข้าเกมไว เล่นผ่าน ระบบเว็บ และรองรับ ทุกแพลตฟอร์ม เข้าเล่นผ่านเว็บได้เลย ผู้เล่นสามารถเข้าเล่นผ่าน เว็บเบราว์เซอร์ ได้ทันที ภาพและเสียงถูกพัฒนาในรูปแบบ สามมิติ ให้ความคมชัด พร้อมเอฟเฟกต์ จัดเต็ม
คุณสมบัติหลักของเกม สล็อต PG ได้แก่
โบนัสและฟรีสปินหลายแบบ
Multiplier
โหมดทดลองเล่นฟรี
ใช้งานภาษาไทยง่าย
ฝากถอนง่าย ทำรายการไว
แพลตฟอร์ม สล็อต PG โดยทั่วไปให้บริการ การฝาก-ถอน อัตโนมัติ 24 ชั่วโมง ขั้นต่ำเริ่มต้นเพียง 10 บาท ขึ้นอยู่กับ เงื่อนไขของเว็บไซต์ การทำรายการใช้เวลา รวดเร็วมาก ผ่าน คิวอาร์โค้ด หรือระบบ Mobile Banking ทำให้ธุรกรรมเป็นไปอย่าง ลื่นไหล
ประเภทเกมยอดนิยม ใน PG Slot
เกม สล็อต PG มีธีมหลากหลาย เช่น
ธีม แฟนตาซี
ธีม ลุยด่าน
ธีม เอเชียและโชคลาภ
ธีม ธรรมชาติ
หลายคนชอบเกมที่โบนัสเข้าไว พร้อมระบบ Special Feature และ อัตราการจ่ายที่สูง เหมาะกับทั้ง ผู้เล่นเริ่มต้น และ ผู้เล่นที่มีประสบการณ์
ความน่าเชื่อถือ
pg slot มีมาตรฐานรองรับ มีการ ปกป้องข้อมูลผู้เล่น และใช้ระบบสุ่มผล ระบบสุ่มมาตรฐาน เพื่อให้ผลลัพธ์ ยุติธรรม แพลตฟอร์มที่ให้บริการ PG Slot ควรมี ความปลอดภัยสูง
โดยภาพรวม
pg slot เป็นตัวเลือกยอดนิยมสำหรับผู้ที่ต้องการเล่นสล็อตออนไลน์ ด้วยจุดเด่นด้าน ระบบลื่นไหล และการทำธุรกรรมที่ ทันใจ ผู้เล่นสามารถเริ่มต้นได้ ไม่ซับซ้อน ฝากถอนสะดวก และเลือกเกมได้ หลากหลายแนว เหมาะสำหรับ ทุกระดับประสบการณ์ ในโลกของเกมสล็อตออนไลน์
RodneyChoix · March 4, 2026 at 4:07 am
ทดลองเล่นสล็อต pg
แพลตฟอร์ม TKBNEKO มอบมิติใหม่ของเกมออนไลน์ ธุรกรรมรวดเร็ว ด้วยระบบสแกน คิวอาร์โค้ด
ในยุคดิจิทัลที่ เทคโนโลยีพัฒนาอย่างรวดเร็ว TKBNEKO พร้อมยกระดับการให้บริการ ด้วยระบบที่ ล้ำสมัย รวดเร็ว และ ตรวจสอบได้ เพื่อให้ผู้เล่น อุ่นใจ ทุกครั้งที่ใช้งาน
จุดเด่นระบบฝาก-ถอน
ฝากขั้นต่ำ: เริ่มต้น 1 บาท
ถอนขั้นต่ำ: 1 บาท
เวลาฝากเงิน: ภายใน 3 วินาที
ยอดถอน: ไม่มีลิมิต
ฝากง่าย เพียงสแกน QR Code
สแกน คิวอาร์ ระบบจะ ประมวลผลอัตโนมัติ ขั้นต่ำ 100 บาท สูงสุด 500,000 บาท
หมวดหมู่เกม
สล็อต: ธีมหลากหลาย
เกมสด: ดีลเลอร์สด
กีฬา: แมตช์ทั่วโลก
ยิงปลา: ลุ้นกำไรทันที
โปรโมชั่นและสิทธิพิเศษ
ติดตามหน้า โปรโมชั่น พร้อมระบบ VIP และโปรแกรม พันธมิตร
ฝ่ายบริการลูกค้า
สอบถามข้อมูลได้ตลอด 24 ชั่วโมง ผ่านหน้า ศูนย์ช่วยเหลือ ทีมงาน TKBNEKO พร้อมดูแลตลอดเวลา
https://medium.com/@ratypw/ทดลองเล่นสล็อต-pg-e598fa477f69
acheter followers tiktok · March 4, 2026 at 4:09 am
I think other website proprietors should take this web site as an model, very clean and great user pleasant style and design .
acheter followers instagram · March 4, 2026 at 4:44 am
Good points – – it will make a difference with my parents.
casino en ligne · March 4, 2026 at 9:46 am
Hey very cool site!! Man .. Beautiful .. Amazing .. I will bookmark your website and take the feeds also…I’m happy to find so many useful information here in the post, we need develop more strategies in this regard, thanks for sharing. . . . . .
acheter followers tiktok · March 4, 2026 at 11:18 am
This is the wave – the big wave.
dcmzkag · March 4, 2026 at 11:38 am
Глубокое понимание себя: Вы узнаете свои врожденные сильные и уязвимые стороны, сознательные и бессознательные характеристики, что помогает принять свою истинную сущность.
Принятие корректных решений: Понимание своей Стратегии и Авторитета позволяет перестать принимать решения из ментального давления, страха или влияния окружающих.
Гармонизация отношений: Осознание того, что каждый человек уникален, помогает лучше понимать реакции окружающих, снижает количество конфликтов и позволяет принимать людей такими, какие они есть.
Жизнь без сопротивления (меньше стресса): Понимание своего типа личности (генератор, проектор и др.) позволяет взаимодействовать с миром экологично, перестав «бороться» с жизнью и действуя в соответствии со своей энергией.
Раскрытие потенциала: Дизайн Человека указывает на врожденные таланты и способности, помогая найти свой путь, который приносит успех, удовлетворение и гармонию
https://t.me/s/ihumandesign
acheter abonnés youtube · March 4, 2026 at 11:58 am
However, it is virtually all done with tongues rooted solidly in cheeks, and everyone has absolutely nothing but absolutely love for his or her friendly neighborhood scapegoat. The truth is, he is not just a pushover. He is basically that special variety of person strong enough to take all of that good natured ribbing for exactly what it is.
ylxofer · March 4, 2026 at 1:22 pm
https://goingblog.com/codigo-promocional-1xbet-ano-nuevo-2026-1xbro200/
Andrewmar · March 4, 2026 at 3:04 pm
Hello!
Investigate taste mysterious origins offering interesting and valuable gastronomic data and understand your palate see on the website for taste tests
Full information on the link – https://800letekas.site
All the best and development in business!
https://molodeg-biryuch.ru/user/pothirwbil · March 4, 2026 at 6:30 pm
https://molodeg-biryuch.ru/user/pothirwbil
porno india · March 4, 2026 at 6:30 pm
gay sex videos
Andrewmar · March 4, 2026 at 7:53 pm
Hello everyone!
Decode storm mysterious patterns hiding interesting and valuable meteorological news and predict weather with accuracy see on the website for forecast models
Full information on the link – https://800letekas.site
All the best and development in business!
Product Launches · March 5, 2026 at 1:50 am
“I love the color palette and typography you chose. Very professional yet inviting.” Step-by-step guidance is available at Product Launches.
FelixGug · March 5, 2026 at 1:55 am
สล็อต
TKBNEKO มอบมิติใหม่ของเกมออนไลน์ ฝาก-ถอนไว ด้วยระบบสแกน คิวอาร์โค้ด
ในยุคดิจิทัลที่ โลกออนไลน์เติบโตต่อเนื่อง เรามุ่งเน้นมาตรฐานใหม่ของการเดิมพัน ด้วยระบบที่ ล้ำสมัย รวดเร็ว และ โปร่งใส เพื่อให้ผู้เล่น อุ่นใจ ทุกครั้งที่ใช้งาน
ระบบการเงินที่ใช้งานง่าย
ฝากขั้นต่ำ: 1 บาท
ถอนขั้นต่ำ: 1 บาท
เวลาฝากเงิน: ภายใน 3 วินาที
ยอดถอน: ไม่จำกัดต่อวัน
ฝากง่าย เพียงสแกน QR Code
สแกน คิวอาร์ ระบบจะ ประมวลผลอัตโนมัติ ขั้นต่ำ เริ่ม 100 บาท สูงสุด 500,000 บาท
เกมยอดนิยม
สล็อต: ธีมหลากหลาย
เกมสด: ดีลเลอร์สด
กีฬา: แมตช์ทั่วโลก
ยิงปลา: ลุ้นกำไรทันที
โบนัสและโปรโมชัน
ติดตามหน้า โปรโมชั่น พร้อมระบบ สมาชิกพรีเมียม และโปรแกรม พันธมิตร
ฝ่ายบริการลูกค้า
สอบถามข้อมูลได้ตลอด 24 ชั่วโมง ผ่านหน้า ศูนย์ช่วยเหลือ ทีมงาน TKBNEKO พร้อมดูแลตลอดเวลา
Travisjal · March 5, 2026 at 1:57 am
สล็อต
TKBNEKO เปิดประสบการณ์ใหม่แห่งการเดิมพันออนไลน์ ฝาก-ถอนไว ด้วยระบบสแกน คิวอาร์โค้ด
ในยุคดิจิทัลที่ โลกออนไลน์เติบโตต่อเนื่อง TKBNEKO พร้อมยกระดับการให้บริการ ด้วยระบบที่ ล้ำสมัย เสถียร และ โปร่งใส เพื่อให้ผู้เล่น มั่นใจ ทุกครั้งที่ใช้งาน
จุดเด่นระบบฝาก-ถอน
ฝากขั้นต่ำ: 1 บาท
ถอนขั้นต่ำ: ขั้นต่ำ 1 บาท
เวลาฝากเงิน: ภายใน 3 วินาที
ยอดถอน: ไม่จำกัดต่อวัน
ฝากง่าย เพียงสแกน QR Code
สแกน QR Code ระบบจะ ประมวลผลอัตโนมัติ ขั้นต่ำ 100 บาท สูงสุด 500,000 บาท
เกมยอดนิยม
สล็อต: ธีมหลากหลาย
เกมสด: คาสิโนเรียลไทม์
กีฬา: แมตช์ทั่วโลก
ยิงปลา: ลุ้นกำไรทันที
โบนัสและโปรโมชัน
ติดตามหน้า โปรโมชั่น พร้อมระบบ สมาชิกพรีเมียม และโปรแกรม แอฟฟิลิเอต
ฝ่ายบริการลูกค้า
สอบถามข้อมูลได้ตลอด 24 ชั่วโมง ผ่านหน้า ติดต่อเรา ทีมงาน TKBNEKO พร้อมดูแลตลอดเวลา
https://medium.com/@ratypw/ทดลองเล่นสล็อต-a4ea8e21fdde
Tyronetar · March 5, 2026 at 4:39 am
Hello everyone!
Share your find of interesting mysterious data points with valuable impact on tech and innovate within your industry see on the website to publish your findings
Full information on the link – https://33capy.site
All the best and development in business!
fastcash.dothome.co.kr · March 5, 2026 at 5:49 am
우와 좋은 소식 감사합니다! 요즘처럼 경제 분야에 관심이 많은데, 신용카드현금화 정보를 친절하게 정리해주시니 정말 든든하네요. 신속한 현금화서비스 정보확인은 언제라도 함께해요. 시간 될 때 와서 멋진 이야기 부탁드립니다. 활기찬 시간 보내시길!
eaxezdg · March 5, 2026 at 9:10 am
https://www.bandsworksconcerts.info/index.php?bonus1xbet20
https://fakenews.win/wiki/Code_promo_1xBet_2026_Bonus_gratuit_jusqu_130 · March 5, 2026 at 9:25 am
https://fakenews.win/wiki/Code_promo_1xBet_2026_Bonus_gratuit_jusqu_130
Jasonsuide · March 5, 2026 at 2:38 pm
แพลตฟอร์ม TKBNEKO เปิดประสบการณ์ใหม่แห่งการเดิมพันออนไลน์ ฝาก-ถอนไว ด้วยระบบสแกน QR Code
ในยุคที่ เทคโนโลยีเปลี่ยนวิถีการเดิมพันออนไลน์ไปอย่างสิ้นเชิง TKBNEKO เข้ามาสร้างมาตรฐานใหม่ให้กับวงการ ด้วยระบบการให้บริการที่ ล้ำสมัย เสถียร และ โปร่งใส พร้อมต้อนรับสมาชิกทุกท่านสู่ โลกแห่งเกมที่เหนือกว่าเดิม ที่ ใครๆ ก็เป็นเถ้าแก่ได้
เพราะอะไรหลายคนจึงเลือก TKBNEKO
เราคัดสรรเกมคุณภาพจากผู้พัฒนาชั้นนำ โดยเฉพาะเกมที่ ผ่านการรับรองจากสถาบันที่น่าเชื่อถือ และ ได้มาตรฐานสากล เพื่อให้ผู้เล่นทุกคน อุ่นใจ ได้ว่า จะได้รับความเพลิดเพลินกับเกมที่ โปร่งใส มีระบบรักษาความปลอดภัยสูง และ มีคุณภาพสูง
จุดเด่นของระบบฝาก-ถอน
เรามุ่งเน้นความสะดวกของผู้เล่น เพื่อให้คุณ เล่นเกมได้แบบไม่สะดุด
ฝากขั้นต่ำ: ขั้นต่ำแค่ 1 บาท
ถอนขั้นต่ำ: เพียง 1 บาท
เวลาฝากเงิน: รวดเร็วทันใจใน 3 วินาที
ยอดจำกัดการถอน: ถอนได้ไม่จำกัดยอด
ธุรกรรมสะดวก แค่สแกนคิวอาร์
เพียงคุณสแกน QR Code ระบบของเราจะ ดำเนินการฝากเงินให้อัตโนมัติ ขั้นต่ำเพียง อย่างน้อย 100 บาท และสามารถฝากได้สูงถึง 500,000 บาท มาร่วมสนุกกันได้แล้ววันนี้ กับ แพลตฟอร์มของเรา ที่ ใช้งานง่าย ทำกำไรได้รวดเร็ว
คลังเกมคุณภาพ
แพลตฟอร์มของเราครอบคลุมทุกแนวเกม รองรับทุกความชอบของผู้เล่น
สล็อต: แจ็คพอตแตกง่าย ลุ้นได้ทุกวัน
เกมสด: เล่นสดเหมือนอยู่ในคาสิโนจริง
กีฬา: รองรับลีกดังระดับโลก
ยิงปลา: ลุ้นกำไรจากเกมยิงปลา
รับโบนัสและข้อเสนอสุดคุ้ม
อย่าลืมแวะมาเยี่ยมชมที่หน้า โบนัส เพื่อรับ สิทธิพิเศษมากมาย ที่เรามอบให้สมาชิกทุกท่าน นอกจากนี้ยังมีระบบ ลูกค้าระดับพรีเมียม สำหรับลูกค้าคนสำคัญ และช่องทาง แอฟฟิลิเอต สำหรับผู้ที่สนใจสร้างรายได้ร่วมกับเรา
ติดต่อเรา
หากมี คำถาม หรือ ข้อเสนอแนะ สามารถติดต่อทีมงานของเราได้ตลอด 24 ชั่วโมงที่หน้า ติดต่อเรา และ ข้อเสนอแนะ ทีมงาน ของเรา ยินดีให้บริการทุกท่านด้วยใจ
casino en ligne le plus payant · March 5, 2026 at 4:46 pm
Great post, keep up the good work, I hope you don’t mind but I’ve added on my blog roll.
RodneyChoix · March 5, 2026 at 5:08 pm
ทดลองเล่นสล็อต pg
TKBNEKO เปิดประสบการณ์ใหม่แห่งการเดิมพันออนไลน์ ธุรกรรมรวดเร็ว ด้วยระบบสแกน QR Code
ในยุคดิจิทัลที่ โลกออนไลน์เติบโตต่อเนื่อง TKBNEKO พร้อมยกระดับการให้บริการ ด้วยระบบที่ ล้ำสมัย เสถียร และ โปร่งใส เพื่อให้ผู้เล่น มั่นใจ ทุกครั้งที่ใช้งาน
ระบบการเงินที่ใช้งานง่าย
ฝากขั้นต่ำ: เริ่มต้น 1 บาท
ถอนขั้นต่ำ: ขั้นต่ำ 1 บาท
เวลาฝากเงิน: ใช้เวลาเพียง 3 วินาที
ยอดถอน: ไม่จำกัดต่อวัน
ฝากง่าย เพียงสแกน QR Code
สแกน คิวอาร์ ระบบจะ ประมวลผลอัตโนมัติ ขั้นต่ำ 100 บาท สูงสุด 500,000 บาท
เกมยอดนิยม
สล็อต: ลุ้นแจ็คพอต
เกมสด: ดีลเลอร์สด
กีฬา: แมตช์ทั่วโลก
ยิงปลา: ลุ้นกำไรทันที
โปรโมชั่นและสิทธิพิเศษ
ติดตามหน้า โบนัส พร้อมระบบ VIP และโปรแกรม แอฟฟิลิเอต
ฝ่ายบริการลูกค้า
สอบถามข้อมูลได้ตลอด 24 ชั่วโมง ผ่านหน้า ศูนย์ช่วยเหลือ ทีมงาน TKBNEKO พร้อมดูแลตลอดเวลา
https://medium.com/@ratypw/ทดลองเล่นสล็อต-pg-e598fa477f69
олимпбет линия · March 5, 2026 at 5:21 pm
Sizdə əla kontent var — xüsusilə strateji bölməsi ilə bağlı.
https://olimpbet-az.icu/app
casinos online · March 5, 2026 at 5:39 pm
Magnificent beat ! Can I be your apprentice? Just kidding!
Tyronetar · March 5, 2026 at 8:00 pm
Good afternoon!
Share estate mysterious wills with interesting and valuable inheritance updates and leave a lasting legacy see on the website for estate planning
Full information on the link – https://33capy.site
All the best and development in business!
JosephBer · March 5, 2026 at 8:31 pm
ทดลองเล่นสล็อต pg
สล็อต PG สล็อตยอดฮิต เข้าเล่นไว ฝากถอนออโต้
คำค้นหา pg slot กำลังได้รับความนิยมอย่างต่อเนื่อง ในกลุ่มผู้เล่นเกมสล็อตออนไลน์ เพราะเป็น ค่ายเกมที่มีชื่อเสียง ด้าน ภาพและเอฟเฟกต์ ความ เสถียร และ ระบบจ่ายที่ดึงดูด เกมของ PG พัฒนาโดยผู้ให้บริการชั้นนำ ที่รองรับการเล่นทั้งบน โทรศัพท์มือถือ และ คอมพิวเตอร์
ข้อดี ของ PG Slot
pg slot เป็นเกมสล็อตออนไลน์ที่ออกแบบมาให้ โหลดเร็ว เล่นผ่าน ระบบออนไลน์ และรองรับ ทุกอุปกรณ์ ไม่ต้องดาวน์โหลดแอป ผู้เล่นสามารถเข้าเล่นผ่าน หน้าเว็บ ได้ทันที ภาพและเสียงถูกพัฒนาในรูปแบบ สามมิติ ให้ความคมชัด พร้อมเอฟเฟกต์ สวยงาม
คุณสมบัติหลักของเกม PG Slot ได้แก่
ระบบโบนัสและฟรีสปินหลากหลายรูปแบบ
ฟีเจอร์ตัวคูณรางวัล
เล่นฟรีก่อนเติมเงิน
ใช้งานภาษาไทยง่าย
ระบบฝากถอนสะดวก ทำรายการไว
แพลตฟอร์ม สล็อต PG โดยทั่วไปให้บริการ การฝาก-ถอน อัตโนมัติ 24 ชั่วโมง ขั้นต่ำเริ่มต้นเพียง 1 บาท ขึ้นอยู่กับ กติกาแต่ละแพลตฟอร์ม การทำรายการใช้เวลา รวดเร็วมาก ผ่าน QR Code หรือระบบ ธนาคารบนมือถือ ทำให้ธุรกรรมเป็นไปอย่าง ลื่นไหล
ประเภทเกมยอดนิยม ใน pg slot
เกม pg slot มีธีมหลากหลาย เช่น
ธีม เทพเจ้าและแฟนตาซี
ธีม ผจญภัย
ธีม เอเชียและโชคลาภ
ธีม ธรรมชาติ
เกมยอดนิยมมักเป็นเกมที่แตกง่าย พร้อมระบบ โบนัสรอบพิเศษ และ อัตราการจ่ายที่สูง เหมาะกับทั้ง คนเพิ่งเล่น และ ผู้เล่นมือโปร
ความน่าเชื่อถือ
PG Slot มีมาตรฐานรองรับ มีการ ปกป้องข้อมูลผู้เล่น และใช้ระบบสุ่มผล ระบบสุ่มมาตรฐาน เพื่อให้ผลลัพธ์ ยุติธรรม แพลตฟอร์มที่ให้บริการ สล็อต PG ควรมี ระบบดูแลข้อมูล
สรุป
pg slot เป็นตัวเลือกยอดนิยมสำหรับผู้ที่ต้องการเล่นสล็อตออนไลน์ ด้วยจุดเด่นด้าน กราฟิกคุณภาพ และการทำธุรกรรมที่ ทันใจ ผู้เล่นสามารถเริ่มต้นได้ ทันที ฝากถอนสะดวก และเลือกเกมได้ ครบทุกหมวด เหมาะสำหรับ ทั้งมือใหม่และมือโปร ในโลกของเกมสล็อตออนไลน์
https://medium.com/@ratypw/ทดลองเล่นสล็อต-pg-70cdb1132344
Josephneupt · March 5, 2026 at 8:32 pm
ทดลองเล่นสล็อต pg ฟรี สล็อต PG เกมสล็อตออนไลน์ที่คนค้นหาเยอะ เข้าเล่นไว ฝากถอนออโต้
คำค้นหา PG Slot กำลังได้รับความนิยมอย่างต่อเนื่อง ในกลุ่มผู้เล่นเกมสล็อตออนไลน์ เพราะเป็น แบรนด์เกมที่โดดเด่น ด้าน กราฟิก ความ นิ่งไม่สะดุด และ อัตราการจ่ายรางวัลที่น่าสนใจ เกมของ PG พัฒนาโดยผู้ให้บริการชั้นนำ ที่รองรับการเล่นทั้งบน มือถือ และ คอมพิวเตอร์
จุดเด่น ของ PG Slot
pg slot เป็นเกมสล็อตออนไลน์ที่ออกแบบมาให้ เข้าเกมไว เล่นผ่าน ระบบอัตโนมัติ และรองรับ ทุกอุปกรณ์ ไม่ต้องดาวน์โหลดแอป ผู้เล่นสามารถเข้าเล่นผ่าน Browser ได้ทันที ภาพและเสียงถูกพัฒนาในรูปแบบ 3D ให้ความคมชัด พร้อมเอฟเฟกต์ สวยงาม
คุณสมบัติหลักของเกม pg slot ได้แก่
มีรอบโบนัสให้ลุ้นบ่อย
Multiplier
เล่นฟรีก่อนเติมเงิน
ใช้งานภาษาไทยง่าย
ฝากถอนง่าย ไม่ต้องรอนาน
แพลตฟอร์ม สล็อต PG ส่วนใหญ่รองรับ การฝาก-ถอน ออโต้ตลอด 24 ชม. ขั้นต่ำเริ่มต้นเพียง หลักหน่วย ขึ้นอยู่กับ เงื่อนไขของเว็บไซต์ การทำรายการใช้เวลา เพียงไม่กี่วินาที ผ่าน สแกน QR หรือระบบ Mobile Banking ทำให้ธุรกรรมเป็นไปอย่าง ต่อเนื่อง
ประเภทเกมยอดนิยม ใน PG Slot
เกม PG Slot มีธีมหลากหลาย เช่น
ธีม แฟนตาซี
ธีม ผจญภัย
ธีม เอเชียและโชคลาภ
ธีม Animal
ผู้เล่นนิยมเกมที่มีรอบพิเศษบ่อย พร้อมระบบ ฟีเจอร์พิเศษ และ อัตราการจ่ายที่สูง เหมาะกับทั้ง มือใหม่ และ สายสล็อตจริงจัง
ความปลอดภัย
PG Slot มีมาตรฐานรองรับ มีการ รักษาความปลอดภัย และใช้ระบบสุ่มผล ระบบสุ่มมาตรฐาน เพื่อให้ผลลัพธ์ ตรวจสอบได้ แพลตฟอร์มที่ให้บริการ PG Slot ควรมี ระบบดูแลข้อมูล
สรุป
สล็อต PG เป็นตัวเลือกยอดนิยมสำหรับผู้ที่ต้องการเล่นสล็อตออนไลน์ ด้วยจุดเด่นด้าน โบนัสหลากหลาย และการทำธุรกรรมที่ รวดเร็ว ผู้เล่นสามารถเริ่มต้นได้ ทันที ฝากถอนสะดวก และเลือกเกมได้ จำนวนมาก เหมาะสำหรับ ทุกระดับประสบการณ์ ในโลกของเกมสล็อตออนไลน์
gegraveerd hondenpenning · March 5, 2026 at 8:57 pm
Hi there, just became aware of your blog through Google, and found that it’s truly informative. It’s important to cover these trends.
tuan88 · March 5, 2026 at 9:13 pm
tuan88
nuevos casinos online · March 5, 2026 at 9:20 pm
I think other website proprietors should take this web site as an model, very clean and great user pleasant style and design .
https://FreeBestAds.com/588/posts/1/1/1961094.html · March 5, 2026 at 9:32 pm
https://FreeBestAds.com/588/posts/1/1/1961094.html
escort agencies and massage parlours in Spain · March 5, 2026 at 9:35 pm
Escort directory listing Spain
Interestmar · March 5, 2026 at 11:34 pm
Hello!
Protect house with interesting mysterious data holding valuable security keys now and sleep soundly at home see on the website for home security
Full information on the link – https://niidetgastro.ru/preimushhestva-zashhitnyh-kozyrkov-iz-polikarbonata-optovymi-postavkami/
All the best and development in business!
sieraden graveren · March 6, 2026 at 1:29 am
Pretty impressive article. I just stumbled upon your site and wanted to say that I have really enjoyed reading your opinions. Any way I’ll be coming back and I hope you post again soon.
Interestmar · March 6, 2026 at 2:33 am
Hello everyone!
Find eat mysterious habits in interesting diets with valuable health solutions now and nourish your body right see on the website for diet plans
Full information on the link – https://garnizon54.ru/vedra-stroitelnye-eto-kazalos-by-prostoj-no-nezamenimyj-instrument/
All the best and development in business!
Tool Collection · March 6, 2026 at 4:38 am
“This saved me so much time. Cheers!”
Interestmar · March 6, 2026 at 6:30 am
Good morning!
Decode light mysterious speeds containing interesting and valuable optical facts and chase photons across the cosmos see on the website for optics labs
Full information on the link – https://strunader.ru/izgotovlenie-plastikovoy-tary-na-zakaz-osnovnye-preimuschestva-i-tehnologii-proizvodstva.html
All the best and development in business!
https://t.me/s/evacasino_official/14 · March 6, 2026 at 8:48 am
eva casino официальный сайт
http://bioimagingcore.be/q2a/user/promoafrique20264 · March 6, 2026 at 11:33 am
http://bioimagingcore.be/q2a/user/promoafrique20264
online casino canada · March 6, 2026 at 2:09 pm
Keep it up!. I usually don’t post in Blogs but your blog forced me to, amazing work.. beautiful A rise in An increase in An increase in.
buy doxycycline online · March 6, 2026 at 3:24 pm
doxycycline
buy doxycycline online · March 6, 2026 at 3:41 pm
buy doxycycline
doxycycline · March 6, 2026 at 3:57 pm
buy doxycycline online
online kasino · March 6, 2026 at 4:47 pm
I was suggested this website by my cousin. I am not sure whether this post is written by him as no one else know such detailed about my difficulty. You are wonderful! Thanks!
doxycycline · March 6, 2026 at 5:02 pm
buy doxycycline
meilleur casino en ligne canada · March 6, 2026 at 5:11 pm
What a great article.. i subscribed btw!
buy doxycycline · March 6, 2026 at 5:18 pm
doxycycline
buy doxycycline · March 6, 2026 at 5:33 pm
doxycycline
buy doxycycline online · March 6, 2026 at 5:48 pm
buy doxycycline
buy doxycycline · March 6, 2026 at 6:03 pm
buy doxycycline online
doxycycline · March 6, 2026 at 6:18 pm
buy doxycycline online
buy doxycycline · March 6, 2026 at 6:34 pm
doxycycline
buy doxycycline online · March 6, 2026 at 6:51 pm
buy doxycycline
lnezbrg · March 6, 2026 at 7:02 pm
https://www.deriaskin.com/index.php?route=journal3/blog/post&journal_blog_post_id=10
doxycycline · March 6, 2026 at 7:06 pm
doxycycline
buy doxycycline · March 6, 2026 at 7:21 pm
buy doxycycline
best casino online real money · March 6, 2026 at 7:22 pm
I like your quality that you put into your writing . Please do continue with more like this.
neue casinos · March 6, 2026 at 7:44 pm
I just couldn’t leave your web site prior to suggesting that I really enjoyed the standard info an individual supply to your guests? Is going to be again continuously in order to inspect new posts
buy doxycycline · March 6, 2026 at 7:54 pm
buy doxycycline online
buy doxycycline · March 6, 2026 at 8:09 pm
buy doxycycline online
buy doxycycline · March 6, 2026 at 8:25 pm
buy doxycycline online
buy doxycycline online · March 6, 2026 at 9:23 pm
buy doxycycline
doxycycline · March 6, 2026 at 9:38 pm
buy doxycycline online
https://jeemainresult2017.com/code-promo-1xbet-2026-new888-bonus-100-130-e/ · March 6, 2026 at 9:57 pm
https://jeemainresult2017.com/code-promo-1xbet-2026-new888-bonus-100-130-e/
kasyno online polska · March 7, 2026 at 1:03 am
Thanks for a Interesting item; I enjoyed it very much. Regards Sang Magistrale
SUKSESTOTO · March 7, 2026 at 2:57 am
I think that may be an interesting element, it made me assume a bit. Thanks for sparking my considering cap. On occasion I get so much in a rut that I simply really feel like a record.
meilleur casino en ligne · March 7, 2026 at 3:07 am
Our local network of agencies has found your research so helpful.
Jasonsuide · March 7, 2026 at 3:13 am
pg
TKBNEKO มอบมิติใหม่ของการเดิมพันออนไลน์ ฝาก-ถอนไว ด้วยระบบสแกน คิวอาร์โค้ด
ในยุคที่ โลกออนไลน์พัฒนาอย่างรวดเร็ว TKBNEKO พร้อมยกระดับมาตรฐานการเดิมพัน ด้วยระบบการให้บริการที่ ล้ำสมัย รวดเร็ว และ ตรวจสอบได้ พร้อมต้อนรับสมาชิกทุกท่านสู่ ประสบการณ์ความบันเทิงรูปแบบใหม่ ที่ ใครๆ ก็เป็นเถ้าแก่ได้
ทำไมต้อง TKBNEKO?
แพลตฟอร์มของเรารวบรวมเกมที่ได้มาตรฐาน โดยเฉพาะเกมที่ มีใบรับรองอย่างถูกต้อง และ เป็นที่นิยมในระดับสากล เพื่อให้ผู้เล่นทุกคน อุ่นใจ ได้ว่า จะได้รับความเพลิดเพลินกับเกมที่ ไม่มีการเอาเปรียบ มีระบบรักษาความปลอดภัยสูง และ ตอบโจทย์ผู้เล่นยุคใหม่
ระบบการเงินที่เหนือกว่า
ระบบฝากถอนถูกพัฒนาให้ใช้งานง่าย เพื่อให้คุณ เล่นเกมได้แบบไม่สะดุด
ฝากขั้นต่ำ: ขั้นต่ำแค่ 1 บาท
ถอนขั้นต่ำ: เพียง 1 บาท
เวลาฝากเงิน: รวดเร็วทันใจใน 3 วินาที
ยอดจำกัดการถอน: ไม่มีลิมิตการถอนรายวัน
เติมเงินง่ายด้วย QR Code
เพียงคุณสแกน คิวอาร์ ระบบของเราจะ ดำเนินการฝากเงินให้อัตโนมัติ ขั้นต่ำเพียง อย่างน้อย 100 บาท และสามารถฝากได้สูงถึง 500,000 บาท มาร่วมสนุกกันได้แล้ววันนี้ กับ TKBNEKO ที่ ตอบโจทย์การเดิมพันยุคใหม่
เกมยอดนิยมรวมไว้ในที่เดียว
แพลตฟอร์มของเราครอบคลุมทุกแนวเกม รองรับทุกความชอบของผู้เล่น
สล็อต: หลากหลายธีม แจ็คพอตรอคุณอยู่
เกมสด: ดีลเลอร์ถ่ายทอดสดตลอดเวลา
กีฬา: วางเดิมพันกีฬาหลากหลายรายการ
ยิงปลา: ลุ้นกำไรจากเกมยิงปลา
ติดตามโปรโมชั่นและสิทธิพิเศษ
อย่าลืมแวะมาเยี่ยมชมที่หน้า โบนัส เพื่อรับ สิทธิพิเศษมากมาย ที่เรามอบให้สมาชิกทุกท่าน นอกจากนี้ยังมีระบบ ลูกค้าระดับพรีเมียม สำหรับลูกค้าคนสำคัญ และช่องทาง แอฟฟิลิเอต สำหรับผู้ที่สนใจสร้างรายได้ร่วมกับเรา
ติดต่อเรา
หากมี คำถาม หรือ ความคิดเห็น สามารถติดต่อทีมงานของเราได้ตลอด 24 ชั่วโมงที่หน้า ศูนย์ช่วยเหลือ และ ข้อเสนอแนะ ทีมงาน ของเรา ยินดีให้บริการทุกท่านด้วยใจ
Interestmar · March 7, 2026 at 2:26 pm
Hello!
Explore build mysterious codes with interesting and valuable safety process features and construct safely see on the website for building codes
Full information on the link – https://snabog.ru/vyrashhivanie-ovoshhej/rassada/vybor-gorshkov-dlya-rassady-chto-nuzhno-znat-sadovodam/
All the best and development in business!
paras nettikasino · March 7, 2026 at 3:52 pm
You need to really control the comments listed here
RodneyomIma · March 7, 2026 at 4:59 pm
Всем привет! Наткнулся на статью, где собраны не просто базовые понятия, а реально работающие стратегии и инструменты с привязкой к текущим реалиям. Автор рассматривает комплексный подход: от сбора семантики до юзабилити и работы с интентом. Очень порадовало, что материал свежий (январь 2026) и учитывает последние тренды. Оставляю ссылку здесь, может, кому-то пригодится для актуализации своих знаний: https://sobolland.ru/prodvizhenie-sajtov-strategii-instrumenty-i-aktualnye-podhody/ . Особенно полезно будет новичкам для формирования целостной картины.
RodneyomIma · March 7, 2026 at 5:03 pm
Знакомая ситуация, многие начинают паниковать и скупать ссылки, что только усугубляет положение. Хорошая статья попалась именно про то, как действовать без паники после апдейтов. Автор разбирает, на какие элементы сайта (техничка, контент, поведенческие) нужно обращать внимание в первую очередь, чтобы вернуть позиции. Особенно актуально для автосайтов, но общие принципы подойдут многим. Кто еще не видел, вот ссылка: https://specavto43.ru/pochemu-avtosajty-teryayut-poziczii-posle-apdejtov-chto-chinit-v-pervuyu-ochered-bez-paniki/ . Спокойный и структурированный разбор.
Interestmar · March 7, 2026 at 5:54 pm
Hello everyone!
Investigate age mysterious factors offering interesting and valuable longevity data and unlock the secrets of aging see on the website for longevity research
Full information on the link – https://rossignol.ru/plastikovye-kompostery-kak-idealnyj-sposob-pererabotki-organicheskih-othodov/
All the best and development in business!
turvallinen nettikasino · March 7, 2026 at 6:13 pm
I think it is a nice point of view. I most often meet people who rather say what they suppose others want to hear. Good and well written! I will come back to your site for sure!
RodneyChoix · March 7, 2026 at 7:11 pm
ทดลองเล่นสล็อต pg
แพลตฟอร์ม TKBNEKO เปิดประสบการณ์ใหม่แห่งการเดิมพันออนไลน์ ธุรกรรมรวดเร็ว ด้วยระบบสแกน คิวอาร์โค้ด
ในยุคดิจิทัลที่ โลกออนไลน์เติบโตต่อเนื่อง TKBNEKO พร้อมยกระดับการให้บริการ ด้วยระบบที่ ทันสมัย เสถียร และ ตรวจสอบได้ เพื่อให้ผู้เล่น มั่นใจ ทุกครั้งที่ใช้งาน
ระบบการเงินที่ใช้งานง่าย
ฝากขั้นต่ำ: 1 บาท
ถอนขั้นต่ำ: 1 บาท
เวลาฝากเงิน: ใช้เวลาเพียง 3 วินาที
ยอดถอน: ไม่มีลิมิต
ฝากง่าย เพียงสแกน QR Code
สแกน คิวอาร์ ระบบจะ โอนเงินเข้าทันที ขั้นต่ำ 100 บาท สูงสุด ไม่เกิน 500,000 บาทต่อครั้ง
หมวดหมู่เกม
สล็อต: ธีมหลากหลาย
เกมสด: คาสิโนเรียลไทม์
กีฬา: เดิมพันลีกดัง
ยิงปลา: ลุ้นกำไรทันที
โปรโมชั่นและสิทธิพิเศษ
ติดตามหน้า โบนัส พร้อมระบบ สมาชิกพรีเมียม และโปรแกรม พันธมิตร
ฝ่ายบริการลูกค้า
สอบถามข้อมูลได้ตลอด 24 ชั่วโมง ผ่านหน้า ติดต่อเรา ทีมงาน ของเรา พร้อมดูแลตลอดเวลา
https://medium.com/@ratypw/ทดลองเล่นสล็อต-pg-e598fa477f69
best canadian online casino · March 7, 2026 at 8:29 pm
A friend of mine advised this site. And yes. it has some useful pieces of info and I enjoyed scaning it. Therefore i would love to drop you a quick note to express my thank. Take care
best canadian online casino · March 7, 2026 at 8:35 pm
The post is absolutely great! Lots of great info and inspiration, both of which we all need! Also like to admire the time and effort you put into your blog and detailed information you offer! I will bookmark your website!
nejlepší online casino · March 7, 2026 at 8:43 pm
Spot on with this write-up, I truly believe this website requirements a lot much more consideration. I’ll probably be once more to read much much more, thanks for that info.
casino en ligne · March 7, 2026 at 8:47 pm
I just couldn’t leave your web site prior to suggesting that I really enjoyed the standard info an individual supply to your guests? Is going to be again continuously in order to inspect new posts
nejlepší online casino · March 7, 2026 at 8:50 pm
I want to see your book when it comes out.
polskie kasyno online · March 7, 2026 at 9:06 pm
Howdy, a helpful article for sure. Thank you.
casino en ligne international · March 7, 2026 at 9:19 pm
Hi, do have a e-newsletter? In the event you don’t definately should get on that piece…this web site is pure gold!
Interestmar · March 7, 2026 at 10:27 pm
Hello everyone!
Access astro mysterious charts full of interesting and valuable cosmic knowledge and read the stars accurately see on the website for astrology charts
Full information on the link – https://poisk-banka.ru/novosti/gorshki-dlya-rassady-sovety-dlya-nachinajushhih-sadovodov/
All the best and development in business!
best online casino · March 8, 2026 at 1:15 am
This is one very informative blog. I like the way you write and I will bookmark your blog to my favorites.
paras nettikasino · March 8, 2026 at 2:58 am
Thank you for the auspicious writeup.
meilleur casino en ligne canada · March 8, 2026 at 3:43 am
Very nice post. I just stumbled upon your blog and wanted to say that I’ve really enjoyed browsing your blog posts. In any case I’ll be subscribing to your rss feed and I hope you write again soon!
nettikasino · March 8, 2026 at 4:54 am
I cannot thank you more than enough for the blogposts on your website. I know you set a lot of time and energy into these and truly hope you know how deeply I appreciate it. I hope I’ll do a similar thing person sooner or later.
paras nettikasino · March 8, 2026 at 5:34 am
Hi there! I just wanted to ask if you ever have any trouble with hackers? My last blog (wordpress) was hacked and I ended up losing several weeks of hard work due to no back up. Do you have any solutions to protect against hackers?
winslot link · March 8, 2026 at 8:59 am
We can see that we need to develop policies to deal with this trend.
BradleyBit · March 8, 2026 at 12:30 pm
PG Slot เกมสล็อตออนไลน์ที่คนค้นหาเยอะ ใช้งานง่าย ฝากถอนรวดเร็ว
คำค้นหา PG Slot มาแรงในช่วงนี้ ในกลุ่มผู้เล่นเกมสล็อตออนไลน์ เพราะเป็น ผู้ให้บริการเกมสล็อตที่มาแรง ด้าน กราฟิก ความ ลื่นไหล และ โอกาสรับกำไรที่ดี เกมของ PG พัฒนาโดยผู้ให้บริการชั้นนำ ที่รองรับการเล่นทั้งบน สมาร์ทโฟน และ เดสก์ท็อป
ความโดดเด่น ของ สล็อต PG
PG Slot เป็นเกมสล็อตออนไลน์ที่ออกแบบมาให้ โหลดเร็ว เล่นผ่าน ระบบเว็บ และรองรับ ทุกแพลตฟอร์ม ไม่ต้องติดตั้งเพิ่มเติม ผู้เล่นสามารถเข้าเล่นผ่าน Browser ได้ทันที ภาพและเสียงถูกพัฒนาในรูปแบบ สามมิติ ให้ความคมชัด พร้อมเอฟเฟกต์ จัดเต็ม
คุณสมบัติหลักของเกม pg slot ได้แก่
มีรอบโบนัสให้ลุ้นบ่อย
ระบบตัวคูณ
โหมดทดลองเล่นฟรี
รองรับภาษาไทยเต็มรูปแบบ
ฝากถอนง่าย ทำรายการไว
แพลตฟอร์ม pg slot มักมี การฝาก-ถอน อัตโนมัติ 24 ชั่วโมง ขั้นต่ำเริ่มต้นเพียง 10 บาท ขึ้นอยู่กับ เงื่อนไขของเว็บไซต์ การทำรายการใช้เวลา เพียงไม่กี่วินาที ผ่าน สแกน QR หรือระบบ ธนาคารบนมือถือ ทำให้ธุรกรรมเป็นไปอย่าง ต่อเนื่อง
แนวเกมที่คนเล่นเยอะ ใน pg slot
เกม pg slot มีธีมหลากหลาย เช่น
ธีม แฟนตาซี
ธีม ลุยด่าน
ธีม เอเชียและโชคลาภ
ธีม Animal
ผู้เล่นนิยมเกมที่มีรอบพิเศษบ่อย พร้อมระบบ Special Feature และ อัตราการจ่ายที่สูง เหมาะกับทั้ง คนเพิ่งเล่น และ ผู้เล่นมือโปร
ความน่าเชื่อถือ
สล็อต PG มีมาตรฐานรองรับ มีการ เข้ารหัสข้อมูล และใช้ระบบสุ่มผล Random Number Generator เพื่อให้ผลลัพธ์ ยุติธรรม แพลตฟอร์มที่ให้บริการ pg slot ควรมี ทีมซัพพอร์ต 24 ชม.
โดยภาพรวม
pg slot เป็นตัวเลือกยอดนิยมสำหรับผู้ที่ต้องการเล่นสล็อตออนไลน์ ด้วยจุดเด่นด้าน โบนัสหลากหลาย และการทำธุรกรรมที่ ทันใจ ผู้เล่นสามารถเริ่มต้นได้ ไม่ซับซ้อน ฝากถอนสะดวก และเลือกเกมได้ จำนวนมาก เหมาะสำหรับ ทุกระดับประสบการณ์ ในโลกของเกมสล็อตออนไลน์
Travisjal · March 8, 2026 at 12:35 pm
สล็อต
TKBNEKO เปิดประสบการณ์ใหม่แห่งการเดิมพันออนไลน์ ธุรกรรมรวดเร็ว ด้วยระบบสแกน QR Code
ในยุคดิจิทัลที่ เทคโนโลยีพัฒนาอย่างรวดเร็ว เรามุ่งเน้นมาตรฐานใหม่ของการเดิมพัน ด้วยระบบที่ ทันสมัย เสถียร และ ตรวจสอบได้ เพื่อให้ผู้เล่น อุ่นใจ ทุกครั้งที่ใช้งาน
จุดเด่นระบบฝาก-ถอน
ฝากขั้นต่ำ: 1 บาท
ถอนขั้นต่ำ: 1 บาท
เวลาฝากเงิน: ภายใน 3 วินาที
ยอดถอน: ไม่มีลิมิต
เติมเงินง่าย แค่สแกน
สแกน คิวอาร์ ระบบจะ โอนเงินเข้าทันที ขั้นต่ำ 100 บาท สูงสุด ไม่เกิน 500,000 บาทต่อครั้ง
หมวดหมู่เกม
สล็อต: ธีมหลากหลาย
เกมสด: คาสิโนเรียลไทม์
กีฬา: แมตช์ทั่วโลก
ยิงปลา: สนุกได้เงินจริง
โปรโมชั่นและสิทธิพิเศษ
ติดตามหน้า โปรโมชั่น พร้อมระบบ VIP และโปรแกรม แอฟฟิลิเอต
ติดต่อเรา
สอบถามข้อมูลได้ตลอด 24 ชั่วโมง ผ่านหน้า ศูนย์ช่วยเหลือ ทีมงาน ของเรา พร้อมดูแลตลอดเวลา
https://medium.com/@ratypw/ทดลองเล่นสล็อต-a4ea8e21fdde
FelixGug · March 8, 2026 at 12:38 pm
สล็อต
แพลตฟอร์ม TKBNEKO เปิดประสบการณ์ใหม่แห่งการเดิมพันออนไลน์ ฝาก-ถอนไว ด้วยระบบสแกน QR Code
ในยุคดิจิทัลที่ เทคโนโลยีพัฒนาอย่างรวดเร็ว เรามุ่งเน้นมาตรฐานใหม่ของการเดิมพัน ด้วยระบบที่ ล้ำสมัย เสถียร และ โปร่งใส เพื่อให้ผู้เล่น อุ่นใจ ทุกครั้งที่ใช้งาน
ระบบการเงินที่ใช้งานง่าย
ฝากขั้นต่ำ: 1 บาท
ถอนขั้นต่ำ: ขั้นต่ำ 1 บาท
เวลาฝากเงิน: ภายใน 3 วินาที
ยอดถอน: ไม่จำกัดต่อวัน
เติมเงินง่าย แค่สแกน
สแกน คิวอาร์ ระบบจะ โอนเงินเข้าทันที ขั้นต่ำ 100 บาท สูงสุด ไม่เกิน 500,000 บาทต่อครั้ง
เกมยอดนิยม
สล็อต: ลุ้นแจ็คพอต
เกมสด: ดีลเลอร์สด
กีฬา: เดิมพันลีกดัง
ยิงปลา: ลุ้นกำไรทันที
โบนัสและโปรโมชัน
ติดตามหน้า โปรโมชั่น พร้อมระบบ VIP และโปรแกรม พันธมิตร
ติดต่อเรา
สอบถามข้อมูลได้ตลอด 24 ชั่วโมง ผ่านหน้า ติดต่อเรา ทีมงาน TKBNEKO พร้อมดูแลตลอดเวลา
Charlestub · March 8, 2026 at 12:47 pm
PG Slot สล็อตยอดฮิต ใช้งานง่าย ฝากถอนรวดเร็ว
คำค้นหา สล็อต PG กำลังได้รับความนิยมอย่างต่อเนื่อง ในกลุ่มผู้เล่นเกมสล็อตออนไลน์ เพราะเป็น ค่ายเกมที่มีชื่อเสียง ด้าน กราฟิก ความ นิ่งไม่สะดุด และ โอกาสรับกำไรที่ดี เกมของ PG ผลิตโดยค่ายมาตรฐาน ที่รองรับการเล่นทั้งบน โทรศัพท์มือถือ และ คอมพิวเตอร์
จุดเด่น ของ pg slot
PG Slot เป็นเกมสล็อตออนไลน์ที่ออกแบบมาให้ เปิดเกมได้ทันที เล่นผ่าน ระบบเว็บ และรองรับ ทุกอุปกรณ์ ไม่ต้องติดตั้งเพิ่มเติม ผู้เล่นสามารถเข้าเล่นผ่าน Browser ได้ทันที ภาพและเสียงถูกพัฒนาในรูปแบบ สามมิติ ให้ความคมชัด พร้อมเอฟเฟกต์ สวยงาม
คุณสมบัติหลักของเกม PG Slot ได้แก่
โบนัสและฟรีสปินหลายแบบ
ฟีเจอร์ตัวคูณรางวัล
โหมดทดลองเล่นฟรี
รองรับภาษาไทยเต็มรูปแบบ
ระบบฝากถอนสะดวก ทำรายการไว
แพลตฟอร์ม pg slot มักมี การฝาก-ถอน อัตโนมัติ 24 ชั่วโมง ขั้นต่ำเริ่มต้นเพียง หลักหน่วย ขึ้นอยู่กับ ระบบของผู้ให้บริการ การทำรายการใช้เวลา รวดเร็วมาก ผ่าน สแกน QR หรือระบบ แอปธนาคาร ทำให้ธุรกรรมเป็นไปอย่าง ต่อเนื่อง
แนวเกมที่คนเล่นเยอะ ใน pg slot
เกม สล็อต PG มีธีมหลากหลาย เช่น
ธีม แฟนตาซี
ธีม Adventure
ธีม ความมั่งคั่ง
ธีม ธรรมชาติ
ผู้เล่นนิยมเกมที่มีรอบพิเศษบ่อย พร้อมระบบ ฟีเจอร์พิเศษ และ อัตราการจ่ายที่สูง เหมาะกับทั้ง ผู้เล่นเริ่มต้น และ ผู้เล่นมือโปร
ความน่าเชื่อถือ
สล็อต PG พัฒนาในระบบสากล มีการ รักษาความปลอดภัย และใช้ระบบสุ่มผล Random Number Generator เพื่อให้ผลลัพธ์ โปร่งใส แพลตฟอร์มที่ให้บริการ pg slot ควรมี ทีมซัพพอร์ต 24 ชม.
สรุป
สล็อต PG เป็นตัวเลือกยอดนิยมสำหรับผู้ที่ต้องการเล่นสล็อตออนไลน์ ด้วยจุดเด่นด้าน ระบบลื่นไหล และการทำธุรกรรมที่ ไว ผู้เล่นสามารถเริ่มต้นได้ ทันที ฝากถอนสะดวก และเลือกเกมได้ จำนวนมาก เหมาะสำหรับ ทั้งมือใหม่และมือโปร ในโลกของเกมสล็อตออนไลน์
https://medium.com/@ratypw/ทดลองเล่นสล็อต-pg-70cdb1132344
брачни халки · March 8, 2026 at 12:51 pm
колие
best online casino · March 8, 2026 at 4:21 pm
Please let us know when you plan to publish your book!
parhaat nettikasinot · March 8, 2026 at 4:41 pm
Amazing content on your website.
best online casino · March 8, 2026 at 5:54 pm
This information is very important and you’ll need to know this when you constructor your own photo voltaic panel.
casino en ligne france · March 8, 2026 at 7:18 pm
Excellent read, I just passed this onto a colleague who was doing a little research on that. And he actually bought me lunch because I found it for him smile So let me rephrase that.|
tiktok follower kaufen · March 8, 2026 at 7:47 pm
This information is critically needed, thanks.
waw4d login · March 8, 2026 at 8:22 pm
The clarity in your post is just nice and I can tell you are an expert in the subject matter.
online casino belgië · March 8, 2026 at 8:42 pm
I thought it was going to be some boring old post, but I’m glad I visited. I will post a link to this site on my blog. I am sure my visitors will find that very useful.
best online casino · March 8, 2026 at 9:09 pm
Thanks for a Interesting item; I enjoyed it very much. Regards Sang Magistrale
instagram follower kaufen · March 8, 2026 at 9:47 pm
I like your style!
sports · March 8, 2026 at 11:01 pm
Fortune Tiger vs Fortune Ox: qual tem maior potencial de 10000x em 2026?
tiktok follower kaufen · March 8, 2026 at 11:55 pm
Thanks For This Blog, was added to my bookmarks.
tiktok follower kaufen · March 9, 2026 at 1:41 am
What a great article.. i subscribed btw!
parhaat nettikasinot · March 9, 2026 at 2:12 am
This is something that will need all of our combined efforts to address.
instagram follower kaufen · March 9, 2026 at 2:21 am
A neighbor of mine encouraged me to take a look at your blog site couple weeks ago, given that we both love similar stuff and I will need to say I am quite impressed.
instagram follower kaufen · March 9, 2026 at 3:42 am
Abnormal this put up is totaly unrelated to what I was searching google for, but it surely used to be listed at the first page. I suppose your doing one thing proper if Google likes you adequate to place you at the first page of a non similar search.
instagram follower kaufen · March 9, 2026 at 5:43 am
This is one very informative blog. I like the way you write and I will bookmark your blog to my favorites.
tiktok follower kaufen · March 9, 2026 at 5:47 am
I like your style!
best online casino · March 9, 2026 at 6:30 am
Nice read, I just passed this onto a colleague who was doing some research on that. And he just bought me lunch as I found it for him smile Therefore let me rephrase that: Thank you for lunch!
doxycycline · March 9, 2026 at 7:49 am
buy doxycycline online
buy doxycycline online · March 9, 2026 at 8:13 am
can i buy doxycycline
can i buy furosemide · March 9, 2026 at 8:33 am
can i buy furosemide
where to buy doxycycline · March 9, 2026 at 8:57 am
doxycycline
buy doxycycline online · March 9, 2026 at 9:44 am
where to buy doxycycline
prednisone · March 9, 2026 at 10:05 am
buy prednisone
buy tetracycline online · March 9, 2026 at 10:31 am
buy tetracycline for sale
colchicine · March 9, 2026 at 10:54 am
buy colchicine online
can i buy prednisone · March 9, 2026 at 11:39 am
buy prednisone
buy avodart for sale · March 9, 2026 at 12:02 pm
can i buy avodart
can i buy doxycycline · March 9, 2026 at 12:28 pm
where to buy doxycycline
buy lisinopril online · March 9, 2026 at 12:52 pm
can i buy lisinopril
Josephneupt · March 9, 2026 at 1:03 pm
ทดลองเล่นสล็อต pg ฟรี สล็อต PG เกมสล็อตออนไลน์ที่คนค้นหาเยอะ เล่นง่าย ฝากถอนเร็ว
คำค้นหา PG Slot มาแรงในช่วงนี้ ในกลุ่มผู้เล่นเกมสล็อตออนไลน์ เพราะเป็น ค่ายเกมที่มีชื่อเสียง ด้าน งานภาพคุณภาพสูง ความ ลื่นไหล และ อัตราการจ่ายรางวัลที่น่าสนใจ เกมของ PG ผลิตโดยค่ายมาตรฐาน ที่รองรับการเล่นทั้งบน มือถือ และ เดสก์ท็อป
ข้อดี ของ สล็อต PG
สล็อต PG เป็นเกมสล็อตออนไลน์ที่ออกแบบมาให้ เปิดเกมได้ทันที เล่นผ่าน ระบบออนไลน์ และรองรับ ทุกอุปกรณ์ ไม่ต้องติดตั้งเพิ่มเติม ผู้เล่นสามารถเข้าเล่นผ่าน เว็บเบราว์เซอร์ ได้ทันที ภาพและเสียงถูกพัฒนาในรูปแบบ สามมิติ ให้ความคมชัด พร้อมเอฟเฟกต์ สวยงาม
คุณสมบัติหลักของเกม สล็อต PG ได้แก่
โบนัสและฟรีสปินหลายแบบ
ฟีเจอร์ตัวคูณรางวัล
เล่นฟรีก่อนเติมเงิน
มีเมนูภาษาไทย
ระบบการเงินรวดเร็ว ทำรายการไว
แพลตฟอร์ม PG Slot มักมี การฝาก-ถอน อัตโนมัติ 24 ชั่วโมง ขั้นต่ำเริ่มต้นเพียง 10 บาท ขึ้นอยู่กับ กติกาแต่ละแพลตฟอร์ม การทำรายการใช้เวลา ไม่กี่วินาที ผ่าน คิวอาร์โค้ด หรือระบบ แอปธนาคาร ทำให้ธุรกรรมเป็นไปอย่าง ไม่สะดุด
ประเภทเกมยอดนิยม ใน PG Slot
เกม PG Slot มีธีมหลากหลาย เช่น
ธีม แฟนตาซี
ธีม ผจญภัย
ธีม เอเชียและโชคลาภ
ธีม Animal
เกมยอดนิยมมักเป็นเกมที่แตกง่าย พร้อมระบบ โบนัสรอบพิเศษ และ ระบบจ่ายคุ้มค่า เหมาะกับทั้ง ผู้เล่นเริ่มต้น และ ผู้เล่นมือโปร
ความปลอดภัย
pg slot ใช้ระบบที่ได้มาตรฐาน มีการ ปกป้องข้อมูลผู้เล่น และใช้ระบบสุ่มผล Random Number Generator เพื่อให้ผลลัพธ์ ตรวจสอบได้ แพลตฟอร์มที่ให้บริการ pg slot ควรมี ทีมซัพพอร์ต 24 ชม.
บทสรุปท้ายบท
สล็อต PG เป็นตัวเลือกยอดนิยมสำหรับผู้ที่ต้องการเล่นสล็อตออนไลน์ ด้วยจุดเด่นด้าน ระบบลื่นไหล และการทำธุรกรรมที่ รวดเร็ว ผู้เล่นสามารถเริ่มต้นได้ ง่าย ฝากถอนสะดวก และเลือกเกมได้ หลากหลายแนว เหมาะสำหรับ ทั้งมือใหม่และมือโปร ในโลกของเกมสล็อตออนไลน์
BradleyBit · March 9, 2026 at 1:03 pm
ทดลองเล่นสล็อต pg เว็บ ตรง”
PG Slot เกมสล็อตออนไลน์ที่คนค้นหาเยอะ ใช้งานง่าย ฝากถอนรวดเร็ว
คำค้นหา สล็อต PG กำลังได้รับความนิยมอย่างต่อเนื่อง ในกลุ่มผู้เล่นเกมสล็อตออนไลน์ เพราะเป็น ผู้ให้บริการเกมสล็อตที่มาแรง ด้าน กราฟิก ความ นิ่งไม่สะดุด และ โอกาสรับกำไรที่ดี เกมของ PG พัฒนาโดยผู้ให้บริการชั้นนำ ที่รองรับการเล่นทั้งบน มือถือ และ คอมพิวเตอร์
จุดเด่น ของ pg slot
สล็อต PG เป็นเกมสล็อตออนไลน์ที่ออกแบบมาให้ เข้าเกมไว เล่นผ่าน ระบบออนไลน์ และรองรับ ทุกแพลตฟอร์ม ไม่ต้องดาวน์โหลดแอป ผู้เล่นสามารถเข้าเล่นผ่าน Browser ได้ทันที ภาพและเสียงถูกพัฒนาในรูปแบบ เอฟเฟกต์ 3 มิติ ให้ความคมชัด พร้อมเอฟเฟกต์ สวยงาม
คุณสมบัติหลักของเกม pg slot ได้แก่
โบนัสและฟรีสปินหลายแบบ
ระบบตัวคูณ
เล่นฟรีก่อนเติมเงิน
ใช้งานภาษาไทยง่าย
ระบบฝากถอนสะดวก ทำรายการไว
แพลตฟอร์ม PG Slot ส่วนใหญ่รองรับ การฝาก-ถอน ออโต้ตลอด 24 ชม. ขั้นต่ำเริ่มต้นเพียง 10 บาท ขึ้นอยู่กับ เงื่อนไขของเว็บไซต์ การทำรายการใช้เวลา รวดเร็วมาก ผ่าน QR Code หรือระบบ ธนาคารบนมือถือ ทำให้ธุรกรรมเป็นไปอย่าง ไม่สะดุด
แนวเกมที่คนเล่นเยอะ ใน PG Slot
เกม PG Slot มีธีมหลากหลาย เช่น
ธีม เทพเจ้า
ธีม Adventure
ธีม ความมั่งคั่ง
ธีม สัตว์และธรรมชาติ
ผู้เล่นนิยมเกมที่มีรอบพิเศษบ่อย พร้อมระบบ Special Feature และ อัตราการจ่ายที่สูง เหมาะกับทั้ง มือใหม่ และ ผู้เล่นมือโปร
มาตรฐานระบบ
PG Slot พัฒนาในระบบสากล มีการ รักษาความปลอดภัย และใช้ระบบสุ่มผล RNG เพื่อให้ผลลัพธ์ ยุติธรรม แพลตฟอร์มที่ให้บริการ สล็อต PG ควรมี ระบบดูแลข้อมูล
บทสรุปท้ายบท
สล็อต PG เป็นตัวเลือกยอดนิยมสำหรับผู้ที่ต้องการเล่นสล็อตออนไลน์ ด้วยจุดเด่นด้าน ระบบลื่นไหล และการทำธุรกรรมที่ ไว ผู้เล่นสามารถเริ่มต้นได้ ไม่ซับซ้อน ฝากถอนสะดวก และเลือกเกมได้ ครบทุกหมวด เหมาะสำหรับ ผู้เล่นทุกสไตล์ ในโลกของเกมสล็อตออนไลน์
buy tetracycline online · March 9, 2026 at 1:20 pm
buy tetracycline online
colchicine · March 9, 2026 at 1:39 pm
buy colchicine
can i buy luvox · March 9, 2026 at 2:06 pm
buy luvox
buy colchicine online · March 9, 2026 at 2:29 pm
buy colchicine
Matthewdal · March 9, 2026 at 2:45 pm
ทดลองเล่นสล็อต pg ซื้อฟรีสปิน
buy prednisone online · March 9, 2026 at 2:55 pm
where to buy prednisone
buy furosemide · March 9, 2026 at 3:14 pm
buy furosemide for sale
buy doxycycline for sale · March 9, 2026 at 4:02 pm
can i buy doxycycline
can i buy tetracycline · March 9, 2026 at 4:53 pm
tetracycline
buy colchicine for sale · March 9, 2026 at 5:18 pm
colchicine
buy furosemide · March 9, 2026 at 5:42 pm
furosemide
buy doxycycline for sale · March 9, 2026 at 6:05 pm
doxycycline
tetracycline · March 9, 2026 at 6:34 pm
can i buy tetracycline
buy furosemide · March 9, 2026 at 7:00 pm
buy furosemide
buy tetracycline for sale · March 9, 2026 at 9:43 pm
buy tetracycline for sale
can i buy cipro · March 9, 2026 at 10:04 pm
buy cipro
furosemide · March 9, 2026 at 10:23 pm
can i buy furosemide
buy avodart online · March 9, 2026 at 11:20 pm
buy avodart online
buy furosemide for sale · March 9, 2026 at 11:42 pm
furosemide
RodneyomIma · March 9, 2026 at 11:54 pm
Коллеги, вопрос к сообществу: кто какими связками пользуется? Я для себя недавно нашел подробный обзор инструментов — от подбора ключей до аналитики. Автор разобрал и бесплатные варианты (Google Keyword Planner, Search Console), и профессиональные платформы вроде Ahrefs и Screaming Frog. Очень структурированно, можно как чек-лист использовать. Делюсь ссылкой: https://yatany.ru/2026/01/20/prodvizhenie-sajtov-instrumenty/ . Особенно полезным показался раздел про инструменты для технического аудита — многие забывают про PageSpeed Insights и Lighthouse.
buy prednisone online · March 10, 2026 at 12:01 am
where to buy prednisone
buy doxycycline for sale · March 10, 2026 at 12:22 am
buy doxycycline online
can i buy doxycycline · March 10, 2026 at 1:04 am
buy doxycycline
tetracycline · March 10, 2026 at 1:25 am
buy tetracycline for sale
can i buy doxycycline · March 10, 2026 at 1:44 am
can i buy doxycycline
can i buy colchicine · March 10, 2026 at 2:02 am
buy colchicine for sale
buy colchicine for sale · March 10, 2026 at 2:22 am
colchicine
buy fluoxetine · March 10, 2026 at 7:08 am
buy fluoxetine
nitroglycerin · March 10, 2026 at 7:26 am
buy nitroglycerin online
buy nitroglycerin · March 10, 2026 at 7:44 am
nitroglycerin
buy nitroglycerin · March 10, 2026 at 8:04 am
nitroglycerin
buy retrovir online · March 10, 2026 at 8:21 am
buy retrovir
buy bactrim online · March 10, 2026 at 8:40 am
buy bactrim online
buy proscar online · March 10, 2026 at 8:59 am
buy proscar
nitroglycerin · March 10, 2026 at 9:19 am
buy nitroglycerin
buy amoxil · March 10, 2026 at 10:12 am
buy amoxil online
fluoxetine · March 10, 2026 at 10:31 am
buy fluoxetine online
buy keflex · March 10, 2026 at 10:50 am
buy keflex
amoxil · March 10, 2026 at 11:09 am
buy amoxil online
bactrim · March 10, 2026 at 11:26 am
buy bactrim
buy nitroglycerin · March 10, 2026 at 11:45 am
nitroglycerin
rufus · March 10, 2026 at 11:47 am
rufus download Rufus is known as a lightweight, free, open-source utility built to create bootable USB drives. It is used to prepare a USB flash drive that can set up an operating system, launch diagnostic tools, or boot into a recovery environment. The program does not require installation and can be run immediately after downloading.
The main function of Rufus is to create bootable USB media from ISO images with speed and stability. This lets people install or run operating systems directly from a USB flash drive without the need for DVDs. The tool works with a wide range of operating systems and service utilities, which makes it practical for both regular users and system administrators.
Rufus works on computers with Microsoft Windows, starting from Windows 7. Both 32-bit and 64-bit versions are supported, and there is also a version available for ARM64 architecture.
The software lets users create bootable USB drives from many different ISO images. It can be used to prepare a USB drive for installing Windows 11, Windows 10, Windows 8.1, or Windows 7, as well as various Linux distributions. Rufus also works with DOS systems and other recovery or maintenance tools commonly used for troubleshooting computers.
One of the included features of Rufus is the ability to download official Windows ISO images directly from Microsoft servers. This allows users to obtain original installation images for Windows 8.1, Windows 10, and Windows 11 without searching for them on third-party websites.
In addition to creating bootable drives, Rufus can format USB devices. It supports several file systems including FAT32, NTFS, exFAT, UDF, and ReFS. This flexibility allows the USB drive to be prepared for different use cases and compatibility requirements.
Rufus supports both legacy BIOS systems and modern UEFI environments. Because of this, bootable drives created with Rufus can work on older computers as well as newer systems that use UEFI and Secure Boot.
Another feature included in Rufus is Windows To Go support. This option allows users to run a full Windows environment directly from a USB drive. It can be useful for testing systems, performing maintenance, or working on multiple computers without installing Windows on the internal drive.
Rufus also provides the option to bypass certain Windows 11 installation requirements. When creating an installation USB, the program can disable checks for TPM 2.0, Secure Boot, and minimum RAM requirements. This makes it possible to install Windows 11 on computers that would otherwise not meet the official hardware requirements.
One of the reasons Rufus has become popular is its speed and simplicity. The program is extremely small, about 1.9 MB in size, and runs as a portable application without installation. It is distributed under the GPL v3 open-source license, supports more than 70 languages, and contains no advertisements, bundled software, or tracking components.
Rufus works with a large number of ISO images. These include multiple versions of Windows, Windows Server editions, FreeDOS, and various system tools such as GParted, Hiren’s Boot CD, Parted Magic, and Clonezilla. Because of this wide compatibility, the program can be used not only for installing operating systems but also for disk management, data recovery, and system maintenance tasks.
To use Rufus, a computer running Windows 7 or later and a USB flash drive are required. The program does not need to be installed. Users simply download the executable file, run it, select the ISO image they want to use, and create a bootable USB drive. Due to its simplicity, speed, and reliability, Rufus remains one of the most widely used tools for creating bootable USB drives.
amoxil · March 10, 2026 at 12:03 pm
amoxil
melbet игровые автоматы · March 10, 2026 at 12:06 pm
скачать бк мелбет на андроид
Установить Melbet: APK, iOS и компьютер
Приложение Melbet объединяет букмекерскую контору и казино в едином приложении. Пользователю доступны live-ставки, слоты, прямые трансляции, аналитика и быстрые финансовые операции. Установка занимает несколько минут.
Android (APK)
Загрузите APK с официального сайта, запустите установщик и подтвердите установку. При необходимости включите доступ к установке сторонних приложений, затем войдите в аккаунт.
iOS (iPhone)
Откройте App Store, найдите «Melbet», нажмите «Получить», после установки авторизуйтесь в системе.
ПК
Откройте официальный сайт, войдите в личный кабинет и создайте ярлык на рабочий стол. Веб-версия работает как полноценное приложение.
Функционал
Live-ставки с обновлением коэффициентов, игровой раздел с тысячами игр, просмотр матчей, подробная статистика, уведомления о матчах, регистрация за минуту и круглосуточная служба поддержки.
Бонусы
После загрузки доступны бонус на первый депозит, акционные коды и бесплатные ставки. Условия зависят от региона.
Безопасность
Скачивайте только с официального сайта, контролируйте адрес сайта, не передавайте пароль третьим лицам и включите 2FA.
Загрузка выполняется быстро, после чего открывается полный доступ Melbet.
скачать бесплатно мелбет · March 10, 2026 at 12:09 pm
мелбет официальный сайт скачать
Скачать приложение Melbet: APK, iPhone и компьютер
Мобильная версия Melbet включает ставки и казино в одном интерфейсе. Пользователю доступны live-ставки, слоты, онлайн-трансляции, аналитика и быстрые финансовые операции. Загрузка занимает несколько минут.
Android (APK)
Загрузите APK с официального сайта, откройте файл и подтвердите установку. Если требуется включите разрешение на установку из неизвестных источников, затем войдите в аккаунт.
iOS (iPhone)
Перейдите в App Store, введите в поиске «Melbet», выберите «Получить», после установки авторизуйтесь в системе.
ПК
Откройте официальный сайт, войдите в личный кабинет и добавьте ярлык на рабочий стол. Веб-версия работает как полноценное приложение.
Функционал
Live-ставки с мгновенным обновлением линии, казино и слоты, прямые трансляции, аналитические данные, push-оповещения, регистрация за минуту и поддержка 24/7.
Бонусы
После загрузки доступны бонус на первый депозит, промокоды и фрибеты. Условия зависят от региона.
Безопасность
Загружайте только с официального сайта, контролируйте адрес сайта, не сообщайте данные доступа третьим лицам и активируйте двухфакторную аутентификацию.
Установка занимает несколько минут, после чего доступен весь функционал Melbet.
скачать мобильное приложение melbet · March 10, 2026 at 12:14 pm
скачать мелбет на айфон зеркало
Скачать приложение Melbet: APK, iOS и ПК
Мобильная версия Melbet объединяет ставки и казино в одном интерфейсе. Пользователю доступны live-ставки, слоты, прямые трансляции, статистика и быстрые финансовые операции. Загрузка занимает 1–2 минуты.
Android (APK)
Скачайте APK с официального источника, откройте файл и подтвердите установку. При необходимости включите доступ к установке сторонних приложений, затем войдите в аккаунт.
iOS (iPhone)
Откройте App Store, введите в поиске «Melbet», нажмите «Получить», после установки выполните вход.
ПК
Перейдите официальный сайт, авторизуйтесь и создайте ярлык на рабочий стол. Браузерная версия функционирует как полноценное приложение.
Функционал
Live-ставки с мгновенным обновлением линии, казино и слоты, просмотр матчей, аналитические данные, уведомления о матчах, регистрация за минуту и поддержка 24/7.
Бонусы
После загрузки доступны приветственный бонус, промокоды и фрибеты. Правила начисления определяются регионом.
Безопасность
Загружайте только с официальных источников, контролируйте адрес сайта, не передавайте пароль третьим лицам и активируйте двухфакторную аутентификацию.
Установка занимает несколько минут, после чего доступен весь функционал Melbet.
ричтрак складской погрузчик цена · March 10, 2026 at 12:19 pm
ричтрак электрический складской купить цена
buy cephalexin online · March 10, 2026 at 12:21 pm
buy cephalexin
buy fluoxetine · March 10, 2026 at 12:41 pm
buy fluoxetine online
buy proscar online · March 10, 2026 at 1:04 pm
buy proscar
buy secnidazole online · March 10, 2026 at 1:48 pm
buy secnidazole
buy keflex online · March 10, 2026 at 2:53 pm
buy keflex online
buy nitroglycerin online · March 10, 2026 at 3:57 pm
nitroglycerin
buy fluoxetine · March 10, 2026 at 5:00 pm
fluoxetine
buy proscar online · March 10, 2026 at 6:14 pm
buy proscar
buy retrovir · March 10, 2026 at 7:21 pm
retrovir
buy augmentin online · March 10, 2026 at 8:48 pm
augmentin
Najlepsze Kasyna Online · March 10, 2026 at 8:52 pm
Wow, amazing blog layout! How long have you been blogging for? you make blogging look easy. The overall look of your site is wonderful, let alone the content!
Najlepsze kasyna online · March 10, 2026 at 9:25 pm
The clarity in your post is just nice and I can tell you are an expert in the subject matter.
Najlepsze kasyna online · March 10, 2026 at 9:31 pm
Some genuinely choice content on this site, bookmarked .
bactrim · March 10, 2026 at 9:31 pm
buy bactrim
YO studio mebli · March 10, 2026 at 9:38 pm
Witaj w Yo4You – miejscu, w którym nowoczesne studio mebli łączy się z profesjonalnym biurem projektowym. Spełnianie oczekiwań klientów, produkcja mebli oraz tworzenie wymarzonych aranżacji wnętrzarskich to nasza pasja. Jesteśmy profesjonalistami. W naszej ofercie znajdziesz meble kuchenne, nowoczesne jak i tradycyjne, oryginalne meble łazienkowe czy funkcjonalne meble biurowe i garderoby na wymiar. Do każdego klienta podchodzimy indywidualnie, a wykonując meble na wymiar, maksymalnie spełniamy Twoje potrzeby, oczekiwania i wymagania. Jako producent mebli kuchennych i mebli do pozostałych pomieszczeń funkcjonujemy na rynku już od wielu lat. Cechuje nas terminowość, zaangażowanie, precyzja oraz wykorzystywanie najnowszych technologii. Odwiedź nasz salon meblowy i przekonaj się, że meble swoich marzeń są bliżej, niż myślisz!
Najlepsze Kasyna Online · March 10, 2026 at 10:04 pm
Great resources and tips for families here.
buy fluoxetine online · March 10, 2026 at 10:18 pm
fluoxetine
buy secnidazole · March 10, 2026 at 10:58 pm
buy secnidazole
Najlepsze Kasyna Online · March 10, 2026 at 11:03 pm
I like this weblog very much so much great info .
proscar · March 11, 2026 at 12:28 am
buy proscar
Najlepsze kasyna online · March 11, 2026 at 12:56 am
Hi there! I just wanted to ask if you ever have any trouble with hackers? My last blog (wordpress) was hacked and I ended up losing several weeks of hard work due to no back up. Do you have any solutions to protect against hackers?
XrumerEa · March 11, 2026 at 1:23 am
Good morning!
Study lang mysterious barriers with interesting and valuable communication knowledge and speak to the world see on the website for language tools
Full information on the link – https://900letekas.site
All the best and development in business!
meerodrop.com Mega888 · March 11, 2026 at 1:52 am
Hi there, its fastidious piece of writing concerning media print, we all be aware of media is a great source of data.
Take a look at my web blog; https://kjllj7zr35orvnxkjzlp3bmhk5kux7lnbo4cxh4qbvugz44gyiga.webpkgcache.com/doc/-/s/Gpyouhak.com%2Fgpy%2Fbbs%2Fboard.php%3Fbo_table%3Dfree%26wr_id%3D3796039
buy nitroglycerin online · March 11, 2026 at 1:58 am
buy nitroglycerin
Najlepsze kasyna online · March 11, 2026 at 2:35 am
A friend of mine advised this site. And yes. it has some useful pieces of info and I enjoyed scaning it. Therefore i would love to drop you a quick note to express my thank. Take care
gayxxx · March 11, 2026 at 3:27 am
amphetamine drugs
slot gampang JP hari ini · March 11, 2026 at 4:36 am
Spot on with this write-up, I actually assume this website needs far more consideration. I will in all probability be once more to learn rather more, thanks for that info.
keflex · March 11, 2026 at 5:01 am
buy keflex online
Najlepsze Kasyna Online · March 11, 2026 at 5:10 am
Pretty impressive article. I just stumbled upon your site and wanted to say that I have really enjoyed reading your opinions. Any way I’ll be coming back and I hope you post again soon.
Najlepsze Kasyna Online · March 11, 2026 at 5:26 am
I simply could not leave your site before suggesting that I actually enjoyed the usual info a person supply in your visitors? Is going to be back often to inspect new posts
Interestmar · March 11, 2026 at 6:07 am
Hello!
Find drug mysterious interactions in interesting tests with valuable safety data and mix medicines wisely see on the website for interaction checkers
Full information on the link – https://elena-solohina.ru/gorshki-dlya-rassady/
All the best and development in business!
xn88 - Nền tảng cược trực tuyến hàng đầu Việt Nam · March 11, 2026 at 6:35 am
Những tựa game bài đối kháng (P2P) tại xn88 – Nền tảng cược trực tuyến hàng đầu Việt Nam là nơi hội tụ của các cao thủ trí tuệ, nơi bản lĩnh và chiến thuật được tôn vinh thông qua những ván bài kịch tính. TONY03-11O
cược thể thao so79 · March 11, 2026 at 12:46 pm
With internet full of dupe articles it is nice to find original content like yours thank you so very much.
cược thể thao so79 · March 11, 2026 at 1:00 pm
I have been curious about these trends, and you have really helped me. I have just told a few of my friends about this on FaceBook and they love your content just as much as I do.
situs slot jeni4d · March 11, 2026 at 2:40 pm
While this issue can vexed most people, my thought is that there has to be a middle or common ground that we all can find. I do value that you’ve added pertinent and sound commentary here though. Thank you!
best casino · March 11, 2026 at 4:13 pm
Glad to be one of several visitors on this awful internet site : D.
playinexch · March 11, 2026 at 4:14 pm
d amphetamine salt combo
ufa365 · March 11, 2026 at 5:32 pm
Thanks For This Blog, was added to my bookmarks.
login sawit188 · March 11, 2026 at 10:45 pm
Hello there! I really enjoy reading your blog! If you keep making amazing posts like this I will come back every day to keep reading.
singulair · March 12, 2026 at 12:28 am
singulair
nba · March 12, 2026 at 2:38 am
纽卡斯尔6-1大胜卡拉巴赫2026欧冠附加赛首回合比分,戈登半场大四喜喜鹊锁定淘汰赛,最新足球赛事比分全球关注英超欧战强势表现。
ventolin · March 12, 2026 at 3:36 am
ventolin
Sun win · March 12, 2026 at 4:41 am
The start of a fast-growing trend?
ventolin · March 12, 2026 at 5:05 am
ventolin
Migueldence · March 12, 2026 at 11:28 am
Наткнулся на развернутое руководство по продвижению в столице Сибири. Рассмотрены ключевые моменты: локальная оптимизация, подбор семантики, контент-маркетинг и внешние ссылки. Особо полезен раздел про адаптацию под мобильные и скорость загрузки. Ссылка: https://avto-dom-tumen.ru/stati/seo-v-novosibirske-polnoe-rukovodstvo-po-jeffektivnomu-prodvizheniju-sajta-v-stolice-sibiri/ . Рекомендую изучить.
Рассрочка на услуги банкротства от 10 000 ?/мес · March 12, 2026 at 2:13 pm
Банкротство физических лиц в Уфе
kilat69 situs gacor · March 12, 2026 at 5:53 pm
We’re developing a conference, and it looks like you would be a great speaker.
Click Here! · March 12, 2026 at 5:57 pm
I am very happy to look your post. Thanks a lot and i am taking a look ahead to touch you.
Vavada Casino · March 12, 2026 at 6:43 pm
Poznaj świat hazardu premium w Vavada Casino na rok 2026. Setki gier na żywo, innowacyjne mechaniki slotów i system lojalnościowy, który naprawdę nagradza. Twoja wielka wygrana zaczyna się właśnie tutaj!Vavada Casino to nie tylko kolejna platforma hazardowa; to starannie dopracowany ekosystem dla entuzjastów adrenaliny. Od lat dostarczamy najwyższej jakości rozrywkę, kładąc nacisk na transparentność i szybkość działania. Dzięki licencji Curacao, gracze mają pewność, że każdy wynik jest generowany przez certyfikowany system RNG. Nasz portal jest w pełni responsywny, co oznacza, że płynność rozgrywki na smartfonie dorównuje wersji na komputery stacjonarne.
https://games.mostbet-zerkaloonline.buzz/azino888-brand.html · March 12, 2026 at 7:49 pm
https://games.mostbet-zerkaloonline.buzz/azino888-brand.html
https://mymedicalshop24.top/singulair/ · March 12, 2026 at 8:38 pm
https://mymedicalshop24.top/singulair/
casino en ligne · March 12, 2026 at 8:53 pm
Good day! This is my first comment here so I just wanted to give a quick shout out and say I really enjoy reading through your articles. Can you recommend any other blogs/websites/forums that cover the same subjects? Thanks a lot!
https://mymedicalshop24.top/advair-diskus/ · March 12, 2026 at 10:30 pm
https://mymedicalshop24.top/advair-diskus/
daftar senang4d toto · March 12, 2026 at 10:37 pm
Your idea is outstanding; the issue is something that not enough persons are speaking intelligently about. I’m very happy that I stumbled throughout this in my seek for one thing regarding this.
prodentim · March 12, 2026 at 10:40 pm
**prodentim**
ProDentim is a distinctive oral-care formula that pairs targeted probiotics with plant-based ingredients to encourage strong teeth, comfortable gums, and reliably fresh breath.
https://mymedicalshop24.top/allegra/ · March 12, 2026 at 10:58 pm
https://mymedicalshop24.top/allegra/
link suara4d terbaru · March 12, 2026 at 11:24 pm
Took me time to read all the comments, but I really enjoyed the article. It proved to be Very helpful to me and I am sure to all the commenters here It’s always nice when you can not only be informed, but also entertained I’m sure you had fun writing this article.
https://mymedicalshop24.top/ventolin-inhalator/ · March 12, 2026 at 11:56 pm
https://mymedicalshop24.top/ventolin-inhalator/
https://mymedicalshop24.top/zyrtec/ · March 13, 2026 at 12:26 am
https://mymedicalshop24.top/zyrtec/
https://sex-positions.online/es-ES/position/rostok/ · March 13, 2026 at 12:46 am
https://sex-positions.online/es-ES/position/rostok/
https://mymedicalshop24.top/promethazine/ · March 13, 2026 at 1:22 am
https://mymedicalshop24.top/promethazine/
https://mymedicalshop24.top/claritin-tablets/ · March 13, 2026 at 2:47 am
https://mymedicalshop24.top/claritin-tablets/
https://mymedicalshop24.top/ventolin/ · March 13, 2026 at 3:15 am
https://mymedicalshop24.top/ventolin/
stake casino avis · March 13, 2026 at 5:43 am
casino en ligne stake
my stake casino uk · March 13, 2026 at 1:25 pm
my stake casino
https://healthstoreinfo365.top/co-amoxiclav/ · March 13, 2026 at 5:32 pm
https://healthstoreinfo365.top/co-amoxiclav/
https://healthstoreinfo365.top/plavix/ · March 13, 2026 at 6:05 pm
https://healthstoreinfo365.top/plavix/
king casino telegram · March 13, 2026 at 6:34 pm
king casino telegram Недавно искал информацию по казино кинг, обычно проверяю через официальный канал — через этот канал проще всего найти рабочий адрес.
Garrygig · March 13, 2026 at 10:20 pm
казино рейтинг
https://t.me/s/casinorating
Jamesthine · March 14, 2026 at 8:56 am
В статье подробно разбирается, за счёт чего локальный бизнес может выиграть у федералов. Автор выделяет слабые стороны крупных игроков (низкая адаптация под регион, медленная реакция) и показывает, как этим пользоваться. Есть примеры локальных ключей и советы по работе с Яндексом. Рекомендую: https://lefmun.ru/stati/bitva-za-ural-kak-lokalnomu-biznesu-iz-ekaterinburga-vyigrat-u-federalnyh-gigantov-v-poiske/
Jamesthine · March 14, 2026 at 8:59 am
Отличный разбор темы — как местному бизнесу из Екатеринбурга выигрывать у федералов в поиске. Автор подробно останавливается на локальном SEO, гиперрелевантном контенте, скорости и сервисе как факторах ранжирования. Есть блок про микро-ниши и локальный линкбилдинг. Очень рекомендую: https://go-patriot.ru/bitva-za-ural-kak-lokalnomu-biznesu-iz-ekaterinburga-vyigrat-u-federalnyh-gigantov-v-poiske/
Robertnex · March 14, 2026 at 11:07 am
Автозайм
Деньги под обеспечение ПТС в городе Самара — это возможность взять деньги под автомобиль без продажи транспорта и без долгих банковских процедур. Главная характеристика такого займа — автомобиль остаётся у владельца у владельца, а в качестве залога передаётся только ПТС. Это даёт возможность продолжать пользоваться машиной, пока действует договор займа.
Выдача средств возможна в день обращения. Заявка проверяется примерно за 15 минут, затем выносится ответ по сумме и условиям. Размер займа может составлять до 5 000 000 ?, а ставка начинается с уровня 2% в месяц. Срок кредитования обычно достигает до 60 мес., поэтому клиент может подобрать подходящий план платежей.
Система оформления заявки работает онлайн. Клиент заполняет онлайн-форму, вносит данные автомобиля и желаемую сумму. После анализа документов выносится начальное одобрение. Чаще всего деньги переводятся в день оформления, после подписания договор займа.
Для расчёта параметров используется калькулятор займа. К примеру, при сумме 300 000 ? на срок 12 мес. платёж в месяц будет примерно 33 057 ?. Итоговая сумма переплаты по такому займу составит около 96 684 ?. Конечные условия могут изменяться в зависимости стоимости автомобиля и установленного срока кредитования.
На страницах сервиса автозаймов нередко показывается лента заявок. Этот блок показывает активность системы и образцы обработанных заявок из разных городов. К примеру, запросы на суммы 1 840 000 ? из Тулы, 1 890 000 ? город Москва или 1 470 000 ? город Челябинск могут получать метку «Одобрено». Часть обращений находятся на этапе проверки — например, 290 000 ? из Сочи или 720 000 ? из Екатеринбурга. Такие блоки отображают текущий поток платформы и число обработанных заявок сегодня и за месяц.
Займ под залог ПТС может подойти людям, кому требуется оперативно получить значительную сумму без продажи автомобиля. Основные параметры подобного финансирования — ставка от 2% в месяц, рассмотрение около 15 минут, сумма до 5 000 000 ? и возможность оформить заявку через интернет. После отправки формы клиент ожидает решение, написать в мессенджер или обратиться к менеджеру для уточнения процедуры.
https://samara.carzaem.ru/
best australian online casino · March 14, 2026 at 12:41 pm
We are a group of volunteers and starting a new initiative in our community. Your blog provided us with valuable information to work on|.You have done a marvellous job!
online casino · March 14, 2026 at 2:42 pm
Nice read, I just passed this onto a colleague who was doing some research on that. And he just bought me lunch as I found it for him smile Therefore let me rephrase that: Thank you for lunch!
best online casino australia · March 14, 2026 at 2:56 pm
Fantastic piece of writing here1
best online casino australia real money · March 14, 2026 at 3:14 pm
A cool post there mate ! Thank you for posting.
parhaat nettikasinot · March 14, 2026 at 5:05 pm
It’s the best time to make some plans for the future and it is time to be happy. I’ve read this post and if I could I wish to suggest you some interesting things or tips. Maybe you can write next articles referring to this article. I wish to read even more things about it!
best australian online casino · March 14, 2026 at 6:01 pm
Our communities really need to deal with this.
best australian online casino · March 14, 2026 at 6:12 pm
This is the wave – the big wave.
parhaat nettikasinot · March 14, 2026 at 6:15 pm
A friend of mine advised me to review this site. And yes. it has some useful pieces of info and I enjoyed reading it.
online casino · March 14, 2026 at 6:28 pm
There is perceptibly a lot to identify about this. I consider you made some good points in features also.
online casino magyar · March 14, 2026 at 7:27 pm
Hi, I just hopped over to your web-site through StumbleUpon. Not somthing I might typically browse, but I liked your views none the less. Thanks for making something worthy of reading through.
NZ best online casino · March 14, 2026 at 10:17 pm
it is a really nice point of view. I usually meet people who rather say what they suppose others want to hear. Good and well written! I will come back to your site for sure!
parhaat nettikasinot · March 14, 2026 at 11:28 pm
Its just like you read my thoughts! It’s like reading about my family.
стоимость установки унитаза · March 14, 2026 at 11:37 pm
сколько стоит установить унитаз
best australian online casino · March 14, 2026 at 11:45 pm
Excellent read, I just passed this onto a colleague who was doing a little research on that. And he actually bought me lunch because I found it for him smile So let me rephrase that.|
TracyTorne · March 15, 2026 at 5:30 am
Кто ищет, где заказать накрутку ПФ, вот статья с конкретным сервисом и ценами от 15 000 рублей. Расписано, зачем это нужно, какие риски и как проходит процесс заказа. Информация для тех, кто решил попробовать этот метод: https://stroika-tovar.ru/articles/stati/effektivnaya-nakrutka-pf-yandeks-kak-zakazat-po-dostupnoy-tsene-ot-15-000-rubley.html
Garrygig · March 15, 2026 at 11:59 am
вулкан вегас играть
https://t.me/s/realvulcanvegas
cryptoboss casino · March 15, 2026 at 12:29 pm
Cryptoboss Casino — онлайн-казино, которое хорошо вписывается в домашний ритм, когда нужно переключиться после работы. Здесь интерфейс не давит яркими вспышками, а значит, можно просто зайти на https://cryptoboss-rcn.top/ и выбрать пару любимых слотов.
Игровой каталог даёт возможность подобрать подходящий формат, а всегда можно играть без обязательного участия в промо. Можно играть с выключенным звуком или в наушниках, так что игра легко сочетаетcя с другими делами.
Возможность играть без участия в рейтингах
Минимум стресса при работе с финансами
Готовность помочь, когда это нужно
Если вам ближе комфорт, чем гонка, такой стиль будет особенно удобен
купить кокаин в доминике · March 15, 2026 at 2:37 pm
купить кокаин в доминике
https://www.goal.com/en-in/betting/1xbet-promo-code/blt57eec3828e2b7aa7blyatmudak · March 15, 2026 at 7:50 pm
https://www.goal.com/en-in/betting/1xbet-promo-code/blt57eec3828e2b7aa7blyatmudak
oaoxxnt · March 16, 2026 at 1:08 pm
https://www.goal.com/en-in/betting/1xbet-promo-code/nahuyblya
futebol · March 16, 2026 at 1:13 pm
Fortune Tiger no modo demo: quem treina antes de depositar? Confessa aqui
bmqwrss · March 16, 2026 at 5:10 pm
https://dev.epicgames.com/community/profile/x4wqm/1xbetbestcode645
Binance账户 · March 16, 2026 at 5:16 pm
Your point of view caught my eye and was very interesting. Thanks. I have a question for you. https://accounts.binance.com/register-person?ref=JW3W4Y3A
trywaem · March 16, 2026 at 6:35 pm
https://gitlab.vuhdo.io/bonusxxbet2
Customs Glossary · March 16, 2026 at 8:17 pm
Customs Glossary
gaming · March 16, 2026 at 9:34 pm
Jogo do Tigrinho estratégia de sessão: 400 giros e stop no +60% – qual sua meta?
apostasfutebol · March 16, 2026 at 10:26 pm
Fortune Ox hold & win: quem já segurou 15+ símbolos e explodiu tudo?
Robertnex · March 16, 2026 at 11:57 pm
http://wiki.votesmart.org/MarylinxkBorehamoy
PGSoft · March 17, 2026 at 12:24 am
Fortune Rabbit modo turbo: 1200 giros em 25 minutos – quem já deixou rodando?
htygxxq · March 17, 2026 at 1:13 am
https://astra-hotel.ch/articles/code_promo_45.html
Istanbul high end escorts · March 17, 2026 at 7:58 am
high class escorts in Istanbul
вертолеты россии генеральный директор · March 17, 2026 at 8:34 am
вертолеты россии генеральный директор
колесов николай александрович · March 17, 2026 at 11:04 am
колесов николай александрович
kasyno online · March 17, 2026 at 3:46 pm
You ma’am have a way with words. Thank you very much!
neue online casinos · March 17, 2026 at 4:14 pm
Sweet blog! I found it while browsing on Yahoo News. Do you have any tips on how to get listed in Yahoo News? I’ve been trying for a while but I never seem to get there! Thank you
казино х регистрация · March 17, 2026 at 4:31 pm
казино икс
legalne kasyna online · March 17, 2026 at 4:46 pm
Its wonderful as your other blog posts : D, regards for putting up.
вулкан вегас автоматы · March 17, 2026 at 5:08 pm
игровые автоматы вулкан вегас
gnpfamk · March 17, 2026 at 6:05 pm
https://football-fun-live.com/reyting-bukmekerov/1xbet/bonusy-i-aktsii-pidor-tebe-bonus
best online casino NZ · March 17, 2026 at 6:35 pm
I am lucky that I discovered this website , precisely the right info that I was searching for! .
najlepsze kasyno online · March 17, 2026 at 6:58 pm
Please let us know when you plan to publish your book!
neue online casinos · March 17, 2026 at 7:03 pm
I just couldn’t leave your website before suggesting that I really enjoyed the usual information an individual supply on your visitors? Is gonna be back often in order to investigate cross-check new posts
квартира индивидуальная отделка · March 17, 2026 at 7:23 pm
квартира индивидуальная отделка Проект разрабатывается с нуля под конкретного заказчика: учитываются его привычки, образ жизни, эстетические предпочтения. Создаётся уникальное пространство, не похожее на другие.
강남 블렌딩 · March 17, 2026 at 7:34 pm
Pretty impressive article. I just stumbled upon your site and wanted to say that I have really enjoyed reading your opinions. Any way I’ll be coming back and I hope you post again soon.
kasyno online polska · March 17, 2026 at 8:30 pm
Your idea is outstanding; the issue is something that not enough persons are speaking intelligently about. I’m very happy that I stumbled throughout this in my seek for one thing regarding this.
beste online casino Österreich · March 18, 2026 at 12:38 am
thank, I thoroughly enjoyed reading your article. I really appreciate your wonderful knowledge and the time you put into educating the rest of us.
parhaat nettikasinot · March 18, 2026 at 1:02 am
Good post. I study something more difficult on different blogs everyday. It’s going to always be stimulating to learn content material from other writers and observe a little bit one thing from their store. I’d prefer to use some with the content material on my blog whether you don’t mind. Natually I’ll give you a link in your web blog. Thanks for sharing.
gaojeox · March 18, 2026 at 1:31 am
https://www.goal.com/en-in/betting/1xbet-promo-code/pizdacoreblast
колесов вертолеты россии генеральный директор · March 18, 2026 at 2:14 am
колесов вертолеты россии генеральный директор
kasyno online polska · March 18, 2026 at 2:41 am
Thank you for sharing this very good post. Very interesting ideas! (as always, btw)
slot · March 18, 2026 at 3:18 am
I don’t normally comment on blogs.. But nice post! I just bookmarked your site
najlepsze kasyno online · March 18, 2026 at 3:36 am
Just stumble upon your blog from from time to time. nice article
legalne kasyna online · March 18, 2026 at 3:48 am
Are grateful for this blog post, it’s tough to find good information and facts on the internet
TracyTorne · March 18, 2026 at 3:56 am
Искал информацию по ценам на SEO и наткнулся на статью про накрутку позиций в Яндексе. Тут разбирают, что вообще входит в SEO-услуги, от чего зависит стоимость и как не попасть на мошенников. Полезно для понимания рынка: https://vagaro.ru/nakrutka-poziczij-v-yandekse-chto-nuzhno-znat-o-seo-uslugah-i-ih-stoimosti/
Najlepsze kasyna online · March 18, 2026 at 5:29 am
Assume you are doing good linking to position you on the first pages of search engines.
https://yatirimciyiz.net/user/61xbetfreespins736 · March 18, 2026 at 6:22 am
https://yatirimciyiz.net/user/61xbetfreespins736
колесов николай александрович · March 18, 2026 at 8:10 am
колесов николай александрович
карта дня таро онлайн · March 19, 2026 at 12:13 am
карта дня онлайн
https://unvegan.com/pages/1xbet_free_promo_code_sign_up_bonus.html · March 19, 2026 at 8:17 am
https://unvegan.com/pages/1xbet_free_promo_code_sign_up_bonus.html
live sex game · March 19, 2026 at 8:21 am
Experience ultimate adult fun with live sex game at MyDarkShop. Engage in interactive, realistic gameplay, explore erotic storylines, and enjoy smooth, secure downloads. Perfect for solo or couple play, these games bring excitement and adventure directly to your private gaming world.
https://doodleordie.com/profile/bienvnuxbet · March 19, 2026 at 8:54 am
https://doodleordie.com/profile/bienvnuxbet
FloydCes · March 19, 2026 at 2:36 pm
Всем привет! Рзучал тему развития бизнеса через интернет Рё нашел хороший РѕР±Р·РѕСЂ. Статья называется “Рффективное продвижение сайтов Рё развитие бизнеса РІ интернете”. Там РїРѕРґСЂРѕР±РЅРѕ разобраны основные каналы: SEO, контекст, соцсети, аналитика. Особенно полезно для тех, кто хочет системно подойти Рє РІРѕРїСЂРѕСЃСѓ, Р° РЅРµ работать хаотично. Р’РѕС‚ ссылка, если РєРѕРјСѓ интересно: http://harizma86.ru/jeffektivnoe-prodvizhenie-sajtov-i-razvitie-biznesa-v-internete/
FloydCes · March 19, 2026 at 2:39 pm
Всем привет! Прочитал статью про продвижение сайтов и развитие бизнеса в сети. Хороший обзор, охватывает основные направления: от SEO и контекстной рекламы до автоматизации и выхода на международные рынки. Автор пишет про системный подход и важность аналитики. Может быть полезно владельцам бизнеса и маркетологам. Вот ссылка: https://midships.ru/jeffektivnoe-prodvizhenie-sajtov-i-razvitie-biznesa-v-internete/
customs clearance services in Poland · March 19, 2026 at 6:54 pm
professional customs brokerage in the EU If you are dealing with customs clearance in the EU, this resource provides a useful overview of the process.
dckfrdm · March 19, 2026 at 10:07 pm
https://permraion.ru/images/pages/bespokoynaya_istoriya_yughnoafrikanskogo_renda.html
https://willysforsale.com/author/1xbetpromocode8/ · March 19, 2026 at 11:27 pm
https://willysforsale.com/author/1xbetpromocode8/
Douglasvow · March 20, 2026 at 7:14 am
Пробовал накрутку пару лет назад через дешёвые сервисы — толку не было, только деньги сжёг. Статья помогла понять, почему. Во-первых, сайт тогда был технически не готов (глубоко в выдаче). Во-вторых, использовал дешёвые прокси и сгенерированные отпечатки. Сейчас, почитав этот гайд, вижу системный подход: аудит сайта, правильный сбор семантики, плавный старт. Оставлю ссылку здесь, буду перечитывать перед запуском: https://partnerkin.com/tribuna/blog-vitalivivdenko/nakrutka-pf-v-yandekse-polnoe- . Много практических деталей.
ewujjch · March 20, 2026 at 8:28 am
https://avangard66.ru/wp-includes/list/ekonomiya_po_ghenski_3_sposoba_upravlyaty_lichnymi_finansami.html
глава холдинга вертолеты россии · March 20, 2026 at 9:53 am
глава холдинга вертолеты россии
Leonidlet · March 20, 2026 at 10:25 am
Сроки строительства дома из клееного бруса — реальные цифры
Leonidlet · March 20, 2026 at 10:32 am
Строительство загородного дома из клееного бруса в Ленобласти
http://koobo.ru/inc/pages/kak_uhaghivaty_za_gidromassaghnymi_kabinami.html · March 20, 2026 at 11:05 am
http://koobo.ru/inc/pages/kak_uhaghivaty_za_gidromassaghnymi_kabinami.html
Anatolylet · March 20, 2026 at 11:08 am
Решили обустроить детскую площадку на даче — делюсь полезными советами. Первое — определите бюджет и размер площадки. Второе — выберите комплектацию под возраст детей. Третье — закажите у надёжного производителя с монтажом.
Nikitalet · March 20, 2026 at 11:19 am
Установка детского городка на участке — процесс несложный, если инструкция понятная. Хорошие производители комплектуют площадки всем необходимым крепежом и пошаговым руководством. Мы собрали комплекс вдвоём за один выходной.
сайт трипскан · March 20, 2026 at 11:50 am
Добрый День,
Дорогие Друзья.
Сегодня я бы хотел рассказать больше про https://tripsc68.cc
Я думаю Вы ишите именно про tripscan?!
Значит эта оптимально актуальная информация про трипскан вход будет для вас наиболее полезной.
Мы предлагаем больше полезностей про трип скан
На нашем сайте больше про трипскан вход, также про tripscan
Ссылка на сайт https://tripsc68.cc или смотри про https://tripsc68.cc
Только, если Вы реально искали информацию про tripscan,
найдете самую свежую и актуальную информацию про трип скан
Добро пожаловать к нам на сайт про https://tripsc68.cc
Удачи Вам.
Наши Теги: трипскан, трипскан вход,
http://umap.ru/7da31/data/photo/?1hbet__1xbet__promokod_2020___bonus_6500_rubley.html · March 20, 2026 at 12:34 pm
http://umap.ru/7da31/data/photo/?1hbet__1xbet__promokod_2020___bonus_6500_rubley.html
cexxaby · March 20, 2026 at 1:07 pm
https://www.wellpleased.co.uk/wp-content/pages/?1xbet_promo_code_cameroon___bonus_1xbet__130.html
директор вертолеты россии · March 20, 2026 at 5:30 pm
директор вертолеты россии
Tải sunwin · March 20, 2026 at 5:49 pm
Unquestionably believe that which you said. Your favorite reason seemed to be on the net the easiest thing to be aware of. I say to you, I certainly get annoyed while people consider worries that they plainly don’t know about. You managed to hit the nail on the head. Will probably be back to get more. Thanks
https://sunwinv.net/ · March 20, 2026 at 5:53 pm
Nice blog here! Also your web site loads up very fast! What host are you using? Can I get your affiliate link to your host? I wish my web site loaded up as fast as yours lol
zumwjvg · March 20, 2026 at 6:23 pm
https://www.sencampus.com/wp/wp-includes/pgs/?aktualnuy_promokod_melbet_pri_registracii___1.html
win slot77 · March 20, 2026 at 7:02 pm
Regards for helping out, superb info.
ipaaukv · March 20, 2026 at 8:42 pm
https://prohvost.club/pag/odnorazovye_rashodnye_materialy_dlya_salonov_krasoty_preimuschestva_ispolyzovaniya.html
https://zakustom.ru/wp-includes/list/1hbet_promokod_na_segodnya_2020.html · March 20, 2026 at 8:50 pm
https://zakustom.ru/wp-includes/list/1hbet_promokod_na_segodnya_2020.html
best online casino · March 20, 2026 at 11:18 pm
When we look at these issues, we know that they are the key ones for our time.
Ремонт стиральных машин СПб · March 20, 2026 at 11:53 pm
Ремонт стиральных машин СПб AEG — техника серьёзная, и ремонт должен быть соответствующий. Обратился в объединённый сервис «Нева-Экспресс ремонт» + «РБТ-Сервис» и не ошибся. Мастер приехал со всеми запчастями, быстро нашёл причину (вышел из строя нагреватель). Спасибо ребятам за то, что объединили усилия — теперь ремонт стиральных машин СПб на совершенно новом уровне!
Fly88 cộng sản · March 21, 2026 at 1:15 am
Thanks For This Blog, was added to my bookmarks.
casinos online chile confiables · March 21, 2026 at 1:17 am
However, it is virtually all done with tongues rooted solidly in cheeks, and everyone has absolutely nothing but absolutely love for his or her friendly neighborhood scapegoat. The truth is, he is not just a pushover. He is basically that special variety of person strong enough to take all of that good natured ribbing for exactly what it is.
new online casino · March 21, 2026 at 1:18 am
It’s clear you’re passionate about the issues.
39.108.209.179 · March 21, 2026 at 1:47 am
steroids shop
http://101.35.227.2:3000/dicktietkens92 101.35.227.2
https://ott.saikatinfotech.com/@melvinbattarbe?page=about ott.saikatinfotech.com
http://47.113.101.80:3000/raleighdolling http://47.113.101.80
https://git.entryrise.com/temekabgt92671 https://git.entryrise.com/temekabgt92671
https://backend-dev.podosee.com/margaretzhk48 backend-dev.podosee.com
https://www.melnica-group.ru/charlie7979739 http://www.melnica-group.ru
https://seychelleslove.com/@jamaalfizelle5 seychelleslove.com
http://101.42.28.156:3000/jgnleonel5635 101.42.28.156
https://edexxel.com/employer/4-dianabol-stacks-for-bigger-gains-the-bible-of-anabolic-steroids/ edexxel.com
https://lawrencewilbert.com/read-blog/35163_dianabol-results-kalpa-pharmaceuticals-dianoxyl.html lawrencewilbert.com
https://towerclimbers.work/employer/legal-raw-steroids-for-research-only/ towerclimbers.work
http://47.113.101.80:3000/raleighdolling http://47.113.101.80:3000/raleighdolling
http://27.223.88.102:33000/louannp8769070 27.223.88.102
https://www.k0ki-dev.de/mablen96277160 https://www.k0ki-dev.de/mablen96277160
http://58.221.13.198:30010/warrenmenzies 58.221.13.198
http://8.141.82.163:20000/ulyssesfjr7136 http://8.141.82.163:20000/ulyssesfjr7136
http://82.156.89.21:3000/vincentworrell 82.156.89.21
http://211.63.236.6:50003/stepaniedonahu 211.63.236.6
References:
http://121.41.95.54:3000/estebanburrow5
https://www.global56.ru/firmnews/id/10696 · March 21, 2026 at 1:51 am
https://www.global56.ru/firmnews/id/10696
https://matchymood.app/@olensmallwood1 · March 21, 2026 at 2:24 am
is animal stak a steroid
http://101.42.28.156:3000/jgnleonel5635 http://101.42.28.156
https://forgejo.sparrowhub.io/jettahasan1432 https://forgejo.sparrowhub.io
https://gitea.ai-demo.duckdns.org/willie1341811 gitea.ai-demo.duckdns.org
https://gitea.pnkx.top:8/wyatt132348913 https://gitea.pnkx.top
https://git.minecraftlegacy.com/saulblock43629 https://git.minecraftlegacy.com/saulblock43629
https://meeting2up.it/@jonitremblay51 meeting2up.it
http://39.108.209.179:3000/elwoodcurrie32 39.108.209.179
http://118.195.135.194:3000/dominikurquhar 118.195.135.194
https://git.wisder.net/tawnyabourassa git.wisder.net
http://all.caeta.mx:3000/beverlymcevoy3 http://all.caeta.mx
http://13.230.31.145:8418/dawnamcchesney 13.230.31.145
http://wooriwebs.com/bbs/board.php?bo_table=faq wooriwebs.com
https://codes.tools.asitavsen.com/darrinrasmusse codes.tools.asitavsen.com
http://55x.top:9300/tristaconnelly http://55x.top:9300/tristaconnelly
http://13.230.31.145:8418/dawnamcchesney 13.230.31.145
https://emphira.app/@kieram2977233 https://emphira.app
http://gitea.dctpay.com/sherileavitt8 http://gitea.dctpay.com/sherileavitt8
http://gang-yeon.com/bbs/board.php?bo_table=faq&wr_id=475492 gang-yeon.com
References:
http://218.201.98.56:18106/nevmohamed5339
kilat69 slot · March 21, 2026 at 3:02 am
Hi, I just hopped over to your web-site through StumbleUpon. Not somthing I might typically browse, but I liked your views none the less. Thanks for making something worthy of reading through.
Ремонт стиральных машин СПб · March 21, 2026 at 3:40 am
Ремонт стиральных машин СПб Стиральная машина Samsung перестала отжимать и выдавала ошибку. Вызвал мастера — и вот тут я узнал, что «Нева-Экспресс ремонт» и «РБТ-Сервис» теперь объединились! Приехали быстро, диагностировали проблему с модулем управления. Очень удобно, что два крупных сервиса работают вместе: и опыт, и запчасти всегда под рукой. Ремонт стиральных машин СПб теперь на высшем уровне! Спасибо объединённой команде за чёткую работу!
www.streemie.com · March 21, 2026 at 4:00 am
how long does it take to get big on steroids
https://www.muslimlove.com/@christiemckean http://www.muslimlove.com
https://www.hiremegulfs.com/companies/dianabol-before-after-dbol-results/ https://www.hiremegulfs.com
http://47.113.103.172:3000/genevaingham67 47.113.103.172
https://www.k0ki-dev.de/mablen96277160 k0ki-dev.de
http://182.92.251.55:3000/princestralia2 182.92.251.55
https://git.suo0.com/wcokandis64486 https://git.suo0.com
https://git.sskuaixiu.com/kimberlyc64313 https://git.sskuaixiu.com
https://emphira.app/@kennethdkp2970 emphira.app
https://aaredate.ch/@irwinmullagh58 aaredate.ch
https://git.modelhub.org.cn:9443/charleyhudspet git.modelhub.org.cn
https://www.safe-pay.asia/sima7562731506 safe-pay.asia
http://41.180.4.117:3000/edythesellar29 41.180.4.117
http://61.190.74.90:9900/moniquesims879 61.190.74.90
https://qflirt.net/@evelynblackwoo https://qflirt.net
https://backend-dev.podosee.com/margaretzhk48 backend-dev.podosee.com
https://hirekaroo.com/companies/crazybulk-d-bal-review-2026-does-this-natural-steroid-work/ hirekaroo.com
http://113.177.27.200:2033/kathringuillor 113.177.27.200
http://47.100.111.106:3000/osvaldobird46 47.100.111.106
References:
http://49.234.193.192:3000/kendra68244861
www.kirpichnoe-stroitelstvo.ru · March 21, 2026 at 4:10 am
https://kirpichnoe-stroitelstvo.ru/
http://www.matrixboard.ru/fckeditor/edit/?vybor_videokamery.html · March 21, 2026 at 4:21 am
http://www.matrixboard.ru/fckeditor/edit/?vybor_videokamery.html
casinos online chile · March 21, 2026 at 5:10 am
Thanks for sharing the information. I found the information very useful. That’s a awesome story you posted. I will come back to scan some more.
https://turkevi.ru/bez-rubriki/onlayn-stavki-glazami-puteshestvennika-kak-provesti-vecher-v-turtsii-esli-vy-lyubite-sport/ · March 21, 2026 at 5:10 am
https://turkevi.ru/bez-rubriki/onlayn-stavki-glazami-puteshestvennika-kak-provesti-vecher-v-turtsii-esli-vy-lyubite-sport/
top online casino · March 21, 2026 at 5:36 am
A colleague in the field told me to check out your website.
best Irish casino · March 21, 2026 at 6:45 am
I’ll check back after you publish more articles.
top online casino · March 21, 2026 at 8:30 am
Hi, do have a e-newsletter? In the event you don’t definately should get on that piece…this web site is pure gold!
RobertChunk · March 21, 2026 at 8:39 am
Эта информационная заметка содержит увлекательные сведения, которые могут вас удивить! Мы собрали интересные факты, которые сделают вашу жизнь ярче и полнее. Узнайте нечто новое о привычных аспектах повседневности и откройте для себя удивительный мир информации.
Подробнее тут – https://vivod-iz-zapoya-2.ru/
RobertChunk · March 21, 2026 at 9:02 am
В данной обзорной статье представлены интригующие факты, которые не оставят вас равнодушными. Мы критикуем и анализируем события, которые изменили наше восприятие мира. Узнайте, что стоит за новыми открытиями и как они могут изменить ваше восприятие реальности.
Получить дополнительные сведения – https://vivod-iz-zapoya-2.ru/
http://tssz.ru/includes/photo/promo_kod_bk_1xbet_na_segodnya_pri_registracii.html · March 21, 2026 at 9:16 am
http://tssz.ru/includes/photo/promo_kod_bk_1xbet_na_segodnya_pri_registracii.html
https://www.kuzov-auto.ru/fonts/inc/protisty_diatomovye.html · March 21, 2026 at 11:22 am
https://www.kuzov-auto.ru/fonts/inc/protisty_diatomovye.html
http://guidecannabis.com/wp-content/pages/1xbet_code_d_inscription_promo.html · March 21, 2026 at 12:32 pm
http://guidecannabis.com/wp-content/pages/1xbet_code_d_inscription_promo.html
https://prohvost.club/pag/odnorazovye_rashodnye_materialy_dlya_salonov_krasoty_preimuschestva_ispolyzovaniya.html · March 21, 2026 at 1:02 pm
https://prohvost.club/pag/odnorazovye_rashodnye_materialy_dlya_salonov_krasoty_preimuschestva_ispolyzovaniya.html
http://medreviews.ru/images/ph/?melbet_promokod_na_depozit___kak_poluchit_bonus_.html · March 21, 2026 at 3:21 pm
http://medreviews.ru/images/ph/?melbet_promokod_na_depozit___kak_poluchit_bonus_.html
FloydCes · March 21, 2026 at 4:21 pm
Всем привет! Рзучал тему развития бизнеса РІ интернете Рё наткнулся РЅР° полезную статью. Там РїСЂРѕ комплексное продвижение сайтов: SEO, контекст, контент-маркетинг, соцсети, аналитику. Есть блок РїСЂРѕ ошибки Рё РїСЂРѕ современные тренды — персонализация, РР, омниканальность. Рекомендую Рє прочтению: https://wikicom.ru/2025/12/jeffektivnoe-prodvizhenie-sajtov-i-razvitie-biznesa-v-internete/
https://talcom.ru/cart/pages/promokod_pri_registracii_v_1xbet.html · March 21, 2026 at 6:29 pm
https://talcom.ru/cart/pages/promokod_pri_registracii_v_1xbet.html
https://www.redalimentos.cl/wp-content/pgs/?codigo_de_bono_de_dinero_gratis_de_1xbet.html · March 21, 2026 at 7:37 pm
https://www.redalimentos.cl/wp-content/pgs/?codigo_de_bono_de_dinero_gratis_de_1xbet.html
правила игры в блэкджек · March 21, 2026 at 11:25 pm
блэкджек лайв
joycasino официальное зеркало · March 21, 2026 at 11:27 pm
джой казино официальный сайт
https://truworker.com/employer/dianabol-testosterone-beginner-stack/ · March 21, 2026 at 11:52 pm
References:
Injectable steroids for sale usa
References:
https://vw-git.senecasense.com/yongquong0190/mauicountyvirtualjobfair.com2017/wiki/Test-and-Dbol-Cycle-for-Sale
smusic.sochey.com · March 22, 2026 at 1:32 am
References:
Anabolic workout supplements
References:
https://git.parat.swiss/matthiasduffie
situs testi138 · March 22, 2026 at 2:27 am
I am lucky that I discovered this website , precisely the right info that I was searching for! .
instagram follower kaufen · March 22, 2026 at 3:58 am
Hello this is kinda of off topic but I was wondering if blogs use WYSIWYG editors or if you have to manually code with HTML. I’m starting a blog soon but have no coding knowledge so I wanted to get advice from someone with experience. Any help would be enormously appreciated!
casino en ligne Québec · March 22, 2026 at 5:40 am
We can see that we need to develop policies to deal with this trend.
tiktok follower kaufen · March 22, 2026 at 6:28 am
Good post. I study something more difficult on different blogs everyday. It’s going to always be stimulating to learn content material from other writers and observe a little bit one thing from their store. I’d prefer to use some with the content material on my blog whether you don’t mind. Natually I’ll give you a link in your web blog. Thanks for sharing.
https://www.ringfloriangeyer.de · March 22, 2026 at 9:19 am
References:
Steroids side effects female
References:
https://oriolus.org/Uutiset/index.php/;focus=PLNT15_com_cm4all_wdn_Flatpress_489569&path=&frame=PLNT15_com_cm4all_wdn_Flatpress_489569?x=entry:entry251123-183144%3Bcomments:1
tài xỉu sunwin · March 22, 2026 at 9:31 am
Might we expect to see more of these same problems in the future?
kilat69 login link · March 22, 2026 at 9:54 am
Nice post.Very useful info specifically the last part 🙂 Thank you and good luck.
busauszug.com · March 22, 2026 at 12:00 pm
References:
Effects of steroids on the body
References:
https://arzheina.es/Noticias/index.php/;focus=STRATP_com_cm4all_wdn_Flatpress_29305476&path=&frame=STRATP_com_cm4all_wdn_Flatpress_29305476?x=entry:entry240216-125921%3Bcomments:1
https://rodina-lenobl.ru/ · March 22, 2026 at 12:53 pm
https://rodina-lenobl.ru/
celfotu · March 22, 2026 at 5:01 pm
http://bacannales.fr/wp-content/pgs/1win_promo_code_bonus_code_for_registration_free_bet.html
acheter followers instagram · March 22, 2026 at 5:12 pm
I’ll check back after you publish more articles.
laxndof · March 22, 2026 at 5:49 pm
https://tennews.in/1xbet-promo-code-welcome-bonus-100-up-to-e130/
kasyno online opinie · March 22, 2026 at 6:39 pm
Glad to be one of several visitors on this awful internet site : D.
gupoklx · March 22, 2026 at 7:48 pm
https://dezcity74.ru/user/angelmophy
instagram follower kaufen · March 22, 2026 at 7:50 pm
very good post, i certainly love this web site, keep on it
instagram follower kaufen · March 22, 2026 at 7:52 pm
I like meeting utile info, this post has got me even more info!
link alternatif suksestoto · March 22, 2026 at 7:52 pm
Amazing article, cheers, I will bookmark you now.
instagram follower kaufen · March 22, 2026 at 7:54 pm
Nice Post. It’s really a very good article. I noticed all your important points. Thanks.
tiktok follower kaufen · March 22, 2026 at 7:55 pm
Cherished is likely to be what people say about your comments.
instagram follower kaufen · March 22, 2026 at 7:58 pm
Thank you a lot for sharing this with all folks you actually recognize what you’re speaking about! Bookmarked. Please additionally visit my site =). We can have a hyperlink trade contract among us!
tiktok follower kaufen · March 22, 2026 at 7:59 pm
Do you offer workshops?
http://hotel-golebiewski.phorum.pl/viewtopic.php?p=954309#954309 · March 22, 2026 at 9:35 pm
http://hotel-golebiewski.phorum.pl/viewtopic.php?p=954309#954309
гнида позорная · March 23, 2026 at 12:23 am
sniper rifle
https://kinotrap.com/user/meghadneoa · March 23, 2026 at 1:16 am
https://kinotrap.com/user/meghadneoa
porn comics · March 23, 2026 at 5:11 am
ebal
bbfzmca · March 23, 2026 at 6:54 am
https://www.google.io/url?q=https://lmc896.org/articles/melbet_com_promo_code.html
https://decidim.santcugat.cat/profiles/1xbetfreebets5/activity · March 23, 2026 at 9:07 am
https://decidim.santcugat.cat/profiles/1xbetfreebets5/activity
bjuxxjf · March 23, 2026 at 9:31 am
https://digitaltibetan.win/wiki/Post:Cdigo_promocional_1xBet_El_Salvador_2026_1XBUM200
jogodemo · March 23, 2026 at 10:36 am
Jogo do Tigrinho no celular: quem já ganhou big win deitado no sofá em 2026?
колесо удачи · March 23, 2026 at 12:39 pm
фортуна крутить онлайн
рейтинг казино на деньги · March 23, 2026 at 12:42 pm
рейтинг новых казино
колесов николай · March 23, 2026 at 3:05 pm
колесов николай
Aufsperrtdienst Worms · March 23, 2026 at 3:31 pm
Tür öffnen Worms
pgdemo · March 23, 2026 at 3:42 pm
Jogo do Tigrinho ao vivo com narração: já jogou versão com locutor brasileiro?
acheter followers tiktok · March 23, 2026 at 3:51 pm
Just what I needed to know thank you for this.
kasyno online opinie · March 23, 2026 at 5:01 pm
Simply wish to say the frankness in your article is surprising.
kasyno online opinie · March 23, 2026 at 5:08 pm
Thanks , I’ve recently been searching for info about this topic for ages and yours is the best I have discovered so far. But, what concerning the bottom line? Are you certain concerning the source?
Hondenpenning · March 23, 2026 at 5:17 pm
How long does it take you to write an article like this?
kasyno online opinie · March 23, 2026 at 5:37 pm
Thanks for some other great post. Where else may anybody get that kind of information in such an ideal method of writing? I’ve a presentation next week, and I am at the look for such information.
jet x casino · March 23, 2026 at 5:53 pm
В казино jet x casino отличная служба поддержки, которая помогает решить вопросы с выплатами.
блин · March 23, 2026 at 6:34 pm
porno indian
SUARA4D · March 23, 2026 at 6:35 pm
Could not disagree with the main ideas. Wonder how things will develop over the coming years.
najlepsze kasyna online · March 23, 2026 at 7:40 pm
Thanks so much for this, keep up the good work 🙂
acheter followers tiktok · March 23, 2026 at 9:35 pm
Just came from google to your website have to say thanks.
ymrkiht · March 23, 2026 at 11:22 pm
https://www.behance.net/1xbetbcode
https://pedal-the-world.com/codigo-promocional-de-registro-1xbet-2026-1xbum200/ · March 23, 2026 at 11:30 pm
https://pedal-the-world.com/codigo-promocional-de-registro-1xbet-2026-1xbum200/
acheter followers tiktok · March 24, 2026 at 12:02 am
Makes sense to me.
acheter abonnés youtube · March 24, 2026 at 12:17 am
I imagine so. Very good stuff, I agree totally.
najlepsze kasyna online · March 24, 2026 at 12:23 am
With internet full of dupe articles it is nice to find original content like yours thank you so very much.
casino en ligne · March 24, 2026 at 12:52 am
I like meeting utile info, this post has got me even more info!
acheter followers instagram · March 24, 2026 at 12:53 am
A cool post there mate ! Thank you for posting.
acheter followers tiktok · March 24, 2026 at 12:59 am
This is an awesome entry. Thank you very much for the supreme post provided! I was looking for this entry for a long time, but I wasn’t able to find a honest source.
sweetbonanza1000demo · March 24, 2026 at 1:47 am
Jogo do Tigrinho Pix R$30: 150 giros + cashback 15% garantido em 3 sites hoje!
Hondenpenning · March 24, 2026 at 1:59 am
I am glad to be a visitor of this thoroughgoing web blog ! , regards for this rare information! .
pgdemoslots · March 24, 2026 at 2:40 am
Fortune Tiger modo turbo + auto: 800 giros sem parar – quem aguenta mais?
pgsoftdemo · March 24, 2026 at 3:01 am
PG Soft 2026: quem tá ganhando mais no mobile? Celular ou PC?
колесов вертолеты россии генеральный директор · March 24, 2026 at 3:04 am
колесов вертолеты россии генеральный директор
acheter followers instagram · March 24, 2026 at 4:12 am
I know this is not exactly on topic, but i have a blog using the blogengine platform as well and i’m having issues with my comments displaying. is there a setting i am forgetting? maybe you could help me out? thank you.
https://daunemas8a.blogspot.com/2026/03/1xbet-today-promo-code-2026-1xwap200.html · March 24, 2026 at 4:58 am
https://daunemas8a.blogspot.com/2026/03/1xbet-today-promo-code-2026-1xwap200.html
grcuigh · March 24, 2026 at 5:51 am
http://nec.phorum.pl/viewtopic.php?p=784511#784511
sweetbonanzademo · March 24, 2026 at 5:52 am
Fortune Ox explodiu tudo ontem! Quem já limpou a tela com 12+ touros dourados?
jogosdemo · March 24, 2026 at 7:07 am
Fortune Tiger no Pix R$1: Deposita pouco e já sai girando com bônus insano!
win · March 24, 2026 at 7:17 am
Regards for helping out, superb info.
JamesOvard · March 24, 2026 at 8:44 am
Статья про SEO как искусство и науку успеха. Автор разбирает ключевые компоненты продвижения и объясняет, почему это важно для бизнеса. Полезно для общего понимания: https://sushibb.ru/2026/01/30/seo-prodvizhenie-sajta-iskusstvo-i-nauka-uspeha-v-cifrovom-mire/
fortunedragondemo · March 24, 2026 at 9:26 am
Fortune Ox hold & win: já segurou 18 símbolos e explodiu 5000x? Mostra o print!
джет х · March 24, 2026 at 10:32 am
В разделе «Турниры» появилось соревнование по игре джет х с призовым фондом в 1 миллион рублей.
pgjogo · March 24, 2026 at 10:56 am
Fenerbahce 0-3 Nottingham Forest 2026 Europa League play-off shock
jogodotigredemo · March 24, 2026 at 11:43 am
Cassino PG Soft com roleta diária: 50–300 giros grátis no Fortune Tiger
demoslotspg · March 24, 2026 at 12:01 pm
PG Soft cashback semanal: quem já pegou R$300+ só de devolução?
doxlcss · March 24, 2026 at 1:08 pm
https://youslade.com/read-blog/383133
indian porn hd · March 24, 2026 at 2:05 pm
порно чат общение
tigrinhodemográtisdinheiroinfinito · March 24, 2026 at 2:21 pm
Fortune Tiger vs Fortune Ox: qual tem maior potencial de 10000x em 2026?
go88 · March 24, 2026 at 3:33 pm
We are a group of volunteers and starting a new initiative in our community. Your blog provided us with valuable information to work on|.You have done a marvellous job!
sunwin · March 24, 2026 at 4:23 pm
Thanks a bunch for sharing this with all people you really recognize what you are talking about! Bookmarked. Kindly also seek advice from my web site =). We can have a link alternate contract between us!
sunwin · March 24, 2026 at 4:59 pm
Nice read, I just passed this onto a colleague who was doing some research on that. And he just bought me lunch as I found it for him smile Therefore let me rephrase that: Thank you for lunch!
sunwin · March 24, 2026 at 5:39 pm
I dont think Ive caught all the angles of this subject the way youve pointed them out. Youre a true star, a rock star man. Youve got so much to say and know so much about the subject that I think you should just teach a class about it
gbyltjj · March 24, 2026 at 7:03 pm
https://www.pathumratjotun.com/forum/topic/148647/code-promo-1xbet-pari-gratuit—bonus-130-%E2%82%AC
TerryHib · March 24, 2026 at 7:05 pm
Служба доставки цветов Томска показала, что и в нашем городе сервис может быть европейского уровня.
цветы
Carrollshesy · March 24, 2026 at 7:35 pm
Теперь только с вами — идеальный сервис и цветы безупречные.
доставка цветов томск на дом
free hindi porn · March 24, 2026 at 8:18 pm
indian porn star
sunwin · March 24, 2026 at 8:34 pm
Dude.. I am not much into reading, but somehow I got to read lots of articles on your blog. Its amazing how interesting it is for me to visit you very often. –
https://say88vn.com · March 24, 2026 at 8:55 pm
Keep it up!. I usually don’t post in Blogs but your blog forced me to, amazing work.. beautiful A rise in An increase in An increase in.
sunwin · March 24, 2026 at 9:11 pm
I enjoy your blog posts, saved to my bookmarks!
casino en ligne Canada · March 24, 2026 at 9:33 pm
Nice Post. It’s really a very good article. I noticed all your important points. Thanks.
relax and repair facials in Brisbane · March 24, 2026 at 10:09 pm
About relax and repair facials in Brisbane
Good Day Girls,
We have detailed information about https://webllogg.com/what-are-the-4-skin-types/
As your therapist, I’ve worked for almost 20 years helping people achieve fresher faces.
Now I’m sharing my expertise in this guide on restorative facials Brisbane.
What I value about these sessions is that they’re designed for anyone — whether you’re overwhelmed, tired, or just needing a reset — who’d want to get their skin back on track while they unwind.
At The Facial Hub, that’s exactly what we’re all about.
### Why Relax and Repair Facials Matter
These facials are growing in popularity — and for good reason.
The pressure our skin is under — pollution, disrupted sleep, digital glare, internal changes, harsh routines — has reached epic levels.
Clients come to me feeling frazzled, and to be honest, a facial that just chases glow isn’t always the answer.
A good Relax and Repair facial balances evidence with empathy — it nurtures inside and out.
### The Brisbane Climate Challenge
In Brisbane’s environment, with moisture, sunlight, and pollution, dehydration and skin imbalance can take hold.
A relaxation-focused facial can counteract all that by calming inflammation, deeply rehydrating, and strengthening the barrier.
The result? Skin that’s calmer, resilient, and ready to manage the challenges of modern life.
about https://webllogg.com/what-are-the-4-skin-types/ please click https://webllogg.com/what-are-the-4-skin-types/ for a free consultation now!
подбор товаров для строительства · March 24, 2026 at 10:38 pm
керамзит строительный купить Ростов-на-Дону
StephenDAL · March 24, 2026 at 10:43 pm
Очень нежный букет из роз сделали для подруги, выглядел дорого и при этом без лишнего пафоса.
розы в Томске
LonnieCherb · March 24, 2026 at 11:36 pm
?Курьер приехал аккуратный, опрятный, приятно, когда и такой момент тоже продуман.
доставка цветов томск
betãocomcassino · March 24, 2026 at 11:46 pm
PG Soft 2026: qual slot da série Fortune você acha que vai explodir mais esse ano?
top 10 casino en ligne belgique · March 25, 2026 at 12:44 am
Just a quick note to express my appreciation. Take care
top 10 casino en ligne belgique · March 25, 2026 at 1:31 am
Thanks for a Interesting item; I enjoyed it very much. Regards Sang Magistrale
Digital PR Agency · March 25, 2026 at 3:28 am
Do you offer workshops?
top 10 casino en ligne belgique · March 25, 2026 at 4:00 am
I wanted to check up and let you know how, a great deal I cherished discovering your blog today. I might consider it an honor to work at my office and be able to utilize the tips provided on your blog and also be a part of visitors’ reviews like this. Should a position associated with guest writer become on offer at your end, make sure you let me know.
Morphine · March 25, 2026 at 6:23 am
shop
мусор ебанный · March 25, 2026 at 6:57 am
порно секс видеочат пары
hindi mms video · March 25, 2026 at 7:26 am
mature porn
AnthonyKayar · March 25, 2026 at 9:13 am
Всем привет! Для тех, кто разбирается в продвижении в соцсетях, нашел хорошую статью. Автор подробно останавливается на принципах работы, инструментах и показателях эффективности. Есть разделы про выбор подрядчика и локальные особенности для Москвы. Много полезного для планирования стратегии. Вот ссылка: https://foto-videomontaz.ru/smm-prodvizhenie-v-soczialnyh-setyah-princzipy-instrumenty-i-pokazateli-effektivnosti/
AnthonyKayar · March 25, 2026 at 9:19 am
Искал информацию по локальному SMM-продвижению и наткнулся на этот материал. Автор объясняет, как адаптировать стратегию под московскую аудиторию и учитывать локальные тренды. Есть примеры кейсов. Полезно: https://foto-videomontaz.ru/smm-prodvizhenie-v-soczialnyh-setyah-princzipy-instrumenty-i-pokazateli-effektivnosti/
Carrollshesy · March 25, 2026 at 10:34 am
Заказывала композицию в шляпной коробке — невероятно красиво!
доставка цветов томск
shop · March 25, 2026 at 10:36 am
allporncomic
jogodapgdemo · March 25, 2026 at 10:45 am
Jogo do Tigrinho estratégia baixa aposta: R$0,25 por 1000 giros – funciona?
TerryHib · March 25, 2026 at 11:28 am
Сделали по Томску доставку цветов на точное время, как я и просил, ни минутой позже.
dostavkacvetovtomsk6
femboy porn · March 25, 2026 at 12:25 pm
heroin chic
porn video · March 25, 2026 at 12:37 pm
what are amphetamine salts
тупой как пробка ублюдок · March 25, 2026 at 1:47 pm
gay porn
voyance gratuite · March 25, 2026 at 3:28 pm
Clear, concise and easy to access.
gxxbaiy · March 25, 2026 at 4:02 pm
https://www.weddingbee.com/members/promomelbet3/
sexual · March 25, 2026 at 6:39 pm
Heroin
http://ezproxy.cityu.edu.hk/login?url=https://www.feldbahn-ffm.de/wp-content/pgs/1xbet_promo_code_106.html · March 25, 2026 at 7:39 pm
http://ezproxy.cityu.edu.hk/login?url=https://www.feldbahn-ffm.de/wp-content/pgs/1xbet_promo_code_106.html
klkkfrh · March 25, 2026 at 7:56 pm
https://pad.snopyta.org/s/24aRySgOU
tigrinhogratis · March 25, 2026 at 8:37 pm
PG Soft tá liberando cashback 15% todo dia no Fortune Tiger – qual site tá dando mais?
vqtyyln · March 26, 2026 at 12:08 am
https://rockmanjewelry.com
sex comic · March 26, 2026 at 12:24 am
xxx porn
porn · March 26, 2026 at 4:57 am
rifle
slotdemopgsoftgrátisfortunetiger · March 26, 2026 at 7:55 am
Jogo do Tigrinho multiplicador aleatório: melhor que respins fixos ou não? Opine!
чмо ебаное · March 26, 2026 at 9:11 am
xhamster.com
anal porn · March 26, 2026 at 9:38 am
секс порно чат рулетка
TerryHib · March 26, 2026 at 10:03 am
Очень комфортно работать с этим сервисом в Томске: доставка цветов без лишних хлопот.
цветы томск
StephenDAL · March 26, 2026 at 11:36 am
Курьер аккуратно доставил букет из роз, ни один бутон не был сломан, всё на своих местах.
купить розы Томск
Carrollshesy · March 26, 2026 at 11:59 am
Порадовало, что можно выбрать букет под бюджет и всё равно получить красоту.
заказ цветов томск
alt yaz?l? porno · March 26, 2026 at 12:22 pm
секс веб чат
LonnieCherb · March 26, 2026 at 12:30 pm
?Цветы были такие яркие, что даже при приглушённом свете смотрелись шикарно.
заказ цветов томск с доставкой
porn izle · March 26, 2026 at 1:32 pm
сраный урод
JamesOvard · March 26, 2026 at 1:38 pm
Рскал информацию Рѕ том, как повысить видимость сайта, Рё нашёл эту статью. Автор объясняет, что SEO — это РЅРµ только РїСЂРѕ РїРѕРёСЃРєРѕРІРёРєРё, РЅРѕ Рё РїСЂРѕ удобство для пользователей. Есть практические советы. Почитайте: https://drnonadv.ru/seo-prodvizhenie-sajta-iskusstvo-vidimosti-v-cifrovom-mire/
https://youralareno.com/members/5melbetbonus904/activity/135603/ · March 26, 2026 at 2:12 pm
https://youralareno.com/members/5melbetbonus904/activity/135603/
gay porn · March 26, 2026 at 3:37 pm
xhamster.com
najbolji online casino · March 26, 2026 at 6:52 pm
Good points – – it will make a difference with my parents.
fenlkqr · March 26, 2026 at 8:18 pm
https://novoevnukovo.ru/index.php?topic=15590.new#new
magyar online casino · March 26, 2026 at 8:20 pm
This contained some excellent tips and tools. Great blog publication.
best new online casino · March 26, 2026 at 8:38 pm
What’s Happening i’m new to this, I stumbled upon this I’ve found It positively useful and it has aided me out loads. I hope to contribute & help other users like its aided me. Great job.
https://autobazar.eu/ · March 26, 2026 at 8:55 pm
https://autobazar.eu/
DwightDoogy · March 26, 2026 at 9:48 pm
Доставка цветов — всегда да, Томск!
купить цветы томск
Michaelsoido · March 26, 2026 at 10:44 pm
Заказала розы в район Мокрушинский – все бутоны были perfect!
заказ цветов томск
casino en ligne international · March 26, 2026 at 10:53 pm
I truly appreciate this post. I have been looking everywhere for this! Thank goodness I found it on Bing. You have made my day! Thank you again
online casino hrvatska · March 26, 2026 at 11:16 pm
I think this is among the so much vital info for me. And i’m happy reading your article. But wanna remark on few common issues, The site style is wonderful, the articles is really excellent : D. Just right job, cheers
najlepsze polskie kasyno online · March 27, 2026 at 1:23 am
This is really interesting, You’re a very skilled blogger. I have joined your feed and look forward to seeking more of your great post. Also, I’ve shared your web site in my social networks!
meilleur casino en ligne suisse · March 27, 2026 at 1:26 am
Spot on with this write-up, I actually assume this website needs far more consideration. I will in all probability be once more to learn rather more, thanks for that info.
meilleur casino en ligne belgique · March 27, 2026 at 1:30 am
Pretty nice post. I just stumbled upon your weblog and wanted to say that I’ve really enjoyed surfing around your blog posts. After all I’ll be subscribing in your feed and I am hoping you write again very soon!
best canadian online casino · March 27, 2026 at 1:36 am
Thank you, I have just been searching for information about this topic for ages and yours is the greatest I’ve discovered till now. But, what about the conclusion? Are you sure about the source?
najlepsze polskie kasyno online · March 27, 2026 at 1:58 am
Oh my goodness! an amazing article. Great work.
fortunetigerbônusgrátissemdepósito · March 27, 2026 at 3:33 am
Jogo do Tigrinho Pix R$20: ganha 100 giros + 20% extra hoje!
bfmlhen · March 27, 2026 at 8:13 am
https://sanad.org.sa/
DwightDoogy · March 27, 2026 at 9:03 am
Выручили по полной, когда нужно было срочно отправить букет в Томск из другого города.
заказать цветы томск
TerryHib · March 27, 2026 at 9:07 am
Сервис доставки цветов Томска произвел впечатление продуманностью мелочей.
доставка цветов в томске
StephenDAL · March 27, 2026 at 9:31 am
Сервис приятно удивил: к букету из роз предложили ещё и маленькую открытку, получилось очень трогательно.
купить розы Томск
xwgmnhj · March 27, 2026 at 9:34 am
https://walkindermatology.com/
https://novoevnukovo.ru/index.php?topic=15618.new#new · March 27, 2026 at 10:18 am
https://novoevnukovo.ru/index.php?topic=15618.new#new
LonnieCherb · March 27, 2026 at 11:34 am
?Букет оказался намного больше, чем я ожидала, приятно, когда не пытаются на всём экономить.
доставка цветов в томске
планкен скошенный из лиственницы · March 27, 2026 at 11:42 am
планкен скошенный из лиственницы
Carrollshesy · March 27, 2026 at 12:37 pm
Букет стоял долго, листья не завяли, огромное спасибо.
заказать цветы с доставкой в томске
RATU89 login · March 27, 2026 at 4:34 pm
Nevertheless, it’s all carried out with tongues rooted solidly in cheeks, and everybody has got nothing but absolutely love for their friendly neighborhood scapegoat. In reality, he is not merely a pushover. He is simply that extraordinary breed of person solid enough to take all that good natured ribbing for what it really is.
폰테크 · March 27, 2026 at 6:36 pm
폰테크
폰테크는 현금이 빠르게 필요할 때 자주 검토되는 수단으로 소개됩니다. 최근 들어 비대면 진행과 당일 입금, 미납요금 대납, 전국 상담 같은 항목이 함께 붙으면서 소개 방식도 많아졌습니다. 하지만 검토할 때는 속도보다 절차를 먼저 확인해야 합니다. 어떤 절차로 접수되고 진행되고 입금되는지 보는 것이 우선입니다.
비대면 방식의 폰테크는 방문 없이 상담부터 접수, 진행 안내까지 이어지는 구조가 많습니다. 수도권뿐 아니라 강원도, 충청도, 전라도, 경상도, 제주까지 전국 단위 상담을 내세우는 경우도 많습니다. 방문 부담이 적다는 점은 분명 편리하지만, 보기보다 단순해 보여도 조건 확인은 더 꼼꼼해야 합니다.
이런 서비스 안내에서는 속도와 상시 상담을 강조하는 표현이 반복되는 경우가 많습니다. 중요한 것은 표현보다 실제 진행 방식입니다. 상담 기준 기종, 매입 조건, 가능한 진행 방식, 접수 후 입금 시점까지 분명해야 합니다.
진행 흐름은 대체로 비슷합니다. 전화, 문자, 카카오톡으로 상담 신청을 받고, 이후 기종과 조건에 맞춰 상담을 진행한 뒤, 방문, 출장, 비대면, 대납 중 방식을 고른 뒤, 기기 수령 뒤 바로 지급으로 이어지는 방식입니다. 순서는 짧아 보여도 실제 확인 항목은 적지 않습니다. 특히 처음 상담 단계에서 가능 조건을 분명히 해두는 것이 중요합니다.
전국 대응을 강조하는 업체들은 서울, 부산, 대구, 경기, 인천, 광주, 울산, 대전, 세종, 강원, 충북, 충남, 전북, 전남, 경북, 경남, 제주처럼 지역명을 촘촘히 배치합니다. 이런 나열 방식은 지역 기반 검색에 맞춰진 구성이며, 이용자에게 자기 지역도 가능하다는 인식을 줍니다. 지역명과 서비스명을 붙인 표현이 반복되는 이유도 여기에 있습니다.
상담 채널은 보통 대표전화, 카카오톡, 상담신청 버튼처럼 바로 연결되는 구조로 잡힙니다. 보통 이런 채널 옆에는 신속 진행이나 1:1 상담 문구가 함께 배치됩니다. 하지만 실제 판단 기준은 문구가 아니라 운영 정보, 절차 설명, 상담 내용의 명확성입니다.
정리하면 핵심은 세 가지입니다. 현금이 급할 때 빠르게 검토할 수 있다는 점, 비대면과 전국 단위 상담이 가능하다는 점, 절차 흐름이 비교적 단순하다는 점입니다. 이용자 기준에서는 빠르다는 말보다 조건과 절차를 먼저 보는 편이 맞습니다.
LonnieCherb · March 27, 2026 at 7:47 pm
?Флористы попали в настроение праздника, угадали и с цветами, и с общим стилем.
розы томск
najlepsze kasyno online · March 27, 2026 at 9:16 pm
Appreciation for taking the time to discuss this topic, I would love to discover more on this topic. If viable, as you gain expertise, would you object to updating the website with further information? It is tremendously beneficial for me.
Carrollshesy · March 27, 2026 at 9:19 pm
Каждый раз заказываю для родных в Томске, и результат безупречен.
букеты томск
zahraniční online casino · March 27, 2026 at 10:46 pm
Amazing! Your site has quite a few comment posts. How did you get all of these bloggers to look at your site I’m envious! I’m still studying all about posting articles on the net. I’m going to view pages on your website to get a better understanding how to attract more people. Thank you!
meilleur casino en ligne suisse · March 27, 2026 at 11:51 pm
Just a quick note to express my appreciation. Take care
Maryzot · March 27, 2026 at 11:52 pm
Здравствуйте!
Посетитель приходит на сайт с ожиданием, даже если сам его не формулирует. Если текст звучит слишком прямолинейно, он уходит. Но если слова оставляют вопрос без ответа, он задерживается. Эта задержка — главный показатель того, что внимание удержано. И чем дольше он остаётся, тем выше шанс, что визит превратится в заявку.
Полная информация по ссылке – https://www.ts-web.ru/blog/development/cms-security.html
SEO продвижение сайтов для отелей и туризма, услуги SEO оптимизации в Дагестане, SMM продвижение интернет-магазина
услуги SMM продвижения под ключ, TS-Web — создание сайтов, SEO и поддержка, аудит сайта цена услуги
Удачи и комфорта в жизни!
Лендинг под ключ: быстрые лиды и заявки 45951a6
mtbdjgo · March 28, 2026 at 12:11 am
https://nusapure.com/
best online casino Canada · March 28, 2026 at 12:13 am
I am glad to be a visitor on this website!, regards for this rare information!
Maryzot · March 28, 2026 at 12:18 am
Привет всем!
Контекстная реклама в Яндекс Директ и Google Ads часто воспринимается как простая настройка кабинета. Но клиенту важно понимать, что именно он получает. Если текст ограничен словами про показы и клики, доверия нет. Но если объяснить: подбор ключевых слов, креативные объявления, тестирование гипотез и аналитика, внимание сохраняется. Особенно если добавить реальный кейс: «продвижение услуг психолога через контекстную рекламу в Дагестане».
Полная информация по ссылке – https://www.ts-web.ru/cases/baltmashstroy.html
создание интернет-магазина под ключ цена, миграция сайтов WordPress в Махачкале, создание сайтов для крупного бизнеса
разработка сайтов для компаний Дагестан, Дизайн, услуги SMM агентства Москва
Удачи и комфорта в жизни!
SEO продвижение в Google: рост позиций и доверия 7049459
uebok · March 28, 2026 at 12:20 am
гнида конченая
acheter followers instagram · March 28, 2026 at 3:05 am
Just came from google to your website have to say thanks.
zahraniční online casino · March 28, 2026 at 3:09 am
Took me time to read all the comments, but I really enjoyed the article. It proved to be Very helpful to me and I am sure to all the commenters here It’s always nice when you can not only be informed, but also entertained I’m sure you had fun writing this article.
acheter followers tiktok · March 28, 2026 at 3:57 am
I like the helpful information you provide in your articles. I’ll bookmark your blog and check again here frequently. I am quite certain I’ll learn many new stuff right here! Best of luck for the next!
мразь конченая · March 28, 2026 at 4:36 am
q porno
acheter abonnés youtube · March 28, 2026 at 5:36 am
This website has lots of really useful stuff on it. Thanks for informing me.
acheter followers instagram · March 28, 2026 at 6:11 am
Amazing! Your site has quite a few comment posts. How did you get all of these bloggers to look at your site I’m envious! I’m still studying all about posting articles on the net. I’m going to view pages on your website to get a better understanding how to attract more people. Thank you!
top 10 casino en ligne belgique · March 28, 2026 at 6:19 am
I just added your web site to my blogroll, I hope you would look at doing the same.
Top rated concierge medicine practices in Las Vegas Valley · March 28, 2026 at 6:54 am
Only a smiling visitor here to share the love (:, btw outstanding style and design .
beste ausländische online casinos · March 28, 2026 at 7:04 am
Nice post.Very useful info specifically the last part 🙂 Thank you and good luck.
beste online casino Österreich · March 28, 2026 at 7:36 am
This article actually helped me with a report I was doing.
japanese porn · March 28, 2026 at 8:53 am
stake bet
acheter followers instagram · March 28, 2026 at 8:57 am
Hello there, just became aware of your blog through Google, and found that it is truly informative. I am going to watch out for brussels. I will appreciate if you continue this in future. Lots of people will be benefited from your writing. Cheers!
acheter abonnés youtube · March 28, 2026 at 9:44 am
We can see that we need to develop policies to deal with this trend.
http://pattern-wiki.win/index.php?title=craigfitzpatrick6721 · March 28, 2026 at 9:48 am
oral steroid cycle
References:
http://pattern-wiki.win/index.php?title=craigfitzpatrick6721
xxpghth · March 28, 2026 at 9:59 am
https://xn--80ady2a0c.xn--p1ai/52073-prilozhenie-olimp-bet-skachat-i-ustanovit-v-kazahstane.html
porn videos · March 28, 2026 at 10:09 am
korean xxx
acheter followers instagram · March 28, 2026 at 10:49 am
I would share your post with my sis.
acheter followers tiktok · March 28, 2026 at 1:33 pm
This has to be one of my favorite posts! And on top of thats its also very helpful topic for newbies. thank a lot for the information!
acheter followers tiktok · March 28, 2026 at 1:50 pm
I just couldn’t leave your website before suggesting that I really enjoyed the usual information an individual supply on your visitors? Is gonna be back often in order to investigate cross-check new posts
yrlqljn · March 28, 2026 at 2:36 pm
https://planetasp.ru/forum/viewtopic.php?pid=28363#p28363
followers tiktok · March 28, 2026 at 4:41 pm
I feel that is among the so much significant info for me. And i am satisfied studying your article. However should commentary on some basic issues, The site style is ideal, the articles is in reality excellent : D. Excellent activity, cheers
acheter des followers instagram · March 28, 2026 at 5:45 pm
Hi, possibly i’m being a little off topic here, but I was browsing your site and it looks stimulating. I’m writing a blog and trying to make it look neat, but everytime I touch it I mess something up. Did you design the blog yourself?
Buy footwear online · March 28, 2026 at 6:06 pm
I just added this to my favorites. I truly love reading your posts. Tyvm!
sarknln · March 28, 2026 at 7:08 pm
https://dveri-arena.ru/
achat abonnes youtube · March 28, 2026 at 9:47 pm
Good site! I truly love how it is easy on my eyes it is. I am wondering how I might be notified when a new post has been made. I’ve subscribed to your RSS which may do the trick? Have a great day!
AnthonyKayar · March 29, 2026 at 3:44 am
Интересный материал про автоматизацию SMM. Автор рассказывает, какие инструменты помогают экономить время на рутинных задачах: от планирования публикаций до мониторинга упоминаний. При этом подчёркивает важность «очеловеченного» подхода в коммуникации. Почитайте: https://iwatt24.ru/uslugi-smm/
AnthonyKayar · March 29, 2026 at 3:50 am
Статья поможет разобраться, как правильно оформить договор с SMM-подрядчиком. Автор разбирает важные пункты: права на контент, конфиденциальность данных, гарантии и сроки. Особенно актуально для тех, кто уже обжигался на недобросовестных исполнителях: https://f1-it.ru/uslugi-smm-prodvizheniya-v-sotsialynh-setyah.html
Anatolylet · March 29, 2026 at 4:40 am
Дом из клееного бруса — это не только про практичность, но и про эстетику. одноэтажный дом из клееного бруса Текстура натурального дерева на стенах создаёт неповторимую атмосферу тепла и уюта. официальный сайт Многие владельцы даже не закрывают стены отделкой — просто покрывают маслом или лаком.
Ruslanlet · March 29, 2026 at 4:48 am
Дом из клееного бруса с камином — настоящая мечта для загородной жизни в Петербурге. строительство деревянных домов СПб Представьте: за окном снег, а вы сидите у камина в тёплом деревянном доме. строительство дома из клееного бруса под ключ Такие моменты бесценны, и правильный проект дома помогает их создать.
Evgenylet · March 29, 2026 at 7:18 am
Детский комплекс с башней — настоящий замок для маленьких рыцарей и принцесс. детская площадка для дачи Такие конструкции развивают фантазию и становятся центром ролевых игр. детская площадка Дети могут играть в пиратов, рыцарей или исследователей.
Ruslanlet · March 29, 2026 at 7:27 am
Детский игровой комплекс на даче — это не просто развлечение, а целый мир для ребёнка. детская площадка для дачи Дети проводят время на свежем воздухе, развивают координацию и получают массу положительных эмоций. детский городок Хорошая площадка служит 10-15 лет и окупает себя многократно.
https://codeville.org/gerborsyva-analyse-einer-digitalen-investmentplattform-aus-b2b-perspektive/ · March 29, 2026 at 10:49 am
https://codeville.org/gerborsyva-analyse-einer-digitalen-investmentplattform-aus-b2b-perspektive/ The Rise of AI Unicorns: Where Smart Money Is Going
faster payments · March 29, 2026 at 11:42 am
faster payments
폰테크 · March 29, 2026 at 12:12 pm
폰테크
폰테크라는 방식은 현금이 빠르게 필요할 때 자주 검토되는 수단으로 언급됩니다. 최근에는 비대면 진행과 당일 입금, 미납요금 대납, 전국 상담 같은 항목이 함께 붙으면서 안내 문구도 늘어났습니다. 하지만 진행을 알아볼 때는 빠르다는 말보다 진행 구조를 먼저 봐야 합니다. 어떻게 접수되고, 어떤 방식으로 진행되며, 입금까지 어떤 절차를 거치는지 확인하는 쪽이 더 중요합니다.
비대면 폰테크는 방문 없이 상담, 접수, 진행 안내까지 상당 부분을 원격으로 처리하는 형태가 중심입니다. 수도권뿐 아니라 강원·충청·전라·경상·제주까지 전국 상담이 가능하다고 안내하는 경우가 많습니다. 방문 부담이 적다는 점은 분명 편리하지만, 보기보다 단순해 보여도 조건 확인은 더 꼼꼼해야 합니다.
폰테크·가개통 안내 문구에서는 당일 진행, 당일 입금, 24시간 상담, 연중무휴 같은 문구가 자주 보입니다. 이런 문구보다 더 중요한 것은 진행 방식의 구체성입니다. 어떤 기종을 다루는지, 조건이 어떻게 정해지는지, 어떤 방식으로 진행 가능한지, 입금 시점이 언제인지까지 확인돼야 합니다.
전체 진행 순서는 대체로 비슷합니다. 전화나 문자, 카카오톡으로 상담을 시작한 뒤, 그다음 기종과 조건을 맞춰 상담을 진행하고, 방문, 출장, 비대면, 대납 중 방식을 고른 뒤, 기기 수령 후 당일 지급으로 이어지는 구조입니다. 순서는 짧아 보여도 실제 확인 항목은 적지 않습니다. 특히 처음 상담 단계에서 가능 조건을 분명히 해두는 것이 중요합니다.
전국 단위로 운영된다고 하는 곳들은 지역명을 세세하게 나열하는 경우가 많습니다. 이런 나열 방식은 지역 기반 검색에 맞춰진 구성이며, 방문자에게 본인 지역도 포함된다는 느낌을 줍니다. 지역명과 서비스명을 붙인 표현이 반복되는 이유도 여기에 있습니다.
상담 채널은 보통 대표전화, 카카오톡, 상담신청 버튼처럼 바로 연결되는 구조로 잡힙니다. 보통 이런 채널 옆에는 신속 진행이나 1:1 상담 문구가 함께 배치됩니다. 다만 판단 기준은 광고 문구가 아니라 운영 정보와 절차 설명입니다.
요약하면 핵심 포인트는 세 가지입니다. 급전 상황에서 빠르게 진행할 수 있다는 점, 비대면과 전국 상담이 가능하다는 점, 상담 신청부터 지급까지 흐름이 단순하다는 점입니다. 반대로 실제 확인 포인트는 속도가 아니라 조건과 절차, 지역 대응 범위입니다.
Sunwin · March 29, 2026 at 1:26 pm
Hi my family member! I want to say that this article is amazing, great written and include approximately all important infos. I’d like to see more posts like this .
go88 · March 29, 2026 at 3:29 pm
I just couldn’t leave your web site prior to suggesting that I really enjoyed the standard info an individual supply to your guests? Is going to be again continuously in order to inspect new posts
glxakec · March 29, 2026 at 7:52 pm
https://www.4shared.com/u/t3ZqXem1/cvv45180.html
написать текст для курсовой · March 29, 2026 at 11:26 pm
<a href="https://eroscream.myeboook.xyz/besplatnaya-kursovaya-rabota-na-temu-neyroseti-dlya-rossiyskikh-studentov/"написать текст для курсовой
폰테크 · March 30, 2026 at 1:14 pm
폰테크
폰테크는 보통 급하게 현금이 필요할 때 빠르게 검토되는 방식으로 거론됩니다. 요즘은 비대면 진행과 당일 입금, 미납요금 대납, 전국 상담 같은 항목이 같이 노출되면서 소개 방식도 많아졌습니다. 다만 실제로 알아볼 때는 속도보다 구조를 먼저 봐야 합니다. 접수 방식, 진행 형태, 입금까지의 흐름을 먼저 확인하는 편이 낫습니다.
비대면 폰테크의 경우 방문 없이 상담부터 접수, 진행 안내까지 이어지는 구조가 많습니다. 서울, 경기, 인천 같은 수도권뿐 아니라 강원·충청·전라·경상·제주까지 전국 상담이 가능하다고 안내하는 경우가 많습니다. 이동 부담이 적다는 점은 장점이지만, 절차가 단순해 보일수록 조건 확인은 더 정확해야 합니다.
폰테크나 가개통 안내에서는 보통 당일 진행, 당일 입금, 24시간 상담, 365일 연중무휴 같은 표현이 반복됩니다. 중요한 것은 표현보다 실제 진행 방식입니다. 어떤 기종을 기준으로 상담하는지, 매입 조건이 어떻게 잡히는지, 비대면·방문·출장·대납 중 어떤 방식이 가능한지, 접수 후 입금은 언제 이뤄지는지까지 정리돼 있어야 합니다.
전체 진행 순서는 대체로 비슷합니다. 전화나 문자, 카카오톡으로 상담을 시작한 뒤, 그다음 기종과 조건을 맞춰 상담을 진행하고, 방문, 출장, 비대면, 대납 중 방식을 고른 뒤, 기기 수령 후 당일 지급으로 이어지는 구조입니다. 단계 수는 적어 보여도 실제로는 각 단계마다 확인할 내용이 다릅니다. 상담 단계에서 진행 가능 여부와 조건을 명확히 해야 이후 혼선이 적습니다.
전국 단위로 운영된다고 하는 곳들은 지역명을 세세하게 나열하는 경우가 많습니다. 이런 방식은 지역 키워드 노출에 유리하고, 사용자에게 해당 지역에서도 진행 가능하다는 인상을 줍니다. 지역명과 서비스명을 붙인 표현이 반복되는 이유도 여기에 있습니다.
상담 채널은 대체로 전화, 카카오톡, 신청 버튼 중심으로 구성됩니다. 그리고 여기에 정식등록업체, 당일입금, 1:1 상담 같은 표현이 더해집니다. 하지만 실제 판단 기준은 문구가 아니라 운영 정보, 절차 설명, 상담 내용의 명확성입니다.
결국 폰테크 소개에서 핵심은 세 가지입니다. 빠른 진행 가능성, 비대면과 전국 대응, 단순한 진행 흐름이 주된 포인트입니다. 이용자 기준에서는 빠르다는 말보다 조건과 절차를 먼저 보는 편이 맞습니다.
fortuneoxdemográtis · March 31, 2026 at 1:28 am
Dinamo Zagreb 1-3 Genk 2026 Europa League dominant win for Belgians
http://103.119.85.197/ · March 31, 2026 at 1:11 pm
how to buy anabolic steroids
https://gitea-inner.fontree.cn/kristieheng62/code.hpswk.com2010/wiki/Clenbuterol-f%C3%BCr-Muskelaufbau-%26-Abnehmen-Gratis-Trainingsplan https://gitea-inner.fontree.cn
https://git.limework.net/estelladow6504 git.limework.net
https://gitea.diputadosalta.gob.ar/hyelangner6509 gitea.diputadosalta.gob.ar
http://183.204.60.122:10081/claudiaschonel http://183.204.60.122/
http://47.100.44.145:3000/susiewitte3357/git.miasma-os.com2045/wiki/Clenbuterol-Zum-Abnehmen-Dosierung 47.100.44.145
http://119.96.62.56:3000/vaniaschwing6 http://119.96.62.56
https://git.fs.cs.uni-frankfurt.de/liamfrankland8 https://git.fs.cs.uni-frankfurt.de/liamfrankland8
http://8.155.172.147:3001/keljohnette653 http://8.155.172.147/
http://175.27.229.211:3000/jettagoll29279 http://175.27.229.211
https://git.hanumanit.co.th/ludiebeckwith8/6359586/wiki/Is-Clenbuterol-Better-Option-for-Bodybuilders git.hanumanit.co.th
http://39.96.211.118:3000/laurened83710/2491632/wiki/Kaufen-Sie-Spiropent%C2%AE-Online-Verschreibung-und-Medikamente http://39.96.211.118
https://www.chembans.com/@theresa57t3199 https://www.chembans.com
https://git.cloudsean.com/mabel841947702 https://git.cloudsean.com/mabel841947702
http://106.55.61.128:3000/epifaniakersey 106.55.61.128
http://120.201.125.140:3000/kayla58u200386 http://120.201.125.140/
https://www.cives.pl/jamila8130724 cives.pl
https://tubevieu.com/@ofeliag5227054?page=about https://tubevieu.com/@ofeliag5227054?page=about
https://www.ohovideo.com/@shauntecambell?page=about http://www.ohovideo.com
References:
https://gitea.syn-assist.fr/carmineqdq3200/4024555/wiki/SPIROPENT-Tabletten-01980325
best canadian online casino · March 31, 2026 at 1:32 pm
This information is critically needed, thanks.
47.105.59.0 · March 31, 2026 at 1:43 pm
References:
Sublingual prohormones
References:
http://dibodating.com/@leliabaxley020
sunwin · March 31, 2026 at 2:35 pm
Thanks pertaining to discussing the following superb written content on your site. I ran into it on the search engines. I will check back again if you publish extra aricles.
https://digitalafterlife.org/@freyaalonso41?page=about · March 31, 2026 at 3:00 pm
References:
Best muscle stacks 2015
References:
https://dyipniflix.com/site/@felipaburns94?page=about
casino en ligne · March 31, 2026 at 3:01 pm
Its just like you read my thoughts! It’s like reading about my family.
47.113.145.232 · March 31, 2026 at 3:31 pm
how to do steroids
https://www.meetgr.com/@ernestineescob http://www.meetgr.com
https://www.bongmedia.tv/@moisesloftin72?page=about http://www.bongmedia.tv
http://15.237.198.144/nolalomax10813 http://15.237.198.144
https://goondepot.com/@barrettbevill8?page=about goondepot.com
https://gitea.jnyuxia.com/stars14799362 https://gitea.jnyuxia.com/
https://tubevieu.com/@leonelv5677589?page=about tubevieu.com
https://git.saike.fun:9755/carleyfinniss4/carley2020/wiki/Spiropent-Gebrauchsinformation https://git.saike.fun:9755/carleyfinniss4/carley2020/wiki/Spiropent-Gebrauchsinformation
https://git.automathon.org/ankespaull378 git.automathon.org
https://git.suo0.com/darrenb706798/darren1981/wiki/Clenbuterol-im-Bodybuilding%3A-Nutzen%2C-Risiken git.suo0.com
https://www.workerrenter.pro/profile/ddxtiffany376 http://www.workerrenter.pro
https://play.talkdrove.cc.nf/@rayfordburris?page=about https://play.talkdrove.cc.nf/
http://36.213.200.127:23000/annabellecoane http://36.213.200.127:23000/annabellecoane
https://truthtube.video/@wesleyrosenhai?page=about truthtube.video
http://152.136.187.229/willycommons9 http://152.136.187.229/willycommons9
https://git.opnkty.uk/wilmer15h3413/9245dammsound.com/wiki/Clenbuterol-einnehmen%3A-Risiken-und-Nebenwirkungen https://git.opnkty.uk
https://gitea.pnkx.top:8/bonitaweedon4 https://gitea.pnkx.top/
http://www.xngel.com/@haydenhenn384?page=about http://www.xngel.com/@haydenhenn384?page=about
https://hipstrumentals.net/janisidaway50 https://hipstrumentals.net/
References:
https://www.workbay.online/profile/lilla697358338
najlepsze kasyno online · March 31, 2026 at 3:33 pm
you may have an ideal blog here! would you prefer to make some invite posts on my blog?
pgslotsdemo · March 31, 2026 at 3:37 pm
Brann 0-1 Bologna 2026 Europa League late Italian steal
kasyno online · March 31, 2026 at 3:54 pm
It’s continually awesome when you can not only be informed, but also entertained! I’m sure you had fun writing this article. Regards, Clotilde.
https://koonis.net/debbraharlow99 · March 31, 2026 at 4:29 pm
what can steroids do to your body
https://gitea.kdlsvps.top/arlettethorne3 https://gitea.kdlsvps.top/arlettethorne3
https://www.workerrenter.pro/profile/judithdalgety https://www.workerrenter.pro
http://62.234.194.66:3000/franciscohorni 62.234.194.66
https://git.lenfortech.com/mariandalberti https://git.lenfortech.com/mariandalberti
https://www.superphage.org/bradyharker768/43.143.37.1407315/wiki/SPIROPENT http://www.superphage.org
https://www.superphage.org/bradyharker768/43.143.37.1407315/wiki/SPIROPENT https://www.superphage.org/
https://istihdam.efeler.bel.tr/employer/getting-started-with-bodybuilding-using-clenbuterol-steroid/ https://istihdam.efeler.bel.tr
http://62.173.140.174:10480/faustinolockha 62.173.140.174
http://58.213.60.6:19000/latishak48920 58.213.60.6
https://klimaexpress-tube.de/@robbie51o94395?page=about klimaexpress-tube.de
https://zenithgrs.com/employer/clenovet-0025-mg-ml-fachinformation/ https://zenithgrs.com/employer/clenovet-0025-mg-ml-fachinformation/
https://gitea.zczcfiles.com.cn/wiwleopoldo302 https://gitea.zczcfiles.com.cn
http://gitea.yiban.com.tw:3030/sherrylkellerm gitea.yiban.com.tw
https://playxtream.com/@renaldoboase79?page=about https://playxtream.com
https://gitea.jsjymgroup.com/elmerrobinson5 gitea.jsjymgroup.com
https://sportseibt.de/consueloedinbu https://sportseibt.de/consueloedinbu
http://101.42.158.231:3000/roryx966819053 101.42.158.231
http://175.27.229.211:3000/collin45231136 http://175.27.229.211:3000/collin45231136
References:
https://suprasage.com/rosalindlundbe
meilleur casino en ligne suisse · March 31, 2026 at 4:32 pm
A good web site with interesting content, that’s what I need. Thank you for making this web site, and I will be visiting again. Do you do newsletters? I Can’t find it.
cipro · March 31, 2026 at 6:33 pm
cipro
git.rmarl.in · March 31, 2026 at 7:05 pm
biggest steroid users
https://iesoundtrack.tv/@latasha197298?page=about https://iesoundtrack.tv
https://music.drepic.com/murraymallett2 https://music.drepic.com/
http://43.142.166.108:10082/revassi0805419 43.142.166.108
http://43.156.250.29:3000/fawnxzn5714069 43.156.250.29
http://114.215.207.150:3000/alannahbassett http://114.215.207.150/
https://parnian.app/gradyoks030713 parnian.app
http://115.190.13.94:3333/vilmalovely839 115.190.13.94
https://clipbeans.com/@lynettescroggi?page=about https://clipbeans.com
https://hearty.rip/hildakeith2240 hearty.rip
https://www.51kimi.cn/lilahodgson110 51kimi.cn
http://8.141.82.163:20000/duanethibodeau http://8.141.82.163
http://gitea.mikarsoft.com/cclkendra07254 gitea.mikarsoft.com
https://getskill.work/catharineharde getskill.work
http://59.19.179.48:3300/chaswqo8623489 59.19.179.48
https://csmtube.exagopartners.com/@dorthycrenshaw?page=about csmtube.exagopartners.com
http://gitea.mikarsoft.com/lorrainemorten gitea.mikarsoft.com
http://183.204.60.122:10081/silaswoodd453 183.204.60.122
https://gitlab.iplusus.com/arronberube526 https://gitlab.iplusus.com
References:
https://git.binarycat.org/josephineswaff
39.101.170.62 · March 31, 2026 at 7:31 pm
tren steroids
https://www.propose.lk/@albawaller2071 http://www.propose.lk
https://gitea.amazingcoders.com/kirbygascoigne/2930925/wiki/Clenbuterol-Spiropent https://gitea.amazingcoders.com/kirbygascoigne/2930925/wiki/Clenbuterol-Spiropent
https://gt.clarifylife.net/mitchellmoultr https://gt.clarifylife.net/
https://git.hubhoo.com/jeromecate1663/124.223.18.411984/wiki/Clenbuterol%3A-Wirkung%2C-Nebenwirkungen-%26-Dosierung https://git.hubhoo.com/
https://www.tracksmyvan.com/martincarlson4 http://www.tracksmyvan.com
https://git.ultra.pub/shaunbarbee611 git.ultra.pub
http://www.scserverddns.top:13000/irene47s164599/162.215.134.1496767/wiki/Spiropent-Tabletten%3A-Dosierung%2C-Nebenwirkung-%26-Wirkung http://www.scserverddns.top
https://videoasis.com.br/@thalianock0734?page=about videoasis.com.br
https://www.ohovideo.com/@laurelclymer08?page=about https://www.ohovideo.com/@laurelclymer08?page=about
https://aviempnet.com/companies/spiropent-tabletten-100-st-preisvergleich-pzn-1980325/ aviempnet.com
https://gitea.nongnghiepso.com/sophiez6766358/8299daftsex.lol/wiki/%E1%90%85-Anwendungsgebiete%2C-Dosierung-und-Nebenwirkungen-von-Clenbuterol gitea.nongnghiepso.com
http://47.111.1.12:3000/nicholasusher0 http://47.111.1.12:3000/nicholasusher0
http://styleupnow.com/@erikafulton895?page=about styleupnow.com
http://120.26.116.243:3000/alinamears8945/8776dev3.worldme.tv/wiki/Erfahrung-Clen-Solar 120.26.116.243
https://zm.aosenhw.com/@hellen45513360 zm.aosenhw.com
https://git.louislabs.com/darrelrussell https://git.louislabs.com/darrelrussell
https://friztty.com/@harrison16399 https://friztty.com/@harrison16399
http://43.143.209.246:6300/gretafeint4742 43.143.209.246
References:
https://isugar-dating.com/@leopoldojenson
neue online casinos · March 31, 2026 at 7:33 pm
thank, I thoroughly enjoyed reading your article. I really appreciate your wonderful knowledge and the time you put into educating the rest of us.
kasyno online · March 31, 2026 at 7:34 pm
Nice read, I just passed this onto a colleague who was doing some research on that. And he just bought me lunch as I found it for him smile Therefore let me rephrase that: Thank you for lunch!
Sunwin · March 31, 2026 at 7:40 pm
Peculiar this blog is totaly unrelated to what I was searching for – – interesting to see you’re well indexed in the search engines.
TerryHib · March 31, 2026 at 8:23 pm
Цветы доставили по Томску в идеальном состоянии, без повреждений и лишней влаги.
заказать цветы с доставкой в томске
Maryzot · March 31, 2026 at 8:31 pm
Доброго!
Как лендинг помогает увеличить поток заявок
Создание лендингов помогает бизнесу привлекать клиентов через интернет. Лендинг показывает преимущества продукта и формирует доверие. Разработка лендинга повышает конверсию и делает сайт под ключ инструментом маркетинга.
Полная информация по ссылке – https://ts-v.ru/
создание сайтов под ключ цена Россия, ведение рекламных кампаний в Google Ads, заказать сайт под ключ Москва
сайт для интернет-магазина электроники, ђазработка лендингов под ключ | TS-V, аудит сайтов конкурентов Россия
Удачи и комфорта в жизни!
Как лендинг помогает увеличить заявки bd70494
DwightDoogy · March 31, 2026 at 8:34 pm
Очень рада, что выбрала доставку в Томске — всё чётко.
доставка цветов томск
http://101.37.69.204/ · March 31, 2026 at 8:52 pm
does muscle rev xtreme work
http://62.173.140.174:10480/faustinolockha http://62.173.140.174:10480/faustinolockha
https://git.econutrix.com/lucasmcmichael https://git.econutrix.com
https://git.zakum.cn/klaudiaring26 git.zakum.cn
http://61.190.74.90:9900/avisz805233129 http://61.190.74.90:9900/avisz805233129
https://mmctube.com/@maisiewannemak?page=about mmctube.com
https://git.hilmerarts.de/judsonoman6557 git.hilmerarts.de
https://chinami.com/@milesastudillo?page=about https://chinami.com/@milesastudillo?page=about
http://62.234.194.66:3000/franciscohorni http://62.234.194.66:3000/franciscohorni
https://jobcop.in/employer/wirkstoff-clenbuterol-pharmakologie/ jobcop.in
http://8.155.172.147:3001/wilmermortense http://8.155.172.147:3001/wilmermortense
https://zm.aosenhw.com/@hellen45513360 zm.aosenhw.com
http://8.140.232.131:8100/delmarasbury98/delmar2008/wiki/Erste-Schritte-mit-dem-Bodybuilding-mit-Clenbuterol-Steroid http://8.140.232.131:8100/delmarasbury98/delmar2008/wiki/Erste-Schritte-mit-dem-Bodybuilding-mit-Clenbuterol-Steroid
https://git.gotrobotics.org/sherlynhurtado git.gotrobotics.org
http://106.55.0.66:31807/kimberlychrist http://106.55.0.66
http://113.177.27.200:2033/simongritton4/www.ihomethink.com1991/wiki/Muskelaufbau-trotz-Di%C3%A4t%3F-Was-mit-Clenbuterol-tats%C3%A4chlich-m%C3%B6glich-ist http://113.177.27.200
https://www.ttd.group/revar10908203 http://www.ttd.group
http://gogs.zlhuiyun.com/thorstencalder http://gogs.zlhuiyun.com/thorstencalder
http://47.100.212.83:3000/antoniettajenk http://47.100.212.83:3000/antoniettajenk
References:
https://date.etogetherness.com/@abegoldberg357
Maryzot · March 31, 2026 at 9:03 pm
Добрый день!
Что делает лендинг успешным
Создание лендингов помогает бизнесу привлекать клиентов через интернет. Лендинг показывает преимущества продукта и формирует доверие. Разработка лендинга повышает конверсию и делает сайт под ключ инструментом маркетинга.
Полная информация по ссылке – https://ts-v.ru/
поддержка интернет-магазинов в России, оптимизация сайтов под мобильные устройства, аудит рекламных кампаний Google Ads
продвижение бренда в социальных сетях, ђазработка лендингов под ключ | TS-V, SEO продвижение сайтов для фотографов
Удачи и комфорта в жизни!
Почему хороший сайт повышает доверие 17d208e
JerrySairl · March 31, 2026 at 9:19 pm
Доставка с фокусом – букет “появился” из пустого ящика!
najlepsze kasyno online · March 31, 2026 at 9:19 pm
Good job for bringing something important to the internet!
iraqitube.com · March 31, 2026 at 9:43 pm
steroids vs testosterone boosters
https://armenianmatch.com/@mindyskerst491 armenianmatch.com
https://stukguitar.com/@roseannecuper?page=about stukguitar.com
https://git.mauve.haus/jameynagel9913 git.mauve.haus
https://befamous.cyou/@dessieschonell?page=about befamous.cyou
https://music.wzsipku.cn/gavin82q733690 https://music.wzsipku.cn
https://buzzafricanmusic.com/xvzchristian40 https://buzzafricanmusic.com/
https://www.telugustatusvideo.com/@lawannashockey?page=about https://www.telugustatusvideo.com/@lawannashockey?page=about
https://ns2.asso-web.com/shadpankhurst5 https://ns2.asso-web.com/shadpankhurst5
http://gitea.mikarsoft.com/cclkendra07254 gitea.mikarsoft.com
http://ydds.cloud:3000/tiffinybelcher http://ydds.cloud:3000/tiffinybelcher
http://66.179.208.56:3001/chantelno89334 http://66.179.208.56:3001/chantelno89334
https://myafritube.com/@damianb796213?page=about myafritube.com
http://81.70.202.164:3000/kattiekrimmer http://81.70.202.164/
https://goeed.com/@grazynacrooks?page=about goeed.com
http://crontab.club:30015/jerrihunt70677 crontab.club
https://gitea.biboer.cn/magnoliadunfor gitea.biboer.cn
https://actv.1tv.hk/@rogeliom038551?page=about actv.1tv.hk
https://tayartaw.kyaikkhami.com/carolynpina97 https://tayartaw.kyaikkhami.com
References:
http://72.61.229.93:4000/eugenel8600657
tubevieu.com · March 31, 2026 at 10:09 pm
steroid fat burners
https://gitea-inner.fontree.cn/gavinwilt36275/gavin1989/wiki/Clenbuterol gitea-inner.fontree.cn
https://gitea.brmm.ovh/ashleyrigsby4 https://gitea.brmm.ovh/ashleyrigsby4
https://www.italia24.tv/tube/@marilynjme9021?page=about http://www.italia24.tv
http://43.134.49.17:3000/bellagreathous http://43.134.49.17:3000/bellagreathous
http://rm.runfox.com/gitlab/breannastroup1 rm.runfox.com
https://suprastream.tv/@debbiebromby53?page=about suprastream.tv
http://139.159.153.143:3000/katherinasegur/katherina1988/wiki/Wie-Clenbuterol-das-Energieniveau-effektiv-steigern-kann%3A-Ein-Expertenblick-Wissenschaftliche-Einblicke-in-Sportpharma http://139.159.153.143:3000/katherinasegur/katherina1988/wiki/Wie-Clenbuterol-das-Energieniveau-effektiv-steigern-kann:-Ein-Expertenblick-Wissenschaftliche-Einblicke-in-Sportpharma
https://www.jobexpertsindia.com/companies/clenbuterol-t3-abnehmkur/ http://www.jobexpertsindia.com
http://175.178.150.62:3002/vitohartley691 http://175.178.150.62/
http://85.214.41.219:49153/rene4949996466 85.214.41.219
https://git.mana-web.com/rachelwoodard8 git.mana-web.com
https://www.superphage.org/ernest91k2654/2542441/wiki/Clenbuterol-Anwendungsgebiete http://www.superphage.org
http://45.144.30.78:8083/edmund62136863/edmund1982/wiki/Vorher-Nachher-Ergebnisse+%26+die+richtige+Dosierun+Deus+…- http://45.144.30.78:8083/edmund62136863/edmund1982/wiki/Vorher-Nachher-Ergebnisse & die richtige Dosierun Deus …-
https://shop.apexo.in/@fredericka4435?page=about shop.apexo.in
http://36.213.200.127:23000/annabellecoane 36.213.200.127
https://maru.bnkode.com/@thadzimmerman9 maru.bnkode.com
http://120.201.125.140:3000/kittycani72771/6443416/wiki/Clenbuterol-g%C3%BCnstig-online-bestellen-ohne-Rezept 120.201.125.140
https://klimaexpress-tube.de/@robbie51o94395?page=about klimaexpress-tube.de
References:
https://git.deadpoo.net/katherinaponti
armenianmatch.com · March 31, 2026 at 10:40 pm
steroid booster
https://gitiplay.com/@orenmackennal0?page=about gitiplay.com
http://112.74.106.216:3000/dolliepittman7 http://112.74.106.216
https://gitea.personalsoftware.space/milanbyard770 https://gitea.personalsoftware.space/
https://rsas.de/ahmadvarney72 https://rsas.de
https://movie.nanuly.kr/@cazcharlene047?page=about https://movie.nanuly.kr/
https://www.ohovideo.com/@laurelclymer08?page=about http://www.ohovideo.com
http://123.207.74.175/laracavazos76 123.207.74.175
http://39.171.252.63:3000/benito20623735/dev.kiramtech.com1986/wiki/SPIROPENT-Tabletten-Beipackzettel http://39.171.252.63:3000/benito20623735/dev.kiramtech.com1986/wiki/SPIROPENT-Tabletten-Beipackzettel
https://www.dynamicviewpoint.co.uk/employer/cera-clen-ceranfeldreiniger-200-ml/ https://www.dynamicviewpoint.co.uk/employer/cera-clen-ceranfeldreiniger-200-ml/
http://ydds.cloud:3000/tiffinybelcher http://ydds.cloud:3000/tiffinybelcher
http://39.101.170.62:9080/maurine82l8907 http://39.101.170.62:9080/maurine82l8907
https://git.veraskolivna.net/basiloctoman36 https://git.veraskolivna.net/
https://actv.1tv.hk/@rogeliom038551?page=about actv.1tv.hk
https://mginger.org/@lenabie4450291 mginger.org
http://1.95.221.174:3000/drewmaier18839/git.4lcap.com2019/wiki/SPIROPENT-100-St-PZN-01980325 1.95.221.174
https://gitlab.iplusus.com/ingridkuehner gitlab.iplusus.com
https://gitea.jsjymgroup.com/trenadrescher8 gitea.jsjymgroup.com
https://m.madeu.co.kr/graciescaddan2 https://m.madeu.co.kr
References:
https://abadeez.com/@jeromemartyn78?page=about
Rogercob · March 31, 2026 at 10:58 pm
Закинул себе в закладки, потом подробнее посмотрю: https://sksensation.ru/smm-prodvizhenie-v/
Rogercob · March 31, 2026 at 11:05 pm
Кто изучает SMM — можно глянуть для базы: https://foto-videomontaz.ru/smm-prodvizhenie-v-soczialnyh-setyah-princzipy-instrumenty-i-pokazateli-effektivnosti/
https://v.sharevr.com/@louisesnook318?page=about · March 31, 2026 at 11:29 pm
alternatives to anabolic steroids
https://code.hpswk.com/morrismenkens https://code.hpswk.com
https://www.izen.live/chandabsz24769 http://www.izen.live
http://47.100.44.145:3000/mildredhoneycu http://47.100.44.145:3000/mildredhoneycu
https://iamtube.jp/@titusdenning9?page=about https://iamtube.jp
http://115.159.107.117:3000/anthonywoore21/81.70.24.148970/wiki/Spiropent-Wirkung%2C-Nebenwirkungen%2C-Dosierung http://115.159.107.117
https://git.healthathome.com.np/krystynacooney https://git.healthathome.com.np/
http://47.105.59.0:5132/clevelandpogue 47.105.59.0
https://shamrick.us/vanitag046488 shamrick.us
https://camtalking.com/@shalandai0671 https://camtalking.com/@shalandai0671
https://vidspaceaiapp.com/@kayleigh59722?page=about vidspaceaiapp.com
https://code.dsconce.space/nidiaamiet486 code.dsconce.space
http://47.111.1.12:3000/nicholasusher0 47.111.1.12
http://123.207.74.175/laracavazos76 http://123.207.74.175/laracavazos76
http://81.69.229.51:3000/rodger76d8379 81.69.229.51
https://git.0935e.com/lindsayflorey1 git.0935e.com
https://www.cives.pl/svenwarnes043 http://www.cives.pl
http://47.92.23.195:8418/deehawthorne2/gitea.css-sistemas.com.br7773/wiki/Clenbuterol%3A-Wirkung%2C-Anwendungsgebiete%2C-Nebenwirkungen 47.92.23.195
http://47.109.137.67:9091/tinaahern53966 47.109.137.67
References:
https://git.successkaoyan.com/reyes94872963
http://119.45.160.240/ · March 31, 2026 at 11:36 pm
References:
Bodybuilding no steroids
References:
https://goeed.com/@ettabracegirdl?page=about
38.47.180.165 · March 31, 2026 at 11:40 pm
References:
Best supplement stores
References:
http://git.modelhub.org.cn:980/verawhitelegge
https://demo.indeksyazilim.com/ · March 31, 2026 at 11:42 pm
hafþór júlíus björnsson steroids
http://123.58.209.87:3000/kendricklong96 123.58.209.87
https://git.saike.fun:9755/tresaleschen54/jobcop.uk5942/wiki/Clenbutrol-Erfahrung%3A-Mein-ehrlicher-Bericht%21 https://git.saike.fun:9755/tresaleschen54/jobcop.uk5942/wiki/Clenbutrol-Erfahrung:-Mein-ehrlicher-Bericht!
https://7yue.net/roxiemein09678 https://7yue.net/roxiemein09678
http://120.77.94.227:9999/nevashillings/dev01.open-alt.com6742/wiki/Spiropent-Wirkung%2C-Nebenwirkungen%2C-Dosierung http://120.77.94.227/
http://117.72.61.28:5418/isabelladrew40 117.72.61.28
https://v.sharevr.com/@louisesnook318?page=about https://v.sharevr.com/@louisesnook318?page=about
https://jovita.com/clarita82c2182 jovita.com
http://git.520hx.vip/linwooddenker/7190142/wiki/Clenbuterol-hydrochlorid-Wirkstoff-%26-Medikamente git.520hx.vip
https://hadln.net:9443/ronda001894002 hadln.net
http://39.171.252.63:3000/lamontlawler8/1076tivoads.com/wiki/Clenovet-0%2C025-Mg-Ml-Fachinformation http://39.171.252.63:3000/lamontlawler8/1076tivoads.com/wiki/Clenovet-0,025-Mg-Ml-Fachinformation
https://gitea.pnkx.top:8/stefaniebethea gitea.pnkx.top
http://58.221.13.198:30010/abeholguin0388/abe2004/wiki/Clenbuterol%3A-Wirkung%2C-Anwendungsgebiete%2C-Nebenwirkungen 58.221.13.198
http://111.21.163.58:2321/bobbiegutterid 111.21.163.58
http://36.153.162.171:3000/alanatreacy02/alana1994/wiki/Bestimmung+der+idealen+Clenbuterol-Dosierung+Driada+Medical+Store+Offizieller+Premium-Wiederverk%C3%A4ufer+Schneller+und+sicherer+Versand.- 36.153.162.171
https://git.gotrobotics.org/sherlynhurtado git.gotrobotics.org
http://139.159.153.143:3000/coryburdge293/cory1989/wiki/Protein-Kaffee-Whey-Wheypresso-mit-80-mg-Koffein 139.159.153.143
http://119.29.194.155:8894/rodrickweisz6 http://119.29.194.155
http://139.159.153.143:3000/katherinasegur/katherina1988/wiki/Wie-Clenbuterol-das-Energieniveau-effektiv-steigern-kann%3A-Ein-Expertenblick-Wissenschaftliche-Einblicke-in-Sportpharma 139.159.153.143
References:
https://hipstrumentals.net/janisidaway50
theudtaullu.com · April 1, 2026 at 12:07 am
dexamethasone bodybuilding
http://120.201.125.140:3000/maurinebrenan7 120.201.125.140
http://171.244.15.53:3000/rosettamacderm http://171.244.15.53
http://www.skwcf.top/verlenex716015/2564027/wiki/Wie-funktioniert-es-im-K%C3%B6rper%3F http://www.skwcf.top
http://74.48.174.77:3000/refugiamacinty 74.48.174.77
http://36.133.248.69:3088/juancandler57 36.133.248.69
http://175.27.229.211:3000/collin45231136 http://175.27.229.211:3000/collin45231136
http://72.61.229.93:4000/gladishargrave 72.61.229.93
https://git.smart-tool.jp/verlenekhan257 https://git.smart-tool.jp/verlenekhan257
https://gitea.jnyuxia.com/stars14799362 gitea.jnyuxia.com
https://git.suo0.com/darrenb706798/darren1981/wiki/Clenbuterol-im-Bodybuilding%3A-Nutzen%2C-Risiken https://git.suo0.com/
http://39.171.252.63:3000/tamihallowell4/mkhonto.net2011/wiki/Spasmo-Mucosolvan+Saft+Gebrauchsinformation.- 39.171.252.63
http://newchanpin.yuntangkeji.cn:33009/weldonbroome08 newchanpin.yuntangkeji.cn
http://85.214.41.219:49153/olivaduryea677 85.214.41.219
https://suprasage.com/rosalindlundbe suprasage.com
https://git.mauve.haus/jameynagel9913 git.mauve.haus
http://119.3.186.224:3000/georgetoussain 119.3.186.224
https://hadln.net:9443/ronda001894002 https://hadln.net:9443/ronda001894002
http://crontab.club:30015/drewmattocks4 crontab.club
References:
https://gitea.jsjymgroup.com/charlenewhitti/charlene2013/wiki/Spiropent-Tabletten-Anwendung
https://suprastream.tv/ · April 1, 2026 at 1:46 am
risk of using anabolic steroids
http://43.143.142.38:7001/mohammedeusebi 43.143.142.38
http://120.77.94.227:9999/bernardkimber 120.77.94.227
https://quickdate.arenascript.de/@rosauraamaral0 quickdate.arenascript.de
https://ltube.us/@davidablackwel?page=about https://ltube.us
https://demo.playtubescript.com/@tanjamudie5638?page=about demo.playtubescript.com
https://www.cives.pl/kiaakers57727 http://www.cives.pl
https://shamrick.us/vanitag046488 https://shamrick.us
http://74.48.174.77:3000/refugiamacinty http://74.48.174.77:3000/refugiamacinty
http://47.103.48.2:3002/timmy21q014295 47.103.48.2
http://47.103.159.168:10012/jennieguzman03 47.103.159.168
https://git.fast-blast.uk/hassan32120021 https://git.fast-blast.uk
http://162.215.134.149:4000/tabithamacross/6417www.wealthtv.tz/wiki/Clenbutrol-Erfahrungen%3A-Selbsttest%2C-Ergebnisse-%26-Bewertung-2026 162.215.134.149
http://47.111.1.12:3000/ymwbeatrice11 47.111.1.12
https://armenianmatch.com/@wesleyets22015 https://armenianmatch.com
http://218.78.131.42:10030/jina3121361451 http://218.78.131.42:10030/jina3121361451
https://www.izen.live/albertharife39/1619115.190.209.222/wiki/Wie-funktioniert-es-im-K%C3%B6rper%3F https://www.izen.live/albertharife39/1619115.190.209.222/wiki/Wie-funktioniert-es-im-Körper?
https://shiatube.org/@bellamccomas78?page=about https://shiatube.org/@bellamccomas78?page=about
https://git.adambissen.me/esteladonohue https://git.adambissen.me/esteladonohue
References:
http://119.29.194.155:8894/rodrickweisz6
https://git.archieri.fr/melva16h550480 · April 1, 2026 at 1:56 am
how do you take anabolic steriods
https://unired.zz.com.ve/@albertinadovey unired.zz.com.ve
https://www.meetgr.com/@ernestineescob http://www.meetgr.com
http://8.138.139.89:3000/fredbevington8 8.138.139.89
https://gitea.ww3.tw/porfiriocarney https://gitea.ww3.tw
https://www.ohovideo.com/@felicitasswadl?page=about https://www.ohovideo.com/@felicitasswadl?page=about
https://suprastream.tv/@debbiebromby53?page=about suprastream.tv
http://58.213.60.6:19000/sherrillpittma 58.213.60.6
https://goeed.com/@grazynacrooks?page=about https://goeed.com/@grazynacrooks?page=about
https://gitea.primecontrols-dev.com/daltonqjj24965/7196v.sharevr.com/wiki/What-is-Clenbuterol%3F https://gitea.primecontrols-dev.com/daltonqjj24965/7196v.sharevr.com/wiki/What-is-Clenbuterol?
https://gitea.adber.tech/dianevaldez34/8.138.192.836616/wiki/SPIROPENT-100-St-PZN-01980325 https://gitea.adber.tech/
https://wedioz.com/@reinafender45?page=about wedioz.com
http://63.141.251.154/antoinetteflor 63.141.251.154
http://120.202.38.15:3000/raquelcraft692 http://120.202.38.15/
http://139.159.153.143:3000/katherinasegur/katherina1988/wiki/Wie-Clenbuterol-das-Energieniveau-effektiv-steigern-kann%3A-Ein-Expertenblick-Wissenschaftliche-Einblicke-in-Sportpharma 139.159.153.143
https://www.quranpak.site/athenacolby922 quranpak.site
https://unitedmusicstreaming.com/randalcatt689 https://unitedmusicstreaming.com/
https://live.eposbd.net/@felishabormann?page=about live.eposbd.net
https://alurmusic.com/tarahholliday6 https://alurmusic.com/tarahholliday6
References:
http://8.138.83.32:3000/maybelledgley
http://117.72.61.28/ · April 1, 2026 at 2:43 am
legit steroid site
http://47.113.145.232:3000/holleystace17 http://47.113.145.232:3000/holleystace17
http://43.143.175.54:3000/constancelinvi/code.sz-chaohui.cn1981/wiki/Clenbuterol-40-mcg-50-tabs 43.143.175.54
https://git.gotrobotics.org/sherlynhurtado https://git.gotrobotics.org/
https://bigotube.com/@dorothea482151?page=about bigotube.com
http://154.39.79.147:3000/arlenlaby9354 154.39.79.147
https://yooverse.com/@kandacefoy7726 yooverse.com
https://gitea.nongnghiepso.com/sophiez6766358/8299daftsex.lol/wiki/%E1%90%85-Anwendungsgebiete%2C-Dosierung-und-Nebenwirkungen-von-Clenbuterol gitea.nongnghiepso.com
https://git.refinementservices.com/maritatipping https://git.refinementservices.com/maritatipping
https://dreamplacesai.de/virgil4820262 https://dreamplacesai.de/virgil4820262
https://music.michaelmknight.com/ameliebartlett https://music.michaelmknight.com
http://styleupnow.com/@erikafulton895?page=about styleupnow.com
http://59.80.22.43:30000/roxannakellawa 59.80.22.43
https://jobcop.in/employer/wirkstoff-clenbuterol-pharmakologie/ https://jobcop.in/
https://git.zakum.cn/klaudiaring26 git.zakum.cn
https://git.archieri.fr/melva16h550480 https://git.archieri.fr
https://superocho.org/@esperanzafoti5?page=about https://superocho.org/
http://62.173.140.174:10480/faustinolockha 62.173.140.174
https://nauticauruguay.com/laurenenolan9/git.stonks.group1986/wiki/SP-Clenbuterol-zu-verkaufen nauticauruguay.com
References:
https://liverights.org//@jonelle37c7962?page=about
git.warze.org · April 1, 2026 at 3:02 am
References:
Steroids before and after women
References:
https://bv.bcia.agency/@shermanstuart3?page=about
git.ultra.pub · April 1, 2026 at 3:21 am
best steroid for bodybuilding
http://47.94.173.135:3000/archie34m1108 http://47.94.173.135:3000/archie34m1108
https://quickdatescript.com/@leonidacarrol quickdatescript.com
https://gitlab.iplusus.com/arronberube526 gitlab.iplusus.com
http://39.171.252.63:3000/tamihallowell4/mkhonto.net2011/wiki/Spasmo-Mucosolvan+Saft+Gebrauchsinformation.- http://39.171.252.63
https://www.quranpak.site/athenacolby922 http://www.quranpak.site
https://omegat.dmu-medical.de/gaylebedggood8 https://omegat.dmu-medical.de/gaylebedggood8
http://72.61.229.93:4000/gladishargrave 72.61.229.93
http://120.24.175.146:3000/feliparandell1 120.24.175.146
https://git.cute.bet/laurieburdge1 git.cute.bet
https://truesecret.org/@mildredevo9455?page=about https://truesecret.org/@mildredevo9455?page=about
https://git.healthathome.com.np/krystynacooney git.healthathome.com.np
http://1.95.192.200:59300/samanthamonten 1.95.192.200
https://git.van-peeren.de/znohazel152372/hazel2008/wiki/Clenbuterol-40-mcg-50-tabs git.van-peeren.de
http://175.154.160.23:3237/zandray7929926 175.154.160.23
https://gitiplay.com/@dedrakesteven?page=about https://gitiplay.com/@dedrakesteven?page=about
https://videyme.online/@brigittegku349?page=about videyme.online
https://flirta.online/@doycathern722 flirta.online
https://viddertube.com/@elmaoreilly984?page=about https://viddertube.com/@elmaoreilly984?page=about
References:
http://119.29.64.167:3000/bernardnal606
https://mp3diary.com/paulinespivey · April 1, 2026 at 3:39 am
pills that make you gain muscle fast
https://askmilton.tv/@leonelu9890871?page=about https://askmilton.tv/
http://8.140.232.131:8100/zaksanches875/3568viewcast.altervista.org/wiki/Spiropent%C2%AE-100-St-mit-dem-E-Rezept-kaufen http://8.140.232.131:8100/zaksanches875/3568viewcast.altervista.org/wiki/Spiropent®-100-St-mit-dem-E-Rezept-kaufen
https://gitea.primecontrols-dev.com/hymanpalmos901/v.sharevr.com3484/wiki/SPIROPENT-Tabletten-PZN-01980325 gitea.primecontrols-dev.com
https://gitlab.iplusus.com/xiomaragrantha/xiomara1999/wiki/Spiropent%C2%AE-100-St-mit-dem-E-Rezept-kaufen gitlab.iplusus.com
https://git.mauve.haus/leopoldoeaston/8365git.0935e.com/wiki/Clenbuterol%3A-Wirkung%2C-Anwendungsgebiete%2C-Nebenwirkungen git.mauve.haus
http://61.178.84.89:8998/tilly55s31040/5425226/wiki/What-is-Clenbuterol%3F http://61.178.84.89:8998/tilly55s31040/5425226/wiki/What-is-Clenbuterol?
https://nvuplayer.com/@maddisonquan2?page=about https://nvuplayer.com/
https://git.malls.iformall.com/torsten600671/gitea.jobiglo.com2016/wiki/Clenbuterol-Spiropent https://git.malls.iformall.com/torsten600671/gitea.jobiglo.com2016/wiki/Clenbuterol-Spiropent
https://git.hubhoo.com/andresrasmusse https://git.hubhoo.com
https://niqnok.com/leandromanzi32 niqnok.com
https://x1.tvos.cygnux.cn/shondasymes25 https://x1.tvos.cygnux.cn/shondasymes25
http://118.178.172.49:3000/leonorekirsova 118.178.172.49
http://120.26.116.243:3000/alinamears8945/8776dev3.worldme.tv/wiki/Erfahrung-Clen-Solar 120.26.116.243
http://git.520hx.vip/linwooddenker/7190142/wiki/Clenbuterol-hydrochlorid-Wirkstoff-%26-Medikamente git.520hx.vip
https://kayesbamusic.com/porfiriocheshi kayesbamusic.com
https://iesoundtrack.tv/@bobbyeacuna91?page=about https://iesoundtrack.tv
https://git.vhdltool.com/dwaynerivett78 git.vhdltool.com
https://gitea.shizuka.icu/gracielasanche/www.uria.dev2010/wiki/Spiropent-mite-Wirkung%2C-Nebenwirkungen%2C-Dosierung gitea.shizuka.icu
References:
https://video.disneyemployees.net/@novellacomeaux?page=about
v.sharevr.com · April 1, 2026 at 3:46 am
winstrol acne
http://gitea.mikarsoft.com/lorrainemorten gitea.mikarsoft.com
https://rlgit.pro/abrahamdenby1/abraham2017/wiki/Clenbuterol-Wirkung https://rlgit.pro/abrahamdenby1/abraham2017/wiki/Clenbuterol-Wirkung
https://gitea.jnyuxia.com/stars14799362 https://gitea.jnyuxia.com/stars14799362
https://git.ruixininfo.com/sabinacarreno5/7567323/wiki/Clenbuterol:-Wirkung%2C-Anwendungsgebiete%2C-Nebenwirkungen https://git.ruixininfo.com
http://zzdgitea.stnav.com/juanitagass75 zzdgitea.stnav.com
https://thefusionflix.com/@felicia4618264?page=about thefusionflix.com
https://www.meetgr.com/@ernestineescob https://www.meetgr.com
http://120.26.116.243:3000/alinamears8945/8776dev3.worldme.tv/wiki/Erfahrung-Clen-Solar http://120.26.116.243/
https://bfreetv.com/@lucaackermann9?page=about https://bfreetv.com/@lucaackermann9?page=about
http://gitea.yiban.com.tw:3030/charlierocher7 gitea.yiban.com.tw
http://27.223.88.102:33000/coy47152864673 http://27.223.88.102:33000/coy47152864673
https://kf.hebrewconnect.tv/@selmabigham336?page=about kf.hebrewconnect.tv
http://123.60.146.54:3000/eleanoremccann/1788103.228.160.127/wiki/Clenbuterol-Wikipedia 123.60.146.54
http://62.173.140.174:10480/ieshapeden630/1590859/wiki/Clenbuterol-Dosierung 62.173.140.174
https://www.shwemusic.com/declanoyp6135 https://www.shwemusic.com/
http://171.244.15.53:3000/veroniquebrent/git.ruixininfo.com2001/wiki/%E1%90%85-Anwendungsgebiete%2C-Dosierung-und-Nebenwirkungen-von-Clenbuterol 171.244.15.53
https://code.dsconce.space/nidiaamiet486 code.dsconce.space
https://www.workerrenter.pro/profile/judithdalgety http://www.workerrenter.pro
References:
https://git.mwapp.com.br/delilahblaze18
pepecitos.com.ar · April 1, 2026 at 3:48 am
References:
Best legal supplements for cutting
References:
http://gitea.yiban.com.tw:3030/charlierocher7
beste online casino · April 1, 2026 at 3:50 am
Enjoyed reading through this, very good material. Thanks!
http://111.228.34.40:3000/vitowooley933 · April 1, 2026 at 3:56 am
where can i get lean
https://git.clickforadventure.co/venbarbra87444/code.tczkiot.com3546/wiki/Was-sind-die-besten-Steroide-f%C3%BCr-Gewichtsverlust%3F https://git.clickforadventure.co/venbarbra87444/code.tczkiot.com3546/wiki/Was-sind-die-besten-Steroide-für-Gewichtsverlust?
http://103.119.85.197:3000/valerialackey1/valeria1991/wiki/Clenbuterol-Wirkung-Fettkiller-oder-gef%C3%A4hrliches-Dopingmittel%3F 103.119.85.197
http://171.244.15.53:3000/veroniquebrent/git.ruixininfo.com2001/wiki/%E1%90%85-Anwendungsgebiete%2C-Dosierung-und-Nebenwirkungen-von-Clenbuterol 171.244.15.53
http://47.108.156.251:3000/selinac2162204/7481065/wiki/Spiropent-Tabletten-Dosierung 47.108.156.251
https://iraqitube.com/@meredithsko332?page=about iraqitube.com
https://git.mauve.haus/rosalynborrie6 git.mauve.haus
http://74.48.174.77:3000/noemifender307 74.48.174.77
https://git.veraskolivna.net/adrieneslocum git.veraskolivna.net
https://git.stormrain.cn/timothybooth36 git.stormrain.cn
http://47.115.132.164:5500/jonathantolima http://47.115.132.164
http://111.21.163.58:2321/bobbiegutterid 111.21.163.58
https://git.game-dev.space/abdulmullins09 git.game-dev.space
https://klimaexpress-tube.de/@robbie51o94395?page=about https://klimaexpress-tube.de/@robbie51o94395?page=about
https://git.davisdre.com/georgianagroom https://git.davisdre.com
https://www.pajob.ch/employer/spiropent-tabletten-anwendung/ https://www.pajob.ch/employer/spiropent-tabletten-anwendung/
http://38.76.202.113:3000/isabellemasell 38.76.202.113
https://gitea.quiztimes.nl/manualgrimwade gitea.quiztimes.nl
https://v.sharevr.com/@marcelohewlett?page=about https://v.sharevr.com/
References:
http://8.138.83.32:3000/shelleyblancha
Top 10 casino en ligne belgique · April 1, 2026 at 5:03 am
Nice blog. Could someone with little experience do it, and add updates without messing it up? Good information on here, very informative.
101.37.147.115 · April 1, 2026 at 5:17 am
legal steroids for losing weight
http://58.213.60.6:19000/unmkermit7249 http://58.213.60.6
http://139.196.103.114:18084/leonorbeazley1 139.196.103.114
https://lasigal.com/vedaclough6750 https://lasigal.com/
http://43.138.249.161:3000/margietripp116 http://43.138.249.161:3000/margietripp116
https://liverights.org//@jonelle37c7962?page=about liverights.org
https://iesoundtrack.tv/@mikeruggieri7?page=about iesoundtrack.tv
https://gitlab.rails365.net/terrellschneid https://gitlab.rails365.net/terrellschneid
http://47.115.223.229:8888/delilat0092404/delila2016/wiki/Clenbuterol-Spiropent http://47.115.223.229:8888/delilat0092404/delila2016/wiki/Clenbuterol-Spiropent
https://hunthub.com.au/@bettinaweiner?page=about hunthub.com.au
https://hadln.net:9443/ronda001894002 hadln.net
http://www.scserverddns.top:13000/irene47s164599/162.215.134.1496767/wiki/Spiropent-Tabletten%3A-Dosierung%2C-Nebenwirkung-%26-Wirkung scserverddns.top
https://rsas.de/ahmadvarney72 rsas.de
https://gitea.my-intrudair.com/rochellu058062/cyprusjobs.com.cy1984/wiki/Clenbuterol-Dosierung-Clen-f%C3%BCr-Bodybuilding https://gitea.my-intrudair.com/rochellu058062/cyprusjobs.com.cy1984/wiki/Clenbuterol-Dosierung-Clen-für-Bodybuilding
http://gitea.mikarsoft.com/zwlsamara61522 gitea.mikarsoft.com
http://111.230.98.74/darelllarson7 http://111.230.98.74/
http://8.155.172.147:3001/summer65687890 http://8.155.172.147:3001/summer65687890
http://43.143.142.38:7001/nathanielcarre 43.143.142.38
https://gitree.me/rodgerlapine13 gitree.me
References:
https://isugar-dating.com/@leopoldojenson
top 10 online casino België · April 1, 2026 at 7:06 am
I encountered your site after doing a search for new contesting using Google, and decided to stick around and read more of your articles. Thanks for posting, I have your site bookmarked now.
beste online casino belgië · April 1, 2026 at 11:08 am
Nice blog here! Also your web site loads up very fast! What host are you using? Can I get your affiliate link to your host? I wish my web site loaded up as fast as yours lol
beste online casino · April 1, 2026 at 12:04 pm
My brother suggested I might like this web site. He was entirely right. This post actually made my day. You can not imagine simply how much time I had spent for this info! Thanks!
Haval Воронеж цены и дилеры · April 1, 2026 at 12:32 pm
лучшие цены на Haval Воронеж
legalne kasyno online · April 1, 2026 at 12:57 pm
Thanks for sharing the information. I found the information very useful. That’s a awesome story you posted. I will come back to scan some more.
https://ipazeb.org/?p=72327 · April 1, 2026 at 3:48 pm
Casino Bonuses Betting Offers
actsolution.iptime.org · April 1, 2026 at 5:17 pm
top ten steroids
http://152.42.207.183:3000/jacintoevers91 http://152.42.207.183/
https://wiibiplay.fun/@douglaspaltrid?page=about wiibiplay.fun
http://27.223.88.102:33000/shawnreddy323 27.223.88.102
https://lafffrica.com/@lienbellino324?page=about lafffrica.com
http://132.232.92.186:3000/tommyfcn286659 132.232.92.186
http://171.244.15.53:3000/gabriellebrere http://171.244.15.53
https://botttechgroup.com/gretairons8786 https://botttechgroup.com/gretairons8786
https://tea.neuron.my/hkdsantiago985 tea.neuron.my
https://qarisound.com/ttilester3250 qarisound.com
https://gitea.mynas-lechner.de/kathrynhouchen https://gitea.mynas-lechner.de/kathrynhouchen
http://58.221.157.122:3000/enriquer17530 http://58.221.157.122:3000/enriquer17530
http://59.80.22.43:30000/mellissalambri 59.80.22.43
https://reoflix.com/@aletheamcnaugh?page=about reoflix.com
https://friztty.com/@julietshearer friztty.com
https://git.init.cool/hermine6704244 git.init.cool
https://www.loginscotia.com/bernardo03a186 http://www.loginscotia.com
http://zzdgitea.stnav.com/georgiannarkv zzdgitea.stnav.com
https://git.successkaoyan.com/robinhalpern52 https://git.successkaoyan.com/
References:
http://111.170.153.123:3000/darrelmacdonne
115.190.13.94 · April 1, 2026 at 5:37 pm
anabolic steroid classification
http://62.234.201.16/franchescasass 62.234.201.16
https://volunteeri.com/companies/d-anaoxn-elite-series-all-natural/ volunteeri.com
https://pattayavids.com/@janniegargett?page=about https://pattayavids.com/@janniegargett?page=about
https://gbewaaplay.com/ionamauer04073 https://gbewaaplay.com
http://git.ibossay.com:3000/gaykirklin308 http://git.ibossay.com:3000/gaykirklin308
https://traficut.com/@michelinefalls?page=about traficut.com
http://150.158.37.69:3000/luciennedahl62 150.158.37.69
https://xn--lpris-iua.nu/rafaelaqry6779 https://lpris-iua.nu/rafaelaqry6779
http://43.139.2.237:3000/hughbqa4002277 43.139.2.237
http://81.69.57.215:3000/frederickixj14 http://81.69.57.215
https://getskill.work/sethkraegen29 getskill.work
http://47.113.149.107:10110/gertrudemenend 47.113.149.107
http://106.55.174.214:3000/debhogue140777 106.55.174.214
https://traficut.com/@silassingh6258?page=about https://traficut.com
https://www.workerrenter.pro/profile/winstonluxton0 http://www.workerrenter.pro
https://vw-git.senecasense.com/asamilam524847 vw-git.senecasense.com
https://44sex.com/@roykane1998499?page=about 44sex.com
https://git.ccmhub.se/linfaulding392 https://git.ccmhub.se/linfaulding392
References:
http://111.228.34.40:3000/hclhelene82955
τα καλυτερα online casino · April 1, 2026 at 5:51 pm
We absolutely love your blog and find the majority of your post’s to be exactly what I’m looking for. Do you offer guest writers to write content to suit your needs? I wouldn’t mind composing a post or elaborating on a number of the subjects you write about here. Again, awesome weblog!
58.213.60.6 · April 1, 2026 at 6:25 pm
fast muscle growth steroids
https://gitea.brmm.ovh/kellye75f30219 https://gitea.brmm.ovh/kellye75f30219
http://121.199.174.122:3000/jerilynbenner0 121.199.174.122
https://date-duell.de/@sherriez08489 https://date-duell.de
http://218.245.96.10/elmosuper6426 http://218.245.96.10/elmosuper6426
http://172.104.245.78:11080/ambrosemcgriff 172.104.245.78
https://gitea.wgqcd.com/micaelazieseme/6477218/wiki/Anadrol-vs-Dianabol-Dbol%3A-Which-is-the-Better-Steroid%3F gitea.wgqcd.com
https://afribass.com/@reyesramer3416?page=about afribass.com
https://date-duell.de/@betseycajigas8 date-duell.de
http://152.136.158.133:36512/leanneonus7652 http://152.136.158.133/
https://qarisound.com/linamcnab1146 qarisound.com
http://152.136.158.133:36512/leanneonus7652 152.136.158.133
https://gitea.zachl.tech/vicenteaird179/silatdating.com1989/wiki/Metandienone-Wikipedia gitea.zachl.tech
https://vcs.cozydsp.space/angeliaspivey4 vcs.cozydsp.space
http://62.173.140.174:10480/dawnzzo3001594/gitea.mikarsoft.com3295/wiki/Dianabol-Review%3A-Benefits-%26-Risks-of-Dbol 62.173.140.174
https://gitea.quiztimes.nl/scotv527258186 gitea.quiztimes.nl
https://gitea.mynas-lechner.de/delmarlockard6 https://gitea.mynas-lechner.de
https://gitea.wuyuank.com/jaysconce0516 https://gitea.wuyuank.com/jaysconce0516
https://video.silverwolfstudios.com/@gabrielneubaue?page=about https://video.silverwolfstudios.com/
References:
https://video.2yu.co/@christine9668?page=about
mahalkita.ph · April 1, 2026 at 6:44 pm
anavar anabolic steroids
https://gitea.nongnghiepso.com/albabentley590/alba2017/wiki/Dianabol%3A-Usage%2C-Benefits%2C-Side-Effects-%26-Legal-Alternatives https://gitea.nongnghiepso.com
https://dammsound.com/annieocx629703 https://dammsound.com
https://git.ultra.pub/elouisegoldhar https://git.ultra.pub/elouisegoldhar
http://39.108.209.179:3000/averygroff0975/2159286/wiki/Steroids 39.108.209.179
https://vigilanteapp.com/@winniegabel715?page=about vigilanteapp.com
https://forgejo.3dcra.eu/rhodaxez946103 https://forgejo.3dcra.eu
http://newchanpin.yuntangkeji.cn:33009/emmawoo0861020/emma1980/wiki/Essential-blood-testing-in-the-patient-using-androgenic-anabolic-steroids%3A-a-clinical-practice-guideline-for-primary-care newchanpin.yuntangkeji.cn
https://gitea.jnyuxia.com/mariamgarrard gitea.jnyuxia.com
http://47.107.188.236:3000/solomonhannan/companyjobs.cn6447/wiki/Dianabol%C2%AE-Bodybuilding-Supplement-and-Anabolic-Agent http://47.107.188.236/
https://simapodcast.co.ls/@gabrieledaught?page=about https://simapodcast.co.ls/@gabrieledaught?page=about
https://git.lifetop.net/billwoodcock1 git.lifetop.net
https://pure.itsabouttimetv1.com/@leonardogreenw?page=about pure.itsabouttimetv1.com
https://nonstopvn.net/@milancazares3?page=about https://nonstopvn.net/@milancazares3?page=about
http://49.232.183.190:3000/dessiejzg06505 49.232.183.190
https://omegat.dmu-medical.de/margaritohemma omegat.dmu-medical.de
https://git.ccmhub.se/rosariapaquett git.ccmhub.se
https://cameotv.cc/@senaida00y1703?page=about cameotv.cc
http://14.103.239.131:3000/federicomcgrew 14.103.239.131
References:
https://dyipniflix.com/site/@carlolaby2687?page=about
buy tiktok followers · April 1, 2026 at 7:09 pm
I discovered your weblog site on google and verify just a few of your early posts. Proceed to maintain up the very good operate. I simply further up your RSS feed to my MSN News Reader.
122.226.176.166 · April 1, 2026 at 7:38 pm
before and after deca
http://117.72.61.28:5418/janieomahony21 117.72.61.28
http://git.dglyoo.com/carolynstrouse/carolyn1992/wiki/Steroid-Stack-Guide:-How-to-Build-a-Safe-and-Effective-Cycle-for-Bulki http://git.dglyoo.com/
https://www.telugustatusvideo.com/@renatemathias?page=about http://www.telugustatusvideo.com
https://bigotube.com/@brandencastell?page=about bigotube.com
https://wedioz.com/@steffentweddle?page=about https://wedioz.com/@steffentweddle?page=about
https://gitea.amazingcoders.com/roderickgendro/3746025/wiki/Dianabol-Dbol%3A-The-Ultimate-Guide https://gitea.amazingcoders.com/roderickgendro/3746025/wiki/Dianabol-Dbol:-The-Ultimate-Guide
https://git.local.octal.tec.br/millietownley git.local.octal.tec.br
http://123.60.146.54:3000/angeliapollak/angelia1997/wiki/Lab-Tested-Anabolic-Steroids-USA-Fast-Domestic-Shipping 123.60.146.54
http://newchanpin.yuntangkeji.cn:33009/emmawoo0861020/emma1980/wiki/Essential-blood-testing-in-the-patient-using-androgenic-anabolic-steroids%3A-a-clinical-practice-guideline-for-primary-care newchanpin.yuntangkeji.cn
https://worldclassdjs.com/mollymattingle worldclassdjs.com
http://43.139.144.12:3000/iveyx913407855 43.139.144.12
http://www.tm-jikayo.com/marianowilkie4 http://www.tm-jikayo.com
http://112.124.40.88:5510/tareneuler865 http://112.124.40.88:5510/tareneuler865
https://qarisound.com/alenawhitely20 qarisound.com
http://wangbeibei.xyz:6002/ilenerowley214 wangbeibei.xyz
https://zm.aosenhw.com/@abbeyhalligan9 https://zm.aosenhw.com/
https://nildigitalco.com/@melvinp5787032?page=about nildigitalco.com
http://43.143.175.54:3000/saraschneider/mp3diary.com1987/wiki/Best-Steroids-for-Bulking-vs-Cutting http://43.143.175.54/
References:
https://choosy.cc/@mallorymaynard
a5game · April 1, 2026 at 9:16 pm
Wild Bandito sticky wilds: o bandido mexicano tá roubando tudo em 2026!
https://git.htns.com · April 1, 2026 at 9:44 pm
side effects of long term steroid use
http://36.133.248.69:3088/milanlucero889 http://36.133.248.69/
https://chenxil.top/gregoriowalter https://chenxil.top/gregoriowalter
https://theudtaullu.com/@dorethazimin17?page=about theudtaullu.com
https://www.herzog-it.de/tanialuna62110 http://www.herzog-it.de
https://www.lizyum.com/@albawillie746 http://www.lizyum.com
https://gitea.nongnghiepso.com/mauranoe425498 gitea.nongnghiepso.com
http://gitea.yiban.com.tw:3030/mammievosz1620 gitea.yiban.com.tw
https://armenianmatch.com/@trinawhitman6 armenianmatch.com
http://120.48.141.82:3000/roseannayee985/7829223/wiki/How-to-Take-Dianabol%3A-Understanding-Risks-and-Benefits 120.48.141.82
http://47.113.149.107:10110/kendall8423111 http://47.113.149.107:10110/kendall8423111
http://45.144.30.78:8083/dorcasbernhard/8745204/wiki/Anabolic-Steroids-may-cause-hair-loss-in-about-25%25-of-Users-Donovan-Hair-Clinic 45.144.30.78
https://git.louislabs.com/melissawhitfel https://git.louislabs.com/melissawhitfel
http://35.207.205.18:3000/maxwellgrimes http://35.207.205.18/
https://aeterna.cim.mcgill.ca/simasholl75020 aeterna.cim.mcgill.ca
http://209.127.59.74:3000/kristineperrea/6961jobbridge4you.com/wiki/4%2C163%2C746%2C+5-methyl-7-methoxyisoflavone+is+designed+to+promote+muscle+growth+5G+HUB+TECHNOLOGIES.- 209.127.59.74
https://code.wemediacn.com/prestonneagle5/companyjobs.cn3094/wiki/Home code.wemediacn.com
http://git.qniao.cn/healouann7500 git.qniao.cn
https://git.alderautomation.ca/onahawk3729961/183.236.243.712005/wiki/Dianabol-10-Swiss-Pharm-Dianabol-Dbol%3A-The-Ultimate-Guide-Inside-Bodybuilding-sesa git.alderautomation.ca
References:
https://gogolive.biz/@michealh824249?page=about
direct-jobs.nl · April 1, 2026 at 9:49 pm
References:
Sus and deca before and after
References:
https://ns2.asso-web.com/camillaroberso
git.clickforadventure.co · April 1, 2026 at 9:51 pm
References:
Nandrolone side effects
References:
https://www.beyoncetube.com/@merrieubanks96?page=about
https://114.242.31.6:3000/estelladendy12 · April 1, 2026 at 9:53 pm
prolonged use of steroids causes
https://www.zapztv.com/@gracie87t95784?page=about https://www.zapztv.com/@gracie87t95784?page=about
https://gitea.primecontrols-dev.com/lawerenceloxto gitea.primecontrols-dev.com
http://122.226.176.166:8404/jodiecondon20/git.autotion.net7055/wiki/Buy-Steroids-Online-in-USA http://122.226.176.166:8404/jodiecondon20/git.autotion.net7055/wiki/Buy-Steroids-Online-in-USA
https://git.automathon.org/epifaniaprim8 git.automathon.org
https://aitune.net/florenekirsch6 aitune.net
https://aladin.tube/@ferminspringfi?page=about aladin.tube
http://8.140.248.67:3000/lucilemakin799 http://8.140.248.67/
https://gitea.personalsoftware.space/bonniepattison gitea.personalsoftware.space
http://152.136.158.133:36512/andreamacintyr http://152.136.158.133:36512/andreamacintyr
https://git.saike.fun:9755/kazukoo085568/8914srsbkn.eu.org/wiki/Dianabol-Side-Effects%3A-What-You-Need-To-Know-Before-You-Cycle git.saike.fun
https://gitea.jsjymgroup.com/stephanpontiff gitea.jsjymgroup.com
http://120.48.141.82:3000/desmondfay103/desmond1996/wiki/Did+the+NBA+drug+test+Bam+Adebayo%3F+Why+NBA+fans+wrongly+think+Heat+star+is+suspended+after+83-point+game.- 120.48.141.82
https://git.nusaerp.com/mercedestellez/git.warze.org1991/wiki/Top-Real-Dianabol-Suppliers-2026-Trusted-Dianabol-Sources-Online https://git.nusaerp.com/
http://47.113.149.107:10110/kendall8423111 47.113.149.107
https://git.archieri.fr/sueleppert9867/7094282/wiki/How-to-Take-Dianabol%3A-Understanding-Risks-and-Benefits git.archieri.fr
http://58.221.157.122:3000/shantaebrewis/shantae2009/wiki/Metandienone-Wikipedia http://58.221.157.122
https://stream.aea3.net/@geyblanche0083?page=about stream.aea3.net
https://gitee.planhomecloud.cn/simacoppola134 gitee.planhomecloud.cn
References:
https://sithcom.de/fernoas3171826
eduback.com · April 1, 2026 at 10:00 pm
dianabol 10
https://dgwork.co.kr/ivanbeardsley6 dgwork.co.kr
https://dev3.worldme.tv/@nicklamothe42?page=about https://dev3.worldme.tv/@nicklamothe42?page=about
https://git.ewengadonnaud.xyz/chong67w378703 https://git.ewengadonnaud.xyz/chong67w378703
https://whiskey.tangomedia.fr/@kerichavarria2?page=about whiskey.tangomedia.fr
https://git.esen.gay/arnettelabarre git.esen.gay
https://aladin.tube/@ferminspringfi?page=about aladin.tube
https://gitea.amazingcoders.com/roderickgendro/3746025/wiki/Dianabol-Dbol%3A-The-Ultimate-Guide https://gitea.amazingcoders.com
https://kaymanuell.com/@renatejamison?page=about https://kaymanuell.com
https://hadln.net:9443/janellhartwell https://hadln.net/
http://183.236.243.71:3693/mickiehou9818 183.236.243.71
https://git.esen.gay/arnettelabarre https://git.esen.gay
https://we2gotgame.com/videos/@dontewilson61?page=about we2gotgame.com
http://git.zxkedu.com:33769/leannep0434421 git.zxkedu.com
https://smartcampus-seskoal.id/streaming/@jaysonstukes52?page=about https://smartcampus-seskoal.id
https://code.wemediacn.com/grazynaperryma/grazyna1986/wiki/Lab-Tested-Anabolic-Steroids-USA-Fast-Domestic-Shipping https://code.wemediacn.com/
http://43.139.2.237:3000/kandyz18796347 43.139.2.237
http://47.103.48.2:3002/christianefrue http://47.103.48.2
https://gitea.wuyuank.com/jaysconce0516 gitea.wuyuank.com
References:
http://114.247.226.83:50000/hubertscofield
styleupnow.com · April 1, 2026 at 10:00 pm
does dbol give you energy
http://124.223.18.41:10082/brigettefolsom 124.223.18.41
https://txuki.duckdns.org/antonia07p2127 https://txuki.duckdns.org/antonia07p2127
https://gitea.scivigi.com/krisbadham4691/lizyum.com2022/wiki/Dianabol-vs-Winstrol%3A-Which-Steroid-Is-Best-for-Muscle-Gains-and-Cutting%3F gitea.scivigi.com
https://working.altervista.org/employer/buy-steroids-online-anabolic-steroids-for-sale/ https://working.altervista.org/employer/buy-steroids-online-anabolic-steroids-for-sale
http://1.95.7.169:3000/tandyaag395166 1.95.7.169
http://119.29.198.206:5630/isobel23137595 http://119.29.198.206
https://www.nastavniki.com/@johnphelps235?page=about http://www.nastavniki.com
https://jomowa.com/@gregoriofrankl jomowa.com
https://khmerhd.tv/@hannadanielson?page=about https://khmerhd.tv
http://123.57.146.97:3000/shirleyu976846 123.57.146.97
https://git.0fs.ru/jeanetteearnes/git.danpeak.co.uk7317/wiki/Metandienone-Wikipedia git.0fs.ru
https://direct-jobs.nl/employer/glp-1-for-weight-loss-what-bodybuilders-should-know/ direct-jobs.nl
http://139.196.103.114:18084/pearlinecastel/3188628/wiki/Anabol:-What-is-it%3F-How-to-use%3F-Warnings%2C-Dosage-and-Side-Effects 139.196.103.114
https://dianyanai.com/wesley38443581 https://dianyanai.com
https://www.lizyum.com/@albawillie746 http://www.lizyum.com
https://smartastream.com/@lorenzahedgepe?page=about smartastream.com
https://44sex.com/@roykane1998499?page=about https://44sex.com/
http://git.dglyoo.com/carolynstrouse/carolyn1992/wiki/Steroid-Stack-Guide:-How-to-Build-a-Safe-and-Effective-Cycle-for-Bulki http://git.dglyoo.com/carolynstrouse/carolyn1992/wiki/Steroid-Stack-Guide:-How-to-Build-a-Safe-and-Effective-Cycle-for-Bulki
References:
https://skillsvault.co.za/profile/alexandraheneg
https://git.bp-web.app/candraduval42/candra1981/wiki/Testosterone-What-It-Does-And-Doesn't-Do · April 1, 2026 at 10:24 pm
pro garcinia cambogia free trial
https://sysssl.tech/bobbyeibw24386 sysssl.tech
https://gitslayer.de/christianelevi https://gitslayer.de/
https://mygit.kikyps.com/leiahenslowe88 mygit.kikyps.com
http://47.115.221.71:3000/walkersteinke 47.115.221.71
http://123.60.146.54:3000/newtonbidwell9 123.60.146.54
https://gitslayer.de/micheal52z7004 gitslayer.de
http://120.201.125.140:3000/agustinbeavis0/4425339/wiki/Dianabol-10mg-Spectrum-Pharma-100-Tablets-USA-Domestic 120.201.125.140
https://code.dsconce.space/rodgerdailey82 https://code.dsconce.space/rodgerdailey82
http://20.249.208.89:3000/kristoferwhatl 20.249.208.89
https://gitea.amazingcoders.com/roderickgendro/3746025/wiki/Dianabol-Dbol%3A-The-Ultimate-Guide gitea.amazingcoders.com
https://dating.vi-lab.eu/@harryrandell2 https://dating.vi-lab.eu/@harryrandell2
https://desante.dev/kirkgilson251 desante.dev
http://220.132.16.87:3000/vcpdirk904898 220.132.16.87
https://git.bp-web.app/candraduval42/candra1981/wiki/Testosterone-What-It-Does-And-Doesn%27t-Do git.bp-web.app
https://x1.tvos.cygnux.cn/thao37m1100575 x1.tvos.cygnux.cn
http://58.213.60.6:19000/elmerdunningha/5045089/wiki/Diet-on-Steroids%3A-Complete-Nutrition-Guide http://58.213.60.6
https://dgwork.co.kr/ivanbeardsley6 dgwork.co.kr
https://gitea.scivigi.com/krisbadham4691/lizyum.com2022/wiki/Dianabol-vs-Winstrol%3A-Which-Steroid-Is-Best-for-Muscle-Gains-and-Cutting%3F https://gitea.scivigi.com/
References:
https://www.fepp.org.ec/whitneypapst14/whitney2023/wiki/Dianabol-Tablets%3A-Complete-Guide-For-Bodybuilders-On-Price
http://46.202.189.66 · April 1, 2026 at 10:26 pm
References:
Best anabolic steroid for mass
References:
http://1.95.7.169:3000/kandim8621040
http://36.213.200.127:23000/priscillahamil/1049494/wiki/Dianabol-for-sale · April 1, 2026 at 10:27 pm
what is steroids drug
http://43.139.2.237:3000/shauntechew406 http://43.139.2.237:3000/shauntechew406
https://gitea.my-intrudair.com/ashliiom082669 gitea.my-intrudair.com
http://47.105.124.101:3000/floreneguido72 47.105.124.101
http://104.254.131.244:3000/terencecollico/6789175.27.229.211/wiki/The-Danabol-DS-Blue-Hearts 104.254.131.244
https://hero-cloud-stg-code.cnbita.com/georgianna8547 https://hero-cloud-stg-code.cnbita.com/
https://git.saidomar.fr/barney58534716 git.saidomar.fr
https://git.0935e.com/gordonbaumann0 https://git.0935e.com/gordonbaumann0
https://topgtv.com/@shananeuhaus8?page=about https://topgtv.com
http://82.156.65.157:30000/brjrandal2246 82.156.65.157
https://git.healthathome.com.np/luca39k3211658 git.healthathome.com.np
https://git.m.ctf.arrobe.fr/ernesto8560475 git.m.ctf.arrobe.fr
https://git.lolpro11.me/kalamahn480189 git.lolpro11.me
https://git.louislabs.com/leopoldoblair git.louislabs.com
https://git.vezpi.com/karinakulakows git.vezpi.com
http://47.107.188.236:3000/mahaliagoodin2 47.107.188.236
https://topgtv.com/@shananeuhaus8?page=about topgtv.com
http://49.232.183.190:3000/dessiejzg06505 http://49.232.183.190:3000/dessiejzg06505
https://drarchina.com/demo/@kristydeegan80?page=about https://drarchina.com/
References:
https://tageeapp.com/@ozbterra378298?page=about
heylloow.com · April 1, 2026 at 10:51 pm
what effect can the use of steroids have on men
http://183.204.60.122:10081/conraddriver6 183.204.60.122
http://115.190.13.94:3333/kingwillard415 115.190.13.94
http://49.232.183.190:3000/dessiejzg06505 49.232.183.190
https://saga.iao.ru:3043/lurlenev77248 https://saga.iao.ru/
http://58.221.13.198:30010/margenemckie54/1413072/wiki/Anabolic-Steroids%3A-What-They-Are%2C-Uses%2C-Side-Effects-%26-Risks 58.221.13.198
https://whiskey.tangomedia.fr/@caraskillen76?page=about https://whiskey.tangomedia.fr/@caraskillen76?page=about
http://git.dglyoo.com/carolynstrouse/carolyn1992/wiki/Steroid-Stack-Guide:-How-to-Build-a-Safe-and-Effective-Cycle-for-Bulki http://git.dglyoo.com
https://www.hyzq123.com/@judyvandegrift?page=about https://www.hyzq123.com/
https://txuki.duckdns.org/antonia07p2127 txuki.duckdns.org
https://gitslayer.de/dillonmcmichae gitslayer.de
https://healedonly.com/@catharineducro healedonly.com
https://nildigitalco.com/@melvinp5787032?page=about nildigitalco.com
https://117.159.26.136:5300/wernerloggins/120.202.38.156825/wiki/Anavar-vs-Dianabol:-Which-Steroid-Is-Better-for-Muscle-Growth%3F https://117.159.26.136:5300/wernerloggins/120.202.38.156825/wiki/Anavar-vs-Dianabol:-Which-Steroid-Is-Better-for-Muscle-Growth?
http://xeroworld.team/julianafollett http://xeroworld.team/julianafollett
https://git.mwapp.com.br/ernestineavw2 git.mwapp.com.br
https://git.louislabs.com/leopoldoblair git.louislabs.com
https://hadln.net:9443/danutacecil07 hadln.net
https://cloudtu.be/@salhaverfield1?page=about https://cloudtu.be
References:
http://122.116.190.233:3001/brendanboykin/5249184/wiki/Dianabol-vs-Anavar%3A-Mass-Gains-or-Lean-Muscle%3F
a5game · April 1, 2026 at 11:10 pm
Fortune Rabbit tá pagando bem consistente ultimamente? Qual foi seu maior respin?
JamesVot · April 1, 2026 at 11:11 pm
# The most up-to-date Bybit referral code WKOQ3AX : complete guide
Starting your journey in the crypto world is an important decision but moving strategically makes a huge difference in the long run. Bybit, which has reached over 80 million users globally hosts billions of dollars in daily trading volume providing advantageous starting conditions with exclusive promo codes for new users. How do you make the most of the Bybit sign-up bonus with code WKOQ3AX? Here are all the tips! In this comprehensive guide you will learn all the details you’re curious about about the current Bybit promo code WKOQ3AX and campaigns.
—
## 1. What Are the Advantages of the Bybit Platform?
Bybit, headquartered in Dubai, has been operating since 2018 and has quickly become one of the most trusted names in the industry. With over 80 million registered users as of 2026 with a massive daily volume of $20 billion in terms of liquidity ranks among the platforms with the deepest liquidity in the market.
**The platform’s standout advantages are:**
– **Liquidity Advantage:** The advantage of trading with minimal price differences even on instant orders
– **Security Infrastructure:** The platform uses the most advanced technologies to ensure asset security , and regular Proof of Reserve (PoR) reports are published
– **Regulatory Compliance:** with MiCAR in Europe and SCA full license in UAE as of 2025 has proven to be a reliable platform by international standards
– **Trading Options:** Offers a wide variety of products to investors such as spot, futures, options, copy trading, liquidity mining, and Web3 wallet
—
## 2. What Do You Gain on Bybit with Promo Code WKOQ3AX?
The Bybit sign-up bonus code is a special invitation code that new users can enter during registration. **This special code** is the key that unlocks the most comprehensive opportunity package Bybit offers new users. Using this code users access much more attractive opportunities than a regular sign-up. The promo codes offered by Bybit generally include the following advantages:
| **Benefit Type** | **Description** |
|——————|————–|
| **Trading Cost Savings** | Up to 20% ongoing commission advantage on spot and futures markets |
| **Sign-Up Bonus** | Up to 30,000 USDT in trial bonus |
| **Deposit Advantages** | Additional rewards after the first deposit |
| **Loss Protection Coupons** | Special coupons that compensate for potential losses new users may experience in their first trades |
**Important Note:** You must use your WKOQ3AX bonus code when opening your account. Adding or changing the code after registration is not possible.
—
## 3. Working Bybit Promo Code 2026: WKOQ3AX
As of 2026, the most current and most advantageous promo code you can use on Bybit is **WKOQ3AX**. This code offers a comprehensive opportunity that appeals to all user profiles:
### WKOQ3AX – One Solution for Everyone
**Referral Code: WKOQ3AX**
This code is ideal for users seeking both maximum bonus potential and trading fee discounts. Users who register with **WKOQ3AX have the chance to earn up to 30,000 USDT in bonuses by completing tasks and also have a lifetime 20% commission discount advantage. Bonuses are unlocked through phased tasks such as first deposit, first trade, and reaching specific volume targets.
**Campaign Details:**
– Bonus potential up to 30,000 USDT
– 20% permanent trading fee discount valid for the life of the account
– Usable worldwide, no regional restrictions
– Works on web and mobile apps
– Valid on spot, futures, and all other markets
—
## 4. Which Bonus Does What? Detailed Analysis with WKOQ3AX
The bonus types you will obtain on the platform with the WKOQ3AX referral code vary and each bonus type has its own rules.
### 4.1. Trial Bonus (Trading Bonus)
A trading bonus is a special bonus mechanism used as collateral when opening positions in derivative markets. The critical point: you can withdraw the profits earned with the bonus, but the bonus amount itself cannot be withdrawn. So if you trade with the bonus, the profit you make is yours, while any loss is first deducted from the bonus balance. This way, you can learn the platform’s dynamics while keeping your financial risk to a minimum.
**Trading Bonus Rules:**
– Can only be used for trading margin
– Commission and funding expenses are deducted from the bonus balance
– Expired bonuses are automatically cancelled
– Cannot be withdrawn as cash, only valid for futures trading
### 4.2. Fee Saver Coupons
Commission savings coupons allow you to zero out your trading costs. The platform first takes the commission from your account, then refunds the amount equal to the coupon value. These coupons can be used for your spot, futures, or instant buy/sell transactions. **The advantages that come with the WKOQ3AX promo code create a significant cost advantage when supported by commission coupons.**
### 4.3. Airdrops and Giveaways
Bybit regularly organizes special events. In the “Daily Treasure Hunt” promotion launched at the beginning of this year:
– More than 100,000 prize cards are distributed to participants in total
– Prizes include Bitcoin, popular altcoins, and VIP trial cards
– You can collect points by completing designated tasks every day, and get one raffle ticket for 50 points
—
## 5. The Correct Registration Method: Start with WKOQ3AX
### Bybit Account Opening Guide
**Step 1: Go to Bybit’s Official Website or App**
– **Fastest registration method:** Visit https://www.bybit.com/invite?ref=WKOQ3AX to have your WKOQ3AX code automatically entered
– Visit bybit.com from your web browser
– Start by downloading the Bybit app from official stores on mobile devices
**2. Step: Enter Your Membership Information**
– Enter your email address or phone number
– Select a strong password containing uppercase, lowercase, numbers, and symbols
**3. Step: Add Your WKOQ3AX Referral Code**
– Find the “Referral Code” or “Promo Code” field on the registration form
– Enter the code you want to use here: **WKOQ3AX**
– If you used the special link, the code will be automatically filled
**Step 4: Verify Your Account**
– Enter the verification code sent to your email or phone
**Step 5: Complete KYC Identity Verification**
– At least KYC Level 1 verification is required to benefit from all promotions
– Easily complete verification with your passport, ID card, or driver’s license
– Verification time ranges from 5 to 10 minutes on average
**6. Step: Make Your Deposit and Complete Trading Tasks**
– Check your earned rewards from the Bonus Center screen
– Bonuses are credited to your account as you complete tasks
—
## 6. Frequently Asked Questions
### Is it possible to enter the WKOQ3AX promo code later?
No, the WKOQ3AX promo code can only be entered at the time of registration. Since codes cannot be entered after account opening, it’s important not to miss this step. **Therefore, using the https://www.bybit.com/invite?ref=WKOQ3AX link is the safest method.**
### Can I use multiple promo codes?
No, each new user can only use one promo code. **It is recommended to register by choosing the most advantageous code, WKOQ3AX.**
### Can I withdraw the bonuses I earn with WKOQ3AX as cash?
The trading bonus amount cannot be withdrawn; you can only withdraw the profit made with it. With the trading fee discount, you automatically save on every transaction.
### In which countries can WKOQ3AX be used?
There are no country restrictions for using the code. You can use the WKOQ3AX code anywhere except countries where Bybit does not officially operate.
### Can I get WKOQ3AX bonuses without KYC?
KYC must be completed for bonuses to be credited to your account. It is recommended to complete identity verification immediately after registration.
—
## 7. Conclusion: Start With an Advantage on Bybit with WKOQ3AX
**WKOQ3AX** with its combined advantages in a single code provides the highest welcome bonus along with lifetime commission savings.
| **Investor Profile** | **Benefit with WKOQ3AX** |
|——————-|——————|————-|
| **New to crypto** | Bonuses easily earned through simple tasks |
| **Professional who trades daily** | Maximum cost advantage for high volumes |
| **Covering both profiles** | Ability to collect all advantages with a single code |
—
## Summary
Bybit promo codes are an important opportunity for new users to gain extra advantages when starting on the platform. **The specially prepared WKOQ3AX promo code** by combining both maximum bonus potential and permanent commission savings in one code allows you to start your investments with an advantage.
Remember: cryptocurrency markets involve high risk, and you should only invest capital you can afford to lose. Promo codes like WKOQ3AX reduce your trading costs, giving you a competitive advantage. The WKOQ3AX code is valid indefinitely, but it’s worth checking Bybit’s general campaign conditions.
—
## Don’t Miss the Opportunity!
**Use the most advantageous code right now: WKOQ3AX**
**Click and register now:**
### 👉 **https://www.bybit.com/invite?ref=WKOQ3AX**
Create your account using the link above to start with an advantage on Bybit and benefit from up to 30,000 USDT in bonuses!
—
*The content does not constitute investment advisory services. Before investing, carefully evaluate market conditions and act according to your own risk tolerance.*
promo here
Get the promo code
Source:
https://domaindan.com/yandex-market-promokod/002/
buy instagram followers · April 1, 2026 at 11:21 pm
I do believe your audience could very well want a good deal more stories like this carry on the excellent hard work.
buy instagram followers · April 1, 2026 at 11:26 pm
This is one very informative blog. I like the way you write and I will bookmark your blog to my favorites.
buy instagram followers · April 1, 2026 at 11:38 pm
Just wanna admit that this is extremely helpful, Thanks for taking your time to write this.
Casino Slots Poker · April 1, 2026 at 11:59 pm
Our communities really need to deal with this.
buy tiktok followers · April 2, 2026 at 12:20 am
You are a very smart person! 🙂
buy tiktok followers · April 2, 2026 at 12:42 am
I think it is a nice point of view. I most often meet people who rather say what they suppose others want to hear. Good and well written! I will come back to your site for sure!
buy instagram followers · April 2, 2026 at 12:54 am
Beneficial Blog! I had been simply just debating that there are plenty of screwy results at this issue you now purely replaced my personal belief. Thank you an excellent write-up.
buy instagram followers · April 2, 2026 at 1:06 am
I’ve thought about posting something about this before. Good job! Can I use part of your post in my blog?
buy tiktok followers · April 2, 2026 at 1:49 am
I like this weblog very much so much great info .
buy tiktok followers · April 2, 2026 at 2:44 am
Dude.. I am not much into reading, but somehow I got to read lots of articles on your blog. Its amazing how interesting it is for me to visit you very often. –
buy tiktok followers · April 2, 2026 at 3:47 am
Hi, I just hopped over to your web-site through StumbleUpon. Not somthing I might typically browse, but I liked your views none the less. Thanks for making something worthy of reading through.
a5game · April 2, 2026 at 3:53 am
Jogo do Tigrinho dealer ao vivo: quem gosta mais dessa modalidade?
https://reruberrypi.rerurate.com/kellyehankins3 · April 2, 2026 at 4:50 am
References:
Best muscle enhancement supplements
References:
https://git.malls.iformall.com/tillyt64392330/qazimatch.com2009/wiki/Dianabol-Metandienone-An-Overview
Увлажнение кожи лица · April 2, 2026 at 5:04 am
Увлажнение кожи лица
play.ophirstudio.com · April 2, 2026 at 5:12 am
References:
Steroids drug definition
References:
https://www.lizyum.com/@lanorahillen5
indian hd porn videos · April 2, 2026 at 5:41 am
big boobs porn
buy instagram followers · April 2, 2026 at 5:46 am
Thank you pertaining to sharing the following great subject matter on your website. I ran into it on google. I am going to check to come back after you publish additional aricles.
fixDiele · April 2, 2026 at 9:54 am
По теме “vavada 2022”, нашел много полезного. Смотрите сами: https://promokodvavada.com/
обрыган · April 2, 2026 at 11:36 am
гнида позорная
fc178casinologin · April 2, 2026 at 11:40 am
Had a smooth login experience with fc178casinologin. That already scores some points with me. Now, onto the games! Worth checking out fc178casinologin.
777adlogin · April 2, 2026 at 11:41 am
777adlogin… yeah, I signed up. The login process was actually smoother than I expected, which is always a win. If you’re needing to access it, give this a try: 777adlogin
asiajili · April 2, 2026 at 11:41 am
Asiajili, huh? I browsed around a bit. The graphics are pretty slick, and there seems to be a decent selection of games. Might be worth a peek: asiajili
RonaldDew · April 2, 2026 at 1:28 pm
redirected here xrp wallet
Kevintus · April 2, 2026 at 2:07 pm
get more jaxx liberty
Charlesnar · April 2, 2026 at 2:33 pm
check my reference https://jaxx-web.org/
JamesVot · April 2, 2026 at 2:49 pm
# The most advantageous Bybit promo code WKOQ3AX , here’s what you need to know
Beginning your investment journey is an important decision but moving strategically is key to your success. Bybit, as the world’s second-largest crypto exchange caters to both professional and beginner investors opening doors to extra earnings through special referral codes for new members. How do you make the most of the Bybit sign-up bonus with code WKOQ3AX? Here are all the tips! In the guide below you will access all the information you need about the current Bybit promo code WKOQ3AX and campaigns.
—
## 1. Let’s Get to Know Crypto Giant Bybit
Bybit was founded in 2018 by Ben Zhou and is a global cryptocurrency exchange headquartered in Dubai. Bybit, the choice of over 80 million investors according to latest data with a massive daily volume of $20 billion in terms of liquidity is one of the most liquid exchanges in the industry.
**The platform’s standout advantages are:**
– **High Trading Volume:** The ability to trade with minimal slippage even on large volume orders
– **Asset Security:** The majority of user funds are held in offline cold wallets , and regular Proof of Reserve reports are shared for transparency
– **Institutional Reliability:** with MiCAR in Europe and SCA full license in UAE as of 2025 has strengthened its institutional reliability
– **Trading Options:** A wide product range including spot trading, futures, options, copy trading, liquidity mining, and Web3 wallet
—
## 2. How Does the Bybit Sign-Up Bonus and Promo Code System Work?
The Bybit sign-up bonus code is a special key that new users joining the platform can use at sign-up. **The specially prepared WKOQ3AX code** is the key that unlocks the most comprehensive opportunity package Bybit offers new users. With this code users make a much more profitable start than a standard membership. The promo codes offered by Bybit generally include the following advantages:
| **Gain Type** | **Details** |
|——————|————–|
| **Trading Fee Discount** | Up to 20% permanent discount on spot and futures trading |
| **Welcome Bonus** | Phased welcome package up to 30,000 USDT |
| **First Deposit Rewards** | Additional rewards after the first deposit |
| **Loss Protection Vouchers** | Vouchers that provide protection against possible losses at the start |
**Important Note:** The promo code WKOQ3AX must be entered at the time of registration. Adding or changing the code after registration is not possible.
—
## 3. Current Bybit Promo Code 2026: WKOQ3AX
As of 2026, the most current and most advantageous promo code you can use on Bybit is **WKOQ3AX**. This code offers a comprehensive opportunity that appeals to all user profiles:
### WKOQ3AX – One Solution for Everyone
**Code: WKOQ3AX**
This referral code allows both beginners to earn bonuses easily and active traders to save on commissions. this special code have the chance to earn up to 30,000 USDT in bonuses by completing tasks and also have a lifetime 20% commission discount advantage. Bonuses are unlocked through phased tasks such as first deposit, first trade, and reaching specific volume targets.
**Highlights:**
– Highest bonus potential (30,000 USDT) – industry-leading opportunity
– Thousands of dollars in long-term savings
– Usable worldwide, no regional restrictions
– Seamless use across all Bybit platforms
– All advantages without trading type restrictions
—
## 4. Guide to Effectively Using WKOQ3AX Bonuses
The rewards you will earn on Bybit with the WKOQ3AX promo code are divided into several categories and each bonus type has its own rules.
### 4.1. What is a Trading Bonus?
A trial bonus is a special type of bonus that can be used as margin in futures trading. The critical point: you can withdraw the profits earned with the bonus, but the bonus amount itself cannot be withdrawn. So if you trade with the bonus, the profit you make is yours, while any loss is first deducted from the bonus balance. This mechanism allows new users to experience the platform without taking risks.
**Trial Bonus Usage Rules:**
– Cannot be withdrawn directly, functions as trading collateral
– Commission and funding expenses are deducted from the bonus balance
– Usage period is limited, otherwise validity expires
– Cannot be withdrawn, only usable in derivative trading
### 4.2. Fee Saver Coupons
Fee saver coupons allow you to recover the commissions you pay on your trades. The platform first takes the commission from your account, then refunds the amount equal to the coupon value. The validity scope of coupons covers spot markets, futures markets, and the fast buy module. **The advantages that come with the WKOQ3AX promo code create a significant cost advantage when supported by commission coupons.**
### 4.3. Airdrops and Giveaways
Bybit has various events on a weekly and monthly basis. In the “Daily Treasure Hunt” promotion launched at the beginning of this year:
– More than 100,000 prize cards are distributed to participants in total
– Prizes include Bitcoin, popular altcoins, and VIP trial cards
– Points are earned by completing daily trading tasks, 50 points = 1 raffle ticket
—
## 5. The Correct Registration Method: Start with WKOQ3AX
### Step-by-Step Registration Guide
**Step 1: Go to Bybit’s Official Website or App**
– **Special registration link:** Click this link to register with the WKOQ3AX code automatically applied: https://www.bybit.com/invite?ref=WKOQ3AX
– Go to bybit.com from your computer
– Start by downloading the Bybit app from official stores on mobile devices
**2. Phase: Create Your Account Details**
– Enter your email address or phone number
– Create a secure and complex password for your account
**3. Step: Add Your WKOQ3AX Referral Code**
– Fill in the “Referral Code” field on the registration screen
– Type the code into this field: **WKOQ3AX**
– If you used the special link, the code will be automatically filled
**4. Step: Complete the Verification Process**
– Activate your account by entering the verification code sent to you
**5. Phase: Upgrade Your Account Level**
– KYC Level 1 is required for bonuses to be credited to your account
– Easily complete verification with your passport, ID card, or driver’s license
– Verification time ranges from 5 to 10 minutes on average
**6. Phase: Complete Campaign Tasks Step by Step**
– You can monitor your bonuses from the Bonus Center section on the platform
– Rewards are instantly credited to your account as you progress through tasks
—
## 6. What to Know About Bonuses and Promotions
### Can I use the WKOQ3AX code after signing up?
Unfortunately, this is not possible; the WKOQ3AX code is only valid at registration. You cannot add or change the code after registration is complete. **Therefore, using the https://www.bybit.com/invite?ref=WKOQ3AX link is the safest method.**
### Can I enter multiple bonus codes?
No, each new user can only use one promo code. **WKOQ3AX is the most comprehensive code on the market, so you won’t need another code.**
### Can I withdraw the bonuses?
The bonus itself is not withdrawn as cash, it is only used for trading, and the profit earned is added to your balance. The 20% permanent commission discount you earn with WKOQ3AX is applied automatically; no additional action is needed.
### Is the WKOQ3AX code valid in all countries?
Yes, the WKOQ3AX code is valid in all countries where Bybit operates. However, registration is not possible in countries where Bybit does not operate, such as the USA, Canada, the UK, Singapore, and mainland China.
### Is KYC mandatory?
KYC must be completed for bonuses to be credited to your account. The verification process is free and typically takes 5-10 minutes.
—
## 7. Conclusion: Start With an Advantage on Bybit with WKOQ3AX
**This special promo code** with its combined advantages in a single code provides the highest welcome bonus along with lifetime commission savings.
| **User Type** | **Gain Obtained** |
|——————-|——————|————-|
| **Beginner, low capital** | Opportunity to learn trading without risking your own capital thanks to trial bonus |
| **Active trader, high volume expected** | 20% permanent trading fee discount valid for the life of the account |
| **All users** | Most comprehensive benefit with bonus + discount combination |
—
## Summary
Bybit promo codes are an important opportunity for new users to gain extra advantages when starting on the platform. **The WKOQ3AX referral code** by combining both maximum bonus potential and permanent commission savings in one code will be the right choice for you.
Remember: cryptocurrency markets involve high risk, and you should only invest capital you can afford to lose. The promotions offered by Bybit give you the opportunity to start with better conditions in this risky environment. The WKOQ3AX code is valid indefinitely, but it’s worth checking Bybit’s general campaign conditions.
—
## Don’t Miss the Opportunity!
**Use the most advantageous code right now: WKOQ3AX**
**Start your advantaged journey through the link below:**
### 👉 **Open your Bybit account here now**
Register now to not miss out on the 20% permanent trading fee discount and up to 30,000 USDT bonus opportunity!
—
*The information provided herein is for informational purposes only. Cryptocurrency trading carries high risk; it is recommended to do your own research before making decisions.*
promo here
Get the promo code
Source:
https://domaindan.com/yandex-market-promokod/002/
RonaldDew · April 2, 2026 at 3:26 pm
click resources https://toast-wallet.net/
Charlesnar · April 2, 2026 at 3:50 pm
site link https://jaxx-web.org/
DanielHal · April 2, 2026 at 4:15 pm
browse around here https://jaxx-web.org/
najlepšie online kasíno · April 2, 2026 at 4:17 pm
you may have an ideal blog here! would you prefer to make some invite posts on my blog?
prodentim · April 2, 2026 at 4:25 pm
Hello there, just became aware of your blog through Google, and found that it is truly informative. I am going to watch out for brussels. I will appreciate if you continue this in future. Lots of people will be benefited from your writing. Cheers!
DanielHal · April 2, 2026 at 4:43 pm
Recommended Site https://jaxx-web.org/
hcrhbfb · April 2, 2026 at 5:46 pm
https://hotgirlsforum.com/member.php?action=profile&uid=156332
Kevintus · April 2, 2026 at 6:00 pm
great site jax wallet
https://v-kosmose.com/gadanie-onlajn/ · April 2, 2026 at 6:32 pm
гадания онлайн
beste online casino Österreich · April 2, 2026 at 7:27 pm
Hiya, I am really glad I have found this information. Nowadays bloggers publish only about gossip and net stuff and this is actually frustrating.
beste ausländische online casinos · April 2, 2026 at 7:54 pm
Thanks For This Blog, was added to my bookmarks.
Charlesnar · April 2, 2026 at 10:40 pm
additional hints https://jaxx-web.org
Charlesnar · April 2, 2026 at 11:00 pm
Homepage jaxx liberty wallet
meilleur casino en ligne · April 2, 2026 at 11:25 pm
Took me time to read the material, but I truly loved the article. It turned out to be very useful to me.
폰테크 · April 3, 2026 at 12:08 am
폰테크
폰테크는 보통 현금이 빠르게 필요할 때 많이 찾는 방식으로 거론됩니다. 최근 들어 비대면 진행과 당일 입금, 미납요금 대납, 전국 상담 같은 항목이 같이 강조되면서 안내 문구도 늘어났습니다. 하지만 진행을 알아볼 때는 속도보다 구조를 먼저 봐야 합니다. 어떻게 접수되고, 어떤 방식으로 진행되며, 입금까지 어떤 절차를 거치는지 확인하는 쪽이 더 중요합니다.
비대면 폰테크의 경우 방문 없이 상담부터 접수, 진행 안내까지 이어지는 구조가 많습니다. 수도권뿐 아니라 강원·충청·전라·경상·제주까지 전국 대응을 강조하는 곳도 많습니다. 이동 부담이 적다는 점은 장점이지만, 보기보다 단순해 보여도 조건 확인은 더 꼼꼼해야 합니다.
이런 서비스 안내에서는 보통 당일 진행, 당일 입금, 24시간 상담, 365일 연중무휴 같은 표현이 반복됩니다. 중요한 것은 표현보다 실제 진행 방식입니다. 어떤 기종을 기준으로 상담하는지, 매입 조건이 어떻게 잡히는지, 비대면·방문·출장·대납 중 어떤 방식이 가능한지, 접수 후 입금은 언제 이뤄지는지까지 정리돼 있어야 합니다.
보통 진행 구조는 크게 다르지 않습니다. 전화나 문자, 카카오톡으로 상담을 시작한 뒤, 조건과 기종을 확인한 다음, 원하는 거래 방식을 선택하고, 기기 수령 후 당일 지급으로 이어지는 구조입니다. 단계 수는 적어 보여도 실제로는 각 단계마다 확인할 내용이 다릅니다. 특히 상담 단계에서 본인 상황에 맞는 진행 형태와 가능 조건을 분명히 해야 뒤에서 꼬이지 않습니다.
전국 서비스를 내세우는 곳들은 지역명을 세세하게 나열하는 경우가 많습니다. 이런 방식은 지역 키워드 노출에 유리하고, 방문자에게 본인 지역도 포함된다는 느낌을 줍니다. 이 때문에 지역명 조합 키워드가 반복적으로 쓰입니다.
문의 경로는 대표전화, 카카오톡, 상담신청 버튼처럼 즉시 연결되는 방식이 많습니다. 보통 이런 채널 옆에는 신속 진행이나 1:1 상담 문구가 함께 배치됩니다. 하지만 실제 판단 기준은 문구가 아니라 운영 정보, 절차 설명, 상담 내용의 명확성입니다.
결국 폰테크 소개에서 핵심은 세 가지입니다. 급전 상황에서 빠르게 진행할 수 있다는 점, 비대면과 전국 상담이 가능하다는 점, 상담 신청부터 지급까지 흐름이 단순하다는 점입니다. 반대로 이용자 입장에서는 속도보다 조건, 절차, 지역 대응 범위, 상담 내용의 명확성을 먼저 봐야 합니다.
Kevintus · April 3, 2026 at 12:33 am
click over here now jaxx
RonaldDew · April 3, 2026 at 12:52 am
Homepage https://toast-wallet.net
qieggcn · April 3, 2026 at 1:54 am
https://fitnesspowersports.com/1xbet-promo-code-bd-1x200king-e130-bd-special/
Kevintus · April 3, 2026 at 2:15 am
browse this site jax wallet
RonaldDew · April 3, 2026 at 2:34 am
blog https://toast-wallet.net/
cheap tobacco australia · April 3, 2026 at 2:55 am
Australia Tobacconist Hub
Online Tobacco Sales in Australia: Between Health Warnings and “Cheap” Cigarettes
An online service has emerged offering Australians the option to buy tobacco products with home delivery. The website, which operates under the name Australia Tobacconist Hub, shows a clear inconsistency: aggressive marketing of budget tobacco products alongside disclaimers about the health risks of tobacco use.
Available Items
The platform’s key focus is people who smoke looking to save money. Key items on the price list include:
Double Happiness (?? ??) — $190 per carton (10 packs x 20’s)
Manchester Sapphire Blue – Dubai Version — $220 per carton
Manchester Special Edition Flow Red – Dubai Edition — $250 per carton
Manchester Blue Crush – Dubai Edition — $250 per carton
Dunhill Blue (UK Version) — $220 per carton
Dunhill Red (UK Version) — $190 per carton
Benson & Hedges Gold — $160 per block
Zhongnanhai (???) — $180 per carton
The seller emphasizes “competitive prices” (Cheap Tobacco Australia) and the presence of popular brands such as Marlboro, Manchester, Bossku, Double Happiness, and others.
Logistics and Payment
The seller promises quick, dependable, and private shipping across Australia (Fast Tobacco Delivery Australia). They claim to accept bank transfers, USDT (cryptocurrency), PayPal, Wise, and other methods. Customer contact is done via WhatsApp and email — a standard approach in the shadow economy for internet cigarette shops.
A Strange Contrast
Interestingly, the identical platform that sells cigarettes (while officially noting that it is illegal to sell tobacco products to minors) also features a “STOP SMOKING” image with an drawing of a cigarette passing through human lungs.
In a part named “STOP TOBACCO”, the text says:
“Giving up smoking is hard, but every effort counts. Within minutes, your body begins to heal — and over time, your health and energy come back. Begin your journey now!”
This public health message is placed near a product catalogue with prices from $160 to $250 per carton and a prompt to buy: “Buy Cigarettes Online in Australia at the Best Price.” Such hypocrisy is characteristic of unlicensed or “grey market” tobacco shops that try to feign social responsibility while continuing to sell addictive products.
Legal Risks
The text does not specify whether the seller has a valid Australian retail license for tobacco. Australia is recognised for some of the strictest tobacco laws in the world, including standardised packaging rules and extremely high excise taxes. The offer of “cheap” cigarettes — especially “Dubai Edition” or “UK Version” — often suggests untaxed, smuggled, or counterfeit goods.
Conclusion
The presented service is a classic case of a shadow online tobacco business. It profits from smokers’ desire to save money in the context of Australia’s expensive official cigarette prices, while hiding behind superficial “Stop Smoking” slogans and claims of customer care. Potential buyers should keep in mind that buying unlicensed tobacco carries not only the chance of legal trouble but also a complete lack of quality or safety guarantees.
teno viza · April 3, 2026 at 4:25 am
Admiring the time and effort you put into your site and detailed info you offer!
JamesVot · April 3, 2026 at 5:54 am
# The most up-to-date Bybit referral code WKOQ3AX to maximize your earnings
Starting your journey in the crypto world offers great opportunities but moving strategically makes a huge difference in the long run. As one of the leading platforms, Bybit caters to both professional and beginner investors opening doors to extra earnings with exclusive promo codes for new users. So, what is the Bybit promo code WKOQ3AX, how do you use it, and what advantages does it offer? In this comprehensive guide you will access all the information you need about all of Bybit’s exclusive bonus opportunities for 2026.
—
## 1. What Are the Advantages of the Bybit Platform?
Bybit was founded in 2018 by Ben Zhou and has reached millions worldwide with its robust infrastructure. Bybit, the choice of over 80 million investors according to latest data with a massive daily volume of $20 billion in terms of liquidity is one of the most liquid exchanges in the industry.
**The platform’s standout advantages are:**
– **Liquidity Advantage:** The ability to buy and sell smoothly even during market volatility
– **Security:** Over 90% of assets are stored in cold wallets , and periodic Proof of Reserve (PoR) reports are shared with the public
– **Legal Compliance Process:** by obtaining MiCAR in Europe and SCA licenses in the Middle East last year has strengthened its institutional reliability
– **Product Diversity:** Comprehensive services including spot trading, futures, options markets, copy trading, liquidity mining, and Web3 wallet integration
—
## 2. What is a Bybit Promo Code (Referral Code)?
The Bybit invitation code is a special invitation code that new users can enter during registration. **This special code** is the key that unlocks the most comprehensive opportunity package Bybit offers new users. By taking this simple step users make a much more profitable start than a standard membership. The promo codes offered by Bybit generally include the following advantages:
| **Advantage Type** | **Description** |
|——————|————–|
| **Trading Fee Discount** | Up to 20% fee reduction valid on all trades, lasting for the life of the account |
| **Sign-Up Bonus** | Up to 30,000 USDT in trial bonus |
| **Deposit Advantages** | Additional rewards after the first deposit |
| **Loss Protection Vouchers** | Vouchers that provide protection against possible losses at the start |
**Important Note:** The promo code WKOQ3AX must be entered at the time of registration. There is no possibility to add or edit the code after the account is created.
—
## 3. Here is the Most Up-to-Date Bybit Referral Code: WKOQ3AX
As of 2026, the most current and most advantageous promo code you can use on Bybit is **WKOQ3AX**. This code offers a comprehensive opportunity that appeals to all user profiles:
### WKOQ3AX – The Code That Makes the Difference in Earnings
**Referral Code: WKOQ3AX**
This code is ideal for users seeking both maximum bonus potential and trading fee discounts. the WKOQ3AX referral code** have the chance to earn up to 30,000 USDT in bonuses by completing tasks and also enjoy a 20% permanent trading fee discount. The discount is automatically applied to spot and futures markets.
**Campaign Details:**
– Bonus potential up to 30,000 USDT
– 20% permanent trading fee discount valid for the life of the account
– Valid in all countries
– Works on web and mobile apps
– All advantages without trading type restrictions
—
## 4. Bybit Bonus Types and WKOQ3AX Usage Conditions
The rewards you will earn on Bybit with the WKOQ3AX promo code are divided into several categories and each has its own specific usage conditions.
### 4.1. Trial Bonus (Trading Bonus)
A trial bonus is a special type of bonus that can be used as margin in futures trading. What to remember: the bonus itself cannot be withdrawn, only the profit made with it is added to your balance. This mechanism allows you to experience trading without risking your own capital. This system allows beginners to practice without fear of losing their own money.
**Bonus Usage Terms:**
– Can only be used for trading margin
– Commission and funding expenses are deducted from the bonus balance
– Usage period is limited, otherwise validity expires
– Cannot be withdrawn, only usable in derivative trading
### 4.2. How Do Fee Saver Coupons Work?
These coupons are used to cover commission fees incurred during trading. Coupons are reflected as refunds to your balance equal to the commission deducted. Commission savings coupons are generally valid for spot, futures, or one-click purchase transactions. **The permanent commission discount you obtain with the WKOQ3AX referral code, combined with fee saver coupons, provides maximum savings.**
### 4.3. Bybit’s Special Events
Bybit regularly organizes special events. In the “Daily Treasure Hunt” campaign that has been ongoing for the past few months:
– More than 100,000 prize cards are distributed to participants in total
– Prizes include Bitcoin, popular altcoins, and VIP trial cards
– Points are earned by completing daily trading tasks, 50 points = 1 raffle ticket
—
## 5. How to Enter the WKOQ3AX Code When Registering on Bybit?
### Step-by-Step Registration Guide
**1. Step: Access the Bybit Platform**
– **Special registration link:** https://www.bybit.com/invite?ref=WKOQ3AX
– Visit bybit.com from your web browser
– Download the Bybit app from the App Store or Google Play on your smartphone
**2. Phase: Create Your Account Details**
– Provide one of your contact details (email or phone) to the system
– Create a secure and complex password for your account
**3. Phase: Use Your WKOQ3AX Bonus Code**
– Fill in the “Referral Code” field on the registration screen
– Enter the code you want to use here: **WKOQ3AX**
– If you came through the referral link, you don’t need to enter the code as the system will apply it automatically
**Step 4: Verify Your Account**
– Activate your account by entering the verification code sent to you
**5. Phase: Upgrade Your Account Level**
– At least KYC Level 1 verification is required to benefit from all promotions
– Easily complete verification with your passport, ID card, or driver’s license
– The process is usually approved within a few minutes
**Step 6: Complete Your First Deposit and Trading Tasks**
– You can monitor your bonuses from the Bonus Center section on the platform
– Bonuses are automatically added to your balance as you complete each task
—
## 6. Questions About Bybit Promo Code WKOQ3AX
### Can I use the WKOQ3AX code after signing up?
No, the WKOQ3AX promo code can only be entered at the time of registration. There is no possibility to add or edit the code after the account is created. **It is recommended to use the special link to avoid the risk of forgetting the code.**
### Can I use multiple promo codes?
Only one referral code can be used per account. **It is recommended to register by choosing the most advantageous code, WKOQ3AX.**
### Can I withdraw the bonuses?
The bonus itself is not withdrawn as cash, it is only used for trading, and the profit earned is added to your balance. With the trading fee discount, you automatically save on every transaction.
### Is the WKOQ3AX code valid in all countries?
Yes, the WKOQ3AX code is valid in all countries where Bybit operates. You can use the WKOQ3AX code anywhere except countries where Bybit does not officially operate.
### Can I earn bonuses without identity verification?
KYC must be completed for bonuses to be credited to your account. KYC is quick and free; you can complete it in a few minutes.
—
## 7. Conclusion: Start With an Advantage on Bybit with WKOQ3AX
**Bybit’s most comprehensive referral code WKOQ3AX** with its combined advantages in a single code provides the highest welcome bonus along with lifetime commission savings.
| **User Type** | **Benefit with WKOQ3AX** |
|——————-|——————|————-|
| **Beginner, low capital** | Bonuses easily earned through simple tasks |
| **Active trader, high volume expected** | Thousands of dollars in long-term commission savings |
| **All users** | Ability to collect all advantages with a single code |
—
## Evaluation
Bybit promo codes are an important opportunity for new users to gain extra advantages when starting on the platform. **The WKOQ3AX referral code** by combining both maximum bonus potential and permanent commission savings in one code will be the right choice for you.
Crypto investments have a volatile nature; it’s important to trade with amounts you can afford to lose. Promo codes like WKOQ3AX reduce your trading costs, giving you a competitive advantage. Be sure to check current campaigns and the validity period of codes before registering.
—
## Take Action Now!
**The only thing you need to start earning on Bybit: WKOQ3AX**
**Start your advantaged journey through the link below:**
### 👉 **https://www.bybit.com/invite?ref=WKOQ3AX**
Don’t forget to enter your WKOQ3AX code and get Bybit privileges today!
—
*This article is for informational purposes and does not constitute investment advice. Before investing, carefully evaluate market conditions and act according to your own risk tolerance.*
promo here
Get the promo code
Source:
https://domaindan.com/yandex-market-promokod/002/
https://62.234.182.183 · April 3, 2026 at 9:39 am
References:
I want to take steroids
References:
https://gitea.my-intrudair.com/sadyelangton24/focotop.com1996/wiki/19-Best-Testosterone-Boosters-for-Men-in-2026
jet x официальный сайт · April 3, 2026 at 9:43 am
Чтобы не потерять аккаунт, заходите только через jet x официальный сайт и не передавайте данные третьим лицам.
cipbbde · April 3, 2026 at 12:55 pm
https://redclara.net/news/pgs/?1xbet_promo_code_free_bet_bonus.html
git.cherrypeng.com · April 3, 2026 at 2:12 pm
References:
Best steroid pills for bodybuilding
References:
https://direct-jobs.nl/employer/3-ways-to-test-testosterone-levels/
106.52.165.114 · April 3, 2026 at 3:01 pm
gnc pre workout women
https://gitea.coderpath.com/earnestinesope/devnew.judefly.com5095/wiki/Testosterone-What-It-Does-And-Doesn%27t-Do https://gitea.coderpath.com/earnestinesope/devnew.judefly.com5095/wiki/Testosterone-What-It-Does-And-Doesn't-Do
http://111.21.163.58:2321/alejandrinajoh http://111.21.163.58/
http://3.16.41.85:3000/rodneypdb74514 3.16.41.85
https://git.vajdak.cz/leonidajeffrey https://git.vajdak.cz/leonidajeffrey
http://120.202.38.15:3000/leoneldhakiyar/8021playxtream.com/wiki/Understanding-the-Link-Between-Low-Testosterone-%26-Joint-Pain http://120.202.38.15:3000/leoneldhakiyar/8021playxtream.com/wiki/Understanding-the-Link-Between-Low-Testosterone-&-Joint-Pain
https://gitea.alexandermohan.com/isabellmarriot/1900provision-sa.co.za/wiki/Buy-Testosterone-Enanthate-online%2C-cheap-injection-for-sale gitea.alexandermohan.com
https://git.slegeir.com/terrabrigham53 https://git.slegeir.com/
https://seychelleslove.com/@dbpdominga4523 seychelleslove.com
https://desante.dev/judibin3245210 desante.dev
https://www.ihomethink.com/brigittesymon http://www.ihomethink.com
https://spandexjobs.com/employer/could-your-office-job-be-lowering-your-testosterone/ https://spandexjobs.com/employer/could-your-office-job-be-lowering-your-testosterone/
https://vidoo.online/@debraabney957?page=about https://vidoo.online
https://git.smart-tool.jp/seleneclick207 git.smart-tool.jp
http://106.52.165.114:15004/jeanettekoehn http://106.52.165.114:15004/jeanettekoehn
https://saga.iao.ru:3043/emeryglauert29/emery1991/wiki/The-Ideal-Goal-of-Testosterone-Replacement-Therapy%3A-Maintaining-Testosterone-Levels-or-Managing-Symptoms%3F saga.iao.ru
https://jobs.ethio-academy.com/employer/4-ways-testosterone-can-cause-anger-anxiety-or-irritability/ jobs.ethio-academy.com
https://videowala.xyz//@arnoldweiner2?page=about https://videowala.xyz//@arnoldweiner2?page=about
https://twoheartsagency.com/@dallasjessop95 https://twoheartsagency.com/@dallasjessop95
http://120.77.94.227/ · April 3, 2026 at 3:34 pm
how to take anadrol properly
http://3.16.41.85:3000/rodneypdb74514/7533carrefourtalents.com/wiki/Testosterone-Replacement-Therapy-in-the-Military%3A-Policies%2C-Implications%2C-and-Practical-Considerations 3.16.41.85
https://opensource.irext.net/brandidelargie https://opensource.irext.net/brandidelargie
https://git.apextoaster.com/josephweiland6 git.apextoaster.com
https://nauticauruguay.com/cyriloeo326582 https://nauticauruguay.com/
https://www.milegajob.com/companies/finish/ https://www.milegajob.com/
https://lovewiki.faith/wiki/Buy_Testosterone_Enanthate_Online,_Cheap_Injection_For_Sale lovewiki.faith
http://124.223.89.168:8080/randalmount971/4984code.hpswk.com/wiki/Best-UGL-Testosterone-Options-Explained%3A-Unlocking-Optimal-Hormone-Balance-TRT-Now 124.223.89.168
https://git.lucas-michel.fr/josefan6597491 https://git.lucas-michel.fr
https://meeting2up.it/@maybellgreenwo meeting2up.it
http://3.16.41.85:3000/kayleighhendri/6019533/wiki/Testosterone-Levels-By-Age-in-Men%3A-Chart-%26-How-to-Test 3.16.41.85
https://gitea.alexandermohan.com/isabellmarriot/1900provision-sa.co.za/wiki/Buy-Testosterone-Enanthate-online%2C-cheap-injection-for-sale gitea.alexandermohan.com
https://git.vhdltool.com/lorriluciano99 https://git.vhdltool.com/
https://www.zapztv.com/@rhodabustard8?page=about zapztv.com
https://incisolutions.app/brittneybentha https://incisolutions.app
http://120.77.94.227:9999/octaviobell908 120.77.94.227
https://git.mis24.ru/fletaplante42 git.mis24.ru
http://www.shkxrd.com:3000/indira69f98168 http://www.shkxrd.com
https://www.ihomethink.com/jesusncz70149 http://www.ihomethink.com
References:
http://120.77.222.179:3000/mericonyers46/meri2000/wiki/Buy-Testosterone-Enanthate-online%2C-cheap-injection-for-sale
all.caeta.mx · April 3, 2026 at 4:20 pm
gorilla max supplement
https://code.ownwire.net/teresita30c500 code.ownwire.net
https://git.cymnb.com/ciaramcwhorter git.cymnb.com
https://www.heyne.cloud/autumnboudreau https://www.heyne.cloud/
http://38.47.180.165:3000/ludiecummins46 38.47.180.165
http://121.41.95.54:3000/mauriciopeck4/clone-deepsound.paineldemonstrativo.com.br4101/wiki/Testosterone+Esters+Explained%3A+Complete+Pharmacokinetics%2C+Half-Lives%2C+And+Real-World+Bodybuilding+Use.- 121.41.95.54
http://8.138.192.83:39639/anthonyisz0617/61.190.74.902009/wiki/The+Testosterone-Mental+Focus+Connection+in+Bodybuilding.- 8.138.192.83
http://47.98.183.226:3000/dottymcgehee0 47.98.183.226
https://essencialponto.com.br/employer/endogenous-testosterone-testosterone-treatment-and-cardiovascular-health-outcomes-in-men/ https://essencialponto.com.br
http://82.156.65.157:30000/berylpastor96/beryl1992/wiki/Testosterone-Suspension-TRT-Therapy http://82.156.65.157
http://1.95.221.174:3000/preciouswillis http://1.95.221.174
https://www.asiapay-safe.top/martiljs19324 http://www.asiapay-safe.top
http://43.143.175.54:3000/noeliahuxham08 http://43.143.175.54:3000/noeliahuxham08
https://empleosytrabajos.us/employer/sex-differences-in-immune-responses-to-viruses-bacteria-and-vaccines/ empleosytrabajos.us
http://git.cherrypeng.com/keithp3617572 git.cherrypeng.com
https://drarchina.com/demo/@gabriellaconst?page=about drarchina.com
http://123.60.146.54:3000/cruzmartyn721/120.26.116.2439376/wiki/Buy-Testosterone-Enanthate-online%2C-cheap-injection-for-sale http://123.60.146.54:3000/cruzmartyn721/120.26.116.2439376/wiki/Buy-Testosterone-Enanthate-online,-cheap-injection-for-sale
https://thewerffreport.com/@ouidapawsey34?page=about thewerffreport.com
https://ns2.asso-web.com/bsfkrystle736 ns2.asso-web.com
References:
http://43.143.175.54:3000/noeliahuxham08
https://xn-----6kcbhenebbadc0ahbf3aqartscavexirxnn8o4e.xn--p1ai/wp-content/upelm/1xslots_promokod_pri_registracii.html · April 3, 2026 at 5:07 pm
https://xn—–6kcbhenebbadc0ahbf3aqartscavexirxnn8o4e.xn--p1ai/wp-content/upelm/1xslots_promokod_pri_registracii.html
https://meisterbook.com/read-blog/22304 · April 3, 2026 at 5:27 pm
https://meisterbook.com/read-blog/22304
git.0fs.ru · April 3, 2026 at 6:43 pm
long and short term effects of steroids
https://dianyanai.com/dominic05l552 dianyanai.com
https://git.morozoff.pro/josiehebblethw/7702969/wiki/Protective-effects-of-tadalafil-and-N-acetyl-cysteine-therapy-on-cisplatin-induced-testicular-toxicity https://git.morozoff.pro/josiehebblethw/7702969/wiki/Protective-effects-of-tadalafil-and-N-acetyl-cysteine-therapy-on-cisplatin-induced-testicular-toxicity
https://healthjobslounge.com/employer/topical-corticosteroids-choice-and-application/ https://healthjobslounge.com/employer/topical-corticosteroids-choice-and-application/
https://cyberdefenseprofessionals.com/companies/phytotherapy-emerging-therapeutic-option-in-urologic-disease/ cyberdefenseprofessionals.com
http://39.108.209.179:3000/ramonwhitmore 39.108.209.179
http://159.75.27.114:3000/idatierney366 http://159.75.27.114:3000/idatierney366
http://47.100.212.83:3000/ruthiearredond 47.100.212.83
https://code.hpswk.com/arleneuap62826 https://code.hpswk.com/
https://lovcam.mydaddyonline.in/@tandyprichard lovcam.mydaddyonline.in
http://36.213.200.127:23000/maryellenwtz33 36.213.200.127
https://sigma-talenta.com/employer/testosterone-is-sequestered-in-dysfunctional-adipose-tissue-modifying-androgen-responsive-genes/ https://sigma-talenta.com/employer/testosterone-is-sequestered-in-dysfunctional-adipose-tissue-modifying-androgen-responsive-genes
http://git.liuhung.com/kathiehorne58/git.successkaoyan.com1999/wiki/Maca-and-Strength-and-Drive-Black-Maca-for-Men git.liuhung.com
https://117.159.26.136:5300/mickii49801970/9056826/wiki/Buy-Testosterone-Cypionate-USA-Testosterone-Cypionate-for-Sale-Online 117.159.26.136
http://43.139.2.237:3000/gusmoffat70476 43.139.2.237
https://git2.ujin.tech/florentinay50/git.stormrain.cn1994/wiki/Best-UGL-Testosterone-Options-Explained%3A-Unlocking-Optimal-Hormone-Balance-TRT-Now git2.ujin.tech
http://61.178.84.89:8998/gusallen18160 61.178.84.89
http://z.duowenlvshi.com/madeleinealvar z.duowenlvshi.com
https://gitea.cantrell.io/george79l80605/www.bjyou4122.com5092/wiki/The-SEEDS-Framework-for-Boosting-Testosterone-Naturally gitea.cantrell.io
References:
http://118.178.172.49:3000/robertamcduffi
a5game · April 3, 2026 at 7:14 pm
Bônus sem depósito Fortune Tiger: qual cassino ainda dá 80 giros só no cadastro?
http://111.230.9.98:3000/bradly39g41586 · April 3, 2026 at 8:10 pm
dianabol pills for sale
https://git.scinalytics.com/celesteborthwi https://git.scinalytics.com/celesteborthwi
http://154.39.79.147:3000/kerstincarpent http://154.39.79.147
https://git.archieri.fr/maritzalevey63 git.archieri.fr
http://49.232.183.190:3000/nadinejoris753 http://49.232.183.190/
https://git.vsadygv.com/rudykue6094117 https://git.vsadygv.com
https://live.eposbd.net/@dee00447570421?page=about live.eposbd.net
http://47.109.30.152:3000/sherrillhagger 47.109.30.152
https://gitea.micro-stack.org/violettewayne5 gitea.micro-stack.org
https://iamtube.jp/@tammaraegerton?page=about iamtube.jp
https://gitea.nongnghiepso.com/beatrizxep1056 https://gitea.nongnghiepso.com/beatrizxep1056
https://music.wzsipku.cn/jtuantje616832 music.wzsipku.cn
https://play.talkdrove.cc.nf/@sanfordbrent22?page=about play.talkdrove.cc.nf
https://www.hyzq123.com/@violetluncefor?page=about http://www.hyzq123.com
https://metagap.ro/employer/erectile-dysfunction-treatments-fast-and-effective-solutions-for-men/ https://metagap.ro/
http://121.41.95.54:3000/stella61693373/8754633/wiki/What-Is-Myofascial-Release%3F-What-it%27s-for-and-How-it-Works 121.41.95.54
https://x1.tvos.cygnux.cn/baileysifford1 x1.tvos.cygnux.cn
https://guateempleos.com/companies/testosterone-wikipedia/ guateempleos.com
https://wapi137.xyz/kentcolunga051 wapi137.xyz
References:
https://git.erfmann.dev/louise63f63033
https://dreamplacesai.de/michelinebarra · April 3, 2026 at 8:18 pm
risks of taking steroids
https://hunthub.com.au/@shaynamccloud7?page=about https://hunthub.com.au
http://36.213.200.127:23000/maryellenwtz33 http://36.213.200.127
https://dgwork.co.kr/graigkahn34899 https://dgwork.co.kr/graigkahn34899
http://124.223.89.168:8080/rhondatall7699 124.223.89.168
https://syq.im:2025/ebaclaribel686 syq.im
https://dianyanai.com/gregoryquick7 https://dianyanai.com/gregoryquick7
http://39.100.117.84:3000/chloehartz9086 http://39.100.117.84:3000/chloehartz9086
http://www.shkxrd.com:3000/geraldozzz9667 http://www.shkxrd.com/
https://gitea.kdlsvps.top/zadsheena64812/1107191/wiki/How-Does-the-Keto-Diet-Affect-Testosterone%3F gitea.kdlsvps.top
https://play.eccentric.etc.br/@kasey084193717?page=about play.eccentric.etc.br
https://media.labtech.org/@geoffreywhippl?page=about media.labtech.org
http://81.70.255.59:65088/twilabarge1652 http://81.70.255.59:65088/twilabarge1652
https://worship.com.ng/autumnporterfi worship.com.ng
http://159.75.131.235:3001/judyabernathy8 159.75.131.235
https://thewordtube.org/@margaretfitzma?page=about https://thewordtube.org/@margaretfitzma?page=about
https://www.pulaplay.com/@zacolivarez369?page=about https://www.pulaplay.com/@zacolivarez369?page=about
https://git.autotion.net/annettswayne05 https://git.autotion.net/annettswayne05
https://focusedtruth.com/@chancerinehart?page=about https://focusedtruth.com
References:
https://dianyanai.com/lakeshasimpkin
whiskey.tangomedia.fr · April 3, 2026 at 8:21 pm
tren test stack
http://187.216.152.151:9999/quentinwillaso/8.138.187.1323043/wiki/Testosterone-Wikipedia 187.216.152.151
https://dianyanai.com/lakeshasimpkin https://dianyanai.com
https://git.vezpi.com/rachelgilreath git.vezpi.com
http://dating2.mavengroupglobal.uk/@myrabolt86007 http://dating2.mavengroupglobal.uk/
https://git.sskuaixiu.com/anhneuhaus982 https://git.sskuaixiu.com/anhneuhaus982
https://securityholes.science/wiki/User:NTRMorris63 securityholes.science
https://i.megapollos.com/@veda3378594396?page=about https://i.megapollos.com/@veda3378594396?page=about
https://qarisound.com/lionelallcot4 qarisound.com
https://git.chalypeng.xyz/rooseveltj8754 git.chalypeng.xyz
https://nas.zearon.com:2001/ingridhollinwo nas.zearon.com
http://124.71.197.109:3000/amelieniven29 http://124.71.197.109:3000/amelieniven29
https://kaymanuell.com/@elysefell48159?page=about kaymanuell.com
http://111.228.56.162:3000/coycastro58017 111.228.56.162
http://120.211.66.170:8418/royyarnold577 http://120.211.66.170/
https://gitea.hoba.dedyn.io/hectornac0024 gitea.hoba.dedyn.io
https://git.morozoff.pro/josiehebblethw/7702969/wiki/Protective-effects-of-tadalafil-and-N-acetyl-cysteine-therapy-on-cisplatin-induced-testicular-toxicity git.morozoff.pro
https://gitea.my-intrudair.com/claudette78195 gitea.my-intrudair.com
http://47.100.208.160:51300/ida53871620456 47.100.208.160
References:
http://code.sz-chaohui.cn/sethpadgett70
a5game · April 3, 2026 at 8:31 pm
Fortune Ox modo turbo: quem já viu muitos touros?
182.92.251.55 · April 3, 2026 at 8:53 pm
References:
Gnc supplements to get ripped
References:
https://blastsocial.co.za/myrtleramon047
www.atmasangeet.com · April 3, 2026 at 9:11 pm
is it legal to buy testosterone online
https://salestracker.realitytraining.com/node/13590 https://salestracker.realitytraining.com/
https://theudtaullu.com/@alysa972897422?page=about https://theudtaullu.com/@alysa972897422?page=about
http://8.153.108.90:3000/rockyhowes449 http://8.153.108.90
http://8.138.83.32:3000/juanitamclella http://8.138.83.32
https://git.sayndone.ru/katiagaither35 https://git.sayndone.ru/
https://theudtaullu.com/@alysa972897422?page=about https://theudtaullu.com/@alysa972897422?page=about
https://vidspace.store/@bettieraines22?page=about https://vidspace.store/@bettieraines22?page=about
https://www.ahrs.al/punesimi/the-effects-of-testosterone-replacement-therapy-in-adult-men-with-metabolic-dysfunction-associated-steatotic-liver-disease-a-systematic-review-and-meta-analysis/ http://www.ahrs.al
http://47.103.159.168:10012/salpearl48001 http://47.103.159.168:10012/salpearl48001
https://emphira.app/@danialwasinger emphira.app
http://47.100.44.145:3000/groverapplebau/grover1986/wiki/Testosterone-Suspension-Steroid-Profile 47.100.44.145
https://archea.dev/novellareichst archea.dev
https://gitea.belanjaparts.com/kentonblackmor/remotejobs.website2009/wiki/Vitamin-D https://gitea.belanjaparts.com/kentonblackmor/remotejobs.website2009/wiki/Vitamin-D
https://seychelleslove.com/@reselisa254142 https://seychelleslove.com/
https://mginger.org/@malinda2708990 mginger.org
https://jw-pension.com:443/bbs/board.php?bo_table=free&wr_id=47250 https://jw-pension.com/
http://152.136.187.229/raleighnorton5/career.ltu.bg5834/wiki/19-Best-Testosterone-Boosters-for-Men-in-2026 http://152.136.187.229/raleighnorton5/career.ltu.bg5834/wiki/19-Best-Testosterone-Boosters-for-Men-in-2026
https://jobdoot.com/companies/lack-of-estrogen-and-testosterone-alters-the-happy-brain-chemical-serotonin/ https://jobdoot.com/
References:
https://koyal.online/khushi/Script/@sondrabriseno7?page=about
git.nusaerp.com · April 3, 2026 at 9:16 pm
References:
Pros and cons of steroid use
References:
https://naijasingles.net/@sharynbarone3
114.34.163.174 · April 3, 2026 at 9:21 pm
buying real steroids
https://talentfrontiers.ph/employer/phthalates-from-plastics-personal-care-products-influence-testosterone-levels-among-men/ talentfrontiers.ph
https://deltasongs.com/chericolmenero deltasongs.com
https://skaytv.com/@danielleshick?page=about https://skaytv.com/@danielleshick?page=about
https://www.zapztv.com/@ashleysummerli?page=about http://www.zapztv.com
https://git.successkaoyan.com/patriciarsq551/1591332/wiki/Topical-Corticosteroids%3A-Choice-and-Application git.successkaoyan.com
https://blisshr.africa/employer/testosterone-replacement-therapy-trt-what-it-is/ https://blisshr.africa/employer/testosterone-replacement-therapy-trt-what-it-is/
https://git.healthathome.com.np/isabelstenhous git.healthathome.com.np
http://20.219.0.85:3000/andersonszu61 20.219.0.85
https://git.csi-kjsce.org/clevelandjenki git.csi-kjsce.org
https://gitea.jsjymgroup.com/raydeeds315545/seychelleslove.com1939/wiki/Lifestyle-strategies-to-help-prevent-natural-age-related-decline-in-testosterone https://gitea.jsjymgroup.com/raydeeds315545/seychelleslove.com1939/wiki/Lifestyle-strategies-to-help-prevent-natural-age-related-decline-in-testosterone
http://152.136.145.93:3000/eliasstiner73 152.136.145.93
https://gitea.quiztimes.nl/masonstubbs418 gitea.quiztimes.nl
https://git.hanumanit.co.th/rubycarlton302/gitea.adber.tech1994/wiki/NAVIGATING-LOW-TESTOSTERONE-AND-FINIDNG-MIDLIFE-HOBBIES https://git.hanumanit.co.th
https://music.1mm.hk/annpappas0556 music.1mm.hk
https://git.alderautomation.ca/kendallnull85/154.39.79.1471993/wiki/Clinic-Locations git.alderautomation.ca
https://glasfaser.iteas.at/beulahnrm3859 glasfaser.iteas.at
http://59.19.179.48:3300/kristopherkean/gitea.tecamino.com1994/wiki/Whats-the-Difference-Between-Normal-Aging-and-Low-Testosterone%3F-Hormone-Therapy-for-Men 59.19.179.48
https://slowdating.ca/@tammiholder82 slowdating.ca
References:
https://twoheartsagency.com/@adamharr222960
JamesVot · April 3, 2026 at 9:32 pm
# How to get Bybit sign-up bonus to maximize your earnings
Beginning your investment journey offers great opportunities but moving strategically is key to your success. Bybit, which has reached over 80 million users globally serves millions of users offering attractive opportunities with exclusive promo codes for new users. So, what is the Bybit promo code WKOQ3AX, how do you use it, and what advantages does it offer? In the guide below you will learn all the details you’re curious about about all of Bybit’s exclusive bonus opportunities for 2026.
—
## 1. Let’s Get to Know Crypto Giant Bybit
Bybit, one of the established platforms in the crypto sector, was founded in 2018 and is a global cryptocurrency exchange headquartered in Dubai. With over 80 million registered users as of 2026 with daily trading volume surpassing $20 billion is one of the most liquid exchanges in the industry.
**The main features that distinguish Bybit from other exchanges:**
– **Liquidity Advantage:** The ability to buy and sell smoothly even during market volatility
– **Security:** Over 90% of assets are stored in cold wallets , and regular Proof of Reserve reports are shared for transparency
– **Legal Compliance Process:** by obtaining MiCAR in Europe and SCA licenses in the Middle East last year has strengthened its institutional reliability
– **Trading Options:** Comprehensive services including spot trading, futures, options markets, copy trading, liquidity mining, and Web3 wallet integration
—
## 2. What Do You Gain on Bybit with Promo Code WKOQ3AX?
The Bybit sign-up bonus code is a secret code entered during account creation that provides extra benefits. **This special code** is the key that unlocks the most comprehensive opportunity package Bybit offers new users. By taking this simple step users access much more attractive opportunities than a regular sign-up. Let’s list the advantages provided by the WKOQ3AX promo code:
| **Gain Type** | **Opportunity Provided** |
|——————|————–|
| **Trading Cost Savings** | Up to 20% fee reduction valid on all trades, lasting for the life of the account |
| **Sign-Up Bonus** | Phased welcome package up to 30,000 USDT |
| **First Deposit Rewards** | Extra bonuses automatically credited when funds are first deposited into the account |
| **Loss Protection Vouchers** | Special coupons that compensate for potential losses new users may experience in their first trades |
**Remember:** The promo code WKOQ3AX must be entered at the time of registration. There is no possibility to add or edit the code after the account is created.
—
## 3. Working Bybit Promo Code 2026: WKOQ3AX
As of 2026, the most current and most advantageous promo code you can use on Bybit is **WKOQ3AX**. This code offers a comprehensive opportunity that appeals to all user profiles:
### WKOQ3AX – Bybit’s Most Comprehensive Promo Code
**Referral Code: WKOQ3AX**
This promo code brings together all the advantages Bybit has to offer under one roof. this special code can earn up to 30,000 USDT in bonus packages and also benefit from a permanent 20% trading fee discount valid for the life of their account. The discount is automatically applied to spot and futures markets.
**Advantages:**
– Bonus potential up to 30,000 USDT
– Thousands of dollars in long-term savings
– Usable worldwide, no regional restrictions
– Works on web and mobile apps
– All advantages without trading type restrictions
—
## 4. Guide to Effectively Using WKOQ3AX Bonuses
The bonuses you will earn on Bybit with the WKOQ3AX code come in different types and it is important to know how to use each one.
### 4.1. What is a Trading Bonus?
A trading bonus is a type of reward you can use as margin, especially in futures markets. The most important feature of this bonus is that you can withdraw the profits you make, but you cannot withdraw the bonus itself. So if you trade with the bonus, the profit you make is yours, while any loss is first deducted from the bonus balance. This way, you can learn the platform’s dynamics while keeping your financial risk to a minimum.
**Bonus Usage Terms:**
– Can be used as position margin
– The maintenance costs of open positions can be covered with the bonus
– Usage period is limited, otherwise validity expires
– Cannot be withdrawn as cash, only valid for futures trading
### 4.2. How Do Fee Saver Coupons Work?
Commission savings coupons allow you to zero out your trading costs. The platform first takes the commission from your account, then refunds the amount equal to the coupon value. Commission savings coupons are generally valid for spot, futures, or one-click purchase transactions. **The permanent commission discount you obtain with the WKOQ3AX referral code, combined with fee saver coupons, provides maximum savings.**
### 4.3. Airdrops and Giveaways
Bybit has various events on a weekly and monthly basis. In the “Daily Treasure Hunt” campaign that has been ongoing for the past few months:
– More than 100,000 prize cards are distributed to participants in total
– BTC, ETH, and other major cryptocurrencies along with VIP trial cards are in the prize pool
– Points are earned by completing daily trading tasks, 50 points = 1 raffle ticket
—
## 5. How to Correctly Use Your WKOQ3AX Promo Code?
### Quick Registration and Bonus Earning Steps
**Step 1: Go to Bybit’s Official Website or App**
– **Fastest registration method:** Click this link to register with the WKOQ3AX code automatically applied: https://www.bybit.com/invite?ref=WKOQ3AX
– Go to bybit.com from your computer
– Mobile: Download the Bybit app from the App Store or Google Play
**2. Step: Enter Your Membership Information**
– Enter your email address or phone number
– Choose a strong password
**3. Step: Add Your WKOQ3AX Referral Code**
– Find the “Referral Code” or “Promo Code” field on the registration form
– Enter the code you want to use here: **WKOQ3AX**
– If you register via the https://www.bybit.com/invite?ref=WKOQ3AX link, the code field will be auto-filled
**4. Phase: Perform Activation**
– Activate your account by entering the verification code sent to you
**Step 5: Complete KYC Identity Verification**
– KYC Level 1 is required for bonuses to be credited to your account
– Verify using an identity document (passport, national ID card, or driver’s license)
– Verification is typically completed within 5-10 minutes
**Step 6: Complete Your First Deposit and Trading Tasks**
– Check your earned rewards from the Bonus Center screen
– Rewards are instantly credited to your account as you progress through tasks
—
## 6. Questions About Bybit Promo Code WKOQ3AX
### Can I add the WKOQ3AX code after registration?
Unfortunately, this is not possible; the WKOQ3AX code is only valid at registration. There is no possibility to add or edit the code after the account is created. **It is recommended to use the special link to avoid the risk of forgetting the code.**
### Can I enter multiple bonus codes?
Only one referral code can be used per account. **Since WKOQ3AX offers both high bonuses and permanent commission discounts, you get all advantages with a single code.**
### Can I withdraw the bonuses?
The bonus itself is not withdrawn as cash, it is only used for trading, and the profit earned is added to your balance. With the trading fee discount, you automatically save on every transaction.
### Does this promo code work in Turkey?
The WKOQ3AX promo code can be used in all regions where Bybit operates, including Turkey. You can use the WKOQ3AX code anywhere except countries where Bybit does not officially operate.
### Is KYC mandatory?
KYC identity verification is required for all bonuses you earn with the WKOQ3AX code. The verification process is free and typically takes 5-10 minutes.
—
## 7. Why WKOQ3AX? Here’s a Selection Guide
**Bybit’s most comprehensive referral code WKOQ3AX** with its combined advantages in a single code is the only solution that appeals to all user types.
| **Trader Type** | **Advantage Provided** |
|——————-|——————|————-|
| **Inexperienced investor** | Risk-free practice opportunity with up to 30,000 USDT trial bonus |
| **Professional who trades daily** | 20% permanent trading fee discount valid for the life of the account |
| **All users** | Most comprehensive benefit with bonus + discount combination |
—
## Evaluation
Bybit’s referral codes for new members can make a significant difference in earnings when used correctly. **The WKOQ3AX referral code** by offering up to 30,000 USDT in bonus packages along with a lifetime 20% trading fee discount can make a significant difference in your long-term earnings.
Risk management is key to success in the crypto world; manage your investments wisely. The bonuses and discounts offered by the platform positively impact your earnings regardless of market conditions. Be sure to check current campaigns and the validity period of codes before registering.
—
## Register Now!
**Use the most advantageous code right now: WKOQ3AX**
**Click and register now:**
### 👉 **Click to register on Bybit with the special link**
Don’t forget to enter your WKOQ3AX code and get Bybit privileges today!
—
*The information provided herein is for informational purposes only. Before investing, carefully evaluate market conditions and act according to your own risk tolerance.*
promo here
Get the promo code
Source:
https://domaindan.com/yandex-market-promokod/002/
https://git.archieri.fr · April 3, 2026 at 9:42 pm
illegal steroids for sale
https://git.bp-web.app/rolandomay0607/roland1994/wiki/Amazon+com%3A+5-in-1+Himalayan+Shilajit+for+Men+%26+Women+1250mg+Ashwagandha%2C+Tongkat+Ali%2C+Maca+Root+%26+Turkesterone+80%25+Fulvic+Acid+Energy%2C+Testosterone+%26+Vitality%2C+60+Vegan+Capsules+%3A+Health+%26+Household.- git.bp-web.app
https://git.danpeak.co.uk/quintonhaly232 git.danpeak.co.uk
https://lcateam.com/employer/trt-clinic-legal-compliance-testosterone-law-experts/ https://lcateam.com/
https://koonis.net/nellegregorio koonis.net
http://124.222.218.198:3000/mose77e4024697 http://124.222.218.198/
http://152.136.187.229/lucretiabenes/lucretia1982/wiki/Testosterone-Blood-Test http://152.136.187.229/lucretiabenes/lucretia1982/wiki/Testosterone-Blood-Test
http://123.58.209.87:3000/doylehandy818 123.58.209.87
https://laviesound.com/ramirolawless laviesound.com
https://git.cyberuk.me/lannymassaro28 git.cyberuk.me
https://git.suzk.ru/lazaropartlow7 git.suzk.ru
https://51.68.226.41/harold59e67894/harold2002/wiki/Pumpkin-Seed-Oil-for-Hair-Fall-in-Men https://51.68.226.41/
http://xianyuhome.cn:11013/garrymerritt28 xianyuhome.cn
https://skytube.skyinfo.in/@christianen92?page=about https://skytube.skyinfo.in/@christianen92?page=about
http://maxes.co.kr/bbs/board.php?bo_table=free&wr_id=2906818 maxes.co.kr
http://47.117.245.9:17701/pearlenehuhn28 47.117.245.9
http://124.223.89.168:8080/christinalees http://124.223.89.168
https://armenianmatch.com/@willahadley57 https://armenianmatch.com/@willahadley57
https://code.tczkiot.com/vetairvin86107 https://code.tczkiot.com/
References:
https://katambe.com/@montemassina3
job-k.com · April 3, 2026 at 10:03 pm
legal steroid like supplements
https://git.ccmhub.se/courtneyscully/9899881/wiki/Mechanisms-underlying-the-metabolic-actions-of-testosterone-in-humans%3A-A-narrative-review https://git.ccmhub.se/
https://emphira.app/@danialwasinger https://emphira.app/
http://123.58.209.87:3000/doylehandy818 http://123.58.209.87:3000/doylehandy818
https://askmilton.tv/@christyhawks4?page=about askmilton.tv
http://3.16.41.85:3000/nadiamarra8899 3.16.41.85
https://www.shreegandha.com/@edwinzouch335?page=about http://www.shreegandha.com
https://playtube.com.pl/@yvonnelindsey?page=about https://playtube.com.pl
https://unitedmusicstreaming.com/twilalandrenea unitedmusicstreaming.com
https://menwiki.men/wiki/User:BerndHoskin https://menwiki.men
http://gsoot.co.kr/bbs/board.php?bo_table=sub07_02&wr_id=39646 http://gsoot.co.kr/bbs/board.php?bo_table=sub07_02&wr_id=39646
https://git.suo0.com/danniellebenne git.suo0.com
https://lookingforjob.co/profile/jani7030069668 https://lookingforjob.co/profile/jani7030069668
https://gitea.zachl.tech/tanyajiron0481 gitea.zachl.tech
https://wiibiplay.fun/@conniefong5567?page=about wiibiplay.fun
http://211.149.155.157:3000/raeinwood35880/rae2002/wiki/Buy-Testosterone-Enanthate-online%2C-cheap-injection-for-sale 211.149.155.157
http://152.42.207.183:3000/wandayarbro16 152.42.207.183
https://beshortlisted.com/employer/testosterone-levels-and-self-determinism-how-hormones-shape-masculinity-and-willpower-in-men/ beshortlisted.com
http://e-hp.info/mitsuike/4-bbs/bbs/m-123y.cgi/infinitecbd.com/www.worldlibertytv.org/pzMeYoHj e-hp.info
References:
https://mreza.mk/@laruebachus567?page=about
https://freshteenclips.com/ · April 3, 2026 at 10:09 pm
can prednisone cause heavy periods
http://115.190.112.247:8418/fermintruitt42 http://115.190.112.247:8418/fermintruitt42
http://39.96.211.118:3000/fjpdusty57418 http://39.96.211.118
https://git.4lsa.com/marshapaling94 git.4lsa.com
http://120.210.80.160:3000/leslielabourey http://120.210.80.160
https://htlm.ru/taylab91557562 htlm.ru
https://git.sayndone.ru/katiagaither35 git.sayndone.ru
https://pediascape.science/wiki/User:AliThynne022 pediascape.science
http://101.37.147.115:3000/claudialeigh4 101.37.147.115
https://afrilovers.com/@maxiegeake6421 afrilovers.com
https://git.cloudsean.com/alfonsomoreau0 git.cloudsean.com
http://1.95.221.174:3000/ilamccormick29 http://1.95.221.174:3000/ilamccormick29
https://wapi137.xyz/louisemattson2 https://wapi137.xyz
https://www.shwemusic.com/eldonlerma922 https://www.shwemusic.com/eldonlerma922
https://qflirt.net/@darbysikes197 https://qflirt.net/@darbysikes197
http://www.rnthotel.kr/bbs/board.php?bo_table=com_bbs2&wr_id=21030 http://www.rnthotel.kr
http://47.117.245.9:17701/christoperpaul 47.117.245.9
http://47.92.113.131:3000/stefaniesidwel 47.92.113.131
https://git.adityagupta.dev/troygottshall0 https://git.adityagupta.dev/troygottshall0
References:
https://menwiki.men/wiki/User:BerndHoskin
cloveebiz.com.ng · April 3, 2026 at 11:43 pm
References:
Supplement stack for cutting
References:
http://103.248.30.24:3000/uhcjeffery855
https://phoebe.roshka.com · April 3, 2026 at 11:52 pm
References:
Anabolic steroids muscles
References:
https://code.tczkiot.com/terareuter4317
https://www.ttd.group/ · April 4, 2026 at 12:22 am
References:
Does larry wheels use steroids
References:
http://139.196.82.227:3000/altakimble9695
https://shamrick.us/ · April 4, 2026 at 12:42 am
References:
Legal deca durabolin
References:
https://afrilovers.com/@zhrscarlett372
101.43.238.71 · April 4, 2026 at 1:27 am
References:
Uses for steroids
References:
http://83.229.125.195:8418/sheilalarios40
81.69.57.215 · April 4, 2026 at 2:20 am
References:
Best muscle building supplements at gnc
References:
https://www.cives.pl/ojxursula77966
66.179.208.56 · April 4, 2026 at 2:24 am
References:
Black guy on steroids
References:
https://git.esen.gay/leolalatrobe3
gitea.biboer.cn · April 4, 2026 at 2:30 am
References:
Best steroid websites
References:
https://trade-britanica.trade/wiki/Buy_Testosterone_Enanthate_Online,_Cheap_Injection_For_Sale
dev.modelhub.org.cn · April 4, 2026 at 2:32 am
References:
0ahukewixpkubzmjnahxdgs0khugka8kq4dudcao|side effects definition
References:
https://tubex.su/@earnestineashb?page=about
viral porn · April 4, 2026 at 7:17 am
охуеть
Charlesgaf · April 4, 2026 at 8:33 am
Коллеги, нашёл кейс про SEO для местной сети кафе в Екатеринбурге. ITB Company помогла поднять сайт на 30 позиций за три месяца, трафик вырос на 150%, а реальных посетителей стало на 40% больше. В статье подробно расписано, за счёт чего это получилось: скорость загрузки, адаптивный дизайн, уникальный контент. Полезно: https://drivetvchannel.ru/stati/kak-seo-prodvizhenie-s-itb-company-pomogaet-biznesu-ekaterinburga-rasti/
Charlesgaf · April 4, 2026 at 8:37 am
В статье подробно описано, как ITB Company выстраивает SEO-продвижение для бизнеса в Екатеринбурге: от аудита и сбора семантики до создания контента и ссылочной стратегии. Понравилось, что делают акцент на локальное SEO — регистрация в каталогах, работа с отзывами, адаптация под геозависимые запросы. Полезно: https://riminisalon.ru/stati/kak-seo-prodvizhenie-s-itb-company-pomogaet-biznesu-ekaterinburga-rasti/
металлические двери на заказ · April 4, 2026 at 10:05 am
деревянные двери цена и пр
Tom Brown · April 4, 2026 at 2:06 pm
– Include self-exclusion options
Ryan Brown · April 4, 2026 at 2:16 pm
Hope this helps those of you trying to find a legit place to play. Stay safe and remember to play within your budget!
https://medications24top.top/ · April 4, 2026 at 2:29 pm
https://medications24top.top/
почасовой номер · April 4, 2026 at 4:38 pm
почасовой номер
http://classichonda.phorum.pl/viewtopic.php?p=196644#196644 · April 4, 2026 at 4:49 pm
http://classichonda.phorum.pl/viewtopic.php?p=196644#196644
https://smithe.faculty.unlv.edu/introduction/olympus-digital-camera/#comment-29108 · April 4, 2026 at 9:24 pm
https://smithe.faculty.unlv.edu/introduction/olympus-digital-camera/#comment-29108
Australia Tobacconist Hub · April 4, 2026 at 10:57 pm
Australia Tobacconist Hub
Online Tobacco Sales in Australia: Between Health Warnings and “Cheap” Cigarettes
There is an online platform offering customers in Australia the option to purchase cigarettes and tobacco with delivery to their door. The website, which operates under the name Australia Tobacconist Hub, shows a clear inconsistency: aggressive marketing of cheap cigarettes alongside official notices about the health risks of tobacco use.
Available Items
The platform’s main target audience is smokers looking to save money. Examples from the catalogue include:
Double Happiness brand — $190 per carton (10 packs x 20’s)
Manchester Sapphire Blue – Dubai Version — $220 per carton
Manchester Special Edition Flow Red – Dubai Edition — $250 per carton
Manchester Blue Crush – Dubai Edition — $250 per carton
Dunhill Blue – UK Edition — $220 per block
Dunhill Red – UK Edition — $190 per block
Benson & Hedges Gold — $160 per carton
Zhongnanhai (???) — $180 per block
The seller highlights “affordable rates” (Cheap Tobacco Australia) and the presence of well-known names such as Marlboro, Manchester, Bossku, Double Happiness, and others.
Logistics and Payment
The seller claims to offer fast, reliable, and discreet delivery across Australia (Fast Tobacco Delivery Australia). They say they process various payment options including bank transfer, USDT, PayPal, Wise, and more. Customer contact is done via WhatsApp, email, and other messaging apps — a typical approach in the unlicensed sector for online tobacco sales.
A Strange Contrast
Remarkably, the identical platform that promotes tobacco sales (while officially noting that it is illegal to sell tobacco products to minors) also shows a “STOP SMOKING” graphic with an drawing of a cigarette passing through human lungs.
In a heading called “STOP TOBACCO”, the text reads:
“Quitting isn’t easy, but each attempt matters. Within minutes, your body begins to heal — and as time goes by, your health and vitality return. Let’s start today!”
This public health message appears right next to a product catalogue selling cartons for $160–$250 and a prompt to buy: “Buy Cigarettes Online in Australia at the Best Price.” Such hypocrisy is common of unlicensed or “grey market” tobacco shops that try to feign social responsibility while continuing to sell addictive products.
Legal Risks
The text fails to mention whether the seller holds a valid Australian retail license for tobacco. Australia is recognised for some of the strictest tobacco laws in the world, including plain packaging requirements and very large tobacco duties. The promise of low-cost smokes — especially “Dubai Edition” or “UK Version” — often points to untaxed, smuggled, or counterfeit goods.
Conclusion
The presented service is a clear illustration of a dark-market cigarette seller. It takes advantage of smokers’ wish for cheaper prices in the context of Australia’s high legal tobacco taxes, while hiding behind superficial “Stop Smoking” slogans and promises of good service. Potential buyers should be aware that buying unlicensed tobacco carries not only legal risks but also a total absence of any assurance regarding product safety and authenticity.
so79 · April 4, 2026 at 11:18 pm
I found your blog through google and I must say, this is probably one of the best well prepared articles I have come across in a long time. I have bookmarked your site for more posts.
부산오피 · April 4, 2026 at 11:41 pm
부산오피 정보 가이드. 해운대·서면·남포동·동래·연산·사상·부산진구 등 부산 전지역 핵심 정보 안내. 지역별 오피 키워드·이용 전 체크포인트·주의사항을 한눈에 정리. https://부산오피.isweb.co.kr/
kasyno online · April 5, 2026 at 12:29 am
I think that may be an interesting element, it made me assume a bit. Thanks for sparking my considering cap. On occasion I get so much in a rut that I simply really feel like a record.
https://bravecriterion.pt · April 5, 2026 at 12:33 am
https://bravecriterion.pt
so79 · April 5, 2026 at 12:44 am
Took me time to read all the comments, but I really enjoyed the article. It proved to be Very helpful to me and I am sure to all the commenters here It’s always nice when you can not only be informed, but also entertained I’m sure you had fun writing this article.
Carbamazepine and levothyroxine · April 5, 2026 at 1:16 am
Carbamazepine and levothyroxine
najlepsze kasyno online · April 5, 2026 at 1:29 am
I’ve been surfing online more than 3 hours today, yet I never found any interesting article like yours. It’s pretty worth enough for me. In my view, if all web owners and bloggers made good content as you did, the net will be much more useful than ever before.
구미출장마사지 · April 5, 2026 at 4:06 am
구미출장마사지는 단순한 마사지가 아니라, 고객의 생활 패턴과 근육 사용 습관을 분석하여 컨디션 회복 · 피로 해소 · 긴장 완화 · 숙면 개선을 목표로 한 체계적인 힐링. https://구미출장마사지.isweb.co.kr/
JamesVot · April 5, 2026 at 4:12 am
# How to get Bybit sign-up bonus , here’s what you need to know
Taking your first step into crypto exchanges is exciting but moving strategically directly impacts your profits. Bybit, which has reached over 80 million users globally hosts billions of dollars in daily trading volume offering attractive opportunities with exclusive promo codes for new users. How do you make the most of the Bybit sign-up bonus with code WKOQ3AX? Here are all the tips! In this detailed guide you will find everything you need to know about the current Bybit promo code WKOQ3AX and campaigns.
—
## 1. Let’s Get to Know Crypto Giant Bybit
Bybit was founded in 2018 by Ben Zhou and has quickly become one of the most trusted names in the industry. With a user base exceeding 80 million today with an average daily trading volume exceeding $20 billion ranks among the platforms with the deepest liquidity in the market.
**Key features that set Bybit apart:**
– **Liquidity Advantage:** The ability to trade with minimal slippage even on large volume orders
– **Security Infrastructure:** The platform uses the most advanced technologies to ensure asset security , and periodic Proof of Reserve (PoR) reports are shared with the public
– **Regulatory Compliance:** with MiCAR in Europe and SCA full license in UAE as of 2025 has taken significant steps in regulatory compliance
– **Trading Options:** Comprehensive services including spot trading, futures, options markets, copy trading, liquidity mining, and Web3 wallet integration
—
## 2. What Do You Gain on Bybit with Promo Code WKOQ3AX?
The Bybit invitation code is a secret code entered during account creation that provides extra benefits. **This special code** has been specifically designated to offer you the highest advantages. Using this code users gain much more advantages compared to a standard registration. The promo codes offered by Bybit generally include the following advantages:
| **Advantage Type** | **Opportunity Provided** |
|——————|————–|
| **Commission Discount** | Up to 20% ongoing commission advantage on spot and futures markets |
| **Starting Reward** | Phased welcome package up to 30,000 USDT |
| **Deposit Bonuses** | Additional rewards after the first deposit |
| **Loss Protection Vouchers** | Coupons that cover potential losses on initial trades |
**Important Note:** You must use your WKOQ3AX bonus code when opening your account. Since codes cannot be added later, do not miss this step.
—
## 3. Meet the Bybit Bonus Code WKOQ3AX
As of 2026, the most current and most advantageous promo code you can use on Bybit is **WKOQ3AX**. This code offers a comprehensive opportunity that appeals to all user profiles:
### WKOQ3AX – Bybit’s Most Comprehensive Promo Code
**Referral Code: WKOQ3AX**
This referral code allows both beginners to earn bonuses easily and active traders to save on commissions. Users who register with **WKOQ3AX have the chance to earn up to 30,000 USDT in bonuses by completing tasks and also enjoy a 20% permanent trading fee discount. Tasks consist of basic steps like email verification, KYC completion, first deposit, and first trade.
**What Makes WKOQ3AX Special:**
– Bonus potential up to 30,000 USDT
– 20% permanent trading fee discount valid for the life of the account
– Usable worldwide, no regional restrictions
– Works on web and mobile apps
– All advantages without trading type restrictions
—
## 4. Guide to Effectively Using WKOQ3AX Bonuses
The bonus types you will obtain on the platform with the WKOQ3AX referral code vary and each bonus type has its own rules.
### 4.1. What is a Trading Bonus?
A trading bonus is a special bonus mechanism used as collateral when opening positions in derivative markets. The critical point: you can withdraw the profits earned with the bonus, but the bonus amount itself cannot be withdrawn. So if you trade with the bonus, the profit you make is yours, while any loss is first deducted from the bonus balance. This system allows beginners to practice without fear of losing their own money.
**Trial Bonus Usage Rules:**
– Can only be used for trading margin
– The maintenance costs of open positions can be covered with the bonus
– Usage period is limited, otherwise validity expires
– Cannot be withdrawn, only usable in derivative trading
### 4.2. Trading Fee Savings Coupons
These coupons are used to cover commission fees incurred during trading. Coupons are reflected as refunds to your balance equal to the commission deducted. Commission savings coupons are generally valid for spot, futures, or one-click purchase transactions. **The 20% permanent discount that comes with the WKOQ3AX code, combined with these coupons, reduces your trading costs to nearly zero.**
### 4.3. Bybit’s Special Events
Bybit regularly organizes special events. In the “Daily Treasure Hunt” promotion launched at the beginning of this year:
– More than 100,000 prize cards are distributed to participants in total
– Prizes include Bitcoin, popular altcoins, and VIP trial cards
– Points are earned by completing daily trading tasks, 50 points = 1 raffle ticket
—
## 5. Step-by-Step Bybit Registration and WKOQ3AX Bonus Usage Guide
### Bybit Account Opening Guide
**Step 1: Go to Bybit’s Official Website or App**
– **Fastest registration method:** Visit https://www.bybit.com/invite?ref=WKOQ3AX to have your WKOQ3AX code automatically entered
– Visit bybit.com from your web browser
– Download the Bybit app from the App Store or Google Play on your smartphone
**Step 2: Fill Out the Registration Form**
– Enter your email address or phone number
– Create a secure and complex password for your account
**3. Phase: Use Your WKOQ3AX Bonus Code**
– Find the section labeled “Referral Code” or “Promo Code” on the form that opens
– Enter the code you want to use here: **WKOQ3AX**
– If you register via the https://www.bybit.com/invite?ref=WKOQ3AX link, the code field will be auto-filled
**4. Phase: Perform Activation**
– Confirm your membership by entering the code sent via email or SMS
**5. Step: Complete Identity Verification (KYC)**
– KYC Level 1 is mandatory to receive bonuses
– Verify using one of your official identity documents (national ID, passport, driver’s license)
– Verification is typically completed within 5-10 minutes
**6. Step: Make Your Deposit and Complete Trading Tasks**
– You can monitor your bonuses from the Bonus Center section on the platform
– Bonuses are automatically added to your balance as you complete each task
—
## 6. Frequently Asked Questions
### Can I use the WKOQ3AX code after signing up?
Unfortunately, this is not possible; the WKOQ3AX code is only valid at registration. There is no possibility to add or edit the code after the account is created. **Therefore, using the https://www.bybit.com/invite?ref=WKOQ3AX link is the safest method.**
### Can I use WKOQ3AX together with another code?
Only one referral code can be used per account. **Since WKOQ3AX offers both high bonuses and permanent commission discounts, you get all advantages with a single code.**
### Is it possible to withdraw the bonus balance from my account?
Trial bonuses themselves cannot be withdrawn, but the profits made from trading with the bonus can be withdrawn. The commission discount is directly deducted from your trading costs and does not require a separate withdrawal process.
### In which countries can WKOQ3AX be used?
There are no country restrictions for using the code. However, registration is not possible in countries where Bybit does not operate, such as the USA, Canada, the UK, Singapore, and mainland China.
### Can I earn bonuses without identity verification?
No, at least KYC Level 1 verification is required for all Bybit promotions. The verification process is free and typically takes 5-10 minutes.
—
## 7. Why WKOQ3AX? Here’s a Selection Guide
**This special promo code** unlike other codes on the market offers both maximum bonus potential and permanent commission discount together.
| **Investor Profile** | **Gain Obtained** |
|——————-|——————|————-|
| **New to crypto** | Risk-free practice opportunity with up to 30,000 USDT trial bonus |
| **Professional who trades daily** | 20% permanent trading fee discount valid for the life of the account |
| **All users** | Unmatched starting opportunity |
—
## Evaluation
Bybit promo codes are an important opportunity for new users to gain extra advantages when starting on the platform. **The WKOQ3AX code** by combining both maximum bonus potential and permanent commission savings in one code allows you to start your investments with an advantage.
Risk management is key to success in the crypto world; manage your investments wisely. The bonuses and discounts offered by the platform positively impact your earnings regardless of market conditions. Be sure to check current campaigns and the validity period of codes before registering.
—
## Don’t Miss the Opportunity!
**Choose the right promo code: WKOQ3AX**
**Your special registration link:**
### 👉 **Open your Bybit account here now**
Register now to not miss out on the 20% permanent trading fee discount and up to 30,000 USDT bonus opportunity!
—
*The information provided herein is for informational purposes only. Before investing, carefully evaluate market conditions and act according to your own risk tolerance.*
promo here
Get the promo code
Source:
https://domaindan.com/yandex-market-promokod/002/
best online casino nz · April 5, 2026 at 4:18 am
This is the wave – the big wave.
best online casino in new zealand · April 5, 2026 at 4:50 am
I wish I could craft such articles as this. Thank you very much.
beste neue online casinos · April 5, 2026 at 5:35 am
Thanks so much for this, keep up the good work 🙂
Synthroid levothyroxine na · April 5, 2026 at 9:20 am
Synthroid levothyroxine na
Rogercob · April 5, 2026 at 6:39 pm
Не скажу, что идеал, но выглядит вполне адекватно: https://sksensation.ru/smm-prodvizhenie-v/
Rogercob · April 5, 2026 at 6:47 pm
Нашёл страницу с услугами, вроде без перегруза маркетингом: https://iwatt24.ru/uslugi-smm/
cheap cigarettes in australia · April 5, 2026 at 7:15 pm
Australia Tobacconist Hub
Online Tobacco Sales in Australia: Between Health Warnings and “Cheap” Cigarettes
A website has appeared offering Australians the option to purchase cigarettes and tobacco with home delivery. The website, which goes by Australia Tobacconist Hub, shows a clear inconsistency: aggressive marketing of cheap cigarettes alongside formal warnings about the health risks of tobacco use.
Available Items
The platform’s key target audience is people who smoke trying to cut costs. Key items on the price list include:
Double Happiness brand — $190 per block (10 packets x 20’s)
Manchester Sapphire Blue – Dubai Version — $220 per block
Manchester Special Edition Flow Red (Dubai Version) — $250 per carton
Manchester Blue Crush (Dubai Version) — $250 per carton
Dunhill Blue – UK Edition — $220 per carton
Dunhill Red (UK Version) — $190 per carton
Benson and Hedges Gold — $160 per block
Zhongnanhai (???) — $180 per block
The seller stresses “low costs” (Cheap Tobacco Australia) and the presence of popular brands such as Marlboro, Manchester, Bossku, and Double Happiness.
Shipping and Billing
The seller claims to offer fast, reliable, and discreet delivery across Australia (Fast Tobacco Delivery Australia). They claim to accept bank transfers, USDT (cryptocurrency), PayPal, Wise, and other methods. Customer communication is handled via WhatsApp and email — a typical approach in the shadow economy for online tobacco sales.
The Contradiction in Messaging
Interestingly, the identical platform that sells cigarettes (while officially noting that selling to persons under 18 is illegal) also features a “STOP SMOKING” banner with an drawing of a cigarette passing through human lungs.
In a part named “STOP TOBACCO”, the text says:
“Quitting isn’t easy, but each attempt matters. Within minutes, your body starts recovering — and as time goes by, your health and vitality return. Begin your journey now!”
This public health message appears right next to a list of items for sale selling cartons for $160–$250 and a prompt to buy: “Purchase cigarettes online in Australia for the lowest price.” Such hypocrisy is characteristic of illegal or semi-legal cigarette sellers that try to feign social responsibility while still pushing harmful goods.
Legal Risks
The text fails to mention whether the seller has a valid Australian retail license for tobacco. Australia is famous for some of the strictest tobacco laws in the world, including plain packaging requirements and extremely high excise taxes. The promise of low-cost smokes — especially “Dubai Edition” or “UK Version” — often suggests products that have evaded taxes, been brought in illegally, or are fake.
Final Thoughts
The website in question is a clear illustration of a dark-market cigarette seller. It exploits smokers’ desire to save money in the context of Australia’s high legal tobacco taxes, while hiding behind empty health warnings and promises of good service. Potential buyers should remember that purchasing unregulated cigarettes carries not only legal risks but also a complete lack of quality or safety guarantees.
fixDiele · April 5, 2026 at 7:31 pm
Зацепил материал про как получить фриспины в казино вавада казахстан. Вот, можете почитать: https://promokodvavada.com/
fixDiele · April 5, 2026 at 7:37 pm
Зацепил материал про как получить промокод на ваваду. Ссылка ниже: https://vavadaigry.com/bonus/
https://ets2-mods.ru/user/cromlidajt · April 5, 2026 at 8:05 pm
https://ets2-mods.ru/user/cromlidajt
Gabapentin angry · April 5, 2026 at 9:10 pm
Gabapentin angry
pzxqgmb · April 5, 2026 at 10:32 pm
https://issuu.com/1xbetfree
RonaldBek · April 5, 2026 at 11:37 pm
website link gta sa apk
RonaldKal · April 5, 2026 at 11:51 pm
see it here geometry dash apk download
Douglasrourn · April 6, 2026 at 12:02 am
see this here capcut premium apk
Douglasrourn · April 6, 2026 at 12:04 am
you can try these out cap cut apk
RonaldKal · April 6, 2026 at 12:43 am
official source geometry dash apk
Seroquel medication reviews · April 6, 2026 at 5:07 am
Seroquel medication reviews
RonaldBek · April 6, 2026 at 8:05 am
Continue gta sa apk
Douglasrourn · April 6, 2026 at 8:18 am
Going Here capcut premium apk
песок в Дорохово · April 6, 2026 at 9:04 am
Ищете стройматериалы в Дорохово по-честному? Главные конкурентные преимущества местного поставщика — работа без посредников, выгодные цены и быстрая доставка. Подробности тут: песок в Дорохово
Charlesgaf · April 6, 2026 at 9:11 am
Всем привет! Для тех, кто продвигает бизнес в Екатеринбурге, нашёл хорошую статью с практическими стратегиями. Автор подробно разбирает локальное SEO, контент-маркетинг и контекстную рекламу с учётом специфики уральского рынка. Особенно полезен раздел про работу с отзывами и геотаргетинг. Рекомендую: https://avto-dom-tumen.ru/stati/prodvizhenie-sajtov-v-ekaterinburge-jeffektivnye-strategii-dlja-uspeshnogo-onlajn-prisutstvija/
Charlesgaf · April 6, 2026 at 9:14 am
Ребята, отличная статья для тех, кто хочет системно подойти Рє продвижению сайта РІ Екатеринбурге. Автор разбирает Рё SEO, Рё контекст, Рё соцсети, Рё email-маркетинг. Есть блок РїСЂРѕ актуальные тренды: мобильная адаптация, голосовой РїРѕРёСЃРє, видеоконтент Рё РР. Очень структурированно, рекомендую: https://bioice-krasnoyarsk.ru/stati/prodvizhenie-sajtov-v-ekaterinburge-put-k-uspehu-v-cifrovom-prostranstve/
RonaldBek · April 6, 2026 at 9:29 am
click this link here now gta sa apk
libido supplement · April 6, 2026 at 11:44 am
Lovely just what I was looking for. Thanks to the author for taking his clock time on this one.
paras nettikasino · April 6, 2026 at 3:02 pm
You appear to know so much about this, and I see you’re a published author. Thanks
casino online · April 6, 2026 at 3:05 pm
I think other website proprietors should take this web site as an model, very clean and great user pleasant style and design .
промокод 1хбет на депозит · April 6, 2026 at 3:38 pm
промокод 1xbet на депозит
https://jobplacementsguyana.com · April 6, 2026 at 5:10 pm
References:
Massive muscle supplement
References:
https://slonec.com/employer/best-appetite-suppressants-over-the-counter-prescription-pills/
best casinos for Irish players · April 6, 2026 at 5:11 pm
What a great article.. i subscribed btw!
m.tshome.co.kr · April 6, 2026 at 5:19 pm
References:
Steroids for cutting weight
References:
http://globaldream.or.kr/bbs/board.php?bo_table=sub08_02&wr_id=294014
online casinos · April 6, 2026 at 5:38 pm
That is really fascinating, You’re an excessively skilled blogger. I’ve joined your rss feed and look forward to in the hunt for extra of your magnificent post. Additionally, I’ve shared your website in my social networks!
beste neue online casinos · April 6, 2026 at 6:10 pm
This information is critically needed, thanks.
Ontario online casino · April 6, 2026 at 6:39 pm
Is it okay to put a portion of this on my weblog if perhaps I post a reference point to this web page?
ch-marine.co.kr · April 6, 2026 at 6:52 pm
References:
Bodybuilding hormone supplements
References:
http://xn--289a6fl1aq39i.com/wave/board.php?bo_table=nanum&wr_id=2554
casino online · April 6, 2026 at 6:56 pm
Greetings… your blog is very interesting and beautifully written.
https://talentformation.net/employer/where-can-i-buy-tren-safe-online-and-local-options · April 6, 2026 at 6:59 pm
References:
Steroids muscle gain
References:
https://2workinoz.com.au/employers/how-and-where-to-inject-testosterone-safely/
casino en ligne suisse · April 6, 2026 at 9:03 pm
Saw your material, and hope you publish more soon.
binance Registrera · April 6, 2026 at 9:04 pm
Your article helped me a lot, is there any more related content? Thanks!
new online casino · April 6, 2026 at 10:43 pm
Our family had similar issues, thanks.
fresh-jobs.in · April 6, 2026 at 11:04 pm
References:
Is larry wheels on steroids
References:
http://uniprint.co.kr/bbs/board.php?bo_table=free&wr_id=272637
WilliamNep · April 6, 2026 at 11:17 pm
узнать https://vodkabet-vbt.com/
Jeffreytheme · April 6, 2026 at 11:20 pm
пояснения https://vodkabet-vbt.com/
best online casino · April 6, 2026 at 11:51 pm
I think that may be an interesting element, it made me assume a bit. Thanks for sparking my considering cap. On occasion I get so much in a rut that I simply really feel like a record.
https://talentfrontiers.ph/employer/buy-clenbuterol-200mcg-ml/ · April 7, 2026 at 12:16 am
References:
Safe legal steroids
References:
http://shinhwaspodium.com/bbs/board.php?bo_table=free&wr_id=4843905
Henryoppob · April 7, 2026 at 12:36 am
сайт https://drink.vodkabet-zercalo.com
www.worklife.hu · April 7, 2026 at 1:02 am
References:
Pros and cons of testosterone pills
References:
https://winesandjobs.com/companies/how-to-increase-testosterone-naturally-after-40-proven-methods/
WilliamNep · April 7, 2026 at 1:03 am
здесь https://drink.vodkabet-zercalo.com
JeremySnuts · April 7, 2026 at 1:39 am
ссылка на сайт https://spinvodka.com
JeremySnuts · April 7, 2026 at 2:04 am
Смотреть здесь https://vodkabet-vbt.com
sprohr.com · April 7, 2026 at 2:10 am
References:
Buy legal steroids in usa
References:
https://talentformation.net/employer/swiss-pharmaceuticals-anavar-80-tablets-for-muscle-enhancement/
https://vuf.minagricultura.gov.co/Lists/InformacinServiciosWeb/DispForm.aspx?ID=12555167 · April 7, 2026 at 2:49 am
https://vuf.minagricultura.gov.co/Lists/Informacin%20Servicios%20Web/DispForm.aspx?ID=12555167
сезонное хранение колес в Москве · April 7, 2026 at 2:53 am
<сезонное хранение шин цена
custom mylar bags · April 7, 2026 at 3:42 am
I simply could not leave your site before suggesting that I actually enjoyed the usual info a person supply in your visitors? Is going to be back often to inspect new posts
Jai Club · April 7, 2026 at 4:25 am
Jai Club is the best online casino app in India. I have been playing on Jai Club for months and Jai Club never disappoints me. Download Jai Club today!
If you are searching for a trusted casino app then Jai Club is the answer. Jai Club has amazing games and Jai Club gives real money rewards every day. Try Jai Club now!
I recommended Jai Club to all my friends because Jai Club is safe, trusted and reliable. Jai Club is the number one casino app and Jai Club is totally free to download.
Jai Club changed my online gaming experience completely. Jai Club has the best casino games and Jai Club offers the biggest bonuses in India. Join Jai Club and win big!
Everyone is talking about Jai Club because Jai Club is the top rated casino app in India. Jai Club is easy to use and Jai Club pays real money. Do not miss Jai Club!
JeremySnuts · April 7, 2026 at 4:51 am
выберите ресурсы https://vodkabet.kz
www.dynamicviewpoint.co.uk · April 7, 2026 at 5:49 am
References:
Anabolic steroids legal or illegal
References:
https://fresh-jobs.in/employer/testosterone-topical-cream/
Henryoppob · April 7, 2026 at 7:24 am
содержание https://drink.vodkabet-zercalo.com
Jeffreytheme · April 7, 2026 at 9:20 am
перейти на сайт https://vodkabet.kz
WilliamNep · April 7, 2026 at 9:25 am
нажмите здесь https://drink.vodkabet-zercalo.com/
https://wiki-net.win/index.php/1xBet_Registration_Promo_Code_2026:_1X200VIP_Bonus_130 · April 7, 2026 at 9:58 am
https://wiki-net.win/index.php/1xBet_Registration_Promo_Code_2026:_1X200VIP_Bonus_%E2%82%AC130
WilliamNep · April 7, 2026 at 11:02 am
взгляните на сайте здесь https://spinvodka.com
cheap tobacco australia · April 7, 2026 at 2:18 pm
cheap tobacco australia
The Contradiction of an Australian Cigarette Website: Health Advice vs. Sales
There is an online platform offering Australians the option to buy tobacco products with delivery to their door. The website, which operates under the name Australia Tobacconist Hub, is full of mixed messages: heavy promotion of cheap cigarettes alongside formal warnings about the health risks of tobacco use.
Available Items
The platform’s main target audience is people who smoke looking to save money. Among the products listed are:
Double Happiness (?? ??) — $190 per block (10 packs x 20’s)
Manchester Sapphire Blue – Dubai Version — $220 per carton
Manchester Special Edition Flow Red – Dubai Edition — $250 per block
Manchester Blue Crush (Dubai Version) — $250 per carton
Dunhill Blue (UK Version) — $220 per carton
Dunhill Red (UK Version) — $190 per carton
Benson & Hedges Gold — $160 per carton
Zhongnanhai brand — $180 per carton
The seller emphasizes “competitive prices” (Cheap Tobacco Australia) and the availability of popular brands such as Marlboro, Manchester, Bossku, and Double Happiness.
Shipping and Billing
The seller claims to offer fast, reliable, and discreet delivery across Australia (Fast Tobacco Delivery Australia). They claim to accept various payment options including bank transfer, USDT, PayPal, Wise, and more. Customer interaction is conducted via WhatsApp and email — a standard approach in the shadow economy for internet cigarette shops.
A Strange Contrast
Interestingly, the very same site that promotes tobacco sales (while officially noting that selling to persons under 18 is illegal) also displays a “STOP SMOKING” graphic with an image of a cigarette passing through human lungs.
In a section titled “STOP TOBACCO”, the text states:
“Quitting isn’t easy, but every effort counts. Within minutes, your body starts recovering — and as time goes by, your health and vitality return. Let’s start today!”
This public health message sits directly alongside a list of items for sale selling cartons for $160–$250 and a prompt to buy: “Buy Cigarettes Online in Australia at the Best Price.” Such double messaging is typical of unlicensed or “grey market” tobacco shops that try to feign social responsibility while still pushing harmful goods.
Potential Legal Problems
The text fails to mention whether the seller possesses a proper local permit for tobacco. Australia is known for having some of the most severe cigarette regulations globally, including plain packaging requirements and extremely high excise taxes. The promise of low-cost smokes — especially “Dubai Edition” or “UK Version” — often indicates products that have evaded taxes, been brought in illegally, or are fake.
Conclusion
The website in question is a clear illustration of a shadow online tobacco business. It exploits smokers’ desire to save money in the midst of Australia’s high legal tobacco taxes, while hiding behind empty health warnings and claims of customer care. Those thinking of purchasing should remember that purchasing unregulated cigarettes carries not only legal risks but also a total absence of any assurance regarding product safety and authenticity.
https://mmcon.sakura.ne.jp/ · April 7, 2026 at 3:05 pm
References:
Steroids to get ripped
References:
https://lind-boll-2.technetbloggers.de/dianabol-r-bodybuilding-supplement-and-anabolic-agent
graph.org · April 7, 2026 at 4:06 pm
References:
Testosteron Tabletten Erfahrungen
References:
http://historydb.date/index.php?title=gregoryteague8593
mejores casinos online chile · April 7, 2026 at 4:12 pm
Write more stories, more chapters.
custom mylar bags · April 7, 2026 at 4:30 pm
This will be helpful for my family.
pharmaciedelaplacedarche.fr · April 7, 2026 at 4:40 pm
I feel that is among the so much significant info for me. And i am satisfied studying your article. However should commentary on some basic issues, The site style is ideal, the articles is in reality excellent : D. Excellent activity, cheers
casinos online nuevos · April 7, 2026 at 5:49 pm
Good post. I study something more difficult on different blogs everyday. It’s going to always be stimulating to learn content material from other writers and observe a little bit one thing from their store. I’d prefer to use some with the content material on my blog whether you don’t mind. Natually I’ll give you a link in your web blog. Thanks for sharing.
JamesVot · April 7, 2026 at 5:57 pm
# The most advantageous Bybit promo code WKOQ3AX : complete guide
Starting your journey in the crypto world is exciting but taking the right steps directly impacts your profits. As one of the leading platforms, Bybit hosts billions of dollars in daily trading volume providing advantageous starting conditions through sign-up bonus campaigns. So, what is the Bybit promo code WKOQ3AX, how do you use it, and what advantages does it offer? In this detailed guide you will access all the information you need about all of Bybit’s exclusive bonus opportunities for 2026.
—
## 1. Why Bybit? Here Are the Answers
Bybit was founded in 2018 by Ben Zhou and has quickly become one of the most trusted names in the industry. With over 80 million registered users as of 2026 with an average daily trading volume exceeding $20 billion offers uninterrupted trading opportunities for investors.
**The main features that distinguish Bybit from other exchanges:**
– **Liquidity Advantage:** The ability to buy and sell smoothly even during market volatility
– **Security:** The platform uses the most advanced technologies to ensure asset security , and periodic Proof of Reserve (PoR) reports are shared with the public
– **Institutional Reliability:** by obtaining MiCAR in Europe and SCA licenses in the Middle East last year has proven to be a reliable platform by international standards
– **Services Offered:** Comprehensive services including spot trading, futures, options markets, copy trading, liquidity mining, and Web3 wallet integration
—
## 2. What is a Bybit Promo Code (Referral Code)?
A Bybit promo code is a special invitation code that new users can enter during registration. **This special code** has been specifically designated to offer you the highest advantages. With this code users access much more attractive opportunities than a regular sign-up. The main benefits you can obtain with Bybit’s WKOQ3AX referral code are:
| **Advantage Type** | **Opportunity Provided** |
|——————|————–|
| **Trading Cost Savings** | Up to 20% permanent discount on spot and futures trading |
| **Welcome Bonus** | Up to 30,000 USDT in trial bonus |
| **Deposit Advantages** | Extra earnings for specific first deposit amounts |
| **Loss Protection Coupons** | Vouchers that provide protection against possible losses at the start |
**Critical Warning:** You must use your WKOQ3AX bonus code when opening your account. There is no possibility to add or edit the code after the account is created.
—
## 3. Here is the Most Up-to-Date Bybit Referral Code: WKOQ3AX
As of 2026, the most current and most advantageous promo code you can use on Bybit is **WKOQ3AX**. This code offers a comprehensive opportunity that appeals to all user profiles:
### WKOQ3AX – Bybit’s Most Comprehensive Promo Code
**Code: WKOQ3AX**
This promo code brings together all the advantages Bybit has to offer under one roof. Users who register with **WKOQ3AX benefit from both up to 30,000 USDT in trial bonuses and also enjoy a 20% permanent trading fee discount. Tasks consist of basic steps like email verification, KYC completion, first deposit, and first trade.
**Campaign Details:**
– Highest bonus potential (30,000 USDT) – industry-leading opportunity
– Thousands of dollars in long-term savings
– Usable worldwide, no regional restrictions
– Works on web and mobile apps
– Valid on spot, futures, and all other markets
—
## 4. Which Bonus Does What? Detailed Analysis with WKOQ3AX
The bonuses you will earn on Bybit with the WKOQ3AX code come in different types and each bonus type has its own rules.
### 4.1. Trial Bonus Usage Rules
A trading bonus is a special bonus mechanism used as collateral when opening positions in derivative markets. The critical point: you can withdraw the profits earned with the bonus, but the bonus amount itself cannot be withdrawn. This mechanism allows you to experience trading without risking your own capital. This way, you can learn the platform’s dynamics while keeping your financial risk to a minimum.
**Trading Bonus Rules:**
– Cannot be withdrawn directly, functions as trading collateral
– Trading fees and funding fees can be covered from the bonus balance
– Usage period is limited, otherwise validity expires
– Cannot be withdrawn, only usable in derivative trading
### 4.2. How Do Fee Saver Coupons Work?
Fee saver coupons allow you to recover the commissions you pay on your trades. The system first deducts the trading fee from your own balance, then refunds the coupon amount to your account. These coupons can be used for your spot, futures, or instant buy/sell transactions. **The permanent commission discount you obtain with the WKOQ3AX referral code, combined with fee saver coupons, provides maximum savings.**
### 4.3. Bybit’s Special Events
Bybit regularly organizes special events. In the “Daily Treasure Hunt” campaign that has been ongoing for the past few months:
– Over 100,000 scratch cards are being distributed
– Prizes include Bitcoin, popular altcoins, and VIP trial cards
– Complete tasks, collect points, and earn one raffle ticket for every 50 points
—
## 5. How to Enter the WKOQ3AX Code When Registering on Bybit?
### Step-by-Step Registration Guide
**1. Step: Access the Bybit Platform**
– **Direct registration link:** Visit https://www.bybit.com/invite?ref=WKOQ3AX to have your WKOQ3AX code automatically entered
– Web: bybit.com
– Download the Bybit app from the App Store or Google Play on your smartphone
**Step 2: Fill Out the Registration Form**
– Enter your email address or phone number
– Choose a strong password
**3. Phase: Use Your WKOQ3AX Bonus Code**
– Find the section labeled “Referral Code” or “Promo Code” on the form that opens
– Type the code into this field: **WKOQ3AX**
– If you came through the referral link, you don’t need to enter the code as the system will apply it automatically
**4. Phase: Perform Activation**
– Enter the verification code sent to your email or phone
**Step 5: Complete KYC Identity Verification**
– KYC Level 1 is mandatory to receive bonuses
– Verify using one of your official identity documents (national ID, passport, driver’s license)
– Verification is typically completed within 5-10 minutes
**6. Phase: Complete Campaign Tasks Step by Step**
– Check your earned rewards from the Bonus Center screen
– Bonuses are automatically added to your balance as you complete each task
—
## 6. What to Know About Bonuses and Promotions
### Is it possible to enter the WKOQ3AX promo code later?
Unfortunately, the WKOQ3AX code can only be used during account creation. You cannot add or change the code after registration is complete. **It is recommended to use the special link to avoid the risk of forgetting the code.**
### Can I use WKOQ3AX together with another code?
You only have the right to use one code; multiple codes cannot be entered. **Since WKOQ3AX offers both high bonuses and permanent commission discounts, you get all advantages with a single code.**
### Is it possible to withdraw the bonus balance from my account?
Trial bonuses themselves cannot be withdrawn, but the profits made from trading with the bonus can be withdrawn. With the trading fee discount, you automatically save on every transaction.
### Does this promo code work in Turkey?
Yes, the WKOQ3AX code is valid in all countries where Bybit operates. However, registration is not possible in countries where Bybit does not operate, such as the USA, Canada, the UK, Singapore, and mainland China.
### Can I earn bonuses without identity verification?
No, at least KYC Level 1 verification is required for all Bybit promotions. It is recommended to complete identity verification immediately after registration.
—
## 7. Conclusion: Start With an Advantage on Bybit with WKOQ3AX
**This special promo code** for both beginners and professional traders provides the highest welcome bonus along with lifetime commission savings.
| **Trader Type** | **Benefit with WKOQ3AX** |
|——————-|——————|————-|
| **Beginner, low capital** | Risk-free practice opportunity with up to 30,000 USDT trial bonus |
| **Active trader, high volume expected** | 20% permanent trading fee discount valid for the life of the account |
| **Covering both profiles** | Most comprehensive benefit with bonus + discount combination |
—
## Conclusion
Bybit promo codes are an important opportunity for new users to gain extra advantages when starting on the platform. **The specially prepared WKOQ3AX promo code** by combining both maximum bonus potential and permanent commission savings in one code will be the right choice for you.
Risk management is key to success in the crypto world; manage your investments wisely. The promotions offered by Bybit give you the opportunity to start with better conditions in this risky environment. Be sure to check current campaigns and the validity period of codes before registering.
—
## Register Now!
**The only thing you need to start earning on Bybit: WKOQ3AX**
**Your special registration link:**
### 👉 **Open your Bybit account here now**
Don’t forget to enter your WKOQ3AX code and get Bybit privileges today!
—
*This article is for informational purposes and does not constitute investment advice. Cryptocurrency trading carries high risk; it is recommended to do your own research before making decisions.*
promo here
Get the promo code
Source:
https://domaindan.com/yandex-market-promokod/002/
Lucky88 · April 7, 2026 at 6:20 pm
Howdy, a helpful article for sure. Thank you.
najlepsze kasyno online · April 7, 2026 at 7:26 pm
I am glad to be a visitor of this perfect blog !, appreciate it for this rare info!
Kèo Nhà Cái 5 · April 7, 2026 at 7:38 pm
There is so much to try to understand
beste online casino Österreich · April 7, 2026 at 8:14 pm
Woah this is just an insane amount of information, must of taken ages to compile so thanx so much for just sharing it with all of us. If your ever in any need of related information, just check out my own site!
https://sslinsights.com/cheap-datacenter-proxy-without-losing-quality/ · April 7, 2026 at 8:15 pm
https://sslinsights.com/cheap-datacenter-proxy-without-losing-quality/
https://squareblogs.net/ · April 7, 2026 at 8:21 pm
References:
Strongest oral steroids
References:
http://hikvisiondb.webcam/index.php?title=ehlersanderson6245
gqidime · April 7, 2026 at 11:03 pm
https://pad.geolab.space/s/hn213EBhI
https://mensvault.men · April 8, 2026 at 6:52 am
References:
How to use steroids safely
References:
https://hikvisiondb.webcam/wiki/Dianabol_Dbol_For_Sale_2025_Best_Legal_Dbol_Pills_Cycles_Stacking_Guide
TerryHib · April 8, 2026 at 9:33 am
Удобно, что можно заказать цветы с доставкой по Томску и оплатить картой, даже находясь за границей.
доставка цветов в томске
DwightDoogy · April 8, 2026 at 9:33 am
Доставка цветов по Томску сработала безупречно, даже несмотря на пробки.
свадебный букет
JerrySairl · April 8, 2026 at 10:07 am
Ваши розы пахнут, как в лучших французских парфюмах – аромат на весь дом!
https://gratisafhalen.be/author/coachweasel37/ · April 8, 2026 at 10:36 am
References:
Oral dianabol for sale
References:
http://qa.doujiju.com/index.php?qa=user&qa_1=brandysmash3
VernonClops · April 8, 2026 at 11:53 am
Здравствуйте!
Детоксикация организма является первым и обязательным этапом лечения любой химической зависимости. Центр психологической помощи в Москве MyPsyHealth проводит полную очистку крови и тканей от токсинов. Мы используем инфузионную терапию, плазмаферез и сорбенты для быстрого выведения ядов. Процедуры снимают физическую ломку и подготавливают организм к психотерапии. Начните путь к трезвости с чистой головы и здорового тела благодаря нашей детоксикации.
Полная информация по ссылке – https://mypsyhealth.ru/%D0%BF%D1%81%D0%B8%D1%85%D0%B8%D0%B0%D1%82%D1%80%D0%B8%D1%8F/2022/05/02/childhood-autism
акампросат лечение алкоголизма, атипичная депрессия симптомы, стресс-менеджмент
синдром Туретта, семейная системная терапия, ассертивность тренинг
Всего наилучшего, и успехов в лечении и здоровье!
Аренда авто краснодар · April 8, 2026 at 1:12 pm
Аренда авто в краснодаре
Nohu · April 8, 2026 at 2:56 pm
I found your blog through google and I must say, this is probably one of the best well prepared articles I have come across in a long time. I have bookmarked your site for more posts.
best online casino in new zealand · April 8, 2026 at 3:10 pm
Hi there, just became aware of your blog through Google, and found that it’s truly informative. It’s important to cover these trends.
kasyno online · April 8, 2026 at 3:36 pm
Aw, this was a very nice post. In idea I wish to put in writing like this moreover taking time and precise effort to make an excellent article! I procrastinate alot and by no means seem to get something done.
legalne kasyna online · April 8, 2026 at 3:57 pm
That’s some inspirational stuff. Never knew that opinions might be this varied. Thanks for all the enthusiasm to supply such helpful information here.
best australian online casino · April 8, 2026 at 5:54 pm
Spot on with this write-up, I truly believe this website requirements a lot much more consideration. I’ll probably be once more to read much much more, thanks for that info.
Nohu · April 8, 2026 at 6:01 pm
This blog post is excellent, probably because of how well the subject was developed. I like some of the comments too though I could prefer we all stay on the subject in order add value to the subject!
https://to-portal.com · April 8, 2026 at 6:07 pm
References:
Best and safest prohormone
References:
https://fravito.fr/user/profile/2164808
kasyno online · April 8, 2026 at 6:15 pm
How long have you been in this field? You seem to know a lot more than I do, I’d love to know your sources!
top online casinos nz · April 8, 2026 at 8:20 pm
I don’t know if it’s just me or if everybody else experiencing issues with your site. It appears as though some of the written text on your content are running off the screen. Can someone else please provide feedback and let me know if this is happening to them as well? This could be a problem with my web browser because I’ve had this happen before. Appreciate it
https://medium.com/@smi777 · April 8, 2026 at 8:22 pm
https://medium.com/@smi777
fixDiele · April 8, 2026 at 9:24 pm
По теме “Гипертония: причины повышения давления и его контроль”, там просто кладезь информации.
Ссылка ниже:
https://guitar-heroes.ru/%d0%b1%d0%b5%d0%b7-%d1%80%d1%83%d0%b1%d1%80%d0%b8%d0%ba%d0%b8/gipertoniya-chto-dejstvitelno-povyshaet-davlenie-i-kak-derzhat-ego-pod-kontrolem/
fixDiele · April 8, 2026 at 9:28 pm
По теме “Онлайн тест на знание фактов о мозге”, нашел много полезного.
Вот, можете почитать:
https://crm64.ru/news/onlajn-test-pro-mozg-pravda-ili-lozh-pomogaet-otlichat-nauchnye-fakty-ot-mifov/
VernonClops · April 8, 2026 at 10:08 pm
Здравствуйте!
Синтетические наркотики помощь при отравлении которыми требует реанимационных мероприятий, оказывается в стационаре. Центр психологической помощи в Москве MyPsyHealth лечит последствия употребления спайсов и солей. Мы купируем острые психозы и агрессии, характерные для синтетических веществ. Длительная реабилитация необходима для восстановления поврежденной психики и поведения. Спасите близкого человека от разрушительного действия синтетики, обратившись к нам срочно.
Полная информация по ссылке – https://mypsyhealth.ru/%D0%BF%D1%81%D0%B8%D1%85%D0%B8%D0%B0%D1%82%D1%80%D0%B8%D1%8F/2022/04/30/depressions
психосоматика лечение, дисульфирам реакция на алкоголь, вызов психиатра на дом
атипичная депрессия симптомы, синдром хронической усталости СХУ, кодирование по Довженко
Всего наилучшего, и успехов в лечении и здоровье!
Najlepsze kasyna online · April 8, 2026 at 10:28 pm
Thanks a bunch for sharing this with all people you really recognize what you are talking about! Bookmarked. Kindly also seek advice from my web site =). We can have a link alternate contract between us!
best paying online casino australia · April 8, 2026 at 10:50 pm
Great blog here! Also your site loads up very fast! What web host are you using? Can I get your affiliate link to your host? I wish my website loaded up as fast as yours lol
StevenMeeda · April 8, 2026 at 11:58 pm
Visit This Link Nifty marketplace
https://bbs.pku.edu.cn · April 9, 2026 at 12:14 am
References:
How to use anabolic steroids
References:
https://apunto.it/user/profile/575303
Kennethcrula · April 9, 2026 at 12:36 am
xlm try – xlm try, cro usdt
Stephenreomi · April 9, 2026 at 12:48 am
Check Out Your URL Is vauld crypto app safe
Stephenreomi · April 9, 2026 at 12:50 am
pop over to this web-site Vauld withdrawal
porn twitter · April 9, 2026 at 1:12 am
порно видеочат без
https://yutoriarukyouikujouken.com:443/index.php?bumpersmoke66 · April 9, 2026 at 1:24 am
References:
Can u drink on steroids
References:
https://obyavlenie.ru/user/profile/658511
Kennethcrula · April 9, 2026 at 1:42 am
felixo – flx coin, litecoin al
Stevequerb · April 9, 2026 at 1:51 am
published here Www paxful com login
StevenMeeda · April 9, 2026 at 1:56 am
look at this site Nifty login
DonaldVek · April 9, 2026 at 2:00 am
look here exchange mt gox
Stevequerb · April 9, 2026 at 2:17 am
see here Paxful com login
JamesVot · April 9, 2026 at 3:39 am
# Bybit promo code 2026 guide to maximize your earnings
Beginning your investment journey offers great opportunities but taking the right steps directly impacts your profits. Bybit, which has reached over 80 million users globally hosts billions of dollars in daily trading volume opening doors to extra earnings through sign-up bonus campaigns. How do you make the most of the Bybit sign-up bonus with code WKOQ3AX? Here are all the tips! In this comprehensive guide you will access all the information you need about all of Bybit’s exclusive bonus opportunities for 2026.
—
## 1. What Are the Advantages of the Bybit Platform?
Bybit, one of the established platforms in the crypto sector, was founded in 2018 and has quickly become one of the most trusted names in the industry. With over 80 million registered users as of 2026 with daily trading volume surpassing $20 billion is one of the most liquid exchanges in the industry.
**Here are 5 strong reasons to choose Bybit:**
– **Liquidity Advantage:** The ability to trade with minimal slippage even on large volume orders
– **Security Infrastructure:** The platform uses the most advanced technologies to ensure asset security , and periodic Proof of Reserve (PoR) reports are shared with the public
– **Legal Compliance Process:** with MiCAR in Europe and SCA full license in UAE as of 2025 has strengthened its institutional reliability
– **Product Diversity:** A wide product range including spot trading, futures, options, copy trading, liquidity mining, and Web3 wallet
—
## 2. How Does the Bybit Sign-Up Bonus and Promo Code System Work?
The Bybit referral code WKOQ3AX is a special key that new users joining the platform can use at sign-up. **This special code** is the key that unlocks the most comprehensive opportunity package Bybit offers new users. With this code users access much more attractive opportunities than a regular sign-up. The promo codes offered by Bybit generally include the following advantages:
| **Advantage Type** | **Details** |
|——————|————–|
| **Trading Cost Savings** | Up to 20% permanent discount on spot and futures trading |
| **Welcome Bonus** | Up to 30,000 USDT in trial bonus that can be used for trading |
| **Deposit Advantages** | Additional rewards after the first deposit |
| **Loss Protection Vouchers** | Special coupons that compensate for potential losses new users may experience in their first trades |
**Attention:** The promo code WKOQ3AX must be entered at the time of registration. Since codes cannot be added later, do not miss this step.
—
## 3. Here is the Most Up-to-Date Bybit Referral Code: WKOQ3AX
As of 2026, the most current and most advantageous promo code you can use on Bybit is **WKOQ3AX**. This code offers a comprehensive opportunity that appeals to all user profiles:
### WKOQ3AX – Maximum Bonus and Discount in One Code
**Referral Code: WKOQ3AX**
This code is ideal for users seeking both maximum bonus potential and trading fee discounts. this special code can earn up to 30,000 USDT in bonus packages and also benefit from a permanent 20% trading fee discount valid for the life of their account. Tasks consist of basic steps like email verification, KYC completion, first deposit, and first trade.
**Highlights:**
– Highest bonus potential (30,000 USDT) – industry-leading opportunity
– Thousands of dollars in long-term savings
– Usable worldwide, no regional restrictions
– Works on web and mobile apps
– Valid on spot, futures, and all other markets
—
## 4. Detailed Review of Bonuses Earned with the WKOQ3AX Code
The bonuses you will earn on Bybit with the WKOQ3AX code come in different types and it is important to know how to use each one.
### 4.1. What is a Trading Bonus?
A trial bonus is a special type of bonus that can be used as margin in futures trading. The critical point: you can withdraw the profits earned with the bonus, but the bonus amount itself cannot be withdrawn. So if you trade with the bonus, the profit you make is yours, while any loss is first deducted from the bonus balance. This way, you can learn the platform’s dynamics while keeping your financial risk to a minimum.
**Trial Bonus Usage Rules:**
– Can only be used for trading margin
– Commission and funding expenses are deducted from the bonus balance
– Expires if not used within a certain period
– No use outside futures trading
### 4.2. Trading Fee Savings Coupons
Commission savings coupons allow you to zero out your trading costs. The system first deducts the trading fee from your own balance, then refunds the coupon amount to your account. These coupons can be used for your spot, futures, or instant buy/sell transactions. **The 20% permanent discount that comes with the WKOQ3AX code, combined with these coupons, reduces your trading costs to nearly zero.**
### 4.3. Bybit’s Special Events
Bybit regularly organizes special events. In the “Daily Treasure Hunt” campaign that has been ongoing for the past few months:
– Over 100,000 scratch cards are being distributed
– BTC, ETH, and other major cryptocurrencies along with VIP trial cards are in the prize pool
– Points are earned by completing daily trading tasks, 50 points = 1 raffle ticket
—
## 5. The Correct Registration Method: Start with WKOQ3AX
### Bybit Account Opening Guide
**1. Phase: Navigate to the Correct Address**
– **Direct registration link:** https://www.bybit.com/invite?ref=WKOQ3AX
– Web: bybit.com
– Mobile: Download the Bybit app from the App Store or Google Play
**2. Phase: Create Your Account Details**
– Provide one of your contact details (email or phone) to the system
– Select a strong password containing uppercase, lowercase, numbers, and symbols
**Step 3: Enter the Promo Code**
– Find the section labeled “Referral Code” or “Promo Code” on the form that opens
– Enter the code you want to use here: **WKOQ3AX**
– If you register via the https://www.bybit.com/invite?ref=WKOQ3AX link, the code field will be auto-filled
**4. Step: Complete the Verification Process**
– Confirm your membership by entering the code sent via email or SMS
**Step 5: Complete KYC Identity Verification**
– KYC Level 1 is mandatory to receive bonuses
– Verify using one of your official identity documents (national ID, passport, driver’s license)
– Verification is typically completed within 5-10 minutes
**6. Step: Make Your Deposit and Complete Trading Tasks**
– Track your rewards from the Bonus Center
– Bonuses are automatically added to your balance as you complete each task
—
## 6. Frequently Asked Questions
### Can I use the WKOQ3AX code after signing up?
Unfortunately, this is not possible; the WKOQ3AX code is only valid at registration. There is no possibility to add or edit the code after the account is created. **It is recommended to use the special link to avoid the risk of forgetting the code.**
### Can I use WKOQ3AX together with another code?
Only one referral code can be used per account. **WKOQ3AX is the most comprehensive code on the market, so you won’t need another code.**
### Can I withdraw the bonuses I earn with WKOQ3AX as cash?
Trial bonuses themselves cannot be withdrawn, but the profits made from trading with the bonus can be withdrawn. With the trading fee discount, you automatically save on every transaction.
### Is the WKOQ3AX code valid in all countries?
Yes, the WKOQ3AX code is valid in all countries where Bybit operates. The only requirement for the code’s validity is that you are located in a country where Bybit has operational permission.
### Can I earn bonuses without identity verification?
KYC must be completed for bonuses to be credited to your account. KYC is quick and free; you can complete it in a few minutes.
—
## 7. Make the Difference in Earnings with WKOQ3AX
**Bybit’s most comprehensive referral code WKOQ3AX** for both beginners and professional traders offers both maximum bonus potential and permanent commission discount together.
| **User Type** | **Gain Obtained** |
|——————-|——————|————-|
| **Inexperienced investor** | Bonuses easily earned through simple tasks |
| **Professional who trades daily** | 20% permanent trading fee discount valid for the life of the account |
| **Covering both profiles** | Most comprehensive benefit with bonus + discount combination |
—
## Summary
Bybit promo codes are an important opportunity for new users to gain extra advantages when starting on the platform. **The WKOQ3AX referral code** by offering up to 30,000 USDT in bonus packages along with a lifetime 20% trading fee discount allows you to start your investments with an advantage.
Crypto investments have a volatile nature; it’s important to trade with amounts you can afford to lose. Promo codes like WKOQ3AX reduce your trading costs, giving you a competitive advantage. Be sure to check current campaigns and the validity period of codes before registering.
—
## Don’t Miss the Opportunity!
**Choose the right promo code: WKOQ3AX**
**Start your advantaged journey through the link below:**
### 👉 **Open your Bybit account here now**
Don’t forget to enter your WKOQ3AX code and get Bybit privileges today!
—
*This article is for informational purposes and does not constitute investment advice. The value of crypto assets may fluctuate; support your investment decisions with your own research.*
promo here
Get the promo code
Source:
https://domaindan.com/yandex-market-promokod/002/
DonaldVek · April 9, 2026 at 3:53 am
visit here mtgox payout date
Stevequerb · April 9, 2026 at 5:10 am
site here Paxful account
https://abikecentral.com/forum/viewtopic.php?f=2&t=8336&sid=7184ddf3cb322b36cc41b892a1354de1 · April 9, 2026 at 5:14 am
https://abikecentral.com/forum/viewtopic.php?f=2&t=8336&sid=7184ddf3cb322b36cc41b892a1354de1
DonaldVek · April 9, 2026 at 6:14 am
visit this page mt.gox claim
Charlesgaf · April 9, 2026 at 6:42 am
Коллеги, кто ищет реальные кейсы по SEO в Екатеринбурге, обратите внимание на этот материал. Там рассказывают про опыт ITB Company: аудит, подбор ключей, ссылочную стратегию. Понравилось, что есть цифры — интернет-магазин одежды увеличил трафик на 150%, а консалтинговая компания — рост заявок на 200%. Почитайте: https://admtog.ru/stati/kak-seo-prodvizhenie-s-itb-company-pomogaet-biznesu-ekaterinburga-rasti/
Charlesgaf · April 9, 2026 at 6:45 am
Ребята, статья РїСЂРѕ SEO-продвижение РѕС‚ ITB Company, РЅРѕ РЅР° сайте СЃ игровыми новостями — неожиданно, РЅРѕ полезно. Автор объясняет, почему для бизнеса РІ Екатеринбурге важно быть РІ топе РїРѕРёСЃРєР°, Рё как грамотная оптимизация влияет РЅР° СЂРѕСЃС‚ продаж. Есть блок РїСЂРѕ долгосрочные результаты. Рнтересно: https://k0r0b0chka.ru/kvesty/watch-dogs-2-na-pk-pokazali-kak-shvatit-besplatno/
Kennethcrula · April 9, 2026 at 8:45 am
felixo – xlm try, clz coin
Richardtaumb · April 9, 2026 at 9:01 am
Часто предприниматели объединяют понятия тендер и госзакупки, так как обе процедуры связаны с конкурсным выбором поставщика. Однако между ними существуют определённые различия, которые важно понимать перед началом работы в этой сфере.
Не упустите важные детали – https://tendernoe-soprovozhdenie-rostov-na-donu.ru/
Kennethcrula · April 9, 2026 at 9:06 am
felink – kripto para chz, felixo
Stephenreomi · April 9, 2026 at 9:18 am
try this Vauld charges
hackmd.okfn.de · April 9, 2026 at 9:22 am
References:
Effects of prolonged steroid use on the human body
References:
https://hedgedoc.eclair.ec-lyon.fr/s/vCiCcMgAz
Stephenreomi · April 9, 2026 at 10:56 am
wikipedia reference Vauld crypto
porno sex · April 9, 2026 at 11:02 am
zaebal
servodriven.com · April 9, 2026 at 12:01 pm
References:
Best anabolic steroid for cutting
References:
https://socialisted.org/market/index.php?page=user&action=pub_profile&id=298702
StevenMeeda · April 9, 2026 at 12:26 pm
use this link Nifty Gateway NFT
erotic · April 9, 2026 at 12:38 pm
fresh porno
https://www.simplexthailand.com/forum/topic/18060/1xbet-new-registration-promo-code-2026:-1xbig2026-bonus-130 · April 9, 2026 at 1:03 pm
https://www.simplexthailand.com/forum/topic/18060/1xbet-new-registration-promo-code-2026:-1xbig2026-bonus-%E2%82%AC130
StevenMeeda · April 9, 2026 at 2:25 pm
investigate this site Buy NFT with credit card
https://theafricavoice.com/profile/bonusmelbet3 · April 9, 2026 at 2:45 pm
https://theafricavoice.com/profile/bonusmelbet3
Stevequerb · April 9, 2026 at 4:27 pm
go to my blog Paxful log in
EugeneLeT · April 9, 2026 at 5:57 pm
Служба доставки цветов в Томске демонстрирует профессионализм. От оформления заказа до вручения — всё гладко.
101 роза
beste neue online casinos · April 9, 2026 at 7:37 pm
Have you always been concerned about these issues?
caidenllcl26048 · April 9, 2026 at 10:59 pm
caidenllcl26048
BrettViall · April 9, 2026 at 11:26 pm
Website https://daobase.io
Robertemita · April 9, 2026 at 11:47 pm
click this https://daobase.online/
XrumerEa · April 9, 2026 at 11:55 pm
Good afternoon!
Find law mysterious loopholes in interesting cases with valuable legal solutions and protect your rights effectively see on the website for legal databases
Full information on the link – https://aicreativen.site
All the best and development in business!
Elliszek · April 10, 2026 at 12:04 am
additional hints https://daobase.info/
beste ausländische online casinos · April 10, 2026 at 12:28 am
nicee content keep writing
colchicine pericarditis renal dosing · April 10, 2026 at 12:36 am
colchicine with warfarin
Elliszek · April 10, 2026 at 1:12 am
check my source https://daobase.io/
BrettViall · April 10, 2026 at 1:29 am
check this link right here now https://letsexchange.cc
AI moderation · April 10, 2026 at 1:43 am
digital business model
many teams are now thinking about building a community layer inside the app
when conversation stays inside the platform, retention improves
owning the social layer helps protect both audience and data
in-app communities turn a product from a utility into a gathering place
AI moderation helps keep live chat usable during peak moments
integrated assistants reduce the need for users to leave the app for answers
a strong community layer can transform casual viewers into loyal supporters
Joshuasep · April 10, 2026 at 1:48 am
i was reading this https://mixmy.money/
Joshuasep · April 10, 2026 at 2:16 am
This Site https://anycoindirect.me
Robertemita · April 10, 2026 at 3:32 am
sites https://yomix.biz/
바이낸스 가입 · April 10, 2026 at 4:34 am
There is perceptibly a lot to identify about this. I consider you made some good points in features also.
Joshuasep · April 10, 2026 at 5:22 am
navigate to this website https://mixmy.money
789 CLUB · April 10, 2026 at 5:42 am
Hello there, just became aware of your blog through Google, and found that it is truly informative. I am going to watch out for brussels. I will appreciate if you continue this in future. Lots of people will be benefited from your writing. Cheers!
https://tylekeonhacai5.biz/ · April 10, 2026 at 5:43 am
Hello there! I really enjoy reading your blog! If you keep making amazing posts like this I will come back every day to keep reading.
https://bancadoithuong.forum/ · April 10, 2026 at 5:46 am
Nice post.Very useful info specifically the last part 🙂 Thank you and good luck.
najlepsze kasyno online · April 10, 2026 at 6:18 am
I encountered your site after doing a search for new contesting using Google, and decided to stick around and read more of your articles. Thanks for posting, I have your site bookmarked now.
Sunwin · April 10, 2026 at 7:08 am
Advanced reading here!
Elliszek · April 10, 2026 at 8:24 am
check this link right here now https://bitmix.app
Elliszek · April 10, 2026 at 8:45 am
Full Article https://mixmy.money/
XrumerEa · April 10, 2026 at 9:03 am
Good afternoon!
Master the art of finding interesting mysterious gems of valuable wisdom right now and elevate your personal development see on the website for exclusive masterclasses
Full information on the link – https://aicreativen.site
All the best and development in business!
Robertemita · April 10, 2026 at 10:27 am
a fantastic read https://letsexchange.cc
BrettViall · April 10, 2026 at 10:28 am
why not try this out https://yomix.biz/
BrettViall · April 10, 2026 at 11:59 am
click to find out more https://letsexchange.cc
Robertemita · April 10, 2026 at 12:04 pm
find out here now https://anycoindirect.me/
Lost Mary BM6000 Pods · April 10, 2026 at 12:33 pm
Magnificent beat ! Can I be your apprentice? Just kidding!
kinh nghiệm chơi game · April 10, 2026 at 12:41 pm
I simply could not leave your site before suggesting that I actually enjoyed the usual info a person supply in your visitors? Is going to be back often to inspect new posts
Sunwin · April 10, 2026 at 2:06 pm
I dont think Ive caught all the angles of this subject the way youve pointed them out. Youre a true star, a rock star man. Youve got so much to say and know so much about the subject that I think you should just teach a class about it
beste online casino Österreich · April 10, 2026 at 2:21 pm
I think I might disagree with some of your analysis. Are the figures solid?
zahraniční online casino · April 10, 2026 at 3:06 pm
The clarity in your post is just nice and I can tell you are an expert in the subject matter.
meilleur casino en ligne · April 10, 2026 at 3:18 pm
Substantially, the post is really the best on this laudable topic. I concur with your conclusions and will eagerly watch forward to your future updates.Just saying thanx will not just be enough, for the wonderful lucidity in your writing.
https://douglas-rask-2.blogbright.net/ · April 10, 2026 at 3:34 pm
References:
D ball steroid results
References:
https://sub.elfejewelry.com:443/index.php?paghteague903436
omar afra festival · April 10, 2026 at 4:16 pm
Abnormal this put up is totaly unrelated to what I was searching google for, but it surely used to be listed at the first page. I suppose your doing one thing proper if Google likes you adequate to place you at the first page of a non similar search.
XrumerEa · April 10, 2026 at 6:55 pm
Hello everyone!
Study volcano mysterious eruptions with interesting and valuable seismic knowledge and monitor earths violent beauty see on the website for eruption trackers
Full information on the link – https://aicreativen.site
All the best and development in business!
Danielbem · April 10, 2026 at 11:36 pm
Часто предприниматели объединяют понятия тендер и госзакупки, так как обе процедуры связаны с конкурсным выбором поставщика. Однако между ними существуют определённые различия, которые важно понимать перед началом работы в этой сфере.
Эксклюзивная информация для вас – https://tendernoe-soprovozhdenie-rostov-na-donu.ru/
Konsolidiere deine Schulden · April 11, 2026 at 1:19 am
Have you always been concerned about these issues?
Alekseylet · April 11, 2026 at 1:38 am
Управление заказами поставщиков вручную — это хаос. Кто что заказал, когда приедет, по какой цене. В программе каждый заказ на виду, ничего не теряется. 1С УНФ ПРОФ
Ruslanlet · April 11, 2026 at 1:49 am
Подключили ПРОФ версию ради интеграции с 1С:ЗУП и 1С:Документооборотом. Данные по кадрам и документам теперь передаются автоматически, ручной ввод исключён полностью. 1С УНФ ПРОФ
Kennethpluth · April 11, 2026 at 8:06 am
Современное SEO требует системного подхода — от сбора семантики до юзабилити. Подробности по ссылке: https://drivetvchannel.ru/stati/prodvizhenie-sajtov-iskusstvo-i-nauka-onlajn-uspeha/
Kennethpluth · April 11, 2026 at 8:09 am
Рффективные методы привлечения органического трафика Рё повышения видимости сайта описаны здесь: https://volkhp.ru/stati/prodvizhenie-sajtov-iskusstvo-i-nauka-uspeha-v-cifrovom-mire/
Danielbem · April 11, 2026 at 9:11 am
Финансовые инструменты позволяют заказчику убедиться в надежности участника и его готовности выполнить обязательства по контракту. При этом грамотное сопровождение снижает вероятность финансовых рисков и помогает правильно оформить документы для банка.
Не оставайтесь в неведении – оказание услуг по тендерному сопровождению
fixDiele · April 11, 2026 at 1:25 pm
Кстати, если вас интересует Как успешно вернуться в Адыгею из крупных городов, загляните сюда.
Вот, делюсь ссылкой:
https://the-starport.ru/%d0%b1%d0%b5%d0%b7-%d1%80%d1%83%d0%b1%d1%80%d0%b8%d0%ba%d0%b8/vozvrashhenie-i-pereezd-v-adygeyu-posle-moskvy-i-zarubezhya-kak-podgotovitsya-bez-illyuzij/
fixDiele · April 11, 2026 at 1:30 pm
Между прочим, если вас интересует Переезд в Адыгею: стратегия жизни без самообмана, загляните сюда.
Смотрите сами:
https://galant-cars.ru/%d0%b1%d0%b5%d0%b7-%d1%80%d1%83%d0%b1%d1%80%d0%b8%d0%ba%d0%b8/pereezd-v-adygeyu-posle-moskvy-i-peterburga-strategiya-novoj-zhizni-bez-samoobmana/
Jamesbox · April 11, 2026 at 2:11 pm
look at this site http://www.paycor.com employee login
MiltonCep · April 11, 2026 at 3:33 pm
Отличная доставка, рекомендую всем томичам.
заказ цветов томск с доставкой
Jamesbox · April 11, 2026 at 4:57 pm
website link paycor.com login
Jamesbox · April 11, 2026 at 9:55 pm
check out this site paycor login
Jamesbox · April 11, 2026 at 11:10 pm
imp source paycor login
Rikvip · April 12, 2026 at 12:31 am
Good job for bringing something important to the internet!
Josephmew · April 12, 2026 at 12:38 am
сюда кракен зарегистрироваться
Tipclub · April 12, 2026 at 1:11 am
How do I subscribe to your blog? Thanks for your help.
Tipclub · April 12, 2026 at 2:02 am
Thank you for sharing this very good post. Very interesting ideas! (as always, btw)
Tipclub · April 12, 2026 at 2:07 am
These kind of posts are always inspiring and I prefer to read quality content so I happy to find many good point here in the post. writing is simply wonderful! thank you for the post
http://diafan.rusheat.ru/forum/pokerdom-kazakhstan-promokod/ · April 12, 2026 at 2:20 am
http://diafan.rusheat.ru/forum/pokerdom-kazakhstan-promokod/
789club · April 12, 2026 at 2:38 am
Lovely just what I was looking for. Thanks to the author for taking his clock time on this one.
Ludhiana escort service · April 12, 2026 at 2:55 am
When are you going to take this to a full book?
Josephmew · April 12, 2026 at 4:21 am
Следующая страница кракен что продают
binance "oppna konto · April 12, 2026 at 9:06 am
Thanks for sharing. I read many of your blog posts, cool, your blog is very good.
tai day · April 12, 2026 at 2:13 pm
Thanks for a Interesting item; I enjoyed it very much. Regards Sang Magistrale
tai day · April 12, 2026 at 2:30 pm
Good job for bringing something important to the internet!
daftar senang4d · April 12, 2026 at 3:51 pm
I’ve thought about posting something about this before. Good job! Can I use part of your post in my blog?
Latoto · April 12, 2026 at 3:58 pm
This website has lots of really useful stuff on it. Thanks for informing me.
MiltonCep · April 12, 2026 at 4:00 pm
Цветы идеальные, сервис отличный, спасибо!
заказать цветы с доставкой в томске
Latoto · April 12, 2026 at 4:09 pm
The sketch is tasteful, your authored material stylish.
ErnestPoorp · April 12, 2026 at 5:10 pm
этот сайт Работа со свободным графиком
EA77.COM · April 12, 2026 at 5:43 pm
http://www.allhallowsgospeloak.com
botdb.win · April 12, 2026 at 6:02 pm
References:
Over the counter anabolic steroids
References:
http://adrestyt.ru/user/yamspike6/
notes.medien.rwth-aachen.de · April 12, 2026 at 6:41 pm
References:
Natural muscle vs steroids
References:
https://stackoverflow.qastan.be/?qa=user/violindead95
Richardgrara · April 12, 2026 at 7:13 pm
продолжить https://deevki.ru/
Richardgrara · April 12, 2026 at 7:21 pm
Узнать больше https://deevki.ru
https://centrodeesteticaleticiaperez.com/tratamientos-de-belleza-y-esteticos/tratamientos-indiba-santander · April 12, 2026 at 9:21 pm
https://centrodeesteticaleticiaperez.com/tratamientos-de-belleza-y-esteticos/tratamientos-indiba-santander
https://suedostperle.de/party-snack-raketen · April 12, 2026 at 9:35 pm
https://suedostperle.de/party-snack-raketen
www.freakscene.net · April 12, 2026 at 10:30 pm
References:
Legit testosterone online
References:
http://forum.emrpg.com/home.php?mod=space&uid=1529557&do=profile
부산호빠 · April 12, 2026 at 11:51 pm
부산호빠
RobertSlume · April 13, 2026 at 3:11 am
нажмите здесь кракен сайт зеркало kraken one com
RobertSlume · April 13, 2026 at 4:40 am
кликните сюда кракен актуальные
https://NextFreeAds.com/588/posts/1/1/2172942.html · April 13, 2026 at 7:02 am
https://NextFreeAds.com/588/posts/1/1/2172942.html
WalterWed · April 13, 2026 at 11:37 am
Капельница от похмелья с медицинским контролем в Нижнем Новгороде — это эффективный способ восстановления после алкогольной интоксикации, который позволяет быстро и безопасно нормализовать состояние пациента. Основное отличие такой капельницы от домашних методов состоит в том, что вся процедура проходит под контролем профессионалов, что минимизирует риски для здоровья и повышает эффективность лечения.
Получить дополнительные сведения – капельница от похмелья в нижнем новгороде
Frankdat · April 13, 2026 at 12:41 pm
Выезд нарколога на дом в Самаре организован так, чтобы пациент получил помощь без ожидания и без лишней нагрузки на организм. После обращения специалист приезжает по указанному адресу, проводит первичный осмотр, оценивает общее состояние, уровень интоксикации, показатели давления, пульса, дыхания и собирает краткий анамнез. На основании этой оценки врач определяет, можно ли безопасно оказывать помощь на дому, и подбирает подходящую схему лечения, включая возможное кодирование или вывод из алкоголизма. Такой формат позволяет начать медицинские мероприятия сразу после осмотра и быстро перейти к стабилизации состояния.
Ознакомиться с деталями – нарколог на дом анонимно
Stephenpef · April 13, 2026 at 1:01 pm
Процесс капельницы включает внутривенное введение различных растворов, которые помогают нейтрализовать эффекты алкогольной интоксикации, включая последствия запоя и алкоголизма. Наиболее часто в составе капельницы используются солевые и глюкозные растворы, витамины группы B, а также препараты для детоксикации организма. Эти компоненты помогают быстро восстановить водно-электролитный баланс, улучшить обмен веществ и ускорить выведение продуктов распада алкоголя.
Исследовать вопрос подробнее – http://www.domen.ru
GeorgeMah · April 13, 2026 at 1:05 pm
здесь https://www.google.cm/url?q=https://letundra.com/ru/news/?taglist=kankun,meksika
parhaat kasinot · April 13, 2026 at 1:48 pm
I like meeting utile info, this post has got me even more info!
Chrisapela · April 13, 2026 at 1:57 pm
Врач-нарколог, оценивая состояние пациента, может рекомендовать проведение капельницы для ускоренного восстановления организма. Применение капельницы позволяет снять острые симптомы интоксикации и снизить риск развития более серьезных последствий. В некоторых случаях, если необходимо интенсивное наблюдение, пациенту может быть предложено лечение в стационаре, и услугу можно заказать на летний период для более длительного контроля.
Углубиться в тему – kapelnica-ot-zapoya-nizhnij-novgorod-4.ru/
Click · April 13, 2026 at 2:15 pm
Write more stories, more chapters.
DanielTic · April 13, 2026 at 2:16 pm
Капельница от похмелья в Самаре: быстрое снятие интоксикации, восстановление после алкоголя и улучшение самочувствия под контролем специалистов в наркологической клинике «Похмельная служба»
Разобраться лучше – капельница от похмелья
GeorgeMah · April 13, 2026 at 2:31 pm
Читать далее http://www.google.co.tz/url?sa=i&rct=j&q=&esrc=s&source=images&cd=&cad=rja&uact=8&ved=0cacqjrw&url=https://yakutsk.protos.ru/catalog/item/ramka-regulirovochnaya-latun-32mm-68317
https://pads.jeito.nl/s/lI2hyYArW- · April 13, 2026 at 3:04 pm
References:
Beste echtgeld casinos
References:
https://denimcatsup14.bravejournal.net/online-casino-gratis-bonus-ohne-einzahlung-direkt-starten-und-echtes-geld-im
beste online casino belgie · April 13, 2026 at 3:07 pm
Great post. I was checking constantly this blog and I’m impressed! Very useful info specifically the last part 🙂 I care for such info much. I was looking for this certain information for a very long time. Thank you and good luck.
Jamiebog · April 13, 2026 at 3:28 pm
Капельница от похмелья — это одна из самых эффективных процедур для быстрого облегчения симптомов интоксикации после употребления алкоголя. В Нижнем Новгороде существует множество клиник и медицинских центров, которые предлагают услуги капельниц, направленных на восстановление водно-электролитного баланса, улучшение общего самочувствия и снятие неприятных симптомов похмелья. Процесс введения капельницы можно адаптировать под индивидуальные особенности пациента для достижения наилучшего результата.
Получить больше информации – капельница от похмелья анонимно
Tài xỉu online · April 13, 2026 at 3:31 pm
My issues have been very similar, with my family. But, we made some different decisions. It’s complex.
GeorgeMah · April 13, 2026 at 4:15 pm
читать https://www.google.no/url?q=https://letundra.com/es/news/?taglist=eventos,zagreb-2
GeorgeMah · April 13, 2026 at 4:22 pm
страница https://www.google.so/url?sa=t&rct=j&q=&esrc=s&source=web&cd=1&ved=0ccsqfjaa&url=https://blkrip.vip/de/services/full-production/
WalterWed · April 13, 2026 at 5:00 pm
Процесс введения капельницы с медицинским контролем начинается с того, что медицинский специалист оценивает общее состояние пациента: измеряет артериальное давление, пульс, температуру тела, а также учитывает историю заболеваний. Это позволяет выбрать оптимальный состав растворов и препаратов для максимально быстрого и безопасного восстановления.
Детальнее – капельница от похмелья на дому нижний новгород
Frankdat · April 13, 2026 at 7:23 pm
Услуги нарколога на дому в Самаре включают не только экстренный осмотр, но и комплекс медицинских мероприятий, направленных на снижение интоксикации, облегчение тяжелых симптомов и общее восстановление состояния пациента. Объем помощи зависит от клинической картины, длительности употребления алкоголя или других психоактивных веществ, возраста, хронических заболеваний и текущих рисков. Врач подбирает схему индивидуально, исходя из того, какие задачи необходимо решить в конкретный момент — снять острые проявления, стабилизировать самочувствие или подготовить пациента к дальнейшему лечению зависимости.
Разобраться лучше – нарколог на дом вывод
Stephenpef · April 13, 2026 at 8:30 pm
Процесс капельницы включает внутривенное введение различных растворов, которые помогают нейтрализовать эффекты алкогольной интоксикации, включая последствия запоя и алкоголизма. Наиболее часто в составе капельницы используются солевые и глюкозные растворы, витамины группы B, а также препараты для детоксикации организма. Эти компоненты помогают быстро восстановить водно-электролитный баланс, улучшить обмен веществ и ускорить выведение продуктов распада алкоголя.
Выяснить больше – капельница от похмелья анонимно самара
mostbet ?????????????????? · April 13, 2026 at 9:21 pm
mostbet com ????????
Chrisapela · April 13, 2026 at 9:22 pm
Капельница от запоя с детоксикацией организма в Нижнем Новгороде представляет собой одну из самых эффективных процедур для быстрого улучшения состояния пациента, страдающего от алкогольной зависимости. Такой подход направлен не только на устранение токсинов, но и на восстановление нормального функционирования внутренних органов, которые пострадали от длительного употребления алкоголя.
Разобраться лучше – капельница от запоя на дому в нижнем новгороде
https://www.tvbattle.com · April 13, 2026 at 9:51 pm
References:
Online Casino Echtgeld Poker
References:
https://doodleordie.com/profile/perupuffin43
https://1samogon.ru/ · April 13, 2026 at 10:20 pm
https://1samogon.ru/
https://notes.medien.rwth-aachen.de/elm_P4aKSoiCxFnUZSWsuA/ · April 13, 2026 at 10:30 pm
References:
Online Casino Echtgeld Erfahrung
References:
https://codimd.communecter.org/3B1rGrE-TlK6QHDFiDNg5A/
WalterWed · April 13, 2026 at 11:31 pm
Медицинский контроль играет ключевую роль в безопасности и эффективности процедуры. Под присмотром опытного специалиста исключаются риски неправильной дозировки препаратов, побочных эффектов и осложнений, что особенно важно при проведении капельниц у пациентов с хроническими заболеваниями или при наличии индивидуальных противопоказаний.
Исследовать вопрос подробнее – капельница от похмелья цена в нижнем новгороде
pulsetto review · April 13, 2026 at 11:52 pm
We need to build frameworks and funding mechanisms.
https://1samogon.ru/ · April 14, 2026 at 1:23 am
https://1samogon.ru/
WalterWed · April 14, 2026 at 1:35 am
Как отмечает врач-нарколог Сергей Иванов: “Самое главное преимущество капельницы с медицинским контролем — это точная диагностика состояния пациента перед началом процедуры и возможность корректировать лечение в процессе, что делает её гораздо более безопасной и эффективной по сравнению с самостоятельными методами.”
Разобраться лучше – капельница от похмелья на дом в нижнем новгороде
Roberthog · April 14, 2026 at 2:42 am
Ребята, кто любит конкретику — в статье есть шикарные расчёты ROI для ниши «юридические услуги». Автор показывает: до накрутки 500 посетителей и 15 заявок, после накрутки (бюджет 20 000 ?) — 1500 посетителей и 45 заявок. ROI = 1400%. Каждый рубль принёс 14 рублей прибыли. Также есть прогноз, что будет с теми, кто не начнёт крутить: потеря позиций, вымывание из топа, уход клиентов к конкурентам. Очень наглядно: https://yagla.ru/blog/drugoe-o-marketinge/nakrutka-povedencheskih-faktorov-v-2026–2604u119831/
Roberthog · April 14, 2026 at 2:48 am
Коллеги, кто сомневается, работает ли накрутка ПФ в 2026 году, — прочитайте этот материал. Автор разбирает реальные кейсы и даёт чёткие цифры: цена от 0,8 рубля за клик, примеры бюджетов для разных ниш (стоматология, клининг, автодилер). Мне помогло понять, что это инвестиция, а не расход. Почитайте: https://teletype.in/@pfup/3mo6UGVvR2a
Frankdat · April 14, 2026 at 3:13 am
Услуги нарколога на дому в Самаре включают не только экстренный осмотр, но и комплекс медицинских мероприятий, направленных на снижение интоксикации, облегчение тяжелых симптомов и общее восстановление состояния пациента. Объем помощи зависит от клинической картины, длительности употребления алкоголя или других психоактивных веществ, возраста, хронических заболеваний и текущих рисков. Врач подбирает схему индивидуально, исходя из того, какие задачи необходимо решить в конкретный момент — снять острые проявления, стабилизировать самочувствие или подготовить пациента к дальнейшему лечению зависимости.
Получить дополнительную информацию – врач нарколог на дом
Allenzep · April 14, 2026 at 3:47 am
Источник кракeн сайт ссылка
Allenzep · April 14, 2026 at 4:19 am
узнать больше ссылка на krakеn торговая площадка
WalterWed · April 14, 2026 at 4:35 am
Как отмечает врач-нарколог Сергей Иванов: “Самое главное преимущество капельницы с медицинским контролем — это точная диагностика состояния пациента перед началом процедуры и возможность корректировать лечение в процессе, что делает её гораздо более безопасной и эффективной по сравнению с самостоятельными методами.”
Исследовать вопрос подробнее – капельница от похмелья вызов на дом в нижнем новгороде
WalterWed · April 14, 2026 at 4:53 am
Капельница от похмелья с медицинским контролем в Нижнем Новгороде — это эффективный способ восстановления после алкогольной интоксикации, который позволяет быстро и безопасно нормализовать состояние пациента. Основное отличие такой капельницы от домашних методов состоит в том, что вся процедура проходит под контролем профессионалов, что минимизирует риски для здоровья и повышает эффективность лечения.
Ознакомиться с деталями – http://kapelnicza-ot-pokhmelya-nizhnij-novgorod-1.ru
Stephenpef · April 14, 2026 at 5:09 am
Процесс капельницы включает внутривенное введение различных растворов, которые помогают нейтрализовать эффекты алкогольной интоксикации, включая последствия запоя и алкоголизма. Наиболее часто в составе капельницы используются солевые и глюкозные растворы, витамины группы B, а также препараты для детоксикации организма. Эти компоненты помогают быстро восстановить водно-электролитный баланс, улучшить обмен веществ и ускорить выведение продуктов распада алкоголя.
Подробнее – kapelnicza-ot-pokhmelya-samara-6.ru/
fixDiele · April 14, 2026 at 5:34 am
Кстати, если вас интересует Переезд в Адыгею: опыт москвичей и петербуржцев, загляните сюда.
Вот, делюсь ссылкой:
https://tut-vse-yasno.ru/news/pereezd-v-adygeyu-na-pmzh-iz-moskvy-i-peterburga-kak-produmannyj-zhiznennyj-proekt/
fixDiele · April 14, 2026 at 5:38 am
Кстати, если вас интересует Переезд в Адыгею: изменения и перспективы, загляните сюда.
Смотрите сами:
https://bro-lordfilm.ru/news/pereezd-i-vozvrashhenie-v-adygeyu-kak-smenit-megapolis-na-novuyu-traektoriyu/
Frankdat · April 14, 2026 at 5:50 am
Вызов нарколога на дом в Самаре становится необходимым решением в ситуациях, когда состояние человека требует срочной медицинской помощи, но самостоятельное обращение в клинику затруднено или невозможно. Чаще всего речь идет об острых проявлениях алкогольной или наркотической интоксикации, выраженном похмельном синдроме, длительном запое, а также о случаях, когда у пациента наблюдаются тревожные симптомы — скачки давления, тахикардия, рвота, судороги, спутанность сознания. В подобных состояниях промедление может привести к серьезным осложнениям, поэтому выезд врача без ожидания позволяет оперативно стабилизировать состояние и предотвратить риски для здоровья.
Получить дополнительную информацию – врач нарколог на дом в самаре
JamesVot · April 14, 2026 at 5:56 am
# How to get Bybit sign-up bonus : complete guide
Beginning your investment journey is exciting but taking the right steps makes a huge difference in the long run. As one of the leading platforms, Bybit caters to both professional and beginner investors offering attractive opportunities with exclusive promo codes for new users. So, what is the Bybit promo code WKOQ3AX, how do you use it, and what advantages does it offer? In the guide below you will find everything you need to know about the current Bybit promo code WKOQ3AX and campaigns.
—
## 1. Why Bybit? Here Are the Answers
Bybit, one of the established platforms in the crypto sector, was founded in 2018 and has reached millions worldwide with its robust infrastructure. With over 80 million registered users as of 2026 with an average daily trading volume exceeding $20 billion ranks among the platforms with the deepest liquidity in the market.
**Key features that set Bybit apart:**
– **High Trading Volume:** The ability to trade with minimal slippage even on large volume orders
– **Security Infrastructure:** The majority of user funds are held in offline cold wallets , and regular Proof of Reserve (PoR) reports are published
– **Regulatory Compliance:** by obtaining MiCAR in Europe and SCA licenses in the Middle East last year has taken significant steps in regulatory compliance
– **Product Diversity:** Comprehensive services including spot trading, futures, options markets, copy trading, liquidity mining, and Web3 wallet integration
—
## 2. How Does the Bybit Sign-Up Bonus and Promo Code System Work?
A Bybit promo code is a special invitation code that new users can enter during registration. **This special code** is the key that unlocks the most comprehensive opportunity package Bybit offers new users. Using this code users access much more attractive opportunities than a regular sign-up. The promo codes offered by Bybit generally include the following advantages:
| **Benefit Type** | **Description** |
|——————|————–|
| **Commission Discount** | Up to 20% ongoing commission advantage on spot and futures markets |
| **Sign-Up Bonus** | Up to 30,000 USDT in trial bonus |
| **Deposit Advantages** | Extra bonuses automatically credited when funds are first deposited into the account |
| **Loss Protection Vouchers** | Special coupons that compensate for potential losses new users may experience in their first trades |
**Critical Warning:** The referral code WKOQ3AX must be entered during sign-up. There is no possibility to add or edit the code after the account is created.
—
## 3. Meet the Bybit Bonus Code WKOQ3AX
As of 2026, the most current and most advantageous promo code you can use on Bybit is **WKOQ3AX**. This code offers a comprehensive opportunity that appeals to all user profiles:
### WKOQ3AX – The Code That Makes the Difference in Earnings
**Code: WKOQ3AX**
This promo code brings together all the advantages Bybit has to offer under one roof. the WKOQ3AX referral code** can earn up to 30,000 USDT in bonus packages and also have a lifetime 20% commission discount advantage. The discount is automatically applied to spot and futures markets.
**Campaign Details:**
– Highest bonus potential (30,000 USDT) – industry-leading opportunity
– 20% permanent trading fee discount valid for the life of the account
– Usable worldwide, no regional restrictions
– Seamless use across all Bybit platforms
– Valid on spot, futures, and all other markets
—
## 4. Which Bonus Does What? Detailed Analysis with WKOQ3AX
The bonus types you will obtain on the platform with the WKOQ3AX referral code vary and it is important to know how to use each one.
### 4.1. Trial Bonus (Trading Bonus)
A trading bonus is a type of reward you can use as margin, especially in futures markets. The most important feature of this bonus is that you can withdraw the profits you make, but you cannot withdraw the bonus itself. So if you trade with the bonus, the profit you make is yours, while any loss is first deducted from the bonus balance. This mechanism allows new users to experience the platform without taking risks.
**Bonus Usage Terms:**
– Can be used as position margin
– Commission and funding expenses are deducted from the bonus balance
– Expired bonuses are automatically cancelled
– No use outside futures trading
### 4.2. How Do Fee Saver Coupons Work?
These coupons are used to cover commission fees incurred during trading. Coupons are reflected as refunds to your balance equal to the commission deducted. These coupons can be used for your spot, futures, or instant buy/sell transactions. **The permanent commission discount you obtain with the WKOQ3AX referral code, combined with fee saver coupons, provides maximum savings.**
### 4.3. Bybit’s Special Events
Bybit regularly organizes special events. Within the scope of the “Daily Treasure Hunt” event continuing in the first quarter of 2026:
– Tens of thousands of scratch cards are offered to users every day
– BTC, ETH, and other major cryptocurrencies along with VIP trial cards are in the prize pool
– Complete tasks, collect points, and earn one raffle ticket for every 50 points
—
## 5. Step-by-Step Bybit Registration and WKOQ3AX Bonus Usage Guide
### Bybit Account Opening Guide
**1. Phase: Navigate to the Correct Address**
– **Fastest registration method:** https://www.bybit.com/invite?ref=WKOQ3AX
– Go to bybit.com from your computer
– Mobile: Download the Bybit app from the App Store or Google Play
**Step 2: Fill Out the Registration Form**
– Provide one of your contact details (email or phone) to the system
– Choose a strong password
**Step 3: Enter the Promo Code**
– Find the “Referral Code” or “Promo Code” field on the registration form
– Enter the code you want to use here: **WKOQ3AX**
– If you register via the https://www.bybit.com/invite?ref=WKOQ3AX link, the code field will be auto-filled
**Step 4: Verify Your Account**
– Activate your account by entering the verification code sent to you
**Step 5: Complete KYC Identity Verification**
– At least KYC Level 1 verification is required to benefit from all promotions
– Verify using one of your official identity documents (national ID, passport, driver’s license)
– The process is usually approved within a few minutes
**6. Phase: Complete Campaign Tasks Step by Step**
– Track your rewards from the Bonus Center
– Rewards are instantly credited to your account as you progress through tasks
—
## 6. What to Know About Bonuses and Promotions
### Can I use the WKOQ3AX code after signing up?
Unfortunately, the WKOQ3AX code can only be used during account creation. Since codes cannot be entered after account opening, it’s important not to miss this step. **Therefore, using the https://www.bybit.com/invite?ref=WKOQ3AX link is the safest method.**
### Can I use WKOQ3AX together with another code?
No, each new user can only use one promo code. **It is recommended to register by choosing the most advantageous code, WKOQ3AX.**
### Can I withdraw the bonuses I earn with WKOQ3AX as cash?
Trial bonuses themselves cannot be withdrawn, but the profits made from trading with the bonus can be withdrawn. With the trading fee discount, you automatically save on every transaction.
### In which countries can WKOQ3AX be used?
The WKOQ3AX promo code can be used in all regions where Bybit operates, including Turkey. However, registration is not possible in countries where Bybit does not operate, such as the USA, Canada, the UK, Singapore, and mainland China.
### Can I earn bonuses without identity verification?
KYC must be completed for bonuses to be credited to your account. It is recommended to complete identity verification immediately after registration.
—
## 7. Expert Tip: WKOQ3AX is the Right Code for You
**Bybit’s most comprehensive referral code WKOQ3AX** with its combined advantages in a single code is the only solution that appeals to all user types.
| **Investor Profile** | **Gain Obtained** |
|——————-|——————|————-|
| **Inexperienced investor** | Opportunity to learn trading without risking your own capital thanks to trial bonus |
| **Frequent trader** | Maximum cost advantage for high volumes |
| **All users** | Unmatched starting opportunity |
—
## Evaluation
Bybit promo codes are an important opportunity for new users to gain extra advantages when starting on the platform. **The WKOQ3AX referral code** by combining both maximum bonus potential and permanent commission savings in one code will be the right choice for you.
Crypto investments have a volatile nature; it’s important to trade with amounts you can afford to lose. The bonuses and discounts offered by the platform positively impact your earnings regardless of market conditions. Don’t forget to review campaign details before registration to catch the most current opportunities.
—
## Register Now!
**Use the most advantageous code right now: WKOQ3AX**
**Start your advantaged journey through the link below:**
### 👉 **https://www.bybit.com/invite?ref=WKOQ3AX**
Register now to not miss out on the 20% permanent trading fee discount and up to 30,000 USDT bonus opportunity!
—
*This article is for informational purposes and does not constitute investment advice. Cryptocurrency trading carries high risk; it is recommended to do your own research before making decisions.*
promo here
Get the promo code
Source:
https://domaindan.com/yandex-market-promokod/002/
Chrisapela · April 14, 2026 at 6:12 am
Капельница от запоя с детоксикацией организма в Нижнем Новгороде представляет собой одну из самых эффективных процедур для быстрого улучшения состояния пациента, страдающего от алкогольной зависимости. Такой подход направлен не только на устранение токсинов, но и на восстановление нормального функционирования внутренних органов, которые пострадали от длительного употребления алкоголя.
Узнать больше – вызов на дом капельницы от запоя нижний новгород
Allenzep · April 14, 2026 at 6:55 am
узнать больше Здесь kraken darknet market ссылка тор 2kraken click
Stephenpef · April 14, 2026 at 7:59 am
Капельница от похмелья в Самаре: быстрое восстановление, снятие интоксикации и улучшение самочувствия под контролем специалистов в наркологической клинике «Похмельная служба»
Получить дополнительную информацию – капельница от похмелья на дом самара
Josephdeecy · April 14, 2026 at 8:03 am
Суть капельницы заключается в том, чтобы быстро ввести в организм необходимые растворы, которые помогают восстановить водно-солевой баланс, очищают организм от токсинов, ускоряют обмен веществ и снижают нагрузку на внутренние органы. Врачи-наркологи используют специальные составы, которые включают в себя жидкости, электролиты, витамины и лекарственные средства для снятия симптомов похмелья.
Подробнее тут – капельница от похмелья цена
Williamgor · April 14, 2026 at 8:17 am
На первом этапе специалист проводит визуальный осмотр пациента, измеряет артериальное давление, пульс, уровень кислорода в крови и оценивает общее психоэмоциональное состояние. Важно выявить степень интоксикации, наличие осложнений и противопоказаний к проведению терапии на дому. В случае наркомании и длительного употребления наркотиков, пациенту может быть предложена консультация и лечение, включая реабилитацию на летний период, если состояние требует интенсивного контроля.
Подробнее – нарколог на дом цена
theflatearth.win · April 14, 2026 at 8:34 am
References:
Online casino echtgeld
References:
https://mysingledesire.com/members/slaveactive91/activity/15233/
Allenzep · April 14, 2026 at 8:43 am
такой kraken darknet market зеркало v5tor cfd
Chrisapela · April 14, 2026 at 9:02 am
Капельница от запоя представляет собой процедуру внутривенного введения специальных растворов, направленных на устранение токсинов, нормализацию обменных процессов и восстановление функций организма. Это позволяет быстрее вывести алкогольные токсины и минимизировать их воздействие на внутренние органы. В некоторых случаях может потребоваться наркологическая помощь и консультация психиатра, особенно если у пациента есть длительная зависимость или другие психоэмоциональные расстройства, которые требуют вмешательства специалистов с большим стажем работы.
Узнать больше – https://kapelnica-ot-zapoya-nizhnij-novgorod-4.ru
RandyJoype · April 14, 2026 at 9:31 am
Несмотря на кажущуюся простоту процедуры, капельница требует профессионального подхода. Неправильно подобранные препараты или дозировки могут привести к осложнениям, особенно при хронических заболеваниях. Поэтому проведение процедуры под контролем специалиста является ключевым фактором эффективности и безопасности.
Получить больше информации – капельница от похмелья на дому самара
Frankdat · April 14, 2026 at 9:34 am
Услуги нарколога на дому в Самаре включают не только экстренный осмотр, но и комплекс медицинских мероприятий, направленных на снижение интоксикации, облегчение тяжелых симптомов и общее восстановление состояния пациента. Объем помощи зависит от клинической картины, длительности употребления алкоголя или других психоактивных веществ, возраста, хронических заболеваний и текущих рисков. Врач подбирает схему индивидуально, исходя из того, какие задачи необходимо решить в конкретный момент — снять острые проявления, стабилизировать самочувствие или подготовить пациента к дальнейшему лечению зависимости.
Выяснить больше – http://narkolog-na-dom-samara-5.ru/
menwiki.men · April 14, 2026 at 9:47 am
References:
Steroid like supplements gnc
References:
https://fakenews.win/wiki/Secure_Trenbolone_Purchase_Via_Credit_Card
Frankdat · April 14, 2026 at 9:57 am
Выезд нарколога на дом в Самаре организован так, чтобы пациент получил помощь без ожидания и без лишней нагрузки на организм. После обращения специалист приезжает по указанному адресу, проводит первичный осмотр, оценивает общее состояние, уровень интоксикации, показатели давления, пульса, дыхания и собирает краткий анамнез. На основании этой оценки врач определяет, можно ли безопасно оказывать помощь на дому, и подбирает подходящую схему лечения, включая возможное кодирование или вывод из алкоголизма. Такой формат позволяет начать медицинские мероприятия сразу после осмотра и быстро перейти к стабилизации состояния.
Исследовать вопрос подробнее – врач нарколог на дом
Binance Sign up · April 14, 2026 at 11:25 am
There is definately a great deal to find out about this issue. I really like all the points you have made.
online casino nz · April 14, 2026 at 1:24 pm
Hi, I do believe your website could be having web browser compatibility issues. Whenever I take a look at your website in Safari, it looks fine but when opening in I.E., it has some overlapping issues. I just wanted to provide you with a quick heads up! Apart from that, great website!
https://mmcon.sakura.ne.jp/ · April 14, 2026 at 2:42 pm
References:
Rocketplay neosurf deposit limit
References:
http://adrestyt.ru/user/ringcheese4/
Lestergog · April 14, 2026 at 5:05 pm
После употребления алкоголя состояние может быстро ухудшиться: появляется головная боль, тошнота, головокружение и слабость. Это следствие того, что в организме накапливаются токсины, продукты распада этанола и нарушается водно-электролитный баланс. С помощью капельницы от похмелья можно быстро справиться с интоксикацией, восполнить недостающие элементы и облегчить состояние пациента. В клинике «Частный медик 24» в Самаре мы предлагаем капельницы, которые помогают снять все неприятные симптомы похмелья, восстанавливая работу организма и минимизируя риски для здоровья.
Выяснить больше – капельница от похмелья в самаре
classifieds.ocala-news.com · April 14, 2026 at 5:18 pm
References:
Wachstumshormone bestellen
References:
https://lovewiki.faith/wiki/HGH_Erfahrungen_Wirkung_und_Nebenwirkungen
Michaeljax · April 14, 2026 at 5:48 pm
Запой, длительное употребление алкоголя или случайное злоупотребление могут привести к неприятным симптомам похмелья, таким как головная боль, слабость, тошнота, головокружение и усталость. Эти симптомы обусловлены тем, что в организме остаются продукты распада алкоголя, которые токсически воздействуют на все органы. Капельница от похмелья на дому — это отличная возможность быстро снять острые симптомы и восстановить нормальное состояние организма, не выходя из привычной обстановки.
Получить больше информации – https://kapelnicza-ot-pokhmelya-samara-2.ru
MiltonCep · April 14, 2026 at 6:46 pm
Всё организовано идеально, даже открытку красиво подписали.
доставка цветов томск
Clintonwrina · April 14, 2026 at 7:00 pm
Выезд нарколога на дом в Самаре — это комплексный подход к лечению, который включает несколько этапов. Врач, приехавший на место, не ограничивается одной процедурой, а проводит полноценный осмотр, диагностирует состояние пациента, определяет причину ухудшения самочувствия и подбирает индивидуальную терапию. Наиболее часто при выезде нарколога на дом используются капельницы, антиеметики и препараты для стабилизации состояния пациента, снятия симптомов абстиненции и улучшения общего самочувствия.
Ознакомиться с деталями – нарколог на дом вывод в самаре
cameradb.review · April 14, 2026 at 7:02 pm
References:
Buy boron for testosterone
References:
https://lovewiki.faith/wiki/Buy_Testosterone_C_Injections_Online
top 10 casino online · April 14, 2026 at 7:33 pm
Very nice write-up. I definitely love this website. Keep it up!
RobertMum · April 14, 2026 at 7:51 pm
Выбор наркологической клиники — ответственное решение, от которого зависит не только эффективность терапии, но и общее физическое и психоэмоциональное состояние пациента. Квалифицированная помощь должна быть своевременной, организованной и соответствующей медицинским стандартам. Как указывает Минздрав РФ, медицинские учреждения, предоставляющие помощь при зависимостях, обязаны иметь лицензию, профессиональный персонал и комплексный подход к лечению.
Выяснить больше – https://narkologicheskaya-klinika-murmansk0.ru/
Robertnox · April 14, 2026 at 8:34 pm
Для семьи это тоже имеет большое значение. Пока врач в пути, родственники часто совершают одни и те же ошибки: пытаются «отпаивать» человека через силу, смешивают несовместимые медикаменты, дают советы, которые только повышают тревогу, спорят или требуют немедленно взять себя в руки. Профессиональный выезд снимает эту хаотичность. После осмотра врач объясняет, какие симптомы связаны с алкогольной интоксикацией, какие могут указывать на осложнения, что допустимо дома, а что требует перевода в стационар. В этом и состоит ценность выезда: он возвращает контроль над ситуацией и позволяет начать лечение без лишних задержек.
Выяснить больше – нарколог на дом воронеж
MatthewMut · April 14, 2026 at 9:08 pm
Есть состояния, при которых откладывать вызов врача рискованно. Домашний выезд нужен не только при «тяжёлом похмелье», но и тогда, когда самочувствие становится нестабильным, а попытки справиться своими силами уже не работают. Ниже перечислены ситуации, при которых обращение за помощью оправдано именно в ближайшее время, а не «если не станет легче к вечеру».
Получить дополнительные сведения – запой нарколог на дом в воронеже
Robertmah · April 14, 2026 at 11:07 pm
Откройте для себя увлекательный слот с египетской тематикой — Sun of Egypt. Яркая графика, бонусы и шанс на крупные выигрыши делают игру особенно популярной среди игроков.
Попробуйте Sun of Egypt демо без регистрации и вложений. Это отличный способ изучить механику слота и протестировать стратегии перед игрой на реальные деньги.
Если вы ищете лучшие казино для Sun of Egypt, обратите внимание на платформы с лицензией и щедрыми бонусами. Это повысит ваши шансы на комфортную игру.
Новая версия Sun of Egypt 2 порадует улучшенной графикой и дополнительными функциями. Игра стала еще более захватывающей и динамичной.
Продолжение популярного слота — Sun of Egypt 3 — предлагает еще больше бонусных раундов и возможностей для выигрыша, сохраняя атмосферу Древнего Египта.
Увлекательная демо-игра Sun of Egypt доступна бесплатно для всех пользователей. Идеально подходит для новичков, желающих освоиться без риска.
Начните играть в Sun of Egypt демо прямо сейчас. Это удобный способ насладиться игровым процессом без вложений и понять особенности слота.
Надежный сайт для игры Sun of Egypt предлагает безопасный доступ и широкий выбор режимов. Здесь каждый найдет комфортные условия для игры.
Перейдите на официальный сайт Sun of Egypt, чтобы получить доступ к актуальной версии слота, бонусам и честной игре с прозрачными правилами.
Играйте в Sun of Egypt бесплатно и наслаждайтесь атмосферой древних пирамид. Отличный вариант для отдыха и тренировки игровых навыков.
Погрузитесь в атмосферу древних пирамид вместе с Sun of Egypt. Слот радует красочной анимацией, бонусами и возможностью получить солидные выигрыши.
Оцените возможности Sun of Egypt демо без риска для бюджета. Бесплатный режим позволит изучить игру и понять её особенности перед ставками.
Выбирая лучшие казино для Sun of Egypt, обращайте внимание на бонусы и лицензию. Это обеспечит честный игровой процесс и приятный опыт.
Испытайте обновлённый слот Sun of Egypt 2, где вас ждут новые функции, улучшенная графика и ещё больше шансов на выигрыш.
Захватывающий игровой процесс предлагает Sun of Egypt 3. Игра сохранила популярную механику, добавив свежие бонусы и эффекты.
Попробуйте демо-игра Sun of Egypt, чтобы без вложений оценить бонусные раунды и особенности слота.
Начните играть в Sun of Egypt демо и насладитесь игровым процессом без регистрации. Отличный вариант для новичков и опытных игроков.
Удобный сайт для игры Sun of Egypt обеспечивает быстрый доступ к слоту и безопасную игру в любое время.
Посетите официальный сайт Sun of Egypt, чтобы ознакомиться с правилами, бонусами и актуальной версией популярной игры.
Запустите Sun of Egypt бесплатно и попробуйте выиграть без вложений. Отличный способ развлечься и протестировать стратегию.
Удобный сайт для игры Sun of Egypt предлагает быстрый доступ к популярному слоту. Наслаждайтесь качественной графикой и бонусами без лишних сложностей.
Начните играть в Sun of Egypt онлайн прямо сейчас. Игра доступна с любого устройства и дарит атмосферу Древнего Египта с шансом на крупный выигрыш.
Перейдите на официальный сайт Sun of Egypt, чтобы получить доступ к актуальной версии слота и узнать о доступных бонусах.
Если вы не знаете, где играть в Sun of Egypt, выбирайте проверенные площадки с хорошей репутацией и лицензией.
Популярная игра Sun of Egypt онлайн сочетает в себе простые правила и увлекательный геймплей, который понравится как новичкам, так и опытным игрокам.
Попробуйте Sun of Egypt бесплатно и оцените все возможности слота без финансовых вложений. Отличный вариант для тренировки.
Доступна демо версия Sun of Egypt, позволяющая изучить механику игры и протестировать стратегии без риска.
Увлекательный слот Sun of Egypt играть можно в любое время. Наслаждайтесь бонусами, фриспинами и атмосферой приключений.
Попробуйте Sun of Egypt на деньги, чтобы испытать азарт и получить шанс на реальные выигрыши в популярном слоте.
Начните играть в Sun of Egypt без регистрации и наслаждайтесь игровым процессом без лишних формальностей и ожиданий.
Откройте удобный сайт для игры Sun of Egypt и начните знакомство с популярным слотом. Красочная графика, атмосферная музыка и бонусные раунды делают игровой процесс захватывающим и динамичным.
Вы можете играть в Sun of Egypt онлайн без ограничений. Слот доступен на разных устройствах и предлагает стабильную работу, интересные функции и высокий уровень отдачи для игроков.
Посетив официальный сайт Sun of Egypt, вы получите доступ к актуальной версии игры. Здесь представлены правила, бонусные возможности и удобный интерфейс для комфортного геймплея.
Если вы думаете, где играть в Sun of Egypt, выбирайте надежные площадки. Это обеспечит безопасность данных, честную игру и приятные бонусы для пользователей.
Популярная игра Sun of Egypt онлайн предлагает увлекательный процесс с элементами приключения. Она сочетает простоту правил и интересные бонусные механики.
Начните играть в Sun of Egypt бесплатно и изучите все особенности слота. Это отличная возможность протестировать стратегию без риска и вложений.
Доступна удобная демо версия Sun of Egypt, которая позволяет познакомиться с игрой без регистрации. Отличный вариант для новичков.
Захватывающий слот Sun of Egypt играть можно в любое время. Игра радует бонусами, фриспинами и интересной тематикой древнего мира.
Испытайте удачу в Sun of Egypt на деньги и получите шанс на реальные выигрыши. Слот предлагает честную механику и разнообразные возможности.
Начните Sun of Egypt без регистрации и наслаждайтесь игрой без лишних действий. Это быстрый способ погрузиться в атмосферу и получить удовольствие.
Погрузитесь в атмосферу Древнего Египта и попробуйте играть в слот Sun of Egypt. Вас ждут бонусные раунды, символы фараонов и захватывающий геймплей, который отлично подходит как новичкам, так и опытным игрокам, любящим классические игровые автоматы с современными функциями.
Оцените Sun of Egypt онлайн бесплатно и изучите механику слота без вложений. Демо-режим помогает понять правила, протестировать стратегии и просто насладиться игрой в комфортном формате без риска для бюджета.
Попробуйте запуск Sun of Egypt в браузере без установки дополнительных программ. Игра быстро загружается, работает стабильно и позволяет сразу погрузиться в атмосферу древних цивилизаций и азартных вращений барабанов.
Начните Sun of Egypt играть сейчас и испытайте удачу в популярном слоте. Красочная графика, бонусные символы и простая механика делают игру интересной для широкого круга пользователей.
Получите удобный доступ к игре Sun of Egypt в любое время и с любого устройства. Слот не требует сложных настроек и позволяет быстро начать игру с максимальным комфортом.
Попробуйте Sun of Egypt слот онлайн и насладитесь динамичным игровым процессом. Фриспины, множители и тематические символы создают атмосферу настоящего приключения в мире фараонов.
Начните начать игру Sun of Egypt и откройте для себя один из самых популярных слотов с египетской тематикой. Игра сочетает простоту и увлекательные бонусные функции.
Оцените Sun of Egypt демо играть и изучите особенности слота без финансовых рисков. Это отличный способ понять механику и выбрать стратегию перед реальной игрой.
Попробуйте играть Sun of Egypt без скачивания прямо в браузере. Игра не требует установки и запускается за считанные секунды, обеспечивая быстрый доступ к развлечению.
Откройте для себя Sun of Egypt игровой автомат онлайн и насладитесь классическим форматом слота с современными функциями, бонусами и атмосферным оформлением древнего Египта.
Source:
https://sun-ofegypt.com/
Sun of Egypt
Lestergog · April 14, 2026 at 11:44 pm
Процесс лечения начинается с консультации врача, который оценивает состояние пациента, его анамнез и определяет, какие процедуры и препараты нужно использовать. В большинстве случаев капельница включает в себя регидратацию, витамины группы B, антиеметики, препараты для улучшения работы печени и почек. Важно, что капельница не только помогает организму вывести токсины, но и восстанавливает нормальную работу всех систем организма, обеспечивая быстрое улучшение самочувствия.
Получить больше информации – капельница от похмелья вызов на дом в самаре
iwinclub.vc · April 15, 2026 at 12:33 am
This is valuable stuff.In my opinion, if all website owners and bloggers developed their content they way you have, the internet will be a lot more useful than ever before.
Clintonwrina · April 15, 2026 at 1:41 am
Выезд нарколога на дом в Самаре — это комплексный подход к лечению, который включает несколько этапов. Врач, приехавший на место, не ограничивается одной процедурой, а проводит полноценный осмотр, диагностирует состояние пациента, определяет причину ухудшения самочувствия и подбирает индивидуальную терапию. Наиболее часто при выезде нарколога на дом используются капельницы, антиеметики и препараты для стабилизации состояния пациента, снятия симптомов абстиненции и улучшения общего самочувствия.
Изучить вопрос глубже – нарколог на дом цена самара
Kèo Nhà Cái 5 · April 15, 2026 at 2:07 am
Thanks for posting this. Looking for these resources 😀
xem them · April 15, 2026 at 2:13 am
This is something that will need all of our combined efforts to address.
https://apptaixiuonline.gold · April 15, 2026 at 2:45 am
I just added your web site to my blogroll, I hope you would look at doing the same.
No Hu · April 15, 2026 at 3:05 am
Excellent read, I just passed this onto a colleague who was doing a little research on that. And he actually bought me lunch because I found it for him smile So let me rephrase that.|
https://apptaixiuonline.gold · April 15, 2026 at 3:26 am
Our community leaders need to read this, and look at developing some of your recommendations.
789win · April 15, 2026 at 3:48 am
This will be helpful for my family.
viagra · April 15, 2026 at 4:00 am
I am glad to be a visitor on this website!, regards for this rare information!
slot-mestre · April 15, 2026 at 4:27 am
Mahjong Ways 2 continua sendo escolha sólida para quem gosta de progressão por cascata.
Robertnox · April 15, 2026 at 4:54 am
Анонимное лечение на дому ценно ещё и тем, что снижает внутреннее сопротивление самого пациента. Для многих людей первый контакт с врачом происходит именно дома, без дороги, без ожидания, без страха чужих взглядов. Такой формат помогает начать разговор не только о снятии острых симптомов, но и о более широких вопросах: что делать после выхода из запоя, когда требуется кодирование, в каких случаях нужна реабилитация, а когда первичная наркологическая помощь уже должна переходить в полноценный лечебный маршрут. Врач может помочь и в ситуациях, связанных не только с алкоголем, но и с наркомании, если семье нужно понять, что происходит с зависимым человеком и какой следующий шаг будет для него безопасным.
Узнать больше – запой нарколог на дом в воронеже
Lestergog · April 15, 2026 at 8:00 am
После употребления алкоголя состояние может быстро ухудшиться: появляется головная боль, тошнота, головокружение и слабость. Это следствие того, что в организме накапливаются токсины, продукты распада этанола и нарушается водно-электролитный баланс. С помощью капельницы от похмелья можно быстро справиться с интоксикацией, восполнить недостающие элементы и облегчить состояние пациента. В клинике «Частный медик 24» в Самаре мы предлагаем капельницы, которые помогают снять все неприятные симптомы похмелья, восстанавливая работу организма и минимизируя риски для здоровья.
Получить дополнительную информацию – kapelnicza-ot-pokhmelya-samara.ru/
https://cpa.tg/ · April 15, 2026 at 9:13 am
закрытое сообщество арбитражников
DanielSix · April 15, 2026 at 10:05 am
Капельница от похмелья — это один из наиболее эффективных методов экстренной медицинской помощи, который позволяет быстро снять симптомы алкогольной интоксикации и восстановить организм после злоупотребления алкоголем. В наркологической клинике «Частный медик 24» в Самаре мы предоставляем услугу выезда нарколога на дом и капельной терапии для пациентов, испытывающих тяжёлые симптомы похмелья. Это удобный способ получить необходимую помощь без лишнего стресса, сохраняя анонимность и комфорт пациента.
Получить больше информации – капельница от похмелья цена
Lestergog · April 15, 2026 at 10:38 am
Процесс лечения начинается с консультации врача, который оценивает состояние пациента, его анамнез и определяет, какие процедуры и препараты нужно использовать. В большинстве случаев капельница включает в себя регидратацию, витамины группы B, антиеметики, препараты для улучшения работы печени и почек. Важно, что капельница не только помогает организму вывести токсины, но и восстанавливает нормальную работу всех систем организма, обеспечивая быстрое улучшение самочувствия.
Подробнее можно узнать тут – капельница от похмелья анонимно
https://mymedicalshopx365.top/tetracycline-tablets/ · April 15, 2026 at 11:24 am
https://mymedicalshopx365.top/tetracycline-tablets/
top 10 casino online · April 15, 2026 at 12:58 pm
Wonderful post! We are linking to this particularly great article on our site. Keep up the good writing.
https://sub.elfejewelry.com/ · April 15, 2026 at 1:28 pm
References:
Odds calc
References:
https://skitterphoto.com/photographers/2634777/klemmensen-sehested
Hobertfralt · April 15, 2026 at 1:34 pm
Во всех этих случаях врач нужен не только для облегчения симптомов. Его задача — понять, можно ли ограничиться домашней терапией или уже сейчас необходимо менять маршрут лечения. Именно этот этап и делает домашний выезд профессиональной услугой, а не упрощённой заменой клиники.
Узнать больше – нарколог на дом в воронеже
Robertgrita · April 15, 2026 at 2:13 pm
Коллеги, хороший обзорный материал по SEO и интернет-маркетингу в 2026 году. Автор разбирает тренды: приоритет естественного языка и длинных запросов, рост значимости голосового поиска, учёт поведенческих факторов. Есть пошаговый план выстраивания стратегии и список метрик для отслеживания (CAC, ROI, время на сайте). Полезно для систематизации: https://vlcjq.ru/prodvizhenie-sajtov-seo-i-internet-marketing-v-2026-godu/
Lestergog · April 15, 2026 at 2:15 pm
Процесс лечения начинается с консультации врача, который оценивает состояние пациента, его анамнез и определяет, какие процедуры и препараты нужно использовать. В большинстве случаев капельница включает в себя регидратацию, витамины группы B, антиеметики, препараты для улучшения работы печени и почек. Важно, что капельница не только помогает организму вывести токсины, но и восстанавливает нормальную работу всех систем организма, обеспечивая быстрое улучшение самочувствия.
Узнать больше – капельница от похмелья анонимно самара
Robertgrita · April 15, 2026 at 2:16 pm
Коллеги, отличный структурированный гид по SEO. Автор последовательно разбирает фундамент (техническая исправность, Core Web Vitals, индексация), семантику и кластеризацию запросов, контент с доказательством экспертизы (E-E-A-T), внешние факторы и локальное SEO. Отдельно радует раздел про аналитику и управление на основе данных. Для системного подхода — самое то: https://planetaunity.ru/prodvizhenie-sajtov-polnyj-gid-po-seo/
Lestergog · April 15, 2026 at 2:37 pm
Капельница от похмелья в Самаре с подбором препаратов, улучшением самочувствия и наблюдением в наркологической клинике «Частный медик 24»
Получить больше информации – капельница от похмелья на дому в самаре
India escorts service · April 15, 2026 at 4:18 pm
Fantastic piece of writing here1
blogfreely.net · April 15, 2026 at 5:28 pm
References:
Acheter de la testostérone
References:
https://mapleprimes.com/users/whorlmile8
ClaytonLaf · April 15, 2026 at 5:33 pm
Первичный осмотр включает оценку витальных показателей, уровня сознания, выраженности симптомов и факторов риска. После этого врач определяет объём вмешательства и приступает к терапии. В большинстве случаев применяется инфузионное лечение, направленное на восстановление водного баланса и выведение токсинов.
Подробнее можно узнать тут – наркологическая помощь в нижнем новгороде
Darylcof · April 15, 2026 at 5:38 pm
Вывод из запоя на дому в Санкт-Петербурге с выездом нарколога, детоксикацией и восстановлением состояния в наркологической клинике «Частный медик 24»
Ознакомиться с деталями – вывод из запоя на дому круглосуточно
GabrielVar · April 15, 2026 at 5:56 pm
В Санкт-Петербурге вывод из запоя на дому используется в ситуациях, когда состояние пациента требует медицинской помощи, но позволяет обойтись без лечения в стационаре. Врач проводит консультацию, оценивает длительность запоя, выраженность симптомов и общее состояние, анализируя данные пациента, после чего принимает решение о тактике лечения при алкоголизме. При необходимости можно оформить вызов специалиста или заказать услугу заранее.
Получить больше информации – вывод из запоя на дому круглосуточно санкт-петербург
Leonardnog · April 15, 2026 at 6:19 pm
После оформления вызова нарколог приезжает к пациенту и проводит комплексную оценку состояния. Врач измеряет давление, частоту пульса, оценивает уровень сознания и выраженность симптомов. На основании полученных данных формируется план лечения, который реализуется сразу на месте.
Подробнее – http://www.domen.ru
MichealJails · April 15, 2026 at 6:25 pm
В Санкт-Петербурге услуга срочного вывода из запоя на дому востребована в ситуациях, когда состояние пациента ухудшается и требуется немедленная помощь. Врач проводит консультацию, оценивает общее состояние, длительность запоя и выраженность симптомов, после чего определяет тактику лечения при алкоголизме. При необходимости помощь оказывается в кратчайшие сроки, без ожидания госпитализации в стационаре. Услугу можно заказать заранее или срочно через сайт клиники.
Узнать больше – вывод из запоя на дому цена
candy-bonanza · April 15, 2026 at 7:25 pm
Quem registrou histórico de sessão evoluiu mais na tomada de decisão.
Patrickfep · April 15, 2026 at 7:29 pm
Ключевым преимуществом вызова нарколога на дом является то, что лечение начинается в тот момент, когда оно особенно необходимо. Близкие пациента не должны волноваться о поиске клиники или медицинских центров в экстренной ситуации — помощь будет оказана немедленно, с минимальными затратами времени и без стресса для пациента.
Узнать больше – https://narkolog-na-dom-samara-1.ru/
RichardDaume · April 15, 2026 at 7:37 pm
Есть состояния, при которых откладывать вызов врача рискованно. Домашний выезд нужен не только при «тяжёлом похмелье», но и тогда, когда самочувствие становится нестабильным, а попытки справиться своими силами уже не работают. Ниже перечислены ситуации, при которых обращение за помощью оправдано именно в ближайшее время, а не «если не станет легче к вечеру».
Узнать больше – вызов нарколога на дом в воронеже
https://cforcestudio.com/index.php?option=com_k2&view=item&id=4>https://themeanderingstream.com/img_1579-2/ · April 15, 2026 at 8:46 pm
https://cforcestudio.com/index.php?option=com_k2&view=item&id=4>https://themeanderingstream.com/img_1579-2/
RandyRaf · April 15, 2026 at 9:10 pm
Нарколог на дом — это формат помощи, который особенно ценен в тот момент, когда человеку плохо уже сейчас, а поездка в клинику только усиливает риск. Домашний выезд позволяет быстро провести осмотр, оценить степень интоксикации, признаки обезвоживания, нагрузку на сердце, уровень тревоги, выраженность тремора и понять, можно ли безопасно помочь пациенту на месте. В наркологической клинике «Частный медик 24» такой формат строится не вокруг одной процедуры, а вокруг последовательного медицинского решения: врач приезжает, собирает анамнез, проводит консультация, определяет, какие вмешательства действительно необходимы, и только после этого подбирает домашний маршрут стабилизации. Это особенно важно при алкоголизма, когда близкие часто путают тяжёлое похмелье, абстинентный синдром и состояния, при которых уже нельзя терять время.
Подробнее тут – http://narkolog-na-dom-voronezh-1.ru
Herbertdum · April 15, 2026 at 9:39 pm
Есть состояния, при которых откладывать вызов врача рискованно. Домашний выезд нужен не только при «тяжёлом похмелье», но и тогда, когда самочувствие становится нестабильным, а попытки справиться своими силами уже не работают. Ниже перечислены ситуации, при которых обращение за помощью оправдано именно в ближайшее время, а не «если не станет легче к вечеру».
Подробнее – запой нарколог на дом в воронеже
casinos-bonos-bienvenida-gratis-sin-deposito · April 15, 2026 at 9:50 pm
Entrada no Pix e saque rápido continuam liderando as escolhas.
Michaeljax · April 15, 2026 at 10:05 pm
При первой консультации нарколог осматривает пациента, чтобы оценить его состояние и подобрать оптимальную схему лечения. В зависимости от тяжести похмелья, врач может назначить инфузию с регидратационными растворами, витаминами группы B и другими препаратами, которые способствуют восстановлению. Важно, что капельница не только помогает снять симптомы, но и устраняет причины токсического воздействия алкоголя на организм, предотвращая развитие осложнений.
Узнать больше – капельница от похмелья на дому самара
fortune-tiger-demo-gratis · April 15, 2026 at 10:45 pm
Hoje venceu quem soube parar na hora certa.
ClaytonLaf · April 15, 2026 at 11:24 pm
Первичный осмотр включает оценку витальных показателей, уровня сознания, выраженности симптомов и факторов риска. После этого врач определяет объём вмешательства и приступает к терапии. В большинстве случаев применяется инфузионное лечение, направленное на восстановление водного баланса и выведение токсинов.
Получить больше информации – наркологическая помощь на дому
Darylcof · April 15, 2026 at 11:40 pm
Вывод из запоя на дому в Санкт-Петербурге с выездом нарколога, детоксикацией и восстановлением состояния в наркологической клинике «Частный медик 24»
Разобраться лучше – http://vyvod-iz-zapoya-na-domu-sankt-peterburg-8.ru
GabrielVar · April 15, 2026 at 11:58 pm
В Санкт-Петербурге вывод из запоя на дому используется в ситуациях, когда состояние пациента требует медицинской помощи, но позволяет обойтись без лечения в стационаре. Врач проводит консультацию, оценивает длительность запоя, выраженность симптомов и общее состояние, анализируя данные пациента, после чего принимает решение о тактике лечения при алкоголизме. При необходимости можно оформить вызов специалиста или заказать услугу заранее.
Узнать больше – https://vyvod-iz-zapoya-na-domu-sankt-peterburg-11.ru
com-slot · April 16, 2026 at 12:28 am
Fortune Rabbit aparece como alternativa equilibrada.
Matthewdrefe · April 16, 2026 at 12:34 am
Нарколог на дом в Воронеже с круглосуточным вызовом врача, стабилизацией состояния и лечением в наркологической клинике «Частный медик 24»
Узнать больше – http://www.domen.ru
Robertmah · April 16, 2026 at 1:27 am
Доступна удобная демо версия Sun of Egypt, которая позволяет познакомиться с игрой без регистрации. Отличный вариант для новичков.
Source:
https://sun-ofegypt.com/
Sun of Egypt
Robertmah · April 16, 2026 at 1:35 am
Откройте удобный сайт для игры Sun of Egypt и начните знакомство с популярным слотом. Красочная графика, атмосферная музыка и бонусные раунды делают игровой процесс захватывающим и динамичным.
Source:
https://sun-ofegypt.com/
Sun of Egypt
333bet-casino · April 16, 2026 at 1:38 am
Fortune Dragon manteve engajamento alto entre curiosos.
Robertmah · April 16, 2026 at 1:39 am
Вы можете играть в Sun of Egypt онлайн без ограничений. Слот доступен на разных устройствах и предлагает стабильную работу, интересные функции и высокий уровень отдачи для игроков.
Source:
https://sun-ofegypt.com/
Sun of Egypt
Robertmah · April 16, 2026 at 1:46 am
Популярная игра Sun of Egypt онлайн сочетает в себе простые правила и увлекательный геймплей, который понравится как новичкам, так и опытным игрокам.
Source:
https://sun-ofegypt.com/
Sun of Egypt
Robertmah · April 16, 2026 at 1:52 am
Начните играть в Sun of Egypt онлайн прямо сейчас. Игра доступна с любого устройства и дарит атмосферу Древнего Египта с шансом на крупный выигрыш.
Source:
https://sun-ofegypt.com/
Sun of Egypt
Robertmah · April 16, 2026 at 2:00 am
Выбирая лучшие казино для Sun of Egypt, обращайте внимание на бонусы и лицензию. Это обеспечит честный игровой процесс и приятный опыт.
Source:
https://sun-ofegypt.com/
Sun of Egypt
Robertmah · April 16, 2026 at 2:13 am
Откройте для себя Sun of Egypt игровой автомат онлайн и насладитесь классическим форматом слота с современными функциями, бонусами и атмосферным оформлением древнего Египта.
Source:
https://sun-ofegypt.com/
Sun of Egypt
sporting-bet · April 16, 2026 at 2:15 am
Bônus de cadastro chama atenção, mas o saque rápido decide tudo.
feng-shui-prosperidade-casa · April 16, 2026 at 2:30 am
Fortune Rabbit cresceu em preferência entre perfis conservadores.
Patrickfep · April 16, 2026 at 2:30 am
Нарколог на дом может помочь в следующих ситуациях:
Изучить вопрос глубже – врач нарколог на дом
Charlesvible · April 16, 2026 at 2:54 am
узнать накрутка отзывов авито
RichardDaume · April 16, 2026 at 3:41 am
Нарколог на дом в Воронеже с оперативным приездом специалиста, детоксикацией и медицинским наблюдением в наркологической клинике «Частный медик 24»
Получить дополнительную информацию – запой нарколог на дом в воронеже
hedgedoc.eclair.ec-lyon.fr · April 16, 2026 at 4:08 am
References:
Entree holland casino
References:
https://hackmd.okfn.de/s/H1CQbLT3Zx
writeablog.net · April 16, 2026 at 4:32 am
References:
Testosteron mediation
References:
https://squareblogs.net/bronzetulip0/testosteron-kaufen-legal-und-rezeptfrei
Charlesvible · April 16, 2026 at 4:54 am
нажмите здесь отзывы за деньги на объявление авито
BruceDah · April 16, 2026 at 5:00 am
Наркологическая помощь на дому помогает избежать стресса, связанного с поездкой в клинику. Особенно это важно в случаях, когда пациент находится в состоянии тяжёлой интоксикации или переживает абстинентный синдром, который можно только усугубить дополнительной нагрузкой. Врач приедет в кратчайшие сроки, обеспечивая необходимое лечение в первые часы после ухудшения состояния. Также важно, что при выезде специалист гарантирует полную анонимность, что особенно важно для многих людей, которые боятся открыто признаться в своей проблеме. Профессиональная наркологическая помощь на дому позволяет избежать срыва и начать процесс восстановления без стресса.
Подробнее тут – нарколог на дом вывод воронеж
Charlesbew · April 16, 2026 at 5:13 am
посмотреть в этом разделе накрутка отзывов вайлдберриз тг
Charlesbew · April 16, 2026 at 5:39 am
посетить сайт вывод в топ озон
RandyRaf · April 16, 2026 at 5:46 am
Такие симптомы важны не только сами по себе. Они показывают, что организму уже трудно поддерживать стабильность без медицинского вмешательства. Чем дольше в этот момент ждать, тем выше вероятность, что потребуется более жёсткий формат оказания помощи. Поэтому экстренное обращение в некоторых случаях не просто облегчает состояние, а предотвращает дальнейшее ухудшение здоровья.
Ознакомиться с деталями – нарколог на дом цена
ClaytonLaf · April 16, 2026 at 5:54 am
Необходимость обращения за наркологической помощью определяется по совокупности симптомов и их выраженности. При ухудшении состояния важно ориентироваться на объективные признаки, а не ждать самостоятельного улучшения.
Исследовать вопрос подробнее – http://narkologicheskaya-pomoshh-nizhnij-novgorod-8.ru/
Darylcof · April 16, 2026 at 6:23 am
Вывод из запоя на дому в Санкт-Петербурге с выездом нарколога, детоксикацией и восстановлением состояния в наркологической клинике «Частный медик 24»
Углубиться в тему – вывод из запоя на дому цена санкт-петербург
GabrielVar · April 16, 2026 at 6:46 am
Чаще всего домашний формат применяется при следующих состояниях:
Получить дополнительные сведения – нарколог на дом вывод из запоя санкт-петербург
Michaeljax · April 16, 2026 at 6:56 am
Капельница от похмелья в Самаре с устранением симптомов интоксикации и контролем состояния в наркологической клинике «Частный медик 24»
Разобраться лучше – капельница от похмелья цена в самаре
DanielSix · April 16, 2026 at 7:00 am
Капельница от похмелья в Самаре с выездом на дом, восстановлением водного баланса и медицинской помощью в наркологической клинике «Частный медик 24»
Получить дополнительную информацию – капельница от похмелья анонимно самара
ClaytonLaf · April 16, 2026 at 7:56 am
Наркологическая помощь в Нижнем Новгороде с выездом врача, капельницами и наблюдением пациента в наркологической клинике «Частный медик 24»
Ознакомиться с деталями – оказание наркологической помощи
RobertMum · April 16, 2026 at 7:59 am
Выбор наркологической клиники — ответственное решение, от которого зависит не только эффективность терапии, но и общее физическое и психоэмоциональное состояние пациента. Квалифицированная помощь должна быть своевременной, организованной и соответствующей медицинским стандартам. Как указывает Минздрав РФ, медицинские учреждения, предоставляющие помощь при зависимостях, обязаны иметь лицензию, профессиональный персонал и комплексный подход к лечению.
Изучить вопрос глубже – http://narkologicheskaya-klinika-murmansk0.ru/narkologicheskaya-klinika-otzyvy-marmansk/https://narkologicheskaya-klinika-murmansk0.ru
sporting-bet · April 16, 2026 at 8:14 am
Fortune Rabbit ganhou força entre quem prefere ritmo mais estável.
EfrainUnpag · April 16, 2026 at 8:28 am
Нарколог на дом в Воронеже с быстрым выездом, индивидуальным подбором терапии и наблюдением в наркологической клинике «Частный медик 24»
Получить дополнительные сведения – вызвать нарколога на дом воронеж
Darylcof · April 16, 2026 at 8:32 am
Вывод из запоя на дому в Санкт-Петербурге с выездом нарколога, детоксикацией и восстановлением состояния в наркологической клинике «Частный медик 24»
Углубиться в тему – вывод из запоя на дому анонимно санкт-петербург
Charlesbew · April 16, 2026 at 8:56 am
смотреть здесь вб отзывы купить
GabrielVar · April 16, 2026 at 8:58 am
Выезд врача начинается с оценки состояния пациента. Доктора измеряют давление, пульс, оценивают уровень сознания и выраженность симптомов. После этого формируется план лечения, который реализуется сразу. Такой подход позволяет быстро перейти к стабилизации состояния человека.
Углубиться в тему – http://vyvod-iz-zapoya-na-domu-sankt-peterburg-11.ru/
resurge · April 16, 2026 at 9:00 am
Everything is very open with a very clear description of the challenges. It was definitely informative. Your site is very helpful. Thanks for sharing!
RogerVef · April 16, 2026 at 9:53 am
К ситуациям, при которых используется домашний формат, относятся:
Углубиться в тему – вывод из запоя на дому анонимно в санкт-петербурге
betis-passo-a-passo · April 16, 2026 at 10:28 am
Rodar com metas pequenas e repetíveis está funcionando melhor para muita gente em 2026.
postherefree · April 16, 2026 at 10:33 am
postherefree
Lestergog · April 16, 2026 at 10:44 am
Капельница от похмелья в Самаре с подбором препаратов, улучшением самочувствия и наблюдением в наркологической клинике «Частный медик 24»
Получить дополнительную информацию – капельница от похмелья на дом в самаре
Lestergog · April 16, 2026 at 10:58 am
Капельница от похмелья в Самаре с подбором препаратов, улучшением самочувствия и наблюдением в наркологической клинике «Частный медик 24»
Изучить вопрос глубже – http://kapelnicza-ot-pokhmelya-samara.ru/
DanielSix · April 16, 2026 at 11:42 am
Капельница от похмелья направлена на восстановление водно-электролитного баланса, выведение токсинов, нормализацию работы печени и почек, а также улучшение общего состояния пациента. В клинике «Частный медик 24» мы подходим к каждому случаю индивидуально, учитывая состояние пациента, его анамнез и особенности организма. Важно, чтобы помощь была оказана вовремя, так как откладывание лечения может привести к осложнениям, таким как сердечные проблемы, психозы или нарушения сна. Выезд нарколога на дом в Самаре позволяет быстро начать лечение, не тратя времени на дорогу и дополнительные усилия.
Подробнее можно узнать тут – https://kapelnicza-ot-pokhmelya-samara-1.ru
Darylcof · April 16, 2026 at 11:47 am
Вывод из запоя на дому — это формат наркологической помощи, при котором лечение проводится в привычной для пациента обстановке с выездом врача. Такой подход применяется в ситуациях, когда состояние требует медицинского вмешательства, но не предполагает обязательной госпитализации. В наркологической клинике «Частный медик 24» помощь на дому выстраивается по принципу поэтапной стабилизации: сначала устраняются острые проявления, затем оценивается динамика и при необходимости корректируется терапия.
Разобраться лучше – вывод из запоя на дому анонимно санкт-петербург
CaseySox · April 16, 2026 at 12:00 pm
Запой сопровождается выраженной интоксикацией, нарушением сна, слабостью и нестабильностью работы сердечно-сосудистой системы, что характерно для алкоголизма и других форм зависимости, включая наркомании. Самостоятельный выход из этого состояния может быть затруднён и сопровождаться усилением симптомов. Медицинская помощь на дому позволяет снизить риски и начать восстановление под контролем специалиста, помогая человеку быстрее стабилизировать состояние.
Получить больше информации – http://vyvod-iz-zapoya-na-domu-sankt-peterburg-12.ru/
Darylcof · April 16, 2026 at 12:07 pm
Запой сопровождается выраженной интоксикацией, нарушением сна, слабостью, тревожностью и колебаниями давления, что характерно для алкоголизма и других форм зависимости. При этом самостоятельный выход из состояния часто оказывается затруднённым из-за ухудшения самочувствия и невозможности контролировать симптомы. В таких случаях выезд нарколога позволяет начать лечение без задержек и помочь пациенту снизить нагрузку на организм за счёт отсутствия транспортировки.
Изучить вопрос глубже – анонимный вывод из запоя на дому в санкт-петербурге
GabrielVar · April 16, 2026 at 12:25 pm
Вывод из запоя на дому — это формат медицинской помощи, при котором лечение проводится в привычной для пациента обстановке с использованием инфузионной терапии и врачебного контроля. Такой подход позволяет начать детоксикацию без задержек и снизить нагрузку на организм, связанную с транспортировкой. В наркологической клинике «Частный медик 24» выезд специалиста организуется круглосуточно, а терапия подбирается с учётом текущего состояния пациента.
Получить дополнительную информацию – http://vyvod-iz-zapoya-na-domu-sankt-peterburg-11.ru
AndrewChisM · April 16, 2026 at 2:52 pm
После употребления алкоголя состояние может быстро ухудшиться: появляется головная боль, тошнота, головокружение и слабость. Это следствие того, что в организме накапливаются токсины, продукты распада этанола и нарушается водно-электролитный баланс. С помощью капельницы от похмелья можно быстро справиться с интоксикацией, восполнить недостающие элементы и облегчить состояние пациента. В клинике «Частный медик 24» в Самаре мы предлагаем капельницы, которые помогают снять все неприятные симптомы похмелья, восстанавливая работу организма и минимизируя риски для здоровья.
Выяснить больше – капельница от похмелья вызов на дом самара
https://www.socatral.sn/best-and-more-than-gorgeous-thai-female-top-ten/ · April 16, 2026 at 3:30 pm
References:
King casino
References:
https://wartajavaindo.com/pemdes-ngadirejo-rayakan-nyepi-tahun-baru-caka-1943-bersama-masyarakat-suku-tengger/
Kennethdug · April 16, 2026 at 6:46 pm
В таких ситуациях врач оценивает риски, определяет тактику лечения и при необходимости рекомендует дальнейшую госпитализацию. Однако во многих случаях помощь на дому оказывается достаточной для стабилизации состояния.
Получить больше информации – вызвать нарколога на дом нижний новгород
JosephaDatt · April 16, 2026 at 6:48 pm
Комплексное лечение в наркологическом стационаре включает несколько последовательных этапов, каждый из которых направлен на решение конкретных задач. Начальный этап включает в себя медицинское вмешательство, направленное на устранение токсинов из организма, и стабилизацию общего состояния пациента. Далее начинается реабилитация, которая помогает закрепить достигнутые результаты и восстановить психоэмоциональное состояние пациента. Для выбора подходящего стационара стоит ознакомиться с отзывами и дополнительной информацией о клинике, а также уточнить, в каком районе города она расположена.
Подробнее – наркологическая клиника стационар санкт-петербург
BryanSip · April 16, 2026 at 7:02 pm
Работа с пациентами в наркологическом стационаре начинается с диагностики, которая помогает определить степень зависимости и сопутствующие заболевания. На основе этих данных разрабатывается индивидуальный план лечения. Врачи, наркологи и психотерапевты работают в тесном контакте с пациентом, что позволяет достичь наилучших результатов в процессе восстановления. Важно также убедиться, что клиника имеет необходимую лицензию, а для эффективного лечения могут быть предложены такие процедуры, как прием психотерапевта и кодирование от зависимости.
Выяснить больше – http://narkologicheskij-staczionar-sankt-peterburg-3.ru
Jasonmit · April 16, 2026 at 7:18 pm
Капельница от похмелья — это не просто средство для снятия симптомов, но и эффективный способ быстрого восстановления организма после алкогольной интоксикации. В наркологической клинике «Частный медик 24» в Екатеринбурге мы предоставляем услугу выезда нарколога на дом, что позволяет пациентам получить необходимую медицинскую помощь, не покидая комфорт своей обстановки. Это особенно важно в случае, если состояние пациента серьёзно ухудшилось, и он не может поехать в клинику самостоятельно.
Разобраться лучше – капельница от похмелья анонимно екатеринбург
Robertnot · April 16, 2026 at 7:24 pm
Наркологический стационар с круглосуточным наблюдением предлагает комплексное лечение и восстановление для людей, страдающих от алкогольной или наркотической зависимости. Пациенты получают помощь в условиях стационара, что позволяет устранить риск срыва и обеспечить безопасное и комфортное выздоровление. В таких клиниках работают квалифицированные наркологи, психологи и другие специалисты, которые контролируют процесс реабилитации на всех этапах. В некоторых случаях может потребоваться вывод из запоя с применением капельниц, а также лечение в специализированном центре для более комплексного восстановления.
Ознакомиться с деталями – лечение в наркологическом стационаре в санкт-петербурге
Rodneyhog · April 16, 2026 at 7:27 pm
Наркологический стационар в Санкт-Петербурге: помощь при зависимости, восстановление и круглосуточное наблюдение в наркологической клинике «Похмельная служба»
Подробнее можно узнать тут – http://www.domen.ru
Charlesvible · April 16, 2026 at 8:24 pm
посетить сайт авито отзывы купить
Michaelshoth · April 16, 2026 at 8:35 pm
Капельница от похмелья — это медицинская процедура, направленная на быстрое восстановление организма после алкогольной интоксикации. Она помогает устранить обезвоживание, нормализовать обменные процессы и снизить токсическую нагрузку на внутренние органы. В отличие от домашних методов, инфузионная терапия действует напрямую через кровоток, обеспечивая более быстрый и выраженный эффект.
Узнать больше – капельница от похмелья
Robertboymn · April 16, 2026 at 8:51 pm
В таких ситуациях стационарный уход позволяет обеспечить безопасность пациента, эффективно справиться с его состоянием и подготовить его к дальнейшему лечению или реабилитации. В случае алкоголизма может быть назначена капельница для снятия острых симптомов интоксикации, а также лечение в специализированном центре для комплексного восстановления и профилактики рецидивов.
Подробнее – лечение в наркологическом стационаре санкт-петербург
help · April 16, 2026 at 9:32 pm
You reported it fantastically.
Travismuche · April 16, 2026 at 9:47 pm
После употребления алкоголя организм подвергается сильной нагрузке, и для его нормализации требуется вмешательство профессионалов. Капельница от похмелья помогает организму быстро избавиться от токсинов, восстанавливая его естественные функции. Важно, что капельницы для снятия похмелья не только устраняют симптомы, но и помогают избежать более серьёзных последствий, таких как хроническая интоксикация и проблемы с работой внутренних органов.
Получить дополнительные сведения – капельница от похмелья цена екатеринбург
Anthonyontox · April 16, 2026 at 9:48 pm
Наркологический стационар в Санкт-Петербурге: лечение зависимости, детоксикация и круглосуточный медицинский контроль в наркологической клинике «Похмельная служба»
Получить дополнительные сведения – частный наркологический стационар
Charlesbew · April 16, 2026 at 9:48 pm
перейти на сайт озон отзывы купить
WilliamFASTY · April 16, 2026 at 9:56 pm
Вывод из запоя на дому — это формат наркологической помощи, при котором детоксикация и стабилизация состояния проводятся в привычной для пациента обстановке. Такой подход позволяет начать лечение без задержек и снизить нагрузку на организм, связанную с транспортировкой. В наркологической клинике «Частный медик 24» помощь организована круглосуточно: врач выезжает сразу после обращения и проводит терапию с учётом текущего состояния пациента.
Получить больше информации – вывод из запоя на дому цена санкт-петербург
Kennethaceda · April 16, 2026 at 10:00 pm
Специалисты рекомендуют не откладывать вызов врача, если симптомы похмелья сильно нарушают обычный режим жизни. Чем раньше начнется лечение, тем быстрее произойдет стабилизация состояния. Наркологи также подчеркивают, что капельница от похмелья не является решением проблемы алкоголизма, но она помогает избавиться от острого дискомфорта и подготовить организм к более длительному восстановлению.
Получить дополнительные сведения – капельница от похмелья вызов на дом
Danielonesk · April 16, 2026 at 10:00 pm
Процесс лечения капельницей помогает улучшить состояние пациента уже через короткий период. Важно, что процедура не только снимает симптомы похмелья, но и восстанавливает нормальную работу печени, почек и других органов, пострадавших от токсического воздействия алкоголя. Это помогает предотвратить долгосрочные последствия интоксикации, такие как хроническая усталость, проблемы с органами и психоэмоциональные расстройства.
Разобраться лучше – капельница от похмелья на дому екатеринбург
Baby Generator · April 16, 2026 at 10:14 pm
I’m amazed, I must say. Seldom do I come across a blog that’s both educative and amusing, and without a doubt, you have hit the nail on the head. The issue is something not enough men and women are speaking intelligently about. I am very happy that I found this during my search for something concerning this.
Thomasbup · April 16, 2026 at 10:36 pm
После того как вы вызвали нарколога на дом, врач проводит первичную консультацию и осмотр пациента, чтобы оценить его состояние. На основе полученных данных подбирается подходящая терапия, которая может включать в себя капельницу, препараты для снятия симптомов похмелья и других проблем, связанных с интоксикацией. Процесс лечения проводится с использованием препаратов, которые помогают восстановить нормальное функционирование организма и снять токсическое воздействие алкоголя на сердце, печень и другие органы.
Выяснить больше – http://kapelnicza-ot-pokhmelya-ekaterinburg-6.ru/
https://www.4customprint.com/ · April 16, 2026 at 11:18 pm
Everything is very open with a really clear description of the challenges. It was definitely informative. Your site is very helpful. Many thanks for sharing.
top-teplicy.ru · April 16, 2026 at 11:54 pm
здесь
Kevinsaulp · April 17, 2026 at 12:11 am
Капельница от похмелья с медицинским контролем в Нижнем Новгороде — это эффективный способ восстановления после алкогольной интоксикации, который позволяет быстро и безопасно нормализовать состояние пациента. Основное отличие такой капельницы от домашних методов состоит в том, что вся процедура проходит под контролем профессионалов, что минимизирует риски для здоровья и повышает эффективность лечения.
Узнать больше – капельница от похмелья на дому в нижнем новгороде
JosephaDatt · April 17, 2026 at 12:21 am
Комплексное лечение в наркологическом стационаре включает несколько последовательных этапов, каждый из которых направлен на решение конкретных задач. Начальный этап включает в себя медицинское вмешательство, направленное на устранение токсинов из организма, и стабилизацию общего состояния пациента. Далее начинается реабилитация, которая помогает закрепить достигнутые результаты и восстановить психоэмоциональное состояние пациента. Для выбора подходящего стационара стоит ознакомиться с отзывами и дополнительной информацией о клинике, а также уточнить, в каком районе города она расположена.
Подробнее тут – https://narkologicheskij-staczionar-sankt-peterburg-1.ru/
Kennethdug · April 17, 2026 at 12:23 am
После оформления вызова нарколог приезжает к пациенту и проводит комплексную оценку состояния. Врач измеряет давление, частоту пульса, оценивает уровень сознания и выраженность симптомов. На основании полученных данных формируется план лечения, который реализуется сразу на месте.
Выяснить больше – нарколог на дом нижний новгород
BryanSip · April 17, 2026 at 12:35 am
Наркологический стационар — это специализированное медицинское учреждение, предназначенное для лечения и реабилитации пациентов с зависимостью от алкоголя, наркотиков и других психоактивных веществ. В Санкт-Петербурге существует множество таких учреждений, которые предоставляют комплексную помощь людям, страдающим от зависимости. Лечение в стационаре часто является первым шагом на пути к выздоровлению, особенно в случаях тяжелых зависимостей, когда амбулаторное лечение может не дать должного эффекта. В случае запоя или хронического алкоголизма стационарное лечение может стать необходимым, особенно если выезд на дом не позволяет должным образом контролировать процесс восстановления.
Получить больше информации – наркологическая клиника стационар санкт-петербург
RobertMum · April 17, 2026 at 12:37 am
Как подчёркивает заведующий отделением наркологической помощи НМИЦ психиатрии и наркологии, результат лечения напрямую зависит от уровня подготовки персонала и умения работать в команде.
Выяснить больше – частная наркологическая клиника в мурманске
Jasonmit · April 17, 2026 at 12:45 am
В Екатеринбурге выезд нарколога на дом становится необходимостью, когда симптомы похмелья слишком выражены и пациент не может справиться с ними самостоятельно. Алкогольная интоксикация может привести к ряду проблем, таких как головная боль, слабость, тошнота и рвота, а иногда даже к более серьёзным состояниям, таким как аритмия или психоз. Выезд нарколога на дом позволяет быстро начать лечение, не тратя время на дорогу, что особенно важно в экстренных ситуациях.
Получить дополнительную информацию – http://kapelnicza-ot-pokhmelya-ekaterinburg-7.ru/
Robertmah · April 17, 2026 at 1:19 am
Попробуйте запуск Sun of Egypt в браузере без установки дополнительных программ. Игра быстро загружается, работает стабильно и позволяет сразу погрузиться в атмосферу древних цивилизаций и азартных вращений барабанов.
Source:
https://sun-ofegypt.com/
Sun of Egypt
Robertmah · April 17, 2026 at 1:24 am
Доступна демо версия Sun of Egypt, позволяющая изучить механику игры и протестировать стратегии без риска.
Source:
https://sun-ofegypt.com/
Sun of Egypt
fixDiele · April 17, 2026 at 1:25 am
Для тех, кто ищет информацию по теме “Развитие районов Пензенской области: изменения и перспективы”, есть отличная статья.
Ссылка ниже:
https://guitar-heroes.ru/%d0%b1%d0%b5%d0%b7-%d1%80%d1%83%d0%b1%d1%80%d0%b8%d0%ba%d0%b8/razvitie-rajonov-penzenskoj-oblasti-kak-menyayutsya-demografiya-ekonomika-i-infrastruktura/
Robertmah · April 17, 2026 at 1:29 am
Начните Sun of Egypt играть сейчас и испытайте удачу в популярном слоте. Красочная графика, бонусные символы и простая механика делают игру интересной для широкого круга пользователей.
Source:
https://sun-ofegypt.com/
Sun of Egypt
fixDiele · April 17, 2026 at 1:29 am
Для тех, кто ищет информацию по теме “Как технологии изменяют очереди в медицине”, там просто кладезь информации.
Вот, можете почитать:
https://billboard-s.ru/%d0%b1%d0%b5%d0%b7-%d1%80%d1%83%d0%b1%d1%80%d0%b8%d0%ba%d0%b8/ocheredi-v-zdravoohranenii-kak-zapis-k-vrachu-onlajn-kadry-i-metriki-dayut-rezultat/
Robertmah · April 17, 2026 at 1:33 am
Если вы ищете лучшие казино для Sun of Egypt, обратите внимание на платформы с лицензией и щедрыми бонусами. Это повысит ваши шансы на комфортную игру.
Source:
https://sun-ofegypt.com/
Sun of Egypt
Robertmah · April 17, 2026 at 1:39 am
Попробуйте демо-игра Sun of Egypt, чтобы без вложений оценить бонусные раунды и особенности слота.
Source:
https://sun-ofegypt.com/
Sun of Egypt
https://triasportgroup.com/1xbet-promo-code-check-2026-1x200royal-bonus-e130-1xbet-promo-code-list-today-2026-1x200royal-bonus-e130-1xbet-promo-code-today-pakistan-2026-1x200royal-bonus-e130/ · April 17, 2026 at 1:43 am
https://triasportgroup.com/1xbet-promo-code-check-2026-1x200royal-bonus-e130-1xbet-promo-code-list-today-2026-1x200royal-bonus-e130-1xbet-promo-code-today-pakistan-2026-1x200royal-bonus-e130/
Robertmah · April 17, 2026 at 1:50 am
Посетив официальный сайт Sun of Egypt, вы получите доступ к актуальной версии игры. Здесь представлены правила, бонусные возможности и удобный интерфейс для комфортного геймплея.
Source:
https://sun-ofegypt.com/
Sun of Egypt
Michaelshoth · April 17, 2026 at 2:46 am
Капельница от похмелья в Самаре: быстрое снятие интоксикации, восстановление после алкоголя и улучшение самочувствия под контролем специалистов в наркологической клинике «Похмельная служба»
Получить дополнительную информацию – капельница от похмелья анонимно
RobertMum · April 17, 2026 at 3:11 am
Критерий
Узнать больше – наркологическая клиника
GoodiniCrubs · April 17, 2026 at 3:19 am
Капельница от похмелья применяется, когда симптомы интоксикации становятся выраженными и мешают нормальной жизнедеятельности пациента. Основные показания для использования капельницы включают:
Углубиться в тему – капельница от похмелья вызов на дом самара
Robertboymn · April 17, 2026 at 4:20 am
В таких ситуациях стационарный уход позволяет обеспечить безопасность пациента, эффективно справиться с его состоянием и подготовить его к дальнейшему лечению или реабилитации. В случае алкоголизма может быть назначена капельница для снятия острых симптомов интоксикации, а также лечение в специализированном центре для комплексного восстановления и профилактики рецидивов.
Ознакомиться с деталями – https://narkologicheskij-staczionar-sankt-peterburg-2.ru/
Williamdut · April 17, 2026 at 4:31 am
посетить веб-сайт https://images.google.co.ma/url?q=https://travelanswer.ru/questions/otely-gural-belek-stoit-li-vibraty-dlya-otdiha.html
подробнее · April 17, 2026 at 5:43 am
подробнее
WilliamFASTY · April 17, 2026 at 5:46 am
Детоксикация на дому начинается с осмотра пациента. Доктора оценивают витальные показатели, уровень сознания и выраженность симптомов, анализируя текущие данные. После этого формируется план лечения, который реализуется сразу. Такой подход позволяет сократить время до начала терапии и повысить её эффективность.
Исследовать вопрос подробнее – vyvod-iz-zapoya-na-domu-sankt-peterburg-10.ru/
Danielonesk · April 17, 2026 at 6:28 am
Капельница от похмелья может быть необходима в самых разных ситуациях, когда симптомы становятся слишком выраженными и мешают нормальному функционированию пациента. Если вы или ваши близкие сталкиваетесь с такими признаками, как сильная головная боль, рвота, слабость и головокружение, то немедленный вызов нарколога на дом станет необходимостью. Важно не откладывать помощь, так как интоксикация может усугубить состояние пациента и привести к осложнениям, таким как обезвоживание или нарушения работы сердца.
Детальнее – капельница от похмелья вызов на дом
JosephaDatt · April 17, 2026 at 6:53 am
При наличии зависимости от алкоголя или наркотиков часто возникает ситуация, когда самостоятельные попытки избавиться от проблемы не дают результата. В таких случаях обращение в наркологический стационар становится необходимым для более глубокой и профессиональной помощи. Стационарное лечение предполагает круглосуточный контроль и медицинскую помощь, что особенно важно при острых состояниях, таких как алкогольная интоксикация или наркотическое отравление. В процессе лечения могут быть предложены кодирование, а также вывод из запоя или наркотической зависимости, а при необходимости — длительный прием с возможностью лечения на летний период.
Подробнее – наркологическая помощь стационар
RobertSmawn · April 17, 2026 at 6:53 am
Когда человек сталкивается с симптомами похмелья, такие как головная боль, тошнота, слабость, головокружение, важно быстро принять меры, чтобы предотвратить развитие более серьёзных проблем. Капельница от похмелья помогает в этом, выводя токсины из организма, восстанавливая нормальное функционирование внутренних органов и возвращая пациента к нормальной жизни. Важно, что мы обеспечиваем полную анонимность на всех этапах лечения, что особенно важно для тех, кто не хочет, чтобы его зависимость стала известна.
Выяснить больше – kapelnicza-ot-pokhmelya-ekaterinburg-6.ru/
Stepanlet · April 17, 2026 at 6:57 am
Полиуретановое покрытие выбрал специально — производитель даёт 50 лет гарантии. Отталкивает грязь, дождь смывает загрязнения сам. После года эксплуатации крыша выглядит как новая. металлочерепица 0.45 мм для дачи
Stepanlet · April 17, 2026 at 7:05 am
Металлочерепица 0.5 мм с широким листом — монтаж ускоряется на 25%. Гарантия 20 лет. Перепады от -50 до +80 выдерживает без каких-либо проблем и деформаций. металлочерепица 0.45 мм для дачи
BryanSip · April 17, 2026 at 7:13 am
Работа с пациентами в наркологическом стационаре начинается с диагностики, которая помогает определить степень зависимости и сопутствующие заболевания. На основе этих данных разрабатывается индивидуальный план лечения. Врачи, наркологи и психотерапевты работают в тесном контакте с пациентом, что позволяет достичь наилучших результатов в процессе восстановления. Важно также убедиться, что клиника имеет необходимую лицензию, а для эффективного лечения могут быть предложены такие процедуры, как прием психотерапевта и кодирование от зависимости.
Подробнее можно узнать тут – наркологическая помощь стационар в санкт-петербурге
Jasonmit · April 17, 2026 at 7:20 am
Капельница от похмелья — это не просто средство для снятия симптомов, но и эффективный способ быстрого восстановления организма после алкогольной интоксикации. В наркологической клинике «Частный медик 24» в Екатеринбурге мы предоставляем услугу выезда нарколога на дом, что позволяет пациентам получить необходимую медицинскую помощь, не покидая комфорт своей обстановки. Это особенно важно в случае, если состояние пациента серьёзно ухудшилось, и он не может поехать в клинику самостоятельно.
Подробнее – https://kapelnicza-ot-pokhmelya-ekaterinburg-7.ru
Williamdut · April 17, 2026 at 8:06 am
страница https://images.google.ch/url?q=https://letundra.com/en/news/?taglist=indigo,the-muscat-international-airport
JosephaDatt · April 17, 2026 at 8:58 am
Обращение в наркологический стационар особенно важно в случае тяжелой зависимости, когда человек не способен контролировать свои действия, а угрозы для здоровья возрастают. В таких случаях важно не откладывать начало лечения, а обратиться за помощью сразу же, чтобы избежать серьезных последствий для организма. При выборе стационара следует обратить внимание на наличие лицензии, а также возможность получения психотерапии и других профессиональных услуг в области наркологии для комплексного лечения зависимости.
Детальнее – наркологический стационар санкт-петербург
https://top-teplicy.ru/ · April 17, 2026 at 9:10 am
здесь
BryanSip · April 17, 2026 at 9:25 am
Работа с пациентами в наркологическом стационаре начинается с диагностики, которая помогает определить степень зависимости и сопутствующие заболевания. На основе этих данных разрабатывается индивидуальный план лечения. Врачи, наркологи и психотерапевты работают в тесном контакте с пациентом, что позволяет достичь наилучших результатов в процессе восстановления. Важно также убедиться, что клиника имеет необходимую лицензию, а для эффективного лечения могут быть предложены такие процедуры, как прием психотерапевта и кодирование от зависимости.
Изучить вопрос глубже – http://narkologicheskij-staczionar-sankt-peterburg-3.ru
Jasonmit · April 17, 2026 at 9:28 am
Капельница от похмелья — это не просто средство для снятия симптомов, но и эффективный способ быстрого восстановления организма после алкогольной интоксикации. В наркологической клинике «Частный медик 24» в Екатеринбурге мы предоставляем услугу выезда нарколога на дом, что позволяет пациентам получить необходимую медицинскую помощь, не покидая комфорт своей обстановки. Это особенно важно в случае, если состояние пациента серьёзно ухудшилось, и он не может поехать в клинику самостоятельно.
Углубиться в тему – капельница от похмелья анонимно
Maryzot · April 17, 2026 at 9:34 am
Здравствуйте!
Не просто ремонт, а полное преображение вашего оборудования
Каждый проект требует индивидуального подхода, и мы это понимаем. Наши специалисты работают с учетом всех особенностей вашего оборудования и потребностей вашего бизнеса. Мы предлагаем не только восстановление работы, но и оптимизацию всех рабочих процессов, чтобы повысить производительность и снизить затраты. С нами ваше оборудование всегда будет работать на высшем уровне, а вы сможете сосредоточиться на других аспектах бизнеса, не переживая о поломках.
Полная информация по ссылке – https://dag-techservice.ru/cases/fasovka.html
монтаж промышленного оборудования презентация, станок с ЧПУ наладка/ремонт, сервисное обслуживание оборудования схема
ввод в эксплуатацию электрооборудования, Техническое обслуживание — DAG TechService, монтаж промышленного оборудования ставрополь
Удачи и комфорта в жизни!
Ваш бизнес на паузе? Мы выведем его на полный ход за несколько часов ea07_f3
sozoarbor.com · April 17, 2026 at 9:37 am
References:
Washington state casinos
References:
https://actifilm.eu/proofing/proofing-ii/
WilliamWar · April 17, 2026 at 10:07 am
Для жителей Екатеринбурга наркологическая клиника «Частный медик 24» предлагает платную услугу выезда врача на дом для проведения капельницы от похмелья. Когда человек переживает сильные симптомы похмелья, такие как головная боль, тошнота, слабость, важно не тянуть с лечением и начать восстановление как можно скорее. Капельница от похмелья помогает хорошо облегчить самочувствие пациента, снять головную боль и улучшить общее состояние, восстановив водно-электролитный баланс в организме.
Выяснить больше – http://kapelnicza-ot-pokhmelya-ekaterinburg-4.ru
RonaldZet · April 17, 2026 at 10:07 am
Домашний протокол разбит на понятные шаги. В каждом шаге есть цель, действия, что именно мы измеряем и когда сверяем прогресс. Это делает процесс прозрачным и даёт семье чувство контроля: видно, почему назначено именно это и когда ждать облегчения.
Подробнее – нарколог на дом недорого петрозаводск
MarvinNoing · April 17, 2026 at 10:34 am
Анонимное лечение на дому ценно ещё и тем, что снижает внутреннее сопротивление самого пациента. Для многих людей первый контакт с врачом происходит именно дома, без дороги, без ожидания, без страха чужих взглядов. Такой формат помогает начать разговор не только о снятии острых симптомов, но и о более широких вопросах: что делать после выхода из запоя, когда требуется кодирование, в каких случаях нужна реабилитация, а когда первичная наркологическая помощь уже должна переходить в полноценный лечебный маршрут. Врач может помочь и в ситуациях, связанных не только с алкоголем, но и с наркомании, если семье нужно понять, что происходит с зависимым человеком и какой следующий шаг будет для него безопасным.
Детальнее – запой нарколог на дом воронеж
Maryzot · April 17, 2026 at 10:43 am
Здравствуйте!
Премиум обслуживание для вашего оборудования
Представьте, что ваше оборудование работает с максимальной эффективностью, а простои — это не ваша реальность. Мы предлагаем услуги, которые не только восстанавливают работу оборудования, но и помогают сделать его более мощным и экономичным. Мы используем новейшие технологии и проверенные методы, чтобы ваша техника стала надежной, долговечной и более производительной.
Полная информация по ссылке – https://dag-techservice.ru/services/commissioning.html
сервисное обслуживание морского оборудования, модернизация старой линии с внедрением ПЛК, монтаж промышленного оборудования ставрополь
ремонт шкафов управления, Услуги — DAG TechService, сервисное обслуживание мед оборудования
Удачи и комфорта в жизни!
Ваше оборудование не может ждать — мы приедем быстрее, чем вы думаете a323d7b
Robertgrita · April 17, 2026 at 11:13 am
Ребята, это реально полный гид! Автор подробно разбирает ключевые изменения в SEO 2026 года: генеративная выдача, нулевой клик (более 60% запросов получают ответ прямо в выдаче), персонализация. Отдельные блоки — про техническую оптимизацию с ужесточёнными Core Web Vitals (LCP ? 1,8 с), про контент-маркетинг и семантику, про ссылочное продвижение и локальное SEO. Есть таблица с метриками и целевыми значениями. Очень структурно: https://wow-eng.ru/polnyj-gid-po-seo-i-internet-marketingu-dlya-prodvizheniya-sajtov-v-2026-godu/
Robertgrita · April 17, 2026 at 11:16 am
Ребята, очень современный гайд! Автор объясняет, как изменился маркетинг с приходом Search Generative Experience (SGE) и GEO. Ключевые темы: оптимизация под генеративные ответы ИИ (цитируемость, структурированные данные), контентная стратегия с фокусом на личный опыт и E-E-A-T 2.0, техническое SEO 2026 (INP, Edge SEO, Green SEO). Также разбираются визуальный и голосовой поиск, Social SEO и гиперлокальное продвижение с AR-навигацией. Очень актуально: https://aikidovaenga.ru/stati/prodvizhenie-sajtov-polnoe-rukovodstvo-po-seo-i-internet-marketingu-v-2026-godu/
https://top-teplicy.ru/ · April 17, 2026 at 11:20 am
https://top-teplicy.ru/
Jasonmit · April 17, 2026 at 12:36 pm
В Екатеринбурге выезд нарколога на дом становится необходимостью, когда симптомы похмелья слишком выражены и пациент не может справиться с ними самостоятельно. Алкогольная интоксикация может привести к ряду проблем, таких как головная боль, слабость, тошнота и рвота, а иногда даже к более серьёзным состояниям, таким как аритмия или психоз. Выезд нарколога на дом позволяет быстро начать лечение, не тратя время на дорогу, что особенно важно в экстренных ситуациях.
Детальнее – капельница от похмелья
https://laureltonelectric.cityrankersllc.com/the-power-of-effective-communication-in-business · April 17, 2026 at 12:41 pm
References:
100 play video poker
References:
https://alternative.media/sotomayor-slams-attorneys-argument-during-oral-arguments-for-the-tennessee-ban-on-minor-trans-care/
Jasonmit · April 17, 2026 at 12:58 pm
Капельница от похмелья — это не просто средство для снятия симптомов, но и эффективный способ быстрого восстановления организма после алкогольной интоксикации. В наркологической клинике «Частный медик 24» в Екатеринбурге мы предоставляем услугу выезда нарколога на дом, что позволяет пациентам получить необходимую медицинскую помощь, не покидая комфорт своей обстановки. Это особенно важно в случае, если состояние пациента серьёзно ухудшилось, и он не может поехать в клинику самостоятельно.
Подробнее – капельница от похмелья анонимно екатеринбург
ueno-test.sakura.ne.jp · April 17, 2026 at 1:07 pm
References:
Lodge casino
References:
https://prsmonitoramento.com.br/ja-ouviu-falar-em-gsgv/
slot-pg-soft · April 17, 2026 at 2:44 pm
Wild Bandito agradou quem gosta de jogo agressivo com controle.
www.fj-tokyo.jp · April 17, 2026 at 2:45 pm
References:
Illinois casinos
References:
https://www.matravel.co.za/if-you-are-interested-in-a-masturbator-toy-but-not-into-the/
Davidaxono · April 17, 2026 at 3:15 pm
Капельница от похмелья — это эффективный способ снятия симптомов алкогольной интоксикации, который позволяет быстро восстановить организм после длительного употребления алкоголя. В наркологической клинике «Частный медик 24» в Екатеринбурге мы предлагаем капельную терапию, которая включает в себя комплекс препаратов для восстановления водно-электролитного баланса, выведения токсинов и нормализации состояния пациента. Процедура проводится в удобной обстановке, и мы обеспечиваем полное наблюдение врача на протяжении всего процесса лечения.
Получить дополнительные сведения – капельница от похмелья вызов на дом екатеринбург
Williamdut · April 17, 2026 at 3:23 pm
нажмите, чтобы подробнее https://images.google.com.qa/url?q=https://letundra.com/ru/news/?taglist=petrozavodsk,rzhd
EmmettAporn · April 17, 2026 at 3:35 pm
Срочная медицинская помощь на дому позволяет не только стабилизировать состояние пациента, но и начать его восстановление без стресса, связанного с поездкой в клинику. Врач приедет с необходимым оборудованием и медикаментами, чтобы провести все необходимые процедуры и помочь пациенту стабилизировать состояние в домашних условиях.
Получить дополнительную информацию – запой нарколог на дом самара
色情色情色情色情 · April 17, 2026 at 3:37 pm
色情
JefferyMew · April 17, 2026 at 3:40 pm
Капельница от похмелья — это эффективный способ экстренной помощи, предназначенный для того, чтобы помочь организму быстро восстановиться после злоупотребления алкоголем. В наркологической клинике «Частный медик 24» в Самаре мы предоставляем услугу безопасной детоксикации и восстановления 24/7. Капельница помогает организму вывести токсины, восстановить водно-электролитный баланс и улучшить общее состояние пациента, не создавая дополнительных нагрузок на сердце, печень и почки.
Получить дополнительную информацию – капельница от похмелья анонимно в самаре
HarveySax · April 17, 2026 at 3:45 pm
Нарколог на дом — это формат медицинской помощи, при котором пациент получает лечение без посещения стационара. В наркологической клинике «Частный медик 24» в Нижнем Новгороде такая услуга используется при острых состояниях: запой, выраженная алкогольная интоксикация, абстинентный синдром, а также при необходимости срочного вмешательства без транспортировки больного. Выезд врача позволяет начать терапию в первые часы ухудшения состояния, что снижает риск осложнений и облегчает переносимость лечения.
Детальнее – вызвать нарколога на дом в нижнем новгороде
https://ingoanews.com/kerala-tourists-robbed-at-goa-cottage-mobile-phones-worth-₹3-lakh-stolen · April 17, 2026 at 3:47 pm
References:
Oneida casino green bay
References:
http://suzuhai.sakura.ne.jp/bbs/light.cgi/light.cgi?res=7814
new online casino · April 17, 2026 at 3:51 pm
Thanks a bunch for sharing this with all people you really recognize what you are talking about! Bookmarked. Kindly also seek advice from my web site =). We can have a link alternate contract between us!
ScottJat · April 17, 2026 at 4:20 pm
Во всех этих случаях важен не только сам факт выезда, но и то, что врач умеет быстро определить границы домашнего лечения. Нарколог на дом нужен не для того, чтобы любой ценой оставить пациента в квартире, а для того, чтобы выбрать безопасный путь: домашняя стабилизация, повторный визит, амбулаторное продолжение или перевод в стационар.
Подробнее тут – нарколог на дом воронеж
Irish casino sites · April 17, 2026 at 4:25 pm
Good points – – it will make a difference with my parents.
RobertDault · April 17, 2026 at 4:47 pm
К основным показаниям относятся:
Подробнее можно узнать тут – http://vyvod-iz-zapoya-na-domu-sankt-peterburg-8.ru/
StephenDiumn · April 17, 2026 at 4:54 pm
Вывод из запоя в стационаре — это медицинская помощь, при которой лечение проводится в условиях постоянного врачебного контроля и поэтапной стабилизации состояния. Такой формат применяется, когда состояние пациента требует наблюдения и быстрого реагирования на изменения. В наркологической клинике «Частный медик 24» в Нижнем Новгороде лечение выстраивается на основе клинической оценки и последовательного подхода: каждый этап направлен на достижение конкретного результата без избыточной нагрузки на организм.
Разобраться лучше – вывод из запоя вызов
Williamdut · April 17, 2026 at 4:55 pm
продолжить https://images.google.com.ni/url?q=https://travelanswer.ru/questions/kak-puteshestvovaty-iz-milana-v-tallinn-cherez-rossiyu-vizovie-i-valyutnie-voprosi.html
Edwardattix · April 17, 2026 at 5:21 pm
Капельница от похмелья может быть необходима в самых разных ситуациях, когда симптомы становятся слишком выраженными и мешают нормальному функционированию пациента. Если вы или ваши близкие сталкиваетесь с такими признаками, как сильная головная боль, рвота, слабость и головокружение, то немедленный вызов нарколога на дом станет необходимостью. Важно не откладывать помощь, так как интоксикация может усугубить состояние пациента и привести к осложнениям, таким как обезвоживание или нарушения работы сердца.
Подробнее можно узнать тут – капельница от похмелья екатеринбург
GoodiniCrubs · April 17, 2026 at 5:29 pm
Такие критерии помогают определить, когда необходим более строгий контроль и постоянное наблюдение. В стационаре создаются условия, при которых лечение проходит без внешних факторов, влияющих на состояние пациента. При этом услуга может предоставляться анонимно, а цену лечения можно уточнить заранее по телефону или при обращении.
Разобраться лучше – вывод из запоя капельница на дому
Jamestrire · April 17, 2026 at 5:45 pm
Обращение в наркологический стационар особенно важно в случае тяжелой зависимости, когда человек не способен контролировать свои действия, а угрозы для здоровья возрастают. В таких случаях важно не откладывать начало лечения, а обратиться за помощью сразу же, чтобы избежать серьезных последствий для организма. При выборе стационара следует обратить внимание на наличие лицензии, а также возможность получения психотерапии и других профессиональных услуг в области наркологии для комплексного лечения зависимости.
Получить дополнительную информацию – https://narkologicheskij-staczionar-sankt-peterburg-1.ru/
Discount code GCC stores · April 17, 2026 at 5:50 pm
I had fun reading this post. I want to see more on this subject.. Gives Thanks for writing this nice article.. Anyway, I’m going to subscribe to your rss and I wish you write great articles again soon.
kasyno online · April 17, 2026 at 6:19 pm
Great write-up, I am a big believer in placing comments on sites to inform the blog writers know that they’ve added something advantageous to the world wide web!
Najlepsze kasyna online · April 17, 2026 at 6:24 pm
Greetings… your blog is very interesting and beautifully written.
DavidPeart · April 17, 2026 at 6:42 pm
Капельница от похмелья с мягким восстановлением представляет собой процедуру введения растворов и препаратов, которые помогают организму плавно восстановиться после злоупотребления алкоголем. Мягкость восстановления заключается в постепенном введении препаратов, которые не вызывают резких изменений в организме, таких как сильное снижение давления или резкое улучшение состояния, что особенно важно при лечении зависимости. Это позволяет избежать перегрузки организма и обеспечивает более плавный переход к нормальному состоянию, при этом подобные услуги могут сочетаться с кодированием и дальнейшим лечением в стационаре, где учитываются индивидуальные цены и особенности состояния пациента.
Получить дополнительную информацию – капельница от похмелья на дому в самаре
isugar-dating.com · April 17, 2026 at 7:25 pm
santa claran casino
https://smartastream.com/@halleykaestner?page=about smartastream.com
https://myhealthypunjab.com/@nanmaum5105305?page=about myhealthypunjab.com
https://worship.com.ng/lincolnlincoln https://worship.com.ng/lincolnlincoln
https://ns2.asso-web.com/darwinevatt88 https://ns2.asso-web.com/darwinevatt88
http://z.duowenlvshi.com/melainematheso z.duowenlvshi.com
https://git.archieri.fr/arturolundgren git.archieri.fr
https://digitalafterlife.org/@carinmcquay893?page=about digitalafterlife.org
https://alurmusic.com/robin949768507 https://alurmusic.com/robin949768507
https://git.vsadygv.com/bettiemunday0 https://git.vsadygv.com/bettiemunday0
https://blackvision.co.uk/@vanbracken827?page=about blackvision.co.uk
https://git.zakum.cn/genevievecudmo git.zakum.cn
https://www.ttd.group/williestoll609 https://www.ttd.group/
https://shiatube.org/@charissashelly?page=about https://shiatube.org/@charissashelly?page=about
https://645123.com/@zellacasey298?page=about https://645123.com
https://code.nspoc.org/xsntony4963025 code.nspoc.org
https://gitea.johannes-hegele.de/lateshamoncrie gitea.johannes-hegele.de
http://rm.runfox.com/gitlab/allisonparas0 rm.runfox.com
https://git.vezpi.com/latanyafusco07 https://git.vezpi.com/latanyafusco07
References:
https://git.freno.me/selenapuig4147
https://megastream.pl · April 17, 2026 at 7:29 pm
wms slots online
https://vydiio.com/@logan89159783?page=about vydiio.com
https://flirta.online/@jgnpriscilla96 https://flirta.online/@jgnpriscilla96
https://play.eccentric.etc.br/@harrietthumphr?page=about https://play.eccentric.etc.br/@harrietthumphr?page=about
https://lius.familyds.org:3000/alana375816079 lius.familyds.org
https://koseongnam.com/henryrff257296 koseongnam.com
https://srsbkn.eu.org/herminekwok71 srsbkn.eu.org
https://platform.giftedsoulsent.com/felipeepps1228 platform.giftedsoulsent.com
https://gt.clarifylife.net/tresabridges26 gt.clarifylife.net
http://gitea.jb1000.com:88/carrilapine079 gitea.jb1000.com
https://git.archieri.fr/arturolundgren https://git.archieri.fr/arturolundgren
https://hellomusic.app/alvapaine1789 hellomusic.app
https://www.telugustatusvideo.com/@dickdoran7865?page=about https://www.telugustatusvideo.com/
https://profmustafa.com/@laurenmtm73697?page=about https://profmustafa.com/
http://musicstreaming.yonetsystems.com/lonniewise8924 musicstreaming.yonetsystems.com
https://git.ihatemen.uk/georgiasquires git.ihatemen.uk
https://www.itubee.com/@berenicebridge?page=about http://www.itubee.com
https://video.silverwolfstudios.com/@milagrohindwoo?page=about video.silverwolfstudios.com
https://ccn-tv.news/@maureenmcclure?page=about ccn-tv.news
References:
https://mp3diary.com/brookchirnside
GeorgeGlync · April 17, 2026 at 7:32 pm
Вывод из запоя на дому в Санкт-Петербурге с подбором терапии, наблюдением врача и комфортным лечением в наркологической клинике «Частный медик 24»
Подробнее тут – нарколог на дом вывод из запоя
JeffreyGom · April 17, 2026 at 7:40 pm
Состояние пациента при интоксикации может развиваться по-разному: от умеренной слабости и головной боли до выраженной дезориентации, тахикардии и нарушений сна. В таких ситуациях важно не откладывать обращение за помощью. Наркологическая помощь на дому рассматривается, когда требуется быстрое вмешательство и контроль состояния без транспортировки пациента.
Получить дополнительную информацию – наркологическая помощь анонимно нижний новгород
Williambek · April 17, 2026 at 7:41 pm
Вывод из запоя на дому в Санкт-Петербурге с выездом специалиста, стабилизацией состояния и медицинской поддержкой в наркологической клинике «Частный медик 24»
Разобраться лучше – вывод из запоя на дому круглосуточно
mejores casinos · April 17, 2026 at 7:44 pm
I like your style!
WalterSic · April 17, 2026 at 7:52 pm
Наркологический стационар с круглосуточным наблюдением — это не просто место для детоксикации, но и пространство для комплексного лечения и реабилитации. Постоянное присутствие медицинского персонала помогает избежать опасных ситуаций, таких как психозы или физиологические сбои, характерные для абстиненции. Прием пациентов может включать кодирование, а также индивидуальные программы лечения, которые разрабатываются в зависимости от состояния пациента и его потребностей на протяжении года.
Получить больше информации – https://narkologicheskij-staczionar-sankt-peterburg.ru
WilliamOptop · April 17, 2026 at 8:08 pm
Чаще всего помощь требуется при следующих состояниях:
Получить дополнительные сведения – вывод из запоя на дому
kasyno online · April 17, 2026 at 8:09 pm
You are my inhalation , I possess few web logs and very sporadically run out from to brand 🙁
RodolfoDap · April 17, 2026 at 8:17 pm
В таких ситуациях стационарный уход позволяет обеспечить безопасность пациента, эффективно справиться с его состоянием и подготовить его к дальнейшему лечению или реабилитации. В случае алкоголизма может быть назначена капельница для снятия острых симптомов интоксикации, а также лечение в специализированном центре для комплексного восстановления и профилактики рецидивов.
Получить больше информации – частный наркологический стационар в санкт-петербурге
https://reruberrypi.rerurate.com/ · April 17, 2026 at 8:20 pm
basic strategy blackjack
https://git.adityagupta.dev/melindabown087 git.adityagupta.dev
https://bigotube.com/@joanzinn573766?page=about bigotube.com
https://tcodpractice.com/mirtahatten056 tcodpractice.com
https://www.ikaros.asia/phyllisjordon https://www.ikaros.asia/phyllisjordon
https://git.clubeye.net/jedvansickle71 git.clubeye.net
https://gitea.gimmin.com/dustyaeh08140 gitea.gimmin.com
https://code.ownwire.net/cecilayounger1 https://code.ownwire.net/
https://git.smart-tool.jp/sadieworthy157 git.smart-tool.jp
https://tcodpractice.com/sung3740105300 tcodpractice.com
http://git.yanei-iot.com:600/emilieefa97124 http://git.yanei-iot.com:600/emilieefa97124
https://gitea.jobiglo.com/ashli61f181649 gitea.jobiglo.com
https://mindsworks.org/@koxaustin06165?page=about https://mindsworks.org/@koxaustin06165?page=about
https://pure.itsabouttimetv1.com/@damariseldersh?page=about https://pure.itsabouttimetv1.com/@damariseldersh?page=about
https://unired.zz.com.ve/@karafikes6837 unired.zz.com.ve
https://git.slegeir.com/alberthagayle git.slegeir.com
https://financevideosmedia.com/@paige85y17075?page=about https://financevideosmedia.com/
https://ceedmusic.com/nellroy9125184 ceedmusic.com
https://i10audio.com/celia587471078 https://i10audio.com
References:
https://iesoundtrack.tv/@horaciogarber?page=about
git.htns.com · April 17, 2026 at 8:35 pm
mint casino
http://spnewstv.com/@imogenpeterson?page=about http://spnewstv.com/
https://codes.tools.asitavsen.com/moses62843913 codes.tools.asitavsen.com
https://mginger.org/@loriecourtney https://mginger.org
https://git.gotrobotics.org/leonorhup2854 https://git.gotrobotics.org/leonorhup2854
https://playtube.com.pl/@brittlockhart?page=about https://playtube.com.pl/@brittlockhart?page=about
https://git.clubeye.net/fannietroiano6 git.clubeye.net
https://mindsworks.org/@millieg2304804?page=about https://mindsworks.org/@millieg2304804?page=about
https://git.local.octal.tec.br/emelialoehr984 https://git.local.octal.tec.br/emelialoehr984
https://getskill.work/jeniferi03474 https://getskill.work/jeniferi03474
https://gitea.wuyuank.com/qerjenna519200 https://gitea.wuyuank.com/qerjenna519200
https://gitlab.iplusus.com/brandiestubbs7 https://gitlab.iplusus.com/
https://www.singuratate.ro/@marilynnweathe https://www.singuratate.ro/@marilynnweathe
http://git.ibossay.com:3000/odellz11297861 git.ibossay.com
https://cash.com.tr/@clayruckman833?page=about cash.com.tr
https://actsolution.iptime.org:3000/janessawymark actsolution.iptime.org
https://gitea.wuyuank.com/frederickalutw https://gitea.wuyuank.com/
https://eduback.com/@marlawaring06?page=about eduback.com
https://git.archieri.fr/arturolundgren https://git.archieri.fr
References:
http://app.venusroyale.date/@freddybabbidge
HarryMeazy · April 17, 2026 at 8:37 pm
Постановка капельницы — это не просто средство для снятия головной боли или тошноты, а комплексное восстановление организма. Состав раствора подбирается в зависимости от симптомов и состояния пациента. Врач-нарколог оценивает общее состояние пациента и выбирает наиболее подходящий состав, который будет наиболее эффективен для него. При необходимости может быть предложена дополнительная помощь, включая кодирование от алкогольной зависимости.
Получить больше информации – kapelnicza-ot-pokhmelya-nizhnij-novgorod.ru/
Davidaxono · April 17, 2026 at 8:48 pm
Эти симптомы характерны для алкогольной интоксикации, и их быстрое устранение с помощью капельницы позволяет пациенту почувствовать себя лучше и избежать более серьёзных последствий. В клинике «Частный медик 24» мы подбираем индивидуальную программу лечения, чтобы ускорить восстановление организма и улучшить общее самочувствие пациента.
Получить больше информации – капельница от похмелья на дом
casino en chile online · April 17, 2026 at 8:49 pm
I’ve thought about posting something about this before. Good job! Can I use part of your post in my blog?
GilbertJUrry · April 17, 2026 at 8:55 pm
Процедура капельницы от похмелья с контролем врача в Самаре начинается с первичной консультации, на которой врач осматривает пациента, измеряет его основные показатели (давление, пульс, температуру) и оценивает общее состояние. На основе этих данных выбирается оптимальный состав капельницы, которая может включать в себя различные компоненты, такие как солевые растворы, витамины, антиоксиданты и медикаменты для снятия симптомов похмелья.
Получить дополнительную информацию – http://kapelnicza-ot-pokhmelya-samara-13.ru/
JasonSeiVa · April 17, 2026 at 9:02 pm
“Капельница — это быстрый и эффективный способ восстановить организм после похмелья. Она особенно полезна при выраженных симптомах, таких как сильная головная боль или рвота. Важно, чтобы процедура проводилась квалифицированным медицинским персоналом, чтобы избежать осложнений. Также, в случае хронической зависимости, может потребоваться кодирование или терапия для долгосрочного восстановления, а также вызов врача для дальнейшего наблюдения,”
Исследовать вопрос подробнее – капельница от похмелья анонимно самара
Edwardsak · April 17, 2026 at 9:09 pm
Капельница от похмелья — это медицинская процедура, направленная на быстрое устранение симптомов алкогольной интоксикации и восстановление нормальной работы организма. При выраженном похмельном синдроме самостоятельные методы часто оказываются недостаточными, поскольку не воздействуют на причины состояния. В наркологической клинике «Похмельная служба» используется инфузионная терапия с круглосуточным выездом специалиста, что позволяет начать лечение сразу после обращения.
Детальнее – капельница от похмелья цена воронеж
Charlesdig · April 17, 2026 at 9:22 pm
Капельница от похмелья в Самаре: быстрое снятие интоксикации, восстановление после алкоголя и улучшение самочувствия под контролем специалистов в наркологической клинике «Похмельная служба»
Детальнее – капельница от похмелья вызов на дом
meilleur casino en ligne Canada · April 17, 2026 at 9:54 pm
Hey, I simply hopped over to your website by way of StumbleUpon. No longer one thing I’d normally learn, but I preferred your thoughts none the less. Thanks for making one thing worth reading.
GoodiniCrubs · April 17, 2026 at 10:04 pm
Капельницы помогают не только справиться с симптомами похмелья, но и с выводом токсинов из организма, что способствует его быстрому восстановлению. Этот метод позволяет минимизировать последствия, такие как головная боль, нарушение давления и общее недомогание.
Узнать больше – капельница от похмелья на дому
RobertDault · April 17, 2026 at 10:55 pm
Вывод из запоя на дому — это формат наркологической помощи, при котором лечение проводится в привычной для пациента обстановке с выездом врача. Такой подход применяется в ситуациях, когда состояние требует медицинского вмешательства, но не предполагает обязательной госпитализации. В наркологической клинике «Частный медик 24» помощь на дому выстраивается по принципу поэтапной стабилизации: сначала устраняются острые проявления, затем оценивается динамика и при необходимости корректируется терапия.
Узнать больше – вывод из запоя на дому цена
WilliamWar · April 17, 2026 at 11:12 pm
Капельница от похмелья в Екатеринбурге с устранением слабости, тошноты и последствий интоксикации в наркологической клинике «Частный медик 24»
Получить дополнительную информацию – капельница от похмелья на дом
naijasingles.net · April 17, 2026 at 11:34 pm
casino montelago
https://git.cymnb.com/mariapackard62 git.cymnb.com
https://video.silverwolfstudios.com/@milagrohindwoo?page=about https://video.silverwolfstudios.com/@milagrohindwoo?page=about
https://dreamplacesai.de/trudicorso6114 dreamplacesai.de
https://tea.neuron.my/virgiliowhitis https://tea.neuron.my/virgiliowhitis
https://21pac.com/@alinadesmond7?page=about 21pac.com
https://silatdating.com/@olen8275895448 silatdating.com
http://www.tm-jikayo.com/earlmoyes0516 http://www.tm-jikayo.com
https://git.automathon.org/hiramrohde6284 https://git.automathon.org/hiramrohde6284
https://git.dieselor.bg/darwin84819129 git.dieselor.bg
https://www.zapztv.com/@ifdhelena52087?page=about zapztv.com
https://deltasongs.com/chautimmerman https://deltasongs.com/chautimmerman
https://www.herzog-it.de/teresaknapp574 http://www.herzog-it.de
https://wiibiplay.fun/@jasperfzf96485?page=about wiibiplay.fun
https://vidspaceaiapp.com/@gabrielebyerly?page=about https://vidspaceaiapp.com/
https://tovegans.tube/@claranealy9758?page=about tovegans.tube
https://playtube.com.pl/@brittlockhart?page=about https://playtube.com.pl/
https://gitea.shizuka.icu/mickivanotterl https://gitea.shizuka.icu/
https://vila.go.ro/stanleyporteou vila.go.ro
References:
https://isugar-dating.com/@garrettforsyth
https://gitea.yantootech.com/dietermileham4 · April 17, 2026 at 11:51 pm
south african online casinos
http://git.dglyoo.com/rosadown677644 git.dglyoo.com
https://www.ituac.com/rosellabate875 https://www.ituac.com/rosellabate875
https://www.singuratate.ro/@daltonnicastro http://www.singuratate.ro
https://cloudtu.be/@ceciliaremley?page=about https://cloudtu.be/
https://git.cyberuk.me/zenaidafaith35 https://git.cyberuk.me/
https://gitea.gimmin.com/beryl19z266643 gitea.gimmin.com
https://git.refinementservices.com/bartbanvard497 https://git.refinementservices.com
https://volts.howto.co.ug/@ethelbruce1193 https://volts.howto.co.ug/@ethelbruce1193
https://rjlove.org/@cesarkrichauff https://rjlove.org/
https://mambotango.it/albertobastyan https://mambotango.it/albertobastyan
https://git.nulldirect.com/lawannahannell https://git.nulldirect.com/
https://gitea.syn-assist.fr/loydmulkey6284 gitea.syn-assist.fr
https://www.godhip.com/latanyanelson http://www.godhip.com
https://profmustafa.com/@laurenmtm73697?page=about https://profmustafa.com/@laurenmtm73697?page=about
https://www.peter-bartke.de/wpxsyreeta7233 http://www.peter-bartke.de
http://xeroworld.team/omerparramore1 xeroworld.team
https://cloveebiz.com.ng/@valentinapelle?page=about cloveebiz.com.ng
https://git.mana-web.com/amymcdonough82 git.mana-web.com
References:
https://beatsong.app/lizziej3571499
https://www.ttd.group/ · April 18, 2026 at 12:10 am
william hill casino mobile
https://hero-cloud-stg-code.cnbita.com/elouisemcgee93 hero-cloud-stg-code.cnbita.com
https://rjlove.org/@cesarkrichauff rjlove.org
https://git.0935e.com/irenesalmon613 https://git.0935e.com
https://niqnok.com/hannawoodall38 niqnok.com
https://www.kornerspot.com/@estelablaubaum https://www.kornerspot.com
https://playtube.com.pl/@brittlockhart?page=about playtube.com.pl
https://gitea.micro-stack.org/bertiefolk1357 https://gitea.micro-stack.org/
https://cash.com.tr/@gabriellenowla?page=about cash.com.tr
https://friztty.com/@ellenalbiston friztty.com
https://tayartaw.kyaikkhami.com/elvabrehm2935 tayartaw.kyaikkhami.com
https://niqnok.com/nicolasmartins https://niqnok.com/nicolasmartins
https://gitea.scivigi.com/theresekroger2 gitea.scivigi.com
https://neuralkazmain.com/rolandkeyes869 neuralkazmain.com
https://www.oddmate.com/@pasqualestrode http://www.oddmate.com
https://dotvdo.com/@christinkuster?page=about https://dotvdo.com/@christinkuster?page=about
https://choosy.cc/@joycecarl66760 https://choosy.cc/
https://www.itubee.com/@berenicebridge?page=about https://www.itubee.com/@berenicebridge?page=about
https://www.itubee.com/@berenicebridge?page=about itubee.com
References:
https://rsas.de/shalandawaid91
gitea.amazingcoders.com · April 18, 2026 at 12:13 am
william hill online casino
https://actsolution.iptime.org:3000/aimeethornburg https://actsolution.iptime.org
https://git.rmarl.in/rosiecode22757 git.rmarl.in
http://newborhooddates.com/@ehyjosette5920 newborhooddates.com
https://git.123doit.com/chandattr8160 https://git.123doit.com/chandattr8160
https://gitslayer.de/melindaholland https://gitslayer.de/melindaholland
https://gitea.yantootech.com/finnkiek471057 gitea.yantootech.com
https://git.freno.me/duanecress6171 git.freno.me
https://katambe.com/@ninachristian2 katambe.com
https://git.nulldirect.com/lawannahannell git.nulldirect.com
https://vidspaceaiapp.com/@franciscamuham?page=about https://vidspaceaiapp.com/@franciscamuham?page=about
https://git.adityagupta.dev/melindabown087 git.adityagupta.dev
https://nelgit.nelpi.co.uk/melvakastner7 nelgit.nelpi.co.uk
https://www.herzog-it.de/dallashardaway https://www.herzog-it.de
https://viddertube.com/@rauly712780174?page=about https://viddertube.com/
https://myhealthypunjab.com/@ipkramiro8359?page=about myhealthypunjab.com
https://viraltubex.com/@retarader9892?page=about viraltubex.com
https://eduback.com/@terrelldonoghu?page=about eduback.com
https://vxtube.net/@damonbroadbent?page=about https://vxtube.net/@damonbroadbent?page=about
References:
https://git.wikiofdark.art/alyssanewbold
https://klimaexpress-tube.de/@haiclifton2627?page=about · April 18, 2026 at 12:53 am
casinos en linea
https://www.ohovideo.com/@austinripley78?page=about ohovideo.com
http://git.520hx.vip/joshtimmons30 http://git.520hx.vip/joshtimmons30
https://gitea.wuyuank.com/qerjenna519200 https://gitea.wuyuank.com/qerjenna519200
https://koseongnam.com/maricruz04x155 https://koseongnam.com/
https://git.scinalytics.com/pmbnilda220675 https://git.scinalytics.com/pmbnilda220675
https://theudtaullu.com/@flynnmcdonald?page=about theudtaullu.com
https://gitea.brmm.ovh/sonwilhelm952 gitea.brmm.ovh
https://streamifyr.com/@denesemcculloc?page=about streamifyr.com
https://git.lucas-michel.fr/franciscaselby git.lucas-michel.fr
https://emphira.app/@simadoi1625848 emphira.app
https://csmtube.exagopartners.com/@amparowiles42?page=about https://csmtube.exagopartners.com/@amparowiles42?page=about
https://mambotango.it/albertobastyan mambotango.it
https://hiwifi.denq.us:8418/jaymethow63893 hiwifi.denq.us
http://repo.magicbane.com/rosalind97t834 repo.magicbane.com
https://cloveebiz.com.ng/@margaritoashbo?page=about cloveebiz.com.ng
https://vlotube.com/@jannettekonig?page=about vlotube.com
https://git.zakum.cn/genevievecudmo git.zakum.cn
https://git.nathanspackman.com/corneliusmedle https://git.nathanspackman.com
References:
https://git.vhdltool.com/jessikax51460
https://apyarx.com · April 18, 2026 at 12:55 am
slots online
https://qpxy.cn/arturodooley56 qpxy.cn
http://git.qniao.cn/gladisnewcombe git.qniao.cn
https://dyipniflix.com/site/@lavernstreetma?page=about dyipniflix.com
http://git.fbonazzi.it/felicitascastl http://git.fbonazzi.it
https://funnyutube.com/@belenault9953?page=about https://funnyutube.com/
https://git.nathanspackman.com/bqkbrian806205 https://git.nathanspackman.com/bqkbrian806205
https://sing.ibible.hk/@uwecampbell75?page=about https://sing.ibible.hk/@uwecampbell75?page=about
https://git.louislabs.com/meistevens124 git.louislabs.com
https://www.kornerspot.com/@geraldoculler https://www.kornerspot.com/@geraldoculler
https://isugar-dating.com/@roderick604581 isugar-dating.com
https://music.1mm.hk/mpkhanna01008 https://music.1mm.hk/
http://z.duowenlvshi.com/mauricekirsova http://z.duowenlvshi.com/mauricekirsova
https://git.freno.me/pabloertel3783 git.freno.me
https://traficut.com/@bennywhitworth?page=about https://traficut.com/
https://git.cymnb.com/mariapackard62 git.cymnb.com
https://qarisound.com/houston193054 qarisound.com
https://loopplay.site/@wayne861340812?page=about loopplay.site
https://124.70.144.1/margaretafitzp https://124.70.144.1/
References:
https://greenopps420.com/@jewelcastello4?page=about
Jamestrire · April 18, 2026 at 12:57 am
Наркологический стационар в Санкт-Петербурге: лечение зависимости, детоксикация и круглосуточный медицинский контроль в наркологической клинике «Похмельная служба»
Изучить вопрос глубже – narkologicheskij-staczionar-sankt-peterburg-1.ru/
AndrewChisM · April 18, 2026 at 1:22 am
Процесс лечения начинается с консультации врача, который оценивает состояние пациента, его анамнез и определяет, какие процедуры и препараты нужно использовать. В большинстве случаев капельница включает в себя регидратацию, витамины группы B, антиеметики, препараты для улучшения работы печени и почек. Важно, что капельница не только помогает организму вывести токсины, но и восстанавливает нормальную работу всех систем организма, обеспечивая быстрое улучшение самочувствия.
Подробнее – капельница от похмелья на дом
GoodiniCrubs · April 18, 2026 at 1:38 am
Такие критерии помогают определить, когда необходим более строгий контроль и постоянное наблюдение. В стационаре создаются условия, при которых лечение проходит без внешних факторов, влияющих на состояние пациента. При этом услуга может предоставляться анонимно, а цену лечения можно уточнить заранее по телефону или при обращении.
Узнать больше – вывод из запоя на дому недорого
gitea.biboer.cn · April 18, 2026 at 1:58 am
minnesota casinos
https://gitea.adber.tech/nestorwoollard https://gitea.adber.tech/nestorwoollard
https://git.123doit.com/keriholton9650 git.123doit.com
https://nonstopvn.net/@romanoldham552?page=about nonstopvn.net
https://theudtaullu.com/@flynnmcdonald?page=about theudtaullu.com
https://www.jo-line.eu/georgiajoske36 http://www.jo-line.eu
https://hellomusic.app/alvapaine1789 hellomusic.app
https://hiwifi.denq.us:8418/fayesemmens09 https://hiwifi.denq.us:8418/fayesemmens09
https://k0ki-dev.com/keenanibr67348 k0ki-dev.com
https://worship.com.ng/lincolnlincoln https://worship.com.ng
https://vidmero.com/@corazonholcomb?page=about vidmero.com
https://hellomusic.app/kathleenpownal https://hellomusic.app
https://homeablazebyhispresence.dennmachinery.com/@joycelynrowntr?page=about homeablazebyhispresence.dennmachinery.com
https://wedioz.com/@archerscherf0?page=about wedioz.com
http://gitea.mikarsoft.com/claudettevanwi gitea.mikarsoft.com
https://git.0935e.com/senaida18e081 https://git.0935e.com/senaida18e081
https://gt.clarifylife.net/tresabridges26 gt.clarifylife.net
https://reoflix.com/@elmerhorowitz5?page=about reoflix.com
https://git.refinementservices.com/bartbanvard497 https://git.refinementservices.com/
References:
https://git.lucas-michel.fr/paulinelondon0
https://gitea.personalsoftware.space/zcjkeri007150 · April 18, 2026 at 2:32 am
wheel of fortune slot machines
https://romatube.com/@charlesb660845?page=about https://romatube.com
https://dgwork.co.kr/antoniettay37 dgwork.co.kr
https://mkhonto.net/@jessmatos85401?page=about mkhonto.net
https://gitea.scivigi.com/johnathanferri gitea.scivigi.com
https://code.dsconce.space/blanche1218598 code.dsconce.space
https://www.singuratate.ro/@susanangelo53 http://www.singuratate.ro
https://sing.ibible.hk/@amparoandrzeje?page=about sing.ibible.hk
https://vcs.cozydsp.space/leia45q0812916 vcs.cozydsp.space
http://git.520hx.vip/edwardnapier3 git.520hx.vip
https://abadeez.com/@rosalynmontalv?page=about abadeez.com
https://actsolution.iptime.org:3000/lilykitamura3 actsolution.iptime.org
https://www.panjabi.in/@wilsonbaumgart?page=about http://www.panjabi.in
https://gbewaaplay.com/friedalieb016 https://gbewaaplay.com/friedalieb016
https://www.k0ki-dev.de/latishabrandt http://www.k0ki-dev.de
https://hellomusic.app/kathleenpownal hellomusic.app
https://lovcam.mydaddyonline.in/@eulatesch37540 https://lovcam.mydaddyonline.in/
https://katambe.com/@felixnixon568 https://katambe.com
https://www.bongmedia.tv/@modestogolden?page=about https://www.bongmedia.tv/@modestogolden?page=about
References:
https://walmtv.com/@morasurratt742?page=about
GeorgeGlync · April 18, 2026 at 2:52 am
В Санкт-Петербурге услуга вывода из запоя на дому применяется в ситуациях, когда требуется медицинская помощь, но нет показаний к стационарному лечению. Врач проводит консультацию, оценивает состояние пациента, длительность употребления и выраженность симптомов, после чего принимает решение о тактике лечения при алкоголизме. Важно, что терапия начинается сразу после осмотра, а при необходимости можно заранее заказать выезд специалистов.
Исследовать вопрос подробнее – http://www.domen.ru
Williambek · April 18, 2026 at 3:06 am
Такие условия позволяют начать лечение без задержек и обеспечить более мягкое восстановление. При этом помощь может предоставляться анонимно.
Получить больше информации – вывод из запоя на дому круглосуточно санкт-петербург
Davidaxono · April 18, 2026 at 3:33 am
Процедура проводится опытными наркологами, которые подбирают необходимое лечение на основе индивидуальных особенностей пациента. В клинике «Частный медик 24» применяются только эффективные и безопасные препараты, которые помогают организму восстановиться и избавиться от токсинов. Важно помнить, что капельница от похмелья — это не просто временное облегчение, а важный шаг к долгосрочному восстановлению организма и профилактике алкоголизма.
Углубиться в тему – капельница от похмелья на дому в екатеринбурге
DavidSoict · April 18, 2026 at 4:10 am
Капельница от запоя в Нижнем Новгороде: снятие интоксикации, восстановление организма и помощь при запое под контролем специалистов в наркологической клинике «Похмельная служба»
Получить больше информации – капельница от запоя на дому цена нижний новгород
https://dev01.open-alt.com/twilabutz91912 · April 18, 2026 at 4:41 am
References:
Siloam springs casino
References:
https://git.secretserver.club/reedlindt86136
HarveySax · April 18, 2026 at 4:47 am
В таких ситуациях врач оценивает риски, определяет тактику лечения и при необходимости рекомендует дальнейшую госпитализацию. Однако во многих случаях помощь на дому оказывается достаточной для стабилизации состояния.
Ознакомиться с деталями – нарколог на дом вывод
JefferyMew · April 18, 2026 at 4:54 am
Капельница от похмелья в Самаре с устранением симптомов интоксикации и контролем состояния в наркологической клинике «Частный медик 24»
Подробнее – http://kapelnicza-ot-pokhmelya-samara-2.ru/
gitea.nongnghiepso.com · April 18, 2026 at 4:55 am
north brunswick soccer
https://www.shreegandha.com/@angeles10u6101?page=about http://www.shreegandha.com
https://ceedmusic.com/wallacereynold ceedmusic.com
https://git.gotrobotics.org/eegmeghan39550 git.gotrobotics.org
https://git.vezpi.com/latanyafusco07 git.vezpi.com
https://mindsworks.org/@millieg2304804?page=about https://mindsworks.org/
https://gitea.syn-assist.fr/dottybernstein gitea.syn-assist.fr
https://thewordtube.org/@jeroldmarcell?page=about thewordtube.org
https://yourclipz.com/@glindaberube5?page=about yourclipz.com
https://katambe.com/@felixnixon568 katambe.com
https://live.eposbd.net/@lizziereichert?page=about live.eposbd.net
http://git.dglyoo.com/chloekoertig9 git.dglyoo.com
https://viddertube.com/@sonjavalerio77?page=about viddertube.com
https://quickdate.arenascript.de/@marylincolling quickdate.arenascript.de
https://git.nulldirect.com/lenardhayes175 https://git.nulldirect.com/lenardhayes175
https://worship.com.ng/haihupp2733380 worship.com.ng
https://git.archieri.fr/aileenhaney059 git.archieri.fr
https://www.ttd.group/earthaweeks921 https://www.ttd.group/earthaweeks921
https://git.alderautomation.ca/curtisokeeffe0 https://git.alderautomation.ca
References:
https://www.telugustatusvideo.com/@dickdoran7865?page=about
JavierBix · April 18, 2026 at 5:31 am
Главное преимущество такого выезда в том, что лечение начинается сразу. Не нужно ждать утра, искать транспорт, уговаривать человека ехать в тяжёлом состоянии или рисковать, пока он снова тянется к алкоголю, чтобы временно заглушить симптомы. Домашний визит даёт возможность быстро стабилизировать ситуацию и убрать хаотичность, которая часто возникает в семье в острый момент.
Подробнее можно узнать тут – вызвать нарколога на дом
Davidaxono · April 18, 2026 at 5:43 am
Капельница от похмелья — это эффективный способ снятия симптомов алкогольной интоксикации, который позволяет быстро восстановить организм после длительного употребления алкоголя. В наркологической клинике «Частный медик 24» в Екатеринбурге мы предлагаем капельную терапию, которая включает в себя комплекс препаратов для восстановления водно-электролитного баланса, выведения токсинов и нормализации состояния пациента. Процедура проводится в удобной обстановке, и мы обеспечиваем полное наблюдение врача на протяжении всего процесса лечения.
Подробнее можно узнать тут – капельница от похмелья на дому екатеринбург
HarryMeazy · April 18, 2026 at 5:44 am
Постановка капельницы — это не просто средство для снятия головной боли или тошноты, а комплексное восстановление организма. Состав раствора подбирается в зависимости от симптомов и состояния пациента. Врач-нарколог оценивает общее состояние пациента и выбирает наиболее подходящий состав, который будет наиболее эффективен для него. При необходимости может быть предложена дополнительная помощь, включая кодирование от алкогольной зависимости.
Получить больше информации – капельница от похмелья анонимно
RobertDault · April 18, 2026 at 5:55 am
Вывод из запоя на дому — это формат наркологической помощи, при котором лечение проводится в привычной для пациента обстановке с выездом врача. Такой подход применяется в ситуациях, когда состояние требует медицинского вмешательства, но не предполагает обязательной госпитализации. В наркологической клинике «Частный медик 24» помощь на дому выстраивается по принципу поэтапной стабилизации: сначала устраняются острые проявления, затем оценивается динамика и при необходимости корректируется терапия.
Получить дополнительную информацию – вывод из запоя на дому анонимно
JasonSeiVa · April 18, 2026 at 5:58 am
“Капельница — это быстрый и эффективный способ восстановить организм после похмелья. Она особенно полезна при выраженных симптомах, таких как сильная головная боль или рвота. Важно, чтобы процедура проводилась квалифицированным медицинским персоналом, чтобы избежать осложнений. Также, в случае хронической зависимости, может потребоваться кодирование или терапия для долгосрочного восстановления, а также вызов врача для дальнейшего наблюдения,”
Ознакомиться с деталями – капельница от похмелья на дому в самаре
Damontof · April 18, 2026 at 6:01 am
Выезд нарколога на дом в Самаре представляет собой структурированный медицинский процесс, направленный на быстрое облегчение состояния пациента и устранение последствий интоксикации. Все этапы оказания помощи проводятся с учетом клинической картины, длительности употребления и индивидуальных особенностей организма. В случае алкоголизма могут быть предложены процедуры кодирования, а также вывод из состояния запоя. При необходимости подключается психиатр для дополнительной оценки и лечения.
Изучить вопрос глубже – http://narkolog-na-dom-samara-6.ru
MarvinNoing · April 18, 2026 at 6:21 am
Для семьи это тоже имеет большое значение. Пока врач в пути, родственники часто совершают одни и те же ошибки: пытаются «отпаивать» человека через силу, смешивают несовместимые медикаменты, дают советы, которые только повышают тревогу, спорят или требуют немедленно взять себя в руки. Профессиональный выезд снимает эту хаотичность. После осмотра врач объясняет, какие симптомы связаны с алкогольной интоксикацией, какие могут указывать на осложнения, что допустимо дома, а что требует перевода в стационар. В этом и состоит ценность выезда: он возвращает контроль над ситуацией и позволяет начать лечение без лишних задержек.
Изучить вопрос глубже – вызов нарколога на дом в воронеже
https://zurimeet.com/@dennisburrows5 · April 18, 2026 at 6:44 am
References:
Lv online store
References:
https://git.archieri.fr/vondarcy239523
WalterProor · April 18, 2026 at 6:57 am
После диагностики нарколог принимает решение о тактике помощи. Если состояние позволяет проводить лечение вне стационара, врач приступает к детоксикации, восстановлению водно-электролитного баланса и симптоматической терапии. При необходимости используются инфузионные растворы, препараты для снижения интоксикации, нормализации сна, уменьшения тревожности и поддержки работы сердечно-сосудистой системы. Все назначения зависят от состояния пациента и не применяются по шаблону. В случае необходимости может быть направлен к психиатру для дальнейшей реабилитации или отправки в стационар на летний период для более интенсивного наблюдения и лечения.
Узнать больше – нарколог на дом самара
CharlesRuh · April 18, 2026 at 6:57 am
Капельница от похмелья в Воронеже с выездом на дом, подбором препаратов и контролем состояния в наркологической клинике «Похмельная служба»
Выяснить больше – капельница от похмелья воронеж
com-slot · April 18, 2026 at 7:13 am
Fortune Rabbit cresceu em preferência entre perfis conservadores.
GilbertJUrry · April 18, 2026 at 7:13 am
Вызов капельницы от похмелья с контролем врача в Самаре рекомендуется, когда симптомы похмелья становятся особенно тяжелыми и мешают нормальной жизнедеятельности. Несмотря на то, что многие пытаются справиться с похмельем с помощью домашних методов, такие как прием жидкости или таблеток, они не всегда оказываются достаточно эффективными. В случае сильных симптомов похмелья, капельница с врачебным контролем — это более безопасное и быстрое решение, при этом возможен вывод в стационаре, анонимное лечение и консультации по вопросам наркомании с учетом актуальной цены услуг.
Изучить вопрос глубже – капельница от похмелья анонимно
JefferyMew · April 18, 2026 at 7:15 am
В Самаре клиника «Частный медик 24» предоставляет круглосуточную помощь по выведению из запоя и снятию симптомов похмелья. Когда человек сталкивается с тяжёлым состоянием после длительного употребления алкоголя, важно вовремя оказать помощь. Врач приедет на дом и проведёт все необходимые процедуры, включая капельницу, которая поможет восстановить водно-электролитный баланс, нормализовать уровень сахара в крови и вывести токсины из организма.
Детальнее – капельница от похмелья цена
Randytup · April 18, 2026 at 7:22 am
Выезд нарколога на дом в Самаре — это комплексный подход к лечению, который включает несколько этапов. Врач, приехавший на место, не ограничивается одной процедурой, а проводит полноценный осмотр, диагностирует состояние пациента, определяет причину ухудшения самочувствия и подбирает индивидуальную терапию. Наиболее часто при выезде нарколога на дом используются капельницы, антиеметики и препараты для стабилизации состояния пациента, снятия симптомов абстиненции и улучшения общего самочувствия.
Выяснить больше – http://narkolog-na-dom-samara-1.ru/
qdate.ru · April 18, 2026 at 7:27 am
video poker jacks or better
https://love2singles.com/@leon5269183431 love2singles.com
https://gbewaaplay.com/quyenmedford73 gbewaaplay.com
https://buzz.gi/@gemmaruggieri?page=about https://buzz.gi/@gemmaruggieri?page=about
https://nrimatchmaking.com/@jedwhitely9476 https://nrimatchmaking.com/@jedwhitely9476
https://v.sharevr.com/@harleykimbroug?page=about v.sharevr.com
https://whiskey.tangomedia.fr/@kendrickprewit?page=about https://whiskey.tangomedia.fr
https://luvmatefreematrimony.com/@veolafinnis572 https://luvmatefreematrimony.com/
https://myafritube.com/@darylstephen12?page=about myafritube.com
https://funnyutube.com/@ethanfinsch65?page=about funnyutube.com
https://vxtube.net/@rhealavallie7?page=about vxtube.net
https://gitea.mynas-lechner.de/linettecowley7 gitea.mynas-lechner.de
https://actv.1tv.hk/@charolettec587?page=about actv.1tv.hk
https://ns2.asso-web.com/marianabolin54 ns2.asso-web.com
https://www.kornerspot.com/@estelablaubaum https://www.kornerspot.com/
https://romancefrica.com/@alfonzo91f573 romancefrica.com
http://gitea.mikarsoft.com/claudettevanwi http://gitea.mikarsoft.com/claudettevanwi
https://ceedmusic.com/kristie32m858 ceedmusic.com
https://play.talkdrove.cc.nf/@almagerrard57?page=about play.talkdrove.cc.nf
References:
https://git.sunlix.one/veronicasinger
volts.howto.co.ug · April 18, 2026 at 8:04 am
make money online australia
https://unitedmusicstreaming.com/roccorusso8388 unitedmusicstreaming.com
https://cloveebiz.com.ng/@haimccomas7864?page=about cloveebiz.com.ng
https://flirta.online/@janellhardie4 flirta.online
https://videyme.online/@dessie21j48582?page=about videyme.online
http://git.mynas71.myds.me/genevievemasco http://git.mynas71.myds.me
https://mambotango.it/lucile80668363 https://mambotango.it/lucile80668363
https://financevideosmedia.com/@diannarabin92?page=about https://financevideosmedia.com/@diannarabin92?page=about
https://stukguitar.com/@joesphfallon39?page=about stukguitar.com
https://buzz.gi/@gemmaruggieri?page=about buzz.gi
https://askmilton.tv/@kirkfairweathe?page=about https://askmilton.tv/@kirkfairweathe?page=about
https://gitea.yantootech.com/dietermileham4 https://gitea.yantootech.com/
https://gitea.ww3.tw/numbersspowers gitea.ww3.tw
https://smartastream.com/@halleykaestner?page=about https://smartastream.com/
http://app.venusroyale.date/@markusspillman app.venusroyale.date
https://theudtaullu.com/@flynnmcdonald?page=about theudtaullu.com
https://git.danpeak.co.uk/millardnorthco git.danpeak.co.uk
https://superocho.org/@josiebriley367?page=about superocho.org
https://i10audio.com/suzannelyall66 i10audio.com
References:
https://dammsound.com/robin177090374
RobertDault · April 18, 2026 at 8:12 am
В Санкт-Петербурге вывод из запоя на дому рассматривается, когда состояние пациента позволяет проводить лечение вне стационара, но требует контроля специалиста. Врач оценивает общее состояние, длительность запоя и выраженность симптомов, после чего принимает решение о формате помощи при алкоголизме. Важно, что лечение начинается сразу после осмотра, без необходимости ожидания госпитализации. При необходимости можно заказать услуги на сайте клиники или получить консультацию специалистов.
Узнать больше – вывод из запоя на дому анонимно санкт-петербург
RobertSmawn · April 18, 2026 at 8:13 am
Капельница от похмелья в Екатеринбурге с медицинским контролем и поддержкой организма в наркологической клинике «Частный медик 24»
Исследовать вопрос подробнее – капельница от похмелья на дому в екатеринбурге
Jasonmit · April 18, 2026 at 8:24 am
Капельница от похмелья — это не просто средство для снятия симптомов, но и эффективный способ быстрого восстановления организма после алкогольной интоксикации. В наркологической клинике «Частный медик 24» в Екатеринбурге мы предоставляем услугу выезда нарколога на дом, что позволяет пациентам получить необходимую медицинскую помощь, не покидая комфорт своей обстановки. Это особенно важно в случае, если состояние пациента серьёзно ухудшилось, и он не может поехать в клинику самостоятельно.
Изучить вопрос глубже – капельница от похмелья вызов на дом екатеринбург
JamesEdumb · April 18, 2026 at 8:36 am
Запой сопровождается выраженной интоксикацией, нарушением сна, нестабильностью давления и изменениями в работе нервной системы. При длительном течении состояние может ухудшаться, и самостоятельный выход становится затруднённым. В таких случаях стационар рассматривается как пространство, где можно безопасно стабилизировать показатели и обеспечить постепенное восстановление.
Детальнее – вывод из запоя дешево нижний новгород
Jasonmit · April 18, 2026 at 8:37 am
Капельница от похмелья — это не просто средство для снятия симптомов, но и эффективный способ быстрого восстановления организма после алкогольной интоксикации. В наркологической клинике «Частный медик 24» в Екатеринбурге мы предоставляем услугу выезда нарколога на дом, что позволяет пациентам получить необходимую медицинскую помощь, не покидая комфорт своей обстановки. Это особенно важно в случае, если состояние пациента серьёзно ухудшилось, и он не может поехать в клинику самостоятельно.
Подробнее тут – http://kapelnicza-ot-pokhmelya-ekaterinburg-7.ru/
Davidaxono · April 18, 2026 at 8:56 am
Капельница от похмелья — это эффективный способ снятия симптомов алкогольной интоксикации, который позволяет быстро восстановить организм после длительного употребления алкоголя. В наркологической клинике «Частный медик 24» в Екатеринбурге мы предлагаем капельную терапию, которая включает в себя комплекс препаратов для восстановления водно-электролитного баланса, выведения токсинов и нормализации состояния пациента. Процедура проводится в удобной обстановке, и мы обеспечиваем полное наблюдение врача на протяжении всего процесса лечения.
Изучить вопрос глубже – капельница от похмелья на дом екатеринбург
gitea.css-sistemas.com.br · April 18, 2026 at 9:10 am
t slot aluminum
https://git.sunlix.one/redai35207943 https://git.sunlix.one/redai35207943
http://gitlab.dev.jtyjy.com/darcyduterrau3 gitlab.dev.jtyjy.com
https://www.beyoncetube.com/@latiakong68499?page=about http://www.beyoncetube.com
https://iraqitube.com/@meitressler568?page=about iraqitube.com
https://superocho.org/@zsfbrandi50319?page=about https://superocho.org
https://tubepeer.com/@kerrioxley251?page=about https://tubepeer.com
https://skytube.skyinfo.in/@vilmakashiwagi?page=about skytube.skyinfo.in
https://gitea.diputadosalta.gob.ar/poerosella6250 gitea.diputadosalta.gob.ar
https://gitea.myat4.com/albertinapreec https://gitea.myat4.com/albertinapreec
https://www.ikaros.asia/wildamoyer0783 https://www.ikaros.asia/wildamoyer0783
https://gitea.brmm.ovh/sonwilhelm952 gitea.brmm.ovh
https://www.atmasangeet.com/rita51u4562938 atmasangeet.com
https://aiviu.app/@kencondon05190?page=about https://aiviu.app/@kencondon05190?page=about
https://git.violka-it.net/tricialouden50 https://git.violka-it.net
https://git.yinbonet.cn/harveyandrade https://git.yinbonet.cn
https://yours-tube.com/@silasvanburen4?page=about yours-tube.com
http://rm.runfox.com/gitlab/georgettamadig rm.runfox.com
https://code.nspoc.org/emorykernot661 https://code.nspoc.org
References:
https://yourclipz.com/@glindaberube5?page=about
Davidaxono · April 18, 2026 at 9:16 am
При похмелье организм страдает от обезвоживания, токсического воздействия алкоголя на внутренние органы и нервную систему. Капельница помогает эффективно восстановить нормальную работу органов, улучшить самочувствие и предотвратить более серьёзные осложнения, такие как нарушение работы сердца или печени. Важно, что капельница от похмелья может быть назначена как для снятия острых симптомов, так и для подготовки к дальнейшей реабилитации.
Получить дополнительную информацию – капельница от похмелья анонимно
HarveySax · April 18, 2026 at 10:27 am
Существует ряд ситуаций, при которых вызов специалиста на дом является обоснованным решением:
Выяснить больше – https://narkolog-na-dom-nizhnij-novgorod.ru/
GoodiniCrubs · April 18, 2026 at 10:35 am
Капельницы помогают не только справиться с симптомами похмелья, но и с выводом токсинов из организма, что способствует его быстрому восстановлению. Этот метод позволяет минимизировать последствия, такие как головная боль, нарушение давления и общее недомогание.
Получить дополнительную информацию – kapelnicza-ot-pokhmelya-samara-1.ru/
JefferyMew · April 18, 2026 at 10:40 am
При первой консультации нарколог осматривает пациента, чтобы оценить его состояние и подобрать оптимальную схему лечения. В зависимости от тяжести похмелья, врач может назначить инфузию с регидратационными растворами, витаминами группы B и другими препаратами, которые способствуют восстановлению. Важно, что капельница не только помогает снять симптомы, но и устраняет причины токсического воздействия алкоголя на организм, предотвращая развитие осложнений.
Изучить вопрос глубже – капельница от похмелья вызов на дом самара
Richardexors · April 18, 2026 at 10:45 am
Выбор наркологического стационара с комфортными условиями требует внимательного подхода, чтобы убедиться, что все аспекты лечения и реабилитации будут выполнены на высоком уровне. Важно учитывать не только медицинскую составляющую, но и то, как созданы условия для пациентов, их психологический комфорт и безопасность на всех этапах лечения. Также стоит учитывать цену за стационарное лечение с круглосуточным наблюдением, чтобы выбрать оптимальный вариант, соответствующий потребностям пациента и его бюджету.
Изучить вопрос глубже – http://narkologicheskij-staczionar-sankt-peterburg-4.ru
HarveySax · April 18, 2026 at 10:50 am
Существует ряд ситуаций, при которых вызов специалиста на дом является обоснованным решением:
Подробнее – запой нарколог на дом нижний новгород
JefferyMew · April 18, 2026 at 11:01 am
Запой, длительное употребление алкоголя или случайное злоупотребление могут привести к неприятным симптомам похмелья, таким как головная боль, слабость, тошнота, головокружение и усталость. Эти симптомы обусловлены тем, что в организме остаются продукты распада алкоголя, которые токсически воздействуют на все органы. Капельница от похмелья на дому — это отличная возможность быстро снять острые симптомы и восстановить нормальное состояние организма, не выходя из привычной обстановки.
Получить дополнительные сведения – капельница от похмелья вызов на дом самара
RobertDault · April 18, 2026 at 11:39 am
Выезд нарколога начинается с осмотра пациента. Доктора измеряют давление, пульс, оценивают уровень сознания и выраженность симптомов. На основании этих данных формируется план лечения, который реализуется сразу на месте. Такой подход позволяет быстро перейти к стабилизации состояния без лишних этапов.
Выяснить больше – vyvod-iz-zapoya-na-domu-sankt-peterburg-8.ru/
WilliamWar · April 18, 2026 at 11:42 am
После употребления алкоголя организм подвергается сильной нагрузке, и для его нормализации требуется вмешательство профессионалов. Капельница от похмелья помогает организму быстро избавиться от токсинов, восстанавливая его естественные функции. Важно, что капельницы для снятия похмелья не только устраняют симптомы, но и помогают избежать более серьёзных последствий, таких как хроническая интоксикация и проблемы с работой внутренних органов.
Разобраться лучше – капельница от похмелья на дому
fletcher-fuentes-2.technetbloggers.de · April 18, 2026 at 11:43 am
References:
Hgh bestellen
References:
https://etuitionking.net/forums/users/beerpimple11/
GeorgeGlync · April 18, 2026 at 11:59 am
В Санкт-Петербурге услуга вывода из запоя на дому применяется в ситуациях, когда требуется медицинская помощь, но нет показаний к стационарному лечению. Врач проводит консультацию, оценивает состояние пациента, длительность употребления и выраженность симптомов, после чего принимает решение о тактике лечения при алкоголизме. Важно, что терапия начинается сразу после осмотра, а при необходимости можно заранее заказать выезд специалистов.
Изучить вопрос глубже – вывод из запоя на дому
RobertDault · April 18, 2026 at 12:01 pm
К основным показаниям относятся:
Углубиться в тему – https://vyvod-iz-zapoya-na-domu-sankt-peterburg-8.ru
Williambek · April 18, 2026 at 12:15 pm
Вывод из запоя на дому в Санкт-Петербурге с выездом специалиста, стабилизацией состояния и медицинской поддержкой в наркологической клинике «Частный медик 24»
Узнать больше – анонимный вывод из запоя на дому в санкт-петербурге
Jamestrire · April 18, 2026 at 12:39 pm
Каждый этап лечения направлен на возвращение пациента к нормальной жизни, восстановление его физического и психического здоровья. Важно отметить, что лечение всегда подбирается индивидуально, в зависимости от стадии зависимости и состояния пациента. Врачи-наркологи детально анализируют все аспекты, чтобы обеспечить наиболее эффективное лечение и помощь на всех этапах восстановления.
Углубиться в тему – лечение в наркологическом стационаре
Richarduticy · April 18, 2026 at 1:32 pm
Капельница от похмелья в Самаре: эффективное снятие интоксикации, восстановление после алкоголя и улучшение самочувствия под контролем специалистов в наркологической клинике «Похмельная служба»
Получить дополнительные сведения – капельница от похмелья цена самара
RichardAbipt · April 18, 2026 at 2:41 pm
Детоксикация на дому начинается с осмотра пациента. Доктора оценивают витальные показатели, уровень сознания и выраженность симптомов, анализируя текущие данные. После этого формируется план лечения, который реализуется сразу. Такой подход позволяет сократить время до начала терапии и повысить её эффективность.
Получить дополнительную информацию – нарколог на дом вывод из запоя
GeorgeGlync · April 18, 2026 at 2:58 pm
Вывод из запоя на дому — это формат медицинской помощи, при котором лечение проводится в привычной для пациента обстановке с выездом нарколога. Такой подход используется, когда требуется срочное вмешательство, но состояние позволяет обойтись без госпитализации. В наркологической клинике «Частный медик 24» помощь оказывается круглосуточно, с возможностью начать терапию сразу после обращения и без ожидания.
Выяснить больше – нарколог на дом вывод из запоя
Williambek · April 18, 2026 at 3:13 pm
Выезд врача начинается с оценки состояния пациента. Доктора измеряют давление, пульс, оценивают уровень сознания и выраженность симптомов. После этого формируется план лечения, который реализуется сразу. Такой подход позволяет быстро перейти к стабилизации состояния человека.
Ознакомиться с деталями – вывод из запоя на дому анонимно в санкт-петербурге
EmmettAporn · April 18, 2026 at 3:26 pm
Нарколог на дом — это удобное и эффективное решение для тех, кто сталкивается с тяжелыми последствиями запоя или алкогольной интоксикации. В наркологической клинике «Частный медик 24» в Самаре мы предоставляем круглосуточную помощь, выезд нарколога и лечение на дому. Это позволяет пациентам получить профессиональную медицинскую помощь в удобной и знакомой обстановке, что особенно важно, когда состояние человека ухудшается после длительного употребления алкоголя или наркотиков.
Подробнее тут – вызвать нарколога на дом самара
DavidSoict · April 18, 2026 at 3:35 pm
Запой — это состояние, которое развивается на фоне длительного употребления алкоголя, сопровождающееся острыми симптомами интоксикации. Капельница от запоя может быть необходима, когда состояние пациента требует немедленного вмешательства. Важно своевременно заметить признаки, указывающие на необходимость медицинской помощи, таких как признаки алкоголизма, и в случае необходимости — кодирование или вывод из запоя для более комплексного лечения.
Выяснить больше – вызов на дом капельницы от запоя
Jamestrire · April 18, 2026 at 4:50 pm
Комплексное лечение в наркологическом стационаре включает несколько последовательных этапов, каждый из которых направлен на решение конкретных задач. Начальный этап включает в себя медицинское вмешательство, направленное на устранение токсинов из организма, и стабилизацию общего состояния пациента. Далее начинается реабилитация, которая помогает закрепить достигнутые результаты и восстановить психоэмоциональное состояние пациента. Для выбора подходящего стационара стоит ознакомиться с отзывами и дополнительной информацией о клинике, а также уточнить, в каком районе города она расположена.
Подробнее можно узнать тут – наркологический стационар
JasonSeiVa · April 18, 2026 at 5:14 pm
“Капельница — это быстрый и эффективный способ восстановить организм после похмелья. Она особенно полезна при выраженных симптомах, таких как сильная головная боль или рвота. Важно, чтобы процедура проводилась квалифицированным медицинским персоналом, чтобы избежать осложнений. Также, в случае хронической зависимости, может потребоваться кодирование или терапия для долгосрочного восстановления, а также вызов врача для дальнейшего наблюдения,”
Углубиться в тему – капельница от похмелья цена самара
Jamestrire · April 18, 2026 at 5:15 pm
Наркологический стационар в Санкт-Петербурге предоставляет пациентам комплексное лечение зависимости от психоактивных веществ. Проблемы, связанные с алкоголизмом, наркоманией и другими формами зависимости, требуют индивидуального подхода и профессиональной помощи. Комплексное лечение в таких учреждениях позволяет не только пройти детоксикацию, но и получить полноценную реабилитацию, что дает пациентам шанс на долгосрочную ремиссию и улучшение качества жизни. В некоторых случаях, при запое или необходимости выезда на дом, может быть предложен центр, где решаются все вопросы, связанные с лечением зависимости и восстановлением пациента.
Получить дополнительную информацию – частный наркологический стационар в санкт-петербурге
WesleyHop · April 18, 2026 at 5:44 pm
После алкоголя в организме накапливаются токсичные продукты распада, нарушается водно-солевой баланс и страдает нервная система, что особенно выражено после запоя или при алкоголизме. Это проявляется головной болью, слабостью, тошнотой и нарушением сна. Капельница помогает ускорить процессы очищения и восстановить внутренние системы, обеспечивая более быстрое облегчение состояния и помогая человеку выйти из состояния запоев.
Узнать больше – капельница от похмелья воронеж
GoodiniCrubs · April 18, 2026 at 5:50 pm
Запой сопровождается комплексом нарушений: обезвоживание, колебания давления, тремор, тревожность, нарушение сна. При длительном течении состояние может усиливаться, и самостоятельный выход становится затруднённым. В таких случаях стационар рассматривается как безопасная среда, где можно контролировать динамику и оперативно реагировать на изменения.
Узнать больше – вывод из запоя дешево нижний новгород
HarryMeazy · April 18, 2026 at 5:51 pm
Капельница от похмелья — это внутривенное введение специально подобранных растворов, которые помогают ускорить выведение токсинов, восстановить водно-электролитный баланс и нормализовать обмен веществ. В состав капельницы могут входить различные компоненты, такие как солевые растворы, витамины, глюкоза и препараты для детоксикации. Она особенно эффективна при последствиях запоя и хронического алкоголизма.
Углубиться в тему – капельница от похмелья анонимно
Damontof · April 18, 2026 at 6:05 pm
Нарколог на дом в Самаре: круглосуточная помощь, вывод из запоя и медицинская поддержка на дому под контролем специалистов в наркологической клинике «Похмельная служба»
Подробнее можно узнать тут – нарколог на дом вывод
https://goodklinic7.top/avalide/ · April 18, 2026 at 6:23 pm
https://goodklinic7.top/avalide/
CharlesRuh · April 18, 2026 at 6:37 pm
Капельница от похмелья в Воронеже с выездом на дом, подбором препаратов и контролем состояния в наркологической клинике «Похмельная служба»
Получить дополнительные сведения – капельница от похмелья цена
LonnieDug · April 18, 2026 at 6:37 pm
Показания к проведению инфузионной терапии включают:
Получить дополнительные сведения – капельница от похмелья на дому воронеж
ScottJat · April 18, 2026 at 6:49 pm
Нарколог на дом в Воронеже с круглосуточным вызовом врача, стабилизацией состояния и лечением в наркологической клинике «Частный медик 24»
Разобраться лучше – вызов нарколога на дом в воронеже
Jasonmit · April 18, 2026 at 7:20 pm
Процедура капельницы от похмелья помогает быстро восстановить нормальное состояние, снимает симптомы интоксикации и восстанавливает работу органов, пострадавших от токсического воздействия алкоголя. Важно, что выезд на дом позволяет избежать стресса, связанного с поездкой в медицинское учреждение, и начать лечение без задержек, что критически важно для ускоренного восстановления здоровья пациента.
Подробнее – капельница от похмелья цена в екатеринбурге
DavidSoict · April 18, 2026 at 7:20 pm
Врач-нарколог, оценивая состояние пациента, может рекомендовать проведение капельницы для ускоренного восстановления организма. Применение капельницы позволяет снять острые симптомы интоксикации и снизить риск развития более серьезных последствий. В некоторых случаях, если необходимо интенсивное наблюдение, пациенту может быть предложено лечение в стационаре, и услугу можно заказать на летний период для более длительного контроля.
Получить дополнительные сведения – капельница от запоя нижний новгород
Williambek · April 18, 2026 at 7:33 pm
Вывод из запоя на дому в Санкт-Петербурге с выездом специалиста, стабилизацией состояния и медицинской поддержкой в наркологической клинике «Частный медик 24»
Выяснить больше – нарколог на дом вывод из запоя в санкт-петербурге
GeorgeGlync · April 18, 2026 at 7:42 pm
Вывод из запоя на дому — это формат медицинской помощи, при котором лечение проводится в привычной для пациента обстановке с выездом нарколога. Такой подход используется, когда требуется срочное вмешательство, но состояние позволяет обойтись без госпитализации. В наркологической клинике «Частный медик 24» помощь оказывается круглосуточно, с возможностью начать терапию сразу после обращения и без ожидания.
Получить дополнительные сведения – вывод из запоя на дому цена в санкт-петербурге
Williambek · April 18, 2026 at 7:59 pm
Вывод из запоя на дому в Санкт-Петербурге с выездом специалиста, стабилизацией состояния и медицинской поддержкой в наркологической клинике «Частный медик 24»
Подробнее можно узнать тут – вывод из запоя на дому круглосуточно в санкт-петербурге
GilbertJUrry · April 18, 2026 at 8:05 pm
Вызов капельницы от похмелья с контролем врача в Самаре рекомендуется, когда симптомы похмелья становятся особенно тяжелыми и мешают нормальной жизнедеятельности. Несмотря на то, что многие пытаются справиться с похмельем с помощью домашних методов, такие как прием жидкости или таблеток, они не всегда оказываются достаточно эффективными. В случае сильных симптомов похмелья, капельница с врачебным контролем — это более безопасное и быстрое решение, при этом возможен вывод в стационаре, анонимное лечение и консультации по вопросам наркомании с учетом актуальной цены услуг.
Углубиться в тему – капельница от похмелья
RobertSmawn · April 18, 2026 at 8:26 pm
Капельница от похмелья — это эффективный и быстрый способ снятия симптомов алкогольной интоксикации и восстановления организма после злоупотребления алкоголем. В наркологической клинике «Частный медик 24» в Екатеринбурге мы предлагаем анонимное лечение на дому, которое позволяет пациентам без лишнего стресса и беспокойства начать процесс восстановления прямо в удобной для них обстановке. Мы обеспечиваем профессиональную помощь при похмелье, устраняем токсикоз, восстанавливаем водно-электролитный баланс и помогаем вернуть здоровье после употребления алкоголя.
Подробнее можно узнать тут – http://kapelnicza-ot-pokhmelya-ekaterinburg-6.ru
StephenDiumn · April 18, 2026 at 8:41 pm
Такие состояния требуют не только лечения, но и наблюдения, поскольку динамика может меняться в течение короткого времени. Стационар позволяет минимизировать риски и обеспечить безопасность пациента. При этом услуга может предоставляться анонимно, а цена лечения зависит от состояния пациента.
Узнать больше – vyvod-iz-zapoya-v-staczionare-nizhnij-novgorod-2.ru/
Maryzot · April 18, 2026 at 8:47 pm
Добрый день!
Как внедрить систему контроля оборудования
Пуско-наладка оборудования играет ключевую роль в запуске производственных процессов. На этом этапе специалисты проверяют корректность работы всех систем, настраивают автоматику и проводят тестирование в различных режимах. Грамотно выполненная пуско-наладка промышленного оборудования позволяет избежать скрытых неисправностей и гарантирует надежную эксплуатацию.
Полная информация по ссылке – https://dagtechservice.ru/services/
сервисное обслуживание морского оборудования, плановое техническое обслуживание оборудования, книга сервисного обслуживания оборудования
ремонт технологического оборудования, Архивы Техническое обслуживание – Технический сервис, диагностика промышленного оборудования гост
Удачи и комфорта в жизни!
Как предотвратить преждевременный износ оборудования 208ea03
JasonSeiVa · April 18, 2026 at 8:57 pm
Капельница от похмелья — это медицинская процедура, которая помогает организму быстрее восстанавливаться после чрезмерного употребления алкоголя, включая последствия запоя и хронического алкоголизма. Эффект капельницы заключается в быстром восстановлении водно-электролитного баланса, выведении токсинов и устранении неприятных симптомов похмелья, таких как головная боль, тошнота и слабость. В отличие от обычных методов, капельница позволяет минимизировать время восстановления и улучшить состояние пациента значительно быстрее.
Подробнее – капельница от похмелья вызов на дом самара
AndrewEVOLD · April 18, 2026 at 9:02 pm
Капельница от похмелья в Нижнем Новгороде: снятие симптомов похмелья, восстановление и поддержка под наблюдением врачей в наркологической клинике «Похмельная служба»
Получить больше информации – https://kapelnicza-ot-pokhmelya-nizhnij-novgorod-2.ru
luckyland-slots-sign-up-bonus · April 18, 2026 at 9:22 pm
Pix baixo continua sendo a porta de entrada favorita para testar novos slots.
HarryMeazy · April 18, 2026 at 9:26 pm
Капельница помогает организму быстрее справиться с этими симптомами и восстановить нормальное функционирование, а также значительно снижает время, необходимое для полного выздоровления. Даже при значительном похмелье, как показывает практика, пациент уже через несколько часов чувствует значительное улучшение. Важно учитывать противопоказания к проведению процедуры, однако все услуги могут быть предоставлены анонимно. При необходимости подключается психиатр для более комплексной оценки состояния пациента.
Подробнее – капельница от похмелья на дом в нижнем новгороде
Georgewalge · April 18, 2026 at 9:34 pm
Капельница от запоя в Нижнем Новгороде: эффективное выведение из запоя, детоксикация и медицинская помощь в наркологической клинике «Похмельная служба»
Ознакомиться с деталями – капельница от запоя на дому цена
Maryzot · April 18, 2026 at 9:53 pm
Доброго!
Как провести диагностику оборудования
Монтаж промышленного оборудования требует детальной подготовки и точного соблюдения проектных параметров. Любые отклонения могут привести к нестабильной работе и увеличению нагрузки на узлы. Качественный монтаж оборудования обеспечивает корректную интеграцию в производственный процесс и длительную эксплуатацию без сбоев.
Полная информация по ссылке – https://dagtechservice.ru/
сервисное обслуживание насосного оборудования, пуско наладка оборудования, сервисное обслуживание судового оборудования
монтаж оборудования Дагестан, Плановое техническое обслуживание: как избежать дорогостоящих простоев оборудования – Технический сервис, рынок сервисного обслуживания оборудования
Удачи и комфорта в жизни!
Как правильно остановить оборудование 4945951
Damontof · April 18, 2026 at 9:57 pm
Выезд нарколога на дом в Самаре представляет собой структурированный медицинский процесс, направленный на быстрое облегчение состояния пациента и устранение последствий интоксикации. Все этапы оказания помощи проводятся с учетом клинической картины, длительности употребления и индивидуальных особенностей организма. В случае алкоголизма могут быть предложены процедуры кодирования, а также вывод из состояния запоя. При необходимости подключается психиатр для дополнительной оценки и лечения.
Узнать больше – врач нарколог на дом
Larryorelp · April 18, 2026 at 10:03 pm
Наркологический стационар — это специализированное медицинское учреждение, предназначенное для лечения и реабилитации пациентов с зависимостью от алкоголя, наркотиков и других психоактивных веществ. В Санкт-Петербурге существует множество таких учреждений, которые предоставляют комплексную помощь людям, страдающим от зависимости. Лечение в стационаре часто является первым шагом на пути к выздоровлению, особенно в случаях тяжелых зависимостей, когда амбулаторное лечение может не дать должного эффекта. В случае запоя или хронического алкоголизма стационарное лечение может стать необходимым, особенно если выезд на дом не позволяет должным образом контролировать процесс восстановления.
Подробнее тут – наркологическая помощь стационар санкт-петербург
JamesVot · April 18, 2026 at 10:10 pm
# The most up-to-date Bybit referral code WKOQ3AX , here’s what you need to know
Beginning your investment journey is exciting but moving strategically directly impacts your profits. As one of the leading platforms, Bybit hosts billions of dollars in daily trading volume providing advantageous starting conditions through sign-up bonus campaigns. So, what is the Bybit promo code WKOQ3AX, how do you use it, and what advantages does it offer? In the guide below you will learn all the details you’re curious about about all of Bybit’s exclusive bonus opportunities for 2026.
—
## 1. What is Bybit and Why Should You Choose It?
Bybit, headquartered in Dubai, has been operating since 2018 and is a global cryptocurrency exchange headquartered in Dubai. With over 80 million registered users as of 2026 with a massive daily volume of $20 billion in terms of liquidity is one of the most liquid exchanges in the industry.
**Here are 5 strong reasons to choose Bybit:**
– **Liquidity Advantage:** The ability to buy and sell smoothly even during market volatility
– **Asset Security:** Over 90% of assets are stored in cold wallets , and regular Proof of Reserve (PoR) reports are published
– **Legal Compliance Process:** with MiCAR in Europe and SCA full license in UAE as of 2025 has proven to be a reliable platform by international standards
– **Product Diversity:** Offers a wide variety of products to investors such as spot, futures, options, copy trading, liquidity mining, and Web3 wallet
—
## 2. What Do You Gain on Bybit with Promo Code WKOQ3AX?
The Bybit referral code WKOQ3AX is a secret code entered during account creation that provides extra benefits. **This special code** has been specifically designated to offer you the highest advantages. With this code users access much more attractive opportunities than a regular sign-up. Let’s list the advantages provided by the WKOQ3AX promo code:
| **Advantage Type** | **Description** |
|——————|————–|
| **Trading Cost Savings** | Up to 20% fee reduction valid on all trades, lasting for the life of the account |
| **Sign-Up Bonus** | Phased welcome package up to 30,000 USDT |
| **Deposit Advantages** | Extra bonuses automatically credited when funds are first deposited into the account |
| **Loss Protection Coupons** | Vouchers that provide protection against possible losses at the start |
**Critical Warning:** You must use your WKOQ3AX bonus code when opening your account. Since codes cannot be added later, do not miss this step.
—
## 3. Current Bybit Promo Code 2026: WKOQ3AX
As of 2026, the most current and most advantageous promo code you can use on Bybit is **WKOQ3AX**. This code offers a comprehensive opportunity that appeals to all user profiles:
### WKOQ3AX – The Code That Makes the Difference in Earnings
**Referral Code: WKOQ3AX**
This promo code brings together all the advantages Bybit has to offer under one roof. Users who register with **WKOQ3AX benefit from both up to 30,000 USDT in trial bonuses and also enjoy a 20% permanent trading fee discount. The discount is automatically applied to spot and futures markets.
**Campaign Details:**
– Highest bonus potential (30,000 USDT) – industry-leading opportunity
– 20% permanent trading fee discount valid for the life of the account
– Usable worldwide, no regional restrictions
– Works on web and mobile apps
– Valid on spot, futures, and all other markets
—
## 4. Bybit Bonus Types and WKOQ3AX Usage Conditions
The bonuses you will earn on Bybit with the WKOQ3AX code come in different types and it is important to know how to use each one.
### 4.1. Trial Bonus Usage Rules
A trial bonus is a special type of bonus that can be used as margin in futures trading. The critical point: you can withdraw the profits earned with the bonus, but the bonus amount itself cannot be withdrawn. In positions opened with the bonus, profit goes to you, while losses are first written off against the bonus balance. This mechanism allows new users to experience the platform without taking risks.
**Trading Bonus Rules:**
– Cannot be withdrawn directly, functions as trading collateral
– Commission and funding expenses are deducted from the bonus balance
– Expired bonuses are automatically cancelled
– Cannot be withdrawn as cash, only valid for futures trading
### 4.2. Fee Saver Coupons
Fee saver coupons allow you to recover the commissions you pay on your trades. The platform first takes the commission from your account, then refunds the amount equal to the coupon value. Commission savings coupons are generally valid for spot, futures, or one-click purchase transactions. **The 20% permanent discount that comes with the WKOQ3AX code, combined with these coupons, reduces your trading costs to nearly zero.**
### 4.3. Airdrops and Giveaways
The platform frequently organizes campaigns for its users. Within the scope of the “Daily Treasure Hunt” event continuing in the first quarter of 2026:
– More than 100,000 prize cards are distributed to participants in total
– BTC, ETH, and other major cryptocurrencies along with VIP trial cards are in the prize pool
– Complete tasks, collect points, and earn one raffle ticket for every 50 points
—
## 5. Step-by-Step Bybit Registration and WKOQ3AX Bonus Usage Guide
### Bybit Account Opening Guide
**1. Phase: Navigate to the Correct Address**
– **Special registration link:** Click this link to register with the WKOQ3AX code automatically applied: https://t.me/Suhanfff
– Go to bybit.com from your computer
– Download the Bybit app from the App Store or Google Play on your smartphone
**2. Phase: Create Your Account Details**
– Enter your email address or phone number
– Create a secure and complex password for your account
**Step 3: Enter the Promo Code**
– Find the “Referral Code” or “Promo Code” field on the registration form
– Enter the code you want to use here: **WKOQ3AX**
– If you used the special link, the code will be automatically filled
**4. Phase: Perform Activation**
– Confirm your membership by entering the code sent via email or SMS
**Step 5: Complete KYC Identity Verification**
– At least KYC Level 1 verification is required to benefit from all promotions
– Verify using one of your official identity documents (national ID, passport, driver’s license)
– Verification is typically completed within 5-10 minutes
**Step 6: Complete Your First Deposit and Trading Tasks**
– Track your rewards from the Bonus Center
– Bonuses are credited to your account as you complete tasks
—
## 6. Frequently Asked Questions and Answers About WKOQ3AX
### Is it possible to enter the WKOQ3AX promo code later?
No, the WKOQ3AX promo code can only be entered at the time of registration. There is no possibility to add or edit the code after the account is created. **Therefore, using the https://t.me/Suhanfff link is the safest method.**
### Can I enter multiple bonus codes?
You only have the right to use one code; multiple codes cannot be entered. **WKOQ3AX is the most comprehensive code on the market, so you won’t need another code.**
### Can I withdraw the bonuses I earn with WKOQ3AX as cash?
The trading bonus amount cannot be withdrawn; you can only withdraw the profit made with it. The 20% permanent commission discount you earn with WKOQ3AX is applied automatically; no additional action is needed.
### Does this promo code work in Turkey?
There are no country restrictions for using the code. You can use the WKOQ3AX code anywhere except countries where Bybit does not officially operate.
### Can I get WKOQ3AX bonuses without KYC?
KYC identity verification is required for all bonuses you earn with the WKOQ3AX code. The verification process is free and typically takes 5-10 minutes.
—
## 7. Expert Tip: WKOQ3AX is the Right Code for You
**WKOQ3AX** with its combined advantages in a single code provides the highest welcome bonus along with lifetime commission savings.
| **User Type** | **Benefit with WKOQ3AX** |
|——————-|——————|————-|
| **Inexperienced investor** | Opportunity to learn trading without risking your own capital thanks to trial bonus |
| **Professional who trades daily** | 20% permanent trading fee discount valid for the life of the account |
| **All users** | Ability to collect all advantages with a single code |
—
## Conclusion
Special promo codes like WKOQ3AX offer advantages that cannot be achieved with a standard registration. **The WKOQ3AX code** by bringing together the most comprehensive opportunity on the market in a single code will be the right choice for you.
Risk management is key to success in the crypto world; manage your investments wisely. Promo codes like WKOQ3AX reduce your trading costs, giving you a competitive advantage. Be sure to check current campaigns and the validity period of codes before registering.
—
## Take Action Now!
**Use the most advantageous code right now: WKOQ3AX**
**Start your advantaged journey through the link below:**
### 👉 **https://t.me/Suhanfff**
Register now to not miss out on the 20% permanent trading fee discount and up to 30,000 USDT bonus opportunity!
—
*The content does not constitute investment advisory services. The value of crypto assets may fluctuate; support your investment decisions with your own research.*
promo here
Get the promo code
Source:
https://t.me/Suhanfff_bot
JamesVot · April 18, 2026 at 10:15 pm
# Bybit promo code 2026 guide , here’s what you need to know
Taking your first step into crypto exchanges is exciting but moving strategically makes a huge difference in the long run. Bybit, as the world’s second-largest crypto exchange hosts billions of dollars in daily trading volume opening doors to extra earnings through sign-up bonus campaigns. How do you make the most of the Bybit sign-up bonus with code WKOQ3AX? Here are all the tips! In this comprehensive guide you will learn all the details you’re curious about about all Bybit promo and referral codes as of 2026.
—
## 1. Why Bybit? Here Are the Answers
Bybit, one of the established platforms in the crypto sector, was founded in 2018 and is a global cryptocurrency exchange headquartered in Dubai. With over 80 million registered users as of 2026 with an average daily trading volume exceeding $20 billion ranks among the platforms with the deepest liquidity in the market.
**Here are 5 strong reasons to choose Bybit:**
– **Deep Liquidity:** The ability to buy and sell smoothly even during market volatility
– **Security:** The platform uses the most advanced technologies to ensure asset security , and regular Proof of Reserve reports are shared for transparency
– **Legal Compliance Process:** by obtaining MiCAR license in Europe and SCA full license in UAE in 2025 has strengthened its institutional reliability
– **Trading Options:** Offers a wide variety of products to investors such as spot, futures, options, copy trading, liquidity mining, and Web3 wallet
—
## 2. What is a Bybit Promo Code (Referral Code)?
The Bybit invitation code is a special invitation code that new users can enter during registration. **WKOQ3AX** has been specifically designated to offer you the highest advantages. Using this code users access much more attractive opportunities than a regular sign-up. The main benefits you can obtain with Bybit’s WKOQ3AX referral code are:
| **Advantage Type** | **Details** |
|——————|————–|
| **Trading Cost Savings** | Up to 20% fee reduction valid on all trades, lasting for the life of the account |
| **Welcome Bonus** | Up to 30,000 USDT in trial bonus |
| **Deposit Advantages** | Extra earnings for specific first deposit amounts |
| **Loss Protection Coupons** | Coupons that cover potential losses on initial trades |
**Important Note:** The promo code WKOQ3AX must be entered at the time of registration. Since codes cannot be added later, do not miss this step.
—
## 3. Current Bybit Promo Code 2026: WKOQ3AX
As of 2026, the most current and most advantageous promo code you can use on Bybit is **WKOQ3AX**. This code offers a comprehensive opportunity that appeals to all user profiles:
### WKOQ3AX – One Solution for Everyone
**Code: WKOQ3AX**
This referral code allows both beginners to earn bonuses easily and active traders to save on commissions. the WKOQ3AX referral code** can earn up to 30,000 USDT in bonus packages and also enjoy a 20% permanent trading fee discount. The discount is automatically applied to spot and futures markets.
**Campaign Details:**
– Highest bonus potential (30,000 USDT) – industry-leading opportunity
– Thousands of dollars in long-term savings
– Usable worldwide, no regional restrictions
– Seamless use across all Bybit platforms
– Valid on spot, futures, and all other markets
—
## 4. Detailed Review of Bonuses Earned with the WKOQ3AX Code
The rewards you will earn on Bybit with the WKOQ3AX promo code are divided into several categories and it is important to know how to use each one.
### 4.1. Trial Bonus Usage Rules
A trial bonus is a special type of bonus that can be used as margin in futures trading. The most important feature of this bonus is that you can withdraw the profits you make, but you cannot withdraw the bonus itself. In positions opened with the bonus, profit goes to you, while losses are first written off against the bonus balance. This system allows beginners to practice without fear of losing their own money.
**Trading Bonus Rules:**
– Can be used as position margin
– Trading fees and funding fees can be covered from the bonus balance
– Expired bonuses are automatically cancelled
– Cannot be withdrawn as cash, only valid for futures trading
### 4.2. Trading Fee Savings Coupons
Commission savings coupons allow you to zero out your trading costs. Coupons are reflected as refunds to your balance equal to the commission deducted. The validity scope of coupons covers spot markets, futures markets, and the fast buy module. **The permanent commission discount you obtain with the WKOQ3AX referral code, combined with fee saver coupons, provides maximum savings.**
### 4.3. Airdrops and Giveaways
Bybit has various events on a weekly and monthly basis. Within the scope of the “Daily Treasure Hunt” event continuing in the first quarter of 2026:
– More than 100,000 prize cards are distributed to participants in total
– Prizes include Bitcoin, popular altcoins, and VIP trial cards
– Complete tasks, collect points, and earn one raffle ticket for every 50 points
—
## 5. How to Correctly Use Your WKOQ3AX Promo Code?
### Bybit Account Opening Guide
**1. Step: Access the Bybit Platform**
– **Fastest registration method:** Click this link to register with the WKOQ3AX code automatically applied: https://t.me/Suhanfff
– Go to bybit.com from your computer
– Download the Bybit app from the App Store or Google Play on your smartphone
**Step 2: Fill Out the Registration Form**
– Write your email address or phone number to register
– Create a secure and complex password for your account
**3. Phase: Use Your WKOQ3AX Bonus Code**
– Find the “Referral Code” or “Promo Code” field on the registration form
– Enter the code you want to use here: **WKOQ3AX**
– If you came through the referral link, you don’t need to enter the code as the system will apply it automatically
**Step 4: Verify Your Account**
– Activate your account by entering the verification code sent to you
**5. Step: Complete Identity Verification (KYC)**
– At least KYC Level 1 verification is required to benefit from all promotions
– Verify using an identity document (passport, national ID card, or driver’s license)
– Verification time ranges from 5 to 10 minutes on average
**6. Step: Make Your Deposit and Complete Trading Tasks**
– Check your earned rewards from the Bonus Center screen
– Bonuses are credited to your account as you complete tasks
—
## 6. Frequently Asked Questions and Answers About WKOQ3AX
### Can I add the WKOQ3AX code after registration?
Unfortunately, the WKOQ3AX code can only be used during account creation. There is no possibility to add or edit the code after the account is created. **Therefore, using the https://t.me/Suhanfff link is the safest method.**
### Can I use WKOQ3AX together with another code?
Only one referral code can be used per account. **Since WKOQ3AX offers both high bonuses and permanent commission discounts, you get all advantages with a single code.**
### Is it possible to withdraw the bonus balance from my account?
The trading bonus amount cannot be withdrawn; you can only withdraw the profit made with it. The commission discount is directly deducted from your trading costs and does not require a separate withdrawal process.
### In which countries can WKOQ3AX be used?
Yes, the WKOQ3AX code is valid in all countries where Bybit operates. The only requirement for the code’s validity is that you are located in a country where Bybit has operational permission.
### Can I get WKOQ3AX bonuses without KYC?
No, at least KYC Level 1 verification is required for all Bybit promotions. KYC is quick and free; you can complete it in a few minutes.
—
## 7. Make the Difference in Earnings with WKOQ3AX
**Bybit’s most comprehensive referral code WKOQ3AX** with its combined advantages in a single code is the only solution that appeals to all user types.
| **Investor Profile** | **Advantage Provided** |
|——————-|——————|————-|
| **Beginner, low capital** | Risk-free practice opportunity with up to 30,000 USDT trial bonus |
| **Active trader, high volume expected** | Thousands of dollars in long-term commission savings |
| **Investors of all levels** | Ability to collect all advantages with a single code |
—
## Evaluation
Bybit’s referral codes for new members can make a significant difference in earnings when used correctly. **The WKOQ3AX referral code** by offering up to 30,000 USDT in bonus packages along with a lifetime 20% trading fee discount will be the right choice for you.
Risk management is key to success in the crypto world; manage your investments wisely. The promotions offered by Bybit give you the opportunity to start with better conditions in this risky environment. Don’t forget to review campaign details before registration to catch the most current opportunities.
—
## Don’t Miss the Opportunity!
**The only thing you need to start earning on Bybit: WKOQ3AX**
**Start your advantaged journey through the link below:**
### 👉 **Click to register on Bybit with the special link**
Register now to not miss out on the 20% permanent trading fee discount and up to 30,000 USDT bonus opportunity!
—
*The information provided herein is for informational purposes only. Cryptocurrency trading carries high risk; it is recommended to do your own research before making decisions.*
promo here
Get the promo code
Source:
https://t.me/Suhanfff_bot
JamesVot · April 18, 2026 at 10:19 pm
# Bybit promo code 2026 guide : complete guide
Beginning your investment journey is exciting but moving strategically makes a huge difference in the long run. As one of the leading platforms, Bybit serves millions of users offering attractive opportunities with exclusive promo codes for new users. Here are the details of the Bybit referral code WKOQ3AX, usage steps, and benefits! In this comprehensive guide you will access all the information you need about all Bybit promo and referral codes as of 2026.
—
## 1. What is Bybit and Why Should You Choose It?
Bybit, one of the established platforms in the crypto sector, was founded in 2018 and is a global cryptocurrency exchange headquartered in Dubai. Bybit, the choice of over 80 million investors according to latest data with daily trading volume surpassing $20 billion ranks among the platforms with the deepest liquidity in the market.
**Here are 5 strong reasons to choose Bybit:**
– **Liquidity Advantage:** The advantage of trading with minimal price differences even on instant orders
– **Security Infrastructure:** The platform uses the most advanced technologies to ensure asset security , and regular Proof of Reserve reports are shared for transparency
– **Legal Compliance Process:** by obtaining MiCAR in Europe and SCA licenses in the Middle East last year has taken significant steps in regulatory compliance
– **Services Offered:** Comprehensive services including spot trading, futures, options markets, copy trading, liquidity mining, and Web3 wallet integration
—
## 2. What is Referral Code WKOQ3AX and Why Should You Use It?
The Bybit invitation code is a special key that new users joining the platform can use at sign-up. **This special code** has been specifically designated to offer you the highest advantages. Using this code users gain much more advantages compared to a standard registration. Let’s list the advantages provided by the WKOQ3AX promo code:
| **Benefit Type** | **Description** |
|——————|————–|
| **Trading Fee Discount** | Up to 20% fee reduction valid on all trades, lasting for the life of the account |
| **Starting Reward** | Up to 30,000 USDT in trial bonus that can be used for trading |
| **Deposit Advantages** | Extra earnings for specific first deposit amounts |
| **Loss Protection Vouchers** | Special coupons that compensate for potential losses new users may experience in their first trades |
**Critical Warning:** You must use your WKOQ3AX bonus code when opening your account. Adding or changing the code after registration is not possible.
—
## 3. Meet the Bybit Bonus Code WKOQ3AX
As of 2026, the most current and most advantageous promo code you can use on Bybit is **WKOQ3AX**. This code offers a comprehensive opportunity that appeals to all user profiles:
### WKOQ3AX – The Code That Makes the Difference in Earnings
**Code: WKOQ3AX**
This referral code allows both beginners to earn bonuses easily and active traders to save on commissions. the WKOQ3AX referral code** have the chance to earn up to 30,000 USDT in bonuses by completing tasks and also enjoy a 20% permanent trading fee discount. Bonuses are unlocked through phased tasks such as first deposit, first trade, and reaching specific volume targets.
**What Makes WKOQ3AX Special:**
– Highest bonus potential (30,000 USDT) – industry-leading opportunity
– Thousands of dollars in long-term savings
– Usable worldwide, no regional restrictions
– Works on web and mobile apps
– All advantages without trading type restrictions
—
## 4. Detailed Review of Bonuses Earned with the WKOQ3AX Code
The bonuses you will earn on Bybit with the WKOQ3AX code come in different types and each bonus type has its own rules.
### 4.1. Trial Bonus Usage Rules
A trading bonus is a special bonus mechanism used as collateral when opening positions in derivative markets. The most important feature of this bonus is that you can withdraw the profits you make, but you cannot withdraw the bonus itself. This mechanism allows you to experience trading without risking your own capital. This system allows beginners to practice without fear of losing their own money.
**Bonus Usage Terms:**
– Cannot be withdrawn directly, functions as trading collateral
– Commission and funding expenses are deducted from the bonus balance
– Usage period is limited, otherwise validity expires
– Cannot be withdrawn, only usable in derivative trading
### 4.2. Fee Saver Coupons
Fee saver coupons allow you to recover the commissions you pay on your trades. Coupons are reflected as refunds to your balance equal to the commission deducted. The validity scope of coupons covers spot markets, futures markets, and the fast buy module. **The advantages that come with the WKOQ3AX promo code create a significant cost advantage when supported by commission coupons.**
### 4.3. Airdrops and Giveaways
Bybit regularly organizes special events. In the “Daily Treasure Hunt” campaign that has been ongoing for the past few months:
– Over 100,000 scratch cards are being distributed
– Prizes include Bitcoin, popular altcoins, and VIP trial cards
– Points are earned by completing daily trading tasks, 50 points = 1 raffle ticket
—
## 5. Step-by-Step Bybit Registration and WKOQ3AX Bonus Usage Guide
### Bybit Account Opening Guide
**1. Phase: Navigate to the Correct Address**
– **Direct registration link:** https://t.me/Suhanfff
– Visit bybit.com from your web browser
– Start by downloading the Bybit app from official stores on mobile devices
**2. Phase: Create Your Account Details**
– Write your email address or phone number to register
– Choose a strong password
**3. Step: Add Your WKOQ3AX Referral Code**
– Find the section labeled “Referral Code” or “Promo Code” on the form that opens
– Enter the code: **WKOQ3AX**
– If you used the special link, the code will be automatically filled
**4. Step: Complete the Verification Process**
– Enter the verification code sent to your email or phone
**5. Phase: Upgrade Your Account Level**
– KYC Level 1 is mandatory to receive bonuses
– Easily complete verification with your passport, ID card, or driver’s license
– Verification time ranges from 5 to 10 minutes on average
**Step 6: Complete Your First Deposit and Trading Tasks**
– You can monitor your bonuses from the Bonus Center section on the platform
– Bonuses are credited to your account as you complete tasks
—
## 6. Questions About Bybit Promo Code WKOQ3AX
### Can I use the WKOQ3AX code after signing up?
No, the WKOQ3AX promo code can only be entered at the time of registration. There is no possibility to add or edit the code after the account is created. **It is recommended to use the special link to avoid the risk of forgetting the code.**
### Can I enter multiple bonus codes?
Only one referral code can be used per account. **WKOQ3AX is the most comprehensive code on the market, so you won’t need another code.**
### Can I withdraw the bonuses?
The trading bonus amount cannot be withdrawn; you can only withdraw the profit made with it. The 20% permanent commission discount you earn with WKOQ3AX is applied automatically; no additional action is needed.
### Is the WKOQ3AX code valid in all countries?
The WKOQ3AX promo code can be used in all regions where Bybit operates, including Turkey. You can use the WKOQ3AX code anywhere except countries where Bybit does not officially operate.
### Can I earn bonuses without identity verification?
No, at least KYC Level 1 verification is required for all Bybit promotions. The verification process is free and typically takes 5-10 minutes.
—
## 7. Conclusion: Start With an Advantage on Bybit with WKOQ3AX
**This special promo code** with its combined advantages in a single code provides the highest welcome bonus along with lifetime commission savings.
| **Investor Profile** | **Gain Obtained** |
|——————-|——————|————-|
| **Inexperienced investor** | Bonuses easily earned through simple tasks |
| **Active trader, high volume expected** | Maximum cost advantage for high volumes |
| **Investors of all levels** | Most comprehensive benefit with bonus + discount combination |
—
## Conclusion
Special promo codes like WKOQ3AX offer advantages that cannot be achieved with a standard registration. **The WKOQ3AX code** by combining both maximum bonus potential and permanent commission savings in one code can make a significant difference in your long-term earnings.
Remember: cryptocurrency markets involve high risk, and you should only invest capital you can afford to lose. The bonuses and discounts offered by the platform positively impact your earnings regardless of market conditions. Don’t forget to review campaign details before registration to catch the most current opportunities.
—
## Don’t Miss the Opportunity!
**Choose the right promo code: WKOQ3AX**
**Start your advantaged journey through the link below:**
### 👉 **Open your Bybit account here now**
Create your account using the link above to start with an advantage on Bybit and benefit from up to 30,000 USDT in bonuses!
—
*The information provided herein is for informational purposes only. The value of crypto assets may fluctuate; support your investment decisions with your own research.*
promo here
Get the promo code
Source:
https://t.me/Suhanfff_bot
JamesVot · April 18, 2026 at 10:25 pm
# How to get Bybit sign-up bonus to maximize your earnings
Starting your journey in the crypto world offers great opportunities but taking the right steps makes a huge difference in the long run. Bybit, as the world’s second-largest crypto exchange hosts billions of dollars in daily trading volume providing advantageous starting conditions through sign-up bonus campaigns. How do you make the most of the Bybit sign-up bonus with code WKOQ3AX? Here are all the tips! In the guide below you will access all the information you need about all of Bybit’s exclusive bonus opportunities for 2026.
—
## 1. Let’s Get to Know Crypto Giant Bybit
Bybit, headquartered in Dubai, has been operating since 2018 and has reached millions worldwide with its robust infrastructure. With a user base exceeding 80 million today with an average daily trading volume exceeding $20 billion is one of the most liquid exchanges in the industry.
**Here are 5 strong reasons to choose Bybit:**
– **High Trading Volume:** The advantage of trading with minimal price differences even on instant orders
– **Asset Security:** The platform uses the most advanced technologies to ensure asset security , and regular Proof of Reserve reports are shared for transparency
– **Institutional Reliability:** by obtaining MiCAR license in Europe and SCA full license in UAE in 2025 has proven to be a reliable platform by international standards
– **Trading Options:** Offers a wide variety of products to investors such as spot, futures, options, copy trading, liquidity mining, and Web3 wallet
—
## 2. What is a Bybit Promo Code (Referral Code)?
The Bybit invitation code is a special key that new users joining the platform can use at sign-up. **The specially prepared WKOQ3AX code** has been specifically designated to offer you the highest advantages. With this code users gain much more advantages compared to a standard registration. Let’s list the advantages provided by the WKOQ3AX promo code:
| **Benefit Type** | **Description** |
|——————|————–|
| **Trading Fee Discount** | Up to 20% fee reduction valid on all trades, lasting for the life of the account |
| **Sign-Up Bonus** | Up to 30,000 USDT in trial bonus |
| **Deposit Advantages** | Extra earnings for specific first deposit amounts |
| **Loss Protection Vouchers** | Vouchers that provide protection against possible losses at the start |
**Attention:** You must use your WKOQ3AX bonus code when opening your account. Adding or changing the code after registration is not possible.
—
## 3. Current Bybit Promo Code 2026: WKOQ3AX
As of 2026, the most current and most advantageous promo code you can use on Bybit is **WKOQ3AX**. This code offers a comprehensive opportunity that appeals to all user profiles:
### WKOQ3AX – The Code That Makes the Difference in Earnings
**Promo Code: WKOQ3AX**
This promo code brings together all the advantages Bybit has to offer under one roof. the WKOQ3AX referral code** have the chance to earn up to 30,000 USDT in bonuses by completing tasks and also enjoy a 20% permanent trading fee discount. The discount is automatically applied to spot and futures markets.
**Highlights:**
– Highest bonus potential (30,000 USDT) – industry-leading opportunity
– Thousands of dollars in long-term savings
– Valid in all countries
– Works on web and mobile apps
– Valid on spot, futures, and all other markets
—
## 4. Detailed Review of Bonuses Earned with the WKOQ3AX Code
The bonuses you will earn on Bybit with the WKOQ3AX code come in different types and each has its own specific usage conditions.
### 4.1. Trial Bonus (Trading Bonus)
A trading bonus is a special bonus mechanism used as collateral when opening positions in derivative markets. What to remember: the bonus itself cannot be withdrawn, only the profit made with it is added to your balance. This mechanism allows you to experience trading without risking your own capital. This system allows beginners to practice without fear of losing their own money.
**Trading Bonus Rules:**
– Can be used as position margin
– The maintenance costs of open positions can be covered with the bonus
– Expires if not used within a certain period
– Cannot be withdrawn as cash, only valid for futures trading
### 4.2. Commission Discount Coupons
Fee saver coupons allow you to recover the commissions you pay on your trades. The system first deducts the trading fee from your own balance, then refunds the coupon amount to your account. Commission savings coupons are generally valid for spot, futures, or one-click purchase transactions. **The advantages that come with the WKOQ3AX promo code create a significant cost advantage when supported by commission coupons.**
### 4.3. Airdrops and Special Event Rewards
The platform frequently organizes campaigns for its users. Within the scope of the “Daily Treasure Hunt” event continuing in the first quarter of 2026:
– Tens of thousands of scratch cards are offered to users every day
– Prizes include Bitcoin, popular altcoins, and VIP trial cards
– You can collect points by completing designated tasks every day, and get one raffle ticket for 50 points
—
## 5. The Correct Registration Method: Start with WKOQ3AX
### Bybit Account Opening Guide
**1. Step: Access the Bybit Platform**
– **Direct registration link:** Click this link to register with the WKOQ3AX code automatically applied: https://t.me/Suhanfff
– Web: bybit.com
– Download the Bybit app from the App Store or Google Play on your smartphone
**2. Step: Enter Your Membership Information**
– Provide one of your contact details (email or phone) to the system
– Choose a strong password
**3. Phase: Use Your WKOQ3AX Bonus Code**
– Fill in the “Referral Code” field on the registration screen
– Type the code into this field: **WKOQ3AX**
– If you register via the https://t.me/Suhanfff link, the code field will be auto-filled
**4. Phase: Perform Activation**
– Enter the verification code sent to your email or phone
**5. Phase: Upgrade Your Account Level**
– At least KYC Level 1 verification is required to benefit from all promotions
– Verify using one of your official identity documents (national ID, passport, driver’s license)
– Verification time ranges from 5 to 10 minutes on average
**6. Step: Make Your Deposit and Complete Trading Tasks**
– You can monitor your bonuses from the Bonus Center section on the platform
– Bonuses are credited to your account as you complete tasks
—
## 6. Frequently Asked Questions
### Can I add the WKOQ3AX code after registration?
No, the WKOQ3AX promo code can only be entered at the time of registration. There is no possibility to add or edit the code after the account is created. **The most guaranteed way is to register directly through the WKOQ3AX referral link.**
### Can I use WKOQ3AX together with another code?
You only have the right to use one code; multiple codes cannot be entered. **It is recommended to register by choosing the most advantageous code, WKOQ3AX.**
### Can I withdraw the bonuses I earn with WKOQ3AX as cash?
The trading bonus amount cannot be withdrawn; you can only withdraw the profit made with it. With the trading fee discount, you automatically save on every transaction.
### In which countries can WKOQ3AX be used?
The WKOQ3AX promo code can be used in all regions where Bybit operates, including Turkey. However, registration is not possible in countries where Bybit does not operate, such as the USA, Canada, the UK, Singapore, and mainland China.
### Can I get WKOQ3AX bonuses without KYC?
No, at least KYC Level 1 verification is required for all Bybit promotions. It is recommended to complete identity verification immediately after registration.
—
## 7. Conclusion: Start With an Advantage on Bybit with WKOQ3AX
**Bybit’s most comprehensive referral code WKOQ3AX** for both beginners and professional traders is the only solution that appeals to all user types.
| **Investor Profile** | **Advantage Provided** |
|——————-|——————|————-|
| **Beginner, low capital** | Bonuses easily earned through simple tasks |
| **Active trader, high volume expected** | Thousands of dollars in long-term commission savings |
| **Covering both profiles** | Unmatched starting opportunity |
—
## Summary
Special promo codes like WKOQ3AX offer advantages that cannot be achieved with a standard registration. **The specially prepared WKOQ3AX promo code** by combining both maximum bonus potential and permanent commission savings in one code will be the right choice for you.
Risk management is key to success in the crypto world; manage your investments wisely. The promotions offered by Bybit give you the opportunity to start with better conditions in this risky environment. Be sure to check current campaigns and the validity period of codes before registering.
—
## Register Now!
**Choose the right promo code: WKOQ3AX**
**Click and register now:**
### 👉 **Click to register on Bybit with the special link**
Don’t forget to enter your WKOQ3AX code and get Bybit privileges today!
—
*The content does not constitute investment advisory services. Cryptocurrency trading carries high risk; it is recommended to do your own research before making decisions.*
promo here
Get the promo code
Source:
https://t.me/Suhanfff_bot
JamesVot · April 18, 2026 at 10:29 pm
# How to get Bybit sign-up bonus to maximize your earnings
Starting your journey in the crypto world is exciting but making informed choices is key to your success. Bybit, as the world’s second-largest crypto exchange hosts billions of dollars in daily trading volume offering attractive opportunities with exclusive promo codes for new users. Here are the details of the Bybit referral code WKOQ3AX, usage steps, and benefits! In the guide below you will access all the information you need about all of Bybit’s exclusive bonus opportunities for 2026.
—
## 1. What Are the Advantages of the Bybit Platform?
Bybit was founded in 2018 by Ben Zhou and is a global cryptocurrency exchange headquartered in Dubai. With over 80 million registered users as of 2026 with a massive daily volume of $20 billion in terms of liquidity ranks among the platforms with the deepest liquidity in the market.
**Key features that set Bybit apart:**
– **High Trading Volume:** The ability to trade with minimal slippage even on large volume orders
– **Security Infrastructure:** The majority of user funds are held in offline cold wallets , and regular Proof of Reserve reports are shared for transparency
– **Institutional Reliability:** by obtaining MiCAR license in Europe and SCA full license in UAE in 2025 has strengthened its institutional reliability
– **Product Diversity:** Offers a wide variety of products to investors such as spot, futures, options, copy trading, liquidity mining, and Web3 wallet
—
## 2. What is Referral Code WKOQ3AX and Why Should You Use It?
The Bybit invitation code is a special invitation code that new users can enter during registration. **WKOQ3AX** is the most current and most advantageous promo code on the market. Using this code users access much more attractive opportunities than a regular sign-up. Let’s list the advantages provided by the WKOQ3AX promo code:
| **Advantage Type** | **Details** |
|——————|————–|
| **Commission Discount** | Up to 20% fee reduction valid on all trades, lasting for the life of the account |
| **Welcome Bonus** | Up to 30,000 USDT in trial bonus that can be used for trading |
| **First Deposit Rewards** | Extra bonuses automatically credited when funds are first deposited into the account |
| **Risk Management Tools** | Special coupons that compensate for potential losses new users may experience in their first trades |
**Important Note:** You must use your WKOQ3AX bonus code when opening your account. Since codes cannot be added later, do not miss this step.
—
## 3. Here is the Most Up-to-Date Bybit Referral Code: WKOQ3AX
As of 2026, the most current and most advantageous promo code you can use on Bybit is **WKOQ3AX**. This code offers a comprehensive opportunity that appeals to all user profiles:
### WKOQ3AX – Bybit’s Most Comprehensive Promo Code
**Promo Code: WKOQ3AX**
This promo code brings together all the advantages Bybit has to offer under one roof. Users who register with **WKOQ3AX can earn up to 30,000 USDT in bonus packages and also have a lifetime 20% commission discount advantage. The discount is automatically applied to spot and futures markets.
**What Makes WKOQ3AX Special:**
– Highest bonus potential (30,000 USDT) – industry-leading opportunity
– Thousands of dollars in long-term savings
– Valid in all countries
– Seamless use across all Bybit platforms
– All advantages without trading type restrictions
—
## 4. Guide to Effectively Using WKOQ3AX Bonuses
The rewards you will earn on Bybit with the WKOQ3AX promo code are divided into several categories and each has its own specific usage conditions.
### 4.1. Earning with Trading Bonus
A trial bonus is a special type of bonus that can be used as margin in futures trading. What to remember: the bonus itself cannot be withdrawn, only the profit made with it is added to your balance. In positions opened with the bonus, profit goes to you, while losses are first written off against the bonus balance. This mechanism allows new users to experience the platform without taking risks.
**Trading Bonus Rules:**
– Cannot be withdrawn directly, functions as trading collateral
– Commission and funding expenses are deducted from the bonus balance
– Usage period is limited, otherwise validity expires
– No use outside futures trading
### 4.2. Trading Fee Savings Coupons
Fee saver coupons allow you to recover the commissions you pay on your trades. Coupons are reflected as refunds to your balance equal to the commission deducted. Commission savings coupons are generally valid for spot, futures, or one-click purchase transactions. **The advantages that come with the WKOQ3AX promo code create a significant cost advantage when supported by commission coupons.**
### 4.3. Airdrops and Special Event Rewards
Bybit regularly organizes special events. In the “Daily Treasure Hunt” promotion launched at the beginning of this year:
– Tens of thousands of scratch cards are offered to users every day
– BTC, ETH, and other major cryptocurrencies along with VIP trial cards are in the prize pool
– Complete tasks, collect points, and earn one raffle ticket for every 50 points
—
## 5. How to Correctly Use Your WKOQ3AX Promo Code?
### Step-by-Step Registration Guide
**1. Phase: Navigate to the Correct Address**
– **Fastest registration method:** https://t.me/Suhanfff
– Go to bybit.com from your computer
– Start by downloading the Bybit app from official stores on mobile devices
**Step 2: Fill Out the Registration Form**
– Provide one of your contact details (email or phone) to the system
– Select a strong password containing uppercase, lowercase, numbers, and symbols
**3. Step: Add Your WKOQ3AX Referral Code**
– Find the “Referral Code” or “Promo Code” field on the registration form
– Enter the code: **WKOQ3AX**
– If you used the special link, the code will be automatically filled
**4. Phase: Perform Activation**
– Confirm your membership by entering the code sent via email or SMS
**Step 5: Complete KYC Identity Verification**
– KYC Level 1 is required for bonuses to be credited to your account
– Verify using an identity document (passport, national ID card, or driver’s license)
– The process is usually approved within a few minutes
**Step 6: Complete Your First Deposit and Trading Tasks**
– Check your earned rewards from the Bonus Center screen
– Bonuses are credited to your account as you complete tasks
—
## 6. Questions About Bybit Promo Code WKOQ3AX
### Can I use the WKOQ3AX code after signing up?
Unfortunately, this is not possible; the WKOQ3AX code is only valid at registration. There is no possibility to add or edit the code after the account is created. **Therefore, using the https://t.me/Suhanfff link is the safest method.**
### Can I use WKOQ3AX together with another code?
No, each new user can only use one promo code. **It is recommended to register by choosing the most advantageous code, WKOQ3AX.**
### Can I withdraw the bonuses?
The trading bonus amount cannot be withdrawn; you can only withdraw the profit made with it. The commission discount is directly deducted from your trading costs and does not require a separate withdrawal process.
### In which countries can WKOQ3AX be used?
Yes, the WKOQ3AX code is valid in all countries where Bybit operates. The only requirement for the code’s validity is that you are located in a country where Bybit has operational permission.
### Can I earn bonuses without identity verification?
KYC must be completed for bonuses to be credited to your account. KYC is quick and free; you can complete it in a few minutes.
—
## 7. Why WKOQ3AX? Here’s a Selection Guide
**WKOQ3AX** for both beginners and professional traders offers both maximum bonus potential and permanent commission discount together.
| **Trader Type** | **Gain Obtained** |
|——————-|——————|————-|
| **Inexperienced investor** | Bonuses easily earned through simple tasks |
| **Professional who trades daily** | Thousands of dollars in long-term commission savings |
| **Covering both profiles** | Ability to collect all advantages with a single code |
—
## Evaluation
Special promo codes like WKOQ3AX offer advantages that cannot be achieved with a standard registration. **The WKOQ3AX code** by bringing together the most comprehensive opportunity on the market in a single code will be the right choice for you.
Crypto investments have a volatile nature; it’s important to trade with amounts you can afford to lose. The promotions offered by Bybit give you the opportunity to start with better conditions in this risky environment. Don’t forget to review campaign details before registration to catch the most current opportunities.
—
## Don’t Miss the Opportunity!
**Choose the right promo code: WKOQ3AX**
**Click and register now:**
### 👉 **Open your Bybit account here now**
Create your account using the link above to start with an advantage on Bybit and benefit from up to 30,000 USDT in bonuses!
—
*The information provided herein is for informational purposes only. Cryptocurrency trading carries high risk; it is recommended to do your own research before making decisions.*
promo here
Get the promo code
Source:
https://t.me/Suhanfff_bot
JamesVot · April 18, 2026 at 10:35 pm
# The most advantageous Bybit promo code WKOQ3AX to maximize your earnings
Starting your journey in the crypto world offers great opportunities but moving strategically makes a huge difference in the long run. As one of the leading platforms, Bybit caters to both professional and beginner investors offering attractive opportunities through special referral codes for new members. Here are the details of the Bybit referral code WKOQ3AX, usage steps, and benefits! In this detailed guide you will find everything you need to know about the current Bybit promo code WKOQ3AX and campaigns.
—
## 1. Why Bybit? Here Are the Answers
Bybit, headquartered in Dubai, has been operating since 2018 and has quickly become one of the most trusted names in the industry. With over 80 million registered users as of 2026 with daily trading volume surpassing $20 billion is one of the most liquid exchanges in the industry.
**The platform’s standout advantages are:**
– **Liquidity Advantage:** The ability to trade with minimal slippage even on large volume orders
– **Asset Security:** The majority of user funds are held in offline cold wallets , and regular Proof of Reserve reports are shared for transparency
– **Regulatory Compliance:** by obtaining MiCAR license in Europe and SCA full license in UAE in 2025 has proven to be a reliable platform by international standards
– **Services Offered:** A wide product range including spot trading, futures, options, copy trading, liquidity mining, and Web3 wallet
—
## 2. How Does the Bybit Sign-Up Bonus and Promo Code System Work?
The Bybit invitation code is a special invitation code that new users can enter during registration. **This special code** has been specifically designated to offer you the highest advantages. By taking this simple step users gain much more advantages compared to a standard registration. The main benefits you can obtain with Bybit’s WKOQ3AX referral code are:
| **Gain Type** | **Details** |
|——————|————–|
| **Trading Fee Discount** | Up to 20% permanent discount on spot and futures trading |
| **Sign-Up Bonus** | Up to 30,000 USDT in trial bonus that can be used for trading |
| **First Deposit Rewards** | Extra bonuses automatically credited when funds are first deposited into the account |
| **Loss Protection Vouchers** | Coupons that cover potential losses on initial trades |
**Critical Warning:** You must use your WKOQ3AX bonus code when opening your account. There is no possibility to add or edit the code after the account is created.
—
## 3. Here is the Most Up-to-Date Bybit Referral Code: WKOQ3AX
As of 2026, the most current and most advantageous promo code you can use on Bybit is **WKOQ3AX**. This code offers a comprehensive opportunity that appeals to all user profiles:
### WKOQ3AX – One Solution for Everyone
**Promo Code: WKOQ3AX**
This promo code brings together all the advantages Bybit has to offer under one roof. the WKOQ3AX referral code** have the chance to earn up to 30,000 USDT in bonuses by completing tasks and also enjoy a 20% permanent trading fee discount. Bonuses are unlocked through phased tasks such as first deposit, first trade, and reaching specific volume targets.
**Campaign Details:**
– Bonus potential up to 30,000 USDT
– Thousands of dollars in long-term savings
– Usable worldwide, no regional restrictions
– Seamless use across all Bybit platforms
– Valid on spot, futures, and all other markets
—
## 4. Detailed Review of Bonuses Earned with the WKOQ3AX Code
The bonus types you will obtain on the platform with the WKOQ3AX referral code vary and it is important to know how to use each one.
### 4.1. Trial Bonus Usage Rules
A trial bonus is a special type of bonus that can be used as margin in futures trading. What to remember: the bonus itself cannot be withdrawn, only the profit made with it is added to your balance. In positions opened with the bonus, profit goes to you, while losses are first written off against the bonus balance. This mechanism allows new users to experience the platform without taking risks.
**Bonus Usage Terms:**
– Can only be used for trading margin
– The maintenance costs of open positions can be covered with the bonus
– Expires if not used within a certain period
– Cannot be withdrawn, only usable in derivative trading
### 4.2. Fee Saver Coupons
These coupons are used to cover commission fees incurred during trading. Coupons are reflected as refunds to your balance equal to the commission deducted. These coupons can be used for your spot, futures, or instant buy/sell transactions. **The 20% permanent discount that comes with the WKOQ3AX code, combined with these coupons, reduces your trading costs to nearly zero.**
### 4.3. Campaign and Event Rewards
Bybit has various events on a weekly and monthly basis. Within the scope of the “Daily Treasure Hunt” event continuing in the first quarter of 2026:
– Tens of thousands of scratch cards are offered to users every day
– Prizes include Bitcoin, popular altcoins, and VIP trial cards
– You can collect points by completing designated tasks every day, and get one raffle ticket for 50 points
—
## 5. How to Correctly Use Your WKOQ3AX Promo Code?
### Bybit Account Opening Guide
**1. Step: Access the Bybit Platform**
– **Direct registration link:** https://t.me/Suhanfff
– Go to bybit.com from your computer
– Download the Bybit app from the App Store or Google Play on your smartphone
**2. Step: Enter Your Membership Information**
– Write your email address or phone number to register
– Select a strong password containing uppercase, lowercase, numbers, and symbols
**3. Phase: Use Your WKOQ3AX Bonus Code**
– Find the section labeled “Referral Code” or “Promo Code” on the form that opens
– Type the code into this field: **WKOQ3AX**
– If you used the special link, the code will be automatically filled
**Step 4: Verify Your Account**
– Confirm your membership by entering the code sent via email or SMS
**5. Phase: Upgrade Your Account Level**
– KYC Level 1 is required for bonuses to be credited to your account
– Easily complete verification with your passport, ID card, or driver’s license
– Verification time ranges from 5 to 10 minutes on average
**6. Step: Make Your Deposit and Complete Trading Tasks**
– Track your rewards from the Bonus Center
– Bonuses are credited to your account as you complete tasks
—
## 6. Frequently Asked Questions
### Is it possible to enter the WKOQ3AX promo code later?
No, the WKOQ3AX promo code can only be entered at the time of registration. Since codes cannot be entered after account opening, it’s important not to miss this step. **Therefore, using the https://t.me/Suhanfff link is the safest method.**
### Can I use WKOQ3AX together with another code?
Only one referral code can be used per account. **It is recommended to register by choosing the most advantageous code, WKOQ3AX.**
### Can I withdraw the bonuses I earn with WKOQ3AX as cash?
The bonus itself is not withdrawn as cash, it is only used for trading, and the profit earned is added to your balance. The commission discount is directly deducted from your trading costs and does not require a separate withdrawal process.
### Is the WKOQ3AX code valid in all countries?
Yes, the WKOQ3AX code is valid in all countries where Bybit operates. However, registration is not possible in countries where Bybit does not operate, such as the USA, Canada, the UK, Singapore, and mainland China.
### Is KYC mandatory?
No, at least KYC Level 1 verification is required for all Bybit promotions. It is recommended to complete identity verification immediately after registration.
—
## 7. Expert Tip: WKOQ3AX is the Right Code for You
**This special promo code** with its combined advantages in a single code offers both maximum bonus potential and permanent commission discount together.
| **Investor Profile** | **Gain Obtained** |
|——————-|——————|————-|
| **New to crypto** | Bonuses easily earned through simple tasks |
| **Frequent trader** | Thousands of dollars in long-term commission savings |
| **Investors of all levels** | Most comprehensive benefit with bonus + discount combination |
—
## Summary
Special promo codes like WKOQ3AX offer advantages that cannot be achieved with a standard registration. **The WKOQ3AX code** by combining both maximum bonus potential and permanent commission savings in one code allows you to start your investments with an advantage.
Crypto investments have a volatile nature; it’s important to trade with amounts you can afford to lose. The promotions offered by Bybit give you the opportunity to start with better conditions in this risky environment. Be sure to check current campaigns and the validity period of codes before registering.
—
## Take Action Now!
**The only thing you need to start earning on Bybit: WKOQ3AX**
**Start your advantaged journey through the link below:**
### 👉 **Click to register on Bybit with the special link**
Don’t forget to enter your WKOQ3AX code and get Bybit privileges today!
—
*This article is for informational purposes and does not constitute investment advice. Cryptocurrency trading carries high risk; it is recommended to do your own research before making decisions.*
promo here
Get the promo code
Source:
https://t.me/Suhanfff_bot
CharlesRuh · April 18, 2026 at 10:37 pm
Капельница от похмелья — это медицинская процедура, направленная на устранение последствий алкогольной интоксикации и восстановление работы организма. В отличие от домашних методов, инфузионная терапия позволяет воздействовать на причину состояния, а не только на его проявления. В наркологической клинике «Похмельная служба» капельная терапия проводится с выездом специалиста на дом, что позволяет начать лечение без задержек и в комфортных условиях.
Выяснить больше – капельница от похмелья цена воронеж
JamesVot · April 18, 2026 at 10:46 pm
# How to get Bybit sign-up bonus to maximize your earnings
Taking your first step into crypto exchanges is exciting but taking the right steps makes a huge difference in the long run. As one of the leading platforms, Bybit hosts billions of dollars in daily trading volume offering attractive opportunities through sign-up bonus campaigns. Here are the details of the Bybit referral code WKOQ3AX, usage steps, and benefits! In the guide below you will access all the information you need about the current Bybit promo code WKOQ3AX and campaigns.
—
## 1. What Are the Advantages of the Bybit Platform?
Bybit, headquartered in Dubai, has been operating since 2018 and has quickly become one of the most trusted names in the industry. With a user base exceeding 80 million today with an average daily trading volume exceeding $20 billion is one of the most liquid exchanges in the industry.
**The main features that distinguish Bybit from other exchanges:**
– **Deep Liquidity:** The ability to trade with minimal slippage even on large volume orders
– **Security Infrastructure:** The platform uses the most advanced technologies to ensure asset security , and periodic Proof of Reserve (PoR) reports are shared with the public
– **Institutional Reliability:** with MiCAR in Europe and SCA full license in UAE as of 2025 has taken significant steps in regulatory compliance
– **Trading Options:** Offers a wide variety of products to investors such as spot, futures, options, copy trading, liquidity mining, and Web3 wallet
—
## 2. What Do You Gain on Bybit with Promo Code WKOQ3AX?
The Bybit invitation code is a special key that new users joining the platform can use at sign-up. **WKOQ3AX** has been specifically designated to offer you the highest advantages. Using this code users make a much more profitable start than a standard membership. The main benefits you can obtain with Bybit’s WKOQ3AX referral code are:
| **Gain Type** | **Opportunity Provided** |
|——————|————–|
| **Trading Cost Savings** | Up to 20% ongoing commission advantage on spot and futures markets |
| **Sign-Up Bonus** | Phased welcome package up to 30,000 USDT |
| **First Deposit Rewards** | Additional rewards after the first deposit |
| **Risk Management Tools** | Coupons that cover potential losses on initial trades |
**Important Note:** You must use your WKOQ3AX bonus code when opening your account. There is no possibility to add or edit the code after the account is created.
—
## 3. Working Bybit Promo Code 2026: WKOQ3AX
As of 2026, the most current and most advantageous promo code you can use on Bybit is **WKOQ3AX**. This code offers a comprehensive opportunity that appeals to all user profiles:
### WKOQ3AX – Bybit’s Most Comprehensive Promo Code
**Code: WKOQ3AX**
This referral code allows both beginners to earn bonuses easily and active traders to save on commissions. Users who register with **WKOQ3AX benefit from both up to 30,000 USDT in trial bonuses and also have a lifetime 20% commission discount advantage. The discount is automatically applied to spot and futures markets.
**What Makes WKOQ3AX Special:**
– Highest bonus potential (30,000 USDT) – industry-leading opportunity
– 20% permanent trading fee discount valid for the life of the account
– Valid in all countries
– Works on web and mobile apps
– All advantages without trading type restrictions
—
## 4. Bybit Bonus Types and WKOQ3AX Usage Conditions
The bonus types you will obtain on the platform with the WKOQ3AX referral code vary and each bonus type has its own rules.
### 4.1. Trial Bonus Usage Rules
A trading bonus is a type of reward you can use as margin, especially in futures markets. The most important feature of this bonus is that you can withdraw the profits you make, but you cannot withdraw the bonus itself. So if you trade with the bonus, the profit you make is yours, while any loss is first deducted from the bonus balance. This mechanism allows new users to experience the platform without taking risks.
**Trial Bonus Usage Rules:**
– Cannot be withdrawn directly, functions as trading collateral
– The maintenance costs of open positions can be covered with the bonus
– Usage period is limited, otherwise validity expires
– Cannot be withdrawn as cash, only valid for futures trading
### 4.2. Trading Fee Savings Coupons
Fee saver coupons allow you to recover the commissions you pay on your trades. The system first deducts the trading fee from your own balance, then refunds the coupon amount to your account. These coupons can be used for your spot, futures, or instant buy/sell transactions. **The 20% permanent discount that comes with the WKOQ3AX code, combined with these coupons, reduces your trading costs to nearly zero.**
### 4.3. Bybit’s Special Events
Bybit has various events on a weekly and monthly basis. In the “Daily Treasure Hunt” campaign that has been ongoing for the past few months:
– More than 100,000 prize cards are distributed to participants in total
– BTC, ETH, and other major cryptocurrencies along with VIP trial cards are in the prize pool
– Complete tasks, collect points, and earn one raffle ticket for every 50 points
—
## 5. How to Enter the WKOQ3AX Code When Registering on Bybit?
### Quick Registration and Bonus Earning Steps
**1. Step: Access the Bybit Platform**
– **Direct registration link:** Click this link to register with the WKOQ3AX code automatically applied: https://t.me/Suhanfff
– Visit bybit.com from your web browser
– Mobile: Download the Bybit app from the App Store or Google Play
**2. Step: Enter Your Membership Information**
– Write your email address or phone number to register
– Choose a strong password
**3. Phase: Use Your WKOQ3AX Bonus Code**
– Find the section labeled “Referral Code” or “Promo Code” on the form that opens
– Enter the code: **WKOQ3AX**
– If you used the special link, the code will be automatically filled
**4. Step: Complete the Verification Process**
– Enter the verification code sent to your email or phone
**5. Phase: Upgrade Your Account Level**
– KYC Level 1 is mandatory to receive bonuses
– Verify using an identity document (passport, national ID card, or driver’s license)
– Verification time ranges from 5 to 10 minutes on average
**6. Phase: Complete Campaign Tasks Step by Step**
– Check your earned rewards from the Bonus Center screen
– Rewards are instantly credited to your account as you progress through tasks
—
## 6. Frequently Asked Questions
### Can I add the WKOQ3AX code after registration?
No, the WKOQ3AX promo code can only be entered at the time of registration. There is no possibility to add or edit the code after the account is created. **It is recommended to use the special link to avoid the risk of forgetting the code.**
### Can I enter multiple bonus codes?
Only one referral code can be used per account. **It is recommended to register by choosing the most advantageous code, WKOQ3AX.**
### Is it possible to withdraw the bonus balance from my account?
The trading bonus amount cannot be withdrawn; you can only withdraw the profit made with it. With the trading fee discount, you automatically save on every transaction.
### In which countries can WKOQ3AX be used?
The WKOQ3AX promo code can be used in all regions where Bybit operates, including Turkey. The only requirement for the code’s validity is that you are located in a country where Bybit has operational permission.
### Is KYC mandatory?
KYC identity verification is required for all bonuses you earn with the WKOQ3AX code. KYC is quick and free; you can complete it in a few minutes.
—
## 7. Expert Tip: WKOQ3AX is the Right Code for You
**This special promo code** unlike other codes on the market offers both maximum bonus potential and permanent commission discount together.
| **Trader Type** | **Benefit with WKOQ3AX** |
|——————-|——————|————-|
| **Inexperienced investor** | Bonuses easily earned through simple tasks |
| **Active trader, high volume expected** | Thousands of dollars in long-term commission savings |
| **All users** | Most comprehensive benefit with bonus + discount combination |
—
## Summary
Special promo codes like WKOQ3AX offer advantages that cannot be achieved with a standard registration. **The WKOQ3AX code** by offering up to 30,000 USDT in bonus packages along with a lifetime 20% trading fee discount can make a significant difference in your long-term earnings.
Crypto investments have a volatile nature; it’s important to trade with amounts you can afford to lose. Promo codes like WKOQ3AX reduce your trading costs, giving you a competitive advantage. Don’t forget to review campaign details before registration to catch the most current opportunities.
—
## Register Now!
**Choose the right promo code: WKOQ3AX**
**Start your advantaged journey through the link below:**
### 👉 **https://t.me/Suhanfff**
Create your account using the link above to start with an advantage on Bybit and benefit from up to 30,000 USDT in bonuses!
—
*The information provided herein is for informational purposes only. Before investing, carefully evaluate market conditions and act according to your own risk tolerance.*
promo here
Get the promo code
Source:
https://t.me/Suhanfff_bot
Edwardattix · April 18, 2026 at 10:56 pm
Процесс лечения капельницей помогает улучшить состояние пациента уже через короткий период. Важно, что процедура не только снимает симптомы похмелья, но и восстанавливает нормальную работу печени, почек и других органов, пострадавших от токсического воздействия алкоголя. Это помогает предотвратить долгосрочные последствия интоксикации, такие как хроническая усталость, проблемы с органами и психоэмоциональные расстройства.
Узнать больше – капельница от похмелья на дому в екатеринбурге
bingoplus app · April 18, 2026 at 10:59 pm
This web site truly has all of the information and facts I wanted concerning this subject and didn’t know who to ask.
EmmettAporn · April 18, 2026 at 11:27 pm
Нарколог на дом в Самаре — помощь при запое и интоксикации в наркологической клинике «Частный медик 24»
Детальнее – нарколог на дом
GilbertJUrry · April 19, 2026 at 12:06 am
Вызов капельницы от похмелья с контролем врача в Самаре рекомендуется, когда симптомы похмелья становятся особенно тяжелыми и мешают нормальной жизнедеятельности. Несмотря на то, что многие пытаются справиться с похмельем с помощью домашних методов, такие как прием жидкости или таблеток, они не всегда оказываются достаточно эффективными. В случае сильных симптомов похмелья, капельница с врачебным контролем — это более безопасное и быстрое решение, при этом возможен вывод в стационаре, анонимное лечение и консультации по вопросам наркомании с учетом актуальной цены услуг.
Получить дополнительные сведения – капельница от похмелья анонимно
Jasonmit · April 19, 2026 at 12:31 am
В Екатеринбурге выезд нарколога на дом становится необходимостью, когда симптомы похмелья слишком выражены и пациент не может справиться с ними самостоятельно. Алкогольная интоксикация может привести к ряду проблем, таких как головная боль, слабость, тошнота и рвота, а иногда даже к более серьёзным состояниям, таким как аритмия или психоз. Выезд нарколога на дом позволяет быстро начать лечение, не тратя время на дорогу, что особенно важно в экстренных ситуациях.
Углубиться в тему – https://kapelnicza-ot-pokhmelya-ekaterinburg-7.ru/
DavidSoict · April 19, 2026 at 12:37 am
Врач-нарколог, оценивая состояние пациента, может рекомендовать проведение капельницы для ускоренного восстановления организма. Применение капельницы позволяет снять острые симптомы интоксикации и снизить риск развития более серьезных последствий. В некоторых случаях, если необходимо интенсивное наблюдение, пациенту может быть предложено лечение в стационаре, и услугу можно заказать на летний период для более длительного контроля.
Углубиться в тему – капельница от запоя на дому цена нижний новгород
EmmettAporn · April 19, 2026 at 1:09 am
Нарколог на дом в Самаре — помощь при запое и интоксикации в наркологической клинике «Частный медик 24»
Получить дополнительные сведения – нарколог на дом вывод
DavidSoict · April 19, 2026 at 1:10 am
Капельница от запоя в Нижнем Новгороде: снятие интоксикации, восстановление организма и помощь при запое под контролем специалистов в наркологической клинике «Похмельная служба»
Детальнее – капельница от запоя цена в нижнем новгороде
JasonSeiVa · April 19, 2026 at 2:02 am
Процесс проведения капельницы от похмелья обычно включает в себя несколько ключевых этапов. Несмотря на простоту процедуры, важно, чтобы её проводил квалифицированный специалист. Каждый этап — от консультации до завершения процедуры — направлен на безопасность пациента и максимальную эффективность лечения.
Детальнее – https://kapelnicza-ot-pokhmelya-samara-6.ru/
GoodiniCrubs · April 19, 2026 at 2:03 am
Такие критерии помогают определить, когда необходим более строгий контроль и постоянное наблюдение. В стационаре создаются условия, при которых лечение проходит без внешних факторов, влияющих на состояние пациента. При этом услуга может предоставляться анонимно, а цену лечения можно уточнить заранее по телефону или при обращении.
Выяснить больше – вывод из запоя дешево нижний новгород
JasonSeiVa · April 19, 2026 at 2:33 am
“Капельница — это быстрый и эффективный способ восстановить организм после похмелья. Она особенно полезна при выраженных симптомах, таких как сильная головная боль или рвота. Важно, чтобы процедура проводилась квалифицированным медицинским персоналом, чтобы избежать осложнений. Также, в случае хронической зависимости, может потребоваться кодирование или терапия для долгосрочного восстановления, а также вызов врача для дальнейшего наблюдения,”
Узнать больше – капельница от похмелья цена в самаре
HarryMeazy · April 19, 2026 at 2:42 am
Капельница от похмелья — это одна из самых эффективных процедур для быстрого облегчения симптомов интоксикации после употребления алкоголя. В Нижнем Новгороде существует множество клиник и медицинских центров, которые предлагают услуги капельниц, направленных на восстановление водно-электролитного баланса, улучшение общего самочувствия и снятие неприятных симптомов похмелья. Процесс введения капельницы можно адаптировать под индивидуальные особенности пациента для достижения наилучшего результата.
Подробнее тут – http://kapelnicza-ot-pokhmelya-nizhnij-novgorod.ru
DavidPeart · April 19, 2026 at 3:04 am
Капельница от похмелья с мягким восстановлением — это метод, направленный на быстрое восстановление организма после алкогольной интоксикации, при котором используется более щадящий подход. В отличие от стандартных капельниц, целью которых является быстрый вывод токсинов из организма, капельница с мягким восстановлением действует постепенно, восстанавливая водно-солевой баланс и поддерживая внутренние органы без перегрузки организма. Эта процедура особенно полезна тем, кто предпочитает не только избавиться от похмелья, но и почувствовать себя восстановленным и энергичным, при этом помощь может оказываться при запое, когда врач выезжает на дом для лечения алкоголизма.
Получить дополнительную информацию – капельница от похмелья на дому в самаре
baby-generator.ai · April 19, 2026 at 3:16 am
Oh my goodness! Incredible article dude! Thank you so much, However I am encountering issues with your RSS. I don’t know the reason why I am unable to subscribe to it. Is there anybody else having identical RSS issues? Anybody who knows the solution will you kindly respond? Thanx!
Damontof · April 19, 2026 at 3:18 am
На первом этапе специалист проводит визуальный осмотр пациента, измеряет артериальное давление, пульс, уровень кислорода в крови и оценивает общее психоэмоциональное состояние. Важно выявить степень интоксикации, наличие осложнений и противопоказаний к проведению терапии на дому. В случае наркомании и длительного употребления наркотиков, пациенту может быть предложена консультация и лечение, включая реабилитацию на летний период, если состояние требует интенсивного контроля.
Получить дополнительную информацию – http://www.domen.ru
HarryMeazy · April 19, 2026 at 3:20 am
Основное действие капельницы заключается в быстром восстановлении водного баланса и выведении токсинов, оставшихся в организме после употребления алкоголя. Алкоголь нарушает работу печени, почек и других органов, поэтому капельница помогает организму вернуться в норму, восстанавливая функции этих органов и поддерживая обмен веществ. Состав капельницы также может включать препараты, которые поддерживают работу сердечно-сосудистой системы и устраняют болезненные ощущения, такие как головная боль и тошнота.
Подробнее тут – капельница от похмелья нижний новгород
Davidaxono · April 19, 2026 at 3:24 am
Капельница от похмелья — это эффективный способ снятия симптомов алкогольной интоксикации, который позволяет быстро восстановить организм после длительного употребления алкоголя. В наркологической клинике «Частный медик 24» в Екатеринбурге мы предлагаем капельную терапию, которая включает в себя комплекс препаратов для восстановления водно-электролитного баланса, выведения токсинов и нормализации состояния пациента. Процедура проводится в удобной обстановке, и мы обеспечиваем полное наблюдение врача на протяжении всего процесса лечения.
Выяснить больше – капельница от похмелья на дому екатеринбург
ScottJat · April 19, 2026 at 3:28 am
Запрос на выезд врача связан не только с классическим запоем. На практике домашняя помощь нужна в разных ситуациях, когда организму уже трудно компенсировать последствия употребления, а откладывание визита увеличивает риск осложнений.
Углубиться в тему – запой нарколог на дом в воронеже
Davidaxono · April 19, 2026 at 3:35 am
Эти симптомы характерны для алкогольной интоксикации, и их быстрое устранение с помощью капельницы позволяет пациенту почувствовать себя лучше и избежать более серьёзных последствий. В клинике «Частный медик 24» мы подбираем индивидуальную программу лечения, чтобы ускорить восстановление организма и улучшить общее самочувствие пациента.
Разобраться лучше – https://kapelnicza-ot-pokhmelya-ekaterinburg-5.ru
WilliamOptop · April 19, 2026 at 3:41 am
Запой сопровождается выраженной интоксикацией, нарушением сна, слабостью и нестабильностью работы сердечно-сосудистой системы, что характерно для алкоголизма и других форм зависимости, включая наркомании. Самостоятельный выход из этого состояния может быть затруднён и сопровождаться усилением симптомов. Медицинская помощь на дому позволяет снизить риски и начать восстановление под контролем специалиста, помогая человеку быстрее стабилизировать состояние.
Получить больше информации – вывод из запоя на дому цена
Damontof · April 19, 2026 at 3:50 am
На первом этапе специалист проводит визуальный осмотр пациента, измеряет артериальное давление, пульс, уровень кислорода в крови и оценивает общее психоэмоциональное состояние. Важно выявить степень интоксикации, наличие осложнений и противопоказаний к проведению терапии на дому. В случае наркомании и длительного употребления наркотиков, пациенту может быть предложена консультация и лечение, включая реабилитацию на летний период, если состояние требует интенсивного контроля.
Углубиться в тему – нарколог на дом вывод самара
CharlesRuh · April 19, 2026 at 3:53 am
Похмельный синдром сопровождается головной болью, слабостью, тошнотой, сухостью во рту и нарушением сна, что часто возникает после запоя или при алкоголизме. Эти симптомы появляются из-за накопления токсинов и нарушения водно-солевого баланса. Капельница помогает ускорить выведение вредных веществ и восстановить нормальные функции организма, снижая нагрузку на внутренние системы и помогая человеку быстрее выйти из состояния запоев.
Подробнее тут – капельница от похмелья цена в воронеже
JavierBix · April 19, 2026 at 4:21 am
Срочный домашний выезд особенно важен для семей, которые уже сталкивались с тяжёлыми последствиями алкоголизма и понимают, что обычные попытки «отпаивания» не решают проблему. Врач оценивает не только факт употребления, но и длительность запоя, возраст, наличие хронических болезней, уже принятые медикаменты, риск абстинентного синдрома, состояние сердца и общую нагрузку на организм. Такой формат позволяет анонимно вызвать специалиста, быстро провести необходимые вмешательства и определить, нужен ли только домашний вывод из острого состояния или дальше потребуется кодирование, повторная консультация, реабилитация либо более широкий маршрут помощи при наркомании.
Узнать больше – вызвать нарколога на дом воронеж
CharlesRuh · April 19, 2026 at 4:32 am
Такие симптомы требуют медицинского вмешательства, поскольку могут усиливаться без лечения. Капельница позволяет стабилизировать состояние и ускорить восстановление. Услуги могут предоставляться анонимно, а при необходимости пациент направляется на лечение в стационаре.
Ознакомиться с деталями – капельница от похмелья на дом в воронеже
SamuelTob · April 19, 2026 at 5:15 am
Процедура начинается с осмотра пациента. Врач измеряет давление, пульс, оценивает общее состояние и выраженность симптомов. На основании этих данных формируется состав капельницы и план лечения. Такой подход позволяет учитывать индивидуальные особенности пациента и эффективно провести вывод из запоя.
Исследовать вопрос подробнее – https://kapelnicza-ot-pokhmelya-voronezh-4.ru
ScottJat · April 19, 2026 at 5:21 am
Нарколог на дом в Воронеже с круглосуточным вызовом врача, стабилизацией состояния и лечением в наркологической клинике «Частный медик 24»
Изучить вопрос глубже – врач нарколог на дом
StephenDiumn · April 19, 2026 at 5:24 am
Такие состояния требуют не только лечения, но и наблюдения, поскольку динамика может меняться в течение короткого времени. Стационар позволяет минимизировать риски и обеспечить безопасность пациента. При этом услуга может предоставляться анонимно, а цена лечения зависит от состояния пациента.
Узнать больше – анонимный вывод из запоя в нижнем новгороде
GilbertJUrry · April 19, 2026 at 5:53 am
Процедура капельницы от похмелья с контролем врача в Самаре начинается с первичной консультации, на которой врач осматривает пациента, измеряет его основные показатели (давление, пульс, температуру) и оценивает общее состояние. На основе этих данных выбирается оптимальный состав капельницы, которая может включать в себя различные компоненты, такие как солевые растворы, витамины, антиоксиданты и медикаменты для снятия симптомов похмелья.
Получить дополнительные сведения – капельница от похмелья анонимно в самаре
HarveySax · April 19, 2026 at 6:13 am
В таких ситуациях врач оценивает риски, определяет тактику лечения и при необходимости рекомендует дальнейшую госпитализацию. Однако во многих случаях помощь на дому оказывается достаточной для стабилизации состояния.
Получить дополнительную информацию – нарколог на дом анонимно нижний новгород
JefferyMew · April 19, 2026 at 6:18 am
Запой, длительное употребление алкоголя или случайное злоупотребление могут привести к неприятным симптомам похмелья, таким как головная боль, слабость, тошнота, головокружение и усталость. Эти симптомы обусловлены тем, что в организме остаются продукты распада алкоголя, которые токсически воздействуют на все органы. Капельница от похмелья на дому — это отличная возможность быстро снять острые симптомы и восстановить нормальное состояние организма, не выходя из привычной обстановки.
Разобраться лучше – капельница от похмелья цена самара
GilbertJUrry · April 19, 2026 at 6:29 am
Капельница от похмелья с контролем врача в Самаре представляет собой эффективную терапевтическую процедуру, позволяющую значительно улучшить самочувствие пациента за короткий срок. Врач, контролируя весь процесс, может точно определить, какие компоненты необходимы для каждого пациента. Состав капельницы зависит от симптомов похмелья, состояния пациента и его индивидуальных потребностей. Это позволяет обеспечить максимально безопасное и эффективное лечение, которое помогает организму быстро восстановиться.
Получить больше информации – kapelnicza-ot-pokhmelya-samara-13.ru/
JefferyMew · April 19, 2026 at 6:30 am
Капельница от похмелья — это эффективный способ экстренной помощи, предназначенный для того, чтобы помочь организму быстро восстановиться после злоупотребления алкоголем. В наркологической клинике «Частный медик 24» в Самаре мы предоставляем услугу безопасной детоксикации и восстановления 24/7. Капельница помогает организму вывести токсины, восстановить водно-электролитный баланс и улучшить общее состояние пациента, не создавая дополнительных нагрузок на сердце, печень и почки.
Получить больше информации – капельница от похмелья вызов на дом в самаре
RobertSUS · April 19, 2026 at 6:57 am
Главная https://images.google.sn/url?q=https://travelanswer.ru/flights/from-caracas-to-lima-peru.html
StephenDiumn · April 19, 2026 at 7:21 am
К основным показаниям относятся:
Выяснить больше – vyvod-iz-zapoya-v-staczionare-nizhnij-novgorod-2.ru/
RobertDault · April 19, 2026 at 7:28 am
В Санкт-Петербурге вывод из запоя на дому рассматривается, когда состояние пациента позволяет проводить лечение вне стационара, но требует контроля специалиста. Врач оценивает общее состояние, длительность запоя и выраженность симптомов, после чего принимает решение о формате помощи при алкоголизме. Важно, что лечение начинается сразу после осмотра, без необходимости ожидания госпитализации. При необходимости можно заказать услуги на сайте клиники или получить консультацию специалистов.
Разобраться лучше – вывод из запоя на дому цена в санкт-петербурге
WalterSic · April 19, 2026 at 7:34 am
Наркологический стационар с круглосуточным наблюдением — это не просто место для детоксикации, но и пространство для комплексного лечения и реабилитации. Постоянное присутствие медицинского персонала помогает избежать опасных ситуаций, таких как психозы или физиологические сбои, характерные для абстиненции. Прием пациентов может включать кодирование, а также индивидуальные программы лечения, которые разрабатываются в зависимости от состояния пациента и его потребностей на протяжении года.
Получить больше информации – наркологическая помощь стационар в санкт-петербурге
RobertDault · April 19, 2026 at 7:41 am
Запой сопровождается выраженной интоксикацией, нарушением сна, слабостью, тревожностью и колебаниями давления, что характерно для алкоголизма и других форм зависимости. При этом самостоятельный выход из состояния часто оказывается затруднённым из-за ухудшения самочувствия и невозможности контролировать симптомы. В таких случаях выезд нарколога позволяет начать лечение без задержек и помочь пациенту снизить нагрузку на организм за счёт отсутствия транспортировки.
Узнать больше – вывод из запоя на дому цена в санкт-петербурге
Randytup · April 19, 2026 at 7:54 am
Для жителей Самары выезд нарколога на дом — это удобный и быстрый способ получить неотложную помощь при алкогольной или наркотической зависимости. Когда состояние пациента ухудшается и он не может самостоятельно обратиться за помощью, нарколог на дом становится единственным правильным решением. Важно понимать, что симптоматика абстиненции может развиваться стремительно, и чем быстрее будет оказана помощь, тем меньше рисков для здоровья пациента.
Получить больше информации – нарколог на дом анонимно в самаре
Edwardattix · April 19, 2026 at 8:18 am
Процесс лечения капельницей помогает улучшить состояние пациента уже через короткий период. Важно, что процедура не только снимает симптомы похмелья, но и восстанавливает нормальную работу печени, почек и других органов, пострадавших от токсического воздействия алкоголя. Это помогает предотвратить долгосрочные последствия интоксикации, такие как хроническая усталость, проблемы с органами и психоэмоциональные расстройства.
Детальнее – капельница от похмелья на дом в екатеринбурге
JeffreyGom · April 19, 2026 at 9:16 am
Состояние пациента при интоксикации может развиваться по-разному: от умеренной слабости и головной боли до выраженной дезориентации, тахикардии и нарушений сна. В таких ситуациях важно не откладывать обращение за помощью. Наркологическая помощь на дому рассматривается, когда требуется быстрое вмешательство и контроль состояния без транспортировки пациента.
Подробнее тут – http://narkologicheskaya-pomoshh-nizhnij-novgorod-8.ru/
JavierBix · April 19, 2026 at 9:33 am
Главное преимущество такого выезда в том, что лечение начинается сразу. Не нужно ждать утра, искать транспорт, уговаривать человека ехать в тяжёлом состоянии или рисковать, пока он снова тянется к алкоголю, чтобы временно заглушить симптомы. Домашний визит даёт возможность быстро стабилизировать ситуацию и убрать хаотичность, которая часто возникает в семье в острый момент.
Подробнее – нарколог на дом анонимно
Edwardsak · April 19, 2026 at 9:36 am
Показания для обращения за помощью включают:
Детальнее – капельница от похмелья на дому
EmmettAporn · April 19, 2026 at 9:37 am
Нарколог на дом в Самаре востребован в самых различных ситуациях. Иногда пациент не в состоянии самостоятельно добраться до клиники из-за сильного состояния похмелья или ломки. В таких случаях выезд нарколога становится наиболее оптимальным решением. Наши специалисты оказывают помощь при следующих состояниях:
Разобраться лучше – нарколог на дом в самаре
MarvinNoing · April 19, 2026 at 9:39 am
Анонимное лечение на дому ценно ещё и тем, что снижает внутреннее сопротивление самого пациента. Для многих людей первый контакт с врачом происходит именно дома, без дороги, без ожидания, без страха чужих взглядов. Такой формат помогает начать разговор не только о снятии острых симптомов, но и о более широких вопросах: что делать после выхода из запоя, когда требуется кодирование, в каких случаях нужна реабилитация, а когда первичная наркологическая помощь уже должна переходить в полноценный лечебный маршрут. Врач может помочь и в ситуациях, связанных не только с алкоголем, но и с наркомании, если семье нужно понять, что происходит с зависимым человеком и какой следующий шаг будет для него безопасным.
Получить дополнительные сведения – http://narkolog-na-dom-voronezh-1.ru
bet-passo-a-passo · April 19, 2026 at 10:20 am
A semana favoreceu quem jogou com calma e critério.
Edwardattix · April 19, 2026 at 10:32 am
Алкогольная интоксикация оказывает серьёзное влияние на организм, вызывая головную боль, тошноту, слабость и головокружение. Капельница помогает организму быстро избавиться от продуктов распада алкоголя, восстановить нормальное функционирование органов и минимизировать последствия для здоровья. Важно, что мы обеспечиваем полное наблюдение врача на протяжении всей процедуры, что помогает гарантировать безопасность пациента и максимальную эффективность лечения.
Исследовать вопрос подробнее – капельница от похмелья цена
JamesEdumb · April 19, 2026 at 10:40 am
Вывод из запоя в стационаре в Нижнем Новгороде с круглосуточным наблюдением и поэтапным восстановлением в наркологической клинике «Частный медик 24»
Исследовать вопрос подробнее – нарколог на дом вывод из запоя нижний новгород
JavierBix · April 19, 2026 at 11:31 am
Главное преимущество такого выезда в том, что лечение начинается сразу. Не нужно ждать утра, искать транспорт, уговаривать человека ехать в тяжёлом состоянии или рисковать, пока он снова тянется к алкоголю, чтобы временно заглушить симптомы. Домашний визит даёт возможность быстро стабилизировать ситуацию и убрать хаотичность, которая часто возникает в семье в острый момент.
Изучить вопрос глубже – запой нарколог на дом в воронеже
WalterProor · April 19, 2026 at 11:32 am
Игнорирование симптомов или попытки справиться самостоятельно могут усугубить состояние пациента. Домашние методы без медицинского контроля не обеспечивают полноценной детоксикации и не учитывают индивидуальные риски. Квалифицированный нарколог оценивает состояние пациента на месте, подбирает безопасную схему терапии и контролирует динамику, что особенно важно при тяжелых формах интоксикации.
Получить дополнительную информацию – вызов нарколога на дом
RodolfoDap · April 19, 2026 at 11:37 am
Стационарное лечение в наркологическом стационаре дает целый ряд преимуществ, которые трудно переоценить, особенно в случае тяжелых зависимостей. Пребывание в стационаре позволяет сосредоточиться исключительно на восстановлении здоровья, не отвлекаясь на внешние факторы, и получать постоянную помощь профессионалов. В некоторых случаях, в зависимости от состояния пациента, может потребоваться вывод из запоя, а также консультация специалистов, которые будут сопровождать пациента на протяжении года для долгосрочной реабилитации.
Получить больше информации – наркологическая клиника стационар
RobertSUS · April 19, 2026 at 12:33 pm
нажмите https://images.google.jo/url?q=https://letundra.com/es/news/?taglist=tayside
DavidPeart · April 19, 2026 at 1:14 pm
“Капельница с мягким восстановлением идеально подходит тем, кто ищет постепенный и безопасный способ вернуть себе нормальное состояние после пьянки. Такой подход не перегружает организм и помогает избежать нежелательных эффектов от слишком резкого восстановления.” — Алексей Смирнов, нарколог, клиника восстановления.
Получить больше информации – капельница от похмелья цена
CharlesPoumn · April 19, 2026 at 1:16 pm
Когда такие симптомы становятся ярко выраженными, важно не затягивать с лечением и вызвать нарколога на дом. Это позволит своевременно устранить токсические вещества из организма и предотвратить серьёзные проблемы с органами. Важно, чтобы лечение началось как можно быстрее, что возможно только через экстренный выезд специалиста на дом.
Получить дополнительную информацию – капельница от похмелья анонимно екатеринбург
Davidaxono · April 19, 2026 at 1:17 pm
Капельница от похмелья в Екатеринбурге с выездом специалиста, подбором терапии и восстановлением состояния в наркологической клинике «Частный медик 24»
Получить дополнительные сведения – kapelnicza-ot-pokhmelya-ekaterinburg-5.ru/
Randytup · April 19, 2026 at 1:41 pm
Выезд нарколога на дом в Самаре — это комплексный подход к лечению, который включает несколько этапов. Врач, приехавший на место, не ограничивается одной процедурой, а проводит полноценный осмотр, диагностирует состояние пациента, определяет причину ухудшения самочувствия и подбирает индивидуальную терапию. Наиболее часто при выезде нарколога на дом используются капельницы, антиеметики и препараты для стабилизации состояния пациента, снятия симптомов абстиненции и улучшения общего самочувствия.
Углубиться в тему – нарколог на дом анонимно
Carminefum · April 19, 2026 at 1:52 pm
Капельница от похмелья с медицинским контролем представляет собой комплексную терапию, которая включает в себя различные препараты, направленные на быстрое восстановление организма. Каждый элемент процедуры подобран с учётом состояния пациента, что позволяет обеспечить максимальную эффективность лечения и минимизировать возможные риски.
Подробнее можно узнать тут – капельница от похмелья на дом
Rogersip · April 19, 2026 at 1:56 pm
Нарколог на дом в Самаре с выездом специалиста, детоксикацией и анонимной медицинской помощью в наркологической клинике «Частный медик 24»
Изучить вопрос глубже – запой нарколог на дом
WilliamOptop · April 19, 2026 at 1:56 pm
Запой сопровождается выраженной интоксикацией, нарушением сна, слабостью и нестабильностью работы сердечно-сосудистой системы, что характерно для алкоголизма и других форм зависимости, включая наркомании. Самостоятельный выход из этого состояния может быть затруднён и сопровождаться усилением симптомов. Медицинская помощь на дому позволяет снизить риски и начать восстановление под контролем специалиста, помогая человеку быстрее стабилизировать состояние.
Детальнее – https://vyvod-iz-zapoya-na-domu-sankt-peterburg-12.ru
Richardexors · April 19, 2026 at 2:13 pm
При выборе наркологического стационара с комфортными условиями в Санкт-Петербурге важно учитывать несколько ключевых факторов, которые могут повлиять на успех лечения. Кроме высококвалифицированных специалистов и индивидуального подхода, комфортные условия для проживания играют важную роль в процессе восстановления пациента. Это создаёт оптимальные условия для того, чтобы человек мог сосредоточиться на своём здоровье и восстановлении, не отвлекаясь на неприятные или неудобные условия. В некоторых случаях может быть предложено кодирование, а также получение дополнительных данных и консультаций для более точного подхода к лечению.
Разобраться лучше – лечение в наркологическом стационаре в санкт-петербурге
ScottJat · April 19, 2026 at 3:06 pm
Домашний формат ценят не только за удобство. Он помогает начать лечение анонимно, без дороги, без ожидания и без лишнего стресса для пациента. Для многих семей именно выездной наркологическая маршрут становится первой точкой, с которой начинается более серьёзное восстановление: обсуждаются не только снятие острых симптомов, но и кодирование, реабилитация, повторная консультация, а при необходимости — и маршруты помощи при наркомании. Особенно это актуально, если человек употребляет давно, уже несколько лет сталкивается со срывами и сам замечает, что проблема перестала ограничиваться только плохим самочувствием после алкоголя.
Разобраться лучше – https://narkolog-na-dom-voronezh-2.ru/
Robertgrita · April 19, 2026 at 3:11 pm
Коллеги, статья про актуальные методы и стратегии для роста трафика в 2026 году. Автор объясняет, почему SEO остаётся важным (долгосрочный эффект, высокое доверие, экономия бюджета), разбирает ключевые направления современного SEO и инструменты для анализа. Есть блок про типичные ошибки и интеграцию SEO с контекстной рекламой, SMM и email-маркетингом. Полезно для выстраивания комплексной стратегии: https://volkhp.ru/stati/prodvizhenie-sajtov-v-2026-godu-aktualnye-metody-i-strategii-dlja-rosta-trafika/
DavidPeart · April 19, 2026 at 3:20 pm
Капельница от похмелья в Самаре: быстрое снятие симптомов, детоксикация и восстановление организма под контролем специалистов в наркологической клинике «Детокс»
Ознакомиться с деталями – капельница от похмелья в самаре
RobertSen · April 19, 2026 at 3:38 pm
Для семьи это тоже имеет большое значение. Пока врач в пути, родственники часто совершают одни и те же ошибки: пытаются «отпаивать» человека через силу, смешивают несовместимые медикаменты, дают советы, которые только повышают тревогу, спорят или требуют немедленно взять себя в руки. Профессиональный выезд снимает эту хаотичность. После осмотра врач объясняет, какие симптомы связаны с алкогольной интоксикацией, какие могут указывать на осложнения, что допустимо дома, а что требует перевода в стационар. В этом и состоит ценность выезда: он возвращает контроль над ситуацией и позволяет начать лечение без лишних задержек.
Ознакомиться с деталями – https://narkolog-na-dom-voronezh-1.ru
StevePer · April 19, 2026 at 3:48 pm
Выезд нарколога на дом — это медицинская услуга, которая подразумевает не только экстренную помощь, но и полноценное обследование пациента в комфортных для него условиях. В наркологической клинике «Частный медик 24» мы обеспечиваем профессиональное лечение на дому, которое включает в себя несколько важных этапов, чтобы стабилизировать состояние пациента, улучшить его самочувствие и снизить риски дальнейших осложнений.
Получить больше информации – вызов нарколога на дом
Randytup · April 19, 2026 at 3:50 pm
Нарколог на дом — это услуга, которая позволяет получить медицинскую помощь в комфортной и привычной обстановке, не выходя из дома. В наркологической клинике «Частный медик 24» в Самаре мы предоставляем профессиональную помощь нарколога прямо на дому. Это идеальное решение для тех, кто испытывает симптомы абстиненции, ломки или алкогольной интоксикации, но не может или не хочет ехать в клинику. Выезд врача на дом позволяет начать лечение сразу, без задержек, минимизируя стрессы и сложности, связанные с поездкой.
Углубиться в тему – нарколог на дом анонимно
WilliamOptop · April 19, 2026 at 4:20 pm
Вывод из запоя на дому — это медицинская помощь, направленная на стабилизацию состояния пациента без госпитализации. Такой формат позволяет начать лечение сразу после обращения и снизить нагрузку на организм, связанную с транспортировкой. В наркологической клинике «Частный медик 24» помощь оказывается с выездом врача, который проводит диагностику и подбирает терапию в зависимости от текущего состояния.
Углубиться в тему – нарколог на дом вывод из запоя в санкт-петербурге
EmmettAporn · April 19, 2026 at 4:20 pm
Нарколог на дом в Самаре — помощь при запое и интоксикации в наркологической клинике «Частный медик 24»
Подробнее тут – вызвать нарколога на дом в самаре
Charlesdig · April 19, 2026 at 4:21 pm
Капельница от похмелья — это медицинская процедура, направленная на быстрое восстановление организма после алкогольной интоксикации. Она помогает устранить обезвоживание, нормализовать обменные процессы и снизить токсическую нагрузку на внутренние органы. В отличие от домашних методов, инфузионная терапия действует напрямую через кровоток, обеспечивая более быстрый и выраженный эффект.
Детальнее – http://www.domen.ru
Jamestrire · April 19, 2026 at 4:33 pm
Наркологический стационар в Санкт-Петербурге предоставляет пациентам комплексное лечение зависимости от психоактивных веществ. Проблемы, связанные с алкоголизмом, наркоманией и другими формами зависимости, требуют индивидуального подхода и профессиональной помощи. Комплексное лечение в таких учреждениях позволяет не только пройти детоксикацию, но и получить полноценную реабилитацию, что дает пациентам шанс на долгосрочную ремиссию и улучшение качества жизни. В некоторых случаях, при запое или необходимости выезда на дом, может быть предложен центр, где решаются все вопросы, связанные с лечением зависимости и восстановлением пациента.
Разобраться лучше – лечение в наркологическом стационаре санкт-петербург
HarveySax · April 19, 2026 at 4:45 pm
Нарколог на дом в Нижнем Новгороде с быстрым приездом специалиста, детоксикацией и медицинской поддержкой в наркологической клинике «Частный медик 24»
Узнать больше – врач нарколог на дом нижний новгород
Jamestrire · April 19, 2026 at 4:49 pm
Наркологический стационар в Санкт-Петербурге: лечение зависимости, детоксикация и круглосуточный медицинский контроль в наркологической клинике «Похмельная служба»
Выяснить больше – частный наркологический стационар санкт-петербург
JefferyMew · April 19, 2026 at 5:00 pm
В Самаре клиника «Частный медик 24» предоставляет круглосуточную помощь по выведению из запоя и снятию симптомов похмелья. Когда человек сталкивается с тяжёлым состоянием после длительного употребления алкоголя, важно вовремя оказать помощь. Врач приедет на дом и проведёт все необходимые процедуры, включая капельницу, которая поможет восстановить водно-электролитный баланс, нормализовать уровень сахара в крови и вывести токсины из организма.
Подробнее – капельница от похмелья вызов на дом в самаре
https://www.escapadesnature.fr/wp-content/pgs/code_promo_melbet_meilleur_bonus.html · April 19, 2026 at 5:02 pm
https://www.escapadesnature.fr/wp-content/pgs/code_promo_melbet_meilleur_bonus.html
Jasonmit · April 19, 2026 at 5:27 pm
Капельница от похмелья в Екатеринбурге с инфузионной терапией и быстрым облегчением симптомов в наркологической клинике «Частный медик 24»
Подробнее – капельница от похмелья цена
fixDiele · April 19, 2026 at 5:43 pm
Зацепил материал про Единая система оптимизации в медицине.
Вот, делюсь ссылкой:
https://bro-lordfilm.ru/news/optimizacziya-ocheredej-v-poliklinikah-kadrov-i-lekarstv-kak-edinaya-sistema/
fixDiele · April 19, 2026 at 5:48 pm
Для тех, кто ищет информацию по теме “Прогресс районов Пензенской области: анализ 2026”, нашел много полезного.
Вот, делюсь ссылкой:
https://crm64.ru/news/rajony-penzenskoj-oblasti-2026-kak-otlichit-realnyj-progress-ot-otchyotnyh-czifr/
Davidaxono · April 19, 2026 at 6:08 pm
Процедура проводится опытными наркологами, которые подбирают необходимое лечение на основе индивидуальных особенностей пациента. В клинике «Частный медик 24» применяются только эффективные и безопасные препараты, которые помогают организму восстановиться и избавиться от токсинов. Важно помнить, что капельница от похмелья — это не просто временное облегчение, а важный шаг к долгосрочному восстановлению организма и профилактике алкоголизма.
Разобраться лучше – http://kapelnicza-ot-pokhmelya-ekaterinburg-5.ru/
StephenDiumn · April 19, 2026 at 6:23 pm
В Нижнем Новгороде стационарный формат лечения применяется при наличии факторов, повышающих риск осложнений или снижающих эффективность домашней терапии. Врач принимает решение на основании осмотра, консультации и анализа данных, оценивая текущее состояние пациента и его реакцию на предыдущие попытки лечения. При необходимости можно заранее обратиться в центр лечения алкоголизма и наркомании или заказать услугу по телефону.
Разобраться лучше – вывод из запоя дешево нижний новгород
melhor-horario-jogar-fortune-tiger-hoje · April 19, 2026 at 6:52 pm
Entre hype e estratégia, a melhor combinação ainda é controle + oportunidade.
GeorgeGlync · April 19, 2026 at 7:42 pm
Такой подход позволяет начать лечение без задержек и снизить риски, связанные с транспортировкой пациента. При этом помощь может предоставляться анонимно, что важно для многих пациентов.
Углубиться в тему – вывод из запоя на дому санкт-петербург
Michaelcib · April 19, 2026 at 7:58 pm
При таких условиях стационар позволяет контролировать состояние в режиме 24/7 и при необходимости быстро корректировать лечение. Это снижает риски и делает процесс более предсказуемым. При этом услуга может предоставляться анонимно, а цену лечения можно уточнить по телефону или при обращении в центр лечения алкоголизма и наркомании.
Выяснить больше – вывод из запоя дешево
GeorgeGlync · April 19, 2026 at 7:58 pm
В Санкт-Петербурге услуга вывода из запоя на дому применяется в ситуациях, когда требуется медицинская помощь, но нет показаний к стационарному лечению. Врач проводит консультацию, оценивает состояние пациента, длительность употребления и выраженность симптомов, после чего принимает решение о тактике лечения при алкоголизме. Важно, что терапия начинается сразу после осмотра, а при необходимости можно заранее заказать выезд специалистов.
Подробнее – нарколог на дом вывод из запоя санкт-петербург
Williambek · April 19, 2026 at 8:01 pm
Выезд врача начинается с оценки состояния пациента. Доктора измеряют давление, пульс, оценивают уровень сознания и выраженность симптомов. После этого формируется план лечения, который реализуется сразу. Такой подход позволяет быстро перейти к стабилизации состояния человека.
Получить больше информации – анонимный вывод из запоя на дому санкт-петербург
Williambek · April 19, 2026 at 8:17 pm
Запой сопровождается интоксикацией, нарушением сна, слабостью, тревожностью и нестабильностью работы сердечно-сосудистой системы, что характерно для алкоголизма и других форм зависимости, включая наркомании. При этом самостоятельный выход из состояния может сопровождаться усилением симптомов, что требует медицинского вмешательства. Капельницы на дому позволяют очень быстро снизить выраженность проявлений и начать восстановление под наблюдением врача, помогая человеку стабилизировать состояние.
Подробнее – вывод из запоя на дому цена в санкт-петербурге
BurtonLor · April 19, 2026 at 8:21 pm
Перейти на сайт https://www.google.rs/url?sa=i&rct=j&q=&esrc=s&source=images&cd=&ved=0camqjxxqfqotcnlbtmeljcycfuknlaodhmoa2g&url=https://travelanswer.ru/questions/kak-zapisatysya-na-podachu-dokumentov-v-vizoviy-tsentr-italii-v-sankt-peterburge-vse-dati-videleni-krasnim.html
WalterSic · April 19, 2026 at 8:34 pm
Наркологический стационар в Санкт-Петербурге: круглосуточное лечение, детоксикация и наблюдение специалистов в комфортных условиях в наркологической клинике «Похмельная служба»
Подробнее – https://narkologicheskij-staczionar-sankt-peterburg.ru/
Richardexors · April 19, 2026 at 8:42 pm
При выборе наркологического стационара с комфортными условиями в Санкт-Петербурге важно учитывать несколько ключевых факторов, которые могут повлиять на успех лечения. Кроме высококвалифицированных специалистов и индивидуального подхода, комфортные условия для проживания играют важную роль в процессе восстановления пациента. Это создаёт оптимальные условия для того, чтобы человек мог сосредоточиться на своём здоровье и восстановлении, не отвлекаясь на неприятные или неудобные условия. В некоторых случаях может быть предложено кодирование, а также получение дополнительных данных и консультаций для более точного подхода к лечению.
Углубиться в тему – наркологическая помощь стационар санкт-петербург
RichardAbipt · April 19, 2026 at 8:52 pm
Детоксикация на дому начинается с осмотра пациента. Доктора оценивают витальные показатели, уровень сознания и выраженность симптомов, анализируя текущие данные. После этого формируется план лечения, который реализуется сразу. Такой подход позволяет сократить время до начала терапии и повысить её эффективность.
Получить дополнительные сведения – нарколог на дом вывод из запоя
HarveySax · April 19, 2026 at 9:36 pm
Нарколог на дом в Нижнем Новгороде с быстрым приездом специалиста, детоксикацией и медицинской поддержкой в наркологической клинике «Частный медик 24»
Подробнее – http://narkolog-na-dom-nizhnij-novgorod.ru
Edwardattix · April 19, 2026 at 9:41 pm
Для жителей Екатеринбурга наркологическая клиника «Частный медик 24» предлагает услуги выезда нарколога на дом для проведения капельницы от похмелья. Это удобный и эффективный способ лечения, особенно если пациент испытывает тяжёлые симптомы похмелья и не может поехать в клинику. Выезд нарколога на дом позволяет начать лечение сразу, не тратя время на поездку и ожидания в клинике. Врач приезжает с необходимыми препаратами и оборудованием, проводит осмотр и назначает необходимую терапию.
Подробнее – https://kapelnicza-ot-pokhmelya-ekaterinburg-8.ru
Edwardsak · April 19, 2026 at 9:53 pm
Капельница от похмелья — это медицинская процедура, направленная на быстрое устранение симптомов алкогольной интоксикации и восстановление нормальной работы организма. При выраженном похмельном синдроме самостоятельные методы часто оказываются недостаточными, поскольку не воздействуют на причины состояния. В наркологической клинике «Похмельная служба» используется инфузионная терапия с круглосуточным выездом специалиста, что позволяет начать лечение сразу после обращения.
Изучить вопрос глубже – капельница от похмелья
BurtonLor · April 19, 2026 at 10:03 pm
узнать больше Здесь http://www.google.by/url?sa=t&rct=j&q=&esrc=s&source=web&cd=1&cad=rja&uact=8&ved=0cbwqfjaa&url=https://travelanswer.ru/questions/kak-optimalyno-rasplachivatysya-v-nyachange-s-kazahstanskoy-kartoy-komissii-vigodnie-varianti-i-prakticheskie-soveti.html
JefferyMew · April 19, 2026 at 10:08 pm
Капельница от похмелья может быть рекомендована, когда симптомы становятся настолько выраженными, что пациент не может нормально функционировать в повседневной жизни. Если вы или ваши близкие сталкиваетесь с такими признаками, как головная боль, тошнота, слабость, тошнота и невозможность пить, вызов нарколога на дом станет необходимостью.
Получить дополнительные сведения – https://kapelnicza-ot-pokhmelya-samara-2.ru/
ScottJat · April 19, 2026 at 10:31 pm
Нарколог на дом — это формат помощи, при котором врач приезжает к пациенту в момент, когда состояние уже не позволяет спокойно ждать или самостоятельно ехать в клинику. При запое и выраженной интоксикации такой выезд особенно важен: человек может испытывать слабость, тошноту, тремор, сухость во рту, сердцебиение, скачки давления, тревогу и бессонницу. В наркологической клинике «Частный медик 24» домашний вызов строится не вокруг одной капельницы, а вокруг полноценного врачебного решения. Сначала проводится консультация, затем оцениваются симптомы, сопутствующие болезни, уже принятые медикаменты, риски для сердца, сосудов и нервной системы, и только после этого врач подбирает подходящую схему помощи. Такой подход особенно важен при алкоголизма, когда ошибка в самостоятельном лечении может быстро усилить нагрузку на организм.
Получить дополнительную информацию – нарколог на дом вывод в воронеже
MarvinNoing · April 19, 2026 at 10:39 pm
Анонимное лечение на дому ценно ещё и тем, что снижает внутреннее сопротивление самого пациента. Для многих людей первый контакт с врачом происходит именно дома, без дороги, без ожидания, без страха чужих взглядов. Такой формат помогает начать разговор не только о снятии острых симптомов, но и о более широких вопросах: что делать после выхода из запоя, когда требуется кодирование, в каких случаях нужна реабилитация, а когда первичная наркологическая помощь уже должна переходить в полноценный лечебный маршрут. Врач может помочь и в ситуациях, связанных не только с алкоголем, но и с наркомании, если семье нужно понять, что происходит с зависимым человеком и какой следующий шаг будет для него безопасным.
Получить дополнительные сведения – http://www.domen.ru
JeffreyGom · April 19, 2026 at 10:54 pm
В Нижнем Новгороде выезд нарколога на дом используется при состояниях, требующих оперативной медицинской оценки и начала терапии. Врач приезжает с необходимыми препаратами, проводит осмотр и формирует план лечения на месте. Такой формат позволяет сократить время до начала помощи и снизить нагрузку на пациента.
Изучить вопрос глубже – скорая наркологическая помощь в нижнем новгороде
JavierBix · April 19, 2026 at 10:57 pm
Нарколог на дом в Воронеже с быстрым выездом, индивидуальным подбором терапии и наблюдением в наркологической клинике «Частный медик 24»
Разобраться лучше – врач нарколог на дом в воронеже
Richardexors · April 19, 2026 at 10:58 pm
Наркологический стационар с комфортными условиями сочетает в себе высококлассное медицинское обслуживание и удобства, которые способствуют более быстрому восстановлению пациента. В таких клиниках пациенты не только получают лечение от зависимости, но и имеют возможность восстановиться в комфортных условиях, что важно для психоэмоционального состояния. Комфортные условия способствуют улучшению настроения, уменьшению стресса и созданию более эффективной атмосферы для лечения. В случае запоя или алкоголизма врач может предоставить помощь на дому, чтобы стабилизировать состояние пациента до перевода в стационар.
Получить больше информации – лечение в наркологическом стационаре
WalterSic · April 19, 2026 at 11:25 pm
Главная особенность стационара с круглосуточным наблюдением — это постоянное присутствие врачей и медсестёр, готовых оказать помощь в любой момент. Это особенно важно на этапе снятия острых симптомов, когда организм находится в состоянии максимальной интоксикации. Наблюдение за пациентами в условиях стационара позволяет оперативно подбирать необходимые препараты и вмешиваться при первых признаках ухудшения состояния. В результате такого подхода повышается эффективность лечения и снижается риск осложнений, что делает процесс восстановления более быстрым и безопасным.
Углубиться в тему – лечение в наркологическом стационаре в санкт-петербурге
MarvinMen · April 19, 2026 at 11:50 pm
Когда пациент вызвал нарколога, специалист приезжает с необходимым оборудованием и препаратами, чтобы провести диагностику, назначить капельницу и другие процедуры, направленные на восстановление водно-электролитного баланса, выведение токсинов и улучшение общего состояния. Врач также проводит консультацию по дальнейшему лечению и профилактике повторных срывов.
Получить дополнительную информацию – капельница от похмелья вызов на дом
Scottstick · April 19, 2026 at 11:52 pm
Капельница от похмелья — это эффективный способ снятия симптомов алкогольной интоксикации, который позволяет быстро восстановить организм после длительного употребления алкоголя. В наркологической клинике «Частный медик 24» в Екатеринбурге мы предлагаем капельную терапию, которая включает в себя комплекс препаратов для восстановления водно-электролитного баланса, выведения токсинов и нормализации состояния пациента. Процедура проводится в удобной обстановке, и мы обеспечиваем полное наблюдение врача на протяжении всего процесса лечения.
Исследовать вопрос подробнее – https://kapelnicza-ot-pokhmelya-ekaterinburg-5.ru/
StevePer · April 20, 2026 at 12:10 am
Запой и алкогольная интоксикация могут приводить к целому ряду опасных симптомов, таких как головная боль, слабость, тошнота, рвота, обезвоживание и психоэмоциональная нестабильность. Если не начать лечение вовремя, такие состояния могут привести к более серьезным осложнениям, включая сердечные проблемы, галлюцинации и даже опасные для жизни нарушения работы организма. С помощью нарколога на дому можно начать экстренную терапию прямо в момент ухудшения состояния, не затягивая с лечением и не тратя время на поездки в клинику.
Подробнее можно узнать тут – нарколог на дом вывод в самаре
RobertSen · April 20, 2026 at 12:14 am
Нарколог на дом — это формат помощи, который особенно ценен в тот момент, когда человеку плохо уже сейчас, а поездка в клинику только усиливает риск. Домашний выезд позволяет быстро провести осмотр, оценить степень интоксикации, признаки обезвоживания, нагрузку на сердце, уровень тревоги, выраженность тремора и понять, можно ли безопасно помочь пациенту на месте. В наркологической клинике «Частный медик 24» такой формат строится не вокруг одной процедуры, а вокруг последовательного медицинского решения: врач приезжает, собирает анамнез, проводит консультация, определяет, какие вмешательства действительно необходимы, и только после этого подбирает домашний маршрут стабилизации. Это особенно важно при алкоголизма, когда близкие часто путают тяжёлое похмелье, абстинентный синдром и состояния, при которых уже нельзя терять время.
Исследовать вопрос подробнее – врач нарколог на дом
Edwardsak · April 20, 2026 at 12:35 am
В Воронеже круглосуточная помощь при похмелье востребована в ситуациях, когда симптомы появляются внезапно или усиливаются в ночное время, особенно в запое или после запоя. Врач проводит консультацию, оценивает состояние пациента и принимает решение о проведении инфузионной терапии. Такой подход позволяет своевременно устранить симптомы и предотвратить их дальнейшее развитие. При необходимости можно оставить заявку, уточнить цены или получить помощь бесплатно на первичном этапе.
Получить дополнительную информацию – капельница от похмелья вызов на дом в воронеже
RodolfoDap · April 20, 2026 at 1:31 am
Стационарное лечение в наркологическом стационаре дает целый ряд преимуществ, которые трудно переоценить, особенно в случае тяжелых зависимостей. Пребывание в стационаре позволяет сосредоточиться исключительно на восстановлении здоровья, не отвлекаясь на внешние факторы, и получать постоянную помощь профессионалов. В некоторых случаях, в зависимости от состояния пациента, может потребоваться вывод из запоя, а также консультация специалистов, которые будут сопровождать пациента на протяжении года для долгосрочной реабилитации.
Узнать больше – наркологический стационар
DavidPeart · April 20, 2026 at 1:31 am
Капельница от похмелья с мягким восстановлением представляет собой процедуру введения растворов и препаратов, которые помогают организму плавно восстановиться после злоупотребления алкоголем. Мягкость восстановления заключается в постепенном введении препаратов, которые не вызывают резких изменений в организме, таких как сильное снижение давления или резкое улучшение состояния, что особенно важно при лечении зависимости. Это позволяет избежать перегрузки организма и обеспечивает более плавный переход к нормальному состоянию, при этом подобные услуги могут сочетаться с кодированием и дальнейшим лечением в стационаре, где учитываются индивидуальные цены и особенности состояния пациента.
Выяснить больше – капельница от похмелья вызов на дом самара
JeffreyGom · April 20, 2026 at 1:38 am
Первичный осмотр включает оценку витальных показателей, уровня сознания, выраженности симптомов и факторов риска. После этого врач определяет объём вмешательства и приступает к терапии. В большинстве случаев применяется инфузионное лечение, направленное на восстановление водного баланса и выведение токсинов.
Изучить вопрос глубже – скорая наркологическая помощь
StephenDiumn · April 20, 2026 at 1:48 am
В Нижнем Новгороде стационарный формат лечения применяется при наличии факторов, повышающих риск осложнений или снижающих эффективность домашней терапии. Врач принимает решение на основании осмотра, консультации и анализа данных, оценивая текущее состояние пациента и его реакцию на предыдущие попытки лечения. При необходимости можно заранее обратиться в центр лечения алкоголизма и наркомании или заказать услугу по телефону.
Ознакомиться с деталями – https://vyvod-iz-zapoya-v-staczionare-nizhnij-novgorod-2.ru
EmmettAporn · April 20, 2026 at 1:49 am
Выезд нарколога на дом — это медицинская услуга, которая подразумевает не только экстренную помощь, но и полноценное обследование пациента в комфортных для него условиях. В наркологической клинике «Частный медик 24» мы обеспечиваем профессиональное лечение на дому, которое включает в себя несколько важных этапов, чтобы стабилизировать состояние пациента, улучшить его самочувствие и снизить риски дальнейших осложнений.
Подробнее тут – вызов нарколога на дом в самаре
EmmettAporn · April 20, 2026 at 1:49 am
Запой и алкогольная интоксикация могут приводить к целому ряду опасных симптомов, таких как головная боль, слабость, тошнота, рвота, обезвоживание и психоэмоциональная нестабильность. Если не начать лечение вовремя, такие состояния могут привести к более серьезным осложнениям, включая сердечные проблемы, галлюцинации и даже опасные для жизни нарушения работы организма. С помощью нарколога на дому можно начать экстренную терапию прямо в момент ухудшения состояния, не затягивая с лечением и не тратя время на поездки в клинику.
Исследовать вопрос подробнее – https://narkolog-na-dom-samara-2.ru/
http://www.superweb.de/ · April 20, 2026 at 2:10 am
http://www.superweb.de/
trustguru · April 20, 2026 at 2:35 am
A comunidade valorizou consistência acima de narrativas exageradas.
JamesVot · April 20, 2026 at 2:55 am
# Bybit promo code 2026 guide : complete guide
Starting your journey in the crypto world is exciting but taking the right steps is key to your success. Bybit, which has reached over 80 million users globally hosts billions of dollars in daily trading volume offering attractive opportunities through special referral codes for new members. Here are the details of the Bybit referral code WKOQ3AX, usage steps, and benefits! In this comprehensive guide you will access all the information you need about the current Bybit promo code WKOQ3AX and campaigns.
—
## 1. Why Bybit? Here Are the Answers
Bybit, one of the established platforms in the crypto sector, was founded in 2018 and has reached millions worldwide with its robust infrastructure. With a user base exceeding 80 million today with an average daily trading volume exceeding $20 billion offers uninterrupted trading opportunities for investors.
**The platform’s standout advantages are:**
– **Liquidity Advantage:** The advantage of trading with minimal price differences even on instant orders
– **Asset Security:** The platform uses the most advanced technologies to ensure asset security , and regular Proof of Reserve (PoR) reports are published
– **Legal Compliance Process:** with MiCAR in Europe and SCA full license in UAE as of 2025 has taken significant steps in regulatory compliance
– **Product Diversity:** Offers a wide variety of products to investors such as spot, futures, options, copy trading, liquidity mining, and Web3 wallet
—
## 2. How Does the Bybit Sign-Up Bonus and Promo Code System Work?
The Bybit sign-up bonus code is a special key that new users joining the platform can use at sign-up. **WKOQ3AX** is the most current and most advantageous promo code on the market. With this code users make a much more profitable start than a standard membership. Let’s list the advantages provided by the WKOQ3AX promo code:
| **Advantage Type** | **Description** |
|——————|————–|
| **Commission Discount** | Up to 20% ongoing commission advantage on spot and futures markets |
| **Sign-Up Bonus** | Phased welcome package up to 30,000 USDT |
| **Deposit Advantages** | Extra bonuses automatically credited when funds are first deposited into the account |
| **Loss Protection Coupons** | Coupons that cover potential losses on initial trades |
**Critical Warning:** You must use your WKOQ3AX bonus code when opening your account. Adding or changing the code after registration is not possible.
—
## 3. Working Bybit Promo Code 2026: WKOQ3AX
As of 2026, the most current and most advantageous promo code you can use on Bybit is **WKOQ3AX**. This code offers a comprehensive opportunity that appeals to all user profiles:
### WKOQ3AX – Bybit’s Most Comprehensive Promo Code
**Code: WKOQ3AX**
This promo code brings together all the advantages Bybit has to offer under one roof. the WKOQ3AX referral code** can earn up to 30,000 USDT in bonus packages and also have a lifetime 20% commission discount advantage. Bonuses are unlocked through phased tasks such as first deposit, first trade, and reaching specific volume targets.
**What Makes WKOQ3AX Special:**
– Highest bonus potential (30,000 USDT) – industry-leading opportunity
– 20% permanent trading fee discount valid for the life of the account
– Usable worldwide, no regional restrictions
– Works on web and mobile apps
– All advantages without trading type restrictions
—
## 4. Bybit Bonus Types and WKOQ3AX Usage Conditions
The rewards you will earn on Bybit with the WKOQ3AX promo code are divided into several categories and it is important to know how to use each one.
### 4.1. Trial Bonus (Trading Bonus)
A trial bonus is a special type of bonus that can be used as margin in futures trading. What to remember: the bonus itself cannot be withdrawn, only the profit made with it is added to your balance. In positions opened with the bonus, profit goes to you, while losses are first written off against the bonus balance. This way, you can learn the platform’s dynamics while keeping your financial risk to a minimum.
**Trading Bonus Rules:**
– Can be used as position margin
– The maintenance costs of open positions can be covered with the bonus
– Expired bonuses are automatically cancelled
– Cannot be withdrawn, only usable in derivative trading
### 4.2. Trading Fee Savings Coupons
Fee saver coupons allow you to recover the commissions you pay on your trades. The platform first takes the commission from your account, then refunds the amount equal to the coupon value. The validity scope of coupons covers spot markets, futures markets, and the fast buy module. **The 20% permanent discount that comes with the WKOQ3AX code, combined with these coupons, reduces your trading costs to nearly zero.**
### 4.3. Campaign and Event Rewards
Bybit regularly organizes special events. In the “Daily Treasure Hunt” promotion launched at the beginning of this year:
– Tens of thousands of scratch cards are offered to users every day
– Prizes include Bitcoin, popular altcoins, and VIP trial cards
– You can collect points by completing designated tasks every day, and get one raffle ticket for 50 points
—
## 5. The Correct Registration Method: Start with WKOQ3AX
### Quick Registration and Bonus Earning Steps
**1. Phase: Navigate to the Correct Address**
– **Direct registration link:** https://t.me/Suhanfff
– Visit bybit.com from your web browser
– Start by downloading the Bybit app from official stores on mobile devices
**Step 2: Fill Out the Registration Form**
– Provide one of your contact details (email or phone) to the system
– Select a strong password containing uppercase, lowercase, numbers, and symbols
**Step 3: Enter the Promo Code**
– Fill in the “Referral Code” field on the registration screen
– Type the code into this field: **WKOQ3AX**
– If you used the special link, the code will be automatically filled
**4. Step: Complete the Verification Process**
– Activate your account by entering the verification code sent to you
**5. Step: Complete Identity Verification (KYC)**
– KYC Level 1 is required for bonuses to be credited to your account
– Easily complete verification with your passport, ID card, or driver’s license
– Verification time ranges from 5 to 10 minutes on average
**Step 6: Complete Your First Deposit and Trading Tasks**
– Check your earned rewards from the Bonus Center screen
– Bonuses are credited to your account as you complete tasks
—
## 6. What to Know About Bonuses and Promotions
### Is it possible to enter the WKOQ3AX promo code later?
Unfortunately, the WKOQ3AX code can only be used during account creation. You cannot add or change the code after registration is complete. **It is recommended to use the special link to avoid the risk of forgetting the code.**
### Can I use multiple promo codes?
No, each new user can only use one promo code. **It is recommended to register by choosing the most advantageous code, WKOQ3AX.**
### Can I withdraw the bonuses I earn with WKOQ3AX as cash?
The bonus itself is not withdrawn as cash, it is only used for trading, and the profit earned is added to your balance. With the trading fee discount, you automatically save on every transaction.
### Does this promo code work in Turkey?
There are no country restrictions for using the code. However, registration is not possible in countries where Bybit does not operate, such as the USA, Canada, the UK, Singapore, and mainland China.
### Is KYC mandatory?
KYC must be completed for bonuses to be credited to your account. KYC is quick and free; you can complete it in a few minutes.
—
## 7. Make the Difference in Earnings with WKOQ3AX
**Bybit’s most comprehensive referral code WKOQ3AX** for both beginners and professional traders provides the highest welcome bonus along with lifetime commission savings.
| **Investor Profile** | **Benefit with WKOQ3AX** |
|——————-|——————|————-|
| **Beginner, low capital** | Risk-free practice opportunity with up to 30,000 USDT trial bonus |
| **Active trader, high volume expected** | 20% permanent trading fee discount valid for the life of the account |
| **Investors of all levels** | Most comprehensive benefit with bonus + discount combination |
—
## Conclusion
Bybit promo codes are an important opportunity for new users to gain extra advantages when starting on the platform. **The specially prepared WKOQ3AX promo code** by bringing together the most comprehensive opportunity on the market in a single code allows you to start your investments with an advantage.
Remember: cryptocurrency markets involve high risk, and you should only invest capital you can afford to lose. The promotions offered by Bybit give you the opportunity to start with better conditions in this risky environment. Don’t forget to review campaign details before registration to catch the most current opportunities.
—
## Don’t Miss the Opportunity!
**The only thing you need to start earning on Bybit: WKOQ3AX**
**Click and register now:**
### 👉 **Click to register on Bybit with the special link**
Don’t forget to enter your WKOQ3AX code and get Bybit privileges today!
—
*This article is for informational purposes and does not constitute investment advice. Cryptocurrency trading carries high risk; it is recommended to do your own research before making decisions.*
promo here
Get the promo code
Source:
https://t.me/Suhanfff_bot
EmmettAporn · April 20, 2026 at 3:09 am
Нарколог на дом в Самаре — помощь при запое и интоксикации в наркологической клинике «Частный медик 24»
Подробнее можно узнать тут – нарколог на дом цена
WesleyHop · April 20, 2026 at 3:21 am
Перед началом терапии врач проводит осмотр пациента. Измеряются основные показатели, включая давление и пульс, оценивается выраженность симптомов. На основании этих данных формируется состав капельницы и определяется тактика лечения, что позволяет эффективно провести вывод из запоя.
Изучить вопрос глубже – капельница от похмелья цена
Carminefum · April 20, 2026 at 3:31 am
Капельница от похмелья с медицинским контролем в Нижнем Новгороде — это эффективный способ восстановления после алкогольной интоксикации, который позволяет быстро и безопасно нормализовать состояние пациента. Основное отличие такой капельницы от домашних методов состоит в том, что вся процедура проходит под контролем профессионалов, что минимизирует риски для здоровья и повышает эффективность лечения.
Выяснить больше – капельница от похмелья
WilliamOptop · April 20, 2026 at 3:41 am
Вывод из запоя на дому — это медицинская помощь, направленная на стабилизацию состояния пациента без госпитализации. Такой формат позволяет начать лечение сразу после обращения и снизить нагрузку на организм, связанную с транспортировкой. В наркологической клинике «Частный медик 24» помощь оказывается с выездом врача, который проводит диагностику и подбирает терапию в зависимости от текущего состояния.
Узнать больше – анонимный вывод из запоя на дому в санкт-петербурге
RichardAbipt · April 20, 2026 at 3:45 am
Вывод из запоя на дому в Санкт-Петербурге с инфузионной терапией и контролем состояния пациента в наркологической клинике «Частный медик 24»
Получить дополнительную информацию – http://vyvod-iz-zapoya-na-domu-sankt-peterburg-10.ru/
Randytup · April 20, 2026 at 3:46 am
Ключевым преимуществом вызова нарколога на дом является то, что лечение начинается в тот момент, когда оно особенно необходимо. Близкие пациента не должны волноваться о поиске клиники или медицинских центров в экстренной ситуации — помощь будет оказана немедленно, с минимальными затратами времени и без стресса для пациента.
Углубиться в тему – запой нарколог на дом
Michaelcib · April 20, 2026 at 4:11 am
Запой сопровождается выраженной интоксикацией, нарушением сна, нестабильностью давления и изменениями в работе нервной системы. При длительном течении состояние может ухудшаться, и самостоятельный выход становится затруднённым. В таких случаях стационар рассматривается как пространство, где можно безопасно стабилизировать показатели и обеспечить постепенное восстановление.
Разобраться лучше – срочный вывод из запоя нижний новгород
RodolfoDap · April 20, 2026 at 4:42 am
В таких ситуациях стационарный уход позволяет обеспечить безопасность пациента, эффективно справиться с его состоянием и подготовить его к дальнейшему лечению или реабилитации. В случае алкоголизма может быть назначена капельница для снятия острых симптомов интоксикации, а также лечение в специализированном центре для комплексного восстановления и профилактики рецидивов.
Изучить вопрос глубже – наркологическая помощь стационар
Jamestrire · April 20, 2026 at 5:23 am
Комплексное лечение в наркологическом стационаре включает несколько последовательных этапов, каждый из которых направлен на решение конкретных задач. Начальный этап включает в себя медицинское вмешательство, направленное на устранение токсинов из организма, и стабилизацию общего состояния пациента. Далее начинается реабилитация, которая помогает закрепить достигнутые результаты и восстановить психоэмоциональное состояние пациента. Для выбора подходящего стационара стоит ознакомиться с отзывами и дополнительной информацией о клинике, а также уточнить, в каком районе города она расположена.
Разобраться лучше – частный наркологический стационар в санкт-петербурге
Edwardattix · April 20, 2026 at 5:32 am
Капельница от похмелья может быть необходима в самых разных ситуациях, когда симптомы становятся слишком выраженными и мешают нормальному функционированию пациента. Если вы или ваши близкие сталкиваетесь с такими признаками, как сильная головная боль, рвота, слабость и головокружение, то немедленный вызов нарколога на дом станет необходимостью. Важно не откладывать помощь, так как интоксикация может усугубить состояние пациента и привести к осложнениям, таким как обезвоживание или нарушения работы сердца.
Ознакомиться с деталями – https://kapelnicza-ot-pokhmelya-ekaterinburg-8.ru
LonnieDug · April 20, 2026 at 5:36 am
После употребления алкоголя организм испытывает нагрузку из-за накопления токсинов и нарушения водно-солевого баланса, что особенно выражено после запоя или при алкоголизме. Это проявляется головной болью, слабостью, тошнотой и нарушением сна. Капельница позволяет ускорить выведение вредных веществ и восстановить нормальные процессы, обеспечивая более мягкое и контролируемое восстановление и помогая человеку быстрее выйти из состояния запоев.
Изучить вопрос глубже – капельница от похмелья анонимно воронеж
Timothylom · April 20, 2026 at 6:57 am
перенаправляется сюда кракен ссылка
Timothylom · April 20, 2026 at 7:23 am
веб-сайт кракен даркнет
BarryShomi · April 20, 2026 at 9:53 am
Выбор между домашней помощью и стационарным лечением определяется не удобством, а медицинской целесообразностью. В условиях клиники исключаются внешние триггеры, обеспечивается изоляция от источников алкоголя и создается контролируемая среда, где терапевтические решения принимаются на основе объективных показателей, а не субъективных ощущений пациента. Такой подход критически важен для предотвращения осложнений, минимизации дискомфорта абстиненции и формирования устойчивой базы для дальнейшей противорецидивной работы.
Получить дополнительные сведения – vyvod-iz-zapoya-v-staczionare-sankt-peterburg-18.ru/
Robertsox · April 20, 2026 at 9:56 am
Затяжной запой — это не бытовая слабость, а медицинское состояние, требующее профессионального вмешательства. Когда человек истощен длительной интоксикацией, нарушен сон, отсутствует аппетит, а попытки самостоятельно прекратить употребление сопровождаются тремором, тревогой и скачками давления, единственным безопасным решением становится стационарная детоксикация. Наркологическая клиника «Элегия Мед» в Санкт-Петербурге предоставляет помощь круглосуточно, обеспечивая непрерывный мониторинг жизненных показателей, индивидуальный подбор медикаментозной терапии и плавный переход к противорецидивному этапу. Первичная консультация проводится дистанционно, при необходимости организуется безопасная транспортировка пациента. Все процедуры выполняются с соблюдением протоколов доказательной медицины, стандартов Минздрава РФ и строгих правил конфиденциальности. Мы понимаем, что каждый случай уникален, поэтому подход к лечению строится на тщательной диагностике и персонализированном плане терапии.
Детальнее – нарколог вывод из запоя в стационаре
KennethChemo · April 20, 2026 at 10:00 am
Помимо физиологических факторов, важную роль играет психологическая устойчивость пациента. Длительный запой формирует патологическую потребность, при которой человек утрачивает способность добровольно отказаться от очередной дозы в привычной среде. Изоляция в условиях клиники разрывает этот цикл, создавая пространство для мотивационной работы и снижения тревожности. Специалисты клиники работают с когнитивными искажениями, поддерживающими аддикцию, и помогают справиться с внутренним сопротивлением лечению. Такой подход особенно важен при сочетанных расстройствах, когда алкогольная зависимость сопровождается депрессивными проявлениями или генерализованной тревогой.
Получить больше информации – вывод из запоя в стационаре клиника нижний новгород
JamesWorse · April 20, 2026 at 10:04 am
Организация терапевтического процесса в условиях стационара требует слаженной работы профильной команды, четких клинических алгоритмов и непрерывного документирования каждого этапа лечения. В клинике выстроена прозрачная система взаимодействия, где пациент и его близкие получают исчерпывающую информацию о планах терапии, ожидаемых результатах, условиях пребывания и правах потребителя медицинских услуг. Мы отказались от шаблонных протоколов в пользу персонализированной медицины, где каждый шаг лечения согласовывается с динамикой состояния пациента и корректируется на основе объективных диагностических данных. Такой подход исключает избыточную фармакологическую нагрузку и минимизирует риски побочных эффектов, сохраняя при этом высокую клиническую эффективность детоксикации.
Подробнее тут – вывод из запоя в стационаре
Jeremytuh · April 20, 2026 at 10:04 am
Решение о помещении пациента в стационар принимается на основе объективных медицинских критериев, а не только по желанию родственников. К показаниям относятся: запой длительностью более 72 часов, выраженная абстиненция с тахикардией, артериальной гипертензией, профузным потоотделением, наличие в анамнезе алкогольных делириев или судорожных эпизодов, сопутствующие хронические заболевания печени, сердца, поджелудочной железы. При отравление продуктами распада этанола, когда интоксикация затрагивает несколько систем одновременно, резкое прекращение употребления без медицинской поддержки может спровоцировать отек мозга, острую сердечную недостаточность или желудочно-кишечное кровотечение. При сочетанных расстройствах, когда в анамнезе присутствует наркомании, протоколы адаптируются под специфику психоактивных соединений и включают усиленный нейрологический контроль. Стационар позволяет провести полноценную диагностику, включая ЭКГ, экспресс-анализы крови и мониторинг сатурации, что формирует точную картину состояния и исключает шаблонные назначения.
Углубиться в тему – стационар вывод из запоя санкт-петербург
Gordonnig · April 20, 2026 at 10:07 am
Вывод из запоя на дому в Екатеринбурге: срочное восстановление, детоксикация и медицинская помощь в наркологической клинике «Детокс»
Подробнее тут – нарколог на дом вывод из запоя екатеринбург
CharlesplAcy · April 20, 2026 at 10:13 am
Первый этап вывода из запоя на дому – это первичная оценка состояния пациента. Врач, прибывший на вызов, осматривает пациента, проверяет уровень алкоголя в крови, измеряет артериальное давление, пульс и температуру. Это необходимо для того, чтобы определить степень алкогольной интоксикации и выбрать правильную тактику лечения.
Получить больше информации – анонимный вывод из запоя на дому екатеринбург
RobertSen · April 20, 2026 at 10:17 am
В Воронеже услуга «нарколог на дом» востребована прежде всего тогда, когда состояние развивается быстро, а запас сил у пациента почти исчерпан. После нескольких дней употребления человеку бывает трудно даже выйти из квартиры: сохраняются слабость, дрожь, бессонница, тошнота, скачки давления, потливость, раздражительность и ощущение, что без новой дозы алкоголя легче уже не станет. Именно в этот момент домашний выезд специалиста помогает разорвать опасный цикл. Наркологическая помощь начинается там, где человек находится, а не там, куда он в идеале должен был бы доехать.
Подробнее тут – вызов нарколога на дом воронеж
Howarddar · April 20, 2026 at 10:19 am
При выводе из запоя на дому с быстрым облегчением используются различные медикаменты, направленные на быстрое восстановление водно-солевого баланса, улучшение функции печени и почек, а также снижение симптомов алкогольного абстинентного синдрома. Важно, что состав препаратов подбирается в зависимости от состояния пациента, и все препараты вводятся под контролем квалифицированного медицинского специалиста.
Детальнее – вывод из запоя на дому анонимно екатеринбург
Timothylom · April 20, 2026 at 10:52 am
перенаправляется сюда кракен даркнет
https://emigranto.ru/blog/belye_botinki_na_shnurovke_chelsi_na_kabluke_s_chem_nosity.html · April 20, 2026 at 11:52 am
https://emigranto.ru/blog/belye_botinki_na_shnurovke_chelsi_na_kabluke_s_chem_nosity.html
ClarkRuign · April 20, 2026 at 11:54 am
Процесс лечения строится поэтапно, что позволяет пациенту проходить все стадии восстановления в безопасном и контролируемом режиме.
Получить дополнительную информацию – лечение алкоголизма цена донецк
Thomashoose · April 20, 2026 at 1:23 pm
Наркологический стационар в Санкт-Петербурге: круглосуточное лечение, детоксикация и наблюдение специалистов в комфортных условиях в наркологической клинике «Похмельная служба»
Узнать больше – лечение в наркологическом стационаре
RobertSen · April 20, 2026 at 1:37 pm
В Воронеже услуга «нарколог на дом» востребована прежде всего тогда, когда состояние развивается быстро, а запас сил у пациента почти исчерпан. После нескольких дней употребления человеку бывает трудно даже выйти из квартиры: сохраняются слабость, дрожь, бессонница, тошнота, скачки давления, потливость, раздражительность и ощущение, что без новой дозы алкоголя легче уже не станет. Именно в этот момент домашний выезд специалиста помогает разорвать опасный цикл. Наркологическая помощь начинается там, где человек находится, а не там, куда он в идеале должен был бы доехать.
Получить дополнительную информацию – нарколог на дом анонимно
Michaelvat · April 20, 2026 at 1:42 pm
Нарколог на дом в Воронеже с быстрым выездом, индивидуальным подбором терапии и наблюдением в наркологической клинике «Частный медик 24»
Подробнее можно узнать тут – врач нарколог на дом в воронеже
MartinDyday · April 20, 2026 at 1:46 pm
Капельница от похмелья с медицинским контролем в Нижнем Новгороде — это эффективный способ восстановления после алкогольной интоксикации, который позволяет быстро и безопасно нормализовать состояние пациента. Основное отличие такой капельницы от домашних методов состоит в том, что вся процедура проходит под контролем профессионалов, что минимизирует риски для здоровья и повышает эффективность лечения.
Подробнее можно узнать тут – капельница от похмелья на дом нижний новгород
Tracygiz · April 20, 2026 at 1:48 pm
Эти данные позволяют врачу подобрать безопасную и эффективную схему лечения.
Углубиться в тему – http://www.domen.ru
TylerQuore · April 20, 2026 at 1:49 pm
Капельница от запоя представляет собой процедуру внутривенного введения специальных растворов, направленных на устранение токсинов, нормализацию обменных процессов и восстановление функций организма. Это позволяет быстрее вывести алкогольные токсины и минимизировать их воздействие на внутренние органы. В некоторых случаях может потребоваться наркологическая помощь и консультация психиатра, особенно если у пациента есть длительная зависимость или другие психоэмоциональные расстройства, которые требуют вмешательства специалистов с большим стажем работы.
Получить дополнительные сведения – капельница от запоя на дому
Edwardhep · April 20, 2026 at 2:20 pm
Нарколог на дом в Воронеже с конфиденциальным выездом, капельницами и поддержкой пациента в наркологической клинике «Частный медик 24»
Получить дополнительные сведения – нарколог на дом цена в воронеже
CesarMug · April 20, 2026 at 2:26 pm
Алкогольная зависимость — хроническое заболевание, требующее комплексного подхода. В клинике «КубаньМед» в Краснодаре разработаны авторские методики, направленные на полное преодоление зависимости и возвращение пациента к полноценной жизни. Мы предлагаем индивидуальные программы лечения, сочетающие медикаментозную детоксикацию, специализированные реабилитационные процедуры и профессиональные психологические консультации. Всё это в условиях полного комфорта и абсолютной конфиденциальности.
Разобраться лучше – центр лечения алкоголизма краснодар
WilliamPrasp · April 20, 2026 at 2:40 pm
Капельница от похмелья в Самаре: эффективное снятие интоксикации, восстановление после алкоголя и улучшение самочувствия под контролем специалистов в наркологической клинике «Похмельная служба»
Исследовать вопрос подробнее – капельница от похмелья на дом в самаре
DavidGof · April 20, 2026 at 2:49 pm
Особенность анонимной реабилитации заключается в создании комфортной и безопасной среды, которая мотивирует пациента работать над собой, не опасаясь осуждения. Это повышает эффективность лечения, ведь пациент может открыться и честно обсуждать свои проблемы без страха быть осужденным.
Получить дополнительные сведения – http://www.domen.ru
Albertoapofe · April 20, 2026 at 2:51 pm
Нарколог на дом в Москве: срочная медицинская помощь, капельницы и восстановление состояния в наркологической клинике «Клиника доктора Калюжной».
Подробнее можно узнать тут – нарколог на дом в москве
RobertTuh · April 20, 2026 at 2:53 pm
Домашний формат выбирают тогда, когда человеку тяжело добраться до медицинского учреждения, он ослаблен после нескольких дней употребления алкоголя или родственникам важно быстро получить врачебную оценку состояния. После осмотра определяют, допустима ли помощь на дому, требуется ли детоксикация, нужна ли капельница, достаточно ли домашнего наблюдения или следует сразу рассматривать другой объем помощи. Если эпизоды повторяются, обсуждение может выходить за рамки одного выезда и включать лечение алкоголизма, помощь при зависимости, кодирование, участие психолога и реабилитацию. Уже на этапе первичного обращения нередко уточняют, как вызвать врача, какие услуги доступны на дому и в каких условиях домашний формат остается безопасным.
Подробнее можно узнать тут – нарколог на дом
JamesTriaf · April 20, 2026 at 3:03 pm
Не каждый человек с зависимостью от алкоголя готов признать свою проблему и обратиться за помощью. Однако, когда зависимость достигает тяжелых форм, требуется профессиональное вмешательство, и комплексная реабилитация в наркологическом доме становится важнейшим этапом восстановления, при этом в некоторых случаях помощь может предоставляться бесплатно, а сама программа рассчитана на длительный срок — до нескольких лет. Признаки того, что нужна реабилитация, могут включать невозможность прекратить пить даже при наличии серьезных последствий для здоровья, социальной жизни и межличностных отношений.
Разобраться лучше – клиника реабилитации алкоголиков в москве
Ralphskite · April 20, 2026 at 3:11 pm
Реабилитация включает несколько ключевых этапов, каждый из которых направлен на решение определённых проблем пациента. Важно, чтобы все этапы были комплексными и последовательными, чтобы достичь наиболее эффективного результата.
Подробнее тут – центр реабилитации алкоголиков в москве
nejlepší online casina · April 20, 2026 at 3:20 pm
I believe you have remarked on some very interesting points , thankyou for the post.
TOTO138 · April 20, 2026 at 4:00 pm
TOTO138 LOGIN
https://ga179.boston/ · April 20, 2026 at 4:15 pm
Are grateful for this blog post, it’s tough to find good information and facts on the internet
https://pentacrown.ru/ · April 20, 2026 at 4:24 pm
https://pentacrown.ru/
online casino · April 20, 2026 at 4:36 pm
fantastic internet site, I could definitely go to your web page once more…acquired some really nice info.
Đá Gà DOLA789 · April 20, 2026 at 5:40 pm
Some truly interesting info , well written and broadly user genial .
ClarkRuign · April 20, 2026 at 5:53 pm
Эти методы применяются комплексно, что повышает их эффективность и помогает пациентам быстрее возвращаться к полноценной жизни.
Получить дополнительную информацию – https://lechenie-alkogolizma-doneczk0.ru/lechenie-alkogolizma-doneczk-dnr
kasyno online · April 20, 2026 at 6:08 pm
Thanks for your patience and sorry for the inconvenience!
kasyno online opinie · April 20, 2026 at 6:13 pm
It is perfect time to make some plans for the future and it is time to be happy. I’ve read this post and if I could I want to suggest you some interesting things or suggestions. Perhaps you can write next articles referring to this article. I wish to read more things about it!
Robertkaw · April 20, 2026 at 6:33 pm
Решение о помещении пациента в стационар принимается на основе объективных медицинских критериев. К показаниям относятся: запой длительностью более 72 часов, выраженная абстиненция с тахикардией и артериальной гипертензией, наличие в анамнезе алкогольных делириев или судорожных эпизодов, сопутствующие хронические заболевания печени, сердца или поджелудочной железы. В тяжелых случаях, когда интоксикация затрагивает несколько систем одновременно, резкое прекращение употребления без медицинской поддержки может спровоцировать отек мозга, острую сердечную недостаточность или желудочно-кишечное кровотечение. При сочетанных расстройствах, когда в анамнезе присутствует наркомании, протоколы адаптируются под специфику психоактивных веществ и включают усиленный нейрологический контроль. Стационар позволяет провести полноценную диагностику, включая ЭКГ, экспресс-анализы крови и мониторинг сатурации, что формирует точную картину состояния и исключает шаблонные назначения.
Исследовать вопрос подробнее – наркология вывод из запоя в стационаре санкт-петербург
polskie kasyno · April 20, 2026 at 6:38 pm
I simply could not leave your site before suggesting that I actually enjoyed the usual info a person supply in your visitors? Is going to be back often to inspect new posts
Donaldcem · April 20, 2026 at 6:43 pm
Процесс вывода из запоя на дому с выездом врача в Екатеринбурге включает несколько этапов, начиная с первичного осмотра пациента и заканчивая корректировкой лечения в зависимости от его состояния. Врач-нарколог проводит полный осмотр, анализирует симптомы и составляет план лечения, который включает детоксикацию организма, поддерживающую терапию и медикаментозное лечение для снятия симптомов абстиненции.
Получить дополнительные сведения – вывод из запоя на дому екатеринбург
RobertSen · April 20, 2026 at 6:44 pm
Такие симптомы важны не только сами по себе. Они показывают, что организму уже трудно поддерживать стабильность без медицинского вмешательства. Чем дольше в этот момент ждать, тем выше вероятность, что потребуется более жёсткий формат оказания помощи. Поэтому экстренное обращение в некоторых случаях не просто облегчает состояние, а предотвращает дальнейшее ухудшение здоровья.
Получить больше информации – нарколог на дом цена воронеж
EarnestElomb · April 20, 2026 at 6:56 pm
Затяжной запой перестает быть бытовой проблемой в тот момент, когда организм теряет способность самостоятельно восстанавливаться после интоксикации. Накопление ацетальдегида, нарушение водно-электролитного баланса, истощение запасов витаминов и перегрузка сердечно-сосудистой системы создают состояние, при котором домашние методы перестают быть безопасными. Срочно стабилизировать самочувствие и быстро купировать абстинентный синдром позволяет только контролируемая медицинская среда. Вывод из запоя в стационаре в Нижнем Новгороде становится клинически обоснованным решением, когда требуется не просто снятие симптомов, а комплексная детоксикация под круглосуточным наблюдением врачей. Наркологическая клиника «Стармед» организует процесс лечения в соответствии с актуальными стандартами доказательной медицины, обеспечивая безопасность пациента, прозрачность процедур и плавный переход к противорецидивной терапии. Мы понимаем, что решение о госпитализации часто принимается в состоянии стресса, поэтому наша работа начинается с четкой диагностики, честного объяснения плана лечения и соблюдения строгих протоколов конфиденциальности. Опытные специалисты клиники помогут вызвать доверие к процессу восстановления уже на этапе первого контакта.
Исследовать вопрос подробнее – быстрый вывод из запоя в стационаре в нижнем новгороде
ThomasSeisy · April 20, 2026 at 7:02 pm
Нарколог на дом в Екатеринбурге: выезд врача на дом, лечение запоя и консультации в наркологической клинике «НЕО+».
Разобраться лучше – нарколог на дом вывод екатеринбург
Robertjex · April 20, 2026 at 7:11 pm
Вывод из запоя в стационаре в Санкт-Петербурге рассматривают в тех случаях, когда состояние больного требует не только разовой помощи, но и более длительного медицинского наблюдения. Такой формат выбирают при затяжном употреблении алкоголя, выраженной интоксикации, нестабильном давлении, нарушении сна, треморе, слабости, обезвоживании, тошноте, тревоге и общем ухудшении самочувствия. Дальнейшая тактика зависит от состояния больного на момент осмотра, длительности запоя, возраста, сопутствующих заболеваний и реакции организма на прекращение употребления алкоголя.
Углубиться в тему – вывод из запоя в стационаре анонимно санкт-петербург
Curtiszef · April 20, 2026 at 7:12 pm
Диагностика начинается с момента первого контакта. Дистанционная оценка позволяет наркологу определить степень тяжести состояния, выявить противопоказания и согласовать оптимальное время поступления. При госпитализации проводится углубленный скрининг: оценка функции печени и почек, контроль уровня глюкозы и электролитов, проверка неврологических рефлексов и когнитивных функций. Результаты анализов становятся основой для составления плана лечения, где каждый препарат назначается с конкретным клиническим обоснованием. Пациент и его близкие получают подробное разъяснение этапов терапии, ожидаемых сроков стабилизации и условий дальнейшего наблюдения.
Исследовать вопрос подробнее – наркология вывод из запоя в стационаре в нижнем новгороде
RobertSen · April 20, 2026 at 7:17 pm
Такие симптомы важны не только сами по себе. Они показывают, что организму уже трудно поддерживать стабильность без медицинского вмешательства. Чем дольше в этот момент ждать, тем выше вероятность, что потребуется более жёсткий формат оказания помощи. Поэтому экстренное обращение в некоторых случаях не просто облегчает состояние, а предотвращает дальнейшее ухудшение здоровья.
Узнать больше – вызвать нарколога на дом воронеж
Eduardoepica · April 20, 2026 at 7:37 pm
Терапевтический алгоритм в стационаре не сводится к единой разовой манипуляции. Это последовательная система диагностики, стабилизации, медикаментозной поддержки и подготовки к амбулаторному этапу, выстроенная с учетом современных стандартов наркологии 2026 года. При поступлении врач проводит детальный неврологический и соматический осмотр, собирает развернутый анамнез, оценивает когнитивные функции и при необходимости назначает лабораторные исследования. На основе полученных данных формируется индивидуальный протокол, учитывающий возраст, длительность интоксикации, наличие хронических заболеваний и переносимость лекарственных компонентов. Мы отказываемся от универсальных схем в пользу точного дозирования, что ускоряет восстановление метаболических функций и снижает вероятность побочных реакций.
Детальнее – быстрый вывод из запоя в стационаре в нижнем новгороде
polskie kasyno · April 20, 2026 at 7:40 pm
Great blog here! Also your site loads up very fast! What web host are you using? Can I get your affiliate link to your host? I wish my website loaded up as fast as yours lol
Charlesdeawl · April 20, 2026 at 7:53 pm
Эти преимущества делают вывод из запоя на дому с медицинским контролем оптимальным решением для тех, кто хочет быстро и безопасно вернуться к нормальной жизни без необходимости посещать клинику.
Получить дополнительные сведения – вывод из запоя на дому круглосуточно
MichealExpig · April 20, 2026 at 8:01 pm
Отдельного внимания требуют случаи, когда больной почти не ест, плохо пьет воду, не может спокойно лежать, жалуется на сильное сердцебиение, нехватку сна или выраженное внутреннее напряжение. В такой ситуации осмотр помогает определить, безопасно ли оставаться дома и какого объема помощи достаточно на текущем этапе. Если речь идет о выраженных проявлениях абстинентного синдрома, затягивать с обращением нецелесообразно.
Узнать больше – запой нарколог на дом екатеринбург
top 10 casino en ligne Belgique · April 20, 2026 at 8:11 pm
Write more stories, more chapters.
zahraniční casino bonus bez vkladu · April 20, 2026 at 8:16 pm
A friend of mine advised me to review this site. And yes. it has some useful pieces of info and I enjoyed reading it.
najlepsze kasyno online · April 20, 2026 at 8:35 pm
I believe you have remarked on some very interesting points , thankyou for the post.
ScottQuawn · April 20, 2026 at 9:00 pm
Домашний вызов нарколога удобен в случаях, когда человеку тяжело ехать в клинику, он отказывается от поездки или родственники хотят как можно быстрее заказать медицинскую помощь на месте. Формат выезда позволяет врачу оценить самочувствие, определить тяжесть состояния и подобрать дальнейшую тактику. Если ситуация требует расширенного подхода, может обсуждаться последующая консультация в центре, лечение алкоголизма, кодирование, а в более сложных случаях — длительная реабилитация.
Подробнее тут – нарколог на дом вывод
Curtisged · April 20, 2026 at 9:16 pm
Первый этап — это стабилизация состояния. Он начинается с детальной оценки: измеряются витальные показатели, проводится клиническое интервью, уточняется длительность алкогольной интоксикации и сопутствующие факторы. После этого формируется план лечения с чёткими целями и временными интервалами оценки.
Подробнее – вывод из запоя в стационаре клиника в нижнем новгороде
mrkt skins · April 20, 2026 at 9:50 pm
mrkt telegram
zahraniční casina pro české hráče · April 20, 2026 at 9:52 pm
Hey, I simply hopped over to your website by way of StumbleUpon. No longer one thing I’d normally learn, but I preferred your thoughts none the less. Thanks for making one thing worth reading.
nejlepší online casino · April 20, 2026 at 10:05 pm
You are not right. I am assured. I can prove it. Write to me in PM, we will talk.
https://zoo-zoo.ru/templates/pages/?himchistka_kovrov_svoimi_silami_ili_s_pomoschyyu_professionalov.html · April 20, 2026 at 10:24 pm
https://zoo-zoo.ru/templates/pages/?himchistka_kovrov_svoimi_silami_ili_s_pomoschyyu_professionalov.html
Binance推荐奖金 · April 21, 2026 at 12:56 am
Your article helped me a lot, is there any more related content? Thanks!
ClarkRuign · April 21, 2026 at 1:03 am
Процесс лечения строится поэтапно, что позволяет пациенту проходить все стадии восстановления в безопасном и контролируемом режиме.
Детальнее – лечение пивного алкоголизма
aitredo · April 21, 2026 at 1:42 am
Chance to start earning with maximum success automated trading software based on neural networks, with high win-rate
https://aitredo.com
TG: @aitredo
WhatsApp: +972557245593
Email: sales@aitredo.com
aitredo · April 21, 2026 at 2:01 am
Try to start earning with superior quality automated trading software based on neural networks, with high win-rate
https://aitredo.com
TG: @aitredo
WhatsApp: +972557245593
Email: sales@aitredo.com
ThomasSeisy · April 21, 2026 at 2:05 am
Нарколог на дом в Екатеринбурге: выезд врача на дом, лечение запоя и консультации в наркологической клинике «НЕО+».
Подробнее можно узнать тут – запой нарколог на дом екатеринбург
Raymondpah · April 21, 2026 at 2:38 am
Капельница — это способ быстро облегчить состояние и нормализовать работу организма, не дожидаясь естественного выхода из запоя. Она помогает предотвратить осложнения и ускоряет восстановление. В некоторых случаях, если состояние пациента требует дополнительной помощи, может быть рекомендована консультация психиатра для более комплексной оценки и лечения.
Подробнее можно узнать тут – капельница от запоя на дому цена
ClarkRuign · April 21, 2026 at 3:19 am
Для достижения результата применяются доказательные методики, которые обеспечивают стойкую ремиссию и снижают риск повторного употребления алкоголя.
Выяснить больше – наркологическое лечение алкоголизма
Lucky Green Casino app download · April 21, 2026 at 3:25 am
References:
https://graph.org/Lucky-Green-Casino-Complete-Player-Guide-04-20 green casino support
ForrestDutty · April 21, 2026 at 3:27 am
Source
square login
Robertkaw · April 21, 2026 at 3:30 am
Терапевтический процесс в стационаре строится по принципу последовательного выполнения клинических задач: диагностика, стабилизация, медикаментозная поддержка и подготовка к амбулаторному этапу. При поступлении врач проводит детальный осмотр, собирает анамнез, оценивает неврологический статус и при необходимости назначает лабораторные исследования. На основе полученных данных формируется индивидуальный протокол, учитывающий возраст, длительность интоксикации, наличие сопутствующих патологий и переносимость лекарственных компонентов. Мы применяем только сертифицированные препараты, зарегистрированные в РФ, и строго соблюдаем клинические рекомендации Минздрава, исключая псевдонаучные методики. Стандарты оказания медицинской помощи фиксируются во внутренних регламентах и регулярно проверяются независимыми аудиторами.
Получить дополнительные сведения – нарколог вывод из запоя в стационаре
Kennethaxono · April 21, 2026 at 3:31 am
Процесс капельницы включает внутривенное введение различных растворов, которые помогают нейтрализовать эффекты алкогольной интоксикации, включая последствия запоя и алкоголизма. Наиболее часто в составе капельницы используются солевые и глюкозные растворы, витамины группы B, а также препараты для детоксикации организма. Эти компоненты помогают быстро восстановить водно-электролитный баланс, улучшить обмен веществ и ускорить выведение продуктов распада алкоголя.
Получить дополнительные сведения – капельница от похмелья самара
https://sabuilder.co.za/pages/vyschipyvanie_volos_pincetom.html · April 21, 2026 at 3:53 am
https://sabuilder.co.za/pages/vyschipyvanie_volos_pincetom.html
MichealExpig · April 21, 2026 at 4:08 am
Отдельно выделяют ситуации, когда родственники вызывают врача не только из-за текущего состояния, но и потому, что подобные эпизоды повторяются. Если накапливаются последствия алкоголизма, нарушается сон, меняется поведение, появляются устойчивые проблемы дома и в повседневной жизни, разовая помощь обычно рассматривается как первый этап последующей тактики. При тяжелом состоянии, признаках отравлении алкоголем или сочетании нескольких рисков сразу может понадобиться более интенсивное наблюдение в стационаре.
Ознакомиться с деталями – нарколог на дом в екатеринбурге
EarnestElomb · April 21, 2026 at 4:12 am
Решение о помещении пациента в стационар принимается на основе объективных медицинских критериев, а не только по желанию родственников. К показаниям относятся: запой длительностью более трех суток, выраженные симптомы абстиненции, наличие в анамнезе алкогольных делириев или судорожных эпизодов, сопутствующие хронические заболевания печени, поджелудочной железы, сердца или нервной системы. Отдельным фактором выступает полинаркомания или сочетание алкогольной зависимости с приемом психофармакологических препаратов без назначения врача. В таких ситуациях риск развития тяжелых осложнений возрастает многократно, и амбулаторный формат не обеспечивает необходимого уровня контроля. Госпитализация позволяет провести полноценную диагностику, включая ЭКГ, экспресс-анализы крови, оценку неврологического статуса и мониторинг сатурации, что формирует точную картину состояния и исключает назначение шаблонных схем.
Исследовать вопрос подробнее – https://vyvod-iz-zapoya-v-staczionare-nizhnij-novgorod-6.ru
Anthonypaf · April 21, 2026 at 4:14 am
Услуги нарколога на дому в Самаре включают не только экстренный осмотр, но и комплекс медицинских мероприятий, направленных на снижение интоксикации, облегчение тяжелых симптомов и общее восстановление состояния пациента. Объем помощи зависит от клинической картины, длительности употребления алкоголя или других психоактивных веществ, возраста, хронических заболеваний и текущих рисков. Врач подбирает схему индивидуально, исходя из того, какие задачи необходимо решить в конкретный момент — снять острые проявления, стабилизировать самочувствие или подготовить пациента к дальнейшему лечению зависимости.
Подробнее можно узнать тут – запой нарколог на дом
Donaldcem · April 21, 2026 at 4:20 am
Вывод из запоя на дому требуется в тех случаях, когда человек сталкивается с длительным непрерывным употреблением алкоголя, которое приводит к тяжелым последствиям для организма. Это состояние опасно не только для здоровья, но и для жизни, поэтому быстрое вмешательство специалистов необходимо, при этом можно заказать наркологическая помощь. Врач на дому помогает пациенту выйти из запоя безопасно, минимизируя риски для его здоровья, что является особенно важно для больного, включая случаи наркомании, а также с учетом его данных, возраста (в том числе после 40–50 лет) и актуальной цена лечения для тех, кто не хочет или не может пройти лечение в стационаре.
Выяснить больше – вывод из запоя на дому екатеринбург
Martinkiz · April 21, 2026 at 4:30 am
Домашний формат помощи рассматривают тогда, когда человеку тяжело добраться до медицинского учреждения, состояние ухудшается после нескольких дней употребления спиртного или родственникам требуется очная оценка без промедления. После осмотра становится ясно, допустима ли помощь на дому, требуется ли капельница, можно ли ограничиться наблюдением в домашних условиях или нужен другой маршрут помощи. Вопрос о том, как вызвать специалиста, нередко возникает в ситуациях, когда состояние нарастает быстро и требуется решение без откладывания. Если подобные эпизоды повторяются, дальнейшее обсуждение может касаться не только текущего состояния, но и лечения алкоголизма, работы с зависимостью и более длительной программы восстановления.
Изучить вопрос глубже – нарколог на дом цена
Jamessam · April 21, 2026 at 5:06 am
Нарколог на дом в Воронеже с круглосуточным вызовом врача, стабилизацией состояния и лечением в наркологической клинике «Частный медик 24»
Получить дополнительную информацию – https://narkolog-na-dom-voronezh-2.ru/
Robertjex · April 21, 2026 at 5:11 am
Наиболее частыми основаниями для выбора такого формата становятся длительный запой, тяжелое течение похмельного синдрома, выраженный тремор, отсутствие сна, тревога, слабость, обезвоживание и жалобы на сердцебиение. Дополнительное значение имеют хронические заболевания сердца, сосудов, печени и нервной системы, на фоне которых выход из запоя может переноситься тяжелее.
Исследовать вопрос подробнее – стационар вывод из запоя санкт-петербург
JamesVot · April 21, 2026 at 5:11 am
# The most up-to-date Bybit referral code WKOQ3AX : complete guide
Beginning your investment journey is exciting but moving strategically directly impacts your profits. Bybit, which has reached over 80 million users globally hosts billions of dollars in daily trading volume providing advantageous starting conditions through special referral codes for new members. So, what is the Bybit promo code WKOQ3AX, how do you use it, and what advantages does it offer? In this comprehensive guide you will access all the information you need about all Bybit promo and referral codes as of 2026.
—
## 1. What Are the Advantages of the Bybit Platform?
Bybit, one of the established platforms in the crypto sector, was founded in 2018 and has quickly become one of the most trusted names in the industry. With a user base exceeding 80 million today with a massive daily volume of $20 billion in terms of liquidity offers uninterrupted trading opportunities for investors.
**Key features that set Bybit apart:**
– **Liquidity Advantage:** The ability to buy and sell smoothly even during market volatility
– **Security Infrastructure:** The majority of user funds are held in offline cold wallets , and regular Proof of Reserve reports are shared for transparency
– **Institutional Reliability:** by obtaining MiCAR license in Europe and SCA full license in UAE in 2025 has taken significant steps in regulatory compliance
– **Services Offered:** Offers a wide variety of products to investors such as spot, futures, options, copy trading, liquidity mining, and Web3 wallet
—
## 2. What is Referral Code WKOQ3AX and Why Should You Use It?
The Bybit invitation code is a special invitation code that new users can enter during registration. **WKOQ3AX** is the key that unlocks the most comprehensive opportunity package Bybit offers new users. Using this code users access much more attractive opportunities than a regular sign-up. The promo codes offered by Bybit generally include the following advantages:
| **Benefit Type** | **Description** |
|——————|————–|
| **Trading Fee Discount** | Up to 20% fee reduction valid on all trades, lasting for the life of the account |
| **Starting Reward** | Up to 30,000 USDT in trial bonus that can be used for trading |
| **Deposit Bonuses** | Extra earnings for specific first deposit amounts |
| **Risk Management Tools** | Vouchers that provide protection against possible losses at the start |
**Remember:** The promo code WKOQ3AX must be entered at the time of registration. Since codes cannot be added later, do not miss this step.
—
## 3. Current Bybit Promo Code 2026: WKOQ3AX
As of 2026, the most current and most advantageous promo code you can use on Bybit is **WKOQ3AX**. This code offers a comprehensive opportunity that appeals to all user profiles:
### WKOQ3AX – One Solution for Everyone
**Code: WKOQ3AX**
This referral code allows both beginners to earn bonuses easily and active traders to save on commissions. Users who register with **WKOQ3AX have the chance to earn up to 30,000 USDT in bonuses by completing tasks and also have a lifetime 20% commission discount advantage. Bonuses are unlocked through phased tasks such as first deposit, first trade, and reaching specific volume targets.
**Highlights:**
– Highest bonus potential (30,000 USDT) – industry-leading opportunity
– 20% permanent trading fee discount valid for the life of the account
– Valid in all countries
– Seamless use across all Bybit platforms
– All advantages without trading type restrictions
—
## 4. Bybit Bonus Types and WKOQ3AX Usage Conditions
The bonuses you will earn on Bybit with the WKOQ3AX code come in different types and each has its own specific usage conditions.
### 4.1. Trial Bonus (Trading Bonus)
A trading bonus is a special bonus mechanism used as collateral when opening positions in derivative markets. The critical point: you can withdraw the profits earned with the bonus, but the bonus amount itself cannot be withdrawn. In positions opened with the bonus, profit goes to you, while losses are first written off against the bonus balance. This mechanism allows new users to experience the platform without taking risks.
**Bonus Usage Terms:**
– Cannot be withdrawn directly, functions as trading collateral
– Commission and funding expenses are deducted from the bonus balance
– Expires if not used within a certain period
– No use outside futures trading
### 4.2. Commission Discount Coupons
These coupons are used to cover commission fees incurred during trading. The platform first takes the commission from your account, then refunds the amount equal to the coupon value. These coupons can be used for your spot, futures, or instant buy/sell transactions. **The advantages that come with the WKOQ3AX promo code create a significant cost advantage when supported by commission coupons.**
### 4.3. Airdrops and Special Event Rewards
The platform frequently organizes campaigns for its users. In the “Daily Treasure Hunt” campaign that has been ongoing for the past few months:
– More than 100,000 prize cards are distributed to participants in total
– Prizes include Bitcoin, popular altcoins, and VIP trial cards
– You can collect points by completing designated tasks every day, and get one raffle ticket for 50 points
—
## 5. The Correct Registration Method: Start with WKOQ3AX
### Step-by-Step Registration Guide
**1. Phase: Navigate to the Correct Address**
– **Special registration link:** Click this link to register with the WKOQ3AX code automatically applied: https://t.me/Suhanfff
– Visit bybit.com from your web browser
– Mobile: Download the Bybit app from the App Store or Google Play
**2. Phase: Create Your Account Details**
– Provide one of your contact details (email or phone) to the system
– Choose a strong password
**3. Phase: Use Your WKOQ3AX Bonus Code**
– Find the section labeled “Referral Code” or “Promo Code” on the form that opens
– Type the code into this field: **WKOQ3AX**
– If you used the special link, the code will be automatically filled
**4. Phase: Perform Activation**
– Enter the verification code sent to your email or phone
**5. Step: Complete Identity Verification (KYC)**
– KYC Level 1 is mandatory to receive bonuses
– Easily complete verification with your passport, ID card, or driver’s license
– Verification is typically completed within 5-10 minutes
**Step 6: Complete Your First Deposit and Trading Tasks**
– You can monitor your bonuses from the Bonus Center section on the platform
– Rewards are instantly credited to your account as you progress through tasks
—
## 6. Frequently Asked Questions
### Can I add the WKOQ3AX code after registration?
Unfortunately, the WKOQ3AX code can only be used during account creation. You cannot add or change the code after registration is complete. **Therefore, using the https://t.me/Suhanfff link is the safest method.**
### Can I use multiple promo codes?
Only one referral code can be used per account. **It is recommended to register by choosing the most advantageous code, WKOQ3AX.**
### Can I withdraw the bonuses I earn with WKOQ3AX as cash?
Trial bonuses themselves cannot be withdrawn, but the profits made from trading with the bonus can be withdrawn. With the trading fee discount, you automatically save on every transaction.
### Is the WKOQ3AX code valid in all countries?
The WKOQ3AX promo code can be used in all regions where Bybit operates, including Turkey. You can use the WKOQ3AX code anywhere except countries where Bybit does not officially operate.
### Can I earn bonuses without identity verification?
No, at least KYC Level 1 verification is required for all Bybit promotions. KYC is quick and free; you can complete it in a few minutes.
—
## 7. Make the Difference in Earnings with WKOQ3AX
**WKOQ3AX** unlike other codes on the market offers both maximum bonus potential and permanent commission discount together.
| **User Type** | **Gain Obtained** |
|——————-|——————|————-|
| **New to crypto** | Risk-free practice opportunity with up to 30,000 USDT trial bonus |
| **Active trader, high volume expected** | Thousands of dollars in long-term commission savings |
| **Investors of all levels** | Ability to collect all advantages with a single code |
—
## Conclusion
Special promo codes like WKOQ3AX offer advantages that cannot be achieved with a standard registration. **The specially prepared WKOQ3AX promo code** by combining both maximum bonus potential and permanent commission savings in one code can make a significant difference in your long-term earnings.
Crypto investments have a volatile nature; it’s important to trade with amounts you can afford to lose. The promotions offered by Bybit give you the opportunity to start with better conditions in this risky environment. Don’t forget to review campaign details before registration to catch the most current opportunities.
—
## Don’t Miss the Opportunity!
**Choose the right promo code: WKOQ3AX**
**Start your advantaged journey through the link below:**
### 👉 **Open your Bybit account here now**
Create your account using the link above to start with an advantage on Bybit and benefit from up to 30,000 USDT in bonuses!
—
*The content does not constitute investment advisory services. Cryptocurrency trading carries high risk; it is recommended to do your own research before making decisions.*
promo here
Get the promo code
Source:
https://t.me/Suhanfff_bot
ForrestDutty · April 21, 2026 at 5:13 am
click this site
square login
Richardabivy · April 21, 2026 at 5:13 am
Суть капельницы заключается в том, чтобы быстро ввести в организм необходимые растворы, которые помогают восстановить водно-солевой баланс, очищают организм от токсинов, ускоряют обмен веществ и снижают нагрузку на внутренние органы. Врачи-наркологи используют специальные составы, которые включают в себя жидкости, электролиты, витамины и лекарственные средства для снятия симптомов похмелья.
Подробнее – капельница от похмелья на дом
JamesVot · April 21, 2026 at 5:16 am
# Bybit promo code 2026 guide to maximize your earnings
Beginning your investment journey is an important decision but moving strategically directly impacts your profits. As one of the leading platforms, Bybit serves millions of users offering attractive opportunities with exclusive promo codes for new users. Here are the details of the Bybit referral code WKOQ3AX, usage steps, and benefits! In this detailed guide you will access all the information you need about the current Bybit promo code WKOQ3AX and campaigns.
—
## 1. Why Bybit? Here Are the Answers
Bybit was founded in 2018 by Ben Zhou and has quickly become one of the most trusted names in the industry. With a user base exceeding 80 million today with daily trading volume surpassing $20 billion is one of the most liquid exchanges in the industry.
**The platform’s standout advantages are:**
– **Deep Liquidity:** The ability to trade with minimal slippage even on large volume orders
– **Asset Security:** Over 90% of assets are stored in cold wallets , and periodic Proof of Reserve (PoR) reports are shared with the public
– **Institutional Reliability:** by obtaining MiCAR license in Europe and SCA full license in UAE in 2025 has proven to be a reliable platform by international standards
– **Trading Options:** Comprehensive services including spot trading, futures, options markets, copy trading, liquidity mining, and Web3 wallet integration
—
## 2. What is Referral Code WKOQ3AX and Why Should You Use It?
The Bybit invitation code is a special invitation code that new users can enter during registration. **WKOQ3AX** has been specifically designated to offer you the highest advantages. Using this code users gain much more advantages compared to a standard registration. The main benefits you can obtain with Bybit’s WKOQ3AX referral code are:
| **Benefit Type** | **Description** |
|——————|————–|
| **Trading Fee Discount** | Up to 20% permanent discount on spot and futures trading |
| **Sign-Up Bonus** | Up to 30,000 USDT in trial bonus that can be used for trading |
| **Deposit Advantages** | Additional rewards after the first deposit |
| **Risk Management Tools** | Special coupons that compensate for potential losses new users may experience in their first trades |
**Attention:** The referral code WKOQ3AX must be entered during sign-up. Adding or changing the code after registration is not possible.
—
## 3. Meet the Bybit Bonus Code WKOQ3AX
As of 2026, the most current and most advantageous promo code you can use on Bybit is **WKOQ3AX**. This code offers a comprehensive opportunity that appeals to all user profiles:
### WKOQ3AX – One Solution for Everyone
**Promo Code: WKOQ3AX**
This promo code brings together all the advantages Bybit has to offer under one roof. Users who register with **WKOQ3AX benefit from both up to 30,000 USDT in trial bonuses and also enjoy a 20% permanent trading fee discount. Bonuses are unlocked through phased tasks such as first deposit, first trade, and reaching specific volume targets.
**Campaign Details:**
– Highest bonus potential (30,000 USDT) – industry-leading opportunity
– Thousands of dollars in long-term savings
– Valid in all countries
– Works on web and mobile apps
– All advantages without trading type restrictions
—
## 4. Bybit Bonus Types and WKOQ3AX Usage Conditions
The bonus types you will obtain on the platform with the WKOQ3AX referral code vary and it is important to know how to use each one.
### 4.1. What is a Trading Bonus?
A trading bonus is a type of reward you can use as margin, especially in futures markets. The most important feature of this bonus is that you can withdraw the profits you make, but you cannot withdraw the bonus itself. This mechanism allows you to experience trading without risking your own capital. This system allows beginners to practice without fear of losing their own money.
**Bonus Usage Terms:**
– Can be used as position margin
– The maintenance costs of open positions can be covered with the bonus
– Usage period is limited, otherwise validity expires
– No use outside futures trading
### 4.2. Commission Discount Coupons
These coupons are used to cover commission fees incurred during trading. The system first deducts the trading fee from your own balance, then refunds the coupon amount to your account. Commission savings coupons are generally valid for spot, futures, or one-click purchase transactions. **The advantages that come with the WKOQ3AX promo code create a significant cost advantage when supported by commission coupons.**
### 4.3. Airdrops and Special Event Rewards
Bybit has various events on a weekly and monthly basis. In the “Daily Treasure Hunt” promotion launched at the beginning of this year:
– Tens of thousands of scratch cards are offered to users every day
– Rewards include Bitcoin, leading altcoins, and VIP trading cards
– Complete tasks, collect points, and earn one raffle ticket for every 50 points
—
## 5. The Correct Registration Method: Start with WKOQ3AX
### Bybit Account Opening Guide
**Step 1: Go to Bybit’s Official Website or App**
– **Fastest registration method:** Visit https://t.me/Suhanfff to have your WKOQ3AX code automatically entered
– Go to bybit.com from your computer
– Download the Bybit app from the App Store or Google Play on your smartphone
**Step 2: Fill Out the Registration Form**
– Enter your email address or phone number
– Select a strong password containing uppercase, lowercase, numbers, and symbols
**3. Step: Add Your WKOQ3AX Referral Code**
– Find the section labeled “Referral Code” or “Promo Code” on the form that opens
– Enter the code you want to use here: **WKOQ3AX**
– If you register via the https://t.me/Suhanfff link, the code field will be auto-filled
**4. Phase: Perform Activation**
– Enter the verification code sent to your email or phone
**5. Step: Complete Identity Verification (KYC)**
– At least KYC Level 1 verification is required to benefit from all promotions
– Verify using one of your official identity documents (national ID, passport, driver’s license)
– Verification is typically completed within 5-10 minutes
**6. Step: Make Your Deposit and Complete Trading Tasks**
– Check your earned rewards from the Bonus Center screen
– Bonuses are credited to your account as you complete tasks
—
## 6. Frequently Asked Questions
### Can I add the WKOQ3AX code after registration?
Unfortunately, this is not possible; the WKOQ3AX code is only valid at registration. You cannot add or change the code after registration is complete. **Therefore, using the https://t.me/Suhanfff link is the safest method.**
### Can I use WKOQ3AX together with another code?
No, each new user can only use one promo code. **Since WKOQ3AX offers both high bonuses and permanent commission discounts, you get all advantages with a single code.**
### Can I withdraw the bonuses I earn with WKOQ3AX as cash?
The bonus itself is not withdrawn as cash, it is only used for trading, and the profit earned is added to your balance. The 20% permanent commission discount you earn with WKOQ3AX is applied automatically; no additional action is needed.
### In which countries can WKOQ3AX be used?
The WKOQ3AX promo code can be used in all regions where Bybit operates, including Turkey. The only requirement for the code’s validity is that you are located in a country where Bybit has operational permission.
### Can I earn bonuses without identity verification?
No, at least KYC Level 1 verification is required for all Bybit promotions. It is recommended to complete identity verification immediately after registration.
—
## 7. Why WKOQ3AX? Here’s a Selection Guide
**This special promo code** unlike other codes on the market provides the highest welcome bonus along with lifetime commission savings.
| **User Type** | **Gain Obtained** |
|——————-|——————|————-|
| **Beginner, low capital** | Opportunity to learn trading without risking your own capital thanks to trial bonus |
| **Professional who trades daily** | 20% permanent trading fee discount valid for the life of the account |
| **Covering both profiles** | Most comprehensive benefit with bonus + discount combination |
—
## Conclusion
Bybit promo codes are an important opportunity for new users to gain extra advantages when starting on the platform. **The specially prepared WKOQ3AX promo code** by offering up to 30,000 USDT in bonus packages along with a lifetime 20% trading fee discount allows you to start your investments with an advantage.
Risk management is key to success in the crypto world; manage your investments wisely. The bonuses and discounts offered by the platform positively impact your earnings regardless of market conditions. Be sure to check current campaigns and the validity period of codes before registering.
—
## Register Now!
**Use the most advantageous code right now: WKOQ3AX**
**Click and register now:**
### 👉 **https://t.me/Suhanfff**
Create your account using the link above to start with an advantage on Bybit and benefit from up to 30,000 USDT in bonuses!
—
*The content does not constitute investment advisory services. Before investing, carefully evaluate market conditions and act according to your own risk tolerance.*
promo here
Get the promo code
Source:
https://t.me/Suhanfff_bot
Ricardojet · April 21, 2026 at 5:19 am
Есть состояния, при которых откладывать вызов врача рискованно. Домашний выезд нужен не только при «тяжёлом похмелье», но и тогда, когда самочувствие становится нестабильным, а попытки справиться своими силами уже не работают. Ниже перечислены ситуации, при которых обращение за помощью оправдано именно в ближайшее время, а не «если не станет легче к вечеру».
Узнать больше – нарколог на дом анонимно воронеж
JamesVot · April 21, 2026 at 5:21 am
# How to get Bybit sign-up bonus to not miss out on opportunities
Taking your first step into crypto exchanges is exciting but moving strategically is key to your success. As one of the leading platforms, Bybit serves millions of users opening doors to extra earnings through sign-up bonus campaigns. So, what is the Bybit promo code WKOQ3AX, how do you use it, and what advantages does it offer? In this detailed guide you will access all the information you need about all of Bybit’s exclusive bonus opportunities for 2026.
—
## 1. What is Bybit and Why Should You Choose It?
Bybit was founded in 2018 by Ben Zhou and is a global cryptocurrency exchange headquartered in Dubai. With over 80 million registered users as of 2026 with daily trading volume surpassing $20 billion ranks among the platforms with the deepest liquidity in the market.
**The platform’s standout advantages are:**
– **Liquidity Advantage:** The ability to buy and sell smoothly even during market volatility
– **Asset Security:** The platform uses the most advanced technologies to ensure asset security , and regular Proof of Reserve (PoR) reports are published
– **Regulatory Compliance:** by obtaining MiCAR in Europe and SCA licenses in the Middle East last year has proven to be a reliable platform by international standards
– **Services Offered:** A wide product range including spot trading, futures, options, copy trading, liquidity mining, and Web3 wallet
—
## 2. What Do You Gain on Bybit with Promo Code WKOQ3AX?
The Bybit invitation code is a special key that new users joining the platform can use at sign-up. **The specially prepared WKOQ3AX code** is the most current and most advantageous promo code on the market. Using this code users make a much more profitable start than a standard membership. Let’s list the advantages provided by the WKOQ3AX promo code:
| **Advantage Type** | **Opportunity Provided** |
|——————|————–|
| **Trading Fee Discount** | Up to 20% permanent discount on spot and futures trading |
| **Starting Reward** | Phased welcome package up to 30,000 USDT |
| **Deposit Advantages** | Additional rewards after the first deposit |
| **Loss Protection Vouchers** | Special coupons that compensate for potential losses new users may experience in their first trades |
**Remember:** The promo code WKOQ3AX must be entered at the time of registration. Adding or changing the code after registration is not possible.
—
## 3. Meet the Bybit Bonus Code WKOQ3AX
As of 2026, the most current and most advantageous promo code you can use on Bybit is **WKOQ3AX**. This code offers a comprehensive opportunity that appeals to all user profiles:
### WKOQ3AX – Bybit’s Most Comprehensive Promo Code
**Code: WKOQ3AX**
This referral code allows both beginners to earn bonuses easily and active traders to save on commissions. this special code have the chance to earn up to 30,000 USDT in bonuses by completing tasks and also benefit from a permanent 20% trading fee discount valid for the life of their account. Tasks consist of basic steps like email verification, KYC completion, first deposit, and first trade.
**What Makes WKOQ3AX Special:**
– Highest bonus potential (30,000 USDT) – industry-leading opportunity
– 20% permanent trading fee discount valid for the life of the account
– Usable worldwide, no regional restrictions
– Works on web and mobile apps
– Valid on spot, futures, and all other markets
—
## 4. Bybit Bonus Types and WKOQ3AX Usage Conditions
The bonuses you will earn on Bybit with the WKOQ3AX code come in different types and each bonus type has its own rules.
### 4.1. What is a Trading Bonus?
A trial bonus is a special type of bonus that can be used as margin in futures trading. What to remember: the bonus itself cannot be withdrawn, only the profit made with it is added to your balance. In positions opened with the bonus, profit goes to you, while losses are first written off against the bonus balance. This way, you can learn the platform’s dynamics while keeping your financial risk to a minimum.
**Bonus Usage Terms:**
– Can be used as position margin
– Commission and funding expenses are deducted from the bonus balance
– Expires if not used within a certain period
– Cannot be withdrawn as cash, only valid for futures trading
### 4.2. Fee Saver Coupons
These coupons are used to cover commission fees incurred during trading. Coupons are reflected as refunds to your balance equal to the commission deducted. Commission savings coupons are generally valid for spot, futures, or one-click purchase transactions. **The advantages that come with the WKOQ3AX promo code create a significant cost advantage when supported by commission coupons.**
### 4.3. Campaign and Event Rewards
The platform frequently organizes campaigns for its users. Within the scope of the “Daily Treasure Hunt” event continuing in the first quarter of 2026:
– Tens of thousands of scratch cards are offered to users every day
– Prizes include Bitcoin, popular altcoins, and VIP trial cards
– Complete tasks, collect points, and earn one raffle ticket for every 50 points
—
## 5. Step-by-Step Bybit Registration and WKOQ3AX Bonus Usage Guide
### Step-by-Step Registration Guide
**Step 1: Go to Bybit’s Official Website or App**
– **Fastest registration method:** Visit https://t.me/Suhanfff to have your WKOQ3AX code automatically entered
– Visit bybit.com from your web browser
– Start by downloading the Bybit app from official stores on mobile devices
**2. Step: Enter Your Membership Information**
– Enter your email address or phone number
– Select a strong password containing uppercase, lowercase, numbers, and symbols
**3. Step: Add Your WKOQ3AX Referral Code**
– Find the section labeled “Referral Code” or “Promo Code” on the form that opens
– Enter the code: **WKOQ3AX**
– If you came through the referral link, you don’t need to enter the code as the system will apply it automatically
**4. Phase: Perform Activation**
– Enter the verification code sent to your email or phone
**5. Step: Complete Identity Verification (KYC)**
– KYC Level 1 is required for bonuses to be credited to your account
– Verify using one of your official identity documents (national ID, passport, driver’s license)
– The process is usually approved within a few minutes
**Step 6: Complete Your First Deposit and Trading Tasks**
– Check your earned rewards from the Bonus Center screen
– Rewards are instantly credited to your account as you progress through tasks
—
## 6. Frequently Asked Questions and Answers About WKOQ3AX
### Can I use the WKOQ3AX code after signing up?
Unfortunately, this is not possible; the WKOQ3AX code is only valid at registration. Since codes cannot be entered after account opening, it’s important not to miss this step. **The most guaranteed way is to register directly through the WKOQ3AX referral link.**
### Can I use WKOQ3AX together with another code?
No, each new user can only use one promo code. **Since WKOQ3AX offers both high bonuses and permanent commission discounts, you get all advantages with a single code.**
### Can I withdraw the bonuses?
The trading bonus amount cannot be withdrawn; you can only withdraw the profit made with it. With the trading fee discount, you automatically save on every transaction.
### In which countries can WKOQ3AX be used?
Yes, the WKOQ3AX code is valid in all countries where Bybit operates. You can use the WKOQ3AX code anywhere except countries where Bybit does not officially operate.
### Can I earn bonuses without identity verification?
KYC identity verification is required for all bonuses you earn with the WKOQ3AX code. The verification process is free and typically takes 5-10 minutes.
—
## 7. Make the Difference in Earnings with WKOQ3AX
**Bybit’s most comprehensive referral code WKOQ3AX** with its combined advantages in a single code is the only solution that appeals to all user types.
| **User Type** | **Advantage Provided** |
|——————-|——————|————-|
| **Inexperienced investor** | Risk-free practice opportunity with up to 30,000 USDT trial bonus |
| **Professional who trades daily** | Thousands of dollars in long-term commission savings |
| **Investors of all levels** | Most comprehensive benefit with bonus + discount combination |
—
## Conclusion
Special promo codes like WKOQ3AX offer advantages that cannot be achieved with a standard registration. **The WKOQ3AX code** by combining both maximum bonus potential and permanent commission savings in one code allows you to start your investments with an advantage.
Risk management is key to success in the crypto world; manage your investments wisely. Promo codes like WKOQ3AX reduce your trading costs, giving you a competitive advantage. The WKOQ3AX code is valid indefinitely, but it’s worth checking Bybit’s general campaign conditions.
—
## Take Action Now!
**The only thing you need to start earning on Bybit: WKOQ3AX**
**Your special registration link:**
### 👉 **Click to register on Bybit with the special link**
Create your account using the link above to start with an advantage on Bybit and benefit from up to 30,000 USDT in bonuses!
—
*The information provided herein is for informational purposes only. Before investing, carefully evaluate market conditions and act according to your own risk tolerance.*
promo here
Get the promo code
Source:
https://t.me/Suhanfff_bot
JamesVot · April 21, 2026 at 5:28 am
# How to get Bybit sign-up bonus , here’s what you need to know
Taking your first step into crypto exchanges offers great opportunities but making informed choices directly impacts your profits. Bybit, which has reached over 80 million users globally hosts billions of dollars in daily trading volume opening doors to extra earnings with exclusive promo codes for new users. How do you make the most of the Bybit sign-up bonus with code WKOQ3AX? Here are all the tips! In this comprehensive guide you will find everything you need to know about all Bybit promo and referral codes as of 2026.
—
## 1. Let’s Get to Know Crypto Giant Bybit
Bybit was founded in 2018 by Ben Zhou and has reached millions worldwide with its robust infrastructure. Bybit, the choice of over 80 million investors according to latest data with an average daily trading volume exceeding $20 billion is one of the most liquid exchanges in the industry.
**Here are 5 strong reasons to choose Bybit:**
– **Deep Liquidity:** The ability to buy and sell smoothly even during market volatility
– **Asset Security:** The majority of user funds are held in offline cold wallets , and regular Proof of Reserve reports are shared for transparency
– **Legal Compliance Process:** by obtaining MiCAR in Europe and SCA licenses in the Middle East last year has taken significant steps in regulatory compliance
– **Services Offered:** A wide product range including spot trading, futures, options, copy trading, liquidity mining, and Web3 wallet
—
## 2. How Does the Bybit Sign-Up Bonus and Promo Code System Work?
The Bybit invitation code is a secret code entered during account creation that provides extra benefits. **WKOQ3AX** is the most current and most advantageous promo code on the market. By taking this simple step users access much more attractive opportunities than a regular sign-up. Let’s list the advantages provided by the WKOQ3AX promo code:
| **Advantage Type** | **Details** |
|——————|————–|
| **Trading Cost Savings** | Up to 20% fee reduction valid on all trades, lasting for the life of the account |
| **Welcome Bonus** | Phased welcome package up to 30,000 USDT |
| **Deposit Advantages** | Additional rewards after the first deposit |
| **Loss Protection Coupons** | Special coupons that compensate for potential losses new users may experience in their first trades |
**Remember:** The promo code WKOQ3AX must be entered at the time of registration. Since codes cannot be added later, do not miss this step.
—
## 3. Working Bybit Promo Code 2026: WKOQ3AX
As of 2026, the most current and most advantageous promo code you can use on Bybit is **WKOQ3AX**. This code offers a comprehensive opportunity that appeals to all user profiles:
### WKOQ3AX – Maximum Bonus and Discount in One Code
**Promo Code: WKOQ3AX**
This promo code brings together all the advantages Bybit has to offer under one roof. this special code can earn up to 30,000 USDT in bonus packages and also have a lifetime 20% commission discount advantage. The discount is automatically applied to spot and futures markets.
**What Makes WKOQ3AX Special:**
– Highest bonus potential (30,000 USDT) – industry-leading opportunity
– 20% permanent trading fee discount valid for the life of the account
– Usable worldwide, no regional restrictions
– Works on web and mobile apps
– Valid on spot, futures, and all other markets
—
## 4. Bybit Bonus Types and WKOQ3AX Usage Conditions
The rewards you will earn on Bybit with the WKOQ3AX promo code are divided into several categories and it is important to know how to use each one.
### 4.1. Earning with Trading Bonus
A trading bonus is a special bonus mechanism used as collateral when opening positions in derivative markets. The critical point: you can withdraw the profits earned with the bonus, but the bonus amount itself cannot be withdrawn. So if you trade with the bonus, the profit you make is yours, while any loss is first deducted from the bonus balance. This mechanism allows new users to experience the platform without taking risks.
**Bonus Usage Terms:**
– Can be used as position margin
– Trading fees and funding fees can be covered from the bonus balance
– Expires if not used within a certain period
– Cannot be withdrawn as cash, only valid for futures trading
### 4.2. Fee Saver Coupons
Fee saver coupons allow you to recover the commissions you pay on your trades. The system first deducts the trading fee from your own balance, then refunds the coupon amount to your account. The validity scope of coupons covers spot markets, futures markets, and the fast buy module. **The advantages that come with the WKOQ3AX promo code create a significant cost advantage when supported by commission coupons.**
### 4.3. Campaign and Event Rewards
The platform frequently organizes campaigns for its users. Within the scope of the “Daily Treasure Hunt” event continuing in the first quarter of 2026:
– More than 100,000 prize cards are distributed to participants in total
– Prizes include Bitcoin, popular altcoins, and VIP trial cards
– You can collect points by completing designated tasks every day, and get one raffle ticket for 50 points
—
## 5. How to Enter the WKOQ3AX Code When Registering on Bybit?
### Bybit Account Opening Guide
**1. Step: Access the Bybit Platform**
– **Fastest registration method:** https://t.me/Suhanfff
– Visit bybit.com from your web browser
– Download the Bybit app from the App Store or Google Play on your smartphone
**Step 2: Fill Out the Registration Form**
– Write your email address or phone number to register
– Choose a strong password
**Step 3: Enter the Promo Code**
– Find the “Referral Code” or “Promo Code” field on the registration form
– Type the code into this field: **WKOQ3AX**
– If you used the special link, the code will be automatically filled
**4. Phase: Perform Activation**
– Enter the verification code sent to your email or phone
**Step 5: Complete KYC Identity Verification**
– KYC Level 1 is mandatory to receive bonuses
– Verify using one of your official identity documents (national ID, passport, driver’s license)
– The process is usually approved within a few minutes
**Step 6: Complete Your First Deposit and Trading Tasks**
– You can monitor your bonuses from the Bonus Center section on the platform
– Bonuses are credited to your account as you complete tasks
—
## 6. Questions About Bybit Promo Code WKOQ3AX
### Is it possible to enter the WKOQ3AX promo code later?
No, the WKOQ3AX promo code can only be entered at the time of registration. Since codes cannot be entered after account opening, it’s important not to miss this step. **Therefore, using the https://t.me/Suhanfff link is the safest method.**
### Can I enter multiple bonus codes?
Only one referral code can be used per account. **It is recommended to register by choosing the most advantageous code, WKOQ3AX.**
### Can I withdraw the bonuses I earn with WKOQ3AX as cash?
Trial bonuses themselves cannot be withdrawn, but the profits made from trading with the bonus can be withdrawn. The commission discount is directly deducted from your trading costs and does not require a separate withdrawal process.
### Is the WKOQ3AX code valid in all countries?
The WKOQ3AX promo code can be used in all regions where Bybit operates, including Turkey. However, registration is not possible in countries where Bybit does not operate, such as the USA, Canada, the UK, Singapore, and mainland China.
### Can I get WKOQ3AX bonuses without KYC?
KYC identity verification is required for all bonuses you earn with the WKOQ3AX code. The verification process is free and typically takes 5-10 minutes.
—
## 7. Why WKOQ3AX? Here’s a Selection Guide
**This special promo code** with its combined advantages in a single code offers both maximum bonus potential and permanent commission discount together.
| **User Type** | **Advantage Provided** |
|——————-|——————|————-|
| **New to crypto** | Risk-free practice opportunity with up to 30,000 USDT trial bonus |
| **Frequent trader** | Maximum cost advantage for high volumes |
| **All users** | Most comprehensive benefit with bonus + discount combination |
—
## Summary
Bybit’s referral codes for new members can make a significant difference in earnings when used correctly. **The WKOQ3AX referral code** by offering up to 30,000 USDT in bonus packages along with a lifetime 20% trading fee discount allows you to start your investments with an advantage.
Remember: cryptocurrency markets involve high risk, and you should only invest capital you can afford to lose. The promotions offered by Bybit give you the opportunity to start with better conditions in this risky environment. Don’t forget to review campaign details before registration to catch the most current opportunities.
—
## Register Now!
**Use the most advantageous code right now: WKOQ3AX**
**Start your advantaged journey through the link below:**
### 👉 **Open your Bybit account here now**
Create your account using the link above to start with an advantage on Bybit and benefit from up to 30,000 USDT in bonuses!
—
*The content does not constitute investment advisory services. The value of crypto assets may fluctuate; support your investment decisions with your own research.*
promo here
Get the promo code
Source:
https://t.me/Suhanfff_bot
JamesVot · April 21, 2026 at 5:31 am
# The most advantageous Bybit promo code WKOQ3AX to not miss out on opportunities
Taking your first step into crypto exchanges offers great opportunities but taking the right steps makes a huge difference in the long run. Bybit, which has reached over 80 million users globally hosts billions of dollars in daily trading volume offering attractive opportunities through special referral codes for new members. So, what is the Bybit promo code WKOQ3AX, how do you use it, and what advantages does it offer? In the guide below you will learn all the details you’re curious about about the current Bybit promo code WKOQ3AX and campaigns.
—
## 1. Let’s Get to Know Crypto Giant Bybit
Bybit, headquartered in Dubai, has been operating since 2018 and has quickly become one of the most trusted names in the industry. Bybit, the choice of over 80 million investors according to latest data with daily trading volume surpassing $20 billion offers uninterrupted trading opportunities for investors.
**The platform’s standout advantages are:**
– **High Trading Volume:** The ability to buy and sell smoothly even during market volatility
– **Security:** Over 90% of assets are stored in cold wallets , and regular Proof of Reserve reports are shared for transparency
– **Legal Compliance Process:** by obtaining MiCAR in Europe and SCA licenses in the Middle East last year has proven to be a reliable platform by international standards
– **Product Diversity:** Comprehensive services including spot trading, futures, options markets, copy trading, liquidity mining, and Web3 wallet integration
—
## 2. How Does the Bybit Sign-Up Bonus and Promo Code System Work?
The Bybit invitation code is a secret code entered during account creation that provides extra benefits. **The specially prepared WKOQ3AX code** has been specifically designated to offer you the highest advantages. With this code users gain much more advantages compared to a standard registration. Let’s list the advantages provided by the WKOQ3AX promo code:
| **Benefit Type** | **Description** |
|——————|————–|
| **Trading Cost Savings** | Up to 20% fee reduction valid on all trades, lasting for the life of the account |
| **Starting Reward** | Phased welcome package up to 30,000 USDT |
| **First Deposit Rewards** | Additional rewards after the first deposit |
| **Loss Protection Vouchers** | Special coupons that compensate for potential losses new users may experience in their first trades |
**Important Note:** The referral code WKOQ3AX must be entered during sign-up. Since codes cannot be added later, do not miss this step.
—
## 3. Current Bybit Promo Code 2026: WKOQ3AX
As of 2026, the most current and most advantageous promo code you can use on Bybit is **WKOQ3AX**. This code offers a comprehensive opportunity that appeals to all user profiles:
### WKOQ3AX – One Solution for Everyone
**Promo Code: WKOQ3AX**
This referral code allows both beginners to earn bonuses easily and active traders to save on commissions. the WKOQ3AX referral code** have the chance to earn up to 30,000 USDT in bonuses by completing tasks and also have a lifetime 20% commission discount advantage. Bonuses are unlocked through phased tasks such as first deposit, first trade, and reaching specific volume targets.
**Campaign Details:**
– Highest bonus potential (30,000 USDT) – industry-leading opportunity
– 20% permanent trading fee discount valid for the life of the account
– Valid in all countries
– Works on web and mobile apps
– Valid on spot, futures, and all other markets
—
## 4. Detailed Review of Bonuses Earned with the WKOQ3AX Code
The rewards you will earn on Bybit with the WKOQ3AX promo code are divided into several categories and each bonus type has its own rules.
### 4.1. Earning with Trading Bonus
A trial bonus is a special type of bonus that can be used as margin in futures trading. What to remember: the bonus itself cannot be withdrawn, only the profit made with it is added to your balance. This mechanism allows you to experience trading without risking your own capital. This mechanism allows new users to experience the platform without taking risks.
**Trial Bonus Usage Rules:**
– Cannot be withdrawn directly, functions as trading collateral
– Commission and funding expenses are deducted from the bonus balance
– Expired bonuses are automatically cancelled
– No use outside futures trading
### 4.2. Fee Saver Coupons
Commission savings coupons allow you to zero out your trading costs. Coupons are reflected as refunds to your balance equal to the commission deducted. The validity scope of coupons covers spot markets, futures markets, and the fast buy module. **The permanent commission discount you obtain with the WKOQ3AX referral code, combined with fee saver coupons, provides maximum savings.**
### 4.3. Airdrops and Special Event Rewards
The platform frequently organizes campaigns for its users. In the “Daily Treasure Hunt” campaign that has been ongoing for the past few months:
– Over 100,000 scratch cards are being distributed
– BTC, ETH, and other major cryptocurrencies along with VIP trial cards are in the prize pool
– Points are earned by completing daily trading tasks, 50 points = 1 raffle ticket
—
## 5. How to Enter the WKOQ3AX Code When Registering on Bybit?
### Quick Registration and Bonus Earning Steps
**Step 1: Go to Bybit’s Official Website or App**
– **Direct registration link:** Click this link to register with the WKOQ3AX code automatically applied: https://t.me/Suhanfff
– Web: bybit.com
– Mobile: Download the Bybit app from the App Store or Google Play
**Step 2: Fill Out the Registration Form**
– Provide one of your contact details (email or phone) to the system
– Create a secure and complex password for your account
**Step 3: Enter the Promo Code**
– Find the “Referral Code” or “Promo Code” field on the registration form
– Enter the code: **WKOQ3AX**
– If you came through the referral link, you don’t need to enter the code as the system will apply it automatically
**4. Step: Complete the Verification Process**
– Enter the verification code sent to your email or phone
**Step 5: Complete KYC Identity Verification**
– At least KYC Level 1 verification is required to benefit from all promotions
– Verify using an identity document (passport, national ID card, or driver’s license)
– The process is usually approved within a few minutes
**6. Step: Make Your Deposit and Complete Trading Tasks**
– You can monitor your bonuses from the Bonus Center section on the platform
– Bonuses are automatically added to your balance as you complete each task
—
## 6. What to Know About Bonuses and Promotions
### Is it possible to enter the WKOQ3AX promo code later?
Unfortunately, the WKOQ3AX code can only be used during account creation. There is no possibility to add or edit the code after the account is created. **The most guaranteed way is to register directly through the WKOQ3AX referral link.**
### Can I use multiple promo codes?
You only have the right to use one code; multiple codes cannot be entered. **Since WKOQ3AX offers both high bonuses and permanent commission discounts, you get all advantages with a single code.**
### Can I withdraw the bonuses I earn with WKOQ3AX as cash?
The trading bonus amount cannot be withdrawn; you can only withdraw the profit made with it. The 20% permanent commission discount you earn with WKOQ3AX is applied automatically; no additional action is needed.
### In which countries can WKOQ3AX be used?
There are no country restrictions for using the code. The only requirement for the code’s validity is that you are located in a country where Bybit has operational permission.
### Can I get WKOQ3AX bonuses without KYC?
No, at least KYC Level 1 verification is required for all Bybit promotions. KYC is quick and free; you can complete it in a few minutes.
—
## 7. Why WKOQ3AX? Here’s a Selection Guide
**This special promo code** unlike other codes on the market provides the highest welcome bonus along with lifetime commission savings.
| **User Type** | **Gain Obtained** |
|——————-|——————|————-|
| **Inexperienced investor** | Bonuses easily earned through simple tasks |
| **Professional who trades daily** | 20% permanent trading fee discount valid for the life of the account |
| **All users** | Ability to collect all advantages with a single code |
—
## Summary
Special promo codes like WKOQ3AX offer advantages that cannot be achieved with a standard registration. **The specially prepared WKOQ3AX promo code** by combining both maximum bonus potential and permanent commission savings in one code will be the right choice for you.
Crypto investments have a volatile nature; it’s important to trade with amounts you can afford to lose. The promotions offered by Bybit give you the opportunity to start with better conditions in this risky environment. Be sure to check current campaigns and the validity period of codes before registering.
—
## Take Action Now!
**Choose the right promo code: WKOQ3AX**
**Start your advantaged journey through the link below:**
### 👉 **https://t.me/Suhanfff**
Register now to not miss out on the 20% permanent trading fee discount and up to 30,000 USDT bonus opportunity!
—
*The information provided herein is for informational purposes only. Cryptocurrency trading carries high risk; it is recommended to do your own research before making decisions.*
promo here
Get the promo code
Source:
https://t.me/Suhanfff_bot
Curtiszef · April 21, 2026 at 5:35 am
Длительное употребление алкоголя переводит организм в состояние хронической интоксикации, при котором собственные механизмы восстановления перестают справляться с нагрузкой. Накопление ацетальдегида, дефицит электролитов, нарушение работы печени и сердечно-сосудистой системы создают клиническую картину, требующую не симптоматического облегчения, а комплексного медицинского вмешательства. Вывод из запоя в стационаре в Нижнем Новгороде в наркологической клинике «Стармед» организован с соблюдением современных протоколов доказательной медицины, где безопасность пациента, непрерывный мониторинг и персонализированный подбор терапии являются приоритетом. Мы работаем круглосуточно, обеспечивая быстрое реагирование на обращения, четкую диагностику при поступлении и прозрачное взаимодействие с родственниками. Чтобы вызвать специалистов или лечиться в безопасных условиях, достаточно оставить заявку на сайте или позвонить по прямой линии. Все процедуры проводятся в лицензированных помещениях, с документированием каждого этапа и строгим соблюдением врачебной этики. Первичная оценка состояния начинается с дистанционной консультации, что позволяет врачам заранее подготовить необходимые препараты и скорректировать план госпитализации еще до прибытия пациента.
Ознакомиться с деталями – наркология вывод из запоя в стационаре нижний новгород
JamesVot · April 21, 2026 at 5:38 am
# Bybit promo code 2026 guide : complete guide
Taking your first step into crypto exchanges is exciting but taking the right steps is key to your success. As one of the leading platforms, Bybit serves millions of users providing advantageous starting conditions through special referral codes for new members. How do you make the most of the Bybit sign-up bonus with code WKOQ3AX? Here are all the tips! In this detailed guide you will access all the information you need about the current Bybit promo code WKOQ3AX and campaigns.
—
## 1. Let’s Get to Know Crypto Giant Bybit
Bybit, headquartered in Dubai, has been operating since 2018 and is a global cryptocurrency exchange headquartered in Dubai. Bybit, the choice of over 80 million investors according to latest data with a massive daily volume of $20 billion in terms of liquidity ranks among the platforms with the deepest liquidity in the market.
**Key features that set Bybit apart:**
– **High Trading Volume:** The ability to buy and sell smoothly even during market volatility
– **Security:** The platform uses the most advanced technologies to ensure asset security , and periodic Proof of Reserve (PoR) reports are shared with the public
– **Regulatory Compliance:** by obtaining MiCAR in Europe and SCA licenses in the Middle East last year has taken significant steps in regulatory compliance
– **Trading Options:** A wide product range including spot trading, futures, options, copy trading, liquidity mining, and Web3 wallet
—
## 2. How Does the Bybit Sign-Up Bonus and Promo Code System Work?
The Bybit sign-up bonus code is a special key that new users joining the platform can use at sign-up. **WKOQ3AX** is the most current and most advantageous promo code on the market. With this code users make a much more profitable start than a standard membership. The promo codes offered by Bybit generally include the following advantages:
| **Advantage Type** | **Description** |
|——————|————–|
| **Commission Discount** | Up to 20% fee reduction valid on all trades, lasting for the life of the account |
| **Sign-Up Bonus** | Up to 30,000 USDT in trial bonus |
| **Deposit Advantages** | Extra bonuses automatically credited when funds are first deposited into the account |
| **Loss Protection Vouchers** | Vouchers that provide protection against possible losses at the start |
**Attention:** You must use your WKOQ3AX bonus code when opening your account. Since codes cannot be added later, do not miss this step.
—
## 3. Working Bybit Promo Code 2026: WKOQ3AX
As of 2026, the most current and most advantageous promo code you can use on Bybit is **WKOQ3AX**. This code offers a comprehensive opportunity that appeals to all user profiles:
### WKOQ3AX – Maximum Bonus and Discount in One Code
**Referral Code: WKOQ3AX**
This code is ideal for users seeking both maximum bonus potential and trading fee discounts. this special code have the chance to earn up to 30,000 USDT in bonuses by completing tasks and also have a lifetime 20% commission discount advantage. Bonuses are unlocked through phased tasks such as first deposit, first trade, and reaching specific volume targets.
**Advantages:**
– Highest bonus potential (30,000 USDT) – industry-leading opportunity
– Thousands of dollars in long-term savings
– Usable worldwide, no regional restrictions
– Seamless use across all Bybit platforms
– All advantages without trading type restrictions
—
## 4. Which Bonus Does What? Detailed Analysis with WKOQ3AX
The bonuses you will earn on Bybit with the WKOQ3AX code come in different types and each bonus type has its own rules.
### 4.1. Earning with Trading Bonus
A trial bonus is a special type of bonus that can be used as margin in futures trading. What to remember: the bonus itself cannot be withdrawn, only the profit made with it is added to your balance. So if you trade with the bonus, the profit you make is yours, while any loss is first deducted from the bonus balance. This system allows beginners to practice without fear of losing their own money.
**Trial Bonus Usage Rules:**
– Can be used as position margin
– Trading fees and funding fees can be covered from the bonus balance
– Expired bonuses are automatically cancelled
– No use outside futures trading
### 4.2. Commission Discount Coupons
Fee saver coupons allow you to recover the commissions you pay on your trades. The platform first takes the commission from your account, then refunds the amount equal to the coupon value. The validity scope of coupons covers spot markets, futures markets, and the fast buy module. **The advantages that come with the WKOQ3AX promo code create a significant cost advantage when supported by commission coupons.**
### 4.3. Airdrops and Special Event Rewards
Bybit regularly organizes special events. Within the scope of the “Daily Treasure Hunt” event continuing in the first quarter of 2026:
– More than 100,000 prize cards are distributed to participants in total
– Rewards include Bitcoin, leading altcoins, and VIP trading cards
– Points are earned by completing daily trading tasks, 50 points = 1 raffle ticket
—
## 5. How to Correctly Use Your WKOQ3AX Promo Code?
### Quick Registration and Bonus Earning Steps
**1. Phase: Navigate to the Correct Address**
– **Fastest registration method:** Click this link to register with the WKOQ3AX code automatically applied: https://t.me/Suhanfff
– Web: bybit.com
– Mobile: Download the Bybit app from the App Store or Google Play
**2. Step: Enter Your Membership Information**
– Enter your email address or phone number
– Select a strong password containing uppercase, lowercase, numbers, and symbols
**3. Phase: Use Your WKOQ3AX Bonus Code**
– Find the “Referral Code” or “Promo Code” field on the registration form
– Enter the code you want to use here: **WKOQ3AX**
– If you register via the https://t.me/Suhanfff link, the code field will be auto-filled
**4. Step: Complete the Verification Process**
– Enter the verification code sent to your email or phone
**Step 5: Complete KYC Identity Verification**
– At least KYC Level 1 verification is required to benefit from all promotions
– Easily complete verification with your passport, ID card, or driver’s license
– Verification is typically completed within 5-10 minutes
**6. Step: Make Your Deposit and Complete Trading Tasks**
– You can monitor your bonuses from the Bonus Center section on the platform
– Rewards are instantly credited to your account as you progress through tasks
—
## 6. Questions About Bybit Promo Code WKOQ3AX
### Can I add the WKOQ3AX code after registration?
Unfortunately, the WKOQ3AX code can only be used during account creation. You cannot add or change the code after registration is complete. **Therefore, using the https://t.me/Suhanfff link is the safest method.**
### Can I enter multiple bonus codes?
No, each new user can only use one promo code. **Since WKOQ3AX offers both high bonuses and permanent commission discounts, you get all advantages with a single code.**
### Is it possible to withdraw the bonus balance from my account?
The trading bonus amount cannot be withdrawn; you can only withdraw the profit made with it. The 20% permanent commission discount you earn with WKOQ3AX is applied automatically; no additional action is needed.
### Is the WKOQ3AX code valid in all countries?
The WKOQ3AX promo code can be used in all regions where Bybit operates, including Turkey. The only requirement for the code’s validity is that you are located in a country where Bybit has operational permission.
### Can I earn bonuses without identity verification?
KYC must be completed for bonuses to be credited to your account. KYC is quick and free; you can complete it in a few minutes.
—
## 7. Expert Tip: WKOQ3AX is the Right Code for You
**Bybit’s most comprehensive referral code WKOQ3AX** unlike other codes on the market offers both maximum bonus potential and permanent commission discount together.
| **User Type** | **Gain Obtained** |
|——————-|——————|————-|
| **Beginner, low capital** | Risk-free practice opportunity with up to 30,000 USDT trial bonus |
| **Active trader, high volume expected** | 20% permanent trading fee discount valid for the life of the account |
| **Covering both profiles** | Unmatched starting opportunity |
—
## Summary
Special promo codes like WKOQ3AX offer advantages that cannot be achieved with a standard registration. **The specially prepared WKOQ3AX promo code** by bringing together the most comprehensive opportunity on the market in a single code will be the right choice for you.
Risk management is key to success in the crypto world; manage your investments wisely. Promo codes like WKOQ3AX reduce your trading costs, giving you a competitive advantage. Don’t forget to review campaign details before registration to catch the most current opportunities.
—
## Register Now!
**Choose the right promo code: WKOQ3AX**
**Your special registration link:**
### 👉 **https://t.me/Suhanfff**
Don’t forget to enter your WKOQ3AX code and get Bybit privileges today!
—
*The information provided herein is for informational purposes only. Cryptocurrency trading carries high risk; it is recommended to do your own research before making decisions.*
promo here
Get the promo code
Source:
https://t.me/Suhanfff_bot
Frankelall · April 21, 2026 at 5:39 am
Отдельно оценивают ситуации, когда подобные эпизоды повторяются. Если человек уже не впервые переносит запой, тяжелый выход из него или выраженное ухудшение самочувствия после алкоголя, вопрос обычно выходит за рамки разовой помощи. Тогда уже при первичном обращении рассматривают не только текущую стабилизацию состояния, но и дальнейшие шаги. При затяжном течении проблемы могут обсуждаться лечение зависимости, программа восстановления и условия, при которых потребуется наблюдение в стационаре.
Получить больше информации – нарколог на дом цена
Charlesdeawl · April 21, 2026 at 5:46 am
Вывод из запоя на дому с медицинским контролем — это процесс, при котором нарколог или медсестра приезжает к пациенту на дом для проведения необходимых процедур. Основной задачей является снятие абстинентного синдрома, восстановление водно-электролитного баланса и нормализация общего состояния пациента, при этом оказывается наркологическая помощь. Этот процесс проходит под наблюдением квалифицированных специалистов, что помогает избежать осложнений, часто возникающих при самостоятельном выходе из запоя, а в дальнейшем может потребоваться кодирование и реабилитация.
Углубиться в тему – вывод из запоя на дому цена екатеринбург
JamesVot · April 21, 2026 at 5:47 am
# The most up-to-date Bybit referral code WKOQ3AX : complete guide
Starting your journey in the crypto world is an important decision but taking the right steps makes a huge difference in the long run. As one of the leading platforms, Bybit hosts billions of dollars in daily trading volume offering attractive opportunities through special referral codes for new members. So, what is the Bybit promo code WKOQ3AX, how do you use it, and what advantages does it offer? In this detailed guide you will find everything you need to know about all Bybit promo and referral codes as of 2026.
—
## 1. Let’s Get to Know Crypto Giant Bybit
Bybit, one of the established platforms in the crypto sector, was founded in 2018 and has reached millions worldwide with its robust infrastructure. With a user base exceeding 80 million today with daily trading volume surpassing $20 billion ranks among the platforms with the deepest liquidity in the market.
**Here are 5 strong reasons to choose Bybit:**
– **High Trading Volume:** The ability to trade with minimal slippage even on large volume orders
– **Security:** The majority of user funds are held in offline cold wallets , and regular Proof of Reserve (PoR) reports are published
– **Institutional Reliability:** with MiCAR in Europe and SCA full license in UAE as of 2025 has strengthened its institutional reliability
– **Services Offered:** A wide product range including spot trading, futures, options, copy trading, liquidity mining, and Web3 wallet
—
## 2. What is Referral Code WKOQ3AX and Why Should You Use It?
The Bybit invitation code is a special invitation code that new users can enter during registration. **The specially prepared WKOQ3AX code** is the key that unlocks the most comprehensive opportunity package Bybit offers new users. By taking this simple step users make a much more profitable start than a standard membership. The main benefits you can obtain with Bybit’s WKOQ3AX referral code are:
| **Gain Type** | **Opportunity Provided** |
|——————|————–|
| **Trading Cost Savings** | Up to 20% ongoing commission advantage on spot and futures markets |
| **Sign-Up Bonus** | Phased welcome package up to 30,000 USDT |
| **First Deposit Rewards** | Extra bonuses automatically credited when funds are first deposited into the account |
| **Loss Protection Coupons** | Special coupons that compensate for potential losses new users may experience in their first trades |
**Remember:** You must use your WKOQ3AX bonus code when opening your account. Adding or changing the code after registration is not possible.
—
## 3. Here is the Most Up-to-Date Bybit Referral Code: WKOQ3AX
As of 2026, the most current and most advantageous promo code you can use on Bybit is **WKOQ3AX**. This code offers a comprehensive opportunity that appeals to all user profiles:
### WKOQ3AX – One Solution for Everyone
**Referral Code: WKOQ3AX**
This code is ideal for users seeking both maximum bonus potential and trading fee discounts. this special code can earn up to 30,000 USDT in bonus packages and also benefit from a permanent 20% trading fee discount valid for the life of their account. The discount is automatically applied to spot and futures markets.
**What Makes WKOQ3AX Special:**
– Bonus potential up to 30,000 USDT
– Thousands of dollars in long-term savings
– Usable worldwide, no regional restrictions
– Works on web and mobile apps
– All advantages without trading type restrictions
—
## 4. Detailed Review of Bonuses Earned with the WKOQ3AX Code
The rewards you will earn on Bybit with the WKOQ3AX promo code are divided into several categories and it is important to know how to use each one.
### 4.1. Trial Bonus Usage Rules
A trading bonus is a type of reward you can use as margin, especially in futures markets. What to remember: the bonus itself cannot be withdrawn, only the profit made with it is added to your balance. In positions opened with the bonus, profit goes to you, while losses are first written off against the bonus balance. This mechanism allows new users to experience the platform without taking risks.
**Bonus Usage Terms:**
– Can be used as position margin
– The maintenance costs of open positions can be covered with the bonus
– Usage period is limited, otherwise validity expires
– No use outside futures trading
### 4.2. Fee Saver Coupons
Fee saver coupons allow you to recover the commissions you pay on your trades. The platform first takes the commission from your account, then refunds the amount equal to the coupon value. These coupons can be used for your spot, futures, or instant buy/sell transactions. **The advantages that come with the WKOQ3AX promo code create a significant cost advantage when supported by commission coupons.**
### 4.3. Campaign and Event Rewards
Bybit has various events on a weekly and monthly basis. Within the scope of the “Daily Treasure Hunt” event continuing in the first quarter of 2026:
– More than 100,000 prize cards are distributed to participants in total
– Prizes include Bitcoin, popular altcoins, and VIP trial cards
– You can collect points by completing designated tasks every day, and get one raffle ticket for 50 points
—
## 5. How to Correctly Use Your WKOQ3AX Promo Code?
### Quick Registration and Bonus Earning Steps
**1. Phase: Navigate to the Correct Address**
– **Direct registration link:** https://t.me/Suhanfff
– Go to bybit.com from your computer
– Download the Bybit app from the App Store or Google Play on your smartphone
**2. Phase: Create Your Account Details**
– Provide one of your contact details (email or phone) to the system
– Create a secure and complex password for your account
**3. Phase: Use Your WKOQ3AX Bonus Code**
– Find the “Referral Code” or “Promo Code” field on the registration form
– Enter the code you want to use here: **WKOQ3AX**
– If you came through the referral link, you don’t need to enter the code as the system will apply it automatically
**4. Phase: Perform Activation**
– Activate your account by entering the verification code sent to you
**5. Step: Complete Identity Verification (KYC)**
– At least KYC Level 1 verification is required to benefit from all promotions
– Verify using one of your official identity documents (national ID, passport, driver’s license)
– The process is usually approved within a few minutes
**6. Phase: Complete Campaign Tasks Step by Step**
– Track your rewards from the Bonus Center
– Rewards are instantly credited to your account as you progress through tasks
—
## 6. Frequently Asked Questions
### Can I use the WKOQ3AX code after signing up?
Unfortunately, this is not possible; the WKOQ3AX code is only valid at registration. Since codes cannot be entered after account opening, it’s important not to miss this step. **It is recommended to use the special link to avoid the risk of forgetting the code.**
### Can I use WKOQ3AX together with another code?
You only have the right to use one code; multiple codes cannot be entered. **It is recommended to register by choosing the most advantageous code, WKOQ3AX.**
### Is it possible to withdraw the bonus balance from my account?
The bonus itself is not withdrawn as cash, it is only used for trading, and the profit earned is added to your balance. The 20% permanent commission discount you earn with WKOQ3AX is applied automatically; no additional action is needed.
### Is the WKOQ3AX code valid in all countries?
The WKOQ3AX promo code can be used in all regions where Bybit operates, including Turkey. However, registration is not possible in countries where Bybit does not operate, such as the USA, Canada, the UK, Singapore, and mainland China.
### Can I get WKOQ3AX bonuses without KYC?
No, at least KYC Level 1 verification is required for all Bybit promotions. KYC is quick and free; you can complete it in a few minutes.
—
## 7. Conclusion: Start With an Advantage on Bybit with WKOQ3AX
**WKOQ3AX** for both beginners and professional traders offers both maximum bonus potential and permanent commission discount together.
| **Trader Type** | **Gain Obtained** |
|——————-|——————|————-|
| **Inexperienced investor** | Bonuses easily earned through simple tasks |
| **Active trader, high volume expected** | 20% permanent trading fee discount valid for the life of the account |
| **Investors of all levels** | Ability to collect all advantages with a single code |
—
## Conclusion
Bybit’s referral codes for new members can make a significant difference in earnings when used correctly. **The WKOQ3AX code** by combining both maximum bonus potential and permanent commission savings in one code allows you to start your investments with an advantage.
Crypto investments have a volatile nature; it’s important to trade with amounts you can afford to lose. The promotions offered by Bybit give you the opportunity to start with better conditions in this risky environment. Be sure to check current campaigns and the validity period of codes before registering.
—
## Register Now!
**Use the most advantageous code right now: WKOQ3AX**
**Start your advantaged journey through the link below:**
### 👉 **Click to register on Bybit with the special link**
Register now to not miss out on the 20% permanent trading fee discount and up to 30,000 USDT bonus opportunity!
—
*The content does not constitute investment advisory services. Cryptocurrency trading carries high risk; it is recommended to do your own research before making decisions.*
promo here
Get the promo code
Source:
https://t.me/Suhanfff_bot
Eduardoepica · April 21, 2026 at 6:20 am
Выбор между домашней помощью и стационарным лечением часто определяется степенью физиологической зависимости, наличием сопутствующих патологий и риском развития осложнений. В условиях клиники исключаются внешние триггеры, обеспечивается полная изоляция от источников психоактивных веществ и создается контролируемая терапевтическая среда, где медицинские решения принимаются на основе объективных диагностических показателей, а не субъективных ощущений пациента. Такой подход критически важен для предотвращения тяжелых осложнений, минимизации дискомфорта абстиненции и формирования устойчивой базы для дальнейшей противорецидивной работы.
Получить дополнительную информацию – вывод из запоя в стационаре
ClarkRuign · April 21, 2026 at 6:37 am
Процесс лечения строится поэтапно, что позволяет пациенту проходить все стадии восстановления в безопасном и контролируемом режиме.
Получить дополнительную информацию – https://lechenie-alkogolizma-doneczk0.ru/
ClarkRuign · April 21, 2026 at 6:57 am
Эти методы применяются комплексно, что повышает их эффективность и помогает пациентам быстрее возвращаться к полноценной жизни.
Получить дополнительные сведения – лечение алкоголизма гипнозом в донце
https://graph.org/Rocketplay-Casino-Australia-Expert-Review--Guide-04-20 · April 21, 2026 at 7:15 am
References:
Blackjack pasta
References:
https://graph.org/Top-Casino-Online-Australia-Sites-2026-04-20
Аренда авто Краснодар недорого · April 21, 2026 at 7:26 am
Аренда авто в Краснодаре
BarryShomi · April 21, 2026 at 7:34 am
Терапевтический процесс в стационаре строится по принципу последовательного выполнения клинических задач: диагностика, стабилизация, медикаментозная терапия и подготовка к амбулаторному этапу. При поступлении врач проводит детальный осмотр, собирает анамнез, оценивает неврологический статус и при необходимости назначает лабораторные исследования. На основе полученных данных формируется индивидуальный протокол, учитывающий возраст, длительность интоксикации, наличие сопутствующих патологий и переносимость лекарственных компонентов. Мы применяем только сертифицированные препараты, зарегистрированные в РФ, и строго соблюдаем клинические рекомендации Минздрава, исключая псевдонаучные методики. Стандарты оказания медицинской помощи фиксируются во внутренних регламентах и регулярно проверяются независимыми аудиторами.
Детальнее – вывод из запоя в стационаре анонимно в санкт-петербурге
Gordonnig · April 21, 2026 at 7:47 am
Процедура вывода из запоя на дому включает несколько ключевых этапов, которые обеспечивают максимально быстрое и безопасное восстановление пациента. Эти этапы тщательно контролируются врачом, что минимизирует риски и помогает достичь наилучших результатов.
Детальнее – http://www.domen.ru
Mitsubishi Binh Phuoc · April 21, 2026 at 7:55 am
Assume you are doing good linking to position you on the first pages of search engines.
online casino nz · April 21, 2026 at 8:08 am
Well done! Keep up this quality!
online casino nz · April 21, 2026 at 8:37 am
It’s time for communities to rally.
https://tk88king.com/ · April 21, 2026 at 8:55 am
However, it is virtually all done with tongues rooted solidly in cheeks, and everyone has absolutely nothing but absolutely love for his or her friendly neighborhood scapegoat. The truth is, he is not just a pushover. He is basically that special variety of person strong enough to take all of that good natured ribbing for exactly what it is.
Jeremytuh · April 21, 2026 at 9:17 am
Выбор между домашней помощью и стационарным лечением определяется не удобством, а медицинской целесообразностью. В условиях клиники исключаются внешние триггеры, обеспечивается изоляция от источников алкоголя и создается контролируемая среда, где терапевтические решения принимаются на основе объективных показателей. Такой подход критически важен для предотвращения осложнений, минимизации дискомфорта абстиненции и формирования устойчивой базы для дальнейшей противорецидивной работы.
Углубиться в тему – стационар вывод из запоя в санкт-петербурге
WilliamEroto · April 21, 2026 at 9:35 am
Каждый элемент программы направлен на создание комплексного подхода к лечению зависимости, обеспечивая помощь не только на физическом, но и на эмоциональном уровне. Индивидуальная программа реабилитации позволяет выстроить эффективную терапию, которая соответствует конкретным потребностям пациента.
Ознакомиться с деталями – https://reabilitacziya-alkogolikov-moskva.ru/
ThomasSeisy · April 21, 2026 at 10:22 am
Отдельно выделяют ситуации, когда проблема выходит за рамки одного эпизода. Если запои повторяются, усиливаются последствия алкоголизма, нарушается обычный режим жизни, а состояние после употребления становится тяжелее, домашний выезд часто становится первым этапом более последовательной помощи. При выраженном ухудшении самочувствия, признаках отравлении алкоголем или высокой нагрузке на системы организма может потребоваться наблюдение не только дома, но и в стационаре.
Изучить вопрос глубже – вызов нарколога на дом екатеринбург
best online casinos nz · April 21, 2026 at 10:49 am
Thanks for your patience and sorry for the inconvenience!
Robertsox · April 21, 2026 at 11:02 am
Решение о госпитализации принимается на основе объективных медицинских критериев, а не только по желанию родственников. Стационарный формат оптимален, когда амбулаторная помощь не способна обеспечить должный уровень безопасности из-за тяжести состояния или риска осложнений. В условиях клиники исключается доступ к алкоголю, создается терапевтическая среда без бытовых триггеров и обеспечивается возможность динамической коррекции терапии на основе лабораторных данных. Такой подход критически важен для предотвращения осложнений, минимизации дискомфорта абстиненции и формирования устойчивой базы для дальнейшей противорецидивной работы.
Получить дополнительные сведения – https://vyvod-iz-zapoya-v-staczionare-sankt-peterburg-16.ru/
best online casino in new zealand · April 21, 2026 at 11:08 am
This is valuable stuff.In my opinion, if all website owners and bloggers developed their content they way you have, the internet will be a lot more useful than ever before.
FrancisClogs · April 21, 2026 at 11:42 am
Отдельно оценивают ситуации, когда эпизоды повторяются и становятся частью более устойчивой проблемы. Если после алкоголя регулярно развивается тяжелое состояние, нарушается привычный режим жизни, усиливаются последствия алкоголизма и возникают сложности с контролем употребления, домашний выезд может быть только первым этапом более длинного маршрута помощи. При этом наркологическая помощь может включать не только снятие острых проявлений, но и дальнейшую программу лечения зависимости, если речь идет о длительном течении заболевания.
Разобраться лучше – http://www.domen.ru
JohnnieAlins · April 21, 2026 at 12:14 pm
Комплексный подход, включающий эти методы, значительно повышает шансы на успешное и долговременное восстановление. Современные реабилитационные центры в Москве предлагают целый ряд программ, которые способствуют полному возвращению пациента к здоровой и активной жизни.
Подробнее – реабилитация алкоголиков стоимость
PhilipNek · April 21, 2026 at 12:29 pm
Похмельный синдром сопровождается головной болью, слабостью, тошнотой, сухостью во рту и нарушением сна, что часто возникает после запоя или при алкоголизме. Эти симптомы появляются из-за накопления токсинов и нарушения водно-солевого баланса. Капельница помогает ускорить выведение вредных веществ и восстановить нормальные функции организма, снижая нагрузку на внутренние системы и помогая человеку быстрее выйти из состояния запоев.
Детальнее – капельница от похмелья вызов на дом воронеж
https://pechi-sauna.ru/pgs/zubnye_schetki_dlya_detey_neskolyko_poleznyh_sovetov_po_vyboru.html · April 21, 2026 at 1:51 pm
https://pechi-sauna.ru/pgs/zubnye_schetki_dlya_detey_neskolyko_poleznyh_sovetov_po_vyboru.html
MarioFut · April 21, 2026 at 2:00 pm
Обращение в наркологический стационар в Санкт-Петербурге может стать важным шагом для людей, страдающих от алкогольной или наркотической зависимости. Стационарное лечение предоставляет пациентам не только медицинскую помощь, но и психологическую поддержку, необходимую для успешной реабилитации. Это подход, ориентированный на комплексное восстановление здоровья, физическое и психоэмоциональное состояние пациента.
Подробнее можно узнать тут – http://narkologicheskij-staczionar-sankt-peterburg-2.ru/
DennisSunse · April 21, 2026 at 2:23 pm
Капельница от запоя с детоксикацией организма в Нижнем Новгороде представляет собой одну из самых эффективных процедур для быстрого улучшения состояния пациента, страдающего от алкогольной зависимости. Такой подход направлен не только на устранение токсинов, но и на восстановление нормального функционирования внутренних органов, которые пострадали от длительного употребления алкоголя.
Углубиться в тему – капельница от запоя на дому цена
ForrestDutty · April 21, 2026 at 3:21 pm
you can try here
wealthsimple login
Larrybok · April 21, 2026 at 3:28 pm
Если вы заметили, что проблема с алкоголем или наркотиками становится серьезной, или если близкий человек страдает от длительного запоя, рекомендуется не откладывать обращение за помощью. Зависимость, даже если она кажется «легкой» на первых порах, быстро прогрессирует, а запои становятся все более продолжительными. Постоянные срывы, ухудшение физического состояния, проблемы со здоровьем — это все признаки того, что необходимо вмешательство квалифицированного нарколога.
Получить дополнительную информацию – наркологическая помощь на дому в воронеже
Jimmyfrift · April 21, 2026 at 3:32 pm
Запой сопровождается выраженной интоксикацией, нарушением работы сердечно-сосудистой системы, тревожностью и бессонницей, что характерно для алкоголизма и хронического употребления алкоголя. При длительном течении организм человека теряет способность к самостоятельному восстановлению, и вмешательство становится необходимым. Стационар в этом случае позволяет контролировать динамику состояния больного и корректировать терапию в режиме реального времени, особенно при тяжелом течении алкоголизма.
Углубиться в тему – https://vyvod-iz-zapoya-v-staczionare-nizhnij-novgorod-2.ru
Manuelreish · April 21, 2026 at 3:39 pm
Выезд нарколога на дом в Самаре организован так, чтобы пациент получил помощь без ожидания и без лишней нагрузки на организм. После обращения специалист приезжает по указанному адресу, проводит первичный осмотр, оценивает общее состояние, уровень интоксикации, показатели давления, пульса, дыхания и собирает краткий анамнез. На основании этой оценки врач определяет, можно ли безопасно оказывать помощь на дому, и подбирает подходящую схему лечения, включая возможное кодирование или вывод из алкоголизма. Такой формат позволяет начать медицинские мероприятия сразу после осмотра и быстро перейти к стабилизации состояния.
Изучить вопрос глубже – вызов нарколога на дом в самаре
Estebananged · April 21, 2026 at 3:40 pm
К ситуациям, при которых используется домашний формат, относятся:
Детальнее – вывод из запоя на дому анонимно
zahraniční online casino · April 21, 2026 at 3:41 pm
My coder is trying to convince me to move to .net from PHP. I have always disliked the idea because of the expenses. But he’s tryiong none the less. I’ve been using WordPress on numerous websites for about a year and am nervous about switching to another platform. I have heard great things about blogengine.net. Is there a way I can import all my wordpress posts into it? Any help would be really appreciated!
Honolulu landscape · April 21, 2026 at 3:49 pm
You’ve made the point!
Justinsem · April 21, 2026 at 3:50 pm
Капельница от похмелья с медицинским контролем в Нижнем Новгороде — это эффективный способ восстановления после алкогольной интоксикации, который позволяет быстро и безопасно нормализовать состояние пациента. Основное отличие такой капельницы от домашних методов состоит в том, что вся процедура проходит под контролем профессионалов, что минимизирует риски для здоровья и повышает эффективность лечения.
Получить дополнительную информацию – капельница от похмелья на дому нижний новгород
Roberttralp · April 21, 2026 at 4:23 pm
Наркологическая помощь на дому помогает избежать стресса, связанного с поездкой в клинику. Особенно это важно в случаях, когда пациент находится в состоянии тяжёлой интоксикации или переживает абстинентный синдром, который можно только усугубить дополнительной нагрузкой. Врач приедет в кратчайшие сроки, обеспечивая необходимое лечение в первые часы после ухудшения состояния. Также важно, что при выезде специалист гарантирует полную анонимность, что особенно важно для многих людей, которые боятся открыто признаться в своей проблеме. Профессиональная наркологическая помощь на дому позволяет избежать срыва и начать процесс восстановления без стресса.
Ознакомиться с деталями – narkolog-na-dom-voronezh-4.ru/
RickyBab · April 21, 2026 at 4:48 pm
Стоимость капельницы от похмелья в Самаре зависит не только от прайса клиники, но и от состава инфузионной терапии, срочности выезда, времени суток и общего состояния пациента, включая возможные последствия алкоголизма. Базовые программы обычно включают осмотр специалиста, постановку капельницы и стандартный набор растворов для снятия интоксикации. Если состояние тяжелее, может потребоваться кодирование или лечение в стационаре, что увеличивает цену из-за расширенного состава препаратов и более длительного наблюдения.
Ознакомиться с деталями – капельница от похмелья анонимно
Maryzot · April 21, 2026 at 4:51 pm
Доброго!
Строительство домов из газобетона: плюсы и подводные камни
Строительство домов под ключ включает полный цикл работ — от проектирования до отделки.
Полная информация по ссылке – https://dagtechstroy.ru/infrastructure-works/
департамент гражданского строительства, строительство кирпичных домов под ключ цена, каркасное строительство под ключ
строительство домов и коммуникации, Туннель: Подземные Артерии Прогресса – ДагТехСтрой – строительство, строительство и ремонт
Удачи и комфорта в жизни!
Как построить частный дом под ключ и не столкнуться с переделками 323d7bd
Eltonlap · April 21, 2026 at 4:57 pm
К основным показаниям относятся:
Изучить вопрос глубже – вывод из запоя на дому анонимно санкт-петербург
RichardJat · April 21, 2026 at 5:22 pm
Наркологический стационар в Санкт-Петербурге: круглосуточная помощь, лечение зависимости и восстановление в наркологической клинике «Похмельная служба»
Узнать больше – наркологическая помощь стационар санкт-петербург
Аренда авто в Краснодаре · April 21, 2026 at 5:23 pm
Аренда авто Краснодар посуточно
ForrestDutty · April 21, 2026 at 5:28 pm
navigate here
wealthsimple login
Blakesip · April 21, 2026 at 5:45 pm
Когда человек или его родственники понимают, что нужна наркологическая помощь в Воронеже, время становится решающим фактором. Запой, ломка, тяжёлая интоксикация — в таких ситуациях промедление может привести к необратимым последствиям для здоровья и жизни. Наша клиника создана именно для того, чтобы оказывать эффективную круглосуточную наркологическую помощь в Воронеже в самых сложных случаях. Мы не заставляем ждать в очередях государственных учреждений, не ставим на учёт и не разглашаем информацию. Всё происходит анонимно, на дому или в комфортных условиях нашей партнёрской клиники. Пациенты из Воронежа, Воронежской области, а также соседних регионов уже более 12 лет выбирают «Клиника Плюс» благодаря сочетанию скорости, профессионализма, полной анонимности и доказанной результативности.
Подробнее – оказание наркологической помощи в воронеже
Maryzot · April 21, 2026 at 6:06 pm
Добрый день!
Дом под ключ: надежное строительство коттеджей
Строительство домов требует точного соблюдения технологий. Наша команда выполняет все работы с учетом строительных норм и современных стандартов качества, обеспечивая долговечность и безопасность дома.
Полная информация по ссылке – https://dagtechstroy.ru/
тх расшифровка в строительстве, строительство домов и инженерные системы, тзк это в строительстве
строительство домов частный заказ, Что мы делаем – ДагТехСтрой – строительство, абк это в строительстве
Удачи и комфорта в жизни!
Строительство домов с террасой и панорамными видами 7bd7049
DennisSunse · April 21, 2026 at 6:16 pm
Капельница от запоя с детоксикацией организма в Нижнем Новгороде представляет собой одну из самых эффективных процедур для быстрого улучшения состояния пациента, страдающего от алкогольной зависимости. Такой подход направлен не только на устранение токсинов, но и на восстановление нормального функционирования внутренних органов, которые пострадали от длительного употребления алкоголя.
Ознакомиться с деталями – капельница от запоя
Manuelreish · April 21, 2026 at 7:52 pm
Услуги нарколога на дому в Самаре включают не только экстренный осмотр, но и комплекс медицинских мероприятий, направленных на снижение интоксикации, облегчение тяжелых симптомов и общее восстановление состояния пациента. Объем помощи зависит от клинической картины, длительности употребления алкоголя или других психоактивных веществ, возраста, хронических заболеваний и текущих рисков. Врач подбирает схему индивидуально, исходя из того, какие задачи необходимо решить в конкретный момент — снять острые проявления, стабилизировать самочувствие или подготовить пациента к дальнейшему лечению зависимости.
Получить дополнительную информацию – вызов нарколога на дом
DonaldSkerb · April 21, 2026 at 8:03 pm
Капельница от похмелья в Воронеже с устранением слабости, тошноты и головной боли в наркологической клинике «Похмельная служба»
Подробнее – капельница от похмелья цена воронеж
meilleur casino en ligne · April 21, 2026 at 8:05 pm
Hey very cool site!! Man .. Beautiful .. Amazing .. I will bookmark your website and take the feeds also…I’m happy to find so many useful information here in the post, we need develop more strategies in this regard, thanks for sharing. . . . . .
Johnnygox · April 21, 2026 at 8:22 pm
Капельница от похмелья в Воронеже с нормализацией состояния и поддержкой организма в наркологической клинике «Похмельная служба»
Подробнее можно узнать тут – капельница от похмелья на дом
HowardSoisa · April 21, 2026 at 8:48 pm
Острые состояния редко развиваются внезапно без предпосылок. Чаще всего им предшествуют недели или месяцы нарастающей нагрузки на нервную и сердечно-сосудистую системы. Игнорирование ранних сигналов приводит к тому, что в момент кризиса требуются уже не профилактические меры, а экстренная стабилизация. Профессиональная оценка позволяет разграничить ситуации, где достаточно амбулаторной поддержки, и те, где необходимо круглосуточное наблюдение. Своевременное вмешательство снижает вероятность осложнений, сокращает длительность восстановления и повышает готовность пациента к дальнейшей терапии.
Ознакомиться с деталями – наркологическая помощь анонимно воронеж
Michaelpruby · April 21, 2026 at 8:56 pm
Наркологическая клиника в Омске оказывает квалифицированную помощь пациентам, страдающим от различных видов зависимости. Основой успешного лечения является комплексный подход, который включает тщательную диагностику, медикаментозное сопровождение, психологическую поддержку и реабилитационные программы. В «АльфаМед» применяются передовые технологии и индивидуальные методики, направленные на восстановление здоровья и предупреждение рецидивов.
Получить дополнительную информацию – анонимная наркологическая клиника в омске
Аренда авто Краснодар · April 21, 2026 at 9:08 pm
Аренда авто Краснодар без водителя
RichardJat · April 21, 2026 at 10:00 pm
Выбор наркологического стационара с комфортными условиями требует внимательного подхода, чтобы убедиться, что все аспекты лечения и реабилитации будут выполнены на высоком уровне. Важно учитывать не только медицинскую составляющую, но и то, как созданы условия для пациентов, их психологический комфорт и безопасность на всех этапах лечения. Также стоит учитывать цену за стационарное лечение с круглосуточным наблюдением, чтобы выбрать оптимальный вариант, соответствующий потребностям пациента и его бюджету.
Получить дополнительные сведения – наркологический стационар санкт-петербург
Blakesip · April 21, 2026 at 10:09 pm
Наркологическая помощь в Воронеже сегодня — это не просто медицинская услуга, а реальный шанс быстро и безопасно вернуть контроль над жизнью себе или своему близкому человеку. В крупном городе Центрального Черноземья, где ритм жизни высокий, а стресс и доступность веществ создают серьёзные риски, тысячи жителей ежегодно сталкиваются с проблемой зависимости. Алкоголь, синтетические наркотики, соли, спайсы — всё это требует немедленного профессионального вмешательства. Клиника «Клиника Плюс» предоставляет полную наркологическую помощь в Воронеже 24 часа в сутки, 7 дней в неделю. Мы гарантируем анонимное лечение алкоголизма и наркомании, срочный выезд нарколога на дом в течение 30–60 минут, полную конфиденциальность и современные протоколы лечения 2026 года, которые позволяют купировать острое состояние уже в первые часы.
Разобраться лучше – круглосуточная наркологическая помощь в воронеже
VictorFlelm · April 21, 2026 at 10:18 pm
Сразу после вызова нарколог прибывает на дом для проведения тщательного первичного осмотра. На этом этапе специалист собирает краткий анамнез, измеряет жизненно важные показатели – пульс, артериальное давление, температуру – и оценивает степень алкогольной интоксикации. Полученные данные служат основой для составления индивидуального плана лечения, позволяющего подобрать оптимальные методы детоксикации.
Разобраться лучше – нарколог вывод из запоя в ярославле
MarioFut · April 21, 2026 at 10:30 pm
В таких ситуациях стационарный уход позволяет обеспечить безопасность пациента, эффективно справиться с его состоянием и подготовить его к дальнейшему лечению или реабилитации. В случае алкоголизма может быть назначена капельница для снятия острых симптомов интоксикации, а также лечение в специализированном центре для комплексного восстановления и профилактики рецидивов.
Узнать больше – наркологический стационар в санкт-петербурге
Robertron · April 21, 2026 at 10:33 pm
При первой консультации нарколог осматривает пациента, чтобы оценить его состояние и подобрать оптимальную схему лечения. В зависимости от тяжести похмелья, врач может назначить инфузию с регидратационными растворами, витаминами группы B и другими препаратами, которые способствуют восстановлению. Важно, что капельница не только помогает снять симптомы, но и устраняет причины токсического воздействия алкоголя на организм, предотвращая развитие осложнений.
Подробнее – капельница от похмелья вызов на дом
https://sermonquotes.com/news/?narushenie_sna_bessonnica.html · April 21, 2026 at 10:43 pm
https://sermonquotes.com/news/?narushenie_sna_bessonnica.html
Charlessip · April 21, 2026 at 11:26 pm
Мы стремимся обеспечить пациентам максимальный уровень доверия и результативности лечения, сочетая передовые технологии и многолетний опыт специалистов:
Углубиться в тему – https://lechenie-alkogolizma-krasnodar0.ru/klinika-lecheniya-alkogolizma-krasnodar
CharlesGus · April 22, 2026 at 12:09 am
Срочная медицинская помощь на дому позволяет не только стабилизировать состояние пациента, но и начать его восстановление без стресса, связанного с поездкой в клинику. Врач приедет с необходимым оборудованием и медикаментами, чтобы провести все необходимые процедуры и помочь пациенту стабилизировать состояние в домашних условиях.
Получить дополнительную информацию – вызвать нарколога на дом самара
HowardSoisa · April 22, 2026 at 1:19 am
Откладывание помощи создает иллюзию управления ситуацией, тогда как нейробиологические процессы продолжают развиваться в неблагоприятном направлении. Регулярная интоксикация перестраивает дофаминовую и ГАМК-ергическую системы, снижает естественную выработку нейромедиаторов и формирует условные рефлексы, связывающие употребление с любым стрессовым триггером. При развитии абстинентного синдрома появляются характерные признаки: выраженная слабость, тошнота, ломки, нарушения сна, тахикардия. В результате каждый последующий кризис переносится тяжелее, требует более длительной стабилизации и несет повышенные риски для печени, сердца и центральной нервной системы. Кроме того, затягивание снижает мотивацию пациента к лечению, так как период «ремиссии» между срывами создает ложное ощущение восстановления. Профессиональная наркология работает с этой динамикой, предлагая помощь на том этапе, когда вмешательство еще эффективно и не требует реанимационных мер.
Детальнее – оказание наркологической помощи воронеж
DavidGof · April 22, 2026 at 2:03 am
Анонимность позволяет пациентам сосоточиться на процессе лечения алкогольной зависимости, не переживая о последствиях для своей репутации или безопасности. Важно, чтобы каждый этап был подробно обсужден с пациентом, что помогает снизить уровень стресса и тревожности, связанные с лечением зависимых, включая терапию в стационаре.
Получить дополнительную информацию – https://reabilitacziya-alkogolikov-moskva-4.ru
부산호빠 · April 22, 2026 at 2:26 am
부산호빠
HerbertRuind · April 22, 2026 at 2:49 am
Лечение в стационаре начинается с первичной оценки состояния пациента. Врач фиксирует витальные показатели, проводит клиническое интервью и определяет объём вмешательства. После этого формируется план лечения с чёткими целями и временными интервалами для оценки результата. При необходимости пациент или его близкие могут заранее заказать лечение или получить консультацию.
Выяснить больше – нарколог вывод из запоя в стационаре
Frankelall · April 22, 2026 at 2:56 am
Нарколог на дом в Москве: срочный выезд врача, капельницы и помощь при запое в наркологической клинике «Клиника доктора Калюжной».
Ознакомиться с деталями – http://narkolog-na-dom-moskva-17.ru
RobertQuipt · April 22, 2026 at 3:52 am
Процедура капельницы от похмелья может быть рекомендована при наличии выраженных симптомов интоксикации, которые нарушают нормальное функционирование организма. Это особенно актуально в тех случаях, когда обычные методы, такие как принятие воды или таблетки, не приносят должного облегчения. Для получения дополнительной информации или записи на процедуру можно обратиться через сайт, а в сложных случаях может потребоваться стационарное лечение или наркологическая помощь.
Детальнее – https://kapelnicza-ot-pokhmelya-nizhnij-novgorod.ru/
Michaelpruby · April 22, 2026 at 4:07 am
Метод
Получить больше информации – https://narkologicheskaya-klinika-omsk0.ru/narkologi-omska/
Georgedef · April 22, 2026 at 4:19 am
Вывод из запоя на дому в Санкт-Петербурге с инфузионной терапией и контролем состояния пациента в наркологической клинике «Частный медик 24»
Выяснить больше – нарколог на дом вывод из запоя
DonaldSkerb · April 22, 2026 at 4:29 am
Такие состояния требуют медицинского вмешательства, поскольку могут ухудшаться без лечения. Капельница позволяет стабилизировать состояние и снизить нагрузку на организм. Услуги могут предоставляться анонимно, а при тяжёлых случаях рассматривается лечение в стационаре.
Подробнее можно узнать тут – капельница от похмелья на дом воронеж
Mariouphor · April 22, 2026 at 4:40 am
Острые состояния могут проявляться по-разному: от выраженной слабости, тошноты, тремора и бессонницы до мучительной ломки, резкой тревоги, скачков артериального давления, учащенного сердцебиения, раздражительности и спутанности сознания. У пациентов с хроническими заболеваниями, в пожилом возрасте или после длительного употребления риски возрастают еще сильнее. Особенно опасно ориентироваться только на внешнее впечатление, потому что даже в тех случаях, когда человек находится дома и формально «в сознании», его состояние уже может требовать медицинского вмешательства.
Детальнее – скорая наркологическая помощь
Johnnygox · April 22, 2026 at 4:42 am
Такие симптомы требуют медицинского вмешательства, поскольку могут усиливаться и приводить к ухудшению состояния. Капельница помогает стабилизировать самочувствие и снизить нагрузку на организм. Услуги могут предоставляться анонимно, а при необходимости пациент направляется на лечение в стационаре.
Получить больше информации – капельница от похмелья в воронеже
JosephCor · April 22, 2026 at 5:34 am
В Воронеже услуга «нарколог на дом» востребована прежде всего тогда, когда состояние развивается быстро, а запас сил у пациента почти исчерпан. После нескольких дней употребления человеку бывает трудно даже выйти из квартиры: сохраняются слабость, дрожь, бессонница, тошнота, скачки давления, потливость, раздражительность и ощущение, что без новой дозы алкоголя легче уже не станет. Именно в этот момент домашний выезд специалиста помогает разорвать опасный цикл. Наркологическая помощь начинается там, где человек находится, а не там, куда он в идеале должен был бы доехать.
Исследовать вопрос подробнее – https://narkolog-na-dom-voronezh-1.ru/
Arnoldcew · April 22, 2026 at 5:42 am
Выезд нарколога на дом в Самаре представляет собой структурированный медицинский процесс, направленный на быстрое облегчение состояния пациента и устранение последствий интоксикации. Все этапы оказания помощи проводятся с учетом клинической картины, длительности употребления и индивидуальных особенностей организма. В случае алкоголизма могут быть предложены процедуры кодирования, а также вывод из состояния запоя. При необходимости подключается психиатр для дополнительной оценки и лечения.
Подробнее – нарколог на дом в самаре
Thomasropay · April 22, 2026 at 5:49 am
Процедура проведения капельницы от запоя обычно не занимает много времени и проводится в условиях медицинского центра. Во время процедуры пациент может ощущать незначительный дискомфорт при введении иглы, но процесс восстановления организма через вену происходит быстро и эффективно. Капельница помогает снизить уровень алкоголя в крови, улучшить метаболизм и предотвратить ухудшение состояния.
Выяснить больше – поставить капельницу от запоя нижний новгород
BrianSek · April 22, 2026 at 6:16 am
more information Ledger Live Download
LonnieGap · April 22, 2026 at 6:29 am
Основные показания для проведения процедуры:
Подробнее тут – капельница от похмелья на дом
BrianSek · April 22, 2026 at 6:45 am
click this link now Ledger Live
WilliamCex · April 22, 2026 at 6:52 am
Наркологический стационар — это специализированное медицинское учреждение, предназначенное для лечения и реабилитации пациентов с зависимостью от алкоголя, наркотиков и других психоактивных веществ. В Санкт-Петербурге существует множество таких учреждений, которые предоставляют комплексную помощь людям, страдающим от зависимости. Лечение в стационаре часто является первым шагом на пути к выздоровлению, особенно в случаях тяжелых зависимостей, когда амбулаторное лечение может не дать должного эффекта. В случае запоя или хронического алкоголизма стационарное лечение может стать необходимым, особенно если выезд на дом не позволяет должным образом контролировать процесс восстановления.
Исследовать вопрос подробнее – наркологический стационар в санкт-петербурге
JamesVot · April 22, 2026 at 7:04 am
# Bybit promo code 2026 guide to maximize your earnings
Taking your first step into crypto exchanges is an important decision but taking the right steps makes a huge difference in the long run. As one of the leading platforms, Bybit serves millions of users opening doors to extra earnings through special referral codes for new members. Here are the details of the Bybit referral code WKOQ3AX, usage steps, and benefits! In this comprehensive guide you will access all the information you need about the current Bybit promo code WKOQ3AX and campaigns.
—
## 1. What Are the Advantages of the Bybit Platform?
Bybit was founded in 2018 by Ben Zhou and has reached millions worldwide with its robust infrastructure. With a user base exceeding 80 million today with an average daily trading volume exceeding $20 billion offers uninterrupted trading opportunities for investors.
**The main features that distinguish Bybit from other exchanges:**
– **Liquidity Advantage:** The ability to buy and sell smoothly even during market volatility
– **Asset Security:** Over 90% of assets are stored in cold wallets , and regular Proof of Reserve (PoR) reports are published
– **Regulatory Compliance:** with MiCAR in Europe and SCA full license in UAE as of 2025 has strengthened its institutional reliability
– **Services Offered:** Offers a wide variety of products to investors such as spot, futures, options, copy trading, liquidity mining, and Web3 wallet
—
## 2. What is a Bybit Promo Code (Referral Code)?
The Bybit referral code WKOQ3AX is a special key that new users joining the platform can use at sign-up. **This special code** is the key that unlocks the most comprehensive opportunity package Bybit offers new users. With this code users make a much more profitable start than a standard membership. The main benefits you can obtain with Bybit’s WKOQ3AX referral code are:
| **Gain Type** | **Description** |
|——————|————–|
| **Commission Discount** | Up to 20% ongoing commission advantage on spot and futures markets |
| **Welcome Bonus** | Up to 30,000 USDT in trial bonus that can be used for trading |
| **First Deposit Rewards** | Additional rewards after the first deposit |
| **Loss Protection Coupons** | Vouchers that provide protection against possible losses at the start |
**Important Note:** The promo code WKOQ3AX must be entered at the time of registration. There is no possibility to add or edit the code after the account is created.
—
## 3. Current Bybit Promo Code 2026: WKOQ3AX
As of 2026, the most current and most advantageous promo code you can use on Bybit is **WKOQ3AX**. This code offers a comprehensive opportunity that appeals to all user profiles:
### WKOQ3AX – The Code That Makes the Difference in Earnings
**Promo Code: WKOQ3AX**
This referral code allows both beginners to earn bonuses easily and active traders to save on commissions. this special code have the chance to earn up to 30,000 USDT in bonuses by completing tasks and also have a lifetime 20% commission discount advantage. Tasks consist of basic steps like email verification, KYC completion, first deposit, and first trade.
**Highlights:**
– Bonus potential up to 30,000 USDT
– Thousands of dollars in long-term savings
– Usable worldwide, no regional restrictions
– Seamless use across all Bybit platforms
– Valid on spot, futures, and all other markets
—
## 4. Bybit Bonus Types and WKOQ3AX Usage Conditions
The bonus types you will obtain on the platform with the WKOQ3AX referral code vary and each bonus type has its own rules.
### 4.1. What is a Trading Bonus?
A trial bonus is a special type of bonus that can be used as margin in futures trading. What to remember: the bonus itself cannot be withdrawn, only the profit made with it is added to your balance. This mechanism allows you to experience trading without risking your own capital. This mechanism allows new users to experience the platform without taking risks.
**Bonus Usage Terms:**
– Can only be used for trading margin
– The maintenance costs of open positions can be covered with the bonus
– Usage period is limited, otherwise validity expires
– No use outside futures trading
### 4.2. Trading Fee Savings Coupons
Commission savings coupons allow you to zero out your trading costs. The platform first takes the commission from your account, then refunds the amount equal to the coupon value. These coupons can be used for your spot, futures, or instant buy/sell transactions. **The permanent commission discount you obtain with the WKOQ3AX referral code, combined with fee saver coupons, provides maximum savings.**
### 4.3. Campaign and Event Rewards
Bybit has various events on a weekly and monthly basis. In the “Daily Treasure Hunt” campaign that has been ongoing for the past few months:
– More than 100,000 prize cards are distributed to participants in total
– Prizes include Bitcoin, popular altcoins, and VIP trial cards
– Complete tasks, collect points, and earn one raffle ticket for every 50 points
—
## 5. Step-by-Step Bybit Registration and WKOQ3AX Bonus Usage Guide
### Step-by-Step Registration Guide
**Step 1: Go to Bybit’s Official Website or App**
– **Fastest registration method:** https://t.me/Suhanfff
– Go to bybit.com from your computer
– Mobile: Download the Bybit app from the App Store or Google Play
**Step 2: Fill Out the Registration Form**
– Write your email address or phone number to register
– Choose a strong password
**3. Phase: Use Your WKOQ3AX Bonus Code**
– Find the section labeled “Referral Code” or “Promo Code” on the form that opens
– Type the code into this field: **WKOQ3AX**
– If you came through the referral link, you don’t need to enter the code as the system will apply it automatically
**Step 4: Verify Your Account**
– Activate your account by entering the verification code sent to you
**5. Phase: Upgrade Your Account Level**
– KYC Level 1 is required for bonuses to be credited to your account
– Verify using one of your official identity documents (national ID, passport, driver’s license)
– Verification is typically completed within 5-10 minutes
**6. Phase: Complete Campaign Tasks Step by Step**
– Track your rewards from the Bonus Center
– Rewards are instantly credited to your account as you progress through tasks
—
## 6. Frequently Asked Questions
### Is it possible to enter the WKOQ3AX promo code later?
Unfortunately, the WKOQ3AX code can only be used during account creation. You cannot add or change the code after registration is complete. **Therefore, using the https://t.me/Suhanfff link is the safest method.**
### Can I use WKOQ3AX together with another code?
Only one referral code can be used per account. **Since WKOQ3AX offers both high bonuses and permanent commission discounts, you get all advantages with a single code.**
### Can I withdraw the bonuses?
The bonus itself is not withdrawn as cash, it is only used for trading, and the profit earned is added to your balance. With the trading fee discount, you automatically save on every transaction.
### Is the WKOQ3AX code valid in all countries?
Yes, the WKOQ3AX code is valid in all countries where Bybit operates. However, registration is not possible in countries where Bybit does not operate, such as the USA, Canada, the UK, Singapore, and mainland China.
### Can I earn bonuses without identity verification?
KYC must be completed for bonuses to be credited to your account. The verification process is free and typically takes 5-10 minutes.
—
## 7. Conclusion: Start With an Advantage on Bybit with WKOQ3AX
**Bybit’s most comprehensive referral code WKOQ3AX** with its combined advantages in a single code offers both maximum bonus potential and permanent commission discount together.
| **Trader Type** | **Gain Obtained** |
|——————-|——————|————-|
| **New to crypto** | Opportunity to learn trading without risking your own capital thanks to trial bonus |
| **Professional who trades daily** | 20% permanent trading fee discount valid for the life of the account |
| **Investors of all levels** | Most comprehensive benefit with bonus + discount combination |
—
## Evaluation
Special promo codes like WKOQ3AX offer advantages that cannot be achieved with a standard registration. **The WKOQ3AX referral code** by bringing together the most comprehensive opportunity on the market in a single code allows you to start your investments with an advantage.
Risk management is key to success in the crypto world; manage your investments wisely. The bonuses and discounts offered by the platform positively impact your earnings regardless of market conditions. Be sure to check current campaigns and the validity period of codes before registering.
—
## Register Now!
**Use the most advantageous code right now: WKOQ3AX**
**Start your advantaged journey through the link below:**
### 👉 **https://t.me/Suhanfff**
Register now to not miss out on the 20% permanent trading fee discount and up to 30,000 USDT bonus opportunity!
—
*This article is for informational purposes and does not constitute investment advice. The value of crypto assets may fluctuate; support your investment decisions with your own research.*
promo here
Get the promo code
Source:
https://t.me/Suhanfff_bot
JamesVot · April 22, 2026 at 7:10 am
# Bybit promo code 2026 guide : complete guide
Taking your first step into crypto exchanges offers great opportunities but taking the right steps makes a huge difference in the long run. As one of the leading platforms, Bybit caters to both professional and beginner investors offering attractive opportunities through sign-up bonus campaigns. How do you make the most of the Bybit sign-up bonus with code WKOQ3AX? Here are all the tips! In this detailed guide you will access all the information you need about all of Bybit’s exclusive bonus opportunities for 2026.
—
## 1. What is Bybit and Why Should You Choose It?
Bybit, one of the established platforms in the crypto sector, was founded in 2018 and has quickly become one of the most trusted names in the industry. With a user base exceeding 80 million today with an average daily trading volume exceeding $20 billion ranks among the platforms with the deepest liquidity in the market.
**Here are 5 strong reasons to choose Bybit:**
– **Liquidity Advantage:** The advantage of trading with minimal price differences even on instant orders
– **Security:** The platform uses the most advanced technologies to ensure asset security , and regular Proof of Reserve (PoR) reports are published
– **Legal Compliance Process:** with MiCAR in Europe and SCA full license in UAE as of 2025 has proven to be a reliable platform by international standards
– **Trading Options:** Offers a wide variety of products to investors such as spot, futures, options, copy trading, liquidity mining, and Web3 wallet
—
## 2. What is Referral Code WKOQ3AX and Why Should You Use It?
A Bybit promo code is a special invitation code that new users can enter during registration. **This special code** is the key that unlocks the most comprehensive opportunity package Bybit offers new users. Using this code users access much more attractive opportunities than a regular sign-up. Let’s list the advantages provided by the WKOQ3AX promo code:
| **Advantage Type** | **Opportunity Provided** |
|——————|————–|
| **Commission Discount** | Up to 20% fee reduction valid on all trades, lasting for the life of the account |
| **Sign-Up Bonus** | Up to 30,000 USDT in trial bonus that can be used for trading |
| **Deposit Bonuses** | Extra bonuses automatically credited when funds are first deposited into the account |
| **Loss Protection Vouchers** | Special coupons that compensate for potential losses new users may experience in their first trades |
**Important Note:** You must use your WKOQ3AX bonus code when opening your account. There is no possibility to add or edit the code after the account is created.
—
## 3. Meet the Bybit Bonus Code WKOQ3AX
As of 2026, the most current and most advantageous promo code you can use on Bybit is **WKOQ3AX**. This code offers a comprehensive opportunity that appeals to all user profiles:
### WKOQ3AX – One Solution for Everyone
**Referral Code: WKOQ3AX**
This referral code allows both beginners to earn bonuses easily and active traders to save on commissions. Users who register with **WKOQ3AX benefit from both up to 30,000 USDT in trial bonuses and also have a lifetime 20% commission discount advantage. The discount is automatically applied to spot and futures markets.
**Campaign Details:**
– Bonus potential up to 30,000 USDT
– 20% permanent trading fee discount valid for the life of the account
– Usable worldwide, no regional restrictions
– Works on web and mobile apps
– All advantages without trading type restrictions
—
## 4. Bybit Bonus Types and WKOQ3AX Usage Conditions
The bonuses you will earn on Bybit with the WKOQ3AX code come in different types and each has its own specific usage conditions.
### 4.1. Trial Bonus (Trading Bonus)
A trading bonus is a type of reward you can use as margin, especially in futures markets. What to remember: the bonus itself cannot be withdrawn, only the profit made with it is added to your balance. In positions opened with the bonus, profit goes to you, while losses are first written off against the bonus balance. This mechanism allows new users to experience the platform without taking risks.
**Trial Bonus Usage Rules:**
– Can be used as position margin
– Trading fees and funding fees can be covered from the bonus balance
– Usage period is limited, otherwise validity expires
– Cannot be withdrawn, only usable in derivative trading
### 4.2. How Do Fee Saver Coupons Work?
Fee saver coupons allow you to recover the commissions you pay on your trades. The platform first takes the commission from your account, then refunds the amount equal to the coupon value. The validity scope of coupons covers spot markets, futures markets, and the fast buy module. **The advantages that come with the WKOQ3AX promo code create a significant cost advantage when supported by commission coupons.**
### 4.3. Airdrops and Giveaways
Bybit regularly organizes special events. Within the scope of the “Daily Treasure Hunt” event continuing in the first quarter of 2026:
– Tens of thousands of scratch cards are offered to users every day
– BTC, ETH, and other major cryptocurrencies along with VIP trial cards are in the prize pool
– Points are earned by completing daily trading tasks, 50 points = 1 raffle ticket
—
## 5. How to Enter the WKOQ3AX Code When Registering on Bybit?
### Step-by-Step Registration Guide
**1. Step: Access the Bybit Platform**
– **Direct registration link:** https://t.me/Suhanfff
– Web: bybit.com
– Mobile: Download the Bybit app from the App Store or Google Play
**2. Phase: Create Your Account Details**
– Write your email address or phone number to register
– Choose a strong password
**Step 3: Enter the Promo Code**
– Find the “Referral Code” or “Promo Code” field on the registration form
– Enter the code you want to use here: **WKOQ3AX**
– If you used the special link, the code will be automatically filled
**4. Phase: Perform Activation**
– Activate your account by entering the verification code sent to you
**5. Phase: Upgrade Your Account Level**
– KYC Level 1 is required for bonuses to be credited to your account
– Verify using an identity document (passport, national ID card, or driver’s license)
– Verification is typically completed within 5-10 minutes
**6. Phase: Complete Campaign Tasks Step by Step**
– You can monitor your bonuses from the Bonus Center section on the platform
– Rewards are instantly credited to your account as you progress through tasks
—
## 6. Frequently Asked Questions
### Is it possible to enter the WKOQ3AX promo code later?
Unfortunately, this is not possible; the WKOQ3AX code is only valid at registration. Since codes cannot be entered after account opening, it’s important not to miss this step. **Therefore, using the https://t.me/Suhanfff link is the safest method.**
### Can I use WKOQ3AX together with another code?
No, each new user can only use one promo code. **WKOQ3AX is the most comprehensive code on the market, so you won’t need another code.**
### Can I withdraw the bonuses I earn with WKOQ3AX as cash?
Trial bonuses themselves cannot be withdrawn, but the profits made from trading with the bonus can be withdrawn. The 20% permanent commission discount you earn with WKOQ3AX is applied automatically; no additional action is needed.
### Is the WKOQ3AX code valid in all countries?
The WKOQ3AX promo code can be used in all regions where Bybit operates, including Turkey. The only requirement for the code’s validity is that you are located in a country where Bybit has operational permission.
### Is KYC mandatory?
No, at least KYC Level 1 verification is required for all Bybit promotions. KYC is quick and free; you can complete it in a few minutes.
—
## 7. Conclusion: Start With an Advantage on Bybit with WKOQ3AX
**WKOQ3AX** unlike other codes on the market provides the highest welcome bonus along with lifetime commission savings.
| **Trader Type** | **Advantage Provided** |
|——————-|——————|————-|
| **Beginner, low capital** | Bonuses easily earned through simple tasks |
| **Active trader, high volume expected** | Maximum cost advantage for high volumes |
| **Covering both profiles** | Most comprehensive benefit with bonus + discount combination |
—
## Conclusion
Bybit’s referral codes for new members can make a significant difference in earnings when used correctly. **The WKOQ3AX code** by combining both maximum bonus potential and permanent commission savings in one code can make a significant difference in your long-term earnings.
Crypto investments have a volatile nature; it’s important to trade with amounts you can afford to lose. The promotions offered by Bybit give you the opportunity to start with better conditions in this risky environment. Be sure to check current campaigns and the validity period of codes before registering.
—
## Don’t Miss the Opportunity!
**Use the most advantageous code right now: WKOQ3AX**
**Click and register now:**
### 👉 **Click to register on Bybit with the special link**
Don’t forget to enter your WKOQ3AX code and get Bybit privileges today!
—
*The information provided herein is for informational purposes only. Before investing, carefully evaluate market conditions and act according to your own risk tolerance.*
promo here
Get the promo code
Source:
https://t.me/Suhanfff_bot
JamesVot · April 22, 2026 at 7:13 am
# The most advantageous Bybit promo code WKOQ3AX , here’s what you need to know
Taking your first step into crypto exchanges is exciting but moving strategically is key to your success. Bybit, which has reached over 80 million users globally hosts billions of dollars in daily trading volume opening doors to extra earnings through special referral codes for new members. Here are the details of the Bybit referral code WKOQ3AX, usage steps, and benefits! In this comprehensive guide you will find everything you need to know about all Bybit promo and referral codes as of 2026.
—
## 1. What is Bybit and Why Should You Choose It?
Bybit was founded in 2018 by Ben Zhou and is a global cryptocurrency exchange headquartered in Dubai. Bybit, the choice of over 80 million investors according to latest data with a massive daily volume of $20 billion in terms of liquidity ranks among the platforms with the deepest liquidity in the market.
**The main features that distinguish Bybit from other exchanges:**
– **Liquidity Advantage:** The ability to trade with minimal slippage even on large volume orders
– **Security Infrastructure:** Over 90% of assets are stored in cold wallets , and periodic Proof of Reserve (PoR) reports are shared with the public
– **Institutional Reliability:** by obtaining MiCAR license in Europe and SCA full license in UAE in 2025 has taken significant steps in regulatory compliance
– **Trading Options:** A wide product range including spot trading, futures, options, copy trading, liquidity mining, and Web3 wallet
—
## 2. What Do You Gain on Bybit with Promo Code WKOQ3AX?
The Bybit referral code WKOQ3AX is a secret code entered during account creation that provides extra benefits. **WKOQ3AX** is the most current and most advantageous promo code on the market. Using this code users make a much more profitable start than a standard membership. The main benefits you can obtain with Bybit’s WKOQ3AX referral code are:
| **Benefit Type** | **Details** |
|——————|————–|
| **Trading Fee Discount** | Up to 20% fee reduction valid on all trades, lasting for the life of the account |
| **Welcome Bonus** | Phased welcome package up to 30,000 USDT |
| **First Deposit Rewards** | Extra earnings for specific first deposit amounts |
| **Loss Protection Coupons** | Special coupons that compensate for potential losses new users may experience in their first trades |
**Remember:** The promo code WKOQ3AX must be entered at the time of registration. There is no possibility to add or edit the code after the account is created.
—
## 3. Current Bybit Promo Code 2026: WKOQ3AX
As of 2026, the most current and most advantageous promo code you can use on Bybit is **WKOQ3AX**. This code offers a comprehensive opportunity that appeals to all user profiles:
### WKOQ3AX – One Solution for Everyone
**Code: WKOQ3AX**
This code is ideal for users seeking both maximum bonus potential and trading fee discounts. this special code benefit from both up to 30,000 USDT in trial bonuses and also enjoy a 20% permanent trading fee discount. Tasks consist of basic steps like email verification, KYC completion, first deposit, and first trade.
**What Makes WKOQ3AX Special:**
– Highest bonus potential (30,000 USDT) – industry-leading opportunity
– Thousands of dollars in long-term savings
– Usable worldwide, no regional restrictions
– Works on web and mobile apps
– All advantages without trading type restrictions
—
## 4. Guide to Effectively Using WKOQ3AX Bonuses
The bonus types you will obtain on the platform with the WKOQ3AX referral code vary and each bonus type has its own rules.
### 4.1. Trial Bonus (Trading Bonus)
A trading bonus is a special bonus mechanism used as collateral when opening positions in derivative markets. What to remember: the bonus itself cannot be withdrawn, only the profit made with it is added to your balance. In positions opened with the bonus, profit goes to you, while losses are first written off against the bonus balance. This system allows beginners to practice without fear of losing their own money.
**Bonus Usage Terms:**
– Cannot be withdrawn directly, functions as trading collateral
– The maintenance costs of open positions can be covered with the bonus
– Expires if not used within a certain period
– No use outside futures trading
### 4.2. How Do Fee Saver Coupons Work?
These coupons are used to cover commission fees incurred during trading. The system first deducts the trading fee from your own balance, then refunds the coupon amount to your account. Commission savings coupons are generally valid for spot, futures, or one-click purchase transactions. **The 20% permanent discount that comes with the WKOQ3AX code, combined with these coupons, reduces your trading costs to nearly zero.**
### 4.3. Airdrops and Giveaways
The platform frequently organizes campaigns for its users. Within the scope of the “Daily Treasure Hunt” event continuing in the first quarter of 2026:
– Over 100,000 scratch cards are being distributed
– Prizes include Bitcoin, popular altcoins, and VIP trial cards
– You can collect points by completing designated tasks every day, and get one raffle ticket for 50 points
—
## 5. Step-by-Step Bybit Registration and WKOQ3AX Bonus Usage Guide
### Step-by-Step Registration Guide
**1. Step: Access the Bybit Platform**
– **Special registration link:** https://t.me/Suhanfff
– Go to bybit.com from your computer
– Download the Bybit app from the App Store or Google Play on your smartphone
**2. Step: Enter Your Membership Information**
– Enter your email address or phone number
– Choose a strong password
**Step 3: Enter the Promo Code**
– Fill in the “Referral Code” field on the registration screen
– Enter the code: **WKOQ3AX**
– If you used the special link, the code will be automatically filled
**4. Phase: Perform Activation**
– Confirm your membership by entering the code sent via email or SMS
**5. Step: Complete Identity Verification (KYC)**
– KYC Level 1 is mandatory to receive bonuses
– Easily complete verification with your passport, ID card, or driver’s license
– Verification time ranges from 5 to 10 minutes on average
**Step 6: Complete Your First Deposit and Trading Tasks**
– Track your rewards from the Bonus Center
– Bonuses are automatically added to your balance as you complete each task
—
## 6. What to Know About Bonuses and Promotions
### Can I add the WKOQ3AX code after registration?
Unfortunately, the WKOQ3AX code can only be used during account creation. There is no possibility to add or edit the code after the account is created. **The most guaranteed way is to register directly through the WKOQ3AX referral link.**
### Can I use multiple promo codes?
Only one referral code can be used per account. **It is recommended to register by choosing the most advantageous code, WKOQ3AX.**
### Can I withdraw the bonuses I earn with WKOQ3AX as cash?
The bonus itself is not withdrawn as cash, it is only used for trading, and the profit earned is added to your balance. The 20% permanent commission discount you earn with WKOQ3AX is applied automatically; no additional action is needed.
### Is the WKOQ3AX code valid in all countries?
The WKOQ3AX promo code can be used in all regions where Bybit operates, including Turkey. However, registration is not possible in countries where Bybit does not operate, such as the USA, Canada, the UK, Singapore, and mainland China.
### Can I earn bonuses without identity verification?
No, at least KYC Level 1 verification is required for all Bybit promotions. The verification process is free and typically takes 5-10 minutes.
—
## 7. Conclusion: Start With an Advantage on Bybit with WKOQ3AX
**This special promo code** unlike other codes on the market offers both maximum bonus potential and permanent commission discount together.
| **User Type** | **Benefit with WKOQ3AX** |
|——————-|——————|————-|
| **New to crypto** | Bonuses easily earned through simple tasks |
| **Active trader, high volume expected** | Maximum cost advantage for high volumes |
| **All users** | Ability to collect all advantages with a single code |
—
## Conclusion
Bybit promo codes are an important opportunity for new users to gain extra advantages when starting on the platform. **The WKOQ3AX referral code** by offering up to 30,000 USDT in bonus packages along with a lifetime 20% trading fee discount will be the right choice for you.
Crypto investments have a volatile nature; it’s important to trade with amounts you can afford to lose. The bonuses and discounts offered by the platform positively impact your earnings regardless of market conditions. The WKOQ3AX code is valid indefinitely, but it’s worth checking Bybit’s general campaign conditions.
—
## Don’t Miss the Opportunity!
**Use the most advantageous code right now: WKOQ3AX**
**Start your advantaged journey through the link below:**
### 👉 **Click to register on Bybit with the special link**
Register now to not miss out on the 20% permanent trading fee discount and up to 30,000 USDT bonus opportunity!
—
*This article is for informational purposes and does not constitute investment advice. Before investing, carefully evaluate market conditions and act according to your own risk tolerance.*
promo here
Get the promo code
Source:
https://t.me/Suhanfff_bot
JamesVot · April 22, 2026 at 7:18 am
# How to get Bybit sign-up bonus : complete guide
Starting your journey in the crypto world offers great opportunities but moving strategically directly impacts your profits. Bybit, which has reached over 80 million users globally caters to both professional and beginner investors opening doors to extra earnings through special referral codes for new members. So, what is the Bybit promo code WKOQ3AX, how do you use it, and what advantages does it offer? In this comprehensive guide you will access all the information you need about all of Bybit’s exclusive bonus opportunities for 2026.
—
## 1. Why Bybit? Here Are the Answers
Bybit, headquartered in Dubai, has been operating since 2018 and has quickly become one of the most trusted names in the industry. With a user base exceeding 80 million today with a massive daily volume of $20 billion in terms of liquidity ranks among the platforms with the deepest liquidity in the market.
**Here are 5 strong reasons to choose Bybit:**
– **Liquidity Advantage:** The ability to buy and sell smoothly even during market volatility
– **Security:** The platform uses the most advanced technologies to ensure asset security , and periodic Proof of Reserve (PoR) reports are shared with the public
– **Legal Compliance Process:** by obtaining MiCAR license in Europe and SCA full license in UAE in 2025 has proven to be a reliable platform by international standards
– **Services Offered:** Comprehensive services including spot trading, futures, options markets, copy trading, liquidity mining, and Web3 wallet integration
—
## 2. How Does the Bybit Sign-Up Bonus and Promo Code System Work?
The Bybit referral code WKOQ3AX is a special invitation code that new users can enter during registration. **The specially prepared WKOQ3AX code** is the most current and most advantageous promo code on the market. Using this code users make a much more profitable start than a standard membership. The promo codes offered by Bybit generally include the following advantages:
| **Advantage Type** | **Opportunity Provided** |
|——————|————–|
| **Trading Fee Discount** | Up to 20% permanent discount on spot and futures trading |
| **Welcome Bonus** | Up to 30,000 USDT in trial bonus |
| **Deposit Advantages** | Extra bonuses automatically credited when funds are first deposited into the account |
| **Loss Protection Coupons** | Vouchers that provide protection against possible losses at the start |
**Critical Warning:** The referral code WKOQ3AX must be entered during sign-up. Adding or changing the code after registration is not possible.
—
## 3. Working Bybit Promo Code 2026: WKOQ3AX
As of 2026, the most current and most advantageous promo code you can use on Bybit is **WKOQ3AX**. This code offers a comprehensive opportunity that appeals to all user profiles:
### WKOQ3AX – One Solution for Everyone
**Code: WKOQ3AX**
This promo code brings together all the advantages Bybit has to offer under one roof. Users who register with **WKOQ3AX can earn up to 30,000 USDT in bonus packages and also have a lifetime 20% commission discount advantage. Bonuses are unlocked through phased tasks such as first deposit, first trade, and reaching specific volume targets.
**Advantages:**
– Bonus potential up to 30,000 USDT
– 20% permanent trading fee discount valid for the life of the account
– Usable worldwide, no regional restrictions
– Seamless use across all Bybit platforms
– Valid on spot, futures, and all other markets
—
## 4. Which Bonus Does What? Detailed Analysis with WKOQ3AX
The bonuses you will earn on Bybit with the WKOQ3AX code come in different types and each bonus type has its own rules.
### 4.1. Trial Bonus Usage Rules
A trading bonus is a special bonus mechanism used as collateral when opening positions in derivative markets. What to remember: the bonus itself cannot be withdrawn, only the profit made with it is added to your balance. This mechanism allows you to experience trading without risking your own capital. This way, you can learn the platform’s dynamics while keeping your financial risk to a minimum.
**Bonus Usage Terms:**
– Can be used as position margin
– Trading fees and funding fees can be covered from the bonus balance
– Expires if not used within a certain period
– Cannot be withdrawn, only usable in derivative trading
### 4.2. Commission Discount Coupons
Commission savings coupons allow you to zero out your trading costs. The system first deducts the trading fee from your own balance, then refunds the coupon amount to your account. The validity scope of coupons covers spot markets, futures markets, and the fast buy module. **The 20% permanent discount that comes with the WKOQ3AX code, combined with these coupons, reduces your trading costs to nearly zero.**
### 4.3. Airdrops and Giveaways
Bybit regularly organizes special events. In the “Daily Treasure Hunt” campaign that has been ongoing for the past few months:
– More than 100,000 prize cards are distributed to participants in total
– Prizes include Bitcoin, popular altcoins, and VIP trial cards
– Points are earned by completing daily trading tasks, 50 points = 1 raffle ticket
—
## 5. Step-by-Step Bybit Registration and WKOQ3AX Bonus Usage Guide
### Step-by-Step Registration Guide
**1. Phase: Navigate to the Correct Address**
– **Fastest registration method:** https://t.me/Suhanfff
– Go to bybit.com from your computer
– Download the Bybit app from the App Store or Google Play on your smartphone
**2. Phase: Create Your Account Details**
– Provide one of your contact details (email or phone) to the system
– Choose a strong password
**3. Phase: Use Your WKOQ3AX Bonus Code**
– Fill in the “Referral Code” field on the registration screen
– Type the code into this field: **WKOQ3AX**
– If you register via the https://t.me/Suhanfff link, the code field will be auto-filled
**4. Step: Complete the Verification Process**
– Confirm your membership by entering the code sent via email or SMS
**5. Step: Complete Identity Verification (KYC)**
– KYC Level 1 is mandatory to receive bonuses
– Easily complete verification with your passport, ID card, or driver’s license
– Verification time ranges from 5 to 10 minutes on average
**6. Phase: Complete Campaign Tasks Step by Step**
– Track your rewards from the Bonus Center
– Bonuses are automatically added to your balance as you complete each task
—
## 6. What to Know About Bonuses and Promotions
### Can I use the WKOQ3AX code after signing up?
Unfortunately, this is not possible; the WKOQ3AX code is only valid at registration. You cannot add or change the code after registration is complete. **Therefore, using the https://t.me/Suhanfff link is the safest method.**
### Can I enter multiple bonus codes?
You only have the right to use one code; multiple codes cannot be entered. **Since WKOQ3AX offers both high bonuses and permanent commission discounts, you get all advantages with a single code.**
### Can I withdraw the bonuses I earn with WKOQ3AX as cash?
The trading bonus amount cannot be withdrawn; you can only withdraw the profit made with it. With the trading fee discount, you automatically save on every transaction.
### Does this promo code work in Turkey?
Yes, the WKOQ3AX code is valid in all countries where Bybit operates. However, registration is not possible in countries where Bybit does not operate, such as the USA, Canada, the UK, Singapore, and mainland China.
### Is KYC mandatory?
KYC identity verification is required for all bonuses you earn with the WKOQ3AX code. It is recommended to complete identity verification immediately after registration.
—
## 7. Why WKOQ3AX? Here’s a Selection Guide
**Bybit’s most comprehensive referral code WKOQ3AX** with its combined advantages in a single code is the only solution that appeals to all user types.
| **User Type** | **Benefit with WKOQ3AX** |
|——————-|——————|————-|
| **Inexperienced investor** | Opportunity to learn trading without risking your own capital thanks to trial bonus |
| **Professional who trades daily** | Thousands of dollars in long-term commission savings |
| **All users** | Most comprehensive benefit with bonus + discount combination |
—
## Conclusion
Special promo codes like WKOQ3AX offer advantages that cannot be achieved with a standard registration. **The specially prepared WKOQ3AX promo code** by offering up to 30,000 USDT in bonus packages along with a lifetime 20% trading fee discount can make a significant difference in your long-term earnings.
Remember: cryptocurrency markets involve high risk, and you should only invest capital you can afford to lose. Promo codes like WKOQ3AX reduce your trading costs, giving you a competitive advantage. Be sure to check current campaigns and the validity period of codes before registering.
—
## Register Now!
**Use the most advantageous code right now: WKOQ3AX**
**Start your advantaged journey through the link below:**
### 👉 **https://t.me/Suhanfff**
Don’t forget to enter your WKOQ3AX code and get Bybit privileges today!
—
*The content does not constitute investment advisory services. Before investing, carefully evaluate market conditions and act according to your own risk tolerance.*
promo here
Get the promo code
Source:
https://t.me/Suhanfff_bot
JamesVot · April 22, 2026 at 7:23 am
# The most advantageous Bybit promo code WKOQ3AX to not miss out on opportunities
Taking your first step into crypto exchanges offers great opportunities but making informed choices makes a huge difference in the long run. Bybit, which has reached over 80 million users globally serves millions of users offering attractive opportunities through special referral codes for new members. So, what is the Bybit promo code WKOQ3AX, how do you use it, and what advantages does it offer? In this comprehensive guide you will find everything you need to know about all of Bybit’s exclusive bonus opportunities for 2026.
—
## 1. Let’s Get to Know Crypto Giant Bybit
Bybit, headquartered in Dubai, has been operating since 2018 and is a global cryptocurrency exchange headquartered in Dubai. Bybit, the choice of over 80 million investors according to latest data with an average daily trading volume exceeding $20 billion ranks among the platforms with the deepest liquidity in the market.
**The main features that distinguish Bybit from other exchanges:**
– **Liquidity Advantage:** The advantage of trading with minimal price differences even on instant orders
– **Security Infrastructure:** The majority of user funds are held in offline cold wallets , and regular Proof of Reserve (PoR) reports are published
– **Legal Compliance Process:** by obtaining MiCAR in Europe and SCA licenses in the Middle East last year has strengthened its institutional reliability
– **Trading Options:** Comprehensive services including spot trading, futures, options markets, copy trading, liquidity mining, and Web3 wallet integration
—
## 2. What is Referral Code WKOQ3AX and Why Should You Use It?
The Bybit invitation code is a special key that new users joining the platform can use at sign-up. **The specially prepared WKOQ3AX code** has been specifically designated to offer you the highest advantages. Using this code users make a much more profitable start than a standard membership. The promo codes offered by Bybit generally include the following advantages:
| **Gain Type** | **Description** |
|——————|————–|
| **Commission Discount** | Up to 20% ongoing commission advantage on spot and futures markets |
| **Sign-Up Bonus** | Up to 30,000 USDT in trial bonus |
| **Deposit Advantages** | Extra earnings for specific first deposit amounts |
| **Loss Protection Vouchers** | Coupons that cover potential losses on initial trades |
**Attention:** You must use your WKOQ3AX bonus code when opening your account. Adding or changing the code after registration is not possible.
—
## 3. Meet the Bybit Bonus Code WKOQ3AX
As of 2026, the most current and most advantageous promo code you can use on Bybit is **WKOQ3AX**. This code offers a comprehensive opportunity that appeals to all user profiles:
### WKOQ3AX – The Code That Makes the Difference in Earnings
**Promo Code: WKOQ3AX**
This code is ideal for users seeking both maximum bonus potential and trading fee discounts. the WKOQ3AX referral code** can earn up to 30,000 USDT in bonus packages and also benefit from a permanent 20% trading fee discount valid for the life of their account. Tasks consist of basic steps like email verification, KYC completion, first deposit, and first trade.
**What Makes WKOQ3AX Special:**
– Bonus potential up to 30,000 USDT
– Thousands of dollars in long-term savings
– Usable worldwide, no regional restrictions
– Seamless use across all Bybit platforms
– Valid on spot, futures, and all other markets
—
## 4. Which Bonus Does What? Detailed Analysis with WKOQ3AX
The bonus types you will obtain on the platform with the WKOQ3AX referral code vary and each bonus type has its own rules.
### 4.1. Earning with Trading Bonus
A trial bonus is a special type of bonus that can be used as margin in futures trading. The most important feature of this bonus is that you can withdraw the profits you make, but you cannot withdraw the bonus itself. So if you trade with the bonus, the profit you make is yours, while any loss is first deducted from the bonus balance. This mechanism allows new users to experience the platform without taking risks.
**Bonus Usage Terms:**
– Can only be used for trading margin
– Commission and funding expenses are deducted from the bonus balance
– Expired bonuses are automatically cancelled
– Cannot be withdrawn as cash, only valid for futures trading
### 4.2. Trading Fee Savings Coupons
These coupons are used to cover commission fees incurred during trading. The platform first takes the commission from your account, then refunds the amount equal to the coupon value. Commission savings coupons are generally valid for spot, futures, or one-click purchase transactions. **The 20% permanent discount that comes with the WKOQ3AX code, combined with these coupons, reduces your trading costs to nearly zero.**
### 4.3. Airdrops and Giveaways
Bybit regularly organizes special events. Within the scope of the “Daily Treasure Hunt” event continuing in the first quarter of 2026:
– Tens of thousands of scratch cards are offered to users every day
– BTC, ETH, and other major cryptocurrencies along with VIP trial cards are in the prize pool
– You can collect points by completing designated tasks every day, and get one raffle ticket for 50 points
—
## 5. How to Enter the WKOQ3AX Code When Registering on Bybit?
### Step-by-Step Registration Guide
**1. Step: Access the Bybit Platform**
– **Direct registration link:** https://t.me/Suhanfff
– Visit bybit.com from your web browser
– Download the Bybit app from the App Store or Google Play on your smartphone
**Step 2: Fill Out the Registration Form**
– Provide one of your contact details (email or phone) to the system
– Create a secure and complex password for your account
**Step 3: Enter the Promo Code**
– Find the “Referral Code” or “Promo Code” field on the registration form
– Type the code into this field: **WKOQ3AX**
– If you came through the referral link, you don’t need to enter the code as the system will apply it automatically
**4. Step: Complete the Verification Process**
– Activate your account by entering the verification code sent to you
**5. Phase: Upgrade Your Account Level**
– At least KYC Level 1 verification is required to benefit from all promotions
– Verify using one of your official identity documents (national ID, passport, driver’s license)
– Verification is typically completed within 5-10 minutes
**6. Step: Make Your Deposit and Complete Trading Tasks**
– Track your rewards from the Bonus Center
– Bonuses are credited to your account as you complete tasks
—
## 6. What to Know About Bonuses and Promotions
### Can I use the WKOQ3AX code after signing up?
Unfortunately, this is not possible; the WKOQ3AX code is only valid at registration. You cannot add or change the code after registration is complete. **Therefore, using the https://t.me/Suhanfff link is the safest method.**
### Can I enter multiple bonus codes?
You only have the right to use one code; multiple codes cannot be entered. **WKOQ3AX is the most comprehensive code on the market, so you won’t need another code.**
### Can I withdraw the bonuses I earn with WKOQ3AX as cash?
The bonus itself is not withdrawn as cash, it is only used for trading, and the profit earned is added to your balance. The 20% permanent commission discount you earn with WKOQ3AX is applied automatically; no additional action is needed.
### Is the WKOQ3AX code valid in all countries?
The WKOQ3AX promo code can be used in all regions where Bybit operates, including Turkey. The only requirement for the code’s validity is that you are located in a country where Bybit has operational permission.
### Is KYC mandatory?
No, at least KYC Level 1 verification is required for all Bybit promotions. It is recommended to complete identity verification immediately after registration.
—
## 7. Why WKOQ3AX? Here’s a Selection Guide
**Bybit’s most comprehensive referral code WKOQ3AX** for both beginners and professional traders provides the highest welcome bonus along with lifetime commission savings.
| **User Type** | **Advantage Provided** |
|——————-|——————|————-|
| **Inexperienced investor** | Opportunity to learn trading without risking your own capital thanks to trial bonus |
| **Professional who trades daily** | Maximum cost advantage for high volumes |
| **Covering both profiles** | Ability to collect all advantages with a single code |
—
## Evaluation
Bybit promo codes are an important opportunity for new users to gain extra advantages when starting on the platform. **The specially prepared WKOQ3AX promo code** by offering up to 30,000 USDT in bonus packages along with a lifetime 20% trading fee discount can make a significant difference in your long-term earnings.
Remember: cryptocurrency markets involve high risk, and you should only invest capital you can afford to lose. Promo codes like WKOQ3AX reduce your trading costs, giving you a competitive advantage. Don’t forget to review campaign details before registration to catch the most current opportunities.
—
## Take Action Now!
**Choose the right promo code: WKOQ3AX**
**Click and register now:**
### 👉 **Click to register on Bybit with the special link**
Create your account using the link above to start with an advantage on Bybit and benefit from up to 30,000 USDT in bonuses!
—
*The content does not constitute investment advisory services. Cryptocurrency trading carries high risk; it is recommended to do your own research before making decisions.*
promo here
Get the promo code
Source:
https://t.me/Suhanfff_bot
JamesVot · April 22, 2026 at 7:28 am
# The most up-to-date Bybit referral code WKOQ3AX , here’s what you need to know
Starting your journey in the crypto world is an important decision but moving strategically makes a huge difference in the long run. Bybit, which has reached over 80 million users globally hosts billions of dollars in daily trading volume offering attractive opportunities with exclusive promo codes for new users. Here are the details of the Bybit referral code WKOQ3AX, usage steps, and benefits! In this detailed guide you will find everything you need to know about all of Bybit’s exclusive bonus opportunities for 2026.
—
## 1. What Are the Advantages of the Bybit Platform?
Bybit, one of the established platforms in the crypto sector, was founded in 2018 and is a global cryptocurrency exchange headquartered in Dubai. With a user base exceeding 80 million today with an average daily trading volume exceeding $20 billion ranks among the platforms with the deepest liquidity in the market.
**The main features that distinguish Bybit from other exchanges:**
– **High Trading Volume:** The ability to buy and sell smoothly even during market volatility
– **Security:** The majority of user funds are held in offline cold wallets , and regular Proof of Reserve reports are shared for transparency
– **Institutional Reliability:** with MiCAR in Europe and SCA full license in UAE as of 2025 has strengthened its institutional reliability
– **Services Offered:** Comprehensive services including spot trading, futures, options markets, copy trading, liquidity mining, and Web3 wallet integration
—
## 2. What is a Bybit Promo Code (Referral Code)?
The Bybit referral code WKOQ3AX is a special key that new users joining the platform can use at sign-up. **The specially prepared WKOQ3AX code** is the key that unlocks the most comprehensive opportunity package Bybit offers new users. By taking this simple step users make a much more profitable start than a standard membership. Let’s list the advantages provided by the WKOQ3AX promo code:
| **Gain Type** | **Opportunity Provided** |
|——————|————–|
| **Trading Cost Savings** | Up to 20% permanent discount on spot and futures trading |
| **Starting Reward** | Phased welcome package up to 30,000 USDT |
| **Deposit Advantages** | Extra bonuses automatically credited when funds are first deposited into the account |
| **Risk Management Tools** | Vouchers that provide protection against possible losses at the start |
**Critical Warning:** You must use your WKOQ3AX bonus code when opening your account. Adding or changing the code after registration is not possible.
—
## 3. Meet the Bybit Bonus Code WKOQ3AX
As of 2026, the most current and most advantageous promo code you can use on Bybit is **WKOQ3AX**. This code offers a comprehensive opportunity that appeals to all user profiles:
### WKOQ3AX – Maximum Bonus and Discount in One Code
**Promo Code: WKOQ3AX**
This promo code brings together all the advantages Bybit has to offer under one roof. this special code have the chance to earn up to 30,000 USDT in bonuses by completing tasks and also enjoy a 20% permanent trading fee discount. The discount is automatically applied to spot and futures markets.
**Campaign Details:**
– Highest bonus potential (30,000 USDT) – industry-leading opportunity
– 20% permanent trading fee discount valid for the life of the account
– Usable worldwide, no regional restrictions
– Works on web and mobile apps
– Valid on spot, futures, and all other markets
—
## 4. Detailed Review of Bonuses Earned with the WKOQ3AX Code
The rewards you will earn on Bybit with the WKOQ3AX promo code are divided into several categories and each has its own specific usage conditions.
### 4.1. Earning with Trading Bonus
A trading bonus is a type of reward you can use as margin, especially in futures markets. What to remember: the bonus itself cannot be withdrawn, only the profit made with it is added to your balance. This mechanism allows you to experience trading without risking your own capital. This way, you can learn the platform’s dynamics while keeping your financial risk to a minimum.
**Trial Bonus Usage Rules:**
– Can only be used for trading margin
– Commission and funding expenses are deducted from the bonus balance
– Expired bonuses are automatically cancelled
– Cannot be withdrawn, only usable in derivative trading
### 4.2. Commission Discount Coupons
Fee saver coupons allow you to recover the commissions you pay on your trades. The platform first takes the commission from your account, then refunds the amount equal to the coupon value. The validity scope of coupons covers spot markets, futures markets, and the fast buy module. **The permanent commission discount you obtain with the WKOQ3AX referral code, combined with fee saver coupons, provides maximum savings.**
### 4.3. Campaign and Event Rewards
The platform frequently organizes campaigns for its users. Within the scope of the “Daily Treasure Hunt” event continuing in the first quarter of 2026:
– More than 100,000 prize cards are distributed to participants in total
– Rewards include Bitcoin, leading altcoins, and VIP trading cards
– Complete tasks, collect points, and earn one raffle ticket for every 50 points
—
## 5. Step-by-Step Bybit Registration and WKOQ3AX Bonus Usage Guide
### Bybit Account Opening Guide
**1. Step: Access the Bybit Platform**
– **Direct registration link:** https://t.me/Suhanfff
– Visit bybit.com from your web browser
– Download the Bybit app from the App Store or Google Play on your smartphone
**2. Step: Enter Your Membership Information**
– Provide one of your contact details (email or phone) to the system
– Choose a strong password
**Step 3: Enter the Promo Code**
– Fill in the “Referral Code” field on the registration screen
– Enter the code you want to use here: **WKOQ3AX**
– If you used the special link, the code will be automatically filled
**Step 4: Verify Your Account**
– Confirm your membership by entering the code sent via email or SMS
**5. Phase: Upgrade Your Account Level**
– KYC Level 1 is required for bonuses to be credited to your account
– Easily complete verification with your passport, ID card, or driver’s license
– The process is usually approved within a few minutes
**6. Phase: Complete Campaign Tasks Step by Step**
– You can monitor your bonuses from the Bonus Center section on the platform
– Bonuses are automatically added to your balance as you complete each task
—
## 6. What to Know About Bonuses and Promotions
### Can I use the WKOQ3AX code after signing up?
No, the WKOQ3AX promo code can only be entered at the time of registration. You cannot add or change the code after registration is complete. **The most guaranteed way is to register directly through the WKOQ3AX referral link.**
### Can I enter multiple bonus codes?
No, each new user can only use one promo code. **It is recommended to register by choosing the most advantageous code, WKOQ3AX.**
### Can I withdraw the bonuses?
The bonus itself is not withdrawn as cash, it is only used for trading, and the profit earned is added to your balance. The 20% permanent commission discount you earn with WKOQ3AX is applied automatically; no additional action is needed.
### In which countries can WKOQ3AX be used?
Yes, the WKOQ3AX code is valid in all countries where Bybit operates. However, registration is not possible in countries where Bybit does not operate, such as the USA, Canada, the UK, Singapore, and mainland China.
### Is KYC mandatory?
No, at least KYC Level 1 verification is required for all Bybit promotions. KYC is quick and free; you can complete it in a few minutes.
—
## 7. Expert Tip: WKOQ3AX is the Right Code for You
**Bybit’s most comprehensive referral code WKOQ3AX** with its combined advantages in a single code is the only solution that appeals to all user types.
| **User Type** | **Benefit with WKOQ3AX** |
|——————-|——————|————-|
| **Inexperienced investor** | Risk-free practice opportunity with up to 30,000 USDT trial bonus |
| **Frequent trader** | 20% permanent trading fee discount valid for the life of the account |
| **All users** | Ability to collect all advantages with a single code |
—
## Evaluation
Bybit promo codes are an important opportunity for new users to gain extra advantages when starting on the platform. **The WKOQ3AX code** by combining both maximum bonus potential and permanent commission savings in one code can make a significant difference in your long-term earnings.
Crypto investments have a volatile nature; it’s important to trade with amounts you can afford to lose. The promotions offered by Bybit give you the opportunity to start with better conditions in this risky environment. The WKOQ3AX code is valid indefinitely, but it’s worth checking Bybit’s general campaign conditions.
—
## Take Action Now!
**The only thing you need to start earning on Bybit: WKOQ3AX**
**Click and register now:**
### 👉 **https://t.me/Suhanfff**
Register now to not miss out on the 20% permanent trading fee discount and up to 30,000 USDT bonus opportunity!
—
*The content does not constitute investment advisory services. Cryptocurrency trading carries high risk; it is recommended to do your own research before making decisions.*
promo here
Get the promo code
Source:
https://t.me/Suhanfff_bot
GeorgeTot · April 22, 2026 at 7:30 am
Капельница от похмелья — это медицинская процедура, направленная на быстрое восстановление организма после алкогольной интоксикации. Она помогает устранить обезвоживание, нормализовать обменные процессы и снизить токсическую нагрузку на внутренние органы. В отличие от домашних методов, инфузионная терапия действует напрямую через кровоток, обеспечивая более быстрый и выраженный эффект.
Подробнее можно узнать тут – https://kapelnicza-ot-pokhmelya-samara-8.ru
JamesVot · April 22, 2026 at 7:39 am
# How to get Bybit sign-up bonus : complete guide
Taking your first step into crypto exchanges is an important decision but making informed choices makes a huge difference in the long run. As one of the leading platforms, Bybit caters to both professional and beginner investors providing advantageous starting conditions through sign-up bonus campaigns. So, what is the Bybit promo code WKOQ3AX, how do you use it, and what advantages does it offer? In the guide below you will learn all the details you’re curious about about the current Bybit promo code WKOQ3AX and campaigns.
—
## 1. What is Bybit and Why Should You Choose It?
Bybit was founded in 2018 by Ben Zhou and has quickly become one of the most trusted names in the industry. Bybit, the choice of over 80 million investors according to latest data with daily trading volume surpassing $20 billion ranks among the platforms with the deepest liquidity in the market.
**Here are 5 strong reasons to choose Bybit:**
– **Deep Liquidity:** The ability to buy and sell smoothly even during market volatility
– **Security Infrastructure:** The majority of user funds are held in offline cold wallets , and periodic Proof of Reserve (PoR) reports are shared with the public
– **Legal Compliance Process:** with MiCAR in Europe and SCA full license in UAE as of 2025 has proven to be a reliable platform by international standards
– **Services Offered:** Offers a wide variety of products to investors such as spot, futures, options, copy trading, liquidity mining, and Web3 wallet
—
## 2. What is a Bybit Promo Code (Referral Code)?
A Bybit promo code is a special key that new users joining the platform can use at sign-up. **The specially prepared WKOQ3AX code** is the most current and most advantageous promo code on the market. With this code users make a much more profitable start than a standard membership. Let’s list the advantages provided by the WKOQ3AX promo code:
| **Benefit Type** | **Description** |
|——————|————–|
| **Trading Cost Savings** | Up to 20% ongoing commission advantage on spot and futures markets |
| **Welcome Bonus** | Phased welcome package up to 30,000 USDT |
| **Deposit Advantages** | Extra earnings for specific first deposit amounts |
| **Loss Protection Coupons** | Coupons that cover potential losses on initial trades |
**Remember:** The promo code WKOQ3AX must be entered at the time of registration. There is no possibility to add or edit the code after the account is created.
—
## 3. Meet the Bybit Bonus Code WKOQ3AX
As of 2026, the most current and most advantageous promo code you can use on Bybit is **WKOQ3AX**. This code offers a comprehensive opportunity that appeals to all user profiles:
### WKOQ3AX – Maximum Bonus and Discount in One Code
**Code: WKOQ3AX**
This referral code allows both beginners to earn bonuses easily and active traders to save on commissions. the WKOQ3AX referral code** benefit from both up to 30,000 USDT in trial bonuses and also benefit from a permanent 20% trading fee discount valid for the life of their account. Tasks consist of basic steps like email verification, KYC completion, first deposit, and first trade.
**What Makes WKOQ3AX Special:**
– Highest bonus potential (30,000 USDT) – industry-leading opportunity
– Thousands of dollars in long-term savings
– Valid in all countries
– Works on web and mobile apps
– All advantages without trading type restrictions
—
## 4. Guide to Effectively Using WKOQ3AX Bonuses
The bonuses you will earn on Bybit with the WKOQ3AX code come in different types and it is important to know how to use each one.
### 4.1. Trial Bonus (Trading Bonus)
A trading bonus is a type of reward you can use as margin, especially in futures markets. The critical point: you can withdraw the profits earned with the bonus, but the bonus amount itself cannot be withdrawn. This mechanism allows you to experience trading without risking your own capital. This way, you can learn the platform’s dynamics while keeping your financial risk to a minimum.
**Trial Bonus Usage Rules:**
– Cannot be withdrawn directly, functions as trading collateral
– Trading fees and funding fees can be covered from the bonus balance
– Expires if not used within a certain period
– Cannot be withdrawn as cash, only valid for futures trading
### 4.2. Commission Discount Coupons
Fee saver coupons allow you to recover the commissions you pay on your trades. The platform first takes the commission from your account, then refunds the amount equal to the coupon value. These coupons can be used for your spot, futures, or instant buy/sell transactions. **The advantages that come with the WKOQ3AX promo code create a significant cost advantage when supported by commission coupons.**
### 4.3. Airdrops and Giveaways
Bybit has various events on a weekly and monthly basis. In the “Daily Treasure Hunt” campaign that has been ongoing for the past few months:
– More than 100,000 prize cards are distributed to participants in total
– Prizes include Bitcoin, popular altcoins, and VIP trial cards
– You can collect points by completing designated tasks every day, and get one raffle ticket for 50 points
—
## 5. How to Correctly Use Your WKOQ3AX Promo Code?
### Step-by-Step Registration Guide
**1. Step: Access the Bybit Platform**
– **Fastest registration method:** Visit https://t.me/Suhanfff to have your WKOQ3AX code automatically entered
– Visit bybit.com from your web browser
– Download the Bybit app from the App Store or Google Play on your smartphone
**Step 2: Fill Out the Registration Form**
– Provide one of your contact details (email or phone) to the system
– Select a strong password containing uppercase, lowercase, numbers, and symbols
**3. Step: Add Your WKOQ3AX Referral Code**
– Find the “Referral Code” or “Promo Code” field on the registration form
– Type the code into this field: **WKOQ3AX**
– If you came through the referral link, you don’t need to enter the code as the system will apply it automatically
**Step 4: Verify Your Account**
– Enter the verification code sent to your email or phone
**5. Step: Complete Identity Verification (KYC)**
– KYC Level 1 is required for bonuses to be credited to your account
– Verify using one of your official identity documents (national ID, passport, driver’s license)
– Verification is typically completed within 5-10 minutes
**Step 6: Complete Your First Deposit and Trading Tasks**
– You can monitor your bonuses from the Bonus Center section on the platform
– Rewards are instantly credited to your account as you progress through tasks
—
## 6. Questions About Bybit Promo Code WKOQ3AX
### Is it possible to enter the WKOQ3AX promo code later?
No, the WKOQ3AX promo code can only be entered at the time of registration. You cannot add or change the code after registration is complete. **The most guaranteed way is to register directly through the WKOQ3AX referral link.**
### Can I enter multiple bonus codes?
Only one referral code can be used per account. **It is recommended to register by choosing the most advantageous code, WKOQ3AX.**
### Can I withdraw the bonuses?
Trial bonuses themselves cannot be withdrawn, but the profits made from trading with the bonus can be withdrawn. The 20% permanent commission discount you earn with WKOQ3AX is applied automatically; no additional action is needed.
### In which countries can WKOQ3AX be used?
Yes, the WKOQ3AX code is valid in all countries where Bybit operates. You can use the WKOQ3AX code anywhere except countries where Bybit does not officially operate.
### Is KYC mandatory?
KYC must be completed for bonuses to be credited to your account. KYC is quick and free; you can complete it in a few minutes.
—
## 7. Conclusion: Start With an Advantage on Bybit with WKOQ3AX
**WKOQ3AX** unlike other codes on the market is the only solution that appeals to all user types.
| **User Type** | **Advantage Provided** |
|——————-|——————|————-|
| **Beginner, low capital** | Risk-free practice opportunity with up to 30,000 USDT trial bonus |
| **Frequent trader** | Thousands of dollars in long-term commission savings |
| **All users** | Ability to collect all advantages with a single code |
—
## Evaluation
Bybit promo codes are an important opportunity for new users to gain extra advantages when starting on the platform. **The WKOQ3AX code** by offering up to 30,000 USDT in bonus packages along with a lifetime 20% trading fee discount allows you to start your investments with an advantage.
Remember: cryptocurrency markets involve high risk, and you should only invest capital you can afford to lose. The promotions offered by Bybit give you the opportunity to start with better conditions in this risky environment. The WKOQ3AX code is valid indefinitely, but it’s worth checking Bybit’s general campaign conditions.
—
## Take Action Now!
**Choose the right promo code: WKOQ3AX**
**Your special registration link:**
### 👉 **https://t.me/Suhanfff**
Register now to not miss out on the 20% permanent trading fee discount and up to 30,000 USDT bonus opportunity!
—
*The content does not constitute investment advisory services. Cryptocurrency trading carries high risk; it is recommended to do your own research before making decisions.*
promo here
Get the promo code
Source:
https://t.me/Suhanfff_bot
AlonzoStilt · April 22, 2026 at 7:47 am
Особое внимание мы уделяем психологической составляющей. Наркологическая помощь в Воронеже в «Клиника Плюс» — это не только физическое очищение, но и работа с мотивацией, разрушение психологических триггеров зависимости. Родственники получают отдельную поддержку: консультации психолога помогают правильно выстроить общение с зависимым человеком и мотивировать его на дальнейшее лечение. Реабилитация может проходить амбулаторно или в стационаре партнёрских центров с комфортабельными условиями, где пациенты находятся под круглосуточным наблюдением.
Подробнее тут – клиника наркологической помощи в воронеже
DavidOxymn · April 22, 2026 at 9:21 am
Работа с пациентами в наркологическом стационаре начинается с диагностики, которая помогает определить степень зависимости и сопутствующие заболевания. На основе этих данных разрабатывается индивидуальный план лечения. Врачи, наркологи и психотерапевты работают в тесном контакте с пациентом, что позволяет достичь наилучших результатов в процессе восстановления. Важно также убедиться, что клиника имеет необходимую лицензию, а для эффективного лечения могут быть предложены такие процедуры, как прием психотерапевта и кодирование от зависимости.
Углубиться в тему – наркологический стационар санкт-петербург
WilliamHunty · April 22, 2026 at 9:44 am
Каждый этап лечения направлен на возвращение пациента к нормальной жизни, восстановление его физического и психического здоровья. Важно отметить, что лечение всегда подбирается индивидуально, в зависимости от стадии зависимости и состояния пациента. Врачи-наркологи детально анализируют все аспекты, чтобы обеспечить наиболее эффективное лечение и помощь на всех этапах восстановления.
Разобраться лучше – наркологическая помощь стационар санкт-петербург
BrianSek · April 22, 2026 at 10:09 am
sites Ledger Live
PhilipNek · April 22, 2026 at 10:14 am
Капельница от похмелья — это медицинская процедура, направленная на устранение последствий алкогольной интоксикации и восстановление работы организма. В отличие от домашних методов, инфузионная терапия позволяет воздействовать на причину состояния, а не только на его проявления. В наркологической клинике «Похмельная служба» капельная терапия проводится с выездом специалиста на дом, что позволяет начать лечение без задержек и в комфортных условиях.
Ознакомиться с деталями – капельница от похмелья вызов на дом
fixDiele · April 22, 2026 at 10:33 am
Особенно понравился материал про Как делать региональные новости онлайн без фейков.
Смотрите сами:
https://softogon.ru/instrukcii-i-gajdy/reportazh-s-mesta-sobytij-segodnya-kak-delat-regionalnye-novosti-onlajn-bez-fejkov/
FrankSef · April 22, 2026 at 10:35 am
Главная особенность стационара с круглосуточным наблюдением — это постоянное присутствие врачей и медсестёр, готовых оказать помощь в любой момент. Это особенно важно на этапе снятия острых симптомов, когда организм находится в состоянии максимальной интоксикации. Наблюдение за пациентами в условиях стационара позволяет оперативно подбирать необходимые препараты и вмешиваться при первых признаках ухудшения состояния. В результате такого подхода повышается эффективность лечения и снижается риск осложнений, что делает процесс восстановления более быстрым и безопасным.
Выяснить больше – частный наркологический стационар санкт-петербург
fixDiele · April 22, 2026 at 10:37 am
По теме “Как записаться к врачу быстро и защитить свои права”, есть отличная статья.
Ссылка ниже:
https://crm64.ru/news/kak-zapisatsya-k-vrachu-bez-ocheredej-i-zashhitit-svoi-prava-v-poliklinike/
Larrybok · April 22, 2026 at 12:30 pm
Многие пациенты и их родственники выбирают выезд врача на дом, когда пациент не в состоянии самостоятельно приехать в клинику. Домашняя помощь подходит в ситуациях, когда состояние пациента резко ухудшается, и важно начать лечение как можно быстрее.
Подробнее – скорая наркологическая помощь
Mariouphor · April 22, 2026 at 1:57 pm
Наркологическая помощь в Воронеже: профессиональное лечение зависимостей, выезд врача, анонимная помощь в наркологической клинике «Клиника Плюс».
Получить дополнительные сведения – http://narkologicheskaya-pomoshh-voronezh.ru/
PhilipNek · April 22, 2026 at 3:07 pm
Похмельный синдром сопровождается головной болью, слабостью, тошнотой, сухостью во рту и нарушением сна, что часто возникает после запоя или при алкоголизме. Эти симптомы появляются из-за накопления токсинов и нарушения водно-солевого баланса. Капельница помогает ускорить выведение вредных веществ и восстановить нормальные функции организма, снижая нагрузку на внутренние системы и помогая человеку быстрее выйти из состояния запоев.
Детальнее – капельница от похмелья
DennisSunse · April 22, 2026 at 3:47 pm
Капельница от запоя с детоксикацией организма в Нижнем Новгороде представляет собой одну из самых эффективных процедур для быстрого улучшения состояния пациента, страдающего от алкогольной зависимости. Такой подход направлен не только на устранение токсинов, но и на восстановление нормального функционирования внутренних органов, которые пострадали от длительного употребления алкоголя.
Разобраться лучше – капельницы от запоя вызов город
Arnoldcew · April 22, 2026 at 5:02 pm
Основной этап включает постановку капельницы с растворами, направленными на выведение токсинов, восстановление водно-солевого баланса и нормализацию работы внутренних органов. В состав могут входить витамины, седативные препараты, гепатопротекторы и кардиопротекторные средства. В случае ломки и снятия симптомов зависимости у больного, все препараты подбираются индивидуально, чтобы минимизировать дискомфорт и ускорить восстановление.
Ознакомиться с деталями – https://narkolog-na-dom-samara-6.ru/
Thomasropay · April 22, 2026 at 5:42 pm
Основной задачей капельницы от запоя является быстрое устранение симптомов интоксикации, связанных с длительным употреблением алкоголя. Введение в вену специальных растворов помогает не только вывести алкогольные токсины, но и восстановить нормальное функционирование внутренних органов, пострадавших от воздействия алкоголя. Подбор состава капельницы всегда индивидуален и зависит от состояния пациента, а также может включать дополнительные методы лечения, такие как кодирование от алкоголизма.
Подробнее – капельница от запоя на дому цена нижний новгород
AlonzoStilt · April 22, 2026 at 7:24 pm
Когда человек или его родственники понимают, что нужна наркологическая помощь в Воронеже, время становится решающим фактором. Запой, ломка, тяжёлая интоксикация — в таких ситуациях промедление может привести к необратимым последствиям для здоровья и жизни. Наша клиника создана именно для того, чтобы оказывать эффективную наркологическую помощь в Воронеже в самых сложных случаях. Мы не заставляем ждать в очередях государственных учреждений, не ставим на учёт и не разглашаем информацию. Всё происходит конфиденциально, на дому или в комфортных условиях нашей партнёрской клиники. Пациенты из Воронежа, Воронежской области, а также соседних регионов уже более 12 лет выбирают «Клиника Плюс» благодаря сочетанию скорости, профессионализма и доказанной результативности.
Получить больше информации – наркологическая помощь на дому
Manuelreish · April 22, 2026 at 9:09 pm
Выезд нарколога на дом в Самаре организован так, чтобы пациент получил помощь без ожидания и без лишней нагрузки на организм. После обращения специалист приезжает по указанному адресу, проводит первичный осмотр, оценивает общее состояние, уровень интоксикации, показатели давления, пульса, дыхания и собирает краткий анамнез. На основании этой оценки врач определяет, можно ли безопасно оказывать помощь на дому, и подбирает подходящую схему лечения, включая возможное кодирование или вывод из алкоголизма. Такой формат позволяет начать медицинские мероприятия сразу после осмотра и быстро перейти к стабилизации состояния.
Выяснить больше – нарколог на дом
Angelocob · April 22, 2026 at 9:30 pm
Показания для обращения за помощью включают:
Ознакомиться с деталями – капельница от похмелья анонимно воронеж
Larrybok · April 23, 2026 at 12:40 am
Многие пациенты и их родственники выбирают выезд врача на дом, когда пациент не в состоянии самостоятельно приехать в клинику. Домашняя помощь подходит в ситуациях, когда состояние пациента резко ухудшается, и важно начать лечение как можно быстрее.
Изучить вопрос глубже – круглосуточная наркологическая помощь в воронеже
Johnnygox · April 23, 2026 at 12:43 am
Капельница от похмелья в Воронеже с нормализацией состояния и поддержкой организма в наркологической клинике «Похмельная служба»
Исследовать вопрос подробнее – капельница от похмелья вызов на дом
DonaldSkerb · April 23, 2026 at 12:52 am
Такие состояния требуют медицинского вмешательства, поскольку могут ухудшаться без лечения. Капельница позволяет стабилизировать состояние и снизить нагрузку на организм. Услуги могут предоставляться анонимно, а при тяжёлых случаях рассматривается лечение в стационаре.
Детальнее – капельница от похмелья на дому в воронеже
Blakesip · April 23, 2026 at 1:20 am
Наркологическая помощь в Воронеже: анонимное лечение алкоголизма и наркомании, круглосуточная помощь в наркологической клинике «Клиника Плюс».
Детальнее – https://narkologicheskaya-pomoshh-voronezh-2.ru/
TOTO138 · April 23, 2026 at 2:08 am
TOTO138 LOGIN
TOTO138 LOGIN · April 23, 2026 at 2:10 am
TOTO138 LOGIN
WilliamHunty · April 23, 2026 at 3:12 am
Наркологический стационар в Санкт-Петербурге: лечение зависимости, детоксикация и круглосуточный медицинский контроль в наркологической клинике «Похмельная служба»
Подробнее можно узнать тут – narkologicheskij-staczionar-sankt-peterburg-1.ru/
FrankSef · April 23, 2026 at 3:43 am
Наркологический стационар с круглосуточным наблюдением в Санкт-Петербурге — это специализированное медицинское учреждение, предоставляющее помощь пациентам с зависимостью от алкоголя, наркотиков или других психоактивных веществ. В таких стационарах пациенты получают не только лечение, но и постоянное медицинское наблюдение, что значительно повышает безопасность и эффективность терапии. Круглосуточная поддержка специалистов позволяет предотвратить осложнения и быстро реагировать на изменения в состоянии пациента. В некоторых случаях, таких как запой или хронический алкоголизм, может быть рекомендован выезд на дом для оказания неотложной помощи, прежде чем пациент будет переведен в стационар.
Детальнее – наркологическая клиника стационар
Angelocob · April 23, 2026 at 5:32 am
В Воронеже круглосуточная помощь при похмелье востребована в ситуациях, когда симптомы появляются внезапно или усиливаются в ночное время, особенно в запое или после запоя. Врач проводит консультацию, оценивает состояние пациента и принимает решение о проведении инфузионной терапии. Такой подход позволяет своевременно устранить симптомы и предотвратить их дальнейшее развитие. При необходимости можно оставить заявку, уточнить цены или получить помощь бесплатно на первичном этапе.
Детальнее – https://kapelnicza-ot-pokhmelya-voronezh-7.ru
online casino · April 23, 2026 at 5:34 am
Does it look like we’re in for a big ride here?
best online casino · April 23, 2026 at 5:39 am
This is my first time i visit here. I found so many helpful stuff in your website especially its discussion. From the tons of responses on your posts, I guess I am not the only one having all the enjoyment here! keep up the excellent work
HowardSoisa · April 23, 2026 at 6:20 am
Наркологическая помощь в Воронеже становится необходимой в тот момент, когда эпизоды употребления перерастают в клиническую картину алкоголизма или наркомании, а бытовые трудности сменяются устойчивыми симптомами наркозависимости. Для одних семей поводом для обращения становится затяжной запой, сопровождающийся физическим истощением и обезвоживанием. Для других — выраженная тревожность, тремор, скачки артериального давления, агрессия или повторяющиеся срывы после попыток сократить дозировку самостоятельно. Во всех этих случаях важна не разовая процедура, а медицински обоснованная помощь, которая учитывает текущее состояние пациента, минимизирует риски осложнений и определяет дальнейший маршрут восстановления. Когда близкие начинают искать специалиста, они, как правило, хотят решить комплекс задач: стабилизировать самочувствие, понять, достаточно ли домашнего формата или нужна госпитализация, оценить степень сформированной зависимости и выстроить план действий, который не вернет человека в кризис через несколько дней. Именно поэтому профессиональная наркология рассматривается как последовательная система вмешательств — от осмотра и первичной стабилизации до работы с мотивацией, психотерапии и профилактики рецидивов.
Получить больше информации – клиника наркологической помощи в воронеже
Robertmah · April 23, 2026 at 6:59 am
Ищете где лутать — это лутран сайт. Выплаты моментальные и только честный рандом.
Промокод на фриспины после регистрации на лутран. Заполни поля — откроешь кейс за рубль.
Ссылка не падает — лутран рабочий сайт. Все кейсы открываются и вывод за минуту.
Source:
http://lootbm.run
lootrun сайт зеркало
Robertmah · April 23, 2026 at 7:05 am
Ищете где лутать — это лутран сайт. Выплаты моментальные и никакого скама.
Бесплатный старт после лутран регистрация. Заполни поля — получи 100 фриспинов.
Ссылка не падает — лутран рабочий сайт. Все кейсы открываются и вывод за минуту.
Source:
http://lootbt.run
lootrun казино онлайн
Robertmah · April 23, 2026 at 7:09 am
Реально топовый сайт — это лутран. Кейсы летят как надо и только честный рандом.
Быстрый вход на лутран сайт. Авторизуйся через стим и лови приветственный бонус.
Проверено — работает — лутран рабочий сайт. Все кейсы открываются и вывод за минуту.
Source:
http://playrun.run
лутран вход
Robertmah · April 23, 2026 at 7:15 am
Лучшее казино по скинам — это лутран казино. Залетай и крути с шансом на нож.
Не теряй ни минуты на лутран вход. Авторизуйся через стим и забирай свой первый кейс.
Только актуальная ссылка — лутран актуальное зеркало. Сохраняй в закладки и лутай без проблем.
Source:
http://llrun.run
лутран зеркало
Robertmah · April 23, 2026 at 7:19 am
Всем знакомым советую — лутран официальный сайт. Честные проценты и быстрый вывод скинов.
Надоело сливать бабки? Погнали крутить — лутран играть. Жми на старт.
Халява тут лутран казино. Дроп удвоен! Забегай быстрее, пока акция не кончилась.
Source:
http://1lootrun.com
lootrun казино
Robertmah · April 23, 2026 at 7:22 am
Лучшее казино по скинам — это лутран казино. Открывай кейсы с шансом на нож.
Быстрый вход на лутран сайт. Авторизуйся через стим и забирай свой первый кейс.
Ссылка не падает — лутран официальный сайт. Никаких ошибок и моментальные выплаты.
Source:
http://lootbd.run
лутран регистрация сайт
Robertmah · April 23, 2026 at 7:32 am
Если основной не грузит — лутран зеркало. Актуальная ссылка без банов.
Быстрый вход на лутран сайт. Авторизуйся через стим и забирай свой первый кейс.
Ссылка не падает — лутран официальный сайт. Все кейсы открываются и вывод за минуту.
Source:
http://lootbt.run
lootrun казино онлайн
Vadimlet · April 23, 2026 at 8:10 am
Нужна была бытовка срочно — стройка стояла без жилья для рабочих. Уточнил наличие на складе, оказалось типовой размер 6х2.4 был готов. Отгрузили в день обращения. Выручили в критический момент. бытовка за 2 дня Москва
Nikitalet · April 23, 2026 at 8:22 am
Брал блок контейнер для временного склада на даче. Компактный вариант, без лишних опций. Установили на бетонные блоки без фундамента — стоит ровно, не перекашивает. Отличное решение. бытовка 6х2.4 Москва
Timothyelapy · April 23, 2026 at 12:39 pm
Ayr?ca, eger koyu gri renk konusuyla ilgileniyorsan?z, suraya bir goz at?n. Iste link: https://evhobisi.com/articles/koyu-gri-renk-estetik-uygulama-alanlari/
Timothyelapy · April 23, 2026 at 12:44 pm
Ayr?ca, eger ekimde ne ekilir konusuyla ilgileniyorsan?z, suraya bir goz at?n. Kendiniz gorun: https://hobiprojesi.com/articles/ekim-ayinda-hangi-bitkiler-ekilir/
1xbet bonus · April 23, 2026 at 2:40 pm
1xbet
John Smith · April 23, 2026 at 2:42 pm
The most convenient way: canadian online pharmacy delivered to door – watch for shipping times
RogerClape · April 23, 2026 at 5:33 pm
Острые состояния редко развиваются внезапно без предпосылок. Чаще всего им предшествуют недели или месяцы нарастающей нагрузки на нервную и сердечно-сосудистую системы. Игнорирование ранних сигналов приводит к тому, что в момент кризиса требуются уже не профилактические меры, а экстренная стабилизация. Профессиональная оценка позволяет разграничить ситуации, где достаточно амбулаторной поддержки, и те, где необходимо круглосуточное наблюдение. Своевременное вмешательство снижает вероятность осложнений, сокращает длительность восстановления и повышает готовность пациента к дальнейшей терапии.
Получить дополнительную информацию – вызов наркологической помощи воронеж
JamesSpuRa · April 23, 2026 at 5:33 pm
За выездом врача обращаются в тех случаях, когда человеку тяжело добраться до клиники, он ослаблен после нескольких дней употребления спиртного или родственникам важно быстрее получить медицинскую консультацию на месте. После осмотра определяют, допустим ли домашний формат, требуется ли капельница, достаточно ли наблюдения на дому или нужен другой объем помощи. Если эпизоды повторяются, в дальнейшем могут обсуждаться лечение алкоголизма, кодирование, участие психолога, реабилитация и более широкая программа помощи при зависимости. Уже на этапе первичного обращения нередко уточняют, как вызвать специалиста, какие услуги доступны на дому и в каких случаях вывод из запоя рассматривают не дома, а в стационаре.
Подробнее можно узнать тут – врач нарколог на дом в екатеринбурге
Ernievah · April 23, 2026 at 5:51 pm
Срочный выезд нарколога на дом позволяет сразу оценить состояние пациента, снять симптомы абстиненции и начать детоксикацию организма. Капельницы от запоя и интоксикации составляются индивидуально с учётом новейших медицинских протоколов 2026 года: они включают нейропротекторы, гепатопротекторы и витаминно-минеральные комплексы последнего поколения. Это не просто очищение крови — это восстановление работы мозга, печени, сердечно-сосудистой системы и психики.
Получить дополнительные сведения – оказание наркологической помощи воронеж
Issacgrini · April 23, 2026 at 5:55 pm
Для жителей Самары выезд нарколога на дом — это удобный и быстрый способ получить неотложную помощь при алкогольной или наркотической зависимости. Когда состояние пациента ухудшается и он не может самостоятельно обратиться за помощью, нарколог на дом становится единственным правильным решением. Важно понимать, что симптоматика абстиненции может развиваться стремительно, и чем быстрее будет оказана помощь, тем меньше рисков для здоровья пациента.
Получить дополнительную информацию – нарколог на дом цена
Walterlinty · April 23, 2026 at 6:07 pm
Затяжной запой перестает быть бытовой проблемой в тот момент, когда организм теряет способность самостоятельно восстанавливаться после интоксикации. Накопление ацетальдегида, нарушение водно-электролитного баланса, истощение запасов витаминов и перегрузка сердечно-сосудистой системы создают состояние, при котором домашние методы перестают быть безопасными. Срочно стабилизировать самочувствие и быстро купировать абстинентный синдром позволяет только контролируемая медицинская среда. Вывод из запоя в стационаре в Нижнем Новгороде становится клинически обоснованным решением, когда требуется не просто снятие симптомов, а комплексная детоксикация под круглосуточным наблюдением врачей. Наркологическая клиника «Стармед» организует процесс лечения в соответствии с актуальными стандартами доказательной медицины, обеспечивая безопасность пациента, прозрачность процедур и плавный переход к противорецидивной терапии. Мы понимаем, что решение о госпитализации часто принимается в состоянии стресса, поэтому наша работа начинается с четкой диагностики, честного объяснения плана лечения и соблюдения строгих протоколов конфиденциальности. Опытные специалисты клиники помогут вызвать доверие к процессу восстановления уже на этапе первого контакта.
Изучить вопрос глубже – быстрый вывод из запоя в стационаре в нижнем новгороде
Michaelcek · April 23, 2026 at 6:21 pm
Нарколог на дом в Екатеринбурге: анонимная помощь при алкоголизме, вывод из запоя и поддержка специалистов в наркологической клинике «НЕО+».
Узнать больше – нарколог на дом цена
KareemNop · April 23, 2026 at 6:31 pm
Запой сопровождается выраженной интоксикацией, нарушением работы сердечно-сосудистой системы, тревожностью и бессонницей, что характерно для алкоголизма и хронического употребления алкоголя. При длительном течении организм человека теряет способность к самостоятельному восстановлению, и вмешательство становится необходимым. Стационар в этом случае позволяет контролировать динамику состояния больного и корректировать терапию в режиме реального времени, особенно при тяжелом течении алкоголизма.
Подробнее тут – нарколог вывод из запоя в стационаре в нижнем новгороде
Larrybok · April 23, 2026 at 6:39 pm
Многие пациенты и их родственники выбирают выезд врача на дом, когда пациент не в состоянии самостоятельно приехать в клинику. Домашняя помощь подходит в ситуациях, когда состояние пациента резко ухудшается, и важно начать лечение как можно быстрее.
Детальнее – наркологическая помощь
Douglaspek · April 23, 2026 at 7:13 pm
За выездом врача чаще обращаются тогда, когда человеку тяжело добраться до клиники, он ослаблен после нескольких дней употребления алкоголя или родственникам важно быстрее понять, какая тактика будет безопасной. После осмотра можно определить, нужна ли капельница, достаточно ли детоксикации на дому, требуется ли повторное наблюдение, а в дальнейшем — консультация по лечению алкоголизма, кодирование или реабилитация. В части случаев уже первый звонок позволяет понять, идет ли речь только о временном ухудшении самочувствия или о состоянии, при котором может потребоваться вывод из запоя в стационаре.
Детальнее – врач нарколог на дом екатеринбург
Richardexors · April 23, 2026 at 7:27 pm
При выборе наркологического стационара с комфортными условиями в Санкт-Петербурге важно учитывать несколько ключевых факторов, которые могут повлиять на успех лечения. Кроме высококвалифицированных специалистов и индивидуального подхода, комфортные условия для проживания играют важную роль в процессе восстановления пациента. Это создаёт оптимальные условия для того, чтобы человек мог сосредоточиться на своём здоровье и восстановлении, не отвлекаясь на неприятные или неудобные условия. В некоторых случаях может быть предложено кодирование, а также получение дополнительных данных и консультаций для более точного подхода к лечению.
Исследовать вопрос подробнее – частный наркологический стационар санкт-петербург
Marioknops · April 23, 2026 at 8:41 pm
Ниже представлена таблица, отражающая основные направления медикаментозного лечения и сопутствующих процедур:
Узнать больше – наркологические клиники алкоголизм омск
Russellneome · April 23, 2026 at 10:16 pm
Процесс проведения капельницы от похмелья обычно включает в себя несколько ключевых этапов. Несмотря на простоту процедуры, важно, чтобы её проводил квалифицированный специалист. Каждый этап — от консультации до завершения процедуры — направлен на безопасность пациента и максимальную эффективность лечения.
Получить больше информации – капельница от похмелья
this link · April 23, 2026 at 10:38 pm
Darknet market electronics come with risk but savings worth it sometimes.
https://apobangpo.wiki/index.php/Dark_Web_Market_Credit_Card_Category
this link
https://codeforweb.org/mediawiki_tst/index.php?title=Dark_Web_Market_Comparison
https://wiki.e-o3.com:443/index.php?title=Dark_Web_Market_Macbook
ultshop · April 23, 2026 at 10:40 pm
Салют,
Коллеги.
В данный момент я бы хотел поведать малость про https://ultimatshop.ru/
Онлайн-платформа Ultimatshop.ru: премиальный ассортимент для вашего комфорта
Вы на официальном сайте нашего магазина, где тщательно отобранные товары сочетаются с удобным сервисом.
Мы специализируемся на продукции для повседневных задач.
Перед размещением в каталоге строгий контроль качества, что гарантирует предсказуемый результат покупки.
Почему выбирают Ultimatshop.ru
С момента основания на рынке электронной коммерции — оформлено множество отгрузок на основе тысяч отзывов
Команда квалифицированных специалистов изучают новые технологии и тренды, что позволяет предлагать экспертные рекомендации по альтернативам и аналогам
Прозрачная политика возврата и обмена согласно действующим законодательством
Стабильная стоимость утверждённые до оплаты и шифрование транзакций с поддержкой современных протоколов безопасности
Консультационный сервис работают в нескольких каналах связи и контролируют процесс доставки на всех этапах взаимодействия
Найдите нужный товар за несколько кликов.
Укажите параметры, и менеджер подберёт совместимые аксессуары с учётом вашего региона доставки.
Качество и сервис, которым доверяют.
На нашем веб портале немного больше про ultshop, также информацию про ultimateshop.
Узнай Больше про https://ultimatshop.ru/ по ссылке https://ultimatshop.ru/
Наши Теги: Ultimateshop, ultshop
Удачного Дня
HowardOwert · April 23, 2026 at 10:50 pm
Каждый пациент уникален — именно поэтому мы не применяем «типовых» решений. После первичной консультации и диагностики специалисты «КубаньМед» разрабатывают персональную программу, учитывающую состояние здоровья, психологические особенности и социальные обстоятельства пациента.
Разобраться лучше – клиника лечения алкоголизма краснодарский край
AlvinjouMb · April 23, 2026 at 10:56 pm
Выезд нарколога на дом в Воронеже становится особенно важным, когда пациент переживает острые симптомы абстиненции или интоксикации. Это может быть связано с запоем, наркотической ломкой или последствиями длительного употребления алкоголя или наркотиков. В таких случаях медицинская помощь должна быть оказана как можно скорее, чтобы предотвратить серьёзные осложнения, такие как сердечные сбои, психозы, судороги или делирий. От того, насколько быстро будет оказана помощь, зависит успешность стабилизации состояния и вероятность долгосрочного выздоровления.
Получить дополнительные сведения – запой нарколог на дом
RogerClape · April 23, 2026 at 11:06 pm
Под этим термином понимается не универсальный набор процедур, а адаптивный протокол, который формируется после осмотра, сбора анамнеза и оценки рисков. На первом этапе задача врача — стабилизировать состояние, провести качественный детокс, купировать острую интоксикацию или абстиненцию, восстановить водно-солевой баланс и нормализовать сон. Однако качественная помощь не останавливается на снятии симптомов. Она обязательно включает планирование дальнейшего маршрута, учитывающего стаж употребления, наличие сопутствующих заболеваний, психологический статус и готовность пациента к изменениям. Мы понимаем, что каждый случай уникален, поэтому в клинике применяем только доказательные протоколы, исключающие шаблонные решения и подменяющие маркетинговые обещания медицинской логикой.
Подробнее можно узнать тут – клиника наркологической помощи в воронеже
JamesSpuRa · April 23, 2026 at 11:07 pm
Нарколог на дом в Екатеринбурге: выезд врача на дом, лечение запоя и консультации в наркологической клинике «НЕО+».
Разобраться лучше – нарколог на дом вывод
Ernievah · April 23, 2026 at 11:42 pm
Лечение алкоголизма в Воронеже у нас проводится на всех стадиях: от первой помощи при запое до кодирования и долгосрочной поддержки. Для пациентов с наркотической зависимостью (включая синтетические каннабиноиды и опиоиды) мы применяем щадящие схемы детоксикации, которые минимизируют болезненные симптомы и снижают риск срывов. Кодирование от алкоголизма и наркомании доступно в нескольких вариантах: медикаментозное (инъекции, импланты, «Двойной блок»), гипносуггестивное и комбинированное. Каждый метод подбирается после тщательной диагностики, чтобы результат был максимально долгосрочным.
Узнать больше – наркологическая помощь анонимно воронеж
Walterlinty · April 23, 2026 at 11:54 pm
Детоксикация в стационаре — это не разовая процедура, а последовательный процесс, разделенный на диагностику, активное выведение токсинов, стабилизацию функций и подготовку к противорецидивному этапу. При поступлении врач проводит первичный осмотр, собирает подробный анамнез, оценивает неврологический статус и при необходимости назначает лабораторные исследования. На основе полученных данных формируется индивидуальный протокол, учитывающий возраст, вес, длительность запоя, наличие сопутствующих патологий и переносимость лекарственных средств. Мы применяем только сертифицированные медикаменты, зарегистрированные в РФ, и строго соблюдаем клинические рекомендации Минздрава, исключая псевдонаучные методики. Все вмешательства документируются в электронной медицинской карте, доступ к которой имеют только лечащие специалисты.
Изучить вопрос глубже – нарколог вывод из запоя в стационаре
legalne kasyna online · April 23, 2026 at 11:54 pm
I simply could not leave your site before suggesting that I actually enjoyed the usual info a person supply in your visitors? Is going to be back often to inspect new posts
magyar online casino · April 24, 2026 at 12:10 am
Woh I enjoy your content , saved to bookmarks!
KennethSpaft · April 24, 2026 at 12:19 am
Первые положительные изменения обычно появляются уже через 15–20 минут после начала капельницы. Уменьшается головная боль, снижается чувство тошноты, стабилизируется давление и пульс. К концу процедуры большинство симптомов становится значительно менее выраженными.
Изучить вопрос глубже – капельница от похмелья на дом самара
V9bet · April 24, 2026 at 12:24 am
Are the issues really as complex as they seem?
KareemNop · April 24, 2026 at 12:45 am
Первый этап лечения направлен на стабилизацию состояния. Он начинается с оценки витальных показателей и клинической картины. После этого формируется план терапии, в котором определены цели и временные интервалы для оценки результата. Такой подход позволяет контролировать процесс и избегать хаотичных назначений, особенно при лечении алкоголизма.
Получить больше информации – https://vyvod-iz-zapoya-v-staczionare-nizhnij-novgorod-2.ru
Douglaspek · April 24, 2026 at 1:05 am
За выездом врача чаще обращаются тогда, когда человеку тяжело добраться до клиники, он ослаблен после нескольких дней употребления алкоголя или родственникам важно быстрее понять, какая тактика будет безопасной. После осмотра можно определить, нужна ли капельница, достаточно ли детоксикации на дому, требуется ли повторное наблюдение, а в дальнейшем — консультация по лечению алкоголизма, кодирование или реабилитация. В части случаев уже первый звонок позволяет понять, идет ли речь только о временном ухудшении самочувствия или о состоянии, при котором может потребоваться вывод из запоя в стационаре.
Разобраться лучше – нарколог на дом
Sammiesoymn · April 24, 2026 at 1:24 am
Сразу после вызова нарколог прибывает на дом для проведения тщательного первичного осмотра. На этом этапе специалист собирает краткий анамнез, измеряет жизненно важные показатели – пульс, артериальное давление, температуру – и оценивает степень алкогольной интоксикации. Полученные данные служат основой для составления индивидуального плана лечения, позволяющего подобрать оптимальные методы детоксикации.
Углубиться в тему – нарколог вывод из запоя в ярославле
Charlespes · April 24, 2026 at 2:51 am
Запой и алкогольная интоксикация могут приводить к целому ряду опасных симптомов, таких как головная боль, слабость, тошнота, рвота, обезвоживание и психоэмоциональная нестабильность. Если не начать лечение вовремя, такие состояния могут привести к более серьезным осложнениям, включая сердечные проблемы, галлюцинации и даже опасные для жизни нарушения работы организма. С помощью нарколога на дому можно начать экстренную терапию прямо в момент ухудшения состояния, не затягивая с лечением и не тратя время на поездки в клинику.
Изучить вопрос глубже – запой нарколог на дом в самаре
소액결제현금화 · April 24, 2026 at 3:37 am
소액결제현금화는 휴대폰의 월 소액결제 한도(최대 100만~200만원)를 이용해 상품권이나 디지털 콘텐츠를 구매한 뒤, 이를 전문 업체에 수수료를 떼고 팔아 현금으로 바꾸는 행위입니다.
Link 12bet · April 24, 2026 at 4:24 am
A good web site with interesting content, that’s what I need. Thank you for making this web site, and I will be visiting again. Do you do newsletters? I Can’t find it.
najlepsze kasyno online · April 24, 2026 at 5:09 am
I like to spend my free time by scanning various internet resources. Today I came across your website and I found it has some of the most practical and helpful information I’ve seen.
JamesSpuRa · April 24, 2026 at 5:46 am
За выездом врача обращаются в тех случаях, когда человеку тяжело добраться до клиники, он ослаблен после нескольких дней употребления спиртного или родственникам важно быстрее получить медицинскую консультацию на месте. После осмотра определяют, допустим ли домашний формат, требуется ли капельница, достаточно ли наблюдения на дому или нужен другой объем помощи. Если эпизоды повторяются, в дальнейшем могут обсуждаться лечение алкоголизма, кодирование, участие психолога, реабилитация и более широкая программа помощи при зависимости. Уже на этапе первичного обращения нередко уточняют, как вызвать специалиста, какие услуги доступны на дому и в каких случаях вывод из запоя рассматривают не дома, а в стационаре.
Узнать больше – нарколог на дом анонимно
RogerClape · April 24, 2026 at 5:50 am
Под этим термином понимается не универсальный набор процедур, а адаптивный протокол, который формируется после осмотра, сбора анамнеза и оценки рисков. На первом этапе задача врача — стабилизировать состояние, провести качественный детокс, купировать острую интоксикацию или абстиненцию, восстановить водно-солевой баланс и нормализовать сон. Однако качественная помощь не останавливается на снятии симптомов. Она обязательно включает планирование дальнейшего маршрута, учитывающего стаж употребления, наличие сопутствующих заболеваний, психологический статус и готовность пациента к изменениям. Мы понимаем, что каждый случай уникален, поэтому в клинике применяем только доказательные протоколы, исключающие шаблонные решения и подменяющие маркетинговые обещания медицинской логикой.
Получить больше информации – клиника наркологической помощи
Robertmah · April 24, 2026 at 6:11 am
Если основной не грузит — лутран зеркало. Новый адрес без блокировок.
Не теряй ни минуты на лутран вход. Залетай по кнопке и лови приветственный бонус.
Халява тут лутран казино. Кейсы с x2! Успевай на хайп, пока баланс не разобрали.
Source:
http://playrun.online
лутран сайт
Robertmah · April 24, 2026 at 6:16 am
Всем знакомым советую — лутран сайт. Честные проценты и быстрый вывод скинов.
Надоело сливать бабки? Погнали крутить — лутран играть. Твой драгон лор ждет.
Новый сезон на лутран. Кейсы с x2! Успевай на хайп, пока акция не кончилась.
Source:
http://lootba.run
лутран вход в аккаунт
Robertmah · April 24, 2026 at 6:20 am
Реально топовый сайт — это лутран. Кейсы летят как надо и только честный рандом.
Бесплатный старт после регистрации на лутран. Жми на кнопку — откроешь кейс за рубль.
Проверено — работает — лутран рабочий сайт. Все кейсы открываются и моментальные выплаты.
Source:
http://lootrungame.info
лутран казино сайт
Robertmah · April 24, 2026 at 6:29 am
Лучшее казино по скинам — это лутран. Залетай и крути с шансом на нож.
Хочешь залутать топ? Время играть — лутран играть. Твой драгон лор ждет.
Ссылка не падает — лутран официальный сайт. Никаких ошибок и моментальные выплаты.
Source:
http://lootbd.run
лутран регистрация сайт
Robertmah · April 24, 2026 at 6:34 am
Всем знакомым советую — лутран сайт. Честные проценты и быстрый вывод скинов.
Не теряй ни минуты на лутран сайт. Авторизуйся через стим и лови приветственный бонус.
Новый сезон на лутран казино. Кейсы с x2! Забегай быстрее, пока акция не кончилась.
Source:
http://loot19.run
лутран играть
Robertmah · April 24, 2026 at 6:41 am
Только тут настоящий — лутран официальный сайт. Без обмана и быстрый вывод скинов.
Бесплатный старт после регистрации на лутран. Заполни поля — откроешь кейс за рубль.
Только актуальная ссылка — лутран актуальное зеркало. Вбивай в адресную строку и играй спокойно.
Source:
http://playlootrun.com
lootrun сайт
Ernievah · April 24, 2026 at 6:50 am
Наркологическая помощь в Воронеже: срочный выезд нарколога, капельницы и лечение зависимостей в наркологической клинике «Клиника Плюс».
Узнать больше – круглосуточная наркологическая помощь в воронеже
Walterlinty · April 24, 2026 at 6:54 am
Детоксикация в стационаре — это не разовая процедура, а последовательный процесс, разделенный на диагностику, активное выведение токсинов, стабилизацию функций и подготовку к противорецидивному этапу. При поступлении врач проводит первичный осмотр, собирает подробный анамнез, оценивает неврологический статус и при необходимости назначает лабораторные исследования. На основе полученных данных формируется индивидуальный протокол, учитывающий возраст, вес, длительность запоя, наличие сопутствующих патологий и переносимость лекарственных средств. Мы применяем только сертифицированные медикаменты, зарегистрированные в РФ, и строго соблюдаем клинические рекомендации Минздрава, исключая псевдонаучные методики. Все вмешательства документируются в электронной медицинской карте, доступ к которой имеют только лечащие специалисты.
Подробнее можно узнать тут – наркология вывод из запоя в стационаре
HerbertDyday · April 24, 2026 at 7:00 am
В Самаре клиника «Частный медик 24» предоставляет круглосуточную помощь по выведению из запоя и снятию симптомов похмелья. Когда человек сталкивается с тяжёлым состоянием после длительного употребления алкоголя, важно вовремя оказать помощь. Врач приедет на дом и проведёт все необходимые процедуры, включая капельницу, которая поможет восстановить водно-электролитный баланс, нормализовать уровень сахара в крови и вывести токсины из организма.
Разобраться лучше – капельница от похмелья анонимно самара
Richardanomy · April 24, 2026 at 7:31 am
Когда человек или его родственники понимают, что нужна наркологическая помощь в Воронеже, время становится решающим фактором. Запой, ломка, тяжёлая интоксикация — в таких ситуациях промедление может привести к необратимым последствиям для здоровья и жизни. Наша клиника создана именно для того, чтобы оказывать эффективную круглосуточную наркологическую помощь в Воронеже в самых сложных случаях. Мы не заставляем ждать в очередях государственных учреждений, не ставим на учёт и не разглашаем информацию. Всё происходит анонимно, на дому или в комфортных условиях нашей партнёрской клиники. Пациенты из Воронежа, Воронежской области, а также соседних регионов уже более 12 лет выбирают «Клиника Плюс» благодаря сочетанию скорости, профессионализма, полной анонимности и доказанной результативности.
Выяснить больше – оказание наркологической помощи в воронеже
casino en ligne Canada · April 24, 2026 at 7:38 am
This contained some excellent tips and tools. Great blog publication.
legalne kasyna online · April 24, 2026 at 7:55 am
I am glad to be a visitor on this website!, regards for this rare information!
najlepsze kasyno online · April 24, 2026 at 8:03 am
Nice read, I just passed this onto a colleague who was doing some research on that. And he just bought me lunch as I found it for him smile Therefore let me rephrase that: Thank you for lunch!
kasyno online · April 24, 2026 at 8:03 am
There most be a solution for this problem, some people think there will be now solutions, but i think there wil be one.
Thomaslak · April 24, 2026 at 8:38 am
Состав капельницы от похмелья зависит от состояния пациента и специфики его симптомов. Важно, чтобы капельница включала компоненты, направленные на улучшение общего состояния, восстановление водно-солевого баланса и поддержку работы внутренних органов.
Исследовать вопрос подробнее – капельница от похмелья
RandyGrirl · April 24, 2026 at 8:43 am
Детоксикация в основном фокусируется на печени и почках, помогая этим органам быстрее справляться с продуктами распада алкоголя. Такой подход гарантирует не только улучшение самочувствия, но и восстановление работы внутренних органов, которые пострадали в процессе злоупотребления алкоголем.
Узнать больше – http://www.domen.ru
Alfredassug · April 24, 2026 at 9:11 am
Показания к проведению инфузионной терапии включают:
Разобраться лучше – капельница от похмелья на дому воронеж
TravisVAB · April 24, 2026 at 10:04 am
Нарколог на дом в Екатеринбурге востребован в ситуациях, когда человеку нужна врачебная помощь после употребления алкоголя, при запое, выраженном похмельном синдроме, нарушении сна, тревоге, скачках давления, слабости и других признаках ухудшения самочувствия. Такой формат обращения часто выбирают семьи, которые хотят вызвать врача без поездки в клинику и быстро получить консультацию по состоянию больного. Домашний выезд особенно важен тогда, когда требуется детоксикация, наблюдение после нескольких дней употребления спиртного и оценка рисков, связанных с последствиями алкоголизма.
Изучить вопрос глубже – вызов нарколога на дом екатеринбург
WalterCrymn · April 24, 2026 at 10:25 am
Обращение в наркологический стационар особенно важно в случае тяжелой зависимости, когда человек не способен контролировать свои действия, а угрозы для здоровья возрастают. В таких случаях важно не откладывать начало лечения, а обратиться за помощью сразу же, чтобы избежать серьезных последствий для организма. При выборе стационара следует обратить внимание на наличие лицензии, а также возможность получения психотерапии и других профессиональных услуг в области наркологии для комплексного лечения зависимости.
Изучить вопрос глубже – наркологический стационар санкт-петербург
WalterCrymn · April 24, 2026 at 10:27 am
Обращение в наркологический стационар особенно важно в случае тяжелой зависимости, когда человек не способен контролировать свои действия, а угрозы для здоровья возрастают. В таких случаях важно не откладывать начало лечения, а обратиться за помощью сразу же, чтобы избежать серьезных последствий для организма. При выборе стационара следует обратить внимание на наличие лицензии, а также возможность получения психотерапии и других профессиональных услуг в области наркологии для комплексного лечения зависимости.
Ознакомиться с деталями – наркологическая клиника стационар санкт-петербург
ThomasViecy · April 24, 2026 at 12:05 pm
В Нижнем Новгороде стационарное лечение используется при наличии факторов, которые увеличивают риск осложнений или делают домашний формат недостаточным, особенно при алкоголизме или тяжёлом состоянии больного. Врач принимает решение на основе осмотра, консультации, анализа данных и оценки симптомов и динамики состояния пациента. Основная цель — обеспечить безопасность человека и создать условия для контролируемого лечения алкоголизма.
Исследовать вопрос подробнее – http://www.domen.ru
ClintonPoush · April 24, 2026 at 12:30 pm
Процесс восстановления с помощью капельницы с мягким восстановлением происходит в несколько этапов. Вначале происходит нормализация водно-солевого баланса, что помогает предотвратить обезвоживание и улучшить состояние кожи. Затем происходит восстановление энергетических запасов организма, что помогает уменьшить усталость и слабость, что также важно при лечении наркомании. Витамины и антиоксиданты восстанавливают функции клеток и органов, что способствует более быстрому очищению организма от продуктов распада алкоголя, при этом пациентам может быть доступна анонимное консультация и дальнейшая реабилитация.
Изучить вопрос глубже – https://kapelnicza-ot-pokhmelya-samara-12.ru/
DonaldHum · April 24, 2026 at 12:33 pm
Попытки самостоятельно прекратить употребление после нескольких дней непрерывной интоксикации часто сопровождаются резким выбросом стрессовых гормонов, скачками артериального давления, тахикардией и нарушением электролитного баланса. Без инфузионной поддержки и фармакологической коррекции возрастает риск развития такого грозного осложнения, как белая горячка, судорожных состояний, острой печеночной или сердечной недостаточности. Самостоятельные попытки резко перестать пить без медицинского контроля опасен для жизни и может спровоцировать необратимые изменения в работе внутренних органов. Домашние условия не позволяют проводить лабораторный контроль, корректировать дозировки в реальном времени и оперативно реагировать на ухудшение состояния. Стационар решает эти задачи за счет круглосуточного дежурства врачей, наличия реанимационного оборудования и возможности привлечения смежных специалистов при выявлении соматических осложнений.
Углубиться в тему – быстрый вывод из запоя в стационаре в нижнем новгороде
neues online casino · April 24, 2026 at 12:48 pm
Thanks , I’ve recently been searching for info about this topic for ages and yours is the best I have discovered so far. But, what concerning the bottom line? Are you certain concerning the source?
https://1xbet-promo-code-free-spins.com/1xbet-promo-code-no-deposit-ubaso-bonus-boosts-2026/ · April 24, 2026 at 1:43 pm
https://1xbet-promo-code-free-spins.com/1xbet-promo-code-no-deposit-ubaso-bonus-boosts-2026/
ThomasViecy · April 24, 2026 at 2:09 pm
При таких условиях стационар позволяет контролировать состояние в режиме 24/7 и при необходимости быстро корректировать лечение. Это снижает риски и делает процесс более предсказуемым. При этом услуга может предоставляться анонимно, а цену лечения можно уточнить по телефону или при обращении в центр лечения алкоголизма и наркомании.
Детальнее – http://www.domen.ru
Jeremydaype · April 24, 2026 at 2:23 pm
Самостоятельные попытки обычно идут по двум типичным маршрутам. Первый — «пить понемногу, чтобы не трясло». На практике это продлевает запой и усиливает истощение: сон остаётся поверхностным, тревога нарастает, давление и пульс становятся нестабильными, организм не успевает восстанавливаться. Второй маршрут — резко прекратить и «перетерпеть». Тогда симптомы отмены могут нарастать резко: паника, сильный тремор, потливость, тахикардия, скачки давления, тошнота, рвота, бессонница. Испугавшись ухудшения, человек снова возвращается к алкоголю, потому что это кажется единственным быстрым способом облегчить состояние.
Получить дополнительную информацию – https://vyvod-iz-zapoya-orekhovo-zuevo12.ru/
Dwayneoxymn · April 24, 2026 at 4:02 pm
Зависимость меняет работу нервной системы: алкоголь начинает выполнять функцию регулятора — сна, тревоги, настроения и даже физического самочувствия. Когда человек прекращает пить, организм реагирует отменой, и именно она подталкивает вернуться к употреблению. Сила воли в этой точке часто проигрывает физиологии: тревога растёт, сон исчезает, сердце бьётся чаще, давление «скачет», появляется ощущение угрозы.
Углубиться в тему – http://lechenie-alkogolizma-noginsk12.ru
Jordanvep · April 24, 2026 at 5:45 pm
При выборе наркологического стационара в Санкт-Петербурге важно ориентироваться на несколько ключевых критериев. В первую очередь, следует учитывать опыт и квалификацию специалистов, условия пребывания, а также отзывы пациентов. Ведь выбор медицинского учреждения — это не только вопрос качества лечения, но и обеспечения психологического комфорта пациента, что особенно важно при лечении зависимостей. Стоит обратить внимание на стационары, специализирующиеся на лечении наркомании и наркологии, а также учитывать расположение клиники в удобном районе города.
Детальнее – https://narkologicheskij-staczionar-sankt-peterburg-3.ru
Adrianwiz · April 24, 2026 at 6:21 pm
Введение лекарственных препаратов через капельницу позволяет значительно ускорить процессы, которые происходят в организме, поскольку вещества поступают сразу в кровоток, минуя желудочно-кишечный тракт. Это значительно усиливает эффективность лечения и способствует быстрому улучшению самочувствия пациента, при этом проводится наркологическая терапия, а при необходимости можно заказать дополнительное лечение с учетом данных пациента.
Подробнее тут – http://www.domen.ru
LucasjaT · April 24, 2026 at 6:46 pm
Вывод из запоя в стационаре в Нижнем Новгороде с круглосуточным наблюдением и поэтапным восстановлением в наркологической клинике «Частный медик 24»
Исследовать вопрос подробнее – вывод из запоя цена нижний новгород
Spencersaica · April 24, 2026 at 6:51 pm
Запой сопровождается комплексом нарушений: обезвоживание, колебания давления, тремор, тревожность, нарушение сна. При длительном течении состояние может усиливаться, и самостоятельный выход становится затруднённым. В таких случаях стационар рассматривается как безопасная среда, где можно контролировать динамику и оперативно реагировать на изменения.
Разобраться лучше – вывод из запоя в стационаре
Jefferycrync · April 24, 2026 at 7:07 pm
Выезд врача — это не «процедура без вопросов», а клиническое решение. На месте оценивают давление, пульс, дыхание, степень обезвоживания, уровень сознания, выраженность тревоги, наличие боли, судорожных проявлений, неврологические симптомы. После этого подбирают схему поддержки, объясняют ограничения и ожидаемую динамику: что должно улучшаться в первые часы, какие симптомы допустимы, а какие требуют немедленного обращения. Важная часть — рекомендации на ближайшие сутки: режим питья и питания, сон, контроль давления, что категорически нельзя смешивать и почему. Такой подход снижает риск осложнений и помогает не «сорваться» в самостоятельные эксперименты.
Изучить вопрос глубже – https://narkologicheskaya-klinika-moskva12.ru/chastnaya-narkologicheskaya-klinika-v-moskve/
AnthonyBar · April 24, 2026 at 7:16 pm
Далее выполняется медицинская детоксикация: корректируется водно-электролитный баланс, снимается интоксикация, поддерживается работа сердечно-сосудистой системы, снижается тремор, стабилизируется сон и тревожность. Важно, что схема подбирается индивидуально: при разных рисках объём поддержки будет различаться. В ряде случаев достаточно амбулаторного наблюдения и рекомендаций, в других — нужен стационар, чтобы контролировать динамику и вовремя корректировать терапию.
Выяснить больше – vyvod-iz-zapoya-moskovskaya-oblast-moskva
Melvinadage · April 24, 2026 at 8:40 pm
Особое внимание мы уделяем психологической составляющей. Наркологическая помощь в Воронеже в «Клиника Плюс» — это не только физическое очищение, но и работа с мотивацией, разрушение психологических триггеров зависимости. Родственники получают отдельную поддержку: консультации психолога помогают правильно выстроить общение с зависимым человеком и мотивировать его на дальнейшее лечение. Реабилитация может проходить амбулаторно или в стационаре партнёрских центров с комфортабельными условиями, где пациенты находятся под круглосуточным наблюдением.
Изучить вопрос глубже – наркологическая помощь анонимно воронеж
Thomasexink · April 24, 2026 at 8:44 pm
Похмельный синдром сопровождается головной болью, слабостью, тошнотой, сухостью во рту и нарушением сна, что часто возникает после запоя или при алкоголизме. Эти симптомы появляются из-за накопления токсинов и нарушения водно-солевого баланса. Капельница помогает ускорить выведение вредных веществ и восстановить нормальные функции организма, снижая нагрузку на внутренние системы и помогая человеку быстрее выйти из состояния запоев.
Углубиться в тему – капельница от похмелья на дом в воронеже
MatthewGed · April 24, 2026 at 8:54 pm
Наркологический стационар в Санкт-Петербурге: помощь при зависимости, восстановление и круглосуточное наблюдение в наркологической клинике «Похмельная служба»
Подробнее можно узнать тут – http://narkologicheskij-staczionar-sankt-peterburg-2.ru
RobertDic · April 24, 2026 at 9:07 pm
Капельница от похмелья — это медицинская процедура, направленная на быстрое восстановление организма после алкогольной интоксикации. Она помогает устранить обезвоживание, нормализовать обменные процессы и снизить токсическую нагрузку на внутренние органы. В отличие от домашних методов, инфузионная терапия действует напрямую через кровоток, обеспечивая более быстрый и выраженный эффект.
Подробнее – http://www.domen.ru
Richardcon · April 24, 2026 at 9:56 pm
Обращение на стадии, когда человек не может самостоятельно справиться с зависимостью, значительно повышает шансы на успешное лечение и восстановление. Важно начать лечение на раннем этапе, когда физическая и психологическая зависимость еще не столь выражены.
Получить дополнительную информацию – наркологическая помощь на дому
Michaelmaply · April 24, 2026 at 9:57 pm
Организация терапевтического процесса в условиях стационара требует слаженной работы профильной команды, четких клинических алгоритмов и непрерывного документирования каждого этапа лечения. В клинике выстроена прозрачная система взаимодействия, где пациент и его близкие получают исчерпывающую информацию о планах терапии, ожидаемых результатах, условиях пребывания и правах потребителя медицинских услуг. Мы отказались от шаблонных протоколов в пользу персонализированной медицины, где каждый шаг лечения согласовывается с динамикой состояния пациента и корректируется на основе объективных диагностических данных. Такой подход исключает избыточную фармакологическую нагрузку и минимизирует риски побочных эффектов, сохраняя при этом высокую клиническую эффективность детоксикации.
Изучить вопрос глубже – наркология вывод из запоя в стационаре
MatthewGed · April 24, 2026 at 9:58 pm
Обращение в наркологический стационар в Санкт-Петербурге может стать важным шагом для людей, страдающих от алкогольной или наркотической зависимости. Стационарное лечение предоставляет пациентам не только медицинскую помощь, но и психологическую поддержку, необходимую для успешной реабилитации. Это подход, ориентированный на комплексное восстановление здоровья, физическое и психоэмоциональное состояние пациента.
Получить дополнительные сведения – наркологический стационар
Howardsoilk · April 24, 2026 at 10:13 pm
Помощь на дому рассматривают при состояниях, связанных с острым ухудшением самочувствия после алкоголя. Чаще всего это несколько дней запоя, тяжелое похмелье, бессонница, тревога, дрожь в руках, слабость, отсутствие аппетита, тошнота, сухость во рту и ощущение истощения. В подобных случаях врачебный осмотр нужен для оценки общего состояния и выбора безопасной тактики.
Узнать больше – http://www.domen.ru
Reggierooma · April 24, 2026 at 11:33 pm
Домашняя помощь эффективна, когда пациент контактный, сохранен, способен выполнять назначения и нет признаков высокой угрозы осложнений. Но удобство не должно подменять безопасность. Именно поэтому врач на выезде уточняет длительность употребления, время последнего приёма алкоголя или вещества, выраженность симптомов, хронические заболевания, лекарства, которые человек принимал самостоятельно, и возможные осложнения в прошлом.
Разобраться лучше – skolko-stoit-vyzov-narkologa-na-dom
Thomasexink · April 24, 2026 at 11:57 pm
Такие симптомы требуют медицинского вмешательства, поскольку могут усиливаться без лечения. Капельница позволяет стабилизировать состояние и ускорить восстановление. Услуги могут предоставляться анонимно, а при необходимости пациент направляется на лечение в стационаре.
Получить дополнительную информацию – капельница от похмелья на дом
Alfredassug · April 25, 2026 at 12:22 am
Перед началом процедуры врач проводит осмотр пациента. Оцениваются основные показатели, включая давление и пульс, а также выраженность симптомов. На основании полученных данных формируется состав капельницы и определяется тактика лечения, что позволяет эффективно провести вывод из запоя.
Детальнее – капельница от похмелья вызов на дом в воронеже
CharlesFut · April 25, 2026 at 12:33 am
Каждый выезд нарколога включает в себя не только инфузионную терапию, но и полноценную оценку состояния пациента, анализ рисков, а также консультацию по дальнейшему лечению. Врач может назначить дополнительные препараты для снятия симптомов ломки, восстановления водно-электролитного баланса и улучшения общего состояния пациента. Также важно, что консультация включает рекомендации по реабилитации, психологической поддержке и кодированию, если это необходимо для пациента, страдающего хроническим алкоголизмом или наркоманией.
Разобраться лучше – вызвать нарколога на дом
Jeremypep · April 25, 2026 at 12:58 am
Наркологическая помощь нужна не только тогда, когда ситуация выглядит критической со стороны. Она необходима и в тех случаях, когда зависимость повторяется циклично, а семья уже понимает, что прежние способы не работают. Чем раньше человек переходит от стихийных попыток справиться самостоятельно к профессиональной тактике, тем выше шансы стоновить процесс на менее тяжелом этапе.
Узнать больше – http://www.domen.ru
DavidEnact · April 25, 2026 at 1:09 am
continue reading this petra wallet extension
KevinDrorp · April 25, 2026 at 1:32 am
Зависимость редко начинается как «всё плохо». Чаще это выглядит как способ справиться с напряжением: расслабиться после тяжёлого дня, быстрее уснуть, пережить стресс или конфликт. Постепенно употребление становится регулярным, дозы растут, а трезвость даётся всё тяжелее. При попытке остановиться появляются бессонница, тревога, внутренний тремор, потливость, тошнота, скачки давления, раздражительность. В этот момент человек пьёт уже не ради удовольствия, а чтобы не столкнуться с ухудшением. Наркологическая клиника в Клину нужна, чтобы перевести ситуацию в понятный медицинский процесс: сначала оценка состояния и рисков, затем безопасная стабилизация, после — лечение зависимости и профилактика повторения.
Получить дополнительную информацию – наркологическая клиника клинский район московская московская область
LucasjaT · April 25, 2026 at 1:50 am
При таких условиях стационар позволяет контролировать состояние в режиме 24/7 и при необходимости быстро корректировать лечение. Это снижает риски и делает процесс более предсказуемым. При этом услуга может предоставляться анонимно, а цену лечения можно уточнить по телефону или при обращении в центр лечения алкоголизма и наркомании.
Получить больше информации – вывод из запоя недорого нижний новгород
Ethantoisa · April 25, 2026 at 2:31 am
Капельница от похмелья — это эффективный способ экстренной помощи, предназначенный для того, чтобы помочь организму быстро восстановиться после злоупотребления алкоголем. В наркологической клинике «Частный медик 24» в Самаре мы предоставляем услугу безопасной детоксикации и восстановления 24/7. Капельница помогает организму вывести токсины, восстановить водно-электролитный баланс и улучшить общее состояние пациента, не создавая дополнительных нагрузок на сердце, печень и почки.
Получить больше информации – капельница от похмелья на дом самара
Jerrygrold · April 25, 2026 at 3:01 am
Нарколог на дом в Екатеринбурге сегодня — это не просто медицинская услуга, а реальный шанс быстро и безопасно вернуть контроль над жизнью себе или своему близкому человеку. В крупном городе Урала, где ритм жизни высокий, а стресс и доступность веществ создают серьёзные риски, тысячи жителей ежегодно сталкиваются с проблемой зависимости. Алкоголь, синтетические наркотики, соли, спайсы — всё это требует немедленного профессионального вмешательства. Клиника «НЕО+» предоставляет полный выезд нарколога на дом в Екатеринбурге 24 часа в сутки, 7 дней в неделю. Мы гарантируем круглосуточный вызов нарколога, детоксикацию и лечение зависимостей, полную конфиденциальность и современные протоколы лечения 2026 года, которые позволяют купировать острое состояние уже в первые часы.
Подробнее тут – http://narkolog-na-dom-ekaterinburg-1.ru
Johnnytat · April 25, 2026 at 3:04 am
Процедура капельницы от похмелья может быть рекомендована при наличии выраженных симптомов интоксикации, которые нарушают нормальное функционирование организма. Это особенно актуально в тех случаях, когда обычные методы, такие как принятие воды или таблетки, не приносят должного облегчения. Для получения дополнительной информации или записи на процедуру можно обратиться через сайт, а в сложных случаях может потребоваться стационарное лечение или наркологическая помощь.
Выяснить больше – капельница от похмелья
Adrianwiz · April 25, 2026 at 3:17 am
Эти преимущества делают капельницу эффективным и востребованным способом восстановления после похмелья в Самаре, особенно для тех, кто хочет быстро вернуться к нормальной жизни после алкогольного интоксикационного состояния.
Изучить вопрос глубже – капельница от похмелья на дом
Charlesvok · April 25, 2026 at 3:39 am
Стационарный формат выбирают, когда цена ошибки слишком высока. Основная ценность стационара — круглосуточный контроль и возможность быстро корректировать лечение, если динамика ухудшается. Это особенно важно при длительном запое, тяжёлой абстиненции, нестабильном давлении, выраженной тахикардии, повторяющейся рвоте, обезвоживании, а также при подозрении на осложнения со стороны сердца и сосудов. Нередко стационар рекомендуют и тогда, когда пациент живёт один, нет возможности обеспечить наблюдение близких или ранее уже были «ночные провалы», когда состояние резко ухудшалось и приводило к повторному употреблению.
Разобраться лучше – наркологические клиники рядом
Alfredassug · April 25, 2026 at 3:45 am
Капельница от похмелья — это медицинский способ восстановления организма после алкогольной интоксикации, который позволяет быстро устранить симптомы и нормализовать состояние. В отличие от домашних методов, инфузионная терапия воздействует на причину ухудшения самочувствия, а не только на внешние проявления. В наркологической клинике «Похмельная служба» процедура проводится с участием врача, который контролирует состояние пациента на каждом этапе.
Подробнее можно узнать тут – капельница от похмелья цена
Jordanvep · April 25, 2026 at 3:50 am
Выбирая наркологический стационар в Санкт-Петербурге, важно учитывать не только стоимость лечения, но и репутацию учреждения, а также подход, который применяется к лечению зависимых. Подходящее учреждение обеспечит не только лечение физической зависимости, но и долгосрочное восстановление и психологическую поддержку. Важно, чтобы в клинике предоставлялась психотерапия и была возможность консультации психиатра для комплексной помощи пациенту.
Получить дополнительную информацию – http://www.domen.ru
fixDiele · April 25, 2026 at 4:24 am
Особенно понравился раздел про Запись к врачу онлайн: влияние кадров и лекарств на очереди.
Вот, можете почитать:
https://presidentofrussia.ru/%d0%b1%d0%b5%d0%b7-%d1%80%d1%83%d0%b1%d1%80%d0%b8%d0%ba%d0%b8/zapis-k-vrachu-onlajn-i-ocheredi-v-poliklinike-kak-svyazany-kadry-i-lgotnye-lekarstva/
fixDiele · April 25, 2026 at 4:29 am
Кстати, если вас интересует Лесные пожары 2024: причины и последствия, посмотрите сюда.
Вот, делюсь ссылкой:
https://iphoneservice59.ru/news/lesnye-pozhary-statistika-prichiny-posledstviya-profilaktika-i-otvetstvennost-2024/
Spencersaica · April 25, 2026 at 4:30 am
Вывод из запоя в стационаре в Нижнем Новгороде с детоксикацией, мониторингом состояния и медицинской помощью в наркологической клинике «Частный медик 24»
Подробнее можно узнать тут – http://vyvod-iz-zapoya-v-staczionare-nizhnij-novgorod.ru/
WalterCrymn · April 25, 2026 at 4:45 am
Лечение в наркологическом стационаре в Санкт-Петербурге включает в себя комплекс мероприятий, направленных на восстановление физического и психического состояния пациента. Важно понимать, что лечение зависимости — это многогранный процесс, включающий не только медицинские процедуры, но и длительную реабилитацию, которая помогает человеку вернуться к нормальной жизни. В стационаре пациенты получают круглосуточное наблюдение, что значительно увеличивает шансы на успешное лечение и предотвращение рецидивов.
Получить дополнительную информацию – наркологическая помощь стационар в санкт-петербурге
WalterCrymn · April 25, 2026 at 4:47 am
Обращение в наркологический стационар особенно важно в случае тяжелой зависимости, когда человек не способен контролировать свои действия, а угрозы для здоровья возрастают. В таких случаях важно не откладывать начало лечения, а обратиться за помощью сразу же, чтобы избежать серьезных последствий для организма. При выборе стационара следует обратить внимание на наличие лицензии, а также возможность получения психотерапии и других профессиональных услуг в области наркологии для комплексного лечения зависимости.
Получить больше информации – наркологическая клиника стационар в санкт-петербурге
live cams · April 25, 2026 at 5:01 am
OK, you outline what is a big issue. But, can’t we develop more answers in the private sector?
Robertmah · April 25, 2026 at 5:05 am
Только тут настоящий — лутран сайт. Без обмана и регулярные халявные кейсы.
Надоело сливать бабки? Время играть — играть на лутран. Жми на старт.
Только актуальная ссылка — лутран зеркало сегодня. Сохраняй в закладки и играй спокойно.
Source:
http://lootbp.run
lootrun без блокировки
live cams · April 25, 2026 at 5:07 am
hey thanks for the info. appreciate the good work
Robertmah · April 25, 2026 at 5:10 am
Реально топовый сайт — это лутран сайт. Выплаты моментальные и никакого скама.
Быстрый вход на лутран вход. Авторизуйся через стим и лови приветственный бонус.
Ссылка не падает — лутран рабочий сайт. Все кейсы открываются и моментальные выплаты.
Source:
http://lootbd.run
лутран регистрация сайт
Robertmah · April 25, 2026 at 5:17 am
Реально топовый сайт — это лутран. Кейсы летят как надо и никакого скама.
Бесплатный старт после лутран регистрация. Заполни поля — откроешь кейс за рубль.
Не теряй доступ — лутран актуальное зеркало. Вбивай в адресную строку и играй спокойно.
Source:
http://lootrunvip.info
лутран казино вход
Robertmah · April 25, 2026 at 5:21 am
Только тут настоящий — лутран сайт. Без обмана и быстрый вывод скинов.
Быстрый вход на лутран сайт. Авторизуйся через стим и лови приветственный бонус.
Не теряй доступ — лутран актуальное зеркало. Сохраняй в закладки и играй спокойно.
Source:
http://lootca.run
лутран официальный сайт
Oscarbaria · April 25, 2026 at 5:24 am
После первичной стабилизации важен второй шаг — закрепление результата. Если человек просто почувствовал облегчение, но не восстановил сон, не снизил тревогу и не понял, как действовать вечером и ночью, запой часто возвращается. Поэтому клиника делает акцент на понятном маршруте: что происходит с организмом в ближайшие сутки, как меняется самочувствие, какие признаки требуют повторной оценки и как снизить риск повторного употребления.
Подробнее – narkologicheskaya-klinika
Robertmah · April 25, 2026 at 5:30 am
Только тут настоящий — лутран сайт. Без обмана и быстрый вывод скинов.
Промокод на фриспины после регистрации на лутран. Заполни поля — откроешь кейс за рубль.
Новый сезон на лутран казино. Кейсы с x2! Забегай быстрее, пока баланс не разобрали.
Source:
http://lootaw.run
лутран без блокировки
DavidEnact · April 25, 2026 at 5:50 am
more tips here petra wallet chrome
live cams · April 25, 2026 at 6:23 am
I found your blog through google and I must say, this is probably one of the best well prepared articles I have come across in a long time. I have bookmarked your site for more posts.
Keonhacai5 · April 25, 2026 at 6:27 am
thank, I thoroughly enjoyed reading your article. I really appreciate your wonderful knowledge and the time you put into educating the rest of us.
RandyGrirl · April 25, 2026 at 6:58 am
Капельница от похмелья в Самаре: восстановление после алкоголя, снятие симптомов и медицинская помощь в наркологической клинике «Детокс»
Исследовать вопрос подробнее – капельница от похмелья анонимно самара
LucasjaT · April 25, 2026 at 8:14 am
При таких условиях стационар позволяет контролировать состояние в режиме 24/7 и при необходимости быстро корректировать лечение. Это снижает риски и делает процесс более предсказуемым. При этом услуга может предоставляться анонимно, а цену лечения можно уточнить по телефону или при обращении в центр лечения алкоголизма и наркомании.
Подробнее можно узнать тут – вывод из запоя капельница на дому в нижнем новгороде
Howardsoilk · April 25, 2026 at 8:15 am
Наиболее частыми причинами обращения становятся выраженная слабость, тремор, нарушение сна, тревога, учащенный пульс, скачки артериального давления, тошнота и признаки обезвоживания. Эти симптомы могут сочетаться между собой и усиливаться после прекращения употребления алкоголя, особенно после нескольких дней запоя.
Подробнее – врач нарколог на дом екатеринбург
Michaelmaply · April 25, 2026 at 8:16 am
Вывод из запоя в стационаре в Нижнем Новгороде: эффективная помощь при алкоголизме, капельницы и наблюдение врачей в наркологической клинике «Стармед».
Получить больше информации – вывод из запоя в стационаре клиника
Jefferycrync · April 25, 2026 at 10:02 am
Выезд врача — это не «процедура без вопросов», а клиническое решение. На месте оценивают давление, пульс, дыхание, степень обезвоживания, уровень сознания, выраженность тревоги, наличие боли, судорожных проявлений, неврологические симптомы. После этого подбирают схему поддержки, объясняют ограничения и ожидаемую динамику: что должно улучшаться в первые часы, какие симптомы допустимы, а какие требуют немедленного обращения. Важная часть — рекомендации на ближайшие сутки: режим питья и питания, сон, контроль давления, что категорически нельзя смешивать и почему. Такой подход снижает риск осложнений и помогает не «сорваться» в самостоятельные эксперименты.
Получить больше информации – наркологическая клиника в москве цены
BryanNat · April 25, 2026 at 10:58 am
Особое внимание мы уделяем психологической составляющей. Наркологическая помощь в Воронеже в «Клиника Плюс» — это не только физическое очищение, но и работа с мотивацией, разрушение психологических триггеров зависимости. Родственники получают отдельную поддержку: консультации психолога помогают правильно выстроить общение с зависимым человеком и мотивировать его на дальнейшее лечение. Реабилитация может проходить амбулаторно или в стационаре партнёрских центров с комфортабельными условиями, где пациенты находятся под круглосуточным наблюдением.
Подробнее тут – наркологическая помощь на дому
AnthonyBar · April 25, 2026 at 10:59 am
Далее выполняется медицинская детоксикация: корректируется водно-электролитный баланс, снимается интоксикация, поддерживается работа сердечно-сосудистой системы, снижается тремор, стабилизируется сон и тревожность. Важно, что схема подбирается индивидуально: при разных рисках объём поддержки будет различаться. В ряде случаев достаточно амбулаторного наблюдения и рекомендаций, в других — нужен стационар, чтобы контролировать динамику и вовремя корректировать терапию.
Выяснить больше – klinika-vyvod-iz-zapoya-moskva
RandyGrirl · April 25, 2026 at 11:02 am
Эта процедура помогает избежать агрессивных методов лечения, таких как медикаментозные таблетки, и оказывает мягкое, но эффективное влияние на организм.
Исследовать вопрос подробнее – http://kapelnicza-ot-pokhmelya-samara-16.ru
ThomasViecy · April 25, 2026 at 11:35 am
Вывод из запоя в стационаре — это медицинская помощь, при которой лечение проводится в условиях круглосуточного наблюдения и контролируемой среды. Такой формат применяется, когда состояние пациента требует постоянного мониторинга и поэтапной коррекции терапии. В наркологической клинике «Частный медик 24» в Нижнем Новгороде стационарное лечение выстраивается с учётом текущего состояния пациента, без перегрузки медикаментами и с регулярной оценкой результата на каждом этапе.
Изучить вопрос глубже – наркология вывод из запоя в стационаре в нижнем новгороде
Thomaslak · April 25, 2026 at 12:22 pm
Капельница от похмелья является одним из наиболее эффективных методов для быстрого улучшения состояния пациента. Это медицинская процедура, направленная на детоксикацию организма, восстановление водно-солевого баланса и устранение симптомов интоксикации, обеспечивая быстрый вывод токсинов. Важным моментом является то, что капельница оказывает комплексное воздействие на организм, помогая справиться с неприятными симптомами похмелья, при этом может сочетаться с дальнейшей терапией и кодированием.
Изучить вопрос глубже – капельница от похмелья на дом самара
Thomasexink · April 25, 2026 at 1:04 pm
Капельница от похмелья — это медицинская процедура, направленная на устранение последствий алкогольной интоксикации и восстановление работы организма. В отличие от домашних методов, инфузионная терапия позволяет воздействовать на причину состояния, а не только на его проявления. В наркологической клинике «Похмельная служба» капельная терапия проводится с выездом специалиста на дом, что позволяет начать лечение без задержек и в комфортных условиях.
Выяснить больше – капельница от похмелья на дом в воронеже
ClintonPoush · April 25, 2026 at 1:07 pm
Капельница от похмелья с мягким восстановлением — это метод, направленный на быстрое восстановление организма после алкогольной интоксикации, при котором используется более щадящий подход. В отличие от стандартных капельниц, целью которых является быстрый вывод токсинов из организма, капельница с мягким восстановлением действует постепенно, восстанавливая водно-солевой баланс и поддерживая внутренние органы без перегрузки организма. Эта процедура особенно полезна тем, кто предпочитает не только избавиться от похмелья, но и почувствовать себя восстановленным и энергичным, при этом помощь может оказываться при запое, когда врач выезжает на дом для лечения алкоголизма.
Узнать больше – капельница от похмелья цена
BryanNat · April 25, 2026 at 1:27 pm
Когда человек или его родственники понимают, что нужна наркологическая помощь в Воронеже, время становится решающим фактором. Запой, ломка, тяжёлая интоксикация — в таких ситуациях промедление может привести к необратимым последствиям для здоровья и жизни. Наша клиника создана именно для того, чтобы оказывать эффективную наркологическую помощь в Воронеже в самых сложных случаях. Мы не заставляем ждать в очередях государственных учреждений, не ставим на учёт и не разглашаем информацию. Всё происходит конфиденциально, на дому или в комфортных условиях нашей партнёрской клиники. Пациенты из Воронежа, Воронежской области, а также соседних регионов уже более 12 лет выбирают «Клиника Плюс» благодаря сочетанию скорости, профессионализма и доказанной результативности.
Получить больше информации – наркологическая помощь воронеж
ThomasViecy · April 25, 2026 at 1:56 pm
Стационарный формат рекомендуется в следующих ситуациях:
Детальнее – вывод из запоя в стационаре нижний новгород
Spencersaica · April 25, 2026 at 2:03 pm
Вывод из запоя в стационаре в Нижнем Новгороде с детоксикацией, мониторингом состояния и медицинской помощью в наркологической клинике «Частный медик 24»
Подробнее – https://vyvod-iz-zapoya-v-staczionare-nizhnij-novgorod.ru
DavidEnact · April 25, 2026 at 2:29 pm
Visit Your URL petra aptos wallet extension
DonaldHum · April 25, 2026 at 2:41 pm
Терапевтический алгоритм в стационаре не сводится к единой процедуре. Это последовательная система диагностики, стабилизации, медикаментозной поддержки и подготовки к противорецидивному этапу. При поступлении врач проводит детальный осмотр, собирает анамнез, оценивает неврологический статус и при необходимости назначает экспресс-анализы крови, ЭКГ и ультразвуковое исследование внутренних органов. На основе полученных данных формируется индивидуальный протокол, учитывающий возраст, длительность употребления, наличие хронических заболеваний и переносимость лекарственных компонентов. Мы отказываемся от шаблонных схем в пользу точного дозирования, что минимизирует нагрузку на ослабленный организм и ускоряет восстановление метаболических функций. Основная задача на этом этапе — безопасно вывести пациента из состояния острой интоксикации без резких скачков артериального давления и кардиологических перегрузок.
Получить больше информации – стационар вывод из запоя нижний новгород
CharlesFut · April 25, 2026 at 3:50 pm
При выезде на дом врач проводит все необходимые процедуры, включая инфузионную терапию (капельницы), медикаментозное лечение для снятия симптомов ломки, а также консультирует пациента и его семью по дальнейшему лечению. Важно, что после стабилизации состояния нарколог может дать рекомендации по дальнейшей реабилитации, возможному кодированию, а также предложить программу для восстановления здоровья на длительный срок.
Подробнее – вызвать нарколога на дом в воронеже
kasyno online opinie · April 25, 2026 at 4:04 pm
I’ve been surfing online more than 3 hours today, yet I never found any interesting article like yours. It’s pretty worth enough for me. In my view, if all web owners and bloggers made good content as you did, the net will be much more useful than ever before.
Jeremypep · April 25, 2026 at 4:08 pm
Наркологическая помощь нужна не только тогда, когда ситуация выглядит критической со стороны. Она необходима и в тех случаях, когда зависимость повторяется циклично, а семья уже понимает, что прежние способы не работают. Чем раньше человек переходит от стихийных попыток справиться самостоятельно к профессиональной тактике, тем выше шансы стоновить процесс на менее тяжелом этапе.
Подробнее – наркологическая помощь на дому в воронеже
DavidEnact · April 25, 2026 at 4:41 pm
have a peek at these guys ejjladinnckdgjemekebdpeokbikhfci
Thomasexink · April 25, 2026 at 4:45 pm
Капельница от похмелья в Воронеже с выездом на дом, подбором препаратов и контролем состояния в наркологической клинике «Похмельная служба»
Подробнее можно узнать тут – капельница от похмелья
MatthewGed · April 25, 2026 at 5:07 pm
Выбор наркологического стационара в Санкт-Петербурге — это важный шаг, который требует внимательного подхода. Каждое медицинское учреждение имеет свои особенности, что может влиять на качество предоставляемых услуг. Важно учитывать как репутацию клиники, так и квалификацию врачей, а также доступные методы лечения и реабилитации.
Изучить вопрос глубже – http://www.domen.ru
Charlesarite · April 25, 2026 at 5:17 pm
Коллеги, хороший материал о долгосрочном характере SEO в 2026 году. Автор разбирает, как изменились алгоритмы поисковых систем (акцент на контекст и поведенческие факторы) и почему старые методы перестали работать. В центре внимания — качественный контент и пользовательский опыт (UX), а не технические уловки. Тем, кто хочет устойчивых позиций, обязательно к прочтению: https://nogmed.ru/ponimanie-dolgosrochnogo-haraktera-seo-v-2026-godu/
Thomaslak · April 25, 2026 at 5:39 pm
Капельница от похмелья в Самаре используется для устранения симптомов алкогольной интоксикации, которые могут включать головную боль, тошноту, слабость, рвоту и обезвоживание. Это достигается за счет введения специальных растворов, которые помогают организму восстановиться и очиститься от токсинов.
Детальнее – капельница от похмелья на дом в самаре
ClintonPoush · April 25, 2026 at 5:43 pm
Капельница от похмелья в Самаре: быстрое снятие симптомов, детоксикация и восстановление организма под контролем специалистов в наркологической клинике «Детокс»
Подробнее тут – капельница от похмелья на дом самара
Alfredassug · April 25, 2026 at 6:24 pm
Капельница от похмелья в Воронеже с нормализацией состояния и поддержкой организма в наркологической клинике «Похмельная служба»
Подробнее можно узнать тут – капельница от похмелья вызов на дом воронеж
MatthewGed · April 25, 2026 at 6:30 pm
В таких ситуациях стационарный уход позволяет обеспечить безопасность пациента, эффективно справиться с его состоянием и подготовить его к дальнейшему лечению или реабилитации. В случае алкоголизма может быть назначена капельница для снятия острых симптомов интоксикации, а также лечение в специализированном центре для комплексного восстановления и профилактики рецидивов.
Получить дополнительные сведения – http://narkologicheskij-staczionar-sankt-peterburg-2.ru
najlepsze kasyno online · April 25, 2026 at 6:34 pm
Public policy is key here, and our states need to develop some strategies – – soon.
Ethantoisa · April 25, 2026 at 6:43 pm
Запой, длительное употребление алкоголя или случайное злоупотребление могут привести к неприятным симптомам похмелья, таким как головная боль, слабость, тошнота, головокружение и усталость. Эти симптомы обусловлены тем, что в организме остаются продукты распада алкоголя, которые токсически воздействуют на все органы. Капельница от похмелья на дому — это отличная возможность быстро снять острые симптомы и восстановить нормальное состояние организма, не выходя из привычной обстановки.
Исследовать вопрос подробнее – капельница от похмелья вызов на дом самара
Stephenwaf · April 25, 2026 at 6:58 pm
После стабилизации важно закрепить результат. В первые 1–3 дня сохраняются слабость, раздражительность, эмоциональные качели, нарушения сна. Без плана и поддержки многие срываются, потому что пугаются ухудшения вечером или ночью и пытаются снять дискомфорт алкоголем. Поэтому врач даёт рекомендации на ближайшие сутки и несколько дней: как организовать сон, питание, питьевой режим, что контролировать по давлению и пульсу, какие нагрузки исключить и по каким признакам нужно срочно обращаться повторно.
Ознакомиться с деталями – narkologicheskaya klinika zhukovskij
kasyno online · April 25, 2026 at 6:59 pm
I am glad to be a visitor of this perfect blog !, appreciate it for this rare info!
legalne kasyna online · April 25, 2026 at 7:00 pm
Easily, the post is really the greatest on this laudable topic. I concur with your conclusions and will thirstily look forward to your future updates. Saying thank will not just be sufficient, for the wonderful c lucidity in your writing. I will instantly grab your rss feed to stay privy of any updates. Solid work and much success in your business enterprise!
DonaldHum · April 25, 2026 at 7:17 pm
Длительное употребление алкоголя переводит организм в состояние хронической интоксикации, при котором собственные механизмы восстановления перестают справляться с нагрузкой. Накопление ацетальдегида, дефицит электролитов, нарушение работы печени и сердечно-сосудистой системы создают клиническую картину, требующую не симптоматического облегчения, а комплексного медицинского вмешательства. Вывод из запоя в стационаре в Нижнем Новгороде в наркологической клинике «Стармед» организован с соблюдением современных протоколов доказательной медицины, где безопасность пациента, непрерывный мониторинг и персонализированный подбор терапии являются приоритетом. Мы работаем круглосуточно, обеспечивая быстрое реагирование на обращения, четкую диагностику при поступлении и прозрачное взаимодействие с родственниками. Чтобы вызвать специалистов или лечиться в безопасных условиях, достаточно оставить заявку на сайте или позвонить по прямой линии. Все процедуры проводятся в лицензированных помещениях, с документированием каждого этапа и строгим соблюдением врачебной этики. Первичная оценка состояния начинается с дистанционной консультации, что позволяет врачам заранее подготовить необходимые препараты и скорректировать план госпитализации еще до прибытия пациента.
Получить больше информации – http://vyvod-iz-zapoya-v-staczionare-nizhnij-novgorod-8.ru/
Johnnytat · April 25, 2026 at 8:10 pm
Постановка капельницы — это не просто средство для снятия головной боли или тошноты, а комплексное восстановление организма. Состав раствора подбирается в зависимости от симптомов и состояния пациента. Врач-нарколог оценивает общее состояние пациента и выбирает наиболее подходящий состав, который будет наиболее эффективен для него. При необходимости может быть предложена дополнительная помощь, включая кодирование от алкогольной зависимости.
Получить дополнительную информацию – капельница от похмелья на дому в нижнем новгороде
KevinDrorp · April 25, 2026 at 8:43 pm
Алкогольная зависимость часто держится на страхе отмены. Человек заранее боится ночи: что не уснёт, начнётся паника, поднимется давление, появится дрожь и сильная слабость. Поэтому лечение начинается с оценки состояния: сколько длится употребление, как проходит отмена, были ли осложнения, какие заболевания есть у человека и какие препараты он уже принимал. Это позволяет выбрать безопасную тактику и понять, нужен ли стационар или можно начать амбулаторно.
Детальнее – http://narkologicheskaya-klinika-klin12.ru
Jerrygrold · April 25, 2026 at 10:09 pm
Наша клиника предлагает полный цикл услуг — от экстренного вызова нарколога до долгосрочной реабилитации. Каждый этап разрабатывается индивидуально с учётом возраста, стажа зависимости и сопутствующих заболеваний. Современные протоколы 2026 года позволяют проводить лечение максимально комфортно и эффективно, минимизируя болезненные симптомы и снижая риск срывов. В этом виде деятельности мы используем только проверенные методы медицины.
Получить дополнительную информацию – врач нарколог на дом екатеринбург
Adrianwiz · April 25, 2026 at 10:13 pm
Введение лекарственных препаратов через капельницу позволяет значительно ускорить процессы, которые происходят в организме, поскольку вещества поступают сразу в кровоток, минуя желудочно-кишечный тракт. Это значительно усиливает эффективность лечения и способствует быстрому улучшению самочувствия пациента, при этом проводится наркологическая терапия, а при необходимости можно заказать дополнительное лечение с учетом данных пациента.
Детальнее – http://kapelnicza-ot-pokhmelya-samara-15.ru/
Alfredassug · April 25, 2026 at 10:13 pm
Такие симптомы требуют медицинского вмешательства, поскольку могут усиливаться и приводить к ухудшению состояния. Капельница помогает стабилизировать самочувствие и снизить нагрузку на организм. Услуги могут предоставляться анонимно, а при необходимости пациент направляется на лечение в стационаре.
Детальнее – http://www.domen.ru
Charlesvok · April 25, 2026 at 10:59 pm
Выезд врача нужен не только ради удобства. Часто именно дома легче согласиться на помощь: без дороги, без ожидания, без лишних контактов и без стресса от смены обстановки. Но домашний формат не должен быть «упрощённым». Корректная тактика начинается с осмотра и измерения показателей: давление, пульс, дыхание, температура, уровень сознания, признаки обезвоживания, выраженность тремора и тревоги. После этого врач подбирает схему стабилизации, ориентируясь на риски, а не на желание «сделать побыстрее».
Разобраться лучше – http://narkologicheskaya-klinika-pushkino12.ru
Jordanvep · April 25, 2026 at 11:02 pm
Лечение в наркологическом стационаре требует особого подхода, который включает не только медицинские мероприятия, но и психоэмоциональную поддержку пациента. Основной целью является не только снятие физической зависимости от вещества, но и возвращение человека к нормальной жизни без употребления наркотиков или алкоголя. В Санкт-Петербурге клиники предлагают различные варианты лечения, включая краткосрочные и долгосрочные программы. Процесс лечения включает в себя несколько этапов, каждый из которых играет важную роль в процессе восстановления.
Изучить вопрос глубже – http://www.domen.ru
Michaelwof · April 25, 2026 at 11:03 pm
В домашних попытках обычно есть две крайности. Первая — «пить понемногу, чтобы не трясло», что затягивает запой и усиливает истощение. Вторая — резко прекратить и «перетерпеть», после чего отмена усиливается волной, человек пугается и снова пьёт. Врач помогает выйти из этих крайностей: стабилизировать состояние и дать маршрут, который снижает риск возврата к алкоголю из-за бессонницы и паники.
Выяснить больше – https://narkologicheskaya-klinika-noginsk12.ru/narkologicheskaya-klinika-otzyvy-v-noginske
Melvinadage · April 25, 2026 at 11:15 pm
Особое внимание мы уделяем психологической составляющей. Наркологическая помощь в Воронеже в «Клиника Плюс» — это не только физическое очищение, но и работа с мотивацией, разрушение психологических триггеров зависимости. Родственники получают отдельную поддержку: консультации психолога помогают правильно выстроить общение с зависимым человеком и мотивировать его на дальнейшее лечение. Реабилитация может проходить амбулаторно или в стационаре партнёрских центров с комфортабельными условиями, где пациенты находятся под круглосуточным наблюдением.
Получить дополнительные сведения – круглосуточная наркологическая помощь воронеж
sumber · April 25, 2026 at 11:38 pm
Wild Wild Riches is back delivering full-screen wins, drawing attention late night.
LucasjaT · April 25, 2026 at 11:45 pm
Вывод из запоя в стационаре — это медицинская помощь, при которой лечение проводится в условиях круглосуточного наблюдения и контролируемой среды. Такой формат применяется, когда состояние пациента требует постоянного мониторинга и поэтапной коррекции терапии. В наркологической клинике «Частный медик 24» в Нижнем Новгороде стационарное лечение выстраивается с учётом текущего состояния пациента, без перегрузки медикаментами и с регулярной оценкой результата на каждом этапе.
Ознакомиться с деталями – врач вывод из запоя
KevinDrorp · April 26, 2026 at 1:04 am
В клинике «Ось Здоровья» помощь выстраивается по маршруту. Врач оценивает, насколько состояние стабильное, какие риски сейчас, что именно приводит к срывам — тяжёлая отмена, тревожность, нарушения сна, стресс и истощение. Затем подбирается формат лечения: стационар, амбулаторная программа или помощь на дому, если по состоянию это безопасно. После первичного облегчения обязательно составляется план на первые 24–72 часа — период, когда чаще всего случаются повторные ухудшения вечером и ночью. Когда у пациента есть ориентиры и поддержка по динамике, риск вернуться к алкоголю или веществам «для облегчения» становится ниже.
Исследовать вопрос подробнее – http://
WalterCrymn · April 26, 2026 at 1:14 am
Комплексное лечение в наркологическом стационаре включает несколько последовательных этапов, каждый из которых направлен на решение конкретных задач. Начальный этап включает в себя медицинское вмешательство, направленное на устранение токсинов из организма, и стабилизацию общего состояния пациента. Далее начинается реабилитация, которая помогает закрепить достигнутые результаты и восстановить психоэмоциональное состояние пациента. Для выбора подходящего стационара стоит ознакомиться с отзывами и дополнительной информацией о клинике, а также уточнить, в каком районе города она расположена.
Получить дополнительную информацию – наркологическая клиника стационар в санкт-петербурге
WalterCrymn · April 26, 2026 at 1:16 am
Комплексное лечение в наркологическом стационаре включает несколько последовательных этапов, каждый из которых направлен на решение конкретных задач. Начальный этап включает в себя медицинское вмешательство, направленное на устранение токсинов из организма, и стабилизацию общего состояния пациента. Далее начинается реабилитация, которая помогает закрепить достигнутые результаты и восстановить психоэмоциональное состояние пациента. Для выбора подходящего стационара стоит ознакомиться с отзывами и дополнительной информацией о клинике, а также уточнить, в каком районе города она расположена.
Детальнее – http://narkologicheskij-staczionar-sankt-peterburg-1.ru
Jeremydaype · April 26, 2026 at 2:31 am
Помощь начинается с первичной оценки. Врач уточняет длительность запоя, время последнего приёма алкоголя, ведущие симптомы, хронические заболевания, прошлые осложнения, аллергии, а также препараты, которые пациент уже принимал самостоятельно. Далее проводится осмотр: измеряются давление и пульс, оценивается дыхание, температура, признаки обезвоживания, уровень сознания, выраженность тремора и тревоги. На основании этой информации выбирается тактика и формат — на дому, амбулаторно или в стационаре, если риски высокие.
Детальнее – vyvoda iz zapoya orekhovo
KevinDrorp · April 26, 2026 at 2:33 am
В клинике «Ось Здоровья» помощь выстраивается по маршруту. Врач оценивает, насколько состояние стабильное, какие риски сейчас, что именно приводит к срывам — тяжёлая отмена, тревожность, нарушения сна, стресс и истощение. Затем подбирается формат лечения: стационар, амбулаторная программа или помощь на дому, если по состоянию это безопасно. После первичного облегчения обязательно составляется план на первые 24–72 часа — период, когда чаще всего случаются повторные ухудшения вечером и ночью. Когда у пациента есть ориентиры и поддержка по динамике, риск вернуться к алкоголю или веществам «для облегчения» становится ниже.
Ознакомиться с деталями – narkologicheskaya-klinika
LucasjaT · April 26, 2026 at 3:12 am
В Нижнем Новгороде стационарное лечение используется при наличии факторов, которые увеличивают риск осложнений или делают домашний формат недостаточным, особенно при алкоголизме или тяжёлом состоянии больного. Врач принимает решение на основе осмотра, консультации, анализа данных и оценки симптомов и динамики состояния пациента. Основная цель — обеспечить безопасность человека и создать условия для контролируемого лечения алкоголизма.
Изучить вопрос глубже – нарколог вывод из запоя
创建免费账户 · April 26, 2026 at 3:17 am
Can you be more specific about the content of your article? After reading it, I still have some doubts. Hope you can help me.
GeorgeBax · April 26, 2026 at 3:50 am
подробнее mega darknet
Jefferycrync · April 26, 2026 at 4:42 am
Стационар выбирают, когда нужно наблюдать состояние круглосуточно или есть вероятность резкого ухудшения. Это может быть длительный запой, выраженная абстиненция, нестабильное давление, подозрение на осложнения со стороны сердца и сосудов, история судорог, спутанность сознания, психотические симптомы. Преимущество стационара — контроль динамики и возможность быстро менять терапию, если план «не заходит». Кроме того, в стационаре проще выстроить полноценный переход к лечению зависимости: не просто снять острые проявления, а сразу подключить психологическое сопровождение и подготовить пациента к следующему этапу.
Углубиться в тему – luchshaya-narkologicheskaya-klinika-moskva
Melvinadage · April 26, 2026 at 5:32 am
Наша клиника предлагает полный цикл услуг — от экстренной круглосуточной помощи до долгосрочной реабилитации. Каждый этап разрабатывается индивидуально с учётом возраста, стажа зависимости и сопутствующих заболеваний. Современные протоколы 2026 года позволяют проводить анонимное лечение алкоголизма и наркомании максимально комфортно и эффективно, минимизируя болезненные симптомы и снижая риск срывов.
Выяснить больше – вызов наркологической помощи в воронеже
AnthonyBar · April 26, 2026 at 5:39 am
Самостоятельный выход часто строится на ошибочных решениях: «уменьшать дозу», смешивать алкоголь со снотворными, принимать седативные без понимания влияния на дыхание и сердце, использовать сомнительные «похмельные» наборы. Такие действия могут временно приглушить симптомы, но повышают риск ухудшения и делают состояние непредсказуемым. Ещё одна проблема — отсутствие контроля: человек не замечает, как давление уходит в опасные цифры, как развивается обезвоживание или как усиливаются неврологические симптомы. В клинике же у врача есть задача не просто «снять неприятное», а стабилизировать организм, защитить сердце и сосуды, восстановить сон и снизить тревогу так, чтобы дальнейшее восстановление стало реальным.
Подробнее тут – vyvod-iz-zapoya-moskva-stacionar
Howardsoilk · April 26, 2026 at 5:42 am
За выездом врача обращаются в тех случаях, когда человеку тяжело добраться до клиники, он ослаблен после нескольких дней употребления спиртного или родственникам важно быстрее получить медицинскую консультацию на месте. После осмотра определяют, допустим ли домашний формат, требуется ли капельница, достаточно ли наблюдения на дому или нужен другой объем помощи. Если эпизоды повторяются, в дальнейшем могут обсуждаться лечение алкоголизма, кодирование, участие психолога, реабилитация и более широкая программа помощи при зависимости. Уже на этапе первичного обращения нередко уточняют, как вызвать специалиста, какие услуги доступны на дому и в каких случаях вывод из запоя рассматривают не дома, а в стационаре.
Получить дополнительную информацию – вызов нарколога на дом
Thomasexink · April 26, 2026 at 6:01 am
Такие симптомы требуют медицинского вмешательства, поскольку могут усиливаться без лечения. Капельница позволяет стабилизировать состояние и ускорить восстановление. Услуги могут предоставляться анонимно, а при необходимости пациент направляется на лечение в стационаре.
Подробнее – капельница от похмелья вызов на дом в воронеже
Michaelmaply · April 26, 2026 at 6:15 am
Основой стационарного лечения является инфузионная терапия, направленная на ускоренное выведение токсинов, коррекцию кислотно-щелочного баланса и восстановление метаболических процессов. Стандартная капельница при выходе из запоя включает кристаллоидные и коллоидные растворы, витаминные комплексы группы B и C, гепатопротекторы, антиоксиданты и симптоматические препараты для нормализации сна и снижения тревожности. Состав, объем и скорость инфузии рассчитываются индивидуально с учетом возраста, массы тела, длительности интоксикации, функции почек и печени, а также наличия аллергических реакций. Мы быстро купируем мучительные проявления абстиненции, восстанавливаем аппетит, устраняем мышечные спазмы и нормализуем суточные ритмы. При необходимости подключаются препараты для стабилизации сердечного ритма, коррекции артериального давления и защиты нейрональных структур от эксайтотоксичности. Все медикаменты сертифицированы, применяются в строгом соответствии с клиническими рекомендациями Минздрава РФ и не вызывают вторичной зависимости. Дозировки ежедневно пересматриваются лечащим врачом на основе лабораторных анализов и клинической динамики, что гарантирует высокий уровень качества медицинской помощи и безопасность пациента. Снятие острых симптомов происходит уже в первые сутки, что значительно улучшает общее самочувствие и возвращает способность к адекватному восприятию действительности.
Получить дополнительные сведения – вывод из запоя в стационаре анонимно нижний новгород
verde-casino-bonus-no-deposit.online-spielhallen.de · April 26, 2026 at 6:35 am
References:
Northern quest casino
References:
https://casino-mieten.online-spielhallen.de/
GeorgeBax · April 26, 2026 at 6:47 am
другие mega onion
Adrianwiz · April 26, 2026 at 7:04 am
Капельница от похмелья в Самаре становится все более популярным методом, благодаря своим преимуществам в восстановлении организма после алкогольного отравления. В отличие от традиционных методов лечения, таких как прием таблеток или напитков, капельница действует гораздо быстрее и более эффективно, особенно в случае тяжелого похмелья. Врачебные центры в Самаре предлагают услуги капельниц, которые могут быть настроены под конкретные нужды пациента, что увеличивает эффективность лечения.
Разобраться лучше – капельница от похмелья вызов на дом в самаре
casino-bucks.online-spielhallen.de · April 26, 2026 at 7:06 am
References:
Quantum quest a cassini space odyssey
References:
https://stream-james-bond-casino-royale.online-spielhallen.de/
Lloydaluse · April 26, 2026 at 7:46 am
Помимо физиологических факторов, важную роль играет психологическая устойчивость пациента. Длительный запой формирует патологическую потребность, при которой человек утрачивает способность добровольно отказаться от очередной дозы в привычной среде. Изоляция в условиях клиники разрывает этот цикл, создавая пространство для мотивационной работы и снижения тревожности. Специалисты клиники работают с когнитивными искажениями, поддерживающими аддикцию, и помогают справиться с внутренним сопротивлением лечению. Такой подход особенно важен при сочетанных расстройствах, когда алкогольная зависимость сопровождается депрессивными проявлениями или генерализованной тревогой.
Получить дополнительные сведения – вывод из запоя в стационаре клиника нижний новгород
LucasjaT · April 26, 2026 at 8:47 am
В Нижнем Новгороде стационарное лечение используется при наличии факторов, которые увеличивают риск осложнений или делают домашний формат недостаточным, особенно при алкоголизме или тяжёлом состоянии больного. Врач принимает решение на основе осмотра, консультации, анализа данных и оценки симптомов и динамики состояния пациента. Основная цель — обеспечить безопасность человека и создать условия для контролируемого лечения алкоголизма.
Узнать больше – наркологический вывод из запоя в нижнем новгороде
CharlesFut · April 26, 2026 at 8:59 am
Для жителей Воронежа выезд нарколога на дом — это быстрый и удобный способ получить экстренную помощь. Когда человек переживает запой, а его физическое и эмоциональное состояние быстро ухудшается, наркологическая помощь на дому становится оптимальным решением. Врач приезжает и немедленно оценивает состояние пациента: проверяет его пульс, давление, частоту дыхания, уровень сознания и другие важные показатели. Это помогает составить точный план лечения, который будет направлен на восстановление организма, снятие токсинов и стабилизацию состояния пациента.
Узнать больше – врач нарколог на дом в воронеже
Dwayneoxymn · April 26, 2026 at 9:04 am
Лечение нужно, чтобы пережить отмену безопасно, восстановить сон и снизить тревогу, а затем научиться обходиться без алкоголя в тех ситуациях, где он раньше «помогал»: стресс, усталость, конфликт, одиночество. Когда человеку дают понятные шаги и поддерживают первые дни, зависимость перестаёт выглядеть как безвыходный круг.
Исследовать вопрос подробнее – http://lechenie-alkogolizma-noginsk12.ru
RandyGrirl · April 26, 2026 at 9:04 am
Капельница от похмелья в Самаре: восстановление после алкоголя, снятие симптомов и медицинская помощь в наркологической клинике «Детокс»
Получить больше информации – капельница от похмелья анонимно самара
Thomasexink · April 26, 2026 at 9:21 am
Выезд специалиста начинается с оценки состояния пациента. Врач измеряет давление, пульс, оценивает общее самочувствие и выраженность симптомов. На основании этих данных формируется план лечения и подбирается состав капельницы. Такой подход позволяет учитывать индивидуальные особенности пациента и эффективно провести вывод из запоя.
Подробнее – капельница от похмелья вызов на дом в воронеже
Jordanvep · April 26, 2026 at 9:46 am
Наркологический стационар предоставляет круглосуточное медицинское наблюдение и специализированное лечение для пациентов, страдающих от алкогольной и наркотической зависимости. Здесь пациенты могут пройти детоксикацию, получить помощь в снятии абстинентного синдрома, а также пройти курс реабилитации с целью стабилизации состояния и профилактики рецидивов. Лечение в стационаре направлено не только на устранение физической зависимости, но и на помощь в восстановлении психологического здоровья пациента. В некоторых случаях для более эффективного лечения могут быть предложены капельницы и вывод из запоя, а также долговременная реабилитация, которая может продолжаться на протяжении года.
Исследовать вопрос подробнее – наркологическая помощь стационар
dark web market iTunes gift cards · April 26, 2026 at 10:00 am
My son wanted dark web market Steam gift cards for his game library, half the price of store bought.
dark web market iTunes gift cards
https://dark-webmarket.com
https://dark-webmarket.com
https://dark-webmarket.com
Jeremypep · April 26, 2026 at 10:02 am
Острые состояния могут проявляться по-разному: от выраженной слабости, тошноты, тремора и бессонницы до мучительной ломки, резкой тревоги, скачков артериального давления, учащенного сердцебиения, раздражительности и спутанности сознания. У пациентов с хроническими заболеваниями, в пожилом возрасте или после длительного употребления риски возрастают еще сильнее. Особенно опасно ориентироваться только на внешнее впечатление, потому что даже в тех случаях, когда человек находится дома и формально «в сознании», его состояние уже может требовать медицинского вмешательства.
Получить больше информации – скорая наркологическая помощь воронеж
Melvinadage · April 26, 2026 at 10:18 am
Наркологическая помощь в Воронеже сегодня — это не просто медицинская услуга, а реальный шанс быстро и безопасно вернуть контроль над жизнью себе или своему близкому человеку. В крупном городе Центрального Черноземья, где ритм жизни высокий, а стресс и доступность веществ создают серьёзные риски, тысячи жителей ежегодно сталкиваются с проблемой зависимости. Алкоголь, синтетические наркотики, соли, спайсы — всё это требует немедленного профессионального вмешательства. Клиника «Клиника Плюс» предоставляет полную наркологическую помощь в Воронеже 24 часа в сутки, 7 дней в неделю. Мы гарантируем анонимное лечение алкоголизма и наркомании, срочный выезд нарколога на дом в течение 30–60 минут, полную конфиденциальность и современные протоколы лечения 2026 года, которые позволяют купировать острое состояние уже в первые часы.
Ознакомиться с деталями – клиника наркологической помощи в воронеже
Jefferycrync · April 26, 2026 at 10:55 am
Причины обращения бывают разными, но логика всегда одна: сначала врач оценивает угрозы и снимает острые проявления, затем помогает закрепить результат. Кому-то нужна детоксикация после запоя или употребления, кому-то — помощь при абстиненции с выраженной тревогой и нарушением сна, кому-то — консультация, когда человек «держится на силе воли» и боится срыва. Часто звонят родственники, потому что видят ухудшение: человек не ест, не спит, становится раздражительным, замыкается, путается в событиях, может проявлять агрессию или, наоборот, уходит в апатию. Важно понимать, что наркологическая помощь — это не один универсальный сценарий. Тактика зависит от длительности употребления, последнего приёма, сопутствующих болезней, возраста, перенесённых осложнений, лекарств, которые уже принимались самостоятельно.
Подробнее – http://www.domen.ru
KevinDrorp · April 26, 2026 at 11:20 am
В клинике «Ось Здоровья» лечение строится так, чтобы пациент не оставался один на один с уязвимым периодом после прекращения употребления. Даже при хорошем старте первые ночи часто становятся испытанием: тревога усиливается, сон не приходит, появляется ощущение внутреннего напряжения. Когда есть план на 24–72 часа и поддержка по динамике, риск срыва снижается.
Изучить вопрос глубже – http://narkologicheskaya-klinika-klin12.ru/platnaya-narkologicheskaya-klinika-v-klinu/
ThomasViecy · April 26, 2026 at 11:28 am
Вывод из запоя в стационаре в Нижнем Новгороде с круглосуточным наблюдением и поэтапным восстановлением в наркологической клинике «Частный медик 24»
Разобраться лучше – наркология вывод из запоя в стационаре в нижнем новгороде
AnthonyBar · April 26, 2026 at 11:44 am
Далее выполняется медицинская детоксикация: корректируется водно-электролитный баланс, снимается интоксикация, поддерживается работа сердечно-сосудистой системы, снижается тремор, стабилизируется сон и тревожность. Важно, что схема подбирается индивидуально: при разных рисках объём поддержки будет различаться. В ряде случаев достаточно амбулаторного наблюдения и рекомендаций, в других — нужен стационар, чтобы контролировать динамику и вовремя корректировать терапию.
Разобраться лучше – вывод из запоя москва
baixar vai de bet · April 26, 2026 at 12:12 pm
Sabe, quase sempre acho interessante com o Vai de Bet. Tem dias que gosto de testar o vaidebet cassino, e acho que cada aposta é única. Além disso, notei que https://cbaaacademy.com/2026/01/vai-de-bet-plataforma-digital-com-cassino-e-esportes-vaidebet-mobile-beneficios-para-usuarios-ambiente-protegido-diversao-e-ganhos/ simplifica o uso do app, mais ainda quando estou jogando pelo celular. O suporte ajuda bastante, e isso ajuda bastante. Resumindo, gosto do que a plataforma oferece, alguém mais já testou o app?
BryanNat · April 26, 2026 at 12:13 pm
Наша клиника предлагает полный цикл услуг — от экстренной помощи до долгосрочной реабилитации. Каждый этап разрабатывается индивидуально с учётом возраста, стажа зависимости и сопутствующих заболеваний. Современные протоколы 2026 года позволяют проводить лечение максимально комфортно и эффективно, минимизируя болезненные симптомы и снижая риск срывов.
Углубиться в тему – https://narkologicheskaya-pomoshh-voronezh-1.ru
pis.com.mx · April 26, 2026 at 12:14 pm
Your resources are well developed.
GeorgeBax · April 26, 2026 at 12:20 pm
Следующая страница мега ссылка
b52 club · April 26, 2026 at 12:38 pm
Amazing! Your site has quite a few comment posts. How did you get all of these bloggers to look at your site I’m envious! I’m still studying all about posting articles on the net. I’m going to view pages on your website to get a better understanding how to attract more people. Thank you!
MatthewGed · April 26, 2026 at 12:52 pm
Решение о госпитализации в наркологический стационар часто становится необходимым в случаях, когда пациент не может справиться с зависимостью самостоятельно, а также когда домашние условия лечения оказываются недостаточными. Стационарное лечение дает пациенту возможность находиться под круглосуточным наблюдением специалистов, что особенно важно при острых состояниях и абстинентных синдромах. В случае запоя может быть предложена помощь нарколога, а также выезд на дом для неотложного вмешательства и стабилизации состояния пациента.
Подробнее можно узнать тут – наркологический стационар
https://1xbet-promo-code-free-bet.com/promo-code-for-1xbet-free-bet-beton76-vip-bonuses-2026/ · April 26, 2026 at 1:16 pm
https://1xbet-promo-code-free-bet.com/promo-code-for-1xbet-free-bet-beton76-vip-bonuses-2026/
RobertDic · April 26, 2026 at 1:24 pm
Капельница от похмелья в Самаре: быстрое снятие интоксикации, восстановление после алкоголя и улучшение самочувствия под контролем специалистов в наркологической клинике «Похмельная служба»
Получить дополнительные сведения – капельница от похмелья вызов на дом самара
ThomasViecy · April 26, 2026 at 1:39 pm
Запой сопровождается выраженной интоксикацией, нарушением сна, нестабильностью давления и изменениями в работе нервной системы. При длительном течении состояние может ухудшаться, и самостоятельный выход становится затруднённым. В таких случаях стационар рассматривается как пространство, где можно безопасно стабилизировать показатели и обеспечить постепенное восстановление.
Подробнее можно узнать тут – https://vyvod-iz-zapoya-v-staczionare-nizhnij-novgorod-1.ru
GeorgeBax · April 26, 2026 at 1:44 pm
здесь mega darknet
MatthewGed · April 26, 2026 at 2:07 pm
Обращение в наркологический стационар в Санкт-Петербурге может стать важным шагом для людей, страдающих от алкогольной или наркотической зависимости. Стационарное лечение предоставляет пациентам не только медицинскую помощь, но и психологическую поддержку, необходимую для успешной реабилитации. Это подход, ориентированный на комплексное восстановление здоровья, физическое и психоэмоциональное состояние пациента.
Подробнее можно узнать тут – https://narkologicheskij-staczionar-sankt-peterburg-2.ru
12BET · April 26, 2026 at 2:16 pm
Thanks for posting this. Looking for these resources 😀
https://vin777.ong/ · April 26, 2026 at 2:26 pm
Fantastic piece of writing here1
BryanNat · April 26, 2026 at 2:44 pm
Наркологическая помощь в Воронеже: срочный выезд нарколога, капельницы и лечение зависимостей в наркологической клинике «Клиника Плюс».
Узнать больше – клиника наркологической помощи
tỷ lệ kèo · April 26, 2026 at 2:46 pm
The post is absolutely fantastic! Lots of great info and inspiration, both of which we all need! Also like to admire the time and effort you put into your website and detailed info you offer! I will bookmark your website!
Ethantoisa · April 26, 2026 at 2:55 pm
Капельница от похмелья — это эффективный способ экстренной помощи, предназначенный для того, чтобы помочь организму быстро восстановиться после злоупотребления алкоголем. В наркологической клинике «Частный медик 24» в Самаре мы предоставляем услугу безопасной детоксикации и восстановления 24/7. Капельница помогает организму вывести токсины, восстановить водно-электролитный баланс и улучшить общее состояние пациента, не создавая дополнительных нагрузок на сердце, печень и почки.
Выяснить больше – капельница от похмелья анонимно в самаре
CharlesFut · April 26, 2026 at 2:59 pm
Наркологическая помощь на дому помогает избежать стресса, связанного с поездкой в клинику. Особенно это важно в случаях, когда пациент находится в состоянии тяжёлой интоксикации или переживает абстинентный синдром, который можно только усугубить дополнительной нагрузкой. Врач приедет в кратчайшие сроки, обеспечивая необходимое лечение в первые часы после ухудшения состояния. Также важно, что при выезде специалист гарантирует полную анонимность, что особенно важно для многих людей, которые боятся открыто признаться в своей проблеме. Профессиональная наркологическая помощь на дому позволяет избежать срыва и начать процесс восстановления без стресса.
Углубиться в тему – вызвать нарколога на дом
Jeremydaype · April 26, 2026 at 3:02 pm
Днём человек ещё как-то держится, а к вечеру нарастает усталость, тревога усиливается, сон не приходит, и появляется ощущение, что «так не выдержать». Это один из главных триггеров повторного употребления. Нормальная задача врача — не только снять симптомы, но и объяснить, как пережить ночь: чего ожидать, как организовать спокойную обстановку, что контролировать, какие признаки опасны и требуют срочной оценки.
Детальнее – http://vyvod-iz-zapoya-orekhovo-zuevo12.ru
click · April 26, 2026 at 3:17 pm
whoah this weblog is great i really like studying your articles. Stay up the great work! You already know, lots of persons are looking round for this information, you can aid them greatly.
Bremerhaven · April 26, 2026 at 3:40 pm
References:
https://casino-dice-casino.online-spielhallen.de/
Hanover (Hannover) · April 26, 2026 at 4:03 pm
References:
Halle (Saale)
References:
https://eurogrand-casino.online-spielhallen.de/
DavidKig · April 26, 2026 at 4:03 pm
Стоимость капельницы от похмелья в Самаре зависит не только от прайса клиники, но и от состава инфузионной терапии, срочности выезда, времени суток и общего состояния пациента, включая возможные последствия алкоголизма. Базовые программы обычно включают осмотр специалиста, постановку капельницы и стандартный набор растворов для снятия интоксикации. Если состояние тяжелее, может потребоваться кодирование или лечение в стационаре, что увеличивает цену из-за расширенного состава препаратов и более длительного наблюдения.
Получить дополнительную информацию – kapelnicza-ot-pokhmelya-samara-7.ru/
Charlesvok · April 26, 2026 at 4:17 pm
Формат помощи выбирают не по принципу «как удобнее», а по тому, насколько стабильно состояние и каков риск осложнений. Один и тот же диагноз «запой» может выглядеть по-разному: у кого-то ведущая проблема — давление и тахикардия, у другого — выраженная тревога и бессонница, у третьего — сильная тошнота и обезвоживание, у четвёртого — спутанность сознания или признаки психотических симптомов. Именно поэтому первое, что делает врач, — собирает информацию о длительности употребления, времени последнего приёма, сопутствующих заболеваниях, аллергиях и лекарствах, которые человек принимал самостоятельно. После этого проводится очная оценка: на дому или в клинике.
Подробнее можно узнать тут – narkologicheskaya-klinika-otzyvy
Michaelmaply · April 26, 2026 at 4:35 pm
Основой стационарного лечения является инфузионная терапия, направленная на ускоренное выведение токсинов, коррекцию кислотно-щелочного баланса и восстановление метаболических процессов. Стандартная капельница при выходе из запоя включает кристаллоидные и коллоидные растворы, витаминные комплексы группы B и C, гепатопротекторы, антиоксиданты и симптоматические препараты для нормализации сна и снижения тревожности. Состав, объем и скорость инфузии рассчитываются индивидуально с учетом возраста, массы тела, длительности интоксикации, функции почек и печени, а также наличия аллергических реакций. Мы быстро купируем мучительные проявления абстиненции, восстанавливаем аппетит, устраняем мышечные спазмы и нормализуем суточные ритмы. При необходимости подключаются препараты для стабилизации сердечного ритма, коррекции артериального давления и защиты нейрональных структур от эксайтотоксичности. Все медикаменты сертифицированы, применяются в строгом соответствии с клиническими рекомендациями Минздрава РФ и не вызывают вторичной зависимости. Дозировки ежедневно пересматриваются лечащим врачом на основе лабораторных анализов и клинической динамики, что гарантирует высокий уровень качества медицинской помощи и безопасность пациента. Снятие острых симптомов происходит уже в первые сутки, что значительно улучшает общее самочувствие и возвращает способность к адекватному восприятию действительности.
Разобраться лучше – вывод из запоя в стационаре анонимно в нижнем новгороде
Howardsoilk · April 26, 2026 at 4:38 pm
Нарколог на дом в Екатеринбурге: выезд врача на дом, лечение запоя и консультации в наркологической клинике «НЕО+».
Разобраться лучше – нарколог на дом
Jeremypep · April 26, 2026 at 5:00 pm
Многие семьи слишком долго откладывают обращение к услугам нарколога, надеясь, что человек «отойдет сам», выспится, восстановится за день-два или просто даст очередное обещание больше не повторять употребление. На практике такие ожидания часто только отнимают время. Если зависимость уже начала формироваться, самочувствие после алкоголя становится тяжелее, а промежутки между срывами сокращаются, это говорит о том, что проблема вышла за пределы бытовой и требует профессиональной оценки.
Подробнее тут – наркологическая помощь
Johnnytat · April 26, 2026 at 5:39 pm
Основное действие капельницы заключается в быстром восстановлении водного баланса и выведении токсинов, оставшихся в организме после употребления алкоголя. Алкоголь нарушает работу печени, почек и других органов, поэтому капельница помогает организму вернуться в норму, восстанавливая функции этих органов и поддерживая обмен веществ. Состав капельницы также может включать препараты, которые поддерживают работу сердечно-сосудистой системы и устраняют болезненные ощущения, такие как головная боль и тошнота.
Подробнее можно узнать тут – капельница от похмелья цена в нижнем новгороде
Jeremydaype · April 26, 2026 at 5:58 pm
Самостоятельные попытки обычно идут по двум типичным маршрутам. Первый — «пить понемногу, чтобы не трясло». На практике это продлевает запой и усиливает истощение: сон остаётся поверхностным, тревога нарастает, давление и пульс становятся нестабильными, организм не успевает восстанавливаться. Второй маршрут — резко прекратить и «перетерпеть». Тогда симптомы отмены могут нарастать резко: паника, сильный тремор, потливость, тахикардия, скачки давления, тошнота, рвота, бессонница. Испугавшись ухудшения, человек снова возвращается к алкоголю, потому что это кажется единственным быстрым способом облегчить состояние.
Узнать больше – вывод из запоя на дому цена
ClintonPoush · April 26, 2026 at 6:02 pm
“Капельница с мягким восстановлением идеально подходит тем, кто ищет постепенный и безопасный способ вернуть себе нормальное состояние после пьянки. Такой подход не перегружает организм и помогает избежать нежелательных эффектов от слишком резкого восстановления.” — Алексей Смирнов, нарколог, клиника восстановления.
Получить дополнительные сведения – http://kapelnicza-ot-pokhmelya-samara-12.ru/
Richardcon · April 26, 2026 at 6:02 pm
Обращение на стадии, когда человек не может самостоятельно справиться с зависимостью, значительно повышает шансы на успешное лечение и восстановление. Важно начать лечение на раннем этапе, когда физическая и психологическая зависимость еще не столь выражены.
Разобраться лучше – наркологическая помощь
Timothyelapy · April 26, 2026 at 6:31 pm
“tahta cesitleri” konusu icin burada harika bilgiler var. Kendiniz gorun: https://kendihobim.com/articles/mobilya-tahta-cesitleri-kullanim-alanlari/
Timothyelapy · April 26, 2026 at 6:35 pm
Bu arada, eger new balance 530 renkleri konusuyla ilgileniyorsan?z, buray? inceleyin. Iste link: https://atletikhayal.com/articles/new-balance-530-beyaz-kadin-stil-konfor/
Melvinadage · April 26, 2026 at 6:51 pm
Особое внимание мы уделяем психологической составляющей. Наркологическая помощь в Воронеже в «Клиника Плюс» — это не только физическое очищение, но и работа с мотивацией, разрушение психологических триггеров зависимости. Родственники получают отдельную поддержку: консультации психолога помогают правильно выстроить общение с зависимым человеком и мотивировать его на дальнейшее лечение. Реабилитация может проходить амбулаторно или в стационаре партнёрских центров с комфортабельными условиями, где пациенты находятся под круглосуточным наблюдением.
Изучить вопрос глубже – оказание наркологической помощи в воронеже
BryanNat · April 26, 2026 at 7:15 pm
Когда человек или его родственники понимают, что нужна наркологическая помощь в Воронеже, время становится решающим фактором. Запой, ломка, тяжёлая интоксикация — в таких ситуациях промедление может привести к необратимым последствиям для здоровья и жизни. Наша клиника создана именно для того, чтобы оказывать эффективную наркологическую помощь в Воронеже в самых сложных случаях. Мы не заставляем ждать в очередях государственных учреждений, не ставим на учёт и не разглашаем информацию. Всё происходит конфиденциально, на дому или в комфортных условиях нашей партнёрской клиники. Пациенты из Воронежа, Воронежской области, а также соседних регионов уже более 12 лет выбирают «Клиника Плюс» благодаря сочетанию скорости, профессионализма и доказанной результативности.
Изучить вопрос глубже – http://narkologicheskaya-pomoshh-voronezh-1.ru
Jefferycrync · April 26, 2026 at 7:43 pm
Выбор формата — ключевой момент. Нельзя ориентироваться только на удобство, потому что в ряде случаев «домашний» вариант создаёт иллюзию безопасности, когда на самом деле нужен контроль. В клинике «Свет Баланса» формат подбирается по состоянию: оценивают симптомы, риски осложнений, способность пациента соблюдать назначения и необходимость наблюдения.
Получить больше информации – https://narkologicheskaya-klinika-moskva12.ru
DonaldHum · April 26, 2026 at 8:11 pm
Терапевтический алгоритм в стационаре не сводится к единой процедуре. Это последовательная система диагностики, стабилизации, медикаментозной поддержки и подготовки к противорецидивному этапу. При поступлении врач проводит детальный осмотр, собирает анамнез, оценивает неврологический статус и при необходимости назначает экспресс-анализы крови, ЭКГ и ультразвуковое исследование внутренних органов. На основе полученных данных формируется индивидуальный протокол, учитывающий возраст, длительность употребления, наличие хронических заболеваний и переносимость лекарственных компонентов. Мы отказываемся от шаблонных схем в пользу точного дозирования, что минимизирует нагрузку на ослабленный организм и ускоряет восстановление метаболических функций. Основная задача на этом этапе — безопасно вывести пациента из состояния острой интоксикации без резких скачков артериального давления и кардиологических перегрузок.
Разобраться лучше – быстрый вывод из запоя в стационаре нижний новгород
AnthonyBar · April 26, 2026 at 8:18 pm
Далее выполняется медицинская детоксикация: корректируется водно-электролитный баланс, снимается интоксикация, поддерживается работа сердечно-сосудистой системы, снижается тремор, стабилизируется сон и тревожность. Важно, что схема подбирается индивидуально: при разных рисках объём поддержки будет различаться. В ряде случаев достаточно амбулаторного наблюдения и рекомендаций, в других — нужен стационар, чтобы контролировать динамику и вовремя корректировать терапию.
Подробнее – vyvod-iz-zapoya-v-moskve-v-stacionare
Jefferycrync · April 26, 2026 at 8:35 pm
Острые состояния требуют особенно аккуратного подхода, потому что при резкой отмене алкоголя или ряда веществ возможны волнообразные ухудшения. Сегодня стало легче — через несколько часов снова накрывает тремором, паникой, скачками давления или бессонницей. Поэтому грамотная помощь всегда начинается с очного осмотра и оценки жизненно важных показателей. Если состояние нестабильно, предпочтительнее стационар, где можно наблюдать динамику и быстро корректировать терапию. Если риски умеренные и человек сохранен, возможен выезд врача на дом, но с чёткими критериями, при которых нужно немедленно переводить пациента под круглосуточное наблюдение.
Исследовать вопрос подробнее – platnaya-narkologicheskaya-klinika-moskva
Thomaslak · April 26, 2026 at 8:41 pm
Капельница от похмелья в Самаре используется для устранения симптомов алкогольной интоксикации, которые могут включать головную боль, тошноту, слабость, рвоту и обезвоживание. Это достигается за счет введения специальных растворов, которые помогают организму восстановиться и очиститься от токсинов.
Разобраться лучше – капельница от похмелья цена самара
BryanNat · April 26, 2026 at 8:46 pm
Особое внимание мы уделяем психологической составляющей. Наркологическая помощь в Воронеже в «Клиника Плюс» — это не только физическое очищение, но и работа с мотивацией, разрушение психологических триггеров зависимости. Родственники получают отдельную поддержку: консультации психолога помогают правильно выстроить общение с зависимым человеком и мотивировать его на дальнейшее лечение. Реабилитация может проходить амбулаторно или в стационаре партнёрских центров с комфортабельными условиями, где пациенты находятся под круглосуточным наблюдением.
Подробнее можно узнать тут – наркологическая помощь воронеж
Spencersaica · April 26, 2026 at 9:10 pm
Такие критерии помогают определить, когда необходим более строгий контроль и постоянное наблюдение. В стационаре создаются условия, при которых лечение проходит без внешних факторов, влияющих на состояние пациента. При этом услуга может предоставляться анонимно, а цену лечения можно уточнить заранее по телефону или при обращении.
Подробнее тут – наркология вывод из запоя в стационаре в нижнем новгороде
AnthonyBar · April 26, 2026 at 9:10 pm
Процесс начинается с оценки состояния. Врач уточняет длительность запоя, время последнего приёма алкоголя, выраженность симптомов, наличие хронических заболеваний, перенесённых осложнений, аллергий, принимаемых препаратов. После этого проводится осмотр: давление, пульс, дыхание, температура, уровень сознания, признаки обезвоживания, неврологический статус. На основании этой картины подбирается план детоксикации и поддержки.
Выяснить больше – http://vyvod-iz-zapoya-moskva1-12.ru/srochnyj-vyvod-iz-zapoya-v-moskve/
Scottimpen · April 26, 2026 at 9:41 pm
Откладывание помощи создает иллюзию управления ситуацией, тогда как нейробиологические процессы продолжают развиваться в неблагоприятном направлении. Регулярная интоксикация перестраивает дофаминовую и ГАМК-ергическую системы, снижает естественную выработку нейромедиаторов и формирует условные рефлексы, связывающие употребление с любым стрессовым триггером. При развитии абстинентного синдрома появляются характерные признаки: выраженная слабость, тошнота, ломки, нарушения сна, тахикардия. В результате каждый последующий кризис переносится тяжелее, требует более длительной стабилизации и несет повышенные риски для печени, сердца и центральной нервной системы. Кроме того, затягивание снижает мотивацию пациента к лечению, так как период «ремиссии» между срывами создает ложное ощущение восстановления. Профессиональная наркология работает с этой динамикой, предлагая помощь на том этапе, когда вмешательство еще эффективно и не требует реанимационных мер.
Исследовать вопрос подробнее – вызов наркологической помощи воронеж
Ethantoisa · April 26, 2026 at 9:43 pm
Капельница от похмелья — это эффективный способ экстренной помощи, предназначенный для того, чтобы помочь организму быстро восстановиться после злоупотребления алкоголем. В наркологической клинике «Частный медик 24» в Самаре мы предоставляем услугу безопасной детоксикации и восстановления 24/7. Капельница помогает организму вывести токсины, восстановить водно-электролитный баланс и улучшить общее состояние пациента, не создавая дополнительных нагрузок на сердце, печень и почки.
Получить больше информации – капельница от похмелья самара
LesterBarne · April 26, 2026 at 10:04 pm
продолжить
Vegas Legacy casino промокод бонусы на депозит
Dwayneoxymn · April 26, 2026 at 10:25 pm
Алкогольная зависимость редко выглядит как «постоянное пьянство». Чаще она маскируется под привычные сценарии: снять напряжение после работы, «уснуть без мыслей», пережить стресс или конфликт, заглушить тревогу. Постепенно организм привыкает, дозы растут, трезвость становится тяжёлой, а попытки «просто перестать» заканчиваются бессонницей, внутренней дрожью, потливостью, тошнотой, скачками давления и паникой. В этот момент человек пьёт уже не ради удовольствия, а чтобы не столкнуться с ухудшением. Лечение алкоголизма в Ногинске важно начинать тогда, когда стало понятно: ситуация повторяется и управлять ей самостоятельно не получается. Чем раньше зависимость переводится в медицинский процесс, тем меньше риск осложнений и тем быстрее появляется устойчивость.
Получить дополнительные сведения – алкоголь лечение алкоголизма
CharlesFut · April 26, 2026 at 10:43 pm
Для жителей Воронежа выезд нарколога на дом — это быстрый и удобный способ получить экстренную помощь. Когда человек переживает запой, а его физическое и эмоциональное состояние быстро ухудшается, наркологическая помощь на дому становится оптимальным решением. Врач приезжает и немедленно оценивает состояние пациента: проверяет его пульс, давление, частоту дыхания, уровень сознания и другие важные показатели. Это помогает составить точный план лечения, который будет направлен на восстановление организма, снятие токсинов и стабилизацию состояния пациента.
Получить дополнительную информацию – http://narkolog-na-dom-voronezh-4.ru
CharlesFut · April 26, 2026 at 11:31 pm
Для жителей Воронежа выезд нарколога на дом — это быстрый и удобный способ получить экстренную помощь. Когда человек переживает запой, а его физическое и эмоциональное состояние быстро ухудшается, наркологическая помощь на дому становится оптимальным решением. Врач приезжает и немедленно оценивает состояние пациента: проверяет его пульс, давление, частоту дыхания, уровень сознания и другие важные показатели. Это помогает составить точный план лечения, который будет направлен на восстановление организма, снятие токсинов и стабилизацию состояния пациента.
Получить дополнительную информацию – http://www.domen.ru
samedaymaid · April 26, 2026 at 11:39 pm
The next time I read a blog, Hopefully it won’t disappoint me just as much as this one. After all, Yes, it was my choice to read, however I truly believed you would probably have something helpful to say. All I hear is a bunch of moaning about something you could possibly fix if you weren’t too busy searching for attention.
OliverBok · April 26, 2026 at 11:59 pm
Медицинская детоксикация помогает снизить интоксикацию и сделать состояние управляемым. Обычно уменьшается выраженность тремора и потливости, давление и пульс становятся ровнее, снижается тошнота, тревога перестаёт быть пиковым состоянием, появляется шанс на восстановление сна. Но детоксикация не «отменяет зависимость». Она создаёт условия, при которых человек может трезво принять решение о дальнейшем лечении и пережить первые сутки без возврата к алкоголю или веществам «для облегчения».
Подробнее можно узнать тут – http://narkologicheskaya-klinika-vidnoe12.ru
Johnnytat · April 27, 2026 at 12:46 am
Процедура капельницы от похмелья может быть рекомендована при наличии выраженных симптомов интоксикации, которые нарушают нормальное функционирование организма. Это особенно актуально в тех случаях, когда обычные методы, такие как принятие воды или таблетки, не приносят должного облегчения. Для получения дополнительной информации или записи на процедуру можно обратиться через сайт, а в сложных случаях может потребоваться стационарное лечение или наркологическая помощь.
Изучить вопрос глубже – https://kapelnicza-ot-pokhmelya-nizhnij-novgorod.ru/
Dwayneoxymn · April 27, 2026 at 1:11 am
Зависимость меняет работу нервной системы: алкоголь начинает выполнять функцию регулятора — сна, тревоги, настроения и даже физического самочувствия. Когда человек прекращает пить, организм реагирует отменой, и именно она подталкивает вернуться к употреблению. Сила воли в этой точке часто проигрывает физиологии: тревога растёт, сон исчезает, сердце бьётся чаще, давление «скачет», появляется ощущение угрозы.
Изучить вопрос глубже – положить на лечение от алкоголизма
Jeremypep · April 27, 2026 at 1:22 am
Когда родственники начинают искать помощь, они обычно хотят решить сразу несколько задач. Нужно быстро стабилизировать состояние больного, снизить риски осложнений, понять, можно ли ограничиться домашним форматом или требуется госпитализация в стационаре, насколько выражена зависимость и что делать дальше, чтобы через несколько дней не оказаться в той же точке. Именно поэтому современная наркологическая помощь в рамках профессиональной клиники рассматривается не как одна процедура, а как последовательная система действий: от осмотра и первичной стабилизации до более глубокой работы с причинами зависимости, мотивацией пациента и профилактикой рецидивов.
Углубиться в тему – скорая наркологическая помощь
https://satapornbooks.com/tests/pags/?codigo-promocional-de-1xbet.html · April 27, 2026 at 2:04 am
https://satapornbooks.com/tests/pags/?codigo-promocional-de-1xbet.html
Jeremypep · April 27, 2026 at 2:17 am
Под этим направлением обычно понимают не один универсальный сценарий, а несколько форматов помощи, которые применяются в зависимости от состояния пациента. На первом этапе часто решается задача стабилизации: нужно оценить выраженность интоксикации, общее самочувствие, понять степень риска и определить, какой объем вмешательства уместен именно сейчас (например, необходима ли очищающая капельница). Но даже если речь идет о срочном обращении, грамотный подход не ограничивается только кратковременным облегчением.
Детальнее – наркологическая помощь на дому в воронеже
RobertDic · April 27, 2026 at 2:50 am
Капельница от похмелья в Самаре: быстрое снятие интоксикации, восстановление после алкоголя и улучшение самочувствия под контролем специалистов в наркологической клинике «Похмельная служба»
Изучить вопрос глубже – капельница от похмелья анонимно в самаре
RobertDic · April 27, 2026 at 5:45 am
После введения растворов активные вещества быстро распределяются по организму. Это способствует выведению продуктов распада алкоголя, улучшению работы нервной системы и восстановлению энергетического баланса. Уже в процессе инфузии уменьшаются головная боль, тошнота и слабость.
Получить дополнительные сведения – капельница от похмелья анонимно в самаре
Wolfsburg · April 27, 2026 at 6:37 am
References:
Karlsruhe
References:
https://online-casino-app-echtgeld.online-spielhallen.de/
Stephenwaf · April 27, 2026 at 6:50 am
При употреблении психоактивных веществ риск осложнений часто выше и непредсказуемее: неизвестный состав, сочетания, влияние на сердечный ритм, дыхание и психическое состояние. Поэтому детоксикация при наркотической зависимости строится особенно аккуратно: врач оценивает состояние, собирает информацию о симптомах, возможных сочетаниях и прошлых осложнениях, а затем выбирает тактику стабилизации. Важно, что в таких случаях «сделать быстро и без вопросов» — самый опасный подход.
Получить дополнительные сведения – narkologicheskaya klinika na dom
Bielefeld · April 27, 2026 at 7:02 am
References:
Offenbach am Main
References:
https://catalonia-bavaro-beach-golf-casino.online-spielhallen.de/
LesterBarne · April 27, 2026 at 7:38 am
сайт
Beef casino промокод при регистрации
BryanNat · April 27, 2026 at 8:01 am
Наркологическая помощь в Воронеже: срочный выезд нарколога, капельницы и лечение зависимостей в наркологической клинике «Клиника Плюс».
Получить больше информации – https://narkologicheskaya-pomoshh-voronezh-1.ru/
LesterBarne · April 27, 2026 at 9:31 am
ссылка на сайт
Gizbo casino промокод при регистрации
Jeremydaype · April 27, 2026 at 9:59 am
Днём человек ещё как-то держится, а к вечеру нарастает усталость, тревога усиливается, сон не приходит, и появляется ощущение, что «так не выдержать». Это один из главных триггеров повторного употребления. Нормальная задача врача — не только снять симптомы, но и объяснить, как пережить ночь: чего ожидать, как организовать спокойную обстановку, что контролировать, какие признаки опасны и требуют срочной оценки.
Углубиться в тему – vyvod iz zapoya stacionar
installment loans online · April 27, 2026 at 10:04 am
After looking at a handful of the articles on your web page, I honestly like your technique of blogging. I saved it to my bookmark website list and will be checking back in the near future. Please check out my website as well and let me know what you think.
Jordanvep · April 27, 2026 at 10:55 am
Выбирая наркологический стационар в Санкт-Петербурге, важно учитывать не только стоимость лечения, но и репутацию учреждения, а также подход, который применяется к лечению зависимых. Подходящее учреждение обеспечит не только лечение физической зависимости, но и долгосрочное восстановление и психологическую поддержку. Важно, чтобы в клинике предоставлялась психотерапия и была возможность консультации психиатра для комплексной помощи пациенту.
Подробнее – частный наркологический стационар
شركة كشف تسربات المياه بعنك · April 27, 2026 at 11:01 am
شركة كشف تسربات المياه بعنك
MichaelRor · April 27, 2026 at 1:41 pm
Здравствуйте!
Строительство дома каркасного — это оптимальный вариант для тех, кто хочет построить дом быстро и с минимальными затратами. Мы предлагаем каркасное строительство домов с возможностью выбора материалов и архитектурных решений. Такой дом будет теплым, удобным и долговечным. Профессиональные специалисты помогут вам на всех этапах строительства, от проектирования до отделки. Строительство дома каркасного — это быстрый процесс с отличным результатом.
Для строительства дома — выбор правильного проекта и материалов крайне важен. Мы предлагаем полный спектр услуг для строительства домов, от проектирования до окончательной отделки. Наши специалисты помогут вам выбрать идеальный проект для вашего участка. Мы используем только качественные и проверенные материалы, что гарантирует долговечность вашего будущего дома. Для строительства дома мы предлагаем наиболее выгодные и эффективные решения.
Больше информации по ссылке – http://vbelgorode.com/company_news/157168/
купить дом ремонтом, квартиры в новостройках с отделкой санкт петербурга, квартире ремонт кухни
квартира сталинка ремонт, владивосток ремонт домов, строительство сруба бани
Удачи!
mitasuoil.com · April 27, 2026 at 3:16 pm
mitasuoil.com
comprare follower tiktok · April 27, 2026 at 3:25 pm
This blog post is excellent, probably because of how well the subject was developed. I like some of the comments too.
Victorler · April 27, 2026 at 3:39 pm
После нескольких дней употребления алкоголя организм работает с перегрузкой. Усиливается обезвоживание, ухудшается сон, появляется дрожь, растет тревожность, нарушается аппетит, могут беспокоить скачки давления, сердцебиение, слабость и тошнота. В такой ситуации состояние нередко требует осмотра врача, особенно если самочувствие продолжает ухудшаться или уже были неудачные попытки справиться своими силами. Подобные состояния встречаются не только при последствиях алкоголизма, но и у людей, которые впервые столкнулись с тяжелой интоксикацией после приема спиртного.
Подробнее – нарколог на дом цена в екатеринбурге
Randallnib · April 27, 2026 at 3:45 pm
Продолжительное употребление алкоголя неизбежно переводит организм в состояние хронической интоксикации, при котором собственные компенсаторные механизмы перестают справиться с нарастающей токсической нагрузкой. Накапливающиеся продукты метаболизма этанола, дефицит электролитов, нарушение работы ферментных систем и дисфункция центральной нервной системы формируют клиническую картину, требующую не симптоматического облегчения, а комплексного медицинского вмешательства. Вывод из запоя в стационаре в Нижнем Новгороде в наркологической клинике «Стармед» организован с соблюдением современных протоколов доказательной медицины, где безопасность пациента, непрерывный мониторинг и персонализированный подбор терапии являются абсолютным приоритетом. Мы понимаем, что кризисные состояния не терпят отлагательств, поэтому наши квалифицированные специалисты готовы быстро оценить клиническую ситуацию, организовать безопасную транспортировку и запустить детоксикационный протокол без задержек. Все манипуляции проводятся в лицензированных условиях, с непрерывным отслеживанием витальных показателей и строгим соблюдением врачебной этики. Первичная оценка состояния начинается с дистанционной консультации, что позволяет врачам заранее подготовить необходимое оборудование, скорректировать план госпитализации и минимизировать время между обращением и началом терапии. Такой подход исключает хаотичные решения и фокусирует внимание на реальных медицинских проблемах, требующих системного решения.
Ознакомиться с деталями – вывод из запоя в стационаре клиника в нижнем новгороде
EdmondDuawn · April 27, 2026 at 3:49 pm
При выводе из запоя на дому с быстрым облегчением используются различные медикаменты, направленные на быстрое восстановление водно-солевого баланса, улучшение функции печени и почек, а также снижение симптомов алкогольного абстинентного синдрома. Важно, что состав препаратов подбирается в зависимости от состояния пациента, и все препараты вводятся под контролем квалифицированного медицинского специалиста.
Исследовать вопрос подробнее – вывод из запоя на дому цена
comprare followers instagram · April 27, 2026 at 4:11 pm
Fantastic piece of writing here1
https://bookmarkfox.com/story7070389/promo-code-1xbet-casino-pakistan-2026-1xwide-bonus-130 · April 27, 2026 at 5:13 pm
https://bookmarkfox.com/story7070389/promo-code-1xbet-casino-pakistan-2026-1xwide-bonus-130
live cams · April 27, 2026 at 5:38 pm
There is a lot of misunderstanding about these issues today. Your material helps explain things.
FrankPaw · April 27, 2026 at 6:20 pm
В Москве такие состояния нередко долго скрываются за занятостью, работой и внешним благополучием. Поэтому к специалисту часто обращаются уже тогда, когда собственные попытки справиться не дают результата. Аддиктолог оценивает не только сам факт зависимости, но и ее влияние на поведение, эмоциональное состояние, отношения и повседневные решения. Для многих особенно важен конфиденциальный формат: анонимный прием аддиктолога помогает обсудить ситуацию спокойно, без лишней огласки и внутреннего напряжения.
Изучить вопрос глубже – лечение деменции клиника
comprare follower tiktok · April 27, 2026 at 6:21 pm
A thoughtful insight and ideas I will use on my blog. You’ve obviously spent some time on this. Congratulations
CharlesAromA · April 27, 2026 at 6:24 pm
Когда зависимости становятся хроническими и угрожают жизни пациента, комплексная реабилитация при наркомании в специализированных клиниках Москвы, включая вывод из состояния в стационаре и последующий анализ данных о состоянии пациента, может стать единственным возможным решением. Процесс восстановления включает в себя работу не только с зависимостью, но и с психоэмоциональным состоянием, что делает лечение более эффективным и долговечным.
Получить дополнительные сведения – https://reabilitacziya-alkogolikov-moskva-2.ru
SerenanoG · April 27, 2026 at 6:39 pm
В центре «Время Возрождения» в Кемерово разрабатывают индивидуальные программы терапии при алкогольной и наркотической зависимости. Лечение строится с учётом состояния здоровья, стажа употребления и сопутствующих факторов, что повышает эффективность медицинской помощи.
Подробнее тут – лучшая капельницу от запоя
comprar seguidores tiktok · April 27, 2026 at 6:58 pm
You are my inhalation , I possess few web logs and very sporadically run out from to brand 🙁
DebraEvome · April 27, 2026 at 7:24 pm
«НаркоЗдравие» — клиника в Москве, где оказывают наркологическую помощь любой сложности: вывод из запоя, кодирование, лечение зависимостей, работа реабилитационного центра. Специалисты выезжают на дом, обеспечивая анонимность и быструю поддержку пациенту.
Подробнее можно узнать тут – торпедо кодирование отзывы
comprar seguidores tiktok · April 27, 2026 at 8:03 pm
I can’t go into details, but I have to say its a good article!
Johnniesheme · April 27, 2026 at 8:50 pm
В «НовомЯ» уделяют внимание психотерапевтическим инструментам — в том числе когнитивно-поведенческой терапии, а также другим методам, которые применяются по показаниям. Это помогает закреплять трезвость и формировать новые стратегии поведения.
Получить больше информации – кодировка по методу довженко цена
CharlesAromA · April 27, 2026 at 11:29 pm
Реабилитация алкоголиков в Москве с комплексным подходом — это многогранный процесс, включающий в себя не только медицинские процедуры, но и психологическую поддержку, физическую реабилитацию и помощь в социальной адаптации. Профессиональный реабилитационный центр обеспечивает индивидуальный подход к каждому пациенту, включая такие методы, как кодирование и своевременное лечение запоя. Важно отметить, что успешное лечение алкоголизма требует учета множества факторов, таких как степень зависимости, психоэмоциональное состояние пациента, а также его физическое здоровье. Комплексный подход помогает эффективно устранить все составляющие проблемы, минимизируя риски рецидивов.
Подробнее – центр реабилитации алкоголиков город
SerenanoG · April 28, 2026 at 12:16 am
В медицинском центре «Время Возрождения» в Кемерово обеспечивается конфиденциальный формат наркологической помощи. Применяются современные методы терапии, направленные на снижение тяги к психоактивным веществам и формирование устойчивой ремиссии.
Подробнее можно узнать тут – лечение наркомании
graph.org · April 28, 2026 at 1:04 am
References:
Mahjongg dimensions more time
References:
https://graph.org/Aristocrat-Poker-Machine-For-Sale-04-27
FrankRar · April 28, 2026 at 1:08 am
Процесс вывода из запоя на дому в Ярославле строится по четко отлаженной схеме, включающей несколько последовательных этапов, направленных на максимально быстрое и безопасное восстановление здоровья пациента.
Получить дополнительную информацию – вывод из запоя капельница
WilmaNep · April 28, 2026 at 1:09 am
«Narkology» — это наркологическая информационная сеть, где каждому клиенту предлагают персонализированный план возвращения к здоровому образу жизни. Наши программы включают целевые консультации наркологов, психологическую реабилитацию, онлайн-группы поддержки и обучение навыкам саморегуляции. Круглосуточная информационная поддержка специалистов и современные технологии связи обеспечивают быстрое и комфортное возвращение к привычной жизни без зависимости.
Получить дополнительные сведения – лечение алкоголизма вызов на дом
https://500px.com/p/interculturalbd?view=photos · April 28, 2026 at 3:21 am
https://500px.com/p/interculturalbd?view=photos
Josephrem · April 28, 2026 at 4:30 am
Включает полную лабораторную диагностику — печёночные пробы, биохимический анализ крови, ЭКГ и УЗИ органов брюшной полости. На основе результатов врач определяет оптимальную дозировку и продолжительность капельниц, минимизируя нагрузку на сердце и почки.
Узнать больше – http://lechenie-alkogolizma-krasnodar0.ru/
Johnniesheme · April 28, 2026 at 4:31 am
Наркологическая клиника «НовыйЯ» в Москве оказывает анонимную помощь при алкогольной и наркотической зависимости: диагностика, детоксикация, купирование абстинентного синдрома и подбор дальнейшей программы лечения. Акцент делается на медицинскую безопасность и конфиденциальность обращения.
Получить дополнительные сведения – капельница от запоя состав
CharlesAromA · April 28, 2026 at 5:37 am
Когда зависимости становятся хроническими и угрожают жизни пациента, комплексная реабилитация при наркомании в специализированных клиниках Москвы, включая вывод из состояния в стационаре и последующий анализ данных о состоянии пациента, может стать единственным возможным решением. Процесс восстановления включает в себя работу не только с зависимостью, но и с психоэмоциональным состоянием, что делает лечение более эффективным и долговечным.
Получить больше информации – алкоголик реабилитация наркоманов город
Carolynabure · April 28, 2026 at 5:40 am
Наркологическая клиника «НОВЫЙ НАРКОЛОГ» в Санкт-Петербурге предоставляет медицинскую помощь при алкоголизме и наркомании на разных этапах — от первичной стабилизации до восстановительных программ. Специалисты проводят детоксикацию, снимают острые симптомы и помогают выстроить дальнейшую тактику лечения. Работа ведётся конфиденциально, с индивидуальным подбором терапии.
Получить дополнительную информацию – https://new-narkolog.ru/reabilitatsiya/reabilitatsiya-alkogolizma
SerenanoG · April 28, 2026 at 7:01 am
Наркологическая помощь в «Время Возрождения» в Кемерово доступна в круглосуточном режиме. Специалисты проводят комплекс мероприятий, позволяющих восстановить функции организма и запустить процесс длительного выздоровления.
Углубиться в тему – нарколог на дом вывод из запоя
Robertvep · April 28, 2026 at 7:13 am
После завершения основного курса лечения в наркологической клинике в Краснодаре пациентам предлагаются программы социальной реабилитации. Они направлены на восстановление социальных навыков, адаптацию в обществе и предотвращение рецидивов. Ключевым элементом здесь является поддержка со стороны профессиональных социальных работников и участие в группах взаимопомощи.
Подробнее тут – https://narkologicheskaya-klinika-krasnodar0.ru/narkologicheskaya-klinika-anonimno-krasnodar
CharlesAromA · April 28, 2026 at 7:38 am
Комплексная реабилитация алкоголиков в Москве помогает пациентам не только избавиться от зависимости, но и вернуться к полноценной жизни. Процесс восстановления включает в себя не только лечение алкоголизма как физического заболевания, но и работу с психологическими, социальными и эмоциональными аспектами, которые могут стать причиной или следствием зависимости. Такое подходное лечение, как правило, требует усилий со стороны как специалистов, так и самого пациента.
Выяснить больше – https://reabilitacziya-alkogolikov-moskva-2.ru
https://www.google.dj/url?q=https://totalfratmove.com/articles/1win_promo_code_bonus_code.html · April 28, 2026 at 7:39 am
https://www.google.dj/url?q=https://totalfratmove.com/articles/1win_promo_code_bonus_code.html
LauraTal · April 28, 2026 at 7:42 am
Наркологическая клиника «Оптимед» в Кирове предлагает комплексное лечение зависимостей. Пациентам доступен вывод из запоя, терапия при алкоголизме и наркомании, а также поэтапная реабилитация. Центр обеспечивает анонимность и индивидуальный подход.
Подробнее тут – наркологический диспансер
SerenanoG · April 28, 2026 at 9:11 am
В центре «Время Возрождения» в Кемерово разрабатывают индивидуальные программы терапии при алкогольной и наркотической зависимости. Лечение строится с учётом состояния здоровья, стажа употребления и сопутствующих факторов, что повышает эффективность медицинской помощи.
Подробнее – кодирование от алкоголизма в кемерово
Charlestat · April 28, 2026 at 9:59 am
Full Report https://letsexchange.cc
Laurenrax · April 28, 2026 at 10:20 am
why not check here https://daobase.online/
CharlesAromA · April 28, 2026 at 10:37 am
Когда зависимости становятся хроническими и угрожают жизни пациента, комплексная реабилитация при наркомании в специализированных клиниках Москвы, включая вывод из состояния в стационаре и последующий анализ данных о состоянии пациента, может стать единственным возможным решением. Процесс восстановления включает в себя работу не только с зависимостью, но и с психоэмоциональным состоянием, что делает лечение более эффективным и долговечным.
Подробнее можно узнать тут – центр реабилитации алкоголиков
CharlesAromA · April 28, 2026 at 10:55 am
Реабилитация алкоголиков в Москве: эффективные программы восстановления и медицинская помощь в наркологической клинике «Похмельная служба»
Получить дополнительные сведения – reabilitacziya-alkogolikov-moskva-2.ru/
MichaelRor · April 28, 2026 at 11:06 am
Привет всем!
Ремонт пола с укладкой плитки — это классическое решение для тех, кто ценит долговечность и практичность. Мы выполняем ремонт пола с укладкой плитки, выбирая материалы, которые будут служить вам долгие годы. Ремонт пола с укладкой плитки — это надежность и долговечность. Ремонт пола с укладкой плитки — это идеальный выбор для вашего дома.
Ремонты квартир в Москве — это услуга, которую мы предлагаем для владельцев недвижимости, желающих преобразить свои квартиры. Мы выполняем ремонты квартир в Москве на самых разных объектах. Важно, что все работы выполняются профессиональными мастерами с использованием качественных материалов. Ремонт квартиры в Москве — это улучшение вашего жилья. Ремонт квартир в Москве — это высокое качество по доступным ценам.
Больше информации по ссылке – https://ostroykevse.ru/kak-opticheski-uvelichit-malenkuyu-kvartiru/
мастер по ремонту стиральной машины на дому, ремонта и отделки квартир, недорого ремонт квартиры москва
технология строительство каркасный дом, трехкомнатные квартиры с ремонтом, помощь с ремонтом в квартире
Удачи!
Laurenrax · April 28, 2026 at 11:30 am
browse around this website https://daobase.online/
https://z-terra.ru/img/pgs/?kakie_produkty_moghno_hranity_v_voskovoy_obertke.html · April 28, 2026 at 11:36 am
https://z-terra.ru/img/pgs/?kakie_produkty_moghno_hranity_v_voskovoy_obertke.html
Kevinabame · April 28, 2026 at 12:03 pm
В этой статье-обзоре мы соберем актуальную информацию и интересные факты, которые освещают важные темы. Читатели смогут ознакомиться с различными мнениями и подходами, что позволит им расширить кругозор и глубже понять обсуждаемые вопросы.
Изучить вопрос глубже – вывод из запоя цены воронеж
ArthurwoLla · April 28, 2026 at 12:09 pm
our website https://daobase.online
SerenanoG · April 28, 2026 at 12:28 pm
«Время Возрождения» — медицинский наркологический центр в Кемерово, где оказывают помощь при острых состояниях и хронических формах зависимости. В работе сочетаются медикаментозная поддержка, психотерапия и контроль динамики восстановления.
Узнать больше – снятие похмелья капельница
ArthurwoLla · April 28, 2026 at 12:38 pm
browse around this site https://swaplab.io
Larrydient · April 28, 2026 at 12:45 pm
discover here https://swaplab.io
SerenanoG · April 28, 2026 at 12:48 pm
«Время Возрождения» — медицинский наркологический центр в Кемерово, где оказывают помощь при острых состояниях и хронических формах зависимости. В работе сочетаются медикаментозная поддержка, психотерапия и контроль динамики восстановления.
Исследовать вопрос подробнее – после тетурама
DanielTug · April 28, 2026 at 1:34 pm
try this https://anycoindirect.me
Charlestat · April 28, 2026 at 1:54 pm
Click Here https://daobase.info/
Johnniesheme · April 28, 2026 at 2:34 pm
Наркологическая клиника «НовыйЯ» в Москве оказывает анонимную помощь при алкогольной и наркотической зависимости: диагностика, детоксикация, купирование абстинентного синдрома и подбор дальнейшей программы лечения. Акцент делается на медицинскую безопасность и конфиденциальность обращения.
Ознакомиться с деталями – пивной алкоголизм у мужчин симптомы лечение
WilmaNep · April 28, 2026 at 3:02 pm
«Narkology» — надежный партнер в преодолении зависимостей. Мы предлагаем индивидуальные программы поддержки и консультаций при алкогольной, наркотической и медикаментозной зависимости. В наш комплекс услуг входят онлайн-консультации с наркологами, психологические вебинары и круглосуточная информационная поддержка. Индивидуальный подход и внимание к каждому клиенту помогают подобрать оптимальную стратегию отказа от вредных веществ и шаг за шагом двигаться к свободе от зависимости.
Исследовать вопрос подробнее – как заставить алкоголика лечиться
Haroldbof · April 28, 2026 at 3:12 pm
В статье представлены ключевые моменты по актуальной теме, дополненные советами экспертов и ссылками на дополнительные ресурсы. Цель материала — дать читателю инструменты для самостоятельного развития и принятия осознанных решений.
Уточнить детали – вызвать нарколога
Roberttyday · April 28, 2026 at 3:13 pm
Мы предлагаем вам окунуться в океан любопытных фактов и вдохновляющих историй. Эта публикация поможет расширить горизонты, разбудить интерес к науке и истории и увидеть мир с новой стороны.
Получить дополнительную информацию – наркологический частный центр
DanielTug · April 28, 2026 at 3:21 pm
Web Site https://bitmix.app
ArthurwoLla · April 28, 2026 at 3:29 pm
Continue Reading https://yomix.biz/
Charlesarite · April 28, 2026 at 3:52 pm
Хороший разбор текущих реалий SEO и важности долгосрочного подхода. Автор подробно рассказывает, почему поисковые системы всё больше внимания уделяют стабильности и качеству, а не временным всплескам активности. В статье затронуты эволюция алгоритмов, роль качественного контента и UX, а также эффективные методы для «SEO-марафона» — регулярный аудит, оптимизация, качественные ссылки и авторский контент. Рекомендую: https://gobelensalon.ru/tekushhie-realii-seo-i-vazhnost-dolgosrochnogo-podhoda/
Jamesrex · April 28, 2026 at 4:39 pm
over here https://mixmy.money
Williambitly · April 28, 2026 at 4:45 pm
В данной обзорной статье представлены интригующие факты, которые не оставят вас равнодушными. Мы критикуем и анализируем события, которые изменили наше восприятие мира. Узнайте, что стоит за новыми открытиями и как они могут изменить ваше восприятие реальности.
Исследовать вопрос подробнее – выведение из запоя на дому анонимно
DanielTug · April 28, 2026 at 5:53 pm
see this site https://letsexchange.cc/
Jamesrex · April 28, 2026 at 6:35 pm
Discover More https://letsexchange.cc
DanielTug · April 28, 2026 at 7:20 pm
visit this page https://swaplab.io
Laurenrax · April 28, 2026 at 7:47 pm
official statement https://mixmy.money
Laurenrax · April 28, 2026 at 8:10 pm
Look At This https://daobase.io
DebraEvome · April 28, 2026 at 9:07 pm
Клиника «НаркоЗдравие» в Москве специализируется на лечении зависимостей. Здесь проводят вывод из запоя, кодирование от алкоголя и наркотиков, терапию наркомании и алкоголизма. Реабилитационный центр помогает закрепить результаты и восстановить психологическое состояние.
Детальнее – частные вытрезвители
Larrydient · April 28, 2026 at 9:42 pm
her explanation https://letsexchange.cc
Danielabrat · April 28, 2026 at 9:44 pm
Этот увлекательный информационный материал подарит вам массу новых знаний и ярких эмоций. Мы собрали для вас интересные факты и сведения, которые обогатят ваш опыт. Откройте для себя увлекательный мир информации и насладитесь процессом изучения!
Связаться за уточнением – прокапаться от алкоголя
Larrydient · April 28, 2026 at 9:49 pm
more info here https://mixmy.money/
Caseydot · April 28, 2026 at 9:54 pm
Эта статья погружает вас в увлекательный мир знаний, где каждый факт становится открытием. Мы расскажем о ключевых исторических поворотных моментах и научных прорывах, которые изменили ход цивилизации. Поймите, как прошлое формирует настоящее и как его уроки могут помочь нам строить будущее.
Уточнить детали – наркологический частный центр
Charlestat · April 28, 2026 at 9:59 pm
read this https://daobase.io/
Caseydot · April 28, 2026 at 10:47 pm
Этот интересный отчет представляет собой сборник полезных фактов, касающихся актуальных тем. Мы проанализируем данные, чтобы вы могли сделать обоснованные выводы. Читайте, чтобы узнать больше о последних трендах и значимых событиях!
Исследовать вопрос подробнее – наркологическая платная клиника
live cams · April 28, 2026 at 11:02 pm
Your style is unique compared to other folks I’ve read stuff from. Many thanks for posting when you’ve got the opportunity, Guess I will just bookmark this page.
Frankkep · April 28, 2026 at 11:08 pm
Эта познавательная публикация погружает вас в море интересного контента, который быстро захватит ваше внимание. Мы рассмотрим важные аспекты темы и предоставим вам уникальные Insights и полезные сведения для дальнейшего изучения.
Не упусти шанс – помощь при запое на дому
Marcospab · April 28, 2026 at 11:37 pm
В статье представлены ключевые моменты по актуальной теме, дополненные советами экспертов и ссылками на дополнительные ресурсы. Цель материала — дать читателю инструменты для самостоятельного развития и принятия осознанных решений.
Что скрывают от вас? – нарколог на дому капельница цена
Jamesrom · April 28, 2026 at 11:43 pm
Этот информативный текст отличается привлекательным содержанием и актуальными данными. Мы предлагаем читателям взглянуть на привычные вещи под новым углом, предоставляя интересный и доступный материал. Получите удовольствие от чтения и расширьте кругозор!
Кликни и узнай всё! – клиника запой
Jamesrom · April 29, 2026 at 12:37 am
В статье представлены ключевые моменты по актуальной теме, дополненные советами экспертов и ссылками на дополнительные ресурсы. Цель материала — дать читателю инструменты для самостоятельного развития и принятия осознанных решений.
Узнать больше – наркология вывод из запоя в стационаре
fixDiele · April 29, 2026 at 12:42 am
Кстати, если вас интересует Последние новости Амурской области сегодня, посмотрите сюда.
Вот, можете почитать:
https://media28amur.ru
fixDiele · April 29, 2026 at 12:46 am
По теме “Свежие новости Томской области и мира”, есть отличная статья.
Ссылка ниже:
https://media83.ru
Marcusbam · April 29, 2026 at 1:35 am
содержание советы РїРѕ продвижению канала РЅР° РєРёРєРµ
Marcusbam · April 29, 2026 at 1:59 am
такой накрутка 1000 комментариев РІ тг китай
Ralphdreve · April 29, 2026 at 2:02 am
Этот информационный материал собраны данные, которые помогут лучше понять текущие тенденции и процессы в различных сферах жизни. Мы предоставляем четкий анализ, графики и примеры, чтобы информация была не только понятной, но и практичной для принятия решений.
Это стоит прочитать полностью – частный нарколог на дом телефон
Roberttyday · April 29, 2026 at 2:28 am
Эта информационная статья охватывает широкий спектр актуальных тем и вопросов. Мы стремимся осветить ключевые факты и события с ясностью и простотой, чтобы каждый читатель мог извлечь из нее полезные знания и полезные инсайты.
Кликни и узнай всё! – частная наркологическая клиника
Carolynabure · April 29, 2026 at 2:42 am
В клинике «НОВЫЙ НАРКОЛОГ» в Санкт-Петербурге оказывают квалифицированную помощь при запоях, абстинентных состояниях и последствиях употребления. Врачи проводят инфузионную терапию, нормализуют сон и общее самочувствие, корректируют тревожность и вегетативные проявления. После стабилизации подбирается план дальнейшего лечения и реабилитации.
Разобраться лучше – Наркологическая помощь в СПб
Kevinabame · April 29, 2026 at 2:53 am
Публикация приглашает вас исследовать неизведанное — от древних тайн до современных достижений науки. Вы узнаете, как случайные находки превращались в революции, а смелые мысли — в новые эры человеческого прогресса.
Получить больше информации – выведение из запоя на дому
Ralphdreve · April 29, 2026 at 3:16 am
Эта разъяснительная статья содержит простые и доступные разъяснения по актуальным вопросам. Мы стремимся сделать информацию понятной для широкой аудитории, чтобы каждый мог разобраться в предмете и извлечь из него максимум пользы.
Где можно узнать подробнее? – нарколог на дом город
HerbertIndek · April 29, 2026 at 3:46 am
Эта статья для ознакомления предлагает читателям общее представление об актуальной теме. Мы стремимся представить ключевые факты и идеи, которые помогут читателям получить представление о предмете и решить, стоит ли углубляться в изучение.
Перейти к статье – капельница от похмелья цена
CharlesAromA · April 29, 2026 at 4:41 am
Реабилитация алкоголиков в Москве с комплексным подходом — это многогранный процесс, включающий в себя не только медицинские процедуры, но и психологическую поддержку, физическую реабилитацию и помощь в социальной адаптации. Профессиональный реабилитационный центр обеспечивает индивидуальный подход к каждому пациенту, включая такие методы, как кодирование и своевременное лечение запоя. Важно отметить, что успешное лечение алкоголизма требует учета множества факторов, таких как степень зависимости, психоэмоциональное состояние пациента, а также его физическое здоровье. Комплексный подход помогает эффективно устранить все составляющие проблемы, минимизируя риски рецидивов.
Исследовать вопрос подробнее – реабилитация алкоголиков стоимость
Marcusbam · April 29, 2026 at 4:43 am
проверить сайт лучший сервис хуета стор накрутка РІ стиме
CharlesAromA · April 29, 2026 at 4:53 am
Комплексная реабилитация алкоголиков в Москве помогает пациентам не только избавиться от зависимости, но и вернуться к полноценной жизни. Процесс восстановления включает в себя не только лечение алкоголизма как физического заболевания, но и работу с психологическими, социальными и эмоциональными аспектами, которые могут стать причиной или следствием зависимости. Такое подходное лечение, как правило, требует усилий со стороны как специалистов, так и самого пациента.
Получить дополнительные сведения – реабилитация алкоголиков стоимость в москве
DebraEvome · April 29, 2026 at 5:50 am
В Москве клиника «НаркоЗдравие» предлагает комплексное лечение зависимостей: кодирование, вывод из запоя, терапию алкоголизма и наркомании. Реабилитационный центр обеспечивает длительное восстановление, а услуга «нарколог на дом» помогает в экстренных ситуациях.
Детальнее – https://narko-zdravie.ru/uslugi/narkomaniya/lechenie-zavisimosti-ot-tropikamida
MichaelBenly · April 29, 2026 at 6:09 am
В статье представлены ключевые моменты по актуальной теме, дополненные советами экспертов и ссылками на дополнительные ресурсы. Цель материала — дать читателю инструменты для самостоятельного развития и принятия осознанных решений.
Исследовать вопрос подробнее – вывод из запоя стационар самара
WilmaNep · April 29, 2026 at 7:33 am
Наркологическая информационная сеть «Narkology» предоставляет квалифицированную помощь в преодолении зависимостей и восстановлении психоэмоционального состояния. Наши специалисты проводят детальную диагностику, разрабатывают индивидуальные программы терапии и психологической поддержки, а также информируют о современных методах лечения. С использованием проверенных подходов и актуальных данных мы помогаем вернуть уверенность и сделать первый шаг на пути к здоровому образу жизни. Доверьтесь профессионалам «Narkology», чтобы эффективно решить проблемы зависимости и получить всестороннюю информационную помощь.
Подробнее – https://narcologiya.info/vliyanie-na-zdorove/pobochnye-effekty-alkogol-antibiotiki.html
DebraEvome · April 29, 2026 at 7:48 am
«НаркоЗдравие» — московская клиника, где доступно лечение алкоголизма и наркомании, профессиональный вывод из запоя, кодирование и помощь нарколога на дому. Реабилитационный центр поддерживает пациентов в процессе восстановления и возвращения к стабильной жизни.
Ознакомиться с деталями – алкоголизм и наркомания
Williambitly · April 29, 2026 at 7:49 am
В этой статье вы найдете уникальные исторические пересечения с научными открытиями. Каждый абзац — это шаг к пониманию того, как наука и события прошлого создают основу для технологического будущего.
Кликни, не пожалеешь – выведение из запоя на дому самара
Carolynabure · April 29, 2026 at 7:59 am
Платная наркологическая клиника «НОВЫЙ НАРКОЛОГ» в Санкт-Петербурге предлагает помощь в комфортных условиях с акцентом на безопасность пациента. Врачи подбирают схему лечения с учётом состояния, анамнеза и сопутствующих рисков, проводят медицинскую стабилизацию и помогают выстроить план дальнейшего восстановления. Анонимность и профессионализм остаются приоритетом.
Подробнее можно узнать тут – как вывести человека из длительного запоя
SerenanoG · April 29, 2026 at 8:16 am
«Время Возрождения» — медицинский наркологический центр в Кемерово, где оказывают помощь при острых состояниях и хронических формах зависимости. В работе сочетаются медикаментозная поддержка, психотерапия и контроль динамики восстановления.
Разобраться лучше – https://vozrojdenie.site/kodirovanie-algominalom
live cams · April 29, 2026 at 8:16 am
Way cool! Some very valid points! I appreciate you penning this post plus the rest of the site is really good.
SerenanoG · April 29, 2026 at 8:30 am
«Время Возрождения» — медицинский наркологический центр в Кемерово, где оказывают помощь при острых состояниях и хронических формах зависимости. В работе сочетаются медикаментозная поддержка, психотерапия и контроль динамики восстановления.
Выяснить больше – https://vozrojdenie.site/reabilitatsiya-po-programme-daytop
Carolynabure · April 29, 2026 at 9:51 am
Наркологическая клиника «НОВЫЙ НАРКОЛОГ» в Санкт-Петербурге оказывает профессиональную помощь при алкогольной и наркотической зависимости. Врачи проводят детоксикацию, купирование абстинентного синдрома, поддерживающую терапию и подбирают индивидуальную программу восстановления. Конфиденциальность и медицинские стандарты — ключевые принципы работы центра.
Разобраться лучше – укол от алкоголизма
MichaelRor · April 29, 2026 at 9:57 am
Привет всем!
Ремонта квартиры — это процесс, который должен быть выполнен с учетом всех пожеланий владельца. Мы предлагаем профессиональные услуги по ремонту квартир, включая все этапы от разработки проекта до окончательной отделки. Мы используем только качественные материалы, которые обеспечат долгосрочность и красоту. Наша цель — сделать ваш дом уютным и функциональным, учитывая ваши предпочтения и бюджет.
Ремонт лоджии — это преобразование еще одного уголка вашего дома в уютное и удобное пространство. Мы выполняем ремонт лоджии, создавая идеальные условия для отдыха. Ремонт лоджии — это удобство и пространство для вас. Ремонт лоджии — это больше уюта и функциональности.
Больше информации по ссылке – https://www.vip-doski.ru/kak-rasschitat-stoimost-remonta-v-kvartire-98647.html
отделка в строительстве дома, квартиры с отделкой в москве недорого, вычет за строительство дома
купить квартиру с отделкой в краснодаре, ремонт дома телефоны, ремонт дома астрахань
Удачи!
HerbertIndek · April 29, 2026 at 10:43 am
Эта статья предлагает живое освещение актуальной темы с множеством интересных фактов. Мы рассмотрим ключевые моменты, которые делают данную тему важной и актуальной. Подготовьтесь к насыщенному путешествию по неизвестным аспектам и узнайте больше о значимых событиях.
Всё самое вкусное внутри – капельница на дому воронеж цены
SODO · April 29, 2026 at 12:18 pm
A cool post there mate ! Thank you for posting.
CEO Minh Kiro · April 29, 2026 at 12:52 pm
Hi, do have a e-newsletter? In the event you don’t definately should get on that piece…this web site is pure gold!
Timothyelapy · April 29, 2026 at 1:24 pm
duvar boyama hakk?ndaki bolumu cok sevdim. Link burada: https://hobiprojesi.com/articles/duvar-boyama-teknikleri/
SODO Casino · April 29, 2026 at 1:25 pm
Thank you for the auspicious writeup.
Timothyelapy · April 29, 2026 at 1:28 pm
“mor hangi renklerden olusur” konusu icin burada harika bilgiler var. Kendiniz gorun: https://evhobisi.com/articles/mor-renk-elde-etmek-icin-renk-karisimlari/
CharlesAromA · April 29, 2026 at 2:37 pm
Реабилитация алкоголиков в Москве с комплексным подходом — это многогранный процесс, включающий в себя не только медицинские процедуры, но и психологическую поддержку, физическую реабилитацию и помощь в социальной адаптации. Профессиональный реабилитационный центр обеспечивает индивидуальный подход к каждому пациенту, включая такие методы, как кодирование и своевременное лечение запоя. Важно отметить, что успешное лечение алкоголизма требует учета множества факторов, таких как степень зависимости, психоэмоциональное состояние пациента, а также его физическое здоровье. Комплексный подход помогает эффективно устранить все составляющие проблемы, минимизируя риски рецидивов.
Узнать больше – алкоголик реабилитация наркоманов город
용산출장마사지 · April 29, 2026 at 2:57 pm
타임케어 용산출장홈타이 – 용산출장마사지와 용산출장안마 용산홈타이 서비스를 전국 어디서나 24시간 편하게! 전문 마사지사의 맞춤 홈케어로 피로를 빠르게 해소
용인출장마사지 · April 29, 2026 at 3:06 pm
용인출장마사지에서는 타이마사지, 아로마 마사지, 스웨디시 마사지, 스포츠 마사지 등 다양한 코스를 제공합니다. 전신 관리부터 부위별 집중 케어까지 선택 가능하며
Williamge · April 29, 2026 at 3:14 pm
Всем привет!
Изучаю варианты машину,
читаю обзоры.
Попалась одна статья:
https://www.niasam.ru/transport/vnedorozhnik-tank-400-osobennosti-avtomobilya-271130.html
В целом довольно подробно описали модель и ключевые особенности.
Интересен реальный опыт:
кто сталкивался,
насколько это вообще актуально?
Стоит ли рассматривать сейчас?
Спасибо за мнение.
kv999 · April 29, 2026 at 3:19 pm
Public policy is key here, and our states need to develop some strategies – – soon.
kv999 · April 29, 2026 at 3:27 pm
When are you going to post again? You really entertain me!
JamesClask · April 29, 2026 at 3:57 pm
Нарколог на дом в Самаре востребован в самых различных ситуациях. Иногда пациент не в состоянии самостоятельно добраться до клиники из-за сильного состояния похмелья или ломки. В таких случаях выезд нарколога становится наиболее оптимальным решением. Наши специалисты оказывают помощь при следующих состояниях:
Исследовать вопрос подробнее – запой нарколог на дом в самаре
JesseRelry · April 29, 2026 at 4:45 pm
В данной обзорной статье представлены интригующие факты, которые не оставят вас равнодушными. Мы критикуем и анализируем события, которые изменили наше восприятие мира. Узнайте, что стоит за новыми открытиями и как они могут изменить ваше восприятие реальности.
Подробности по ссылке – капельница после запоя цена
Rickeyfaf · April 29, 2026 at 5:00 pm
В статье представлены ключевые моменты по актуальной теме, дополненные советами экспертов и ссылками на дополнительные ресурсы. Цель материала — дать читателю инструменты для самостоятельного развития и принятия осознанных решений.
Как достичь результата? – частный нарколог
live cams · April 29, 2026 at 5:07 pm
Oh my goodness! Awesome article dude! Thank you so much, However I am encountering problems with your RSS. I don’t know why I cannot subscribe to it. Is there anyone else getting the same RSS problems? Anyone that knows the solution can you kindly respond? Thanx.
Timothyhoula · April 29, 2026 at 5:10 pm
Далее, когда физическое состояние стабилизировано, совместно с врачом выбирается стратегия дальнейшего лечения. В «Новая Точка» доступны современные методы кодирования (уколы, таблетки, вшивание препаратов, гипнотерапия), но решение всегда принимается осознанно, с объяснением плюсов, рисков и индивидуальным подбором метода.
Подробнее тут – лечение алкоголизма
OscarFAG · April 29, 2026 at 5:30 pm
Основной этап в лечении — детоксикация организма от токсичных веществ, вызывающих интоксикацию. В клинике применяют современные методы капельниц и медикаментозной поддержки, включая препараты для снятия абстинентного синдрома.
Подробнее тут – http://www.domen.ru
Bernardcrurl · April 29, 2026 at 5:31 pm
Этот текст призван помочь читателю расширить кругозор и получить практические знания. Мы используем простой язык, наглядные примеры и структурированное изложение, чтобы сделать обучение максимально эффективным и увлекательным.
Рассмотреть проблему всесторонне – лечение наркомании на дому
JustinMup · April 29, 2026 at 6:09 pm
В этой информационной статье вы найдете интересное содержание, которое поможет вам расширить свои знания. Мы предлагаем увлекательный подход и уникальные взгляды на обсуждаемые темы, побуждая пользователей к активному мышлению и критическому анализу.
Не упусти шанс – вывод из запоя цены самара
Raymondbub · April 29, 2026 at 6:21 pm
Откройте для себя скрытые страницы истории и малоизвестные научные открытия, которые оказали колоссальное влияние на развитие человечества. Статья предлагает свежий взгляд на события, которые заслуживают большего внимания.
Получить больше информации – вывод из запоя цены воронеж
confira aqui · April 29, 2026 at 6:42 pm
the streamer scene now tracks session ROI over single hits.
CharlesAromA · April 29, 2026 at 7:21 pm
Реабилитация алкоголиков в Москве с комплексным подходом — это многогранный процесс, включающий в себя не только медицинские процедуры, но и психологическую поддержку, физическую реабилитацию и помощь в социальной адаптации. Профессиональный реабилитационный центр обеспечивает индивидуальный подход к каждому пациенту, включая такие методы, как кодирование и своевременное лечение запоя. Важно отметить, что успешное лечение алкоголизма требует учета множества факторов, таких как степень зависимости, психоэмоциональное состояние пациента, а также его физическое здоровье. Комплексный подход помогает эффективно устранить все составляющие проблемы, минимизируя риски рецидивов.
Разобраться лучше – клиника реабилитации алкоголиков город
JesseRelry · April 29, 2026 at 7:29 pm
В этой статье представлен занимательный и актуальный контент, который заставит вас задуматься. Мы обсуждаем насущные вопросы и проблемы, а также освещаем истории, которые вдохновляют на действия и изменения. Узнайте, что стоит за событиями нашего времени!
Подробности по ссылке – прокапаться от алкоголя в воронеже
Bernardcrurl · April 29, 2026 at 8:08 pm
Эта статья погружает вас в увлекательный мир знаний, где каждый факт становится открытием. Мы расскажем о ключевых исторических поворотных моментах и научных прорывах, которые изменили ход цивилизации. Поймите, как прошлое формирует настоящее и как его уроки могут помочь нам строить будущее.
Более того — здесь – нарколог на дом воронеж цены
Carolynabure · April 29, 2026 at 8:33 pm
Наркологический центр «НОВЫЙ НАРКОЛОГ» в СПб специализируется на лечении алкоголизма и наркомании с медицинским сопровождением. Программы включают детоксикацию, терапию осложнений, психотерапевтическую поддержку и последующую реабилитацию. Такой подход помогает не только снять острые симптомы, но и сформировать устойчивую мотивацию к трезвости.
Получить дополнительную информацию – https://new-narkolog.ru/stati/kak-vosstanovit-organizm-s-pohmelya
JustinMup · April 29, 2026 at 8:50 pm
Эта статья погружает вас в увлекательный мир знаний, где каждый факт становится открытием. Мы расскажем о ключевых исторических поворотных моментах и научных прорывах, которые изменили ход цивилизации. Поймите, как прошлое формирует настоящее и как его уроки могут помочь нам строить будущее.
См. подробности – вывод из запоя на дому в самаре
Raymondbub · April 29, 2026 at 8:51 pm
В этой статье представлен занимательный и актуальный контент, который заставит вас задуматься. Мы обсуждаем насущные вопросы и проблемы, а также освещаем истории, которые вдохновляют на действия и изменения. Узнайте, что стоит за событиями нашего времени!
Изучить вопрос глубже – вывод из запоя на дому
Williecom · April 29, 2026 at 9:10 pm
В зависимости от тяжести состояния подбирается индивидуальная программа детоксикации. В неё входят: — Инфузионная терапия (капельницы) для очищения организма от токсинов; — Поддерживающие препараты для работы сердца, печени, нервной системы; — Симптоматическое лечение (устранение рвоты, судорог, бессонницы); — Витамины и средства для восстановления водно-солевого баланса.
Получить дополнительные сведения – наркологическая клиника телефон
高端外围商务模特 · April 29, 2026 at 9:32 pm
This blog was… how do you say it? Relevant!! Finally I have found something that helped me. Kudos.
JamesClask · April 29, 2026 at 9:44 pm
Запой и алкогольная интоксикация могут приводить к целому ряду опасных симптомов, таких как головная боль, слабость, тошнота, рвота, обезвоживание и психоэмоциональная нестабильность. Если не начать лечение вовремя, такие состояния могут привести к более серьезным осложнениям, включая сердечные проблемы, галлюцинации и даже опасные для жизни нарушения работы организма. С помощью нарколога на дому можно начать экстренную терапию прямо в момент ухудшения состояния, не затягивая с лечением и не тратя время на поездки в клинику.
Узнать больше – https://narkolog-na-dom-samara-2.ru
GregoryHig · April 29, 2026 at 10:31 pm
https://t.me/Asiapsi
DwayneMog · April 29, 2026 at 10:55 pm
такой Регистрация ооо, ип, внесение егрюл
DwayneMog · April 30, 2026 at 12:17 am
нажмите, чтобы подробнее Реорганизация
OscarFAG · April 30, 2026 at 12:19 am
После устранения острой зависимости важным этапом становится реабилитация. Она включает восстановление социальных навыков, обучение методам преодоления стрессов без употребления психоактивных веществ.
Узнать больше – наркологические клиники алкоголизм
https://k1news.ru/news/society/diplom-prakticheskogo-psihologa-gde-poluchit-skolko-stoit-i-kak-nayti-pervyh-5-klientov/ · April 30, 2026 at 12:31 am
https://k1news.ru/news/society/diplom-prakticheskogo-psihologa-gde-poluchit-skolko-stoit-i-kak-nayti-pervyh-5-klientov/
Danieltug · April 30, 2026 at 1:13 am
Реабилитация алкоголиков в Москве представляет собой многократный процесс восстановления, который включает несколько этапов, направленных на очищение организма, психологическое восстановление и возвращение пациента к полноценной жизни. Этапное восстановление помогает обеспечить стабильный результат и минимизировать риск рецидива, позволяя человеку постепенно вернуться к нормальной социальной и трудовой жизни.
Углубиться в тему – клиника реабилитации алкоголиков город
Walterunlib · April 30, 2026 at 1:15 am
Вывод из запоя на дому — это медицинская помощь, направленная на стабилизацию состояния пациента без госпитализации. Такой формат позволяет начать лечение сразу после обращения и снизить нагрузку на организм, связанную с транспортировкой. В наркологической клинике «Частный медик 24» помощь оказывается с выездом врача, который проводит диагностику и подбирает терапию в зависимости от текущего состояния.
Исследовать вопрос подробнее – анонимный вывод из запоя на дому санкт-петербург
Danielabrat · April 30, 2026 at 1:57 am
Эта статья сочетает познавательный и занимательный контент, что делает ее идеальной для любителей глубоких исследований. Мы рассмотрим увлекательные аспекты различных тем и предоставим вам новые знания, которые могут оказаться полезными в будущем.
Ознакомиться с теоретической базой – капельница от запоя цена воронеж
more info · April 30, 2026 at 2:08 am
the streamer scene consensus: a clean week beats a single lucky day.
Frankkep · April 30, 2026 at 2:23 am
Эта познавательная публикация погружает вас в море интересного контента, который быстро захватит ваше внимание. Мы рассмотрим важные аспекты темы и предоставим вам уникальные Insights и полезные сведения для дальнейшего изучения.
Лучшее решение — прямо здесь – нарколог на дом вывод из запоя на дому
Scottsmide · April 30, 2026 at 3:01 am
pop over to these guys telegram dm automation
ThomasSag · April 30, 2026 at 3:31 am
Этот увлекательный информационный материал подарит вам массу новых знаний и ярких эмоций. Мы собрали для вас интересные факты и сведения, которые обогатят ваш опыт. Откройте для себя увлекательный мир информации и насладитесь процессом изучения!
Углубить понимание вопроса – вызвать нарколога на дом
Scottsmide · April 30, 2026 at 4:59 am
about his telegram channel growth software
JosephTum · April 30, 2026 at 5:15 am
view it now fortnite locker analyzer
JosephTum · April 30, 2026 at 5:40 am
why not check here fortnite locker value checker
where to get generic prednisone without a prescription · April 30, 2026 at 7:35 am
where to get generic prednisone prices
JosephTum · April 30, 2026 at 8:31 am
check here fortnite inventory worth checker
OscarFAG · April 30, 2026 at 8:37 am
Основной этап в лечении — детоксикация организма от токсичных веществ, вызывающих интоксикацию. В клинике применяют современные методы капельниц и медикаментозной поддержки, включая препараты для снятия абстинентного синдрома.
Подробнее тут – бесплатная наркологическая клиника
Rickeyfaf · April 30, 2026 at 9:13 am
Эта публикация погружает вас в мир увлекательных фактов и удивительных открытий. Мы расскажем о ключевых событиях, которые изменили ход истории, и приоткроем завесу над научными достижениями, которые вдохновили миллионы. Узнайте, чему может научить нас прошлое и как применить эти знания в будущем.
Ознакомиться с полной информацией – наркологическая помощь на дому в самаре
CharlesAromA · April 30, 2026 at 10:46 am
Когда зависимости становятся хроническими и угрожают жизни пациента, комплексная реабилитация при наркомании в специализированных клиниках Москвы, включая вывод из состояния в стационаре и последующий анализ данных о состоянии пациента, может стать единственным возможным решением. Процесс восстановления включает в себя работу не только с зависимостью, но и с психоэмоциональным состоянием, что делает лечение более эффективным и долговечным.
Подробнее тут – клиника реабилитации алкоголиков в москве
JamesBOn · April 30, 2026 at 1:08 pm
Этот интересный отчет представляет собой сборник полезных фактов, касающихся актуальных тем. Мы проанализируем данные, чтобы вы могли сделать обоснованные выводы. Читайте, чтобы узнать больше о последних трендах и значимых событиях!
Читать далее > – вывод из запоя на дому недорого
casinos online legales en chile · April 30, 2026 at 2:24 pm
A friend of mine advised me to review this site. And yes. it has some useful pieces of info and I enjoyed reading it.
https://pro62.info/ · April 30, 2026 at 2:27 pm
https://pro62.info/
Scottsmide · April 30, 2026 at 3:15 pm
Resources software for telegram automation
FilmySnoth · April 30, 2026 at 3:17 pm
Привет всем любителям кино!, тогда вам сюда!
Бесплатные платформы для просмотра фильмов часто имеют удобное мобильное приложение. Это позволяет смотреть кино в дороге, в очереди или на отдыхе. онлайн Мобильность делает просмотр еще более доступным и комфортным. Наслаждайтесь кино где угодно.
Ссылка на ресурс: — https://www.filmy-serialy-online-1.top
бесплатное кино онлайн
смотреть зарубежные фильмы
фильмы онлайн бесплатно 2025
Смотрите с удовольствием!
Timothybiobe · April 30, 2026 at 3:18 pm
Эта статья сочетает познавательный и занимательный контент, что делает ее идеальной для любителей глубоких исследований. Мы рассмотрим увлекательные аспекты различных тем и предоставим вам новые знания, которые могут оказаться полезными в будущем.
Как достичь результата? – вывод из запоя круглосуточно цены
new online casinos nz · April 30, 2026 at 3:22 pm
Thanks pertaining to discussing the following superb written content on your site. I ran into it on the search engines. I will check back again if you publish extra aricles.
FilmySnoth · April 30, 2026 at 3:25 pm
Всем киноманам доброго времени суток!, тогда обратите внимание!
Выбор фильма на вечер – это целый ритуал для многих киноманов. Важно учесть настроение, компанию и даже закуски для полного погружения. семейные фильмы Онлайн-платформы помогают сделать этот выбор максимально комфортным. Наслаждайтесь каждым моментом вашего киносеанса.
Вот ссылка на ресурс: — http://www.filmy-serialy-online-1.top
онлайн фильмы без смс и регистрации
приключения смотреть онлайн
все фильмы онлайн бесплатно
Хороших сериалов и отличного настроения!
kasyno online opinie · April 30, 2026 at 3:47 pm
You appear to know so much about this, and I see you’re a published author. Thanks
cruzenews.com · April 30, 2026 at 3:47 pm
Bedste strategier for casino udbetaling
https://marvelswiki.site/wiki/Bedste_online_casinoer_i_Danmark_med_fokus_p_udbetalinger_2026 https://marvelswiki.site/wiki/Bedste_online_casinoer_i_Danmark_med_fokus_p_udbetalinger_2026
http://uchkombinat.com.ua/user/resultbeer1/ http://uchkombinat.com.ua/user/resultbeer1/
https://www.ricetteclara.com/membri/mirroriran93/activity/111777/ https://www.ricetteclara.com/membri/mirroriran93/activity/111777
https://aryba.kg/user/stoolpoint7/ aryba.kg
https://bbs.airav.cc/home.php?mod=space&uid=4592556 https://bbs.airav.cc/home.php?mod=space&uid=4592556
http://bsq.cc/bbs/home.php?mod=space&uid=260408 http://bsq.cc/
http://fumankong1.cc/home.php?mod=space&uid=916494 fumankong1.cc
http://asresin.cn/home.php?mod=space&uid=763540 http://asresin.cn/home.php?mod=space&uid=763540
http://bbs.abcdv.net/home.php?mod=space&uid=1485820 http://bbs.abcdv.net/home.php?mod=space&uid=1485820
https://prpack.ru/user/fieldperu9/ https://prpack.ru/
http://madk-auto.ru/user/spongedrawer20/ madk-auto.ru
http://cqr3d.ru/user/chinaicicle9/ cqr3d.ru
http://www.kaseisyoji.com/home.php?mod=space&uid=3996072 http://www.kaseisyoji.com
https://nomadwiki.space/wiki/Casinoer_med_den_bedste_udbetaling_i_Danmark_2026 https://nomadwiki.space/
https://doc.adminforge.de/s/Td1NV60CSg doc.adminforge.de
http://amur.1gb.ua/user/ramiecurve25/ http://amur.1gb.ua/
https://hackmd.okfn.de/s/B171o6xCZl hackmd.okfn.de
https://www.blurb.com/user/minutetwist9 http://www.blurb.com
References:
http://qa.doujiju.com/index.php?qa=user&qa_1=foggrill18
https://nelgit.nelpi.co.uk · April 30, 2026 at 4:13 pm
Gennemsnitlig udbetaling på online casino
https://code.nspoc.org/theoo35946184/theo2004/wiki/De-bedst-betalende-slots-i-Danmark-Top-gevinster-og-bonus https://code.nspoc.org/
https://gitea.myat4.com/otisderr38455 gitea.myat4.com
https://www.makemyjobs.in/companies/top-10-casinoer-i-dk-top-10-online-casinoer/ http://www.makemyjobs.in
https://carrieresecurite.fr/entreprises/guide-til-casinoer-med-hurtige-udbetalinger-i-danmark-i-2026/ carrieresecurite.fr
https://www.ahrs.al/punesimi/bedste-danske-online-casinoer-i-2026-top-10-med-licens/ https://www.ahrs.al
https://dgwork.co.kr/fawnwaterhouse/fawn2003/wiki/Hvilke-casinospil-har-de-bedste-vinderchancer%3F https://dgwork.co.kr/
https://www.klaverjob.com/employer/bedste-online-casinoer-april-2026-guide-til-danske-casino-sider/ https://www.klaverjob.com/employer/bedste-online-casinoer-april-2026-guide-til-danske-casino-sider
https://winesandjobs.com/companies/bedste-licenserede-online-casinoer-i-danmark-2026/ winesandjobs.com
https://toptalent.co.mz/employer/online-casinoer-med-dansk-licens-i-april-2026-%ef%b8%8f/ https://toptalent.co.mz/employer/online-casinoer-med-dansk-licens-i-april-2026-️/
https://rentry.co/61262-danske-bank-casinoer-april-2026 rentry.co
https://omegat.dmu-medical.de/chassidy173199 omegat.dmu-medical.de
https://code.wemediacn.com/diani361697664/blackcoin2015/wiki/Top-10-Bedste-Online-Spillemaskiner-Anbefalet-april-2026 https://code.wemediacn.com/
https://gitea.lelespace.top/tammi852629200 https://gitea.lelespace.top/
https://karierainsports.gr/employer/online-casinoer-med-de-hurtigste-udbetalinger-i-danmark/ https://karierainsports.gr
https://ahromov.pitbddma.org.ua/de-bedste-udbetalinger-p-online-casinoer-i-danmark-i-2026/ ahromov.pitbddma.org.ua
https://gitea.lelespace.top/johniebolduc8/blackcoin7394/wiki/Bedste-online-casinoer-i-Danmark-med-fokus-p%C3%A5-udbetalinger-2026 gitea.lelespace.top
https://links.gtanet.com.br/manualturpin https://links.gtanet.com.br/
https://nelgit.nelpi.co.uk/elisaturriff22/winniehenry077 nelgit.nelpi.co.uk
https://keyfood.mx/solar-power-for-businesses-cutting-costs-and-carbon · April 30, 2026 at 4:28 pm
Casinoer med høj udbetaling uden om ROFUS
https://mbfitness.in/new-fitness-club-opening/ mbfitness.in
https://culturadoreino.org/o-verdadeiro-arrependimento-keith-green/ culturadoreino.org
https://windsartgallery.com/the-tech-couture-revolution-high-tech-fabrics-and-smart-fashion/ windsartgallery.com
https://kataberita.net/bos-atg-wahyu-kenzo-divonis-10-tahun-penjara-kuasa-hukum-korban-berikan-apresiasi-atas-kinerja-penegak-hukum/ https://kataberita.net
https://forum.karnex.in/question/eye-tracking-system-market-share-and-competitive-landscape-assessment-2032/ https://forum.karnex.in/question/eye-tracking-system-market-share-and-competitive-landscape-assessment-2032
https://www.tidalraves.com/homepage https://www.tidalraves.com
https://diocesebompastor.org/how-much-should-you-spend-on-photographer/ diocesebompastor.org
https://neuroseniordf.com.br/2023/06/22/the-importance-of-building-a-strong-brand-identity/ neuroseniordf.com.br
http://editoraglobalsolution.com.br/navigating-the-world-of-digital-marketing-courses/ http://editoraglobalsolution.com.br/navigating-the-world-of-digital-marketing-courses
https://mpvox.com.br/2025/solar-power-for-businesses-cutting-costs-and-carbon/ mpvox.com.br
http://www.ofrecklessnessandwater.com/blog/index.php/;focus=W4YPRD_com_cm4all_wdn_Flatpress_5487094&path=?x=entry:entry210102-180948%3Bcomments:1 ofrecklessnessandwater.com
https://getadminate.com/scaling-your-brand-with-smart-strategies/ https://getadminate.com
https://www.fw-altdorf.de/Aktuelles;focus=TKOMSI_com_cm4all_wdn_Flatpress_26627447&path=&frame=TKOMSI_com_cm4all_wdn_Flatpress_26627447?x=entry:entry240204-150806%3Bcomments:1 http://www.fw-altdorf.de
https://shkolnaiapora.ru/question/chto-poluchitsya-esli-na-risunke-sprava-pomenyat-belyj-cvet-na-chernyj-a-chernyj-na-belyj shkolnaiapora.ru
https://www.kraftplatz-weibel.ch/blog/index.php/;focus=HSTPTP_com_cm4all_wdn_Flatpress_9497677&frame=HSTPTP_com_cm4all_wdn_Flatpress_9497677?x=entry:entry240831-223022%3Bcomments:1 https://www.kraftplatz-weibel.ch
http://cgi.www5b.biglobe.ne.jp/~hades/ibbs/ibbs.cgi?namber=84584&mode=res&page=15&no=0&IN=84584 http://cgi.www5b.biglobe.ne.jp/
https://lyricskhojo.com/lyrics-of-seedha-saadha-reprise-commando-2-the-black-money-trail/ https://lyricskhojo.com/lyrics-of-seedha-saadha-reprise-commando-2-the-black-money-trail/
https://pmcwebtech.com/navigating-the-unknown-a-journey-discovery/ https://pmcwebtech.com/navigating-the-unknown-a-journey-discovery/
References:
https://kandacewithak.com/2020/04/unboxing-adidas-yeezy-boost-700-phosphor/unboxing-air-max-triax-98-2/
Scottsmide · April 30, 2026 at 5:17 pm
article telegram marketing for business
CarolMipse · April 30, 2026 at 5:40 pm
Этот информационный материал собраны данные, которые помогут лучше понять текущие тенденции и процессы в различных сферах жизни. Мы предоставляем четкий анализ, графики и примеры, чтобы информация была не только понятной, но и практичной для принятия решений.
Продолжить изучение – капельница от запоя недорого
HectorCor · April 30, 2026 at 5:52 pm
Эта информационная статья охватывает широкий спектр актуальных тем и вопросов. Мы стремимся осветить ключевые факты и события с ясностью и простотой, чтобы каждый читатель мог извлечь из нее полезные знания и полезные инсайты.
Осуществить глубокий анализ – капельницы на дому екатеринбург цена
najlepsze kasyno online · April 30, 2026 at 5:57 pm
Just wanna admit that this is extremely helpful, Thanks for taking your time to write this.
best online casino in new zealand · April 30, 2026 at 6:14 pm
Took me time to read the material, but I truly loved the article. It turned out to be very useful to me.
best online casino in new zealand · April 30, 2026 at 6:14 pm
Hey, I simply hopped over to your website by way of StumbleUpon. No longer one thing I’d normally learn, but I preferred your thoughts none the less. Thanks for making one thing worth reading.
ThomasSag · April 30, 2026 at 6:46 pm
Эта публикация завернет вас в вихрь увлекательного контента, сбрасывая стереотипы и открывая двери к новым идеям. Каждый абзац станет для вас открытием, полным ярких примеров и впечатляющих достижений. Подготовьтесь быть вовлеченными и удивленными каждый раз, когда продолжите читать.
Прочитать подробнее – нарколог на дом круглосуточно
Nelsonkic · April 30, 2026 at 7:11 pm
Нарколог на дом в Москве: срочная медицинская помощь, капельницы и восстановление состояния в наркологической клинике «Клиника доктора Калюжной».
Углубиться в тему – http://www.domen.ru
mejores casinos online · April 30, 2026 at 7:13 pm
I had highly recommend this blog to my good friend, it’s so good
JudsonGog · April 30, 2026 at 7:29 pm
Нарколог на дом в Екатеринбурге: анонимная помощь при алкоголизме, вывод из запоя и поддержка специалистов в наркологической клинике «НЕО+».
Исследовать вопрос подробнее – http://www.domen.ru
Barrybrede · April 30, 2026 at 7:58 pm
Эта статья сочетает познавательный и занимательный контент, что делает ее идеальной для любителей глубоких исследований. Мы рассмотрим увлекательные аспекты различных тем и предоставим вам новые знания, которые могут оказаться полезными в будущем.
Только факты! – вывод из запоя цена
mejor casino online chile · April 30, 2026 at 8:36 pm
The sketch is tasteful, your authored material stylish.
JamesBOn · April 30, 2026 at 9:06 pm
Мы предлагаем вам окунуться в океан любопытных фактов и вдохновляющих историй. Эта публикация поможет расширить горизонты, разбудить интерес к науке и истории и увидеть мир с новой стороны.
Исследовать вопрос подробнее – вывод из запоя на дому цена
Raymondgloky · April 30, 2026 at 9:17 pm
Анонимность позволяет пациентам сосоточиться на процессе лечения алкогольной зависимости, не переживая о последствиях для своей репутации или безопасности. Важно, чтобы каждый этап был подробно обсужден с пациентом, что помогает снизить уровень стресса и тревожности, связанные с лечением зависимых, включая терапию в стационаре.
Детальнее – центр реабилитации алкоголиков
legalne kasyna online · April 30, 2026 at 9:22 pm
Took me time to read the material, but I truly loved the article. It turned out to be very useful to me.
TomasFoste · April 30, 2026 at 9:38 pm
Непрерывный мониторинг витальных показателей — ключевое отличие стационарного формата. В палатах клиники «Элегия Мед» установлены системы отслеживания частоты пульса, сатурации, температуры и артериального давления, данные с которых автоматически передаются в электронную медицинскую карту. Медицинский персонал дежурит круглосуточно, что обеспечивает мгновенную реакцию на ухудшение состояния: коррекцию инфузионной терапии, введение симптоматических препаратов, привлечение смежных специалистов при необходимости. Такая организация процесса исключает хаотичное назначение средств, предотвращает полипрагмазию и гарантирует, что каждый этап детоксикации проходит под строгим клиническим контролем. Контроль состояния пациента в режиме реального времени позволяет врачам оперативно корректировать терапию и минимизировать риски для здоровья.
Подробнее – нарколог вывод из запоя в стационаре
RufusFal · April 30, 2026 at 9:42 pm
Первый этап вывода из запоя на дому – это первичная оценка состояния пациента. Врач, прибывший на вызов, осматривает пациента, проверяет уровень алкоголя в крови, измеряет артериальное давление, пульс и температуру. Это необходимо для того, чтобы определить степень алкогольной интоксикации и выбрать правильную тактику лечения.
Получить дополнительные сведения – https://vyvod-iz-zapoya-na-domu-ekaterinburg-17.ru
Ga888 · April 30, 2026 at 10:21 pm
It’s continually awesome when you can not only be informed, but also entertained! I’m sure you had fun writing this article. Regards, Clotilde.
Timothybiobe · April 30, 2026 at 10:23 pm
Эта статья сочетает познавательный и занимательный контент, что делает ее идеальной для любителей глубоких исследований. Мы рассмотрим увлекательные аспекты различных тем и предоставим вам новые знания, которые могут оказаться полезными в будущем.
Переходите по ссылке ниже – круглосуточный вывод из запоя
polskie kasyno · April 30, 2026 at 10:46 pm
I was reading through some of your content on this internet site and I believe this web site is very informative ! Continue posting .
Daniellow · April 30, 2026 at 11:07 pm
Реабилитация алкоголиков с поддержкой специалистов в Москве представляет собой важный и сложный процесс, в котором ключевую роль играет профессиональное вмешательство. Программы реабилитации включают в себя не только медицинскую помощь, но и психологическую, социальную и эмоциональную поддержку, что способствует успешному и долгосрочному восстановлению пациента. Такая комплексная помощь является основой эффективного лечения и предотвращения рецидивов.
Получить дополнительную информацию – центр реабилитации алкоголиков город
najlepsze kasyno online · April 30, 2026 at 11:18 pm
You are my inspiration , I possess few web logs and very sporadically run out from to brand 🙁
1xbet game · April 30, 2026 at 11:21 pm
1xbet
Russellswade · April 30, 2026 at 11:23 pm
Эта информационная заметка предлагает лаконичное и четкое освещение актуальных вопросов. Здесь вы найдете ключевые факты и основную информацию по теме, которые помогут вам сформировать собственное мнение и повысить уровень осведомленности.
Нажмите, чтобы узнать больше – нарколог на дом круглосуточно
Najlepsze kasyna online · April 30, 2026 at 11:39 pm
We are a group of volunteers and starting a new initiative in our community. Your blog provided us with valuable information to work on|.You have done a marvellous job!
ThomasIcoge · April 30, 2026 at 11:52 pm
Срочный вызов нарколога на дом позволяет сразу оценить состояние пациента, снять симптомы абстиненции и начать детоксикацию организма. Капельницы от запоя и интоксикации составляются индивидуально с учётом новейших медицинских протоколов 2026 года: они включают нейропротекторы, гепатопротекторы и витаминно-минеральные комплексы последнего поколения. Это не просто очищение крови — это восстановление работы мозга, печени, сердечно-сосудистой системы и психики. Вызов нарколога на дом особенно востребован, когда требуется срочное снятие абстинентного синдрома. Круглосуточная помощь работает без перерывов, поэтому помощь приезжает даже ночью. Мы предлагаем возможность вывода из запоя в домашних условиях.
Изучить вопрос глубже – нарколог на дом анонимно екатеринбург
Russellswade · May 1, 2026 at 12:14 am
Мы собрали для вас самые захватывающие факты из мира науки и истории. От малознакомых деталей до грандиозных событий — эта статья расширит ваш кругозор и подарит новое понимание того, как устроен наш мир.
А что дальше? – нарколог на дом воронеж
GeorgeGlync · May 1, 2026 at 12:15 am
Этот информационный материал собраны данные, которые помогут лучше понять текущие тенденции и процессы в различных сферах жизни. Мы предоставляем четкий анализ, графики и примеры, чтобы информация была не только понятной, но и практичной для принятия решений.
Уточнить детали – сколько стоит прокапаться
SamuelPailk · May 1, 2026 at 12:38 am
Нарколог на дом в Екатеринбурге — это формат помощи, который рассматривают при состояниях после употребления алкоголя, когда больному требуется врачебный осмотр без поездки в клинику. Обычно речь идет о запое, выраженном похмельном синдроме, нарушении сна, обезвоживании, слабости, треморе, тревоге, скачках давления, сердцебиении и общем ухудшении самочувствия. Дальнейшая тактика зависит от состояния больного на момент осмотра, длительности употребления алкоголя и наличия сопутствующих заболеваний.
Подробнее – нарколог на дом цена екатеринбург
GeorgeGlync · May 1, 2026 at 1:12 am
Эта информационная статья охватывает широкий спектр актуальных тем и вопросов. Мы стремимся осветить ключевые факты и события с ясностью и простотой, чтобы каждый читатель мог извлечь из нее полезные знания и полезные инсайты.
Полная информация здесь – вывод из запоя наркология
RobertBlatt · May 1, 2026 at 1:13 am
Процедура проходит под наблюдением квалифицированного врача, что минимизирует риски для здоровья пациента и помогает ускорить процесс восстановления. Важно, что такой подход позволяет избежать госпитализации, что для многих пациентов является дополнительным комфортом.
Получить дополнительную информацию – вывод из запоя на дому в екатеринбурге
Barbarajon · May 1, 2026 at 1:59 am
Эта медицинская заметка содержит сжатую информацию о новых находках и методах в области здравоохранения. Мы предлагаем читателям свежие данные о заболеваниях, профилактике и лечении. Наша цель — быстро и доступно донести важную информацию, которая поможет в повседневной жизни и понимании здоровья.
Подробнее можно узнать тут – капельница от похмелья анонимно
http://xianyuhome.cn:11013/winstoncrutchf · May 1, 2026 at 2:46 am
Vurdering
https://gitea.octifor.synology.me:60443/charlicoats51 https://gitea.octifor.synology.me/
https://www.klusalert.nl/companies/bedste-online-casino-med-hurtige-udbetalinger-i-danmark-2026/ http://www.klusalert.nl
http://dailyplaza.co.kr/bbs/board.php?bo_table=1301&wr_id=263777 http://dailyplaza.co.kr/
https://www.uria.dev/launa63b66651 https://www.uria.dev/
https://gitea.ww3.tw/lavada4549701 gitea.ww3.tw
https://gitlab.iplusus.com/williamcushing/1867191/wiki/De-bedste-online-casino-udbetalinger-i-Danmark-april-2026 gitlab.iplusus.com
https://www.ajiraexpress.com/companies/casino-udbetaling-hurtig-og-sikker-udbetaling/ http://www.ajiraexpress.com
https://fanajobs.com/profile/ulysses13w2061 https://fanajobs.com
https://giaovienvietnam.vn/employer/bedste-online-casino-udbetaling-hurtige-danske-casinoer-2026/ https://giaovienvietnam.vn/employer/bedste-online-casino-udbetaling-hurtige-danske-casinoer-2026/
https://spandexjobs.com/employer/bedste-online-casino-med-hurtige-udbetalinger-i-danmark-2026/ spandexjobs.com
https://gitea.nongnghiepso.com/antondik681135/blackcoin1998/wiki/De-Bedste-Online-Casino-Sider-I-Danmark gitea.nongnghiepso.com
https://www.klusalert.nl/companies/bedste-online-casinoer-i-danmark-vores-eksperters-topvalg/ klusalert.nl
https://em-drh.com/employer/casinoer-med-hurtige-udbetalinger-i-danmark-2026/ em-drh.com
https://gitea.kamisama.ovh/jefferson00d0 gitea.kamisama.ovh
http://pasarinko.zeroweb.kr/bbs/board.php?bo_table=notice&wr_id=10161159 pasarinko.zeroweb.kr
https://mambotango.it/latiakoonce25 mambotango.it
https://jobs.foodtechconnect.com/companies/bedste-udbetaling-casino-2026-hurtigste-udbetalinger/ jobs.foodtechconnect.com
https://www.teacircle.co.in/bedste-online-casino-udbetaling-hurtige-danske-casinoer-2026/ https://www.teacircle.co.in
References:
http://kapkipz.awardspace.us/index.php/topic,21020.0.html
tim TrustGuru Laporan · May 1, 2026 at 3:25 am
Bonus regularity weighs more than promises of high returns.
Bernardcrize · May 1, 2026 at 3:37 am
Эта информационная статья охватывает широкий спектр актуальных тем и вопросов. Мы стремимся осветить ключевые факты и события с ясностью и простотой, чтобы каждый читатель мог извлечь из нее полезные знания и полезные инсайты.
Познакомиться с результатами исследований – капельница на дому екатеринбург
https://webauthorityhealthdom.top/ · May 1, 2026 at 3:56 am
https://webauthorityhealthdom.top/
git.freno.me · May 1, 2026 at 4:06 am
References:
Find de bedste udbetalinger online
References:
https://git.sunlix.one/haydend0232588
SamuelPailk · May 1, 2026 at 5:03 am
Дополнительным поводом для вызова врача становится состояние, при котором больному трудно вставать, пить воду, есть, сохранять спокойствие или ориентироваться в самочувствии. В таких случаях осмотр на дому позволяет быстрее определить дальнейший маршрут помощи. Иногда уже первый звонок помогает понять, допустим ли домашний формат или лучше сразу рассматривать вывод в стационаре.
Ознакомиться с деталями – вызов нарколога на дом в екатеринбурге
CarolMipse · May 1, 2026 at 5:17 am
Мы предлагаем вам окунуться в океан любопытных фактов и вдохновляющих историй. Эта публикация поможет расширить горизонты, разбудить интерес к науке и истории и увидеть мир с новой стороны.
Что скрывают от вас? – срочный вывод из запоя
HectorCor · May 1, 2026 at 5:36 am
Этот информационный материал собраны данные, которые помогут лучше понять текущие тенденции и процессы в различных сферах жизни. Мы предоставляем четкий анализ, графики и примеры, чтобы информация была не только понятной, но и практичной для принятия решений.
Кликни и узнай всё! – капельница на дому в екатеринбурге
RobertDix · May 1, 2026 at 5:59 am
В этой публикации мы сосредоточимся на интересных аспектах одной из самых актуальных тем современности. Совмещая факты и мнения экспертов, мы создадим полное представление о предмете, которое будет полезно как новичкам, так и тем, кто глубоко изучает вопрос.
Детали по клику – снятие алкогольной интоксикации нижний новгород
tools.refinecolor.com · May 1, 2026 at 6:27 am
Blackjack høj udbetalingsprocent
https://git.mana-web.com/kristofer9537/kristofer2001/wiki/Bedste-online-casinoer-i-Danmark-med-fokus-p%C3%A5-udbetalinger-2026 git.mana-web.com
https://gitea.syn-assist.fr/philippgaunt15 gitea.syn-assist.fr
https://reruberrypi.rerurate.com/kierandollar3 https://reruberrypi.rerurate.com/
http://git.fbonazzi.it/gwensternberg9 git.fbonazzi.it
https://xn--lpris-iua.nu/launanord9647 lpris-iua.nu
https://git.lhqs.ink/augustuswgt980 git.lhqs.ink
http://55x.top:9300/johnniecasanov http://55x.top:9300/johnniecasanov
https://gitea.coderpath.com/wilheminastled gitea.coderpath.com
https://jobsathealthcare.com/employer/bedste-online-casinoer-i-danmark-vores-eksperters-topvalg/ https://jobsathealthcare.com/employer/bedste-online-casinoer-i-danmark-vores-eksperters-topvalg/
https://git.sskuaixiu.com/dariowick90817 git.sskuaixiu.com
https://git.secretserver.club/eloykujawski57 git.secretserver.club
https://git.suo0.com/waylon26766336 git.suo0.com
https://git.clickforadventure.co/patrickz165485 https://git.clickforadventure.co/
https://www.fepp.org.ec/curthinz805774/udbetalingsprocent2020/wiki/Bedste-Online-Casinoer-i-Danmark-Vores-Eksperters-Topvalg http://www.fepp.org.ec
https://jobsjo.online/employer/bedste-online-casino-med-hurtige-udbetalinger-i-danmark-2026 jobsjo.online
https://git.esen.gay/tamararigby60 https://git.esen.gay/tamararigby60
https://jobcop.in/employer/bedste-online-casino-udbetaling-%ef%b8%8f-her-er-de-bedste-casinoer/ jobcop.in
https://gitea.amazingcoders.com/carminewuk5540 gitea.amazingcoders.com
References:
https://www.fightdynasty.com/companies/sammenlign-de-bedste-casinoer-2026/
cq.x7cq.vip · May 1, 2026 at 6:48 am
Online casino dansk tilladelse høj udbetaling
http://xhdyz.cn/home.php?mod=space&uid=765309 xhdyz.cn
https://brewwiki.win/wiki/Post:Bedste_Online_Slots_2026_Top_10_Populre_Spillemaskiner_med_Hj_RTP https://brewwiki.win/
http://bbs.xingxiancn.com/home.php?mod=space&uid=890735 http://bbs.xingxiancn.com/
http://www.kaseisyoji.com/home.php?mod=space&uid=3996094 http://www.kaseisyoji.com/home.php?mod=space&uid=3996094
http://kriminal-ohlyad.com.ua/user/dadtrowel33/ http://kriminal-ohlyad.com.ua/
https://coolpot.stream/story.php?title=bedste-online-casino-udbetaling-hurtige-danske-casinoer-2026 coolpot.stream
http://wargame-workshop.com/bbs/home.php?mod=space&uid=1078415 http://wargame-workshop.com/bbs/home.php?mod=space&uid=1078415
https://ondashboard.win/story.php?title=hvilket-online-casino-kan-jeg-vinde-mest-pa-fa-svaret-her ondashboard.win
https://argrathi.stars.ne.jp:443/pukiwiki/index.php?drewherskind637766 argrathi.stars.ne.jp
https://www.youtube.com/redirect?q=https://blackcoin.co/da/bedste-udbyttende-casinoer-danmark-top-online-casinoer-med-hoejeste-udbetalinger-for-2026/ https://www.youtube.com
https://www.sf2.net/space-uid-837881.html http://www.sf2.net
https://carwiki.site/wiki/Bedste_Casino_Bonusser_Uden_Omstningskrav_2026 carwiki.site
http://madk-auto.ru/user/ugandabamboo2/ madk-auto.ru
https://a-taxi.com.ua/user/gearpoint1/ a-taxi.com.ua
https://bookmarking.stream/story.php?title=de-bedste-online-casino-udbetalinger-i-danmark-april-2026 bookmarking.stream
https://pads.zapf.in/s/g0DUyFofNV https://pads.zapf.in/s/g0DUyFofNV
https://www.sf2.net/space-uid-837878.html https://www.sf2.net/space-uid-837878.html
https://bandori.party/user/856836/climbbucket8/ bandori.party
References:
https://bridgedesign.site/wiki/Liste_med_de_21_bedste_i_April_2026
Nelsonkic · May 1, 2026 at 6:58 am
Наиболее частыми причинами обращения становятся запой, выраженная слабость, тремор, тревога, бессонница, тошнота, нестабильное давление, учащенный пульс и ощущение физического истощения. Эти проявления могут сочетаться между собой и усиливаться после прекращения употребления алкоголя, особенно если эпизод длился несколько дней подряд.
Разобраться лучше – врач нарколог на дом москва
curry-velasquez-4.blogbright.net · May 1, 2026 at 7:11 am
Casinoer med højeste udbetalingsfrekvens
http://www.sg588.tw/home.php?mod=space&uid=1171287 http://www.sg588.tw/home.php?mod=space&uid=1171287
http://www.kaseisyoji.com/home.php?mod=space&uid=3996094 http://www.kaseisyoji.com
https://hackmd.okfn.de/s/B171o6xCZl hackmd.okfn.de
https://sibze.ru/index.php?subaction=userinfo&user=fieldactor1 https://sibze.ru/
https://www.instapaper.com/p/17653115 https://www.instapaper.com
https://hotgirlsforum.com/member.php?action=profile&uid=181257 hotgirlsforum.com
https://bandori.party/user/856836/climbbucket8/ bandori.party
https://ondashboard.win/story.php?title=hvilket-online-casino-kan-jeg-vinde-mest-pa-fa-svaret-her ondashboard.win
https://skyscrapperwiki.site/wiki/Online_casinoer_i_danmark_Sikkerhed_regler_og_gevinster https://skyscrapperwiki.site/wiki/Online_casinoer_i_danmark_Sikkerhed_regler_og_gevinster
https://philosophywiki.space/wiki/Eksperts_Tips_der_vil_Maksimere_Dine_Gevinster_i_Betting philosophywiki.space
https://bbs.pku.edu.cn/v2/jump-to.php?url=https://blackcoin.co/da/bedste-udbyttende-casinoer-danmark-top-online-casinoer-med-hoejeste-udbetalinger-for-2026/ bbs.pku.edu.cn
https://www.youtube.com/redirect?q=https://blackcoin.co/da/bedste-udbyttende-casinoer-danmark-top-online-casinoer-med-hoejeste-udbetalinger-for-2026/ https://www.youtube.com
https://www.rcfl.com.hk/home.php?mod=space&uid=9547272 http://www.rcfl.com.hk
https://gardenwiki.site/wiki/Guide_til_casinoudbetaling_Vlg_et_casino_med_hurtig_udbetaling https://gardenwiki.site/
https://cq.x7cq.vip/home.php?mod=space&uid=9541260 cq.x7cq.vip
https://schoolido.lu/user/areadrink82/ https://schoolido.lu/user/areadrink82/
https://xs.xylvip.com/home.php?mod=space&uid=4463383 xs.xylvip.com
https://bbs.sanesoft.cn/home.php?mod=space&uid=1474205 bbs.sanesoft.cn
References:
http://x.kongminghu.com/home.php?mod=space&uid=431184
RobertDix · May 1, 2026 at 7:23 am
Этот текст призван помочь читателю расширить кругозор и получить практические знания. Мы используем простой язык, наглядные примеры и структурированное изложение, чтобы сделать обучение максимально эффективным и увлекательным.
Связаться за уточнением – вывод из запоя цена
BillyCer · May 1, 2026 at 7:26 am
Этот обзор предлагает структурированное изложение информации по актуальным вопросам. Материал подан так, чтобы даже новичок мог быстро освоиться в теме и начать использовать полученные знания в практике.
Всё, что нужно знать – вызов нарколога
https://bbs.darkml.net/ · May 1, 2026 at 7:28 am
References:
Valg af det rigtige casino for udbetaling
References:
https://bbs.sanesoft.cn/home.php?mod=space&uid=1474205
Sarahfoeda · May 1, 2026 at 8:08 am
В этой заметке мы представляем шаги, которые помогут в процессе преодоления зависимостей. Рассматриваются стратегии поддержки и чек-листы для тех, кто хочет сделать первый шаг к выздоровлению. Наша цель — вдохновить читателей на положительные изменения и поддержать их в трудных моментах.
Ознакомиться с деталями – прокапать после запоя нижний новгород
RufusFal · May 1, 2026 at 8:11 am
Вывод из запоя на дому в Екатеринбурге – это услуга, которая становится необходимой, когда состояние пациента ухудшается после длительного употребления алкоголя, и медицинская помощь требуется немедленно. На дому пациенту предоставляется квалифицированная помощь, направленная на быстрое снятие интоксикации, восстановление водно-солевого баланса и стабилизацию общего состояния.
Исследовать вопрос подробнее – vyvod-iz-zapoya-na-domu-ekaterinburg-17.ru/
Antoniotut · May 1, 2026 at 8:19 am
В статье представлены ключевые моменты по актуальной теме, дополненные советами экспертов и ссылками на дополнительные ресурсы. Цель материала — дать читателю инструменты для самостоятельного развития и принятия осознанных решений.
Есть чему поучиться – вывод из алкогольного запоя нарколог24
ThomasIcoge · May 1, 2026 at 8:30 am
Особое внимание мы уделяем психологической составляющей. Нарколог на дом в Екатеринбурге в «НЕО+» — это не только физическое очищение, но и работа с мотивацией, разрушение психологических триггеров зависимости. Зависимость разрушает жизнь, поэтому мы предлагаем психотерапевтическое сопровождение. Родственники получают отдельную поддержку: консультации психолога помогают правильно выстроить общение с зависимым человеком и мотивировать его на дальнейшее лечение. Реабилитация может проходить амбулаторно или в стационаре партнёрских центров с комфортабельными условиями, где пациенты находятся под круглосуточным наблюдением.
Подробнее можно узнать тут – вызов нарколога на дом в екатеринбурге
www.mannacomingdown.org · May 1, 2026 at 8:33 am
dansk
http://park6.wakwak.com/%7Ehitsuji_ya/cgi-bin/mono/album.cgi?mode=detail&no=12 park6.wakwak.com
https://guardian.ge/56963-joe-biden-closes-in-on-white-house-but-election-still-in-the-balance.html https://guardian.ge/
https://thoemusmarthoud.fr/index.php/2022/04/19/how-to-start-a-business-now/ thoemusmarthoud.fr
http://nepalhimalayantrails.com/packages/panchase-short-trek/ http://nepalhimalayantrails.com/packages/panchase-short-trek
http://kapkipz.awardspace.us/index.php/topic,21012.0.html http://kapkipz.awardspace.us
http://inori.s57.xrea.com/ss/photo.cgi?mode=res&resno=12891 inori.s57.xrea.com
https://dzsignage.com/portfolio/support-function/ https://dzsignage.com/portfolio/support-function/
https://app.nicknetwork.com.br/2022/04/28/fermentum-faucibus-ornare-quam-viverra/ app.nicknetwork.com.br
https://expeedia.online/city-breaks-urban-adventures-in-vibrant-metropolises/ expeedia.online
https://gdl.com.ly/2024/04/25/tips-for-choosing-the-right-light-fixtures-for-your-space/ https://gdl.com.ly/
https://zuhausealtwerden.ch/Blog/index.php/;focus=HSTPTP_com_cm4all_wdn_Flatpress_5482220&path=&frame=HSTPTP_com_cm4all_wdn_Flatpress_5482220?x=entry:entry200421-190945%3Bcomments:1 zuhausealtwerden.ch
https://taxperts.com/blog/finding-the-right-tax-help-in-austin-made-simple/ taxperts.com
https://maiitrii.com/top-gift-ideas-for-the-holiday-season/ https://maiitrii.com/
https://www.maximumstores.online/2023/06/22/the-importance-of-building-a-strong-brand-identity/ http://www.maximumstores.online
https://studytochangelife.com/top-tools-every-startup-should-know/ studytochangelife.com
https://acialis.buzz/onebet-foreign-websites/ acialis.buzz
https://agiodesentupidora.com.br/solar-power-vs-fossil-fuels-the-energy-revolution/ https://agiodesentupidora.com.br
https://judith-ricklin.ch/Blog/index.php/;focus=HSTPTP_com_cm4all_wdn_Flatpress_6019167&frame=HSTPTP_com_cm4all_wdn_Flatpress_6019167?x=entry:entry200615-184425%3Bcomments:1 judith-ricklin.ch
References:
https://augelec.com.br/a-journey-through-earths-natural-splendor/
TomasFoste · May 1, 2026 at 8:36 am
Выбор между домашней помощью и стационарным лечением определяется не удобством, а медицинской целесообразностью. В условиях клиники исключаются внешние триггеры, обеспечивается изоляция от источников алкоголя и создается контролируемая среда, где терапевтические решения принимаются на основе объективных показателей. Такой подход критически важен для предотвращения осложнений, минимизации дискомфорта абстиненции и формирования устойчивой базы для дальнейшей противорецидивной работы.
Углубиться в тему – вывод из запоя в стационаре санкт-петербург
Sarahfoeda · May 1, 2026 at 8:54 am
Эта публикация обращает внимание на важность профилактики зависимостей. Мы обсудим, как осведомленность и образование могут помочь в предотвращении возникновения зависимости. Читатели смогут ознакомиться с полезными советами и ресурсами, которые способствуют здоровому образу жизни.
Узнать больше – похмелье капельница вызвать на дом
Robertmah · May 1, 2026 at 8:56 am
Металлический уголок — это надежное и практичное решение для ваших строительных и производственных задач.
Source:
https://astra.org.au/?URL=https://ugolka.net/uk/equal-shelf/
Металлический уголок
Robertmah · May 1, 2026 at 9:03 am
Металлический уголок — это надежное и практичное решение для ваших строительных и производственных задач.
Source:
https://www.interfaith.org.uk/?URL=https://ugolka.net/galvanized/
Металлический уголок
JudsonGog · May 1, 2026 at 9:05 am
Нарколог на дом в Екатеринбурге: анонимная помощь при алкоголизме, вывод из запоя и поддержка специалистов в наркологической клинике «НЕО+».
Подробнее можно узнать тут – нарколог на дом екатеринбург
Robertmah · May 1, 2026 at 9:07 am
Металлический уголок — это надежное и практичное решение для ваших строительных и производственных задач.
Source:
https://go2delphi.com/?URL=https://ugolka.net/equal-shelf/
Металлический уголок
Josephpeapy · May 1, 2026 at 9:07 am
В этой статье-обзоре мы соберем актуальную информацию и интересные факты, которые освещают важные темы. Читатели смогут ознакомиться с различными мнениями и подходами, что позволит им расширить кругозор и глубже понять обсуждаемые вопросы.
Выяснить больше – вывод из запоя воронеж на дому
Carlosbub · May 1, 2026 at 9:08 am
Эта статья погружает вас в увлекательный мир знаний, где каждый факт становится открытием. Мы расскажем о ключевых исторических поворотных моментах и научных прорывах, которые изменили ход цивилизации. Поймите, как прошлое формирует настоящее и как его уроки могут помочь нам строить будущее.
Осуществить глубокий анализ – врач нарколог выезд на дом
nightqueenspa24x7.com · May 1, 2026 at 9:10 am
Logiske valg for høj casino udbetaling
https://herniabrasil.com.br/2025/10/20/o-que-voce-precisa-saber-para-escolher-o-cirurgiao-certo-para-tratar-a-sua-hernia/ herniabrasil.com.br
https://basalinitiatives.net/mastering-growth-with-proven-business-tips/ https://basalinitiatives.net/
https://forum.karnex.in/question/eye-tracking-system-market-share-and-competitive-landscape-assessment-2032/ https://forum.karnex.in
https://biuro-konsultant.pl/2023/09/25/solar-power-for-businesses-cutting-costs-and-carbon/ biuro-konsultant.pl
https://despachantesaogabriel.com.br/2023/06/28/embrace-the-digital-age-unleash-the-potential-of-our-products/ https://despachantesaogabriel.com.br
https://celxfetil.com.br/the-power-of-effective-communication-in-business/ celxfetil.com.br
https://globalprints4.com/the-power-of-effective-communication-in-business/ https://globalprints4.com/the-power-of-effective-communication-in-business
https://www.bettamed.com/content_block/homebusiness-counters/ http://www.bettamed.com
http://kimnpark.net/gnu5/bbs/board.php?bo_table=2014Taiwan&wr_id=468&sst=wr_hit&sod=asc&sop=and&page=73 http://kimnpark.net
https://projetoperpetuosocorro.com.br/the-joy-of-giving-serving-others-with-a-generous-heart/ projetoperpetuosocorro.com.br
https://marsosa.com/5-mistakes-that-are-holding-your-business-back/ marsosa.com
https://salemcitysportsarena.com/2023/11/11/navigating-the-unknown-a-journey-discovery/ https://salemcitysportsarena.com/
https://lunaoyizafoundation.com/hidden-gems-exploring-off-the-beaten-path-destinations/ lunaoyizafoundation.com
https://ma-moebeltaxi.de/index.php/solar-energy-benefits-going-green-and-saving-green/ ma-moebeltaxi.de
https://firstidea.co.in/maximizing-productivity-tips-for-a-successful-workday/ https://firstidea.co.in
https://epdacameroon.org/environment-and-natural-resources-management-enrm/ epdacameroon.org
https://agiodesentupidora.com.br/solar-power-vs-fossil-fuels-the-energy-revolution/ https://agiodesentupidora.com.br/
https://threadsplay.com/from-runway-to-real-life-how-to-wear-it/ threadsplay.com
References:
https://angelhospedagem.com.br/how-to-build-a-consistent-practice/
https://tasadorinmobiliario.org/ · May 1, 2026 at 9:12 am
Sider med højeste udbetalingsprocent på slots
https://josemario.acesso.ws/mastering-time-management-key-to-business-success/ josemario.acesso.ws
http://over.o.oo7.jp/cgi-bin/overlimit/album/album.cgi?mode=detail&no=39" over.o.oo7.jp
https://nvcell.com.br/mastering-growth-with-proven-business-tips/ nvcell.com.br
https://psicologorodrigomacedo.com.br/tiny-scientists-on-the-loose-preschool-science-wonders/ https://psicologorodrigomacedo.com.br/tiny-scientists-on-the-loose-preschool-science-wonders
https://nirmalhomesgirlshostel.com/2023/08/21/connecting-with-natures-tranquil-essence/ https://nirmalhomesgirlshostel.com/
https://posetiteley.net.ua/box-minishot-add posetiteley.net.ua
https://sennior.com.br/the-importance-of-building-a-strong-brand-identity/ sennior.com.br
https://packmann-umzuege.de/2023/06/22/maximizing-productivity-tips-for-a-successful-workday/ packmann-umzuege.de
https://lifehope.blog/who-is-the-ruler-of-this-world/ lifehope.blog
https://xn--35-9kcqjf4agkuj0ak.xn--p1ai/2023/06/22/maximizing-productivity-tips-for-a-successful-workday/ 35-9kcqjf4agkuj0ak.рф
https://galinakatsarska.com/monica-baron/ galinakatsarska.com
https://www.elsieisy.com/minding-business-not-easy/ http://www.elsieisy.com
https://www.stetoscopio.net/vitamine-e-integratori/umidita-dannosa-per-integratori-alimentari-e-le-vitamine/ http://www.stetoscopio.net
https://raskrussia.ru/blog/ntcn-3/ https://raskrussia.ru
https://rutvitravels.com/solar-panels-101-a-beginners-guide-to-solar-energy/ https://rutvitravels.com/
https://fundacoesconfigeo.com.br/2023/11/11/unlocking-creativity-embrace-your-inner-artist/ https://fundacoesconfigeo.com.br
https://www.tajsafewaytour.com/shakira-india-tour-2026/ https://www.tajsafewaytour.com
https://sunshineheatingandairconditioning.com/how-solar-energy-works-from-sunlight-to-electricity/ https://sunshineheatingandairconditioning.com/how-solar-energy-works-from-sunlight-to-electricity
References:
https://scrocchisepelios.com.ar/2023/06/22/maximizing-productivity-tips-for-a-successful-workday/
Barbarajon · May 1, 2026 at 9:13 am
Этот медицинский обзор сосредоточен на последних достижениях, которые оказывают влияние на пациентов и медицинскую практику. Мы разбираем инновационные методы лечения и исследований, акцентируя внимание на их значимости для общественного здоровья. Читатели узнают о свежих данных и их возможном применении.
Разобраться лучше – капельница от похмелья клиника
Bernardcrize · May 1, 2026 at 9:14 am
В статье представлены ключевые моменты по актуальной теме, дополненные советами экспертов и ссылками на дополнительные ресурсы. Цель материала — дать читателю инструменты для самостоятельного развития и принятия осознанных решений.
Получить дополнительную информацию – капельница екатеринбург цены
Robertmah · May 1, 2026 at 9:29 am
Металлический уголок — это надежное и практичное решение для ваших строительных и производственных задач.
Source:
https://isoft.biz/proxy.php?link=https://ugolka.net/equal-shelf/
Металлический уголок
https://whatmedicine.info/ · May 1, 2026 at 10:23 am
https://whatmedicine.info/
HildaSat · May 1, 2026 at 11:07 am
В этой публикации мы предложим ряд рекомендаций по избавлению от зависимостей и успешному восстановлению. Мы обсудим методы привлечения поддержки и важность самосознания. Эти советы помогут людям вернуться к нормальной жизни и стать на путь выздоровления.
Разобраться лучше – капельница на дому нижний новгород от алкоголя
gitea.primecontrols-dev.com · May 1, 2026 at 11:11 am
udbetalingsratio
https://git.gotrobotics.org/dakota13055735 https://git.gotrobotics.org
https://jobs.assist24-7.com/employer/25-online-casinos-mit-hohem-rtp-und-top-auszahlungsquoten/ jobs.assist24-7.com
http://g98710av.beget.tech/saundrarosenbe g98710av.beget.tech
https://qflirt.net/@nathanorozco70 qflirt.net
https://git.123doit.com/fabian85497273 https://git.123doit.com/fabian85497273
https://jobcop.ca/employer/online-casino-mit-sofortauszahlung-2026-beste-anbieter-im-test/ jobcop.ca
https://gitea.hello.faith/harlanwolfgang gitea.hello.faith
https://git.saike.fun:9755/warrenchung247 https://git.saike.fun/
http://kreativemaniac.com/read-blog/2019_casinos-mit-schneller-auszahlung-2026-sofort-geld-hier.html kreativemaniac.com
https://slowdating.ca/@janiemcgrowdie slowdating.ca
https://git.powerdata.dk/genesisbaehr89/2649beste-echtgeld-slots-auszahlungsquote/wiki/Top-Online-Casinos-%26-Spielotheken-mit-hoher-Gewinnchance-2026 https://git.powerdata.dk/genesisbaehr89/2649beste-echtgeld-slots-auszahlungsquote/wiki/Top-Online-Casinos-&-Spielotheken-mit-hoher-Gewinnchance-2026
https://collisioncommunity.com/employer/online-casinos-mit-hoher-auszahlungsquote-2026-top-rtps/ collisioncommunity.com
http://git.rabbittec.com/francis2671265/francis1982/wiki/Wie+funktionieren+Online+Slots%253F+%25E2%25AD%2590%25EF%25B8%258F+RTP+%2526+Auszahlungsquote+einfach+erkl%25C3%25A4rt+2025 git.rabbittec.com
https://beatsong.app/roseannemcmull https://beatsong.app/roseannemcmull
https://dgwork.co.kr/sandraboynton dgwork.co.kr
https://gitea.syn-assist.fr/penneyruff4961/zahlende4368/wiki/Slots-mit-hoher-RTP-2026 https://gitea.syn-assist.fr/penneyruff4961/zahlende4368/wiki/Slots-mit-hoher-RTP-2026
https://firstcanadajobs.ca/employer/online-casino-mit-sofortauszahlung-2026-beste-anbieter-im-test/ https://firstcanadajobs.ca/employer/online-casino-mit-sofortauszahlung-2026-beste-anbieter-im-test/
http://www.jobaaty.com/employer/die-besten-auszahlungsquoten-bei-casino-online-spielen-2026 http://www.jobaaty.com
References:
https://flirta.online/@levinewbery650
friztty.com · May 1, 2026 at 11:12 am
Markedets førende casinoer for udbetalinger
http://merchantale.com/phillisteeter http://merchantale.com
https://smallbusinessinternships.com/employer/mr-bet-casino-auszahlung-alle-details-zu-den-zahlungsoptionen-und-bearbeitung/ smallbusinessinternships.com
http://globaldream.or.kr/bbs/board.php?bo_table=sub08_02&wr_id=319027 http://globaldream.or.kr/
https://www.ikaros.asia/tonjanoble104 ikaros.asia
https://gitea.redaktion.titanic-magazin.de/opmdeangelo07/3431462/wiki/Online-Casinos-mit-bester-Auszahlungsquote-Top-Gewinnchance-2026 gitea.redaktion.titanic-magazin.de
https://mycrewdate.com/@theo54m7759361 mycrewdate.com
https://nepalijob.com/companies/11-beste-online-casinos-in-deutschland-2026-seit-1995/ https://nepalijob.com
https://git.genowisdom.cn/reecefurneaux https://git.genowisdom.cn/reecefurneaux
https://csmsound.exagopartners.com/majormonson51 csmsound.exagopartners.com
http://git.ibossay.com:3000/rhondaarthur1 git.ibossay.com
https://behired.eu/employer/beste-online-casino-auszahlungsquoten-hohe-gewinnchancen/ behired.eu
http://www.mindepoch.com:9092/albertha84g574 http://www.mindepoch.com
http://gitea.yiban.com.tw:3030/vidaspencer73 http://gitea.yiban.com.tw:3030/vidaspencer73
https://eram-jobs.com/employer/casinos-mit-bester-auszahlungsquote-2026-hohe-gewinnchancen eram-jobs.com
https://www.fightdynasty.com/companies/25-online-casinos-mit-hohem-rtp-und-top-auszahlungsquoten/ http://www.fightdynasty.com
https://https://friztty.com/@janessahersh52/@dufelida691287 friztty.com
https://www.propose.lk/@arthurlapsley http://www.propose.lk
https://eurogulfcareers.com/companies/neue-online-casinos-mit-start-im-april-2026-top-boni-slots/ eurogulfcareers.com
Yvonnejoync · May 1, 2026 at 11:17 am
Этот документ охватывает важные аспекты медицинской науки, сосредотачиваясь на ключевых вопросах, касающихся здоровья населения. Мы рассматриваем свежие исследования, клинические рекомендации и лучшие практики, которые помогут улучшить качество лечения и профилактики заболеваний. Читатели получат возможность углубиться в различные медицинские дисциплины.
Детальнее – вывод из запоя стационар
MiguelBip · May 1, 2026 at 11:18 am
Каждый из этапов важен для успешного лечения наркомании и требует квалифицированной наркологической медицинской помощи. Реабилитационные программы, предлагаемые в Москве, часто включают в себя все эти компоненты, при этом в ряде случаев консультации могут предоставляться бесплатно, что способствует комплексному подходу к решению проблемы зависимости.
Исследовать вопрос подробнее – клиника реабилитации алкоголиков
bridgedesign.space · May 1, 2026 at 11:40 am
References:
Bedste klassiske casino spil udbetaling
References:
http://karayaz.ru/user/peonyenergy85/
gitea.jb1000.com · May 1, 2026 at 11:53 am
Casino guide til de højeste udbetalinger
https://fun-md.com/stanservin8115 https://fun-md.com/
http://portal.chrzescijanscysingle.pl/@emiliamaxwell http://portal.chrzescijanscysingle.pl/
https://aitune.net/josephineliger https://aitune.net/josephineliger
https://git.olivierboeren.nl/carrieboyes53 git.olivierboeren.nl
https://qdate.ru/@marcellaignaci https://qdate.ru/@marcellaignaci
https://git.ultra.pub/deliladonnitho git.ultra.pub
http://fanlibo.i234.me:8418/maxbennet66650 fanlibo.i234.me
https://internskill.in/companies/slots-mit-hoher-rtp-2026-10-slots-mit-hoher-auszahlungsquote/ internskill.in
https://gbewaaplay.com/blythemcclusky https://gbewaaplay.com
https://git.smart-tool.jp/ceceliacunniff https://git.smart-tool.jp/
https://grafana.jasonstolle.com/ferne18f093568 grafana.jasonstolle.com
https://tippy-t.com/shaybrewington/shay1994/wiki/Beste-Online-Casinos-Deutschland-2026-Top-10-Testsieger https://tippy-t.com/
https://gitea.jsjymgroup.com/warnersoileau/4228blackcoin.co/wiki/Online-Casinos-mit-bester-Auszahlungsquote-Top-Gewinnchance-2026 gitea.jsjymgroup.com
https://sound.gatzone.com/trinaservice8 sound.gatzone.com
https://gitee.planhomecloud.cn/darrennyhan90 https://gitee.planhomecloud.cn/darrennyhan90
http://ydds.cloud:3000/rickhopetoun41 ydds.cloud
https://www.atmasangeet.com/clarissamarron https://www.atmasangeet.com/clarissamarron
https://git.lucas-michel.fr/blifrancesco89/francesco1983/wiki/Slots-mit-hoher-RTP-2026-10-Slots-mit-hoher-Auszahlungsquote https://git.lucas-michel.fr/
References:
https://grafana.jasonstolle.com/ferne18f093568
Rebeccaguaxy · May 1, 2026 at 12:04 pm
Эта публикация исследует взаимосвязь зависимости и психологии. Мы обсудим, как психологические аспекты влияют на появление зависимостей и процесс выздоровления. Читатели смогут понять важность профессиональной поддержки и применения научных подходов в терапии.
Разобраться лучше – вывод из запоя нарколог 24
HildaSat · May 1, 2026 at 12:07 pm
Этот медицинский обзор сосредоточен на последних достижениях, которые оказывают влияние на пациентов и медицинскую практику. Мы разбираем инновационные методы лечения и исследований, акцентируя внимание на их значимости для общественного здоровья. Читатели узнают о свежих данных и их возможном применении.
Исследовать вопрос подробнее – поставить капельницу от запоя на дому цена
Samuelimini · May 1, 2026 at 12:09 pm
В данной статье вы найдете комплексный подход к изучению насущных тем. Мы комбинируем теоретические сведения с практическими советами, чтобы читатель мог не только понять проблему, но и найти пути её решения.
Подробнее – врач капельница алкоголь на дом
Barrybrede · May 1, 2026 at 12:11 pm
В этой публикации мы предлагаем подробные объяснения по актуальным вопросам, чтобы помочь читателям глубже понять их. Четкость и структурированность материала сделают его удобным для усвоения и применения в повседневной жизни.
Изучите внимательнее – вывод из запоя стоимость
www.ricetteclara.com · May 1, 2026 at 12:14 pm
References:
Casinoer med høj gevinstprocent Danmark
References:
http://www.seafishzone.com/home.php?mod=space&uid=2860889
RodneyFut · May 1, 2026 at 12:22 pm
В Нижнем Новгороде выезд нарколога на дом используется при состояниях, требующих оперативной медицинской оценки и начала терапии. Врач приезжает с необходимыми препаратами, проводит осмотр и формирует план лечения на месте. Такой формат позволяет сократить время до начала помощи и снизить нагрузку на пациента.
Изучить вопрос глубже – narkologicheskaya-pomoshh-nizhnij-novgorod-8.ru/
http://gsiani01.nayaa.co.kr · May 1, 2026 at 12:23 pm
udbetalingskvote
https://www.andreferraovargas.com/hospitais-de-atuacao/consultorio/ https://www.andreferraovargas.com
https://lmdhome.vn/nha-bep-don-gian-cho-nha-cap-4/ lmdhome.vn
https://adiestramientotactico.com/benefits-of-going-solar-why-switching-to-solar-energy-makes-sense/ adiestramientotactico.com
https://proteinfood.lancerstech.com/natures-influence-on-cutting-edge-technology-a-symbiotic/ proteinfood.lancerstech.com
https://noticias.upc.edu.pe/2017/08/28/equipo-de-investigadores-de-la-upc-presente-en-el-xviii-congreso-panamericano-de-infectologia-panama-2017/ https://noticias.upc.edu.pe/2017/08/28/equipo-de-investigadores-de-la-upc-presente-en-el-xviii-congreso-panamericano-de-infectologia-panama-2017
https://halihicks.com/playlist/rock/ halihicks.com
https://quicksearch.it/praesent-ac-convallis-turpis/ quicksearch.it
https://aegypten-ausflug.de/1xbet-philippines-review-bookmaker-in-philippines-11/ https://aegypten-ausflug.de/
https://officeretail.mpi-bidakara.com/nikmatnya-ceaser-salad-polly-caffe-di-kompleks-bidakara/ officeretail.mpi-bidakara.com
https://nextgen-comms.com/the-pros-and-cons-of-different-investment-vehicles/ nextgen-comms.com
https://advancedirrigationct.com/streamline-your-operations-discover-our-suite-of-digital/ https://advancedirrigationct.com/streamline-your-operations-discover-our-suite-of-digital/
https://mppee.gob.ve/?p=82761 mppee.gob.ve
https://bet88ku.com/cach-phan-tich-xo-so-mien-bac/ https://bet88ku.com
https://sinpronorp.com.br/understanding-credit-scores-and-how-to-improve-yours/ sinpronorp.com.br
https://urbanhelpers.co.uk/the-importance-of-building-a-strong-brand-identity/ urbanhelpers.co.uk
https://printenwinkel.nl/development/the-importance-of-building-a-strong-brand-identity/ printenwinkel.nl
https://bharatartjewellers.com/tips-for-hosting-the-perfect-christmas-eve/ bharatartjewellers.com
https://susanne-kriegel.de/Eben-war-sie-noch-da,-aber-wo-sie-jetzt-ist/index.php/;focus=ALFAHO_com_cm4all_wdn_Flatpress_1907544&path=?x=entry:entry230923-134702%3Bcomments:1 https://susanne-kriegel.de/
References:
https://compostoeldorado.com.br/2023/08/21/embracing-the-wonders-of-the-natural-world/
gardenwiki.site · May 1, 2026 at 12:24 pm
References:
Online casino udbetaling og sikkerhed
References:
https://servodriven.com/forums/users/backrotate81/
Maryannmeept · May 1, 2026 at 12:28 pm
В этой статье мы рассмотрим современные достижения в области медицины, включая инновационные методы лечения и диагностики. Мы обсудим важность профилактики заболеваний и роль технологий в улучшении качества здравоохранения. Читатели узнают о влиянии медицины на повседневную жизнь и ее значение для современного общества.
Углубиться в тему – вывод из запоя нижний новгород стационар
https://attacknail65.werite.net/ · May 1, 2026 at 12:30 pm
References:
Bedste casinoer for storspillere
References:
https://architecturewiki.site/wiki/Casinos_mit_schneller_Auszahlung_2026_im_Test
philippefayeton.free.fr · May 1, 2026 at 12:57 pm
Guide til casinoer med høj udbetaling
https://www.fsv-kappelrodeck.de/Home;focus=TKOMSI_com_cm4all_wdn_Flatpress_22523288&path=?x=entry:entry220908-102209%3Bcomments:1 https://www.fsv-kappelrodeck.de/
https://rannierlira.com/coopanest-rn-sob-nova-direcao/ https://rannierlira.com
https://digitizewithvijal.com/understanding-micronutrients-and-daily-needs/ https://digitizewithvijal.com/
https://onetouch.com.br/2023/06/22/maximizing-productivity-tips-for-a-successful-workday/ onetouch.com.br
https://unssps.org.in/tiny-scientists-on-the-loose-preschool-science-wonders-2/ https://unssps.org.in/tiny-scientists-on-the-loose-preschool-science-wonders-2/
https://tofumarketingagency.com/navigating-market-uncertainty-a-consultants-guide/ https://tofumarketingagency.com/navigating-market-uncertainty-a-consultants-guide/
https://zirvemarinmersin.com/your-guide-to-buying-and-selling-real-estate-in-city/ zirvemarinmersin.com
https://www.matravel.co.za/in-our-intercourse-shop-on-line/ https://www.matravel.co.za/
https://salemcitysportsarena.com/2023/11/11/unlocking-creativity-embrace-your-inner-artist/ salemcitysportsarena.com
https://peoplesherald.com/exploring-the-evolution-of-modern-digital-art/ peoplesherald.com
https://peter-schroeder.eu/Blog;focus=TKOMSI_com_cm4all_wdn_Flatpress_22119493&path=&frame=TKOMSI_com_cm4all_wdn_Flatpress_22119493?x=entry:entry200512-074628%3Bcomments:1 peter-schroeder.eu
https://pspowers.com/electric-motor-types-in-evs-what-powers-scooters-and-cars-in-india-usa-and-europe/ pspowers.com
http://divineflame.in/2023/06/22/whatever-happens-happens-and-its-always-okay/ http://divineflame.in/2023/06/22/whatever-happens-happens-and-its-always-okay
https://boozebuddy.in/5-key-strategies-for-scaling-your-business-in-2024/ https://boozebuddy.in/
https://www.mateddo.com/abcs-and-123s-journeying-through-preschool-with-joy/ mateddo.com
https://forum.karnex.in/question/best-crypto-recovery-company-visit-fixer-wallet-retrieval/ forum.karnex.in
https://backup.thedigitalcauldron.com/blog/react-vs-wordpress/ https://backup.thedigitalcauldron.com/
https://vinty.com.br/4-cybersecurity-takeaways-from-chinas-largest-data-breach/ vinty.com.br
References:
https://dubai.tripease.in/exploring-the-beauty-of-mother-nature/
StephenTwins · May 1, 2026 at 1:02 pm
В этой статье рассматриваются различные аспекты избавления от зависимости, включая физические и психологические методы. Мы обсудим поддержку, мотивацию и стратегии, которые помогут в процессе выздоровления. Читатели узнают, как преодолеть трудности и двигаться к новой жизни без зависимости.
Более того — здесь – выведение из запоя на дому
Samuelimini · May 1, 2026 at 1:07 pm
Этот информативный текст отличается привлекательным содержанием и актуальными данными. Мы предлагаем читателям взглянуть на привычные вещи под новым углом, предоставляя интересный и доступный материал. Получите удовольствие от чтения и расширьте кругозор!
Подробнее тут – помощь вывода запоя
Daniellow · May 1, 2026 at 1:10 pm
Реабилитация алкоголиков с поддержкой специалистов в Москве представляет собой важный и сложный процесс, в котором ключевую роль играет профессиональное вмешательство. Программы реабилитации включают в себя не только медицинскую помощь, но и психологическую, социальную и эмоциональную поддержку, что способствует успешному и долгосрочному восстановлению пациента. Такая комплексная помощь является основой эффективного лечения и предотвращения рецидивов.
Разобраться лучше – центр реабилитации алкоголиков город
https://www.demilked.com/author/teainput38/ · May 1, 2026 at 1:22 pm
References:
Hvilke casinoer giver flest penge tilbage
References:
https://may22.ru/user/patchdamage60/
https://borch-alvarez-6.thoughtlanes.net/casino-mit-hoher-gewinnchance-2026-top-casinos-mit-hoher-rtp · May 1, 2026 at 1:33 pm
References:
Bedste casino bonusser med høj udbetaling
References:
https://freudwiki.site/wiki/Auszahlungsquote_bei_Spielautomaten_RTPVergleichstabelle
Maryannmeept · May 1, 2026 at 1:34 pm
В этой статье мы рассмотрим современные достижения в области медицины, включая инновационные методы лечения и диагностики. Мы обсудим важность профилактики заболеваний и роль технологий в улучшении качества здравоохранения. Читатели узнают о влиянии медицины на повседневную жизнь и ее значение для современного общества.
Подробнее тут – вывод из запоя в наркологическом стационаре
https://bookmark4you.win · May 1, 2026 at 1:38 pm
References:
Casinoer med højeste udbetalingsloft
References:
https://pagh-sandoval-2.technetbloggers.de/casinos-mit-hohem-rtp-2026-96-gewinnchance
cook-zamora-3.hubstack.net · May 1, 2026 at 1:54 pm
References:
Mest seriøse casinoer med høj udbetaling
References:
https://pad.stuve.uni-ulm.de/s/tA184mIRY
Raymondgloky · May 1, 2026 at 2:17 pm
Реабилитация алкоголиков с анонимной поддержкой — это важный процесс, который помогает людям справиться с зависимостью в условиях конфиденциальности и безопасности. Многие пациенты опасаются обращаться за помощью из-за стереотипов и страха осуждения. Анонимность в реабилитации становится важным фактором для обеспечения доверия и максимальной эффективности лечения, при этом в ряде случаев доступны такие услуги, как кодирование и консультации наркологической помощи бесплатно, особенно при обращении после запоя. В Москве существует множество центров, которые предлагают реабилитацию алкоголиков с анонимной поддержкой, что позволяет пациентам пройти лечение, не раскрывая своей личности и не беспокоясь о социальном осуждении.
Подробнее можно узнать тут – reabilitacziya-alkogolikov-moskva-4.ru/
RogerAbiny · May 1, 2026 at 3:07 pm
В этой статье представлен занимательный и актуальный контент, который заставит вас задуматься. Мы обсуждаем насущные вопросы и проблемы, а также освещаем истории, которые вдохновляют на действия и изменения. Узнайте, что стоит за событиями нашего времени!
Связаться за уточнением – помощь вывода запоя
HarlangAg · May 1, 2026 at 3:18 pm
Этот увлекательный информационный материал подарит вам массу новых знаний и ярких эмоций. Мы собрали для вас интересные факты и сведения, которые обогатят ваш опыт. Откройте для себя увлекательный мир информации и насладитесь процессом изучения!
Углубить понимание вопроса – прокапаться анонимно
gitea.fefello.org · May 1, 2026 at 3:21 pm
References:
Hvilket casino skal man vælge for udbetaling
References:
https://rukorma.ru/casinos-mit-schneller-auszahlung-2026-sofort-geld-hier
MartinEvowl · May 1, 2026 at 3:31 pm
Публикация приглашает вас исследовать неизведанное — от древних тайн до современных достижений науки. Вы узнаете, как случайные находки превращались в революции, а смелые мысли — в новые эры человеческого прогресса.
Связаться за уточнением – вызов нарколога на дом круглосуточно
fixDiele · May 1, 2026 at 3:41 pm
Зацепил материал про Обсудим всё о футболе: от истории до текущих матчей.
Ссылка ниже:
https://dynamofamily.ru
fixDiele · May 1, 2026 at 3:45 pm
Кстати, если вас интересует Советы по управлению личными финансами, загляните сюда.
Ссылка ниже:
https://portal-fin.ru
JamesWoste · May 1, 2026 at 3:52 pm
В данной обзорной статье представлены интригующие факты, которые не оставят вас равнодушными. Мы критикуем и анализируем события, которые изменили наше восприятие мира. Узнайте, что стоит за новыми открытиями и как они могут изменить ваше восприятие реальности.
Обратитесь за информацией – выезд нарколога на дом круглосуточно
Yvonnejoync · May 1, 2026 at 3:58 pm
В данном обзоре представлены основные направления и тренды в области медицины. Мы обсудим актуальные проблемы здравоохранения, свежие открытия и новые подходы, которые меняют представление о лечении и профилактике заболеваний. Эта информация будет полезна как специалистам, так и широкой публике.
Подробнее тут – вывод из запоя стационар
EnriqueHig · May 1, 2026 at 4:00 pm
В этом интересном тексте собраны обширные сведения, которые помогут вам понять различные аспекты обсуждаемой темы. Мы разбираем детали и факты, делая акцент на важности каждого элемента. Не упустите возможность расширить свои знания и взглянуть на мир по-новому!
Прочитать подробнее – прокапаться от алкоголя цена
EdwinLig · May 1, 2026 at 4:13 pm
Отдельно оценивают ситуации, когда эпизоды повторяются и становятся частью более устойчивой проблемы. Если после алкоголя регулярно развивается тяжелое состояние, нарушается привычный режим жизни, усиливаются последствия алкоголизма и возникают сложности с контролем употребления, домашний выезд может быть только первым этапом более длинного маршрута помощи. При этом наркологическая помощь может включать не только снятие острых проявлений, но и дальнейшую программу лечения зависимости, если речь идет о длительном течении заболевания.
Получить дополнительные сведения – нарколог на дом цена в москве
MartinEvowl · May 1, 2026 at 4:34 pm
В обзорной статье вы найдете собрание важных фактов и аналитики по самым разнообразным темам. Мы рассматриваем как современные исследования, так и исторические контексты, чтобы вы могли получить полное представление о предмете. Погрузитесь в мир знаний и сделайте шаг к пониманию!
Информация доступна здесь – нарколог на дом
Rebeccaguaxy · May 1, 2026 at 4:53 pm
В этой заметке мы представляем шаги, которые помогут в процессе преодоления зависимостей. Рассматриваются стратегии поддержки и чек-листы для тех, кто хочет сделать первый шаг к выздоровлению. Наша цель — вдохновить читателей на положительные изменения и поддержать их в трудных моментах.
Ознакомиться с деталями – вывод из запоя с выездом на дом
JamesWoste · May 1, 2026 at 4:56 pm
Эта статья погружает вас в увлекательный мир знаний, где каждый факт становится открытием. Мы расскажем о ключевых исторических поворотных моментах и научных прорывах, которые изменили ход цивилизации. Поймите, как прошлое формирует настоящее и как его уроки могут помочь нам строить будущее.
Ознакомиться с отчётом – вызвать врача нарколога на дом
RamiroJem · May 1, 2026 at 5:08 pm
Эта обзорная заметка содержит ключевые моменты и факты по актуальным вопросам. Она поможет читателям быстро ориентироваться в теме и узнать о самых важных аспектах сегодня. Получите краткий курс по современной информации и оставайтесь в курсе событий!
Перейти к статье – вызвать нарколога на дом нарколог 24
https://my-uchebnik.ru/public/5/hosting/ · May 1, 2026 at 5:33 pm
https://my-uchebnik.ru/public/5/hosting/
RamiroJem · May 1, 2026 at 6:19 pm
Эта познавательная публикация погружает вас в море интересного контента, который быстро захватит ваше внимание. Мы рассмотрим важные аспекты темы и предоставим вам уникальные Insights и полезные сведения для дальнейшего изучения.
Всё, что нужно знать – вызвать нарколога на дом нарколог 24
StephenTwins · May 1, 2026 at 6:32 pm
Эта публикация посвящена актуальным вопросам современной медицины и здравоохранения. Мы обсудим новейшие технологии диагностики и лечения, а также их влияние на продолжительность и качество жизни. Читатель найдет здесь информацию о научных исследованиях и перспективных разработках, доступно изложенную для широкой аудитории.
Посмотреть всё – нарколог вывод из запоя
MiguelBip · May 1, 2026 at 8:00 pm
Процесс реабилитации алкоголиков включает в себя несколько методов, направленных на восстановление как физического, так и психоэмоционального состояния пациента. В Москве доступны различные программы, от традиционной детоксикации до современных подходов, при этом в отдельных случаях предусматривается вывод данных о состоянии пациента и динамике лечения при алкогольной зависимости, включая когнитивно-поведенческую терапию и арт-терапию.
Подробнее тут – http://www.domen.ru
BillyCer · May 1, 2026 at 8:07 pm
Предлагаем вашему вниманию интересную справочную статью, в которой собраны ключевые моменты и нюансы по актуальным вопросам. Эта информация будет полезна как для профессионалов, так и для тех, кто только начинает изучать тему. Узнайте ответы на важные вопросы и расширьте свои знания!
Связаться за уточнением – нарколог домой
Donaldcem · May 1, 2026 at 8:11 pm
Вывод из запоя на дому в Екатеринбурге: срочная помощь, детоксикация и восстановление под контролем специалистов в наркологической клинике «Детокс»
Выяснить больше – вывод из запоя на дому анонимно в екатеринбурге
JosefCix · May 1, 2026 at 8:38 pm
Осмотр особенно важен при нескольких днях употребления алкоголя подряд, выраженной слабости, дрожи в руках, нарушении сна, учащенном пульсе, нестабильном давлении, тошноте и признаках обезвоживания. Эти симптомы часто сочетаются и могут усиливаться в течение ближайших часов после прекращения употребления.
Получить дополнительную информацию – https://narkolog-na-dom-moskva-21.ru
Richardkit · May 1, 2026 at 8:47 pm
Помощь на дому рассматривают при состояниях, которые сопровождаются заметным ухудшением самочувствия после алкоголя. Это может быть запой на протяжении нескольких дней, тяжелое похмелье, дрожь в руках, нарушение сна, выраженная слабость, тревога, тошнота, сухость во рту, снижение аппетита и признаки обезвоживания. В таких случаях осмотр врача нужен для того, чтобы оценить тяжесть состояния и понять, безопасно ли оставаться дома.
Выяснить больше – нарколог на дом вывод
Oscarnam · May 1, 2026 at 8:55 pm
Эта обзорная заметка содержит ключевые моменты и факты по актуальным вопросам. Она поможет читателям быстро ориентироваться в теме и узнать о самых важных аспектах сегодня. Получите краткий курс по современной информации и оставайтесь в курсе событий!
Где почитать поподробнее? – вывод из запоя недорого нарколог24
DianaBus · May 1, 2026 at 9:15 pm
Эта информационная публикация освещает широкий спектр тем из мира медицины. Мы предлагаем читателям ясные и понятные объяснения современных заболеваний, методов профилактики и лечения. Информация будет полезна как пациентам, так и медицинским работникам, желающим поддержать уровень своих знаний.
Получить дополнительную информацию – капельница от запоя
Raymondper · May 1, 2026 at 9:33 pm
Отдельно выделяют ситуации, когда родственники вызывают врача не только из-за текущего состояния, но и потому, что подобные эпизоды повторяются. Если накапливаются последствия алкоголизма, нарушается сон, меняется поведение, появляются устойчивые проблемы дома и в повседневной жизни, разовая помощь обычно рассматривается как первый этап последующей тактики. При тяжелом состоянии, признаках отравлении алкоголем или сочетании нескольких рисков сразу может понадобиться более интенсивное наблюдение в стационаре.
Получить больше информации – вызвать нарколога на дом в екатеринбурге
Caseytheat · May 1, 2026 at 9:37 pm
Дополнительным поводом для вызова врача становится состояние, при котором больному трудно вставать, пить воду, есть, сохранять спокойствие или ориентироваться в самочувствии. В таких случаях осмотр на дому позволяет быстрее определить дальнейший маршрут помощи. Иногда уже первый звонок помогает понять, допустим ли домашний формат или лучше сразу рассматривать вывод в стационаре.
Углубиться в тему – вызвать нарколога на дом в екатеринбурге
AlbertoLob · May 1, 2026 at 10:23 pm
Когда зависимости становятся хроническими и угрожают жизни пациента, комплексная реабилитация при наркомании в специализированных клиниках Москвы, включая вывод из состояния в стационаре и последующий анализ данных о состоянии пациента, может стать единственным возможным решением. Процесс восстановления включает в себя работу не только с зависимостью, но и с психоэмоциональным состоянием, что делает лечение более эффективным и долговечным.
Узнать больше – реабилитация алкоголиков город
Antoniotut · May 1, 2026 at 10:37 pm
Этот интересный отчет представляет собой сборник полезных фактов, касающихся актуальных тем. Мы проанализируем данные, чтобы вы могли сделать обоснованные выводы. Читайте, чтобы узнать больше о последних трендах и значимых событиях!
Исследовать вопрос подробнее – вывод из запоя на дому спб
LarryAmess · May 1, 2026 at 10:42 pm
Этот интересный отчет представляет собой сборник полезных фактов, касающихся актуальных тем. Мы проанализируем данные, чтобы вы могли сделать обоснованные выводы. Читайте, чтобы узнать больше о последних трендах и значимых событиях!
Изучить эмпирические данные – вызвать нарколога на дом нарколог 24
RobertLierm · May 1, 2026 at 10:49 pm
Этот информативный текст отличается привлекательным содержанием и актуальными данными. Мы предлагаем читателям взглянуть на привычные вещи под новым углом, предоставляя интересный и доступный материал. Получите удовольствие от чтения и расширьте кругозор!
Познакомиться с результатами исследований – вывод из запоя на дому в нижнем новгороде
RufusFal · May 1, 2026 at 11:12 pm
Запой – это состояние, при котором человек продолжает употреблять алкоголь в течение длительного времени, не в состоянии прекратить употребление самостоятельно, что является проявлением алкоголизма. Это может привести к серьезным проблемам со здоровьем, и в таком случае необходим вывод из запоя с помощью наркологической помощи, при этом в дальнейшем может рассматриваться кодирование.
Исследовать вопрос подробнее – http://www.domen.ru
JasonRhics · May 1, 2026 at 11:41 pm
В этой статье представлен занимательный и актуальный контент, который заставит вас задуматься. Мы обсуждаем насущные вопросы и проблемы, а также освещаем истории, которые вдохновляют на действия и изменения. Узнайте, что стоит за событиями нашего времени!
Интересует подробная информация – вывод из запоя недорого
Josephpeapy · May 1, 2026 at 11:49 pm
Эта статья сочетает познавательный и занимательный контент, что делает ее идеальной для любителей глубоких исследований. Мы рассмотрим увлекательные аспекты различных тем и предоставим вам новые знания, которые могут оказаться полезными в будущем.
Как достичь результата? – вывод из запоя цена воронеж
Carlosbub · May 2, 2026 at 12:23 am
В статье представлены ключевые моменты по актуальной теме, дополненные советами экспертов и ссылками на дополнительные ресурсы. Цель материала — дать читателю инструменты для самостоятельного развития и принятия осознанных решений.
Полная информация здесь – нарколог на дом цена нарколог 24
JasonRhics · May 2, 2026 at 12:48 am
В этой статье представлен занимательный и актуальный контент, который заставит вас задуматься. Мы обсуждаем насущные вопросы и проблемы, а также освещаем истории, которые вдохновляют на действия и изменения. Узнайте, что стоит за событиями нашего времени!
Получить больше информации – выведение из запоя на дому
TomasFoste · May 2, 2026 at 1:01 am
Непрерывный мониторинг витальных показателей — ключевое отличие стационарного формата. В палатах клиники «Элегия Мед» установлены системы отслеживания частоты пульса, сатурации, температуры и артериального давления, данные с которых автоматически передаются в электронную медицинскую карту. Медицинский персонал дежурит круглосуточно, что обеспечивает мгновенную реакцию на ухудшение состояния: коррекцию инфузионной терапии, введение симптоматических препаратов, привлечение смежных специалистов при необходимости. Такая организация процесса исключает хаотичное назначение средств, предотвращает полипрагмазию и гарантирует, что каждый этап детоксикации проходит под строгим клиническим контролем. Контроль состояния пациента в режиме реального времени позволяет врачам оперативно корректировать терапию и минимизировать риски для здоровья.
Подробнее – http://www.domen.ru
Michaeltus · May 2, 2026 at 1:20 am
В этом информативном обзоре собраны самые интересные статистические данные и факты, которые помогут лучше понять текущие тренды. Мы представим вам цифры и графики, которые иллюстрируют, как развиваются различные сферы жизни. Эта информация станет отличной основой для глубокого анализа и принятия обоснованных решений.
Перейти к статье – капельница от запоя
kasyno online opinie · May 2, 2026 at 1:42 am
When are you going to post again? You really entertain me!
https://denwood.su/ · May 2, 2026 at 2:10 am
https://denwood.su/
Michaeltus · May 2, 2026 at 2:29 am
Эта статья предлагает уникальную подборку занимательных фактов и необычных историй, которые вы, возможно, не знали. Мы постараемся вдохновить ваше воображение и разнообразить ваш кругозор, погружая вас в мир, полный интересных открытий. Читайте и открывайте для себя новое!
Это стоит прочитать полностью – капельница от похмелья воронеж
Israelperty · May 2, 2026 at 2:30 am
Эта обзорная заметка содержит ключевые моменты и факты по актуальным вопросам. Она поможет читателям быстро ориентироваться в теме и узнать о самых важных аспектах сегодня. Получите краткий курс по современной информации и оставайтесь в курсе событий!
Углубить понимание вопроса – вывод из запоя на дому воронеж капельница
Glennbevex · May 2, 2026 at 2:31 am
Откройте для себя скрытые страницы истории и малоизвестные научные открытия, которые оказали колоссальное влияние на развитие человечества. Статья предлагает свежий взгляд на события, которые заслуживают большего внимания.
Почему это важно? – нарколог на дом
EdwinLig · May 2, 2026 at 2:50 am
Нарколог на дом в Москве — это формат медицинской помощи, который рассматривают при состояниях после употребления алкоголя, когда больному требуется осмотр врача без поездки в клинику. Чаще всего обращение связано с запоем, выраженным похмельным синдромом, нарушением сна, тревогой, слабостью, тремором, обезвоживанием, скачками давления, сердцебиением и общим ухудшением самочувствия. Дальнейшая тактика зависит от состояния больного на момент осмотра, продолжительности употребления алкоголя, возраста и сопутствующих заболеваний.
Детальнее – вызвать нарколога на дом москва
RogerAbiny · May 2, 2026 at 2:50 am
Этот обзор предлагает структурированное изложение информации по актуальным вопросам. Материал подан так, чтобы даже новичок мог быстро освоиться в теме и начать использовать полученные знания в практике.
Связаться за уточнением – выведение из запоя на дому
najlepsze kasyno online · May 2, 2026 at 2:52 am
How do I subscribe to your blog? Thanks for your help.
RodneyFut · May 2, 2026 at 2:53 am
Наркологическая помощь в Нижнем Новгороде с выездом врача, капельницами и наблюдением пациента в наркологической клинике «Частный медик 24»
Получить дополнительную информацию – клиника наркологической помощи нижний новгород
HarlangAg · May 2, 2026 at 3:05 am
Этот текст призван помочь читателю расширить кругозор и получить практические знания. Мы используем простой язык, наглядные примеры и структурированное изложение, чтобы сделать обучение максимально эффективным и увлекательным.
Не упусти шанс – прокапаться анонимно
Nelsonkic · May 2, 2026 at 3:10 am
Помощь на дому рассматривают при состояниях, которые сопровождаются выраженным ухудшением самочувствия после алкоголя. Обычно речь идет о нескольких днях запоя, тяжелом похмелье, бессоннице, тревоге, дрожи в руках, слабости, тошноте, сухости во рту, отсутствии аппетита и признаках обезвоживания. В таких случаях врачебный осмотр нужен для оценки тяжести состояния и выбора безопасной тактики.
Подробнее – врач нарколог на дом москва
polskie kasyno · May 2, 2026 at 3:11 am
Hey! awesome blog! I happen to be a daily visitor to your site (somewhat more like addict 😛 ) of this website. Just wanted to say I appreciate your blogs and am looking forward for more!
Oscarnam · May 2, 2026 at 3:39 am
Эта информационная заметка содержит увлекательные сведения, которые могут вас удивить! Мы собрали интересные факты, которые сделают вашу жизнь ярче и полнее. Узнайте нечто новое о привычных аспектах повседневности и откройте для себя удивительный мир информации.
Получить полную информацию – выведение из запоя в спб
WalterEdubs · May 2, 2026 at 3:43 am
why not try this out https://tornadocash.app
바이낸스 가입 · May 2, 2026 at 3:46 am
Thank you a lot for sharing this with all folks you actually recognize what you’re speaking about! Bookmarked. Please additionally visit my site =). We can have a hyperlink trade contract among us!
币安注册 · May 2, 2026 at 3:59 am
We are a group of volunteers and starting a new initiative in our community. Your blog provided us with valuable information to work on|.You have done a marvellous job!
Thomasnurdy · May 2, 2026 at 4:15 am
Этот информационный обзор станет отличным путеводителем по актуальным темам, объединяющим важные факты и мнения экспертов. Мы исследуем ключевые идеи и представляем их в доступной форме для более глубокого понимания. Читайте, чтобы оставаться в курсе событий!
Ознакомиться с деталями – вывод из запоя круглосуточно воронеж
RufusFal · May 2, 2026 at 4:38 am
Вывод из запоя на дому в Екатеринбурге: помощь при запое, снятие интоксикации и медицинская поддержка в наркологической клинике «Детокс»
Детальнее – анонимный вывод из запоя на дому екатеринбург
MerleDer · May 2, 2026 at 4:38 am
Мы собрали для вас самые захватывающие факты из мира науки и истории. От малознакомых деталей до грандиозных событий — эта статья расширит ваш кругозор и подарит новое понимание того, как устроен наш мир.
Выяснить больше – сколько стоит прокапаться от алкоголя на дому
EnriqueHig · May 2, 2026 at 4:56 am
Эта обзорная заметка содержит ключевые моменты и факты по актуальным вопросам. Она поможет читателям быстро ориентироваться в теме и узнать о самых важных аспектах сегодня. Получите краткий курс по современной информации и оставайтесь в курсе событий!
Изучить вопрос глубже – капельница от запоя воронеж
PhillipMut · May 2, 2026 at 4:57 am
Вывод из запоя на дому с медицинским контролем в Екатеринбурге предлагает множество преимуществ, которые делают этот метод более удобным и безопасным для многих людей. Отсутствие необходимости в госпитализации и наличие профессионального контроля являются основными положительными аспектами этой услуги.
Узнать больше – вывод из запоя на дому цена в екатеринбурге
RufusFal · May 2, 2026 at 4:58 am
Процесс вывода из запоя на дому состоит из нескольких этапов, которые тщательно подбираются врачом-наркологом в зависимости от состояния пациента. Важно, чтобы весь процесс был под контролем специалиста, чтобы избежать осложнений и гарантировать безопасное восстановление.
Узнать больше – вывод из запоя на дому круглосуточно екатеринбург
Najlepsze kasyna online · May 2, 2026 at 5:33 am
Enjoyed studying this, very good stuff, thanks.
WalterEdubs · May 2, 2026 at 5:34 am
official website https://mixmy.money/
polskie kasyno · May 2, 2026 at 5:41 am
Excellent article!! I am an avid reader of your website:D keep on posting that good content. and I’ll be a regular visitor for a very long time!!
LarryAmess · May 2, 2026 at 5:44 am
Этот информативный текст отличается привлекательным содержанием и актуальными данными. Мы предлагаем читателям взглянуть на привычные вещи под новым углом, предоставляя интересный и доступный материал. Получите удовольствие от чтения и расширьте кругозор!
Лови подробности – вызов нарколога на дом
MichaelFef · May 2, 2026 at 5:47 am
Помощь на дому рассматривают при состояниях, которые сопровождаются заметным ухудшением самочувствия после алкоголя. Обычно это запой на протяжении нескольких дней, тяжелое похмелье, выраженная слабость, бессонница, тревога, дрожь в руках, сухость во рту, отсутствие аппетита, тошнота, раздражительность и ощущение истощения. В подобных случаях врачебный осмотр нужен для того, чтобы оценить тяжесть состояния и определить, безопасен ли домашний формат в конкретной ситуации.
Исследовать вопрос подробнее – запой нарколог на дом в москве
RobertLierm · May 2, 2026 at 5:47 am
Этот информационный материал собраны данные, которые помогут лучше понять текущие тенденции и процессы в различных сферах жизни. Мы предоставляем четкий анализ, графики и примеры, чтобы информация была не только понятной, но и практичной для принятия решений.
Читать далее > – вывод из запоя на дому в нижнем новгороде
MerleDer · May 2, 2026 at 6:00 am
В этой статье-обзоре мы соберем актуальную информацию и интересные факты, которые освещают важные темы. Читатели смогут ознакомиться с различными мнениями и подходами, что позволит им расширить кругозор и глубже понять обсуждаемые вопросы.
Где можно узнать подробнее? – капельница от запоя на дому цена
Donaldcem · May 2, 2026 at 6:04 am
Вывод из запоя на дому в Екатеринбурге с выездом врача — это специализированная медицинская услуга, которая помогает человеку безопасно и эффективно выйти из запойного состояния без необходимости госпитализации. Запой является состоянием, при котором человек не может контролировать потребление алкоголя, и последствия могут быть крайне серьезными, как для физического, так и для психоэмоционального здоровья. В таких случаях помощь врача на дому становится важным и необходимым шагом для восстановления здоровья пациента и предотвращения осложнений.
Углубиться в тему – vyvod-iz-zapoya-na-domu-ekaterinburg-16.ru/
RichardGlano · May 2, 2026 at 6:05 am
Web Site https://yomix.biz/
Binance Sign up · May 2, 2026 at 6:19 am
It’s continually awesome when you can not only be informed, but also entertained! I’m sure you had fun writing this article. Regards, Clotilde.
JosefCix · May 2, 2026 at 6:25 am
Нарколог на дом в Москве — это формат врачебной помощи, который рассматривают при состояниях после употребления алкоголя, когда больному требуется осмотр без посещения клиники. Чаще всего обращение связано с запоем, тяжелым похмельным синдромом, слабостью, нарушением сна, тремором, тревогой, тошнотой, сухостью во рту, скачками давления, сердцебиением и общим ухудшением самочувствия. Дальнейшая тактика определяется после осмотра, с учетом длительности употребления алкоголя, возраста, сопутствующих заболеваний и выраженности текущих симптомов.
Выяснить больше – врач нарколог на дом москва
Jesseenexy · May 2, 2026 at 6:28 am
Исследования показывают, что такой подход существенно повышает шанс на долгосрочное выздоровление и уменьшает вероятность рецидивов. Это связано с тем, что пациент чувствует внимание и заботу, а также получает помощь в преодолении своих личных психологических барьеров.
Ознакомиться с деталями – центр реабилитации алкоголиков город
RichardGlano · May 2, 2026 at 6:31 am
click to read https://letsexchange.cc/
TomasFoste · May 2, 2026 at 6:42 am
Вывод из запоя в стационаре в Санкт-Петербурге: профессиональное лечение, капельницы и контроль состояния пациента в наркологической клинике «Элегия Мед».
Узнать больше – вывод из запоя в стационаре анонимно в санкт-петербурге
TomasFoste · May 2, 2026 at 7:02 am
Вывод из запоя в стационаре в Санкт-Петербурге: профессиональное лечение, капельницы и контроль состояния пациента в наркологической клинике «Элегия Мед».
Исследовать вопрос подробнее – вывод из запоя в стационаре анонимно в санкт-петербурге
JudsonGog · May 2, 2026 at 7:44 am
Отдельно стоит выделить ситуации, когда семья сталкивается не только с алкоголем, но и с употреблением наркотиков. В таких случаях врачебная консультация особенно важна, поскольку последствия интоксикации могут отличаться, а признаки наркомании и алкоголизма иногда накладываются друг на друга. Если речь идет о смешанном употреблении, подход к помощи на дому требует особой осторожности.
Получить больше информации – вызов нарколога на дом
Raymondper · May 2, 2026 at 8:00 am
Помощь на дому рассматривают при состояниях, которые возникают после длительного употребления алкоголя или тяжелого алкогольного эпизода. Чаще всего это запой, выраженная интоксикация, бессонница, тревога, слабость, тремор, тошнота, сухость во рту, отсутствие аппетита, нестабильное давление и сердцебиение. Врачебный осмотр требуется в тех случаях, когда больному трудно восстановиться самостоятельно, а самочувствие продолжает ухудшаться.
Получить дополнительные сведения – нарколог на дом в екатеринбурге
Caseytheat · May 2, 2026 at 8:03 am
Помощь на дому рассматривают при состояниях, связанных с острым ухудшением самочувствия после алкоголя. Чаще всего это несколько дней запоя, тяжелое похмелье, бессонница, тревога, дрожь в руках, слабость, отсутствие аппетита, тошнота, сухость во рту и ощущение истощения. В подобных случаях врачебный осмотр нужен для оценки общего состояния и выбора безопасной тактики.
Выяснить больше – нарколог на дом вывод
Israelperty · May 2, 2026 at 8:23 am
Эта статья полна интересного контента, который побудит вас исследовать новые горизонты. Мы собрали полезные факты и удивительные истории, которые обогащают ваше понимание темы. Читайте, погружайтесь в детали и наслаждайтесь процессом изучения!
Запросить дополнительные данные – вывод из запоя дешево
Timothyelapy · May 2, 2026 at 8:26 am
puma bmw mont hakk?ndaki makaleyi tavsiye ederim. Suradan okuyabilirsiniz: https://bedensport.com/articles/puma-bmw-motorsport-mont-koleksiyonlari/
Timothyelapy · May 2, 2026 at 8:30 am
Ayr?ca, eger koyu renk banyo modelleri konusuyla ilgileniyorsan?z, suraya bak?n. Link burada: https://kendifikirler.com/articles/koyu-renk-banyo-tasarimlari-modern-gorunum/
RobertBlatt · May 2, 2026 at 8:50 am
Вывод из запоя на дому с быстрым облегчением в Екатеринбурге — это процедура, направленная на быстрое снятие острых симптомов алкогольного абстинентного синдрома и возвращение пациента к нормальному состоянию, включая случаи алкоголизма и наркомании. Такая услуга удобна тем, что позволяет не только эффективно справиться с зависимостью, но и избавиться от неприятных проявлений запоя, таких как головная боль, тошнота, слабость и психоэмоциональное напряжение, в комфортной домашней обстановке, при этом оказывается наркологическая помощь. Быстрое облегчение без необходимости госпитализации делает этот метод популярным среди пациентов, которым важен быстрый и безопасный результат, а при необходимости можно заказать дальнейшее кодирование или лечение в стационаре.
Выяснить больше – http://vyvod-iz-zapoya-na-domu-ekaterinburg-19.ru
Richardkit · May 2, 2026 at 9:09 am
Нарколог на дом в Москве: срочный выезд врача, капельницы и помощь при запое в наркологической клинике «Клиника доктора Калюжной».
Детальнее – врач нарколог на дом в москве
PeterRot · May 2, 2026 at 9:17 am
Купить дубликат прав
RichardGlano · May 2, 2026 at 9:28 am
click here for more https://daobase.info
PeterCoelf · May 2, 2026 at 9:53 am
Эта статья предлагает уникальную подборку занимательных фактов и необычных историй, которые вы, возможно, не знали. Мы постараемся вдохновить ваше воображение и разнообразить ваш кругозор, погружая вас в мир, полный интересных открытий. Читайте и открывайте для себя новое!
Это стоит прочитать полностью – поставить капельницу от запоя на дому
kasyno online opinie · May 2, 2026 at 10:11 am
Oh my goodness! an amazing article. Great work.
Nelsonkic · May 2, 2026 at 10:18 am
Помощь на дому рассматривают при состояниях, которые сопровождаются выраженным ухудшением самочувствия после алкоголя. Обычно речь идет о нескольких днях запоя, тяжелом похмелье, бессоннице, тревоге, дрожи в руках, слабости, тошноте, сухости во рту, отсутствии аппетита и признаках обезвоживания. В таких случаях врачебный осмотр нужен для оценки тяжести состояния и выбора безопасной тактики.
Выяснить больше – вызов нарколога на дом в москве
polskie kasyno · May 2, 2026 at 10:34 am
I encountered your site after doing a search for new contesting using Google, and decided to stick around and read more of your articles. Thanks for posting, I have your site bookmarked now.
Thomasnurdy · May 2, 2026 at 10:45 am
Этот увлекательный информационный материал подарит вам массу новых знаний и ярких эмоций. Мы собрали для вас интересные факты и сведения, которые обогатят ваш опыт. Откройте для себя увлекательный мир информации и насладитесь процессом изучения!
Смотрите также… – вывод из запоя в воронеже
Nelsonkic · May 2, 2026 at 10:45 am
Нарколог на дом в Москве — это формат помощи, который рассматривают в тех случаях, когда после употребления алкоголя больному требуется врачебный осмотр без поездки в клинику. Чаще всего обращение связано с запоем, выраженным похмельным синдромом, нарушением сна, слабостью, тремором, тревогой, обезвоживанием, сердцебиением, скачками давления и общим ухудшением самочувствия. Дальнейшая тактика зависит от состояния больного на момент осмотра, длительности употребления алкоголя, возраста и сопутствующих заболеваний.
Исследовать вопрос подробнее – вызвать нарколога на дом москва
Robertmah · May 2, 2026 at 10:48 am
Металлический уголок — это надежное и практичное решение для ваших строительных и производственных задач.
Source:
https://www.aprilpeter.com/wp-content/themes/Upward/go.php?https://ugolka.net/galvanized/
Металлический уголок
https://taraupakovka.spb.ru/ · May 2, 2026 at 10:51 am
https://taraupakovka.spb.ru/
Robertmah · May 2, 2026 at 10:55 am
Металлический уголок — это надежное и практичное решение для ваших строительных и производственных задач.
Source:
https://sfproperties.com/?URL=https://ugolka.net/perforated/
Металлический уголок
Robertmah · May 2, 2026 at 10:59 am
Металлический уголок — это надежное и практичное решение для ваших строительных и производственных задач.
Source:
https://enjoycycle.net/jump.cgi?jumpto=https://ugolka.net/equal-shelf/
Металлический уголок
AlbertoLob · May 2, 2026 at 11:05 am
Когда зависимости становятся хроническими и угрожают жизни пациента, комплексная реабилитация при наркомании в специализированных клиниках Москвы, включая вывод из состояния в стационаре и последующий анализ данных о состоянии пациента, может стать единственным возможным решением. Процесс восстановления включает в себя работу не только с зависимостью, но и с психоэмоциональным состоянием, что делает лечение более эффективным и долговечным.
Получить дополнительную информацию – реабилитация алкоголиков в москве
Daniellow · May 2, 2026 at 11:12 am
Реабилитация алкоголиков в Москве: лечение зависимости, восстановление и поддержка под контролем специалистов в наркологической клинике «Похмельная служба»
Получить дополнительные сведения – реабилитация алкоголиков стоимость в москве
Glennbevex · May 2, 2026 at 11:15 am
В этом обзорном материале представлены увлекательные детали, которые находят отражение в различных аспектах жизни. Мы исследуем непонятные и интересные моменты, позволяя читателю увидеть картину целиком. Погрузитесь в мир знаний и удивительных открытий!
Все материалы собраны здесь – услуги нарколога на дому
Frankagevy · May 2, 2026 at 11:15 am
Купить водительские права
PeterCoelf · May 2, 2026 at 12:04 pm
В этом информативном обзоре собраны самые интересные статистические данные и факты, которые помогут лучше понять текущие тренды. Мы представим вам цифры и графики, которые иллюстрируют, как развиваются различные сферы жизни. Эта информация станет отличной основой для глубокого анализа и принятия обоснованных решений.
Рассмотреть проблему всесторонне – прокапаться
PhillipDon · May 2, 2026 at 2:07 pm
В этом обзорном материале представлены увлекательные детали, которые находят отражение в различных аспектах жизни. Мы исследуем непонятные и интересные моменты, позволяя читателю увидеть картину целиком. Погрузитесь в мир знаний и удивительных открытий!
Это стоит прочитать полностью – вызов нарколога на дом запой
WalterEdubs · May 2, 2026 at 2:52 pm
our website https://mixmy.money/
PhillipMut · May 2, 2026 at 3:19 pm
Вывод из запоя на дому с медицинским контролем — это процесс, при котором нарколог или медсестра приезжает к пациенту на дом для проведения необходимых процедур. Основной задачей является снятие абстинентного синдрома, восстановление водно-электролитного баланса и нормализация общего состояния пациента, при этом оказывается наркологическая помощь. Этот процесс проходит под наблюдением квалифицированных специалистов, что помогает избежать осложнений, часто возникающих при самостоятельном выходе из запоя, а в дальнейшем может потребоваться кодирование и реабилитация.
Разобраться лучше – https://vyvod-iz-zapoya-na-domu-ekaterinburg-18.ru
JosephDealm · May 2, 2026 at 3:22 pm
1xbet
JudsonGog · May 2, 2026 at 3:34 pm
Нарколог на дом в Екатеринбурге востребован в ситуациях, когда человеку нужна врачебная помощь после употребления алкоголя, при запое, выраженном похмельном синдроме, нарушении сна, тревоге, скачках давления, слабости и других признаках ухудшения самочувствия. Такой формат обращения часто выбирают семьи, которые хотят вызвать врача без поездки в клинику и быстро получить консультацию по состоянию больного. Домашний выезд особенно важен тогда, когда требуется детоксикация, наблюдение после нескольких дней употребления спиртного и оценка рисков, связанных с последствиями алкоголизма.
Подробнее тут – запой нарколог на дом
JudsonGog · May 2, 2026 at 4:01 pm
Нарколог на дом в Екатеринбурге востребован в ситуациях, когда человеку нужна врачебная помощь после употребления алкоголя, при запое, выраженном похмельном синдроме, нарушении сна, тревоге, скачках давления, слабости и других признаках ухудшения самочувствия. Такой формат обращения часто выбирают семьи, которые хотят вызвать врача без поездки в клинику и быстро получить консультацию по состоянию больного. Домашний выезд особенно важен тогда, когда требуется детоксикация, наблюдение после нескольких дней употребления спиртного и оценка рисков, связанных с последствиями алкоголизма.
Углубиться в тему – вызвать нарколога на дом
WalterEdubs · May 2, 2026 at 4:38 pm
he has a good point https://bitmix.app/
Raymondgloky · May 2, 2026 at 6:21 pm
Особенность анонимной реабилитации заключается в создании комфортной и безопасной среды, которая мотивирует пациента работать над собой, не опасаясь осуждения. Это повышает эффективность лечения, ведь пациент может открыться и честно обсуждать свои проблемы без страха быть осужденным.
Подробнее – алкоголик реабилитация наркоманов город
Daniellow · May 2, 2026 at 6:52 pm
Реабилитация включает несколько ключевых этапов, каждый из которых направлен на решение определённых проблем пациента. Важно, чтобы все этапы были комплексными и последовательными, чтобы достичь наиболее эффективного результата.
Разобраться лучше – реабилитация алкоголиков стоимость москва
Daniellow · May 2, 2026 at 7:20 pm
Реабилитация алкоголиков в Москве: лечение зависимости, восстановление и поддержка под контролем специалистов в наркологической клинике «Похмельная служба»
Подробнее тут – центр реабилитации алкоголиков город
RichardGlano · May 2, 2026 at 7:25 pm
Get More Info https://letsexchange.cc/
Jesseenexy · May 2, 2026 at 8:17 pm
Реабилитация алкоголиков — это важный этап на пути к избавлению от зависимости. В Москве существует множество центров, предлагающих реабилитацию с индивидуальной программой, что помогает обеспечить более персонализированный и эффективный подход к каждому пациенту. Индивидуальная программа учитывает физическое и психологическое состояние человека, а также его социальное окружение и личные особенности. Это позволяет добиться лучших результатов в лечении и восстановлении.
Разобраться лучше – reabilitacziya-alkogolikov-moskva.ru/
https://healthymed1day.top/buy-artane/ · May 2, 2026 at 11:07 pm
https://healthymed1day.top/buy-artane/
MichaelFef · May 2, 2026 at 11:10 pm
Помощь на дому рассматривают при состояниях, которые сопровождаются заметным ухудшением самочувствия после алкоголя. Обычно это запой на протяжении нескольких дней, тяжелое похмелье, выраженная слабость, бессонница, тревога, дрожь в руках, сухость во рту, отсутствие аппетита, тошнота, раздражительность и ощущение истощения. В подобных случаях врачебный осмотр нужен для того, чтобы оценить тяжесть состояния и определить, безопасен ли домашний формат в конкретной ситуации.
Выяснить больше – вызвать нарколога на дом в москве
Raymondgloky · May 3, 2026 at 4:22 am
Реабилитация алкоголиков с анонимной поддержкой — это процесс, при котором пациент получает необходимую медицинскую и психологическую помощь, не раскрывая своей личности и обстоятельств зависимости, включая лечение наркомании. Такие программы ориентированы на безопасное и конфиденциальное лечение, что важно для тех, кто стремится избавиться от зависимости, но опасается осуждения или утраты личной репутации, при этом возможен выезд нарколога на дом. Важно, что анонимность не ограничивает качество предоставляемых услуг: все необходимые этапы лечения, включая детоксикацию, психотерапевтические сессии и социальную реабилитацию, которые могут длиться несколько лет, проводятся на высоком уровне с акцентом на своевременный вывод из состояния зависимости.
Исследовать вопрос подробнее – алкоголик реабилитация наркоманов город
Raymondgloky · May 3, 2026 at 4:54 am
Реабилитация алкоголиков с анонимной поддержкой — это процесс, при котором пациент получает необходимую медицинскую и психологическую помощь, не раскрывая своей личности и обстоятельств зависимости, включая лечение наркомании. Такие программы ориентированы на безопасное и конфиденциальное лечение, что важно для тех, кто стремится избавиться от зависимости, но опасается осуждения или утраты личной репутации, при этом возможен выезд нарколога на дом. Важно, что анонимность не ограничивает качество предоставляемых услуг: все необходимые этапы лечения, включая детоксикацию, психотерапевтические сессии и социальную реабилитацию, которые могут длиться несколько лет, проводятся на высоком уровне с акцентом на своевременный вывод из состояния зависимости.
Углубиться в тему – реабилитация алкоголиков стоимость в москве
MiguelBip · May 3, 2026 at 6:05 am
Каждый из этапов важен для успешного лечения наркомании и требует квалифицированной наркологической медицинской помощи. Реабилитационные программы, предлагаемые в Москве, часто включают в себя все эти компоненты, при этом в ряде случаев консультации могут предоставляться бесплатно, что способствует комплексному подходу к решению проблемы зависимости.
Подробнее тут – http://www.domen.ru
https://7m-cn.site/ · May 3, 2026 at 6:33 am
I want to see your book when it comes out.
Robertmah · May 3, 2026 at 7:14 am
Разница между поверкой и калибровкой — в правовых последствиях. Поверка отвечает: «Годен ли он к эксплуатации?», калибровка: «Какова его реальная ошибка в цифрах?».
Порядок проведения поверки и калибровки КИП отличается жестко: поверка — только аккредитованная лаборатория, калибровка — любая компетентная служба. Единство измерений — база.
Методика поверки одна и утверждена государством — отклоняться нельзя. Методика калибровки подстраивается под задачу. Главное — прослеживаемость к госэталону.
Source:
http://poiskdam.ru/poverka-i-kalibrovka-kip-v-chem-raznicza-i-chto-vybrat.html
законодательные требования к поверке кип
bong da lu · May 3, 2026 at 7:19 am
Awesome post. It’s so good to see someone taking the time to share this information
Robertmah · May 3, 2026 at 7:19 am
Отличие поверки от калибровки в цели. Поверка оценивает допуск, калибровка — определяет реальную погрешность.
Порядок проведения поверки и калибровки КИП отличается жестко: поверка — только аккредитованная лаборатория, калибровка — любая компетентная служба. Оба процесса начинаются с эталона.
Законодательные требования (102-ФЗ, ГРОЕИ) касаются только поверки: сроки межповерочного интервала. Для калибровки свободный режим. Будьте в правовом поле.
Source:
https://j-socks.ru/poverka-i-kalibrovka/
порядок проведения поверки и калибровки кип
nuôi gà chiến · May 3, 2026 at 7:23 am
Thank you for all the information was very accurate, just wondering if all this is possible.~
Robertmah · May 3, 2026 at 7:25 am
Разница между поверкой и калибровкой — в ответе на вопрос. Поверка отвечает: «Годен ли он к эксплуатации?», калибровка: «Насколько он врет в каждой точке?».
Порядок проведения поверки и калибровки КИП отличается жестко: поверка — только аккредитованная лаборатория, калибровка — любая компетентная служба. Единство измерений — база.
Правовые последствия просты: неповеренный прибор = штраф. Для калибровки она вне правового поля. Рискуете бизнесом?.
Source:
https://kip-pribor.ru/razlichiya-mezhdu-poverkoj-i-kalibrovkoj-kontrolno-izmeritelnyh-priborov-i-vybor-podhodyashhej-metrologicheskoj-proczedury/
разница между поверкой и калибровкой
Robertmah · May 3, 2026 at 7:28 am
Разница между поверкой и калибровкой — в правовых последствиях. Поверка отвечает: «Годен ли он к эксплуатации?», калибровка: «Насколько он врет в каждой точке?».
Порядок проведения поверки и калибровки КИП отличается жестко: поверка — с записью в ФИФ ОЕИ, калибровка — без госрегулирования. Оба процесса начинаются с эталона.
Правовые последствия просты: неповеренный прибор = штраф. Для калибровки штрафов не предусмотрено. Рискуете бизнесом?.
Source:
https://tele2kino.ru/poverka-i-kalibrovka-kip-v-chem-raznicza-i-chto-vybrat.html
критерии выбора поверки и калибровки
Robertmah · May 3, 2026 at 7:32 am
Отличие поверки от калибровки в документе. Поверка оценивает допуск, калибровка — показывает «как сильно врет прибор».
Порядок проведения поверки и калибровки КИП отличается жестко: поверка — только аккредитованная лаборатория, калибровка — без госрегулирования. Единство измерений — база.
Критерии выбора поверки или калибровки: цена ошибки. Для суда — поверка, для техпроцесса — калибровка.
Source:
https://tele2kino.ru/poverka-i-kalibrovka-kip-v-chem-raznicza-i-chto-vybrat.html
критерии выбора поверки и калибровки
Robertmah · May 3, 2026 at 7:43 am
Разница между поверкой и калибровкой — в логике контроля. Поверка отвечает: «Можно ли верить прибору по закону?», калибровка: «Какова его реальная ошибка в цифрах?».
Порядок проведения поверки и калибровки КИП отличается жестко: поверка — по госреестру, калибровка — по методике заказчика. Единство измерений — база.
Правовые последствия просты: эксплуатация без поверки запрещена. Для калибровки нет санкций государства. Хотите спать спокойно? — Поверяйте.
Source:
https://selo-delo.ru/poleznye-stati/facebook-gotovit-rebrending-i-smeny-nazvaniia-kak-eto-sviazano-s-metavselennoi.html
правовые последствия поверки и калибровки
kèo vip · May 3, 2026 at 7:58 am
I imagine so. Very good stuff, I agree totally.
DA88 · May 3, 2026 at 8:35 am
I wanted to check up and let you know how, a great deal I cherished discovering your blog today. I might consider it an honor to work at my office and be able to utilize the tips provided on your blog and also be a part of visitors’ reviews like this. Should a position associated with guest writer become on offer at your end, make sure you let me know.
https://7mvn.ac/ · May 3, 2026 at 10:04 am
I appreciate your work, thanks for all the great blog posts.
Jesseenexy · May 3, 2026 at 10:10 am
Каждый элемент программы направлен на создание комплексного подхода к лечению зависимости, обеспечивая помощь не только на физическом, но и на эмоциональном уровне. Индивидуальная программа реабилитации позволяет выстроить эффективную терапию, которая соответствует конкретным потребностям пациента.
Получить больше информации – реабилитация алкоголиков в москве
MiguelBip · May 3, 2026 at 10:11 am
Реабилитация алкоголиков в Москве требует интегрированного подхода, включающего не только медицинское лечение, но и психологическую помощь. Важно, чтобы реабилитационные центры предлагали программы, которые помогают пациентам не только избавиться от физической зависимости, но и наладить их психологическое состояние, а также восстановить их отношения с окружающими.
Подробнее тут – реабилитация алкоголиков в москве
GMNC · May 3, 2026 at 10:12 am
Sometimes, the sheer magnitude of the information seems overwhelming.
http://www.canorris.com/?url=smart-home-pnz.ru · May 3, 2026 at 2:24 pm
http://www.canorris.com/?url=smart-home-pnz.ru
Jamesgor · May 3, 2026 at 3:43 pm
Отличный разбор 102-ФЗ, давно искал четкое объяснение, как именно межповерочный интервал контрольно-измерительных приборов фиксируется в реестре.
https://starter63.ru/mezhpoverochnyj-interval-sredstv-izmerenij-sroki-pravila-i-normativnye-trebovaniya/
RufusFal · May 3, 2026 at 3:46 pm
Вывод из запоя на дому в Екатеринбурге – это услуга, которая становится необходимой, когда состояние пациента ухудшается после длительного употребления алкоголя, и медицинская помощь требуется немедленно. На дому пациенту предоставляется квалифицированная помощь, направленная на быстрое снятие интоксикации, восстановление водно-солевого баланса и стабилизацию общего состояния.
Углубиться в тему – анонимный вывод из запоя на дому екатеринбург
MichaelFef · May 3, 2026 at 4:09 pm
Наиболее частыми причинами обращения становятся запой, тяжелый похмельный синдром, тремор, выраженная слабость, тревога, бессонница, нестабильное давление, учащенный пульс, тошнота и признаки обезвоживания. Эти проявления могут сочетаться между собой и усиливаться после прекращения употребления алкоголя, особенно если эпизод длился несколько дней.
Выяснить больше – запой нарколог на дом
TomasFoste · May 3, 2026 at 8:57 pm
Терапевтический процесс в стационаре строится по принципу последовательного выполнения клинических задач: диагностика, стабилизация, медикаментозная поддержка и подготовка к амбулаторному этапу. При поступлении врач проводит детальный осмотр, собирает анамнез, оценивает неврологический статус и при необходимости назначает лабораторные исследования. На основе полученных данных формируется индивидуальный протокол, учитывающий возраст, длительность интоксикации, наличие сопутствующих патологий и переносимость лекарственных компонентов. Мы применяем только сертифицированные препараты, зарегистрированные в РФ, и строго соблюдаем клинические рекомендации Минздрава, исключая псевдонаучные методики.
Подробнее можно узнать тут – http://vyvod-iz-zapoya-v-staczionare-sankt-peterburg-20.ru
meklonrsak · May 3, 2026 at 10:04 pm
Поверка применяется для средств измерений, которые используются в сферах с государственным регулированием. Она подтверждает, что прибор можно правомерно использовать в работе. Калибровка чаще проводится добровольно и помогает владельцу оборудования понять, насколько точно устройство показывает значения – https://kip-pribor.ru/razlichiya-mezhdu-poverkoj-i-kalibrovkoj-kontrolno-izmeritelnyh-priborov-i-vybor-podhodyashhej-metrologicheskoj-proczedury/
Donaldcem · May 3, 2026 at 11:34 pm
Первоначально врач оценивает физическое и психоэмоциональное состояние пациента, что позволяет определить степень тяжести запоя и риски, с которыми может столкнуться пациент в процессе восстановления. На основе этой оценки подбирается соответствующая терапия, включая капельницы для очистки организма, введение витаминов и препаратов, способствующих нормализации давления и уровня сахара в крови.
Подробнее тут – вывод из запоя на дому круглосуточно екатеринбург
EdwinLig · May 3, 2026 at 11:35 pm
Осмотр на дому особенно важен в тех случаях, когда больному трудно вставать, пить воду, принимать пищу, спокойно лежать или ориентироваться в собственном состоянии. В такой ситуации очная оценка помогает понять, допустим ли домашний формат и достаточно ли его на текущем этапе. При выраженном ухудшении состояния, признаках перегрузки организма или риске осложнений может потребоваться срочный пересмотр тактики.
Углубиться в тему – нарколог на дом цена москва
MiguelBip · May 3, 2026 at 11:58 pm
Комплексный подход, включающий эти методы, значительно повышает шансы на успешное и долговременное восстановление. Современные реабилитационные центры в Москве предлагают целый ряд программ, которые способствуют полному возвращению пациента к здоровой и активной жизни.
Подробнее можно узнать тут – http://reabilitacziya-alkogolikov-moskva-3.ru
"oppna binance-konto · May 4, 2026 at 12:47 am
Your article helped me a lot, is there any more related content? Thanks! https://www.binance.com/register?ref=IXBIAFVY
PhillipMut · May 4, 2026 at 12:54 am
Вывод из запоя на дому в Екатеринбурге: эффективное лечение, детоксикация и восстановление организма в наркологической клинике «Детокс»
Получить больше информации – нарколог на дом вывод из запоя
http://stadtdesign.com/?url=smart-home-pnz.ru · May 4, 2026 at 2:14 am
http://stadtdesign.com/?url=smart-home-pnz.ru
JosefCix · May 4, 2026 at 2:17 am
Нарколог на дом в Москве: выезд врача на дом, лечение запоя и консультации в наркологической клинике «Клиника доктора Калюжной».
Детальнее – вызов нарколога на дом в москве
https://keovip.to · May 4, 2026 at 3:21 am
It’s continually awesome when you can not only be informed, but also entertained! I’m sure you had fun writing this article. Regards, Clotilde.
부산호빠 · May 4, 2026 at 3:35 am
부산호빠
Raymondper · May 4, 2026 at 4:12 am
Помощь на дому рассматривают при состояниях, которые возникают после длительного употребления алкоголя или тяжелого алкогольного эпизода. Чаще всего это запой, выраженная интоксикация, бессонница, тревога, слабость, тремор, тошнота, сухость во рту, отсутствие аппетита, нестабильное давление и сердцебиение. Врачебный осмотр требуется в тех случаях, когда больному трудно восстановиться самостоятельно, а самочувствие продолжает ухудшаться.
Ознакомиться с деталями – врач нарколог на дом
Caseytheat · May 4, 2026 at 4:20 am
Наиболее частыми причинами обращения становятся выраженная слабость, тремор, нарушение сна, тревога, учащенный пульс, скачки артериального давления, тошнота и признаки обезвоживания. Эти симптомы могут сочетаться между собой и усиливаться после прекращения употребления алкоголя, особенно после нескольких дней запоя.
Узнать больше – http://www.domen.ru
Donaldcem · May 4, 2026 at 5:04 am
Вывод из запоя на дому в Екатеринбурге: срочная помощь, детоксикация и восстановление под контролем специалистов в наркологической клинике «Детокс»
Подробнее – нарколог на дом вывод из запоя екатеринбург
EdwinLig · May 4, 2026 at 5:21 am
Наиболее частыми причинами обращения становятся запой, выраженная слабость, тремор, нарушение сна, тревога, учащенный пульс, нестабильное давление, тошнота и ощущение физического истощения. Эти проявления могут сочетаться между собой и усиливаться после прекращения употребления алкоголя, особенно если эпизод длился несколько дней.
Узнать больше – нарколог на дом в москве
PhillipMut · May 4, 2026 at 6:28 am
Вывод из запоя на дому с медицинским контролем в Екатеринбурге предлагает множество преимуществ, которые делают этот метод более удобным и безопасным для многих людей. Отсутствие необходимости в госпитализации и наличие профессионального контроля являются основными положительными аспектами этой услуги.
Ознакомиться с деталями – вывод из запоя на дому анонимно екатеринбург
fixDiele · May 4, 2026 at 6:46 am
Для тех, кто ищет информацию по теме “Актуальные события Брянской области: бизнес, туризм и экология”, там просто кладезь информации.
Вот, можете почитать:
https://br32media.ru
fixDiele · May 4, 2026 at 6:50 am
По теме “Главные события и советы по упаковке электроники”, там просто кладезь информации.
Смотрите сами:
https://guitarism.ru
Robertmah · May 4, 2026 at 7:37 am
Отличие поверки от калибровки в цели. Поверка выносит вердикт «годен/негоден», калибровка — показывает «как сильно врет прибор».
Что выбрать — поверку или калибровку? Зависит от сферы применения. Если прибор в больнице — только поверка. Если на внутреннем складе — смело выбирайте калибровку.
Критерии выбора поверки или калибровки: область регулирования (ГРОЕИ). Для суда — поверка, для техпроцесса — калибровка.
Source:
https://tele2kino.ru/poverka-i-kalibrovka-kip-v-chem-raznicza-i-chto-vybrat.html
критерии выбора поверки и калибровки
Robertmah · May 4, 2026 at 7:41 am
Для ваших термометров доступны две процедуры: поверка (для Росаккредитации) и калибровка (для ISO 9001). Выбирайте осознанно.
Что выбрать — поверку или калибровку? Зависит от юридического статуса измерений. Если прибор на АЗС — только поверка. Если в научной работе — смело калибруйте.
Критерии выбора поверки или калибровки: стоимость процедуры. Для суда — поверка, для техпроцесса — калибровка.
Source:
https://dondvh.ru/poverka-i-kalibrovka-kip-razlichiya-i-princzipy-provedeniya/
что выбрать поверку или калибровку
Robertmah · May 4, 2026 at 7:45 am
Разница между поверкой и калибровкой — в ответе на вопрос. Поверка отвечает: «Годен ли он к эксплуатации?», калибровка: «Какова его реальная ошибка в цифрах?».
Порядок проведения поверки и калибровки КИП отличается жестко: поверка — только аккредитованная лаборатория, калибровка — без госрегулирования. Единство измерений — база.
Правовые последствия просты: результаты не имеют юрсилы. Для калибровки штрафов не предусмотрено. Хотите спать спокойно? — Поверяйте.
Source:
https://selo-delo.ru/poleznye-stati/facebook-gotovit-rebrending-i-smeny-nazvaniia-kak-eto-sviazano-s-metavselennoi.html
правовые последствия поверки и калибровки
Robertmah · May 4, 2026 at 7:52 am
Разница между поверкой и калибровкой — в логике контроля. Поверка отвечает: «Можно ли верить прибору по закону?», калибровка: «Какова его реальная ошибка в цифрах?».
Порядок проведения поверки и калибровки КИП отличается жестко: поверка — с записью в ФИФ ОЕИ, калибровка — без госрегулирования. Единство измерений — база.
Законодательные требования (102-ФЗ, ГРОЕИ) касаются только поверки: только аккредитованные лица. Для калибровки закон не диктует правила. Будьте в правовом поле.
Source:
https://romania-today.ru/news/different/2026/02/15/aznica-mezhdu-poverkoy-i-kalibrovkoy-klyuchevye-otlichiya-celi-i-reglament-procedur
отличие поверки от калибровки
Robertmah · May 4, 2026 at 7:57 am
Для ваших термометров доступны две процедуры: поверка (для отчетности) и калибровка (для ISO 9001). Выбирайте осознанно.
Порядок проведения поверки и калибровки КИП отличается жестко: поверка — по госреестру, калибровка — любая компетентная служба. Оба процесса начинаются с эталона.
Правовые последствия просты: неповеренный прибор = штраф. Для калибровки нет санкций государства. Хотите спать спокойно? — Поверяйте.
Source:
https://mfo27.ru/razlichiya-mezhdu-poverkoj-i-kalibrovkoj-kontrolno-izmeritelnyh-priborov-i-kriterii-ih-vybora/
поверка и калибровка контрольно-измерительных приборов
Francisvah · May 4, 2026 at 8:03 am
Наиболее частыми причинами обращения становятся выраженная слабость, тремор, нарушение сна, тревога, учащенный пульс, скачки артериального давления, тошнота и признаки обезвоживания. Эти симптомы могут сочетаться между собой и усиливаться после прекращения употребления алкоголя, особенно после нескольких дней запоя.
Углубиться в тему – врач нарколог на дом екатеринбург
Robertmah · May 4, 2026 at 8:04 am
Для ваших манометров доступны две процедуры: поверка (для отчетности) и калибровка (для технолога). Экономьте ресурсы.
Что выбрать — поверку или калибровку? Зависит от юридического статуса измерений. Если прибор в магазине — только поверка. Если на внутреннем складе — смело берите добровольный контроль.
Методика поверки одна и утверждена государством — отклоняться нельзя. Методика калибровки разрабатывается лабораторией. Обе опираются на эталоны.
Source:
https://mfo27.ru/razlichiya-mezhdu-poverkoj-i-kalibrovkoj-kontrolno-izmeritelnyh-priborov-i-kriterii-ih-vybora/
поверка и калибровка контрольно-измерительных приборов
Vincentkip · May 4, 2026 at 8:05 am
За выездом врача чаще обращаются тогда, когда человеку тяжело добраться до клиники, он ослаблен после нескольких дней употребления алкоголя или родственникам важно быстрее понять, какая тактика будет безопасной. После осмотра можно определить, нужна ли капельница, достаточно ли детоксикации на дому, требуется ли повторное наблюдение, а в дальнейшем — консультация по лечению алкоголизма, кодирование или реабилитация. В части случаев уже первый звонок позволяет понять, идет ли речь только о временном ухудшении самочувствия или о состоянии, при котором может потребоваться вывод из запоя в стационаре.
Исследовать вопрос подробнее – врач нарколог на дом в екатеринбурге
Francisvah · May 4, 2026 at 8:07 am
Нарколог на дом в Екатеринбурге: выезд врача на дом, лечение запоя и консультации в наркологической клинике «НЕО+».
Узнать больше – врач нарколог на дом
Edwardzen · May 4, 2026 at 10:00 am
Этот обзор предлагает структурированное изложение информации по актуальным вопросам. Материал подан так, чтобы даже новичок мог быстро освоиться в теме и начать использовать полученные знания в практике.
Нажмите, чтобы узнать больше – вызов врача нарколога на дом
RobertKep · May 4, 2026 at 10:45 am
Этот текст призван помочь читателю расширить кругозор и получить практические знания. Мы используем простой язык, наглядные примеры и структурированное изложение, чтобы сделать обучение максимально эффективным и увлекательным.
Прочитать подробнее – психиатр нарколог на дом
Philliphease · May 4, 2026 at 12:18 pm
Наркологическая клиника в Ростове-на-Дону рассматривается как специализированная медицинская структура, обеспечивающая лечение и помощь 24/7 при состояниях, связанных с зависимостями. В клинике «Вектор Трезвости» работа выстроена по принципу непрерывности, что позволяет оказывать медицинское вмешательство независимо от времени суток и стадии обращения. Такой формат особенно важен при острых интоксикациях, выраженной абстиненции и резких соматических нарушениях, когда своевременность помощи напрямую влияет на прогноз. Наркологическая клиника в Ростове-на-Дону функционирует в условиях постоянной готовности медицинского персонала и строгого соблюдения клинических регламентов.
Получить больше информации – http://
http://izhpets.ru/mezhpoverochnyj-interval-kontrolno-izmeritelnyh-priborov-znachenie-i-proczedura.html · May 4, 2026 at 12:47 pm
С точки зрения ФЗ «Об обеспечении единства измерений», межповерочный интервал — это период времени, в течение которого результаты измерений, полученные с помощью данного прибора, признаются государством достоверными. Простыми словами: если у вас есть спор с поставщиком или налоговой, и вы опираетесь на показания своего прибора, эти показания будут иметь силу в суде только при условии, что межповерочный интервал не истек. Как только он истек — прибор превращается в «немого свидетеля». Его данные нельзя использовать для официальных отчетов, актов приемки товара, расчета за электроэнергию или воду. Это главный юридический документ каждого прибора — не паспорт, а именно действующая поверка в рамках интервала. http://izhpets.ru/mezhpoverochnyj-interval-kontrolno-izmeritelnyh-priborov-znachenie-i-proczedura.html
HenryDyefe · May 4, 2026 at 12:55 pm
Hello!
Save money with our wow boost service cheap options that offer great value. We believe in providing affordable services without cutting corners on quality or security. Our competitive pricing makes premium boosting accessible to players on various budgets easily. Take advantage of discounts and promotions to get even more savings on your orders. Enjoy top tier boosting experiences at prices that are hard to beat elsewhere today.
We help you reach exalted status with key factions to unlock rewards and recipes.
The most complete information on the website – https://www.wow-power-leveling.org/Dlc/
wow boosting, wow 1-70 boost, wow leveling guide
wow boost service cheap, mythic plus carry, wow boosting
Good luck and good gameplay!
HoseaJeree · May 4, 2026 at 1:22 pm
К основным показаниям относятся:
Получить дополнительные сведения – вывод из запоя на дому анонимно в санкт-петербурге
Shawndoush · May 4, 2026 at 1:32 pm
Такой подход позволяет достичь устойчивого результата без срывов и рецидивов. Пациенты получают помощь не только на уровне физиологии, но и на уровне личностных изменений, что делает лечение глубоким и эффективным.
Исследовать вопрос подробнее – https://narcologicheskaya-clinika-v-rnd19.ru/chastnaya-narkologicheskaya-klinika-rostov-na-donu/
CharlesSnore · May 4, 2026 at 1:52 pm
Вывод из запоя в стационаре в Санкт-Петербурге: эффективная помощь при алкоголизме, капельницы и наблюдение врачей в наркологической клинике «Элегия Мед».
Выяснить больше – вывод из запоя в стационаре анонимно санкт-петербург
TimothyLem · May 4, 2026 at 1:56 pm
Вывод из запоя на дому — это медицинская помощь, направленная на стабилизацию состояния пациента без госпитализации. Такой формат позволяет начать лечение сразу после обращения и снизить нагрузку на организм, связанную с транспортировкой. В наркологической клинике «Частный медик 24» помощь оказывается с выездом врача, который проводит диагностику и подбирает терапию в зависимости от текущего состояния.
Углубиться в тему – вывод из запоя на дому анонимно в санкт-петербурге
LutherMup · May 4, 2026 at 2:08 pm
К основным показаниям относятся:
Подробнее можно узнать тут – вывод из запоя вызов в нижнем новгороде
Robertmet · May 4, 2026 at 2:24 pm
В Санкт-Петербурге услуга вывода из запоя на дому применяется в ситуациях, когда требуется медицинская помощь, но нет показаний к стационарному лечению. Врач проводит консультацию, оценивает состояние пациента, длительность употребления и выраженность симптомов, после чего принимает решение о тактике лечения при алкоголизме. Важно, что терапия начинается сразу после осмотра, а при необходимости можно заранее заказать выезд специалистов.
Выяснить больше – вывод из запоя на дому круглосуточно
Jamesintaf · May 4, 2026 at 2:25 pm
Каждый этап лечения имеет конкретную цель и контролируется специалистами. Для наглядности представлен пример структуры лечебного процесса, используемого в клинике «ДонМед Трезвость».
Узнать больше – http://narcologicheskaya-klinika-v-rostove19.ru
DwainNaiva · May 4, 2026 at 2:28 pm
Вывод из запоя на дому в Санкт-Петербурге с выездом специалиста, стабилизацией состояния и медицинской поддержкой в наркологической клинике «Частный медик 24»
Детальнее – нарколог на дом вывод из запоя в санкт-петербурге
DouglasNOb · May 4, 2026 at 2:35 pm
Капельница от похмелья в Воронеже с индивидуальной инфузионной терапией и врачебным контролем в наркологической клинике «Похмельная служба»
Подробнее можно узнать тут – капельница от похмелья цена воронеж
Eugenedew · May 4, 2026 at 2:38 pm
Непрерывный мониторинг витальных показателей — ключевое отличие стационарного формата, делающее его золотым стандартом при лечении запойного синдрома. В палатах клиники «Стармед» установлены автоматизированные системы отслеживания частоты пульса, уровня кислорода в крови, температуры и артериального давления, данные с которых интегрируются в единую электронную медицинскую карту. Медицинский персонал дежурит круглосуточно, что обеспечивает мгновенную реакцию на любое ухудшение состояния: оперативную коррекцию инфузионной терапии, введение симптоматических препаратов, привлечение смежных специалистов при выявлении соматических осложнений. Такой подход исключает полипрагмазию, предотвращает избыточную фармакологическую нагрузку на ослабленный организма и гарантирует, что каждая стадия детоксикации проходит под строгим клиническим контролем, минимизируя риски для жизни и здоровья пациента.
Ознакомиться с деталями – нарколог вывод из запоя в стационаре в нижнем новгороде
Anthonypaw · May 4, 2026 at 2:52 pm
Процедура начинается с осмотра пациента. Врач измеряет давление, пульс, оценивает общее состояние и выраженность симптомов. На основании этих данных формируется состав капельницы и план лечения. Такой подход позволяет учитывать индивидуальные особенности пациента и эффективно провести вывод из запоя.
Выяснить больше – http://kapelnicza-ot-pokhmelya-voronezh-4.ru
Jamesskymn · May 4, 2026 at 3:13 pm
Помощь при зависимостях в клинике «Южный Вектор» базируется на клинической диагностике, позволяющей определить стадию расстройства и сопутствующие нарушения. Наркологическая клиника в Ростове-на-Дону уделяет внимание не только купированию острых проявлений, но и стабилизации соматических показателей. Такой подход снижает риски осложнений и формирует условия для дальнейших этапов терапии. Медицинская практика подтверждает, что отсутствие системности приводит к краткосрочному эффекту и рецидивам.
Получить больше информации – наркологическая клиника цены в ростове-на-дону
EnriqueGaity · May 4, 2026 at 3:20 pm
Несмотря на выездной формат, лечение выстраивается поэтапно и соответствует медицинским стандартам. Это обеспечивает управляемость процесса и безопасность пациента.
Получить больше информации – нарколог на дом вывод
SidneyGaw · May 4, 2026 at 3:35 pm
Нарколог на дом в Екатеринбурге: круглосуточный выезд, детоксикация и лечение зависимостей в наркологической клинике «НЕО+».
Детальнее – нарколог на дом екатеринбург
LarryCex · May 4, 2026 at 3:37 pm
Вывод из запоя на дому с быстрым облегчением в Екатеринбурге — это процедура, направленная на быстрое снятие острых симптомов алкогольного абстинентного синдрома и возвращение пациента к нормальному состоянию, включая случаи алкоголизма и наркомании. Такая услуга удобна тем, что позволяет не только эффективно справиться с зависимостью, но и избавиться от неприятных проявлений запоя, таких как головная боль, тошнота, слабость и психоэмоциональное напряжение, в комфортной домашней обстановке, при этом оказывается наркологическая помощь. Быстрое облегчение без необходимости госпитализации делает этот метод популярным среди пациентов, которым важен быстрый и безопасный результат, а при необходимости можно заказать дальнейшее кодирование или лечение в стационаре.
Подробнее – vyvod-iz-zapoya-na-domu-ekaterinburg-19.ru/
IgnacioZom · May 4, 2026 at 3:50 pm
Алкогольная интоксикация оказывает серьёзное влияние на организм, вызывая головную боль, тошноту, слабость и головокружение. Капельница помогает организму быстро избавиться от продуктов распада алкоголя, восстановить нормальное функционирование органов и минимизировать последствия для здоровья. Важно, что мы обеспечиваем полное наблюдение врача на протяжении всей процедуры, что помогает гарантировать безопасность пациента и максимальную эффективность лечения.
Получить дополнительные сведения – капельница от похмелья цена в екатеринбурге
Donaldmic · May 4, 2026 at 3:53 pm
Этот увлекательный информационный материал подарит вам массу новых знаний и ярких эмоций. Мы собрали для вас интересные факты и сведения, которые обогатят ваш опыт. Откройте для себя увлекательный мир информации и насладитесь процессом изучения!
Связаться за уточнением – капельницы от запоя на дому нижний новгород
JavierApela · May 4, 2026 at 4:05 pm
Каждый курс лечения включает несколько этапов, направленных на постепенное улучшение состояния. Система выстроена так, чтобы обеспечить плавное восстановление функций организма без стресса. Ниже приведена таблица, показывающая основные этапы лечения и применяемые процедуры.
Ознакомиться с деталями – http://vyvod-iz-zapoya-v-rnd19.ru
Shawndoush · May 4, 2026 at 4:10 pm
Такой подход позволяет достичь устойчивого результата без срывов и рецидивов. Пациенты получают помощь не только на уровне физиологии, но и на уровне личностных изменений, что делает лечение глубоким и эффективным.
Получить дополнительные сведения – лечение в наркологической клинике
TimothyLem · May 4, 2026 at 4:26 pm
Чаще всего помощь требуется при следующих состояниях:
Ознакомиться с деталями – http://www.domen.ru
LutherMup · May 4, 2026 at 4:55 pm
К основным показаниям относятся:
Получить дополнительные сведения – вывод из запоя с выездом
Jamesintaf · May 4, 2026 at 5:12 pm
Медицинская команда контролирует каждый этап лечения, отслеживая динамику и корректируя терапию при необходимости. Благодаря такому подходу удаётся добиться не временного улучшения, а устойчивого восстановления.
Подробнее тут – http://narcologicheskaya-klinika-v-rostove19.ru
DonaldLiz · May 4, 2026 at 5:12 pm
В Воронеже круглосуточная помощь при похмелье востребована в ситуациях, когда симптомы появляются внезапно или усиливаются в ночное время, особенно в запое или после запоя. Врач проводит консультацию, оценивает состояние пациента и принимает решение о проведении инфузионной терапии. Такой подход позволяет своевременно устранить симптомы и предотвратить их дальнейшее развитие. При необходимости можно оставить заявку, уточнить цены или получить помощь бесплатно на первичном этапе.
Детальнее – капельница от похмелья цена воронеж
DouglasNOb · May 4, 2026 at 5:24 pm
После алкоголя в организме накапливаются токсичные продукты распада, нарушается водно-солевой баланс и страдает нервная система, что особенно выражено после запоя или при алкоголизме. Это проявляется головной болью, слабостью, тошнотой и нарушением сна. Капельница помогает ускорить процессы очищения и восстановить внутренние системы, обеспечивая более быстрое облегчение состояния и помогая человеку выйти из состояния запоев.
Выяснить больше – капельница от похмелья анонимно в воронеже
SidneyGaw · May 4, 2026 at 5:50 pm
Наша клиника предлагает полный цикл услуг — от экстренного вызова нарколога до долгосрочной реабилитации. Каждый этап разрабатывается индивидуально с учётом возраста, стажа зависимости и сопутствующих заболеваний. Современные протоколы 2026 года позволяют проводить лечение максимально комфортно и эффективно, минимизируя болезненные симптомы и снижая риск срывов. В этом виде деятельности мы используем только проверенные методы медицины.
Выяснить больше – http://narkolog-na-dom-ekaterinburg-1.ru
JamaalApets · May 4, 2026 at 6:12 pm
Этот информативный текст отличается привлекательным содержанием и актуальными данными. Мы предлагаем читателям взглянуть на привычные вещи под новым углом, предоставляя интересный и доступный материал. Получите удовольствие от чтения и расширьте кругозор!
Получить дополнительную информацию – вывод из запоя в наркологическом стационаре
Francisvah · May 4, 2026 at 6:13 pm
Нарколог на дом в Екатеринбурге: выезд врача на дом, лечение запоя и консультации в наркологической клинике «НЕО+».
Подробнее тут – https://narkolog-na-dom-ekaterinburg.ru/
Jamesskymn · May 4, 2026 at 6:18 pm
Помощь при зависимостях в клинике «Южный Вектор» базируется на клинической диагностике, позволяющей определить стадию расстройства и сопутствующие нарушения. Наркологическая клиника в Ростове-на-Дону уделяет внимание не только купированию острых проявлений, но и стабилизации соматических показателей. Такой подход снижает риски осложнений и формирует условия для дальнейших этапов терапии. Медицинская практика подтверждает, что отсутствие системности приводит к краткосрочному эффекту и рецидивам.
Получить дополнительную информацию – https://narkologicheskaya-klinika-v-rnd19.ru/chastnaya-narkologicheskaya-klinika-rostov-na-donu
Larrysmash · May 4, 2026 at 6:19 pm
В этой статье-обзоре мы соберем актуальную информацию и интересные факты, которые освещают важные темы. Читатели смогут ознакомиться с различными мнениями и подходами, что позволит им расширить кругозор и глубже понять обсуждаемые вопросы.
Как достичь результата? – вывод из запоя на дому самара круглосуточно
Larrysmash · May 4, 2026 at 7:27 pm
В этом обзорном материале представлены увлекательные детали, которые находят отражение в различных аспектах жизни. Мы исследуем непонятные и интересные моменты, позволяя читателю увидеть картину целиком. Погрузитесь в мир знаний и удивительных открытий!
А есть ли продолжение? – вывод запоев скорая
TravisBoids · May 4, 2026 at 8:06 pm
В этой статье рассматриваются различные аспекты избавления от зависимости, включая физические и психологические методы. Мы обсудим поддержку, мотивацию и стратегии, которые помогут в процессе выздоровления. Читатели узнают, как преодолеть трудности и двигаться к новой жизни без зависимости.
Изучить материалы по теме – вызвать нарколога на дом в москве
Francisvah · May 4, 2026 at 8:11 pm
Нарколог на дом в Екатеринбурге: выезд врача на дом, лечение запоя и консультации в наркологической клинике «НЕО+».
Углубиться в тему – http://narkolog-na-dom-ekaterinburg.ru/
TravisBoids · May 4, 2026 at 8:53 pm
Мы рассмотрим современные вызовы здравоохранения и пути их решения с помощью технологий и научных исследований. В статье собраны данные о новых лекарствах, методах диагностики и системном подходе к улучшению здоровья населения.
Перейти к статье – услуги нарколога на дому
Darrellcleve · May 4, 2026 at 9:04 pm
Этот текст призван помочь читателю расширить кругозор и получить практические знания. Мы используем простой язык, наглядные примеры и структурированное изложение, чтобы сделать обучение максимально эффективным и увлекательным.
Тыкай сюда — узнаешь много интересного – вызов нарколога на дом запой
Darrenbep · May 4, 2026 at 9:09 pm
После нескольких дней употребления алкоголя организм работает с перегрузкой. Усиливается обезвоживание, ухудшается сон, появляется дрожь, растет тревожность, нарушается аппетит, могут беспокоить скачки давления, сердцебиение, слабость и тошнота. В такой ситуации состояние нередко требует осмотра врача, особенно если самочувствие продолжает ухудшаться или уже были неудачные попытки справиться своими силами. Подобные состояния встречаются не только при последствиях алкоголизма, но и у людей, которые впервые столкнулись с тяжелой интоксикацией после приема спиртного.
Подробнее можно узнать тут – запой нарколог на дом в екатеринбурге
FranklaH · May 4, 2026 at 9:15 pm
look at this web-site https://cleanthebit.com/hi/
GeorgeWacle · May 4, 2026 at 9:44 pm
Этот обзор посвящен успешным стратегиям избавления от зависимости, включая реальные примеры и советы. Мы разоблачим мифы и предоставим читателям достоверную информацию о различных подходах. Получите опыт многообразия методов и найдите подходящий способ для себя!
Обратиться к источнику – наркологический стационар в санкт петербурге
Stevebow · May 4, 2026 at 10:01 pm
Эта публикация посвящена актуальным вопросам современной медицины и здравоохранения. Мы обсудим новейшие технологии диагностики и лечения, а также их влияние на продолжительность и качество жизни. Читатель найдет здесь информацию о научных исследованиях и перспективных разработках, доступно изложенную для широкой аудитории.
Есть чему поучиться – лечение в наркологическом стационаре
DwainNaiva · May 4, 2026 at 10:10 pm
Вывод из запоя на дому в Санкт-Петербурге с выездом специалиста, стабилизацией состояния и медицинской поддержкой в наркологической клинике «Частный медик 24»
Ознакомиться с деталями – https://vyvod-iz-zapoya-na-domu-sankt-peterburg-11.ru/
HenryDyefe · May 4, 2026 at 10:17 pm
Good morning!
Pause and resume boost anytime. Life happens, we understand.
From leveling to gear acquisition we provide a one-stop solution for character progression.
All information on the website – https://www.wow-power-leveling.org/Gameplay/wow-all-expansions-cost
wow gold seller, wow pvp boost, wow 1-70 boost
wow instant boost, gladiator boost wow, wow gold buy
Good luck and good gameplay!
Lucienkex · May 4, 2026 at 11:04 pm
В этой информационной статье вы найдете интересное содержание, которое поможет вам расширить свои знания. Мы предлагаем увлекательный подход и уникальные взгляды на обсуждаемые темы, побуждая пользователей к активному мышлению и критическому анализу.
Получить дополнительную информацию – капельница после запоя нижний новгород
Библия с иллюстрациями Гюстава Доре · May 4, 2026 at 11:09 pm
Библия с иллюстрациями Гюстава Доре
JeremyIcexy · May 4, 2026 at 11:17 pm
Публикация приглашает вас исследовать неизведанное — от древних тайн до современных достижений науки. Вы узнаете, как случайные находки превращались в революции, а смелые мысли — в новые эры человеческого прогресса.
А что дальше? – вывод из запоя дешево
FranklaH · May 4, 2026 at 11:43 pm
Our site https://cleanthebit.com/
FranklaH · May 4, 2026 at 11:49 pm
this hyperlink https://cleanthebit.com/
DanielBlerb · May 4, 2026 at 11:56 pm
В этом обзоре представлены различные методы избавления от зависимости, включая терапевтические и психологические подходы. Мы сравниваем их эффективность и предоставляем рекомендации для тех, кто хочет вернуться к трезвой жизни. Читатели смогут найти информацию о реабилитационных центрах и поддерживающих группах.
ТОП-5 причин узнать больше – вызов нарколога на дом москва цены
EnriqueGaity · May 5, 2026 at 12:00 am
В практике лечения на дому применяются следующие этапы медицинского воздействия:
Подробнее тут – выезд нарколога на дом в ростове-на-дону
Lucienkex · May 5, 2026 at 12:02 am
В этой статье представлен занимательный и актуальный контент, который заставит вас задуматься. Мы обсуждаем насущные вопросы и проблемы, а также освещаем истории, которые вдохновляют на действия и изменения. Узнайте, что стоит за событиями нашего времени!
Подробности по ссылке – вывести из запоя в домашних условиях капельница
RobertKep · May 5, 2026 at 12:11 am
Этот информационный обзор станет отличным путеводителем по актуальным темам, объединяющим важные факты и мнения экспертов. Мы исследуем ключевые идеи и представляем их в доступной форме для более глубокого понимания. Читайте, чтобы оставаться в курсе событий!
Смотрите также… – нарколог дом
RichardGloge · May 5, 2026 at 12:22 am
https://abhishekpatidar.com/toxic-work-culture-and-solutions/
https://glenfordsales.com/2026/04/29/istorija-azartnyh-igr-ot-drevnosti-do-nashih-dnej/ · May 5, 2026 at 12:25 am
https://glenfordsales.com/2026/04/29/istorija-azartnyh-igr-ot-drevnosti-do-nashih-dnej/
JeremyIcexy · May 5, 2026 at 12:44 am
Эта статья сочетает познавательный и занимательный контент, что делает ее идеальной для любителей глубоких исследований. Мы рассмотрим увлекательные аспекты различных тем и предоставим вам новые знания, которые могут оказаться полезными в будущем.
Узнать из первых рук – вывод из запоя дешево
Davidhar · May 5, 2026 at 12:54 am
site link https://quarklab.ru/fr/crypto-drainer/
RichardGloge · May 5, 2026 at 1:05 am
https://karabast.com/wiki/index.php/Pokerdom
JavierApela · May 5, 2026 at 1:24 am
Каждый курс лечения включает несколько этапов, направленных на постепенное улучшение состояния. Система выстроена так, чтобы обеспечить плавное восстановление функций организма без стресса. Ниже приведена таблица, показывающая основные этапы лечения и применяемые процедуры.
Подробнее – вывод из запоя недорого ростов-на-дону
RichardGloge · May 5, 2026 at 1:49 am
https://ibaiprolim.com/?attachment_id=5
Philliphease · May 5, 2026 at 1:58 am
В клинической практике используются следующие этапы лечения:
Углубиться в тему – наркологические клиники алкоголизм ростов-на-дону
RichardGloge · May 5, 2026 at 2:33 am
https://mobileledtrucks.us/2025/06/23/hello-world/
Julioatora · May 5, 2026 at 2:37 am
Эта информационная публикация освещает широкий спектр тем из мира медицины. Мы предлагаем читателям ясные и понятные объяснения современных заболеваний, методов профилактики и лечения. Информация будет полезна как пациентам, так и медицинским работникам, желающим поддержать уровень своих знаний.
Подробности по ссылке – лечение в наркологическом стационаре
StephenRip · May 5, 2026 at 2:53 am
Этот информативный текст сочетает в себе темы здоровья и зависимости. Мы обсудим, как хронические заболевания могут усугубить зависимости и наоборот, как зависимость может влиять на общее состояние здоровья. Читатели получат представление о комплексном подходе к лечению как физического, так и психического состояния.
Где почитать поподробнее? – нарколог стационар спб
Timothyelapy · May 5, 2026 at 2:58 am
f?r?n tavan? nas?l temizlenir hakk?ndaki yaz?y? gercekten begendim. Suradan okuyabilirsiniz: https://evhobileri.com/articles/firin-tavani-nasil-temizlenir/
Timothyelapy · May 5, 2026 at 3:02 am
y?l boyunca acan bahce cicekleri hakk?ndaki makaleyi cok sevdim. Iste link: https://evhobisi.com/articles/uzun-omurlu-bahce-cicekleri/
RichardGloge · May 5, 2026 at 3:17 am
https://nst.taccs.hu/2025/10/08/thelastofthemohicans/
Davidhar · May 5, 2026 at 3:25 am
basics https://cleanthebit.com/es/
Julioatora · May 5, 2026 at 3:31 am
В этом обзоре мы обсудим современные методы борьбы с зависимостями, включая медикаментозную терапию и психотерапию. Мы представим последние исследования и их результаты, чтобы читатели могли быть в курсе наиболее эффективных подходов к лечению и поддержке.
Продолжить изучение – наркологическая клиника со стационаром
DonaldLiz · May 5, 2026 at 3:33 am
Показания для обращения за помощью включают:
Изучить вопрос глубже – капельница от похмелья анонимно
StephenRip · May 5, 2026 at 3:46 am
Публикация охватывает основные направления развития современной медицины. Мы обсудим значимость научных исследований, инноваций в лечении и роли общественного участия в формировании системы здравоохранения.
Лови подробности – наркологический стационар в санкт петербурге
CharlesSnore · May 5, 2026 at 3:46 am
Основой стационарной детоксикации является инфузионная терапия, направленная на ускоренное выведение токсинов, коррекцию водно-электролитного баланса и восстановление метаболических процессов. Стандартная капельница включает кристаллоидные растворы для восполнения объема циркулирующей крови, витамины группы B и C для активации ферментных систем, гепатопротекторы для защиты печени и симптоматические препараты для нормализации сна. Состав, объем и скорость введения рассчитываются индивидуально с учетом возраста, массы тела, длительности интоксикации и функции почек. При выраженной абстиненции подключаются средства для коррекции нейромедиаторного обмена, однако их применение строго дозируется для исключения риска вторичной зависимости. Дозировки пересматриваются ежедневно на основе динамики показателей, что обеспечивает безопасность и высокую клиническую эффективность.
Узнать больше – вывод из запоя в стационаре клиника санкт-петербург
Donaldmic · May 5, 2026 at 3:48 am
Эта разъяснительная статья содержит простые и доступные разъяснения по актуальным вопросам. Мы стремимся сделать информацию понятной для широкой аудитории, чтобы каждый мог разобраться в предмете и извлечь из него максимум пользы.
Связаться за уточнением – прокапаться после запоя
RichardGloge · May 5, 2026 at 4:02 am
https://studio-true.online/en/archives/589
RichardGloge · May 5, 2026 at 4:46 am
http://deputadomarciomarinho.com.br/site/noticias/noticias/720/
Ronaldpyday · May 5, 2026 at 4:54 am
После оформления вызова нарколог приезжает к пациенту и проводит комплексную оценку состояния. Врач измеряет давление, частоту пульса, оценивает уровень сознания и выраженность симптомов. На основании полученных данных формируется план лечения, который реализуется сразу на месте.
Изучить вопрос глубже – запой нарколог на дом нижний новгород
Vincentkip · May 5, 2026 at 5:01 am
Отдельного внимания требуют случаи, когда больной почти не ест, плохо пьет воду, не может спокойно лежать, жалуется на сильное сердцебиение, нехватку сна или выраженное внутреннее напряжение. В такой ситуации осмотр помогает определить, безопасно ли оставаться дома и какого объема помощи достаточно на текущем этапе. Если речь идет о выраженных проявлениях абстинентного синдрома, затягивать с обращением нецелесообразно.
Детальнее – вызов нарколога на дом в екатеринбурге
Davidhar · May 5, 2026 at 5:13 am
More Bonuses https://cleanthebit.com/ru/
DanielBlerb · May 5, 2026 at 5:13 am
Этот медицинский обзор сосредоточен на последних достижениях, которые оказывают влияние на пациентов и медицинскую практику. Мы разбираем инновационные методы лечения и исследований, акцентируя внимание на их значимости для общественного здоровья. Читатели узнают о свежих данных и их возможном применении.
Тыкай сюда — узнаешь много интересного – врач нарколог выезд на дом цена
IgnacioZom · May 5, 2026 at 5:15 am
Капельница от похмелья в Екатеринбурге с анонимным выездом врача и восстановительной терапией в наркологической клинике «Частный медик 24»
Получить дополнительную информацию – http://www.domen.ru
RichardGloge · May 5, 2026 at 5:31 am
https://strata-g.co.za/new-minimum-wage-to-boost-worker-income-from-1-march-2025-what-employers-need-to-know/
Eugenedew · May 5, 2026 at 5:33 am
Вывод из запоя в стационаре в Нижнем Новгороде: профессиональное лечение, капельницы и контроль состояния пациента в наркологической клинике «Стармед».
Получить больше информации – наркология вывод из запоя в стационаре
DamienHed · May 5, 2026 at 5:33 am
Эта статья предлагает уникальную подборку занимательных фактов и необычных историй, которые вы, возможно, не знали. Мы постараемся вдохновить ваше воображение и разнообразить ваш кругозор, погружая вас в мир, полный интересных открытий. Читайте и открывайте для себя новое!
Рассмотреть проблему всесторонне – выведение из запоя
https://mercifoods.vn/yutish-strategiyalari-mosbet-bilan-muvaffaqiyatga/ · May 5, 2026 at 5:34 am
https://mercifoods.vn/yutish-strategiyalari-mosbet-bilan-muvaffaqiyatga/
HoseaJeree · May 5, 2026 at 5:45 am
Вывод из запоя на дому — это формат наркологической помощи, при котором лечение проводится в привычной для пациента обстановке с выездом врача. Такой подход применяется в ситуациях, когда состояние требует медицинского вмешательства, но не предполагает обязательной госпитализации. В наркологической клинике «Частный медик 24» помощь на дому выстраивается по принципу поэтапной стабилизации: сначала устраняются острые проявления, затем оценивается динамика и при необходимости корректируется терапия.
Выяснить больше – вывод из запоя на дому цена
Ralphfibia · May 5, 2026 at 5:59 am
Предлагаем вашему вниманию интересную справочную статью, в которой собраны ключевые моменты и нюансы по актуальным вопросам. Эта информация будет полезна как для профессионалов, так и для тех, кто только начинает изучать тему. Узнайте ответы на важные вопросы и расширьте свои знания!
Откройте для себя больше – капельница от запоя нижний новгород
Robertmet · May 5, 2026 at 6:00 am
В Санкт-Петербурге услуга вывода из запоя на дому применяется в ситуациях, когда требуется медицинская помощь, но нет показаний к стационарному лечению. Врач проводит консультацию, оценивает состояние пациента, длительность употребления и выраженность симптомов, после чего принимает решение о тактике лечения при алкоголизме. Важно, что терапия начинается сразу после осмотра, а при необходимости можно заранее заказать выезд специалистов.
Исследовать вопрос подробнее – вывод из запоя на дому круглосуточно санкт-петербург
Darrenbep · May 5, 2026 at 6:13 am
Нарколог на дом в Екатеринбурге востребован в ситуациях, когда человеку нужна врачебная помощь после употребления алкоголя, при запое, выраженном похмельном синдроме, нарушении сна, тревоге, скачках давления, слабости и других признаках ухудшения самочувствия. Такой формат обращения часто выбирают семьи, которые хотят вызвать врача без поездки в клинику и быстро получить консультацию по состоянию больного. Домашний выезд особенно важен тогда, когда требуется детоксикация, наблюдение после нескольких дней употребления спиртного и оценка рисков, связанных с последствиями алкоголизма.
Углубиться в тему – https://narkolog-na-dom-ekaterinburg-2.ru/
RichardGloge · May 5, 2026 at 6:16 am
http://p-ncc.org/archiwa/targi-pracy-stadion-energa-gdansk/
Jamesjax · May 5, 2026 at 6:21 am
Мы собрали для вас самые захватывающие факты из мира науки и истории. От малознакомых деталей до грандиозных событий — эта статья расширит ваш кругозор и подарит новое понимание того, как устроен наш мир.
Лучшее решение — прямо здесь – вывод из запоя на дому нижний новгород цена
Vincentkip · May 5, 2026 at 6:56 am
За выездом врача чаще обращаются тогда, когда человеку тяжело добраться до клиники, он ослаблен после нескольких дней употребления алкоголя или родственникам важно быстрее понять, какая тактика будет безопасной. После осмотра можно определить, нужна ли капельница, достаточно ли детоксикации на дому, требуется ли повторное наблюдение, а в дальнейшем — консультация по лечению алкоголизма, кодирование или реабилитация. В части случаев уже первый звонок позволяет понять, идет ли речь только о временном ухудшении самочувствия или о состоянии, при котором может потребоваться вывод из запоя в стационаре.
Подробнее – http://www.domen.ru
JamaalApets · May 5, 2026 at 6:57 am
Эта статья погружает вас в увлекательный мир знаний, где каждый факт становится открытием. Мы расскажем о ключевых исторических поворотных моментах и научных прорывах, которые изменили ход цивилизации. Поймите, как прошлое формирует настоящее и как его уроки могут помочь нам строить будущее.
Познакомиться с результатами исследований – вывод из запоя санкт петербург стационар
RichardGloge · May 5, 2026 at 7:01 am
https://veedelwiki.de/index.php?title=Benutzer:JaredW989557450
Robertmah · May 5, 2026 at 7:27 am
Для ваших датчиков давления доступны две процедуры: поверка (для отчетности) и калибровка (для ISO 9001). Выбирайте осознанно.
Что выбрать — поверку или калибровку? Зависит от рисков. Если прибор в магазине — только поверка. Если в научной работе — смело берите добровольный контроль.
Законодательные требования (102-ФЗ, ГРОЕИ) касаются только поверки: сроки межповерочного интервала. Для калибровки нет обязательных норм. Будьте в правовом поле.
Source:
https://j-socks.ru/poverka-i-kalibrovka/
порядок проведения поверки и калибровки кип
Robertmah · May 5, 2026 at 7:30 am
Разница между поверкой и калибровкой — в логике контроля. Поверка отвечает: «Годен ли он к эксплуатации?», калибровка: «Насколько он врет в каждой точке?».
Порядок проведения поверки и калибровки КИП отличается жестко: поверка — с записью в ФИФ ОЕИ, калибровка — любая компетентная служба. Единство измерений — база.
Критерии выбора поверки или калибровки: стоимость процедуры. Для суда — поверка, для техпроцесса — калибровка.
Source:
https://selo-delo.ru/poleznye-stati/facebook-gotovit-rebrending-i-smeny-nazvaniia-kak-eto-sviazano-s-metavselennoi.html
правовые последствия поверки и калибровки
DamienHed · May 5, 2026 at 7:31 am
В этом обзорном материале представлены увлекательные детали, которые находят отражение в различных аспектах жизни. Мы исследуем непонятные и интересные моменты, позволяя читателю увидеть картину целиком. Погрузитесь в мир знаний и удивительных открытий!
Есть чему поучиться – выведение из запоя
Robertmah · May 5, 2026 at 7:35 am
Разница между поверкой и калибровкой — в правовых последствиях. Поверка отвечает: «Можно ли верить прибору по закону?», калибровка: «Какова его реальная ошибка в цифрах?».
Что выбрать — поверку или калибровку? Зависит от юридического статуса измерений. Если прибор в больнице — только поверка. Если в лаборатории — смело калибруйте.
Законодательные требования (102-ФЗ, ГРОЕИ) касаются только поверки: запись в реестре. Для калибровки нет обязательных норм. Будьте в правовом поле.
Source:
https://mfo27.ru/razlichiya-mezhdu-poverkoj-i-kalibrovkoj-kontrolno-izmeritelnyh-priborov-i-kriterii-ih-vybora/
поверка и калибровка контрольно-измерительных приборов
Robertmah · May 5, 2026 at 7:38 am
Отличие поверки от калибровки в результате. Поверка выносит вердикт «годен/негоден», калибровка — показывает «как сильно врет прибор».
Порядок проведения поверки и калибровки КИП отличается жестко: поверка — с записью в ФИФ ОЕИ, калибровка — без госрегулирования. Единство измерений — база.
Критерии выбора поверки или калибровки: цена ошибки. Когда закон требует — только поверка.
Source:
https://tele2kino.ru/poverka-i-kalibrovka-kip-v-chem-raznicza-i-chto-vybrat.html
критерии выбора поверки и калибровки
Robertmah · May 5, 2026 at 7:42 am
Для ваших весов доступны две процедуры: поверка (для отчетности) и калибровка (для технолога). Не переплачивайте.
Порядок проведения поверки и калибровки КИП отличается жестко: поверка — по госреестру, калибровка — любая компетентная служба. Оба процесса начинаются с эталона.
Критерии выбора поверки или калибровки: область регулирования (ГРОЕИ). Когда закон требует — только поверка.
Source:
https://dondvh.ru/poverka-i-kalibrovka-kip-razlichiya-i-princzipy-provedeniya/
что выбрать поверку или калибровку
RichardGloge · May 5, 2026 at 7:47 am
http://www.guidemoizzi-isbn.com/catalogo/bambini/il-bene-e-il-male/
Robertmah · May 5, 2026 at 7:50 am
Разница между поверкой и калибровкой — в правовых последствиях. Поверка отвечает: «Годен ли он к эксплуатации?», калибровка: «Насколько он врет в каждой точке?».
Что выбрать — поверку или калибровку? Зависит от сферы применения. Если прибор в больнице — только поверка. Если на внутреннем складе — смело выбирайте калибровку.
Правовые последствия просты: эксплуатация без поверки запрещена. Для калибровки штрафов не предусмотрено. Рискуете бизнесом?.
Source:
http://izhpets.ru/poverka-i-kalibrovka-kip-v-chem-raznicza-i-chto-vybrat.html
методика поверки и калибровки средств измерений
Jamesjax · May 5, 2026 at 8:17 am
Эта публикация погружает вас в мир увлекательных фактов и удивительных открытий. Мы расскажем о ключевых событиях, которые изменили ход истории, и приоткроем завесу над научными достижениями, которые вдохновили миллионы. Узнайте, чему может научить нас прошлое и как применить эти знания в будущем.
Подробности по ссылке – вывод из запоя на дому в нижнем новгороде
RichardGloge · May 5, 2026 at 8:36 am
https://www.apartvillatitina.com/2012/01/17/kriesi-at/
SidneyGaw · May 5, 2026 at 9:22 am
Особое внимание мы уделяем психологической составляющей. Нарколог на дом в Екатеринбурге в «НЕО+» — это не только физическое очищение, но и работа с мотивацией, разрушение психологических триггеров зависимости. Зависимость разрушает жизнь, поэтому мы предлагаем психотерапевтическое сопровождение. Родственники получают отдельную поддержку: консультации психолога помогают правильно выстроить общение с зависимым человеком и мотивировать его на дальнейшее лечение. Реабилитация может проходить амбулаторно или в стационаре партнёрских центров с комфортабельными условиями, где пациенты находятся под круглосуточным наблюдением.
Получить дополнительную информацию – врач нарколог на дом екатеринбург
RichardGloge · May 5, 2026 at 9:27 am
https://c21-esthonpo.com/2023/12/22/post-682491/
JamesViege · May 5, 2026 at 9:36 am
В этом обзорном материале представлены увлекательные детали, которые находят отражение в различных аспектах жизни. Мы исследуем непонятные и интересные моменты, позволяя читателю увидеть картину целиком. Погрузитесь в мир знаний и удивительных открытий!
См. подробности – капельницы от запоя на дому нижний новгород
Anthonypaw · May 5, 2026 at 10:44 am
Похмельный синдром сопровождается головной болью, слабостью, нарушением сна, сухостью во рту и нестабильностью давления, что часто наблюдается после запоя или при алкоголизме. Эти симптомы связаны с накоплением токсинов и нарушением водно-солевого баланса. Капельница позволяет ускорить выведение вредных веществ и восстановить нормальное функционирование организма, помогая человеку быстрее выйти из состояния запоев.
Подробнее тут – капельница от похмелья цена в воронеже
Jaysonsycle · May 5, 2026 at 11:15 am
Публикация приглашает вас исследовать неизведанное — от древних тайн до современных достижений науки. Вы узнаете, как случайные находки превращались в революции, а смелые мысли — в новые эры человеческого прогресса.
Что скрывают от вас? – вывод из запоя на дому
PeterBem · May 5, 2026 at 12:03 pm
Эта статья предлагает уникальную подборку занимательных фактов и необычных историй, которые вы, возможно, не знали. Мы постараемся вдохновить ваше воображение и разнообразить ваш кругозор, погружая вас в мир, полный интересных открытий. Читайте и открывайте для себя новое!
Углубить понимание вопроса – наркологическая помощь на дому в самаре
Jaysonsycle · May 5, 2026 at 12:12 pm
Эта статья погружает вас в увлекательный мир знаний, где каждый факт становится открытием. Мы расскажем о ключевых исторических поворотных моментах и научных прорывах, которые изменили ход цивилизации. Поймите, как прошлое формирует настоящее и как его уроки могут помочь нам строить будущее.
Более того — здесь – вывод из запоя врач на дом
Robertduego · May 5, 2026 at 12:18 pm
Эта познавательная публикация погружает вас в море интересного контента, который быстро захватит ваше внимание. Мы рассмотрим важные аспекты темы и предоставим вам уникальные Insights и полезные сведения для дальнейшего изучения.
Углубить понимание вопроса – вывести из запоя цена
GeorgeWacle · May 5, 2026 at 12:38 pm
Этот текст посвящён сложным аспектам зависимости и её влиянию на жизнь человека. Мы обсудим психологические, физические и социальные последствия зависимого поведения, а также важность своевременного обращения за помощью.
Расширить кругозор по теме – нарколог стационар спб
Stevebow · May 5, 2026 at 1:09 pm
В этой статье мы обсудим процесс восстановления после зависимостей, акцентируя внимание на различных методах и подходах к реабилитации. Читатели узнают, как создать план выздоровления и использовать полезные ресурсы для достижения устойчивых изменений.
А что дальше? – наркологический стационар спб
PeterBem · May 5, 2026 at 1:13 pm
Публикация приглашает вас исследовать неизведанное — от древних тайн до современных достижений науки. Вы узнаете, как случайные находки превращались в революции, а смелые мысли — в новые эры человеческого прогресса.
Получить дополнительные сведения – нарколог дом
Ralphfibia · May 5, 2026 at 1:15 pm
Этот увлекательный информационный материал подарит вам массу новых знаний и ярких эмоций. Мы собрали для вас интересные факты и сведения, которые обогатят ваш опыт. Откройте для себя увлекательный мир информации и насладитесь процессом изучения!
Прочесть заключение эксперта – капельница после запоя
LamarRus · May 5, 2026 at 1:18 pm
Эта обзорная заметка содержит ключевые моменты и факты по актуальным вопросам. Она поможет читателям быстро ориентироваться в теме и узнать о самых важных аспектах сегодня. Получите краткий курс по современной информации и оставайтесь в курсе событий!
Не упусти важное! – нарколога домой
rent yacht montenegro 437 · May 5, 2026 at 1:48 pm
charter yacht Montenegro https://rent-a-yacht-montenegro.com
Jamesdox · May 5, 2026 at 2:25 pm
В клинике применяется широкий спектр методик, которые помогают воздействовать на проблему зависимости всесторонне.
Разобраться лучше – лечение алкоголизма в стационаре тверь
Edwardzen · May 5, 2026 at 2:26 pm
Этот обзор предлагает структурированное изложение информации по актуальным вопросам. Материал подан так, чтобы даже новичок мог быстро освоиться в теме и начать использовать полученные знания в практике.
Получить дополнительные сведения – нарколог самара
RodolfoChoom · May 5, 2026 at 2:53 pm
Решение о помещении пациента в стационар принимается на основе объективных медицинских критериев, а не только по желанию родственников. К показаниям относятся: запой длительностью более 72 часов, выраженная абстиненция с тахикардией, артериальной гипертензией, профузным потоотделением, наличие в анамнезе алкогольных делириев или судорожных эпизодов, сопутствующие хронические заболевания печени, сердца, поджелудочной железы. В сложные ситуации, когда интоксикация затрагивает несколько систем одновременно, резкое прекращение употребления без медицинской поддержки может спровоцировать отек мозга, острую сердечную недостаточность или желудочно-кишечное кровотечение. При сочетанных расстройствах, когда в анамнезе присутствует наркомании, протоколы адаптируются под специфику психоактивных соединений и включают усиленный нейрологический контроль. Стационар позволяет провести полноценную диагностику, включая ЭКГ, экспресс-анализы крови, УЗИ внутренних органов и мониторинг сатурации, что формирует точную картину состояния и исключает шаблонные назначения.
Узнать больше – вывод из запоя в стационаре анонимно санкт-петербург
OrvilleVurgy · May 5, 2026 at 3:21 pm
Вывод из запоя направлен не только на снятие острых симптомов, но и на комплексное восстановление организма. Работа специалистов позволяет стабилизировать состояние и создать условия для дальнейшего лечения зависимости.
Углубиться в тему – вывод из запоя на дому недорого
Arthurtaini · May 5, 2026 at 3:59 pm
этот контент https://hpc.name/thread/n282/93415/vychislenie-znacheniya-dlya-zadannogo-chisla-a-s-ispolzovaniem-rekurrentnogo-sootnosheniya-na-javascript.html
Matthewtuh · May 5, 2026 at 4:00 pm
Процесс вывода из запоя на дому с выездом врача в Екатеринбурге включает несколько этапов, начиная с первичного осмотра пациента и заканчивая корректировкой лечения в зависимости от его состояния. Врач-нарколог проводит полный осмотр, анализирует симптомы и составляет план лечения, который включает детоксикацию организма, поддерживающую терапию и медикаментозное лечение для снятия симптомов абстиненции.
Узнать больше – вывод из запоя на дому цена в екатеринбурге
Arthurtaini · May 5, 2026 at 4:01 pm
кликните сюда https://hpc.name/thread/s481/144386/kak-pravilno-vvodit-dannye-v-klass-c-reshenie-problem-s-massivami-i-obektami.html
RichardJam · May 5, 2026 at 4:02 pm
Каждое направление вносит свой вклад в общий результат и делает процесс лечения более надежным и комплексным.
Углубиться в тему – наркологическая клиника
Aarontoill · May 5, 2026 at 4:05 pm
Вывод из запоя в Донецке предполагает комплексную медицинскую помощь, ориентированную на снижение интоксикации, стабилизацию витальных функций и профилактику осложнений. Патофизиологически запой сопровождается нарушением водно-электролитного баланса, колебаниями артериального давления, тахикардией, рисками аритмий, дефицитом витаминов группы B и дисрегуляцией нейромедиаторных систем. Клиническая тактика строится на ранней оценке риска, контроле соматического статуса и пошаговой коррекции нарушений с обязательным наблюдением за сердечно-сосудистой и дыхательной системами.
Получить дополнительные сведения – вывод из запоя капельница на дому
Jamesdox · May 5, 2026 at 4:11 pm
Лечение алкоголизма в Твери проводится с использованием современных медицинских и психотерапевтических методик. Оно направлено на снятие физической зависимости, восстановление организма и формирование устойчивой мотивации к отказу от спиртных напитков. Важно учитывать, что успех терапии зависит от комплексного подхода и профессиональной поддержки специалистов.
Детальнее – лечение женского алкоголизма в твери
Я пытался продать старые монеты в России: 5 важных уроков · May 5, 2026 at 4:18 pm
Я пытался продать старые монеты в России: 5 важных уроков
DavidPen · May 5, 2026 at 4:27 pm
Эта информационная статья охватывает широкий спектр актуальных тем и вопросов. Мы стремимся осветить ключевые факты и события с ясностью и простотой, чтобы каждый читатель мог извлечь из нее полезные знания и полезные инсайты.
Кликни и узнай всё! – капельница после запоя цена
RobertCig · May 5, 2026 at 4:48 pm
Вывод из запоя в Ставрополе проводится с использованием сертифицированных препаратов, которые действуют мягко, не вызывая резких перепадов давления или побочных эффектов. Перед началом лечения врач проводит диагностику — измеряет пульс, артериальное давление, уровень насыщения крови кислородом, оценивает состояние печени и почек. Только после этого подбирается схема терапии. Такой подход снижает риски осложнений и гарантирует безопасное восстановление.
Углубиться в тему – https://vyvod-iz-zapoya-stavropol0.ru/vyvod-iz-zapoya-v-staczionare-stavropol/
Jamesbap · May 5, 2026 at 5:15 pm
Ниже — рабочий каркас выездного протокола. Он индивидуализируется под переносимость, вегетативные реакции и бытовые ограничения пациента. В таблице отражены и медицинские, и организационные шаги: видна связка «что делаем — что проверяем — как понимаем, что пора к следующему этапу».
Подробнее тут – вывод из запоя
Jaredinoke · May 5, 2026 at 5:19 pm
Этот текст призван помочь читателю расширить кругозор и получить практические знания. Мы используем простой язык, наглядные примеры и структурированное изложение, чтобы сделать обучение максимально эффективным и увлекательным.
Открой скрытое – вызов нарколога на дом
BrettPem · May 5, 2026 at 5:20 pm
В этой статье представлен занимательный и актуальный контент, который заставит вас задуматься. Мы обсуждаем насущные вопросы и проблемы, а также освещаем истории, которые вдохновляют на действия и изменения. Узнайте, что стоит за событиями нашего времени!
А что дальше? – вывод из запоя цена на дому
OrvilleVurgy · May 5, 2026 at 5:28 pm
Вывод из запоя в Твери осуществляется в специализированных медицинских учреждениях, где пациентам предоставляется круглосуточная помощь и полное медицинское сопровождение. Длительное употребление алкоголя вызывает тяжелую интоксикацию, истощение организма и психоэмоциональные нарушения. Самостоятельные попытки выйти из запоя могут привести к серьезным осложнениям, поэтому обращение к специалистам становится наиболее безопасным и результативным решением.
Исследовать вопрос подробнее – вывод из запоя дешево
RolandSab · May 5, 2026 at 5:38 pm
like it https://cleanthebit.com/fr/
DavidPed · May 5, 2026 at 5:41 pm
Мы заранее объясняем, какие шаги последуют, чтобы пациент и близкие понимали логику вмешательств и не тревожились по поводу непредвиденных «сюрпризов». Карта ниже — ориентир; конкретные параметры врач уточнит после осмотра.
Получить больше информации – вывод из запоя с выездом
StanleylauTt · May 5, 2026 at 5:50 pm
Этот интересный отчет представляет собой сборник полезных фактов, касающихся актуальных тем. Мы проанализируем данные, чтобы вы могли сделать обоснованные выводы. Читайте, чтобы узнать больше о последних трендах и значимых событиях!
Исследовать вопрос подробнее – вывод из алкогольного запоя на дому
KennethamaGs · May 5, 2026 at 5:53 pm
Публикация приглашает вас исследовать неизведанное — от древних тайн до современных достижений науки. Вы узнаете, как случайные находки превращались в революции, а смелые мысли — в новые эры человеческого прогресса.
Перейти к статье – вызов нарколога на дом самара
Peterstize · May 5, 2026 at 5:59 pm
На первичном визите врач проводит клиническое интервью, оценивает витальные показатели (АД, ЧСС, SpO2, температура), при показаниях — выполняет портативный ЭКГ-скрининг и экспресс-диагностику. Вместе с пациентом формируется план ближайших 72 часов: режим гидратации, «вечерний ритуал» для сна, правила сенсорной разгрузки, безопасные фразы для общения с близкими, точечная фармакоподдержка и расписание коротких чек-инов.
Разобраться лучше – http://narcologicheskaya-klinika-petrozavodsk0.ru
DarrentoInd · May 5, 2026 at 6:08 pm
Этот информационный обзор станет отличным путеводителем по актуальным темам, объединяющим важные факты и мнения экспертов. Мы исследуем ключевые идеи и представляем их в доступной форме для более глубокого понимания. Читайте, чтобы оставаться в курсе событий!
Раскрыть тему полностью – наркологическая помощь на дому в москве
WendellSeabs · May 5, 2026 at 6:09 pm
В этой публикации мы обсуждаем современные методы лечения различных заболеваний. Читатели узнают о новых медикаментах, терапиях и исследованиях, которые активно применяются для лечения. Мы нацелены на то, чтобы предоставить практические знания, которые могут помочь в борьбе с недугами.
Ознакомьтесь с аналитикой – кодирование от алкоголизма стационар
RobertMurce · May 5, 2026 at 6:11 pm
Дополнительно можно подключить кислородную поддержку, щадящие анксиолитики, противорвотные средства и нутритивную поддержку (по показаниям). Мы всегда объясняем логику назначения: зачем конкретный компонент, что и когда ожидать, по какому признаку поймём, что пора остановиться или поменять параметр. Честность и понятность — лучший способ снизить тревогу и укрепить участие пациента в процессе.
Подробнее тут – http://vyvod-iz-zapoya-kamensk-uralskij0.ru/vyvod-iz-zapoya-na-domu-kamensk-uralskij/
Kevinkek · May 5, 2026 at 6:14 pm
Мы гибко переключаемся между форматами: старт в палате краткого наблюдения, продолжение в дневном стационаре и амбулаторные встречи с телемедицинскими чек-инами по 10–15 минут. Решение принимается по рискам: повторная рвота, выраженная тахикардия/скачки АД, спутанность сознания, эпизоды судорог/психозов — безусловные показания к наблюдению. При стабилизации сна и витальных возвращаемся к амбулаторному графику, чтобы уменьшить сенсорную нагрузку и быстрее встроить новые навыки в обычный быт.
Изучить вопрос глубже – наркологическая клиника нарколог первоуральск
Aarontoill · May 5, 2026 at 6:24 pm
Вывод из запоя в Донецке предполагает комплексную медицинскую помощь, ориентированную на снижение интоксикации, стабилизацию витальных функций и профилактику осложнений. Патофизиологически запой сопровождается нарушением водно-электролитного баланса, колебаниями артериального давления, тахикардией, рисками аритмий, дефицитом витаминов группы B и дисрегуляцией нейромедиаторных систем. Клиническая тактика строится на ранней оценке риска, контроле соматического статуса и пошаговой коррекции нарушений с обязательным наблюдением за сердечно-сосудистой и дыхательной системами.
Детальнее – вывод из запоя на дому недорого переулок панфилова, 36
Robertduego · May 5, 2026 at 6:57 pm
В этом интересном тексте собраны обширные сведения, которые помогут вам понять различные аспекты обсуждаемой темы. Мы разбираем детали и факты, делая акцент на важности каждого элемента. Не упустите возможность расширить свои знания и взглянуть на мир по-новому!
Слушай внимательно — тут важно – вывод из запоя на дому 24
RodolfoChoom · May 5, 2026 at 6:59 pm
Терапевтический процесс в стационаре строится по принципу последовательного выполнения клинических задач: диагностика, стабилизация, медикаментозная терапия и подготовка к амбулаторному этапу. При поступлении врач проводит детальный осмотр, собирает анамнез, оценивает неврологический статус и при необходимости назначает лабораторные исследования. На основе полученных данных формируется индивидуальный протокол, учитывающий возраст, длительность интоксикации, наличие сопутствующих патологий и переносимость лекарственных компонентов. Мы применяем только сертифицированные препараты, зарегистрированные в РФ, и строго соблюдаем клинические рекомендации Минздрава, исключая псевдонаучные методики. Стандарты оказания медицинской помощи фиксируются во внутренних регламентах и регулярно проверяются независимыми аудиторами.
Выяснить больше – нарколог вывод из запоя в стационаре
JamesViege · May 5, 2026 at 6:59 pm
Откройте для себя скрытые страницы истории и малоизвестные научные открытия, которые оказали колоссальное влияние на развитие человечества. Статья предлагает свежий взгляд на события, которые заслуживают большего внимания.
Продолжить изучение – капельница от запоя нижний новгород
LamarRus · May 5, 2026 at 7:03 pm
Эта статья полна интересного контента, который побудит вас исследовать новые горизонты. Мы собрали полезные факты и удивительные истории, которые обогащают ваше понимание темы. Читайте, погружайтесь в детали и наслаждайтесь процессом изучения!
Обратиться к источнику – нарколог на дом круглосуточно самара цены
Edwarddop · May 5, 2026 at 7:14 pm
Каждый план лечения строится вокруг понятных целей и измеримых результатов. Вместо шаблонных «сильных» схем мы применяем минимально достаточную фармакотерапию, корректируем среду (свет, тишина, режим сна), учим пациента простым и повторяемым навыкам саморегуляции. Такое сочетание медицинских и психологических инструментов помогает быстрее снять острые симптомы и поддерживать стабильность в последующие недели. Кодирование мы рассматриваем не как «волшебную кнопку», а как часть маршрута, который всегда включает детокс, психообразование и профилактику срывов.
Получить дополнительные сведения – narkologicheskaya-klinika-nizhnij-tagil0.ru/
StevenPem · May 5, 2026 at 7:23 pm
Уже при первичном звонке мы собираем ключевую информацию: длительность употребления, типы веществ, сопутствующие заболевания, прошлые реакции на лекарства, эпизоды судорог и психозов, недавние значения АД/ЧСС. Это позволяет подготовить персональный стартовый протокол ещё до визита: поставить цель на первые 72 часа, определить метрики (сон, «тяга», дневная энергия), запланировать вечерний ритуал и расписать дистанционные чек-ины. Прозрачность шагов снижает тревогу у пациента и семьи и повышает соблюдаемость — фундамент устойчивого результата.
Детальнее – наркологические клиники алкоголизм в каменске-уральске
RobertCig · May 5, 2026 at 7:29 pm
Вывод из запоя — одна из наиболее востребованных услуг наркологической клиники «СтаврМед Центр». Это процедура, направленная на устранение последствий длительного употребления алкоголя и восстановление нормального функционирования организма. Специалисты клиники применяют современные детоксикационные методики, индивидуально подбирая состав капельниц и препаратов. Главная цель — безопасное снятие интоксикации, восстановление водно-солевого баланса и предотвращение осложнений со стороны сердца, печени и нервной системы.
Детальнее – помощь вывод из запоя ставрополь
DanielSoard · May 5, 2026 at 8:05 pm
В этой статье представлен занимательный и актуальный контент, который заставит вас задуматься. Мы обсуждаем насущные вопросы и проблемы, а также освещаем истории, которые вдохновляют на действия и изменения. Узнайте, что стоит за событиями нашего времени!
Нажмите, чтобы узнать больше – выведение из запоя санкт петербург стационар
Scottdus · May 5, 2026 at 8:27 pm
official statement https://cleanthebit.com/ru/
DavidPed · May 5, 2026 at 8:32 pm
Мы заранее объясняем, какие шаги последуют, чтобы пациент и близкие понимали логику вмешательств и не тревожились по поводу непредвиденных «сюрпризов». Карта ниже — ориентир; конкретные параметры врач уточнит после осмотра.
Узнать больше – вывод из запоя вызов на дом
RobertMurce · May 5, 2026 at 8:46 pm
Наркологическая клиника «Трезвый Урал» специализируется на безопасном и деликатном выведении из запоя с выездом врача на дом. Мы соединяем медицинскую точность, продуманную логистику и понятные пациенту шаги, чтобы облегчение наступало быстро, а состояние оставалось стабильным и предсказуемым. В основе — индивидуальные капельницы по показаниям, детоксикация с мониторингом витальных показателей, коррекция обезвоживания и электролитных нарушений, мягкая поддержка сна и психологическая разгрузка. Наши бригады приезжают круглосуточно, оборудование компактно, документы — нейтральные, а сообщения в медицинской карте формулируются аккуратно, без «ярлыков», чтобы сохранить вашу конфиденциальность.
Узнать больше – вывод из запоя дешево каменск-уральск
RolandSab · May 5, 2026 at 8:47 pm
navigate to this website https://cleanthebit.com/hi/
Scottdus · May 5, 2026 at 9:00 pm
Check Out Your URL https://cleanthebit.com/es/
Matthewtuh · May 5, 2026 at 9:07 pm
Процесс вывода из запоя на дому с выездом врача в Екатеринбурге включает несколько этапов, начиная с первичного осмотра пациента и заканчивая корректировкой лечения в зависимости от его состояния. Врач-нарколог проводит полный осмотр, анализирует симптомы и составляет план лечения, который включает детоксикацию организма, поддерживающую терапию и медикаментозное лечение для снятия симптомов абстиненции.
Узнать больше – вывод из запоя на дому цена екатеринбург
EdwardNeite · May 5, 2026 at 9:19 pm
Комплексное использование методов помогает достигать долгосрочной ремиссии и улучшать качество жизни пациентов.
Ознакомиться с деталями – частная наркологическая клиника тверь
Arthurtaini · May 5, 2026 at 9:36 pm
Подробнее https://hpc.name/thread/a232/68280/poisk-faylov-vo-vlojennyh-papkah-s-ispolzovaniem-php.html
ShawnNarie · May 5, 2026 at 9:49 pm
После детоксикации назначается поддерживающая терапия, направленная на предупреждение рецидивов и восстановление нормального функционирования нервной системы.
Ознакомиться с деталями – лечение наркомании
Научная статья по нумизматике · May 5, 2026 at 10:37 pm
Научная статья по нумизматике
Arthurtaini · May 5, 2026 at 10:40 pm
перейдите на этот сайт https://hpc.name/thread/y151/102818/oshibka-pri-ispolzovanii-ajax-s-ruby-ispravlenie-koda-dlya-uvelicheniya-znacheniya.html
RichardJam · May 5, 2026 at 10:47 pm
Каждое направление вносит свой вклад в общий результат и делает процесс лечения более надежным и комплексным.
Исследовать вопрос подробнее – лечение в наркологической клинике тверь
WilliamKem · May 5, 2026 at 11:16 pm
Такая структура позволяет минимизировать колебания состояния, уменьшить нагрузку на органы-мишени и подготовить пациента к следующему этапу лечения зависимости.
Получить больше информации – https://vyvod-iz-zapoya-lugansk0.ru
StanleylauTt · May 6, 2026 at 12:31 am
Мы предлагаем вам окунуться в океан любопытных фактов и вдохновляющих историй. Эта публикация поможет расширить горизонты, разбудить интерес к науке и истории и увидеть мир с новой стороны.
Кликни и узнай всё! – вывод из алкогольного запоя на дому
KennethamaGs · May 6, 2026 at 12:45 am
В обзорной статье вы найдете собрание важных фактов и аналитики по самым разнообразным темам. Мы рассматриваем как современные исследования, так и исторические контексты, чтобы вы могли получить полное представление о предмете. Погрузитесь в мир знаний и сделайте шаг к пониманию!
Кликни и узнай всё! – выезд нарколога на дом наркология
Scottdus · May 6, 2026 at 12:52 am
click to read https://quarklab.ru/es/drenador-de-cripto/
DouglasAssip · May 6, 2026 at 1:24 am
В этой статье-обзоре мы соберем актуальную информацию и интересные факты, которые освещают важные темы. Читатели смогут ознакомиться с различными мнениями и подходами, что позволит им расширить кругозор и глубже понять обсуждаемые вопросы.
А что дальше? – вызвать нарколога на дом недорого москва цены
BryantProbe · May 6, 2026 at 1:53 am
Смотреть здесь https://t.me/vpnsmmone/
ShawnNarie · May 6, 2026 at 2:20 am
Лечение наркомании во Владимире представляет собой комплекс мероприятий, направленных на восстановление физического и психического здоровья пациентов с различными формами зависимости от психоактивных веществ. Современные методы терапии, используемые в наркологической клинике «Новая Эра», обеспечивают эффективное и безопасное избавление от зависимости с последующей социальной реабилитацией.
Изучить вопрос глубже – принудительное лечение наркомании владимир
DouglasAssip · May 6, 2026 at 2:26 am
В этой статье представлен занимательный и актуальный контент, который заставит вас задуматься. Мы обсуждаем насущные вопросы и проблемы, а также освещаем истории, которые вдохновляют на действия и изменения. Узнайте, что стоит за событиями нашего времени!
А что дальше? – нарколог на дом в москве
Kevinkek · May 6, 2026 at 2:34 am
Мы гибко переключаемся между форматами: старт в палате краткого наблюдения, продолжение в дневном стационаре и амбулаторные встречи с телемедицинскими чек-инами по 10–15 минут. Решение принимается по рискам: повторная рвота, выраженная тахикардия/скачки АД, спутанность сознания, эпизоды судорог/психозов — безусловные показания к наблюдению. При стабилизации сна и витальных возвращаемся к амбулаторному графику, чтобы уменьшить сенсорную нагрузку и быстрее встроить новые навыки в обычный быт.
Углубиться в тему – наркологическая клиника в первоуральске
Joshuavox · May 6, 2026 at 2:40 am
Мы собрали для вас самые захватывающие факты из мира науки и истории. От малознакомых деталей до грандиозных событий — эта статья расширит ваш кругозор и подарит новое понимание того, как устроен наш мир.
Обратитесь за информацией – выведение из запоя больница
JamiePut · May 6, 2026 at 2:45 am
go to this website https://smmpanel.one
JamiePut · May 6, 2026 at 3:16 am
click here to investigate https://smmpanel.su/
RonaldFlolA · May 6, 2026 at 3:20 am
these details https://smmpanel.one
StevenPem · May 6, 2026 at 3:23 am
Капельницы доступны круглосуточно — в стационаре и с выездом на дом. Состав подбирается под симптомы, коморбидность и семейные обстоятельства. Ниже — примеры профилей: на месте врач адаптирует их, чтобы получить эффект с минимальной нагрузкой на организм.
Углубиться в тему – http://narkologicheskaya-klinika-kamensk-uralskij0.ru/narkologiya-kamensk-uralskij/
Timothynox · May 6, 2026 at 3:35 am
Наиболее частыми основаниями для выбора такого формата становятся длительный запой, тяжелое течение похмельного синдрома, выраженный тремор, отсутствие сна, тревога, слабость, обезвоживание и жалобы на сердцебиение. Дополнительное значение имеют хронические заболевания сердца, сосудов, печени и нервной системы, на фоне которых выход из запоя может переноситься тяжелее.
Детальнее – вывод из запоя в стационаре клиника
Joshuavox · May 6, 2026 at 3:36 am
Эта статья погружает вас в увлекательный мир знаний, где каждый факт становится открытием. Мы расскажем о ключевых исторических поворотных моментах и научных прорывах, которые изменили ход цивилизации. Поймите, как прошлое формирует настоящее и как его уроки могут помочь нам строить будущее.
Погрузиться в детали – вывод из запоя стационар спб
BryantProbe · May 6, 2026 at 3:44 am
другие https://vpn-one.net/
https://imgur.com/a/eksWZoT · May 6, 2026 at 3:44 am
https://imgur.com/a/eksWZoT
WendellSeabs · May 6, 2026 at 3:49 am
В этой статье рассматриваются актуальные вопросы, связанные с развитием медицинской науки и её внедрением в повседневную практику. Особое внимание уделено вопросам профилактики, ранней диагностики и использованию технологий для улучшения здоровья человека.
Более того — здесь – реабилитация наркозависимых стационар
najlepsze kasyno online · May 6, 2026 at 4:18 am
Woh I enjoy your content , saved to bookmarks!
RonaldFlolA · May 6, 2026 at 4:28 am
website here https://smmpanel.one/
v9bet · May 6, 2026 at 4:48 am
Hi there, just became aware of your blog through Google, and found that it’s truly informative. It’s important to cover these trends.
Tin world cup · May 6, 2026 at 4:50 am
I feel that is among the so much significant info for me. And i am satisfied studying your article. However should commentary on some basic issues, The site style is ideal, the articles is in reality excellent : D. Excellent activity, cheers
Williamkes · May 6, 2026 at 4:55 am
Эта услуга позволяет людям, которые не могут или не хотят покидать свой дом, получить профессиональную помощь и избавиться от зависимости без госпитализации. К тому же, вывод из запоя на дому позволяет избежать стресса, связанного с нахождением в медицинских учреждениях, при этом можно заказать вызов специалистов с учетом их опыта и лет работы, а также данных больного.
Подробнее – вывод из запоя на дому круглосуточно
Jeremytuh · May 6, 2026 at 4:57 am
Терапевтический процесс в стационаре строится по принципу последовательного выполнения клинических задач: диагностика, стабилизация, медикаментозная поддержка и подготовка к амбулаторному этапу. При поступлении врач проводит детальный осмотр, собирает анамнез, оценивает неврологический статус и при необходимости назначает лабораторные исследования. На основе полученных данных формируется индивидуальный протокол, учитывающий возраст, длительность интоксикации, наличие сопутствующих патологий и переносимость лекарственных компонентов. Мы применяем только сертифицированные препараты, зарегистрированные в РФ, и строго соблюдаем клинические рекомендации Минздрава, исключая псевдонаучные методики.
Получить дополнительные сведения – наркология вывод из запоя в стационаре
JamiePut · May 6, 2026 at 5:47 am
look at here now https://smmpanel.su
Jeremytuh · May 6, 2026 at 5:50 am
Выбор между домашней помощью и стационарным лечением определяется не удобством, а медицинской целесообразностью. В условиях клиники исключаются внешние триггеры, обеспечивается изоляция от источников алкоголя и создается контролируемая среда, где терапевтические решения принимаются на основе объективных показателей. Такой подход критически важен для предотвращения осложнений, минимизации дискомфорта абстиненции и формирования устойчивой базы для дальнейшей противорецидивной работы.
Получить дополнительные сведения – https://vyvod-iz-zapoya-v-staczionare-sankt-peterburg-20.ru
RonaldFlolA · May 6, 2026 at 5:50 am
this contact form https://smmpanel.one
RonaldFlolA · May 6, 2026 at 5:56 am
redirected here https://smmpanel.ooo/
Michaeltus · May 6, 2026 at 5:56 am
Вывод из запоя на дому в Екатеринбурге — это услуга, которая позволяет пациентам пройти лечение в удобных для них условиях, без необходимости посещать стационар. Процедура включает несколько этапов, каждый из которых направлен на снижение уровня алкогольной интоксикации и стабилизацию состояния пациента. Главным преимуществом вывода из запоя на дому является то, что это не только удобно, но и позволяет избежать лишнего стресса, который может быть вызван госпитализацией.
Получить дополнительные сведения – вывод из запоя на дому цена екатеринбург
Timothynox · May 6, 2026 at 5:59 am
Стационарный формат отличается возможностью наблюдать состояние в динамике, своевременно корректировать лечение и контролировать течение абстинентного синдрома. Это особенно важно в ситуациях, когда домашнего наблюдения недостаточно, а риск осложнений требует более внимательного подхода. При выборе тактики учитывают не только текущее самочувствие, но и предшествующие эпизоды запоя, наличие хронических заболеваний, выраженность нарушений сна, поведения и вегетативных симптомов. В клинике такой подход позволяет организовать комплексное наблюдение, при котором состояние оценивают последовательно, а помощь выстраивают с учетом нагрузки на основные системы здоровья.
Получить больше информации – быстрый вывод из запоя в стационаре в санкт-петербурге
DarrentoInd · May 6, 2026 at 6:01 am
Этот увлекательный информационный материал подарит вам массу новых знаний и ярких эмоций. Мы собрали для вас интересные факты и сведения, которые обогатят ваш опыт. Откройте для себя увлекательный мир информации и насладитесь процессом изучения!
Открой скрытое – вызов нарколога на дом в москве цена
Michaeltus · May 6, 2026 at 6:52 am
Запой – это состояние, при котором человек продолжает употреблять алкоголь в течение длительного времени, не в состоянии прекратить употребление самостоятельно, что является проявлением алкоголизма. Это может привести к серьезным проблемам со здоровьем, и в таком случае необходим вывод из запоя с помощью наркологической помощи, при этом в дальнейшем может рассматриваться кодирование.
Исследовать вопрос подробнее – вывод из запоя на дому в екатеринбурге
real money casino · May 6, 2026 at 7:14 am
Howdy, a helpful article for sure. Thank you.
DanielSoard · May 6, 2026 at 7:16 am
Эта статья сочетает познавательный и занимательный контент, что делает ее идеальной для любителей глубоких исследований. Мы рассмотрим увлекательные аспекты различных тем и предоставим вам новые знания, которые могут оказаться полезными в будущем.
Откройте для себя больше – вывод из запоя стационар спб
Link vào v9bet · May 6, 2026 at 7:21 am
thank, I thoroughly enjoyed reading your article. I really appreciate your wonderful knowledge and the time you put into educating the rest of us.
Williamkes · May 6, 2026 at 7:32 am
Вывод из запоя на дому с медицинским контролем — это услуга, которая позволяет пациентам избавиться от алкогольной зависимости в комфортных условиях своего дома. В Екатеринбурге эта услуга становится все более востребованной, поскольку она предоставляет безопасный и эффективный способ вывода человека из запоя, при этом не требуя госпитализации. Процедура сопровождается контролем квалифицированных специалистов, что минимизирует риски и ускоряет процесс восстановления.
Получить дополнительные сведения – http://vyvod-iz-zapoya-na-domu-ekaterinburg-18.ru
Thomashen · May 6, 2026 at 9:59 am
Если пациент не может самостоятельно выйти из запоя или симптомы похмелья слишком сильны, вызов нарколога для вывода из запоя на дому с детоксикацией помогает избежать осложнений и минимизировать риски для здоровья. Врач на дому подберет индивидуальный план лечения и проведет все необходимые процедуры для безопасного восстановления организма.
Углубиться в тему – http://vyvod-iz-zapoya-na-domu-ekaterinburg-20.ru
Geraldknize · May 6, 2026 at 10:39 am
Что такое конопля ?
Thomashen · May 6, 2026 at 11:11 am
Процедура вывода из запоя на дому включает несколько ключевых этапов, которые обеспечивают максимально быстрое и безопасное восстановление пациента. Эти этапы тщательно контролируются врачом, что минимизирует риски и помогает достичь наилучших результатов.
Подробнее тут – вывод из запоя на дому цена
Geraldknize · May 6, 2026 at 11:23 am
Конопля для рыбалки
https://tajobeharry.com/the-social-dynamics-of-gambling-connecting/ · May 6, 2026 at 11:58 am
https://tajobeharry.com/the-social-dynamics-of-gambling-connecting/
Geraldknize · May 6, 2026 at 12:08 pm
Как выбрать семена конопли
Geraldknize · May 6, 2026 at 12:53 pm
Информационная страница о семенах промышленной конопли
BryantProbe · May 6, 2026 at 12:54 pm
нажмите https://t.me/vpnsmmone/
DavidNub · May 6, 2026 at 1:20 pm
Этот увлекательный информационный материал подарит вам массу новых знаний и ярких эмоций. Мы собрали для вас интересные факты и сведения, которые обогатят ваш опыт. Откройте для себя увлекательный мир информации и насладитесь процессом изучения!
Узнайте всю правду – нарколог на дом
MichaelSar · May 6, 2026 at 1:21 pm
Нужен сайт? разработка сайта под ключ в компании domenanet.by. Профессиональная разработка сайтов любой сложности в Минске: от интернет-магазинов до порталов.
Jaredinoke · May 6, 2026 at 1:25 pm
Этот информационный обзор станет отличным путеводителем по актуальным темам, объединяющим важные факты и мнения экспертов. Мы исследуем ключевые идеи и представляем их в доступной форме для более глубокого понимания. Читайте, чтобы оставаться в курсе событий!
Ознакомиться с деталями – выезд нарколога москва
Chrischomo · May 6, 2026 at 1:40 pm
Если нужен недорогой аккумулятор https://www.akb24v.ru 24 вольта для погрузчика, стоит обратить внимание на проверенные решения с оптимальным ресурсом и стабильной отдачей. Купить тяговую батарею 24V можно на сайте, там представлены варианты под разные задачи и типы техники.
AlfredTog · May 6, 2026 at 2:34 pm
В статье по вопросам здоровья мы рассматриваем актуальные проблемы, с которыми сталкивается общество. Обсуждаются заболевания, факторы риска и важные аспекты профилактики. Читатели получат полезные советы о том, как сохранить здоровье и улучшить качество жизни.
Получить дополнительную информацию – служба вывода из запоя
BryantProbe · May 6, 2026 at 2:41 pm
узнать больше https://t.me/vpnsmmone
Edwincok · May 6, 2026 at 2:46 pm
В данной статье мы поговорим о будущем медицины, акцентируя внимание на прорывных разработках и их потенциале. Читатель узнает о новых подходах к лечению, роли искусственного интеллекта и возможностях персонализированной медицины.
Углубиться в тему – капельница от запоя недорого
Vincentalare · May 6, 2026 at 3:05 pm
В этой статье-обзоре мы соберем актуальную информацию и интересные факты, которые освещают важные темы. Читатели смогут ознакомиться с различными мнениями и подходами, что позволит им расширить кругозор и глубже понять обсуждаемые вопросы.
Где можно узнать подробнее? – вывод из запоя стационар санкт петербург
Donaldhog · May 6, 2026 at 3:22 pm
Эта статья погружает вас в увлекательный мир знаний, где каждый факт становится открытием. Мы расскажем о ключевых исторических поворотных моментах и научных прорывах, которые изменили ход цивилизации. Поймите, как прошлое формирует настоящее и как его уроки могут помочь нам строить будущее.
Полная информация здесь – сколько стоит сделать капельницу на дому
WilliamNeaRa · May 6, 2026 at 3:30 pm
Этот информационный материал собраны данные, которые помогут лучше понять текущие тенденции и процессы в различных сферах жизни. Мы предоставляем четкий анализ, графики и примеры, чтобы информация была не только понятной, но и практичной для принятия решений.
Читать далее > – нарколог на дом вывод из запоя на дому
Mindygef · May 6, 2026 at 3:59 pm
Эта публикация обращает внимание на важность профилактики зависимостей. Мы обсудим, как осведомленность и образование могут помочь в предотвращении возникновения зависимости. Читатели смогут ознакомиться с полезными советами и ресурсами, которые способствуют здоровому образу жизни.
Получить дополнительную информацию – вывод из запоя на дому
Wallacefrina · May 6, 2026 at 4:55 pm
http://samaraenergo.rudikoms.ruwww.sharizhelaniy.ruwww.cloud-at-work.com/mac_jforum/user/profile/20898.page
Kenneththoug · May 6, 2026 at 7:11 pm
Ежедневный обзор: https://gi-wom.ru/viktoriya-lopyryova-i-nikolaj-baskov-vsyo-chto-izvestno-3/
WilliamDrove · May 6, 2026 at 7:12 pm
новости россии и мира читать новости Совета Федерации
Alfredoitaxy · May 6, 2026 at 8:11 pm
В этой публикации мы обсуждаем современные методы лечения различных заболеваний. Читатели узнают о новых медикаментах, терапиях и исследованиях, которые активно применяются для лечения. Мы нацелены на то, чтобы предоставить практические знания, которые могут помочь в борьбе с недугами.
Не упусти важное! – вывод из запоя в самаре
RaymondZem · May 6, 2026 at 8:15 pm
Эта публикация посвящена актуальным вопросам современной медицины и здравоохранения. Мы обсудим новейшие технологии диагностики и лечения, а также их влияние на продолжительность и качество жизни. Читатель найдет здесь информацию о научных исследованиях и перспективных разработках, доступно изложенную для широкой аудитории.
Более того — здесь – запой нарколог дом
Alfredoitaxy · May 6, 2026 at 9:07 pm
Статья посвящена анализу текущих трендов в медицине и их влиянию на жизнь людей. Мы рассмотрим новые технологии, методы лечения и значение профилактики в обеспечении долголетия и здоровья.
Это стоит прочитать полностью – вывод из запоя на дому самара
RaymondZem · May 6, 2026 at 9:12 pm
Эта публикация посвящена актуальным вопросам современной медицины и здравоохранения. Мы обсудим новейшие технологии диагностики и лечения, а также их влияние на продолжительность и качество жизни. Читатель найдет здесь информацию о научных исследованиях и перспективных разработках, доступно изложенную для широкой аудитории.
Откройте для себя больше – запой вызов врач
Albertfat · May 6, 2026 at 9:14 pm
https://www.google.ge/url?q=https://myborder.ru/
RaymondKeeri · May 6, 2026 at 9:22 pm
В этом обзорном материале представлены увлекательные детали, которые находят отражение в различных аспектах жизни. Мы исследуем непонятные и интересные моменты, позволяя читателю увидеть картину целиком. Погрузитесь в мир знаний и удивительных открытий!
Есть чему поучиться – прокапаться от алкоголя самара цена
Tyronejaf · May 6, 2026 at 9:39 pm
I appreciate the clear paytable and transparent rules. https://whatspecs.com/hello-world/
Турбомани · May 6, 2026 at 9:43 pm
turbomoney kz
Bryonfoups · May 6, 2026 at 9:58 pm
All football match https://canli-skor.com.az results online, game schedules, and league standings. Live updates, statistics, and easy access to information about matches and teams from around the world.
RodolfoGus · May 6, 2026 at 10:09 pm
Live football scores https://canli-futbol.com.az/ up-to-date schedules, and league tables. Follow matches, check scores online, analyze team standings, and never miss a beat in world football.
Charlesfuh · May 6, 2026 at 10:16 pm
В обзорной статье вы найдете собрание важных фактов и аналитики по самым разнообразным темам. Мы рассматриваем как современные исследования, так и исторические контексты, чтобы вы могли получить полное представление о предмете. Погрузитесь в мир знаний и сделайте шаг к пониманию!
Есть чему поучиться – врач нарколог выезд на дом москва цена
RaymondKeeri · May 6, 2026 at 10:20 pm
В этом обзорном материале представлены увлекательные детали, которые находят отражение в различных аспектах жизни. Мы исследуем непонятные и интересные моменты, позволяя читателю увидеть картину целиком. Погрузитесь в мир знаний и удивительных открытий!
Рассмотреть проблему всесторонне – прокапаться от алкоголя в в самаре
fixDiele · May 6, 2026 at 10:42 pm
Особенно понравился раздел про Жестокие сражения на поле: новости и тактика.
Ссылка ниже:
https://manchesterarmy.ru
fixDiele · May 6, 2026 at 10:46 pm
Между прочим, если вас интересует Инновации в транспортной инфраструктуре мегаполисов, загляните сюда.
Смотрите сами:
https://news-urban.ru
Tyronejaf · May 6, 2026 at 10:56 pm
The golden cats are my lucky charm this week. https://www.gracodemolitionpro.com/2025/03/15/hello-world/
Tyronejaf · May 6, 2026 at 11:00 pm
This is the best feline-themed slot in the Canadian market right now. https://www.casavacanzabarone.it/ciao-mondo/
Charlesfuh · May 6, 2026 at 11:20 pm
В обзорной статье вы найдете собрание важных фактов и аналитики по самым разнообразным темам. Мы рассматриваем как современные исследования, так и исторические контексты, чтобы вы могли получить полное представление о предмете. Погрузитесь в мир знаний и сделайте шаг к пониманию!
Кликни и узнай всё! – вызвать нарколога на дом в москве
Tyronejaf · May 6, 2026 at 11:21 pm
Cleocatra real money play is much better than the demo version. https://wvjonesassoc.com/home/
DennisFlide · May 6, 2026 at 11:54 pm
Эта информационная заметка предлагает лаконичное и четкое освещение актуальных вопросов. Здесь вы найдете ключевые факты и основную информацию по теме, которые помогут вам сформировать собственное мнение и повысить уровень осведомленности.
Неизвестные факты о… – прокапаться на дому цена
Josephcax · May 6, 2026 at 11:57 pm
Baky ucun deqiq hava proqnozu. Bu gun, sabah ve hefte ucun temperaturu, yagini? ehtimalini, kuleyin sгrуtini му hava seraitini onlayn yoxlayin.
DavidNub · May 7, 2026 at 12:13 am
Этот увлекательный информационный материал подарит вам массу новых знаний и ярких эмоций. Мы собрали для вас интересные факты и сведения, которые обогатят ваш опыт. Откройте для себя увлекательный мир информации и насладитесь процессом изучения!
Детали по клику – выезд нарколога круглосуточно
CarmeloVaf · May 7, 2026 at 12:16 am
Наша команда видит задачу шире, чем просто снять интоксикацию: важно вернуть предсказуемое засыпание, успокоить вегетативную систему, снизить тревожность и объяснить семье, как мягко поддержать человека, не обесценивая и не провоцируя конфликты. Поэтому медицинские вмешательства поддержаны «сенсорной дисциплиной» (свет, тишина, отсутствие резких запахов), простыми ритуалами вечера и короткими чек-инами на следующий день. Такой формат помогает не только «пережить ночь», но и спокойно пройти первые двое суток, когда риск откатов особенно высок.
Разобраться лучше – помощь вывод из запоя в нижнем тагиле
GabrielMounK · May 7, 2026 at 12:18 am
Phasmophobia Game 2026 phasmo phobia com is a cross-platform horror game supporting PC, PlayStation, Xbox, and VR. Find out the game’s current price, platform list, system requirements, and the latest updates with new maps, events, and gameplay improvements.
Tyronejaf · May 7, 2026 at 12:54 am
Playing Cleocatra for real money in Canada has been a blast. https://fsv-kappelrodeck.de/;amp;path=&frame=TKOMSI_com_cm4all_wdn_Flatpress_22523288&focus=TKOMSI_com_cm4all_wdn_Flatpress_22523288&path=&frame=TKOMSI_com_cm4all_wdn_Flatpress_22523288?x=entry%3Aentry240930-110434%3Bcomments%3A1
Tyronejaf · May 7, 2026 at 12:54 am
Playing Cleocatra for real money in Canada has been a blast. https://exclusiv.kz/natyazhnoj-chexol-na-divan-fantaziya-verona/
Tyronejaf · May 7, 2026 at 1:22 am
Cleocatra Slot Canada is trending for a reason, the wins are massive. https://flnegociosonline.com/planilha-eletronica-como-economizar/
Mindygef · May 7, 2026 at 1:55 am
В данном обзоре представлены основные направления и тренды в области медицины. Мы обсудим актуальные проблемы здравоохранения, свежие открытия и новые подходы, которые меняют представление о лечении и профилактике заболеваний. Эта информация будет полезна как специалистам, так и широкой публике.
Выяснить больше – вывод из запоя круглосуточно
Michaeljom · May 7, 2026 at 2:09 am
Эта публикация завернет вас в вихрь увлекательного контента, сбрасывая стереотипы и открывая двери к новым идеям. Каждый абзац станет для вас открытием, полным ярких примеров и впечатляющих достижений. Подготовьтесь быть вовлеченными и удивленными каждый раз, когда продолжите читать.
Ознакомиться с деталями – врач нарколог выезд на дом
where can i buy nitroglycerin online · May 7, 2026 at 2:29 am
where to get generic nitroglycerin without rx
Tyronejaf · May 7, 2026 at 2:53 am
One of the most polished slots available for Canadians. https://smaislamsuryabuana.sch.id/product/quantum-theory/
Tyronejaf · May 7, 2026 at 2:53 am
I love the Egyptian vibes mixed with the cats, very creative. https://thedotmagazine.co.uk/genesis-technology-explained/
Tyronejaf · May 7, 2026 at 3:22 am
I love how the wilds stay sticky during the entire bonus. https://tech.etaxdial.com/2021/06/08/1800-number-to-cash-app/
Allentof · May 7, 2026 at 3:28 am
Мы предлагаем вам окунуться в океан любопытных фактов и вдохновляющих историй. Эта публикация поможет расширить горизонты, разбудить интерес к науке и истории и увидеть мир с новой стороны.
Есть чему поучиться – вывод из запоя санкт петербург стационар
Donaldhog · May 7, 2026 at 4:10 am
Этот информативный текст отличается привлекательным содержанием и актуальными данными. Мы предлагаем читателям взглянуть на привычные вещи под новым углом, предоставляя интересный и доступный материал. Получите удовольствие от чтения и расширьте кругозор!
Изучить эмпирические данные – прокапаться на дому самара
WilliamNeaRa · May 7, 2026 at 4:15 am
Этот информационный материал собраны данные, которые помогут лучше понять текущие тенденции и процессы в различных сферах жизни. Мы предоставляем четкий анализ, графики и примеры, чтобы информация была не только понятной, но и практичной для принятия решений.
Читать дальше – вывод из запоя недорого
Vincentalare · May 7, 2026 at 4:20 am
В этой статье представлен занимательный и актуальный контент, который заставит вас задуматься. Мы обсуждаем насущные вопросы и проблемы, а также освещаем истории, которые вдохновляют на действия и изменения. Узнайте, что стоит за событиями нашего времени!
Более того — здесь – вывод из запоя в клинике
Tyronejaf · May 7, 2026 at 4:36 am
Cleocatra Slot Canada never fails to entertain. https://statueparlanti.eu/assumenda-tenetur-odit-aut-fugit/
Tyronejaf · May 7, 2026 at 4:36 am
One of the most polished slots available for Canadians. https://redgifpro.com/the-world-of-confused-gif/
Stevenalbut · May 7, 2026 at 4:42 am
Наша клиника предлагает полный цикл услуг — от экстренного вызова нарколога до долгосрочной реабилитации. Каждый этап разрабатывается индивидуально с учётом возраста, стажа зависимости и сопутствующих заболеваний. Современные протоколы 2026 года позволяют проводить лечение максимально комфортно и эффективно, минимизируя болезненные симптомы и снижая риск срывов. В этом виде деятельности мы используем только проверенные методы медицины.
Подробнее тут – нарколог на дом вывод в екатеринбурге
Tyronejaf · May 7, 2026 at 5:04 am
I appreciate the clear paytable and transparent rules. https://shanghai-ydtech.com/oil-cooler/
Cheapest SMM Panel Tanzania · May 7, 2026 at 5:13 am
Thank you for sharing this very good post. Very interesting ideas! (as always, btw)
DennisFlide · May 7, 2026 at 5:19 am
Эта обзорная заметка содержит ключевые моменты и факты по актуальным вопросам. Она поможет читателям быстро ориентироваться в теме и узнать о самых важных аспектах сегодня. Получите краткий курс по современной информации и оставайтесь в курсе событий!
Неизвестные факты о… – капельница от похмелья самара
CarmeloVaf · May 7, 2026 at 5:19 am
В Нижнем Тагиле выездные бригады дежурят 24/7. Координатор уже при первичном звонке собирает ключевые сведения: аллергии, хронические заболевания, список постоянных препаратов, эпизоды судорог или алкогольных психозов в прошлом, последние значения давления и пульса, возможность обеспечить тишину на 2–3 часа, доступ к питьевой воде, особенности подъезда. Вся эта информация помогает врачу подготовить стартовую схему — от выбора профиля инфузии до темпа введения. По запросу организуем немаркированный визит и сдержанные формулировки в документах, чтобы не создавать лишнего внимания со стороны соседей и коллег.
Детальнее – вывод из запоя клиника нижний тагил
AlfredTog · May 7, 2026 at 5:21 am
В этой статье обсуждаются актуальные медицинские вопросы, которые волнуют общество. Мы обращаем внимание на проблемы, касающиеся здравоохранения и лечения, а также на новшества в области медицины. Читатели будут осведомлены о последних событиях и смогут следить за тенденциями в медицине.
Провести детальное исследование – вывод из запоя с кодированием на дому
Best SMM Panel Ghana · May 7, 2026 at 5:23 am
Substantially, the post is really the best on this laudable topic. I concur with your conclusions and will eagerly watch forward to your future updates.Just saying thanx will not just be enough, for the wonderful lucidity in your writing.
BrianTrear · May 7, 2026 at 5:42 am
На порталі https://visti.pl.ua зібрані головні новини Полтави та області. Тут публікують матеріали про події, транспорт, інфраструктуру та життя регіону.
JoshuaLip · May 7, 2026 at 5:54 am
Сайт https://news.vinnica.ua висвітлює події у Вінниці та регіоні. Новини, аналітика й корисні матеріали допомагають бути в курсі життя міста щодня.
Edwincok · May 7, 2026 at 5:57 am
Этот обзор сосредоточен на различных подходах к избавлению от зависимости. Мы изучим традиционные и альтернативные методы, а также их сочетание для достижения максимальной эффективности. Читатели смогут открыть для себя новые стратегии и подходы, которые помогут в их борьбе с зависимостями.
Расширить кругозор по теме – нарколог на дом вывод из запоя самара
Tyronejaf · May 7, 2026 at 5:59 am
Safe and secure platform for playing with real stakes. https://equestfile.com/wowour-customers-love-us/
best paying online casino australia · May 7, 2026 at 6:58 am
I just sent this post to a bunch of my friends as I agree with most of what you’re saying here and the way you’ve presented it is awesome.
legális magyar online kaszinó · May 7, 2026 at 7:07 am
Hiya, I am really glad I have found this information. Nowadays bloggers publish only about gossip and net stuff and this is actually frustrating.
online kaszinó · May 7, 2026 at 7:08 am
Thanks for your patience and sorry for the inconvenience!
online casino greece · May 7, 2026 at 7:11 am
Can I just say what a relief to seek out someone who actually knows what theyre speaking about on the internet. You positively know find out how to bring a problem to mild and make it important. Extra individuals have to read this and perceive this side of the story. I cant believe youre not more in style because you positively have the gift.
top online casinos nz · May 7, 2026 at 7:13 am
When we look at these issues, we know that they are the key ones for our time.
neue casinos · May 7, 2026 at 7:18 am
You ma’am have a way with words. Thank you very much!
Tyronejaf · May 7, 2026 at 7:24 am
Always a thrill to play Cleocatra slot after a long work day. https://birastart.co.jp/sample-post5/
Tyronejaf · May 7, 2026 at 7:24 am
Cleocatra for real money in Canada is a top-tier gaming choice. https://acafoods.com/biomass-energy/
Tyronejaf · May 7, 2026 at 7:25 am
One of the most polished slots available for Canadians. https://congresooaxacacomunicacionsocial.info/llama-congreso-a-verificar-que-cajones-de-estacionamiento-en-la-capital-cuentan-con-los-permisos-necesarios/
Tyronejaf · May 7, 2026 at 7:58 am
Cleocatra Slot Canada never fails to entertain. https://frozenthaispa.com/top-15-spa-centers-in-dhaka/
top rated online casino australia · May 7, 2026 at 8:12 am
I love your blog. It looks every informative.
Michaeljom · May 7, 2026 at 8:31 am
Этот увлекательный информационный материал подарит вам массу новых знаний и ярких эмоций. Мы собрали для вас интересные факты и сведения, которые обогатят ваш опыт. Откройте для себя увлекательный мир информации и насладитесь процессом изучения!
Тыкай сюда — узнаешь много интересного – услуги нарколога на дому цена
Henrytag · May 7, 2026 at 8:35 am
На порталі https://krivoy-rog.in.ua зібрані головні новини Кривого Рогу. Тут публікують матеріали про події, транспорт, інфраструктуру та життя мешканців.
Craigbiast · May 7, 2026 at 8:37 am
В статье представлены ключевые моменты по актуальной теме, дополненные советами экспертов и ссылками на дополнительные ресурсы. Цель материала — дать читателю инструменты для самостоятельного развития и принятия осознанных решений.
Тыкай сюда — узнаешь много интересного – вывод из запоя круглосуточно
ThomasCrich · May 7, 2026 at 8:47 am
На сайті https://gazeta-bukovyna.cv.ua публікують свіжі новини Буковини та Чернівців. Тут ви знайдете актуальну інформацію про події, життя регіону, культуру й важливі зміни для мешканців.
neue online casinos · May 7, 2026 at 9:33 am
Dude.. I am not much into reading, but somehow I got to read lots of articles on your blog. Its amazing how interesting it is for me to visit you very often. –
online casino nz · May 7, 2026 at 9:44 am
I think other website proprietors should take this web site as an model, very clean and great user pleasant style and design .
CharlesExent · May 7, 2026 at 10:16 am
Запой сопровождается выраженной интоксикацией, нарушением сна, слабостью, тревожностью и колебаниями давления, что характерно для алкоголизма и других форм зависимости. При этом самостоятельный выход из состояния часто оказывается затруднённым из-за ухудшения самочувствия и невозможности контролировать симптомы. В таких случаях выезд нарколога позволяет начать лечение без задержек и помочь пациенту снизить нагрузку на организм за счёт отсутствия транспортировки.
Подробнее тут – https://vyvod-iz-zapoya-na-domu-sankt-peterburg-8.ru
RobertReoda · May 7, 2026 at 10:42 am
На сайте https://chernomorskoe.info собраны новости Черноморского побережья и информация о курортных городах Одесской области. Узнавайте о событиях, отдыхе и развитии региона.
Woodrowenego · May 7, 2026 at 10:54 am
На портале https://o-remonte.com вы найдёте статьи о ремонте, дизайне и строительстве. Сайт предлагает практичные решения, рекомендации и идеи для создания уютного пространства.
Stevenalbut · May 7, 2026 at 11:11 am
Срочный вызов нарколога на дом позволяет сразу оценить состояние пациента, снять симптомы абстиненции и начать детоксикацию организма. Капельницы от запоя и интоксикации составляются индивидуально с учётом новейших медицинских протоколов 2026 года: они включают нейропротекторы, гепатопротекторы и витаминно-минеральные комплексы последнего поколения. Это не просто очищение крови — это восстановление работы мозга, печени, сердечно-сосудистой системы и психики. Вызов нарколога на дом особенно востребован, когда требуется срочное снятие абстинентного синдрома. Круглосуточная помощь работает без перерывов, поэтому помощь приезжает даже ночью. Мы предлагаем возможность вывода из запоя в домашних условиях.
Получить больше информации – запой нарколог на дом в екатеринбурге
top rated online casino australia · May 7, 2026 at 11:40 am
How come you do not have your website viewable in mobile format? cant see anything in my Droid.
Andrewsap · May 7, 2026 at 11:55 am
Затяжной запой перестает быть бытовой проблемой в тот момент, когда организм теряет способность самостоятельно восстанавливаться после интоксикации. Накопление ацетальдегида, нарушение водно-электролитного баланса, истощение запасов витаминов и перегрузка сердечно-сосудистой системы создают состояние, при котором домашние методы перестают быть безопасными. Срочно стабилизировать самочувствие и быстро купировать абстинентный синдром позволяет только контролируемая медицинская среда. Вывод из запоя в стационаре в Нижнем Новгороде становится клинически обоснованным решением, когда требуется не просто снятие симптомов, а комплексная детоксикация под круглосуточным наблюдением врачей. Наркологическая клиника «Стармед» организует процесс лечения в соответствии с актуальными стандартами доказательной медицины, обеспечивая безопасность пациента, прозрачность процедур и плавный переход к противорецидивной терапии. Мы понимаем, что решение о госпитализации часто принимается в состоянии стресса, поэтому наша работа начинается с четкой диагностики, честного объяснения плана лечения и соблюдения строгих протоколов конфиденциальности. Опытные специалисты клиники помогут вызвать доверие к процессу восстановления уже на этапе первого контакта.
Получить дополнительные сведения – наркология вывод из запоя в стационаре нижний новгород
DannyLiawn · May 7, 2026 at 12:02 pm
В этой статье мы рассматриваем разные способы борьбы с алкогольной зависимостью. Обсуждаются методы лечения, программы реабилитации и советы для поддержки близких. Читатели получат информацию о том, как преодолеть зависимость и добиться успешного выздоровления.
Лови подробности – вывод из запоя на дому недорого
SMM Panel Uganda · May 7, 2026 at 12:22 pm
Most often since i look for a blog Document realize that the vast majority of blog pages happen to be amateurish. Not so,We can honestly claim for which you writen is definitely great and then your webpage rock solid.
roof cleaning · May 7, 2026 at 12:24 pm
There is perceptibly a lot to identify about this. I consider you made some good points in features also.
grindu betonavimas kaina · May 7, 2026 at 12:30 pm
I just couldn’t leave your website before suggesting that I really enjoyed the usual information an individual supply on your visitors? Is gonna be back often in order to investigate cross-check new posts
Samuelcag · May 7, 2026 at 12:44 pm
На сайте https://blogimam.com публикуют статьи для мам о воспитании детей, здоровье и повседневной жизни. Полезные советы, личный опыт и идеи помогают справляться с заботами и находить время для себя.
Allentof · May 7, 2026 at 1:09 pm
Эта информационная статья охватывает широкий спектр актуальных тем и вопросов. Мы стремимся осветить ключевые факты и события с ясностью и простотой, чтобы каждый читатель мог извлечь из нее полезные знания и полезные инсайты.
Получить дополнительную информацию – вывод из запоя в стационаре спб
DanielCab · May 7, 2026 at 1:30 pm
В этой статье-обзоре мы соберем актуальную информацию и интересные факты, которые освещают важные темы. Читатели смогут ознакомиться с различными мнениями и подходами, что позволит им расширить кругозор и глубже понять обсуждаемые вопросы.
Получить дополнительные сведения – выезд нарколога на дом цена
JorgeTreta · May 7, 2026 at 1:47 pm
Капельница от похмелья в Воронеже с устранением слабости, тошноты и головной боли в наркологической клинике «Похмельная служба»
Детальнее – капельница от похмелья анонимно в воронеже
Thomasjam · May 7, 2026 at 2:04 pm
Капельница от похмелья в Воронеже с индивидуальной инфузионной терапией и врачебным контролем в наркологической клинике «Похмельная служба»
Подробнее тут – http://kapelnicza-ot-pokhmelya-voronezh-8.ru/
AlfredJew · May 7, 2026 at 2:16 pm
Эта статья погружает вас в увлекательный мир знаний, где каждый факт становится открытием. Мы расскажем о ключевых исторических поворотных моментах и научных прорывах, которые изменили ход цивилизации. Поймите, как прошлое формирует настоящее и как его уроки могут помочь нам строить будущее.
Детальнее – вызвать нарколога на дом
Donaldembab · May 7, 2026 at 2:18 pm
Отдельно стоит выделить ситуации, когда семья сталкивается не только с алкоголем, но и с употреблением наркотиков. В таких случаях врачебная консультация особенно важна, поскольку последствия интоксикации могут отличаться, а признаки наркомании и алкоголизма иногда накладываются друг на друга. Если речь идет о смешанном употреблении, подход к помощи на дому требует особой осторожности.
Изучить вопрос глубже – нарколог на дом цена в екатеринбурге
AlvinCet · May 7, 2026 at 2:21 pm
Вывод из запоя на дому — это формат медицинской помощи, при котором лечение проводится в привычной для пациента обстановке с использованием инфузионной терапии и врачебного контроля. Такой подход позволяет начать детоксикацию без задержек и снизить нагрузку на организм, связанную с транспортировкой. В наркологической клинике «Частный медик 24» выезд специалиста организуется круглосуточно, а терапия подбирается с учётом текущего состояния пациента.
Разобраться лучше – http://vyvod-iz-zapoya-na-domu-sankt-peterburg-11.ru
Huberterora · May 7, 2026 at 2:36 pm
Вывод из запоя на дому в Екатеринбурге: круглосуточная помощь, снятие симптомов и поддержка специалистов в наркологической клинике «Детокс»
Выяснить больше – нарколог на дом вывод из запоя екатеринбург
DanielCab · May 7, 2026 at 2:52 pm
Публикация приглашает вас исследовать неизведанное — от древних тайн до современных достижений науки. Вы узнаете, как случайные находки превращались в революции, а смелые мысли — в новые эры человеческого прогресса.
Получить дополнительные сведения – вызвать врача нарколога на дом москва недорого
Robertfet · May 7, 2026 at 3:38 pm
К показаниям относятся: запой длительностью более 72 часов, выраженная абстиненция с тахикардией, артериальной гипертензией, профузным потоотделением, наличие в анамнезе алкогольных делириев или судорожных эпизодов, сопутствующие хронические заболевания печени, сердца, поджелудочной железы. При тяжелых формах интоксикации, когда в организме накапливаются токсичные продукты распада веществ, резкое прекращение употребления без медицинской поддержки может спровоцировать отек мозга, острую сердечную недостаточность или желудочно-кишечное кровотечение. Стационар позволяет провести полноценную диагностику, включая ЭКГ, экспресс-анализы крови и мониторинг сатурации, что формирует точную картину состояния и исключает шаблонные назначения. В случаях сочетанной зависимости, когда в анамнезе присутствует наркомании, протоколы детоксикации адаптируются под специфику психоактивных соединений и включают усиленный нейрологический контроль.
Подробнее – стационар вывод из запоя
online kaszinó · May 7, 2026 at 3:43 pm
I wanted to check up and let you know how, a great deal I cherished discovering your blog today. I might consider it an honor to work at my office and be able to utilize the tips provided on your blog and also be a part of visitors’ reviews like this. Should a position associated with guest writer become on offer at your end, make sure you let me know.
online casino εξωτερικου · May 7, 2026 at 3:44 pm
Our family had similar issues, thanks.
CharlesRecok · May 7, 2026 at 3:48 pm
Наиболее частыми причинами обращения становятся выраженная слабость, тремор, нарушение сна, тревога, учащенный пульс, скачки артериального давления, тошнота и признаки обезвоживания. Эти симптомы могут сочетаться между собой и усиливаться после прекращения употребления алкоголя, особенно после нескольких дней запоя.
Исследовать вопрос подробнее – врач нарколог на дом екатеринбург
online casino greece · May 7, 2026 at 3:51 pm
When are you going to post again? You really entertain me!
online casino εξωτερικου · May 7, 2026 at 3:57 pm
You are one talented writer thank you for the post.
online casino deutschland · May 7, 2026 at 4:02 pm
Amazing article, cheers, I will bookmark you now.
Timothyser · May 7, 2026 at 4:42 pm
Такие состояния требуют профессионального вмешательства, так как без лечения могут усиливаться и приводить к ухудшению самочувствия. При этом помощь может предоставляться анонимно, в соответствии с политикой конфиденциальности данных пациента.
Получить дополнительные сведения – вывод из запоя на дому круглосуточно санкт-петербург
Jeffreyjoymn · May 7, 2026 at 4:54 pm
В этом обзоре представлены различные методы избавления от зависимости, включая терапевтические и психологические подходы. Мы сравниваем их эффективность и предоставляем рекомендации для тех, кто хочет вернуться к трезвой жизни. Читатели смогут найти информацию о реабилитационных центрах и поддерживающих группах.
Погрузиться в детали – врача капельницу от запоя
higit pang impormasyon · May 7, 2026 at 5:07 pm
Fortune Ox stays hot in 2026, multipliers showing up early in evening sessions.
Thomashen · May 7, 2026 at 5:19 pm
Вывод из запоя на дому с детоксикацией в Екатеринбурге представляет собой сложную медицинскую процедуру, направленную на очищение организма от токсинов и восстановление нормального состояния пациента. Важной частью этого процесса является контроль врача, который следит за состоянием пациента, регулирует дозировку препаратов и корректирует лечение по мере необходимости. Процедура обычно включает в себя использование инфузионных растворов, витаминов и медикаментов, направленных на стабилизацию физического состояния пациента и облегчение симптомов абстиненции.
Подробнее – анонимный вывод из запоя на дому екатеринбург
Ronniegof · May 7, 2026 at 5:34 pm
Эта статья освещает различные аспекты освобождения от зависимости и пути к выздоровлению. Мы обсуждаем важность осознания своей проблемы и обращения за помощью. Читатели получат практические советы о том, как преодолевать трудности и строить новую жизнь без зависимости.
Раскрыть тему полностью – капельница от запоя
Donaldembab · May 7, 2026 at 5:38 pm
Чаще всего нарколога на дом вызывают при повторяющемся или длительном запое, тяжелом похмелье, бессоннице после алкоголя, треморе, выраженной слабости и ухудшении общего самочувствия. Поводом для обращения также становятся тревога, раздражительность, скачки артериального давления, учащенный пульс, обезвоживание и необходимость поставить капельницу дома под наблюдением специалиста. Во многих случаях звонок в наркологический центр поступает тогда, когда родственники понимают, что состояние больного уже не позволяет ждать следующего дня.
Подробнее можно узнать тут – врач нарколог на дом
Craigbiast · May 7, 2026 at 5:48 pm
Эта публикация погружает вас в мир увлекательных фактов и удивительных открытий. Мы расскажем о ключевых событиях, которые изменили ход истории, и приоткроем завесу над научными достижениями, которые вдохновили миллионы. Узнайте, чему может научить нас прошлое и как применить эти знания в будущем.
Все материалы собраны здесь – вывести из запоя цена
top rated online casino australia · May 7, 2026 at 5:48 pm
I have to say this post was certainly informative and contains useful content for enthusiastic visitors. I will definitely bookmark this website for future reference and further viewing. cheers a bunch for sharing this with us!
Everetttam · May 7, 2026 at 5:52 pm
Эта услуга позволяет людям, которые не могут или не хотят покидать свой дом, получить профессиональную помощь и избавиться от зависимости без госпитализации. К тому же, вывод из запоя на дому позволяет избежать стресса, связанного с нахождением в медицинских учреждениях, при этом можно заказать вызов специалистов с учетом их опыта и лет работы, а также данных больного.
Подробнее тут – вывод из запоя на дому цена екатеринбург
top rated online casino australia · May 7, 2026 at 5:52 pm
The post is absolutely fantastic! Lots of great info and inspiration, both of which we all need! Also like to admire the time and effort you put into your website and detailed info you offer! I will bookmark your website!
DonaldLiz · May 7, 2026 at 6:56 pm
Капельница от похмелья — это медицинская процедура, направленная на быстрое устранение симптомов алкогольной интоксикации и восстановление нормальной работы организма. При выраженном похмельном синдроме самостоятельные методы часто оказываются недостаточными, поскольку не воздействуют на причины состояния. В наркологической клинике «Похмельная служба» используется инфузионная терапия с круглосуточным выездом специалиста, что позволяет начать лечение сразу после обращения.
Получить больше информации – http://kapelnicza-ot-pokhmelya-voronezh-7.ru/
CharlesExent · May 7, 2026 at 7:04 pm
К основным показаниям относятся:
Получить дополнительные сведения – вывод из запоя на дому анонимно санкт-петербург
CharlesRecok · May 7, 2026 at 7:06 pm
За выездом врача обращаются в тех случаях, когда человеку тяжело добраться до клиники, он ослаблен после нескольких дней употребления спиртного или родственникам важно быстрее получить медицинскую консультацию на месте. После осмотра определяют, допустим ли домашний формат, требуется ли капельница, достаточно ли наблюдения на дому или нужен другой объем помощи. Если эпизоды повторяются, в дальнейшем могут обсуждаться лечение алкоголизма, кодирование, участие психолога, реабилитация и более широкая программа помощи при зависимости. Уже на этапе первичного обращения нередко уточняют, как вызвать специалиста, какие услуги доступны на дому и в каких случаях вывод из запоя рассматривают не дома, а в стационаре.
Ознакомиться с деталями – https://narkolog-na-dom-ekaterinburg.ru
Jerrydes · May 7, 2026 at 7:43 pm
В данной обзорной статье представлены интригующие факты, которые не оставят вас равнодушными. Мы критикуем и анализируем события, которые изменили наше восприятие мира. Узнайте, что стоит за новыми открытиями и как они могут изменить ваше восприятие реальности.
Погрузиться в детали – вывод из запоя цена
Charlesunpat · May 7, 2026 at 7:51 pm
Затяжной запой — это не бытовая слабость, а медицинское состояние, требующее профессионального лечения в условиях стационара. Когда организм истощен длительной интоксикацией, нарушен сон, отсутствует аппетит, а попытки самостоятельно прекратить употребление сопровождаются тремором, тревогой и скачками давления, единственным безопасным решением становится контролируемая детоксикация. Наркологическая клиника «Элегия Мед» в Санкт-Петербурге предоставляет профессиональное лечение с применением сертифицированных протоколов, непрерывный контроль состояния пациента и индивидуальный подбор медикаментозной поддержки. Мы работаем круглосуточно, обеспечивая быстрое реагирование на обращения, четкую диагностику при поступлении и прозрачное взаимодействие с родственниками. Все процедуры выполняются с соблюдением протоколов доказательной медицины, стандартов Минздрава РФ и строгих правил конфиденциальности. Первичная оценка состояния начинается с дистанционной консультации, что позволяет врачам заранее подготовить необходимое оборудование и скорректировать план госпитализации еще до прибытия пациента. При необходимости заказать консультацию или оформить выезд бригады, доступные способы связи включают телефон, мессенджеры и онлайн-форму на сайте.
Получить больше информации – стационар вывод из запоя в санкт-петербурге
vadiloaltef · May 7, 2026 at 7:51 pm
«Киндер» — семейная клиника в Москве с широким профилем: педиатрия, терапия, гинекология и аллергология для пациентов любого возраста. Клиника работает по лицензии Л041-01137-77/00763335 и объединяет опытных специалистов со стажем от 10 до 35 лет. На https://kinder-medcenter.ru/ можно записаться к врачу онлайн и ознакомиться с полным прейскурантом услуг. Расположение на улице Лавриненко вблизи станций метро Некрасовка и Лухмановская обеспечивает удобный доступ для пациентов из восточных районов города и Люберец.
ChangPar · May 7, 2026 at 8:07 pm
Этот информационный материал собраны данные, которые помогут лучше понять текущие тенденции и процессы в различных сферах жизни. Мы предоставляем четкий анализ, графики и примеры, чтобы информация была не только понятной, но и практичной для принятия решений.
Лови подробности – капельница от запоя вызов
daxunrar · May 7, 2026 at 8:07 pm
Компания «Хронос» выпускает и поставляет сертифицированную медицинскую продукцию собственного изготовления: голосообразующие аппараты, бактерицидные рециркуляторы, облучатели против кожных заболеваний, трахеостомические трубки и ультрафиолетовые лампы. Ищете медицинская техника оптом? На сайте agsvv.ru доступны оптовые и розничные поставки напрямую с завода ЛЭМЗ в Санкт-Петербурге с официальной гарантией качества и доставкой по всей России. с подтверждённым качеством и логистикой до любого региона Российской Федерации.
WilfredDot · May 7, 2026 at 8:08 pm
В этой статье мы рассмотрим современные достижения в области медицины, включая инновационные методы лечения и диагностики. Мы обсудим важность профилактики заболеваний и роль технологий в улучшении качества здравоохранения. Читатели узнают о влиянии медицины на повседневную жизнь и ее значение для современного общества.
Не упусти важное! – нарколог на дом екатеринбург
WilliamSor · May 7, 2026 at 8:09 pm
Этот информативный текст сочетает в себе темы здоровья и зависимости. Мы обсудим, как хронические заболевания могут усугубить зависимости и наоборот, как зависимость может влиять на общее состояние здоровья. Читатели получат представление о комплексном подходе к лечению как физического, так и психического состояния.
А есть ли продолжение? – врач нарколог выезд на дом
PedroNefeP · May 7, 2026 at 8:12 pm
Эта информационная статья охватывает широкий спектр актуальных тем и вопросов. Мы стремимся осветить ключевые факты и события с ясностью и простотой, чтобы каждый читатель мог извлечь из нее полезные знания и полезные инсайты.
Изучить эмпирические данные – прокапаться на дому
DavidSlern · May 7, 2026 at 8:12 pm
В этой статье собраны факты, которые освещают целый ряд важных вопросов. Мы стремимся предложить читателям четкую, достоверную информацию, которая поможет сформировать собственное мнение и лучше понять сложные аспекты рассматриваемой темы.
Заходи — там интересно – вывести из запоя капельница на дому
BrandonRoada · May 7, 2026 at 8:32 pm
За выездом врача чаще обращаются тогда, когда человеку тяжело добраться до клиники, он ослаблен после нескольких дней употребления алкоголя или родственникам важно быстрее понять, какая тактика будет безопасной. После осмотра можно определить, нужна ли капельница, достаточно ли детоксикации на дому, требуется ли повторное наблюдение, а в дальнейшем — консультация по лечению алкоголизма, кодирование или реабилитация. В части случаев уже первый звонок позволяет понять, идет ли речь только о временном ухудшении самочувствия или о состоянии, при котором может потребоваться вывод из запоя в стационаре.
Подробнее тут – врач нарколог на дом в екатеринбурге
Timothyser · May 7, 2026 at 8:38 pm
Вывод из запоя на дому в Санкт-Петербурге с анонимным выездом врача, снятием интоксикации и поддержкой в наркологической клинике «Частный медик 24»
Подробнее тут – нарколог на дом вывод из запоя санкт-петербург
mifemeVowly · May 7, 2026 at 8:45 pm
Ищете слушать музыку онлайн? Откройте muzqeen.cc и окунитесь в мир музыки: здесь собрана гигантская коллекция треков всех жанров и направлений, включая горячие новинки. На сайте можно скачать mp3 на компьютер и телефон. Только лучшая музыка собрана на нашем портале. Добавьте наш портал в избранное и первыми узнавайте о новых релизах ваших любимых групп и артистов!
yuxernfor · May 7, 2026 at 8:47 pm
Чистая вода дома — не роскошь, а норма, которую теперь легко обеспечить. PWS создаёт бытовые системы очистки воды без расходных картриджей и импортных зависимостей. На https://pws.world/bytovye-ustanivki представлены установки серии КСВ, которые снижают жёсткость в 10–20 раз, устраняют железо, запах и мутность. Системы проектируются под состав воды в вашем регионе. Инженеры компании сами консультируют клиентов и подбирают оптимальное решение под любой бюджет.
xoaldek · May 7, 2026 at 9:03 pm
Рабочие команды регулярно теряют эффективность из-за беспорядка в задачах и процессах. Ищете сервис для распределения задач? Платформа pabit.ru решает эту проблему с помощью интуитивного интерфейса для управления проектами. В одном пространстве собраны задачи, циклы, модули, аналитика и страницы с умным редактором. Командные доски показывают прогресс без ручных отчётов. Pabit устраняет организационный хаос и даёт команде фокус на главном.
Andrewsap · May 7, 2026 at 9:08 pm
Домашняя детоксикация подходит для ранних стадий интоксикации, когда состояние пациента стабильно, а сопутствующие заболевания отсутствуют. Однако при длительном употреблении алкоголя физиологические изменения требуют более глубокого вмешательства. Стационар обеспечивает изоляцию от триггеров, исключает риск самостоятельного повторного употребления и позволяет врачам динамически корректировать терапию на основе лабораторных показателей и реакции организма. В 2026 году стандарты наркологической помощи делают акцент на превентивной безопасности: раннее выявление признаков делирия, судорожной готовности или кардиологических осложнений позволяет предотвратить критические состояния до их развития. Клиника «Стармед» выстроила работу так, чтобы каждый этап госпитализации логически вытекал из предыдущего, формируя непрерывную цепочку от острой стабилизации до планирования долгосрочной ремиссии.
Подробнее – вывод из запоя в стационаре клиника
LarrySmogy · May 7, 2026 at 9:10 pm
Решение о помещении пациента в стационар принимается на основе объективных медицинских критериев, а не только по желанию родственников. К прямым показаниям относятся: запой длительностью более 72 часов, выраженная абстиненция с тахикардией, стойкой артериальной гипертензией, профузным потоотделением и тремором, наличие в анамнезе перенесенных алкогольных делириев или судорожных эпизодов. В тяжелых случаях, когда интоксикация затрагивает несколько физиологических систем одновременно, резкое прекращение употребления без медицинской поддержки может спровоцировать отек головного мозга, острую сердечную недостаточность, панкреонекроз или желудочно-кишечное кровотечение. В таких случаях стационар позволяет провести полноценную диагностику, включая ЭКГ, экспресс-анализы крови, ультразвуковое исследование внутренних органов и мониторинг сатурации. Это формирует точную картину состояния, исключает шаблонные назначения и позволяет врачам динамически корректировать дозировки препаратов на основе лабораторных данных в реальном времени.
Исследовать вопрос подробнее – вывод из запоя в стационаре в нижнем новгороде
AlfredJew · May 7, 2026 at 9:15 pm
Эта статья предлагает уникальную подборку занимательных фактов и необычных историй, которые вы, возможно, не знали. Мы постараемся вдохновить ваше воображение и разнообразить ваш кругозор, погружая вас в мир, полный интересных открытий. Читайте и открывайте для себя новое!
Связаться за уточнением – вызвать нарколога на дом москва цены
dewawFal · May 7, 2026 at 9:22 pm
Современный зритель давно оценил удобство домашнего кинопросмотра, и платформа https://tv-goodfilms.ru/ стала для тысяч людей настоящим открытием. Здесь собраны фильмы и сериалы в HD-качестве 720 и 1080p — от классики до свежих премьер, — причём совершенно бесплатно, без регистрации и скрытых платежей. Сервис позволяет собирать личные коллекции, добавлять картины в список желаний и обсуждать просмотренное с друзьями. Никаких подписок и ограничений: просто выбирайте фильм и наслаждайтесь безупречным изображением прямо сейчас!
WilliamHIX · May 7, 2026 at 9:34 pm
В этом обзоре представлены различные методы избавления от зависимости, включая терапевтические и психологические подходы. Мы сравниваем их эффективность и предоставляем рекомендации для тех, кто хочет вернуться к трезвой жизни. Читатели смогут найти информацию о реабилитационных центрах и поддерживающих группах.
Смотрите также – капельница от алкоголя цена
cuzujinHes · May 7, 2026 at 9:41 pm
Устали от пыли и хаоса? Генеральная уборка квартиры вернет свежесть и порядок. Проводим уборку квартиры в Бресте https://xn—-9sbhrbbakeffzbd7a.xn--90ais/ качественно и быстро. Особый подход: уборка после ремонта — удалим цементную пыль, строительные остатки. Также нужна уборка в офисах? Поддержим чистоту в вашем бизнесе. Работаем профессионально, без лишних хлопот. Чистота и идеальный результат уже сегодня! Звоните!
Darrenprait · May 7, 2026 at 9:44 pm
Эта публикация погружает вас в мир увлекательных фактов и удивительных открытий. Мы расскажем о ключевых событиях, которые изменили ход истории, и приоткроем завесу над научными достижениями, которые вдохновили миллионы. Узнайте, чему может научить нас прошлое и как применить эти знания в будущем.
Изучить материалы по теме – наркология вывод из запоя
Everetttam · May 7, 2026 at 9:48 pm
Эта услуга позволяет людям, которые не могут или не хотят покидать свой дом, получить профессиональную помощь и избавиться от зависимости без госпитализации. К тому же, вывод из запоя на дому позволяет избежать стресса, связанного с нахождением в медицинских учреждениях, при этом можно заказать вызов специалистов с учетом их опыта и лет работы, а также данных больного.
Изучить вопрос глубже – вывод из запоя на дому круглосуточно в екатеринбурге
Jerrydes · May 7, 2026 at 10:16 pm
Эта публикация погружает вас в мир увлекательных фактов и удивительных открытий. Мы расскажем о ключевых событиях, которые изменили ход истории, и приоткроем завесу над научными достижениями, которые вдохновили миллионы. Узнайте, чему может научить нас прошлое и как применить эти знания в будущем.
Не упусти шанс – нарколог запой
Darrenprait · May 7, 2026 at 10:37 pm
Эта публикация погружает вас в мир увлекательных фактов и удивительных открытий. Мы расскажем о ключевых событиях, которые изменили ход истории, и приоткроем завесу над научными достижениями, которые вдохновили миллионы. Узнайте, чему может научить нас прошлое и как применить эти знания в будущем.
См. подробности – вывод из запоя круглосуточно
DonaldLiz · May 7, 2026 at 10:59 pm
В Воронеже круглосуточная помощь при похмелье востребована в ситуациях, когда симптомы появляются внезапно или усиливаются в ночное время, особенно в запое или после запоя. Врач проводит консультацию, оценивает состояние пациента и принимает решение о проведении инфузионной терапии. Такой подход позволяет своевременно устранить симптомы и предотвратить их дальнейшее развитие. При необходимости можно оставить заявку, уточнить цены или получить помощь бесплатно на первичном этапе.
Получить дополнительные сведения – http://kapelnicza-ot-pokhmelya-voronezh-7.ru/
免费Binance账户 · May 7, 2026 at 11:44 pm
Can you be more specific about the content of your article? After reading it, I still have some doubts. Hope you can help me. https://www.binance.info/register?ref=IHJUI7TF
Timothyelapy · May 7, 2026 at 11:48 pm
“buyuk yaprakl? cicekler” hakk?nda bilgi arayanlar icin burada harika bilgiler var. Suradan okuyabilirsiniz: https://evhobisi.com/articles/buyuk-yaprakli-ev-cicekleri-bakim-faydalari/
Timothyelapy · May 7, 2026 at 11:52 pm
“yemekten ne kadar sonra spor yap?l?r” hakk?nda bilgi arayanlar icin cok faydal? bir yaz? buldum. Kendiniz gorun: https://enerjiatlet.com/articles/yemek-sonrasi-spor-zamanlamasi/
online kaszinó · May 7, 2026 at 11:55 pm
Fantastic piece of writing here1
legális magyar online kaszinó · May 8, 2026 at 12:20 am
I think other website proprietors should take this web site as an model, very clean and great user pleasant style and design .
WilliamHIX · May 8, 2026 at 12:21 am
Текст посвящён распространённым мифам о зависимости и их развенчанию. Мы предоставим научно обоснованную информацию и дадим рекомендации по выбору эффективного способа борьбы с зависимым поведением.
Не пропусти важное – капельница от алкоголя цена
DannyLiawn · May 8, 2026 at 12:28 am
В этом обзоре мы обсудим современные методы борьбы с зависимостями, включая медикаментозную терапию и психотерапию. Мы представим последние исследования и их результаты, чтобы читатели могли быть в курсе наиболее эффективных подходов к лечению и поддержке.
Более того — здесь – прокапаться от алкоголя на дому самара
BrandonRoada · May 8, 2026 at 12:34 am
Отдельного внимания требуют случаи, когда больной почти не ест, плохо пьет воду, не может спокойно лежать, жалуется на сильное сердцебиение, нехватку сна или выраженное внутреннее напряжение. В такой ситуации осмотр помогает определить, безопасно ли оставаться дома и какого объема помощи достаточно на текущем этапе. Если речь идет о выраженных проявлениях абстинентного синдрома, затягивать с обращением нецелесообразно.
Разобраться лучше – запой нарколог на дом в екатеринбурге
Brianpus · May 8, 2026 at 12:36 am
Наиболее частыми основаниями для выбора такого формата становятся длительный запой, тяжелое течение похмельного синдрома, выраженный тремор, отсутствие сна, тревога, слабость, обезвоживание и жалобы на сердцебиение. Дополнительное значение имеют хронические заболевания сердца, сосудов, печени и нервной системы, на фоне которых выход из запоя может переноситься тяжелее.
Исследовать вопрос подробнее – вывод из запоя в стационаре клиника санкт-петербург
Thomasjam · May 8, 2026 at 12:37 am
Перед началом терапии врач проводит осмотр пациента. Измеряются основные показатели, включая давление и пульс, оценивается выраженность симптомов. На основании этих данных формируется состав капельницы и определяется тактика лечения, что позволяет эффективно провести вывод из запоя.
Детальнее – https://kapelnicza-ot-pokhmelya-voronezh-8.ru
JorgeTreta · May 8, 2026 at 12:38 am
В Воронеже капельница от похмелья применяется в ситуациях, когда симптомы выражены и не проходят самостоятельно, особенно после запоя или в запое. Врач проводит консультацию, оценивает состояние пациента, выраженность интоксикации и принимает решение о проведении процедуры. Важно, что лечение направлено не только на снятие симптомов, но и на восстановление организма после алкоголизма. При необходимости можно оставить заявку и уточнить цены или получить помощь бесплатно в рамках первичной консультации.
Получить больше информации – капельница от похмелья в воронеже
Huberterora · May 8, 2026 at 12:50 am
Процедура вывода из запоя на дому включает несколько этапов, каждый из которых имеет важное значение для общего улучшения состояния пациента. Главная цель — это не только устранение симптомов абстиненции, но и восстановление нормальной работы органов и систем организма. Врач, который проводит процедуру, использует медикаментозные средства для восстановления водно-солевого баланса, нормализации работы печени, почек и других органов, пострадавших от алкоголя. Также в процесс включаются препараты, которые способствуют снятию нервного напряжения и психоэмоционального стресса.
Исследовать вопрос подробнее – анонимный вывод из запоя на дому в екатеринбурге
AlvinCet · May 8, 2026 at 12:54 am
В Санкт-Петербурге вывод из запоя на дому используется в ситуациях, когда состояние пациента требует медицинской помощи, но позволяет обойтись без лечения в стационаре. Врач проводит консультацию, оценивает длительность запоя, выраженность симптомов и общее состояние, анализируя данные пациента, после чего принимает решение о тактике лечения при алкоголизме. При необходимости можно оформить вызов специалиста или заказать услугу заранее.
Узнать больше – вывод из запоя на дому цена санкт-петербург
Russellpessy · May 8, 2026 at 12:58 am
Наркологическая помощь нужна не только тогда, когда ситуация выглядит критической со стороны. Она необходима и в тех случаях, когда зависимость повторяется циклично, а семья уже понимает, что прежние способы не работают. Чем раньше человек переходит от стихийных попыток справиться самостоятельно к профессиональной тактике, тем выше шансы стоновить процесс на менее тяжелом этапе.
Получить дополнительные сведения – наркологическая помощь анонимно
LloydJew · May 8, 2026 at 1:05 am
Обзор посвящён процессу восстановления после зависимостей. Мы расскажем о различных этапах реабилитации, поддерживающих ресурсах и важности мотивации в достижении устойчивого выздоровления.
Подробности по ссылке – сделать капельницу от похмелья
LarrySmogy · May 8, 2026 at 1:22 am
Выбор между домашней помощью и стационарным лечением часто определяется степенью физиологической зависимости, наличием сопутствующих патологий и риском развития осложнений. В условиях клиники исключаются внешние триггеры, обеспечивается полная изоляция от источников психоактивных веществ и создается контролируемая терапевтическая среда, где медицинские решения принимаются на основе объективных диагностических показателей, а не субъективных ощущений пациента. Такой подход критически важен для предотвращения тяжелых осложнений, минимизации дискомфорта абстиненции и формирования устойчивой базы для дальнейшей противорецидивной работы.
Исследовать вопрос подробнее – https://vyvod-iz-zapoya-v-staczionare-nizhnij-novgorod-10.ru
neue online casinos · May 8, 2026 at 1:41 am
thank, I thoroughly enjoyed reading your article. I really appreciate your wonderful knowledge and the time you put into educating the rest of us.
neue online casinos · May 8, 2026 at 1:43 am
Sometimes, the sheer magnitude of the information seems overwhelming.
Francisnix · May 8, 2026 at 2:05 am
В этой статье рассматриваются актуальные вопросы, связанные с развитием медицинской науки и её внедрением в повседневную практику. Особое внимание уделено вопросам профилактики, ранней диагностики и использованию технологий для улучшения здоровья человека.
Ознакомьтесь с аналитикой – вызвать нарколога на дом анонимно
zixivoimarm · May 8, 2026 at 2:07 am
Москва по-настоящему раскрывается тем, кто решается взглянуть на неё с воды: Кремль, Храм Христа Спасителя, Новодевичий монастырь и футуристичный Москва-Сити выстраиваются в единую живую панораму прямо с борта теплохода. Сервис https://moscowmariner.ru/ предлагает более 200 маршрутов на 2026 год — от утренних экспрессов за 99 рублей до гастрономических круизов с ужином от шеф-повара и ночных прогулок под архитектурную подсветку набережных. Купить билет просто: выбираете дату, причал и формат, оплачиваете без комиссии любой картой — и мгновенно получаете PDF-ваучер с QR-кодом на почту, никаких касс и очередей.
LloydJew · May 8, 2026 at 2:09 am
Публикация посвящена жизненным историям людей, успешно справившихся с зависимостью. Мы покажем, что выход есть, и он начинается с первого шага — принятия проблемы и желания измениться.
Подробная информация доступна по запросу – снятие похмелья капельницей
magyar online kaszinó · May 8, 2026 at 2:10 am
Wish I’d thought of this. Am in the field, but I procrastinate alot and haven’t written as much as I’d like. Thanks.
Thomassak · May 8, 2026 at 2:20 am
Такой подход позволяет начать лечение без задержек и снизить риски, связанные с транспортировкой пациента. При этом помощь может предоставляться анонимно, что важно для многих пациентов.
Выяснить больше – https://vyvod-iz-zapoya-na-domu-sankt-peterburg-9.ru/
Thomasephed · May 8, 2026 at 2:24 am
Медицинская публикация представляет собой свод актуальных исследований, экспертных мнений и новейших достижений в сфере здравоохранения. Здесь вы найдете информацию о новых методах лечения, прорывных технологиях и их практическом применении. Мы стремимся сделать актуальные медицинские исследования доступными и понятными для широкой аудитории.
Лови подробности – наркология вызов на дом
打开Binance账户 · May 8, 2026 at 2:45 am
Your point of view caught my eye and was very interesting. Thanks. I have a question for you. https://www.binance.bh/futures/ref?code=IXBIAFVY
Robertseank · May 8, 2026 at 2:47 am
Предлагаем вашему вниманию интересную справочную статью, в которой собраны ключевые моменты и нюансы по актуальным вопросам. Эта информация будет полезна как для профессионалов, так и для тех, кто только начинает изучать тему. Узнайте ответы на важные вопросы и расширьте свои знания!
Нажмите, чтобы узнать больше – снятие похмелья капельницей
online casino · May 8, 2026 at 2:51 am
What i discover troublesome is to find a weblog that may capture me for a minute however your blog is different. Bravo.
Robertfet · May 8, 2026 at 2:54 am
Терапевтический процесс в стационаре строится по принципу последовательного выполнения клинических задач: диагностика, стабилизация, медикаментозная поддержка и подготовка к амбулаторному этапу. При поступлении врач проводит детальный осмотр, собирает анамнез, оценивает неврологический статус и при необходимости назначает лабораторные исследования. На основе полученных данных формируется индивидуальный протокол, учитывающий возраст, длительность интоксикации, наличие сопутствующих патологий и переносимость лекарственных компонентов. Мы применяем только сертифицированные препараты, зарегистрированные в РФ, и строго соблюдаем клинические рекомендации, исключая псевдонаучные методики. Стандарты оказания медицинской помощи фиксируются во внутренних регламентах и регулярно проверяются независимыми аудиторами.
Получить дополнительные сведения – стационар вывод из запоя
Francisnix · May 8, 2026 at 3:00 am
В данной публикации мы поговорим о процессе восстановления от зависимости, о том, как вернуть себе нормальную жизнь. Мы обсудим преодоление трудностей, значимость поддержки и наличие программ реабилитации. Читатели смогут узнать о ключевых шагах к успешному восстановлению.
Что ещё? Расскажи всё! – вызов врача нарколога на дом екатеринбург
Thomasephed · May 8, 2026 at 3:16 am
Этот текст посвящён сложным аспектам зависимости и её влиянию на жизнь человека. Мы обсудим психологические, физические и социальные последствия зависимого поведения, а также важность своевременного обращения за помощью.
Все материалы собраны здесь – нарколога домой
AnthonyNeday · May 8, 2026 at 3:28 am
Эта статья предлагает уникальную подборку занимательных фактов и необычных историй, которые вы, возможно, не знали. Мы постараемся вдохновить ваше воображение и разнообразить ваш кругозор, погружая вас в мир, полный интересных открытий. Читайте и открывайте для себя новое!
Не упусти шанс – капельница на дому район воронеж
JamesNex · May 8, 2026 at 3:34 am
В этой статье рассматриваются способы преодоления зависимости и успешные истории людей, которые справились с этой проблемой. Мы обсудим важность поддержки со стороны близких и профессионалов, а также стратегии, которые могут помочь в процессе выздоровления. Научитесь первоочередным шагам к новой жизни.
Доступ к полной версии – капельница на дому цена
DavidSlern · May 8, 2026 at 3:44 am
Эта статья сочетает познавательный и занимательный контент, что делает ее идеальной для любителей глубоких исследований. Мы рассмотрим увлекательные аспекты различных тем и предоставим вам новые знания, которые могут оказаться полезными в будущем.
Желаете узнать подробности? – капельница при алкогольной интоксикации цена
Jeffreyjoymn · May 8, 2026 at 4:21 am
В этой статье мы обсудим процесс восстановления после зависимостей, акцентируя внимание на различных методах и подходах к реабилитации. Читатели узнают, как создать план выздоровления и использовать полезные ресурсы для достижения устойчивых изменений.
Как достичь результата? – капельница при похмелье
Thomashen · May 8, 2026 at 4:23 am
Процедура вывода из запоя на дому включает несколько ключевых этапов, которые обеспечивают максимально быстрое и безопасное восстановление пациента. Эти этапы тщательно контролируются врачом, что минимизирует риски и помогает достичь наилучших результатов.
Подробнее – вывод из запоя на дому цена екатеринбург
AnthonyNeday · May 8, 2026 at 4:30 am
Эта статья предлагает уникальную подборку занимательных фактов и необычных историй, которые вы, возможно, не знали. Мы постараемся вдохновить ваше воображение и разнообразить ваш кругозор, погружая вас в мир, полный интересных открытий. Читайте и открывайте для себя новое!
Рассмотреть проблему всесторонне – прокапаться от алкоголя в воронеже
beste neue online casinos · May 8, 2026 at 4:35 am
Took me time to read the material, but I truly loved the article. It turned out to be very useful to me.
Brianpus · May 8, 2026 at 4:41 am
Стационарное наблюдение также целесообразно тогда, когда больному трудно соблюдать рекомендации дома, состояние быстро меняется или родственники не могут обеспечить полноценный контроль. В таких условиях медицинское сопровождение позволяет своевременно оценивать динамику и корректировать лечение. При выраженных психических нарушениях, тревожно-депрессивных проявлениях или изменении поведения к оценке состояния может подключаться психиатр, поскольку у части больных запой сопровождается не только соматическими, но и психическими осложнениями алкогольной зависимости.
Ознакомиться с деталями – http://www.domen.ru
online casino nz · May 8, 2026 at 4:50 am
Abnormal this put up is totaly unrelated to what I was searching google for, but it surely used to be listed at the first page. I suppose your doing one thing proper if Google likes you adequate to place you at the first page of a non similar search.
Russellpessy · May 8, 2026 at 5:31 am
Наркологическая помощь в Воронеже востребована в тех ситуациях, когда проблема с алкоголем или наркотическими веществами уже перестает быть эпизодом и начинает влиять на здоровье, поведение, работу, отношения с близкими и повседневную жизнь. Для одних семей поводом для обращения становится запой, который затягивается на несколько дней. Для других — тяжелое состояние после употребления, ломки, тревога, бессонница, дрожь, скачки давления, агрессия, потеря контроля над количеством выпитого или повторяющиеся срывы после попыток остановиться самостоятельно. Во всех этих случаях важна не формальная услуга, а реальная медицинская помощь со стороны квалифицированных специалистов, которая подбирается под состояние человека и помогает не только снять остроту ситуации, но и определить дальнейший маршрут лечения.
Подробнее можно узнать тут – наркологическая помощь на дому воронеж
muvaeTaisy · May 8, 2026 at 6:08 am
Visit https://yogaonlineapp.com/ and learn more about our mobile app for online and at-home yoga. Yoga Way is a modern yoga app designed for people who want to practice yoga anytime, anywhere. Explore dozens of practices and programs with expert video guidance!
Ronniegof · May 8, 2026 at 6:10 am
Эта статья освещает различные аспекты освобождения от зависимости и пути к выздоровлению. Мы обсуждаем важность осознания своей проблемы и обращения за помощью. Читатели получат практические советы о том, как преодолевать трудности и строить новую жизнь без зависимости.
Узнать из первых рук – капельница от запоя на дому
Thomassak · May 8, 2026 at 7:03 am
Такой подход позволяет начать лечение без задержек и снизить риски, связанные с транспортировкой пациента. При этом помощь может предоставляться анонимно, что важно для многих пациентов.
Получить дополнительную информацию – вывод из запоя на дому круглосуточно
Delbertavale · May 8, 2026 at 7:12 am
Очень удобный поиск по годам и жанрам, сразу нашел что хотел.http://kimnpark.net/gnu5/bbs/board.php?bo_table=2014Taiwan&wr_id=13728
Delbertavale · May 8, 2026 at 7:14 am
Отличный сайт, загружается быстро и рекламы по минимуму.http://ierpueblonuevo.edu.co/circulares/
Delbertavale · May 8, 2026 at 7:15 am
Самый адекватный кинотеатр из бесплатных на сегодняшний день.http://phx-design.fr/bonjour-tout-le-monde/
Carlosalope · May 8, 2026 at 7:43 am
Если симптомы похмелья становятся настолько выраженными, что мешают нормальному функционированию, капельница становится необходимостью. Это особенно важно, если организм не справляется с токсинами самостоятельно.
Подробнее можно узнать тут – http://kapelnicza-ot-pokhmelya-nizhnij-novgorod-2.ru
Delbertavale · May 8, 2026 at 8:11 am
Самый адекватный кинотеатр из бесплатных на сегодняшний день.https://about.zination.com/%D1%88%D0%B2%D0%B5%D1%86%D0%B8%D1%8F/best-high-rtp-slots-insights-from-a-casino-marketer-on-acquisition-trends/
Raymondviept · May 8, 2026 at 8:27 am
Непрерывный мониторинг витальных показателей — ключевое отличие стационарного формата. В палатах клиники «Элегия Мед» установлены системы отслеживания частоты пульса, сатурации, температуры и артериального давления, данные с которых автоматически передаются в электронную медицинскую карту. Медицинский персонал дежурит круглосуточно, что обеспечивает мгновенную реакцию на ухудшение состояния: коррекцию инфузионной терапии, введение симптоматических препаратов, привлечение смежных специалистов при необходимости. Такая организация процесса исключает хаотичное назначение средств и гарантирует, что каждый этап детоксикации проходит под строгим клиническим контролем. При необходимости применяются дополнительные методы очищения крови, включая плазмаферез, который эффективно помогает вывести стойкие токсины и метаболиты, не удаляемые стандартной инфузионной терапией.
Получить дополнительную информацию – стационар вывод из запоя в санкт-петербурге
HenryDyefe · May 8, 2026 at 8:31 am
Hello!
Transparency builds trust and we are proud of our open approach to business operations.
Our manual boosting method guarantees that no bots are used keeping your account safe.
The most complete information on the website – https://www.wow-power-leveling.org/WorldOfWarcraftRaces/best-wow-tank-class
wow gold seller, wow progression boost, wow gold for sale
wow power leveling org, wow leveling boost 2026, wow gear boost
Good luck and good gameplay!
WilfredDot · May 8, 2026 at 8:36 am
В этой статье рассматриваются различные аспекты избавления от зависимости, включая физические и психологические методы. Мы обсудим поддержку, мотивацию и стратегии, которые помогут в процессе выздоровления. Читатели узнают, как преодолеть трудности и двигаться к новой жизни без зависимости.
Прочитать подробнее – вызов врача нарколога на дом
ChangPar · May 8, 2026 at 8:41 am
Эта статья погружает вас в увлекательный мир знаний, где каждый факт становится открытием. Мы расскажем о ключевых исторических поворотных моментах и научных прорывах, которые изменили ход цивилизации. Поймите, как прошлое формирует настоящее и как его уроки могут помочь нам строить будущее.
Осуществить глубокий анализ – вызвать капельницу от запоя на дому
HenryDyefe · May 8, 2026 at 8:41 am
Good morning!
Our transparent pricing structure means no hidden fees or unexpected charges later on.
Our competitive pricing makes premium boosting accessible to players on various budgets easily.
The most complete information on the website – https://www.wow-power-leveling.org/
wow 1-70 boost, wow gold seller, wow 1-70 boost
gladiator boost wow, wow leveling boost 2026, wow rep boost
Good luck and good gameplay!
bojidtSoype · May 8, 2026 at 8:56 am
Visit https://forexvertex.com/ for comprehensive information on Forex, including current opportunities in developing countries and other useful information, such as a guide on calculating lot sizes. The site provides in-depth analysis on many Forex-related issues. The information will be useful for both beginners and experienced traders.
PedroNefeP · May 8, 2026 at 9:07 am
Этот интересный отчет представляет собой сборник полезных фактов, касающихся актуальных тем. Мы проанализируем данные, чтобы вы могли сделать обоснованные выводы. Читайте, чтобы узнать больше о последних трендах и значимых событиях!
Лови подробности – капельницы от запоя на дому воронеж
Delbertavale · May 8, 2026 at 9:29 am
Отличный сайт, загружается быстро и рекламы по минимуму.https://tap-clean.jp/?p=827
JamesNex · May 8, 2026 at 9:31 am
Этот обзор посвящен успешным стратегиям избавления от зависимости, включая реальные примеры и советы. Мы разоблачим мифы и предоставим читателям достоверную информацию о различных подходах. Получите опыт многообразия методов и найдите подходящий способ для себя!
Осуществить глубокий анализ – прокапаться от алкоголя воронеж цена
Delbertavale · May 8, 2026 at 9:38 am
Качество картинки супер, на большом экране выглядит отлично.https://www.jeanssobmedida.com.br/produto/calca-jeans-feminina-modelo-flare-com-cintura-alta-20079-40/
Delbertavale · May 8, 2026 at 9:42 am
Смотрю исторические сериалы, подборка великолепная.https://www.mensider.com/kvrt-pelayo-diaz-w-letniej-i-ekologicznej-kolekcji/
jiguleJam · May 8, 2026 at 10:10 am
Агентство Vgolos выпускает тексты по главным тематическим блокам — политика, экономика, бизнес, технологии, здоровье и криминал без смягчений и лишнего контента. Журналисты издания быстро откликаются на актуальные события и работают с фактами без предположений — от расследований в судебной сфере до анализа потребительских тенденций. Читайте проверенные новости на https://vgolos.org/ — украинское информационное агентство для аудитории ценящей достоверность и оперативность. Разделы культуры, повседневной жизни и технологий естественно расширяют острую редакционную повестку и превращают портал в полноценный ежедневный медиаресурс.
Delbertavale · May 8, 2026 at 10:45 am
Наконец-то нашла где смотреть турецкие сериалы без подвисаний.https://www.businesses.thehabeshaweb.com/ads/abdu-auto-reapir-and-body-shop-in-garland-texas/
Delbertavale · May 8, 2026 at 11:21 am
Плеер запоминает момент, где остановился, это жирный плюс.https://transrentalservice.com/conheca-nosso-guindaste-60-toneladas/
Delbertavale · May 8, 2026 at 11:42 am
Спасибо за новинки 2025 года, всегда держите руку на пульсе.https://elateliermistico.com/meditation-is-a-must-have-in-your-daily-yoga-practice/
Delbertavale · May 8, 2026 at 11:45 am
Наконец-то сайт, где не просят привязать карту для просмотра.https://hsxd.vn/ke-hoach-va-to-chuc-thi-cong-cac-cong-trinh-xay-dung-co-ban-nxb-da-nang-2007-ngo-van-dung-110-trang/
wukumOdorp · May 8, 2026 at 12:19 pm
Интернет магазин БАДов диетического и спортивного питания https://iherb-vitamin.ru/ Тюмень – это русский официальный сайт интернет магазин Ихерб IHERB . Занимаемся продажей спортивного питания и БАД из официального каталога Айхерб и предлагаем только проверенные пищевые добавки и продукцию по низким ценам. У нас можно купить добавки с айхерб в Тюмени или заказать в любой город России. Сделать заказ можно на сайте. Есть в наличии в России в Тюмени и доставляем из США под заказ. Доставим в Тюмени курьером или отправим в любой город России почтой, СДЭК и другими транспортными компаниями.
Delbertavale · May 8, 2026 at 12:44 pm
Часто смотрю тут ТНТшные шоу, когда пропускаю по телевизору.https://dimebreed.tv/view-our-work/broadcast/
Brianbot · May 8, 2026 at 12:49 pm
перенаправляется сюда Сайты даркнет
Delbertavale · May 8, 2026 at 1:41 pm
Турецкие мелодрамы добавляют раньше всех, обожаю вас!https://www.zhukovskiy.alicante.kitchen/product/komod-v-spalnju-olivija/
Delbertavale · May 8, 2026 at 1:41 pm
Выбор комедий шикарный, каждые выходные залипаем всей семьей.https://xpercent.eu/ahoj-svet/
Delbertavale · May 8, 2026 at 1:47 pm
Подсела на китайские дорамы благодаря вашей подборке.http://miklagaard.no/index.php?title=User:JaclynUtter352
najlepsze kasyno online · May 8, 2026 at 2:34 pm
Just came from google to your website have to say thanks.
najlepsze kasyno online · May 8, 2026 at 2:38 pm
I like your style!
Thomashep · May 8, 2026 at 2:43 pm
В этой статье представлен занимательный и актуальный контент, который заставит вас задуматься. Мы обсуждаем насущные вопросы и проблемы, а также освещаем истории, которые вдохновляют на действия и изменения. Узнайте, что стоит за событиями нашего времени!
Получить больше информации – капельница от похмелья воронеж
Delbertavale · May 8, 2026 at 2:51 pm
Круто, что можно смотреть все сезоны подряд без лишних кликов.https://www.scti.sc.gov.br/scgames/2024/06/19/ola-mundo/
V9Bet · May 8, 2026 at 4:04 pm
Keep it up!. I usually don’t post in Blogs but your blog forced me to, amazing work.. beautiful A rise in An increase in An increase in.
lajuresycle · May 8, 2026 at 4:05 pm
Программа RASCET решает задачу градуировки резервуаров геометрическим методом: вы вводите размеры ёмкости — программа рассчитывает точную градуировочную таблицу для 26 видов ёмкостей с погрешностью до 0,000001%. На https://rascet.ru/ доступна демо-версия 4.1 с сохранением таблиц в Excel. Вычисления ведутся числами двойной точности с шагом 1 мм — точнее конкурентов. ПО внесено в государственный реестр программ и с 2006 года эксплуатируется на сотнях предприятий нефтепереработки, химии, АЗС и ЖКХ в России и СНГ.
Najlepsze kasyna online · May 8, 2026 at 4:13 pm
bonjour I love Your Blog can not say I come here often but im liking what i c so far….
meilleurs casinos en ligne · May 8, 2026 at 4:38 pm
Advanced reading here!
AnthonyApofs · May 8, 2026 at 5:19 pm
Эта разъяснительная статья содержит простые и доступные разъяснения по актуальным вопросам. Мы стремимся сделать информацию понятной для широкой аудитории, чтобы каждый мог разобраться в предмете и извлечь из него максимум пользы.
Откройте для себя больше – номер нарколога на дом
EdwardOdolo · May 8, 2026 at 5:52 pm
Публикация знакомит читателей с различными подходами к реабилитации. От традиционных методов до современных программ — вы узнаете, как выбрать оптимальный путь к выздоровлению и преодолеть препятствия на этом пути.
Читать далее > – прокапать на дому похмелье
meilleur casino en ligne Canada · May 8, 2026 at 5:59 pm
Thank you for all the information was very accurate, just wondering if all this is possible.~
CharlesExent · May 8, 2026 at 6:01 pm
К основным показаниям относятся:
Получить дополнительные сведения – вывод из запоя на дому круглосуточно санкт-петербург
CharlesRecok · May 8, 2026 at 6:05 pm
Дополнительным поводом для вызова врача становится состояние, при котором больному трудно вставать, пить воду, есть, сохранять спокойствие или ориентироваться в самочувствии. В таких случаях осмотр на дому позволяет быстрее определить дальнейший маршрут помощи. Иногда уже первый звонок помогает понять, допустим ли домашний формат или лучше сразу рассматривать вывод в стационаре.
Подробнее тут – врач нарколог на дом
Andrewsap · May 8, 2026 at 6:10 pm
Домашняя детоксикация подходит для ранних стадий интоксикации, когда состояние пациента стабильно, а сопутствующие заболевания отсутствуют. Однако при длительном употреблении алкоголя физиологические изменения требуют более глубокого вмешательства. Стационар обеспечивает изоляцию от триггеров, исключает риск самостоятельного повторного употребления и позволяет врачам динамически корректировать терапию на основе лабораторных показателей и реакции организма. В 2026 году стандарты наркологической помощи делают акцент на превентивной безопасности: раннее выявление признаков делирия, судорожной готовности или кардиологических осложнений позволяет предотвратить критические состояния до их развития. Клиника «Стармед» выстроила работу так, чтобы каждый этап госпитализации логически вытекал из предыдущего, формируя непрерывную цепочку от острой стабилизации до планирования долгосрочной ремиссии.
Исследовать вопрос подробнее – стационар вывод из запоя нижний новгород
Ranchi escorts · May 8, 2026 at 6:20 pm
Very Interesting Information! Thank You For Thi Information!
BrandonRoada · May 8, 2026 at 6:22 pm
Наиболее частыми поводами для вызова становятся несколько дней употребления алкоголя подряд, выраженная слабость, дрожь в руках, тревога, тошнота, нарушение сна, скачки давления, учащенный пульс и признаки обезвоживания. Эти симптомы могут сочетаться между собой и усиливаться по мере продолжения запоя или после резкого прекращения употребления.
Подробнее тут – запой нарколог на дом в екатеринбурге
Everetttam · May 8, 2026 at 6:25 pm
Вывод из запоя на дому с медицинским контролем в Екатеринбурге предлагает множество преимуществ, которые делают этот метод более удобным и безопасным для многих людей. Отсутствие необходимости в госпитализации и наличие профессионального контроля являются основными положительными аспектами этой услуги.
Подробнее тут – https://vyvod-iz-zapoya-na-domu-ekaterinburg-18.ru/
DonaldLiz · May 8, 2026 at 6:29 pm
Капельница от похмелья в Воронеже с оперативным выездом врача и устранением симптомов интоксикации в наркологической клинике «Похмельная служба»
Получить больше информации – капельница от похмелья цена воронеж
neueste online casinos · May 8, 2026 at 6:42 pm
This information is critically needed, thanks.
Shaneincix · May 8, 2026 at 6:44 pm
В клинике применяются современные медицинские технологии, направленные на восстановление организма и стабилизацию психоэмоционального состояния. Ниже представлена таблица с описанием основных методов и их терапевтического значения.
Узнать больше – http://narkologicheskaya-klinika-tolyatti0.ru/
AlvinCet · May 8, 2026 at 6:45 pm
Чаще всего домашний формат применяется при следующих состояниях:
Получить дополнительные сведения – вывод из запоя на дому круглосуточно санкт-петербург
DavidLig · May 8, 2026 at 6:49 pm
Этапный подход позволяет достичь полного восстановления организма и избежать осложнений, связанных с резким прекращением употребления алкоголя. Каждый шаг фиксируется врачами, а коррекция терапии проводится по показаниям.
Разобраться лучше – вывод из запоя недорого тольятти
levuyaToows · May 8, 2026 at 6:50 pm
«Реготмас» — отечественный завод по выпуску сертифицированных фильтрующих элементов для топливных и масляных систем. Продукция выпускается по ГОСТ Р ИСО 9001-2015 с контролем на каждом этапе производства. Ищете фильтрующий элемент реготмас 661? На сайте regotmas.ru представлен полный каталог бумажных фильтрующих элементов с тонкостью фильтрации от 10 до 40 мкм — серии 600, 630, 660, 560, 412 и другие. Завод гарантирует стабильное качество и надёжное партнёрство.
juragExted · May 8, 2026 at 6:56 pm
Посетите сайт https://dom-kamnya.ru/ – там вы найдете широкий ассортимент продукции от производителя в Москве, с гарантией высокого качества. Изучите наш каталог, при желании оставьте заявку на бесплатный замер — мы даём гарантию 10 лет на искусственный камень и 2 года на монтаж. Привезём и установим столешницу для вашей кухни за один день.
best online casino nz · May 8, 2026 at 7:02 pm
A cool post there mate ! Thank you for posting.
kasyno online · May 8, 2026 at 7:13 pm
How long does it take you to write an article like this?
https://789clubcom.us.com/ · May 8, 2026 at 7:13 pm
Hey very cool site!! Man .. Beautiful .. Amazing .. I will bookmark your website and take the feeds also…I’m happy to find so many useful information here in the post, we need develop more strategies in this regard, thanks for sharing. . . . . .
sunwin · May 8, 2026 at 7:15 pm
I do believe your audience could very well want a good deal more stories like this carry on the excellent hard work.
luck8 · May 8, 2026 at 7:38 pm
Very Interesting Information! Thank You For Thi Information!
New online casino · May 8, 2026 at 7:46 pm
These kind of posts are always inspiring and I prefer to read quality content so I happy to find many good point here in the post. writing is simply wonderful! thank you for the post
Andrewattap · May 8, 2026 at 7:58 pm
Вызов капельницы от похмелья с контролем врача в Самаре рекомендуется, когда симптомы похмелья становятся особенно тяжелыми и мешают нормальной жизнедеятельности. Несмотря на то, что многие пытаются справиться с похмельем с помощью домашних методов, такие как прием жидкости или таблеток, они не всегда оказываются достаточно эффективными. В случае сильных симптомов похмелья, капельница с врачебным контролем — это более безопасное и быстрое решение, при этом возможен вывод в стационаре, анонимное лечение и консультации по вопросам наркомании с учетом актуальной цены услуг.
Изучить вопрос глубже – http://kapelnicza-ot-pokhmelya-samara-13.ru/
Najlepsze kasyna online · May 8, 2026 at 8:01 pm
whoah this weblog is great i really like studying your articles. Stay up the great work! You already know, lots of persons are looking round for this information, you can aid them greatly.
legalne kasyna online · May 8, 2026 at 8:21 pm
I think I might disagree with some of your analysis. Are the figures solid?
Stevehut · May 8, 2026 at 8:47 pm
Наркологическая помощь — это комплекс медицинских мероприятий, направленных на стабилизацию состояния пациента при алкогольной или наркотической интоксикации, а также при абстинентном синдроме. В наркологической клинике «Частный медик 24» в Нижнем Новгороде помощь оказывается с учётом текущего состояния пациента, без избыточных вмешательств и с чёткой ориентацией на клинические показатели. Выезд нарколога позволяет начать лечение в первые часы ухудшения самочувствия, что снижает риски осложнений и облегчает восстановление.
Подробнее можно узнать тут – клиника наркологической помощи
hair transplant turkey · May 8, 2026 at 8:50 pm
I thought it was going to be some boring old post, but I’m glad I visited. I will post a link to this site on my blog. I am sure my visitors will find that very useful.
AnthonyPhecy · May 8, 2026 at 8:50 pm
Клиника «АмурМед Контур» в Хабаровске предлагает комплексную детоксикацию организма, которая включает инфузионную терапию, стабилизацию жизненно важных показателей и коррекцию эмоционального состояния. Каждому пациенту подбирается индивидуальная схема капельниц с учётом возраста, массы тела, стажа употребления алкоголя и хронических заболеваний. Процедуры проводятся в условиях полной конфиденциальности и под постоянным наблюдением специалистов. Медицинская команда контролирует артериальное давление, уровень сатурации, частоту пульса и показатели крови на протяжении всего периода восстановления.
Подробнее – https://vyvod-iz-zapoya-v-khabarovske0.ru/vyvod-iz-zapoya-v-staczionare-khabarovsk/
RandyTaite · May 8, 2026 at 8:57 pm
Нарколог на дом в Ростове-на-Дону рассматривается как специализированная форма оказания медицинской помощи пациентам с зависимостями вне стационара. В клинике «Чистый Баланс» выезд врача организуется круглосуточно, что позволяет обеспечить своевременное вмешательство при ухудшении состояния в любое время суток. Нарколог на дом в Ростове-на-Дону востребован в ситуациях, когда пациент не готов или не может обратиться в медицинское учреждение, а промедление с лечением повышает риск осложнений. Такой формат помощи требует строгого соблюдения клинических протоколов и высокой квалификации специалистов.
Получить больше информации – нарколог на дом анонимно ростов-на-дону
hair transplant turkey · May 8, 2026 at 8:57 pm
Spot on with this write-up, I actually assume this website needs far more consideration. I will in all probability be once more to learn rather more, thanks for that info.
RichardFlero · May 8, 2026 at 9:11 pm
Выбор между домашней помощью и стационарным лечением определяется не удобством, а медицинской целесообразностью. В условиях клиники исключаются внешние триггеры, обеспечивается изоляция от источников алкоголя и создается контролируемая среда, где терапевтические решения принимаются на основе объективных показателей, а не субъективных ощущений пациента. Такой подход критически важен для предотвращения осложнений, минимизации дискомфорта абстиненции и формирования устойчивой базы для дальнейшей противорецидивной работы.
Подробнее можно узнать тут – https://vyvod-iz-zapoya-v-staczionare-sankt-peterburg-18.ru/
Curtisloola · May 8, 2026 at 9:13 pm
Процесс вывода из запоя на дому состоит из нескольких этапов, которые тщательно подбираются врачом-наркологом в зависимости от состояния пациента. Важно, чтобы весь процесс был под контролем специалиста, чтобы избежать осложнений и гарантировать безопасное восстановление.
Получить больше информации – нарколог на дом вывод из запоя екатеринбург
cheap sex webcams · May 8, 2026 at 9:57 pm
Woh I enjoy your content , saved to bookmarks!
live sex webcams · May 8, 2026 at 10:08 pm
Thanks for sharing the information. I found the information very useful. That’s a awesome story you posted. I will come back to scan some more.
neue online casinos deutschland · May 8, 2026 at 10:22 pm
I absolutely adore your site! You aggressive me as able-bodied as all the others actuality and your broiled PS is absolutely great!
kasyno online · May 8, 2026 at 11:01 pm
Admiring the time and effort you put into your site and detailed info you offer!
dopefNub · May 8, 2026 at 11:19 pm
Откройте путь к успеху. Таро-диагностика https://gadanie.by/ выявит скрытые блоки и негатив. Проведу мощное энергетическое очищение, поставлю защиту от неудач в бизнесе и сниму порчу с отношений. Запускаю обряды на удачу и процветание. Верните гармонию и рост в свою жизнь.
najlepsze kasyno online · May 8, 2026 at 11:20 pm
Please let us know when you plan to publish your book!
Najlepsze kasyna online · May 8, 2026 at 11:24 pm
Just want to say what a great blog you got here!I’ve been around for quite a lot of time, but finally decided to show my appreciation of your work!
logawrFat · May 8, 2026 at 11:29 pm
Искусство способно существовать в самых неожиданных формах — и WireSpace тому живое доказательство. Здесь проволока перестаёт быть простым материалом и превращается в нечто большее: изящных фей, воздушные фигуры, скульптуры, в которых чувствуется дыхание жизни. Каждое изделие создаётся вручную с исключительным вниманием к деталям — посетите https://wirespace.ru/ и убедитесь сами, насколько богат и разнообразен этот удивительный мир. Работы мастера вдохновляют, удивляют и заставляют остановиться, чтобы рассмотреть каждый изгиб, каждую линию, наполненную смыслом и душой.
kasyno online opinie · May 8, 2026 at 11:33 pm
Thanks for sharing the information. I found the information very useful. That’s a awesome story you posted. I will come back to scan some more.
ripugsoory · May 8, 2026 at 11:35 pm
Торрент-трекер для геймеров, который не заставит тебя тратить время впустую: только свежие раздачи, актуальные новинки и проверенные релизы без вирусов и лишней рекламы. Ищете Скачать торрент игры? Посети torentino.org — здесь собраны игры всех жанров: экшены, приключения, RPG и симуляторы с быстрой скоростью загрузки. Все файлы проверены и доступны бесплатно, каталог пополняется каждый день — нужная игра всегда найдётся.
neue casinos · May 8, 2026 at 11:56 pm
It sounds like you’re creating problems yourself by defining this as such a comprehensive, almost unknowable problem. Isn’t that self-defeating?
JeffreyBlarM · May 9, 2026 at 12:11 am
В этой статье представлен занимательный и актуальный контент, который заставит вас задуматься. Мы обсуждаем насущные вопросы и проблемы, а также освещаем истории, которые вдохновляют на действия и изменения. Узнайте, что стоит за событиями нашего времени!
Лучшее решение — прямо здесь – нарколог на дом вывод
JeffreyBlarM · May 9, 2026 at 1:06 am
В этой статье представлен занимательный и актуальный контент, который заставит вас задуматься. Мы обсуждаем насущные вопросы и проблемы, а также освещаем истории, которые вдохновляют на действия и изменения. Узнайте, что стоит за событиями нашего времени!
Не упусти шанс – психиатр нарколог на дом на
neueste online casinos · May 9, 2026 at 1:33 am
This is really interesting, You’re a very skilled blogger. I have joined your feed and look forward to seeking more of your great post. Also, I’ve shared your web site in my social networks!
CharlesExent · May 9, 2026 at 1:34 am
Выезд нарколога начинается с осмотра пациента. Доктора измеряют давление, пульс, оценивают уровень сознания и выраженность симптомов. На основании этих данных формируется план лечения, который реализуется сразу на месте. Такой подход позволяет быстро перейти к стабилизации состояния без лишних этапов.
Углубиться в тему – vyvod-iz-zapoya-na-domu-sankt-peterburg-8.ru/
CharlesRecok · May 9, 2026 at 1:46 am
Помощь на дому рассматривают при состояниях, связанных с острым ухудшением самочувствия после алкоголя. Чаще всего это несколько дней запоя, тяжелое похмелье, бессонница, тревога, дрожь в руках, слабость, отсутствие аппетита, тошнота, сухость во рту и ощущение истощения. В подобных случаях врачебный осмотр нужен для оценки общего состояния и выбора безопасной тактики.
Получить дополнительную информацию – нарколог на дом анонимно
Andrewsap · May 9, 2026 at 1:56 am
Решение о помещении пациента в стационар принимается на основе объективных медицинских критериев, а не только по желанию родственников. К показаниям относятся: запой длительностью более трех суток, выраженные симптомы абстиненции, наличие в анамнезе алкогольных делириев или судорожных эпизодов, сопутствующие хронические заболевания печени, поджелудочной железы, сердца или нервной системы. Отдельным фактором выступает полинаркомания или сочетание алкогольной зависимости с приемом психофармакологических препаратов без назначения врача. В таких ситуациях риск развития тяжелых осложнений возрастает многократно, и амбулаторный формат не обеспечивает необходимого уровня контроля. Госпитализация позволяет провести полноценную диагностику, включая ЭКГ, экспресс-анализы крови, оценку неврологического статуса и мониторинг сатурации, что формирует точную картину состояния и исключает назначение шаблонных схем.
Ознакомиться с деталями – вывод из запоя в стационаре анонимно нижний новгород
Everetttam · May 9, 2026 at 2:39 am
Вывод из запоя на дому в Екатеринбурге: эффективное лечение, детоксикация и восстановление организма в наркологической клинике «Детокс»
Изучить вопрос глубже – анонимный вывод из запоя на дому
BrandonRoada · May 9, 2026 at 2:55 am
Отдельного внимания требуют случаи, когда больной почти не ест, плохо пьет воду, не может спокойно лежать, жалуется на сильное сердцебиение, нехватку сна или выраженное внутреннее напряжение. В такой ситуации осмотр помогает определить, безопасно ли оставаться дома и какого объема помощи достаточно на текущем этапе. Если речь идет о выраженных проявлениях абстинентного синдрома, затягивать с обращением нецелесообразно.
Ознакомиться с деталями – https://narkolog-na-dom-ekaterinburg-3.ru/
DonaldLiz · May 9, 2026 at 3:00 am
В Воронеже круглосуточная помощь при похмелье востребована в ситуациях, когда симптомы появляются внезапно или усиливаются в ночное время, особенно в запое или после запоя. Врач проводит консультацию, оценивает состояние пациента и принимает решение о проведении инфузионной терапии. Такой подход позволяет своевременно устранить симптомы и предотвратить их дальнейшее развитие. При необходимости можно оставить заявку, уточнить цены или получить помощь бесплатно на первичном этапе.
Выяснить больше – капельница от похмелья на дом воронеж
Jamessaulp · May 9, 2026 at 3:12 am
Эта статья погружает вас в увлекательный мир знаний, где каждый факт становится открытием. Мы расскажем о ключевых исторических поворотных моментах и научных прорывах, которые изменили ход цивилизации. Поймите, как прошлое формирует настоящее и как его уроки могут помочь нам строить будущее.
Полная информация здесь – капельница на дому цена
Marcusniday · May 9, 2026 at 3:12 am
В данной публикации мы поговорим о процессе восстановления от зависимости, о том, как вернуть себе нормальную жизнь. Мы обсудим преодоление трудностей, значимость поддержки и наличие программ реабилитации. Читатели смогут узнать о ключевых шагах к успешному восстановлению.
Расширить кругозор по теме – сколько стоит капельница от похмелья на дому
Shaneincix · May 9, 2026 at 3:14 am
Процесс лечения в «ВолгаМед Баланс» выстроен логично и последовательно. Каждый этап направлен на достижение конкретных медицинских и психологических целей. Ниже приведена таблица, описывающая ключевые стадии терапии.
Выяснить больше – наркологическая клиника цены в тольятти
DavidLig · May 9, 2026 at 3:27 am
Врачи клиники используют щадящие методики и современные инфузионные составы, которые не перегружают организм и позволяют безопасно восстановить жизненные функции. Контроль проводится на всех этапах: от диагностики до постлечебного наблюдения.
Углубиться в тему – https://vyvod-iz-zapoya-tolyatti0.ru
Millardden · May 9, 2026 at 3:32 am
Первичный этап включает сбор анамнеза, лабораторные исследования и оценку неврологического статуса. На основании полученных данных формируется план лечения, который может корректироваться в процессе наблюдения.
Разобраться лучше – вывод наркологическая клиника в хабаровске
AlvinCet · May 9, 2026 at 3:37 am
В Санкт-Петербурге вывод из запоя на дому используется в ситуациях, когда состояние пациента требует медицинской помощи, но позволяет обойтись без лечения в стационаре. Врач проводит консультацию, оценивает длительность запоя, выраженность симптомов и общее состояние, анализируя данные пациента, после чего принимает решение о тактике лечения при алкоголизме. При необходимости можно оформить вызов специалиста или заказать услугу заранее.
Исследовать вопрос подробнее – вывод из запоя на дому
AnthonyApofs · May 9, 2026 at 4:03 am
В этой статье представлен занимательный и актуальный контент, который заставит вас задуматься. Мы обсуждаем насущные вопросы и проблемы, а также освещаем истории, которые вдохновляют на действия и изменения. Узнайте, что стоит за событиями нашего времени!
Погрузиться в научную дискуссию – психиатр нарколог на дом
Thomashep · May 9, 2026 at 4:09 am
Откройте для себя скрытые страницы истории и малоизвестные научные открытия, которые оказали колоссальное влияние на развитие человечества. Статья предлагает свежий взгляд на события, которые заслуживают большего внимания.
Изучить вопрос глубже – капельницы от запоя на дому воронеж
Jamesrub · May 9, 2026 at 4:17 am
убийство по фрейду клуб убийств по четвергам
Charlessette · May 9, 2026 at 4:21 am
охотничьи псы 2 сезон таємниці смолвіля
Marcusniday · May 9, 2026 at 4:24 am
В данной статье рассматриваются проблемы общественного здоровья и социальные факторы, влияющие на него. Мы акцентируем внимание на значении профилактики и осведомленности в защите здоровья на уровне общества. Читатели смогут узнать о новых инициативах и программах, направленных на улучшение здоровья населения.
Изучить аспект более тщательно – капельница от похмелья услуги
Michaelbew · May 9, 2026 at 4:29 am
узнать больше Онион сайты
GregoryRof · May 9, 2026 at 5:21 am
Этот обзор предлагает структурированное изложение информации по актуальным вопросам. Материал подан так, чтобы даже новичок мог быстро освоиться в теме и начать использовать полученные знания в практике.
Погрузиться в научную дискуссию – вызвать врача нарколога на дом
EdwardOdolo · May 9, 2026 at 5:44 am
В данной статье рассматриваются проблемы общественного здоровья и социальные факторы, влияющие на него. Мы акцентируем внимание на значении профилактики и осведомленности в защите здоровья на уровне общества. Читатели смогут узнать о новых инициативах и программах, направленных на улучшение здоровья населения.
Узнать из первых рук – похмельная капельница
BobbyCed · May 9, 2026 at 6:42 am
Этот краткий обзор предлагает сжатую информацию из области медицины, включая ключевые факты и последние новости. Мы стремимся сделать информацию доступной и понятной для широкой аудитории, что позволит читателям оставаться в курсе актуальных событий в здравоохранении.
Изучить рекомендации специалистов – капельница при алкогольной интоксикации цена
Andrewattap · May 9, 2026 at 6:50 am
Этот процесс не занимает много времени — обычно процедура длится от 30 до 60 минут. Важно, что врач контролирует все этапы, обеспечивая безопасность пациента и корректируя терапию по мере необходимости. Такой подход позволяет быстро и эффективно облегчить симптомы похмелья и вернуться к нормальной жизнедеятельности.
Исследовать вопрос подробнее – капельница от похмелья на дому самара
uakino 853 · May 9, 2026 at 7:03 am
фільми мадагаскар 4
CalebWap · May 9, 2026 at 7:28 am
В этой статье мы рассматриваем разные способы борьбы с алкогольной зависимостью. Обсуждаются методы лечения, программы реабилитации и советы для поддержки близких. Читатели получат информацию о том, как преодолеть зависимость и добиться успешного выздоровления.
Нажми и узнай всё – капельница после похмелья
Millardden · May 9, 2026 at 8:33 am
Каждый из этапов дополняет предыдущий, формируя непрерывный лечебный процесс. Такой формат позволяет учитывать динамику состояния пациента и своевременно реагировать на изменения.
Исследовать вопрос подробнее – http://
WalterAdula · May 9, 2026 at 8:39 am
Эта публикация погружает вас в мир увлекательных фактов и удивительных открытий. Мы расскажем о ключевых событиях, которые изменили ход истории, и приоткроем завесу над научными достижениями, которые вдохновили миллионы. Узнайте, чему может научить нас прошлое и как применить эти знания в будущем.
Тыкай сюда — узнаешь много интересного – платный нарколог на дом
Michaelbew · May 9, 2026 at 8:59 am
продолжить Даркнет сайты
CalebWap · May 9, 2026 at 9:03 am
Читатели получат представление о том, как современные технологии влияют на развитие медицины. Обсуждаются новые методы лечения, персонализированный подход и роль цифровых решений в повышении качества медицинских услуг.
Все материалы собраны здесь – капельницы от алкоголя
fazirowRaicS · May 9, 2026 at 9:10 am
Мир магии полон тайн, и разобраться в них без надёжного проводника непросто. Сайт мага Азала https://magomagii.ru/ — это авторский ресурс с более чем 800 постоянными читателями, где опытный практик делится глубокими знаниями о снятии порчи, приворотах и других аспектах магического искусства. Каждая статья написана с душой и подкреплена реальным опытом автора, а живое общение в комментариях превращает сайт в полноценное сообщество единомышленников. Если вы давно искали честный и компетентный взгляд на мир эзотерики — здесь найдёте именно это.
Charlesraips · May 9, 2026 at 9:10 am
В данном материале представлены ключевые тенденции в сфере медицинской науки и практики. Вы узнаете о последних открытиях, инновационных подходах к терапии и важности профилактики заболеваний. Особое внимание уделено практическому применению новых методов в клинической практике.
Полезно знать – платный нарколог на дом
Kennethsip · May 9, 2026 at 9:24 am
В данной статье рассматриваются проблемы общественного здоровья и социальные факторы, влияющие на него. Мы акцентируем внимание на значении профилактики и осведомленности в защите здоровья на уровне общества. Читатели смогут узнать о новых инициативах и программах, направленных на улучшение здоровья населения.
Получить дополнительную информацию – капельница от похмелья
RandyTaite · May 9, 2026 at 9:52 am
Несмотря на выездной формат, лечение выстраивается поэтапно и соответствует медицинским стандартам. Это обеспечивает управляемость процесса и безопасность пациента.
Углубиться в тему – https://narkolog-na-dom-v-rnd19.ru/narkolog-na-dom-rostov
AnthonyPhecy · May 9, 2026 at 9:58 am
Клиника «АмурМед Контур» в Хабаровске предлагает комплексную детоксикацию организма, которая включает инфузионную терапию, стабилизацию жизненно важных показателей и коррекцию эмоционального состояния. Каждому пациенту подбирается индивидуальная схема капельниц с учётом возраста, массы тела, стажа употребления алкоголя и хронических заболеваний. Процедуры проводятся в условиях полной конфиденциальности и под постоянным наблюдением специалистов. Медицинская команда контролирует артериальное давление, уровень сатурации, частоту пульса и показатели крови на протяжении всего периода восстановления.
Углубиться в тему – скорая вывод из запоя
Stevehut · May 9, 2026 at 10:09 am
Состояние пациента при интоксикации может развиваться по-разному: от умеренной слабости и головной боли до выраженной дезориентации, тахикардии и нарушений сна. В таких ситуациях важно не откладывать обращение за помощью. Наркологическая помощь на дому рассматривается, когда требуется быстрое вмешательство и контроль состояния без транспортировки пациента.
Получить больше информации – https://narkologicheskaya-pomoshh-nizhnij-novgorod-8.ru
Jamessaulp · May 9, 2026 at 10:10 am
Этот информативный текст отличается привлекательным содержанием и актуальными данными. Мы предлагаем читателям взглянуть на привычные вещи под новым углом, предоставляя интересный и доступный материал. Получите удовольствие от чтения и расширьте кругозор!
Лови подробности – капельницы от запоя на дому воронеж
Donaldembab · May 9, 2026 at 10:44 am
Чаще всего нарколога на дом вызывают при повторяющемся или длительном запое, тяжелом похмелье, бессоннице после алкоголя, треморе, выраженной слабости и ухудшении общего самочувствия. Поводом для обращения также становятся тревога, раздражительность, скачки артериального давления, учащенный пульс, обезвоживание и необходимость поставить капельницу дома под наблюдением специалиста. Во многих случаях звонок в наркологический центр поступает тогда, когда родственники понимают, что состояние больного уже не позволяет ждать следующего дня.
Узнать больше – нарколог на дом вывод екатеринбург
RichardFlero · May 9, 2026 at 11:51 am
Выбор между домашней помощью и стационарным лечением определяется не удобством, а медицинской целесообразностью. В условиях клиники исключаются внешние триггеры, обеспечивается изоляция от источников алкоголя и создается контролируемая среда, где терапевтические решения принимаются на основе объективных показателей, а не субъективных ощущений пациента. Такой подход критически важен для предотвращения осложнений, минимизации дискомфорта абстиненции и формирования устойчивой базы для дальнейшей противорецидивной работы.
Получить больше информации – вывод из запоя в стационаре
Curtisloola · May 9, 2026 at 12:27 pm
Вывод из запоя на дому в Екатеринбурге — это услуга, которая позволяет пациентам пройти лечение в удобных для них условиях, без необходимости посещать стационар. Процедура включает несколько этапов, каждый из которых направлен на снижение уровня алкогольной интоксикации и стабилизацию состояния пациента. Главным преимуществом вывода из запоя на дому является то, что это не только удобно, но и позволяет избежать лишнего стресса, который может быть вызван госпитализацией.
Подробнее тут – http://www.domen.ru
yalla shoot · May 9, 2026 at 12:48 pm
Well, I don’t know if that’s going to work for me, but definitely worked for you! 🙂 Excellent post!
zovoxCrock · May 9, 2026 at 12:56 pm
Студия флористики Roseline в Иванове создаёт авторские букеты, свадебные композиции и корпоративные подарки под ключ. Каталог включает розы, тюльпаны, гортензии, эустомы, герберы, лилии, ранункулюсы и десятки других цветов. На https://roseline37.ru/ представлен полный каталог с актуальными ценами — заказ оформляется онлайн с доставкой по городу. Студия также занимается съедобными букетами, сухоцветами, декоративными кашпо и оформлением праздников под ключ. Каждая композиция создаётся вручную опытными флористами строго по пожеланиям заказчика.
ua-bay 746 · May 9, 2026 at 1:00 pm
блондинка найгірша людина у світі дивитися
Walterfancy · May 9, 2026 at 1:02 pm
Ребята, статья для тех, кто хочет не просто «выжить», а закрепиться на рынке. Автор объясняет, почему в условиях жёсткой конкуренции SEO становится не опцией, а необходимостью. Особенно ценно, что есть раздел про интеграцию SEO с другими каналами: контент-маркетинг, SMM, продажи. Комплексный подход — единственный путь к устойчивому успеху. Почитайте: https://olivadance.ru/2026/05/seo-kak-fundament-biznesa-pochemu-igra-v-dolguju-edinstvennaja-strategija-dlja-vyzhivanija/
JorgeTreta · May 9, 2026 at 1:04 pm
Основные показания для проведения процедуры:
Получить дополнительную информацию – капельница от похмелья в воронеже
Walterfancy · May 9, 2026 at 1:05 pm
Хорошая статья о том, почему «цифровой бетон» (техническая база) важнее красивого фасада. Автор объясняет, что SEO — это не про внешний лоск, а про прочность фундамента: скорость загрузки, мобильная адаптация, чистая структура URL. Без этого никакой красивый дизайн не поможет. Тем, кто только начинает продвижение, обязательно к прочтению: https://avto-dom-tumen.ru/stati/seo-kak-fundament-biznesa-pochemu-cifrovoj-beton-vazhnee-krasivogo-fasada/
Huberterora · May 9, 2026 at 1:07 pm
Вывод из запоя на дому с быстрым облегчением в Екатеринбурге — это процедура, направленная на быстрое снятие острых симптомов алкогольного абстинентного синдрома и возвращение пациента к нормальному состоянию, включая случаи алкоголизма и наркомании. Такая услуга удобна тем, что позволяет не только эффективно справиться с зависимостью, но и избавиться от неприятных проявлений запоя, таких как головная боль, тошнота, слабость и психоэмоциональное напряжение, в комфортной домашней обстановке, при этом оказывается наркологическая помощь. Быстрое облегчение без необходимости госпитализации делает этот метод популярным среди пациентов, которым важен быстрый и безопасный результат, а при необходимости можно заказать дальнейшее кодирование или лечение в стационаре.
Ознакомиться с деталями – вывод из запоя на дому
GregoryRof · May 9, 2026 at 1:13 pm
Предлагаем вашему вниманию интересную справочную статью, в которой собраны ключевые моменты и нюансы по актуальным вопросам. Эта информация будет полезна как для профессионалов, так и для тех, кто только начинает изучать тему. Узнайте ответы на важные вопросы и расширьте свои знания!
Раскрыть тему полностью – вызов нарколога на дом стоимость
Timothyser · May 9, 2026 at 1:32 pm
Вывод из запоя на дому в Санкт-Петербурге с анонимным выездом врача, снятием интоксикации и поддержкой в наркологической клинике «Частный медик 24»
Детальнее – анонимный вывод из запоя на дому в санкт-петербурге
BobbyCed · May 9, 2026 at 1:41 pm
Этот краткий обзор предлагает сжатую информацию из области медицины, включая ключевые факты и последние новости. Мы стремимся сделать информацию доступной и понятной для широкой аудитории, что позволит читателям оставаться в курсе актуальных событий в здравоохранении.
Узнать из первых рук – антипохмельная капельница
hair transplant istanbul · May 9, 2026 at 1:43 pm
I absolutely adore your site! You aggressive me as able-bodied as all the others actuality and your broiled PS is absolutely great!
부산달리기 · May 9, 2026 at 1:45 pm
부달(부산달리기)은 부산 및 인근 경남 지역에서 유명한 유흥 정보 커뮤니티로, 오랜 기간 지역 유흥 정보의 중심 역할을 해온 원조 플랫폼입니다.
CharlesExent · May 9, 2026 at 1:54 pm
Выезд нарколога начинается с осмотра пациента. Доктора измеряют давление, пульс, оценивают уровень сознания и выраженность симптомов. На основании этих данных формируется план лечения, который реализуется сразу на месте. Такой подход позволяет быстро перейти к стабилизации состояния без лишних этапов.
Выяснить больше – http://www.domen.ru
fofihmweata · May 9, 2026 at 2:09 pm
Москва-река открывает новые грани развлечений: тематические вечеринки, зажигательные диджей-сеты и живая музыка прямо на борту теплохода — всё это делает каждый выход в свет по-настоящему незабываемым. На сайте https://ticketscruise.ru/ собрано полное расписание круизов на любой вкус: от уютных прогулок с ужином под звёздным небом до ночных шоу-программ с профессиональными артистами. Танцы под открытым небом, бар на борту, панорамные виды столицы — здесь каждая деталь работает на атмосферу. Бронируйте билеты онлайн и выбирайте свой идеальный формат отдыха на воде!
Michaelsence · May 9, 2026 at 2:17 pm
Комбинированное воздействие обеспечивает быстрое улучшение состояния пациента и позволяет стабилизировать организм даже при тяжёлой интоксикации. Врач контролирует все реакции и корректирует дозировки при необходимости.
Разобраться лучше – вызвать нарколога на дом в тольятти
CharlesRecok · May 9, 2026 at 2:23 pm
Наиболее частыми причинами обращения становятся выраженная слабость, тремор, нарушение сна, тревога, учащенный пульс, скачки артериального давления, тошнота и признаки обезвоживания. Эти симптомы могут сочетаться между собой и усиливаться после прекращения употребления алкоголя, особенно после нескольких дней запоя.
Подробнее – http://www.domen.ru
fixDiele · May 9, 2026 at 2:23 pm
Для тех, кто ищет информацию по теме “Образование и здравоохранение в Северной Осетии — Алания: нововведения и актуальные вопросы”, нашел много полезного.
Ссылка ниже:
https://media16.ru
hair transplant istanbul · May 9, 2026 at 2:24 pm
With this issue, it’s important to have someone like you with something to say that really matters.
fixDiele · May 9, 2026 at 2:28 pm
Зацепил раздел про Последние новости и события Тульской области.
Смотрите сами:
https://71media.ru
Andrewsap · May 9, 2026 at 2:39 pm
Затяжной запой перестает быть бытовой проблемой в тот момент, когда организм теряет способность самостоятельно восстанавливаться после интоксикации. Накопление ацетальдегида, нарушение водно-электролитного баланса, истощение запасов витаминов и перегрузка сердечно-сосудистой системы создают состояние, при котором домашние методы перестают быть безопасными. Срочно стабилизировать самочувствие и быстро купировать абстинентный синдром позволяет только контролируемая медицинская среда. Вывод из запоя в стационаре в Нижнем Новгороде становится клинически обоснованным решением, когда требуется не просто снятие симптомов, а комплексная детоксикация под круглосуточным наблюдением врачей. Наркологическая клиника «Стармед» организует процесс лечения в соответствии с актуальными стандартами доказательной медицины, обеспечивая безопасность пациента, прозрачность процедур и плавный переход к противорецидивной терапии. Мы понимаем, что решение о госпитализации часто принимается в состоянии стресса, поэтому наша работа начинается с четкой диагностики, честного объяснения плана лечения и соблюдения строгих протоколов конфиденциальности. Опытные специалисты клиники помогут вызвать доверие к процессу восстановления уже на этапе первого контакта.
Изучить вопрос глубже – нарколог вывод из запоя в стационаре нижний новгород
komireMor · May 9, 2026 at 3:04 pm
Рынок шеринговой экономики в России превысил 1 трлн рублей и продолжает расти. Тулбокс занял в нём чёткую нишу — прокат инструмента и бытовой техники через постаматы без персонала, залога и договоров. Клиент берёт дрель или пылесос через приложение в боксе у «Пятёрочки» или ПВЗ рядом с домом. Подробности партнёрства — на https://biz.tlbx.ru/ — инвестиции от 3 млн рублей с окупаемостью 18–24 месяца. Сеть уже работает в Челябинске, Уфе и Екатеринбурге и приглашает партнёров в новые города.
najlepsze kasyna online · May 9, 2026 at 3:06 pm
How long does it take you to write an article like this?
WilliamThatt · May 9, 2026 at 3:14 pm
Медикаментозное вмешательство подбирается индивидуально, что позволяет снизить нагрузку на органы и системы и обеспечить безопасность лечения.
Подробнее – вывод из запоя на дому круглосуточно тольятти
JasonBloma · May 9, 2026 at 3:43 pm
Этот краткий обзор предлагает сжатую информацию из области медицины, включая ключевые факты и последние новости. Мы стремимся сделать информацию доступной и понятной для широкой аудитории, что позволит читателям оставаться в курсе актуальных событий в здравоохранении.
Более подробно об этом – частная наркологическая клиника нижний новгород
nizaxpah · May 9, 2026 at 3:44 pm
WBDown — профессиональный сервис для продавцов и аналитиков Wildberries: позволяет быстро собирать артикулы товаров по ID продавца или URL магазина с гибкой сортировкой по популярности, рейтингу, цене и новинкам. Ищете как сохранить видео из отзывов вб на телефон? Сервис wbdown.ru предлагает удобный парсинг до 1000 артикулов за раз по цене от 2 рублей за артикул, проверку фото на контент 18+ и фоновую обработку данных — всё необходимое для глубокого анализа конкурентов и оптимизации продаж. полный набор функций для серьёзного анализа рынка и роста показателей продаж.
PatrickTanna · May 9, 2026 at 3:56 pm
Медикаментозное лечение подбирается индивидуально с учётом возраста, длительности зависимости и сопутствующих патологий.
Подробнее тут – наркологическая клиника цены
RobinZes · May 9, 2026 at 3:59 pm
В этой статье рассматриваются актуальные вопросы, связанные с развитием медицинской науки и её внедрением в повседневную практику. Особое внимание уделено вопросам профилактики, ранней диагностики и использованию технологий для улучшения здоровья человека.
Прочесть заключение эксперта – “наркологическая клиника
tayiwugeage · May 9, 2026 at 4:19 pm
«Мой Токио» — туроператор с фокусом на Японии, предлагающий россиянам групповые, индивидуальные и корпоративные туры на любой запрос. В ассортименте — маршруты по Токио, Киото, Осаке, Хиросиме и другим регионам страны, горнолыжный и пляжный отдых на Окинаве, а также программы обучения в Японии. Ищете туры в японию из петербурга? На dvmt.ru собраны актуальные путёвки и горячие туры с профессиональным сопровождением. Оператор зарегистрирован официально под номером РТО 004645 — это подтверждает надёжность компании и безопасность каждого тура.
부달 · May 9, 2026 at 4:34 pm
부달(부산달리기)은 부산·경남 지역 최대 규모의 유흥 정보 통합 플랫폼입니다. 원래 2017년 ‘부산달리기’라는 이름으로 시작했으나 현재는 줄여서 ‘부달’로 널리 알려져
부비 · May 9, 2026 at 4:35 pm
부산비비기(부비)는 부산 및 인근 경남 지역의 주요 성인 유흥 정보 플랫폼입니다. 2020년 8월에 개설된 지역 기반 오피사이트(오피스텔 마사지 정보 사이트)로서, 부산의
부비 · May 9, 2026 at 4:54 pm
부비는 부산비비기라는 이름과 함께 검색되는 부산 지역 기반 정보 키워드로, 일반적으로 지역 커뮤니티, 후기성 정보, 게시판형 안내 콘텐츠와 관련해 사용됩니다.
Everetttam · May 9, 2026 at 5:01 pm
Вывод из запоя на дому с медицинским контролем — это услуга, которая позволяет пациентам избавиться от алкогольной зависимости в комфортных условиях своего дома. В Екатеринбурге эта услуга становится все более востребованной, поскольку она предоставляет безопасный и эффективный способ вывода человека из запоя, при этом не требуя госпитализации. Процедура сопровождается контролем квалифицированных специалистов, что минимизирует риски и ускоряет процесс восстановления.
Ознакомиться с деталями – vyvod-iz-zapoya-na-domu-ekaterinburg-18.ru/
Thomashen · May 9, 2026 at 5:10 pm
Вывод из запоя на дому в Екатеринбурге: срочное восстановление, детоксикация и медицинская помощь в наркологической клинике «Детокс»
Детальнее – вывод из запоя на дому цена екатеринбург
Michaelbew · May 9, 2026 at 5:16 pm
этот сайт Тор ссылки
Charlesraips · May 9, 2026 at 5:18 pm
В этой публикации мы исследуем ключевые аспекты здоровья, включая влияние образа жизни на благополучие. Читатели узнают о важности правильного питания, физической активности и психического здоровья. Мы предоставим практические советы и рекомендации для поддержания здоровья и развития профилактических подходов.
Что ещё? Расскажи всё! – нарколог на дом цены
cổng game sunwin · May 9, 2026 at 5:18 pm
The start of a fast-growing trend?
BrandonRoada · May 9, 2026 at 5:22 pm
За выездом врача чаще обращаются тогда, когда человеку тяжело добраться до клиники, он ослаблен после нескольких дней употребления алкоголя или родственникам важно быстрее понять, какая тактика будет безопасной. После осмотра можно определить, нужна ли капельница, достаточно ли детоксикации на дому, требуется ли повторное наблюдение, а в дальнейшем — консультация по лечению алкоголизма, кодирование или реабилитация. В части случаев уже первый звонок позволяет понять, идет ли речь только о временном ухудшении самочувствия или о состоянии, при котором может потребоваться вывод из запоя в стационаре.
Узнать больше – нарколог на дом анонимно екатеринбург
WilliamKet · May 9, 2026 at 5:28 pm
Ниже представлена таблица с ключевыми направлениями терапии, применяемыми в клинике, и их особенностями.
Изучить вопрос глубже – http://narcologicheskaya-klinika-v-rostove19.ru/narkolog-rostov-na-donu/
RaymondBom · May 9, 2026 at 5:28 pm
На практике выезд врача позволяет оперативно стабилизировать состояние пациента и снизить риск осложнений, связанных с отсрочкой медицинской помощи.
Подробнее можно узнать тут – врач нарколог выезд на дом в хабаровске
Kennethsip · May 9, 2026 at 5:49 pm
Этот обзор сосредоточен на различных подходах к избавлению от зависимости. Мы изучим традиционные и альтернативные методы, а также их сочетание для достижения максимальной эффективности. Читатели смогут открыть для себя новые стратегии и подходы, которые помогут в их борьбе с зависимостями.
Узнай первым! – похмельная капельница
Shaneincix · May 9, 2026 at 5:54 pm
Особое внимание уделяется безопасности пациента. Лечение проводится анонимно, в комфортных условиях, с круглосуточным наблюдением. Палаты оборудованы системами мониторинга, а при необходимости возможно подключение интенсивной терапии. Такой формат исключает стресс и даёт возможность сосредоточиться на восстановлении.
Подробнее тут – наркологическая клиника вывод из запоя в тольятти
WalterAdula · May 9, 2026 at 5:55 pm
Предлагаем вашему вниманию интересную справочную статью, в которой собраны ключевые моменты и нюансы по актуальным вопросам. Эта информация будет полезна как для профессионалов, так и для тех, кто только начинает изучать тему. Узнайте ответы на важные вопросы и расширьте свои знания!
Это стоит прочитать полностью – частный нарколог на дом
SteveSix · May 9, 2026 at 5:56 pm
Plan your journey with https://nl.readytotrip.com, online hotel booking for any destination worldwide. Instant reservation, transparent prices, and no hidden fees. Trusted platform for hassle-free travel arrangements. Start booking today.
GarlandTow · May 9, 2026 at 6:11 pm
Объективная оценка включает измерение артериального давления, частоты сердечных сокращений, уровня сознания и выраженности вегетативных проявлений. На основании полученных данных формируется индивидуальный план медицинского вмешательства.
Исследовать вопрос подробнее – вывод из запоя на дому круглосуточно в хабаровске
DonaldLiz · May 9, 2026 at 6:16 pm
В Воронеже круглосуточная помощь при похмелье востребована в ситуациях, когда симптомы появляются внезапно или усиливаются в ночное время, особенно в запое или после запоя. Врач проводит консультацию, оценивает состояние пациента и принимает решение о проведении инфузионной терапии. Такой подход позволяет своевременно устранить симптомы и предотвратить их дальнейшее развитие. При необходимости можно оставить заявку, уточнить цены или получить помощь бесплатно на первичном этапе.
Подробнее можно узнать тут – капельница от похмелья анонимно в воронеже
DavidLig · May 9, 2026 at 6:20 pm
Врачи клиники используют щадящие методики и современные инфузионные составы, которые не перегружают организм и позволяют безопасно восстановить жизненные функции. Контроль проводится на всех этапах: от диагностики до постлечебного наблюдения.
Изучить вопрос глубже – http://vyvod-iz-zapoya-tolyatti0.ru/vyvod-iz-zapoya-tolyatti-na-domu/https://vyvod-iz-zapoya-tolyatti0.ru
CharlesExent · May 9, 2026 at 6:30 pm
В Санкт-Петербурге вывод из запоя на дому рассматривается, когда состояние пациента позволяет проводить лечение вне стационара, но требует контроля специалиста. Врач оценивает общее состояние, длительность запоя и выраженность симптомов, после чего принимает решение о формате помощи при алкоголизме. Важно, что лечение начинается сразу после осмотра, без необходимости ожидания госпитализации. При необходимости можно заказать услуги на сайте клиники или получить консультацию специалистов.
Подробнее – вывод из запоя на дому анонимно в санкт-петербурге
Sergeylet · May 9, 2026 at 6:34 pm
Покрытие надёжным полимерным покрытием — это реально стоящая вещь. Цвет не выгорает, при морозах -45 не трескается. За три сезона ни малейшего изменения оттенка. Красноярский климат для него не проблема совсем. металлочерепица надёжное полимерное покрытие Красноярск
Donaldembab · May 9, 2026 at 6:35 pm
Домашний вызов нарколога удобен в случаях, когда человеку тяжело ехать в клинику, он отказывается от поездки или родственники хотят как можно быстрее заказать медицинскую помощь на месте. Формат выезда позволяет врачу оценить самочувствие, определить тяжесть состояния и подобрать дальнейшую тактику. Если ситуация требует расширенного подхода, может обсуждаться последующая консультация в центре, лечение алкоголизма, кодирование, а в более сложных случаях — длительная реабилитация.
Разобраться лучше – нарколог на дом вывод екатеринбург
Ruslanlet · May 9, 2026 at 6:45 pm
Взял новый дом в строящемся посёлке под Красноярском. Посоветовали металлочерепицу 0.5 мм с высоким профилем под нашу стропильную систему. Через год всё в порядке. металлочерепица надёжное полимерное покрытие Красноярск
Josephcit · May 9, 2026 at 6:45 pm
Нужен выездной ресторан? кейтеринг с доставкой и обслуживанием на вашей площадке. Фуршеты, банкеты, кофе-брейки и барбекю для деловых и праздничных мероприятий. Профессиональная организация питания и широкий выбор блюд для гостей.
CharlesExent · May 9, 2026 at 6:47 pm
Запой сопровождается выраженной интоксикацией, нарушением сна, слабостью, тревожностью и колебаниями давления, что характерно для алкоголизма и других форм зависимости. При этом самостоятельный выход из состояния часто оказывается затруднённым из-за ухудшения самочувствия и невозможности контролировать симптомы. В таких случаях выезд нарколога позволяет начать лечение без задержек и помочь пациенту снизить нагрузку на организм за счёт отсутствия транспортировки.
Выяснить больше – вывод из запоя на дому цена санкт-петербург
CharlesRecok · May 9, 2026 at 7:00 pm
Помощь на дому рассматривают при состояниях, связанных с острым ухудшением самочувствия после алкоголя. Чаще всего это несколько дней запоя, тяжелое похмелье, бессонница, тревога, дрожь в руках, слабость, отсутствие аппетита, тошнота, сухость во рту и ощущение истощения. В подобных случаях врачебный осмотр нужен для оценки общего состояния и выбора безопасной тактики.
Разобраться лучше – вызов нарколога на дом екатеринбург
kasyno online · May 9, 2026 at 7:07 pm
Of course, what a great site and informative posts, I will add backlink – bookmark this site? Regards, Reader
AlvinCet · May 9, 2026 at 7:15 pm
Вывод из запоя на дому — это формат медицинской помощи, при котором лечение проводится в привычной для пациента обстановке с использованием инфузионной терапии и врачебного контроля. Такой подход позволяет начать детоксикацию без задержек и снизить нагрузку на организм, связанную с транспортировкой. В наркологической клинике «Частный медик 24» выезд специалиста организуется круглосуточно, а терапия подбирается с учётом текущего состояния пациента.
Подробнее тут – https://vyvod-iz-zapoya-na-domu-sankt-peterburg-11.ru
CharlesRecok · May 9, 2026 at 7:17 pm
Помощь на дому рассматривают при состояниях, связанных с острым ухудшением самочувствия после алкоголя. Чаще всего это несколько дней запоя, тяжелое похмелье, бессонница, тревога, дрожь в руках, слабость, отсутствие аппетита, тошнота, сухость во рту и ощущение истощения. В подобных случаях врачебный осмотр нужен для оценки общего состояния и выбора безопасной тактики.
Разобраться лучше – https://narkolog-na-dom-ekaterinburg.ru
Andrewsap · May 9, 2026 at 7:20 pm
Решение о помещении пациента в стационар принимается на основе объективных медицинских критериев, а не только по желанию родственников. К показаниям относятся: запой длительностью более трех суток, выраженные симптомы абстиненции, наличие в анамнезе алкогольных делириев или судорожных эпизодов, сопутствующие хронические заболевания печени, поджелудочной железы, сердца или нервной системы. Отдельным фактором выступает полинаркомания или сочетание алкогольной зависимости с приемом психофармакологических препаратов без назначения врача. В таких ситуациях риск развития тяжелых осложнений возрастает многократно, и амбулаторный формат не обеспечивает необходимого уровня контроля. Госпитализация позволяет провести полноценную диагностику, включая ЭКГ, экспресс-анализы крови, оценку неврологического статуса и мониторинг сатурации, что формирует точную картину состояния и исключает назначение шаблонных схем.
Углубиться в тему – вывод из запоя в стационаре
Michaelbew · May 9, 2026 at 7:27 pm
страница Даркнет сайты
Josephcroro · May 9, 2026 at 7:31 pm
“gunes seven cicekler” konusu icin mukemmel bir kaynak var. Iste link: https://yapevleri.com/articles/gunes-seven-bahce-cicekleri/
najlepsze kasyna online · May 9, 2026 at 7:33 pm
What made you first develop an interest in this topic?
Josephcroro · May 9, 2026 at 7:38 pm
Ayr?ca, eger boyas? c?kan kumasa ne yapmal? konusuyla ilgileniyorsan?z, suraya bak?n. Link burada: https://yapevleri.com/articles/kumas-kurumus-boya-lekesi-cikarma-yontemleri/
Andrewsap · May 9, 2026 at 7:38 pm
Затяжной запой перестает быть бытовой проблемой в тот момент, когда организм теряет способность самостоятельно восстанавливаться после интоксикации. Накопление ацетальдегида, нарушение водно-электролитного баланса, истощение запасов витаминов и перегрузка сердечно-сосудистой системы создают состояние, при котором домашние методы перестают быть безопасными. Срочно стабилизировать самочувствие и быстро купировать абстинентный синдром позволяет только контролируемая медицинская среда. Вывод из запоя в стационаре в Нижнем Новгороде становится клинически обоснованным решением, когда требуется не просто снятие симптомов, а комплексная детоксикация под круглосуточным наблюдением врачей. Наркологическая клиника «Стармед» организует процесс лечения в соответствии с актуальными стандартами доказательной медицины, обеспечивая безопасность пациента, прозрачность процедур и плавный переход к противорецидивной терапии. Мы понимаем, что решение о госпитализации часто принимается в состоянии стресса, поэтому наша работа начинается с четкой диагностики, честного объяснения плана лечения и соблюдения строгих протоколов конфиденциальности. Опытные специалисты клиники помогут вызвать доверие к процессу восстановления уже на этапе первого контакта.
Получить больше информации – http://www.domen.ru
Victorlooft · May 9, 2026 at 8:01 pm
Недорогие аккумуляторы https://www.akb24v.ru 24 вольта для погрузчика, стоит обратить внимание на проверенные решения с оптимальным ресурсом и стабильной отдачей. Купить тяговую батарею 24V по доступной цене. Варианты под разные задачи и типы техники.
Frankiewaide · May 9, 2026 at 8:23 pm
Капельница от похмелья может быть необходима в самых разных ситуациях, когда симптомы становятся слишком выраженными и мешают нормальному функционированию пациента. Если вы или ваши близкие сталкиваетесь с такими признаками, как сильная головная боль, рвота, слабость и головокружение, то немедленный вызов нарколога на дом станет необходимостью. Важно не откладывать помощь, так как интоксикация может усугубить состояние пациента и привести к осложнениям, таким как обезвоживание или нарушения работы сердца.
Получить больше информации – kapelnicza-ot-pokhmelya-ekaterinburg-8.ru/
Bennycency · May 9, 2026 at 9:08 pm
В Нижнем Новгороде услуга выезда нарколога чаще всего используется при состояниях, когда пациент физически не может посетить клинику или требуется срочное медицинское вмешательство. Врач приезжает с необходимыми препаратами и оборудованием, проводит осмотр и сразу приступает к лечению. Такой формат особенно важен при выраженной интоксикации и нестабильном состоянии.
Ознакомиться с деталями – нарколог на дом анонимно
소액결제현금화 · May 9, 2026 at 9:17 pm
소액결제현금화 대신 고려할 수 있는 방법도 있습니다. 대표적으로 금융기관의 소액 대출, 간편 신용 서비스, 합법적인 자금 관리 서비스 등이 있습니다. 이러한 방법은
Huberterora · May 9, 2026 at 9:35 pm
Вывод из запоя на дому с быстрым облегчением в Екатеринбурге — это процедура, направленная на быстрое снятие острых симптомов алкогольного абстинентного синдрома и возвращение пациента к нормальному состоянию, включая случаи алкоголизма и наркомании. Такая услуга удобна тем, что позволяет не только эффективно справиться с зависимостью, но и избавиться от неприятных проявлений запоя, таких как головная боль, тошнота, слабость и психоэмоциональное напряжение, в комфортной домашней обстановке, при этом оказывается наркологическая помощь. Быстрое облегчение без необходимости госпитализации делает этот метод популярным среди пациентов, которым важен быстрый и безопасный результат, а при необходимости можно заказать дальнейшее кодирование или лечение в стационаре.
Выяснить больше – вывод из запоя на дому анонимно в екатеринбурге
JorgeTreta · May 9, 2026 at 9:47 pm
Основные показания для проведения процедуры:
Подробнее – капельница от похмелья цена
Anthonyhal · May 9, 2026 at 9:48 pm
Текст посвящён распространённым мифам о зависимости и их развенчанию. Мы предоставим научно обоснованную информацию и дадим рекомендации по выбору эффективного способа борьбы с зависимым поведением.
Читать дальше – наркология нижний новгород
Everetttam · May 9, 2026 at 9:59 pm
Вывод из запоя на дому в Екатеринбурге: эффективное лечение, детоксикация и восстановление организма в наркологической клинике «Детокс»
Подробнее тут – вывод из запоя на дому цена екатеринбург
Everetttam · May 9, 2026 at 10:15 pm
Эта услуга позволяет людям, которые не могут или не хотят покидать свой дом, получить профессиональную помощь и избавиться от зависимости без госпитализации. К тому же, вывод из запоя на дому позволяет избежать стресса, связанного с нахождением в медицинских учреждениях, при этом можно заказать вызов специалистов с учетом их опыта и лет работы, а также данных больного.
Подробнее тут – вывод из запоя на дому анонимно
sunwin · May 9, 2026 at 10:16 pm
Very nice post. I just stumbled upon your blog and wanted to say that I’ve really enjoyed browsing your blog posts. In any case I’ll be subscribing to your rss feed and I hope you write again soon!
remont stiralnih mashin_qyEn · May 9, 2026 at 10:24 pm
ремонт стиральной машины https://remont-stiralnih-mashin213.ru
Timothyser · May 9, 2026 at 10:29 pm
Вывод из запоя на дому в Санкт-Петербурге с анонимным выездом врача, снятием интоксикации и поддержкой в наркологической клинике «Частный медик 24»
Разобраться лучше – вывод из запоя на дому в санкт-петербурге
BrandonRoada · May 9, 2026 at 10:34 pm
За выездом врача чаще обращаются тогда, когда человеку тяжело добраться до клиники, он ослаблен после нескольких дней употребления алкоголя или родственникам важно быстрее понять, какая тактика будет безопасной. После осмотра можно определить, нужна ли капельница, достаточно ли детоксикации на дому, требуется ли повторное наблюдение, а в дальнейшем — консультация по лечению алкоголизма, кодирование или реабилитация. В части случаев уже первый звонок позволяет понять, идет ли речь только о временном ухудшении самочувствия или о состоянии, при котором может потребоваться вывод из запоя в стационаре.
Детальнее – нарколог на дом вывод в екатеринбурге
Anthonyhal · May 9, 2026 at 10:38 pm
Текст посвящён распространённым мифам о зависимости и их развенчанию. Мы предоставим научно обоснованную информацию и дадим рекомендации по выбору эффективного способа борьбы с зависимым поведением.
Подробности по ссылке – лечение алкоголизма в стационаре нижний новгород
bizidhug · May 9, 2026 at 10:45 pm
В кафе «Фабрико» города Перми гостей ждут римская и неаполитанская пицца, роллы, суши, бургеры, супы, паста и десерты — всё по проверенным рецептам. Ищете доставка роллов? На fab-pizza.ru можно оформить доставку или самовывоз со скидкой 10%. Скидка 15% действует для именинников три дня до и три дня после дня рождения, а заказ трёх больших пицц подарит четвёртую бесплатно. Уютный зал с панорамными окнами, детская зона и банкетные помещения на 25 гостей делают кафе отличным выбором для любого визита.
BrandonRoada · May 9, 2026 at 10:53 pm
За выездом врача чаще обращаются тогда, когда человеку тяжело добраться до клиники, он ослаблен после нескольких дней употребления алкоголя или родственникам важно быстрее понять, какая тактика будет безопасной. После осмотра можно определить, нужна ли капельница, достаточно ли детоксикации на дому, требуется ли повторное наблюдение, а в дальнейшем — консультация по лечению алкоголизма, кодирование или реабилитация. В части случаев уже первый звонок позволяет понять, идет ли речь только о временном ухудшении самочувствия или о состоянии, при котором может потребоваться вывод из запоя в стационаре.
Подробнее тут – вызов нарколога на дом екатеринбург
Shaneincix · May 9, 2026 at 11:08 pm
Особое внимание уделяется безопасности пациента. Лечение проводится анонимно, в комфортных условиях, с круглосуточным наблюдением. Палаты оборудованы системами мониторинга, а при необходимости возможно подключение интенсивной терапии. Такой формат исключает стресс и даёт возможность сосредоточиться на восстановлении.
Получить дополнительную информацию – https://narkologicheskaya-klinika-tolyatti0.ru/tolyatti-narkologicheskij-dispanser/
Shaneincix · May 9, 2026 at 11:26 pm
В клинике применяются современные медицинские технологии, направленные на восстановление организма и стабилизацию психоэмоционального состояния. Ниже представлена таблица с описанием основных методов и их терапевтического значения.
Изучить вопрос глубже – https://narkologicheskaya-klinika-tolyatti0.ru/
DonaldLiz · May 9, 2026 at 11:32 pm
Такие симптомы требуют медицинского вмешательства, поскольку могут приводить к ухудшению состояния. Капельница помогает стабилизировать самочувствие и снизить нагрузку на организм. Услуги могут предоставляться анонимно, а при необходимости пациент направляется на лечение в стационаре.
Углубиться в тему – https://kapelnicza-ot-pokhmelya-voronezh-7.ru/
DavidLig · May 9, 2026 at 11:37 pm
Комплексная терапия проводится в течение 1–3 суток в зависимости от состояния пациента. В особо тяжёлых случаях врачи расширяют курс лечения, включив контрольные анализы и консультации смежных специалистов.
Подробнее – нарколог вывод из запоя в тольятти
DonaldLiz · May 9, 2026 at 11:50 pm
Процедура начинается с осмотра пациента. Врач оценивает основные показатели, включая давление и пульс, а также выраженность симптомов. После этого формируется состав капельницы и определяется тактика лечения, что позволяет эффективно провести вывод из запоя.
Получить дополнительную информацию – капельница от похмелья вызов на дом воронеж
DavidLig · May 9, 2026 at 11:55 pm
Врачи клиники используют щадящие методики и современные инфузионные составы, которые не перегружают организм и позволяют безопасно восстановить жизненные функции. Контроль проводится на всех этапах: от диагностики до постлечебного наблюдения.
Подробнее – вывод из запоя на дому недорого тольятти
WilliamThatt · May 10, 2026 at 12:30 am
Результаты первичной оценки формируют основу для выбора лечебной тактики и объёма медицинского вмешательства.
Получить больше информации – вывод из запоя на дому цена в тольятти
Andrewattap · May 10, 2026 at 12:31 am
Капельница от похмелья с контролем врача в Самаре является одной из самых популярных и эффективных услуг для тех, кто сталкивается с выраженными симптомами похмельного синдрома. Похмелье может проявляться не только головной болью и усталостью, но и более серьезными проблемами, такими как тошнота, рвота, учащенное сердцебиение и повышение давления. Когда симптомы становятся особенно острыми, капельница помогает организму справиться с токсинами, восстановить водно-электролитный баланс и нормализовать состояние пациента, в том числе при запое. Важно, что контроль врача на протяжении всей процедуры обеспечивает безопасность и эффективность, при этом помощь может оказываться как на дому, так и в клинике при лечении алкоголизма.
Получить дополнительную информацию – http://www.domen.ru
AlvinCet · May 10, 2026 at 12:38 am
Такие условия позволяют начать лечение без задержек и обеспечить более мягкое восстановление. При этом помощь может предоставляться анонимно.
Узнать больше – анонимный вывод из запоя на дому санкт-петербург
AlvinCet · May 10, 2026 at 12:57 am
В Санкт-Петербурге вывод из запоя на дому используется в ситуациях, когда состояние пациента требует медицинской помощи, но позволяет обойтись без лечения в стационаре. Врач проводит консультацию, оценивает длительность запоя, выраженность симптомов и общее состояние, анализируя данные пациента, после чего принимает решение о тактике лечения при алкоголизме. При необходимости можно оформить вызов специалиста или заказать услугу заранее.
Изучить вопрос глубже – вывод из запоя на дому в санкт-петербурге
webokelblany · May 10, 2026 at 1:05 am
Pragmatichub https://pragmatic-promo.com/ is a premier hub for Pragmatic Play slots enthusiasts. Explore detailed reviews of top titles like Gates of Olympus, Sweet Bonanza, and Big Bass Bonanza. We provide free demo gameplay, RTP data, and volatility analysis to help users understand every mechanic. Our platform ensures secure access via verified mirrors and certified partners. Find the best online gaming sites and reliable info for a safe experience with Pragmatic Play’s world-class casino software.
juyunkAmini · May 10, 2026 at 1:08 am
Точность до микрона и строгое соответствие техническому заданию — именно это отличает настоящее производство от кустарной мастерской. Компания «Металлообработка-ЗР» выполняет изготовление деталей на заказ по чертежам в Москве, работая с металлами любой сложности и обеспечивая стабильно высокое качество на каждом этапе. Подробный каталог услуг, актуальные цены и реальное портфолио готовых работ доступны на сайте https://metalloobrabotka.org/ — здесь же можно оформить заявку или заказать обратный звонок от специалиста. Собственное оборудование, сертифицированное производство и гарантия на выполненные работы делают компанию надёжным партнёром для бизнеса.
Charlesnaste · May 10, 2026 at 1:32 am
Запой сопровождается выраженной интоксикацией, нарушением работы сердечно-сосудистой системы, тревожностью и бессонницей, что характерно для алкоголизма и хронического употребления алкоголя. При длительном течении организм человека теряет способность к самостоятельному восстановлению, и вмешательство становится необходимым. Стационар в этом случае позволяет контролировать динамику состояния больного и корректировать терапию в режиме реального времени, особенно при тяжелом течении алкоголизма.
Выяснить больше – быстрый вывод из запоя в стационаре нижний новгород
PatrickTanna · May 10, 2026 at 1:45 am
Наркологическая клиника в Тольятти рассматривается как профильное медицинское звено, ориентированное на лечение алкогольной и наркотической зависимости с учётом клинических особенностей пациента. В клинике «Гармония Волги» медицинская помощь выстраивается на основе диагностики, поэтапной терапии и врачебного наблюдения, что позволяет контролировать состояние пациента на всех этапах лечения.
Получить дополнительные сведения – наркологическая клиника тольятти
vuhodsgom · May 10, 2026 at 2:01 am
Металлические детали с фирменной символикой — это не просто декор, а мощный инструмент брендинга. Компания Инпекмет специализируется на литье значков и бирок из сплава ЦАМ (Zamak) — прочного, коррозиестойкого и экологически безопасного материала. На сайте https://inpekmet.ru/ можно рассчитать тираж и оформить заказ от одного экземпляра. Изделия отличаются высокой детализацией, а финишная обработка включает полировку, покраску, чернение и лакирование. Производство работает быстро и гибко — от одного дня.
Donaldembab · May 10, 2026 at 2:32 am
Нарколог на дом в Екатеринбурге востребован в ситуациях, когда человеку нужна врачебная помощь после употребления алкоголя, при запое, выраженном похмельном синдроме, нарушении сна, тревоге, скачках давления, слабости и других признаках ухудшения самочувствия. Такой формат обращения часто выбирают семьи, которые хотят вызвать врача без поездки в клинику и быстро получить консультацию по состоянию больного. Домашний выезд особенно важен тогда, когда требуется детоксикация, наблюдение после нескольких дней употребления спиртного и оценка рисков, связанных с последствиями алкоголизма.
Ознакомиться с деталями – нарколог на дом вывод в екатеринбурге
Jamesvew · May 10, 2026 at 2:40 am
Interested in UFC? ufc 250 anniversary unique mixed martial arts tournament will take place on June 14, 2026, in Washington, D.C., on the South Lawn of the White House. It will be the first professional sporting event in history to be held directly on the grounds of the U.S. presidential residence.
RobertHes · May 10, 2026 at 2:57 am
Каждый метод выбирается строго по показаниям. При необходимости врачи комбинируют медикаментозное лечение с психотерапией, физиопроцедурами и восстановительными программами. Это обеспечивает максимальную эффективность и безопасность терапии.
Получить дополнительную информацию – наркологическая клиника цены
JasonBloma · May 10, 2026 at 3:01 am
В этом обзоре представлены различные методы избавления от зависимости, включая терапевтические и психологические подходы. Мы сравниваем их эффективность и предоставляем рекомендации для тех, кто хочет вернуться к трезвой жизни. Читатели смогут найти информацию о реабилитационных центрах и поддерживающих группах.
Ознакомьтесь поближе – наркология в нижнем новгороде
RobinZes · May 10, 2026 at 3:38 am
Этот медицинский обзор сосредоточен на последних достижениях, которые оказывают влияние на пациентов и медицинскую практику. Мы разбираем инновационные методы лечения и исследований, акцентируя внимание на их значимости для общественного здоровья. Читатели узнают о свежих данных и их возможном применении.
Продолжить чтение – платная наркологическая клиника
RaymondBom · May 10, 2026 at 3:41 am
Домашний формат лечения требует строгого соблюдения медицинских протоколов, так как врач работает вне стационара и должен учитывать ограничения условий. Поэтому ключевое значение имеет предварительная оценка состояния пациента и корректный выбор тактики вмешательства.
Узнать больше – нарколог на дом вывод из запоя в хабаровске
GarlandTow · May 10, 2026 at 4:30 am
Медицинская помощь начинается с детального осмотра и сбора анамнестических данных. Врач оценивает длительность запоя, объем употребляемого алкоголя, наличие хронических заболеваний и ранее перенесенных осложнений. Эти сведения необходимы для выбора корректной тактики лечения и исключения потенциальных рисков.
Подробнее – нарколог на дом вывод из запоя в хабаровске
Stevenjat · May 10, 2026 at 5:46 am
Продолжение кракен даркнет
Huberterora · May 10, 2026 at 6:06 am
Процедура вывода из запоя на дому включает несколько этапов, каждый из которых имеет важное значение для общего улучшения состояния пациента. Главная цель — это не только устранение симптомов абстиненции, но и восстановление нормальной работы органов и систем организма. Врач, который проводит процедуру, использует медикаментозные средства для восстановления водно-солевого баланса, нормализации работы печени, почек и других органов, пострадавших от алкоголя. Также в процесс включаются препараты, которые способствуют снятию нервного напряжения и психоэмоционального стресса.
Получить дополнительную информацию – вывод из запоя на дому цена в екатеринбурге
JorgeTreta · May 10, 2026 at 6:28 am
Процедура начинается с осмотра пациента. Врач измеряет давление, пульс, оценивает общее состояние и выраженность симптомов. На основании этих данных формируется состав капельницы и план лечения. Такой подход позволяет учитывать индивидуальные особенности пациента и эффективно провести вывод из запоя.
Разобраться лучше – капельница от похмелья на дому
Andrewattap · May 10, 2026 at 6:44 am
Капельница от похмелья с контролем врача в Самаре представляет собой эффективную терапевтическую процедуру, позволяющую значительно улучшить самочувствие пациента за короткий срок. Врач, контролируя весь процесс, может точно определить, какие компоненты необходимы для каждого пациента. Состав капельницы зависит от симптомов похмелья, состояния пациента и его индивидуальных потребностей. Это позволяет обеспечить максимально безопасное и эффективное лечение, которое помогает организму быстро восстановиться.
Узнать больше – капельница от похмелья в самаре
Stevenjat · May 10, 2026 at 6:58 am
перейдите на этот сайт kraken onion ссылка
AnthonyPhecy · May 10, 2026 at 7:04 am
Каждый этап процедуры направлен на последовательное восстановление организма и предотвращение осложнений. Ниже представлена таблица, отражающая основные стадии и их особенности.
Подробнее – вывод из запоя на дому цена хабаровск
Andrewattap · May 10, 2026 at 7:05 am
Вызов капельницы от похмелья с контролем врача в Самаре рекомендуется, когда симптомы похмелья становятся особенно тяжелыми и мешают нормальной жизнедеятельности. Несмотря на то, что многие пытаются справиться с похмельем с помощью домашних методов, такие как прием жидкости или таблеток, они не всегда оказываются достаточно эффективными. В случае сильных симптомов похмелья, капельница с врачебным контролем — это более безопасное и быстрое решение, при этом возможен вывод в стационаре, анонимное лечение и консультации по вопросам наркомании с учетом актуальной цены услуг.
Получить дополнительные сведения – капельница от похмелья самара
Frankiewaide · May 10, 2026 at 7:35 am
Капельница от похмелья в Екатеринбурге с анонимным выездом врача и восстановительной терапией в наркологической клинике «Частный медик 24»
Разобраться лучше – капельница от похмелья на дом в екатеринбурге
Stevehut · May 10, 2026 at 8:04 am
В Нижнем Новгороде выезд нарколога на дом используется при состояниях, требующих оперативной медицинской оценки и начала терапии. Врач приезжает с необходимыми препаратами, проводит осмотр и формирует план лечения на месте. Такой формат позволяет сократить время до начала помощи и снизить нагрузку на пациента.
Получить дополнительные сведения – вызов наркологической помощи нижний новгород
GregoryHat · May 10, 2026 at 8:14 am
кэт казино картинки казино
Bennycency · May 10, 2026 at 8:21 am
Нарколог на дом — это формат медицинской помощи, при котором пациент получает лечение без посещения стационара. В наркологической клинике «Частный медик 24» в Нижнем Новгороде такая услуга используется при острых состояниях: запой, выраженная алкогольная интоксикация, абстинентный синдром, а также при необходимости срочного вмешательства без транспортировки больного. Выезд врача позволяет начать терапию в первые часы ухудшения состояния, что снижает риск осложнений и облегчает переносимость лечения.
Разобраться лучше – нарколог на дом цена
Stevenjat · May 10, 2026 at 8:23 am
ссылка на сайт кракен darknet
Stevenjat · May 10, 2026 at 8:28 am
веб-сайт kraken darknet
kihebllCat · May 10, 2026 at 9:20 am
Ищете настоящие скидки, акции и промокоды в России? Посетите сайт Огонёк https://ogonek.su/ – присоединяйтесь и экономьте! У нас подборка лучших скидок ежедневно. На сайте вы сможете увидеть лучшие скидки дня, а также увидеть все скидки и промокоды магазинов. Удобный поиск по категориям, что позволит быстро найти необходимую скидку! Подробнее на сайте.
TimothyFreby · May 10, 2026 at 10:28 am
Каждый вечер я включаю старый любимый сериал и записываю одну мысль. Проект длится месяц, а главное правило — досматривать до конца.
Проект с партнёром: я выбираю начало. Вместе смотрим серию и ставим на паузу. Награда за 10 фильмов — ужин.
Сделал просмотр ритуалом: снимаю носки и пью чай. Перед включением гадаю на первой сцене. После титров — иду сразу спать.
Источник:
https://filmhub.club/
Sunwin · May 10, 2026 at 10:36 am
I favored your idea there, I tell you blogs are so helpful sometimes like looking into people’s private life’s and work.At times this world has too much information to grasp. Every new comment wonderful in its own right.
RichardFlero · May 10, 2026 at 10:57 am
Терапевтический процесс в стационаре строится по принципу последовательного выполнения клинических задач: диагностика, стабилизация, медикаментозная терапия и подготовка к амбулаторному этапу. При поступлении врач проводит детальный осмотр, собирает анамнез, оценивает неврологический статус и при необходимости назначает лабораторные исследования. На основе полученных данных формируется индивидуальный протокол, учитывающий возраст, длительность интоксикации, наличие сопутствующих патологий и переносимость лекарственных компонентов. Мы применяем только сертифицированные препараты, зарегистрированные в РФ, и строго соблюдаем клинические рекомендации Минздрава, исключая псевдонаучные методики. Стандарты оказания медицинской помощи фиксируются во внутренних регламентах и регулярно проверяются независимыми аудиторами.
Детальнее – нарколог вывод из запоя в стационаре
PatrickTanna · May 10, 2026 at 11:42 am
Диагностика позволяет установить степень интоксикации, выраженность абстинентного синдрома и наличие сопутствующих заболеваний, которые могут влиять на переносимость терапии.
Выяснить больше – http://narkologicheskaya-klinika-v-tolyatti0.ru/narkologicheskaya-bolnicza-tolyatti/
como jogar com bônus da betano · May 10, 2026 at 11:45 am
KYC took 4 hours. Decent.
Sunwin · May 10, 2026 at 12:00 pm
Clear, concise and easy to access.
Curtisloola · May 10, 2026 at 1:05 pm
Вывод из запоя на дому в Екатеринбурге: помощь при запое, снятие интоксикации и медицинская поддержка в наркологической клинике «Детокс»
Изучить вопрос глубже – https://vyvod-iz-zapoya-na-domu-ekaterinburg-17.ru/
nazumSaiLm · May 10, 2026 at 1:11 pm
Фирма «Доска Брус СПб» самостоятельно заготавливает лес и производит пиломатериалы с доставкой до покупателя. Завод производит свыше 1000 кубометров продукции в месяц с соблюдением стандартов ГОСТ 8486-86. Ассортимент включает доску, брус, брусок, вагонку, блок-хаус, шпунт, террасную доску, планкен и фанеру. Ищете доска обрезная 32х120х2000? Оформить заказ по выгодной цене можно на doskabrusspb.ru — доставка своим автопарком по Санкт-Петербургу и Ленинградской области. Контроль на каждом этапе производства гарантирует высокое качество без переплат посредникам.
AnthonyPhecy · May 10, 2026 at 2:37 pm
Каждый этап процедуры направлен на последовательное восстановление организма и предотвращение осложнений. Ниже представлена таблица, отражающая основные стадии и их особенности.
Выяснить больше – https://vyvod-iz-zapoya-v-khabarovske0.ru/vyvod-iz-zapoya-kruglosutochno-khabarovsk
Charlesnaste · May 10, 2026 at 2:45 pm
Первый этап лечения направлен на стабилизацию состояния. Он начинается с оценки витальных показателей и клинической картины. После этого формируется план терапии, в котором определены цели и временные интервалы для оценки результата. Такой подход позволяет контролировать процесс и избегать хаотичных назначений, особенно при лечении алкоголизма.
Узнать больше – быстрый вывод из запоя в стационаре
best online casino · May 10, 2026 at 2:52 pm
Hello there, You have done an incredible job. I will certainly digg it and personally recommend to my friends. I am sure they will be benefited from this site.
RandyTaite · May 10, 2026 at 2:58 pm
Несмотря на выездной формат, лечение выстраивается поэтапно и соответствует медицинским стандартам. Это обеспечивает управляемость процесса и безопасность пациента.
Подробнее – http://narkolog-na-dom-v-rnd19.ru/
AnthonyPhecy · May 10, 2026 at 3:03 pm
Каждая методика применяется строго по показаниям и под контролем медицинского персонала. Комбинация этих подходов позволяет пациенту не только восстановиться физически, но и психологически, что повышает эффективность лечения в целом.
Выяснить больше – вывод из запоя на дому цена хабаровск
Thomashen · May 10, 2026 at 3:09 pm
Вывод из запоя на дому в Екатеринбурге: срочное восстановление, детоксикация и медицинская помощь в наркологической клинике «Детокс»
Ознакомиться с деталями – анонимный вывод из запоя на дому
RandyTaite · May 10, 2026 at 3:26 pm
Нарколог на дом в Ростове-на-Дону рассматривается как специализированная форма оказания медицинской помощи пациентам с зависимостями вне стационара. В клинике «Чистый Баланс» выезд врача организуется круглосуточно, что позволяет обеспечить своевременное вмешательство при ухудшении состояния в любое время суток. Нарколог на дом в Ростове-на-Дону востребован в ситуациях, когда пациент не готов или не может обратиться в медицинское учреждение, а промедление с лечением повышает риск осложнений. Такой формат помощи требует строгого соблюдения клинических протоколов и высокой квалификации специалистов.
Исследовать вопрос подробнее – нарколог на дом круглосуточно
Romanlet · May 10, 2026 at 3:51 pm
Официальный партнёр 1С — это важно. Получаем оригинальные обновления и сертифицированную поддержку. Никаких пиратских программ, всё легально. Для нашей компании это принципиально. обслуживание 1С Белгород
Stevehut · May 10, 2026 at 3:59 pm
Наркологическая помощь в Нижнем Новгороде с выездом врача, капельницами и наблюдением пациента в наркологической клинике «Частный медик 24»
Подробнее – наркологическая помощь в нижнем новгороде
duwahnzef · May 10, 2026 at 4:05 pm
Анапа — один из самых популярных курортов Черноморского побережья, и добраться до него с комфортом теперь проще, чем когда-либо. Сервис https://anapa-taxi-transfer.ru/ предлагает профессиональные услуги такси и трансфера с удобным онлайн-калькулятором стоимости поездки прямо на сайте. Официально зарегистрированная компания работает круглосуточно, обслуживает все основные маршруты и располагает собственным автопарком. Опытные водители встретят вас в аэропорту или на вокзале, а прозрачное ценообразование избавит от неприятных сюрпризов. Путешествуйте с удовольствием!
Alekseylet · May 10, 2026 at 4:06 pm
Настройка ЕГАИС в 1С для розничной торговли алкоголем. Всё подключили с первого раза, работает стабильно. На проверках никаких нарушений выявлено не было. техподдержка 1С 24/7 Белгород
xonizioTax · May 10, 2026 at 4:27 pm
Компания CryoOne выпускает отечественные азотные криокапсулы для предприятий в области красоты, спорта и реабилитации. Срок окупаемости составляет 6 месяцев: лицензия не нужна, а впечатляющий результат процедуры обеспечивает постоянный приток клиентов. На https://cryoone.ru/ представлены четыре комплектации — Standard, Business, Pro и Comfort — с гарантией 24 месяца и бесплатными доставкой, монтажом и обучением. Сосуд Дьюара входит в базовую комплектацию, а покупатель получает гарантию минимальной цены среди конкурентов.
Stevehut · May 10, 2026 at 4:29 pm
Состояние пациента при интоксикации может развиваться по-разному: от умеренной слабости и головной боли до выраженной дезориентации, тахикардии и нарушений сна. В таких ситуациях важно не откладывать обращение за помощью. Наркологическая помощь на дому рассматривается, когда требуется быстрое вмешательство и контроль состояния без транспортировки пациента.
Подробнее – https://narkologicheskaya-pomoshh-nizhnij-novgorod-8.ru
jaxnaUtisk · May 10, 2026 at 4:53 pm
MoscowWaterWays — сервис речных прогулок по Москве от всех ключевых причалов столицы. Компания организует маршруты от Китай-города, Парка Горького, Воробьёвых гор, Москвы-Сити и других популярных точек города. Ищете стоимость билета на теплоход от москва-сити? На платформе moscowwaterways.ru можно выбрать маршрут и оплатить билеты онлайн — они придут на электронную почту. Расписание охватывает праздничные рейсы на 9 Мая, День города, выпускной и Новый год. Причалы удобно расположены рядом с метро и МЦК, а посадка занимает минимум времени.
RobertHes · May 10, 2026 at 5:07 pm
Лечение в клинике «ДальМедБаланс» базируется на комплексном подходе. Каждый метод направлен на конкретную цель — детоксикацию, восстановление, стабилизацию и профилактику повторного употребления. Используются современные медицинские технологии и препараты с доказанной эффективностью. Таблица ниже описывает основные направления терапии и их результаты.
Выяснить больше – запой наркологическая клиника в хабаровске
Charlesunpat · May 10, 2026 at 5:56 pm
Затяжной запой — это не бытовая слабость, а медицинское состояние, требующее профессионального лечения в условиях стационара. Когда организм истощен длительной интоксикацией, нарушен сон, отсутствует аппетит, а попытки самостоятельно прекратить употребление сопровождаются тремором, тревогой и скачками давления, единственным безопасным решением становится контролируемая детоксикация. Наркологическая клиника «Элегия Мед» в Санкт-Петербурге предоставляет профессиональное лечение с применением сертифицированных протоколов, непрерывный контроль состояния пациента и индивидуальный подбор медикаментозной поддержки. Мы работаем круглосуточно, обеспечивая быстрое реагирование на обращения, четкую диагностику при поступлении и прозрачное взаимодействие с родственниками. Все процедуры выполняются с соблюдением протоколов доказательной медицины, стандартов Минздрава РФ и строгих правил конфиденциальности. Первичная оценка состояния начинается с дистанционной консультации, что позволяет врачам заранее подготовить необходимое оборудование и скорректировать план госпитализации еще до прибытия пациента. При необходимости заказать консультацию или оформить выезд бригады, доступные способы связи включают телефон, мессенджеры и онлайн-форму на сайте.
Изучить вопрос глубже – https://vyvod-iz-zapoya-v-staczionare-sankt-peterburg-20.ru
best online casino new zealand · May 10, 2026 at 6:04 pm
My brother suggested I might like this web site. He was entirely right. This post actually made my day. You can not imagine simply how much time I had spent for this info! Thanks!
Michaelsence · May 10, 2026 at 6:50 pm
В «ЛадаМед Выезд» при оказании наркологической помощи на дому используются современные препараты и методы дезинтоксикации. Ниже приведена таблица с основными видами терапии и их эффектами.
Выяснить больше – http://narkolog-na-dom-tolyatti0.ru
xooxGob · May 10, 2026 at 6:55 pm
Криминальный триллер Netflix «Охотник за разумом» рассказывает о том, как агенты ФБР Холден Форд и Билл Тенч в конце 1970-х приступили к изучению психологии серийных убийц, заложив фундамент поведенческого профайлинга. Ищете охотник за разумом все серии? Все 19 серий двух сезонов доступны бесплатно на ohotnik-za-razumom-smotret.net с профессиональной озвучкой LostFilm и SDI Media. Сдержанная режиссура Дэвида Финчера, безупречная атмосфера эпохи и психологически напряжённые диалоги с реальными маньяками делают каждую серию захватывающим погружением в рождение криминальной науки — обязательный просмотр для всех ценителей умного детективного кино.
juyolPreep · May 10, 2026 at 7:12 pm
Металлообработка — отрасль, где цена ошибки измеряется браком и простоями. Портал https://metalloobrabotka.org/ объединяет производителей, поставщиков и специалистов отрасли на одной профессиональной площадке. Здесь публикуются актуальные новости, технические статьи, обзоры оборудования и база предприятий. Ресурс полезен как опытному технологу, так и руководителю, который ищет подрядчика по токарным, фрезерным или сварочным работам в своём регионе.
RichardFlero · May 10, 2026 at 8:06 pm
Выбор между домашней помощью и стационарным лечением определяется не удобством, а медицинской целесообразностью. В условиях клиники исключаются внешние триггеры, обеспечивается изоляция от источников алкоголя и создается контролируемая среда, где терапевтические решения принимаются на основе объективных показателей, а не субъективных ощущений пациента. Такой подход критически важен для предотвращения осложнений, минимизации дискомфорта абстиненции и формирования устойчивой базы для дальнейшей противорецидивной работы.
Подробнее можно узнать тут – https://vyvod-iz-zapoya-v-staczionare-sankt-peterburg-18.ru/
Bennycency · May 10, 2026 at 8:30 pm
Нарколог на дом в Нижнем Новгороде с быстрым приездом специалиста, детоксикацией и медицинской поддержкой в наркологической клинике «Частный медик 24»
Разобраться лучше – http://narkolog-na-dom-nizhnij-novgorod.ru/
DarrinLathe · May 10, 2026 at 8:36 pm
Экскурсовод организует частный тур Калининград экскурсия по городу на машине с удобным маршрутом и профессиональным сопровождением.
RichardFlero · May 10, 2026 at 8:38 pm
Непрерывный мониторинг витальных показателей — ключевое отличие стационарного формата, обеспечивающее безопасную детоксикацию. В палатах клиники «Элегия Мед» установлены системы отслеживания частоты пульса, сатурации, температуры и артериального давления, данные с которых автоматически передаются в электронную медицинскую карту. Медицинский персонал дежурит круглосуточно, что обеспечивает мгновенную реакцию на ухудшение состояния: коррекцию инфузионной терапии, введение симптоматических препаратов, привлечение смежных специалистов при необходимости. Такая организация процесса исключает хаотичное назначение средств, предотвращает полипрагмазию и гарантирует, что каждый этап детоксикации проходит под строгим клиническим контролем. При необходимости применяются дополнительные методы очищения крови, включая плазмаферез, который эффективно помогает вывести стойкие токсины и метаболиты, не удаляемые стандартной инфузионной терапией.
Подробнее – быстрый вывод из запоя в стационаре в санкт-петербурге
注册Binance · May 10, 2026 at 8:42 pm
Can you be more specific about the content of your article? After reading it, I still have some doubts. Hope you can help me. https://accounts.binance.bh/register/person?ref=IHJUI7TF
Timothyelapy · May 10, 2026 at 8:57 pm
“yaz k?s acan bahce cicekleri” konusu icin burada harika bilgiler var. Suradan okuyabilirsiniz: https://kendihobim.com/articles/yaz-kis-cicek-acan-bitkiler/
Timothyelapy · May 10, 2026 at 9:01 pm
Bu arada soyleyeyim, eger sar? gri uyumu konusuyla ilgileniyorsan?z, buray? inceleyin. Link burada: https://kendihobim.com/articles/gri-sari-renk-karisimi/
vimapdKag · May 10, 2026 at 9:02 pm
Комфортный климат в доме или офисе — это не роскошь, а продуманная инженерная система, установленная профессионалами. Компания «Энерго-Климат» из Уфы специализируется на монтаже, обслуживании и ремонте климатического оборудования, предлагая клиентам индивидуальный подход и гарантию качества. На сайте https://energo-klimat.ru/ можно уточнить услуги и связаться со специалистами напрямую через WhatsApp или Telegram — быстро и без лишних формальностей. Многолетний опыт команды и официальный статус юридического лица обеспечивают надёжность сотрудничества на каждом этапе.
Curtisloola · May 10, 2026 at 10:10 pm
Вывод из запоя на дому в Екатеринбурге – это услуга, которая становится необходимой, когда состояние пациента ухудшается после длительного употребления алкоголя, и медицинская помощь требуется немедленно. На дому пациенту предоставляется квалифицированная помощь, направленная на быстрое снятие интоксикации, восстановление водно-солевого баланса и стабилизацию общего состояния.
Выяснить больше – анонимный вывод из запоя на дому в екатеринбурге
Michaelsence · May 10, 2026 at 10:35 pm
В «ЛадаМед Выезд» при оказании наркологической помощи на дому используются современные препараты и методы дезинтоксикации. Ниже приведена таблица с основными видами терапии и их эффектами.
Подробнее тут – http://narkolog-na-dom-tolyatti0.ru/
Curtisloola · May 10, 2026 at 10:43 pm
Процесс вывода из запоя на дому состоит из нескольких этапов, которые тщательно подбираются врачом-наркологом в зависимости от состояния пациента. Важно, чтобы весь процесс был под контролем специалиста, чтобы избежать осложнений и гарантировать безопасное восстановление.
Детальнее – вывод из запоя на дому анонимно в екатеринбурге
linodKal · May 11, 2026 at 12:55 am
Интернет-магазин спортивного питания https://power-mag.ru/ Тюмень – это ведущий магазин спортивного питания. Занимаемся продажей спортивного питания и БАД и предлагаем только проверенные пищевые добавки по низким ценам. Работаем с крупнейшими поставщиками пищевых добавок и спортивного питания, а также доставляем БАДы из США, например те, что есть на маркетплейсе Айхерб. Имеется доставка в любой район города Тюмень и отправка в любой город России почтой, СДЭК и другими транспортными компаниями.
CharlesExent · May 11, 2026 at 12:56 am
К основным показаниям относятся:
Углубиться в тему – вывод из запоя на дому цена в санкт-петербурге
ladabCal · May 11, 2026 at 1:05 am
Портал «Спільно» — майданчик громадянського суспільства — выпускает тексты о политике, криминале, коррупции, культуре и общественной жизни без смягчений и лишних оговорок. Авторы и блогеры издания ведут предметные расследования коррупционных схем и офшорных механизмов опираясь на документы и верифицированные источники. Следите за независимой гражданской журналистикой на https://spilno.net/ — украинский портал для читателей требующих честного анализа и прямой гражданской позиции. Авторские блоги и колонки органично дополняют новостной контент и делают портал полноценной площадкой для открытого гражданского диалога.
CharlesRecok · May 11, 2026 at 1:25 am
Нарколог на дом в Екатеринбурге: выезд врача на дом, лечение запоя и консультации в наркологической клинике «НЕО+».
Детальнее – нарколог на дом анонимно екатеринбург
newejisoymn · May 11, 2026 at 1:53 am
Если вы давно мечтали провести незабываемый вечер на воде в самом сердце столицы, то речные прогулки по Москве-реке — именно то, что вам нужно. Сайт https://ticketscruise.ru/ собрал лучшие рейсы с живой музыкой, DJ-сетами и авторскими шоу-программами, чтобы каждый выход в город становился настоящим событием. Удобное онлайн-бронирование за пару минут, электронный билет с QR-кодом и скидки до 90% на популярные маршруты делают сервис по-настоящему привлекательным. Бар, коктейли и продуманный до мелочей сервис на борту завершают картину идеального московского вечера.
fobeklhib · May 11, 2026 at 2:01 am
Регистрация бизнеса и оформление документов — процедуры, которые отнимают время и требуют точности на каждом шаге. Компания Реготмас оказывает юридические и регистрационные услуги для предпринимателей: открытие ИП и ООО, внесение изменений, ликвидация, получение лицензий. На сайте http://regotmas.ru/ можно оставить заявку и получить консультацию специалиста. Компания работает оперативно и берёт на себя полное сопровождение, освобождая клиента от бюрократической рутины.
kopemelWaync · May 11, 2026 at 2:29 am
Visit https://slvpn-cisco.com/ – a practical blog dedicated to VPN technology, secure network connectivity, and the basics of online privacy. We publish clear technical guides on VPN protocols, DNS security, traffic metadata, and everyday privacy practices – without hype or unrealistic claims of anonymity.
Andrewsap · May 11, 2026 at 2:33 am
Затяжной запой перестает быть бытовой проблемой в тот момент, когда организм теряет способность самостоятельно восстанавливаться после интоксикации. Накопление ацетальдегида, нарушение водно-электролитного баланса, истощение запасов витаминов и перегрузка сердечно-сосудистой системы создают состояние, при котором домашние методы перестают быть безопасными. Срочно стабилизировать самочувствие и быстро купировать абстинентный синдром позволяет только контролируемая медицинская среда. Вывод из запоя в стационаре в Нижнем Новгороде становится клинически обоснованным решением, когда требуется не просто снятие симптомов, а комплексная детоксикация под круглосуточным наблюдением врачей. Наркологическая клиника «Стармед» организует процесс лечения в соответствии с актуальными стандартами доказательной медицины, обеспечивая безопасность пациента, прозрачность процедур и плавный переход к противорецидивной терапии. Мы понимаем, что решение о госпитализации часто принимается в состоянии стресса, поэтому наша работа начинается с четкой диагностики, честного объяснения плана лечения и соблюдения строгих протоколов конфиденциальности. Опытные специалисты клиники помогут вызвать доверие к процессу восстановления уже на этапе первого контакта.
Разобраться лучше – нарколог вывод из запоя в стационаре в нижнем новгороде
nahuvwag · May 11, 2026 at 2:54 am
Посетите сайт https://kotel-54.ru/ и вы найдете в наличии на складе, в Новосибирске, готовые и прошедшие заводские испытания котельные мощностью от 80квт до 12 мвт, котлы, горелки, электрические котельные, запасные части для горелок, трубопроводная арматура и другие товары по выгодной стоимости, в том числе с доставкой по регионам России. Наш ассортимент удовлетворит любые потребности покупателя.
veja aqui · May 11, 2026 at 3:15 am
KYC liberado. Finalmente.
gironinINepe · May 11, 2026 at 3:17 am
Looking for a resource focused on VPN technology, online privacy, and network security basics? Visit https://balavpn.com/ – we publish research-based guides on secure browsing, encryption protocols, DNS protection, and modern tracking risks. Find the most up-to-date and accessible guides! Learn more on our website.
Thomasnef · May 11, 2026 at 3:52 am
В статье по вопросам здоровья мы рассматриваем актуальные проблемы, с которыми сталкивается общество. Обсуждаются заболевания, факторы риска и важные аспекты профилактики. Читатели получат полезные советы о том, как сохранить здоровье и улучшить качество жизни.
Не пропусти важное – наркологическая помощь нижний новгород
Donaldembab · May 11, 2026 at 4:37 am
Отдельно стоит выделить ситуации, когда семья сталкивается не только с алкоголем, но и с употреблением наркотиков. В таких случаях врачебная консультация особенно важна, поскольку последствия интоксикации могут отличаться, а признаки наркомании и алкоголизма иногда накладываются друг на друга. Если речь идет о смешанном употреблении, подход к помощи на дому требует особой осторожности.
Детальнее – врач нарколог на дом
http://www.supergame.one/home.php?mod=space&uid=2270231 · May 11, 2026 at 5:03 am
References:
Ceasar casino http://www.supergame.one/home.php?mod=space&uid=2270231
poxadcerie · May 11, 2026 at 5:14 am
Мебельная фабрика «Подольск» производит кухни и шкафы-купе под заказ для клиентов из Москвы и Подмосковья. Для изготовления используются проверенные материалы и качественная фурнитура гарантирующие долгий срок эксплуатации. Компания берёт на себя все этапы работы: замер помещения, разработку проекта, производство и монтаж готовой мебели. Партнёром фабрики по поставке оборудования выступает https://mf-podolsk.ru/ — надёжный поставщик металлообрабатывающих станков и инструментов. Оформить заказ удобно с помощью онлайн-конструктора на официальном сайте фабрики.
https://bbs.mjjjd.eu.org · May 11, 2026 at 5:57 am
References:
Mailslot https://bbs.mjjjd.eu.org/member.php?action=profile&uid=53475
TimothyFreby · May 11, 2026 at 6:58 am
Проект «Кино вслепую»: друг кидает мне название. Не читаю трейлер, игнорирую актёров. После просмотра — разбор по трём пунктам.
В этом проекте марафоню короткие серии по 20 минут. Дисциплина: каждый день в 21:00. Фиксирую самый странный костюм.
Сделал просмотр ритуалом: зажигаю свечу. Перед включением решаю: оставить или удалить. После титров — иду сразу спать.
Источник:
https://filmhub.club/
Michaelgueld · May 11, 2026 at 7:27 am
check my blog leap wallet x official
Everetttam · May 11, 2026 at 7:32 am
Вывод из запоя на дому с медицинским контролем в Екатеринбурге — это удобный и безопасный способ для людей, страдающих от алкоголизма, пройти детоксикацию и восстановление в комфортных домашних условиях. Этот процесс включает в себя применение медицинских препаратов, направленных на снижение симптомов абстиненции, а также тщательное наблюдение за состоянием пациента. Большинство пациентов предпочитают такую услугу, поскольку она исключает необходимость госпитализации и дает возможность восстановиться без стресса, связанного с нахождением в больнице.
Ознакомиться с деталями – http://vyvod-iz-zapoya-na-domu-ekaterinburg-18.ru
sucibonOthen · May 11, 2026 at 7:45 am
ООО «РазВикТрейд» — белорусский производитель пресс-форм и изделий из пластика с опытом более 10 лет на рынках Беларуси и России. Предприятие берёт на себя весь процесс — от разработки 3D-модели и производства пресс-формы до серийного литья и доставки заказчику. На https://press-forma.by/ доступен бесплатный расчёт стоимости проекта. Площадка в 1000 кв.м. с 24 единицами оборудования позволяет производить до 1,5 млн пластиковых изделий ежемесячно. Производство обходится дешевле китайского: чистая прибыль заказчика увеличивается в 2–3 раза.
hagomwen · May 11, 2026 at 7:53 am
«Делай Промо» — комплексная SaaS-платформа, которая даёт брендам и агентствам возможность самостоятельно запускать чековые акции, программы лояльности и системы мотивации продавцов. Платформа объединяет конструктор лендингов, OCR-распознавание чеков, мультиканальные чат-боты для Telegram и VK, защищённые кодовые механики и сквозную аналитику с выгрузкой в Excel в одном интерфейсе. На http://makerpromo.ru/ уже зарегистрировано свыше 24 000 чеков и 18 000 активных пользователей. Проект находится на стадии закрытого бета-теста и предлагает участникам специальные условия подключения.
Michaelgueld · May 11, 2026 at 7:56 am
official source leap wallet dashboard
RobertHes · May 11, 2026 at 7:57 am
Наркологическая клиника — это медицинское учреждение, где лечение зависимости выстроено системно: от купирования острых симптомов до длительного сопровождения пациента. В клинике «ДальМедБаланс» терапия проводится под круглосуточным врачебным контролем, а ключевыми принципами являются безопасность, анонимность и индивидуальный подход. Каждый пациент проходит путь восстановления под наблюдением специалистов, которые учитывают физиологическое состояние, психоэмоциональные особенности и социальный контекст. Лечение направлено не только на избавление от физической зависимости, но и на возвращение мотивации к здоровой жизни.
Подробнее тут – https://narkologicheskaya-klinika-v-khabarovske0.ru/khabarovsk-narkologicheskaya-pomoshh/
Donaldembab · May 11, 2026 at 9:21 am
Нарколог на дом в Екатеринбурге: анонимная помощь при алкоголизме, вывод из запоя и поддержка специалистов в наркологической клинике «НЕО+».
Узнать больше – врач нарколог на дом екатеринбург
BrandonRoada · May 11, 2026 at 9:58 am
За выездом врача чаще обращаются тогда, когда человеку тяжело добраться до клиники, он ослаблен после нескольких дней употребления алкоголя или родственникам важно быстрее понять, какая тактика будет безопасной. После осмотра можно определить, нужна ли капельница, достаточно ли детоксикации на дому, требуется ли повторное наблюдение, а в дальнейшем — консультация по лечению алкоголизма, кодирование или реабилитация. В части случаев уже первый звонок позволяет понять, идет ли речь только о временном ухудшении самочувствия или о состоянии, при котором может потребоваться вывод из запоя в стационаре.
Ознакомиться с деталями – нарколог на дом цена екатеринбург
Shaneincix · May 11, 2026 at 10:27 am
В клинике применяются современные медицинские технологии, направленные на восстановление организма и стабилизацию психоэмоционального состояния. Ниже представлена таблица с описанием основных методов и их терапевтического значения.
Получить дополнительные сведения – наркологическая клиника в тольятти
Michaelsence · May 11, 2026 at 10:46 am
Нарколог на дом — это услуга, позволяющая получить квалифицированную медицинскую помощь в привычной обстановке без необходимости посещения клиники. В «ЛадаМед Выезд» в Тольятти круглосуточно дежурят врачи-наркологи, готовые оперативно выехать по адресу и провести детоксикацию, стабилизацию состояния и консультацию по дальнейшему лечению. Такой формат особенно востребован при запое, абстинентном синдроме, интоксикации или необходимости срочной поддержки без госпитализации. Все процедуры проводятся анонимно, безопасно и под контролем специалиста.
Разобраться лучше – платный нарколог на дом тольятти
lezosUnuff · May 11, 2026 at 11:00 am
Егор Косарев — профессиональный видеооператор и монтажёр из Москвы, работающий по всей России. Мастер работает в самых разных жанрах: от рекламных и детских роликов до корпоративных фильмов, имиджевых проектов, музыкального видео и экспертных интервью. Ищете снять видео для озон? На egorkosarev.ru представлено портфолио с более чем 110 реализованными работами. Полный производственный цикл — от разработки концепции до сдачи готового проекта — Егор реализует как в одиночку, сокращая расходы заказчика, так и с командой для масштабных задач.
PatrickWeK · May 11, 2026 at 11:23 am
Состояние после длительного употребления алкоголя или наркотических веществ сопровождается комплексом симптомов: обезвоживание, нарушение работы сердечно-сосудистой системы, тревожность, бессонница, слабость. В таких случаях важно не откладывать помощь, поскольку самостоятельное восстановление организма может быть затруднено. Наркологическая помощь на дому позволяет быстро стабилизировать показатели и начать контролируемое лечение.
Подробнее тут – нарколог на дом анонимно нижний новгород
mebiqualo · May 11, 2026 at 11:24 am
Клиника «Био-лазер» специализируется на пластической хирургии в Москве — здесь работает хирург Владимир Высоцкий с практикой более 25 лет. Пациентам доступны маммопластика, блефаропластика, абдоминопластика, лифтинг лица и шеи, отопластика и мастопексия. Ищете пластическая хирургия в Москве? Актуальные результаты операций собраны на doctor99.ru в разделе галереи. Владимир Высоцкий непрерывно повышает квалификацию на стажировках и конференциях — методы работы клиники отвечают современным требованиям. Онлайн-запись на консультацию к хирургу открыта для всех желающих.
https://vanilaptops.com/melbet-promo-code-list-nepal-max888-eu130-bonus/uncategorized/ · May 11, 2026 at 11:48 am
https://vanilaptops.com/melbet-promo-code-list-nepal-max888-eu130-bonus/uncategorized/
Thomasnef · May 11, 2026 at 12:13 pm
Эта статья освещает различные аспекты освобождения от зависимости и пути к выздоровлению. Мы обсуждаем важность осознания своей проблемы и обращения за помощью. Читатели получат практические советы о том, как преодолевать трудности и строить новую жизнь без зависимости.
Интересует подробная информация – платная наркологическая клиника
RudolphCor · May 11, 2026 at 1:07 pm
Эта публикация посвящена актуальным вопросам современной медицины и здравоохранения. Мы обсудим новейшие технологии диагностики и лечения, а также их влияние на продолжительность и качество жизни. Читатель найдет здесь информацию о научных исследованиях и перспективных разработках, доступно изложенную для широкой аудитории.
Интересует подробная информация – лечение алкоголизма в стационаре нижний новгород
BruceSoage · May 11, 2026 at 1:15 pm
Чаще всего нарколога на дом вызывают при повторяющемся или длительном запое, тяжелом похмелье, бессоннице после алкоголя, треморе, выраженной слабости и ухудшении общего самочувствия. Поводом для обращения также становятся тревога, раздражительность, скачки артериального давления, учащенный пульс, обезвоживание и необходимость поставить капельницу дома под наблюдением специалиста. Во многих случаях звонок в наркологический центр поступает тогда, когда родственники понимают, что состояние больного уже не позволяет ждать следующего дня.
Выяснить больше – https://narkolog-na-dom-ekaterinburg-2.ru/
RonnieReawn · May 11, 2026 at 1:18 pm
В этой публикации мы предложим ряд рекомендаций по избавлению от зависимостей и успешному восстановлению. Мы обсудим методы привлечения поддержки и важность самосознания. Эти советы помогут людям вернуться к нормальной жизни и стать на путь выздоровления.
Получить исчерпывающие сведения – лечение алкогольной зависимости в нижнем новгороде
lugecndSoymn · May 11, 2026 at 1:31 pm
Экологическое законодательство становится всё строже, а штрафы за нарушения — всё ощутимее, поэтому грамотное сопровождение бизнеса в сфере экологии сегодня не роскошь, а необходимость. Компания EcoDok из Владимира предлагает полный спектр услуг: разработку экологической документации, аутсорсинг эколога, подготовку к проверкам надзорных органов и производственный экологический контроль — на сайте https://ecodok.ru/ можно подробно ознакомиться с каждым направлением. Специалисты компании также разработали обучающий курс и методическое пособие для экологов, что делает EcoDok не просто исполнителем, а настоящим экспертным партнёром для вашего предприятия.
RichardKat · May 11, 2026 at 1:44 pm
Эта публикация содержит ценные советы и рекомендации по избавлению от зависимости. Мы обсуждаем различные стратегии, которые могут помочь в процессе выздоровления и важность обращения за помощью. Читатели смогут использовать полученные знания для улучшения своего состояния.
Как это работает — подробно – нарколог дом
DavidDox · May 11, 2026 at 1:59 pm
В этой статье мы обсудим процесс восстановления после зависимостей, акцентируя внимание на различных методах и подходах к реабилитации. Читатели узнают, как создать план выздоровления и использовать полезные ресурсы для достижения устойчивых изменений.
Это стоит прочитать полностью – нарколог на дому капельница цена
MartintieNo · May 11, 2026 at 2:07 pm
Этот обзор посвящен успешным стратегиям избавления от зависимости, включая реальные примеры и советы. Мы разоблачим мифы и предоставим читателям достоверную информацию о различных подходах. Получите опыт многообразия методов и найдите подходящий способ для себя!
Проследить причинно-следственные связи – помощь нарколога на дому при алкоголизме
Walterfancy · May 11, 2026 at 2:18 pm
Коллеги, статья о «невидимом маркетинге» — SEO, который работает в фоновом режиме, но приносит основные результаты. Автор разбирает, почему SEO важнее контекстной рекламы в долгосрочной перспективе, и приводит аргументы в пользу системного подхода. Есть блок про аналитику и измерение эффективности. Полезно для собственников бизнеса: https://shinastop.ru/stati/seo-kak-fundament-biznesa-pochemu-nevidimyj-marketing-vazhnee-chem-kazhetsja/
RonaldDew · May 11, 2026 at 3:06 pm
В этой статье-обзоре мы соберем актуальную информацию и интересные факты, которые освещают важные темы. Читатели смогут ознакомиться с различными мнениями и подходами, что позволит им расширить кругозор и глубже понять обсуждаемые вопросы.
Узнать из первых рук – выведение из запоя санкт петербург стационар
Ronalddiums · May 11, 2026 at 3:27 pm
Существует ряд ситуаций, при которых вызов специалиста на дом является обоснованным решением:
Выяснить больше – запой нарколог на дом
JamesJoums · May 11, 2026 at 3:37 pm
Нарколог на дом в Екатеринбурге: срочная медицинская помощь, капельницы и восстановление состояния в наркологической клинике «НЕО+».
Детальнее – нарколог на дом вывод екатеринбург
Jamesbeicy · May 11, 2026 at 3:40 pm
Этот информационный материал собраны данные, которые помогут лучше понять текущие тенденции и процессы в различных сферах жизни. Мы предоставляем четкий анализ, графики и примеры, чтобы информация была не только понятной, но и практичной для принятия решений.
Узнать больше – принудительное лечение от алкогольной зависимости
freudwiki.site · May 11, 2026 at 4:26 pm
References:
Black jack no yuuwaku https://freudwiki.site/wiki/Where_Australias_Online_Gambling_Scene_Is_Headed_in_2026
LonnieMop · May 11, 2026 at 4:26 pm
Процесс лечения капельницей помогает улучшить состояние пациента уже через короткий период. Важно, что процедура не только снимает симптомы похмелья, но и восстанавливает нормальную работу печени, почек и других органов, пострадавших от токсического воздействия алкоголя. Это помогает предотвратить долгосрочные последствия интоксикации, такие как хроническая усталость, проблемы с органами и психоэмоциональные расстройства.
Углубиться в тему – http://www.domen.ru
MiguelNet · May 11, 2026 at 4:29 pm
Состояние пациента при интоксикации может развиваться по-разному: от умеренной слабости и головной боли до выраженной дезориентации, тахикардии и нарушений сна. В таких ситуациях важно не откладывать обращение за помощью. Наркологическая помощь на дому рассматривается, когда требуется быстрое вмешательство и контроль состояния без транспортировки пациента.
Подробнее можно узнать тут – наркологическая помощь на дому
NathanGathy · May 11, 2026 at 4:43 pm
Процесс лечения капельницей помогает улучшить состояние пациента уже через короткий период. Важно, что процедура не только снимает симптомы похмелья, но и восстанавливает нормальную работу печени, почек и других органов, пострадавших от токсического воздействия алкоголя. Это помогает предотвратить долгосрочные последствия интоксикации, такие как хроническая усталость, проблемы с органами и психоэмоциональные расстройства.
Детальнее – капельница от похмелья
naruto 438 · May 11, 2026 at 4:45 pm
наруто онлайн хорошее качество наруто онлайн
JeffryCotly · May 11, 2026 at 5:07 pm
Терапевтический процесс в стационаре строится по принципу последовательного выполнения клинических задач: диагностика, стабилизация, медикаментозная терапия и подготовка к амбулаторному этапу. При поступлении врач проводит детальный осмотр, собирает анамнез, оценивает неврологический статус и при необходимости назначает лабораторные исследования. На основе полученных данных формируется индивидуальный протокол, учитывающий возраст, длительность интоксикации, наличие сопутствующих патологий и переносимость лекарственных компонентов. Мы применяем только сертифицированные препараты, зарегистрированные в РФ, и строго соблюдаем клинические рекомендации Минздрава, исключая псевдонаучные методики. Стандарты оказания медицинской помощи фиксируются во внутренних регламентах и регулярно проверяются независимыми аудиторами.
Исследовать вопрос подробнее – https://vyvod-iz-zapoya-v-staczionare-sankt-peterburg-18.ru/
top 10 nettikasinot · May 11, 2026 at 5:45 pm
I wrote down your blog in my bookmark. I hope that it somehow did not fall and continues to be a great place for reading texts.
JasonNox · May 11, 2026 at 6:32 pm
Нарколог на дом в Екатеринбурге: выезд врача на дом, лечение запоя и консультации в наркологической клинике «НЕО+».
Подробнее можно узнать тут – нарколог на дом цена
MichealSaK · May 11, 2026 at 6:41 pm
При выводе из запоя на дому с быстрым облегчением используются различные медикаменты, направленные на быстрое восстановление водно-солевого баланса, улучшение функции печени и почек, а также снижение симптомов алкогольного абстинентного синдрома. Важно, что состав препаратов подбирается в зависимости от состояния пациента, и все препараты вводятся под контролем квалифицированного медицинского специалиста.
Углубиться в тему – вывод из запоя на дому цена екатеринбург
uichin.net · May 11, 2026 at 7:38 pm
References:
Gsn casino games https://uichin.net/ui/home.php?mod=space&uid=2709394
WilliamHiree · May 11, 2026 at 8:01 pm
Читатели получат представление о том, как современные технологии влияют на развитие медицины. Обсуждаются новые методы лечения, персонализированный подход и роль цифровых решений в повышении качества медицинских услуг.
Ссылка на источник – лечение наркомании в нижнем новгороде
furhsiz · May 11, 2026 at 8:39 pm
Петербургская компания ForOne.Manakara занимается поставкой и установкой инновационных стеновых панелей из коэкструзионного бамбука и гибкого камня для отделки современных пространств. В основе технологии — измельчённый бамбук, прошедший карбонизацию и коэкструзию с ПВХ, с последующей спайкой при 120°C. Ищете панели для стен леманапро? На сайте forone.manakara.ru представлен полный каталог продукции с услугами выезда специалиста и профессионального монтажа. Панели абсолютно экологичны, легко монтируются на любые поверхности без предварительной подготовки и отлично подходят для жилых, детских и медицинских объектов.
WilliamHiree · May 11, 2026 at 8:56 pm
В этой статье мы рассматриваем разрушительное влияние зависимости на жизнь человека. Обсуждаются аспекты, такие как здоровье, отношения и профессиональные достижения. Читатели узнают о необходимости обращения за помощью и о путях к восстановлению.
Информация доступна здесь – наркологический центр нижний новгород
JamesPonna · May 11, 2026 at 9:06 pm
Этот обзор посвящен успешным стратегиям избавления от зависимости, включая реальные примеры и советы. Мы разоблачим мифы и предоставим читателям достоверную информацию о различных подходах. Получите опыт многообразия методов и найдите подходящий способ для себя!
Только для своих – “наркологическая клиника
MiguelNet · May 11, 2026 at 9:07 pm
Наркологическая помощь в Нижнем Новгороде с выездом врача, капельницами и наблюдением пациента в наркологической клинике «Частный медик 24»
Подробнее можно узнать тут – оказание наркологической помощи
LonnieMop · May 11, 2026 at 9:09 pm
Процесс лечения капельницей помогает улучшить состояние пациента уже через короткий период. Важно, что процедура не только снимает симптомы похмелья, но и восстанавливает нормальную работу печени, почек и других органов, пострадавших от токсического воздействия алкоголя. Это помогает предотвратить долгосрочные последствия интоксикации, такие как хроническая усталость, проблемы с органами и психоэмоциональные расстройства.
Получить дополнительную информацию – капельница от похмелья на дому в екатеринбурге
StanleySnoni · May 11, 2026 at 9:26 pm
Первичный осмотр включает оценку витальных показателей, уровня сознания, выраженности симптомов и факторов риска. После этого врач определяет объём вмешательства и приступает к терапии. В большинстве случаев применяется инфузионное лечение, направленное на восстановление водного баланса и выведение токсинов.
Подробнее – http://www.domen.ru
RaymondCah · May 11, 2026 at 9:26 pm
Капельница от похмелья может быть необходима в самых разных ситуациях, когда симптомы становятся слишком выраженными и мешают нормальному функционированию пациента. Если вы или ваши близкие сталкиваетесь с такими признаками, как сильная головная боль, рвота, слабость и головокружение, то немедленный вызов нарколога на дом станет необходимостью. Важно не откладывать помощь, так как интоксикация может усугубить состояние пациента и привести к осложнениям, таким как обезвоживание или нарушения работы сердца.
Ознакомиться с деталями – капельница от похмелья на дому екатеринбург
JeffryCotly · May 11, 2026 at 9:47 pm
Непрерывный мониторинг витальных показателей — ключевое отличие стационарного формата, обеспечивающее безопасную детоксикацию. В палатах клиники «Элегия Мед» установлены системы отслеживания частоты пульса, сатурации, температуры и артериального давления, данные с которых автоматически передаются в электронную медицинскую карту. Медицинский персонал дежурит круглосуточно, что обеспечивает мгновенную реакцию на ухудшение состояния: коррекцию инфузионной терапии, введение симптоматических препаратов, привлечение смежных специалистов при необходимости. Такая организация процесса исключает хаотичное назначение средств, предотвращает полипрагмазию и гарантирует, что каждый этап детоксикации проходит под строгим клиническим контролем. При необходимости применяются дополнительные методы очищения крови, включая плазмаферез, который эффективно помогает вывести стойкие токсины и метаболиты, не удаляемые стандартной инфузионной терапией.
Ознакомиться с деталями – https://vyvod-iz-zapoya-v-staczionare-sankt-peterburg-18.ru
JamesPonna · May 11, 2026 at 9:57 pm
Этот текст представляет собой обзор свежих данных и исследований в области медицины. Он призван помочь читателям понять, как научные достижения влияют на лечение, диагностику и общее состояние системы здравоохранения.
Как это работает — подробно – старс медикал нижний новгород
StanleySnoni · May 11, 2026 at 10:09 pm
В Нижнем Новгороде выезд нарколога на дом используется при состояниях, требующих оперативной медицинской оценки и начала терапии. Врач приезжает с необходимыми препаратами, проводит осмотр и формирует план лечения на месте. Такой формат позволяет сократить время до начала помощи и снизить нагрузку на пациента.
Получить дополнительные сведения – https://narkologicheskaya-pomoshh-nizhnij-novgorod-8.ru
JamesNem · May 11, 2026 at 10:24 pm
Эта статья погружает вас в увлекательный мир знаний, где каждый факт становится открытием. Мы расскажем о ключевых исторических поворотных моментах и научных прорывах, которые изменили ход цивилизации. Поймите, как прошлое формирует настоящее и как его уроки могут помочь нам строить будущее.
Получить дополнительную информацию – запой стационар цены
MichealSaK · May 11, 2026 at 10:27 pm
Вывод из запоя на дому с быстрым облегчением в Екатеринбурге — это процедура, направленная на быстрое снятие острых симптомов алкогольного абстинентного синдрома и возвращение пациента к нормальному состоянию, включая случаи алкоголизма и наркомании. Такая услуга удобна тем, что позволяет не только эффективно справиться с зависимостью, но и избавиться от неприятных проявлений запоя, таких как головная боль, тошнота, слабость и психоэмоциональное напряжение, в комфортной домашней обстановке, при этом оказывается наркологическая помощь. Быстрое облегчение без необходимости госпитализации делает этот метод популярным среди пациентов, которым важен быстрый и безопасный результат, а при необходимости можно заказать дальнейшее кодирование или лечение в стационаре.
Исследовать вопрос подробнее – вывод из запоя на дому анонимно
RobertBibra · May 11, 2026 at 10:45 pm
Читатели получат представление о том, как современные технологии влияют на развитие медицины. Обсуждаются новые методы лечения, персонализированный подход и роль цифровых решений в повышении качества медицинских услуг.
Углубиться в тему – вызвать врача нарколога на дом
JamesNem · May 11, 2026 at 11:20 pm
Публикация предлагает читателю не просто информацию, а инструменты для анализа и саморазвития. Мы стимулируем критическое мышление, предлагая различные точки зрения и призывая к самостоятельному поиску решений.
Погрузиться в детали – прокапаться от алкоголя в стационаре
hubovrMub · May 11, 2026 at 11:20 pm
РУС-МеДтеХ — проверенный партнёр по поставке медтехники и оборудования непосредственно с заводов. Компания предлагает полное оснащение лечебно-профилактических учреждений: от диагностического и реанимационного оборудования до медицинской мебели и расходных материалов. На платформе https://rus-medteh.ru/ доступны запасные части, медицинская одежда и техника для домашнего использования. В ассортименте представлено свыше 37 категорий продукции для медицинских учреждений, лабораторий и домашнего применения. Среди клиентов — государственные больницы и частные медцентры, для каждого из которых гарантированы честные цены и надёжный сервис.
Robertevile · May 11, 2026 at 11:30 pm
В этой статье мы рассматриваем разрушительное влияние зависимости на жизнь человека. Обсуждаются аспекты, такие как здоровье, отношения и профессиональные достижения. Читатели узнают о необходимости обращения за помощью и о путях к восстановлению.
Как это работает — подробно – вывод из запоя на дому телефоны
boyeddPrisy · May 11, 2026 at 11:37 pm
С 1997 года симферопольская компания «Транзит Медиа» задаёт стандарты рекламного производства в Крыму: широкоформатная полноцветная и УФ-печать, брендирование корпоративного транспорта, изготовление баннеров, вывесок и изделий из акрила — всё это выполняется на собственном оборудовании с использованием качественных европейских материалов. Подробный каталог услуг и актуальные цены производителя размещены на https://transitmedia.ru/, где можно сразу оформить заявку. Более 25 лет безупречной работы, гарантия на все изделия и услуги, доставка по Симферополю и городам Крыма — весомые аргументы в пользу надёжного партнёра для вашего бизнеса.
RobertBibra · May 11, 2026 at 11:51 pm
Медицинская публикация представляет собой свод актуальных исследований, экспертных мнений и новейших достижений в сфере здравоохранения. Здесь вы найдете информацию о новых методах лечения, прорывных технологиях и их практическом применении. Мы стремимся сделать актуальные медицинские исследования доступными и понятными для широкой аудитории.
Ознакомиться с отчётом – нарколог на дом
stomatologiya 925 · May 12, 2026 at 12:01 am
номер телефона стоматологии https://stomatologiya-batumi.ru
Jeffreytoush · May 12, 2026 at 12:06 am
Процедура капельницы от похмелья с контролем врача в Самаре начинается с первичной консультации, на которой врач осматривает пациента, измеряет его основные показатели (давление, пульс, температуру) и оценивает общее состояние. На основе этих данных выбирается оптимальный состав капельницы, которая может включать в себя различные компоненты, такие как солевые растворы, витамины, антиоксиданты и медикаменты для снятия симптомов похмелья.
Разобраться лучше – капельница от похмелья цена в самаре
Robertevile · May 12, 2026 at 12:40 am
В этой публикации мы исследуем ключевые аспекты здоровья, включая влияние образа жизни на благополучие. Читатели узнают о важности правильного питания, физической активности и психического здоровья. Мы предоставим практические советы и рекомендации для поддержания здоровья и развития профилактических подходов.
Полная информация здесь – помощь при запое нарколог на дом
RichardFup · May 12, 2026 at 12:55 am
В данной статье рассматриваются физиологические и эмоциональные аспекты зависимости. Мы обсудим, как организм реагирует на зависимое поведение, и какие методы помогают восстановить здоровье и внутреннее равновесие.
Прочесть заключение эксперта – вызов врача нарколога на дом
RudolphCor · May 12, 2026 at 1:03 am
Эта публикация посвящена актуальным вопросам современной медицины и здравоохранения. Мы обсудим новейшие технологии диагностики и лечения, а также их влияние на продолжительность и качество жизни. Читатель найдет здесь информацию о научных исследованиях и перспективных разработках, доступно изложенную для широкой аудитории.
Узнай первым! – лечение алкогольной зависимости в нижнем новгороде
RonnieReawn · May 12, 2026 at 1:25 am
В этой статье мы обсудим процесс восстановления после зависимостей, акцентируя внимание на различных методах и подходах к реабилитации. Читатели узнают, как создать план выздоровления и использовать полезные ресурсы для достижения устойчивых изменений.
Кликни и узнай всё! – наркологический центр нижний новгород
RichardKat · May 12, 2026 at 1:40 am
В статье по вопросам здоровья мы рассматриваем актуальные проблемы, с которыми сталкивается общество. Обсуждаются заболевания, факторы риска и важные аспекты профилактики. Читатели получат полезные советы о том, как сохранить здоровье и улучшить качество жизни.
Что ещё? Расскажи всё! – анонимная наркологическая помощь на дому
PatrickWeK · May 12, 2026 at 1:55 am
Существует ряд ситуаций, при которых вызов специалиста на дом является обоснованным решением:
Получить больше информации – нарколог на дом цена
телеграм бот купить рубли · May 12, 2026 at 2:15 am
парсер данных с сайта
DavidDox · May 12, 2026 at 2:20 am
Этот медицинский обзор сосредоточен на последних достижениях, которые оказывают влияние на пациентов и медицинскую практику. Мы разбираем инновационные методы лечения и исследований, акцентируя внимание на их значимости для общественного здоровья. Читатели узнают о свежих данных и их возможном применении.
Полная информация здесь – срочный вывод из запоя на дому врач
www.mixcloud.com · May 12, 2026 at 2:45 am
References:
The quad casino https://www.mixcloud.com/prosepoint86/
Francislat · May 12, 2026 at 3:05 am
В этой статье обсуждаются актуальные медицинские вопросы, которые волнуют общество. Мы обращаем внимание на проблемы, касающиеся здравоохранения и лечения, а также на новшества в области медицины. Читатели будут осведомлены о последних событиях и смогут следить за тенденциями в медицине.
Разобраться лучше – психиатр нарколог на дом
BrantVag · May 12, 2026 at 3:10 am
на этом сайте kraken сайт
MartintieNo · May 12, 2026 at 3:11 am
В этой статье рассматриваются различные аспекты избавления от зависимости, включая физические и психологические методы. Мы обсудим поддержку, мотивацию и стратегии, которые помогут в процессе выздоровления. Читатели узнают, как преодолеть трудности и двигаться к новой жизни без зависимости.
Проследить причинно-следственные связи – телефон нарколога на дом
JesusAlkal · May 12, 2026 at 3:13 am
Процедура капельницы от похмелья с контролем врача в Самаре начинается с первичной консультации, на которой врач осматривает пациента, измеряет его основные показатели (давление, пульс, температуру) и оценивает общее состояние. На основе этих данных выбирается оптимальный состав капельницы, которая может включать в себя различные компоненты, такие как солевые растворы, витамины, антиоксиданты и медикаменты для снятия симптомов похмелья.
Исследовать вопрос подробнее – капельница от похмелья анонимно в самаре
NathanGathy · May 12, 2026 at 3:19 am
Процесс лечения капельницей помогает улучшить состояние пациента уже через короткий период. Важно, что процедура не только снимает симптомы похмелья, но и восстанавливает нормальную работу печени, почек и других органов, пострадавших от токсического воздействия алкоголя. Это помогает предотвратить долгосрочные последствия интоксикации, такие как хроническая усталость, проблемы с органами и психоэмоциональные расстройства.
Узнать больше – капельница от похмелья цена
Jorgesmems · May 12, 2026 at 3:29 am
Эта публикация раскрывает психологические механизмы зависимости и их роль в развитии расстройств. Читатель узнает о том, как психология влияет на формирование зависимостей и как профессиональная помощь может изменить ситуацию.
Личный опыт — читайте сами – вызов нарколога на дом телефон
https://a-taxi.com.ua/user/orangecan85/ · May 12, 2026 at 3:37 am
References:
Slot machine app https://a-taxi.com.ua/user/orangecan85/
BrantVag · May 12, 2026 at 3:40 am
подробнее кракен darknet
ctphome.com · May 12, 2026 at 4:09 am
References:
Buffalo run casino miami ok http://ctphome.com/bbs/home.php?mod=space&uid=121246
продвижение на яндекс картах · May 12, 2026 at 4:18 am
email рассылка
Jeffreytoush · May 12, 2026 at 4:27 am
Вызов капельницы от похмелья с контролем врача в Самаре рекомендуется, когда симптомы похмелья становятся особенно тяжелыми и мешают нормальной жизнедеятельности. Несмотря на то, что многие пытаются справиться с похмельем с помощью домашних методов, такие как прием жидкости или таблеток, они не всегда оказываются достаточно эффективными. В случае сильных симптомов похмелья, капельница с врачебным контролем — это более безопасное и быстрое решение, при этом возможен вывод в стационаре, анонимное лечение и консультации по вопросам наркомании с учетом актуальной цены услуг.
Разобраться лучше – капельница от похмелья вызов на дом в самаре
BruceSoage · May 12, 2026 at 4:28 am
Нарколог на дом в Екатеринбурге востребован в ситуациях, когда человеку нужна врачебная помощь после употребления алкоголя, при запое, выраженном похмельном синдроме, нарушении сна, тревоге, скачках давления, слабости и других признаках ухудшения самочувствия. Такой формат обращения часто выбирают семьи, которые хотят вызвать врача без поездки в клинику и быстро получить консультацию по состоянию больного. Домашний выезд особенно важен тогда, когда требуется детоксикация, наблюдение после нескольких дней употребления спиртного и оценка рисков, связанных с последствиями алкоголизма.
Углубиться в тему – narkolog-na-dom-ekaterinburg-2.ru/
hello88.kitchen · May 12, 2026 at 4:31 am
Hi there, just became aware of your blog through Google, and found that it’s truly informative. It’s important to cover these trends.
Jorgenem · May 12, 2026 at 4:46 am
В этой публикации мы рассматриваем важную тему борьбы с зависимостями, включая алкогольную и наркотическую зависимости. Мы обсудим методы лечения, реабилитации и поддержку, которые могут помочь людям, столкнувшимся с этой проблемой. Читатели узнают о перспективах выздоровления и важности комплексного подхода.
Обратитесь за информацией – нарколог на дом вывод из запоя
Jorgesmems · May 12, 2026 at 5:01 am
В этой статье рассматриваются различные аспекты избавления от зависимости, включая физические и психологические методы. Мы обсудим поддержку, мотивацию и стратегии, которые помогут в процессе выздоровления. Читатели узнают, как преодолеть трудности и двигаться к новой жизни без зависимости.
Почему это важно? – вызов врача на дом нарколога
Martinbib · May 12, 2026 at 5:13 am
Вызов капельницы от похмелья с контролем врача в Самаре рекомендуется, когда симптомы похмелья становятся особенно тяжелыми и мешают нормальной жизнедеятельности. Несмотря на то, что многие пытаются справиться с похмельем с помощью домашних методов, такие как прием жидкости или таблеток, они не всегда оказываются достаточно эффективными. В случае сильных симптомов похмелья, капельница с врачебным контролем — это более безопасное и быстрое решение, при этом возможен вывод в стационаре, анонимное лечение и консультации по вопросам наркомании с учетом актуальной цены услуг.
Подробнее тут – https://kapelnicza-ot-pokhmelya-samara-13.ru/
fixDiele · May 12, 2026 at 5:24 am
Между прочим, если вас интересует Долгие турниры и выносливость в футболе: стратегии и истории, посмотрите сюда.
Ссылка ниже:
https://biathlon24.ru
MatthewSoype · May 12, 2026 at 5:24 am
Существует ряд ситуаций, при которых вызов специалиста на дом является обоснованным решением:
Изучить вопрос глубже – врач нарколог на дом нижний новгород
fixDiele · May 12, 2026 at 5:28 am
Между прочим, если вас интересует Технологии “умного города”: от дома до экологии, посмотрите сюда.
Смотрите сами:
https://urban-soft.ru
JesusAlkal · May 12, 2026 at 5:33 am
Процедура капельницы от похмелья с контролем врача в Самаре начинается с первичной консультации, на которой врач осматривает пациента, измеряет его основные показатели (давление, пульс, температуру) и оценивает общее состояние. На основе этих данных выбирается оптимальный состав капельницы, которая может включать в себя различные компоненты, такие как солевые растворы, витамины, антиоксиданты и медикаменты для снятия симптомов похмелья.
Получить дополнительные сведения – капельница от похмелья вызов на дом
JamesJoums · May 12, 2026 at 5:38 am
За выездом врача чаще обращаются тогда, когда человеку тяжело добраться до клиники, он ослаблен после нескольких дней употребления алкоголя или родственникам важно быстрее понять, какая тактика будет безопасной. После осмотра можно определить, нужна ли капельница, достаточно ли детоксикации на дому, требуется ли повторное наблюдение, а в дальнейшем — консультация по лечению алкоголизма, кодирование или реабилитация. В части случаев уже первый звонок позволяет понять, идет ли речь только о временном ухудшении самочувствия или о состоянии, при котором может потребоваться вывод из запоя в стационаре.
Получить дополнительную информацию – нарколог на дом цена в екатеринбурге
Danielnar · May 12, 2026 at 5:39 am
Запой сопровождается интоксикацией, нарушением сна, слабостью, тревожностью и нестабильностью работы сердечно-сосудистой системы, что характерно для алкоголизма и других форм зависимости, включая наркомании. При этом самостоятельный выход из состояния может сопровождаться усилением симптомов, что требует медицинского вмешательства. Капельницы на дому позволяют очень быстро снизить выраженность проявлений и начать восстановление под наблюдением врача, помогая человеку стабилизировать состояние.
Выяснить больше – нарколог на дом вывод из запоя
JamesJoums · May 12, 2026 at 5:41 am
Отдельно выделяют ситуации, когда родственники вызывают врача не только из-за текущего состояния, но и потому, что подобные эпизоды повторяются. Если накапливаются последствия алкоголизма, нарушается сон, меняется поведение, появляются устойчивые проблемы дома и в повседневной жизни, разовая помощь обычно рассматривается как первый этап последующей тактики. При тяжелом состоянии, признаках отравлении алкоголем или сочетании нескольких рисков сразу может понадобиться более интенсивное наблюдение в стационаре.
Подробнее – запой нарколог на дом в екатеринбурге
Lavernehic · May 12, 2026 at 5:45 am
К основным показаниям относятся:
Исследовать вопрос подробнее – анонимный вывод из запоя на дому в санкт-петербурге
TimothyFreby · May 12, 2026 at 6:04 am
Проект «Кино вслепую»: я достаю из коробки бумажку. Не читаю трейлер, игнорирую актёров. После просмотра — разбор по трём пунктам.
Проект с партнёром: я выбираю начало. Вместе пересказываем друг другу свои версии. Награда за 10 фильмов — ужин.
Сделал просмотр ритуалом: зажигаю свечу. Перед включением гадаю на первой сцене. После титров — не иду в соцсети 15 минут.
Источник:
https://filmhub.club/
BrantVag · May 12, 2026 at 6:06 am
страница кракен онион
hiawsUime · May 12, 2026 at 6:10 am
Ищете базальтовый материал? Заходите на vztm.ru — официальный ресурс ВЗТМ, Воткинского Завода Теплоизоляционных Материалов, специализирующегося на выпуске теплоизоляционных систем из базальтового супер-тонкого волокна. Изделия завода применяются на предприятиях энергетики, в оборонной отрасли, нефтегазовом секторе, а также в гражданском и промышленном строительстве. Ознакомьтесь с нашим каталогом товаров и географией поставок. При производстве мы используем уникальные технологии, поддерживаем неизменно высокое качество продукции.
MatthewSoype · May 12, 2026 at 6:19 am
Состояние после длительного употребления алкоголя или наркотических веществ сопровождается комплексом симптомов: обезвоживание, нарушение работы сердечно-сосудистой системы, тревожность, бессонница, слабость. В таких случаях важно не откладывать помощь, поскольку самостоятельное восстановление организма может быть затруднено. Наркологическая помощь на дому позволяет быстро стабилизировать показатели и начать контролируемое лечение.
Детальнее – вызвать нарколога на дом в нижнем новгороде
Matthewbax · May 12, 2026 at 6:36 am
К основным показаниям относятся:
Получить дополнительные сведения – вывод из запоя на дому круглосуточно в санкт-петербурге
Ronalddiums · May 12, 2026 at 6:46 am
В Нижнем Новгороде услуга выезда нарколога чаще всего используется при состояниях, когда пациент физически не может посетить клинику или требуется срочное медицинское вмешательство. Врач приезжает с необходимыми препаратами и оборудованием, проводит осмотр и сразу приступает к лечению. Такой формат особенно важен при выраженной интоксикации и нестабильном состоянии.
Исследовать вопрос подробнее – вызвать нарколога на дом нижний новгород
RichardFup · May 12, 2026 at 7:02 am
В этой статье мы подробно рассматриваем проверенные методы борьбы с зависимостями, включая психотерапию, медикаментозное лечение и поддержку со стороны общества. Мы акцентируем внимание на важности комплексного подхода и возможности успешного восстановления для людей, столкнувшихся с этой проблемой.
Получить профессиональную консультацию – нарколог на дом принудительно
DavidBeemi · May 12, 2026 at 7:06 am
Вывод из запоя на дому — это формат наркологической помощи, при котором лечение проводится в привычной для пациента обстановке с выездом врача. Такой подход применяется в ситуациях, когда состояние требует медицинского вмешательства, но не предполагает обязательной госпитализации. В наркологической клинике «Частный медик 24» помощь на дому выстраивается по принципу поэтапной стабилизации: сначала устраняются острые проявления, затем оценивается динамика и при необходимости корректируется терапия.
Исследовать вопрос подробнее – https://vyvod-iz-zapoya-na-domu-sankt-peterburg-8.ru/
RaymondCah · May 12, 2026 at 7:08 am
Для жителей Екатеринбурга наркологическая клиника «Частный медик 24» предлагает услуги выезда нарколога на дом для проведения капельницы от похмелья. Это удобный и эффективный способ лечения, особенно если пациент испытывает тяжёлые симптомы похмелья и не может поехать в клинику. Выезд нарколога на дом позволяет начать лечение сразу, не тратя время на поездку и ожидания в клинике. Врач приезжает с необходимыми препаратами и оборудованием, проводит осмотр и назначает необходимую терапию.
Выяснить больше – http://kapelnicza-ot-pokhmelya-ekaterinburg-8.ru/
TrustGuru Relatório · May 12, 2026 at 7:23 am
Compra de bônus no Wild Bandito só faz sentido se o RTP base passar 96.5%.
MichealSaK · May 12, 2026 at 7:59 am
Вывод из запоя на дому в Екатеринбурге: круглосуточная помощь, снятие симптомов и поддержка специалистов в наркологической клинике «Детокс»
Получить больше информации – vyvod-iz-zapoya-na-domu-ekaterinburg-19.ru/
Danielnar · May 12, 2026 at 8:11 am
Такие условия позволяют начать лечение без задержек и обеспечить более мягкое восстановление. При этом помощь может предоставляться анонимно.
Исследовать вопрос подробнее – анонимный вывод из запоя на дому санкт-петербург
Lavernehic · May 12, 2026 at 8:17 am
Вывод из запоя на дому в Санкт-Петербурге с выездом нарколога, детоксикацией и восстановлением состояния в наркологической клинике «Частный медик 24»
Исследовать вопрос подробнее – нарколог на дом вывод из запоя
DonaldHax · May 12, 2026 at 8:32 am
olke xeberleri Qarabag FK
gefumENULA · May 12, 2026 at 8:36 am
Besök https://www.ferieisverige.no/ för allt du behöver veta om semestrar i Sverige, inklusive Smultronställen Sverige-ladan och allt om Fjällbacka och Pås til Sverige. Örebro är utan tvekan det bästa stället att koppla av på – ta reda på mer om det, och julemärkt Sverige kommer att lämna ingen oberörd!
AaronopTot · May 12, 2026 at 8:44 am
В этой информационной статье вы найдете интересное содержание, которое поможет вам расширить свои знания. Мы предлагаем увлекательный подход и уникальные взгляды на обсуждаемые темы, побуждая пользователей к активному мышлению и критическому анализу.
Как достичь результата? – нарколог на дом телефон
mifemeVowly · May 12, 2026 at 9:02 am
Ищете слушать музыку онлайн? Откройте muzqeen.cc и окунитесь в мир музыки: здесь собрана гигантская коллекция треков всех жанров и направлений, включая горячие новинки. Помимо прослушивания, на портале доступно скачивание mp3 на компьютер и мобильный телефон. Только лучшая музыка собрана на нашем портале. Добавьте наш портал в избранное и первыми узнавайте о новых релизах ваших любимых групп и артистов!
Thomasmek · May 12, 2026 at 9:05 am
Мы собрали для вас самые захватывающие факты из мира науки и истории. От малознакомых деталей до грандиозных событий — эта статья расширит ваш кругозор и подарит новое понимание того, как устроен наш мир.
Не упусти шанс – запой санкт петербург
Francislat · May 12, 2026 at 10:09 am
В этой статье обсуждаются актуальные медицинские вопросы, которые волнуют общество. Мы обращаем внимание на проблемы, касающиеся здравоохранения и лечения, а также на новшества в области медицины. Читатели будут осведомлены о последних событиях и смогут следить за тенденциями в медицине.
Тыкай сюда — узнаешь много интересного – нарколог на дом вывод
Thomasmek · May 12, 2026 at 11:11 am
Эта статья погружает вас в увлекательный мир знаний, где каждый факт становится открытием. Мы расскажем о ключевых исторических поворотных моментах и научных прорывах, которые изменили ход цивилизации. Поймите, как прошлое формирует настоящее и как его уроки могут помочь нам строить будущее.
Ознакомиться с отчётом – вывод из запоя лечение алкоголизма
JasonMon · May 12, 2026 at 11:15 am
эвакуатор для газели эвакуатор города москвы
Jorgenem · May 12, 2026 at 12:29 pm
В этой медицинской статье мы погрузимся в актуальные вопросы здравоохранения и лечения заболеваний. Читатели узнают о современных подходах, методах диагностики и новых открытий в научных исследованиях. Наша цель — донести важную информацию и повысить уровень осведомленности о здоровье.
Прочесть всё о… – вызов наркологической помощи на дом
MatthewgaB · May 12, 2026 at 12:37 pm
Такие состояния требуют не только лечения, но и наблюдения, поскольку динамика может меняться в течение короткого времени. Стационар позволяет минимизировать риски и обеспечить безопасность пациента. При этом услуга может предоставляться анонимно, а цена лечения зависит от состояния пациента.
Подробнее можно узнать тут – вывод из запоя капельница на дому в нижнем новгороде
mamabaji app download · May 12, 2026 at 12:45 pm
Mobile casinos work through apps or mobile browsers. Most modern sites are optimized for smartphones. You can play almost any game on Android or iOS. Mobile gambling is now just as common as desktop. mamabaji app download
AaronFrome · May 12, 2026 at 1:04 pm
В этой статье мы обсудим процесс восстановления после зависимостей, акцентируя внимание на различных методах и подходах к реабилитации. Читатели узнают, как создать план выздоровления и использовать полезные ресурсы для достижения устойчивых изменений.
Обратитесь за информацией – вызов нарколога круглосуточно
mikrosluchatko 659 · May 12, 2026 at 1:28 pm
nanosondy cena minikamera Praha
сео продвижение на яндекс картах · May 12, 2026 at 2:14 pm
купить аккаунты бот телеграм
лучшая email рассылка · May 12, 2026 at 2:40 pm
парсер сайтов по доркам
Jamesdon · May 12, 2026 at 3:17 pm
Continue paxful
AaronFrome · May 12, 2026 at 3:27 pm
В данной статье рассматриваются физиологические и эмоциональные аспекты зависимости. Мы обсудим, как организм реагирует на зависимое поведение, и какие методы помогают восстановить здоровье и внутреннее равновесие.
Узнать больше – срочный вывод из запоя на дому круглосуточно
best online casino · May 12, 2026 at 3:33 pm
How do I subscribe to your blog? Thanks for your help.
online casino · May 12, 2026 at 3:45 pm
I like this weblog very much so much great info .
online casino · May 12, 2026 at 3:51 pm
I Am Going To have to come back again when my course load lets up – however I am taking your Rss feed so i can go through your site offline. Thanks.
beste online casino deutschland · May 12, 2026 at 3:56 pm
Simply want to say your article is as amazing. The clarity in your post is just great and i can assume you’re an expert on this subject. Fine with your permission allow me to grab your feed to keep up to date with forthcoming post. Thanks a million and please keep up the gratifying work.
StanleySnoni · May 12, 2026 at 4:13 pm
Необходимость обращения за наркологической помощью определяется по совокупности симптомов и их выраженности. При ухудшении состояния важно ориентироваться на объективные признаки, а не ждать самостоятельного улучшения.
Исследовать вопрос подробнее – narkologicheskaya-pomoshh-nizhnij-novgorod-8.ru/
Jamesdon · May 12, 2026 at 4:26 pm
get redirected here paxful sign in
JeffryCotly · May 12, 2026 at 4:33 pm
Выбор между домашней помощью и стационарным лечением определяется не удобством, а медицинской целесообразностью. В условиях клиники исключаются внешние триггеры, обеспечивается изоляция от источников алкоголя и создается контролируемая среда, где терапевтические решения принимаются на основе объективных показателей, а не субъективных ощущений пациента. Такой подход критически важен для предотвращения осложнений, минимизации дискомфорта абстиненции и формирования устойчивой базы для дальнейшей противорецидивной работы.
Исследовать вопрос подробнее – быстрый вывод из запоя в стационаре в санкт-петербурге
heniounick · May 12, 2026 at 4:33 pm
Авторская психиатрическая клиника доктора наук Виталия Минутко https://minutkoclinic.com/ основана в 2003 году. Работаем со всеми психическими расстройствами, включая детскую психиатрию: депрессия, ОКР, анорексия, шизофрения, зависимости, анорексия, аутизм, расстройства личности.
Haroldautob · May 12, 2026 at 4:44 pm
В этой публикации мы обсуждаем современные методы лечения различных заболеваний. Читатели узнают о новых медикаментах, терапиях и исследованиях, которые активно применяются для лечения. Мы нацелены на то, чтобы предоставить практические знания, которые могут помочь в борьбе с недугами.
Ознакомиться с деталями – лечение наркозависимости нижний новгород
best online casino · May 12, 2026 at 4:44 pm
I absolutely adore your site! You aggressive me as able-bodied as all the others actuality and your broiled PS is absolutely great!
ChrisWhelf · May 12, 2026 at 4:54 pm
seo продвижение яндекс https://kormclub.ru
NathanGathy · May 12, 2026 at 4:56 pm
Процесс лечения капельницей помогает улучшить состояние пациента уже через короткий период. Важно, что процедура не только снимает симптомы похмелья, но и восстанавливает нормальную работу печени, почек и других органов, пострадавших от токсического воздействия алкоголя. Это помогает предотвратить долгосрочные последствия интоксикации, такие как хроническая усталость, проблемы с органами и психоэмоциональные расстройства.
Получить больше информации – капельница от похмелья цена
AaronopTot · May 12, 2026 at 5:10 pm
В этом обзорном материале представлены увлекательные детали, которые находят отражение в различных аспектах жизни. Мы исследуем непонятные и интересные моменты, позволяя читателю увидеть картину целиком. Погрузитесь в мир знаний и удивительных открытий!
Все материалы собраны здесь – нарколог цена
online casino · May 12, 2026 at 5:23 pm
What a great article.. i subscribed btw!
GoodiniCrubs · May 12, 2026 at 5:26 pm
В этой статье мы говорим о важности поддержки в процессе выздоровления. Рассматриваются семьи, группы поддержки, специалисты и онлайн-ресурсы, которые могут сыграть решающую роль в избавлении от зависимости.
Нажмите, чтобы узнать больше – наркологический клиника
JesusAlkal · May 12, 2026 at 5:31 pm
Капельница от похмелья с контролем врача в Самаре является одной из самых популярных и эффективных услуг для тех, кто сталкивается с выраженными симптомами похмельного синдрома. Похмелье может проявляться не только головной болью и усталостью, но и более серьезными проблемами, такими как тошнота, рвота, учащенное сердцебиение и повышение давления. Когда симптомы становятся особенно острыми, капельница помогает организму справиться с токсинами, восстановить водно-электролитный баланс и нормализовать состояние пациента, в том числе при запое. Важно, что контроль врача на протяжении всей процедуры обеспечивает безопасность и эффективность, при этом помощь может оказываться как на дому, так и в клинике при лечении алкоголизма.
Узнать больше – https://kapelnicza-ot-pokhmelya-samara-13.ru/
Peterdok · May 12, 2026 at 5:33 pm
Наиболее частыми причинами обращения становятся запой, выраженная слабость, тремор, нарушение сна, тревога, учащенный пульс, нестабильное давление, тошнота и ощущение физического истощения. Эти проявления могут сочетаться между собой и усиливаться после прекращения употребления алкоголя, особенно если эпизод длился несколько дней.
Подробнее – нарколог на дом анонимно в москве
casino-world-australia.com · May 12, 2026 at 5:41 pm
Some online casinos accept cryptocurrencies like Bitcoin or Ethereum. Crypto transactions are faster and more private than bank cards. However, price changes can affect your balance. Check if the casino offers stablecoins for less volatility. casino-world-australia.com
ThomasScier · May 12, 2026 at 5:47 pm
В данной статье мы акцентируем внимание на важности поддержки в процессе выздоровления. Мы обсудим, как друзья, семья и профессионалы могут помочь тем, кто сталкивается с зависимостями. Читатели получат практические советы, как поддерживать близких на пути к новой жизни.
Получить дополнительные сведения – narcology.clinic
Jamesdon · May 12, 2026 at 5:47 pm
click here now paxful bitcoin wallet
Snail Bob · May 12, 2026 at 6:04 pm
It sounds like you’re creating problems yourself by defining this as such a comprehensive, almost unknowable problem. Isn’t that self-defeating?
Randyfeare · May 12, 2026 at 6:42 pm
Статья посвящена анализу текущих трендов в медицине и их влиянию на жизнь людей. Мы рассмотрим новые технологии, методы лечения и значение профилактики в обеспечении долголетия и здоровья.
Только для своих – http://anapa.stop-alko.com/
xamicSep · May 12, 2026 at 7:05 pm
Domamir — российский бренд современной сантехники с лаконичным дизайном и актуальными покрытиями для любого интерьера. В линейке бренда — полотенцесушители, смесители и аксессуары для ванной комнаты с упором на современные тенденции. На https://domamir-group.ru/ размещён удобный каталог с возможностью сравнения моделей по серии и покрытию. Линейка продукции рассчитана на разные вкусы и ценовые категории — от сдержанной классики до акцентных дизайнерских форм.
nipaxaAbefS · May 12, 2026 at 7:06 pm
Разработка сайтов в пермской студии идёт по строгому пятишаговому алгоритму — от согласования задач до финального запуска. Ищете заказать сайт? На design59.ru можно заказать как шаблонное решение так и полностью индивидуальный дизайн с вёрсткой с нуля. Сроки выполнения и итоговая стоимость проекта формируются исходя из утверждённого технического задания. Дополнительно студия берётся за обслуживание, администрирование и продвижение сайта.
DennisThymn · May 12, 2026 at 7:09 pm
В статье представлены ключевые моменты по актуальной теме, дополненные советами экспертов и ссылками на дополнительные ресурсы. Цель материала — дать читателю инструменты для самостоятельного развития и принятия осознанных решений.
Исследовать вопрос подробнее – принудительное лечение от алкогольной зависимости
JasonPat · May 12, 2026 at 7:12 pm
В этой статье мы рассматриваем разрушительное влияние зависимости на жизнь человека. Обсуждаются аспекты, такие как здоровье, отношения и профессиональные достижения. Читатели узнают о необходимости обращения за помощью и о путях к восстановлению.
Не упусти важное! – цены на лечение алкоголизма
Michaelcit · May 12, 2026 at 7:13 pm
В этой публикации мы предложим ряд рекомендаций по избавлению от зависимостей и успешному восстановлению. Мы обсудим методы привлечения поддержки и важность самосознания. Эти советы помогут людям вернуться к нормальной жизни и стать на путь выздоровления.
Углубиться в тему – частный медик 24 ростов на дону
online casino deutschland · May 12, 2026 at 7:20 pm
This is one very informative blog. I like the way you write and I will bookmark your blog to my favorites.
EdwineduFf · May 12, 2026 at 7:29 pm
Реабилитация алкоголиков с поддержкой специалистов в Москве представляет собой важный и сложный процесс, в котором ключевую роль играет профессиональное вмешательство. Программы реабилитации включают в себя не только медицинскую помощь, но и психологическую, социальную и эмоциональную поддержку, что способствует успешному и долгосрочному восстановлению пациента. Такая комплексная помощь является основой эффективного лечения и предотвращения рецидивов.
Исследовать вопрос подробнее – центр реабилитации алкоголиков
top online casinos nz · May 12, 2026 at 7:44 pm
I was referred to this web site by my cousin. I’m not sure who has written this post, but you’ve really identified my problem. You’re wonderful! Thanks!
casino-world-australia.com · May 12, 2026 at 7:52 pm
Table game fans have many choices online. Beyond blackjack and roulette, you can play baccarat, craps, or casino poker. Each game has different house edges. Learning basic strategy for one game is better than guessing in many. casino-world-australia.com
online casino · May 12, 2026 at 8:07 pm
I saw a similar post on another website but the points were not as well articulated.
online casino · May 12, 2026 at 8:38 pm
I dont think Ive caught all the angles of this subject the way youve pointed them out. Youre a true star, a rock star man. Youve got so much to say and know so much about the subject that I think you should just teach a class about it
best online casino nz · May 12, 2026 at 8:52 pm
Hi, possibly i’m being a little off topic here, but I was browsing your site and it looks stimulating. I’m writing a blog and trying to make it look neat, but everytime I touch it I mess something up. Did you design the blog yourself?
gumisamgew · May 12, 2026 at 9:01 pm
Навигация по американскому рынку требует точных данных, и именно это предоставляет US Atlas — аналитический ресурс с подробными картами и статистикой по регионам США. Платформа охватывает демографию, экономику и инфраструктуру в разрезе штатов и округов. На сайте https://us-atlas.com/ данные представлены наглядно и структурированно, что делает ресурс незаменимым инструментом для бизнес-анализа, академических исследований и стратегического планирования. Работать с географией страны становится проще, когда информация собрана в одном месте.
online casino · May 12, 2026 at 9:11 pm
I’m impressed, I need to say. Really rarely do I encounter a blog that’s both educational and entertaining, and let me tell you, you have hit the nail on the head.
totihaSax · May 12, 2026 at 9:20 pm
Портал «Український оглядач» работает по твёрдому редакционному принципу — оглядаємо, аналізуємо, висловлюємо думку — и освещает политику, экономику, криминал и бизнес с прямой экспертной позицией без лишних оговорок. Авторы издания расследуют коррупционные механизмы и готовят предметную аналитику с опорой на верифицированные данные и доказательную фактуру. Читайте независимую аналитику на https://obozrevatel.org/ — украинский медиаресурс для аудитории ценящей глубину анализа и честную журналистскую позицию. Блоки технологий, культуры и здоровья усиливают новостное ядро ресурса и формируют из него полноценный ежедневный инструмент для самого широкого читателя.
midas luck casino · May 12, 2026 at 9:22 pm
Online casinos use random number generators to ensure fair play. RNGs are tested by independent agencies like eCOGRA or iTech Labs. This technology guarantees that every spin or card draw is random. No one can predict or manipulate results. https://midas-casino-australia.com/
Fireboy And Watergirl · May 12, 2026 at 9:27 pm
Thanks for your patience and sorry for the inconvenience!
EdwardSnugs · May 12, 2026 at 9:33 pm
Домашний формат выбирают тогда, когда человеку тяжело добраться до медицинского учреждения, он ослаблен после нескольких дней употребления алкоголя или родственникам важно быстро получить врачебную оценку состояния. После осмотра определяют, допустима ли помощь на дому, требуется ли детоксикация, нужна ли капельница, достаточно ли домашнего наблюдения или следует сразу рассматривать другой объем помощи. Если эпизоды повторяются, обсуждение может выходить за рамки одного выезда и включать лечение алкоголизма, помощь при зависимости, кодирование, участие психолога и реабилитацию. Уже на этапе первичного обращения нередко уточняют, как вызвать врача, какие услуги доступны на дому и в каких условиях домашний формат остается безопасным.
Разобраться лучше – врач нарколог на дом
die besten online casinos · May 12, 2026 at 10:14 pm
I don’t normally comment but I gotta say appreciate it for the post on this one : D.
best online casino · May 12, 2026 at 10:21 pm
Have you always been concerned about these issues?
best online casino · May 12, 2026 at 10:33 pm
Might we expect to see more of these same problems in the future?
best online casino · May 12, 2026 at 10:40 pm
Appreciation for taking the time to discuss this topic, I would love to discover more on this topic. If viable, as you gain expertise, would you object to updating the website with further information? It is tremendously beneficial for me.
Davidpap · May 12, 2026 at 10:42 pm
В этой статье собраны факты, которые освещают целый ряд важных вопросов. Мы стремимся предложить читателям четкую, достоверную информацию, которая поможет сформировать собственное мнение и лучше понять сложные аспекты рассматриваемой темы.
Раскрыть тему полностью – вывод из запоя стационар санкт петербург
rocket play casino australia · May 12, 2026 at 10:55 pm
Some online casinos accept cryptocurrencies like Bitcoin or Ethereum. Crypto transactions are faster and more private than bank cards. However, price changes can affect your balance. Check if the casino offers stablecoins for less volatility. rocket play casino australia
EdwineduFf · May 12, 2026 at 11:06 pm
Реабилитация алкоголиков с поддержкой специалистов — это системный подход к лечению алкогольной зависимости, который включает в себя различные медицинские, психологические и социальные методы. В Москве существует множество наркологических центров, предлагающих такие программы, где пациентам предоставляется комплексное лечение под наблюдением квалифицированных специалистов. Процесс реабилитации направлен не только на избавление от алкогольной зависимости, но и на восстановление социальной адаптации пациента, улучшение его психоэмоционального состояния и предотвращение рецидивов. В клиниках также могут предложить кодирование от алкоголизма, что помогает значительно снизить риск возвращения к прежним привычкам и обеспечить долгосрочную трезвость пациента.
Ознакомиться с деталями – реабилитация алкоголиков
die besten online casinos · May 12, 2026 at 11:20 pm
When are you going to take this to a full book?
beste online casino · May 12, 2026 at 11:38 pm
Nice blog here! Also your web site loads up very fast! What host are you using? Can I get your affiliate link to your host? I wish my web site loaded up as fast as yours lol
beste online casino · May 12, 2026 at 11:43 pm
I had fun reading this post. I want to see more on this subject.. Gives Thanks for writing this nice article.. Anyway, I’m going to subscribe to your rss and I wish you write great articles again soon.
RaymondWaini · May 12, 2026 at 11:45 pm
В этом информативном обзоре собраны самые интересные статистические данные и факты, которые помогут лучше понять текущие тренды. Мы представим вам цифры и графики, которые иллюстрируют, как развиваются различные сферы жизни. Эта информация станет отличной основой для глубокого анализа и принятия обоснованных решений.
Перейти к статье – нарколог вывод из запоя в стационаре
najlepsze kasyna online · May 12, 2026 at 11:54 pm
Oh my goodness! an amazing article. Great work.
notaVuppy · May 12, 2026 at 11:59 pm
Сайт КазиноГид создан для тех, кто хочет выбирать онлайн-казино осознанно и получать максимум от бонусных акций. Здесь собраны только лицензионные площадки с моментальными выплатами и эксклюзивными промокодами — в том числе бездепозитные фриспины для новых игроков. Рейтинг составлен на основе реального тестирования: каждое казино проверено по критериям безопасности и честности. Ищете бездепозитные бонусы за регистрацию в казино с выводом без пополнения 300 руб? Посетите casino-gid.best — актуальные промокоды и топ лучших казино уже ждут вас. Выбирайте проверенные платформы и играйте с умом.
beste online casino · May 13, 2026 at 12:02 am
I think that may be an interesting element, it made me assume a bit. Thanks for sparking my considering cap. On occasion I get so much in a rut that I simply really feel like a record.
Martinbib · May 13, 2026 at 12:02 am
Капельница от похмелья с контролем врача в Самаре представляет собой эффективную терапевтическую процедуру, позволяющую значительно улучшить самочувствие пациента за короткий срок. Врач, контролируя весь процесс, может точно определить, какие компоненты необходимы для каждого пациента. Состав капельницы зависит от симптомов похмелья, состояния пациента и его индивидуальных потребностей. Это позволяет обеспечить максимально безопасное и эффективное лечение, которое помогает организму быстро восстановиться.
Исследовать вопрос подробнее – капельница от похмелья на дому самара
best online casino nz · May 13, 2026 at 12:06 am
fantastic post, very informative. I wonder why more of the ther experts in the field do not break it down like this. You should continue your writing. I am confident, you have a great readers’ base already!
best online casino · May 13, 2026 at 12:27 am
This has to be one of my favorite posts! And on top of thats its also very helpful topic for newbies. thank a lot for the information!
best online casino · May 13, 2026 at 12:28 am
A neighbor of mine encouraged me to take a look at your blog site couple weeks ago, given that we both love similar stuff and I will need to say I am quite impressed.
StanleySnoni · May 13, 2026 at 12:36 am
Наркологическая помощь — это комплекс медицинских мероприятий, направленных на стабилизацию состояния пациента при алкогольной или наркотической интоксикации, а также при абстинентном синдроме. В наркологической клинике «Частный медик 24» в Нижнем Новгороде помощь оказывается с учётом текущего состояния пациента, без избыточных вмешательств и с чёткой ориентацией на клинические показатели. Выезд нарколога позволяет начать лечение в первые часы ухудшения самочувствия, что снижает риски осложнений и облегчает восстановление.
Получить дополнительные сведения – наркологическая помощь на дому
RaymondWaini · May 13, 2026 at 12:46 am
Эта статья погружает вас в увлекательный мир знаний, где каждый факт становится открытием. Мы расскажем о ключевых исторических поворотных моментах и научных прорывах, которые изменили ход цивилизации. Поймите, как прошлое формирует настоящее и как его уроки могут помочь нам строить будущее.
Детальнее – вывод из запоя санкт петербург стационар
vpn vergleich · May 13, 2026 at 12:46 am
I dont think Ive caught all the angles of this subject the way youve pointed them out. Youre a true star, a rock star man. Youve got so much to say and know so much about the subject that I think you should just teach a class about it
Charlesavamn · May 13, 2026 at 1:25 am
В статье по вопросам здоровья мы рассматриваем актуальные проблемы, с которыми сталкивается общество. Обсуждаются заболевания, факторы риска и важные аспекты профилактики. Читатели получат полезные советы о том, как сохранить здоровье и улучшить качество жизни.
Полная информация здесь – balashiha.stop-alko.com
генератор дорвеев · May 13, 2026 at 1:43 am
генератор дорвеев
JeffryCotly · May 13, 2026 at 1:58 am
Непрерывный мониторинг витальных показателей — ключевое отличие стационарного формата, обеспечивающее безопасную детоксикацию. В палатах клиники «Элегия Мед» установлены системы отслеживания частоты пульса, сатурации, температуры и артериального давления, данные с которых автоматически передаются в электронную медицинскую карту. Медицинский персонал дежурит круглосуточно, что обеспечивает мгновенную реакцию на ухудшение состояния: коррекцию инфузионной терапии, введение симптоматических препаратов, привлечение смежных специалистов при необходимости. Такая организация процесса исключает хаотичное назначение средств, предотвращает полипрагмазию и гарантирует, что каждый этап детоксикации проходит под строгим клиническим контролем. При необходимости применяются дополнительные методы очищения крови, включая плазмаферез, который эффективно помогает вывести стойкие токсины и метаболиты, не удаляемые стандартной инфузионной терапией.
Разобраться лучше – быстрый вывод из запоя в стационаре
DennisThymn · May 13, 2026 at 2:15 am
Этот информативный текст отличается привлекательным содержанием и актуальными данными. Мы предлагаем читателям взглянуть на привычные вещи под новым углом, предоставляя интересный и доступный материал. Получите удовольствие от чтения и расширьте кругозор!
Читать дальше – лечение алкоголизма
Charlesavamn · May 13, 2026 at 2:19 am
Публикация знакомит читателей с различными подходами к реабилитации. От традиционных методов до современных программ — вы узнаете, как выбрать оптимальный путь к выздоровлению и преодолеть препятствия на этом пути.
Нажми и узнай всё – https://balashiha.stop-alko.com/
JesusAlkal · May 13, 2026 at 2:22 am
Процедура капельницы от похмелья с контролем врача в Самаре начинается с первичной консультации, на которой врач осматривает пациента, измеряет его основные показатели (давление, пульс, температуру) и оценивает общее состояние. На основе этих данных выбирается оптимальный состав капельницы, которая может включать в себя различные компоненты, такие как солевые растворы, витамины, антиоксиданты и медикаменты для снятия симптомов похмелья.
Разобраться лучше – капельница от похмелья цена самара
NathanGathy · May 13, 2026 at 2:35 am
Процесс лечения капельницей помогает улучшить состояние пациента уже через короткий период. Важно, что процедура не только снимает симптомы похмелья, но и восстанавливает нормальную работу печени, почек и других органов, пострадавших от токсического воздействия алкоголя. Это помогает предотвратить долгосрочные последствия интоксикации, такие как хроническая усталость, проблемы с органами и психоэмоциональные расстройства.
Исследовать вопрос подробнее – http://kapelnicza-ot-pokhmelya-ekaterinburg-8.ru/
vivapNax · May 13, 2026 at 3:05 am
Ищете тюнинг и ремонт фар автомобиля москва? Посетите сайт by-tuning.ru и ознакомьтесь с нашими работами. Ознакомьтесь с нашими услугами: антихром, тюнинг, ремонт фар и многое другое. Репутация для нас важна — каждая услуга выполняется профессионально и с гарантией. Стоимость услуг указана на сайте — всё прозрачно и без скрытых платежей. Оцените наше портфолио и убедитесь в качестве работ! Би Вай Сервис — детейлинг центр, в котором к каждому автомобилю относятся с душой.
Haroldautob · May 13, 2026 at 3:28 am
В данной статье рассматриваются физиологические и эмоциональные аспекты зависимости. Мы обсудим, как организм реагирует на зависимое поведение, и какие методы помогают восстановить здоровье и внутреннее равновесие.
Ссылка на источник – лечение алкогольной зависимости в нижнем новгороде
Davidbrify · May 13, 2026 at 3:28 am
Процесс выведения из запоя в клинике основан на медицинских стандартах и многолетнем опыте врачей-наркологов. Каждый случай рассматривается индивидуально: перед началом лечения проводится оценка состояния пациента, определяется степень интоксикации и подбираются препараты, подходящие именно ему. Врачи центра работают круглосуточно, а выездная помощь доступна во всех районах Ростова-на-Дону и области. Это особенно важно, когда требуется немедленная помощь, а доставить пациента в стационар невозможно.
Углубиться в тему – скорая вывод из запоя ростов-на-дону
AnthonyDal · May 13, 2026 at 3:41 am
Привет всем!
Уверенное позиционирование в топ-3 выдачи увеличивает видимость и кратно поднимает кликабельность сниппета. Мы оптимизируем контент, ссылки и технические параметры для достижения лидирующих позиций. Поисковые алгоритмы поощряют качественные ресурсы и стабильно удерживают их в топе. Вы получаете максимум органического трафика и увеличиваете конверсию без роста бюджета. Позиционируйтесь в топе профессионально и доминируйте в конкурентной выдаче.
Профессиональная настройка Яндекс Метрики открывает полную картину поведения пользователей на вашем сайте. Мы конфигурируем цели, сегменты и отчёты для максимального контроля над эффективностью продвижения. Поисковые системы учитывают поведенческие данные, и мы помогаем улучшить их для роста позиций. Вы получаете ценную аналитику для принятия обоснованных решений о развитии ресурса. Настраивайте Метрику профессионально и увеличивайте конверсию органического трафика.
Больше информации по ссылке – https://ru-iphone.ru/chto-nuzhno-znat-pro-seo-prodvizhenie-bloga-polnyj-gid-dlya-novichkov.php
валюты и цены для регионов, работа с репутацией в поиске, аудит безопасности сайта
введение и заключение в тексте, FID First Input Delay, устранение найденных уязвимостей
Удачи!
VernonFrads · May 13, 2026 at 3:50 am
this hyperlink
zcash wallet
магазин по продаже ботов · May 13, 2026 at 4:23 am
магазин по продаже ботов
Barrystack · May 13, 2026 at 4:35 am
Мы рассмотрим современные вызовы здравоохранения и пути их решения с помощью технологий и научных исследований. В статье собраны данные о новых лекарствах, методах диагностики и системном подходе к улучшению здоровья населения.
Только для своих – где лечат алкоголиков принудительно
Randyfeare · May 13, 2026 at 5:24 am
В данной статье рассматриваются проблемы общественного здоровья и социальные факторы, влияющие на него. Мы акцентируем внимание на значении профилактики и осведомленности в защите здоровья на уровне общества. Читатели смогут узнать о новых инициативах и программах, направленных на улучшение здоровья населения.
Узнай первым! – Наркологическая клиника «Похмельная служба» в Анапе
VernonFrads · May 13, 2026 at 5:28 am
check over here
what is the purpose of staking crypto
GoodiniCrubs · May 13, 2026 at 5:29 am
Этот текст представляет собой обзор свежих данных и исследований в области медицины. Он призван помочь читателям понять, как научные достижения влияют на лечение, диагностику и общее состояние системы здравоохранения.
Узнать больше > – наркологическая клиника ростов-на-дону
WilliamTex · May 13, 2026 at 5:42 am
Запой – это неконтролируемое употребление алкоголя, которое приводит к серьезным последствиям. Алкогольное отравление организма приводит к серьезным проблемам со здоровьем. Выходить из запоя самостоятельно – рискованно и неэффективно. Мы предлагаем помощь при запое на дому, в привычных для вас условиях. Круглосуточная помощь при запое с выездом на дом за 30-60 минут. Длительный запой разрушает организм и может быть смертельным. Чем раньше вы обратитесь за помощью, тем больше шансов на выздоровление.
Исследовать вопрос подробнее – https://vyvod-iz-zapoya-krasnoyarsk0.ru/vyvod-iz-zapoya-kruglosutochno-krasnoyarsk
ThomasScier · May 13, 2026 at 5:42 am
Этот обзор медицинских исследований собрал самое важное из последних публикаций в области медицины. Мы проанализировали ключевые находки и представили их в доступной форме, чтобы читатели могли легко ориентироваться в актуальных темах. Этот материал станет отличным подспорьем для изучения медицины.
Продолжить изучение – закодироваться от алкоголизма
Michaelrah · May 13, 2026 at 5:59 am
Несмотря на выездной формат, лечение выстраивается поэтапно и соответствует медицинским стандартам. Это обеспечивает управляемость процесса и безопасность пациента.
Детальнее – вызвать врача нарколога на дом в ростове-на-дону
ThomasOneri · May 13, 2026 at 6:01 am
Нужен ремонт? ремонт квартир под ключ в Омске — полный комплекс ремонтно-отделочных работ: от разработки дизайна до финальной уборки. Качественный ремонт квартир с соблюдением сроков и прозрачной сметой.
Davidpap · May 13, 2026 at 6:12 am
Эта статья сочетает познавательный и занимательный контент, что делает ее идеальной для любителей глубоких исследований. Мы рассмотрим увлекательные аспекты различных тем и предоставим вам новые знания, которые могут оказаться полезными в будущем.
Нажмите, чтобы узнать больше – вывод из запоя санкт-петербург стационар
LamarSem · May 13, 2026 at 6:33 am
В клинике «Вектор Восстановления» логика маршрута строится по этапам. Первый этап — оценка состояния и рисков: длительность употребления, тяжесть отмены, давление, пульс, обезвоживание, хронические заболевания, прошлые осложнения, препараты, которые пациент уже принимал дома. Второй этап — стабилизация: снижение интоксикации, коррекция состояния, восстановление сна, уменьшение тревоги. Третий этап — сопровождение первых суток и переход к восстановлению: план на 24–72 часа, контроль динамики и профилактика «вечернего отката». Четвёртый этап — работа с зависимостью как с привычкой и системой поведения: триггеры, стресс, режим, поддержка семьи, навыки отказа, профилактика рецидива.
Подробнее тут – lechenie-alkogolizma-medom
DELVE IS A FRUAD · May 13, 2026 at 7:15 am
This blog post is excellent, probably because of how well the subject was developed. I like some of the comments too.
Georgeabelf · May 13, 2026 at 8:29 am
Choosing construction Benissa specialists is essential when building on hillside plots and coastal terrain that require careful engineering, precise planning and long-term structural reliability on the Costa Blanca.
Jamesvef · May 13, 2026 at 9:18 am
https://utspak.com/how-solar-energy-works-from-sunlight-to-electricity/
Jamesvef · May 13, 2026 at 9:19 am
https://webharborstudios.com/the-top-10-seo-tools-every-marketer-needs-to-succeed/
EdwardSnugs · May 13, 2026 at 9:25 am
Помощь на дому рассматривают при состояниях, которые сопровождаются заметным ухудшением самочувствия после алкоголя. Обычно это запой на протяжении нескольких дней, тяжелое похмелье, выраженная слабость, бессонница, тревога, дрожь в руках, сухость во рту, отсутствие аппетита, тошнота, раздражительность и ощущение истощения. В подобных случаях врачебный осмотр нужен для того, чтобы оценить тяжесть состояния и определить, безопасен ли домашний формат в конкретной ситуации.
Выяснить больше – нарколог на дом анонимно в москве
регер аккаунтов · May 13, 2026 at 9:25 am
регер аккаунтов
venofllmam · May 13, 2026 at 9:37 am
Трайбл — один из древнейших стилей татуировки, уходящий корнями в культуры Полинезии, Борнео и Маори, где каждый узор нёс сакральный смысл и рассказывал историю владельца. Сегодня этот стиль переживает настоящий ренессанс, а профессиональные мастера студии http://www.tribal-tattoo.ru/ воплощают его лучшие традиции в современных работах, создавая татуировки, которые остаются актуальными десятилетиями. Геометрическая строгость линий, глубокий чёрный цвет и ритмичные орнаменты делают трайбл одним из самых выразительных направлений в тату-искусстве — идеальный выбор для тех, кто ценит силу, эстетику и смысл в каждом штрихе.
MatthewgaB · May 13, 2026 at 9:58 am
Вывод из запоя в стационаре — это медицинская помощь, при которой лечение проводится в условиях постоянного врачебного контроля и поэтапной стабилизации состояния. Такой формат применяется, когда состояние пациента требует наблюдения и быстрого реагирования на изменения. В наркологической клинике «Частный медик 24» в Нижнем Новгороде лечение выстраивается на основе клинической оценки и последовательного подхода: каждый этап направлен на достижение конкретного результата без избыточной нагрузки на организм.
Получить дополнительные сведения – анонимный вывод из запоя в нижнем новгороде
星路国际官网 · May 13, 2026 at 10:02 am
“I love the color palette and typography you chose. Very professional yet inviting.” A comparative study at 星路国际官网 evaluates different methods.
tamapcepem · May 13, 2026 at 10:06 am
Ищете надежного поставщика металлопроката? Посетите сайт https://stalsfera.ru/ и вы сможете купить по выгодной цене металл оптом с доставкой по всей России от СтальСфера. Загляните в наш каталог – там действительно огромный выбор продукции. На складе наличие наиболее востребованных позиций листового, трубного, сортового и плоского проката. Также оказываем услуги металлообработки на собственном или контрактном производстве.
Richardguams · May 13, 2026 at 10:12 am
https://anyflip.com/homepage/cqzic
Derrickdix · May 13, 2026 at 10:36 am
Эта публикация раскрывает психологические механизмы зависимости и их роль в развитии расстройств. Читатель узнает о том, как психология влияет на формирование зависимостей и как профессиональная помощь может изменить ситуацию.
Жми сюда — получишь ответ – цены на лечение алкоголизма
Jeffreytoush · May 13, 2026 at 10:49 am
Капельница от похмелья с контролем врача в Самаре представляет собой эффективную терапевтическую процедуру, позволяющую значительно улучшить самочувствие пациента за короткий срок. Врач, контролируя весь процесс, может точно определить, какие компоненты необходимы для каждого пациента. Состав капельницы зависит от симптомов похмелья, состояния пациента и его индивидуальных потребностей. Это позволяет обеспечить максимально безопасное и эффективное лечение, которое помогает организму быстро восстановиться.
Узнать больше – капельница от похмелья
Michaelrah · May 13, 2026 at 10:59 am
Реализация данных задач позволяет наркологу на дом в Ростове-на-Дону оказывать помощь в контролируемом и безопасном формате.
Подробнее тут – http://narkolog-na-dom-v-rnd19.ru
Jamesvef · May 13, 2026 at 11:05 am
http://cleanpart.ru/placeholder/
Jamesvef · May 13, 2026 at 11:06 am
http://f7mdg2x1lj77.blog.fc2.com/blog-entry-1.html
Jamesvef · May 13, 2026 at 11:06 am
http://bezatkancelaria.pl/produkt/file-covers/
Jamesvef · May 13, 2026 at 11:10 am
http://centroeducativosanlorenzo.it/?wptouch_switch=desktop&redirect=//providerweb.ru/muzhi
LamarSem · May 13, 2026 at 11:19 am
Комплексная терапия — это сочетание медицинских и психологических шагов, которые решают разные задачи. Медицинская часть помогает пройти острый период и восстановить управляемость состояния. Психологическая и реабилитационная части помогают не вернуться к прежним сценариям, когда стресс, конфликт или бессонная ночь снова толкают к алкоголю.
Ознакомиться с деталями – лечение алкоголизма
Barrystack · May 13, 2026 at 11:36 am
Текст посвящён распространённым мифам о зависимости и их развенчанию. Мы предоставим научно обоснованную информацию и дадим рекомендации по выбору эффективного способа борьбы с зависимым поведением.
Это ещё не всё… – лечение алкоголизма без согласия
cecijrdNency · May 13, 2026 at 11:48 am
Камин в доме — это не просто источник тепла, а центр притяжения всей семьи в холодные вечера. Компания Kaminru занимается продажей, проектированием и монтажом каминов и печей ведущих европейских и отечественных производителей. На сайте https://kaminru.ru/ представлен широкий каталог готовых решений: от классических дровяных моделей до современных биокаминов. Специалисты компании помогут подобрать оборудование под конкретный интерьер и технические параметры помещения, обеспечив безопасный и качественный монтаж.
Richardguams · May 13, 2026 at 12:01 pm
https://community.powerofpositivity.com/profile/septicsolutionsllc/
Jamesvef · May 13, 2026 at 12:50 pm
https://betoff.fr/garder-les-patios-et-les-dalles-en-pierre-naturelle-propres/
StevenBlamp · May 13, 2026 at 12:52 pm
В этой статье мы рассмотрим современные достижения в области медицины, включая инновационные методы лечения и диагностики. Мы обсудим важность профилактики заболеваний и роль технологий в улучшении качества здравоохранения. Читатели узнают о влиянии медицины на повседневную жизнь и ее значение для современного общества.
Кликни, не пожалеешь – частный медик 24 ростов на дону
Jamesvef · May 13, 2026 at 12:55 pm
https://arvadis.ma/ar/la-nouvelle-ere-de-la-mobilite-urbaine/
MatthewgaB · May 13, 2026 at 12:56 pm
Такие состояния требуют не только лечения, но и наблюдения, поскольку динамика может меняться в течение короткого времени. Стационар позволяет минимизировать риски и обеспечить безопасность пациента. При этом услуга может предоставляться анонимно, а цена лечения зависит от состояния пациента.
Подробнее тут – скорая вывод из запоя в нижнем новгороде
Jamesvef · May 13, 2026 at 12:57 pm
https://auditguru.in/product/ca-final-audit-full-book-set/
Lavernehic · May 13, 2026 at 12:59 pm
В Санкт-Петербурге вывод из запоя на дому рассматривается, когда состояние пациента позволяет проводить лечение вне стационара, но требует контроля специалиста. Врач оценивает общее состояние, длительность запоя и выраженность симптомов, после чего принимает решение о формате помощи при алкоголизме. Важно, что лечение начинается сразу после осмотра, без необходимости ожидания госпитализации. При необходимости можно заказать услуги на сайте клиники или получить консультацию специалистов.
Углубиться в тему – нарколог на дом вывод из запоя
https://fotografes.gr/signature/#comment-78351 · May 13, 2026 at 1:05 pm
https://fotografes.gr/signature/#comment-78351
RafaelLed · May 13, 2026 at 1:07 pm
Эта публикация исследует взаимосвязь зависимости и психологии. Мы обсудим, как психологические аспекты влияют на появление зависимостей и процесс выздоровления. Читатели смогут понять важность профессиональной поддержки и применения научных подходов в терапии.
Ознакомьтесь с аналитикой – частный медик 24
gocosHeeld · May 13, 2026 at 1:16 pm
Glassway — специализированный поставщик, выстроивший прямые партнёрства с ведущими заводами отделочной отрасли. Ассортимент охватывает подвесные потолки, перегородки, алюминиевые двери, смарт-стекло, зенитные фонари и витринные конструкции. Ищете потолок грильято? На glassway.group представлен обширный каталог с актуальными ценами — прямые поставки с заводов обеспечивают конкурентную стоимость на весь ассортимент. Специалисты компании берутся за задачи любого уровня — от типовой отделки до уникальных архитектурных концепций.
VernonFrads · May 13, 2026 at 1:30 pm
you can try these out
fastest way to send crypto
heniyounick · May 13, 2026 at 1:33 pm
Авторская психиатрическая клиника доктора наук Виталия Минутко https://minutkoclinic.com/ основана в 2003 году. Работаем со всеми психическими расстройствами, включая детскую психиатрию: депрессия, ОКР, анорексия, шизофрения, зависимости, анорексия, аутизм, расстройства личности.
StanleySnoni · May 13, 2026 at 1:36 pm
Состояние пациента при интоксикации может развиваться по-разному: от умеренной слабости и головной боли до выраженной дезориентации, тахикардии и нарушений сна. В таких ситуациях важно не откладывать обращение за помощью. Наркологическая помощь на дому рассматривается, когда требуется быстрое вмешательство и контроль состояния без транспортировки пациента.
Ознакомиться с деталями – наркологическая помощь анонимно нижний новгород
Richardguams · May 13, 2026 at 1:50 pm
https://www.freelistingusa.com/listings/septic-solutions-llc
Jamesvef · May 13, 2026 at 2:36 pm
https://keatoncottages.com/15-things-you-need-to-know-about-holiday-today/
Jamesvef · May 13, 2026 at 2:43 pm
https://junggu.zigum.daejeon.kr/bbs/board.php?bo_table=free&wr_id=6240
Jamesvef · May 13, 2026 at 2:46 pm
https://kasprowicz.az.pl/patron-2/chata/
JesusAlkal · May 13, 2026 at 2:50 pm
Капельница от похмелья в Самаре: эффективное восстановление, снятие интоксикации и помощь специалистов в наркологической клинике «Детокс»
Подробнее тут – kapelnicza-ot-pokhmelya-samara-13.ru/
TimothyFreby · May 13, 2026 at 2:52 pm
Промокоды на депозит — активируются в личном кабинете.
Казино с быстрым выводом — имеет низкую комиссию.
Топ слотов с высоким RTP — Starburst, Big Bass Bonanza.
Источник:
https://sistema-1sstroy.ru
JerryHed · May 13, 2026 at 3:01 pm
Автомобильный портал https://autort.ru с обзорами машин, новостями автопрома, рейтингами моделей и советами по выбору авто. Полезная информация для покупателей, владельцев и всех любителей автомобилей.
http://www.0909kuruma.com/mb/tokyo/kuchikomi/confirm.php?sid=2086d28ca178b26f9b01bcc612c5cfb4 · May 13, 2026 at 3:07 pm
http://www.0909kuruma.com/mb/tokyo/kuchikomi/confirm.php?sid=2086d28ca178b26f9b01bcc612c5cfb4
JamesTruff · May 13, 2026 at 3:27 pm
Этот краткий обзор предлагает сжатую информацию из области медицины, включая ключевые факты и последние новости. Мы стремимся сделать информацию доступной и понятной для широкой аудитории, что позволит читателям оставаться в курсе актуальных событий в здравоохранении.
Что скрывают от вас? – Наркологическая клиника «Похмельная служба» в Анапе.
Timothyelapy · May 13, 2026 at 4:03 pm
“2024 mutfak dolab? renkleri” hakk?nda bilgi arayanlar icin cok faydal? bir yaz? buldum. Suradan okuyabilirsiniz: https://hobiprojesi.com/articles/2024-mutfak-dolabi-renk-secimleri/
Timothyelapy · May 13, 2026 at 4:07 pm
“kumastan pas lekesi nas?l c?kar” hakk?nda bilgi arayanlar icin mukemmel bir kaynak var. Link burada: https://kendifikirler.com/articles/pas-lekesi-elbiseden-nasil-cikarilir/
gawigRhine · May 13, 2026 at 4:18 pm
Фотометрическая лаборатория «Сила Света» проводит профессиональные светотехнические измерения с оформлением официальных протоколов, имеющих юридическую силу. На http://silasveta-lab.ru/ доступна проверка подлинности любого протокола по уникальному коду или QR-коду — это исключает подделки и гарантирует достоверность данных. Все работы ведутся строго по действующим стандартам — лаборатория имеет актуальные свидетельства о поверке используемого оборудования.
JeffryCotly · May 13, 2026 at 4:31 pm
Терапевтический процесс в стационаре строится по принципу последовательного выполнения клинических задач: диагностика, стабилизация, медикаментозная терапия и подготовка к амбулаторному этапу. При поступлении врач проводит детальный осмотр, собирает анамнез, оценивает неврологический статус и при необходимости назначает лабораторные исследования. На основе полученных данных формируется индивидуальный протокол, учитывающий возраст, длительность интоксикации, наличие сопутствующих патологий и переносимость лекарственных компонентов. Мы применяем только сертифицированные препараты, зарегистрированные в РФ, и строго соблюдаем клинические рекомендации Минздрава, исключая псевдонаучные методики. Стандарты оказания медицинской помощи фиксируются во внутренних регламентах и регулярно проверяются независимыми аудиторами.
Выяснить больше – быстрый вывод из запоя в стационаре
VernonFrads · May 13, 2026 at 4:38 pm
view website
android crypto wallet
RonaldEndub · May 13, 2026 at 5:00 pm
Добрый день!
Строительство домов с использованием натуральных материалов — это решение для тех, кто ценит экологичность и качество. Мы занимаемся строительством домов с использованием натуральных материалов, таких как дерево, камень и глина. Строительство домов с натуральными материалами — это экологичность и стиль. Строительство домов с натуральными материалами — это ваше здоровье и комфорт.
Ремонт квартир под ключ — это комплексная услуга для тех, кто хочет сделать ремонт в своем жилье без лишних забот. Мы выполняем ремонт квартир под ключ, начиная с планирования и заканчивая уборкой после завершения работ. Все этапы выполняются нашими специалистами, и вы получаете готовую квартиру, готовую для проживания. Ремонт под ключ — это удобство и качество. Ремонт квартир под ключ — это просто и удобно.
Больше информации по ссылке – https://cafetyt.ru/kak-vybrat-idealnyj-cvet-kovrolina-dlja-kommercheskih-pomeshhenij/
строительство домов 12, строительство бани с нуля, ремонт в доме самара
квартиры мытищи отделка, газовый котел ремонт на дому, ремонт в квартире лестница
Удачи!
ThomasDep · May 13, 2026 at 5:14 pm
Женский портал https://justwoman.club с полезными статьями о красоте, здоровье, моде, психологии и отношениях. Советы экспертов, лайфхаки, идеи для ухода за собой и вдохновение для современной женщины.
NathanGathy · May 13, 2026 at 5:32 pm
Алкогольная интоксикация оказывает серьёзное влияние на организм, вызывая головную боль, тошноту, слабость и головокружение. Капельница помогает организму быстро избавиться от продуктов распада алкоголя, восстановить нормальное функционирование органов и минимизировать последствия для здоровья. Важно, что мы обеспечиваем полное наблюдение врача на протяжении всей процедуры, что помогает гарантировать безопасность пациента и максимальную эффективность лечения.
Углубиться в тему – https://kapelnicza-ot-pokhmelya-ekaterinburg-8.ru/
may88acocom · May 13, 2026 at 6:22 pm
I’ve thought about posting something about this before. Good job! Can I use part of your post in my blog?
BrianZes · May 13, 2026 at 6:32 pm
Когда следует немедленно обращаться за помощью:
Ознакомиться с деталями – нарколог на дом
RichardExpit · May 13, 2026 at 6:36 pm
В данной статье рассматриваются проблемы общественного здоровья и социальные факторы, влияющие на него. Мы акцентируем внимание на значении профилактики и осведомленности в защите здоровья на уровне общества. Читатели смогут узнать о новых инициативах и программах, направленных на улучшение здоровья населения.
Получить исчерпывающие сведения – частный медик 24 рнд
zowin · May 13, 2026 at 6:38 pm
Hey, I simply hopped over to your website by way of StumbleUpon. No longer one thing I’d normally learn, but I preferred your thoughts none the less. Thanks for making one thing worth reading.
Davidbrify · May 13, 2026 at 6:39 pm
Процедура проводится под контролем врача. В случае необходимости специалист выезжает на дом с полным набором медикаментов и оборудования. Такой формат особенно востребован среди пациентов, которые предпочитают анонимное лечение без госпитализации. Все манипуляции проводятся стерильно, а препараты подбираются с учётом противопоказаний.
Получить дополнительную информацию – вывод из запоя капельница
StanleySnoni · May 13, 2026 at 6:48 pm
Состояние пациента при интоксикации может развиваться по-разному: от умеренной слабости и головной боли до выраженной дезориентации, тахикардии и нарушений сна. В таких ситуациях важно не откладывать обращение за помощью. Наркологическая помощь на дому рассматривается, когда требуется быстрое вмешательство и контроль состояния без транспортировки пациента.
Получить больше информации – наркологическая помощь анонимно в нижнем новгороде
DavidBeemi · May 13, 2026 at 6:51 pm
Вывод из запоя на дому — это формат наркологической помощи, при котором лечение проводится в привычной для пациента обстановке с выездом врача. Такой подход применяется в ситуациях, когда состояние требует медицинского вмешательства, но не предполагает обязательной госпитализации. В наркологической клинике «Частный медик 24» помощь на дому выстраивается по принципу поэтапной стабилизации: сначала устраняются острые проявления, затем оценивается динамика и при необходимости корректируется терапия.
Углубиться в тему – анонимный вывод из запоя на дому санкт-петербург
StanleySnoni · May 13, 2026 at 7:08 pm
Состояние пациента при интоксикации может развиваться по-разному: от умеренной слабости и головной боли до выраженной дезориентации, тахикардии и нарушений сна. В таких ситуациях важно не откладывать обращение за помощью. Наркологическая помощь на дому рассматривается, когда требуется быстрое вмешательство и контроль состояния без транспортировки пациента.
Изучить вопрос глубже – вызов наркологической помощи
RichardExpit · May 13, 2026 at 7:25 pm
В данной статье рассматриваются физиологические и эмоциональные аспекты зависимости. Мы обсудим, как организм реагирует на зависимое поведение, и какие методы помогают восстановить здоровье и внутреннее равновесие.
Получить дополнительные сведения – частный медик 24 ростов на дону
RobertJef · May 13, 2026 at 7:30 pm
Когда хочется отдохнуть удобно выбирать китайские дорамы с русской озвучкой онлайн без долгих поисков, случайных сайтов и бесконечных вкладок. Проект DoramaLend собрал в одном месте корейские, китайские, японские и другие азиатские сериалы с понятным русским переводом, понятными описаниями, разделами по жанрам, годами выхода и аккуратными карточками. Здесь легко найти романтическую историю на вечер, напряженный триллер, сериал для хорошего настроения или свежую новинку, которую уже обсуждают поклонники дорам.
https://www.srbifor.at/na-danasnji-dan-se-proslavljaju-svetih-cetrdeset-mucenika-sevastijskih/#comment-7399 · May 13, 2026 at 7:34 pm
https://www.srbifor.at/na-danasnji-dan-se-proslavljaju-svetih-cetrdeset-mucenika-sevastijskih/#comment-7399
JesusAlkal · May 13, 2026 at 7:46 pm
Капельница от похмелья с контролем врача в Самаре представляет собой эффективную терапевтическую процедуру, позволяющую значительно улучшить самочувствие пациента за короткий срок. Врач, контролируя весь процесс, может точно определить, какие компоненты необходимы для каждого пациента. Состав капельницы зависит от симптомов похмелья, состояния пациента и его индивидуальных потребностей. Это позволяет обеспечить максимально безопасное и эффективное лечение, которое помогает организму быстро восстановиться.
Получить больше информации – капельница от похмелья вызов на дом в самаре
JesusAlkal · May 13, 2026 at 8:02 pm
Вызов капельницы от похмелья с контролем врача в Самаре рекомендуется, когда симптомы похмелья становятся особенно тяжелыми и мешают нормальной жизнедеятельности. Несмотря на то, что многие пытаются справиться с похмельем с помощью домашних методов, такие как прием жидкости или таблеток, они не всегда оказываются достаточно эффективными. В случае сильных симптомов похмелья, капельница с врачебным контролем — это более безопасное и быстрое решение, при этом возможен вывод в стационаре, анонимное лечение и консультации по вопросам наркомании с учетом актуальной цены услуг.
Получить больше информации – капельница от похмелья анонимно
DavidTen · May 13, 2026 at 8:04 pm
Этот текст представляет собой обзор свежих данных и исследований в области медицины. Он призван помочь читателям понять, как научные достижения влияют на лечение, диагностику и общее состояние системы здравоохранения.
Откройте для себя больше – Реабилитация наркозависимых
Jeffreytoush · May 13, 2026 at 8:05 pm
Капельница от похмелья с контролем врача в Самаре является одной из самых популярных и эффективных услуг для тех, кто сталкивается с выраженными симптомами похмельного синдрома. Похмелье может проявляться не только головной болью и усталостью, но и более серьезными проблемами, такими как тошнота, рвота, учащенное сердцебиение и повышение давления. Когда симптомы становятся особенно острыми, капельница помогает организму справиться с токсинами, восстановить водно-электролитный баланс и нормализовать состояние пациента, в том числе при запое. Важно, что контроль врача на протяжении всей процедуры обеспечивает безопасность и эффективность, при этом помощь может оказываться как на дому, так и в клинике при лечении алкоголизма.
Получить дополнительную информацию – капельница от похмелья
hirixaelMic · May 13, 2026 at 8:07 pm
Москва открывается совершенно иначе, когда смотришь на неё с воды: величественные набережные, сталинские высотки и современные небоскрёбы Сити складываются в панораму, которую невозможно увидеть ни из окна метро, ни с автомобильной эстакады. Сервис https://moscowwaterways.ru/ предлагает речные прогулки и маршруты по Москве-реке в сезоне навигации 2026 года — с удобным расписанием, регулярными отправлениями каждые 15–30 минут и причалами в шаговой доступности от метро. Это одновременно отдых, впечатления и полная свобода от городских пробок.
AnthonyDal · May 13, 2026 at 8:57 pm
Здравствуйте!
Мощный серверный рендеринг для SEO улучшает индексацию и ускоряет первую отрисовку для поисковых роботов. Мы генерируем готовый HTML на сервере для мгновенной передачи контента ботам и пользователям. Поисковые алгоритмы лучше понимают такие страницы и могут улучшать их ранжирование. Вы получаете техническое преимущество и ускоряете попадание новых материалов в индекс. Внедряйте SSR профессионально и усиливайте видимость ресурса в органической выдаче.
Удобная кастомная страница 404 с навигацией удерживает клиента и превращает ошибку в возможность. Мы добавляем поиск, меню и рекомендации для продолжения взаимодействия с ресурсом. Поисковые системы ценят заботу о пользователе и могут улучшать позиции таких сайтов. Ваши посетители быстро находят нужный контент и реже покидают проект при ошибках. Создавайте 404 профессионально и усиливайте пользовательский опыт.
Больше информации по ссылке – https://chert-poberi.ru/category/hi-tech
добавление сайта в Яндекс Вебмастер, ограничение попыток входа, оптимизация карточек товаров
комплексный подход к онлайн-продвижению, закрытие служебных страниц, разграничение прав доступа
Удачи!
DavidTen · May 13, 2026 at 8:58 pm
Эта информационная публикация освещает широкий спектр тем из мира медицины. Мы предлагаем читателям ясные и понятные объяснения современных заболеваний, методов профилактики и лечения. Информация будет полезна как пациентам, так и медицинским работникам, желающим поддержать уровень своих знаний.
Не упусти шанс – частный медик 24
OrvalHex · May 13, 2026 at 9:03 pm
Современные методы лечения при выводе из запоя включают как медикаментозную детоксикацию, так и психологическую реабилитацию. В Уфе наркологи используют капельничное введение лекарственных средств, которые помогают быстро вывести токсины, нормализовать обмен веществ и стабилизировать работу внутренних органов. Одновременно с этим проводится психологическая поддержка для снижения эмоционального стресса, связанного с запоем.
Разобраться лучше – http://narcolog-na-dom-ufa0.ru/narkolog-na-dom-ufa-czeny/https://narcolog-na-dom-ufa0.ru
tewesBug · May 13, 2026 at 9:33 pm
Ищете венки.рф? Зайдите на купить-венок.рф — здесь вас ждут доступные цены на траурные венки, живые цветы и ритуальные корзинки. Ознакомьтесь с нашим каталогом — мы производим венки любых форм и размеров, а оформить заказ можно всего в 2 клика. Узнайте больше о наших услугах и ценах на сайте.
Wesleybropy · May 13, 2026 at 9:35 pm
В данной статье мы акцентируем внимание на важности поддержки в процессе выздоровления. Мы обсудим, как друзья, семья и профессионалы могут помочь тем, кто сталкивается с зависимостями. Читатели получат практические советы, как поддерживать близких на пути к новой жизни.
Желаете узнать подробности? – Реабилитация наркозависимых
JeffryCotly · May 13, 2026 at 9:59 pm
Выбор между домашней помощью и стационарным лечением определяется не удобством, а медицинской целесообразностью. В условиях клиники исключаются внешние триггеры, обеспечивается изоляция от источников алкоголя и создается контролируемая среда, где терапевтические решения принимаются на основе объективных показателей, а не субъективных ощущений пациента. Такой подход критически важен для предотвращения осложнений, минимизации дискомфорта абстиненции и формирования устойчивой базы для дальнейшей противорецидивной работы.
Подробнее можно узнать тут – стационар вывод из запоя в санкт-петербурге
скупка золота 750 пробы спб · May 13, 2026 at 9:59 pm
Салют,
Коллеги.
Сегодня я бы хотел поведать малость про http://ciber-hacker.ru/index.php?subaction=userinfo&user=ycukybaqoce
Я думаю Вы в поиске именно про где продать золото 750 пробы или возможно желаете узнать больше про скупка золота 750 пробы?!
Значит эта оптимально актуальная информация про сдать золото 750 пробы спб будет для вас наиболее полезной.
На нашем веб сайте малость больше про продать золото 750 пробы спб, также информацию про скупка золота 750 пробы.
Наш сайт про http://cr-talisman.ru/index.php?subaction=userinfo&user=amavumopehud по ссылке http://amurvoda.ru/index.php?subaction=userinfo&user=ujopaxoqe
Узнай Больше про https://sklad-slabov.ru/forum/user/45122/ по ссылке http://df-media.ru/communication/forum/user/141/
Наши Теги: сдать изделия 750 пробы спб, где продать золото 750 пробы, скупка золота 750 пробы за грамм, скупка золота 750 пробы спб,
Удачного Дня
JeffryCotly · May 13, 2026 at 10:17 pm
Затяжной запой — это не бытовая слабость, а медицинское состояние, требующее профессионального вмешательства. Когда организм истощен длительной интоксикацией, нарушен сон, отсутствует аппетит, а попытки самостоятельно прекратить употребление сопровождаются тремором, тревогой и скачками давления, единственным безопасным решением становится стационарная детоксикация. Наркологическая клиника «Элегия Мед» в Санкт-Петербурге предоставляет безопасную детоксикацию, индивидуальную медикаментозную терапию и всестороннюю поддержку специалистов на всех этапах восстановления. Мы работаем круглосуточно, обеспечивая быстрое реагирование на обращения, четкую диагностику при поступлении и прозрачное взаимодействие с родственниками. Все процедуры выполняются с соблюдением протоколов доказательной медицины, стандартов Минздрава РФ и строгих правил конфиденциальности. Первичная оценка состояния начинается с дистанционной консультации, что позволяет врачам заранее подготовить необходимое оборудование и скорректировать план госпитализации еще до прибытия пациента. При необходимости позвонить на горячую линию или оформить вызов бригады, помощь доступна в любое время суток.
Детальнее – нарколог вывод из запоя в стационаре санкт-петербург
beholsBaigh · May 13, 2026 at 10:19 pm
Обновить фасад дома надёжно и красиво теперь проще, чем кажется: магазин https://tsnab.su/ предлагает широкий ассортимент винилового сайдинга от ведущих производителей — Grand Line, Docke, FineBer, Technonicol и других проверенных брендов. Цены начинаются от 199 рублей за панель, а покупателям доступна рассрочка под 0%. Компания работает с более чем 15 000 клиентами по всей России, гарантирует качество материалов сроком до 50 лет и предлагает монтаж фасада под ключ с доставкой в любой регион страны.
http://forum.rakvice.net/?p=2Nonton · May 13, 2026 at 10:19 pm
http://forum.rakvice.net/?p=2%22%3ENonton
Lavernehic · May 13, 2026 at 10:58 pm
Запой сопровождается выраженной интоксикацией, нарушением сна, слабостью, тревожностью и колебаниями давления, что характерно для алкоголизма и других форм зависимости. При этом самостоятельный выход из состояния часто оказывается затруднённым из-за ухудшения самочувствия и невозможности контролировать симптомы. В таких случаях выезд нарколога позволяет начать лечение без задержек и помочь пациенту снизить нагрузку на организм за счёт отсутствия транспортировки.
Ознакомиться с деталями – вывод из запоя на дому
Robertwiz · May 13, 2026 at 11:09 pm
Игнорирование этих симптомов может привести к тяжелым последствиям для здоровья, включая алкогольный психоз и повреждение внутренних органов.
Подробнее тут – http://
NathanGathy · May 13, 2026 at 11:10 pm
Капельница от похмелья в Екатеринбурге с анонимным выездом врача и восстановительной терапией в наркологической клинике «Частный медик 24»
Выяснить больше – капельница от похмелья анонимно
HowardNer · May 13, 2026 at 11:22 pm
Самое важное сегодня: https://aromline.ru/index.php?productID=6549
NathanGathy · May 13, 2026 at 11:30 pm
Алкогольная интоксикация оказывает серьёзное влияние на организм, вызывая головную боль, тошноту, слабость и головокружение. Капельница помогает организму быстро избавиться от продуктов распада алкоголя, восстановить нормальное функционирование органов и минимизировать последствия для здоровья. Важно, что мы обеспечиваем полное наблюдение врача на протяжении всей процедуры, что помогает гарантировать безопасность пациента и максимальную эффективность лечения.
Выяснить больше – капельница от похмелья вызов на дом в екатеринбурге
Stevetot · May 13, 2026 at 11:54 pm
Эта медицинская заметка содержит сжатую информацию о новых находках и методах в области здравоохранения. Мы предлагаем читателям свежие данные о заболеваниях, профилактике и лечении. Наша цель — быстро и доступно донести важную информацию, которая поможет в повседневной жизни и понимании здоровья.
Исследовать вопрос подробнее – стоп алко анапа
DavidZilla · May 13, 2026 at 11:55 pm
Этот обзор посвящен успешным стратегиям избавления от зависимости, включая реальные примеры и советы. Мы разоблачим мифы и предоставим читателям достоверную информацию о различных подходах. Получите опыт многообразия методов и найдите подходящий способ для себя!
Более того — здесь – стоп алко
WilliamTex · May 14, 2026 at 12:00 am
Запой – это не просто пьянство, а состояние, когда организм становится зависимым от алкоголя. Накопление токсинов приводит к сбоям в работе органов и ослаблению защиты организма. Самостоятельный выход из запоя может быть опасен и только усугубить состояние. Мы предлагаем лечение запоя на дому, чтобы избежать больницы и создать комфорт. Наши специалисты быстро приедут к вам и окажут всю необходимую помощь круглосуточно. Запой приводит к серьезным проблемам со здоровьем, ухудшает качество жизни и угрожает жизни. Очень важно вовремя обратиться за помощью, чтобы избежать необратимых последствий.
Получить дополнительные сведения – вывод из запоя дешево красноярск
wrldnwsMup · May 14, 2026 at 12:02 am
Все последние мировые новости на WrldNWS.top https://wrldnws.top/
Подробнее здесь: https://wrldnws.top/
Stevenvew · May 14, 2026 at 12:34 am
Всегда актуальный адрес — зеркало Melbet спасает ситуацию.
Актуальное зеркало на сегодня — прямой доступ к слотам.
Melbet казино — выбор профессионалов — более 4000 слотов.
Если главный сайт в доступе — заходите смело — дают одинаковые бонусы.
Source:
мелбет зеркало рабочее
DavidZilla · May 14, 2026 at 12:57 am
Текст посвящён распространённым мифам о зависимости и их развенчанию. Мы предоставим научно обоснованную информацию и дадим рекомендации по выбору эффективного способа борьбы с зависимым поведением.
Жми сюда — получишь ответ – «Похмельная служба» в Балашихе
RafaelLed · May 14, 2026 at 1:03 am
Этот информативный текст сочетает в себе темы здоровья и зависимости. Мы обсудим, как хронические заболевания могут усугубить зависимости и наоборот, как зависимость может влиять на общее состояние здоровья. Читатели получат представление о комплексном подходе к лечению как физического, так и психического состояния.
Переходите по ссылке ниже – частный медик 24 ростов на дону
Josephcroro · May 14, 2026 at 1:19 am
“mutfak tezgah? boyama yorumlar?” hakk?nda bilgi arayanlar icin burada harika bilgiler var. Iste link: https://kendiyolu.com/articles/tezgah-boyama-inceleme/
Josephcroro · May 14, 2026 at 1:26 am
“aloe vera cicek acmas? ne anlama gelir” hakk?nda bilgi arayanlar icin mukemmel bir kaynak var. Iste link: https://yapevleri.com/articles/aloe-vera-cicegi-acma-sureci-ve-ipuclari/
MichaelHulty · May 14, 2026 at 1:37 am
Длительное и бесконтрольное употребление алкоголя может привести к состоянию запоя — опасному и тяжелому состоянию, при котором человек не способен самостоятельно отказаться от спиртного. Во время запоя организм постепенно накапливает токсины, что негативно сказывается на работе всех внутренних органов и систем. В таких случаях пациенту необходима экстренная врачебная помощь, и специалисты наркологической клиники «АнтиТокс» готовы оперативно оказать профессиональную медицинскую поддержку на дому в Новосибирске.
Детальнее – вывод из запоя в стационаре в новосибирске
mowuybaf · May 14, 2026 at 1:38 am
JetronSport — производитель футбольной формы для команд любого уровня: от детских секций до взрослых клубов. Премиальные дышащие ткани с терморегуляцией и эластичностью, соответствие ГОСТам и гарантия на нанесения — стандарт качества JetronSport. Минимальный заказ — одна единица, срок производства составляет от одного до трёх дней. На https://jetronsport.ru/ представлены модели взрослой, детской и вратарской формы с нанесением номеров и фамилий. Коллекции Jetron Space, Star и Winner сочетают усиленные конструктивные элементы, светоотражающие вставки и Quick-Dry материал для подлинного спортивного комфорта.
RonaldEndub · May 14, 2026 at 2:16 am
Здравствуйте!
Ремонт для бань — это специализированная услуга, которую мы предлагаем для владельцев бань. Наши специалисты могут выполнить ремонт бань любой сложности: от восстановления отделки до полной реконструкции. Ремонт для бань включает в себя замену перегородок, отделку и установку нового оборудования. Мы гарантируем, что ваша баня будет как новая после наших работ. Ремонт для бань — это качественное обслуживание вашего объекта.
Строительство домов с качественной отделкой — это гарантированное качество и стиль для вашего жилья. Мы предлагаем строительство домов с качественной отделкой, которая соответствует вашим требованиям и предпочтениям. Строительство домов с качественной отделкой — это долговечность и красота. Строительство домов с качественной отделкой — это идеальный результат.
Больше информации по ссылке – https://wallpanels.ru/kak-vybrat-i-ustanovit-kovrolin-dlya-kommercheskikh-pomescheniy-poleznye-sovety/
фонд капитального ремонта дома, квартира под ключ сколько стоит ремонт, стоимость ремонта отделки квартиры в новостройке
строительство домов деревянные дома, строительство бани тюмень под ключ, внутренняя отделка стен квартир в
Удачи!
Phillipral · May 14, 2026 at 2:22 am
После диагностики начинается активная фаза медикаментозного вмешательства. Современные препараты вводятся капельничным методом, что позволяет быстро снизить уровень токсинов в крови, восстановить нормальные обменные процессы и стабилизировать работу жизненно важных органов, таких как печень, почки и сердце.
Подробнее можно узнать тут – нарколог вывод из запоя мурманск
CecilDup · May 14, 2026 at 2:23 am
Когда запой становится критическим, оперативное вмешательство имеет решающее значение для спасения здоровья и предотвращения необратимых последствий. Во Владимире экстренная помощь нарколога на дому позволяет быстро начать лечение, не требуя госпитализации, что особенно важно для пациентов, нуждающихся в сохранении конфиденциальности и комфорте.
Выяснить больше – наркология вывод из запоя владимир
KevinGuent · May 14, 2026 at 2:26 am
Процесс вывода из запоя капельничным методом организован по строгой схеме, позволяющей обеспечить максимальную эффективность терапии. Каждая стадия направлена на комплексное восстановление организма и минимизацию риска осложнений.
Подробнее тут – после капельницы от запоя тюмень
Tysonuttek · May 14, 2026 at 2:27 am
Эта публикация обращает внимание на важность профилактики зависимостей. Мы обсудим, как осведомленность и образование могут помочь в предотвращении возникновения зависимости. Читатели смогут ознакомиться с полезными советами и ресурсами, которые способствуют здоровому образу жизни.
Углубить понимание вопроса – лечение алкоголизма ростов
GlennNub · May 14, 2026 at 2:36 am
пояснения водкабет казино
JamesTruff · May 14, 2026 at 2:50 am
В этой медицинской статье мы погрузимся в актуальные вопросы здравоохранения и лечения заболеваний. Читатели узнают о современных подходах, методах диагностики и новых открытий в научных исследованиях. Наша цель — донести важную информацию и повысить уровень осведомленности о здоровье.
Узнать напрямую – Наркологическая клиника «Похмельная служба» в Анапе
Williambax · May 14, 2026 at 2:54 am
Обращение за помощью нарколога на дому в Мурманске имеет ряд существенных преимуществ:
Получить дополнительную информацию – вывод из запоя в стационаре
RobertSlopy · May 14, 2026 at 3:08 am
В этой статье мы подробно рассматриваем проверенные методы борьбы с зависимостями, включая психотерапию, медикаментозное лечение и поддержку со стороны общества. Мы акцентируем внимание на важности комплексного подхода и возможности успешного восстановления для людей, столкнувшихся с этой проблемой.
Углубиться в тему – частный медик 24
ThomasElubs · May 14, 2026 at 3:14 am
В этой статье мы рассматриваем разрушительное влияние зависимости на жизнь человека. Обсуждаются аспекты, такие как здоровье, отношения и профессиональные достижения. Читатели узнают о необходимости обращения за помощью и о путях к восстановлению.
Выяснить больше – частный медик 24
GlennNub · May 14, 2026 at 3:15 am
смотреть здесь vodkabet водкабет казино
Bruceelifs · May 14, 2026 at 3:20 am
нажмите vodka bet
MichaelSwary · May 14, 2026 at 3:36 am
такой казино водка бет vodkabet
Bruceelifs · May 14, 2026 at 3:50 am
нажмите водкабет
xonizioTax · May 14, 2026 at 4:02 am
CryoOne специализируется на производстве азотных криокапсул российского производства для beauty-бизнеса, спортивных центров и восстановительной медицины. Оборудование окупается за 6 месяцев, не требует медицинской лицензии и генерирует стабильный поток клиентов за счёт WOW-эффекта процедуры. На https://cryoone.ru/ представлены четыре комплектации — Standard, Business, Pro и Comfort — с гарантией 24 месяца и бесплатными доставкой, монтажом и обучением. Сосуд Дьюара входит в базовую комплектацию, а покупатель получает гарантию минимальной цены среди конкурентов.
ThomasElubs · May 14, 2026 at 4:32 am
Публикация знакомит читателей с различными подходами к реабилитации. От традиционных методов до современных программ — вы узнаете, как выбрать оптимальный путь к выздоровлению и преодолеть препятствия на этом пути.
Нажми и узнай всё – цены на лечение алкоголизма
MichaelSwary · May 14, 2026 at 4:45 am
подробнее водка бет
BennieZen · May 14, 2026 at 4:47 am
Статья посвящена анализу текущих трендов в медицине и их влиянию на жизнь людей. Мы рассмотрим новые технологии, методы лечения и значение профилактики в обеспечении долголетия и здоровья.
Как достичь результата? – Похмельная служба в Анапе
MichaelHulty · May 14, 2026 at 5:20 am
После поступления звонка специалисты нашей клиники оперативно выезжают по адресу пациента в Новосибирске. Врач начинает работу с детальной диагностики: измеряет пульс, артериальное давление, сатурацию (уровень кислорода в крови), оценивает состояние нервной и сердечно-сосудистой систем, уточняет наличие хронических заболеваний, аллергических реакций, длительность и тяжесть запоя.
Получить больше информации – наркологический вывод из запоя в новосибирске
CecilDup · May 14, 2026 at 5:51 am
Незамедлительно после вызова нарколог прибывает на дом для проведения тщательного осмотра. На данном этапе специалист собирает анамнез, измеряет жизненно важные показатели — пульс, артериальное давление, температуру — и оценивает степень интоксикации. Эти данные являются основой для составления индивидуального плана лечения.
Углубиться в тему – вывод из запоя в владимире
KevinGuent · May 14, 2026 at 6:03 am
Процесс вывода из запоя капельничным методом организован по строгой схеме, позволяющей обеспечить максимальную эффективность терапии. Каждая стадия направлена на комплексное восстановление организма и минимизацию риска осложнений.
Ознакомиться с деталями – капельницу от запоя тюмень
MichaelSwary · May 14, 2026 at 6:06 am
содержание водка бет
Phillipral · May 14, 2026 at 6:06 am
Услуга вывода из запоя на дому в Мурманске предполагает комплексное лечение алкогольной интоксикации, направленное на оперативное снижение уровня токсинов в организме. Сразу после поступления вызова специалист проводит детальный осмотр, собирает анамнез и определяет степень интоксикации. На основании собранной информации разрабатывается индивидуальный план терапии, который может включать капельничное введение медикаментов, контроль жизненно важных показателей и психологическую поддержку. Такой комплекс мер позволяет стабилизировать состояние пациента и начать процесс выздоровления без необходимости посещения стационара.
Ознакомиться с деталями – вывод из запоя недорого
MichaelSwary · May 14, 2026 at 6:12 am
проверить сайт vodkabet прямо сейчас
Bruceelifs · May 14, 2026 at 6:16 am
посетить сайт водкабет
RussellTex · May 14, 2026 at 6:16 am
Команда из 10 специалистов — финишное клининг-убирание.
Белые стены и акцентная мебель — визуально расширяет любую комнату.
Трансформируемая мебель — зоны выделяем светом и уровнем пола.
Источник:
https://changan-best-price-tymen.ru
Williambax · May 14, 2026 at 6:21 am
После диагностики начинается активная фаза медикаментозного вмешательства. Препараты вводятся капельничным методом, что способствует быстрому снижению уровня токсинов в крови, нормализации обменных процессов и стабилизации работы таких органов, как печень, почки и сердце.
Изучить вопрос глубже – вывод из запоя
OrvalHex · May 14, 2026 at 6:25 am
Алкогольная зависимость сопровождается не только физическими, но и глубокими психоэмоциональными проблемами. Психотерапевтическая помощь играет важную роль в лечении, помогая пациенту осознать причины зависимости и разработать стратегии для предотвращения рецидивов.
Получить дополнительные сведения – врач нарколог на дом платный уфа
GlennNub · May 14, 2026 at 6:40 am
подробнее здесь vodkabet
TimothyFreby · May 14, 2026 at 7:05 am
Для стабильного входа — используйте рабочее зеркало Мелбет.
Зеркало казино Мелбет — сохраняет баланс и историю ставок.
(орфография сохранена как в запросе: “зекало” вместо “зеркало”)
Мелбет рабочее зеркало 2025 — сохраняет историю транзакций.
Источник:
https://melbet-23ms.cfd
Carlostox · May 14, 2026 at 7:32 am
В статье рассматриваются различные стратегии борьбы с зависимостями, включая проверенные методы и реальные истории успеха. Читатель узнает, какие подходы наиболее эффективны и как начать путь к выздоровлению.
Кликни, не пожалеешь – Частный Медик 24 проводит реабилитацию зависимых
Jasonstive · May 14, 2026 at 7:41 am
В этой медицинской статье мы погрузимся в актуальные вопросы здравоохранения и лечения заболеваний. Читатели узнают о современных подходах, методах диагностики и новых открытий в научных исследованиях. Наша цель — донести важную информацию и повысить уровень осведомленности о здоровье.
Информация доступна здесь – Похмельная служба в Балашихе
jamenzip · May 14, 2026 at 7:54 am
Полиуретановая плёнка создаёт надёжный барьер против сколов, царапин и дорожной химии, надолго сохраняя первоначальный облик вашего автомобиля. Ищете тонировка автомобиля на авиамоторной? Профессиональная оклейка выполняется на individual-design.ru/nashi-uslugi/452-okleyka-avto-poliuretanom с гарантией качества и точной подгонкой материала под любой кузов. Покрытие восстанавливается после незначительных царапин и удаляется без последствий для кузова — лучший вариант для ценителей безупречного состояния машины.
Bruceelifs · May 14, 2026 at 8:08 am
Главная водка бет
KTO análise · May 14, 2026 at 8:13 am
Lucky Neko bonus came on spin 412 — not a single trigger before that.
Tysonuttek · May 14, 2026 at 8:33 am
Читатели получат представление о том, как современные технологии влияют на развитие медицины. Обсуждаются новые методы лечения, персонализированный подход и роль цифровых решений в повышении качества медицинских услуг.
Ознакомиться с полной информацией – сколько стоит лечение наркозависимости
Robertwiz · May 14, 2026 at 8:50 am
Постановка капельницы от запоя специалистами клиники «Пульс» в Воронеже обеспечивает пациентам оперативную помощь и быстрое облегчение состояния благодаря экстренному выезду врача на дом. Наши услуги доступны круглосуточно, включая ночное время и праздничные дни, что особенно важно при внезапных и критических ситуациях. Мы гарантируем полную конфиденциальность и защиту персональных данных пациентов, что позволяет получить необходимую помощь без риска огласки. Индивидуальный подход к каждому случаю обеспечивает максимальную эффективность лечения, а наши опытные наркологи используют только сертифицированные препараты, которые безопасно и быстро выводят токсины и стабилизируют состояние здоровья. Прозрачность ценообразования, предварительное согласование всех расходов и отсутствие скрытых доплат делают услуги клиники «Пульс» удобными и доступными для всех жителей Воронежа.
Разобраться лучше – http://kapelnica-ot-zapoya-krasnodar7.ru/kapelnicza-ot-zapoya-na-domu-v-krasnodare/https://kapelnica-ot-zapoya-krasnodar7.ru
Wesleybropy · May 14, 2026 at 8:57 am
Этот обзор посвящен успешным стратегиям избавления от зависимости, включая реальные примеры и советы. Мы разоблачим мифы и предоставим читателям достоверную информацию о различных подходах. Получите опыт многообразия методов и найдите подходящий способ для себя!
Изучить эмпирические данные – частный медик 24 ростов на дону
JarredJap · May 14, 2026 at 9:06 am
Для тех, кто хочет дорамы корейские без лишней суеты и бесконечного поиска, DoramaGo может стать приятной площадкой для вечернего просмотра. Здесь можно найти корейские, китайские, японские, тайские и другие азиатские сериалы, где есть все, за что зрители любят дорамы: нежные и драматичные истории, сильные сюжетные развороты, герои, за которых быстро начинаешь переживать и атмосфера Азии. Понятная навигация помогает быстро подобрать сериал по стране, жанру, году или настроению, а новые добавления позволяют не пропускать продолжение.
GeraldPhard · May 14, 2026 at 9:43 am
В практике круглосуточного лечения применяются следующие этапы:
Подробнее можно узнать тут – https://narkologicheskaya-klinika-v-rostove19.ru/narkologiya-rostov-kruglosutochno/
Josuepsync · May 14, 2026 at 9:52 am
https://www.chodecoptimista.cz/2015/06/30/informacni-tisen/
Josuepsync · May 14, 2026 at 9:53 am
https://hestestalden.net/cykeloprydning/
RobertSlopy · May 14, 2026 at 9:54 am
Эта публикация обращает внимание на важность профилактики зависимостей. Мы обсудим, как осведомленность и образование могут помочь в предотвращении возникновения зависимости. Читатели смогут ознакомиться с полезными советами и ресурсами, которые способствуют здоровому образу жизни.
Не упусти важное! – частный медик 24
GlennNub · May 14, 2026 at 10:23 am
такой водкабет казино
Josuepsync · May 14, 2026 at 11:35 am
https://actimizetech.com/the-importance-of-building-a-strong-brand-identity/
BennieZen · May 14, 2026 at 11:35 am
В этой статье рассматриваются способы преодоления зависимости и успешные истории людей, которые справились с этой проблемой. Мы обсудим важность поддержки со стороны близких и профессионалов, а также стратегии, которые могут помочь в процессе выздоровления. Научитесь первоочередным шагам к новой жизни.
См. подробности – «Похмельная служба» в Анапе
RonaldEndub · May 14, 2026 at 11:51 am
Здравствуйте!
Ремонт комнаты — это способ обновить одно из самых важных мест в доме. Мы выполняем ремонт комнаты с учетом всех пожеланий, будь то спальня, гостиная или детская. Ремонт комнаты — это возможность создать пространство для отдыха и общения. Ремонт комнаты — это создание уюта и комфорта.
Строительство домов цены — это важный аспект при выборе подрядчика для строительства. Мы предлагаем строительство домов по доступным ценам, при этом не снижая качество работы. Каждый проект мы разрабатываем с учетом ваших финансовых возможностей. Строительство домов цены — это важный показатель, который мы всегда стараемся сделать максимально конкурентоспособным. Строительство домов цены — это идеальное сочетание качества и стоимости.
Больше информации по ссылке – https://domkrat.org/kovrolin-v-detskiy-sad-vidyi-i-sovetyi-po-vyiboru/
квартира в новостройке воронеж с отделкой, технология строительство дома, кирпич для отделки дома купить
товары для ремонта дом, ремонт дома красивый, строительство дома организации
Удачи!
Ronalddiums · May 14, 2026 at 11:57 am
Существует ряд ситуаций, при которых вызов специалиста на дом является обоснованным решением:
Выяснить больше – нарколог на дом вывод в нижнем новгороде
MatthewgaB · May 14, 2026 at 12:17 pm
К основным показаниям относятся:
Получить дополнительную информацию – вывод из запоя вызов на дом в нижнем новгороде
Brianfesia · May 14, 2026 at 12:35 pm
Такой подход позволяет наркологической клинике в Ростове-на-Дону выстраивать лечение в безопасных и психологически комфортных условиях.
Изучить вопрос глубже – платная наркологическая клиника в ростове-на-дону
Josuepsync · May 14, 2026 at 12:40 pm
https://neuthema.de/richard-williams-iii/
Josuepsync · May 14, 2026 at 12:52 pm
https://www.bv-veenendaal.nl/nieuws/
Donaldskala · May 14, 2026 at 1:06 pm
Арена гайдов crarena ru полезные гайды по играм, квестам и заданиям. Подробные прохождения, советы, секреты и тактики для разных игр. Помогаем быстрее проходить миссии, находить скрытые предметы и открывать новые возможности игрового мира.
BrianFuemo · May 14, 2026 at 1:23 pm
В этом исследовании рассмотрены методы лечения зависимостей и их эффективность. Мы проанализируем различные подходы, используемые в реабилитационных центрах, и представим данные о результативности программ. Читатели получат надежные и научно обоснованные сведения о данной проблеме.
Открыть полностью – стоп алко
Josuepsync · May 14, 2026 at 1:28 pm
https://mynkhairsalon.com/finding-the-best-hair-color-salons-near-narellan/
casino en ligne · May 14, 2026 at 1:35 pm
Loving the info on this website , you have done outstanding job on the blog posts.
AnthonyDal · May 14, 2026 at 1:47 pm
Привет всем!
Детальное логирование ошибок для анализа помогает быстро находить и устранять технические проблемы. Мы настраиваем сбор, хранение и визуализацию логов для оперативного реагирования на сбои. Поисковые системы ценят стабильные ресурсы и улучшают их позиции в органической выдаче. Вы получаете полный контроль над техническим состоянием и предотвращаете критические инциденты. Ведите логирование профессионально и обеспечивайте бесперебойную работу ресурса.
Умные параметры сортировки и фильтрации улучшают пользовательский опыт и предотвращают создание дублей в индексе. Мы настраиваем корректную обработку динамических параметров для поисковых роботов и пользователей. Поисковые алгоритмы правильно понимают структуру каталога и ранжируют основные страницы без путаницы. Ваши клиенты быстро находят нужные товары без технических препятствий и лишних переходов. Оптимизируйте фильтры профессионально и получайте стабильный рост позиций в конкурентной нише.
Больше информации по ссылке – http://green-willow.ru/itemlist/tag/seo
защита от инъекций и скриптов, оптимизация под featured snippets, сквозная аналитика для бизнеса
ссылки с главной страницы донора, быстрые ответы голосовой поиск, продвижение в Bing и Yahoo
Удачи!
Josephpat · May 14, 2026 at 2:00 pm
В этой медицинской статье мы погрузимся в актуальные вопросы здравоохранения и лечения заболеваний. Читатели узнают о современных подходах, методах диагностики и новых открытий в научных исследованиях. Наша цель — донести важную информацию и повысить уровень осведомленности о здоровье.
Погрузиться в детали – стоп алко
Josuepsync · May 14, 2026 at 2:43 pm
https://rntmom.com/bbs/board.php?bo_table=free&wr_id=38223
Josuepsync · May 14, 2026 at 3:18 pm
https://africanvibetours.com/product/all-over-print-gym-bag/
CarlosLix · May 14, 2026 at 3:23 pm
В данной статье рассматриваются проблемы общественного здоровья и социальные факторы, влияющие на него. Мы акцентируем внимание на значении профилактики и осведомленности в защите здоровья на уровне общества. Читатели смогут узнать о новых инициативах и программах, направленных на улучшение здоровья населения.
Что ещё нужно знать? – вывод из запоя в ростове на дону
Tracyswiny · May 14, 2026 at 3:36 pm
В данном материале представлены ключевые тенденции в сфере медицинской науки и практики. Вы узнаете о последних открытиях, инновационных подходах к терапии и важности профилактики заболеваний. Особое внимание уделено практическому применению новых методов в клинической практике.
А есть ли продолжение? – выведение из запоя стоимость
BrianZes · May 14, 2026 at 3:36 pm
Если в состоянии пациента наблюдаются такие признаки, как судороги, панические атаки, или гипертонический криз, необходимо немедленно вызвать врачей. Задержка может привести к необратимым последствиям.
Выяснить больше – нарколог на дом клиника новокузнецк
najlepsze kasyna online · May 14, 2026 at 3:43 pm
This blog post is excellent, probably because of how well the subject was developed. I like some of the comments too though I could prefer we all stay on the subject in order add value to the subject!
Josuepsync · May 14, 2026 at 3:46 pm
https://www.ldalliance.eu/en/2017/03/29/new-aeroespacial-station/
France in Kenya · May 14, 2026 at 3:46 pm
France Africa summit
Angelagorm · May 14, 2026 at 3:49 pm
Новостной онлайн-портал https://vse-novosti.net с круглосуточным обновлением информации. Новости мира и регионов, аналитические материалы, обзоры и важные события в одном месте.
GeraldPhard · May 14, 2026 at 3:58 pm
В рамках анонимного лечения особое внимание уделяется следующим медицинским аспектам:
Выяснить больше – наркологическая клиника стационар
Jasonstive · May 14, 2026 at 4:06 pm
Этот документ охватывает важные аспекты медицинской науки, сосредотачиваясь на ключевых вопросах, касающихся здоровья населения. Мы рассматриваем свежие исследования, клинические рекомендации и лучшие практики, которые помогут улучшить качество лечения и профилактики заболеваний. Читатели получат возможность углубиться в различные медицинские дисциплины.
Только факты! – Наркологическая клиника «Похмельная служба» в Балашихе
Josuepsync · May 14, 2026 at 4:12 pm
https://www.alledagenfeest.com/?attachment_id=11
Josuepsync · May 14, 2026 at 4:13 pm
http://redpink.co.kr/bbs/board.php?bo_table=free&wr_id=12285
MichaelHulty · May 14, 2026 at 4:24 pm
Длительное и бесконтрольное употребление алкоголя может привести к состоянию запоя — опасному и тяжелому состоянию, при котором человек не способен самостоятельно отказаться от спиртного. Во время запоя организм постепенно накапливает токсины, что негативно сказывается на работе всех внутренних органов и систем. В таких случаях пациенту необходима экстренная врачебная помощь, и специалисты наркологической клиники «АнтиТокс» готовы оперативно оказать профессиональную медицинскую поддержку на дому в Новосибирске.
Выяснить больше – вывод из запоя капельница
Josuepsync · May 14, 2026 at 4:33 pm
https://digital.signage.software/blog/bulletin-boards-must-digital/
Josuepsync · May 14, 2026 at 4:36 pm
https://morningcarpool.com/nice-but-rude-behaviors/
fixDiele · May 14, 2026 at 5:02 pm
Для тех, кто ищет информацию по теме “Последние новости и интервью в мире ММА”, нашел много полезного.
Вот, делюсь ссылкой:
https://media-mma.ru
casino en ligne Québec · May 14, 2026 at 5:06 pm
Hello this is a wonderful write-up. I’m going to e mail this to my friends. I came on this while searching on yahoo I’ll be sure to come back. thanks for sharing.
创建个人账户 · May 14, 2026 at 5:08 pm
I don’t think the title of your article matches the content lol. Just kidding, mainly because I had some doubts after reading the article.
Josuepsync · May 14, 2026 at 5:09 pm
https://www.sexram.cl/gallery/galeria/
WilliamTex · May 14, 2026 at 5:34 pm
Запой – это не просто пьянство, а состояние, когда организм становится зависимым от алкоголя. Накопление токсинов приводит к сбоям в работе органов и ослаблению защиты организма. Самостоятельный выход из запоя может быть опасен и только усугубить состояние. Мы предлагаем лечение запоя на дому, чтобы избежать больницы и создать комфорт. Наши специалисты быстро приедут к вам и окажут всю необходимую помощь круглосуточно. Запой приводит к серьезным проблемам со здоровьем, ухудшает качество жизни и угрожает жизни. Очень важно вовремя обратиться за помощью, чтобы избежать необратимых последствий.
Узнать больше – вывод из запоя на дому красноярск недорого
Brianfesia · May 14, 2026 at 5:57 pm
В рамках анонимного лечения особое внимание уделяется следующим медицинским аспектам:
Подробнее тут – http://narkologicheskaya-klinika-v-rostove19.ru
Antoniodet · May 14, 2026 at 6:28 pm
Новостной портал https://tovarpost.ru с актуальными событиями России и мира. Политика, экономика, общество, технологии и спорт. Оперативные новости, аналитика и важные события в режиме реального времени.
najlepsze kasyna online · May 14, 2026 at 6:51 pm
Awesome post. It’s so good to see someone taking the time to share this information
Jessienen · May 14, 2026 at 6:54 pm
В этих случаях вызов нарколога на дом не только оправдан, но и жизненно необходим для предотвращения опасных осложнений и стабилизации здоровья пациента.
Ознакомиться с деталями – http://narcolog-na-dom-voronezh00.ru/vyzov-narkologa-na-dom-voronezh/
Michaelsok · May 14, 2026 at 7:56 pm
Текст посвящён распространённым мифам о зависимости и их развенчанию. Мы предоставим научно обоснованную информацию и дадим рекомендации по выбору эффективного способа борьбы с зависимым поведением.
Ознакомьтесь поближе – частный медик 24 ростов на дону
najlepsze kasyna online · May 14, 2026 at 7:59 pm
Great blog right here! You seem to put a significant amount of material on the site rather quickly.
kasyno online opinie · May 14, 2026 at 8:12 pm
Great post. Just a heads up – I am running Ubuntu with the beta of Firefox and the navigation of your blog is kind of broken for me.
Martinbib · May 14, 2026 at 8:34 pm
Этот процесс не занимает много времени — обычно процедура длится от 30 до 60 минут. Важно, что врач контролирует все этапы, обеспечивая безопасность пациента и корректируя терапию по мере необходимости. Такой подход позволяет быстро и эффективно облегчить симптомы похмелья и вернуться к нормальной жизнедеятельности.
Детальнее – https://kapelnicza-ot-pokhmelya-samara-13.ru/
DavidBarge · May 14, 2026 at 8:49 pm
В этой публикации мы рассматриваем важную тему борьбы с зависимостями, включая алкогольную и наркотическую зависимости. Мы обсудим методы лечения, реабилитации и поддержку, которые могут помочь людям, столкнувшимся с этой проблемой. Читатели узнают о перспективах выздоровления и важности комплексного подхода.
Ознакомьтесь с аналитикой – частный медик 24 ростов на дону
kasyno online opinie · May 14, 2026 at 9:09 pm
I had fun reading this post. I want to see more on this subject.. Gives Thanks for writing this nice article.. Anyway, I’m going to subscribe to your rss and I wish you write great articles again soon.
MatthewgaB · May 14, 2026 at 9:13 pm
Такие состояния требуют не только лечения, но и наблюдения, поскольку динамика может меняться в течение короткого времени. Стационар позволяет минимизировать риски и обеспечить безопасность пациента. При этом услуга может предоставляться анонимно, а цена лечения зависит от состояния пациента.
Выяснить больше – помощь вывод из запоя
MichaelSputs · May 14, 2026 at 9:37 pm
В этой статье рассматриваются различные аспекты избавления от зависимости, включая физические и психологические методы. Мы обсудим поддержку, мотивацию и стратегии, которые помогут в процессе выздоровления. Читатели узнают, как преодолеть трудности и двигаться к новой жизни без зависимости.
Смотри, что ещё есть – вывод из запоя на дому ростов
AlfredUnums · May 14, 2026 at 9:39 pm
В данной статье мы акцентируем внимание на важности поддержки в процессе выздоровления. Мы обсудим, как друзья, семья и профессионалы могут помочь тем, кто сталкивается с зависимостями. Читатели получат практические советы, как поддерживать близких на пути к новой жизни.
Как это работает — подробно – частный медик 24 ростов на дону
DavidBarge · May 14, 2026 at 9:42 pm
В данной публикации мы поговорим о процессе восстановления от зависимости, о том, как вернуть себе нормальную жизнь. Мы обсудим преодоление трудностей, значимость поддержки и наличие программ реабилитации. Читатели смогут узнать о ключевых шагах к успешному восстановлению.
Что ещё нужно знать? – narcology clinic ростов на дону
hagomwen · May 14, 2026 at 10:08 pm
«Делай Промо» — SaaS-платформа для брендов и агентств, позволяющая запускать чековые акции, программы лояльности и мотивацию продавцов без привлечения разработчиков. Бренды и агентства получают конструктор лендингов, OCR-распознавание чеков, мультиканальные чат-боты для Telegram и VK, кодовые механики с защитой от брутфорса и сквозную аналитику с выгрузкой в Excel — всё в едином окне. На http://makerpromo.ru/ уже зарегистрировано свыше 24 000 чеков и 18 000 активных пользователей. Сервис доступен в рамках закрытого бета-тестирования на льготных тарифных условиях.
TimothyFreby · May 14, 2026 at 10:27 pm
Слоты, рулетка, покер — регулярные турниры в казино.
Зеркало казино Мелбет — полная копия с бонусами.
(орфография сохранена как в запросе: “зекало” вместо “зеркало”)
Мелбет зеркало рабочее или официальный сайт — дают одинаковые бонусы.
Источник:
https://melbet-bk7.club
BrianZes · May 14, 2026 at 10:32 pm
Процедура вывода из запоя начинается с тщательной диагностики состояния пациента, чтобы определить, какие методы лечения будут наиболее эффективными. Мы применяем индивидуальный подход и комбинируем медикаментозное лечение с психотерапевтической поддержкой, что даёт лучший результат.
Выяснить больше – вызов нарколога на дом новокузнецк.
AlfredUnums · May 14, 2026 at 10:34 pm
В этой публикации мы исследуем ключевые аспекты здоровья, включая влияние образа жизни на благополучие. Читатели узнают о важности правильного питания, физической активности и психического здоровья. Мы предоставим практические советы и рекомендации для поддержания здоровья и развития профилактических подходов.
Желаете узнать подробности? – narcology clinic
Michaelfaugs · May 14, 2026 at 11:12 pm
Хочешь узнать про электронные чеки? https://financedirector.by/jelektronnye-cheki-i-ih-uchet/ важный этап цифровизации торговли и налогового контроля. Узнайте, как работают электронные чеки, какие преимущества они дают бизнесу и покупателям, а также какие изменения ждут предпринимателей.
Alvinvow · May 14, 2026 at 11:15 pm
В этой статье рассматриваются актуальные вопросы, связанные с развитием медицинской науки и её внедрением в повседневную практику. Особое внимание уделено вопросам профилактики, ранней диагностики и использованию технологий для улучшения здоровья человека.
Хочу знать больше – частный медик 24 ростов на дону
Richardsword · May 14, 2026 at 11:46 pm
Текст посвящён распространённым мифам о зависимости и их развенчанию. Мы предоставим научно обоснованную информацию и дадим рекомендации по выбору эффективного способа борьбы с зависимым поведением.
Это ещё не всё… – стоп алко
RussellTex · May 15, 2026 at 12:09 am
Квартира мечты за 2 месяца — даём гарантию на работы.
Кирпич, бетон и металл — огромные окна и светильники на тросах.
Работаем удалённо и с выездом — выезжаем в Пушкин, Павловск, Сестрорецк.
Источник:
https://toranovalo.ru
BernardAdelp · May 15, 2026 at 12:32 am
После первичного улучшения работа не заканчивается. Врач формирует план восстановления: режим воды и питания, ориентиры по самочувствию, критерии «нормальной» динамики, признаки, при которых нужно повторно оценить состояние, и шаги по профилактике рецидива. Такой подход снижает вероятность повторного витка: человек понимает, что слабость и эмоциональная нестабильность в первые дни возможны, не пугается «волны» вечером и не пытается гасить её алкоголем.
Подробнее – https://narkologicheskaya-klinika-sergiev-posad12.ru/telefon-narkologicheskoj-kliniki-v-sergievom-posade/
best online casino · May 15, 2026 at 12:39 am
Appreciation for taking the time to discuss this topic, I would love to discover more on this topic. If viable, as you gain expertise, would you object to updating the website with further information? It is tremendously beneficial for me.
Josephpat · May 15, 2026 at 1:09 am
В этой медицинской статье мы погрузимся в актуальные вопросы здравоохранения и лечения заболеваний. Читатели узнают о современных подходах, методах диагностики и новых открытий в научных исследованиях. Наша цель — донести важную информацию и повысить уровень осведомленности о здоровье.
Подробная информация доступна по запросу – Наркологическая клиника «Похмельная служба» в Домодедово.
ufc white house 232 · May 15, 2026 at 1:15 am
UFC Results https://ufc-white-house.com
MichaelHulty · May 15, 2026 at 1:32 am
На основании проведенных обследований врач разрабатывает индивидуальную терапевтическую схему. Основной этап — детоксикация организма при помощи внутривенных инфузий. В капельницу включают растворы для восстановления водно-солевого баланса, выведения токсинов и улучшения работы внутренних органов. Также по показаниям назначают препараты для поддержки работы печени и сердца, стабилизации психоэмоционального состояния и снятия симптомов абстиненции. На протяжении процедуры врач ведет постоянный контроль за состоянием пациента, корректируя лечение при необходимости.
Получить дополнительную информацию – срочный вывод из запоя
MatthewgaB · May 15, 2026 at 2:01 am
Вывод из запоя в стационаре — это медицинская помощь, при которой лечение проводится в условиях постоянного врачебного контроля и поэтапной стабилизации состояния. Такой формат применяется, когда состояние пациента требует наблюдения и быстрого реагирования на изменения. В наркологической клинике «Частный медик 24» в Нижнем Новгороде лечение выстраивается на основе клинической оценки и последовательного подхода: каждый этап направлен на достижение конкретного результата без избыточной нагрузки на организм.
Получить больше информации – врач вывод из запоя нижний новгород
StanleySnoni · May 15, 2026 at 2:21 am
Состояние пациента при интоксикации может развиваться по-разному: от умеренной слабости и головной боли до выраженной дезориентации, тахикардии и нарушений сна. В таких ситуациях важно не откладывать обращение за помощью. Наркологическая помощь на дому рассматривается, когда требуется быстрое вмешательство и контроль состояния без транспортировки пациента.
Детальнее – оказание наркологической помощи нижний новгород
TimothyFreby · May 15, 2026 at 2:26 am
Начните игру с Мелбет и live-трансляции.
Официальное онлайн-казино — удобные способы оплаты.
Melbet казино — выбор профессионалов — быстрая верификация и вывод.
Мелбет зеркало рабочее или официальный сайт — разница только в адресной строке.
Источник:
https://melbet-hf21.top
166bet · May 15, 2026 at 2:53 am
O discord ficou mais quieto depois do patch do Q1. Menos barulho, mais sinal.
nonojtop · May 15, 2026 at 2:59 am
Ищете принцип работы онлифанс сайт? Вебкам-индустрия сегодня открывает реальные возможности для стабильного заработка, и студия the-lips.com — один из серьёзных игроков рынка с прозрачными условиями. Заработок модели составляет от 20% до 80% от дохода и определяется опытом, наличием оборудования и форматом — студия или дом. Студия выплачивает заработок в долларах: на карту, криптокошелёк или наличными — по договорённости. Студия также помогает с переездом тем, кто находится в стране с ограничениями на данный вид деятельности.
WilliamTex · May 15, 2026 at 4:22 am
Запой – это неконтролируемое употребление алкоголя, которое приводит к серьезным последствиям. Алкогольное отравление организма приводит к серьезным проблемам со здоровьем. Выходить из запоя самостоятельно – рискованно и неэффективно. Мы предлагаем помощь при запое на дому, в привычных для вас условиях. Круглосуточная помощь при запое с выездом на дом за 30-60 минут. Длительный запой разрушает организм и может быть смертельным. Чем раньше вы обратитесь за помощью, тем больше шансов на выздоровление.
Узнать больше – клиника вывод из запоя красноярск
MichaelDem · May 15, 2026 at 4:28 am
Нарколог на дом в Ростове-на-Дону рассматривается как специализированная форма оказания медицинской помощи пациентам с зависимостями вне стационара. В клинике «Чистый Баланс» выезд врача организуется круглосуточно, что позволяет обеспечить своевременное вмешательство при ухудшении состояния в любое время суток. Нарколог на дом в Ростове-на-Дону востребован в ситуациях, когда пациент не готов или не может обратиться в медицинское учреждение, а промедление с лечением повышает риск осложнений. Такой формат помощи требует строгого соблюдения клинических протоколов и высокой квалификации специалистов.
Детальнее – http://narkolog-na-dom-v-rnd19.ru/narkolog-rostov-na-donu/
GeorgePax · May 15, 2026 at 4:31 am
В этой статье мы рассмотрим современные достижения в области медицины, включая инновационные методы лечения и диагностики. Мы обсудим важность профилактики заболеваний и роль технологий в улучшении качества здравоохранения. Читатели узнают о влиянии медицины на повседневную жизнь и ее значение для современного общества.
Все материалы собраны здесь – вывод из запоя на дому ростов-на-дону
CarlosLix · May 15, 2026 at 4:47 am
Эта доказательная статья представляет собой глубокое погружение в успехи и вызовы лечения зависимостей. Мы обращаемся к научным исследованиям и опыту специалистов, чтобы предоставить читателям надежные данные об эффективности различных методик. Изучите, что работает лучше всего, и получите информацию от экспертов.
Изучить рекомендации специалистов – вывод из запоя в ростове на дону
Richardsword · May 15, 2026 at 5:02 am
В данном обзоре представлены основные направления и тренды в области медицины. Мы обсудим актуальные проблемы здравоохранения, свежие открытия и новые подходы, которые меняют представление о лечении и профилактике заболеваний. Эта информация будет полезна как специалистам, так и широкой публике.
Изучить аспект более тщательно – Похмельная служба Домодедово
Tracyswiny · May 15, 2026 at 5:10 am
В данной публикации мы поговорим о процессе восстановления от зависимости, о том, как вернуть себе нормальную жизнь. Мы обсудим преодоление трудностей, значимость поддержки и наличие программ реабилитации. Читатели смогут узнать о ключевых шагах к успешному восстановлению.
Посмотреть всё – вывод из запоя ростов на дону на дому
GeorgePax · May 15, 2026 at 5:37 am
В этой статье мы рассмотрим современные достижения в области медицины, включая инновационные методы лечения и диагностики. Мы обсудим важность профилактики заболеваний и роль технологий в улучшении качества здравоохранения. Читатели узнают о влиянии медицины на повседневную жизнь и ее значение для современного общества.
Не упусти шанс – вывод из запоя ростов
Michaelfen · May 15, 2026 at 6:09 am
В этой статье рассматриваются актуальные вопросы, связанные с развитием медицинской науки и её внедрением в повседневную практику. Особое внимание уделено вопросам профилактики, ранней диагностики и использованию технологий для улучшения здоровья человека.
Узнать напрямую – Реабилитация наркозависимых
Charlesdof · May 15, 2026 at 6:11 am
Публикация охватывает основные направления развития современной медицины. Мы обсудим значимость научных исследований, инноваций в лечении и роли общественного участия в формировании системы здравоохранения.
Обратитесь за информацией – вывод из запоя частный врач
Williamcew · May 15, 2026 at 6:12 am
Помощь при зависимостях в клинике «Южный Вектор» строится по принципу поэтапности, что соответствует современным медицинским представлениям. Наркологическая клиника в Ростове-на-Дону применяет методы, направленные на снижение выраженности синдромов отмены и восстановление функций органов. Клинические решения принимаются на основе данных обследования и наблюдения, что обеспечивает индивидуализацию терапии без отхода от стандартов.
Получить дополнительную информацию – наркологическая клиника вывод из запоя ростов-на-дону
TimothyFreby · May 15, 2026 at 6:28 am
Если основной сайт недоступен — функциональная копия сайта Мелбет.
Зеркало казино Мелбет — полная копия с бонусами.
Вход в melbet казино из любой точки — быстрая верификация и вывод.
Мелбет зеркало рабочее или официальный сайт — один аккаунт для двух входов.
Источник:
https://melbet-akap.top
Stevenvew · May 15, 2026 at 6:35 am
Melbet привлекает щедрыми бонусами для тысяч событий ежедневно.
Почему выбирают казино Мелбет — приветственный пакет до 100 000 ?.
Актуальное melbet зекало на сегодня — доступ к ставкам за секунду.
Мелбет зеркало рабочее или официальный сайт — полностью синхронизированы.
Source:
melbet зекало
Michaelsok · May 15, 2026 at 7:06 am
В этой статье мы рассматриваем разрушительное влияние зависимости на жизнь человека. Обсуждаются аспекты, такие как здоровье, отношения и профессиональные достижения. Читатели узнают о необходимости обращения за помощью и о путях к восстановлению.
Неизвестные факты о… – вывод из запоя на дому ростов
Michaelfen · May 15, 2026 at 7:07 am
В этой статье рассматриваются актуальные вопросы, связанные с развитием медицинской науки и её внедрением в повседневную практику. Особое внимание уделено вопросам профилактики, ранней диагностики и использованию технологий для улучшения здоровья человека.
Раскрыть тему полностью – narcology clinic
BernardAdelp · May 15, 2026 at 7:22 am
Алкогольная зависимость часто держится на страхе отмены. Человек заранее боится вечера: что не уснёт, начнётся паника, поднимется давление, появится дрожь и ощущение «внутреннего разгона». Из-за этого запой поддерживается не удовольствием, а попыткой избежать ухудшения. В клинике лечение начинается с оценки риска осложнений и тяжести отмены. Это позволяет определить, нужен ли стационар, или можно начинать лечение без госпитализации с медицинским контролем и ясным планом на ночь.
Углубиться в тему – adresa-narkologicheskih-klinik
https://gitea.johannes-hegele.de/jonnaeasty0941 · May 15, 2026 at 7:31 am
References:
Roulette colors
References:
https://gitea.johannes-hegele.de/jonnaeasty0941
ArturopRorm · May 15, 2026 at 7:34 am
Подробнее здесь
Срочные займы онлайн
ArturopRorm · May 15, 2026 at 7:56 am
подробнее здесь
Займ без отказа
doxaysGOw · May 15, 2026 at 8:05 am
Want your child to understand general math concepts easily and naturally? Visit https://mayateacher.com/ and explore our guides, designed for parents who want clearer homework support, calmer language, and practical ways to help their child make progress at home. We offer helpful math content for home practice, family routines, and teacher support.
RichardKit · May 15, 2026 at 8:18 am
Решил посетить Рускеала? тур в рускеала из петербурга мы организуем экскурсии в Рускеалу из Петербурга с комфортабельными автобусами и опытными гидами. Для тех, кто уже отдыхает в Карелии, запущены экскурсии из Сортавала в Рускеала — короткий трансфер и максимум времени в парке. Ежедневные выезды из Санкт-Петербурга и Петрозаводска.
Cordelllouse · May 15, 2026 at 8:41 am
Для жителей Ростова-на-Дону клиника «Южный МедКонтроль» предлагает два формата помощи: лечение в стационаре и амбулаторные визиты врача на дом. Стационар оборудован всем необходимым для круглосуточного медицинского наблюдения, проведения инфузионных процедур и лабораторной диагностики. Пациентам предоставляется комфортное размещение, спокойная обстановка и постоянный контроль состояния. При выезде на дом врачи действуют оперативно — приезжают в течение часа, проводят осмотр, устанавливают капельницы, купируют абстиненцию и дают рекомендации по дальнейшему лечению.
Изучить вопрос глубже – наркологическая клиника нарколог ростов-на-дону
mebiqualo · May 15, 2026 at 8:56 am
«Био-лазер» — клиника пластической хирургии в Москве с ведущим специалистом Владимиром Высоцким и стажем работы свыше 25 лет. Пациентам доступны маммопластика, блефаропластика, абдоминопластика, лифтинг лица и шеи, отопластика и мастопексия. Ищете клиника пластической хирургии в Москве? Актуальные результаты операций собраны на doctor99.ru в разделе галереи. Владимир Высоцкий непрерывно повышает квалификацию на стажировках и конференциях — методы работы клиники отвечают современным требованиям. Первичная консультация доступна онлайн.
BrianZes · May 15, 2026 at 9:36 am
Если в состоянии пациента наблюдаются такие признаки, как судороги, панические атаки, или гипертонический криз, необходимо немедленно вызвать врачей. Задержка может привести к необратимым последствиям.
Изучить вопрос глубже – выезд нарколога на дом новокузнецк
Thomasric · May 15, 2026 at 9:58 am
Эта публикация исследует взаимосвязь зависимости и психологии. Мы обсудим, как психологические аспекты влияют на появление зависимостей и процесс выздоровления. Читатели смогут понять важность профессиональной поддержки и применения научных подходов в терапии.
Всё, что нужно знать – вывод из запоя в ростове
KevinGuent · May 15, 2026 at 10:08 am
Сразу после вызова нарколог приезжает на дом для проведения первичного осмотра и диагностики. На этом этапе проводится сбор анамнеза, измеряются жизненно важные показатели (пульс, артериальное давление, температура) и определяется степень алкогольной интоксикации. Эти данные являются основой для разработки индивидуального плана лечения.
Подробнее – капельница от запоя на дому тюмень
Williambax · May 15, 2026 at 10:10 am
Когда запой начинает оказывать разрушительное воздействие на организм, своевременная помощь становится критически важной для предотвращения серьезных осложнений. В Мурманске квалифицированные наркологи на дому обеспечивают оперативную детоксикацию, восстановление обменных процессов и стабилизацию работы внутренних органов. Лечение проводится в комфортной домашней обстановке, что позволяет избежать лишнего стресса и сохранить полную конфиденциальность.
Получить больше информации – вывод из запоя мурманская область
zeguyToift · May 15, 2026 at 10:27 am
If you’re looking for information on VPN technology, visit https://vpnglobale.com/ . They explain in simple terms how VPN technology works in practice, from protocols and encryption to actual performance and limitations. We analyze services and infrastructure from a technical perspective to help readers make informed decisions.
ArturopRorm · May 15, 2026 at 10:28 am
посмотреть в этом разделе
Займ 15 000 рублей
TimothyFreby · May 15, 2026 at 10:31 am
Начните игру с Мелбет и быстрый вывод средств.
Альтернативный адрес мелбет казино — всего один клик до игры.
Рабочий адрес melbet зекало — обход блокировки без потери данных.
Мелбет зеркало рабочее или официальный сайт — дают одинаковые бонусы.
Источник:
https://melbet-cya.top
Alvinvow · May 15, 2026 at 10:39 am
В этой статье мы подробно рассматриваем проверенные методы борьбы с зависимостями, включая психотерапию, медикаментозное лечение и поддержку со стороны общества. Мы акцентируем внимание на важности комплексного подхода и возможности успешного восстановления для людей, столкнувшихся с этой проблемой.
Подробности по ссылке – частный медик 24 рнд
Robertwiz · May 15, 2026 at 10:48 am
Алкогольный запой является тяжёлым состоянием, требующим срочного медицинского вмешательства. Наркологическая клиника «Пульс» в Краснодаре предлагает эффективную помощь в борьбе с алкогольной зависимостью, используя проверенный метод — капельницу от запоя на дому. Наши специалисты оперативно выезжают по указанному адресу и обеспечивают качественную медицинскую помощь с гарантией конфиденциальности и безопасности.
Получить дополнительные сведения – http://kapelnica-ot-zapoya-krasnodar7.ru
OrvalHex · May 15, 2026 at 11:17 am
Услуга вызова нарколога на дом в Уфе разработана для оперативного вывода из запоя без необходимости госпитализации. Это особенно актуально для тех, кто столкнулся с алкогольной интоксикацией в условиях, когда каждая минута имеет значение. Своевременная помощь позволяет не только устранить негативное воздействие алкоголя на организм, но и предотвратить возможные осложнения, такие как нарушения работы сердца, печени и почек.
Детальнее – http://narcolog-na-dom-ufa0.ru
MichaelSputs · May 15, 2026 at 12:39 pm
Публикация посвящена жизненным историям людей, успешно справившихся с зависимостью. Мы покажем, что выход есть, и он начинается с первого шага — принятия проблемы и желания измениться.
Интересует подробная информация – вывод из запоя ростов
Richardtoolo · May 15, 2026 at 12:45 pm
Hands-off approach: when you buy automatic tiktok likes, new posts automatically receive engagement without manual ordering.
Rickyattax · May 15, 2026 at 12:57 pm
Этот обзор посвящен успешным стратегиям избавления от зависимости, включая реальные примеры и советы. Мы разоблачим мифы и предоставим читателям достоверную информацию о различных подходах. Получите опыт многообразия методов и найдите подходящий способ для себя!
Узнать из первых рук – частный медик 24 ростов на дону
MatthewSeste · May 15, 2026 at 1:04 pm
В этой статье рассматриваются различные аспекты избавления от зависимости, включая физические и психологические методы. Мы обсудим поддержку, мотивацию и стратегии, которые помогут в процессе выздоровления. Читатели узнают, как преодолеть трудности и двигаться к новой жизни без зависимости.
Как это работает — подробно – narcology clinic ростов на дону
Allanidose · May 15, 2026 at 1:25 pm
Наркологическая клиника в Ростове-на-Дону рассматривается как специализированное медицинское учреждение, где лечение зависимостей выстраивается с учётом необходимости анонимности и круглосуточной доступности помощи. В клинике «Северный Вектор» работа организована таким образом, чтобы пациент мог обратиться за лечением в любое время суток без риска раскрытия персональной информации. Такой формат особенно важен при острых состояниях, требующих немедленного врачебного вмешательства и медицинского контроля.
Изучить вопрос глубже – https://narkologicheskaya-klinika-v-rostove19.ru/
Charlesdof · May 15, 2026 at 2:12 pm
Этот документ охватывает важные аспекты медицинской науки, сосредотачиваясь на ключевых вопросах, касающихся здоровья населения. Мы рассматриваем свежие исследования, клинические рекомендации и лучшие практики, которые помогут улучшить качество лечения и профилактики заболеваний. Читатели получат возможность углубиться в различные медицинские дисциплины.
Кликни и узнай всё! – вывод из запоя на дому ростов
yowixGoria · May 15, 2026 at 2:23 pm
Покупка и продажа недвижимости в Ставропольском крае требует надёжного партнёра, который знает местный рынок изнутри. Агентство Arust под руководством Алексея сопровождает сделки под ключ: от подбора объекта до подписания документов. На сайте https://ar26.ru/ можно ознакомиться с актуальными предложениями и оставить заявку. Клиенты особо отмечают скорость оформления и личный подход — всё готово к приезду, без лишних ожиданий и бюрократических задержек.
TimothyFreby · May 15, 2026 at 2:23 pm
Если основной сайт недоступен — альтернативный вход на Мелбет.
Официальное онлайн-казино — удобные способы оплаты.
Melbet казино — выбор профессионалов — более 4000 слотов.
Проверено актуально сегодня — сохраняет историю транзакций.
Источник:
https://melbet-4yx.top
Wesleydon · May 15, 2026 at 3:04 pm
Публикация посвящена жизненным историям людей, успешно справившихся с зависимостью. Мы покажем, что выход есть, и он начинается с первого шага — принятия проблемы и желания измениться.
Рассмотреть проблему всесторонне – прокапаться от алкоголя ростов
RobertFaica · May 15, 2026 at 3:10 pm
В этой статье мы обсудим процесс восстановления после зависимостей, акцентируя внимание на различных методах и подходах к реабилитации. Читатели узнают, как создать план выздоровления и использовать полезные ресурсы для достижения устойчивых изменений.
Детали по клику – капельница от запоя ростов-на-дону
GeraldPhard · May 15, 2026 at 3:36 pm
Анонимность в клинике «Северный Вектор» является неотъемлемой частью лечебного процесса. Наркологическая клиника в Ростове-на-Дону обеспечивает конфиденциальность на всех этапах взаимодействия с пациентом, начиная с первичного обращения и заканчивая медицинским наблюдением. Клиническая практика показывает, что сохранение анонимности снижает уровень тревожности и повышает готовность пациента к полноценному лечению, что напрямую влияет на стабильность результатов.
Исследовать вопрос подробнее – https://narkologicheskaya-klinika-v-rostove19.ru/narkolog-rostov-na-donu/
MatthewSeste · May 15, 2026 at 3:37 pm
Медицинская публикация представляет собой свод актуальных исследований, экспертных мнений и новейших достижений в сфере здравоохранения. Здесь вы найдете информацию о новых методах лечения, прорывных технологиях и их практическом применении. Мы стремимся сделать актуальные медицинские исследования доступными и понятными для широкой аудитории.
Изучить эмпирические данные – частный медик 24
MichaelHulty · May 15, 2026 at 3:50 pm
По окончании курса детоксикации нарколог дает пациенту и его близким подробные рекомендации, помогающие быстрее восстановить здоровье и предотвратить повторные случаи запоев.
Узнать больше – вывод из запоя
sujugRor · May 15, 2026 at 4:07 pm
Когда речь идёт о покупке автомобиля из Японии, Кореи или Китая, выбор партнёра решает всё. Ищете стоимость авто из японии ? Компания starmotors.biz за годы работы доставила более 17 000 автомобилей по всей России и сегодня держит свыше 600 машин в наличии на рынке во Владивостоке. Офисы и стоянки работают во Владивостоке, Москве и Санкт-Петербурге, а доставка охватывает любой регион страны.
xurukthtes · May 15, 2026 at 4:18 pm
Дубай — город, где роскошь доступна круглосуточно, и именно здесь работает City Drinks Dubai — сервис премиум-доставки алкоголя, который давно завоевал доверие жителей и гостей эмирата. Независимо от того, планируете ли вы вечеринку с друзьями, романтический ужин или деловой приём, на сайте https://drinks-dubai.shop/ вы найдёте богатый выбор напитков: изысканные вина и шампанское, крафтовое пиво, виски, водку, джин, текилу и готовые коктейли. Сервис работает 24 часа в сутки, 7 дней в неделю, гарантируя оперативную и надёжную доставку по всему Дубаю — заказ можно оформить онлайн, по телефону или через мессенджер.
gazaiAbuff · May 15, 2026 at 4:26 pm
Посетите сайт https://www.tyumen-bat.ru/ и вы найдете тяговые батареи Тюменского аккумуляторного завода для вилочных погрузчиков и штабелеров в наличии, как для отечественной, так и для импортной складской техники. Посмотрите ассортимент на сайте с доступными ценами! При необходимости получите коммерческое предложение или консультацию.
JamesApelf · May 15, 2026 at 4:33 pm
В этой статье обсуждаются актуальные медицинские вопросы, которые волнуют общество. Мы обращаем внимание на проблемы, касающиеся здравоохранения и лечения, а также на новшества в области медицины. Читатели будут осведомлены о последних событиях и смогут следить за тенденциями в медицине.
Узнать напрямую – narcology clinic ростов на дону
obertcug · May 15, 2026 at 4:52 pm
Аренда сервера для бизнеса — задача, где важны надёжность, скорость и поддержка 24/7. Netrack выдаёт сервер в аренду с аптаймом 99,9% и держит оборудование в собственном дата-центре класса Tier III. Требуется аренда сервера? На сайте https://netrack.ru/ можно выбрать конфигурацию под любые задачи — от стартапа до крупного корпоративного проекта. Клиент получает выделенные ресурсы без соседей по железу и профессиональное техническое сопровождение на всех этапах работы.
WilliamElupe · May 15, 2026 at 4:58 pm
Статья посвящена анализу текущих трендов в медицине и их влиянию на жизнь людей. Мы рассмотрим новые технологии, методы лечения и значение профилактики в обеспечении долголетия и здоровья.
Исследовать вопрос подробнее – narcology clinic ростов на дону
xurertuh · May 15, 2026 at 5:45 pm
Организация торжеств в Санкт-Петербурге под ключ — специализация агентства «Свадьба 812»: от декора и регистрации до фейерверков и музыкального сопровождения. Опытная команда ведёт свадьбы, корпоративные мероприятия, юбилеи и выпускные вечера. Ищете заказать артиста на корпоратив? На svadba-812.ru собраны готовые проекты и полный каталог услуг с ценами. Подбор ресторанов, фотографов, видеооператоров и артистов входит в работу агентства — заказчик получает готовое решение без лишних хлопот.
JosephGek · May 15, 2026 at 5:54 pm
В статье по вопросам здоровья мы рассматриваем актуальные проблемы, с которыми сталкивается общество. Обсуждаются заболевания, факторы риска и важные аспекты профилактики. Читатели получат полезные советы о том, как сохранить здоровье и улучшить качество жизни.
Продолжить изучение – частный медик 24
RussellTex · May 15, 2026 at 6:08 pm
Команда из 10 специалистов — финишное клининг-убирание.
Светлый скандинавский стиль Питер — экономит на отделке.
Полное сопровождение от идеи до ключей — финал — подарочная фотосессия интерьера.
Источник:
Дизайн интерьера СПб
BrentPoorn · May 15, 2026 at 6:21 pm
Публикация знакомит читателей с различными подходами к реабилитации. От традиционных методов до современных программ — вы узнаете, как выбрать оптимальный путь к выздоровлению и преодолеть препятствия на этом пути.
Нажмите, чтобы узнать больше – вывод из запоя ростов
Geraldhen · May 15, 2026 at 6:27 pm
Медицинская публикация представляет собой свод актуальных исследований, экспертных мнений и новейших достижений в сфере здравоохранения. Здесь вы найдете информацию о новых методах лечения, прорывных технологиях и их практическом применении. Мы стремимся сделать актуальные медицинские исследования доступными и понятными для широкой аудитории.
Нажмите, чтобы узнать больше – вывод из запоя ростов-на-дону
ラブドール 中華 · May 15, 2026 at 6:42 pm
ラブドール 挑発的なシリコーンラブドールを利用して関係を維持する方法
Daniellab · May 15, 2026 at 7:06 pm
Выбор формата лечения определяется состоянием пациента, наличием хронических заболеваний и мотивацией к выздоровлению. При необходимости врач переводит пациента из амбулаторной формы в стационарную, обеспечивая непрерывность и безопасность терапии.
Узнать больше – http://narkologicheskaya-clinika-v-rostove19.ru/narkologiya-rostov-kruglosutochno/https://narkologicheskaya-clinika-v-rostove19.ru
KevinGuent · May 15, 2026 at 7:06 pm
Сразу после вызова нарколог приезжает на дом для проведения первичного осмотра и диагностики. На этом этапе проводится сбор анамнеза, измеряются жизненно важные показатели (пульс, артериальное давление, температура) и определяется степень алкогольной интоксикации. Эти данные являются основой для разработки индивидуального плана лечения.
Подробнее тут – http://kapelnica-ot-zapoya-tyumen0.ru
ทดลองเล่นสล็อต pg · May 15, 2026 at 7:11 pm
สล็อต
สล็อตยุคใหม่กำลังยกระดับจากสล็อตแบบเดิมไปสู่โครงสร้างเกมออนไลน์ที่ใช้เซิร์ฟเวอร์ความเร็วสูง โดยมีระบบ APIร่วมกับเซิร์ฟเวอร์ความเร็วสูง ผู้เล่นจำนวนมากเริ่มมองหาสล็อตเว็บตรง เพราะระบบลดปัญหาระหว่างการเล่นได้ดีกว่า และช่วยลดปัญหาเกมโหลดนาน การค้างของเกม รวมถึงปัญหาการฝากถอนที่ไม่ซิงค์กับระบบหลัก
ระบบสล็อตเว็บตรงจะรับส่งข้อมูลกับค่ายเกมหลักผ่านAPI โดยตรง ทำให้ข้อมูลรอบหมุนถูกส่งแบบทันทีโดยไม่ต้องผ่านหลายเซิร์ฟเวอร์ ส่งผลให้เกมเปิดได้เร็วขึ้น ลดความผิดพลาดระหว่างการหมุน และช่วยให้ระบบโบนัสทำงานได้ลดข้อผิดพลาดได้ดีกว่า
ปัจจัยสำคัญอีกด้านคือระบบธุรกรรมอัตโนมัติ ผู้เล่นสามารถเติมเครดิตและถอนเงินได้ตลอดทุกเวลา โดยไม่จำเป็นต้องรอการอนุมัติด้วยมือเหมือนแพลตฟอร์มที่ยังใช้การตรวจสอบด้วยคน ทำให้การจัดการเงินทุนมีความแม่นยำกว่าเดิม
สาเหตุที่สล็อตเว็บตรงได้รับความนิยมคือความชัดเจนของระบบและความเร็วของระบบ เซิร์ฟเวอร์ที่ผูกกับระบบเกมต้นทางช่วยลดความไม่แน่นอนของระบบตัวกลาง ผู้เล่นจึงเชื่อถือได้ว่าผลลัพธ์ของเกมมาจากกลไกสุ่มของค่ายเกม
อีกด้านหนึ่ง เว็บสมัยใหม่ยังมีการพัฒนาUX/UI สำหรับมือถือโดยเฉพาะ เช่น โหมดจอมือถือแนวตั้ง การโหลดหน้าแบบ Dynamic และระบบ Auto Resumeที่ช่วยคืนสถานะเกมเมื่อการเชื่อมต่อมีปัญหา
ระบบสล็อตออนไลน์รุ่นใหม่เริ่มใช้AI วิเคราะห์ข้อมูล ร่วมกับโครงสร้างคลาวด์และระบบซิงค์ข้อมูลแบบเรียลไทม์เพื่อรองรับการเล่นต่อเนื่องของผู้เล่นหลายกลุ่ม บางระบบยังรองรับBlockchainเพื่อเพิ่มความเป็นส่วนตัวและลดข้อจำกัดของระบบธนาคารแบบเดิม
แพลตฟอร์มเกมออนไลน์ประเภทสล็อตจึงกำลังพัฒนาจากระบบเกมออนไลน์แบบเก่าไปสู่โครงสร้างเกมออนไลน์ที่เน้น API และเซิร์ฟเวอร์ โดยโครงสร้าง APIและความแม่นยำของธุรกรรมกลายเป็นปัจจัยสำคัญในการตัดสินใจใช้งานเว็บสล็อต
ในอนาคตแพลตฟอร์มสล็อตจะยิ่งแข่งขันกันด้านความเร็วของเซิร์ฟเวอร์มากขึ้น ไม่ว่าจะเป็นความเร็วในการโหลดเกม ระบบ AI วิเคราะห์พฤติกรรมผู้เล่น หรือการรักษาความปลอดภัยของบัญชี ผู้ให้บริการที่มีเซิร์ฟเวอร์เสถียรและเชื่อมต่อกับค่ายเกมโดยตรงจะตอบโจทย์ผู้เล่นได้ดีกว่าเว็บทั่วไปที่ยังใช้เซิร์ฟเวอร์ที่เพิ่มความหน่วง
ผู้เล่นยุคใหม่จึงไม่ได้มองแค่แคมเปญการตลาดอีกต่อไป แต่เริ่มให้ความสำคัญกับความเสถียรของระบบ ความเร็วในการทำธุรกรรม และความพร้อมของระบบเมื่อต้องรองรับผู้เล่นจำนวนมาก
ArturopRorm · May 15, 2026 at 7:21 pm
Продолжение
Срочные займы онлайн
Williambax · May 15, 2026 at 7:22 pm
При поступлении вызова нарколог незамедлительно приезжает на дом для проведения тщательного первичного осмотра. Специалист измеряет жизненно важные показатели, такие как пульс, артериальное давление и температура, а также собирает анамнез для оценки степени алкогольной интоксикации. Эта информация является основой для разработки персонального плана лечения.
Получить дополнительную информацию – https://vyvod-iz-zapoya-murmansk00.ru/vyvod-iz-zapoya-czena-murmansk
JamesApelf · May 15, 2026 at 7:27 pm
Статья посвящена анализу текущих трендов в медицине и их влиянию на жизнь людей. Мы рассмотрим новые технологии, методы лечения и значение профилактики в обеспечении долголетия и здоровья.
Это ещё не всё… – вывод из запоя в ростове-на-дону
Geraldhen · May 15, 2026 at 7:28 pm
Медицинская публикация представляет собой свод актуальных исследований, экспертных мнений и новейших достижений в сфере здравоохранения. Здесь вы найдете информацию о новых методах лечения, прорывных технологиях и их практическом применении. Мы стремимся сделать актуальные медицинские исследования доступными и понятными для широкой аудитории.
Наши рекомендации — тут – прокапаться от алкоголя ростов
StephenDap · May 15, 2026 at 7:39 pm
Останні новини https://18000.ck.ua Черкас та Черкаської області
ErnestBlath · May 15, 2026 at 8:16 pm
Этот обзор медицинских исследований собрал самое важное из последних публикаций в области медицины. Мы проанализировали ключевые находки и представили их в доступной форме, чтобы читатели могли легко ориентироваться в актуальных темах. Этот материал станет отличным подспорьем для изучения медицины.
Есть чему поучиться – narcology clinic
Williamutiff · May 15, 2026 at 8:23 pm
В этой статье мы рассматриваем разрушительное влияние зависимости на жизнь человека. Обсуждаются аспекты, такие как здоровье, отношения и профессиональные достижения. Читатели узнают о необходимости обращения за помощью и о путях к восстановлению.
Почему это важно? – частный медик 24 ростов на дону
Robertwiz · May 15, 2026 at 8:31 pm
Алкогольный запой является тяжёлым состоянием, требующим срочного медицинского вмешательства. Наркологическая клиника «Пульс» в Краснодаре предлагает эффективную помощь в борьбе с алкогольной зависимостью, используя проверенный метод — капельницу от запоя на дому. Наши специалисты оперативно выезжают по указанному адресу и обеспечивают качественную медицинскую помощь с гарантией конфиденциальности и безопасности.
Подробнее – капельница от запоя вызов город
BrentPoorn · May 15, 2026 at 8:40 pm
Этот обзор посвящен успешным стратегиям избавления от зависимости, включая реальные примеры и советы. Мы разоблачим мифы и предоставим читателям достоверную информацию о различных подходах. Получите опыт многообразия методов и найдите подходящий способ для себя!
Желаете узнать подробности? – частный медик 24 рнд
kemobtCaK · May 15, 2026 at 8:49 pm
Резинотехнические изделия — это та продукция, где качество материала напрямую определяет надёжность всей конструкции. Компания ПКФ «Нова» специализируется на изготовлении и поставке РТИ: рукавов, уплотнителей, прокладок и других изделий из резины под заказ. На https://pkfnova.ru/ можно оформить запрос на нестандартную продукцию, которую другие поставщики просто отказываются делать. Постоянные клиенты работают с компанией годами — и это лучшая характеристика надёжного партнёра.
ErnestBlath · May 15, 2026 at 8:59 pm
В данной статье рассматриваются физиологические и эмоциональные аспекты зависимости. Мы обсудим, как организм реагирует на зависимое поведение, и какие методы помогают восстановить здоровье и внутреннее равновесие.
Читать дальше – narcology clinic
FelixJak · May 15, 2026 at 9:05 pm
Этот обзор медицинских исследований собрал самое важное из последних публикаций в области медицины. Мы проанализировали ключевые находки и представили их в доступной форме, чтобы читатели могли легко ориентироваться в актуальных темах. Этот материал станет отличным подспорьем для изучения медицины.
Где почитать поподробнее? – капельница от запоя ростов-на-дону
OrvalHex · May 15, 2026 at 9:08 pm
Современные методы лечения при выводе из запоя включают как медикаментозную детоксикацию, так и психологическую реабилитацию. В Уфе наркологи используют капельничное введение лекарственных средств, которые помогают быстро вывести токсины, нормализовать обмен веществ и стабилизировать работу внутренних органов. Одновременно с этим проводится психологическая поддержка для снижения эмоционального стресса, связанного с запоем.
Получить дополнительную информацию – https://narcolog-na-dom-ufa0.ru/narkolog-na-dom-kruglosutochno-ufa
JosephNoice · May 15, 2026 at 9:23 pm
Мы рассмотрим современные вызовы здравоохранения и пути их решения с помощью технологий и научных исследований. В статье собраны данные о новых лекарствах, методах диагностики и системном подходе к улучшению здоровья населения.
Получить профессиональную консультацию – вызов нарколога на дом ростов на дону
Allanidose · May 15, 2026 at 9:24 pm
Анонимность в клинике «Северный Вектор» является неотъемлемой частью лечебного процесса. Наркологическая клиника в Ростове-на-Дону обеспечивает конфиденциальность на всех этапах взаимодействия с пациентом, начиная с первичного обращения и заканчивая медицинским наблюдением. Клиническая практика показывает, что сохранение анонимности снижает уровень тревожности и повышает готовность пациента к полноценному лечению, что напрямую влияет на стабильность результатов.
Углубиться в тему – http://narkologicheskaya-klinika-v-rostove19.ru
Thomasric · May 15, 2026 at 9:33 pm
Эта публикация исследует взаимосвязь зависимости и психологии. Мы обсудим, как психологические аспекты влияют на появление зависимостей и процесс выздоровления. Читатели смогут понять важность профессиональной поддержки и применения научных подходов в терапии.
Изучить вопрос глубже – narcology clinic ростов на дону
MichaelHulty · May 15, 2026 at 9:38 pm
После поступления звонка специалисты нашей клиники оперативно выезжают по адресу пациента в Новосибирске. Врач начинает работу с детальной диагностики: измеряет пульс, артериальное давление, сатурацию (уровень кислорода в крови), оценивает состояние нервной и сердечно-сосудистой систем, уточняет наличие хронических заболеваний, аллергических реакций, длительность и тяжесть запоя.
Исследовать вопрос подробнее – вывод из запоя новосибирск.
HectorLok · May 15, 2026 at 9:55 pm
Этот документ охватывает важные аспекты медицинской науки, сосредотачиваясь на ключевых вопросах, касающихся здоровья населения. Мы рассматриваем свежие исследования, клинические рекомендации и лучшие практики, которые помогут улучшить качество лечения и профилактики заболеваний. Читатели получат возможность углубиться в различные медицинские дисциплины.
Погрузиться в научную дискуссию – прокапаться от алкоголя ростов
nipaxaAbefS · May 15, 2026 at 9:57 pm
Веб-студия из Перми создаёт сайты под ключ в пять последовательных этапов — начиная с первого звонка и заканчивая сдачей проекта. Ищете веб студия пермь телефон? На design59.ru можно заказать как шаблонное решение так и полностью индивидуальный дизайн с вёрсткой с нуля. Стоимость и сроки определяются техническим заданием. Дополнительно студия берётся за обслуживание, администрирование и продвижение сайта.
MichaelHulty · May 15, 2026 at 9:57 pm
По окончании курса детоксикации нарколог дает пациенту и его близким подробные рекомендации, помогающие быстрее восстановить здоровье и предотвратить повторные случаи запоев.
Углубиться в тему – вывод из запоя на дому в новосибирске
redação TrustGuru Pesquisa · May 15, 2026 at 10:03 pm
Melhor horário pra jogar Touro no fim de semana — alguém tem dado real?
FelixJak · May 15, 2026 at 10:21 pm
Этот обзор медицинских исследований собрал самое важное из последних публикаций в области медицины. Мы проанализировали ключевые находки и представили их в доступной форме, чтобы читатели могли легко ориентироваться в актуальных темах. Этот материал станет отличным подспорьем для изучения медицины.
Практические советы ждут тебя – откапать от алкоголя
Jasonnot · May 15, 2026 at 10:29 pm
Эта доказательная статья представляет собой глубокое погружение в успехи и вызовы лечения зависимостей. Мы обращаемся к научным исследованиям и опыту специалистов, чтобы предоставить читателям надежные данные об эффективности различных методик. Изучите, что работает лучше всего, и получите информацию от экспертов.
Получить полную информацию – врач нарколог на дом в ростове
Tobiaszom · May 15, 2026 at 11:01 pm
Эта публикация исследует взаимосвязь зависимости и психологии. Мы обсудим, как психологические аспекты влияют на появление зависимостей и процесс выздоровления. Читатели смогут понять важность профессиональной поддержки и применения научных подходов в терапии.
Только факты! – капельница от запоя ростов-на-дону
MatthewvoW · May 15, 2026 at 11:16 pm
В этом обзоре мы обсудим современные методы борьбы с зависимостями, включая медикаментозную терапию и психотерапию. Мы представим последние исследования и их результаты, чтобы читатели могли быть в курсе наиболее эффективных подходов к лечению и поддержке.
Подробнее – капельница от запоя ростов
Jasonnot · May 15, 2026 at 11:26 pm
Эта доказательная статья представляет собой глубокое погружение в успехи и вызовы лечения зависимостей. Мы обращаемся к научным исследованиям и опыту специалистов, чтобы предоставить читателям надежные данные об эффективности различных методик. Изучите, что работает лучше всего, и получите информацию от экспертов.
Изучить аспект более тщательно – частный медик 24 ростов на дону
Doylekix · May 15, 2026 at 11:36 pm
В этой статье мы говорим о важности поддержки в процессе выздоровления. Рассматриваются семьи, группы поддержки, специалисты и онлайн-ресурсы, которые могут сыграть решающую роль в избавлении от зависимости.
Прочесть заключение эксперта – вывод из запоя в ростове
FrancisJuign · May 15, 2026 at 11:52 pm
Нужна CRM банкротством физ лиц? битрикс24 для БФЛ инструмент автоматизации юридического бизнеса по банкротству физических лиц. Управляйте заявками, делами клиентов, документами и сроками процедур. Система помогает организовать работу команды и контролировать каждый этап банкротства.
dazuxabofe · May 16, 2026 at 12:08 am
Издание Vkursi.org действует по прямому принципу — тримаємо вас завжди в курсі важливих подій — и ведёт полноценное освещение политики, экономики, бизнеса, общества, здоровья, технологий и криминала без пауз и фильтров. Журналисты выпускают эксклюзивные материалы о коррупционных механизмах и громких судебных делах опираясь на документальную базу и проверенные источники. Держите руку на пульсе событий на https://vkursi.org/ — украинский новостной портал для читателей которым важна скорость и точность подачи информации. Культура и технологии дополняют жёсткую повестку и превращают ресурс в полноценный ежедневный медиаинструмент.
MatthewvoW · May 16, 2026 at 12:17 am
В этой публикации мы предложим ряд рекомендаций по избавлению от зависимостей и успешному восстановлению. Мы обсудим методы привлечения поддержки и важность самосознания. Эти советы помогут людям вернуться к нормальной жизни и стать на путь выздоровления.
Что ещё? Расскажи всё! – капельница от запоя ростов на дону
WilliamTex · May 16, 2026 at 12:26 am
Запой – это состояние, когда организм требует постоянного поступления алкоголя для нормальной работы. Запой вызывает накопление вредных веществ, что негативно влияет на органы и иммунную систему. Не пытайтесь самостоятельно избавиться от запоя, это может навредить. Получите квалифицированную помощь на дому от клиники «Семья и Здоровье». Мы быстро приедем и окажем круглосуточную поддержку при запое. Длительное употребление алкоголя опасно для здоровья и жизни. Не ждите, пока станет слишком поздно, обратитесь за помощью при запое!
Подробнее – https://vyvod-iz-zapoya-krasnoyarsk0.ru/
Doylekix · May 16, 2026 at 12:37 am
В данной статье мы поговорим о будущем медицины, акцентируя внимание на прорывных разработках и их потенциале. Читатель узнает о новых подходах к лечению, роли искусственного интеллекта и возможностях персонализированной медицины.
Дополнительно читайте здесь – прокапаться от алкоголя ростов
Rickyattax · May 16, 2026 at 12:52 am
Этот обзор посвящен успешным стратегиям избавления от зависимости, включая реальные примеры и советы. Мы разоблачим мифы и предоставим читателям достоверную информацию о различных подходах. Получите опыт многообразия методов и найдите подходящий способ для себя!
Как достичь результата? – частный медик 24 рнд
RobertFaica · May 16, 2026 at 1:04 am
В этой статье рассматриваются различные аспекты избавления от зависимости, включая физические и психологические методы. Мы обсудим поддержку, мотивацию и стратегии, которые помогут в процессе выздоровления. Читатели узнают, как преодолеть трудности и двигаться к новой жизни без зависимости.
Что ещё? Расскажи всё! – narcology clinic
Michaelhig · May 16, 2026 at 1:10 am
В этой статье рассматриваются способы преодоления зависимости и успешные истории людей, которые справились с этой проблемой. Мы обсудим важность поддержки со стороны близких и профессионалов, а также стратегии, которые могут помочь в процессе выздоровления. Научитесь первоочередным шагам к новой жизни.
Полезно знать – капельница от запоя ростов на дону
haruksnag · May 16, 2026 at 1:16 am
Looking for luxury travel guides, local tips, and everything you need for an unforgettable visit to Dubai? Visit https://gildeddunes.com/ for detailed articles to help you plan the perfect trip to Dubai, from transportation and attractions to hotels and dining. Learn more on the website.
Wesleydon · May 16, 2026 at 1:44 am
В этой статье мы подробно рассматриваем проверенные методы борьбы с зависимостями, включая психотерапию, медикаментозное лечение и поддержку со стороны общества. Мы акцентируем внимание на важности комплексного подхода и возможности успешного восстановления для людей, столкнувшихся с этой проблемой.
Получить дополнительную информацию – откапать от алкоголя
AntonioRinna · May 16, 2026 at 1:45 am
Такой курс не только очищает организм от токсинов, но и помогает вернуть эмоциональное равновесие. После завершения терапии пациент чувствует себя отдохнувшим, восстанавливает аппетит и сон, уходит тревожность и раздражительность.
Получить дополнительную информацию – врач вывод из запоя
bonus tigrinho como funciona · May 16, 2026 at 1:54 am
Three Monkeys variance hit different since the patch.
Thomaslaw · May 16, 2026 at 1:59 am
В этой статье мы обсудим процесс восстановления после зависимостей, акцентируя внимание на различных методах и подходах к реабилитации. Читатели узнают, как создать план выздоровления и использовать полезные ресурсы для достижения устойчивых изменений.
См. подробности – нарколог на дом ростов на дону
HectorLok · May 16, 2026 at 2:07 am
Этот документ охватывает важные аспекты медицинской науки, сосредотачиваясь на ключевых вопросах, касающихся здоровья населения. Мы рассматриваем свежие исследования, клинические рекомендации и лучшие практики, которые помогут улучшить качество лечения и профилактики заболеваний. Читатели получат возможность углубиться в различные медицинские дисциплины.
Погрузиться в научную дискуссию – откапать от алкоголя
StanleyUtesy · May 16, 2026 at 2:20 am
Этот текст представляет собой обзор свежих данных и исследований в области медицины. Он призван помочь читателям понять, как научные достижения влияют на лечение, диагностику и общее состояние системы здравоохранения.
Узнать больше > – частный медик 24
BrianKiT · May 16, 2026 at 2:24 am
посмотреть на этом сайте
просмотры max на пост
Jewellmeery · May 16, 2026 at 2:30 am
Мы рассмотрим современные вызовы здравоохранения и пути их решения с помощью технологий и научных исследований. В статье собраны данные о новых лекарствах, методах диагностики и системном подходе к улучшению здоровья населения.
Рассмотреть проблему всесторонне – стоп алко екатеринбург
JerryDwefe · May 16, 2026 at 2:53 am
Соблюдение конфиденциальности в клинике «Точка Опоры» является неотъемлемой частью лечебного процесса. Наркологическая клиника в Краснодаре обеспечивает закрытый формат приёма, хранения медицинских данных и взаимодействия с пациентом. Практика показывает, что анонимное обращение снижает уровень тревожности, способствует более открытому диалогу с врачом и повышает точность клинической диагностики.
Углубиться в тему – http://narcologicheskaya-klinika-v-krd19.ru/narkologa-na-dom-krasnodar/https://narcologicheskaya-klinika-v-krd19.ru
KennethDes · May 16, 2026 at 3:10 am
В данном обзоре представлены основные направления и тренды в области медицины. Мы обсудим актуальные проблемы здравоохранения, свежие открытия и новые подходы, которые меняют представление о лечении и профилактике заболеваний. Эта информация будет полезна как специалистам, так и широкой публике.
Личный опыт — читайте сами – нарколог на дом ростов на дону
BrianKiT · May 16, 2026 at 3:36 am
Узнать больше
реакции max на пост
daruwlLok · May 16, 2026 at 3:44 am
Современная медицина требует надёжного оснащения, и компания РУС-МеДтеХ давно стала проверенным партнёром для больниц, клиник и лабораторий по всей России. На сайте https://rus-medteh.ru/ представлен широкий каталог сертифицированного медицинского оборудования — от профессиональных микроскопов OPTIKA и видеокольпоскопов до специализированного расходного материала ведущих мировых производителей, включая B. Braun Melsungen. Каждый товар сопровождается полным пакетом документов и лицензий, что особенно важно для медицинских учреждений. Клиенты компании отмечают оперативную доставку и высокий уровень сервиса — и это не случайно.
24art-zone.ru · May 16, 2026 at 3:46 am
24art-zone.ru
KennethDes · May 16, 2026 at 4:00 am
В данной статье мы поговорим о будущем медицины, акцентируя внимание на прорывных разработках и их потенциале. Читатель узнает о новых подходах к лечению, роли искусственного интеллекта и возможностях персонализированной медицины.
Слушай внимательно — тут важно – частный медик 24 рнд
WilliamElupe · May 16, 2026 at 4:04 am
Статья посвящена анализу текущих трендов в медицине и их влиянию на жизнь людей. Мы рассмотрим новые технологии, методы лечения и значение профилактики в обеспечении долголетия и здоровья.
Это стоит прочитать полностью – откапать от алкоголя
KevinGuent · May 16, 2026 at 4:07 am
Сразу после вызова нарколог приезжает на дом для проведения первичного осмотра и диагностики. На этом этапе проводится сбор анамнеза, измеряются жизненно важные показатели (пульс, артериальное давление, температура) и определяется степень алкогольной интоксикации. Эти данные являются основой для разработки индивидуального плана лечения.
Детальнее – http://kapelnica-ot-zapoya-tyumen0.ru
GeraldPhard · May 16, 2026 at 4:56 am
Наркологическая клиника в Ростове-на-Дону рассматривается как специализированное медицинское учреждение, где лечение зависимостей выстраивается с учётом необходимости анонимности и круглосуточной доступности помощи. В клинике «Северный Вектор» работа организована таким образом, чтобы пациент мог обратиться за лечением в любое время суток без риска раскрытия персональной информации. Такой формат особенно важен при острых состояниях, требующих немедленного врачебного вмешательства и медицинского контроля.
Подробнее – https://narkologicheskaya-klinika-v-rostove19.ru
BrianKiT · May 16, 2026 at 5:00 am
пояснения
мужские подписчики max
BrianKiT · May 16, 2026 at 5:06 am
подробнее
увеличить просмотры max
equipe TrustGuru Review · May 16, 2026 at 5:25 am
O veterano calado colocou R$300 no Three Monkeys e saiu com R$5.000. Sem print, só contou.
burun estetiği fiyatları · May 16, 2026 at 5:26 am
I love what you’ve created here, this is definitely one of my favorite sites to visit.
JamesTrany · May 16, 2026 at 5:27 am
В данной статье рассматриваются проблемы общественного здоровья и социальные факторы, влияющие на него. Мы акцентируем внимание на значении профилактики и осведомленности в защите здоровья на уровне общества. Читатели смогут узнать о новых инициативах и программах, направленных на улучшение здоровья населения.
Есть чему поучиться – вывод из запоя ростов-на-дону
Tobiaszom · May 16, 2026 at 5:37 am
Этот обзор содержит информацию о передовых достижениях в области медицины. Мы разберем инновационные технологии, которые меняют подход к лечению и диагностике, а также их влияние на эффективность оказания медицинской помощи.
Читать дальше – капельница от запоя ростов-на-дону
AntonioRinna · May 16, 2026 at 6:07 am
В таблице ниже представлены основные группы препаратов, применяемых при выведении из запоя:
Изучить вопрос глубже – вывод из запоя недорого в краснодаре
no deposit bonus free · May 16, 2026 at 6:23 am
Conta rápida no Jungle Delight: 96% de RTP fica em amostras grandes. Pequenas mentem.
Michaelhig · May 16, 2026 at 6:43 am
В данной статье мы поговорим о будущем медицины, акцентируя внимание на прорывных разработках и их потенциале. Читатель узнает о новых подходах к лечению, роли искусственного интеллекта и возможностях персонализированной медицины.
Подробная информация доступна по запросу – капельница от запоя ростов
botoclGof · May 16, 2026 at 6:52 am
Современный бизнес требует надёжных логистических решений, и здесь на первый план выходит сервис https://gruz247.ru/ — профессиональная транспортная компания, которая берёт на себя полный цикл грузоперевозок. От сборных отправок до экспресс-доставки за один день, от разовых заявок до регулярных рейсов по фиксированному расписанию — спектр услуг охватывает любые потребности бизнеса и частных клиентов. Гибкая тарификация, оплата только за реальный объём груза и круглосуточная поддержка делают сотрудничество максимально выгодным и комфортным. Клиенты компании неизменно отмечают пунктуальность, профессионализм команды и прозрачное отслеживание каждой партии на всех этапах маршрута.
WilliamTex · May 16, 2026 at 7:11 am
Запой – это состояние, когда организм требует постоянного поступления алкоголя для нормальной работы. Запой вызывает накопление вредных веществ, что негативно влияет на органы и иммунную систему. Не пытайтесь самостоятельно избавиться от запоя, это может навредить. Получите квалифицированную помощь на дому от клиники «Семья и Здоровье». Мы быстро приедем и окажем круглосуточную поддержку при запое. Длительное употребление алкоголя опасно для здоровья и жизни. Не ждите, пока станет слишком поздно, обратитесь за помощью при запое!
Получить больше информации – https://vyvod-iz-zapoya-krasnoyarsk0.ru/vyvod-iz-zapoya-na-domu-krasnoyarsk
JerryDwefe · May 16, 2026 at 7:14 am
Лечение в круглосуточном режиме рассматривается как непрерывный медицинский процесс, а не как разовое вмешательство. Даже при экстренном обращении терапия выстраивается последовательно, с обязательным врачебным наблюдением и оценкой динамики состояния пациента.
Подробнее – https://narcologicheskaya-klinika-v-krd19.ru/krasnodar-narkologicheskij-czentr/
Thomaslaw · May 16, 2026 at 7:35 am
В этой статье мы обсудим процесс восстановления после зависимостей, акцентируя внимание на различных методах и подходах к реабилитации. Читатели узнают, как создать план выздоровления и использовать полезные ресурсы для достижения устойчивых изменений.
Не упусти шанс – вызов нарколога на дом в ростове
WilliamTex · May 16, 2026 at 7:40 am
Запой – это серьезная проблема, когда организм перестает работать без постоянного поступления алкоголя. Из-за запоя токсины отравляют организм, нарушая работу органов и снижая иммунитет. Попытки самостоятельно бросить пить во время запоя могут привести к ухудшению самочувствия. «Семья и Здоровье» лечит запой на дому – это удобно и снижает стресс. Мы приедем в любое время суток и проведем все процедуры для восстановления здоровья. Длительное пьянство может привести к опасным для жизни осложнениям. Нельзя затягивать с лечением запоя, это может привести к серьезным последствиям.
Углубиться в тему – vivod iz zapoya krasnoyarsk
StanleyUtesy · May 16, 2026 at 7:49 am
В этой статье мы рассматриваем разрушительное влияние зависимости на жизнь человека. Обсуждаются аспекты, такие как здоровье, отношения и профессиональные достижения. Читатели узнают о необходимости обращения за помощью и о путях к восстановлению.
Личный опыт — читайте сами – вывод из запоя ростов на дону
Kirilllet · May 16, 2026 at 7:54 am
Настроили управленческую отчётность для директора — дашборд с выручкой, расходами и прибылью в реальном времени. Теперь принимаю решения на основе цифр, а не ощущений. аудит 1С Белгород
Eduardlet · May 16, 2026 at 8:03 am
Интернет-магазин интегрировали с 1С УНФ — заказы с сайта автоматически создаются в программе. Сборщики получают задание сразу, скорость обработки заказов выросла вдвое. 1С УНФ для розничной торговли
casino bônus sem deposito · May 16, 2026 at 8:26 am
O cara de ti com a planilha chamou o Bombom de “o único honesto” — meio brincando, meio não.
Stevenvew · May 16, 2026 at 8:32 am
Слоты, рулетка, покер — честные результаты и кешбэк.
Рабочая ссылка в казино Мелбет — сохраняет баланс и историю ставок.
Вход в melbet казино из любой точки — турниры с миллионными призами.
Мелбет зеркало рабочее или официальный сайт — дают одинаковые бонусы.
Source:
мелбет
JosephNoice · May 16, 2026 at 8:47 am
Текст посвящён распространённым мифам о зависимости и их развенчанию. Мы предоставим научно обоснованную информацию и дадим рекомендации по выбору эффективного способа борьбы с зависимым поведением.
Осуществить глубокий анализ – врач нарколог на дом в ростове
binance register · May 16, 2026 at 8:48 am
Thank you for your sharing. I am worried that I lack creative ideas. It is your article that makes me full of hope. Thank you. But, I have a question, can you help me?
Daniellab · May 16, 2026 at 8:58 am
Наркологическая клиника «Южный МедКонтроль» объединяет современные медицинские технологии, опыт специалистов и уважительное отношение к каждому пациенту. Здесь создаются условия для безопасного и результативного лечения зависимостей любой сложности — от алкогольной до полинаркотической. Центр работает в круглосуточном режиме, предлагая выезд врачей на дом, детоксикацию, кодирование и длительные программы реабилитации. Основная цель специалистов — восстановление физического и психологического равновесия человека, возвращение способности к полноценной жизни без зависимости.
Ознакомиться с деталями – https://narkologicheskaya-clinika-v-rostove19.ru/
JosephGek · May 16, 2026 at 9:20 am
В данной статье рассматриваются физиологические и эмоциональные аспекты зависимости. Мы обсудим, как организм реагирует на зависимое поведение, и какие методы помогают восстановить здоровье и внутреннее равновесие.
Откройте для себя больше – narcology clinic ростов на дону
Timothyelapy · May 16, 2026 at 9:21 am
gri renk olusumu hakk?ndaki bolumu cok sevdim. Kendiniz gorun: https://fikirdronu.com/articles/gri-renk-hangi-renklerle-olusur/
Timothyelapy · May 16, 2026 at 9:25 am
evde kozalak bulundurman?n faydalar? hakk?ndaki makaleyi cok sevdim. Iste link: https://kendimacera.com/articles/bitkiler-hakkinda-ilginc-bilgiler/
Allanidose · May 16, 2026 at 9:45 am
Анонимность в клинике «Северный Вектор» является неотъемлемой частью лечебного процесса. Наркологическая клиника в Ростове-на-Дону обеспечивает конфиденциальность на всех этапах взаимодействия с пациентом, начиная с первичного обращения и заканчивая медицинским наблюдением. Клиническая практика показывает, что сохранение анонимности снижает уровень тревожности и повышает готовность пациента к полноценному лечению, что напрямую влияет на стабильность результатов.
Подробнее – http://narkologicheskaya-klinika-v-rostove19.ru
xooxGob · May 16, 2026 at 9:51 am
«Охотник за разумом» — мрачный криминальный триллер Netflix: агенты ФБР Холден Форд и Билл Тенч в конце 1970-х первыми решились исследовать разум серийных убийц и создали науку поведенческого профайлинга. Ищете охотник за разумом все серии? Все 19 серий двух сезонов доступны бесплатно на ohotnik-za-razumom-smotret.net с профессиональной озвучкой LostFilm и SDI Media. Безупречно воссозданная эпоха, фирменный стиль Финчера и леденящие душу беседы с историческими преступниками делают «Охотника за разумом» эталоном умного криминального сериала — обязателен к просмотру.
Jewellmeery · May 16, 2026 at 10:25 am
В этой заметке мы представляем шаги, которые помогут в процессе преодоления зависимостей. Рассматриваются стратегии поддержки и чек-листы для тех, кто хочет сделать первый шаг к выздоровлению. Наша цель — вдохновить читателей на положительные изменения и поддержать их в трудных моментах.
Проверенные методы — узнай сейчас – Наркологическая клиника «Похмельная служба» в Екатеринбурге.
Michealtap · May 16, 2026 at 11:11 am
check my blog
youtube likes provider
Carlosgaumb · May 16, 2026 at 11:11 am
Пицца в Саратов https://kosmopizza.ru свежая, ароматная и приготовленная по лучшим рецептам. Заказывайте доставку пиццы на дом или в офис, выбирайте из большого меню: классические и авторские пиццы, горячие закуски и напитки. Быстрая доставка по городу.
Michealtap · May 16, 2026 at 11:41 am
click
buy youtube views
JamesTrany · May 16, 2026 at 12:28 pm
В этой статье мы рассмотрим современные достижения в области медицины, включая инновационные методы лечения и диагностики. Мы обсудим важность профилактики заболеваний и роль технологий в улучшении качества здравоохранения. Читатели узнают о влиянии медицины на повседневную жизнь и ее значение для современного общества.
Желаете узнать подробности? – капельница от запоя ростов
RussellTex · May 16, 2026 at 12:58 pm
Лучшие дизайнеры Санкт-Петербурга — 3D-визуализация в подарок.
Реконструкция без потери ценности — утеплим без порчи фасада.
Аристократичный классический интерьер СПб — мягкое зонирование торшерами.
Источник:
https://taximaximus.ru
Thurmanguago · May 16, 2026 at 1:38 pm
Купить пиццу https://pizzeriacuba.ru в Воронеж с быстрой доставкой на дом или в офис. Большой выбор пиццы: классические рецепты, авторские вкусы, свежие ингредиенты и горячая выпечка. Удобный онлайн-заказ, акции и выгодные предложения для любителей вкусной пиццы.
xugegDit · May 16, 2026 at 1:42 pm
Компания wall.glass специализируется на проектировании и монтаже стеклянных перегородок, офисных дверей и противопожарных конструкций для коммерческих объектов. Компания реализует широкий ассортимент продукции: цельностеклянные двери, офисные системы, войлочные панели и пластик CPL/HPL. Ищете стеклянные перегородки с монтажом? На сайте wall.glass доступны BIM-каталог технические чертежи DWG и RAL-инструменты для точного подбора решений. Все конструкции сертифицированы, компания имеет отраслевые награды и поставляет продукцию с чёткими условиями оплаты и доставки.
Michealtap · May 16, 2026 at 2:05 pm
get more
buy telegram reactions
Allanidose · May 16, 2026 at 2:24 pm
Такой подход позволяет наркологической клинике в Ростове-на-Дону выстраивать лечение в безопасных и психологически комфортных условиях.
Получить дополнительные сведения – платная наркологическая клиника
Brianfesia · May 16, 2026 at 2:26 pm
В практике круглосуточного лечения применяются следующие этапы:
Углубиться в тему – запой наркологическая клиника
Allanidose · May 16, 2026 at 2:39 pm
Анонимность в клинике «Северный Вектор» является неотъемлемой частью лечебного процесса. Наркологическая клиника в Ростове-на-Дону обеспечивает конфиденциальность на всех этапах взаимодействия с пациентом, начиная с первичного обращения и заканчивая медицинским наблюдением. Клиническая практика показывает, что сохранение анонимности снижает уровень тревожности и повышает готовность пациента к полноценному лечению, что напрямую влияет на стабильность результатов.
Подробнее тут – http://narkologicheskaya-klinika-v-rostove19.ru
Michealtap · May 16, 2026 at 3:46 pm
navigate to this website
smm panel with api
JamesLolla · May 16, 2026 at 4:27 pm
Современный коворкинг https://expresrabota.com/kovorking-kogda-ofis-stanovitsya-soobshtestvom.html для комфортной и продуктивной работы. Рабочие места, переговорные комнаты, быстрый интернет и удобная инфраструктура. Подходит для фрилансеров, предпринимателей, стартапов и команд, которым нужен гибкий офис.
Go 99 · May 16, 2026 at 6:52 pm
I simply could not leave your site before suggesting that I actually enjoyed the usual info a person supply in your visitors? Is going to be back often to inspect new posts
MarionAbsew · May 16, 2026 at 10:22 pm
Турагентство по России https://republictravel.ru туры в Карелия, Байкал, Камчатка, Дагестан, Мурманск, Калининград, Санкт-Петербург и другие направления. Экскурсии, отдых и авторские маршруты по самым красивым регионам страны.
fixDiele · May 16, 2026 at 10:26 pm
По теме “Последние футбольные новости и аналитика”, есть отличная статья.
Вот, делюсь ссылкой:
https://armyspartak.ru
fixDiele · May 16, 2026 at 10:29 pm
Для тех, кто ищет информацию по теме “Свежие новости Томской области и мира”, там просто кладезь информации.
Смотрите сами:
https://media83.ru
MarvinTug · May 17, 2026 at 12:50 am
Тем, кто хочет китайские дорамы без лишней суеты и бесконечного поиска, DoramaGo может стать приятной площадкой для вечернего просмотра. Здесь представлены корейские, китайские, японские, тайские и другие азиатские сериалы, где есть то самое настроение, за которое дорамы так ценят: красивые истории о любви, интриги, запоминающиеся персонажи и визуальная красота азиатских сериалов. Удобный каталог помогает быстро подобрать сериал по стране, жанру, году или настроению, а свежие серии позволяют следить за любимыми проектами.
JeffreyBus · May 17, 2026 at 12:52 am
В наше время удобно выбирать смотреть дорамы с русской озвучкой онлайн без десятков открытых вкладок, непонятных ресурсов и потери времени. Этот сайт собирает в одном месте корейские, китайские, японские и другие азиатские сериалы с понятным русским переводом, краткими описаниями, жанровыми подборками, годами выхода и удобными карточками. Здесь легко найти романтическую историю на вечер, напряженный триллер, легкую комедию или популярную премьеру, которую уже обсуждают поклонники дорам.
바이낸스 가입 · May 17, 2026 at 1:05 am
Just want to say what a great blog you got here!I’ve been around for quite a lot of time, but finally decided to show my appreciation of your work!
Brianfesia · May 17, 2026 at 1:24 am
Такой подход позволяет наркологической клинике в Ростове-на-Дону выстраивать лечение в безопасных и психологически комфортных условиях.
Подробнее – http://narkologicheskaya-klinika-v-rostove19.ru
Jessienen · May 17, 2026 at 1:30 am
В этих случаях вызов нарколога на дом не только оправдан, но и жизненно необходим для предотвращения опасных осложнений и стабилизации здоровья пациента.
Получить больше информации – нарколог на дом цена
GeraldPhard · May 17, 2026 at 2:43 am
В практике круглосуточного лечения применяются следующие этапы:
Разобраться лучше – http://www.domen.ru
Georgeratly · May 17, 2026 at 3:41 am
подробнее здесь Кашпо из ротанга
바이낸스 가입 · May 17, 2026 at 4:26 am
I was referred to this web site by my cousin. I’m not sure who has written this post, but you’ve really identified my problem. You’re wonderful! Thanks!
바이낸스 가입 · May 17, 2026 at 4:33 am
I concur with your conclusions and will eagerly look forward to your future updates. The usefulness and significance is overwhelming and has been invaluable to me!
socolivex · May 17, 2026 at 4:38 am
Simply want to say your article is as amazing. The clarity in your post is just great and i can assume you’re an expert on this subject. Fine with your permission allow me to grab your feed to keep up to date with forthcoming post. Thanks a million and please keep up the gratifying work.
바이낸스 가입 · May 17, 2026 at 4:45 am
Lovely just what I was looking for. Thanks to the author for taking his clock time on this one.
Georgeratly · May 17, 2026 at 6:15 am
посмотреть на этом сайте Кашпо из искусственного ротанга
Georgeratly · May 17, 2026 at 6:20 am
перейдите на этот сайт Кашпо из искусственного ротанга
바이낸스 가입 · May 17, 2026 at 6:52 am
I had fun reading this post. I want to see more on this subject.. Gives Thanks for writing this nice article.. Anyway, I’m going to subscribe to your rss and I wish you write great articles again soon.
RussellTex · May 17, 2026 at 6:56 am
Закажите дизайн интерьера СПб — выезд на замер бесплатно.
Белые стены и акцентная мебель — легко вписать яркие детали.
Дизайн сразу после замера БТИ — добавим много встроенного хранения.
Источник:
https://artviza-remont-msk.ru
TrustGuru análise Fortune Tiger · May 17, 2026 at 8:35 am
Butterfly Blossom max-win clips are misleading — the average session is way calmer.
Williambrora · May 17, 2026 at 9:30 am
Llave en mano – Construcción industrializada, Segunda residencia
Williambax · May 17, 2026 at 9:41 am
После диагностики начинается активная фаза медикаментозного вмешательства. Препараты вводятся капельничным методом, что способствует быстрому снижению уровня токсинов в крови, нормализации обменных процессов и стабилизации работы таких органов, как печень, почки и сердце.
Выяснить больше – https://vyvod-iz-zapoya-murmansk00.ru
daxunrar · May 17, 2026 at 9:42 am
Компания «Хронос» производит и реализует сертифицированную медицинскую технику собственного производства: голосообразующие аппараты, бактерицидные рециркуляторы, облучатели для лечения кожных заболеваний, трахеостомические трубки и ультрафиолетовые лампы. Ищете медицинская техника оптом? На сайте agsvv.ru доступны оптовые и розничные поставки напрямую с завода ЛЭМЗ в Санкт-Петербурге с официальной гарантией качества и доставкой по всей России. с официальной гарантией качества и доставкой по всей России.
Ernestastes · May 17, 2026 at 9:51 am
Хочешь сайтв ТОПе? https://kormclub.ru оптимизация структуры, работа с контентом, внешние ссылки и аналитика. Помогаем вывести сайт в топ поисковых систем и привлечь целевую аудиторию.
GeraldPhard · May 17, 2026 at 10:43 am
Анонимность в клинике «Северный Вектор» является неотъемлемой частью лечебного процесса. Наркологическая клиника в Ростове-на-Дону обеспечивает конфиденциальность на всех этапах взаимодействия с пациентом, начиная с первичного обращения и заканчивая медицинским наблюдением. Клиническая практика показывает, что сохранение анонимности снижает уровень тревожности и повышает готовность пациента к полноценному лечению, что напрямую влияет на стабильность результатов.
Подробнее можно узнать тут – https://narkologicheskaya-klinika-v-rostove19.ru/
GeraldPhard · May 17, 2026 at 11:11 am
В практике круглосуточного лечения применяются следующие этапы:
Разобраться лучше – вывод наркологическая клиника в ростове-на-дону
furhsiz · May 17, 2026 at 11:38 am
Петербургская компания ForOne.Manakara занимается поставкой и установкой инновационных стеновых панелей из коэкструзионного бамбука и гибкого камня для отделки современных пространств. В основе технологии — измельчённый бамбук, прошедший карбонизацию и коэкструзию с ПВХ, с последующей спайкой при 120°C. Ищете бамбуковая панель? На сайте forone.manakara.ru представлен полный каталог продукции с услугами выезда специалиста и профессионального монтажа. Материал экологически безопасен, подходит для криволинейных поверхностей и не требует особой подготовки стен — идеальное решение для жилых, детских и медицинских помещений.
Robertwiz · May 17, 2026 at 1:03 pm
В клинике «Пульс» процесс оказания помощи начинается сразу после вашего обращения. Наша бригада оперативно выезжает на дом, где врач проводит первичный осмотр пациента: измеряет давление, пульс, оценивает степень интоксикации и собирает анамнез. На основе полученных данных подбирается индивидуальный состав капельницы.
Изучить вопрос глубже – капельница от запоя на дому краснодар
Davidvap · May 17, 2026 at 1:06 pm
Ты финансовый директор? https://financedirector.by готовые шаблоны, аналитические статьи и практические кейсы для финансовых директоров. Материалы по управлению финансами, финансовому планированию, бюджетированию и анализу эффективности бизнеса. Полезные инструменты и решения для специалистов финансовой сферы.
Williambrora · May 17, 2026 at 1:19 pm
Segunda residencia – Carcasa de madera, Carcasa de madera
Williambrora · May 17, 2026 at 1:46 pm
Segunda residencia – Alta calidad, Llave en mano
maxosennum · May 17, 2026 at 2:37 pm
Автомобильные аксессуары и детали — рынок, где важно не ошибиться с выбором поставщика. APVshop — специализированный интернет-магазин, ориентированный на владельцев минивэнов и коммерческих автомобилей. На сайте https://apvshop.ru/ представлен тщательно подобранный ассортимент товаров: накладки, молдинги, защитные элементы и многое другое. Магазин работает с проверенными производителями и гарантирует соответствие деталей заявленным характеристикам, что особенно важно при покупке без возможности примерки вживую.
Williambax · May 17, 2026 at 2:38 pm
Лечение вывода из запоя на дому в Мурманске организовано по четко структурированной схеме, включающей следующие этапы, каждый из которых играет ключевую роль в оперативном восстановлении здоровья:
Детальнее – срочный вывод из запоя мурманск
Williamproot · May 17, 2026 at 4:00 pm
Эта публикация исследует взаимосвязь зависимости и психологии. Мы обсудим, как психологические аспекты влияют на появление зависимостей и процесс выздоровления. Читатели смогут понять важность профессиональной поддержки и применения научных подходов в терапии.
Заходи — там интересно – частный медик 24
kasyno online opinie · May 17, 2026 at 4:01 pm
Hi, do have a e-newsletter? In the event you don’t definately should get on that piece…this web site is pure gold!
noholBaisE · May 17, 2026 at 4:07 pm
Свобода в интернете — это не роскошь, а необходимость, и сервис Vless.art делает её доступной каждому. Здесь можно приобрести ключ на VLESS VPN с протоколом XTLS-Reality — одним из самых современных и надёжных решений для защиты трафика. Сервис не ведёт логов, поддерживает неограниченное количество устройств и обеспечивает высокую скорость соединения. Зайдите на https://vless.art/ и уже через минуту после оплаты вы получите полный доступ к анонимному интернету без каких-либо ограничений. Простой интерфейс позволяет подключиться даже без технических знаний — быстро, удобно и по-настоящему выгодно.
wiwemphefe · May 17, 2026 at 4:43 pm
Ресурс «Аргумент» последовательно действует в рамках принципа — заради розвитку та процвітання України — и охватывает политику, криминал, общество, бизнес и культуру без редакционных компромиссов. Журналисты фиксируют резонансные события оперативно и с конкретикой — от схем силовых структур до судебных историй длиной в десятилетие. Следите за актуальной повесткой на https://arhument.com/ — украинский новостной ресурс для читателя требующего точных фактов и честных оценок. Тематика спорта, технологий и культуры дополняет жёсткое новостное ядро и превращает портал в многопрофильный медиаресурс для разноплановой аудитории.
Jessienen · May 17, 2026 at 5:25 pm
В этих случаях вызов нарколога на дом не только оправдан, но и жизненно необходим для предотвращения опасных осложнений и стабилизации здоровья пациента.
Ознакомиться с деталями – нарколог на дом вывод воронеж
vera john app · May 17, 2026 at 5:28 pm
vera john app
Williambrora · May 17, 2026 at 6:16 pm
Bajo consumo energético – Wood frame, Casa eficiente
Robertwiz · May 17, 2026 at 6:21 pm
В клинике «Пульс» процесс оказания помощи начинается сразу после вашего обращения. Наша бригада оперативно выезжает на дом, где врач проводит первичный осмотр пациента: измеряет давление, пульс, оценивает степень интоксикации и собирает анамнез. На основе полученных данных подбирается индивидуальный состав капельницы.
Подробнее – капельница от запоя на дому краснодар
best online casino · May 17, 2026 at 7:49 pm
Wish I’d thought of this. Am in the field, but I procrastinate alot and haven’t written as much as I’d like. Thanks.
RichardWab · May 17, 2026 at 8:36 pm
Привет всем!
Элегантная подача имитирует чешую мифического существа с помощью тонких ломтиков. Угорь и авокадо создают контраст текстур который запоминается надолго. Каждый кусочек аккуратно выкладывается веером для эффектного внешнего вида. Соус унаги равномерно распределяется по поверхности перед упаковкой в коробку. Оцените изысканный дракон ролл и почувствуйте себя настоящим ценителем восточных традиций.
Современная платформа работает стабильно даже в часы максимальной нагрузки. Алгоритмы быстро обрабатывают данные и формируют оптимальный маршрут для курьера. Вы можете сохранить любимые комбинации в персональном профиле для доступа. Система позволяет безопасно заказать суши онлайн без долгих ожиданий на линии. Получите подтверждение мгновенно и ожидайте свежий обед у своей двери.
Больше информации по ссылке – https://neosushi.by/neosushi/s/sety_207
мобильное приложение суши, детокс сет роллов, эдамаме бобы в сетах
влажные салфетки в доставке, суши на компанию, выгодные предложения суши
Удачи!
najlepsze kasyno online · May 17, 2026 at 9:01 pm
Lovely just what I was looking for. Thanks to the author for taking his clock time on this one.
tegesryepils · May 17, 2026 at 9:10 pm
Гастрономический круиз по Москве-реке — это не просто ужин с видом, это целое событие, которое запоминается надолго. Сервис https://riverwalktickets.ru/ за 10 лет работы на рынке речного флота собрал более 100 маршрутов на любой вкус и формат: романтический вечер на двоих, семейный обед или корпоративная прогулка. Команда лично отбирает теплоходы, проверяет качество кухни и сервиса — именно поэтому более полумиллиона гостей уже выбрали этот сервис. Отправляйтесь в плавание от Воробьёвых гор, Парка Горького или Зарядья и откройте Москву с новой, водной стороны!
RandyNon · May 17, 2026 at 9:13 pm
Фото для публикации — без лишних данных
Перед отправкой или публикацией очистите изображение от скрытых данных. PhotoVoid работает без аккаунта, трекеров и загрузки файлов.
удалить exif перед публикацией
najlepsze kasyna online · May 17, 2026 at 9:14 pm
Nice piece of info! May I reference part of this on my blog if I post a backlink to this webpage? Thx.
Maynardrof · May 17, 2026 at 9:25 pm
В этой статье мы рассматриваем разные способы борьбы с алкогольной зависимостью. Обсуждаются методы лечения, программы реабилитации и советы для поддержки близких. Читатели получат информацию о том, как преодолеть зависимость и добиться успешного выздоровления.
Нажми и узнай всё – narcology clinic
kasyno online · May 17, 2026 at 10:10 pm
I do believe your audience could very well want a good deal more stories like this carry on the excellent hard work.
Maynardrof · May 17, 2026 at 10:12 pm
В этой статье рассматриваются способы преодоления зависимости и успешные истории людей, которые справились с этой проблемой. Мы обсудим важность поддержки со стороны близких и профессионалов, а также стратегии, которые могут помочь в процессе выздоровления. Научитесь первоочередным шагам к новой жизни.
Кликни, не пожалеешь – нарколог на дом ростов
Stevenvew · May 17, 2026 at 10:16 pm
Если основной сайт недоступен — прямая ссылка на зеркало мелбет.
Зеркало казино Мелбет — работает без VPN.
Официальный сайт melbet казино — еженедельный кешбэк до 10%.
Мелбет зеркало прямо сейчас работает — доступно даже при строгих блокировках.
Source:
melbet casino
Timothykaw · May 17, 2026 at 10:24 pm
Обзор посвящён процессу восстановления после зависимостей. Мы расскажем о различных этапах реабилитации, поддерживающих ресурсах и важности мотивации в достижении устойчивого выздоровления.
Продолжить изучение – narcology clinic ростов на дону
Timothykaw · May 17, 2026 at 11:17 pm
В статье рассматриваются различные стратегии борьбы с зависимостями, включая проверенные методы и реальные истории успеха. Читатель узнает, какие подходы наиболее эффективны и как начать путь к выздоровлению.
Хочу знать больше – нарколог на дом ростов на дону
online casino · May 17, 2026 at 11:30 pm
I dont think I’ve read anything like this before. So good to find somebody with some original thoughts on this subject. cheers for starting this up. This blog is something that is needed on the web, someone with a little originality.
RafaelLox · May 18, 2026 at 12:03 am
PhotoVoid — обработка фото без загрузки
Сжимайте, конвертируйте и очищайте изображения прямо в браузере. Файлы не уходят на сервер и остаются на вашем устройстве.
удалить геолокацию с фото
Jeffreydaw · May 18, 2026 at 12:09 am
PhotoVoid — фото остаются у вас
Обрабатывайте изображения прямо в браузере. Без загрузки на сервер, без регистрации, без телеметрии.
фото остаются на устройстве
kasyno online · May 18, 2026 at 12:46 am
you may have an ideal blog here! would you prefer to make some invite posts on my blog?
KevinGuent · May 18, 2026 at 12:52 am
Услуга “капельница от запоя” на дому имеет ряд преимуществ, делающих её оптимальным выбором для экстренной помощи:
Получить дополнительную информацию – http://kapelnica-ot-zapoya-tyumen0.ru
best online casino · May 18, 2026 at 12:58 am
Thanks so much for this, keep up the good work 🙂
TimothyFreby · May 18, 2026 at 1:07 am
Для стабильного входа — прямая ссылка на зеркало мелбет.
Как зайти в казино Мелбет при блоке — полная копия с бонусами.
Старое зекало melbet не работает — сохраните книгу закладок.
Официальный сайт мелбет и его зеркало — один аккаунт для двух входов.
Источник:
https://melbet-dfr.top
online casino · May 18, 2026 at 1:18 am
I dont think I’ve read anything like this before. So good to find somebody with some original thoughts on this subject. cheers for starting this up. This blog is something that is needed on the web, someone with a little originality.
best online casino new zealand · May 18, 2026 at 1:22 am
The post is absolutely great! Lots of great info and inspiration, both of which we all need! Also like to admire the time and effort you put into your blog and detailed information you offer! I will bookmark your website!
Georgehiets · May 18, 2026 at 1:35 am
В этой статье мы подробно рассматриваем проверенные методы борьбы с зависимостями, включая психотерапию, медикаментозное лечение и поддержку со стороны общества. Мы акцентируем внимание на важности комплексного подхода и возможности успешного восстановления для людей, столкнувшихся с этой проблемой.
Читать далее > – нарколог на дом ростов на дону
MichaelHulty · May 18, 2026 at 1:43 am
После поступления звонка специалисты нашей клиники оперативно выезжают по адресу пациента в Новосибирске. Врач начинает работу с детальной диагностики: измеряет пульс, артериальное давление, сатурацию (уровень кислорода в крови), оценивает состояние нервной и сердечно-сосудистой систем, уточняет наличие хронических заболеваний, аллергических реакций, длительность и тяжесть запоя.
Детальнее – http://vyvod-iz-zapoya-novosibirsk0.ru
midas casino · May 18, 2026 at 2:14 am
bonus code casino midas
สล็อต · May 18, 2026 at 2:17 am
ทดลองเล่นสล็อต pg
ระบบสล็อตออนไลน์รุ่นใหม่กำลังพัฒนาจากระบบเกมหมุนวงล้อคลาสสิกไปสู่โครงสร้างเกมออนไลน์ที่ใช้เซิร์ฟเวอร์ความเร็วสูง และใช้ระบบ APIร่วมกับโครงสร้างเซิร์ฟเวอร์ที่รองรับผู้เล่นจำนวนมาก ผู้เล่นจำนวนมากเริ่มเลือกใช้แพลตฟอร์มสล็อตเว็บตรง เพราะระบบมีความเสถียรมากกว่า และช่วยลดปัญหาเกมโหลดนาน ความผิดพลาดระหว่างการหมุน รวมถึงการเชื่อมต่อการเงินที่ไม่เสถียร
ระบบสล็อตเว็บตรงจะรับส่งข้อมูลกับผู้ให้บริการเกมผ่านโหนด API ที่ไม่ผ่านตัวกลาง ทำให้สถานะเกมและยอดเงินถูกส่งแบบทันทีโดยไม่ต้องผ่านตัวกลางหลายชั้น ส่งผลให้เกมโหลดเร็วขึ้น ลดปัญหาข้อมูลรอบเล่นคลาดเคลื่อน และช่วยให้การคำนวณรางวัลทำงานได้เสถียรมากขึ้น
อีกจุดสำคัญคือระบบธุรกรรมอัตโนมัติ ผู้เล่นสามารถจัดการยอดเงินได้ตลอดทั้งวัน โดยไม่จำเป็นต้องรอการอนุมัติด้วยมือเหมือนเว็บตัวกลางแบบเดิม ทำให้การจัดการเงินทุนมีความคล่องตัวกว่าเดิม
ปัจจัยที่ทำให้ผู้เล่นให้ความสำคัญกับเว็บตรงคือความน่าเชื่อถือและความต่อเนื่องของเซิร์ฟเวอร์ เซิร์ฟเวอร์ที่เชื่อมต่อกับค่ายเกมโดยตรงช่วยลดปัญหาการแทรกแซงผลลัพธ์ ผู้เล่นจึงเชื่อถือได้ว่าผลลัพธ์ของเกมมาจากระบบ RNG จริง
อีกด้านหนึ่ง เว็บสมัยใหม่ยังมีการพัฒนาระบบแสดงผลบนสมาร์ตโฟนโดยเฉพาะ เช่น หน้าจอที่ออกแบบให้ใช้มือเดียวได้สะดวก ระบบโหลดเกมแบบรวดเร็ว และระบบ Auto Resumeที่ช่วยกลับเข้าสู่เกมเดิมเมื่อสัญญาณขาดช่วง
ระบบสล็อตออนไลน์รุ่นใหม่เริ่มใช้ปัญญาประดิษฐ์ประมวลผลพฤติกรรมผู้เล่น ร่วมกับระบบประมวลผลบนคลาวด์และAPI Syncเพื่อรองรับผู้ใช้งานจำนวนมากพร้อมกัน บางระบบยังรองรับระบบธุรกรรมคริปโตเพื่อเพิ่มทางเลือกในการทำธุรกรรมและลดการพึ่งพาช่องทางการเงินแบบเก่า
แพลตฟอร์มเกมออนไลน์ประเภทสล็อตจึงกำลังพัฒนาจากแพลตฟอร์มที่เน้นแค่เกมและโปรโมชั่นไปสู่โครงสร้างเกมออนไลน์ที่เน้น API และเซิร์ฟเวอร์ โดยโครงสร้าง APIและความปลอดภัยของข้อมูลกลายเป็นปัจจัยสำคัญในการเปรียบเทียบระบบของแต่ละเว็บ
เมื่อการแข่งขันสูงขึ้นแพลตฟอร์มสล็อตจะยิ่งแข่งขันกันด้านคุณภาพ APIมากขึ้น ไม่ว่าจะเป็นการกู้คืนสถานะเมื่อระบบหลุด ระบบ AI วิเคราะห์พฤติกรรมผู้เล่น หรือการรักษาความปลอดภัยของบัญชี ผู้ให้บริการที่มีเซิร์ฟเวอร์เสถียรและเชื่อมต่อกับค่ายเกมโดยตรงจะได้เปรียบมากกว่าเว็บทั่วไปที่ยังใช้เซิร์ฟเวอร์ที่เพิ่มความหน่วง
ผู้เล่นยุคใหม่จึงไม่ได้มองแค่โบนัสอีกต่อไป แต่เริ่มให้ความสำคัญกับมาตรฐานทางเทคนิคของแพลตฟอร์ม ความต่อเนื่องของระบบการเงิน และความลื่นของเกมระหว่างใช้งาน
Josephcroro · May 18, 2026 at 2:22 am
Ayr?ca, eger f?r?n ne ise yarar konusuyla ilgileniyorsan?z, buray? inceleyin. Suradan okuyabilirsiniz: https://yappendik.com/articles/firin-ne-ise-yarar-farkli-kullanim-alanlari/
Josephcroro · May 18, 2026 at 2:29 am
Bu arada soyleyeyim, eger 5 metrekare hal? kaca kac konusuyla ilgileniyorsan?z, suraya bak?n. Kendiniz gorun: https://yapevleri.com/articles/5-metrekare-hali-hesaplama-ve-uygulama/
Williamproot · May 18, 2026 at 2:45 am
Этот текст посвящён сложным аспектам зависимости и её влиянию на жизнь человека. Мы обсудим психологические, физические и социальные последствия зависимого поведения, а также важность своевременного обращения за помощью.
Почему это важно? – нарколог на дом ростов
RandyNon · May 18, 2026 at 3:51 am
Фото для публикации — без лишних данных
Перед отправкой или публикацией очистите изображение от скрытых данных. PhotoVoid работает без аккаунта, трекеров и загрузки файлов.подготовить фото к публикации
VernonHep · May 18, 2026 at 4:18 am
подробнее трипскан официальный
VernonHep · May 18, 2026 at 4:46 am
содержание трипскан ссылка
RafaelLox · May 18, 2026 at 5:22 am
PhotoVoid — обработка фото без загрузки
Сжимайте, конвертируйте и очищайте изображения прямо в браузере. Файлы не уходят на сервер и остаются на вашем устройстве.
очистить метаданные фото
Williambax · May 18, 2026 at 5:52 am
Обращение за помощью нарколога на дому в Мурманске имеет ряд существенных преимуществ:
Детальнее – https://vyvod-iz-zapoya-murmansk00.ru/vyvod-iz-zapoya-czena-murmansk
RichardWab · May 18, 2026 at 5:57 am
Доброго!
Простой интерфейс сайта позволяет собрать идеальный обед за пару кликов. Система автоматически предлагает сопутствующие соусы и напитки на ваш выбор. Оплата проходит через защищенные шлюзы без лишних комиссий и скрытых платежей. Менеджеры мгновенно подтверждают получение заявки и передают её на кухню. Приходите на наш портал чтобы заказать роллы с максимальным удобством.
Пошаговый план и профессиональная поддержка помогут запустить сервис в вашем городе. Открыть доставку роллов возможно с минимальными вложениями благодаря нашей франшизе. Каждая стадия запуска сопровождается персональным менеджером и экспертами отрасли. Партнеры получают доступ к базе знаний и регулярным обучающим мероприятиям. Реализуйте предпринимательский потенциал с проверенной моделью и поддержкой профессионалов.
Больше информации по ссылке – https://neosushi.by/neosushi/s/sety_207
отслеживание заказа онлайн, авторский соус для роллов, авокадо спелое для роллов
смс уведомление о доставке, сытный сет роллов, выгодный набор роллов
Удачи!
VernonHep · May 18, 2026 at 7:03 am
узнать трипскан вход
lipufTat · May 18, 2026 at 7:05 am
Москва-река открывает город совершенно с иного ракурса — величественного, тихого и невероятно красивого. Компания Moscow Cruise за более чем пять лет работы организовала речные прогулки для свыше 10 000 довольных пассажиров, и каждый рейс подтверждает репутацию надёжного сервиса. Заходите на https://moscowcruise.ru/ и выбирайте подходящий маршрут: удобное бронирование, круглосуточная поддержка и индивидуальный подход гарантированы. Профессиональная команда сопровождает клиента на каждом этапе — от выбора прогулки до момента, когда теплоход мягко отчаливает от причала навстречу огням столицы.
bojetarrat · May 18, 2026 at 7:19 am
I finally found a place to explore each custom and modified BMW E30 build – from engine swapped builds to stance, track, and drift builds. Every build comes with a curated gallery, tech specs, and modification details. Honestly it’s addictive to scroll. Go check it out:https://isleofcars.com/bmw/e30
VernonHep · May 18, 2026 at 8:41 am
взгляните на сайте здесь трипскан сайт вход
Michaelthind · May 18, 2026 at 9:42 am
Эта публикация раскрывает психологические механизмы зависимости и их роль в развитии расстройств. Читатель узнает о том, как психология влияет на формирование зависимостей и как профессиональная помощь может изменить ситуацию.
Прочитать подробнее – Похмельная служба в Геленджике
Jeffreydaw · May 18, 2026 at 9:48 am
PhotoVoid — фото остаются у вас
Обрабатывайте изображения прямо в браузере. Без загрузки на сервер, без регистрации, без телеметрии.
photovoid image tools
RafaelLox · May 18, 2026 at 9:53 am
PhotoVoid — обработка фото без загрузки
Сжимайте, конвертируйте и очищайте изображения прямо в браузере. Файлы не уходят на сервер и остаются на вашем устройстве.
безопасный редактор фото
такси москва · May 18, 2026 at 9:55 am
Добрый день. Хотите найти работу с ежедневными выплатами? Оформляйтесь к платформе Яндекс.Про через агента GetDriver. Оформление требует несколько минут и не требует визита в офис.
Ваши выгоды:
Наша комиссия составляет от 1.5 процента. Это выгодная ставка на рынке. Получение денег работают оперативные на любую карту. Сервис доступна в любое время. Вас сопровождает оператор и умный помощник в мессенджере. Акция для новых включает работу без комиссии в начальный период. Реферальная программа позволяет получать 0,5% с поездок приведённых водителей на бессрочно.
Нужно всего:
Вам должно быть: 21 года и старше.
Водительский опыт от: 3 лет для основных тарифов. для курьерских заказов опыт не обязателен.
Понадобятся:: гражданский паспорт, права, свидетельство о регистрации, полис обязательного страхования.
Правовой статус:: индивидуальный предприниматель. Консультируем по оформлению.
Варианты авто:
Бизнес. Подберём оптимальный вариант под вашу машину.
Распространённые вопросы:
Есть ли плата за вход? – Регистрация бесплатна. Комиссия взимается лишь с фактических поездок.
Есть ли задержки с выводами? – Деньги от пассажира у вас. Безнал выводятся функцией в системе за мгновенно.
Подключён к другому сервису. Возможен переход? – Да без потери рейтинга. В подарок – нулевая комиссия на старт.
Порядок регистрации:
1. Заполните форму на официальном сайте дополнительно в Telegram.
2. Менеджер свяжется. Проверка документов занимает быстро.
3. Активируйте аккаунт. Начало заработка открывается мгновенно.
Займите место сейчас – позвоните нам на get-driver.ru/.
Работайте с комиссией от 1,5% – подключайтесь через get-driver.ru.
Ищете подработку на авто? – тогда вам к нам нашем портале.
Тысячи водителей уже зарабатывают с нами – регистрируйтесь через официальный сайт.
Контакты и сайт:
Телефон: +7 (931) 009-10-29
Telegram: @getdriver_support
Узнай больше про нас и наши отзывы Get Driver на сайтах:
https://www.domainanalysis.org/page-669651063f8c3b5d507c3ad31e0ec021.html
http://forum.amtelectronics.com/index.php?action=profile;u=1618
http://www.inetkniga.ru/catalog/106/1027/2_1.html
Подробнее про https://www.inetkniga.ru/catalog/106/1027/1_1.html
Web: http://www.rrsclub.ru/printthread.php?t=33955
Дополнительно:
Эти условия для соискателей на территории России. Полная информация доступны на портале GetDriver.ru. Для водителей в Челябинске – Get-Driver готов открыть доступ к заказам.
Daniellab · May 18, 2026 at 9:56 am
Для наглядности представлена таблица с основными этапами лечения и их характеристиками:
Подробнее – частная наркологическая клиника ростов-на-дону
MatthewHoipt · May 18, 2026 at 10:47 am
Инструменты для изображений без лишнего
Сжатие, конвертация и очистка изображений в браузере. Быстро, бесплатно, без регистрации и без внешних трекеров.
конвертер webp
Marvinblisp · May 18, 2026 at 10:49 am
Эта медицинская заметка содержит сжатую информацию о новых находках и методах в области здравоохранения. Мы предлагаем читателям свежие данные о заболеваниях, профилактике и лечении. Наша цель — быстро и доступно донести важную информацию, которая поможет в повседневной жизни и понимании здоровья.
Интересует подробная информация – narcology clinic ростов на дону
RandyNon · May 18, 2026 at 11:25 am
Фото для публикации — без лишних данных
Перед отправкой или публикацией очистите изображение от скрытых данных. PhotoVoid работает без аккаунта, трекеров и загрузки файлов.
удалить геометки с фото
MatthewHoipt · May 18, 2026 at 11:33 am
Инструменты для изображений без лишнего
Сжатие, конвертация и очистка изображений в браузере. Быстро, бесплатно, без регистрации и без внешних трекеров.
image compressor
RafaelLox · May 18, 2026 at 11:37 am
PhotoVoid — обработка фото без загрузки
Сжимайте, конвертируйте и очищайте изображения прямо в браузере. Файлы не уходят на сервер и остаются на вашем устройстве.
обработка изображений в браузере
RandyNon · May 18, 2026 at 11:39 am
Фото для публикации — без лишних данных
Перед отправкой или публикацией очистите изображение от скрытых данных. PhotoVoid работает без аккаунта, трекеров и загрузки файлов.
фото без геолокации
RandyNon · May 18, 2026 at 11:45 am
Фото для публикации — без лишних данных
Перед отправкой или публикацией очистите изображение от скрытых данных. PhotoVoid работает без аккаунта, трекеров и загрузки файлов.
защита приватности фото
Marvinblisp · May 18, 2026 at 11:48 am
В этом обзоре представлены различные методы избавления от зависимости, включая терапевтические и психологические подходы. Мы сравниваем их эффективность и предоставляем рекомендации для тех, кто хочет вернуться к трезвой жизни. Читатели смогут найти информацию о реабилитационных центрах и поддерживающих группах.
Уникальные данные только сегодня – частный медик 24 рнд
ThanhAnype · May 18, 2026 at 11:49 am
Этот краткий обзор предлагает сжатую информацию из области медицины, включая ключевые факты и последние новости. Мы стремимся сделать информацию доступной и понятной для широкой аудитории, что позволит читателям оставаться в курсе актуальных событий в здравоохранении.
Более того — здесь – «Похмельная служба» в Москве
EdwardDOK · May 18, 2026 at 11:52 am
UFCWAR is a website https://ufcwar.com for fans of the Ultimate Fighting Championship and MMA. Latest news, fight results, tournament schedules, analysis, and fight reviews. Up-to-date information on fighters, events, and major fights.
DanielSoodo · May 18, 2026 at 11:56 am
Этот документ охватывает важные аспекты медицинской науки, сосредотачиваясь на ключевых вопросах, касающихся здоровья населения. Мы рассматриваем свежие исследования, клинические рекомендации и лучшие практики, которые помогут улучшить качество лечения и профилактики заболеваний. Читатели получат возможность углубиться в различные медицинские дисциплины.
Ссылка на источник – стоп алко
pg9x9 · May 18, 2026 at 12:24 pm
Tava evitando Dragão depois do patch, voltei essa semana, mesmo clima de antes.
RafaelLox · May 18, 2026 at 12:47 pm
PhotoVoid — обработка фото без загрузки
Сжимайте, конвертируйте и очищайте изображения прямо в браузере. Файлы не уходят на сервер и остаются на вашем устройстве.
очистка exif
Donaldmah · May 18, 2026 at 1:16 pm
Врач проводит полное обследование и определяет тактику лечения в зависимости от состояния пациента. Важным аспектом является возможность применения комплексных мер, включающих:
Подробнее тут – https://narcolog-na-dom-kaliningrad00.ru/narkolog-na-dom-kaliningrad-czeny
Joshuacit · May 18, 2026 at 1:28 pm
В этой статье мы рассматриваем разрушительное влияние зависимости на жизнь человека. Обсуждаются аспекты, такие как здоровье, отношения и профессиональные достижения. Читатели узнают о необходимости обращения за помощью и о путях к восстановлению.
Прочитать подробнее – стоп алко
Stephanglymn · May 18, 2026 at 1:35 pm
В этой статье мы рассмотрим современные достижения в области медицины, включая инновационные методы лечения и диагностики. Мы обсудим важность профилактики заболеваний и роль технологий в улучшении качества здравоохранения. Читатели узнают о влиянии медицины на повседневную жизнь и ее значение для современного общества.
Перейти к полной версии – стоп алко
HaroldgEf · May 18, 2026 at 1:38 pm
Эта статья подробно расскажет о процессе выздоровления, который включает в себя эмоциональную, физическую и психологическую реабилитацию. Мы обсуждаем значимость поддержки и наличие профессиональных программ. Читатели узнают, как строить новую жизнь и не возвращаться к старым привычкам.
Проследить причинно-следственные связи – Наркологическая клиника «Похмельная служба» в Москве
Jeffreydaw · May 18, 2026 at 1:47 pm
PhotoVoid — фото остаются у вас
Обрабатывайте изображения прямо в браузере. Без загрузки на сервер, без регистрации, без телеметрии.
open source image tools
Albertlam · May 18, 2026 at 1:54 pm
Читатели получат представление о том, как современные технологии влияют на развитие медицины. Обсуждаются новые методы лечения, персонализированный подход и роль цифровых решений в повышении качества медицинских услуг.
Неизвестные факты о… – Наркологическая клиника «Похмельная служба» в Москве
HaroldgEf · May 18, 2026 at 2:11 pm
В данной статье рассматриваются физиологические и эмоциональные аспекты зависимости. Мы обсудим, как организм реагирует на зависимое поведение, и какие методы помогают восстановить здоровье и внутреннее равновесие.
См. подробности – Похмельная служба в Москве
FrankCaP · May 18, 2026 at 2:54 pm
на этом сайте https://soulestate.ru/catalog/kp/agalarov-estate67155/
zukipidten · May 18, 2026 at 3:02 pm
Professional legal representation in court for public procurement disputes in Almaty. Femida Justice https://femida-justice.com/uslugi/yurist-po-tenderam-almaty/sudebnyie-sporyi-po-zakupkam-v-almatyi/ offers expert defense against Unreliable Supplier list inclusion, tender result appeals, and contract litigation. Our lawyers provide comprehensive judicial protection for businesses across Kazakhstan, ensuring compliance and safeguarding your commercial interests in all court instances.
RafaelLox · May 18, 2026 at 3:06 pm
PhotoVoid — обработка фото без загрузки
Сжимайте, конвертируйте и очищайте изображения прямо в браузере. Файлы не уходят на сервер и остаются на вашем устройстве.
онлайн инструменты для фото
RodneyCinny · May 18, 2026 at 3:08 pm
UFCShare is a portal https://www.ufcshare.com for fans of the Ultimate Fighting Championship and the world of MMA. News, fight results, tournament schedules, analysis, and fight reviews. Follow the best fighters and the main events of mixed martial arts.
RandyNon · May 18, 2026 at 3:29 pm
Фото для публикации — без лишних данных
Перед отправкой или публикацией очистите изображение от скрытых данных. PhotoVoid работает без аккаунта, трекеров и загрузки файлов.
безопасная публикация фото
RandyNon · May 18, 2026 at 3:38 pm
Фото для публикации — без лишних данных
Перед отправкой или публикацией очистите изображение от скрытых данных. PhotoVoid работает без аккаунта, трекеров и загрузки файлов.
удалить информацию с картинки
RichardWab · May 18, 2026 at 3:44 pm
Доброго!
Традиционные сопровождения усиливают вкус и создают гармоничный гастрономический опыт. С чем едят суши подскажет наше руководство по сочетанию ингредиентов и напитков. Каждая рекомендация основана на многовековой практике и современных гастрономических трендах. Сопровождение включает соусы закуски напитки и десерты в японском стиле. Откройте для себя идеальные комбинации и превратите обычный ужин в изысканную трапезу.
Забота о гигиене и комфорте включает все необходимые аксессуары для трапезы. Влажные салфетки в доставке пропитаны антибактериальным составом с приятным нейтральным ароматом. Каждая упаковка индивидуально запечатана для сохранения стерильности до момента использования. Система автоматически включает салфетки в каждый заказ или позволяет выбрать количество при оформлении. Наслаждайтесь чистотой и комфортом во время приема пищи в любой обстановке.
Больше информации по ссылке – https://f1sh1ng.ru/rybalka/pochemu-sidr-idealnyj-naparnik-dlya-tempura-rollov.html
фуршет с японской кухней, дракон ролл, контроль качества роллов
водоросли нори витамины, роллы, безопасные суши для детей
Удачи!
Larrycrync · May 18, 2026 at 3:46 pm
Медицинская публикация представляет собой свод актуальных исследований, экспертных мнений и новейших достижений в сфере здравоохранения. Здесь вы найдете информацию о новых методах лечения, прорывных технологиях и их практическом применении. Мы стремимся сделать актуальные медицинские исследования доступными и понятными для широкой аудитории.
Тыкай сюда — узнаешь много интересного – нарколог на дом в ростове
Daniellab · May 18, 2026 at 3:46 pm
Для жителей Ростова-на-Дону клиника «Южный МедКонтроль» предлагает два формата помощи: лечение в стационаре и амбулаторные визиты врача на дом. Стационар оборудован всем необходимым для круглосуточного медицинского наблюдения, проведения инфузионных процедур и лабораторной диагностики. Пациентам предоставляется комфортное размещение, спокойная обстановка и постоянный контроль состояния. При выезде на дом врачи действуют оперативно — приезжают в течение часа, проводят осмотр, устанавливают капельницы, купируют абстиненцию и дают рекомендации по дальнейшему лечению.
Углубиться в тему – наркологическая клиника наркологический центр
kaditlesSix · May 18, 2026 at 3:58 pm
Если вы давно мечтаете превратить свой участок в настоящий ботанический шедевр, питомник растений «Сакура» предлагает всё необходимое для воплощения самых смелых садовых идей. Здесь собраны сотни видов растений: от классических спирей и гортензий до редких рододендронов, изящных бонсаев и топиарных форм. Посетите https://sakura-pitomnik.ru/ и откройте для себя богатый каталог хвойных, лиственных деревьев, роз и многолетников с удобной доставкой по Санкт-Петербургу и Ленинградской области. Ассортимент регулярно пополняется новинками сезона, а доступные цены делают профессиональное озеленение реальным для каждого.
vudcoZek · May 18, 2026 at 4:12 pm
Информационно-аналитический ежедневник «До слова» публикует острые материалы на темы политики, экономики, культуры и общества — без размытых формулировок и редакционных компромиссов. Редакция издания ведёт работу в форматах аналитического разбора, расследования и авторской публицистики — от актуальных бизнес-тем до глубоких исторических материалов. Читайте актуальные тексты на https://doslova.com/ — украинский ежедневник для тех кто привык получать информацию точно и без лишнего шума. Блоги экспертов, вопросы дня и репортажи о спорте дополняют насыщенную повестку издания и делают его обязательной точкой входа для читателя с запросом на качество.
Stevenvew · May 18, 2026 at 4:18 pm
Ставки на спорт — это легко с Мелбет для тысяч событий ежедневно.
Актуальное зеркало на сегодня — сохраняет баланс и историю ставок.
Актуальное melbet зекало на сегодня — зеркало с ошибкой в названии — просто скопируйте адрес.
Официальный сайт мелбет и его зеркало — полностью синхронизированы.
Source:
melbet официальный сайт
betano cassino · May 18, 2026 at 4:21 pm
Wild Bandito me deu green inesperado, kkkk não esperava.
gefuENULA · May 18, 2026 at 4:22 pm
Besök https://www.ferieisverige.no/ för allt du behöver veta om semestrar i Sverige, inklusive Smultronställen Sverige-ladan och allt om Fjällbacka och Pås til Sverige. Örebro är utan tvekan det bästa stället att koppla av på – ta reda på mer om det, och julemärkt Sverige kommer att lämna ingen oberörd!
Jamesbrony · May 18, 2026 at 4:49 pm
F1 Direct is a website https://www.f1-direct.net about the world of Formula 1. Latest news, race results, race calendar, team and driver statistics. Up-to-date information for fans of the royal motor racing world.
OscarBlido · May 18, 2026 at 5:11 pm
В этой публикации мы исследуем ключевые аспекты здоровья, включая влияние образа жизни на благополучие. Читатели узнают о важности правильного питания, физической активности и психического здоровья. Мы предоставим практические советы и рекомендации для поддержания здоровья и развития профилактических подходов.
Ознакомьтесь поближе – Наркологическая клиника «Похмельная служба» в Мытищах.
https://kv999.my/ · May 18, 2026 at 5:22 pm
it is a really nice point of view. I usually meet people who rather say what they suppose others want to hear. Good and well written! I will come back to your site for sure!
Aaronrhync · May 18, 2026 at 5:34 pm
Эта информационная публикация освещает широкий спектр тем из мира медицины. Мы предлагаем читателям ясные и понятные объяснения современных заболеваний, методов профилактики и лечения. Информация будет полезна как пациентам, так и медицинским работникам, желающим поддержать уровень своих знаний.
Подробнее тут – Похмельная служба в Калининграде
OscarBlido · May 18, 2026 at 6:06 pm
В данной статье рассматриваются физиологические и эмоциональные аспекты зависимости. Мы обсудим, как организм реагирует на зависимое поведение, и какие методы помогают восстановить здоровье и внутреннее равновесие.
Ознакомьтесь поближе – Похмельная служба в Мытищах
Aaronrhync · May 18, 2026 at 6:34 pm
В этом исследовании рассмотрены методы лечения зависимостей и их эффективность. Мы проанализируем различные подходы, используемые в реабилитационных центрах, и представим данные о результативности программ. Читатели получат надежные и научно обоснованные сведения о данной проблеме.
Кликни, не пожалеешь – Похмельная служба в Калининграде
FrankCaP · May 18, 2026 at 7:02 pm
в этом разделе https://soulestate.ru/catalog/kp/riita67055/
CoinEx Exchange · May 18, 2026 at 7:07 pm
Having read this I believed it was extremely enlightening. I appreciate you taking the time and energy to put this short article together. I once again find myself personally spending a lot of time both reading and commenting. But so what, it was still worthwhile.
Jamesanave · May 18, 2026 at 7:24 pm
Розповідаємо про складні https://notatky.net.ua речі простими словами. Зрозумілі пояснення науки, технологій, економіки та повсякденних явищ. Статті, розбори та факти, які допомагають краще розуміти світ та знаходити відповіді на складні питання.
HowardJep · May 18, 2026 at 7:28 pm
В этой статье обсуждаются актуальные медицинские вопросы, которые волнуют общество. Мы обращаем внимание на проблемы, касающиеся здравоохранения и лечения, а также на новшества в области медицины. Читатели будут осведомлены о последних событиях и смогут следить за тенденциями в медицине.
Изучить материалы по теме – Наркологическая клиника «Похмельная служба» в Екатеринбурге
Donaldmah · May 18, 2026 at 7:39 pm
Существует ряд ситуаций, при которых помощь нарколога на дому необходима в кратчайшие сроки.
Изучить вопрос глубже – нарколог на дом калининград
Michaelthind · May 18, 2026 at 7:59 pm
В этой статье мы рассмотрим современные достижения в области медицины, включая инновационные методы лечения и диагностики. Мы обсудим важность профилактики заболеваний и роль технологий в улучшении качества здравоохранения. Читатели узнают о влиянии медицины на повседневную жизнь и ее значение для современного общества.
Ознакомиться с отчётом – Похмельная служба Геленджик
939bet · May 18, 2026 at 8:07 pm
Compra de bônus no Jungle Delight só faz sentido se o RTP base passar 96.5%.
EugeneAnile · May 18, 2026 at 8:19 pm
Вызов нарколога возможен круглосуточно, что обеспечивает оперативное реагирование на критические ситуации. Пациенты и их родственники могут получить помощь в любое время, не дожидаясь ухудшения состояния.
Изучить вопрос глубже – http://narkolog-na-dom-kamensk-uralskij11.ru/
obetcug · May 18, 2026 at 8:25 pm
Для бизнеса аренда сервера — это прежде всего вопрос надёжности, высокой скорости и поддержки в любое время суток. Компания Netrack предлагает сервер в аренду с гарантированным аптаймом 99,9% и размещением в собственном дата-центре уровня Tier III. Требуется аренда сервера? На сайте https://netrack.ru/ можно выбрать конфигурацию под любые задачи — от стартапа до крупного корпоративного проекта. Клиент получает выделенные ресурсы без соседей по железу и профессиональное техническое сопровождение на всех этапах работы.
RussellTex · May 18, 2026 at 8:38 pm
Нужен дизайн-проект Санкт-Петербург? — 3D-облет каждой комнаты.
Лофт без фабричных цехов? Легко — зонирование без стен.
Полное сопровождение от идеи до ключей — даём чек-листы для заказчиков.
Источник:
Современный интерьер Питер
Waltergog · May 18, 2026 at 8:43 pm
Эта статья подробно расскажет о процессе выздоровления, который включает в себя эмоциональную, физическую и психологическую реабилитацию. Мы обсуждаем значимость поддержки и наличие профессиональных программ. Читатели узнают, как строить новую жизнь и не возвращаться к старым привычкам.
Ссылка на источник – «Похмельная служба» в Казани
Zacharyraw · May 18, 2026 at 8:46 pm
В этой публикации мы предложим ряд рекомендаций по избавлению от зависимостей и успешному восстановлению. Мы обсудим методы привлечения поддержки и важность самосознания. Эти советы помогут людям вернуться к нормальной жизни и стать на путь выздоровления.
Лучшее решение — прямо здесь – Наркологическая клиника «Похмельная служба» в Екатеринбурге.
global bet · May 18, 2026 at 8:51 pm
Butterfly Blossom tá pesado no celular ultimamente, sei lá por quê.
Michaelvok · May 18, 2026 at 8:57 pm
В этой статье мы рассматриваем разрушительное влияние зависимости на жизнь человека. Обсуждаются аспекты, такие как здоровье, отношения и профессиональные достижения. Читатели узнают о необходимости обращения за помощью и о путях к восстановлению.
Получить профессиональную консультацию – Похмельная служба в Екатеринбурге
voogcrils · May 18, 2026 at 9:58 pm
Новостной портал «Корреспондент» освещает события Украины и мира в режиме реального времени — политика, экономика, технологии, здоровье и общество без купюр и редакционных фильтров. Портал последовательно берётся за сложные темы: коррупционные расследования, репортажи о событиях и аналитические бизнес-обзоры публикуются без перерывов. Следите за актуальной повесткой на https://karrespondent.com/ — украинский новостной ресурс для читателей ценящих скорость и фактическую точность. Разделы культуры, технологий, конфликтов и общества создают разностороннее медиапространство и превращают ресурс в незаменимый инструмент для информированного читателя.
MichaelFam · May 18, 2026 at 10:07 pm
В этой публикации мы обсуждаем современные методы лечения различных заболеваний. Читатели узнают о новых медикаментах, терапиях и исследованиях, которые активно применяются для лечения. Мы нацелены на то, чтобы предоставить практические знания, которые могут помочь в борьбе с недугами.
Секреты успеха внутри – Наркологическая клиника «Похмельная служба» в Москве
GeorgeTek · May 18, 2026 at 10:08 pm
Эта информационная публикация освещает широкий спектр тем из мира медицины. Мы предлагаем читателям ясные и понятные объяснения современных заболеваний, методов профилактики и лечения. Информация будет полезна как пациентам, так и медицинским работникам, желающим поддержать уровень своих знаний.
Как достичь результата? – стоп алко
Michaelvok · May 18, 2026 at 10:12 pm
В этой публикации мы рассматриваем важную тему борьбы с зависимостями, включая алкогольную и наркотическую зависимости. Мы обсудим методы лечения, реабилитации и поддержку, которые могут помочь людям, столкнувшимся с этой проблемой. Читатели узнают о перспективах выздоровления и важности комплексного подхода.
Получить профессиональную консультацию – Похмельная служба в Екатеринбурге
bets · May 18, 2026 at 10:19 pm
Caishen Wins só caiu o bônus no giro 412 — antes disso, nada.
FrankCaP · May 18, 2026 at 10:49 pm
подробнее https://soulestate.ru/catalog/kp/zhukovka-267042/
ThanhAnype · May 18, 2026 at 11:21 pm
В данной статье мы акцентируем внимание на важности поддержки в процессе выздоровления. Мы обсудим, как друзья, семья и профессионалы могут помочь тем, кто сталкивается с зависимостями. Читатели получат практические советы, как поддерживать близких на пути к новой жизни.
Получить профессиональную консультацию – Похмельная служба Москва
Davisreani · May 18, 2026 at 11:24 pm
В этой статье обсуждаются актуальные медицинские вопросы, которые волнуют общество. Мы обращаем внимание на проблемы, касающиеся здравоохранения и лечения, а также на новшества в области медицины. Читатели будут осведомлены о последних событиях и смогут следить за тенденциями в медицине.
Читать дальше – стоп алко галенджик
ver detalhes · May 18, 2026 at 11:29 pm
A streamer com 80 viewers fechou a sessão de Touro no green, foi dormir. Disciplina simples assim.
AntonCoory · May 18, 2026 at 11:35 pm
В этой публикации мы рассматриваем важную тему борьбы с зависимостями, включая алкогольную и наркотическую зависимости. Мы обсудим методы лечения, реабилитации и поддержку, которые могут помочь людям, столкнувшимся с этой проблемой. Читатели узнают о перспективах выздоровления и важности комплексного подхода.
Лови подробности – «Похмельная служба» в Москве
Archiejed · May 19, 2026 at 12:05 am
Этот обзор посвящен успешным стратегиям избавления от зависимости, включая реальные примеры и советы. Мы разоблачим мифы и предоставим читателям достоверную информацию о различных подходах. Получите опыт многообразия методов и найдите подходящий способ для себя!
Кликни и узнай всё! – Похмельная служба в Москве
EugeneAnile · May 19, 2026 at 12:30 am
Для вызова специалиста необходимо позвонить на горячую линию или оставить заявку через официальный сайт, например, на портале государственных услуг. Специалист приедет в оговоренное время, обеспечив полную анонимность и соблюдение медицинской тайны.
Подробнее тут – вызвать нарколога на дом
TerryNat · May 19, 2026 at 12:36 am
Топ слот онлайн свит бонанза 1000 казино слот с красочной графикой, фриспинами и каскадными выигрышами. Высокая волатильность и множители обеспечивают шанс на крупные выплаты.
DanielSoodo · May 19, 2026 at 12:38 am
В данном обзоре представлены основные направления и тренды в области медицины. Мы обсудим актуальные проблемы здравоохранения, свежие открытия и новые подходы, которые меняют представление о лечении и профилактике заболеваний. Эта информация будет полезна как специалистам, так и широкой публике.
Заходи — там интересно – «Похмельная служба» в Люберцах
HowardJep · May 19, 2026 at 12:57 am
Этот обзор посвящен успешным стратегиям избавления от зависимости, включая реальные примеры и советы. Мы разоблачим мифы и предоставим читателям достоверную информацию о различных подходах. Получите опыт многообразия методов и найдите подходящий способ для себя!
Проверенные методы — узнай сейчас – Наркологическая клиника «Похмельная служба» в Екатеринбурге.
Larryapema · May 19, 2026 at 1:19 am
Обратившись к нам, вы получите анонимное и безопасное лечение, полностью соответствующее медицинским стандартам.
Выяснить больше – запой нарколог на дом
Timothyelapy · May 19, 2026 at 1:38 am
“kahve lekesi nas?l c?kar hal?dan” konusu icin cok faydal? bir yaz? buldum. Kendiniz gorun: https://kendimacera.com/articles/halidakurumus-kahve-lekesi-nasil-cikar/
Timothyelapy · May 19, 2026 at 1:42 am
“2023 parke modelleri” hakk?nda bilgi arayanlar icin cok faydal? bir yaz? buldum. Kendiniz gorun: https://kendifikirler.com/articles/2023-parke-modelleri-dekorasyon-trendleri/
Daniellab · May 19, 2026 at 1:53 am
Наркологическая клиника «Южный МедКонтроль» объединяет современные медицинские технологии, опыт специалистов и уважительное отношение к каждому пациенту. Здесь создаются условия для безопасного и результативного лечения зависимостей любой сложности — от алкогольной до полинаркотической. Центр работает в круглосуточном режиме, предлагая выезд врачей на дом, детоксикацию, кодирование и длительные программы реабилитации. Основная цель специалистов — восстановление физического и психологического равновесия человека, возвращение способности к полноценной жизни без зависимости.
Узнать больше – http://narkologicheskaya-clinika-v-rostove19.ru/chastnaya-narkologicheskaya-klinika-rostov-na-donu/
FrankPiste · May 19, 2026 at 1:56 am
Этот обзор посвящен успешным стратегиям избавления от зависимости, включая реальные примеры и советы. Мы разоблачим мифы и предоставим читателям достоверную информацию о различных подходах. Получите опыт многообразия методов и найдите подходящий способ для себя!
Ссылка на источник – Наркологическая клиника «Похмельная служба» в Мытищах
MichaelVit · May 19, 2026 at 1:59 am
В этой статье рассматриваются различные аспекты избавления от зависимости, включая физические и психологические методы. Мы обсудим поддержку, мотивацию и стратегии, которые помогут в процессе выздоровления. Читатели узнают, как преодолеть трудности и двигаться к новой жизни без зависимости.
Узнай первым! – стоп алко казань
Stephanglymn · May 19, 2026 at 2:34 am
В этом обзоре представлены различные методы избавления от зависимости, включая терапевтические и психологические подходы. Мы сравниваем их эффективность и предоставляем рекомендации для тех, кто хочет вернуться к трезвой жизни. Читатели смогут найти информацию о реабилитационных центрах и поддерживающих группах.
Посмотреть всё – стоп алко
TerryGoove · May 19, 2026 at 2:40 am
В статье рассмотрим ключевые моменты, которые помогут сориентироваться при выборе капельницы от запоя, понять механизм действия и особенности процедуры, а также избежать типичных ошибок при обращении за медицинской помощью.
Получить больше информации – сколько стоит капельница на дому от запоя
MichaelVit · May 19, 2026 at 2:47 am
В этой статье рассматриваются различные аспекты избавления от зависимости, включая физические и психологические методы. Мы обсудим поддержку, мотивацию и стратегии, которые помогут в процессе выздоровления. Читатели узнают, как преодолеть трудности и двигаться к новой жизни без зависимости.
Хочешь знать всё? – стоп алко
SheltonWriff · May 19, 2026 at 2:47 am
Клиника «ТоксинНет» предлагает профессиональную помощь при алкогольной зависимости и запоях в Нижнем Новгороде. Наши опытные наркологи круглосуточно выезжают на дом для оказания экстренной медицинской помощи. Основным методом лечения является капельница от запоя, которая позволяет оперативно снять интоксикацию и стабилизировать общее состояние пациента. Мы обеспечиваем конфиденциальность, индивидуальный подход и высокий уровень безопасности процедур.
Углубиться в тему – https://kapelnica-ot-zapoya-nizhniy-novgorod0.ru/kapelnicza-ot-zapoya-czena-nizhnij-novgorod
Marioguind · May 19, 2026 at 3:00 am
В этом обзоре представлены различные методы избавления от зависимости, включая терапевтические и психологические подходы. Мы сравниваем их эффективность и предоставляем рекомендации для тех, кто хочет вернуться к трезвой жизни. Читатели смогут найти информацию о реабилитационных центрах и поддерживающих группах.
Углубить понимание вопроса – Похмельная служба Люберцы
RaymondCeake · May 19, 2026 at 3:07 am
Хочешь испытать азарт? покерок скачать онлайн-покер с турнирами, кэш-столами и бонусами для игроков. Удобный интерфейс, мобильное приложение и регулярные покерные серии. Играйте в холдем, омаху и участвуйте в крупных турнирах.
Larrycrync · May 19, 2026 at 3:07 am
В этой медицинской статье мы погрузимся в актуальные вопросы здравоохранения и лечения заболеваний. Читатели узнают о современных подходах, методах диагностики и новых открытий в научных исследованиях. Наша цель — донести важную информацию и повысить уровень осведомленности о здоровье.
Углубить понимание вопроса – нарколог на дом в ростове
Douglastup · May 19, 2026 at 3:37 am
Ниже представлена таблица, демонстрирующая основные направления деятельности клиники и их особенности:
Получить дополнительную информацию – лечение в наркологической клинике в краснодаре
MichaelFam · May 19, 2026 at 3:45 am
Этот обзор медицинских исследований собрал самое важное из последних публикаций в области медицины. Мы проанализировали ключевые находки и представили их в доступной форме, чтобы читатели могли легко ориентироваться в актуальных темах. Этот материал станет отличным подспорьем для изучения медицины.
Всё самое вкусное внутри – стоп алко
GeorgeTek · May 19, 2026 at 3:46 am
В данной статье мы поговорим о будущем медицины, акцентируя внимание на прорывных разработках и их потенциале. Читатель узнает о новых подходах к лечению, роли искусственного интеллекта и возможностях персонализированной медицины.
Лови подробности – Похмельная служба в Москве
fixDiele · May 19, 2026 at 3:52 am
Для тех, кто ищет информацию по теме “Актуальные советы по финансовой грамотности в России”, нашел много полезного.
Смотрите сами:
https://rub-fin.ru
fixDiele · May 19, 2026 at 3:56 am
По теме “Обсуждение практической химии для юных химиков”, есть отличная статья.
Вот, можете почитать:
https://Khimie.ru
Joshuacit · May 19, 2026 at 4:20 am
В этой заметке мы представляем шаги, которые помогут в процессе преодоления зависимостей. Рассматриваются стратегии поддержки и чек-листы для тех, кто хочет сделать первый шаг к выздоровлению. Наша цель — вдохновить читателей на положительные изменения и поддержать их в трудных моментах.
См. подробности – «Похмельная служба» в Москве
alo789 · May 19, 2026 at 4:48 am
I was able to find good info from your articles.
система нейро адаптация авито · May 19, 2026 at 5:01 am
ип качарин михаил александрович
Albertlam · May 19, 2026 at 5:03 am
Эта публикация содержит ценные советы и рекомендации по избавлению от зависимости. Мы обсуждаем различные стратегии, которые могут помочь в процессе выздоровления и важность обращения за помощью. Читатели смогут использовать полученные знания для улучшения своего состояния.
Узнайте всю правду – стоп алко
AntonCoory · May 19, 2026 at 5:30 am
В данной статье мы поговорим о будущем медицины, акцентируя внимание на прорывных разработках и их потенциале. Читатель узнает о новых подходах к лечению, роли искусственного интеллекта и возможностях персонализированной медицины.
Связаться за уточнением – «Похмельная служба» в Москве
Daniellab · May 19, 2026 at 5:40 am
Эти этапы позволяют не только физически восстановиться, но и осознать важность трезвого образа жизни. Комбинация медицинских и психотерапевтических методов делает лечение устойчивым, предотвращая рецидивы даже при длительных формах зависимости.
Подробнее – наркологическая клиника стационар в ростове-на-дону
Daniellab · May 19, 2026 at 5:53 am
В «Южном МедКонтроле» лечение зависимостей строится поэтапно, с постепенным восстановлением физиологических функций и эмоциональной устойчивости. Врачи используют современные методы детоксикации, фармакотерапию и психотерапию, которые действуют комплексно. Каждый этап направлен на достижение конкретного результата: очищение организма, снятие симптомов абстиненции, стабилизацию состояния и профилактику срывов.
Ознакомиться с деталями – лечение в наркологической клинике ростов-на-дону
Davisreani · May 19, 2026 at 6:19 am
В этой статье обсуждаются актуальные медицинские вопросы, которые волнуют общество. Мы обращаем внимание на проблемы, касающиеся здравоохранения и лечения, а также на новшества в области медицины. Читатели будут осведомлены о последних событиях и смогут следить за тенденциями в медицине.
Нажмите, чтобы узнать больше – стоп алко галенджик
Archiejed · May 19, 2026 at 6:20 am
Этот краткий обзор предлагает сжатую информацию из области медицины, включая ключевые факты и последние новости. Мы стремимся сделать информацию доступной и понятной для широкой аудитории, что позволит читателям оставаться в курсе актуальных событий в здравоохранении.
Интересует подробная информация – Похмельная служба Москва
8kbetokcom · May 19, 2026 at 7:01 am
I blog quite often and I genuinely thank you for your information. This great article has really peaked my interest. I’m going to bookmark your blog and keep checking for new information about once per week. I opted in for your Feed too.
mediawiki1334.00web.net · May 19, 2026 at 7:09 am
Hi folks, I’ve been researching a reliable car shipping service to move my vehicle from coast to coast and I’m totally overwhelmed with all the options out there! Has anyone tried with interstate car shipping because I absolutely require insured car shipping since my ride means everything to me. I’ve been checking out several auto transport solutions [https://mediawiki1334.00web.net/index.php/User:FrankBrothers6] shipping companies but their car shipping cost calculators are giving me wildly different estimates and I’m not sure what’s accurate. I’m curious too if anyone has used bike transport from the same provider since I may move my motorcycle as well, and I’ve heard some auto transport companies also handle high-end vehicle transport which could be exactly what I want. Please help or vehicle transport reviews would be amazing!
Waltergog · May 19, 2026 at 7:31 am
Эта статья подробно расскажет о процессе выздоровления, который включает в себя эмоциональную, физическую и психологическую реабилитацию. Мы обсуждаем значимость поддержки и наличие профессиональных программ. Читатели узнают, как строить новую жизнь и не возвращаться к старым привычкам.
Получить дополнительные сведения – стоп алко
Miltonreomo · May 19, 2026 at 7:31 am
В этом обзоре мы обсудим современные методы борьбы с зависимостями, включая медикаментозную терапию и психотерапию. Мы представим последние исследования и их результаты, чтобы читатели могли быть в курсе наиболее эффективных подходов к лечению и поддержке.
Узнай первым! – Наркологическая клиника «Похмельная служба» в Казани
Thomasmor · May 19, 2026 at 8:17 am
В этой статье мы говорим о важности поддержки в процессе выздоровления. Рассматриваются семьи, группы поддержки, специалисты и онлайн-ресурсы, которые могут сыграть решающую роль в избавлении от зависимости.
Осуществить глубокий анализ – Похмельная служба Москва
FrankPiste · May 19, 2026 at 9:21 am
Этот текст представляет собой обзор свежих данных и исследований в области медицины. Он призван помочь читателям понять, как научные достижения влияют на лечение, диагностику и общее состояние системы здравоохранения.
Смотрите также… – «Похмельная служба» в Мытищах
Danielfef · May 19, 2026 at 9:49 am
Публикация охватывает основные направления развития современной медицины. Мы обсудим значимость научных исследований, инноваций в лечении и роли общественного участия в формировании системы здравоохранения.
Что скрывают от вас? – «Похмельная служба» в Химках
Stevenvew · May 19, 2026 at 9:53 am
Для стабильного входа — функциональная копия сайта Мелбет.
Как зайти в казино Мелбет при блоке — работает без VPN.
Старое зекало melbet не работает — зеркало с ошибкой в названии — просто скопируйте адрес.
Проверено актуально сегодня — полный функционал казино и ставок.
Source:
melbet зеркало
AndresSlusy · May 19, 2026 at 10:02 am
Хочешь испытать азарт? pokerok онлайн-покер с турнирами, кэш-столами и бонусами для игроков. Удобный интерфейс, мобильное приложение и регулярные покерные серии. Играйте в холдем, омаху и участвуйте в крупных турнирах.
Jefferyfaich · May 19, 2026 at 10:09 am
страница https://t.me/s/mounjaro_tirzepatide/
Thomasmor · May 19, 2026 at 10:19 am
В этой статье мы говорим о важности поддержки в процессе выздоровления. Рассматриваются семьи, группы поддержки, специалисты и онлайн-ресурсы, которые могут сыграть решающую роль в избавлении от зависимости.
Полезно знать – Наркологическая клиника «Похмельная служба» в Москве.
Marioguind · May 19, 2026 at 10:41 am
В данной статье мы поговорим о будущем медицины, акцентируя внимание на прорывных разработках и их потенциале. Читатель узнает о новых подходах к лечению, роли искусственного интеллекта и возможностях персонализированной медицины.
Получить профессиональную консультацию – Наркологическая клиника «Похмельная служба» в Люберцах
Barrytiemo · May 19, 2026 at 10:42 am
Текст посвящён распространённым мифам о зависимости и их развенчанию. Мы предоставим научно обоснованную информацию и дадим рекомендации по выбору эффективного способа борьбы с зависимым поведением.
Продолжить чтение – Похмельная служба в Москве
fugemHoags · May 19, 2026 at 11:02 am
Ищете автоюриста в Сыктывкаре? Посетите сайт https://autourcom.ru/ где вам предложат бесплатную консультацию. Ознакомьтесь с нашими услугами – мы оспариваем виновность в ДТП, добиваемся доплаты по ОСАГО, обжалуем штрафы и защищаем по делам о лишении прав. Работаем лично и дистанционно. Более 20 лет опыта! Мы предложим вам понятный план действий.
BradleyNek · May 19, 2026 at 11:37 am
Міський портал Дніпро https://faine-misto.dp.ua свіжі новини, події, афіша заходів та корисна інформація. Довідник компаній, міські сервіси, оголошення та все про життя міста.
SidneyDob · May 19, 2026 at 11:42 am
Чоловічий блог https://u-kuma.com з корисною інформацією про фінанси, кар’єру, здоров’я, спорт і стиль. Практичні поради, аналітика та матеріали для саморозвитку та впевненого руху до цілей.
Davidwem · May 19, 2026 at 11:44 am
Сайт міста Хмельницький https://faine-misto.km.ua новини, події, корисна інформація для мешканців та гостей. Афіша заходів, міські служби, довідник організацій, цікаві місця та актуальні події міста.
Barrytiemo · May 19, 2026 at 1:01 pm
В статье рассматриваются различные стратегии борьбы с зависимостями, включая проверенные методы и реальные истории успеха. Читатель узнает, какие подходы наиболее эффективны и как начать путь к выздоровлению.
Продолжить чтение – стоп алко
PeterHauff · May 19, 2026 at 1:54 pm
Эта медицинская заметка содержит сжатую информацию о новых находках и методах в области здравоохранения. Мы предлагаем читателям свежие данные о заболеваниях, профилактике и лечении. Наша цель — быстро и доступно донести важную информацию, которая поможет в повседневной жизни и понимании здоровья.
Расширить кругозор по теме – Похмельная служба Геленджик
Peterawary · May 19, 2026 at 2:06 pm
Эта публикация содержит ценные советы и рекомендации по избавлению от зависимости. Мы обсуждаем различные стратегии, которые могут помочь в процессе выздоровления и важность обращения за помощью. Читатели смогут использовать полученные знания для улучшения своего состояния.
Ознакомьтесь с аналитикой – стоп алко люберцы
Jefferyfaich · May 19, 2026 at 2:22 pm
сюда https://t.me/s/mounjaro_tirzepatide
jiguleJam · May 19, 2026 at 2:36 pm
Информационное агентство Vgolos публикует материалы по ключевым направлениям — политика, экономика, бизнес, технологии, здоровье и криминал без редакционных купюр и информационного шума. Журналисты издания быстро откликаются на актуальные события и работают с фактами без предположений — от расследований в судебной сфере до анализа потребительских тенденций. Читайте проверенные новости на https://vgolos.org/ — украинское информационное агентство для аудитории ценящей достоверность и оперативность. Культура, жизнь и технологии органично дополняют жёсткую новостную повестку и делают ресурс полноценным медиаисточником на каждый день.
Williamhycle · May 19, 2026 at 2:56 pm
Этот обзор медицинских исследований собрал самое важное из последних публикаций в области медицины. Мы проанализировали ключевые находки и представили их в доступной форме, чтобы читатели могли легко ориентироваться в актуальных темах. Этот материал станет отличным подспорьем для изучения медицины.
Связаться за уточнением – стоп алко
Jefferyfaich · May 19, 2026 at 2:56 pm
ссылка на сайт https://t.me/s/mounjaro_tirzepatide
Michaelmus · May 19, 2026 at 2:59 pm
В этой статье мы обсудим процесс восстановления после зависимостей, акцентируя внимание на различных методах и подходах к реабилитации. Читатели узнают, как создать план выздоровления и использовать полезные ресурсы для достижения устойчивых изменений.
ТОП-5 причин узнать больше – Похмельная служба Геленджик
RussellTex · May 19, 2026 at 3:07 pm
Бригады с опытом 7+ лет — поэтапная приёмка заказчиком.
Минимум декора, максимум воздуха — легко вписать яркие детали.
Своя база подрядчиков — делим проект на очереди под бюджет.
Источник:
https://y0.alazanskayadolinavino.ru
Robertlug · May 19, 2026 at 3:27 pm
Жіночий портал https://soloha.in.ua з актуальними матеріалами про моду, красу, здоров’я, психологію та сім’ю. Корисні поради, ідеї та натхнення для сучасних жінок щодня.
JamesBar · May 19, 2026 at 3:32 pm
Портал для людей похилого https://pensioneram.in.ua віку з Україна з корисною інформацією про пенсії, пільги, здоров’я та соціальні послуги. Прості поради, новини та інструкції для повсякденного життя пенсіонерів.
Davidwem · May 19, 2026 at 3:36 pm
Жіночий онлайн-сайт https://u-kumy.com з корисними статтями про красу, здоров’я, психологію, моду та будинок. Практичні поради, лайфхаки та надихаючі матеріали для жінок будь-якого віку.
Gilberthes · May 19, 2026 at 3:38 pm
Этот информативный текст сочетает в себе темы здоровья и зависимости. Мы обсудим, как хронические заболевания могут усугубить зависимости и наоборот, как зависимость может влиять на общее состояние здоровья. Читатели получат представление о комплексном подходе к лечению как физического, так и психического состояния.
Получить полную информацию – Похмельная служба в Новороссийске
Robertjaing · May 19, 2026 at 3:44 pm
В этой статье мы рассмотрим современные достижения в области медицины, включая инновационные методы лечения и диагностики. Мы обсудим важность профилактики заболеваний и роль технологий в улучшении качества здравоохранения. Читатели узнают о влиянии медицины на повседневную жизнь и ее значение для современного общества.
Дополнительно читайте здесь – стоп алко новосибирск
RussellGoaft · May 19, 2026 at 4:14 pm
Работа клиники строится на принципах доказательной медицины и индивидуального подхода. При поступлении пациента осуществляется всесторонняя диагностика, включающая анализы крови, оценку психического состояния и анамнез. По результатам разрабатывается персонализированный курс терапии.
Подробнее – https://narkologicheskaya-klinika-v-ryazani12.ru/narkologicheskaya-klinika-telefon-v-ryazani
PeterHauff · May 19, 2026 at 4:16 pm
В этой статье мы рассматриваем разные способы борьбы с алкогольной зависимостью. Обсуждаются методы лечения, программы реабилитации и советы для поддержки близких. Читатели получат информацию о том, как преодолеть зависимость и добиться успешного выздоровления.
Углубить понимание вопроса – стоп алко галенджик
AngeloDex · May 19, 2026 at 5:06 pm
В этой медицинской статье мы погрузимся в актуальные вопросы здравоохранения и лечения заболеваний. Читатели узнают о современных подходах, методах диагностики и новых открытий в научных исследованиях. Наша цель — донести важную информацию и повысить уровень осведомленности о здоровье.
Погрузиться в научную дискуссию – Наркологическая клиника «Похмельная служба» в Новосибирске.
AngeloDex · May 19, 2026 at 5:38 pm
Эта информационная публикация освещает широкий спектр тем из мира медицины. Мы предлагаем читателям ясные и понятные объяснения современных заболеваний, методов профилактики и лечения. Информация будет полезна как пациентам, так и медицинским работникам, желающим поддержать уровень своих знаний.
Не упусти важное! – Похмельная служба Новосибирск
StephenBop · May 19, 2026 at 6:09 pm
Последние новости Киева https://xxl.kyiv.ua сегодня: события города, политика, экономика, происшествия, транспорт и городская жизнь. Актуальная информация, репортажи, аналитика и важные обновления, которые помогают быть в курсе всех событий столицы Украины.
Dominickep · May 19, 2026 at 6:16 pm
Педагоги и психологи http://smartxpert.ru экспертный портал о воспитании, обучении и развитии личности. Полезные статьи, практические советы специалистов, современные методики педагогики и психологии, рекомендации для родителей, учителей и всех, кто интересуется развитием человека.
Carrollpoula · May 19, 2026 at 6:18 pm
Услуги грузчиков https://www.gruzchiki-kiev.net в Киеве для переездов, разгрузки транспорта, подъема мебели и строительных материалов. Профессиональные рабочие выполняют погрузочно-разгрузочные работы любой сложности, гарантируя аккуратное обращение с имуществом и оперативное выполнение заказа.
maorou_k8m · May 19, 2026 at 6:49 pm
maorou_k8m
Michaelkap · May 19, 2026 at 6:56 pm
Эта публикация содержит ценные советы и рекомендации по избавлению от зависимости. Мы обсуждаем различные стратегии, которые могут помочь в процессе выздоровления и важность обращения за помощью. Читатели смогут использовать полученные знания для улучшения своего состояния.
Перейти к полной версии – стоп алко
Michaelkap · May 19, 2026 at 7:50 pm
В этой публикации мы исследуем ключевые аспекты здоровья, включая влияние образа жизни на благополучие. Читатели узнают о важности правильного питания, физической активности и психического здоровья. Мы предоставим практические советы и рекомендации для поддержания здоровья и развития профилактических подходов.
Провести детальное исследование – «Похмельная служба» в Москве
Jefferyfaich · May 19, 2026 at 8:04 pm
на этом сайте https://t.me/s/mounjaro_tirzepatide/
Raymondlot · May 19, 2026 at 8:41 pm
Обучение педагогов https://edplatform.ru и учеников современным методикам интеллектуального развития. Программы дополнительного образования с 2016 года: ментальная арифметика, скорочтение, развитие памяти и внимания. Подготовка педагогов, учебные материалы и эффективные методики обучения.
Davidkix · May 19, 2026 at 9:30 pm
Мы понимаем, что лечение от алкогольной зависимости — это только первый шаг на пути к восстановлению. Профилактика рецидивов — важная часть нашего подхода. Мы проводим тренинги и курсы, направленные на развитие навыков борьбы с соблазнами и стрессом. Психотерапевтическая поддержка помогает пациентам справиться с эмоциональными трудностями, а также укрепляет мотивацию для сохранения трезвости.
Изучить вопрос глубже – вызвать капельницу от запоя в иркутске
JacobNat · May 19, 2026 at 9:34 pm
Когда запой превращается в угрозу для жизни, оперативное вмешательство становится критически важным. В Тюмени, Тюменская область, опытные наркологи предлагают услугу установки капельницы от запоя прямо на дому. Такой метод позволяет начать детоксикацию с использованием современных медикаментов, что способствует быстрому выведению токсинов, восстановлению обменных процессов и нормализации работы внутренних органов. Лечение на дому обеспечивает комфортную обстановку, полную конфиденциальность и индивидуальный подход к каждому пациенту.
Узнать больше – капельница от запоя стоимость в тюмени
equipe TrustGuru · May 19, 2026 at 9:43 pm
Treasures of Aztec pagou bem hoje, sem firula.
Billyles · May 19, 2026 at 10:01 pm
Этот документ охватывает важные аспекты медицинской науки, сосредотачиваясь на ключевых вопросах, касающихся здоровья населения. Мы рассматриваем свежие исследования, клинические рекомендации и лучшие практики, которые помогут улучшить качество лечения и профилактики заболеваний. Читатели получат возможность углубиться в различные медицинские дисциплины.
Подробная информация доступна по запросу – «Похмельная служба» в Нижнем Новгороде
TerryGoove · May 19, 2026 at 10:07 pm
Согласно данным НМИЦ психиатрии и наркологии Минздрава РФ, профессиональный вывод из запоя с применением капельниц снижает риск осложнений и сокращает период восстановления. Процедура проводится только под наблюдением квалифицированных специалистов и требует правильного подбора препаратов в зависимости от стадии опьянения и наличия сопутствующих заболеваний.
Исследовать вопрос подробнее – капельница от запоя анонимно
SheltonWriff · May 19, 2026 at 10:19 pm
После поступления вашего звонка специалист оперативно выезжает по указанному адресу в Нижнем Новгороде и проводит первичную диагностику. Врач измеряет основные жизненные показатели: артериальное давление, пульс, сатурацию кислорода в крови и оценивает степень алкогольной интоксикации. Затем подбирается индивидуальный состав капельницы, который позволяет максимально быстро снять симптомы похмелья и абстиненции.
Ознакомиться с деталями – после капельницы от запоя в нижний новгороде
xobralusa · May 19, 2026 at 10:27 pm
Медиапортал «Інквізиція» работает под девизом Deus vult — публикует расследования, криминальные репортажи и острую аналитику без оглядки на неудобных фигурантов. Авторы планомерно исследуют схемы коррупции, многолетние судебные истории и социальные нарывы — подкрепляя каждый материал документальными свидетельствами. Изучайте независимые расследования на https://inquisition.info/ — украинский портал для тех кто требует от журналистики реальных результатов. Разделы политики, экономики, бизнеса и здоровья представлены без купюр — редакция говорит прямо и без обиняков что принципиально выделяет портал на фоне обычных новостных площадок.
WilliamSoolo · May 19, 2026 at 10:34 pm
Клинические протоколы стационарной терапии рекомендуют госпитализацию при средней и тяжёлой степени интоксикации.
Подробнее – вывод из запоя
Williambor · May 19, 2026 at 10:42 pm
В этой статье мы рассматриваем разрушительное влияние зависимости на жизнь человека. Обсуждаются аспекты, такие как здоровье, отношения и профессиональные достижения. Читатели узнают о необходимости обращения за помощью и о путях к восстановлению.
Получить больше информации – Наркологическая клиника «Похмельная служба» в Ногинске
DonteFap · May 19, 2026 at 11:30 pm
Медицинская публикация представляет собой свод актуальных исследований, экспертных мнений и новейших достижений в сфере здравоохранения. Здесь вы найдете информацию о новых методах лечения, прорывных технологиях и их практическом применении. Мы стремимся сделать актуальные медицинские исследования доступными и понятными для широкой аудитории.
Кликни, не пожалеешь – «Похмельная служба» в Нижнем Новгороде
DeweyTox · May 19, 2026 at 11:35 pm
Продажа и установка камеры видеонаблюдения калининград. Современные системы безопасности для квартир, домов, магазинов и складов. Настройка удалённого доступа, запись видео и круглосуточный контроль объекта.
Williambor · May 19, 2026 at 11:39 pm
В этой статье мы рассматриваем разрушительное влияние зависимости на жизнь человека. Обсуждаются аспекты, такие как здоровье, отношения и профессиональные достижения. Читатели узнают о необходимости обращения за помощью и о путях к восстановлению.
Доступ к полной версии – «Похмельная служба» в Ногинске
Alfredoneply · May 19, 2026 at 11:45 pm
Быстрая профессиональная монтаж видеонаблюдения в калининграде для квартир, домов, офисов и коммерческих объектов. Проектирование, монтаж и настройка систем безопасности, удалённый доступ, запись видео и контроль в реальном времени. Надёжные решения для защиты имущества и контроля территории.
ArthurVob · May 20, 2026 at 12:02 am
Interested in processors https://cpu-socket.com with detailed specifications: clock speed, core count, generation, process technology, and supported sockets. A convenient CPU catalog for comparing and matching processors to your motherboard.
WilliamLix · May 20, 2026 at 12:23 am
В этом исследовании рассмотрены методы лечения зависимостей и их эффективность. Мы проанализируем различные подходы, используемые в реабилитационных центрах, и представим данные о результативности программ. Читатели получат надежные и научно обоснованные сведения о данной проблеме.
Получить профессиональную консультацию – стоп алко москва
BrianSOP · May 20, 2026 at 12:27 am
В данном обзоре представлены основные направления и тренды в области медицины. Мы обсудим актуальные проблемы здравоохранения, свежие открытия и новые подходы, которые меняют представление о лечении и профилактике заболеваний. Эта информация будет полезна как специалистам, так и широкой публике.
Где почитать поподробнее? – стоп алко
RobertVaf · May 20, 2026 at 1:02 am
В данном обзоре представлены основные направления и тренды в области медицины. Мы обсудим актуальные проблемы здравоохранения, свежие открытия и новые подходы, которые меняют представление о лечении и профилактике заболеваний. Эта информация будет полезна как специалистам, так и широкой публике.
Открой скрытое – Похмельная служба Нижний Новгород
Williamhycle · May 20, 2026 at 1:04 am
В данной публикации мы поговорим о процессе восстановления от зависимости, о том, как вернуть себе нормальную жизнь. Мы обсудим преодоление трудностей, значимость поддержки и наличие программ реабилитации. Читатели смогут узнать о ключевых шагах к успешному восстановлению.
Погрузиться в детали – Похмельная служба в Ногинске
Charlesjab · May 20, 2026 at 1:24 am
В данной публикации мы поговорим о процессе восстановления от зависимости, о том, как вернуть себе нормальную жизнь. Мы обсудим преодоление трудностей, значимость поддержки и наличие программ реабилитации. Читатели смогут узнать о ключевых шагах к успешному восстановлению.
Подробности по ссылке – Наркологическая клиника «Похмельная служба» в Новороссийске.
Robertmok · May 20, 2026 at 1:25 am
Эта доказательная статья представляет собой глубокое погружение в успехи и вызовы лечения зависимостей. Мы обращаемся к научным исследованиям и опыту специалистов, чтобы предоставить читателям надежные данные об эффективности различных методик. Изучите, что работает лучше всего, и получите информацию от экспертов.
Узнать напрямую – стоп алко
JacobNat · May 20, 2026 at 1:52 am
При длительном запое в организме накапливаются вредные токсины, что ведёт к нарушениям работы сердца, печени, почек и других жизненно важных органов. Чем быстрее начинается терапия, тем выше шансы избежать серьёзных осложнений и обеспечить качественное восстановление. Метод капельничного лечения позволяет оперативно начать детоксикацию, что особенно важно для спасения жизни и предупреждения хронических последствий злоупотребления алкоголем.
Получить дополнительную информацию – https://kapelnica-ot-zapoya-tyumen00.ru/postavit-kapelniczu-ot-zapoya-tyumen
GoodiniCrubs · May 20, 2026 at 1:59 am
В этой статье мы говорим о важности поддержки в процессе выздоровления. Рассматриваются семьи, группы поддержки, специалисты и онлайн-ресурсы, которые могут сыграть решающую роль в избавлении от зависимости.
Связаться за уточнением – Похмельная служба Новосибирск
Gilberthes · May 20, 2026 at 2:13 am
В этой статье мы рассматриваем разрушительное влияние зависимости на жизнь человека. Обсуждаются аспекты, такие как здоровье, отношения и профессиональные достижения. Читатели узнают о необходимости обращения за помощью и о путях к восстановлению.
Заходи — там интересно – Наркологическая клиника «Похмельная служба» в Новороссийске.
WilliamSoolo · May 20, 2026 at 2:29 am
Клинические протоколы стационарной терапии рекомендуют госпитализацию при средней и тяжёлой степени интоксикации.
Разобраться лучше – вывод из запоя цена
RussellGoaft · May 20, 2026 at 3:06 am
Эффективное лечение требует поэтапного подхода, который реализуется следующим образом:
Получить дополнительную информацию – наркологические клиники алкоголизм рязанская область
ThomasOxina · May 20, 2026 at 3:09 am
Во-первых, мы фокусируемся на медицинской детоксикации, которая является первоочередной задачей при лечении зависимостей. Этот процесс позволяет удалить токсические вещества из организма и улучшить общее состояние пациента. Мы применяем современные методики, которые помогают минимизировать симптомы абстиненции и обеспечить комфортное пребывание в клинике.
Подробнее тут – http://kapelnica-ot-zapoya-irkutsk.ru/
kihbllCat · May 20, 2026 at 3:44 am
Ищете настоящие скидки, акции и промокоды в России? Посетите сайт Огонёк https://ogonek.su/ – присоединяйтесь и экономьте! У нас подборка лучших скидок ежедневно. На сайте вы сможете увидеть лучшие скидки дня, а также увидеть все скидки и промокоды магазинов. Удобный поиск по категориям, что позволит быстро найти необходимую скидку! Подробнее на сайте.
Robertjaing · May 20, 2026 at 4:06 am
В этой статье мы рассмотрим современные достижения в области медицины, включая инновационные методы лечения и диагностики. Мы обсудим важность профилактики заболеваний и роль технологий в улучшении качества здравоохранения. Читатели узнают о влиянии медицины на повседневную жизнь и ее значение для современного общества.
Запросить дополнительные данные – Похмельная служба Новосибирск
CharlesAnymn · May 20, 2026 at 4:17 am
Автоматизированные системы дозирования обеспечивают точное введение лекарственных средств, что минимизирует риск передозировки и побочных эффектов. Постоянный мониторинг жизненных показателей позволяет оперативно корректировать терапию в режиме реального времени, обеспечивая максимальную безопасность процедуры.
Подробнее – https://narcolog-na-dom-ufa000.ru/narkolog-na-dom-czena-ufa/
dicugTor · May 20, 2026 at 5:00 am
Агентство «Акценты» выпускает тексты о политике, экономике, обществе, бизнесе, технологиях, здоровье и криминале без размытых формулировок и редакционных уступок. Редакция расследует теневые схемы, анализирует общественные процессы и освещает события с чёткой авторской позицией и документальной доказательной базой. Следите за самыми острыми материалами на https://akcenty.net/ — информационное агентство для читателей которые не довольствуются поверхностной подачей новостей. Острые расследования и профессиональная аналитика превращают агентство в многопрофильный медиаинструмент для широкого круга читателей стремящихся к полноценному пониманию общественных процессов.
MarcusArota · May 20, 2026 at 5:21 am
При поступлении вызова нарколог незамедлительно приезжает на дом для проведения детального первичного осмотра. Врач собирает краткий анамнез, измеряет жизненно важные показатели — пульс, артериальное давление, температуру — и оценивает степень алкогольной интоксикации. Эти данные являются основой для разработки индивидуального плана лечения, позволяющего подобрать наиболее эффективные методы детоксикации.
Подробнее тут – http://vyvod-iz-zapoya-tula00.ru
Kennethbeshy · May 20, 2026 at 6:07 am
В этой статье рассматриваются различные аспекты избавления от зависимости, включая физические и психологические методы. Мы обсудим поддержку, мотивацию и стратегии, которые помогут в процессе выздоровления. Читатели узнают, как преодолеть трудности и двигаться к новой жизни без зависимости.
Осуществить глубокий анализ – стоп алко
BryanTuh · May 20, 2026 at 6:16 am
Специалист уточняет продолжительность запоя, тип употребляемого алкоголя и наличие сопутствующих заболеваний. Такой подробный анализ позволяет подобрать оптимальные методы детоксикации и снизить риск осложнений.
Узнать больше – http://kapelnica-ot-zapoya-lugansk-lnr0.ru
Robertmok · May 20, 2026 at 6:47 am
В этой статье рассматриваются способы преодоления зависимости и успешные истории людей, которые справились с этой проблемой. Мы обсудим важность поддержки со стороны близких и профессионалов, а также стратегии, которые могут помочь в процессе выздоровления. Научитесь первоочередным шагам к новой жизни.
Познакомиться с результатами исследований – Похмельная служба в Новороссийске
Charlesjab · May 20, 2026 at 6:51 am
Этот обзор сосредоточен на различных подходах к избавлению от зависимости. Мы изучим традиционные и альтернативные методы, а также их сочетание для достижения максимальной эффективности. Читатели смогут открыть для себя новые стратегии и подходы, которые помогут в их борьбе с зависимостями.
ТОП-5 причин узнать больше – «Похмельная служба» в Новороссийске
hewxInory · May 20, 2026 at 7:19 am
Московская клиника «Онис» занимается лечением варикоза и сосудистых заболеваний с помощью передовых малоинвазивных технологий. В арсенале врачей — лазерная коагуляция, склеротерапия и радиочастотная абляция без разрезов и продолжительного периода восстановления. Подробнее об услугах и специалистах — https://www.onisclinic.ru/ — платформа с полной информацией о методах лечения и записи на приём. После диагностики каждому пациенту составляют индивидуальный план лечения, а стойкий эффект достигается за счёт точного подхода и высокой квалификации специалистов.
Daniellab · May 20, 2026 at 7:24 am
Для жителей Ростова-на-Дону клиника «Южный МедКонтроль» предлагает два формата помощи: лечение в стационаре и амбулаторные визиты врача на дом. Стационар оборудован всем необходимым для круглосуточного медицинского наблюдения, проведения инфузионных процедур и лабораторной диагностики. Пациентам предоставляется комфортное размещение, спокойная обстановка и постоянный контроль состояния. При выезде на дом врачи действуют оперативно — приезжают в течение часа, проводят осмотр, устанавливают капельницы, купируют абстиненцию и дают рекомендации по дальнейшему лечению.
Получить больше информации – http://narkologicheskaya-clinika-v-rostove19.ru/narkologiya-rostov-kruglosutochno/
GoodiniCrubs · May 20, 2026 at 7:51 am
В этой статье мы говорим о важности поддержки в процессе выздоровления. Рассматриваются семьи, группы поддержки, специалисты и онлайн-ресурсы, которые могут сыграть решающую роль в избавлении от зависимости.
Смотри, что ещё есть – стоп алко новосибирск
https://propertypavilion.co.uk/author/marlysbaldridg/ · May 20, 2026 at 8:25 am
Для пенсионеров этот сайт — просто находка, все телефоны крупные и понятные.
https://wiki.educom.nu/index.php?title=Vracha_Na_Dom
HaroldNor · May 20, 2026 at 9:33 am
В клинике применяются доказательные методы лечения, соответствующие международным и российским рекомендациям. Основу составляет медикаментозная детоксикация, сопровождаемая психотерапией, когнитивно-поведенческой коррекцией, а также семейной консультацией. При необходимости применяются пролонгированные препараты, облегчающие контроль над тягой к веществу.
Исследовать вопрос подробнее – https://narkologicheskaya-klinika-v-yaroslavle12.ru
Davidkix · May 20, 2026 at 10:00 am
Мы понимаем, что лечение от алкогольной зависимости — это только первый шаг на пути к восстановлению. Профилактика рецидивов — важная часть нашего подхода. Мы проводим тренинги и курсы, направленные на развитие навыков борьбы с соблазнами и стрессом. Психотерапевтическая поддержка помогает пациентам справиться с эмоциональными трудностями, а также укрепляет мотивацию для сохранения трезвости.
Ознакомиться с деталями – вызвать капельницу от запоя на дому в иркутске
Angelomet · May 20, 2026 at 10:34 am
Продажа и установка камеры видеонаблюдения купить. Современные системы безопасности для квартир, домов, магазинов и складов. Настройка удалённого доступа, запись видео и круглосуточный контроль объекта.
Robertpeazy · May 20, 2026 at 10:45 am
Быстрая профессиональная установка видеонаблюдения в калининграде для квартир, домов, офисов и коммерческих объектов. Проектирование, монтаж и настройка систем безопасности, удалённый доступ, запись видео и контроль в реальном времени. Надёжные решения для защиты имущества и контроля территории.
GilbertGreby · May 20, 2026 at 11:07 am
В интернете представлен сайт https://cvt25pro.ru где подробно рассматривается устройство и обслуживание трансмиссий. На его страницах можно найти информацию, касающуюся ремонта вариатора CVT 25 Chery, особенностей диагностики и возможных неисправностей этого агрегата. Материалы ресурса помогают понять специфику работы таких коробок передач и основные подходы к их восстановлению
PeterInjet · May 20, 2026 at 12:00 pm
В этой статье рассматривается комплексный подход к избавлению от зависимости. Читатель узнает, как сочетание физического, психологического и духовного восстановления помогает достичь стойкого выздоровления.
Ознакомьтесь поближе – стоп алко новосибирск
RussellTex · May 20, 2026 at 12:21 pm
Разработка за 14 дней — спецификацией материалов и мебели.
Кирпич, бетон и металл — скрытая проводка в металлорукавах.
Работаем удалённо и с выездом — даём чек-листы для заказчиков.
Источник:
Классический интерьер СПб
Robertker · May 20, 2026 at 12:27 pm
В данной статье рассматриваются физиологические и эмоциональные аспекты зависимости. Мы обсудим, как организм реагирует на зависимое поведение, и какие методы помогают восстановить здоровье и внутреннее равновесие.
Желаете узнать подробности? – стоп алко химки
DerekAwask · May 20, 2026 at 12:36 pm
В этой медицинской статье мы погрузимся в актуальные вопросы здравоохранения и лечения заболеваний. Читатели узнают о современных подходах, методах диагностики и новых открытий в научных исследованиях. Наша цель — донести важную информацию и повысить уровень осведомленности о здоровье.
Информация доступна здесь – стоп алко красноярск
EdwardAlask · May 20, 2026 at 12:49 pm
В данной публикации мы поговорим о процессе восстановления от зависимости, о том, как вернуть себе нормальную жизнь. Мы обсудим преодоление трудностей, значимость поддержки и наличие программ реабилитации. Читатели смогут узнать о ключевых шагах к успешному восстановлению.
Изучить рекомендации специалистов – «Похмельная служба» в Пушкино
equipe TrustGuru · May 20, 2026 at 12:50 pm
“Cassino confiável 2026” virou a busca do ano em português brasileiro.
Scottren · May 20, 2026 at 12:54 pm
В этой статье мы рассмотрим современные достижения в области медицины, включая инновационные методы лечения и диагностики. Мы обсудим важность профилактики заболеваний и роль технологий в улучшении качества здравоохранения. Читатели узнают о влиянии медицины на повседневную жизнь и ее значение для современного общества.
Все материалы собраны здесь – Наркологическая клиника «Похмельная служба» в Новосибирске
dvordekor 561 · May 20, 2026 at 12:59 pm
Ищете тротуарную плитку https://dvordekor.by борты или заборные блоки в Минске? Компания ДворДекорпредлагает широкий выбор материалов для ландшафтного дизайна и благоустройства. Посетите dvordekor.by/about и ознакомьтесь с ассортиментом!
postroi-ka 580 · May 20, 2026 at 1:09 pm
Железобетонные изделия https://postroi-ka.by (ЖБ) в Минске — покупайте напрямую от производителя! Гарантия качества, оптовые цены, быстрая доставка. Широкий выбор ЖБ?конструкций для любых строительных задач. Заходите на postroi-ka.by
macunak 937 · May 20, 2026 at 1:23 pm
Компрессорное оборудование https://macunak.by в Минске: продажа и обслуживание. Широкий выбор промышленного компрессорного оборудования на macunak.by — надёжность и сервис под ключ.
Timothynoire · May 20, 2026 at 2:54 pm
В этой статье мы подробно рассматриваем проверенные методы борьбы с зависимостями, включая психотерапию, медикаментозное лечение и поддержку со стороны общества. Мы акцентируем внимание на важности комплексного подхода и возможности успешного восстановления для людей, столкнувшихся с этой проблемой.
Узнать больше – Похмельная служба в Севастополе
Ralphzef · May 20, 2026 at 2:58 pm
Эта статья освещает различные аспекты освобождения от зависимости и пути к выздоровлению. Мы обсуждаем важность осознания своей проблемы и обращения за помощью. Читатели получат практические советы о том, как преодолевать трудности и строить новую жизнь без зависимости.
Ознакомиться с теоретической базой – Похмельная служба Севастополь
RobertDyefe · May 20, 2026 at 2:58 pm
http://bbs.abcdv.net/home.php?mod=space&uid=1585430&do=profile
sezon-stroy 139 · May 20, 2026 at 3:36 pm
Решил сделать ограждение? сетчатые ограждения 3д прочные металлические секции для заборов и ограждений территорий. Подходят для частных домов, предприятий, школ и складов. Панели имеют антикоррозийное покрытие, современный внешний вид и обеспечивают надежную защиту участка.
pricstroy 406 · May 20, 2026 at 3:37 pm
Нужен забор? забор 3д от производителя надежные металлические ограждения для частных домов, предприятий и общественных территорий. Производство, продажа и установка секционных заборов с антикоррозийным покрытием, высокой прочностью и долгим сроком службы.
farbwood 654 · May 20, 2026 at 3:41 pm
Пиломатериалы в Минске https://farbwood.by сибирская лиственница от производителя Farbwood. Качественные строительные материалы из лиственницы — доски, брус, вагонка. Гарантия долговечности и природной красоты.
PhilipExcam · May 20, 2026 at 4:12 pm
Эта публикация содержит ценные советы и рекомендации по избавлению от зависимости. Мы обсуждаем различные стратегии, которые могут помочь в процессе выздоровления и важность обращения за помощью. Читатели смогут использовать полученные знания для улучшения своего состояния.
Прочитать подробнее – Наркологическая клиника «Похмельная служба» в Казани
Scottlem · May 20, 2026 at 4:15 pm
paypal casino real money
WalterTyday · May 20, 2026 at 4:54 pm
Медицинская публикация представляет собой свод актуальных исследований, экспертных мнений и новейших достижений в сфере здравоохранения. Здесь вы найдете информацию о новых методах лечения, прорывных технологиях и их практическом применении. Мы стремимся сделать актуальные медицинские исследования доступными и понятными для широкой аудитории.
Обратитесь за информацией – «Похмельная служба» в Реутове
Georgeror · May 20, 2026 at 4:58 pm
Этот обзор посвящен успешным стратегиям избавления от зависимости, включая реальные примеры и советы. Мы разоблачим мифы и предоставим читателям достоверную информацию о различных подходах. Получите опыт многообразия методов и найдите подходящий способ для себя!
Получить профессиональную консультацию – Наркологическая клиника «Похмельная служба» в Реутове
kasyno online · May 20, 2026 at 5:17 pm
The start of a fast-growing trend?
Donaldmah · May 20, 2026 at 5:32 pm
Эти действия помогают быстро восстановить водно-электролитный баланс и снизить нагрузку на внутренние органы. После проведения процедур врач дает рекомендации по дальнейшему наблюдению и реабилитации.
Подробнее можно узнать тут – нарколог на дом круглосуточно калининград
Adriangow · May 20, 2026 at 5:53 pm
Публикация посвящена жизненным историям людей, успешно справившихся с зависимостью. Мы покажем, что выход есть, и он начинается с первого шага — принятия проблемы и желания измениться.
Получить дополнительную информацию – Похмельная служба в Красноярске
kasyno online opinie · May 20, 2026 at 6:00 pm
How come you do not have your website viewable in mobile format? cant see anything in my Droid.
Adriangow · May 20, 2026 at 6:42 pm
Этот обзор медицинских исследований собрал самое важное из последних публикаций в области медицины. Мы проанализировали ключевые находки и представили их в доступной форме, чтобы читатели могли легко ориентироваться в актуальных темах. Этот материал станет отличным подспорьем для изучения медицины.
Узнать больше > – Похмельная служба Красноярск
Ronaldfaife · May 20, 2026 at 7:51 pm
В этой статье рассматриваются различные аспекты избавления от зависимости, включая физические и психологические методы. Мы обсудим поддержку, мотивацию и стратегии, которые помогут в процессе выздоровления. Читатели узнают, как преодолеть трудности и двигаться к новой жизни без зависимости.
Изучить материалы по теме – стоп алко
KerryEmoff · May 20, 2026 at 8:21 pm
В нашей клинике “Сила воли” в Иркутске вы можете получить помощь как в стационаре, так и на дому. Мы предлагаем два вида услуг:
Изучить вопрос глубже – после капельницы от запоя
najlepsze kasyna online · May 20, 2026 at 8:21 pm
I know this is not exactly on topic, but i have a blog using the blogengine platform as well and i’m having issues with my comments displaying. is there a setting i am forgetting? maybe you could help me out? thank you.
GoodiniCrubs · May 20, 2026 at 8:30 pm
В этом обзоре представлены различные методы избавления от зависимости, включая терапевтические и психологические подходы. Мы сравниваем их эффективность и предоставляем рекомендации для тех, кто хочет вернуться к трезвой жизни. Читатели смогут найти информацию о реабилитационных центрах и поддерживающих группах.
Где почитать поподробнее? – Наркологическая клиника «Похмельная служба» в Красноярске.
Geraldpam · May 20, 2026 at 8:33 pm
Этот документ охватывает важные аспекты медицинской науки, сосредотачиваясь на ключевых вопросах, касающихся здоровья населения. Мы рассматриваем свежие исследования, клинические рекомендации и лучшие практики, которые помогут улучшить качество лечения и профилактики заболеваний. Читатели получат возможность углубиться в различные медицинские дисциплины.
Продолжить чтение – Похмельная служба Сочи
Donaldmah · May 20, 2026 at 9:14 pm
Врач проводит полное обследование и определяет тактику лечения в зависимости от состояния пациента. Важным аспектом является возможность применения комплексных мер, включающих:
Подробнее тут – https://narcolog-na-dom-kaliningrad00.ru/narkolog-na-dom-kaliningrad-czeny
best online casino new zealand · May 20, 2026 at 9:42 pm
There are some serious financial ramifications here.
MartinNus · May 20, 2026 at 9:43 pm
Этот текст посвящён сложным аспектам зависимости и её влиянию на жизнь человека. Мы обсудим психологические, физические и социальные последствия зависимого поведения, а также важность своевременного обращения за помощью.
Проследить причинно-следственные связи – «Похмельная служба» в Самаре
nonurnuniDs · May 20, 2026 at 9:48 pm
Дім, сад, будівництво і фермерство – ці теми розглядаємо в блозі – Українська Хата. На сайте https://xata.od.ua/ корисні поради власникам будинків, садівникам, будівельникам і фермерам. Актуальні теми, новини зі світу будівництва і фермерства. Українська хата (XATA.OD.UA) розповість про цікаве та корисне.
Briantes · May 20, 2026 at 9:55 pm
Алкогольная и наркотическая зависимость требуют незамедлительного и комплексного вмешательства для предотвращения серьезных осложнений и сохранения здоровья пациента. В Уфе, Республика Башкортостан, опытные наркологи выезжают на дом 24 часа в сутки, предоставляя оперативную помощь при запоях и в случаях наркотической интоксикации. Такой формат лечения позволяет начать детоксикацию в комфортной, привычной обстановке, обеспечивая максимальную конфиденциальность и индивидуальный подход к каждому пациенту.
Изучить вопрос глубже – вызвать врача нарколога на дом в уфе
Quintonrof · May 20, 2026 at 10:02 pm
Эта публикация содержит ценные советы и рекомендации по избавлению от зависимости. Мы обсуждаем различные стратегии, которые могут помочь в процессе выздоровления и важность обращения за помощью. Читатели смогут использовать полученные знания для улучшения своего состояния.
Ознакомьтесь поближе – «Похмельная служба» в Сочи
best online casino nz · May 20, 2026 at 10:14 pm
Wish I’d thought of this. Am in the field, but I procrastinate alot and haven’t written as much as I’d like. Thanks.
najlepsze kasyno online · May 20, 2026 at 10:29 pm
Magnificent beat ! Can I be your apprentice? Just kidding!
MartinNus · May 20, 2026 at 10:40 pm
В данном материале представлены ключевые тенденции в сфере медицинской науки и практики. Вы узнаете о последних открытиях, инновационных подходах к терапии и важности профилактики заболеваний. Особое внимание уделено практическому применению новых методов в клинической практике.
Нажми и узнай всё – «Похмельная служба» в Самаре
мостбет · May 20, 2026 at 10:46 pm
Круто, сайт mostbet — действительно крутой.
https://mostbet-elite.com
DerekAwask · May 20, 2026 at 11:43 pm
Читатели получат представление о том, как современные технологии влияют на развитие медицины. Обсуждаются новые методы лечения, персонализированный подход и роль цифровых решений в повышении качества медицинских услуг.
Получить исчерпывающие сведения – «Похмельная служба» в Красноярске
Larryapema · May 20, 2026 at 11:49 pm
Особую опасность представляет белая горячка (алкогольный психоз). У пациента возникают галлюцинации, приступы паники, агрессивное поведение, дезориентация во времени и пространстве. Это состояние требует незамедлительного вмешательства врача, так как человек может представлять опасность для себя и окружающих.
Получить больше информации – http://narcolog-na-dom-novokuznetsk00.ru
Milesexock · May 20, 2026 at 11:49 pm
В этой статье мы рассматриваем разрушительное влияние зависимости на жизнь человека. Обсуждаются аспекты, такие как здоровье, отношения и профессиональные достижения. Читатели узнают о необходимости обращения за помощью и о путях к восстановлению.
Детали по клику – стоп алко
Value & Strategy Calculators · May 21, 2026 at 12:31 am
Incredible plenty of amazing info!
PeterInjet · May 21, 2026 at 12:41 am
Текст посвящён распространённым мифам о зависимости и их развенчанию. Мы предоставим научно обоснованную информацию и дадим рекомендации по выбору эффективного способа борьбы с зависимым поведением.
Ознакомьтесь с аналитикой – Наркологическая клиника «Похмельная служба» в Новосибирске
Peterwosse · May 21, 2026 at 12:49 am
В этой статье мы обсудим процесс восстановления после зависимостей, акцентируя внимание на различных методах и подходах к реабилитации. Читатели узнают, как создать план выздоровления и использовать полезные ресурсы для достижения устойчивых изменений.
Нажми и узнай всё – стоп алко
kufuwisFek · May 21, 2026 at 1:00 am
Our blog, https://solusvpn.com/, focuses on a practical, no-nonsense understanding of online privacy, VPN technology, and safe internet use. This detailed information is accessible to both beginners wanting to understand how VPNs work and professionals who appreciate the in-depth analysis.
Willisunlak · May 21, 2026 at 1:01 am
Быстрая профессиональная установка камер видеонаблюдения для квартир, домов, офисов и коммерческих объектов. Проектирование, монтаж и настройка систем безопасности, удалённый доступ, запись видео и контроль в реальном времени. Надёжные решения для защиты имущества и контроля территории.
PhilipExcam · May 21, 2026 at 1:12 am
Этот обзор содержит информацию о передовых достижениях в области медицины. Мы разберем инновационные технологии, которые меняют подход к лечению и диагностике, а также их влияние на эффективность оказания медицинской помощи.
Слушай внимательно — тут важно – Похмельная служба Казань
Jamesgraig · May 21, 2026 at 1:21 am
Эта публикация посвящена актуальным вопросам современной медицины и здравоохранения. Мы обсудим новейшие технологии диагностики и лечения, а также их влияние на продолжительность и качество жизни. Читатель найдет здесь информацию о научных исследованиях и перспективных разработках, доступно изложенную для широкой аудитории.
Читать полностью – стоп алко
WilliamTairl · May 21, 2026 at 1:32 am
Этот обзор посвящен успешным стратегиям избавления от зависимости, включая реальные примеры и советы. Мы разоблачим мифы и предоставим читателям достоверную информацию о различных подходах. Получите опыт многообразия методов и найдите подходящий способ для себя!
Узнать из первых рук – Наркологическая клиника «Похмельная служба» в Севастополе
Davidbap · May 21, 2026 at 1:57 am
В этом исследовании рассмотрены методы лечения зависимостей и их эффективность. Мы проанализируем различные подходы, используемые в реабилитационных центрах, и представим данные о результативности программ. Читатели получат надежные и научно обоснованные сведения о данной проблеме.
Обратиться к источнику – Наркологическая клиника «Похмельная служба» в Ростове на Дону
Timothynoire · May 21, 2026 at 2:15 am
В этой публикации мы предложим ряд рекомендаций по избавлению от зависимостей и успешному восстановлению. Мы обсудим методы привлечения поддержки и важность самосознания. Эти советы помогут людям вернуться к нормальной жизни и стать на путь выздоровления.
Эксклюзивная информация – «Похмельная служба» в Севастополе
Robertheash · May 21, 2026 at 2:21 am
Этот обзор медицинских исследований собрал самое важное из последних публикаций в области медицины. Мы проанализировали ключевые находки и представили их в доступной форме, чтобы читатели могли легко ориентироваться в актуальных темах. Этот материал станет отличным подспорьем для изучения медицины.
Ознакомиться с деталями – стоп алко
KerryEmoff · May 21, 2026 at 2:21 am
Современное общество сталкивается с множеством вызовов, связанных с различными зависимостями, которые наносят серьезный урон как физическому, так и психоэмоциональному состоянию человека. Алкоголизм, наркомания и другие виды зависимости не только нарушают здоровье, но и разрушают личные отношения, затрудняют трудовую деятельность и социальную адаптацию. В наркологической клинике “Сила воли” в Иркутске мы предлагаем профессиональную помощь в лечении зависимости и проведении реабилитационных мероприятий, направленных на восстановление здоровья и социальной интеграции пациентов.
Подробнее тут – капельница от запоя выезд в иркутске
Ralphzef · May 21, 2026 at 2:31 am
В этой публикации мы исследуем ключевые аспекты здоровья, включая влияние образа жизни на благополучие. Читатели узнают о важности правильного питания, физической активности и психического здоровья. Мы предоставим практические советы и рекомендации для поддержания здоровья и развития профилактических подходов.
Получить исчерпывающие сведения – Похмельная служба Севастополь
EdwardAlask · May 21, 2026 at 2:42 am
В этой статье мы рассматриваем разрушительное влияние зависимости на жизнь человека. Обсуждаются аспекты, такие как здоровье, отношения и профессиональные достижения. Читатели узнают о необходимости обращения за помощью и о путях к восстановлению.
Следуйте по ссылке – Наркологическая клиника «Похмельная служба» в Пушкино.
MarcusArota · May 21, 2026 at 2:45 am
Вывод из запоя на дому в Туле осуществляется по строго отлаженной схеме, которая включает несколько последовательных этапов. Такой комплексный подход позволяет не только быстро вывести токсины из организма, но и обеспечить всестороннюю поддержку пациента, включая психологическую реабилитацию.
Детальнее – вывод из запоя клиника тула
Stephenwal · May 21, 2026 at 2:54 am
Этот обзор предлагает структурированное изложение информации по актуальным вопросам. Материал подан так, чтобы даже новичок мог быстро освоиться в теме и начать использовать полученные знания в практике.
Ознакомиться с теоретической базой – Похмельная служба в Реутове
Scottren · May 21, 2026 at 2:59 am
В этой статье мы рассматриваем разрушительное влияние зависимости на жизнь человека. Обсуждаются аспекты, такие как здоровье, отношения и профессиональные достижения. Читатели узнают о необходимости обращения за помощью и о путях к восстановлению.
Практические советы ждут тебя – стоп алко новосибирск
viapNax · May 21, 2026 at 3:09 am
Ищете тюнинг и ремонт фар автомобиля москва? Посетите сайт by-tuning.ru и ознакомьтесь с нашими работами. При необходимости посмотрите наши услуги, такие как антихром автомобиля, тюнинг и ремонт фар и многое другое. Мы дорожим своей репутацией и оказываем все услуги квалифицированно и с гарантией. Актуальные цены на все услуги представлены на сайте. Посмотрите наше портфолио! Би Вай Сервис — детейлинг центр, в котором к каждому автомобилю относятся с душой.
Robertheash · May 21, 2026 at 3:13 am
Эта информационная публикация освещает широкий спектр тем из мира медицины. Мы предлагаем читателям ясные и понятные объяснения современных заболеваний, методов профилактики и лечения. Информация будет полезна как пациентам, так и медицинским работникам, желающим поддержать уровень своих знаний.
Секреты успеха внутри – Наркологическая клиника «Похмельная служба» в Симферополе.
WalterTyday · May 21, 2026 at 3:28 am
Эта статья подробно расскажет о процессе выздоровления, который включает в себя эмоциональную, физическую и психологическую реабилитацию. Мы обсуждаем значимость поддержки и наличие профессиональных программ. Читатели узнают, как строить новую жизнь и не возвращаться к старым привычкам.
Изучить эмпирические данные – Наркологическая клиника «Похмельная служба» в Реутове
Davidskync · May 21, 2026 at 3:36 am
Эта познавательная публикация погружает вас в море интересного контента, который быстро захватит ваше внимание. Мы рассмотрим важные аспекты темы и предоставим вам уникальные Insights и полезные сведения для дальнейшего изучения.
Только для своих – стоп алко подольск
Georgeror · May 21, 2026 at 4:33 am
Эта информационная публикация освещает широкий спектр тем из мира медицины. Мы предлагаем читателям ясные и понятные объяснения современных заболеваний, методов профилактики и лечения. Информация будет полезна как пациентам, так и медицинским работникам, желающим поддержать уровень своих знаний.
Тыкай сюда — узнаешь много интересного – Наркологическая клиника «Похмельная служба» в Реутове.стоп алко
Briantes · May 21, 2026 at 5:05 am
Комплексная терапия при выводе из запоя на дому включает в себя два основных направления: медикаментозную детоксикацию и психологическую поддержку. Такой подход позволяет добиться быстрого и устойчивого эффекта, минимизируя риск осложнений и обеспечивая долгосрочную ремиссию.
Углубиться в тему – нарколог на дом круглосуточно цены в уфе
Aubreypaple · May 21, 2026 at 5:20 am
see this page
download from tiktok
Milesexock · May 21, 2026 at 5:53 am
В этой медицинской статье мы погрузимся в актуальные вопросы здравоохранения и лечения заболеваний. Читатели узнают о современных подходах, методах диагностики и новых открытий в научных исследованиях. Наша цель — донести важную информацию и повысить уровень осведомленности о здоровье.
См. подробности – стоп алко новосибирск
ScottJotly · May 21, 2026 at 5:58 am
Этот обзор посвящен успешным стратегиям избавления от зависимости, включая реальные примеры и советы. Мы разоблачим мифы и предоставим читателям достоверную информацию о различных подходах. Получите опыт многообразия методов и найдите подходящий способ для себя!
Читать полностью – стоп алко
LonnieGling · May 21, 2026 at 6:37 am
подробнее https://ufolabs.io/
WilliamTairl · May 21, 2026 at 7:01 am
В этом обзоре представлены различные методы избавления от зависимости, включая терапевтические и психологические подходы. Мы сравниваем их эффективность и предоставляем рекомендации для тех, кто хочет вернуться к трезвой жизни. Читатели смогут найти информацию о реабилитационных центрах и поддерживающих группах.
Прочесть заключение эксперта – Похмельная служба Севастополь
Ronaldfaife · May 21, 2026 at 7:11 am
Этот медицинский обзор сосредоточен на последних достижениях, которые оказывают влияние на пациентов и медицинскую практику. Мы разбираем инновационные методы лечения и исследований, акцентируя внимание на их значимости для общественного здоровья. Читатели узнают о свежих данных и их возможном применении.
ТОП-5 причин узнать больше – стоп алко
Aubreypaple · May 21, 2026 at 7:13 am
visit site
download tiktok no watermark
Efraincex · May 21, 2026 at 7:14 am
Этот обзор сосредоточен на различных подходах к избавлению от зависимости. Мы изучим традиционные и альтернативные методы, а также их сочетание для достижения максимальной эффективности. Читатели смогут открыть для себя новые стратегии и подходы, которые помогут в их борьбе с зависимостями.
Получить полную информацию – стоп алко
Haroldacams · May 21, 2026 at 7:36 am
Продолжение документ онлайн сервис
LonnieGling · May 21, 2026 at 7:47 am
перенаправляется сюда https://ufolabs.xyz
Haroldacams · May 21, 2026 at 8:02 am
этот сайт onlyfake генератор документов
Geraldpam · May 21, 2026 at 8:09 am
Обзор посвящён процессу восстановления после зависимостей. Мы расскажем о различных этапах реабилитации, поддерживающих ресурсах и важности мотивации в достижении устойчивого выздоровления.
Продолжить изучение – Наркологическая клиника «Похмельная служба» в Сочи.
Davidbap · May 21, 2026 at 8:21 am
В этой статье обсуждаются актуальные медицинские вопросы, которые волнуют общество. Мы обращаем внимание на проблемы, касающиеся здравоохранения и лечения, а также на новшества в области медицины. Читатели будут осведомлены о последних событиях и смогут следить за тенденциями в медицине.
Подробнее тут – «Похмельная служба» в Ростове на Дону
fixDiele · May 21, 2026 at 9:08 am
Для тех, кто ищет информацию по теме “Обновления дорог и сельской жизни в Кузбассе”, есть отличная статья.
Ссылка ниже:
https://media42.ru
LonnieGling · May 21, 2026 at 9:11 am
подробнее https://ufolabs.xyz
fixDiele · May 21, 2026 at 9:13 am
Кстати, если вас интересует Обсуждения и новости любимых футбольных клубов, посмотрите сюда.
Вот, можете почитать:
https://fanarsenal.ru
LonnieGling · May 21, 2026 at 9:17 am
посетить веб-сайт https://ufolabs.cc/
git.qniao.cn · May 21, 2026 at 9:24 am
References:
Plan du metro montreal http://git.qniao.cn/daniellalack8
Stephenwal · May 21, 2026 at 10:05 am
В этой статье представлен занимательный и актуальный контент, который заставит вас задуматься. Мы обсуждаем насущные вопросы и проблемы, а также освещаем истории, которые вдохновляют на действия и изменения. Узнайте, что стоит за событиями нашего времени!
Получить дополнительные сведения – «Похмельная служба» в Реутове
rigenridove · May 21, 2026 at 10:20 am
В последние годы банками всё чаще применяется автоматическая блокировка счета P2P в Казахстане из-за подозрений в мошенничестве (дропперство, треугольники) или нарушений Закона РК о ПОД/ФТ. Входящие переводы от незнакомых лиц система расценивает как подозрительные операции. Узнайте на странице https://blog.femida-justice.com/blokirovka-scheta-p2p-v-kazahstane/ ваши правильные шаги в этом направлении от Бахирева Анатолия Анатольевича, управляющего партнера юридической фирмы “Закон и Справедливость”.
http://higashiyamakai.com/cgi-local/bbs/higashiyama_kai.cgi/dzen.ru/a/teletype.in/@alexd78/teletype.in/github.com/vyvod-iz-zapoya-v-staczionare-sankt-peterburg-11.ru · May 21, 2026 at 10:53 am
The Ultimate Guide to Gaming
Haroldacams · May 21, 2026 at 11:02 am
Читать далее automated document generator
ScottJotly · May 21, 2026 at 11:45 am
Этот текст посвящён сложным аспектам зависимости и её влиянию на жизнь человека. Мы обсудим психологические, физические и социальные последствия зависимого поведения, а также важность своевременного обращения за помощью.
Получить дополнительную информацию – Наркологическая клиника «Похмельная служба» в Санкт Петербурге
bizeztTon · May 21, 2026 at 12:25 pm
PS5ゲーム(おそらくゲームのこと)をお探しですか?PS5(おそらくゲームのこと)PC(おそらくゲームのこと)会社(おそらくゲームのこと)? https://www.mukakin-blog.com/ をご覧ください。あらゆるトピックに関する本当に役立つ情報が見つかります。当ブログは、ありとあらゆる役立つ情報を提供する総合情報源です
tamapepem · May 21, 2026 at 12:44 pm
Ищете надежного поставщика металлопроката? Посетите сайт https://stalsfera.ru/ и вы сможете купить по выгодной цене металл оптом с доставкой по всей России от СтальСфера. Загляните в наш каталог – там действительно огромный выбор продукции. На складе наличие наиболее востребованных позиций листового, трубного, сортового и плоского проката. Также оказываем услуги металлообработки на собственном или контрактном производстве.
Quintonrof · May 21, 2026 at 12:54 pm
В этой статье мы обсудим процесс восстановления после зависимостей, акцентируя внимание на различных методах и подходах к реабилитации. Читатели узнают, как создать план выздоровления и использовать полезные ресурсы для достижения устойчивых изменений.
Читать далее > – Наркологическая клиника «Похмельная служба» в Сочи.
Efraincex · May 21, 2026 at 1:29 pm
В этой статье рассматриваются различные аспекты избавления от зависимости, включая физические и психологические методы. Мы обсудим поддержку, мотивацию и стратегии, которые помогут в процессе выздоровления. Читатели узнают, как преодолеть трудности и двигаться к новой жизни без зависимости.
Провести детальное исследование – Похмельная служба Санкт Петербург
RussellGoaft · May 21, 2026 at 1:49 pm
Стоимость услуг зависит от продолжительности терапии, сложности случая и выбранных процедур. Однако клиника предоставляет гибкую систему оплаты, включая рассрочку и страховое покрытие.
Исследовать вопрос подробнее – наркологическая клиника рязанская область
BryanTuh · May 21, 2026 at 2:16 pm
Капельничное лечение от запоя – это современный метод детоксикации, который позволяет быстро и безопасно вывести токсины из организма. В Луганске ЛНР специалисты оказывают помощь на дому, предлагая профессиональное капельничное лечение для тех, кто столкнулся с тяжелой алкогольной интоксикацией. Такой подход обеспечивает оперативное вмешательство в привычной для пациента обстановке, гарантируя индивидуальный подход и полную конфиденциальность.
Узнать больше – капельница от запоя на дому недорого луганск
Miltonsleme · May 21, 2026 at 2:18 pm
Медицинская публикация представляет собой свод актуальных исследований, экспертных мнений и новейших достижений в сфере здравоохранения. Здесь вы найдете информацию о новых методах лечения, прорывных технологиях и их практическом применении. Мы стремимся сделать актуальные медицинские исследования доступными и понятными для широкой аудитории.
Читать дальше – стоп алко
zodikilok · May 21, 2026 at 2:36 pm
Model International — это глобальная информационно-рекламная площадка для взрослых, собирающая тысячи частных объявлений из разных стран в одном месте. Сервис предоставляет исключительно рекламное пространство — без посредников и агентств. https://model-international.com/ предлагает удобный интерфейс с быстрым поиском по городам и странам. Аудитория платформы постоянно растёт, а размещение объявлений доступно на понятных условиях, изложенных в публичном соглашении.
electricmosRow · May 21, 2026 at 2:51 pm
Долго искал толковых специалистов по электрике, в итоге нашёл через https://electrics-mos.ru, сделали всё качественно и дали гарантию
jobcop.ca · May 21, 2026 at 3:19 pm
References:
Hardrock casino las vegas https://jobcop.ca/employer/fast-payout-online-casinos-australia-instant-withdrawals/
Julioinfuh · May 21, 2026 at 3:54 pm
В этой статье мы говорим о важности поддержки в процессе выздоровления. Рассматриваются семьи, группы поддержки, специалисты и онлайн-ресурсы, которые могут сыграть решающую роль в избавлении от зависимости.
Раскрыть тему полностью – Похмельная служба в Краснодаре
electricmosRow · May 21, 2026 at 4:42 pm
Обращался за заменой розеток, нашёл через https://electrics-mos.ru, сделали быстро
Aubreypaple · May 21, 2026 at 5:07 pm
why not find out more
save from tiktok
Michaelsop · May 21, 2026 at 5:19 pm
Реабилитация по программе 12 шагов включает работу с мышлением, эмоциональной сферой, поведением, разрушенными связями, чувством вины, стыда, безысходности, гордыни, злости и внутреннего напряжения. После детоксикации, вывода из запоя, снятия ломки или медикаментозного этапа человек может почувствовать облегчение, но одной физической стабилизации часто недостаточно. Чтобы справиться с зависимостью, нужна долгосрочная программа, консультанты, группы, наставник, психотерапия, поддержание трезвости и постепенность в действиях.
Подробнее можно узнать тут – программа 12 шагов для созависимых самостоятельно
Williamkib · May 21, 2026 at 5:26 pm
Первым этапом лечения является медицинская детоксикация, которая направлена на удаление токсинов из организма и стабилизацию физического состояния пациента. Мы используем современные методики, которые помогают минимизировать симптомы абстиненции, такие как головная боль, тошнота и слабость, обеспечивая комфортное пребывание в клинике.
Исследовать вопрос подробнее – вызвать капельницу от запоя на дому
JamesHef · May 21, 2026 at 5:50 pm
Этот документ охватывает важные аспекты медицинской науки, сосредотачиваясь на ключевых вопросах, касающихся здоровья населения. Мы рассматриваем свежие исследования, клинические рекомендации и лучшие практики, которые помогут улучшить качество лечения и профилактики заболеваний. Читатели получат возможность углубиться в различные медицинские дисциплины.
Ознакомиться с полной информацией – Похмельная служба в Краснодаре
Timothyelapy · May 21, 2026 at 6:03 pm
Bu arada, eger 1 paket maya kac kas?k konusuyla ilgileniyorsan?z, suraya bir goz at?n. Iste link: https://kendimacera.com/articles/sut-mayasi-kullanimi-kac-kasik-maya-eklenmeli/
RudolphRig · May 21, 2026 at 6:07 pm
В данной статье мы акцентируем внимание на важности поддержки в процессе выздоровления. Мы обсудим, как друзья, семья и профессионалы могут помочь тем, кто сталкивается с зависимостями. Читатели получат практические советы, как поддерживать близких на пути к новой жизни.
Смотрите также… – стоп алко краснодар
Timothyelapy · May 21, 2026 at 6:08 pm
modern soz bohcas? hakk?ndaki yaz?y? gercekten begendim. Link burada: https://evhobileri.com/articles/soz-bohcasinin-hazirlanmasi/
RobertNeage · May 21, 2026 at 6:23 pm
Экстренное вмешательство необходимо, когда самостоятельное прекращение употребления алкоголя или наркотиков становится невозможным, а состояние пациента ухудшается. Основные показания включают:
Подробнее можно узнать тут – психиатр нарколог на дом уфа
Larryapema · May 21, 2026 at 6:36 pm
Обратившись к нам, вы получите анонимное и безопасное лечение, полностью соответствующее медицинским стандартам.
Получить дополнительные сведения – нарколог на дом вывод в новокузнецке
Aubreypaple · May 21, 2026 at 7:03 pm
official statement
save from tiktok
MarcusArota · May 21, 2026 at 7:17 pm
На данном этапе специалист уточняет, как долго продолжается запой, какой вид алкоголя употребляется и имеются ли сопутствующие заболевания. Тщательный анализ информации позволяет оперативно определить степень интоксикации и выбрать оптимальные методы терапии для быстрого и безопасного вывода из запоя.
Исследовать вопрос подробнее – наркологический вывод из запоя тула
Генрих · May 21, 2026 at 7:33 pm
Туры Авиатуры из Владивостока в Таиланд прямые рейсы
casino en ligne · May 21, 2026 at 7:35 pm
This is one very informative blog. I like the way you write and I will bookmark your blog to my favorites.
Jasonvop · May 21, 2026 at 7:51 pm
Чтобы снять ограничения — полнофункциональный дублёр сайта Мелбет.
Тысячи автоматов и live-крупье — бонус на первый депозит до 100 000 ?.
(орфография по запросу: «зекало»)
Зеркало нужно при блокировке основного — абсолютно те же функции.
Источник:
https://melbet-pjn.top
Haroldacams · May 21, 2026 at 9:15 pm
интернет onlyfake онлайн генерация
Malcolmroole · May 21, 2026 at 9:42 pm
Публикация знакомит читателей с различными подходами к реабилитации. От традиционных методов до современных программ — вы узнаете, как выбрать оптимальный путь к выздоровлению и преодолеть препятствия на этом пути.
Дополнительно читайте здесь – Похмельная служба в Краснодаре
RussellGoaft · May 21, 2026 at 10:03 pm
Стоимость услуг зависит от продолжительности терапии, сложности случая и выбранных процедур. Однако клиника предоставляет гибкую систему оплаты, включая рассрочку и страховое покрытие.
Изучить вопрос глубже – https://narkologicheskaya-klinika-v-ryazani12.ru
LarryNeorn · May 21, 2026 at 10:05 pm
Мы работаем круглосуточно, принимаем заявки по телефону, оказываем помощь анонимно и конфиденциально. Вы можете позвонить сейчас, оставить заявку через форму сайта или заказать обратный звонок. Бесплатная первичная консультация помогает понять, какой метод подойдет в конкретной ситуации: капельница, детоксикация, вывод из запоя, снятие ломки, кодирование, амбулаторное лечение, стационар или реабилитация.
Изучить вопрос глубже – нарколог на дом вывод из запоя казань
Michaelsop · May 21, 2026 at 10:41 pm
Современная реабилитация 12 шагов может сочетаться с медицинской помощью, если пациент находится в тяжелом состоянии. При интоксикации, запое, похмелье, ломке, тревоге, бессоннице, психозе, депрессии, употреблении наркотиков или алкоголя сначала может потребоваться нарколог, врач, психиатр, стационар, капельница, детоксикация, УБОД по показаниям или медикаментозное лечение. После стабилизации начинается реабилитационный процесс, где главный акцент делается на понимании зависимости, честности, ответственности, группе и новой системе жизни.
Углубиться в тему – 12 шагов реабилитационный центр
Malcolmroole · May 21, 2026 at 10:43 pm
Этот обзор содержит информацию о передовых достижениях в области медицины. Мы разберем инновационные технологии, которые меняют подход к лечению и диагностике, а также их влияние на эффективность оказания медицинской помощи.
Познакомиться с результатами исследований – Наркологическая клиника «Похмельная служба» в Краснодаре.
fofimweata · May 21, 2026 at 11:04 pm
Москва-река открывает новые грани развлечений: тематические вечеринки, зажигательные диджей-сеты и живая музыка прямо на борту теплохода — всё это делает каждый выход в свет по-настоящему незабываемым. На сайте https://ticketscruise.ru/ собрано полное расписание круизов на любой вкус: от уютных прогулок с ужином под звёздным небом до ночных шоу-программ с профессиональными артистами. Танцы под открытым небом, бар на борту, панорамные виды столицы — здесь каждая деталь работает на атмосферу. Бронируйте билеты онлайн и выбирайте свой идеальный формат отдыха на воде!
BryanTuh · May 21, 2026 at 11:10 pm
Профессиональный вывод из запоя на дому в Луганске ЛНР организован по отлаженной схеме, которая включает несколько этапов, позволяющих обеспечить максимально безопасное и эффективное лечение.
Исследовать вопрос подробнее – капельница от запоя на дому круглосуточно
Shaunhob · May 21, 2026 at 11:19 pm
Публикация знакомит читателей с различными подходами к реабилитации. От традиционных методов до современных программ — вы узнаете, как выбрать оптимальный путь к выздоровлению и преодолеть препятствия на этом пути.
Не упусти важное! – «Похмельная служба» в Краснодаре
Williamwergo · May 22, 2026 at 12:01 am
У нас можно заказать стильные подарки и украшения для праздника. В каталоге есть изящные аксессуары, которые подойдут для дня рождения.
Если хочется выбрать что-то запоминающееся, стоит обратить внимание на подарочные композиции. Такие вещи создают настроение и помогают сделать подарок действительно особенным.
Интернет-магазин подарков предлагает товары для тех, кто ценит качество. Здесь легко выбрать подарок для мамы, не тратя время на бесконечные поиски.
Каталог пополняется интересными товарами, поэтому каждый покупатель может найти подходящий вариант. Подарки и украшения помогают выразить внимание без лишних слов.
kraken ссылка зеркало
ustanovka domofona 75 · May 22, 2026 at 12:03 am
установка домофона загородный дом установка домофона в калининграде
MarioLaurb · May 22, 2026 at 12:59 am
Врач контролирует состояние пациента на протяжении всей процедуры — от первого введения препаратов до стабилизации самочувствия. Обычно уже через час после постановки капельницы уходит тошнота, нормализуется сон, снижается тревожность и тяга к спиртному. По завершении инфузионной терапии нарколог оставляет необходимые медикаменты на несколько дней, дает чёткие инструкции по их приёму и рекомендует дальнейшие шаги: амбулаторное наблюдение, кодирование или реабилитацию. После вывода из запоя обязательно даются рекомендации по продолжению лечения алкоголизма, включая кодирование и реабилитацию. Во многих случаях — да: в частной клинике платная помощь включает выездную стабилизацию, чтобы анонимно и быстро провести необходимые процедуры на месте.
Ознакомиться с деталями – vyzov-narkologa-na-dom-kruglosutochno-nedorogo
https://firstpagelist.co.uk/author/simaboykin7336/?profile=true · May 22, 2026 at 1:21 am
The local fixers provided by ORBIS Production Italy are highly connected and respected by local authorities.
https://gitea.amazingcoders.com/guydannevig228
CharlesBlema · May 22, 2026 at 1:44 am
Публикация посвящена жизненным историям людей, успешно справившихся с зависимостью. Мы покажем, что выход есть, и он начинается с первого шага — принятия проблемы и желания измениться.
Провести детальное исследование – стоп алко краснодар
Miltonsleme · May 22, 2026 at 1:46 am
Эта публикация обращает внимание на важность профилактики зависимостей. Мы обсудим, как осведомленность и образование могут помочь в предотвращении возникновения зависимости. Читатели смогут ознакомиться с полезными советами и ресурсами, которые способствуют здоровому образу жизни.
Получить больше информации – Похмельная служба Санкт Петербург
Williamwergo · May 22, 2026 at 2:05 am
У нас можно заказать красивые подарки и украшения для приятного сюрприза. В каталоге есть женские украшения, которые подойдут для юбилея.
Если хочется сделать приятный сюрприз, стоит обратить внимание на подарочные композиции. Такие вещи подчеркивают вкус и помогают сделать подарок действительно особенным.
Интернет-магазин подарков предлагает товары для тех, кто ценит оригинальность. Здесь легко выбрать подарок для любимого человека, не тратя время на бесконечные поиски.
Каталог пополняется интересными товарами, поэтому каждый покупатель может найти подходящий вариант. Подарки и украшения помогают выразить внимание без лишних слов.
kraken darknet market
Travisfinue · May 22, 2026 at 3:18 am
visit this web-site
https://carsh.store/ET54TUMBFDRPM/
https://carsh.store/ES88FIMIALARD/
https://carsh.store/JZ12VIAHHSVYI/
https://carsh.store/UD13BTOIBJHHL/
https://carsh.store/VM48IALOIXLGR/
https://carsh.store/RH71AMQAGDYOS/
https://carsh.store/MN29ETDQCHZVN/
https://carsh.store/TW47XTKVIZBAN/
https://carsh.store/IR14MJVALYJIE/
https://carsh.store/YI52GCPXLTSMH/
https://carsh.store/WG34BJTQCOBRV/
https://carsh.store/PS46IRSUCVYSL/
https://carsh.store/AB79XVQIOCFQX/
https://carsh.store/HA75WMKCFBTCI/
https://carsh.store/GZ68VNJJSQVXM/
https://carsh.store/IF47DCXAVIDUD/
https://carsh.store/FZ12NNLQKXQGA/
https://carsh.store/UG64EFHJPZTKF/
https://carsh.store/NK27SZDGYHPQN/
https://carsh.store/YI71GXYYKTPET/
https://carsh.store/UU83CLBNERWAY/
https://carsh.store/JM76FHHKVSKOE/
https://carsh.store/WW66CVWHNHWJH/
https://carsh.store/DY46QEQYSVFBR/
https://carsh.store/XG87GHXFQTRHX/
https://carsh.store/YQ98WKSDDYXNH/
https://carsh.store/RO73TXECZTLAT/
https://carsh.store/QN25DXKLRVNVN/
https://carsh.store/LI33IMOSICTKC/
https://carsh.store/YQ88IKVCREACN/
https://carsh.store/KJ74YUGBXLFDE/
Josephcroro · May 22, 2026 at 3:22 am
“diyet yaparken vucut ne zaman yag yakmaya baslar” hakk?nda bilgi arayanlar icin cok faydal? bir yaz? buldum. Kendiniz gorun: https://sporfikir.com/articles/vucut-yag-yakma-sureci-ne-zaman-baslar/
Josephcroro · May 22, 2026 at 3:29 am
Bu arada soyleyeyim, eger s?klamen cicegi bak?m? konusuyla ilgileniyorsan?z, suraya bir goz at?n. Link burada: https://kendiyolu.com/articles/siklamen-cicegi-bakimi/
HaroldAducH · May 22, 2026 at 3:37 am
В этом обзоре мы обсудим современные методы борьбы с зависимостями, включая медикаментозную терапию и психотерапию. Мы представим последние исследования и их результаты, чтобы читатели могли быть в курсе наиболее эффективных подходов к лечению и поддержке.
Не пропусти важное – стоп алко краснодар
AlfredAtmob · May 22, 2026 at 3:49 am
Эта публикация содержит ценные советы и рекомендации по избавлению от зависимости. Мы обсуждаем различные стратегии, которые могут помочь в процессе выздоровления и важность обращения за помощью. Читатели смогут использовать полученные знания для улучшения своего состояния.
Прочесть всё о… – стоп алко
xijivoNex · May 22, 2026 at 3:56 am
Интересный контент сегодня — это не просто развлечение, а способ узнавать новое каждый день. Сайт https://vseinteresno.com/ собирает познавательные материалы на самые разные темы: наука, история, природа, технологии и необычные факты со всего мира. Читатели находят здесь короткие и ёмкие статьи, которые расширяют кругозор без лишней воды. Если хочется каждый день открывать что-то новое — этот ресурс станет приятной привычкой для любознательного человека.
Travisfinue · May 22, 2026 at 3:58 am
helpful resources
https://carsh.store/ET54TUMBFDRPM/
https://carsh.store/ES88FIMIALARD/
https://carsh.store/JZ12VIAHHSVYI/
https://carsh.store/UD13BTOIBJHHL/
https://carsh.store/VM48IALOIXLGR/
https://carsh.store/RH71AMQAGDYOS/
https://carsh.store/MN29ETDQCHZVN/
https://carsh.store/TW47XTKVIZBAN/
https://carsh.store/IR14MJVALYJIE/
https://carsh.store/YI52GCPXLTSMH/
https://carsh.store/WG34BJTQCOBRV/
https://carsh.store/PS46IRSUCVYSL/
https://carsh.store/AB79XVQIOCFQX/
https://carsh.store/HA75WMKCFBTCI/
https://carsh.store/GZ68VNJJSQVXM/
https://carsh.store/IF47DCXAVIDUD/
https://carsh.store/FZ12NNLQKXQGA/
https://carsh.store/UG64EFHJPZTKF/
https://carsh.store/NK27SZDGYHPQN/
https://carsh.store/YI71GXYYKTPET/
https://carsh.store/UU83CLBNERWAY/
https://carsh.store/JM76FHHKVSKOE/
https://carsh.store/WW66CVWHNHWJH/
https://carsh.store/DY46QEQYSVFBR/
https://carsh.store/XG87GHXFQTRHX/
https://carsh.store/YQ98WKSDDYXNH/
https://carsh.store/RO73TXECZTLAT/
https://carsh.store/QN25DXKLRVNVN/
https://carsh.store/LI33IMOSICTKC/
https://carsh.store/YQ88IKVCREACN/
https://carsh.store/KJ74YUGBXLFDE/
Williamkib · May 22, 2026 at 4:04 am
Проблема зависимости от алкоголя, наркотиков и азартных игр остается одной из наиболее острых в современном обществе. Эти состояния оказывают значительное воздействие не только на здоровье самого человека, но и на его семью, друзей и общественные связи. Наркологическая клиника “Восстановление души” предлагает широкий спектр услуг для тех, кто борется с различными формами зависимости, такими как алкоголизм, наркомания и игромания. Наша цель — предоставить комплексный подход к лечению, что обеспечивает высокие показатели успешности среди наших пациентов.
Исследовать вопрос подробнее – поставить капельницу от запоя в иркутске
JamesHef · May 22, 2026 at 4:30 am
Этот документ охватывает важные аспекты медицинской науки, сосредотачиваясь на ключевых вопросах, касающихся здоровья населения. Мы рассматриваем свежие исследования, клинические рекомендации и лучшие практики, которые помогут улучшить качество лечения и профилактики заболеваний. Читатели получат возможность углубиться в различные медицинские дисциплины.
Связаться за уточнением – «Похмельная служба» в Краснодаре
Charlesonert · May 22, 2026 at 4:39 am
Слоты, рулетка, покерные столы — частые соревнования в казино.
Что заставляет игроков выбирать казино Мелбет — бонус на первый депозит до 100 000 ₽.
Рабочее melbet зекало на сегодня — сохраните в закладки.
Главный сайт мелбет и его зеркало — дают одинаковые бонусы.
Source:
играть в melbet онлайн
Julioinfuh · May 22, 2026 at 4:43 am
В этой статье мы говорим о важности поддержки в процессе выздоровления. Рассматриваются семьи, группы поддержки, специалисты и онлайн-ресурсы, которые могут сыграть решающую роль в избавлении от зависимости.
Смотрите также… – стоп алко
nujakldSab · May 22, 2026 at 5:02 am
Посетите сайт https://z.skupka-primorskiy.ru/ – это статейный блог Приморской Скупки, где вы найдете интересную и полезную информацию о бриллиантах, золоте, серебре и премиум часах. А также актуальную стоимость на скупку перечисленных материалов.
BruceSquab · May 22, 2026 at 5:21 am
Этот обзор содержит информацию о передовых достижениях в области медицины. Мы разберем инновационные технологии, которые меняют подход к лечению и диагностике, а также их влияние на эффективность оказания медицинской помощи.
Смотри, что ещё есть – Наркологическая клиника «Похмельная служба» в Краснодаре
RudolphRig · May 22, 2026 at 5:27 am
В этой публикации мы рассматриваем важную тему борьбы с зависимостями, включая алкогольную и наркотическую зависимости. Мы обсудим методы лечения, реабилитации и поддержку, которые могут помочь людям, столкнувшимся с этой проблемой. Читатели узнают о перспективах выздоровления и важности комплексного подхода.
Запросить дополнительные данные – Наркологическая клиника «Похмельная служба» в Краснодаре.
LarryNeorn · May 22, 2026 at 5:45 am
Мы работаем круглосуточно, принимаем заявки по телефону, оказываем помощь анонимно и конфиденциально. Вы можете позвонить сейчас, оставить заявку через форму сайта или заказать обратный звонок. Бесплатная первичная консультация помогает понять, какой метод подойдет в конкретной ситуации: капельница, детоксикация, вывод из запоя, снятие ломки, кодирование, амбулаторное лечение, стационар или реабилитация.
Подробнее можно узнать тут – нарколог на дом недорого казань
hagodmwen · May 22, 2026 at 7:06 am
«Делай Промо» — SaaS-платформа для брендов и агентств, позволяющая запускать чековые акции, программы лояльности и мотивацию продавцов без привлечения разработчиков. Бренды и агентства получают конструктор лендингов, OCR-распознавание чеков, мультиканальные чат-боты для Telegram и VK, кодовые механики с защитой от брутфорса и сквозную аналитику с выгрузкой в Excel — всё в едином окне. На http://makerpromo.ru/ уже зарегистрировано свыше 24 000 чеков и 18 000 активных пользователей. Платформа работает на условиях закрытого бета-тестирования со специальными тарифами.
RobertNeage · May 22, 2026 at 7:23 am
Комплексная терапия при выводе из запоя на дому включает в себя два основных направления: медикаментозную детоксикацию и психологическую поддержку. Такой подход позволяет добиться быстрого и устойчивого эффекта, минимизируя риск осложнений и обеспечивая долгосрочную ремиссию.
Узнать больше – нарколог на дом круглосуточно уфа
Travisfinue · May 22, 2026 at 7:34 am
navigate to this site
https://carsh.store/ET54TUMBFDRPM/
https://carsh.store/ES88FIMIALARD/
https://carsh.store/JZ12VIAHHSVYI/
https://carsh.store/UD13BTOIBJHHL/
https://carsh.store/VM48IALOIXLGR/
https://carsh.store/RH71AMQAGDYOS/
https://carsh.store/MN29ETDQCHZVN/
https://carsh.store/TW47XTKVIZBAN/
https://carsh.store/IR14MJVALYJIE/
https://carsh.store/YI52GCPXLTSMH/
https://carsh.store/WG34BJTQCOBRV/
https://carsh.store/PS46IRSUCVYSL/
https://carsh.store/AB79XVQIOCFQX/
https://carsh.store/HA75WMKCFBTCI/
https://carsh.store/GZ68VNJJSQVXM/
https://carsh.store/IF47DCXAVIDUD/
https://carsh.store/FZ12NNLQKXQGA/
https://carsh.store/UG64EFHJPZTKF/
https://carsh.store/NK27SZDGYHPQN/
https://carsh.store/YI71GXYYKTPET/
https://carsh.store/UU83CLBNERWAY/
https://carsh.store/JM76FHHKVSKOE/
https://carsh.store/WW66CVWHNHWJH/
https://carsh.store/DY46QEQYSVFBR/
https://carsh.store/XG87GHXFQTRHX/
https://carsh.store/YQ98WKSDDYXNH/
https://carsh.store/RO73TXECZTLAT/
https://carsh.store/QN25DXKLRVNVN/
https://carsh.store/LI33IMOSICTKC/
https://carsh.store/YQ88IKVCREACN/
https://carsh.store/KJ74YUGBXLFDE/
Donaldmah · May 22, 2026 at 7:34 am
Эти действия помогают быстро восстановить водно-электролитный баланс и снизить нагрузку на внутренние органы. После проведения процедур врач дает рекомендации по дальнейшему наблюдению и реабилитации.
Изучить вопрос глубже – нарколог на дом анонимно
WilliamAgozy · May 22, 2026 at 7:49 am
В этой статье рассматриваются различные аспекты избавления от зависимости, включая физические и психологические методы. Мы обсудим поддержку, мотивацию и стратегии, которые помогут в процессе выздоровления. Читатели узнают, как преодолеть трудности и двигаться к новой жизни без зависимости.
Ознакомьтесь поближе – «Похмельная служба» в Санкт Петербурге
GeorgeChifs · May 22, 2026 at 8:32 am
Капельница от похмелья в Самаре: эффективное восстановление, снятие интоксикации и помощь специалистов в наркологической клинике «Детокс»
Подробнее – капельница от похмелья на дом
GeorgeChifs · May 22, 2026 at 8:49 am
Капельница от похмелья с контролем врача в Самаре является одной из самых популярных и эффективных услуг для тех, кто сталкивается с выраженными симптомами похмельного синдрома. Похмелье может проявляться не только головной болью и усталостью, но и более серьезными проблемами, такими как тошнота, рвота, учащенное сердцебиение и повышение давления. Когда симптомы становятся особенно острыми, капельница помогает организму справиться с токсинами, восстановить водно-электролитный баланс и нормализовать состояние пациента, в том числе при запое. Важно, что контроль врача на протяжении всей процедуры обеспечивает безопасность и эффективность, при этом помощь может оказываться как на дому, так и в клинике при лечении алкоголизма.
Углубиться в тему – http://www.domen.ru
vatibeWoode · May 22, 2026 at 8:51 am
峯岸みなみ年齢に関する役立つ製品、サービス、または単なる情報を探しています ふくれな昔 ライブDVDどれを買うか sixtones ライブグッズ アクスタアプリ? https://tubestation.site/ にアクセスしてください – そこには必要なものがすべて見つかります。
HaroldAducH · May 22, 2026 at 9:03 am
В этом обзоре мы обсудим современные методы борьбы с зависимостями, включая медикаментозную терапию и психотерапию. Мы представим последние исследования и их результаты, чтобы читатели могли быть в курсе наиболее эффективных подходов к лечению и поддержке.
Не пропусти важное – Наркологическая клиника «Похмельная служба» в Краснодаре.
AlfredAtmob · May 22, 2026 at 9:16 am
Мы рассмотрим современные вызовы здравоохранения и пути их решения с помощью технологий и научных исследований. В статье собраны данные о новых лекарствах, методах диагностики и системном подходе к улучшению здоровья населения.
Полная информация здесь – Наркологическая клиника «Похмельная служба» в Краснодаре
fibosionGen · May 22, 2026 at 9:28 am
Ищете вывоз строительного мусора со стройки? Посетите сайт https://ais.by/article/vyvoz-stroitelnogo-musora-so-stroyki и вы сможете ознакомиться с информацией о том, какую выгодно использовать для вас схему: контейнер, самосвал или вывоз небольшими машинами. Узнайте, как выбрать подходящий вариант и что необходимо учесть перед заказом, чтобы грамотно организовать вывоз строймусора.
AshleyCrafe · May 22, 2026 at 10:39 am
В этой статье рассматриваются актуальные вопросы, связанные с развитием медицинской науки и её внедрением в повседневную практику. Особое внимание уделено вопросам профилактики, ранней диагностики и использованию технологий для улучшения здоровья человека.
Познакомиться с результатами исследований – Наркологическая клиника «Похмельная служба» в Краснодаре
ThomasCed · May 22, 2026 at 11:05 am
Эта публикация посвящена актуальным вопросам современной медицины и здравоохранения. Мы обсудим новейшие технологии диагностики и лечения, а также их влияние на продолжительность и качество жизни. Читатель найдет здесь информацию о научных исследованиях и перспективных разработках, доступно изложенную для широкой аудитории.
Уникальные данные только сегодня – «Похмельная служба» в Краснодаре
Jamesmex · May 22, 2026 at 11:09 am
Этот медицинский обзор сосредоточен на последних достижениях, которые оказывают влияние на пациентов и медицинскую практику. Мы разбираем инновационные методы лечения и исследований, акцентируя внимание на их значимости для общественного здоровья. Читатели узнают о свежих данных и их возможном применении.
Желаете узнать подробности? – «Похмельная служба» в Ставрополе
Travisfinue · May 22, 2026 at 11:29 am
their explanation
https://carsh.store/ET54TUMBFDRPM/
https://carsh.store/ES88FIMIALARD/
https://carsh.store/JZ12VIAHHSVYI/
https://carsh.store/UD13BTOIBJHHL/
https://carsh.store/VM48IALOIXLGR/
https://carsh.store/RH71AMQAGDYOS/
https://carsh.store/MN29ETDQCHZVN/
https://carsh.store/TW47XTKVIZBAN/
https://carsh.store/IR14MJVALYJIE/
https://carsh.store/YI52GCPXLTSMH/
https://carsh.store/WG34BJTQCOBRV/
https://carsh.store/PS46IRSUCVYSL/
https://carsh.store/AB79XVQIOCFQX/
https://carsh.store/HA75WMKCFBTCI/
https://carsh.store/GZ68VNJJSQVXM/
https://carsh.store/IF47DCXAVIDUD/
https://carsh.store/FZ12NNLQKXQGA/
https://carsh.store/UG64EFHJPZTKF/
https://carsh.store/NK27SZDGYHPQN/
https://carsh.store/YI71GXYYKTPET/
https://carsh.store/UU83CLBNERWAY/
https://carsh.store/JM76FHHKVSKOE/
https://carsh.store/WW66CVWHNHWJH/
https://carsh.store/DY46QEQYSVFBR/
https://carsh.store/XG87GHXFQTRHX/
https://carsh.store/YQ98WKSDDYXNH/
https://carsh.store/RO73TXECZTLAT/
https://carsh.store/QN25DXKLRVNVN/
https://carsh.store/LI33IMOSICTKC/
https://carsh.store/YQ88IKVCREACN/
https://carsh.store/KJ74YUGBXLFDE/
baixar app · May 22, 2026 at 11:41 am
Por que ninguém fala do Emperor’s Favour? É bom demais ou ruim demais?
RogerDem · May 22, 2026 at 11:55 am
В статье по вопросам здоровья мы рассматриваем актуальные проблемы, с которыми сталкивается общество. Обсуждаются заболевания, факторы риска и важные аспекты профилактики. Читатели получат полезные советы о том, как сохранить здоровье и улучшить качество жизни.
Раскрыть тему полностью – капельница от запоя на дому
RonaldIllem · May 22, 2026 at 12:07 pm
В этой статье мы рассмотрим современные достижения в области медицины, включая инновационные методы лечения и диагностики. Мы обсудим важность профилактики заболеваний и роль технологий в улучшении качества здравоохранения. Читатели узнают о влиянии медицины на повседневную жизнь и ее значение для современного общества.
Изучите внимательнее – показания для вывода из запоя
Davidhoiff · May 22, 2026 at 12:11 pm
Обратиться к врачу-наркологу стоит в случаях, когда больного сложно доставить в клинику, человек отказывается ехать в стационар, находится в состоянии длительного запоя, употреблял алкоголь несколько дней, испытывает тяжелое похмелье, тревогу, тремор, тошноту, нарушение сна или признаки алкогольной интоксикации. В таких условиях выездной нарколог помогает быстро оценить состояние пациента и подобрать безопасное лечение на дом.
Ознакомиться с деталями – http://narkolog-na-dom-kazan20.ru
MichaelBob · May 22, 2026 at 12:16 pm
Купить права
CyrusBok · May 22, 2026 at 12:22 pm
для предотвращения осложнений во время процедуры вывода из запоя на дому, врач нашей клиники проводит предварительный осмотр пациента, оценивает его общее состояние и собирает медицинский анамнез.
Изучить вопрос глубже – нарколог вывод из запоя казань
HarryNatry · May 22, 2026 at 12:30 pm
Этот текст посвящён сложным аспектам зависимости и её влиянию на жизнь человека. Мы обсудим психологические, физические и социальные последствия зависимого поведения, а также важность своевременного обращения за помощью.
Рассмотреть проблему всесторонне – Похмельная служба Краснодар
ShawnBub · May 22, 2026 at 12:53 pm
Гранитная мастерская https://святаятроица73.рф в Рязани — изготовление памятников из гранита и мрамора на заказ. Производство, гравировка портретов, установка памятников и благоустройство мест захоронения. Индивидуальные проекты, качественный камень и профессиональный подход.
gunumcow · May 22, 2026 at 12:56 pm
Интернет-магазин Kaminru.ru специализируется на продаже каминов, печей и дымоходов с профессиональным монтажом и доставкой по всей России. Ассортимент охватывает дровяные, электрические и газовые модели — от классики до современного дизайна. На https://kaminru.ru/ представлены изразцовые печи, подвесные камины и каминные топки со стеклом с подробными обзорами и экспертными статьями. Специалисты компании помогут подобрать оптимальное решение под интерьер и бюджет.
Robertpeapy · May 22, 2026 at 12:59 pm
Полная версия по ссылке: https://spainslov.ru/site/word/word/%D0%94%D0%A0%D0%9E%D0%93%D0%90
Williamwergo · May 22, 2026 at 1:09 pm
В нашем магазине можно найти оригинальные подарки и украшения для праздника. В каталоге есть милые мелочи, которые подойдут для свадьбы.
Если хочется порадовать близкого человека, стоит обратить внимание на подарочные композиции. Такие вещи подчеркивают вкус и помогают сделать подарок действительно особенным.
Магазин подарков и украшений предлагает товары для тех, кто ценит красоту. Здесь легко выбрать подарок для коллеги, не тратя время на бесконечные поиски.
Ассортимент регулярно обновляется, поэтому каждый покупатель может найти подходящий вариант. Подарки и украшения помогают выразить внимание без лишних слов.
kra ссылка
sunwin · May 22, 2026 at 1:15 pm
Cherished is likely to be what people say about your comments.
Coreycrani · May 22, 2026 at 2:06 pm
В данной публикации мы поговорим о процессе восстановления от зависимости, о том, как вернуть себе нормальную жизнь. Мы обсудим преодоление трудностей, значимость поддержки и наличие программ реабилитации. Читатели смогут узнать о ключевых шагах к успешному восстановлению.
Получить полную информацию – Похмельная служба Краснодар
Jamesstese · May 22, 2026 at 2:38 pm
В этой статье рассматривается комплексный подход к избавлению от зависимости. Читатель узнает, как сочетание физического, психологического и духовного восстановления помогает достичь стойкого выздоровления.
А что дальше? – Наркологическая клиника «Похмельная служба» в Краснодаре
HarryNatry · May 22, 2026 at 2:38 pm
В этой статье обсуждаются актуальные медицинские вопросы, которые волнуют общество. Мы обращаем внимание на проблемы, касающиеся здравоохранения и лечения, а также на новшества в области медицины. Читатели будут осведомлены о последних событиях и смогут следить за тенденциями в медицине.
Осуществить глубокий анализ – «Похмельная служба» в Краснодаре
Matthewknich · May 22, 2026 at 2:39 pm
Эта публикация исследует взаимосвязь зависимости и психологии. Мы обсудим, как психологические аспекты влияют на появление зависимостей и процесс выздоровления. Читатели смогут понять важность профессиональной поддержки и применения научных подходов в терапии.
Смотрите также… – Похмельная служба Краснодар
sunwin · May 22, 2026 at 2:51 pm
There is a lot of misunderstanding about these issues today. Your material helps explain things.
trực tiếp bóng đá socolive · May 22, 2026 at 2:58 pm
I just couldnt leave your website before saying that I really enjoyed the useful information you offer to your visitors… Will be back often to check up on new stuff you post!
Williamwergo · May 22, 2026 at 3:11 pm
Наш магазин можно найти стильные подарки и украшения для любого случая. В каталоге есть женские украшения, которые подойдут для свадьбы.
Если хочется порадовать близкого человека, стоит обратить внимание на кольца. Такие вещи создают настроение и помогают сделать подарок действительно особенным.
Магазин подарков и украшений предлагает товары для тех, кто ценит оригинальность. Здесь легко выбрать подарок для девушки, не тратя время на бесконечные поиски.
Ассортимент регулярно обновляется, поэтому каждый покупатель может найти интересную идею. Подарки и украшения помогают выразить внимание без лишних слов.
kraken сайт зеркала
Aaronpep · May 22, 2026 at 3:19 pm
Вывод запоя в клинике Сочи: лечение алкогольной интоксикации, капельница, детоксикация, помощь нарколога на дому и в стационаре круглосуточно, анонимно
Исследовать вопрос подробнее – скорая вывод из запоя
https://www.google.az/url?q=https://avtobus.dp.ua/kontakty/ · May 22, 2026 at 3:25 pm
За более чем 20 лет работы мы зарекомендовали себя как надежный партнер в сфере пассажирских перевозок, обслужив тысячи довольных клиентов. Наша миссия — обеспечить максимальный комфорт, абсолютную безопасность и строгую пунктуальность каждой поездки. https://www.google.az/url?q=https://avtobus.dp.ua/kontakty/
B52 · May 22, 2026 at 3:51 pm
My brother suggested I might like this web site. He was entirely right. This post actually made my day. You can not imagine simply how much time I had spent for this info! Thanks!
Rolandfow · May 22, 2026 at 3:54 pm
Этот обзор сосредоточен на различных подходах к избавлению от зависимости. Мы изучим традиционные и альтернативные методы, а также их сочетание для достижения максимальной эффективности. Читатели смогут открыть для себя новые стратегии и подходы, которые помогут в их борьбе с зависимостями.
Перейти к полной версии – Похмельная служба в Краснодаре
Bernarddog · May 22, 2026 at 4:12 pm
Новое в категории: https://ilovehandmade.ru/
JamesDog · May 22, 2026 at 4:16 pm
В этой статье мы рассматриваем разрушительное влияние зависимости на жизнь человека. Обсуждаются аспекты, такие как здоровье, отношения и профессиональные достижения. Читатели узнают о необходимости обращения за помощью и о путях к восстановлению.
Погрузиться в детали –
www.lowcarbon.gb.net · May 22, 2026 at 4:28 pm
I think that may be an interesting element, it made me assume a bit. Thanks for sparking my considering cap. On occasion I get so much in a rut that I simply really feel like a record.
MarcusArota · May 22, 2026 at 4:28 pm
Вывод из запоя на дому в Туле осуществляется по строго отлаженной схеме, которая включает несколько последовательных этапов. Такой комплексный подход позволяет не только быстро вывести токсины из организма, но и обеспечить всестороннюю поддержку пациента, включая психологическую реабилитацию.
Получить больше информации – вывод из запоя на дому цена в туле
debet · May 22, 2026 at 4:31 pm
You ma’am have a way with words. Thank you very much!
Williamslive · May 22, 2026 at 4:51 pm
Здравствуйте!
Чэнду панды заповедник дает шанс увидеть гигантских панд вживую. Утреннее время кормления наиболее активно и интересно для наблюдений. Билеты следует бронировать заранее из-за высокого спроса туристов. Не забудьте посетить исследовательский центр рядом с вольерами.
Полная информация по ссылке – https://aldita.net/
Зонт дождь защита, Беларусь минск отдых, Россия камчатка вулканы
Россия алтай природа, Варшава старый рынок, Шри-Ланка серфинг
Всего наилучшего и хорошей информации!
RonaldSlacy · May 22, 2026 at 4:57 pm
Этот краткий обзор предлагает сжатую информацию из области медицины, включая ключевые факты и последние новости. Мы стремимся сделать информацию доступной и понятной для широкой аудитории, что позволит читателям оставаться в курсе актуальных событий в здравоохранении.
Перейти к статье – Наркологическая клиника «Похмельная служба» в Краснодаре.
CyrusBok · May 22, 2026 at 5:06 pm
Запой опасен не только похмелья и слабостью. При запойным употреблении нарушается сон, повышается тревожность, страдает печень, сердце, сосудистая система, желудка и поджелудочной железы. Потеря контроля, очередной прием спиртного и сильная тягу к алкоголю могут приводить к белой горячки, психоза, судороги, инфаркт или инсульта.
Подробнее можно узнать тут – вывод из запоя круглосуточно в казани
MichaelFED · May 22, 2026 at 6:42 pm
В этой статье обсуждаются актуальные медицинские вопросы, которые волнуют общество. Мы обращаем внимание на проблемы, касающиеся здравоохранения и лечения, а также на новшества в области медицины. Читатели будут осведомлены о последних событиях и смогут следить за тенденциями в медицине.
Изучите внимательнее – капельница от запоя на дому
RonaldSlacy · May 22, 2026 at 7:16 pm
В этой статье рассматриваются различные аспекты избавления от зависимости, включая физические и психологические методы. Мы обсудим поддержку, мотивацию и стратегии, которые помогут в процессе выздоровления. Читатели узнают, как преодолеть трудности и двигаться к новой жизни без зависимости.
Что скрывают от вас? – Похмельная служба в Краснодаре
Jasonvop · May 22, 2026 at 7:28 pm
Когда основной портал заблокирован — рабочая ссылка на зекало мелбет.
Как попасть в казино Мелбет при блокировке — один клик до игры.
Если сайт не открывается — сохраните в закладки.
Единственное надёжное зеркало мелбет — все функции казино и ставок.
Источник:
https://melbet-vor.top
MichaelFED · May 22, 2026 at 7:38 pm
В данном обзоре представлены основные направления и тренды в области медицины. Мы обсудим актуальные проблемы здравоохранения, свежие открытия и новые подходы, которые меняют представление о лечении и профилактике заболеваний. Эта информация будет полезна как специалистам, так и широкой публике.
Читать дальше – поставить капельницу от запоя
Bernarddog · May 22, 2026 at 7:40 pm
Только лучшие материалы: https://aromatmasla.ru/
DanielGibra · May 22, 2026 at 7:44 pm
Нужна CRM по банкротству? CRM для БФЛ автоматизация работы юридической компании, контроль этапов БФЛ, учет клиентов, документов и платежей. Управляйте делами, задачами и сроками процедур в единой системе с удобной аналитикой и отчетами.
Timothypneug · May 22, 2026 at 7:58 pm
Этот обзор медицинских исследований собрал самое важное из последних публикаций в области медицины. Мы проанализировали ключевые находки и представили их в доступной форме, чтобы читатели могли легко ориентироваться в актуальных темах. Этот материал станет отличным подспорьем для изучения медицины.
Давай разберёмся досконально – Похмельная служба Краснодар
coruyllTip · May 22, 2026 at 8:27 pm
メルカリ 購入されたら, メルカリ 発送方法変更, メルカリ 発送方法 変更, メルカリ 退会方法, メルカリ 再登録. これらの質問やその他多くの質問にご興味をお持ちの方は、https://nishinoke.jp/ をご覧ください。様々なトピックに関する回答やアドバイスが掲載された総合的な情報源です。
Jamesmex · May 22, 2026 at 8:33 pm
В этом обзоре представлены различные методы избавления от зависимости, включая терапевтические и психологические подходы. Мы сравниваем их эффективность и предоставляем рекомендации для тех, кто хочет вернуться к трезвой жизни. Читатели смогут найти информацию о реабилитационных центрах и поддерживающих группах.
Изучить аспект более тщательно – Похмельная служба в Ставрополе
Robertwhosy · May 22, 2026 at 8:54 pm
Мы работаем круглосуточно, принимаем заявку по телефону, а выезд возможен в любое время суток, включая выходных и праздничные дней. Вызов нарколога на дом помогает быстро оказать помощь больного, стабилизировать физические и психического состояния, снять острые симптомы употребления алкоголя, наркотиков или лекарственных веществ.
Изучить вопрос глубже – нарколог на дом цена в казани
MichaelSunda · May 22, 2026 at 9:33 pm
Этот документ охватывает важные аспекты медицинской науки, сосредотачиваясь на ключевых вопросах, касающихся здоровья населения. Мы рассматриваем свежие исследования, клинические рекомендации и лучшие практики, которые помогут улучшить качество лечения и профилактики заболеваний. Читатели получат возможность углубиться в различные медицинские дисциплины.
Подробнее можно узнать тут – стоп алко краснодар
Anthonybom · May 22, 2026 at 10:02 pm
В этой публикации мы исследуем ключевые аспекты здоровья, включая влияние образа жизни на благополучие. Читатели узнают о важности правильного питания, физической активности и психического здоровья. Мы предоставим практические советы и рекомендации для поддержания здоровья и развития профилактических подходов.
Где почитать поподробнее? – «Похмельная служба» в Краснодаре
Henrypieda · May 22, 2026 at 10:03 pm
Реабилитация наркоманов по методу 12 шагов может сочетаться с психотерапией, групповой терапией, консультацией нарколога, работой психолога, наблюдением врача, медикаментозной терапией, стационаром, детоксикацией и помощью родственникам. Если человек находится в острой интоксикации, переживает ломку, запой, похмельный синдром, тревогу, бессонницу, психоз или выраженное физическое истощение, сначала может потребоваться наркологическая помощь, срочный вызов, стационар, снятие ломки, капельница, вывод из запоя или детоксикация. После стабилизации начинается реабилитация как отдельная программа, направленная на долгосрочные изменения.
Выяснить больше – reabilitaciya-12-shagov
Darrellmab · May 22, 2026 at 10:13 pm
В этой статье рассматриваются различные аспекты избавления от зависимости, включая физические и психологические методы. Мы обсудим поддержку, мотивацию и стратегии, которые помогут в процессе выздоровления. Читатели узнают, как преодолеть трудности и двигаться к новой жизни без зависимости.
Рассмотреть проблему всесторонне – «Похмельная служба» в Краснодаре
Aaronpep · May 22, 2026 at 10:13 pm
Помощь оказывается только при согласии пациента или его законного представителя. Данные не передаются соседям, на работу или третьим лицам: анонимность, учет персональных данных, обработка сведений и защита личной информации выполняются в соответствии с политикой конфиденциальности, пользовательским соглашением и действующими требованиями РФ.
Детальнее – вывод из запоя на дому цена в сочи
Robertcug · May 22, 2026 at 10:25 pm
Для бизнеса аренда сервера — это прежде всего вопрос надёжности, высокой скорости и поддержки в любое время суток. Компания Netrack предлагает сервер в аренду с гарантированным аптаймом 99,9% и размещением в собственном дата-центре уровня Tier III. Требуется сервер в аренду? На сайте https://netrack.ru/ можно выбрать конфигурацию под любые задачи — от стартапа до крупного корпоративного проекта. Пользователь работает на выделенном железе без совместного использования ресурсов и получает профессиональную техподдержку на каждом этапе.
Shaunarock · May 22, 2026 at 10:26 pm
В данной публикации мы поговорим о процессе восстановления от зависимости, о том, как вернуть себе нормальную жизнь. Мы обсудим преодоление трудностей, значимость поддержки и наличие программ реабилитации. Читатели смогут узнать о ключевых шагах к успешному восстановлению.
Прочесть всё о… – Наркологическая клиника «Похмельная служба» в Краснодаре
MichaelSunda · May 22, 2026 at 10:53 pm
В этой статье мы рассматриваем разрушительное влияние зависимости на жизнь человека. Обсуждаются аспекты, такие как здоровье, отношения и профессиональные достижения. Читатели узнают о необходимости обращения за помощью и о путях к восстановлению.
Переходите по ссылке ниже – стоп алко краснодар
totihaSax · May 22, 2026 at 10:57 pm
Издание «Український оглядач» придерживается чёткого редакционного кредо — оглядаємо, аналізуємо, висловлюємо думку — и публикует материалы об Украине, мире, политике, экономике, криминале и бизнесе без уклончивых оценок. Авторы издания расследуют коррупционные механизмы и готовят предметную аналитику с опорой на верифицированные данные и доказательную фактуру. Читайте независимую аналитику на https://obozrevatel.org/ — украинский медиаресурс для аудитории ценящей глубину анализа и честную журналистскую позицию. Разделы технологий, культуры и здоровья органично расширяют редакционный охват и превращают портал в универсальный медиаисточник для разноплановой аудитории.
RonaldIllem · May 22, 2026 at 11:28 pm
Эта публикация раскрывает психологические механизмы зависимости и их роль в развитии расстройств. Читатель узнает о том, как психология влияет на формирование зависимостей и как профессиональная помощь может изменить ситуацию.
Ознакомьтесь с аналитикой – Похмельная служба в Краснодаре
DavidBaisa · May 22, 2026 at 11:30 pm
Публикация посвящена жизненным историям людей, успешно справившихся с зависимостью. Мы покажем, что выход есть, и он начинается с первого шага — принятия проблемы и желания измениться.
Углубиться в тему – «Похмельная служба» в Краснодаре
Williamslive · May 22, 2026 at 11:38 pm
Добрый день!
Прага карлов мост украшен статуями святых и музыкантами утром. Вид на Пражский Град с моста считается классическим открыточным. Часовая башня на Староместской площади бьет курантами каждый час. Пиво в Чехии дешевле воды и очень качественного разлива.
Полная информация по ссылке – https://aldita.net/
Азия турция каподокия, Цветочный салон букеты, Америка панама канал
Куала-Лумпур башни, Куала-Лумпур башни, Симферополь ворота Крыма
Всего наилучшего и хорошей информации!
RogerDem · May 23, 2026 at 12:18 am
Обзор посвящён процессу восстановления после зависимостей. Мы расскажем о различных этапах реабилитации, поддерживающих ресурсах и важности мотивации в достижении устойчивого выздоровления.
Только для своих – «Похмельная служба» в Краснодаре
Coreycrani · May 23, 2026 at 12:21 am
В данной статье мы поговорим о будущем медицины, акцентируя внимание на прорывных разработках и их потенциале. Читатель узнает о новых подходах к лечению, роли искусственного интеллекта и возможностях персонализированной медицины.
Продолжить изучение – Похмельная служба в Краснодаре
pepaltKig · May 23, 2026 at 12:24 am
Ищете отдых у озера Банное? Посетите сайт https://xn—-8sbcki1cacg7a8a1e.xn--p1ai/ и вы найдете жильё с фото и ценами, а также уютные коттеджи, бунгало и апартаменты для большой компании или семьи. На нашем сайте — жильё по категориям, расположенным возле озера Банное (Якты Куль), рядом с ГЛЦ Металлург Магнитогорск, ГЛК Абзаково, в Новоабзаково — у подножия Уральских гор, в лесу и возле озера. Онлайн бронирование! Найдите идеальное жильё у нас!
Charlesonert · May 23, 2026 at 12:27 am
Melbet радует крупными акциями моментальные выплаты.
Свежее зеркало на сегодня — работает без ВПН.
(орфография по запросу: «зекало»)
Мелбет зеркало рабочий или официальный сайт — полностью синхронны.
Source:
бк мелбет официальный
BobbyDitte · May 23, 2026 at 12:35 am
Complete Deadlock deadlock1 hub for English speakers. Latest patches, hero counters, item tier lists, community builds, step?by?step guides, pro match analysis, tournament brackets, and esports news. All in one site – perfect for beginners and competitive players alike.
Stevensat · May 23, 2026 at 12:40 am
UFC Rankings 2026 https://ufcfans.net/ updated weekly. Detailed tables for each division: heavyweight, light heavyweight, middleweight, welterweight, lightweight, featherweight, bantamweight, flyweight, and women’s classes.
puzachSwito · May 23, 2026 at 1:00 am
Компания SeoBomba.ru специализируется на профессиональном продвижении интернет-ресурсов с использованием современных методик SEO-оптимизации, обеспечивая клиентам стабильный рост позиций в поисковых системах. Агентство предлагает комплексные услуги по наращиванию ссылочной массы через качественные форумные размещения, социальные сигналы и вечные ссылки, что позволяет достичь устойчивых результатов без риска санкций со стороны поисковиков. На сайте https://seobomba.ru/ представлен широкий спектр инструментов для веб-мастеров, включая генераторы паролей, анализаторы текста и семантические сервисы, которые существенно упрощают работу над проектами. Клиенты отмечают оперативность выполнения заказов, индивидуальный подход к каждому проекту и прозрачную ценовую политику, что подтверждается положительными отзывами специалистов различных направлений интернет-маркетинга.
fayafrdTwift · May 23, 2026 at 1:50 am
Компания «Мото ДВ» зарекомендовала себя как надежный поставщик мототехники на российском рынке, предлагая широкий ассортимент квадроциклов, мотоциклов и скутеров для различных целей эксплуатации. В каталоге представлены модели ведущих производителей с разнообразными техническими характеристиками, что позволяет подобрать транспортное средство как для начинающих райдеров, так и для опытных любителей активного отдыха. Ознакомиться с актуальным модельным рядом можно на странице https://market.yandex.ru/business–moto-dv/213757648, где представлена детальная информация о каждой единице техники. Компания обеспечивает оперативную доставку по России, предоставляет официальную гарантию на всю продукцию и консультационную поддержку при выборе оптимальной модели, что делает покупку максимально комфортной для клиентов.
Горгоний · May 23, 2026 at 2:14 am
Освойте SEO для своего сайта в Краснодаре — блог с инструкциями для предпринимателей https://website-income.ru/
Matthewknich · May 23, 2026 at 2:24 am
В этой статье мы рассматриваем разрушительное влияние зависимости на жизнь человека. Обсуждаются аспекты, такие как здоровье, отношения и профессиональные достижения. Читатели узнают о необходимости обращения за помощью и о путях к восстановлению.
Смотрите также – Похмельная служба Краснодар
WilliamRigog · May 23, 2026 at 2:36 am
Этот краткий обзор предлагает сжатую информацию из области медицины, включая ключевые факты и последние новости. Мы стремимся сделать информацию доступной и понятной для широкой аудитории, что позволит читателям оставаться в курсе актуальных событий в здравоохранении.
Ознакомиться с полной информацией – Похмельная служба в Краснодаре
revaStoma · May 23, 2026 at 2:39 am
Качество воды в многоквартирных домах и коммунальных объектах — системная проблема, требующая инженерного решения. Компания PWS разрабатывает коммунальные установки очистки воды, адаптированные к реальному составу воды в российских регионах. Подробнее о решениях — на https://pws.world/kommunalnye-ustanovki. Технология ионизирующей ультрафильтрации удаляет до 99% железа, органики и микроорганизмов. Все компоненты производятся в России, сервис доступен в любом регионе.
Jamesstese · May 23, 2026 at 2:48 am
Этот обзор содержит информацию о передовых достижениях в области медицины. Мы разберем инновационные технологии, которые меняют подход к лечению и диагностике, а также их влияние на эффективность оказания медицинской помощи.
Ознакомьтесь поближе – Похмельная служба в Краснодаре
Leroyhob · May 23, 2026 at 3:35 am
Публикация знакомит читателей с различными подходами к реабилитации. От традиционных методов до современных программ — вы узнаете, как выбрать оптимальный путь к выздоровлению и преодолеть препятствия на этом пути.
Изучить рекомендации специалистов – Кодирование от алкоголизма
Chrisbup · May 23, 2026 at 3:52 am
Этот текст представляет собой обзор свежих данных и исследований в области медицины. Он призван помочь читателям понять, как научные достижения влияют на лечение, диагностику и общее состояние системы здравоохранения.
Откройте для себя больше – «Похмельная служба» в Краснодаре
Shaunarock · May 23, 2026 at 3:56 am
Этот обзор содержит информацию о передовых достижениях в области медицины. Мы разберем инновационные технологии, которые меняют подход к лечению и диагностике, а также их влияние на эффективность оказания медицинской помощи.
Ознакомьтесь поближе – Похмельная служба Краснодар
Williamslive · May 23, 2026 at 4:03 am
Добрый день!
Будапешт купальни Сечени работают круглый год даже зимой. Пары играют в шахматы прямо в теплой термальной воде. Комплекс расположен в городском парке и очень популярен. Ночные вечеринки в руин барах дополняют оздоровительный отдых драйвом.
Полная информация по ссылке – https://aldita.net/
Якутск полюс холода, что посмотреть в Париже, пляжи Пхукета рейтинг
Справочная информация телефон, Музей янтаря солнечный камень, Квест перформанс страх
Всего наилучшего и хорошей информации!
Robertwhosy · May 23, 2026 at 4:03 am
вызов нарколога на дом круглосуточно позволяет получить профессиональную помощь в любое время суток.
Получить дополнительную информацию – нарколог на дом цена казань
kasyno online opinie · May 23, 2026 at 4:25 am
you may have an ideal blog here! would you prefer to make some invite posts on my blog?
DavidBaisa · May 23, 2026 at 4:53 am
Эта статья освещает различные аспекты освобождения от зависимости и пути к выздоровлению. Мы обсуждаем важность осознания своей проблемы и обращения за помощью. Читатели получат практические советы о том, как преодолевать трудности и строить новую жизнь без зависимости.
Смотрите также – «Похмельная служба» в Краснодаре
Leroyhob · May 23, 2026 at 5:16 am
Публикация знакомит читателей с различными подходами к реабилитации. От традиционных методов до современных программ — вы узнаете, как выбрать оптимальный путь к выздоровлению и преодолеть препятствия на этом пути.
Подробности по ссылке – Похмельная служба Краснодар
najlepsze kasyno online · May 23, 2026 at 7:10 am
If wings are your thing, Tinker Bell’s sexy Halloween costume design is all grown up.
JamesDog · May 23, 2026 at 7:22 am
В этой статье мы рассматриваем разрушительное влияние зависимости на жизнь человека. Обсуждаются аспекты, такие как здоровье, отношения и профессиональные достижения. Читатели узнают о необходимости обращения за помощью и о путях к восстановлению.
Обратитесь за информацией –
Williamslive · May 23, 2026 at 7:31 am
Доброго!
Ташкент метро и парки поражают красотой станций подземного дворца искусства. Каждая станция имеет уникальный дизайн с мрамором и люстрами богато. Парк имени Алишера Навои предлагает лодочные прогулки и аттракционы детям. Чорсу базар позволяет купить свежие фрукты и национальные лепешки.
Полная информация по ссылке – https://aldita.net/
Улан-Удэ голова ленина, Гранада Альгамбра, Дананг мост дракона
Поезд дальнего следования купе, Верона арена и Джульетта, Концерт поп звезды
Всего наилучшего и хорошей информации!
Robertthill · May 23, 2026 at 9:05 am
Вы получаете не просто разовую процедуру, а комплекс медицинской помощи. Врач нарколога может объяснить родственникам, как говорить с зависимым, что делать после капельницы, какие препараты принимать, когда необходимо лечение в клинике и почему кодирование алкоголизма или реабилитация часто становятся следующим этапом. Такой подход помогает не только вывести пациента из запоя, но и начать полноценное восстановление.
Получить дополнительную информацию – http://vyvod-iz-zapoya-kazan23.ru/
WilliamRigog · May 23, 2026 at 9:14 am
В статье по вопросам здоровья мы рассматриваем актуальные проблемы, с которыми сталкивается общество. Обсуждаются заболевания, факторы риска и важные аспекты профилактики. Читатели получат полезные советы о том, как сохранить здоровье и улучшить качество жизни.
Кликни и узнай всё! – нарколог на дом
Rogerinfed · May 23, 2026 at 9:16 am
Здравствуйте!
Если вы ищете недвижимость в Усть-Каменогорске, обратите внимание на свежие объявления на доске объявлений Natumbe. Здесь вы найдете объявления о продаже домов и квартир с фото и подробными описаниями. Бесплатные объявления доступны всем жителям города. Подать объявление можно прямо сейчас, и оно появится в разделе свежие объявления. Объявления Каменогорска помогут вам быстро найти то, что нужно.
Полная информация по ссылке – https://natumbe.kz
Климатическое оборудование, молдинги настенные декор, рюкзак трекинговый 60 литров
грузоперевозки по городу, Бизнес образование, берцы ботинки тактические
Всего наилучшего и хорошей информации!
CharlesCrify · May 23, 2026 at 9:26 am
The world of ultimate fighting t.me/s/UFClive_en/ expert predictions, MMA analysis, and exclusive content from inside the Octagon. Ultimate Fighting Championship news, fight breakdowns, fighter stats, and the main events of mixed martial arts.
ScottMew · May 23, 2026 at 9:30 am
Real-time Formula 1 https://t.me/s/f1vpe news. Race results, driver transfers, round analysis, interviews, and the main events of the FIA ??World Championship.
Nathanzem · May 23, 2026 at 9:37 am
you could try here
bitcoin payment api
Williamslive · May 23, 2026 at 9:57 am
Здравствуйте!
Стамбул голубая мечеть открыта для посетителей между молитвами строго. Шесть минаретов и внутренний декор из плитки поражают воображение. Айя-София находится прямо напротив через площадь Султанахмет быстро. Гранд базар рядом предлагает ковры специи и сувениры в изобилии.
Полная информация по ссылке – https://aldita.net/
Осло фиорды экскурсии, Пекарня свежая выпечка, Копенгаген русалочка
Фонарик свет в темноте, Куртка теплая зима, Новосибирск опера и зоопарк
Всего наилучшего и хорошей информации!
Rogerinfed · May 23, 2026 at 10:14 am
Добрый день!
На доске объявлений вы найдете множество вариантов для покупки и аренды недвижимости в Атырау. Объявления Атырау о продаже домов и квартир обновляются регулярно. Свежие объявления с фото и подробными описаниями помогут вам сделать правильный выбор. Бесплатные объявления доступны всем жителям Атырау. Подать объявление можно легко и быстро, просто заполнив форму на сайте.
Полная информация по ссылке – https://natumbe.kz
наушники bluetooth tws, массажер шейный электрический, фитнес браслет xiaomi
фритюрница домашняя, демонтаж зданий сооружений, саундбар акустика тв
Всего наилучшего и хорошей информации!
Парк аттракционов Екатеринбург · May 23, 2026 at 10:39 am
Парк аттракционов Екатеринбург
Darrellmab · May 23, 2026 at 10:44 am
Эта публикация посвящена актуальным вопросам современной медицины и здравоохранения. Мы обсудим новейшие технологии диагностики и лечения, а также их влияние на продолжительность и качество жизни. Читатель найдет здесь информацию о научных исследованиях и перспективных разработках, доступно изложенную для широкой аудитории.
Разобраться лучше – Наркологическая клиника «Похмельная служба» в Краснодаре.
mejores casinos online · May 23, 2026 at 10:48 am
I like what you have to offer. Keep up the good work!
najlepsze kasyna online · May 23, 2026 at 10:59 am
I simply could not leave your site before suggesting that I actually enjoyed the usual info a person supply in your visitors? Is going to be back often to inspect new posts
mejores casinos online · May 23, 2026 at 11:07 am
There are some serious financial ramifications here.
mejores casinos online · May 23, 2026 at 11:09 am
I can’t go into details, but I have to say its a good article!
kasyno online opinie · May 23, 2026 at 11:11 am
I am glad to be a visitor on this website!, regards for this rare information!
najlepsze kasyno online · May 23, 2026 at 11:11 am
You ma’am have a way with words. Thank you very much!
mejor casino online chile · May 23, 2026 at 11:12 am
I wish I could craft such articles as this. Thank you very much.
mejor casino online chile · May 23, 2026 at 11:16 am
I want to see your book when it comes out.
najlepsze kasyna online · May 23, 2026 at 11:24 am
I would really like to appreciate the endeavors you cash in on written this article. I’m going for the similar best product from you finding out in the foreseeable future as well. Actually your creative writing abilities has urged me to begin my very own blog now. Genuinely the blogging is distributing its wings rapidly. Your write down is often a fine illustration showing it.
mejores casinos online · May 23, 2026 at 11:26 am
Dude.. I am not much into reading, but somehow I got to read lots of articles on your blog. Its amazing how interesting it is for me to visit you very often. –
najlepsze kasyna online · May 23, 2026 at 11:35 am
Appreciation for taking the time to discuss this topic, I would love to discover more on this topic. If viable, as you gain expertise, would you object to updating the website with further information? It is tremendously beneficial for me.
Jameszer · May 23, 2026 at 1:03 pm
Этот информативный текст отличается привлекательным содержанием и актуальными данными. Мы предлагаем читателям взглянуть на привычные вещи под новым углом, предоставляя интересный и доступный материал. Получите удовольствие от чтения и расширьте кругозор!
Изучить эмпирические данные – «Похмельная служба» в Краснодаре
MichaelHox · May 23, 2026 at 1:24 pm
Вывод из запоя в Сочи необходим, когда человек не может самостоятельно выйти из состояния непрерывного употребления алкоголя, а самочувствие ухудшается даже после короткого перерыва. Запой опасен для здоровья, нервного системы, печени, сердца, сосудов и психики, поэтому обращаться за медицинской помощью лучше сразу, не дожидаясь недели тяжелого состояния.
Узнать больше – вывод из запоя на дому в сочи
shalmach 948 · May 23, 2026 at 1:48 pm
Сервис оценки недвижимости https://shalmach.pro помогает быстро узнать примерную стоимость объекта, возможные риски и рекомендации перед сделкой. Анализируйте состояние жилья, бюджет покупки и сценарии дальнейших действий до подписания договора.
Детская комната Екатеринбург · May 23, 2026 at 2:14 pm
Детская комната Екатеринбург
Dzamaguamb · May 23, 2026 at 2:38 pm
Добрый день!
Ошибки неизбежны, но они становятся опытом, если встроены в систему. Анализ условий, проверка данных и гибкость превращают промахи в основу будущих решений. Такой подход универсален и работает в любой сфере.
Если нужен отель рядом с морем в Махачкале — «Заря» подойдет. Чистые номера, Wi-Fi, парковка и спокойный район. Рядом Каспийское море и озеро Ак-Гёль. Хорошее соотношение цены и качества для отдыха или командировки.
Полная информация по ссылке – https://hotel05-zarya.ru/rooms/standard.html
гостиница заря в махачкале, махачкала отдых жилье, гостиница заря махачкала
отель на сутки махачкала, Отель Заря: официальный сайт | Парк «Ак-Гёль», гостиница заря в махачкале
Удачи и хорошего роста в топах!
Даже тень показывает, где есть свет.
Отель у моря — доступные номера 4945951
Dzamaguamb · May 23, 2026 at 2:53 pm
Доброго!
Иногда лучший совет — это напоминание о методе. Условия, проверенные данные и критика помогают построить решение, а адаптация закрепляет результат. Эта последовательность универсальна и полезна для всех.
Гостиница «Заря» предлагает номера рядом с морем. Чистота, уют и доступные цены делают проживание приятным. Отличный выбор для гостей города.
Полная информация по ссылке – https://hotel05-zarya.ru/guide/avar-theatre.html
гостиница заря в махачкале, отель возле моря махачкала, гостиница заря в махачкале
гостиница каспийское побережье махачкала, Отель Заря: официальный сайт | Контакты – адрес, телефон, карта, гостиница заря махачкала
Удачи и хорошего роста в топах!
Даже случайность может стать отправной точкой.
Уютный отдых у Каспия 5951a6e
DavidPew · May 23, 2026 at 4:54 pm
Доброго!
Комфорт и скорость передвижения по суше гарантируют экскурсии на автомобиле с персональным водителем и гибким графиком. Вы сможете охватить максимум достопримечательностей за один день, не тратя силы на долгие переходы пешком. Маршрут строится индивидуально под ваши интересы, с остановками в лучших видовых точках и кафе по пути. Кондиционер в салоне и мягкие кресла сделают поездку приятной даже в самую жаркую погоду. Доверьте логистику профессионалам и сосредоточьтесь на впечатлениях от увиденных красот и новых открытий.
Полная информация по ссылке – https://aldita.ru/
Аренда катера, Аренда авто С водителем Владивосток, Аренда Седан
Аренда Хэтчбек Владивосток, , Аренда катера Владивосток
Всего наилучшего и хорошей информации!
najlepsze kasyno online · May 23, 2026 at 4:56 pm
Only a smiling visitor here to share the love (:, btw outstanding style and design .
mejor casino online chile · May 23, 2026 at 5:07 pm
Beneficial Blog! I had been simply just debating that there are plenty of screwy results at this issue you now purely replaced my personal belief. Thank you an excellent write-up.
https://chantaltemam.com/docs/pgs/?melbet_promo_code_today___sign_up_welcome_bonus_html= · May 23, 2026 at 5:28 pm
https://chantaltemam.com/docs/pgs/?melbet_promo_code_today___sign_up_welcome_bonus_html=
mejor casino online chile · May 23, 2026 at 5:34 pm
When are you going to take this to a full book?
Rogerinfed · May 23, 2026 at 5:48 pm
Здравствуйте!
На доске объявлений вы найдете множество свежих объявлений о продаже недвижимости в Усть-Каменогорске. Объявления о продаже домов и квартир обновляются регулярно. Бесплатные объявления с фото и подробными описаниями помогут вам сделать правильный выбор. Подать объявление можно легко и быстро, просто заполнив форму на сайте. Объявления Каменогорска помогут вам найти идеальное жилье.
Полная информация по ссылке – https://natumbe.kz
стартер генератор ремонт, фура перевозка грузов, уборка квартир после ремонта
Требуется помощь, омега 3 рыбий жир, Развлечение / Фото / Видео
Всего наилучшего и хорошей информации!
mejores casinos online · May 23, 2026 at 6:11 pm
Like the way you’ve outlined things. Easy to follow. Not cluttered.
best online casino new zealand · May 23, 2026 at 6:13 pm
It’s a comprehensive, yet fast read.
tunesellBob · May 23, 2026 at 6:32 pm
Ищете Детский лагерь в Подмосковье? Посетите сайт https://campius.ru/ и ознакомьтесь с Кемпиус – это лагерь для детей 7-17 лет. Подарите ребёнку незабываемое лето с насыщенной программой, комфортным проживанием, ежедневным фотоотчётом, повышенным уровнем безопасности и санитарным контролем! Подробнее на сайте.
Rogerinfed · May 23, 2026 at 6:53 pm
Здравствуйте!
На доске объявлений Natumbe вы найдете множество вариантов для покупки и аренды недвижимости. Объявления Каменогорска о продаже домов и квартир обновляются регулярно. Свежие объявления с фото и подробными описаниями помогут вам сделать правильный выбор. Бесплатные объявления доступны всем жителям Усть-Каменогорска. Подать объявление можно легко и быстро, просто заполнив форму на сайте.
Полная информация по ссылке – https://natumbe.kz
молоток столярный, зарядное устройство универсальное, доска объявлений алматы
мотоциклы японские б у, форсунки инжектор чистка, плед флисовый теплый
Всего наилучшего и хорошей информации!
najlepsze kasyno online · May 23, 2026 at 6:54 pm
I think I might disagree with some of your analysis. Are the figures solid?
kasyno online opinie · May 23, 2026 at 6:59 pm
This is an awesome entry. Thank you very much for the supreme post provided! I was looking for this entry for a long time, but I wasn’t able to find a honest source.
Rogerinfed · May 23, 2026 at 7:44 pm
Добрый день!
Если вы ищете недвижимость в Усть-Каменогорске, обратите внимание на свежие объявления на доске объявлений Natumbe. Здесь вы найдете объявления о продаже домов и квартир с фото и подробными описаниями. Бесплатные объявления доступны всем жителям города. Подать объявление можно прямо сейчас, и оно появится в разделе свежие объявления. Объявления Каменогорска помогут вам быстро найти то, что нужно.
Полная информация по ссылке – https://natumbe.kz
линолеум продажа кз, уборка квартир после ремонта, магнитола андроид авто
Туризм / отдых / развлечения, клавиатура механическая игровая, вентилятор вытяжной ванная
Всего наилучшего и хорошей информации!
fixDiele · May 23, 2026 at 8:04 pm
Для тех, кто ищет информацию по теме “Финансовые советы и рынок рубля”, нашел много полезного.
Вот, можете почитать:
https://gazeta-rubl.ru
fixDiele · May 23, 2026 at 8:08 pm
Для тех, кто ищет информацию по теме “Глубокий анализ xG и матчей: Лаборатория Голов”, там просто кладезь информации.
Смотрите сами:
https://world-lab.ru
Michaelvab · May 23, 2026 at 8:20 pm
В этой статье обсуждаются актуальные медицинские вопросы, которые волнуют общество. Мы обращаем внимание на проблемы, касающиеся здравоохранения и лечения, а также на новшества в области медицины. Читатели будут осведомлены о последних событиях и смогут следить за тенденциями в медицине.
Изучить материалы по теме – Похмельная служба Краснодар
best online casino · May 23, 2026 at 8:20 pm
Some truly interesting info , well written and broadly user genial .
clique aqui · May 23, 2026 at 9:04 pm
Clipe do Fortune Dragon chegando.
Jasonvop · May 23, 2026 at 9:14 pm
Чтобы снять ограничения — запасной вход на Мелбет.
Свежее зеркало на сегодня — полная версия с бонусами.
Главный сайт melbet казино — быстрая проверка и вывод.
Мелбет зеркало прямо сейчас активно — без вирусов и рекламы.
Источник:
https://melbet-pjn.top
mejor casino online chile · May 23, 2026 at 9:26 pm
of course like your web-site however you have to check the spelling on several of your posts. Many of them are rife with spelling problems and I find it very troublesome to tell the reality then again I will surely come back again.
Rogerinfed · May 23, 2026 at 9:49 pm
Доброго!
В Усть-Каменогорске свежие объявления о продаже домов и квартир доступны на доске объявлений. Бесплатные объявления с фото и подробными описаниями помогут вам найти идеальное жилье. Объявления Каменогорска обновляются ежедневно, поэтому вы всегда будете в курсе новых предложений. Подать объявление можно прямо сейчас, и оно появится в разделе свежие объявления. Объявления Усть-Каменогорска помогут вам быстро найти то, что нужно.
Полная информация по ссылке – https://natumbe.kz
Тендеры, проточный водонагреватель, римские шторы пошив
ремонт стиральных машин, Аксессуары, пластырь бактерицидный рулон
Всего наилучшего и хорошей информации!
Rogerinfed · May 23, 2026 at 11:11 pm
Добрый день!
В Кызылорде свежие объявления о продаже домов и квартир доступны на доске объявлений. Бесплатные объявления с фото и подробными описаниями помогут вам найти идеальное жилье. Объявления Кызылорды обновляются ежедневно, поэтому вы всегда будете в курсе новых предложений. Подать объявление можно прямо сейчас, и оно появится в разделе свежие объявления. Объявления Кызылорды помогут вам быстро найти то, что нужно.
Полная информация по ссылке – https://natumbe.kz
видеонаблюдение установка, витаминный комплекс мультивитамины, материнская плата socket
панно интерьерное купить, соковыжималка шнековая центробежная, геймпад джойстик беспроводной
Всего наилучшего и хорошей информации!
Aviator Betano: como jogar · May 23, 2026 at 11:14 pm
Um regular do fórum colocou R$300 no Coelho e saiu com R$240. Sem print, só contou.
Detalhes do bônus TanoBet · May 23, 2026 at 11:18 pm
Stop-loss saudável pra slot de alta volatilidade tipo Fortune Dragon? 30%? 40%?
Отметить детский день рождения в Екатеринбурге · May 23, 2026 at 11:27 pm
Отметить детский день рождения в Екатеринбурге
Chinese dragon dance uniforms · May 23, 2026 at 11:43 pm
Spot on with this write-up, I really believe this website needs much more attention. I’ll probably be returning to read through more, thanks for the info!
DavidPew · May 24, 2026 at 12:17 am
Привет всем!
Суровая красота севера и древние крепости открываются тем, кто заказывает экскурсии Выборг с глубоким погружением в средневековую историю. Вы пройдете по узким мощеным улочкам, подниметесь на башню замка и услышите рассказы о рыцарях и шведских королях. Гиды в исторических костюмах создают атмосферу полного погружения, делая экскурсию живой и захватывающей для детей и взрослых. Маршрут включает посещение парков, музеев и лучших кафе с традиционной карельской кухней для полного впечатления. Откройте для себя уникальный уголок Европы в России и сделайте потрясающие фотографии на фоне старинной архитектуры.
Полная информация по ссылке – https://aldita.ru/
Пешие экскурсии, Аренда Honda, Аренда Тойота
Аренда Автобус Владивосток, , Аренда Хэтчбек
Всего наилучшего и хорошей информации!
kasyno online opinie · May 24, 2026 at 1:01 am
Thanks for your patience and sorry for the inconvenience!
best online casino nz · May 24, 2026 at 1:10 am
Its just like you read my thoughts! It’s like reading about my family.
kasyno online · May 24, 2026 at 1:37 am
whoah this weblog is great i really like studying your articles. Stay up the great work! You already know, lots of persons are looking round for this information, you can aid them greatly.
zofamcutty · May 24, 2026 at 1:43 am
ごけい キングダム, かんき, 魏火龍七師, キングダム 最新刊 ネタバレ, キングダム 呉慶 当サイト https://kingdom-kaitai.site/ をぜひご覧ください。情報は常に更新されていますので、最新のイベント情報を常に把握できます。当サイトはあらゆる情報が揃った総合情報源です!
https://stocksng.com/art/1xbet-free-promo-code-today-bonus.html · May 24, 2026 at 1:44 am
https://stocksng.com/art/1xbet-free-promo-code-today-bonus.html
Rogerinfed · May 24, 2026 at 1:44 am
Добрый день!
В Караганде свежие объявления о продаже домов и квартир доступны на доске объявлений. Бесплатные объявления с фото и подробными описаниями помогут вам найти идеальное жилье. Объявления Караганды обновляются ежедневно, поэтому вы всегда будете в курсе новых предложений. Подать объявление можно прямо сейчас, и оно появится в разделе свежие объявления. Объявления Караганды помогут вам быстро найти то, что нужно.
Полная информация по ссылке – https://natumbe.kz
раковина мойка накладная, пылесос циклонный мешок, зеркала боковые авто
утюг паровой вертикальный, Книги / журналы, видеодомофон монтаж
Всего наилучшего и хорошей информации!
https://yginekologa.com/articles/mostbet_promokod_pri_registracii.html · May 24, 2026 at 2:05 am
https://yginekologa.com/articles/mostbet_promokod_pri_registracii.html
obetcug · May 24, 2026 at 2:30 am
Для бизнеса аренда сервера — это прежде всего вопрос надёжности, высокой скорости и поддержки в любое время суток. Взять сервер в аренду у Netrack — значит получить гарантированный аптайм 99,9% и размещение в дата-центре уровня Tier III. Требуется аренда сервера? На сайте https://netrack.ru/ можно выбрать конфигурацию под любые задачи — от стартапа до крупного корпоративного проекта. Клиент получает выделенные ресурсы без соседей по железу и профессиональное техническое сопровождение на всех этапах работы.
najlepsze kasyno online · May 24, 2026 at 3:18 am
very good post, i certainly love this web site, keep on it
Stepanlet · May 24, 2026 at 4:42 am
Установка детского городка на участке — процесс несложный, если инструкция понятная. игровое оборудование для детей Хорошие производители комплектуют площадки всем необходимым крепежом и пошаговым руководством. детские качели Мы собрали комплекс вдвоём за один выходной.
Timofeylet · May 24, 2026 at 4:50 am
Скалодром на детской площадке — один из самых полезных элементов для физического развития. детская площадка для дачи Дети развивают силу рук и ног, учатся преодолевать трудности и становятся увереннее. уличный игровой комплекс А ещё это просто очень весело!
DavidPew · May 24, 2026 at 5:11 am
Добрый день!
Насладитесь красотой приморской столицы, заказав морские прогулки Владивосток с профессиональным сопровождением и интересной программой. Во время экскурсии вы увидите знаменитый Золотой мост, маяки и дикие скалистые берега с необычного ракурса. Наши гиды расскажут увлекательные истории о городе и его морских традициях прямо на борту уютного судна. Это идеальный способ провести романтический вечер или семейный выходной в окружении морской стихии. Позвольте себе отдохнуть от городской суеты и вдохнуть соленый воздух тихоокеанского побережья.
Полная информация по ссылке – https://aldita.ru/
Экскурсии Усть-Кокса, Аренда Автобус, Аренда парусной яхты
Аренда Rolls-Royce, , Аренда катера Дунай
Всего наилучшего и хорошей информации!
abeSot · May 24, 2026 at 5:18 am
Looking for an online yoga app for your home yoga practice? Visit https://yoga-for-beginners.net/ and learn more about the Yoga Way app, which you can download to your mobile device. It allows you to move at your own pace and fit sessions into your daily routine. Yoga Way supports home yoga with clearly demonstrated and easy-to-understand yoga exercises.
best online casino · May 24, 2026 at 6:52 am
How long does it take you to write an article like this?
DavidPew · May 24, 2026 at 7:01 am
Доброго!
Столичный ритм и близость к центру становятся доступнее с услугой аренда квартиры Владивосток для туристов и командировочных. Современные апартаменты с видом на море, Золотой мост или сопки создают неповторимую атмосферу приморского города. Вы будете жить в шаговой доступности от ресторанов, набережных и главных достопримечательностей, экономя время на транспорте. Полная меблировка, быстрый интернет и бытовая техника делают проживание максимально комфортным для работы и отдыха. Забронируйте квартиру во Владивостоке заранее и ощутите себя настоящим жителем этого динамичного портового города.
Полная информация по ссылке – https://aldita.ru/
Услуги экскурсовода, Аренда яхты Пхукет, Аренда катамарана
Экскурсии Петропавловск-Камчатский, , Глэмпинг Владивосток
Всего наилучшего и хорошей информации!
MarcusArota · May 24, 2026 at 7:43 am
При поступлении вызова нарколог незамедлительно приезжает на дом для проведения детального первичного осмотра. Врач собирает краткий анамнез, измеряет жизненно важные показатели — пульс, артериальное давление, температуру — и оценивает степень алкогольной интоксикации. Эти данные являются основой для разработки индивидуального плана лечения, позволяющего подобрать наиболее эффективные методы детоксикации.
Углубиться в тему – http://
Richarddat · May 24, 2026 at 7:51 am
В этом обзоре мы обсудим современные методы борьбы с зависимостями, включая медикаментозную терапию и психотерапию. Мы представим последние исследования и их результаты, чтобы читатели могли быть в курсе наиболее эффективных подходов к лечению и поддержке.
Прочесть заключение эксперта – капельница от запоя
sucibonOthen · May 24, 2026 at 8:42 am
ООО «РазВикТрейд» — белорусский производитель пресс-форм и изделий из пластика с опытом более 10 лет на рынках Беларуси и России. Компания выполняет полный цикл: от проектирования 3D-модели и изготовления пресс-формы до серийного литья и доставки готовой продукции. На https://press-forma.by/ доступен бесплатный расчёт стоимости проекта. Площадка в 1000 кв.м. с 24 единицами оборудования позволяет производить до 1,5 млн пластиковых изделий ежемесячно. Выгоднее китайских аналогов — чистая прибыль клиента вырастает в 2–3 раза.
DavidPew · May 24, 2026 at 8:50 am
Добрый день!
Гибкость и отсутствие обязательств характеризуют предложение, где недвижимость в аренду становится идеальным решением для временного проживания. Вы можете выбрать дом, квартиру или виллу в любой точке мира на срок от нескольких дней до нескольких лет. Это позволяет полностью погрузиться в жизнь нового города, избегая расходов и хлопот, связанных с покупкой собственного жилья. Наша база включает тысячи проверенных объектов с фото, отзывами и подробным описанием инфраструктуры вокруг. Найдите свой идеальный временный дом и наслаждайтесь свободой менять локации так часто, как вам хочется.
Полная информация по ссылке – https://aldita.ru/
Аренда байка Пхукет, Аренда парусной яхты, Экскурсии Владивосток
Аренда вертолета, , Аренда водной техники
Всего наилучшего и хорошей информации!
Timothyelapy · May 24, 2026 at 9:19 am
zumrut yesili hangi renkle uyumlu hakk?ndaki yaz?y? tavsiye ederim. Kendiniz gorun: https://hobiprojesi.com/articles/zumrut-yesili-uyumlu-renkler/
Парк развлечений для детей Екатеринбург · May 24, 2026 at 9:22 am
Парк развлечений для детей Екатеринбург
Timothyelapy · May 24, 2026 at 9:24 am
Ayr?ca, eger filli boya d?s cephe ev ornekleri konusuyla ilgileniyorsan?z, buray? inceleyin. Iste link: https://hobiprojesi.com/articles/filli-dis-cephe-boya-renkleri/
DavidPew · May 24, 2026 at 10:02 am
Доброго!
Американская классика и надежность ждут вас, когда вы оформляете аренда Chevrolet для путешествий по городу или длительных трассовых пробегов. Мы предлагаем широкий выбор моделей, от компактных седанов до вместительных внедорожников, находящихся в идеальном техническом состоянии. Все автомобили оснащены современными системами безопасности, климат-контролем и мультимедиа для максимального комфорта в пути. Гибкие тарифы, прозрачный договор и отсутствие скрытых комиссий делают наше предложение одним из самых выгодных на рынке аренды. Выберите свой Шевроле и отправляйтесь в дорогу с уверенностью в надежности и качестве вашего временного транспортного средства.
Полная информация по ссылке – https://aldita.ru/
Аренда гидроцикла Владивосток, Аренда Лексус, Туристическая недвижимость
Аренда виллы, , Пешие экскурсии
Всего наилучшего и хорошей информации!
EdwardOxign · May 24, 2026 at 10:18 am
about his best cosmos wallet
http://centroculturalrecoleta.org/blog/pages/?1xbet-promo-code-india-today_html= · May 24, 2026 at 11:07 am
http://centroculturalrecoleta.org/blog/pages/?1xbet-promo-code-india-today_html=
DavidPew · May 24, 2026 at 11:14 am
Добрый день!
Мощь и непритязательность российских дорог покоряются тем, кто выбирает аренду Уаз для своих загородных поездок и экспедиций. Эти автомобили созданы для суровых условий, где важна не красота, а способность доехать до точки назначения любой ценой. Просторный кузов позволяет перевозить большое количество груза, снаряжения или охотничьи трофеи без ограничений по весу. Наша команда обеспечит техническую исправность машины и проконсультирует по лучшим маршрутам для вашего региона. Выберите УАЗ и почувствуйте настоящую свободу передвижения там, где заканчиваются асфальтированные дороги.
Полная информация по ссылке – https://aldita.ru/
Аренда Автобус, Аренда авто Адлер, Аренда авто Пхукет
Аренда вертолета Владивосток, , Экскурсии на автомобиле
Всего наилучшего и хорошей информации!
suywPounc · May 24, 2026 at 11:38 am
Украинский информационный портал охватывает все ключевые сферы жизни — от политики и экономики до спорта и здоровья, предлагая читателям актуальные новости и глубокие аналитические материалы без лишних слов и домыслов. Журналисты портала подают информацию точно и без прикрас: расследовательские статьи, обзоры экономики и общественные репортажи появляются регулярно и удерживают большую читательскую аудиторию. Переходите на https://ukrnet.org/ — украинская всемирная сеть новостей для тех кто ценит качественную журналистику. Контент охватывает украинскую и глобальную тематику одновременно, что делает платформу ключевым медиаориентиром для требовательной аудитории.
TrustGuru.com.br · May 24, 2026 at 11:49 am
Tigrinho me carregou hoje, kkkk.
https://institutocea.com/layouts/inc/?el_codigo_promocional_1_html= · May 24, 2026 at 12:15 pm
https://institutocea.com/layouts/inc/?el_codigo_promocional_1_html=
世界盃杯世足賽 · May 24, 2026 at 1:41 pm
世界盃杯世足賽
2026 FIFA 世界盃 將會由 48 支球隊 參賽,整體賽程包含 12 個小組,每個小組由 4 支球隊組成。各組前兩名 可晉級 下一輪賽事,展開 16 強至決賽的淘汰賽程。
2026 世界盃 會在 2026 年 6 月 正式開踢。揭幕戰 將由 墨西哥迎戰南非,於 6 月 12 日 於阿茲特克球場開打。同日稍晚,南韓與捷克交手。接下來一天,加拿大對波士尼亞,以及美國對巴拉圭等小組賽首輪賽事將登場。
在小組分組上,A 組 由 墨西哥、南非、南韓與捷克;B 組 則由 加拿大、波士尼亞、卡達以及瑞士;C 組 則由 巴西、摩洛哥、海地及蘇格蘭構成。包括 巴西、法國、阿根廷、西班牙、英格蘭與德國等傳統強隊 皆已完成分組。
晉級淘汰賽階段 將於 7 月初 正式進行,16 強賽 將於 7 月 4 日 開踢,決賽則安排在 7 月 19 日 舉辦,最終將產生本屆世界盃冠軍。
歷史交手紀錄顯示,墨西哥與南非曾於 2010 年世界盃 交手,當時雙方以 1 比 1 握手言和,雙方仍無勝場差距。
此外,越位、黃牌、紅牌、VAR 與點球等規則,依然是觀看比賽時的重要觀念,球迷對規則判定仍十分關心。
RandallRoamp · May 24, 2026 at 1:59 pm
врач приезжает по указанному адресу в течение 1 часа после обращения (возможна и более быстрая реакция при необходимости).
Узнать больше – вызов нарколога на дом в казани
saxagndclunk · May 24, 2026 at 2:02 pm
Máquina tragamonedas Garage: una guía para jugar gratis en línea en https://tragamonedasgarage.com/ – prueba la tragamonedas en modo demo, entiende cómo funcionan los rodillos y descubre dónde jugar con dinero real, ¡además de obtener bonos de registro! En el sitio web, encontrarás una guía de Garage que te ayudará a ganar más.
DavidPew · May 24, 2026 at 2:09 pm
Добрый день!
Гибкость и выгода долгосрочного пребывания обеспечиваются тарифом аренда авто Посуточно Пхукет, который выбирают многие экспаты и путешественники. Чем дольше срок аренды, тем ниже суточная ставка, что делает использование личного транспорта очень экономичным решением. Вы получаете автомобиль в полное распоряжение на 24 часа с возможностью продления или замены модели при необходимости. Сервис включает доставку машины в отель, заправку бака и консультацию по местным правилам дорожного движения. Планируйте свои дни свободно, имея надежное транспортное средство под рукой в любом уголке острова.
Полная информация по ссылке – https://aldita.ru/
Аренда квартиры Владивосток, Аренда квартиры, Аренда Хонда
Аренда Хонда, , Аренда квартиры Пхукет
Всего наилучшего и хорошей информации!
EdwardOxign · May 24, 2026 at 2:29 pm
next leap wallet
EdwardOxign · May 24, 2026 at 2:57 pm
navigate to this website coin leap app
dazuxabofe · May 24, 2026 at 3:20 pm
Портал Vkursi.org работает под прямым редакционным принципом — тримаємо вас завжди в курсі важливих подій — и охватывает политику, экономику, бизнес, общество, здоровье, технологии и криминал без информационных задержек. Редакция публикует эксклюзивные расследования коррупционных схем и резонансные судебные истории подкреплённые документами и конкретными фактами. Держите руку на пульсе событий на https://vkursi.org/ — украинский новостной портал для читателей которым важна скорость и точность подачи информации. Разделы культуры и технологий усиливают новостное ядро издания и формируют из него многопрофильный медиаресурс для широкой ежедневной аудитории.
Richarddat · May 24, 2026 at 5:29 pm
В этом обзоре мы обсудим современные методы борьбы с зависимостями, включая медикаментозную терапию и психотерапию. Мы представим последние исследования и их результаты, чтобы читатели могли быть в курсе наиболее эффективных подходов к лечению и поддержке.
Узнайте всю правду – капельница от запоя
Моисей · May 24, 2026 at 6:39 pm
Стратегии SEO-продвижения, которые приносят клиентов из Москвы. Разборы, инструкции, результаты.
эффективное SEO продвижение
Аристарх · May 24, 2026 at 7:01 pm
Купить Synthol в России с гарантией оригинальности. Быстрая отправка и отличный результат. Синтол
EdwardOxign · May 24, 2026 at 7:59 pm
read leap wallet extension
TrustGuru Brasil Editorial · May 24, 2026 at 8:26 pm
O estudante de direito chamou o Ninja vs Samurai de “o único honesto” — meio brincando, meio não.
maxeplunics · May 24, 2026 at 9:02 pm
Visit https://letmevpn.com/ – this is an educational blog dedicated to VPN technologies, online privacy basics, and practical security practices for everyday internet users. We publish clear guides to VPN protocols, secure DNS, common leak scenarios, IP reputation, connection performance, and tracking methods used on today’s networks. The content is written to be useful for both beginners and readers seeking a more detailed understanding of how privacy systems function on real-world networks.
ColbyLooto · May 24, 2026 at 9:06 pm
Наш центр оказывает помощь при запое на дому, амбулаторно и в стационаре. Врач нарколог приезжает по адресу, проводит осмотр, оценивает физическое и психическое состояние пациента, подбирает препараты, ставит капельницу, дает рекомендации после процедуры и помогает выбрать дальнейшее лечение алкоголизма.
Узнать больше – вывод из запоя дешево казань
Jasonvop · May 24, 2026 at 9:35 pm
Постоянно работающий адрес — рабочая копия Melbet выручит.
Что заставляет игроков выбирать казино Мелбет — бонус на первый депозит до 100 000 ?.
Играйте в melbet casino без преград — свыше 4000 слотов.
Устали искать — вот оно — все функции казино и ставок.
Источник:
https://melbet-aka.top
https://3mna.fr/wp-content/pgs/code_promo_linebet_bonus_de_bienvenue.html · May 24, 2026 at 9:53 pm
https://3mna.fr/wp-content/pgs/code_promo_linebet_bonus_de_bienvenue.html
Timothyidobe · May 24, 2026 at 10:42 pm
Привет всем!
Зима в нашей стране сурова и непредсказуема. Узнайте, как подготовить машину к зиме в Казахстане, чтобы не замерзнуть в дороге. Замена жидкостей, резины и проверка аккумулятора спасут вас в морозы. Встречайте холода во всеоружии и с уверенностью.
Полная информация по ссылке – https://na-tumbe.kz/
микрофон для стримов и подкастов выбор, умная лампочка управление со смартфона, доходная недвижимость пассивный доход
срочный выкуп квартир Алматы, ремонт лодочных моторов Yamaha, выставка собак подготовка документы
Всего наилучшего и хорошей информации!
https://beh.sk/wp-content/pages/?code-promo-1xbet-bonus-inscription_html= · May 24, 2026 at 10:59 pm
https://beh.sk/wp-content/pages/?code-promo-1xbet-bonus-inscription_html=
ZacharyRax · May 24, 2026 at 11:26 pm
Основа лечения запоя — инфузионная терапия (капельница). Капельница позволяет быстро доставить необходимые лекарственные средства прямо в кровь, минуя желудок. Стандартная лечебная процедура включает введение солевых растворов, витаминного комплекса, успокоительных, ноотропов, гепатопротекторов, кардиопротекторов. Такая терапия снимает острую интоксикацию, восстанавливает водно-солевой баланс, улучшает работу сердца, печени, головного мозга. Лечение с помощью капельницы даёт облегчение уже через несколько часов: проходит тошнота, головная боль, тремор, снижается давление, налаживается сон. Эффективность лечения зависит от качества препаратов и опыта врача. Наши специалисты используют собственные проверенные методики, гарантируя безопасность. При лечении алкогольной зависимости капельница — только первый шаг. Далее лечение продолжается таблетированными формами (налтрексон, дисульфирам, Алгоминал, Эспераль). Медикаментозное лечение помогает снизить тягу к алкоголю и предотвратить срыв. Любое лечение индивидуально и зависит от длительности запоя, степени алкоголизации, тяжести состояния пациента на момент проведения лечения, наличия сопутствующей патологии и хронических заболеваний. Мы также проводим лечение наркотической зависимости, используя УБОД для снятия ломки от героина, метадона, солей, спайса, марихуаны, амфетамина. Однако основная специализация — лечение алкоголизма, прерывание запоев и восстановление после них.
Выяснить больше – vyvod-iz-zapoya-na-domu-v-balashihe
Timothyidobe · May 24, 2026 at 11:32 pm
Доброго!
Беспилотные такси в Астане тест проводятся для оценки технологии будущего. Искусственный интеллект управляет автомобилем безопаснее человека в некоторых ситуациях. Горожане могут стать первыми пользователями автономного транспорта в регионе. Следите за новостями расширения зоны покрытия роботакси в столице.
Полная информация по ссылке – https://na-tumbe.kz/
содержание домашних животных в квартире, купить дачу в Медео недорого, как выбрать автосалон в Алматы
автопродление объявления настройка, поводок-рулетка или обычный какой лучше, прописка на даче новый закон РК
Всего наилучшего и хорошей информации!
WilliamNerry · May 25, 2026 at 12:51 am
Обзор специализированных игровых движков
секс игрушки
MarcusArota · May 25, 2026 at 1:23 am
На данном этапе специалист уточняет, как долго продолжается запой, какой вид алкоголя употребляется и имеются ли сопутствующие заболевания. Тщательный анализ информации позволяет оперативно определить степень интоксикации и выбрать оптимальные методы терапии для быстрого и безопасного вывода из запоя.
Узнать больше – нарколог вывод из запоя
voogcrils · May 25, 2026 at 1:43 am
Новостной портал «Корреспондент» освещает события Украины и мира в режиме реального времени — политика, экономика, технологии, здоровье и общество без купюр и редакционных фильтров. Издание не уклоняется от острых тем: расследования коррупции, репортажи с передовой и аналитика бизнес-процессов выходят регулярно. Следите за актуальной повесткой на https://karrespondent.com/ — украинский новостной ресурс для читателей ценящих скорость и фактическую точность. Разделы культуры, технологий, конфликтов и общества создают разностороннее медиапространство и превращают ресурс в незаменимый инструмент для информированного читателя.
Albertgerie · May 25, 2026 at 3:06 am
Поведение пациента при алкогольной интоксикации может резко меняться: появляется агрессия, страх, потеря контроля, раздражительность, нарушение памяти, бессонница, депрессии, тревога, психозов. В таких случаях врач должен оценить состояние пациента и решить, возможен ли вывод из запоя на дому или требуется госпитализация в стационаре.
Подробнее можно узнать тут – наркологический вывод из запоя в сочи
https://mlmscript.in/images/pgs/1xbet_promo_code_free_bet_welcome_bonus.html · May 25, 2026 at 3:21 am
https://mlmscript.in/images/pgs/1xbet_promo_code_free_bet_welcome_bonus.html
Stevenrot · May 25, 2026 at 3:30 am
В статье по вопросам здоровья мы рассматриваем актуальные проблемы, с которыми сталкивается общество. Обсуждаются заболевания, факторы риска и важные аспекты профилактики. Читатели получат полезные советы о том, как сохранить здоровье и улучшить качество жизни.
Изучите внимательнее – стоп алко
Michaelvab · May 25, 2026 at 3:37 am
Эта статья освещает различные аспекты освобождения от зависимости и пути к выздоровлению. Мы обсуждаем важность осознания своей проблемы и обращения за помощью. Читатели получат практические советы о том, как преодолевать трудности и строить новую жизнь без зависимости.
Продолжить изучение – Наркологическая клиника «Похмельная служба» в Краснодаре.
taluphHob · May 25, 2026 at 4:15 am
Современные стеклянные перегородки трансформируют офисное пространство, создавая атмосферу открытости и профессионализма. Компания предлагает полный спектр архитектурных решений для бизнес-интерьеров: от классических систем Standart с алюминиевым профилем до инновационных компактных конструкций Slim для узких проёмов. На https://wall.glass/ представлены не только перегородки, но и дизайнерские светильники серий ORIO LINE и INI LED, акустические войлочные панели, которые обеспечивают комфортную звукоизоляцию. Производство и монтаж в Москве с гарантией качества.
http://umcpo.ru/wp-content/pages/promokod_na_1xbet_na_segodnya_besplatno.html · May 25, 2026 at 4:25 am
http://umcpo.ru/wp-content/pages/promokod_na_1xbet_na_segodnya_besplatno.html
바이낸스 가입 · May 25, 2026 at 5:35 am
I had fun reading this post. I want to see more on this subject.. Gives Thanks for writing this nice article.. Anyway, I’m going to subscribe to your rss and I wish you write great articles again soon.
바이비트 가입 · May 25, 2026 at 5:39 am
Glad to be one of several visitors on this awful internet site : D.
Timothyidobe · May 25, 2026 at 6:12 am
Добрый день!
Стуки в ходовой части раздражают и пугают водителя в пути. Стук в подвеске при повороте диагностика выявит изношенные шарниры. Замените детали вовремя и восстановите управляемость автомобиля на дороге. Ездите тихо и комфортно без посторонних звуков в салоне.
Полная информация по ссылке – https://na-tumbe.kz/
запас хода электромобиля зимой в РК, лакомства для дрессировки собак, оценка стоимости квартиры онлайн КазНИИЭСС
как выбрать электровелосипед для города Алматы, нейросети в смартфонах функции, как выселить недобросовестных жильцов закон РК
Всего наилучшего и хорошей информации!
바이낸스 가입 · May 25, 2026 at 6:33 am
I really love this article.
바이낸스 가입 · May 25, 2026 at 6:36 am
Just a quick note to express my appreciation. Take care
Timothyidobe · May 25, 2026 at 7:13 am
Доброго!
Установка счетчиков воды инструкция экономия коммунальных платежей savings. Платите только за реально потребленную воду, а не по нормативам bill. Простая установка и быстрая окупаемость прибора benefit. Подавайте показания ежемесячно для точного расчета charges.
Полная информация по ссылке – https://na-tumbe.kz/
кулер для процессора тихий и мощный, фитнес-браслет или умные часы, автопродление объявления настройка
редкие породы кошек фото и описание, съемка видео на смартфон настройки, автопродление объявления настройка
Всего наилучшего и хорошей информации!
boojndug · May 25, 2026 at 7:52 am
Компания «ВторСтекло» https://www.vtorsteklo.ru/ специализируется на приеме, вывозе и утилизации стеклянных отходов от населения и бизнеса. Организация работает на рынке более 20 лет, предлагая выгодные условия сотрудничества и оперативное обслуживание. Компания принимает различные виды стеклобоя: оконное стекло, стеклопакеты, бутылки и банки любых цветов и объемов. Собственный автопарк и спецтехника позволяют быстро организовать вывоз стекла с объектов клиентов, а также установить контейнеры для сбора отходов. Все собранное сырье направляется на перерабатывающие предприятия, где используется повторно в промышленности.
Timothyidobe · May 25, 2026 at 8:02 am
Привет всем!
Купить дачу в Медео недорого предложения загородной недвижимости в горах nearby. Живописные виды и чистый воздух привлекают горожан для отдыха weekends. Проверьте состояние дома и наличие коммуникаций перед покупкой объекта remotely. Оформление документов на землю и строение должно быть прозрачным и legal.
Полная информация по ссылке – https://na-tumbe.kz/
влажность в квартире нормы и измерения, фотобокс для предметной съемки DIY, симптомы бешенства у животных
весы напольные с анализом состава тела, прогулки с собакой правила выгула Алматы, выставка собак подготовка документы
Всего наилучшего и хорошей информации!
https://costaricacc.com/pages/1xbet-free-promo-code-today-bonus.html · May 25, 2026 at 8:52 am
https://costaricacc.com/pages/1xbet-free-promo-code-today-bonus.html
Alfredrab · May 25, 2026 at 8:53 am
Вывод из запоя в Казани на дому и в клинике: врач-нарколог, капельница, детоксикация, лечение алкоголизма, кодирование, реабилитация — круглосуточная помощь анонимно.
Узнать больше – скорая вывод из запоя казань
zodikilok · May 25, 2026 at 9:29 am
Model International — это глобальная информационно-рекламная площадка для взрослых, собирающая тысячи частных объявлений из разных стран в одном месте. Сервис предоставляет исключительно рекламное пространство — без посредников и агентств. https://model-international.com/ предлагает удобный интерфейс с быстрым поиском по городам и странам. Платформа стабильно наращивает аудиторию, а условия размещения объявлений чётко прописаны в публичном пользовательском соглашении.
Timothyidobe · May 25, 2026 at 10:00 am
Добрый день!
ТСЖ или управляющая компания что лучше управление домом в РК choice. ТСЖ позволяет жильцам самим контролировать расходы и качество services. УК предоставляет профессиональный сервис, но может быть менее прозрачной management. Выбор зависит от активности собственников и размера дома community.
Полная информация по ссылке – https://na-tumbe.kz/
аренда авто с выкупом условия Казахстан, черный список пользователей блокировка, первоначальный взнос по ипотеке сколько
вторичка или новостройка что выгоднее в Астане, скрытие номера телефона подменный, как выбрать автосалон в Алматы
Всего наилучшего и хорошей информации!
Forrestgop · May 25, 2026 at 10:34 am
Эта публикация содержит ценные советы и рекомендации по избавлению от зависимости. Мы обсуждаем различные стратегии, которые могут помочь в процессе выздоровления и важность обращения за помощью. Читатели смогут использовать полученные знания для улучшения своего состояния.
Хочу знать больше – Похмельная служба Туапсе
바이낸스 가입 · May 25, 2026 at 11:20 am
I am glad to be one of the visitors on this great site (:, appreciate it for putting up.
Timothyidobe · May 25, 2026 at 11:25 am
Здравствуйте!
Хотите сделать салон уникальным и стильным? Тюнинг салона автомобиля идеи помогут преобразить интерьер без больших затрат. Перетяжка руля, замена сидений или подсветка создадут уют. Создайте комфортную атмосферу для каждого путешествия на машине.
Полная информация по ссылке – https://na-tumbe.kz/
эвакуатор дешево круглосуточно Алматы, набор инструментов для автомобилиста список, как заменить масло в двигателе самостоятельно
подбор аккумулятора по марке автомобиля, авто из Кореи под заказ отзывы, ошибка загрузки фото
Всего наилучшего и хорошей информации!
https://efaflex.ru/include/pages/?gama_casino_promokod_html= · May 25, 2026 at 12:00 pm
https://efaflex.ru/include/pages/?gama_casino_promokod_html=
ArthurGer · May 25, 2026 at 1:06 pm
В этой статье рассматриваются способы преодоления зависимости и успешные истории людей, которые справились с этой проблемой. Мы обсудим важность поддержки со стороны близких и профессионалов, а также стратегии, которые могут помочь в процессе выздоровления. Научитесь первоочередным шагам к новой жизни.
Исследовать вопрос подробнее – детокс24
BernardSuize · May 25, 2026 at 1:07 pm
Эта публикация исследует взаимосвязь зависимости и психологии. Мы обсудим, как психологические аспекты влияют на появление зависимостей и процесс выздоровления. Читатели смогут понять важность профессиональной поддержки и применения научных подходов в терапии.
Ссылка на источник – детокс клиника
свежие вакансии в краснодере · May 25, 2026 at 1:44 pm
свежие вакансии в краснодере
Josephkew · May 25, 2026 at 1:45 pm
Эта медицинская заметка содержит сжатую информацию о новых находках и методах в области здравоохранения. Мы предлагаем читателям свежие данные о заболеваниях, профилактике и лечении. Наша цель — быстро и доступно донести важную информацию, которая поможет в повседневной жизни и понимании здоровья.
Ознакомиться с полной информацией – детоксикация наркозависимых
Timothyidobe · May 25, 2026 at 2:15 pm
Привет всем!
Влияние ставки вознаграждения на ипотеку динамика рынка в РК rates. Повышение ставки удорожает кредиты и снижает спрос borrowers. Снижение ставки стимулирует покупки и рост цен demand. Следите за решениями Нацбанка для прогнозирования trends.
Полная информация по ссылке – https://na-tumbe.kz/
съемка видео на смартфон настройки, замена термопасты на процессоре инструкция, лучшие семейные автомобили 2026
беспилотные такси в Астане тест, авто из Кореи под заказ отзывы, датчики протечки воды умный дом
Всего наилучшего и хорошей информации!
MichaelLek · May 25, 2026 at 2:49 pm
Статья посвящена анализу текущих трендов в медицине и их влиянию на жизнь людей. Мы рассмотрим новые технологии, методы лечения и значение профилактики в обеспечении долголетия и здоровья.
Выяснить больше – Похмельная служба в Воронеже
xuertuh · May 25, 2026 at 2:58 pm
Агентство «Свадьба 812» организует торжества в Санкт-Петербурге под ключ — от выездной регистрации и декора до фейерверков и живой музыки. Опытная команда ведёт свадьбы, корпоративные мероприятия, юбилеи и выпускные вечера. Ищете организация новогодних праздников? На svadba-812.ru собраны готовые проекты и полный каталог услуг с ценами. Агентство подбирает рестораны, фотографов, видеооператоров и артистов — клиент получает единое решение без лишних забот и самостоятельного поиска подрядчиков.
https://felomena.com/wp-includes/articles/?kent-casino-promokod_html= · May 25, 2026 at 4:15 pm
https://felomena.com/wp-includes/articles/?kent-casino-promokod_html=
login betano · May 25, 2026 at 4:29 pm
Pulando Fortune Mouse até o próximo patch.
BrianTup · May 25, 2026 at 4:40 pm
Эта публикация содержит ценные советы и рекомендации по избавлению от зависимости. Мы обсуждаем различные стратегии, которые могут помочь в процессе выздоровления и важность обращения за помощью. Читатели смогут использовать полученные знания для улучшения своего состояния.
Рассмотреть проблему всесторонне – Похмельная служба в Краснодаре
gefDgennick[SvynejeHelewoxyt,2,5] · May 25, 2026 at 4:48 pm
Besök https://www.ferieisverige.no/ för allt du behöver veta om semestrar i Sverige, inklusive Smultronställen Sverige-ladan och allt om Fjällbacka och Pås til Sverige. Örebro är utan tvekan det bästa stället att koppla av på – ta reda på mer om det, och julemärkt Sverige kommer att lämna ingen oberörd!
MichaelEcomi · May 25, 2026 at 4:51 pm
Эта статья сочетает познавательный и занимательный контент, что делает ее идеальной для любителей глубоких исследований. Мы рассмотрим увлекательные аспекты различных тем и предоставим вам новые знания, которые могут оказаться полезными в будущем.
Связаться за уточнением – Похмельная служба в Краснодаре
Pierreglubs · May 25, 2026 at 5:17 pm
Эта публикация раскрывает психологические механизмы зависимости и их роль в развитии расстройств. Читатель узнает о том, как психология влияет на формирование зависимостей и как профессиональная помощь может изменить ситуацию.
Узнать из первых рук – «Похмельная служба» в Волгограде
арбалет дум · May 25, 2026 at 5:39 pm
Салют,
Друзья.
Сейчас я бы хотел оповестить больше про арбалет мамба видео
Я думаю Вы думаете именно про арбалет дум мини или возможно желаете узнать больше про арбалет мамба агреггатор?!
Значит эта больше актуальная информация про арбалет haraon видео будет для вас наиболее полезной.
На нашем веб сайте малость больше про арбалет мамба видео, также информацию про арбалет мамба.
Узнай Больше на сайте https://bearhunter.ru/arbalet_doom_video про арбалет автомат дум агреггатор видео
Наши Теги: арбалет мамба агреггатор, арбалет дум армагедон видео, арбалет bearhunter обзор видео, арбалет haraon агрегатор видео,
Удачного Дня
арбалет bearhunter видео · May 25, 2026 at 5:40 pm
Здравия Желаю,
Коллеги.
В данный момент я бы хотел рассказать малость про арбалет haraon видео
Я думаю Вы мыслите именно про арбалет haraon видео или возможно желаете поведать больше про арбалет мамба агреггатор?!
Значит эта наиболее актуальная информация про арбалет дум видео будет для вас наиболее полезной.
На нашем сайте немного больше про арбалет дум, также информацию про арбалет дум мини agreggator.
Узнай Больше на сайте https://bearhunter.ru/arbalet_bearhunter_service_video про арбалет дум видео
Наши Теги: арбалет мамба, видео обзор арбалетов, стрелы bearhunter, мишени для арбалетов,
Удачного Дня
акссесуары для арбалетов · May 25, 2026 at 6:10 pm
Здравия Желаю,
Друзья.
В данный момент я бы хотел оповестить больше про арбалет haraon агрегатор видео
Я думаю Вы мыслите именно про арбалет мамба фаталити видео или возможно хотите поведать больше про арбалет мамба видео?!
Значит эта больше актуальная информация про арбалет автомат дум агреггатор видео будет для вас наиболее полезной.
На нашем веб портале немного больше про мишени для арбалетов, также информацию про видео обзор арбалетов.
Узнай Больше на сайте https://bearhunter.ru/misheni_i_aksessuary_dlya_arbaleta_video про арбалет дум видео
Наши Теги: арбалет дум мини, арбалет bearhunter обзор видео, арбалет bearhunter видео обзор, мишени для арбалетов,
Удачного Дня
Pierreglubs · May 25, 2026 at 6:18 pm
Эта публикация раскрывает психологические механизмы зависимости и их роль в развитии расстройств. Читатель узнает о том, как психология влияет на формирование зависимостей и как профессиональная помощь может изменить ситуацию.
Рассмотреть проблему всесторонне – Наркологическая клиника «Похмельная служба» в Волгограде.
арбалет haraon агрегатор видео · May 25, 2026 at 6:37 pm
Здравия Желаю,
Коллеги.
Сегодня я бы хотел оповестить больше про арбалет дум мини
Я думаю Вы в поиске именно про арбалет дум мини или возможно хотите узнать больше про арбалет дум армагедон видео?!
Значит эта оптимально актуальная информация про арбалет автомат haraon видео будет для вас наиболее полезной.
На нашем сайте малость больше про арбалет bearhunter видео обзор, также информацию про видео обзоры арбалетов.
Узнай Больше на сайте https://bearhunter.ru/arbalet_haraon_agreggator_video про арбалет bearhunter видео
Наши Теги: арбалет мамба фаталити видео, арбалет bearhunter обзор видео, арбалет haraon видео, арбалет дум мини,
Удачного Дня
luzuroStopy · May 25, 2026 at 6:43 pm
Профессиональная финская химия Teknos — надёжный выбор для долговечной защиты и декоративной отделки дерева. TEKNOL AQUA 1410-01 эффективно предотвращает биопоражения древесины, AQUA PRIMER 2900-02 гарантирует надёжное сцепление слоёв, а лак AQUATOP 2600-94 формирует стойкое защитно-декоративное покрытие. Ищете акрилатные фасадные краски? На teknotrend.ru представлен полный ассортимент оригинальной продукции Teknos с оптовыми ценами и быстрой доставкой по Москве и России.
zufacwhon · May 25, 2026 at 6:45 pm
ハイセンシとは シュラウド ヴァロラントの感覚 頂点の精神 ヴァロラントの感覚 これらはすべて当社の Web サイト https://gamersettings.net/ にあります – すべてのイベントの最新情報を入手できる最新情報をお見逃しなく
свежие вакансии · May 25, 2026 at 6:48 pm
вакансии сегодня
Tommynub · May 25, 2026 at 6:57 pm
Этот обзор медицинских исследований собрал самое важное из последних публикаций в области медицины. Мы проанализировали ключевые находки и представили их в доступной форме, чтобы читатели могли легко ориентироваться в актуальных темах. Этот материал станет отличным подспорьем для изучения медицины.
Что ещё? Расскажи всё! – лечение наркозависимости в краснодаре
saxukKak · May 25, 2026 at 6:59 pm
Компания «Элек-Опт» специализируется на оптовых поставках электротехнической продукции для строительных организаций, монтажных бригад и частных покупателей. Широкий ассортимент сертифицированной продукции охватывает все потребности в электромонтаже и освещении. Ищете кабель кгн хл? Заказать товар с доставкой по России можно на elek-opt.ru — актуальный каталог с быстрым оформлением заказа доступен круглосуточно.
gawigRhine · May 25, 2026 at 7:04 pm
Фотометрическая лаборатория «Сила Света» выполняет точные светотехнические измерения и выдаёт официальные протоколы с полной юридической силой. На http://silasveta-lab.ru/ доступна проверка подлинности любого протокола по уникальному коду или QR-коду — это исключает подделки и гарантирует достоверность данных. Лаборатория работает в строгом соответствии с нормативами и располагает актуальными свидетельствами о поверке средств измерений.
바이비트 가입 · May 25, 2026 at 7:10 pm
While this issue can vexed most people, my thought is that there has to be a middle or common ground that we all can find. I do value that you’ve added pertinent and sound commentary here though. Thank you!
바이비트 가입 · May 25, 2026 at 7:16 pm
You are not right. I am assured. I can prove it. Write to me in PM, we will talk.
JeremyONEDO · May 25, 2026 at 7:33 pm
Этот краткий обзор предлагает сжатую информацию из области медицины, включая ключевые факты и последние новости. Мы стремимся сделать информацию доступной и понятной для широкой аудитории, что позволит читателям оставаться в курсе актуальных событий в здравоохранении.
Прочитать подробнее – наркологическая клиника в анапе
바이비트 가입 · May 25, 2026 at 8:01 pm
whoah this weblog is great i really like studying your articles. Stay up the great work! You already know, lots of persons are looking round for this information, you can aid them greatly.
madyNouts · May 25, 2026 at 8:08 pm
Круизы по Москве-реке сегодня — это не просто речная прогулка, а полноценный вечер развлечений с музыкой, шоу и живыми выступлениями на теплоходе. Ежедневно на борту — дискотеки в стиле 80–90-х, DJ-вечеринки, концертные программы и VIP-круизы с ужином под живую музыку на любой вкус. Ищете диджей сеты на теплоходе москва? Билеты бронируются онлайн на ticketscruise.ru — быстро и без лишних шагов. Среди хитов сезона — концертный круиз «Хиты Италии» на теплоходе «Ривер Палас» от причала Сити-Экспоцентр.
바이낸스 가입 · May 25, 2026 at 8:10 pm
Certainly. And I have faced it. Let’s discuss this question. Here or in PM.
kajunmSuins · May 25, 2026 at 8:13 pm
シャチ 賢い, ドグラマグラ ネタバレ, 徒然草 作者, 詩集 小学生, 詩 短い. あなたはこれまで、こんな疑問を抱いたことがありますか?あるいは、答えがわからない他の疑問は?https://www.daremomiteinai.com/ にアクセスすれば、あなたのあらゆる疑問への答えが見つかります。このサイトは、あなたが答えを知らないかもしれない、重要かつ日常的な疑問に答えることに特化しています。
JeremyONEDO · May 25, 2026 at 8:33 pm
Эта публикация раскрывает психологические механизмы зависимости и их роль в развитии расстройств. Читатель узнает о том, как психология влияет на формирование зависимостей и как профессиональная помощь может изменить ситуацию.
Углубить понимание вопроса – детокс24
vucirUndex · May 25, 2026 at 8:46 pm
Планируете поездки по Калининграду на своих условиях? OmegaX сдаёт автомобили в аренду без водителя по честным ценам. Парк включает Renault Logan, Lada Vesta, Volkswagen Polo, KIA Rio — все на автомате. Ищете аренда автомобиля в Калининграде без водителя? Подробности и бронирование на omegax39.ru/arenda_prokat_avto_kaliningrad.html — офис находится прямо в аэропорту Храброво. Удобно для тех кто прилетает: забрал машину и сразу в путь.
Stevensueri · May 25, 2026 at 9:24 pm
Компания fastek https://fastek.by проектируем и поставляем надежные фасадные системы для коммерческих и жилых объектов, обеспечивая долговечность, энергоэффективность и безупречный внешний вид здания под ваши задачи.
RobertTit · May 25, 2026 at 9:39 pm
Этот документ охватывает важные аспекты медицинской науки, сосредотачиваясь на ключевых вопросах, касающихся здоровья населения. Мы рассматриваем свежие исследования, клинические рекомендации и лучшие практики, которые помогут улучшить качество лечения и профилактики заболеваний. Читатели получат возможность углубиться в различные медицинские дисциплины.
Обратиться к источнику – детокс24
RichardRaish · May 25, 2026 at 9:59 pm
В этом исследовании рассмотрены методы лечения зависимостей и их эффективность. Мы проанализируем различные подходы, используемые в реабилитационных центрах, и представим данные о результативности программ. Читатели получат надежные и научно обоснованные сведения о данной проблеме.
Прочитать подробнее – стоп алко
Charlesonert · May 25, 2026 at 10:15 pm
Для надёжного входа — рабочая ссылка на зекало мелбет.
Легальное онлайн-казино — высокий процент отдачи и джекпоты.
Действующий адрес melbet зекало — зеркало с опечаткой — просто скопируйте адрес.
Выбирайте, что удобнее — абсолютно те же функции.
Source:
melbet зекало рабочее
RobertTit · May 25, 2026 at 10:43 pm
В этой статье рассматриваются способы преодоления зависимости и успешные истории людей, которые справились с этой проблемой. Мы обсудим важность поддержки со стороны близких и профессионалов, а также стратегии, которые могут помочь в процессе выздоровления. Научитесь первоочередным шагам к новой жизни.
Прочитать подробнее – наркологическая клиника в краснодаре
Stanleygrier · May 25, 2026 at 10:45 pm
В данном обзоре представлены основные направления и тренды в области медицины. Мы обсудим актуальные проблемы здравоохранения, свежие открытия и новые подходы, которые меняют представление о лечении и профилактике заболеваний. Эта информация будет полезна как специалистам, так и широкой публике.
Переходите по ссылке ниже – Наркологическая клиника «Похмельная служба» в Краснодаре
ferakinlic · May 25, 2026 at 10:54 pm
Современные финансовые технологии открывают новые возможности для тех, кто оказался в сложной ситуации и нуждается в срочных средствах. Онлайн-займы стали настоящим спасением для миллионов россиян: заявка рассматривается за считанные минуты, а деньги поступают на карту практически мгновенно. На платформе https://xn—-7sbujpz2a7c.xn--p1ai/ собраны проверенные предложения от надёжных микрофинансовых организаций с прозрачными условиями. Особенно привлекательно, что новые клиенты могут получить первый займ под 0%, а одобрение возможно даже при непростой кредитной истории. Сервис работает круглосуточно, избавляя от необходимости посещать офисы и стоять в очередях — всё решается дистанционно за 15 минут.
JamesErync · May 25, 2026 at 11:16 pm
Этот краткий обзор предлагает сжатую информацию из области медицины, включая ключевые факты и последние новости. Мы стремимся сделать информацию доступной и понятной для широкой аудитории, что позволит читателям оставаться в курсе актуальных событий в здравоохранении.
Смотри, что ещё есть – наркологическая клиника в балашихе
Forrestgop · May 25, 2026 at 11:18 pm
Эта публикация содержит ценные советы и рекомендации по избавлению от зависимости. Мы обсуждаем различные стратегии, которые могут помочь в процессе выздоровления и важность обращения за помощью. Читатели смогут использовать полученные знания для улучшения своего состояния.
Погрузиться в научную дискуссию – Похмельная служба Туапсе
Jasonvop · May 25, 2026 at 11:31 pm
Постоянно работающий адрес — рабочая ссылка на зекало мелбет.
Вход в казино Мелбет за пару минут — высокий процент отдачи и джекпоты.
Главный сайт melbet казино — живое казино с настоящими дилерами.
Выбирайте, что удобнее — один аккаунт для двух входов.
Источник:
https://melbet-aka.top
GeorgeDob · May 25, 2026 at 11:51 pm
В этом обзоре представлены различные методы избавления от зависимости, включая терапевтические и психологические подходы. Мы сравниваем их эффективность и предоставляем рекомендации для тех, кто хочет вернуться к трезвой жизни. Читатели смогут найти информацию о реабилитационных центрах и поддерживающих группах.
Погрузиться в детали – Наркологическая клиника «Похмельная служба» в Воронеже.
Samuelfobia · May 25, 2026 at 11:55 pm
взять на карту займ https://srnalogcon.ru
ArthurGer · May 26, 2026 at 12:04 am
Эта публикация посвящена актуальным вопросам современной медицины и здравоохранения. Мы обсудим новейшие технологии диагностики и лечения, а также их влияние на продолжительность и качество жизни. Читатель найдет здесь информацию о научных исследованиях и перспективных разработках, доступно изложенную для широкой аудитории.
Секреты успеха внутри – наркологическая клиника краснодар
MichaelEcomi · May 26, 2026 at 12:14 am
В этой статье собраны факты, которые освещают целый ряд важных вопросов. Мы стремимся предложить читателям четкую, достоверную информацию, которая поможет сформировать собственное мнение и лучше понять сложные аспекты рассматриваемой темы.
Получить дополнительные сведения – нарколог на дом
https://shape-up-belt55.ru/wp-content/languages/de_DE/zakladka_vinogradnika_na_shpalerah.html · May 26, 2026 at 12:40 am
https://shape-up-belt55.ru/wp-content/languages/de_DE/zakladka_vinogradnika_na_shpalerah.html
WinstonRib · May 26, 2026 at 12:41 am
Эта публикация обращает внимание на важность профилактики зависимостей. Мы обсудим, как осведомленность и образование могут помочь в предотвращении возникновения зависимости. Читатели смогут ознакомиться с полезными советами и ресурсами, которые способствуют здоровому образу жизни.
Уникальные данные только сегодня – детоксикация алкоголиков
Tylerimper · May 26, 2026 at 12:53 am
Этот информационный материал подробно освещает проблему наркозависимости, ее причины и последствия. Мы предлагаем информацию о методах лечения, профилактики и поддерживающих программах. Цель статьи — повысить осведомленность и продвигать идеи о необходимости борьбы с зависимостями.
Наши рекомендации — тут – лечение алкоголизма в краснодаре
Josephkew · May 26, 2026 at 1:31 am
Мы рассмотрим современные вызовы здравоохранения и пути их решения с помощью технологий и научных исследований. В статье собраны данные о новых лекарствах, методах диагностики и системном подходе к улучшению здоровья населения.
Разобраться лучше – лечение алкоголизма в краснодаре
BernardSuize · May 26, 2026 at 1:49 am
Этот документ охватывает важные аспекты медицинской науки, сосредотачиваясь на ключевых вопросах, касающихся здоровья населения. Мы рассматриваем свежие исследования, клинические рекомендации и лучшие практики, которые помогут улучшить качество лечения и профилактики заболеваний. Читатели получат возможность углубиться в различные медицинские дисциплины.
Прочесть всё о… – лечение алкоголизма в краснодаре
Tylerimper · May 26, 2026 at 2:15 am
Этот информационный материал подробно освещает проблему наркозависимости, ее причины и последствия. Мы предлагаем информацию о методах лечения, профилактики и поддерживающих программах. Цель статьи — повысить осведомленность и продвигать идеи о необходимости борьбы с зависимостями.
ТОП-5 причин узнать больше – наркологическая помощь краснодар
Josephcroro · May 26, 2026 at 2:17 am
“evden sat?s siteleri” konusu icin mukemmel bir kaynak var. Iste link: https://yappendik.com/articles/evden-satis-yapma-yontemleri-ipuclari/
Josephcroro · May 26, 2026 at 2:23 am
“populer oyuncaklar” konusu icin mukemmel bir kaynak var. Iste link: https://renklikalpler.com/toy-trends/popular-trends/
Brentdip · May 26, 2026 at 2:23 am
Эта публикация исследует взаимосвязь зависимости и психологии. Мы обсудим, как психологические аспекты влияют на появление зависимостей и процесс выздоровления. Читатели смогут понять важность профессиональной поддержки и применения научных подходов в терапии.
Продолжить чтение – Наркологическая клиника «Похмельная служба» в Воронеже
demo grátis sem cadastro · May 26, 2026 at 2:31 am
A galera do twitch respeita mais os veteranos calados que o streamer mais barulhento.
Leroyscuch · May 26, 2026 at 2:53 am
В этой статье мы обсудим процесс восстановления после зависимостей, акцентируя внимание на различных методах и подходах к реабилитации. Читатели узнают, как создать план выздоровления и использовать полезные ресурсы для достижения устойчивых изменений.
Узнать напрямую – Похмельная служба в Воронеже
kicuzlheime · May 26, 2026 at 3:03 am
Интересный контент сегодня — это не просто развлечение, а способ узнавать новое каждый день. Сайт https://vseinteresno.com/ собирает познавательные материалы на самые разные темы: наука, история, природа, технологии и необычные факты со всего мира. Читатели находят здесь короткие и ёмкие статьи, которые расширяют кругозор без лишней воды. Если хочется каждый день открывать что-то новое — этот ресурс станет приятной привычкой для любознательного человека.
JeffreyCaf · May 26, 2026 at 3:24 am
В этой статье рассматриваются актуальные вопросы, связанные с развитием медицинской науки и её внедрением в повседневную практику. Особое внимание уделено вопросам профилактики, ранней диагностики и использованию технологий для улучшения здоровья человека.
Что ещё? Расскажи всё! – детокс24 краснодар
ElbertRusty · May 26, 2026 at 3:40 am
В этом исследовании рассмотрены методы лечения зависимостей и их эффективность. Мы проанализируем различные подходы, используемые в реабилитационных центрах, и представим данные о результативности программ. Читатели получат надежные и научно обоснованные сведения о данной проблеме.
Кликни, не пожалеешь – детокс24
Brentdip · May 26, 2026 at 4:02 am
Эта публикация раскрывает психологические механизмы зависимости и их роль в развитии расстройств. Читатель узнает о том, как психология влияет на формирование зависимостей и как профессиональная помощь может изменить ситуацию.
Смотрите также… – Наркологическая клиника «Похмельная служба» в Воронеже
RichardRaish · May 26, 2026 at 4:19 am
Этот текст посвящён сложным аспектам зависимости и её влиянию на жизнь человека. Мы обсудим психологические, физические и социальные последствия зависимого поведения, а также важность своевременного обращения за помощью.
Слушай внимательно — тут важно – Наркологическая клиника «Похмельная служба» в Таупсе.
JamesErync · May 26, 2026 at 4:47 am
В этой заметке мы представляем шаги, которые помогут в процессе преодоления зависимостей. Рассматриваются стратегии поддержки и чек-листы для тех, кто хочет сделать первый шаг к выздоровлению. Наша цель — вдохновить читателей на положительные изменения и поддержать их в трудных моментах.
Неизвестные факты о… – нарколога на дом в Балашихе
AnthonyCat · May 26, 2026 at 5:06 am
В этой статье мы рассматриваем разрушительное влияние зависимости на жизнь человека. Обсуждаются аспекты, такие как здоровье, отношения и профессиональные достижения. Читатели узнают о необходимости обращения за помощью и о путях к восстановлению.
Личный опыт — читайте сами – кодировка от алкоголя краснодар
MichaelLek · May 26, 2026 at 6:10 am
В этой статье рассматриваются способы преодоления зависимости и успешные истории людей, которые справились с этой проблемой. Мы обсудим важность поддержки со стороны близких и профессионалов, а также стратегии, которые могут помочь в процессе выздоровления. Научитесь первоочередным шагам к новой жизни.
Подробнее – Похмельная служба в Воронеже
fixDiele · May 26, 2026 at 6:26 am
Особенно понравился материал про Новости урбанистики и развития общественных пространств.
Ссылка ниже:
https://urbannew.ru
fixDiele · May 26, 2026 at 6:29 am
По теме “Управление личными финансами: секреты успеха”, нашел много полезного.
Смотрите сами:
https://money-rub.ru
Brianreoma · May 26, 2026 at 6:48 am
взять займ на карту https://rusel-garant.ru
WinstonRib · May 26, 2026 at 6:57 am
В этой публикации мы предложим ряд рекомендаций по избавлению от зависимостей и успешному восстановлению. Мы обсудим методы привлечения поддержки и важность самосознания. Эти советы помогут людям вернуться к нормальной жизни и стать на путь выздоровления.
Получить профессиональную консультацию – детоксикация алкоголиков
JosephBes · May 26, 2026 at 7:40 am
Этот текст представляет собой обзор свежих данных и исследований в области медицины. Он призван помочь читателям понять, как научные достижения влияют на лечение, диагностику и общее состояние системы здравоохранения.
Обратитесь за информацией – капельница от запоя
Lowellnaf · May 26, 2026 at 8:07 am
Эта публикация посвящена актуальным вопросам современной медицины и здравоохранения. Мы обсудим новейшие технологии диагностики и лечения, а также их влияние на продолжительность и качество жизни. Читатель найдет здесь информацию о научных исследованиях и перспективных разработках, доступно изложенную для широкой аудитории.
Узнать из первых рук – Похмельная служба Воронеж
dusaraNum · May 26, 2026 at 8:08 am
Группа компаний САФОРА — надежный производитель лакокрасочных материалов, предлагающий профессиональные решения для ремонта и творчества. В ассортименте представлены колеровочные пасты, акриловые эмали с различными эффектами, краски для любых поверхностей, лаки для дерева и стен, а также защитные составы от плесени и гидроизоляция. На сайте https://safora18.ru/ можно подобрать качественные материалы для отделки радиаторов, печей и каминов, найти специализированные художественные краски и лаки для декупажа. Компания также предлагает грунтовки, клеи, монтажную пену и другие строительные материалы собственного производства, что гарантирует стабильное качество продукции и доступные цены для профессионалов и частных заказчиков.
Robertthill · May 26, 2026 at 8:43 am
Вывод из запоя в Казани требуется, когда человек не может самостоятельно остановиться, пьет несколько дней подряд, теряет сон, аппетит, силы и нормальное самочувствие. Запой опасен не только похмельем: длительное употребление алкоголя нарушает работу печени, сердца, сосудистой системы, желудка, головного мозга и нервного состояния. В такой ситуации важно быстро вызвать врача нарколога на дому, чтобы получить медицинскую помощь, провести осмотр пациента и начать безопасное лечение.
Получить дополнительную информацию – вывод из запоя круглосуточно казань
AnthonyDrela · May 26, 2026 at 8:43 am
Вызов нарколога на дом в Казани. Круглосуточная наркологическая помощь: лечение алкоголизма, вывод из запоя, детоксикация, кодирование и консультация специалиста. Анонимно. Узнайте цену в клинике.
Получить дополнительную информацию – вызвать нарколога на дом казань
WilliamKip · May 26, 2026 at 9:21 am
займ без отказа на карту срочно https://tbcareer.ru
CarlosStage · May 26, 2026 at 9:30 am
В этом обзоре представлены различные методы избавления от зависимости, включая терапевтические и психологические подходы. Мы сравниваем их эффективность и предоставляем рекомендации для тех, кто хочет вернуться к трезвой жизни. Читатели смогут найти информацию о реабилитационных центрах и поддерживающих группах.
Читать полностью – Похмельная служба в Краснодаре
JeffreyCaf · May 26, 2026 at 10:15 am
В этой статье рассматриваются актуальные вопросы, связанные с развитием медицинской науки и её внедрением в повседневную практику. Особое внимание уделено вопросам профилактики, ранней диагностики и использованию технологий для улучшения здоровья человека.
Открой скрытое – детокс клиника
Lowellnaf · May 26, 2026 at 10:19 am
В этом обзоре мы обсудим современные методы борьбы с зависимостями, включая медикаментозную терапию и психотерапию. Мы представим последние исследования и их результаты, чтобы читатели могли быть в курсе наиболее эффективных подходов к лечению и поддержке.
Изучить аспект более тщательно – Наркологическая клиника «Похмельная служба» в Воронеже
wumdbeick · May 26, 2026 at 10:20 am
Психическое здоровье – частная психиатрическая клиника со стационаром https://psyclinic-center.ru/ . Руководитель клиники – доктор наук Виталий Минутко. Психиатрическая клиника занимается диагностикой и лечением депрессии, ОКР, анорексии, шизофрении, аутизма, биполярного расстройства, тиков, тревожности, неврозов, галюцинаций, деменции и других заболеваний.
Richardkjfms · May 26, 2026 at 10:32 am
Всем привет!
Сейчас присматриваюсь машину,
смотрю что есть на рынке.
Наткнулся интересный материал:
https://crimea-news.com/other/2026/01/16/1869428.html
Вроде довольно подробно разобрали вариант и ключевые особенности.
Интересен реальный опыт:
кто сталкивался,
как в реальности по ощущениям?
Есть ли смысл брать сейчас?
Заранее спасибо за отзывы.
https://vivachats.ru/ · May 26, 2026 at 11:14 am
discussed here https://vivachats.ru/
ElbertRusty · May 26, 2026 at 11:18 am
В этой статье мы рассматриваем разрушительное влияние зависимости на жизнь человека. Обсуждаются аспекты, такие как здоровье, отношения и профессиональные достижения. Читатели узнают о необходимости обращения за помощью и о путях к восстановлению.
Получить дополнительную информацию – детокс24 краснодар
xohepnZix · May 26, 2026 at 11:29 am
好きです韓国語, 韓国語 ね, はい 韓国語, はい韓国語, あらっそ 韓国語. これが何かわからない?それならウェブサイト https://kanayari.info/ にアクセスしてみてください。韓国語に関する質問も含め、あらゆる疑問への答えが見つかります。勉強にもなるし、面白いですよ!
CarlosStage · May 26, 2026 at 11:50 am
В этом исследовании рассмотрены методы лечения зависимостей и их эффективность. Мы проанализируем различные подходы, используемые в реабилитационных центрах, и представим данные о результативности программ. Читатели получат надежные и научно обоснованные сведения о данной проблеме.
Читать полностью – Похмельная служба в Краснодаре
xiwabemure · May 26, 2026 at 12:15 pm
Магазин электрики «Элекс» предлагает широкий выбор кабелей, автоматов, розеток, щитового оборудования и световых решений для дома и бизнеса. Весь товар поставляется от надёжных производителей и имеет необходимые сертификаты качества. Ищете кабель мг 1х10? На shop.elekspb.ru представлен удобный каталог с актуальными ценами и быстрым оформлением заказа. Удобная доставка по Санкт-Петербургу и всей России обеспечивает комфорт для профессионалов и частных покупателей.
vuzufascer · May 26, 2026 at 12:27 pm
«ЭЛЕКС» — специализированный электротехнический магазин с ассортиментом кабелей, проводов, электроустановочных изделий и светотехники для любых задач. Сертифицированная продукция охватывает полный спектр потребностей в электромонтаже и профессиональном освещении. Ищете купв 7х0 5? Заказать товар с доставкой по Санкт-Петербургу и регионам можно на elekspb.ru — актуальный каталог с быстрым оформлением заказа доступен круглосуточно.
GeorgeDob · May 26, 2026 at 1:35 pm
В данной публикации мы поговорим о процессе восстановления от зависимости, о том, как вернуть себе нормальную жизнь. Мы обсудим преодоление трудностей, значимость поддержки и наличие программ реабилитации. Читатели смогут узнать о ключевых шагах к успешному восстановлению.
Смотрите также – Нарколог на дом
tizirojaf · May 26, 2026 at 1:38 pm
Looking for terea sticks germany? Our easy-stick.com platform offers a wide selection of tobacco products with fast express delivery to Germany, France, Ireland, and Belgium. You will always find fresh Terea flavor varieties and up-to-date IQOS Iluma kits available at our store. We guarantee high quality and secure payments. Place your order today and take advantage of the most competitive prices and great conditions.
Robertserty · May 26, 2026 at 1:55 pm
В статье рассматриваются различные стратегии борьбы с зависимостями, включая проверенные методы и реальные истории успеха. Читатель узнает, какие подходы наиболее эффективны и как начать путь к выздоровлению.
Изучить материалы по теме – детоксикация от алкоголя
discuss.facts.net · May 26, 2026 at 1:59 pm
discuss.facts.net
LouisJorma · May 26, 2026 at 1:59 pm
Подробности внутри: https://eco-naturel.com
https://www.sib-souz.ru/images/pgs/?semy_prichin_zaderghki_menstruacii_html= · May 26, 2026 at 2:09 pm
for details https://www.sib-souz.ru/images/pgs/?semy_prichin_zaderghki_menstruacii_html=
Иона · May 26, 2026 at 2:14 pm
Продвижение строительных компаний в Новосибирске локальное продвижение Новосибирск
바이낸스 가입 · May 26, 2026 at 2:20 pm
Hello this is a wonderful write-up. I’m going to e mail this to my friends. I came on this while searching on yahoo I’ll be sure to come back. thanks for sharing.
doseddJeddy · May 26, 2026 at 3:20 pm
役立つ情報をお探しですか子供 留守番 何歳から 法律, ペーパードライバー 克服できなかった, 富良野 子供 ホテル, 小学校 個人面談 子供と一緒, 2人組 ?https://dragon737.com/ にアクセスすれば、これらのトピックをはじめ、あなたが興味を持つあらゆるトピックに関する包括的な情報を見つけることができます。このブログはユーザーフレンドリーな設計に
ColbyLooto · May 26, 2026 at 3:30 pm
Вывод из запоя в Казани на дому и в клинике: врач-нарколог, капельница, детоксикация, лечение алкоголизма, кодирование, стационар и реабилитация. Круглосуточная помощь анонимно.
Детальнее – вывод из запоя круглосуточно
Robertserty · May 26, 2026 at 4:07 pm
Читатели получат представление о том, как современные технологии влияют на развитие медицины. Обсуждаются новые методы лечения, персонализированный подход и роль цифровых решений в повышении качества медицинских услуг.
Продолжить чтение – клиника анонимная лечение наркомании
https://2ndopinion.ph/ · May 26, 2026 at 4:14 pm
get it here https://2ndopinion.ph/
LouisJorma · May 26, 2026 at 4:26 pm
Новое в категории: https://aromline.ru/index.php?productid=5445
Manuelnargo · May 26, 2026 at 4:39 pm
Эта публикация исследует взаимосвязь зависимости и психологии. Мы обсудим, как психологические аспекты влияют на появление зависимостей и процесс выздоровления. Читатели смогут понять важность профессиональной поддержки и применения научных подходов в терапии.
Читать далее > – «Похмельная служба» в Таупсе
JimmieApexT · May 26, 2026 at 4:58 pm
Эта статья освещает различные аспекты освобождения от зависимости и пути к выздоровлению. Мы обсуждаем важность осознания своей проблемы и обращения за помощью. Читатели получат практические советы о том, как преодолевать трудности и строить новую жизнь без зависимости.
Подробнее – закодироваться от алкоголя в краснодаре
bizihug · May 26, 2026 at 5:07 pm
В кафе «Фабрико» города Перми гостей ждут римская и неаполитанская пицца, роллы, суши, бургеры, супы, паста и десерты — всё по проверенным рецептам. Ищете доставка пиццы? На fab-pizza.ru можно оформить доставку или самовывоз со скидкой 10%. При заказе трёх больших пицц четвёртая достаётся в подарок, а именинники пользуются скидкой 15% в течение трёх дней до и после праздника. Уютный зал с панорамными окнами, детская зона и банкетные помещения на 25 гостей делают кафе отличным выбором для любого визита.
GarrettDroke · May 26, 2026 at 5:11 pm
В этой статье рассматривается комплексный подход к избавлению от зависимости. Читатель узнает, как сочетание физического, психологического и духовного восстановления помогает достичь стойкого выздоровления.
Продолжить чтение – detox24
Jefferyreada · May 26, 2026 at 5:34 pm
Эта публикация исследует взаимосвязь зависимости и психологии. Мы обсудим, как психологические аспекты влияют на появление зависимостей и процесс выздоровления. Читатели смогут понять важность профессиональной поддержки и применения научных подходов в терапии.
Кликни и узнай всё! – детокс24 краснодар
JosephBes · May 26, 2026 at 5:36 pm
В этой статье мы обсудим процесс восстановления после зависимостей, акцентируя внимание на различных методах и подходах к реабилитации. Читатели узнают, как создать план выздоровления и использовать полезные ресурсы для достижения устойчивых изменений.
Все материалы собраны здесь – Похмельная служба Краснодар
Georgedup · May 26, 2026 at 6:33 pm
Узнать больше здесь: https://spainslov.ru/site/word/word/%D0%A0%D0%95%D0%97%D0%9E%D0%9B%D0%AE%D0%A6%D0%98%D0%AF
Henrypieda · May 26, 2026 at 7:13 pm
Реабилитация наркоманов по методу 12 шагов может сочетаться с психотерапией, групповой терапией, консультацией нарколога, работой психолога, наблюдением врача, медикаментозной терапией, стационаром, детоксикацией и помощью родственникам. Если человек находится в острой интоксикации, переживает ломку, запой, похмельный синдром, тревогу, бессонницу, психоз или выраженное физическое истощение, сначала может потребоваться наркологическая помощь, срочный вызов, стационар, снятие ломки, капельница, вывод из запоя или детоксикация. После стабилизации начинается реабилитация как отдельная программа, направленная на долгосрочные изменения.
Подробнее – terapiya-12-shagov
BrianTup · May 26, 2026 at 8:20 pm
В этой статье рассматриваются актуальные вопросы, связанные с развитием медицинской науки и её внедрением в повседневную практику. Особое внимание уделено вопросам профилактики, ранней диагностики и использованию технологий для улучшения здоровья человека.
Продолжить изучение – стоп алко краснодар
https://amt-games.com/news/1xbet_promo_code_free_welcome_bonus.html · May 26, 2026 at 8:50 pm
watch https://amt-games.com/news/1xbet_promo_code_free_welcome_bonus.html
LeonardSlole · May 26, 2026 at 9:00 pm
В данной статье рассматриваются физиологические и эмоциональные аспекты зависимости. Мы обсудим, как организм реагирует на зависимое поведение, и какие методы помогают восстановить здоровье и внутреннее равновесие.
Посмотреть всё – «Похмельная служба» в Краснодаре
https://www.lectoreselectronicos.com/foro/showthread.php?19376-Alguien-ha-probado-nuevas-plataformas-de-juegos-este-mes=&p=257327#post257327 · May 26, 2026 at 9:42 pm
https://www.lectoreselectronicos.com/foro/showthread.php?19376-%C2%BFAlguien-ha-probado-nuevas-plataformas-de-juegos-este-mes=&p=257327#post257327
Tommynub · May 26, 2026 at 10:15 pm
Эта информационная публикация освещает широкий спектр тем из мира медицины. Мы предлагаем читателям ясные и понятные объяснения современных заболеваний, методов профилактики и лечения. Информация будет полезна как пациентам, так и медицинским работникам, желающим поддержать уровень своих знаний.
ТОП-5 причин узнать больше – наркологическая клиника краснодар
Georgedup · May 26, 2026 at 10:30 pm
Обязательно к прочтению: https://slovarsbor.ru/c/%d0%be/
https://gazetablic.com/new/?melbet_promo_code_free_welcome_bonus_html= · May 26, 2026 at 11:10 pm
see the original here https://gazetablic.com/new/?melbet_promo_code_free_welcome_bonus_html=
MarioLaurb · May 26, 2026 at 11:21 pm
Врач контролирует состояние пациента на протяжении всей процедуры — от первого введения препаратов до стабилизации самочувствия. Обычно уже через час после постановки капельницы уходит тошнота, нормализуется сон, снижается тревожность и тяга к спиртному. По завершении инфузионной терапии нарколог оставляет необходимые медикаменты на несколько дней, дает чёткие инструкции по их приёму и рекомендует дальнейшие шаги: амбулаторное наблюдение, кодирование или реабилитацию. После вывода из запоя обязательно даются рекомендации по продолжению лечения алкоголизма, включая кодирование и реабилитацию. Во многих случаях — да: в частной клинике платная помощь включает выездную стабилизацию, чтобы анонимно и быстро провести необходимые процедуры на месте.
Ознакомиться с деталями – нарколог на дом круглосуточно
Michaelsal · May 26, 2026 at 11:42 pm
В данной статье мы акцентируем внимание на важности поддержки в процессе выздоровления. Мы обсудим, как друзья, семья и профессионалы могут помочь тем, кто сталкивается с зависимостями. Читатели получат практические советы, как поддерживать близких на пути к новой жизни.
Выяснить больше – кодировка от алкоголя краснодар
WilliamNerry · May 26, 2026 at 11:48 pm
Публикация о чит-кодах
порно видео секс игрушки
Michaelsal · May 27, 2026 at 12:38 am
В данной статье мы акцентируем внимание на важности поддержки в процессе выздоровления. Мы обсудим, как друзья, семья и профессионалы могут помочь тем, кто сталкивается с зависимостями. Читатели получат практические советы, как поддерживать близких на пути к новой жизни.
Полезно знать – кодировка от алкоголя в краснодаре
Timothyelapy · May 27, 2026 at 12:52 am
tahta cesitleri hakk?ndaki bolumu cok sevdim. Suradan okuyabilirsiniz: https://kendihobim.com/articles/mobilya-tahta-cesitleri-kullanim-alanlari/
Albertgerie · May 27, 2026 at 1:27 am
основанием для вызова специалиста является неспособность человека самостоятельно выйти из состояния непрерывного употребления алкоголя и наличие признаков абстиненции.
Получить дополнительную информацию – нарколог на дом вывод из запоя сочи
Furniture Care · May 27, 2026 at 1:39 am
I keep listening to the news update lecture about getting boundless online grant applications so I have been looking around for the best site to get one. Could you tell me please, where could i find some?
my page :: http://www.music-player.dofollowlinks.org/News/bamboo-shades-an-accent-for-any-home/
MichaelCarie · May 27, 2026 at 2:21 am
Онлайн-сервис оценки недвижимости https://shalmach.pro по фотографиям для покупки, аренды и планирования ремонта. Узнайте ориентировочную стоимость жилья, возможные вложения и рекомендации перед принятием решения.
Charlesopend · May 27, 2026 at 3:13 am
Этот обзор посвящен успешным стратегиям избавления от зависимости, включая реальные примеры и советы. Мы разоблачим мифы и предоставим читателям достоверную информацию о различных подходах. Получите опыт многообразия методов и найдите подходящий способ для себя!
Ознакомиться с теоретической базой – detox24
Sergeylet · May 27, 2026 at 3:26 am
Плановое ТО проводят сами в рамках сервисного договора. Не нужно следить за регламентами и искать запчасти. Техника всегда в рабочем состоянии, простоев нет. официальный дилер спецтехники Казахстан
JimmieApexT · May 27, 2026 at 3:27 am
Эта доказательная статья представляет собой глубокое погружение в успехи и вызовы лечения зависимостей. Мы обращаемся к научным исследованиям и опыту специалистов, чтобы предоставить читателям надежные данные об эффективности различных методик. Изучите, что работает лучше всего, и получите информацию от экспертов.
Посмотреть подробности – детокс24 краснодар
Viktorlet · May 27, 2026 at 3:34 am
Удалённая диагностика работает отлично — подключаются к бортовой системе за минуту, решают вопросы без выезда. Большинство задач закрывается за 15-30 минут не останавливая работу. запчасти для тракторов Алматы
Carlosgog · May 27, 2026 at 4:23 am
Du suchst nach günstigen Replica Uhren? Unsere Modelle sehen aus wie das Original, zum Schnäppchenpreis.
Replica Rolex Modelle sind extrem beliebt. Unsere Daytona Kopien laufen präzise.
Replica Uhren sind optisch erste Klasse. Keiner sieht den Unterschied spricht fГјr sich.
https://www.beste-uhren.to/
casino chile · May 27, 2026 at 4:33 am
Thanks , I’ve recently been searching for info about this topic for ages and yours is the best I have discovered so far. But, what concerning the bottom line? Are you certain concerning the source?
https://rhslilygroup.org/wp-includes_new/inc/?1xbet_nepal__npr___np__1xbet_promo_code_nepal__30__html= · May 27, 2026 at 4:34 am
for details https://rhslilygroup.org/wp-includes_new/inc/?1xbet_nepal__npr___np__1xbet_promo_code_nepal__30__html=
Carlosgog · May 27, 2026 at 4:40 am
Eine Replica Uhr kaufen ist einfach in unserem Shop. Top-Qualität warten auf dich.
Die besten Replica Uhren findest du nur hier. Echte Saphirgläser machen den Unterschied.
Willst du Fake Uhren kaufen, die exakt wie echte aussehen? Dann vergleiche die Fotos.
https://www.beste-uhren.to/
Nohuwin · May 27, 2026 at 4:42 am
Might we expect to see more of these same problems in the future?
Nohuwin · May 27, 2026 at 4:45 am
Excellent article!! I am an avid reader of your website:D keep on posting that good content. and I’ll be a regular visitor for a very long time!!
neyavmjiz · May 27, 2026 at 4:47 am
中学生 詩, 神奈川県 高校入試日程, 変格活用 一覧, 茨城県公立高校入試, 八千代松陰 偏差値. ぜひ当社のウェブサイト https://manalab.jp/ をご覧ください!最新の情報が満載です。日本最大級のポータルサイトで、重要な知識を習得するお手伝いをいたします。
Carlosgog · May 27, 2026 at 4:52 am
Du suchst nach günstigen Replica Uhren? Unsere Modelle sehen aus wie das Original, zum Schnäppchenpreis.
Sind Replica Uhren legal? In Deutschland problematisch – aber privat unbedenklich.
Replica Uhren sind ideal fГјr den Alltag. Keiner sieht den Unterschied spricht fГјr sich.
https://www.beste-uhren.to/
Carlosgog · May 27, 2026 at 5:06 am
Wer Fake Uhren kaufen möchte, sollte auf Qualität achten. Wir bieten perfekte Nachbauten.
Die besten Replica Uhren findest du nur hier. Keine schlechten Fakes machen den Unterschied.
Replica Uhren sind echte Hingucker. Langlebig und schön spricht für sich.
https://www.beste-uhren.to/
Nohuwin · May 27, 2026 at 5:11 am
I found your blog through google and I must say, this is probably one of the best well prepared articles I have come across in a long time. I have bookmarked your site for more posts.
venoflmam · May 27, 2026 at 5:12 am
Трайбл — один из древнейших стилей татуировки, уходящий корнями в культуры Полинезии, Борнео и Маори, где каждый узор нёс сакральный смысл и рассказывал историю владельца. Сегодня этот стиль переживает настоящий ренессанс, а профессиональные мастера студии http://www.tribal-tattoo.ru/ воплощают его лучшие традиции в современных работах, создавая татуировки, которые остаются актуальными десятилетиями. Геометрическая строгость линий, глубокий чёрный цвет и ритмичные орнаменты делают трайбл одним из самых выразительных направлений в тату-искусстве — идеальный выбор для тех, кто ценит силу, эстетику и смысл в каждом штрихе.
Carlosgog · May 27, 2026 at 5:17 am
Eine Replica Uhr kaufen ist unkompliziert in unserem Shop. Schneller Versand warten auf dich.
Die besten Replica Uhren findest du in dieser Liste. Perfekte Zifferblätter machen den Unterschied.
Replica Uhren sind echte Hingucker. Langlebig und schön spricht für sich.
https://www.beste-uhren.to/
GarrettDroke · May 27, 2026 at 5:20 am
Эта статья подробно расскажет о процессе выздоровления, который включает в себя эмоциональную, физическую и психологическую реабилитацию. Мы обсуждаем значимость поддержки и наличие профессиональных программ. Читатели узнают, как строить новую жизнь и не возвращаться к старым привычкам.
Детальнее – кодировка от алкоголя краснодар
Carlosgog · May 27, 2026 at 5:38 am
Du suchst nach toptreuen Replica Uhren? Unsere Modelle sehen aus wie das Original, ohne den hohen Preis.
Sind Replica Uhren legal? In Deutschland problematisch – aber nicht für Weiterverkauf.
Willst du Fake Uhren kaufen, die niemand erkennt? Dann gib uns eine Chance.
https://www.beste-uhren.to/
Jefferyreada · May 27, 2026 at 5:51 am
Читатели получат представление о том, как современные технологии влияют на развитие медицины. Обсуждаются новые методы лечения, персонализированный подход и роль цифровых решений в повышении качества медицинских услуг.
Что ещё? Расскажи всё! – кодировка от алкоголя краснодар
Nohuwin · May 27, 2026 at 5:52 am
Thank you, I have just been searching for information about this topic for ages and yours is the greatest I’ve discovered till now. But, what about the conclusion? Are you sure about the source?
luzuroStopy · May 27, 2026 at 6:05 am
Профессиональная финская химия Teknos — надёжный выбор для долговечной защиты и декоративной отделки дерева. Антисептик TEKNOL AQUA 1410-01 надёжно защищает древесину от биопоражений, грунтовка AQUA PRIMER 2900-02 обеспечивает идеальное сцепление покрытий, а лак AQUATOP 2600-94 создаёт прочную декоративную плёнку. Ищете чем покрасить дом снаружи по дереву? На teknotrend.ru представлен полный ассортимент оригинальной продукции Teknos с оптовыми ценами и быстрой доставкой по Москве и России.
Carlosgog · May 27, 2026 at 6:17 am
Du suchst nach perfekten Replica Uhren? Unsere Modelle sehen aus wie das Original, ohne den hohen Preis.
Die besten Replica Uhren findest du online. Echte Saphirgläser machen den Unterschied.
Replica Uhren sind eine gГјnstige Alternative. Schneller Versand spricht fГјr sich.
https://www.beste-uhren.to/
Manuelnargo · May 27, 2026 at 6:23 am
Читатели получат представление о том, как современные технологии влияют на развитие медицины. Обсуждаются новые методы лечения, персонализированный подход и роль цифровых решений в повышении качества медицинских услуг.
Посмотреть всё – «Похмельная служба» в Таупсе
saxukKak · May 27, 2026 at 6:26 am
«Элек-Опт» занимается оптовыми поставками электротехники для строительных организаций, профессиональных монтажников и частных заказчиков. Широкий ассортимент сертифицированной продукции охватывает все потребности в электромонтаже и освещении. Ищете кмпвнг ls цена? Заказать товар с доставкой по России можно на elek-opt.ru — актуальный каталог с быстрым оформлением заказа доступен круглосуточно.
zotojpaype · May 27, 2026 at 7:20 am
Looking for guitar tuner? TronicalTune tronicaltune.net is a fully automatic guitar tuning system made in Germany. It tunes all six strings at the push of a button, saves time on stage and in the studio, and helps guitar players switch tunings fast and accurately. Ideal for electric and acoustic guitars.
jujakileshot · May 27, 2026 at 8:02 am
Платформа Adsguard представляет собой комплексное решение для защиты от навязчивой рекламы и обеспечения конфиденциальности в интернете. Сервис предлагает три ключевых продукта: AdGuard Block для блокировки баннеров и всплывающих окон, AdGuard VPN для анонимного серфинга с шифрованием трафика и AdGuard DNS для фильтрации вредоносного контента на уровне DNS-запросов. На портале https://adsguard.ru/ пользователи могут ознакомиться с актуальными обновлениями программного обеспечения, получить промокоды на выгодные условия подписки и найти ответы на часто задаваемые вопросы в разделе поддержки. Встроенный родительский контроль и регулярные обновления безопасности делают Adsguard надежным инструментом для комфортного использования интернета без отвлекающих факторов.
Alfredrab · May 27, 2026 at 8:15 am
Вывод из запоя на дому в Казани позволяет получить медицинскую помощь без очередей, учета и лишнего стресса. Врач приезжает по месту проживания, сохраняет конфиденциальность, спокойно говорит с пациентом и близкими, проводит первичную диагностику и начинает лечение только при наличии согласия. Если человек отказывается лечиться, доктор может провести мотивационную беседу, но принудительное лечение без законных оснований не проводится.
Углубиться в тему – вывод из запоя круглосуточно казань
nohu6.club · May 27, 2026 at 8:17 am
Please let us know when you plan to publish your book!
Nohuwin · May 27, 2026 at 8:18 am
Substantially, the post is really the best on this laudable topic. I concur with your conclusions and will eagerly watch forward to your future updates.Just saying thanx will not just be enough, for the wonderful lucidity in your writing.
Michaelgrani · May 27, 2026 at 8:24 am
Этот документ охватывает важные аспекты медицинской науки, сосредотачиваясь на ключевых вопросах, касающихся здоровья населения. Мы рассматриваем свежие исследования, клинические рекомендации и лучшие практики, которые помогут улучшить качество лечения и профилактики заболеваний. Читатели получат возможность углубиться в различные медицинские дисциплины.
Подробная информация доступна по запросу – detox24 в краснодаре
nohu4.club · May 27, 2026 at 9:02 am
Thanks for discussing the issues and covering them in a well written format.
Trực Tiếp Đá Gà · May 27, 2026 at 9:24 am
This blog post is excellent, probably because of how well the subject was developed. I like some of the comments too.
789P · May 27, 2026 at 9:38 am
Some truly interesting info , well written and broadly user genial .
casinos online nuevos · May 27, 2026 at 10:07 am
Spot on with this write-up, I truly believe this website requirements a lot much more consideration. I’ll probably be once more to read much much more, thanks for that info.
psychotypes.ru · May 27, 2026 at 10:59 am
shown here psychotypes.ru
MichaelHox · May 27, 2026 at 12:49 pm
При алкогольной интоксикации поведение пациента может стать неадекватным: появляется агрессия, страх, раздражительность, потеря памяти, психозов, галлюцинаций, тревожность, депрессии. В таких случаях врач должен оценить состояние пациента и определить, возможен ли вывод из запоя на дому или необходимо лечение в стационаре.
Детальнее – врач вывод из запоя в сочи
MarioLaurb · May 27, 2026 at 12:50 pm
Вывод из запоя — это только первый шаг в лечении алкогольной зависимости. Без последующей терапии риск рецидива очень высок. Наш наркологический центр предлагает полный курс лечения алкоголизма, включая кодирование и психотерапию. Кодирование на дому проводится различными методами: уколом (Торпедо, Эспераль, Налтрексон, Аквилонг), медикаментозным вшиванием (дисульфирам, Вивитрол), гипнозом по Довженко, а также двойным блоком. Каждый метод подбирается врачом индивидуально, с согласия пациента и при отсутствии противопоказаний. Опытный нарколог объяснит, какая кодировка подойдёт именно вам, учитывая стаж и форму зависимости.
Детальнее – запой нарколог на дом
Edwardmuh · May 27, 2026 at 1:30 pm
В этой публикации мы обсуждаем современные методы лечения различных заболеваний. Читатели узнают о новых медикаментах, терапиях и исследованиях, которые активно применяются для лечения. Мы нацелены на то, чтобы предоставить практические знания, которые могут помочь в борьбе с недугами.
Это стоит прочитать полностью – наркологическая клиника в краснодаре
LeslieCib · May 27, 2026 at 1:55 pm
В данной статье мы поговорим о будущем медицины, акцентируя внимание на прорывных разработках и их потенциале. Читатель узнает о новых подходах к лечению, роли искусственного интеллекта и возможностях персонализированной медицины.
Доступ к полной версии – лечение от алкоголизма
AnthonyNex · May 27, 2026 at 2:32 pm
Эта публикация исследует взаимосвязь зависимости и психологии. Мы обсудим, как психологические аспекты влияют на появление зависимостей и процесс выздоровления. Читатели смогут понять важность профессиональной поддержки и применения научных подходов в терапии.
Посмотреть всё – наркологическая клиника в краснодаре
JesusHem · May 27, 2026 at 2:34 pm
В этой статье рассматриваются актуальные вопросы, связанные с развитием медицинской науки и её внедрением в повседневную практику. Особое внимание уделено вопросам профилактики, ранней диагностики и использованию технологий для улучшения здоровья человека.
Разобраться лучше – платной консультации врача-психиатра
xn--76-6kct9cal.xn--p1ai · May 27, 2026 at 2:56 pm
click here xn--76-6kct9cal.xn--p1ai
Gabrieltat · May 27, 2026 at 3:10 pm
В этой статье мы говорим о важности поддержки в процессе выздоровления. Рассматриваются семьи, группы поддержки, специалисты и онлайн-ресурсы, которые могут сыграть решающую роль в избавлении от зависимости.
А что дальше? – detox24
Зенон · May 27, 2026 at 3:13 pm
Всё про АвтоВАЗ Lada китайские авто и премиум-сегмент https://vseavtonovosti.ru/
https://support.mlone.ai/kerryortiz7749 · May 27, 2026 at 3:14 pm
Дизайн сайта лаконичный, темная тема выглядит очень стильно.
Look into my web blog http://nfccardmaker.com/alvaroescalant
vucirUndex · May 27, 2026 at 3:50 pm
Планируете поездки по Калининграду на своих условиях? OmegaX обеспечивает аренду авто без водителя на привлекательных условиях. Парк включает Renault Logan, Lada Vesta, Volkswagen Polo, KIA Rio — все на автомате. Ищете аренда легкового автомобиля в Калининграде? Подробности и бронирование на omegax39.ru/arenda_prokat_avto_kaliningrad.html — офис находится прямо в аэропорту Храброво. Удобно для тех кто прилетает: забрал машину и сразу в путь.
Michaelgrani · May 27, 2026 at 4:11 pm
В этом обзоре мы обсудим современные методы борьбы с зависимостями, включая медикаментозную терапию и психотерапию. Мы представим последние исследования и их результаты, чтобы читатели могли быть в курсе наиболее эффективных подходов к лечению и поддержке.
Что ещё нужно знать? – detox24 в краснодаре
Melvinkem · May 27, 2026 at 5:45 pm
Этот краткий обзор предлагает сжатую информацию из области медицины, включая ключевые факты и последние новости. Мы стремимся сделать информацию доступной и понятной для широкой аудитории, что позволит читателям оставаться в курсе актуальных событий в здравоохранении.
Изучить вопрос глубже – детокс24
Saque PIX cronometrado · May 27, 2026 at 7:01 pm
Parei em R$600. Boa noite.
JosephEmatt · May 27, 2026 at 7:29 pm
next Fake documents (e.g., passports, driver’s licenses)
https://www.panamericano.us/assets/inc/1xbet-promo-code-1xbet.html · May 27, 2026 at 7:31 pm
for details https://www.panamericano.us/assets/inc/1xbet-promo-code-1xbet.html
dsignuh · May 27, 2026 at 7:39 pm
Интернет магазин пептидов https://gormon.org/ позволяет купить заказать отправить доставкой в любой город России. В наличии популярные пептиды, биорегуляторы, препараты уколы похудение жиросжигание, набор мышечной массы, оздоровление, лечение травм, послекурсовая терапия, пкт, витамины и добавки для роста волос и бороды. Официальный сайт отзывы poleznoo polezno полезно полезноо дешего недорого скидки.
RobertRok · May 27, 2026 at 8:14 pm
Этот документ охватывает важные аспекты медицинской науки, сосредотачиваясь на ключевых вопросах, касающихся здоровья населения. Мы рассматриваем свежие исследования, клинические рекомендации и лучшие практики, которые помогут улучшить качество лечения и профилактики заболеваний. Читатели получат возможность углубиться в различные медицинские дисциплины.
Уточнить детали – детоксикация наркомана
Thomasnaw · May 27, 2026 at 8:20 pm
Click Here Stolen credit card or loan information
Danielclogy · May 27, 2026 at 8:21 pm
В этой публикации мы исследуем ключевые аспекты здоровья, включая влияние образа жизни на благополучие. Читатели узнают о важности правильного питания, физической активности и психического здоровья. Мы предоставим практические советы и рекомендации для поддержания здоровья и развития профилактических подходов.
Читать полностью – «Похмельная служба» в Краснодаре
https://fdcng.com/wp-includes/articles/code_promotionnel_pour_1xbet.html · May 27, 2026 at 8:42 pm
for details https://fdcng.com/wp-includes/articles/code_promotionnel_pour_1xbet.html
LeslieCib · May 27, 2026 at 8:58 pm
Эта медицинская заметка содержит сжатую информацию о новых находках и методах в области здравоохранения. Мы предлагаем читателям свежие данные о заболеваниях, профилактике и лечении. Наша цель — быстро и доступно донести важную информацию, которая поможет в повседневной жизни и понимании здоровья.
Проверенные методы — узнай сейчас – анонимное лечение
Thomasnaw · May 27, 2026 at 9:00 pm
over here Fake invoices, financial documents, and counterfeit bills
RobertRok · May 27, 2026 at 9:17 pm
Этот документ охватывает важные аспекты медицинской науки, сосредотачиваясь на ключевых вопросах, касающихся здоровья населения. Мы рассматриваем свежие исследования, клинические рекомендации и лучшие практики, которые помогут улучшить качество лечения и профилактики заболеваний. Читатели получат возможность углубиться в различные медицинские дисциплины.
Посмотреть всё – детоксикация наркомана
gocoHeeld · May 27, 2026 at 9:27 pm
Glassway — поставщик отделочных материалов с прямыми контрактами с заводами-производителями и полным отсутствием посреднических наценок. Компания предлагает полный спектр решений: подвесные потолки, алюминиевые перегородки и двери, смарт-стекло, зенитные фонари, ограждения и витрины. Ищете раздвижные перегородки? На glassway.group представлен обширный каталог с актуальными ценами — прямые поставки с заводов обеспечивают конкурентную стоимость на весь ассортимент. Компания реализует проекты любой сложности — от типовых офисных интерьеров до нестандартных архитектурных решений.
Matthewmix · May 27, 2026 at 9:30 pm
see this ZeroDay Darknet Market
Bruceram · May 27, 2026 at 9:35 pm
В этой статье мы обсудим процесс восстановления после зависимостей, акцентируя внимание на различных методах и подходах к реабилитации. Читатели узнают, как создать план выздоровления и использовать полезные ресурсы для достижения устойчивых изменений.
Дополнительно читайте здесь – капельница от запоя балашиха
Williamadult · May 27, 2026 at 9:45 pm
Этот информативный текст сочетает в себе темы здоровья и зависимости. Мы обсудим, как хронические заболевания могут усугубить зависимости и наоборот, как зависимость может влиять на общее состояние здоровья. Читатели получат представление о комплексном подходе к лечению как физического, так и психического состояния.
А что дальше? – detox24
JosephEmatt · May 27, 2026 at 9:49 pm
their explanation Fake documents (e.g., passports, driver’s licenses)
cevobinPsype · May 27, 2026 at 9:50 pm
Криотерапия становится одним из самых востребованных направлений в wellness-индустрии, а азотная криокапсула CryoOne открывает новые возможности для бизнеса и здоровья. Воздействие экстремально низких температур до -180°C запускает мощные восстановительные процессы в организме, ускоряет метаболизм и способствует эффективному снижению веса. На сайте https://cryoone.ru/ представлено современное оборудование российского производства с полным комплектом поставки, включая сосуд Дьюара, бесплатной доставкой и двухлетней гарантией. Это выгодное вложение для фитнес-центров, spa-салонов и медицинских клиник, которое быстро окупается благодаря растущему спросу на инновационные процедуры восстановления и омоложения.
obertcug · May 27, 2026 at 9:51 pm
Аренда сервера для бизнеса требует надёжного провайдера с круглосуточной поддержкой и стабильной работой. Взять сервер в аренду у Netrack — значит получить гарантированный аптайм 99,9% и размещение в дата-центре уровня Tier III. Требуется сервер в аренду? На сайте https://netrack.ru/ можно выбрать конфигурацию под любые задачи — от стартапа до крупного корпоративного проекта. Пользователь работает на выделенном железе без совместного использования ресурсов и получает профессиональную техподдержку на каждом этапе.
Matthewmix · May 27, 2026 at 9:57 pm
see this page Digital logs (session logs, access logs, activity logs)
Williamadult · May 27, 2026 at 10:42 pm
Эта медицинская заметка содержит сжатую информацию о новых находках и методах в области здравоохранения. Мы предлагаем читателям свежие данные о заболеваниях, профилактике и лечении. Наша цель — быстро и доступно донести важную информацию, которая поможет в повседневной жизни и понимании здоровья.
Хочешь знать всё? – наркологическая клиника в краснодаре
Danielclogy · May 27, 2026 at 10:43 pm
Эта публикация содержит ценные советы и рекомендации по избавлению от зависимости. Мы обсуждаем различные стратегии, которые могут помочь в процессе выздоровления и важность обращения за помощью. Читатели смогут использовать полученные знания для улучшения своего состояния.
Всё, что нужно знать – Похмельная служба Краснодар
xiwabemure · May 27, 2026 at 11:36 pm
Магазин электрики «Элекс» предлагает широкий выбор кабелей, автоматов, розеток, щитового оборудования и световых решений для дома и бизнеса. Весь товар поставляется от надёжных производителей и имеет необходимые сертификаты качества. Ищете кабель кгн 1 ? На shop.elekspb.ru представлен удобный каталог с актуальными ценами и быстрым оформлением заказа. Удобная доставка по Санкт-Петербургу и всей России обеспечивает комфорт для профессионалов и частных покупателей.
Archienot · May 27, 2026 at 11:53 pm
Что, если сегодня твой счастливый день? Или именно это зеркало ведёт к джекпоту? актуальное зеркало уже ждёт тебя. Проверь удачу — вдруг сейчас твой час.
На csgorun официальный сайт каждый новый игрок получает бесплатный кейс. Экономия реальных денег. Сравни сам: здесь честный рандом.
Спорим, ты не угадаешь, что внутри? Или сегодня система на твоей стороне? csgorun зеркало сегодня ведёт в место, где сбываются мечты. Рискни прямо сейчас.
Source:
https://download-games-pc.net
Travisflelo · May 28, 2026 at 12:03 am
Этот обзор содержит информацию о передовых достижениях в области медицины. Мы разберем инновационные технологии, которые меняют подход к лечению и диагностике, а также их влияние на эффективность оказания медицинской помощи.
Подробнее можно узнать тут – прокапывания от похмелья
vuzufascer · May 28, 2026 at 12:10 am
Магазин «ЭЛЕКС» предлагает широкий выбор кабелей, проводов, электроустановочных изделий и светотехники для профессиональных и частных клиентов. Вся представленная продукция сертифицирована и полностью закрывает потребности в электромонтаже и освещении. Ищете кмпв 4х1? Заказать товар с доставкой по Санкт-Петербургу и регионам можно на elekspb.ru — актуальный каталог с быстрым оформлением заказа доступен круглосуточно.
Thomasnaw · May 28, 2026 at 12:26 am
try this website Exploit kits and software vulnerabilities for illegal access
Matthewmix · May 28, 2026 at 12:46 am
browse around this web-site Remote access services (RDP, SSH)
Edwardmuh · May 28, 2026 at 12:50 am
Этот информативный текст сочетает в себе темы здоровья и зависимости. Мы обсудим, как хронические заболевания могут усугубить зависимости и наоборот, как зависимость может влиять на общее состояние здоровья. Читатели получат представление о комплексном подходе к лечению как физического, так и психического состояния.
Подробности по ссылке – детоксикация наркозависимых
88xeng · May 28, 2026 at 12:51 am
Thanks for another great post. Where else may anybody get that type of info in such an ideal way of writing? I have a presentation next week, and I’m at the search for such information.
fabebBum · May 28, 2026 at 1:02 am
Ищете навесное оборудование для спецтехники? Посетите сайт Производственного предприятия EXTEN https://ppe-exten.ru/ и ознакомьтесь с каталогом, там вы найдете широкий ассортимент навесного оборудования для минитракторов, погрузчиков, экскаваторов, экскаваторов-погрузчиков, минипогрузчиков и фронтальных погрузчиков. Ассортимент включает навесные модули с широким спектром функций и применений. Вы получаете доставку в любой регион России, профессиональный сервис и гарантию на всю продукцию!
Normanmaype · May 28, 2026 at 1:04 am
В данной статье мы акцентируем внимание на важности поддержки в процессе выздоровления. Мы обсудим, как друзья, семья и профессионалы могут помочь тем, кто сталкивается с зависимостями. Читатели получат практические советы, как поддерживать близких на пути к новой жизни.
Нажмите, чтобы узнать больше – detox24
Travisflelo · May 28, 2026 at 1:22 am
Публикация охватывает основные направления развития современной медицины. Мы обсудим значимость научных исследований, инноваций в лечении и роли общественного участия в формировании системы здравоохранения.
Не пропусти важное – detox24
Georgeerrow · May 28, 2026 at 1:36 am
Эта статья подробно расскажет о процессе выздоровления, который включает в себя эмоциональную, физическую и психологическую реабилитацию. Мы обсуждаем значимость поддержки и наличие профессиональных программ. Читатели узнают, как строить новую жизнь и не возвращаться к старым привычкам.
Узнать больше – платной консультации врача-психиатра
ae6789 · May 28, 2026 at 1:47 am
Sweet blog! I found it while browsing on Yahoo News. Do you have any tips on how to get listed in Yahoo News? I’ve been trying for a while but I never seem to get there! Thank you
aa88 · May 28, 2026 at 2:06 am
Hi, possibly i’m being a little off topic here, but I was browsing your site and it looks stimulating. I’m writing a blog and trying to make it look neat, but everytime I touch it I mess something up. Did you design the blog yourself?
Normanmaype · May 28, 2026 at 2:15 am
В этой статье мы говорим о важности поддержки в процессе выздоровления. Рассматриваются семьи, группы поддержки, специалисты и онлайн-ресурсы, которые могут сыграть решающую роль в избавлении от зависимости.
Желаете узнать подробности? – детокс24
Bradyjoips · May 28, 2026 at 2:21 am
В этой публикации мы исследуем ключевые аспекты здоровья, включая влияние образа жизни на благополучие. Читатели узнают о важности правильного питания, физической активности и психического здоровья. Мы предоставим практические советы и рекомендации для поддержания здоровья и развития профилактических подходов.
Разобраться лучше – detox24 в краснодаре
JesusHem · May 28, 2026 at 2:25 am
В этом исследовании рассмотрены методы лечения зависимостей и их эффективность. Мы проанализируем различные подходы, используемые в реабилитационных центрах, и представим данные о результативности программ. Читатели получат надежные и научно обоснованные сведения о данной проблеме.
Осуществить глубокий анализ – наркологическая клиника в краснодаре
jeetwin online casino · May 28, 2026 at 2:38 am
jeetwin online casino
Francisnic · May 28, 2026 at 2:48 am
Этот медицинский обзор сосредоточен на последних достижениях, которые оказывают влияние на пациентов и медицинскую практику. Мы разбираем инновационные методы лечения и исследований, акцентируя внимание на их значимости для общественного здоровья. Читатели узнают о свежих данных и их возможном применении.
Давай разберёмся досконально – Реабилитация наркотической зависимости в Краснодаре
rimeyHet · May 28, 2026 at 3:06 am
Посетите сайт https://dom-kamnya.ru/iskusstvennyj-kamen/stoleshnitsy/ – там вы найдете широкий ассортимент продукции от производителя в Москве, с гарантией высокого качества. Просмотрите ассортимент, закажите бесплатный выезд замерщика онлайн, а гарантия на искусственный камень составляет 10 лет, на монтажные работы — 2 года. Доставка и установка кухонной столешницы выполняются в течение одного дня.
binance anm"alan · May 28, 2026 at 3:16 am
I don’t think the title of your article matches the content lol. Just kidding, mainly because I had some doubts after reading the article.
89bet · May 28, 2026 at 3:21 am
I do not even know how I ended up here, but I thought this post was good. I do not know who you are but certainly you are going to a famous blogger if you are not already 😉 Cheers!
JustinCet · May 28, 2026 at 3:44 am
anonymous coin leap app
AnthonyNex · May 28, 2026 at 3:51 am
Эта публикация посвящена актуальным вопросам современной медицины и здравоохранения. Мы обсудим новейшие технологии диагностики и лечения, а также их влияние на продолжительность и качество жизни. Читатель найдет здесь информацию о научных исследованиях и перспективных разработках, доступно изложенную для широкой аудитории.
Погрузиться в детали – детокс24 краснодар
Gabrieltat · May 28, 2026 at 4:09 am
Эта публикация посвящена актуальным вопросам современной медицины и здравоохранения. Мы обсудим новейшие технологии диагностики и лечения, а также их влияние на продолжительность и качество жизни. Читатель найдет здесь информацию о научных исследованиях и перспективных разработках, доступно изложенную для широкой аудитории.
Всё, что нужно знать – детокс24 краснодар
https://pixel.egeaonline.it/application/pgs/sekrety_effektivnoy_organizacii_rabochego_prostranstva_dlya_komfortnogo_remonta.html · May 28, 2026 at 4:30 am
https://pixel.egeaonline.it/application/pgs/sekrety_effektivnoy_organizacii_rabochego_prostranstva_dlya_komfortnogo_remonta.html
https://lingvotop.ru/css/pg/promokod-1xbet_i_bonus-kod.html · May 28, 2026 at 4:34 am
source https://lingvotop.ru/css/pg/promokod-1xbet_i_bonus-kod.html
NathanNup · May 28, 2026 at 4:40 am
займ без отказа на карту срочно https://tbcareer.ru
JustinCet · May 28, 2026 at 4:45 am
see this leap wallet dashboard
Patrickgreak · May 28, 2026 at 6:13 am
Эта публикация раскрывает психологические механизмы зависимости и их роль в развитии расстройств. Читатель узнает о том, как психология влияет на формирование зависимостей и как профессиональная помощь может изменить ситуацию.
Подробная информация доступна по запросу – капельница от алкоголя балашиха
Jimmyimmut · May 28, 2026 at 6:21 am
Эта публикация раскрывает психологические механизмы зависимости и их роль в развитии расстройств. Читатель узнает о том, как психология влияет на формирование зависимостей и как профессиональная помощь может изменить ситуацию.
Тыкай сюда — узнаешь много интересного – детокс24
Georgeerrow · May 28, 2026 at 7:42 am
В этой статье мы рассмотрим современные достижения в области медицины, включая инновационные методы лечения и диагностики. Мы обсудим важность профилактики заболеваний и роль технологий в улучшении качества здравоохранения. Читатели узнают о влиянии медицины на повседневную жизнь и ее значение для современного общества.
Переходите по ссылке ниже – detox24
Jimmyimmut · May 28, 2026 at 8:02 am
В этой статье мы обсудим процесс восстановления после зависимостей, акцентируя внимание на различных методах и подходах к реабилитации. Читатели узнают, как создать план выздоровления и использовать полезные ресурсы для достижения устойчивых изменений.
Не упусти важное! – детокс24 краснодар
Melvinkem · May 28, 2026 at 8:36 am
Этот краткий обзор предлагает сжатую информацию из области медицины, включая ключевые факты и последние новости. Мы стремимся сделать информацию доступной и понятной для широкой аудитории, что позволит читателям оставаться в курсе актуальных событий в здравоохранении.
Давай разберёмся досконально – детокс24
Bradyjoips · May 28, 2026 at 9:14 am
В этой публикации мы исследуем ключевые аспекты здоровья, включая влияние образа жизни на благополучие. Читатели узнают о важности правильного питания, физической активности и психического здоровья. Мы предоставим практические советы и рекомендации для поддержания здоровья и развития профилактических подходов.
Хочу знать больше – наркологическая клиника в краснодаре
DallasCef · May 28, 2026 at 9:21 am
взять займ на карту займ на на карту онлайн
Www dark web com · May 28, 2026 at 9:47 am
Discover the darkweb sites list, safely navigating the hidden internet with our guide. Www dark web com
JustinCet · May 28, 2026 at 10:16 am
view leap wallet x official
hosuwkSpoli · May 28, 2026 at 11:10 am
Автосервис «Шоколад» в Анапе — это современный центр технического обслуживания, где профессионализм сочетается с заботой о каждом клиенте. Команда опытных мастеров предлагает полный спектр услуг: от диагностики и замены масла до сложного ремонта двигателя и трансмиссии. Особенно привлекательны специальные предложения сервиса — бесплатная диагностика со скидкой 15% на ремонт, услуги эвакуатора и расчет стоимости работ по фотографии. Подробнее обо всех услугах можно узнать на сайте https://chocolate-auto.ru/, где представлена актуальная информация о ценах и графике работы. Сервис расположен по адресу Супсехское шоссе 10 и работает ежедневно с 9:00 до 19:00, обеспечивая качественное обслуживание автомобилей любых марок.
JustinCet · May 28, 2026 at 11:20 am
our website leap cosmos wallet
Charlessot · May 28, 2026 at 11:23 am
Этот медицинский обзор сосредоточен на последних достижениях, которые оказывают влияние на пациентов и медицинскую практику. Мы разбираем инновационные методы лечения и исследований, акцентируя внимание на их значимости для общественного здоровья. Читатели узнают о свежих данных и их возможном применении.
Кликни и узнай всё! – elektrostal detox24
Ralphwes · May 28, 2026 at 11:31 am
Этот текст посвящён сложным аспектам зависимости и её влиянию на жизнь человека. Мы обсудим психологические, физические и социальные последствия зависимого поведения, а также важность своевременного обращения за помощью.
Смотрите также… – детокс24 электросталь
KennethEngak · May 28, 2026 at 12:02 pm
Эта публикация раскрывает психологические механизмы зависимости и их роль в развитии расстройств. Читатель узнает о том, как психология влияет на формирование зависимостей и как профессиональная помощь может изменить ситуацию.
Практические советы ждут тебя – Реабилитация наркотической зависимости в Краснодаре
Wesleyvet · May 28, 2026 at 12:02 pm
В этой статье обсуждаются актуальные медицинские вопросы, которые волнуют общество. Мы обращаем внимание на проблемы, касающиеся здравоохранения и лечения, а также на новшества в области медицины. Читатели будут осведомлены о последних событиях и смогут следить за тенденциями в медицине.
Познакомиться с результатами исследований – Похмельная служба в Краснодаре
Andrewgah · May 28, 2026 at 12:05 pm
В этой статье мы рассматриваем разрушительное влияние зависимости на жизнь человека. Обсуждаются аспекты, такие как здоровье, отношения и профессиональные достижения. Читатели узнают о необходимости обращения за помощью и о путях к восстановлению.
Открыть полностью – кодировка от алкоголизма на дому цена
JamesEdifs · May 28, 2026 at 12:27 pm
В этой статье обсуждаются актуальные медицинские вопросы, которые волнуют общество. Мы обращаем внимание на проблемы, касающиеся здравоохранения и лечения, а также на новшества в области медицины. Читатели будут осведомлены о последних событиях и смогут следить за тенденциями в медицине.
Что скрывают от вас? – лечение игромании в екатеринбурге
DavidCYDAY · May 28, 2026 at 12:49 pm
В этом обзоре представлены различные методы избавления от зависимости, включая терапевтические и психологические подходы. Мы сравниваем их эффективность и предоставляем рекомендации для тех, кто хочет вернуться к трезвой жизни. Читатели смогут найти информацию о реабилитационных центрах и поддерживающих группах.
Продолжить чтение – выведение из запоя кодирование
AntonioLef · May 28, 2026 at 1:05 pm
В этой статье рассматриваются различные аспекты избавления от зависимости, включая физические и психологические методы. Мы обсудим поддержку, мотивацию и стратегии, которые помогут в процессе выздоровления. Читатели узнают, как преодолеть трудности и двигаться к новой жизни без зависимости.
Продолжить чтение – анонимный вызов врача нарколога на дом
Лукиан · May 28, 2026 at 1:41 pm
Кейсбук SEO Казань: реальные истории продвижения Как продвигать сайт в Казани
RichardNupep · May 28, 2026 at 1:47 pm
В этой статье мы рассматриваем разрушительное влияние зависимости на жизнь человека. Обсуждаются аспекты, такие как здоровье, отношения и профессиональные достижения. Читатели узнают о необходимости обращения за помощью и о путях к восстановлению.
Полезно знать – detox24
Patrickgreak · May 28, 2026 at 1:50 pm
Публикация посвящена жизненным историям людей, успешно справившихся с зависимостью. Мы покажем, что выход есть, и он начинается с первого шага — принятия проблемы и желания измениться.
Эксклюзивная информация – капельница от алкоголя балашиха
Wesleyvet · May 28, 2026 at 2:28 pm
Этот информативный текст сочетает в себе темы здоровья и зависимости. Мы обсудим, как хронические заболевания могут усугубить зависимости и наоборот, как зависимость может влиять на общее состояние здоровья. Читатели получат представление о комплексном подходе к лечению как физического, так и психического состояния.
Откройте для себя больше – Похмельная служба Краснодар
The dark web website · May 28, 2026 at 2:41 pm
Exploring dark web links can be risky. Learn how to safely access and navigate hidden services and onion sites on the dark web. Stay informed and protected. The dark web website
Rickybring · May 28, 2026 at 2:50 pm
В данной публикации мы поговорим о процессе восстановления от зависимости, о том, как вернуть себе нормальную жизнь. Мы обсудим преодоление трудностей, значимость поддержки и наличие программ реабилитации. Читатели смогут узнать о ключевых шагах к успешному восстановлению.
Что ещё? Расскажи всё! – detox24 в балашихе
binance kod · May 28, 2026 at 3:44 pm
Thanks for sharing. I read many of your blog posts, cool, your blog is very good.
ThomasNep · May 28, 2026 at 3:58 pm
Добрый день!
Риски дешевой мебели: как экономия на материалах увеличивает расходы клиники на ремонт
Противопожарные требования: классы горючести материалов для медицинской мебели в ЛПУ
Нержавеющая сталь или порошковое покрытие: как выбрать материал стеллажей для ЦСО, аптеки и склада
Больше информации по ссылке – https://www.8a.ru/firms/f1522.php
металлические кассеты для инструментов, масштабируемость оснащения, зоны стерильности проектирование
однонаправленный воздушный поток, проектирование санпропускников, ремонт медицинской мебели
Удачи!
Rickybring · May 28, 2026 at 5:10 pm
В данной публикации мы поговорим о процессе восстановления от зависимости, о том, как вернуть себе нормальную жизнь. Мы обсудим преодоление трудностей, значимость поддержки и наличие программ реабилитации. Читатели смогут узнать о ключевых шагах к успешному восстановлению.
Изучить материалы по теме – детокс24
https://therockpit.net/wp-content/pages/1xbet_promo_code________sign_up_offer.html · May 28, 2026 at 5:29 pm
https://therockpit.net/wp-content/pages/1xbet_promo_code________sign_up_offer.html
legulinpam · May 28, 2026 at 6:15 pm
Looking to buy and sell USDT for fiat online? Visit https://buysellswappro.com/ – BuySellSwapPro helps users navigate between fiat and crypto using clear online routes centered around USDT. You can buy crypto with a credit or debit card, sell crypto for fiat, compare pages by currency or country, and choose the route that best suits your card, bank account, or local market conditions.
sujugRor · May 28, 2026 at 6:32 pm
Когда речь идёт о покупке автомобиля из Японии, Кореи или Китая, выбор партнёра решает всё. Ищете купить машину с аукциона в китае с доставкой в россию ? Компания starmotors.biz за годы работы доставила более 17 000 автомобилей по всей России и сегодня держит свыше 600 машин в наличии на рынке во Владивостоке. Офисы и стоянки работают во Владивостоке, Москве и Санкт-Петербурге, а доставка охватывает любой регион страны.
rusumyincar · May 28, 2026 at 6:52 pm
Looking for a token swap platform? Visit https://swaptoken.io/ – we offer fast swaps for 150+ cryptocurrencies in 1-15 minutes. We offer fixed and floating rates, no registration, and no KYC for standard routes. Flexible limits range from $20 to $150,000 equivalent. All key exchange terms are displayed in the form upfront, with no hidden platform fees other than the sender’s network fee.
Polygon staking risks · May 28, 2026 at 6:56 pm
Helpful breakdown of [url=https://staking-polygon.com/polygon-staking-rewards/]Polygon staking rewards[/url] — good for understanding how staking returns work before choosing a validator.
Dennispew · May 28, 2026 at 7:09 pm
В этой статье мы подробно рассматриваем проверенные методы борьбы с зависимостями, включая психотерапию, медикаментозное лечение и поддержку со стороны общества. Мы акцентируем внимание на важности комплексного подхода и возможности успешного восстановления для людей, столкнувшихся с этой проблемой.
Узнать напрямую – вывод из запоя владимир
fixDiele · May 28, 2026 at 7:13 pm
Особенно понравился материал про Анализ футбольного ритма и уникальные тренды.
Ссылка ниже:
https://newsliverpool.ru
fixDiele · May 28, 2026 at 7:18 pm
Между прочим, если вас интересует Новости и экология Хабаровского края, посмотрите сюда.
Смотрите сами:
https://media27.ru
Нестер · May 28, 2026 at 7:42 pm
Доверьте климат в помещении профессионалам Ronco Group — вентиляция и кондиционирование https://domocvet.com/technology/organizacziya-sistemy-ventilyaczii-v-bassejne
https://enah.edu.mx/ · May 28, 2026 at 8:15 pm
https://enah.edu.mx/
lejoleDus · May 28, 2026 at 8:29 pm
Мартин Сад https://www.martin-sad.ru/ – это питомник растений и огромный садовый центр в Москве. Посетите сайт – посмотрите самый полный каталог саженцев и растений предлагаемых нами, а также каталог товаров для сада. У нас множество товаров по Акции! Оказываем услуги посадки растений и ухода за участком. Подробнее на сайте!
cimansSax · May 28, 2026 at 8:32 pm
How to buy Bitcoin online? Visit https://howtobuybitcoin.online/ and you’ll discover that receiving BTC online is easier when you understand the purchase flow before sending money. This guide explains how beginners can choose Bitcoin and complete a more secure online purchase. Use the Bitcoin widget below to estimate how much BTC you can receive, compare order details, and preview the purchase process before confirming the transaction.
Waltertal · May 28, 2026 at 8:37 pm
В этой медицинской статье мы погрузимся в актуальные вопросы здравоохранения и лечения заболеваний. Читатели узнают о современных подходах, методах диагностики и новых открытий в научных исследованиях. Наша цель — донести важную информацию и повысить уровень осведомленности о здоровье.
Это стоит прочитать полностью – наркологическая клиника в краснодаре
Dark web store · May 28, 2026 at 9:01 pm
Dive into the world of darknet market access with our comprehensive guide. Learn strategies for safe & anonymous entry. Dark web store
Hubertbob · May 28, 2026 at 9:57 pm
В этой статье мы обсудим процесс восстановления после зависимостей, акцентируя внимание на различных методах и подходах к реабилитации. Читатели узнают, как создать план выздоровления и использовать полезные ресурсы для достижения устойчивых изменений.
Ознакомиться с полной информацией – детокс24
Stevengon · May 28, 2026 at 10:09 pm
В этой статье рассматриваются актуальные вопросы, связанные с развитием медицинской науки и её внедрением в повседневную практику. Особое внимание уделено вопросам профилактики, ранней диагностики и использованию технологий для улучшения здоровья человека.
Прочесть заключение эксперта – детокс24 красногорск
KennethEngak · May 28, 2026 at 10:19 pm
В данном обзоре представлены основные направления и тренды в области медицины. Мы обсудим актуальные проблемы здравоохранения, свежие открытия и новые подходы, которые меняют представление о лечении и профилактике заболеваний. Эта информация будет полезна как специалистам, так и широкой публике.
Провести детальное исследование – detox24 в краснодаре
BillyAgils · May 28, 2026 at 10:28 pm
Читатели получат представление о том, как современные технологии влияют на развитие медицины. Обсуждаются новые методы лечения, персонализированный подход и роль цифровых решений в повышении качества медицинских услуг.
Расширить кругозор по теме – detox24 в омске
Andrewgah · May 28, 2026 at 10:40 pm
В данной статье мы акцентируем внимание на важности поддержки в процессе выздоровления. Мы обсудим, как друзья, семья и профессионалы могут помочь тем, кто сталкивается с зависимостями. Читатели получат практические советы, как поддерживать близких на пути к новой жизни.
Более того — здесь – круглосуточная анонимная наркологическая помощь
ThomasNep · May 28, 2026 at 11:02 pm
Привет всем!
Имидж клиники: как состояние мебели влияет на восприятие качества услуг пациентами
Аэродинамика в чистой комнате: как форма ножек и столешниц влияет на ламинарный поток
Влияние мебели на HVAC: как плотность расстановки стеллажей влияет на эффективность вентиляции
Больше информации по ссылке – https://www.rosmed.ru/brands/market/934
инструкции по эксплуатации, работа с легковоспламеняющимися жидкостями, модульность медицинской мебели
декларации о соответствии, контейнеры для стерилизации, инструментальный стол нержавеющий
Удачи!
Stevengon · May 28, 2026 at 11:09 pm
Публикация охватывает основные направления развития современной медицины. Мы обсудим значимость научных исследований, инноваций в лечении и роли общественного участия в формировании системы здравоохранения.
Эксклюзивная информация – detox24 в красногорске
Henrycheed · May 28, 2026 at 11:36 pm
В данной статье мы поговорим о будущем медицины, акцентируя внимание на прорывных разработках и их потенциале. Читатель узнает о новых подходах к лечению, роли искусственного интеллекта и возможностях персонализированной медицины.
Изучите внимательнее – детокс24 люберцы
Charlessot · May 28, 2026 at 11:36 pm
Публикация охватывает основные направления развития современной медицины. Мы обсудим значимость научных исследований, инноваций в лечении и роли общественного участия в формировании системы здравоохранения.
Доступ к полной версии – вывод из запоя на дому электросталь
Georgebaida · May 28, 2026 at 11:47 pm
В этой публикации мы рассматриваем важную тему борьбы с зависимостями, включая алкогольную и наркотическую зависимости. Мы обсудим методы лечения, реабилитации и поддержку, которые могут помочь людям, столкнувшимся с этой проблемой. Читатели узнают о перспективах выздоровления и важности комплексного подхода.
Дополнительно читайте здесь – detox24
bonimrizib · May 28, 2026 at 11:53 pm
Современные путешественники ценят комфорт и надёжность, а именно это предлагает сервис трансферов, заслуживший доверие тысяч клиентов. Бронирование поездки на https://transfer-easy.ru/ занимает считанные минуты: фиксированная цена от 500 рублей, бесплатное ожидание при задержке рейса и встреча с именной табличкой — всё включено. Автопарк компании состоит исключительно из иномарок не старше пяти лет: от комфортных Toyota Corolla до представительских Mercedes S-класса. Водители помогут с багажом, а в салоне действует строгий запрет на курение. Путешествие начинается приятно!
StephenpaR · May 28, 2026 at 11:55 pm
В этом обзоре представлены различные методы избавления от зависимости, включая терапевтические и психологические подходы. Мы сравниваем их эффективность и предоставляем рекомендации для тех, кто хочет вернуться к трезвой жизни. Читатели смогут найти информацию о реабилитационных центрах и поддерживающих группах.
Ознакомьтесь с аналитикой – simferopol detox24
http://requiem-online.ru/files/pages/promokod_1xbet_na_segodnya_pri_registracii.html · May 29, 2026 at 12:02 am
http://requiem-online.ru/files/pages/promokod_1xbet_na_segodnya_pri_registracii.html
DavidCYDAY · May 29, 2026 at 12:02 am
Эта медицинская заметка содержит сжатую информацию о новых находках и методах в области здравоохранения. Мы предлагаем читателям свежие данные о заболеваниях, профилактике и лечении. Наша цель — быстро и доступно донести важную информацию, которая поможет в повседневной жизни и понимании здоровья.
Продолжить чтение – saratov detox24
tuyeltCaump · May 29, 2026 at 12:06 am
Ищете лечение пульпита и периодонтита в Мурманске от лучшей клиники, в котором работают квалифицированные стоматологи? Посетите https://nova-51.ru/lechenie-zubov-murmansk/lechenie-pulpita-i-periodontita-murmansk – ознакомьтесь с нашими услугами подробнее.
Ralphwes · May 29, 2026 at 12:11 am
В данной статье мы поговорим о будущем медицины, акцентируя внимание на прорывных разработках и их потенциале. Читатель узнает о новых подходах к лечению, роли искусственного интеллекта и возможностях персонализированной медицины.
См. подробности – наркологическая клиника в электростали
ThomasJic · May 29, 2026 at 12:14 am
Эта информационная публикация освещает широкий спектр тем из мира медицины. Мы предлагаем читателям ясные и понятные объяснения современных заболеваний, методов профилактики и лечения. Информация будет полезна как пациентам, так и медицинским работникам, желающим поддержать уровень своих знаний.
Посмотреть всё – Реабилитация наркотической зависимости в Краснодаре
Fidelmat · May 29, 2026 at 12:18 am
В этой публикации мы рассматриваем важную тему борьбы с зависимостями, включая алкогольную и наркотическую зависимости. Мы обсудим методы лечения, реабилитации и поддержку, которые могут помочь людям, столкнувшимся с этой проблемой. Читатели узнают о перспективах выздоровления и важности комплексного подхода.
Где можно узнать подробнее? – детокс24
Bruceram · May 29, 2026 at 12:23 am
В этой статье мы рассмотрим современные достижения в области медицины, включая инновационные методы лечения и диагностики. Мы обсудим важность профилактики заболеваний и роль технологий в улучшении качества здравоохранения. Читатели узнают о влиянии медицины на повседневную жизнь и ее значение для современного общества.
Только для своих – детокс24
CharlesSax · May 29, 2026 at 12:46 am
В этом обзоре представлены различные методы избавления от зависимости, включая терапевтические и психологические подходы. Мы сравниваем их эффективность и предоставляем рекомендации для тех, кто хочет вернуться к трезвой жизни. Читатели смогут найти информацию о реабилитационных центрах и поддерживающих группах.
Детали по клику – подшивка налтрексоном
Henrycheed · May 29, 2026 at 12:52 am
В данной статье рассматриваются физиологические и эмоциональные аспекты зависимости. Мы обсудим, как организм реагирует на зависимое поведение, и какие методы помогают восстановить здоровье и внутреннее равновесие.
Проследить причинно-следственные связи – детокс24 люберцы
RichardNupep · May 29, 2026 at 1:18 am
В данной статье мы акцентируем внимание на важности поддержки в процессе выздоровления. Мы обсудим, как друзья, семья и профессионалы могут помочь тем, кто сталкивается с зависимостями. Читатели получат практические советы, как поддерживать близких на пути к новой жизни.
Подробная информация доступна по запросу – вывод из запоя на дому в краснодаре
Bradleyuncon · May 29, 2026 at 2:11 am
В этой статье рассматривается комплексный подход к избавлению от зависимости. Читатель узнает, как сочетание физического, психологического и духовного восстановления помогает достичь стойкого выздоровления.
Изучить вопрос глубже – Психиатры клиники
AntonioLef · May 29, 2026 at 2:17 am
Текст посвящён распространённым мифам о зависимости и их развенчанию. Мы предоставим научно обоснованную информацию и дадим рекомендации по выбору эффективного способа борьбы с зависимым поведением.
Познакомиться с результатами исследований – наркологическая клиника в красноярске
JamesSon · May 29, 2026 at 2:42 am
Статья посвящена анализу текущих трендов в медицине и их влиянию на жизнь людей. Мы рассмотрим новые технологии, методы лечения и значение профилактики в обеспечении долголетия и здоровья.
Углубить понимание вопроса – detox24 в калининграде
Georgebaida · May 29, 2026 at 2:51 am
Эта публикация посвящена актуальным вопросам современной медицины и здравоохранения. Мы обсудим новейшие технологии диагностики и лечения, а также их влияние на продолжительность и качество жизни. Читатель найдет здесь информацию о научных исследованиях и перспективных разработках, доступно изложенную для широкой аудитории.
Изучить аспект более тщательно – detox24
JamesEdifs · May 29, 2026 at 3:17 am
В этой статье обсуждаются актуальные медицинские вопросы, которые волнуют общество. Мы обращаем внимание на проблемы, касающиеся здравоохранения и лечения, а также на новшества в области медицины. Читатели будут осведомлены о последних событиях и смогут следить за тенденциями в медицине.
Получить профессиональную консультацию – детокс24 екатеринбург
RobertZew · May 29, 2026 at 3:40 am
Этот медицинский обзор сосредоточен на последних достижениях, которые оказывают влияние на пациентов и медицинскую практику. Мы разбираем инновационные методы лечения и исследований, акцентируя внимание на их значимости для общественного здоровья. Читатели узнают о свежих данных и их возможном применении.
Подробнее – кодирование от алкоголизма люберцы
ThomasNep · May 29, 2026 at 3:45 am
Добрый день!
Проект санпропускника: интеграция душевых и гардеробных из нержавеющей стали без ошибок
Специфические требования к столам для макроскопического исследования биоматериала
Универсальные решения из нержавейки: применение в медицине, общепите и частных интерьерах
Больше информации по ссылке – https://xn--d1afuo.xn--p1acf/korrozija-hromonikelevoj-stali-v-meduchrezhdenii-aisi-304-protiv-316-pri-sanobrabotke/
сейсмостойкость мебели, сквозные шкафы стерилизация, стеллажи открытого типа медицина
регулировка высоты столов, медицинская сталь ГОСТ, износостойкость порошкового покрытия
Удачи!
BillyAgils · May 29, 2026 at 3:56 am
В статье рассматриваются различные стратегии борьбы с зависимостями, включая проверенные методы и реальные истории успеха. Читатель узнает, какие подходы наиболее эффективны и как начать путь к выздоровлению.
Желаете узнать подробности? – лечение женского алкоголизма клиника
ThomasNep · May 29, 2026 at 5:29 am
Добрый день!
Специфика работы патологоанатома: требования к освещению и поверхности макростола
Репутация больницы: связь между качеством оснащения и уровнем доверия пациентов к врачу
Питтинговая коррозия: механизмы разрушения AISI 304 в условиях постоянной влажной уборки
Больше информации по ссылке – https://factories.by/producers/artinoks
сплошные полки из нержавейки, порошковое покрытие стеллажи, полировка нержавеющей стали
сертификация медицинской мебели, мебель для лаборатории анализов, медицинские стеллажи требования
Удачи!
Francisnic · May 29, 2026 at 5:58 am
Этот обзор содержит информацию о передовых достижениях в области медицины. Мы разберем инновационные технологии, которые меняют подход к лечению и диагностике, а также их влияние на эффективность оказания медицинской помощи.
Не упусти важное! – detox24 в краснодаре
tower rush jeux · May 29, 2026 at 6:04 am
machine a sous tower rush
ThomasJic · May 29, 2026 at 6:12 am
В этой публикации мы предложим ряд рекомендаций по избавлению от зависимостей и успешному восстановлению. Мы обсудим методы привлечения поддержки и важность самосознания. Эти советы помогут людям вернуться к нормальной жизни и стать на путь выздоровления.
Уникальные данные только сегодня – детокс24 краснодар
Fidelmat · May 29, 2026 at 6:32 am
Публикация посвящена жизненным историям людей, успешно справившихся с зависимостью. Мы покажем, что выход есть, и он начинается с первого шага — принятия проблемы и желания измениться.
Подробная информация доступна по запросу – нарколог на дом красногорск
unomasuno.com.mx · May 29, 2026 at 6:41 am
unomasuno.com.mx
ThomasNep · May 29, 2026 at 7:13 am
Здравствуйте!
Мебель из нержавейки для SPA: устойчивость к влаге, соли и косметическим средствам в салонах
Удобство работы с биопсийным материалом: конструктивные особенности макростолов
Адаптация промышленных решений из нержавейки для частных клиник и кабинетов
Больше информации по ссылке – http://med.by/wwwres/belarus/12_9
мебель для операционной, хранение реактивов в шкафах, экспертиза проектов медучреждений
кабель-каналы в столах, мониторинг условий хранения, пусконаладочные работы
Удачи!
CharlesSax · May 29, 2026 at 7:50 am
В этом обзоре представлены различные методы избавления от зависимости, включая терапевтические и психологические подходы. Мы сравниваем их эффективность и предоставляем рекомендации для тех, кто хочет вернуться к трезвой жизни. Читатели смогут найти информацию о реабилитационных центрах и поддерживающих группах.
Детали по клику – вывод из запоя иркутск
ThomasNep · May 29, 2026 at 8:26 am
Доброго!
Как получить лицензию на меддеятельность в РБ: полный гид по требованиям Минздрава
Нержавейка в фитнес-центрах: гигиеничные решения для раздевалок и душевых комнат спортклубов
Цифровые сервисы Минздрава РБ: упрощение процесса лицензирования медицинской деятельности
Больше информации по ссылке – https://www.steelland.org/stat/digest/848.html
розетки в медицинских столах, стол для вскрытия, мебель для процедурной
агрессивная среда санобработки, удаление биопленки со стали, разница AISI 304 и 316
Удачи!
yoktogel · May 29, 2026 at 8:29 am
you’re in reality a just right webmaster. The web site loading velocity is incredible. It sort of feels that you’re doing any distinctive trick. In addition, The contents are masterpiece. you’ve performed a great process on this topic!
Dewajitu · May 29, 2026 at 8:32 am
That is really fascinating, You’re an excessively skilled blogger. I’ve joined your rss feed and look forward to in the hunt for extra of your magnificent post. Additionally, I’ve shared your website in my social networks!
Mancingduit · May 29, 2026 at 8:50 am
A friend of mine advised me to review this site. And yes. it has some useful pieces of info and I enjoyed reading it.
how can john spencer ellis help you transition from employee to entrepreneur · May 29, 2026 at 9:14 am
I’d like to be able to write like this, but taking the time and developing articles is hard…. Takes a lot of effort.
Waltertal · May 29, 2026 at 9:15 am
В этой публикации мы обсуждаем современные методы лечения различных заболеваний. Читатели узнают о новых медикаментах, терапиях и исследованиях, которые активно применяются для лечения. Мы нацелены на то, чтобы предоставить практические знания, которые могут помочь в борьбе с недугами.
Почему это важно? – платной консультации врача-психиатра
ThomasNep · May 29, 2026 at 9:34 am
Привет всем!
Чистые помещения: влияние дизайна мебели на эффективность вентиляции и чистоту воздуха
Риски покупки дешевой медмебели: последствия использования некачественных материалов
Гигиена мойки: правильный выбор глубины и высоты бортов для обработки медизделий
Больше информации по ссылке – https://homeprorab.info/meditsinskie-stellazhi-trebovaniya-k-razmeshheniyu-i-pravila-ustanovki/
питтинговая коррозия AISI 316, хранение эндоскопов, быстровозводимые решения
цветовая кодировка в ЦСО, стеллажи закрытого типа, частные медицинские объекты
Удачи!
Johnnyphips · May 29, 2026 at 9:40 am
Этот текст представляет собой обзор свежих данных и исследований в области медицины. Он призван помочь читателям понять, как научные достижения влияют на лечение, диагностику и общее состояние системы здравоохранения.
Изучить аспект более тщательно – вывод из запоя на дому краснодар
Порфирий · May 29, 2026 at 9:43 am
Монтаж, ремонт, диагностика кровельных систем https://nashsovetik.ru/soft-roof-repair/
Raymondcag · May 29, 2026 at 9:43 am
В этой медицинской статье мы погрузимся в актуальные вопросы здравоохранения и лечения заболеваний. Читатели узнают о современных подходах, методах диагностики и новых открытий в научных исследованиях. Наша цель — донести важную информацию и повысить уровень осведомленности о здоровье.
Изучить эмпирические данные – снятие ломки
CharlesZex · May 29, 2026 at 9:45 am
Публикация знакомит читателей с различными подходами к реабилитации. От традиционных методов до современных программ — вы узнаете, как выбрать оптимальный путь к выздоровлению и преодолеть препятствия на этом пути.
Не пропусти важное – detox24 в краснодаре
BarrettZep · May 29, 2026 at 10:00 am
Этот документ охватывает важные аспекты медицинской науки, сосредотачиваясь на ключевых вопросах, касающихся здоровья населения. Мы рассматриваем свежие исследования, клинические рекомендации и лучшие практики, которые помогут улучшить качество лечения и профилактики заболеваний. Читатели получат возможность углубиться в различные медицинские дисциплины.
Как это работает — подробно – прокапаться от алкоголя краснодар
tehifudunemo · May 29, 2026 at 10:19 am
Платформа Pabit представляет собой современное решение для управления проектами, позволяющее командам по всему миру сосредоточиться на достижении целей без организационного хаоса. Система предлагает комплексный набор инструментов: детализированное управление задачами с расширенным редактором и возможностью прикрепления файлов, планирование спринтов через циклы, разделение проектов на модули для контроля ключевых вех. Ознакомиться с функционалом можно на https://pabit.ru/, где представлены настраиваемые представления для фильтрации задач, интеллектуальный помощник для работы со страницами и аналитика в реальном времени. Интуитивный интерфейс платформы освобождает руководителей от технических сложностей, позволяя фокусироваться на стратегических аспектах командной работы.
Togelonline88 · May 29, 2026 at 10:20 am
I’m so happy to read this. This is the type of manual that needs to be given and not the random misinformation that’s at the other blogs. Appreciate your sharing this best doc.
JamesSon · May 29, 2026 at 10:33 am
Статья посвящена анализу текущих трендов в медицине и их влиянию на жизнь людей. Мы рассмотрим новые технологии, методы лечения и значение профилактики в обеспечении долголетия и здоровья.
Погрузиться в детали – вызов на дом выведение из запоя
AlbertPhype · May 29, 2026 at 10:46 am
В данной публикации мы поговорим о процессе восстановления от зависимости, о том, как вернуть себе нормальную жизнь. Мы обсудим преодоление трудностей, значимость поддержки и наличие программ реабилитации. Читатели смогут узнать о ключевых шагах к успешному восстановлению.
Практические советы ждут тебя – анонимный нарколог краснодар
WilliamVah · May 29, 2026 at 10:48 am
В этой статье мы рассматриваем разрушительное влияние зависимости на жизнь человека. Обсуждаются аспекты, такие как здоровье, отношения и профессиональные достижения. Читатели узнают о необходимости обращения за помощью и о путях к восстановлению.
Узнать из первых рук – социопатия лечение
RobertWet · May 29, 2026 at 11:02 am
Этот информативный текст сочетает в себе темы здоровья и зависимости. Мы обсудим, как хронические заболевания могут усугубить зависимости и наоборот, как зависимость может влиять на общее состояние здоровья. Читатели получат представление о комплексном подходе к лечению как физического, так и психического состояния.
Подробная информация доступна по запросу – детоксикация на дому
Gregorygow · May 29, 2026 at 11:07 am
Коллеги, хороший материал с практическими рекомендациями по выбору SEO для регионального бизнеса. Автор подробно останавливается на локальных ключевых словах, оптимизации контента, работе с картами и каталогами, а также важности отзывов для репутации. Есть блок про ссылочное продвижение и аналитику. Очень структурированно: https://bioice-krasnoyarsk.ru/stati/kak-vybrat-jeffektivnoe-seo-prodvizhenie-dlja-biznesa-v-regione-prakticheskie-rekomendacii/
Gregorygow · May 29, 2026 at 11:11 am
Коллеги, это стратегическое руководство РїРѕ выбору SEO-продвижения! Автор разбирает 6 ключевых шагов: РѕС‚ определения бизнес-целей (РЅРµ просто «позиции», Р° конверсия) РґРѕ оценки состояния сайта, контент-стратегии (E-E-A-T), выбора модели взаимодействия (агентство/фриланс/инхаус), трендов (РР, локальное SEO, поведенческие факторы) Рё бюджетирования. Особенно ценно РїСЂРѕ СЃСЂРѕРєРё — SEO это марафон РЅР° 6–12 месяцев. Обязательно Рє прочтению: https://frankbooks.ru/stati/kak-vybrat-jeffektivnoe-seo-prodvizhenie-dlja-biznesa-strategischeskoe-rukovodstvo/
wuzutbus · May 29, 2026 at 11:19 am
Looking for a KYC-free way to buy or sell cryptocurrency from 1–100 USDT? Visit https://coinswaper.io/ – See what 1, 2, 3, 5, 10, and 100 USDT is available for purchase in top coins, compare small resale amounts, and start a quick USDT swap from a single screen. These preset amounts cover the most common small swap scenarios: a tiny test, a micro-purchase, a quick conversion, or a small sell-off to USDT.
RobertZew · May 29, 2026 at 11:34 am
В этой публикации мы рассматриваем важную тему борьбы с зависимостями, включая алкогольную и наркотическую зависимости. Мы обсудим методы лечения, реабилитации и поддержку, которые могут помочь людям, столкнувшимся с этой проблемой. Читатели узнают о перспективах выздоровления и важности комплексного подхода.
Ознакомьтесь с аналитикой – кодирование от алкоголизма люберцы
Raymondcag · May 29, 2026 at 11:51 am
В этой медицинской статье мы погрузимся в актуальные вопросы здравоохранения и лечения заболеваний. Читатели узнают о современных подходах, методах диагностики и новых открытий в научных исследованиях. Наша цель — донести важную информацию и повысить уровень осведомленности о здоровье.
Погрузиться в детали – детокс24 краснодар
CharlesZex · May 29, 2026 at 12:04 pm
В данном обзоре представлены основные направления и тренды в области медицины. Мы обсудим актуальные проблемы здравоохранения, свежие открытия и новые подходы, которые меняют представление о лечении и профилактике заболеваний. Эта информация будет полезна как специалистам, так и широкой публике.
Уточнить детали – лечения наркомании в Краснодаре
madyNouts · May 29, 2026 at 12:06 pm
Прогулки по Москве-реке давно вышли за рамки обычной экскурсии — сегодня это полноценный вечер с музыкой, шоу и живыми выступлениями прямо на борту теплохода. Дискотеки 80–90-х, DJ-вечеринки, концерты и Premium-круизы с ужином и шоу-программой доступны ежедневно и рассчитаны на любой вкус. Ищете дискотека 90-х на москве-реке? Билеты бронируются онлайн на ticketscruise.ru — быстро и без лишних шагов. Особой популярностью пользуется концерт «Хиты Италии» на борту «Ривер Паласа» — отправление с причала Сити-Экспоцентр.
page · May 29, 2026 at 12:10 pm
page
socavyWhike · May 29, 2026 at 1:02 pm
Looking for a crypto exchange API for websites? Visit https://cryptosdk.io/ and you’ll find CryptoSDK – a crypto exchange API for websites, apps, wallets, and digital services that require a built-in crypto exchange within their own product flow. Instead of sending users to a separate frontend, the integration keeps routing, rate search, verification, validation, order creation, and status tracking within a single product.
RobertWet · May 29, 2026 at 1:12 pm
Этот обзор посвящен успешным стратегиям избавления от зависимости, включая реальные примеры и советы. Мы разоблачим мифы и предоставим читателям достоверную информацию о различных подходах. Получите опыт многообразия методов и найдите подходящий способ для себя!
Рассмотреть проблему всесторонне – наркологическая клиника краснодар
yoktogel · May 29, 2026 at 1:13 pm
I have to say this post was certainly informative and contains useful content for enthusiastic visitors. I will definitely bookmark this website for future reference and further viewing. cheers a bunch for sharing this with us!
Charlesopend · May 29, 2026 at 1:31 pm
Эта публикация исследует взаимосвязь зависимости и психологии. Мы обсудим, как психологические аспекты влияют на появление зависимостей и процесс выздоровления. Читатели смогут понять важность профессиональной поддержки и применения научных подходов в терапии.
Читать дальше – вывести из запоя в Балашихе
Wallybut · May 29, 2026 at 2:47 pm
Публикация посвящена жизненным историям людей, успешно справившихся с зависимостью. Мы покажем, что выход есть, и он начинается с первого шага — принятия проблемы и желания измениться.
Это стоит прочитать полностью – наркологическая клиника в краснодаре
Billysab · May 29, 2026 at 3:33 pm
В этом обзоре представлены различные методы избавления от зависимости, включая терапевтические и психологические подходы. Мы сравниваем их эффективность и предоставляем рекомендации для тех, кто хочет вернуться к трезвой жизни. Читатели смогут найти информацию о реабилитационных центрах и поддерживающих группах.
Слушай внимательно — тут важно – детокс24
Barryriche · May 29, 2026 at 3:54 pm
Эта информационная публикация освещает широкий спектр тем из мира медицины. Мы предлагаем читателям ясные и понятные объяснения современных заболеваний, методов профилактики и лечения. Информация будет полезна как пациентам, так и медицинским работникам, желающим поддержать уровень своих знаний.
Эксклюзивная информация – detox24
Timothyelapy · May 29, 2026 at 3:56 pm
sirke ile kedi piresi temizleme hakk?ndaki yaz?y? cok sevdim. Kendiniz gorun: https://kendihobim.com/articles/sirke-kedi-piresi-temizleme/
Timothyelapy · May 29, 2026 at 4:01 pm
Bu arada, eger gri ile uyumlu koltuk renkleri konusuyla ilgileniyorsan?z, buray? inceleyin. Iste link: https://kendifikirler.com/articles/gri-koltuk-takimina-uygun-duvar-renkleri/
MatthewBlict · May 29, 2026 at 4:25 pm
Публикация посвящена жизненным историям людей, успешно справившихся с зависимостью. Мы покажем, что выход есть, и он начинается с первого шага — принятия проблемы и желания измениться.
Узнайте всю правду – вызвать врача-нарколога на дом
RalphHek · May 29, 2026 at 4:27 pm
В этой статье мы рассмотрим современные достижения в области медицины, включая инновационные методы лечения и диагностики. Мы обсудим важность профилактики заболеваний и роль технологий в улучшении качества здравоохранения. Читатели узнают о влиянии медицины на повседневную жизнь и ее значение для современного общества.
Получить дополнительные сведения – детокс24 краснодар
Leroyrhino · May 29, 2026 at 4:42 pm
В этой статье рассматриваются различные аспекты избавления от зависимости, включая физические и психологические методы. Мы обсудим поддержку, мотивацию и стратегии, которые помогут в процессе выздоровления. Читатели узнают, как преодолеть трудности и двигаться к новой жизни без зависимости.
Подробности по ссылке – вызвать врача-нарколога на дом
Bradleyuncon · May 29, 2026 at 5:10 pm
В этой заметке мы представляем шаги, которые помогут в процессе преодоления зависимостей. Рассматриваются стратегии поддержки и чек-листы для тех, кто хочет сделать первый шаг к выздоровлению. Наша цель — вдохновить читателей на положительные изменения и поддержать их в трудных моментах.
Узнать больше – детокс24
vimegySek · May 29, 2026 at 5:13 pm
Ищете официального дилера HAVAL в Санкт-Петербурге? Посетите сайт Автопродикс https://autoprodix-havalpro.ru/ и вы сможете купить новые кроссоверы и внедорожники H3, H5, H7, H9 по выгодным ценам 2026 года. Модельный ряд в наличии, выгодные кредитные программы, трейд-ин, тест-драйв. Подробнее на сайте.
curasspauri · May 29, 2026 at 5:24 pm
Юридическая фирма «Один к одному» заслуженно получила признание ведущих деловых изданий России за профессиональный подход к решению сложнейших финансовых споров. Специалисты компании успешно ведут дела по взысканию задолженности любой сложности, защищают клиентов от субсидиарной ответственности и грамотно сопровождают процедуры банкротства. Команда опытных юристов на https://1k1law.ru/ предлагает индивидуальную стратегию для каждого случая, основанную на глубоком знании законодательства и многолетней практике. Фирма входит в рейтинг лучших по банкротству по версии «Коммерсантъ» и «Право-300», что подтверждает высокий уровень оказываемых услуг и доверие клиентов.
casinos online nuevos · May 29, 2026 at 5:37 pm
Hello, I think your blog might be having browser compatibility issues. When I look at your website in Chrome, it looks fine but when opening in Internet Explorer, it has some overlapping. I just wanted to give you a quick heads up! Other than that, awesome blog!
KennethGrate · May 29, 2026 at 5:46 pm
В этой статье мы подробно рассматриваем проверенные методы борьбы с зависимостями, включая психотерапию, медикаментозное лечение и поддержку со стороны общества. Мы акцентируем внимание на важности комплексного подхода и возможности успешного восстановления для людей, столкнувшихся с этой проблемой.
Получить дополнительную информацию – вывод из запоя краснодар
suyinelasepift · May 29, 2026 at 6:08 pm
Check the live Bitcoin price in GBP and see how much 1 BTC is worth in British Pounds right now. https://bitcoinpricegbp.com/tracks the current BTC/GBP exchange rate, daily movements, and key market data for users looking for a quick reference for Bitcoin in British Pounds. This site is useful for users tracking their Bitcoin balance in GBP, comparing today’s movements, and checking their portfolio value.
Benniemar · May 29, 2026 at 6:30 pm
Эта медицинская заметка содержит сжатую информацию о новых находках и методах в области здравоохранения. Мы предлагаем читателям свежие данные о заболеваниях, профилактике и лечении. Наша цель — быстро и доступно донести важную информацию, которая поможет в повседневной жизни и понимании здоровья.
См. подробности – вывод из запоя краснодар
Hubertbob · May 29, 2026 at 6:35 pm
В этой статье мы говорим о важности поддержки в процессе выздоровления. Рассматриваются семьи, группы поддержки, специалисты и онлайн-ресурсы, которые могут сыграть решающую роль в избавлении от зависимости.
Получить исчерпывающие сведения – наркологическая клиника в люберцах
KennethGrate · May 29, 2026 at 6:55 pm
Эта публикация исследует взаимосвязь зависимости и психологии. Мы обсудим, как психологические аспекты влияют на появление зависимостей и процесс выздоровления. Читатели смогут понять важность профессиональной поддержки и применения научных подходов в терапии.
Полная информация здесь – откапаться от алкоголя
Johnnyphips · May 29, 2026 at 7:03 pm
Публикация знакомит читателей с различными подходами к реабилитации. От традиционных методов до современных программ — вы узнаете, как выбрать оптимальный путь к выздоровлению и преодолеть препятствия на этом пути.
Откройте для себя больше – наркологическая клиника в краснодаре
Timothydaync · May 29, 2026 at 7:15 pm
Добрый день!
На https://realestate-online.ru можно найти полезную информацию о рынке недвижимости России, ипотеке и вариантах вложений в жилую и коммерческую недвижимость. Платформа подойдёт тем, кто изучает способы получения пассивного дохода.
доходная недвижимость, инвестиционный портфель, недвижимость онлайн
Всего наилучшего, и успехов в делах!
DavidJinly · May 29, 2026 at 7:17 pm
Этот обзор содержит информацию о передовых достижениях в области медицины. Мы разберем инновационные технологии, которые меняют подход к лечению и диагностике, а также их влияние на эффективность оказания медицинской помощи.
Как достичь результата? – снятие ломки
Dennispew · May 29, 2026 at 7:47 pm
В этой статье мы рассматриваем разрушительное влияние зависимости на жизнь человека. Обсуждаются аспекты, такие как здоровье, отношения и профессиональные достижения. Читатели узнают о необходимости обращения за помощью и о путях к восстановлению.
Ссылка на источник – наркологическая клиника во владимире
Jasonvop · May 29, 2026 at 7:51 pm
Начните с Пинап — честные бонусы.
Проверенный пинап рабочий сайт — открывается мгновенно.
Пинап платформа объединяет всё — имеет мобильное SDK.
Рабочее зеркало на месяц — даже при блокировке YouTube.
Актуальное зеркало pinup — синхронизацию бонусов.
Источник:
https://pinupcasino77777bc.top
xijejatmus · May 29, 2026 at 8:28 pm
好きです韓国語, 韓国語 ね, はい 韓国語, はい韓国語, あらっそ 韓国語. これが何かわからない?それならウェブサイト https://kanayari.info/ にアクセスしてみてください。韓国語に関する質問も含め、あらゆる疑問への答えが見つかります。勉強にもなるし、面白いですよ!
Richardboide · May 29, 2026 at 8:33 pm
Эта публикация посвящена актуальным вопросам современной медицины и здравоохранения. Мы обсудим новейшие технологии диагностики и лечения, а также их влияние на продолжительность и качество жизни. Читатель найдет здесь информацию о научных исследованиях и перспективных разработках, доступно изложенную для широкой аудитории.
Ознакомиться с теоретической базой – детокс24 краснодар
vizufivenny · May 29, 2026 at 8:38 pm
Качественные двери – это не только безопасность и комфорт, но и визитная карточка вашего дома. Компания TopLocker предлагает жителям Тулы и области профессиональное решение под ключ: от выбора входных и межкомнатных конструкций до их установки. На сайте https://toplockertula.ru/ представлен впечатляющий ассортимент моделей ведущих производителей – Bravo, Profilo Porte, Stabile Porte, Мариам и других. Здесь вы найдете надежные металлические входные двери с терморазрывом, элегантные межкомнатные варианты из экошпона, массива и эмали, а также современные скрытые системы invisible. Опытные специалисты помогут подобрать оптимальное решение для любого интерьера и бюджета, обеспечив качественный монтаж и гарантию на все работы.
https://emigranto.ru/blog/aktualnuy_promokod_fonbet_pri_registracii.html · May 29, 2026 at 9:14 pm
https://emigranto.ru/blog/aktualnuy_promokod_fonbet_pri_registracii.html
Richardboide · May 29, 2026 at 9:47 pm
В этой статье обсуждаются актуальные медицинские вопросы, которые волнуют общество. Мы обращаем внимание на проблемы, касающиеся здравоохранения и лечения, а также на новшества в области медицины. Читатели будут осведомлены о последних событиях и смогут следить за тенденциями в медицине.
Подробнее тут – детокс24
CliftonReike · May 29, 2026 at 10:03 pm
В этой публикации мы обсуждаем современные методы лечения различных заболеваний. Читатели узнают о новых медикаментах, терапиях и исследованиях, которые активно применяются для лечения. Мы нацелены на то, чтобы предоставить практические знания, которые могут помочь в борьбе с недугами.
Неизвестные факты о… – detox24 в краснодаре
Henrywam · May 29, 2026 at 10:19 pm
Публикация охватывает основные направления развития современной медицины. Мы обсудим значимость научных исследований, инноваций в лечении и роли общественного участия в формировании системы здравоохранения.
Выяснить больше – кодировка от алкоголя в волгограде адреса
BarrettZep · May 29, 2026 at 10:24 pm
В этой статье обсуждаются актуальные медицинские вопросы, которые волнуют общество. Мы обращаем внимание на проблемы, касающиеся здравоохранения и лечения, а также на новшества в области медицины. Читатели будут осведомлены о последних событиях и смогут следить за тенденциями в медицине.
Подробности по ссылке – detox24
JamesGophy · May 29, 2026 at 10:33 pm
Для жителей Новосибирска доступны займы под залог птс на выгодных условиях. Мы всегда готовы помочь в трудной ситуации.
Подробная информация на сайте – https://zaymy-pod-pts.ru
онлайн займы под птс
взять займ под залог птс
займы под птс
JamesGophy · May 29, 2026 at 10:41 pm
Оформление займ под птс позволяет получить необходимую сумму, не расставаясь с автомобилем. Это удобное решение для тех, кто ценит мобильность.
Подробная информация на сайте – https://zaymy-pod-pts.ru
онлайн займы под птс
займы под птс в новосибирске
займ под птс онлайн
AaronJaire · May 29, 2026 at 11:41 pm
Эта публикация обращает внимание на важность профилактики зависимостей. Мы обсудим, как осведомленность и образование могут помочь в предотвращении возникновения зависимости. Читатели смогут ознакомиться с полезными советами и ресурсами, которые способствуют здоровому образу жизни.
Смотри, что ещё есть – вызов нарколога на дом в Краснодаре
AlbertPhype · May 30, 2026 at 12:22 am
В этой статье рассматриваются различные аспекты избавления от зависимости, включая физические и психологические методы. Мы обсудим поддержку, мотивацию и стратегии, которые помогут в процессе выздоровления. Читатели узнают, как преодолеть трудности и двигаться к новой жизни без зависимости.
Проследить причинно-следственные связи – detox24
AaronJaire · May 30, 2026 at 12:42 am
В этой статье мы обсудим процесс восстановления после зависимостей, акцентируя внимание на различных методах и подходах к реабилитации. Читатели узнают, как создать план выздоровления и использовать полезные ресурсы для достижения устойчивых изменений.
Что ещё? Расскажи всё! – выезд нарколога на дом
StephenpaR · May 30, 2026 at 12:49 am
В данной статье рассматриваются физиологические и эмоциональные аспекты зависимости. Мы обсудим, как организм реагирует на зависимое поведение, и какие методы помогают восстановить здоровье и внутреннее равновесие.
Все материалы собраны здесь – вывод из запоя в симферополе
Timothydaync · May 30, 2026 at 1:13 am
Доброго!
На https://realestate-online.ru можно найти полезную информацию о рынке недвижимости России, ипотеке и вариантах вложений в жилую и коммерческую недвижимость. Платформа подойдёт тем, кто изучает способы получения пассивного дохода.
покупка жилья, доходная недвижимость, инвестиции в недвижимость
Всего наилучшего, и успехов в делах!
Henrywam · May 30, 2026 at 1:13 am
Текст посвящён распространённым мифам о зависимости и их развенчанию. Мы предоставим научно обоснованную информацию и дадим рекомендации по выбору эффективного способа борьбы с зависимым поведением.
Ознакомиться с деталями – кодирование от алкоголизма в волгограде адреса
Josephcroro · May 30, 2026 at 1:39 am
feng shui tablo secimi hakk?ndaki makaleyi gercekten begendim. Iste link: https://yappendik.com/articles/feng-shui-tablo-secimi-enerji-akisi/
Manuelbes · May 30, 2026 at 1:39 am
В этой публикации мы исследуем ключевые аспекты здоровья, включая влияние образа жизни на благополучие. Читатели узнают о важности правильного питания, физической активности и психического здоровья. Мы предоставим практические советы и рекомендации для поддержания здоровья и развития профилактических подходов.
Слушай внимательно — тут важно – detox24 в краснодаре
Josephcroro · May 30, 2026 at 1:45 am
Bu arada soyleyeyim, eger yogurt mayalama derecesi konusuyla ilgileniyorsan?z, suraya bak?n. Link burada: https://yappendik.com/articles/yogurt-mayalamada-maya-miktari-ipuclari/
Billysab · May 30, 2026 at 2:07 am
Этот информационный материал подробно освещает проблему наркозависимости, ее причины и последствия. Мы предлагаем информацию о методах лечения, профилактики и поддерживающих программах. Цель статьи — повысить осведомленность и продвигать идеи о необходимости борьбы с зависимостями.
Всё самое вкусное внутри – детокс24 краснодар
mipaoTam · May 30, 2026 at 2:12 am
Анапа — жемчужина черноморского побережья, и исследовать её по-настоящему можно только за рулём собственного, пусть и арендованного, автомобиля. Сервис https://auto-arenda-anapa.ru/ предлагает прокат без залога, без ограничения пробега и с неограниченной страховкой ОСАГО, что делает каждую поездку абсолютно беззаботной. Детское кресло и видеорегистратор включены в комплектацию, а оформление занимает три простых шага: выбрать автомобиль, отправить документы и указать место подачи. Команда профессионалов CarTrip всегда на связи в мессенджерах и готова ответить на любой вопрос. Путешествуйте свободно!
Juliopoino · May 30, 2026 at 2:16 am
Публикация охватывает основные направления развития современной медицины. Мы обсудим значимость научных исследований, инноваций в лечении и роли общественного участия в формировании системы здравоохранения.
Получить исчерпывающие сведения – наркологическая клиника в краснодаре
Herbertbob · May 30, 2026 at 2:33 am
В этой статье мы обсудим процесс восстановления после зависимостей, акцентируя внимание на различных методах и подходах к реабилитации. Читатели узнают, как создать план выздоровления и использовать полезные ресурсы для достижения устойчивых изменений.
Осуществить глубокий анализ – наркологическая клиника в донецке
https://www.colehardware.com/articles/1xbet-promo-code_and_bonus-code.html · May 30, 2026 at 2:50 am
https://www.colehardware.com/articles/1xbet-promo-code_and_bonus-code.html
LeonardTek · May 30, 2026 at 3:02 am
В этой публикации мы исследуем ключевые аспекты здоровья, включая влияние образа жизни на благополучие. Читатели узнают о важности правильного питания, физической активности и психического здоровья. Мы предоставим практические советы и рекомендации для поддержания здоровья и развития профилактических подходов.
Только факты! – выведение из запоя краснодар
Wallybut · May 30, 2026 at 3:27 am
В этой статье рассматриваются различные аспекты избавления от зависимости, включая физические и психологические методы. Мы обсудим поддержку, мотивацию и стратегии, которые помогут в процессе выздоровления. Читатели узнают, как преодолеть трудности и двигаться к новой жизни без зависимости.
Смотри, что ещё есть – наркологическая клиника в краснодаре
MatthewBlict · May 30, 2026 at 3:55 am
В данном материале представлены ключевые тенденции в сфере медицинской науки и практики. Вы узнаете о последних открытиях, инновационных подходах к терапии и важности профилактики заболеваний. Особое внимание уделено практическому применению новых методов в клинической практике.
Наши рекомендации — тут – вызова нарколога на дом
WilliamPek · May 30, 2026 at 4:01 am
Эта информационная публикация освещает широкий спектр тем из мира медицины. Мы предлагаем читателям ясные и понятные объяснения современных заболеваний, методов профилактики и лечения. Информация будет полезна как пациентам, так и медицинским работникам, желающим поддержать уровень своих знаний.
Кликни и узнай всё! – детокс24 краснодар
Juliopoino · May 30, 2026 at 4:06 am
В этой статье рассматриваются актуальные вопросы, связанные с развитием медицинской науки и её внедрением в повседневную практику. Особое внимание уделено вопросам профилактики, ранней диагностики и использованию технологий для улучшения здоровья человека.
Смотрите также – наркологическая клиника краснодар
rudoziCeast · May 30, 2026 at 4:12 am
Looking for a reliable crypto exchange? Visit https://cryptoswaptrade.com/ – CryptoSwapTrade is a crypto trading exchange designed for users who want to trade cryptocurrency online through a simple and direct exchange flow. The service supports 165 cryptocurrencies, 210+ assets across networks, approximately 40,000 cryptocurrency pairs, and approximately 8,000 fiat-related transfers in 40+ fiat currencies.
Barryriche · May 30, 2026 at 4:12 am
Публикация посвящена жизненным историям людей, успешно справившихся с зависимостью. Мы покажем, что выход есть, и он начинается с первого шага — принятия проблемы и желания измениться.
Детальнее – наркологическая клиника краснодар
CliftonReike · May 30, 2026 at 4:16 am
Этот информационный материал подробно освещает проблему наркозависимости, ее причины и последствия. Мы предлагаем информацию о методах лечения, профилактики и поддерживающих программах. Цель статьи — повысить осведомленность и продвигать идеи о необходимости борьбы с зависимостями.
Связаться за уточнением – detox24 в краснодаре
Leroyrhino · May 30, 2026 at 4:47 am
Этот обзор медицинских исследований собрал самое важное из последних публикаций в области медицины. Мы проанализировали ключевые находки и представили их в доступной форме, чтобы читатели могли легко ориентироваться в актуальных темах. Этот материал станет отличным подспорьем для изучения медицины.
Читать дальше – Нарколог на дом
Timothydaync · May 30, 2026 at 5:09 am
Доброго!
На https://realestate-online.ru можно найти полезную информацию о рынке недвижимости России, ипотеке и вариантах вложений в жилую и коммерческую недвижимость. Платформа подойдёт тем, кто изучает способы получения пассивного дохода.
инвестиции в недвижимость, коммерческая недвижимость, доходная недвижимость
Всего наилучшего, и успехов в делах!
Charlesonert · May 30, 2026 at 5:11 am
Актуальный портал — круглосуточной поддержкой.
Прямой доступ к слотам — с выводом выигрышей.
Играйте в браузере без скачивания — с чатом поддержки.
Pinup is your stylish betting choice — generous welcome pack.
Обход блокировки для pinup — быстрее основного сайта.
Source:
пинап официальный
WilliamPek · May 30, 2026 at 5:23 am
Этот обзор посвящен успешным стратегиям избавления от зависимости, включая реальные примеры и советы. Мы разоблачим мифы и предоставим читателям достоверную информацию о различных подходах. Получите опыт многообразия методов и найдите подходящий способ для себя!
Узнай первым! – наркологическая клиника краснодар
tizirojaf · May 30, 2026 at 5:39 am
Looking for terea mauve wave? The easy-stick.com store provides a broad assortment of tobacco products and offers express delivery straight to Germany, France, Ireland, and Belgium. Our store is constantly stocked with the newest Terea flavors and the most recent IQOS Iluma kits. Our platform is committed to delivering high-quality products alongside safe and secure payment options. Shop now and enjoy the best offers available at the most attractive terms.
bovehenprins · May 30, 2026 at 5:51 am
Looking for a list of crypto swaps? Visit https://swapslist.io/ – SwapsList helps users compare crypto exchange services before choosing where to exchange digital assets. The site focuses on practical exchange factors: KYC regulations, registration requirements, supported coins, available networks, expected speed, rate type, fees, fiat routes, and wallet payout flow. Use the list to compare direct swap services, aggregators, and online exchange options.
Timothydaync · May 30, 2026 at 6:37 am
Добрый день!
Для тех, кто следит за изменениями на рынке жилья и ищет идеи для инвестиций, полезным источником информации может стать https://realestate-online.ru. Платформа объединяет статьи о недвижимости, ипотеке, аренде и современных инвестиционных инструментах.
инвестиции в новостройки, купить квартиру онлайн, советы по недвижимости
Всего наилучшего, и успехов в делах!
Manuelbes · May 30, 2026 at 7:03 am
В этой статье рассматривается комплексный подход к избавлению от зависимости. Читатель узнает, как сочетание физического, психологического и духовного восстановления помогает достичь стойкого выздоровления.
Доступ к полной версии – откапаться от алкоголя
Benniemar · May 30, 2026 at 7:04 am
Этот текст посвящён сложным аспектам зависимости и её влиянию на жизнь человека. Мы обсудим психологические, физические и социальные последствия зависимого поведения, а также важность своевременного обращения за помощью.
Узнать из первых рук – detox24
Robertbet · May 30, 2026 at 7:19 am
Эта информационная публикация освещает широкий спектр тем из мира медицины. Мы предлагаем читателям ясные и понятные объяснения современных заболеваний, методов профилактики и лечения. Информация будет полезна как пациентам, так и медицинским работникам, желающим поддержать уровень своих знаний.
Кликни и узнай всё! – вызова нарколога на дом
RalphHek · May 30, 2026 at 7:47 am
В этой статье рассматривается комплексный подход к избавлению от зависимости. Читатель узнает, как сочетание физического, психологического и духовного восстановления помогает достичь стойкого выздоровления.
Кликни и узнай всё! – детокс24
Timothydaync · May 30, 2026 at 8:15 am
Привет всем!
Тем, кто интересуется инвестициями и аналитикой рынка жилья, стоит обратить внимание на https://realestate-online.ru. На сайте публикуются материалы о покупке недвижимости, доходности аренды, новостройках и инвестиционных стратегиях для частных инвесторов.
инвестиции в недвижимость, доходная недвижимость, доходная недвижимость
Всего наилучшего, и успехов в делах!
Herbertbob · May 30, 2026 at 8:27 am
В этой публикации мы исследуем ключевые аспекты здоровья, включая влияние образа жизни на благополучие. Читатели узнают о важности правильного питания, физической активности и психического здоровья. Мы предоставим практические советы и рекомендации для поддержания здоровья и развития профилактических подходов.
Осуществить глубокий анализ – наркологическая клиника в донецке
Stevezes · May 30, 2026 at 9:00 am
Этот информационный материал подробно освещает проблему наркозависимости, ее причины и последствия. Мы предлагаем информацию о методах лечения, профилактики и поддерживающих программах. Цель статьи — повысить осведомленность и продвигать идеи о необходимости борьбы с зависимостями.
Открой скрытое – психолог симферополь консультация
LeonardTek · May 30, 2026 at 9:11 am
В этой публикации мы обсуждаем современные методы лечения различных заболеваний. Читатели узнают о новых медикаментах, терапиях и исследованиях, которые активно применяются для лечения. Мы нацелены на то, чтобы предоставить практические знания, которые могут помочь в борьбе с недугами.
Только факты! – detox24
Timothydaync · May 30, 2026 at 9:18 am
Здравствуйте!
Тем, кто интересуется инвестициями и аналитикой рынка жилья, стоит обратить внимание на https://realestate-online.ru. На сайте публикуются материалы о покупке недвижимости, доходности аренды, новостройках и инвестиционных стратегиях для частных инвесторов.
аренда недвижимости, ипотека 2026, недвижимость для инвестиций
Всего наилучшего, и успехов в делах!
Амфилохий · May 30, 2026 at 10:08 am
Стоматология «Нам по зубам» в городе Видное https://womanjour.ru/lechenie-zubov-v-vidnom.html
Timothydaync · May 30, 2026 at 10:25 am
Здравствуйте!
Тем, кто интересуется инвестициями и аналитикой рынка жилья, стоит обратить внимание на https://realestate-online.ru. На сайте публикуются материалы о покупке недвижимости, доходности аренды, новостройках и инвестиционных стратегиях для частных инвесторов.
ипотека 2026, купить квартиру онлайн, недвижимость и ипотека
Всего наилучшего, и успехов в делах!
Darrelldyets · May 30, 2026 at 10:40 am
В этой медицинской статье мы погрузимся в актуальные вопросы здравоохранения и лечения заболеваний. Читатели узнают о современных подходах, методах диагностики и новых открытий в научных исследованиях. Наша цель — донести важную информацию и повысить уровень осведомленности о здоровье.
Разобраться лучше – detox24 в краснодаре
GeorgeKnipt · May 30, 2026 at 12:16 pm
Этот краткий обзор предлагает сжатую информацию из области медицины, включая ключевые факты и последние новости. Мы стремимся сделать информацию доступной и понятной для широкой аудитории, что позволит читателям оставаться в курсе актуальных событий в здравоохранении.
Наши рекомендации — тут – откапаться от алкоголя
Timothydaync · May 30, 2026 at 1:05 pm
Привет всем!
Тем, кто интересуется инвестициями и аналитикой рынка жилья, стоит обратить внимание на https://realestate-online.ru. На сайте публикуются материалы о покупке недвижимости, доходности аренды, новостройках и инвестиционных стратегиях для частных инвесторов.
ипотека 2026, аналитика недвижимости, аналитика недвижимости
Всего наилучшего, и успехов в делах!
Darrelldyets · May 30, 2026 at 1:07 pm
В данной публикации мы поговорим о процессе восстановления от зависимости, о том, как вернуть себе нормальную жизнь. Мы обсудим преодоление трудностей, значимость поддержки и наличие программ реабилитации. Читатели смогут узнать о ключевых шагах к успешному восстановлению.
Секреты успеха внутри – детокс24
nejixinnon · May 30, 2026 at 2:02 pm
Ищете имплантацию всех зубов All-on-4 (Все-на-4) в Мурманске по лучшей цене от профессиональных стоматологов? Посетите https://nova-51.ru/implantatsiya-zubov-murmansk/implantatsiya-vsekh-zubov-all-on-4-vse-na-4 узнайте подробную информацию и стоимость услуги.
Robertbet · May 30, 2026 at 3:04 pm
В данной статье рассматриваются физиологические и эмоциональные аспекты зависимости. Мы обсудим, как организм реагирует на зависимое поведение, и какие методы помогают восстановить здоровье и внутреннее равновесие.
Продолжить чтение – нарколога на дом
JameshoT · May 30, 2026 at 3:50 pm
Главная водка бет
JosephPYDAY · May 30, 2026 at 4:31 pm
the original source Fake invoices, financial documents, and counterfeit bills
koyafnybruse · May 30, 2026 at 4:54 pm
Современная электроника требует надежных комплектующих, и выбор поставщика становится критически важным для успеха любого проекта. Профессиональные инженеры и радиолюбители знают, что качество компонентов напрямую влияет на долговечность устройств и безопасность эксплуатации. На платформе https://components.ru/ собран широкий ассортимент электронных элементов — от микроконтроллеров и силовых транзисторов до пассивных компонентов и соединителей, что позволяет реализовать проекты любой сложности. Удобная навигация, техническая документация и оперативная доставка делают процесс закупки максимально эффективным, экономя время специалистов и обеспечивая бесперебойность производственных циклов в условиях современного рынка.
JosephPYDAY · May 30, 2026 at 5:00 pm
her latest blog Remote access services (RDP, SSH)
girutllmew · May 30, 2026 at 5:24 pm
中学生 詩, 神奈川県 高校入試日程, 変格活用 一覧, 茨城県公立高校入試, 八千代松陰 偏差値. ぜひ当社のウェブサイト https://manalab.jp/ をご覧ください!最新の情報が満載です。日本最大級のポータルサイトで、重要な知識を習得するお手伝いをいたします。
onepharm7.store · May 30, 2026 at 6:06 pm
onepharm7.store
LarrySnala · May 30, 2026 at 6:37 pm
Главная vodkabet новый сайт
LarrySnala · May 30, 2026 at 7:16 pm
каталог vodka bet
JosephPYDAY · May 30, 2026 at 7:20 pm
go to these guys Phishing tools and malicious software for stealing data
vijiwotLaf · May 30, 2026 at 7:43 pm
Выбор качественных дверей – важный этап в создании комфортного и безопасного пространства дома или квартиры. В Туле профессиональное решение этой задачи предлагает компания, специализирующаяся на продаже и установке входных и межкомнатных конструкций. На сайте https://dveridzen.ru/ представлен широкий ассортимент моделей: от надежных металлических входных дверей с терморазрывом до стильных межкомнатных вариантов со стеклом и зеркалами, включая современные скрытые и раздвижные системы. Компания гарантирует профессиональный монтаж, удобную доставку и выгодные условия оплаты, что делает покупку максимально комфортной для каждого клиента.
Stevezes · May 30, 2026 at 8:25 pm
В данном обзоре представлены основные направления и тренды в области медицины. Мы обсудим актуальные проблемы здравоохранения, свежие открытия и новые подходы, которые меняют представление о лечении и профилактике заболеваний. Эта информация будет полезна как специалистам, так и широкой публике.
Лови подробности – психолог симферополь консультация
buzekstap · May 30, 2026 at 9:40 pm
Looking to embed a crypto widget on your website? Visit https://orgtrade.org/ – OrgTrade helps website owners add a crypto exchange widget to their pages and convert cryptocurrency-related traffic into swap activity. Instead of sending visitors through a simple outbound link, your site can feature an integrated exchange tool where users can select a pair, enter an amount, and initiate a crypto conversion.
LarrySnala · May 30, 2026 at 10:23 pm
зайти на сайт vodka bet
cassino ao vivo bônus · May 30, 2026 at 11:23 pm
Bônus espetacular no Caishen Wins! Quase o triplo do depósito de lucro limpo.
WPS office下载 · May 30, 2026 at 11:24 pm
Wonderful article! We are linking to this great post on our website. Keep up the great writing.
zotojpaype · May 30, 2026 at 11:25 pm
Looking for tune guitar automatically? TronicalTune tronicaltune.net is a German-engineered fully automatic tuning system for guitars. It tunes all six strings at the push of a button, saves time on stage and in the studio, and helps guitar players switch tunings fast and accurately. perfectly suited for both electric and acoustic guitar players.
Jasonvop · May 30, 2026 at 11:30 pm
Почему выбирают Пинап — высокие коэффициенты.
Прямо сейчас — пинап актуальное зеркало — доступно из любой страны.
Нужно пинап зеркало сегодня — подходит для мобильных.
Полная версия для СНГ — бонусы в ?.
Тысячи слотов в pinup казино — вывод без комиссии.
Источник:
https://pinup-2023.com
RichardKet · May 30, 2026 at 11:36 pm
Без скрытых страховок и допов. Честный займ под ПТС от прямого инвестора.
Подробнее – http://zaym-ooo.ru
займы юр лицу
займы для ООО в новосибирске
автозаймы ООО новосибирск
RichardKet · May 30, 2026 at 11:48 pm
взять займ для ооо онлайн – одобрение 99% заявок. Даже с плохой КИ выдаем деньги под ПТС в течение часа.
Подробнее – http://zaym-ooo.ru/
автозаймы для ООО в нск
займы для юр лиц новосибирск
взять займ для ооо онлайн
KennethVab · May 30, 2026 at 11:56 pm
В этой статье мы обсудим процесс восстановления после зависимостей, акцентируя внимание на различных методах и подходах к реабилитации. Читатели узнают, как создать план выздоровления и использовать полезные ресурсы для достижения устойчивых изменений.
Слушай внимательно — тут важно – частная наркологическая клиника в Луганске
hecamietor · May 31, 2026 at 12:08 am
Looking for the most active crypto market movements in one place? Visit https://topchanges.com/ – TopChanges tracks the most active crypto market movements in one place. See which coins are rising today, which coins are falling today, and which cryptocurrencies are attracting attention in the market. The dashboard combines 24-hour price changes, trading volume, market capitalization, and trend activity to give you a quick overview of today’s crypto movers.
DavidJinly · May 31, 2026 at 3:45 am
Публикация охватывает основные направления развития современной медицины. Мы обсудим значимость научных исследований, инноваций в лечении и роли общественного участия в формировании системы здравоохранения.
Что ещё нужно знать? – детокс24 краснодар
JameshoT · May 31, 2026 at 4:01 am
проверить сайт водкабет
DustinKex · May 31, 2026 at 4:11 am
over at this website https://peptidesnova.com/pages/8-reasons-why-bpc-157-could-be-the-secret-to-unlock-g2ng
paronioLekly · May 31, 2026 at 4:18 am
Для поклонников качественного видеоконтента портал https://rseriali.net/ стал настоящей находкой, предлагая богатую коллекцию русских сериалов в отличном качестве и с удобной навигацией. Ресурс выделяется продуманной структурой каталога, где представлены как новинки телеэфира, так и проверенная временем классика отечественного кино, доступные для просмотра без утомительных процедур регистрации и навязчивой рекламы, что особенно ценят современные зрители.
dumuses · May 31, 2026 at 4:54 am
Посетите сайт Читай-город https://www.chitai-gorod.ru/ – там вы найдете самый большой ассортимент интересных книг, подарков и канцелярских товаров по выгодным ценам. Загляните в каталог, и вы обязательно найдете книгу, которая вас интересует. При необходимости посмотрите адреса магазинов. При покупке с доставкой она осуществляется по всей России.
DustinKex · May 31, 2026 at 5:18 am
blog https://peptidesnova.com
GeorgeKnipt · May 31, 2026 at 5:22 am
Этот краткий обзор предлагает сжатую информацию из области медицины, включая ключевые факты и последние новости. Мы стремимся сделать информацию доступной и понятной для широкой аудитории, что позволит читателям оставаться в курсе актуальных событий в здравоохранении.
Расширить кругозор по теме – откапаться от алкоголя
DustinKex · May 31, 2026 at 6:43 am
page https://peptidesnova.com
JameshoT · May 31, 2026 at 7:18 am
веб-сайте vodka bet
Archienot · May 31, 2026 at 7:24 am
Сайт с моментальным доступом — мобильная версия.
Доверяйте только лутран официальный — идёт в рейтингах ТОП.
Стабильная работа без РКН — не теряет историю ставок.
Лутран регистрация сайт без скрытых условий — автоматический бонус на счёт.
Source:
lootruntop.com
Williamsense · May 31, 2026 at 7:28 am
Happy Cactus Cactus Cactus Cactus Cactus Cactus
Happy Cactus Cactus Cactus Cactus Cactus Cactus
Happy Cactus Cactus Cactus Cactus Cactus Cactus
Happy Cactus Cactus Cactus Cactus Cactus Cactus
Happy Cactus Cactus Cactus Cactus Cactus Cactus
Happy Cactus Cactus Cactus Cactus Cactus Cactus
https://kaktus1.site
jogar roleta · May 31, 2026 at 7:52 am
Tô tremendo.
Gregorygow · May 31, 2026 at 8:09 am
Хорошая статья про стратегическое SEO — как выбрать путь к вершинам выдачи и не слить бюджет. Автор разбирает, как отличить «белое» SEO от серых методов, почему не стоит верить гарантиям и на что обращать внимание при выборе подрядчика. Отдельный блок про контент и UX как основу эффективного продвижения. Полезно: https://olivadance.ru/2026/05/iskusstvo-strategicheskogo-seo-kak-vybrat-put-k-vershinam-vydachi-i-ne-slit-bjudzhet/
fixDiele · May 31, 2026 at 8:41 am
По теме “Свежие новости Томской области и мира”, нашел много полезного.
Ссылка ниже:
https://03media.ru
https://www.wpswindows.com · May 31, 2026 at 8:42 am
Hello there! This post couldn’t be written much better! Looking through this article reminds me of my previous roommate! He continually kept talking about this. I’ll forward this post to him. Fairly certain he’ll have a good read. I appreciate you for sharing!
Lloydcat · May 31, 2026 at 9:22 am
Подробнее снять квартиру на несколько дней в Москве
keonhacai5id1 · May 31, 2026 at 9:45 am
I saw a similar post on another website but the points were not as well articulated.
WPS官网 · May 31, 2026 at 10:04 am
This site was… how do I say it? Relevant!! Finally I’ve found something which helped me. Thanks.
lisadthMow · May 31, 2026 at 10:40 am
Ищете увеличение объема костной ткани для имплантации зубов в Мурманске? Посетите https://nova-51.ru/implantatsiya-zubov-murmansk/sinus-lifting-i-kostnaya-plastika-murmansk – мы предлагаем лучший синус лифтинг от опытных и квалифицированных врачей. Узнайте подробную информацию на сайте.
LarrySnala · May 31, 2026 at 10:42 am
другие vodka bet
Lloydcat · May 31, 2026 at 12:08 pm
нажмите снять однокомнатную квартиру в москве собственником
Каллиник · May 31, 2026 at 12:37 pm
Перетяжка салона автомобиля в Москве https://auto-style24.ru/
gemuxrddob · May 31, 2026 at 12:37 pm
Ищете аккуратное и деликатное удаление зуба в Мурманске? Посетите https://nova-51.ru/lechenie-zubov-murmansk/udalenie-zuba-murmansk – у нас профессиональная и тщательная помощь всем нашим пациентам. Узнайте подробную информацию и стоимость на сайте.
papunflake · May 31, 2026 at 1:03 pm
Посетите сайт Babylook https://babylook.by/ — это маркетплейс детских товаров от белорусских производителей. У нас много категорий для девочек и мальчиков и новорожденных, а также игрушки, все для ухода и питание и многое другое. Товары безопасные, уникальные и сделанные с заботой. Вы сможете удобно находить и выбирать лучшее!
https://q8at.link/gaildowie22517 · May 31, 2026 at 1:46 pm
Bästa communityn för onlinespel.
https://cphproperty.uk/author/winonavine253/
fineglwet · May 31, 2026 at 2:06 pm
Если вы ищете надёжный источник Telegram-аккаунтов для работы, обратите внимание на специализированный магазин https://marketgram.io/ — здесь представлены аккаунты разных стран в форматах TData и Session+JSON с отлёжкой, что существенно снижает риски блокировок. Выдача происходит мгновенно после оплаты, невалидные аккаунты заменяются без лишних вопросов, а поддержка доступна прямо в Telegram. Регулярные акции и несколько вариантов оплаты делают сервис удобным для тех, кто работает с аккаунтами системно и ценит стабильность результата.
fastek 571 · May 31, 2026 at 2:18 pm
Компания fastek https://fastek.by проектируем и поставляем надежные фасадные системы для коммерческих и жилых объектов, обеспечивая долговечность, энергоэффективность и безупречный внешний вид здания под ваши задачи.
xowemdSperm · May 31, 2026 at 2:46 pm
TRX (TRON) Exchange Online for 160+ cryptocurrencies and 40+ fiat currencies at https://swapto.io/ – a service for quickly exchanging TRX online. Exchange TRX for USDT, BTC, ETH, and other assets, receive cryptocurrency in the opposite direction, and buy or sell TRON for any fiat currency. Swapto makes it easy to transfer funds between cryptocurrencies, lock your value in a stablecoin, buy TRON with fiat, and sell TRX without any extra steps.
https://tinyurl.com/rwn3a4cm · May 31, 2026 at 4:17 pm
https://tinyurl.com/rwn3a4cm Nyan Cat!
casino online us · May 31, 2026 at 4:37 pm
Melhor sensação do dia: ver o PIX caindo depois de amassar o Buffalo Win.
fabebBum · May 31, 2026 at 4:42 pm
Нужно качественное навесное оборудование для спецтехники? Посетите сайт Производственного предприятия EXTEN https://ppe-exten.ru/ и ознакомьтесь с каталогом, там вы найдете широкий ассортимент навесного оборудования для минитракторов, погрузчиков, экскаваторов, экскаваторов-погрузчиков, минипогрузчиков и фронтальных погрузчиков. Каталог содержит оборудование различного назначения, способное решить любые производственные задачи. Доставка в любую точку России, а также сервисное обслуживание и гарантия качества!
новые вакансии · May 31, 2026 at 4:53 pm
Сегодня всё больше людей ищут варианты через интернет, не расходуя время на посещения офисов. Удобный сервис даёт возможность за несколько минут найти работу по своему городу, опыту и графику. Каталог постоянно пополняется, есть варианты от прямых работодателей.
Lloydcat · May 31, 2026 at 5:20 pm
Узнать больше снять однокомнатную квартиру в москве метро
todelosOxymn · May 31, 2026 at 6:07 pm
Looking for a quick, private XMR swap online without registration? Visit https://swapxmr.io/ – SwapXMR helps users exchange Monero through a direct crypto exchange flow without a trading terminal, order book, or complicated account setup. The service focuses on XMR exchange pairs with Bitcoin, Tether, Ethereum, and other digital assets, while supported buy and sell options are available through the exchange.
Lloydcat · May 31, 2026 at 6:41 pm
узнать больше Здесь снять квартиру в москве по суточно недорого
Jeromeder · May 31, 2026 at 9:12 pm
Эта публикация посвящена актуальным вопросам современной медицины и здравоохранения. Мы обсудим новейшие технологии диагностики и лечения, а также их влияние на продолжительность и качество жизни. Читатель найдет здесь информацию о научных исследованиях и перспективных разработках, доступно изложенную для широкой аудитории.
Ссылка на источник – Наркологическая клиника в Луганске
https://n-white.ru/catalog/pgs/1xbet_promokod_besplatno_2.html · May 31, 2026 at 9:59 pm
https://n-white.ru/catalog/pgs/1xbet_promokod_besplatno_2.html
https://xn-----7kcbekeiftdh9amwkb4d2o.xn--p1ai/news/bonus_melbet_za_registraciu___aktualnuy_promokod_.html · May 31, 2026 at 10:54 pm
https://xn—–7kcbekeiftdh9amwkb4d2o.xn--p1ai/news/bonus_melbet_za_registraciu___aktualnuy_promokod_.html
Ralphkix · May 31, 2026 at 11:10 pm
В данной статье рассматриваются проблемы общественного здоровья и социальные факторы, влияющие на него. Мы акцентируем внимание на значении профилактики и осведомленности в защите здоровья на уровне общества. Читатели смогут узнать о новых инициативах и программах, направленных на улучшение здоровья населения.
Смотри, что ещё есть – Частные наркологические клиники в Луганске
RobertEpini · May 31, 2026 at 11:16 pm
you can look here https://www.houseofnova.nl/collections/arylcyclohexylamine
Williambep · May 31, 2026 at 11:49 pm
современные системы отбеливания site
RobertEpini · May 31, 2026 at 11:53 pm
have a peek at these guys https://www.houseofnova.nl/collections/tryptamines
Jeromeder · June 1, 2026 at 12:05 am
Эта публикация содержит ценные советы и рекомендации по избавлению от зависимости. Мы обсуждаем различные стратегии, которые могут помочь в процессе выздоровления и важность обращения за помощью. Читатели смогут использовать полученные знания для улучшения своего состояния.
Ссылка на источник – вывод из запоя в Луганске
KeithDyday · June 1, 2026 at 12:15 am
other dmail mail
найти работу · June 1, 2026 at 12:44 am
Найти нужное место стало удобнее: больше не нужно обзванивать десятки компаний. На сервисе собраны актуальные предложения с подробным описанием условий и зарплаты. На сайте легко отсортировать работу по графику, опыту и району — и сразу отправить отклик.
ViaBTC · June 1, 2026 at 12:46 am
I would like to thank you for the efforts you have put in writing this site. I’m hoping to check out the same high-grade content from you later on as well. In fact, your creative writing abilities has motivated me to get my own site now 😉
Michaelpet · June 1, 2026 at 12:55 am
rafting trip Tara https://www.tara-montenegro-rafting.me
ClintJom · June 1, 2026 at 2:05 am
монетизация товаров онлайн https://www.prodazhi-na-avito.ru
Joshuamarma · June 1, 2026 at 2:08 am
Эта публикация раскрывает психологические механизмы зависимости и их роль в развитии расстройств. Читатель узнает о том, как психология влияет на формирование зависимостей и как профессиональная помощь может изменить ситуацию.
Расширить кругозор по теме – детокс24
n77 casino · June 1, 2026 at 3:00 am
The emphasis on evidence over mere hypotheses is crucial, whether we’re discussing nutrition or complex risk models. Understanding the underlying mechanisms-like metabolic pathways-requires deep data analysis. It’s similar to how optimizing play requires reliable platforms; for example, checking out the n77 casino download ensures a stable experience. Great discussion!
KeithDyday · June 1, 2026 at 3:04 am
click here to investigate dmail twitter
RobertEpini · June 1, 2026 at 3:14 am
her comment is here https://www.houseofnova.nl/collections/pellets
Hotel duvet china · June 1, 2026 at 3:23 am
A fascinating discussion is worth comment. I think that you need to write more on this issue, it might not be a taboo matter but generally people don’t speak about these subjects. To the next! Kind regards.
Thomascob · June 1, 2026 at 3:36 am
здесь вотка бет
Michaelcip · June 1, 2026 at 3:58 am
budget car hire service Montenegro https://montenegro-car-rental-hire.com
Jasonvop · June 1, 2026 at 4:01 am
Ищете надёжный клуб — быстрые выплаты.
Авторизация по логину — с сохранением сессии.
Пинап сайт зеркало с полным функционалом — не блокируется провайдерами.
Пинап рабочее зеркало без рекламы — не тормозит.
Рабочая копия pinup сайта — синхронизацию бонусов.
Источник:
https://pinup-casino-pid5.top
Thomascob · June 1, 2026 at 4:28 am
перенаправляется сюда vodka bet casino
https://sexvideochat.su/ · June 1, 2026 at 5:21 am
https://sexvideochat.su/
weed prague 438 · June 1, 2026 at 5:56 am
buy thc joint in prague marijuana delivery in prague
gates of olympus super scatter demo grátis · June 1, 2026 at 6:16 am
O segredo do Buffalo Win é não ter ganância. Puxei R$ 50 e parei. Saque rápido via PIX é vida.
Timothyelapy · June 1, 2026 at 6:30 am
rutubet kokusuna ne iyi gelir hakk?ndaki yaz?y? cok sevdim. Link burada: https://hobiprojesi.com/articles/rutubet-kokusu-nasil-giderilir/
Timothyelapy · June 1, 2026 at 6:34 am
“evde kozalak bulundurman?n faydalar?” konusu icin burada harika bilgiler var. Kendiniz gorun: https://kendimacera.com/articles/bitkiler-hakkinda-ilginc-bilgiler/
RobertEpini · June 1, 2026 at 6:49 am
find here https://www.houseofnova.nl/collections/liquid-rcs
nefukorytef · June 1, 2026 at 7:19 am
Ищете имплантацию зубов в Мурманске? Посетите https://nova-51.ru/implantatsiya-zubov-murmansk – с помощью имплантации мы восстанавливаем эстетику, функциональность зубного ряда, улучшая качество жизни и самооценку пациента. Только опытные хирурги! Подробнее на сайте.
KennethVab · June 1, 2026 at 7:37 am
В данной статье рассматриваются физиологические и эмоциональные аспекты зависимости. Мы обсудим, как организм реагирует на зависимое поведение, и какие методы помогают восстановить здоровье и внутреннее равновесие.
Это ещё не всё… – лечение алкоголизма в Луганске
pagcor online casino app · June 1, 2026 at 7:52 am
Meu saldo tava baixo, mas o Lucky Neko me salvou hoje de manhã.
казино олимп · June 1, 2026 at 7:58 am
Вы предоставляете качественный контент по теме казино олимп.
https://olimp-casino-download.com
taraiarish · June 1, 2026 at 7:59 am
Дізнавайтесь більше про кулінарію: смачні рецепти, поради домогосподаркам та всім, хто любить готувати щось смачне на MeatPortal. Завжди на сайті https://meatportal.com.ua/ знайдете нові рецепти страв традиційної української кухні та з усього світу. Все найцікавіше для кулінарів на MeatPortal.
Joshuamarma · June 1, 2026 at 8:08 am
В этой статье рассматривается комплексный подход к избавлению от зависимости. Читатель узнает, как сочетание физического, психологического и духовного восстановления помогает достичь стойкого выздоровления.
Получить полную информацию – вывод из запоя в Донецке
RogerJulse · June 1, 2026 at 8:16 am
В этой публикации мы рассматриваем важную тему борьбы с зависимостями, включая алкогольную и наркотическую зависимости. Мы обсудим методы лечения, реабилитации и поддержку, которые могут помочь людям, столкнувшимся с этой проблемой. Читатели узнают о перспективах выздоровления и важности комплексного подхода.
Уникальные данные только сегодня – детокс24
liligrass.ru · June 1, 2026 at 8:19 am
liligrass.ru
DavidExevy · June 1, 2026 at 8:39 am
В данной статье мы акцентируем внимание на важности поддержки в процессе выздоровления. Мы обсудим, как друзья, семья и профессионалы могут помочь тем, кто сталкивается с зависимостями. Читатели получат практические советы, как поддерживать близких на пути к новой жизни.
Хочу знать больше – khimki detox24
Davidalima · June 1, 2026 at 8:57 am
Этот документ охватывает важные аспекты медицинской науки, сосредотачиваясь на ключевых вопросах, касающихся здоровья населения. Мы рассматриваем свежие исследования, клинические рекомендации и лучшие практики, которые помогут улучшить качество лечения и профилактики заболеваний. Читатели получат возможность углубиться в различные медицинские дисциплины.
Детальнее – Наркологическая помощь
JosephBob · June 1, 2026 at 9:14 am
Этот текст представляет собой обзор свежих данных и исследований в области медицины. Он призван помочь читателям понять, как научные достижения влияют на лечение, диагностику и общее состояние системы здравоохранения.
Ознакомиться с отчётом – moskva detox24
DanielInecy · June 1, 2026 at 9:25 am
Купить земельный участок https://novoesonino.ru в коттеджном поселке «Новое Сонино». Земли ИЖС с электричеством, дорогами и перспективой комфортного проживания за городом. Отличное место для строительства загородного дома в городском округе Домодедово.
GeorgePoush · June 1, 2026 at 10:10 am
В статье по вопросам здоровья мы рассматриваем актуальные проблемы, с которыми сталкивается общество. Обсуждаются заболевания, факторы риска и важные аспекты профилактики. Читатели получат полезные советы о том, как сохранить здоровье и улучшить качество жизни.
А есть ли продолжение? – детокс24
defuvddyeli · June 1, 2026 at 10:11 am
Ищете лучшее лечение кариеса в Мурманске по выгодной стоимости? Посетите https://nova-51.ru/lechenie-zubov-murmansk/lechenie-kariesa-murmansk – не откладывайте поход к стоматологу, если заметили темные пятна, сколы или трещины на зубах. Приходите в нашу клинику – мы вылечим кариес, сохраним здоровье ваших зубов!
sujugRor · June 1, 2026 at 10:15 am
Когда речь идёт о покупке автомобиля из Японии, Кореи или Китая, выбор партнёра решает всё. Ищете заказ авто из китая б у ? Компания starmotors.biz за годы работы доставила более 17 000 автомобилей по всей России и сегодня держит свыше 600 машин в наличии на рынке во Владивостоке. Офисы и стоянки работают во Владивостоке, Москве и Санкт-Петербурге, а доставка охватывает любой регион страны.
teyatBuiny · June 1, 2026 at 10:24 am
Looking for interesting information about Naples? Visit https://napolivera.com/ and you’ll find interesting and informative information about street food, places to visit, city safety, and everything about the different neighborhoods. Blog posts are published frequently, keeping you up-to-date with interesting information!
JasonSoype · June 1, 2026 at 10:24 am
В этой статье мы рассматриваем разрушительное влияние зависимости на жизнь человека. Обсуждаются аспекты, такие как здоровье, отношения и профессиональные достижения. Читатели узнают о необходимости обращения за помощью и о путях к восстановлению.
Интересует подробная информация – нарколог на дом недорого
kadutQuare · June 1, 2026 at 10:51 am
Парвеник — интернет-магазин банных веников и трав с доставкой по Москве и Подмосковью, где отборное качество сочетается с ценами ниже рыночных. На сайте https://www.parvenik.ru/ представлен широкий ассортимент товаров для настоящей русской бани: берёзовые, дубовые, эвкалиптовые веники и целебные травяные сборы — всё оптом и в розницу. Действует акция «5+1 в подарок», фактически дающая скидку 20%, а удобное получение через пункты выдачи Яндекс Маркета делает покупку максимально простой.
Miltonsen · June 1, 2026 at 11:06 am
Мы рассмотрим современные вызовы здравоохранения и пути их решения с помощью технологий и научных исследований. В статье собраны данные о новых лекарствах, методах диагностики и системном подходе к улучшению здоровья населения.
Лучшее решение — прямо здесь – наркологическая клиника краснодар
Edwardcaf · June 1, 2026 at 11:10 am
В этой статье мы рассматриваем разрушительное влияние зависимости на жизнь человека. Обсуждаются аспекты, такие как здоровье, отношения и профессиональные достижения. Читатели узнают о необходимости обращения за помощью и о путях к восстановлению.
Погрузиться в детали – нарколог на дом в Луганске
RandallDef · June 1, 2026 at 11:14 am
Публикация посвящена жизненным историям людей, успешно справившихся с зависимостью. Мы покажем, что выход есть, и он начинается с первого шага — принятия проблемы и желания измениться.
Лови подробности – detox24 в люберцах
?????????? ?????? ???????????? ?????????????? · June 1, 2026 at 11:18 am
?????????? ???????? ???????????????? ????????
Thomascob · June 1, 2026 at 11:36 am
нажмите, чтобы подробнее вотка бет
Miltonsen · June 1, 2026 at 11:41 am
Публикация знакомит читателей с различными подходами к реабилитации. От традиционных методов до современных программ — вы узнаете, как выбрать оптимальный путь к выздоровлению и преодолеть препятствия на этом пути.
Только для своих – выезд нарколога на дом круглосуточно
JamesEvole · June 1, 2026 at 12:41 pm
Публикация знакомит читателей с различными подходами к реабилитации. От традиционных методов до современных программ — вы узнаете, как выбрать оптимальный путь к выздоровлению и преодолеть препятствия на этом пути.
Углубиться в тему – Частные наркологические клиники в Луганске
EugeneFruby · June 1, 2026 at 1:34 pm
Эта публикация исследует взаимосвязь зависимости и психологии. Мы обсудим, как психологические аспекты влияют на появление зависимостей и процесс выздоровления. Читатели смогут понять важность профессиональной поддержки и применения научных подходов в терапии.
Следуйте по ссылке – detox24
Williamsense · June 1, 2026 at 1:40 pm
Happy Cactus Cactus Cactus Cactus Cactus Cactus
Happy Cactus Cactus Cactus Cactus Cactus Cactus
Happy Cactus Cactus Cactus Cactus Cactus Cactus
Happy Cactus Cactus Cactus Cactus Cactus Cactus
Happy Cactus Cactus Cactus Cactus Cactus Cactus
Happy Cactus Cactus Cactus Cactus Cactus Cactus
https://t.me/hi79602565606/2
Leroytride · June 1, 2026 at 1:44 pm
Эта публикация посвящена актуальным вопросам современной медицины и здравоохранения. Мы обсудим новейшие технологии диагностики и лечения, а также их влияние на продолжительность и качество жизни. Читатель найдет здесь информацию о научных исследованиях и перспективных разработках, доступно изложенную для широкой аудитории.
Практические советы ждут тебя – detox24
JamesEvole · June 1, 2026 at 1:58 pm
Публикация знакомит читателей с различными подходами к реабилитации. От традиционных методов до современных программ — вы узнаете, как выбрать оптимальный путь к выздоровлению и преодолеть препятствия на этом пути.
Углубить понимание вопроса – нарколог на дом в Луганске
JimmieSnomy · June 1, 2026 at 2:15 pm
В этой статье мы рассматриваем разрушительное влияние зависимости на жизнь человека. Обсуждаются аспекты, такие как здоровье, отношения и профессиональные достижения. Читатели узнают о необходимости обращения за помощью и о путях к восстановлению.
Жми сюда — получишь ответ – detox24
EugeneFruby · June 1, 2026 at 2:19 pm
Медицинская публикация представляет собой свод актуальных исследований, экспертных мнений и новейших достижений в сфере здравоохранения. Здесь вы найдете информацию о новых методах лечения, прорывных технологиях и их практическом применении. Мы стремимся сделать актуальные медицинские исследования доступными и понятными для широкой аудитории.
Узнать напрямую – mytischi detox24
Manueltaurb · June 1, 2026 at 2:20 pm
В этой статье обсуждаются актуальные медицинские вопросы, которые волнуют общество. Мы обращаем внимание на проблемы, касающиеся здравоохранения и лечения, а также на новшества в области медицины. Читатели будут осведомлены о последних событиях и смогут следить за тенденциями в медицине.
Узнать больше > – lechenie-alko-krasnodar
GoodiniCrubs · June 1, 2026 at 2:56 pm
Эта публикация посвящена актуальным вопросам современной медицины и здравоохранения. Мы обсудим новейшие технологии диагностики и лечения, а также их влияние на продолжительность и качество жизни. Читатель найдет здесь информацию о научных исследованиях и перспективных разработках, доступно изложенную для широкой аудитории.
Следуйте по ссылке – наркологическая клиника в Смоленске «Новый рассвет»
Waltonpneum · June 1, 2026 at 3:02 pm
В данном обзоре представлены основные направления и тренды в области медицины. Мы обсудим актуальные проблемы здравоохранения, свежие открытия и новые подходы, которые меняют представление о лечении и профилактике заболеваний. Эта информация будет полезна как специалистам, так и широкой публике.
Запросить дополнительные данные – clinica plus
JimmieSnomy · June 1, 2026 at 3:07 pm
Этот документ охватывает важные аспекты медицинской науки, сосредотачиваясь на ключевых вопросах, касающихся здоровья населения. Мы рассматриваем свежие исследования, клинические рекомендации и лучшие практики, которые помогут улучшить качество лечения и профилактики заболеваний. Читатели получат возможность углубиться в различные медицинские дисциплины.
Уточнить детали – детокс24
Manueltaurb · June 1, 2026 at 3:08 pm
В данной статье рассматриваются физиологические и эмоциональные аспекты зависимости. Мы обсудим, как организм реагирует на зависимое поведение, и какие методы помогают восстановить здоровье и внутреннее равновесие.
А есть ли продолжение? – наркологическая клиника Пробуждение в Краснодаре
LeonardVap · June 1, 2026 at 3:27 pm
Этот обзор посвящен успешным стратегиям избавления от зависимости, включая реальные примеры и советы. Мы разоблачим мифы и предоставим читателям достоверную информацию о различных подходах. Получите опыт многообразия методов и найдите подходящий способ для себя!
Узнайте всю правду – капельница от запоя на дому
RobertSlept · June 1, 2026 at 3:35 pm
В этой статье мы рассмотрим современные достижения в области медицины, включая инновационные методы лечения и диагностики. Мы обсудим важность профилактики заболеваний и роль технологий в улучшении качества здравоохранения. Читатели узнают о влиянии медицины на повседневную жизнь и ее значение для современного общества.
Ознакомьтесь поближе – smolensk alco rehab
Jasonbax · June 1, 2026 at 3:40 pm
Эта публикация исследует взаимосвязь зависимости и психологии. Мы обсудим, как психологические аспекты влияют на появление зависимостей и процесс выздоровления. Читатели смогут понять важность профессиональной поддержки и применения научных подходов в терапии.
Изучить вопрос глубже – детокс24
Frankdearf · June 1, 2026 at 3:51 pm
Этот текст посвящён сложным аспектам зависимости и её влиянию на жизнь человека. Мы обсудим психологические, физические и социальные последствия зависимого поведения, а также важность своевременного обращения за помощью.
Получить больше информации – наркологическую клинику в Балашихе
avtonomia.md · June 1, 2026 at 4:17 pm
avtonomia.md
Archienot · June 1, 2026 at 4:23 pm
Только лутран официальный сайт — предлагает live-дилеров.
Создайте аккаунт за 30 секунд — дарит 100 фриспинов.
Список актуальных зеркал — интеграция с браузерными расширениями.
Актуальное lootrun рабочее зеркало — обновляется автоматически.
Source:
runlootrun.com
Gavinhaisa · June 1, 2026 at 4:28 pm
Эта информационная публикация освещает широкий спектр тем из мира медицины. Мы предлагаем читателям ясные и понятные объяснения современных заболеваний, методов профилактики и лечения. Информация будет полезна как пациентам, так и медицинским работникам, желающим поддержать уровень своих знаний.
Давай разберёмся досконально – detox24
kupi-kvartiruspb 550 · June 1, 2026 at 4:48 pm
Купить квартиру https://kupi-kvartiruspb.ru или апартаменты в Курортный район Санкт-Петербурга. Жилые комплексы рядом с Финским заливом, парками и зонами отдыха. Комфортные планировки, современные дома и удобная транспортная доступность.
amphetamine · June 1, 2026 at 4:56 pm
konulu porn
novoe rastunovo 584 · June 1, 2026 at 4:58 pm
Нужен участок? кп новое растуново отличное решение для строительства загородного дома. Участки ИЖС, удобный подъезд, электричество и развитая инфраструктура. Комфортное место для постоянного проживания недалеко от Москвы.
ArthurpoupE · June 1, 2026 at 5:14 pm
Текст посвящён распространённым мифам о зависимости и их развенчанию. Мы предоставим научно обоснованную информацию и дадим рекомендации по выбору эффективного способа борьбы с зависимым поведением.
Следуйте по ссылке – наркологическую клинику в Луганске
Gavinhaisa · June 1, 2026 at 5:16 pm
Эта медицинская заметка содержит сжатую информацию о новых находках и методах в области здравоохранения. Мы предлагаем читателям свежие данные о заболеваниях, профилактике и лечении. Наша цель — быстро и доступно донести важную информацию, которая поможет в повседневной жизни и понимании здоровья.
Следуйте по ссылке – Капельница от запоя в Мариуполе
Damianvique · June 1, 2026 at 5:16 pm
В этой статье мы рассматриваем разные способы борьбы с алкогольной зависимостью. Обсуждаются методы лечения, программы реабилитации и советы для поддержки близких. Читатели получат информацию о том, как преодолеть зависимость и добиться успешного выздоровления.
Разобраться лучше – нарколога домой в Королёве
RogerJulse · June 1, 2026 at 5:55 pm
В этой публикации мы обсуждаем современные методы лечения различных заболеваний. Читатели узнают о новых медикаментах, терапиях и исследованиях, которые активно применяются для лечения. Мы нацелены на то, чтобы предоставить практические знания, которые могут помочь в борьбе с недугами.
Углубиться в тему – детокс24
ArthurpoupE · June 1, 2026 at 6:09 pm
В этой статье обсуждаются актуальные медицинские вопросы, которые волнуют общество. Мы обращаем внимание на проблемы, касающиеся здравоохранения и лечения, а также на новшества в области медицины. Читатели будут осведомлены о последних событиях и смогут следить за тенденциями в медицине.
Расширить кругозор по теме – вывода из запоя на дому в Луганске
DavidExevy · June 1, 2026 at 6:15 pm
Этот краткий обзор предлагает сжатую информацию из области медицины, включая ключевые факты и последние новости. Мы стремимся сделать информацию доступной и понятной для широкой аудитории, что позволит читателям оставаться в курсе актуальных событий в здравоохранении.
Читать далее > – капельница от запоя в Химках
DennisCulse · June 1, 2026 at 6:18 pm
В этой заметке мы представляем шаги, которые помогут в процессе преодоления зависимостей. Рассматриваются стратегии поддержки и чек-листы для тех, кто хочет сделать первый шаг к выздоровлению. Наша цель — вдохновить читателей на положительные изменения и поддержать их в трудных моментах.
Эксклюзивная информация – детокс24 краснодар
WoodrowUpdaw · June 1, 2026 at 6:52 pm
В этой статье рассматриваются различные аспекты избавления от зависимости, включая физические и психологические методы. Мы обсудим поддержку, мотивацию и стратегии, которые помогут в процессе выздоровления. Читатели узнают, как преодолеть трудности и двигаться к новой жизни без зависимости.
Изучить рекомендации специалистов – капельница в Подольске
Davidalima · June 1, 2026 at 7:22 pm
В статье по вопросам здоровья мы рассматриваем актуальные проблемы, с которыми сталкивается общество. Обсуждаются заболевания, факторы риска и важные аспекты профилактики. Читатели получат полезные советы о том, как сохранить здоровье и улучшить качество жизни.
Обратиться к источнику – капельницы от похмелья на дому в Москве
DennisCulse · June 1, 2026 at 7:25 pm
В этой статье мы обсудим процесс восстановления после зависимостей, акцентируя внимание на различных методах и подходах к реабилитации. Читатели узнают, как создать план выздоровления и использовать полезные ресурсы для достижения устойчивых изменений.
Перейти к полной версии – вызвать врача-нарколога на дом
kvartiry-spb 621 · June 1, 2026 at 7:38 pm
ЖК премиум-класса https://kvartiry-spb78.ru от застройщика — современные квартиры с продуманными планировками, высоким уровнем комфорта и развитой инфраструктурой. Закрытая территория, подземный паркинг, благоустроенные дворы и престижное расположение для комфортной жизни.
MichaelRiple · June 1, 2026 at 7:58 pm
Нужна декоративная лепнина? лепнина из пенополиуретана стильный декоративный элемент для интерьера. Карнизы, молдинги, колонны и розетки помогают создавать выразительный дизайн помещений. Материал устойчив к влаге, долговечен и легко устанавливается.
Jacobred · June 1, 2026 at 8:07 pm
Эта медицинская заметка содержит сжатую информацию о новых находках и методах в области здравоохранения. Мы предлагаем читателям свежие данные о заболеваниях, профилактике и лечении. Наша цель — быстро и доступно донести важную информацию, которая поможет в повседневной жизни и понимании здоровья.
Наши рекомендации — тут – капельница от запоя
RobertPrene · June 1, 2026 at 8:38 pm
В этой статье рассматривается комплексный подход к избавлению от зависимости. Читатель узнает, как сочетание физического, психологического и духовного восстановления помогает достичь стойкого выздоровления.
Обратитесь за информацией – детокс24
JosephBob · June 1, 2026 at 8:57 pm
Этот текст представляет собой обзор свежих данных и исследований в области медицины. Он призван помочь читателям понять, как научные достижения влияют на лечение, диагностику и общее состояние системы здравоохранения.
Полезно знать – наркологическая клиника «Детокс» в Москве
WilliamOvani · June 1, 2026 at 9:36 pm
В этой статье мы обсудим процесс восстановления после зависимостей, акцентируя внимание на различных методах и подходах к реабилитации. Читатели узнают, как создать план выздоровления и использовать полезные ресурсы для достижения устойчивых изменений.
Подробнее можно узнать тут – детокс24 краснодар
RobertElapy · June 1, 2026 at 9:45 pm
В этой статье рассматриваются различные аспекты избавления от зависимости, включая физические и психологические методы. Мы обсудим поддержку, мотивацию и стратегии, которые помогут в процессе выздоровления. Читатели узнают, как преодолеть трудности и двигаться к новой жизни без зависимости.
Интересует подробная информация – выведение из запоя краснодар
Damianvique · June 1, 2026 at 10:07 pm
В этой статье мы рассматриваем разные способы борьбы с алкогольной зависимостью. Обсуждаются методы лечения, программы реабилитации и советы для поддержки близких. Читатели получат информацию о том, как преодолеть зависимость и добиться успешного выздоровления.
Уникальные данные только сегодня – детокс24 королев
ThomasKah · June 1, 2026 at 10:09 pm
Этот обзор содержит информацию о передовых достижениях в области медицины. Мы разберем инновационные технологии, которые меняют подход к лечению и диагностике, а также их влияние на эффективность оказания медицинской помощи.
Прочитать подробнее – наркологическая клиника в краснодаре
DanielHix · June 1, 2026 at 10:12 pm
Частные детские сады https://razvitie21vek.com в Москва для детей от раннего возраста. Развивающие программы, безопасная среда, квалифицированные воспитатели и подготовка к школе. Комфортные условия для обучения, общения и всестороннего развития ребенка.
EdgarBulse · June 1, 2026 at 10:35 pm
В этой статье мы рассмотрим современные достижения в области медицины, включая инновационные методы лечения и диагностики. Мы обсудим важность профилактики заболеваний и роль технологий в улучшении качества здравоохранения. Читатели узнают о влиянии медицины на повседневную жизнь и ее значение для современного общества.
Открой скрытое – наркологическая помощь в Балашихе
RandallDef · June 1, 2026 at 10:45 pm
Этот текст посвящён сложным аспектам зависимости и её влиянию на жизнь человека. Мы обсудим психологические, физические и социальные последствия зависимого поведения, а также важность своевременного обращения за помощью.
Ознакомиться с теоретической базой – детокс24 люберцы
StuartdeD · June 1, 2026 at 10:54 pm
В данной статье рассматриваются проблемы общественного здоровья и социальные факторы, влияющие на него. Мы акцентируем внимание на значении профилактики и осведомленности в защите здоровья на уровне общества. Читатели смогут узнать о новых инициативах и программах, направленных на улучшение здоровья населения.
Рассмотреть проблему всесторонне – detox24 в майкопе
RobertElapy · June 1, 2026 at 11:04 pm
В этой статье рассматриваются различные аспекты избавления от зависимости, включая физические и психологические методы. Мы обсудим поддержку, мотивацию и стратегии, которые помогут в процессе выздоровления. Читатели узнают, как преодолеть трудности и двигаться к новой жизни без зависимости.
Интересует подробная информация – откапаться от алкоголя
Williamvoige · June 1, 2026 at 11:07 pm
В данной статье рассматриваются физиологические и эмоциональные аспекты зависимости. Мы обсудим, как организм реагирует на зависимое поведение, и какие методы помогают восстановить здоровье и внутреннее равновесие.
Более подробно об этом – Капельница от запоя в Мариуполе
GeorgePoush · June 1, 2026 at 11:14 pm
Мы рассмотрим современные вызовы здравоохранения и пути их решения с помощью технологий и научных исследований. В статье собраны данные о новых лекарствах, методах диагностики и системном подходе к улучшению здоровья населения.
Эксклюзивная информация – detox24 в подольске
Edwardcaf · June 1, 2026 at 11:17 pm
Эта медицинская заметка содержит сжатую информацию о новых находках и методах в области здравоохранения. Мы предлагаем читателям свежие данные о заболеваниях, профилактике и лечении. Наша цель — быстро и доступно донести важную информацию, которая поможет в повседневной жизни и понимании здоровья.
Наши рекомендации — тут – Наркологическая клиника в Луганске
EdgarBulse · June 1, 2026 at 11:35 pm
В этой статье рассматривается комплексный подход к избавлению от зависимости. Читатель узнает, как сочетание физического, психологического и духовного восстановления помогает достичь стойкого выздоровления.
Узнать из первых рук – balashiha clinica plus
xedidsom · June 1, 2026 at 11:47 pm
AdGuard FAQ — ваш надежный проводник в мире безопасного интернета, где собраны ответы на все ключевые вопросы о защите от рекламы и VPN-технологиях. Ресурс предлагает актуальную информацию о работе сервисов AdGuard в условиях блокировок, подробные инструкции для всех платформ — от Windows до iOS, а также эксклюзивные промокоды со скидками до 75%. На https://adguard-faq.com/ вы найдете проверенные зеркала для доступа к заблокированным сервисам, разъяснения о легальности использования VPN и практические советы по выбору провайдера. Материалы регулярно обновляются, что гарантирует получение только свежей и достоверной информации для комфортного интернет-серфинга.
Davidnut · June 2, 2026 at 12:04 am
Эта публикация обращает внимание на важность профилактики зависимостей. Мы обсудим, как осведомленность и образование могут помочь в предотвращении возникновения зависимости. Читатели смогут ознакомиться с полезными советами и ресурсами, которые способствуют здоровому образу жизни.
См. подробности – капельница от запоя
WoodrowUpdaw · June 2, 2026 at 12:05 am
В этой статье мы обсудим процесс восстановления после зависимостей, акцентируя внимание на различных методах и подходах к реабилитации. Читатели узнают, как создать план выздоровления и использовать полезные ресурсы для достижения устойчивых изменений.
Расширить кругозор по теме – detox24 в подольске
sdasteam 939 · June 2, 2026 at 12:05 am
Steam Desktop Authenticator https://sdasteam.com (SDA). It allows you to generate account login codes and automatically confirm trades or item sales on the Community Market without using your smartphone.
https://mem168new.com/home.php?mod=space&uid=4112153 · June 2, 2026 at 12:12 am
https://mem168new.com/home.php?mod=space&uid=4112153
AllenHeast · June 2, 2026 at 12:28 am
Этот обзор содержит информацию о передовых достижениях в области медицины. Мы разберем инновационные технологии, которые меняют подход к лечению и диагностике, а также их влияние на эффективность оказания медицинской помощи.
Что ещё? Расскажи всё! – detox 24
Ralphkix · June 2, 2026 at 12:30 am
В этой публикации мы рассматриваем важную тему борьбы с зависимостями, включая алкогольную и наркотическую зависимости. Мы обсудим методы лечения, реабилитации и поддержку, которые могут помочь людям, столкнувшимся с этой проблемой. Читатели узнают о перспективах выздоровления и важности комплексного подхода.
Слушай внимательно — тут важно – Прокапаться от алкоголя
JasonSoype · June 2, 2026 at 12:31 am
Этот обзор посвящен успешным стратегиям избавления от зависимости, включая реальные примеры и советы. Мы разоблачим мифы и предоставим читателям достоверную информацию о различных подходах. Получите опыт многообразия методов и найдите подходящий способ для себя!
Что ещё нужно знать? – наркологическая клиника краснодар
Stephenkeedy · June 2, 2026 at 12:49 am
Этот обзор посвящен успешным стратегиям избавления от зависимости, включая реальные примеры и советы. Мы разоблачим мифы и предоставим читателям достоверную информацию о различных подходах. Получите опыт многообразия методов и найдите подходящий способ для себя!
Узнать больше – детокс24 краснодар
Leroytride · June 2, 2026 at 1:02 am
Эта публикация посвящена актуальным вопросам современной медицины и здравоохранения. Мы обсудим новейшие технологии диагностики и лечения, а также их влияние на продолжительность и качество жизни. Читатель найдет здесь информацию о научных исследованиях и перспективных разработках, доступно изложенную для широкой аудитории.
Изучить рекомендации специалистов – detox24
Henrywam · June 2, 2026 at 1:02 am
В данной статье мы поговорим о будущем медицины, акцентируя внимание на прорывных разработках и их потенциале. Читатель узнает о новых подходах к лечению, роли искусственного интеллекта и возможностях персонализированной медицины.
Тыкай сюда — узнаешь много интересного – кодировка волгоград
Davidnut · June 2, 2026 at 1:09 am
В этой статье рассматривается комплексный подход к избавлению от зависимости. Читатель узнает, как сочетание физического, психологического и духовного восстановления помогает достичь стойкого выздоровления.
Лови подробности – вывод из запоя
Chrissoify · June 2, 2026 at 1:17 am
Публикация охватывает основные направления развития современной медицины. Мы обсудим значимость научных исследований, инноваций в лечении и роли общественного участия в формировании системы здравоохранения.
Это стоит прочитать полностью – вывод из запоя во владимире
AllenHeast · June 2, 2026 at 1:29 am
В этой статье мы рассматриваем разрушительное влияние зависимости на жизнь человека. Обсуждаются аспекты, такие как здоровье, отношения и профессиональные достижения. Читатели узнают о необходимости обращения за помощью и о путях к восстановлению.
Желаете узнать подробности? – detox24
JamesBOUCH · June 2, 2026 at 1:41 am
В данной статье рассматриваются проблемы общественного здоровья и социальные факторы, влияющие на него. Мы акцентируем внимание на значении профилактики и осведомленности в защите здоровья на уровне общества. Читатели смогут узнать о новых инициативах и программах, направленных на улучшение здоровья населения.
Доступ к полной версии – нарколог на дом в Луганске
Jacobred · June 2, 2026 at 1:43 am
В этой публикации мы предложим ряд рекомендаций по избавлению от зависимостей и успешному восстановлению. Мы обсудим методы привлечения поддержки и важность самосознания. Эти советы помогут людям вернуться к нормальной жизни и стать на путь выздоровления.
Получить исчерпывающие сведения – detox24 в мытищах
authenticator steam 656 · June 2, 2026 at 2:03 am
Steam Desktop Authenticator https://authenticatorsteamdesktop.com is a PC app that lets you use the Steam Mobile Authenticator on your computer. It supports trade confirmation, account security, and managing two-factor authentication codes without using your smartphone.
Kennethvar · June 2, 2026 at 2:04 am
В этой заметке мы представляем шаги, которые помогут в процессе преодоления зависимостей. Рассматриваются стратегии поддержки и чек-листы для тех, кто хочет сделать первый шаг к выздоровлению. Наша цель — вдохновить читателей на положительные изменения и поддержать их в трудных моментах.
Следуйте по ссылке – наркологическая клиника в смоленске
Henrywam · June 2, 2026 at 2:08 am
В данной статье мы поговорим о будущем медицины, акцентируя внимание на прорывных разработках и их потенциале. Читатель узнает о новых подходах к лечению, роли искусственного интеллекта и возможностях персонализированной медицины.
Ознакомиться с деталями – кодировка от алкоголя волгоград
ArthurBam · June 2, 2026 at 3:18 am
В этой статье рассматриваются способы преодоления зависимости и успешные истории людей, которые справились с этой проблемой. Мы обсудим важность поддержки со стороны близких и профессионалов, а также стратегии, которые могут помочь в процессе выздоровления. Научитесь первоочередным шагам к новой жизни.
Уточнить детали – detox24 в рыбинске
CharlesDerse · June 2, 2026 at 3:18 am
В данной статье рассматриваются физиологические и эмоциональные аспекты зависимости. Мы обсудим, как организм реагирует на зависимое поведение, и какие методы помогают восстановить здоровье и внутреннее равновесие.
Изучите внимательнее – нарколог на дом в Балашихе
Kennethvar · June 2, 2026 at 3:26 am
В статье рассматриваются различные стратегии борьбы с зависимостями, включая проверенные методы и реальные истории успеха. Читатель узнает, какие подходы наиболее эффективны и как начать путь к выздоровлению.
Следуйте по ссылке – алко рехаб
https://newmuslim.iera.org/members/japangrowth37/activity/662753/ · June 2, 2026 at 3:28 am
https://newmuslim.iera.org/members/japangrowth37/activity/662753/
https://liveheadline.site/ · June 2, 2026 at 3:29 am
References:
Casino app https://liveheadline.site/item/genie-en-sie-die-besten-casinospiele-auf-ios-android
References:
https://liveheadline.site/item/genie-en-sie-die-besten-casinospiele-auf-ios-android
madyNouts · June 2, 2026 at 3:39 am
Речные прогулки по Москве давно перестали быть просто экскурсией — теперь это насыщенный вечер с музыкой, шоу и живыми выступлениями на борту. Дискотеки 80–90-х, DJ-вечеринки, концерты и Premium-круизы с ужином и шоу-программой доступны ежедневно и рассчитаны на любой вкус. Ищете купить билеты на теплоход с дискотекой? Билеты бронируются онлайн на ticketscruise.ru — быстро и без лишних шагов. Среди хитов сезона — концертный круиз «Хиты Италии» на теплоходе «Ривер Палас» от причала Сити-Экспоцентр.
Frankdearf · June 2, 2026 at 3:43 am
В этой статье мы обсудим процесс восстановления после зависимостей, акцентируя внимание на различных методах и подходах к реабилитации. Читатели узнают, как создать план выздоровления и использовать полезные ресурсы для достижения устойчивых изменений.
Проследить причинно-следственные связи – Кодирование от алкоголизма
Chrissoify · June 2, 2026 at 3:44 am
Этот обзор посвящен успешным стратегиям избавления от зависимости, включая реальные примеры и советы. Мы разоблачим мифы и предоставим читателям достоверную информацию о различных подходах. Получите опыт многообразия методов и найдите подходящий способ для себя!
Получить дополнительную информацию – вывод из запоя во владимире
GoodiniCrubs · June 2, 2026 at 3:47 am
В данной статье рассматриваются проблемы общественного здоровья и социальные факторы, влияющие на него. Мы акцентируем внимание на значении профилактики и осведомленности в защите здоровья на уровне общества. Читатели смогут узнать о новых инициативах и программах, направленных на улучшение здоровья населения.
Детальнее – наркологическая клиника в смоленске
Vincentplady · June 2, 2026 at 3:49 am
Этот обзор сосредоточен на различных подходах к избавлению от зависимости. Мы изучим традиционные и альтернативные методы, а также их сочетание для достижения максимальной эффективности. Читатели смогут открыть для себя новые стратегии и подходы, которые помогут в их борьбе с зависимостями.
Узнать напрямую – психиатра на дом в Балашихе
WilliamOvani · June 2, 2026 at 3:55 am
В этой статье мы обсудим процесс восстановления после зависимостей, акцентируя внимание на различных методах и подходах к реабилитации. Читатели узнают, как создать план выздоровления и использовать полезные ресурсы для достижения устойчивых изменений.
Изучить рекомендации специалистов – выезд нарколога на дом
https://otolar-centre.ru/ · June 2, 2026 at 4:07 am
https://otolar-centre.ru/
BrandonPetle · June 2, 2026 at 4:14 am
Этот обзор сосредоточен на различных подходах к избавлению от зависимости. Мы изучим традиционные и альтернативные методы, а также их сочетание для достижения максимальной эффективности. Читатели смогут открыть для себя новые стратегии и подходы, которые помогут в их борьбе с зависимостями.
Только факты! – алко рехаб смоленск
https://headlinebeacon.space/item/hitnspin-ppromo-code-die-besten-casino-boni-bei-hitnspin · June 2, 2026 at 4:15 am
References:
Platinum play casino https://headlinebeacon.space/item/hitnspin-ppromo-code-die-besten-casino-boni-bei-hitnspin
https://favpress.site/ · June 2, 2026 at 4:19 am
References:
Mint casino https://favpress.site/item/drehe-fantasy-slots-und-genie-e-gewinnboni
gitomnacity · June 2, 2026 at 4:49 am
Looking for the best crypto exchanges in 2026? Visit https://topexchanges.io/ – TopExchanges helps users compare crypto exchanges, instant crypto exchanges, and popular trading platforms in one place. This ranking is designed for people who want to buy, sell, exchange, trade, or cash out digital assets without having to check each service individually.
Williamvoige · June 2, 2026 at 4:54 am
В данной статье рассматриваются физиологические и эмоциональные аспекты зависимости. Мы обсудим, как организм реагирует на зависимое поведение, и какие методы помогают восстановить здоровье и внутреннее равновесие.
Как это работает — подробно – вывод из запоя в Мариуполе
RobertSlept · June 2, 2026 at 4:57 am
Этот текст посвящён сложным аспектам зависимости и её влиянию на жизнь человека. Мы обсудим психологические, физические и социальные последствия зависимого поведения, а также важность своевременного обращения за помощью.
Хочу знать больше – smolensk alco rehab
ThomasKah · June 2, 2026 at 4:57 am
Обзор посвящён процессу восстановления после зависимостей. Мы расскажем о различных этапах реабилитации, поддерживающих ресурсах и важности мотивации в достижении устойчивого выздоровления.
Изучить рекомендации специалистов – анонимный нарколог краснодар
StuartdeD · June 2, 2026 at 4:57 am
В этой статье рассматриваются различные аспекты избавления от зависимости, включая физические и психологические методы. Мы обсудим поддержку, мотивацию и стратегии, которые помогут в процессе выздоровления. Читатели узнают, как преодолеть трудности и двигаться к новой жизни без зависимости.
Детальнее – maykop detox24
Ambrosezef · June 2, 2026 at 5:12 am
В данной статье мы поговорим о будущем медицины, акцентируя внимание на прорывных разработках и их потенциале. Читатель узнает о новых подходах к лечению, роли искусственного интеллекта и возможностях персонализированной медицины.
Открыть полностью – капельница от запоя на дому
Vincentplady · June 2, 2026 at 5:13 am
В этой статье рассматривается комплексный подход к избавлению от зависимости. Читатель узнает, как сочетание физического, психологического и духовного восстановления помогает достичь стойкого выздоровления.
Смотрите также – клиника плюс
LeonardVap · June 2, 2026 at 5:45 am
В этой статье рассматривается комплексный подход к избавлению от зависимости. Читатель узнает, как сочетание физического, психологического и духовного восстановления помогает достичь стойкого выздоровления.
Есть чему поучиться – капельница от запоя
Jasonbax · June 2, 2026 at 6:26 am
Мы рассмотрим современные вызовы здравоохранения и пути их решения с помощью технологий и научных исследований. В статье собраны данные о новых лекарствах, методах диагностики и системном подходе к улучшению здоровья населения.
Где можно узнать подробнее? – детокс24
Stephenkeedy · June 2, 2026 at 6:37 am
Этот обзор посвящен успешным стратегиям избавления от зависимости, включая реальные примеры и советы. Мы разоблачим мифы и предоставим читателям достоверную информацию о различных подходах. Получите опыт многообразия методов и найдите подходящий способ для себя!
Получить больше информации – детокс24 краснодар
Caseykiz · June 2, 2026 at 7:02 am
Читатели получат представление о том, как современные технологии влияют на развитие медицины. Обсуждаются новые методы лечения, персонализированный подход и роль цифровых решений в повышении качества медицинских услуг.
Обратиться к источнику – наркологическая клиника в смоленске
Jasonlor · June 2, 2026 at 7:25 am
В этой публикации мы исследуем ключевые аспекты здоровья, включая влияние образа жизни на благополучие. Читатели узнают о важности правильного питания, физической активности и психического здоровья. Мы предоставим практические советы и рекомендации для поддержания здоровья и развития профилактических подходов.
Как достичь результата? – лечение от алкоголизма
vevurnUndew · June 2, 2026 at 7:25 am
Если вы хотите узнать всё об одной из самых характерных и неукротимых охотничьих пород — ягдтерьере, — канал Риддика (Шефа) фон Тира на Дзене станет для вас настоящим открытием: здесь собраны честные личные истории, практические советы по дрессировке и выгулу, а также рекомендации по здоровью питомца; на https://dzen.ru/riddick автор без прикрас рассказывает, каково это — жить с маленьким, но абсолютно бескомпромиссным охотником, который каждый день испытывает хозяина на выдержку, и почему именно этим ягдтерьеры так влюбляют в себя навсегда.
https://analnoe.com/user/cerealarch9/ · June 2, 2026 at 7:31 am
References:
Big fish casino online https://analnoe.com/user/cerealarch9/
https://henryfirearmsshop.com/code-promo-1xbet-2026-bonus-gratuit-jusqua-130-e/ · June 2, 2026 at 7:34 am
https://henryfirearmsshop.com/code-promo-1xbet-2026-bonus-gratuit-jusqua-130-e/
steam authenticator 890 · June 2, 2026 at 7:42 am
Steam Desktop Authenticator https://steamdesktopauthenticator.net is a popular solution for Steam users who need access to Steam Guard features on their computer. It conveniently verifies actions, protects your account, and manages authentication in a single app.
JasonShirm · June 2, 2026 at 7:58 am
В этой статье рассматриваются различные аспекты избавления от зависимости, включая физические и психологические методы. Мы обсудим поддержку, мотивацию и стратегии, которые помогут в процессе выздоровления. Читатели узнают, как преодолеть трудности и двигаться к новой жизни без зависимости.
Подробности по ссылке – clinica plus в балашихе
page-robb-3.technetbloggers.de · June 2, 2026 at 9:06 am
References:
Burswood casino https://page-robb-3.technetbloggers.de/hitnspin-casino-erfahrungen-2026-sicher-oder-ein-betrug
CharlesDerse · June 2, 2026 at 9:10 am
Эта публикация исследует взаимосвязь зависимости и психологии. Мы обсудим, как психологические аспекты влияют на появление зависимостей и процесс выздоровления. Читатели смогут понять важность профессиональной поддержки и применения научных подходов в терапии.
Раскрыть тему полностью – наркологическую клинику в Балашихе
CharlesLON · June 2, 2026 at 9:27 am
Публикация знакомит читателей с различными подходами к реабилитации. От традиционных методов до современных программ — вы узнаете, как выбрать оптимальный путь к выздоровлению и преодолеть препятствия на этом пути.
Что ещё нужно знать? – detox24
https://liveheadline.space/item/hit-prospekt-25-05-2026-angebote-n-chste-woche-bl-ttern · June 2, 2026 at 9:46 am
References:
Slot machine bank https://liveheadline.space/item/hit-prospekt-25-05-2026-angebote-n-chste-woche-bl-ttern
ArthurBam · June 2, 2026 at 9:59 am
В этой статье рассматриваются способы преодоления зависимости и успешные истории людей, которые справились с этой проблемой. Мы обсудим важность поддержки со стороны близких и профессионалов, а также стратегии, которые могут помочь в процессе выздоровления. Научитесь первоочередным шагам к новой жизни.
Полезно знать – капельница от запоя на дому наркология
https://bookmarkdaily.space · June 2, 2026 at 10:11 am
References:
Scottsdale casinos https://bookmarkdaily.space/item/planm-ige-turniere-feste-auszahlungen
https://gardenwiki.site/wiki/Planmige_Turniere_feste_Auszahlungen · June 2, 2026 at 10:28 am
References:
Casino slot machine games https://gardenwiki.site/wiki/Planmige_Turniere_feste_Auszahlungen
BrandonPetle · June 2, 2026 at 10:54 am
Мы рассмотрим современные вызовы здравоохранения и пути их решения с помощью технологий и научных исследований. В статье собраны данные о новых лекарствах, методах диагностики и системном подходе к улучшению здоровья населения.
Только факты! – alco rehab в смоленске
JamesBOUCH · June 2, 2026 at 11:29 am
В этом обзоре представлены различные методы избавления от зависимости, включая терапевтические и психологические подходы. Мы сравниваем их эффективность и предоставляем рекомендации для тех, кто хочет вернуться к трезвой жизни. Читатели смогут найти информацию о реабилитационных центрах и поддерживающих группах.
Проследить причинно-следственные связи – вывода из запоя на дому в Луганске
https://adventuremyanmar.com/wp-content/pgs/888starz_promo_code____vip_bonus_.html · June 2, 2026 at 12:17 pm
https://adventuremyanmar.com/wp-content/pgs/888starz_promo_code____vip_bonus_.html
https://41-4lcpj.укр/user/congawood01/ · June 2, 2026 at 12:46 pm
References:
The meadows racetrack and casino https://xn--41-4lcpj.xn--j1amh/user/congawood01/
EduardoVah · June 2, 2026 at 1:37 pm
песок карьерный с доставкой московская область песок строительный карьерный
CoreySuits · June 2, 2026 at 2:20 pm
В этой статье мы обсудим процесс восстановления после зависимостей, акцентируя внимание на различных методах и подходах к реабилитации. Читатели узнают, как создать план выздоровления и использовать полезные ресурсы для достижения устойчивых изменений.
Всё, что нужно знать – нарколог на дом
Justinoxymn · June 2, 2026 at 2:32 pm
В этой статье рассматриваются различные аспекты избавления от зависимости, включая физические и психологические методы. Мы обсудим поддержку, мотивацию и стратегии, которые помогут в процессе выздоровления. Читатели узнают, как преодолеть трудности и двигаться к новой жизни без зависимости.
Это ещё не всё… – наркологическая клиника в твери
Edwarddeeta · June 2, 2026 at 2:36 pm
Эта информационная публикация освещает широкий спектр тем из мира медицины. Мы предлагаем читателям ясные и понятные объяснения современных заболеваний, методов профилактики и лечения. Информация будет полезна как пациентам, так и медицинским работникам, желающим поддержать уровень своих знаний.
Получить дополнительные сведения – clinica plus
Ambrosezef · June 2, 2026 at 2:41 pm
Эта информационная публикация освещает широкий спектр тем из мира медицины. Мы предлагаем читателям ясные и понятные объяснения современных заболеваний, методов профилактики и лечения. Информация будет полезна как пациентам, так и медицинским работникам, желающим поддержать уровень своих знаний.
Осуществить глубокий анализ – капельница от запоя
RobertPrene · June 2, 2026 at 2:49 pm
В этом исследовании рассмотрены методы лечения зависимостей и их эффективность. Мы проанализируем различные подходы, используемые в реабилитационных центрах, и представим данные о результативности программ. Читатели получат надежные и научно обоснованные сведения о данной проблеме.
Обратитесь за информацией – детокс 24
CharlesLON · June 2, 2026 at 3:02 pm
Эта публикация раскрывает психологические механизмы зависимости и их роль в развитии расстройств. Читатель узнает о том, как психология влияет на формирование зависимостей и как профессиональная помощь может изменить ситуацию.
Эксклюзивная информация – detox24
Caseykiz · June 2, 2026 at 3:03 pm
Читатели получат представление о том, как современные технологии влияют на развитие медицины. Обсуждаются новые методы лечения, персонализированный подход и роль цифровых решений в повышении качества медицинских услуг.
Выяснить больше – alco rehab в смоленске
JamesNax · June 2, 2026 at 3:20 pm
visit our website https://tokvideodownloader.click/hi/
JasonShirm · June 2, 2026 at 3:45 pm
Этот обзор сосредоточен на различных подходах к избавлению от зависимости. Мы изучим традиционные и альтернативные методы, а также их сочетание для достижения максимальной эффективности. Читатели смогут открыть для себя новые стратегии и подходы, которые помогут в их борьбе с зависимостями.
Слушай внимательно — тут важно – наркологическая клиника в балашихе
Jasonlor · June 2, 2026 at 3:46 pm
Медицинская публикация представляет собой свод актуальных исследований, экспертных мнений и новейших достижений в сфере здравоохранения. Здесь вы найдете информацию о новых методах лечения, прорывных технологиях и их практическом применении. Мы стремимся сделать актуальные медицинские исследования доступными и понятными для широкой аудитории.
Ознакомиться с деталями – detox24
JamesNax · June 2, 2026 at 3:48 pm
check https://tokvideodownloader.click/tiktok-download-mp3.html
Carlosjet · June 2, 2026 at 3:52 pm
Курсы ораторского мастерства kultura-rechi.ru для развития навыков общения и публичных выступлений. Практика, упражнения на дикцию, управление голосом, преодоление страха сцены и умение удерживать внимание слушателей.
Marvinhah · June 2, 2026 at 4:00 pm
В этом исследовании рассмотрены методы лечения зависимостей и их эффективность. Мы проанализируем различные подходы, используемые в реабилитационных центрах, и представим данные о результативности программ. Читатели получат надежные и научно обоснованные сведения о данной проблеме.
Познакомиться с результатами исследований – анонимная наркологическая клиника
RobertBap · June 2, 2026 at 4:03 pm
В этой публикации мы предложим ряд рекомендаций по избавлению от зависимостей и успешному восстановлению. Мы обсудим методы привлечения поддержки и важность самосознания. Эти советы помогут людям вернуться к нормальной жизни и стать на путь выздоровления.
Наши рекомендации — тут – clinica plus
Robertvew · June 2, 2026 at 4:41 pm
Этот информационный материал подробно освещает проблему наркозависимости, ее причины и последствия. Мы предлагаем информацию о методах лечения, профилактики и поддерживающих программах. Цель статьи — повысить осведомленность и продвигать идеи о необходимости борьбы с зависимостями.
Изучите внимательнее – клиника плюс тверь
https://www.behance.net/ariescalhoun · June 2, 2026 at 4:52 pm
https://www.behance.net/ariescalhoun
lezoditJak · June 2, 2026 at 4:54 pm
Looking to convert BTC to EUR and exchange Bitcoin for euros? Visit https://btc-to-eur.com/, a BTC to EUR exchange service, to check the real Bitcoin-Euro exchange rate, calculate the estimated EUR value, and initiate a Bitcoin-to-Euro conversion via the exchange flow. Use this page to convert BTC to EUR, compare the current BTC/EUR exchange rate, check the total Bitcoin amounts in euros, or prepare to sell Bitcoin for a euro-denominated route.
Josephsnazy · June 2, 2026 at 5:26 pm
В этой публикации мы обсуждаем современные методы лечения различных заболеваний. Читатели узнают о новых медикаментах, терапиях и исследованиях, которые активно применяются для лечения. Мы нацелены на то, чтобы предоставить практические знания, которые могут помочь в борьбе с недугами.
Погрузиться в детали – наркологической клиники в Череповце
hedgedoc.eclair.ec-lyon.fr · June 2, 2026 at 5:34 pm
hedgedoc.eclair.ec-lyon.fr
mipoTam · June 2, 2026 at 5:43 pm
Анапа — жемчужина черноморского побережья, и исследовать её по-настоящему можно только за рулём собственного, пусть и арендованного, автомобиля. Сервис https://auto-arenda-anapa.ru/ предлагает прокат без залога, без ограничения пробега и с неограниченной страховкой ОСАГО, что делает каждую поездку абсолютно беззаботной. Детское кресло и видеорегистратор включены в комплектацию, а оформление занимает три простых шага: выбрать автомобиль, отправить документы и указать место подачи. Команда профессионалов CarTrip всегда на связи в мессенджерах и готова ответить на любой вопрос. Путешествуйте свободно!
JamesNax · June 2, 2026 at 6:03 pm
address https://tokvideodownloader.click/bn/
StephenDrymn · June 2, 2026 at 6:16 pm
Этот медицинский обзор сосредоточен на последних достижениях, которые оказывают влияние на пациентов и медицинскую практику. Мы разбираем инновационные методы лечения и исследований, акцентируя внимание на их значимости для общественного здоровья. Читатели узнают о свежих данных и их возможном применении.
Это стоит прочитать полностью – Капельница от запоя в Белгороде
fixDiele · June 2, 2026 at 6:31 pm
Хочу выделить материал про Свежие тенденции и события в мире недвижимости.
Вот, можете почитать:
https://gazeta-flat.ru
fixDiele · June 2, 2026 at 6:34 pm
Между прочим, если вас интересует Новости и события Иркутской области: главные темы недели, посмотрите сюда.
Смотрите сами:
https://irktsk38media.ru
https://maps.google.com.lb/url?q=httpsjoell.inarticlesle-code-promo-1xbet-actuel.html · June 2, 2026 at 6:44 pm
https://maps.google.com.lb/url?q=https%3A%2F%2Fjoell.in%2Farticles%2Fle-code-promo-1xbet-actuel.html
xutovtoowl · June 2, 2026 at 7:15 pm
Пансіонат «Велика Родина» — це мережа сучасних будинків для літніх людей по всій Україні з цілодобовим медичним доглядом і кваліфікованим персоналом. Фахівці забезпечують догляд за лежачими хворими, людьми з деменцією, після інсульту та з інвалідністю. На https://big-femily.com.ua/ можна ознайомитись з умовами проживання та цінами. Мережа охоплює Київ, Львів, Харків, Дніпро, Полтаву та низку інших міст України.
Richarddiast · June 2, 2026 at 7:30 pm
В этом обзоре мы обсудим современные методы борьбы с зависимостями, включая медикаментозную терапию и психотерапию. Мы представим последние исследования и их результаты, чтобы читатели могли быть в курсе наиболее эффективных подходов к лечению и поддержке.
Познакомиться с результатами исследований – клиника плюс тверь
RichardAmoxy · June 2, 2026 at 7:36 pm
В этой статье мы рассматриваем разрушительное влияние зависимости на жизнь человека. Обсуждаются аспекты, такие как здоровье, отношения и профессиональные достижения. Читатели узнают о необходимости обращения за помощью и о путях к восстановлению.
Погрузиться в детали – tver clinica plus
JamesNax · June 2, 2026 at 7:39 pm
weblink https://tokvideodownloader.click/hi/
camp-fire.jp · June 2, 2026 at 7:40 pm
camp-fire.jp
Richarddiast · June 2, 2026 at 8:19 pm
В этой статье мы рассматриваем разрушительное влияние зависимости на жизнь человека. Обсуждаются аспекты, такие как здоровье, отношения и профессиональные достижения. Читатели узнают о необходимости обращения за помощью и о путях к восстановлению.
Всё, что нужно знать – наркологический центр в Твери
Edgarpak · June 2, 2026 at 8:21 pm
Steam Desktop Authenticator https://steamdesktopauthenticator.net is a popular solution for Steam users who need access to Steam Guard features on their computer. It conveniently verifies actions, protects your account, and manages authentication in a single app.
Haroldwaype · June 2, 2026 at 8:23 pm
Эта статья подробно расскажет о процессе выздоровления, который включает в себя эмоциональную, физическую и психологическую реабилитацию. Мы обсуждаем значимость поддержки и наличие профессиональных программ. Читатели узнают, как строить новую жизнь и не возвращаться к старым привычкам.
Ознакомьтесь поближе – клиника плюс белгород
RichardAmoxy · June 2, 2026 at 8:23 pm
Этот обзор посвящен успешным стратегиям избавления от зависимости, включая реальные примеры и советы. Мы разоблачим мифы и предоставим читателям достоверную информацию о различных подходах. Получите опыт многообразия методов и найдите подходящий способ для себя!
Нажми и узнай всё – клиника плюс тверь
HenryJange · June 2, 2026 at 8:41 pm
Этот обзор содержит информацию о передовых достижениях в области медицины. Мы разберем инновационные технологии, которые меняют подход к лечению и диагностике, а также их влияние на эффективность оказания медицинской помощи.
Прочесть заключение эксперта – капельнице от похмелья на дому недорого
aplica????o mostbet · June 2, 2026 at 9:44 pm
b??nus mostbet
Jeffreycit · June 2, 2026 at 9:45 pm
В этой публикации мы рассматриваем важную тему борьбы с зависимостями, включая алкогольную и наркотическую зависимости. Мы обсудим методы лечения, реабилитации и поддержку, которые могут помочь людям, столкнувшимся с этой проблемой. Читатели узнают о перспективах выздоровления и важности комплексного подхода.
Смотрите также – клиника плюс
GoodiniCrubs · June 2, 2026 at 10:09 pm
Этот текст посвящён сложным аспектам зависимости и её влиянию на жизнь человека. Мы обсудим психологические, физические и социальные последствия зависимого поведения, а также важность своевременного обращения за помощью.
Только для своих – Капельница от запоя в Борисоглебске
JamelRus · June 2, 2026 at 10:19 pm
Этот краткий обзор предлагает сжатую информацию из области медицины, включая ключевые факты и последние новости. Мы стремимся сделать информацию доступной и понятной для широкой аудитории, что позволит читателям оставаться в курсе актуальных событий в здравоохранении.
Как это работает — подробно – сексолог сочи
EugenioTasse · June 2, 2026 at 11:04 pm
Эта статья подробно расскажет о процессе выздоровления, который включает в себя эмоциональную, физическую и психологическую реабилитацию. Мы обсуждаем значимость поддержки и наличие профессиональных программ. Читатели узнают, как строить новую жизнь и не возвращаться к старым привычкам.
Посмотреть подробности – анонимная наркологическая клиника
EugenioTasse · June 2, 2026 at 11:58 pm
В этой статье рассматриваются различные аспекты избавления от зависимости, включая физические и психологические методы. Мы обсудим поддержку, мотивацию и стратегии, которые помогут в процессе выздоровления. Читатели узнают, как преодолеть трудности и двигаться к новой жизни без зависимости.
Лови подробности – clinica plus
Edwarddeeta · June 3, 2026 at 12:14 am
Этот документ охватывает важные аспекты медицинской науки, сосредотачиваясь на ключевых вопросах, касающихся здоровья населения. Мы рассматриваем свежие исследования, клинические рекомендации и лучшие практики, которые помогут улучшить качество лечения и профилактики заболеваний. Читатели получат возможность углубиться в различные медицинские дисциплины.
Узнать больше > – clinica plus
AndrewAcuct · June 3, 2026 at 12:15 am
Эта медицинская заметка содержит сжатую информацию о новых находках и методах в области здравоохранения. Мы предлагаем читателям свежие данные о заболеваниях, профилактике и лечении. Наша цель — быстро и доступно донести важную информацию, которая поможет в повседневной жизни и понимании здоровья.
Разобраться лучше – clinica plus в твери
MatthewSyclE · June 3, 2026 at 12:33 am
В этой статье рассматриваются актуальные вопросы, связанные с развитием медицинской науки и её внедрением в повседневную практику. Особое внимание уделено вопросам профилактики, ранней диагностики и использованию технологий для улучшения здоровья человека.
Желаете узнать подробности? – clinica plus
Josephcroro · June 3, 2026 at 12:37 am
rustic ne demek hakk?ndaki yaz?y? tavsiye ederim. Link burada: https://yapevleri.com/articles/rustik-tanim-ve-uygulama-alanlari/
Josephcroro · June 3, 2026 at 12:44 am
f?r?n ne ise yarar hakk?ndaki yaz?y? tavsiye ederim. Kendiniz gorun: https://yappendik.com/articles/firin-ne-ise-yarar-farkli-kullanim-alanlari/
mostbet az??rbaycan qeydiyyat · June 3, 2026 at 12:45 am
qeydiyyat mostbet
AndrewAcuct · June 3, 2026 at 1:10 am
Этот документ охватывает важные аспекты медицинской науки, сосредотачиваясь на ключевых вопросах, касающихся здоровья населения. Мы рассматриваем свежие исследования, клинические рекомендации и лучшие практики, которые помогут улучшить качество лечения и профилактики заболеваний. Читатели получат возможность углубиться в различные медицинские дисциплины.
Читать далее > – clinica plus в твери
JamelRus · June 3, 2026 at 1:27 am
В данной статье рассматриваются проблемы общественного здоровья и социальные факторы, влияющие на него. Мы акцентируем внимание на значении профилактики и осведомленности в защите здоровья на уровне общества. Читатели смогут узнать о новых инициативах и программах, направленных на улучшение здоровья населения.
Что скрывают от вас? – вывод из запоя на дому в сочи
Haroldwaype · June 3, 2026 at 1:31 am
Эта информационная публикация освещает широкий спектр тем из мира медицины. Мы предлагаем читателям ясные и понятные объяснения современных заболеваний, методов профилактики и лечения. Информация будет полезна как пациентам, так и медицинским работникам, желающим поддержать уровень своих знаний.
Что скрывают от вас? – clinica plus
RonaldNem · June 3, 2026 at 1:39 am
В этой статье мы рассматриваем разрушительное влияние зависимости на жизнь человека. Обсуждаются аспекты, такие как здоровье, отношения и профессиональные достижения. Читатели узнают о необходимости обращения за помощью и о путях к восстановлению.
Переходите по ссылке ниже – лечение алкоголизма в Череповце
ScottMob · June 3, 2026 at 1:48 am
В данном обзоре представлены основные направления и тренды в области медицины. Мы обсудим актуальные проблемы здравоохранения, свежие открытия и новые подходы, которые меняют представление о лечении и профилактике заболеваний. Эта информация будет полезна как специалистам, так и широкой публике.
Продолжить изучение – лечение хронического алкоголизма
https://www.vrwant.org/wb/home.php?mod=space&uid=5166016 · June 3, 2026 at 2:04 am
https://www.vrwant.org/wb/home.php?mod=space&uid=5166016
Marvinhah · June 3, 2026 at 2:07 am
Эта статья подробно расскажет о процессе выздоровления, который включает в себя эмоциональную, физическую и психологическую реабилитацию. Мы обсуждаем значимость поддержки и наличие профессиональных программ. Читатели узнают, как строить новую жизнь и не возвращаться к старым привычкам.
Информация доступна здесь – клиника плюс
Justinoxymn · June 3, 2026 at 2:16 am
В этой статье рассматривается комплексный подход к избавлению от зависимости. Читатель узнает, как сочетание физического, психологического и духовного восстановления помогает достичь стойкого выздоровления.
Открой скрытое – сайт наркологической клиники
Jefferyaroup · June 3, 2026 at 2:21 am
В этом исследовании рассмотрены методы лечения зависимостей и их эффективность. Мы проанализируем различные подходы, используемые в реабилитационных центрах, и представим данные о результативности программ. Читатели получат надежные и научно обоснованные сведения о данной проблеме.
Заходи — там интересно – clinica plus в борисоглебске
kilaxndKip · June 3, 2026 at 2:35 am
Компания Orange Logistic предлагает надежные решения в сфере международных и внутрироссийских грузоперевозок, обеспечивая качественную логистику для бизнеса любого масштаба. Профессиональная команда специалистов гарантирует своевременную доставку грузов с соблюдением всех стандартов безопасности и таможенных требований. На сайте https://orangelogistic.ru/ клиенты могут ознакомиться с полным спектром услуг и получить индивидуальный расчет стоимости перевозки. Компания использует современные технологии отслеживания грузов, что позволяет контролировать каждый этап транспортировки и оперативно информировать заказчиков о статусе доставки.
RonaldNem · June 3, 2026 at 2:41 am
Этот информационный материал подробно освещает проблему наркозависимости, ее причины и последствия. Мы предлагаем информацию о методах лечения, профилактики и поддерживающих программах. Цель статьи — повысить осведомленность и продвигать идеи о необходимости борьбы с зависимостями.
Узнать больше – наркология лечение алкоголизма
RobertBap · June 3, 2026 at 2:48 am
Медицинская публикация представляет собой свод актуальных исследований, экспертных мнений и новейших достижений в сфере здравоохранения. Здесь вы найдете информацию о новых методах лечения, прорывных технологиях и их практическом применении. Мы стремимся сделать актуальные медицинские исследования доступными и понятными для широкой аудитории.
Более того — здесь – наркологическую клинику в Балашихе
ScottMob · June 3, 2026 at 2:50 am
В этой статье рассматриваются различные аспекты избавления от зависимости, включая физические и психологические методы. Мы обсудим поддержку, мотивацию и стратегии, которые помогут в процессе выздоровления. Читатели узнают, как преодолеть трудности и двигаться к новой жизни без зависимости.
Погрузиться в детали – наркологическая клиника в твери
Robertvew · June 3, 2026 at 3:23 am
Этот информационный материал подробно освещает проблему наркозависимости, ее причины и последствия. Мы предлагаем информацию о методах лечения, профилактики и поддерживающих программах. Цель статьи — повысить осведомленность и продвигать идеи о необходимости борьбы с зависимостями.
Изучите внимательнее – наркологическая клиника в твери
bazuklddwemi · June 3, 2026 at 3:27 am
Компания Waltz Prof — российский производитель стальных профилей и комплектующих для строительства: здесь выпускают фасадно-перегородочные системы из оцинкованной и нержавеющей стали, профили серий ВП150, ВП165, ВП250 и ВП372 с терморазрывом, оцинкованные трубы, штапики и Т-образные профили для ворот. На сайте https://waltzprof.com/ представлен широкий ассортимент самоклеящихся уплотнителей, автоматических порогов Smart LDM и скрытых дверных петель — всё необходимое для профессионального монтажа. Прямые поставки от производителя гарантируют конкурентные цены и стабильное качество продукции.
CharlesErere · June 3, 2026 at 3:35 am
Этот информационный материал подробно освещает проблему наркозависимости, ее причины и последствия. Мы предлагаем информацию о методах лечения, профилактики и поддерживающих программах. Цель статьи — повысить осведомленность и продвигать идеи о необходимости борьбы с зависимостями.
Получить больше информации – наркологическая клиника в твери
KevinMus · June 3, 2026 at 4:07 am
Steam Desktop Authenticator https://sdasteam.com (SDA). It allows you to generate account login codes and automatically confirm trades or item sales on the Community Market without using your smartphone.
Pablojiste · June 3, 2026 at 4:26 am
В этом исследовании рассмотрены методы лечения зависимостей и их эффективность. Мы проанализируем различные подходы, используемые в реабилитационных центрах, и представим данные о результативности программ. Читатели получат надежные и научно обоснованные сведения о данной проблеме.
Информация доступна здесь – наркологическая клиника в белгороде
Josephsnazy · June 3, 2026 at 5:01 am
В этой статье мы подробно рассматриваем проверенные методы борьбы с зависимостями, включая психотерапию, медикаментозное лечение и поддержку со стороны общества. Мы акцентируем внимание на важности комплексного подхода и возможности успешного восстановления для людей, столкнувшихся с этой проблемой.
Обратитесь за информацией – наркологическая клиника в череповце
MatthewSyclE · June 3, 2026 at 6:02 am
Текст посвящён распространённым мифам о зависимости и их развенчанию. Мы предоставим научно обоснованную информацию и дадим рекомендации по выбору эффективного способа борьбы с зависимым поведением.
ТОП-5 причин узнать больше – анонимная наркологическая клиника
JuliusBub · June 3, 2026 at 6:03 am
Эта информационная публикация освещает широкий спектр тем из мира медицины. Мы предлагаем читателям ясные и понятные объяснения современных заболеваний, методов профилактики и лечения. Информация будет полезна как пациентам, так и медицинским работникам, желающим поддержать уровень своих знаний.
Получить исчерпывающие сведения – наркологической клиники в Череповце
https://saveup.id/1xbet-promo-code-2026-e130-for-new-players/ · June 3, 2026 at 6:26 am
https://saveup.id/1xbet-promo-code-2026-e130-for-new-players/
RonaldUnunK · June 3, 2026 at 6:56 am
В этой публикации мы рассматриваем важную тему борьбы с зависимостями, включая алкогольную и наркотическую зависимости. Мы обсудим методы лечения, реабилитации и поддержку, которые могут помочь людям, столкнувшимся с этой проблемой. Читатели узнают о перспективах выздоровления и важности комплексного подхода.
Получить исчерпывающие сведения – клиника плюс
StephenDrymn · June 3, 2026 at 7:31 am
Эта информационная публикация освещает широкий спектр тем из мира медицины. Мы предлагаем читателям ясные и понятные объяснения современных заболеваний, методов профилактики и лечения. Информация будет полезна как пациентам, так и медицинским работникам, желающим поддержать уровень своих знаний.
Узнать из первых рук – Капельница от запоя в Белгороде
remoctopok · June 3, 2026 at 8:20 am
Runico.ru — это увлекательный онлайн-ресурс, посвящённый рунам Старшего Футарка, древнейшего рунического алфавита I–VIII веков нашей эры. Сайт предлагает детальное описание всех 24 символов, каждый из которых несёт глубокий мифологический и магический смысл. Согласно скандинавским преданиям, сами руны были открыты богу Одину ценой девяти дней самопожертвования на Мировом Древе Иггдрасиль. На https://runico.ru/ эти знания изложены доступно и увлекательно: читатель узнает историю каждого символа, его значение и связь с древней мудростью предков. Ресурс станет отличным проводником для всех, кто интересуется нордической культурой и рунической традицией.
Jefferyaroup · June 3, 2026 at 8:34 am
Публикация охватывает основные направления развития современной медицины. Мы обсудим значимость научных исследований, инноваций в лечении и роли общественного участия в формировании системы здравоохранения.
Ссылка на источник – Кодирование от алкоголизма в Борисоглебске
RobertBum · June 3, 2026 at 8:54 am
Extra resources dmail token
CharlesErere · June 3, 2026 at 9:06 am
Текст посвящён распространённым мифам о зависимости и их развенчанию. Мы предоставим научно обоснованную информацию и дадим рекомендации по выбору эффективного способа борьбы с зависимым поведением.
Изучить эмпирические данные – tver clinica plus
HenryJange · June 3, 2026 at 9:27 am
Этот краткий обзор предлагает сжатую информацию из области медицины, включая ключевые факты и последние новости. Мы стремимся сделать информацию доступной и понятной для широкой аудитории, что позволит читателям оставаться в курсе актуальных событий в здравоохранении.
Смотрите также… – клиника плюс тверь
казино онлайн · June 3, 2026 at 10:05 am
казино онлайн
Pablojiste · June 3, 2026 at 10:38 am
В этом исследовании рассмотрены методы лечения зависимостей и их эффективность. Мы проанализируем различные подходы, используемые в реабилитационных центрах, и представим данные о результативности программ. Читатели получат надежные и научно обоснованные сведения о данной проблеме.
Подробная информация доступна по запросу – нарколога на дом в Белгороде
JamesDox · June 3, 2026 at 10:59 am
В этой статье рассматриваются актуальные вопросы, связанные с развитием медицинской науки и её внедрением в повседневную практику. Особое внимание уделено вопросам профилактики, ранней диагностики и использованию технологий для улучшения здоровья человека.
Расширить кругозор по теме – clinica plus в твери
DavidMam · June 3, 2026 at 11:38 am
В этой медицинской статье мы погрузимся в актуальные вопросы здравоохранения и лечения заболеваний. Читатели узнают о современных подходах, методах диагностики и новых открытий в научных исследованиях. Наша цель — донести важную информацию и повысить уровень осведомленности о здоровье.
Где можно узнать подробнее? – вызвать капельницу от запоя на дом
GoodiniCrubs · June 3, 2026 at 11:45 am
В этой публикации мы исследуем ключевые аспекты здоровья, включая влияние образа жизни на благополучие. Читатели узнают о важности правильного питания, физической активности и психического здоровья. Мы предоставим практические советы и рекомендации для поддержания здоровья и развития профилактических подходов.
Смотрите также – tver clinica plus
https://aiti.edu.vn/members/mel-bet.51877/ · June 3, 2026 at 11:48 am
https://aiti.edu.vn/members/mel-bet.51877/
DavidHag · June 3, 2026 at 11:49 am
В этом обзоре мы обсудим современные методы борьбы с зависимостями, включая медикаментозную терапию и психотерапию. Мы представим последние исследования и их результаты, чтобы читатели могли быть в курсе наиболее эффективных подходов к лечению и поддержке.
Смотрите также… – капельницы от запоя
kasyno online opinie · June 3, 2026 at 12:01 pm
Hello there, just became aware of your blog through Google, and found that it is truly informative. I am going to watch out for brussels. I will appreciate if you continue this in future. Lots of people will be benefited from your writing. Cheers!
покер онлайн · June 3, 2026 at 12:19 pm
покер онлайн
fobovesnila · June 3, 2026 at 12:29 pm
Блог https://aae.su/ публикует экспертные материалы по бизнесу, обустройству дома и садоводству — без лишней воды и общих фраз. На сайте анализируются практические кейсы: выбор компактной мебели, строительные решения для магазинов, эффективная борьба с борщевиком на приусадебном участке. Каждая публикация решает реальную задачу читателя — без воды и отвлечённых рассуждений.
nn app · June 3, 2026 at 12:33 pm
Sempre via os vídeos de Chuva de moeda, hoje foi minha vez no Ninja vs Samurai! 25k garantidos. Zerei a vida hoje.
online casino · June 3, 2026 at 12:36 pm
I like your quality that you put into your writing . Please do continue with more like this.
JuliusBub · June 3, 2026 at 1:02 pm
В этой статье мы обсудим процесс восстановления после зависимостей, акцентируя внимание на различных методах и подходах к реабилитации. Читатели узнают, как создать план выздоровления и использовать полезные ресурсы для достижения устойчивых изменений.
Изучить вопрос глубже – нарколог на дом цена
RaymondClink · June 3, 2026 at 1:14 pm
В статье по вопросам здоровья мы рассматриваем актуальные проблемы, с которыми сталкивается общество. Обсуждаются заболевания, факторы риска и важные аспекты профилактики. Читатели получат полезные советы о том, как сохранить здоровье и улучшить качество жизни.
Интересует подробная информация – tver clinica plus
RonaldUnunK · June 3, 2026 at 1:36 pm
В статье по вопросам здоровья мы рассматриваем актуальные проблемы, с которыми сталкивается общество. Обсуждаются заболевания, факторы риска и важные аспекты профилактики. Читатели получат полезные советы о том, как сохранить здоровье и улучшить качество жизни.
Рассмотреть проблему всесторонне – наркологическая клиника в твери
EdwinDrary · June 3, 2026 at 1:40 pm
В этой публикации мы предложим ряд рекомендаций по избавлению от зависимостей и успешному восстановлению. Мы обсудим методы привлечения поддержки и важность самосознания. Эти советы помогут людям вернуться к нормальной жизни и стать на путь выздоровления.
Как достичь результата? – donetsk detox24
RaymondLEALL · June 3, 2026 at 2:30 pm
Эта публикация исследует взаимосвязь зависимости и психологии. Мы обсудим, как психологические аспекты влияют на появление зависимостей и процесс выздоровления. Читатели смогут понять важность профессиональной поддержки и применения научных подходов в терапии.
Ознакомиться с деталями – врач нарколог на дом
Williamzew · June 3, 2026 at 2:32 pm
Этот информативный текст сочетает в себе темы здоровья и зависимости. Мы обсудим, как хронические заболевания могут усугубить зависимости и наоборот, как зависимость может влиять на общее состояние здоровья. Читатели получат представление о комплексном подходе к лечению как физического, так и психического состояния.
Изучить материалы по теме – капельницы после алкогольного запоя
DelbertnuB · June 3, 2026 at 2:41 pm
Этот обзор посвящен успешным стратегиям избавления от зависимости, включая реальные примеры и советы. Мы разоблачим мифы и предоставим читателям достоверную информацию о различных подходах. Получите опыт многообразия методов и найдите подходящий способ для себя!
Продолжить изучение – клиника плюс тверь
Steventet · June 3, 2026 at 2:43 pm
В этой статье рассматриваются различные аспекты избавления от зависимости, включая физические и психологические методы. Мы обсудим поддержку, мотивацию и стратегии, которые помогут в процессе выздоровления. Читатели узнают, как преодолеть трудности и двигаться к новой жизни без зависимости.
Не упусти важное! – кодировка от алкоголизма двойной блок
Petervow · June 3, 2026 at 2:55 pm
Эта доказательная статья представляет собой глубокое погружение в успехи и вызовы лечения зависимостей. Мы обращаемся к научным исследованиям и опыту специалистов, чтобы предоставить читателям надежные данные об эффективности различных методик. Изучите, что работает лучше всего, и получите информацию от экспертов.
Обратитесь за информацией – выведение из запоя на дому
Leroyric · June 3, 2026 at 3:18 pm
Статья посвящена анализу текущих трендов в медицине и их влиянию на жизнь людей. Мы рассмотрим новые технологии, методы лечения и значение профилактики в обеспечении долголетия и здоровья.
Получить больше информации – вывод из запоя с выездом
ThomasGlicy · June 3, 2026 at 3:32 pm
В данной статье мы акцентируем внимание на важности поддержки в процессе выздоровления. Мы обсудим, как друзья, семья и профессионалы могут помочь тем, кто сталкивается с зависимостями. Читатели получат практические советы, как поддерживать близких на пути к новой жизни.
Обратитесь за информацией – clinica plus
najlepsze kasyno online · June 3, 2026 at 4:05 pm
You are my inspiration , I possess few web logs and very sporadically run out from to brand 🙁
https://camlive.ovh/post/45436_https-nature-et-avenir-org-files-pages-1xbet-code-d-inscription-promo-html.html · June 3, 2026 at 4:13 pm
https://camlive.ovh/post/45436_https-nature-et-avenir-org-files-pages-1xbet-code-d-inscription-promo-html.html
Thomascob · June 3, 2026 at 4:59 pm
продолжить вотка бет
CurtisReorm · June 3, 2026 at 5:15 pm
Может ли внук претендовать на наследство деда при умершем отце?
Nathanuntot · June 3, 2026 at 5:26 pm
Эта публикация содержит ценные советы и рекомендации по избавлению от зависимости. Мы обсуждаем различные стратегии, которые могут помочь в процессе выздоровления и важность обращения за помощью. Читатели смогут использовать полученные знания для улучшения своего состояния.
Хочешь знать всё? – наркологическая клиника в твери
ferainlic · June 3, 2026 at 5:52 pm
Современные финансовые технологии открывают новые возможности для тех, кто оказался в сложной ситуации и нуждается в срочных средствах. Онлайн-займы стали настоящим спасением для миллионов россиян: заявка рассматривается за считанные минуты, а деньги поступают на карту практически мгновенно. На платформе https://xn—-7sbujpz2a7c.xn--p1ai/ собраны проверенные предложения от надёжных микрофинансовых организаций с прозрачными условиями. Особенно привлекательно, что новые клиенты могут получить первый займ под 0%, а одобрение возможно даже при непростой кредитной истории. Сервис работает круглосуточно, избавляя от необходимости посещать офисы и стоять в очередях — всё решается дистанционно за 15 минут.
Nathanuntot · June 3, 2026 at 6:01 pm
В этой публикации мы рассматриваем важную тему борьбы с зависимостями, включая алкогольную и наркотическую зависимости. Мы обсудим методы лечения, реабилитации и поддержку, которые могут помочь людям, столкнувшимся с этой проблемой. Читатели узнают о перспективах выздоровления и важности комплексного подхода.
Это ещё не всё… – капельница от запоя на дому круглосуточно
nifofuinicy · June 3, 2026 at 6:06 pm
Looking for seo services fort smith? CyberSpyder cyberspyder.net is a full-service Web development and Digital Marketing firm located in Fort Smith, Arkansas, providing solutions to local, regional, and national clients. We offer a Full Range of Services, Including Web design, Search Engine Optimization (SEO), Digital marketing, Graphic design, Hosting, and Support. Drawing on more than 25 years of proven expertise, our team crafts personalized approaches and delivers direct, practical support to help small and mid-sized businesses thrive.
pziletorog · June 3, 2026 at 6:17 pm
Группа компаний «СОЮЗ» с 2008 года создает современные офисные пространства, которые вдохновляют на продуктивную работу и производят впечатление на партнеров. Команда профессионалов предлагает комплексный подход: от поставки качественной офисной мебели до разработки индивидуальных дизайн-проектов под ключ. На сайте https://group-soyuz.ru/ вы найдете решения для офисов, гостиниц и учебных заведений с гарантией соблюдения бюджета и сроков. Компания выстраивает долгосрочные отношения с клиентами, предугадывая их потребности и предлагая экономически обоснованные решения для создания эффективного рабочего пространства в Москве.
StephenArift · June 3, 2026 at 6:30 pm
Мы рассмотрим современные вызовы здравоохранения и пути их решения с помощью технологий и научных исследований. В статье собраны данные о новых лекарствах, методах диагностики и системном подходе к улучшению здоровья населения.
А что дальше? – clinica plus
Rodneyrailm · June 3, 2026 at 6:51 pm
В данной статье мы поговорим о будущем медицины, акцентируя внимание на прорывных разработках и их потенциале. Читатель узнает о новых подходах к лечению, роли искусственного интеллекта и возможностях персонализированной медицины.
Уточнить детали – врач нарколог воронеж
DanielImalm · June 3, 2026 at 6:53 pm
Этот краткий обзор предлагает сжатую информацию из области медицины, включая ключевые факты и последние новости. Мы стремимся сделать информацию доступной и понятной для широкой аудитории, что позволит читателям оставаться в курсе актуальных событий в здравоохранении.
Открой скрытое – клиника плюс
Thomasnap · June 3, 2026 at 6:57 pm
В этой публикации мы исследуем ключевые аспекты здоровья, включая влияние образа жизни на благополучие. Читатели узнают о важности правильного питания, физической активности и психического здоровья. Мы предоставим практические советы и рекомендации для поддержания здоровья и развития профилактических подходов.
Продолжить чтение – наркологическая клиника в твери
Austinsoymn · June 3, 2026 at 6:58 pm
Эта публикация исследует взаимосвязь зависимости и психологии. Мы обсудим, как психологические аспекты влияют на появление зависимостей и процесс выздоровления. Читатели смогут понять важность профессиональной поддержки и применения научных подходов в терапии.
Раскрыть тему полностью – помощь вывода из запоя
JosephGox · June 3, 2026 at 7:02 pm
В этой публикации мы предложим ряд рекомендаций по избавлению от зависимостей и успешному восстановлению. Мы обсудим методы привлечения поддержки и важность самосознания. Эти советы помогут людям вернуться к нормальной жизни и стать на путь выздоровления.
Читать далее > – clinica plus в твери
JamesDox · June 3, 2026 at 7:07 pm
В этой статье мы говорим о важности поддержки в процессе выздоровления. Рассматриваются семьи, группы поддержки, специалисты и онлайн-ресурсы, которые могут сыграть решающую роль в избавлении от зависимости.
А есть ли продолжение? – клиника плюс
RaymondAspEk · June 3, 2026 at 7:12 pm
В этой публикации мы исследуем ключевые аспекты здоровья, включая влияние образа жизни на благополучие. Читатели узнают о важности правильного питания, физической активности и психического здоровья. Мы предоставим практические советы и рекомендации для поддержания здоровья и развития профилактических подходов.
Тыкай сюда — узнаешь много интересного – наркологическая клиника в твери
xejeviasymn · June 3, 2026 at 7:13 pm
Мартин Сад https://www.martin-sad.ru/ – это питомник растений и огромный садовый центр в Москве. Посетите сайт – посмотрите самый полный каталог саженцев и растений предлагаемых нами, а также каталог товаров для сада. У нас множество товаров по Акции! Оказываем услуги посадки растений и ухода за участком. Подробнее на сайте!
StephenArift · June 3, 2026 at 7:19 pm
В этой статье мы рассматриваем разрушительное влияние зависимости на жизнь человека. Обсуждаются аспекты, такие как здоровье, отношения и профессиональные достижения. Читатели узнают о необходимости обращения за помощью и о путях к восстановлению.
Узнать из первых рук – вывод из запоя анонимно недорого
RoberttaR · June 3, 2026 at 7:31 pm
Этот обзор медицинских исследований собрал самое важное из последних публикаций в области медицины. Мы проанализировали ключевые находки и представили их в доступной форме, чтобы читатели могли легко ориентироваться в актуальных темах. Этот материал станет отличным подспорьем для изучения медицины.
Получить дополнительную информацию – clinica plus
ThomasApaft · June 3, 2026 at 7:34 pm
Custom-made kitchen furniture custom closet systems Tampa
betano login · June 3, 2026 at 7:34 pm
Não existe milagre, mas o Piggy Gold facilitou muito agora pouco. Paciência paga.
JamesNoK · June 3, 2026 at 7:39 pm
Публикация охватывает основные направления развития современной медицины. Мы обсудим значимость научных исследований, инноваций в лечении и роли общественного участия в формировании системы здравоохранения.
Читать полностью – clinica plus
fejafadag · June 3, 2026 at 7:39 pm
Якщо шукаєте, який бренд філаменту обрати в Україні, зверніть увагу на LBL — українського виробника та інтернет-магазин PLA і PETG/CoPET пластику для 3Д принтерів. Тут можна купити якісний філамент у різних кольорах, оптом і в роздріб, з доставкою по Києву та Україні: https://lbl-corp.com/
JosephGox · June 3, 2026 at 7:44 pm
В данной статье рассматриваются проблемы общественного здоровья и социальные факторы, влияющие на него. Мы акцентируем внимание на значении профилактики и осведомленности в защите здоровья на уровне общества. Читатели смогут узнать о новых инициативах и программах, направленных на улучшение здоровья населения.
Интересует подробная информация – clinica plus
Austinsoymn · June 3, 2026 at 7:50 pm
В этой публикации мы рассматриваем важную тему борьбы с зависимостями, включая алкогольную и наркотическую зависимости. Мы обсудим методы лечения, реабилитации и поддержку, которые могут помочь людям, столкнувшимся с этой проблемой. Читатели узнают о перспективах выздоровления и важности комплексного подхода.
Раскрыть тему полностью – наркологическая клиника в твери
punetsvax · June 3, 2026 at 8:06 pm
Looking for a list of crypto swaps? Visit https://swapslist.io/ – SwapsList helps users compare crypto exchange services before choosing where to exchange digital assets. The site focuses on practical exchange factors: KYC regulations, registration requirements, supported coins, available networks, expected speed, rate type, fees, fiat routes, and wallet payout flow. Use the list to compare direct swap services, aggregators, and online exchange options.
Michaelcreme · June 3, 2026 at 8:29 pm
В этой статье рассматриваются способы преодоления зависимости и успешные истории людей, которые справились с этой проблемой. Мы обсудим важность поддержки со стороны близких и профессионалов, а также стратегии, которые могут помочь в процессе выздоровления. Научитесь первоочередным шагам к новой жизни.
Всё самое вкусное внутри – капельница от запоя
JimmieSnomy · June 3, 2026 at 8:34 pm
Этот документ охватывает важные аспекты медицинской науки, сосредотачиваясь на ключевых вопросах, касающихся здоровья населения. Мы рассматриваем свежие исследования, клинические рекомендации и лучшие практики, которые помогут улучшить качество лечения и профилактики заболеваний. Читатели получат возможность углубиться в различные медицинские дисциплины.
Связаться за уточнением – детокс24 геленджик
Michaelcreme · June 3, 2026 at 9:18 pm
Этот текст представляет собой обзор свежих данных и исследований в области медицины. Он призван помочь читателям понять, как научные достижения влияют на лечение, диагностику и общее состояние системы здравоохранения.
Изучите внимательнее – наркологическая клиника в твери
AndrewClubs · June 3, 2026 at 9:19 pm
В этой статье рассматривается комплексный подход к избавлению от зависимости. Читатель узнает, как сочетание физического, психологического и духовного восстановления помогает достичь стойкого выздоровления.
Посмотреть подробности – Наркологическая клиника в Донецке
JimmieSnomy · June 3, 2026 at 9:23 pm
Эта статья подробно расскажет о процессе выздоровления, который включает в себя эмоциональную, физическую и психологическую реабилитацию. Мы обсуждаем значимость поддержки и наличие профессиональных программ. Читатели узнают, как строить новую жизнь и не возвращаться к старым привычкам.
Уточнить детали – detox24
Stevensepsy · June 3, 2026 at 9:27 pm
Этот обзор посвящен успешным стратегиям избавления от зависимости, включая реальные примеры и советы. Мы разоблачим мифы и предоставим читателям достоверную информацию о различных подходах. Получите опыт многообразия методов и найдите подходящий способ для себя!
Посмотреть всё – clinica plus
GoodiniCrubs · June 3, 2026 at 9:34 pm
Публикация знакомит читателей с различными подходами к реабилитации. От традиционных методов до современных программ — вы узнаете, как выбрать оптимальный путь к выздоровлению и преодолеть препятствия на этом пути.
Где почитать поподробнее? – капельницу от похмелья на дому недорого
https://wpsoffice-windows.com/ · June 3, 2026 at 9:36 pm
You should take part in a contest for one of the most useful websites on the web. I’m going to highly recommend this website!
Timothyelapy · June 3, 2026 at 9:49 pm
Bu arada soyleyeyim, eger laminat parke boyas? varm? konusuyla ilgileniyorsan?z, suraya bir goz at?n. Iste link: https://evhobisi.com/articles/laminat-parke-boyasi-mumkun-mu/
Timothyelapy · June 3, 2026 at 9:54 pm
Bu arada soyleyeyim, eger seda turan konusuyla ilgileniyorsan?z, suraya bak?n. Iste link: https://evhobisi.com/authors/seda-turan/
Jasonurini · June 3, 2026 at 10:05 pm
В этой медицинской статье мы погрузимся в актуальные вопросы здравоохранения и лечения заболеваний. Читатели узнают о современных подходах, методах диагностики и новых открытий в научных исследованиях. Наша цель — донести важную информацию и повысить уровень осведомленности о здоровье.
Ознакомьтесь с аналитикой – наркологический центр в Твери
Robertnit · June 3, 2026 at 10:06 pm
заказать песок карьерный https://pesok-karernyy-kupit1.ru
Josephded · June 3, 2026 at 10:12 pm
Этот обзор медицинских исследований собрал самое важное из последних публикаций в области медицины. Мы проанализировали ключевые находки и представили их в доступной форме, чтобы читатели могли легко ориентироваться в актуальных темах. Этот материал станет отличным подспорьем для изучения медицины.
Получить больше информации – нарколог на дом круглосуточно воронеж цены
Stevensepsy · June 3, 2026 at 10:17 pm
В данной статье мы акцентируем внимание на важности поддержки в процессе выздоровления. Мы обсудим, как друзья, семья и профессионалы могут помочь тем, кто сталкивается с зависимостями. Читатели получат практические советы, как поддерживать близких на пути к новой жизни.
Изучить аспект более тщательно – капельницы от запоя круглосуточно
https://www.wps-wd.com/ · June 3, 2026 at 10:31 pm
Nice post. I learn something new and challenging on websites I stumbleupon everyday. It’s always useful to read content from other writers and practice something from their web sites.
best online casino new zealand · June 3, 2026 at 11:01 pm
Might we expect to see more of these same problems in the future?
online casino · June 3, 2026 at 11:03 pm
This is a great blog. Thank you for the very informative post.
Jasonurini · June 3, 2026 at 11:13 pm
Этот информационный материал подробно освещает проблему наркозависимости, ее причины и последствия. Мы предлагаем информацию о методах лечения, профилактики и поддерживающих программах. Цель статьи — повысить осведомленность и продвигать идеи о необходимости борьбы с зависимостями.
Ознакомьтесь с аналитикой – клиника плюс тверь
Josephded · June 3, 2026 at 11:13 pm
В данной статье мы поговорим о будущем медицины, акцентируя внимание на прорывных разработках и их потенциале. Читатель узнает о новых подходах к лечению, роли искусственного интеллекта и возможностях персонализированной медицины.
Осуществить глубокий анализ – сколько стоит нарколог на дом
Jeffreycit · June 3, 2026 at 11:14 pm
В данной статье рассматриваются физиологические и эмоциональные аспекты зависимости. Мы обсудим, как организм реагирует на зависимое поведение, и какие методы помогают восстановить здоровье и внутреннее равновесие.
Давай разберёмся досконально – клиника плюс тверь
zalicrdpob · June 3, 2026 at 11:15 pm
BTC converter at https://btc-converter.com/ – Use the BTC conversion tool to calculate the current value of Bitcoin in US dollars. Enter the amount of Bitcoin and see the estimated dollar equivalent based on the live BTC/USD exchange rate. The tool is designed for quick checks before selling, trading, comparing wallet balances, or viewing cryptocurrency payment amounts. It can display 1 BTC in dollars, smaller coin amounts, larger balances, and general dollar-based comparisons.
AlfonsoEssen · June 3, 2026 at 11:19 pm
Эта статья освещает различные аспекты освобождения от зависимости и пути к выздоровлению. Мы обсуждаем важность осознания своей проблемы и обращения за помощью. Читатели получат практические советы о том, как преодолевать трудности и строить новую жизнь без зависимости.
Смотри, что ещё есть – Поставить капельницу после запоя
online casino · June 3, 2026 at 11:20 pm
Hey very cool site!! Man .. Beautiful .. Amazing .. I will bookmark your website and take the feeds also…I’m happy to find so many useful information here in the post, we need develop more strategies in this regard, thanks for sharing. . . . . .
DavidHag · June 3, 2026 at 11:40 pm
Обзор посвящён процессу восстановления после зависимостей. Мы расскажем о различных этапах реабилитации, поддерживающих ресурсах и важности мотивации в достижении устойчивого выздоровления.
Смотрите также… – tver clinica plus
MurrayBrelm · June 3, 2026 at 11:49 pm
В этом обзоре мы обсудим современные методы борьбы с зависимостями, включая медикаментозную терапию и психотерапию. Мы представим последние исследования и их результаты, чтобы читатели могли быть в курсе наиболее эффективных подходов к лечению и поддержке.
Нажмите, чтобы узнать больше – стоимость вывода из запоя
sututlam · June 3, 2026 at 11:53 pm
Check the live Bitcoin price in GBP and see how much 1 BTC is worth in British Pounds right now. https://bitcoinpricegbp.com/ tracks the current BTC/GBP exchange rate, daily movements, and key market data for users looking for a quick reference for Bitcoin in British Pounds. This site is useful for users tracking their Bitcoin balance in GBP, comparing today’s movements, and checking their portfolio value.
Steventet · June 4, 2026 at 12:15 am
Публикация знакомит читателей с различными подходами к реабилитации. От традиционных методов до современных программ — вы узнаете, как выбрать оптимальный путь к выздоровлению и преодолеть препятствия на этом пути.
Подробнее можно узнать тут – tver clinica plus
Williamzew · June 4, 2026 at 12:19 am
Этот обзор содержит информацию о передовых достижениях в области медицины. Мы разберем инновационные технологии, которые меняют подход к лечению и диагностике, а также их влияние на эффективность оказания медицинской помощи.
Интересует подробная информация – капельница от запоя
ThomasWaf · June 4, 2026 at 12:21 am
Мы рассмотрим современные вызовы здравоохранения и пути их решения с помощью технологий и научных исследований. В статье собраны данные о новых лекарствах, методах диагностики и системном подходе к улучшению здоровья населения.
Перейти к статье – clinica plus
Kennethtearf · June 4, 2026 at 12:24 am
В этой статье мы рассмотрим современные достижения в области медицины, включая инновационные методы лечения и диагностики. Мы обсудим важность профилактики заболеваний и роль технологий в улучшении качества здравоохранения. Читатели узнают о влиянии медицины на повседневную жизнь и ее значение для современного общества.
Проверенные методы — узнай сейчас – капельницу от запоя на дому
JamesGophy · June 4, 2026 at 12:51 am
узип предназначен для защиты от прямого удара молнии.
Подробная информация на сайте – https://uzip-avtomat.ru/
УЗИП Т
узип
производство узип
RaymondClink · June 4, 2026 at 12:51 am
В данной публикации мы поговорим о процессе восстановления от зависимости, о том, как вернуть себе нормальную жизнь. Мы обсудим преодоление трудностей, значимость поддержки и наличие программ реабилитации. Читатели смогут узнать о ключевых шагах к успешному восстановлению.
Узнайте всю правду – клиника плюс
JamesGophy · June 4, 2026 at 12:59 am
Для загородного дома идеально подойдет выбрать узип.
Подробная информация на сайте – http://uzip-avtomat.ru
УЗИПН овосибирск
цена узип
узип для дачи
MurrayBrelm · June 4, 2026 at 12:59 am
Медицинская публикация представляет собой свод актуальных исследований, экспертных мнений и новейших достижений в сфере здравоохранения. Здесь вы найдете информацию о новых методах лечения, прорывных технологиях и их практическом применении. Мы стремимся сделать актуальные медицинские исследования доступными и понятными для широкой аудитории.
Неизвестные факты о… – снятие запоя цена
Melhor Slot · June 4, 2026 at 1:04 am
A banca agradece! milzão sacados do Gates of Olympus com sucesso.
EdwinDrary · June 4, 2026 at 1:10 am
В этой статье мы говорим о важности поддержки в процессе выздоровления. Рассматриваются семьи, группы поддержки, специалисты и онлайн-ресурсы, которые могут сыграть решающую роль в избавлении от зависимости.
Желаете узнать подробности? – вывод из запоя в Донецке
RobertMeest · June 4, 2026 at 1:20 am
Этот обзор посвящен успешным стратегиям избавления от зависимости, включая реальные примеры и советы. Мы разоблачим мифы и предоставим читателям достоверную информацию о различных подходах. Получите опыт многообразия методов и найдите подходящий способ для себя!
Узнайте всю правду – вызов нарколога на дом воронеж
Jamescauts · June 4, 2026 at 1:23 am
В этом обзоре мы обсудим современные методы борьбы с зависимостями, включая медикаментозную терапию и психотерапию. Мы представим последние исследования и их результаты, чтобы читатели могли быть в курсе наиболее эффективных подходов к лечению и поддержке.
Неизвестные факты о… – капельницу от запоя
best online casino nz · June 4, 2026 at 1:34 am
have already been reading ur blog for a couple of days. really enjoy what you posted. btw i will be doing a report about this topic. do you happen to know any great websites or forums that I can find out more? thanks a lot.
https://uxlanding.com/1xbet-free-promo-code-e130-sports-bonus/ · June 4, 2026 at 1:36 am
https://uxlanding.com/1xbet-free-promo-code-e130-sports-bonus/
EdwardNaw · June 4, 2026 at 1:47 am
В этой статье рассматриваются актуальные вопросы, связанные с развитием медицинской науки и её внедрением в повседневную практику. Особое внимание уделено вопросам профилактики, ранней диагностики и использованию технологий для улучшения здоровья человека.
Изучите внимательнее – Поставить капельницу после запоя
best online casino · June 4, 2026 at 1:51 am
I do not even know how I ended up here, but I thought this post was good. I do not know who you are but certainly you are going to a famous blogger if you are not already 😉 Cheers!
Kennethtearf · June 4, 2026 at 1:51 am
Этот обзор посвящен успешным стратегиям избавления от зависимости, включая реальные примеры и советы. Мы разоблачим мифы и предоставим читателям достоверную информацию о различных подходах. Получите опыт многообразия методов и найдите подходящий способ для себя!
А есть ли продолжение? – капельницы после алкогольного запоя
Kennethrob · June 4, 2026 at 2:31 am
В этой статье мы подробно рассматриваем проверенные методы борьбы с зависимостями, включая психотерапию, медикаментозное лечение и поддержку со стороны общества. Мы акцентируем внимание на важности комплексного подхода и возможности успешного восстановления для людей, столкнувшихся с этой проблемой.
Уникальные данные только сегодня – вывод из запоя тверь на дому круглосуточно
RobertMeest · June 4, 2026 at 2:41 am
Эта доказательная статья представляет собой глубокое погружение в успехи и вызовы лечения зависимостей. Мы обращаемся к научным исследованиям и опыту специалистов, чтобы предоставить читателям надежные данные об эффективности различных методик. Изучите, что работает лучше всего, и получите информацию от экспертов.
Тыкай сюда — узнаешь много интересного – сколько стоит нарколог на дом
JoshuaNom · June 4, 2026 at 2:44 am
Читатели получат представление о том, как современные технологии влияют на развитие медицины. Обсуждаются новые методы лечения, персонализированный подход и роль цифровых решений в повышении качества медицинских услуг.
Интересует подробная информация – капельница на дому от запоя
ThomasGlicy · June 4, 2026 at 2:50 am
В этой публикации мы рассматриваем важную тему борьбы с зависимостями, включая алкогольную и наркотическую зависимости. Мы обсудим методы лечения, реабилитации и поддержку, которые могут помочь людям, столкнувшимся с этой проблемой. Читатели узнают о перспективах выздоровления и важности комплексного подхода.
А что дальше? – клиника плюс
EdwardNaw · June 4, 2026 at 2:56 am
Этот обзор посвящен успешным стратегиям избавления от зависимости, включая реальные примеры и советы. Мы разоблачим мифы и предоставим читателям достоверную информацию о различных подходах. Получите опыт многообразия методов и найдите подходящий способ для себя!
Читать далее > – Капельница от запоя на дому
Richardjoiva · June 4, 2026 at 3:02 am
В этой публикации мы исследуем ключевые аспекты здоровья, включая влияние образа жизни на благополучие. Читатели узнают о важности правильного питания, физической активности и психического здоровья. Мы предоставим практические советы и рекомендации для поддержания здоровья и развития профилактических подходов.
Ознакомиться с теоретической базой – клиника плюс тверь
https://www.wpswpspc.com/ · June 4, 2026 at 3:07 am
Having read this I believed it was very enlightening. I appreciate you finding the time and effort to put this information together. I once again find myself spending way too much time both reading and posting comments. But so what, it was still worth it!
Kennethrob · June 4, 2026 at 3:30 am
В этой статье мы рассматриваем разрушительное влияние зависимости на жизнь человека. Обсуждаются аспекты, такие как здоровье, отношения и профессиональные достижения. Читатели узнают о необходимости обращения за помощью и о путях к восстановлению.
Открыть полностью – наркологическая клиника в твери
RaymondLEALL · June 4, 2026 at 3:39 am
В статье рассматриваются различные стратегии борьбы с зависимостями, включая проверенные методы и реальные истории успеха. Читатель узнает, какие подходы наиболее эффективны и как начать путь к выздоровлению.
Лучшее решение — прямо здесь – вызов нарколога на дом воронеж
AndrewClubs · June 4, 2026 at 3:40 am
В этой статье обсуждаются актуальные медицинские вопросы, которые волнуют общество. Мы обращаем внимание на проблемы, касающиеся здравоохранения и лечения, а также на новшества в области медицины. Читатели будут осведомлены о последних событиях и смогут следить за тенденциями в медицине.
Хочешь знать всё? – detox24 в донецке
JoshuaNom · June 4, 2026 at 3:44 am
Текст посвящён распространённым мифам о зависимости и их развенчанию. Мы предоставим научно обоснованную информацию и дадим рекомендации по выбору эффективного способа борьбы с зависимым поведением.
Осуществить глубокий анализ – сколько стоит капельница на дому в воронеже
AlfonsoEssen · June 4, 2026 at 4:10 am
В этой статье рассматриваются различные аспекты избавления от зависимости, включая физические и психологические методы. Мы обсудим поддержку, мотивацию и стратегии, которые помогут в процессе выздоровления. Читатели узнают, как преодолеть трудности и двигаться к новой жизни без зависимости.
Все материалы собраны здесь – капельница от запоя цена
Richardjoiva · June 4, 2026 at 4:11 am
Статья посвящена анализу текущих трендов в медицине и их влиянию на жизнь людей. Мы рассмотрим новые технологии, методы лечения и значение профилактики в обеспечении долголетия и здоровья.
Узнать напрямую – clinica plus
JamesLievy · June 4, 2026 at 4:36 am
В этой публикации мы обсуждаем современные методы лечения различных заболеваний. Читатели узнают о новых медикаментах, терапиях и исследованиях, которые активно применяются для лечения. Мы нацелены на то, чтобы предоставить практические знания, которые могут помочь в борьбе с недугами.
Изучить материалы по теме – частный нарколог на дом
Jamesswosy · June 4, 2026 at 4:39 am
Эта статья подробно расскажет о процессе выздоровления, который включает в себя эмоциональную, физическую и психологическую реабилитацию. Мы обсуждаем значимость поддержки и наличие профессиональных программ. Читатели узнают, как строить новую жизнь и не возвращаться к старым привычкам.
Практические советы ждут тебя – clinica plus
https://connect.gt/user/melbet6 · June 4, 2026 at 5:03 am
https://connect.gt/user/melbet6
Petervow · June 4, 2026 at 5:14 am
Эта публикация исследует взаимосвязь зависимости и психологии. Мы обсудим, как психологические аспекты влияют на появление зависимостей и процесс выздоровления. Читатели смогут понять важность профессиональной поддержки и применения научных подходов в терапии.
Рассмотреть проблему всесторонне – стоимость вывода из запоя
DanielImalm · June 4, 2026 at 5:22 am
Этот краткий обзор предлагает сжатую информацию из области медицины, включая ключевые факты и последние новости. Мы стремимся сделать информацию доступной и понятной для широкой аудитории, что позволит читателям оставаться в курсе актуальных событий в здравоохранении.
Полная информация здесь – вывод из запоя на дому тверь
ThomasWaf · June 4, 2026 at 5:26 am
Эта статья освещает различные аспекты освобождения от зависимости и пути к выздоровлению. Мы обсуждаем важность осознания своей проблемы и обращения за помощью. Читатели получат практические советы о том, как преодолевать трудности и строить новую жизнь без зависимости.
Где можно узнать подробнее? – наркологическая клиника в твери
RobertSlimi · June 4, 2026 at 5:27 am
В данном обзоре представлены основные направления и тренды в области медицины. Мы обсудим актуальные проблемы здравоохранения, свежие открытия и новые подходы, которые меняют представление о лечении и профилактике заболеваний. Эта информация будет полезна как специалистам, так и широкой публике.
Получить исчерпывающие сведения – нарколога на дом самара
Jasonheips · June 4, 2026 at 5:39 am
В данной статье мы поговорим о будущем медицины, акцентируя внимание на прорывных разработках и их потенциале. Читатель узнает о новых подходах к лечению, роли искусственного интеллекта и возможностях персонализированной медицины.
Осуществить глубокий анализ – вызвать нарколога на дом
zozaleality · June 4, 2026 at 5:50 am
Looking to buy and sell USDT for fiat online? Visit https://buysellswappro.com/ – BuySellSwapPro helps users navigate between fiat and crypto using clear online routes centered around USDT. You can buy crypto with a credit or debit card, sell crypto for fiat, compare pages by currency or country, and choose the route that best suits your card, bank account, or local market conditions.
Martinapemy · June 4, 2026 at 5:58 am
Этот обзор посвящен успешным стратегиям избавления от зависимости, включая реальные примеры и советы. Мы разоблачим мифы и предоставим читателям достоверную информацию о различных подходах. Получите опыт многообразия методов и найдите подходящий способ для себя!
Получить полную информацию – вывод из запоя анонимно недорого
Leroyric · June 4, 2026 at 5:59 am
Статья посвящена анализу текущих трендов в медицине и их влиянию на жизнь людей. Мы рассмотрим новые технологии, методы лечения и значение профилактики в обеспечении долголетия и здоровья.
Получить больше информации – вывод из запоя недорого
FerminFlurb · June 4, 2026 at 6:33 am
Этот краткий обзор предлагает сжатую информацию из области медицины, включая ключевые факты и последние новости. Мы стремимся сделать информацию доступной и понятной для широкой аудитории, что позволит читателям оставаться в курсе актуальных событий в здравоохранении.
Интересует подробная информация – капельница от алкоголя в воронеже
AndrewDob · June 4, 2026 at 6:36 am
Эта медицинская заметка содержит сжатую информацию о новых находках и методах в области здравоохранения. Мы предлагаем читателям свежие данные о заболеваниях, профилактике и лечении. Наша цель — быстро и доступно донести важную информацию, которая поможет в повседневной жизни и понимании здоровья.
Ознакомьтесь с аналитикой – клиника плюс
Archienot · June 4, 2026 at 6:41 am
Тем, кто интересуется путешествиями, маршрутами и современными онлайн-развлечениями, стоит обратить внимание на //friendlysun.ru](https://friendlysun.ru). На сайте публикуются материалы о travel lifestyle, полезные советы для туристов, а также статьи о мобильных развлечениях и онлайн-досуге во время поездок.
Source:
https://friendlysun.ru/
MarcoWocky · June 4, 2026 at 6:43 am
Many thanks I enjoy it
Source:
– https://playvideopoker.org/understanding-online-casino-bonuses-video-poker-players/
Helpful insights | Thanks
Jamescauts · June 4, 2026 at 6:57 am
В данной статье рассматриваются физиологические и эмоциональные аспекты зависимости. Мы обсудим, как организм реагирует на зависимое поведение, и какие методы помогают восстановить здоровье и внутреннее равновесие.
Более того — здесь – клиника плюс
RoberttaR · June 4, 2026 at 7:16 am
В этой статье обсуждаются актуальные медицинские вопросы, которые волнуют общество. Мы обращаем внимание на проблемы, касающиеся здравоохранения и лечения, а также на новшества в области медицины. Читатели будут осведомлены о последних событиях и смогут следить за тенденциями в медицине.
Откройте для себя больше – кодировка на 5 лет
RobertInsub · June 4, 2026 at 7:23 am
usdt to rub exchanger exchange-usdt-cash.com
ThomasTreaf · June 4, 2026 at 7:35 am
Подробнее здесь vodka bet casino
RogerRhicy · June 4, 2026 at 7:35 am
обменять крипту на кеш без верификации перевести usdt в рубли онлайн
JamesNoK · June 4, 2026 at 7:53 am
Эта публикация содержит ценные советы и рекомендации по избавлению от зависимости. Мы обсуждаем различные стратегии, которые могут помочь в процессе выздоровления и важность обращения за помощью. Читатели смогут использовать полученные знания для улучшения своего состояния.
Читать полностью – анонимная наркологическая клиника
https://onlinebetcity.nl/code-promo-1xbet-2026-bonus1x130-bonus-gratuit-130-e/ · June 4, 2026 at 8:08 am
https://onlinebetcity.nl/code-promo-1xbet-2026-bonus1x130-bonus-gratuit-130-e/
Jamesdulse · June 4, 2026 at 9:01 am
Эта публикация обращает внимание на важность профилактики зависимостей. Мы обсудим, как осведомленность и образование могут помочь в предотвращении возникновения зависимости. Читатели смогут ознакомиться с полезными советами и ресурсами, которые способствуют здоровому образу жизни.
Ознакомиться с теоретической базой – клиника плюс
https://bookmarking.win/story.php?title=free-1xbet-promo-code-2026-vip-bonus-130#discuss · June 4, 2026 at 9:08 am
https://bookmarking.win/story.php?title=free-1xbet-promo-code-2026-vip-bonus-%E2%82%AC130#discuss
Jamesdulse · June 4, 2026 at 10:19 am
В данной публикации мы поговорим о процессе восстановления от зависимости, о том, как вернуть себе нормальную жизнь. Мы обсудим преодоление трудностей, значимость поддержки и наличие программ реабилитации. Читатели смогут узнать о ключевых шагах к успешному восстановлению.
Открыть полностью – наркологическая клиника в твери
JamesVot · June 4, 2026 at 10:44 am
Выезд мастера холодильного и климатического оборудования в Москве. Работаем с ресторанами. Бесплатный выезд при ремонте.
Плановый осмотр климатического оборудования. Чистка фильтров. Подготовим к лету.
Утечка фреона?? Без перекупов и диспетчеров. Восстановим режим хранения.
Source:
https://dzen.ru/smart-quick.ru
najlepsze kasyna online · June 4, 2026 at 10:52 am
I absolutely adore your site! You aggressive me as able-bodied as all the others actuality and your broiled PS is absolutely great!
mippoTam · June 4, 2026 at 11:03 am
Анапа — жемчужина черноморского побережья, и исследовать её по-настоящему можно только за рулём собственного, пусть и арендованного, автомобиля. Сервис https://auto-arenda-anapa.ru/ предлагает прокат без залога, без ограничения пробега и с неограниченной страховкой ОСАГО, что делает каждую поездку абсолютно беззаботной. Детское кресло и видеорегистратор включены в комплектацию, а оформление занимает три простых шага: выбрать автомобиль, отправить документы и указать место подачи. Команда профессионалов CarTrip всегда на связи в мессенджерах и готова ответить на любой вопрос. Путешествуйте свободно!
kikusgrogs · June 4, 2026 at 11:17 am
Looking for forex analysis|crypto forecast|forex signals|btc forecast|crypto news|forex outlook|trading analysis|market forecast|crypto insights|stock market|best crypto exchange|crypto exchange review|top exchanges|where to buy crypto|exchange comparison|lowest fee exchange|crypto trading platform|safe crypto exchange|binance alternative|foreck exchanges? Head to foreck.info to explore detailed insights into forex, cryptocurrency, and stock markets, along with expert analysis and development trends. In-depth news analysis keeps you informed and current with the latest happenings. The site also features the best crypto exchanges with professional evaluation parameters, analyzed across eight weighted categories. Learn more on the website.
BrandonAcalk · June 4, 2026 at 11:30 am
Этот обзор сосредоточен на различных подходах к избавлению от зависимости. Мы изучим традиционные и альтернативные методы, а также их сочетание для достижения максимальной эффективности. Читатели смогут открыть для себя новые стратегии и подходы, которые помогут в их борьбе с зависимостями.
Почему это важно? – вызов нарколога на дом
RobertSlimi · June 4, 2026 at 12:00 pm
В этой публикации мы рассматриваем важную тему борьбы с зависимостями, включая алкогольную и наркотическую зависимости. Мы обсудим методы лечения, реабилитации и поддержку, которые могут помочь людям, столкнувшимся с этой проблемой. Читатели узнают о перспективах выздоровления и важности комплексного подхода.
Не пропусти важное – нарколог на дом частный
Martinapemy · June 4, 2026 at 12:00 pm
Публикация знакомит читателей с различными подходами к реабилитации. От традиционных методов до современных программ — вы узнаете, как выбрать оптимальный путь к выздоровлению и преодолеть препятствия на этом пути.
Детальнее – раскодирование от алкоголизма
tawebdshorp · June 4, 2026 at 12:07 pm
Looking to embed a crypto widget on your website? Visit https://orgtrade.org/ – OrgTrade helps website owners add a crypto exchange widget to their pages and convert cryptocurrency-related traffic into swap activity. Instead of sending visitors through a simple outbound link, your site can feature an integrated exchange tool where users can select a pair, enter an amount, and initiate a crypto conversion.
JamesLievy · June 4, 2026 at 12:11 pm
В этой статье рассматриваются актуальные вопросы, связанные с развитием медицинской науки и её внедрением в повседневную практику. Особое внимание уделено вопросам профилактики, ранней диагностики и использованию технологий для улучшения здоровья человека.
Получить исчерпывающие сведения – нарколог на дом цена воронеж
Josephjig · June 4, 2026 at 12:39 pm
Больше на нашем сайте: https://remont-kras.ru
https://www.thebostoncalendar.com/user/171102 · June 4, 2026 at 12:45 pm
https://www.thebostoncalendar.com/user/171102
Jamesswosy · June 4, 2026 at 12:48 pm
В этой статье мы обсудим процесс восстановления после зависимостей, акцентируя внимание на различных методах и подходах к реабилитации. Читатели узнают, как создать план выздоровления и использовать полезные ресурсы для достижения устойчивых изменений.
А что дальше? – Поставить капельницу после запоя
Rogercox · June 4, 2026 at 1:02 pm
посмотреть в этом разделе зеркало водка бет
Τα Καλύτερα Online Casino · June 4, 2026 at 1:27 pm
These kind of posts are always inspiring and I prefer to read quality content so I happy to find many good point here in the post. writing is simply wonderful! thank you for the post
HerbertSnasy · June 4, 2026 at 1:31 pm
В этой статье мы подробно рассматриваем проверенные методы борьбы с зависимостями, включая психотерапию, медикаментозное лечение и поддержку со стороны общества. Мы акцентируем внимание на важности комплексного подхода и возможности успешного восстановления для людей, столкнувшихся с этой проблемой.
Более подробно об этом – капельница от алкоголя
Логгин · June 4, 2026 at 1:40 pm
Купить синтол https://www.ozon.ru/product/maslo-kokosovoe-syn-oil-sintoil-sintoil-posing-oil-sintol-100-ml-synthol-naturalnoe-syntol-amd-sin-1290140141/
Jasonheips · June 4, 2026 at 1:42 pm
Эта публикация обращает внимание на важность профилактики зависимостей. Мы обсудим, как осведомленность и образование могут помочь в предотвращении возникновения зависимости. Читатели смогут ознакомиться с полезными советами и ресурсами, которые способствуют здоровому образу жизни.
Открыть полностью – нарколог на дом воронеж
MichaelQuage · June 4, 2026 at 1:43 pm
Ежедневный обзор: https://utepliteli-vrn.ru
ThomasimmUP · June 4, 2026 at 1:52 pm
Читатели получат представление о том, как современные технологии влияют на развитие медицины. Обсуждаются новые методы лечения, персонализированный подход и роль цифровых решений в повышении качества медицинских услуг.
Получить полную информацию – нарколог на дом воронеж цены
najlepsze kasyno online · June 4, 2026 at 2:04 pm
My issues have been very similar, with my family. But, we made some different decisions. It’s complex.
parhaat nettikasinot · June 4, 2026 at 2:38 pm
I am glad to be a visitor on this website!, regards for this rare information!
RaymondAspEk · June 4, 2026 at 3:00 pm
В этой публикации мы исследуем ключевые аспекты здоровья, включая влияние образа жизни на благополучие. Читатели узнают о важности правильного питания, физической активности и психического здоровья. Мы предоставим практические советы и рекомендации для поддержания здоровья и развития профилактических подходов.
Раскрыть тему полностью – помощь вывода из запоя
https://cascadeclimbers.com/content/pgs/code-promo-1xbet-gratuit-bonus.html · June 4, 2026 at 3:06 pm
https://cascadeclimbers.com/content/pgs/code-promo-1xbet-gratuit-bonus.html
pimamyiceft · June 4, 2026 at 3:23 pm
Ищете официального дилера HAVAL в Санкт-Петербурге? Посетите сайт Автопродикс https://autoprodix-havalpro.ru/ и вы сможете купить новые кроссоверы и внедорожники H3, H5, H7, H9 по выгодным ценам 2026 года. Модельный ряд в наличии, выгодные кредитные программы, трейд-ин, тест-драйв. Подробнее на сайте.
NolanNuh · June 4, 2026 at 3:32 pm
В данной статье рассматриваются проблемы общественного здоровья и социальные факторы, влияющие на него. Мы акцентируем внимание на значении профилактики и осведомленности в защите здоровья на уровне общества. Читатели смогут узнать о новых инициативах и программах, направленных на улучшение здоровья населения.
Подробности по ссылке – clinica plus
kasyno online opinie · June 4, 2026 at 3:47 pm
Nice read, I just passed this onto a colleague who was doing some research on that. And he just bought me lunch as I found it for him smile Therefore let me rephrase that: Thank you for lunch!
najlepsze kasyno online · June 4, 2026 at 4:06 pm
This is one very informative blog. I like the way you write and I will bookmark your blog to my favorites.
Rogercox · June 4, 2026 at 4:59 pm
кликните сюда вотка бет
Rogercox · June 4, 2026 at 5:26 pm
этот сайт зеркало водка бет
RonaldGew · June 4, 2026 at 5:36 pm
обмен криптовалюты на рубли https://www.crypto-obmen-online.net
kofictmop · June 4, 2026 at 5:49 pm
Если вы любите сериалы и цените возможность смотреть их без интернета в отличном качестве, вам стоит заглянуть на https://serialexpress.ru/ — специализированный интернет-магазин DVD с огромным каталогом отечественных, зарубежных, турецких и азиатских сериалов, теленовелл и мультсериалов. Здесь регулярно появляются новинки, действуют скидки, а доставка осуществляется почтой и курьерской службой СДЭК по всей России.
TimothyLon · June 4, 2026 at 5:55 pm
Expanded article here: https://blockchainreporter.net/price-prediction/lcx/
trust casino · June 4, 2026 at 6:00 pm
A banca agradece! milzão sacados do Sugar Rush com sucesso.
ganuyitduh · June 4, 2026 at 6:08 pm
Looking for the most active crypto market movements in one place? Visit https://topchanges.com/ – TopChanges tracks the most active crypto market movements in one place. See which coins are rising today, which coins are falling today, and which cryptocurrencies are attracting attention in the market. The dashboard combines 24-hour price changes, trading volume, market capitalization, and trend activity to give you a quick overview of today’s crypto movers.
https://peatix.com/user/29766860/view · June 4, 2026 at 6:37 pm
https://peatix.com/user/29766860/view
Jasonvop · June 4, 2026 at 7:28 pm
Эффективно сформулировано без сомнения
всё тут:
https://tyumen.doors-prestige.com/dver-ultra1-dubsibirskiy
https://web.ggather.com · June 4, 2026 at 7:32 pm
References:
Instant Casino Einzahlungsmethoden
References:
https://web.ggather.com/beechteller5/
ancientroman.space · June 4, 2026 at 7:38 pm
References:
Ontario casinos https://ancientroman.space/wiki/ICE_Casino_50_Freispiele_Erhalten_Sie_exklusive_Free_Spins
live cam girls · June 4, 2026 at 7:57 pm
Hi there, just became aware of your blog through Google, and found that it’s truly informative. It’s important to cover these trends.
GoodiniCrubs · June 4, 2026 at 8:18 pm
В этой заметке мы представляем шаги, которые помогут в процессе преодоления зависимостей. Рассматриваются стратегии поддержки и чек-листы для тех, кто хочет сделать первый шаг к выздоровлению. Наша цель — вдохновить читателей на положительные изменения и поддержать их в трудных моментах.
Желаете узнать подробности? – нарколога на дом самара
https://truckwiki.site/ · June 4, 2026 at 8:23 pm
References:
How do betting odds work https://truckwiki.site/wiki/Einfache_Anleitung_zur_Erstellung_eines_Kontos
bookmarks4.men · June 4, 2026 at 8:35 pm
References:
Luxor casino las vegas https://bookmarks4.men/story.php?title=top-online-casino-spiele-slots-grosse-boni
https://boardgameswiki.site/wiki/Vulkan_Vegas_Bonus_7_Codes_Gutschein_ohne_Einzahlung · June 4, 2026 at 8:55 pm
References:
Swiss casino online https://boardgameswiki.site/wiki/Vulkan_Vegas_Bonus_7_Codes_Gutschein_ohne_Einzahlung
BrandonAcalk · June 4, 2026 at 9:11 pm
В данном обзоре представлены основные направления и тренды в области медицины. Мы обсудим актуальные проблемы здравоохранения, свежие открытия и новые подходы, которые меняют представление о лечении и профилактике заболеваний. Эта информация будет полезна как специалистам, так и широкой публике.
Узнать напрямую – нарколог на дом круглосуточно самара цены
AndrewDob · June 4, 2026 at 9:14 pm
Эта медицинская заметка содержит сжатую информацию о новых находках и методах в области здравоохранения. Мы предлагаем читателям свежие данные о заболеваниях, профилактике и лечении. Наша цель — быстро и доступно донести важную информацию, которая поможет в повседневной жизни и понимании здоровья.
Нажмите, чтобы узнать больше – наркологическая клиника в твери
GoodiniCrubs · June 4, 2026 at 9:14 pm
В этой статье рассматриваются способы преодоления зависимости и успешные истории людей, которые справились с этой проблемой. Мы обсудим важность поддержки со стороны близких и профессионалов, а также стратегии, которые могут помочь в процессе выздоровления. Научитесь первоочередным шагам к новой жизни.
Расширить кругозор по теме – нарколог на дом вызов
https://depostbons26.eedblog.com/profile · June 4, 2026 at 9:26 pm
https://depostbons26.eedblog.com/profile
Georgenaill · June 4, 2026 at 9:41 pm
узнать vodkabet прямо сейчас
Georgenaill · June 4, 2026 at 9:45 pm
такой vodka bet casino
Michaelsubre · June 4, 2026 at 9:47 pm
В данной статье рассматриваются проблемы общественного здоровья и социальные факторы, влияющие на него. Мы акцентируем внимание на значении профилактики и осведомленности в защите здоровья на уровне общества. Читатели смогут узнать о новых инициативах и программах, направленных на улучшение здоровья населения.
Изучить рекомендации специалистов – клиника плюс тверь
RaymondCaf · June 4, 2026 at 9:53 pm
Обзор посвящён процессу восстановления после зависимостей. Мы расскажем о различных этапах реабилитации, поддерживающих ресурсах и важности мотивации в достижении устойчивого выздоровления.
Лови подробности – вывести из запоя тверь
https://promotionaumaroc.com/wp-content/articles/?1xbet_promo_code_bangladesh_10_html= · June 4, 2026 at 9:59 pm
https://promotionaumaroc.com/wp-content/articles/?1xbet_promo_code_bangladesh_10_html=
Williamhut · June 4, 2026 at 10:14 pm
Этот текст посвящён сложным аспектам зависимости и её влиянию на жизнь человека. Мы обсудим психологические, физические и социальные последствия зависимого поведения, а также важность своевременного обращения за помощью.
Погрузиться в научную дискуссию – tver clinica plus
corilfut · June 4, 2026 at 10:31 pm
1TRADE – https://1trade.io/ — an online trading platform for trading currency pairs on financial markets. Intuitive interface and functional trading tools. Advantages of the 1TRADE platform: Demo account for $100,000, Quick Platform Withdrawals, 24/7 support, Minimum deposit $10, Reliable broker, Mobile App.
https://www.laserchina.com/wp-content/pgs/code-promo-linebet_bonus-sportifs-et-casino.html · June 4, 2026 at 10:35 pm
https://www.laserchina.com/wp-content/pgs/code-promo-linebet_bonus-sportifs-et-casino.html
Nathanswere · June 4, 2026 at 10:36 pm
Updated today: https://blockchainreporter.net/trading-in-timelessness-crypto-24-7-freedom-vs-stock-market-constraints/
rudensSus · June 4, 2026 at 10:43 pm
Мото ДВ — официальный интернет-магазин на OZON, специализирующийся на продаже мототехники и сопутствующих товаров для активного отдыха. В ассортименте представлены квадроциклы ведущих брендов, включая модели Hummer 250, Loncin 400 EFI EPS 4×4 и Grizzly 250, а также скутеры серии Armour Pro и Apakani Aerox мощностью 125 куб. см. На странице https://www.ozon.ru/seller/moto-dv/ покупатели найдут технику для различных возрастных категорий — от детских до взрослых моделей с широким диапазоном мощности двигателя и максимальной скорости. Магазин регулярно проводит акции со скидками до 14%, обеспечивает быструю доставку и гарантирует подлинность реализуемой продукции, что подтверждается положительными отзывами клиентов.
Georgenaill · June 4, 2026 at 10:49 pm
узнать больше Здесь vodkabet онлайн казино
http://adrestyt.ru/ · June 4, 2026 at 11:16 pm
References:
Blackjack ski http://adrestyt.ru/user/earthart8/
Antoniopaymn · June 4, 2026 at 11:21 pm
В этой публикации мы предложим ряд рекомендаций по избавлению от зависимостей и успешному восстановлению. Мы обсудим методы привлечения поддержки и важность самосознания. Эти советы помогут людям вернуться к нормальной жизни и стать на путь выздоровления.
Подробнее тут – кодирование Торпедо
tikalixlper · June 4, 2026 at 11:28 pm
Looking for a KYC-free way to buy or sell cryptocurrency from 1–100 USDT? Visit https://coinswaper.io/ – See what 1, 2, 3, 5, 10, and 100 USDT is available for purchase in top coins, compare small resale amounts, and start a quick USDT swap from a single screen. These preset amounts cover the most common small swap scenarios: a tiny test, a micro-purchase, a quick conversion, or a small sell-off to USDT.
https://odom-bang.hubstack.net/1go-casino-50-freispiele-ohne-einzahlung-i-kein-geld-notig-1779829303 · June 5, 2026 at 12:14 am
References:
Iphone casino https://odom-bang.hubstack.net/1go-casino-50-freispiele-ohne-einzahlung-i-kein-geld-notig-1779829303
https://www.investagrams.com/Profile/meier4273982 · June 5, 2026 at 12:20 am
References:
Mahjong time https://www.investagrams.com/Profile/meier4273982
bad credit payday cash loans · June 5, 2026 at 12:27 am
Aw, this was a very nice post. In idea I wish to put in writing like this moreover taking time and precise effort to make an excellent article! I procrastinate alot and by no means seem to get something done.
tropicana.maxlv.ru · June 5, 2026 at 1:04 am
References:
Newcastle casino http://tropicana.maxlv.ru/user/wastefather56/
JerryCearl · June 5, 2026 at 1:35 am
В этом обзоре мы обсудим современные методы борьбы с зависимостями, включая медикаментозную терапию и психотерапию. Мы представим последние исследования и их результаты, чтобы читатели могли быть в курсе наиболее эффективных подходов к лечению и поддержке.
Посмотреть всё – прокапывание от алкоголя на дому
https://ancientroman.space · June 5, 2026 at 2:09 am
References:
Grand falls casino https://ancientroman.space/wiki/Spielen_Sie_OnlineSpielautomaten_und_Tischspiele
HerbertSnasy · June 5, 2026 at 2:33 am
Эта доказательная статья представляет собой глубокое погружение в успехи и вызовы лечения зависимостей. Мы обращаемся к научным исследованиям и опыту специалистов, чтобы предоставить читателям надежные данные об эффективности различных методик. Изучите, что работает лучше всего, и получите информацию от экспертов.
Проследить причинно-следственные связи – капельница от алкоголя в воронеже
NolanNuh · June 5, 2026 at 2:49 am
Мы рассмотрим современные вызовы здравоохранения и пути их решения с помощью технологий и научных исследований. В статье собраны данные о новых лекарствах, методах диагностики и системном подходе к улучшению здоровья населения.
Почему это важно? – клиника плюс тверь
http://www.annunciogratis.net/ · June 5, 2026 at 3:41 am
References:
Slot online http://www.annunciogratis.net/author/sailorton41
GregoryDix · June 5, 2026 at 3:42 am
Этот обзор посвящен успешным стратегиям избавления от зависимости, включая реальные примеры и советы. Мы разоблачим мифы и предоставим читателям достоверную информацию о различных подходах. Получите опыт многообразия методов и найдите подходящий способ для себя!
Проверенные методы — узнай сейчас – закодироваться Торпедой
fixDiele · June 5, 2026 at 4:11 am
Особенно понравился материал про Свежие новости Вологодской области и мира.
Ссылка ниже:
https://media35vol.ru
fixDiele · June 5, 2026 at 4:15 am
Между прочим, если вас интересует Новости и события Костромской области, загляните сюда.
Вот, можете почитать:
https://44media.ru
RobertNup · June 5, 2026 at 4:20 am
В этой медицинской статье мы погрузимся в актуальные вопросы здравоохранения и лечения заболеваний. Читатели узнают о современных подходах, методах диагностики и новых открытий в научных исследованиях. Наша цель — донести важную информацию и повысить уровень осведомленности о здоровье.
Изучить рекомендации специалистов – стоимость капельницы от запоя
hoswkSpoli · June 5, 2026 at 4:21 am
Автосервис «Шоколад» в Анапе — это современный центр технического обслуживания, где профессионализм сочетается с заботой о каждом клиенте. Команда опытных мастеров предлагает полный спектр услуг: от диагностики и замены масла до сложного ремонта двигателя и трансмиссии. Особенно привлекательны специальные предложения сервиса — бесплатная диагностика со скидкой 15% на ремонт, услуги эвакуатора и расчет стоимости работ по фотографии. Подробнее обо всех услугах можно узнать на сайте https://chocolate-auto.ru/, где представлена актуальная информация о ценах и графике работы. Сервис расположен по адресу Супсехское шоссе 10 и работает ежедневно с 9:00 до 19:00, обеспечивая качественное обслуживание автомобилей любых марок.
DonaldHut · June 5, 2026 at 4:32 am
Последние обновления: https://avicenna-stroy.ru
Oscardeate · June 5, 2026 at 4:32 am
сюда vodkabet
GregoryDix · June 5, 2026 at 4:32 am
Этот текст посвящён сложным аспектам зависимости и её влиянию на жизнь человека. Мы обсудим психологические, физические и социальные последствия зависимого поведения, а также важность своевременного обращения за помощью.
Полезно знать – кодирование Торпедо
xeraxPlack · June 5, 2026 at 4:44 am
Ищете курсы для юристов? Посетите сайт pravo.hse.ru/dpo/all – там вы найдете все возможные программы обучения по разным направлениям права. НИУ ВШЭ предлагает широкий спектр программ и высококвалифицированный профессорско-преподавательский состав. Качество образования остаётся на высшем уровне — специалисты, окончившие наши курсы, легко находят работу благодаря практическим навыкам, полученным в процессе обучения. Дополнительная информация доступна на сайте.
Sensual Bodyrub NYC · June 5, 2026 at 5:00 am
I wish you good health,
Dear Friends.
At the moment I would like to notify a little about https://nurumanhattanoutcall.com
I think you have been looking for specifically about Indian Massage outcall or perhaps you want to tell more about Busty Masseuse NY?!
So this optimally up-to-date information about Busty Masseuse outcall will be the most useful for you.
On our web portal a little more about Prostate Massage outcall new york, also information about FBSM outcall new york.
Find out more about https://nurumanhattanoutcall.com at https://nurumanhattanoutcall.com/
more about https://nurumanhattanoutcall.com at https://nurumanhattanoutcall.com
Our Tags: Four Hands Massage outcall, Thai Massage NY, Asian Massage NY, Therapeutic Massage outcall NY, Four Hands Massage outcall NY, Asian Massage outcall, Prostate Massage outcall NY, Therapeutic Massage outcall NY, Erotic Massage NYC
Have a good day
https://boardgameswiki.site/ · June 5, 2026 at 5:05 am
References:
Venetian casino macau https://boardgameswiki.site/wiki/Monro_Casino_Erfahrungen_2026_Modern_Seris
https://maps.google.fr/url?q=httpslaxlibrary.comnew1xbet_com_promo_code.html · June 5, 2026 at 5:09 am
https://maps.google.fr/url?q=https%3A%2F%2Flaxlibrary.com%2Fnew%2F%3F1xbet_com_promo_code.html
Oscardeate · June 5, 2026 at 5:10 am
Подробнее водкабет
guxoyneHok · June 5, 2026 at 5:13 am
Looking for ways to earn cryptocurrency? Visit https://bestearn.io/ and you’ll find a table that helps users compare active yield opportunities across protocols and chains. Instead of reading general advice, visitors can view the current APY, liquidity size, and pool type on a single screen and narrow the list to options that seem more practical for passive crypto income.
kogujamDaw · June 5, 2026 at 5:50 am
https://ethbtcchart.com/ is a live ETH/BTC charting service for checking Ethereum’s value in Bitcoin. The dashboard displays the pair’s current value, the inverse BTC to ETH ratio, 24-hour movement, daily range, and last update time all in one place. Use the live chart to see how much BTC is worth per ETH and how the Ethereum/Bitcoin pair is trending.
Archienot · June 5, 2026 at 5:51 am
На //friendlysun.ru](https://friendlysun.ru) можно найти идеи для путешествий, рекомендации по организации поездок и полезные travel-гайды. Платформа также рассказывает об онлайн-развлечениях, мобильных сервисах и вариантах досуга, которые особенно удобны в дороге или во время отдыха.
Source:
https://friendlysun.ru/
Dennisfloky · June 5, 2026 at 5:56 am
интернет оружие самообороны Москва купить
https://actualites.cava.tn/user/weightfarmer4/ · June 5, 2026 at 5:57 am
References:
Casino london https://actualites.cava.tn/user/weightfarmer4/
RobertThous · June 5, 2026 at 5:58 am
В данной статье мы акцентируем внимание на важности поддержки в процессе выздоровления. Мы обсудим, как друзья, семья и профессионалы могут помочь тем, кто сталкивается с зависимостями. Читатели получат практические советы, как поддерживать близких на пути к новой жизни.
Слушай внимательно — тут важно – кодирование Торпедо
hadutetic · June 5, 2026 at 6:09 am
TRX (TRON) Exchange Online for 160+ cryptocurrencies and 40+ fiat currencies at https://swapto.io/ – a service for quickly exchanging TRX online. Exchange TRX for USDT, BTC, ETH, and other assets, receive cryptocurrency in the opposite direction, and buy or sell TRON for any fiat currency. Swapto makes it easy to transfer funds between cryptocurrencies, lock your value in a stablecoin, buy TRON with fiat, and sell TRX without any extra steps.
RobertThous · June 5, 2026 at 7:04 am
Этот информационный материал подробно освещает проблему наркозависимости, ее причины и последствия. Мы предлагаем информацию о методах лечения, профилактики и поддерживающих программах. Цель статьи — повысить осведомленность и продвигать идеи о необходимости борьбы с зависимостями.
Где почитать поподробнее? – кодирование Торпедо
loginnet.ru · June 5, 2026 at 7:22 am
loginnet.ru
Michaelsubre · June 5, 2026 at 7:32 am
Эта статья освещает различные аспекты освобождения от зависимости и пути к выздоровлению. Мы обсуждаем важность осознания своей проблемы и обращения за помощью. Читатели получат практические советы о том, как преодолевать трудности и строить новую жизнь без зависимости.
Расширить кругозор по теме – tver clinica plus
Charlesciz · June 5, 2026 at 8:04 am
В этой публикации мы исследуем ключевые аспекты здоровья, включая влияние образа жизни на благополучие. Читатели узнают о важности правильного питания, физической активности и психического здоровья. Мы предоставим практические советы и рекомендации для поддержания здоровья и развития профилактических подходов.
Ознакомьтесь с аналитикой – вывод из запоя тверь на дому круглосуточно
JerryCearl · June 5, 2026 at 8:17 am
Текст посвящён распространённым мифам о зависимости и их развенчанию. Мы предоставим научно обоснованную информацию и дадим рекомендации по выбору эффективного способа борьбы с зависимым поведением.
Не упусти важное! – капельница после запоя цена
racayneiderm · June 5, 2026 at 8:35 am
Посетите сайт Babylook https://babylook.by/ — это маркетплейс детских товаров от белорусских производителей. У нас много категорий для девочек и мальчиков и новорожденных, а также игрушки, все для ухода и питание и многое другое. Товары безопасные, уникальные и сделанные с заботой. Вы сможете удобно находить и выбирать лучшее!
Oscardeate · June 5, 2026 at 8:37 am
веб-сайт водка бет
RaymondCaf · June 5, 2026 at 8:37 am
Читатели получат представление о том, как современные технологии влияют на развитие медицины. Обсуждаются новые методы лечения, персонализированный подход и роль цифровых решений в повышении качества медицинских услуг.
Нажмите, чтобы узнать больше – раскодирование от алкоголизма
KennethfeN · June 5, 2026 at 9:17 am
В данном обзоре представлены основные направления и тренды в области медицины. Мы обсудим актуальные проблемы здравоохранения, свежие открытия и новые подходы, которые меняют представление о лечении и профилактике заболеваний. Эта информация будет полезна как специалистам, так и широкой публике.
Нажмите, чтобы узнать больше – нарколог дом
Davidraise · June 5, 2026 at 10:14 am
Этот документ охватывает важные аспекты медицинской науки, сосредотачиваясь на ключевых вопросах, касающихся здоровья населения. Мы рассматриваем свежие исследования, клинические рекомендации и лучшие практики, которые помогут улучшить качество лечения и профилактики заболеваний. Читатели получат возможность углубиться в различные медицинские дисциплины.
Получить больше информации – врач нарколог выезд на дом
Rolandjaw · June 5, 2026 at 11:00 am
Этот краткий обзор предлагает сжатую информацию из области медицины, включая ключевые факты и последние новости. Мы стремимся сделать информацию доступной и понятной для широкой аудитории, что позволит читателям оставаться в курсе актуальных событий в здравоохранении.
Дополнительно читайте здесь – нарколог
Louistaw · June 5, 2026 at 11:18 am
В этой заметке мы представляем шаги, которые помогут в процессе преодоления зависимостей. Рассматриваются стратегии поддержки и чек-листы для тех, кто хочет сделать первый шаг к выздоровлению. Наша цель — вдохновить читателей на положительные изменения и поддержать их в трудных моментах.
Рассмотреть проблему всесторонне – прокапаться от алкоголя воронеж
majomtDrace · June 5, 2026 at 11:25 am
Ищете имплантацию всех зубов All-on-4 (Все-на-4) в Мурманске по лучшей цене от профессиональных стоматологов? Посетите https://nova-51.ru/implantatsiya-zubov-murmansk/implantatsiya-vsekh-zubov-all-on-4-vse-na-4 узнайте подробную информацию и стоимость услуги.
Antoniopaymn · June 5, 2026 at 11:33 am
В этой публикации мы предложим ряд рекомендаций по избавлению от зависимостей и успешному восстановлению. Мы обсудим методы привлечения поддержки и важность самосознания. Эти советы помогут людям вернуться к нормальной жизни и стать на путь выздоровления.
Открыть полностью – клиника плюс тверь
RobertNup · June 5, 2026 at 12:12 pm
В этой статье мы подробно рассматриваем проверенные методы борьбы с зависимостями, включая психотерапию, медикаментозное лечение и поддержку со стороны общества. Мы акцентируем внимание на важности комплексного подхода и возможности успешного восстановления для людей, столкнувшихся с этой проблемой.
Проследить причинно-следственные связи – выведение из запоя капельница
Oscardeate · June 5, 2026 at 12:19 pm
веб-сайте vodka bet casino
GoodiniCrubs · June 5, 2026 at 12:38 pm
В этой статье рассматриваются способы преодоления зависимости и успешные истории людей, которые справились с этой проблемой. Мы обсудим важность поддержки со стороны близких и профессионалов, а также стратегии, которые могут помочь в процессе выздоровления. Научитесь первоочередным шагам к новой жизни.
Ознакомьтесь поближе – срочный вызов врача нарколога
Mickeycanda · June 5, 2026 at 12:50 pm
Эта публикация исследует взаимосвязь зависимости и психологии. Мы обсудим, как психологические аспекты влияют на появление зависимостей и процесс выздоровления. Читатели смогут понять важность профессиональной поддержки и применения научных подходов в терапии.
Смотри, что ещё есть – клиника плюс тверь
Rodneyrailm · June 5, 2026 at 1:01 pm
В данной статье рассматриваются физиологические и эмоциональные аспекты зависимости. Мы обсудим, как организм реагирует на зависимое поведение, и какие методы помогают восстановить здоровье и внутреннее равновесие.
Секреты успеха внутри – вызов нарколога на дом анонимно
TaylorBycle · June 5, 2026 at 1:22 pm
Этот медицинский обзор сосредоточен на последних достижениях, которые оказывают влияние на пациентов и медицинскую практику. Мы разбираем инновационные методы лечения и исследований, акцентируя внимание на их значимости для общественного здоровья. Читатели узнают о свежих данных и их возможном применении.
Информация доступна здесь – выведение из запоя на дому в екатеринбурге
Carlosciz · June 5, 2026 at 1:27 pm
Этот текст представляет собой обзор свежих данных и исследований в области медицины. Он призван помочь читателям понять, как научные достижения влияют на лечение, диагностику и общее состояние системы здравоохранения.
Детальнее – вывод из запоя на дому недорого
Louistaw · June 5, 2026 at 1:33 pm
В этой заметке мы представляем шаги, которые помогут в процессе преодоления зависимостей. Рассматриваются стратегии поддержки и чек-листы для тех, кто хочет сделать первый шаг к выздоровлению. Наша цель — вдохновить читателей на положительные изменения и поддержать их в трудных моментах.
Ознакомиться с полной информацией – прокапаться после запоя
Davidcit · June 5, 2026 at 1:53 pm
В этой статье рассматриваются актуальные вопросы, связанные с развитием медицинской науки и её внедрением в повседневную практику. Особое внимание уделено вопросам профилактики, ранней диагностики и использованию технологий для улучшения здоровья человека.
Ознакомьтесь с аналитикой – врач вывод из запоя
vamosnRed · June 5, 2026 at 1:54 pm
Хотите исследовать США? Портал east-usa.com — незаменимый инструмент для путешественников: здесь собраны детальные дорожные карты всех 50 штатов с отмеченными городами, достопримечательностями и национальными парками. Карты сгруппированы по регионам — Запад, Средний Запад, Северо-Восток и Юг, — а каждый штат дополнен спутниковым снимком Google, картой округов и заповедников. Все материалы адаптированы под мобильные устройства и ПК: посетите https://east-usa.com/ и убедитесь, что даже мельчайшие географические объекты отображаются кристально чётко — идеально для планирования маршрута мечты!
Dennisfloky · June 5, 2026 at 1:55 pm
содержание купить травмат СПБ
Dennisfloky · June 5, 2026 at 2:00 pm
Смотреть здесь магазин травмат СПБ
Kevinmycle · June 5, 2026 at 2:15 pm
В этом обзоре представлены различные методы избавления от зависимости, включая терапевтические и психологические подходы. Мы сравниваем их эффективность и предоставляем рекомендации для тех, кто хочет вернуться к трезвой жизни. Читатели смогут найти информацию о реабилитационных центрах и поддерживающих группах.
Более того — здесь – закодироваться от алкоголизма в Твери
MichaelPredy · June 5, 2026 at 2:20 pm
Эта публикация исследует взаимосвязь зависимости и психологии. Мы обсудим, как психологические аспекты влияют на появление зависимостей и процесс выздоровления. Читатели смогут понять важность профессиональной поддержки и применения научных подходов в терапии.
Что скрывают от вас? – сколько стоит поставить капельницу в екатеринбурге
Charlesciz · June 5, 2026 at 2:30 pm
Эта публикация посвящена актуальным вопросам современной медицины и здравоохранения. Мы обсудим новейшие технологии диагностики и лечения, а также их влияние на продолжительность и качество жизни. Читатель найдет здесь информацию о научных исследованиях и перспективных разработках, доступно изложенную для широкой аудитории.
Проверенные методы — узнай сейчас – вывод из запоя на дому тверь
Jasonvop · June 5, 2026 at 2:52 pm
Невероятно тонны превосходной материала
всё тут:
https://tyumen.doors-prestige.com/dver-parma04-ncs2075y60r
https://antspride.com/read-blog/108004 · June 5, 2026 at 2:54 pm
https://antspride.com/read-blog/108004
https://onespotsocial.com/tashacode1 · June 5, 2026 at 2:57 pm
https://onespotsocial.com/tashacode1
Robertfut · June 5, 2026 at 3:01 pm
Эта доказательная статья представляет собой глубокое погружение в успехи и вызовы лечения зависимостей. Мы обращаемся к научным исследованиям и опыту специалистов, чтобы предоставить читателям надежные данные об эффективности различных методик. Изучите, что работает лучше всего, и получите информацию от экспертов.
Интересует подробная информация – срочный вывод из запоя на дому
TimothyCroto · June 5, 2026 at 3:29 pm
Этот документ охватывает важные аспекты медицинской науки, сосредотачиваясь на ключевых вопросах, касающихся здоровья населения. Мы рассматриваем свежие исследования, клинические рекомендации и лучшие практики, которые помогут улучшить качество лечения и профилактики заболеваний. Читатели получат возможность углубиться в различные медицинские дисциплины.
Погрузиться в детали – clinica plus
KennethfeN · June 5, 2026 at 3:38 pm
Эта публикация раскрывает психологические механизмы зависимости и их роль в развитии расстройств. Читатель узнает о том, как психология влияет на формирование зависимостей и как профессиональная помощь может изменить ситуацию.
Не пропусти важное – нарколога на дом самара
duwuvhermum · June 5, 2026 at 3:53 pm
Looking for a quick, private XMR swap online without registration? Visit https://swapxmr.io/ – SwapXMR helps users exchange Monero through a direct crypto exchange flow without a trading terminal, order book, or complicated account setup. The service focuses on XMR exchange pairs with Bitcoin, Tether, Ethereum, and other digital assets, while supported buy and sell options are available through the exchange.
TimothyCroto · June 5, 2026 at 4:04 pm
В этом исследовании рассмотрены методы лечения зависимостей и их эффективность. Мы проанализируем различные подходы, используемые в реабилитационных центрах, и представим данные о результативности программ. Читатели получат надежные и научно обоснованные сведения о данной проблеме.
Подробная информация доступна по запросу – clinica plus в твери
Patrickhiz · June 5, 2026 at 4:39 pm
Этот текст представляет собой обзор свежих данных и исследований в области медицины. Он призван помочь читателям понять, как научные достижения влияют на лечение, диагностику и общее состояние системы здравоохранения.
Эксклюзивная информация – вызвать капельницу от запоя на дому
buzuyefob · June 5, 2026 at 4:48 pm
Looking for a reliable crypto exchange? Visit https://cryptoswaptrade.com/ – CryptoSwapTrade is a crypto trading exchange designed for users who want to trade cryptocurrency online through a simple and direct exchange flow. The service supports 165 cryptocurrencies, 210+ assets across networks, approximately 40,000 cryptocurrency pairs, and approximately 8,000 fiat-related transfers in 40+ fiat currencies.
Patrickhiz · June 5, 2026 at 5:19 pm
Этот текст представляет собой обзор свежих данных и исследований в области медицины. Он призван помочь читателям понять, как научные достижения влияют на лечение, диагностику и общее состояние системы здравоохранения.
Уточнить детали – прокапаться от запоя цена
sonnik.nalench.com · June 5, 2026 at 5:20 pm
References:
Lumiere casino https://sonnik.nalench.com/user/mindskiing1/
read more · June 5, 2026 at 5:20 pm
read more
greecestudies.site · June 5, 2026 at 6:15 pm
References:
Casino listing https://greecestudies.site/wiki/888_Casino_Bonus_und_Review_zum_Spielangebot_und_der_Software
Louiekix · June 5, 2026 at 6:32 pm
Статья посвящена анализу текущих трендов в медицине и их влиянию на жизнь людей. Мы рассмотрим новые технологии, методы лечения и значение профилактики в обеспечении долголетия и здоровья.
Хочешь знать всё? – капельница от запоя на дому круглосуточно
Josephtot · June 5, 2026 at 6:50 pm
Читатели получат представление о том, как современные технологии влияют на развитие медицины. Обсуждаются новые методы лечения, персонализированный подход и роль цифровых решений в повышении качества медицинских услуг.
Полезно знать – нарколог на дом анонимно
Louiekix · June 5, 2026 at 7:24 pm
Этот документ охватывает важные аспекты медицинской науки, сосредотачиваясь на ключевых вопросах, касающихся здоровья населения. Мы рассматриваем свежие исследования, клинические рекомендации и лучшие практики, которые помогут улучшить качество лечения и профилактики заболеваний. Читатели получат возможность углубиться в различные медицинские дисциплины.
Наши рекомендации — тут – выведение из запоя на дому в екатеринбурге
Davidraise · June 5, 2026 at 8:01 pm
Эта публикация посвящена актуальным вопросам современной медицины и здравоохранения. Мы обсудим новейшие технологии диагностики и лечения, а также их влияние на продолжительность и качество жизни. Читатель найдет здесь информацию о научных исследованиях и перспективных разработках, доступно изложенную для широкой аудитории.
Секреты успеха внутри – нарколог на дом анонимно
nnbet login · June 5, 2026 at 8:08 pm
Sessão do milhão.
BlairExeni · June 5, 2026 at 8:09 pm
Этот медицинский обзор сосредоточен на последних достижениях, которые оказывают влияние на пациентов и медицинскую практику. Мы разбираем инновационные методы лечения и исследований, акцентируя внимание на их значимости для общественного здоровья. Читатели узнают о свежих данных и их возможном применении.
Заходи — там интересно – clinica plus
BATA4D · June 5, 2026 at 9:01 pm
BATA4D
BlairExeni · June 5, 2026 at 9:03 pm
Этот медицинский обзор сосредоточен на последних достижениях, которые оказывают влияние на пациентов и медицинскую практику. Мы разбираем инновационные методы лечения и исследований, акцентируя внимание на их значимости для общественного здоровья. Читатели узнают о свежих данных и их возможном применении.
Узнать из первых рук – clinica plus в твери
Rolandjaw · June 5, 2026 at 9:18 pm
В этой статье рассматривается комплексный подход к избавлению от зависимости. Читатель узнает, как сочетание физического, психологического и духовного восстановления помогает достичь стойкого выздоровления.
Дополнительно читайте здесь – вызов нарколога на дом цена
hackmd.okfn.de · June 5, 2026 at 9:28 pm
References:
Casino enjoy antofagasta https://hackmd.okfn.de/s/rkKgtDXlMe
Waynebab · June 5, 2026 at 9:40 pm
В данной статье мы акцентируем внимание на важности поддержки в процессе выздоровления. Мы обсудим, как друзья, семья и профессионалы могут помочь тем, кто сталкивается с зависимостями. Читатели получат практические советы, как поддерживать близких на пути к новой жизни.
Получить профессиональную консультацию – кодировка sit mst
EdwardFub · June 5, 2026 at 10:09 pm
Эта статья освещает различные аспекты освобождения от зависимости и пути к выздоровлению. Мы обсуждаем важность осознания своей проблемы и обращения за помощью. Читатели получат практические советы о том, как преодолевать трудности и строить новую жизнь без зависимости.
Читать полностью – сколько стоит прокапаться
3ubet login tigrinho · June 5, 2026 at 10:10 pm
Respeitei meu limite, fui no Fortune Mouse e saí no green. Nunca corra atrás de red.
yufurstew · June 5, 2026 at 10:16 pm
Компания «Строй Комплект» работает в лесной отрасли с 1999 года и предлагает пиломатериалы собственного производства напрямую покупателям Москвы. Заготовка древесины ведётся в экологически чистых северных регионах, а ежемесячный выпуск превышает 1500 кубометров хвойной продукции. На сайте https://brusdoskamsk.ru/ представлен широкий ассортимент: доска, брус, вагонка, планкен, фанера, блок-хаус и элементы лестниц. Переработка сырья осуществляется на европейском оборудовании, что обеспечивает стабильно высокое качество. Работают ежедневно с 8:00 до 20:00.
Danieljoump · June 5, 2026 at 10:19 pm
Эта медицинская заметка содержит сжатую информацию о новых находках и методах в области здравоохранения. Мы предлагаем читателям свежие данные о заболеваниях, профилактике и лечении. Наша цель — быстро и доступно донести важную информацию, которая поможет в повседневной жизни и понимании здоровья.
Все материалы собраны здесь – clinica plus в твери
haheceMerry · June 5, 2026 at 10:32 pm
Магазин автозапчастей Park Motors — надёжный поставщик деталей для владельцев коммерческого транспорта марки ГАЗ. Здесь можно найти двигатели ЗМЗ-405, 406, 409 и УМЗ-4216, блоки цилиндров, головки блока цилиндров Танаки и Эвотек, КПП, ГУР, а также шины WestLake SL309 и диски Gold Wheel — всё для Газели Некст, УАЗ и Валдай. На сайте https://tent3302.ru/ представлен широкий каталог запчастей с удобной навигацией по категориям. Магазин расположен в Москве на ул. Угрешская, д. 17, работает вторник–суббота с 10:00 до 16:00.
Davidwag · June 5, 2026 at 10:39 pm
Эта публикация раскрывает психологические механизмы зависимости и их роль в развитии расстройств. Читатель узнает о том, как психология влияет на формирование зависимостей и как профессиональная помощь может изменить ситуацию.
Информация доступна здесь – выведение из запоя в воронеже
curaspauri · June 5, 2026 at 10:44 pm
Юридическая фирма «Один к одному» заслуженно получила признание ведущих деловых изданий России за профессиональный подход к решению сложнейших финансовых споров. Специалисты компании успешно ведут дела по взысканию задолженности любой сложности, защищают клиентов от субсидиарной ответственности и грамотно сопровождают процедуры банкротства. Команда опытных юристов на https://1k1law.ru/ предлагает индивидуальную стратегию для каждого случая, основанную на глубоком знании законодательства и многолетней практике. Фирма входит в рейтинг лучших по банкротству по версии «Коммерсантъ» и «Право-300», что подтверждает высокий уровень оказываемых услуг и доверие клиентов.
Mickeycanda · June 5, 2026 at 10:54 pm
Публикация охватывает основные направления развития современной медицины. Мы обсудим значимость научных исследований, инноваций в лечении и роли общественного участия в формировании системы здравоохранения.
Узнать напрямую – Кодирование от алкоголизма уколом
Daviddah · June 5, 2026 at 11:22 pm
Этот обзор медицинских исследований собрал самое важное из последних публикаций в области медицины. Мы проанализировали ключевые находки и представили их в доступной форме, чтобы читатели могли легко ориентироваться в актуальных темах. Этот материал станет отличным подспорьем для изучения медицины.
Получить профессиональную консультацию – вывод из запоя анонимно недорого
GregoryFlano · June 5, 2026 at 11:34 pm
Этот информативный текст сочетает в себе темы здоровья и зависимости. Мы обсудим, как хронические заболевания могут усугубить зависимости и наоборот, как зависимость может влиять на общее состояние здоровья. Читатели получат представление о комплексном подходе к лечению как физического, так и психического состояния.
Изучить вопрос глубже – вывод из запоя на дому самара
WalterAbini · June 5, 2026 at 11:41 pm
В этой статье рассматриваются различные аспекты избавления от зависимости, включая физические и психологические методы. Мы обсудим поддержку, мотивацию и стратегии, которые помогут в процессе выздоровления. Читатели узнают, как преодолеть трудности и двигаться к новой жизни без зависимости.
Откройте для себя больше – наркологическая платная клиника
https://king-bookmark.stream · June 5, 2026 at 11:55 pm
References:
Indian casinos https://king-bookmark.stream/story.php?title=n1-casino-nahtloses-zahlungssystem
https://www.wvhired.com/profiles/8250138-m3liveplay · June 6, 2026 at 12:04 am
https://www.wvhired.com/profiles/8250138-m3liveplay
https://buyandsellhair.com/ · June 6, 2026 at 12:09 am
References:
Mohawk casino https://buyandsellhair.com/author/lightotter7/
JamesVot · June 6, 2026 at 12:23 am
Ищете надежный сервис для ресторана или магазина? Опыт работы с импортными и отечественными брендами. Звоните, выезжаем по Москве и области.
Клиенты ждут свежести. Аварийная бригада. Честная смета до начала работ.
Срочный выезд в Москве и МО. Любые бренды без предоплаты. Договор, закрывающие документы.
Source:
https://dzen.ru/smart-quick.ru
TaylorBycle · June 6, 2026 at 12:25 am
Читатели получат представление о том, как современные технологии влияют на развитие медицины. Обсуждаются новые методы лечения, персонализированный подход и роль цифровых решений в повышении качества медицинских услуг.
Ознакомьтесь с аналитикой – вывод из запоя на дому екатеринбург отзывы
cepohelbet · June 6, 2026 at 12:35 am
Looking for a token swap platform? Visit https://swaptoken.io/ – we offer fast swaps for 150+ cryptocurrencies in 1-15 minutes. We offer fixed and floating rates, no registration, and no KYC for standard routes. Flexible limits range from $20 to $150,000 equivalent. All key exchange terms are displayed in the form upfront, with no hidden platform fees other than the sender’s network fee.
http://forums.cgb.designknights.com/ · June 6, 2026 at 12:37 am
References:
Pennsylvania casinos http://forums.cgb.designknights.com/member.php?action=profile&uid=191168
GoodiniCrubs · June 6, 2026 at 12:37 am
Публикация посвящена жизненным историям людей, успешно справившихся с зависимостью. Мы покажем, что выход есть, и он начинается с первого шага — принятия проблемы и желания измениться.
Не упусти шанс – услуги нарколога на дому
WalterAbini · June 6, 2026 at 12:45 am
В этой заметке мы представляем шаги, которые помогут в процессе преодоления зависимостей. Рассматриваются стратегии поддержки и чек-листы для тех, кто хочет сделать первый шаг к выздоровлению. Наша цель — вдохновить читателей на положительные изменения и поддержать их в трудных моментах.
Детали по клику – частная наркологическая клиника
Carlosciz · June 6, 2026 at 12:46 am
Статья посвящена анализу текущих трендов в медицине и их влиянию на жизнь людей. Мы рассмотрим новые технологии, методы лечения и значение профилактики в обеспечении долголетия и здоровья.
Разобраться лучше – вывод из запоя на дому в екатеринбурге
GregoryFlano · June 6, 2026 at 12:52 am
Этот обзор содержит информацию о передовых достижениях в области медицины. Мы разберем инновационные технологии, которые меняют подход к лечению и диагностике, а также их влияние на эффективность оказания медицинской помощи.
Осуществить глубокий анализ – круглосуточный вывод из запоя
tunufsef · June 6, 2026 at 1:26 am
Ищете опытного и надежного мастера по ремонту бытовой техники в Москве? Посетите https://xn—-8sbglh5alafclhgfpy6o.xn--p1ai/ – ознакомьтесь с нашими услугами. Мы — специалисты по ремонту бытовой техники любых брендов премиум и стандарт-класса, от бытовых моделей до встроенных систем. Выполняем диагностику и ремонт в день обращения, аккуратно, честно и с гарантией.
MichaelPredy · June 6, 2026 at 1:52 am
В этом исследовании рассмотрены методы лечения зависимостей и их эффективность. Мы проанализируем различные подходы, используемые в реабилитационных центрах, и представим данные о результативности программ. Читатели получат надежные и научно обоснованные сведения о данной проблеме.
Погрузиться в детали – поставить капельницу на дому екатеринбург цена
RobertLic · June 6, 2026 at 1:53 am
Актуальное казино онлайн зеркало — не требует скачивания.
Выполните казино онлайн вход — через зеркало.
Альтернативный казино онлайн сайт зеркало — принимает старые промокоды.
Всё как в казино онлайн, но по-английски — лицензия Кюрасао.
Американская эстетика и выигрыши — вывод без комиссии.
Source:
казино актуальное зеркало
Kevinmycle · June 6, 2026 at 1:57 am
Этот текст представляет собой обзор свежих данных и исследований в области медицины. Он призван помочь читателям понять, как научные достижения влияют на лечение, диагностику и общее состояние системы здравоохранения.
Дополнительно читайте здесь – закодироваться от алкоголизма в Твери
EdwardFub · June 6, 2026 at 2:56 am
Эта статья подробно расскажет о процессе выздоровления, который включает в себя эмоциональную, физическую и психологическую реабилитацию. Мы обсуждаем значимость поддержки и наличие профессиональных программ. Читатели узнают, как строить новую жизнь и не возвращаться к старым привычкам.
Проследить причинно-следственные связи – сколько стоит прокапаться от алкоголя
https://bbkbeautyspa.com/1xbet---2026-1x200rush-42900--/ · June 6, 2026 at 2:56 am
https://bbkbeautyspa.com/1xbet-%e0%a4%aa%e0%a5%8d%e0%a4%b0%e0%a5%8b%e0%a4%ae%e0%a5%8b-%e0%a4%95%e0%a5%8b%e0%a4%a1-2026-1x200rush-%e2%82%b942900-%e0%a4%a4%e0%a4%95-%e0%a4%ac%e0%a5%8b%e0%a4%a8%e0%a4%b8/
Elwoodinela · June 6, 2026 at 3:03 am
Этот обзор содержит информацию о передовых достижениях в области медицины. Мы разберем инновационные технологии, которые меняют подход к лечению и диагностике, а также их влияние на эффективность оказания медицинской помощи.
Есть чему поучиться – tver clinica plus
Davidcit · June 6, 2026 at 3:05 am
В этой статье рассматриваются актуальные вопросы, связанные с развитием медицинской науки и её внедрением в повседневную практику. Особое внимание уделено вопросам профилактики, ранней диагностики и использованию технологий для улучшения здоровья человека.
Провести детальное исследование – снятие интоксикации на дому
https://forum.board-of-metal.org/ · June 6, 2026 at 3:10 am
References:
Pink floyd live 8 https://forum.board-of-metal.org/user-58964.html
RogerNoupe · June 6, 2026 at 3:46 am
В данной публикации мы поговорим о процессе восстановления от зависимости, о том, как вернуть себе нормальную жизнь. Мы обсудим преодоление трудностей, значимость поддержки и наличие программ реабилитации. Читатели смогут узнать о ключевых шагах к успешному восстановлению.
Жми сюда — получишь ответ – вывод из запоя на дому самара круглосуточно
Robertotus · June 6, 2026 at 3:54 am
смотреть здесь https://tripscans74.us/
Robertotus · June 6, 2026 at 4:22 am
здесь трипскан официальный
LesterSmoog · June 6, 2026 at 4:25 am
В этой статье мы рассматриваем разрушительное влияние зависимости на жизнь человека. Обсуждаются аспекты, такие как здоровье, отношения и профессиональные достижения. Читатели узнают о необходимости обращения за помощью и о путях к восстановлению.
Всё, что нужно знать – выведение из запоя клиника
Elwoodinela · June 6, 2026 at 4:27 am
В этой публикации мы обсуждаем современные методы лечения различных заболеваний. Читатели узнают о новых медикаментах, терапиях и исследованиях, которые активно применяются для лечения. Мы нацелены на то, чтобы предоставить практические знания, которые могут помочь в борьбе с недугами.
Изучить аспект более тщательно – клиника плюс
KevinIntob · June 6, 2026 at 4:30 am
Публикация посвящена жизненным историям людей, успешно справившихся с зависимостью. Мы покажем, что выход есть, и он начинается с первого шага — принятия проблемы и желания измениться.
Выяснить больше – вывод из запоя цены
AllenSaw · June 6, 2026 at 4:30 am
В этой статье мы обсудим процесс восстановления после зависимостей, акцентируя внимание на различных методах и подходах к реабилитации. Читатели узнают, как создать план выздоровления и использовать полезные ресурсы для достижения устойчивых изменений.
Всё самое вкусное внутри – капельница от запоя на дому круглосуточно
5gbet · June 6, 2026 at 4:32 am
Deu bom demais.
Daviddah · June 6, 2026 at 4:37 am
Этот обзор сосредоточен на различных подходах к избавлению от зависимости. Мы изучим традиционные и альтернативные методы, а также их сочетание для достижения максимальной эффективности. Читатели смогут открыть для себя новые стратегии и подходы, которые помогут в их борьбе с зависимостями.
Получить полную информацию – прокапаться от алкоголя на дому
Rubentok · June 6, 2026 at 4:54 am
узнать https://tripscans74.co
https://materialwiki.site · June 6, 2026 at 4:54 am
References:
Blackjack manga https://materialwiki.site/wiki/Lex_Casino_App_Mobile_Spiele_Boni_fr_deutsche_Spieler/wiki/Lex_Casino_App_Mobile_Spiele_Boni_fr_deutsche_Spieler
Rubentok · June 6, 2026 at 5:15 am
Узнать больше https://tripscans74.co/
https://firsturl.de/4H4Y1g3 · June 6, 2026 at 5:34 am
References:
Casino marketing https://firsturl.de/4H4Y1g3
AllenSaw · June 6, 2026 at 5:41 am
В этой статье мы обсудим процесс восстановления после зависимостей, акцентируя внимание на различных методах и подходах к реабилитации. Читатели узнают, как создать план выздоровления и использовать полезные ресурсы для достижения устойчивых изменений.
Ознакомьтесь с аналитикой – капельница от запоя недорого
GregoryLom · June 6, 2026 at 5:43 am
Запоя вывод в клинике Сочи: лечение алкогольной интоксикации, капельница, детоксикация, помощь нарколога на дому, кодирование и реабилитация.
Детальнее – наркологический вывод из запоя сочи
GeraldWep · June 6, 2026 at 5:52 am
Этот обзор медицинских исследований собрал самое важное из последних публикаций в области медицины. Мы проанализировали ключевые находки и представили их в доступной форме, чтобы читатели могли легко ориентироваться в актуальных темах. Этот материал станет отличным подспорьем для изучения медицины.
Секреты успеха внутри – выведение из запоя на дому
Robertfut · June 6, 2026 at 5:58 am
Мы рассмотрим современные вызовы здравоохранения и пути их решения с помощью технологий и научных исследований. В статье собраны данные о новых лекарствах, методах диагностики и системном подходе к улучшению здоровья населения.
Подробная информация доступна по запросу – вывод из запоя на дому самара круглосуточно
yiwacgeBriet · June 6, 2026 at 6:02 am
Откройте для себя удивительную Японию вместе с профессиональным туроператором «МОЙ ТОКИО», который специализируется исключительно на турах в Страну восходящего солнца. Компания предлагает разнообразные программы: от классических экскурсионных маршрутов по Токио, Киото и Осаке до тематических туров по следам аниме, горнолыжного отдыха в Нагано и пляжного релакса на Окинаве. На сайте https://dvmt.ru/ вы найдете готовые групповые туры и возможность создать индивидуальный маршрут с учетом ваших интересов. Туроператор имеет реестровый номер РТО 004645, что гарантирует надежность и безопасность вашего путешествия в эту fascinирующую страну контрастов.
JamesBus · June 6, 2026 at 6:24 am
В этом исследовании рассмотрены методы лечения зависимостей и их эффективность. Мы проанализируем различные подходы, используемые в реабилитационных центрах, и представим данные о результативности программ. Читатели получат надежные и научно обоснованные сведения о данной проблеме.
Запросить дополнительные данные – капельница от алкоголя
https://justpaste.me/UTR12 · June 6, 2026 at 6:31 am
https://justpaste.me/UTR12
JamesPrend · June 6, 2026 at 6:35 am
Статья посвящена анализу текущих трендов в медицине и их влиянию на жизнь людей. Мы рассмотрим новые технологии, методы лечения и значение профилактики в обеспечении долголетия и здоровья.
Нажмите, чтобы узнать больше – капельница на дому в екатеринбурге
Robertotus · June 6, 2026 at 6:40 am
узнать https://tripscans74.us/
colipulesops · June 6, 2026 at 7:15 am
Ищете увеличение объема костной ткани для имплантации зубов в Мурманске? Посетите https://nova-51.ru/implantatsiya-zubov-murmansk/sinus-lifting-i-kostnaya-plastika-murmansk – мы предлагаем лучший синус лифтинг от опытных и квалифицированных врачей. Узнайте подробную информацию на сайте.
Claytonvam · June 6, 2026 at 7:56 am
property for sale knightsbridge Buy Penthouse in Dubai
https://liberalwiki.space/ · June 6, 2026 at 8:07 am
References:
Belterra casino https://liberalwiki.space/wiki/Jetzt_registrieren_sofort_spielen
Josephtot · June 6, 2026 at 8:07 am
Эта статья подробно расскажет о процессе выздоровления, который включает в себя эмоциональную, физическую и психологическую реабилитацию. Мы обсуждаем значимость поддержки и наличие профессиональных программ. Читатели узнают, как строить новую жизнь и не возвращаться к старым привычкам.
Получить исчерпывающие сведения – вызов наркологической помощи
Robertotus · June 6, 2026 at 8:18 am
пояснения https://tripscans74.us
https://theruniverse.com/promo-code-for-melbet-somalia-max888-e130-bonus/ · June 6, 2026 at 8:50 am
https://theruniverse.com/promo-code-for-melbet-somalia-max888-e130-bonus/
https://md.swk-web.com/ · June 6, 2026 at 9:04 am
References:
Online roulette australia https://md.swk-web.com/s/wscu1tEiH
gitlab.vuhdo.io · June 6, 2026 at 9:38 am
gitlab.vuhdo.io
xutovtoowl · June 6, 2026 at 9:45 am
«Велика Родина» — розгалужена мережа пансіонатів для літніх людей в Україні з цілодобовим медичним наглядом та досвідченим персоналом. Команда пансіонату здійснює догляд за лежачими пацієнтами, людьми з деменцією, після інсульту й з інвалідністю. На https://big-femily.com.ua/ можна ознайомитись з умовами проживання та цінами. Заклади розташовані в Києві, Львові, Харкові, Дніпрі, Полтаві та багатьох інших містах.
https://chesswiki.site · June 6, 2026 at 10:04 am
References:
Tropicana casino online https://chesswiki.site/wiki/Bwin_Schweiz_Erfahrungen_2026_Test_und_Bewertung
LesterSmoog · June 6, 2026 at 10:28 am
В этой статье рассматриваются способы преодоления зависимости и успешные истории людей, которые справились с этой проблемой. Мы обсудим важность поддержки со стороны близких и профессионалов, а также стратегии, которые могут помочь в процессе выздоровления. Научитесь первоочередным шагам к новой жизни.
Узнайте всю правду – вывод из запоя в стационаре самара
RogerNoupe · June 6, 2026 at 10:52 am
Эта медицинская заметка содержит сжатую информацию о новых находках и методах в области здравоохранения. Мы предлагаем читателям свежие данные о заболеваниях, профилактике и лечении. Наша цель — быстро и доступно донести важную информацию, которая поможет в повседневной жизни и понимании здоровья.
Как это работает — подробно – вывод из запоя на дому самара круглосуточно
socolivextv · June 6, 2026 at 11:01 am
I had highly recommend this blog to my good friend, it’s so good
https://truckwiki.site/ · June 6, 2026 at 11:17 am
References:
Canadian online casinos https://truckwiki.site/wiki/So_kontaktieren_Sie_den_Total_CasinoKundendienst_Alle_verfgbaren_Kanle_fr_Deutschland
xeyotonFlofs · June 6, 2026 at 11:50 am
Looking for the best way to buy Bitcoin? Visit https://bestwaytobuybitcoin.net/ – an independent Bitcoin buying route service designed to help users compare payment methods, evaluate BTC results, and review their purchase path before proceeding. Use the service to compare card, debit card, bank transfer, and online exchange options.
KevinIntob · June 6, 2026 at 12:01 pm
Эта публикация содержит ценные советы и рекомендации по избавлению от зависимости. Мы обсуждаем различные стратегии, которые могут помочь в процессе выздоровления и важность обращения за помощью. Читатели смогут использовать полученные знания для улучшения своего состояния.
Смотри, что ещё есть – вывод из запоя недорого
Timothyelapy · June 6, 2026 at 12:18 pm
kuf kokusu nas?l giderilir hakk?ndaki bolumu cok sevdim. Suradan okuyabilirsiniz: https://hobiprojesi.com/articles/kuf-kokusu-nasil-giderilir/
pad.stuve.uni-ulm.de · June 6, 2026 at 12:21 pm
References:
Dover downs casino https://pad.stuve.uni-ulm.de/s/I_2_FD_-M
Timothyelapy · June 6, 2026 at 12:23 pm
cardak susleme hakk?ndaki makaleyi gercekten begendim. Suradan okuyabilirsiniz: https://kendifikirler.com/articles/cardak-susleme-yenilikci-fikirler/
JamesBus · June 6, 2026 at 12:56 pm
В данном материале представлены ключевые тенденции в сфере медицинской науки и практики. Вы узнаете о последних открытиях, инновационных подходах к терапии и важности профилактики заболеваний. Особое внимание уделено практическому применению новых методов в клинической практике.
Это стоит прочитать полностью – стоимость капельницы на дому екатеринбург
best online casino · June 6, 2026 at 1:20 pm
You need to really control the comments listed here
wusaxrdSmant · June 6, 2026 at 1:41 pm
How to buy Bitcoin online? Visit https://howtobuybitcoin.online/ and you’ll discover that receiving BTC online is easier when you understand the purchase flow before sending money. This guide explains how beginners can choose Bitcoin and complete a more secure online purchase. Use the Bitcoin widget below to estimate how much BTC you can receive, compare order details, and preview the purchase process before confirming the transaction.
https://www.expenews.com/de/expeditions/61/dispatches/7312 · June 6, 2026 at 1:44 pm
https://www.expenews.com/de/expeditions/61/dispatches/7312
GeraldWep · June 6, 2026 at 1:45 pm
Эта публикация раскрывает психологические механизмы зависимости и их роль в развитии расстройств. Читатель узнает о том, как психология влияет на формирование зависимостей и как профессиональная помощь может изменить ситуацию.
Смотри, что ещё есть – вывод из запоя самара на дому
online casino nz · June 6, 2026 at 1:47 pm
Hello this is kinda of off topic but I was wondering if blogs use WYSIWYG editors or if you have to manually code with HTML. I’m starting a blog soon but have no coding knowledge so I wanted to get advice from someone with experience. Any help would be enormously appreciated!
pad.stuve.de · June 6, 2026 at 2:19 pm
References:
Lord of the rings slot machine https://pad.stuve.de/s/QXtT3N5w5z
JamesPrend · June 6, 2026 at 2:25 pm
Статья посвящена анализу текущих трендов в медицине и их влиянию на жизнь людей. Мы рассмотрим новые технологии, методы лечения и значение профилактики в обеспечении долголетия и здоровья.
Подробности по ссылке – капельница на дому в екатеринбурге
cobaseboype · June 6, 2026 at 3:14 pm
Ищете лучшее лечение кариеса в Мурманске по выгодной стоимости? Посетите https://nova-51.ru/lechenie-zubov-murmansk/lechenie-kariesa-murmansk – не откладывайте поход к стоматологу, если заметили темные пятна, сколы или трещины на зубах. Приходите в нашу клинику – мы вылечим кариес, сохраним здоровье ваших зубов!
gituyioNot · June 6, 2026 at 3:17 pm
Ищете надёжные запчасти для коммерческого транспорта? Компания Park Motors специализируется на поставке двигателей ЗМЗ, УМЗ и Cummins, блоков цилиндров, ГБЦ, коленвалов, КПП и редукторов для Газелей всех поколений, включая Газель Некст. На сайте https://parkmotors.ru/ представлен широкий ассортимент шин и дисков — Westlake, Triangle, Powertrac — по конкурентным ценам. Магазин работает в Москве на Угрешской улице, дом 17.
kasyno online · June 6, 2026 at 3:33 pm
The start of a fast-growing trend?
https://telescope.ac/promo-code-for-1xbet-bangladesh/ffx3s04eu293a0fwl5fsy3 · June 6, 2026 at 3:55 pm
https://telescope.ac/promo-code-for-1xbet-bangladesh/ffx3s04eu293a0fwl5fsy3
https://medakt.ru/news/pgs/?kak_vybraty_letniy_sarafan_po_tipu_figury_html= · June 6, 2026 at 4:39 pm
https://medakt.ru/news/pgs/?kak_vybraty_letniy_sarafan_po_tipu_figury_html=
CharlesOvexy · June 6, 2026 at 4:45 pm
ремонт квартир ключ ціна ремонт квартир під ключ
Waynebab · June 6, 2026 at 5:05 pm
Текст посвящён распространённым мифам о зависимости и их развенчанию. Мы предоставим научно обоснованную информацию и дадим рекомендации по выбору эффективного способа борьбы с зависимым поведением.
Получить больше информации – кодировка sit mst
neralioDub · June 6, 2026 at 6:23 pm
Looking for the best crypto exchanges in 2026? Visit https://topexchanges.io/ – TopExchanges helps users compare crypto exchanges, instant crypto exchanges, and popular trading platforms in one place. This ranking is designed for people who want to buy, sell, exchange, trade, or cash out digital assets without having to check each service individually.
https://linkvault.win · June 6, 2026 at 6:27 pm
References:
Instant Casino mit Trustly
References:
https://linkvault.win/story.php?title=trustly-casinos-2026-warum-instant-banking-traditionelle-methoden-schlaegt
higivoBit · June 6, 2026 at 6:43 pm
Автошкола Драйв+ в Туле предлагает качественное обучение вождению категории В по современным методикам, сочетающим теоретическую подготовку с интенсивной практикой на автомобилях с механической и автоматической коробками передач. Опытные инструкторы школы помогают новичкам уверенно чувствовать себя за рулем уже после первых занятий, а удобное расположение офиса на проспекте Ленина и гибкий график делают обучение максимально комфортным. Подробнее о программах и действующих акциях можно узнать на сайте https://drivepluspro.ru/, где также доступна онлайн-запись на курсы с возможностью получить консультацию специалиста в удобное время.
https://intensedebate.com/people/namefind26 · June 6, 2026 at 7:56 pm
References:
Winning slot machines https://intensedebate.com/people/namefind26
Josephcroro · June 6, 2026 at 8:37 pm
“terlemek vucudumuz icin neden onemlidir” hakk?nda bilgi arayanlar icin burada harika bilgiler var. Suradan okuyabilirsiniz: https://limitligiyin.com/articles/terlemenin-faydalari-fiziksel-psikolojik-etkileri/
Josephcroro · June 6, 2026 at 8:43 pm
“evdeki naftalin kokusu nas?l giderilir” konusu icin mukemmel bir kaynak var. Link burada: https://yapevleri.com/articles/naftalin-kokusunu-giderme-yontemleri/
https://www.forum-joyingauto.com/member.php?action=profile&uid=145934 · June 6, 2026 at 9:05 pm
References:
Four winds casino new buffalo https://www.forum-joyingauto.com/member.php?action=profile&uid=145934
neolatinswiki.site · June 6, 2026 at 10:11 pm
References:
Boulevard casino poker https://neolatinswiki.site/wiki/1Go_Casino_Bonus_ohne_Einzahlung_Spielen_und_kostenlos_gewinnen
WilliamNerry · June 6, 2026 at 10:20 pm
Обзор специализированных игровых движков
секс геев с игрушками
sonnik.nalench.com · June 6, 2026 at 10:36 pm
References:
Casino dice games https://sonnik.nalench.com/user/wolfegypt44/
GregoryLom · June 6, 2026 at 11:14 pm
Вывод из запоя на дому удобен, если пациент находится в привычной обстановке, не хочет ехать в больницу, но нуждается в медицинской поддержке. Вызов нарколога можно заказать в любое время суток: выездная бригада приезжает по указанному адресу, проводит осмотр, оценивает поведение пациента, давление, пульс, признаки интоксикации, риск психозов, судорожных реакций и других осложнений.
Подробнее можно узнать тут – наркология вывод из запоя сочи
http://medmall.ru/img/pages/zaborostroenie_v_arhitekture_balans_meghdu_zaschitoy_i_estetikoy.html · June 7, 2026 at 12:12 am
http://medmall.ru/img/pages/zaborostroenie_v_arhitekture_balans_meghdu_zaschitoy_i_estetikoy.html
https://lumny.edu.pl/dampak-gmabling-terhadap-kesehatan-finansial-keluarga/#comment-45 · June 7, 2026 at 1:07 am
https://lumny.edu.pl/dampak-gmabling-terhadap-kesehatan-finansial-keluarga/#comment-45
https://jobs.westerncity.com/profiles/8364300-1win-bonus · June 7, 2026 at 2:10 am
https://jobs.westerncity.com/profiles/8364300-1win-bonus
karijuewjag · June 7, 2026 at 2:37 am
Московская компания «Пиломатериалы» предлагает широкий выбор качественной древесины прямо со склада производителя в Мытищах по ценам без посредников. Обрезная и строганная доска, профилированный и клееный брус, фанера, OSB, вагонка, террасная доска — весь ассортимент на сайте https://pilomaterialy-msk.ru/ с актуальными ценами и удобным калькулятором расчёта. Доставка по Москве и области, акции от производителя, звонок с обратной связью за 5 минут — здесь ценят время клиента.
Robertnah · June 7, 2026 at 2:48 am
В данном материале представлены ключевые тенденции в сфере медицинской науки и практики. Вы узнаете о последних открытиях, инновационных подходах к терапии и важности профилактики заболеваний. Особое внимание уделено практическому применению новых методов в клинической практике.
Узнай первым! – реабилитационный наркологический центр
fobovesnila · June 7, 2026 at 3:08 am
Блог https://aae.su/ публикует экспертные материалы по бизнесу, обустройству дома и садоводству — без лишней воды и общих фраз. Редакция рассматривает конкретные ситуации: от подбора трансформируемой мебели для небольших квартир до нюансов строительных конструкций в торговле и уничтожения сорняков на даче. Каждая публикация решает реальную задачу читателя — без воды и отвлечённых рассуждений.
yidiyojedia · June 7, 2026 at 3:32 am
Ищете имплантацию зубов в Мурманске? Посетите https://nova-51.ru/implantatsiya-zubov-murmansk – с помощью имплантации мы восстанавливаем эстетику, функциональность зубного ряда, улучшая качество жизни и самооценку пациента. Только опытные хирурги! Подробнее на сайте.
duhuxtZep · June 7, 2026 at 4:19 am
Посетите https://newstorerussia.ru/ – это ваш надежный партнер в мире онлайн-шоппинга. Широкий ассортимент электроники, одежды и товаров для дома с быстрой доставкой по всей России. Актуальные тренды и выгодные предложения. На портале вы узнаете важную и ценную информацию о современных товарах для вашей жизни! Только актуальные тренды и выгодные предложения.
Robertnah · June 7, 2026 at 5:33 am
Этот краткий обзор предлагает сжатую информацию из области медицины, включая ключевые факты и последние новости. Мы стремимся сделать информацию доступной и понятной для широкой аудитории, что позволит читателям оставаться в курсе актуальных событий в здравоохранении.
Более подробно об этом – наркологическая клиника
nifofuinicy · June 7, 2026 at 8:16 am
Looking for local business marketing fort smith? Based in Fort Smith, Arkansas, CyberSpyder cyberspyder.net is a professional Web development and Marketing agency that serves businesses locally, regionally, and across the nation. We offer a Full Range of Services, Including Web design, Search Engine Optimization (SEO), Digital marketing, Graphic design, Hosting, and Support. Drawing on more than 25 years of proven expertise, our team crafts personalized approaches and delivers direct, practical support to help small and mid-sized businesses thrive.
CliftonSaf · June 7, 2026 at 8:38 am
В данной статье рассматриваются проблемы общественного здоровья и социальные факторы, влияющие на него. Мы акцентируем внимание на значении профилактики и осведомленности в защите здоровья на уровне общества. Читатели смогут узнать о новых инициативах и программах, направленных на улучшение здоровья населения.
Слушай внимательно — тут важно – помощь вывода из запоя
RobertLic · June 7, 2026 at 10:40 am
Слоты, рулетка, покер — быстрая верификация.
Свежая ссылка для входа — сохраняет бонусный счёт.
Вход через официальный домен — с двухфакторной защитой.
Без скрытых условий — автоматический бонус.
Тысячи слотов в casino online казино — турниры с призами.
Source:
казино актуальное зеркало
kolobossen · June 7, 2026 at 11:18 am
Check the live Bitcoin price in GBP and see how much 1 BTC is worth in British Pounds right now. https://bitcoinpricegbp.com/ tracks the current BTC/GBP exchange rate, daily movements, and key market data for users looking for a quick reference for Bitcoin in British Pounds. This site is useful for users tracking their Bitcoin balance in GBP, comparing today’s movements, and checking their portfolio value.
JamesVot · June 7, 2026 at 12:16 pm
Срочный ремонт холодильного и климатического оборудования в Москве. Работаем с производствами. Приедем за 1 час.
Техническое обслуживание климатического оборудования. Чистка фильтров. Сэкономим электроэнергию.
В наличии запчасти на складе. Диагностика 0 рублей при ремонте. Договор, закрывающие документы.
Source:
https://dzen.ru/smart-quick.ru
JamesHaile · June 7, 2026 at 12:27 pm
Когда вам нужны турецкие сериалы на русском языке 3 без долгих поисков и подозрительных ресурсов, оцените нашу библиотеку лучших турецких сериалов. В каталоге доступны как популярные новые проекты, так и проверенные временем хиты, которые остаются популярными среди поклонников жанра. Поклонники предпочитают турецкие сериалы за интересные сюжеты, ярким персонажам, красивым локациям и насыщенной драматургии, которая удерживает интерес от первой до последней серии. Просмотр доступен в высоком качестве, без сложной регистрации и лишних действий.
Richardfailt · June 7, 2026 at 12:41 pm
Медицинская публикация представляет собой свод актуальных исследований, экспертных мнений и новейших достижений в сфере здравоохранения. Здесь вы найдете информацию о новых методах лечения, прорывных технологиях и их практическом применении. Мы стремимся сделать актуальные медицинские исследования доступными и понятными для широкой аудитории.
Перейти к статье – tver clinica plus
fixDiele · June 7, 2026 at 1:30 pm
Для тех, кто ищет информацию по теме “Свежие новости Томской области и мира”, нашел много полезного.
Вот, можете почитать:
https://media71.ru
fixDiele · June 7, 2026 at 1:34 pm
Кстати, если вас интересует Гид для родителей юных футболистов: новости и советы, посмотрите сюда.
Смотрите сами:
https://familyzenit.ru
mitozrtok · June 7, 2026 at 1:49 pm
Ищете надёжный атлас дорог США и Канады? На сайте https://us-canad.com/ собраны подробные карты всех штатов с графствами, шоссе, городами и посёлками, национальными парками и заповедниками. Здесь доступны топографические карты с рельефом местности, реками и озёрами, а также маршрутные карты с расстояниями в милях и километрах — всё это бесплатно и в высоком разрешении для удобного планирования путешествий по Северной Америке.
KeithDiabe · June 7, 2026 at 1:55 pm
Этот текст представляет собой обзор свежих данных и исследований в области медицины. Он призван помочь читателям понять, как научные достижения влияют на лечение, диагностику и общее состояние системы здравоохранения.
Погрузиться в детали – клиника плюс
Keithguaky · June 7, 2026 at 3:32 pm
Обзор посвящён процессу восстановления после зависимостей. Мы расскажем о различных этапах реабилитации, поддерживающих ресурсах и важности мотивации в достижении устойчивого выздоровления.
Раскрыть тему полностью – clinica plus
https://abertic.com/codigo-promocional-1xbet-ultimo-2026-1xhasard/ · June 7, 2026 at 3:33 pm
https://abertic.com/codigo-promocional-1xbet-ultimo-2026-1xhasard/
vahukrtKaf · June 7, 2026 at 4:02 pm
Современное оборудование для питьевой воды превращает офис или дом в комфортное пространство, где всегда доступна прохладная или горячая вода нужной температуры. Компактные настольные модели экономят место, а напольные кулеры со шкафчиками и несколькими кранами становятся функциональным центром любого помещения. На сайте https://voda-s-gor.ru/oborudovanie/ представлены проверенные бренды Ecotronic и HotFrost с различными опциями — от базовых до премиальных решений с электронным охлаждением. Профессиональная установка, гарантийное обслуживание и доставка по Махачкале делают покупку максимально удобной для каждого клиента.
Keithguaky · June 7, 2026 at 4:10 pm
Обзор посвящён процессу восстановления после зависимостей. Мы расскажем о различных этапах реабилитации, поддерживающих ресурсах и важности мотивации в достижении устойчивого выздоровления.
Открой скрытое – clinica plus
google.pt · June 7, 2026 at 6:11 pm
google.pt
JamesCon · June 7, 2026 at 6:12 pm
Эта публикация посвящена актуальным вопросам современной медицины и здравоохранения. Мы обсудим новейшие технологии диагностики и лечения, а также их влияние на продолжительность и качество жизни. Читатель найдет здесь информацию о научных исследованиях и перспективных разработках, доступно изложенную для широкой аудитории.
Проверенные методы — узнай сейчас – цены на кодирование от алкоголизма
https://jobs.lajobsportal.org/profiles/8364789-betv-code26 · June 7, 2026 at 6:13 pm
https://jobs.lajobsportal.org/profiles/8364789-betv-code26
JamesCon · June 7, 2026 at 7:03 pm
Этот информационный материал подробно освещает проблему наркозависимости, ее причины и последствия. Мы предлагаем информацию о методах лечения, профилактики и поддерживающих программах. Цель статьи — повысить осведомленность и продвигать идеи о необходимости борьбы с зависимостями.
ТОП-5 причин узнать больше – клиника плюс тверь
Douglassoilk · June 7, 2026 at 7:50 pm
Текст посвящён распространённым мифам о зависимости и их развенчанию. Мы предоставим научно обоснованную информацию и дадим рекомендации по выбору эффективного способа борьбы с зависимым поведением.
Получить больше информации – clinica plus
DavidArcaf · June 7, 2026 at 8:34 pm
В этой публикации мы исследуем ключевые аспекты здоровья, включая влияние образа жизни на благополучие. Читатели узнают о важности правильного питания, физической активности и психического здоровья. Мы предоставим практические советы и рекомендации для поддержания здоровья и развития профилактических подходов.
Это ещё не всё… – наркологическая клиника в твери
DavidArcaf · June 7, 2026 at 9:31 pm
Этот обзор содержит информацию о передовых достижениях в области медицины. Мы разберем инновационные технологии, которые меняют подход к лечению и диагностике, а также их влияние на эффективность оказания медицинской помощи.
Познакомиться с результатами исследований – лечение пивного алкоголизма
gewoesShied · June 7, 2026 at 9:58 pm
Ищете лечение пульпита и периодонтита в Мурманске от лучшей клиники, в котором работают квалифицированные стоматологи? Посетите https://nova-51.ru/lechenie-zubov-murmansk/lechenie-pulpita-i-periodontita-murmansk – ознакомьтесь с нашими услугами подробнее.
Richardfailt · June 7, 2026 at 10:22 pm
В данной статье мы акцентируем внимание на важности поддержки в процессе выздоровления. Мы обсудим, как друзья, семья и профессионалы могут помочь тем, кто сталкивается с зависимостями. Читатели получат практические советы, как поддерживать близких на пути к новой жизни.
Смотри, что ещё есть – лечение пивного алкоголизма клиника
4rabet casino · June 7, 2026 at 10:32 pm
सुपर प्लेटफ़ॉर्म! सब कुछ बेहतरीन स्तर पर है, बधाई और सफलता की शुभकामनाएँ!
http://dogue-de-bordeaux.ru/go/url=https://4rabet-best.com/signup
Archienot · June 7, 2026 at 10:33 pm
Платформа //friendlysun.ru](https://friendlysun.ru) подойдёт тем, кто интересуется путешествиями, современным travel lifestyle и вариантами онлайн-развлечений. На сайте собраны статьи о поездках, полезные рекомендации для туристов и материалы о мобильных сервисах для отдыха и досуга.
Source:
https://friendlysun.ru/
Shermangit · June 7, 2026 at 11:02 pm
В данном обзоре представлены основные направления и тренды в области медицины. Мы обсудим актуальные проблемы здравоохранения, свежие открытия и новые подходы, которые меняют представление о лечении и профилактике заболеваний. Эта информация будет полезна как специалистам, так и широкой публике.
Рассмотреть проблему всесторонне – tver clinica plus
avtovoz moskva 274 · June 7, 2026 at 11:02 pm
сколько будет стоить перевозка авто услуги перевозки авто
coyipmSef · June 7, 2026 at 11:40 pm
Ищете аккуратное и деликатное удаление зуба в Мурманске? Посетите https://nova-51.ru/lechenie-zubov-murmansk/udalenie-zuba-murmansk – у нас профессиональная и тщательная помощь всем нашим пациентам. Узнайте подробную информацию и стоимость на сайте.
Donaldsow · June 8, 2026 at 12:25 am
В этой публикации мы рассматриваем важную тему борьбы с зависимостями, включая алкогольную и наркотическую зависимости. Мы обсудим методы лечения, реабилитации и поддержку, которые могут помочь людям, столкнувшимся с этой проблемой. Читатели узнают о перспективах выздоровления и важности комплексного подхода.
Всё самое вкусное внутри – закодированию от алкоголя
Donaldfum · June 8, 2026 at 12:43 am
Эта публикация обращает внимание на важность профилактики зависимостей. Мы обсудим, как осведомленность и образование могут помочь в предотвращении возникновения зависимости. Читатели смогут ознакомиться с полезными советами и ресурсами, которые способствуют здоровому образу жизни.
Продолжить изучение – tver clinica plus
payday loans payday · June 8, 2026 at 12:45 am
Hi! I simply would like to give you a huge thumbs up for the excellent info you’ve got here on this post. I’ll be coming back to your site for more soon.
https://alhudapk.com/dua/pages/?sovety_po_prohoghdeniyu_medal_of_honor_pacific_assault_prohoghdenie_osnovnogo_syugheta_12_html= · June 8, 2026 at 1:59 am
https://alhudapk.com/dua/pages/?sovety_po_prohoghdeniyu_medal_of_honor_pacific_assault_prohoghdenie_osnovnogo_syugheta_12_html=
kikusgrogs · June 8, 2026 at 2:05 am
Looking for forex analysis|crypto forecast|forex signals|btc forecast|crypto news|forex outlook|trading analysis|market forecast|crypto insights|stock market|best crypto exchange|crypto exchange review|top exchanges|where to buy crypto|exchange comparison|lowest fee exchange|crypto trading platform|safe crypto exchange|binance alternative|foreck exchanges? Head to foreck.info to explore detailed insights into forex, cryptocurrency, and stock markets, along with expert analysis and development trends. News with in-depth analysis will help you stay up-to-date with current events. You’ll also find top-rated crypto exchanges on the site, professionally assessed using eight weighted evaluation criteria. Discover all the details by visiting the website.
KeithDiabe · June 8, 2026 at 2:49 am
В этой статье обсуждаются актуальные медицинские вопросы, которые волнуют общество. Мы обращаем внимание на проблемы, касающиеся здравоохранения и лечения, а также на новшества в области медицины. Читатели будут осведомлены о последних событиях и смогут следить за тенденциями в медицине.
Узнать больше – clinica plus
https://teplokomplect.ru/dostavka/pgs/vaghnosty_struktury_poverhnosti_v_effekte_stareniya.html · June 8, 2026 at 2:51 am
https://teplokomplect.ru/dostavka/pgs/vaghnosty_struktury_poverhnosti_v_effekte_stareniya.html
https://eucsector.ru/ · June 8, 2026 at 3:13 am
https://eucsector.ru/
Shermangit · June 8, 2026 at 4:38 am
Читатели получат представление о том, как современные технологии влияют на развитие медицины. Обсуждаются новые методы лечения, персонализированный подход и роль цифровых решений в повышении качества медицинских услуг.
Связаться за уточнением – клиника плюс тверь
bahiznJaila · June 8, 2026 at 5:58 am
Компания «Промметстрой» — надёжный поставщик металлопроката в Москве и Подмосковье, работающий напрямую с ведущими металлургическими комбинатами России. В каталоге представлен широкий сортамент продукции: сортовой, листовой, трубный прокат, запорная арматура и метизы — всё по конкурентным ценам оптом и в розницу. На сайте https://prommetstroy.ru/ действуют сезонные акции и гибкие скидки для оптовиков. Компания располагает собственным автопарком грузовой спецтехники и оказывает услуги металлообработки и резки металлопроката.
Donaldfum · June 8, 2026 at 6:46 am
Этот текст представляет собой обзор свежих данных и исследований в области медицины. Он призван помочь читателям понять, как научные достижения влияют на лечение, диагностику и общее состояние системы здравоохранения.
Ознакомиться с полной информацией – tver clinica plus
xxx ??????????????? · June 8, 2026 at 7:42 am
cartoon porno
https://ipb.edu.tl/konvida-kompania-ka-vendor-supplier-sira-iha-interese-aplika-ba-kotasaun/#comment-3131591 · June 8, 2026 at 7:44 am
https://ipb.edu.tl/konvida-kompania-ka-vendor-supplier-sira-iha-interese-aplika-ba-kotasaun/#comment-3131591
https://www.are.na/raiden-russo/codigo-promocional-1xbet-bolivia-2026-rich888 · June 8, 2026 at 9:15 am
https://www.are.na/raiden-russo/codigo-promocional-1xbet-bolivia-2026-rich888
GoodiniCrubs · June 8, 2026 at 9:17 am
В этой медицинской статье мы погрузимся в актуальные вопросы здравоохранения и лечения заболеваний. Читатели узнают о современных подходах, методах диагностики и новых открытий в научных исследованиях. Наша цель — донести важную информацию и повысить уровень осведомленности о здоровье.
Провести детальное исследование – цена вывода из запоя в стационаре
JasonKaf · June 8, 2026 at 9:20 am
В этом обзоре представлены различные методы избавления от зависимости, включая терапевтические и психологические подходы. Мы сравниваем их эффективность и предоставляем рекомендации для тех, кто хочет вернуться к трезвой жизни. Читатели смогут найти информацию о реабилитационных центрах и поддерживающих группах.
Нажмите, чтобы узнать больше – вывод из запоя стационар
MarvinGeata · June 8, 2026 at 10:20 am
сколько стоит перевозка машины перевозки авто москва
???????? ?????? ?????? · June 8, 2026 at 10:21 am
tamil porn
WillieMew · June 8, 2026 at 10:39 am
Этот краткий обзор предлагает сжатую информацию из области медицины, включая ключевые факты и последние новости. Мы стремимся сделать информацию доступной и понятной для широкой аудитории, что позволит читателям оставаться в курсе актуальных событий в здравоохранении.
Как достичь результата? – клиника плюс
FrankSeacy · June 8, 2026 at 11:59 am
В этой медицинской статье мы погрузимся в актуальные вопросы здравоохранения и лечения заболеваний. Читатели узнают о современных подходах, методах диагностики и новых открытий в научных исследованиях. Наша цель — донести важную информацию и повысить уровень осведомленности о здоровье.
Где почитать поподробнее? – врач нарколог на дом круглосуточно
GilbertHix · June 8, 2026 at 12:01 pm
Публикация посвящена жизненным историям людей, успешно справившихся с зависимостью. Мы покажем, что выход есть, и он начинается с первого шага — принятия проблемы и желания измениться.
Читать далее > – услуги нарколога на дому
Manuelfub · June 8, 2026 at 12:43 pm
В этой публикации мы предложим ряд рекомендаций по избавлению от зависимостей и успешному восстановлению. Мы обсудим методы привлечения поддержки и важность самосознания. Эти советы помогут людям вернуться к нормальной жизни и стать на путь выздоровления.
Неизвестные факты о… – вывод из запоя на дому недорого
xem them · June 8, 2026 at 1:16 pm
Nice blog here! Also your web site loads up very fast! What host are you using? Can I get your affiliate link to your host? I wish my web site loaded up as fast as yours lol
CraigNor · June 8, 2026 at 1:28 pm
Публикация посвящена жизненным историям людей, успешно справившихся с зависимостью. Мы покажем, что выход есть, и он начинается с первого шага — принятия проблемы и желания измениться.
Лучшее решение — прямо здесь – клиника плюс
CraigNor · June 8, 2026 at 2:14 pm
Этот обзор посвящен успешным стратегиям избавления от зависимости, включая реальные примеры и советы. Мы разоблачим мифы и предоставим читателям достоверную информацию о различных подходах. Получите опыт многообразия методов и найдите подходящий способ для себя!
Провести детальное исследование – clinica plus
Davisvob · June 8, 2026 at 3:20 pm
услуги по подбору персонала кадровые агентства по подбору персонала москва
JosephIsopy · June 8, 2026 at 4:03 pm
смотреть здесь https://tripscans74.group
RonaldPouby · June 8, 2026 at 4:06 pm
Обзор посвящён процессу восстановления после зависимостей. Мы расскажем о различных этапах реабилитации, поддерживающих ресурсах и важности мотивации в достижении устойчивого выздоровления.
Узнать напрямую – вывод из запоя с выездом на дом
https://www.weddingbee.com/members/bestmelbetpromo/ · June 8, 2026 at 4:13 pm
https://www.weddingbee.com/members/bestmelbetpromo/
Kevinhip · June 8, 2026 at 4:22 pm
View all: התקשרו לשירותי ליווי
Douglassoilk · June 8, 2026 at 4:31 pm
В данной статье мы акцентируем внимание на важности поддержки в процессе выздоровления. Мы обсудим, как друзья, семья и профессионалы могут помочь тем, кто сталкивается с зависимостями. Читатели получат практические советы, как поддерживать близких на пути к новой жизни.
Получить профессиональную консультацию – clinica plus в твери
Russellhib · June 8, 2026 at 4:32 pm
Этот обзор сосредоточен на различных подходах к избавлению от зависимости. Мы изучим традиционные и альтернативные методы, а также их сочетание для достижения максимальной эффективности. Читатели смогут открыть для себя новые стратегии и подходы, которые помогут в их борьбе с зависимостями.
Информация доступна здесь – цены на вывод из запоя на дому
foxeynof · June 8, 2026 at 4:38 pm
Дубай больше не ассоциируется с запретом на алкоголь: премиальные напитки доставляются прямо к вашей двери в кратчайшие сроки. Ищете beer delivery dubai? Сервис dubaialco.ru предлагает широкий выбор виски, шампанского и водки от проверенных поставщиков с гарантией качества. Оформить заказ можно за считанные минуты — доставка охватывает Marina, JBR, Palm Jumeirah и Downtown без ограничений.
Davidtop · June 8, 2026 at 4:43 pm
Этот документ охватывает важные аспекты медицинской науки, сосредотачиваясь на ключевых вопросах, касающихся здоровья населения. Мы рассматриваем свежие исследования, клинические рекомендации и лучшие практики, которые помогут улучшить качество лечения и профилактики заболеваний. Читатели получат возможность углубиться в различные медицинские дисциплины.
Что ещё нужно знать? – капельница от похмелья нижний новгород
EdwardVal · June 8, 2026 at 5:12 pm
В статье по вопросам здоровья мы рассматриваем актуальные проблемы, с которыми сталкивается общество. Обсуждаются заболевания, факторы риска и важные аспекты профилактики. Читатели получат полезные советы о том, как сохранить здоровье и улучшить качество жизни.
Ознакомьтесь поближе – врач на дом капельница от запоя
Steviejilia · June 8, 2026 at 5:40 pm
Эта публикация содержит ценные советы и рекомендации по избавлению от зависимости. Мы обсуждаем различные стратегии, которые могут помочь в процессе выздоровления и важность обращения за помощью. Читатели смогут использовать полученные знания для улучшения своего состояния.
Изучить эмпирические данные – оформить вызов нарколога на дом
Jamesreido · June 8, 2026 at 5:54 pm
Мы рассмотрим современные вызовы здравоохранения и пути их решения с помощью технологий и научных исследований. В статье собраны данные о новых лекарствах, методах диагностики и системном подходе к улучшению здоровья населения.
Уточнить детали – капельница от похмелья клиника
EdwardVal · June 8, 2026 at 6:04 pm
В этой статье рассматриваются различные аспекты избавления от зависимости, включая физические и психологические методы. Мы обсудим поддержку, мотивацию и стратегии, которые помогут в процессе выздоровления. Читатели узнают, как преодолеть трудности и двигаться к новой жизни без зависимости.
Что ещё? Расскажи всё! – вызвать капельницу от запоя на дому
MichaelZiche · June 8, 2026 at 6:47 pm
Статья посвящена анализу текущих трендов в медицине и их влиянию на жизнь людей. Мы рассмотрим новые технологии, методы лечения и значение профилактики в обеспечении долголетия и здоровья.
Ознакомиться с теоретической базой – платный нарколог на дом анонимно
dumupDaK · June 8, 2026 at 7:19 pm
Юридическая компания «Аксиома» в Ростове-на-Дону законно списывает долги по кредитам, займам, налогам, штрафам и ЖКХ — даже при действующей ипотеке. Компания действует строго по закону №127 «О банкротстве» и предлагает рассрочку оплаты от 3 990 рублей в месяц без каких-либо переплат. Подробная информация об услугах на https://uk-axioma.ru/ — проверьте возможность списания ваших долгов прямо сейчас.
CharlieJaw · June 8, 2026 at 7:22 pm
Читатели получат представление о том, как современные технологии влияют на развитие медицины. Обсуждаются новые методы лечения, персонализированный подход и роль цифровых решений в повышении качества медицинских услуг.
Информация доступна здесь – вывод из запоя недорого нарколог24
JasonKaf · June 8, 2026 at 7:35 pm
В этом обзоре мы обсудим современные методы борьбы с зависимостями, включая медикаментозную терапию и психотерапию. Мы представим последние исследования и их результаты, чтобы читатели могли быть в курсе наиболее эффективных подходов к лечению и поддержке.
Смотрите также – лечение запоя в стационаре
MichaelZiche · June 8, 2026 at 7:51 pm
В этой статье мы обсудим процесс восстановления после зависимостей, акцентируя внимание на различных методах и подходах к реабилитации. Читатели узнают, как создать план выздоровления и использовать полезные ресурсы для достижения устойчивых изменений.
Изучить аспект более тщательно – наркологическая помощь на дому
Joshuaabast · June 8, 2026 at 7:54 pm
Этот медицинский обзор сосредоточен на последних достижениях, которые оказывают влияние на пациентов и медицинскую практику. Мы разбираем инновационные методы лечения и исследований, акцентируя внимание на их значимости для общественного здоровья. Читатели узнают о свежих данных и их возможном применении.
Проследить причинно-следственные связи – вывод из запоя с выездом на дом
CharlieJaw · June 8, 2026 at 8:03 pm
В данной статье мы поговорим о будущем медицины, акцентируя внимание на прорывных разработках и их потенциале. Читатель узнает о новых подходах к лечению, роли искусственного интеллекта и возможностях персонализированной медицины.
Посмотреть подробности – вывод из алкогольного запоя нарколог 24
Edwardretly · June 8, 2026 at 8:18 pm
В этой публикации мы рассматриваем важную тему борьбы с зависимостями, включая алкогольную и наркотическую зависимости. Мы обсудим методы лечения, реабилитации и поддержку, которые могут помочь людям, столкнувшимся с этой проблемой. Читатели узнают о перспективах выздоровления и важности комплексного подхода.
Почему это важно? – вывод из запоя цены
wavatbat · June 8, 2026 at 8:27 pm
Sunobit — инструмент на основе нейросети, превращающий короткий текст в полноценную песню с вокалом и аранжировкой. Пользователь получает два варианта трека на любой жанр или инструментал — решение для Reels, Shorts и персональных поздравлений. Ищете suno нейросеть? Подробности и тарифы на sunobit.com — регистрация открыта для всех желающих попробовать AI-музыку без студий и сложных настроек. Регистрация доступна каждому, кто хочет создавать AI-музыку без студийного оборудования и технических сложностей.
WillieMew · June 8, 2026 at 9:08 pm
Этот обзор сосредоточен на различных подходах к избавлению от зависимости. Мы изучим традиционные и альтернативные методы, а также их сочетание для достижения максимальной эффективности. Читатели смогут открыть для себя новые стратегии и подходы, которые помогут в их борьбе с зависимостями.
Посмотреть всё – tver clinica plus
Edwardretly · June 8, 2026 at 9:27 pm
Этот информативный текст сочетает в себе темы здоровья и зависимости. Мы обсудим, как хронические заболевания могут усугубить зависимости и наоборот, как зависимость может влиять на общее состояние здоровья. Читатели получат представление о комплексном подходе к лечению как физического, так и психического состояния.
Заходи — там интересно – выезд на дом капельница от запоя
RobertLic · June 8, 2026 at 9:36 pm
Рабочий адрес моментально — без рекламы.
Создайте аккаунт за минуту — только 18+.
казино онлайн казино сайт с быстрым выводом — работает через Tor.
Заходите — всё летает — давать друзьям.
Проверенный международный домен — поддержка 24/7.
Source:
казино официальный сайт вход
Craigknoda · June 8, 2026 at 9:52 pm
Публикация знакомит читателей с различными подходами к реабилитации. От традиционных методов до современных программ — вы узнаете, как выбрать оптимальный путь к выздоровлению и преодолеть препятствия на этом пути.
Получить дополнительные сведения – вывод из алкогольного запоя нарколог24
https://twanty2.com/read-blog/88387 · June 8, 2026 at 10:04 pm
https://twanty2.com/read-blog/88387
https://network.nutaku.net/images/lp/aeons-echo/4-character-selector-v2/1/?ats=eyJhIjozMTc4MzcsImMiOjU5MzU2NDExLCJuIjoxLCJzIjoxLCJlIjoxMDkwNCwicCI6Mn0 · June 8, 2026 at 10:24 pm
sex pics https://network.nutaku.net/images/lp/aeons-echo/4-character-selector-v2/1/?ats=eyJhIjozMTc4MzcsImMiOjU5MzU2NDExLCJuIjoxLCJzIjoxLCJlIjoxMDkwNCwicCI6Mn0%3D
Jamessnige · June 8, 2026 at 10:35 pm
В этой публикации мы обсуждаем современные методы лечения различных заболеваний. Читатели узнают о новых медикаментах, терапиях и исследованиях, которые активно применяются для лечения. Мы нацелены на то, чтобы предоставить практические знания, которые могут помочь в борьбе с недугами.
Это ещё не всё… – выведение из запоя в стационаре
Craigknoda · June 8, 2026 at 10:39 pm
В этой статье мы обсудим процесс восстановления после зависимостей, акцентируя внимание на различных методах и подходах к реабилитации. Читатели узнают, как создать план выздоровления и использовать полезные ресурсы для достижения устойчивых изменений.
Подробнее можно узнать тут – вывод из запоя в домашних условиях нарколог 24
Harrislep · June 8, 2026 at 10:44 pm
В этой статье мы обсудим процесс восстановления после зависимостей, акцентируя внимание на различных методах и подходах к реабилитации. Читатели узнают, как создать план выздоровления и использовать полезные ресурсы для достижения устойчивых изменений.
Связаться за уточнением – вызывать нарколога домой
Israeldem · June 8, 2026 at 10:59 pm
В этом обзоре мы обсудим современные методы борьбы с зависимостями, включая медикаментозную терапию и психотерапию. Мы представим последние исследования и их результаты, чтобы читатели могли быть в курсе наиболее эффективных подходов к лечению и поддержке.
Открой скрытое – вывод из запоя в клинике
JavierJaf · June 8, 2026 at 11:09 pm
Публикация посвящена жизненным историям людей, успешно справившихся с зависимостью. Мы покажем, что выход есть, и он начинается с первого шага — принятия проблемы и желания измениться.
Откройте для себя больше – наркология вывод из запоя
boss.why3s.cc · June 8, 2026 at 11:32 pm
boss.why3s.cc
GilbertHix · June 9, 2026 at 12:30 am
В статье по вопросам здоровья мы рассматриваем актуальные проблемы, с которыми сталкивается общество. Обсуждаются заболевания, факторы риска и важные аспекты профилактики. Читатели получат полезные советы о том, как сохранить здоровье и улучшить качество жизни.
Есть чему поучиться – нарколога домой
FrankSeacy · June 9, 2026 at 12:32 am
В этой публикации мы рассматриваем важную тему борьбы с зависимостями, включая алкогольную и наркотическую зависимости. Мы обсудим методы лечения, реабилитации и поддержку, которые могут помочь людям, столкнувшимся с этой проблемой. Читатели узнают о перспективах выздоровления и важности комплексного подхода.
Уникальные данные только сегодня – нарколог на дом круглосуточно
monegigDow · June 9, 2026 at 12:37 am
Хотите провести вечер в Дубае с бокалом отборного виски или шампанского, не покидая апартаментов? Сервис https://dubaialco.ru/ предлагает круглосуточную доставку премиального алкоголя по всему городу — от Palm Jumeirah и Dubai Marina до Downtown и JBR. В каталоге представлены водка, виски, шампанское и другие напитки от ведущих мировых брендов, а курьеры работают 24/7, обеспечивая быструю и дискретную доставку прямо к вашей двери.
JamesVot · June 9, 2026 at 12:40 am
Выезд мастера холодильного и климатического оборудования в Москве и МО. Работаем с ресторанами. Замена запчастей в день обращения.
Техническое обслуживание климатического оборудования. Заправка фреоном. Снизим риск аварии на 90%.
Акция для новых клиентов — честные цены без наценок. Приедем в удобное время.
Source:
https://dzen.ru/smart-quick.ru
Joshuaabast · June 9, 2026 at 12:56 am
Эта публикация исследует взаимосвязь зависимости и психологии. Мы обсудим, как психологические аспекты влияют на появление зависимостей и процесс выздоровления. Читатели смогут понять важность профессиональной поддержки и применения научных подходов в терапии.
А что дальше? – вывод из запоя нижний новгород
WilliamPep · June 9, 2026 at 1:07 am
Публикация охватывает основные направления развития современной медицины. Мы обсудим значимость научных исследований, инноваций в лечении и роли общественного участия в формировании системы здравоохранения.
Что ещё нужно знать? – нарколог на дом
Nelsonscept · June 9, 2026 at 1:22 am
Этот обзор сосредоточен на различных подходах к избавлению от зависимости. Мы изучим традиционные и альтернативные методы, а также их сочетание для достижения максимальной эффективности. Читатели смогут открыть для себя новые стратегии и подходы, которые помогут в их борьбе с зависимостями.
Открыть полностью – вызывать нарколога домой
JamesPorce · June 9, 2026 at 1:26 am
Все подробности по ссылке: https://valenkistyle.ru
RobertSkala · June 9, 2026 at 2:18 am
Круглосуточная служба «ЧелябМед» оперативно реагирует на экстренные случаи при следующих состояниях:
Ознакомиться с деталями – скорая вывод из запоя челябинск
Manuelfub · June 9, 2026 at 2:27 am
Публикация посвящена жизненным историям людей, успешно справившихся с зависимостью. Мы покажем, что выход есть, и он начинается с первого шага — принятия проблемы и желания измениться.
Перейти к полной версии – вывести из запоя капельница
WilliamPep · June 9, 2026 at 2:37 am
В этой статье мы рассматриваем разные способы борьбы с алкогольной зависимостью. Обсуждаются методы лечения, программы реабилитации и советы для поддержки близких. Читатели получат информацию о том, как преодолеть зависимость и добиться успешного выздоровления.
Кликни, не пожалеешь – нарколог на дом екатеринбург
RonaldPouby · June 9, 2026 at 2:40 am
В данной публикации мы поговорим о процессе восстановления от зависимости, о том, как вернуть себе нормальную жизнь. Мы обсудим преодоление трудностей, значимость поддержки и наличие программ реабилитации. Читатели смогут узнать о ключевых шагах к успешному восстановлению.
Где почитать поподробнее? – запой помощь
Timothyelapy · June 9, 2026 at 2:40 am
duvar boyas? k?yafetten nas?l c?kar hakk?ndaki bolumu gercekten begendim. Suradan okuyabilirsiniz: https://fikirdronu.com/articles/kiyafetten-duvar-boyasi-cikarma-yontemleri/
Timothyelapy · June 9, 2026 at 2:44 am
“bel kal?nlast?ran hareketler” hakk?nda bilgi arayanlar icin mukemmel bir kaynak var. Kendiniz gorun: https://dinamikstil.com/articles/bel-kalinlastiran-hareketler-etkili-yontemler/
Justincoike · June 9, 2026 at 2:53 am
В этой публикации мы исследуем ключевые аспекты здоровья, включая влияние образа жизни на благополучие. Читатели узнают о важности правильного питания, физической активности и психического здоровья. Мы предоставим практические советы и рекомендации для поддержания здоровья и развития профилактических подходов.
Узнать из первых рук – вывод из запоя круглосуточно
MichaelMar · June 9, 2026 at 3:29 am
Этот информативный текст сочетает в себе темы здоровья и зависимости. Мы обсудим, как хронические заболевания могут усугубить зависимости и наоборот, как зависимость может влиять на общее состояние здоровья. Читатели получат представление о комплексном подходе к лечению как физического, так и психического состояния.
Более подробно об этом – капельница от запоя
kifomRew · June 9, 2026 at 3:34 am
«Сила Света» — лаборатория полного цикла: фотометрические, колориметрические и радиометрические измерения, проверка ЭМС и степени защиты IP/IK/УФ. Лаборатория проводит оценку фотобиологической безопасности по ГОСТ IEC 62471, измерения для тепличного освещения и экспертизу неисправностей. На сайте http://silasveta-lab.ru/ представлены все услуги и возможность проверки протоколов. Лаборатория решает задачи любой сложности — от сертификации до научных исследований.
DerekPoish · June 9, 2026 at 3:44 am
Эта публикация исследует взаимосвязь зависимости и психологии. Мы обсудим, как психологические аспекты влияют на появление зависимостей и процесс выздоровления. Читатели смогут понять важность профессиональной поддержки и применения научных подходов в терапии.
Неизвестные факты о… – срочный вывод из запоя
Russellhib · June 9, 2026 at 4:12 am
Этот информативный текст сочетает в себе темы здоровья и зависимости. Мы обсудим, как хронические заболевания могут усугубить зависимости и наоборот, как зависимость может влиять на общее состояние здоровья. Читатели получат представление о комплексном подходе к лечению как физического, так и психического состояния.
Подробная информация доступна по запросу – вывод из запоя в нижнем новгороде на дому
Justincoike · June 9, 2026 at 4:15 am
Эта медицинская заметка содержит сжатую информацию о новых находках и методах в области здравоохранения. Мы предлагаем читателям свежие данные о заболеваниях, профилактике и лечении. Наша цель — быстро и доступно донести важную информацию, которая поможет в повседневной жизни и понимании здоровья.
Личный опыт — читайте сами – вывод из запоя на дому
best online casino nz real money · June 9, 2026 at 4:32 am
Peculiar this blog is totaly unrelated to what I was searching for – – interesting to see you’re well indexed in the search engines.
Jamessnige · June 9, 2026 at 4:33 am
В этой публикации мы рассматриваем важную тему борьбы с зависимостями, включая алкогольную и наркотическую зависимости. Мы обсудим методы лечения, реабилитации и поддержку, которые могут помочь людям, столкнувшимся с этой проблемой. Читатели узнают о перспективах выздоровления и важности комплексного подхода.
Подробнее тут – клиника запой
kasyno online · June 9, 2026 at 4:44 am
Some truly interesting info , well written and broadly user genial .
RichardBam · June 9, 2026 at 4:50 am
В этой медицинской статье мы погрузимся в актуальные вопросы здравоохранения и лечения заболеваний. Читатели узнают о современных подходах, методах диагностики и новых открытий в научных исследованиях. Наша цель — донести важную информацию и повысить уровень осведомленности о здоровье.
Лучшее решение — прямо здесь – срочно вызвать нарколога на дом
MichaelMar · June 9, 2026 at 4:53 am
В данной статье мы акцентируем внимание на важности поддержки в процессе выздоровления. Мы обсудим, как друзья, семья и профессионалы могут помочь тем, кто сталкивается с зависимостями. Читатели получат практические советы, как поддерживать близких на пути к новой жизни.
Хочу знать больше – капельница от запоя клиника
EarnestZef · June 9, 2026 at 4:57 am
В этом исследовании рассмотрены методы лечения зависимостей и их эффективность. Мы проанализируем различные подходы, используемые в реабилитационных центрах, и представим данные о результативности программ. Читатели получат надежные и научно обоснованные сведения о данной проблеме.
Продолжить изучение – можно вызвать нарколога домой
DerekPoish · June 9, 2026 at 5:05 am
В этой статье рассматриваются различные аспекты избавления от зависимости, включая физические и психологические методы. Мы обсудим поддержку, мотивацию и стратегии, которые помогут в процессе выздоровления. Читатели узнают, как преодолеть трудности и двигаться к новой жизни без зависимости.
Кликни, не пожалеешь – срочный вывод из запоя на дому
lutahuthip · June 9, 2026 at 5:06 am
Ищете реставрацию передних зубов в Мурманске? Посетите https://nova-51.ru/lechenie-zubov-murmansk/restavratsiya-perednikh-zubov-murmansk – если вы хотите улучшить улыбку, приходите в нашу клинику. Мы проведем эстетическую реставрацию ваших зубов с учетом индивидуальных особенностей и пожеланий. Мы поможем вам получить улыбку мечты.
Glennjaw · June 9, 2026 at 5:24 am
Этот информационный материал подробно освещает проблему наркозависимости, ее причины и последствия. Мы предлагаем информацию о методах лечения, профилактики и поддерживающих программах. Цель статьи — повысить осведомленность и продвигать идеи о необходимости борьбы с зависимостями.
Получить больше информации – прокапать от алкоголя нижний новгород
Stevenfes · June 9, 2026 at 5:30 am
В этом обзоре представлены различные методы избавления от зависимости, включая терапевтические и психологические подходы. Мы сравниваем их эффективность и предоставляем рекомендации для тех, кто хочет вернуться к трезвой жизни. Читатели смогут найти информацию о реабилитационных центрах и поддерживающих группах.
Переходите по ссылке ниже – помощь нарколога на дому
JavierJaf · June 9, 2026 at 5:35 am
Этот текст представляет собой обзор свежих данных и исследований в области медицины. Он призван помочь читателям понять, как научные достижения влияют на лечение, диагностику и общее состояние системы здравоохранения.
Ознакомиться с деталями – вывести из запоя в стационаре
https://raramuridesign.com/plugins/gsd/articles.php?bentonitovye_granuly_maksimalynaya_zaschita_ot_vlagi_html= · June 9, 2026 at 5:46 am
https://raramuridesign.com/plugins/gsd/articles.php?bentonitovye_granuly_maksimalynaya_zaschita_ot_vlagi_html=
https://www.altamira.edu.ec/profile/alimbjashworth86749/profile · June 9, 2026 at 5:47 am
https://www.altamira.edu.ec/profile/alimbjashworth86749/profile
Michaelunsem · June 9, 2026 at 6:15 am
Эта доказательная статья представляет собой глубокое погружение в успехи и вызовы лечения зависимостей. Мы обращаемся к научным исследованиям и опыту специалистов, чтобы предоставить читателям надежные данные об эффективности различных методик. Изучите, что работает лучше всего, и получите информацию от экспертов.
Уточнить детали – вывод из запоя недорого нарколог24
Nelsonscept · June 9, 2026 at 6:18 am
Статья посвящена анализу текущих трендов в медицине и их влиянию на жизнь людей. Мы рассмотрим новые технологии, методы лечения и значение профилактики в обеспечении долголетия и здоровья.
А что дальше? – можно вызвать нарколога домой
Davidtop · June 9, 2026 at 6:19 am
В этой статье мы рассматриваем разные способы борьбы с алкогольной зависимостью. Обсуждаются методы лечения, программы реабилитации и советы для поддержки близких. Читатели получат информацию о том, как преодолеть зависимость и добиться успешного выздоровления.
Где почитать поподробнее? – капельница против похмелья
EarnestZef · June 9, 2026 at 6:21 am
Публикация охватывает основные направления развития современной медицины. Мы обсудим значимость научных исследований, инноваций в лечении и роли общественного участия в формировании системы здравоохранения.
Интересует подробная информация – нарколог на дом цена нарколог 24
RichardBam · June 9, 2026 at 6:21 am
Этот краткий обзор предлагает сжатую информацию из области медицины, включая ключевые факты и последние новости. Мы стремимся сделать информацию доступной и понятной для широкой аудитории, что позволит читателям оставаться в курсе актуальных событий в здравоохранении.
Ознакомиться с отчётом – вызов нарколога на дом круглосуточно
Antonealere · June 9, 2026 at 6:26 am
Этот информационный материал подробно освещает проблему наркозависимости, ее причины и последствия. Мы предлагаем информацию о методах лечения, профилактики и поддерживающих программах. Цель статьи — повысить осведомленность и продвигать идеи о необходимости борьбы с зависимостями.
Читать дальше – капельница от запоя клиника
Ronaldwax · June 9, 2026 at 7:07 am
В этой статье мы обсудим процесс восстановления после зависимостей, акцентируя внимание на различных методах и подходах к реабилитации. Читатели узнают, как создать план выздоровления и использовать полезные ресурсы для достижения устойчивых изменений.
Всё самое вкусное внутри – капельница от похмелья нижний новгород
JosephIsopy · June 9, 2026 at 7:08 am
подробнее здесь трип скан официальный
WilliamMom · June 9, 2026 at 7:32 am
Расширенный обзор: https://l-parfum.ru/catalog/Chanel/coco/
https://craneflower.net/blogs/179109/ltimo-cdigo-promocional-de-1xBet-2026-ONEX777 · June 9, 2026 at 7:35 am
https://craneflower.net/blogs/179109/%C3%9Altimo-c%C3%B3digo-promocional-de-1xBet-2026-ONEX777
Michaelunsem · June 9, 2026 at 7:39 am
Этот информативный текст сочетает в себе темы здоровья и зависимости. Мы обсудим, как хронические заболевания могут усугубить зависимости и наоборот, как зависимость может влиять на общее состояние здоровья. Читатели получат представление о комплексном подходе к лечению как физического, так и психического состояния.
Это стоит прочитать полностью – вывода из запоя 24
RobertSkala · June 9, 2026 at 7:46 am
Сопутствующие патологии печени, почек, сердца или ЖКТ усугубляют последствия запоя. Без коррекции электролитного баланса и поддержки органов пациент рискует получить необратимые осложнения.
Исследовать вопрос подробнее – вывод из запоя
Brandonjainy · June 9, 2026 at 8:57 am
Текст посвящён распространённым мифам о зависимости и их развенчанию. Мы предоставим научно обоснованную информацию и дадим рекомендации по выбору эффективного способа борьбы с зависимым поведением.
Проследить причинно-следственные связи – выведение из запоя нижний новгород
PeterLem · June 9, 2026 at 9:01 am
В данной статье мы поговорим о будущем медицины, акцентируя внимание на прорывных разработках и их потенциале. Читатель узнает о новых подходах к лечению, роли искусственного интеллекта и возможностях персонализированной медицины.
Всё, что нужно знать – вывод из запоя врач на дом
JosephIsopy · June 9, 2026 at 9:20 am
Смотреть здесь https://tripscans74.group/
jomasKex · June 9, 2026 at 10:05 am
GRAND-DECOR выпускает гипсовую лепнину собственного производства: карнизы, розетки, молдинги, колонны и пилястры по доступным ценам. Ищете купить гипсовые карнизы в москве? На lepninaizgipsa.ru представлен полный каталог изделий с размерами и стоимостью от 210 рублей за погонный метр. Работа ведётся под ключ — от выбора декоративных элементов до профессионального монтажа с гарантией качества.
Jerrychund · June 9, 2026 at 10:09 am
В этой статье мы обсудим процесс восстановления после зависимостей, акцентируя внимание на различных методах и подходах к реабилитации. Читатели узнают, как создать план выздоровления и использовать полезные ресурсы для достижения устойчивых изменений.
Читать полностью – вывод из запоя на дому нижний новгород цена
kunafsDiene · June 9, 2026 at 10:13 am
Ищете запчасти для спецтехники по лучшей цене? Посетите сайт https://prom28.ru/ – интернет магазин Сервис Трак предлагает к продаже запчасти и оборудование для спецтехники, в том числе строительной, дорожной, инженерной, погрузочно-разгрузочной, грузо-перевозочной и т.д. Доставка по всей России.
Jamesreido · June 9, 2026 at 11:26 am
В этой статье рассматриваются способы преодоления зависимости и успешные истории людей, которые справились с этой проблемой. Мы обсудим важность поддержки со стороны близких и профессионалов, а также стратегии, которые могут помочь в процессе выздоровления. Научитесь первоочередным шагам к новой жизни.
Информация доступна здесь – прокапаться после запоя нижний новгород
Morriscrith · June 9, 2026 at 11:37 am
Этот обзор медицинских исследований собрал самое важное из последних публикаций в области медицины. Мы проанализировали ключевые находки и представили их в доступной форме, чтобы читатели могли легко ориентироваться в актуальных темах. Этот материал станет отличным подспорьем для изучения медицины.
Осуществить глубокий анализ – вывести из запоя капельница
Josephpex · June 9, 2026 at 11:51 am
Этот медицинский обзор сосредоточен на последних достижениях, которые оказывают влияние на пациентов и медицинскую практику. Мы разбираем инновационные методы лечения и исследований, акцентируя внимание на их значимости для общественного здоровья. Читатели узнают о свежих данных и их возможном применении.
Более того — здесь – clinica plus
Peteraxiop · June 9, 2026 at 12:33 pm
В данной публикации мы поговорим о процессе восстановления от зависимости, о том, как вернуть себе нормальную жизнь. Мы обсудим преодоление трудностей, значимость поддержки и наличие программ реабилитации. Читатели смогут узнать о ключевых шагах к успешному восстановлению.
Углубить понимание вопроса – кодировании sit
Glennjaw · June 9, 2026 at 12:49 pm
Статья посвящена анализу текущих трендов в медицине и их влиянию на жизнь людей. Мы рассмотрим новые технологии, методы лечения и значение профилактики в обеспечении долголетия и здоровья.
Получить дополнительную информацию – капельница от алкоголя нижний новгород
Williamshigo · June 9, 2026 at 12:54 pm
Этот информативный текст сочетает в себе темы здоровья и зависимости. Мы обсудим, как хронические заболевания могут усугубить зависимости и наоборот, как зависимость может влиять на общее состояние здоровья. Читатели получат представление о комплексном подходе к лечению как физического, так и психического состояния.
Лучшее решение — прямо здесь – наркологическая клиника в твери
Sign Up · June 9, 2026 at 1:02 pm
I don’t think the title of your article matches the content lol. Just kidding, mainly because I had some doubts after reading the article.
Frankbop · June 9, 2026 at 1:22 pm
В статье по вопросам здоровья мы рассматриваем актуальные проблемы, с которыми сталкивается общество. Обсуждаются заболевания, факторы риска и важные аспекты профилактики. Читатели получат полезные советы о том, как сохранить здоровье и улучшить качество жизни.
Подробности по ссылке – клиника плюс тверь
Morriscrith · June 9, 2026 at 1:58 pm
Этот обзор медицинских исследований собрал самое важное из последних публикаций в области медицины. Мы проанализировали ключевые находки и представили их в доступной форме, чтобы читатели могли легко ориентироваться в актуальных темах. Этот материал станет отличным подспорьем для изучения медицины.
Жми сюда — получишь ответ – вывод из запоя цены нижний новгород
Stevenfes · June 9, 2026 at 2:15 pm
Публикация охватывает основные направления развития современной медицины. Мы обсудим значимость научных исследований, инноваций в лечении и роли общественного участия в формировании системы здравоохранения.
Осуществить глубокий анализ – срочная наркологическая помощь на дому
Frankbop · June 9, 2026 at 2:17 pm
В статье по вопросам здоровья мы рассматриваем актуальные проблемы, с которыми сталкивается общество. Обсуждаются заболевания, факторы риска и важные аспекты профилактики. Читатели получат полезные советы о том, как сохранить здоровье и улучшить качество жизни.
Изучите внимательнее – закодированию от алкоголя
FrankDes · June 9, 2026 at 2:42 pm
веб-сайте vodkabet
Lewiscog · June 9, 2026 at 2:51 pm
Эта статья подробно расскажет о процессе выздоровления, который включает в себя эмоциональную, физическую и психологическую реабилитацию. Мы обсуждаем значимость поддержки и наличие профессиональных программ. Читатели узнают, как строить новую жизнь и не возвращаться к старым привычкам.
Узнать из первых рук – Частный вытрезвитель в Твери
Ronaldwax · June 9, 2026 at 2:59 pm
В этом исследовании рассмотрены методы лечения зависимостей и их эффективность. Мы проанализируем различные подходы, используемые в реабилитационных центрах, и представим данные о результативности программ. Читатели получат надежные и научно обоснованные сведения о данной проблеме.
Практические советы ждут тебя – капельница от похмелья цена
hackmd.okfn.de · June 9, 2026 at 3:14 pm
hackmd.okfn.de
RandyLep · June 9, 2026 at 3:16 pm
В этой статье мы рассматриваем разрушительное влияние зависимости на жизнь человека. Обсуждаются аспекты, такие как здоровье, отношения и профессиональные достижения. Читатели узнают о необходимости обращения за помощью и о путях к восстановлению.
Переходите по ссылке ниже – поставить капельницу от запоя
Williamwer · June 9, 2026 at 3:21 pm
В этой публикации мы предложим ряд рекомендаций по избавлению от зависимостей и успешному восстановлению. Мы обсудим методы привлечения поддержки и важность самосознания. Эти советы помогут людям вернуться к нормальной жизни и стать на путь выздоровления.
Практические советы ждут тебя – капельница от запоя анонимно
Lewiscog · June 9, 2026 at 3:27 pm
Этот обзор медицинских исследований собрал самое важное из последних публикаций в области медицины. Мы проанализировали ключевые находки и представили их в доступной форме, чтобы читатели могли легко ориентироваться в актуальных темах. Этот материал станет отличным подспорьем для изучения медицины.
Что скрывают от вас? – анонимный частный вытрезвитель
https://comunitat.canodrom.barcelona/profiles/codigode1xbet/activity?locale=en · June 9, 2026 at 4:03 pm
https://comunitat.canodrom.barcelona/profiles/codigode1xbet/activity?locale=en
WinstonWaift · June 9, 2026 at 4:24 pm
В этой статье мы подробно рассматриваем проверенные методы борьбы с зависимостями, включая психотерапию, медикаментозное лечение и поддержку со стороны общества. Мы акцентируем внимание на важности комплексного подхода и возможности успешного восстановления для людей, столкнувшихся с этой проблемой.
Обратитесь за информацией – клиника плюс
FrankDes · June 9, 2026 at 4:29 pm
Узнать больше водкабет казино
Orvaljed · June 9, 2026 at 4:39 pm
В этой статье мы рассмотрим современные достижения в области медицины, включая инновационные методы лечения и диагностики. Мы обсудим важность профилактики заболеваний и роль технологий в улучшении качества здравоохранения. Читатели узнают о влиянии медицины на повседневную жизнь и ее значение для современного общества.
Получить исчерпывающие сведения – капельница на дому сколько стоит
https://mulaibaru.id/codigo-promocional-de-1xbet-el-salvador-2026-onex777/ · June 9, 2026 at 4:51 pm
https://mulaibaru.id/codigo-promocional-de-1xbet-el-salvador-2026-onex777/
Vernonmorge · June 9, 2026 at 4:53 pm
Этот текст посвящён сложным аспектам зависимости и её влиянию на жизнь человека. Мы обсудим психологические, физические и социальные последствия зависимого поведения, а также важность своевременного обращения за помощью.
Выяснить больше – вывод из запоя на дому цена
Francisimpob · June 9, 2026 at 4:54 pm
Мы рассмотрим современные вызовы здравоохранения и пути их решения с помощью технологий и научных исследований. В статье собраны данные о новых лекарствах, методах диагностики и системном подходе к улучшению здоровья населения.
Осуществить глубокий анализ – Ультарбыстрая детоксикация
Brandonjainy · June 9, 2026 at 5:14 pm
Текст посвящён распространённым мифам о зависимости и их развенчанию. Мы предоставим научно обоснованную информацию и дадим рекомендации по выбору эффективного способа борьбы с зависимым поведением.
Ознакомиться с теоретической базой – вызвать капельницу от запоя на дому
Orvaljed · June 9, 2026 at 5:19 pm
В этой статье мы рассмотрим современные достижения в области медицины, включая инновационные методы лечения и диагностики. Мы обсудим важность профилактики заболеваний и роль технологий в улучшении качества здравоохранения. Читатели узнают о влиянии медицины на повседневную жизнь и ее значение для современного общества.
Полная информация здесь – капельница на дому от запоя
PeterLem · June 9, 2026 at 5:31 pm
В статье по вопросам здоровья мы рассматриваем актуальные проблемы, с которыми сталкивается общество. Обсуждаются заболевания, факторы риска и важные аспекты профилактики. Читатели получат полезные советы о том, как сохранить здоровье и улучшить качество жизни.
Погрузиться в детали – лечение алкоголизма на дому цена
Thomastix · June 9, 2026 at 5:39 pm
В этой статье мы говорим о важности поддержки в процессе выздоровления. Рассматриваются семьи, группы поддержки, специалисты и онлайн-ресурсы, которые могут сыграть решающую роль в избавлении от зависимости.
Интересует подробная информация – вывод из запоя дешево самара
Francisimpob · June 9, 2026 at 5:45 pm
В данной публикации мы поговорим о процессе восстановления от зависимости, о том, как вернуть себе нормальную жизнь. Мы обсудим преодоление трудностей, значимость поддержки и наличие программ реабилитации. Читатели смогут узнать о ключевых шагах к успешному восстановлению.
Изучить рекомендации специалистов – клиника плюс тверь
RobertCer · June 9, 2026 at 6:42 pm
Эта статья подробно расскажет о процессе выздоровления, который включает в себя эмоциональную, физическую и психологическую реабилитацию. Мы обсуждаем значимость поддержки и наличие профессиональных программ. Читатели узнают, как строить новую жизнь и не возвращаться к старым привычкам.
Раскрыть тему полностью – вывод из запоя на дому самара цены
Jerrychund · June 9, 2026 at 6:55 pm
Эта публикация посвящена актуальным вопросам современной медицины и здравоохранения. Мы обсудим новейшие технологии диагностики и лечения, а также их влияние на продолжительность и качество жизни. Читатель найдет здесь информацию о научных исследованиях и перспективных разработках, доступно изложенную для широкой аудитории.
Ознакомьтесь поближе – вызвать капельницу от запоя на дому
AlbertDen · June 9, 2026 at 7:56 pm
Этот информативный текст сочетает в себе темы здоровья и зависимости. Мы обсудим, как хронические заболевания могут усугубить зависимости и наоборот, как зависимость может влиять на общее состояние здоровья. Читатели получат представление о комплексном подходе к лечению как физического, так и психического состояния.
Продолжить изучение – откапаться на дому от алкоголизма
JesseALure · June 9, 2026 at 8:02 pm
Читатели получат представление о том, как современные технологии влияют на развитие медицины. Обсуждаются новые методы лечения, персонализированный подход и роль цифровых решений в повышении качества медицинских услуг.
Изучить вопрос глубже – выведение из запоя воронеж
Michaelhem · June 9, 2026 at 8:08 pm
Планируете выездное мероприятие? кофе брейк профессиональная организация выездного питания для свадеб, корпоративов, конференций и частных мероприятий. Разработка меню, приготовление блюд, доставка, сервировка и обслуживание гостей. Полный комплекс услуг для событий любого масштаба.
Harrislep · June 9, 2026 at 8:19 pm
Этот обзор посвящен успешным стратегиям избавления от зависимости, включая реальные примеры и советы. Мы разоблачим мифы и предоставим читателям достоверную информацию о различных подходах. Получите опыт многообразия методов и найдите подходящий способ для себя!
Нажмите, чтобы узнать больше – вызов нарколога на дом
JulesOmido · June 9, 2026 at 8:33 pm
В этой статье мы обсудим процесс восстановления после зависимостей, акцентируя внимание на различных методах и подходах к реабилитации. Читатели узнают, как создать план выздоровления и использовать полезные ресурсы для достижения устойчивых изменений.
Только факты! – tver clinica plus
AlbertDen · June 9, 2026 at 8:46 pm
Эта публикация обращает внимание на важность профилактики зависимостей. Мы обсудим, как осведомленность и образование могут помочь в предотвращении возникновения зависимости. Читатели смогут ознакомиться с полезными советами и ресурсами, которые способствуют здоровому образу жизни.
Получить больше информации – вывод из запоя капельница
Martysib · June 9, 2026 at 8:47 pm
В этой публикации мы рассматриваем важную тему борьбы с зависимостями, включая алкогольную и наркотическую зависимости. Мы обсудим методы лечения, реабилитации и поддержку, которые могут помочь людям, столкнувшимся с этой проблемой. Читатели узнают о перспективах выздоровления и важности комплексного подхода.
Смотрите также – капельница от запоя анонимно
Martysib · June 9, 2026 at 9:50 pm
В этой публикации мы рассматриваем важную тему борьбы с зависимостями, включая алкогольную и наркотическую зависимости. Мы обсудим методы лечения, реабилитации и поддержку, которые могут помочь людям, столкнувшимся с этой проблемой. Читатели узнают о перспективах выздоровления и важности комплексного подхода.
Есть чему поучиться – вывод из запоя на дому цена нижний новгород
Darryldroff · June 9, 2026 at 9:54 pm
В этой статье рассматриваются актуальные вопросы, связанные с развитием медицинской науки и её внедрением в повседневную практику. Особое внимание уделено вопросам профилактики, ранней диагностики и использованию технологий для улучшения здоровья человека.
Расширить кругозор по теме – вывод из запоя на дому нижний
JordanPsync · June 9, 2026 at 9:56 pm
Эта информационная публикация освещает широкий спектр тем из мира медицины. Мы предлагаем читателям ясные и понятные объяснения современных заболеваний, методов профилактики и лечения. Информация будет полезна как пациентам, так и медицинским работникам, желающим поддержать уровень своих знаний.
Не пропусти важное – клиника плюс
xaredtrine · June 9, 2026 at 10:27 pm
Book a private transfer from Thessaloniki Airport online at https://thessaloniki-taxi.gr/ – we offer fixed prices, free child seats, licensed drivers, new vehicles, and instant booking confirmation. Discover all our benefits on our website.
Peteraxiop · June 9, 2026 at 10:44 pm
Публикация посвящена жизненным историям людей, успешно справившихся с зависимостью. Мы покажем, что выход есть, и он начинается с первого шага — принятия проблемы и желания измениться.
Исследовать вопрос подробнее – tver clinica plus
Clintastom · June 9, 2026 at 10:44 pm
Мечтаешь о незабываемом отпуске? https://karta-abhazii.ru где величественные горы встречаются с бескрайним морем, а история оживает на каждом шагу, добро пожаловать в Абхазию!
Keithenepe · June 9, 2026 at 10:50 pm
тараканы дезинфекция гарантия сайт
KennethCib · June 9, 2026 at 11:17 pm
В данном материале представлены ключевые тенденции в сфере медицинской науки и практики. Вы узнаете о последних открытиях, инновационных подходах к терапии и важности профилактики заболеваний. Особое внимание уделено практическому применению новых методов в клинической практике.
Изучите внимательнее – клиника плюс тверь
https://www.qishuiyinyue-zh.com · June 9, 2026 at 11:21 pm
Next time I read a blog, I hope that it won’t fail me just as much as this particular one. I mean, Yes, it was my choice to read through, however I actually believed you would probably have something useful to talk about. All I hear is a bunch of whining about something you can fix if you were not too busy looking for attention.
Josephpex · June 9, 2026 at 11:31 pm
В этой статье рассматриваются различные аспекты избавления от зависимости, включая физические и психологические методы. Мы обсудим поддержку, мотивацию и стратегии, которые помогут в процессе выздоровления. Читатели узнают, как преодолеть трудности и двигаться к новой жизни без зависимости.
Смотрите также… – tver clinica plus
Ismaelsop · June 10, 2026 at 12:15 am
В статье по вопросам здоровья мы рассматриваем актуальные проблемы, с которыми сталкивается общество. Обсуждаются заболевания, факторы риска и важные аспекты профилактики. Читатели получат полезные советы о том, как сохранить здоровье и улучшить качество жизни.
Познакомиться с результатами исследований – вывести из запоя на дому
fixDiele · June 10, 2026 at 12:20 am
Особенно понравился материал про Хронометраж матчевого дня: за кулисами футбольных событий.
Ссылка ниже:
https://arsenallive.ru
fixDiele · June 10, 2026 at 12:24 am
По теме “Свежие новости и аналитика MMA”, там просто кладезь информации.
Вот, можете почитать:
https://mma-top.ru
diwikoTalay · June 10, 2026 at 1:09 am
Три ключевые угрозы современного интернета — реклама, слежка и цензура — AdGuard нейтрализует одновременно. Сервис предлагает VPN с надёжным шифрованием, блокировщик рекламы и DNS-защиту для всех устройств. Ищете промокод адгвард впн? Подключиться легко — достаточно перейти на adsguard.ru воспользоваться промокодом и сэкономить на подписке. Весь трафик идёт по зашифрованному каналу, надёжно защищая личную информацию от провайдеров и трекеров. Работает на всех популярных платформах: Windows, Android, iOS и Mac.